User login
Why consults don’t happen
Today our team saw an 89-year-old gentleman on the hospitalist service with dementia, heart failure, atrial fibrillation, chronic kidney disease, and problems falling. His last known fall was less than 3 months ago and resulted in a broken hip requiring surgical intervention. This was his fourth hospitalization in 6 months, yet it was the first time he was seen by our service.
The frequency at which palliative care (PC) consults are ordered in a particular hospital varies widely. Some reasons for this are not easy fixes – PC is not available in each hospital (as was the case in two of this gentleman’s four hospitalizations), many PC teams are available only Monday-Friday, and patient volumes within a hospital ebb and flow with much less predictability than the tides.
However, some of the reasons are amenable to change. These might include the particular group of hospitalists, or one attending physician, utilizing PC consults less frequently than another. Or it may simply be that the connection was not made between the patient’s experience and the usefulness of an early PC consults. Screening tools are one method of decreasing variability in PC involvement as well as increasing the appropriateness of our service for a particular patient.
There are quite a few palliative care screening tools available. Many of them focus on what most of us would expect, which are the most common diagnoses we see (late-stage cancer, HF, cirrhosis, end-stage renal disease, dementia, etc.). Multiple studies have estimated that mature PC programs in large hospitals are consulted on 1%-2% of live discharges. However, we estimate that more than 10% of these discharged patients have palliative needs that go unmet. While it is true that we wish PC could be involved in all of these lives, this large number of people who spend time in the hospital with these diagnoses, coupled with a national shortage of PC providers, translates into an unbalanced equation.
Rather than looking at a specific diagnosis, we suggest incorporating inquiries on the presence of "palliative care–related problems." While these might require more thought or investigation into a patient’s situation, we find them to be more fruitful than using diagnosis alone.
Some examples? Mismatch between the expectations of the medical team vs. patient/family when it comes to prognosis or the goals of care would be one of them. Another might be persistent uncontrolled symptoms despite usual medical management. Family members disagreeing or demonstrating concerns about the goals of care is still another.
Having used various screening tools in multiple hospitals and clinical settings, we suggest the following considerations in setting up your own:
• Stakeholder management: The right services and staff need to agree on this being a way to improve quality of care (we always provide an "opt-out" option for those who don’t want us involved for some reason).
• Start small: Implement these on one unit at a time or limit the diagnoses to one or two conditions only. You can make the criteria less stringent if the PC team’s bandwidth is not too narrow.
• Be flexible: Even by starting small, there will be times that the PC teams are overwhelmed on a particular day leaving the occasional patient who meets criteria unseen. If the consult is urgent, a phone call is appropriate so that an assumption isn’t made that the screening tool will catch 100% of the patients.
• Track data: When using these tools, palliative care teams have been able to show things such as improved Hospital Consumer Assessment of Healthcare Providers and Systems survey results and decreased readmissions. Demonstrate what you’re doing for your institution so that you can expand the units or patients served.
PC screening tools are an effective way to decrease variability and improve quality. For examples of tools that we use, please get in touch. Find our contact info and read earlier columns at ehospitalistnews/Palliatively.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Today our team saw an 89-year-old gentleman on the hospitalist service with dementia, heart failure, atrial fibrillation, chronic kidney disease, and problems falling. His last known fall was less than 3 months ago and resulted in a broken hip requiring surgical intervention. This was his fourth hospitalization in 6 months, yet it was the first time he was seen by our service.
The frequency at which palliative care (PC) consults are ordered in a particular hospital varies widely. Some reasons for this are not easy fixes – PC is not available in each hospital (as was the case in two of this gentleman’s four hospitalizations), many PC teams are available only Monday-Friday, and patient volumes within a hospital ebb and flow with much less predictability than the tides.
However, some of the reasons are amenable to change. These might include the particular group of hospitalists, or one attending physician, utilizing PC consults less frequently than another. Or it may simply be that the connection was not made between the patient’s experience and the usefulness of an early PC consults. Screening tools are one method of decreasing variability in PC involvement as well as increasing the appropriateness of our service for a particular patient.
There are quite a few palliative care screening tools available. Many of them focus on what most of us would expect, which are the most common diagnoses we see (late-stage cancer, HF, cirrhosis, end-stage renal disease, dementia, etc.). Multiple studies have estimated that mature PC programs in large hospitals are consulted on 1%-2% of live discharges. However, we estimate that more than 10% of these discharged patients have palliative needs that go unmet. While it is true that we wish PC could be involved in all of these lives, this large number of people who spend time in the hospital with these diagnoses, coupled with a national shortage of PC providers, translates into an unbalanced equation.
Rather than looking at a specific diagnosis, we suggest incorporating inquiries on the presence of "palliative care–related problems." While these might require more thought or investigation into a patient’s situation, we find them to be more fruitful than using diagnosis alone.
Some examples? Mismatch between the expectations of the medical team vs. patient/family when it comes to prognosis or the goals of care would be one of them. Another might be persistent uncontrolled symptoms despite usual medical management. Family members disagreeing or demonstrating concerns about the goals of care is still another.
Having used various screening tools in multiple hospitals and clinical settings, we suggest the following considerations in setting up your own:
• Stakeholder management: The right services and staff need to agree on this being a way to improve quality of care (we always provide an "opt-out" option for those who don’t want us involved for some reason).
• Start small: Implement these on one unit at a time or limit the diagnoses to one or two conditions only. You can make the criteria less stringent if the PC team’s bandwidth is not too narrow.
• Be flexible: Even by starting small, there will be times that the PC teams are overwhelmed on a particular day leaving the occasional patient who meets criteria unseen. If the consult is urgent, a phone call is appropriate so that an assumption isn’t made that the screening tool will catch 100% of the patients.
• Track data: When using these tools, palliative care teams have been able to show things such as improved Hospital Consumer Assessment of Healthcare Providers and Systems survey results and decreased readmissions. Demonstrate what you’re doing for your institution so that you can expand the units or patients served.
PC screening tools are an effective way to decrease variability and improve quality. For examples of tools that we use, please get in touch. Find our contact info and read earlier columns at ehospitalistnews/Palliatively.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Today our team saw an 89-year-old gentleman on the hospitalist service with dementia, heart failure, atrial fibrillation, chronic kidney disease, and problems falling. His last known fall was less than 3 months ago and resulted in a broken hip requiring surgical intervention. This was his fourth hospitalization in 6 months, yet it was the first time he was seen by our service.
The frequency at which palliative care (PC) consults are ordered in a particular hospital varies widely. Some reasons for this are not easy fixes – PC is not available in each hospital (as was the case in two of this gentleman’s four hospitalizations), many PC teams are available only Monday-Friday, and patient volumes within a hospital ebb and flow with much less predictability than the tides.
However, some of the reasons are amenable to change. These might include the particular group of hospitalists, or one attending physician, utilizing PC consults less frequently than another. Or it may simply be that the connection was not made between the patient’s experience and the usefulness of an early PC consults. Screening tools are one method of decreasing variability in PC involvement as well as increasing the appropriateness of our service for a particular patient.
There are quite a few palliative care screening tools available. Many of them focus on what most of us would expect, which are the most common diagnoses we see (late-stage cancer, HF, cirrhosis, end-stage renal disease, dementia, etc.). Multiple studies have estimated that mature PC programs in large hospitals are consulted on 1%-2% of live discharges. However, we estimate that more than 10% of these discharged patients have palliative needs that go unmet. While it is true that we wish PC could be involved in all of these lives, this large number of people who spend time in the hospital with these diagnoses, coupled with a national shortage of PC providers, translates into an unbalanced equation.
Rather than looking at a specific diagnosis, we suggest incorporating inquiries on the presence of "palliative care–related problems." While these might require more thought or investigation into a patient’s situation, we find them to be more fruitful than using diagnosis alone.
Some examples? Mismatch between the expectations of the medical team vs. patient/family when it comes to prognosis or the goals of care would be one of them. Another might be persistent uncontrolled symptoms despite usual medical management. Family members disagreeing or demonstrating concerns about the goals of care is still another.
Having used various screening tools in multiple hospitals and clinical settings, we suggest the following considerations in setting up your own:
• Stakeholder management: The right services and staff need to agree on this being a way to improve quality of care (we always provide an "opt-out" option for those who don’t want us involved for some reason).
• Start small: Implement these on one unit at a time or limit the diagnoses to one or two conditions only. You can make the criteria less stringent if the PC team’s bandwidth is not too narrow.
• Be flexible: Even by starting small, there will be times that the PC teams are overwhelmed on a particular day leaving the occasional patient who meets criteria unseen. If the consult is urgent, a phone call is appropriate so that an assumption isn’t made that the screening tool will catch 100% of the patients.
• Track data: When using these tools, palliative care teams have been able to show things such as improved Hospital Consumer Assessment of Healthcare Providers and Systems survey results and decreased readmissions. Demonstrate what you’re doing for your institution so that you can expand the units or patients served.
PC screening tools are an effective way to decrease variability and improve quality. For examples of tools that we use, please get in touch. Find our contact info and read earlier columns at ehospitalistnews/Palliatively.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Negotiation: Priceless in good communication
The Society of Hospital Medicine held its annual meeting recently in Las Vegas, and Stephen had the opportunity to speak on the topic of "Family Meetings: The Art and the Evidence." As a special edition of Palliatively Speaking, we thought we would highlight one aspect of this subject, with other elements forthcoming in future pieces.
As a hospitalist, I stumbled and stuttered through many family meetings until I eventually found myself on more comfortable ground. Overall, I found them rewarding when they went well but stressful and deflating when they did not. The latter sensation was enough to create some avoidant behavior on my part.
After a few years of practice, my hospitalist group began shadowing one another periodically on rounds to provide feedback to our colleagues in the hope of improving the quality of our communication skills. It was then that I noticed that one of my partners was a master at these meetings. A real Rembrandt. He had the ability to deliver bad or difficult news without the dynamic in the room becoming inflammatory or out of control.
I will never forget watching him mediate a disagreement between a nurse and a patient suspected of using illicit substances while hospitalized. He flipped an antagonistic, heated situation into one where the patient, nurse, and physician all agreed on putting the past to rest and forging ahead with his proposed plan. We all left the room with a genuine sense that we had mutual purpose. In my admiration I realized that some of these skills must be teachable.
While I didn’t act on learning those communication techniques immediately after that encounter, I would eventually be formally exposed to them during my palliative medicine training. As it turns out, I still have some uncomfortable meetings with patients and families, but they come around much less frequently and when they do I now have a variety of tools to deal with challenges.
My appreciation of these tools doesn’t stop when I walk through the hospital doors each evening. I have found them to be invaluable in my personal life. In fact, learning to communicate better has been a source of renewal for me at work and staves off burnout. These techniques include active listening, motivational interviewing, demonstration of empathy, conflict resolution, and also negotiation. For the Society of Hospital Medicine meeting audience, I dissected negotiation, citing how it and the other skills can inject vitality into your interactions.
In any negotiation, it’s all about the other party. You are the smallest person in the room, the least important.
This is counterintuitive. Oftentimes at work we are trying to convince everyone how important we are. The readmissions committee should implement your plan to reduce recurrent hospitalizations. Your fellow hospitalists should recognize your value and make you the leader of the group. Patients show their appreciation for you making the right diagnosis and averting a medical calamity for them. But when you enter a family meeting, the patient and his or her loved ones are the center stage. To be successful you have to listen more and talk less. Get to understand the pictures in their heads and then summarize those thoughts and ideas back to them to show you’ve listened.
Make emotional payments. I don’t get into the meat of the meeting until I’ve done that with the patient and every family member in the room. No one holds family meetings for patients who are thriving and have outstanding outcomes. We have family meetings to figure out goals in the face of terrible diseases, when elder abuse is a possibility, when insurance-funded resources are depleted, and for a host of other difficult reasons.
This means that everyone in the room is suffering, sacrificing, scared, confused, or worried. Acknowledge them. Hold them up. Thank them. Reflect on similar moments in your life and demonstrate empathy. Apologize when things haven’t gone right for them at your hospital. These payments will pay handsome dividends as your relationship evolves.
Not manipulation. The term negotiation might bring up images of used car salespeople. I strongly disagree. In manipulation, one side wins and the other doesn’t. In negotiation, the goal is improved communication and understanding. Manipulation is about one side of the equation having knowledge that the other side is lacking and using that to achieve its means. Negotiators hope everyone at the table has the same knowledge.
This leads to two key principles of negotiations: transparency and genuineness. Patients and families are excellent at taking the temperature of the room when you sit down to meet with them. Share knowledge. Don’t have any hidden agendas. Following this principle builds trust.
Be incremental. Taking patients from comfortable, familiar territory into that which is uncomfortable or unfamiliar should not be done in one giant leap. Let’s use code status (CS) as an example because of the frequency with which it comes up (though I rarely talk about CS without first understanding the patient’s goals and hopes).
Some patients refuse to talk about CS, so I think incrementally. I ask that they consider talking about CS with me in the future. Very few people refuse to consider something. Two or three days later I ask, "Have you considered talking to me about CS?" That by itself opens up the topic for conversation. In the extremely unusual case where they still won’t engage, I then ask them, "What would it take for you to consider talking to me about this?" More incrementalism.
While this is not nearly an exhaustive list of negotiation techniques, we hope it is stimulating enough that you might be curious enough to learn more on your own and try incorporating this into your practice. If you’re motivated to do so, please feel free to contact us for reading suggestions: E-mail [email protected].
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Dr. Eric Gartman, FCCP, comments: We all have seen these discussions go well and been impressed by those who lead them. However, too often such conversations and family meetings are not actively pursued simply because they are "hard" - they take time and an investment of one's emotional energy. We should follow the example of many medical schools and training programs in recognizing the immense importance of gaining these skills, and foster the desire to be the one that others aim to emulate.
Dr. Eric Gartman, FCCP, comments: We all have seen these discussions go well and been impressed by those who lead them. However, too often such conversations and family meetings are not actively pursued simply because they are "hard" - they take time and an investment of one's emotional energy. We should follow the example of many medical schools and training programs in recognizing the immense importance of gaining these skills, and foster the desire to be the one that others aim to emulate.
Dr. Eric Gartman, FCCP, comments: We all have seen these discussions go well and been impressed by those who lead them. However, too often such conversations and family meetings are not actively pursued simply because they are "hard" - they take time and an investment of one's emotional energy. We should follow the example of many medical schools and training programs in recognizing the immense importance of gaining these skills, and foster the desire to be the one that others aim to emulate.
The Society of Hospital Medicine held its annual meeting recently in Las Vegas, and Stephen had the opportunity to speak on the topic of "Family Meetings: The Art and the Evidence." As a special edition of Palliatively Speaking, we thought we would highlight one aspect of this subject, with other elements forthcoming in future pieces.
As a hospitalist, I stumbled and stuttered through many family meetings until I eventually found myself on more comfortable ground. Overall, I found them rewarding when they went well but stressful and deflating when they did not. The latter sensation was enough to create some avoidant behavior on my part.
After a few years of practice, my hospitalist group began shadowing one another periodically on rounds to provide feedback to our colleagues in the hope of improving the quality of our communication skills. It was then that I noticed that one of my partners was a master at these meetings. A real Rembrandt. He had the ability to deliver bad or difficult news without the dynamic in the room becoming inflammatory or out of control.
