User login
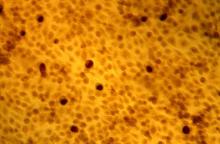
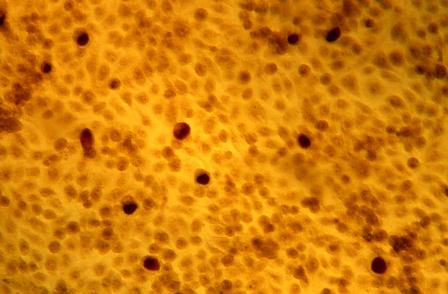
HIV-associated Kaposi sarcoma responds to checkpoint inhibitors
Checkpoint inhibitor therapy is effective for patients with HIV-associated Kaposi sarcoma (KS), a recent study has found.
Partial or complete remission was achieved by a majority of patients; others currently have stable disease lasting longer than 6 months, reported Natalie Galanina, MD, of Rebecca and John Moores Cancer Center at the University of California, San Diego, and her colleagues. Earlier this year, investigators reported similar responses to checkpoint inhibitors in two patients with KS that wasn’t associated with HIV.
“An association has been demonstrated between chronic viral infection, malignancy, and up-regulation of programmed death receptor 1 (PD-1) on CD8+ cytotoxic T-lymphocytes,” the authors wrote in Cancer Immunology Research. In particular, “HIV-specific CD8+ T cells have increased PD-1 expression, which … promotes a cellular milieu conducive to oncogenesis.” These factors, together with the results from the previous study, have suggested that checkpoint inhibitors may be effective for patients with HIV-associated KS.
The retrospective study involved 320 patients treated with immunotherapy at Moores Cancer Center from August 2013 through December 2017. From this group, nine cases of HIV-associated KS were found. Median CD4 count was 256 cells/mcL and median viral load was 20 copies/mL. Eight patients were treated with nivolumab and one was treated with pembrolizumab. Median age was 44 years. All patients were male and receiving antiretroviral therapy.
Six patients (67%) achieved remission, with five attaining partial remission and one attaining complete remission (gastrointestinal disease). Of the remaining three patients, two currently have stable disease lasting longer than 6 months, and one has stable disease lasting longer than 3 months.
Muscle aches, pruritus, and low-grade fever were the most common adverse events. No grade 3 or higher drug-related adverse events occurred.
“Most of our patients received one to four prior lines of therapy but still responded to checkpoint blockade,” the authors wrote. “Our observations suggest that patients with HIV-associated KS have high [response rates] to PD-1 checkpoint blockade, without significant toxicity, even in the presence of low [tumor mutational burden] and/or lack of PD-L1 expression.”
Authors reported compensation from Incyte, Genentech, Merck, Pfizer, and others.
SOURCE: Galanina et al. Cancer Immunol Res. doi: 10.1158/2326-6066.CIR-18-0121.
Checkpoint inhibitor therapy is effective for patients with HIV-associated Kaposi sarcoma (KS), a recent study has found.
Partial or complete remission was achieved by a majority of patients; others currently have stable disease lasting longer than 6 months, reported Natalie Galanina, MD, of Rebecca and John Moores Cancer Center at the University of California, San Diego, and her colleagues. Earlier this year, investigators reported similar responses to checkpoint inhibitors in two patients with KS that wasn’t associated with HIV.
“An association has been demonstrated between chronic viral infection, malignancy, and up-regulation of programmed death receptor 1 (PD-1) on CD8+ cytotoxic T-lymphocytes,” the authors wrote in Cancer Immunology Research. In particular, “HIV-specific CD8+ T cells have increased PD-1 expression, which … promotes a cellular milieu conducive to oncogenesis.” These factors, together with the results from the previous study, have suggested that checkpoint inhibitors may be effective for patients with HIV-associated KS.
The retrospective study involved 320 patients treated with immunotherapy at Moores Cancer Center from August 2013 through December 2017. From this group, nine cases of HIV-associated KS were found. Median CD4 count was 256 cells/mcL and median viral load was 20 copies/mL. Eight patients were treated with nivolumab and one was treated with pembrolizumab. Median age was 44 years. All patients were male and receiving antiretroviral therapy.
Six patients (67%) achieved remission, with five attaining partial remission and one attaining complete remission (gastrointestinal disease). Of the remaining three patients, two currently have stable disease lasting longer than 6 months, and one has stable disease lasting longer than 3 months.
Muscle aches, pruritus, and low-grade fever were the most common adverse events. No grade 3 or higher drug-related adverse events occurred.
“Most of our patients received one to four prior lines of therapy but still responded to checkpoint blockade,” the authors wrote. “Our observations suggest that patients with HIV-associated KS have high [response rates] to PD-1 checkpoint blockade, without significant toxicity, even in the presence of low [tumor mutational burden] and/or lack of PD-L1 expression.”
Authors reported compensation from Incyte, Genentech, Merck, Pfizer, and others.
SOURCE: Galanina et al. Cancer Immunol Res. doi: 10.1158/2326-6066.CIR-18-0121.
Checkpoint inhibitor therapy is effective for patients with HIV-associated Kaposi sarcoma (KS), a recent study has found.
Partial or complete remission was achieved by a majority of patients; others currently have stable disease lasting longer than 6 months, reported Natalie Galanina, MD, of Rebecca and John Moores Cancer Center at the University of California, San Diego, and her colleagues. Earlier this year, investigators reported similar responses to checkpoint inhibitors in two patients with KS that wasn’t associated with HIV.
“An association has been demonstrated between chronic viral infection, malignancy, and up-regulation of programmed death receptor 1 (PD-1) on CD8+ cytotoxic T-lymphocytes,” the authors wrote in Cancer Immunology Research. In particular, “HIV-specific CD8+ T cells have increased PD-1 expression, which … promotes a cellular milieu conducive to oncogenesis.” These factors, together with the results from the previous study, have suggested that checkpoint inhibitors may be effective for patients with HIV-associated KS.
The retrospective study involved 320 patients treated with immunotherapy at Moores Cancer Center from August 2013 through December 2017. From this group, nine cases of HIV-associated KS were found. Median CD4 count was 256 cells/mcL and median viral load was 20 copies/mL. Eight patients were treated with nivolumab and one was treated with pembrolizumab. Median age was 44 years. All patients were male and receiving antiretroviral therapy.
Six patients (67%) achieved remission, with five attaining partial remission and one attaining complete remission (gastrointestinal disease). Of the remaining three patients, two currently have stable disease lasting longer than 6 months, and one has stable disease lasting longer than 3 months.
Muscle aches, pruritus, and low-grade fever were the most common adverse events. No grade 3 or higher drug-related adverse events occurred.
“Most of our patients received one to four prior lines of therapy but still responded to checkpoint blockade,” the authors wrote. “Our observations suggest that patients with HIV-associated KS have high [response rates] to PD-1 checkpoint blockade, without significant toxicity, even in the presence of low [tumor mutational burden] and/or lack of PD-L1 expression.”
Authors reported compensation from Incyte, Genentech, Merck, Pfizer, and others.
SOURCE: Galanina et al. Cancer Immunol Res. doi: 10.1158/2326-6066.CIR-18-0121.
FROM CANCER IMMUNOLOGY RESEARCH
Key clinical point: Checkpoint inhibitor therapy is effective for patients with HIV-associated Kaposi sarcoma.
Major finding: Two-thirds of patients (67%) with HIV-associated Kaposi sarcoma achieved partial or complete remission when treated with immune checkpoint blockade.
Study details: A retrospective study involving nine patients with Kaposi sarcoma treated with either nivolumab or pembrolizumab at the Rebecca and John Moores Cancer Center at the University of California, San Diego, (UCSD) from August 2013 through December 2017.
Disclosures: Authors reported compensation from Incyte, Genentech, Merck, Pfizer, and others.
Source: Galanina et al. Cancer Immunol Res. 2018 Sept 7. doi: 10.1158/2326-6066.CIR-18-0121.
Age cutoff suggested for STI screening in HIV patients
WASHINGTON – Current guidelines recommend a minimum of annual screening for gonorrhea and chlamydia in all sexually active individuals with HIV infection. However, this goal, which is frequently not attained in HIV clinics, may be excessive in certain populations with HIV infection.
In particular, women as well as men who have sex exclusively with women (MSW) may best be served by targeted, age-based screening rather than universal screening, according to a presentation by Susan A. Tuddenham, MD, an assistant professor of medicine at Johns Hopkins University, Baltimore.
“Detection and treatment of gonorrhea and chlamydia in HIV-positive patients in the United States is a priority both because of patient morbidity and because of the potential for these infections to enhance transmission of HIV,” said Dr. Tuddenham.
She and her colleagues assessed data from 16,864 gonorrhea and chlamydia tests of all adults in care at three HIV Research Network sites during 2011-2014. She presented the data at a conference on STD prevention sponsored by the Centers for Disease Control and Prevention.
They assessed the number needed to screen (NNS) in order to identify a single infection across three risk populations of individuals with HIV infection: 1,123 women, 1,236 men who have sex only with women (MSW), and 3,501 men who have sex with men (MSM). NNS was defined as the number of persons tested divided by the number who tested positive and was calculated for the three risk groups for urogenital and extragenital (rectal and pharyngeal) sampling and by age.
Dr. Tuddenham and her colleagues found that NNS based on urogenital screening was similar in all three groups for those individuals aged younger than or equal to 25 years: 15 for women (95% confidence interval, 9-71); 21 for MSW (95% CI, 6-171); and 20 for MSM (95% CI, 12-36). However at ages greater than 25 years, the picture changed, with urogenital NNS increasing to 363 for women (95% CI, 167-1000); 160 for MSW (95% CI, 100-333). For MSM over the age of 25 years, however, the NNS only increased to 46 (95% CI, 38-56).
There were insufficient numbers of extragenital screenings of women and MSW for analysis. But for MSM, rectal NNS was 5 and 10 for those men aged 25 years and younger and those aged over age 25 years, respectively, and pharyngeal NNS was 8 and 20 for the two groups, respectively.
“Our results provide some support for age-based screening cutoffs for women and MSW, with universal screening appropriate for those less than or equal to 25 years of age, and targeted screening for those over 25,” said Dr. Tuddenham. She emphasized the importance of continued universal screening of MSM of all ages for gonorrhea/chlamydia, in particular using extragenital screening as well in order to capture those missed by urogenital screening alone.
Dr. Tuddenham reported that she had no disclosures.
WASHINGTON – Current guidelines recommend a minimum of annual screening for gonorrhea and chlamydia in all sexually active individuals with HIV infection. However, this goal, which is frequently not attained in HIV clinics, may be excessive in certain populations with HIV infection.
In particular, women as well as men who have sex exclusively with women (MSW) may best be served by targeted, age-based screening rather than universal screening, according to a presentation by Susan A. Tuddenham, MD, an assistant professor of medicine at Johns Hopkins University, Baltimore.
“Detection and treatment of gonorrhea and chlamydia in HIV-positive patients in the United States is a priority both because of patient morbidity and because of the potential for these infections to enhance transmission of HIV,” said Dr. Tuddenham.
She and her colleagues assessed data from 16,864 gonorrhea and chlamydia tests of all adults in care at three HIV Research Network sites during 2011-2014. She presented the data at a conference on STD prevention sponsored by the Centers for Disease Control and Prevention.
They assessed the number needed to screen (NNS) in order to identify a single infection across three risk populations of individuals with HIV infection: 1,123 women, 1,236 men who have sex only with women (MSW), and 3,501 men who have sex with men (MSM). NNS was defined as the number of persons tested divided by the number who tested positive and was calculated for the three risk groups for urogenital and extragenital (rectal and pharyngeal) sampling and by age.
Dr. Tuddenham and her colleagues found that NNS based on urogenital screening was similar in all three groups for those individuals aged younger than or equal to 25 years: 15 for women (95% confidence interval, 9-71); 21 for MSW (95% CI, 6-171); and 20 for MSM (95% CI, 12-36). However at ages greater than 25 years, the picture changed, with urogenital NNS increasing to 363 for women (95% CI, 167-1000); 160 for MSW (95% CI, 100-333). For MSM over the age of 25 years, however, the NNS only increased to 46 (95% CI, 38-56).
There were insufficient numbers of extragenital screenings of women and MSW for analysis. But for MSM, rectal NNS was 5 and 10 for those men aged 25 years and younger and those aged over age 25 years, respectively, and pharyngeal NNS was 8 and 20 for the two groups, respectively.
“Our results provide some support for age-based screening cutoffs for women and MSW, with universal screening appropriate for those less than or equal to 25 years of age, and targeted screening for those over 25,” said Dr. Tuddenham. She emphasized the importance of continued universal screening of MSM of all ages for gonorrhea/chlamydia, in particular using extragenital screening as well in order to capture those missed by urogenital screening alone.
Dr. Tuddenham reported that she had no disclosures.
WASHINGTON – Current guidelines recommend a minimum of annual screening for gonorrhea and chlamydia in all sexually active individuals with HIV infection. However, this goal, which is frequently not attained in HIV clinics, may be excessive in certain populations with HIV infection.
In particular, women as well as men who have sex exclusively with women (MSW) may best be served by targeted, age-based screening rather than universal screening, according to a presentation by Susan A. Tuddenham, MD, an assistant professor of medicine at Johns Hopkins University, Baltimore.
“Detection and treatment of gonorrhea and chlamydia in HIV-positive patients in the United States is a priority both because of patient morbidity and because of the potential for these infections to enhance transmission of HIV,” said Dr. Tuddenham.
She and her colleagues assessed data from 16,864 gonorrhea and chlamydia tests of all adults in care at three HIV Research Network sites during 2011-2014. She presented the data at a conference on STD prevention sponsored by the Centers for Disease Control and Prevention.
They assessed the number needed to screen (NNS) in order to identify a single infection across three risk populations of individuals with HIV infection: 1,123 women, 1,236 men who have sex only with women (MSW), and 3,501 men who have sex with men (MSM). NNS was defined as the number of persons tested divided by the number who tested positive and was calculated for the three risk groups for urogenital and extragenital (rectal and pharyngeal) sampling and by age.
Dr. Tuddenham and her colleagues found that NNS based on urogenital screening was similar in all three groups for those individuals aged younger than or equal to 25 years: 15 for women (95% confidence interval, 9-71); 21 for MSW (95% CI, 6-171); and 20 for MSM (95% CI, 12-36). However at ages greater than 25 years, the picture changed, with urogenital NNS increasing to 363 for women (95% CI, 167-1000); 160 for MSW (95% CI, 100-333). For MSM over the age of 25 years, however, the NNS only increased to 46 (95% CI, 38-56).
There were insufficient numbers of extragenital screenings of women and MSW for analysis. But for MSM, rectal NNS was 5 and 10 for those men aged 25 years and younger and those aged over age 25 years, respectively, and pharyngeal NNS was 8 and 20 for the two groups, respectively.
