User login
Company withdraws application for idelalisib
Gilead Sciences International Ltd. recently withdrew its application for European approval of idelalisib (Zydelig) in combination with rituximab and bendamustine for the treatment of relapsed/refractory chronic lymphocytic leukemia (CLL).
Idelalisib is currently approved in the European Union for use in combination with an anti-CD20 monoclonal antibody (rituximab or ofatumumab) to treat adults with CLL who have received at least 1 prior therapy or as first-line treatment of CLL in the presence of 17p deletion or TP53 mutation in patients who are not eligible for any other therapies.
Idelalisib is also approved as monotherapy for adults with follicular lymphoma that is refractory to 2 prior lines of treatment.
In seeking expanded approval for idelalisib, Gilead submitted data from a study (NCT01569295) comparing idelalisib plus bendamustine and rituximab to placebo plus bendamustine and rituximab.
Interim results from this study were published in The Lancet Oncology in March 2017.
Gilead withdrew the application for idelalisib after the European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) had evaluated documentation provided by the company and formulated lists of questions.
Gilead had not responded to the last round of questions at the time of the withdrawal.
At that point, the CHMP was of the provisional opinion that idelalisib should not be approved for use in combination with rituximab and bendamustine in patients with relapsed/refractory CLL.
The CHMP said additional, longer-term data are needed to show the benefits of idelalisib plus rituximab and bendamustine outweigh the risks.
Gilead said its withdrawal of the application was based on the CHMP’s opinion that there was insufficient evidence of a favorable benefit-risk profile.
The company also said the withdrawal does not impact ongoing trials of idelalisib.
Gilead Sciences International Ltd. recently withdrew its application for European approval of idelalisib (Zydelig) in combination with rituximab and bendamustine for the treatment of relapsed/refractory chronic lymphocytic leukemia (CLL).
Idelalisib is currently approved in the European Union for use in combination with an anti-CD20 monoclonal antibody (rituximab or ofatumumab) to treat adults with CLL who have received at least 1 prior therapy or as first-line treatment of CLL in the presence of 17p deletion or TP53 mutation in patients who are not eligible for any other therapies.
Idelalisib is also approved as monotherapy for adults with follicular lymphoma that is refractory to 2 prior lines of treatment.
In seeking expanded approval for idelalisib, Gilead submitted data from a study (NCT01569295) comparing idelalisib plus bendamustine and rituximab to placebo plus bendamustine and rituximab.
Interim results from this study were published in The Lancet Oncology in March 2017.
Gilead withdrew the application for idelalisib after the European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) had evaluated documentation provided by the company and formulated lists of questions.
Gilead had not responded to the last round of questions at the time of the withdrawal.
At that point, the CHMP was of the provisional opinion that idelalisib should not be approved for use in combination with rituximab and bendamustine in patients with relapsed/refractory CLL.
The CHMP said additional, longer-term data are needed to show the benefits of idelalisib plus rituximab and bendamustine outweigh the risks.
Gilead said its withdrawal of the application was based on the CHMP’s opinion that there was insufficient evidence of a favorable benefit-risk profile.
The company also said the withdrawal does not impact ongoing trials of idelalisib.
Gilead Sciences International Ltd. recently withdrew its application for European approval of idelalisib (Zydelig) in combination with rituximab and bendamustine for the treatment of relapsed/refractory chronic lymphocytic leukemia (CLL).
Idelalisib is currently approved in the European Union for use in combination with an anti-CD20 monoclonal antibody (rituximab or ofatumumab) to treat adults with CLL who have received at least 1 prior therapy or as first-line treatment of CLL in the presence of 17p deletion or TP53 mutation in patients who are not eligible for any other therapies.
Idelalisib is also approved as monotherapy for adults with follicular lymphoma that is refractory to 2 prior lines of treatment.
In seeking expanded approval for idelalisib, Gilead submitted data from a study (NCT01569295) comparing idelalisib plus bendamustine and rituximab to placebo plus bendamustine and rituximab.
Interim results from this study were published in The Lancet Oncology in March 2017.
Gilead withdrew the application for idelalisib after the European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) had evaluated documentation provided by the company and formulated lists of questions.
Gilead had not responded to the last round of questions at the time of the withdrawal.
At that point, the CHMP was of the provisional opinion that idelalisib should not be approved for use in combination with rituximab and bendamustine in patients with relapsed/refractory CLL.
The CHMP said additional, longer-term data are needed to show the benefits of idelalisib plus rituximab and bendamustine outweigh the risks.
Gilead said its withdrawal of the application was based on the CHMP’s opinion that there was insufficient evidence of a favorable benefit-risk profile.
The company also said the withdrawal does not impact ongoing trials of idelalisib.
CHMP endorses drug delivery system
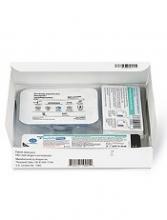
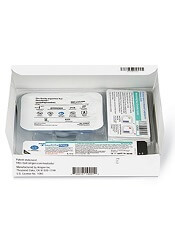
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) has recommended a label variation for Neulasta® (pegfilgrastim) to include the Neulasta® Onpro® Kit.
The Neulasta Onpro Kit is an on-body injector (OBI) delivery system for Neulasta, which is approved in the European Union to reduce the duration of neutropenia and the incidence of febrile neutropenia in adults treated with cytotoxic chemotherapy for malignancy (with the exception of chronic myeloid leukemia and myelodysplastic syndromes).
The Neulasta Onpro Kit includes a specifically designed Neulasta pre-filled syringe along with a single-use OBI. The small, lightweight OBI is applied to a patient’s skin on the same day of chemotherapy.
The OBI is intended to facilitate timed delivery of the correct dose of Neulasta and eliminate the need for patients to return to a healthcare setting the day after they receive chemotherapy.
The CHMP’s opinion on the Neulasta Onpro Kit will be reviewed by the European Commission (EC).
If the EC agrees with the CHMP, the centralized marketing authorization of Neulasta will be updated to include information on the Neulasta Onpro Kit in the drug’s label.
This change will be valid throughout the European Union. Norway, Iceland, and Liechtenstein will make corresponding decisions about Neulasta’s label on the basis of the EC’s decision.
The EC typically makes a decision within 67 days of the CHMP’s recommendation.
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) has recommended a label variation for Neulasta® (pegfilgrastim) to include the Neulasta® Onpro® Kit.
The Neulasta Onpro Kit is an on-body injector (OBI) delivery system for Neulasta, which is approved in the European Union to reduce the duration of neutropenia and the incidence of febrile neutropenia in adults treated with cytotoxic chemotherapy for malignancy (with the exception of chronic myeloid leukemia and myelodysplastic syndromes).
The Neulasta Onpro Kit includes a specifically designed Neulasta pre-filled syringe along with a single-use OBI. The small, lightweight OBI is applied to a patient’s skin on the same day of chemotherapy.
The OBI is intended to facilitate timed delivery of the correct dose of Neulasta and eliminate the need for patients to return to a healthcare setting the day after they receive chemotherapy.
The CHMP’s opinion on the Neulasta Onpro Kit will be reviewed by the European Commission (EC).
If the EC agrees with the CHMP, the centralized marketing authorization of Neulasta will be updated to include information on the Neulasta Onpro Kit in the drug’s label.
This change will be valid throughout the European Union. Norway, Iceland, and Liechtenstein will make corresponding decisions about Neulasta’s label on the basis of the EC’s decision.
The EC typically makes a decision within 67 days of the CHMP’s recommendation.
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) has recommended a label variation for Neulasta® (pegfilgrastim) to include the Neulasta® Onpro® Kit.
The Neulasta Onpro Kit is an on-body injector (OBI) delivery system for Neulasta, which is approved in the European Union to reduce the duration of neutropenia and the incidence of febrile neutropenia in adults treated with cytotoxic chemotherapy for malignancy (with the exception of chronic myeloid leukemia and myelodysplastic syndromes).
The Neulasta Onpro Kit includes a specifically designed Neulasta pre-filled syringe along with a single-use OBI. The small, lightweight OBI is applied to a patient’s skin on the same day of chemotherapy.
The OBI is intended to facilitate timed delivery of the correct dose of Neulasta and eliminate the need for patients to return to a healthcare setting the day after they receive chemotherapy.
The CHMP’s opinion on the Neulasta Onpro Kit will be reviewed by the European Commission (EC).
If the EC agrees with the CHMP, the centralized marketing authorization of Neulasta will be updated to include information on the Neulasta Onpro Kit in the drug’s label.
This change will be valid throughout the European Union. Norway, Iceland, and Liechtenstein will make corresponding decisions about Neulasta’s label on the basis of the EC’s decision.
The EC typically makes a decision within 67 days of the CHMP’s recommendation.
CHMP backs bosutinib for newly diagnosed CML
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) has recommended expanding the approved use of bosutinib (BOSULIF) to include treatment of patients with newly diagnosed, chronic phase, Philadelphia chromosome-positive (Ph+) chronic myelogenous leukemia (CML).
Bosutinib is currently approved in Europe to treat patients with Ph+ CML in chronic, accelerated, or blast phase who have received one or more tyrosine kinase inhibitors and for whom imatinib, nilotinib, and dasatinib are not considered appropriate treatment options.
The CHMP’s opinion on bosutinib will be reviewed by the European Commission (EC). If the EC agrees with the CHMP, the commission will grant a centralized marketing authorization that will be valid in the European Union. Norway, Iceland, and Liechtenstein will make corresponding decisions on the basis of the EC’s decision.
The EC typically makes a decision within 67 days of the CHMP’s recommendation.
The CHMP’s recommendation for bosutinib is based on results from the BFORE trial, which were recently published in the Journal of Clinical Oncology.
The publication included data on 536 patients newly diagnosed with chronic phase CML. They were randomized 1:1 to receive bosutinib (n=268) or imatinib (n=268).
The modified intent-to-treat population included Ph+ patients with e13a2/e14a2 transcripts who had at least 12 months of follow-up. In this group, there were 246 patients in the bosutinib arm and 241 in the imatinib arm.
In the modified intent-to-treat population, the rate of major molecular response at 12 months was 47.2% in the bosutinib arm and 36.9% in the imatinib arm (P=0.02). The rate of complete cytogenetic response was 77.2% and 66.4%, respectively (P<0.008).
In the entire study population, 22.0% of patients receiving bosutinib and 26.8% of those receiving imatinib discontinued treatment—12.7% and 8.7%, respectively, due to drug-related toxicity.
Adverse events that were more common in the bosutinib arm than the imatinib arm included grade 3 or higher diarrhea (7.8% vs 0.8%), increased alanine levels (19% vs 1.5%), increased aspartate levels (9.7% vs 1.9%), cardiovascular events (3% vs 0.4%), and peripheral vascular events (1.5% vs 1.1%).
Cerebrovascular events were more common with imatinib than bosutinib (0.4% and 0%, respectively).
