User login
HE4 tumor marker aids as triage tool in ovarian cancer
MELBOURNE – Measurement of the human epididymis protein 4 (HE4) tumor marker in women presenting with elevated cancer antigen 125 may improve the specificity of testing and help guide referral and management decisions, an investigator reported at the biennial meeting of the International Gynecologic Cancer Society.
Dr. Nithya Ratnavelu, subspeciality fellow at the Northern Gynaecological Oncology Centre in Gateshead, England, presented data from a prospective pilot study which showed the inclusion of HE4 measurement at the time of cancer antigen 125 (CA 125) measurement improved the specificity and positive predictive value of testing.
The study involved 601 women presenting to primary care with vague abdominal symptoms, such as pelvic mass, abdominal pain, bloating, nausea, vomiting, or weight loss, who then had both their CA 125 and HE4 levels tested.
Women with abnormal CA 125 or HE4 were then referred for pelvic ultrasound, which identified two cases of ovarian cancer, both in postmenopausal women with elevated CA 125 and HE4.
The inclusion of HE4 at the time of CA 125 testing improved the specificity of testing from 95% with CA 125 alone to 98.6%, and the positive predictive value from 6.25% with CA 125 alone to 20% with the combined tests.
A total of fifty women presented with elevated HE4 levels, and ten of these also had abnormal CA 125. No cancers were found among the 40 women with elevated HE4 but normal CA 125, and doctors diagnosed one cecal tumor and one endometrial cancer in the 22 women with elevated CA 125 but normal HE4.
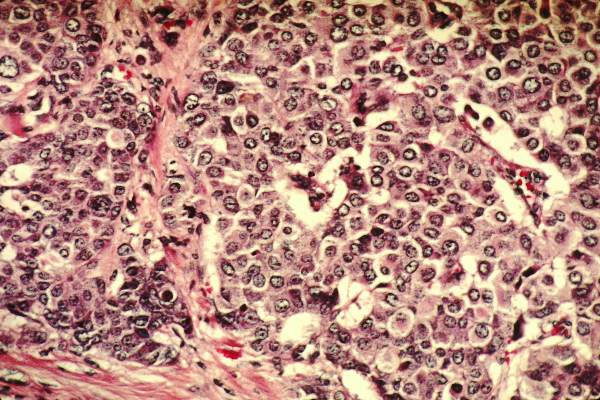
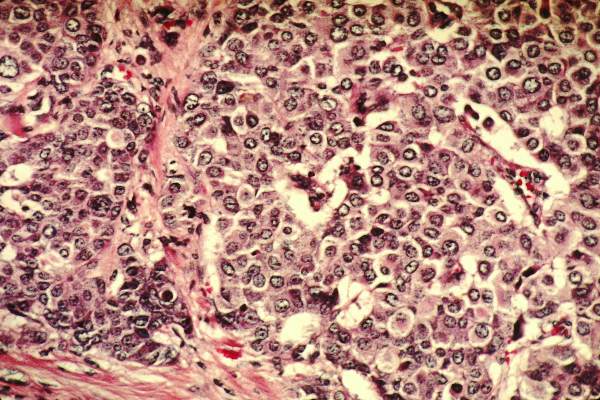
HE4 is a protease inhibitor that is overexpressed in certain histologies including ovarian, endometrial, respiratory, and renal cancers, Dr. Ratnavelu said, and was one of the more frequently investigated tumor markers in ovarian cancer.
While there were only two ovarian cancers found in the study, Dr. Ratnavelu said she had found the HE4 marker useful in her clinical practice.
“We have actually started using it clinically, and in a woman with maybe a slightly raised CA 125, with quite a small pelvic mass, to say instead of a big midline laparotomy, should we maybe just do laparoscopic surgery if your HE4 and ROMA score suggest it’s probably benign,” Dr. Ratnavelu said in an interview.
Another example she gave was of a premenopausal woman with bilateral ovarian cysts and a very high CA 125 but normal HE4, who turned out to have endometriosis rather than ovarian cancer.
“There is the potential here to aid management for community referrals,” Dr. Ratnavelu told the conference.
“Obviously, this is a pilot study, and to draw firm conclusions, further prospective multicenter studies are warranted.
In addition, a poster presented at the conference showed that an algorithm incorporating both HE4 and CA 125 measurements could be used to identify higher-risk patients with newly diagnosed endometrial cancer who were more likely to benefit from referral to specialist gynecologic oncologist services.
When they used cutoff points of a CA 125 greater than 35U/mL and/or an HE4 measurement greater than 111 pm, researchers found the odds of patients having deep myometrial invasion were 11.7 times higher among those with a positive test, compared with a negative test (95% confidence interval, 3.4-39.5; P < .001).
Similarly, patients who met those same cut-offs and had a high body mass index were 8.7 times more likely to require specialized treatment, compared with the negative population (95% CI, 3.7-20.5; P < .001), according to the retrospective cohort study in 200 patients surgically treated for endometrial cancer.
“Using an algorithm to triage higher-risk endometrial cancer patients to specialized centers could contribute to standardizing referral practices, optimizing the use of healthcare resources while improving oncologic outcomes, and overall quality of patient care,” wrote Dr. Eleftheria Kalogera and colleagues from the Mayo Clinic.
Dr. Ratnavelu declared travel expenses from Roche UK. There were no other conflicts of interest declared.
MELBOURNE – Measurement of the human epididymis protein 4 (HE4) tumor marker in women presenting with elevated cancer antigen 125 may improve the specificity of testing and help guide referral and management decisions, an investigator reported at the biennial meeting of the International Gynecologic Cancer Society.
Dr. Nithya Ratnavelu, subspeciality fellow at the Northern Gynaecological Oncology Centre in Gateshead, England, presented data from a prospective pilot study which showed the inclusion of HE4 measurement at the time of cancer antigen 125 (CA 125) measurement improved the specificity and positive predictive value of testing.
The study involved 601 women presenting to primary care with vague abdominal symptoms, such as pelvic mass, abdominal pain, bloating, nausea, vomiting, or weight loss, who then had both their CA 125 and HE4 levels tested.
Women with abnormal CA 125 or HE4 were then referred for pelvic ultrasound, which identified two cases of ovarian cancer, both in postmenopausal women with elevated CA 125 and HE4.
The inclusion of HE4 at the time of CA 125 testing improved the specificity of testing from 95% with CA 125 alone to 98.6%, and the positive predictive value from 6.25% with CA 125 alone to 20% with the combined tests.
A total of fifty women presented with elevated HE4 levels, and ten of these also had abnormal CA 125. No cancers were found among the 40 women with elevated HE4 but normal CA 125, and doctors diagnosed one cecal tumor and one endometrial cancer in the 22 women with elevated CA 125 but normal HE4.
HE4 is a protease inhibitor that is overexpressed in certain histologies including ovarian, endometrial, respiratory, and renal cancers, Dr. Ratnavelu said, and was one of the more frequently investigated tumor markers in ovarian cancer.
While there were only two ovarian cancers found in the study, Dr. Ratnavelu said she had found the HE4 marker useful in her clinical practice.
“We have actually started using it clinically, and in a woman with maybe a slightly raised CA 125, with quite a small pelvic mass, to say instead of a big midline laparotomy, should we maybe just do laparoscopic surgery if your HE4 and ROMA score suggest it’s probably benign,” Dr. Ratnavelu said in an interview.
Another example she gave was of a premenopausal woman with bilateral ovarian cysts and a very high CA 125 but normal HE4, who turned out to have endometriosis rather than ovarian cancer.
“There is the potential here to aid management for community referrals,” Dr. Ratnavelu told the conference.
“Obviously, this is a pilot study, and to draw firm conclusions, further prospective multicenter studies are warranted.
In addition, a poster presented at the conference showed that an algorithm incorporating both HE4 and CA 125 measurements could be used to identify higher-risk patients with newly diagnosed endometrial cancer who were more likely to benefit from referral to specialist gynecologic oncologist services.
When they used cutoff points of a CA 125 greater than 35U/mL and/or an HE4 measurement greater than 111 pm, researchers found the odds of patients having deep myometrial invasion were 11.7 times higher among those with a positive test, compared with a negative test (95% confidence interval, 3.4-39.5; P < .001).
Similarly, patients who met those same cut-offs and had a high body mass index were 8.7 times more likely to require specialized treatment, compared with the negative population (95% CI, 3.7-20.5; P < .001), according to the retrospective cohort study in 200 patients surgically treated for endometrial cancer.
“Using an algorithm to triage higher-risk endometrial cancer patients to specialized centers could contribute to standardizing referral practices, optimizing the use of healthcare resources while improving oncologic outcomes, and overall quality of patient care,” wrote Dr. Eleftheria Kalogera and colleagues from the Mayo Clinic.
Dr. Ratnavelu declared travel expenses from Roche UK. There were no other conflicts of interest declared.
