User login
Memorial and honorary gifts: a special tribute
Did you know you can honor a family member, friend, or colleague whose life has been touched by GI research through a gift to the AGA Research Foundation? Your gift will honor a loved one or yourself and support the AGA Research Awards Program, while giving you a tax benefit.
• Giving now or later. Any charitable gift can be made in honor or memory of someone.
• A gift today. An outright gift will help fund the AGA Research Awards Program. Your gift will assist in furthering basic digestive disease research, which can ultimately advance research into all digestive diseases. The financial benefits include an income tax deduction and possible elimination of capital gains tax. A cash gift of $25,000 or more qualifies for membership in the AGA Legacy Society, which recognizes the foundation’s most generous individual donors.
• A gift through your will or living trust. You can include a bequest in your will or living trust stating that a specific asset, certain dollar amount, or more commonly a percentage of your estate will pass to the AGA Research Foundation at your death in honor of your loved one. A bequest gift of $50,000 or more qualifies for membership in the AGA Legacy Society.
• Named funds. A named fund, which can be named to honor or memorialize a loved one, can be established with a minimum gift of $100,000 over the course of 5 years or through an estate gift. Gifts of cash, appreciated securities, life insurance, or property are gift vehicles that may be used to establish a fund. Donors receive a tax deduction at the time a fund is established and when additional contributions are made to the fund. Because the principal remains intact, the fund will support our mission in perpetuity. The larger the fund, the more impact it has on the program it is designed to benefit.
Your next step
An honorary gift is a wonderful way to acknowledge someone’s vision for the future. To learn more about ways to recognize your honoree, visit our website at www.gastro.org/contribute or contact Stacey Hinton Tuneski at 301-222-4005 or [email protected].
Did you know you can honor a family member, friend, or colleague whose life has been touched by GI research through a gift to the AGA Research Foundation? Your gift will honor a loved one or yourself and support the AGA Research Awards Program, while giving you a tax benefit.
• Giving now or later. Any charitable gift can be made in honor or memory of someone.
• A gift today. An outright gift will help fund the AGA Research Awards Program. Your gift will assist in furthering basic digestive disease research, which can ultimately advance research into all digestive diseases. The financial benefits include an income tax deduction and possible elimination of capital gains tax. A cash gift of $25,000 or more qualifies for membership in the AGA Legacy Society, which recognizes the foundation’s most generous individual donors.
• A gift through your will or living trust. You can include a bequest in your will or living trust stating that a specific asset, certain dollar amount, or more commonly a percentage of your estate will pass to the AGA Research Foundation at your death in honor of your loved one. A bequest gift of $50,000 or more qualifies for membership in the AGA Legacy Society.
• Named funds. A named fund, which can be named to honor or memorialize a loved one, can be established with a minimum gift of $100,000 over the course of 5 years or through an estate gift. Gifts of cash, appreciated securities, life insurance, or property are gift vehicles that may be used to establish a fund. Donors receive a tax deduction at the time a fund is established and when additional contributions are made to the fund. Because the principal remains intact, the fund will support our mission in perpetuity. The larger the fund, the more impact it has on the program it is designed to benefit.
Your next step
An honorary gift is a wonderful way to acknowledge someone’s vision for the future. To learn more about ways to recognize your honoree, visit our website at www.gastro.org/contribute or contact Stacey Hinton Tuneski at 301-222-4005 or [email protected].
Did you know you can honor a family member, friend, or colleague whose life has been touched by GI research through a gift to the AGA Research Foundation? Your gift will honor a loved one or yourself and support the AGA Research Awards Program, while giving you a tax benefit.
• Giving now or later. Any charitable gift can be made in honor or memory of someone.
• A gift today. An outright gift will help fund the AGA Research Awards Program. Your gift will assist in furthering basic digestive disease research, which can ultimately advance research into all digestive diseases. The financial benefits include an income tax deduction and possible elimination of capital gains tax. A cash gift of $25,000 or more qualifies for membership in the AGA Legacy Society, which recognizes the foundation’s most generous individual donors.
• A gift through your will or living trust. You can include a bequest in your will or living trust stating that a specific asset, certain dollar amount, or more commonly a percentage of your estate will pass to the AGA Research Foundation at your death in honor of your loved one. A bequest gift of $50,000 or more qualifies for membership in the AGA Legacy Society.
• Named funds. A named fund, which can be named to honor or memorialize a loved one, can be established with a minimum gift of $100,000 over the course of 5 years or through an estate gift. Gifts of cash, appreciated securities, life insurance, or property are gift vehicles that may be used to establish a fund. Donors receive a tax deduction at the time a fund is established and when additional contributions are made to the fund. Because the principal remains intact, the fund will support our mission in perpetuity. The larger the fund, the more impact it has on the program it is designed to benefit.
Your next step
An honorary gift is a wonderful way to acknowledge someone’s vision for the future. To learn more about ways to recognize your honoree, visit our website at www.gastro.org/contribute or contact Stacey Hinton Tuneski at 301-222-4005 or [email protected].
Apply for AGA’s Tech Summit Shark Tank
Physician entrepreneurs and innovators are invited to apply for the Shark Tank session at the 2016 AGA Tech Summit. Selected participants will receive valuable feedback from a panel of business development leaders, investors, established entrepreneurs, and other strategic partners.
Each participant will be given 5 minutes to present their GI-related innovation or technology. Selection is competitive and is limited to only five slots. Applications must be received no later than Feb. 16, 2016. If an applicant is selected, registration fees will be waived. However, participants will be responsible for their own travel and lodging costs.
Apply for the Shark Tank today at www.gastro.org/techsummit.
The AGA Tech Summit was developed in collaboration with the Society of American Gastrointestinal and Endoscopic Surgeons.
Physician entrepreneurs and innovators are invited to apply for the Shark Tank session at the 2016 AGA Tech Summit. Selected participants will receive valuable feedback from a panel of business development leaders, investors, established entrepreneurs, and other strategic partners.
Each participant will be given 5 minutes to present their GI-related innovation or technology. Selection is competitive and is limited to only five slots. Applications must be received no later than Feb. 16, 2016. If an applicant is selected, registration fees will be waived. However, participants will be responsible for their own travel and lodging costs.
Apply for the Shark Tank today at www.gastro.org/techsummit.
The AGA Tech Summit was developed in collaboration with the Society of American Gastrointestinal and Endoscopic Surgeons.
Physician entrepreneurs and innovators are invited to apply for the Shark Tank session at the 2016 AGA Tech Summit. Selected participants will receive valuable feedback from a panel of business development leaders, investors, established entrepreneurs, and other strategic partners.
Each participant will be given 5 minutes to present their GI-related innovation or technology. Selection is competitive and is limited to only five slots. Applications must be received no later than Feb. 16, 2016. If an applicant is selected, registration fees will be waived. However, participants will be responsible for their own travel and lodging costs.
Apply for the Shark Tank today at www.gastro.org/techsummit.
The AGA Tech Summit was developed in collaboration with the Society of American Gastrointestinal and Endoscopic Surgeons.
Catch the next wave in science, medicine at DDW® 2016
Early bird registration (www.xpressreg.net/register/ddwk0516/attendee/landing.asp?hkey=&ea=&sc=&iq) and housing for Digestive Disease Week® (DDW) 2016 are now open. Register by April 6 to save at least $75 on your registration, receive additional discounts on the sponsoring societies’ courses, and book your hotel.
DDW On Demand (www.ddw.org/attendees/maximize-your-experience/ddw-on-demand), an online-only library that will include nearly 450 hours of nonticketed presentations from DDW 2016, is once again included in the cost of registration.
Registration is also now open for the 2016 AGA Postgraduate Course: Cognitive and Technical Skills for the Gastroenterologist. The course, which is scheduled for May 21 and 22, features six general sessions, 13 clinical challenge sessions, and 12 lunch breakout sessions that will teach you critical updates for 2016. This live activity will be eligible for a maximum of 11.5 AMA PRA Category 1 Credits™.
Additional details, including the program agenda and learning objectives, are available online at www. gastro.org/in-person/2015/10/27/2016-aga-postgraduate-course.
Early bird registration (www.xpressreg.net/register/ddwk0516/attendee/landing.asp?hkey=&ea=&sc=&iq) and housing for Digestive Disease Week® (DDW) 2016 are now open. Register by April 6 to save at least $75 on your registration, receive additional discounts on the sponsoring societies’ courses, and book your hotel.
DDW On Demand (www.ddw.org/attendees/maximize-your-experience/ddw-on-demand), an online-only library that will include nearly 450 hours of nonticketed presentations from DDW 2016, is once again included in the cost of registration.
Registration is also now open for the 2016 AGA Postgraduate Course: Cognitive and Technical Skills for the Gastroenterologist. The course, which is scheduled for May 21 and 22, features six general sessions, 13 clinical challenge sessions, and 12 lunch breakout sessions that will teach you critical updates for 2016. This live activity will be eligible for a maximum of 11.5 AMA PRA Category 1 Credits™.
Additional details, including the program agenda and learning objectives, are available online at www. gastro.org/in-person/2015/10/27/2016-aga-postgraduate-course.
Early bird registration (www.xpressreg.net/register/ddwk0516/attendee/landing.asp?hkey=&ea=&sc=&iq) and housing for Digestive Disease Week® (DDW) 2016 are now open. Register by April 6 to save at least $75 on your registration, receive additional discounts on the sponsoring societies’ courses, and book your hotel.
DDW On Demand (www.ddw.org/attendees/maximize-your-experience/ddw-on-demand), an online-only library that will include nearly 450 hours of nonticketed presentations from DDW 2016, is once again included in the cost of registration.
Registration is also now open for the 2016 AGA Postgraduate Course: Cognitive and Technical Skills for the Gastroenterologist. The course, which is scheduled for May 21 and 22, features six general sessions, 13 clinical challenge sessions, and 12 lunch breakout sessions that will teach you critical updates for 2016. This live activity will be eligible for a maximum of 11.5 AMA PRA Category 1 Credits™.
Additional details, including the program agenda and learning objectives, are available online at www. gastro.org/in-person/2015/10/27/2016-aga-postgraduate-course.
MRD test can predict AML relapse

Photo by William Weinert
A test measuring minimal residual disease (MRD) can help predict relapse in patients with acute myeloid leukemia (AML), according to a study published in NEJM.
Investigators used the test to detect MRD in samples from patients with NPM1-mutated AML who were deemed standard-risk by conventional methods.
The team said the presence of MRD after treatment provided powerful prognostic information independent of other risk factors.
“What we have been able to identify is a group of patients who otherwise would be thought to do quite well, who, in fact, have a very poor prognosis, and who are not well served currently,” said study author Robert Hills, DPhil, of Cardiff University School of Medicine in the UK.
