User login
SHM Report Provides New Insights About Physician Practice Leaders
The Society of Hospital Medicine’s 2012 State of Hospital Medicine report (SOHM) offers new insights about physician practice leaders.
Physician Leader Presence
“Choose a hospitalist leader with the right skills and experience. Selecting the right leader is fundamental to a successful hospitalist practice. These individuals are hard to find. They must be excellent clinically and have superb communication skills.”1
The SOHM survey shows that the vast majority (97%) of hospital medicine groups (HMGs) in the U.S. now have a designated physician leader (see Figure 1). Given this high percentage, examining the outliers is intriguing. Of the 13 adult medicine HMGs that reported not having a physician leader, the large majority were hospital-owned, located in the South region, and situated in non-teaching hospitals. The size of the HMG impacted the presence of a physician leader: 100% of groups with 20 or more full-time equivalents had physician leaders.
Source: 2012 State of Hospital Medicine report
Dedicated Leadership Time
“The medical director of the hospitalist program needs sufficient, non-clinical time to address administrative and leadership issues.”1
The 2007/2008 SOHM survey reported a median of 20% administrative time for physician leaders. In the 2012 survey, the median amount of time was 25% for adult medicine HMGs. The percentages were higher in the East and West regions, in hospital-owned programs, and in non- academic programs. The percentage of protected time also went up with group size.
Compensation
The 2012 SOHM shows median compensation premiums for physician leaders of 20%; that is, leader compensation is 120% of the average salary in their group. The numbers across regions and sizes were remarkably consistent. Overall, it seems that a 15% to 20% compensation premium for hospitalist leaders is standard.
Key Takeaways
No. 1, hospitalist groups need physician hospitalist leaders with protected leadership, but who also work clinically as a hospitalist. Why? Because hospitalists need a leader they respect, someone that they believe understands their specific issues. Unless the physician in charge has worked those 12-hour overnight shifts, argued with the consultants, tried to discharge an ornery patient, received 20 pages in an hour about medication reconciliation, or disagreed with an ED doc about the appropriateness of an admission, it would be hard for that leader to fully understand the stresses hospitalists encounter on a daily basis.
Hospitalist leaders are taking on increasingly important roles to help their organizations realize key performance improvement goals.
Additionally, the roles of outpatient doctors are changing: “Many physicians are no longer able or willing to serve on hospital committees or play a leadership role for the medical staff. Hospitalists have the potential to step in and help address these key issues”1
No. 2, size matters. Given increased responsibilities that include handling focused and ongoing professional practice evaluations, designing pathways to reduce adverse events, counseling, mentoring, disciplining, conducting yearly reviews, and investigating patient and staff complaints, it makes sense that larger programs also have leaders with more protected time and commensurate compensation.
As our healthcare systems ask hospitalists to offer higher reliability and to champion more administrative, safety, and quality projects, HM leaders—who are perfectly placed to organize and manage those projects—need the time and the compensation to do so. To borrow from hospitalist pioneer Bob Wachter, MD, MHM, our future C-suite leaders are percolating in hospitalist programs, learning the skills we will need to participate in the high reliability hospitals of our present and future.
Dr. Lovins is chief of hospital medicine at Middlesex Hospital in Middletown, Conn., and assistant clinical professor of medicine at Yale University School of Medicine. She is a member of SHM’s Practice Analysis Committee.
Reference
The Society of Hospital Medicine’s 2012 State of Hospital Medicine report (SOHM) offers new insights about physician practice leaders.
Physician Leader Presence
“Choose a hospitalist leader with the right skills and experience. Selecting the right leader is fundamental to a successful hospitalist practice. These individuals are hard to find. They must be excellent clinically and have superb communication skills.”1
The SOHM survey shows that the vast majority (97%) of hospital medicine groups (HMGs) in the U.S. now have a designated physician leader (see Figure 1). Given this high percentage, examining the outliers is intriguing. Of the 13 adult medicine HMGs that reported not having a physician leader, the large majority were hospital-owned, located in the South region, and situated in non-teaching hospitals. The size of the HMG impacted the presence of a physician leader: 100% of groups with 20 or more full-time equivalents had physician leaders.
Source: 2012 State of Hospital Medicine report
Dedicated Leadership Time
“The medical director of the hospitalist program needs sufficient, non-clinical time to address administrative and leadership issues.”1
The 2007/2008 SOHM survey reported a median of 20% administrative time for physician leaders. In the 2012 survey, the median amount of time was 25% for adult medicine HMGs. The percentages were higher in the East and West regions, in hospital-owned programs, and in non- academic programs. The percentage of protected time also went up with group size.
Compensation
The 2012 SOHM shows median compensation premiums for physician leaders of 20%; that is, leader compensation is 120% of the average salary in their group. The numbers across regions and sizes were remarkably consistent. Overall, it seems that a 15% to 20% compensation premium for hospitalist leaders is standard.
Key Takeaways
No. 1, hospitalist groups need physician hospitalist leaders with protected leadership, but who also work clinically as a hospitalist. Why? Because hospitalists need a leader they respect, someone that they believe understands their specific issues. Unless the physician in charge has worked those 12-hour overnight shifts, argued with the consultants, tried to discharge an ornery patient, received 20 pages in an hour about medication reconciliation, or disagreed with an ED doc about the appropriateness of an admission, it would be hard for that leader to fully understand the stresses hospitalists encounter on a daily basis.
Hospitalist leaders are taking on increasingly important roles to help their organizations realize key performance improvement goals.
Additionally, the roles of outpatient doctors are changing: “Many physicians are no longer able or willing to serve on hospital committees or play a leadership role for the medical staff. Hospitalists have the potential to step in and help address these key issues”1
No. 2, size matters. Given increased responsibilities that include handling focused and ongoing professional practice evaluations, designing pathways to reduce adverse events, counseling, mentoring, disciplining, conducting yearly reviews, and investigating patient and staff complaints, it makes sense that larger programs also have leaders with more protected time and commensurate compensation.
As our healthcare systems ask hospitalists to offer higher reliability and to champion more administrative, safety, and quality projects, HM leaders—who are perfectly placed to organize and manage those projects—need the time and the compensation to do so. To borrow from hospitalist pioneer Bob Wachter, MD, MHM, our future C-suite leaders are percolating in hospitalist programs, learning the skills we will need to participate in the high reliability hospitals of our present and future.
Dr. Lovins is chief of hospital medicine at Middlesex Hospital in Middletown, Conn., and assistant clinical professor of medicine at Yale University School of Medicine. She is a member of SHM’s Practice Analysis Committee.
Reference
The Society of Hospital Medicine’s 2012 State of Hospital Medicine report (SOHM) offers new insights about physician practice leaders.
Physician Leader Presence
“Choose a hospitalist leader with the right skills and experience. Selecting the right leader is fundamental to a successful hospitalist practice. These individuals are hard to find. They must be excellent clinically and have superb communication skills.”1
The SOHM survey shows that the vast majority (97%) of hospital medicine groups (HMGs) in the U.S. now have a designated physician leader (see Figure 1). Given this high percentage, examining the outliers is intriguing. Of the 13 adult medicine HMGs that reported not having a physician leader, the large majority were hospital-owned, located in the South region, and situated in non-teaching hospitals. The size of the HMG impacted the presence of a physician leader: 100% of groups with 20 or more full-time equivalents had physician leaders.
Source: 2012 State of Hospital Medicine report
Dedicated Leadership Time
“The medical director of the hospitalist program needs sufficient, non-clinical time to address administrative and leadership issues.”1
The 2007/2008 SOHM survey reported a median of 20% administrative time for physician leaders. In the 2012 survey, the median amount of time was 25% for adult medicine HMGs. The percentages were higher in the East and West regions, in hospital-owned programs, and in non- academic programs. The percentage of protected time also went up with group size.
Compensation
The 2012 SOHM shows median compensation premiums for physician leaders of 20%; that is, leader compensation is 120% of the average salary in their group. The numbers across regions and sizes were remarkably consistent. Overall, it seems that a 15% to 20% compensation premium for hospitalist leaders is standard.
Key Takeaways
No. 1, hospitalist groups need physician hospitalist leaders with protected leadership, but who also work clinically as a hospitalist. Why? Because hospitalists need a leader they respect, someone that they believe understands their specific issues. Unless the physician in charge has worked those 12-hour overnight shifts, argued with the consultants, tried to discharge an ornery patient, received 20 pages in an hour about medication reconciliation, or disagreed with an ED doc about the appropriateness of an admission, it would be hard for that leader to fully understand the stresses hospitalists encounter on a daily basis.
Hospitalist leaders are taking on increasingly important roles to help their organizations realize key performance improvement goals.
Additionally, the roles of outpatient doctors are changing: “Many physicians are no longer able or willing to serve on hospital committees or play a leadership role for the medical staff. Hospitalists have the potential to step in and help address these key issues”1
No. 2, size matters. Given increased responsibilities that include handling focused and ongoing professional practice evaluations, designing pathways to reduce adverse events, counseling, mentoring, disciplining, conducting yearly reviews, and investigating patient and staff complaints, it makes sense that larger programs also have leaders with more protected time and commensurate compensation.
As our healthcare systems ask hospitalists to offer higher reliability and to champion more administrative, safety, and quality projects, HM leaders—who are perfectly placed to organize and manage those projects—need the time and the compensation to do so. To borrow from hospitalist pioneer Bob Wachter, MD, MHM, our future C-suite leaders are percolating in hospitalist programs, learning the skills we will need to participate in the high reliability hospitals of our present and future.
Dr. Lovins is chief of hospital medicine at Middlesex Hospital in Middletown, Conn., and assistant clinical professor of medicine at Yale University School of Medicine. She is a member of SHM’s Practice Analysis Committee.