“Our results provide some support for age-based screening cutoffs for women and MSW, with universal screening appropriate for those less than or equal to 25 years of age, and targeted screening for those over 25,” said Dr. Tuddenham. She emphasized the importance of continued universal screening of MSM of all ages for gonorrhea/chlamydia, in particular using extragenital screening as well in order to capture those missed by urogenital screening alone.
Dr. Tuddenham reported that she had no disclosures.
REPORTING FROM THE 2018 STD PREVENTION CONFERENCE
Key clinical point: Men who have sex with men with HIV should be regularly screened for STIs regardless of age.
Major finding: The number needed to screen to detect an STI in individuals infected with HIV aged over 25 years were 363 (women); 160 (men who have sex exclusively with women); and 46 (men who have sex with men).
Study details: Gonorrhea/chlamydia tests were assessed from 16,864 individuals infected with HIV and number needed to screen calculated.
Disclosures: Dr. Tuddenham reported that she had no disclosures.
FDA approves two once-daily HIV drugs
Two once-daily oral HIV-1 medicines have been approved by the Food and Drug Administration, according to Merck: Delstrigo, a fixed-dose combination tablet of doravirine (100 mg), lamivudine (300 mg), and tenofovir disoproxil fumarate (300 mg), and Pifeltro (doravirine, 100 mg). Both drugs are indicated for treating HIV-1 infection in adult patients with no prior antiretroviral treatment.
Pifeltro is a nonnucleoside reverse transcriptase inhibitor to be used in combination with other antiretroviral medicines. Delstrigo contains a boxed warning regarding posttreatment acute exacerbation of hepatitis B infection.
Delstrigo and Pifeltro are not curative, according to the announcement by Merck, which manufactures both drugs.
The FDA approval of Delstrigo was based on findings from the DRIVE-AHEAD trial (NCT02403674), which randomized 728 participants with no history of antiretroviral treatment to receive once daily either Delstrigo or efavirenz/emtricitabine/tenofovir disoproxil fumarate (EFV 600 mg/FTC 200 mg/TDF 300 mg). Delstrigo was associated with sustained viral suppression through 48 weeks, meeting its primary endpoint of noninferior efficacy when compared with EFV/FTC/TDF (84% vs. 81%, respectively), according to Merck.
Pifeltro was approved based on the results of the DRIVE-FORWARD trial (NCT02275780), which randomized 766 participants with no history of antiretroviral treatment to receive either Pifeltro once daily or darunavir 800 mg plus ritonavir 100 mg (DRV+r) once daily, each in combination with either emtricitabine (FTC)/TDF or abacavir (ABC)/lamivudine (3TC), as selected by the investigator. Pifeltro was associated with sustained viral suppression through 48 weeks, meeting its primary endpoint of noninferior efficacy when compared with DRV+r, each in combination with FTC/TDF or ABC/3TC (84% vs. 80%, respectively), according to the Merck announcement.
Two once-daily oral HIV-1 medicines have been approved by the Food and Drug Administration, according to Merck: Delstrigo, a fixed-dose combination tablet of doravirine (100 mg), lamivudine (300 mg), and tenofovir disoproxil fumarate (300 mg), and Pifeltro (doravirine, 100 mg). Both drugs are indicated for treating HIV-1 infection in adult patients with no prior antiretroviral treatment.
Pifeltro is a nonnucleoside reverse transcriptase inhibitor to be used in combination with other antiretroviral medicines. Delstrigo contains a boxed warning regarding posttreatment acute exacerbation of hepatitis B infection.
Delstrigo and Pifeltro are not curative, according to the announcement by Merck, which manufactures both drugs.
The FDA approval of Delstrigo was based on findings from the DRIVE-AHEAD trial (NCT02403674), which randomized 728 participants with no history of antiretroviral treatment to receive once daily either Delstrigo or efavirenz/emtricitabine/tenofovir disoproxil fumarate (EFV 600 mg/FTC 200 mg/TDF 300 mg). Delstrigo was associated with sustained viral suppression through 48 weeks, meeting its primary endpoint of noninferior efficacy when compared with EFV/FTC/TDF (84% vs. 81%, respectively), according to Merck.
Pifeltro was approved based on the results of the DRIVE-FORWARD trial (NCT02275780), which randomized 766 participants with no history of antiretroviral treatment to receive either Pifeltro once daily or darunavir 800 mg plus ritonavir 100 mg (DRV+r) once daily, each in combination with either emtricitabine (FTC)/TDF or abacavir (ABC)/lamivudine (3TC), as selected by the investigator. Pifeltro was associated with sustained viral suppression through 48 weeks, meeting its primary endpoint of noninferior efficacy when compared with DRV+r, each in combination with FTC/TDF or ABC/3TC (84% vs. 80%, respectively), according to the Merck announcement.
Two once-daily oral HIV-1 medicines have been approved by the Food and Drug Administration, according to Merck: Delstrigo, a fixed-dose combination tablet of doravirine (100 mg), lamivudine (300 mg), and tenofovir disoproxil fumarate (300 mg), and Pifeltro (doravirine, 100 mg). Both drugs are indicated for treating HIV-1 infection in adult patients with no prior antiretroviral treatment.
Pifeltro is a nonnucleoside reverse transcriptase inhibitor to be used in combination with other antiretroviral medicines. Delstrigo contains a boxed warning regarding posttreatment acute exacerbation of hepatitis B infection.
Delstrigo and Pifeltro are not curative, according to the announcement by Merck, which manufactures both drugs.
The FDA approval of Delstrigo was based on findings from the DRIVE-AHEAD trial (NCT02403674), which randomized 728 participants with no history of antiretroviral treatment to receive once daily either Delstrigo or efavirenz/emtricitabine/tenofovir disoproxil fumarate (EFV 600 mg/FTC 200 mg/TDF 300 mg). Delstrigo was associated with sustained viral suppression through 48 weeks, meeting its primary endpoint of noninferior efficacy when compared with EFV/FTC/TDF (84% vs. 81%, respectively), according to Merck.
Pifeltro was approved based on the results of the DRIVE-FORWARD trial (NCT02275780), which randomized 766 participants with no history of antiretroviral treatment to receive either Pifeltro once daily or darunavir 800 mg plus ritonavir 100 mg (DRV+r) once daily, each in combination with either emtricitabine (FTC)/TDF or abacavir (ABC)/lamivudine (3TC), as selected by the investigator. Pifeltro was associated with sustained viral suppression through 48 weeks, meeting its primary endpoint of noninferior efficacy when compared with DRV+r, each in combination with FTC/TDF or ABC/3TC (84% vs. 80%, respectively), according to the Merck announcement.
HIV, HBV, and HCV Increase Risks After Joint Replacement
As patients with HIV, hepatitis B (HBV), and hepatitis C (HCV) live longer, more active lives with the help of antiviral treatments, they are now more often having joint replacement surgeries. But HIV, HBV, and HCV can increase the risk of postoperative complications, say researchers from Duke University in North Carolina.
The researchers studied 16,338 patients in 4 cohorts: those with HIV, HBV, HCV, and HIV plus HBV or HCV. They evaluated the patients at 30 days, 90 days, and 2 years after total joint arthroplasty (TJA), comparing their progress with that of a control group.
Patients with HBV and HCV were at risk of both acute and long-term medical and surgical complications. At 90 days and 2 years, the participants had increased risk of pneumonia, sepsis, joint infection, and revision surgery. They also had a greater risk of complications than did patients with HIV, especially for infection, within the first 90 days postsurgery.
Notably, after TJA, patients with HCV had increased risk of acute kidney injury, sepsis, and transfusion at 30 and 90 days. After hip replacement, patients with HBV had a higher risk of acute kidney injury, pneumonia, and transfusion at 30 and 90 days.
Only 364 patients in the study had both HIV and HBV or HBC, but they did have a greater risk of transfusion at 30 and 90 days following both knee and hip surgery.
Following total hip arthroplasty, patients with HIV were more at risk for deep vein thrombosis and transfusion rather than infection. The lower incidence of infection is likely to be related to effective highly active antiretroviral therapy, the researchers say. HIV patients also were more likely to have mechanical complications, such as loosening, periprosthetic fracture, and revision at 90 days, but not at 2 years. Patients with HIV who underwent total knee arthroplasty (TKA) had a higher risk of death at 30 days and medical complications at 90 days. At 2 years, they had a higher risk of periprosthetic joint infection, irrigation and debridement, and revision. The researchers say the higher incidence of mechanical complications can be explained by the younger, more active, and healthy HIV patients in the cohort—the majority were aged younger than 65 years. They also emphasize that the only risk of infection following TJA in their study was 2 years after TKA.
The researchers suggest that their findings could help prompt future guidelines supporting routine screening prior to elective TJA.
Source:
Kildow BJ, Politzer CS, DiLallo M, Bolognesi MP, Seyler TM. J Arthroplasty. 2018;33(suppl 7):S86-S92.
doi: 10.1016/j.arth.2017.10.061.
As patients with HIV, hepatitis B (HBV), and hepatitis C (HCV) live longer, more active lives with the help of antiviral treatments, they are now more often having joint replacement surgeries. But HIV, HBV, and HCV can increase the risk of postoperative complications, say researchers from Duke University in North Carolina.
The researchers studied 16,338 patients in 4 cohorts: those with HIV, HBV, HCV, and HIV plus HBV or HCV. They evaluated the patients at 30 days, 90 days, and 2 years after total joint arthroplasty (TJA), comparing their progress with that of a control group.
Patients with HBV and HCV were at risk of both acute and long-term medical and surgical complications. At 90 days and 2 years, the participants had increased risk of pneumonia, sepsis, joint infection, and revision surgery. They also had a greater risk of complications than did patients with HIV, especially for infection, within the first 90 days postsurgery.
Notably, after TJA, patients with HCV had increased risk of acute kidney injury, sepsis, and transfusion at 30 and 90 days. After hip replacement, patients with HBV had a higher risk of acute kidney injury, pneumonia, and transfusion at 30 and 90 days.
Only 364 patients in the study had both HIV and HBV or HBC, but they did have a greater risk of transfusion at 30 and 90 days following both knee and hip surgery.
Following total hip arthroplasty, patients with HIV were more at risk for deep vein thrombosis and transfusion rather than infection. The lower incidence of infection is likely to be related to effective highly active antiretroviral therapy, the researchers say. HIV patients also were more likely to have mechanical complications, such as loosening, periprosthetic fracture, and revision at 90 days, but not at 2 years. Patients with HIV who underwent total knee arthroplasty (TKA) had a higher risk of death at 30 days and medical complications at 90 days. At 2 years, they had a higher risk of periprosthetic joint infection, irrigation and debridement, and revision. The researchers say the higher incidence of mechanical complications can be explained by the younger, more active, and healthy HIV patients in the cohort—the majority were aged younger than 65 years. They also emphasize that the only risk of infection following TJA in their study was 2 years after TKA.
The researchers suggest that their findings could help prompt future guidelines supporting routine screening prior to elective TJA.
Source:
Kildow BJ, Politzer CS, DiLallo M, Bolognesi MP, Seyler TM. J Arthroplasty. 2018;33(suppl 7):S86-S92.
doi: 10.1016/j.arth.2017.10.061.
As patients with HIV, hepatitis B (HBV), and hepatitis C (HCV) live longer, more active lives with the help of antiviral treatments, they are now more often having joint replacement surgeries. But HIV, HBV, and HCV can increase the risk of postoperative complications, say researchers from Duke University in North Carolina.
The researchers studied 16,338 patients in 4 cohorts: those with HIV, HBV, HCV, and HIV plus HBV or HCV. They evaluated the patients at 30 days, 90 days, and 2 years after total joint arthroplasty (TJA), comparing their progress with that of a control group.
Patients with HBV and HCV were at risk of both acute and long-term medical and surgical complications. At 90 days and 2 years, the participants had increased risk of pneumonia, sepsis, joint infection, and revision surgery. They also had a greater risk of complications than did patients with HIV, especially for infection, within the first 90 days postsurgery.
Notably, after TJA, patients with HCV had increased risk of acute kidney injury, sepsis, and transfusion at 30 and 90 days. After hip replacement, patients with HBV had a higher risk of acute kidney injury, pneumonia, and transfusion at 30 and 90 days.
Only 364 patients in the study had both HIV and HBV or HBC, but they did have a greater risk of transfusion at 30 and 90 days following both knee and hip surgery.
Following total hip arthroplasty, patients with HIV were more at risk for deep vein thrombosis and transfusion rather than infection. The lower incidence of infection is likely to be related to effective highly active antiretroviral therapy, the researchers say. HIV patients also were more likely to have mechanical complications, such as loosening, periprosthetic fracture, and revision at 90 days, but not at 2 years. Patients with HIV who underwent total knee arthroplasty (TKA) had a higher risk of death at 30 days and medical complications at 90 days. At 2 years, they had a higher risk of periprosthetic joint infection, irrigation and debridement, and revision. The researchers say the higher incidence of mechanical complications can be explained by the younger, more active, and healthy HIV patients in the cohort—the majority were aged younger than 65 years. They also emphasize that the only risk of infection following TJA in their study was 2 years after TKA.
The researchers suggest that their findings could help prompt future guidelines supporting routine screening prior to elective TJA.
Source:
Kildow BJ, Politzer CS, DiLallo M, Bolognesi MP, Seyler TM. J Arthroplasty. 2018;33(suppl 7):S86-S92.
doi: 10.1016/j.arth.2017.10.061.
Etravirine Lowers Risk of Hospitalization for Patients With HIV
When all 3 original classes of antiretroviral drugs no longer suppress viral load in a patient with HIV, the next step may be a new drug like etravirine (ETR), a nonnucleoside reverse transcriptase inhibitor (NNRTI). And, according to a French study, that could be a good way of keeping patients out of the hospital.
Using data from the French Hospital Database on HIV (FHDH), researchers analyzed hospitalization rates among heavily treated HIV-1 infected patients on failing regimens between 2005 (etravirine became available in France in 2006) and 2011. They compared 2 groups of patients: those who had received ETR plus a ritonavir-boosted protease inhibitor (PI) and those who had not. The primary endpoint of the study was hospitalization, divided by AIDS-defining cause and non–AIDS-defining cause.
Of 3,884 patients who had been exposed to at least 2 nucleoside reverse transcriptase inhibitors (NRTI), 2 PIs, and 1 NNRTI, 838 received ETR + PI.
During 13,986 person-years of follow-up, there were 2,484 hospitalizations among 956 patients: 617 were from an AIDS-defining cause in 301 patients, and 1,867 from a non–AIDS-defining cause in 828 patients.
The ETR + PI was associated with a 20% reduction in the hospitalization rate, mainly due to the reduction in AIDS hospitalizations. The researchers suggest that the clinical benefit of ETR could be explained by a high rate of virologic suppression (62% at month 6) and excellent tolerability. The FHDH did not include adherence data, but adherence is “unlikely” to explain the better outcome, the researchers say, given that ETR is a twice-daily drug, which may lead to slightly lower adherence than does a once-daily regimen.