“This opens up the exciting prospect that we can do the same for other groups of patients as well.”
For this study, Dr Hills and his colleagues used a reverse-transcriptase quantitative polymerase-chain-reaction assay to detect MRD in 2569 samples (902 bone marrow samples and 1667 peripheral blood samples) from 346 patients with NPM1-mutated AML.
The patients had received 2 cycles of chemotherapy as part of the National Cancer Research Institute AML17 trial. They were treated at centers in the UK, Denmark, and New Zealand. All patients were shown to be at standard risk of relapse using conventional tests.
The investigators found that NPM1-mutated transcripts persisted in the blood of 15% of patients after the second cycle of chemotherapy.
This finding was associated with a greater risk of relapse after 3 years of follow-up.
Eighty-two percent of patients with NPM1-mutated transcripts had relapsed within 3 years, compared to 30% of patients who had no detectable NPM1. The hazard ratio was 4.80 (P<0.001).
Patients with traces of NPM1 also had a lower rate of survival—24%, compared to 75% for patients without detectable NPM1. The hazard ratio was 4.38 (P<0.001).
In multivariate analysis, the presence of MRD was the only significant prognostic factor for relapse or death. The hazard ratios were 5.09 and 4.84, respectively (P<0.001 for both).
The investigators validated these findings in a cohort of 91 patients with NPM1-mutated AML.
The presence of MRD in the blood of these patients was associated with a higher cumulative incidence of relapse—70% vs 31% (P=0.001)—and a lower rate of survival—40% vs 87% (P=0.001)—at 2 years.
The investigators also found that, with sequential monitoring of MRD, a rising level of NPM1-mutated transcripts could predict relapse.
“Conventional methods for guiding treatment for this aggressive type of leukemia are inadequate,” said study author David Grimwade, PhD, of King’s College London in the UK.
“The MRD test is an invaluable tool to assess treatment response and identify those patients for whom chemotherapy is not sufficient and require stem cell transplantation or new treatments.” ![]()

Photo by William Weinert
A test measuring minimal residual disease (MRD) can help predict relapse in patients with acute myeloid leukemia (AML), according to a study published in NEJM.
Investigators used the test to detect MRD in samples from patients with NPM1-mutated AML who were deemed standard-risk by conventional methods.
The team said the presence of MRD after treatment provided powerful prognostic information independent of other risk factors.
“What we have been able to identify is a group of patients who otherwise would be thought to do quite well, who, in fact, have a very poor prognosis, and who are not well served currently,” said study author Robert Hills, DPhil, of Cardiff University School of Medicine in the UK.
“This opens up the exciting prospect that we can do the same for other groups of patients as well.”
For this study, Dr Hills and his colleagues used a reverse-transcriptase quantitative polymerase-chain-reaction assay to detect MRD in 2569 samples (902 bone marrow samples and 1667 peripheral blood samples) from 346 patients with NPM1-mutated AML.
The patients had received 2 cycles of chemotherapy as part of the National Cancer Research Institute AML17 trial. They were treated at centers in the UK, Denmark, and New Zealand. All patients were shown to be at standard risk of relapse using conventional tests.
The investigators found that NPM1-mutated transcripts persisted in the blood of 15% of patients after the second cycle of chemotherapy.
This finding was associated with a greater risk of relapse after 3 years of follow-up.
Eighty-two percent of patients with NPM1-mutated transcripts had relapsed within 3 years, compared to 30% of patients who had no detectable NPM1. The hazard ratio was 4.80 (P<0.001).
Patients with traces of NPM1 also had a lower rate of survival—24%, compared to 75% for patients without detectable NPM1. The hazard ratio was 4.38 (P<0.001).
In multivariate analysis, the presence of MRD was the only significant prognostic factor for relapse or death. The hazard ratios were 5.09 and 4.84, respectively (P<0.001 for both).
The investigators validated these findings in a cohort of 91 patients with NPM1-mutated AML.
The presence of MRD in the blood of these patients was associated with a higher cumulative incidence of relapse—70% vs 31% (P=0.001)—and a lower rate of survival—40% vs 87% (P=0.001)—at 2 years.
The investigators also found that, with sequential monitoring of MRD, a rising level of NPM1-mutated transcripts could predict relapse.
“Conventional methods for guiding treatment for this aggressive type of leukemia are inadequate,” said study author David Grimwade, PhD, of King’s College London in the UK.
“The MRD test is an invaluable tool to assess treatment response and identify those patients for whom chemotherapy is not sufficient and require stem cell transplantation or new treatments.” ![]()

Photo by William Weinert
A test measuring minimal residual disease (MRD) can help predict relapse in patients with acute myeloid leukemia (AML), according to a study published in NEJM.
Investigators used the test to detect MRD in samples from patients with NPM1-mutated AML who were deemed standard-risk by conventional methods.
The team said the presence of MRD after treatment provided powerful prognostic information independent of other risk factors.
“What we have been able to identify is a group of patients who otherwise would be thought to do quite well, who, in fact, have a very poor prognosis, and who are not well served currently,” said study author Robert Hills, DPhil, of Cardiff University School of Medicine in the UK.
“This opens up the exciting prospect that we can do the same for other groups of patients as well.”
For this study, Dr Hills and his colleagues used a reverse-transcriptase quantitative polymerase-chain-reaction assay to detect MRD in 2569 samples (902 bone marrow samples and 1667 peripheral blood samples) from 346 patients with NPM1-mutated AML.
The patients had received 2 cycles of chemotherapy as part of the National Cancer Research Institute AML17 trial. They were treated at centers in the UK, Denmark, and New Zealand. All patients were shown to be at standard risk of relapse using conventional tests.
The investigators found that NPM1-mutated transcripts persisted in the blood of 15% of patients after the second cycle of chemotherapy.
This finding was associated with a greater risk of relapse after 3 years of follow-up.
Eighty-two percent of patients with NPM1-mutated transcripts had relapsed within 3 years, compared to 30% of patients who had no detectable NPM1. The hazard ratio was 4.80 (P<0.001).
Patients with traces of NPM1 also had a lower rate of survival—24%, compared to 75% for patients without detectable NPM1. The hazard ratio was 4.38 (P<0.001).
In multivariate analysis, the presence of MRD was the only significant prognostic factor for relapse or death. The hazard ratios were 5.09 and 4.84, respectively (P<0.001 for both).
The investigators validated these findings in a cohort of 91 patients with NPM1-mutated AML.
The presence of MRD in the blood of these patients was associated with a higher cumulative incidence of relapse—70% vs 31% (P=0.001)—and a lower rate of survival—40% vs 87% (P=0.001)—at 2 years.
The investigators also found that, with sequential monitoring of MRD, a rising level of NPM1-mutated transcripts could predict relapse.
“Conventional methods for guiding treatment for this aggressive type of leukemia are inadequate,” said study author David Grimwade, PhD, of King’s College London in the UK.
“The MRD test is an invaluable tool to assess treatment response and identify those patients for whom chemotherapy is not sufficient and require stem cell transplantation or new treatments.” ![]()
Caprini Score Accurately Predicts Risk of Venous Thromboembolism in Critically Ill Surgical Patients
Clinical question: Is the Caprini risk assessment model (RAM) a valid tool to predict venous thromboembolism (VTE) risk in critically ill surgical patients?
Background: VTE is a major source of morbidity and mortality among hospitalized patients; prevention is critical to reduce morbidity and cut healthcare costs. Risk assessment is important to determine thromboprophylaxis, yet data are lacking regarding an appropriate tool for risk stratification in the critically ill.
Study design: Retrospective cohort.
Setting: University of Michigan Health System; 20-bed surgical ICU at an academic hospital.
Synopsis: This study included 4,844 surgical ICU patients. Primary outcome was VTE during the patient’s hospital admission. A retrospective risk scoring method based on the 2005 Caprini RAM was used to calculate the risk for all patients at the time of ICU admission. Patients were divided into low (Caprini score 0–2), moderate, high, highest, and super-high (Caprini score > 8) risk levels. The incidence of VTE increased in linear fashion with increasing Caprini score.
This study was limited to one academic medical center. The retrospective scoring model limits the ability to identify all patient risk factors. VTE outcomes were reported only for the length of hospitalization and did not include post-discharge follow-up. Replicating this study across a larger patient population and performing a prospective study with follow-up after discharge would address these limitations.
Bottom line: The Caprini risk assessment model is a valid instrument to assess VTE risk in critically ill surgical patients.
Citation: Obi AT, Pannucci CJ, Nackashi A, et al. Validation of the Caprini venous thromboembolism risk assessment model in critically ill surgical patients. JAMA Surg. 2015;150(10):941-948.
Clinical question: Is the Caprini risk assessment model (RAM) a valid tool to predict venous thromboembolism (VTE) risk in critically ill surgical patients?
Background: VTE is a major source of morbidity and mortality among hospitalized patients; prevention is critical to reduce morbidity and cut healthcare costs. Risk assessment is important to determine thromboprophylaxis, yet data are lacking regarding an appropriate tool for risk stratification in the critically ill.
Study design: Retrospective cohort.
Setting: University of Michigan Health System; 20-bed surgical ICU at an academic hospital.
Synopsis: This study included 4,844 surgical ICU patients. Primary outcome was VTE during the patient’s hospital admission. A retrospective risk scoring method based on the 2005 Caprini RAM was used to calculate the risk for all patients at the time of ICU admission. Patients were divided into low (Caprini score 0–2), moderate, high, highest, and super-high (Caprini score > 8) risk levels. The incidence of VTE increased in linear fashion with increasing Caprini score.
This study was limited to one academic medical center. The retrospective scoring model limits the ability to identify all patient risk factors. VTE outcomes were reported only for the length of hospitalization and did not include post-discharge follow-up. Replicating this study across a larger patient population and performing a prospective study with follow-up after discharge would address these limitations.
Bottom line: The Caprini risk assessment model is a valid instrument to assess VTE risk in critically ill surgical patients.
Citation: Obi AT, Pannucci CJ, Nackashi A, et al. Validation of the Caprini venous thromboembolism risk assessment model in critically ill surgical patients. JAMA Surg. 2015;150(10):941-948.
Clinical question: Is the Caprini risk assessment model (RAM) a valid tool to predict venous thromboembolism (VTE) risk in critically ill surgical patients?
Background: VTE is a major source of morbidity and mortality among hospitalized patients; prevention is critical to reduce morbidity and cut healthcare costs. Risk assessment is important to determine thromboprophylaxis, yet data are lacking regarding an appropriate tool for risk stratification in the critically ill.
Study design: Retrospective cohort.
Setting: University of Michigan Health System; 20-bed surgical ICU at an academic hospital.