MELBOURNE – Measurement of the human epididymis protein 4 (HE4) tumor marker in women presenting with elevated cancer antigen 125 may improve the specificity of testing and help guide referral and management decisions, an investigator reported at the biennial meeting of the International Gynecologic Cancer Society.
Dr. Nithya Ratnavelu, subspeciality fellow at the Northern Gynaecological Oncology Centre in Gateshead, England, presented data from a prospective pilot study which showed the inclusion of HE4 measurement at the time of cancer antigen 125 (CA 125) measurement improved the specificity and positive predictive value of testing.
The study involved 601 women presenting to primary care with vague abdominal symptoms, such as pelvic mass, abdominal pain, bloating, nausea, vomiting, or weight loss, who then had both their CA 125 and HE4 levels tested.
Women with abnormal CA 125 or HE4 were then referred for pelvic ultrasound, which identified two cases of ovarian cancer, both in postmenopausal women with elevated CA 125 and HE4.
The inclusion of HE4 at the time of CA 125 testing improved the specificity of testing from 95% with CA 125 alone to 98.6%, and the positive predictive value from 6.25% with CA 125 alone to 20% with the combined tests.
A total of fifty women presented with elevated HE4 levels, and ten of these also had abnormal CA 125. No cancers were found among the 40 women with elevated HE4 but normal CA 125, and doctors diagnosed one cecal tumor and one endometrial cancer in the 22 women with elevated CA 125 but normal HE4.
HE4 is a protease inhibitor that is overexpressed in certain histologies including ovarian, endometrial, respiratory, and renal cancers, Dr. Ratnavelu said, and was one of the more frequently investigated tumor markers in ovarian cancer.
While there were only two ovarian cancers found in the study, Dr. Ratnavelu said she had found the HE4 marker useful in her clinical practice.
“We have actually started using it clinically, and in a woman with maybe a slightly raised CA 125, with quite a small pelvic mass, to say instead of a big midline laparotomy, should we maybe just do laparoscopic surgery if your HE4 and ROMA score suggest it’s probably benign,” Dr. Ratnavelu said in an interview.
Another example she gave was of a premenopausal woman with bilateral ovarian cysts and a very high CA 125 but normal HE4, who turned out to have endometriosis rather than ovarian cancer.
“There is the potential here to aid management for community referrals,” Dr. Ratnavelu told the conference.
“Obviously, this is a pilot study, and to draw firm conclusions, further prospective multicenter studies are warranted.
In addition, a poster presented at the conference showed that an algorithm incorporating both HE4 and CA 125 measurements could be used to identify higher-risk patients with newly diagnosed endometrial cancer who were more likely to benefit from referral to specialist gynecologic oncologist services.
When they used cutoff points of a CA 125 greater than 35U/mL and/or an HE4 measurement greater than 111 pm, researchers found the odds of patients having deep myometrial invasion were 11.7 times higher among those with a positive test, compared with a negative test (95% confidence interval, 3.4-39.5; P < .001).
Similarly, patients who met those same cut-offs and had a high body mass index were 8.7 times more likely to require specialized treatment, compared with the negative population (95% CI, 3.7-20.5; P < .001), according to the retrospective cohort study in 200 patients surgically treated for endometrial cancer.
“Using an algorithm to triage higher-risk endometrial cancer patients to specialized centers could contribute to standardizing referral practices, optimizing the use of healthcare resources while improving oncologic outcomes, and overall quality of patient care,” wrote Dr. Eleftheria Kalogera and colleagues from the Mayo Clinic.
Dr. Ratnavelu declared travel expenses from Roche UK. There were no other conflicts of interest declared.
AT IGCS 2014
Key clinical point: The inclusion of the HE4 tumor marker in assessment of women for ovarian cancer could help guide management and referral decisions.
Major finding: The addition of HE4 to CA 125 measurements improves specificity from 95% to 98.6% and positive predictive value from 6.25% to 20%.
Data source: Prospective pilot study in 601 women presenting to general practice with abdominal symptoms.
Disclosures: The speaker declared travel expenses from Roche UK.
Breast Cancer Relapse Risk Halved Since 1986
Breast cancer outcomes have improved significantly over the past 3 decades, with major gains in relapse-free survival and declines in mortality for all subtypes but particularly HER-2 positive breast cancer, a retrospective case-control study has found.
Researchers compared matched data from 7,178 women referred to the British Columbia Cancer Agency for breast cancer between 1986 and 1992 (C1) and mid-2004 and 2008 (C2) and found the risk of relapse halved in the second cohort, compared to the first, up to year 7 of follow-up, according to a paper published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.57.2461].
While there were similar patterns of disease relapse over time for both the estrogen receptor (ER)-negative and ER-positive patients between the two cohorts, the risk of relapse halved for ER-negative patients in the second cohort relative to the first, while the risk ratio for C2/C1 ranged from 0.26 to 0.56 in ER-positive patients.
“The greatest improvements in outcomes were achieved in the BC subtypes known to be more aggressive, namely the HER2-positive and ER-negative/HER2-negative patients,” wrote Dr. Rachel J.D. Cossetti and colleagues from the Vancouver (B.C.) Cancer Centre.The study was supported by coauthor Dr. Karen A. Gelmon, also of the Vancouver Cancer Centre.
Breast cancer outcomes have improved significantly over the past 3 decades, with major gains in relapse-free survival and declines in mortality for all subtypes but particularly HER-2 positive breast cancer, a retrospective case-control study has found.
Researchers compared matched data from 7,178 women referred to the British Columbia Cancer Agency for breast cancer between 1986 and 1992 (C1) and mid-2004 and 2008 (C2) and found the risk of relapse halved in the second cohort, compared to the first, up to year 7 of follow-up, according to a paper published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.57.2461].
While there were similar patterns of disease relapse over time for both the estrogen receptor (ER)-negative and ER-positive patients between the two cohorts, the risk of relapse halved for ER-negative patients in the second cohort relative to the first, while the risk ratio for C2/C1 ranged from 0.26 to 0.56 in ER-positive patients.
“The greatest improvements in outcomes were achieved in the BC subtypes known to be more aggressive, namely the HER2-positive and ER-negative/HER2-negative patients,” wrote Dr. Rachel J.D. Cossetti and colleagues from the Vancouver (B.C.) Cancer Centre.The study was supported by coauthor Dr. Karen A. Gelmon, also of the Vancouver Cancer Centre.
Breast cancer outcomes have improved significantly over the past 3 decades, with major gains in relapse-free survival and declines in mortality for all subtypes but particularly HER-2 positive breast cancer, a retrospective case-control study has found.
Researchers compared matched data from 7,178 women referred to the British Columbia Cancer Agency for breast cancer between 1986 and 1992 (C1) and mid-2004 and 2008 (C2) and found the risk of relapse halved in the second cohort, compared to the first, up to year 7 of follow-up, according to a paper published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.57.2461].
While there were similar patterns of disease relapse over time for both the estrogen receptor (ER)-negative and ER-positive patients between the two cohorts, the risk of relapse halved for ER-negative patients in the second cohort relative to the first, while the risk ratio for C2/C1 ranged from 0.26 to 0.56 in ER-positive patients.
“The greatest improvements in outcomes were achieved in the BC subtypes known to be more aggressive, namely the HER2-positive and ER-negative/HER2-negative patients,” wrote Dr. Rachel J.D. Cossetti and colleagues from the Vancouver (B.C.) Cancer Centre.The study was supported by coauthor Dr. Karen A. Gelmon, also of the Vancouver Cancer Centre.
FROM JOURNAL OF CLINICAL ONCOLOGY
Breast cancer relapse risk halved since 1986
Breast cancer outcomes have improved significantly over the past 3 decades, with major gains in relapse-free survival and declines in mortality for all subtypes but particularly HER-2 positive breast cancer, a retrospective case-control study has found.
Researchers compared matched data from 7,178 women referred to the British Columbia Cancer Agency for breast cancer between 1986 and 1992 (C1) and mid-2004 and 2008 (C2) and found the risk of relapse halved in the second cohort, compared to the first, up to year 7 of follow-up, according to a paper published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.57.2461].
While there were similar patterns of disease relapse over time for both the estrogen receptor (ER)-negative and ER-positive patients between the two cohorts, the risk of relapse halved for ER-negative patients in the second cohort relative to the first, while the risk ratio for C2/C1 ranged from 0.26 to 0.56 in ER-positive patients.
“The greatest improvements in outcomes were achieved in the BC subtypes known to be more aggressive, namely the HER2-positive and ER-negative/HER2-negative patients,” wrote Dr. Rachel J.D. Cossetti and colleagues from the Vancouver (B.C.) Cancer Centre.The study was supported by coauthor Dr. Karen A. Gelmon, also of the Vancouver Cancer Centre.