I will never forget watching him mediate a disagreement between a nurse and a patient suspected of using illicit substances while hospitalized. He flipped an antagonistic, heated situation into one where the patient, nurse, and physician all agreed on putting the past to rest and forging ahead with his proposed plan. We all left the room with a genuine sense that we had mutual purpose. In my admiration I realized that some of these skills must be teachable.
While I didn’t act on learning those communication techniques immediately after that encounter, I would eventually be formally exposed to them during my palliative medicine training. As it turns out, I still have some uncomfortable meetings with patients and families, but they come around much less frequently and when they do I now have a variety of tools to deal with challenges.
My appreciation of these tools doesn’t stop when I walk through the hospital doors each evening. I have found them to be invaluable in my personal life. In fact, learning to communicate better has been a source of renewal for me at work and staves off burnout. These techniques include active listening, motivational interviewing, demonstration of empathy, conflict resolution, and also negotiation. For the Society of Hospital Medicine meeting audience, I dissected negotiation, citing how it and the other skills can inject vitality into your interactions.
In any negotiation, it’s all about the other party. You are the smallest person in the room, the least important.
This is counterintuitive. Oftentimes at work we are trying to convince everyone how important we are. The readmissions committee should implement your plan to reduce recurrent hospitalizations. Your fellow hospitalists should recognize your value and make you the leader of the group. Patients show their appreciation for you making the right diagnosis and averting a medical calamity for them. But when you enter a family meeting, the patient and his or her loved ones are the center stage. To be successful you have to listen more and talk less. Get to understand the pictures in their heads and then summarize those thoughts and ideas back to them to show you’ve listened.
Make emotional payments. I don’t get into the meat of the meeting until I’ve done that with the patient and every family member in the room. No one holds family meetings for patients who are thriving and have outstanding outcomes. We have family meetings to figure out goals in the face of terrible diseases, when elder abuse is a possibility, when insurance-funded resources are depleted, and for a host of other difficult reasons.
This means that everyone in the room is suffering, sacrificing, scared, confused, or worried. Acknowledge them. Hold them up. Thank them. Reflect on similar moments in your life and demonstrate empathy. Apologize when things haven’t gone right for them at your hospital. These payments will pay handsome dividends as your relationship evolves.
Not manipulation. The term negotiation might bring up images of used car salespeople. I strongly disagree. In manipulation, one side wins and the other doesn’t. In negotiation, the goal is improved communication and understanding. Manipulation is about one side of the equation having knowledge that the other side is lacking and using that to achieve its means. Negotiators hope everyone at the table has the same knowledge.
This leads to two key principles of negotiations: transparency and genuineness. Patients and families are excellent at taking the temperature of the room when you sit down to meet with them. Share knowledge. Don’t have any hidden agendas. Following this principle builds trust.
Be incremental. Taking patients from comfortable, familiar territory into that which is uncomfortable or unfamiliar should not be done in one giant leap. Let’s use code status (CS) as an example because of the frequency with which it comes up (though I rarely talk about CS without first understanding the patient’s goals and hopes).
Some patients refuse to talk about CS, so I think incrementally. I ask that they consider talking about CS with me in the future. Very few people refuse to consider something. Two or three days later I ask, "Have you considered talking to me about CS?" That by itself opens up the topic for conversation. In the extremely unusual case where they still won’t engage, I then ask them, "What would it take for you to consider talking to me about this?" More incrementalism.
While this is not nearly an exhaustive list of negotiation techniques, we hope it is stimulating enough that you might be curious enough to learn more on your own and try incorporating this into your practice. If you’re motivated to do so, please feel free to contact us for reading suggestions: E-mail [email protected].
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
The Society of Hospital Medicine held its annual meeting recently in Las Vegas, and Stephen had the opportunity to speak on the topic of "Family Meetings: The Art and the Evidence." As a special edition of Palliatively Speaking, we thought we would highlight one aspect of this subject, with other elements forthcoming in future pieces.
As a hospitalist, I stumbled and stuttered through many family meetings until I eventually found myself on more comfortable ground. Overall, I found them rewarding when they went well but stressful and deflating when they did not. The latter sensation was enough to create some avoidant behavior on my part.
After a few years of practice, my hospitalist group began shadowing one another periodically on rounds to provide feedback to our colleagues in the hope of improving the quality of our communication skills. It was then that I noticed that one of my partners was a master at these meetings. A real Rembrandt. He had the ability to deliver bad or difficult news without the dynamic in the room becoming inflammatory or out of control.
I will never forget watching him mediate a disagreement between a nurse and a patient suspected of using illicit substances while hospitalized. He flipped an antagonistic, heated situation into one where the patient, nurse, and physician all agreed on putting the past to rest and forging ahead with his proposed plan. We all left the room with a genuine sense that we had mutual purpose. In my admiration I realized that some of these skills must be teachable.
While I didn’t act on learning those communication techniques immediately after that encounter, I would eventually be formally exposed to them during my palliative medicine training. As it turns out, I still have some uncomfortable meetings with patients and families, but they come around much less frequently and when they do I now have a variety of tools to deal with challenges.
My appreciation of these tools doesn’t stop when I walk through the hospital doors each evening. I have found them to be invaluable in my personal life. In fact, learning to communicate better has been a source of renewal for me at work and staves off burnout. These techniques include active listening, motivational interviewing, demonstration of empathy, conflict resolution, and also negotiation. For the Society of Hospital Medicine meeting audience, I dissected negotiation, citing how it and the other skills can inject vitality into your interactions.
In any negotiation, it’s all about the other party. You are the smallest person in the room, the least important.
This is counterintuitive. Oftentimes at work we are trying to convince everyone how important we are. The readmissions committee should implement your plan to reduce recurrent hospitalizations. Your fellow hospitalists should recognize your value and make you the leader of the group. Patients show their appreciation for you making the right diagnosis and averting a medical calamity for them. But when you enter a family meeting, the patient and his or her loved ones are the center stage. To be successful you have to listen more and talk less. Get to understand the pictures in their heads and then summarize those thoughts and ideas back to them to show you’ve listened.
Make emotional payments. I don’t get into the meat of the meeting until I’ve done that with the patient and every family member in the room. No one holds family meetings for patients who are thriving and have outstanding outcomes. We have family meetings to figure out goals in the face of terrible diseases, when elder abuse is a possibility, when insurance-funded resources are depleted, and for a host of other difficult reasons.
This means that everyone in the room is suffering, sacrificing, scared, confused, or worried. Acknowledge them. Hold them up. Thank them. Reflect on similar moments in your life and demonstrate empathy. Apologize when things haven’t gone right for them at your hospital. These payments will pay handsome dividends as your relationship evolves.
Not manipulation. The term negotiation might bring up images of used car salespeople. I strongly disagree. In manipulation, one side wins and the other doesn’t. In negotiation, the goal is improved communication and understanding. Manipulation is about one side of the equation having knowledge that the other side is lacking and using that to achieve its means. Negotiators hope everyone at the table has the same knowledge.
This leads to two key principles of negotiations: transparency and genuineness. Patients and families are excellent at taking the temperature of the room when you sit down to meet with them. Share knowledge. Don’t have any hidden agendas. Following this principle builds trust.
Be incremental. Taking patients from comfortable, familiar territory into that which is uncomfortable or unfamiliar should not be done in one giant leap. Let’s use code status (CS) as an example because of the frequency with which it comes up (though I rarely talk about CS without first understanding the patient’s goals and hopes).
Some patients refuse to talk about CS, so I think incrementally. I ask that they consider talking about CS with me in the future. Very few people refuse to consider something. Two or three days later I ask, "Have you considered talking to me about CS?" That by itself opens up the topic for conversation. In the extremely unusual case where they still won’t engage, I then ask them, "What would it take for you to consider talking to me about this?" More incrementalism.
While this is not nearly an exhaustive list of negotiation techniques, we hope it is stimulating enough that you might be curious enough to learn more on your own and try incorporating this into your practice. If you’re motivated to do so, please feel free to contact us for reading suggestions: E-mail [email protected].
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Negotiation: Priceless in good communication
The Society of Hospital Medicine held its annual meeting recently in Las Vegas, and Stephen had the opportunity to speak on the topic of "Family Meetings: The Art and the Evidence." As a special edition of Palliatively Speaking, we thought we would highlight one aspect of this subject, with other elements forthcoming in future pieces.
As a hospitalist, I stumbled and stuttered through many family meetings until I eventually found myself on more comfortable ground. Overall, I found them rewarding when they went well but stressful and deflating when they did not. The latter sensation was enough to create some avoidant behavior on my part.
After a few years of practice, my hospitalist group began shadowing one another periodically on rounds to provide feedback to our colleagues in the hope of improving the quality of our communication skills. It was then that I noticed that one of my partners was a master at these meetings. A real Rembrandt. He had the ability to deliver bad or difficult news without the dynamic in the room becoming inflammatory or out of control.
I will never forget watching him mediate a disagreement between a nurse and a patient suspected of using illicit substances while hospitalized. He flipped an antagonistic, heated situation into one where the patient, nurse, and physician all agreed on putting the past to rest and forging ahead with his proposed plan. We all left the room with a genuine sense that we had mutual purpose. In my admiration I realized that some of these skills must be teachable.
While I didn’t act on learning those communication techniques immediately after that encounter, I would eventually be formally exposed to them during my palliative medicine training. As it turns out, I still have some uncomfortable meetings with patients and families, but they come around much less frequently and when they do I now have a variety of tools to deal with challenges.
My appreciation of these tools doesn’t stop when I walk through the hospital doors each evening. I have found them to be invaluable in my personal life. In fact, learning to communicate better has been a source of renewal for me at work and staves off burnout. These techniques include active listening, motivational interviewing, demonstration of empathy, conflict resolution, and also negotiation. For the Society of Hospital Medicine meeting audience, I dissected negotiation, citing how it and the other skills can inject vitality into your interactions.
In any negotiation, it’s all about the other party. You are the smallest person in the room, the least important.
This is counterintuitive. Oftentimes at work we are trying to convince everyone how important we are. The readmissions committee should implement your plan to reduce recurrent hospitalizations. Your fellow hospitalists should recognize your value and make you the leader of the group. Patients show their appreciation for you making the right diagnosis and averting a medical calamity for them. But when you enter a family meeting, the patient and his or her loved ones are the center stage. To be successful you have to listen more and talk less. Get to understand the pictures in their heads and then summarize those thoughts and ideas back to them to show you’ve listened.
Make emotional payments. I don’t get into the meat of the meeting until I’ve done that with the patient and every family member in the room. No one holds family meetings for patients who are thriving and have outstanding outcomes. We have family meetings to figure out goals in the face of terrible diseases, when elder abuse is a possibility, when insurance-funded resources are depleted, and for a host of other difficult reasons.
This means that everyone in the room is suffering, sacrificing, scared, confused, or worried. Acknowledge them. Hold them up. Thank them. Reflect on similar moments in your life and demonstrate empathy. Apologize when things haven’t gone right for them at your hospital. These payments will pay handsome dividends as your relationship evolves.
Not manipulation. The term negotiation might bring up images of used car salespeople. I strongly disagree. In manipulation, one side wins and the other doesn’t. In negotiation, the goal is improved communication and understanding. Manipulation is about one side of the equation having knowledge that the other side is lacking and using that to achieve its means. Negotiators hope everyone at the table has the same knowledge.
This leads to two key principles of negotiations: transparency and genuineness. Patients and families are excellent at taking the temperature of the room when you sit down to meet with them. Share knowledge. Don’t have any hidden agendas. Following this principle builds trust.
Be incremental. Taking patients from comfortable, familiar territory into that which is uncomfortable or unfamiliar should not be done in one giant leap. Let’s use code status (CS) as an example because of the frequency with which it comes up (though I rarely talk about CS without first understanding the patient’s goals and hopes).
Some patients refuse to talk about CS, so I think incrementally. I ask that they consider talking about CS with me in the future. Very few people refuse to consider something. Two or three days later I ask, "Have you considered talking to me about CS?" That by itself opens up the topic for conversation. In the extremely unusual case where they still won’t engage, I then ask them, "What would it take for you to consider talking to me about this?" More incrementalism.
While this is not nearly an exhaustive list of negotiation techniques, we hope it is stimulating enough that you might be curious enough to learn more on your own and try incorporating this into your practice. If you’re motivated to do so, please feel free to contact us for reading suggestions: E-mail [email protected].
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
The Society of Hospital Medicine held its annual meeting recently in Las Vegas, and Stephen had the opportunity to speak on the topic of "Family Meetings: The Art and the Evidence." As a special edition of Palliatively Speaking, we thought we would highlight one aspect of this subject, with other elements forthcoming in future pieces.
As a hospitalist, I stumbled and stuttered through many family meetings until I eventually found myself on more comfortable ground. Overall, I found them rewarding when they went well but stressful and deflating when they did not. The latter sensation was enough to create some avoidant behavior on my part.
After a few years of practice, my hospitalist group began shadowing one another periodically on rounds to provide feedback to our colleagues in the hope of improving the quality of our communication skills. It was then that I noticed that one of my partners was a master at these meetings. A real Rembrandt. He had the ability to deliver bad or difficult news without the dynamic in the room becoming inflammatory or out of control.
I will never forget watching him mediate a disagreement between a nurse and a patient suspected of using illicit substances while hospitalized. He flipped an antagonistic, heated situation into one where the patient, nurse, and physician all agreed on putting the past to rest and forging ahead with his proposed plan. We all left the room with a genuine sense that we had mutual purpose. In my admiration I realized that some of these skills must be teachable.
While I didn’t act on learning those communication techniques immediately after that encounter, I would eventually be formally exposed to them during my palliative medicine training. As it turns out, I still have some uncomfortable meetings with patients and families, but they come around much less frequently and when they do I now have a variety of tools to deal with challenges.
My appreciation of these tools doesn’t stop when I walk through the hospital doors each evening. I have found them to be invaluable in my personal life. In fact, learning to communicate better has been a source of renewal for me at work and staves off burnout. These techniques include active listening, motivational interviewing, demonstration of empathy, conflict resolution, and also negotiation. For the Society of Hospital Medicine meeting audience, I dissected negotiation, citing how it and the other skills can inject vitality into your interactions.
In any negotiation, it’s all about the other party. You are the smallest person in the room, the least important.
This is counterintuitive. Oftentimes at work we are trying to convince everyone how important we are. The readmissions committee should implement your plan to reduce recurrent hospitalizations. Your fellow hospitalists should recognize your value and make you the leader of the group. Patients show their appreciation for you making the right diagnosis and averting a medical calamity for them. But when you enter a family meeting, the patient and his or her loved ones are the center stage. To be successful you have to listen more and talk less. Get to understand the pictures in their heads and then summarize those thoughts and ideas back to them to show you’ve listened.
Make emotional payments. I don’t get into the meat of the meeting until I’ve done that with the patient and every family member in the room. No one holds family meetings for patients who are thriving and have outstanding outcomes. We have family meetings to figure out goals in the face of terrible diseases, when elder abuse is a possibility, when insurance-funded resources are depleted, and for a host of other difficult reasons.