Synopsis: This study included 4,844 surgical ICU patients. Primary outcome was VTE during the patient’s hospital admission. A retrospective risk scoring method based on the 2005 Caprini RAM was used to calculate the risk for all patients at the time of ICU admission. Patients were divided into low (Caprini score 0–2), moderate, high, highest, and super-high (Caprini score > 8) risk levels. The incidence of VTE increased in linear fashion with increasing Caprini score.
This study was limited to one academic medical center. The retrospective scoring model limits the ability to identify all patient risk factors. VTE outcomes were reported only for the length of hospitalization and did not include post-discharge follow-up. Replicating this study across a larger patient population and performing a prospective study with follow-up after discharge would address these limitations.
Bottom line: The Caprini risk assessment model is a valid instrument to assess VTE risk in critically ill surgical patients.
Citation: Obi AT, Pannucci CJ, Nackashi A, et al. Validation of the Caprini venous thromboembolism risk assessment model in critically ill surgical patients. JAMA Surg. 2015;150(10):941-948.
Total Knee Replacement Superior to Non-Surgical Intervention
Clinical question: Does total knee replacement followed by a 12-week non-surgical treatment program provide greater pain relief and improvement in function and quality of life than non-surgical treatment alone?
Background: The number of total knee replacements in the U.S. has increased dramatically since the 1970s and is expected to continue to rise. To date, evidence to support the effectiveness of surgical intervention compared to non-surgical intervention is lacking.
Study design: Randomized, controlled trial.
Setting: Aalborg University Hospital Outpatient Clinics, Denmark.
Synopsis: One hundred patients with osteoarthritis were randomly assigned to undergo total knee replacement followed by 12 weeks of non-surgical treatment or to receive only 12 weeks of non-surgical treatment. The non-surgical treatment program consisted of exercise, education, dietary advice, insoles, and pain medication. Change from baseline to 12 months was assessed using the Knee Injury and Osteoarthritis Outcome Score (KOOS).
The total knee replacement group had a significantly greater improvement in the KOOS score than did the non-surgical group. Serious adverse events were more common in the total knee replacement group.
The study did not include a sham-surgery control group. It is unknown whether the KOOS pain subscale is generalizable to patients with severe pain. Additionally, the intensity of non-surgical treatment may have differed between groups.
Bottom line: Total knee replacement followed by non-surgical treatment is more efficacious than non-surgical treatment alone in providing pain relief and improving function and quality of life, but it is associated with higher number of adverse events.
Citation: Skou ST, Roos EM, Laursen MB, et al. A randomized, controlled trial of total knee replacement. N Engl J Med. 2015;373(17):1597-1606.
Clinical question: Does total knee replacement followed by a 12-week non-surgical treatment program provide greater pain relief and improvement in function and quality of life than non-surgical treatment alone?
Background: The number of total knee replacements in the U.S. has increased dramatically since the 1970s and is expected to continue to rise. To date, evidence to support the effectiveness of surgical intervention compared to non-surgical intervention is lacking.
Study design: Randomized, controlled trial.
Setting: Aalborg University Hospital Outpatient Clinics, Denmark.
Synopsis: One hundred patients with osteoarthritis were randomly assigned to undergo total knee replacement followed by 12 weeks of non-surgical treatment or to receive only 12 weeks of non-surgical treatment. The non-surgical treatment program consisted of exercise, education, dietary advice, insoles, and pain medication. Change from baseline to 12 months was assessed using the Knee Injury and Osteoarthritis Outcome Score (KOOS).
The total knee replacement group had a significantly greater improvement in the KOOS score than did the non-surgical group. Serious adverse events were more common in the total knee replacement group.
The study did not include a sham-surgery control group. It is unknown whether the KOOS pain subscale is generalizable to patients with severe pain. Additionally, the intensity of non-surgical treatment may have differed between groups.
Bottom line: Total knee replacement followed by non-surgical treatment is more efficacious than non-surgical treatment alone in providing pain relief and improving function and quality of life, but it is associated with higher number of adverse events.
Citation: Skou ST, Roos EM, Laursen MB, et al. A randomized, controlled trial of total knee replacement. N Engl J Med. 2015;373(17):1597-1606.
Clinical question: Does total knee replacement followed by a 12-week non-surgical treatment program provide greater pain relief and improvement in function and quality of life than non-surgical treatment alone?
Background: The number of total knee replacements in the U.S. has increased dramatically since the 1970s and is expected to continue to rise. To date, evidence to support the effectiveness of surgical intervention compared to non-surgical intervention is lacking.
Study design: Randomized, controlled trial.
Setting: Aalborg University Hospital Outpatient Clinics, Denmark.
Synopsis: One hundred patients with osteoarthritis were randomly assigned to undergo total knee replacement followed by 12 weeks of non-surgical treatment or to receive only 12 weeks of non-surgical treatment. The non-surgical treatment program consisted of exercise, education, dietary advice, insoles, and pain medication. Change from baseline to 12 months was assessed using the Knee Injury and Osteoarthritis Outcome Score (KOOS).
The total knee replacement group had a significantly greater improvement in the KOOS score than did the non-surgical group. Serious adverse events were more common in the total knee replacement group.
The study did not include a sham-surgery control group. It is unknown whether the KOOS pain subscale is generalizable to patients with severe pain. Additionally, the intensity of non-surgical treatment may have differed between groups.
Bottom line: Total knee replacement followed by non-surgical treatment is more efficacious than non-surgical treatment alone in providing pain relief and improving function and quality of life, but it is associated with higher number of adverse events.
Citation: Skou ST, Roos EM, Laursen MB, et al. A randomized, controlled trial of total knee replacement. N Engl J Med. 2015;373(17):1597-1606.
Fertility concerns of AYA cancer survivors

patient and her father
Photo by Rhoda Baer
Results of a small study suggest that adolescent and young adult (AYA) cancer survivors have a range of concerns regarding their fertility.
The female cancer survivors studied were more likely than males to describe feeling distressed and overwhelmed about their fertility.
Females also tended to worry about pregnancy-related health risks and cancer recurrence.
However, AYA cancer survivors of both sexes expressed concerns about genetic risk factors and how infertility might impact their future lives.
Catherine Benedict, PhD, of Memorial Sloan Kettering Cancer Center in New York, New York, and her colleagues conducted this research and reported the results in the Journal of Adolescent and Young Adult Oncology.
The researchers assessed fertility concerns in 43 AYA cancer survivors. They were 16 to 24 at the time of the study, had been diagnosed with cancer between ages 14 and 18, and were at least 6 months post-treatment.
The subjects either completed an individual interview (n=26) or participated in 1 of 4 focus groups (n=17).
Before treatment, 5 of the males had banked sperm, but none of the females took steps to preserve their fertility. More males (50%) than females (39%) reported uncertainty about their fertility.
The researchers identified 3 themes when discussing fertility with the study subjects: fertility concerns, emotions raised when discussing fertility, and strategies used to manage fertility concerns.
Concerns
Some subjects expressed concerns about how potential infertility could affect dating and relationships with partners (8% of males and 20% of females).
Some subjects were concerned about the health risks associated with having children—both risks to the subjects themselves and to any potential children (39% of males and 30% of females).
And some subjects were concerned about how potential infertility would affect their lives going forward (31% of males and 20% of females).
Emotions
When it came to emotions associated with fertility discussions, some subjects said they felt distressed and overwhelmed (23% of males and 30% of females).
However, some subjects said they weren’t concerned about their fertility (31% of males and 15% of females) or they felt hopeful despite the risk of infertility (8% of males and 20% of females).
Managing concerns
The subjects also mentioned a few strategies for managing fertility concerns. Some said they had accepted infertility (23% of males and 15% of females).
Some subjects said they weren’t going to worry about their fertility until they were older and actually wanted to have children (23% of males and 20% of females).
And some subjects said they would rely on assisted reproductive technology if necessary (31% of males and 20% of females).
Dr Benedict and her colleagues said this study suggests AYA cancer survivors may have a number of reproductive concerns and fertility-related distress, which may affect other areas of psychosocial functioning.
So future research should explore how to best incorporate fertility-related informational and support services more fully into survivorship care. ![]()

patient and her father
Photo by Rhoda Baer
Results of a small study suggest that adolescent and young adult (AYA) cancer survivors have a range of concerns regarding their fertility.
The female cancer survivors studied were more likely than males to describe feeling distressed and overwhelmed about their fertility.
Females also tended to worry about pregnancy-related health risks and cancer recurrence.
However, AYA cancer survivors of both sexes expressed concerns about genetic risk factors and how infertility might impact their future lives.
Catherine Benedict, PhD, of Memorial Sloan Kettering Cancer Center in New York, New York, and her colleagues conducted this research and reported the results in the Journal of Adolescent and Young Adult Oncology.
The researchers assessed fertility concerns in 43 AYA cancer survivors. They were 16 to 24 at the time of the study, had been diagnosed with cancer between ages 14 and 18, and were at least 6 months post-treatment.
The subjects either completed an individual interview (n=26) or participated in 1 of 4 focus groups (n=17).
Before treatment, 5 of the males had banked sperm, but none of the females took steps to preserve their fertility. More males (50%) than females (39%) reported uncertainty about their fertility.
The researchers identified 3 themes when discussing fertility with the study subjects: fertility concerns, emotions raised when discussing fertility, and strategies used to manage fertility concerns.
Concerns
Some subjects expressed concerns about how potential infertility could affect dating and relationships with partners (8% of males and 20% of females).
Some subjects were concerned about the health risks associated with having children—both risks to the subjects themselves and to any potential children (39% of males and 30% of females).
And some subjects were concerned about how potential infertility would affect their lives going forward (31% of males and 20% of females).
Emotions
When it came to emotions associated with fertility discussions, some subjects said they felt distressed and overwhelmed (23% of males and 30% of females).
However, some subjects said they weren’t concerned about their fertility (31% of males and 15% of females) or they felt hopeful despite the risk of infertility (8% of males and 20% of females).
Managing concerns
The subjects also mentioned a few strategies for managing fertility concerns. Some said they had accepted infertility (23% of males and 15% of females).
Some subjects said they weren’t going to worry about their fertility until they were older and actually wanted to have children (23% of males and 20% of females).
And some subjects said they would rely on assisted reproductive technology if necessary (31% of males and 20% of females).
Dr Benedict and her colleagues said this study suggests AYA cancer survivors may have a number of reproductive concerns and fertility-related distress, which may affect other areas of psychosocial functioning.
So future research should explore how to best incorporate fertility-related informational and support services more fully into survivorship care. ![]()

patient and her father
Photo by Rhoda Baer
Results of a small study suggest that adolescent and young adult (AYA) cancer survivors have a range of concerns regarding their fertility.
The female cancer survivors studied were more likely than males to describe feeling distressed and overwhelmed about their fertility.
Females also tended to worry about pregnancy-related health risks and cancer recurrence.