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) has recommended expanding the approved use of bosutinib (BOSULIF) to include treatment of patients with newly diagnosed, chronic phase, Philadelphia chromosome-positive (Ph+) chronic myelogenous leukemia (CML).
Bosutinib is currently approved in Europe to treat patients with Ph+ CML in chronic, accelerated, or blast phase who have received one or more tyrosine kinase inhibitors and for whom imatinib, nilotinib, and dasatinib are not considered appropriate treatment options.
The CHMP’s opinion on bosutinib will be reviewed by the European Commission (EC). If the EC agrees with the CHMP, the commission will grant a centralized marketing authorization that will be valid in the European Union. Norway, Iceland, and Liechtenstein will make corresponding decisions on the basis of the EC’s decision.
The EC typically makes a decision within 67 days of the CHMP’s recommendation.
The CHMP’s recommendation for bosutinib is based on results from the BFORE trial, which were recently published in the Journal of Clinical Oncology.
The publication included data on 536 patients newly diagnosed with chronic phase CML. They were randomized 1:1 to receive bosutinib (n=268) or imatinib (n=268).
The modified intent-to-treat population included Ph+ patients with e13a2/e14a2 transcripts who had at least 12 months of follow-up. In this group, there were 246 patients in the bosutinib arm and 241 in the imatinib arm.
In the modified intent-to-treat population, the rate of major molecular response at 12 months was 47.2% in the bosutinib arm and 36.9% in the imatinib arm (P=0.02). The rate of complete cytogenetic response was 77.2% and 66.4%, respectively (P<0.008).
In the entire study population, 22.0% of patients receiving bosutinib and 26.8% of those receiving imatinib discontinued treatment—12.7% and 8.7%, respectively, due to drug-related toxicity.
Adverse events that were more common in the bosutinib arm than the imatinib arm included grade 3 or higher diarrhea (7.8% vs 0.8%), increased alanine levels (19% vs 1.5%), increased aspartate levels (9.7% vs 1.9%), cardiovascular events (3% vs 0.4%), and peripheral vascular events (1.5% vs 1.1%).
Cerebrovascular events were more common with imatinib than bosutinib (0.4% and 0%, respectively).
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) has recommended expanding the approved use of bosutinib (BOSULIF) to include treatment of patients with newly diagnosed, chronic phase, Philadelphia chromosome-positive (Ph+) chronic myelogenous leukemia (CML).
Bosutinib is currently approved in Europe to treat patients with Ph+ CML in chronic, accelerated, or blast phase who have received one or more tyrosine kinase inhibitors and for whom imatinib, nilotinib, and dasatinib are not considered appropriate treatment options.
The CHMP’s opinion on bosutinib will be reviewed by the European Commission (EC). If the EC agrees with the CHMP, the commission will grant a centralized marketing authorization that will be valid in the European Union. Norway, Iceland, and Liechtenstein will make corresponding decisions on the basis of the EC’s decision.
The EC typically makes a decision within 67 days of the CHMP’s recommendation.
The CHMP’s recommendation for bosutinib is based on results from the BFORE trial, which were recently published in the Journal of Clinical Oncology.
The publication included data on 536 patients newly diagnosed with chronic phase CML. They were randomized 1:1 to receive bosutinib (n=268) or imatinib (n=268).
The modified intent-to-treat population included Ph+ patients with e13a2/e14a2 transcripts who had at least 12 months of follow-up. In this group, there were 246 patients in the bosutinib arm and 241 in the imatinib arm.
In the modified intent-to-treat population, the rate of major molecular response at 12 months was 47.2% in the bosutinib arm and 36.9% in the imatinib arm (P=0.02). The rate of complete cytogenetic response was 77.2% and 66.4%, respectively (P<0.008).
In the entire study population, 22.0% of patients receiving bosutinib and 26.8% of those receiving imatinib discontinued treatment—12.7% and 8.7%, respectively, due to drug-related toxicity.
Adverse events that were more common in the bosutinib arm than the imatinib arm included grade 3 or higher diarrhea (7.8% vs 0.8%), increased alanine levels (19% vs 1.5%), increased aspartate levels (9.7% vs 1.9%), cardiovascular events (3% vs 0.4%), and peripheral vascular events (1.5% vs 1.1%).
Cerebrovascular events were more common with imatinib than bosutinib (0.4% and 0%, respectively).
Expanded UCB product can stand alone
SALT LAKE CITY—The expanded umbilical cord blood (UCB) product NiCord can be used as a stand-alone graft, according to research presented at the 2018 BMT Tandem Meetings.
Researchers found that a single NiCord unit provided “robust” engraftment in a phase 1/2 study of patients with high-risk hematologic malignancies.
NiCord recipients had quicker neutrophil and platelet engraftment than matched control subjects who received standard myeloablative UCB transplant (single or double).
Mitchell Horwitz, MD, of the Duke University Medical Center in Durham, North Carolina, presented these results at the meeting as abstract 49.* The research was sponsored by Gamida Cell, the company developing NiCord.
“[NiCord] is an ex vivo expanded cell product that’s derived from an entire unit of umbilical cord blood,” Dr Horwitz explained. “It’s manufactured starting with a CD133-positive selection, which is the progenitor cell population that’s cultured, and a T-cell containing CD133-negative fraction that is provided also at the time of transplant.”
“The culture system contains nicotinamide—that’s the active ingredient in the culture. And that’s supplemented with cytokines—thrombopoietin, IL-6, FLT-3 ligand, and stem cell factor. The culture is 21 days.”
Previous research showed that double UCB transplant including a NiCord unit could provide benefits over standard double UCB transplant. This led Dr Horwitz and his colleagues to wonder if NiCord could be used as a stand-alone graft.
So the team evaluated the safety and efficacy of NiCord alone in 36 adolescents/adults with high-risk hematologic malignancies.
Patients had acute myelogenous leukemia (n=17), acute lymphoblastic leukemia (n=9), myelodysplastic syndrome (n=7), chronic myelogenous leukemia (n=2), and Hodgkin lymphoma (n=1).
Most patients had intermediate (n=15) or high-risk (n=13) disease. They had a median age of 44 (range, 13-63) and a median weight of 75 kg (range, 41-125).
Treatment
For conditioning, 19 patients received thiotepa, busulfan, and fludarabine. Fifteen patients received total body irradiation and fludarabine with or without cyclophosphamide or thiotepa. And 2 patients received clofarabine, fludarabine, and busulfan.
Most patients had a 4/6 human leukocyte antigen (HLA) match (n=26), 8 had a 5/6 HLA match, and 2 had a 6/6 HLA match.
The median total nucleated cell dose was 2.4 x 107/kg prior to expansion of the UCB unit and 3.7 x 107/kg after expansion. The median CD34+ cell dose was 0.2 x 106/kg and 6.3 x 106/kg, respectively.
“CD34 cells were expanded 33-fold in the 3-week culture system,” Dr Horwitz noted. “That translated to a median CD34 dose of 6.3 x 106/kg, a dose comparable to what would be obtained from an adult donor graft.”
Engraftment
There was 1 case of primary graft failure and 2 cases of secondary graft failure. One case of secondary graft failure was associated with an HHV-6 infection, and the other was due to a lethal adenovirus infection.
Of those patients who engrafted, 97% achieved full donor chimerism, and 3% had mixed chimerism.
Dr Horwitz and his colleagues compared engraftment results in the NiCord recipients to results in a cohort of patients from the CIBMTR registry who underwent UCB transplants from 2010 to 2013. They had similar characteristics as the NiCord patients—age, conditioning regimen, disease status, etc.
In total, there were 148 CIBMTR registry patients, 20% of whom received a single UCB unit.
The median time to neutrophil engraftment was 11.5 days (range, 6-26) with NiCord and 21 days in the CIBMTR matched control cohort (P<0.001). The cumulative incidence of neutrophil engraftment was 94.4% and 89.7%, respectively.
The median time to platelet engraftment was 34 days (range, 25-96) with NiCord and 46 days in the CIBMTR controls (P<0.001). The cumulative incidence of platelet engraftment was 80.6% and 67.1%, respectively.
“There’s a median 10-day reduction in neutrophil recovery [and] 12-day reduction in time to platelet recovery [with NiCord],” Dr Horwitz noted. “There is evidence of robust and durable engraftment with a NiCord unit, with one patient now over 7 years from his first transplant on the pilot trial.”
Relapse, survival, and GVHD
Dr Horwitz reported other outcomes in the NiCord recipients without making comparisons to the CIBMTR matched controls.
The estimated 2-year rate of non-relapse mortality in NiCord recipients was 23.8%, and the estimated 2-year incidence of relapse was 33.2%.
The estimated disease-free survival was 49.1% at 1 year and 43.0% at 2 years. The estimated overall survival was 51.2% at 1 year and 2 years.
At 100 days, the rate of grade 2-4 acute GVHD was 44.0%, and the rate of grade 3-4 acute GVHD was 11.1%.
The estimated 1-year rate of mild to severe chronic GVHD was 40.5%, and the estimated 2-year rate of moderate to severe chronic GVHD was 9.8%.
Dr Horwitz said these “promising results” have led to the launch of a phase 3 registration trial in which researchers are comparing NiCord to standard single or double UCB transplant. The trial is open for accrual.
*Information in the abstract differs from the presentation.
SALT LAKE CITY—The expanded umbilical cord blood (UCB) product NiCord can be used as a stand-alone graft, according to research presented at the 2018 BMT Tandem Meetings.
Researchers found that a single NiCord unit provided “robust” engraftment in a phase 1/2 study of patients with high-risk hematologic malignancies.
NiCord recipients had quicker neutrophil and platelet engraftment than matched control subjects who received standard myeloablative UCB transplant (single or double).
Mitchell Horwitz, MD, of the Duke University Medical Center in Durham, North Carolina, presented these results at the meeting as abstract 49.* The research was sponsored by Gamida Cell, the company developing NiCord.
“[NiCord] is an ex vivo expanded cell product that’s derived from an entire unit of umbilical cord blood,” Dr Horwitz explained. “It’s manufactured starting with a CD133-positive selection, which is the progenitor cell population that’s cultured, and a T-cell containing CD133-negative fraction that is provided also at the time of transplant.”
“The culture system contains nicotinamide—that’s the active ingredient in the culture. And that’s supplemented with cytokines—thrombopoietin, IL-6, FLT-3 ligand, and stem cell factor. The culture is 21 days.”
Previous research showed that double UCB transplant including a NiCord unit could provide benefits over standard double UCB transplant. This led Dr Horwitz and his colleagues to wonder if NiCord could be used as a stand-alone graft.
So the team evaluated the safety and efficacy of NiCord alone in 36 adolescents/adults with high-risk hematologic malignancies.
Patients had acute myelogenous leukemia (n=17), acute lymphoblastic leukemia (n=9), myelodysplastic syndrome (n=7), chronic myelogenous leukemia (n=2), and Hodgkin lymphoma (n=1).
Most patients had intermediate (n=15) or high-risk (n=13) disease. They had a median age of 44 (range, 13-63) and a median weight of 75 kg (range, 41-125).
