User login
Damian McNamara is a journalist for Medscape Medical News and MDedge. He worked full-time for MDedge as the Miami Bureau covering a dozen medical specialties during 2001-2012, then as a freelancer for Medscape and MDedge, before being hired on staff by Medscape in 2018. Now the two companies are one. He uses what he learned in school – Damian has a BS in chemistry and an MS in science, health and environmental reporting/journalism. He works out of a home office in Miami, with a 100-pound chocolate lab known to snore under his desk during work hours.
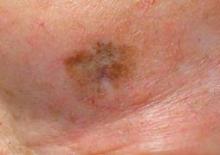
Recent Research Could Refine Treatment of Squamous Cell Carcinoma
ORLANDO – Despite a paucity of recently approved treatments for squamous cell carcinoma, you can use study findings from the past few years to refine your clinical approach, Dr. Suzanne Olbricht said.
"It would be nice if I had some new treatments to discuss, but I don’t. So let’s go through some recent studies," Dr. Olbricht said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Photodynamic Therapy
Investigators, for example, found methyl aminolevulinate photodynamic therapy (MAL-PDT) superior to 5-fluorouracil and cryosurgery for squamous cell carcinoma in situ. In addition, ophthalmologists might start using more imiquimod to treat periorbital skin cancers based on outcomes of a recent case series, Dr. Olbricht said. Other findings support promise for the oral medications cetuximab and capecitabine.
The prospective, randomized study that bolsters use of MAL-PDT included 225 patients with biopsy-confirmed squamous cell carcinoma in situ (Arch. Dermatol. 2006;142:729-35). Researchers found an 80% complete response rate in the MAL-PDT–treated patients at 12 months, compared with a 69% rate with 5-fluorouracil and a 67% rate in patients treated with cryotherapy.
"MAL-PDT was judged [to have the] most acceptable cosmetic outcome," Dr. Olbricht said. She added that 5-fluorouracil is "still a good therapy if some patients prefer to do things at home."
This is a "large study that is worth thinking about," said Dr. Olbricht, chair of the department of dermatology at the Lahey Clinic in Burlington, Mass., and a member of the dermatology faculty at Harvard Medical School, Boston.
Photodynamic therapy (PDT) was associated with a 72% complete response in a smaller study of 30 patients with recurrent tumors of the head and neck (J. Drugs Dermatol. 2010;9:122-6).
These investigators described PDT as effective, tolerable, and associated with good cosmetic results for recurrent squamous cell carcinoma or basal cell carcinoma. One concern, Dr. Olbricht said, is "they did not describe how they did the PDT."
Imiquimod Therapy
Another noteworthy study supports imiquimod for periorbital skin lesions (Orbit 2010;29:83-7). Two patients in this case series had basal cell carcinoma of the eyelid, one had actinic keratosis, and another had intraepidermal squamous cell carcinoma (Bowen’s disease). A fifth patient presented with concomitant squamous cell carcinoma and intraepidermal squamous cell carcinoma. All tumors regressed with a clinical cure at 6-9 months.
"It’s a short follow-up, but your ophthalmologic colleagues will be using imiquimod," Dr. Olbricht said.
Cetuximab and Capecitabine
Oral cetuximab (Erbitux, Imclone) was associated with a complete clinical response for a patient with organ metastases from cutaneous squamous cell carcinoma (Dermatol. Surg. 2010;36:2069-74). Keep two caveats in mind with a cetuximab treatment strategy, Dr. Olbricht said. First, it’s expensive – costing approximately $30,000 for an 8-week series of infusions. Second, cetuximab is effective only for skin cancer patients who do not have a KRAS mutation.
Another treatment showing promise is capecitabine (Xeloda, Hoffmann La Roche), an oral 5-fluorouracil precursor. New lesion development was halted within 6 months for three patients with a history of more than one new squamous cell carcinoma occurrence per month for more than 3 years (Dermatol. Surg. 2009;35:1657-72). Dr. Olbricht noted that hand and foot erythema occurred, which "is supposedly well known with this oral medication."
A meeting attendee asked how Dr. Olbricht manages patients with chronic, multiple squamous cell carcinomas. "I probably have six or seven people for years who come in at least once a month for skin cancer," she replied. "I try to take care of what they have at that moment."
For example, she recently treated a man whose biggest clinical concern is skin cancer 7 years post kidney transplant. "We sent 12 specimens to pathology. We did two Mohs procedures on his face, two excisions on his legs, and the rest were probably electrodesiccation and curettage on his trunk."
"I know I would make more money if I treated each lesion at individual sessions ... but I think this is best approach to this kind of patient," Dr. Olbricht said.
Dr. Olbricht said she had no relevant disclosures.
ORLANDO – Despite a paucity of recently approved treatments for squamous cell carcinoma, you can use study findings from the past few years to refine your clinical approach, Dr. Suzanne Olbricht said.
"It would be nice if I had some new treatments to discuss, but I don’t. So let’s go through some recent studies," Dr. Olbricht said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Photodynamic Therapy
Investigators, for example, found methyl aminolevulinate photodynamic therapy (MAL-PDT) superior to 5-fluorouracil and cryosurgery for squamous cell carcinoma in situ. In addition, ophthalmologists might start using more imiquimod to treat periorbital skin cancers based on outcomes of a recent case series, Dr. Olbricht said. Other findings support promise for the oral medications cetuximab and capecitabine.
The prospective, randomized study that bolsters use of MAL-PDT included 225 patients with biopsy-confirmed squamous cell carcinoma in situ (Arch. Dermatol. 2006;142:729-35). Researchers found an 80% complete response rate in the MAL-PDT–treated patients at 12 months, compared with a 69% rate with 5-fluorouracil and a 67% rate in patients treated with cryotherapy.
"MAL-PDT was judged [to have the] most acceptable cosmetic outcome," Dr. Olbricht said. She added that 5-fluorouracil is "still a good therapy if some patients prefer to do things at home."
This is a "large study that is worth thinking about," said Dr. Olbricht, chair of the department of dermatology at the Lahey Clinic in Burlington, Mass., and a member of the dermatology faculty at Harvard Medical School, Boston.
Photodynamic therapy (PDT) was associated with a 72% complete response in a smaller study of 30 patients with recurrent tumors of the head and neck (J. Drugs Dermatol. 2010;9:122-6).
These investigators described PDT as effective, tolerable, and associated with good cosmetic results for recurrent squamous cell carcinoma or basal cell carcinoma. One concern, Dr. Olbricht said, is "they did not describe how they did the PDT."
Imiquimod Therapy
Another noteworthy study supports imiquimod for periorbital skin lesions (Orbit 2010;29:83-7). Two patients in this case series had basal cell carcinoma of the eyelid, one had actinic keratosis, and another had intraepidermal squamous cell carcinoma (Bowen’s disease). A fifth patient presented with concomitant squamous cell carcinoma and intraepidermal squamous cell carcinoma. All tumors regressed with a clinical cure at 6-9 months.
"It’s a short follow-up, but your ophthalmologic colleagues will be using imiquimod," Dr. Olbricht said.
Cetuximab and Capecitabine
Oral cetuximab (Erbitux, Imclone) was associated with a complete clinical response for a patient with organ metastases from cutaneous squamous cell carcinoma (Dermatol. Surg. 2010;36:2069-74). Keep two caveats in mind with a cetuximab treatment strategy, Dr. Olbricht said. First, it’s expensive – costing approximately $30,000 for an 8-week series of infusions. Second, cetuximab is effective only for skin cancer patients who do not have a KRAS mutation.
Another treatment showing promise is capecitabine (Xeloda, Hoffmann La Roche), an oral 5-fluorouracil precursor. New lesion development was halted within 6 months for three patients with a history of more than one new squamous cell carcinoma occurrence per month for more than 3 years (Dermatol. Surg. 2009;35:1657-72). Dr. Olbricht noted that hand and foot erythema occurred, which "is supposedly well known with this oral medication."
A meeting attendee asked how Dr. Olbricht manages patients with chronic, multiple squamous cell carcinomas. "I probably have six or seven people for years who come in at least once a month for skin cancer," she replied. "I try to take care of what they have at that moment."
For example, she recently treated a man whose biggest clinical concern is skin cancer 7 years post kidney transplant. "We sent 12 specimens to pathology. We did two Mohs procedures on his face, two excisions on his legs, and the rest were probably electrodesiccation and curettage on his trunk."
"I know I would make more money if I treated each lesion at individual sessions ... but I think this is best approach to this kind of patient," Dr. Olbricht said.
Dr. Olbricht said she had no relevant disclosures.
ORLANDO – Despite a paucity of recently approved treatments for squamous cell carcinoma, you can use study findings from the past few years to refine your clinical approach, Dr. Suzanne Olbricht said.
"It would be nice if I had some new treatments to discuss, but I don’t. So let’s go through some recent studies," Dr. Olbricht said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Photodynamic Therapy
Investigators, for example, found methyl aminolevulinate photodynamic therapy (MAL-PDT) superior to 5-fluorouracil and cryosurgery for squamous cell carcinoma in situ. In addition, ophthalmologists might start using more imiquimod to treat periorbital skin cancers based on outcomes of a recent case series, Dr. Olbricht said. Other findings support promise for the oral medications cetuximab and capecitabine.
The prospective, randomized study that bolsters use of MAL-PDT included 225 patients with biopsy-confirmed squamous cell carcinoma in situ (Arch. Dermatol. 2006;142:729-35). Researchers found an 80% complete response rate in the MAL-PDT–treated patients at 12 months, compared with a 69% rate with 5-fluorouracil and a 67% rate in patients treated with cryotherapy.
"MAL-PDT was judged [to have the] most acceptable cosmetic outcome," Dr. Olbricht said. She added that 5-fluorouracil is "still a good therapy if some patients prefer to do things at home."
This is a "large study that is worth thinking about," said Dr. Olbricht, chair of the department of dermatology at the Lahey Clinic in Burlington, Mass., and a member of the dermatology faculty at Harvard Medical School, Boston.
Photodynamic therapy (PDT) was associated with a 72% complete response in a smaller study of 30 patients with recurrent tumors of the head and neck (J. Drugs Dermatol. 2010;9:122-6).
These investigators described PDT as effective, tolerable, and associated with good cosmetic results for recurrent squamous cell carcinoma or basal cell carcinoma. One concern, Dr. Olbricht said, is "they did not describe how they did the PDT."
Imiquimod Therapy
Another noteworthy study supports imiquimod for periorbital skin lesions (Orbit 2010;29:83-7). Two patients in this case series had basal cell carcinoma of the eyelid, one had actinic keratosis, and another had intraepidermal squamous cell carcinoma (Bowen’s disease). A fifth patient presented with concomitant squamous cell carcinoma and intraepidermal squamous cell carcinoma. All tumors regressed with a clinical cure at 6-9 months.
"It’s a short follow-up, but your ophthalmologic colleagues will be using imiquimod," Dr. Olbricht said.
Cetuximab and Capecitabine
Oral cetuximab (Erbitux, Imclone) was associated with a complete clinical response for a patient with organ metastases from cutaneous squamous cell carcinoma (Dermatol. Surg. 2010;36:2069-74). Keep two caveats in mind with a cetuximab treatment strategy, Dr. Olbricht said. First, it’s expensive – costing approximately $30,000 for an 8-week series of infusions. Second, cetuximab is effective only for skin cancer patients who do not have a KRAS mutation.
Another treatment showing promise is capecitabine (Xeloda, Hoffmann La Roche), an oral 5-fluorouracil precursor. New lesion development was halted within 6 months for three patients with a history of more than one new squamous cell carcinoma occurrence per month for more than 3 years (Dermatol. Surg. 2009;35:1657-72). Dr. Olbricht noted that hand and foot erythema occurred, which "is supposedly well known with this oral medication."
A meeting attendee asked how Dr. Olbricht manages patients with chronic, multiple squamous cell carcinomas. "I probably have six or seven people for years who come in at least once a month for skin cancer," she replied. "I try to take care of what they have at that moment."
For example, she recently treated a man whose biggest clinical concern is skin cancer 7 years post kidney transplant. "We sent 12 specimens to pathology. We did two Mohs procedures on his face, two excisions on his legs, and the rest were probably electrodesiccation and curettage on his trunk."
"I know I would make more money if I treated each lesion at individual sessions ... but I think this is best approach to this kind of patient," Dr. Olbricht said.
Dr. Olbricht said she had no relevant disclosures.
EXPERT OPINION FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Dimethyl Fumarate Named 2011 Allergen of the Year
NEW ORLEANS – Dimethyl fumarate – a volatile substance included in shipments of furniture, clothing, and shoes to inhibit growth of mold – earned the distinction as the American Contact Dermatitis Society's 2011 Allergen of the Year.
"We had a difficult decision," Dr. Donald V. Belsito said. "But we decided to go with dimethyl fumarate. It caused an epidemic in Europe starting in 2007."
The substance is now being regulated in Europe, "although apparently some stuff is still sneaking through," Dr. Belsito said. "To date, I know of no cases in the U.S., although Dr. Melanie Pratt has had a few cases in Ontario."
Dimethyl fumarate "produces an extremely severe dermatitis," said Dr. Belsito, a dermatologist in private practice in Shawnee, Kan.
The unlikely story behind identification of this preservative and fungicide demonstrates the benefits of international collaboration, he noted.
First noted by dermatologists in Finland, cases of the severe dermatitis began to appear in Sweden and the U.K. The severe rash, seen predominantly on the backs of the legs, buttocks, and back, was an etiologic mystery. Through extensive sleuth work, Finnish dermatologists determined a common link – each person recently purchased furniture from a particular Chinese manufacturer.