The is the first study, to their knowledge, the researchers say, to focus on the risk of hospitalizations in current clinical practice and to show a positive effect.
Source:
Potard V, Goujard C, Valantin MA, et al. BMC Infect Dis. 2018;8:326.
doi: 10.1186/s12879-018-3231-5.
When all 3 original classes of antiretroviral drugs no longer suppress viral load in a patient with HIV, the next step may be a new drug like etravirine (ETR), a nonnucleoside reverse transcriptase inhibitor (NNRTI). And, according to a French study, that could be a good way of keeping patients out of the hospital.
Using data from the French Hospital Database on HIV (FHDH), researchers analyzed hospitalization rates among heavily treated HIV-1 infected patients on failing regimens between 2005 (etravirine became available in France in 2006) and 2011. They compared 2 groups of patients: those who had received ETR plus a ritonavir-boosted protease inhibitor (PI) and those who had not. The primary endpoint of the study was hospitalization, divided by AIDS-defining cause and non–AIDS-defining cause.
Of 3,884 patients who had been exposed to at least 2 nucleoside reverse transcriptase inhibitors (NRTI), 2 PIs, and 1 NNRTI, 838 received ETR + PI.
During 13,986 person-years of follow-up, there were 2,484 hospitalizations among 956 patients: 617 were from an AIDS-defining cause in 301 patients, and 1,867 from a non–AIDS-defining cause in 828 patients.
The ETR + PI was associated with a 20% reduction in the hospitalization rate, mainly due to the reduction in AIDS hospitalizations. The researchers suggest that the clinical benefit of ETR could be explained by a high rate of virologic suppression (62% at month 6) and excellent tolerability. The FHDH did not include adherence data, but adherence is “unlikely” to explain the better outcome, the researchers say, given that ETR is a twice-daily drug, which may lead to slightly lower adherence than does a once-daily regimen.
The is the first study, to their knowledge, the researchers say, to focus on the risk of hospitalizations in current clinical practice and to show a positive effect.
Source:
Potard V, Goujard C, Valantin MA, et al. BMC Infect Dis. 2018;8:326.
doi: 10.1186/s12879-018-3231-5.
When all 3 original classes of antiretroviral drugs no longer suppress viral load in a patient with HIV, the next step may be a new drug like etravirine (ETR), a nonnucleoside reverse transcriptase inhibitor (NNRTI). And, according to a French study, that could be a good way of keeping patients out of the hospital.
Using data from the French Hospital Database on HIV (FHDH), researchers analyzed hospitalization rates among heavily treated HIV-1 infected patients on failing regimens between 2005 (etravirine became available in France in 2006) and 2011. They compared 2 groups of patients: those who had received ETR plus a ritonavir-boosted protease inhibitor (PI) and those who had not. The primary endpoint of the study was hospitalization, divided by AIDS-defining cause and non–AIDS-defining cause.
Of 3,884 patients who had been exposed to at least 2 nucleoside reverse transcriptase inhibitors (NRTI), 2 PIs, and 1 NNRTI, 838 received ETR + PI.
During 13,986 person-years of follow-up, there were 2,484 hospitalizations among 956 patients: 617 were from an AIDS-defining cause in 301 patients, and 1,867 from a non–AIDS-defining cause in 828 patients.
The ETR + PI was associated with a 20% reduction in the hospitalization rate, mainly due to the reduction in AIDS hospitalizations. The researchers suggest that the clinical benefit of ETR could be explained by a high rate of virologic suppression (62% at month 6) and excellent tolerability. The FHDH did not include adherence data, but adherence is “unlikely” to explain the better outcome, the researchers say, given that ETR is a twice-daily drug, which may lead to slightly lower adherence than does a once-daily regimen.
The is the first study, to their knowledge, the researchers say, to focus on the risk of hospitalizations in current clinical practice and to show a positive effect.
Source:
Potard V, Goujard C, Valantin MA, et al. BMC Infect Dis. 2018;8:326.
doi: 10.1186/s12879-018-3231-5.
Neural-tube defect signal from dolutegravir HIV treatment raises concerns
AMSTERDAM – Over the past couple of years, integrase inhibitors have become the preferred anchor drug worldwide for HIV-treatment regimens. But in May 2018, researchers first reported an unexpected signal that one drug from the class, dolutegravir, showed a statistically significant link with an increased rate of neural-tube defects in neonates born to women in Botswana who had received dolutegravir at the time they conceived.
The data showed a 0.94% incidence of a neonate born with a neural-tube defect (NTD) among 426 HIV-infected women who were taking dolutegravir when they became pregnant. While this surprising finding remains preliminary because of limited number of women studied so far, and although the magnitude of the apparent effect fell somewhat after factoring in no further infants born with an NTD among 170 additional exposed women, the suggestion of an important teratogenic effect from dolutegravir led to a special session during the 22nd International AIDS Conference. The overwhelming consensus from this session seemed to be that the possible excess of NTDs linked with treatment with an integrase strand transfer inhibitor (INSTI) at the start of pregnancy was concerning enough to suggest caution and extra counseling for women of childbearing potential, but it was by no means a reason to derail the worldwide shift to the INSTI drug class as the core agent for treating HIV.
“Dolutegravir has been a beacon of hope for treating HIV,” said Maggie Little, PhD, a professor of philosophy and medical ethicist at Georgetown University in Washington. “Dolutegravir offers substantial benefits to quality of life in addition to reducing women’s mortality.” The new finding of excess NTDs “appears to pit pregnant women against their children. But the numbers never tell us the answer; it’s not arithmetic.” The appropriate public health response should focus on “supporting meaningful choice by women,” Dr. Little said during a talk at the session. “Policies must be made in ongoing consultation with communities of women who live with HIV.”
Rise of the INSTIs
The International AIDS Conference showcased the contrast between the benefits of the INSTIs and their possible perils.
Well before news of the NTD signal came out, the conference program featured a plenary talk from Pedro Cahn, MD, PhD, entitled “Moving into the Integrase Era.” During his talk, Dr. Cahn proclaimed that HIV treatment is “moving toward the integrase world,” and recently featured “unprecedented rollout” in low-income countries. In addition to dolutegravir (Tivicay) the INSTI class includes raltegravir (Isentress), elvitegravir (Vitekta), and bictegravir (Symtuza).
Dr. Cahn attributed the first-line status of the INSTIs to several factors: their higher antiviral activity, compared with every other anti-HIV drug including proven superior efficacy to efavirenz (Sustiva) – the former core drug for antiretroviral regimens, rapid viral suppression, good tolerability with a low rate of treatment discontinuations, good recovery of CD4 cells, a relatively high genetic barrier to selection of HIV resistance mutations with relatively few resistant mutations seen when used in combination regimen’s in treatment-naive patients, and few drug-drug interactions, By mid-2018, dolutegravir or another INSTI had been named part of a first-line HIV treatment regimen by several countries and by the World Health Organization; according to WHO data, by mid-2018 more than half the low- and middle-income countries of the world had endorsed an INSTI-containing regimen including Botswana, Brazil, Kenya, Nigeria, and Uganda, said Dr. Cahn, scientific director of the Huésbed Foundation in Buenos Aires.
One example of the success that dolutegravir has recently shown as first-line treatment came in data reported at the Conference from Brazil. where a three-drug regimen containing dolutegravir plus lamivudine (3TC; Epivir) and tenofovir (TDF; Viread) replaced a triple regimen of efavirenz plus 3TC and TDF as recommended first-line treatment in 2017. Data collected by the Brazilian Ministry of Health during January 2014-June 2017 identified 103,240 people at least 15 years old who received treatment for HIV. The review showed that 85% of people treated with a dolutegravir-containing regimen had successful viral suppression to an undetectable level, compared with 78% of people on the same regimen but with efavirenz instead of dolutegravir, Mariana V. Meireles reported at the conference. Other triple-drug regimens had even lower rates of viral suppression. After researchers controlled for the age, sex, level of adherence, and baseline viral load and CD4 cell count the people who received the dolutegravir-containing regimen had at least a 42% higher rate of undetectable virus compared with any other regimen used by Brazilian patients, said Ms. Meireles, a researcher with the Brazilian Ministry of Health in Brasilia.
Dr. Cahn acknowledged the current concern and uncertainty about INSTIs and NTDs. “Caution and effective contraception are recommended for dolutegravir. The risks and benefits should be compared with other [treatment] options. Women have the right to make informed choices,” he said. Dr. Cahn also highlighted that safety analyses need data from additional early-pregnancy exposures to clearly rule in or rule out a teratogenic effect from dolutegravir. And he stressed that, whether or not the possible NTD link is a class effect remains to be assessed as data from early-pregnancy exposures of women on other INSTIs are currently much more limited than they are those for dolutegravir. He also raised a question voiced by others: Is the effect from dolutegravir somehow mediated by folic acid levels, a dietary component that protects against NTDs? Botswana, the country that generated the NTD data, doesn’t fortify wheat flour or any other food with folic acid, as occurs in the United States, noted Rebecca M. Zash, MD, the researcher who led the Botswana study.
The NTD data
The signal for an NTD link to dolutegravir came from a study run in Botswana designed for a totally different, albeit related purpose. The Tsepamo study launched in 2014 with the goal of assessing the safety of efavirenz-based HIV regimens when used by pregnant women. The study has run at eight of the country’s largest maternity wards, where nearly half of Botswana’s deliveries occur. The midwives at those locations collected data on all women at their clinics, and once Botswana adopted dolutegravir as its anchor drug of choice for treating people infected with HIV in 2017 significant numbers of the women in the Tsepamo study received dolutegravir. Through May 1, 2018, the study had enrolled more than 89,000 women who had 88,755 live births, including nearly 22,000 women infected with HIV (and more than 66,000 without infection), nearly 12,00 of those infected with HIV who received some type of antiretroviral therapy, 5,787 on efavirenz at the time of conception, 2,812 women who started on dolutegravir treatment during pregnancy, and 426 women who were on dolutegravir at the time of conception, said Dr. Zash, an infectious diseases physician at Beth Israel Deaconess Hospital in Boston and codirector of the Reproductive Health for HIV-Infected Populations Study Working Group at the Harvard University Center for AIDS Research in Cambridge, Mass.
A recently published analysis by Dr. Zash and her associates found no difference in the incidence rate of adverse birth outcomes among women who started on either efavirenz or dolutegravir during pregnancy. This analysis also showed that women infected with HIV overall had “mildly increased” rates of both total adverse birth outcomes and severe adverse birth outcomes compared with women without HIV infection (Lancet Glob Health. 2018 Jul;6[7]:e804-e10).
When the researchers looked at NTDs among neonates born to women exposed at conception, they saw a different picture. The entire cohort of nearly 89,000 live births included 86 neonates with an NTD, a 0.1% rate. This included 4 of the 426 births from mothers on dolutegravir at conception, a 0.94% rate, significantly higher than the overall rate. Other comparator NTD rates included a 0,12% incidence among mothers on any anti-HIV drug other than dolutegravir at conception, a 0.09% rate among mothers who were not infected with HIV, and a 0.05% rate among mothers on efavirenz at conception, Dr. Zash and her associates reported in a publication that appeared coincident with her talk at the conference (N Engl J Med. 2018 Jul 24.doi: 10.1056/NEJMc1807653). The NTDs linked with dolutegravir use involved four distinct types of NTD, a finding Dr. Zash called “unusual,” but not unique among teratogens.
During her talk, Dr. Zash further updated the dolutegravir numbers based on extended follow-up of the Botswana cohort during May 1-July 15, during which time two NTDs occurred, one involving an uninfected mother and the second from a mother who started on dolutegravir at 8 weeks’ gestational age, after the time when NTDs occur. Further follow-up also added 170 more neonates born to women exposed to dolutegravir at conception, bringing the total now to 596 births with 4 NTDs or a rate of 0.67%, still significantly elevated, compared with other exposure groups. The Tsepamo study continues, with an additional 10 sites planned to soon join that will boost maternity coverage to 72% of Botswana’s annual births. The next planned analysis is in March 2019, and by then the number of neonates born to women with early dolutegravir exposure should more than double, Dr. Zash predicted.
Modeling the risks and benefits
Identifying a possible excess of NTDs with dolutegravir treatment in adolescent girls and young women doesn’t, of course, tell the whole risk-benefit story for dolutegravir and possibly the other INSTIs. Caitlin Dugdale, MD, an infectious diseases physician at Massachusetts General Hospital in Boston, reported a model she developed to better define the pluses and minuses of dolutegravir treatment, compared with efavirenz. The model used projections for women in South Africa of child-bearing potential infected by HIV over the next 5 years and used data on drug efficacy and harms based on published reports. For example, the ability of the two drugs to produce undetectable viral loads was assumed by the model to be 94% after 48 weeks on treatment with dolutegravir and 86% with efavirenz, based on the rates reported in the phase 3, randomized comparison of dolutegravir- and efavirenz-based regimens in the SINGLE trial, with adjustments for factors such as protocol deviations and mortality that were accounted for in other parts of the model, Dr. Dugdale said. She used estimates for NTD incidence based on the published numbers reported by Dr. Zash.
The results showed that, over the next 5 years, based on just the existing and projected rates of HIV infection, treating all infected women and children with a dolutegravir-based regimen instead of a regimen anchored by efavirenz would result in the benefits of 28,400 fewer deaths among women, 52,800 fewer sexual transmissions of HIV, 5,000 fewer pediatric HIV transmissions, and 1,600 fewer pediatric deaths unrelated to an NTD. On the minus side relying on dolutegravir instead of efavirenz was projected to cause an excess of 10,000 neonates born with an NTD, 8,400 excess pediatric deaths, and overall 5,400 fewer children alive and free from HIV. These projections were based on 3.5 million women on first-line treatment with antiretroviral therapy and 1.1 million children born with HIV exposure.
Dr. Dugdale drew particular attention to the comparison between 28,400 fewer deaths among women when treated with dolutegravir at the cost of 8,400 excess pediatric deaths, but cautioned that this creates “a difficult trade-off to balance.” Findings from the model and other information on HIV treatment options should enter into the decision making of each HIV-infected woman who could become pregnant, she said. It’s important that patients view the risks and benefits not just on a population level but on an individual, personal level, Dr. Dugdale said in a video interview. “The individual woman must balance the risks and benefits for herself and her child.”
“Patients need to decide what is important to them,” agreed Dr. Zash during the conference.
The NTD findings also underscored the importance of better contraception options for HIV-infected women. “This is an opportunity to improve reproductive health and contraception for women, especially in resource-poor countries,” commented Elaine J. Abrams, MD, professor of epidemiology and pediatrics at Columbia University in New York, who cochaired the conference session.
Another lesson from the NTD findings is the importance of tracking the safety of new drugs used when women become pregnant and during pregnancy. The dolutegravir arm of the Tsepamo study “was almost by accident,” noted the Georgetown medical ethicist, Dr. Little. “Every new treatment should be examined in pregnant women and infants,” she added. “Studies like this should not be left to chance. Women deserve an evidence base for medication use across the lifespan including during pregnancy and periconception.”