This means that everyone in the room is suffering, sacrificing, scared, confused, or worried. Acknowledge them. Hold them up. Thank them. Reflect on similar moments in your life and demonstrate empathy. Apologize when things haven’t gone right for them at your hospital. These payments will pay handsome dividends as your relationship evolves.
Not manipulation. The term negotiation might bring up images of used car salespeople. I strongly disagree. In manipulation, one side wins and the other doesn’t. In negotiation, the goal is improved communication and understanding. Manipulation is about one side of the equation having knowledge that the other side is lacking and using that to achieve its means. Negotiators hope everyone at the table has the same knowledge.
This leads to two key principles of negotiations: transparency and genuineness. Patients and families are excellent at taking the temperature of the room when you sit down to meet with them. Share knowledge. Don’t have any hidden agendas. Following this principle builds trust.
Be incremental. Taking patients from comfortable, familiar territory into that which is uncomfortable or unfamiliar should not be done in one giant leap. Let’s use code status (CS) as an example because of the frequency with which it comes up (though I rarely talk about CS without first understanding the patient’s goals and hopes).
Some patients refuse to talk about CS, so I think incrementally. I ask that they consider talking about CS with me in the future. Very few people refuse to consider something. Two or three days later I ask, "Have you considered talking to me about CS?" That by itself opens up the topic for conversation. In the extremely unusual case where they still won’t engage, I then ask them, "What would it take for you to consider talking to me about this?" More incrementalism.
While this is not nearly an exhaustive list of negotiation techniques, we hope it is stimulating enough that you might be curious enough to learn more on your own and try incorporating this into your practice. If you’re motivated to do so, please feel free to contact us for reading suggestions: E-mail [email protected].
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
The Society of Hospital Medicine held its annual meeting recently in Las Vegas, and Stephen had the opportunity to speak on the topic of "Family Meetings: The Art and the Evidence." As a special edition of Palliatively Speaking, we thought we would highlight one aspect of this subject, with other elements forthcoming in future pieces.
As a hospitalist, I stumbled and stuttered through many family meetings until I eventually found myself on more comfortable ground. Overall, I found them rewarding when they went well but stressful and deflating when they did not. The latter sensation was enough to create some avoidant behavior on my part.
After a few years of practice, my hospitalist group began shadowing one another periodically on rounds to provide feedback to our colleagues in the hope of improving the quality of our communication skills. It was then that I noticed that one of my partners was a master at these meetings. A real Rembrandt. He had the ability to deliver bad or difficult news without the dynamic in the room becoming inflammatory or out of control.
I will never forget watching him mediate a disagreement between a nurse and a patient suspected of using illicit substances while hospitalized. He flipped an antagonistic, heated situation into one where the patient, nurse, and physician all agreed on putting the past to rest and forging ahead with his proposed plan. We all left the room with a genuine sense that we had mutual purpose. In my admiration I realized that some of these skills must be teachable.
While I didn’t act on learning those communication techniques immediately after that encounter, I would eventually be formally exposed to them during my palliative medicine training. As it turns out, I still have some uncomfortable meetings with patients and families, but they come around much less frequently and when they do I now have a variety of tools to deal with challenges.
My appreciation of these tools doesn’t stop when I walk through the hospital doors each evening. I have found them to be invaluable in my personal life. In fact, learning to communicate better has been a source of renewal for me at work and staves off burnout. These techniques include active listening, motivational interviewing, demonstration of empathy, conflict resolution, and also negotiation. For the Society of Hospital Medicine meeting audience, I dissected negotiation, citing how it and the other skills can inject vitality into your interactions.
In any negotiation, it’s all about the other party. You are the smallest person in the room, the least important.
This is counterintuitive. Oftentimes at work we are trying to convince everyone how important we are. The readmissions committee should implement your plan to reduce recurrent hospitalizations. Your fellow hospitalists should recognize your value and make you the leader of the group. Patients show their appreciation for you making the right diagnosis and averting a medical calamity for them. But when you enter a family meeting, the patient and his or her loved ones are the center stage. To be successful you have to listen more and talk less. Get to understand the pictures in their heads and then summarize those thoughts and ideas back to them to show you’ve listened.
Make emotional payments. I don’t get into the meat of the meeting until I’ve done that with the patient and every family member in the room. No one holds family meetings for patients who are thriving and have outstanding outcomes. We have family meetings to figure out goals in the face of terrible diseases, when elder abuse is a possibility, when insurance-funded resources are depleted, and for a host of other difficult reasons.
This means that everyone in the room is suffering, sacrificing, scared, confused, or worried. Acknowledge them. Hold them up. Thank them. Reflect on similar moments in your life and demonstrate empathy. Apologize when things haven’t gone right for them at your hospital. These payments will pay handsome dividends as your relationship evolves.
Not manipulation. The term negotiation might bring up images of used car salespeople. I strongly disagree. In manipulation, one side wins and the other doesn’t. In negotiation, the goal is improved communication and understanding. Manipulation is about one side of the equation having knowledge that the other side is lacking and using that to achieve its means. Negotiators hope everyone at the table has the same knowledge.
This leads to two key principles of negotiations: transparency and genuineness. Patients and families are excellent at taking the temperature of the room when you sit down to meet with them. Share knowledge. Don’t have any hidden agendas. Following this principle builds trust.
Be incremental. Taking patients from comfortable, familiar territory into that which is uncomfortable or unfamiliar should not be done in one giant leap. Let’s use code status (CS) as an example because of the frequency with which it comes up (though I rarely talk about CS without first understanding the patient’s goals and hopes).
Some patients refuse to talk about CS, so I think incrementally. I ask that they consider talking about CS with me in the future. Very few people refuse to consider something. Two or three days later I ask, "Have you considered talking to me about CS?" That by itself opens up the topic for conversation. In the extremely unusual case where they still won’t engage, I then ask them, "What would it take for you to consider talking to me about this?" More incrementalism.
While this is not nearly an exhaustive list of negotiation techniques, we hope it is stimulating enough that you might be curious enough to learn more on your own and try incorporating this into your practice. If you’re motivated to do so, please feel free to contact us for reading suggestions: E-mail [email protected].
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
‘One call’ pilot program made chronic pain a priority
Do hospitalists, or anyone who spends time practicing within the hospital setting, feel well equipped to deal with all aspects of an inpatient’s chronic pain? In palliative care, we have training and interest in this field, our program has some resources earmarked for this, and we face chronic pain multiple times a day. Yet, it is difficult to recall a patient encounter in which some piece of the pain plan did not seem bereft of a key element.
Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) data, government agencies and legislation, media, and other avenues call more attention to the escalating problem of the culture and care of chronic pain. And, because the Joint Commission, HCAHPS, and other trackers of pain in the hospital do not distinguish between acute pain and chronic pain, we are challenged with creating approaches to a problem that in many ways is out of our control.
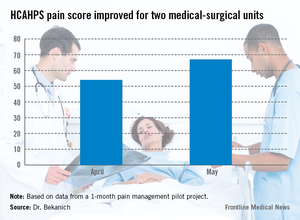
At Seton Medical Center in Austin, Tex., we have proposed and performed a short pilot of a model that allowed us to see where our gaps exist and to think through how to shrink them. Importantly, it made an impression on our leadership to the degree that they are considering a business plan we put forward to make this a permanent part of our institution.
Our pilot project produced data that made us proud as well as demonstrated areas that need improvement. For pain specialties that are hospital based, the response times were excellent. These consults were typically seen within 4 hours of the order being placed. For those specialties that do not have a regular inpatient presence, new consults were often not seen until the next day causing patient frustration. HCAHPS rose during that month (see graphic).
But before exploring the model we have proposed and piloted in conjunction with hospitalists, it is worth examining what we call "pain truths" for chronic pain (CP):
• CP is the most common symptom of many serious or advanced illnesses. While often thought of as a condition associated with cancer, it is now recognized as a part of almost every major illness arising from the failure, or damage to, each major organ. We also have a host of patients with painful conditions that have no clear etiology in areas such as the back, abdomen, and extremities.
• In most cases, CP began long before the patient was hospitalized and has no cure. It is frustrating to be on either side of this equation, because the patient does not always appreciate our limitations, and we can be left feeling less than our best for not being able to solve the problem.
• Hospital operations have not been well equipped to deal with chronic pain. The history of pain control in the hospital is such that we’ve excelled in the perioperative realm and in controlling other forms of acute pain. This is not the case with chronic pain. Whether it is a lack of useful measurements (how helpful is it to use a 10-point pain scale for CP who "feel fine" at a 9 or 10 and rate their pain at 100 out of 10 when they are having an exacerbation?), inadequate access to procedures for CP, or an absence of teams that specialize in tackling it, the number of hospitals fully prepared for CP are indeed few in number.
• No one specialty or provider deals with all facets or forms of pain. This statement frequently elicits surprise. However, no single training tract is available that teaches how to manage medications in medically complex patients, perform procedures, use a variety of counseling techniques, attend to the psychosocial barriers, and improve function via different physical therapies. It takes a diverse team to cover CP from tip to tail.
• The educational and cultural gaps in pain evaluation and management for health care providers are vast. The medical literature is flush with testimonials of this.
• Inpatient incentives for excellence in pain management are evolving from unfavorable to favorable. With reimbursements tied to HCAHPS and readmission, along with a shift toward rewarding value, we have an opportunity to change the balance sheet in resourcing pain teams.
• Comprehensive inpatient management is not possible without a complimentary outpatient component. Without the "safe place to land," patients may as well run into roundabouts that have an equal chance of spilling them out back in the direction of the hospital. These long-term problems need long-term solutions. Frequently, the best we can hope for in the hospital is to deliver a CP patient an experience that highlights the expression of empathy, demonstrates our commitment to continuously trying to help them, and cools off their pain to a tolerable level. The bulk of the work needs to be done outside the hospital walls.
Making a ‘bright spot’
Using these truths to construct a framework for effective inpatient collaborations, we set about piloting the following model. Please note that the purpose of this pilot project was not to have the intervention stand up to the rigors of scrutiny demanded by a clinical trial. Our intent was to see if we could create a "bright spot" for pain management, cobbling together existing resources, with the hope that hospital leadership would support us with new resources should we demonstrate a promising model.
Seton Medical Center is a large, urban hospital with providers from both the community and an academic medical group practice. We sought buy in for this project with the hospitalists, surgeons, pharmacy, nursing staff, and leadership. The pilot lasted for 1 month and took place on two med-surg units. Currently, there is no dedicated pain team in this hospital. The disciplines that provided pain management were anesthesia, behavioral health, palliative care, and physical medicine, and rehabilitation. The proposal to the hospitalists and surgeons was that once the pain team was involved all pain management decisions through the responsible pain team in an attempt to bring clarity and consistency to the pain plan.
• Consults. Consults were triggered one of three ways. All required a physician order and allowed the physician to opt-out if they disagreed with potential consults generated from options 2 or 3.
Option 1 – Traditional route: The provider saw a need for assistance with pain management and puts in the order.
Option 2 – Nurse initiated: The nurse felt as though pain was uncontrolled or there were other concerns about pain.
Option 3 – Patient initiated: After 48 hours of admission, patients experiencing pain were asked if they would like to visit with someone from the pain team.
• Hotline. A pain hotline was set up for a "one call, that’s all" approach. This obviated the need for those calling us to be familiar with which specialty would be most appropriate for managing a specific painful condition. Prior to the start of the pilot, each specialty agreed upon which etiologies of pain they would be primarily responsible for managing. For example, if it was perioperative pain, then anesthesia would be the primary pain service; if the diagnosis was pain that was related to a neoplastic process, then palliative care would be deployed.
• First contact. Initial encounters with the patient were through an advance practice nurse (APN). The APN was familiar with the purview of each specialty. After quickly assessing the patient, the nurse would distribute a leaflet to the patient and families that provided education about pain, including expectations, limitations, and a definition of how the pain team functions. For instance, they were provided with an explanation of why and when we change the route of administration of opioids from IV to PO. The APN would then activate the proper service, which would take ownership of pain management for that patient while they were hospitalized. We frequently involved colleagues from the different pain specialties to provide a comprehensive service. For example, when our team would see a patient with pain related to cirrhosis but they also had poor coping mechanisms, we would involve our behavioral health colleagues.
• Discharge planning. We sought to have a specific pain discharge plan documented in each patient’s progress note prior to leaving the hospital. This included which medications we recommend, the written prescriptions, and who would be responsible for continued management of the pain after discharge. If this were a primary care doctor or specialist that knows the patient we personally contacted that provider to assure that they concurred with our plans. If the patient had no such provider or their provider was uncomfortable managing the pain then we saw them as an outpatient in our respective clinics within 2 weeks of their hospital release.
We constructed our metrics with the awareness that pain scores do not paint a picture reflective of the patient experience or quality of care. We believe that, especially in the CP population, that less emphasis will be placed on pain scores and more attention given to some of these other markers of effectiveness. Metrics included pain scores, patient’s ability to function, satisfaction through HCAHPS, whether or not a documented pain discharge plan was in the medical record, tolerability, safety measures, and pharmacy use. While a detailed analysis of our results is beyond the scope of this piece, we were pleased with our data. For instance, 91% of our patients had a specific pain discharge plan documented.
Creation of a bright spot in the hospital for pain management was not the only benefit. This short pilot project created what we see as elements of sustainability on the nursing staff and providers – getting nurses and physicians on the same page about the goals of pain management, looking at pain through a more refined lens, and building an improved sense of teamwork needed to deliver this complex care.
Our physician colleagues appreciated this service to the point that we had daily requests to include patients in the pilot that were not on the participating units. Response for the program was so enthusiastic that it incurred no additional costs. Everyone who took part did so on a voluntary basis, and those who don’t normally take call at nights or on weekends did so because of their commitment to the cause.
Most importantly, patients and families were grateful, and there was a recurrent feeling that they were well educated about their medications and other aspects of their health care.
Dr. Fredholm and Dr. Bekanich are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin. Share your thoughts with Dr. Bekanich at [email protected].
Do hospitalists, or anyone who spends time practicing within the hospital setting, feel well equipped to deal with all aspects of an inpatient’s chronic pain? In palliative care, we have training and interest in this field, our program has some resources earmarked for this, and we face chronic pain multiple times a day. Yet, it is difficult to recall a patient encounter in which some piece of the pain plan did not seem bereft of a key element.
Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) data, government agencies and legislation, media, and other avenues call more attention to the escalating problem of the culture and care of chronic pain. And, because the Joint Commission, HCAHPS, and other trackers of pain in the hospital do not distinguish between acute pain and chronic pain, we are challenged with creating approaches to a problem that in many ways is out of our control.

At Seton Medical Center in Austin, Tex., we have proposed and performed a short pilot of a model that allowed us to see where our gaps exist and to think through how to shrink them. Importantly, it made an impression on our leadership to the degree that they are considering a business plan we put forward to make this a permanent part of our institution.
Our pilot project produced data that made us proud as well as demonstrated areas that need improvement. For pain specialties that are hospital based, the response times were excellent. These consults were typically seen within 4 hours of the order being placed. For those specialties that do not have a regular inpatient presence, new consults were often not seen until the next day causing patient frustration. HCAHPS rose during that month (see graphic).