Treatment
For conditioning, 19 patients received thiotepa, busulfan, and fludarabine. Fifteen patients received total body irradiation and fludarabine with or without cyclophosphamide or thiotepa. And 2 patients received clofarabine, fludarabine, and busulfan.
Most patients had a 4/6 human leukocyte antigen (HLA) match (n=26), 8 had a 5/6 HLA match, and 2 had a 6/6 HLA match.
The median total nucleated cell dose was 2.4 x 107/kg prior to expansion of the UCB unit and 3.7 x 107/kg after expansion. The median CD34+ cell dose was 0.2 x 106/kg and 6.3 x 106/kg, respectively.
“CD34 cells were expanded 33-fold in the 3-week culture system,” Dr Horwitz noted. “That translated to a median CD34 dose of 6.3 x 106/kg, a dose comparable to what would be obtained from an adult donor graft.”
Engraftment
There was 1 case of primary graft failure and 2 cases of secondary graft failure. One case of secondary graft failure was associated with an HHV-6 infection, and the other was due to a lethal adenovirus infection.
Of those patients who engrafted, 97% achieved full donor chimerism, and 3% had mixed chimerism.
Dr Horwitz and his colleagues compared engraftment results in the NiCord recipients to results in a cohort of patients from the CIBMTR registry who underwent UCB transplants from 2010 to 2013. They had similar characteristics as the NiCord patients—age, conditioning regimen, disease status, etc.
In total, there were 148 CIBMTR registry patients, 20% of whom received a single UCB unit.
The median time to neutrophil engraftment was 11.5 days (range, 6-26) with NiCord and 21 days in the CIBMTR matched control cohort (P<0.001). The cumulative incidence of neutrophil engraftment was 94.4% and 89.7%, respectively.
The median time to platelet engraftment was 34 days (range, 25-96) with NiCord and 46 days in the CIBMTR controls (P<0.001). The cumulative incidence of platelet engraftment was 80.6% and 67.1%, respectively.
“There’s a median 10-day reduction in neutrophil recovery [and] 12-day reduction in time to platelet recovery [with NiCord],” Dr Horwitz noted. “There is evidence of robust and durable engraftment with a NiCord unit, with one patient now over 7 years from his first transplant on the pilot trial.”
Relapse, survival, and GVHD
Dr Horwitz reported other outcomes in the NiCord recipients without making comparisons to the CIBMTR matched controls.
The estimated 2-year rate of non-relapse mortality in NiCord recipients was 23.8%, and the estimated 2-year incidence of relapse was 33.2%.
The estimated disease-free survival was 49.1% at 1 year and 43.0% at 2 years. The estimated overall survival was 51.2% at 1 year and 2 years.
At 100 days, the rate of grade 2-4 acute GVHD was 44.0%, and the rate of grade 3-4 acute GVHD was 11.1%.
The estimated 1-year rate of mild to severe chronic GVHD was 40.5%, and the estimated 2-year rate of moderate to severe chronic GVHD was 9.8%.
Dr Horwitz said these “promising results” have led to the launch of a phase 3 registration trial in which researchers are comparing NiCord to standard single or double UCB transplant. The trial is open for accrual.
*Information in the abstract differs from the presentation.
SALT LAKE CITY—The expanded umbilical cord blood (UCB) product NiCord can be used as a stand-alone graft, according to research presented at the 2018 BMT Tandem Meetings.
Researchers found that a single NiCord unit provided “robust” engraftment in a phase 1/2 study of patients with high-risk hematologic malignancies.
NiCord recipients had quicker neutrophil and platelet engraftment than matched control subjects who received standard myeloablative UCB transplant (single or double).
Mitchell Horwitz, MD, of the Duke University Medical Center in Durham, North Carolina, presented these results at the meeting as abstract 49.* The research was sponsored by Gamida Cell, the company developing NiCord.
“[NiCord] is an ex vivo expanded cell product that’s derived from an entire unit of umbilical cord blood,” Dr Horwitz explained. “It’s manufactured starting with a CD133-positive selection, which is the progenitor cell population that’s cultured, and a T-cell containing CD133-negative fraction that is provided also at the time of transplant.”
“The culture system contains nicotinamide—that’s the active ingredient in the culture. And that’s supplemented with cytokines—thrombopoietin, IL-6, FLT-3 ligand, and stem cell factor. The culture is 21 days.”
Previous research showed that double UCB transplant including a NiCord unit could provide benefits over standard double UCB transplant. This led Dr Horwitz and his colleagues to wonder if NiCord could be used as a stand-alone graft.
So the team evaluated the safety and efficacy of NiCord alone in 36 adolescents/adults with high-risk hematologic malignancies.
Patients had acute myelogenous leukemia (n=17), acute lymphoblastic leukemia (n=9), myelodysplastic syndrome (n=7), chronic myelogenous leukemia (n=2), and Hodgkin lymphoma (n=1).
Most patients had intermediate (n=15) or high-risk (n=13) disease. They had a median age of 44 (range, 13-63) and a median weight of 75 kg (range, 41-125).
Treatment
For conditioning, 19 patients received thiotepa, busulfan, and fludarabine. Fifteen patients received total body irradiation and fludarabine with or without cyclophosphamide or thiotepa. And 2 patients received clofarabine, fludarabine, and busulfan.
Most patients had a 4/6 human leukocyte antigen (HLA) match (n=26), 8 had a 5/6 HLA match, and 2 had a 6/6 HLA match.
The median total nucleated cell dose was 2.4 x 107/kg prior to expansion of the UCB unit and 3.7 x 107/kg after expansion. The median CD34+ cell dose was 0.2 x 106/kg and 6.3 x 106/kg, respectively.
“CD34 cells were expanded 33-fold in the 3-week culture system,” Dr Horwitz noted. “That translated to a median CD34 dose of 6.3 x 106/kg, a dose comparable to what would be obtained from an adult donor graft.”
Engraftment
There was 1 case of primary graft failure and 2 cases of secondary graft failure. One case of secondary graft failure was associated with an HHV-6 infection, and the other was due to a lethal adenovirus infection.
Of those patients who engrafted, 97% achieved full donor chimerism, and 3% had mixed chimerism.
Dr Horwitz and his colleagues compared engraftment results in the NiCord recipients to results in a cohort of patients from the CIBMTR registry who underwent UCB transplants from 2010 to 2013. They had similar characteristics as the NiCord patients—age, conditioning regimen, disease status, etc.
In total, there were 148 CIBMTR registry patients, 20% of whom received a single UCB unit.
The median time to neutrophil engraftment was 11.5 days (range, 6-26) with NiCord and 21 days in the CIBMTR matched control cohort (P<0.001). The cumulative incidence of neutrophil engraftment was 94.4% and 89.7%, respectively.
The median time to platelet engraftment was 34 days (range, 25-96) with NiCord and 46 days in the CIBMTR controls (P<0.001). The cumulative incidence of platelet engraftment was 80.6% and 67.1%, respectively.
“There’s a median 10-day reduction in neutrophil recovery [and] 12-day reduction in time to platelet recovery [with NiCord],” Dr Horwitz noted. “There is evidence of robust and durable engraftment with a NiCord unit, with one patient now over 7 years from his first transplant on the pilot trial.”
Relapse, survival, and GVHD
Dr Horwitz reported other outcomes in the NiCord recipients without making comparisons to the CIBMTR matched controls.
The estimated 2-year rate of non-relapse mortality in NiCord recipients was 23.8%, and the estimated 2-year incidence of relapse was 33.2%.
The estimated disease-free survival was 49.1% at 1 year and 43.0% at 2 years. The estimated overall survival was 51.2% at 1 year and 2 years.
At 100 days, the rate of grade 2-4 acute GVHD was 44.0%, and the rate of grade 3-4 acute GVHD was 11.1%.
The estimated 1-year rate of mild to severe chronic GVHD was 40.5%, and the estimated 2-year rate of moderate to severe chronic GVHD was 9.8%.
Dr Horwitz said these “promising results” have led to the launch of a phase 3 registration trial in which researchers are comparing NiCord to standard single or double UCB transplant. The trial is open for accrual.
*Information in the abstract differs from the presentation.
Baseline stress signals need for psychological help in CLL
, according to a prospective study of 152 patients.
“These findings suggest that integration of psychological intervention for patients who have high cancer-specific stress at baseline might be appropriate for this population,” wrote investigators led by Neha G. Goyal, PhD, a research fellow at Wake Forest University, Winston-Salem, N.C.
The subjects all had relapsed/refractory chronic lymphocytic leukemia (CLL). They filled out mental and physical function questionnaires at baseline, then at months 1, 2, and 5 during a nonrandomized phase 2 trial of ibrutinib (Imbruvica). The findings were published in the Annals of Behavioral Medicine.
Cancer-specific stress – essentially traumatic stress associated with cancer diagnosis, recurrence, and treatment – was assessed by the Impact of Event Scale, a common cancer research tool in which patients rate the intensity of intrusive thoughts and avoidant thoughts and behaviors. A score of 8 – out of a range of 0-64 – was the cut point used to separate patients with low versus high stress; higher scores mean worse symptoms.
“At treatment initiation, cancer-specific stress was associated with higher levels of cognitive-affective depressive symptoms, negative mood, fatigue interference, and sleep problems, and lower mental health quality of life. While patients with higher cancer-specific stress at baseline improved more rapidly on these outcomes ... higher cancer-specific stress at baseline was still associated with poorer psychological outcomes, but not physical outcomes, at 5 months,” the investigators said (Ann Behav Med. 2018 Feb 9. doi: 10.1093/abm/kax004).
For instance, high-stress patients started the trial with mean scores of about 4.5 on the 42-point cognitive-affective subscale of the Beck Depression Inventory; scores improved to about 2.5 after 5 months of treatment. Low-stress patients, however, started and ended the study with scores of about 1.5.
Cancer-specific stress has been associated with poorer outcomes in previous cancer studies, but its impact on CLL hasn’t been clear until now. It might be a particularly bad problem in CLL, because the disease is incurable and patients go through multiple relapses and treatment cycles.
“There has been a call to screen cancer patients to determine those who may be at risk for poor outcomes, and assessment of cancer-specific stress may have clinical utility as an individual difference predictor of psychological responses,” the team noted.
The mean age in the study was 64.1 years; 71% of the subjects were men. The majority were educated beyond high school, and almost all reported significant, supportive relationships. Patients had a median of three prior therapies, but one patients had been through 16.
Dr. Goyal reported having no financial disclosures. One author disclosed ties to Pharmacyclics and Janssen, marketers of ibrutinib. The work was supported by the National Cancer Institute and Pharmacyclics, among others.
, according to a prospective study of 152 patients.
“These findings suggest that integration of psychological intervention for patients who have high cancer-specific stress at baseline might be appropriate for this population,” wrote investigators led by Neha G. Goyal, PhD, a research fellow at Wake Forest University, Winston-Salem, N.C.