Dr. Little, Ms. Meireles, Dr. Zash, and Dr. Dugdale had no disclosures. Dr. Cahn has been an adviser to or speaker for AbbVie, Merck, and ViiV and has received research funding from AbbVie, Merck, ViiV, and Richmond. Dr. Abrams has been an adviser to Merck and ViiV. Viiv is the company that markets dolutegravir.
AMSTERDAM – Over the past couple of years, integrase inhibitors have become the preferred anchor drug worldwide for HIV-treatment regimens. But in May 2018, researchers first reported an unexpected signal that one drug from the class, dolutegravir, showed a statistically significant link with an increased rate of neural-tube defects in neonates born to women in Botswana who had received dolutegravir at the time they conceived.
The data showed a 0.94% incidence of a neonate born with a neural-tube defect (NTD) among 426 HIV-infected women who were taking dolutegravir when they became pregnant. While this surprising finding remains preliminary because of limited number of women studied so far, and although the magnitude of the apparent effect fell somewhat after factoring in no further infants born with an NTD among 170 additional exposed women, the suggestion of an important teratogenic effect from dolutegravir led to a special session during the 22nd International AIDS Conference. The overwhelming consensus from this session seemed to be that the possible excess of NTDs linked with treatment with an integrase strand transfer inhibitor (INSTI) at the start of pregnancy was concerning enough to suggest caution and extra counseling for women of childbearing potential, but it was by no means a reason to derail the worldwide shift to the INSTI drug class as the core agent for treating HIV.
“Dolutegravir has been a beacon of hope for treating HIV,” said Maggie Little, PhD, a professor of philosophy and medical ethicist at Georgetown University in Washington. “Dolutegravir offers substantial benefits to quality of life in addition to reducing women’s mortality.” The new finding of excess NTDs “appears to pit pregnant women against their children. But the numbers never tell us the answer; it’s not arithmetic.” The appropriate public health response should focus on “supporting meaningful choice by women,” Dr. Little said during a talk at the session. “Policies must be made in ongoing consultation with communities of women who live with HIV.”
Rise of the INSTIs
The International AIDS Conference showcased the contrast between the benefits of the INSTIs and their possible perils.
Well before news of the NTD signal came out, the conference program featured a plenary talk from Pedro Cahn, MD, PhD, entitled “Moving into the Integrase Era.” During his talk, Dr. Cahn proclaimed that HIV treatment is “moving toward the integrase world,” and recently featured “unprecedented rollout” in low-income countries. In addition to dolutegravir (Tivicay) the INSTI class includes raltegravir (Isentress), elvitegravir (Vitekta), and bictegravir (Symtuza).
Dr. Cahn attributed the first-line status of the INSTIs to several factors: their higher antiviral activity, compared with every other anti-HIV drug including proven superior efficacy to efavirenz (Sustiva) – the former core drug for antiretroviral regimens, rapid viral suppression, good tolerability with a low rate of treatment discontinuations, good recovery of CD4 cells, a relatively high genetic barrier to selection of HIV resistance mutations with relatively few resistant mutations seen when used in combination regimen’s in treatment-naive patients, and few drug-drug interactions, By mid-2018, dolutegravir or another INSTI had been named part of a first-line HIV treatment regimen by several countries and by the World Health Organization; according to WHO data, by mid-2018 more than half the low- and middle-income countries of the world had endorsed an INSTI-containing regimen including Botswana, Brazil, Kenya, Nigeria, and Uganda, said Dr. Cahn, scientific director of the Huésbed Foundation in Buenos Aires.
One example of the success that dolutegravir has recently shown as first-line treatment came in data reported at the Conference from Brazil. where a three-drug regimen containing dolutegravir plus lamivudine (3TC; Epivir) and tenofovir (TDF; Viread) replaced a triple regimen of efavirenz plus 3TC and TDF as recommended first-line treatment in 2017. Data collected by the Brazilian Ministry of Health during January 2014-June 2017 identified 103,240 people at least 15 years old who received treatment for HIV. The review showed that 85% of people treated with a dolutegravir-containing regimen had successful viral suppression to an undetectable level, compared with 78% of people on the same regimen but with efavirenz instead of dolutegravir, Mariana V. Meireles reported at the conference. Other triple-drug regimens had even lower rates of viral suppression. After researchers controlled for the age, sex, level of adherence, and baseline viral load and CD4 cell count the people who received the dolutegravir-containing regimen had at least a 42% higher rate of undetectable virus compared with any other regimen used by Brazilian patients, said Ms. Meireles, a researcher with the Brazilian Ministry of Health in Brasilia.
Dr. Cahn acknowledged the current concern and uncertainty about INSTIs and NTDs. “Caution and effective contraception are recommended for dolutegravir. The risks and benefits should be compared with other [treatment] options. Women have the right to make informed choices,” he said. Dr. Cahn also highlighted that safety analyses need data from additional early-pregnancy exposures to clearly rule in or rule out a teratogenic effect from dolutegravir. And he stressed that, whether or not the possible NTD link is a class effect remains to be assessed as data from early-pregnancy exposures of women on other INSTIs are currently much more limited than they are those for dolutegravir. He also raised a question voiced by others: Is the effect from dolutegravir somehow mediated by folic acid levels, a dietary component that protects against NTDs? Botswana, the country that generated the NTD data, doesn’t fortify wheat flour or any other food with folic acid, as occurs in the United States, noted Rebecca M. Zash, MD, the researcher who led the Botswana study.
The NTD data
The signal for an NTD link to dolutegravir came from a study run in Botswana designed for a totally different, albeit related purpose. The Tsepamo study launched in 2014 with the goal of assessing the safety of efavirenz-based HIV regimens when used by pregnant women. The study has run at eight of the country’s largest maternity wards, where nearly half of Botswana’s deliveries occur. The midwives at those locations collected data on all women at their clinics, and once Botswana adopted dolutegravir as its anchor drug of choice for treating people infected with HIV in 2017 significant numbers of the women in the Tsepamo study received dolutegravir. Through May 1, 2018, the study had enrolled more than 89,000 women who had 88,755 live births, including nearly 22,000 women infected with HIV (and more than 66,000 without infection), nearly 12,00 of those infected with HIV who received some type of antiretroviral therapy, 5,787 on efavirenz at the time of conception, 2,812 women who started on dolutegravir treatment during pregnancy, and 426 women who were on dolutegravir at the time of conception, said Dr. Zash, an infectious diseases physician at Beth Israel Deaconess Hospital in Boston and codirector of the Reproductive Health for HIV-Infected Populations Study Working Group at the Harvard University Center for AIDS Research in Cambridge, Mass.
A recently published analysis by Dr. Zash and her associates found no difference in the incidence rate of adverse birth outcomes among women who started on either efavirenz or dolutegravir during pregnancy. This analysis also showed that women infected with HIV overall had “mildly increased” rates of both total adverse birth outcomes and severe adverse birth outcomes compared with women without HIV infection (Lancet Glob Health. 2018 Jul;6[7]:e804-e10).
When the researchers looked at NTDs among neonates born to women exposed at conception, they saw a different picture. The entire cohort of nearly 89,000 live births included 86 neonates with an NTD, a 0.1% rate. This included 4 of the 426 births from mothers on dolutegravir at conception, a 0.94% rate, significantly higher than the overall rate. Other comparator NTD rates included a 0,12% incidence among mothers on any anti-HIV drug other than dolutegravir at conception, a 0.09% rate among mothers who were not infected with HIV, and a 0.05% rate among mothers on efavirenz at conception, Dr. Zash and her associates reported in a publication that appeared coincident with her talk at the conference (N Engl J Med. 2018 Jul 24.doi: 10.1056/NEJMc1807653). The NTDs linked with dolutegravir use involved four distinct types of NTD, a finding Dr. Zash called “unusual,” but not unique among teratogens.
During her talk, Dr. Zash further updated the dolutegravir numbers based on extended follow-up of the Botswana cohort during May 1-July 15, during which time two NTDs occurred, one involving an uninfected mother and the second from a mother who started on dolutegravir at 8 weeks’ gestational age, after the time when NTDs occur. Further follow-up also added 170 more neonates born to women exposed to dolutegravir at conception, bringing the total now to 596 births with 4 NTDs or a rate of 0.67%, still significantly elevated, compared with other exposure groups. The Tsepamo study continues, with an additional 10 sites planned to soon join that will boost maternity coverage to 72% of Botswana’s annual births. The next planned analysis is in March 2019, and by then the number of neonates born to women with early dolutegravir exposure should more than double, Dr. Zash predicted.
Modeling the risks and benefits
Identifying a possible excess of NTDs with dolutegravir treatment in adolescent girls and young women doesn’t, of course, tell the whole risk-benefit story for dolutegravir and possibly the other INSTIs. Caitlin Dugdale, MD, an infectious diseases physician at Massachusetts General Hospital in Boston, reported a model she developed to better define the pluses and minuses of dolutegravir treatment, compared with efavirenz. The model used projections for women in South Africa of child-bearing potential infected by HIV over the next 5 years and used data on drug efficacy and harms based on published reports. For example, the ability of the two drugs to produce undetectable viral loads was assumed by the model to be 94% after 48 weeks on treatment with dolutegravir and 86% with efavirenz, based on the rates reported in the phase 3, randomized comparison of dolutegravir- and efavirenz-based regimens in the SINGLE trial, with adjustments for factors such as protocol deviations and mortality that were accounted for in other parts of the model, Dr. Dugdale said. She used estimates for NTD incidence based on the published numbers reported by Dr. Zash.
The results showed that, over the next 5 years, based on just the existing and projected rates of HIV infection, treating all infected women and children with a dolutegravir-based regimen instead of a regimen anchored by efavirenz would result in the benefits of 28,400 fewer deaths among women, 52,800 fewer sexual transmissions of HIV, 5,000 fewer pediatric HIV transmissions, and 1,600 fewer pediatric deaths unrelated to an NTD. On the minus side relying on dolutegravir instead of efavirenz was projected to cause an excess of 10,000 neonates born with an NTD, 8,400 excess pediatric deaths, and overall 5,400 fewer children alive and free from HIV. These projections were based on 3.5 million women on first-line treatment with antiretroviral therapy and 1.1 million children born with HIV exposure.
Dr. Dugdale drew particular attention to the comparison between 28,400 fewer deaths among women when treated with dolutegravir at the cost of 8,400 excess pediatric deaths, but cautioned that this creates “a difficult trade-off to balance.” Findings from the model and other information on HIV treatment options should enter into the decision making of each HIV-infected woman who could become pregnant, she said. It’s important that patients view the risks and benefits not just on a population level but on an individual, personal level, Dr. Dugdale said in a video interview. “The individual woman must balance the risks and benefits for herself and her child.”
“Patients need to decide what is important to them,” agreed Dr. Zash during the conference.
The NTD findings also underscored the importance of better contraception options for HIV-infected women. “This is an opportunity to improve reproductive health and contraception for women, especially in resource-poor countries,” commented Elaine J. Abrams, MD, professor of epidemiology and pediatrics at Columbia University in New York, who cochaired the conference session.
Another lesson from the NTD findings is the importance of tracking the safety of new drugs used when women become pregnant and during pregnancy. The dolutegravir arm of the Tsepamo study “was almost by accident,” noted the Georgetown medical ethicist, Dr. Little. “Every new treatment should be examined in pregnant women and infants,” she added. “Studies like this should not be left to chance. Women deserve an evidence base for medication use across the lifespan including during pregnancy and periconception.”
Dr. Little, Ms. Meireles, Dr. Zash, and Dr. Dugdale had no disclosures. Dr. Cahn has been an adviser to or speaker for AbbVie, Merck, and ViiV and has received research funding from AbbVie, Merck, ViiV, and Richmond. Dr. Abrams has been an adviser to Merck and ViiV. Viiv is the company that markets dolutegravir.
AMSTERDAM – Over the past couple of years, integrase inhibitors have become the preferred anchor drug worldwide for HIV-treatment regimens. But in May 2018, researchers first reported an unexpected signal that one drug from the class, dolutegravir, showed a statistically significant link with an increased rate of neural-tube defects in neonates born to women in Botswana who had received dolutegravir at the time they conceived.
The data showed a 0.94% incidence of a neonate born with a neural-tube defect (NTD) among 426 HIV-infected women who were taking dolutegravir when they became pregnant. While this surprising finding remains preliminary because of limited number of women studied so far, and although the magnitude of the apparent effect fell somewhat after factoring in no further infants born with an NTD among 170 additional exposed women, the suggestion of an important teratogenic effect from dolutegravir led to a special session during the 22nd International AIDS Conference. The overwhelming consensus from this session seemed to be that the possible excess of NTDs linked with treatment with an integrase strand transfer inhibitor (INSTI) at the start of pregnancy was concerning enough to suggest caution and extra counseling for women of childbearing potential, but it was by no means a reason to derail the worldwide shift to the INSTI drug class as the core agent for treating HIV.
“Dolutegravir has been a beacon of hope for treating HIV,” said Maggie Little, PhD, a professor of philosophy and medical ethicist at Georgetown University in Washington. “Dolutegravir offers substantial benefits to quality of life in addition to reducing women’s mortality.” The new finding of excess NTDs “appears to pit pregnant women against their children. But the numbers never tell us the answer; it’s not arithmetic.” The appropriate public health response should focus on “supporting meaningful choice by women,” Dr. Little said during a talk at the session. “Policies must be made in ongoing consultation with communities of women who live with HIV.”
Rise of the INSTIs
The International AIDS Conference showcased the contrast between the benefits of the INSTIs and their possible perils.
Well before news of the NTD signal came out, the conference program featured a plenary talk from Pedro Cahn, MD, PhD, entitled “Moving into the Integrase Era.” During his talk, Dr. Cahn proclaimed that HIV treatment is “moving toward the integrase world,” and recently featured “unprecedented rollout” in low-income countries. In addition to dolutegravir (Tivicay) the INSTI class includes raltegravir (Isentress), elvitegravir (Vitekta), and bictegravir (Symtuza).
Dr. Cahn attributed the first-line status of the INSTIs to several factors: their higher antiviral activity, compared with every other anti-HIV drug including proven superior efficacy to efavirenz (Sustiva) – the former core drug for antiretroviral regimens, rapid viral suppression, good tolerability with a low rate of treatment discontinuations, good recovery of CD4 cells, a relatively high genetic barrier to selection of HIV resistance mutations with relatively few resistant mutations seen when used in combination regimen’s in treatment-naive patients, and few drug-drug interactions, By mid-2018, dolutegravir or another INSTI had been named part of a first-line HIV treatment regimen by several countries and by the World Health Organization; according to WHO data, by mid-2018 more than half the low- and middle-income countries of the world had endorsed an INSTI-containing regimen including Botswana, Brazil, Kenya, Nigeria, and Uganda, said Dr. Cahn, scientific director of the Huésbed Foundation in Buenos Aires.