Reference
Two Hospitalist Groups Join SHM's Hospital Medicine Exchange
HMX: Two New Communities, Lots of New Conversations
More than 2,500 hospitalists have logged in to HMX (www.hmxchange.org) to share their experiences and learn from the experiences of other hospitalists. And now, two other groups of hospitalists have a new reason to check out HMX.
The first community, for family medicine hospitalists, was launched in October. Approximately 10% of SHM’s active members are hospitalists trained in family medicine (HTFM), many of whom are very active within SHM. More than 60 hospitalists trained in family medicine are either Fellows in Hospital Medicine or Senior Fellows in Hospital Medicine.
And, in December, hospitalists who work in post-acute care can work together to tackle the challenges unique to post-acute care. This new community was an outgrowth of SHM’s Post-Acute Care Task Force.
Brendon Shank is SHM’s associate vice president of communications.
HMX: Two New Communities, Lots of New Conversations
More than 2,500 hospitalists have logged in to HMX (www.hmxchange.org) to share their experiences and learn from the experiences of other hospitalists. And now, two other groups of hospitalists have a new reason to check out HMX.
The first community, for family medicine hospitalists, was launched in October. Approximately 10% of SHM’s active members are hospitalists trained in family medicine (HTFM), many of whom are very active within SHM. More than 60 hospitalists trained in family medicine are either Fellows in Hospital Medicine or Senior Fellows in Hospital Medicine.
And, in December, hospitalists who work in post-acute care can work together to tackle the challenges unique to post-acute care. This new community was an outgrowth of SHM’s Post-Acute Care Task Force.
Brendon Shank is SHM’s associate vice president of communications.
HMX: Two New Communities, Lots of New Conversations
More than 2,500 hospitalists have logged in to HMX (www.hmxchange.org) to share their experiences and learn from the experiences of other hospitalists. And now, two other groups of hospitalists have a new reason to check out HMX.
The first community, for family medicine hospitalists, was launched in October. Approximately 10% of SHM’s active members are hospitalists trained in family medicine (HTFM), many of whom are very active within SHM. More than 60 hospitalists trained in family medicine are either Fellows in Hospital Medicine or Senior Fellows in Hospital Medicine.
And, in December, hospitalists who work in post-acute care can work together to tackle the challenges unique to post-acute care. This new community was an outgrowth of SHM’s Post-Acute Care Task Force.
Brendon Shank is SHM’s associate vice president of communications.
Applications Being Accepted for SHM Fellows Program
Fellows Deadline Is Jan. 10, 2014
Thousands of hospitalists across the country have earned the Fellow in Hospital Medicine (FHM) and Senior Fellow in Hospital Medicine (SFHM) designation to set themselves apart in the specialty—and among other hospital-based caregivers.
For the second year, nurse practitioners and physician assistants can also earn the FHM and SFHM designations.
Candidates for FHM and SFHM can now apply online. For more information or to apply, visit www.hospitalmedicine.org/fellows.
Fellows Deadline Is Jan. 10, 2014
Thousands of hospitalists across the country have earned the Fellow in Hospital Medicine (FHM) and Senior Fellow in Hospital Medicine (SFHM) designation to set themselves apart in the specialty—and among other hospital-based caregivers.
For the second year, nurse practitioners and physician assistants can also earn the FHM and SFHM designations.
Candidates for FHM and SFHM can now apply online. For more information or to apply, visit www.hospitalmedicine.org/fellows.
Fellows Deadline Is Jan. 10, 2014
Thousands of hospitalists across the country have earned the Fellow in Hospital Medicine (FHM) and Senior Fellow in Hospital Medicine (SFHM) designation to set themselves apart in the specialty—and among other hospital-based caregivers.
For the second year, nurse practitioners and physician assistants can also earn the FHM and SFHM designations.
Candidates for FHM and SFHM can now apply online. For more information or to apply, visit www.hospitalmedicine.org/fellows.
Submit Your HM14 Scientific Abstracts Soon
HM14: Submit Your Scientific Abstracts Soon
Abstracts are being accepted for SHM’s scientific poster and oral abstract competition, known as Research, Innovations, and Clinical Vignettes (RIV), until Sunday, Dec. 1. Visit the Academic Community page on the SHM website, or, for a full suite of resources for submitting your abstract, go directly to the abstract submission site (https://shm.confex.com/shm/HM14/cfp.cgi) to submit your abstract today.
For more on HM14, the biggest meeting in hospital medicine, visit www.hospitalmedicine2014.org.
Brendon Shank is SHM’s associate vice president of communications.
HM14: Submit Your Scientific Abstracts Soon
Abstracts are being accepted for SHM’s scientific poster and oral abstract competition, known as Research, Innovations, and Clinical Vignettes (RIV), until Sunday, Dec. 1. Visit the Academic Community page on the SHM website, or, for a full suite of resources for submitting your abstract, go directly to the abstract submission site (https://shm.confex.com/shm/HM14/cfp.cgi) to submit your abstract today.
For more on HM14, the biggest meeting in hospital medicine, visit www.hospitalmedicine2014.org.
Brendon Shank is SHM’s associate vice president of communications.
HM14: Submit Your Scientific Abstracts Soon
Abstracts are being accepted for SHM’s scientific poster and oral abstract competition, known as Research, Innovations, and Clinical Vignettes (RIV), until Sunday, Dec. 1. Visit the Academic Community page on the SHM website, or, for a full suite of resources for submitting your abstract, go directly to the abstract submission site (https://shm.confex.com/shm/HM14/cfp.cgi) to submit your abstract today.
For more on HM14, the biggest meeting in hospital medicine, visit www.hospitalmedicine2014.org.
Brendon Shank is SHM’s associate vice president of communications.
Movers and Shakers in Hospital Medicine
Xavier Perez, MD, is the 2013 Hospitalist Medical Director of the Year at TeamHealth. Dr. Perez oversees the hospital medicine program at Sutter Solano Medical Center, a 102-bed acute care center in Vallejo, Calif. Knoxville, Tenn.-based TeamHealth has been partnering with hospital-based providers to provide hospitalist, emergency, and anesthesia staffing since 1979.
Christopher Sharp, MD, has been named the new chief medical information officer at Stanford Hospital and Clinics in Stanford, Calif. Dr. Sharp is hospitalist at Stanford University Medical Center, clinical associate professor of medicine at Stanford University School of Medicine, and chair of the Medical Staff Health Information Management (HIM) Committee.
Business Moves
Hospitalists of Northern Michigan (HNM), based in Traverse City, Mich., has been recognized as one of Modern Healthcare’s 2013 Best Places to Work in Healthcare. The award has honored healthcare employers for economic development, employee satisfaction, and retention for the last six years. HNM provides hospitalist services to six hospitals in four different healthcare systems throughout Northern Michigan.
IPC The Hospitalist Company, based in North Hollywood, Calif., recently announced that it will oversee hospitalist services at Metropolitan Pulmonary and Hospital Medicine, P.C. (MPHM), in Kansas City, Mo. This new agreement will place IPC management into two new Kansas City hospitals. IPC provides hospitalist services to over 350 hospitals in 28 states throughout the country.
WakeMed Health and Hospitals, a Raleigh, N.C.-based healthcare system, now provides pediatric hospitalist services to Central Carolina Hospital (CCH) in Sanford, N.C. WakeMed will begin by staffing three pediatric hospitalists at CCH to establish 24-hour pediatric inpatient care. Central Carolina Hospital is an acute care community hospital that already offers hospitalist services to its adult patients.
Tacoma, Wash.-based Sound Inpatient Physicians has partnered with CHRISTUS Health to provide hospitalist services at seven of its hospitals in Texas and Louisiana. The seven hospitals are CHRISTUS Spohn Hospital Corpus Christi-Shoreline and CHRISTUS Spohn Hospital Corpus Christi-South in Corpus Christi, Texas; CHRISTUS Santa Rosa Hospital-Medical Center and CHRISTUS Santa Rosa Hospital-Westover Hills, both in San Antonio, Texas; CHRISTUS St. Frances Cabrini Hospital in Alexandria, La.; CHRISTUS St. Patrick Hospital in Lake Charles, La.; and CHRISTUS Highland Medical Center in Shreveport, La. Sound now provides hospitalist services to over 70 hospitals throughout the country. CHRISTUS Health is a Catholic hospital system made up of more than 40 hospitals throughout seven U.S. states and six Mexican states.
Carolinas Medical Center–Union in Monroe, N.C., will staff three 24-hour pediatric hospitalists thanks to an agreement with Levine Children’s Hospital in Charlotte, N.C. Both hospitals are part of Carolinas HealthCare System, which is the largest public, non-profit hospital system in North and South Carolina.
Curry General Hospital in Gold Beach, Ore., is offering hospitalist services to inpatients at the flagship hospital of Curry Health Network, which is made up of seven hospitals and outpatient clinics serving the Wild Rivers Coast area of southwestern Oregon.
Xavier Perez, MD, is the 2013 Hospitalist Medical Director of the Year at TeamHealth. Dr. Perez oversees the hospital medicine program at Sutter Solano Medical Center, a 102-bed acute care center in Vallejo, Calif. Knoxville, Tenn.-based TeamHealth has been partnering with hospital-based providers to provide hospitalist, emergency, and anesthesia staffing since 1979.
Christopher Sharp, MD, has been named the new chief medical information officer at Stanford Hospital and Clinics in Stanford, Calif. Dr. Sharp is hospitalist at Stanford University Medical Center, clinical associate professor of medicine at Stanford University School of Medicine, and chair of the Medical Staff Health Information Management (HIM) Committee.
