User login
PI3Kδ/γ inhibitor generates rapid responses in CLL

VIENNA—New research indicates that duvelisib, a dual inhibitor of PI3Kδ and PI3Kγ, can generate rapid partial responses in treatment-naïve patients with chronic lymphocytic leukemia (CLL).
The 18 patients in the expansion cohort of a phase 1 study of duvelisib had a median time to response of 3.7 months, according to iwCLL response criteria.
And 47% of the responses occurred by the first assessment on day 1 of cycle 3.
“One thing that does seem to be different with this drug is that you’re getting your [partial responses] a bit faster than you see with some of the other drugs,” said Susan O’Brien, MD, of UC Irvine Health in Orange, California.
“[W]hat that means in the long run is not completely clear, but there’s no question that the responses are very rapid.”
Dr O’Brien presented these findings at the 20th Congress of the European Hematology Association (abstract S434*). The research was funded by Infinity Pharmaceuticals, Inc., the company developing duvelisib.
Older CLL patients with comorbidities and patients with high-risk genomic alterations, such as 17p deletion and TP53 mutations, often don’t fare well on the standard chemoimmunotherapy. Duvelisib is being developed as a potential alternative for these patients and others with hematologic malignancies.
In the dose-escalation portion of this phase 1 study, duvelisib at 25 mg twice daily was well-tolerated and exhibited clinical activity in relapsed/refractory CLL, even in those patients with TP53 mutations and 17p deletion.
So investigators conducted the expansion cohort with 18 patients who received duvelisib at the same dose in 28-day cycles. Duvelisib is given continuously until patients have an adverse event or lose their response.
Patient demographics
Dr O’Brien said there was nothing unusual about the demographics of the study population, except the risk factors: 83% of the patients were over 65, “which is very different from what you would see in a chemoimmunotherapy trial.”
She noted that the patients’ median age was 74, and 56% of patients had either a 17p deletion or TP53 mutation.
“And that’s very unusual because . . . the percentage of patients with that abnormality in frontline CLL is about 5% to 10%,” she added.
Patients were a median of 3 years (range, 0–9) from their initial diagnosis, 47% had Rai stage 3 or greater disease, 44% had splenomegaly, and 11% had grade 4 cytopenia.
Response
Patients stayed on treatment for a median of 14 months (range, 1–20). Eight (44%) discontinued treatment—6 (33%) due to an adverse event, 1 withdrew consent, and 1 discontinued for other reasons.
The best overall response rate was 88%, which consisted of 15 partial responses. Two patients (12%) had stable disease, and there were no complete responses or cases of progressive disease.
One patient with a TP53 mutation/17p deletion withdrew consent prior to the first efficacy assessment.
“There’s no upfront progression,” Dr O’Brien said, “and the response rate was identical for patients with high-risk disease or 17p deletion.”
The median progression-free survival was not yet reached, and the rate was 92% at 18 months. One patient progressed at cycle 13.
The median overall survival was also not reached, with a 94% survival rate at 18 months. One patient died of progressive disease approximately 5 months after the last dose.
Adverse events
The most frequent adverse events (AEs) occurring in more than 25% of patients were, in order of frequency, diarrhea, rash, cough, neutropenia, peripheral edema, fatigue, nausea, pyrexia, ALT/AST increase, anemia, and dizziness.
Grade 3 AEs included diarrhea (22%), ALT/AST increase (17%), rash (11%), neutropenia (6%), fatigue (6%), and anemia (6%). The only grade 4 AE was neutropenia (28%).
Serious AEs in more than 1 patient included diarrhea (n=3), colitis (n=2), dehydration (n=2), pneumonia (n=2), and pneumonitis (n=2).
The AEs leading to treatment discontinuation were increased ALT/AST, dehydration, and spinal stenosis (all in 1 patient), as well as arthritis, pneumonitis, colitis, diarrhea, and stomatitis.
“We tend to see the transaminitis and the pneumonitis earlier, and then the late toxicity tends to be the diarrhea and colitis,” Dr O’ Brien said. “The one toxicity where I would not be inclined to try and re-treat a patient is pneumonitis, but I do think colitis can be successfully re-treated.”
Pharmacodynamic studies show very rapid inhibition of phosphorylated AKT following treatment, which is sustained throughout the whole first cycle. And following 1 cycle of duvelisib, there is near-complete inhibition of CLL proliferation, as evidenced by the reduction in Ki67.
Given these data, the investigators recommended further development of duvelisib in treatment-naïve CLL. ![]()
*Information in the abstract differs from that presented at the meeting.

VIENNA—New research indicates that duvelisib, a dual inhibitor of PI3Kδ and PI3Kγ, can generate rapid partial responses in treatment-naïve patients with chronic lymphocytic leukemia (CLL).
The 18 patients in the expansion cohort of a phase 1 study of duvelisib had a median time to response of 3.7 months, according to iwCLL response criteria.
And 47% of the responses occurred by the first assessment on day 1 of cycle 3.
“One thing that does seem to be different with this drug is that you’re getting your [partial responses] a bit faster than you see with some of the other drugs,” said Susan O’Brien, MD, of UC Irvine Health in Orange, California.
“[W]hat that means in the long run is not completely clear, but there’s no question that the responses are very rapid.”
Dr O’Brien presented these findings at the 20th Congress of the European Hematology Association (abstract S434*). The research was funded by Infinity Pharmaceuticals, Inc., the company developing duvelisib.
Older CLL patients with comorbidities and patients with high-risk genomic alterations, such as 17p deletion and TP53 mutations, often don’t fare well on the standard chemoimmunotherapy. Duvelisib is being developed as a potential alternative for these patients and others with hematologic malignancies.
In the dose-escalation portion of this phase 1 study, duvelisib at 25 mg twice daily was well-tolerated and exhibited clinical activity in relapsed/refractory CLL, even in those patients with TP53 mutations and 17p deletion.
So investigators conducted the expansion cohort with 18 patients who received duvelisib at the same dose in 28-day cycles. Duvelisib is given continuously until patients have an adverse event or lose their response.
Patient demographics
Dr O’Brien said there was nothing unusual about the demographics of the study population, except the risk factors: 83% of the patients were over 65, “which is very different from what you would see in a chemoimmunotherapy trial.”
She noted that the patients’ median age was 74, and 56% of patients had either a 17p deletion or TP53 mutation.
“And that’s very unusual because . . . the percentage of patients with that abnormality in frontline CLL is about 5% to 10%,” she added.
Patients were a median of 3 years (range, 0–9) from their initial diagnosis, 47% had Rai stage 3 or greater disease, 44% had splenomegaly, and 11% had grade 4 cytopenia.
Response
Patients stayed on treatment for a median of 14 months (range, 1–20). Eight (44%) discontinued treatment—6 (33%) due to an adverse event, 1 withdrew consent, and 1 discontinued for other reasons.
The best overall response rate was 88%, which consisted of 15 partial responses. Two patients (12%) had stable disease, and there were no complete responses or cases of progressive disease.
One patient with a TP53 mutation/17p deletion withdrew consent prior to the first efficacy assessment.
“There’s no upfront progression,” Dr O’Brien said, “and the response rate was identical for patients with high-risk disease or 17p deletion.”
The median progression-free survival was not yet reached, and the rate was 92% at 18 months. One patient progressed at cycle 13.
The median overall survival was also not reached, with a 94% survival rate at 18 months. One patient died of progressive disease approximately 5 months after the last dose.
Adverse events
The most frequent adverse events (AEs) occurring in more than 25% of patients were, in order of frequency, diarrhea, rash, cough, neutropenia, peripheral edema, fatigue, nausea, pyrexia, ALT/AST increase, anemia, and dizziness.
Grade 3 AEs included diarrhea (22%), ALT/AST increase (17%), rash (11%), neutropenia (6%), fatigue (6%), and anemia (6%). The only grade 4 AE was neutropenia (28%).
Serious AEs in more than 1 patient included diarrhea (n=3), colitis (n=2), dehydration (n=2), pneumonia (n=2), and pneumonitis (n=2).
The AEs leading to treatment discontinuation were increased ALT/AST, dehydration, and spinal stenosis (all in 1 patient), as well as arthritis, pneumonitis, colitis, diarrhea, and stomatitis.
“We tend to see the transaminitis and the pneumonitis earlier, and then the late toxicity tends to be the diarrhea and colitis,” Dr O’ Brien said. “The one toxicity where I would not be inclined to try and re-treat a patient is pneumonitis, but I do think colitis can be successfully re-treated.”
Pharmacodynamic studies show very rapid inhibition of phosphorylated AKT following treatment, which is sustained throughout the whole first cycle. And following 1 cycle of duvelisib, there is near-complete inhibition of CLL proliferation, as evidenced by the reduction in Ki67.
Given these data, the investigators recommended further development of duvelisib in treatment-naïve CLL. ![]()
*Information in the abstract differs from that presented at the meeting.

VIENNA—New research indicates that duvelisib, a dual inhibitor of PI3Kδ and PI3Kγ, can generate rapid partial responses in treatment-naïve patients with chronic lymphocytic leukemia (CLL).
The 18 patients in the expansion cohort of a phase 1 study of duvelisib had a median time to response of 3.7 months, according to iwCLL response criteria.
And 47% of the responses occurred by the first assessment on day 1 of cycle 3.
“One thing that does seem to be different with this drug is that you’re getting your [partial responses] a bit faster than you see with some of the other drugs,” said Susan O’Brien, MD, of UC Irvine Health in Orange, California.
“[W]hat that means in the long run is not completely clear, but there’s no question that the responses are very rapid.”
Dr O’Brien presented these findings at the 20th Congress of the European Hematology Association (abstract S434*). The research was funded by Infinity Pharmaceuticals, Inc., the company developing duvelisib.
Older CLL patients with comorbidities and patients with high-risk genomic alterations, such as 17p deletion and TP53 mutations, often don’t fare well on the standard chemoimmunotherapy. Duvelisib is being developed as a potential alternative for these patients and others with hematologic malignancies.
In the dose-escalation portion of this phase 1 study, duvelisib at 25 mg twice daily was well-tolerated and exhibited clinical activity in relapsed/refractory CLL, even in those patients with TP53 mutations and 17p deletion.
So investigators conducted the expansion cohort with 18 patients who received duvelisib at the same dose in 28-day cycles. Duvelisib is given continuously until patients have an adverse event or lose their response.
Patient demographics
Dr O’Brien said there was nothing unusual about the demographics of the study population, except the risk factors: 83% of the patients were over 65, “which is very different from what you would see in a chemoimmunotherapy trial.”
She noted that the patients’ median age was 74, and 56% of patients had either a 17p deletion or TP53 mutation.
“And that’s very unusual because . . . the percentage of patients with that abnormality in frontline CLL is about 5% to 10%,” she added.
Patients were a median of 3 years (range, 0–9) from their initial diagnosis, 47% had Rai stage 3 or greater disease, 44% had splenomegaly, and 11% had grade 4 cytopenia.
Response
Patients stayed on treatment for a median of 14 months (range, 1–20). Eight (44%) discontinued treatment—6 (33%) due to an adverse event, 1 withdrew consent, and 1 discontinued for other reasons.
The best overall response rate was 88%, which consisted of 15 partial responses. Two patients (12%) had stable disease, and there were no complete responses or cases of progressive disease.
One patient with a TP53 mutation/17p deletion withdrew consent prior to the first efficacy assessment.
“There’s no upfront progression,” Dr O’Brien said, “and the response rate was identical for patients with high-risk disease or 17p deletion.”
The median progression-free survival was not yet reached, and the rate was 92% at 18 months. One patient progressed at cycle 13.
The median overall survival was also not reached, with a 94% survival rate at 18 months. One patient died of progressive disease approximately 5 months after the last dose.
Adverse events
The most frequent adverse events (AEs) occurring in more than 25% of patients were, in order of frequency, diarrhea, rash, cough, neutropenia, peripheral edema, fatigue, nausea, pyrexia, ALT/AST increase, anemia, and dizziness.
Grade 3 AEs included diarrhea (22%), ALT/AST increase (17%), rash (11%), neutropenia (6%), fatigue (6%), and anemia (6%). The only grade 4 AE was neutropenia (28%).
Serious AEs in more than 1 patient included diarrhea (n=3), colitis (n=2), dehydration (n=2), pneumonia (n=2), and pneumonitis (n=2).
The AEs leading to treatment discontinuation were increased ALT/AST, dehydration, and spinal stenosis (all in 1 patient), as well as arthritis, pneumonitis, colitis, diarrhea, and stomatitis.
“We tend to see the transaminitis and the pneumonitis earlier, and then the late toxicity tends to be the diarrhea and colitis,” Dr O’ Brien said. “The one toxicity where I would not be inclined to try and re-treat a patient is pneumonitis, but I do think colitis can be successfully re-treated.”
Pharmacodynamic studies show very rapid inhibition of phosphorylated AKT following treatment, which is sustained throughout the whole first cycle. And following 1 cycle of duvelisib, there is near-complete inhibition of CLL proliferation, as evidenced by the reduction in Ki67.
Given these data, the investigators recommended further development of duvelisib in treatment-naïve CLL. ![]()
*Information in the abstract differs from that presented at the meeting.
Drug can produce durable responses in rel/ref PTCL
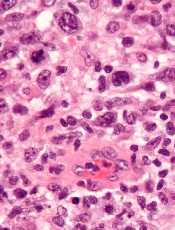
anaplastic large cell lymphoma
The histone deacetylase inhibitor belinostat can produce durable responses in patients with relapsed/refractory peripheral T-cell lymphoma (PTCL), results of the BELIEF study suggest.
The overall response rate (ORR) was low in this heavily pretreated population, at about 26%.
But responses occurred across PTCL subtypes and irrespective of a patient’s prior treatment, and the median duration of response was 13.6 months.
The researchers said toxicity was manageable, and the rate of grade 3/4 thrombocytopenia was low.
“This is a very exciting time in the treatment of patients with PTCL,” said Owen O’Connor, MD, PhD, of Columbia University Medical Center in New York, New York.
“At long last, we finally have tools in the therapeutic armamentarium to help our patients. Belinostat represents the latest drug approved for patients with [relapsed/refractory] PTCL that has relatively few side effects and produces long durations of benefit, even in patients who have received multiple conventional treatments in the past.”
Dr O’Connor and his colleagues reported results with belinostat in the Journal of Clinical Oncology. The research was sponsored by Spectrum Pharmaceuticals, Inc., the company developing belinostat (as Beleodaq).
BELIEF was a single-arm, phase 2 trial that enrolled 129 patients with relapsed/refractory PTCL. One hundred and twenty patients were evaluable. They had a median age of 64 (range, 29-81), and roughly half of patients were female.
PTCL subtypes included PTCL-not otherwise specified (n=77), angioimmunoblastic T-cell lymphoma (n=22), ALK-negative anaplastic large cell lymphoma (n=13), ALK-positive anaplastic large cell lymphoma (n=2), enteropathy-associated T-cell lymphoma (n=2), nasal type extranodal natural killer T-cell lymphoma (n=2), and hepatosplenic T-cell lymphoma (n=2).
The patients had received a median of 2 prior therapies (range, 1-8), including multi-agent and single-agent regimens, as well as transplant.
For this study, the patients received belinostat (1000 mg/m2) as daily, 30-minute infusions on days 1-5 every 21 days until disease progression or unacceptable toxicity.
Response and survival
The study’s primary endpoint was ORR, as assessed by an independent review committee using the International Working Group criteria. The ORR was 25.8% (n=31), including 13 complete responses (10.8%) and 18 partial responses (15%).
The median time to response was 5.6 weeks, and the median duration of response was 13.6 months by International Working Group criteria. The median duration of response based on the date of first response to progressive disease or death was 8.4 months.
Among patients who achieved a complete response, the median duration of response was not reached and exceeded 29 months. The longest ongoing patient response is more than 36 months.
The median progression-free survival was 1.6 months, and the median overall survival was 7.9 months.
Forty-six patients were censored for overall survival because they were alive at the data cutoff point. Seven of these patients continued to receive belinostat. Five were in complete response, 1 had a partial response, and 1 had stable disease.
Twelve patients underwent stem cell transplant after belinostat, and 10 of these patients were still alive at the data cutoff. Their overall survival ranged from 9.4 months to 22.9 months.
Adverse events
Treatment-emergent adverse events (AEs) occurred in 96.9% of patients, and treatment-related AEs occurred in 83.7%. The most common treatment-related AEs were nausea (38.0%), fatigue (28.7%), and vomiting (24.0%). Serious AEs occurred in 47.3% of patients.
Grade 3/4 related AEs were reported in 61.2% of patients, and the most common were anemia (10.9%), thrombocytopenia (7.0%), dyspnea (6.2%), neutropenia (6.2%), fatigue (5.4%), and pneumonia (5.4%).
About 12% of patients underwent a dose reduction due to AEs, 19.4% discontinued treatment due to AEs, and 10.9% of these AEs were considered treatment-related.
Twenty-two patients (17.1%) died, 12 (9.3%) of progressive disease and 10 (7.8%) of AEs. One death was considered related to belinostat. This patient had tolerated 9 cycles of the drug without complications but had elevated liver function tests at the start of cycle 10 that subsequently led to death from toxic liver failure. ![]()