It then became commonly called "sofa dermatitis." A contact allergy to the upholstery fabric was initially suspected. However, no common chemical or fabric was identified among the different pieces of furniture purchased by affected patients.
Dr. Magnus Bruze, an occupational and environmental dermatologist at Malmo University in Sweden, and other investigators took apart the furniture, patch tested 40 affected patients to various components, and eventually identified the culprit: dimethyl fumarate. The allergen was enclosed in packets similar in appearance to silicone packets often labeled "Warning: Do Not Eat."
Dimethyl fumarate is so volatile it can vaporize within 6 weeks. The vapors cause the dermatitis – sometimes spread out and sometimes patchy – after permeating the sofas, clothing, and shoe products during shipment.
Particularly concerning is very low exposure levels to dimethyl fumarate can trigger a reaction, concentrations well below those of common contact dermatitis allergens.
In an unprecedented move, Dr. Belsito revealed the leading contender, at least for now, for the 2012 Allergen of the Year: acrylates and methacrylates. Acrylates and methacrylates are polymers and adhesives. Methacrylate, for example, is used as bone cement for prosthetic devices placed during orthopedic surgery. The ACDS is soliciting feedback from members about naming this class of compounds at their next Allergen of the Year.
Neomcyin was the 2010 Allergen of the Year. Dr. Belsito described neomycin reactions as "common, not readily recognized, and problematic." Neomycin was chosen because of its widespread use as an over-the-counter antibiotic product; its high propensity for cross-reaction with other agents in the aminoglycoside class, including gentamicin, kanamycin, and tobramycin; and because neomycin is included as a preservative in some vaccines. Because a neomycin allergy is not a type 1 IgE-mediated, a reaction results in eczema, not anaphylaxis and death.
Gold was the 2001 Allergen of the Year, and reactions to gold are common and clinically problematic. Bacitracin (2003) and glucocorticosteroids (2005) are other allergens that are both common and clinically relevant. In contrast, thimerosal (2002) is a common but nonrelevant allergen because it has been removed from most products in the United States. A reaction to mixed dialkyl thioureas (2009), used in production of rubber products, is relatively uncommon but important when it occurs.
Dr. Belsito said that he had no relevant disclosures.
NEW ORLEANS – Dimethyl fumarate – a volatile substance included in shipments of furniture, clothing, and shoes to inhibit growth of mold – earned the distinction as the American Contact Dermatitis Society's 2011 Allergen of the Year.
"We had a difficult decision," Dr. Donald V. Belsito said. "But we decided to go with dimethyl fumarate. It caused an epidemic in Europe starting in 2007."
The substance is now being regulated in Europe, "although apparently some stuff is still sneaking through," Dr. Belsito said. "To date, I know of no cases in the U.S., although Dr. Melanie Pratt has had a few cases in Ontario."
Dimethyl fumarate "produces an extremely severe dermatitis," said Dr. Belsito, a dermatologist in private practice in Shawnee, Kan.
The unlikely story behind identification of this preservative and fungicide demonstrates the benefits of international collaboration, he noted.
First noted by dermatologists in Finland, cases of the severe dermatitis began to appear in Sweden and the U.K. The severe rash, seen predominantly on the backs of the legs, buttocks, and back, was an etiologic mystery. Through extensive sleuth work, Finnish dermatologists determined a common link – each person recently purchased furniture from a particular Chinese manufacturer.
It then became commonly called "sofa dermatitis." A contact allergy to the upholstery fabric was initially suspected. However, no common chemical or fabric was identified among the different pieces of furniture purchased by affected patients.
Dr. Magnus Bruze, an occupational and environmental dermatologist at Malmo University in Sweden, and other investigators took apart the furniture, patch tested 40 affected patients to various components, and eventually identified the culprit: dimethyl fumarate. The allergen was enclosed in packets similar in appearance to silicone packets often labeled "Warning: Do Not Eat."
Dimethyl fumarate is so volatile it can vaporize within 6 weeks. The vapors cause the dermatitis – sometimes spread out and sometimes patchy – after permeating the sofas, clothing, and shoe products during shipment.
Particularly concerning is very low exposure levels to dimethyl fumarate can trigger a reaction, concentrations well below those of common contact dermatitis allergens.
In an unprecedented move, Dr. Belsito revealed the leading contender, at least for now, for the 2012 Allergen of the Year: acrylates and methacrylates. Acrylates and methacrylates are polymers and adhesives. Methacrylate, for example, is used as bone cement for prosthetic devices placed during orthopedic surgery. The ACDS is soliciting feedback from members about naming this class of compounds at their next Allergen of the Year.
Neomcyin was the 2010 Allergen of the Year. Dr. Belsito described neomycin reactions as "common, not readily recognized, and problematic." Neomycin was chosen because of its widespread use as an over-the-counter antibiotic product; its high propensity for cross-reaction with other agents in the aminoglycoside class, including gentamicin, kanamycin, and tobramycin; and because neomycin is included as a preservative in some vaccines. Because a neomycin allergy is not a type 1 IgE-mediated, a reaction results in eczema, not anaphylaxis and death.
Gold was the 2001 Allergen of the Year, and reactions to gold are common and clinically problematic. Bacitracin (2003) and glucocorticosteroids (2005) are other allergens that are both common and clinically relevant. In contrast, thimerosal (2002) is a common but nonrelevant allergen because it has been removed from most products in the United States. A reaction to mixed dialkyl thioureas (2009), used in production of rubber products, is relatively uncommon but important when it occurs.
Dr. Belsito said that he had no relevant disclosures.
NEW ORLEANS – Dimethyl fumarate – a volatile substance included in shipments of furniture, clothing, and shoes to inhibit growth of mold – earned the distinction as the American Contact Dermatitis Society's 2011 Allergen of the Year.
"We had a difficult decision," Dr. Donald V. Belsito said. "But we decided to go with dimethyl fumarate. It caused an epidemic in Europe starting in 2007."
The substance is now being regulated in Europe, "although apparently some stuff is still sneaking through," Dr. Belsito said. "To date, I know of no cases in the U.S., although Dr. Melanie Pratt has had a few cases in Ontario."
Dimethyl fumarate "produces an extremely severe dermatitis," said Dr. Belsito, a dermatologist in private practice in Shawnee, Kan.
The unlikely story behind identification of this preservative and fungicide demonstrates the benefits of international collaboration, he noted.
First noted by dermatologists in Finland, cases of the severe dermatitis began to appear in Sweden and the U.K. The severe rash, seen predominantly on the backs of the legs, buttocks, and back, was an etiologic mystery. Through extensive sleuth work, Finnish dermatologists determined a common link – each person recently purchased furniture from a particular Chinese manufacturer.
It then became commonly called "sofa dermatitis." A contact allergy to the upholstery fabric was initially suspected. However, no common chemical or fabric was identified among the different pieces of furniture purchased by affected patients.
Dr. Magnus Bruze, an occupational and environmental dermatologist at Malmo University in Sweden, and other investigators took apart the furniture, patch tested 40 affected patients to various components, and eventually identified the culprit: dimethyl fumarate. The allergen was enclosed in packets similar in appearance to silicone packets often labeled "Warning: Do Not Eat."
Dimethyl fumarate is so volatile it can vaporize within 6 weeks. The vapors cause the dermatitis – sometimes spread out and sometimes patchy – after permeating the sofas, clothing, and shoe products during shipment.
Particularly concerning is very low exposure levels to dimethyl fumarate can trigger a reaction, concentrations well below those of common contact dermatitis allergens.
In an unprecedented move, Dr. Belsito revealed the leading contender, at least for now, for the 2012 Allergen of the Year: acrylates and methacrylates. Acrylates and methacrylates are polymers and adhesives. Methacrylate, for example, is used as bone cement for prosthetic devices placed during orthopedic surgery. The ACDS is soliciting feedback from members about naming this class of compounds at their next Allergen of the Year.
Neomcyin was the 2010 Allergen of the Year. Dr. Belsito described neomycin reactions as "common, not readily recognized, and problematic." Neomycin was chosen because of its widespread use as an over-the-counter antibiotic product; its high propensity for cross-reaction with other agents in the aminoglycoside class, including gentamicin, kanamycin, and tobramycin; and because neomycin is included as a preservative in some vaccines. Because a neomycin allergy is not a type 1 IgE-mediated, a reaction results in eczema, not anaphylaxis and death.
Gold was the 2001 Allergen of the Year, and reactions to gold are common and clinically problematic. Bacitracin (2003) and glucocorticosteroids (2005) are other allergens that are both common and clinically relevant. In contrast, thimerosal (2002) is a common but nonrelevant allergen because it has been removed from most products in the United States. A reaction to mixed dialkyl thioureas (2009), used in production of rubber products, is relatively uncommon but important when it occurs.
Dr. Belsito said that he had no relevant disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN CONTACT DERMATITIS SOCIETY
Dimethyl Fumarate Named 2011 Allergen of the Year
NEW ORLEANS – Dimethyl fumarate – a volatile substance included in shipments of furniture, clothing, and shoes to inhibit growth of mold – earned the distinction as the American Contact Dermatitis Society's 2011 Allergen of the Year.
"We had a difficult decision," Dr. Donald V. Belsito said. "But we decided to go with dimethyl fumarate. It caused an epidemic in Europe starting in 2007."
The substance is now being regulated in Europe, "although apparently some stuff is still sneaking through," Dr. Belsito said. "To date, I know of no cases in the U.S., although Dr. Melanie Pratt has had a few cases in Ontario."
Dimethyl fumarate "produces an extremely severe dermatitis," said Dr. Belsito, a dermatologist in private practice in Shawnee, Kan.
The unlikely story behind identification of this preservative and fungicide demonstrates the benefits of international collaboration, he noted.
First noted by dermatologists in Finland, cases of the severe dermatitis began to appear in Sweden and the U.K. The severe rash, seen predominantly on the backs of the legs, buttocks, and back, was an etiologic mystery. Through extensive sleuth work, Finnish dermatologists determined a common link – each person recently purchased furniture from a particular Chinese manufacturer.
It then became commonly called "sofa dermatitis." A contact allergy to the upholstery fabric was initially suspected. However, no common chemical or fabric was identified among the different pieces of furniture purchased by affected patients.
Dr. Magnus Bruze, an occupational and environmental dermatologist at Malmo University in Sweden, and other investigators took apart the furniture, patch tested 40 affected patients to various components, and eventually identified the culprit: dimethyl fumarate. The allergen was enclosed in packets similar in appearance to silicone packets often labeled "Warning: Do Not Eat."
Dimethyl fumarate is so volatile it can vaporize within 6 weeks. The vapors cause the dermatitis – sometimes spread out and sometimes patchy – after permeating the sofas, clothing, and shoe products during shipment.
Particularly concerning is very low exposure levels to dimethyl fumarate can trigger a reaction, concentrations well below those of common contact dermatitis allergens.
In an unprecedented move, Dr. Belsito revealed the leading contender, at least for now, for the 2012 Allergen of the Year: acrylates and methacrylates. Acrylates and methacrylates are polymers and adhesives. Methacrylate, for example, is used as bone cement for prosthetic devices placed during orthopedic surgery. The ACDS is soliciting feedback from members about naming this class of compounds at their next Allergen of the Year.
Neomcyin was the 2010 Allergen of the Year. Dr. Belsito described neomycin reactions as "common, not readily recognized, and problematic." Neomycin was chosen because of its widespread use as an over-the-counter antibiotic product; its high propensity for cross-reaction with other agents in the aminoglycoside class, including gentamicin, kanamycin, and tobramycin; and because neomycin is included as a preservative in some vaccines. Because a neomycin allergy is not a type 1 IgE-mediated, a reaction results in eczema, not anaphylaxis and death.
Gold was the 2001 Allergen of the Year, and reactions to gold are common and clinically problematic. Bacitracin (2003) and glucocorticosteroids (2005) are other allergens that are both common and clinically relevant. In contrast, thimerosal (2002) is a common but nonrelevant allergen because it has been removed from most products in the United States. A reaction to mixed dialkyl thioureas (2009), used in production of rubber products, is relatively uncommon but important when it occurs.
Dr. Belsito said that he had no relevant disclosures.
NEW ORLEANS – Dimethyl fumarate – a volatile substance included in shipments of furniture, clothing, and shoes to inhibit growth of mold – earned the distinction as the American Contact Dermatitis Society's 2011 Allergen of the Year.
"We had a difficult decision," Dr. Donald V. Belsito said. "But we decided to go with dimethyl fumarate. It caused an epidemic in Europe starting in 2007."
The substance is now being regulated in Europe, "although apparently some stuff is still sneaking through," Dr. Belsito said. "To date, I know of no cases in the U.S., although Dr. Melanie Pratt has had a few cases in Ontario."
Dimethyl fumarate "produces an extremely severe dermatitis," said Dr. Belsito, a dermatologist in private practice in Shawnee, Kan.
The unlikely story behind identification of this preservative and fungicide demonstrates the benefits of international collaboration, he noted.
First noted by dermatologists in Finland, cases of the severe dermatitis began to appear in Sweden and the U.K. The severe rash, seen predominantly on the backs of the legs, buttocks, and back, was an etiologic mystery. Through extensive sleuth work, Finnish dermatologists determined a common link – each person recently purchased furniture from a particular Chinese manufacturer.
It then became commonly called "sofa dermatitis." A contact allergy to the upholstery fabric was initially suspected. However, no common chemical or fabric was identified among the different pieces of furniture purchased by affected patients.
Dr. Magnus Bruze, an occupational and environmental dermatologist at Malmo University in Sweden, and other investigators took apart the furniture, patch tested 40 affected patients to various components, and eventually identified the culprit: dimethyl fumarate. The allergen was enclosed in packets similar in appearance to silicone packets often labeled "Warning: Do Not Eat."