Business Moves
Hospitalists of Northern Michigan (HNM), based in Traverse City, Mich., has been recognized as one of Modern Healthcare’s 2013 Best Places to Work in Healthcare. The award has honored healthcare employers for economic development, employee satisfaction, and retention for the last six years. HNM provides hospitalist services to six hospitals in four different healthcare systems throughout Northern Michigan.
IPC The Hospitalist Company, based in North Hollywood, Calif., recently announced that it will oversee hospitalist services at Metropolitan Pulmonary and Hospital Medicine, P.C. (MPHM), in Kansas City, Mo. This new agreement will place IPC management into two new Kansas City hospitals. IPC provides hospitalist services to over 350 hospitals in 28 states throughout the country.
WakeMed Health and Hospitals, a Raleigh, N.C.-based healthcare system, now provides pediatric hospitalist services to Central Carolina Hospital (CCH) in Sanford, N.C. WakeMed will begin by staffing three pediatric hospitalists at CCH to establish 24-hour pediatric inpatient care. Central Carolina Hospital is an acute care community hospital that already offers hospitalist services to its adult patients.
Tacoma, Wash.-based Sound Inpatient Physicians has partnered with CHRISTUS Health to provide hospitalist services at seven of its hospitals in Texas and Louisiana. The seven hospitals are CHRISTUS Spohn Hospital Corpus Christi-Shoreline and CHRISTUS Spohn Hospital Corpus Christi-South in Corpus Christi, Texas; CHRISTUS Santa Rosa Hospital-Medical Center and CHRISTUS Santa Rosa Hospital-Westover Hills, both in San Antonio, Texas; CHRISTUS St. Frances Cabrini Hospital in Alexandria, La.; CHRISTUS St. Patrick Hospital in Lake Charles, La.; and CHRISTUS Highland Medical Center in Shreveport, La. Sound now provides hospitalist services to over 70 hospitals throughout the country. CHRISTUS Health is a Catholic hospital system made up of more than 40 hospitals throughout seven U.S. states and six Mexican states.
Carolinas Medical Center–Union in Monroe, N.C., will staff three 24-hour pediatric hospitalists thanks to an agreement with Levine Children’s Hospital in Charlotte, N.C. Both hospitals are part of Carolinas HealthCare System, which is the largest public, non-profit hospital system in North and South Carolina.
Curry General Hospital in Gold Beach, Ore., is offering hospitalist services to inpatients at the flagship hospital of Curry Health Network, which is made up of seven hospitals and outpatient clinics serving the Wild Rivers Coast area of southwestern Oregon.
Xavier Perez, MD, is the 2013 Hospitalist Medical Director of the Year at TeamHealth. Dr. Perez oversees the hospital medicine program at Sutter Solano Medical Center, a 102-bed acute care center in Vallejo, Calif. Knoxville, Tenn.-based TeamHealth has been partnering with hospital-based providers to provide hospitalist, emergency, and anesthesia staffing since 1979.
Christopher Sharp, MD, has been named the new chief medical information officer at Stanford Hospital and Clinics in Stanford, Calif. Dr. Sharp is hospitalist at Stanford University Medical Center, clinical associate professor of medicine at Stanford University School of Medicine, and chair of the Medical Staff Health Information Management (HIM) Committee.
Business Moves
Hospitalists of Northern Michigan (HNM), based in Traverse City, Mich., has been recognized as one of Modern Healthcare’s 2013 Best Places to Work in Healthcare. The award has honored healthcare employers for economic development, employee satisfaction, and retention for the last six years. HNM provides hospitalist services to six hospitals in four different healthcare systems throughout Northern Michigan.
IPC The Hospitalist Company, based in North Hollywood, Calif., recently announced that it will oversee hospitalist services at Metropolitan Pulmonary and Hospital Medicine, P.C. (MPHM), in Kansas City, Mo. This new agreement will place IPC management into two new Kansas City hospitals. IPC provides hospitalist services to over 350 hospitals in 28 states throughout the country.
WakeMed Health and Hospitals, a Raleigh, N.C.-based healthcare system, now provides pediatric hospitalist services to Central Carolina Hospital (CCH) in Sanford, N.C. WakeMed will begin by staffing three pediatric hospitalists at CCH to establish 24-hour pediatric inpatient care. Central Carolina Hospital is an acute care community hospital that already offers hospitalist services to its adult patients.
Tacoma, Wash.-based Sound Inpatient Physicians has partnered with CHRISTUS Health to provide hospitalist services at seven of its hospitals in Texas and Louisiana. The seven hospitals are CHRISTUS Spohn Hospital Corpus Christi-Shoreline and CHRISTUS Spohn Hospital Corpus Christi-South in Corpus Christi, Texas; CHRISTUS Santa Rosa Hospital-Medical Center and CHRISTUS Santa Rosa Hospital-Westover Hills, both in San Antonio, Texas; CHRISTUS St. Frances Cabrini Hospital in Alexandria, La.; CHRISTUS St. Patrick Hospital in Lake Charles, La.; and CHRISTUS Highland Medical Center in Shreveport, La. Sound now provides hospitalist services to over 70 hospitals throughout the country. CHRISTUS Health is a Catholic hospital system made up of more than 40 hospitals throughout seven U.S. states and six Mexican states.
Carolinas Medical Center–Union in Monroe, N.C., will staff three 24-hour pediatric hospitalists thanks to an agreement with Levine Children’s Hospital in Charlotte, N.C. Both hospitals are part of Carolinas HealthCare System, which is the largest public, non-profit hospital system in North and South Carolina.
Curry General Hospital in Gold Beach, Ore., is offering hospitalist services to inpatients at the flagship hospital of Curry Health Network, which is made up of seven hospitals and outpatient clinics serving the Wild Rivers Coast area of southwestern Oregon.
Culture Shift Required to Defeat Defensive Medicine
Hospitalist Allen Kachalia, MD, JD, of Brigham and Women’s Hospital in Boston, sees defensive medicine as a source of unnecessary costs—and a threat to patient safety.
In fact, he and his colleagues offered an oral presentation at HM13 earlier this year titled, “Overutilization and Defensive Medicine in U.S. Hospitals: A Randomized National Survey of Hospitalists.” In a survey of 1,020 hospitalists, it was reported that defensive medicine was practiced in 37% of pre-operative evaluations and 58% of syncope cases.
Dr. Kachalia says he understands the pressures that can lead physicians to order unnecessary tests, particularly when patients request them. So what does he say about those requests?
“The answer is a simple one but takes time and effort: If you don’t think that something is clinically indicated, you should talk with the patient, explaining to them why you don’t think it’s necessary,” he says. “And, hopefully, you can come to mutual agreement. Ordering things just for the sake of preventing legal liability is just not the right thing to do.”
Dr. Kachalia says he believes that a paradigm shift in how medical liability is handled in this country is needed to change those habits.
But culture change also takes time.
Bryan Weiss, MBA, managing director of the consulting services practice at Irving, Texas-based MedSynergies, says the first step of that change may be having physicians admit that few doctors know a lot about malpractice issues, because they are typically negotiated, arranged, and paid for by their employers, whether that’s a hospital or large management companies.
“It’s not me versus them,” says Weiss, a Team Hospitalist member. “As a specialty, we need to be in this together, to push the education and awareness that it’s OK not to know, so let’s work together to make it better. But it’s not going to happen overnight.”
Hospitalist Allen Kachalia, MD, JD, of Brigham and Women’s Hospital in Boston, sees defensive medicine as a source of unnecessary costs—and a threat to patient safety.
In fact, he and his colleagues offered an oral presentation at HM13 earlier this year titled, “Overutilization and Defensive Medicine in U.S. Hospitals: A Randomized National Survey of Hospitalists.” In a survey of 1,020 hospitalists, it was reported that defensive medicine was practiced in 37% of pre-operative evaluations and 58% of syncope cases.
Dr. Kachalia says he understands the pressures that can lead physicians to order unnecessary tests, particularly when patients request them. So what does he say about those requests?
“The answer is a simple one but takes time and effort: If you don’t think that something is clinically indicated, you should talk with the patient, explaining to them why you don’t think it’s necessary,” he says. “And, hopefully, you can come to mutual agreement. Ordering things just for the sake of preventing legal liability is just not the right thing to do.”
Dr. Kachalia says he believes that a paradigm shift in how medical liability is handled in this country is needed to change those habits.
But culture change also takes time.
Bryan Weiss, MBA, managing director of the consulting services practice at Irving, Texas-based MedSynergies, says the first step of that change may be having physicians admit that few doctors know a lot about malpractice issues, because they are typically negotiated, arranged, and paid for by their employers, whether that’s a hospital or large management companies.
“It’s not me versus them,” says Weiss, a Team Hospitalist member. “As a specialty, we need to be in this together, to push the education and awareness that it’s OK not to know, so let’s work together to make it better. But it’s not going to happen overnight.”
Hospitalist Allen Kachalia, MD, JD, of Brigham and Women’s Hospital in Boston, sees defensive medicine as a source of unnecessary costs—and a threat to patient safety.
In fact, he and his colleagues offered an oral presentation at HM13 earlier this year titled, “Overutilization and Defensive Medicine in U.S. Hospitals: A Randomized National Survey of Hospitalists.” In a survey of 1,020 hospitalists, it was reported that defensive medicine was practiced in 37% of pre-operative evaluations and 58% of syncope cases.
Dr. Kachalia says he understands the pressures that can lead physicians to order unnecessary tests, particularly when patients request them. So what does he say about those requests?