anaplastic large cell lymphoma
The histone deacetylase inhibitor belinostat can produce durable responses in patients with relapsed/refractory peripheral T-cell lymphoma (PTCL), results of the BELIEF study suggest.
The overall response rate (ORR) was low in this heavily pretreated population, at about 26%.
But responses occurred across PTCL subtypes and irrespective of a patient’s prior treatment, and the median duration of response was 13.6 months.
The researchers said toxicity was manageable, and the rate of grade 3/4 thrombocytopenia was low.
“This is a very exciting time in the treatment of patients with PTCL,” said Owen O’Connor, MD, PhD, of Columbia University Medical Center in New York, New York.
“At long last, we finally have tools in the therapeutic armamentarium to help our patients. Belinostat represents the latest drug approved for patients with [relapsed/refractory] PTCL that has relatively few side effects and produces long durations of benefit, even in patients who have received multiple conventional treatments in the past.”
Dr O’Connor and his colleagues reported results with belinostat in the Journal of Clinical Oncology. The research was sponsored by Spectrum Pharmaceuticals, Inc., the company developing belinostat (as Beleodaq).
BELIEF was a single-arm, phase 2 trial that enrolled 129 patients with relapsed/refractory PTCL. One hundred and twenty patients were evaluable. They had a median age of 64 (range, 29-81), and roughly half of patients were female.
PTCL subtypes included PTCL-not otherwise specified (n=77), angioimmunoblastic T-cell lymphoma (n=22), ALK-negative anaplastic large cell lymphoma (n=13), ALK-positive anaplastic large cell lymphoma (n=2), enteropathy-associated T-cell lymphoma (n=2), nasal type extranodal natural killer T-cell lymphoma (n=2), and hepatosplenic T-cell lymphoma (n=2).
The patients had received a median of 2 prior therapies (range, 1-8), including multi-agent and single-agent regimens, as well as transplant.
For this study, the patients received belinostat (1000 mg/m2) as daily, 30-minute infusions on days 1-5 every 21 days until disease progression or unacceptable toxicity.
Response and survival
The study’s primary endpoint was ORR, as assessed by an independent review committee using the International Working Group criteria. The ORR was 25.8% (n=31), including 13 complete responses (10.8%) and 18 partial responses (15%).
The median time to response was 5.6 weeks, and the median duration of response was 13.6 months by International Working Group criteria. The median duration of response based on the date of first response to progressive disease or death was 8.4 months.
Among patients who achieved a complete response, the median duration of response was not reached and exceeded 29 months. The longest ongoing patient response is more than 36 months.
The median progression-free survival was 1.6 months, and the median overall survival was 7.9 months.
Forty-six patients were censored for overall survival because they were alive at the data cutoff point. Seven of these patients continued to receive belinostat. Five were in complete response, 1 had a partial response, and 1 had stable disease.
Twelve patients underwent stem cell transplant after belinostat, and 10 of these patients were still alive at the data cutoff. Their overall survival ranged from 9.4 months to 22.9 months.
Adverse events
Treatment-emergent adverse events (AEs) occurred in 96.9% of patients, and treatment-related AEs occurred in 83.7%. The most common treatment-related AEs were nausea (38.0%), fatigue (28.7%), and vomiting (24.0%). Serious AEs occurred in 47.3% of patients.
Grade 3/4 related AEs were reported in 61.2% of patients, and the most common were anemia (10.9%), thrombocytopenia (7.0%), dyspnea (6.2%), neutropenia (6.2%), fatigue (5.4%), and pneumonia (5.4%).
About 12% of patients underwent a dose reduction due to AEs, 19.4% discontinued treatment due to AEs, and 10.9% of these AEs were considered treatment-related.
Twenty-two patients (17.1%) died, 12 (9.3%) of progressive disease and 10 (7.8%) of AEs. One death was considered related to belinostat. This patient had tolerated 9 cycles of the drug without complications but had elevated liver function tests at the start of cycle 10 that subsequently led to death from toxic liver failure. ![]()

anaplastic large cell lymphoma
The histone deacetylase inhibitor belinostat can produce durable responses in patients with relapsed/refractory peripheral T-cell lymphoma (PTCL), results of the BELIEF study suggest.
The overall response rate (ORR) was low in this heavily pretreated population, at about 26%.
But responses occurred across PTCL subtypes and irrespective of a patient’s prior treatment, and the median duration of response was 13.6 months.
The researchers said toxicity was manageable, and the rate of grade 3/4 thrombocytopenia was low.
“This is a very exciting time in the treatment of patients with PTCL,” said Owen O’Connor, MD, PhD, of Columbia University Medical Center in New York, New York.
“At long last, we finally have tools in the therapeutic armamentarium to help our patients. Belinostat represents the latest drug approved for patients with [relapsed/refractory] PTCL that has relatively few side effects and produces long durations of benefit, even in patients who have received multiple conventional treatments in the past.”
Dr O’Connor and his colleagues reported results with belinostat in the Journal of Clinical Oncology. The research was sponsored by Spectrum Pharmaceuticals, Inc., the company developing belinostat (as Beleodaq).
BELIEF was a single-arm, phase 2 trial that enrolled 129 patients with relapsed/refractory PTCL. One hundred and twenty patients were evaluable. They had a median age of 64 (range, 29-81), and roughly half of patients were female.
PTCL subtypes included PTCL-not otherwise specified (n=77), angioimmunoblastic T-cell lymphoma (n=22), ALK-negative anaplastic large cell lymphoma (n=13), ALK-positive anaplastic large cell lymphoma (n=2), enteropathy-associated T-cell lymphoma (n=2), nasal type extranodal natural killer T-cell lymphoma (n=2), and hepatosplenic T-cell lymphoma (n=2).
The patients had received a median of 2 prior therapies (range, 1-8), including multi-agent and single-agent regimens, as well as transplant.
For this study, the patients received belinostat (1000 mg/m2) as daily, 30-minute infusions on days 1-5 every 21 days until disease progression or unacceptable toxicity.
Response and survival
The study’s primary endpoint was ORR, as assessed by an independent review committee using the International Working Group criteria. The ORR was 25.8% (n=31), including 13 complete responses (10.8%) and 18 partial responses (15%).
The median time to response was 5.6 weeks, and the median duration of response was 13.6 months by International Working Group criteria. The median duration of response based on the date of first response to progressive disease or death was 8.4 months.
Among patients who achieved a complete response, the median duration of response was not reached and exceeded 29 months. The longest ongoing patient response is more than 36 months.
The median progression-free survival was 1.6 months, and the median overall survival was 7.9 months.
Forty-six patients were censored for overall survival because they were alive at the data cutoff point. Seven of these patients continued to receive belinostat. Five were in complete response, 1 had a partial response, and 1 had stable disease.
Twelve patients underwent stem cell transplant after belinostat, and 10 of these patients were still alive at the data cutoff. Their overall survival ranged from 9.4 months to 22.9 months.
Adverse events
Treatment-emergent adverse events (AEs) occurred in 96.9% of patients, and treatment-related AEs occurred in 83.7%. The most common treatment-related AEs were nausea (38.0%), fatigue (28.7%), and vomiting (24.0%). Serious AEs occurred in 47.3% of patients.
Grade 3/4 related AEs were reported in 61.2% of patients, and the most common were anemia (10.9%), thrombocytopenia (7.0%), dyspnea (6.2%), neutropenia (6.2%), fatigue (5.4%), and pneumonia (5.4%).
About 12% of patients underwent a dose reduction due to AEs, 19.4% discontinued treatment due to AEs, and 10.9% of these AEs were considered treatment-related.
Twenty-two patients (17.1%) died, 12 (9.3%) of progressive disease and 10 (7.8%) of AEs. One death was considered related to belinostat. This patient had tolerated 9 cycles of the drug without complications but had elevated liver function tests at the start of cycle 10 that subsequently led to death from toxic liver failure. ![]()
Team endorses intensified chemo for PET-positive HL

Photo by Rhoda Baer
LUGANO—Long-awaited results of the Intergroup H10 trial in PET-positive Hodgkin lymphoma (HL) patients have shown that intensifying chemotherapy significantly increases 5-year progression-free survival (PFS) and produces a non-significant increase in overall survival (OS).
Switching patients who are PET-positive after 2 cycles of ABVD to escalated BEACOPP and involved-node radiotherapy increased 5-year PFS to 91% and 5-year OS to 96%.
The trial was a cooperative effort of the European Organisation for Research and Treatment of Cancer (EORTC), Lymphoma Study Association (LYSA), and Fondazione Italiana Linfomi (FIL).
The investigators already knew that early FDG-PET scans have prognostic impact. Patients with a negative PET scan after 2 cycles of chemotherapy have very good outcomes, while those with PET-positive interim scans have poor outcomes.
So the team designed the H10 trial to learn whether they could reduce long-term toxicity in the majority of patients and improve outcomes in the unfavorable subgroups.
Results of the primary endpoint—whether chemotherapy alone is as effective as, but less toxic than, combined-modality treatment in PET-negative patients after 2 cycles of ABVD—were published in the Journal of Clinical Oncology.
The secondary endpoint was an improvement in PFS with an early change from ABVD to escalated BEACOPP in stage I or II HL patients who are PET-positive after 2 cycles of ABVD.
John M. M. Raemaekers, MD, PhD, of Radboud University Medical Center in The Netherlands, presented details on the trial’s secondary endpoint at the 13th International Congress on Malignant Lymphoma (no abstract available).
H10 trial design
The investigators enrolled patients with favorable and unfavorable prognostic characteristics.
Unfavorable characteristics consisted of age 50 or older, more than 3 nodal areas, mediastinal-to-thorax ratio of 0.35 or higher, erythrocyte sedimentation rate of 50 mm or greater without B symptoms, or erythrocyte sedimentation rate of 30 mm or greater with B symptoms.
In the standard treatment arm, patients with favorable or unfavorable characteristics were treated similarly. After 2 cycles of ABVD, a PET scan was performed, and, irrespective of the result, patients received combined-modality treatment of ABVD followed by involved-node radiotherapy.
In the experimental arm, patients who were PET-negative had chemotherapy alone without involved-node radiotherapy. PET-negative patients were not discussed further in this presentation.
For the PET-positive patients in the experimental arm, the treatment for those with favorable and unfavorable characteristics was identical.
Patients who were PET-positive after 2 cycles were switched to 2 escalated BEACOPP cycles plus involved-node radiotherapy. Patients were considered PET-positive if they had a Deauville score of 3, 4, or 5.
Randomization
The first patient was enrolled in November 2006 and the last in June 2011. Investigators randomized 1950 patients, 754 with favorable and 1196 with unfavorable characteristics. All patients had untreated, supradiaphragmatic, clinical stage I or II HL.
Nine hundred fifty-four patients were enrolled in the standard arm, 371 with favorable characteristics and 583 with unfavorable. Nine hundred seventy-one patients entered the experimental arm, 376 with favorable and 595 with unfavorable characteristics.
Twenty-five patients were excluded because they did not complete the first 2 cycles of ABVD or did not have a PET scan.
After 2 cycles of ABVD, 361 patients were PET-positive, 192 in the ABVD arm (54 favorable, 138 unfavorable), and 169 in the escalated BEACOPP arm (43 favorable, 126 unfavorable).
The median age was 30 years in both arms (range, 15 to 70), and the investigators followed patients for a median of 4.5 years.
Results
The only grade 3-4 toxicities were hematologic events and infection.
“As expected, the neutropenia, thrombocytopenia, and anemia, grade 3-4, were more frequent in the experimental BEACOPP arm,” Dr Raemaekers said.
The incidence of grade 3-4 neutropenia was 30.3% (ABVD) and 53.5% (BEACOPP), thrombocytopenia was 0% (ABVD) and 19.7% (BEACOPP), and anemia was 0% (ABVD) and 4.9% (BEACOPP).
The incidence of grade 3-4 febrile neutropenia was 1.1% (ABVD) and 23.9% (BEACOPP), and infection without neutropenia was 1.1% (ABVD) and 11.2% (BEACOPP).
Progression or relapse occurred in 18.8% of patients in the ABVD arm and 7.7% in the BEACOPP arm.
There were 18 deaths in the ABVD arm and 7 deaths in the BEACOPP arm. Eleven deaths in the ABVD arm and 3 in the BEACOPP arm were due to progressive disease or relapse.
The investigators also tallied up the number of patients who progressed, relapsed, or died, whichever occurred first. Forty-one patients in the ABVD arm fulfilled one of these criteria, compared to 16 in the BEACOPP arm.
“Progression and relapse had to be established by conventional restaging, including physical exam, chest X-ray, and CT scan,” Dr Raemaekers pointed out. “And it was based on any new lesion or increase by 50% or more in size of previously involved sites.”
Patients in the BEACOPP arm experienced a significantly better PFS than the ABVD arm, with a hazard ratio of 0.42 (P=0.002). The 5-year PFS was 91% in the BEACOPP arm and 77% in the ABVD arm.
The 5-year OS was 89% in the ABVD arm and 96% in the BEACOPP arm, a difference that was not statistically significant.
“But [the trial] was also not powered for overall survival,” Dr Raemaekers said. “[T]here is a hint, at least, that, even in overall survival, the BEACOPP arm is superior to the ABVD arm.”
Based on these findings, the investigators concluded that, despite increased toxicity, physicians should consider intensifying chemotherapy in early PET-positive patients with stage I/II HL in the combined-modality setting. ![]()