One example of the success that dolutegravir has recently shown as first-line treatment came in data reported at the Conference from Brazil. where a three-drug regimen containing dolutegravir plus lamivudine (3TC; Epivir) and tenofovir (TDF; Viread) replaced a triple regimen of efavirenz plus 3TC and TDF as recommended first-line treatment in 2017. Data collected by the Brazilian Ministry of Health during January 2014-June 2017 identified 103,240 people at least 15 years old who received treatment for HIV. The review showed that 85% of people treated with a dolutegravir-containing regimen had successful viral suppression to an undetectable level, compared with 78% of people on the same regimen but with efavirenz instead of dolutegravir, Mariana V. Meireles reported at the conference. Other triple-drug regimens had even lower rates of viral suppression. After researchers controlled for the age, sex, level of adherence, and baseline viral load and CD4 cell count the people who received the dolutegravir-containing regimen had at least a 42% higher rate of undetectable virus compared with any other regimen used by Brazilian patients, said Ms. Meireles, a researcher with the Brazilian Ministry of Health in Brasilia.
Dr. Cahn acknowledged the current concern and uncertainty about INSTIs and NTDs. “Caution and effective contraception are recommended for dolutegravir. The risks and benefits should be compared with other [treatment] options. Women have the right to make informed choices,” he said. Dr. Cahn also highlighted that safety analyses need data from additional early-pregnancy exposures to clearly rule in or rule out a teratogenic effect from dolutegravir. And he stressed that, whether or not the possible NTD link is a class effect remains to be assessed as data from early-pregnancy exposures of women on other INSTIs are currently much more limited than they are those for dolutegravir. He also raised a question voiced by others: Is the effect from dolutegravir somehow mediated by folic acid levels, a dietary component that protects against NTDs? Botswana, the country that generated the NTD data, doesn’t fortify wheat flour or any other food with folic acid, as occurs in the United States, noted Rebecca M. Zash, MD, the researcher who led the Botswana study.
The NTD data
The signal for an NTD link to dolutegravir came from a study run in Botswana designed for a totally different, albeit related purpose. The Tsepamo study launched in 2014 with the goal of assessing the safety of efavirenz-based HIV regimens when used by pregnant women. The study has run at eight of the country’s largest maternity wards, where nearly half of Botswana’s deliveries occur. The midwives at those locations collected data on all women at their clinics, and once Botswana adopted dolutegravir as its anchor drug of choice for treating people infected with HIV in 2017 significant numbers of the women in the Tsepamo study received dolutegravir. Through May 1, 2018, the study had enrolled more than 89,000 women who had 88,755 live births, including nearly 22,000 women infected with HIV (and more than 66,000 without infection), nearly 12,00 of those infected with HIV who received some type of antiretroviral therapy, 5,787 on efavirenz at the time of conception, 2,812 women who started on dolutegravir treatment during pregnancy, and 426 women who were on dolutegravir at the time of conception, said Dr. Zash, an infectious diseases physician at Beth Israel Deaconess Hospital in Boston and codirector of the Reproductive Health for HIV-Infected Populations Study Working Group at the Harvard University Center for AIDS Research in Cambridge, Mass.
A recently published analysis by Dr. Zash and her associates found no difference in the incidence rate of adverse birth outcomes among women who started on either efavirenz or dolutegravir during pregnancy. This analysis also showed that women infected with HIV overall had “mildly increased” rates of both total adverse birth outcomes and severe adverse birth outcomes compared with women without HIV infection (Lancet Glob Health. 2018 Jul;6[7]:e804-e10).
When the researchers looked at NTDs among neonates born to women exposed at conception, they saw a different picture. The entire cohort of nearly 89,000 live births included 86 neonates with an NTD, a 0.1% rate. This included 4 of the 426 births from mothers on dolutegravir at conception, a 0.94% rate, significantly higher than the overall rate. Other comparator NTD rates included a 0,12% incidence among mothers on any anti-HIV drug other than dolutegravir at conception, a 0.09% rate among mothers who were not infected with HIV, and a 0.05% rate among mothers on efavirenz at conception, Dr. Zash and her associates reported in a publication that appeared coincident with her talk at the conference (N Engl J Med. 2018 Jul 24.doi: 10.1056/NEJMc1807653). The NTDs linked with dolutegravir use involved four distinct types of NTD, a finding Dr. Zash called “unusual,” but not unique among teratogens.
During her talk, Dr. Zash further updated the dolutegravir numbers based on extended follow-up of the Botswana cohort during May 1-July 15, during which time two NTDs occurred, one involving an uninfected mother and the second from a mother who started on dolutegravir at 8 weeks’ gestational age, after the time when NTDs occur. Further follow-up also added 170 more neonates born to women exposed to dolutegravir at conception, bringing the total now to 596 births with 4 NTDs or a rate of 0.67%, still significantly elevated, compared with other exposure groups. The Tsepamo study continues, with an additional 10 sites planned to soon join that will boost maternity coverage to 72% of Botswana’s annual births. The next planned analysis is in March 2019, and by then the number of neonates born to women with early dolutegravir exposure should more than double, Dr. Zash predicted.
Modeling the risks and benefits
Identifying a possible excess of NTDs with dolutegravir treatment in adolescent girls and young women doesn’t, of course, tell the whole risk-benefit story for dolutegravir and possibly the other INSTIs. Caitlin Dugdale, MD, an infectious diseases physician at Massachusetts General Hospital in Boston, reported a model she developed to better define the pluses and minuses of dolutegravir treatment, compared with efavirenz. The model used projections for women in South Africa of child-bearing potential infected by HIV over the next 5 years and used data on drug efficacy and harms based on published reports. For example, the ability of the two drugs to produce undetectable viral loads was assumed by the model to be 94% after 48 weeks on treatment with dolutegravir and 86% with efavirenz, based on the rates reported in the phase 3, randomized comparison of dolutegravir- and efavirenz-based regimens in the SINGLE trial, with adjustments for factors such as protocol deviations and mortality that were accounted for in other parts of the model, Dr. Dugdale said. She used estimates for NTD incidence based on the published numbers reported by Dr. Zash.
The results showed that, over the next 5 years, based on just the existing and projected rates of HIV infection, treating all infected women and children with a dolutegravir-based regimen instead of a regimen anchored by efavirenz would result in the benefits of 28,400 fewer deaths among women, 52,800 fewer sexual transmissions of HIV, 5,000 fewer pediatric HIV transmissions, and 1,600 fewer pediatric deaths unrelated to an NTD. On the minus side relying on dolutegravir instead of efavirenz was projected to cause an excess of 10,000 neonates born with an NTD, 8,400 excess pediatric deaths, and overall 5,400 fewer children alive and free from HIV. These projections were based on 3.5 million women on first-line treatment with antiretroviral therapy and 1.1 million children born with HIV exposure.
Dr. Dugdale drew particular attention to the comparison between 28,400 fewer deaths among women when treated with dolutegravir at the cost of 8,400 excess pediatric deaths, but cautioned that this creates “a difficult trade-off to balance.” Findings from the model and other information on HIV treatment options should enter into the decision making of each HIV-infected woman who could become pregnant, she said. It’s important that patients view the risks and benefits not just on a population level but on an individual, personal level, Dr. Dugdale said in a video interview. “The individual woman must balance the risks and benefits for herself and her child.”
“Patients need to decide what is important to them,” agreed Dr. Zash during the conference.
The NTD findings also underscored the importance of better contraception options for HIV-infected women. “This is an opportunity to improve reproductive health and contraception for women, especially in resource-poor countries,” commented Elaine J. Abrams, MD, professor of epidemiology and pediatrics at Columbia University in New York, who cochaired the conference session.
Another lesson from the NTD findings is the importance of tracking the safety of new drugs used when women become pregnant and during pregnancy. The dolutegravir arm of the Tsepamo study “was almost by accident,” noted the Georgetown medical ethicist, Dr. Little. “Every new treatment should be examined in pregnant women and infants,” she added. “Studies like this should not be left to chance. Women deserve an evidence base for medication use across the lifespan including during pregnancy and periconception.”
Dr. Little, Ms. Meireles, Dr. Zash, and Dr. Dugdale had no disclosures. Dr. Cahn has been an adviser to or speaker for AbbVie, Merck, and ViiV and has received research funding from AbbVie, Merck, ViiV, and Richmond. Dr. Abrams has been an adviser to Merck and ViiV. Viiv is the company that markets dolutegravir.
REPORTING FROM AIDS 2018
Ibalizumab shows promise against MDR HIV-1
In combination with an optimized background regimen, the humanized IgG4 monoclonal antibody ibalizumab can reduce viral load and increase CD4 counts in patients with multidrug-resistant HIV type 1 (MDR HIV-1), according to a study published in the New England Journal of Medicine. It does so by binding noncompetitively to CD4 receptors, which can thereby block HIV-1 entry.
TMB-301 (NCT02475629) was a 24-week, open-label, single-group, phase 3 study that included patients with MDR HIV-1. During July 2015 to October 2016, patients first continued on their previous treatment for 7 days, then were given a 2,000-mg loading dose of ibalizumab as monotherapy, and then continued on 800 mg ibalizumab every 14 days plus an individualized regimen that was optimized based on patients’ past treatments for the remainder of the study period.
The primary endpoint was how many patients experienced a decrease in viral load of at least 0.5 log10 copies/mL from baseline to day 14 – that is, after the 7-day control period plus the 7-days ibalizumab monotherapy period. This occurred in 33 of the 40 patients (83%; 95% confidence interval, 67%-93%; P less than .001); in fact, 60% of patients (n = 24) experienced a decrease of at least 1.0 log10 copies/mL during that period, and the mean and median reductions were 1.1 log10 copies/mL. One secondary end point was increase in CD4 counts: The mean increase was 62 cells/mcL, although smaller increases were seen among patients with lower starting counts. Of the 10 patients who exhibited virologic failure or rebound, 9 showed less susceptibility to ibalizumab at week 25 than they had shown at baseline.
At least one adverse event was seen in 32 patients (80%), although most (87%) of those events were mild to moderate in severity, such as diarrhea (20%) and nausea, fatigue, pyrexia, rash, and dizziness (13% each). More serious events (grade 3 or 4) were seen in 28% of patients (n = 11); serious events were seen in nine patients – including immune reconstitution inflammatory syndrome in one. Four patients died during the study, although none of the deaths were believed to have been related to treatment with ibalizumab.
The investigators noted that the study’s limitations – its small size, uncontrolled design, and limited time for analyzing secondary and safety endpoints – were largely related to small number of patients with MDR HIV-1. The investigators noted that, in accordance with HIV treatment guidelines, patients who experience resistance-related treatment failure should be started on a regimen that includes at least two fully active agents; the investigators suggest that the addition of a drug like ibalizumab provides new opportunities for effective treatments in these situations.
This study was originally presented at the Conference on Retroviruses & Opportunistic Infections in partnership with the International Antiviral Society.
The study was supported by the Orphan Products Clinical Trials Grants Program of the Food and Drug Administration and TaiMed, which developed ibalizumab. The authors disclosed ties to various industry entities, including grants, personal fees, nonfinancial support, and other forms of support from TaiMed.
SOURCE: Emu B et al. New Engl J Med. 2018 Aug 16;379(9):645-54.
In combination with an optimized background regimen, the humanized IgG4 monoclonal antibody ibalizumab can reduce viral load and increase CD4 counts in patients with multidrug-resistant HIV type 1 (MDR HIV-1), according to a study published in the New England Journal of Medicine. It does so by binding noncompetitively to CD4 receptors, which can thereby block HIV-1 entry.
TMB-301 (NCT02475629) was a 24-week, open-label, single-group, phase 3 study that included patients with MDR HIV-1. During July 2015 to October 2016, patients first continued on their previous treatment for 7 days, then were given a 2,000-mg loading dose of ibalizumab as monotherapy, and then continued on 800 mg ibalizumab every 14 days plus an individualized regimen that was optimized based on patients’ past treatments for the remainder of the study period.
The primary endpoint was how many patients experienced a decrease in viral load of at least 0.5 log10 copies/mL from baseline to day 14 – that is, after the 7-day control period plus the 7-days ibalizumab monotherapy period. This occurred in 33 of the 40 patients (83%; 95% confidence interval, 67%-93%; P less than .001); in fact, 60% of patients (n = 24) experienced a decrease of at least 1.0 log10 copies/mL during that period, and the mean and median reductions were 1.1 log10 copies/mL. One secondary end point was increase in CD4 counts: The mean increase was 62 cells/mcL, although smaller increases were seen among patients with lower starting counts. Of the 10 patients who exhibited virologic failure or rebound, 9 showed less susceptibility to ibalizumab at week 25 than they had shown at baseline.
At least one adverse event was seen in 32 patients (80%), although most (87%) of those events were mild to moderate in severity, such as diarrhea (20%) and nausea, fatigue, pyrexia, rash, and dizziness (13% each). More serious events (grade 3 or 4) were seen in 28% of patients (n = 11); serious events were seen in nine patients – including immune reconstitution inflammatory syndrome in one. Four patients died during the study, although none of the deaths were believed to have been related to treatment with ibalizumab.
The investigators noted that the study’s limitations – its small size, uncontrolled design, and limited time for analyzing secondary and safety endpoints – were largely related to small number of patients with MDR HIV-1. The investigators noted that, in accordance with HIV treatment guidelines, patients who experience resistance-related treatment failure should be started on a regimen that includes at least two fully active agents; the investigators suggest that the addition of a drug like ibalizumab provides new opportunities for effective treatments in these situations.
This study was originally presented at the Conference on Retroviruses & Opportunistic Infections in partnership with the International Antiviral Society.
The study was supported by the Orphan Products Clinical Trials Grants Program of the Food and Drug Administration and TaiMed, which developed ibalizumab. The authors disclosed ties to various industry entities, including grants, personal fees, nonfinancial support, and other forms of support from TaiMed.
SOURCE: Emu B et al. New Engl J Med. 2018 Aug 16;379(9):645-54.
In combination with an optimized background regimen, the humanized IgG4 monoclonal antibody ibalizumab can reduce viral load and increase CD4 counts in patients with multidrug-resistant HIV type 1 (MDR HIV-1), according to a study published in the New England Journal of Medicine. It does so by binding noncompetitively to CD4 receptors, which can thereby block HIV-1 entry.
TMB-301 (NCT02475629) was a 24-week, open-label, single-group, phase 3 study that included patients with MDR HIV-1. During July 2015 to October 2016, patients first continued on their previous treatment for 7 days, then were given a 2,000-mg loading dose of ibalizumab as monotherapy, and then continued on 800 mg ibalizumab every 14 days plus an individualized regimen that was optimized based on patients’ past treatments for the remainder of the study period.