“The answer is a simple one but takes time and effort: If you don’t think that something is clinically indicated, you should talk with the patient, explaining to them why you don’t think it’s necessary,” he says. “And, hopefully, you can come to mutual agreement. Ordering things just for the sake of preventing legal liability is just not the right thing to do.”
Dr. Kachalia says he believes that a paradigm shift in how medical liability is handled in this country is needed to change those habits.
But culture change also takes time.
Bryan Weiss, MBA, managing director of the consulting services practice at Irving, Texas-based MedSynergies, says the first step of that change may be having physicians admit that few doctors know a lot about malpractice issues, because they are typically negotiated, arranged, and paid for by their employers, whether that’s a hospital or large management companies.
“It’s not me versus them,” says Weiss, a Team Hospitalist member. “As a specialty, we need to be in this together, to push the education and awareness that it’s OK not to know, so let’s work together to make it better. But it’s not going to happen overnight.”
Why Hospitalists Remain Outside Malpractice Insurers' High-Risk Categories, For Now
Source: The Doctors Company
Ten years ago, the national headlines on malpractice insurance were staggering. Media reports catalogued OB-GYNs who proclaimed they were shutting down their private practices in the face of runaway premiums. Surgeons and other proceduralists decried payments tied to lawsuits they’d argue were arbitrary and capricious. And the American Medical Association (AMA) made announcement after announcement about states being in a “malpractice crisis.”
In recent years, premiums have actually dropped and stabilized at levels that most physicians agree are manageable for bottom lines. But, in that time, there has been scant discussion about hospital medicine’s relationship with malpractice. It’s not because the issue isn’t omnipresent for all healthcare practitioners, including the relatively nascent specialty that is HM.
Practice management experts say anecdotally that delayed diagnosis of, or treatment for, a spinal epidural abscess (SEA) is likely to get more than a few hospitalists sued. And, the proliferation of co-management of other specialties—particularly those with higher risk of incidence and higher premiums than internal medicine—open up hospitalists to further liability.
The issue is that at less than 20 years as a specialty, HM is in its infancy when it comes to its interaction with malpractice premiums. Health insurance companies and trade groups that track the insurance industry are just beginning to have enough data on claims, premiums, and payouts to make recommendations on risk factors, risk mitigation, and potential trends.
Still, even in a landscape of limited information, there are a few rules of thumb hospitalist group leaders should live by when it comes to managing exposure to malpractice cases, according to interviews with a half dozen healthcare professionals:
- Know how your coverage works. Is there “tail coverage” that ensures you have protection for incidents that happened at an institution where you no longer practice? Even though hospital-employed physicians rarely have rate discussions directly (the hospital typically covers premiums as part of the compensation package), take the time to learn the basic details.
- Be diligent in documentation. Note concerns in charts when appropriate, and stand up for your point of view. There’s a fine line between picking fights with other physicians involved in a patient’s care and making your concerns known, but don’t be afraid to put your clinical view on the record.
- Avoid the practice of “defensive medicine.” Ordering tests and procedures that aren’t clinically necessary might seem like it can serve as a protection from later lawsuits, but it adds to healthcare costs and is just not the right thing to do, says hospitalist Allen Kachalia, MD, JD, of Brigham and Women’s Hospital in Boston, who has studied the phenomenon (see “Culture Shift Necessary to Defeat “Defensive” Medicine,” on p. 38).
- Recognize the risks associated with co-management. Caring for neurology, cardiology, and other subspecialty patients is a revenue boost for HM groups, but when some of those complex cases have adverse events, the hospitalist who interacted with the patient daily could be included in a lawsuit.
- Focus on communication skills. An analysis of claims data by The Doctors Company (TDC) (www.thedoctors.com), a medical malpractice insurance company exclusively endorsed by SHM, reports that the second most common factor contributing to patient injury by hospitalists is “communication breakdown among healthcare professionals.”
- Manage workloads to avoid burnout. Don’t take on too many patients at the expense of being involved in hospital committees or quality initiatives.
To be sure, many of the same tenets of being a productive hospitalist with high patient satisfaction scores—maintain manageable censuses; focus on patient centeredness; and use checklists, technology, and regimented protocols to reduce adverse events—translate very well to being a lower-risk hospitalist in relation to malpractice cases.
When you’re “thinking of patient satisfaction strategies, also think of them as risk mitigation strategies,” says John Nelson, MD, MHM, FACP, medical director of the hospitalist practice at Overlake Hospital Medical Center in Bellevue, Wash., an SHM co-founder and practice management columnist for The Hospitalist. “They overlap tremendously.”
A History Lesson
Medical malpractice has been around for centuries and has two prevailing goals: 1) to provide monetary remuneration to patients who have been injured via substandard care and 2) to deter that poor treatment through fiscal punishment.
Malpractice lawsuits were not prevalent enough to be a major medical concern until the early 1800s. By the middle of the 19th century, the country hit its first periods of crisis.1 Cycles ebbed and flowed from there, with malpractice premiums causing crises in the 1980s and again in the early 2000s.
continued below...
Now, rates for medical professional liability insurance have been dropping for seven years, and an eighth straight annual decline is expected this year, according to Mike Matray, the editor of trade publication Medical Liability Monitor and the chief content officer of its associated website, www.mymedicalmalpracticeinsurance.com.
“We are in the longest, deepest soft market that the malpractice insurance industry has ever been in,” he says. “Right now, things are really good for the doctors, as far as rates coming down.”
Matray says he understands that declining rates may seem immaterial to a physician who receives an insurance bill that eats into the bottom line. For some specialties, that premium can be as high as $200,000 per physician, per year—or more.
“I’m not saying it isn’t expensive,” he adds. “It’s expensive to run a medical practice. At the same time, medical malpractice insurance is less expensive in today’s dollars than it was in 2005.”
The reduction in rates is multi-faceted. Prominently, state-level tort reforms like non-economic damage caps, health courts, and arbitration hearings are making it harder to bring cases to trial, particularly for lawyers who take cases on contingency. Second, frivolous lawsuits “are making an impression on jury pools,” Matray says, which means fewer filed claims and fewer cases that make it to trial. Third, this soft cycle has outlasted the typical pattern of rates falling for three to four years before rebounding.
“A lot of smart actuaries keep saying this has to change soon, because in a soft market there is a lot of competition,” he says, noting that in order to compete for low rates, insurance companies offer credits to clients and use their own reserve cash piles. “So things are really going to change in the next couple of years.”

—Robin Diamond, senior vice president and chief patient safety officer, The Doctors Company
In Need of Data, Patience
So what does it all mean for hospitalists and HM group leaders looking to be proactive about medical malpractice liability insurance? Patience is required.
For starters, there is no designated premium category for hospitalists. Much like the situation that exists for coding issues, the closest proxy for HM is internal medicine. According to Medical Liability Monitor, the premium paid by internal medicine physicians as of July 1, 2012, varied widely across the country. In South Florida, internal medicine insurance premiums in Miami, Dade, and Broward counties were between $42,000 and $46,000 per year. In South Dakota, one insurer reported rates of just under $4,000 per year. There is no average or median figure available, and Matray notes that actual rates paid can vary from county to county.
Moreover, it is difficult for group leaders or hospital executives to use past history to negotiate rates with insurers because of a shortage of reliable data. In its spring 2013 newsletter, the PIAA (formerly known as the Physician Insurers Association of America) published its first report on hospitalist claims reported to its Data Sharing Project. Of the 92,868 closed claims reported from 2002-2011, just 312, or 0.3%, named hospitalists as the defendant.
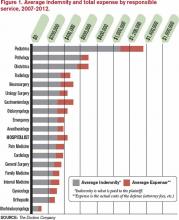
The data also showed that, of those claims, 20% were settled through insurance company payments. Those payments totaled $17.1 million, with an average payout to a claimant (known as the indemnity) of $272,553 per claim. Overall, hospitalists had a 20% paid-to-closed ratio, totaling more than $17.1 million. By comparison, the percent of paid-to-closed claims for all physicians was 29.3%, according to PIAA.
In a separate data set compiled this year by TDC, 34% of allegations against hospitalists were related to missed or failed diagnoses, with 28% tied to “improper management of treatment.” Twelve percent of allegations were the result of either improper medication management or ordering errors.
Robin Diamond, TDC’s senior vice president and chief patient safety officer, says that teasing out trends from the initial data can be challenging. Hospitalists, she says, can deal with so many different patients, diseases, and severity levels that it is difficult to draw conclusions.
“Hospital medicine is different than other specialties, because the hospitalist treats a broad range of patients in an acute care setting—from a pediatric patient to an adult patient with many chronic illnesses,” she says.
Divya Parikh, PIAA’s director of research and loss prevention, says HM group leaders should avoid reading too much into the first batch of data, because it’s a small sample size.
“A big part of that is we feel that a lot of hospitalists are intermingled into the other medical specialties,” she says. “So this becomes a very small subset where they are distinctly identified as hospitalists. And that’s the challenge.”
In particular, Parikh is curious to see whether HM’s rate of claims paid through insurance payments drops from 20% (already below the overall healthcare industry average). “It will be interesting as we proceed...to see if they begin to mitigate areas of risk where we used to see a lot of claims,” she adds. “If you look at a hospital setting, there has been some shift change in what the errors are. And, what you’d hope with hospitalists within these environments who are really owning this specialty, is that you’d see a decrease in that. There would be that connective care. There would be the patient that felt that they had an individual who was their go-to individual throughout their care at a hospital.”
A Peek at the Future
Insurers have begun compiling claims data on hospitalists and are taking a longer-term view of the specialty. TDC, for example, has analyzed its data and identified characteristics it says make a low-risk hospitalist, an analysis the company says is the first of its kind (see Figure 1). The insurer adds that it sees its responsibility as making sure everyone understands the hospitalist’s role within the acute care setting so that its pricing is commensurate with the liability risk.