Photo by Rhoda Baer
LUGANO—Long-awaited results of the Intergroup H10 trial in PET-positive Hodgkin lymphoma (HL) patients have shown that intensifying chemotherapy significantly increases 5-year progression-free survival (PFS) and produces a non-significant increase in overall survival (OS).
Switching patients who are PET-positive after 2 cycles of ABVD to escalated BEACOPP and involved-node radiotherapy increased 5-year PFS to 91% and 5-year OS to 96%.
The trial was a cooperative effort of the European Organisation for Research and Treatment of Cancer (EORTC), Lymphoma Study Association (LYSA), and Fondazione Italiana Linfomi (FIL).
The investigators already knew that early FDG-PET scans have prognostic impact. Patients with a negative PET scan after 2 cycles of chemotherapy have very good outcomes, while those with PET-positive interim scans have poor outcomes.
So the team designed the H10 trial to learn whether they could reduce long-term toxicity in the majority of patients and improve outcomes in the unfavorable subgroups.
Results of the primary endpoint—whether chemotherapy alone is as effective as, but less toxic than, combined-modality treatment in PET-negative patients after 2 cycles of ABVD—were published in the Journal of Clinical Oncology.
The secondary endpoint was an improvement in PFS with an early change from ABVD to escalated BEACOPP in stage I or II HL patients who are PET-positive after 2 cycles of ABVD.
John M. M. Raemaekers, MD, PhD, of Radboud University Medical Center in The Netherlands, presented details on the trial’s secondary endpoint at the 13th International Congress on Malignant Lymphoma (no abstract available).
H10 trial design
The investigators enrolled patients with favorable and unfavorable prognostic characteristics.
Unfavorable characteristics consisted of age 50 or older, more than 3 nodal areas, mediastinal-to-thorax ratio of 0.35 or higher, erythrocyte sedimentation rate of 50 mm or greater without B symptoms, or erythrocyte sedimentation rate of 30 mm or greater with B symptoms.
In the standard treatment arm, patients with favorable or unfavorable characteristics were treated similarly. After 2 cycles of ABVD, a PET scan was performed, and, irrespective of the result, patients received combined-modality treatment of ABVD followed by involved-node radiotherapy.
In the experimental arm, patients who were PET-negative had chemotherapy alone without involved-node radiotherapy. PET-negative patients were not discussed further in this presentation.
For the PET-positive patients in the experimental arm, the treatment for those with favorable and unfavorable characteristics was identical.
Patients who were PET-positive after 2 cycles were switched to 2 escalated BEACOPP cycles plus involved-node radiotherapy. Patients were considered PET-positive if they had a Deauville score of 3, 4, or 5.
Randomization
The first patient was enrolled in November 2006 and the last in June 2011. Investigators randomized 1950 patients, 754 with favorable and 1196 with unfavorable characteristics. All patients had untreated, supradiaphragmatic, clinical stage I or II HL.
Nine hundred fifty-four patients were enrolled in the standard arm, 371 with favorable characteristics and 583 with unfavorable. Nine hundred seventy-one patients entered the experimental arm, 376 with favorable and 595 with unfavorable characteristics.
Twenty-five patients were excluded because they did not complete the first 2 cycles of ABVD or did not have a PET scan.
After 2 cycles of ABVD, 361 patients were PET-positive, 192 in the ABVD arm (54 favorable, 138 unfavorable), and 169 in the escalated BEACOPP arm (43 favorable, 126 unfavorable).
The median age was 30 years in both arms (range, 15 to 70), and the investigators followed patients for a median of 4.5 years.
Results
The only grade 3-4 toxicities were hematologic events and infection.
“As expected, the neutropenia, thrombocytopenia, and anemia, grade 3-4, were more frequent in the experimental BEACOPP arm,” Dr Raemaekers said.
The incidence of grade 3-4 neutropenia was 30.3% (ABVD) and 53.5% (BEACOPP), thrombocytopenia was 0% (ABVD) and 19.7% (BEACOPP), and anemia was 0% (ABVD) and 4.9% (BEACOPP).
The incidence of grade 3-4 febrile neutropenia was 1.1% (ABVD) and 23.9% (BEACOPP), and infection without neutropenia was 1.1% (ABVD) and 11.2% (BEACOPP).
Progression or relapse occurred in 18.8% of patients in the ABVD arm and 7.7% in the BEACOPP arm.
There were 18 deaths in the ABVD arm and 7 deaths in the BEACOPP arm. Eleven deaths in the ABVD arm and 3 in the BEACOPP arm were due to progressive disease or relapse.
The investigators also tallied up the number of patients who progressed, relapsed, or died, whichever occurred first. Forty-one patients in the ABVD arm fulfilled one of these criteria, compared to 16 in the BEACOPP arm.
“Progression and relapse had to be established by conventional restaging, including physical exam, chest X-ray, and CT scan,” Dr Raemaekers pointed out. “And it was based on any new lesion or increase by 50% or more in size of previously involved sites.”
Patients in the BEACOPP arm experienced a significantly better PFS than the ABVD arm, with a hazard ratio of 0.42 (P=0.002). The 5-year PFS was 91% in the BEACOPP arm and 77% in the ABVD arm.
The 5-year OS was 89% in the ABVD arm and 96% in the BEACOPP arm, a difference that was not statistically significant.
“But [the trial] was also not powered for overall survival,” Dr Raemaekers said. “[T]here is a hint, at least, that, even in overall survival, the BEACOPP arm is superior to the ABVD arm.”
Based on these findings, the investigators concluded that, despite increased toxicity, physicians should consider intensifying chemotherapy in early PET-positive patients with stage I/II HL in the combined-modality setting. ![]()

Photo by Rhoda Baer
LUGANO—Long-awaited results of the Intergroup H10 trial in PET-positive Hodgkin lymphoma (HL) patients have shown that intensifying chemotherapy significantly increases 5-year progression-free survival (PFS) and produces a non-significant increase in overall survival (OS).
Switching patients who are PET-positive after 2 cycles of ABVD to escalated BEACOPP and involved-node radiotherapy increased 5-year PFS to 91% and 5-year OS to 96%.
The trial was a cooperative effort of the European Organisation for Research and Treatment of Cancer (EORTC), Lymphoma Study Association (LYSA), and Fondazione Italiana Linfomi (FIL).
The investigators already knew that early FDG-PET scans have prognostic impact. Patients with a negative PET scan after 2 cycles of chemotherapy have very good outcomes, while those with PET-positive interim scans have poor outcomes.
So the team designed the H10 trial to learn whether they could reduce long-term toxicity in the majority of patients and improve outcomes in the unfavorable subgroups.
Results of the primary endpoint—whether chemotherapy alone is as effective as, but less toxic than, combined-modality treatment in PET-negative patients after 2 cycles of ABVD—were published in the Journal of Clinical Oncology.
The secondary endpoint was an improvement in PFS with an early change from ABVD to escalated BEACOPP in stage I or II HL patients who are PET-positive after 2 cycles of ABVD.
John M. M. Raemaekers, MD, PhD, of Radboud University Medical Center in The Netherlands, presented details on the trial’s secondary endpoint at the 13th International Congress on Malignant Lymphoma (no abstract available).
H10 trial design
The investigators enrolled patients with favorable and unfavorable prognostic characteristics.
Unfavorable characteristics consisted of age 50 or older, more than 3 nodal areas, mediastinal-to-thorax ratio of 0.35 or higher, erythrocyte sedimentation rate of 50 mm or greater without B symptoms, or erythrocyte sedimentation rate of 30 mm or greater with B symptoms.
In the standard treatment arm, patients with favorable or unfavorable characteristics were treated similarly. After 2 cycles of ABVD, a PET scan was performed, and, irrespective of the result, patients received combined-modality treatment of ABVD followed by involved-node radiotherapy.
In the experimental arm, patients who were PET-negative had chemotherapy alone without involved-node radiotherapy. PET-negative patients were not discussed further in this presentation.
For the PET-positive patients in the experimental arm, the treatment for those with favorable and unfavorable characteristics was identical.
Patients who were PET-positive after 2 cycles were switched to 2 escalated BEACOPP cycles plus involved-node radiotherapy. Patients were considered PET-positive if they had a Deauville score of 3, 4, or 5.
Randomization
The first patient was enrolled in November 2006 and the last in June 2011. Investigators randomized 1950 patients, 754 with favorable and 1196 with unfavorable characteristics. All patients had untreated, supradiaphragmatic, clinical stage I or II HL.
Nine hundred fifty-four patients were enrolled in the standard arm, 371 with favorable characteristics and 583 with unfavorable. Nine hundred seventy-one patients entered the experimental arm, 376 with favorable and 595 with unfavorable characteristics.
Twenty-five patients were excluded because they did not complete the first 2 cycles of ABVD or did not have a PET scan.
After 2 cycles of ABVD, 361 patients were PET-positive, 192 in the ABVD arm (54 favorable, 138 unfavorable), and 169 in the escalated BEACOPP arm (43 favorable, 126 unfavorable).
The median age was 30 years in both arms (range, 15 to 70), and the investigators followed patients for a median of 4.5 years.
Results
The only grade 3-4 toxicities were hematologic events and infection.
“As expected, the neutropenia, thrombocytopenia, and anemia, grade 3-4, were more frequent in the experimental BEACOPP arm,” Dr Raemaekers said.
The incidence of grade 3-4 neutropenia was 30.3% (ABVD) and 53.5% (BEACOPP), thrombocytopenia was 0% (ABVD) and 19.7% (BEACOPP), and anemia was 0% (ABVD) and 4.9% (BEACOPP).
The incidence of grade 3-4 febrile neutropenia was 1.1% (ABVD) and 23.9% (BEACOPP), and infection without neutropenia was 1.1% (ABVD) and 11.2% (BEACOPP).
Progression or relapse occurred in 18.8% of patients in the ABVD arm and 7.7% in the BEACOPP arm.
There were 18 deaths in the ABVD arm and 7 deaths in the BEACOPP arm. Eleven deaths in the ABVD arm and 3 in the BEACOPP arm were due to progressive disease or relapse.
The investigators also tallied up the number of patients who progressed, relapsed, or died, whichever occurred first. Forty-one patients in the ABVD arm fulfilled one of these criteria, compared to 16 in the BEACOPP arm.
“Progression and relapse had to be established by conventional restaging, including physical exam, chest X-ray, and CT scan,” Dr Raemaekers pointed out. “And it was based on any new lesion or increase by 50% or more in size of previously involved sites.”
Patients in the BEACOPP arm experienced a significantly better PFS than the ABVD arm, with a hazard ratio of 0.42 (P=0.002). The 5-year PFS was 91% in the BEACOPP arm and 77% in the ABVD arm.
The 5-year OS was 89% in the ABVD arm and 96% in the BEACOPP arm, a difference that was not statistically significant.
“But [the trial] was also not powered for overall survival,” Dr Raemaekers said. “[T]here is a hint, at least, that, even in overall survival, the BEACOPP arm is superior to the ABVD arm.”
Based on these findings, the investigators concluded that, despite increased toxicity, physicians should consider intensifying chemotherapy in early PET-positive patients with stage I/II HL in the combined-modality setting. ![]()
‘Radically different’ PI3Kδ inhibitor lacks hepatotoxicity

Photo by Larry Young
LUGANO—Updated phase 1 results with TGR-1202 suggest this next-generation PI3kδ inhibitor lacks the hepatotoxicity associated with other PI3Kδ inhibitors.
Investigators also confirmed that no case of colitis has been reported to date with TGR-1202, and only 2% of evaluable patients on this trial have experienced grade 3-4 diarrhea.
The study is an ongoing, first-in-human trial in patients with relapsed or refractory hematologic malignancies.
Owen O’Connor, MD, PhD, of Columbia University Medical Center in New York, New York, shared results from this trial at the 13th International Congress on Malignant Lymphoma (abstract 038*). The trial is sponsored by TG Therapeutics, Inc., the company developing TGR-1202.
“TGR-1202 is a radically different sort of PI3kδ inhibitor,” Dr O’Connor said. “[I]t’s really a unique chemical entity that is different from the previous 2 structures [idelalisib and duvelisib] that you’ve probably heard something about.”
Study design
This ongoing trial of TGR-1202 is open to patients with hematologic malignancies who relapsed after or were refractory to at least 1 prior treatment regimen. Patients are eligible if they have an ECOG performance status of 2 or less with adequate organ system function, including absolute neutrophil count of 750/μL or greater and platelets of 50,000/μL or greater.
TGR-1202 is dosed orally, once a day in continuous, 28-day cycles. The original dose-escalation portion of the study was a classic 3+3 design, starting at 50 mg and increasing to 1800 mg. Patients who received prior therapy with a PI3K and/or mTOR inhibitor were excluded from the dose-escalation cohorts but were allowed in the expansion cohorts.
Dr O’Connor pointed out that, through cohort 5, TGR-1202 was taken in the fasting state. However, pharmacokinetic studies performed in the fed state revealed that the area under the curve (AUC) and Cmax could be doubled by taking the drug with food. So the expansions in the ongoing 800 mg and 1200 mg cohorts are being conducted in the fed state.
Dr O’Connor also noted that a subsequent, micronized version of TGR-1202 was developed. The micronization “essentially increases the surface area of the formulation, allowing for better bioavailability and markedly increases the AUC and Cmax exposure,” he said.
So the investigators conducted a second escalation with the micronized formulation, starting at 200 mg and increasing to 800 mg. At present, they are enrolling patients to the 800 mg and 1200 mg cohorts conducted in the fed state with the micronized formulation.
Demographics
Dr O’Connor presented data on 66 patients who were evaluable for safety and 51 for efficacy. The patients’ median age was 66 (range, 22–85), and 46 were male.
In all, there were 20 patients with chronic lymphocytic leukemia (CLL), 17 with follicular lymphoma, 10 with diffuse large B-cell lymphoma, 9 with Hodgkin lymphoma, 5 with mantle cell lymphoma, 3 with marginal zone lymphoma, 1 with Waldenström’s macroglobulinemia, and 1 with hairy cell leukemia.
Patients had received a median of 3 prior therapies (range, 1–14), and 36 (55%) had 3 or more prior therapies. Thirty-four patients (52%) were refractory to their prior therapy.
Efficacy
Dr O’Connor reported that higher doses of TGR-1202—1200 mg of the initial formulation and 600 mg or more of the micronized version—demonstrated rapid and profound responses in CLL, follicular lymphoma, and marginal zone lymphoma.
Responses have been limited in diffuse large B-cell lymphoma, Hodgkin lymphoma, and mantle cell lymphoma.
Eighty-eight percent of CLL patients achieved a nodal partial remission, and 63% achieved a response according to iwCLL criteria (Hallek 2008).
Safety and tolerability
Adverse events occurring in more than 10% of patients included nausea (41%), diarrhea (32%), fatigue (32%), headache (23%), vomiting (23%), cough (21%), decreased appetite (17%), rash (17%), constipation (14%), hypokalemia (14%), anemia, dizziness, dyspnea, neutropenia, and pyrexia (12% each), and abdominal pain (11%).
The most common grade 3-4 toxicity was neutropenia, occurring in 11% of patients.
“But other than that, the bulk of the toxicities in terms of grade 3-4 events were relatively modest,” Dr O’Connor said. “[I]t’s worth pointing out that diarrhea grade 3-4 only occurred in about 2% of patients in the population.”
Approximately 50% of patients (n=31) have been on study for more than 6 months, and approximately 30% taking a higher dose level have been on study for 6 months or more. Twenty-five of 37 patients exposed to 800 mg or more of the micronized formulation currently remain on study.
“So this gives you a sense that it is a very well-tolerated drug, with patients staying on for extended periods of time,” Dr O’Connor said.
He added that time on study becomes relevant in assessing some of the gastrointestinal toxicities seen with other PI3Kδ inhibitors, where it seems the median time to gastrointestinal toxicity is beyond 6 months.
“So far, and I’m willing to concede it’s early, but with half the patients being treated for over 6 months, [diarrhea/colitis] seems to be much lower than the experience with the other PI3 kinase inhibitors,” Dr O’Connor said.
“I think one of the more important features of [TGR-1202], and one that allows me to think we might be able to integrate this drug a little more readily into various combination regimens, are the discontinuations due to other adverse events.”
“Only 4% treated with [TGR-1202] had discontinuations secondary to adverse events. [A]nd it looks like the efficacy is in line with what we’d expect with some of the other drugs, but this [study] is actively accruing still.” ![]()
*Information in the abstract differs from that presented at the meeting.