But before exploring the model we have proposed and piloted in conjunction with hospitalists, it is worth examining what we call "pain truths" for chronic pain (CP):
• CP is the most common symptom of many serious or advanced illnesses. While often thought of as a condition associated with cancer, it is now recognized as a part of almost every major illness arising from the failure, or damage to, each major organ. We also have a host of patients with painful conditions that have no clear etiology in areas such as the back, abdomen, and extremities.
• In most cases, CP began long before the patient was hospitalized and has no cure. It is frustrating to be on either side of this equation, because the patient does not always appreciate our limitations, and we can be left feeling less than our best for not being able to solve the problem.
• Hospital operations have not been well equipped to deal with chronic pain. The history of pain control in the hospital is such that we’ve excelled in the perioperative realm and in controlling other forms of acute pain. This is not the case with chronic pain. Whether it is a lack of useful measurements (how helpful is it to use a 10-point pain scale for CP who "feel fine" at a 9 or 10 and rate their pain at 100 out of 10 when they are having an exacerbation?), inadequate access to procedures for CP, or an absence of teams that specialize in tackling it, the number of hospitals fully prepared for CP are indeed few in number.
• No one specialty or provider deals with all facets or forms of pain. This statement frequently elicits surprise. However, no single training tract is available that teaches how to manage medications in medically complex patients, perform procedures, use a variety of counseling techniques, attend to the psychosocial barriers, and improve function via different physical therapies. It takes a diverse team to cover CP from tip to tail.
• The educational and cultural gaps in pain evaluation and management for health care providers are vast. The medical literature is flush with testimonials of this.
• Inpatient incentives for excellence in pain management are evolving from unfavorable to favorable. With reimbursements tied to HCAHPS and readmission, along with a shift toward rewarding value, we have an opportunity to change the balance sheet in resourcing pain teams.
• Comprehensive inpatient management is not possible without a complimentary outpatient component. Without the "safe place to land," patients may as well run into roundabouts that have an equal chance of spilling them out back in the direction of the hospital. These long-term problems need long-term solutions. Frequently, the best we can hope for in the hospital is to deliver a CP patient an experience that highlights the expression of empathy, demonstrates our commitment to continuously trying to help them, and cools off their pain to a tolerable level. The bulk of the work needs to be done outside the hospital walls.
Making a ‘bright spot’
Using these truths to construct a framework for effective inpatient collaborations, we set about piloting the following model. Please note that the purpose of this pilot project was not to have the intervention stand up to the rigors of scrutiny demanded by a clinical trial. Our intent was to see if we could create a "bright spot" for pain management, cobbling together existing resources, with the hope that hospital leadership would support us with new resources should we demonstrate a promising model.
Seton Medical Center is a large, urban hospital with providers from both the community and an academic medical group practice. We sought buy in for this project with the hospitalists, surgeons, pharmacy, nursing staff, and leadership. The pilot lasted for 1 month and took place on two med-surg units. Currently, there is no dedicated pain team in this hospital. The disciplines that provided pain management were anesthesia, behavioral health, palliative care, and physical medicine, and rehabilitation. The proposal to the hospitalists and surgeons was that once the pain team was involved all pain management decisions through the responsible pain team in an attempt to bring clarity and consistency to the pain plan.
• Consults. Consults were triggered one of three ways. All required a physician order and allowed the physician to opt-out if they disagreed with potential consults generated from options 2 or 3.
Option 1 – Traditional route: The provider saw a need for assistance with pain management and puts in the order.
Option 2 – Nurse initiated: The nurse felt as though pain was uncontrolled or there were other concerns about pain.
Option 3 – Patient initiated: After 48 hours of admission, patients experiencing pain were asked if they would like to visit with someone from the pain team.
• Hotline. A pain hotline was set up for a "one call, that’s all" approach. This obviated the need for those calling us to be familiar with which specialty would be most appropriate for managing a specific painful condition. Prior to the start of the pilot, each specialty agreed upon which etiologies of pain they would be primarily responsible for managing. For example, if it was perioperative pain, then anesthesia would be the primary pain service; if the diagnosis was pain that was related to a neoplastic process, then palliative care would be deployed.
• First contact. Initial encounters with the patient were through an advance practice nurse (APN). The APN was familiar with the purview of each specialty. After quickly assessing the patient, the nurse would distribute a leaflet to the patient and families that provided education about pain, including expectations, limitations, and a definition of how the pain team functions. For instance, they were provided with an explanation of why and when we change the route of administration of opioids from IV to PO. The APN would then activate the proper service, which would take ownership of pain management for that patient while they were hospitalized. We frequently involved colleagues from the different pain specialties to provide a comprehensive service. For example, when our team would see a patient with pain related to cirrhosis but they also had poor coping mechanisms, we would involve our behavioral health colleagues.
• Discharge planning. We sought to have a specific pain discharge plan documented in each patient’s progress note prior to leaving the hospital. This included which medications we recommend, the written prescriptions, and who would be responsible for continued management of the pain after discharge. If this were a primary care doctor or specialist that knows the patient we personally contacted that provider to assure that they concurred with our plans. If the patient had no such provider or their provider was uncomfortable managing the pain then we saw them as an outpatient in our respective clinics within 2 weeks of their hospital release.
We constructed our metrics with the awareness that pain scores do not paint a picture reflective of the patient experience or quality of care. We believe that, especially in the CP population, that less emphasis will be placed on pain scores and more attention given to some of these other markers of effectiveness. Metrics included pain scores, patient’s ability to function, satisfaction through HCAHPS, whether or not a documented pain discharge plan was in the medical record, tolerability, safety measures, and pharmacy use. While a detailed analysis of our results is beyond the scope of this piece, we were pleased with our data. For instance, 91% of our patients had a specific pain discharge plan documented.
Creation of a bright spot in the hospital for pain management was not the only benefit. This short pilot project created what we see as elements of sustainability on the nursing staff and providers – getting nurses and physicians on the same page about the goals of pain management, looking at pain through a more refined lens, and building an improved sense of teamwork needed to deliver this complex care.
Our physician colleagues appreciated this service to the point that we had daily requests to include patients in the pilot that were not on the participating units. Response for the program was so enthusiastic that it incurred no additional costs. Everyone who took part did so on a voluntary basis, and those who don’t normally take call at nights or on weekends did so because of their commitment to the cause.
Most importantly, patients and families were grateful, and there was a recurrent feeling that they were well educated about their medications and other aspects of their health care.
Dr. Fredholm and Dr. Bekanich are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin. Share your thoughts with Dr. Bekanich at [email protected].
Do hospitalists, or anyone who spends time practicing within the hospital setting, feel well equipped to deal with all aspects of an inpatient’s chronic pain? In palliative care, we have training and interest in this field, our program has some resources earmarked for this, and we face chronic pain multiple times a day. Yet, it is difficult to recall a patient encounter in which some piece of the pain plan did not seem bereft of a key element.
Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) data, government agencies and legislation, media, and other avenues call more attention to the escalating problem of the culture and care of chronic pain. And, because the Joint Commission, HCAHPS, and other trackers of pain in the hospital do not distinguish between acute pain and chronic pain, we are challenged with creating approaches to a problem that in many ways is out of our control.

At Seton Medical Center in Austin, Tex., we have proposed and performed a short pilot of a model that allowed us to see where our gaps exist and to think through how to shrink them. Importantly, it made an impression on our leadership to the degree that they are considering a business plan we put forward to make this a permanent part of our institution.
Our pilot project produced data that made us proud as well as demonstrated areas that need improvement. For pain specialties that are hospital based, the response times were excellent. These consults were typically seen within 4 hours of the order being placed. For those specialties that do not have a regular inpatient presence, new consults were often not seen until the next day causing patient frustration. HCAHPS rose during that month (see graphic).
But before exploring the model we have proposed and piloted in conjunction with hospitalists, it is worth examining what we call "pain truths" for chronic pain (CP):
• CP is the most common symptom of many serious or advanced illnesses. While often thought of as a condition associated with cancer, it is now recognized as a part of almost every major illness arising from the failure, or damage to, each major organ. We also have a host of patients with painful conditions that have no clear etiology in areas such as the back, abdomen, and extremities.
• In most cases, CP began long before the patient was hospitalized and has no cure. It is frustrating to be on either side of this equation, because the patient does not always appreciate our limitations, and we can be left feeling less than our best for not being able to solve the problem.
• Hospital operations have not been well equipped to deal with chronic pain. The history of pain control in the hospital is such that we’ve excelled in the perioperative realm and in controlling other forms of acute pain. This is not the case with chronic pain. Whether it is a lack of useful measurements (how helpful is it to use a 10-point pain scale for CP who "feel fine" at a 9 or 10 and rate their pain at 100 out of 10 when they are having an exacerbation?), inadequate access to procedures for CP, or an absence of teams that specialize in tackling it, the number of hospitals fully prepared for CP are indeed few in number.
• No one specialty or provider deals with all facets or forms of pain. This statement frequently elicits surprise. However, no single training tract is available that teaches how to manage medications in medically complex patients, perform procedures, use a variety of counseling techniques, attend to the psychosocial barriers, and improve function via different physical therapies. It takes a diverse team to cover CP from tip to tail.
• The educational and cultural gaps in pain evaluation and management for health care providers are vast. The medical literature is flush with testimonials of this.
• Inpatient incentives for excellence in pain management are evolving from unfavorable to favorable. With reimbursements tied to HCAHPS and readmission, along with a shift toward rewarding value, we have an opportunity to change the balance sheet in resourcing pain teams.
• Comprehensive inpatient management is not possible without a complimentary outpatient component. Without the "safe place to land," patients may as well run into roundabouts that have an equal chance of spilling them out back in the direction of the hospital. These long-term problems need long-term solutions. Frequently, the best we can hope for in the hospital is to deliver a CP patient an experience that highlights the expression of empathy, demonstrates our commitment to continuously trying to help them, and cools off their pain to a tolerable level. The bulk of the work needs to be done outside the hospital walls.
Making a ‘bright spot’
Using these truths to construct a framework for effective inpatient collaborations, we set about piloting the following model. Please note that the purpose of this pilot project was not to have the intervention stand up to the rigors of scrutiny demanded by a clinical trial. Our intent was to see if we could create a "bright spot" for pain management, cobbling together existing resources, with the hope that hospital leadership would support us with new resources should we demonstrate a promising model.
Seton Medical Center is a large, urban hospital with providers from both the community and an academic medical group practice. We sought buy in for this project with the hospitalists, surgeons, pharmacy, nursing staff, and leadership. The pilot lasted for 1 month and took place on two med-surg units. Currently, there is no dedicated pain team in this hospital. The disciplines that provided pain management were anesthesia, behavioral health, palliative care, and physical medicine, and rehabilitation. The proposal to the hospitalists and surgeons was that once the pain team was involved all pain management decisions through the responsible pain team in an attempt to bring clarity and consistency to the pain plan.
• Consults. Consults were triggered one of three ways. All required a physician order and allowed the physician to opt-out if they disagreed with potential consults generated from options 2 or 3.
Option 1 – Traditional route: The provider saw a need for assistance with pain management and puts in the order.
Option 2 – Nurse initiated: The nurse felt as though pain was uncontrolled or there were other concerns about pain.
Option 3 – Patient initiated: After 48 hours of admission, patients experiencing pain were asked if they would like to visit with someone from the pain team.
• Hotline. A pain hotline was set up for a "one call, that’s all" approach. This obviated the need for those calling us to be familiar with which specialty would be most appropriate for managing a specific painful condition. Prior to the start of the pilot, each specialty agreed upon which etiologies of pain they would be primarily responsible for managing. For example, if it was perioperative pain, then anesthesia would be the primary pain service; if the diagnosis was pain that was related to a neoplastic process, then palliative care would be deployed.
• First contact. Initial encounters with the patient were through an advance practice nurse (APN). The APN was familiar with the purview of each specialty. After quickly assessing the patient, the nurse would distribute a leaflet to the patient and families that provided education about pain, including expectations, limitations, and a definition of how the pain team functions. For instance, they were provided with an explanation of why and when we change the route of administration of opioids from IV to PO. The APN would then activate the proper service, which would take ownership of pain management for that patient while they were hospitalized. We frequently involved colleagues from the different pain specialties to provide a comprehensive service. For example, when our team would see a patient with pain related to cirrhosis but they also had poor coping mechanisms, we would involve our behavioral health colleagues.
• Discharge planning. We sought to have a specific pain discharge plan documented in each patient’s progress note prior to leaving the hospital. This included which medications we recommend, the written prescriptions, and who would be responsible for continued management of the pain after discharge. If this were a primary care doctor or specialist that knows the patient we personally contacted that provider to assure that they concurred with our plans. If the patient had no such provider or their provider was uncomfortable managing the pain then we saw them as an outpatient in our respective clinics within 2 weeks of their hospital release.
We constructed our metrics with the awareness that pain scores do not paint a picture reflective of the patient experience or quality of care. We believe that, especially in the CP population, that less emphasis will be placed on pain scores and more attention given to some of these other markers of effectiveness. Metrics included pain scores, patient’s ability to function, satisfaction through HCAHPS, whether or not a documented pain discharge plan was in the medical record, tolerability, safety measures, and pharmacy use. While a detailed analysis of our results is beyond the scope of this piece, we were pleased with our data. For instance, 91% of our patients had a specific pain discharge plan documented.
Creation of a bright spot in the hospital for pain management was not the only benefit. This short pilot project created what we see as elements of sustainability on the nursing staff and providers – getting nurses and physicians on the same page about the goals of pain management, looking at pain through a more refined lens, and building an improved sense of teamwork needed to deliver this complex care.
Our physician colleagues appreciated this service to the point that we had daily requests to include patients in the pilot that were not on the participating units. Response for the program was so enthusiastic that it incurred no additional costs. Everyone who took part did so on a voluntary basis, and those who don’t normally take call at nights or on weekends did so because of their commitment to the cause.
Most importantly, patients and families were grateful, and there was a recurrent feeling that they were well educated about their medications and other aspects of their health care.
Dr. Fredholm and Dr. Bekanich are codirectors of Seton Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin. Share your thoughts with Dr. Bekanich at [email protected].
Advance care planning is a good move
Whether we agree or not with the validity of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) or the penalties of high 30-day readmissions, it would be challenging to find a hospitalist group where these measures are not popping up on the dashboard reports. We argue that advance care planning can aid in bending these metrics in a favorable direction.
Approximately 30% of Medicare dollars are spent on the 5% of beneficiaries who die each year (Health Serv. Res. 2004;39:363-75). The last month of life for those Medicare benefits account for one-third of the expenditures. A longitudinal, multi-institutional study looked at whether having a discussion about end-of-life preferences made a difference in quality or cost of care (Arch. Intern. Med. 2009;169:480-8).
Patients were asked "Have you and your doctor discussed any particular wishes you have about the care you would want to receive if you were dying?" For those who answered yes, costs were lower by over 35%, quality of care was rated higher, and people were more likely to spend their final days at home (53.8% vs. 37.8%).
Perhaps the most tested, sophisticated, and celebrated model for advance care planning is practiced throughout the Gunderson Health System in La Crosse, Wis.