Breast cancer outcomes have improved significantly over the past 3 decades, with major gains in relapse-free survival and declines in mortality for all subtypes but particularly HER-2 positive breast cancer, a retrospective case-control study has found.
Researchers compared matched data from 7,178 women referred to the British Columbia Cancer Agency for breast cancer between 1986 and 1992 (C1) and mid-2004 and 2008 (C2) and found the risk of relapse halved in the second cohort, compared to the first, up to year 7 of follow-up, according to a paper published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.57.2461].
While there were similar patterns of disease relapse over time for both the estrogen receptor (ER)-negative and ER-positive patients between the two cohorts, the risk of relapse halved for ER-negative patients in the second cohort relative to the first, while the risk ratio for C2/C1 ranged from 0.26 to 0.56 in ER-positive patients.
“The greatest improvements in outcomes were achieved in the BC subtypes known to be more aggressive, namely the HER2-positive and ER-negative/HER2-negative patients,” wrote Dr. Rachel J.D. Cossetti and colleagues from the Vancouver (B.C.) Cancer Centre.The study was supported by coauthor Dr. Karen A. Gelmon, also of the Vancouver Cancer Centre.
Breast cancer outcomes have improved significantly over the past 3 decades, with major gains in relapse-free survival and declines in mortality for all subtypes but particularly HER-2 positive breast cancer, a retrospective case-control study has found.
Researchers compared matched data from 7,178 women referred to the British Columbia Cancer Agency for breast cancer between 1986 and 1992 (C1) and mid-2004 and 2008 (C2) and found the risk of relapse halved in the second cohort, compared to the first, up to year 7 of follow-up, according to a paper published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.57.2461].
While there were similar patterns of disease relapse over time for both the estrogen receptor (ER)-negative and ER-positive patients between the two cohorts, the risk of relapse halved for ER-negative patients in the second cohort relative to the first, while the risk ratio for C2/C1 ranged from 0.26 to 0.56 in ER-positive patients.
“The greatest improvements in outcomes were achieved in the BC subtypes known to be more aggressive, namely the HER2-positive and ER-negative/HER2-negative patients,” wrote Dr. Rachel J.D. Cossetti and colleagues from the Vancouver (B.C.) Cancer Centre.The study was supported by coauthor Dr. Karen A. Gelmon, also of the Vancouver Cancer Centre.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Breast cancer outcomes have improved significantly over the past 3 decades, with major gains in relapse-free survival and declines in mortality for all subtypes.
Major finding: The risk of relapse has halved for estrogen receptor–negative breast cancer since 1986.
Data source: Retrospective matched cohort study of 7178 women with breast cancer.
Disclosures: The study was supported by author Dr. Karen A. Gelmon.
Multiple biopsies increase sensitivity of colposcopy
Physicians should consider collecting additional biopsies during colposcopy if multiple lesions are present, according to the authors of a study finding the practice increases the detection of high-grade squamous intraepithelial lesions.
An observational study of 690 women referred to colposcopy after abnormal cervical cancer screening results found sensitivity for detecting high-grade squamous intraepithelial lesions (HSILs) increased from 60.6% with a single biopsy to 85.6% with two biopsies and 95.6% with three biopsies.
“The incremental benefit of taking multiple biopsies was present regardless of referral cytology, HPV-16 status, and colposcopic impression; for example, even when there was a high-grade colposcopic impression, a single biopsy did not identify a prevalent HSIL in 35% of the women,” wrote Dr. Nicolas Wentzensen of the National Cancer Institute, Bethesda, Md., and colleagues.
Researchers found an increase in sensitivity of multiple biopsies across a range of subgroups, although the additional biopsies found more disease among women with more severe referral cytology, higher-risk HPV status, and higher-risk colposcopic impression, according to the study, published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.55.9948].
Physicians should consider collecting additional biopsies during colposcopy if multiple lesions are present, according to the authors of a study finding the practice increases the detection of high-grade squamous intraepithelial lesions.
An observational study of 690 women referred to colposcopy after abnormal cervical cancer screening results found sensitivity for detecting high-grade squamous intraepithelial lesions (HSILs) increased from 60.6% with a single biopsy to 85.6% with two biopsies and 95.6% with three biopsies.
“The incremental benefit of taking multiple biopsies was present regardless of referral cytology, HPV-16 status, and colposcopic impression; for example, even when there was a high-grade colposcopic impression, a single biopsy did not identify a prevalent HSIL in 35% of the women,” wrote Dr. Nicolas Wentzensen of the National Cancer Institute, Bethesda, Md., and colleagues.
Researchers found an increase in sensitivity of multiple biopsies across a range of subgroups, although the additional biopsies found more disease among women with more severe referral cytology, higher-risk HPV status, and higher-risk colposcopic impression, according to the study, published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.55.9948].
Physicians should consider collecting additional biopsies during colposcopy if multiple lesions are present, according to the authors of a study finding the practice increases the detection of high-grade squamous intraepithelial lesions.
An observational study of 690 women referred to colposcopy after abnormal cervical cancer screening results found sensitivity for detecting high-grade squamous intraepithelial lesions (HSILs) increased from 60.6% with a single biopsy to 85.6% with two biopsies and 95.6% with three biopsies.
“The incremental benefit of taking multiple biopsies was present regardless of referral cytology, HPV-16 status, and colposcopic impression; for example, even when there was a high-grade colposcopic impression, a single biopsy did not identify a prevalent HSIL in 35% of the women,” wrote Dr. Nicolas Wentzensen of the National Cancer Institute, Bethesda, Md., and colleagues.
Researchers found an increase in sensitivity of multiple biopsies across a range of subgroups, although the additional biopsies found more disease among women with more severe referral cytology, higher-risk HPV status, and higher-risk colposcopic impression, according to the study, published online Nov. 24 in the Journal of Clinical Oncology [doi:10.1200/JCO.2014.55.9948].
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Collecting additional lesion-directed biopsies during colposcopy significantly increases the sensitivity and detection of high-grade squamous intraepithelial lesions.
Major finding: Three biopsies increases the sensitivity of HSIL detection to 95.6%.
Data source: Observational study of 690 women undergoing colposcopy for abnormal cytology.
Disclosures: The study was supported by the Intramural Research Program of the National Cancer Institute.
Bariatric surgery an opportunity to screen for endometrial cancer
MELBOURNE – Bariatric surgery may provide a useful opportunity to screen morbidly obese women for endometrial cancer, according to the presenter of a study showing a 15% prevalence of occult endometrial cancer or atypical hyperplasia in this population.
Speaking at the biennial meeting of the International Gynecologic Cancer Society, Dr. Michelle MacKintosh, clinical research fellow at the Institute of Cancer Sciences at the University of Manchester (England), presented data from a prospective cohort study examining the endometrial effects of weight loss in morbidly obese women.
Among the 67 women so far enrolled and assessed via a regional weight management service, Dr. MacKintosh and her colleagues detected endometrial cancer or atypical endometrial hyperplasia in 10 women; 1 woman presented symptoms suggestive of an underlying endometrial abnormality.
Endometrial biopsies were conducted while the women were under general anesthesia for bariatric surgery, and the researchers also took blood and cervical cytology samples.
Three-quarters of the women were premenopausal, and among those undergoing bariatric surgery, as opposed to a medically-supervised weight management program, the median body mass index was 52.5 kg/m2.
Twelve-month follow-up data showed bariatric surgery–induced weight loss led to a significant reduction in insulin resistance and significant improvements in reproductive function, as measured by sex hormone binding globulin, follicle-stimulating hormone and luteinizing hormone.
The researchers examined the impact of weight loss on levels of Ki67 – a marker of endometrial proliferation that can be used to generate a proliferation index.
“We know that proliferation is a feature of cancer development and we know it increases along that spectrum, so what we wanted to see was if that process appeared to be reversed by weight loss and we thought that looking at the proliferation index would be a way of quantifying that,” Dr. MacKintosh said in an interview.
These analyses are ongoing but Dr. MacKintosh said initial data look promising, with suggestions that endometrial Ki67 expression drops with weight loss.
“The 15% baseline prevalence of endometrial cancer and atypical hyperplasia, which we found in these women, is clinically significant and is far in excess of anything previously been reported,” Dr. MacKintosh said at the conference.
“Ours is the first prospective cohort study to assess blood and endometrial change with weight loss and in answer to the question we posed, we do believe that we can support endometrial screening of such high risk women.”
There were no conflicts of interest declared.
MELBOURNE – Bariatric surgery may provide a useful opportunity to screen morbidly obese women for endometrial cancer, according to the presenter of a study showing a 15% prevalence of occult endometrial cancer or atypical hyperplasia in this population.
Speaking at the biennial meeting of the International Gynecologic Cancer Society, Dr. Michelle MacKintosh, clinical research fellow at the Institute of Cancer Sciences at the University of Manchester (England), presented data from a prospective cohort study examining the endometrial effects of weight loss in morbidly obese women.