Photo by Larry Young
LUGANO—Updated phase 1 results with TGR-1202 suggest this next-generation PI3kδ inhibitor lacks the hepatotoxicity associated with other PI3Kδ inhibitors.
Investigators also confirmed that no case of colitis has been reported to date with TGR-1202, and only 2% of evaluable patients on this trial have experienced grade 3-4 diarrhea.
The study is an ongoing, first-in-human trial in patients with relapsed or refractory hematologic malignancies.
Owen O’Connor, MD, PhD, of Columbia University Medical Center in New York, New York, shared results from this trial at the 13th International Congress on Malignant Lymphoma (abstract 038*). The trial is sponsored by TG Therapeutics, Inc., the company developing TGR-1202.
“TGR-1202 is a radically different sort of PI3kδ inhibitor,” Dr O’Connor said. “[I]t’s really a unique chemical entity that is different from the previous 2 structures [idelalisib and duvelisib] that you’ve probably heard something about.”
Study design
This ongoing trial of TGR-1202 is open to patients with hematologic malignancies who relapsed after or were refractory to at least 1 prior treatment regimen. Patients are eligible if they have an ECOG performance status of 2 or less with adequate organ system function, including absolute neutrophil count of 750/μL or greater and platelets of 50,000/μL or greater.
TGR-1202 is dosed orally, once a day in continuous, 28-day cycles. The original dose-escalation portion of the study was a classic 3+3 design, starting at 50 mg and increasing to 1800 mg. Patients who received prior therapy with a PI3K and/or mTOR inhibitor were excluded from the dose-escalation cohorts but were allowed in the expansion cohorts.
Dr O’Connor pointed out that, through cohort 5, TGR-1202 was taken in the fasting state. However, pharmacokinetic studies performed in the fed state revealed that the area under the curve (AUC) and Cmax could be doubled by taking the drug with food. So the expansions in the ongoing 800 mg and 1200 mg cohorts are being conducted in the fed state.
Dr O’Connor also noted that a subsequent, micronized version of TGR-1202 was developed. The micronization “essentially increases the surface area of the formulation, allowing for better bioavailability and markedly increases the AUC and Cmax exposure,” he said.
So the investigators conducted a second escalation with the micronized formulation, starting at 200 mg and increasing to 800 mg. At present, they are enrolling patients to the 800 mg and 1200 mg cohorts conducted in the fed state with the micronized formulation.
Demographics
Dr O’Connor presented data on 66 patients who were evaluable for safety and 51 for efficacy. The patients’ median age was 66 (range, 22–85), and 46 were male.
In all, there were 20 patients with chronic lymphocytic leukemia (CLL), 17 with follicular lymphoma, 10 with diffuse large B-cell lymphoma, 9 with Hodgkin lymphoma, 5 with mantle cell lymphoma, 3 with marginal zone lymphoma, 1 with Waldenström’s macroglobulinemia, and 1 with hairy cell leukemia.
Patients had received a median of 3 prior therapies (range, 1–14), and 36 (55%) had 3 or more prior therapies. Thirty-four patients (52%) were refractory to their prior therapy.
Efficacy
Dr O’Connor reported that higher doses of TGR-1202—1200 mg of the initial formulation and 600 mg or more of the micronized version—demonstrated rapid and profound responses in CLL, follicular lymphoma, and marginal zone lymphoma.
Responses have been limited in diffuse large B-cell lymphoma, Hodgkin lymphoma, and mantle cell lymphoma.
Eighty-eight percent of CLL patients achieved a nodal partial remission, and 63% achieved a response according to iwCLL criteria (Hallek 2008).
Safety and tolerability
Adverse events occurring in more than 10% of patients included nausea (41%), diarrhea (32%), fatigue (32%), headache (23%), vomiting (23%), cough (21%), decreased appetite (17%), rash (17%), constipation (14%), hypokalemia (14%), anemia, dizziness, dyspnea, neutropenia, and pyrexia (12% each), and abdominal pain (11%).
The most common grade 3-4 toxicity was neutropenia, occurring in 11% of patients.
“But other than that, the bulk of the toxicities in terms of grade 3-4 events were relatively modest,” Dr O’Connor said. “[I]t’s worth pointing out that diarrhea grade 3-4 only occurred in about 2% of patients in the population.”
Approximately 50% of patients (n=31) have been on study for more than 6 months, and approximately 30% taking a higher dose level have been on study for 6 months or more. Twenty-five of 37 patients exposed to 800 mg or more of the micronized formulation currently remain on study.
“So this gives you a sense that it is a very well-tolerated drug, with patients staying on for extended periods of time,” Dr O’Connor said.
He added that time on study becomes relevant in assessing some of the gastrointestinal toxicities seen with other PI3Kδ inhibitors, where it seems the median time to gastrointestinal toxicity is beyond 6 months.
“So far, and I’m willing to concede it’s early, but with half the patients being treated for over 6 months, [diarrhea/colitis] seems to be much lower than the experience with the other PI3 kinase inhibitors,” Dr O’Connor said.
“I think one of the more important features of [TGR-1202], and one that allows me to think we might be able to integrate this drug a little more readily into various combination regimens, are the discontinuations due to other adverse events.”
“Only 4% treated with [TGR-1202] had discontinuations secondary to adverse events. [A]nd it looks like the efficacy is in line with what we’d expect with some of the other drugs, but this [study] is actively accruing still.” ![]()
*Information in the abstract differs from that presented at the meeting.

Photo by Larry Young
LUGANO—Updated phase 1 results with TGR-1202 suggest this next-generation PI3kδ inhibitor lacks the hepatotoxicity associated with other PI3Kδ inhibitors.
Investigators also confirmed that no case of colitis has been reported to date with TGR-1202, and only 2% of evaluable patients on this trial have experienced grade 3-4 diarrhea.
The study is an ongoing, first-in-human trial in patients with relapsed or refractory hematologic malignancies.
Owen O’Connor, MD, PhD, of Columbia University Medical Center in New York, New York, shared results from this trial at the 13th International Congress on Malignant Lymphoma (abstract 038*). The trial is sponsored by TG Therapeutics, Inc., the company developing TGR-1202.
“TGR-1202 is a radically different sort of PI3kδ inhibitor,” Dr O’Connor said. “[I]t’s really a unique chemical entity that is different from the previous 2 structures [idelalisib and duvelisib] that you’ve probably heard something about.”
Study design
This ongoing trial of TGR-1202 is open to patients with hematologic malignancies who relapsed after or were refractory to at least 1 prior treatment regimen. Patients are eligible if they have an ECOG performance status of 2 or less with adequate organ system function, including absolute neutrophil count of 750/μL or greater and platelets of 50,000/μL or greater.
TGR-1202 is dosed orally, once a day in continuous, 28-day cycles. The original dose-escalation portion of the study was a classic 3+3 design, starting at 50 mg and increasing to 1800 mg. Patients who received prior therapy with a PI3K and/or mTOR inhibitor were excluded from the dose-escalation cohorts but were allowed in the expansion cohorts.
Dr O’Connor pointed out that, through cohort 5, TGR-1202 was taken in the fasting state. However, pharmacokinetic studies performed in the fed state revealed that the area under the curve (AUC) and Cmax could be doubled by taking the drug with food. So the expansions in the ongoing 800 mg and 1200 mg cohorts are being conducted in the fed state.
Dr O’Connor also noted that a subsequent, micronized version of TGR-1202 was developed. The micronization “essentially increases the surface area of the formulation, allowing for better bioavailability and markedly increases the AUC and Cmax exposure,” he said.
So the investigators conducted a second escalation with the micronized formulation, starting at 200 mg and increasing to 800 mg. At present, they are enrolling patients to the 800 mg and 1200 mg cohorts conducted in the fed state with the micronized formulation.
Demographics
Dr O’Connor presented data on 66 patients who were evaluable for safety and 51 for efficacy. The patients’ median age was 66 (range, 22–85), and 46 were male.
In all, there were 20 patients with chronic lymphocytic leukemia (CLL), 17 with follicular lymphoma, 10 with diffuse large B-cell lymphoma, 9 with Hodgkin lymphoma, 5 with mantle cell lymphoma, 3 with marginal zone lymphoma, 1 with Waldenström’s macroglobulinemia, and 1 with hairy cell leukemia.
Patients had received a median of 3 prior therapies (range, 1–14), and 36 (55%) had 3 or more prior therapies. Thirty-four patients (52%) were refractory to their prior therapy.
Efficacy
Dr O’Connor reported that higher doses of TGR-1202—1200 mg of the initial formulation and 600 mg or more of the micronized version—demonstrated rapid and profound responses in CLL, follicular lymphoma, and marginal zone lymphoma.
Responses have been limited in diffuse large B-cell lymphoma, Hodgkin lymphoma, and mantle cell lymphoma.
Eighty-eight percent of CLL patients achieved a nodal partial remission, and 63% achieved a response according to iwCLL criteria (Hallek 2008).
Safety and tolerability
Adverse events occurring in more than 10% of patients included nausea (41%), diarrhea (32%), fatigue (32%), headache (23%), vomiting (23%), cough (21%), decreased appetite (17%), rash (17%), constipation (14%), hypokalemia (14%), anemia, dizziness, dyspnea, neutropenia, and pyrexia (12% each), and abdominal pain (11%).
The most common grade 3-4 toxicity was neutropenia, occurring in 11% of patients.
“But other than that, the bulk of the toxicities in terms of grade 3-4 events were relatively modest,” Dr O’Connor said. “[I]t’s worth pointing out that diarrhea grade 3-4 only occurred in about 2% of patients in the population.”
Approximately 50% of patients (n=31) have been on study for more than 6 months, and approximately 30% taking a higher dose level have been on study for 6 months or more. Twenty-five of 37 patients exposed to 800 mg or more of the micronized formulation currently remain on study.
“So this gives you a sense that it is a very well-tolerated drug, with patients staying on for extended periods of time,” Dr O’Connor said.
He added that time on study becomes relevant in assessing some of the gastrointestinal toxicities seen with other PI3Kδ inhibitors, where it seems the median time to gastrointestinal toxicity is beyond 6 months.
“So far, and I’m willing to concede it’s early, but with half the patients being treated for over 6 months, [diarrhea/colitis] seems to be much lower than the experience with the other PI3 kinase inhibitors,” Dr O’Connor said.
“I think one of the more important features of [TGR-1202], and one that allows me to think we might be able to integrate this drug a little more readily into various combination regimens, are the discontinuations due to other adverse events.”
“Only 4% treated with [TGR-1202] had discontinuations secondary to adverse events. [A]nd it looks like the efficacy is in line with what we’d expect with some of the other drugs, but this [study] is actively accruing still.” ![]()
*Information in the abstract differs from that presented at the meeting.
Insecticide can cause NHL, experts say

Photo by John Messina
The insecticide gamma-hexachlorocyclohexane (lindane) is carcinogenic, according to experts from the International Agency for Research on Cancer (IARC), the specialized cancer agency of the World Health Organization.
The experts said they found sufficient evidence that lindane, which is banned or restricted in most countries, can cause non-Hodgkin lymphoma (NHL).
The group also discovered that 2 other chemicals might cause NHL.
The evidence suggests the insecticide dichlorodiphenyltrichloroethane (DDT) is probably carcinogenic, and the herbicide 2,4-dichlorophenoxyacetic acid (2,4-D) is possibly carcinogenic.
A summary of these findings is available in The Lancet Oncology, and the experts’ detailed assessments will be published as Volume 113 of the IARC Monographs.
The group, which consisted of 26 experts convened by the IARC Monographs Programme, reviewed the latest scientific literature on lindane, DDT, and 2,4-D and used their findings to classify these 3 chemicals according to carcinogenicity.
The classification (Group 1, Group 2A, etc.) indicates the strength of the evidence that a substance causes cancer, not the level of risk associated with exposure. The Monographs Programme identifies cancer hazards even when risks are very low at current exposure levels, because new uses or unforeseen exposures could engender risks that are significantly higher.
Lindane
The experts classified lindane as carcinogenic to humans (Group 1), saying they found sufficient evidence that it can cause NHL. Large epidemiological studies of agricultural exposures in the US and Canada showed a 60% increased risk of NHL in people exposed to lindane.
Lindane has been used extensively for insect control, including in agriculture and for the treatment of human lice and scabies. High exposures have occurred among agricultural workers and pesticide applicators. However, the use of lindane is now banned or restricted in most countries.
DDT
The experts classified DDT as probably carcinogenic to humans (Group 2A), saying they found sufficient evidence that DDT causes cancer in experimental animals and limited evidence of DDT’s carcinogenicity in humans.
Epidemiological studies have shown positive associations between exposure to DDT and NHL, testicular cancer, and liver cancer.
There was also strong experimental evidence that DDT can suppress the immune system and disrupt sex hormones. However, overall, there was no association between breast cancer and DDT levels measured in samples of blood or fat.
DDT was introduced for the control of insect-borne diseases during World War II and was later applied widely to eradicate malaria and in agriculture. Most uses of DDT were banned in the 1970s. However, DDT and its breakdown products are highly persistent and can be found in the environment and in animal and human tissues throughout the world.
Exposure to DDT still occurs, mainly through diet. The remaining and essential use of DDT is for disease vector control, mainly for malaria. This use is strictly restricted under the Stockholm Convention.
2,4-D
The experts classified 2,4-D as possibly carcinogenic to humans (Group 2B), saying they had inadequate evidence in humans and limited evidence in experimental animals.
There is strong evidence that 2,4-D induces oxidative stress and moderate evidence that 2,4-D causes immunosuppression, based on in vivo and in vitro studies. However, epidemiological studies did not show strong or consistent increases in the risk of NHL or other cancers in relation to 2,4-D exposure.
Since its introduction in 1945, 2,4-D has been widely used to control weeds in agriculture, forestry, and urban and residential settings. Occupational exposures to 2,4-D can occur during manufacturing and application, and the general population can be exposed through food, water, dust, or residential application, and during spraying. ![]()

Photo by John Messina
The insecticide gamma-hexachlorocyclohexane (lindane) is carcinogenic, according to experts from the International Agency for Research on Cancer (IARC), the specialized cancer agency of the World Health Organization.
The experts said they found sufficient evidence that lindane, which is banned or restricted in most countries, can cause non-Hodgkin lymphoma (NHL).
The group also discovered that 2 other chemicals might cause NHL.
The evidence suggests the insecticide dichlorodiphenyltrichloroethane (DDT) is probably carcinogenic, and the herbicide 2,4-dichlorophenoxyacetic acid (2,4-D) is possibly carcinogenic.
A summary of these findings is available in The Lancet Oncology, and the experts’ detailed assessments will be published as Volume 113 of the IARC Monographs.
The group, which consisted of 26 experts convened by the IARC Monographs Programme, reviewed the latest scientific literature on lindane, DDT, and 2,4-D and used their findings to classify these 3 chemicals according to carcinogenicity.
The classification (Group 1, Group 2A, etc.) indicates the strength of the evidence that a substance causes cancer, not the level of risk associated with exposure. The Monographs Programme identifies cancer hazards even when risks are very low at current exposure levels, because new uses or unforeseen exposures could engender risks that are significantly higher.
Lindane
The experts classified lindane as carcinogenic to humans (Group 1), saying they found sufficient evidence that it can cause NHL. Large epidemiological studies of agricultural exposures in the US and Canada showed a 60% increased risk of NHL in people exposed to lindane.
Lindane has been used extensively for insect control, including in agriculture and for the treatment of human lice and scabies. High exposures have occurred among agricultural workers and pesticide applicators. However, the use of lindane is now banned or restricted in most countries.
DDT
The experts classified DDT as probably carcinogenic to humans (Group 2A), saying they found sufficient evidence that DDT causes cancer in experimental animals and limited evidence of DDT’s carcinogenicity in humans.
Epidemiological studies have shown positive associations between exposure to DDT and NHL, testicular cancer, and liver cancer.
There was also strong experimental evidence that DDT can suppress the immune system and disrupt sex hormones. However, overall, there was no association between breast cancer and DDT levels measured in samples of blood or fat.
DDT was introduced for the control of insect-borne diseases during World War II and was later applied widely to eradicate malaria and in agriculture. Most uses of DDT were banned in the 1970s. However, DDT and its breakdown products are highly persistent and can be found in the environment and in animal and human tissues throughout the world.
Exposure to DDT still occurs, mainly through diet. The remaining and essential use of DDT is for disease vector control, mainly for malaria. This use is strictly restricted under the Stockholm Convention.
2,4-D
The experts classified 2,4-D as possibly carcinogenic to humans (Group 2B), saying they had inadequate evidence in humans and limited evidence in experimental animals.
There is strong evidence that 2,4-D induces oxidative stress and moderate evidence that 2,4-D causes immunosuppression, based on in vivo and in vitro studies. However, epidemiological studies did not show strong or consistent increases in the risk of NHL or other cancers in relation to 2,4-D exposure.
Since its introduction in 1945, 2,4-D has been widely used to control weeds in agriculture, forestry, and urban and residential settings. Occupational exposures to 2,4-D can occur during manufacturing and application, and the general population can be exposed through food, water, dust, or residential application, and during spraying. ![]()

Photo by John Messina
The insecticide gamma-hexachlorocyclohexane (lindane) is carcinogenic, according to experts from the International Agency for Research on Cancer (IARC), the specialized cancer agency of the World Health Organization.
The experts said they found sufficient evidence that lindane, which is banned or restricted in most countries, can cause non-Hodgkin lymphoma (NHL).
The group also discovered that 2 other chemicals might cause NHL.
The evidence suggests the insecticide dichlorodiphenyltrichloroethane (DDT) is probably carcinogenic, and the herbicide 2,4-dichlorophenoxyacetic acid (2,4-D) is possibly carcinogenic.
A summary of these findings is available in The Lancet Oncology, and the experts’ detailed assessments will be published as Volume 113 of the IARC Monographs.
The group, which consisted of 26 experts convened by the IARC Monographs Programme, reviewed the latest scientific literature on lindane, DDT, and 2,4-D and used their findings to classify these 3 chemicals according to carcinogenicity.
The classification (Group 1, Group 2A, etc.) indicates the strength of the evidence that a substance causes cancer, not the level of risk associated with exposure. The Monographs Programme identifies cancer hazards even when risks are very low at current exposure levels, because new uses or unforeseen exposures could engender risks that are significantly higher.
Lindane
The experts classified lindane as carcinogenic to humans (Group 1), saying they found sufficient evidence that it can cause NHL. Large epidemiological studies of agricultural exposures in the US and Canada showed a 60% increased risk of NHL in people exposed to lindane.
Lindane has been used extensively for insect control, including in agriculture and for the treatment of human lice and scabies. High exposures have occurred among agricultural workers and pesticide applicators. However, the use of lindane is now banned or restricted in most countries.
DDT
The experts classified DDT as probably carcinogenic to humans (Group 2A), saying they found sufficient evidence that DDT causes cancer in experimental animals and limited evidence of DDT’s carcinogenicity in humans.
Epidemiological studies have shown positive associations between exposure to DDT and NHL, testicular cancer, and liver cancer.
There was also strong experimental evidence that DDT can suppress the immune system and disrupt sex hormones. However, overall, there was no association between breast cancer and DDT levels measured in samples of blood or fat.
DDT was introduced for the control of insect-borne diseases during World War II and was later applied widely to eradicate malaria and in agriculture. Most uses of DDT were banned in the 1970s. However, DDT and its breakdown products are highly persistent and can be found in the environment and in animal and human tissues throughout the world.
Exposure to DDT still occurs, mainly through diet. The remaining and essential use of DDT is for disease vector control, mainly for malaria. This use is strictly restricted under the Stockholm Convention.
2,4-D
The experts classified 2,4-D as possibly carcinogenic to humans (Group 2B), saying they had inadequate evidence in humans and limited evidence in experimental animals.
There is strong evidence that 2,4-D induces oxidative stress and moderate evidence that 2,4-D causes immunosuppression, based on in vivo and in vitro studies. However, epidemiological studies did not show strong or consistent increases in the risk of NHL or other cancers in relation to 2,4-D exposure.
Since its introduction in 1945, 2,4-D has been widely used to control weeds in agriculture, forestry, and urban and residential settings. Occupational exposures to 2,4-D can occur during manufacturing and application, and the general population can be exposed through food, water, dust, or residential application, and during spraying. ![]()
Nivolumab produces ‘dramatic’ responses in HL

Photo courtesy of UCLA
LUGANO—The PD-1 checkpoint inhibitor nivolumab produces rapid, durable, and, in some cases, “dramatic” responses in Hodgkin lymphoma (HL), according to a speaker at the 13th International Congress on Malignant Lymphoma.
The drug has also produced durable responses in follicular lymphoma (FL), cutaneous T-cell lymphoma (CTCL), and peripheral T-cell lymphoma (PTCL), although patient numbers for these malignancies are small.
John Timmerman, MD, of the University of California, Los Angeles, presented these results from a phase 1 study of patients with relapsed or refractory lymphoid malignancies and chronic HL (abstract 010).
Bristol-Myers Squibb and Ono Pharmaceutical Company are sponsors of the trial.
Original results of the study, with a data cutoff of June 2014, were reported at ASH 2014, with 40 weeks of median follow-up.
The update presented at 13-ICML, with a data lock in April 2015, includes an additional 10 months of data, for a median follow-up of 76 weeks.
Investigators enrolled 105 patients in this dose-escalation study to receive nivolumab at 1 mg/kg, then 3 mg/kg, every 2 weeks for 2 years.
Twenty-three patients had HL. Thirty-one had B-cell non-Hodgkin lymphoma (NHL), including 11 with FL and 10 with diffuse large B-cell lymphoma (DLBCL).
Twenty-three patients had T-cell NHL, including 5 with PTCL and 13 with CTCL/mycosis fungoides (MF). Twenty-seven patients had multiple myeloma (MM), and 1 had chronic myeloid leukemia.
Patients were heavily pretreated. Seventy-eight percent of HL patients and 26% of T-NHL patients had prior brentuximab vedotin. And 78% (HL), 14% (B-NHL), 9% (T-NHL), and 56% (MM) of patients had a prior autologous transplant.
The median number of prior therapies was 5 (range, 2-15) for HL patients and ranged from 1 to 16 for all patients.
The study’s primary endpoint was safety and tolerability, and the secondary endpoint was efficacy.
Safety and tolerability
Ninety-seven percent of patients had an adverse event, 69% of them related to study treatment and 21% of them treatment-related grade 3-4 events.
Fifteen patients (14%) discontinued treatment due to a related adverse event, including 3 with pneumonitis and 1 each with enteritis, stomatitis, pancreatitis, rash, conjunctivitis, sepsis, diplopia, myositis, neutropenia, myelodysplastic syndrome, increased creatinine phosphokinase, and peripheral neuropathy.
“Immune-related adverse events were generally seen early on and generally of low grade,” Dr Timmerman said. “However, it is notable that there were several grade 3 immune-related adverse events that can be seen as far as 6 months out after the start of therapy.”
These included skin, gastrointestinal, and pulmonary events. Most immune-related adverse events (83%) were resolved using protocol-prescribed procedures.
Efficacy
The overall response rate was 87% for HL, 36% for DLBCL, 40% for FL, 15% for CTCL/MF, 40% for PTCL, and 4% for MM.
Dr Timmerman pointed out that, since ASH, 2 additional conversions from partial response (PR) to complete response (CR) occurred in patients with HL. To date, 6 of 23 HL patients have achieved a CR and 14 a PR.
In B-cell NHL, there were additional conversions from PR to CR in DLBCL, while responses remained the same in FL and in the 4 responders with T-cell lymphomas.
“Intriguingly, there has been 1 late CR in the multiple myeloma cohort, which previously had shown no responses,” Dr Timmerman said.
Durability of response
This study suggests PD-1 blockade can produce durable responses in hematologic malignancies, as it does in melanoma and renal cell carcinoma.
In HL, the median response duration at a median follow-up of 86 weeks has not yet been reached, and half (n=10) of the responses are still ongoing.
In FL, CTCL, and PTCL, the median response duration has not been reached at a median follow-up of 81, 43, and 31 weeks, respectively. Of note, there are ongoing responses in at least half of patients in these tumor types.
In HL, none of the 6 patients in CR has progressed, although there have been some progressions in the PR group.
The rapidity of responses is also notable, Dr Timmerman said.
“[I]t’s very interesting that some patients have resolution of symptoms and improvement of symptoms within even 1 day of starting nivolumab therapy,” he said.
And responses to nivolumab in HL “can be very dramatic,” he added, as illustrated in the following case from the Mayo Clinic.
A patient with multiple sites of bulky FDG-avid tumors was scheduled to enter hospice. But first, he entered the nivolumab trial. Within 6 weeks of initiating treatment, he had achieved a near-CR. This response has been maintained for 2 years.
“The occurrence of very durable responses in the PR and CR groups has led us to question whether patients should go on to allogeneic stem cell transplantation after achieving responses with nivolumab or, rather, continue on nivolumab as long as their response remains,” Dr Timmerman said.
He added that an international, phase 2 trial in HL is underway and is accruing briskly.
Nivolumab was awarded breakthrough designation by the US Food and Drug Administration last year. Breakthrough designation is intended to expedite the development and review of drugs for serious or life-threatening conditions. ![]()

Photo courtesy of UCLA
LUGANO—The PD-1 checkpoint inhibitor nivolumab produces rapid, durable, and, in some cases, “dramatic” responses in Hodgkin lymphoma (HL), according to a speaker at the 13th International Congress on Malignant Lymphoma.
The drug has also produced durable responses in follicular lymphoma (FL), cutaneous T-cell lymphoma (CTCL), and peripheral T-cell lymphoma (PTCL), although patient numbers for these malignancies are small.
John Timmerman, MD, of the University of California, Los Angeles, presented these results from a phase 1 study of patients with relapsed or refractory lymphoid malignancies and chronic HL (abstract 010).
Bristol-Myers Squibb and Ono Pharmaceutical Company are sponsors of the trial.
Original results of the study, with a data cutoff of June 2014, were reported at ASH 2014, with 40 weeks of median follow-up.
The update presented at 13-ICML, with a data lock in April 2015, includes an additional 10 months of data, for a median follow-up of 76 weeks.
Investigators enrolled 105 patients in this dose-escalation study to receive nivolumab at 1 mg/kg, then 3 mg/kg, every 2 weeks for 2 years.
Twenty-three patients had HL. Thirty-one had B-cell non-Hodgkin lymphoma (NHL), including 11 with FL and 10 with diffuse large B-cell lymphoma (DLBCL).
Twenty-three patients had T-cell NHL, including 5 with PTCL and 13 with CTCL/mycosis fungoides (MF). Twenty-seven patients had multiple myeloma (MM), and 1 had chronic myeloid leukemia.
Patients were heavily pretreated. Seventy-eight percent of HL patients and 26% of T-NHL patients had prior brentuximab vedotin. And 78% (HL), 14% (B-NHL), 9% (T-NHL), and 56% (MM) of patients had a prior autologous transplant.
The median number of prior therapies was 5 (range, 2-15) for HL patients and ranged from 1 to 16 for all patients.
The study’s primary endpoint was safety and tolerability, and the secondary endpoint was efficacy.
Safety and tolerability
Ninety-seven percent of patients had an adverse event, 69% of them related to study treatment and 21% of them treatment-related grade 3-4 events.
Fifteen patients (14%) discontinued treatment due to a related adverse event, including 3 with pneumonitis and 1 each with enteritis, stomatitis, pancreatitis, rash, conjunctivitis, sepsis, diplopia, myositis, neutropenia, myelodysplastic syndrome, increased creatinine phosphokinase, and peripheral neuropathy.
“Immune-related adverse events were generally seen early on and generally of low grade,” Dr Timmerman said. “However, it is notable that there were several grade 3 immune-related adverse events that can be seen as far as 6 months out after the start of therapy.”
These included skin, gastrointestinal, and pulmonary events. Most immune-related adverse events (83%) were resolved using protocol-prescribed procedures.
Efficacy
The overall response rate was 87% for HL, 36% for DLBCL, 40% for FL, 15% for CTCL/MF, 40% for PTCL, and 4% for MM.
Dr Timmerman pointed out that, since ASH, 2 additional conversions from partial response (PR) to complete response (CR) occurred in patients with HL. To date, 6 of 23 HL patients have achieved a CR and 14 a PR.
In B-cell NHL, there were additional conversions from PR to CR in DLBCL, while responses remained the same in FL and in the 4 responders with T-cell lymphomas.
“Intriguingly, there has been 1 late CR in the multiple myeloma cohort, which previously had shown no responses,” Dr Timmerman said.
Durability of response
This study suggests PD-1 blockade can produce durable responses in hematologic malignancies, as it does in melanoma and renal cell carcinoma.
In HL, the median response duration at a median follow-up of 86 weeks has not yet been reached, and half (n=10) of the responses are still ongoing.
In FL, CTCL, and PTCL, the median response duration has not been reached at a median follow-up of 81, 43, and 31 weeks, respectively. Of note, there are ongoing responses in at least half of patients in these tumor types.
In HL, none of the 6 patients in CR has progressed, although there have been some progressions in the PR group.
The rapidity of responses is also notable, Dr Timmerman said.
“[I]t’s very interesting that some patients have resolution of symptoms and improvement of symptoms within even 1 day of starting nivolumab therapy,” he said.
And responses to nivolumab in HL “can be very dramatic,” he added, as illustrated in the following case from the Mayo Clinic.
A patient with multiple sites of bulky FDG-avid tumors was scheduled to enter hospice. But first, he entered the nivolumab trial. Within 6 weeks of initiating treatment, he had achieved a near-CR. This response has been maintained for 2 years.
“The occurrence of very durable responses in the PR and CR groups has led us to question whether patients should go on to allogeneic stem cell transplantation after achieving responses with nivolumab or, rather, continue on nivolumab as long as their response remains,” Dr Timmerman said.
He added that an international, phase 2 trial in HL is underway and is accruing briskly.
Nivolumab was awarded breakthrough designation by the US Food and Drug Administration last year. Breakthrough designation is intended to expedite the development and review of drugs for serious or life-threatening conditions. ![]()

Photo courtesy of UCLA
LUGANO—The PD-1 checkpoint inhibitor nivolumab produces rapid, durable, and, in some cases, “dramatic” responses in Hodgkin lymphoma (HL), according to a speaker at the 13th International Congress on Malignant Lymphoma.
The drug has also produced durable responses in follicular lymphoma (FL), cutaneous T-cell lymphoma (CTCL), and peripheral T-cell lymphoma (PTCL), although patient numbers for these malignancies are small.
John Timmerman, MD, of the University of California, Los Angeles, presented these results from a phase 1 study of patients with relapsed or refractory lymphoid malignancies and chronic HL (abstract 010).
Bristol-Myers Squibb and Ono Pharmaceutical Company are sponsors of the trial.
Original results of the study, with a data cutoff of June 2014, were reported at ASH 2014, with 40 weeks of median follow-up.
The update presented at 13-ICML, with a data lock in April 2015, includes an additional 10 months of data, for a median follow-up of 76 weeks.
Investigators enrolled 105 patients in this dose-escalation study to receive nivolumab at 1 mg/kg, then 3 mg/kg, every 2 weeks for 2 years.
Twenty-three patients had HL. Thirty-one had B-cell non-Hodgkin lymphoma (NHL), including 11 with FL and 10 with diffuse large B-cell lymphoma (DLBCL).
Twenty-three patients had T-cell NHL, including 5 with PTCL and 13 with CTCL/mycosis fungoides (MF). Twenty-seven patients had multiple myeloma (MM), and 1 had chronic myeloid leukemia.
Patients were heavily pretreated. Seventy-eight percent of HL patients and 26% of T-NHL patients had prior brentuximab vedotin. And 78% (HL), 14% (B-NHL), 9% (T-NHL), and 56% (MM) of patients had a prior autologous transplant.
The median number of prior therapies was 5 (range, 2-15) for HL patients and ranged from 1 to 16 for all patients.
The study’s primary endpoint was safety and tolerability, and the secondary endpoint was efficacy.
Safety and tolerability
Ninety-seven percent of patients had an adverse event, 69% of them related to study treatment and 21% of them treatment-related grade 3-4 events.
Fifteen patients (14%) discontinued treatment due to a related adverse event, including 3 with pneumonitis and 1 each with enteritis, stomatitis, pancreatitis, rash, conjunctivitis, sepsis, diplopia, myositis, neutropenia, myelodysplastic syndrome, increased creatinine phosphokinase, and peripheral neuropathy.
“Immune-related adverse events were generally seen early on and generally of low grade,” Dr Timmerman said. “However, it is notable that there were several grade 3 immune-related adverse events that can be seen as far as 6 months out after the start of therapy.”
These included skin, gastrointestinal, and pulmonary events. Most immune-related adverse events (83%) were resolved using protocol-prescribed procedures.
Efficacy
The overall response rate was 87% for HL, 36% for DLBCL, 40% for FL, 15% for CTCL/MF, 40% for PTCL, and 4% for MM.
Dr Timmerman pointed out that, since ASH, 2 additional conversions from partial response (PR) to complete response (CR) occurred in patients with HL. To date, 6 of 23 HL patients have achieved a CR and 14 a PR.
In B-cell NHL, there were additional conversions from PR to CR in DLBCL, while responses remained the same in FL and in the 4 responders with T-cell lymphomas.
“Intriguingly, there has been 1 late CR in the multiple myeloma cohort, which previously had shown no responses,” Dr Timmerman said.
Durability of response
This study suggests PD-1 blockade can produce durable responses in hematologic malignancies, as it does in melanoma and renal cell carcinoma.
In HL, the median response duration at a median follow-up of 86 weeks has not yet been reached, and half (n=10) of the responses are still ongoing.
In FL, CTCL, and PTCL, the median response duration has not been reached at a median follow-up of 81, 43, and 31 weeks, respectively. Of note, there are ongoing responses in at least half of patients in these tumor types.
In HL, none of the 6 patients in CR has progressed, although there have been some progressions in the PR group.
The rapidity of responses is also notable, Dr Timmerman said.
“[I]t’s very interesting that some patients have resolution of symptoms and improvement of symptoms within even 1 day of starting nivolumab therapy,” he said.
And responses to nivolumab in HL “can be very dramatic,” he added, as illustrated in the following case from the Mayo Clinic.
A patient with multiple sites of bulky FDG-avid tumors was scheduled to enter hospice. But first, he entered the nivolumab trial. Within 6 weeks of initiating treatment, he had achieved a near-CR. This response has been maintained for 2 years.
“The occurrence of very durable responses in the PR and CR groups has led us to question whether patients should go on to allogeneic stem cell transplantation after achieving responses with nivolumab or, rather, continue on nivolumab as long as their response remains,” Dr Timmerman said.
He added that an international, phase 2 trial in HL is underway and is accruing briskly.
Nivolumab was awarded breakthrough designation by the US Food and Drug Administration last year. Breakthrough designation is intended to expedite the development and review of drugs for serious or life-threatening conditions. ![]()
Targeted agent shows early promise for NHL

follicular lymphoma
LUGANO—An anti-CD37 antibody-radionuclide conjugate provides sustained efficacy and a manageable safety profile in patients with relapsed, CD37+ non-Hodgkin lymphoma (NHL), according to researchers.
The drug, 177Lu-DOTA-HH1 (Betalutin), consists of the tumor-specific antibody HH1, which targets the CD37 antigen on the surface of NHL cells, conjugated to the β-emitting isotope lutetium-177 (Lu-177) via the chemical linker DOTA.
In an ongoing, phase 1/2 trial, Betalutin has produced responses in 7 of 12 evaluable patients with relapsed NHL, and 5 of those responses are ongoing.
Grade 3/4 adverse events (AEs) were largely hematologic in nature, and many were transient and reversible. However, grade 3/4 AEs occurred at all 3 dose levels investigated in this study, as did serious AEs.
Arne Kolstad, MD, PhD, of Oslo University Hospital in Norway, and his colleagues reported these results at the 13th International Conference on Malignant Lymphoma (abstract 287*). The study was sponsored by Nordic Nanovector, the company developing Betalutin.
Thus far, the researchers have evaluated 13 patients with relapsed, CD37+ NHL. Twelve patients had a primary diagnosis of follicular lymphoma, and 1 had mantle cell lymphoma (MCL). The patients’ median age was 68 (range, 41-78), and they had received 1 to 8 prior treatments.
In this dose-finding study, the researchers investigated 3 dose levels of Betalutin. Four patients received Betalutin at 10 MBq/kg biweekly, 6 received 15 MBq/kg biweekly, and 3 (including the MCL patient) received 20 MBq/kg biweekly.
All patients received 50 mg of HH1 prior to Betalutin. Patients also received rituximab at 375 mg/m2 on days -28 and -21 (prior to Betalutin on day 0).
Safety and dosing
Dose-limiting toxicities occurred at the 20 MBq/kg biweekly dose, so researchers said 15 MBq/kg biweekly, with HH1 pre-dosing, is the current recommended dose of Betalutin.
Treatment-emergent grade 3 AEs in the 10 MBq/kg group included thrombocytopenia (n=1), neutropenia (n=2), pneumonia (n=1), and pulmonary embolism (n=1). There were no grade 4 AEs in this group.
In the 15 MBq/kg group, 2 patients had grade 3 thrombocytopenia, and 1 had grade 4. One patient each had grade 3 and 4 neutropenia.
Grade 3/4 AEs in the 20 MBq/kg group included grade 4 thrombocytopenia (n=3), grade 3 (n=1) and grade 4 (n=2) neutropenia, and grade 3 epistaxis (n=1).
Serious AEs included pulmonary embolism (1 in the 10 MBq/kg group), pneumonia (1 in the 10 MBq/kg group), atrial fibrillation (2 in the 15 MBq/kg group), thrombocytopenia (1 in the 20 MBq/kg group), and epistaxis (1 in the 20 MBq/kg group).
The researchers said all hematologic AEs were transient and reversible. They also pointed out that 6 patients in this trial have been followed for a year or more, and there have been no secondary malignancies or other events that would suggest long-term toxicity.
Efficacy and next steps
Twelve patients were evaluable for efficacy. Seven patients responded to treatment, including 4 complete responses (CRs) and 3 partial responses. Two patients had stable disease, and 3 progressed. Eight patients had a 50% or greater reduction in tumor volume.
The median response duration has not been reached, and 5 patients’ responses are ongoing. The duration of response in these patients ranges from 6 months to more than 21 months. All 4 patients who achieved a CR (including the MCL patient) are still in CR.
The researchers concluded that Betalutin delivers a highly favorable response rate, with durable clinical responses, and the drug has a predictable and manageable safety profile.
They have opened a new arm of this study to evaluate the safety and efficacy of Betalutin at 15 MBq/kg biweekly and 17.5 MBq/kg biweekly without HH1 pre-dosing. ![]()
*Information in the abstract differs from that presented at the meeting.

follicular lymphoma
LUGANO—An anti-CD37 antibody-radionuclide conjugate provides sustained efficacy and a manageable safety profile in patients with relapsed, CD37+ non-Hodgkin lymphoma (NHL), according to researchers.
The drug, 177Lu-DOTA-HH1 (Betalutin), consists of the tumor-specific antibody HH1, which targets the CD37 antigen on the surface of NHL cells, conjugated to the β-emitting isotope lutetium-177 (Lu-177) via the chemical linker DOTA.
In an ongoing, phase 1/2 trial, Betalutin has produced responses in 7 of 12 evaluable patients with relapsed NHL, and 5 of those responses are ongoing.
Grade 3/4 adverse events (AEs) were largely hematologic in nature, and many were transient and reversible. However, grade 3/4 AEs occurred at all 3 dose levels investigated in this study, as did serious AEs.
Arne Kolstad, MD, PhD, of Oslo University Hospital in Norway, and his colleagues reported these results at the 13th International Conference on Malignant Lymphoma (abstract 287*). The study was sponsored by Nordic Nanovector, the company developing Betalutin.
Thus far, the researchers have evaluated 13 patients with relapsed, CD37+ NHL. Twelve patients had a primary diagnosis of follicular lymphoma, and 1 had mantle cell lymphoma (MCL). The patients’ median age was 68 (range, 41-78), and they had received 1 to 8 prior treatments.
In this dose-finding study, the researchers investigated 3 dose levels of Betalutin. Four patients received Betalutin at 10 MBq/kg biweekly, 6 received 15 MBq/kg biweekly, and 3 (including the MCL patient) received 20 MBq/kg biweekly.
All patients received 50 mg of HH1 prior to Betalutin. Patients also received rituximab at 375 mg/m2 on days -28 and -21 (prior to Betalutin on day 0).
Safety and dosing
Dose-limiting toxicities occurred at the 20 MBq/kg biweekly dose, so researchers said 15 MBq/kg biweekly, with HH1 pre-dosing, is the current recommended dose of Betalutin.
Treatment-emergent grade 3 AEs in the 10 MBq/kg group included thrombocytopenia (n=1), neutropenia (n=2), pneumonia (n=1), and pulmonary embolism (n=1). There were no grade 4 AEs in this group.
In the 15 MBq/kg group, 2 patients had grade 3 thrombocytopenia, and 1 had grade 4. One patient each had grade 3 and 4 neutropenia.
Grade 3/4 AEs in the 20 MBq/kg group included grade 4 thrombocytopenia (n=3), grade 3 (n=1) and grade 4 (n=2) neutropenia, and grade 3 epistaxis (n=1).
Serious AEs included pulmonary embolism (1 in the 10 MBq/kg group), pneumonia (1 in the 10 MBq/kg group), atrial fibrillation (2 in the 15 MBq/kg group), thrombocytopenia (1 in the 20 MBq/kg group), and epistaxis (1 in the 20 MBq/kg group).
The researchers said all hematologic AEs were transient and reversible. They also pointed out that 6 patients in this trial have been followed for a year or more, and there have been no secondary malignancies or other events that would suggest long-term toxicity.
Efficacy and next steps
Twelve patients were evaluable for efficacy. Seven patients responded to treatment, including 4 complete responses (CRs) and 3 partial responses. Two patients had stable disease, and 3 progressed. Eight patients had a 50% or greater reduction in tumor volume.
The median response duration has not been reached, and 5 patients’ responses are ongoing. The duration of response in these patients ranges from 6 months to more than 21 months. All 4 patients who achieved a CR (including the MCL patient) are still in CR.
The researchers concluded that Betalutin delivers a highly favorable response rate, with durable clinical responses, and the drug has a predictable and manageable safety profile.
They have opened a new arm of this study to evaluate the safety and efficacy of Betalutin at 15 MBq/kg biweekly and 17.5 MBq/kg biweekly without HH1 pre-dosing. ![]()
*Information in the abstract differs from that presented at the meeting.

follicular lymphoma
LUGANO—An anti-CD37 antibody-radionuclide conjugate provides sustained efficacy and a manageable safety profile in patients with relapsed, CD37+ non-Hodgkin lymphoma (NHL), according to researchers.
The drug, 177Lu-DOTA-HH1 (Betalutin), consists of the tumor-specific antibody HH1, which targets the CD37 antigen on the surface of NHL cells, conjugated to the β-emitting isotope lutetium-177 (Lu-177) via the chemical linker DOTA.
In an ongoing, phase 1/2 trial, Betalutin has produced responses in 7 of 12 evaluable patients with relapsed NHL, and 5 of those responses are ongoing.
Grade 3/4 adverse events (AEs) were largely hematologic in nature, and many were transient and reversible. However, grade 3/4 AEs occurred at all 3 dose levels investigated in this study, as did serious AEs.
Arne Kolstad, MD, PhD, of Oslo University Hospital in Norway, and his colleagues reported these results at the 13th International Conference on Malignant Lymphoma (abstract 287*). The study was sponsored by Nordic Nanovector, the company developing Betalutin.
Thus far, the researchers have evaluated 13 patients with relapsed, CD37+ NHL. Twelve patients had a primary diagnosis of follicular lymphoma, and 1 had mantle cell lymphoma (MCL). The patients’ median age was 68 (range, 41-78), and they had received 1 to 8 prior treatments.
In this dose-finding study, the researchers investigated 3 dose levels of Betalutin. Four patients received Betalutin at 10 MBq/kg biweekly, 6 received 15 MBq/kg biweekly, and 3 (including the MCL patient) received 20 MBq/kg biweekly.
All patients received 50 mg of HH1 prior to Betalutin. Patients also received rituximab at 375 mg/m2 on days -28 and -21 (prior to Betalutin on day 0).
Safety and dosing
Dose-limiting toxicities occurred at the 20 MBq/kg biweekly dose, so researchers said 15 MBq/kg biweekly, with HH1 pre-dosing, is the current recommended dose of Betalutin.
Treatment-emergent grade 3 AEs in the 10 MBq/kg group included thrombocytopenia (n=1), neutropenia (n=2), pneumonia (n=1), and pulmonary embolism (n=1). There were no grade 4 AEs in this group.
In the 15 MBq/kg group, 2 patients had grade 3 thrombocytopenia, and 1 had grade 4. One patient each had grade 3 and 4 neutropenia.
Grade 3/4 AEs in the 20 MBq/kg group included grade 4 thrombocytopenia (n=3), grade 3 (n=1) and grade 4 (n=2) neutropenia, and grade 3 epistaxis (n=1).
Serious AEs included pulmonary embolism (1 in the 10 MBq/kg group), pneumonia (1 in the 10 MBq/kg group), atrial fibrillation (2 in the 15 MBq/kg group), thrombocytopenia (1 in the 20 MBq/kg group), and epistaxis (1 in the 20 MBq/kg group).
The researchers said all hematologic AEs were transient and reversible. They also pointed out that 6 patients in this trial have been followed for a year or more, and there have been no secondary malignancies or other events that would suggest long-term toxicity.
Efficacy and next steps
Twelve patients were evaluable for efficacy. Seven patients responded to treatment, including 4 complete responses (CRs) and 3 partial responses. Two patients had stable disease, and 3 progressed. Eight patients had a 50% or greater reduction in tumor volume.
The median response duration has not been reached, and 5 patients’ responses are ongoing. The duration of response in these patients ranges from 6 months to more than 21 months. All 4 patients who achieved a CR (including the MCL patient) are still in CR.
The researchers concluded that Betalutin delivers a highly favorable response rate, with durable clinical responses, and the drug has a predictable and manageable safety profile.
They have opened a new arm of this study to evaluate the safety and efficacy of Betalutin at 15 MBq/kg biweekly and 17.5 MBq/kg biweekly without HH1 pre-dosing.
*Information in the abstract differs from that presented at the meeting.
Thiotepa, rituximab improve response in CNS lymphoma

site of 13-ICML
LUGANO—Adding thiotepa and rituximab to the treatment of primary central nervous system (CNS) lymphoma is feasible from a safety perspective and has yielded promising results, according to new research.
An analysis of the IELSG 32 trial—in which patients received methotrexate and cytarabine alone, with rituximab, or with rituximab and thiotepa—has shown the 4-drug regimen improves responses and progression-free survival.
IELSG 32 builds on the foundation of the IELSG 20 trial to determine the best induction therapy for patients with primary CNS lymphoma. In IELSG 20, the complete response (CR) rate was higher among patients receiving high-dose methotrexate and cytarabine than in patients receiving methotrexate alone.
So the researchers decided to investigate whether rituximab and/or thiotepa added to the regimen would impact patient outcome. Rituximab has been associated with improved CR rates in primary CNS lymphoma, and thiotepa is active against aggressive lymphomas. Thiotepa is also able to cross the blood–brain barrier.
Andrés J.M. Ferreri, MD, of IRCCS Ospedale San Raffaele in Milan, Italy, reported the results of this research on behalf of the International Extranodal Lymphoma Study Group (IELSG) at the 13th International Conference on Malignant Lymphoma (abstract 009).
Treatment and toxicity
The investigators randomized 227 patients from 53 centers in 5 countries to 4 cycles of treatment in 3 cohorts:
- Arm A consisted of 4 cycles of methotrexate (3.5 g/m2) on day 1 and cytarabine (2 g/m2) twice a day on days 2 and 3 every 3 weeks.
- Arm B added rituximab (375 mg/m2) on days 5 and 0 to the regimen.
- Arm C added rituximab and thiotepa (30 mg/m2) on day 4 to the regimen.
Eight patients were excluded for various reasons, including incorrect diagnosis. So 219 patients received therapy, 75 in arm A, 69 in arm B, and 75 in arm C.
Patients were a median age of 58 years in arm A and 57 in arms B and C, and the majority were male. More than 80% of patients in all arms were intermediate- or high-risk according to IELSG. And all patients had the diffuse large B-cell lymphoma histotype.
Patients in arm A received 74% of the planned courses, those in arm B received 86%, and those in arm C received 91%. The relative dose intensity across all arms of each drug administered was not significantly different among the arms.
“As expected, hematologic toxicity was common, with grade 4 neutropenia (P=0.01) and thrombocytopenia (P=0.0001) being significantly more common for arm C,” Dr Ferreri said. “However, this was not associated with an increasing array of severe infections, interruptions, toxicity, or toxic deaths.”
Peripheral blood stem cell collection was successful in 94% of patients in arms A and C and 96% of patients in arm B.
Response rates
The overall response rate (ORR) was 72% in IELSG 32, compared to 54% in IELSG 20. But the CR rate was not significantly higher in IELSG 32 than in IELSG 20, at 34% and 31%, respectively.
“There are many explanations for this,” Dr Ferreri said. “But I think it was because there were a significantly greater number of patients with higher IELSG risk [in IELSG 32], a higher proportion of poor-prognosis patients.”
Patients in arm C had significantly higher response rates than patients in the other 2 arms, with a CR rate of 49%, a partial response (PR) rate of 37%, and an ORR of 87%.
This compared to a CR rate of 23% in arm A and 30% in arm B, a PR rate of 31% in arm A and 30% in arm B, and an ORR of 53% in arm A and 74% in arm B.
The investigators also analyzed activity according to IELSG risk.
“Arm C was significantly more active in all the 3 subgroups,” Dr Ferreri observed, “and importantly, the overall response rate and complete remission rate were similar for each arm in the 3 different risk groups.”
Second randomization and survival
One hundred and eighteen patients went on to a second randomization, 35 from arm A, 35 from arm B, and 48 from arm C.
Fifty-nine patients were randomized to the whole-brain radiotherapy cohort, and 59 to the carmustine-thiotepa-autologous stem cell transplant cohort.
At a median follow-up of 21 months, 110 patients remain failure free, 32% from arm A, 54% from arm B, and 65% from arm C. Failure in 97% of the cases was due to primary site involvement, usually the brain.
Fifty-six percent of the patients are still alive, 39% in arm A, 59% in arm B, and 69% in arm C.
Ninety-seven patients died, 73 from lymphoma, 15 from toxicity of the first-line treatment, 2 from toxicity of the salvage regimen, 2 from neurotoxicity, and 5 from other causes.
Dr Ferreri concluded that the MATRIX regimen—the addition of rituximab and thiotepa to methotrexate and cytarabine—was associated with significant improvements in CR rate, ORR, and progression-free and overall survival.
The addition of rituximab and thiotepa did not increase toxicity, with the exception of greater hematologic adverse events, nor did the drugs increase the rates of severe complications. The agents also allowed for high rates of successful stem cell collection.

site of 13-ICML
LUGANO—Adding thiotepa and rituximab to the treatment of primary central nervous system (CNS) lymphoma is feasible from a safety perspective and has yielded promising results, according to new research.
An analysis of the IELSG 32 trial—in which patients received methotrexate and cytarabine alone, with rituximab, or with rituximab and thiotepa—has shown the 4-drug regimen improves responses and progression-free survival.
IELSG 32 builds on the foundation of the IELSG 20 trial to determine the best induction therapy for patients with primary CNS lymphoma. In IELSG 20, the complete response (CR) rate was higher among patients receiving high-dose methotrexate and cytarabine than in patients receiving methotrexate alone.
So the researchers decided to investigate whether rituximab and/or thiotepa added to the regimen would impact patient outcome. Rituximab has been associated with improved CR rates in primary CNS lymphoma, and thiotepa is active against aggressive lymphomas. Thiotepa is also able to cross the blood–brain barrier.
Andrés J.M. Ferreri, MD, of IRCCS Ospedale San Raffaele in Milan, Italy, reported the results of this research on behalf of the International Extranodal Lymphoma Study Group (IELSG) at the 13th International Conference on Malignant Lymphoma (abstract 009).
Treatment and toxicity
The investigators randomized 227 patients from 53 centers in 5 countries to 4 cycles of treatment in 3 cohorts:
- Arm A consisted of 4 cycles of methotrexate (3.5 g/m2) on day 1 and cytarabine (2 g/m2) twice a day on days 2 and 3 every 3 weeks.
- Arm B added rituximab (375 mg/m2) on days 5 and 0 to the regimen.
- Arm C added rituximab and thiotepa (30 mg/m2) on day 4 to the regimen.
Eight patients were excluded for various reasons, including incorrect diagnosis. So 219 patients received therapy, 75 in arm A, 69 in arm B, and 75 in arm C.
Patients were a median age of 58 years in arm A and 57 in arms B and C, and the majority were male. More than 80% of patients in all arms were intermediate- or high-risk according to IELSG. And all patients had the diffuse large B-cell lymphoma histotype.
Patients in arm A received 74% of the planned courses, those in arm B received 86%, and those in arm C received 91%. The relative dose intensity across all arms of each drug administered was not significantly different among the arms.
“As expected, hematologic toxicity was common, with grade 4 neutropenia (P=0.01) and thrombocytopenia (P=0.0001) being significantly more common for arm C,” Dr Ferreri said. “However, this was not associated with an increasing array of severe infections, interruptions, toxicity, or toxic deaths.”
Peripheral blood stem cell collection was successful in 94% of patients in arms A and C and 96% of patients in arm B.
Response rates
The overall response rate (ORR) was 72% in IELSG 32, compared to 54% in IELSG 20. But the CR rate was not significantly higher in IELSG 32 than in IELSG 20, at 34% and 31%, respectively.
“There are many explanations for this,” Dr Ferreri said. “But I think it was because there were a significantly greater number of patients with higher IELSG risk [in IELSG 32], a higher proportion of poor-prognosis patients.”
Patients in arm C had significantly higher response rates than patients in the other 2 arms, with a CR rate of 49%, a partial response (PR) rate of 37%, and an ORR of 87%.
This compared to a CR rate of 23% in arm A and 30% in arm B, a PR rate of 31% in arm A and 30% in arm B, and an ORR of 53% in arm A and 74% in arm B.
The investigators also analyzed activity according to IELSG risk.
“Arm C was significantly more active in all the 3 subgroups,” Dr Ferreri observed, “and importantly, the overall response rate and complete remission rate were similar for each arm in the 3 different risk groups.”
Second randomization and survival
One hundred and eighteen patients went on to a second randomization, 35 from arm A, 35 from arm B, and 48 from arm C.
Fifty-nine patients were randomized to the whole-brain radiotherapy cohort, and 59 to the carmustine-thiotepa-autologous stem cell transplant cohort.
At a median follow-up of 21 months, 110 patients remain failure free, 32% from arm A, 54% from arm B, and 65% from arm C. Failure in 97% of the cases was due to primary site involvement, usually the brain.
Fifty-six percent of the patients are still alive, 39% in arm A, 59% in arm B, and 69% in arm C.
Ninety-seven patients died, 73 from lymphoma, 15 from toxicity of the first-line treatment, 2 from toxicity of the salvage regimen, 2 from neurotoxicity, and 5 from other causes.
Dr Ferreri concluded that the MATRIX regimen—the addition of rituximab and thiotepa to methotrexate and cytarabine—was associated with significant improvements in CR rate, ORR, and progression-free and overall survival.
The addition of rituximab and thiotepa did not increase toxicity, with the exception of greater hematologic adverse events, nor did the drugs increase the rates of severe complications. The agents also allowed for high rates of successful stem cell collection.

site of 13-ICML
LUGANO—Adding thiotepa and rituximab to the treatment of primary central nervous system (CNS) lymphoma is feasible from a safety perspective and has yielded promising results, according to new research.
An analysis of the IELSG 32 trial—in which patients received methotrexate and cytarabine alone, with rituximab, or with rituximab and thiotepa—has shown the 4-drug regimen improves responses and progression-free survival.
IELSG 32 builds on the foundation of the IELSG 20 trial to determine the best induction therapy for patients with primary CNS lymphoma. In IELSG 20, the complete response (CR) rate was higher among patients receiving high-dose methotrexate and cytarabine than in patients receiving methotrexate alone.
So the researchers decided to investigate whether rituximab and/or thiotepa added to the regimen would impact patient outcome. Rituximab has been associated with improved CR rates in primary CNS lymphoma, and thiotepa is active against aggressive lymphomas. Thiotepa is also able to cross the blood–brain barrier.
Andrés J.M. Ferreri, MD, of IRCCS Ospedale San Raffaele in Milan, Italy, reported the results of this research on behalf of the International Extranodal Lymphoma Study Group (IELSG) at the 13th International Conference on Malignant Lymphoma (abstract 009).
Treatment and toxicity
The investigators randomized 227 patients from 53 centers in 5 countries to 4 cycles of treatment in 3 cohorts:
- Arm A consisted of 4 cycles of methotrexate (3.5 g/m2) on day 1 and cytarabine (2 g/m2) twice a day on days 2 and 3 every 3 weeks.
- Arm B added rituximab (375 mg/m2) on days 5 and 0 to the regimen.
- Arm C added rituximab and thiotepa (30 mg/m2) on day 4 to the regimen.
Eight patients were excluded for various reasons, including incorrect diagnosis. So 219 patients received therapy, 75 in arm A, 69 in arm B, and 75 in arm C.
Patients were a median age of 58 years in arm A and 57 in arms B and C, and the majority were male. More than 80% of patients in all arms were intermediate- or high-risk according to IELSG. And all patients had the diffuse large B-cell lymphoma histotype.
Patients in arm A received 74% of the planned courses, those in arm B received 86%, and those in arm C received 91%. The relative dose intensity across all arms of each drug administered was not significantly different among the arms.
“As expected, hematologic toxicity was common, with grade 4 neutropenia (P=0.01) and thrombocytopenia (P=0.0001) being significantly more common for arm C,” Dr Ferreri said. “However, this was not associated with an increasing array of severe infections, interruptions, toxicity, or toxic deaths.”
Peripheral blood stem cell collection was successful in 94% of patients in arms A and C and 96% of patients in arm B.
Response rates
The overall response rate (ORR) was 72% in IELSG 32, compared to 54% in IELSG 20. But the CR rate was not significantly higher in IELSG 32 than in IELSG 20, at 34% and 31%, respectively.
“There are many explanations for this,” Dr Ferreri said. “But I think it was because there were a significantly greater number of patients with higher IELSG risk [in IELSG 32], a higher proportion of poor-prognosis patients.”
Patients in arm C had significantly higher response rates than patients in the other 2 arms, with a CR rate of 49%, a partial response (PR) rate of 37%, and an ORR of 87%.
This compared to a CR rate of 23% in arm A and 30% in arm B, a PR rate of 31% in arm A and 30% in arm B, and an ORR of 53% in arm A and 74% in arm B.
The investigators also analyzed activity according to IELSG risk.
“Arm C was significantly more active in all the 3 subgroups,” Dr Ferreri observed, “and importantly, the overall response rate and complete remission rate were similar for each arm in the 3 different risk groups.”
Second randomization and survival
One hundred and eighteen patients went on to a second randomization, 35 from arm A, 35 from arm B, and 48 from arm C.
Fifty-nine patients were randomized to the whole-brain radiotherapy cohort, and 59 to the carmustine-thiotepa-autologous stem cell transplant cohort.
At a median follow-up of 21 months, 110 patients remain failure free, 32% from arm A, 54% from arm B, and 65% from arm C. Failure in 97% of the cases was due to primary site involvement, usually the brain.
Fifty-six percent of the patients are still alive, 39% in arm A, 59% in arm B, and 69% in arm C.
Ninety-seven patients died, 73 from lymphoma, 15 from toxicity of the first-line treatment, 2 from toxicity of the salvage regimen, 2 from neurotoxicity, and 5 from other causes.
Dr Ferreri concluded that the MATRIX regimen—the addition of rituximab and thiotepa to methotrexate and cytarabine—was associated with significant improvements in CR rate, ORR, and progression-free and overall survival.
The addition of rituximab and thiotepa did not increase toxicity, with the exception of greater hematologic adverse events, nor did the drugs increase the rates of severe complications. The agents also allowed for high rates of successful stem cell collection.
Measuring end-of-life care in oncology practices: learning from the care of the dying
Background There is increased interest among oncology and palliative professionals in providing appropriately timed hospice services for cancer patients. End of life (EoL) metrics have been included in oncology quality programs, but accurate EoL data and benchmarks are hard to obtain.
Objective To improve EoL care by measuring patterns of care among recently deceased patients.
Methods Care utilization among deceased patients was analyzed by using software integrated with patient electronic health records. The data was verified by chart review.
Results Of 179 cancer deaths, tumor registry data differed from chart review in 7% of cases with regard to dates and/or location of death. Institutional EoL metrics were significantly affected by a large number of patients (37%) with advanced illnesses who had clinical diagnoses of cancer made at the end of life, but who had not been managed by oncologists. This population of patients who had not been managed by oncologists was older, less likely to use hospice, and more likely to use the intensive care unit than were oncologist-managed cancer patients. Among the patients of individual oncologists, the median stay in hospice ranged from 6-28 days. Data collection and chart review took an average of 27 minutes per case with combined efforts by a data analyst and oncology practitioner.
Limitations Single institution with comprehensive electronic medical record; some patients were treated outside of the system.
Conclusion Acquiring accurate data on EoL metrics is time consuming. Compared with chart review, other data sources have inaccuracies and include some patients who have not been managed by oncologists. Accurate attribution to individual physicians requires chart review by an experienced clinician.
Click on the PDF icon at the top of this introduction to read the full article.
Background There is increased interest among oncology and palliative professionals in providing appropriately timed hospice services for cancer patients. End of life (EoL) metrics have been included in oncology quality programs, but accurate EoL data and benchmarks are hard to obtain.
Objective To improve EoL care by measuring patterns of care among recently deceased patients.
Methods Care utilization among deceased patients was analyzed by using software integrated with patient electronic health records. The data was verified by chart review.
Results Of 179 cancer deaths, tumor registry data differed from chart review in 7% of cases with regard to dates and/or location of death. Institutional EoL metrics were significantly affected by a large number of patients (37%) with advanced illnesses who had clinical diagnoses of cancer made at the end of life, but who had not been managed by oncologists. This population of patients who had not been managed by oncologists was older, less likely to use hospice, and more likely to use the intensive care unit than were oncologist-managed cancer patients. Among the patients of individual oncologists, the median stay in hospice ranged from 6-28 days. Data collection and chart review took an average of 27 minutes per case with combined efforts by a data analyst and oncology practitioner.
Limitations Single institution with comprehensive electronic medical record; some patients were treated outside of the system.
Conclusion Acquiring accurate data on EoL metrics is time consuming. Compared with chart review, other data sources have inaccuracies and include some patients who have not been managed by oncologists. Accurate attribution to individual physicians requires chart review by an experienced clinician.
Click on the PDF icon at the top of this introduction to read the full article.
Background There is increased interest among oncology and palliative professionals in providing appropriately timed hospice services for cancer patients. End of life (EoL) metrics have been included in oncology quality programs, but accurate EoL data and benchmarks are hard to obtain.
Objective To improve EoL care by measuring patterns of care among recently deceased patients.
Methods Care utilization among deceased patients was analyzed by using software integrated with patient electronic health records. The data was verified by chart review.
Results Of 179 cancer deaths, tumor registry data differed from chart review in 7% of cases with regard to dates and/or location of death. Institutional EoL metrics were significantly affected by a large number of patients (37%) with advanced illnesses who had clinical diagnoses of cancer made at the end of life, but who had not been managed by oncologists. This population of patients who had not been managed by oncologists was older, less likely to use hospice, and more likely to use the intensive care unit than were oncologist-managed cancer patients. Among the patients of individual oncologists, the median stay in hospice ranged from 6-28 days. Data collection and chart review took an average of 27 minutes per case with combined efforts by a data analyst and oncology practitioner.
Limitations Single institution with comprehensive electronic medical record; some patients were treated outside of the system.
Conclusion Acquiring accurate data on EoL metrics is time consuming. Compared with chart review, other data sources have inaccuracies and include some patients who have not been managed by oncologists. Accurate attribution to individual physicians requires chart review by an experienced clinician.
Click on the PDF icon at the top of this introduction to read the full article.
EZH2 inhibitor proves active in rel/ref NHL

LUGANO—The EZH2 inhibitor tazemetostat (EPZ-6438) has shown “meaningful clinical activity” as monotherapy in patients with advanced non-Hodgkin lymphoma (NHL), according to researchers.
In a phase 1 trial, 9 of the 15 evaluable NHL patients achieved an objective response to tazemetostat.
This included 2 ongoing complete responses (CRs), 1 in a patient with diffuse large B-cell lymphoma (DLBCL) and 1 in a patient with follicular lymphoma (FL).
It also included a partial response (PR) in the first treated patient with an EZH2 mutation.
And researchers said the drug was largely well-tolerated, as most adverse events were grade 1 or 2.
“The breadth, depth, and durability of responses seen in NHL patients among multiple histologies continue to impress, as does the safety and tolerability of tazemetostat in this phase 1 study,” said Vincent Ribrag, MD, of Institut Gustave Roussy in Villejuif, France.
“Among the patients in the dose-escalation cohorts, we have seen a noteworthy deepening of responses over time, and, in the first treated patient with an EZH2 tumor mutation, we have seen a partial response, which is very encouraging.”
Dr Ribrag presented these results at the 13th International Conference on Malignant Lymphoma (abstract 145*). The study, which was previously presented at the 26th EORTC-NCI-AACR Symposium on Molecular Targets and Cancer Therapeutics, was sponsored by Epizyme, Inc., the company developing tazemetostat.
The phase 1 trial has enrolled 19 patients with relapsed or refractory B-cell NHL and 26 patients with advanced solid tumors.
Researchers have evaluated 5 cohorts of patients in the dose-escalation portion of the study—100 mg, 200 mg, 400 mg, 800 mg, and 1600 mg—and 2 cohorts—800 mg and 1600 mg—in the dose-expansion phase. All doses of tazemetostat were given twice daily.
The 19 NHL patients had a median age of 61 (range, 24-84) and were heavily pretreated. Eighty-five percent had received 3 or more prior therapies, and 37% had received 5 or more prior therapies.
Thirty-seven percent of patients were refractory to their last prior regimen, and 26% had received a prior autologous hematopoietic stem cell transplant.
Dosing and efficacy
As of June 8, 2015, 15 NHL patients were evaluable for efficacy. Nine had achieved an objective response, including 2 patients with an ongoing CR. All responses were observed between 2 and 10 months on therapy.
Five of the 9 evaluable patients with DLBCL achieved an objective response. One DLBCL patient with a CR remains on study at 18 months of treatment.
Three of 5 evaluable patients with follicular lymphoma (FL) achieved an objective response. One FL patient with a CR remains on study at 13 months, and 1 FL patient with a PR remains on study at 13 months.
The only patient with marginal zone lymphoma achieved a PR and continues on study at 11 months.
One of the 14 patients evaluated for EZH2 status has a specific EZH2 tumor mutation (Y646H). This patient, who had DLBCL that relapsed or was refractory to 6 previous treatment regimens, achieved a PR after 16 weeks of therapy and remains on study.
The recommended phase 2 dose of tazemetostat is 800 mg twice daily.
Adverse events and next steps
All of the 45 enrolled patients were evaluable for safety. Treatment-related adverse events included asthenia (n=10), nausea (n=6), dyspepsia (n=5), thrombocytopenia (n=4), anorexia (n=4), anemia (n=4), vomiting (n=3), constipation (n=2), muscle spasm (n=2), hypertension (n=2), neutropenia (n=2), and elevated transaminase (n=1).
There were 5 grade 3 or higher adverse events related to treatment, including grade 3 anorexia, grade 3 hypertension, grade 3 transaminase elevation, grade 4 thrombocytopenia, and grade 4 neutropenia.
Epizyme plans to report a further update from this trial by the end of this year. The company is now enrolling patients in a phase 2 study of tazemetostat monotherapy in patients with relapsed or refractory NHL, stratified by cell of origin and EZH2 mutation status.
Epizyme is also planning a phase 2 trial of tazemetostat in adults with INI1-deficient solid tumors, a phase 1 study of pediatric patients with INI1-deficient solid tumors, a combination study of tazemetostat with R-CHOP in patients with DLBCL, and a combination study of tazemetostat with a B-cell signaling agent or other emerging targeted therapies for B-cell lymphomas.
*Information in the abstract differs from that presented at the meeting.

LUGANO—The EZH2 inhibitor tazemetostat (EPZ-6438) has shown “meaningful clinical activity” as monotherapy in patients with advanced non-Hodgkin lymphoma (NHL), according to researchers.
In a phase 1 trial, 9 of the 15 evaluable NHL patients achieved an objective response to tazemetostat.
This included 2 ongoing complete responses (CRs), 1 in a patient with diffuse large B-cell lymphoma (DLBCL) and 1 in a patient with follicular lymphoma (FL).
It also included a partial response (PR) in the first treated patient with an EZH2 mutation.
And researchers said the drug was largely well-tolerated, as most adverse events were grade 1 or 2.
“The breadth, depth, and durability of responses seen in NHL patients among multiple histologies continue to impress, as does the safety and tolerability of tazemetostat in this phase 1 study,” said Vincent Ribrag, MD, of Institut Gustave Roussy in Villejuif, France.
“Among the patients in the dose-escalation cohorts, we have seen a noteworthy deepening of responses over time, and, in the first treated patient with an EZH2 tumor mutation, we have seen a partial response, which is very encouraging.”
Dr Ribrag presented these results at the 13th International Conference on Malignant Lymphoma (abstract 145*). The study, which was previously presented at the 26th EORTC-NCI-AACR Symposium on Molecular Targets and Cancer Therapeutics, was sponsored by Epizyme, Inc., the company developing tazemetostat.
The phase 1 trial has enrolled 19 patients with relapsed or refractory B-cell NHL and 26 patients with advanced solid tumors.
Researchers have evaluated 5 cohorts of patients in the dose-escalation portion of the study—100 mg, 200 mg, 400 mg, 800 mg, and 1600 mg—and 2 cohorts—800 mg and 1600 mg—in the dose-expansion phase. All doses of tazemetostat were given twice daily.
The 19 NHL patients had a median age of 61 (range, 24-84) and were heavily pretreated. Eighty-five percent had received 3 or more prior therapies, and 37% had received 5 or more prior therapies.
Thirty-seven percent of patients were refractory to their last prior regimen, and 26% had received a prior autologous hematopoietic stem cell transplant.
Dosing and efficacy
As of June 8, 2015, 15 NHL patients were evaluable for efficacy. Nine had achieved an objective response, including 2 patients with an ongoing CR. All responses were observed between 2 and 10 months on therapy.
Five of the 9 evaluable patients with DLBCL achieved an objective response. One DLBCL patient with a CR remains on study at 18 months of treatment.
Three of 5 evaluable patients with follicular lymphoma (FL) achieved an objective response. One FL patient with a CR remains on study at 13 months, and 1 FL patient with a PR remains on study at 13 months.
The only patient with marginal zone lymphoma achieved a PR and continues on study at 11 months.
One of the 14 patients evaluated for EZH2 status has a specific EZH2 tumor mutation (Y646H). This patient, who had DLBCL that relapsed or was refractory to 6 previous treatment regimens, achieved a PR after 16 weeks of therapy and remains on study.
The recommended phase 2 dose of tazemetostat is 800 mg twice daily.
Adverse events and next steps
All of the 45 enrolled patients were evaluable for safety. Treatment-related adverse events included asthenia (n=10), nausea (n=6), dyspepsia (n=5), thrombocytopenia (n=4), anorexia (n=4), anemia (n=4), vomiting (n=3), constipation (n=2), muscle spasm (n=2), hypertension (n=2), neutropenia (n=2), and elevated transaminase (n=1).
There were 5 grade 3 or higher adverse events related to treatment, including grade 3 anorexia, grade 3 hypertension, grade 3 transaminase elevation, grade 4 thrombocytopenia, and grade 4 neutropenia.
Epizyme plans to report a further update from this trial by the end of this year. The company is now enrolling patients in a phase 2 study of tazemetostat monotherapy in patients with relapsed or refractory NHL, stratified by cell of origin and EZH2 mutation status.
Epizyme is also planning a phase 2 trial of tazemetostat in adults with INI1-deficient solid tumors, a phase 1 study of pediatric patients with INI1-deficient solid tumors, a combination study of tazemetostat with R-CHOP in patients with DLBCL, and a combination study of tazemetostat with a B-cell signaling agent or other emerging targeted therapies for B-cell lymphomas.
*Information in the abstract differs from that presented at the meeting.

LUGANO—The EZH2 inhibitor tazemetostat (EPZ-6438) has shown “meaningful clinical activity” as monotherapy in patients with advanced non-Hodgkin lymphoma (NHL), according to researchers.
In a phase 1 trial, 9 of the 15 evaluable NHL patients achieved an objective response to tazemetostat.
This included 2 ongoing complete responses (CRs), 1 in a patient with diffuse large B-cell lymphoma (DLBCL) and 1 in a patient with follicular lymphoma (FL).
It also included a partial response (PR) in the first treated patient with an EZH2 mutation.
And researchers said the drug was largely well-tolerated, as most adverse events were grade 1 or 2.
“The breadth, depth, and durability of responses seen in NHL patients among multiple histologies continue to impress, as does the safety and tolerability of tazemetostat in this phase 1 study,” said Vincent Ribrag, MD, of Institut Gustave Roussy in Villejuif, France.
“Among the patients in the dose-escalation cohorts, we have seen a noteworthy deepening of responses over time, and, in the first treated patient with an EZH2 tumor mutation, we have seen a partial response, which is very encouraging.”
Dr Ribrag presented these results at the 13th International Conference on Malignant Lymphoma (abstract 145*). The study, which was previously presented at the 26th EORTC-NCI-AACR Symposium on Molecular Targets and Cancer Therapeutics, was sponsored by Epizyme, Inc., the company developing tazemetostat.
The phase 1 trial has enrolled 19 patients with relapsed or refractory B-cell NHL and 26 patients with advanced solid tumors.
Researchers have evaluated 5 cohorts of patients in the dose-escalation portion of the study—100 mg, 200 mg, 400 mg, 800 mg, and 1600 mg—and 2 cohorts—800 mg and 1600 mg—in the dose-expansion phase. All doses of tazemetostat were given twice daily.
The 19 NHL patients had a median age of 61 (range, 24-84) and were heavily pretreated. Eighty-five percent had received 3 or more prior therapies, and 37% had received 5 or more prior therapies.
Thirty-seven percent of patients were refractory to their last prior regimen, and 26% had received a prior autologous hematopoietic stem cell transplant.
Dosing and efficacy
As of June 8, 2015, 15 NHL patients were evaluable for efficacy. Nine had achieved an objective response, including 2 patients with an ongoing CR. All responses were observed between 2 and 10 months on therapy.
Five of the 9 evaluable patients with DLBCL achieved an objective response. One DLBCL patient with a CR remains on study at 18 months of treatment.
Three of 5 evaluable patients with follicular lymphoma (FL) achieved an objective response. One FL patient with a CR remains on study at 13 months, and 1 FL patient with a PR remains on study at 13 months.
The only patient with marginal zone lymphoma achieved a PR and continues on study at 11 months.
One of the 14 patients evaluated for EZH2 status has a specific EZH2 tumor mutation (Y646H). This patient, who had DLBCL that relapsed or was refractory to 6 previous treatment regimens, achieved a PR after 16 weeks of therapy and remains on study.
The recommended phase 2 dose of tazemetostat is 800 mg twice daily.
Adverse events and next steps
All of the 45 enrolled patients were evaluable for safety. Treatment-related adverse events included asthenia (n=10), nausea (n=6), dyspepsia (n=5), thrombocytopenia (n=4), anorexia (n=4), anemia (n=4), vomiting (n=3), constipation (n=2), muscle spasm (n=2), hypertension (n=2), neutropenia (n=2), and elevated transaminase (n=1).
There were 5 grade 3 or higher adverse events related to treatment, including grade 3 anorexia, grade 3 hypertension, grade 3 transaminase elevation, grade 4 thrombocytopenia, and grade 4 neutropenia.
Epizyme plans to report a further update from this trial by the end of this year. The company is now enrolling patients in a phase 2 study of tazemetostat monotherapy in patients with relapsed or refractory NHL, stratified by cell of origin and EZH2 mutation status.
Epizyme is also planning a phase 2 trial of tazemetostat in adults with INI1-deficient solid tumors, a phase 1 study of pediatric patients with INI1-deficient solid tumors, a combination study of tazemetostat with R-CHOP in patients with DLBCL, and a combination study of tazemetostat with a B-cell signaling agent or other emerging targeted therapies for B-cell lymphomas.
*Information in the abstract differs from that presented at the meeting.