In its model, certified advance care planning facilitators (most of whom are nurses) see patients in all venues, from the home to the hospital. They craft disease-specific advance directives with patients and families, the results of which are shared with the patient’s entire community including providers, family members, and others within the community.
Their results, which have been reproduced by other systems using the Gunderson methods, are quite staggering. If we consider the percentage of patients with advanced illnesses who have completed advance directives, the percentage of physicians who are aware of those advance directives, and then have consistency between the directives and which treatments are actually delivered, then we find that national data show us hitting below the 50% mark on all three of these issues (J. Am. Geriatr. Soc. 2010;58:1249-55).
Using Gunderson’s advance care planning program, these metrics all skyrocket to 95% or higher.
The Dartmouth Atlas Study data from 2007 comparing the number of days spent in the hospital and cost of care over the last 2 years of life show the Gunderson numbers are better. Patients spend less than 14 days in the hospital and their cost of care is less than $19,000 over those 2 years. For similar patient populations in other medical centers, the days spent in the hospital are 40-55 and costs exceed $60,000.
In our quest to build the better system, let’s highlight the role of advance care planning and resource it appropriately.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Whether we agree or not with the validity of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) or the penalties of high 30-day readmissions, it would be challenging to find a hospitalist group where these measures are not popping up on the dashboard reports. We argue that advance care planning can aid in bending these metrics in a favorable direction.
Approximately 30% of Medicare dollars are spent on the 5% of beneficiaries who die each year (Health Serv. Res. 2004;39:363-75). The last month of life for those Medicare benefits account for one-third of the expenditures. A longitudinal, multi-institutional study looked at whether having a discussion about end-of-life preferences made a difference in quality or cost of care (Arch. Intern. Med. 2009;169:480-8).
Patients were asked "Have you and your doctor discussed any particular wishes you have about the care you would want to receive if you were dying?" For those who answered yes, costs were lower by over 35%, quality of care was rated higher, and people were more likely to spend their final days at home (53.8% vs. 37.8%).
Perhaps the most tested, sophisticated, and celebrated model for advance care planning is practiced throughout the Gunderson Health System in La Crosse, Wis.
In its model, certified advance care planning facilitators (most of whom are nurses) see patients in all venues, from the home to the hospital. They craft disease-specific advance directives with patients and families, the results of which are shared with the patient’s entire community including providers, family members, and others within the community.
Their results, which have been reproduced by other systems using the Gunderson methods, are quite staggering. If we consider the percentage of patients with advanced illnesses who have completed advance directives, the percentage of physicians who are aware of those advance directives, and then have consistency between the directives and which treatments are actually delivered, then we find that national data show us hitting below the 50% mark on all three of these issues (J. Am. Geriatr. Soc. 2010;58:1249-55).
Using Gunderson’s advance care planning program, these metrics all skyrocket to 95% or higher.
The Dartmouth Atlas Study data from 2007 comparing the number of days spent in the hospital and cost of care over the last 2 years of life show the Gunderson numbers are better. Patients spend less than 14 days in the hospital and their cost of care is less than $19,000 over those 2 years. For similar patient populations in other medical centers, the days spent in the hospital are 40-55 and costs exceed $60,000.
In our quest to build the better system, let’s highlight the role of advance care planning and resource it appropriately.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Whether we agree or not with the validity of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) or the penalties of high 30-day readmissions, it would be challenging to find a hospitalist group where these measures are not popping up on the dashboard reports. We argue that advance care planning can aid in bending these metrics in a favorable direction.
Approximately 30% of Medicare dollars are spent on the 5% of beneficiaries who die each year (Health Serv. Res. 2004;39:363-75). The last month of life for those Medicare benefits account for one-third of the expenditures. A longitudinal, multi-institutional study looked at whether having a discussion about end-of-life preferences made a difference in quality or cost of care (Arch. Intern. Med. 2009;169:480-8).
Patients were asked "Have you and your doctor discussed any particular wishes you have about the care you would want to receive if you were dying?" For those who answered yes, costs were lower by over 35%, quality of care was rated higher, and people were more likely to spend their final days at home (53.8% vs. 37.8%).
Perhaps the most tested, sophisticated, and celebrated model for advance care planning is practiced throughout the Gunderson Health System in La Crosse, Wis.
In its model, certified advance care planning facilitators (most of whom are nurses) see patients in all venues, from the home to the hospital. They craft disease-specific advance directives with patients and families, the results of which are shared with the patient’s entire community including providers, family members, and others within the community.
Their results, which have been reproduced by other systems using the Gunderson methods, are quite staggering. If we consider the percentage of patients with advanced illnesses who have completed advance directives, the percentage of physicians who are aware of those advance directives, and then have consistency between the directives and which treatments are actually delivered, then we find that national data show us hitting below the 50% mark on all three of these issues (J. Am. Geriatr. Soc. 2010;58:1249-55).
Using Gunderson’s advance care planning program, these metrics all skyrocket to 95% or higher.
The Dartmouth Atlas Study data from 2007 comparing the number of days spent in the hospital and cost of care over the last 2 years of life show the Gunderson numbers are better. Patients spend less than 14 days in the hospital and their cost of care is less than $19,000 over those 2 years. For similar patient populations in other medical centers, the days spent in the hospital are 40-55 and costs exceed $60,000.
In our quest to build the better system, let’s highlight the role of advance care planning and resource it appropriately.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Heart failure: an opportunity for palliative care
Heart failure is one of the most common diagnoses encountered in the acute care setting. It afflicts an estimated 5.1 million American adults in 2013 with attendant health care expenditures of $32 billion, and is projected by 2030 to affect 6.4 million Americans at an annual cost of $70 billion. Advances in treatment have extended the lives of patients with HF, yet the 5-year mortality remains around 50% (Circulation 2013:127:e6-e245).
Patients with heart failure (HF) are frequently readmitted within 30 days of hospital discharge, leading the Centers for Medicare and Medicaid Services to include this diagnosis in public reporting and incentive payment programs.
Prognostication can be challenging, with the incidence of sudden death reported as high as 60%. Harbingers of poor prognosis include: inability to achieve euvolemia without symptomatic hypotension or increasing renal insufficiency (GFR less than 20mL/min), need for inotropic support to maintain clinical stability, hospitalization longer than 30 days, and need to reduce angiotensin-converting enzyme inhibitor (ACEI) or beta-blocker therapy due to patient intolerance. HF is often one of several comorbid illnesses, with 45% of decedents in the TIME-CHF study dying of other causes (Am. Heart J. 2010;160:308-14). This prognostic uncertainty generates underinformed patients who are less likely to be involved in shared decision making about their care.
The ACCF/AHA Guideline for the Management of Heart Failure recommend incorporating palliative care into the treatment of patients with HF, but do not provide more specific parameters.
As part of a community-wide effort to standardize and improve the care of patients with HF, we are considering how best to integrate palliation into the continuum of care for this illness. HF patients carry a significant symptom burden. Dyspnea, fatigue, edema, and decreased exercise tolerance are generally well recognized and treated, but patients also experience myalgias, nausea, anorexia, constipation, loss of function, and psychological distress. Systematic assessment and treatment of these symptoms improve quality of life, and may improve survival.
Hospitalists typically encounter HF patients in the chronic disease management phase, receiving guideline directed medical therapy. When symptoms worsen despite optimal management or the patient is diagnosed with a new comorbid illness, consider a palliative care consult. The team will assist the patient and family reassess goals of care, manage symptoms, and construct a preparedness plan. A preparedness plan is a disease-specific advance directive as well as a management plan for expected complications. Preparedness planning begins with assessment of the understanding of the disease process and further education where needed, followed by establishment of goals of care. Goals of care may include prolongation of life, symptom management, improved quality of life, and improved support to family caregivers. Patients identify a surrogate decision maker in the event of incapacity, and complete other advance directives as appropriate. Preferences for CPR are assessed and documented, and a symptom management plan is constructed with input from the cardiology team. This plan is reassessed and updated at times of transition or unanticipated clinical events. HF patients need an outpatient management plan that includes access to a clinician after hours (to forestall avoidable ED visits and readmissions).
At present, palliative care consultations are predominantly available in the acute care hospital setting. Disease education, goals of care and preparedness planning conversations are ideally held in an outpatient setting with a trusted health care provider. True integration of palliative care into the continuum of care for HF will necessitate a combination of collocated palliative care clinicians, primary palliative care education for cardiology clinicians, and realignment of payment incentives. Health care reform efforts such as Accountable Care Organizations and value-based purchasing are intended (in part) to drive this clinical redesign. It remains to be seen whether or not these efforts will succeed.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the UT Southwestern Residency Programs in Austin, Tex. Their respective backgrounds are internal medicine and family medicine. Between the two of them they have extensive hospital medicine experience. Their ongoing work within one of the nation’s Pioneer Accountable Care Organizations puts them in constant collaboration with their hospitalist, general internist, and family medicine colleagues.
Heart failure is one of the most common diagnoses encountered in the acute care setting. It afflicts an estimated 5.1 million American adults in 2013 with attendant health care expenditures of $32 billion, and is projected by 2030 to affect 6.4 million Americans at an annual cost of $70 billion. Advances in treatment have extended the lives of patients with HF, yet the 5-year mortality remains around 50% (Circulation 2013:127:e6-e245).
Patients with heart failure (HF) are frequently readmitted within 30 days of hospital discharge, leading the Centers for Medicare and Medicaid Services to include this diagnosis in public reporting and incentive payment programs.
Prognostication can be challenging, with the incidence of sudden death reported as high as 60%. Harbingers of poor prognosis include: inability to achieve euvolemia without symptomatic hypotension or increasing renal insufficiency (GFR less than 20mL/min), need for inotropic support to maintain clinical stability, hospitalization longer than 30 days, and need to reduce angiotensin-converting enzyme inhibitor (ACEI) or beta-blocker therapy due to patient intolerance. HF is often one of several comorbid illnesses, with 45% of decedents in the TIME-CHF study dying of other causes (Am. Heart J. 2010;160:308-14). This prognostic uncertainty generates underinformed patients who are less likely to be involved in shared decision making about their care.
The ACCF/AHA Guideline for the Management of Heart Failure recommend incorporating palliative care into the treatment of patients with HF, but do not provide more specific parameters.
As part of a community-wide effort to standardize and improve the care of patients with HF, we are considering how best to integrate palliation into the continuum of care for this illness. HF patients carry a significant symptom burden. Dyspnea, fatigue, edema, and decreased exercise tolerance are generally well recognized and treated, but patients also experience myalgias, nausea, anorexia, constipation, loss of function, and psychological distress. Systematic assessment and treatment of these symptoms improve quality of life, and may improve survival.
Hospitalists typically encounter HF patients in the chronic disease management phase, receiving guideline directed medical therapy. When symptoms worsen despite optimal management or the patient is diagnosed with a new comorbid illness, consider a palliative care consult. The team will assist the patient and family reassess goals of care, manage symptoms, and construct a preparedness plan. A preparedness plan is a disease-specific advance directive as well as a management plan for expected complications. Preparedness planning begins with assessment of the understanding of the disease process and further education where needed, followed by establishment of goals of care. Goals of care may include prolongation of life, symptom management, improved quality of life, and improved support to family caregivers. Patients identify a surrogate decision maker in the event of incapacity, and complete other advance directives as appropriate. Preferences for CPR are assessed and documented, and a symptom management plan is constructed with input from the cardiology team. This plan is reassessed and updated at times of transition or unanticipated clinical events. HF patients need an outpatient management plan that includes access to a clinician after hours (to forestall avoidable ED visits and readmissions).
At present, palliative care consultations are predominantly available in the acute care hospital setting. Disease education, goals of care and preparedness planning conversations are ideally held in an outpatient setting with a trusted health care provider. True integration of palliative care into the continuum of care for HF will necessitate a combination of collocated palliative care clinicians, primary palliative care education for cardiology clinicians, and realignment of payment incentives. Health care reform efforts such as Accountable Care Organizations and value-based purchasing are intended (in part) to drive this clinical redesign. It remains to be seen whether or not these efforts will succeed.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the UT Southwestern Residency Programs in Austin, Tex. Their respective backgrounds are internal medicine and family medicine. Between the two of them they have extensive hospital medicine experience. Their ongoing work within one of the nation’s Pioneer Accountable Care Organizations puts them in constant collaboration with their hospitalist, general internist, and family medicine colleagues.
Heart failure is one of the most common diagnoses encountered in the acute care setting. It afflicts an estimated 5.1 million American adults in 2013 with attendant health care expenditures of $32 billion, and is projected by 2030 to affect 6.4 million Americans at an annual cost of $70 billion. Advances in treatment have extended the lives of patients with HF, yet the 5-year mortality remains around 50% (Circulation 2013:127:e6-e245).
Patients with heart failure (HF) are frequently readmitted within 30 days of hospital discharge, leading the Centers for Medicare and Medicaid Services to include this diagnosis in public reporting and incentive payment programs.
Prognostication can be challenging, with the incidence of sudden death reported as high as 60%. Harbingers of poor prognosis include: inability to achieve euvolemia without symptomatic hypotension or increasing renal insufficiency (GFR less than 20mL/min), need for inotropic support to maintain clinical stability, hospitalization longer than 30 days, and need to reduce angiotensin-converting enzyme inhibitor (ACEI) or beta-blocker therapy due to patient intolerance. HF is often one of several comorbid illnesses, with 45% of decedents in the TIME-CHF study dying of other causes (Am. Heart J. 2010;160:308-14). This prognostic uncertainty generates underinformed patients who are less likely to be involved in shared decision making about their care.
The ACCF/AHA Guideline for the Management of Heart Failure recommend incorporating palliative care into the treatment of patients with HF, but do not provide more specific parameters.
As part of a community-wide effort to standardize and improve the care of patients with HF, we are considering how best to integrate palliation into the continuum of care for this illness. HF patients carry a significant symptom burden. Dyspnea, fatigue, edema, and decreased exercise tolerance are generally well recognized and treated, but patients also experience myalgias, nausea, anorexia, constipation, loss of function, and psychological distress. Systematic assessment and treatment of these symptoms improve quality of life, and may improve survival.
Hospitalists typically encounter HF patients in the chronic disease management phase, receiving guideline directed medical therapy. When symptoms worsen despite optimal management or the patient is diagnosed with a new comorbid illness, consider a palliative care consult. The team will assist the patient and family reassess goals of care, manage symptoms, and construct a preparedness plan. A preparedness plan is a disease-specific advance directive as well as a management plan for expected complications. Preparedness planning begins with assessment of the understanding of the disease process and further education where needed, followed by establishment of goals of care. Goals of care may include prolongation of life, symptom management, improved quality of life, and improved support to family caregivers. Patients identify a surrogate decision maker in the event of incapacity, and complete other advance directives as appropriate. Preferences for CPR are assessed and documented, and a symptom management plan is constructed with input from the cardiology team. This plan is reassessed and updated at times of transition or unanticipated clinical events. HF patients need an outpatient management plan that includes access to a clinician after hours (to forestall avoidable ED visits and readmissions).