Among the 67 women so far enrolled and assessed via a regional weight management service, Dr. MacKintosh and her colleagues detected endometrial cancer or atypical endometrial hyperplasia in 10 women; 1 woman presented symptoms suggestive of an underlying endometrial abnormality.
Endometrial biopsies were conducted while the women were under general anesthesia for bariatric surgery, and the researchers also took blood and cervical cytology samples.
Three-quarters of the women were premenopausal, and among those undergoing bariatric surgery, as opposed to a medically-supervised weight management program, the median body mass index was 52.5 kg/m2.
Twelve-month follow-up data showed bariatric surgery–induced weight loss led to a significant reduction in insulin resistance and significant improvements in reproductive function, as measured by sex hormone binding globulin, follicle-stimulating hormone and luteinizing hormone.
The researchers examined the impact of weight loss on levels of Ki67 – a marker of endometrial proliferation that can be used to generate a proliferation index.
“We know that proliferation is a feature of cancer development and we know it increases along that spectrum, so what we wanted to see was if that process appeared to be reversed by weight loss and we thought that looking at the proliferation index would be a way of quantifying that,” Dr. MacKintosh said in an interview.
These analyses are ongoing but Dr. MacKintosh said initial data look promising, with suggestions that endometrial Ki67 expression drops with weight loss.
“The 15% baseline prevalence of endometrial cancer and atypical hyperplasia, which we found in these women, is clinically significant and is far in excess of anything previously been reported,” Dr. MacKintosh said at the conference.
“Ours is the first prospective cohort study to assess blood and endometrial change with weight loss and in answer to the question we posed, we do believe that we can support endometrial screening of such high risk women.”
There were no conflicts of interest declared.
MELBOURNE – Bariatric surgery may provide a useful opportunity to screen morbidly obese women for endometrial cancer, according to the presenter of a study showing a 15% prevalence of occult endometrial cancer or atypical hyperplasia in this population.
Speaking at the biennial meeting of the International Gynecologic Cancer Society, Dr. Michelle MacKintosh, clinical research fellow at the Institute of Cancer Sciences at the University of Manchester (England), presented data from a prospective cohort study examining the endometrial effects of weight loss in morbidly obese women.
Among the 67 women so far enrolled and assessed via a regional weight management service, Dr. MacKintosh and her colleagues detected endometrial cancer or atypical endometrial hyperplasia in 10 women; 1 woman presented symptoms suggestive of an underlying endometrial abnormality.
Endometrial biopsies were conducted while the women were under general anesthesia for bariatric surgery, and the researchers also took blood and cervical cytology samples.
Three-quarters of the women were premenopausal, and among those undergoing bariatric surgery, as opposed to a medically-supervised weight management program, the median body mass index was 52.5 kg/m2.
Twelve-month follow-up data showed bariatric surgery–induced weight loss led to a significant reduction in insulin resistance and significant improvements in reproductive function, as measured by sex hormone binding globulin, follicle-stimulating hormone and luteinizing hormone.
The researchers examined the impact of weight loss on levels of Ki67 – a marker of endometrial proliferation that can be used to generate a proliferation index.
“We know that proliferation is a feature of cancer development and we know it increases along that spectrum, so what we wanted to see was if that process appeared to be reversed by weight loss and we thought that looking at the proliferation index would be a way of quantifying that,” Dr. MacKintosh said in an interview.
These analyses are ongoing but Dr. MacKintosh said initial data look promising, with suggestions that endometrial Ki67 expression drops with weight loss.
“The 15% baseline prevalence of endometrial cancer and atypical hyperplasia, which we found in these women, is clinically significant and is far in excess of anything previously been reported,” Dr. MacKintosh said at the conference.
“Ours is the first prospective cohort study to assess blood and endometrial change with weight loss and in answer to the question we posed, we do believe that we can support endometrial screening of such high risk women.”
There were no conflicts of interest declared.
AT IGCS 2014
Key clinical point: Bariatric surgery may provide a useful opportunity to screen morbidly obese women for endometrial cancer.
Major finding: Fifteen percent of morbidly obese women undergoing bariatric surgery had occult endometrial cancer or atypical hyperplasia.
Data source: Ongoing prospective cohort study of 67 morbidly obese women undergoing bariatric surgery.
Disclosures:There were no conflicts of interest declared.
Patient-led follow-up safe and cost effective
MELBOURNE – Patient-initiated follow-up is a safe, cost-effective alternative to conventional follow-ups every 3 months in patients with gynecological cancer, according to data from a prospective trial presented at the biennial meeting of the International Gynecologic Cancer Society.
Researchers found a much longer time to follow-up among patients who chose patient-initiated follow-up compared with those who elected to remain with conventional follow-up (718 days vs. 386 days), but the median time to death also was longer: 1,035 days in the patient-initiated follow-up group compared with 795 days in the conventional follow-up group.
“What is very clear is that many of our patients want an alternative to conventional follow up,” said Dr. Peter Larsen-Disney of the department of gynecology at Brighton and Sussex University Hospital NHS Trust, Brighton, England.
Dr Larsen-Disney told the conference that he realized patients with a good prognosis after treatment for their gynecological cancers were being given mixed messages by being asked to return for regular follow-up.
“We were saying, ‘there’s every reason to believe you’re cured, you have an excellent prognosis, and we’ll see you every 3 months,’ ” he said.
“The other realization I had was, with the exception of ovarian cancer patients, who we were following up for tumor markers, I believe that I make very few diagnoses of recurrence that the patient didn’t tell me was there.”
After realizing there was little evidence to support follow-up every 3 months in these patients, Dr. Larsen-Disney and his colleagues conducted a prospective study of 997 patients who were offered the choice of conventional follow-up or patient-initiated follow-up.
Patients who chose patient-initiated follow-up were registered in a database, and were provided with disease-specific booklets that outlined the follow-up system, listed details on what symptoms to look out for, and gave information on how to access review if needed.
Patients were able to access a nurse specialist by phone for advice and referrals for other services such as counseling.
Of the 568 patients who registered for patient-initiated follow-up, 71 later switched back to conventional follow-up, mostly at the time of recurrence.
More than half of the patients who registered for patient-initiated follow-up had endometrial cancer, while there were significantly more patients with cervical and vulvar cancer in the conventional follow-up arm than in the patient-initiated follow-up arm, which Dr. Larsen-Disney said partly reflected physician bias.
“We were a little bit reluctant to release the [patients with] very early cervix cancers back into the community because we wanted to follow them up with smears, and ... we weren’t confident that they would get the appropriate smears in the community,” he said.
He said there was no doubt in his mind of the importance of patient-led follow-up to the patients themselves, as well as the fact that it appeared to be a safe, acceptable, and cost-effective alternative to conventional follow-up.
“I think the concerns are that people are nervous that they’re going to miss recurrences and, to be honest, there will be a tiny minority of patients where you will, who won’t present with classical signs of recurrence but I’m not convinced you’d pick them up anyway,” Dr. Larsen-Disney said in an interview.
There were no conflicts of interest declared.
MELBOURNE – Patient-initiated follow-up is a safe, cost-effective alternative to conventional follow-ups every 3 months in patients with gynecological cancer, according to data from a prospective trial presented at the biennial meeting of the International Gynecologic Cancer Society.
Researchers found a much longer time to follow-up among patients who chose patient-initiated follow-up compared with those who elected to remain with conventional follow-up (718 days vs. 386 days), but the median time to death also was longer: 1,035 days in the patient-initiated follow-up group compared with 795 days in the conventional follow-up group.
“What is very clear is that many of our patients want an alternative to conventional follow up,” said Dr. Peter Larsen-Disney of the department of gynecology at Brighton and Sussex University Hospital NHS Trust, Brighton, England.
Dr Larsen-Disney told the conference that he realized patients with a good prognosis after treatment for their gynecological cancers were being given mixed messages by being asked to return for regular follow-up.
“We were saying, ‘there’s every reason to believe you’re cured, you have an excellent prognosis, and we’ll see you every 3 months,’ ” he said.
“The other realization I had was, with the exception of ovarian cancer patients, who we were following up for tumor markers, I believe that I make very few diagnoses of recurrence that the patient didn’t tell me was there.”
After realizing there was little evidence to support follow-up every 3 months in these patients, Dr. Larsen-Disney and his colleagues conducted a prospective study of 997 patients who were offered the choice of conventional follow-up or patient-initiated follow-up.
Patients who chose patient-initiated follow-up were registered in a database, and were provided with disease-specific booklets that outlined the follow-up system, listed details on what symptoms to look out for, and gave information on how to access review if needed.
Patients were able to access a nurse specialist by phone for advice and referrals for other services such as counseling.
