User login
Moderate-to-severe atopic dermatitis: Long-term safety and effectiveness of tralokinumab
Key clinical point: Tralokinumab was well tolerated and maintained long-term disease control for up to 2 years in patients with moderate-to-severe atopic dermatitis (AD).
Major finding: In the safety analysis set (n = 1174), the exposure-adjusted incidence rate of adverse events (AE) was 237.8 events/100 patient-years of exposure and 71.9% of participants reported ≥1 AE of mostly mild or moderate severity. In the efficacy analysis set (n = 345), 82.5% of patients treated with tralokinumab for 2 years maintained ≥75% improvement in the Eczema Area and Severity Index.
Study details: Findings are from the 2-year post hoc interim analysis of the ongoing, 5-year open-label extension trial, ECZTEND, including adult participants with moderate-to-severe AD from previous parent trials who received 300 mg tralokinumab every 2 weeks with or without topical corticosteroids.
Disclosures: The ECZTEND trial was sponsored by LEO Pharma A/S. Three authors declared being employees of LEO Pharma, and other authors reported ties with several sources, including LEO Pharma.
Source: Blauvelt A et al. Long-term 2-year safety and efficacy of tralokinumab in adults with moderate-to-severe atopic dermatitis: Interim analysis of the ECZTEND open-label extension trial. J Am Acad Dermatol. 2022 (Jul 18). Doi: 10.1016/j.jaad.2022.07.019
Key clinical point: Tralokinumab was well tolerated and maintained long-term disease control for up to 2 years in patients with moderate-to-severe atopic dermatitis (AD).
Major finding: In the safety analysis set (n = 1174), the exposure-adjusted incidence rate of adverse events (AE) was 237.8 events/100 patient-years of exposure and 71.9% of participants reported ≥1 AE of mostly mild or moderate severity. In the efficacy analysis set (n = 345), 82.5% of patients treated with tralokinumab for 2 years maintained ≥75% improvement in the Eczema Area and Severity Index.
Study details: Findings are from the 2-year post hoc interim analysis of the ongoing, 5-year open-label extension trial, ECZTEND, including adult participants with moderate-to-severe AD from previous parent trials who received 300 mg tralokinumab every 2 weeks with or without topical corticosteroids.
Disclosures: The ECZTEND trial was sponsored by LEO Pharma A/S. Three authors declared being employees of LEO Pharma, and other authors reported ties with several sources, including LEO Pharma.
Source: Blauvelt A et al. Long-term 2-year safety and efficacy of tralokinumab in adults with moderate-to-severe atopic dermatitis: Interim analysis of the ECZTEND open-label extension trial. J Am Acad Dermatol. 2022 (Jul 18). Doi: 10.1016/j.jaad.2022.07.019
Key clinical point: Tralokinumab was well tolerated and maintained long-term disease control for up to 2 years in patients with moderate-to-severe atopic dermatitis (AD).
Major finding: In the safety analysis set (n = 1174), the exposure-adjusted incidence rate of adverse events (AE) was 237.8 events/100 patient-years of exposure and 71.9% of participants reported ≥1 AE of mostly mild or moderate severity. In the efficacy analysis set (n = 345), 82.5% of patients treated with tralokinumab for 2 years maintained ≥75% improvement in the Eczema Area and Severity Index.
Study details: Findings are from the 2-year post hoc interim analysis of the ongoing, 5-year open-label extension trial, ECZTEND, including adult participants with moderate-to-severe AD from previous parent trials who received 300 mg tralokinumab every 2 weeks with or without topical corticosteroids.
Disclosures: The ECZTEND trial was sponsored by LEO Pharma A/S. Three authors declared being employees of LEO Pharma, and other authors reported ties with several sources, including LEO Pharma.
Source: Blauvelt A et al. Long-term 2-year safety and efficacy of tralokinumab in adults with moderate-to-severe atopic dermatitis: Interim analysis of the ECZTEND open-label extension trial. J Am Acad Dermatol. 2022 (Jul 18). Doi: 10.1016/j.jaad.2022.07.019
Abrocitinib more promising than dupilumab in moderate-to-severe atopic dermatitis
Key clinical point: Abrocitinib was more effective than dupilumab in inducing early itch reduction and controlling disease severity in adults with moderate-to-severe atopic dermatitis (AD) on background topical therapy.
Major finding: A significantly higher proportion of patients in the abrocitinib vs dupilumab group achieved ≥4-point improvement in the Peak Pruritus Numerical Rating Scale score at week 2 (48% vs 26%; P < .0001) and ≥90% improvement in the Eczema Area and Severity Index at week 4 (29% vs 15%; P < .0001). Treatment-emergent adverse events were more frequent in the abrocitinib vs dupilumab group (74% vs 65%).
Study details: Findings are from a phase 3 trial including 727 adults with moderate-to-severe AD who showed inadequate response to medicated topical therapy and were randomly assigned to receive oral abrocitinib or subcutaneous dupilumab for 26 weeks.
Disclosures: This study was funded by Pfizer. Seven authors declared being current or former employees or shareholders of Pfizer or Pfizer Pharma. The other authors reported ties with several sources.
Source: Reich K et al. Efficacy and safety of abrocitinib versus dupilumab in adults with moderate-to-severe atopic dermatitis: A randomised, double-blind, multicentre phase 3 trial. Lancet. 2022;400(10348):273-282 (Jul 23). Doi: 10.1016/S0140-6736(22)01199-0
Key clinical point: Abrocitinib was more effective than dupilumab in inducing early itch reduction and controlling disease severity in adults with moderate-to-severe atopic dermatitis (AD) on background topical therapy.
Major finding: A significantly higher proportion of patients in the abrocitinib vs dupilumab group achieved ≥4-point improvement in the Peak Pruritus Numerical Rating Scale score at week 2 (48% vs 26%; P < .0001) and ≥90% improvement in the Eczema Area and Severity Index at week 4 (29% vs 15%; P < .0001). Treatment-emergent adverse events were more frequent in the abrocitinib vs dupilumab group (74% vs 65%).
Study details: Findings are from a phase 3 trial including 727 adults with moderate-to-severe AD who showed inadequate response to medicated topical therapy and were randomly assigned to receive oral abrocitinib or subcutaneous dupilumab for 26 weeks.
Disclosures: This study was funded by Pfizer. Seven authors declared being current or former employees or shareholders of Pfizer or Pfizer Pharma. The other authors reported ties with several sources.
Source: Reich K et al. Efficacy and safety of abrocitinib versus dupilumab in adults with moderate-to-severe atopic dermatitis: A randomised, double-blind, multicentre phase 3 trial. Lancet. 2022;400(10348):273-282 (Jul 23). Doi: 10.1016/S0140-6736(22)01199-0
Key clinical point: Abrocitinib was more effective than dupilumab in inducing early itch reduction and controlling disease severity in adults with moderate-to-severe atopic dermatitis (AD) on background topical therapy.
Major finding: A significantly higher proportion of patients in the abrocitinib vs dupilumab group achieved ≥4-point improvement in the Peak Pruritus Numerical Rating Scale score at week 2 (48% vs 26%; P < .0001) and ≥90% improvement in the Eczema Area and Severity Index at week 4 (29% vs 15%; P < .0001). Treatment-emergent adverse events were more frequent in the abrocitinib vs dupilumab group (74% vs 65%).
Study details: Findings are from a phase 3 trial including 727 adults with moderate-to-severe AD who showed inadequate response to medicated topical therapy and were randomly assigned to receive oral abrocitinib or subcutaneous dupilumab for 26 weeks.
Disclosures: This study was funded by Pfizer. Seven authors declared being current or former employees or shareholders of Pfizer or Pfizer Pharma. The other authors reported ties with several sources.
Source: Reich K et al. Efficacy and safety of abrocitinib versus dupilumab in adults with moderate-to-severe atopic dermatitis: A randomised, double-blind, multicentre phase 3 trial. Lancet. 2022;400(10348):273-282 (Jul 23). Doi: 10.1016/S0140-6736(22)01199-0
Airway structure in women leads to worse COPD outcomes
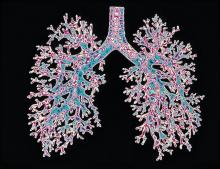
A study aimed at determining whether behind some of the sex differences in chronic obstructive airway disease (COPD) prevalence and clinical outcomes lie structural differences in airways found that airway lumen sizes quantified through chest CT were smaller in women than in men.
The findings, published in Radiology, took into account height and lung size. for equivalent changes, compared with men.
Among key findings in a secondary analysis of consecutive participants (9,363 ever-smokers and 420 never-smokers) enrolled in the Genetic Epidemiology of COPD (COPDGene) study, airway lumen dimensions were lower in never-smoker women than in men (segmental lumen diameter, 8.1 mm vs. 9.1 mm; P < .001). Also, ever-smoker women had narrower segmental lumen diameter (7.8 mm ± 0.05 vs. 8.7 mm ± 0.04; P < .001). The investigators found also that a unit change in wall thickness or lumen area resulted in more severe airflow obstruction, more dyspnea, worse respiratory quality of life, lower 6-minute walk distance, and worse survival in women, compared with men.
While COPD is diagnosed more often in men than women, changes in smoking behavior and increasing urbanization have led to COPD prevalence in women fast approaching the rate in men. Although age-adjusted rates for COPD-related deaths have continued to decline in men, in women they have not. Indeed, never-smoking women accounted for two-thirds of COPD in a population-based study.
COPDGene, a prospective, multicenter, observational cohort study, enrolled current and former smokers, as well as never-smokers, aged 45-80 years at 21 clinical centers across the United States from January 2008 to June 2011 with longitudinal follow-up until November 2020. The investigators quantified airway disease through CT imaging using the following metrics: airway wall thickness of segmental airways, wall area percent of segmental airways, the square root of the wall area of a hypothetical airway with 10-mm internal perimeter, total airway count, lumen diameter of segmental airways, airway volume, and airway fractal dimension.
“Not all sex differences in prevalence of COPD have been explained, and structural differences may explain some of these differences. Our findings may have implications for patient selection for clinical trials,” corresponding author Surya P. Bhatt, MD, associate professor of medicine and director of the University of Alabama Imaging Core at Birmingham, said in an interview.
The investigators wrote: “Our findings have implications for airflow limitation and the consequent clinical outcomes. ... We confirmed that men have more emphysema than women with equivalent smoking burden, and our results suggest that the lower reserve conferred by smaller airways predisposes women to develop airflow limitation predominantly through the airway phenotype. All airway remodeling changes were associated with more dyspnea, worse respiratory quality of life, and lower functional capacity in women than in men. The smaller airways in women can result in higher airway resistance and more turbulent airflow, and thus place a higher ventilatory constraint during exertion. Alteration in each airway measure was also associated with worse survival in women than in men, partially explaining the comparable mortality between the sexes for COPD despite the differing degrees of emphysema.”
“I think these findings highlight underappreciated sex differences in the natural history of COPD,” Mohsen Sadatsafavi, MD, PhD, associate professor, faculty of pharmaceutical sciences, at the University of British Columbia, Vancouver, said in an interview. “To me, first and foremost, the Bhatt et al. findings highlight how the ‘one size fits all’ approach to COPD management of using exacerbation history alone to guide preventive therapies is incorrect. These findings have the potential to change the management paradigm of COPD in the long term, but before getting there, I think we need to relate these findings to clinically relevant and patient-reported outcomes.”
