User login
Damian McNamara is a journalist for Medscape Medical News and MDedge. He worked full-time for MDedge as the Miami Bureau covering a dozen medical specialties during 2001-2012, then as a freelancer for Medscape and MDedge, before being hired on staff by Medscape in 2018. Now the two companies are one. He uses what he learned in school – Damian has a BS in chemistry and an MS in science, health and environmental reporting/journalism. He works out of a home office in Miami, with a 100-pound chocolate lab known to snore under his desk during work hours.
Solutions to Challenges of Mohs Surgery for Lentigo Maligna
ORLANDO – Standard surgical margins often are inadequate for lentigo maligna; instead, perimeter excision techniques or Mohs surgery is preferable because these approaches consistently provide high cure rates, according to Dr. Basil S. Cherpelis.
Lentigo maligna is a subtype of melanoma in situ, characterized as an overgrowth of atypical melanocytes with the potential to become lentigo maligna melanoma. "I think of it as the problem child of the melanoma family," Dr. Cherpelis said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"What margin should I use, and if I am going to do Mohs, how can I see margins on frozen sections?" Intraoperative margin control is recommended, but recent literature suggests that standard 5-mm margins are frequently inadequate (Clin. Plast. Surg. 2010;37:35-46; Int. J. Dermatol. 2010;49:482-91).
In general, traditional frozen sections permit only 1% of margins to be assessed. For that reason, Dr. Cherpelis said he prefers permanent processing or Mohs surgery for these patients. With permanent processing, a surgeon leaves a central island of tissue and removes peripheral strips. Excised samples sent to a lab for evaluation typically take several days for results.
"Permanent processing has excellent cure rates. But on the downside, a patient has to wait for pathology results, which can be inconvenient," said Dr. Cherpelis, a cutaneous oncologist at Moffitt Cancer Center at the University of South Florida in Tampa.
In contrast, Mohs micrographic excision and repair are performed on the same day. Because the entire margin is visualized, cure rates are "excellent," Dr. Cherpelis said.
As to why Mohs isn’t more widely used, one possible reason is that it can be difficult to distinguish melanocytes from keratinocytes on frozen section, he said.
Immunohistostains to the rescue: Melanoma antigen recognized by T cells (MART-1) and microphthalmia-associated transcription factor (MITF) staining each has a role.
"MART-1 is a valuable immunostain for melanoma in situ on photodamaged skin," said Dr. L. Frank Glass, a dermatopathologist at Moffitt Cancer Center. MART-1 on frozen sections can provide the same data as permanent processing. "But MART-1 is not a magic bullet," he added. "There can be false positives."
In addition, expertise and teamwork are required with immunohistostains, Dr. Glass said. "The right MART-1 staining takes a technical staff to do it right."
MITF works in frozen sections and produces results similar to permanent sections. Clinicians can use this nuclear immunostain to quantify melanocytes and assess other parameters that distinguish melanoma in situ from solar lentigines or skin with chronic sun damage, for example.
"MITF is particularly useful in combination with MART-1," Dr. Glass said.
Instead of dendritic processes that overlap and look like confluence, MITF reveals discreet melanocytic cells, Dr. Glass said. "You can feel more comfortable calling a case negative with MITF – if it shows no abnormal cytology – in the same patient where the MART-1 shows clumping."
"The bottom line is we are looking for 100% specificity for melanoma," Dr. Glass said. He and his colleagues also are developing cutoff values, based on melanocyte diameter and density, to distinguish melanoma in situ from solar lentigo or sun-damaged skin.
Dr. Cherpelis and Dr. Glass said they had no relevant financial disclosures.
ORLANDO – Standard surgical margins often are inadequate for lentigo maligna; instead, perimeter excision techniques or Mohs surgery is preferable because these approaches consistently provide high cure rates, according to Dr. Basil S. Cherpelis.
Lentigo maligna is a subtype of melanoma in situ, characterized as an overgrowth of atypical melanocytes with the potential to become lentigo maligna melanoma. "I think of it as the problem child of the melanoma family," Dr. Cherpelis said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"What margin should I use, and if I am going to do Mohs, how can I see margins on frozen sections?" Intraoperative margin control is recommended, but recent literature suggests that standard 5-mm margins are frequently inadequate (Clin. Plast. Surg. 2010;37:35-46; Int. J. Dermatol. 2010;49:482-91).
In general, traditional frozen sections permit only 1% of margins to be assessed. For that reason, Dr. Cherpelis said he prefers permanent processing or Mohs surgery for these patients. With permanent processing, a surgeon leaves a central island of tissue and removes peripheral strips. Excised samples sent to a lab for evaluation typically take several days for results.
"Permanent processing has excellent cure rates. But on the downside, a patient has to wait for pathology results, which can be inconvenient," said Dr. Cherpelis, a cutaneous oncologist at Moffitt Cancer Center at the University of South Florida in Tampa.
In contrast, Mohs micrographic excision and repair are performed on the same day. Because the entire margin is visualized, cure rates are "excellent," Dr. Cherpelis said.
As to why Mohs isn’t more widely used, one possible reason is that it can be difficult to distinguish melanocytes from keratinocytes on frozen section, he said.
Immunohistostains to the rescue: Melanoma antigen recognized by T cells (MART-1) and microphthalmia-associated transcription factor (MITF) staining each has a role.
"MART-1 is a valuable immunostain for melanoma in situ on photodamaged skin," said Dr. L. Frank Glass, a dermatopathologist at Moffitt Cancer Center. MART-1 on frozen sections can provide the same data as permanent processing. "But MART-1 is not a magic bullet," he added. "There can be false positives."
In addition, expertise and teamwork are required with immunohistostains, Dr. Glass said. "The right MART-1 staining takes a technical staff to do it right."
MITF works in frozen sections and produces results similar to permanent sections. Clinicians can use this nuclear immunostain to quantify melanocytes and assess other parameters that distinguish melanoma in situ from solar lentigines or skin with chronic sun damage, for example.
"MITF is particularly useful in combination with MART-1," Dr. Glass said.
Instead of dendritic processes that overlap and look like confluence, MITF reveals discreet melanocytic cells, Dr. Glass said. "You can feel more comfortable calling a case negative with MITF – if it shows no abnormal cytology – in the same patient where the MART-1 shows clumping."
"The bottom line is we are looking for 100% specificity for melanoma," Dr. Glass said. He and his colleagues also are developing cutoff values, based on melanocyte diameter and density, to distinguish melanoma in situ from solar lentigo or sun-damaged skin.
Dr. Cherpelis and Dr. Glass said they had no relevant financial disclosures.
ORLANDO – Standard surgical margins often are inadequate for lentigo maligna; instead, perimeter excision techniques or Mohs surgery is preferable because these approaches consistently provide high cure rates, according to Dr. Basil S. Cherpelis.
Lentigo maligna is a subtype of melanoma in situ, characterized as an overgrowth of atypical melanocytes with the potential to become lentigo maligna melanoma. "I think of it as the problem child of the melanoma family," Dr. Cherpelis said at the annual meeting of the Florida Society of Dermatologic Surgeons.
"What margin should I use, and if I am going to do Mohs, how can I see margins on frozen sections?" Intraoperative margin control is recommended, but recent literature suggests that standard 5-mm margins are frequently inadequate (Clin. Plast. Surg. 2010;37:35-46; Int. J. Dermatol. 2010;49:482-91).
In general, traditional frozen sections permit only 1% of margins to be assessed. For that reason, Dr. Cherpelis said he prefers permanent processing or Mohs surgery for these patients. With permanent processing, a surgeon leaves a central island of tissue and removes peripheral strips. Excised samples sent to a lab for evaluation typically take several days for results.
"Permanent processing has excellent cure rates. But on the downside, a patient has to wait for pathology results, which can be inconvenient," said Dr. Cherpelis, a cutaneous oncologist at Moffitt Cancer Center at the University of South Florida in Tampa.
In contrast, Mohs micrographic excision and repair are performed on the same day. Because the entire margin is visualized, cure rates are "excellent," Dr. Cherpelis said.
As to why Mohs isn’t more widely used, one possible reason is that it can be difficult to distinguish melanocytes from keratinocytes on frozen section, he said.
Immunohistostains to the rescue: Melanoma antigen recognized by T cells (MART-1) and microphthalmia-associated transcription factor (MITF) staining each has a role.
"MART-1 is a valuable immunostain for melanoma in situ on photodamaged skin," said Dr. L. Frank Glass, a dermatopathologist at Moffitt Cancer Center. MART-1 on frozen sections can provide the same data as permanent processing. "But MART-1 is not a magic bullet," he added. "There can be false positives."
In addition, expertise and teamwork are required with immunohistostains, Dr. Glass said. "The right MART-1 staining takes a technical staff to do it right."
MITF works in frozen sections and produces results similar to permanent sections. Clinicians can use this nuclear immunostain to quantify melanocytes and assess other parameters that distinguish melanoma in situ from solar lentigines or skin with chronic sun damage, for example.
"MITF is particularly useful in combination with MART-1," Dr. Glass said.
Instead of dendritic processes that overlap and look like confluence, MITF reveals discreet melanocytic cells, Dr. Glass said. "You can feel more comfortable calling a case negative with MITF – if it shows no abnormal cytology – in the same patient where the MART-1 shows clumping."
"The bottom line is we are looking for 100% specificity for melanoma," Dr. Glass said. He and his colleagues also are developing cutoff values, based on melanocyte diameter and density, to distinguish melanoma in situ from solar lentigo or sun-damaged skin.
Dr. Cherpelis and Dr. Glass said they had no relevant financial disclosures.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Future Technologies Hold Promise for Hair Restoration
ORLANDO - Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
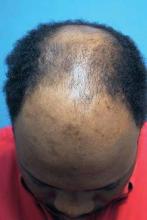
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, England). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
ORLANDO - Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, England). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
ORLANDO - Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, England). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Pearls for Excision and Management of Cylindromas
ORLANDO - Surgical excision is the preferred approach for treating a patient who presents with a cylindroma or with the more extensive familial cylindromatosis, Dr. Leonard Slazinski said.
There are some important distinctions between the two. Cylindromas are benign skin appendage tumors that commonly present as single, slow-growing lesions on the head and neck. Lesions often appear in conjunction with spiradenomas and trichoepitheliomas, they typically are 0.5-6.0 cm in size (although some can grow larger), and they affect females more than males. They arise sporadically with no known inheritance pattern.
The tumor can be excised with careful inspection to ensure removal of all tissue, Dr. Slazinski said. "In my experience, the cylindroma often does have a pseudocapsule, which allows for blunt dissection of the tumor under direct vision."
In contrast, familial cylindromatosis is an inherited autosomal dominant condition characterized by multiple lesions located on the head and neck. Treatment is trickier, as there is no effective field or systemic therapy. Surgery should be considered most effective, but many doctors "are overwhelmed by the number of these lesions," said Dr. Slazinski, a dermatologist in private practice in Sarasota, Fla.
Familial trichoepitheliomas, Brooke-Spiegler syndrome, and familial cylindromatosis share a genetic etiology – a mutation of the CYLD gene on chromosome 16. "Great advances have been made in etiology and cellular mechanisms of familial cylindromatosis and related conditions," Dr. Slazinski said. But "treatment has not advanced to the same degree."