Of the 568 patients who registered for patient-initiated follow-up, 71 later switched back to conventional follow-up, mostly at the time of recurrence.
More than half of the patients who registered for patient-initiated follow-up had endometrial cancer, while there were significantly more patients with cervical and vulvar cancer in the conventional follow-up arm than in the patient-initiated follow-up arm, which Dr. Larsen-Disney said partly reflected physician bias.
“We were a little bit reluctant to release the [patients with] very early cervix cancers back into the community because we wanted to follow them up with smears, and ... we weren’t confident that they would get the appropriate smears in the community,” he said.
He said there was no doubt in his mind of the importance of patient-led follow-up to the patients themselves, as well as the fact that it appeared to be a safe, acceptable, and cost-effective alternative to conventional follow-up.
“I think the concerns are that people are nervous that they’re going to miss recurrences and, to be honest, there will be a tiny minority of patients where you will, who won’t present with classical signs of recurrence but I’m not convinced you’d pick them up anyway,” Dr. Larsen-Disney said in an interview.
There were no conflicts of interest declared.
MELBOURNE – Patient-initiated follow-up is a safe, cost-effective alternative to conventional follow-ups every 3 months in patients with gynecological cancer, according to data from a prospective trial presented at the biennial meeting of the International Gynecologic Cancer Society.
Researchers found a much longer time to follow-up among patients who chose patient-initiated follow-up compared with those who elected to remain with conventional follow-up (718 days vs. 386 days), but the median time to death also was longer: 1,035 days in the patient-initiated follow-up group compared with 795 days in the conventional follow-up group.
“What is very clear is that many of our patients want an alternative to conventional follow up,” said Dr. Peter Larsen-Disney of the department of gynecology at Brighton and Sussex University Hospital NHS Trust, Brighton, England.
Dr Larsen-Disney told the conference that he realized patients with a good prognosis after treatment for their gynecological cancers were being given mixed messages by being asked to return for regular follow-up.
“We were saying, ‘there’s every reason to believe you’re cured, you have an excellent prognosis, and we’ll see you every 3 months,’ ” he said.
“The other realization I had was, with the exception of ovarian cancer patients, who we were following up for tumor markers, I believe that I make very few diagnoses of recurrence that the patient didn’t tell me was there.”
After realizing there was little evidence to support follow-up every 3 months in these patients, Dr. Larsen-Disney and his colleagues conducted a prospective study of 997 patients who were offered the choice of conventional follow-up or patient-initiated follow-up.
Patients who chose patient-initiated follow-up were registered in a database, and were provided with disease-specific booklets that outlined the follow-up system, listed details on what symptoms to look out for, and gave information on how to access review if needed.
Patients were able to access a nurse specialist by phone for advice and referrals for other services such as counseling.
Of the 568 patients who registered for patient-initiated follow-up, 71 later switched back to conventional follow-up, mostly at the time of recurrence.
More than half of the patients who registered for patient-initiated follow-up had endometrial cancer, while there were significantly more patients with cervical and vulvar cancer in the conventional follow-up arm than in the patient-initiated follow-up arm, which Dr. Larsen-Disney said partly reflected physician bias.
“We were a little bit reluctant to release the [patients with] very early cervix cancers back into the community because we wanted to follow them up with smears, and ... we weren’t confident that they would get the appropriate smears in the community,” he said.
He said there was no doubt in his mind of the importance of patient-led follow-up to the patients themselves, as well as the fact that it appeared to be a safe, acceptable, and cost-effective alternative to conventional follow-up.
“I think the concerns are that people are nervous that they’re going to miss recurrences and, to be honest, there will be a tiny minority of patients where you will, who won’t present with classical signs of recurrence but I’m not convinced you’d pick them up anyway,” Dr. Larsen-Disney said in an interview.
There were no conflicts of interest declared.
AT IGCS 2014
Key clinical point: Patient-initiated follow-up is a safe, cost-effective alternative to conventional follow-up every 3 months in patients with gynecological cancer.
Major finding: Patient-led follow-up was associated with a median follow-up of 742 days compared to 386 days with conventional follow-up.
Data source: Prospective study of 997 women with gynecological cancer.
Disclosures: No conflicts of interest declared.
Dabrafenib and trametinib combo boosts melanoma survival
The combination of dabrafenib and trametinib achieves significant improvements in overall survival and progression-free survival in patients with untreated metastatic melanoma compared with treatment with vemurafenib alone, new data suggest.
An open-label randomized phase III trial showed the combination of BRAF inhibitor dabrafenib with MEK inhibitor trametinib in patients with BRAF V600E or V600K mutant melanoma resulted in a significant reduction in death rates at 12 months compared with monotherapy with BRAF inhibitor vemurafenib (HR 0.69, 95% CI 0.53-0.89, P = .005).
Researchers observed a median progression-free survival rate of 11.4 months in the combination arm, compared with 7.3 months in the monotherapy arm (HR 0.56, 95% CI 0.46-0.69, P < .001), according to data presented at the 2014 International Congress for the Society for Melanoma Research.
The most common adverse event was fever, experienced by 53% of patients in the combination arm and 21% of patients in the monotherapy arm; however, there were more grade 3 and 4 adverse events noted among patients treated with vemurafenib alone.
Pyrexia was the most common reason for dose interruption or reduction in the dabrafenib-plus-trametinib group, while rash was the same for the vemurafenib group.
The study, which presented data from a preplanned interim analysis of 704 patients and 222 events, showed an overall response rate of 64% for the combination of dabrafenib and trametinib, and 51% among those treated with vemurafenib alone.
In a paper published simultaneously online Nov. 16 in the New England Journal of Medicine, researchers said that combining a BRAF inhibitor with a MEK inhibitor could address some of the limitations of monotherapy by delaying the development of resistance and reducing the incidence of BRAF inhibitor–induced skin tumors (N. Engl. J. Med. 2014 Nov. 16 [doi: 10.1056/NEJMoa1412690]).
“Together with the previously reported phase II and phase III trials of dabrafenib plus trametinib, as compared with dabrafenib monotherapy, these data provide clear evidence for the benefit of this combination therapy over BRAF monotherapy in prolonging survival,” wrote Dr. Caroline Robert of Institut Gustave Roussy, Paris, and her colleagues.
The researchers noted that more patients in the vemurafenib monotherapy arm received further anticancer therapy than in the combination arm (43% vs. 20%).
The study was supported by GlaxoSmithKline. Some authors declared grants, travel expenses, and personal fees from pharmaceutical companies including GlaxoSmithKline, and several were employees of the company.
The combination of dabrafenib and trametinib achieves significant improvements in overall survival and progression-free survival in patients with untreated metastatic melanoma compared with treatment with vemurafenib alone, new data suggest.
An open-label randomized phase III trial showed the combination of BRAF inhibitor dabrafenib with MEK inhibitor trametinib in patients with BRAF V600E or V600K mutant melanoma resulted in a significant reduction in death rates at 12 months compared with monotherapy with BRAF inhibitor vemurafenib (HR 0.69, 95% CI 0.53-0.89, P = .005).
Researchers observed a median progression-free survival rate of 11.4 months in the combination arm, compared with 7.3 months in the monotherapy arm (HR 0.56, 95% CI 0.46-0.69, P < .001), according to data presented at the 2014 International Congress for the Society for Melanoma Research.
The most common adverse event was fever, experienced by 53% of patients in the combination arm and 21% of patients in the monotherapy arm; however, there were more grade 3 and 4 adverse events noted among patients treated with vemurafenib alone.
Pyrexia was the most common reason for dose interruption or reduction in the dabrafenib-plus-trametinib group, while rash was the same for the vemurafenib group.
The study, which presented data from a preplanned interim analysis of 704 patients and 222 events, showed an overall response rate of 64% for the combination of dabrafenib and trametinib, and 51% among those treated with vemurafenib alone.
In a paper published simultaneously online Nov. 16 in the New England Journal of Medicine, researchers said that combining a BRAF inhibitor with a MEK inhibitor could address some of the limitations of monotherapy by delaying the development of resistance and reducing the incidence of BRAF inhibitor–induced skin tumors (N. Engl. J. Med. 2014 Nov. 16 [doi: 10.1056/NEJMoa1412690]).
“Together with the previously reported phase II and phase III trials of dabrafenib plus trametinib, as compared with dabrafenib monotherapy, these data provide clear evidence for the benefit of this combination therapy over BRAF monotherapy in prolonging survival,” wrote Dr. Caroline Robert of Institut Gustave Roussy, Paris, and her colleagues.
The researchers noted that more patients in the vemurafenib monotherapy arm received further anticancer therapy than in the combination arm (43% vs. 20%).
The study was supported by GlaxoSmithKline. Some authors declared grants, travel expenses, and personal fees from pharmaceutical companies including GlaxoSmithKline, and several were employees of the company.