Dimethyl fumarate is so volatile it can vaporize within 6 weeks. The vapors cause the dermatitis – sometimes spread out and sometimes patchy – after permeating the sofas, clothing, and shoe products during shipment.
Particularly concerning is very low exposure levels to dimethyl fumarate can trigger a reaction, concentrations well below those of common contact dermatitis allergens.
In an unprecedented move, Dr. Belsito revealed the leading contender, at least for now, for the 2012 Allergen of the Year: acrylates and methacrylates. Acrylates and methacrylates are polymers and adhesives. Methacrylate, for example, is used as bone cement for prosthetic devices placed during orthopedic surgery. The ACDS is soliciting feedback from members about naming this class of compounds at their next Allergen of the Year.
Neomcyin was the 2010 Allergen of the Year. Dr. Belsito described neomycin reactions as "common, not readily recognized, and problematic." Neomycin was chosen because of its widespread use as an over-the-counter antibiotic product; its high propensity for cross-reaction with other agents in the aminoglycoside class, including gentamicin, kanamycin, and tobramycin; and because neomycin is included as a preservative in some vaccines. Because a neomycin allergy is not a type 1 IgE-mediated, a reaction results in eczema, not anaphylaxis and death.
Gold was the 2001 Allergen of the Year, and reactions to gold are common and clinically problematic. Bacitracin (2003) and glucocorticosteroids (2005) are other allergens that are both common and clinically relevant. In contrast, thimerosal (2002) is a common but nonrelevant allergen because it has been removed from most products in the United States. A reaction to mixed dialkyl thioureas (2009), used in production of rubber products, is relatively uncommon but important when it occurs.
Dr. Belsito said that he had no relevant disclosures.
NEW ORLEANS – Dimethyl fumarate – a volatile substance included in shipments of furniture, clothing, and shoes to inhibit growth of mold – earned the distinction as the American Contact Dermatitis Society's 2011 Allergen of the Year.
"We had a difficult decision," Dr. Donald V. Belsito said. "But we decided to go with dimethyl fumarate. It caused an epidemic in Europe starting in 2007."
The substance is now being regulated in Europe, "although apparently some stuff is still sneaking through," Dr. Belsito said. "To date, I know of no cases in the U.S., although Dr. Melanie Pratt has had a few cases in Ontario."
Dimethyl fumarate "produces an extremely severe dermatitis," said Dr. Belsito, a dermatologist in private practice in Shawnee, Kan.
The unlikely story behind identification of this preservative and fungicide demonstrates the benefits of international collaboration, he noted.
First noted by dermatologists in Finland, cases of the severe dermatitis began to appear in Sweden and the U.K. The severe rash, seen predominantly on the backs of the legs, buttocks, and back, was an etiologic mystery. Through extensive sleuth work, Finnish dermatologists determined a common link – each person recently purchased furniture from a particular Chinese manufacturer.
It then became commonly called "sofa dermatitis." A contact allergy to the upholstery fabric was initially suspected. However, no common chemical or fabric was identified among the different pieces of furniture purchased by affected patients.
Dr. Magnus Bruze, an occupational and environmental dermatologist at Malmo University in Sweden, and other investigators took apart the furniture, patch tested 40 affected patients to various components, and eventually identified the culprit: dimethyl fumarate. The allergen was enclosed in packets similar in appearance to silicone packets often labeled "Warning: Do Not Eat."
Dimethyl fumarate is so volatile it can vaporize within 6 weeks. The vapors cause the dermatitis – sometimes spread out and sometimes patchy – after permeating the sofas, clothing, and shoe products during shipment.
Particularly concerning is very low exposure levels to dimethyl fumarate can trigger a reaction, concentrations well below those of common contact dermatitis allergens.
In an unprecedented move, Dr. Belsito revealed the leading contender, at least for now, for the 2012 Allergen of the Year: acrylates and methacrylates. Acrylates and methacrylates are polymers and adhesives. Methacrylate, for example, is used as bone cement for prosthetic devices placed during orthopedic surgery. The ACDS is soliciting feedback from members about naming this class of compounds at their next Allergen of the Year.
Neomcyin was the 2010 Allergen of the Year. Dr. Belsito described neomycin reactions as "common, not readily recognized, and problematic." Neomycin was chosen because of its widespread use as an over-the-counter antibiotic product; its high propensity for cross-reaction with other agents in the aminoglycoside class, including gentamicin, kanamycin, and tobramycin; and because neomycin is included as a preservative in some vaccines. Because a neomycin allergy is not a type 1 IgE-mediated, a reaction results in eczema, not anaphylaxis and death.
Gold was the 2001 Allergen of the Year, and reactions to gold are common and clinically problematic. Bacitracin (2003) and glucocorticosteroids (2005) are other allergens that are both common and clinically relevant. In contrast, thimerosal (2002) is a common but nonrelevant allergen because it has been removed from most products in the United States. A reaction to mixed dialkyl thioureas (2009), used in production of rubber products, is relatively uncommon but important when it occurs.
Dr. Belsito said that he had no relevant disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN CONTACT DERMATITIS SOCIETY
Better Survival Reported After EVAR Versus Open AAA Surgery
NAPLES, FLA. – Endovascular aneurysm repair is associated with better long-term survival compared with open abdominal aortic aneurysm surgery, although re-intervention rates for the two techniques were similar in a single-center, retrospective study.
In a registry of 1,066 endovascular aneurysm repair (EVAR) and 920 open abdominal aortic aneurysm (AAA) procedures, all-cause mortality in the first 100 months was 25% following EVAR and 39% after open repair. The mortality disparity was significant, even though the EVAR patients tended to be older and had more comorbidities, such as hypertension or diabetes, Dr. Brenton E. Quinney said at the annual meeting of the Southern Association for Vascular Surgery.
One-year mortality was 16% in the EVAR group and 28% in the open-repair group. At 5 years, mortality rose to 36% and 48%, respectively. "EVAR had better immediate, mid-term, and long-term survival out to 9 years," said Dr. Quinney, a vascular surgery fellow at the University of Alabama at Birmingham.
To compare durability of EVAR vs. open AAA, they examined EVAR cases performed from 1999 to 2009 and open repairs from 1985 to 2009 at the University of Alabama.
Secondary interventions were vascular (aortic graft-related or remote procedures, such as carotid surgery) or nonvascular (incisional or gastrointestinal surgery). "Patients required more secondary vascular procedures after EVAR," Dr. Quinney said. In contrast, "patients required more nonvascular procedures after open AAA repair."
Dr. Quinney and his associates found 12.3% of EVAR versus 5.1% of open surgery cases required graft-related subsequent procedures. "However, when we add GI complications and laparotomy complications, both groups are virtually identical with overall re-intervention rates," Dr. Quinney said. Specifically, 21.9% of the EVAR and 21.1% of the open cases required a re-intervention during the 290-month follow-up (mean, 27 months).
In the EVAR group, the graft-related secondary interventions were mostly minimally invasive transfemoral procedures (131 cases, or 56%). Subsequent nonaortic vascular procedures included 63 cases of infra-inguinal bypass, 13 thoracic aortic aneurysms (TAAs), and 4 gastrointestinal bleed repairs, Dr. Quinney said.
In the open-surgery group, graft-related re-interventions were mostly secondary aneurysm repairs (23 cases). There were also 34 infra-inguinal bypass procedures and 22 TAA repairs in this group. All 97 nonvascular secondary surgeries in the study occurred in patients who initially underwent open surgery.
"What would be your preferred approach to a healthy 54-year-old male patient when this man wants you to make the decision?" asked study discussant Dr. Karthikeshwar Kasirajan, director of clinical research, division of vascular surgery, at Emory University in Atlanta.
"In a 54-year-old with suitable anatomy for AAA, we would probably recommend an EVAR," Dr. Quinney replied.
Potential limitations include the retrospective study design based on nonvascular procedures from medical records and patient reports. Also, the registry at the University of Alabama tracks only procedures, not patients, so "one patient could have had multiple procedures," Dr. Quinney said.
These current findings demonstrating a long-term survival benefit with EVAR differ from results of the Dutch Randomized Endovascular Aneurysm Management (DREAM) trial (N. Engl. J. Med. 2005;352:2398-405). EVAR showed an early postoperative survival advantage versus open repair in the DREAM trial, but "mortality equalized at 1 year," Dr. Quinney said.
Secondary intervention rates in this patient population vary, partly because of different follow-up times, Dr. Quinney said, noting that a comparison of 444 EVAR and 437 open-repair outcomes during a mean 1.8-year follow-up found essentially equivalent rates of secondary interventions (JAMA 2009;302:1535-42). Another study showed a 9.8% re-intervention rate among 543 EVAR cases, compared with 5.8% of 539 open repairs over 4 years (Lancet 2004;364:843-8).
Dr. Quinney said that he had no relevant disclosures. Dr. Kasirajan receives research support from W.L. Gore and Medtronic.
NAPLES, FLA. – Endovascular aneurysm repair is associated with better long-term survival compared with open abdominal aortic aneurysm surgery, although re-intervention rates for the two techniques were similar in a single-center, retrospective study.
In a registry of 1,066 endovascular aneurysm repair (EVAR) and 920 open abdominal aortic aneurysm (AAA) procedures, all-cause mortality in the first 100 months was 25% following EVAR and 39% after open repair. The mortality disparity was significant, even though the EVAR patients tended to be older and had more comorbidities, such as hypertension or diabetes, Dr. Brenton E. Quinney said at the annual meeting of the Southern Association for Vascular Surgery.
One-year mortality was 16% in the EVAR group and 28% in the open-repair group. At 5 years, mortality rose to 36% and 48%, respectively. "EVAR had better immediate, mid-term, and long-term survival out to 9 years," said Dr. Quinney, a vascular surgery fellow at the University of Alabama at Birmingham.
To compare durability of EVAR vs. open AAA, they examined EVAR cases performed from 1999 to 2009 and open repairs from 1985 to 2009 at the University of Alabama.
Secondary interventions were vascular (aortic graft-related or remote procedures, such as carotid surgery) or nonvascular (incisional or gastrointestinal surgery). "Patients required more secondary vascular procedures after EVAR," Dr. Quinney said. In contrast, "patients required more nonvascular procedures after open AAA repair."
Dr. Quinney and his associates found 12.3% of EVAR versus 5.1% of open surgery cases required graft-related subsequent procedures. "However, when we add GI complications and laparotomy complications, both groups are virtually identical with overall re-intervention rates," Dr. Quinney said. Specifically, 21.9% of the EVAR and 21.1% of the open cases required a re-intervention during the 290-month follow-up (mean, 27 months).
In the EVAR group, the graft-related secondary interventions were mostly minimally invasive transfemoral procedures (131 cases, or 56%). Subsequent nonaortic vascular procedures included 63 cases of infra-inguinal bypass, 13 thoracic aortic aneurysms (TAAs), and 4 gastrointestinal bleed repairs, Dr. Quinney said.
In the open-surgery group, graft-related re-interventions were mostly secondary aneurysm repairs (23 cases). There were also 34 infra-inguinal bypass procedures and 22 TAA repairs in this group. All 97 nonvascular secondary surgeries in the study occurred in patients who initially underwent open surgery.
"What would be your preferred approach to a healthy 54-year-old male patient when this man wants you to make the decision?" asked study discussant Dr. Karthikeshwar Kasirajan, director of clinical research, division of vascular surgery, at Emory University in Atlanta.
"In a 54-year-old with suitable anatomy for AAA, we would probably recommend an EVAR," Dr. Quinney replied.
Potential limitations include the retrospective study design based on nonvascular procedures from medical records and patient reports. Also, the registry at the University of Alabama tracks only procedures, not patients, so "one patient could have had multiple procedures," Dr. Quinney said.
These current findings demonstrating a long-term survival benefit with EVAR differ from results of the Dutch Randomized Endovascular Aneurysm Management (DREAM) trial (N. Engl. J. Med. 2005;352:2398-405). EVAR showed an early postoperative survival advantage versus open repair in the DREAM trial, but "mortality equalized at 1 year," Dr. Quinney said.
Secondary intervention rates in this patient population vary, partly because of different follow-up times, Dr. Quinney said, noting that a comparison of 444 EVAR and 437 open-repair outcomes during a mean 1.8-year follow-up found essentially equivalent rates of secondary interventions (JAMA 2009;302:1535-42). Another study showed a 9.8% re-intervention rate among 543 EVAR cases, compared with 5.8% of 539 open repairs over 4 years (Lancet 2004;364:843-8).
Dr. Quinney said that he had no relevant disclosures. Dr. Kasirajan receives research support from W.L. Gore and Medtronic.
NAPLES, FLA. – Endovascular aneurysm repair is associated with better long-term survival compared with open abdominal aortic aneurysm surgery, although re-intervention rates for the two techniques were similar in a single-center, retrospective study.
In a registry of 1,066 endovascular aneurysm repair (EVAR) and 920 open abdominal aortic aneurysm (AAA) procedures, all-cause mortality in the first 100 months was 25% following EVAR and 39% after open repair. The mortality disparity was significant, even though the EVAR patients tended to be older and had more comorbidities, such as hypertension or diabetes, Dr. Brenton E. Quinney said at the annual meeting of the Southern Association for Vascular Surgery.
One-year mortality was 16% in the EVAR group and 28% in the open-repair group. At 5 years, mortality rose to 36% and 48%, respectively. "EVAR had better immediate, mid-term, and long-term survival out to 9 years," said Dr. Quinney, a vascular surgery fellow at the University of Alabama at Birmingham.