The primary endpoint was how many patients experienced a decrease in viral load of at least 0.5 log10 copies/mL from baseline to day 14 – that is, after the 7-day control period plus the 7-days ibalizumab monotherapy period. This occurred in 33 of the 40 patients (83%; 95% confidence interval, 67%-93%; P less than .001); in fact, 60% of patients (n = 24) experienced a decrease of at least 1.0 log10 copies/mL during that period, and the mean and median reductions were 1.1 log10 copies/mL. One secondary end point was increase in CD4 counts: The mean increase was 62 cells/mcL, although smaller increases were seen among patients with lower starting counts. Of the 10 patients who exhibited virologic failure or rebound, 9 showed less susceptibility to ibalizumab at week 25 than they had shown at baseline.
At least one adverse event was seen in 32 patients (80%), although most (87%) of those events were mild to moderate in severity, such as diarrhea (20%) and nausea, fatigue, pyrexia, rash, and dizziness (13% each). More serious events (grade 3 or 4) were seen in 28% of patients (n = 11); serious events were seen in nine patients – including immune reconstitution inflammatory syndrome in one. Four patients died during the study, although none of the deaths were believed to have been related to treatment with ibalizumab.
The investigators noted that the study’s limitations – its small size, uncontrolled design, and limited time for analyzing secondary and safety endpoints – were largely related to small number of patients with MDR HIV-1. The investigators noted that, in accordance with HIV treatment guidelines, patients who experience resistance-related treatment failure should be started on a regimen that includes at least two fully active agents; the investigators suggest that the addition of a drug like ibalizumab provides new opportunities for effective treatments in these situations.
This study was originally presented at the Conference on Retroviruses & Opportunistic Infections in partnership with the International Antiviral Society.
The study was supported by the Orphan Products Clinical Trials Grants Program of the Food and Drug Administration and TaiMed, which developed ibalizumab. The authors disclosed ties to various industry entities, including grants, personal fees, nonfinancial support, and other forms of support from TaiMed.
SOURCE: Emu B et al. New Engl J Med. 2018 Aug 16;379(9):645-54.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
U.S. HIV clinical care fails the hardest hit
AMSTERDAM – The U.S. HIV epidemic during this decade has shown an overall slow but steady decline, with national incidence rates dropping by 5% during 2011-2016. But preventing new HIV infections is clearly falling short for a few, key demographic slices that make up the vast majority of the roughly 40,000 new U.S. HIV cases annually in recent years: black/African American men, Hispanic/Latino men, men who have sex with men (MSM), and young adults aged 25-34 years.
What’s especially glaring in data from the Centers for Disease Control and Prevention are the increasing incidence rates when these groups overlap, compared with falling rates of new HIV infections for most everyone else. The CDC’s numbers for 2010-2015 show statistically significant increases in HIV incidence among MSM aged 25-34 years who are black/African American or Hispanic/Latino. Black/African American MSM accounted for 26% of the total 39,782 U.S. HIV diagnoses in 2016, and Hispanic/Latino MSM accounted for 19%, according to CDC statistics, while all blacks/African Americans accounted for 44% of 2016’s new HIV infections and all Hispanic/Latinos had 25%.
Why are these relatively small demographic subgroups bucking the overall national trend toward fewer infections? Why are their incidence rates so stubbornly high?
A major reason is that the U.S. medical community that delivers HIV prevention, diagnosis, and treatment has fallen short in reaching out to, engaging, and facilitating HIV services to these hardest-hit groups, David Malebranche, MD, said in a plenary talk at the 22nd International AIDS Conference. He cited several factors that contribute to the HIV high-risk populations from getting the care they need.
First, there is HIV stigma, which can be especially acute when accompanied by stigmatization that’s also based on race, ethnicity, and sexual orientation.
“HIV stigma causes difficulties in navigating the HIV treatment cascade. HIV stigma can adversely affect testing behavior, disclosure to sex partners and loved ones, and medical care access,” said Dr. Malebranche, an internal medicine physician and HIV specialist at Morehouse School of Medicine in Atlanta who described himself during his talk as a “ black, same-gender-loving man.” People diagnosed with HIV “will consciously choose to live in a trancelike denial of HIV,” he noted. He also cited criminalization of HIV status as another driver of stigmatization, with 34 states having HIV-specific criminal laws, sentence enhancements, or both.
Beyond HIV status, other stigmas permeate clinics based on race, sex, sexual orientation, immigrant status, and gender identity. A need exists to “study what patients experience in clinics, to identify the barriers to patient engagement and antiretroviral therapy,” but Dr. Malebranche suggested that the HIV medical community is “afraid to evaluate and assess their systems because they’re scared of what they’ll see.” U.S. HIV care has been too focused on scientific advances while “losing sight of the larger social picture,” he maintained.
“The power differential between medical systems and vulnerable communities may be partly responsible for why viral suppressions rates are so low.”
Dr. Malebranche placed much of the blame on the HIV clinical community for failing to engage patients in the most affected demographic groups.
“If a health system or clinic has problems with patient adherence, it needs to self-examine the service it provides. Most research into black MSM and the HIV treatment cascade has looked at what’s wrong in the community first and has only looked at the medical community much later, if at all,” Dr. Malebranche said. “Medical systems say things like ‘they are hard to reach,’ and ‘they don’t trust doctors,’ and ‘they are uneducated.’ Medical systems do this to avoid holding themselves accountable.”
But the people who run these systems often don’t question whether the paperwork is too onerous, certification to receive care is too cumbersome, the location too stigmatizing, and whether the staff is trained in cultural humility. “Blaming the victim doesn’t get us far in public health,” he said. The people who run and staff U.S. HIV programs “should consider the power dynamics created by some of their spaces, employees, and protocols that make them complicit in perpetuating vulnerability, and this may be why patients fall out of care. Don’t call black and same-gender-loving people ‘hard to reach’ just because you don’t know how to reach them,” he said.
In addition to calling for better appreciation of the target populations and better accommodation of their needs, Dr. Malebranche suggested greater use of peer navigators, case managers, social workers, rapid test and treat programs, and attention to overall patient health and not just their HIV status. Fundamentally, he said, the HIV medical community needs to go beyond thinking in terms of just HIV suppression and “practice the art of medicine to keep patients engaged.”
SOURCE: Malebranche D, AIDS 2018, Abstract THPL0107.
AMSTERDAM – The U.S. HIV epidemic during this decade has shown an overall slow but steady decline, with national incidence rates dropping by 5% during 2011-2016. But preventing new HIV infections is clearly falling short for a few, key demographic slices that make up the vast majority of the roughly 40,000 new U.S. HIV cases annually in recent years: black/African American men, Hispanic/Latino men, men who have sex with men (MSM), and young adults aged 25-34 years.
What’s especially glaring in data from the Centers for Disease Control and Prevention are the increasing incidence rates when these groups overlap, compared with falling rates of new HIV infections for most everyone else. The CDC’s numbers for 2010-2015 show statistically significant increases in HIV incidence among MSM aged 25-34 years who are black/African American or Hispanic/Latino. Black/African American MSM accounted for 26% of the total 39,782 U.S. HIV diagnoses in 2016, and Hispanic/Latino MSM accounted for 19%, according to CDC statistics, while all blacks/African Americans accounted for 44% of 2016’s new HIV infections and all Hispanic/Latinos had 25%.
Why are these relatively small demographic subgroups bucking the overall national trend toward fewer infections? Why are their incidence rates so stubbornly high?
A major reason is that the U.S. medical community that delivers HIV prevention, diagnosis, and treatment has fallen short in reaching out to, engaging, and facilitating HIV services to these hardest-hit groups, David Malebranche, MD, said in a plenary talk at the 22nd International AIDS Conference. He cited several factors that contribute to the HIV high-risk populations from getting the care they need.
First, there is HIV stigma, which can be especially acute when accompanied by stigmatization that’s also based on race, ethnicity, and sexual orientation.
“HIV stigma causes difficulties in navigating the HIV treatment cascade. HIV stigma can adversely affect testing behavior, disclosure to sex partners and loved ones, and medical care access,” said Dr. Malebranche, an internal medicine physician and HIV specialist at Morehouse School of Medicine in Atlanta who described himself during his talk as a “ black, same-gender-loving man.” People diagnosed with HIV “will consciously choose to live in a trancelike denial of HIV,” he noted. He also cited criminalization of HIV status as another driver of stigmatization, with 34 states having HIV-specific criminal laws, sentence enhancements, or both.
Beyond HIV status, other stigmas permeate clinics based on race, sex, sexual orientation, immigrant status, and gender identity. A need exists to “study what patients experience in clinics, to identify the barriers to patient engagement and antiretroviral therapy,” but Dr. Malebranche suggested that the HIV medical community is “afraid to evaluate and assess their systems because they’re scared of what they’ll see.” U.S. HIV care has been too focused on scientific advances while “losing sight of the larger social picture,” he maintained.
“The power differential between medical systems and vulnerable communities may be partly responsible for why viral suppressions rates are so low.”
Dr. Malebranche placed much of the blame on the HIV clinical community for failing to engage patients in the most affected demographic groups.
“If a health system or clinic has problems with patient adherence, it needs to self-examine the service it provides. Most research into black MSM and the HIV treatment cascade has looked at what’s wrong in the community first and has only looked at the medical community much later, if at all,” Dr. Malebranche said. “Medical systems say things like ‘they are hard to reach,’ and ‘they don’t trust doctors,’ and ‘they are uneducated.’ Medical systems do this to avoid holding themselves accountable.”
But the people who run these systems often don’t question whether the paperwork is too onerous, certification to receive care is too cumbersome, the location too stigmatizing, and whether the staff is trained in cultural humility. “Blaming the victim doesn’t get us far in public health,” he said. The people who run and staff U.S. HIV programs “should consider the power dynamics created by some of their spaces, employees, and protocols that make them complicit in perpetuating vulnerability, and this may be why patients fall out of care. Don’t call black and same-gender-loving people ‘hard to reach’ just because you don’t know how to reach them,” he said.
In addition to calling for better appreciation of the target populations and better accommodation of their needs, Dr. Malebranche suggested greater use of peer navigators, case managers, social workers, rapid test and treat programs, and attention to overall patient health and not just their HIV status. Fundamentally, he said, the HIV medical community needs to go beyond thinking in terms of just HIV suppression and “practice the art of medicine to keep patients engaged.”
SOURCE: Malebranche D, AIDS 2018, Abstract THPL0107.
AMSTERDAM – The U.S. HIV epidemic during this decade has shown an overall slow but steady decline, with national incidence rates dropping by 5% during 2011-2016. But preventing new HIV infections is clearly falling short for a few, key demographic slices that make up the vast majority of the roughly 40,000 new U.S. HIV cases annually in recent years: black/African American men, Hispanic/Latino men, men who have sex with men (MSM), and young adults aged 25-34 years.
What’s especially glaring in data from the Centers for Disease Control and Prevention are the increasing incidence rates when these groups overlap, compared with falling rates of new HIV infections for most everyone else. The CDC’s numbers for 2010-2015 show statistically significant increases in HIV incidence among MSM aged 25-34 years who are black/African American or Hispanic/Latino. Black/African American MSM accounted for 26% of the total 39,782 U.S. HIV diagnoses in 2016, and Hispanic/Latino MSM accounted for 19%, according to CDC statistics, while all blacks/African Americans accounted for 44% of 2016’s new HIV infections and all Hispanic/Latinos had 25%.
Why are these relatively small demographic subgroups bucking the overall national trend toward fewer infections? Why are their incidence rates so stubbornly high?
A major reason is that the U.S. medical community that delivers HIV prevention, diagnosis, and treatment has fallen short in reaching out to, engaging, and facilitating HIV services to these hardest-hit groups, David Malebranche, MD, said in a plenary talk at the 22nd International AIDS Conference. He cited several factors that contribute to the HIV high-risk populations from getting the care they need.
First, there is HIV stigma, which can be especially acute when accompanied by stigmatization that’s also based on race, ethnicity, and sexual orientation.
“HIV stigma causes difficulties in navigating the HIV treatment cascade. HIV stigma can adversely affect testing behavior, disclosure to sex partners and loved ones, and medical care access,” said Dr. Malebranche, an internal medicine physician and HIV specialist at Morehouse School of Medicine in Atlanta who described himself during his talk as a “ black, same-gender-loving man.” People diagnosed with HIV “will consciously choose to live in a trancelike denial of HIV,” he noted. He also cited criminalization of HIV status as another driver of stigmatization, with 34 states having HIV-specific criminal laws, sentence enhancements, or both.
Beyond HIV status, other stigmas permeate clinics based on race, sex, sexual orientation, immigrant status, and gender identity. A need exists to “study what patients experience in clinics, to identify the barriers to patient engagement and antiretroviral therapy,” but Dr. Malebranche suggested that the HIV medical community is “afraid to evaluate and assess their systems because they’re scared of what they’ll see.” U.S. HIV care has been too focused on scientific advances while “losing sight of the larger social picture,” he maintained.
“The power differential between medical systems and vulnerable communities may be partly responsible for why viral suppressions rates are so low.”
Dr. Malebranche placed much of the blame on the HIV clinical community for failing to engage patients in the most affected demographic groups.
“If a health system or clinic has problems with patient adherence, it needs to self-examine the service it provides. Most research into black MSM and the HIV treatment cascade has looked at what’s wrong in the community first and has only looked at the medical community much later, if at all,” Dr. Malebranche said. “Medical systems say things like ‘they are hard to reach,’ and ‘they don’t trust doctors,’ and ‘they are uneducated.’ Medical systems do this to avoid holding themselves accountable.”
But the people who run these systems often don’t question whether the paperwork is too onerous, certification to receive care is too cumbersome, the location too stigmatizing, and whether the staff is trained in cultural humility. “Blaming the victim doesn’t get us far in public health,” he said. The people who run and staff U.S. HIV programs “should consider the power dynamics created by some of their spaces, employees, and protocols that make them complicit in perpetuating vulnerability, and this may be why patients fall out of care. Don’t call black and same-gender-loving people ‘hard to reach’ just because you don’t know how to reach them,” he said.
In addition to calling for better appreciation of the target populations and better accommodation of their needs, Dr. Malebranche suggested greater use of peer navigators, case managers, social workers, rapid test and treat programs, and attention to overall patient health and not just their HIV status. Fundamentally, he said, the HIV medical community needs to go beyond thinking in terms of just HIV suppression and “practice the art of medicine to keep patients engaged.”
SOURCE: Malebranche D, AIDS 2018, Abstract THPL0107.
REPORTING FROM AIDS 2018
Dolutegravir plus 3TC matches three drugs for HIV control
AMSTERDAM – A two-drug antiretroviral regimen with an integrase inhibitor was noninferior to a standard three-drug regimen for controlling HIV viral load in a pair of identical, phase 3, multicenter, randomized trials with more than 1,400 patients.
The efficacy and safety results seen in the two studies at the primary endpoint follow-up of 48 weeks support the tested combination of the integrase inhibitor dolutegravir (Tivicay) plus the nucleoside reverse transcriptase inhibitor (RTI) lamivudine (3TC, Epivir) as an “effective option,” Pedro Cahn, MD, said at the 22nd International AIDS Conference.