Noting study limitations, the authors stated that a higher proportion of men were active smokers, compared with women, and despite adjustments for smoking status, some of the airway wall differences may be from the impact of active cigarette smoking on airway wall thickness.
Five study authors reported receiving support from various government and industry sources and disclosed conflicts of interest based on relationships with industry. The rest reported no conflicts of interest.
A study aimed at determining whether behind some of the sex differences in chronic obstructive airway disease (COPD) prevalence and clinical outcomes lie structural differences in airways found that airway lumen sizes quantified through chest CT were smaller in women than in men.
The findings, published in Radiology, took into account height and lung size. for equivalent changes, compared with men.
Among key findings in a secondary analysis of consecutive participants (9,363 ever-smokers and 420 never-smokers) enrolled in the Genetic Epidemiology of COPD (COPDGene) study, airway lumen dimensions were lower in never-smoker women than in men (segmental lumen diameter, 8.1 mm vs. 9.1 mm; P < .001). Also, ever-smoker women had narrower segmental lumen diameter (7.8 mm ± 0.05 vs. 8.7 mm ± 0.04; P < .001). The investigators found also that a unit change in wall thickness or lumen area resulted in more severe airflow obstruction, more dyspnea, worse respiratory quality of life, lower 6-minute walk distance, and worse survival in women, compared with men.
While COPD is diagnosed more often in men than women, changes in smoking behavior and increasing urbanization have led to COPD prevalence in women fast approaching the rate in men. Although age-adjusted rates for COPD-related deaths have continued to decline in men, in women they have not. Indeed, never-smoking women accounted for two-thirds of COPD in a population-based study.
COPDGene, a prospective, multicenter, observational cohort study, enrolled current and former smokers, as well as never-smokers, aged 45-80 years at 21 clinical centers across the United States from January 2008 to June 2011 with longitudinal follow-up until November 2020. The investigators quantified airway disease through CT imaging using the following metrics: airway wall thickness of segmental airways, wall area percent of segmental airways, the square root of the wall area of a hypothetical airway with 10-mm internal perimeter, total airway count, lumen diameter of segmental airways, airway volume, and airway fractal dimension.
“Not all sex differences in prevalence of COPD have been explained, and structural differences may explain some of these differences. Our findings may have implications for patient selection for clinical trials,” corresponding author Surya P. Bhatt, MD, associate professor of medicine and director of the University of Alabama Imaging Core at Birmingham, said in an interview.
The investigators wrote: “Our findings have implications for airflow limitation and the consequent clinical outcomes. ... We confirmed that men have more emphysema than women with equivalent smoking burden, and our results suggest that the lower reserve conferred by smaller airways predisposes women to develop airflow limitation predominantly through the airway phenotype. All airway remodeling changes were associated with more dyspnea, worse respiratory quality of life, and lower functional capacity in women than in men. The smaller airways in women can result in higher airway resistance and more turbulent airflow, and thus place a higher ventilatory constraint during exertion. Alteration in each airway measure was also associated with worse survival in women than in men, partially explaining the comparable mortality between the sexes for COPD despite the differing degrees of emphysema.”
“I think these findings highlight underappreciated sex differences in the natural history of COPD,” Mohsen Sadatsafavi, MD, PhD, associate professor, faculty of pharmaceutical sciences, at the University of British Columbia, Vancouver, said in an interview. “To me, first and foremost, the Bhatt et al. findings highlight how the ‘one size fits all’ approach to COPD management of using exacerbation history alone to guide preventive therapies is incorrect. These findings have the potential to change the management paradigm of COPD in the long term, but before getting there, I think we need to relate these findings to clinically relevant and patient-reported outcomes.”
Noting study limitations, the authors stated that a higher proportion of men were active smokers, compared with women, and despite adjustments for smoking status, some of the airway wall differences may be from the impact of active cigarette smoking on airway wall thickness.
Five study authors reported receiving support from various government and industry sources and disclosed conflicts of interest based on relationships with industry. The rest reported no conflicts of interest.
A study aimed at determining whether behind some of the sex differences in chronic obstructive airway disease (COPD) prevalence and clinical outcomes lie structural differences in airways found that airway lumen sizes quantified through chest CT were smaller in women than in men.
The findings, published in Radiology, took into account height and lung size. for equivalent changes, compared with men.
Among key findings in a secondary analysis of consecutive participants (9,363 ever-smokers and 420 never-smokers) enrolled in the Genetic Epidemiology of COPD (COPDGene) study, airway lumen dimensions were lower in never-smoker women than in men (segmental lumen diameter, 8.1 mm vs. 9.1 mm; P < .001). Also, ever-smoker women had narrower segmental lumen diameter (7.8 mm ± 0.05 vs. 8.7 mm ± 0.04; P < .001). The investigators found also that a unit change in wall thickness or lumen area resulted in more severe airflow obstruction, more dyspnea, worse respiratory quality of life, lower 6-minute walk distance, and worse survival in women, compared with men.
While COPD is diagnosed more often in men than women, changes in smoking behavior and increasing urbanization have led to COPD prevalence in women fast approaching the rate in men. Although age-adjusted rates for COPD-related deaths have continued to decline in men, in women they have not. Indeed, never-smoking women accounted for two-thirds of COPD in a population-based study.
COPDGene, a prospective, multicenter, observational cohort study, enrolled current and former smokers, as well as never-smokers, aged 45-80 years at 21 clinical centers across the United States from January 2008 to June 2011 with longitudinal follow-up until November 2020. The investigators quantified airway disease through CT imaging using the following metrics: airway wall thickness of segmental airways, wall area percent of segmental airways, the square root of the wall area of a hypothetical airway with 10-mm internal perimeter, total airway count, lumen diameter of segmental airways, airway volume, and airway fractal dimension.
“Not all sex differences in prevalence of COPD have been explained, and structural differences may explain some of these differences. Our findings may have implications for patient selection for clinical trials,” corresponding author Surya P. Bhatt, MD, associate professor of medicine and director of the University of Alabama Imaging Core at Birmingham, said in an interview.
The investigators wrote: “Our findings have implications for airflow limitation and the consequent clinical outcomes. ... We confirmed that men have more emphysema than women with equivalent smoking burden, and our results suggest that the lower reserve conferred by smaller airways predisposes women to develop airflow limitation predominantly through the airway phenotype. All airway remodeling changes were associated with more dyspnea, worse respiratory quality of life, and lower functional capacity in women than in men. The smaller airways in women can result in higher airway resistance and more turbulent airflow, and thus place a higher ventilatory constraint during exertion. Alteration in each airway measure was also associated with worse survival in women than in men, partially explaining the comparable mortality between the sexes for COPD despite the differing degrees of emphysema.”
“I think these findings highlight underappreciated sex differences in the natural history of COPD,” Mohsen Sadatsafavi, MD, PhD, associate professor, faculty of pharmaceutical sciences, at the University of British Columbia, Vancouver, said in an interview. “To me, first and foremost, the Bhatt et al. findings highlight how the ‘one size fits all’ approach to COPD management of using exacerbation history alone to guide preventive therapies is incorrect. These findings have the potential to change the management paradigm of COPD in the long term, but before getting there, I think we need to relate these findings to clinically relevant and patient-reported outcomes.”
Noting study limitations, the authors stated that a higher proportion of men were active smokers, compared with women, and despite adjustments for smoking status, some of the airway wall differences may be from the impact of active cigarette smoking on airway wall thickness.
Five study authors reported receiving support from various government and industry sources and disclosed conflicts of interest based on relationships with industry. The rest reported no conflicts of interest.
FROM RADIOLOGY
How physicians and their organizations react to online hate
“A sad day. A new low point in the spiral of hate, violence, and lies. Behind every account, there is a person. Do not forget that. In loving memory,” a Twitter user wrote about the death of Lisa-Maria Kellermayr, MD.
“This outcome is very saddening indeed. It should cause everyone to reflect. About interactions in our society, about ‘social’ media, about tolerance, about consideration, and about freedom,” tweeted Dirk Heinrich, MD, chair of the Virchow Association.
The suspected suicide of Dr. Kellermayr, an Austrian vaccinator, is stirring emotions in Germany, too. The active exponent and supporter of COVID-19 measures had been seriously threatened by anti-vaxxers and pandemic deniers. Thousands of people in Vienna said goodbye to her with a solemn vigil.
Dr. Kellermayr, a vaccination campaigner, had received hateful comments and death threats since the start of the pandemic. But a single post on Twitter changed everything. On Nov. 16, 2021, anti-vaxxers held a demonstration outside the Wels-Grieskirchen Hospital. Dr. Kellermayr tweeted in disgust, “Today in Wels: A demonstration by conspiracy theorists spills into the street under the gaze of the authorities and blocks both the main hospital entrance and the Red Cross ambulance exit.”
At the time of her tweet, Dr. Kellermayr was not aware of additional access that had been made available for ambulances. The police reacted to her tweet, calling it a “false report.” As Florian Klenk writes in the Austrian journal Falter, the police basically criticized Dr. Kellermayr publicly, including in front of the 12,000 Twitter users who follow the police on Twitter.
A screenshot of Dr. Kellermayr’s tweet and the authorities’ response went viral on relevant Telegram forums and triggered a flood of hatred. A COVID denier immediately posted her address online.
Dr. Kellermayr deleted her tweet and asked the police to also delete their tweet, but they did not respond, and the tweet remained online. The country physician was inundated with insults, slurs, and death threats. She was beset by alleged patients who came only to disrupt her work, take videos on their cell phones, and share the photos in anti-vaxxer groups. She privately paid for a security guard, who confiscated butterfly knives from multiple “patients” on their way into the waiting room. Dr. Kellermayr looked for help from the medical association, the police, and the Office for the Protection of the Constitution. She made her problem public.
Police recommend supervision
Dr. Kellermayr received emails in which the senders described in detail how they would kill her and her practice team. The physician took the threats seriously; the police did not. The officers investigated. With the evidence that the perpetrators were operating via the dark web, the officers insinuated to Dr. Kellermayr that it was not possible to find them, Klenk reported.
Dr. Kellermayr filed a complaint for the first time on Nov. 22, 2021. The law enforcement authorities in Upper Austria said they did not have domestic jurisdiction. The Austrian authorities launched another investigation. The German prosecution authorities joined the search for those posting death threats on social media. Even the Munich chief public prosecutor’s office and the Berlin public prosecutor’s office investigated the case.
According to some reports, Dr. Kellermayr did not receive police protection; a patrol was sent over from time to time. According to the police, she should “not be afraid,” and if she was, she should just call them. She was also advised to undergo supervision -- in other words, psychological treatment.
Those who had the power to help her provided no support. On the contrary, the spokesperson for the Upper Austria Police said in the Ö1 Mittagsjournal radio program that Dr. Kellermayr was “putting herself in the public eye for her own selfish benefit.” Even Peter Niedermoser, president of the Medical Association of Upper Austria, told the Austrian daily newspaper Standard, “I understand that you have to defend yourself, but it is a whole other question as to whether you have to discuss every topic to excess on Twitter. Sometimes it’s better to step away.”
Leaving Twitter
A German network specialist who hunts pedophiles online offered Dr. Kellermayr her help and was quickly on the trail of suspects, including a neo-Nazi from the Berlin area and a man from Upper Bavaria. Then the Office for the Protection of the Constitution stepped in. Omar Haijawi-Pirchner, head of the Austrian State Security and Intelligence Directorate, stated that the evidence provided by the network specialist would be pursued.