Removal of these lesions is often performed for aesthetic and functional reasons. "These diseases can become quite severe if untreated," Dr. Slazinski said. The psychosocial impact can be great, and patients often become social recluses.
Even with traditional excision, recurrence "is quite high" at approximately 42%, Dr. Slazinski said. Mohs micrographic surgery is used more often for solitary lesions. Other options, depending on the individual presentation, include cryotherapy, curettage, electrosurgery and radiofrequency excision, and true scalp excision with split-thickness grafting, "which is advocated in severe cases."
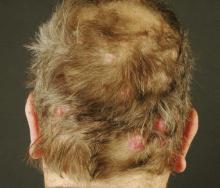
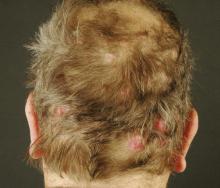
Cylindroma patients often present with pseudoalopecia because the tumor does not grow hair. Scalp cylindromas present a unique challenge, with limited tissue and patients’ desire to spare their hair, Dr. Slazinski said. "Hair cosmesis is often the patient’s greatest concern. Paradoxically, as hair is conserved, [the area] can become a reservoir for future tumor formation."
Some clinicians advocate topical aspirin therapy for familial cylindromatosis, Dr. Slazinski said. There may be "less than stellar results, but my patient is seeing some benefit and wants to continue on compounded, topical salicylic acid."
Dr. Slazinski described a patient with an extensive number of lesions across her face, head, and neck. "I'm blessed to be able to take care of this patient, because no one else has really offered her any possibility of improvement. I’ve taken it on myself to at least try to palliate the situation. I am under no delusion that I can cure her in any way."
Dr. Slazinski said he had no relevant financial disclosures.
ORLANDO - Surgical excision is the preferred approach for treating a patient who presents with a cylindroma or with the more extensive familial cylindromatosis, Dr. Leonard Slazinski said.
There are some important distinctions between the two. Cylindromas are benign skin appendage tumors that commonly present as single, slow-growing lesions on the head and neck. Lesions often appear in conjunction with spiradenomas and trichoepitheliomas, they typically are 0.5-6.0 cm in size (although some can grow larger), and they affect females more than males. They arise sporadically with no known inheritance pattern.
The tumor can be excised with careful inspection to ensure removal of all tissue, Dr. Slazinski said. "In my experience, the cylindroma often does have a pseudocapsule, which allows for blunt dissection of the tumor under direct vision."
In contrast, familial cylindromatosis is an inherited autosomal dominant condition characterized by multiple lesions located on the head and neck. Treatment is trickier, as there is no effective field or systemic therapy. Surgery should be considered most effective, but many doctors "are overwhelmed by the number of these lesions," said Dr. Slazinski, a dermatologist in private practice in Sarasota, Fla.
Familial trichoepitheliomas, Brooke-Spiegler syndrome, and familial cylindromatosis share a genetic etiology – a mutation of the CYLD gene on chromosome 16. "Great advances have been made in etiology and cellular mechanisms of familial cylindromatosis and related conditions," Dr. Slazinski said. But "treatment has not advanced to the same degree."
Removal of these lesions is often performed for aesthetic and functional reasons. "These diseases can become quite severe if untreated," Dr. Slazinski said. The psychosocial impact can be great, and patients often become social recluses.
Even with traditional excision, recurrence "is quite high" at approximately 42%, Dr. Slazinski said. Mohs micrographic surgery is used more often for solitary lesions. Other options, depending on the individual presentation, include cryotherapy, curettage, electrosurgery and radiofrequency excision, and true scalp excision with split-thickness grafting, "which is advocated in severe cases."
Cylindroma patients often present with pseudoalopecia because the tumor does not grow hair. Scalp cylindromas present a unique challenge, with limited tissue and patients’ desire to spare their hair, Dr. Slazinski said. "Hair cosmesis is often the patient’s greatest concern. Paradoxically, as hair is conserved, [the area] can become a reservoir for future tumor formation."
Some clinicians advocate topical aspirin therapy for familial cylindromatosis, Dr. Slazinski said. There may be "less than stellar results, but my patient is seeing some benefit and wants to continue on compounded, topical salicylic acid."
Dr. Slazinski described a patient with an extensive number of lesions across her face, head, and neck. "I'm blessed to be able to take care of this patient, because no one else has really offered her any possibility of improvement. I’ve taken it on myself to at least try to palliate the situation. I am under no delusion that I can cure her in any way."
Dr. Slazinski said he had no relevant financial disclosures.
ORLANDO - Surgical excision is the preferred approach for treating a patient who presents with a cylindroma or with the more extensive familial cylindromatosis, Dr. Leonard Slazinski said.
There are some important distinctions between the two. Cylindromas are benign skin appendage tumors that commonly present as single, slow-growing lesions on the head and neck. Lesions often appear in conjunction with spiradenomas and trichoepitheliomas, they typically are 0.5-6.0 cm in size (although some can grow larger), and they affect females more than males. They arise sporadically with no known inheritance pattern.
The tumor can be excised with careful inspection to ensure removal of all tissue, Dr. Slazinski said. "In my experience, the cylindroma often does have a pseudocapsule, which allows for blunt dissection of the tumor under direct vision."
In contrast, familial cylindromatosis is an inherited autosomal dominant condition characterized by multiple lesions located on the head and neck. Treatment is trickier, as there is no effective field or systemic therapy. Surgery should be considered most effective, but many doctors "are overwhelmed by the number of these lesions," said Dr. Slazinski, a dermatologist in private practice in Sarasota, Fla.
Familial trichoepitheliomas, Brooke-Spiegler syndrome, and familial cylindromatosis share a genetic etiology – a mutation of the CYLD gene on chromosome 16. "Great advances have been made in etiology and cellular mechanisms of familial cylindromatosis and related conditions," Dr. Slazinski said. But "treatment has not advanced to the same degree."
Removal of these lesions is often performed for aesthetic and functional reasons. "These diseases can become quite severe if untreated," Dr. Slazinski said. The psychosocial impact can be great, and patients often become social recluses.
Even with traditional excision, recurrence "is quite high" at approximately 42%, Dr. Slazinski said. Mohs micrographic surgery is used more often for solitary lesions. Other options, depending on the individual presentation, include cryotherapy, curettage, electrosurgery and radiofrequency excision, and true scalp excision with split-thickness grafting, "which is advocated in severe cases."
Cylindroma patients often present with pseudoalopecia because the tumor does not grow hair. Scalp cylindromas present a unique challenge, with limited tissue and patients’ desire to spare their hair, Dr. Slazinski said. "Hair cosmesis is often the patient’s greatest concern. Paradoxically, as hair is conserved, [the area] can become a reservoir for future tumor formation."
Some clinicians advocate topical aspirin therapy for familial cylindromatosis, Dr. Slazinski said. There may be "less than stellar results, but my patient is seeing some benefit and wants to continue on compounded, topical salicylic acid."
Dr. Slazinski described a patient with an extensive number of lesions across her face, head, and neck. "I'm blessed to be able to take care of this patient, because no one else has really offered her any possibility of improvement. I’ve taken it on myself to at least try to palliate the situation. I am under no delusion that I can cure her in any way."
Dr. Slazinski said he had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Pearls for Excision and Management of Cylindromas
ORLANDO – Surgical excision is the preferred approach for treating a patient who presents with a cylindroma or with the more extensive familial cylindromatosis, Dr. Leonard Slazinski said.
There are some important distinctions between the two. Cylindromas are benign skin appendage tumors that commonly present as single, slow-growing lesions on the head and neck. Lesions often appear in conjunction with spiradenomas and trichoepitheliomas, they typically are 0.5 to 6 cm in size (although some can grow larger), and they affect females more than males. They arise sporadically with no known inheritance pattern.
The tumor can be excised with careful inspection to ensure removal of all tissue, Dr. Slazinski said. "In my experience, the cylindroma often does have a pseudocapsule, which allows for blunt dissection of the tumor under direct vision."
In contrast, familial cylindromatosis is an inherited autosomal dominant condition characterized by multiple lesions located on the head and neck. Treatment is trickier, as there is no effective field or systemic therapy. Surgery should be considered most effective, but many doctors "are overwhelmed by the number of these lesions," said Dr. Slazinski, a dermatologist in private practice in Sarasota, Fla.
Familial trichoepitheliomas, Brooke-Spiegler syndrome, and familial cylindromatosis share a genetic etiology – a mutation of the CYLD gene on chromosome 16. "Great advances have been made in etiology and cellular mechanisms of familial cylindromatosis and related conditions," Dr. Slazinski said. But "treatment has not advanced to the same degree."
Removal of these lesions is often performed for aesthetic and functional reasons. "These diseases can become quite severe if untreated," Dr. Slazinski said. The psychosocial impact can be great, and patients often become social recluses.
Even with traditional excision, recurrence "is quite high" at approximately 42%, Dr. Slazinski said. Mohs micrographic surgery is used more often for solitary lesions. Other options, depending on the individual presentation, include cryotherapy, curettage, electrosurgery and radiofrequency excision, and true scalp excision with split-thickness grafting, "which is advocated in severe cases."
Cylindroma patients often present with pseudoalopecia because the tumor does not grow hair. Scalp cylindromas present a unique challenge, with limited tissue and patients’ desire to spare their hair, Dr. Slazinski said. "Hair cosmesis is often the patient’s greatest concern. Paradoxically, as hair is conserved, [the area] can become a reservoir for future tumor formation."
Some clinicians advocate topical aspirin therapy for familial cylindromatosis, Dr. Slazinski said. There may be "less than stellar results, but my patient is seeing some benefit and wants to continue on compounded, topical salicylic acid."
Dr. Slazinski described a patient with an extensive number of lesions across her face, head, and neck. "I’m blessed to be able to take care of this patient, because no one else has really offered her any possibility of improvement. I’ve taken it on myself to at least try to palliate the situation. I am under no delusion that I can cure her in any way."
Dr. Slazinski said he had no relevant financial disclosures.
ORLANDO – Surgical excision is the preferred approach for treating a patient who presents with a cylindroma or with the more extensive familial cylindromatosis, Dr. Leonard Slazinski said.
There are some important distinctions between the two. Cylindromas are benign skin appendage tumors that commonly present as single, slow-growing lesions on the head and neck. Lesions often appear in conjunction with spiradenomas and trichoepitheliomas, they typically are 0.5 to 6 cm in size (although some can grow larger), and they affect females more than males. They arise sporadically with no known inheritance pattern.
The tumor can be excised with careful inspection to ensure removal of all tissue, Dr. Slazinski said. "In my experience, the cylindroma often does have a pseudocapsule, which allows for blunt dissection of the tumor under direct vision."
In contrast, familial cylindromatosis is an inherited autosomal dominant condition characterized by multiple lesions located on the head and neck. Treatment is trickier, as there is no effective field or systemic therapy. Surgery should be considered most effective, but many doctors "are overwhelmed by the number of these lesions," said Dr. Slazinski, a dermatologist in private practice in Sarasota, Fla.