However, AYA cancer survivors of both sexes expressed concerns about genetic risk factors and how infertility might impact their future lives.
Catherine Benedict, PhD, of Memorial Sloan Kettering Cancer Center in New York, New York, and her colleagues conducted this research and reported the results in the Journal of Adolescent and Young Adult Oncology.
The researchers assessed fertility concerns in 43 AYA cancer survivors. They were 16 to 24 at the time of the study, had been diagnosed with cancer between ages 14 and 18, and were at least 6 months post-treatment.
The subjects either completed an individual interview (n=26) or participated in 1 of 4 focus groups (n=17).
Before treatment, 5 of the males had banked sperm, but none of the females took steps to preserve their fertility. More males (50%) than females (39%) reported uncertainty about their fertility.
The researchers identified 3 themes when discussing fertility with the study subjects: fertility concerns, emotions raised when discussing fertility, and strategies used to manage fertility concerns.
Concerns
Some subjects expressed concerns about how potential infertility could affect dating and relationships with partners (8% of males and 20% of females).
Some subjects were concerned about the health risks associated with having children—both risks to the subjects themselves and to any potential children (39% of males and 30% of females).
And some subjects were concerned about how potential infertility would affect their lives going forward (31% of males and 20% of females).
Emotions
When it came to emotions associated with fertility discussions, some subjects said they felt distressed and overwhelmed (23% of males and 30% of females).
However, some subjects said they weren’t concerned about their fertility (31% of males and 15% of females) or they felt hopeful despite the risk of infertility (8% of males and 20% of females).
Managing concerns
The subjects also mentioned a few strategies for managing fertility concerns. Some said they had accepted infertility (23% of males and 15% of females).
Some subjects said they weren’t going to worry about their fertility until they were older and actually wanted to have children (23% of males and 20% of females).
And some subjects said they would rely on assisted reproductive technology if necessary (31% of males and 20% of females).
Dr Benedict and her colleagues said this study suggests AYA cancer survivors may have a number of reproductive concerns and fertility-related distress, which may affect other areas of psychosocial functioning.
So future research should explore how to best incorporate fertility-related informational and support services more fully into survivorship care. ![]()
Gene therapy could treat FVII deficiency

Photo by Julien Valroff
Gene therapy can safely and effectively treat factor VII (FVII) deficiency in dogs, according to research published in Blood.
Three of the 4 dogs treated expressed levels of FVII that would be therapeutic in humans, with long-term stability.
In one dog, the effects have persisted for more than 2.5 years and are ongoing.
In addition, researchers said the therapy appears safe, based on kidney function, liver function, and blood measurements.
The team believes this success in large animals holds considerable potential for a safe, effective, and long-lasting new treatment in humans with FVII deficiency.
“Our finding has great clinical relevance for patients with FVII deficiency,” said Paris Margaritis, DPhil, of The Children’s Hospital of Philadelphia in Pennsylvania.
“These dogs have the type of mutation found in the majority of patients with this disorder, so this approach could lead to a sustained gene therapy in people.”
Dr Margaritis and his colleagues studied dogs with a G96E missense FVII mutation (FVII-G96E), which have less than 1% FVII activity. The researchers said these dogs had undetectable plasmatic antigen by Western blot and therefore represent the most prevalent type of human FVII deficiency.
“We developed a unique animal model of this disease after identifying dogs with naturally occurring FVII deficiency,” Dr Margaritis said. “Our investigations enabled us to design the corrective gene to insert into our virus vector in the current study.”
The researchers tested liver-directed, adeno-associated viral (AAV) serotype 8 vector delivery of a canine FVII zymogen transgene (cFVII) in 4 FVII-G96E dogs, known as Otis, N22, N24, and N25.
The animals received escalating doses of AAV8-cFVII, ranging from 2E11 vg/kg to 4.95E13 vg/kg.
Efficacy
At baseline, all dogs had less than 1% cFVII activity levels. After receiving AAV8-cFVII, they experienced a reduction in prothrombin time that reached a plateau:
- From 121.1± 1.0s to 22.1 ± 3.2s in N24 (4.95E13 vg/kg)
- From 83.5 ± 18.4s to 25.0 ± 3.6s in N22 (2E12 vg/kg)
- From 96.0 ± 5.8s to 28.7 ± 3.7s in N25 (6E11 vg/kg)
- From 124.8 ± 4.6s to 50.4 ± 4.0s in Otis (2E11 vg/kg).
The researchers also observed an increase in cFVII expression for all of the dogs but Otis. Levels of cFVII antigen reached plateaus of:
- 8320 ± 1800 ng/ml in N24, which is 770 ± 167 percent of normal
- 307 ± 56 ng/ml in N22, which is 29.7 ± 6.2 percent of normal
- 170 ± 62 ng/ml in N25, which is 15.7 ± 5.7 percent of normal.
These clinically therapeutic cFVII antigen levels have, thus far, persisted for more than 1 year in N22 and N25 and for 2.6 years in N24.
Safety
The researchers found that measures of liver and kidney function were within the normal range in all of the dogs. Likewise, D-dimer and fibrinogen levels were within the normal range.
The team said these results suggest that continuous cFVII expression—even in N24, which averaged 8.3 μg/ml for 2.6 years—did not result in evident activation of the endogenous coagulation system or induce a chronic pathological state.
N24 did exhibit a transient elevation of anti-cFVII IgG2. However, this response was not inhibitory and did not affect the transgene expression plateau.
The researchers did not detect anti-cFVII IgG2 in the other 3 dogs, nor did the team detect anti-cFVII IgG1 in any of the dogs studied.
“This work is very exciting and promising,” said study author Timothy Nichols, MD, of The University of North Carolina at Chapel Hill.
“The FVII-deficient dogs tolerated the initial gene therapy infusions very well and have had no adverse side effects over several years of follow-up. In other related studies in dogs with hemophilia B, similar positive findings have translated to people with hemophilia B.” ![]()

Photo by Julien Valroff
Gene therapy can safely and effectively treat factor VII (FVII) deficiency in dogs, according to research published in Blood.
Three of the 4 dogs treated expressed levels of FVII that would be therapeutic in humans, with long-term stability.
In one dog, the effects have persisted for more than 2.5 years and are ongoing.
In addition, researchers said the therapy appears safe, based on kidney function, liver function, and blood measurements.
The team believes this success in large animals holds considerable potential for a safe, effective, and long-lasting new treatment in humans with FVII deficiency.
“Our finding has great clinical relevance for patients with FVII deficiency,” said Paris Margaritis, DPhil, of The Children’s Hospital of Philadelphia in Pennsylvania.
“These dogs have the type of mutation found in the majority of patients with this disorder, so this approach could lead to a sustained gene therapy in people.”
Dr Margaritis and his colleagues studied dogs with a G96E missense FVII mutation (FVII-G96E), which have less than 1% FVII activity. The researchers said these dogs had undetectable plasmatic antigen by Western blot and therefore represent the most prevalent type of human FVII deficiency.
“We developed a unique animal model of this disease after identifying dogs with naturally occurring FVII deficiency,” Dr Margaritis said. “Our investigations enabled us to design the corrective gene to insert into our virus vector in the current study.”
The researchers tested liver-directed, adeno-associated viral (AAV) serotype 8 vector delivery of a canine FVII zymogen transgene (cFVII) in 4 FVII-G96E dogs, known as Otis, N22, N24, and N25.
The animals received escalating doses of AAV8-cFVII, ranging from 2E11 vg/kg to 4.95E13 vg/kg.
Efficacy
At baseline, all dogs had less than 1% cFVII activity levels. After receiving AAV8-cFVII, they experienced a reduction in prothrombin time that reached a plateau:
- From 121.1± 1.0s to 22.1 ± 3.2s in N24 (4.95E13 vg/kg)
- From 83.5 ± 18.4s to 25.0 ± 3.6s in N22 (2E12 vg/kg)
- From 96.0 ± 5.8s to 28.7 ± 3.7s in N25 (6E11 vg/kg)
- From 124.8 ± 4.6s to 50.4 ± 4.0s in Otis (2E11 vg/kg).
The researchers also observed an increase in cFVII expression for all of the dogs but Otis. Levels of cFVII antigen reached plateaus of:
- 8320 ± 1800 ng/ml in N24, which is 770 ± 167 percent of normal
- 307 ± 56 ng/ml in N22, which is 29.7 ± 6.2 percent of normal
- 170 ± 62 ng/ml in N25, which is 15.7 ± 5.7 percent of normal.
These clinically therapeutic cFVII antigen levels have, thus far, persisted for more than 1 year in N22 and N25 and for 2.6 years in N24.
Safety
The researchers found that measures of liver and kidney function were within the normal range in all of the dogs. Likewise, D-dimer and fibrinogen levels were within the normal range.
The team said these results suggest that continuous cFVII expression—even in N24, which averaged 8.3 μg/ml for 2.6 years—did not result in evident activation of the endogenous coagulation system or induce a chronic pathological state.
N24 did exhibit a transient elevation of anti-cFVII IgG2. However, this response was not inhibitory and did not affect the transgene expression plateau.
The researchers did not detect anti-cFVII IgG2 in the other 3 dogs, nor did the team detect anti-cFVII IgG1 in any of the dogs studied.
“This work is very exciting and promising,” said study author Timothy Nichols, MD, of The University of North Carolina at Chapel Hill.
“The FVII-deficient dogs tolerated the initial gene therapy infusions very well and have had no adverse side effects over several years of follow-up. In other related studies in dogs with hemophilia B, similar positive findings have translated to people with hemophilia B.” ![]()

Photo by Julien Valroff
Gene therapy can safely and effectively treat factor VII (FVII) deficiency in dogs, according to research published in Blood.
Three of the 4 dogs treated expressed levels of FVII that would be therapeutic in humans, with long-term stability.
In one dog, the effects have persisted for more than 2.5 years and are ongoing.
In addition, researchers said the therapy appears safe, based on kidney function, liver function, and blood measurements.
The team believes this success in large animals holds considerable potential for a safe, effective, and long-lasting new treatment in humans with FVII deficiency.
“Our finding has great clinical relevance for patients with FVII deficiency,” said Paris Margaritis, DPhil, of The Children’s Hospital of Philadelphia in Pennsylvania.
“These dogs have the type of mutation found in the majority of patients with this disorder, so this approach could lead to a sustained gene therapy in people.”
Dr Margaritis and his colleagues studied dogs with a G96E missense FVII mutation (FVII-G96E), which have less than 1% FVII activity. The researchers said these dogs had undetectable plasmatic antigen by Western blot and therefore represent the most prevalent type of human FVII deficiency.
“We developed a unique animal model of this disease after identifying dogs with naturally occurring FVII deficiency,” Dr Margaritis said. “Our investigations enabled us to design the corrective gene to insert into our virus vector in the current study.”