The subjects all had relapsed/refractory chronic lymphocytic leukemia (CLL). They filled out mental and physical function questionnaires at baseline, then at months 1, 2, and 5 during a nonrandomized phase 2 trial of ibrutinib (Imbruvica). The findings were published in the Annals of Behavioral Medicine.
Cancer-specific stress – essentially traumatic stress associated with cancer diagnosis, recurrence, and treatment – was assessed by the Impact of Event Scale, a common cancer research tool in which patients rate the intensity of intrusive thoughts and avoidant thoughts and behaviors. A score of 8 – out of a range of 0-64 – was the cut point used to separate patients with low versus high stress; higher scores mean worse symptoms.
“At treatment initiation, cancer-specific stress was associated with higher levels of cognitive-affective depressive symptoms, negative mood, fatigue interference, and sleep problems, and lower mental health quality of life. While patients with higher cancer-specific stress at baseline improved more rapidly on these outcomes ... higher cancer-specific stress at baseline was still associated with poorer psychological outcomes, but not physical outcomes, at 5 months,” the investigators said (Ann Behav Med. 2018 Feb 9. doi: 10.1093/abm/kax004).
For instance, high-stress patients started the trial with mean scores of about 4.5 on the 42-point cognitive-affective subscale of the Beck Depression Inventory; scores improved to about 2.5 after 5 months of treatment. Low-stress patients, however, started and ended the study with scores of about 1.5.
Cancer-specific stress has been associated with poorer outcomes in previous cancer studies, but its impact on CLL hasn’t been clear until now. It might be a particularly bad problem in CLL, because the disease is incurable and patients go through multiple relapses and treatment cycles.
“There has been a call to screen cancer patients to determine those who may be at risk for poor outcomes, and assessment of cancer-specific stress may have clinical utility as an individual difference predictor of psychological responses,” the team noted.
The mean age in the study was 64.1 years; 71% of the subjects were men. The majority were educated beyond high school, and almost all reported significant, supportive relationships. Patients had a median of three prior therapies, but one patients had been through 16.
Dr. Goyal reported having no financial disclosures. One author disclosed ties to Pharmacyclics and Janssen, marketers of ibrutinib. The work was supported by the National Cancer Institute and Pharmacyclics, among others.
, according to a prospective study of 152 patients.
“These findings suggest that integration of psychological intervention for patients who have high cancer-specific stress at baseline might be appropriate for this population,” wrote investigators led by Neha G. Goyal, PhD, a research fellow at Wake Forest University, Winston-Salem, N.C.
The subjects all had relapsed/refractory chronic lymphocytic leukemia (CLL). They filled out mental and physical function questionnaires at baseline, then at months 1, 2, and 5 during a nonrandomized phase 2 trial of ibrutinib (Imbruvica). The findings were published in the Annals of Behavioral Medicine.
Cancer-specific stress – essentially traumatic stress associated with cancer diagnosis, recurrence, and treatment – was assessed by the Impact of Event Scale, a common cancer research tool in which patients rate the intensity of intrusive thoughts and avoidant thoughts and behaviors. A score of 8 – out of a range of 0-64 – was the cut point used to separate patients with low versus high stress; higher scores mean worse symptoms.
“At treatment initiation, cancer-specific stress was associated with higher levels of cognitive-affective depressive symptoms, negative mood, fatigue interference, and sleep problems, and lower mental health quality of life. While patients with higher cancer-specific stress at baseline improved more rapidly on these outcomes ... higher cancer-specific stress at baseline was still associated with poorer psychological outcomes, but not physical outcomes, at 5 months,” the investigators said (Ann Behav Med. 2018 Feb 9. doi: 10.1093/abm/kax004).
For instance, high-stress patients started the trial with mean scores of about 4.5 on the 42-point cognitive-affective subscale of the Beck Depression Inventory; scores improved to about 2.5 after 5 months of treatment. Low-stress patients, however, started and ended the study with scores of about 1.5.
Cancer-specific stress has been associated with poorer outcomes in previous cancer studies, but its impact on CLL hasn’t been clear until now. It might be a particularly bad problem in CLL, because the disease is incurable and patients go through multiple relapses and treatment cycles.
“There has been a call to screen cancer patients to determine those who may be at risk for poor outcomes, and assessment of cancer-specific stress may have clinical utility as an individual difference predictor of psychological responses,” the team noted.
The mean age in the study was 64.1 years; 71% of the subjects were men. The majority were educated beyond high school, and almost all reported significant, supportive relationships. Patients had a median of three prior therapies, but one patients had been through 16.
Dr. Goyal reported having no financial disclosures. One author disclosed ties to Pharmacyclics and Janssen, marketers of ibrutinib. The work was supported by the National Cancer Institute and Pharmacyclics, among others.
FROM ANNALS OF BEHAVIORAL MEDICINE
‘Remarkable’ survival seen with pretransplant JAK inhibitor
SALT LAKE CITY – The use of Janus kinase (JAK) inhibitor therapy prior to hematopoietic stem cell transplantation is safe and may improve posttransplant survival in patients with myelofibrosis, according to findings from an ongoing prospective phase 2 study.
The 1-year overall survival rate among the 28 initial patients in the single-center study of JAK inhibitor therapy followed by myeloablative or reduced-intensity hematopoietic cell transplantation (HCT) was 93%. The 2-year survival rate was 89%, compared with 54% in a closely matched historical cohort of intermediate-2–risk patients who did not receive pre-HCT JAK inhibitor therapy, Rachel B. Salit, MD, reported at the combined annual meetings of the Center for International Blood & Marrow Transplant Research and the American Society for Blood and Marrow Transplantation.
“So this is pretty exciting for us,” she added, explaining that allogeneic HCT, which is currently indicated only for patients with intermediate-2– or high-risk disease on the Dynamic International Prognostic Scoring System (DIPSS), remains the only curative treatment option for patients with myelofibrosis.
“Transplant outcomes have been associated with DIPSS and DIPSS+ risk scores,” she said, adding that a study demonstrating that association showed a 54% survival rate at 3 years in patients with intermediate-2–risk disease. “Then JAK-2 inhibitors came down the pipe, and they are also indicated for patients with DIPSS intermediate-2– and high-risk disease. They’ve been shown to decrease spleen size, increase quality of life scores, decrease cytokine levels, and improve constitutional symptoms.”
Posttransplant benefits of pre-HCT JAK inhibitor therapy could include improved graft function because of decreased spleen size and cytokines, potentially decreased severe graft-versus-host disease (GVHD), and decreased nonrelapse mortality.
“Our hypothesis was that the use of JAK inhibitors before transplant in patients with myelofibrosis – by decreasing inflammation, improving constitutional symptoms, and reducing splenomegaly – would result in a decreased DIPSS score” and improved posttransplant survival, Dr. Salit said.
Study participants were patients aged 18 years and older (median of 53 years) with primary or secondary myelofibrosis (14 each). About two-thirds of the study participants were men. Prior to JAK inhibitor therapy, 2 patients were low risk, 10 patients were intermediate-1 risk, and 16 patients were intermediate-2 risk according to the DIPSS.
They were given ruxolitinib (Jakafi) for at least 8 weeks prior to HCT (median of 7 months, but up to 3 years), and the treatment was tapered over 1-2 weeks through day 2 or 3 of conditioning chemotherapy, depending on the conditioning regimen. Conditioning regimens were determined by the physician based on donor type.
“After the ruxolitinib, we had 6 patients who were intermediate-1 and 21 who were intermediate-2, so in that way they failed to meet that hypothesis,” Dr. Salit said. This happened because the patients became anemic, so they gained points on their DIPSS scores for declining constitutional symptoms.
Of the 28 participants, 23 received myeloablative HCT, and 5 received reduced-intensity HCT.
“We had a mixture of related, unrelated, and cord blood recipients,” she noted.
At a median follow-up of just over 1 year, and at up to 3 years in some patients, no cases of cytokine release syndrome have occurred with the overlap of ruxolitinib and conditioning chemotherapy, and there have been no graft failures. All patients, including cord blood recipients, engrafted. The median time to engraftment was 19 days, but the range went as high as 35 days. “The 35 was one of our cord blood recipients,” she noted.
Median time to platelet engraftment was 20 days, and median CD3 and CD33 chimerism at day 80 were 88% and 100%, respectively.
Acute grades II-IV GVHD occurred in 70% of patients, but just 15% of these cases were grades III or IV, she said.
Chronic GVHD occurred in 35% of patients, including two severe cases. Two patients relapsed, including one at 6 months with marrow blast and one at 2 years with myeloid sarcoma. Two treatment-related deaths occurred, including one each at days 54 and 81.
The strategy of overlapping a JAK inhibitor with conditioning chemotherapy was safe, and “better in that we haven’t seen any cytokine release syndrome,” she concluded, adding that no graft failures occurred and grades III-IV acute and severe chronic GVHD were encouragingly infrequent.
Future studies should look at the optimal amount of time for JAK inhibitor therapy prior to transplant and whether it’s safe to continue JAK inhibitors through transplant, she said.
“Some of the work in Germany has shown that JAK inhibitors are safe to include up to day 28 through transplant, and that’s something that we’re looking to explore,” she noted.
Dr. Salit reported having no financial disclosures. This study was sponsored by the Fred Hutchinson Cancer Research Center.
SOURCE: Salit R et al. BMT Tandem Meetings, Abstract 17.
SALT LAKE CITY – The use of Janus kinase (JAK) inhibitor therapy prior to hematopoietic stem cell transplantation is safe and may improve posttransplant survival in patients with myelofibrosis, according to findings from an ongoing prospective phase 2 study.
The 1-year overall survival rate among the 28 initial patients in the single-center study of JAK inhibitor therapy followed by myeloablative or reduced-intensity hematopoietic cell transplantation (HCT) was 93%. The 2-year survival rate was 89%, compared with 54% in a closely matched historical cohort of intermediate-2–risk patients who did not receive pre-HCT JAK inhibitor therapy, Rachel B. Salit, MD, reported at the combined annual meetings of the Center for International Blood & Marrow Transplant Research and the American Society for Blood and Marrow Transplantation.
“So this is pretty exciting for us,” she added, explaining that allogeneic HCT, which is currently indicated only for patients with intermediate-2– or high-risk disease on the Dynamic International Prognostic Scoring System (DIPSS), remains the only curative treatment option for patients with myelofibrosis.
“Transplant outcomes have been associated with DIPSS and DIPSS+ risk scores,” she said, adding that a study demonstrating that association showed a 54% survival rate at 3 years in patients with intermediate-2–risk disease. “Then JAK-2 inhibitors came down the pipe, and they are also indicated for patients with DIPSS intermediate-2– and high-risk disease. They’ve been shown to decrease spleen size, increase quality of life scores, decrease cytokine levels, and improve constitutional symptoms.”
Posttransplant benefits of pre-HCT JAK inhibitor therapy could include improved graft function because of decreased spleen size and cytokines, potentially decreased severe graft-versus-host disease (GVHD), and decreased nonrelapse mortality.