The two trials from which he reported results, GEMINI-1 and GEMINI-2, which both compared the dolutegravir (DTG) plus 3TC regimen against DTG plus the nucleotide RTI tenofovir (Viread) and the nucleoside RTI emtricitabine (Emtriva), together showed after 48 weeks on treatment a 91% rate of complete virologic response to DTG plus 3TC with fewer than 50 detectable HIV RNA copies per mL, compared with a 93% complete response among patients on DTG plus tenofovir and emtricitabine. The efficacy of the two-drug regimen fell within the prespecified definition of noninferiority, compared with the three-drug comparator arm, the primary endpoint for both studies, said Dr. Cahn, scientific director of Fundacion Huesped in Buenos Aires, and professor of infectious diseases at Buenos Aires University.
“This is the first time a randomized, controlled trial showed the noninferiority of a two-drug regimen, compared with a three-drug regimen while using an integrase inhibitor as the core drug,” Dr. Cahn said. The goal of cutting the treatment regimen down to two drugs is to “reduce drug burden” and potentially produce fewer adverse effects and reduce cost, he explained.
Integrase strand transport inhibitors like DTG make sense as the core drug because “as a class they quickly reduce viral load” and have several other very attractive properties including good tolerability, a high barrier to resistance mutations, quick recovery of CD4 cell levels, and good adherence by patients, said Dr. Cahn. These advantages apply not only to DTG but also to other drugs in the class: raltegravir (Isentress), elvitegravir (Vitekta), and bictegravir (Biktarvy). Integrase inhibitors have been specified as part of the preferred anti-HIV regimen for most people starting HIV treatment by public health officials in several countries as well as by the World Health Organization in its 2018 revised HIV treatment recommendations.
But Dr. Cahn put a few qualifications on the findings so far for the combination of DTG and 3TC. Its durability has been tested out only to 48 weeks, although during that time no resistant HIV was seen. The studies will continue to follow the patients on dual treatment for as long as 144 weeks, he said. Also, the two-drug regimen should be considered, for the time being, only for patients who match the enrollment criteria for the GEMINI trials: Patients with a viral load no greater than 500,000 RNA copies/mL, no prior treatment, no evidence of preexisting viral resistance to any anti-HIV drugs, and no hepatitis B virus infection or need for hepatitis C virus treatment. Also there is uncertainty about the risk that women who become pregnant while on DTG have for giving birth to an infant with a neural tube defect. A recent report documented preliminary evidence for an increased risk (N Engl J Med. 2018 Jul 24. doi: 10.1056/NEJMc180765).
In addition to its noninferior efficacy, compared with a triple-drug regimen, the dual regimen showed good safety and tolerance, with a 7% incidence of serious adverse events and a 2% rate of events leading to withdrawal of treatment, rates similar to the triple-drug arm. The dual regimen also showed less evidence for renal damage than the triple regimen, including a statistically significant smaller drop in glomerular filtration rate than the triple regimen and no spikes in urine markers of renal damage as occurred on three drugs. Two drugs also induced no increases in markers of bone metabolism, but this happened with three drugs, Dr. Cahn reported.
The combined data from the two GEMINI studies enrolled 1,433 HIV-infected patients at centers in 21 countries including several U.S. centers. Patients averaged about 33 years old, 85% were men, and more than 90% had a CD4 cell count greater than 200 cell/mL at enrollment. Eighty percent had a viral load of no more than 100,00 RNA copies/mL, and the 20% with higher viral loads were stratified in equal numbers into the two treatment arms.
The 91% and 93% virologic response rates in the two treatment arms came in the intention-to-treat analysis and correlated with similar average rises among patients in the two arms in CD4 cell counts after 48 weeks of 224-228 cell/mm3. In the per protocol analysis the virologic response rates were 93% with the dual regimen and 94% with the triple regimen
SOURCE: Cahn P et al. AIDS 2018, Abstract 13210.
AMSTERDAM – A two-drug antiretroviral regimen with an integrase inhibitor was noninferior to a standard three-drug regimen for controlling HIV viral load in a pair of identical, phase 3, multicenter, randomized trials with more than 1,400 patients.
The efficacy and safety results seen in the two studies at the primary endpoint follow-up of 48 weeks support the tested combination of the integrase inhibitor dolutegravir (Tivicay) plus the nucleoside reverse transcriptase inhibitor (RTI) lamivudine (3TC, Epivir) as an “effective option,” Pedro Cahn, MD, said at the 22nd International AIDS Conference.
The two trials from which he reported results, GEMINI-1 and GEMINI-2, which both compared the dolutegravir (DTG) plus 3TC regimen against DTG plus the nucleotide RTI tenofovir (Viread) and the nucleoside RTI emtricitabine (Emtriva), together showed after 48 weeks on treatment a 91% rate of complete virologic response to DTG plus 3TC with fewer than 50 detectable HIV RNA copies per mL, compared with a 93% complete response among patients on DTG plus tenofovir and emtricitabine. The efficacy of the two-drug regimen fell within the prespecified definition of noninferiority, compared with the three-drug comparator arm, the primary endpoint for both studies, said Dr. Cahn, scientific director of Fundacion Huesped in Buenos Aires, and professor of infectious diseases at Buenos Aires University.
“This is the first time a randomized, controlled trial showed the noninferiority of a two-drug regimen, compared with a three-drug regimen while using an integrase inhibitor as the core drug,” Dr. Cahn said. The goal of cutting the treatment regimen down to two drugs is to “reduce drug burden” and potentially produce fewer adverse effects and reduce cost, he explained.
Integrase strand transport inhibitors like DTG make sense as the core drug because “as a class they quickly reduce viral load” and have several other very attractive properties including good tolerability, a high barrier to resistance mutations, quick recovery of CD4 cell levels, and good adherence by patients, said Dr. Cahn. These advantages apply not only to DTG but also to other drugs in the class: raltegravir (Isentress), elvitegravir (Vitekta), and bictegravir (Biktarvy). Integrase inhibitors have been specified as part of the preferred anti-HIV regimen for most people starting HIV treatment by public health officials in several countries as well as by the World Health Organization in its 2018 revised HIV treatment recommendations.
But Dr. Cahn put a few qualifications on the findings so far for the combination of DTG and 3TC. Its durability has been tested out only to 48 weeks, although during that time no resistant HIV was seen. The studies will continue to follow the patients on dual treatment for as long as 144 weeks, he said. Also, the two-drug regimen should be considered, for the time being, only for patients who match the enrollment criteria for the GEMINI trials: Patients with a viral load no greater than 500,000 RNA copies/mL, no prior treatment, no evidence of preexisting viral resistance to any anti-HIV drugs, and no hepatitis B virus infection or need for hepatitis C virus treatment. Also there is uncertainty about the risk that women who become pregnant while on DTG have for giving birth to an infant with a neural tube defect. A recent report documented preliminary evidence for an increased risk (N Engl J Med. 2018 Jul 24. doi: 10.1056/NEJMc180765).
In addition to its noninferior efficacy, compared with a triple-drug regimen, the dual regimen showed good safety and tolerance, with a 7% incidence of serious adverse events and a 2% rate of events leading to withdrawal of treatment, rates similar to the triple-drug arm. The dual regimen also showed less evidence for renal damage than the triple regimen, including a statistically significant smaller drop in glomerular filtration rate than the triple regimen and no spikes in urine markers of renal damage as occurred on three drugs. Two drugs also induced no increases in markers of bone metabolism, but this happened with three drugs, Dr. Cahn reported.
The combined data from the two GEMINI studies enrolled 1,433 HIV-infected patients at centers in 21 countries including several U.S. centers. Patients averaged about 33 years old, 85% were men, and more than 90% had a CD4 cell count greater than 200 cell/mL at enrollment. Eighty percent had a viral load of no more than 100,00 RNA copies/mL, and the 20% with higher viral loads were stratified in equal numbers into the two treatment arms.
The 91% and 93% virologic response rates in the two treatment arms came in the intention-to-treat analysis and correlated with similar average rises among patients in the two arms in CD4 cell counts after 48 weeks of 224-228 cell/mm3. In the per protocol analysis the virologic response rates were 93% with the dual regimen and 94% with the triple regimen
SOURCE: Cahn P et al. AIDS 2018, Abstract 13210.
AMSTERDAM – A two-drug antiretroviral regimen with an integrase inhibitor was noninferior to a standard three-drug regimen for controlling HIV viral load in a pair of identical, phase 3, multicenter, randomized trials with more than 1,400 patients.
The efficacy and safety results seen in the two studies at the primary endpoint follow-up of 48 weeks support the tested combination of the integrase inhibitor dolutegravir (Tivicay) plus the nucleoside reverse transcriptase inhibitor (RTI) lamivudine (3TC, Epivir) as an “effective option,” Pedro Cahn, MD, said at the 22nd International AIDS Conference.
The two trials from which he reported results, GEMINI-1 and GEMINI-2, which both compared the dolutegravir (DTG) plus 3TC regimen against DTG plus the nucleotide RTI tenofovir (Viread) and the nucleoside RTI emtricitabine (Emtriva), together showed after 48 weeks on treatment a 91% rate of complete virologic response to DTG plus 3TC with fewer than 50 detectable HIV RNA copies per mL, compared with a 93% complete response among patients on DTG plus tenofovir and emtricitabine. The efficacy of the two-drug regimen fell within the prespecified definition of noninferiority, compared with the three-drug comparator arm, the primary endpoint for both studies, said Dr. Cahn, scientific director of Fundacion Huesped in Buenos Aires, and professor of infectious diseases at Buenos Aires University.
“This is the first time a randomized, controlled trial showed the noninferiority of a two-drug regimen, compared with a three-drug regimen while using an integrase inhibitor as the core drug,” Dr. Cahn said. The goal of cutting the treatment regimen down to two drugs is to “reduce drug burden” and potentially produce fewer adverse effects and reduce cost, he explained.
Integrase strand transport inhibitors like DTG make sense as the core drug because “as a class they quickly reduce viral load” and have several other very attractive properties including good tolerability, a high barrier to resistance mutations, quick recovery of CD4 cell levels, and good adherence by patients, said Dr. Cahn. These advantages apply not only to DTG but also to other drugs in the class: raltegravir (Isentress), elvitegravir (Vitekta), and bictegravir (Biktarvy). Integrase inhibitors have been specified as part of the preferred anti-HIV regimen for most people starting HIV treatment by public health officials in several countries as well as by the World Health Organization in its 2018 revised HIV treatment recommendations.
But Dr. Cahn put a few qualifications on the findings so far for the combination of DTG and 3TC. Its durability has been tested out only to 48 weeks, although during that time no resistant HIV was seen. The studies will continue to follow the patients on dual treatment for as long as 144 weeks, he said. Also, the two-drug regimen should be considered, for the time being, only for patients who match the enrollment criteria for the GEMINI trials: Patients with a viral load no greater than 500,000 RNA copies/mL, no prior treatment, no evidence of preexisting viral resistance to any anti-HIV drugs, and no hepatitis B virus infection or need for hepatitis C virus treatment. Also there is uncertainty about the risk that women who become pregnant while on DTG have for giving birth to an infant with a neural tube defect. A recent report documented preliminary evidence for an increased risk (N Engl J Med. 2018 Jul 24. doi: 10.1056/NEJMc180765).
In addition to its noninferior efficacy, compared with a triple-drug regimen, the dual regimen showed good safety and tolerance, with a 7% incidence of serious adverse events and a 2% rate of events leading to withdrawal of treatment, rates similar to the triple-drug arm. The dual regimen also showed less evidence for renal damage than the triple regimen, including a statistically significant smaller drop in glomerular filtration rate than the triple regimen and no spikes in urine markers of renal damage as occurred on three drugs. Two drugs also induced no increases in markers of bone metabolism, but this happened with three drugs, Dr. Cahn reported.
The combined data from the two GEMINI studies enrolled 1,433 HIV-infected patients at centers in 21 countries including several U.S. centers. Patients averaged about 33 years old, 85% were men, and more than 90% had a CD4 cell count greater than 200 cell/mL at enrollment. Eighty percent had a viral load of no more than 100,00 RNA copies/mL, and the 20% with higher viral loads were stratified in equal numbers into the two treatment arms.
The 91% and 93% virologic response rates in the two treatment arms came in the intention-to-treat analysis and correlated with similar average rises among patients in the two arms in CD4 cell counts after 48 weeks of 224-228 cell/mm3. In the per protocol analysis the virologic response rates were 93% with the dual regimen and 94% with the triple regimen
SOURCE: Cahn P et al. AIDS 2018, Abstract 13210.
REPORTING FROM AIDS 2018
Key clinical point: The reduction in HIV by dolutegravir plus lamivudine was noninferior to the reduction by dolutegravir plus tenofovir and emtricitabine.
Major finding: HIV levels became undetectable in 91% of patients on dolutegravir plus lamivudine and in 93% on dolutegravir, tenofivir, and emtricitabine.
Study details: GEMINI-1 and GEMINI-2, two identical randomized, multicenter, randomized phase 3 trials with a total of 1,433 HIV-infected patients.
Disclosures: The GEMINI-1 and -2 trials were sponsored by GlaxoSmithKline and Viiv Healthcare, the company that markets dolutegravir (Tivicay). Dr. Cahn has been an advisor to or speaker for Abbvie, Merck, and Viiv, and he has received research funding from Abbvie, Merck, Richmond, and Viiv.
Source: Cahn P et al. AIDS 2018, Abstract 13210.
On-demand and daily PrEP look similar for HIV prevention
AMSTERDAM – Episodic, “on-demand” pre-exposure prophylaxis to prevent transmission of HIV was as effective as daily pre-exposure prophylaxis in a prospective, real-world study of more than 1,100 men who have sex with men in the Paris region.
The results showed very similar performance and complete prevention of new HIV infections in both groups, data that “strengthen the case for on-demand prophylaxis as an alternative to daily PrEP [pre-exposure prophylaxis],” Jean-Michel Molina, MD, said at the 22nd International AIDS Conference.
The evidence for efficacy of on-demand PrEP, used starting a day before through a day after unprotected sex by a man uninfected by HIV, to prevent potential infection “is now good enough for clinicians to counsel people that it is equally effective as daily PrEP and the person can decide” which regimen to use, he said in an interview. “In the future, we’ll use both strategies. We want to make PrEP easy for people to use. We want alternatives so that more people use PrEP, ” said Dr. Molina, professor of infectious diseases at the University of Paris and head of infectious diseases at Saint-Louis Hospital in Paris.
However the study focused on men who have sex with men (MSM) and so the efficacy of on-demand PrEP is not proven for preventing HIV infection during heterosexual sex, including protecting women, Dr. Molina cautioned.
The on-demand PrEP regimen tested by Dr. Molina and his associates uses the same combination of 300 mg tenofovir (Viread) and 200 mg emtricitabine (Emtriva) – formulated into a single pill and marketed as Truvada – as used for daily PrEP.