The researchers tested liver-directed, adeno-associated viral (AAV) serotype 8 vector delivery of a canine FVII zymogen transgene (cFVII) in 4 FVII-G96E dogs, known as Otis, N22, N24, and N25.
The animals received escalating doses of AAV8-cFVII, ranging from 2E11 vg/kg to 4.95E13 vg/kg.
Efficacy
At baseline, all dogs had less than 1% cFVII activity levels. After receiving AAV8-cFVII, they experienced a reduction in prothrombin time that reached a plateau:
- From 121.1± 1.0s to 22.1 ± 3.2s in N24 (4.95E13 vg/kg)
- From 83.5 ± 18.4s to 25.0 ± 3.6s in N22 (2E12 vg/kg)
- From 96.0 ± 5.8s to 28.7 ± 3.7s in N25 (6E11 vg/kg)
- From 124.8 ± 4.6s to 50.4 ± 4.0s in Otis (2E11 vg/kg).
The researchers also observed an increase in cFVII expression for all of the dogs but Otis. Levels of cFVII antigen reached plateaus of:
- 8320 ± 1800 ng/ml in N24, which is 770 ± 167 percent of normal
- 307 ± 56 ng/ml in N22, which is 29.7 ± 6.2 percent of normal
- 170 ± 62 ng/ml in N25, which is 15.7 ± 5.7 percent of normal.
These clinically therapeutic cFVII antigen levels have, thus far, persisted for more than 1 year in N22 and N25 and for 2.6 years in N24.
Safety
The researchers found that measures of liver and kidney function were within the normal range in all of the dogs. Likewise, D-dimer and fibrinogen levels were within the normal range.
The team said these results suggest that continuous cFVII expression—even in N24, which averaged 8.3 μg/ml for 2.6 years—did not result in evident activation of the endogenous coagulation system or induce a chronic pathological state.
N24 did exhibit a transient elevation of anti-cFVII IgG2. However, this response was not inhibitory and did not affect the transgene expression plateau.
The researchers did not detect anti-cFVII IgG2 in the other 3 dogs, nor did the team detect anti-cFVII IgG1 in any of the dogs studied.
“This work is very exciting and promising,” said study author Timothy Nichols, MD, of The University of North Carolina at Chapel Hill.
“The FVII-deficient dogs tolerated the initial gene therapy infusions very well and have had no adverse side effects over several years of follow-up. In other related studies in dogs with hemophilia B, similar positive findings have translated to people with hemophilia B.” ![]()
FDA expands approved use of MM drug

Photo courtesy of Amgen
The US Food and Drug Administration (FDA) has approved the use of carfilzomib (Kyprolis) in combination with dexamethasone or lenalidomide plus dexamethasone to treat patients with relapsed or refractory multiple myeloma (MM) who have received 1 to 3 prior lines of therapy.
The FDA also approved use of carfilzomib as a single agent to treat patients with relapsed or refractory MM who have received 1 or more lines of therapy.
This decision converts to full approval the initial accelerated approval granted for single-agent carfilzomib in July 2012.
In July 2015, the FDA approved the use of carfilzomib in combination with lenalidomide and dexamethasone for the treatment of patients with relapsed MM who have received 1 to 3 prior lines of therapy.
The latest approval of carfilzomib is based on results from the phase 3 ENDEAVOR study.
Trial results
The ENDEAVOR trial included 929 MM patients whose disease had relapsed after 1 to 3 prior therapeutic regimens. The patients received either carfilzomib plus dexamethasone (n=464) or bortezomib plus dexamethasone (n=465) until disease progression.
The primary endpoint was progression-free survival. The median was 18.7 months in the carfilzomib arm and 9.4 months in the bortezomib arm. The hazard ratio was 0.53 (P<0.0001).
Overall survival data are not yet mature and continue to be monitored.
Treatment discontinuation due to adverse events and on-study deaths were comparable between the 2 treatment arms.
However, a number of known adverse events were reported at a higher rate in the carfilzomib arm than the bortezomib arm, including any-grade dyspnea (28% vs 13%), hypertension (25% vs 3%), pyrexia (27% vs 14%), cough (25% vs 15%), cardiac failure (8% vs 3%), and acute renal failure (8% vs 5%).
Carfilzomib is marketed as Kyprolis by Onyx Pharmaceuticals, Inc., a subsidiary of Amgen that holds development and commercialization rights to the drug globally, with the exception of Japan. For more information on the drug, visit www.kyprolis.com. ![]()

Photo courtesy of Amgen
The US Food and Drug Administration (FDA) has approved the use of carfilzomib (Kyprolis) in combination with dexamethasone or lenalidomide plus dexamethasone to treat patients with relapsed or refractory multiple myeloma (MM) who have received 1 to 3 prior lines of therapy.
The FDA also approved use of carfilzomib as a single agent to treat patients with relapsed or refractory MM who have received 1 or more lines of therapy.
This decision converts to full approval the initial accelerated approval granted for single-agent carfilzomib in July 2012.
In July 2015, the FDA approved the use of carfilzomib in combination with lenalidomide and dexamethasone for the treatment of patients with relapsed MM who have received 1 to 3 prior lines of therapy.
The latest approval of carfilzomib is based on results from the phase 3 ENDEAVOR study.
Trial results
The ENDEAVOR trial included 929 MM patients whose disease had relapsed after 1 to 3 prior therapeutic regimens. The patients received either carfilzomib plus dexamethasone (n=464) or bortezomib plus dexamethasone (n=465) until disease progression.
The primary endpoint was progression-free survival. The median was 18.7 months in the carfilzomib arm and 9.4 months in the bortezomib arm. The hazard ratio was 0.53 (P<0.0001).
Overall survival data are not yet mature and continue to be monitored.
Treatment discontinuation due to adverse events and on-study deaths were comparable between the 2 treatment arms.
However, a number of known adverse events were reported at a higher rate in the carfilzomib arm than the bortezomib arm, including any-grade dyspnea (28% vs 13%), hypertension (25% vs 3%), pyrexia (27% vs 14%), cough (25% vs 15%), cardiac failure (8% vs 3%), and acute renal failure (8% vs 5%).
Carfilzomib is marketed as Kyprolis by Onyx Pharmaceuticals, Inc., a subsidiary of Amgen that holds development and commercialization rights to the drug globally, with the exception of Japan. For more information on the drug, visit www.kyprolis.com. ![]()

Photo courtesy of Amgen
The US Food and Drug Administration (FDA) has approved the use of carfilzomib (Kyprolis) in combination with dexamethasone or lenalidomide plus dexamethasone to treat patients with relapsed or refractory multiple myeloma (MM) who have received 1 to 3 prior lines of therapy.
The FDA also approved use of carfilzomib as a single agent to treat patients with relapsed or refractory MM who have received 1 or more lines of therapy.
This decision converts to full approval the initial accelerated approval granted for single-agent carfilzomib in July 2012.
In July 2015, the FDA approved the use of carfilzomib in combination with lenalidomide and dexamethasone for the treatment of patients with relapsed MM who have received 1 to 3 prior lines of therapy.
The latest approval of carfilzomib is based on results from the phase 3 ENDEAVOR study.
Trial results
The ENDEAVOR trial included 929 MM patients whose disease had relapsed after 1 to 3 prior therapeutic regimens. The patients received either carfilzomib plus dexamethasone (n=464) or bortezomib plus dexamethasone (n=465) until disease progression.
The primary endpoint was progression-free survival. The median was 18.7 months in the carfilzomib arm and 9.4 months in the bortezomib arm. The hazard ratio was 0.53 (P<0.0001).
Overall survival data are not yet mature and continue to be monitored.
Treatment discontinuation due to adverse events and on-study deaths were comparable between the 2 treatment arms.
However, a number of known adverse events were reported at a higher rate in the carfilzomib arm than the bortezomib arm, including any-grade dyspnea (28% vs 13%), hypertension (25% vs 3%), pyrexia (27% vs 14%), cough (25% vs 15%), cardiac failure (8% vs 3%), and acute renal failure (8% vs 5%).
Carfilzomib is marketed as Kyprolis by Onyx Pharmaceuticals, Inc., a subsidiary of Amgen that holds development and commercialization rights to the drug globally, with the exception of Japan. For more information on the drug, visit www.kyprolis.com. ![]()
Breakdown
The patient's tachycardia and leukocytosis suggest sepsis. Potential sources include soft tissue infection or osteomyelitis from his sacral ulcers, Clostridium difficile, or a urinary tract infection. Impaired visceral sensation from his spinal cord injury may dampen his response to an intra‐abdominal process, such as mesenteric ischemia or toxic megacolon. Records from other hospitals should be reviewed to assess the acuity of change in his WBC count, hemoglobin, and creatinine. His anemia may be from chronic inflammation (eg, osteomyelitis), renal insufficiency, hemolysis, or occult blood loss, including retroperitoneal and gastrointestinal sources. His kidney injury may be from tubular necrosis in the setting of sepsis or obstructive uropathy related to a neurogenic bladder.
Potential contributors to his PEA and cardiovascular collapse are drug use (cocaine), alcohol withdrawal, infection, hypovolemia, myocardial ischemia, or heart failure. Severe hemorrhage, hyperkalemia, or acidosis from acute kidney injury and sepsis could also account for his cardiac arrest. His paraplegia and hospitalization raise the risk of venous thromboembolism, which can lead to PEA from pulmonary embolus and prolonged hypoxia.
His profound anemia is the likely cause of his PEA arrest and severe lactic acidosis. Massive hemolysis is most likely given no overt evidence of bleeding to account for the precipitous fall in hematocrit. Hemolysis can result from disorders intrinsic or extrinsic to the red blood cell (RBC). Intrinsic defects are usually congenital and involve the membrane, hemoglobin, or metabolic enzymes within the RBC. Extrinsic hemolysis arises from processes that injure the RBC from the outside: antibodies, infections, and mechanical shearing.
A rapidly declining platelet count is seen in microangiopathic hemolytic conditions such as disseminated intravascular coagulation (DIC) or thrombotic thrombocytopenic purpura (TTP), where platelets are consumed along with RBCs; sepsis makes DIC more likely. Autoimmune hemolytic anemia (AIHA) is sometimes accompanied by immune thrombocytopenia. AIHA arises from antibodies that are idiopathic or produced in response to infection, autoimmune conditions (eg, systemic lupus erythematosus), lymphoproliferative disease, or drugs (eg, ‐lactam antibiotics). The antiphospholipid syndrome can lead to thrombocytopenia, hemolysis, and kidney injury. Devitalized tissue in his sacral ulcers may predispose the patient to infection with Clostridium perfringens, which can elaborate enzymes that trigger massive hemolysis.