At the end of June, Dr. Kellermayr closed her practice. The situation was no longer tolerable for her staff, and the costs for security, €100,000 up to that point, were no longer manageable. At the start of July, she announced that she wanted to reopen the practice.
In her suicide note to the Upper Austria State Police Department, she wrote “that there was a lot of talking, but no one did anything.” In her letter to her medical association, she also made it clear that she had felt abandoned.
“Every suicide is a tragedy. This one more so: a woman in need was abandoned by the police and authorities. That is a social failure,” tweeted physicist and author Florian Aigner.
“Threatened. Ruined. Left alone by the state. Because she did her job. Because she got involved. Because she spread information. Because many want to be understanding for the self-styled ‘unconventional thinkers,’ the ‘Querdenker.’ Because many did not want to take the threat seriously. Because we tolerate them,” tweeted the intensive care physician Lämêth.
“Many colleagues using their real names get all of this outside of Twitter too: emails, phone calls, letters, or even visits by radical fanatics. If you are lucky, there is police protection, or a few reports, but often not a lot happens juridically,” tweeted Flow, anesthetist and emergency physician.
“More and more of the people who shaped Twitter by spreading reliable information voluntarily are now backing out. As long as the concept of freedom is abused here for hate and intimidation, individual responsibility can only mean self-defense. Sad,” wrote Christian Lübbers, MD, on Twitter. Since the ENT physician started vaccinating patients against COVID-19, he has been tormented with insults and death threats from anti-vaxxers and COVID deniers, this news organization has reported.
Examples of people who have backed out and deactivated their account are the virologist Isabella Eckerlek, MD, PhD, of the University of Geneva, and Natalie Grams, MD, spokesperson for the Information Network Homeopathy. For a long time, they spread information about COVID-19, corrected false assertions, and were increasingly faced with insults and hostility.
General practitioner Christian Kröner, MD, has repeatedly been the target of threats and insults and has been under police protection from time to time. He made a statement regarding Dr. Kellermayr’s death and has shut down his account for the first time following multiple instances of hostility.
Harassment continues
The hatred, harassment, and slander have not stopped, even after Dr. Kellermayr’s death. Harald Laatsch, who sits in the Berlin house of representatives for the Alternative for Germany party, commented that it seems “much more likely that she could no longer live with the heavy guilt of being a vaccine propagandist.”
“It is repulsive how the Querdenker deride a medical colleague who was driven to death by harassment and violence. She lost her life by saving the lives of others. Others are continuing her work. The state must protect people like her,” tweeted Karl Lauterbach, MD, PhD, who has also been overrun with hate campaigns by Querdenker and COVID deniers.
The page “Ich habe mitgemacht” – Das Archiv für Corona-Unrecht [“I Joined In” – The Archive for COVID Injustice] probably did not help to deescalate the situation on Twitter. Anonymous archivists there collect allegedly ostracizing quotes and share them, along with names. The context in which these statements were given at the time is not mentioned. Some politicians and journalists have given this online pillory the name, “We joined in! We have ostracized, defamed...”
Being humiliated and defamed is par for the course for those who spread information across social media. As doctor and politician Rainer Röver, MD, wrote, “Whoever is involved in spreading information, science, fighting against fake news, and protecting the patients, pupils, clients, or mandates entrusted to them is being shouted down, threatened in writing, or driven to suicide.” The lying, baiting mob is taking over sovereignty of the discussion. According to Röver, the politicians are doing nothing “to actually put a stop to the violent mob.”
For some time now, the Federal Criminal Police Office (BKA) of Germany has considered anti-vaxxers or COVID deniers as a “relevant risk” in connection with attacks on vaccination centers or medical practices.
Increasing aggression
At the start of November last year, participants at the 125th German Medical Assembly demanded that violence against health care professionals be outlawed, Mark Berger, deputy spokesperson of the German Medical Association (BÄK), recollected. At the assembly, various medical associations shared reports of an increase in aggression during the pandemic.
The State Medical Chamber of Physicians of Saxony confirmed threats of violence against physicians, death threats against employees of the Vaccination Committee of Saxony, and criminal damage to medical practices that administer vaccinations. Physicians who administer vaccines in schools receive abuse.
Owing to the increasing amount of aggression, the State Medical Association of Thuringia has set up a special email address as a first point of contact to report violence for those who are affected. “In recent months, we have received a large number of reports from physicians who have received threatening letters in relation to the COVID vaccination, or letters purporting to be liability information or notices of liability,” explained the association. In the cases of which the association becomes aware, a criminal charge is issued most of the time. The investigative proceedings are ongoing.
The State Medical Association of Hesse has devised a reporting form with which it can obtain information on the forms of violence inflicted against physicians and their teams. The reporting is anonymous, and the data are statistically analyzed.
Peter Bobbert, MD, PhD, president of the Berlin Medical Association, provided reports of threat scenarios, “the kind and frequency of which we have never experienced.” He received many messages from physicians asking for help because they had received threatening letters or because their addresses had been posted on social networks.
To date, there have only been isolated cases, said Oliver Erens, MD, spokesperson of the State Medical Association of Baden-Württemberg. “But it is true that some colleagues have already had these kinds of experiences.” Those affected have primarily reported “discussions, debates, and verbal altercations with patients on the topic of the COVID vaccination, compliance with the mask mandate, and other COVID-containment measures – definitely with a high potential for aggression from some of the patients,” said Dr. Erens. Cases of physical violence have not been reported to date.
Above all, there has been a need for advice over the phone, predominantly in the legal department of the regional medical associations. “All physicians and their teams are being recommended by their associations to consistently prosecute any cases of threat of, or use of, violence against them,” Dr. Erens said. In October 2021, the University of Heidelberg started a study on the victimization of physicians. The analysis is ongoing.
Staying on Twitter
Lübbers considered leaving Twitter but decided against it. “I decided not to do it and to carry on spreading information about pseudo-medicine and vaccination. I see this as necessary civic courage and will not give way to hate,” Lübbers tweeted.
As understandable as any departure is, “we must not surrender Twitter to the trolls and harassers. Who is still here? #Iamstaying,” wrote Flow. Others wrote, “I will stay on Twitter as a physician. With my real name, too. [...] We must not surrender it to the Querdenker, idiots, Nazis, and enemies of freedom.”
“We need people to share information, we need voices of reason, just as Kellermayr was. How can you say that it would be better to remain silent? Does everyone who is against idiocy, Querdenker, and conspiracy theorists now have to remain silent?” asked Janos Hegedüs, MD, in his podcast.
Hegedüs, who uncovers fake news about COVID-19 and vaccination, was and remains a frequent target of insults and threats. His attempts to take action against them has had only limited success. His conclusion is sobering. “If you decide to spread information, you should know: You are alone. You will get all of the hate and when you have a problem with it, no one will help you.”
Media attorney Chan-jo Jun, who for many years has taken a stand against hate and harassment, has deactivated his Twitter account. However, this is not a retreat, as he clarified in an interview with the German radio station Deutschlandfunk. “I do not intend to give up the fight against hate, harassment, and misinformation, but I will do it in a different place.”
He sees Dr. Kellermayr’s death as a turning point. “I thought that we had learned something after Lübcke [i.e., politician Walter Lübcke, who was murdered by a neo-Nazi]. But we are seeing that the death of a political opponent is not just the goal, but also a success for the other side. And that is shocking.”
The judicial means of taking action against hate are still not effective, said Mr. Jun. He also sees the platform operators as responsible, since they are not obliged to remove unlawful content. “German law and the German constitution hold no sway on Twitter.”
Right-wing extremism
What happened to Lisa-Maria Kellermayr is the same as targeted terrorism. An organized group set out to annihilate her. Social psychologist Pia Lamberty has spoken, in the context of COVID, about a pandemic of violence, the threatening nature of which has barely been recognized, both in the virtual and analog world.
In an article for the Jüdische Allgemeine, Dr. Lamberty criticizes the fact that “the mistakes made with Pegida [i.e., a far-right, Islamophobic political movement in Germany] are being made once again” in the classification of Querdenker and COVID deniers. From the very start, the protests against the COVID measures have been a rallying point in the mobilization of right-wing extremists. “The Querdenker movement is unifying radical, right-wing extremist elements. Antisemitism and racism were always welcome.” Still, the right-wing extremist motivation has not been clearly labeled as such.
The classification is not just a question of statistics. “It is also about analyzing the potential for danger and deriving political measures from this. And there is an urgent need for action here: The right-wing extremists will utilize the climate crisis, but also the war in Ukraine, attacks against refugees, and LGBTQ rights for further mobilization. Rather than the state, the focus of the attacks will be people who are labeled as the bogeyman. This also must be clearly labeled for what it is,” said Dr. Lamberty.
She wrote on Twitter, “The COVID-related attacks that took place in the last two years will not simply stop, they will shift. If we do not want more and more people to stop expressing themselves publicly, something urgently has to happen.” She added, “Once more: The next few months will be very difficult. This will probably also be accompanied by an increased level of threat for socially engaged people. More protection is urgently required.”
A version of this article first appeared on Medscape.com.
This article was translated from the Medscape German edition.
“A sad day. A new low point in the spiral of hate, violence, and lies. Behind every account, there is a person. Do not forget that. In loving memory,” a Twitter user wrote about the death of Lisa-Maria Kellermayr, MD.
“This outcome is very saddening indeed. It should cause everyone to reflect. About interactions in our society, about ‘social’ media, about tolerance, about consideration, and about freedom,” tweeted Dirk Heinrich, MD, chair of the Virchow Association.
The suspected suicide of Dr. Kellermayr, an Austrian vaccinator, is stirring emotions in Germany, too. The active exponent and supporter of COVID-19 measures had been seriously threatened by anti-vaxxers and pandemic deniers. Thousands of people in Vienna said goodbye to her with a solemn vigil.
Dr. Kellermayr, a vaccination campaigner, had received hateful comments and death threats since the start of the pandemic. But a single post on Twitter changed everything. On Nov. 16, 2021, anti-vaxxers held a demonstration outside the Wels-Grieskirchen Hospital. Dr. Kellermayr tweeted in disgust, “Today in Wels: A demonstration by conspiracy theorists spills into the street under the gaze of the authorities and blocks both the main hospital entrance and the Red Cross ambulance exit.”
At the time of her tweet, Dr. Kellermayr was not aware of additional access that had been made available for ambulances. The police reacted to her tweet, calling it a “false report.” As Florian Klenk writes in the Austrian journal Falter, the police basically criticized Dr. Kellermayr publicly, including in front of the 12,000 Twitter users who follow the police on Twitter.
A screenshot of Dr. Kellermayr’s tweet and the authorities’ response went viral on relevant Telegram forums and triggered a flood of hatred. A COVID denier immediately posted her address online.
Dr. Kellermayr deleted her tweet and asked the police to also delete their tweet, but they did not respond, and the tweet remained online. The country physician was inundated with insults, slurs, and death threats. She was beset by alleged patients who came only to disrupt her work, take videos on their cell phones, and share the photos in anti-vaxxer groups. She privately paid for a security guard, who confiscated butterfly knives from multiple “patients” on their way into the waiting room. Dr. Kellermayr looked for help from the medical association, the police, and the Office for the Protection of the Constitution. She made her problem public.