At present, palliative care consultations are predominantly available in the acute care hospital setting. Disease education, goals of care and preparedness planning conversations are ideally held in an outpatient setting with a trusted health care provider. True integration of palliative care into the continuum of care for HF will necessitate a combination of collocated palliative care clinicians, primary palliative care education for cardiology clinicians, and realignment of payment incentives. Health care reform efforts such as Accountable Care Organizations and value-based purchasing are intended (in part) to drive this clinical redesign. It remains to be seen whether or not these efforts will succeed.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Palliative Care, part of the UT Southwestern Residency Programs in Austin, Tex. Their respective backgrounds are internal medicine and family medicine. Between the two of them they have extensive hospital medicine experience. Their ongoing work within one of the nation’s Pioneer Accountable Care Organizations puts them in constant collaboration with their hospitalist, general internist, and family medicine colleagues.
Advance care planning is a measurably good move
Whether we agree or not with the validity of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) or the penalties of high 30-day readmissions, it would be challenging to find a hospitalist group where these measures are not popping up on the dashboard reports. Can advance care planning aid in bending these metrics in a favorable direction? We would argue in the affirmative.
Approximately 30% of Medicare dollars are spent on the 5% of beneficiaries who die each year (Health Serv. Res. 2004;39:363-75). The last month of life for those Medicare benefits account for one-third of the expenditures. A longitudinal, multi-institutional study following more than 600 incurable cancer patients looked at whether having a discussion about end-of-life preferences made a difference in quality or cost of care (Arch. Intern. Med. 2009;169:480-8).
Baseline end-of-life discussions were documented with a single question: "Have you and your doctor discussed any particular wishes you have about the care you would want to receive if you were dying?" For those who answered yes, not only did costs turn out to be lower by over 35% but quality of care was rated by family members to be higher and people were more likely to spend their final days at home rather than in the hospital (53.8% vs. 37.8%).
This is particularly impressive against the backdrop, demonstrated in many studies, that, when these conversations do occur they last for only a few minutes, the patients don’t have an opportunity to adequately express themselves, caregivers are left wanting more information, and details on specific elements of choices for care are scant.
Perhaps the most tested, sophisticated, and celebrated model for advance care planning is practiced throughout the Gunderson Health System in La Crosse, Wis.
In its model, certified advance care planning facilitators (most of whom are nurses) see patients in all venues, from the home to the hospital. They craft disease-specific advance directives with patients and families, the results of which are shared with the patient’s entire community including providers, family members, and others within the community.
Their results, which have been reproduced by other systems using the Gunderson methods, are quite staggering. If we consider the percentage of patients with advanced illnesses who have completed advance directives, the percentage of physicians who are aware of those advance directives, and then have consistency between the directives and which treatments are actually delivered, then we find that national data show us hitting below the 50% mark on all three of these issues (J. Am. Geriatr. Soc. 2010;58:1249-55).
Using Gunderson’s advance care planning program, these metrics all skyrocket to 95% or higher.
Translation? When using the Dartmouth Atlas Study data from 2007 to compare the number of days spent in the hospital and cost of care over the last 2 years of life, the Gunderson numbers are far more attractive. Their patients spend less than 14 days in the hospital and their cost of care is less than $19,000 over those 2 years. For similar patient populations in other medical centers, the days spent in the hospital are 40-55 and costs exceed $60,000 during the same period of time.
In our quest to build the better system, let’s highlight the role of advance care planning and resource it appropriately.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Whether we agree or not with the validity of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) or the penalties of high 30-day readmissions, it would be challenging to find a hospitalist group where these measures are not popping up on the dashboard reports. Can advance care planning aid in bending these metrics in a favorable direction? We would argue in the affirmative.
Approximately 30% of Medicare dollars are spent on the 5% of beneficiaries who die each year (Health Serv. Res. 2004;39:363-75). The last month of life for those Medicare benefits account for one-third of the expenditures. A longitudinal, multi-institutional study following more than 600 incurable cancer patients looked at whether having a discussion about end-of-life preferences made a difference in quality or cost of care (Arch. Intern. Med. 2009;169:480-8).
Baseline end-of-life discussions were documented with a single question: "Have you and your doctor discussed any particular wishes you have about the care you would want to receive if you were dying?" For those who answered yes, not only did costs turn out to be lower by over 35% but quality of care was rated by family members to be higher and people were more likely to spend their final days at home rather than in the hospital (53.8% vs. 37.8%).
This is particularly impressive against the backdrop, demonstrated in many studies, that, when these conversations do occur they last for only a few minutes, the patients don’t have an opportunity to adequately express themselves, caregivers are left wanting more information, and details on specific elements of choices for care are scant.
Perhaps the most tested, sophisticated, and celebrated model for advance care planning is practiced throughout the Gunderson Health System in La Crosse, Wis.
In its model, certified advance care planning facilitators (most of whom are nurses) see patients in all venues, from the home to the hospital. They craft disease-specific advance directives with patients and families, the results of which are shared with the patient’s entire community including providers, family members, and others within the community.
Their results, which have been reproduced by other systems using the Gunderson methods, are quite staggering. If we consider the percentage of patients with advanced illnesses who have completed advance directives, the percentage of physicians who are aware of those advance directives, and then have consistency between the directives and which treatments are actually delivered, then we find that national data show us hitting below the 50% mark on all three of these issues (J. Am. Geriatr. Soc. 2010;58:1249-55).
Using Gunderson’s advance care planning program, these metrics all skyrocket to 95% or higher.
Translation? When using the Dartmouth Atlas Study data from 2007 to compare the number of days spent in the hospital and cost of care over the last 2 years of life, the Gunderson numbers are far more attractive. Their patients spend less than 14 days in the hospital and their cost of care is less than $19,000 over those 2 years. For similar patient populations in other medical centers, the days spent in the hospital are 40-55 and costs exceed $60,000 during the same period of time.
In our quest to build the better system, let’s highlight the role of advance care planning and resource it appropriately.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Whether we agree or not with the validity of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) or the penalties of high 30-day readmissions, it would be challenging to find a hospitalist group where these measures are not popping up on the dashboard reports. Can advance care planning aid in bending these metrics in a favorable direction? We would argue in the affirmative.
Approximately 30% of Medicare dollars are spent on the 5% of beneficiaries who die each year (Health Serv. Res. 2004;39:363-75). The last month of life for those Medicare benefits account for one-third of the expenditures. A longitudinal, multi-institutional study following more than 600 incurable cancer patients looked at whether having a discussion about end-of-life preferences made a difference in quality or cost of care (Arch. Intern. Med. 2009;169:480-8).
Baseline end-of-life discussions were documented with a single question: "Have you and your doctor discussed any particular wishes you have about the care you would want to receive if you were dying?" For those who answered yes, not only did costs turn out to be lower by over 35% but quality of care was rated by family members to be higher and people were more likely to spend their final days at home rather than in the hospital (53.8% vs. 37.8%).
This is particularly impressive against the backdrop, demonstrated in many studies, that, when these conversations do occur they last for only a few minutes, the patients don’t have an opportunity to adequately express themselves, caregivers are left wanting more information, and details on specific elements of choices for care are scant.
Perhaps the most tested, sophisticated, and celebrated model for advance care planning is practiced throughout the Gunderson Health System in La Crosse, Wis.
In its model, certified advance care planning facilitators (most of whom are nurses) see patients in all venues, from the home to the hospital. They craft disease-specific advance directives with patients and families, the results of which are shared with the patient’s entire community including providers, family members, and others within the community.
Their results, which have been reproduced by other systems using the Gunderson methods, are quite staggering. If we consider the percentage of patients with advanced illnesses who have completed advance directives, the percentage of physicians who are aware of those advance directives, and then have consistency between the directives and which treatments are actually delivered, then we find that national data show us hitting below the 50% mark on all three of these issues (J. Am. Geriatr. Soc. 2010;58:1249-55).
Using Gunderson’s advance care planning program, these metrics all skyrocket to 95% or higher.
Translation? When using the Dartmouth Atlas Study data from 2007 to compare the number of days spent in the hospital and cost of care over the last 2 years of life, the Gunderson numbers are far more attractive. Their patients spend less than 14 days in the hospital and their cost of care is less than $19,000 over those 2 years. For similar patient populations in other medical centers, the days spent in the hospital are 40-55 and costs exceed $60,000 during the same period of time.
In our quest to build the better system, let’s highlight the role of advance care planning and resource it appropriately.
Dr. Bekanich and Dr. Fredholm are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Readmission: Symptom or problem?
Among the myriad efforts at performance improvement in our hospital system, none loom larger than those aimed at preventing readmissions. While clinicians have long known that patients’ outcomes suffer when they are readmitted to the acute care hospital, now hospital outcomes will also suffer – financially, by up to 2% of Medicare billings for FY 2014, with greater penalties in future years.
Our system expects to lose $575,000 for FY 2013, when the penalty is a more modest 1% of Medicare billings. Efforts to prevent readmissions to date have focused primarily on finding and eliminating process gaps: Have we adequately educated the patient and family about medications, treatments, follow-up appointments? Are there transportation challenges? Can the patient afford and obtain medications? National efforts have addressed the most common gaps. These efforts are very effective for the patient whose illness trajectory is one of slow and steady improvement.
As patients enter the final phase of a serious illness, the trajectory is progressive decline, despite available treatments. Trajectory of decline is characterized by functional decline, loss of lean body mass, and the need for frequent medical care (hospitalization, ED and physician visits). These patients have multiple transitions between and among health care settings. Recent analysis of data from the Centers for Medicare and Medicaid Services was discouraging: Though hospice at time of death doubled between 2000 and 2009, nearly a third of those patients were in hospice 3 or fewer days. Forty percent of those short-stay patients were discharged to hospice from an ICU. Fourteen percent of Medicare decedents in 2009 had at least one transition of care in the last 3 days of life (JAMA 309:470-77).
On the palliative care service, we encounter a group of patients who are frequently readmitted, not because of process gaps, but because they are too ill to live well outside of the hospital without significant assistance. For these patients, the readmission is a symptom, not the problem.
The problem is that the patient is dying. How can we better manage the transition away from acute care for the patient whose death is expected? Often these patients are readmitted because we have not provided an alternative to hospital admission for the next crisis. Medicare skilled nursing facilities, and long-term acute care and rehabilitation hospitals, are designed to care for patients whose conditions are improving, and as a result, they rapidly transfer declining patients back to the acute care hospital.
Hospice, as an interdisciplinary 24-hour model of care, is uniquely positioned to treat symptoms and assist the patient and family to cope with distress and grief. Hospices are required to provide respite to caregivers as well as options for inpatient care when the patient’s symptoms cannot be reasonably managed in another setting. Hospice admission within 30 days of death significantly reduces the likelihood of 30-day readmission, subsequent ICU admission, and death in the hospital (Health Aff. 2013;32:552-61). Greater reduction in the likelihood of these outcomes is seen with hospice admission at least 53 days before death. Ironically, hospice patients have demonstrated longer life expectancy than their disease-matched counterparts (J. Pain Symptom Manage. 2007;33:238-46).
Patients with serious, progressive illness need concrete information about the natural history of the illness, its expected course and prognosis, and the potential impact of proposed treatments on morbidity as well as mortality. Understanding what is expected in the illness often alters the choices patients make about treatment and postacute care. After disease education, a patient and family can select goals of care and treatment options that align with their preferences. When asked, most laypersons prefer to die at home, comfortably, with their family. For these patients, the question is not "Do you want to die?" but "How do you want to die?" These conversations are difficult for all involved (physician, patient, family), but allow patients to make truly informed decisions about their care, and to decide what is most important as death approaches.
Lacking complete information, patients are often subjected to a merry-go-round of transfers between the acute and postacute environments, with increased caregiver stress. Attention to goals of care results in fewer readmissions, higher satisfaction, and better outcomes for patients and health care organizations.
Palliative care teams can provide consultative assistance with these conversations, and may be available to provide additional training to health care providers as well. If your institution does not have a palliative care team, look to a board-certified palliative medicine clinician in your community (often the hospice medical director) for consultation and guidance.
Dr. Fredholm and Dr. Bekanich are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Among the myriad efforts at performance improvement in our hospital system, none loom larger than those aimed at preventing readmissions. While clinicians have long known that patients’ outcomes suffer when they are readmitted to the acute care hospital, now hospital outcomes will also suffer – financially, by up to 2% of Medicare billings for FY 2014, with greater penalties in future years.
Our system expects to lose $575,000 for FY 2013, when the penalty is a more modest 1% of Medicare billings. Efforts to prevent readmissions to date have focused primarily on finding and eliminating process gaps: Have we adequately educated the patient and family about medications, treatments, follow-up appointments? Are there transportation challenges? Can the patient afford and obtain medications? National efforts have addressed the most common gaps. These efforts are very effective for the patient whose illness trajectory is one of slow and steady improvement.
As patients enter the final phase of a serious illness, the trajectory is progressive decline, despite available treatments. Trajectory of decline is characterized by functional decline, loss of lean body mass, and the need for frequent medical care (hospitalization, ED and physician visits). These patients have multiple transitions between and among health care settings. Recent analysis of data from the Centers for Medicare and Medicaid Services was discouraging: Though hospice at time of death doubled between 2000 and 2009, nearly a third of those patients were in hospice 3 or fewer days. Forty percent of those short-stay patients were discharged to hospice from an ICU. Fourteen percent of Medicare decedents in 2009 had at least one transition of care in the last 3 days of life (JAMA 309:470-77).
On the palliative care service, we encounter a group of patients who are frequently readmitted, not because of process gaps, but because they are too ill to live well outside of the hospital without significant assistance. For these patients, the readmission is a symptom, not the problem.
The problem is that the patient is dying. How can we better manage the transition away from acute care for the patient whose death is expected? Often these patients are readmitted because we have not provided an alternative to hospital admission for the next crisis. Medicare skilled nursing facilities, and long-term acute care and rehabilitation hospitals, are designed to care for patients whose conditions are improving, and as a result, they rapidly transfer declining patients back to the acute care hospital.
Hospice, as an interdisciplinary 24-hour model of care, is uniquely positioned to treat symptoms and assist the patient and family to cope with distress and grief. Hospices are required to provide respite to caregivers as well as options for inpatient care when the patient’s symptoms cannot be reasonably managed in another setting. Hospice admission within 30 days of death significantly reduces the likelihood of 30-day readmission, subsequent ICU admission, and death in the hospital (Health Aff. 2013;32:552-61). Greater reduction in the likelihood of these outcomes is seen with hospice admission at least 53 days before death. Ironically, hospice patients have demonstrated longer life expectancy than their disease-matched counterparts (J. Pain Symptom Manage. 2007;33:238-46).
Patients with serious, progressive illness need concrete information about the natural history of the illness, its expected course and prognosis, and the potential impact of proposed treatments on morbidity as well as mortality. Understanding what is expected in the illness often alters the choices patients make about treatment and postacute care. After disease education, a patient and family can select goals of care and treatment options that align with their preferences. When asked, most laypersons prefer to die at home, comfortably, with their family. For these patients, the question is not "Do you want to die?" but "How do you want to die?" These conversations are difficult for all involved (physician, patient, family), but allow patients to make truly informed decisions about their care, and to decide what is most important as death approaches.
Lacking complete information, patients are often subjected to a merry-go-round of transfers between the acute and postacute environments, with increased caregiver stress. Attention to goals of care results in fewer readmissions, higher satisfaction, and better outcomes for patients and health care organizations.