The combination of dabrafenib and trametinib achieves significant improvements in overall survival and progression-free survival in patients with untreated metastatic melanoma compared with treatment with vemurafenib alone, new data suggest.
An open-label randomized phase III trial showed the combination of BRAF inhibitor dabrafenib with MEK inhibitor trametinib in patients with BRAF V600E or V600K mutant melanoma resulted in a significant reduction in death rates at 12 months compared with monotherapy with BRAF inhibitor vemurafenib (HR 0.69, 95% CI 0.53-0.89, P = .005).
Researchers observed a median progression-free survival rate of 11.4 months in the combination arm, compared with 7.3 months in the monotherapy arm (HR 0.56, 95% CI 0.46-0.69, P < .001), according to data presented at the 2014 International Congress for the Society for Melanoma Research.
The most common adverse event was fever, experienced by 53% of patients in the combination arm and 21% of patients in the monotherapy arm; however, there were more grade 3 and 4 adverse events noted among patients treated with vemurafenib alone.
Pyrexia was the most common reason for dose interruption or reduction in the dabrafenib-plus-trametinib group, while rash was the same for the vemurafenib group.
The study, which presented data from a preplanned interim analysis of 704 patients and 222 events, showed an overall response rate of 64% for the combination of dabrafenib and trametinib, and 51% among those treated with vemurafenib alone.
In a paper published simultaneously online Nov. 16 in the New England Journal of Medicine, researchers said that combining a BRAF inhibitor with a MEK inhibitor could address some of the limitations of monotherapy by delaying the development of resistance and reducing the incidence of BRAF inhibitor–induced skin tumors (N. Engl. J. Med. 2014 Nov. 16 [doi: 10.1056/NEJMoa1412690]).
“Together with the previously reported phase II and phase III trials of dabrafenib plus trametinib, as compared with dabrafenib monotherapy, these data provide clear evidence for the benefit of this combination therapy over BRAF monotherapy in prolonging survival,” wrote Dr. Caroline Robert of Institut Gustave Roussy, Paris, and her colleagues.
The researchers noted that more patients in the vemurafenib monotherapy arm received further anticancer therapy than in the combination arm (43% vs. 20%).
The study was supported by GlaxoSmithKline. Some authors declared grants, travel expenses, and personal fees from pharmaceutical companies including GlaxoSmithKline, and several were employees of the company.
FROM THE SMR INTERNATIONAL CONGRESS
Key clinical point: The combination of dabrafenib and trametinib boosts overall survival and progression-free survival compared with vemurafenib alone in metastatic BRAF V600E or V600K mutant melanoma.
Major finding: Dabrafenib plus trametinib achieved a 31% reduction in mortality at 12 months compared with vemurafenib.
Data source: Preplanned interim analysis from an open-label randomized phase III trial of 704 patients with untreated, metastatic melanoma.
Disclosures: Several of the researchers disclosed ties with GlaxoSmithKline, which funded the study.
Nivolumab bests dacarbazine for melanoma survival
Nivolumab achieves significant improvements in overall survival and progression-free survival compared with conventional chemotherapy in untreated patients with advanced melanoma, regardless of PD-L1 status, according to data presented at the International Congress for the Society for Melanoma Research.
Data from a randomized, double-blind, placebo-controlled phase III trial showed patients treated with nivolumab – a PD-1 immune checkpoint inhibitor – showed there was a 58% lower incidence of death at 1 year among patients treated with nivolumab compared with those treated with dacarbazine (72.9% vs. 42.1% HR 0.42, 95% CI 0.25-0.73, P < .001).
Median progression-free survival was 5.1 months in the nivolumab arm compared with 2.2 months in the dacarbazine group (HR for death or disease progression: 0.43, 95% CI 0.34-0.56, P < .001). The results were published simultaneously online Nov. 16 in the New England Journal of Medicine.
Researchers randomly assigned 418 previously untreated patients with BRAF mutation-negative advanced melanoma to nivolumab plus placebo, and dacarbazine plus placebo, finding an objective response rate of 40% in patients receiving nivolumab compared with 13.9% in the dacarbazine group.
While PD-L1-positive patients treated with nivolumab showed a greater median response rate compared with PD-L1-negative or indeterminate patients (52.7% vs. 33.1%), both still achieved greater response than either subgroup treated with dacarbazine (N. Engl. J. Med. 2014 Nov. 16 [doi:10.1056/NEJMoa1412082]).
The overall incidence of treatment-related adverse events was similar in the two study arms, although there was a higher incidence of treatment-related grade 3 and 4 adverse events, such as gastrointestinal and hematologic events, in the dacarbazine group.
“It has generally been accepted that immunotherapy is associated with long-term responses in a subset of patients, whereas targeted therapies, such as BRAF inhibitors, are associated with high response rates and a rapid effect, but the responses are often short-lived,” wrote Dr. Caroline Robert of Institut Gustave Roussy, Paris, and her colleagues.
“The present study shows nivolumab is associated with a high response rate, a rapid median time to response (2.1 months, which is similar to the time to response for dacarbazine), and a durable response (the median duration of response was not reached but the duration of follow-up was short),” the investigators said.
The study was supported by Bristol Myers-Squibb. Some authors declared grants, travel expenses, and personal fees from pharmaceutical companies including Bristol Myers-Squibb, and several were employees of the company.
Nivolumab achieves significant improvements in overall survival and progression-free survival compared with conventional chemotherapy in untreated patients with advanced melanoma, regardless of PD-L1 status, according to data presented at the International Congress for the Society for Melanoma Research.
Data from a randomized, double-blind, placebo-controlled phase III trial showed patients treated with nivolumab – a PD-1 immune checkpoint inhibitor – showed there was a 58% lower incidence of death at 1 year among patients treated with nivolumab compared with those treated with dacarbazine (72.9% vs. 42.1% HR 0.42, 95% CI 0.25-0.73, P < .001).
Median progression-free survival was 5.1 months in the nivolumab arm compared with 2.2 months in the dacarbazine group (HR for death or disease progression: 0.43, 95% CI 0.34-0.56, P < .001). The results were published simultaneously online Nov. 16 in the New England Journal of Medicine.
Researchers randomly assigned 418 previously untreated patients with BRAF mutation-negative advanced melanoma to nivolumab plus placebo, and dacarbazine plus placebo, finding an objective response rate of 40% in patients receiving nivolumab compared with 13.9% in the dacarbazine group.
While PD-L1-positive patients treated with nivolumab showed a greater median response rate compared with PD-L1-negative or indeterminate patients (52.7% vs. 33.1%), both still achieved greater response than either subgroup treated with dacarbazine (N. Engl. J. Med. 2014 Nov. 16 [doi:10.1056/NEJMoa1412082]).
The overall incidence of treatment-related adverse events was similar in the two study arms, although there was a higher incidence of treatment-related grade 3 and 4 adverse events, such as gastrointestinal and hematologic events, in the dacarbazine group.
“It has generally been accepted that immunotherapy is associated with long-term responses in a subset of patients, whereas targeted therapies, such as BRAF inhibitors, are associated with high response rates and a rapid effect, but the responses are often short-lived,” wrote Dr. Caroline Robert of Institut Gustave Roussy, Paris, and her colleagues.
“The present study shows nivolumab is associated with a high response rate, a rapid median time to response (2.1 months, which is similar to the time to response for dacarbazine), and a durable response (the median duration of response was not reached but the duration of follow-up was short),” the investigators said.
The study was supported by Bristol Myers-Squibb. Some authors declared grants, travel expenses, and personal fees from pharmaceutical companies including Bristol Myers-Squibb, and several were employees of the company.
Nivolumab achieves significant improvements in overall survival and progression-free survival compared with conventional chemotherapy in untreated patients with advanced melanoma, regardless of PD-L1 status, according to data presented at the International Congress for the Society for Melanoma Research.
Data from a randomized, double-blind, placebo-controlled phase III trial showed patients treated with nivolumab – a PD-1 immune checkpoint inhibitor – showed there was a 58% lower incidence of death at 1 year among patients treated with nivolumab compared with those treated with dacarbazine (72.9% vs. 42.1% HR 0.42, 95% CI 0.25-0.73, P < .001).
Median progression-free survival was 5.1 months in the nivolumab arm compared with 2.2 months in the dacarbazine group (HR for death or disease progression: 0.43, 95% CI 0.34-0.56, P < .001). The results were published simultaneously online Nov. 16 in the New England Journal of Medicine.
Researchers randomly assigned 418 previously untreated patients with BRAF mutation-negative advanced melanoma to nivolumab plus placebo, and dacarbazine plus placebo, finding an objective response rate of 40% in patients receiving nivolumab compared with 13.9% in the dacarbazine group.