Police recommend supervision
Dr. Kellermayr received emails in which the senders described in detail how they would kill her and her practice team. The physician took the threats seriously; the police did not. The officers investigated. With the evidence that the perpetrators were operating via the dark web, the officers insinuated to Dr. Kellermayr that it was not possible to find them, Klenk reported.
Dr. Kellermayr filed a complaint for the first time on Nov. 22, 2021. The law enforcement authorities in Upper Austria said they did not have domestic jurisdiction. The Austrian authorities launched another investigation. The German prosecution authorities joined the search for those posting death threats on social media. Even the Munich chief public prosecutor’s office and the Berlin public prosecutor’s office investigated the case.
According to some reports, Dr. Kellermayr did not receive police protection; a patrol was sent over from time to time. According to the police, she should “not be afraid,” and if she was, she should just call them. She was also advised to undergo supervision -- in other words, psychological treatment.
Those who had the power to help her provided no support. On the contrary, the spokesperson for the Upper Austria Police said in the Ö1 Mittagsjournal radio program that Dr. Kellermayr was “putting herself in the public eye for her own selfish benefit.” Even Peter Niedermoser, president of the Medical Association of Upper Austria, told the Austrian daily newspaper Standard, “I understand that you have to defend yourself, but it is a whole other question as to whether you have to discuss every topic to excess on Twitter. Sometimes it’s better to step away.”
Leaving Twitter
A German network specialist who hunts pedophiles online offered Dr. Kellermayr her help and was quickly on the trail of suspects, including a neo-Nazi from the Berlin area and a man from Upper Bavaria. Then the Office for the Protection of the Constitution stepped in. Omar Haijawi-Pirchner, head of the Austrian State Security and Intelligence Directorate, stated that the evidence provided by the network specialist would be pursued.
At the end of June, Dr. Kellermayr closed her practice. The situation was no longer tolerable for her staff, and the costs for security, €100,000 up to that point, were no longer manageable. At the start of July, she announced that she wanted to reopen the practice.
In her suicide note to the Upper Austria State Police Department, she wrote “that there was a lot of talking, but no one did anything.” In her letter to her medical association, she also made it clear that she had felt abandoned.
“Every suicide is a tragedy. This one more so: a woman in need was abandoned by the police and authorities. That is a social failure,” tweeted physicist and author Florian Aigner.
“Threatened. Ruined. Left alone by the state. Because she did her job. Because she got involved. Because she spread information. Because many want to be understanding for the self-styled ‘unconventional thinkers,’ the ‘Querdenker.’ Because many did not want to take the threat seriously. Because we tolerate them,” tweeted the intensive care physician Lämêth.
“Many colleagues using their real names get all of this outside of Twitter too: emails, phone calls, letters, or even visits by radical fanatics. If you are lucky, there is police protection, or a few reports, but often not a lot happens juridically,” tweeted Flow, anesthetist and emergency physician.
“More and more of the people who shaped Twitter by spreading reliable information voluntarily are now backing out. As long as the concept of freedom is abused here for hate and intimidation, individual responsibility can only mean self-defense. Sad,” wrote Christian Lübbers, MD, on Twitter. Since the ENT physician started vaccinating patients against COVID-19, he has been tormented with insults and death threats from anti-vaxxers and COVID deniers, this news organization has reported.
Examples of people who have backed out and deactivated their account are the virologist Isabella Eckerlek, MD, PhD, of the University of Geneva, and Natalie Grams, MD, spokesperson for the Information Network Homeopathy. For a long time, they spread information about COVID-19, corrected false assertions, and were increasingly faced with insults and hostility.
General practitioner Christian Kröner, MD, has repeatedly been the target of threats and insults and has been under police protection from time to time. He made a statement regarding Dr. Kellermayr’s death and has shut down his account for the first time following multiple instances of hostility.
Harassment continues
The hatred, harassment, and slander have not stopped, even after Dr. Kellermayr’s death. Harald Laatsch, who sits in the Berlin house of representatives for the Alternative for Germany party, commented that it seems “much more likely that she could no longer live with the heavy guilt of being a vaccine propagandist.”
“It is repulsive how the Querdenker deride a medical colleague who was driven to death by harassment and violence. She lost her life by saving the lives of others. Others are continuing her work. The state must protect people like her,” tweeted Karl Lauterbach, MD, PhD, who has also been overrun with hate campaigns by Querdenker and COVID deniers.
The page “Ich habe mitgemacht” – Das Archiv für Corona-Unrecht [“I Joined In” – The Archive for COVID Injustice] probably did not help to deescalate the situation on Twitter. Anonymous archivists there collect allegedly ostracizing quotes and share them, along with names. The context in which these statements were given at the time is not mentioned. Some politicians and journalists have given this online pillory the name, “We joined in! We have ostracized, defamed...”
Being humiliated and defamed is par for the course for those who spread information across social media. As doctor and politician Rainer Röver, MD, wrote, “Whoever is involved in spreading information, science, fighting against fake news, and protecting the patients, pupils, clients, or mandates entrusted to them is being shouted down, threatened in writing, or driven to suicide.” The lying, baiting mob is taking over sovereignty of the discussion. According to Röver, the politicians are doing nothing “to actually put a stop to the violent mob.”
For some time now, the Federal Criminal Police Office (BKA) of Germany has considered anti-vaxxers or COVID deniers as a “relevant risk” in connection with attacks on vaccination centers or medical practices.
Increasing aggression
At the start of November last year, participants at the 125th German Medical Assembly demanded that violence against health care professionals be outlawed, Mark Berger, deputy spokesperson of the German Medical Association (BÄK), recollected. At the assembly, various medical associations shared reports of an increase in aggression during the pandemic.
The State Medical Chamber of Physicians of Saxony confirmed threats of violence against physicians, death threats against employees of the Vaccination Committee of Saxony, and criminal damage to medical practices that administer vaccinations. Physicians who administer vaccines in schools receive abuse.
Owing to the increasing amount of aggression, the State Medical Association of Thuringia has set up a special email address as a first point of contact to report violence for those who are affected. “In recent months, we have received a large number of reports from physicians who have received threatening letters in relation to the COVID vaccination, or letters purporting to be liability information or notices of liability,” explained the association. In the cases of which the association becomes aware, a criminal charge is issued most of the time. The investigative proceedings are ongoing.
The State Medical Association of Hesse has devised a reporting form with which it can obtain information on the forms of violence inflicted against physicians and their teams. The reporting is anonymous, and the data are statistically analyzed.
Peter Bobbert, MD, PhD, president of the Berlin Medical Association, provided reports of threat scenarios, “the kind and frequency of which we have never experienced.” He received many messages from physicians asking for help because they had received threatening letters or because their addresses had been posted on social networks.
To date, there have only been isolated cases, said Oliver Erens, MD, spokesperson of the State Medical Association of Baden-Württemberg. “But it is true that some colleagues have already had these kinds of experiences.” Those affected have primarily reported “discussions, debates, and verbal altercations with patients on the topic of the COVID vaccination, compliance with the mask mandate, and other COVID-containment measures – definitely with a high potential for aggression from some of the patients,” said Dr. Erens. Cases of physical violence have not been reported to date.
Above all, there has been a need for advice over the phone, predominantly in the legal department of the regional medical associations. “All physicians and their teams are being recommended by their associations to consistently prosecute any cases of threat of, or use of, violence against them,” Dr. Erens said. In October 2021, the University of Heidelberg started a study on the victimization of physicians. The analysis is ongoing.
Staying on Twitter
Lübbers considered leaving Twitter but decided against it. “I decided not to do it and to carry on spreading information about pseudo-medicine and vaccination. I see this as necessary civic courage and will not give way to hate,” Lübbers tweeted.
As understandable as any departure is, “we must not surrender Twitter to the trolls and harassers. Who is still here? #Iamstaying,” wrote Flow. Others wrote, “I will stay on Twitter as a physician. With my real name, too. [...] We must not surrender it to the Querdenker, idiots, Nazis, and enemies of freedom.”
“We need people to share information, we need voices of reason, just as Kellermayr was. How can you say that it would be better to remain silent? Does everyone who is against idiocy, Querdenker, and conspiracy theorists now have to remain silent?” asked Janos Hegedüs, MD, in his podcast.
Hegedüs, who uncovers fake news about COVID-19 and vaccination, was and remains a frequent target of insults and threats. His attempts to take action against them has had only limited success. His conclusion is sobering. “If you decide to spread information, you should know: You are alone. You will get all of the hate and when you have a problem with it, no one will help you.”
Media attorney Chan-jo Jun, who for many years has taken a stand against hate and harassment, has deactivated his Twitter account. However, this is not a retreat, as he clarified in an interview with the German radio station Deutschlandfunk. “I do not intend to give up the fight against hate, harassment, and misinformation, but I will do it in a different place.”
He sees Dr. Kellermayr’s death as a turning point. “I thought that we had learned something after Lübcke [i.e., politician Walter Lübcke, who was murdered by a neo-Nazi]. But we are seeing that the death of a political opponent is not just the goal, but also a success for the other side. And that is shocking.”
The judicial means of taking action against hate are still not effective, said Mr. Jun. He also sees the platform operators as responsible, since they are not obliged to remove unlawful content. “German law and the German constitution hold no sway on Twitter.”
Right-wing extremism
What happened to Lisa-Maria Kellermayr is the same as targeted terrorism. An organized group set out to annihilate her. Social psychologist Pia Lamberty has spoken, in the context of COVID, about a pandemic of violence, the threatening nature of which has barely been recognized, both in the virtual and analog world.
In an article for the Jüdische Allgemeine, Dr. Lamberty criticizes the fact that “the mistakes made with Pegida [i.e., a far-right, Islamophobic political movement in Germany] are being made once again” in the classification of Querdenker and COVID deniers. From the very start, the protests against the COVID measures have been a rallying point in the mobilization of right-wing extremists. “The Querdenker movement is unifying radical, right-wing extremist elements. Antisemitism and racism were always welcome.” Still, the right-wing extremist motivation has not been clearly labeled as such.
The classification is not just a question of statistics. “It is also about analyzing the potential for danger and deriving political measures from this. And there is an urgent need for action here: The right-wing extremists will utilize the climate crisis, but also the war in Ukraine, attacks against refugees, and LGBTQ rights for further mobilization. Rather than the state, the focus of the attacks will be people who are labeled as the bogeyman. This also must be clearly labeled for what it is,” said Dr. Lamberty.
She wrote on Twitter, “The COVID-related attacks that took place in the last two years will not simply stop, they will shift. If we do not want more and more people to stop expressing themselves publicly, something urgently has to happen.” She added, “Once more: The next few months will be very difficult. This will probably also be accompanied by an increased level of threat for socially engaged people. More protection is urgently required.”
A version of this article first appeared on Medscape.com.
This article was translated from the Medscape German edition.
“A sad day. A new low point in the spiral of hate, violence, and lies. Behind every account, there is a person. Do not forget that. In loving memory,” a Twitter user wrote about the death of Lisa-Maria Kellermayr, MD.
“This outcome is very saddening indeed. It should cause everyone to reflect. About interactions in our society, about ‘social’ media, about tolerance, about consideration, and about freedom,” tweeted Dirk Heinrich, MD, chair of the Virchow Association.
The suspected suicide of Dr. Kellermayr, an Austrian vaccinator, is stirring emotions in Germany, too. The active exponent and supporter of COVID-19 measures had been seriously threatened by anti-vaxxers and pandemic deniers. Thousands of people in Vienna said goodbye to her with a solemn vigil.
Dr. Kellermayr, a vaccination campaigner, had received hateful comments and death threats since the start of the pandemic. But a single post on Twitter changed everything. On Nov. 16, 2021, anti-vaxxers held a demonstration outside the Wels-Grieskirchen Hospital. Dr. Kellermayr tweeted in disgust, “Today in Wels: A demonstration by conspiracy theorists spills into the street under the gaze of the authorities and blocks both the main hospital entrance and the Red Cross ambulance exit.”
At the time of her tweet, Dr. Kellermayr was not aware of additional access that had been made available for ambulances. The police reacted to her tweet, calling it a “false report.” As Florian Klenk writes in the Austrian journal Falter, the police basically criticized Dr. Kellermayr publicly, including in front of the 12,000 Twitter users who follow the police on Twitter.
A screenshot of Dr. Kellermayr’s tweet and the authorities’ response went viral on relevant Telegram forums and triggered a flood of hatred. A COVID denier immediately posted her address online.
Dr. Kellermayr deleted her tweet and asked the police to also delete their tweet, but they did not respond, and the tweet remained online. The country physician was inundated with insults, slurs, and death threats. She was beset by alleged patients who came only to disrupt her work, take videos on their cell phones, and share the photos in anti-vaxxer groups. She privately paid for a security guard, who confiscated butterfly knives from multiple “patients” on their way into the waiting room. Dr. Kellermayr looked for help from the medical association, the police, and the Office for the Protection of the Constitution. She made her problem public.
Police recommend supervision
Dr. Kellermayr received emails in which the senders described in detail how they would kill her and her practice team. The physician took the threats seriously; the police did not. The officers investigated. With the evidence that the perpetrators were operating via the dark web, the officers insinuated to Dr. Kellermayr that it was not possible to find them, Klenk reported.
Dr. Kellermayr filed a complaint for the first time on Nov. 22, 2021. The law enforcement authorities in Upper Austria said they did not have domestic jurisdiction. The Austrian authorities launched another investigation. The German prosecution authorities joined the search for those posting death threats on social media. Even the Munich chief public prosecutor’s office and the Berlin public prosecutor’s office investigated the case.
According to some reports, Dr. Kellermayr did not receive police protection; a patrol was sent over from time to time. According to the police, she should “not be afraid,” and if she was, she should just call them. She was also advised to undergo supervision -- in other words, psychological treatment.
Those who had the power to help her provided no support. On the contrary, the spokesperson for the Upper Austria Police said in the Ö1 Mittagsjournal radio program that Dr. Kellermayr was “putting herself in the public eye for her own selfish benefit.” Even Peter Niedermoser, president of the Medical Association of Upper Austria, told the Austrian daily newspaper Standard, “I understand that you have to defend yourself, but it is a whole other question as to whether you have to discuss every topic to excess on Twitter. Sometimes it’s better to step away.”
Leaving Twitter
A German network specialist who hunts pedophiles online offered Dr. Kellermayr her help and was quickly on the trail of suspects, including a neo-Nazi from the Berlin area and a man from Upper Bavaria. Then the Office for the Protection of the Constitution stepped in. Omar Haijawi-Pirchner, head of the Austrian State Security and Intelligence Directorate, stated that the evidence provided by the network specialist would be pursued.
At the end of June, Dr. Kellermayr closed her practice. The situation was no longer tolerable for her staff, and the costs for security, €100,000 up to that point, were no longer manageable. At the start of July, she announced that she wanted to reopen the practice.
In her suicide note to the Upper Austria State Police Department, she wrote “that there was a lot of talking, but no one did anything.” In her letter to her medical association, she also made it clear that she had felt abandoned.
“Every suicide is a tragedy. This one more so: a woman in need was abandoned by the police and authorities. That is a social failure,” tweeted physicist and author Florian Aigner.
“Threatened. Ruined. Left alone by the state. Because she did her job. Because she got involved. Because she spread information. Because many want to be understanding for the self-styled ‘unconventional thinkers,’ the ‘Querdenker.’ Because many did not want to take the threat seriously. Because we tolerate them,” tweeted the intensive care physician Lämêth.
“Many colleagues using their real names get all of this outside of Twitter too: emails, phone calls, letters, or even visits by radical fanatics. If you are lucky, there is police protection, or a few reports, but often not a lot happens juridically,” tweeted Flow, anesthetist and emergency physician.
“More and more of the people who shaped Twitter by spreading reliable information voluntarily are now backing out. As long as the concept of freedom is abused here for hate and intimidation, individual responsibility can only mean self-defense. Sad,” wrote Christian Lübbers, MD, on Twitter. Since the ENT physician started vaccinating patients against COVID-19, he has been tormented with insults and death threats from anti-vaxxers and COVID deniers, this news organization has reported.
Examples of people who have backed out and deactivated their account are the virologist Isabella Eckerlek, MD, PhD, of the University of Geneva, and Natalie Grams, MD, spokesperson for the Information Network Homeopathy. For a long time, they spread information about COVID-19, corrected false assertions, and were increasingly faced with insults and hostility.
General practitioner Christian Kröner, MD, has repeatedly been the target of threats and insults and has been under police protection from time to time. He made a statement regarding Dr. Kellermayr’s death and has shut down his account for the first time following multiple instances of hostility.
Harassment continues
The hatred, harassment, and slander have not stopped, even after Dr. Kellermayr’s death. Harald Laatsch, who sits in the Berlin house of representatives for the Alternative for Germany party, commented that it seems “much more likely that she could no longer live with the heavy guilt of being a vaccine propagandist.”
“It is repulsive how the Querdenker deride a medical colleague who was driven to death by harassment and violence. She lost her life by saving the lives of others. Others are continuing her work. The state must protect people like her,” tweeted Karl Lauterbach, MD, PhD, who has also been overrun with hate campaigns by Querdenker and COVID deniers.
The page “Ich habe mitgemacht” – Das Archiv für Corona-Unrecht [“I Joined In” – The Archive for COVID Injustice] probably did not help to deescalate the situation on Twitter. Anonymous archivists there collect allegedly ostracizing quotes and share them, along with names. The context in which these statements were given at the time is not mentioned. Some politicians and journalists have given this online pillory the name, “We joined in! We have ostracized, defamed...”
Being humiliated and defamed is par for the course for those who spread information across social media. As doctor and politician Rainer Röver, MD, wrote, “Whoever is involved in spreading information, science, fighting against fake news, and protecting the patients, pupils, clients, or mandates entrusted to them is being shouted down, threatened in writing, or driven to suicide.” The lying, baiting mob is taking over sovereignty of the discussion. According to Röver, the politicians are doing nothing “to actually put a stop to the violent mob.”
For some time now, the Federal Criminal Police Office (BKA) of Germany has considered anti-vaxxers or COVID deniers as a “relevant risk” in connection with attacks on vaccination centers or medical practices.
Increasing aggression
At the start of November last year, participants at the 125th German Medical Assembly demanded that violence against health care professionals be outlawed, Mark Berger, deputy spokesperson of the German Medical Association (BÄK), recollected. At the assembly, various medical associations shared reports of an increase in aggression during the pandemic.
The State Medical Chamber of Physicians of Saxony confirmed threats of violence against physicians, death threats against employees of the Vaccination Committee of Saxony, and criminal damage to medical practices that administer vaccinations. Physicians who administer vaccines in schools receive abuse.
Owing to the increasing amount of aggression, the State Medical Association of Thuringia has set up a special email address as a first point of contact to report violence for those who are affected. “In recent months, we have received a large number of reports from physicians who have received threatening letters in relation to the COVID vaccination, or letters purporting to be liability information or notices of liability,” explained the association. In the cases of which the association becomes aware, a criminal charge is issued most of the time. The investigative proceedings are ongoing.
The State Medical Association of Hesse has devised a reporting form with which it can obtain information on the forms of violence inflicted against physicians and their teams. The reporting is anonymous, and the data are statistically analyzed.
Peter Bobbert, MD, PhD, president of the Berlin Medical Association, provided reports of threat scenarios, “the kind and frequency of which we have never experienced.” He received many messages from physicians asking for help because they had received threatening letters or because their addresses had been posted on social networks.
To date, there have only been isolated cases, said Oliver Erens, MD, spokesperson of the State Medical Association of Baden-Württemberg. “But it is true that some colleagues have already had these kinds of experiences.” Those affected have primarily reported “discussions, debates, and verbal altercations with patients on the topic of the COVID vaccination, compliance with the mask mandate, and other COVID-containment measures – definitely with a high potential for aggression from some of the patients,” said Dr. Erens. Cases of physical violence have not been reported to date.
Above all, there has been a need for advice over the phone, predominantly in the legal department of the regional medical associations. “All physicians and their teams are being recommended by their associations to consistently prosecute any cases of threat of, or use of, violence against them,” Dr. Erens said. In October 2021, the University of Heidelberg started a study on the victimization of physicians. The analysis is ongoing.
Staying on Twitter
Lübbers considered leaving Twitter but decided against it. “I decided not to do it and to carry on spreading information about pseudo-medicine and vaccination. I see this as necessary civic courage and will not give way to hate,” Lübbers tweeted.
As understandable as any departure is, “we must not surrender Twitter to the trolls and harassers. Who is still here? #Iamstaying,” wrote Flow. Others wrote, “I will stay on Twitter as a physician. With my real name, too. [...] We must not surrender it to the Querdenker, idiots, Nazis, and enemies of freedom.”
“We need people to share information, we need voices of reason, just as Kellermayr was. How can you say that it would be better to remain silent? Does everyone who is against idiocy, Querdenker, and conspiracy theorists now have to remain silent?” asked Janos Hegedüs, MD, in his podcast.
Hegedüs, who uncovers fake news about COVID-19 and vaccination, was and remains a frequent target of insults and threats. His attempts to take action against them has had only limited success. His conclusion is sobering. “If you decide to spread information, you should know: You are alone. You will get all of the hate and when you have a problem with it, no one will help you.”
Media attorney Chan-jo Jun, who for many years has taken a stand against hate and harassment, has deactivated his Twitter account. However, this is not a retreat, as he clarified in an interview with the German radio station Deutschlandfunk. “I do not intend to give up the fight against hate, harassment, and misinformation, but I will do it in a different place.”
He sees Dr. Kellermayr’s death as a turning point. “I thought that we had learned something after Lübcke [i.e., politician Walter Lübcke, who was murdered by a neo-Nazi]. But we are seeing that the death of a political opponent is not just the goal, but also a success for the other side. And that is shocking.”
The judicial means of taking action against hate are still not effective, said Mr. Jun. He also sees the platform operators as responsible, since they are not obliged to remove unlawful content. “German law and the German constitution hold no sway on Twitter.”
Right-wing extremism
What happened to Lisa-Maria Kellermayr is the same as targeted terrorism. An organized group set out to annihilate her. Social psychologist Pia Lamberty has spoken, in the context of COVID, about a pandemic of violence, the threatening nature of which has barely been recognized, both in the virtual and analog world.
In an article for the Jüdische Allgemeine, Dr. Lamberty criticizes the fact that “the mistakes made with Pegida [i.e., a far-right, Islamophobic political movement in Germany] are being made once again” in the classification of Querdenker and COVID deniers. From the very start, the protests against the COVID measures have been a rallying point in the mobilization of right-wing extremists. “The Querdenker movement is unifying radical, right-wing extremist elements. Antisemitism and racism were always welcome.” Still, the right-wing extremist motivation has not been clearly labeled as such.
The classification is not just a question of statistics. “It is also about analyzing the potential for danger and deriving political measures from this. And there is an urgent need for action here: The right-wing extremists will utilize the climate crisis, but also the war in Ukraine, attacks against refugees, and LGBTQ rights for further mobilization. Rather than the state, the focus of the attacks will be people who are labeled as the bogeyman. This also must be clearly labeled for what it is,” said Dr. Lamberty.
She wrote on Twitter, “The COVID-related attacks that took place in the last two years will not simply stop, they will shift. If we do not want more and more people to stop expressing themselves publicly, something urgently has to happen.” She added, “Once more: The next few months will be very difficult. This will probably also be accompanied by an increased level of threat for socially engaged people. More protection is urgently required.”
A version of this article first appeared on Medscape.com.
This article was translated from the Medscape German edition.
Words, now actions: How medical associations try to fulfill pledges to combat racism in health care
– from health care outcomes, from the level and quality of patient treatment, from their own memberships. How have those pronouncements translated into programs that could have, or even have had, positive impacts?
For this article, this news organization asked several associations about tangible actions behind their vows to combat racism in health care. Meanwhile, a recent Medscape report focused on the degree to which physicians prioritize racial disparities as a leading social issue.
American Academy of Family Physicians
The American Academy of Family Physicians’ approach is to integrate diversity, equity, and inclusion (DEI) efforts into all existing and new projects rather than tackle racial disparities as a discrete problem.
“Our policies, our advocacy efforts, everything our commissions and staff do ... is through a lens of diversity, equity, and inclusiveness,” said AAFP Board Chair Ada D. Stewart, MD, FAAP.
That lens is ground by a DEI center the AAFP created in 2017. Run by AAFP staff, members, and chapters, the center focuses on five areas: policy, education and training, practice, diversifying the workplace, and strategic partnerships.
The center has established a special project called EveryONE to provide AAFP members with relevant research, policy templates, and other resources to address patient needs. One example is the Neighborhood Navigator, an online tool that shows food, housing, transportation, and other needs in a patient’s neighborhood.
Meanwhile, the DEI center has created training programs for AAFP members on topics like unconscious and implicit racial biases. And the AAFP has implemented several relevant governing policies regarding pushes to improve childbirth conditions and limit race-based treatment, among other areas.
In January, the AAFP established a new DEI commission for family medicine to set the academy’s agenda on racial issues moving forward. “We only had 10 physician positions available on the commission, and over 100 individuals applied, which gave us comfort that we were going in the right direction,” Dr. Stewart said.
Association of American Medical Colleges
The Association of American Medical Colleges, which represents nearly 600 U.S. and Canadian medical schools and teaching hospitals, has a “longstanding” focus on racial equity, said Philip Alberti, founder of the AAMC Center for Health Justice. However, in 2020 that focus became more detailed and layered.
Those layers include:
- Encouraging self-reflection by members on how personal racial biases and stereotypes can lead to systemic racism in health care.
- Working on the AAMC organizational structure. Priorities range from hiring a consultant to help guide antiracism efforts, to establishing a DEI council and advisors, to regularly seeking input from staff. In 2021, the AAMC launched a Center for Health Justice to work more closely with communities.
- Ramping up collaboration with national and local academic medicine organizations and partners. As one example, the AAMC and American Medical Association released a guide for physicians and health care professionals on language that could be interpreted as racist or disrespectful.
- Continuing to be outspoken about racial disparities in health care in society generally.
Meanwhile, the AAMC is supporting more specific, localized health equity efforts in cities such as Cincinnati and Boston.
Cincinnati Children’s Hospital research has found that children in poor neighborhoods are five times more likely to need hospital stays. AAMC members have helped identify “hot spots” for social needs among children and focused specifically on two neighborhoods in the city. The initiative has roped in partnerships with community and social service organizations as well as health care providers, and proponents say the number of child hospital stays in those neighborhoods has dropped by 20%.
Boston Medical Center researchers learned that Black and Latino patients experiencing problems with heart failure were less likely to be referred to a cardiologist. AAMC members assisted with a program to encourage physicians to make medically necessary referrals more often.
National Health Council
The National Health Council, an umbrella association of health organizations, similarly has made a “commitment, not just around policy work but anytime and anything the NHC is doing, to build around trying to identify and solve issues of health equity,” CEO Randall Rutta said.
The NHC has identified four strategic policy areas including race and in 2021 issued a statement signed by 45 other health care organizations vowing to take on systemic racism and advance equity, through public policy and law.
In relation to policy, Mr. Rutta said his organization is lobbying Congress and federal agencies to diversify clinical trials.
“We want to make sure that clinical trials are inclusive of people from different racial and ethnic groups, in order to understand how [they are] affected by a particular condition,” he said. “As you would imagine, some conditions hit certain groups harder than others for genetic or other reasons, or it may just be a reflection of other disparities that occur across health care.”
The organization has issued suggestions for policy change in the Food and Drug Administration’s clinical trial policy and separately targeted telemedicine policy to promote equity and greater patient access. For example, one initiative aims to ensure patients’ privacy and civil rights as telemedicine’s popularity grows after the COVID-19 pandemic. The NHC presented the initiative in a congressional briefing last year.
American Public Health Association
The American Public Health Association says it started focusing on racial disparities in health care in 2015, following a series of racially fueled violent acts. The APHA started with a four-part webinar series on racism in health (more than 10,000 live participants and 40,000 replays to date).
Shortly afterward, then-APHA President Camara Jones, MD, MPH, PhD, launched a national campaign encouraging APHA members, affiliates, and partners to name and address racism as a determinant of health.
More recently in 2021, the APHA adopted a “Truth, Racial Healing & Transformation” guiding framework and “Healing Through Policy” initiative that offer local leaders policy templates and best practices.
“We have identified a suite of policies that have actually been implemented successfully and are advancing racial equity,” said Regina Davis Moss, APHA’s associate executive director of health policy and practice. “You can’t advance health without having a policy that supports it.”
Montgomery County, Md., is one community that has used the framework (for racial equity training of county employees). Leaders in Evanston, Ill., also used it in crafting a resolution to end structural racism in the city.
A version of this article first appeared on Medscape.com.
– from health care outcomes, from the level and quality of patient treatment, from their own memberships. How have those pronouncements translated into programs that could have, or even have had, positive impacts?
For this article, this news organization asked several associations about tangible actions behind their vows to combat racism in health care. Meanwhile, a recent Medscape report focused on the degree to which physicians prioritize racial disparities as a leading social issue.
American Academy of Family Physicians
The American Academy of Family Physicians’ approach is to integrate diversity, equity, and inclusion (DEI) efforts into all existing and new projects rather than tackle racial disparities as a discrete problem.
“Our policies, our advocacy efforts, everything our commissions and staff do ... is through a lens of diversity, equity, and inclusiveness,” said AAFP Board Chair Ada D. Stewart, MD, FAAP.
That lens is ground by a DEI center the AAFP created in 2017. Run by AAFP staff, members, and chapters, the center focuses on five areas: policy, education and training, practice, diversifying the workplace, and strategic partnerships.
The center has established a special project called EveryONE to provide AAFP members with relevant research, policy templates, and other resources to address patient needs. One example is the Neighborhood Navigator, an online tool that shows food, housing, transportation, and other needs in a patient’s neighborhood.
Meanwhile, the DEI center has created training programs for AAFP members on topics like unconscious and implicit racial biases. And the AAFP has implemented several relevant governing policies regarding pushes to improve childbirth conditions and limit race-based treatment, among other areas.
In January, the AAFP established a new DEI commission for family medicine to set the academy’s agenda on racial issues moving forward. “We only had 10 physician positions available on the commission, and over 100 individuals applied, which gave us comfort that we were going in the right direction,” Dr. Stewart said.
Association of American Medical Colleges
The Association of American Medical Colleges, which represents nearly 600 U.S. and Canadian medical schools and teaching hospitals, has a “longstanding” focus on racial equity, said Philip Alberti, founder of the AAMC Center for Health Justice. However, in 2020 that focus became more detailed and layered.
Those layers include:
- Encouraging self-reflection by members on how personal racial biases and stereotypes can lead to systemic racism in health care.
- Working on the AAMC organizational structure. Priorities range from hiring a consultant to help guide antiracism efforts, to establishing a DEI council and advisors, to regularly seeking input from staff. In 2021, the AAMC launched a Center for Health Justice to work more closely with communities.
- Ramping up collaboration with national and local academic medicine organizations and partners. As one example, the AAMC and American Medical Association released a guide for physicians and health care professionals on language that could be interpreted as racist or disrespectful.
- Continuing to be outspoken about racial disparities in health care in society generally.
Meanwhile, the AAMC is supporting more specific, localized health equity efforts in cities such as Cincinnati and Boston.
Cincinnati Children’s Hospital research has found that children in poor neighborhoods are five times more likely to need hospital stays. AAMC members have helped identify “hot spots” for social needs among children and focused specifically on two neighborhoods in the city. The initiative has roped in partnerships with community and social service organizations as well as health care providers, and proponents say the number of child hospital stays in those neighborhoods has dropped by 20%.
Boston Medical Center researchers learned that Black and Latino patients experiencing problems with heart failure were less likely to be referred to a cardiologist. AAMC members assisted with a program to encourage physicians to make medically necessary referrals more often.
National Health Council
The National Health Council, an umbrella association of health organizations, similarly has made a “commitment, not just around policy work but anytime and anything the NHC is doing, to build around trying to identify and solve issues of health equity,” CEO Randall Rutta said.
The NHC has identified four strategic policy areas including race and in 2021 issued a statement signed by 45 other health care organizations vowing to take on systemic racism and advance equity, through public policy and law.
In relation to policy, Mr. Rutta said his organization is lobbying Congress and federal agencies to diversify clinical trials.
“We want to make sure that clinical trials are inclusive of people from different racial and ethnic groups, in order to understand how [they are] affected by a particular condition,” he said. “As you would imagine, some conditions hit certain groups harder than others for genetic or other reasons, or it may just be a reflection of other disparities that occur across health care.”
The organization has issued suggestions for policy change in the Food and Drug Administration’s clinical trial policy and separately targeted telemedicine policy to promote equity and greater patient access. For example, one initiative aims to ensure patients’ privacy and civil rights as telemedicine’s popularity grows after the COVID-19 pandemic. The NHC presented the initiative in a congressional briefing last year.
American Public Health Association
The American Public Health Association says it started focusing on racial disparities in health care in 2015, following a series of racially fueled violent acts. The APHA started with a four-part webinar series on racism in health (more than 10,000 live participants and 40,000 replays to date).
Shortly afterward, then-APHA President Camara Jones, MD, MPH, PhD, launched a national campaign encouraging APHA members, affiliates, and partners to name and address racism as a determinant of health.
More recently in 2021, the APHA adopted a “Truth, Racial Healing & Transformation” guiding framework and “Healing Through Policy” initiative that offer local leaders policy templates and best practices.
“We have identified a suite of policies that have actually been implemented successfully and are advancing racial equity,” said Regina Davis Moss, APHA’s associate executive director of health policy and practice. “You can’t advance health without having a policy that supports it.”
Montgomery County, Md., is one community that has used the framework (for racial equity training of county employees). Leaders in Evanston, Ill., also used it in crafting a resolution to end structural racism in the city.
A version of this article first appeared on Medscape.com.
– from health care outcomes, from the level and quality of patient treatment, from their own memberships. How have those pronouncements translated into programs that could have, or even have had, positive impacts?
For this article, this news organization asked several associations about tangible actions behind their vows to combat racism in health care. Meanwhile, a recent Medscape report focused on the degree to which physicians prioritize racial disparities as a leading social issue.
American Academy of Family Physicians
The American Academy of Family Physicians’ approach is to integrate diversity, equity, and inclusion (DEI) efforts into all existing and new projects rather than tackle racial disparities as a discrete problem.
“Our policies, our advocacy efforts, everything our commissions and staff do ... is through a lens of diversity, equity, and inclusiveness,” said AAFP Board Chair Ada D. Stewart, MD, FAAP.
That lens is ground by a DEI center the AAFP created in 2017. Run by AAFP staff, members, and chapters, the center focuses on five areas: policy, education and training, practice, diversifying the workplace, and strategic partnerships.
The center has established a special project called EveryONE to provide AAFP members with relevant research, policy templates, and other resources to address patient needs. One example is the Neighborhood Navigator, an online tool that shows food, housing, transportation, and other needs in a patient’s neighborhood.
Meanwhile, the DEI center has created training programs for AAFP members on topics like unconscious and implicit racial biases. And the AAFP has implemented several relevant governing policies regarding pushes to improve childbirth conditions and limit race-based treatment, among other areas.
In January, the AAFP established a new DEI commission for family medicine to set the academy’s agenda on racial issues moving forward. “We only had 10 physician positions available on the commission, and over 100 individuals applied, which gave us comfort that we were going in the right direction,” Dr. Stewart said.
Association of American Medical Colleges
The Association of American Medical Colleges, which represents nearly 600 U.S. and Canadian medical schools and teaching hospitals, has a “longstanding” focus on racial equity, said Philip Alberti, founder of the AAMC Center for Health Justice. However, in 2020 that focus became more detailed and layered.
Those layers include:
- Encouraging self-reflection by members on how personal racial biases and stereotypes can lead to systemic racism in health care.
- Working on the AAMC organizational structure. Priorities range from hiring a consultant to help guide antiracism efforts, to establishing a DEI council and advisors, to regularly seeking input from staff. In 2021, the AAMC launched a Center for Health Justice to work more closely with communities.
- Ramping up collaboration with national and local academic medicine organizations and partners. As one example, the AAMC and American Medical Association released a guide for physicians and health care professionals on language that could be interpreted as racist or disrespectful.
- Continuing to be outspoken about racial disparities in health care in society generally.
Meanwhile, the AAMC is supporting more specific, localized health equity efforts in cities such as Cincinnati and Boston.
Cincinnati Children’s Hospital research has found that children in poor neighborhoods are five times more likely to need hospital stays. AAMC members have helped identify “hot spots” for social needs among children and focused specifically on two neighborhoods in the city. The initiative has roped in partnerships with community and social service organizations as well as health care providers, and proponents say the number of child hospital stays in those neighborhoods has dropped by 20%.
Boston Medical Center researchers learned that Black and Latino patients experiencing problems with heart failure were less likely to be referred to a cardiologist. AAMC members assisted with a program to encourage physicians to make medically necessary referrals more often.
National Health Council
The National Health Council, an umbrella association of health organizations, similarly has made a “commitment, not just around policy work but anytime and anything the NHC is doing, to build around trying to identify and solve issues of health equity,” CEO Randall Rutta said.
The NHC has identified four strategic policy areas including race and in 2021 issued a statement signed by 45 other health care organizations vowing to take on systemic racism and advance equity, through public policy and law.
In relation to policy, Mr. Rutta said his organization is lobbying Congress and federal agencies to diversify clinical trials.
“We want to make sure that clinical trials are inclusive of people from different racial and ethnic groups, in order to understand how [they are] affected by a particular condition,” he said. “As you would imagine, some conditions hit certain groups harder than others for genetic or other reasons, or it may just be a reflection of other disparities that occur across health care.”
The organization has issued suggestions for policy change in the Food and Drug Administration’s clinical trial policy and separately targeted telemedicine policy to promote equity and greater patient access. For example, one initiative aims to ensure patients’ privacy and civil rights as telemedicine’s popularity grows after the COVID-19 pandemic. The NHC presented the initiative in a congressional briefing last year.
American Public Health Association
The American Public Health Association says it started focusing on racial disparities in health care in 2015, following a series of racially fueled violent acts. The APHA started with a four-part webinar series on racism in health (more than 10,000 live participants and 40,000 replays to date).
Shortly afterward, then-APHA President Camara Jones, MD, MPH, PhD, launched a national campaign encouraging APHA members, affiliates, and partners to name and address racism as a determinant of health.
More recently in 2021, the APHA adopted a “Truth, Racial Healing & Transformation” guiding framework and “Healing Through Policy” initiative that offer local leaders policy templates and best practices.
“We have identified a suite of policies that have actually been implemented successfully and are advancing racial equity,” said Regina Davis Moss, APHA’s associate executive director of health policy and practice. “You can’t advance health without having a policy that supports it.”
Montgomery County, Md., is one community that has used the framework (for racial equity training of county employees). Leaders in Evanston, Ill., also used it in crafting a resolution to end structural racism in the city.
A version of this article first appeared on Medscape.com.
ctDNA predicts outcomes in CRC after surgery and ACT
Key clinical point: Compared with circulating tumor DNA (ctDNA)-negative patients, ctDNA-positive patients are at a higher risk for recurrence and have a poorer prognosis for recurrence-free survival (RFS) after colorectal cancer (CRC) surgery and adjuvant chemotherapy (ACT).
Major finding: After CRC surgery and ACT, ctDNA-positive vs -negative patients were at a higher risk for CRC recurrence (relative risk [RR] 4.43 and RR 5.77, respectively; both P < .05) and had a worse prognosis for RFS (adjusted hazard ratio, 10.74 and adjusted RR 22.09, respectively; both P < .05).
Study details: This was a meta-analysis of 14 studies including 2393 patients who underwent radical R0 resection for primary CRC.
Disclosures: The study did not receive any funding. The authors declared no conflicts of interest.
Source: Mi J et al. Circulation tumour DNA in predicting recurrence and prognosis in operable colorectal cancer patients: A meta-analysis. Eur J Clin Invest. 2022 (Jul 20). Doi: 10.1111/eci.13842
Key clinical point: Compared with circulating tumor DNA (ctDNA)-negative patients, ctDNA-positive patients are at a higher risk for recurrence and have a poorer prognosis for recurrence-free survival (RFS) after colorectal cancer (CRC) surgery and adjuvant chemotherapy (ACT).
Major finding: After CRC surgery and ACT, ctDNA-positive vs -negative patients were at a higher risk for CRC recurrence (relative risk [RR] 4.43 and RR 5.77, respectively; both P < .05) and had a worse prognosis for RFS (adjusted hazard ratio, 10.74 and adjusted RR 22.09, respectively; both P < .05).
Study details: This was a meta-analysis of 14 studies including 2393 patients who underwent radical R0 resection for primary CRC.
Disclosures: The study did not receive any funding. The authors declared no conflicts of interest.
Source: Mi J et al. Circulation tumour DNA in predicting recurrence and prognosis in operable colorectal cancer patients: A meta-analysis. Eur J Clin Invest. 2022 (Jul 20). Doi: 10.1111/eci.13842
Key clinical point: Compared with circulating tumor DNA (ctDNA)-negative patients, ctDNA-positive patients are at a higher risk for recurrence and have a poorer prognosis for recurrence-free survival (RFS) after colorectal cancer (CRC) surgery and adjuvant chemotherapy (ACT).
Major finding: After CRC surgery and ACT, ctDNA-positive vs -negative patients were at a higher risk for CRC recurrence (relative risk [RR] 4.43 and RR 5.77, respectively; both P < .05) and had a worse prognosis for RFS (adjusted hazard ratio, 10.74 and adjusted RR 22.09, respectively; both P < .05).
Study details: This was a meta-analysis of 14 studies including 2393 patients who underwent radical R0 resection for primary CRC.
Disclosures: The study did not receive any funding. The authors declared no conflicts of interest.
Source: Mi J et al. Circulation tumour DNA in predicting recurrence and prognosis in operable colorectal cancer patients: A meta-analysis. Eur J Clin Invest. 2022 (Jul 20). Doi: 10.1111/eci.13842
Metformin use not linked with CRC incidence in T2D patients on evading time-related biases
Key clinical point: After considering time-related biases such as immortal time bias (ITB), metformin use is nonsignificantly associated with subsequent colorectal cancer (CRC) incidence in patients with type‑2 diabetes (T2D).
Major finding: Time-dependent Cox regression, landmark, or nested case-control analysis did not reveal a significant association between metformin use and CRC incidence, with hazard ratios (95% CI) for metformin ever-use (≥90 days of metformin prescription throughout follow-up) being 0.88 (0.68-1.13), 0.86 (0.65-1.12), and 1.10 (0.86-1.40), respectively, and those for average metformin prescription days/year being 0.97 (0.90-1.04), 0.95 (0.88-1.04), and 1.02 (0.95-1.10), respectively.
Study details: This observational study employed statistical methods that avoid ITB to analyze the real-world data of 41,533 patients newly diagnosed with T2D who were cancer-free at T2D diagnosis from a prospectively maintained cohort.
Disclosures: No source of funding was disclosed. The authors reported no conflicts of interest.
Source: Zhang HS et al. Metformin use is not associated with colorectal cancer incidence in type-2 diabetes patients: Evidence from methods that avoid immortal time bias. Int J Colorectal Dis. 2022;37:1827–1834 (Jul 14). Doi: 10.1007/s00384-022-04212-9
Key clinical point: After considering time-related biases such as immortal time bias (ITB), metformin use is nonsignificantly associated with subsequent colorectal cancer (CRC) incidence in patients with type‑2 diabetes (T2D).
Major finding: Time-dependent Cox regression, landmark, or nested case-control analysis did not reveal a significant association between metformin use and CRC incidence, with hazard ratios (95% CI) for metformin ever-use (≥90 days of metformin prescription throughout follow-up) being 0.88 (0.68-1.13), 0.86 (0.65-1.12), and 1.10 (0.86-1.40), respectively, and those for average metformin prescription days/year being 0.97 (0.90-1.04), 0.95 (0.88-1.04), and 1.02 (0.95-1.10), respectively.
Study details: This observational study employed statistical methods that avoid ITB to analyze the real-world data of 41,533 patients newly diagnosed with T2D who were cancer-free at T2D diagnosis from a prospectively maintained cohort.
Disclosures: No source of funding was disclosed. The authors reported no conflicts of interest.
Source: Zhang HS et al. Metformin use is not associated with colorectal cancer incidence in type-2 diabetes patients: Evidence from methods that avoid immortal time bias. Int J Colorectal Dis. 2022;37:1827–1834 (Jul 14). Doi: 10.1007/s00384-022-04212-9
Key clinical point: After considering time-related biases such as immortal time bias (ITB), metformin use is nonsignificantly associated with subsequent colorectal cancer (CRC) incidence in patients with type‑2 diabetes (T2D).
Major finding: Time-dependent Cox regression, landmark, or nested case-control analysis did not reveal a significant association between metformin use and CRC incidence, with hazard ratios (95% CI) for metformin ever-use (≥90 days of metformin prescription throughout follow-up) being 0.88 (0.68-1.13), 0.86 (0.65-1.12), and 1.10 (0.86-1.40), respectively, and those for average metformin prescription days/year being 0.97 (0.90-1.04), 0.95 (0.88-1.04), and 1.02 (0.95-1.10), respectively.
Study details: This observational study employed statistical methods that avoid ITB to analyze the real-world data of 41,533 patients newly diagnosed with T2D who were cancer-free at T2D diagnosis from a prospectively maintained cohort.
Disclosures: No source of funding was disclosed. The authors reported no conflicts of interest.
Source: Zhang HS et al. Metformin use is not associated with colorectal cancer incidence in type-2 diabetes patients: Evidence from methods that avoid immortal time bias. Int J Colorectal Dis. 2022;37:1827–1834 (Jul 14). Doi: 10.1007/s00384-022-04212-9
Metastatic CRC: Foods rich in vegetable fats prolong survival
Key clinical point: The risk for all-cause mortality and cancer progression or death is lower among patients with metastatic colorectal cancer (CRC) and a higher intake of vegetable fats.
Major finding: Patients with the highest (23.5% kcal/day; interquartile range [IQR] 21.6%-25.7% kcal/day) vs lowest (11.6% kcal/day; IQR 10.1%-12.7% kcal/day) median intake of vegetable fats showed a lower risk for all-cause mortality (adjusted hazard ratio [aHR] 0.79; 95% CI 0.63-1.00) and cancer progression or death (aHR 0.71; 95% CI 0.57-0.88).
Study details: Findings are from a prospective analysis that included 1149 patients with metastatic CRC from the CALGB 80405 (Alliance)/SWOG 80405 study.
Disclosures: This study was supported by the US National Cancer Institute of the National Institutes of Health and partly by Bristol Myers Squibb, Genentech, Pfizer, and Sanofi. Some authors declared serving as advisory board members or consultants for or receiving research support or payments for research advice or services from various sources, including Pfizer and Genentech.
Source: Van Blarigan EL et al. Dietary fat in relation to all-cause mortality and cancer progression and death among people with metastatic colorectal cancer: Data from CALGB 80405 (Alliance)/SWOG 80405. Int J Cancer. 2022 (Jul 29). Doi: 10.1002/ijc.34230
Key clinical point: The risk for all-cause mortality and cancer progression or death is lower among patients with metastatic colorectal cancer (CRC) and a higher intake of vegetable fats.
Major finding: Patients with the highest (23.5% kcal/day; interquartile range [IQR] 21.6%-25.7% kcal/day) vs lowest (11.6% kcal/day; IQR 10.1%-12.7% kcal/day) median intake of vegetable fats showed a lower risk for all-cause mortality (adjusted hazard ratio [aHR] 0.79; 95% CI 0.63-1.00) and cancer progression or death (aHR 0.71; 95% CI 0.57-0.88).
Study details: Findings are from a prospective analysis that included 1149 patients with metastatic CRC from the CALGB 80405 (Alliance)/SWOG 80405 study.
Disclosures: This study was supported by the US National Cancer Institute of the National Institutes of Health and partly by Bristol Myers Squibb, Genentech, Pfizer, and Sanofi. Some authors declared serving as advisory board members or consultants for or receiving research support or payments for research advice or services from various sources, including Pfizer and Genentech.
Source: Van Blarigan EL et al. Dietary fat in relation to all-cause mortality and cancer progression and death among people with metastatic colorectal cancer: Data from CALGB 80405 (Alliance)/SWOG 80405. Int J Cancer. 2022 (Jul 29). Doi: 10.1002/ijc.34230
Key clinical point: The risk for all-cause mortality and cancer progression or death is lower among patients with metastatic colorectal cancer (CRC) and a higher intake of vegetable fats.
Major finding: Patients with the highest (23.5% kcal/day; interquartile range [IQR] 21.6%-25.7% kcal/day) vs lowest (11.6% kcal/day; IQR 10.1%-12.7% kcal/day) median intake of vegetable fats showed a lower risk for all-cause mortality (adjusted hazard ratio [aHR] 0.79; 95% CI 0.63-1.00) and cancer progression or death (aHR 0.71; 95% CI 0.57-0.88).
Study details: Findings are from a prospective analysis that included 1149 patients with metastatic CRC from the CALGB 80405 (Alliance)/SWOG 80405 study.
Disclosures: This study was supported by the US National Cancer Institute of the National Institutes of Health and partly by Bristol Myers Squibb, Genentech, Pfizer, and Sanofi. Some authors declared serving as advisory board members or consultants for or receiving research support or payments for research advice or services from various sources, including Pfizer and Genentech.
Source: Van Blarigan EL et al. Dietary fat in relation to all-cause mortality and cancer progression and death among people with metastatic colorectal cancer: Data from CALGB 80405 (Alliance)/SWOG 80405. Int J Cancer. 2022 (Jul 29). Doi: 10.1002/ijc.34230
How efficient is neoadjuvant chemotherapy in mismatch repair deficient colon cancer?
Key clinical point: Neoadjuvant chemotherapy (NCT) is associated with higher carcinoembryonic antigen (CEA) levels and multiorgan resection rates owing to larger postoperative tumor size in patients with mismatch repair deficient (dMMR) colon cancer.
Major finding: Patients who received vs did not receive NCT had a higher incidence of abnormal CEA levels (51.6% vs 17.4%; P < .001) and multiorgan resection rate (38.7% vs 16.8%; P = .006) and larger postoperative tumor diameters (7.26 vs 6.21; P = .033).
Study details: This retrospective study analyzed the data of 335 patients with dMMR colon cancer who did (n = 31) or did not (n = 304) receive neoadjuvant chemotherapy after radical surgery.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Yunlong W et al. The efficiency of neoadjuvant chemotherapy in colon cancer with mismatch repair deficiency. Cancer Med. 2022 (Jul 29). Doi: 10.1002/cam4.5076
Key clinical point: Neoadjuvant chemotherapy (NCT) is associated with higher carcinoembryonic antigen (CEA) levels and multiorgan resection rates owing to larger postoperative tumor size in patients with mismatch repair deficient (dMMR) colon cancer.
Major finding: Patients who received vs did not receive NCT had a higher incidence of abnormal CEA levels (51.6% vs 17.4%; P < .001) and multiorgan resection rate (38.7% vs 16.8%; P = .006) and larger postoperative tumor diameters (7.26 vs 6.21; P = .033).
Study details: This retrospective study analyzed the data of 335 patients with dMMR colon cancer who did (n = 31) or did not (n = 304) receive neoadjuvant chemotherapy after radical surgery.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Yunlong W et al. The efficiency of neoadjuvant chemotherapy in colon cancer with mismatch repair deficiency. Cancer Med. 2022 (Jul 29). Doi: 10.1002/cam4.5076
Key clinical point: Neoadjuvant chemotherapy (NCT) is associated with higher carcinoembryonic antigen (CEA) levels and multiorgan resection rates owing to larger postoperative tumor size in patients with mismatch repair deficient (dMMR) colon cancer.
Major finding: Patients who received vs did not receive NCT had a higher incidence of abnormal CEA levels (51.6% vs 17.4%; P < .001) and multiorgan resection rate (38.7% vs 16.8%; P = .006) and larger postoperative tumor diameters (7.26 vs 6.21; P = .033).
Study details: This retrospective study analyzed the data of 335 patients with dMMR colon cancer who did (n = 31) or did not (n = 304) receive neoadjuvant chemotherapy after radical surgery.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Yunlong W et al. The efficiency of neoadjuvant chemotherapy in colon cancer with mismatch repair deficiency. Cancer Med. 2022 (Jul 29). Doi: 10.1002/cam4.5076
Specific clinical features indicate more timely prediagnostic investigations or referral for CRC
Key clinical point: An increase in consultation rates for colorectal cancer (CRC)-relevant symptoms and abnormal blood test results in the 2-year prediagnosis period hint at early initiation of specific investigations or referrals, thereby accelerating the diagnosis and treatment in some patients with symptomatic CRC.
Major finding: The earliest clinical feature to show increased recording rate from the baseline was rectal bleeding, at 10 months before colon cancer diagnosis (95% CI 8.3-11.7) and 8 months before rectal cancer diagnosis (95% CI 6.1-9.9). The rate of abnormal blood measurements (low hemoglobin levels, high platelet counts, etc) recorded increased from 9 months prediagnosis.
Study details: Findings are from a retrospective study that analyzed linked primary care and cancer registry data of patients with colon (n = 5033) or rectal (2516) cancer.
Disclosures: This study was supported by the National Institute for Health Research School for Primary Care Research and linked to the CanTest Collaborative funded by Cancer Research UK. Four authors are a part of the CanTest Collaborative.
Source: Moullet M et al. Pre-diagnostic clinical features and blood tests in patients with colorectal cancer: a retrospective linked-data study. Br J Gen Pract. 2022;72(721):e556-e563 (Jul 28). Doi: 10.3399/BJGP.2021.0563
Key clinical point: An increase in consultation rates for colorectal cancer (CRC)-relevant symptoms and abnormal blood test results in the 2-year prediagnosis period hint at early initiation of specific investigations or referrals, thereby accelerating the diagnosis and treatment in some patients with symptomatic CRC.
Major finding: The earliest clinical feature to show increased recording rate from the baseline was rectal bleeding, at 10 months before colon cancer diagnosis (95% CI 8.3-11.7) and 8 months before rectal cancer diagnosis (95% CI 6.1-9.9). The rate of abnormal blood measurements (low hemoglobin levels, high platelet counts, etc) recorded increased from 9 months prediagnosis.
Study details: Findings are from a retrospective study that analyzed linked primary care and cancer registry data of patients with colon (n = 5033) or rectal (2516) cancer.
Disclosures: This study was supported by the National Institute for Health Research School for Primary Care Research and linked to the CanTest Collaborative funded by Cancer Research UK. Four authors are a part of the CanTest Collaborative.
Source: Moullet M et al. Pre-diagnostic clinical features and blood tests in patients with colorectal cancer: a retrospective linked-data study. Br J Gen Pract. 2022;72(721):e556-e563 (Jul 28). Doi: 10.3399/BJGP.2021.0563
Key clinical point: An increase in consultation rates for colorectal cancer (CRC)-relevant symptoms and abnormal blood test results in the 2-year prediagnosis period hint at early initiation of specific investigations or referrals, thereby accelerating the diagnosis and treatment in some patients with symptomatic CRC.
Major finding: The earliest clinical feature to show increased recording rate from the baseline was rectal bleeding, at 10 months before colon cancer diagnosis (95% CI 8.3-11.7) and 8 months before rectal cancer diagnosis (95% CI 6.1-9.9). The rate of abnormal blood measurements (low hemoglobin levels, high platelet counts, etc) recorded increased from 9 months prediagnosis.
Study details: Findings are from a retrospective study that analyzed linked primary care and cancer registry data of patients with colon (n = 5033) or rectal (2516) cancer.
Disclosures: This study was supported by the National Institute for Health Research School for Primary Care Research and linked to the CanTest Collaborative funded by Cancer Research UK. Four authors are a part of the CanTest Collaborative.
Source: Moullet M et al. Pre-diagnostic clinical features and blood tests in patients with colorectal cancer: a retrospective linked-data study. Br J Gen Pract. 2022;72(721):e556-e563 (Jul 28). Doi: 10.3399/BJGP.2021.0563