Because automated hemoglobin measurement is performed by spectrophotometry (light absorption and scatter), high concentrations of poorly soluble autoantibodies can increase the turbidity of the sample and preclude the measurement of hemoglobin concentration. This could lead to the report of interfering substances.
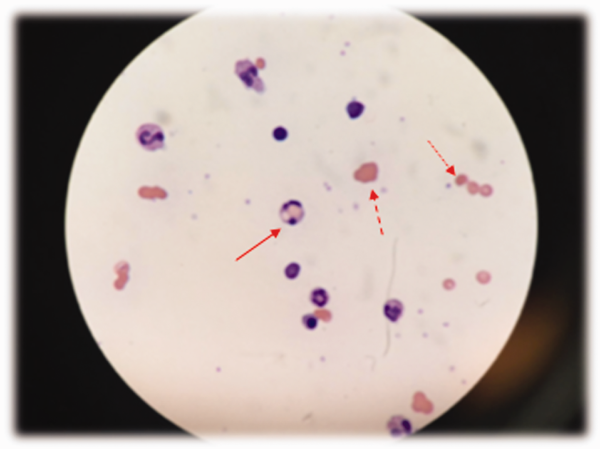
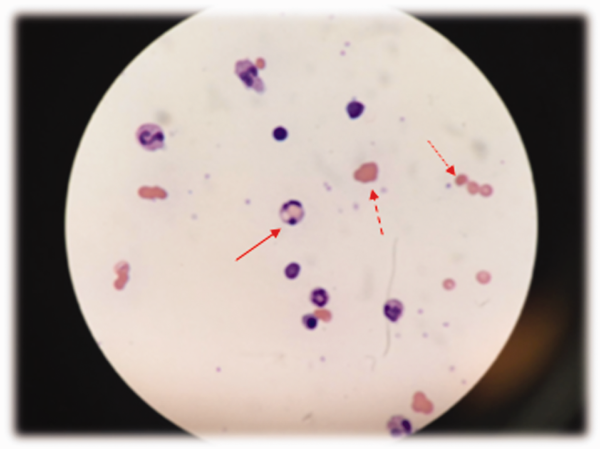
Low haptoglobin, elevated LDH, and hyperbilirubinemia confirm hemolysis. A more robust reticulocytosis is expected in the face of profound anemia, but the patient may also suffer from a concomitant hypoproliferative state (eg, nutritional deficiency). More likely, the rapidity of his decline outpaced the marrow's response, which can be delayed by days.
The most common cause of a combined elevation of the INR/PT and aPTT in a critically ill patient is DIC. Although no schistocytes were detected on the peripheral smear, they can be absent in up to 50% of DIC cases. TTP is associated with hemolytic anemia, kidney injury, and thrombocytopenia, but it generally does not cause coagulopathy.
The combination of red cell agglutination and hemophagocytosis suggests that the RBCs are coated with autoantibodies that cross‐link the cells and make them targets for phagocytosis by neutrophils in the circulation. This is distinct from the hemophagocytic syndrome, a rare immune activation syndrome characterized by macrophage phagocytosis of RBCs in the reticuloendothelial system. The blood smear also shows microspherocytes, which are seen in AIHA and hereditary spherocytosis.
Acute tubular necrosis could result from sepsis, ischemic injury from DIC, hypotension during cardiac arrest, or heme pigment toxicity. Urine sediment should be reviewed for dysmorphic RBCs or RBC casts that would indicate glomerulonephritis (eg, from an underlying autoimmune process associated with AIHA).
Urine hemoglobin that is disproportionate to the degree of hematuria suggests hemoglobinuria, which in turn defines the hemolysis as intravascular. Processes that directly lyse RBCs in circulation via mechanical shearing, activation of complement, infection of the RBC, or enzymatic or oxidative destruction of the membrane cause intravascular hemolysis. Leading considerations include microangiopathy (eg, DIC, TTP), clostridial sepsis, and AIHA.
AIHA can be broadly classified as warm or cold. Warm AIHA is caused by immunoglobulin IgG antibodies that bind most avidly at body temperature. Because warm AIHA does not activate complement, patients present with evidence of extravascular hemolysis that is typically chronic and mild to moderate in severity. It does not typically cause the acute, fulminant, intravascular hemolytic condition seen here.
Cold AIHA is characterized by autoantibodies that bind at lower temperatures and comes in 2 forms: cold agglutinin disease and (rarely) paroxysmal cold hemoglobinuria (PCH). Cold agglutinins are most often IgM antibodies produced in response to infection (Mycoplasma pneumoniae, infectious mononucleosis), drugs, or a hematologic malignancy. These IgM antibodies bind RBCs, causing them to agglutinate, and fix complement (including C3) to the surface of RBCs when blood circulates to cooler parts of the body. This results in complement activation, formation of the membrane attack complex, and intravascular hemolysis when bound and activated complement is present in large numbers. Acute infection can increase the complement available for binding to the surface of RBCs. Through a slightly different mechanism, PCH causes intravascular hemolysis through direct IgG activation of complement fixed to the surface of RBCs. During a hemolytic episode the direct antibody test (DAT) is positive using anti‐C3 and negative for IgG.
Based on the patient's clinical evidence of intravascular hemolysis and a suspected autoimmune etiology, the leading diagnosis at this time is cold AIHA.
The DAT detects IgG or complement adherent to RBCs. This patient has tested positive for both IgG and C3, though much more strongly for IgG, suggesting an unusual ability of the patient's IgG to activate complement. The phenomenon of mixed AIHA, in which the patient has both warm‐ and cold‐reacting antibodies, is rare.
Regarding infections associated with AIHA, there is no cough or rash to suggest M pneumoniae, and there is no sore throat, fever, lymphadenopathy, splenomegaly, or atypical lymphocytosis to suggest infectious mononucleosis. He should be tested for human immunodeficiency virus, which is also associated with AIHA. His leukocytosis may raise suspicion for an underlying hematologic malignancy, but he does not have blasts, dysplastic leukocytes, or lymphocytosis on his peripheral blood smear. Systemic lupus erythematosus can be associated with AIHA, thrombocytopenia, and renal failure, but he lacks the more common clinical manifestations of rash, arthralgias, and fever.
Drug‐induced immune hemolytic anemia (DIIHA) can cause both the clinical and serologic profile of an AIHA, as seen here. DIIHA can be distinguished from mixed AIHA if hemolysis abates with discontinuation of an offending drug. His deterioration is temporally associated with drug administration at the time of admission. Cephalosporins and ‐lactams (e.g., piperacillin) are the most common causes of DIIHA, and ‐lactamases such as tazobactam have also been implicated. By exclusion of other causes, DIIHA secondary to piperacillin is most likely responsible for his massive intravascular hemolysis.
COMMENTARY
This case illustrates a dramatic presentation of fulminant intravascular hemolysis secondary to piperacillin. The incidence of DIIHA is estimated to be 1 in 1 million.[1] Historically, methyldopa and high‐dose penicillin have been responsible for the majority of cases,[2] but in recent years complex penicillins, including piperacillin, and second‐ and third‐generation cephalosporins have been implicated.[3, 4] Cases of DIIHA are often underdiagnosed or misdiagnosed, as smoldering or less severe cases may not be recognized or are attributed to other causes.
A positive DAT, suggesting immunoglobulin and/or complement binding to RBCs, is the most reliable laboratory finding in DIIHA.[5] However, a positive DAT does not identify the source of the antigen and may result in misattribution of the immune hemolysis to autoimmunity rather than to a drug. Repeated or continued administration of the offending drug (as in this case) may perpetuate or worsen the hemolysis. Drug‐specific antibody tests may help to confirm the diagnosis, but these tests are complex and take significant time for specialized laboratories to run.
Severe hemolysis should be considered when a patient has a sudden and dramatic drop in his hemoglobin level in the absence of bleeding. Because DIIHA can be rapidly progressive, discontinuing a suspected culprit drug is the most important diagnostic and therapeutic measure. Typically, when an offending drug is stopped, the hemolysis stops as well. The time course over which this occurs depends on the rapidity of drug clearance.[4] Hemodialysis or plasmapheresis may be required in cases where the medication is renally excreted, particularly in cases of concomitant kidney injury. Evidence supporting corticosteroid use in DIIHA is limited, as the offending agent is usually discontinued by the time corticosteroids are initiated.[4]
This patient's DAT confirmed both IgG and complement activation, consistent with DIIHA caused by an immune complexlike reaction. This mechanism involves the antibody binding to a mixed epitope of the drug and a RBC membrane glycoprotein.[6] The offending drug was stopped only when review of his medical records established a clear temporal association between antibiotic administration and prior hemolysis.
The 2009 Health Information Technology for Economic and Clinical Health Act created an electronic health record (EHR) incentive program (meaningful use criteria).[7] By 2012, only 6% of hospitals met all of the stage 2 criteria, which include EHR interoperability across health systems.[8] The patient's preceding hemolytic event was described in records faxed by the outside hospitals, but without EHR interoperability, the treating clinicians did not have timely access to this information. Instead, the familiar manual process of obtaining outside records involving signed forms, phone calls, fax machines, and reams of paper progressed at its usual pace. Real‐time access to health records might have guided providers to select an alternative antibiotic regimen. Instead, a communication breakdown contributed to a catastrophic drug reaction and to this tragic patient outcome.
KEY TEACHING POINTS
- In a patient presenting with acute hemolysis and a positive DAT, consider DIIHA.
- Both piperacillin and tazobactam can cause a severe, complement‐mediated immune hemolytic anemia (DIIHA).
- Drug‐induced antibodies are detected by direct antiglobulin testing, but a complete medication history is the key to diagnosis.
- Management of drug‐induced hemolytic anemia involves immediate discontinuation of the culprit medication, supportive care, and potentially corticosteroids, plasmapheresis, and/or hemodialysis to expedite removal of the offending agent.
- EHR interoperability may provide timely access to important health information across different hospitals, expedite health information exchange, and reduce adverse patient outcomes that stem from communication delays.
This case was submitted anonymously to AHRQ WebM&M on July 18, 2014, and was accepted on August 7, 2014. The case and WebM&M commentary were published online on October 26, 2015.[9] This separate commentary on the same case was later submitted to the Journal of Hospital Medicine on September 2, 2015, accepted on November 24, 2015, and published on January 22, 2016. The 2 publications are written by different authors, and although they reference the same case, they make different but valuable points.
Disclosure
Nothing to report.
The patient's tachycardia and leukocytosis suggest sepsis. Potential sources include soft tissue infection or osteomyelitis from his sacral ulcers, Clostridium difficile, or a urinary tract infection. Impaired visceral sensation from his spinal cord injury may dampen his response to an intra‐abdominal process, such as mesenteric ischemia or toxic megacolon. Records from other hospitals should be reviewed to assess the acuity of change in his WBC count, hemoglobin, and creatinine. His anemia may be from chronic inflammation (eg, osteomyelitis), renal insufficiency, hemolysis, or occult blood loss, including retroperitoneal and gastrointestinal sources. His kidney injury may be from tubular necrosis in the setting of sepsis or obstructive uropathy related to a neurogenic bladder.