Source: The Doctors Company
“We’re looking at the systems within the hospitalist group, as well as how well that group is integrating with the hospital where they’re practicing,” Diamond says. “What kind of patient mix is this particular hospitalist group seeing in that particular hospital, because it can be different in a large healthcare corporation in Manhattan, New York, from a community hospital in rural Texas.”
The growing popularity of hospitalists taking on co-management responsibilities for other specialties is another trend to keep an eye on, as it creates what insurers call “vicarious liability.” Working together in teams with other specialties can improve communication, reduce errors during transitions of care, and create better outcomes. However, in instances where there are problems, being on a care team means hospitalists can open themselves to liability. To mitigate that risk, hospitalists can look to other groups that have dealt with shared liability issues in the past, Parikh says.
“Historically, you would have seen it with anesthesiology,” she explains. “And one huge improvement anesthesiologists have made when a patient comes in for a surgery now is they come out, introduce themselves, say hello, and tell you what’s going on. They put a face to the name, so that it’s not just a no-name anesthesiologist who gets included in the lawsuit as well because they’re naming everybody in the group.”
But, holistically, the best long-term mitigation strategy appears to be tort reform and new ways of looking at the way in which healthcare liability issues are handled in the U.S., says Anupam Jena, MD, PhD, assistant professor of healthcare policy and medicine at Harvard Medical School, and an internist at Massachusetts General Hospital, both in Boston. Dr. Jena says that there is limited evidence that enacted malpractice reforms have produced more than a 2% to 5% reduction in healthcare spending compared to states that have not.2 Instead, healthcare leaders should push for the elimination of defensive medicine, which he says contributes the lion’s share of the estimated $50 billion annual cost of malpractice liability across the country.
“Do I think the country is in a malpractice crisis? No,” he says. “Do I think that defensive medicine is larger than we think it is? Yes.
“If physicians practice as they felt they should practice without ordering extra tests and procedures, my guess would be you could reduce healthcare spending by substantially more than $50 billion.”
Richard Quinn is a freelance writer in New Jersey.
References
- Spiegel AD, Kavaler F. America’s first medical malpractice crisis, 1835-1865. J Community Health. 1997;22:283-308.
- Chandra A, Jena A, Seabury, S. Defensive medicine may be costlier than it seems. The Wall Street Journal website. http://online.wsj.com/article/SB10001424127887323701904578280112638373302.html. Accessed September 21, 2013.
Source: The Doctors Company
Ten years ago, the national headlines on malpractice insurance were staggering. Media reports catalogued OB-GYNs who proclaimed they were shutting down their private practices in the face of runaway premiums. Surgeons and other proceduralists decried payments tied to lawsuits they’d argue were arbitrary and capricious. And the American Medical Association (AMA) made announcement after announcement about states being in a “malpractice crisis.”
In recent years, premiums have actually dropped and stabilized at levels that most physicians agree are manageable for bottom lines. But, in that time, there has been scant discussion about hospital medicine’s relationship with malpractice. It’s not because the issue isn’t omnipresent for all healthcare practitioners, including the relatively nascent specialty that is HM.
Practice management experts say anecdotally that delayed diagnosis of, or treatment for, a spinal epidural abscess (SEA) is likely to get more than a few hospitalists sued. And, the proliferation of co-management of other specialties—particularly those with higher risk of incidence and higher premiums than internal medicine—open up hospitalists to further liability.
The issue is that at less than 20 years as a specialty, HM is in its infancy when it comes to its interaction with malpractice premiums. Health insurance companies and trade groups that track the insurance industry are just beginning to have enough data on claims, premiums, and payouts to make recommendations on risk factors, risk mitigation, and potential trends.
Still, even in a landscape of limited information, there are a few rules of thumb hospitalist group leaders should live by when it comes to managing exposure to malpractice cases, according to interviews with a half dozen healthcare professionals:
- Know how your coverage works. Is there “tail coverage” that ensures you have protection for incidents that happened at an institution where you no longer practice? Even though hospital-employed physicians rarely have rate discussions directly (the hospital typically covers premiums as part of the compensation package), take the time to learn the basic details.
- Be diligent in documentation. Note concerns in charts when appropriate, and stand up for your point of view. There’s a fine line between picking fights with other physicians involved in a patient’s care and making your concerns known, but don’t be afraid to put your clinical view on the record.
- Avoid the practice of “defensive medicine.” Ordering tests and procedures that aren’t clinically necessary might seem like it can serve as a protection from later lawsuits, but it adds to healthcare costs and is just not the right thing to do, says hospitalist Allen Kachalia, MD, JD, of Brigham and Women’s Hospital in Boston, who has studied the phenomenon (see “Culture Shift Necessary to Defeat “Defensive” Medicine,” on p. 38).
- Recognize the risks associated with co-management. Caring for neurology, cardiology, and other subspecialty patients is a revenue boost for HM groups, but when some of those complex cases have adverse events, the hospitalist who interacted with the patient daily could be included in a lawsuit.
- Focus on communication skills. An analysis of claims data by The Doctors Company (TDC) (www.thedoctors.com), a medical malpractice insurance company exclusively endorsed by SHM, reports that the second most common factor contributing to patient injury by hospitalists is “communication breakdown among healthcare professionals.”
- Manage workloads to avoid burnout. Don’t take on too many patients at the expense of being involved in hospital committees or quality initiatives.
To be sure, many of the same tenets of being a productive hospitalist with high patient satisfaction scores—maintain manageable censuses; focus on patient centeredness; and use checklists, technology, and regimented protocols to reduce adverse events—translate very well to being a lower-risk hospitalist in relation to malpractice cases.
When you’re “thinking of patient satisfaction strategies, also think of them as risk mitigation strategies,” says John Nelson, MD, MHM, FACP, medical director of the hospitalist practice at Overlake Hospital Medical Center in Bellevue, Wash., an SHM co-founder and practice management columnist for The Hospitalist. “They overlap tremendously.”
A History Lesson
Medical malpractice has been around for centuries and has two prevailing goals: 1) to provide monetary remuneration to patients who have been injured via substandard care and 2) to deter that poor treatment through fiscal punishment.
Malpractice lawsuits were not prevalent enough to be a major medical concern until the early 1800s. By the middle of the 19th century, the country hit its first periods of crisis.1 Cycles ebbed and flowed from there, with malpractice premiums causing crises in the 1980s and again in the early 2000s.
continued below...
Now, rates for medical professional liability insurance have been dropping for seven years, and an eighth straight annual decline is expected this year, according to Mike Matray, the editor of trade publication Medical Liability Monitor and the chief content officer of its associated website, www.mymedicalmalpracticeinsurance.com.
“We are in the longest, deepest soft market that the malpractice insurance industry has ever been in,” he says. “Right now, things are really good for the doctors, as far as rates coming down.”
Matray says he understands that declining rates may seem immaterial to a physician who receives an insurance bill that eats into the bottom line. For some specialties, that premium can be as high as $200,000 per physician, per year—or more.
“I’m not saying it isn’t expensive,” he adds. “It’s expensive to run a medical practice. At the same time, medical malpractice insurance is less expensive in today’s dollars than it was in 2005.”
The reduction in rates is multi-faceted. Prominently, state-level tort reforms like non-economic damage caps, health courts, and arbitration hearings are making it harder to bring cases to trial, particularly for lawyers who take cases on contingency. Second, frivolous lawsuits “are making an impression on jury pools,” Matray says, which means fewer filed claims and fewer cases that make it to trial. Third, this soft cycle has outlasted the typical pattern of rates falling for three to four years before rebounding.
“A lot of smart actuaries keep saying this has to change soon, because in a soft market there is a lot of competition,” he says, noting that in order to compete for low rates, insurance companies offer credits to clients and use their own reserve cash piles. “So things are really going to change in the next couple of years.”

—Robin Diamond, senior vice president and chief patient safety officer, The Doctors Company
In Need of Data, Patience
So what does it all mean for hospitalists and HM group leaders looking to be proactive about medical malpractice liability insurance? Patience is required.
For starters, there is no designated premium category for hospitalists. Much like the situation that exists for coding issues, the closest proxy for HM is internal medicine. According to Medical Liability Monitor, the premium paid by internal medicine physicians as of July 1, 2012, varied widely across the country. In South Florida, internal medicine insurance premiums in Miami, Dade, and Broward counties were between $42,000 and $46,000 per year. In South Dakota, one insurer reported rates of just under $4,000 per year. There is no average or median figure available, and Matray notes that actual rates paid can vary from county to county.
Moreover, it is difficult for group leaders or hospital executives to use past history to negotiate rates with insurers because of a shortage of reliable data. In its spring 2013 newsletter, the PIAA (formerly known as the Physician Insurers Association of America) published its first report on hospitalist claims reported to its Data Sharing Project. Of the 92,868 closed claims reported from 2002-2011, just 312, or 0.3%, named hospitalists as the defendant.
The data also showed that, of those claims, 20% were settled through insurance company payments. Those payments totaled $17.1 million, with an average payout to a claimant (known as the indemnity) of $272,553 per claim. Overall, hospitalists had a 20% paid-to-closed ratio, totaling more than $17.1 million. By comparison, the percent of paid-to-closed claims for all physicians was 29.3%, according to PIAA.
In a separate data set compiled this year by TDC, 34% of allegations against hospitalists were related to missed or failed diagnoses, with 28% tied to “improper management of treatment.” Twelve percent of allegations were the result of either improper medication management or ordering errors.