To compare durability of EVAR vs. open AAA, they examined EVAR cases performed from 1999 to 2009 and open repairs from 1985 to 2009 at the University of Alabama.
Secondary interventions were vascular (aortic graft-related or remote procedures, such as carotid surgery) or nonvascular (incisional or gastrointestinal surgery). "Patients required more secondary vascular procedures after EVAR," Dr. Quinney said. In contrast, "patients required more nonvascular procedures after open AAA repair."
Dr. Quinney and his associates found 12.3% of EVAR versus 5.1% of open surgery cases required graft-related subsequent procedures. "However, when we add GI complications and laparotomy complications, both groups are virtually identical with overall re-intervention rates," Dr. Quinney said. Specifically, 21.9% of the EVAR and 21.1% of the open cases required a re-intervention during the 290-month follow-up (mean, 27 months).
In the EVAR group, the graft-related secondary interventions were mostly minimally invasive transfemoral procedures (131 cases, or 56%). Subsequent nonaortic vascular procedures included 63 cases of infra-inguinal bypass, 13 thoracic aortic aneurysms (TAAs), and 4 gastrointestinal bleed repairs, Dr. Quinney said.
In the open-surgery group, graft-related re-interventions were mostly secondary aneurysm repairs (23 cases). There were also 34 infra-inguinal bypass procedures and 22 TAA repairs in this group. All 97 nonvascular secondary surgeries in the study occurred in patients who initially underwent open surgery.
"What would be your preferred approach to a healthy 54-year-old male patient when this man wants you to make the decision?" asked study discussant Dr. Karthikeshwar Kasirajan, director of clinical research, division of vascular surgery, at Emory University in Atlanta.
"In a 54-year-old with suitable anatomy for AAA, we would probably recommend an EVAR," Dr. Quinney replied.
Potential limitations include the retrospective study design based on nonvascular procedures from medical records and patient reports. Also, the registry at the University of Alabama tracks only procedures, not patients, so "one patient could have had multiple procedures," Dr. Quinney said.
These current findings demonstrating a long-term survival benefit with EVAR differ from results of the Dutch Randomized Endovascular Aneurysm Management (DREAM) trial (N. Engl. J. Med. 2005;352:2398-405). EVAR showed an early postoperative survival advantage versus open repair in the DREAM trial, but "mortality equalized at 1 year," Dr. Quinney said.
Secondary intervention rates in this patient population vary, partly because of different follow-up times, Dr. Quinney said, noting that a comparison of 444 EVAR and 437 open-repair outcomes during a mean 1.8-year follow-up found essentially equivalent rates of secondary interventions (JAMA 2009;302:1535-42). Another study showed a 9.8% re-intervention rate among 543 EVAR cases, compared with 5.8% of 539 open repairs over 4 years (Lancet 2004;364:843-8).
Dr. Quinney said that he had no relevant disclosures. Dr. Kasirajan receives research support from W.L. Gore and Medtronic.
Better Survival Reported After EVAR Versus Open AAA Surgery
NAPLES, FLA. – Endovascular aneurysm repair is associated with better long-term survival compared with open abdominal aortic aneurysm surgery, although re-intervention rates for the two techniques were similar in a single-center, retrospective study.
In a registry of 1,066 endovascular aneurysm repair (EVAR) and 920 open abdominal aortic aneurysm (AAA) procedures, all-cause mortality in the first 100 months was 25% following EVAR and 39% after open repair. The mortality disparity was significant, even though the EVAR patients tended to be older and had more comorbidities, such as hypertension or diabetes, Dr. Brenton E. Quinney said at the annual meeting of the Southern Association for Vascular Surgery.
One-year mortality was 16% in the EVAR group and 28% in the open-repair group. At 5 years, mortality rose to 36% and 48%, respectively. "EVAR had better immediate, mid-term, and long-term survival out to 9 years," said Dr. Quinney, a vascular surgery fellow at the University of Alabama at Birmingham.
To compare durability of EVAR vs. open AAA, they examined EVAR cases performed from 1999 to 2009 and open repairs from 1985 to 2009 at the University of Alabama.
Secondary interventions were vascular (aortic graft-related or remote procedures, such as carotid surgery) or nonvascular (incisional or gastrointestinal surgery). "Patients required more secondary vascular procedures after EVAR," Dr. Quinney said. In contrast, "patients required more nonvascular procedures after open AAA repair."
Dr. Quinney and his associates found 12.3% of EVAR versus 5.1% of open surgery cases required graft-related subsequent procedures. "However, when we add GI complications and laparotomy complications, both groups are virtually identical with overall re-intervention rates," Dr. Quinney said. Specifically, 21.9% of the EVAR and 21.1% of the open cases required a re-intervention during the 290-month follow-up (mean, 27 months).
In the EVAR group, the graft-related secondary interventions were mostly minimally invasive transfemoral procedures (131 cases, or 56%). Subsequent nonaortic vascular procedures included 63 cases of infra-inguinal bypass, 13 thoracic aortic aneurysms (TAAs), and 4 gastrointestinal bleed repairs, Dr. Quinney said.
In the open-surgery group, graft-related re-interventions were mostly secondary aneurysm repairs (23 cases). There were also 34 infra-inguinal bypass procedures and 22 TAA repairs in this group. All 97 nonvascular secondary surgeries in the study occurred in patients who initially underwent open surgery.
"What would be your preferred approach to a healthy 54-year-old male patient when this man wants you to make the decision?" asked study discussant Dr. Karthikeshwar Kasirajan, director of clinical research, division of vascular surgery, at Emory University in Atlanta.
"In a 54-year-old with suitable anatomy for AAA, we would probably recommend an EVAR," Dr. Quinney replied.
Potential limitations include the retrospective study design based on nonvascular procedures from medical records and patient reports. Also, the registry at the University of Alabama tracks only procedures, not patients, so "one patient could have had multiple procedures," Dr. Quinney said.
These current findings demonstrating a long-term survival benefit with EVAR differ from results of the Dutch Randomized Endovascular Aneurysm Management (DREAM) trial (N. Engl. J. Med. 2005;352:2398-405). EVAR showed an early postoperative survival advantage versus open repair in the DREAM trial, but "mortality equalized at 1 year," Dr. Quinney said.
Secondary intervention rates in this patient population vary, partly because of different follow-up times, Dr. Quinney said, noting that a comparison of 444 EVAR and 437 open-repair outcomes during a mean 1.8-year follow-up found essentially equivalent rates of secondary interventions (JAMA 2009;302:1535-42). Another study showed a 9.8% re-intervention rate among 543 EVAR cases, compared with 5.8% of 539 open repairs over 4 years (Lancet 2004;364:843-8).
Dr. Quinney said that he had no relevant disclosures. Dr. Kasirajan receives research support from W.L. Gore and Medtronic.
NAPLES, FLA. – Endovascular aneurysm repair is associated with better long-term survival compared with open abdominal aortic aneurysm surgery, although re-intervention rates for the two techniques were similar in a single-center, retrospective study.
In a registry of 1,066 endovascular aneurysm repair (EVAR) and 920 open abdominal aortic aneurysm (AAA) procedures, all-cause mortality in the first 100 months was 25% following EVAR and 39% after open repair. The mortality disparity was significant, even though the EVAR patients tended to be older and had more comorbidities, such as hypertension or diabetes, Dr. Brenton E. Quinney said at the annual meeting of the Southern Association for Vascular Surgery.
One-year mortality was 16% in the EVAR group and 28% in the open-repair group. At 5 years, mortality rose to 36% and 48%, respectively. "EVAR had better immediate, mid-term, and long-term survival out to 9 years," said Dr. Quinney, a vascular surgery fellow at the University of Alabama at Birmingham.
To compare durability of EVAR vs. open AAA, they examined EVAR cases performed from 1999 to 2009 and open repairs from 1985 to 2009 at the University of Alabama.
Secondary interventions were vascular (aortic graft-related or remote procedures, such as carotid surgery) or nonvascular (incisional or gastrointestinal surgery). "Patients required more secondary vascular procedures after EVAR," Dr. Quinney said. In contrast, "patients required more nonvascular procedures after open AAA repair."
Dr. Quinney and his associates found 12.3% of EVAR versus 5.1% of open surgery cases required graft-related subsequent procedures. "However, when we add GI complications and laparotomy complications, both groups are virtually identical with overall re-intervention rates," Dr. Quinney said. Specifically, 21.9% of the EVAR and 21.1% of the open cases required a re-intervention during the 290-month follow-up (mean, 27 months).
In the EVAR group, the graft-related secondary interventions were mostly minimally invasive transfemoral procedures (131 cases, or 56%). Subsequent nonaortic vascular procedures included 63 cases of infra-inguinal bypass, 13 thoracic aortic aneurysms (TAAs), and 4 gastrointestinal bleed repairs, Dr. Quinney said.
In the open-surgery group, graft-related re-interventions were mostly secondary aneurysm repairs (23 cases). There were also 34 infra-inguinal bypass procedures and 22 TAA repairs in this group. All 97 nonvascular secondary surgeries in the study occurred in patients who initially underwent open surgery.
"What would be your preferred approach to a healthy 54-year-old male patient when this man wants you to make the decision?" asked study discussant Dr. Karthikeshwar Kasirajan, director of clinical research, division of vascular surgery, at Emory University in Atlanta.
"In a 54-year-old with suitable anatomy for AAA, we would probably recommend an EVAR," Dr. Quinney replied.
Potential limitations include the retrospective study design based on nonvascular procedures from medical records and patient reports. Also, the registry at the University of Alabama tracks only procedures, not patients, so "one patient could have had multiple procedures," Dr. Quinney said.
These current findings demonstrating a long-term survival benefit with EVAR differ from results of the Dutch Randomized Endovascular Aneurysm Management (DREAM) trial (N. Engl. J. Med. 2005;352:2398-405). EVAR showed an early postoperative survival advantage versus open repair in the DREAM trial, but "mortality equalized at 1 year," Dr. Quinney said.
Secondary intervention rates in this patient population vary, partly because of different follow-up times, Dr. Quinney said, noting that a comparison of 444 EVAR and 437 open-repair outcomes during a mean 1.8-year follow-up found essentially equivalent rates of secondary interventions (JAMA 2009;302:1535-42). Another study showed a 9.8% re-intervention rate among 543 EVAR cases, compared with 5.8% of 539 open repairs over 4 years (Lancet 2004;364:843-8).
Dr. Quinney said that he had no relevant disclosures. Dr. Kasirajan receives research support from W.L. Gore and Medtronic.
NAPLES, FLA. – Endovascular aneurysm repair is associated with better long-term survival compared with open abdominal aortic aneurysm surgery, although re-intervention rates for the two techniques were similar in a single-center, retrospective study.
In a registry of 1,066 endovascular aneurysm repair (EVAR) and 920 open abdominal aortic aneurysm (AAA) procedures, all-cause mortality in the first 100 months was 25% following EVAR and 39% after open repair. The mortality disparity was significant, even though the EVAR patients tended to be older and had more comorbidities, such as hypertension or diabetes, Dr. Brenton E. Quinney said at the annual meeting of the Southern Association for Vascular Surgery.
One-year mortality was 16% in the EVAR group and 28% in the open-repair group. At 5 years, mortality rose to 36% and 48%, respectively. "EVAR had better immediate, mid-term, and long-term survival out to 9 years," said Dr. Quinney, a vascular surgery fellow at the University of Alabama at Birmingham.
To compare durability of EVAR vs. open AAA, they examined EVAR cases performed from 1999 to 2009 and open repairs from 1985 to 2009 at the University of Alabama.
Secondary interventions were vascular (aortic graft-related or remote procedures, such as carotid surgery) or nonvascular (incisional or gastrointestinal surgery). "Patients required more secondary vascular procedures after EVAR," Dr. Quinney said. In contrast, "patients required more nonvascular procedures after open AAA repair."
Dr. Quinney and his associates found 12.3% of EVAR versus 5.1% of open surgery cases required graft-related subsequent procedures. "However, when we add GI complications and laparotomy complications, both groups are virtually identical with overall re-intervention rates," Dr. Quinney said. Specifically, 21.9% of the EVAR and 21.1% of the open cases required a re-intervention during the 290-month follow-up (mean, 27 months).
In the EVAR group, the graft-related secondary interventions were mostly minimally invasive transfemoral procedures (131 cases, or 56%). Subsequent nonaortic vascular procedures included 63 cases of infra-inguinal bypass, 13 thoracic aortic aneurysms (TAAs), and 4 gastrointestinal bleed repairs, Dr. Quinney said.
In the open-surgery group, graft-related re-interventions were mostly secondary aneurysm repairs (23 cases). There were also 34 infra-inguinal bypass procedures and 22 TAA repairs in this group. All 97 nonvascular secondary surgeries in the study occurred in patients who initially underwent open surgery.
"What would be your preferred approach to a healthy 54-year-old male patient when this man wants you to make the decision?" asked study discussant Dr. Karthikeshwar Kasirajan, director of clinical research, division of vascular surgery, at Emory University in Atlanta.
"In a 54-year-old with suitable anatomy for AAA, we would probably recommend an EVAR," Dr. Quinney replied.
Potential limitations include the retrospective study design based on nonvascular procedures from medical records and patient reports. Also, the registry at the University of Alabama tracks only procedures, not patients, so "one patient could have had multiple procedures," Dr. Quinney said.
These current findings demonstrating a long-term survival benefit with EVAR differ from results of the Dutch Randomized Endovascular Aneurysm Management (DREAM) trial (N. Engl. J. Med. 2005;352:2398-405). EVAR showed an early postoperative survival advantage versus open repair in the DREAM trial, but "mortality equalized at 1 year," Dr. Quinney said.