Palliative care teams can provide consultative assistance with these conversations, and may be available to provide additional training to health care providers as well. If your institution does not have a palliative care team, look to a board-certified palliative medicine clinician in your community (often the hospice medical director) for consultation and guidance.
Dr. Fredholm and Dr. Bekanich are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Among the myriad efforts at performance improvement in our hospital system, none loom larger than those aimed at preventing readmissions. While clinicians have long known that patients’ outcomes suffer when they are readmitted to the acute care hospital, now hospital outcomes will also suffer – financially, by up to 2% of Medicare billings for FY 2014, with greater penalties in future years.
Our system expects to lose $575,000 for FY 2013, when the penalty is a more modest 1% of Medicare billings. Efforts to prevent readmissions to date have focused primarily on finding and eliminating process gaps: Have we adequately educated the patient and family about medications, treatments, follow-up appointments? Are there transportation challenges? Can the patient afford and obtain medications? National efforts have addressed the most common gaps. These efforts are very effective for the patient whose illness trajectory is one of slow and steady improvement.
As patients enter the final phase of a serious illness, the trajectory is progressive decline, despite available treatments. Trajectory of decline is characterized by functional decline, loss of lean body mass, and the need for frequent medical care (hospitalization, ED and physician visits). These patients have multiple transitions between and among health care settings. Recent analysis of data from the Centers for Medicare and Medicaid Services was discouraging: Though hospice at time of death doubled between 2000 and 2009, nearly a third of those patients were in hospice 3 or fewer days. Forty percent of those short-stay patients were discharged to hospice from an ICU. Fourteen percent of Medicare decedents in 2009 had at least one transition of care in the last 3 days of life (JAMA 309:470-77).
On the palliative care service, we encounter a group of patients who are frequently readmitted, not because of process gaps, but because they are too ill to live well outside of the hospital without significant assistance. For these patients, the readmission is a symptom, not the problem.
The problem is that the patient is dying. How can we better manage the transition away from acute care for the patient whose death is expected? Often these patients are readmitted because we have not provided an alternative to hospital admission for the next crisis. Medicare skilled nursing facilities, and long-term acute care and rehabilitation hospitals, are designed to care for patients whose conditions are improving, and as a result, they rapidly transfer declining patients back to the acute care hospital.
Hospice, as an interdisciplinary 24-hour model of care, is uniquely positioned to treat symptoms and assist the patient and family to cope with distress and grief. Hospices are required to provide respite to caregivers as well as options for inpatient care when the patient’s symptoms cannot be reasonably managed in another setting. Hospice admission within 30 days of death significantly reduces the likelihood of 30-day readmission, subsequent ICU admission, and death in the hospital (Health Aff. 2013;32:552-61). Greater reduction in the likelihood of these outcomes is seen with hospice admission at least 53 days before death. Ironically, hospice patients have demonstrated longer life expectancy than their disease-matched counterparts (J. Pain Symptom Manage. 2007;33:238-46).
Patients with serious, progressive illness need concrete information about the natural history of the illness, its expected course and prognosis, and the potential impact of proposed treatments on morbidity as well as mortality. Understanding what is expected in the illness often alters the choices patients make about treatment and postacute care. After disease education, a patient and family can select goals of care and treatment options that align with their preferences. When asked, most laypersons prefer to die at home, comfortably, with their family. For these patients, the question is not "Do you want to die?" but "How do you want to die?" These conversations are difficult for all involved (physician, patient, family), but allow patients to make truly informed decisions about their care, and to decide what is most important as death approaches.
Lacking complete information, patients are often subjected to a merry-go-round of transfers between the acute and postacute environments, with increased caregiver stress. Attention to goals of care results in fewer readmissions, higher satisfaction, and better outcomes for patients and health care organizations.
Palliative care teams can provide consultative assistance with these conversations, and may be available to provide additional training to health care providers as well. If your institution does not have a palliative care team, look to a board-certified palliative medicine clinician in your community (often the hospice medical director) for consultation and guidance.
Dr. Fredholm and Dr. Bekanich are codirectors of Seton Health Palliative Care, part of the University of Texas Southwestern Residency Programs in Austin.
Evidence-based restraint
Metastatic lung cancer: a dreaded diagnosis with high symptom burden and universally fatal outcome.
For the patient we recently cared for alongside the hospitalist and oncologist, it also comes with inevitable readmissions. On the third such hospitalization over a period of 6 months, with the advent of adult respiratory distress syndrome, acute kidney injury, and pancytopenia (thought by oncology to be a new hematologic malignancy), our patient was clearly nearing the end of life.
Yet there we stood hearing the family talk of intubation, dialysis, and even future chemotherapy while the patient required daily infusions of platelets and red cells, experienced delirium, and was unable to wean off bilevel positive airway pressure. This family did not request escalation of treatments. The seemingly endless array of options under discussion were offered to them by well-intentioned, caring physicians.
Evidence-based practice (EBP) has been a driver for much of what we do. Can we say the opposite is equally true? Does EBP govern what we do not offer patients and families, with a similar conviction and frequency? If we are to be successful in reconstructing health care delivery to provide safe, comprehensive care that leaves no one behind, then tending to what is unwanted, unnecessary, and nonbeneficial is a vital part of the strategy.
We propose using the term evidence-based restraint (EBR) as a counterpart to evidence-based practice. Evidence of the harms of overdiagnosis and overtreatment is mounting—leading to efforts such as the Choosing Wisely campaign and the Affordable Care Act’s emphasis on comparative effectiveness research. Yet when faced with a dying patient, many physicians seem compelled to offer treatments that are nonbeneficial at best, demonstrably harmful at worst. Overtreatment is remunerated in multiple ways: financial, personal satisfaction, patient and family appreciation. The harms of overtreatment are not yet widely recognized by health care professionals or laypersons, particularly when erroneously viewed as potentially curative treatment.
One piece of EBR that is likely to be challenging for all is telling patients and families "no." Health care professionals don’t want to destroy hope even when redirecting hope is a necessity. Conflict is frequently avoided, amicability in provider-patient relationships is strongly desired, and always looming is the possibility of lawsuits should disagreements lead to outcomes that do not meet family expectations. However, if we do not support one another in saying "no," then the engine of change will stall. One example of where to begin is cardiopulmonary resuscitation status. In JAMA, the authors of an opinion piece titled, "Time to Revise the Approach to Determining Cardiopulmonary Resuscitation Status," challenge us by saying that it is "not only ethical, but also imperative, that CPR not be offered" to those deemed to receive no benefit from it (2011;307:917-8). Paths to compassionately resolve patient and family wishes that are misaligned with the evidence include changes in hospital policy, ethics consultation, and a multidisciplinary approach. Additionally, physicians will need training and support for engaging in difficult conversations.
There are brave and bold voices championing EBR and garnering more attention as it surfs the rising tide of the Affordable Care Act. While only 1.5 years old, "Bending the Cost Curve in Cancer Care," a Sounding Board piece from the New England Journal of Medicine by Dr. Thomas J. Smith and Dr. Bruce E. Hillner, is already considered a seminal work (2011; 364:2060-5.)
In their discussion of bending the cost curve in cancer care, they call for restraint in oncologists’ behavior, attitude, and practice that artfully not only curtails spending, but delivers more patient-centered care. Health care systems should be looking to realign incentives to reward oncologists for seeing these adjustments put into action. Similar thought processes around cardiology, critical care, neurology, and other disciplines are currently in development.
Evidence-based restraint will not win the day easily or quickly. With limited resources and a growing population, it is imperative that we seek to provide care that is cost effective and beneficial, and available to all.
Metastatic lung cancer: a dreaded diagnosis with high symptom burden and universally fatal outcome.
For the patient we recently cared for alongside the hospitalist and oncologist, it also comes with inevitable readmissions. On the third such hospitalization over a period of 6 months, with the advent of adult respiratory distress syndrome, acute kidney injury, and pancytopenia (thought by oncology to be a new hematologic malignancy), our patient was clearly nearing the end of life.
Yet there we stood hearing the family talk of intubation, dialysis, and even future chemotherapy while the patient required daily infusions of platelets and red cells, experienced delirium, and was unable to wean off bilevel positive airway pressure. This family did not request escalation of treatments. The seemingly endless array of options under discussion were offered to them by well-intentioned, caring physicians.
Evidence-based practice (EBP) has been a driver for much of what we do. Can we say the opposite is equally true? Does EBP govern what we do not offer patients and families, with a similar conviction and frequency? If we are to be successful in reconstructing health care delivery to provide safe, comprehensive care that leaves no one behind, then tending to what is unwanted, unnecessary, and nonbeneficial is a vital part of the strategy.
We propose using the term evidence-based restraint (EBR) as a counterpart to evidence-based practice. Evidence of the harms of overdiagnosis and overtreatment is mounting—leading to efforts such as the Choosing Wisely campaign and the Affordable Care Act’s emphasis on comparative effectiveness research. Yet when faced with a dying patient, many physicians seem compelled to offer treatments that are nonbeneficial at best, demonstrably harmful at worst. Overtreatment is remunerated in multiple ways: financial, personal satisfaction, patient and family appreciation. The harms of overtreatment are not yet widely recognized by health care professionals or laypersons, particularly when erroneously viewed as potentially curative treatment.
One piece of EBR that is likely to be challenging for all is telling patients and families "no." Health care professionals don’t want to destroy hope even when redirecting hope is a necessity. Conflict is frequently avoided, amicability in provider-patient relationships is strongly desired, and always looming is the possibility of lawsuits should disagreements lead to outcomes that do not meet family expectations. However, if we do not support one another in saying "no," then the engine of change will stall. One example of where to begin is cardiopulmonary resuscitation status. In JAMA, the authors of an opinion piece titled, "Time to Revise the Approach to Determining Cardiopulmonary Resuscitation Status," challenge us by saying that it is "not only ethical, but also imperative, that CPR not be offered" to those deemed to receive no benefit from it (2011;307:917-8). Paths to compassionately resolve patient and family wishes that are misaligned with the evidence include changes in hospital policy, ethics consultation, and a multidisciplinary approach. Additionally, physicians will need training and support for engaging in difficult conversations.
There are brave and bold voices championing EBR and garnering more attention as it surfs the rising tide of the Affordable Care Act. While only 1.5 years old, "Bending the Cost Curve in Cancer Care," a Sounding Board piece from the New England Journal of Medicine by Dr. Thomas J. Smith and Dr. Bruce E. Hillner, is already considered a seminal work (2011; 364:2060-5.)
In their discussion of bending the cost curve in cancer care, they call for restraint in oncologists’ behavior, attitude, and practice that artfully not only curtails spending, but delivers more patient-centered care. Health care systems should be looking to realign incentives to reward oncologists for seeing these adjustments put into action. Similar thought processes around cardiology, critical care, neurology, and other disciplines are currently in development.
Evidence-based restraint will not win the day easily or quickly. With limited resources and a growing population, it is imperative that we seek to provide care that is cost effective and beneficial, and available to all.
Metastatic lung cancer: a dreaded diagnosis with high symptom burden and universally fatal outcome.
For the patient we recently cared for alongside the hospitalist and oncologist, it also comes with inevitable readmissions. On the third such hospitalization over a period of 6 months, with the advent of adult respiratory distress syndrome, acute kidney injury, and pancytopenia (thought by oncology to be a new hematologic malignancy), our patient was clearly nearing the end of life.
Yet there we stood hearing the family talk of intubation, dialysis, and even future chemotherapy while the patient required daily infusions of platelets and red cells, experienced delirium, and was unable to wean off bilevel positive airway pressure. This family did not request escalation of treatments. The seemingly endless array of options under discussion were offered to them by well-intentioned, caring physicians.
Evidence-based practice (EBP) has been a driver for much of what we do. Can we say the opposite is equally true? Does EBP govern what we do not offer patients and families, with a similar conviction and frequency? If we are to be successful in reconstructing health care delivery to provide safe, comprehensive care that leaves no one behind, then tending to what is unwanted, unnecessary, and nonbeneficial is a vital part of the strategy.
We propose using the term evidence-based restraint (EBR) as a counterpart to evidence-based practice. Evidence of the harms of overdiagnosis and overtreatment is mounting—leading to efforts such as the Choosing Wisely campaign and the Affordable Care Act’s emphasis on comparative effectiveness research. Yet when faced with a dying patient, many physicians seem compelled to offer treatments that are nonbeneficial at best, demonstrably harmful at worst. Overtreatment is remunerated in multiple ways: financial, personal satisfaction, patient and family appreciation. The harms of overtreatment are not yet widely recognized by health care professionals or laypersons, particularly when erroneously viewed as potentially curative treatment.
One piece of EBR that is likely to be challenging for all is telling patients and families "no." Health care professionals don’t want to destroy hope even when redirecting hope is a necessity. Conflict is frequently avoided, amicability in provider-patient relationships is strongly desired, and always looming is the possibility of lawsuits should disagreements lead to outcomes that do not meet family expectations. However, if we do not support one another in saying "no," then the engine of change will stall. One example of where to begin is cardiopulmonary resuscitation status. In JAMA, the authors of an opinion piece titled, "Time to Revise the Approach to Determining Cardiopulmonary Resuscitation Status," challenge us by saying that it is "not only ethical, but also imperative, that CPR not be offered" to those deemed to receive no benefit from it (2011;307:917-8). Paths to compassionately resolve patient and family wishes that are misaligned with the evidence include changes in hospital policy, ethics consultation, and a multidisciplinary approach. Additionally, physicians will need training and support for engaging in difficult conversations.
There are brave and bold voices championing EBR and garnering more attention as it surfs the rising tide of the Affordable Care Act. While only 1.5 years old, "Bending the Cost Curve in Cancer Care," a Sounding Board piece from the New England Journal of Medicine by Dr. Thomas J. Smith and Dr. Bruce E. Hillner, is already considered a seminal work (2011; 364:2060-5.)
In their discussion of bending the cost curve in cancer care, they call for restraint in oncologists’ behavior, attitude, and practice that artfully not only curtails spending, but delivers more patient-centered care. Health care systems should be looking to realign incentives to reward oncologists for seeing these adjustments put into action. Similar thought processes around cardiology, critical care, neurology, and other disciplines are currently in development.
Evidence-based restraint will not win the day easily or quickly. With limited resources and a growing population, it is imperative that we seek to provide care that is cost effective and beneficial, and available to all.
Awareness Is Top Weapon Against Delirium
I expect that [insert patient name here] will have a hospital stay measured in a period of days. During that time we will do our best to prevent complications of hospitalization, which include things such as blood clots and infections. We will also do our best to quickly recognize and treat those complications that do occur such as confusion or pain." This is a conversation I have with the majority of patients’ families when their medically complicated loved one is hospitalized.
I was certain that one gentleman, who has esophageal cancer with metastasis to the spine causing cord compression, would suffer from delirium during his hospital stay. His advanced age, multiple comorbidities, urgent surgery, intensive-care unit stay, and the medications he required to control his pain -- which initially included a fentanyl PCA (patient-controlled analgesia) and was later augmented by a ketamine infusion -- all seemed to put him at high risk for this. Yet, even during his time on our ketamine protocol he had clear and appropriate conversations with our team.