Robin Diamond, TDC’s senior vice president and chief patient safety officer, says that teasing out trends from the initial data can be challenging. Hospitalists, she says, can deal with so many different patients, diseases, and severity levels that it is difficult to draw conclusions.
“Hospital medicine is different than other specialties, because the hospitalist treats a broad range of patients in an acute care setting—from a pediatric patient to an adult patient with many chronic illnesses,” she says.
Divya Parikh, PIAA’s director of research and loss prevention, says HM group leaders should avoid reading too much into the first batch of data, because it’s a small sample size.
“A big part of that is we feel that a lot of hospitalists are intermingled into the other medical specialties,” she says. “So this becomes a very small subset where they are distinctly identified as hospitalists. And that’s the challenge.”
In particular, Parikh is curious to see whether HM’s rate of claims paid through insurance payments drops from 20% (already below the overall healthcare industry average). “It will be interesting as we proceed...to see if they begin to mitigate areas of risk where we used to see a lot of claims,” she adds. “If you look at a hospital setting, there has been some shift change in what the errors are. And, what you’d hope with hospitalists within these environments who are really owning this specialty, is that you’d see a decrease in that. There would be that connective care. There would be the patient that felt that they had an individual who was their go-to individual throughout their care at a hospital.”
A Peek at the Future
Insurers have begun compiling claims data on hospitalists and are taking a longer-term view of the specialty. TDC, for example, has analyzed its data and identified characteristics it says make a low-risk hospitalist, an analysis the company says is the first of its kind (see Figure 1). The insurer adds that it sees its responsibility as making sure everyone understands the hospitalist’s role within the acute care setting so that its pricing is commensurate with the liability risk.
Source: The Doctors Company
“We’re looking at the systems within the hospitalist group, as well as how well that group is integrating with the hospital where they’re practicing,” Diamond says. “What kind of patient mix is this particular hospitalist group seeing in that particular hospital, because it can be different in a large healthcare corporation in Manhattan, New York, from a community hospital in rural Texas.”
The growing popularity of hospitalists taking on co-management responsibilities for other specialties is another trend to keep an eye on, as it creates what insurers call “vicarious liability.” Working together in teams with other specialties can improve communication, reduce errors during transitions of care, and create better outcomes. However, in instances where there are problems, being on a care team means hospitalists can open themselves to liability. To mitigate that risk, hospitalists can look to other groups that have dealt with shared liability issues in the past, Parikh says.
“Historically, you would have seen it with anesthesiology,” she explains. “And one huge improvement anesthesiologists have made when a patient comes in for a surgery now is they come out, introduce themselves, say hello, and tell you what’s going on. They put a face to the name, so that it’s not just a no-name anesthesiologist who gets included in the lawsuit as well because they’re naming everybody in the group.”
But, holistically, the best long-term mitigation strategy appears to be tort reform and new ways of looking at the way in which healthcare liability issues are handled in the U.S., says Anupam Jena, MD, PhD, assistant professor of healthcare policy and medicine at Harvard Medical School, and an internist at Massachusetts General Hospital, both in Boston. Dr. Jena says that there is limited evidence that enacted malpractice reforms have produced more than a 2% to 5% reduction in healthcare spending compared to states that have not.2 Instead, healthcare leaders should push for the elimination of defensive medicine, which he says contributes the lion’s share of the estimated $50 billion annual cost of malpractice liability across the country.
“Do I think the country is in a malpractice crisis? No,” he says. “Do I think that defensive medicine is larger than we think it is? Yes.
“If physicians practice as they felt they should practice without ordering extra tests and procedures, my guess would be you could reduce healthcare spending by substantially more than $50 billion.”
Richard Quinn is a freelance writer in New Jersey.
References
- Spiegel AD, Kavaler F. America’s first medical malpractice crisis, 1835-1865. J Community Health. 1997;22:283-308.
- Chandra A, Jena A, Seabury, S. Defensive medicine may be costlier than it seems. The Wall Street Journal website. http://online.wsj.com/article/SB10001424127887323701904578280112638373302.html. Accessed September 21, 2013.
Source: The Doctors Company
Ten years ago, the national headlines on malpractice insurance were staggering. Media reports catalogued OB-GYNs who proclaimed they were shutting down their private practices in the face of runaway premiums. Surgeons and other proceduralists decried payments tied to lawsuits they’d argue were arbitrary and capricious. And the American Medical Association (AMA) made announcement after announcement about states being in a “malpractice crisis.”
In recent years, premiums have actually dropped and stabilized at levels that most physicians agree are manageable for bottom lines. But, in that time, there has been scant discussion about hospital medicine’s relationship with malpractice. It’s not because the issue isn’t omnipresent for all healthcare practitioners, including the relatively nascent specialty that is HM.
Practice management experts say anecdotally that delayed diagnosis of, or treatment for, a spinal epidural abscess (SEA) is likely to get more than a few hospitalists sued. And, the proliferation of co-management of other specialties—particularly those with higher risk of incidence and higher premiums than internal medicine—open up hospitalists to further liability.
The issue is that at less than 20 years as a specialty, HM is in its infancy when it comes to its interaction with malpractice premiums. Health insurance companies and trade groups that track the insurance industry are just beginning to have enough data on claims, premiums, and payouts to make recommendations on risk factors, risk mitigation, and potential trends.
Still, even in a landscape of limited information, there are a few rules of thumb hospitalist group leaders should live by when it comes to managing exposure to malpractice cases, according to interviews with a half dozen healthcare professionals:
- Know how your coverage works. Is there “tail coverage” that ensures you have protection for incidents that happened at an institution where you no longer practice? Even though hospital-employed physicians rarely have rate discussions directly (the hospital typically covers premiums as part of the compensation package), take the time to learn the basic details.
- Be diligent in documentation. Note concerns in charts when appropriate, and stand up for your point of view. There’s a fine line between picking fights with other physicians involved in a patient’s care and making your concerns known, but don’t be afraid to put your clinical view on the record.
- Avoid the practice of “defensive medicine.” Ordering tests and procedures that aren’t clinically necessary might seem like it can serve as a protection from later lawsuits, but it adds to healthcare costs and is just not the right thing to do, says hospitalist Allen Kachalia, MD, JD, of Brigham and Women’s Hospital in Boston, who has studied the phenomenon (see “Culture Shift Necessary to Defeat “Defensive” Medicine,” on p. 38).
- Recognize the risks associated with co-management. Caring for neurology, cardiology, and other subspecialty patients is a revenue boost for HM groups, but when some of those complex cases have adverse events, the hospitalist who interacted with the patient daily could be included in a lawsuit.
- Focus on communication skills. An analysis of claims data by The Doctors Company (TDC) (www.thedoctors.com), a medical malpractice insurance company exclusively endorsed by SHM, reports that the second most common factor contributing to patient injury by hospitalists is “communication breakdown among healthcare professionals.”
- Manage workloads to avoid burnout. Don’t take on too many patients at the expense of being involved in hospital committees or quality initiatives.
To be sure, many of the same tenets of being a productive hospitalist with high patient satisfaction scores—maintain manageable censuses; focus on patient centeredness; and use checklists, technology, and regimented protocols to reduce adverse events—translate very well to being a lower-risk hospitalist in relation to malpractice cases.
When you’re “thinking of patient satisfaction strategies, also think of them as risk mitigation strategies,” says John Nelson, MD, MHM, FACP, medical director of the hospitalist practice at Overlake Hospital Medical Center in Bellevue, Wash., an SHM co-founder and practice management columnist for The Hospitalist. “They overlap tremendously.”
A History Lesson
Medical malpractice has been around for centuries and has two prevailing goals: 1) to provide monetary remuneration to patients who have been injured via substandard care and 2) to deter that poor treatment through fiscal punishment.
Malpractice lawsuits were not prevalent enough to be a major medical concern until the early 1800s. By the middle of the 19th century, the country hit its first periods of crisis.1 Cycles ebbed and flowed from there, with malpractice premiums causing crises in the 1980s and again in the early 2000s.
continued below...
Now, rates for medical professional liability insurance have been dropping for seven years, and an eighth straight annual decline is expected this year, according to Mike Matray, the editor of trade publication Medical Liability Monitor and the chief content officer of its associated website, www.mymedicalmalpracticeinsurance.com.
“We are in the longest, deepest soft market that the malpractice insurance industry has ever been in,” he says. “Right now, things are really good for the doctors, as far as rates coming down.”
Matray says he understands that declining rates may seem immaterial to a physician who receives an insurance bill that eats into the bottom line. For some specialties, that premium can be as high as $200,000 per physician, per year—or more.
“I’m not saying it isn’t expensive,” he adds. “It’s expensive to run a medical practice. At the same time, medical malpractice insurance is less expensive in today’s dollars than it was in 2005.”
The reduction in rates is multi-faceted. Prominently, state-level tort reforms like non-economic damage caps, health courts, and arbitration hearings are making it harder to bring cases to trial, particularly for lawyers who take cases on contingency. Second, frivolous lawsuits “are making an impression on jury pools,” Matray says, which means fewer filed claims and fewer cases that make it to trial. Third, this soft cycle has outlasted the typical pattern of rates falling for three to four years before rebounding.
“A lot of smart actuaries keep saying this has to change soon, because in a soft market there is a lot of competition,” he says, noting that in order to compete for low rates, insurance companies offer credits to clients and use their own reserve cash piles. “So things are really going to change in the next couple of years.”

—Robin Diamond, senior vice president and chief patient safety officer, The Doctors Company
In Need of Data, Patience
So what does it all mean for hospitalists and HM group leaders looking to be proactive about medical malpractice liability insurance? Patience is required.