“Our hypothesis was that the use of JAK inhibitors before transplant in patients with myelofibrosis – by decreasing inflammation, improving constitutional symptoms, and reducing splenomegaly – would result in a decreased DIPSS score” and improved posttransplant survival, Dr. Salit said.
Study participants were patients aged 18 years and older (median of 53 years) with primary or secondary myelofibrosis (14 each). About two-thirds of the study participants were men. Prior to JAK inhibitor therapy, 2 patients were low risk, 10 patients were intermediate-1 risk, and 16 patients were intermediate-2 risk according to the DIPSS.
They were given ruxolitinib (Jakafi) for at least 8 weeks prior to HCT (median of 7 months, but up to 3 years), and the treatment was tapered over 1-2 weeks through day 2 or 3 of conditioning chemotherapy, depending on the conditioning regimen. Conditioning regimens were determined by the physician based on donor type.
“After the ruxolitinib, we had 6 patients who were intermediate-1 and 21 who were intermediate-2, so in that way they failed to meet that hypothesis,” Dr. Salit said. This happened because the patients became anemic, so they gained points on their DIPSS scores for declining constitutional symptoms.
Of the 28 participants, 23 received myeloablative HCT, and 5 received reduced-intensity HCT.
“We had a mixture of related, unrelated, and cord blood recipients,” she noted.
At a median follow-up of just over 1 year, and at up to 3 years in some patients, no cases of cytokine release syndrome have occurred with the overlap of ruxolitinib and conditioning chemotherapy, and there have been no graft failures. All patients, including cord blood recipients, engrafted. The median time to engraftment was 19 days, but the range went as high as 35 days. “The 35 was one of our cord blood recipients,” she noted.
Median time to platelet engraftment was 20 days, and median CD3 and CD33 chimerism at day 80 were 88% and 100%, respectively.
Acute grades II-IV GVHD occurred in 70% of patients, but just 15% of these cases were grades III or IV, she said.
Chronic GVHD occurred in 35% of patients, including two severe cases. Two patients relapsed, including one at 6 months with marrow blast and one at 2 years with myeloid sarcoma. Two treatment-related deaths occurred, including one each at days 54 and 81.
The strategy of overlapping a JAK inhibitor with conditioning chemotherapy was safe, and “better in that we haven’t seen any cytokine release syndrome,” she concluded, adding that no graft failures occurred and grades III-IV acute and severe chronic GVHD were encouragingly infrequent.
Future studies should look at the optimal amount of time for JAK inhibitor therapy prior to transplant and whether it’s safe to continue JAK inhibitors through transplant, she said.
“Some of the work in Germany has shown that JAK inhibitors are safe to include up to day 28 through transplant, and that’s something that we’re looking to explore,” she noted.
Dr. Salit reported having no financial disclosures. This study was sponsored by the Fred Hutchinson Cancer Research Center.
SOURCE: Salit R et al. BMT Tandem Meetings, Abstract 17.
SALT LAKE CITY – The use of Janus kinase (JAK) inhibitor therapy prior to hematopoietic stem cell transplantation is safe and may improve posttransplant survival in patients with myelofibrosis, according to findings from an ongoing prospective phase 2 study.
The 1-year overall survival rate among the 28 initial patients in the single-center study of JAK inhibitor therapy followed by myeloablative or reduced-intensity hematopoietic cell transplantation (HCT) was 93%. The 2-year survival rate was 89%, compared with 54% in a closely matched historical cohort of intermediate-2–risk patients who did not receive pre-HCT JAK inhibitor therapy, Rachel B. Salit, MD, reported at the combined annual meetings of the Center for International Blood & Marrow Transplant Research and the American Society for Blood and Marrow Transplantation.
“So this is pretty exciting for us,” she added, explaining that allogeneic HCT, which is currently indicated only for patients with intermediate-2– or high-risk disease on the Dynamic International Prognostic Scoring System (DIPSS), remains the only curative treatment option for patients with myelofibrosis.
“Transplant outcomes have been associated with DIPSS and DIPSS+ risk scores,” she said, adding that a study demonstrating that association showed a 54% survival rate at 3 years in patients with intermediate-2–risk disease. “Then JAK-2 inhibitors came down the pipe, and they are also indicated for patients with DIPSS intermediate-2– and high-risk disease. They’ve been shown to decrease spleen size, increase quality of life scores, decrease cytokine levels, and improve constitutional symptoms.”
Posttransplant benefits of pre-HCT JAK inhibitor therapy could include improved graft function because of decreased spleen size and cytokines, potentially decreased severe graft-versus-host disease (GVHD), and decreased nonrelapse mortality.
“Our hypothesis was that the use of JAK inhibitors before transplant in patients with myelofibrosis – by decreasing inflammation, improving constitutional symptoms, and reducing splenomegaly – would result in a decreased DIPSS score” and improved posttransplant survival, Dr. Salit said.
Study participants were patients aged 18 years and older (median of 53 years) with primary or secondary myelofibrosis (14 each). About two-thirds of the study participants were men. Prior to JAK inhibitor therapy, 2 patients were low risk, 10 patients were intermediate-1 risk, and 16 patients were intermediate-2 risk according to the DIPSS.
They were given ruxolitinib (Jakafi) for at least 8 weeks prior to HCT (median of 7 months, but up to 3 years), and the treatment was tapered over 1-2 weeks through day 2 or 3 of conditioning chemotherapy, depending on the conditioning regimen. Conditioning regimens were determined by the physician based on donor type.
“After the ruxolitinib, we had 6 patients who were intermediate-1 and 21 who were intermediate-2, so in that way they failed to meet that hypothesis,” Dr. Salit said. This happened because the patients became anemic, so they gained points on their DIPSS scores for declining constitutional symptoms.
Of the 28 participants, 23 received myeloablative HCT, and 5 received reduced-intensity HCT.
“We had a mixture of related, unrelated, and cord blood recipients,” she noted.
At a median follow-up of just over 1 year, and at up to 3 years in some patients, no cases of cytokine release syndrome have occurred with the overlap of ruxolitinib and conditioning chemotherapy, and there have been no graft failures. All patients, including cord blood recipients, engrafted. The median time to engraftment was 19 days, but the range went as high as 35 days. “The 35 was one of our cord blood recipients,” she noted.
Median time to platelet engraftment was 20 days, and median CD3 and CD33 chimerism at day 80 were 88% and 100%, respectively.
Acute grades II-IV GVHD occurred in 70% of patients, but just 15% of these cases were grades III or IV, she said.
Chronic GVHD occurred in 35% of patients, including two severe cases. Two patients relapsed, including one at 6 months with marrow blast and one at 2 years with myeloid sarcoma. Two treatment-related deaths occurred, including one each at days 54 and 81.
The strategy of overlapping a JAK inhibitor with conditioning chemotherapy was safe, and “better in that we haven’t seen any cytokine release syndrome,” she concluded, adding that no graft failures occurred and grades III-IV acute and severe chronic GVHD were encouragingly infrequent.
Future studies should look at the optimal amount of time for JAK inhibitor therapy prior to transplant and whether it’s safe to continue JAK inhibitors through transplant, she said.
“Some of the work in Germany has shown that JAK inhibitors are safe to include up to day 28 through transplant, and that’s something that we’re looking to explore,” she noted.
Dr. Salit reported having no financial disclosures. This study was sponsored by the Fred Hutchinson Cancer Research Center.
SOURCE: Salit R et al. BMT Tandem Meetings, Abstract 17.
REPORTING FROM THE 2018 BMT TANDEM MEETINGS
Key clinical point:
Major finding: The 2-year overall survival rate was 89%.
Study details: Findings in 28 patients from an ongoing prospective phase 2 study.
Disclosures: Dr. Salit reported having no financial disclosures. The study was sponsored by the Fred Hutchinson Cancer Research Center in Seattle.
Source: Salit R et al. BMT Tandem Meetings, Abstract 17.
Tamibarotene shows strong results in high-risk APL patients
ATLANTA – Maintenance therapy with the synthetic retinoid tamibarotene is more effective than all-trans retinoic acid (ATRA), for decreasing the relapse rate in patients with acute promyelocytic leukemia (APL) – a subtype of acute myeloid leukemia, according to 7-year findings from the JALSG-APL204 randomized controlled trial.
The relapse-free survival findings were particularly pronounced among high-risk patients with leukocyte counts of at least 10,000 per microliter, Akihiro Takeshita, MD, PhD, reported at the annual meeting of the American Society of Hematology.
“These results could lead to a new strategy for the treatment of high-risk patients, which is one of the recent priority issues in the treatment of APL,” said Dr. Takeshita of Hamamatsu (Japan) University.
Of 344 eligible patients aged 15-70 years with newly diagnosed APL and documented cytogenetic and/or molecular evidence of chromosomal translocation t(15;17) or PML/RAR-alpha gene expression, 269 entered the maintenance phase of the study after completing three courses of consolidation therapy and were assigned to receive ATRA or tamibarotene. At a mean follow-up of 7 years, the relapse-free survival rate was 84% in the 135 patients in the ATRA arm, compared with 93% among the 134 patients in the tamibarotene arm.
The difference between the groups was statistically significant, but an even greater difference was seen when the analysis was restricted to 52 high-risk patients with an initial leukocyte count of at least 10,000 per microliter (62% vs. 89%).
Both treatments were generally well tolerated, Dr. Takeshita reported.
Study subjects received ATRA at a daily dose of 45 mg/m2 for remission induction. Once complete remission was achieved, they received chemotherapy based on their initial leukocyte and blast count in the peripheral blood. Those who achieved molecular remission after consolidation chemotherapy were included in the current maintenance phase of the study. During this phase, ATRA was given at a daily dose of 45 mg/m2 divided into 3 doses for 14 days, and tamibarotene was given at a daily dose of 6 mg/m2 divided into 2 doses for 14 days. Each cycle of treatment was repeated every 3 months for 2 years.
Adverse events included secondary hematopoietic disorders in 12 cases, malignancies in 9 cases, and late cardiac complications of grade 3 or higher in 5 cases, but no significant difference in the rates of these events was seen between the two treatment groups, Dr. Takeshita noted.
Tamibarotene was studied in this trial because, compared with ATRA, it has been shown to have about a 10-fold increase in potency for inducing in vitro differentiation of NB-4 cells, enhanced chemical stability, and low affinity for cellular RA-binding protein.
“The clinical efficacy of tamibarotene for the treatment of APL has also been reported,” Dr. Takeshita added.
In the initial phases of the trial, no difference was seen between ATRA and tamibarotene with respect to 4-year relapse-free survival, but there did appear to be improved efficacy with tamibarotene in high-risk patients, which warranted further investigation, he said.
The current findings demonstrate the efficacy of tamibarotene vs. ATRA for decreasing the relapse rate at the 7-year observation point, and confirm the benefit in high-risk patients that was seen in earlier analyses, he concluded.
Dr. Takeshita reported receiving research funding from Chugai Pharmaceutical, Astellas Pharma, Pfizer Japan, and Takeda Pharmaceutical.
SOURCE: Takeshita A et al., ASH 2017, abstract 642.
ATLANTA – Maintenance therapy with the synthetic retinoid tamibarotene is more effective than all-trans retinoic acid (ATRA), for decreasing the relapse rate in patients with acute promyelocytic leukemia (APL) – a subtype of acute myeloid leukemia, according to 7-year findings from the JALSG-APL204 randomized controlled trial.
The relapse-free survival findings were particularly pronounced among high-risk patients with leukocyte counts of at least 10,000 per microliter, Akihiro Takeshita, MD, PhD, reported at the annual meeting of the American Society of Hematology.
“These results could lead to a new strategy for the treatment of high-risk patients, which is one of the recent priority issues in the treatment of APL,” said Dr. Takeshita of Hamamatsu (Japan) University.
Of 344 eligible patients aged 15-70 years with newly diagnosed APL and documented cytogenetic and/or molecular evidence of chromosomal translocation t(15;17) or PML/RAR-alpha gene expression, 269 entered the maintenance phase of the study after completing three courses of consolidation therapy and were assigned to receive ATRA or tamibarotene. At a mean follow-up of 7 years, the relapse-free survival rate was 84% in the 135 patients in the ATRA arm, compared with 93% among the 134 patients in the tamibarotene arm.
The difference between the groups was statistically significant, but an even greater difference was seen when the analysis was restricted to 52 high-risk patients with an initial leukocyte count of at least 10,000 per microliter (62% vs. 89%).
Both treatments were generally well tolerated, Dr. Takeshita reported.
Study subjects received ATRA at a daily dose of 45 mg/m2 for remission induction. Once complete remission was achieved, they received chemotherapy based on their initial leukocyte and blast count in the peripheral blood. Those who achieved molecular remission after consolidation chemotherapy were included in the current maintenance phase of the study. During this phase, ATRA was given at a daily dose of 45 mg/m2 divided into 3 doses for 14 days, and tamibarotene was given at a daily dose of 6 mg/m2 divided into 2 doses for 14 days. Each cycle of treatment was repeated every 3 months for 2 years.
Adverse events included secondary hematopoietic disorders in 12 cases, malignancies in 9 cases, and late cardiac complications of grade 3 or higher in 5 cases, but no significant difference in the rates of these events was seen between the two treatment groups, Dr. Takeshita noted.
Tamibarotene was studied in this trial because, compared with ATRA, it has been shown to have about a 10-fold increase in potency for inducing in vitro differentiation of NB-4 cells, enhanced chemical stability, and low affinity for cellular RA-binding protein.
“The clinical efficacy of tamibarotene for the treatment of APL has also been reported,” Dr. Takeshita added.
In the initial phases of the trial, no difference was seen between ATRA and tamibarotene with respect to 4-year relapse-free survival, but there did appear to be improved efficacy with tamibarotene in high-risk patients, which warranted further investigation, he said.
The current findings demonstrate the efficacy of tamibarotene vs. ATRA for decreasing the relapse rate at the 7-year observation point, and confirm the benefit in high-risk patients that was seen in earlier analyses, he concluded.
Dr. Takeshita reported receiving research funding from Chugai Pharmaceutical, Astellas Pharma, Pfizer Japan, and Takeda Pharmaceutical.
SOURCE: Takeshita A et al., ASH 2017, abstract 642.
ATLANTA – Maintenance therapy with the synthetic retinoid tamibarotene is more effective than all-trans retinoic acid (ATRA), for decreasing the relapse rate in patients with acute promyelocytic leukemia (APL) – a subtype of acute myeloid leukemia, according to 7-year findings from the JALSG-APL204 randomized controlled trial.
The relapse-free survival findings were particularly pronounced among high-risk patients with leukocyte counts of at least 10,000 per microliter, Akihiro Takeshita, MD, PhD, reported at the annual meeting of the American Society of Hematology.
“These results could lead to a new strategy for the treatment of high-risk patients, which is one of the recent priority issues in the treatment of APL,” said Dr. Takeshita of Hamamatsu (Japan) University.
Of 344 eligible patients aged 15-70 years with newly diagnosed APL and documented cytogenetic and/or molecular evidence of chromosomal translocation t(15;17) or PML/RAR-alpha gene expression, 269 entered the maintenance phase of the study after completing three courses of consolidation therapy and were assigned to receive ATRA or tamibarotene. At a mean follow-up of 7 years, the relapse-free survival rate was 84% in the 135 patients in the ATRA arm, compared with 93% among the 134 patients in the tamibarotene arm.
The difference between the groups was statistically significant, but an even greater difference was seen when the analysis was restricted to 52 high-risk patients with an initial leukocyte count of at least 10,000 per microliter (62% vs. 89%).
Both treatments were generally well tolerated, Dr. Takeshita reported.
Study subjects received ATRA at a daily dose of 45 mg/m2 for remission induction. Once complete remission was achieved, they received chemotherapy based on their initial leukocyte and blast count in the peripheral blood. Those who achieved molecular remission after consolidation chemotherapy were included in the current maintenance phase of the study. During this phase, ATRA was given at a daily dose of 45 mg/m2 divided into 3 doses for 14 days, and tamibarotene was given at a daily dose of 6 mg/m2 divided into 2 doses for 14 days. Each cycle of treatment was repeated every 3 months for 2 years.
Adverse events included secondary hematopoietic disorders in 12 cases, malignancies in 9 cases, and late cardiac complications of grade 3 or higher in 5 cases, but no significant difference in the rates of these events was seen between the two treatment groups, Dr. Takeshita noted.
Tamibarotene was studied in this trial because, compared with ATRA, it has been shown to have about a 10-fold increase in potency for inducing in vitro differentiation of NB-4 cells, enhanced chemical stability, and low affinity for cellular RA-binding protein.
“The clinical efficacy of tamibarotene for the treatment of APL has also been reported,” Dr. Takeshita added.
In the initial phases of the trial, no difference was seen between ATRA and tamibarotene with respect to 4-year relapse-free survival, but there did appear to be improved efficacy with tamibarotene in high-risk patients, which warranted further investigation, he said.
The current findings demonstrate the efficacy of tamibarotene vs. ATRA for decreasing the relapse rate at the 7-year observation point, and confirm the benefit in high-risk patients that was seen in earlier analyses, he concluded.
Dr. Takeshita reported receiving research funding from Chugai Pharmaceutical, Astellas Pharma, Pfizer Japan, and Takeda Pharmaceutical.
SOURCE: Takeshita A et al., ASH 2017, abstract 642.
REPORTING FROM ASH 2017
Key clinical point:
Major finding: The 7-year relapse-free survival was 62% vs. 89% with ATRA vs. tamibarotene in high-risk patients.
Study details: Long-term maintenance results in 344 patients from a randomized controlled trial.
Disclosures: Dr. Takeshita reported receiving research funding from Chugai Pharmaceutical, Astellas Pharma, Pfizer Japan, and Takeda Pharmaceutical.
Source: Takeshita A et al. ASH 2017, abstract 642.
AYA cancer patients lost to follow-up
ORLANDO—Many adolescent and young adult (AYA) cancer survivors don’t continue with follow-up care, according to a new study.
Researchers analyzed nearly 2400 AYAs diagnosed with cancer between 2000 and 2015 and found that 37% of these patients had no follow-up visits since 2015.
The proportion of patients with follow-up visits in 2016 did not vary according to cancer type or insurance status, but it did vary according to patients’ time since last cancer treatment.
These findings were presented at the 2018 Cancer Survivorship Symposium (abstract 29).
“Many adolescents and young adults are unaware of what their long-term risks are after they have finished their cancer treatment,” said study investigator Lynda M. Beaupin, MD, of the Roswell Park Cancer Institute in Buffalo, New York.
“Doctors and other healthcare providers need to be more diligent in letting these patients know about future potential side effects and health risks that could occur based on certain aspects of their cancer treatment.”
In a previous study, Dr Beaupin and her colleagues conducted a focus group discussion with 27 AYAs, ages 18 to 39, to query them about the major barriers that prevented them from seeking follow-up care.
Among the factors mentioned were poor communication with their oncologists, ongoing problems in adjusting to life as a cancer survivor, and loss of health insurance.
As a follow-up to that focus group session, the investigators looked at a larger group of AYAs who were treated at Roswell Park Comprehensive Cancer Center.
The team analyzed data from the cancer center’s tumor registry, which included information on a patient’s current age, age at cancer diagnosis, gender, date of diagnosis, date of most recent doctor visit, and type of cancer.
The investigators also looked at patient-provided information on follow-up doctor appointments and insurance status for 2 cohorts of AYA cancer survivors. Patients in cohort A were diagnosed with cancer between 2010 and 2014, and patients in cohort B were diagnosed between 2005 and 2009.
The most common types of cancer were leukemia/lymphoma, melanoma, germ cell tumors, and thyroid and breast cancers.
Findings
There were 2367 patients, ages 18 to 39, who were diagnosed with cancer between 2000 and 2015.
Thirty-seven percent of these patients did not have a follow-up visit since 2015.
There was no difference in follow-up contact according to cancer type or insurance status. However, length of time since patients’ final cancer treatment was a factor in not scheduling a follow-up appointment.
Regardless of insurance status, 33% of cohort A (diagnosed 2010-2014) and 48% of cohort B (diagnosed 2005-2009) did not have a follow-up visit in 2016.
Among insured patients, 33% of those in cohort A and 47% of those in cohort B did not have a visit in 2016. Among uninsured patients, the percentages were 39% and 46%, respectively.
Next steps
The investigators hope to conduct future studies looking at other factors that may affect AYAs’ willingness to seek follow-up care, such as employment status, distance to a cancer center, whether they are getting tested or treated at a facility other than a cancer center, and how AYAs perceive their current quality of life.
“These patients have the potential to live a normal lifespan, and we need to educate them to become their own advocates so they may receive follow-up care on a regular basis,” Dr Beaupin said.
“We hope they continue to receive that follow-up at an established cancer center that has the facilities to assess cardiac health and provide rehabilitation if needed. There are now established survivorship programs nationwide that can provide follow-up care for those who have completed treatment.”
This study was supported by the National Cancer Institute.
ORLANDO—Many adolescent and young adult (AYA) cancer survivors don’t continue with follow-up care, according to a new study.
Researchers analyzed nearly 2400 AYAs diagnosed with cancer between 2000 and 2015 and found that 37% of these patients had no follow-up visits since 2015.
The proportion of patients with follow-up visits in 2016 did not vary according to cancer type or insurance status, but it did vary according to patients’ time since last cancer treatment.
These findings were presented at the 2018 Cancer Survivorship Symposium (abstract 29).
“Many adolescents and young adults are unaware of what their long-term risks are after they have finished their cancer treatment,” said study investigator Lynda M. Beaupin, MD, of the Roswell Park Cancer Institute in Buffalo, New York.
“Doctors and other healthcare providers need to be more diligent in letting these patients know about future potential side effects and health risks that could occur based on certain aspects of their cancer treatment.”
In a previous study, Dr Beaupin and her colleagues conducted a focus group discussion with 27 AYAs, ages 18 to 39, to query them about the major barriers that prevented them from seeking follow-up care.
Among the factors mentioned were poor communication with their oncologists, ongoing problems in adjusting to life as a cancer survivor, and loss of health insurance.
As a follow-up to that focus group session, the investigators looked at a larger group of AYAs who were treated at Roswell Park Comprehensive Cancer Center.
The team analyzed data from the cancer center’s tumor registry, which included information on a patient’s current age, age at cancer diagnosis, gender, date of diagnosis, date of most recent doctor visit, and type of cancer.
The investigators also looked at patient-provided information on follow-up doctor appointments and insurance status for 2 cohorts of AYA cancer survivors. Patients in cohort A were diagnosed with cancer between 2010 and 2014, and patients in cohort B were diagnosed between 2005 and 2009.
The most common types of cancer were leukemia/lymphoma, melanoma, germ cell tumors, and thyroid and breast cancers.
Findings
There were 2367 patients, ages 18 to 39, who were diagnosed with cancer between 2000 and 2015.
Thirty-seven percent of these patients did not have a follow-up visit since 2015.
There was no difference in follow-up contact according to cancer type or insurance status. However, length of time since patients’ final cancer treatment was a factor in not scheduling a follow-up appointment.
Regardless of insurance status, 33% of cohort A (diagnosed 2010-2014) and 48% of cohort B (diagnosed 2005-2009) did not have a follow-up visit in 2016.
Among insured patients, 33% of those in cohort A and 47% of those in cohort B did not have a visit in 2016. Among uninsured patients, the percentages were 39% and 46%, respectively.
Next steps
The investigators hope to conduct future studies looking at other factors that may affect AYAs’ willingness to seek follow-up care, such as employment status, distance to a cancer center, whether they are getting tested or treated at a facility other than a cancer center, and how AYAs perceive their current quality of life.
“These patients have the potential to live a normal lifespan, and we need to educate them to become their own advocates so they may receive follow-up care on a regular basis,” Dr Beaupin said.
“We hope they continue to receive that follow-up at an established cancer center that has the facilities to assess cardiac health and provide rehabilitation if needed. There are now established survivorship programs nationwide that can provide follow-up care for those who have completed treatment.”
This study was supported by the National Cancer Institute.
ORLANDO—Many adolescent and young adult (AYA) cancer survivors don’t continue with follow-up care, according to a new study.
Researchers analyzed nearly 2400 AYAs diagnosed with cancer between 2000 and 2015 and found that 37% of these patients had no follow-up visits since 2015.
The proportion of patients with follow-up visits in 2016 did not vary according to cancer type or insurance status, but it did vary according to patients’ time since last cancer treatment.
These findings were presented at the 2018 Cancer Survivorship Symposium (abstract 29).
“Many adolescents and young adults are unaware of what their long-term risks are after they have finished their cancer treatment,” said study investigator Lynda M. Beaupin, MD, of the Roswell Park Cancer Institute in Buffalo, New York.
“Doctors and other healthcare providers need to be more diligent in letting these patients know about future potential side effects and health risks that could occur based on certain aspects of their cancer treatment.”
In a previous study, Dr Beaupin and her colleagues conducted a focus group discussion with 27 AYAs, ages 18 to 39, to query them about the major barriers that prevented them from seeking follow-up care.
Among the factors mentioned were poor communication with their oncologists, ongoing problems in adjusting to life as a cancer survivor, and loss of health insurance.
As a follow-up to that focus group session, the investigators looked at a larger group of AYAs who were treated at Roswell Park Comprehensive Cancer Center.
The team analyzed data from the cancer center’s tumor registry, which included information on a patient’s current age, age at cancer diagnosis, gender, date of diagnosis, date of most recent doctor visit, and type of cancer.
The investigators also looked at patient-provided information on follow-up doctor appointments and insurance status for 2 cohorts of AYA cancer survivors. Patients in cohort A were diagnosed with cancer between 2010 and 2014, and patients in cohort B were diagnosed between 2005 and 2009.
The most common types of cancer were leukemia/lymphoma, melanoma, germ cell tumors, and thyroid and breast cancers.
Findings
There were 2367 patients, ages 18 to 39, who were diagnosed with cancer between 2000 and 2015.
Thirty-seven percent of these patients did not have a follow-up visit since 2015.
There was no difference in follow-up contact according to cancer type or insurance status. However, length of time since patients’ final cancer treatment was a factor in not scheduling a follow-up appointment.
Regardless of insurance status, 33% of cohort A (diagnosed 2010-2014) and 48% of cohort B (diagnosed 2005-2009) did not have a follow-up visit in 2016.
Among insured patients, 33% of those in cohort A and 47% of those in cohort B did not have a visit in 2016. Among uninsured patients, the percentages were 39% and 46%, respectively.
Next steps
The investigators hope to conduct future studies looking at other factors that may affect AYAs’ willingness to seek follow-up care, such as employment status, distance to a cancer center, whether they are getting tested or treated at a facility other than a cancer center, and how AYAs perceive their current quality of life.
“These patients have the potential to live a normal lifespan, and we need to educate them to become their own advocates so they may receive follow-up care on a regular basis,” Dr Beaupin said.
“We hope they continue to receive that follow-up at an established cancer center that has the facilities to assess cardiac health and provide rehabilitation if needed. There are now established survivorship programs nationwide that can provide follow-up care for those who have completed treatment.”
This study was supported by the National Cancer Institute.
Intervention helps kids stay active after cancer treatment
ORLANDO—Results of a pilot study suggest a web-based, reward-driven intervention can motivate adolescent cancer survivors to stay physically active.
Time spent performing moderate-to-vigorous physical activity (MVPA) increased by an average of 5 minutes a week for subjects who were randomized to the intervention.
For control subjects, MVPA decreased by an average of 24 minutes a week.
These findings were presented at the 2018 Cancer Survivorship Symposium (abstract 102).
“Compared to the general population, childhood cancer survivors have an increased risk for obesity and metabolic syndrome, conditions that can lead to heart disease, stroke, and diabetes, so it is really important that they are physically active,” said study investigator Carrie R. Howell, PhD, of St. Jude Children’s Research Hospital in Memphis, Tennessee.
“By intervening in this young age group, we hope to help kids develop healthy exercise habits for life.”
Dr Howell and her colleagues studied cancer survivors, ages 11 to 15, who were no longer receiving cancer treatment and were physically active less than 60 minutes a day.
The subjects were randomized to the intervention or to a control group. Controls received a wearable activity monitor and an educational handout with information about the importance of physical activity and examples of activities.
The intervention group received the handout and activity monitor but also had access to an interactive website. On at least a weekly basis, subjects would connect their monitor to a computer and log their activity through the website. Upon achieving certain thresholds of activity, they received rewards, such as T-shirts and gift cards by mail.
At the beginning and end of the study, participants visited St. Jude for an assessment of their physical fitness (strength, flexibility, and endurance) and neurocognitive measures (attention and memory), as well as health-related quality of life (assessed using the Pediatric Quality of Life Inventory questionnaire).
Results
Seventy-eight cancer survivors completed the 24-week study, 53 of them in the intervention group and 25 in the control group.
MVPA increased by an average of 4.7 minutes per week in the intervention group and decreased by an average of 24.3 minutes per week in the control group.
“In this age group, it is common to see a decrease in physical activity over time, even among healthy kids,” Dr Howell said. “Therefore, we are encouraged that our intervention was successful at maintaining physical activity levels, but a longer program may be needed to create lasting exercise habits.”
In addition to increases in MVPA, the intervention group had the following improvements in fitness:
- Increase in hand grip strength from an average of 19.9 kg to 21.0 kg
- Increase in number of push-ups from an average of 15 to 18
- Increase in number of sit-ups from an average of 11 to 14.
Furthermore, subjects in the intervention group saw their verbal fluency z-score increase by an average of 0.13 points and their general cognition z-score increase by an average of 0.23 points.
Their quality of life scores increased as well. Both overall quality of life and physical-function-related quality of life scores increased from an average of 74.2 to 78.0.
Control subjects had no significant changes in fitness, neurocognitive measures, or quality of life.
This study was supported by the National Cancer Institute, the American Lebanese Syrian Associated Charities, and HopeLab.
Based on the results of this study, the investigators have designed a larger trial (ALTE1631) to test a web-based physical activity intervention. They hope to enroll 384 survivors of childhood acute lymphoblastic leukemia at institutions across the US. The intervention will last a year, with follow-up at 18 months.
Further down the line, the investigators plan to explore the relationship between physical activity and cognition.
ORLANDO—Results of a pilot study suggest a web-based, reward-driven intervention can motivate adolescent cancer survivors to stay physically active.
Time spent performing moderate-to-vigorous physical activity (MVPA) increased by an average of 5 minutes a week for subjects who were randomized to the intervention.
For control subjects, MVPA decreased by an average of 24 minutes a week.
These findings were presented at the 2018 Cancer Survivorship Symposium (abstract 102).
“Compared to the general population, childhood cancer survivors have an increased risk for obesity and metabolic syndrome, conditions that can lead to heart disease, stroke, and diabetes, so it is really important that they are physically active,” said study investigator Carrie R. Howell, PhD, of St. Jude Children’s Research Hospital in Memphis, Tennessee.
“By intervening in this young age group, we hope to help kids develop healthy exercise habits for life.”
Dr Howell and her colleagues studied cancer survivors, ages 11 to 15, who were no longer receiving cancer treatment and were physically active less than 60 minutes a day.
The subjects were randomized to the intervention or to a control group. Controls received a wearable activity monitor and an educational handout with information about the importance of physical activity and examples of activities.
The intervention group received the handout and activity monitor but also had access to an interactive website. On at least a weekly basis, subjects would connect their monitor to a computer and log their activity through the website. Upon achieving certain thresholds of activity, they received rewards, such as T-shirts and gift cards by mail.
At the beginning and end of the study, participants visited St. Jude for an assessment of their physical fitness (strength, flexibility, and endurance) and neurocognitive measures (attention and memory), as well as health-related quality of life (assessed using the Pediatric Quality of Life Inventory questionnaire).
Results
Seventy-eight cancer survivors completed the 24-week study, 53 of them in the intervention group and 25 in the control group.
MVPA increased by an average of 4.7 minutes per week in the intervention group and decreased by an average of 24.3 minutes per week in the control group.
“In this age group, it is common to see a decrease in physical activity over time, even among healthy kids,” Dr Howell said. “Therefore, we are encouraged that our intervention was successful at maintaining physical activity levels, but a longer program may be needed to create lasting exercise habits.”
In addition to increases in MVPA, the intervention group had the following improvements in fitness:
- Increase in hand grip strength from an average of 19.9 kg to 21.0 kg
- Increase in number of push-ups from an average of 15 to 18
- Increase in number of sit-ups from an average of 11 to 14.
Furthermore, subjects in the intervention group saw their verbal fluency z-score increase by an average of 0.13 points and their general cognition z-score increase by an average of 0.23 points.
Their quality of life scores increased as well. Both overall quality of life and physical-function-related quality of life scores increased from an average of 74.2 to 78.0.
Control subjects had no significant changes in fitness, neurocognitive measures, or quality of life.
This study was supported by the National Cancer Institute, the American Lebanese Syrian Associated Charities, and HopeLab.
Based on the results of this study, the investigators have designed a larger trial (ALTE1631) to test a web-based physical activity intervention. They hope to enroll 384 survivors of childhood acute lymphoblastic leukemia at institutions across the US. The intervention will last a year, with follow-up at 18 months.
Further down the line, the investigators plan to explore the relationship between physical activity and cognition.
ORLANDO—Results of a pilot study suggest a web-based, reward-driven intervention can motivate adolescent cancer survivors to stay physically active.
Time spent performing moderate-to-vigorous physical activity (MVPA) increased by an average of 5 minutes a week for subjects who were randomized to the intervention.
For control subjects, MVPA decreased by an average of 24 minutes a week.
These findings were presented at the 2018 Cancer Survivorship Symposium (abstract 102).
“Compared to the general population, childhood cancer survivors have an increased risk for obesity and metabolic syndrome, conditions that can lead to heart disease, stroke, and diabetes, so it is really important that they are physically active,” said study investigator Carrie R. Howell, PhD, of St. Jude Children’s Research Hospital in Memphis, Tennessee.
“By intervening in this young age group, we hope to help kids develop healthy exercise habits for life.”
Dr Howell and her colleagues studied cancer survivors, ages 11 to 15, who were no longer receiving cancer treatment and were physically active less than 60 minutes a day.
The subjects were randomized to the intervention or to a control group. Controls received a wearable activity monitor and an educational handout with information about the importance of physical activity and examples of activities.
The intervention group received the handout and activity monitor but also had access to an interactive website. On at least a weekly basis, subjects would connect their monitor to a computer and log their activity through the website. Upon achieving certain thresholds of activity, they received rewards, such as T-shirts and gift cards by mail.
At the beginning and end of the study, participants visited St. Jude for an assessment of their physical fitness (strength, flexibility, and endurance) and neurocognitive measures (attention and memory), as well as health-related quality of life (assessed using the Pediatric Quality of Life Inventory questionnaire).
Results
Seventy-eight cancer survivors completed the 24-week study, 53 of them in the intervention group and 25 in the control group.
MVPA increased by an average of 4.7 minutes per week in the intervention group and decreased by an average of 24.3 minutes per week in the control group.
“In this age group, it is common to see a decrease in physical activity over time, even among healthy kids,” Dr Howell said. “Therefore, we are encouraged that our intervention was successful at maintaining physical activity levels, but a longer program may be needed to create lasting exercise habits.”
In addition to increases in MVPA, the intervention group had the following improvements in fitness:
- Increase in hand grip strength from an average of 19.9 kg to 21.0 kg
- Increase in number of push-ups from an average of 15 to 18
- Increase in number of sit-ups from an average of 11 to 14.
Furthermore, subjects in the intervention group saw their verbal fluency z-score increase by an average of 0.13 points and their general cognition z-score increase by an average of 0.23 points.
Their quality of life scores increased as well. Both overall quality of life and physical-function-related quality of life scores increased from an average of 74.2 to 78.0.
Control subjects had no significant changes in fitness, neurocognitive measures, or quality of life.
This study was supported by the National Cancer Institute, the American Lebanese Syrian Associated Charities, and HopeLab.
Based on the results of this study, the investigators have designed a larger trial (ALTE1631) to test a web-based physical activity intervention. They hope to enroll 384 survivors of childhood acute lymphoblastic leukemia at institutions across the US. The intervention will last a year, with follow-up at 18 months.
Further down the line, the investigators plan to explore the relationship between physical activity and cognition.
Study reveals lack of sexual aids for cancer survivors
ORLANDO—A new study suggests many US cancer centers do not have therapeutic aids for patients who experience sexual dysfunction after cancer treatment.
Of 25 cancer centers polled, 80% said they had no sexual aids available on site for men, and 64% said they had no such aids for women.
Sharon Bober, PhD, of the Dana-Farber Cancer Institute in Boston, Massachusetts, and her colleagues presented this research at the 2018 Cancer Survivorship Symposium (abstract 134*).
“[P]roviding sexual aids is one step toward treating sexual health like any other aspect of survivorship care,” Dr Bober said.
“It should be no different than providing wigs and head coverings to women who have lost their hair due to chemotherapy. It’s important to give patients the message that regaining sexual health is a perfectly valid and life-affirming aspect of regaining overall quality of life.”
Dr Bober and her colleagues conducted this study to determine the availability of sexual aids at 25 National Cancer Institute-designated cancer centers.
The researchers called these centers posing as a spouse, adult child, or sibling of a patient. The team made separate calls to ask about sexual aids for women and those for men.
Women’s sexual aids
Twenty-four percent of cancer centers (n=6) said they had sexual aids for women, 64% (n=16) did not, and 12% of centers were unreachable (n=3).
The most common aids were personal lubrication, vaginal moisturizer, and vaginal dilators—all of which were available at 5 centers.
Three centers had vibrators, 2 had books/pamphlets, 2 had pelvic floor exercisers, and 2 had product lists.
Men’s sexual aids
Twelve percent of cancer centers (n=3) said they had sexual aids for men, 80% (n=20) did not, and 8% (n=2) were unreachable.
Two centers said they had personal lubrication available for men, 2 had penile support rings, 1 had vacuum erection devices, and 1 had books/pamphlets.
Next steps
Now, Dr Bober and her colleagues hope to query the other 44 National Cancer Institute-designated cancer centers to see what products they are selling and perhaps conduct patient surveys to find out what types of resources are most useful for cancer survivors.
“What we really need to do is go to the centers that are successfully providing sexual health products and find out how they promote and provide resources to their patients,” Dr Bober said.
“We can’t keep the conversation at the 10,000-foot level. We need to talk concretely about how to partner with providers to make sexual health resources, including sexual health aids, available so cancer survivors can get the help that they need.”
*Information presented differs from the abstract.
ORLANDO—A new study suggests many US cancer centers do not have therapeutic aids for patients who experience sexual dysfunction after cancer treatment.
Of 25 cancer centers polled, 80% said they had no sexual aids available on site for men, and 64% said they had no such aids for women.
Sharon Bober, PhD, of the Dana-Farber Cancer Institute in Boston, Massachusetts, and her colleagues presented this research at the 2018 Cancer Survivorship Symposium (abstract 134*).
“[P]roviding sexual aids is one step toward treating sexual health like any other aspect of survivorship care,” Dr Bober said.
“It should be no different than providing wigs and head coverings to women who have lost their hair due to chemotherapy. It’s important to give patients the message that regaining sexual health is a perfectly valid and life-affirming aspect of regaining overall quality of life.”
Dr Bober and her colleagues conducted this study to determine the availability of sexual aids at 25 National Cancer Institute-designated cancer centers.
The researchers called these centers posing as a spouse, adult child, or sibling of a patient. The team made separate calls to ask about sexual aids for women and those for men.
Women’s sexual aids
Twenty-four percent of cancer centers (n=6) said they had sexual aids for women, 64% (n=16) did not, and 12% of centers were unreachable (n=3).
The most common aids were personal lubrication, vaginal moisturizer, and vaginal dilators—all of which were available at 5 centers.
Three centers had vibrators, 2 had books/pamphlets, 2 had pelvic floor exercisers, and 2 had product lists.
Men’s sexual aids
Twelve percent of cancer centers (n=3) said they had sexual aids for men, 80% (n=20) did not, and 8% (n=2) were unreachable.
Two centers said they had personal lubrication available for men, 2 had penile support rings, 1 had vacuum erection devices, and 1 had books/pamphlets.
Next steps
Now, Dr Bober and her colleagues hope to query the other 44 National Cancer Institute-designated cancer centers to see what products they are selling and perhaps conduct patient surveys to find out what types of resources are most useful for cancer survivors.
“What we really need to do is go to the centers that are successfully providing sexual health products and find out how they promote and provide resources to their patients,” Dr Bober said.
“We can’t keep the conversation at the 10,000-foot level. We need to talk concretely about how to partner with providers to make sexual health resources, including sexual health aids, available so cancer survivors can get the help that they need.”
*Information presented differs from the abstract.
ORLANDO—A new study suggests many US cancer centers do not have therapeutic aids for patients who experience sexual dysfunction after cancer treatment.
Of 25 cancer centers polled, 80% said they had no sexual aids available on site for men, and 64% said they had no such aids for women.
Sharon Bober, PhD, of the Dana-Farber Cancer Institute in Boston, Massachusetts, and her colleagues presented this research at the 2018 Cancer Survivorship Symposium (abstract 134*).
“[P]roviding sexual aids is one step toward treating sexual health like any other aspect of survivorship care,” Dr Bober said.
“It should be no different than providing wigs and head coverings to women who have lost their hair due to chemotherapy. It’s important to give patients the message that regaining sexual health is a perfectly valid and life-affirming aspect of regaining overall quality of life.”
Dr Bober and her colleagues conducted this study to determine the availability of sexual aids at 25 National Cancer Institute-designated cancer centers.
The researchers called these centers posing as a spouse, adult child, or sibling of a patient. The team made separate calls to ask about sexual aids for women and those for men.
Women’s sexual aids
Twenty-four percent of cancer centers (n=6) said they had sexual aids for women, 64% (n=16) did not, and 12% of centers were unreachable (n=3).
The most common aids were personal lubrication, vaginal moisturizer, and vaginal dilators—all of which were available at 5 centers.
Three centers had vibrators, 2 had books/pamphlets, 2 had pelvic floor exercisers, and 2 had product lists.
Men’s sexual aids
Twelve percent of cancer centers (n=3) said they had sexual aids for men, 80% (n=20) did not, and 8% (n=2) were unreachable.
Two centers said they had personal lubrication available for men, 2 had penile support rings, 1 had vacuum erection devices, and 1 had books/pamphlets.
Next steps
Now, Dr Bober and her colleagues hope to query the other 44 National Cancer Institute-designated cancer centers to see what products they are selling and perhaps conduct patient surveys to find out what types of resources are most useful for cancer survivors.
“What we really need to do is go to the centers that are successfully providing sexual health products and find out how they promote and provide resources to their patients,” Dr Bober said.
“We can’t keep the conversation at the 10,000-foot level. We need to talk concretely about how to partner with providers to make sexual health resources, including sexual health aids, available so cancer survivors can get the help that they need.”
*Information presented differs from the abstract.