Potential contributors to his PEA and cardiovascular collapse are drug use (cocaine), alcohol withdrawal, infection, hypovolemia, myocardial ischemia, or heart failure. Severe hemorrhage, hyperkalemia, or acidosis from acute kidney injury and sepsis could also account for his cardiac arrest. His paraplegia and hospitalization raise the risk of venous thromboembolism, which can lead to PEA from pulmonary embolus and prolonged hypoxia.
His profound anemia is the likely cause of his PEA arrest and severe lactic acidosis. Massive hemolysis is most likely given no overt evidence of bleeding to account for the precipitous fall in hematocrit. Hemolysis can result from disorders intrinsic or extrinsic to the red blood cell (RBC). Intrinsic defects are usually congenital and involve the membrane, hemoglobin, or metabolic enzymes within the RBC. Extrinsic hemolysis arises from processes that injure the RBC from the outside: antibodies, infections, and mechanical shearing.
A rapidly declining platelet count is seen in microangiopathic hemolytic conditions such as disseminated intravascular coagulation (DIC) or thrombotic thrombocytopenic purpura (TTP), where platelets are consumed along with RBCs; sepsis makes DIC more likely. Autoimmune hemolytic anemia (AIHA) is sometimes accompanied by immune thrombocytopenia. AIHA arises from antibodies that are idiopathic or produced in response to infection, autoimmune conditions (eg, systemic lupus erythematosus), lymphoproliferative disease, or drugs (eg, ‐lactam antibiotics). The antiphospholipid syndrome can lead to thrombocytopenia, hemolysis, and kidney injury. Devitalized tissue in his sacral ulcers may predispose the patient to infection with Clostridium perfringens, which can elaborate enzymes that trigger massive hemolysis.
Because automated hemoglobin measurement is performed by spectrophotometry (light absorption and scatter), high concentrations of poorly soluble autoantibodies can increase the turbidity of the sample and preclude the measurement of hemoglobin concentration. This could lead to the report of interfering substances.

Low haptoglobin, elevated LDH, and hyperbilirubinemia confirm hemolysis. A more robust reticulocytosis is expected in the face of profound anemia, but the patient may also suffer from a concomitant hypoproliferative state (eg, nutritional deficiency). More likely, the rapidity of his decline outpaced the marrow's response, which can be delayed by days.
The most common cause of a combined elevation of the INR/PT and aPTT in a critically ill patient is DIC. Although no schistocytes were detected on the peripheral smear, they can be absent in up to 50% of DIC cases. TTP is associated with hemolytic anemia, kidney injury, and thrombocytopenia, but it generally does not cause coagulopathy.
The combination of red cell agglutination and hemophagocytosis suggests that the RBCs are coated with autoantibodies that cross‐link the cells and make them targets for phagocytosis by neutrophils in the circulation. This is distinct from the hemophagocytic syndrome, a rare immune activation syndrome characterized by macrophage phagocytosis of RBCs in the reticuloendothelial system. The blood smear also shows microspherocytes, which are seen in AIHA and hereditary spherocytosis.
Acute tubular necrosis could result from sepsis, ischemic injury from DIC, hypotension during cardiac arrest, or heme pigment toxicity. Urine sediment should be reviewed for dysmorphic RBCs or RBC casts that would indicate glomerulonephritis (eg, from an underlying autoimmune process associated with AIHA).
Urine hemoglobin that is disproportionate to the degree of hematuria suggests hemoglobinuria, which in turn defines the hemolysis as intravascular. Processes that directly lyse RBCs in circulation via mechanical shearing, activation of complement, infection of the RBC, or enzymatic or oxidative destruction of the membrane cause intravascular hemolysis. Leading considerations include microangiopathy (eg, DIC, TTP), clostridial sepsis, and AIHA.
AIHA can be broadly classified as warm or cold. Warm AIHA is caused by immunoglobulin IgG antibodies that bind most avidly at body temperature. Because warm AIHA does not activate complement, patients present with evidence of extravascular hemolysis that is typically chronic and mild to moderate in severity. It does not typically cause the acute, fulminant, intravascular hemolytic condition seen here.
Cold AIHA is characterized by autoantibodies that bind at lower temperatures and comes in 2 forms: cold agglutinin disease and (rarely) paroxysmal cold hemoglobinuria (PCH). Cold agglutinins are most often IgM antibodies produced in response to infection (Mycoplasma pneumoniae, infectious mononucleosis), drugs, or a hematologic malignancy. These IgM antibodies bind RBCs, causing them to agglutinate, and fix complement (including C3) to the surface of RBCs when blood circulates to cooler parts of the body. This results in complement activation, formation of the membrane attack complex, and intravascular hemolysis when bound and activated complement is present in large numbers. Acute infection can increase the complement available for binding to the surface of RBCs. Through a slightly different mechanism, PCH causes intravascular hemolysis through direct IgG activation of complement fixed to the surface of RBCs. During a hemolytic episode the direct antibody test (DAT) is positive using anti‐C3 and negative for IgG.
Based on the patient's clinical evidence of intravascular hemolysis and a suspected autoimmune etiology, the leading diagnosis at this time is cold AIHA.
The DAT detects IgG or complement adherent to RBCs. This patient has tested positive for both IgG and C3, though much more strongly for IgG, suggesting an unusual ability of the patient's IgG to activate complement. The phenomenon of mixed AIHA, in which the patient has both warm‐ and cold‐reacting antibodies, is rare.
Regarding infections associated with AIHA, there is no cough or rash to suggest M pneumoniae, and there is no sore throat, fever, lymphadenopathy, splenomegaly, or atypical lymphocytosis to suggest infectious mononucleosis. He should be tested for human immunodeficiency virus, which is also associated with AIHA. His leukocytosis may raise suspicion for an underlying hematologic malignancy, but he does not have blasts, dysplastic leukocytes, or lymphocytosis on his peripheral blood smear. Systemic lupus erythematosus can be associated with AIHA, thrombocytopenia, and renal failure, but he lacks the more common clinical manifestations of rash, arthralgias, and fever.
Drug‐induced immune hemolytic anemia (DIIHA) can cause both the clinical and serologic profile of an AIHA, as seen here. DIIHA can be distinguished from mixed AIHA if hemolysis abates with discontinuation of an offending drug. His deterioration is temporally associated with drug administration at the time of admission. Cephalosporins and ‐lactams (e.g., piperacillin) are the most common causes of DIIHA, and ‐lactamases such as tazobactam have also been implicated. By exclusion of other causes, DIIHA secondary to piperacillin is most likely responsible for his massive intravascular hemolysis.
COMMENTARY
This case illustrates a dramatic presentation of fulminant intravascular hemolysis secondary to piperacillin. The incidence of DIIHA is estimated to be 1 in 1 million.[1] Historically, methyldopa and high‐dose penicillin have been responsible for the majority of cases,[2] but in recent years complex penicillins, including piperacillin, and second‐ and third‐generation cephalosporins have been implicated.[3, 4] Cases of DIIHA are often underdiagnosed or misdiagnosed, as smoldering or less severe cases may not be recognized or are attributed to other causes.
A positive DAT, suggesting immunoglobulin and/or complement binding to RBCs, is the most reliable laboratory finding in DIIHA.[5] However, a positive DAT does not identify the source of the antigen and may result in misattribution of the immune hemolysis to autoimmunity rather than to a drug. Repeated or continued administration of the offending drug (as in this case) may perpetuate or worsen the hemolysis. Drug‐specific antibody tests may help to confirm the diagnosis, but these tests are complex and take significant time for specialized laboratories to run.
Severe hemolysis should be considered when a patient has a sudden and dramatic drop in his hemoglobin level in the absence of bleeding. Because DIIHA can be rapidly progressive, discontinuing a suspected culprit drug is the most important diagnostic and therapeutic measure. Typically, when an offending drug is stopped, the hemolysis stops as well. The time course over which this occurs depends on the rapidity of drug clearance.[4] Hemodialysis or plasmapheresis may be required in cases where the medication is renally excreted, particularly in cases of concomitant kidney injury. Evidence supporting corticosteroid use in DIIHA is limited, as the offending agent is usually discontinued by the time corticosteroids are initiated.[4]
This patient's DAT confirmed both IgG and complement activation, consistent with DIIHA caused by an immune complexlike reaction. This mechanism involves the antibody binding to a mixed epitope of the drug and a RBC membrane glycoprotein.[6] The offending drug was stopped only when review of his medical records established a clear temporal association between antibiotic administration and prior hemolysis.
The 2009 Health Information Technology for Economic and Clinical Health Act created an electronic health record (EHR) incentive program (meaningful use criteria).[7] By 2012, only 6% of hospitals met all of the stage 2 criteria, which include EHR interoperability across health systems.[8] The patient's preceding hemolytic event was described in records faxed by the outside hospitals, but without EHR interoperability, the treating clinicians did not have timely access to this information. Instead, the familiar manual process of obtaining outside records involving signed forms, phone calls, fax machines, and reams of paper progressed at its usual pace. Real‐time access to health records might have guided providers to select an alternative antibiotic regimen. Instead, a communication breakdown contributed to a catastrophic drug reaction and to this tragic patient outcome.
KEY TEACHING POINTS
- In a patient presenting with acute hemolysis and a positive DAT, consider DIIHA.
- Both piperacillin and tazobactam can cause a severe, complement‐mediated immune hemolytic anemia (DIIHA).
- Drug‐induced antibodies are detected by direct antiglobulin testing, but a complete medication history is the key to diagnosis.
- Management of drug‐induced hemolytic anemia involves immediate discontinuation of the culprit medication, supportive care, and potentially corticosteroids, plasmapheresis, and/or hemodialysis to expedite removal of the offending agent.
- EHR interoperability may provide timely access to important health information across different hospitals, expedite health information exchange, and reduce adverse patient outcomes that stem from communication delays.
This case was submitted anonymously to AHRQ WebM&M on July 18, 2014, and was accepted on August 7, 2014. The case and WebM&M commentary were published online on October 26, 2015.[9] This separate commentary on the same case was later submitted to the Journal of Hospital Medicine on September 2, 2015, accepted on November 24, 2015, and published on January 22, 2016. The 2 publications are written by different authors, and although they reference the same case, they make different but valuable points.
Disclosure
Nothing to report.