For starters, there is no designated premium category for hospitalists. Much like the situation that exists for coding issues, the closest proxy for HM is internal medicine. According to Medical Liability Monitor, the premium paid by internal medicine physicians as of July 1, 2012, varied widely across the country. In South Florida, internal medicine insurance premiums in Miami, Dade, and Broward counties were between $42,000 and $46,000 per year. In South Dakota, one insurer reported rates of just under $4,000 per year. There is no average or median figure available, and Matray notes that actual rates paid can vary from county to county.
Moreover, it is difficult for group leaders or hospital executives to use past history to negotiate rates with insurers because of a shortage of reliable data. In its spring 2013 newsletter, the PIAA (formerly known as the Physician Insurers Association of America) published its first report on hospitalist claims reported to its Data Sharing Project. Of the 92,868 closed claims reported from 2002-2011, just 312, or 0.3%, named hospitalists as the defendant.
The data also showed that, of those claims, 20% were settled through insurance company payments. Those payments totaled $17.1 million, with an average payout to a claimant (known as the indemnity) of $272,553 per claim. Overall, hospitalists had a 20% paid-to-closed ratio, totaling more than $17.1 million. By comparison, the percent of paid-to-closed claims for all physicians was 29.3%, according to PIAA.
In a separate data set compiled this year by TDC, 34% of allegations against hospitalists were related to missed or failed diagnoses, with 28% tied to “improper management of treatment.” Twelve percent of allegations were the result of either improper medication management or ordering errors.
Robin Diamond, TDC’s senior vice president and chief patient safety officer, says that teasing out trends from the initial data can be challenging. Hospitalists, she says, can deal with so many different patients, diseases, and severity levels that it is difficult to draw conclusions.
“Hospital medicine is different than other specialties, because the hospitalist treats a broad range of patients in an acute care setting—from a pediatric patient to an adult patient with many chronic illnesses,” she says.
Divya Parikh, PIAA’s director of research and loss prevention, says HM group leaders should avoid reading too much into the first batch of data, because it’s a small sample size.
“A big part of that is we feel that a lot of hospitalists are intermingled into the other medical specialties,” she says. “So this becomes a very small subset where they are distinctly identified as hospitalists. And that’s the challenge.”
In particular, Parikh is curious to see whether HM’s rate of claims paid through insurance payments drops from 20% (already below the overall healthcare industry average). “It will be interesting as we proceed...to see if they begin to mitigate areas of risk where we used to see a lot of claims,” she adds. “If you look at a hospital setting, there has been some shift change in what the errors are. And, what you’d hope with hospitalists within these environments who are really owning this specialty, is that you’d see a decrease in that. There would be that connective care. There would be the patient that felt that they had an individual who was their go-to individual throughout their care at a hospital.”
A Peek at the Future
Insurers have begun compiling claims data on hospitalists and are taking a longer-term view of the specialty. TDC, for example, has analyzed its data and identified characteristics it says make a low-risk hospitalist, an analysis the company says is the first of its kind (see Figure 1). The insurer adds that it sees its responsibility as making sure everyone understands the hospitalist’s role within the acute care setting so that its pricing is commensurate with the liability risk.
Source: The Doctors Company
“We’re looking at the systems within the hospitalist group, as well as how well that group is integrating with the hospital where they’re practicing,” Diamond says. “What kind of patient mix is this particular hospitalist group seeing in that particular hospital, because it can be different in a large healthcare corporation in Manhattan, New York, from a community hospital in rural Texas.”
The growing popularity of hospitalists taking on co-management responsibilities for other specialties is another trend to keep an eye on, as it creates what insurers call “vicarious liability.” Working together in teams with other specialties can improve communication, reduce errors during transitions of care, and create better outcomes. However, in instances where there are problems, being on a care team means hospitalists can open themselves to liability. To mitigate that risk, hospitalists can look to other groups that have dealt with shared liability issues in the past, Parikh says.
“Historically, you would have seen it with anesthesiology,” she explains. “And one huge improvement anesthesiologists have made when a patient comes in for a surgery now is they come out, introduce themselves, say hello, and tell you what’s going on. They put a face to the name, so that it’s not just a no-name anesthesiologist who gets included in the lawsuit as well because they’re naming everybody in the group.”
But, holistically, the best long-term mitigation strategy appears to be tort reform and new ways of looking at the way in which healthcare liability issues are handled in the U.S., says Anupam Jena, MD, PhD, assistant professor of healthcare policy and medicine at Harvard Medical School, and an internist at Massachusetts General Hospital, both in Boston. Dr. Jena says that there is limited evidence that enacted malpractice reforms have produced more than a 2% to 5% reduction in healthcare spending compared to states that have not.2 Instead, healthcare leaders should push for the elimination of defensive medicine, which he says contributes the lion’s share of the estimated $50 billion annual cost of malpractice liability across the country.
“Do I think the country is in a malpractice crisis? No,” he says. “Do I think that defensive medicine is larger than we think it is? Yes.
“If physicians practice as they felt they should practice without ordering extra tests and procedures, my guess would be you could reduce healthcare spending by substantially more than $50 billion.”
Richard Quinn is a freelance writer in New Jersey.
References
- Spiegel AD, Kavaler F. America’s first medical malpractice crisis, 1835-1865. J Community Health. 1997;22:283-308.
- Chandra A, Jena A, Seabury, S. Defensive medicine may be costlier than it seems. The Wall Street Journal website. http://online.wsj.com/article/SB10001424127887323701904578280112638373302.html. Accessed September 21, 2013.
Agency Funding for Healthcare Research Could Benefit Hospital Medicine
David O. Meltzer, MD, PhD, MHM, wants hospitalists to take advantage of the recent announcement by the Patient-Centered Outcomes Research Institute (PCORI) that it intends to award $300 million by the end of this year, and more in the future. And if that means calling him directly, go for it.
Dr. Meltzer, chief of the section of hospital medicine at the University of Chicago, is a member of PCORI's methodology committee. He says in a question-and-answer session with The Hospitalist that PCORI could be a valuable resource and funding source for hospitalist researchers.
Question: What should hospitalists know about PCORI?
Answer: PCORI is focused on figuring out how to improve the effectiveness of healthcare, and it is placing a strong emphasis on the importance of engaging patients and other stakeholders in that process. Also, PCORI is trying to ensure that research recognizes the potential differences between patient subgroups, and even individual patients, to the maximum degree possible.
Q: Given PCORI's focus on outcomes, how can HM researchers pitch the type of projects that would be eligible for funding?
A: They should focus on questions that matter to patients, and engage diverse stakeholders and patients in identifying those questions.
Q: How helpful for the specialty is it to have a leading member involved with the institute?
A: PCORI is becoming an important funder of research in the United States, and I think all specialties need to know about it. PCORI is working hard to get the word out to all specialties, but I hope my colleagues in hospital medicine will feel free to call if I can help them interpret PCORI's guidance about how they can best engage with it. TH
Visit our website for more information on patient-centered care.
David O. Meltzer, MD, PhD, MHM, wants hospitalists to take advantage of the recent announcement by the Patient-Centered Outcomes Research Institute (PCORI) that it intends to award $300 million by the end of this year, and more in the future. And if that means calling him directly, go for it.
Dr. Meltzer, chief of the section of hospital medicine at the University of Chicago, is a member of PCORI's methodology committee. He says in a question-and-answer session with The Hospitalist that PCORI could be a valuable resource and funding source for hospitalist researchers.
Question: What should hospitalists know about PCORI?
Answer: PCORI is focused on figuring out how to improve the effectiveness of healthcare, and it is placing a strong emphasis on the importance of engaging patients and other stakeholders in that process. Also, PCORI is trying to ensure that research recognizes the potential differences between patient subgroups, and even individual patients, to the maximum degree possible.
Q: Given PCORI's focus on outcomes, how can HM researchers pitch the type of projects that would be eligible for funding?
A: They should focus on questions that matter to patients, and engage diverse stakeholders and patients in identifying those questions.
Q: How helpful for the specialty is it to have a leading member involved with the institute?
A: PCORI is becoming an important funder of research in the United States, and I think all specialties need to know about it. PCORI is working hard to get the word out to all specialties, but I hope my colleagues in hospital medicine will feel free to call if I can help them interpret PCORI's guidance about how they can best engage with it. TH
Visit our website for more information on patient-centered care.
David O. Meltzer, MD, PhD, MHM, wants hospitalists to take advantage of the recent announcement by the Patient-Centered Outcomes Research Institute (PCORI) that it intends to award $300 million by the end of this year, and more in the future. And if that means calling him directly, go for it.
Dr. Meltzer, chief of the section of hospital medicine at the University of Chicago, is a member of PCORI's methodology committee. He says in a question-and-answer session with The Hospitalist that PCORI could be a valuable resource and funding source for hospitalist researchers.
Question: What should hospitalists know about PCORI?
Answer: PCORI is focused on figuring out how to improve the effectiveness of healthcare, and it is placing a strong emphasis on the importance of engaging patients and other stakeholders in that process. Also, PCORI is trying to ensure that research recognizes the potential differences between patient subgroups, and even individual patients, to the maximum degree possible.
Q: Given PCORI's focus on outcomes, how can HM researchers pitch the type of projects that would be eligible for funding?
A: They should focus on questions that matter to patients, and engage diverse stakeholders and patients in identifying those questions.
Q: How helpful for the specialty is it to have a leading member involved with the institute?
A: PCORI is becoming an important funder of research in the United States, and I think all specialties need to know about it. PCORI is working hard to get the word out to all specialties, but I hope my colleagues in hospital medicine will feel free to call if I can help them interpret PCORI's guidance about how they can best engage with it. TH
Visit our website for more information on patient-centered care.
Readmission Rates Not Effective Quality Measure of Pediatric Patient Care
A new study in Pediatrics finds limited use for hospital readmission rates as a meaningful quality measure when it comes to pediatric patient care.
By examining 30- and 60-day readmission rates for 958 hospitals that admit children for seven common inpatient conditions, researchers found very few that could be considered either high or low performers. In addition, pediatric 30-day readmission rates overall were low, at less than 10% for all conditions.
Naomi Bardach, MD, MAS, department of pediatrics at the University of California at San Francisco and the report's lead author, emphasizes that her study was a statistical analysis of readmission rates without assessing whether they should be a focus for quality improvement. "They might be useful for larger efforts, such as multi-institution collaboratives to improve care for a given condition," Dr. Bardach says. "But it is clear that readmission rates are not useful for comparing individual hospital performance."
An accompanying editorial noted that delaying hospital discharges even by four hours in an attempt to forestall readmissions could prove more costly in the end.
Although much of the national focus on 30-day hospital readmissions has been on the Medicare-age population, the pediatric realm is getting more attention, Dr. Bardach says. For example, the Children's Health Insurance Program Reauthorization Act of 2009 funded seven research cooperatives to develop core measures for assessing the state of children’s healthcare quality. TH
Visit our website for more information about pediatric readmissions rates.
A new study in Pediatrics finds limited use for hospital readmission rates as a meaningful quality measure when it comes to pediatric patient care.
By examining 30- and 60-day readmission rates for 958 hospitals that admit children for seven common inpatient conditions, researchers found very few that could be considered either high or low performers. In addition, pediatric 30-day readmission rates overall were low, at less than 10% for all conditions.
Naomi Bardach, MD, MAS, department of pediatrics at the University of California at San Francisco and the report's lead author, emphasizes that her study was a statistical analysis of readmission rates without assessing whether they should be a focus for quality improvement. "They might be useful for larger efforts, such as multi-institution collaboratives to improve care for a given condition," Dr. Bardach says. "But it is clear that readmission rates are not useful for comparing individual hospital performance."
An accompanying editorial noted that delaying hospital discharges even by four hours in an attempt to forestall readmissions could prove more costly in the end.
Although much of the national focus on 30-day hospital readmissions has been on the Medicare-age population, the pediatric realm is getting more attention, Dr. Bardach says. For example, the Children's Health Insurance Program Reauthorization Act of 2009 funded seven research cooperatives to develop core measures for assessing the state of children’s healthcare quality. TH
Visit our website for more information about pediatric readmissions rates.
A new study in Pediatrics finds limited use for hospital readmission rates as a meaningful quality measure when it comes to pediatric patient care.
By examining 30- and 60-day readmission rates for 958 hospitals that admit children for seven common inpatient conditions, researchers found very few that could be considered either high or low performers. In addition, pediatric 30-day readmission rates overall were low, at less than 10% for all conditions.
Naomi Bardach, MD, MAS, department of pediatrics at the University of California at San Francisco and the report's lead author, emphasizes that her study was a statistical analysis of readmission rates without assessing whether they should be a focus for quality improvement. "They might be useful for larger efforts, such as multi-institution collaboratives to improve care for a given condition," Dr. Bardach says. "But it is clear that readmission rates are not useful for comparing individual hospital performance."
An accompanying editorial noted that delaying hospital discharges even by four hours in an attempt to forestall readmissions could prove more costly in the end.
Although much of the national focus on 30-day hospital readmissions has been on the Medicare-age population, the pediatric realm is getting more attention, Dr. Bardach says. For example, the Children's Health Insurance Program Reauthorization Act of 2009 funded seven research cooperatives to develop core measures for assessing the state of children’s healthcare quality. TH
Visit our website for more information about pediatric readmissions rates.
Coordinated Care Approach May Be Best for Patients with Heart Failure
A new study that found no association between increased levels of hospitalist or cardiologist care and improved 30-day outcomes in older patients with heart failure might mean a coordinated approach is best, says the report’s lead author.
“Associations Between Use of the Hospitalist Model and Quality of Care and Outcomes of Older Patients Hospitalized for Heart Failure,” published in JACC Heart Failure, analyzed data from a heart-failure registry that included 31,505 Medicare beneficiaries in 166 hospitals.
After multivariable adjustment, researchers found that a 10% increase in the use of hospitalists was not related to an improvement in 30-day readmission rates, but it was linked to a slight increase in mortality (risk ratio: 1.03; 95% confidence interval [CI]: 1.00 to 1.06) and a decrease in length of stay (0.09 days; 95% CI: 0.02 to 0.16).
Similar results for 30-day readmission rates were found when care was associated with a 10% increase in the use of cardiologists, prompting lead author and cardiologist Robb Kociol, MD, to suggest that perhaps a hybrid model using both HM and cardiologist specialists may improve outcomes.
"Comanagement, or commingling of hospitalist and cardiologist care, in these patients may improve at least adherence to measures we know are associated with improved quality of care," says Dr. Kociol, director of advanced-heart-failure and ventricular-assist devices at the CardioVascular Institute at Beth Israel Deaconess Medical Center in Boston.
The paper also reported that increased use of hospitalists in hospitals with high use of cardiologists was associated with improved defect-free adherence to a composite of heart failure performance measures (risk ratio: 1.03; 95% CI: 1.01 to 1.06). Dr. Kociol says further research is needed to tease out just how a hybrid model of hospitalist-cardiologist care would work.
"One model might be that all of these patients are cared for by hospitalists with automatic cardiology consultation," he adds. "Or maybe we find a way to risk-stratify which patients are under the hospitalist service and which patients are cared for by cardiologists. None of those questions are answered in this analysis, but the paper does suggest there may be something that needs to be studied further."
Visit our website for more information on hospitalists’ impact on patient outcomes.
A new study that found no association between increased levels of hospitalist or cardiologist care and improved 30-day outcomes in older patients with heart failure might mean a coordinated approach is best, says the report’s lead author.
“Associations Between Use of the Hospitalist Model and Quality of Care and Outcomes of Older Patients Hospitalized for Heart Failure,” published in JACC Heart Failure, analyzed data from a heart-failure registry that included 31,505 Medicare beneficiaries in 166 hospitals.
After multivariable adjustment, researchers found that a 10% increase in the use of hospitalists was not related to an improvement in 30-day readmission rates, but it was linked to a slight increase in mortality (risk ratio: 1.03; 95% confidence interval [CI]: 1.00 to 1.06) and a decrease in length of stay (0.09 days; 95% CI: 0.02 to 0.16).
Similar results for 30-day readmission rates were found when care was associated with a 10% increase in the use of cardiologists, prompting lead author and cardiologist Robb Kociol, MD, to suggest that perhaps a hybrid model using both HM and cardiologist specialists may improve outcomes.
"Comanagement, or commingling of hospitalist and cardiologist care, in these patients may improve at least adherence to measures we know are associated with improved quality of care," says Dr. Kociol, director of advanced-heart-failure and ventricular-assist devices at the CardioVascular Institute at Beth Israel Deaconess Medical Center in Boston.
The paper also reported that increased use of hospitalists in hospitals with high use of cardiologists was associated with improved defect-free adherence to a composite of heart failure performance measures (risk ratio: 1.03; 95% CI: 1.01 to 1.06). Dr. Kociol says further research is needed to tease out just how a hybrid model of hospitalist-cardiologist care would work.
"One model might be that all of these patients are cared for by hospitalists with automatic cardiology consultation," he adds. "Or maybe we find a way to risk-stratify which patients are under the hospitalist service and which patients are cared for by cardiologists. None of those questions are answered in this analysis, but the paper does suggest there may be something that needs to be studied further."
Visit our website for more information on hospitalists’ impact on patient outcomes.
A new study that found no association between increased levels of hospitalist or cardiologist care and improved 30-day outcomes in older patients with heart failure might mean a coordinated approach is best, says the report’s lead author.
“Associations Between Use of the Hospitalist Model and Quality of Care and Outcomes of Older Patients Hospitalized for Heart Failure,” published in JACC Heart Failure, analyzed data from a heart-failure registry that included 31,505 Medicare beneficiaries in 166 hospitals.
After multivariable adjustment, researchers found that a 10% increase in the use of hospitalists was not related to an improvement in 30-day readmission rates, but it was linked to a slight increase in mortality (risk ratio: 1.03; 95% confidence interval [CI]: 1.00 to 1.06) and a decrease in length of stay (0.09 days; 95% CI: 0.02 to 0.16).
Similar results for 30-day readmission rates were found when care was associated with a 10% increase in the use of cardiologists, prompting lead author and cardiologist Robb Kociol, MD, to suggest that perhaps a hybrid model using both HM and cardiologist specialists may improve outcomes.
"Comanagement, or commingling of hospitalist and cardiologist care, in these patients may improve at least adherence to measures we know are associated with improved quality of care," says Dr. Kociol, director of advanced-heart-failure and ventricular-assist devices at the CardioVascular Institute at Beth Israel Deaconess Medical Center in Boston.
The paper also reported that increased use of hospitalists in hospitals with high use of cardiologists was associated with improved defect-free adherence to a composite of heart failure performance measures (risk ratio: 1.03; 95% CI: 1.01 to 1.06). Dr. Kociol says further research is needed to tease out just how a hybrid model of hospitalist-cardiologist care would work.
"One model might be that all of these patients are cared for by hospitalists with automatic cardiology consultation," he adds. "Or maybe we find a way to risk-stratify which patients are under the hospitalist service and which patients are cared for by cardiologists. None of those questions are answered in this analysis, but the paper does suggest there may be something that needs to be studied further."
Visit our website for more information on hospitalists’ impact on patient outcomes.