Secondary intervention rates in this patient population vary, partly because of different follow-up times, Dr. Quinney said, noting that a comparison of 444 EVAR and 437 open-repair outcomes during a mean 1.8-year follow-up found essentially equivalent rates of secondary interventions (JAMA 2009;302:1535-42). Another study showed a 9.8% re-intervention rate among 543 EVAR cases, compared with 5.8% of 539 open repairs over 4 years (Lancet 2004;364:843-8).
Dr. Quinney said that he had no relevant disclosures. Dr. Kasirajan receives research support from W.L. Gore and Medtronic.
Major Finding: All-cause mortality was 25% following endovascular aneurysm repair versus 39% after open surgery in 100-month follow-up.
Data Source: Retrospective study of 1,066 endovascular and 920 open aneurysm procedures.
Disclosures: Dr. Quinney said he had no relevant disclosures.
Targeted Interventions Improve Hip Fracture Outcomes
Major Finding: Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (odds ratio = 0.19).
Data Source: The Hip Fracture Intervention Trial (HIPFIT) compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions versus 62 randomized to usual care (6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies).
Disclosures: Dr. Singh said she had no relevant financial disclosures.
NEW ORLEANS — Compared with usual care after hip fracture, a comprehensive and targeted intervention that includes high-intensity progressive resistance training over 12 months lowers mortality, decreases nursing home admissions, improves activities of daily living dependency, and decreases the use of assistive devices, according to a randomized, controlled trial.
“It is possible to change the most important outcomes for these people,” Dr. Maria A. Fiatarone Singh said.
Functional dependency, however, did not significantly differ between groups.
Many facets of hip fractures have been studied, from pharmacologic prevention of osteoporosis to acute hospital interventions to fracture rehabilitation. “Although we've done a lot of studies, we still have not figured out how to prevent people from entering a nursing home or dying,” said Dr. Singh, professor of medicine and chair of exercise and sport science at the University of Sydney.
So Dr. Singh and her colleagues launched the Hip Fracture Intervention Trial (HIPFIT). They compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions vs. 62 patients randomized to usual care. She presented results at the meeting.
Intervention was associated with an 84% reduction in the likelihood of nursing home admission (odds ratio, 0.16), compared with usual care, Dr. Singh explained. In absolute numbers, 5 intervention patients (8%) and 12 control patients (19%) were admitted to a nursing home during the 12 months of follow-up.
“Hip fracture is associated with chronic pain, reduced mobility, disability, and increasing degree of dependence. After hip fracture, 10%–20% of formerly community-dwelling people require long-term nursing home care,” Dr. Singh said.
Four intervention patients and eight usual-care patients died. Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (OR = 0.19). Cardiovascular disease, infection, and stroke were among the causes.
Dr. Singh and her associates hypothesized that long-term disability and nursing home utilization after hip fracture would be reduced by targeted, multifactorial intervention aimed at the primary risk factors. They chose modifiable risk factors to make application of their findings more practical, including sarcopenia/muscle weakness, poor balance or gait, malnutrition or weight loss, vitamin D insufficiency, and vision concerns.
All intervention group participants received hip protectors and supervised, high-intensity, progressive resistance training for 12 months. The protocol included seven exercises designed for both upper and lower body strength. A meeting attendee questioned how patients were able to exercise after hip fracture. The intervention began with an isometric measure of strength and actual strength training started about 6 months after fracture, Dr. Singh replied.
Balance training exercises were progressive as well. As tasks were mastered, participants graduated to a more difficult level. For example, if a person could balance holding on to something with two hands, next they progressed to one hand and then to one finger.
Interventions were added for individual participants as needed, up to a total of 13. Treatment of depression, nutritional supplementation, medication management, and vision assessment are examples. Some participants received home assessment and referral to community services. Others received interventions to address risk and/or fear of falling, low self-efficacy, and polypharmacy.
Evaluations were done at baseline and at 4 and 12 months after fracture, with regular review by geriatricians, general practitioners, and ophthalmologists.
Usual care included 6–12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies.
Even though overall functional dependency did not differ significantly, intervention was associated with significantly less decline in some functional dependency KATZ scores (total, continence, and transfer) at 12 months, compared with their prefracture baseline.
In the current study, after the researchers controlled for age, there was less of a decline in function for total KATZ score, transfer change, and continence change if patients were in intervention group vs. usual care, Dr. Singh said.
At baseline, the community-dwelling participants were 69% female; mean age, 79 years; 83% at nutritional risk; 88% vitamin D insufficient; 90% living independently (vs. 10% in nursing homes); and 38% were cognitively impaired. A total 45% were depressed. The mean number of chronic diseases was 3.4. The usual-care group reported worse bodily pain, the only significant difference between groups.
There were no adverse events, except for some musculoskeletal soreness after activity, said Dr. Singh, who is also a senior research associate at Harvard University and a visiting scientist for the Jean Mayer USDA Human Nutrition Research Centre on Aging at Tufts University, all in Boston.
Resistance training was 1 of 13 interventions that kept hip fracture patients out of nursing homes.
Source ©Martinan/Fotolia.com
Major Finding: Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (odds ratio = 0.19).
Data Source: The Hip Fracture Intervention Trial (HIPFIT) compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions versus 62 randomized to usual care (6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies).
Disclosures: Dr. Singh said she had no relevant financial disclosures.
NEW ORLEANS — Compared with usual care after hip fracture, a comprehensive and targeted intervention that includes high-intensity progressive resistance training over 12 months lowers mortality, decreases nursing home admissions, improves activities of daily living dependency, and decreases the use of assistive devices, according to a randomized, controlled trial.
“It is possible to change the most important outcomes for these people,” Dr. Maria A. Fiatarone Singh said.
Functional dependency, however, did not significantly differ between groups.
Many facets of hip fractures have been studied, from pharmacologic prevention of osteoporosis to acute hospital interventions to fracture rehabilitation. “Although we've done a lot of studies, we still have not figured out how to prevent people from entering a nursing home or dying,” said Dr. Singh, professor of medicine and chair of exercise and sport science at the University of Sydney.
So Dr. Singh and her colleagues launched the Hip Fracture Intervention Trial (HIPFIT). They compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions vs. 62 patients randomized to usual care. She presented results at the meeting.
Intervention was associated with an 84% reduction in the likelihood of nursing home admission (odds ratio, 0.16), compared with usual care, Dr. Singh explained. In absolute numbers, 5 intervention patients (8%) and 12 control patients (19%) were admitted to a nursing home during the 12 months of follow-up.
“Hip fracture is associated with chronic pain, reduced mobility, disability, and increasing degree of dependence. After hip fracture, 10%–20% of formerly community-dwelling people require long-term nursing home care,” Dr. Singh said.
Four intervention patients and eight usual-care patients died. Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (OR = 0.19). Cardiovascular disease, infection, and stroke were among the causes.
Dr. Singh and her associates hypothesized that long-term disability and nursing home utilization after hip fracture would be reduced by targeted, multifactorial intervention aimed at the primary risk factors. They chose modifiable risk factors to make application of their findings more practical, including sarcopenia/muscle weakness, poor balance or gait, malnutrition or weight loss, vitamin D insufficiency, and vision concerns.
All intervention group participants received hip protectors and supervised, high-intensity, progressive resistance training for 12 months. The protocol included seven exercises designed for both upper and lower body strength. A meeting attendee questioned how patients were able to exercise after hip fracture. The intervention began with an isometric measure of strength and actual strength training started about 6 months after fracture, Dr. Singh replied.
Balance training exercises were progressive as well. As tasks were mastered, participants graduated to a more difficult level. For example, if a person could balance holding on to something with two hands, next they progressed to one hand and then to one finger.
Interventions were added for individual participants as needed, up to a total of 13. Treatment of depression, nutritional supplementation, medication management, and vision assessment are examples. Some participants received home assessment and referral to community services. Others received interventions to address risk and/or fear of falling, low self-efficacy, and polypharmacy.
Evaluations were done at baseline and at 4 and 12 months after fracture, with regular review by geriatricians, general practitioners, and ophthalmologists.
Usual care included 6–12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies.
Even though overall functional dependency did not differ significantly, intervention was associated with significantly less decline in some functional dependency KATZ scores (total, continence, and transfer) at 12 months, compared with their prefracture baseline.
In the current study, after the researchers controlled for age, there was less of a decline in function for total KATZ score, transfer change, and continence change if patients were in intervention group vs. usual care, Dr. Singh said.
At baseline, the community-dwelling participants were 69% female; mean age, 79 years; 83% at nutritional risk; 88% vitamin D insufficient; 90% living independently (vs. 10% in nursing homes); and 38% were cognitively impaired. A total 45% were depressed. The mean number of chronic diseases was 3.4. The usual-care group reported worse bodily pain, the only significant difference between groups.
There were no adverse events, except for some musculoskeletal soreness after activity, said Dr. Singh, who is also a senior research associate at Harvard University and a visiting scientist for the Jean Mayer USDA Human Nutrition Research Centre on Aging at Tufts University, all in Boston.
Resistance training was 1 of 13 interventions that kept hip fracture patients out of nursing homes.
Source ©Martinan/Fotolia.com
Major Finding: Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (odds ratio = 0.19).
Data Source: The Hip Fracture Intervention Trial (HIPFIT) compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions versus 62 randomized to usual care (6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies).
Disclosures: Dr. Singh said she had no relevant financial disclosures.
NEW ORLEANS — Compared with usual care after hip fracture, a comprehensive and targeted intervention that includes high-intensity progressive resistance training over 12 months lowers mortality, decreases nursing home admissions, improves activities of daily living dependency, and decreases the use of assistive devices, according to a randomized, controlled trial.
“It is possible to change the most important outcomes for these people,” Dr. Maria A. Fiatarone Singh said.
Functional dependency, however, did not significantly differ between groups.
Many facets of hip fractures have been studied, from pharmacologic prevention of osteoporosis to acute hospital interventions to fracture rehabilitation. “Although we've done a lot of studies, we still have not figured out how to prevent people from entering a nursing home or dying,” said Dr. Singh, professor of medicine and chair of exercise and sport science at the University of Sydney.
So Dr. Singh and her colleagues launched the Hip Fracture Intervention Trial (HIPFIT). They compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions vs. 62 patients randomized to usual care. She presented results at the meeting.
Intervention was associated with an 84% reduction in the likelihood of nursing home admission (odds ratio, 0.16), compared with usual care, Dr. Singh explained. In absolute numbers, 5 intervention patients (8%) and 12 control patients (19%) were admitted to a nursing home during the 12 months of follow-up.
“Hip fracture is associated with chronic pain, reduced mobility, disability, and increasing degree of dependence. After hip fracture, 10%–20% of formerly community-dwelling people require long-term nursing home care,” Dr. Singh said.
Four intervention patients and eight usual-care patients died. Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (OR = 0.19). Cardiovascular disease, infection, and stroke were among the causes.
Dr. Singh and her associates hypothesized that long-term disability and nursing home utilization after hip fracture would be reduced by targeted, multifactorial intervention aimed at the primary risk factors. They chose modifiable risk factors to make application of their findings more practical, including sarcopenia/muscle weakness, poor balance or gait, malnutrition or weight loss, vitamin D insufficiency, and vision concerns.
All intervention group participants received hip protectors and supervised, high-intensity, progressive resistance training for 12 months. The protocol included seven exercises designed for both upper and lower body strength. A meeting attendee questioned how patients were able to exercise after hip fracture. The intervention began with an isometric measure of strength and actual strength training started about 6 months after fracture, Dr. Singh replied.
Balance training exercises were progressive as well. As tasks were mastered, participants graduated to a more difficult level. For example, if a person could balance holding on to something with two hands, next they progressed to one hand and then to one finger.
Interventions were added for individual participants as needed, up to a total of 13. Treatment of depression, nutritional supplementation, medication management, and vision assessment are examples. Some participants received home assessment and referral to community services. Others received interventions to address risk and/or fear of falling, low self-efficacy, and polypharmacy.
Evaluations were done at baseline and at 4 and 12 months after fracture, with regular review by geriatricians, general practitioners, and ophthalmologists.
Usual care included 6–12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies.
Even though overall functional dependency did not differ significantly, intervention was associated with significantly less decline in some functional dependency KATZ scores (total, continence, and transfer) at 12 months, compared with their prefracture baseline.
In the current study, after the researchers controlled for age, there was less of a decline in function for total KATZ score, transfer change, and continence change if patients were in intervention group vs. usual care, Dr. Singh said.
At baseline, the community-dwelling participants were 69% female; mean age, 79 years; 83% at nutritional risk; 88% vitamin D insufficient; 90% living independently (vs. 10% in nursing homes); and 38% were cognitively impaired. A total 45% were depressed. The mean number of chronic diseases was 3.4. The usual-care group reported worse bodily pain, the only significant difference between groups.
There were no adverse events, except for some musculoskeletal soreness after activity, said Dr. Singh, who is also a senior research associate at Harvard University and a visiting scientist for the Jean Mayer USDA Human Nutrition Research Centre on Aging at Tufts University, all in Boston.
Resistance training was 1 of 13 interventions that kept hip fracture patients out of nursing homes.
Source ©Martinan/Fotolia.com
From the Annual Meeting of the Gerontological Society of America
Beyond the Convention Center: Dermatologists Give Back
With more than a hundred dermatologists and other volunteers signed up to help, Thursday's (Feb. 3) "Dermatology in Action" project is expected to be a great success and help to a local community in New Orleans still recovering from Hurricane Katrina, American Academy of Dermatology president William D. James said in an interview.