The patient's tachycardia and leukocytosis suggest sepsis. Potential sources include soft tissue infection or osteomyelitis from his sacral ulcers, Clostridium difficile, or a urinary tract infection. Impaired visceral sensation from his spinal cord injury may dampen his response to an intra‐abdominal process, such as mesenteric ischemia or toxic megacolon. Records from other hospitals should be reviewed to assess the acuity of change in his WBC count, hemoglobin, and creatinine. His anemia may be from chronic inflammation (eg, osteomyelitis), renal insufficiency, hemolysis, or occult blood loss, including retroperitoneal and gastrointestinal sources. His kidney injury may be from tubular necrosis in the setting of sepsis or obstructive uropathy related to a neurogenic bladder.
Potential contributors to his PEA and cardiovascular collapse are drug use (cocaine), alcohol withdrawal, infection, hypovolemia, myocardial ischemia, or heart failure. Severe hemorrhage, hyperkalemia, or acidosis from acute kidney injury and sepsis could also account for his cardiac arrest. His paraplegia and hospitalization raise the risk of venous thromboembolism, which can lead to PEA from pulmonary embolus and prolonged hypoxia.
His profound anemia is the likely cause of his PEA arrest and severe lactic acidosis. Massive hemolysis is most likely given no overt evidence of bleeding to account for the precipitous fall in hematocrit. Hemolysis can result from disorders intrinsic or extrinsic to the red blood cell (RBC). Intrinsic defects are usually congenital and involve the membrane, hemoglobin, or metabolic enzymes within the RBC. Extrinsic hemolysis arises from processes that injure the RBC from the outside: antibodies, infections, and mechanical shearing.
A rapidly declining platelet count is seen in microangiopathic hemolytic conditions such as disseminated intravascular coagulation (DIC) or thrombotic thrombocytopenic purpura (TTP), where platelets are consumed along with RBCs; sepsis makes DIC more likely. Autoimmune hemolytic anemia (AIHA) is sometimes accompanied by immune thrombocytopenia. AIHA arises from antibodies that are idiopathic or produced in response to infection, autoimmune conditions (eg, systemic lupus erythematosus), lymphoproliferative disease, or drugs (eg, ‐lactam antibiotics). The antiphospholipid syndrome can lead to thrombocytopenia, hemolysis, and kidney injury. Devitalized tissue in his sacral ulcers may predispose the patient to infection with Clostridium perfringens, which can elaborate enzymes that trigger massive hemolysis.
Because automated hemoglobin measurement is performed by spectrophotometry (light absorption and scatter), high concentrations of poorly soluble autoantibodies can increase the turbidity of the sample and preclude the measurement of hemoglobin concentration. This could lead to the report of interfering substances.

Low haptoglobin, elevated LDH, and hyperbilirubinemia confirm hemolysis. A more robust reticulocytosis is expected in the face of profound anemia, but the patient may also suffer from a concomitant hypoproliferative state (eg, nutritional deficiency). More likely, the rapidity of his decline outpaced the marrow's response, which can be delayed by days.
The most common cause of a combined elevation of the INR/PT and aPTT in a critically ill patient is DIC. Although no schistocytes were detected on the peripheral smear, they can be absent in up to 50% of DIC cases. TTP is associated with hemolytic anemia, kidney injury, and thrombocytopenia, but it generally does not cause coagulopathy.
The combination of red cell agglutination and hemophagocytosis suggests that the RBCs are coated with autoantibodies that cross‐link the cells and make them targets for phagocytosis by neutrophils in the circulation. This is distinct from the hemophagocytic syndrome, a rare immune activation syndrome characterized by macrophage phagocytosis of RBCs in the reticuloendothelial system. The blood smear also shows microspherocytes, which are seen in AIHA and hereditary spherocytosis.
Acute tubular necrosis could result from sepsis, ischemic injury from DIC, hypotension during cardiac arrest, or heme pigment toxicity. Urine sediment should be reviewed for dysmorphic RBCs or RBC casts that would indicate glomerulonephritis (eg, from an underlying autoimmune process associated with AIHA).
Urine hemoglobin that is disproportionate to the degree of hematuria suggests hemoglobinuria, which in turn defines the hemolysis as intravascular. Processes that directly lyse RBCs in circulation via mechanical shearing, activation of complement, infection of the RBC, or enzymatic or oxidative destruction of the membrane cause intravascular hemolysis. Leading considerations include microangiopathy (eg, DIC, TTP), clostridial sepsis, and AIHA.
AIHA can be broadly classified as warm or cold. Warm AIHA is caused by immunoglobulin IgG antibodies that bind most avidly at body temperature. Because warm AIHA does not activate complement, patients present with evidence of extravascular hemolysis that is typically chronic and mild to moderate in severity. It does not typically cause the acute, fulminant, intravascular hemolytic condition seen here.
Cold AIHA is characterized by autoantibodies that bind at lower temperatures and comes in 2 forms: cold agglutinin disease and (rarely) paroxysmal cold hemoglobinuria (PCH). Cold agglutinins are most often IgM antibodies produced in response to infection (Mycoplasma pneumoniae, infectious mononucleosis), drugs, or a hematologic malignancy. These IgM antibodies bind RBCs, causing them to agglutinate, and fix complement (including C3) to the surface of RBCs when blood circulates to cooler parts of the body. This results in complement activation, formation of the membrane attack complex, and intravascular hemolysis when bound and activated complement is present in large numbers. Acute infection can increase the complement available for binding to the surface of RBCs. Through a slightly different mechanism, PCH causes intravascular hemolysis through direct IgG activation of complement fixed to the surface of RBCs. During a hemolytic episode the direct antibody test (DAT) is positive using anti‐C3 and negative for IgG.
Based on the patient's clinical evidence of intravascular hemolysis and a suspected autoimmune etiology, the leading diagnosis at this time is cold AIHA.
The DAT detects IgG or complement adherent to RBCs. This patient has tested positive for both IgG and C3, though much more strongly for IgG, suggesting an unusual ability of the patient's IgG to activate complement. The phenomenon of mixed AIHA, in which the patient has both warm‐ and cold‐reacting antibodies, is rare.
Regarding infections associated with AIHA, there is no cough or rash to suggest M pneumoniae, and there is no sore throat, fever, lymphadenopathy, splenomegaly, or atypical lymphocytosis to suggest infectious mononucleosis. He should be tested for human immunodeficiency virus, which is also associated with AIHA. His leukocytosis may raise suspicion for an underlying hematologic malignancy, but he does not have blasts, dysplastic leukocytes, or lymphocytosis on his peripheral blood smear. Systemic lupus erythematosus can be associated with AIHA, thrombocytopenia, and renal failure, but he lacks the more common clinical manifestations of rash, arthralgias, and fever.
Drug‐induced immune hemolytic anemia (DIIHA) can cause both the clinical and serologic profile of an AIHA, as seen here. DIIHA can be distinguished from mixed AIHA if hemolysis abates with discontinuation of an offending drug. His deterioration is temporally associated with drug administration at the time of admission. Cephalosporins and ‐lactams (e.g., piperacillin) are the most common causes of DIIHA, and ‐lactamases such as tazobactam have also been implicated. By exclusion of other causes, DIIHA secondary to piperacillin is most likely responsible for his massive intravascular hemolysis.
COMMENTARY
This case illustrates a dramatic presentation of fulminant intravascular hemolysis secondary to piperacillin. The incidence of DIIHA is estimated to be 1 in 1 million.[1] Historically, methyldopa and high‐dose penicillin have been responsible for the majority of cases,[2] but in recent years complex penicillins, including piperacillin, and second‐ and third‐generation cephalosporins have been implicated.[3, 4] Cases of DIIHA are often underdiagnosed or misdiagnosed, as smoldering or less severe cases may not be recognized or are attributed to other causes.
A positive DAT, suggesting immunoglobulin and/or complement binding to RBCs, is the most reliable laboratory finding in DIIHA.[5] However, a positive DAT does not identify the source of the antigen and may result in misattribution of the immune hemolysis to autoimmunity rather than to a drug. Repeated or continued administration of the offending drug (as in this case) may perpetuate or worsen the hemolysis. Drug‐specific antibody tests may help to confirm the diagnosis, but these tests are complex and take significant time for specialized laboratories to run.
Severe hemolysis should be considered when a patient has a sudden and dramatic drop in his hemoglobin level in the absence of bleeding. Because DIIHA can be rapidly progressive, discontinuing a suspected culprit drug is the most important diagnostic and therapeutic measure. Typically, when an offending drug is stopped, the hemolysis stops as well. The time course over which this occurs depends on the rapidity of drug clearance.[4] Hemodialysis or plasmapheresis may be required in cases where the medication is renally excreted, particularly in cases of concomitant kidney injury. Evidence supporting corticosteroid use in DIIHA is limited, as the offending agent is usually discontinued by the time corticosteroids are initiated.[4]
This patient's DAT confirmed both IgG and complement activation, consistent with DIIHA caused by an immune complexlike reaction. This mechanism involves the antibody binding to a mixed epitope of the drug and a RBC membrane glycoprotein.[6] The offending drug was stopped only when review of his medical records established a clear temporal association between antibiotic administration and prior hemolysis.
The 2009 Health Information Technology for Economic and Clinical Health Act created an electronic health record (EHR) incentive program (meaningful use criteria).[7] By 2012, only 6% of hospitals met all of the stage 2 criteria, which include EHR interoperability across health systems.[8] The patient's preceding hemolytic event was described in records faxed by the outside hospitals, but without EHR interoperability, the treating clinicians did not have timely access to this information. Instead, the familiar manual process of obtaining outside records involving signed forms, phone calls, fax machines, and reams of paper progressed at its usual pace. Real‐time access to health records might have guided providers to select an alternative antibiotic regimen. Instead, a communication breakdown contributed to a catastrophic drug reaction and to this tragic patient outcome.
KEY TEACHING POINTS
- In a patient presenting with acute hemolysis and a positive DAT, consider DIIHA.
- Both piperacillin and tazobactam can cause a severe, complement‐mediated immune hemolytic anemia (DIIHA).
- Drug‐induced antibodies are detected by direct antiglobulin testing, but a complete medication history is the key to diagnosis.
- Management of drug‐induced hemolytic anemia involves immediate discontinuation of the culprit medication, supportive care, and potentially corticosteroids, plasmapheresis, and/or hemodialysis to expedite removal of the offending agent.
- EHR interoperability may provide timely access to important health information across different hospitals, expedite health information exchange, and reduce adverse patient outcomes that stem from communication delays.
This case was submitted anonymously to AHRQ WebM&M on July 18, 2014, and was accepted on August 7, 2014. The case and WebM&M commentary were published online on October 26, 2015.[9] This separate commentary on the same case was later submitted to the Journal of Hospital Medicine on September 2, 2015, accepted on November 24, 2015, and published on January 22, 2016. The 2 publications are written by different authors, and although they reference the same case, they make different but valuable points.
Disclosure
Nothing to report.