Another elderly woman, with previously undiagnosed dementia, was living at home with family assistance until coming to the hospital after suffering from a fall at home. During her hospital course she experienced side effects of pain medications and also developed a urinary tract infection. The delirium that ensued was severe. She required ICU admission because of the intense nursing supervision she needed to keep her out of physical restraints.
Eventually, when it was appropriate, she was discharged to a skilled nursing facility rather than home because of the persistent cognitive problems she was experiencing. The emergency room physician who called me about the admission anticipated that the patient could return home less than 24 hours after coming in. She left the hospital almost 2 weeks later.
Delirium in hospitalized patients is a common problem. Its presence is often partnered with extended lengths of stay, escalation of care, and poorer outcomes. Once it occurs, we turn to screening tools and treatment protocols that evidence has shown to be useful. Therefore, it should come as no surprise that a hospital’s approach to delirium management is now recognized as a quality-of-care marker.
Two new studies highlight the impact of delirium and provide a new tool for predicting this condition. They expand our body of knowledge, and one of them may even empower us to possibly head off delirium before it occurs.
The first study is a prospective cohort enrolled between 1991 and 2006 into a patient registry for Alzheimer’s disease (AD). Participants were over the age of 65 years with a clinical diagnosis of AD in this community setting, which included 771 patients. Databases identified those who were hospitalized, experienced delirium, died, or were institutionalized. Cognitive decline was also evaluated and based upon a validated test score.
Forty-eight percent (n = 367) were hospitalized and 25% (n = 194) developed delirium. Patients who did not experience delirium in the hospital had an increased risk of death or requiring institutionalization (relative risks of 4.7 and 6.9, respectively). An even more dramatic increase in risk was noted in those with delirium (RRs of 5.4 and 9.3). Delirium was associated with 6% of deaths, 15% of institutionalizations, and 21% of cognitive declines in hospitalized patients with AD.
This is the first time the relative contributions of hospitalizations and episodes of delirium to adverse outcomes for AD patients have been evaluated. The investigators’ goal of observing outcomes for at least 1 year clearly shows that hospitalization is a danger to this patient population and that the outcomes are worse for those with delirium. At least one in eight patients with AD will have an adverse event or death from hospitalization. This clinical cohort was created by merging multiple databases, so incomplete medical records were a problem. Two other aspects of the study are worth noting. As this study was nonrandomized, the hospitalized patients had lower baseline cognitive function than those who avoided admission. Also, ethnic minorities made up only 5% of the study population and therefore do not represent the U.S. Alzheimer’s community in that regard.
The second work is a multicenter observational study. This entailed the development of the Prediction of Delirium in ICU Patients (PRE-DELIRIC) model in a prospective cohort of 1,613 patients, a temporal validation in a second prospective cohort in the same hospital using 549 patients, and external validation with a total of 894 patients in four separate hospitals.
The PRE-DELIRIC model contains 10 risk factors: age, APACHE-II (Acute Physiology and Chronic Health Evaluation) score, admission group (consisting of medical, surgical, trauma, and neurological patients), coma, infection, metabolic acidosis, use of sedating medications, morphine use, blood urea nitrogen levels, and urgent admission. The main outcome measured was development of delirium within the ICU. The model’s ability to predict delirium was compared with that of ICU physicians and nurses to independently predicting delirium within 24 hours of admission.
The model’s area under receiver operating characteristics curve (AUROC) was 0.85 pooled across three cohorts (0.87, 0.86, and 0.84 for the first, second, and third cohorts, respectively). The AUROC for both physicians’ and nurses’ predictions of delirium was 0.59. Providers’ predictive accuracy did not differ by level of clinical experience.
PRE-DELIRIC is the first predictive model published for the ICU population experiencing delirium. Study design makes sense for the intention. It is important to note that patients with a history of alcohol abuse and dementia were excluded. It was felt that their risk for developing delirium is high even without consideration of other factors.
The model clearly outperformed the physicians and nurses, who were equally inferior when it came to predicting delirium. It also appears that this could be an area of medicine where experience is not accompanied by improved accuracy. More experienced clinicians fared no better than their greener colleagues. Limitations included a varied case mix from multiple specialties and inclusion of risk factors that were not based on their systematic review for those associated with delirium.
Both of these studies move us forward. The first should heighten our level of awareness that hospitalization with delirium is a major marker for undesired outcomes. It also should prompt proactive communication with our AD patients’ families about expectations in this scenario. The second should help create a mindset of predicting and preventing delirium rather than our current model, which is to screen and then treat.
Dr. Bekanich is with the department of medicine and is medical director of palliative care at Seton Healthcare in Austin, Tex. To respond to this commentary, e-mail [email protected].
I expect that [insert patient name here] will have a hospital stay measured in a period of days. During that time we will do our best to prevent complications of hospitalization, which include things such as blood clots and infections. We will also do our best to quickly recognize and treat those complications that do occur such as confusion or pain." This is a conversation I have with the majority of patients’ families when their medically complicated loved one is hospitalized.
I was certain that one gentleman, who has esophageal cancer with metastasis to the spine causing cord compression, would suffer from delirium during his hospital stay. His advanced age, multiple comorbidities, urgent surgery, intensive-care unit stay, and the medications he required to control his pain -- which initially included a fentanyl PCA (patient-controlled analgesia) and was later augmented by a ketamine infusion -- all seemed to put him at high risk for this. Yet, even during his time on our ketamine protocol he had clear and appropriate conversations with our team.
Another elderly woman, with previously undiagnosed dementia, was living at home with family assistance until coming to the hospital after suffering from a fall at home. During her hospital course she experienced side effects of pain medications and also developed a urinary tract infection. The delirium that ensued was severe. She required ICU admission because of the intense nursing supervision she needed to keep her out of physical restraints.
Eventually, when it was appropriate, she was discharged to a skilled nursing facility rather than home because of the persistent cognitive problems she was experiencing. The emergency room physician who called me about the admission anticipated that the patient could return home less than 24 hours after coming in. She left the hospital almost 2 weeks later.
Delirium in hospitalized patients is a common problem. Its presence is often partnered with extended lengths of stay, escalation of care, and poorer outcomes. Once it occurs, we turn to screening tools and treatment protocols that evidence has shown to be useful. Therefore, it should come as no surprise that a hospital’s approach to delirium management is now recognized as a quality-of-care marker.
Two new studies highlight the impact of delirium and provide a new tool for predicting this condition. They expand our body of knowledge, and one of them may even empower us to possibly head off delirium before it occurs.
The first study is a prospective cohort enrolled between 1991 and 2006 into a patient registry for Alzheimer’s disease (AD). Participants were over the age of 65 years with a clinical diagnosis of AD in this community setting, which included 771 patients. Databases identified those who were hospitalized, experienced delirium, died, or were institutionalized. Cognitive decline was also evaluated and based upon a validated test score.
Forty-eight percent (n = 367) were hospitalized and 25% (n = 194) developed delirium. Patients who did not experience delirium in the hospital had an increased risk of death or requiring institutionalization (relative risks of 4.7 and 6.9, respectively). An even more dramatic increase in risk was noted in those with delirium (RRs of 5.4 and 9.3). Delirium was associated with 6% of deaths, 15% of institutionalizations, and 21% of cognitive declines in hospitalized patients with AD.
This is the first time the relative contributions of hospitalizations and episodes of delirium to adverse outcomes for AD patients have been evaluated. The investigators’ goal of observing outcomes for at least 1 year clearly shows that hospitalization is a danger to this patient population and that the outcomes are worse for those with delirium. At least one in eight patients with AD will have an adverse event or death from hospitalization. This clinical cohort was created by merging multiple databases, so incomplete medical records were a problem. Two other aspects of the study are worth noting. As this study was nonrandomized, the hospitalized patients had lower baseline cognitive function than those who avoided admission. Also, ethnic minorities made up only 5% of the study population and therefore do not represent the U.S. Alzheimer’s community in that regard.
The second work is a multicenter observational study. This entailed the development of the Prediction of Delirium in ICU Patients (PRE-DELIRIC) model in a prospective cohort of 1,613 patients, a temporal validation in a second prospective cohort in the same hospital using 549 patients, and external validation with a total of 894 patients in four separate hospitals.
The PRE-DELIRIC model contains 10 risk factors: age, APACHE-II (Acute Physiology and Chronic Health Evaluation) score, admission group (consisting of medical, surgical, trauma, and neurological patients), coma, infection, metabolic acidosis, use of sedating medications, morphine use, blood urea nitrogen levels, and urgent admission. The main outcome measured was development of delirium within the ICU. The model’s ability to predict delirium was compared with that of ICU physicians and nurses to independently predicting delirium within 24 hours of admission.
The model’s area under receiver operating characteristics curve (AUROC) was 0.85 pooled across three cohorts (0.87, 0.86, and 0.84 for the first, second, and third cohorts, respectively). The AUROC for both physicians’ and nurses’ predictions of delirium was 0.59. Providers’ predictive accuracy did not differ by level of clinical experience.
PRE-DELIRIC is the first predictive model published for the ICU population experiencing delirium. Study design makes sense for the intention. It is important to note that patients with a history of alcohol abuse and dementia were excluded. It was felt that their risk for developing delirium is high even without consideration of other factors.
The model clearly outperformed the physicians and nurses, who were equally inferior when it came to predicting delirium. It also appears that this could be an area of medicine where experience is not accompanied by improved accuracy. More experienced clinicians fared no better than their greener colleagues. Limitations included a varied case mix from multiple specialties and inclusion of risk factors that were not based on their systematic review for those associated with delirium.
Both of these studies move us forward. The first should heighten our level of awareness that hospitalization with delirium is a major marker for undesired outcomes. It also should prompt proactive communication with our AD patients’ families about expectations in this scenario. The second should help create a mindset of predicting and preventing delirium rather than our current model, which is to screen and then treat.
Dr. Bekanich is with the department of medicine and is medical director of palliative care at Seton Healthcare in Austin, Tex. To respond to this commentary, e-mail [email protected].
I expect that [insert patient name here] will have a hospital stay measured in a period of days. During that time we will do our best to prevent complications of hospitalization, which include things such as blood clots and infections. We will also do our best to quickly recognize and treat those complications that do occur such as confusion or pain." This is a conversation I have with the majority of patients’ families when their medically complicated loved one is hospitalized.
I was certain that one gentleman, who has esophageal cancer with metastasis to the spine causing cord compression, would suffer from delirium during his hospital stay. His advanced age, multiple comorbidities, urgent surgery, intensive-care unit stay, and the medications he required to control his pain -- which initially included a fentanyl PCA (patient-controlled analgesia) and was later augmented by a ketamine infusion -- all seemed to put him at high risk for this. Yet, even during his time on our ketamine protocol he had clear and appropriate conversations with our team.
Another elderly woman, with previously undiagnosed dementia, was living at home with family assistance until coming to the hospital after suffering from a fall at home. During her hospital course she experienced side effects of pain medications and also developed a urinary tract infection. The delirium that ensued was severe. She required ICU admission because of the intense nursing supervision she needed to keep her out of physical restraints.
Eventually, when it was appropriate, she was discharged to a skilled nursing facility rather than home because of the persistent cognitive problems she was experiencing. The emergency room physician who called me about the admission anticipated that the patient could return home less than 24 hours after coming in. She left the hospital almost 2 weeks later.
Delirium in hospitalized patients is a common problem. Its presence is often partnered with extended lengths of stay, escalation of care, and poorer outcomes. Once it occurs, we turn to screening tools and treatment protocols that evidence has shown to be useful. Therefore, it should come as no surprise that a hospital’s approach to delirium management is now recognized as a quality-of-care marker.
Two new studies highlight the impact of delirium and provide a new tool for predicting this condition. They expand our body of knowledge, and one of them may even empower us to possibly head off delirium before it occurs.
The first study is a prospective cohort enrolled between 1991 and 2006 into a patient registry for Alzheimer’s disease (AD). Participants were over the age of 65 years with a clinical diagnosis of AD in this community setting, which included 771 patients. Databases identified those who were hospitalized, experienced delirium, died, or were institutionalized. Cognitive decline was also evaluated and based upon a validated test score.
Forty-eight percent (n = 367) were hospitalized and 25% (n = 194) developed delirium. Patients who did not experience delirium in the hospital had an increased risk of death or requiring institutionalization (relative risks of 4.7 and 6.9, respectively). An even more dramatic increase in risk was noted in those with delirium (RRs of 5.4 and 9.3). Delirium was associated with 6% of deaths, 15% of institutionalizations, and 21% of cognitive declines in hospitalized patients with AD.
This is the first time the relative contributions of hospitalizations and episodes of delirium to adverse outcomes for AD patients have been evaluated. The investigators’ goal of observing outcomes for at least 1 year clearly shows that hospitalization is a danger to this patient population and that the outcomes are worse for those with delirium. At least one in eight patients with AD will have an adverse event or death from hospitalization. This clinical cohort was created by merging multiple databases, so incomplete medical records were a problem. Two other aspects of the study are worth noting. As this study was nonrandomized, the hospitalized patients had lower baseline cognitive function than those who avoided admission. Also, ethnic minorities made up only 5% of the study population and therefore do not represent the U.S. Alzheimer’s community in that regard.
The second work is a multicenter observational study. This entailed the development of the Prediction of Delirium in ICU Patients (PRE-DELIRIC) model in a prospective cohort of 1,613 patients, a temporal validation in a second prospective cohort in the same hospital using 549 patients, and external validation with a total of 894 patients in four separate hospitals.
The PRE-DELIRIC model contains 10 risk factors: age, APACHE-II (Acute Physiology and Chronic Health Evaluation) score, admission group (consisting of medical, surgical, trauma, and neurological patients), coma, infection, metabolic acidosis, use of sedating medications, morphine use, blood urea nitrogen levels, and urgent admission. The main outcome measured was development of delirium within the ICU. The model’s ability to predict delirium was compared with that of ICU physicians and nurses to independently predicting delirium within 24 hours of admission.
The model’s area under receiver operating characteristics curve (AUROC) was 0.85 pooled across three cohorts (0.87, 0.86, and 0.84 for the first, second, and third cohorts, respectively). The AUROC for both physicians’ and nurses’ predictions of delirium was 0.59. Providers’ predictive accuracy did not differ by level of clinical experience.
PRE-DELIRIC is the first predictive model published for the ICU population experiencing delirium. Study design makes sense for the intention. It is important to note that patients with a history of alcohol abuse and dementia were excluded. It was felt that their risk for developing delirium is high even without consideration of other factors.
The model clearly outperformed the physicians and nurses, who were equally inferior when it came to predicting delirium. It also appears that this could be an area of medicine where experience is not accompanied by improved accuracy. More experienced clinicians fared no better than their greener colleagues. Limitations included a varied case mix from multiple specialties and inclusion of risk factors that were not based on their systematic review for those associated with delirium.
Both of these studies move us forward. The first should heighten our level of awareness that hospitalization with delirium is a major marker for undesired outcomes. It also should prompt proactive communication with our AD patients’ families about expectations in this scenario. The second should help create a mindset of predicting and preventing delirium rather than our current model, which is to screen and then treat.
Dr. Bekanich is with the department of medicine and is medical director of palliative care at Seton Healthcare in Austin, Tex. To respond to this commentary, e-mail [email protected].