Familial trichoepitheliomas, Brooke-Spiegler syndrome, and familial cylindromatosis share a genetic etiology – a mutation of the CYLD gene on chromosome 16. "Great advances have been made in etiology and cellular mechanisms of familial cylindromatosis and related conditions," Dr. Slazinski said. But "treatment has not advanced to the same degree."
Removal of these lesions is often performed for aesthetic and functional reasons. "These diseases can become quite severe if untreated," Dr. Slazinski said. The psychosocial impact can be great, and patients often become social recluses.
Even with traditional excision, recurrence "is quite high" at approximately 42%, Dr. Slazinski said. Mohs micrographic surgery is used more often for solitary lesions. Other options, depending on the individual presentation, include cryotherapy, curettage, electrosurgery and radiofrequency excision, and true scalp excision with split-thickness grafting, "which is advocated in severe cases."
Cylindroma patients often present with pseudoalopecia because the tumor does not grow hair. Scalp cylindromas present a unique challenge, with limited tissue and patients’ desire to spare their hair, Dr. Slazinski said. "Hair cosmesis is often the patient’s greatest concern. Paradoxically, as hair is conserved, [the area] can become a reservoir for future tumor formation."
Some clinicians advocate topical aspirin therapy for familial cylindromatosis, Dr. Slazinski said. There may be "less than stellar results, but my patient is seeing some benefit and wants to continue on compounded, topical salicylic acid."
Dr. Slazinski described a patient with an extensive number of lesions across her face, head, and neck. "I’m blessed to be able to take care of this patient, because no one else has really offered her any possibility of improvement. I’ve taken it on myself to at least try to palliate the situation. I am under no delusion that I can cure her in any way."
Dr. Slazinski said he had no relevant financial disclosures.
ORLANDO – Surgical excision is the preferred approach for treating a patient who presents with a cylindroma or with the more extensive familial cylindromatosis, Dr. Leonard Slazinski said.
There are some important distinctions between the two. Cylindromas are benign skin appendage tumors that commonly present as single, slow-growing lesions on the head and neck. Lesions often appear in conjunction with spiradenomas and trichoepitheliomas, they typically are 0.5 to 6 cm in size (although some can grow larger), and they affect females more than males. They arise sporadically with no known inheritance pattern.
The tumor can be excised with careful inspection to ensure removal of all tissue, Dr. Slazinski said. "In my experience, the cylindroma often does have a pseudocapsule, which allows for blunt dissection of the tumor under direct vision."
In contrast, familial cylindromatosis is an inherited autosomal dominant condition characterized by multiple lesions located on the head and neck. Treatment is trickier, as there is no effective field or systemic therapy. Surgery should be considered most effective, but many doctors "are overwhelmed by the number of these lesions," said Dr. Slazinski, a dermatologist in private practice in Sarasota, Fla.
Familial trichoepitheliomas, Brooke-Spiegler syndrome, and familial cylindromatosis share a genetic etiology – a mutation of the CYLD gene on chromosome 16. "Great advances have been made in etiology and cellular mechanisms of familial cylindromatosis and related conditions," Dr. Slazinski said. But "treatment has not advanced to the same degree."
Removal of these lesions is often performed for aesthetic and functional reasons. "These diseases can become quite severe if untreated," Dr. Slazinski said. The psychosocial impact can be great, and patients often become social recluses.
Even with traditional excision, recurrence "is quite high" at approximately 42%, Dr. Slazinski said. Mohs micrographic surgery is used more often for solitary lesions. Other options, depending on the individual presentation, include cryotherapy, curettage, electrosurgery and radiofrequency excision, and true scalp excision with split-thickness grafting, "which is advocated in severe cases."
Cylindroma patients often present with pseudoalopecia because the tumor does not grow hair. Scalp cylindromas present a unique challenge, with limited tissue and patients’ desire to spare their hair, Dr. Slazinski said. "Hair cosmesis is often the patient’s greatest concern. Paradoxically, as hair is conserved, [the area] can become a reservoir for future tumor formation."
Some clinicians advocate topical aspirin therapy for familial cylindromatosis, Dr. Slazinski said. There may be "less than stellar results, but my patient is seeing some benefit and wants to continue on compounded, topical salicylic acid."
Dr. Slazinski described a patient with an extensive number of lesions across her face, head, and neck. "I’m blessed to be able to take care of this patient, because no one else has really offered her any possibility of improvement. I’ve taken it on myself to at least try to palliate the situation. I am under no delusion that I can cure her in any way."
Dr. Slazinski said he had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Future Technologies Hold Promise for Hair Restoration
ORLANDO – Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, U.K.). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
Historically, hair transplantation
ORLANDO – Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, U.K.). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
ORLANDO – Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, U.K.). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
Historically, hair transplantation
Historically, hair transplantation
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Exposure to Maternal Drug Use Disorder Ups Risk for Children
BOCA RATON, Fla. – Exposure to a maternal drug use disorder, particularly during adolescence, significantly increases the risk for development of a drug use disorder in children, according to a follow-up study.
Risk was more than seven times greater for girls exposed to maternal drug use disorder, compared with others without such exposure (odds ratio, 7.04), according to secondary analysis of a study of 262 girls and their family members (Pediatrics 2000;106:792-7).
The initial study included structured psychiatric interviews of these girls, aged 6-17 years, as well as 290 of their siblings and 238 parents. The current study assessed risks for this cohort over 5 years. The average age of girls at 5-year follow-up was 18 years.
Timing of exposure made a significant difference, Dr. Amy M. Yule said. Risk of any offspring developing a drug use disorder was significantly higher if exposure to maternal drug use disorder occurred during adolescence (OR, 3.61), compared with preschool or childhood.
In a practical sense, these findings suggest physicians who treat children screen parents for drug use regularly, Dr. Yule said at the annual meeting of the American Academy of Addiction Psychiatry meeting. "I’m advocating people to ask parents about substance use. This can make a difference in the child’s risk of having a substance use disorder."
You can ask the questions during family history taking, but be sure not to overlook any relevant responses if this is part of a comprehensive initial consultation, said Dr. Yule, a clinical fellow in psychiatry at Harvard Medical School and Massachusetts General Hospital in Boston. Exposures were primarily to cannabis, she added. There was no significant correlation with maternal alcohol use and subsequent child risk.
"The message is also it’s not okay to smoke marijuana in front of your 14-year-old," study coauthor Dr. Timothy E. Wilens said. Dr. Wilens is director of Substance Abuse Services in Pediatric Psychopharmacology, department of psychiatry, at Massachusetts General. "Pediatricians are really good with the ‘No smoking in front of kids’ message."
"The main point is getting people to ask parents if they are using and engaging parents to seek treatment or do a trial of sobriety," Dr. Yule said.
Researchers controlled for familial risk, socioeconomic status, and presence of attention-deficit/hyperactivity disorder (the original study compared 140 children with ADHD to 162 others without). "We looked at exposure only, not at genetic influence," Dr. Yule said. "You cannot change your genetics, but that could also be a [contributing factor]."
Dr. Yule was surprised that their follow-up study did not reveal the same overall associations with substance use disorder exposure cited in the original study. The 2000 study found risk associated with alcohol use, drug use, and both.
The current study focused primarily on risks between mothers and daughters. "I assume the risk is the same for paternal use," Dr. Yule said, although the smaller number of fathers precluded any such official conclusion.
Ideally, pediatricians and other physicians would start screening for parental drug use disorders when the child is in 5th grade, Dr. Wilens said. Even though most children do not start using drugs until age 12 years or older, "we want them to start asking parents about substance use earlier."
Dr. Yule said she had no relevant disclosures. Dr. Wilens is a researcher and consultant for Abbott, Lilly, Merck, and Shire. He is also a researcher for McNeil; a consultant for Astra-Zeneca; and on the speakers bureau for Lilly, McNeil, Novartis, and Shire. He consults and receives research grants from the National Institutes of Health/National Institute for Drug Abuse.
BOCA RATON, Fla. – Exposure to a maternal drug use disorder, particularly during adolescence, significantly increases the risk for development of a drug use disorder in children, according to a follow-up study.
Risk was more than seven times greater for girls exposed to maternal drug use disorder, compared with others without such exposure (odds ratio, 7.04), according to secondary analysis of a study of 262 girls and their family members (Pediatrics 2000;106:792-7).
The initial study included structured psychiatric interviews of these girls, aged 6-17 years, as well as 290 of their siblings and 238 parents. The current study assessed risks for this cohort over 5 years. The average age of girls at 5-year follow-up was 18 years.
Timing of exposure made a significant difference, Dr. Amy M. Yule said. Risk of any offspring developing a drug use disorder was significantly higher if exposure to maternal drug use disorder occurred during adolescence (OR, 3.61), compared with preschool or childhood.
In a practical sense, these findings suggest physicians who treat children screen parents for drug use regularly, Dr. Yule said at the annual meeting of the American Academy of Addiction Psychiatry meeting. "I’m advocating people to ask parents about substance use. This can make a difference in the child’s risk of having a substance use disorder."
You can ask the questions during family history taking, but be sure not to overlook any relevant responses if this is part of a comprehensive initial consultation, said Dr. Yule, a clinical fellow in psychiatry at Harvard Medical School and Massachusetts General Hospital in Boston. Exposures were primarily to cannabis, she added. There was no significant correlation with maternal alcohol use and subsequent child risk.
"The message is also it’s not okay to smoke marijuana in front of your 14-year-old," study coauthor Dr. Timothy E. Wilens said. Dr. Wilens is director of Substance Abuse Services in Pediatric Psychopharmacology, department of psychiatry, at Massachusetts General. "Pediatricians are really good with the ‘No smoking in front of kids’ message."
"The main point is getting people to ask parents if they are using and engaging parents to seek treatment or do a trial of sobriety," Dr. Yule said.
Researchers controlled for familial risk, socioeconomic status, and presence of attention-deficit/hyperactivity disorder (the original study compared 140 children with ADHD to 162 others without). "We looked at exposure only, not at genetic influence," Dr. Yule said. "You cannot change your genetics, but that could also be a [contributing factor]."
Dr. Yule was surprised that their follow-up study did not reveal the same overall associations with substance use disorder exposure cited in the original study. The 2000 study found risk associated with alcohol use, drug use, and both.
The current study focused primarily on risks between mothers and daughters. "I assume the risk is the same for paternal use," Dr. Yule said, although the smaller number of fathers precluded any such official conclusion.
Ideally, pediatricians and other physicians would start screening for parental drug use disorders when the child is in 5th grade, Dr. Wilens said. Even though most children do not start using drugs until age 12 years or older, "we want them to start asking parents about substance use earlier."
Dr. Yule said she had no relevant disclosures. Dr. Wilens is a researcher and consultant for Abbott, Lilly, Merck, and Shire. He is also a researcher for McNeil; a consultant for Astra-Zeneca; and on the speakers bureau for Lilly, McNeil, Novartis, and Shire. He consults and receives research grants from the National Institutes of Health/National Institute for Drug Abuse.
BOCA RATON, Fla. – Exposure to a maternal drug use disorder, particularly during adolescence, significantly increases the risk for development of a drug use disorder in children, according to a follow-up study.