Before the 2010 Summer Academy Meeting, Dr. James and his wife came up with the idea to have the academy donate shade structures to local parks in Chicago.
"I've been thinking about volunteering in a variety of different ways during my presidency," Dr. James said. "We thought it would be nice to leave something behind in the cities where we have our meetings, either something permanent or [through] a volunteer project."
With more time to plan for this year's annual meeting, the community outreach project in New Orleans kept growing. Medical supplies are being donated to help underprivileged patients at the Tulane University Community Health Centers, money is being donated to help the local community, and volunteers will be refurbishing a community center and planting a nearby urban garden at the volunteer event.
"New Orleans seems like an ideal community to give something back to," said Dr. James.
This is the first time the Academy has organized a hands-on volunteer event around a meeting, and the feedback has been very positive, he said. "People are very excited about it." Dr. James will pitch in along with his wife and friends.
The details of the project remained fluid until a couple weeks ago. Based on the number who registered, HandsOn New Orleans, an organization that coordinates local volunteer efforts, suggested several options to the Academy.
"Because we had a good turnout, the opportunity we selected has to do with a community center in the Ninth Ward. That is a part of New Orleans that was fairly hard hit [by Hurricane Katrina]," Dr. James said. The center offers literacy services, job training, recreational facilities, and is a community gathering place. The center also has a small kitchen and living quarters for families in transition.
"The neighborhood does not have a grocery store within biking distance," Dr. James said. "So we decided to help them plant an urban garden space to help people grow their own vegetables. We will remove overgrowth, build raised beds, add soil and mulch, and help them grow their own food."
The volunteers will also leave room for paths to connect the garden to the community center building. Others will help repair the building itself, which has some broken windows and needs some drywall and painting work done, Dr. James said.
Money donated through the Academy Sustaining Fund will help purchase books for the center to facilitate tutoring of local residents.
Unlike the donation of shade structures to parks in Chicago – connected directly to the Academy's sun protection messages – the New Orleans project has wider implications. "This event could be a model for other conventions. One advantage of this project ... is that all groups who hold meetings in New Orleans could do it."
Although this is the first Dermatology in Action project, Dr. James hopes it will not be the last. The volunteer event surrounding this year's annual AAD meeting could become an annual event itself. "If this concept is able to go forward and continues to grow in its impact, it has a lot of potential for the cities where we hold our conventions," he said.
If you missed the opportunity to register, you can still make a difference by donating money or medical supplies. Visit the Dermatology in Action page for more information.
With more than a hundred dermatologists and other volunteers signed up to help, Thursday's (Feb. 3) "Dermatology in Action" project is expected to be a great success and help to a local community in New Orleans still recovering from Hurricane Katrina, American Academy of Dermatology president William D. James said in an interview.
Before the 2010 Summer Academy Meeting, Dr. James and his wife came up with the idea to have the academy donate shade structures to local parks in Chicago.
"I've been thinking about volunteering in a variety of different ways during my presidency," Dr. James said. "We thought it would be nice to leave something behind in the cities where we have our meetings, either something permanent or [through] a volunteer project."
With more time to plan for this year's annual meeting, the community outreach project in New Orleans kept growing. Medical supplies are being donated to help underprivileged patients at the Tulane University Community Health Centers, money is being donated to help the local community, and volunteers will be refurbishing a community center and planting a nearby urban garden at the volunteer event.
"New Orleans seems like an ideal community to give something back to," said Dr. James.
This is the first time the Academy has organized a hands-on volunteer event around a meeting, and the feedback has been very positive, he said. "People are very excited about it." Dr. James will pitch in along with his wife and friends.
The details of the project remained fluid until a couple weeks ago. Based on the number who registered, HandsOn New Orleans, an organization that coordinates local volunteer efforts, suggested several options to the Academy.
"Because we had a good turnout, the opportunity we selected has to do with a community center in the Ninth Ward. That is a part of New Orleans that was fairly hard hit [by Hurricane Katrina]," Dr. James said. The center offers literacy services, job training, recreational facilities, and is a community gathering place. The center also has a small kitchen and living quarters for families in transition.
"The neighborhood does not have a grocery store within biking distance," Dr. James said. "So we decided to help them plant an urban garden space to help people grow their own vegetables. We will remove overgrowth, build raised beds, add soil and mulch, and help them grow their own food."
The volunteers will also leave room for paths to connect the garden to the community center building. Others will help repair the building itself, which has some broken windows and needs some drywall and painting work done, Dr. James said.
Money donated through the Academy Sustaining Fund will help purchase books for the center to facilitate tutoring of local residents.
Unlike the donation of shade structures to parks in Chicago – connected directly to the Academy's sun protection messages – the New Orleans project has wider implications. "This event could be a model for other conventions. One advantage of this project ... is that all groups who hold meetings in New Orleans could do it."
Although this is the first Dermatology in Action project, Dr. James hopes it will not be the last. The volunteer event surrounding this year's annual AAD meeting could become an annual event itself. "If this concept is able to go forward and continues to grow in its impact, it has a lot of potential for the cities where we hold our conventions," he said.
If you missed the opportunity to register, you can still make a difference by donating money or medical supplies. Visit the Dermatology in Action page for more information.
With more than a hundred dermatologists and other volunteers signed up to help, Thursday's (Feb. 3) "Dermatology in Action" project is expected to be a great success and help to a local community in New Orleans still recovering from Hurricane Katrina, American Academy of Dermatology president William D. James said in an interview.
Before the 2010 Summer Academy Meeting, Dr. James and his wife came up with the idea to have the academy donate shade structures to local parks in Chicago.
"I've been thinking about volunteering in a variety of different ways during my presidency," Dr. James said. "We thought it would be nice to leave something behind in the cities where we have our meetings, either something permanent or [through] a volunteer project."
With more time to plan for this year's annual meeting, the community outreach project in New Orleans kept growing. Medical supplies are being donated to help underprivileged patients at the Tulane University Community Health Centers, money is being donated to help the local community, and volunteers will be refurbishing a community center and planting a nearby urban garden at the volunteer event.
"New Orleans seems like an ideal community to give something back to," said Dr. James.
This is the first time the Academy has organized a hands-on volunteer event around a meeting, and the feedback has been very positive, he said. "People are very excited about it." Dr. James will pitch in along with his wife and friends.
The details of the project remained fluid until a couple weeks ago. Based on the number who registered, HandsOn New Orleans, an organization that coordinates local volunteer efforts, suggested several options to the Academy.
"Because we had a good turnout, the opportunity we selected has to do with a community center in the Ninth Ward. That is a part of New Orleans that was fairly hard hit [by Hurricane Katrina]," Dr. James said. The center offers literacy services, job training, recreational facilities, and is a community gathering place. The center also has a small kitchen and living quarters for families in transition.
"The neighborhood does not have a grocery store within biking distance," Dr. James said. "So we decided to help them plant an urban garden space to help people grow their own vegetables. We will remove overgrowth, build raised beds, add soil and mulch, and help them grow their own food."
The volunteers will also leave room for paths to connect the garden to the community center building. Others will help repair the building itself, which has some broken windows and needs some drywall and painting work done, Dr. James said.
Money donated through the Academy Sustaining Fund will help purchase books for the center to facilitate tutoring of local residents.
Unlike the donation of shade structures to parks in Chicago – connected directly to the Academy's sun protection messages – the New Orleans project has wider implications. "This event could be a model for other conventions. One advantage of this project ... is that all groups who hold meetings in New Orleans could do it."
Although this is the first Dermatology in Action project, Dr. James hopes it will not be the last. The volunteer event surrounding this year's annual AAD meeting could become an annual event itself. "If this concept is able to go forward and continues to grow in its impact, it has a lot of potential for the cities where we hold our conventions," he said.
If you missed the opportunity to register, you can still make a difference by donating money or medical supplies. Visit the Dermatology in Action page for more information.
Experts Prefer Mohs for Lentigo Maligna
ORLANDO - Standard surgical margins often are inadequate for lentigo maligna; instead, perimeter excision techniques or Mohs surgery is preferable because these approaches consistently provide high cure rates, according to Dr. Basil S. Cherpelis.
Lentigo maligna is a subtype of melanoma in situ, characterized as an overgrowth of atypical melanocytes with the potential to become lentigo maligna melanoma. "I think of it as the problem child of the melanoma family," Dr. Cherpelis said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"What margin should I use, and if I am going to do Mohs, how can I see margins on frozen sections?" Intraoperative margin control is recommended, but recent literature suggests that standard 5-mm margins are frequently inadequate (Clin. Plast. Surg. 2010;37:35-46; Int. J. Dermatol. 2010;49:482-91).
In general, traditional frozen sections permit only 1% of margins to be assessed. For that reason, Dr. Cherpelis said he prefers permanent processing or Mohs surgery for these patients. With permanent processing, a surgeon leaves a central island of tissue and removes peripheral strips. Excised samples sent to a lab for evaluation typically take several days for results.
"Permanent processing has excellent cure rates. But on the downside, a patient has to wait for pathology results, which can be inconvenient," said Dr. Cherpelis, a cutaneous oncologist at Moffitt Cancer Center at the University of South Florida in Tampa.
In contrast, Mohs micrographic excision and repair are performed on the same day. Because the entire margin is visualized, cure rates are "excellent," Dr. Cherpelis said.
As to why Mohs isn’t more widely used, one possible reason is that it can be difficult to distinguish melanocytes from keratinocytes on frozen section, he said.
Immunohistostains to the rescue: Melanoma antigen recognized by T cells (MART-1) and microphthalmia-associated transcription factor (MITF) staining each has a role.
"MART-1 is a valuable immunostain for melanoma in situ on photodamaged skin," said Dr. L. Frank Glass, a dermatopathologist at Moffitt Cancer Center. MART-1 on frozen sections can provide the same data as permanent processing. "But MART-1 is not a magic bullet," he added. "There can be false positives."
In addition, expertise and teamwork are required with immunohistostains, Dr. Glass said. "The right MART-1 staining takes a technical staff to do it right."
MITF works in frozen sections and produces results similar to permanent sections. Clinicians can use this nuclear immunostain to quantify melanocytes and assess other parameters that distinguish melanoma in situ from solar lentigines or skin with chronic sun damage, for example.
"MITF is particularly useful in combination with MART-1," Dr. Glass said.
Instead of dendritic processes that overlap and look like confluence, MITF reveals discreet melanocytic cells, Dr. Glass said. "You can feel more comfortable calling a case negative with MITF – if it shows no abnormal cytology – in the same patient where the MART-1 shows clumping."
"The bottom line is we are looking for 100% specificity for melanoma," Dr. Glass said. He and his colleagues also are developing cutoff values, based on melanocyte diameter and density, to distinguish melanoma in situ from solar lentigo or sun-damaged skin.
Dr. Cherpelis and Dr. Glass said they had no relevant financial disclosures.
ORLANDO - Standard surgical margins often are inadequate for lentigo maligna; instead, perimeter excision techniques or Mohs surgery is preferable because these approaches consistently provide high cure rates, according to Dr. Basil S. Cherpelis.
Lentigo maligna is a subtype of melanoma in situ, characterized as an overgrowth of atypical melanocytes with the potential to become lentigo maligna melanoma. "I think of it as the problem child of the melanoma family," Dr. Cherpelis said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"What margin should I use, and if I am going to do Mohs, how can I see margins on frozen sections?" Intraoperative margin control is recommended, but recent literature suggests that standard 5-mm margins are frequently inadequate (Clin. Plast. Surg. 2010;37:35-46; Int. J. Dermatol. 2010;49:482-91).
In general, traditional frozen sections permit only 1% of margins to be assessed. For that reason, Dr. Cherpelis said he prefers permanent processing or Mohs surgery for these patients. With permanent processing, a surgeon leaves a central island of tissue and removes peripheral strips. Excised samples sent to a lab for evaluation typically take several days for results.
"Permanent processing has excellent cure rates. But on the downside, a patient has to wait for pathology results, which can be inconvenient," said Dr. Cherpelis, a cutaneous oncologist at Moffitt Cancer Center at the University of South Florida in Tampa.
In contrast, Mohs micrographic excision and repair are performed on the same day. Because the entire margin is visualized, cure rates are "excellent," Dr. Cherpelis said.
As to why Mohs isn’t more widely used, one possible reason is that it can be difficult to distinguish melanocytes from keratinocytes on frozen section, he said.
Immunohistostains to the rescue: Melanoma antigen recognized by T cells (MART-1) and microphthalmia-associated transcription factor (MITF) staining each has a role.
"MART-1 is a valuable immunostain for melanoma in situ on photodamaged skin," said Dr. L. Frank Glass, a dermatopathologist at Moffitt Cancer Center. MART-1 on frozen sections can provide the same data as permanent processing. "But MART-1 is not a magic bullet," he added. "There can be false positives."
In addition, expertise and teamwork are required with immunohistostains, Dr. Glass said. "The right MART-1 staining takes a technical staff to do it right."
MITF works in frozen sections and produces results similar to permanent sections. Clinicians can use this nuclear immunostain to quantify melanocytes and assess other parameters that distinguish melanoma in situ from solar lentigines or skin with chronic sun damage, for example.
"MITF is particularly useful in combination with MART-1," Dr. Glass said.
Instead of dendritic processes that overlap and look like confluence, MITF reveals discreet melanocytic cells, Dr. Glass said. "You can feel more comfortable calling a case negative with MITF – if it shows no abnormal cytology – in the same patient where the MART-1 shows clumping."
"The bottom line is we are looking for 100% specificity for melanoma," Dr. Glass said. He and his colleagues also are developing cutoff values, based on melanocyte diameter and density, to distinguish melanoma in situ from solar lentigo or sun-damaged skin.