For on-demand use patients take two of these pills 2-24 hours prior to their anticipated sexual activity and then 1 pill every 24 hours until the sexual activity stops, with a final pill 24 hours following the last sex event. This translates into an ideal regimen of at least 4 pills total.
The researchers first documented the efficacy of on-demand PrEP in a placebo-controlled study with 400 randomized people that showed the on-demand regimen reduced the rate of new HIV infection by 86%, compared with placebo, among MSM who had unprotected sex (N Engl J Med. 2015 Dec 3;373[23]:2237-46). They designed the current, open-label study, ANRS-PREVENIR (Prevention of HIV in Île-de-France), to further examine the efficacy of and adherence to an on-demand PrEP regimen in a real-world setting and to compare it with daily PrEP.
The study began in May 2017, with a goal of enrolling 3,000 HIV-negative MSM. As of early July 2018, the study had enrolled 1,628 people including 1,102 who had been followed for at least 3 months and for an average of 7 months, including 124 followed for at least 1 year. Participants had a choice of using PrEP in either an on-demand or daily regimen and were allowed to switch from one regimen to the other. At enrollment, 55% opted for the on-demand regimen, and during subsequent months the fraction of participants using an on-demand regimen remained at about half. Based on self-reported use of the regimen, 96% of the men who had opted for on-demand PrEP used it “correctly,” defined as taking at least one pill within 24 hours of their sex event and at least one pill within 24 hours after the event, a rate that was identical to the “correct” usage by participants who opted for daily PrEP. The only substantial difference in PrEP use between the two subgroups was that 19% of men in the on-demand group did not use PrEP prior to at least one sex event, compared with 2% of men in the daily subgroup.
“We need to better understand” why so many participants in the on-demand group failed to use PrEP, admitted Dr. Molina. He speculated that these failures to use PrEP occurred because participants had sex with partners whom they knew were not infected with HIV.
During follow-up, the researchers identified no one who became HIV infected during 949 person-years of follow-up, a level of protection from PrEP that Dr. Molina called “remarkable.” Based on the epidemiology of HIV in the Paris region he estimated that use of PrEP by the participants in the study had prevented what might have otherwise been 85 new HIV infections. During follow-up, participants completely stopped using either daily or on-demand PrEP at a rate of 1.5 discontinuations per 100 person-years.
The incidence of adverse events was similar in the two arms of the study, with no discontinuations because of adverse events, and a 4-5 per 100 person-years incidence of grade 3 or 4 adverse events and an incidence of 2 per 100 person-years of grade 3 or 4 laboratory abnormalities. “The drugs are very well tolerated,” Dr. Molina noted, and a potential reduction in adverse events is not a reason for someone to choose on-demand PrEP instead of daily use. The primary difference is a potentially smaller pill burden: People using on-demand PrEP take on average about half the number of pills as someone on daily PrEP, which could lower the cost of prophylaxis in countries or settings where the person on PrEP has financial responsibility for the drugs. This was not an issue in the current study as the pills are available to people at no charge under the French health coverage system, Dr. Molina noted.
“On-demand PrEP is a viable option. For some people on-demand makes sense,” commented Patrick Sullivan, PhD, a professor of epidemiology at Emory University in Atlanta. It can potentially reduce drug costs, an issue for many Americans, Dr. Sullivan noted in an interview. So far, however, no reported studies have documented the efficacy of on-demand PrEP in a U.S. population, he said.
On-demand PrEP has received endorsement for use by selected people at high risk for HIV infection by public health authorities in the European Union, the United Kingdom, France, Canada, and Australia, Dr. Molina said, and in late July this strategy also received endorsement in revised HIV treatment and prevention recommendations issued by the International Antiviral Society–USA (JAMA. 2018 July 24/31;320[4]:379-96).
ANRS-PREVENIR received no commercial funding. Dr. Molina has been an advisor to Gilead, Merck, Teva, and Viiv and has received research fundings from Gilead.
SOURCE: Molina J-M et al. AIDS 2018, Abstract 13278.
AMSTERDAM – Episodic, “on-demand” pre-exposure prophylaxis to prevent transmission of HIV was as effective as daily pre-exposure prophylaxis in a prospective, real-world study of more than 1,100 men who have sex with men in the Paris region.
The results showed very similar performance and complete prevention of new HIV infections in both groups, data that “strengthen the case for on-demand prophylaxis as an alternative to daily PrEP [pre-exposure prophylaxis],” Jean-Michel Molina, MD, said at the 22nd International AIDS Conference.
The evidence for efficacy of on-demand PrEP, used starting a day before through a day after unprotected sex by a man uninfected by HIV, to prevent potential infection “is now good enough for clinicians to counsel people that it is equally effective as daily PrEP and the person can decide” which regimen to use, he said in an interview. “In the future, we’ll use both strategies. We want to make PrEP easy for people to use. We want alternatives so that more people use PrEP, ” said Dr. Molina, professor of infectious diseases at the University of Paris and head of infectious diseases at Saint-Louis Hospital in Paris.
However the study focused on men who have sex with men (MSM) and so the efficacy of on-demand PrEP is not proven for preventing HIV infection during heterosexual sex, including protecting women, Dr. Molina cautioned.
The on-demand PrEP regimen tested by Dr. Molina and his associates uses the same combination of 300 mg tenofovir (Viread) and 200 mg emtricitabine (Emtriva) – formulated into a single pill and marketed as Truvada – as used for daily PrEP.
For on-demand use patients take two of these pills 2-24 hours prior to their anticipated sexual activity and then 1 pill every 24 hours until the sexual activity stops, with a final pill 24 hours following the last sex event. This translates into an ideal regimen of at least 4 pills total.
The researchers first documented the efficacy of on-demand PrEP in a placebo-controlled study with 400 randomized people that showed the on-demand regimen reduced the rate of new HIV infection by 86%, compared with placebo, among MSM who had unprotected sex (N Engl J Med. 2015 Dec 3;373[23]:2237-46). They designed the current, open-label study, ANRS-PREVENIR (Prevention of HIV in Île-de-France), to further examine the efficacy of and adherence to an on-demand PrEP regimen in a real-world setting and to compare it with daily PrEP.
The study began in May 2017, with a goal of enrolling 3,000 HIV-negative MSM. As of early July 2018, the study had enrolled 1,628 people including 1,102 who had been followed for at least 3 months and for an average of 7 months, including 124 followed for at least 1 year. Participants had a choice of using PrEP in either an on-demand or daily regimen and were allowed to switch from one regimen to the other. At enrollment, 55% opted for the on-demand regimen, and during subsequent months the fraction of participants using an on-demand regimen remained at about half. Based on self-reported use of the regimen, 96% of the men who had opted for on-demand PrEP used it “correctly,” defined as taking at least one pill within 24 hours of their sex event and at least one pill within 24 hours after the event, a rate that was identical to the “correct” usage by participants who opted for daily PrEP. The only substantial difference in PrEP use between the two subgroups was that 19% of men in the on-demand group did not use PrEP prior to at least one sex event, compared with 2% of men in the daily subgroup.
“We need to better understand” why so many participants in the on-demand group failed to use PrEP, admitted Dr. Molina. He speculated that these failures to use PrEP occurred because participants had sex with partners whom they knew were not infected with HIV.
During follow-up, the researchers identified no one who became HIV infected during 949 person-years of follow-up, a level of protection from PrEP that Dr. Molina called “remarkable.” Based on the epidemiology of HIV in the Paris region he estimated that use of PrEP by the participants in the study had prevented what might have otherwise been 85 new HIV infections. During follow-up, participants completely stopped using either daily or on-demand PrEP at a rate of 1.5 discontinuations per 100 person-years.
The incidence of adverse events was similar in the two arms of the study, with no discontinuations because of adverse events, and a 4-5 per 100 person-years incidence of grade 3 or 4 adverse events and an incidence of 2 per 100 person-years of grade 3 or 4 laboratory abnormalities. “The drugs are very well tolerated,” Dr. Molina noted, and a potential reduction in adverse events is not a reason for someone to choose on-demand PrEP instead of daily use. The primary difference is a potentially smaller pill burden: People using on-demand PrEP take on average about half the number of pills as someone on daily PrEP, which could lower the cost of prophylaxis in countries or settings where the person on PrEP has financial responsibility for the drugs. This was not an issue in the current study as the pills are available to people at no charge under the French health coverage system, Dr. Molina noted.
“On-demand PrEP is a viable option. For some people on-demand makes sense,” commented Patrick Sullivan, PhD, a professor of epidemiology at Emory University in Atlanta. It can potentially reduce drug costs, an issue for many Americans, Dr. Sullivan noted in an interview. So far, however, no reported studies have documented the efficacy of on-demand PrEP in a U.S. population, he said.
On-demand PrEP has received endorsement for use by selected people at high risk for HIV infection by public health authorities in the European Union, the United Kingdom, France, Canada, and Australia, Dr. Molina said, and in late July this strategy also received endorsement in revised HIV treatment and prevention recommendations issued by the International Antiviral Society–USA (JAMA. 2018 July 24/31;320[4]:379-96).
ANRS-PREVENIR received no commercial funding. Dr. Molina has been an advisor to Gilead, Merck, Teva, and Viiv and has received research fundings from Gilead.
SOURCE: Molina J-M et al. AIDS 2018, Abstract 13278.
AMSTERDAM – Episodic, “on-demand” pre-exposure prophylaxis to prevent transmission of HIV was as effective as daily pre-exposure prophylaxis in a prospective, real-world study of more than 1,100 men who have sex with men in the Paris region.
The results showed very similar performance and complete prevention of new HIV infections in both groups, data that “strengthen the case for on-demand prophylaxis as an alternative to daily PrEP [pre-exposure prophylaxis],” Jean-Michel Molina, MD, said at the 22nd International AIDS Conference.
The evidence for efficacy of on-demand PrEP, used starting a day before through a day after unprotected sex by a man uninfected by HIV, to prevent potential infection “is now good enough for clinicians to counsel people that it is equally effective as daily PrEP and the person can decide” which regimen to use, he said in an interview. “In the future, we’ll use both strategies. We want to make PrEP easy for people to use. We want alternatives so that more people use PrEP, ” said Dr. Molina, professor of infectious diseases at the University of Paris and head of infectious diseases at Saint-Louis Hospital in Paris.
However the study focused on men who have sex with men (MSM) and so the efficacy of on-demand PrEP is not proven for preventing HIV infection during heterosexual sex, including protecting women, Dr. Molina cautioned.
The on-demand PrEP regimen tested by Dr. Molina and his associates uses the same combination of 300 mg tenofovir (Viread) and 200 mg emtricitabine (Emtriva) – formulated into a single pill and marketed as Truvada – as used for daily PrEP.
For on-demand use patients take two of these pills 2-24 hours prior to their anticipated sexual activity and then 1 pill every 24 hours until the sexual activity stops, with a final pill 24 hours following the last sex event. This translates into an ideal regimen of at least 4 pills total.
The researchers first documented the efficacy of on-demand PrEP in a placebo-controlled study with 400 randomized people that showed the on-demand regimen reduced the rate of new HIV infection by 86%, compared with placebo, among MSM who had unprotected sex (N Engl J Med. 2015 Dec 3;373[23]:2237-46). They designed the current, open-label study, ANRS-PREVENIR (Prevention of HIV in Île-de-France), to further examine the efficacy of and adherence to an on-demand PrEP regimen in a real-world setting and to compare it with daily PrEP.
The study began in May 2017, with a goal of enrolling 3,000 HIV-negative MSM. As of early July 2018, the study had enrolled 1,628 people including 1,102 who had been followed for at least 3 months and for an average of 7 months, including 124 followed for at least 1 year. Participants had a choice of using PrEP in either an on-demand or daily regimen and were allowed to switch from one regimen to the other. At enrollment, 55% opted for the on-demand regimen, and during subsequent months the fraction of participants using an on-demand regimen remained at about half. Based on self-reported use of the regimen, 96% of the men who had opted for on-demand PrEP used it “correctly,” defined as taking at least one pill within 24 hours of their sex event and at least one pill within 24 hours after the event, a rate that was identical to the “correct” usage by participants who opted for daily PrEP. The only substantial difference in PrEP use between the two subgroups was that 19% of men in the on-demand group did not use PrEP prior to at least one sex event, compared with 2% of men in the daily subgroup.
“We need to better understand” why so many participants in the on-demand group failed to use PrEP, admitted Dr. Molina. He speculated that these failures to use PrEP occurred because participants had sex with partners whom they knew were not infected with HIV.
During follow-up, the researchers identified no one who became HIV infected during 949 person-years of follow-up, a level of protection from PrEP that Dr. Molina called “remarkable.” Based on the epidemiology of HIV in the Paris region he estimated that use of PrEP by the participants in the study had prevented what might have otherwise been 85 new HIV infections. During follow-up, participants completely stopped using either daily or on-demand PrEP at a rate of 1.5 discontinuations per 100 person-years.
The incidence of adverse events was similar in the two arms of the study, with no discontinuations because of adverse events, and a 4-5 per 100 person-years incidence of grade 3 or 4 adverse events and an incidence of 2 per 100 person-years of grade 3 or 4 laboratory abnormalities. “The drugs are very well tolerated,” Dr. Molina noted, and a potential reduction in adverse events is not a reason for someone to choose on-demand PrEP instead of daily use. The primary difference is a potentially smaller pill burden: People using on-demand PrEP take on average about half the number of pills as someone on daily PrEP, which could lower the cost of prophylaxis in countries or settings where the person on PrEP has financial responsibility for the drugs. This was not an issue in the current study as the pills are available to people at no charge under the French health coverage system, Dr. Molina noted.
“On-demand PrEP is a viable option. For some people on-demand makes sense,” commented Patrick Sullivan, PhD, a professor of epidemiology at Emory University in Atlanta. It can potentially reduce drug costs, an issue for many Americans, Dr. Sullivan noted in an interview. So far, however, no reported studies have documented the efficacy of on-demand PrEP in a U.S. population, he said.
On-demand PrEP has received endorsement for use by selected people at high risk for HIV infection by public health authorities in the European Union, the United Kingdom, France, Canada, and Australia, Dr. Molina said, and in late July this strategy also received endorsement in revised HIV treatment and prevention recommendations issued by the International Antiviral Society–USA (JAMA. 2018 July 24/31;320[4]:379-96).
ANRS-PREVENIR received no commercial funding. Dr. Molina has been an advisor to Gilead, Merck, Teva, and Viiv and has received research fundings from Gilead.
SOURCE: Molina J-M et al. AIDS 2018, Abstract 13278.
REPORTING FROM AIDS 2018
Key clinical point:
Major finding: Men using on-demand PrEP had no HIV infections during an average 7 months of follow-up.
Study details: ANRS-PREVENIR, a prospective, multicenter, open-label study with 1,102 people followed for at least 3 months.
Disclosures: ANRS-PREVENIR received no commercial funding. Dr. Molina has been an advisor to Gilead, Merck, Teva, and Viiv and has received research fundings from Gilead.
Source: Molina J-M et al. AIDS 2018, Abstract 13278.