While PD-L1-positive patients treated with nivolumab showed a greater median response rate compared with PD-L1-negative or indeterminate patients (52.7% vs. 33.1%), both still achieved greater response than either subgroup treated with dacarbazine (N. Engl. J. Med. 2014 Nov. 16 [doi:10.1056/NEJMoa1412082]).
The overall incidence of treatment-related adverse events was similar in the two study arms, although there was a higher incidence of treatment-related grade 3 and 4 adverse events, such as gastrointestinal and hematologic events, in the dacarbazine group.
“It has generally been accepted that immunotherapy is associated with long-term responses in a subset of patients, whereas targeted therapies, such as BRAF inhibitors, are associated with high response rates and a rapid effect, but the responses are often short-lived,” wrote Dr. Caroline Robert of Institut Gustave Roussy, Paris, and her colleagues.
“The present study shows nivolumab is associated with a high response rate, a rapid median time to response (2.1 months, which is similar to the time to response for dacarbazine), and a durable response (the median duration of response was not reached but the duration of follow-up was short),” the investigators said.
The study was supported by Bristol Myers-Squibb. Some authors declared grants, travel expenses, and personal fees from pharmaceutical companies including Bristol Myers-Squibb, and several were employees of the company.
FROM THE SMR INTERNATIONAL CONGRESS
Key clinical point: Nivolumab achieves significant improvements in overall survival and progression-free survival compared with dacarbazine in untreated patients with advanced melanoma.
Major finding: Nivolumab was associated with a 58% lower incidence of death at 1 year compared with dacarbazine
Data source: Randomized, double-blind, placebo-controlled phase III trial of 418 previously-untreated patients with advanced melanoma.
Disclosures: Several of the researchers disclosed ties with Bristol-Myers Squibb, which funded the study.
Salpingectomy associated with reduced ovarian cancer risk
MELBOURNE – Surgical removal of the fallopian tubes could be a viable option for reducing the risk of ovarian cancer in high-risk women, a speaker said at the biennial meeting of the International Gynecologic Cancer Society.
Dr. Henrik Falconer, head of gynecologic oncology at the Karolinska Institute, Stockholm, said there is an emerging hypothesis that ovarian cancer arises primarily in the fallopian tubes, not in the ovaries, although this is difficult to prove.
Researchers therefore conducted a retrospective, population-based cohort study of women who had previously undergone sterilization; salpingectomy; hysterectomy and bilateral salpingo-oophorectomy; or hysterectomy for a benign indication between 1972 and 2010 in Sweden.
They found that women who had undergone unilateral salpingectomy had a 28% lower risk of ovarian cancer, while those who had undergone bilateral salpingectomy had a 65% lower risk, compared with the general population.
Women who underwent hysterectomy with removal of fallopian tubes and ovaries had the lowest overall risk of ovarian cancer (hazard ratio, 0.06; 95% confidence interval, 0.03-0.12), while those who had hysterectomy alone had a 22% reduction in risk.
Dr. Falconer said a case could be made for proactive removal of the fallopian tubes in women carrying the BRCA mutation, which might then enable a delay in removal of their ovaries.
“Today, we counsel the patients and advise them to take away the tubes and the ovaries, sometimes at 40-45, after they have completed their family planning,” Dr. Falconer said in an interview.
“I think now we could take away the tubes instead earlier, to have risk reduction while they wait to have their ovaries removed, perhaps in their 50s or 60s then, or maybe never.”
This would avoid the morbidity associated with oophorectomy, such as cardiovascular disease and Alzheimer’s disease, Dr. Falconer said, and could not only reduce the risk of cancer but also improve the quality of life in this population of relatively young women.
He also suggested that prophylactic salpingectomy might even be considered in women undergoing sterilization, even if they weren’t necessarily at high risk of ovarian cancer.
The study included data from more than 5 million women, with over 250,000 women exposed to some form of surgery and more than 30,000 cases of ovarian cancer.
One audience member raised concerns about the use of prophylactic salpingectomy in an otherwise healthy population, suggesting that the procedure was not without its risks and could have unintended consequences because of the loss of blood supply to the ovaries.
The study did not control for oral contraceptive use or histological subtypes.
Dr. Falconer declared support from Intuitive Surgical. There were no other conflicts of interest declared.
MELBOURNE – Surgical removal of the fallopian tubes could be a viable option for reducing the risk of ovarian cancer in high-risk women, a speaker said at the biennial meeting of the International Gynecologic Cancer Society.
Dr. Henrik Falconer, head of gynecologic oncology at the Karolinska Institute, Stockholm, said there is an emerging hypothesis that ovarian cancer arises primarily in the fallopian tubes, not in the ovaries, although this is difficult to prove.
Researchers therefore conducted a retrospective, population-based cohort study of women who had previously undergone sterilization; salpingectomy; hysterectomy and bilateral salpingo-oophorectomy; or hysterectomy for a benign indication between 1972 and 2010 in Sweden.
They found that women who had undergone unilateral salpingectomy had a 28% lower risk of ovarian cancer, while those who had undergone bilateral salpingectomy had a 65% lower risk, compared with the general population.
Women who underwent hysterectomy with removal of fallopian tubes and ovaries had the lowest overall risk of ovarian cancer (hazard ratio, 0.06; 95% confidence interval, 0.03-0.12), while those who had hysterectomy alone had a 22% reduction in risk.
Dr. Falconer said a case could be made for proactive removal of the fallopian tubes in women carrying the BRCA mutation, which might then enable a delay in removal of their ovaries.
“Today, we counsel the patients and advise them to take away the tubes and the ovaries, sometimes at 40-45, after they have completed their family planning,” Dr. Falconer said in an interview.
“I think now we could take away the tubes instead earlier, to have risk reduction while they wait to have their ovaries removed, perhaps in their 50s or 60s then, or maybe never.”
This would avoid the morbidity associated with oophorectomy, such as cardiovascular disease and Alzheimer’s disease, Dr. Falconer said, and could not only reduce the risk of cancer but also improve the quality of life in this population of relatively young women.
He also suggested that prophylactic salpingectomy might even be considered in women undergoing sterilization, even if they weren’t necessarily at high risk of ovarian cancer.
The study included data from more than 5 million women, with over 250,000 women exposed to some form of surgery and more than 30,000 cases of ovarian cancer.
One audience member raised concerns about the use of prophylactic salpingectomy in an otherwise healthy population, suggesting that the procedure was not without its risks and could have unintended consequences because of the loss of blood supply to the ovaries.
The study did not control for oral contraceptive use or histological subtypes.
Dr. Falconer declared support from Intuitive Surgical. There were no other conflicts of interest declared.
MELBOURNE – Surgical removal of the fallopian tubes could be a viable option for reducing the risk of ovarian cancer in high-risk women, a speaker said at the biennial meeting of the International Gynecologic Cancer Society.
Dr. Henrik Falconer, head of gynecologic oncology at the Karolinska Institute, Stockholm, said there is an emerging hypothesis that ovarian cancer arises primarily in the fallopian tubes, not in the ovaries, although this is difficult to prove.
Researchers therefore conducted a retrospective, population-based cohort study of women who had previously undergone sterilization; salpingectomy; hysterectomy and bilateral salpingo-oophorectomy; or hysterectomy for a benign indication between 1972 and 2010 in Sweden.
They found that women who had undergone unilateral salpingectomy had a 28% lower risk of ovarian cancer, while those who had undergone bilateral salpingectomy had a 65% lower risk, compared with the general population.
Women who underwent hysterectomy with removal of fallopian tubes and ovaries had the lowest overall risk of ovarian cancer (hazard ratio, 0.06; 95% confidence interval, 0.03-0.12), while those who had hysterectomy alone had a 22% reduction in risk.
Dr. Falconer said a case could be made for proactive removal of the fallopian tubes in women carrying the BRCA mutation, which might then enable a delay in removal of their ovaries.
“Today, we counsel the patients and advise them to take away the tubes and the ovaries, sometimes at 40-45, after they have completed their family planning,” Dr. Falconer said in an interview.
“I think now we could take away the tubes instead earlier, to have risk reduction while they wait to have their ovaries removed, perhaps in their 50s or 60s then, or maybe never.”
This would avoid the morbidity associated with oophorectomy, such as cardiovascular disease and Alzheimer’s disease, Dr. Falconer said, and could not only reduce the risk of cancer but also improve the quality of life in this population of relatively young women.
He also suggested that prophylactic salpingectomy might even be considered in women undergoing sterilization, even if they weren’t necessarily at high risk of ovarian cancer.
The study included data from more than 5 million women, with over 250,000 women exposed to some form of surgery and more than 30,000 cases of ovarian cancer.
One audience member raised concerns about the use of prophylactic salpingectomy in an otherwise healthy population, suggesting that the procedure was not without its risks and could have unintended consequences because of the loss of blood supply to the ovaries.
The study did not control for oral contraceptive use or histological subtypes.