Dr. Cherpelis and Dr. Glass said they had no relevant financial disclosures.
ORLANDO - Standard surgical margins often are inadequate for lentigo maligna; instead, perimeter excision techniques or Mohs surgery is preferable because these approaches consistently provide high cure rates, according to Dr. Basil S. Cherpelis.
Lentigo maligna is a subtype of melanoma in situ, characterized as an overgrowth of atypical melanocytes with the potential to become lentigo maligna melanoma. "I think of it as the problem child of the melanoma family," Dr. Cherpelis said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"What margin should I use, and if I am going to do Mohs, how can I see margins on frozen sections?" Intraoperative margin control is recommended, but recent literature suggests that standard 5-mm margins are frequently inadequate (Clin. Plast. Surg. 2010;37:35-46; Int. J. Dermatol. 2010;49:482-91).
In general, traditional frozen sections permit only 1% of margins to be assessed. For that reason, Dr. Cherpelis said he prefers permanent processing or Mohs surgery for these patients. With permanent processing, a surgeon leaves a central island of tissue and removes peripheral strips. Excised samples sent to a lab for evaluation typically take several days for results.
"Permanent processing has excellent cure rates. But on the downside, a patient has to wait for pathology results, which can be inconvenient," said Dr. Cherpelis, a cutaneous oncologist at Moffitt Cancer Center at the University of South Florida in Tampa.
In contrast, Mohs micrographic excision and repair are performed on the same day. Because the entire margin is visualized, cure rates are "excellent," Dr. Cherpelis said.
As to why Mohs isn’t more widely used, one possible reason is that it can be difficult to distinguish melanocytes from keratinocytes on frozen section, he said.
Immunohistostains to the rescue: Melanoma antigen recognized by T cells (MART-1) and microphthalmia-associated transcription factor (MITF) staining each has a role.
"MART-1 is a valuable immunostain for melanoma in situ on photodamaged skin," said Dr. L. Frank Glass, a dermatopathologist at Moffitt Cancer Center. MART-1 on frozen sections can provide the same data as permanent processing. "But MART-1 is not a magic bullet," he added. "There can be false positives."
In addition, expertise and teamwork are required with immunohistostains, Dr. Glass said. "The right MART-1 staining takes a technical staff to do it right."
MITF works in frozen sections and produces results similar to permanent sections. Clinicians can use this nuclear immunostain to quantify melanocytes and assess other parameters that distinguish melanoma in situ from solar lentigines or skin with chronic sun damage, for example.
"MITF is particularly useful in combination with MART-1," Dr. Glass said.
Instead of dendritic processes that overlap and look like confluence, MITF reveals discreet melanocytic cells, Dr. Glass said. "You can feel more comfortable calling a case negative with MITF – if it shows no abnormal cytology – in the same patient where the MART-1 shows clumping."
"The bottom line is we are looking for 100% specificity for melanoma," Dr. Glass said. He and his colleagues also are developing cutoff values, based on melanocyte diameter and density, to distinguish melanoma in situ from solar lentigo or sun-damaged skin.
Dr. Cherpelis and Dr. Glass said they had no relevant financial disclosures.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Making Waves in Campaign to Decrease Sun Exposure
ORLANDO – Physicians faced unanticipated challenges when they launched a campaign to increase sun-protective behaviors for a high-risk group along the beaches of Australia.
The initiative targeted training programs for junior lifeguards or "nippers," as they are called in Australia. Nippers have multiple risk factors for melanoma, including skin types I and II, summertime sun exposure, and a younger age. "Children are the most vulnerable," Dr. Anthony Dixon said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"I knew I had to do something. Nippers are seen all over Australia. And they don’t wear a lot – they wear funny hats where the ears stick out," said Dr. Dixon, a dermatologic surgeon in private practice Geelong, Victoria. He felt compelled to act after seeing "more and more" of his patients develop skin cancer.
Dr. Dixon and his associates recommended four major changes to the nipper programs, which train children aged 6-12 years to become lifeguards. The recommended changes were:
• Do not hold nipper training between the hours of 11 a.m. and 4 p.m. "UVB is focused toward the middle of the day. We know that, the public does not," Dr. Dixon said. He estimated that nippers would receive less UV exposure during early-morning training.
• The children should wear rash vests, preferably with long sleeves.
• They should also wear broad-brimmed hats while awaiting training exercises
• Sunscreen should be available and reapplied frequently.
"We would all call that ... common sense," said Dr. Dixon. "If only the lifesaving association did what they say in their manual." Their "Public Safety and Aquatic Rescue" manual addresses sun safety on page 15 of its 170 pages. "That is not too bad," he said. It advocates application of sunscreen before sun exposure, for example.
Dr. Dixon and his associates launched the campaign in January 2009 during the peak of summer in the southern hemisphere. Nipper training clubs agreed to the recommendations. However, some programs changed more readily than others, often for unexpected reasons.
For example, the nipper training club at Anglesea Beach did not immediately take to the recommendations, Dr. Dixon said. Program director Peter Foster ("Nipper Pete") briefed the children on the new program while they were standing in full sun. Sunscreen was repeatedly mentioned, but it was not applied until after the briefing. Also, the nippers did not don broad-brimmed hats because they had to wear hats with the sponsor’s name.
Dr. Dixon returned at a later date to observe any progress. "I saw kids at noon wearing only Speedos, [so they had] enormous sun exposure," Dr. Dixon said. "Nipper Pete saw me up on the sand dune with a camera and he panicked." He called the kids over and lectured them.
Sun exposure reduction is not as automatic as other protections, Dr. Dixon said. For example, "if that kid was too far out in the water, Nipper Pete would have gone out, pulled him in, and would have then given him the lecture about going out too deep."
Unbeknownst to Dr. Dixon, initial resistance to moving nipper training at Anglesea Beach to earlier in the morning had to do with a thriving business on the beach. Pressure from a sausage business that was making good money selling lunch to the nippers, their family members, and the trainers impeded the sun safety recommendation. Upon discovering this, Dr. Dixon intervened again. Eventually all parties agreed to conduct training earlier, and for the business to sell donuts instead.
Another nipper training program, in contrast, enacted the recommendations immediately. "The club at Jan Juc Beach decided to change everything with no briefing. They e-mailed the participants beforehand." All the nippers wore bucket hats while waiting for their training exercises, for example.
"So what others said was impossible was being done two beaches down," he said.
Part of the challenge of initiating behavioral changes is a misperception about the relative risk of sun exposure compared with other beach dangers, Dr. Dixon said. When asked about risk factors for death at the beach, "most people would mention drowning first," he said. However, there are 7 deaths from melanoma and 2 deaths from other skin cancers per 100,000 people in Australia each year, compared with 1.2 deaths per 100,000 people for accidental drowning. Put another way, for each person who dies from drowning, 46 Australians die from melanoma.
Other people might cite shark attacks as the greatest danger. In an average year, about four people worldwide die from a shark encounter. A shark attack "is an extremely rare way for humans to die, but when it happens, we all hear about it," Dr. Dixon said. "There are about 5,000 melanoma deaths in Australia for each shark death."
Dr. Dixon said that he did not have any relevant disclosures.
More: Watch live Surfcams from Australia.
ORLANDO – Physicians faced unanticipated challenges when they launched a campaign to increase sun-protective behaviors for a high-risk group along the beaches of Australia.
The initiative targeted training programs for junior lifeguards or "nippers," as they are called in Australia. Nippers have multiple risk factors for melanoma, including skin types I and II, summertime sun exposure, and a younger age. "Children are the most vulnerable," Dr. Anthony Dixon said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"I knew I had to do something. Nippers are seen all over Australia. And they don’t wear a lot – they wear funny hats where the ears stick out," said Dr. Dixon, a dermatologic surgeon in private practice Geelong, Victoria. He felt compelled to act after seeing "more and more" of his patients develop skin cancer.
Dr. Dixon and his associates recommended four major changes to the nipper programs, which train children aged 6-12 years to become lifeguards. The recommended changes were:
• Do not hold nipper training between the hours of 11 a.m. and 4 p.m. "UVB is focused toward the middle of the day. We know that, the public does not," Dr. Dixon said. He estimated that nippers would receive less UV exposure during early-morning training.
• The children should wear rash vests, preferably with long sleeves.
• They should also wear broad-brimmed hats while awaiting training exercises
• Sunscreen should be available and reapplied frequently.
"We would all call that ... common sense," said Dr. Dixon. "If only the lifesaving association did what they say in their manual." Their "Public Safety and Aquatic Rescue" manual addresses sun safety on page 15 of its 170 pages. "That is not too bad," he said. It advocates application of sunscreen before sun exposure, for example.
Dr. Dixon and his associates launched the campaign in January 2009 during the peak of summer in the southern hemisphere. Nipper training clubs agreed to the recommendations. However, some programs changed more readily than others, often for unexpected reasons.
For example, the nipper training club at Anglesea Beach did not immediately take to the recommendations, Dr. Dixon said. Program director Peter Foster ("Nipper Pete") briefed the children on the new program while they were standing in full sun. Sunscreen was repeatedly mentioned, but it was not applied until after the briefing. Also, the nippers did not don broad-brimmed hats because they had to wear hats with the sponsor’s name.
Dr. Dixon returned at a later date to observe any progress. "I saw kids at noon wearing only Speedos, [so they had] enormous sun exposure," Dr. Dixon said. "Nipper Pete saw me up on the sand dune with a camera and he panicked." He called the kids over and lectured them.
Sun exposure reduction is not as automatic as other protections, Dr. Dixon said. For example, "if that kid was too far out in the water, Nipper Pete would have gone out, pulled him in, and would have then given him the lecture about going out too deep."
Unbeknownst to Dr. Dixon, initial resistance to moving nipper training at Anglesea Beach to earlier in the morning had to do with a thriving business on the beach. Pressure from a sausage business that was making good money selling lunch to the nippers, their family members, and the trainers impeded the sun safety recommendation. Upon discovering this, Dr. Dixon intervened again. Eventually all parties agreed to conduct training earlier, and for the business to sell donuts instead.
Another nipper training program, in contrast, enacted the recommendations immediately. "The club at Jan Juc Beach decided to change everything with no briefing. They e-mailed the participants beforehand." All the nippers wore bucket hats while waiting for their training exercises, for example.
"So what others said was impossible was being done two beaches down," he said.
Part of the challenge of initiating behavioral changes is a misperception about the relative risk of sun exposure compared with other beach dangers, Dr. Dixon said. When asked about risk factors for death at the beach, "most people would mention drowning first," he said. However, there are 7 deaths from melanoma and 2 deaths from other skin cancers per 100,000 people in Australia each year, compared with 1.2 deaths per 100,000 people for accidental drowning. Put another way, for each person who dies from drowning, 46 Australians die from melanoma.
Other people might cite shark attacks as the greatest danger. In an average year, about four people worldwide die from a shark encounter. A shark attack "is an extremely rare way for humans to die, but when it happens, we all hear about it," Dr. Dixon said. "There are about 5,000 melanoma deaths in Australia for each shark death."
Dr. Dixon said that he did not have any relevant disclosures.
More: Watch live Surfcams from Australia.
ORLANDO – Physicians faced unanticipated challenges when they launched a campaign to increase sun-protective behaviors for a high-risk group along the beaches of Australia.
The initiative targeted training programs for junior lifeguards or "nippers," as they are called in Australia. Nippers have multiple risk factors for melanoma, including skin types I and II, summertime sun exposure, and a younger age. "Children are the most vulnerable," Dr. Anthony Dixon said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"I knew I had to do something. Nippers are seen all over Australia. And they don’t wear a lot – they wear funny hats where the ears stick out," said Dr. Dixon, a dermatologic surgeon in private practice Geelong, Victoria. He felt compelled to act after seeing "more and more" of his patients develop skin cancer.
Dr. Dixon and his associates recommended four major changes to the nipper programs, which train children aged 6-12 years to become lifeguards. The recommended changes were:
• Do not hold nipper training between the hours of 11 a.m. and 4 p.m. "UVB is focused toward the middle of the day. We know that, the public does not," Dr. Dixon said. He estimated that nippers would receive less UV exposure during early-morning training.
• The children should wear rash vests, preferably with long sleeves.
• They should also wear broad-brimmed hats while awaiting training exercises
• Sunscreen should be available and reapplied frequently.
"We would all call that ... common sense," said Dr. Dixon. "If only the lifesaving association did what they say in their manual." Their "Public Safety and Aquatic Rescue" manual addresses sun safety on page 15 of its 170 pages. "That is not too bad," he said. It advocates application of sunscreen before sun exposure, for example.
Dr. Dixon and his associates launched the campaign in January 2009 during the peak of summer in the southern hemisphere. Nipper training clubs agreed to the recommendations. However, some programs changed more readily than others, often for unexpected reasons.
For example, the nipper training club at Anglesea Beach did not immediately take to the recommendations, Dr. Dixon said. Program director Peter Foster ("Nipper Pete") briefed the children on the new program while they were standing in full sun. Sunscreen was repeatedly mentioned, but it was not applied until after the briefing. Also, the nippers did not don broad-brimmed hats because they had to wear hats with the sponsor’s name.
Dr. Dixon returned at a later date to observe any progress. "I saw kids at noon wearing only Speedos, [so they had] enormous sun exposure," Dr. Dixon said. "Nipper Pete saw me up on the sand dune with a camera and he panicked." He called the kids over and lectured them.
Sun exposure reduction is not as automatic as other protections, Dr. Dixon said. For example, "if that kid was too far out in the water, Nipper Pete would have gone out, pulled him in, and would have then given him the lecture about going out too deep."