Risk was more than seven times greater for girls exposed to maternal drug use disorder, compared with others without such exposure (odds ratio, 7.04), according to secondary analysis of a study of 262 girls and their family members (Pediatrics 2000;106:792-7).
The initial study included structured psychiatric interviews of these girls, aged 6-17 years, as well as 290 of their siblings and 238 parents. The current study assessed risks for this cohort over 5 years. The average age of girls at 5-year follow-up was 18 years.
Timing of exposure made a significant difference, Dr. Amy M. Yule said. Risk of any offspring developing a drug use disorder was significantly higher if exposure to maternal drug use disorder occurred during adolescence (OR, 3.61), compared with preschool or childhood.
In a practical sense, these findings suggest physicians who treat children screen parents for drug use regularly, Dr. Yule said at the annual meeting of the American Academy of Addiction Psychiatry meeting. "I’m advocating people to ask parents about substance use. This can make a difference in the child’s risk of having a substance use disorder."
You can ask the questions during family history taking, but be sure not to overlook any relevant responses if this is part of a comprehensive initial consultation, said Dr. Yule, a clinical fellow in psychiatry at Harvard Medical School and Massachusetts General Hospital in Boston. Exposures were primarily to cannabis, she added. There was no significant correlation with maternal alcohol use and subsequent child risk.
"The message is also it’s not okay to smoke marijuana in front of your 14-year-old," study coauthor Dr. Timothy E. Wilens said. Dr. Wilens is director of Substance Abuse Services in Pediatric Psychopharmacology, department of psychiatry, at Massachusetts General. "Pediatricians are really good with the ‘No smoking in front of kids’ message."
"The main point is getting people to ask parents if they are using and engaging parents to seek treatment or do a trial of sobriety," Dr. Yule said.
Researchers controlled for familial risk, socioeconomic status, and presence of attention-deficit/hyperactivity disorder (the original study compared 140 children with ADHD to 162 others without). "We looked at exposure only, not at genetic influence," Dr. Yule said. "You cannot change your genetics, but that could also be a [contributing factor]."
Dr. Yule was surprised that their follow-up study did not reveal the same overall associations with substance use disorder exposure cited in the original study. The 2000 study found risk associated with alcohol use, drug use, and both.
The current study focused primarily on risks between mothers and daughters. "I assume the risk is the same for paternal use," Dr. Yule said, although the smaller number of fathers precluded any such official conclusion.
Ideally, pediatricians and other physicians would start screening for parental drug use disorders when the child is in 5th grade, Dr. Wilens said. Even though most children do not start using drugs until age 12 years or older, "we want them to start asking parents about substance use earlier."
Dr. Yule said she had no relevant disclosures. Dr. Wilens is a researcher and consultant for Abbott, Lilly, Merck, and Shire. He is also a researcher for McNeil; a consultant for Astra-Zeneca; and on the speakers bureau for Lilly, McNeil, Novartis, and Shire. He consults and receives research grants from the National Institutes of Health/National Institute for Drug Abuse.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ADDICTION PSYCHIATRY
Exposure to Maternal Drug Use Disorder Ups Risk for Children
BOCA RATON, Fla. – Exposure to a maternal drug use disorder, particularly during adolescence, significantly increases the risk for development of a drug use disorder in children, according to a follow-up study.
Risk was more than seven times greater for girls exposed to maternal drug use disorder, compared with others without such exposure (odds ratio, 7.04), according to secondary analysis of a study of 262 girls and their family members (Pediatrics 2000;106:792-7).
The initial study included structured psychiatric interviews of these girls, aged 6-17 years, as well as 290 of their siblings and 238 parents. The current study assessed risks for this cohort over 5 years. The average age of girls at 5-year follow-up was 18 years.
Timing of exposure made a significant difference, Dr. Amy M. Yule said. Risk of any offspring developing a drug use disorder was significantly higher if exposure to maternal drug use disorder occurred during adolescence (OR, 3.61), compared with preschool or childhood.
In a practical sense, these findings suggest physicians who treat children screen parents for drug use regularly, Dr. Yule said at the annual meeting of the American Academy of Addiction Psychiatry meeting. "I’m advocating people to ask parents about substance use. This can make a difference in the child’s risk of having a substance use disorder."
You can ask the questions during family history taking, but be sure not to overlook any relevant responses if this is part of a comprehensive initial consultation, said Dr. Yule, a clinical fellow in psychiatry at Harvard Medical School and Massachusetts General Hospital in Boston. Exposures were primarily to cannabis, she added. There was no significant correlation with maternal alcohol use and subsequent child risk.
"The message is also it’s not okay to smoke marijuana in front of your 14-year-old," study coauthor Dr. Timothy E. Wilens said. Dr. Wilens is director of Substance Abuse Services in Pediatric Psychopharmacology, department of psychiatry, at Massachusetts General. "Pediatricians are really good with the ‘No smoking in front of kids’ message."
"The main point is getting people to ask parents if they are using and engaging parents to seek treatment or do a trial of sobriety," Dr. Yule said.
Researchers controlled for familial risk, socioeconomic status, and presence of attention-deficit/hyperactivity disorder (the original study compared 140 children with ADHD to 162 others without). "We looked at exposure only, not at genetic influence," Dr. Yule said. "You cannot change your genetics, but that could also be a [contributing factor]."
Dr. Yule was surprised that their follow-up study did not reveal the same overall associations with substance use disorder exposure cited in the original study. The 2000 study found risk associated with alcohol use, drug use, and both.
The current study focused primarily on risks between mothers and daughters. "I assume the risk is the same for paternal use," Dr. Yule said, although the smaller number of fathers precluded any such official conclusion.
Ideally, pediatricians and other physicians would start screening for parental drug use disorders when the child is in 5th grade, Dr. Wilens said. Even though most children do not start using drugs until age 12 years or older, "we want them to start asking parents about substance use earlier."
Dr. Yule said she had no relevant disclosures. Dr. Wilens is a researcher and consultant for Abbott, Lilly, Merck, and Shire. He is also a researcher for McNeil; a consultant for Astra-Zeneca; and on the speakers bureau for Lilly, McNeil, Novartis, and Shire. He consults and receives research grants from the National Institutes of Health/National Institute for Drug Abuse.
BOCA RATON, Fla. – Exposure to a maternal drug use disorder, particularly during adolescence, significantly increases the risk for development of a drug use disorder in children, according to a follow-up study.
Risk was more than seven times greater for girls exposed to maternal drug use disorder, compared with others without such exposure (odds ratio, 7.04), according to secondary analysis of a study of 262 girls and their family members (Pediatrics 2000;106:792-7).
The initial study included structured psychiatric interviews of these girls, aged 6-17 years, as well as 290 of their siblings and 238 parents. The current study assessed risks for this cohort over 5 years. The average age of girls at 5-year follow-up was 18 years.
Timing of exposure made a significant difference, Dr. Amy M. Yule said. Risk of any offspring developing a drug use disorder was significantly higher if exposure to maternal drug use disorder occurred during adolescence (OR, 3.61), compared with preschool or childhood.
In a practical sense, these findings suggest physicians who treat children screen parents for drug use regularly, Dr. Yule said at the annual meeting of the American Academy of Addiction Psychiatry meeting. "I’m advocating people to ask parents about substance use. This can make a difference in the child’s risk of having a substance use disorder."
You can ask the questions during family history taking, but be sure not to overlook any relevant responses if this is part of a comprehensive initial consultation, said Dr. Yule, a clinical fellow in psychiatry at Harvard Medical School and Massachusetts General Hospital in Boston. Exposures were primarily to cannabis, she added. There was no significant correlation with maternal alcohol use and subsequent child risk.
"The message is also it’s not okay to smoke marijuana in front of your 14-year-old," study coauthor Dr. Timothy E. Wilens said. Dr. Wilens is director of Substance Abuse Services in Pediatric Psychopharmacology, department of psychiatry, at Massachusetts General. "Pediatricians are really good with the ‘No smoking in front of kids’ message."
"The main point is getting people to ask parents if they are using and engaging parents to seek treatment or do a trial of sobriety," Dr. Yule said.
Researchers controlled for familial risk, socioeconomic status, and presence of attention-deficit/hyperactivity disorder (the original study compared 140 children with ADHD to 162 others without). "We looked at exposure only, not at genetic influence," Dr. Yule said. "You cannot change your genetics, but that could also be a [contributing factor]."
Dr. Yule was surprised that their follow-up study did not reveal the same overall associations with substance use disorder exposure cited in the original study. The 2000 study found risk associated with alcohol use, drug use, and both.
The current study focused primarily on risks between mothers and daughters. "I assume the risk is the same for paternal use," Dr. Yule said, although the smaller number of fathers precluded any such official conclusion.
Ideally, pediatricians and other physicians would start screening for parental drug use disorders when the child is in 5th grade, Dr. Wilens said. Even though most children do not start using drugs until age 12 years or older, "we want them to start asking parents about substance use earlier."
Dr. Yule said she had no relevant disclosures. Dr. Wilens is a researcher and consultant for Abbott, Lilly, Merck, and Shire. He is also a researcher for McNeil; a consultant for Astra-Zeneca; and on the speakers bureau for Lilly, McNeil, Novartis, and Shire. He consults and receives research grants from the National Institutes of Health/National Institute for Drug Abuse.
BOCA RATON, Fla. – Exposure to a maternal drug use disorder, particularly during adolescence, significantly increases the risk for development of a drug use disorder in children, according to a follow-up study.
Risk was more than seven times greater for girls exposed to maternal drug use disorder, compared with others without such exposure (odds ratio, 7.04), according to secondary analysis of a study of 262 girls and their family members (Pediatrics 2000;106:792-7).
The initial study included structured psychiatric interviews of these girls, aged 6-17 years, as well as 290 of their siblings and 238 parents. The current study assessed risks for this cohort over 5 years. The average age of girls at 5-year follow-up was 18 years.
Timing of exposure made a significant difference, Dr. Amy M. Yule said. Risk of any offspring developing a drug use disorder was significantly higher if exposure to maternal drug use disorder occurred during adolescence (OR, 3.61), compared with preschool or childhood.
In a practical sense, these findings suggest physicians who treat children screen parents for drug use regularly, Dr. Yule said at the annual meeting of the American Academy of Addiction Psychiatry meeting. "I’m advocating people to ask parents about substance use. This can make a difference in the child’s risk of having a substance use disorder."
You can ask the questions during family history taking, but be sure not to overlook any relevant responses if this is part of a comprehensive initial consultation, said Dr. Yule, a clinical fellow in psychiatry at Harvard Medical School and Massachusetts General Hospital in Boston. Exposures were primarily to cannabis, she added. There was no significant correlation with maternal alcohol use and subsequent child risk.
"The message is also it’s not okay to smoke marijuana in front of your 14-year-old," study coauthor Dr. Timothy E. Wilens said. Dr. Wilens is director of Substance Abuse Services in Pediatric Psychopharmacology, department of psychiatry, at Massachusetts General. "Pediatricians are really good with the ‘No smoking in front of kids’ message."
"The main point is getting people to ask parents if they are using and engaging parents to seek treatment or do a trial of sobriety," Dr. Yule said.
Researchers controlled for familial risk, socioeconomic status, and presence of attention-deficit/hyperactivity disorder (the original study compared 140 children with ADHD to 162 others without). "We looked at exposure only, not at genetic influence," Dr. Yule said. "You cannot change your genetics, but that could also be a [contributing factor]."
Dr. Yule was surprised that their follow-up study did not reveal the same overall associations with substance use disorder exposure cited in the original study. The 2000 study found risk associated with alcohol use, drug use, and both.
The current study focused primarily on risks between mothers and daughters. "I assume the risk is the same for paternal use," Dr. Yule said, although the smaller number of fathers precluded any such official conclusion.
Ideally, pediatricians and other physicians would start screening for parental drug use disorders when the child is in 5th grade, Dr. Wilens said. Even though most children do not start using drugs until age 12 years or older, "we want them to start asking parents about substance use earlier."
Dr. Yule said she had no relevant disclosures. Dr. Wilens is a researcher and consultant for Abbott, Lilly, Merck, and Shire. He is also a researcher for McNeil; a consultant for Astra-Zeneca; and on the speakers bureau for Lilly, McNeil, Novartis, and Shire. He consults and receives research grants from the National Institutes of Health/National Institute for Drug Abuse.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ADDICTION PSYCHIATRY
Major Finding: Exposure to maternal drug use disorder significantly increases risk of development of same disorder for offspring (odds ratio, 7.04), compared with unexposed children.
Data Source: Secondary analysis of 262 girls and their families followed 5 years after initial study enrollment.
Disclosures: Dr. Amy M. Yule had no relevant disclosures. Dr. Timothy Wilens is a researcher, consultant, and speaker for NIDA and multiple pharmaceutical companies.
Program Improves Hip Fracture Outcomes : Targeted intervention that includes progressive resistance training lowered mortality, dependency.
Major Finding: Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (odds ratio = 0.19).
Data Source: The Hip Fracture Intervention Trial (HIPFIT) compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions versus 62 randomized to usual care (6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies).
Disclosures: Dr. Singh said she had no relevant financial disclosures.
NEW ORLEANS — Compared with usual care after hip fracture, a comprehensive and targeted intervention that includes high-intensity progressive resistance training over 12 months lowers mortality, decreases nursing home admissions, improves activities of daily living dependency, and decreases the use of assistive devices, according to a randomized, controlled trial.
“It is possible to change the most important outcomes for these people,” Dr. Maria A. Fiatarone Singh said.
Functional dependency, however, did not significantly differ between groups.
Many facets of hip fractures have been studied, from pharmacologic prevention of osteoporosis to acute hospital interventions to fracture rehabilitation. “Although we've done a lot of studies, we still have not figured out how to prevent people from entering a nursing home or dying,” said Dr. Singh, professor of medicine and chair of exercise and sport science at the University of Sydney.
So Dr. Singh and her colleagues launched the Hip Fracture Intervention Trial (HIPFIT). They compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions vs. 62 patients randomized to usual care. Intervention was associated with an 84% reduction in the likelihood of nursing home admission (odds ratio, 0.16), compared with usual care, Dr. Singh said. In absolute numbers, 5 intervention patients (8%) and 12 control patients (19%) were admitted to a nursing home during the 12 months of follow-up.
“Hip fracture is associated with chronic pain, reduced mobility, disability, and increasing degree of dependence. After hip fracture, 10%-20% of formerly community-dwelling people require long-term nursing home care,” Dr. Singh said.
Four intervention patients and eight usual-care patients died. Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (OR = 0.19). Cardiovascular disease, infection, and stroke were among the causes.
Dr. Singh and her associates hypothesized that long-term disability and nursing home utilization after hip fracture would be reduced by targeted, multifactorial intervention aimed at the primary risk factors. They chose modifiable risk factors to make application of their findings more practical, including sarcopenia/muscle weakness, poor balance or gait, malnutrition or weight loss, vitamin D insufficiency, and vision concerns.
All intervention group participants received hip protectors and supervised, high-intensity, progressive resistance training for 12 months. The protocol included seven exercises designed for both upper and lower body strength. A meeting attendee questioned how patients were able to exercise after hip fracture. The intervention began with an isometric measure of strength and actual strength training started about 6 months after fracture, Dr. Singh replied.
Balance training exercises were progressive as well. As tasks were mastered, participants graduated to a more difficult level. For example, if a person could balance holding on to something with two hands, next they progressed to one hand and then to one finger.
Interventions were added for individual participants as needed, up to a total of 13. Treatment of depression, nutritional supplementation, medication management, and vision assessment are examples. Some participants received home assessment and referral to community services. Others received interventions to address risk and/or fear of falling, low self-efficacy, and polypharmacy.
Evaluations were done at baseline and at 4 and 12 months after fracture, with regular review by geriatricians, general practitioners, and ophthalmologists.
A meeting attendee asked which interventions were most useful. “Our specific intent was not to break apart the 13 interventions,” Dr. Singh said. She said many were intertwined, for example, vision improvements allowed balance training to be more effective. The effects of strength and balance training were most robust because they were performed twice a week for 12 months.
Usual care included 6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies. “We sent letter to general practitioners if people [in the usual-care group] were depressed, had low vitamin D, or abnormal cognitive function. We did not prescribe for this group,” she said.
Even though overall functional dependency did not differ significantly, intervention was associated with significantly less decline in some functional dependency KATZ scores (total, continence, and transfer) at 12 months, compared with their prefracture baseline. This is relevant, Dr. Singh said, because previous research they did showed that overall function declines for most people after a hip fracture. Only 20% of participants in the Sarcopenia and Hip Fracture Study (SHIP) returned to baseline function at 12 months (J. Gerontol. A. Biol. Sci. Med. Sci. 2009;64:568-74). In the current study, after the researchers controlled for age, there was less of a decline in function for total KATZ score, transfer change, and continence change if patients were in intervention group vs. usual care, according to Dr. Singh.
“Did changes in KATZ activities of daily living total score and scales mediate the nursing home admissions we saw? It seemed to be the case,” Dr. Singh said. “The nursing home residents had greater decline in KATZ function and toileting [continence] scores vs. others.”
All results are based on an intent-to-treat analysis. The dropout rate was low, she said: nine HIPFIT patients and three usual-care patients did not complete follow-up.
At baseline, the community-dwelling participants were 69% female; mean age, 79 years; 83% at nutritional risk; 88% vitamin D insufficient; 90% living independently (vs. 10% in nursing homes); and 38% were cognitively impaired. A total 45% were depressed. The mean number of chronic diseases was 3.4. The usual-care group reported worse bodily pain, the only significant difference between groups. There were no adverse events, except for some musculoskeletal soreness after activity.
Major Finding: Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (odds ratio = 0.19).
Data Source: The Hip Fracture Intervention Trial (HIPFIT) compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions versus 62 randomized to usual care (6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies).
Disclosures: Dr. Singh said she had no relevant financial disclosures.
NEW ORLEANS — Compared with usual care after hip fracture, a comprehensive and targeted intervention that includes high-intensity progressive resistance training over 12 months lowers mortality, decreases nursing home admissions, improves activities of daily living dependency, and decreases the use of assistive devices, according to a randomized, controlled trial.
“It is possible to change the most important outcomes for these people,” Dr. Maria A. Fiatarone Singh said.
Functional dependency, however, did not significantly differ between groups.
Many facets of hip fractures have been studied, from pharmacologic prevention of osteoporosis to acute hospital interventions to fracture rehabilitation. “Although we've done a lot of studies, we still have not figured out how to prevent people from entering a nursing home or dying,” said Dr. Singh, professor of medicine and chair of exercise and sport science at the University of Sydney.
So Dr. Singh and her colleagues launched the Hip Fracture Intervention Trial (HIPFIT). They compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions vs. 62 patients randomized to usual care. Intervention was associated with an 84% reduction in the likelihood of nursing home admission (odds ratio, 0.16), compared with usual care, Dr. Singh said. In absolute numbers, 5 intervention patients (8%) and 12 control patients (19%) were admitted to a nursing home during the 12 months of follow-up.
“Hip fracture is associated with chronic pain, reduced mobility, disability, and increasing degree of dependence. After hip fracture, 10%-20% of formerly community-dwelling people require long-term nursing home care,” Dr. Singh said.
Four intervention patients and eight usual-care patients died. Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (OR = 0.19). Cardiovascular disease, infection, and stroke were among the causes.
Dr. Singh and her associates hypothesized that long-term disability and nursing home utilization after hip fracture would be reduced by targeted, multifactorial intervention aimed at the primary risk factors. They chose modifiable risk factors to make application of their findings more practical, including sarcopenia/muscle weakness, poor balance or gait, malnutrition or weight loss, vitamin D insufficiency, and vision concerns.
All intervention group participants received hip protectors and supervised, high-intensity, progressive resistance training for 12 months. The protocol included seven exercises designed for both upper and lower body strength. A meeting attendee questioned how patients were able to exercise after hip fracture. The intervention began with an isometric measure of strength and actual strength training started about 6 months after fracture, Dr. Singh replied.
Balance training exercises were progressive as well. As tasks were mastered, participants graduated to a more difficult level. For example, if a person could balance holding on to something with two hands, next they progressed to one hand and then to one finger.
Interventions were added for individual participants as needed, up to a total of 13. Treatment of depression, nutritional supplementation, medication management, and vision assessment are examples. Some participants received home assessment and referral to community services. Others received interventions to address risk and/or fear of falling, low self-efficacy, and polypharmacy.
Evaluations were done at baseline and at 4 and 12 months after fracture, with regular review by geriatricians, general practitioners, and ophthalmologists.
A meeting attendee asked which interventions were most useful. “Our specific intent was not to break apart the 13 interventions,” Dr. Singh said. She said many were intertwined, for example, vision improvements allowed balance training to be more effective. The effects of strength and balance training were most robust because they were performed twice a week for 12 months.
Usual care included 6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies. “We sent letter to general practitioners if people [in the usual-care group] were depressed, had low vitamin D, or abnormal cognitive function. We did not prescribe for this group,” she said.
Even though overall functional dependency did not differ significantly, intervention was associated with significantly less decline in some functional dependency KATZ scores (total, continence, and transfer) at 12 months, compared with their prefracture baseline. This is relevant, Dr. Singh said, because previous research they did showed that overall function declines for most people after a hip fracture. Only 20% of participants in the Sarcopenia and Hip Fracture Study (SHIP) returned to baseline function at 12 months (J. Gerontol. A. Biol. Sci. Med. Sci. 2009;64:568-74). In the current study, after the researchers controlled for age, there was less of a decline in function for total KATZ score, transfer change, and continence change if patients were in intervention group vs. usual care, according to Dr. Singh.
“Did changes in KATZ activities of daily living total score and scales mediate the nursing home admissions we saw? It seemed to be the case,” Dr. Singh said. “The nursing home residents had greater decline in KATZ function and toileting [continence] scores vs. others.”
All results are based on an intent-to-treat analysis. The dropout rate was low, she said: nine HIPFIT patients and three usual-care patients did not complete follow-up.
At baseline, the community-dwelling participants were 69% female; mean age, 79 years; 83% at nutritional risk; 88% vitamin D insufficient; 90% living independently (vs. 10% in nursing homes); and 38% were cognitively impaired. A total 45% were depressed. The mean number of chronic diseases was 3.4. The usual-care group reported worse bodily pain, the only significant difference between groups. There were no adverse events, except for some musculoskeletal soreness after activity.
Major Finding: Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (odds ratio = 0.19).
Data Source: The Hip Fracture Intervention Trial (HIPFIT) compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions versus 62 randomized to usual care (6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies).
Disclosures: Dr. Singh said she had no relevant financial disclosures.
NEW ORLEANS — Compared with usual care after hip fracture, a comprehensive and targeted intervention that includes high-intensity progressive resistance training over 12 months lowers mortality, decreases nursing home admissions, improves activities of daily living dependency, and decreases the use of assistive devices, according to a randomized, controlled trial.
“It is possible to change the most important outcomes for these people,” Dr. Maria A. Fiatarone Singh said.
Functional dependency, however, did not significantly differ between groups.
Many facets of hip fractures have been studied, from pharmacologic prevention of osteoporosis to acute hospital interventions to fracture rehabilitation. “Although we've done a lot of studies, we still have not figured out how to prevent people from entering a nursing home or dying,” said Dr. Singh, professor of medicine and chair of exercise and sport science at the University of Sydney.
So Dr. Singh and her colleagues launched the Hip Fracture Intervention Trial (HIPFIT). They compared outcomes for 62 hip fracture patients randomized to resistance training and up to 12 other interventions vs. 62 patients randomized to usual care. Intervention was associated with an 84% reduction in the likelihood of nursing home admission (odds ratio, 0.16), compared with usual care, Dr. Singh said. In absolute numbers, 5 intervention patients (8%) and 12 control patients (19%) were admitted to a nursing home during the 12 months of follow-up.
“Hip fracture is associated with chronic pain, reduced mobility, disability, and increasing degree of dependence. After hip fracture, 10%-20% of formerly community-dwelling people require long-term nursing home care,” Dr. Singh said.
Four intervention patients and eight usual-care patients died. Age-adjusted risk of death was significantly reduced in the intervention group, compared with usual care (OR = 0.19). Cardiovascular disease, infection, and stroke were among the causes.
Dr. Singh and her associates hypothesized that long-term disability and nursing home utilization after hip fracture would be reduced by targeted, multifactorial intervention aimed at the primary risk factors. They chose modifiable risk factors to make application of their findings more practical, including sarcopenia/muscle weakness, poor balance or gait, malnutrition or weight loss, vitamin D insufficiency, and vision concerns.
All intervention group participants received hip protectors and supervised, high-intensity, progressive resistance training for 12 months. The protocol included seven exercises designed for both upper and lower body strength. A meeting attendee questioned how patients were able to exercise after hip fracture. The intervention began with an isometric measure of strength and actual strength training started about 6 months after fracture, Dr. Singh replied.
Balance training exercises were progressive as well. As tasks were mastered, participants graduated to a more difficult level. For example, if a person could balance holding on to something with two hands, next they progressed to one hand and then to one finger.
Interventions were added for individual participants as needed, up to a total of 13. Treatment of depression, nutritional supplementation, medication management, and vision assessment are examples. Some participants received home assessment and referral to community services. Others received interventions to address risk and/or fear of falling, low self-efficacy, and polypharmacy.
Evaluations were done at baseline and at 4 and 12 months after fracture, with regular review by geriatricians, general practitioners, and ophthalmologists.
A meeting attendee asked which interventions were most useful. “Our specific intent was not to break apart the 13 interventions,” Dr. Singh said. She said many were intertwined, for example, vision improvements allowed balance training to be more effective. The effects of strength and balance training were most robust because they were performed twice a week for 12 months.
Usual care included 6-12 weeks of physiotherapy, an orthopedic consult at 6 weeks, and any recommended therapies. “We sent letter to general practitioners if people [in the usual-care group] were depressed, had low vitamin D, or abnormal cognitive function. We did not prescribe for this group,” she said.
Even though overall functional dependency did not differ significantly, intervention was associated with significantly less decline in some functional dependency KATZ scores (total, continence, and transfer) at 12 months, compared with their prefracture baseline. This is relevant, Dr. Singh said, because previous research they did showed that overall function declines for most people after a hip fracture. Only 20% of participants in the Sarcopenia and Hip Fracture Study (SHIP) returned to baseline function at 12 months (J. Gerontol. A. Biol. Sci. Med. Sci. 2009;64:568-74). In the current study, after the researchers controlled for age, there was less of a decline in function for total KATZ score, transfer change, and continence change if patients were in intervention group vs. usual care, according to Dr. Singh.
“Did changes in KATZ activities of daily living total score and scales mediate the nursing home admissions we saw? It seemed to be the case,” Dr. Singh said. “The nursing home residents had greater decline in KATZ function and toileting [continence] scores vs. others.”
All results are based on an intent-to-treat analysis. The dropout rate was low, she said: nine HIPFIT patients and three usual-care patients did not complete follow-up.
At baseline, the community-dwelling participants were 69% female; mean age, 79 years; 83% at nutritional risk; 88% vitamin D insufficient; 90% living independently (vs. 10% in nursing homes); and 38% were cognitively impaired. A total 45% were depressed. The mean number of chronic diseases was 3.4. The usual-care group reported worse bodily pain, the only significant difference between groups. There were no adverse events, except for some musculoskeletal soreness after activity.
Acute Alcohol Withdrawal: DT Risk Higher After Age 65
BOCA RATON, Fla. – Older patients hospitalized with acute alcohol withdrawal experience significantly more delirium tremens and delirium than do inpatients younger than 65 years, according to a retrospective study.
Screen older patients for alcohol consumption and consider medications other than benzodiazepines to treat withdrawal in this population, advised Dr. Jeremy Doniger, a resident at Harvard Longwood Psychiatry in Boston.
"Older people are drinking more than we realize. Be consistent about screening for it," Dr. Doniger said. In fact, with the aging of the population, the number of older adults with an alcohol use disorder is expected to double by 2020 (Brit. Med. J. 2003;327:664-7). A likely outcome is that more older patients will be admitted to hospitals for severe alcohol withdrawal in the future.
"Benzodiazepines can cause delirium, and older patients may be more susceptible [to these effects]," said Dr. Doniger. N-methyl-d-aspartate antagonists, for example, alone or in combination with benzodiazepines, are an effective alternative strategy, he added.
Reports in the literature are mixed as to whether older age predicts worse withdrawal, said Dr. Joji Suzuki, lead study investigator, and director of the Addiction Recovery Program at Brigham and Women’s Hospital and Harvard Medical School, Boston.
To find a more definitive answer, the investigators reviewed the charts of all medical inpatients at Brigham and Women’s Hospital for whom a psychiatry consultation was requested from 2008 to 2010. They identified 141 patients diagnosed and treated for alcohol withdrawal during hospital admission.
They compared 31 older patients to 110 younger ones. "We wanted to know if older patients, those 65 and older, have worse or the same outcomes as younger folks," said Dr. Suzuki. "We found something very striking: that DTs [delirium tremens] or delirium from any cause approaches 50% in older patients," Dr. Suzuki said. "Delirium is very serious, and can be a predictor for death."
Delirium from any cause affected 52% of the older group versus 30% of the younger patients, a statistically significant difference. In addition, 44% of older patients experienced DTs while hospitalized, compared with 20% of younger patients. This disparity also was significantly different.
"Part of it might be severity of comorbidities," Dr. Doniger said. The presence of more severe comorbidities was significantly associated with development of any delirium (odds ratio, 1.2), but not with DTs (OR, 1.13) or withdrawal seizures (OR, 1.02).
Prevalence of withdrawal seizures did not differ significantly between older patients (10%) and younger patients (6%). Nor did hospital length of stay differ significantly. Older patients stayed at Brigham and Women’s Hospital a mean 12.5 days compared with 8.6 days for the younger group.
The take-home message is that "younger patients going through withdrawal will fare about the same or a little worse than someone in a detox setting. But older patients are at greater risk for adverse outcomes, and the longer they stay in the hospital, the higher their risk for not doing well [because of nosocomial infections, falls, and other risk factors]," Dr. Suzuki said.
Inpatients who experienced DTs received significantly higher doses of benzodiazepines than did those who did not. In terms of lorazepam equivalents, the mean dose was 64.6 mg versus 30.5 mg in the non-DT group.
Dr. Doniger said differences in body composition and metabolism could contribute to greater benzodiazepine delirium in older patients because they typically have less water and more fat, which holds medications, and they have slower liver metabolism, he said.
The study was supported in part by the Department of Psychiatry at Harvard Medical School. Dr. Suzuki and Dr. Doniger had no relevant financial disclosures.
BOCA RATON, Fla. – Older patients hospitalized with acute alcohol withdrawal experience significantly more delirium tremens and delirium than do inpatients younger than 65 years, according to a retrospective study.
Screen older patients for alcohol consumption and consider medications other than benzodiazepines to treat withdrawal in this population, advised Dr. Jeremy Doniger, a resident at Harvard Longwood Psychiatry in Boston.
"Older people are drinking more than we realize. Be consistent about screening for it," Dr. Doniger said. In fact, with the aging of the population, the number of older adults with an alcohol use disorder is expected to double by 2020 (Brit. Med. J. 2003;327:664-7). A likely outcome is that more older patients will be admitted to hospitals for severe alcohol withdrawal in the future.
"Benzodiazepines can cause delirium, and older patients may be more susceptible [to these effects]," said Dr. Doniger. N-methyl-d-aspartate antagonists, for example, alone or in combination with benzodiazepines, are an effective alternative strategy, he added.
Reports in the literature are mixed as to whether older age predicts worse withdrawal, said Dr. Joji Suzuki, lead study investigator, and director of the Addiction Recovery Program at Brigham and Women’s Hospital and Harvard Medical School, Boston.
To find a more definitive answer, the investigators reviewed the charts of all medical inpatients at Brigham and Women’s Hospital for whom a psychiatry consultation was requested from 2008 to 2010. They identified 141 patients diagnosed and treated for alcohol withdrawal during hospital admission.
They compared 31 older patients to 110 younger ones. "We wanted to know if older patients, those 65 and older, have worse or the same outcomes as younger folks," said Dr. Suzuki. "We found something very striking: that DTs [delirium tremens] or delirium from any cause approaches 50% in older patients," Dr. Suzuki said. "Delirium is very serious, and can be a predictor for death."
Delirium from any cause affected 52% of the older group versus 30% of the younger patients, a statistically significant difference. In addition, 44% of older patients experienced DTs while hospitalized, compared with 20% of younger patients. This disparity also was significantly different.
"Part of it might be severity of comorbidities," Dr. Doniger said. The presence of more severe comorbidities was significantly associated with development of any delirium (odds ratio, 1.2), but not with DTs (OR, 1.13) or withdrawal seizures (OR, 1.02).
Prevalence of withdrawal seizures did not differ significantly between older patients (10%) and younger patients (6%). Nor did hospital length of stay differ significantly. Older patients stayed at Brigham and Women’s Hospital a mean 12.5 days compared with 8.6 days for the younger group.
The take-home message is that "younger patients going through withdrawal will fare about the same or a little worse than someone in a detox setting. But older patients are at greater risk for adverse outcomes, and the longer they stay in the hospital, the higher their risk for not doing well [because of nosocomial infections, falls, and other risk factors]," Dr. Suzuki said.
Inpatients who experienced DTs received significantly higher doses of benzodiazepines than did those who did not. In terms of lorazepam equivalents, the mean dose was 64.6 mg versus 30.5 mg in the non-DT group.
Dr. Doniger said differences in body composition and metabolism could contribute to greater benzodiazepine delirium in older patients because they typically have less water and more fat, which holds medications, and they have slower liver metabolism, he said.
The study was supported in part by the Department of Psychiatry at Harvard Medical School. Dr. Suzuki and Dr. Doniger had no relevant financial disclosures.
BOCA RATON, Fla. – Older patients hospitalized with acute alcohol withdrawal experience significantly more delirium tremens and delirium than do inpatients younger than 65 years, according to a retrospective study.
Screen older patients for alcohol consumption and consider medications other than benzodiazepines to treat withdrawal in this population, advised Dr. Jeremy Doniger, a resident at Harvard Longwood Psychiatry in Boston.
"Older people are drinking more than we realize. Be consistent about screening for it," Dr. Doniger said. In fact, with the aging of the population, the number of older adults with an alcohol use disorder is expected to double by 2020 (Brit. Med. J. 2003;327:664-7). A likely outcome is that more older patients will be admitted to hospitals for severe alcohol withdrawal in the future.
"Benzodiazepines can cause delirium, and older patients may be more susceptible [to these effects]," said Dr. Doniger. N-methyl-d-aspartate antagonists, for example, alone or in combination with benzodiazepines, are an effective alternative strategy, he added.
Reports in the literature are mixed as to whether older age predicts worse withdrawal, said Dr. Joji Suzuki, lead study investigator, and director of the Addiction Recovery Program at Brigham and Women’s Hospital and Harvard Medical School, Boston.
To find a more definitive answer, the investigators reviewed the charts of all medical inpatients at Brigham and Women’s Hospital for whom a psychiatry consultation was requested from 2008 to 2010. They identified 141 patients diagnosed and treated for alcohol withdrawal during hospital admission.
They compared 31 older patients to 110 younger ones. "We wanted to know if older patients, those 65 and older, have worse or the same outcomes as younger folks," said Dr. Suzuki. "We found something very striking: that DTs [delirium tremens] or delirium from any cause approaches 50% in older patients," Dr. Suzuki said. "Delirium is very serious, and can be a predictor for death."
Delirium from any cause affected 52% of the older group versus 30% of the younger patients, a statistically significant difference. In addition, 44% of older patients experienced DTs while hospitalized, compared with 20% of younger patients. This disparity also was significantly different.
"Part of it might be severity of comorbidities," Dr. Doniger said. The presence of more severe comorbidities was significantly associated with development of any delirium (odds ratio, 1.2), but not with DTs (OR, 1.13) or withdrawal seizures (OR, 1.02).
Prevalence of withdrawal seizures did not differ significantly between older patients (10%) and younger patients (6%). Nor did hospital length of stay differ significantly. Older patients stayed at Brigham and Women’s Hospital a mean 12.5 days compared with 8.6 days for the younger group.
The take-home message is that "younger patients going through withdrawal will fare about the same or a little worse than someone in a detox setting. But older patients are at greater risk for adverse outcomes, and the longer they stay in the hospital, the higher their risk for not doing well [because of nosocomial infections, falls, and other risk factors]," Dr. Suzuki said.
Inpatients who experienced DTs received significantly higher doses of benzodiazepines than did those who did not. In terms of lorazepam equivalents, the mean dose was 64.6 mg versus 30.5 mg in the non-DT group.
Dr. Doniger said differences in body composition and metabolism could contribute to greater benzodiazepine delirium in older patients because they typically have less water and more fat, which holds medications, and they have slower liver metabolism, he said.
The study was supported in part by the Department of Psychiatry at Harvard Medical School. Dr. Suzuki and Dr. Doniger had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ADDICTION PSYCHIATRY
Major Finding: A greater percentage of hospitalized patients 65 and older with alcohol withdrawal experience delirium, 52%, compared with 30% among younger patients.
Data Source: Review of 141 patient charts involving a psychiatry consultation from 2008 to 2010.
Disclosures: Dr. Joji Suzuki and Dr. Jeremy Doniger had no relevant disclosures.
Intensive Outpatient Program Targets Transitional Youth With Addiction
BOCA RATON, Fla. – An intensive outpatient program for transitional age youth with addiction shows promise for increasing treatment engagement and retention.
People aged 18-25 years with addiction are the most challenging to enroll and retain in treatment and, at the same time, have the highest rates of past-month illicit drug use and binge/heavy alcohol use, said Martha T. Kane, Ph.D.
A long-term focus that rewards short-term, smaller successes, and positive peer counseling are among the elements of a new integrated model devised by Dr. Kane and her colleagues at Massachusetts General Hospital in Boston. They combined common elements from several effective treatment modalities, including motivational enhancement therapy, group cognitive-behavioral therapy, and contingency management. There is also recognition of family support and counseling in this underserved, high-risk population.
The program is a work in progress, but early evidence is encouraging. Of 142 youths who initially entered the inpatient Addiction Recovery Management Service (ARMS) between October 2007 and April 2010, 48 enrolled in the intensive outpatient program. A majority, 31 or 65%, completed both intake and a follow-up assessment at 12 weeks, "so something we’re doing is working," Dr. Kane said at the meeting.
Typically 60%-70% of young adults discontinue addiction treatment before completion, said Dr. Kane, ARMS clinical director, Center for Addiction Medicine at Massachusetts General.
"I tell staff and trainees their first priority on day one is to get them to come back," Dr. Kane said. This group is least likely to adhere to continuing care, according to a study of injection drug users (Am. J. Alcohol Drug Abuse 2007;33:217-25).
Completers experienced a 69% increase in the number of days abstinent, 48% fewer days spent "intoxicated all day," and a 32% reduction in days where substance use prevented effective functioning. Other outcomes included a 39% improvement in substance dependence (measured with the Leeds Dependence Questionnaire); a 33% improvement in days bothered by emotional health issues; and a 47% reduction in the number of days where mental health problems prevented effective functioning.
More modest gains were demonstrated on standardized measures, including a 22% improvement in the Beck Depression Inventory; a 13% improvement in State-Trait Anxiety Inventory; and a 5% improvement on State-Trait anger scores. "That is something we need to figure out," Dr. Kane said, "how to make [these] kids less angry."
An average 7 young adults participate in the transitional youth intensive outpatient program at any one time (maximum number is 10). Services are offered 8-10 hours per week over 3-4 days. The intensity of services decreases gradually over the 12-week program. Every participant receives psychiatric evaluation and ongoing medication, as eligible. No medication is on site, but there is a prescriber, Dr. Kane said in response to a question from a meeting attendee.
The program recognizes that transitional youth do not always succeed in adult addiction programs where "these kids are told things will get better," Dr. Kane said. "They don’t have the capacity to wait 6 weeks or more" and instead need a more rapid, positive reinforcement. Patients leave with a goal to improve a small aspect of their life in the first week.
A great deal of flexibility is another feature of the program. Abstinence is not a requirement for enrollment, for example. Partial completion in the program is acknowledged, Dr. Kane said. Also, "if they want to meet at Dunkin’ Donuts instead of our office, we can do a little of that."
Dr. Kane said that it can take a while for some to feel connected to the program. "It’s okay with me if they don’t make another connection for another three weeks." At a minimum, participants are expected to come back to the program when things are not going well. "We never really let go entirely, and they know it."
The psychiatrists, social workers, and care coordinator communicate with the youth via text messaging, e-mail, and telephone. A meeting attendee asked about violating confidentiality. "Little confidential medical information is texted," Dr. Kane said. "We’re not using texting to do clinical care, but to maintain connection in a way that works for them." Examples of text messages are: "How are you today?", "Hope everything is okay," and "Let me know what happened about the job."
An acknowledgement that relapses are likely over time is part of the long-term recovery management approach. Dr. Kane said: "Do not discharge them if they relapse. That doesn’t mean that you tolerate it or ignore it, but incorporate it into your practice."
The program staff recognizes that young adulthood is a time with many development changes, including increased personal freedom and responsibility. For example, they work to help clients effectively manage impulses for autonomy and to successfully communicate with primary care providers, Dr. Kane said. They also learn to communicate during peer counseling. "We get our best outcomes when there are kids who are able to communicate constructively."
An opportunity to practice goal-directed behavior is another component. "We enhance motivation toward a positive outcome rather than avoiding a negative outcome." Getting a job and/or their own apartment, as well as getting parents "off their backs" or to say something nice to them are the main factors that motivate this age group, Dr. Kane said.
There is a focus on positive reinforcement for positive behavior. For example, a girl living in her parents’ basement wanted her own apartment. Her parents were fearful because of her ongoing alcohol use. So program staff worked with her parents to set up a system whereby the parents put money away toward first and last months’ rent on an apartment each week that the girl maintains sobriety. If she fails, she does not lose everything, only the money allotted for that week, Dr. Kane said. "She had 4 straight weeks of sobriety. She is in control and everyone is working toward the same goal."
Multidimensional family therapy is another feature of the program. "What we added to our standard treatment in this population is engagement of families," said Dr. E. Nalan Ward, medical director of the West End Clinic at Massachusetts General.
"Families are the unrecognized factor," Dr. Kane said. "Kids 18-25 still have very active involvements with family."
For example, clinicians work with families to reduce any toxic environmental factors, including parental substance use. Psychological education and skills training (tailored for parents of transitional-age children) also is provided. "Parents learn that kids don’t need the same things from them as they used to," Dr. Kane said. Family participation is important, she added, because even after patients leave treatment they are still involved with their families.
Massachusetts General accepts insurance for the program, including Blue Cross Blue Shield and Massachusetts Behavioral Health (state Medicaid). A donor fund kicks in after insurance benefits and other options are exhausted. Some clients self-pay for a variety of prepackaged service options as well.
Dr. Kane and Dr. Ward had no relevant disclosures.
BOCA RATON, Fla. – An intensive outpatient program for transitional age youth with addiction shows promise for increasing treatment engagement and retention.
People aged 18-25 years with addiction are the most challenging to enroll and retain in treatment and, at the same time, have the highest rates of past-month illicit drug use and binge/heavy alcohol use, said Martha T. Kane, Ph.D.
A long-term focus that rewards short-term, smaller successes, and positive peer counseling are among the elements of a new integrated model devised by Dr. Kane and her colleagues at Massachusetts General Hospital in Boston. They combined common elements from several effective treatment modalities, including motivational enhancement therapy, group cognitive-behavioral therapy, and contingency management. There is also recognition of family support and counseling in this underserved, high-risk population.
The program is a work in progress, but early evidence is encouraging. Of 142 youths who initially entered the inpatient Addiction Recovery Management Service (ARMS) between October 2007 and April 2010, 48 enrolled in the intensive outpatient program. A majority, 31 or 65%, completed both intake and a follow-up assessment at 12 weeks, "so something we’re doing is working," Dr. Kane said at the meeting.
Typically 60%-70% of young adults discontinue addiction treatment before completion, said Dr. Kane, ARMS clinical director, Center for Addiction Medicine at Massachusetts General.
"I tell staff and trainees their first priority on day one is to get them to come back," Dr. Kane said. This group is least likely to adhere to continuing care, according to a study of injection drug users (Am. J. Alcohol Drug Abuse 2007;33:217-25).
Completers experienced a 69% increase in the number of days abstinent, 48% fewer days spent "intoxicated all day," and a 32% reduction in days where substance use prevented effective functioning. Other outcomes included a 39% improvement in substance dependence (measured with the Leeds Dependence Questionnaire); a 33% improvement in days bothered by emotional health issues; and a 47% reduction in the number of days where mental health problems prevented effective functioning.
More modest gains were demonstrated on standardized measures, including a 22% improvement in the Beck Depression Inventory; a 13% improvement in State-Trait Anxiety Inventory; and a 5% improvement on State-Trait anger scores. "That is something we need to figure out," Dr. Kane said, "how to make [these] kids less angry."
An average 7 young adults participate in the transitional youth intensive outpatient program at any one time (maximum number is 10). Services are offered 8-10 hours per week over 3-4 days. The intensity of services decreases gradually over the 12-week program. Every participant receives psychiatric evaluation and ongoing medication, as eligible. No medication is on site, but there is a prescriber, Dr. Kane said in response to a question from a meeting attendee.
The program recognizes that transitional youth do not always succeed in adult addiction programs where "these kids are told things will get better," Dr. Kane said. "They don’t have the capacity to wait 6 weeks or more" and instead need a more rapid, positive reinforcement. Patients leave with a goal to improve a small aspect of their life in the first week.
A great deal of flexibility is another feature of the program. Abstinence is not a requirement for enrollment, for example. Partial completion in the program is acknowledged, Dr. Kane said. Also, "if they want to meet at Dunkin’ Donuts instead of our office, we can do a little of that."
Dr. Kane said that it can take a while for some to feel connected to the program. "It’s okay with me if they don’t make another connection for another three weeks." At a minimum, participants are expected to come back to the program when things are not going well. "We never really let go entirely, and they know it."
The psychiatrists, social workers, and care coordinator communicate with the youth via text messaging, e-mail, and telephone. A meeting attendee asked about violating confidentiality. "Little confidential medical information is texted," Dr. Kane said. "We’re not using texting to do clinical care, but to maintain connection in a way that works for them." Examples of text messages are: "How are you today?", "Hope everything is okay," and "Let me know what happened about the job."
An acknowledgement that relapses are likely over time is part of the long-term recovery management approach. Dr. Kane said: "Do not discharge them if they relapse. That doesn’t mean that you tolerate it or ignore it, but incorporate it into your practice."
The program staff recognizes that young adulthood is a time with many development changes, including increased personal freedom and responsibility. For example, they work to help clients effectively manage impulses for autonomy and to successfully communicate with primary care providers, Dr. Kane said. They also learn to communicate during peer counseling. "We get our best outcomes when there are kids who are able to communicate constructively."
An opportunity to practice goal-directed behavior is another component. "We enhance motivation toward a positive outcome rather than avoiding a negative outcome." Getting a job and/or their own apartment, as well as getting parents "off their backs" or to say something nice to them are the main factors that motivate this age group, Dr. Kane said.
There is a focus on positive reinforcement for positive behavior. For example, a girl living in her parents’ basement wanted her own apartment. Her parents were fearful because of her ongoing alcohol use. So program staff worked with her parents to set up a system whereby the parents put money away toward first and last months’ rent on an apartment each week that the girl maintains sobriety. If she fails, she does not lose everything, only the money allotted for that week, Dr. Kane said. "She had 4 straight weeks of sobriety. She is in control and everyone is working toward the same goal."
Multidimensional family therapy is another feature of the program. "What we added to our standard treatment in this population is engagement of families," said Dr. E. Nalan Ward, medical director of the West End Clinic at Massachusetts General.
"Families are the unrecognized factor," Dr. Kane said. "Kids 18-25 still have very active involvements with family."
For example, clinicians work with families to reduce any toxic environmental factors, including parental substance use. Psychological education and skills training (tailored for parents of transitional-age children) also is provided. "Parents learn that kids don’t need the same things from them as they used to," Dr. Kane said. Family participation is important, she added, because even after patients leave treatment they are still involved with their families.
Massachusetts General accepts insurance for the program, including Blue Cross Blue Shield and Massachusetts Behavioral Health (state Medicaid). A donor fund kicks in after insurance benefits and other options are exhausted. Some clients self-pay for a variety of prepackaged service options as well.
Dr. Kane and Dr. Ward had no relevant disclosures.
BOCA RATON, Fla. – An intensive outpatient program for transitional age youth with addiction shows promise for increasing treatment engagement and retention.
People aged 18-25 years with addiction are the most challenging to enroll and retain in treatment and, at the same time, have the highest rates of past-month illicit drug use and binge/heavy alcohol use, said Martha T. Kane, Ph.D.
A long-term focus that rewards short-term, smaller successes, and positive peer counseling are among the elements of a new integrated model devised by Dr. Kane and her colleagues at Massachusetts General Hospital in Boston. They combined common elements from several effective treatment modalities, including motivational enhancement therapy, group cognitive-behavioral therapy, and contingency management. There is also recognition of family support and counseling in this underserved, high-risk population.
The program is a work in progress, but early evidence is encouraging. Of 142 youths who initially entered the inpatient Addiction Recovery Management Service (ARMS) between October 2007 and April 2010, 48 enrolled in the intensive outpatient program. A majority, 31 or 65%, completed both intake and a follow-up assessment at 12 weeks, "so something we’re doing is working," Dr. Kane said at the meeting.
Typically 60%-70% of young adults discontinue addiction treatment before completion, said Dr. Kane, ARMS clinical director, Center for Addiction Medicine at Massachusetts General.
"I tell staff and trainees their first priority on day one is to get them to come back," Dr. Kane said. This group is least likely to adhere to continuing care, according to a study of injection drug users (Am. J. Alcohol Drug Abuse 2007;33:217-25).
Completers experienced a 69% increase in the number of days abstinent, 48% fewer days spent "intoxicated all day," and a 32% reduction in days where substance use prevented effective functioning. Other outcomes included a 39% improvement in substance dependence (measured with the Leeds Dependence Questionnaire); a 33% improvement in days bothered by emotional health issues; and a 47% reduction in the number of days where mental health problems prevented effective functioning.
More modest gains were demonstrated on standardized measures, including a 22% improvement in the Beck Depression Inventory; a 13% improvement in State-Trait Anxiety Inventory; and a 5% improvement on State-Trait anger scores. "That is something we need to figure out," Dr. Kane said, "how to make [these] kids less angry."
An average 7 young adults participate in the transitional youth intensive outpatient program at any one time (maximum number is 10). Services are offered 8-10 hours per week over 3-4 days. The intensity of services decreases gradually over the 12-week program. Every participant receives psychiatric evaluation and ongoing medication, as eligible. No medication is on site, but there is a prescriber, Dr. Kane said in response to a question from a meeting attendee.
The program recognizes that transitional youth do not always succeed in adult addiction programs where "these kids are told things will get better," Dr. Kane said. "They don’t have the capacity to wait 6 weeks or more" and instead need a more rapid, positive reinforcement. Patients leave with a goal to improve a small aspect of their life in the first week.
A great deal of flexibility is another feature of the program. Abstinence is not a requirement for enrollment, for example. Partial completion in the program is acknowledged, Dr. Kane said. Also, "if they want to meet at Dunkin’ Donuts instead of our office, we can do a little of that."
Dr. Kane said that it can take a while for some to feel connected to the program. "It’s okay with me if they don’t make another connection for another three weeks." At a minimum, participants are expected to come back to the program when things are not going well. "We never really let go entirely, and they know it."
The psychiatrists, social workers, and care coordinator communicate with the youth via text messaging, e-mail, and telephone. A meeting attendee asked about violating confidentiality. "Little confidential medical information is texted," Dr. Kane said. "We’re not using texting to do clinical care, but to maintain connection in a way that works for them." Examples of text messages are: "How are you today?", "Hope everything is okay," and "Let me know what happened about the job."
An acknowledgement that relapses are likely over time is part of the long-term recovery management approach. Dr. Kane said: "Do not discharge them if they relapse. That doesn’t mean that you tolerate it or ignore it, but incorporate it into your practice."
The program staff recognizes that young adulthood is a time with many development changes, including increased personal freedom and responsibility. For example, they work to help clients effectively manage impulses for autonomy and to successfully communicate with primary care providers, Dr. Kane said. They also learn to communicate during peer counseling. "We get our best outcomes when there are kids who are able to communicate constructively."
An opportunity to practice goal-directed behavior is another component. "We enhance motivation toward a positive outcome rather than avoiding a negative outcome." Getting a job and/or their own apartment, as well as getting parents "off their backs" or to say something nice to them are the main factors that motivate this age group, Dr. Kane said.
There is a focus on positive reinforcement for positive behavior. For example, a girl living in her parents’ basement wanted her own apartment. Her parents were fearful because of her ongoing alcohol use. So program staff worked with her parents to set up a system whereby the parents put money away toward first and last months’ rent on an apartment each week that the girl maintains sobriety. If she fails, she does not lose everything, only the money allotted for that week, Dr. Kane said. "She had 4 straight weeks of sobriety. She is in control and everyone is working toward the same goal."
Multidimensional family therapy is another feature of the program. "What we added to our standard treatment in this population is engagement of families," said Dr. E. Nalan Ward, medical director of the West End Clinic at Massachusetts General.
"Families are the unrecognized factor," Dr. Kane said. "Kids 18-25 still have very active involvements with family."
For example, clinicians work with families to reduce any toxic environmental factors, including parental substance use. Psychological education and skills training (tailored for parents of transitional-age children) also is provided. "Parents learn that kids don’t need the same things from them as they used to," Dr. Kane said. Family participation is important, she added, because even after patients leave treatment they are still involved with their families.
Massachusetts General accepts insurance for the program, including Blue Cross Blue Shield and Massachusetts Behavioral Health (state Medicaid). A donor fund kicks in after insurance benefits and other options are exhausted. Some clients self-pay for a variety of prepackaged service options as well.
Dr. Kane and Dr. Ward had no relevant disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ADDICTION PSYCHIATRY
Major Finding: Program completers experienced a 69% increase in the number of days abstinent, 48% fewer days spent "intoxicated all day," and a 32% reduction in days where substance use prevented effective functioning.
Data Source: Study of 48 transition-aged youths who entered intensive outpatient services program at Massachusetts General Hospital between October 2007 and April 2010.
Disclosures: Dr. Kane and Dr. Ward had no relevant disclosures.