Dr. Falconer declared support from Intuitive Surgical. There were no other conflicts of interest declared.
AT IGCS 2014
Key clinical point: Salpingectomy is associated with a significant reduction in the risk of ovarian cancer, even in women who do not have their ovaries removed.
Major finding: Bilateral salpingectomy is associated with a 65% reduction in the risk of ovarian cancer, compared with the general population.
Data source: Retrospective, population-based cohort study.
Disclosures: Dr. Falconer declared support from Intuitive Surgical. There were no other conflicts of interest declared.
No recurrence of cervical cancer seen with simple trachelectomy
MELBOURNE – Simple trachelectomy can achieve fertility-sparing outcomes similar to those obtained from radical trachelectomy in women with early-stage cervical cancer without any increased risk of recurrence, according to a poster presented at the biennial meeting of the International Gynecologic Cancer Society.
A retrospective cohort study of 25 patients who underwent a simple vaginal trachelectomy to remove the cervix after a diagnosis of cervical cancer found that 6 of the 10 patients who declared an intention to conceive were successful in doing so.
“The radical trachelectomy procedures [resulted in] a pregnancy rate between 70% and 80%, so we think the simple trachelectomy will do quite well,” said lead author Dr. Shamitha Kathurusinghe, an obstetrics/gynecology trainee at Royal Women’s Hospital, Melbourne.“We had 10 people with the intention to conceive, and we had 10 pregnancies in 6 patients, and our intention to conceive was about 50%,” she said in an interview.
While the majority of patients in the study sought assisted reproductive technologies, some also conceived naturally.
All pregnancies were treated as high risk, and all patients delivered via cesarean section. Two pregnancies were achieved via a surrogate; there was one first-trimester miscarriage; one ectopic pregnancy; and one second-trimester miscarriage, but the cause was unknown.”
Researchers found no incidence of cancer recurrence during the median 54-month follow-up period, among a group of patients which included 7 with stage IA1 disease, 5 with stage IA2, 11 with stage IB1 disease, and 2 with stage IB2 disease.
The study group included 7 cases of squamous cell carcinoma, 10 adenocarcinomas, 4 adenosquamous tumors, 2 adenosarcomas, and 2 neuroendocrine tumors. In all, 48% of patients were nulliparous prior to the procedure.
Dr. Kathurusinghe said surgical treatments for cervical cancer seemed to be shifting away from more radical toward more conservative approaches.
“What we’ve noticed over time is that the gold standard management is a radical hysterectomy, but we’ve gone back from that and said, maybe we can get away without that, let’s do a radical trachelectomy,” Dr. Kathurusinghe said.
“Now we’re slowly going back and saying we can be a little bit less radical and leave a bit more behind.”
While the study included women with stage IB2 tumors, Dr. Kathurusinghe said the general advice would be to use the more conservative procedure up to stage IB1 tumors only.
“Every patient should be considered on an individual basis by a specialist that’s in that area. Sit down with the patient and decide, does this patient need radical therapy? Is this woman still of a childbearing age, [who] would want to preserve their fertility; and can this be an option for that patient?”
Researchers also found that 15 patients actually had no residual disease on the final histopathology, echoing similar findings from an earlier study.
There were no conflicts of interest declared.
MELBOURNE – Simple trachelectomy can achieve fertility-sparing outcomes similar to those obtained from radical trachelectomy in women with early-stage cervical cancer without any increased risk of recurrence, according to a poster presented at the biennial meeting of the International Gynecologic Cancer Society.
A retrospective cohort study of 25 patients who underwent a simple vaginal trachelectomy to remove the cervix after a diagnosis of cervical cancer found that 6 of the 10 patients who declared an intention to conceive were successful in doing so.
“The radical trachelectomy procedures [resulted in] a pregnancy rate between 70% and 80%, so we think the simple trachelectomy will do quite well,” said lead author Dr. Shamitha Kathurusinghe, an obstetrics/gynecology trainee at Royal Women’s Hospital, Melbourne.“We had 10 people with the intention to conceive, and we had 10 pregnancies in 6 patients, and our intention to conceive was about 50%,” she said in an interview.
While the majority of patients in the study sought assisted reproductive technologies, some also conceived naturally.
All pregnancies were treated as high risk, and all patients delivered via cesarean section. Two pregnancies were achieved via a surrogate; there was one first-trimester miscarriage; one ectopic pregnancy; and one second-trimester miscarriage, but the cause was unknown.”
Researchers found no incidence of cancer recurrence during the median 54-month follow-up period, among a group of patients which included 7 with stage IA1 disease, 5 with stage IA2, 11 with stage IB1 disease, and 2 with stage IB2 disease.
The study group included 7 cases of squamous cell carcinoma, 10 adenocarcinomas, 4 adenosquamous tumors, 2 adenosarcomas, and 2 neuroendocrine tumors. In all, 48% of patients were nulliparous prior to the procedure.
Dr. Kathurusinghe said surgical treatments for cervical cancer seemed to be shifting away from more radical toward more conservative approaches.
“What we’ve noticed over time is that the gold standard management is a radical hysterectomy, but we’ve gone back from that and said, maybe we can get away without that, let’s do a radical trachelectomy,” Dr. Kathurusinghe said.
“Now we’re slowly going back and saying we can be a little bit less radical and leave a bit more behind.”
While the study included women with stage IB2 tumors, Dr. Kathurusinghe said the general advice would be to use the more conservative procedure up to stage IB1 tumors only.
“Every patient should be considered on an individual basis by a specialist that’s in that area. Sit down with the patient and decide, does this patient need radical therapy? Is this woman still of a childbearing age, [who] would want to preserve their fertility; and can this be an option for that patient?”
Researchers also found that 15 patients actually had no residual disease on the final histopathology, echoing similar findings from an earlier study.
There were no conflicts of interest declared.
MELBOURNE – Simple trachelectomy can achieve fertility-sparing outcomes similar to those obtained from radical trachelectomy in women with early-stage cervical cancer without any increased risk of recurrence, according to a poster presented at the biennial meeting of the International Gynecologic Cancer Society.
A retrospective cohort study of 25 patients who underwent a simple vaginal trachelectomy to remove the cervix after a diagnosis of cervical cancer found that 6 of the 10 patients who declared an intention to conceive were successful in doing so.
“The radical trachelectomy procedures [resulted in] a pregnancy rate between 70% and 80%, so we think the simple trachelectomy will do quite well,” said lead author Dr. Shamitha Kathurusinghe, an obstetrics/gynecology trainee at Royal Women’s Hospital, Melbourne.“We had 10 people with the intention to conceive, and we had 10 pregnancies in 6 patients, and our intention to conceive was about 50%,” she said in an interview.
While the majority of patients in the study sought assisted reproductive technologies, some also conceived naturally.
All pregnancies were treated as high risk, and all patients delivered via cesarean section. Two pregnancies were achieved via a surrogate; there was one first-trimester miscarriage; one ectopic pregnancy; and one second-trimester miscarriage, but the cause was unknown.”
Researchers found no incidence of cancer recurrence during the median 54-month follow-up period, among a group of patients which included 7 with stage IA1 disease, 5 with stage IA2, 11 with stage IB1 disease, and 2 with stage IB2 disease.
The study group included 7 cases of squamous cell carcinoma, 10 adenocarcinomas, 4 adenosquamous tumors, 2 adenosarcomas, and 2 neuroendocrine tumors. In all, 48% of patients were nulliparous prior to the procedure.
Dr. Kathurusinghe said surgical treatments for cervical cancer seemed to be shifting away from more radical toward more conservative approaches.
“What we’ve noticed over time is that the gold standard management is a radical hysterectomy, but we’ve gone back from that and said, maybe we can get away without that, let’s do a radical trachelectomy,” Dr. Kathurusinghe said.
“Now we’re slowly going back and saying we can be a little bit less radical and leave a bit more behind.”
While the study included women with stage IB2 tumors, Dr. Kathurusinghe said the general advice would be to use the more conservative procedure up to stage IB1 tumors only.
“Every patient should be considered on an individual basis by a specialist that’s in that area. Sit down with the patient and decide, does this patient need radical therapy? Is this woman still of a childbearing age, [who] would want to preserve their fertility; and can this be an option for that patient?”
Researchers also found that 15 patients actually had no residual disease on the final histopathology, echoing similar findings from an earlier study.
There were no conflicts of interest declared.
AT IGCS 2014
Key clinical point: Simple trachelectomy can achieve fertility-sparing outcomes similar to outcomes obtained from radical trachelectomy, with no increase in recurrence of cervical cancer.
Major finding: Half of women undergoing simple trachelectomy were able to conceive, and without cancer recurrence.
Data source: Retrospective cohort study of 25 patients undergoing simple vaginal trachelectomy for cervical cancer.
Disclosures: There were no conflicts of interest declared.