Unbeknownst to Dr. Dixon, initial resistance to moving nipper training at Anglesea Beach to earlier in the morning had to do with a thriving business on the beach. Pressure from a sausage business that was making good money selling lunch to the nippers, their family members, and the trainers impeded the sun safety recommendation. Upon discovering this, Dr. Dixon intervened again. Eventually all parties agreed to conduct training earlier, and for the business to sell donuts instead.
Another nipper training program, in contrast, enacted the recommendations immediately. "The club at Jan Juc Beach decided to change everything with no briefing. They e-mailed the participants beforehand." All the nippers wore bucket hats while waiting for their training exercises, for example.
"So what others said was impossible was being done two beaches down," he said.
Part of the challenge of initiating behavioral changes is a misperception about the relative risk of sun exposure compared with other beach dangers, Dr. Dixon said. When asked about risk factors for death at the beach, "most people would mention drowning first," he said. However, there are 7 deaths from melanoma and 2 deaths from other skin cancers per 100,000 people in Australia each year, compared with 1.2 deaths per 100,000 people for accidental drowning. Put another way, for each person who dies from drowning, 46 Australians die from melanoma.
Other people might cite shark attacks as the greatest danger. In an average year, about four people worldwide die from a shark encounter. A shark attack "is an extremely rare way for humans to die, but when it happens, we all hear about it," Dr. Dixon said. "There are about 5,000 melanoma deaths in Australia for each shark death."
Dr. Dixon said that he did not have any relevant disclosures.
More: Watch live Surfcams from Australia.
FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Making Waves in Campaign to Decrease Sun Exposure
ORLANDO – Physicians faced unanticipated challenges when they launched a campaign to increase sun-protective behaviors for a high-risk group along the beaches of Australia.
The initiative targeted training programs for junior lifeguards or "nippers," as they are called in Australia. Nippers have multiple risk factors for melanoma, including skin types I and II, summertime sun exposure, and a younger age. "Children are the most vulnerable," Dr. Anthony Dixon said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"I knew I had to do something. Nippers are seen all over Australia. And they don’t wear a lot – they wear funny hats where the ears stick out," said Dr. Dixon, a dermatologic surgeon in private practice Geelong, Victoria. He felt compelled to act after seeing "more and more" of his patients develop skin cancer.
Dr. Dixon and his associates recommended four major changes to the nipper programs, which train children aged 6-12 years to become lifeguards. The recommended changes were:
P Do not hold nipper training between the hours of 11 a.m. and 4 p.m. "UVB is focused toward the middle of the day. We know that, the public does not," Dr. Dixon said. He estimated that nippers would receive less UV exposure during early-morning training.
P The children should wear rash vests, preferably with long sleeves.
P They should also wear broad-brimmed hats while awaiting training exercises
P Sunscreen should be available and reapplied frequently.
"We would all call that … common sense," said Dr. Dixon. "If only the lifesaving association did what they say in their manual." Their "Public Safety and Aquatic Rescue" manual addresses sun safety on page 15 of its 170 pages. "That is not too bad," he said. It advocates application of sunscreen before sun exposure, for example.
Dr. Dixon and his associates launched the campaign in January 2009 during the peak of summer in the southern hemisphere. Nipper training clubs agreed to the recommendations. However, some programs changed more readily than others, often for unexpected reasons.
For example, the nipper training club at Anglesea Beach did not immediately take to the recommendations, Dr. Dixon said. Program director Peter Foster ("Nipper Pete") briefed the children on the new program while they were standing in full sun. Sunscreen was repeatedly mentioned, but it was not applied until after the briefing. Also, the nippers did not don broad-brimmed hats because they had to wear hats with the sponsor’s name.
Dr. Dixon returned at a later date to observe any progress. "I saw kids at noon wearing only Speedos, [so they had] enormous sun exposure," Dr. Dixon said. "Nipper Pete saw me up on the sand dune with a camera and he panicked." He called the kids over and lectured them.
Sun exposure reduction is not as automatic as other protections, Dr. Dixon said. For example, "if that kid was too far out in the water, Nipper Pete would have gone out, pulled him in, and would have then given him the lecture about going out too deep."
Unbeknownst to Dr. Dixon, initial resistance to moving nipper training at Anglesea Beach to earlier in the morning had to do with a thriving business on the beach. Pressure from a sausage business that was making good money selling lunch to the nippers, their family members, and the trainers impeded the sun safety recommendation. Upon discovering this, Dr. Dixon intervened again. Eventually all parties agreed to conduct training earlier, and for the business to sell donuts instead.
Another nipper training program, in contrast, enacted the recommendations immediately. "The club at Jan Juc Beach decided to change everything with no briefing. They e-mailed the participants beforehand." All the nippers wore bucket hats while waiting for their training exercises, for example.
"So what others said was impossible was being done two beaches down," he said.
Part of the challenge of initiating behavioral changes is a misperception about the relative risk of sun exposure compared with other beach dangers, Dr. Dixon said. When asked about risk factors for death at the beach, "most people would mention drowning first," he said. However, there are 7 deaths from melanoma and 2 deaths from other skin cancers per 100,000 people in Australia each year, compared with 1.2 deaths per 100,000 people for accidental drowning. Put another way, for each person who dies from drowning, 46 Australians die from melanoma.
Other people might cite shark attacks as the greatest danger. In an average year, about four people worldwide die from a shark encounter. A shark attack "is an extremely rare way for humans to die, but when it happens, we all hear about it," Dr. Dixon said. "There are about 5,000 melanoma deaths in Australia for each shark death."
Dr. Dixon said that he did not have any relevant disclosures.
Visit http://www.coastalwatch.com for live Surfcams from Australia.
ORLANDO – Physicians faced unanticipated challenges when they launched a campaign to increase sun-protective behaviors for a high-risk group along the beaches of Australia.
The initiative targeted training programs for junior lifeguards or "nippers," as they are called in Australia. Nippers have multiple risk factors for melanoma, including skin types I and II, summertime sun exposure, and a younger age. "Children are the most vulnerable," Dr. Anthony Dixon said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"I knew I had to do something. Nippers are seen all over Australia. And they don’t wear a lot – they wear funny hats where the ears stick out," said Dr. Dixon, a dermatologic surgeon in private practice Geelong, Victoria. He felt compelled to act after seeing "more and more" of his patients develop skin cancer.
Dr. Dixon and his associates recommended four major changes to the nipper programs, which train children aged 6-12 years to become lifeguards. The recommended changes were:
P Do not hold nipper training between the hours of 11 a.m. and 4 p.m. "UVB is focused toward the middle of the day. We know that, the public does not," Dr. Dixon said. He estimated that nippers would receive less UV exposure during early-morning training.
P The children should wear rash vests, preferably with long sleeves.
P They should also wear broad-brimmed hats while awaiting training exercises
P Sunscreen should be available and reapplied frequently.
"We would all call that … common sense," said Dr. Dixon. "If only the lifesaving association did what they say in their manual." Their "Public Safety and Aquatic Rescue" manual addresses sun safety on page 15 of its 170 pages. "That is not too bad," he said. It advocates application of sunscreen before sun exposure, for example.
Dr. Dixon and his associates launched the campaign in January 2009 during the peak of summer in the southern hemisphere. Nipper training clubs agreed to the recommendations. However, some programs changed more readily than others, often for unexpected reasons.
For example, the nipper training club at Anglesea Beach did not immediately take to the recommendations, Dr. Dixon said. Program director Peter Foster ("Nipper Pete") briefed the children on the new program while they were standing in full sun. Sunscreen was repeatedly mentioned, but it was not applied until after the briefing. Also, the nippers did not don broad-brimmed hats because they had to wear hats with the sponsor’s name.
Dr. Dixon returned at a later date to observe any progress. "I saw kids at noon wearing only Speedos, [so they had] enormous sun exposure," Dr. Dixon said. "Nipper Pete saw me up on the sand dune with a camera and he panicked." He called the kids over and lectured them.
Sun exposure reduction is not as automatic as other protections, Dr. Dixon said. For example, "if that kid was too far out in the water, Nipper Pete would have gone out, pulled him in, and would have then given him the lecture about going out too deep."
Unbeknownst to Dr. Dixon, initial resistance to moving nipper training at Anglesea Beach to earlier in the morning had to do with a thriving business on the beach. Pressure from a sausage business that was making good money selling lunch to the nippers, their family members, and the trainers impeded the sun safety recommendation. Upon discovering this, Dr. Dixon intervened again. Eventually all parties agreed to conduct training earlier, and for the business to sell donuts instead.
Another nipper training program, in contrast, enacted the recommendations immediately. "The club at Jan Juc Beach decided to change everything with no briefing. They e-mailed the participants beforehand." All the nippers wore bucket hats while waiting for their training exercises, for example.
"So what others said was impossible was being done two beaches down," he said.
Part of the challenge of initiating behavioral changes is a misperception about the relative risk of sun exposure compared with other beach dangers, Dr. Dixon said. When asked about risk factors for death at the beach, "most people would mention drowning first," he said. However, there are 7 deaths from melanoma and 2 deaths from other skin cancers per 100,000 people in Australia each year, compared with 1.2 deaths per 100,000 people for accidental drowning. Put another way, for each person who dies from drowning, 46 Australians die from melanoma.
Other people might cite shark attacks as the greatest danger. In an average year, about four people worldwide die from a shark encounter. A shark attack "is an extremely rare way for humans to die, but when it happens, we all hear about it," Dr. Dixon said. "There are about 5,000 melanoma deaths in Australia for each shark death."
Dr. Dixon said that he did not have any relevant disclosures.
Visit http://www.coastalwatch.com for live Surfcams from Australia.
ORLANDO – Physicians faced unanticipated challenges when they launched a campaign to increase sun-protective behaviors for a high-risk group along the beaches of Australia.
The initiative targeted training programs for junior lifeguards or "nippers," as they are called in Australia. Nippers have multiple risk factors for melanoma, including skin types I and II, summertime sun exposure, and a younger age. "Children are the most vulnerable," Dr. Anthony Dixon said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"I knew I had to do something. Nippers are seen all over Australia. And they don’t wear a lot – they wear funny hats where the ears stick out," said Dr. Dixon, a dermatologic surgeon in private practice Geelong, Victoria. He felt compelled to act after seeing "more and more" of his patients develop skin cancer.
Dr. Dixon and his associates recommended four major changes to the nipper programs, which train children aged 6-12 years to become lifeguards. The recommended changes were:
P Do not hold nipper training between the hours of 11 a.m. and 4 p.m. "UVB is focused toward the middle of the day. We know that, the public does not," Dr. Dixon said. He estimated that nippers would receive less UV exposure during early-morning training.
P The children should wear rash vests, preferably with long sleeves.
P They should also wear broad-brimmed hats while awaiting training exercises
P Sunscreen should be available and reapplied frequently.
"We would all call that … common sense," said Dr. Dixon. "If only the lifesaving association did what they say in their manual." Their "Public Safety and Aquatic Rescue" manual addresses sun safety on page 15 of its 170 pages. "That is not too bad," he said. It advocates application of sunscreen before sun exposure, for example.
Dr. Dixon and his associates launched the campaign in January 2009 during the peak of summer in the southern hemisphere. Nipper training clubs agreed to the recommendations. However, some programs changed more readily than others, often for unexpected reasons.
For example, the nipper training club at Anglesea Beach did not immediately take to the recommendations, Dr. Dixon said. Program director Peter Foster ("Nipper Pete") briefed the children on the new program while they were standing in full sun. Sunscreen was repeatedly mentioned, but it was not applied until after the briefing. Also, the nippers did not don broad-brimmed hats because they had to wear hats with the sponsor’s name.
Dr. Dixon returned at a later date to observe any progress. "I saw kids at noon wearing only Speedos, [so they had] enormous sun exposure," Dr. Dixon said. "Nipper Pete saw me up on the sand dune with a camera and he panicked." He called the kids over and lectured them.
Sun exposure reduction is not as automatic as other protections, Dr. Dixon said. For example, "if that kid was too far out in the water, Nipper Pete would have gone out, pulled him in, and would have then given him the lecture about going out too deep."
Unbeknownst to Dr. Dixon, initial resistance to moving nipper training at Anglesea Beach to earlier in the morning had to do with a thriving business on the beach. Pressure from a sausage business that was making good money selling lunch to the nippers, their family members, and the trainers impeded the sun safety recommendation. Upon discovering this, Dr. Dixon intervened again. Eventually all parties agreed to conduct training earlier, and for the business to sell donuts instead.
Another nipper training program, in contrast, enacted the recommendations immediately. "The club at Jan Juc Beach decided to change everything with no briefing. They e-mailed the participants beforehand." All the nippers wore bucket hats while waiting for their training exercises, for example.
"So what others said was impossible was being done two beaches down," he said.
Part of the challenge of initiating behavioral changes is a misperception about the relative risk of sun exposure compared with other beach dangers, Dr. Dixon said. When asked about risk factors for death at the beach, "most people would mention drowning first," he said. However, there are 7 deaths from melanoma and 2 deaths from other skin cancers per 100,000 people in Australia each year, compared with 1.2 deaths per 100,000 people for accidental drowning. Put another way, for each person who dies from drowning, 46 Australians die from melanoma.
Other people might cite shark attacks as the greatest danger. In an average year, about four people worldwide die from a shark encounter. A shark attack "is an extremely rare way for humans to die, but when it happens, we all hear about it," Dr. Dixon said. "There are about 5,000 melanoma deaths in Australia for each shark death."
Dr. Dixon said that he did not have any relevant disclosures.
Visit http://www.coastalwatch.com for live Surfcams from Australia.
FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS