User login
Damian McNamara is a journalist for Medscape Medical News and MDedge. He worked full-time for MDedge as the Miami Bureau covering a dozen medical specialties during 2001-2012, then as a freelancer for Medscape and MDedge, before being hired on staff by Medscape in 2018. Now the two companies are one. He uses what he learned in school – Damian has a BS in chemistry and an MS in science, health and environmental reporting/journalism. He works out of a home office in Miami, with a 100-pound chocolate lab known to snore under his desk during work hours.
Nd:YAG Laser Targets Sweat Gland Disorders
CHICAGO – An Nd:YAG laser used for facial fat plasty and laser liposuction treatment has shown promise for targeting axillary bromhidrosis and hyperhidrosis, according to the first prospective, long-term follow-up study for these indications.
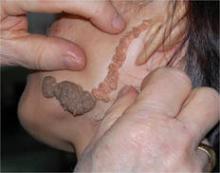
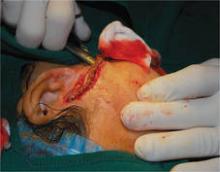
After an iodine starch test at baseline, researchers treated both axillae of 18 patients with the disorders with a 1,444-nm pulsed Nd:YAG laser (AccuSculpt, Lutronic). Each operative field was anesthetized. Participants were then assessed at day 1, 7, 30, 60, and 180 for clinical effects.
"Outcome was good in this study" Dr. Sang Min Yi said. Patients rated 61% of axillary bromhidrosis and 86% of hyperhidrosis results as excellent or good.
Patients judged the severity of their condition at baseline and regular intervals using a 10-point scale (10 being the most severe). For example, average bromhidrosis severity was 1.2 on day 7 and 1.7 on day 60. Patients also rated their average pain severity as 1.2 on day 7 and 0.3 on day 60. Severity of limitation on movement was an average 2.6 on day 7 after treatment and 0.4 on day 60.
Participants also rated the severity of remaining sweating as 1.4 on day 7 and 1.7 on day 60. Overall satisfaction was an average 9 out of 10 on both days 7 and 60. Results at day 180 are pending.
The 1,444-nm pulsed Nd:YAG laser targets apocrine sweat glands in the deep dermis and subcutaneous fat layer. Pulse energy was 175 mJ, pulse rate was 40 Hz, power was 7 watts, and the energy density ranged from 20 J/cm2 to 30 J/cm2.
Other treatments for axillary bromhidrosis and hyperhidrosis include local topical medications, botulinum toxin injections, ultrasonic therapy, and liposuction curettage. However, this laser is one of the best modalities to treat these disorders, said Dr. Yi, of the department of dermatology, Korea University, Ansan Hospital, South Korea.
Most adverse events were temporary and mild. Bullae, mild ecchymoses, and bruises on the operative sites all resolved within 30 days, Dr. Yi said. "The most severe and unwanted complication was skin necrosis." This occurred in two patients. Necrosis is preventable if the tip of the probe is held properly and delivery of excess energy to any unit area is avoided, he noted.
Dr. Yi received research funding from Lutronic, which also funded the study.
CHICAGO – An Nd:YAG laser used for facial fat plasty and laser liposuction treatment has shown promise for targeting axillary bromhidrosis and hyperhidrosis, according to the first prospective, long-term follow-up study for these indications.
After an iodine starch test at baseline, researchers treated both axillae of 18 patients with the disorders with a 1,444-nm pulsed Nd:YAG laser (AccuSculpt, Lutronic). Each operative field was anesthetized. Participants were then assessed at day 1, 7, 30, 60, and 180 for clinical effects.
"Outcome was good in this study" Dr. Sang Min Yi said. Patients rated 61% of axillary bromhidrosis and 86% of hyperhidrosis results as excellent or good.
Patients judged the severity of their condition at baseline and regular intervals using a 10-point scale (10 being the most severe). For example, average bromhidrosis severity was 1.2 on day 7 and 1.7 on day 60. Patients also rated their average pain severity as 1.2 on day 7 and 0.3 on day 60. Severity of limitation on movement was an average 2.6 on day 7 after treatment and 0.4 on day 60.
Participants also rated the severity of remaining sweating as 1.4 on day 7 and 1.7 on day 60. Overall satisfaction was an average 9 out of 10 on both days 7 and 60. Results at day 180 are pending.
The 1,444-nm pulsed Nd:YAG laser targets apocrine sweat glands in the deep dermis and subcutaneous fat layer. Pulse energy was 175 mJ, pulse rate was 40 Hz, power was 7 watts, and the energy density ranged from 20 J/cm2 to 30 J/cm2.
Other treatments for axillary bromhidrosis and hyperhidrosis include local topical medications, botulinum toxin injections, ultrasonic therapy, and liposuction curettage. However, this laser is one of the best modalities to treat these disorders, said Dr. Yi, of the department of dermatology, Korea University, Ansan Hospital, South Korea.
Most adverse events were temporary and mild. Bullae, mild ecchymoses, and bruises on the operative sites all resolved within 30 days, Dr. Yi said. "The most severe and unwanted complication was skin necrosis." This occurred in two patients. Necrosis is preventable if the tip of the probe is held properly and delivery of excess energy to any unit area is avoided, he noted.
Dr. Yi received research funding from Lutronic, which also funded the study.
CHICAGO – An Nd:YAG laser used for facial fat plasty and laser liposuction treatment has shown promise for targeting axillary bromhidrosis and hyperhidrosis, according to the first prospective, long-term follow-up study for these indications.
After an iodine starch test at baseline, researchers treated both axillae of 18 patients with the disorders with a 1,444-nm pulsed Nd:YAG laser (AccuSculpt, Lutronic). Each operative field was anesthetized. Participants were then assessed at day 1, 7, 30, 60, and 180 for clinical effects.
"Outcome was good in this study" Dr. Sang Min Yi said. Patients rated 61% of axillary bromhidrosis and 86% of hyperhidrosis results as excellent or good.
Patients judged the severity of their condition at baseline and regular intervals using a 10-point scale (10 being the most severe). For example, average bromhidrosis severity was 1.2 on day 7 and 1.7 on day 60. Patients also rated their average pain severity as 1.2 on day 7 and 0.3 on day 60. Severity of limitation on movement was an average 2.6 on day 7 after treatment and 0.4 on day 60.
Participants also rated the severity of remaining sweating as 1.4 on day 7 and 1.7 on day 60. Overall satisfaction was an average 9 out of 10 on both days 7 and 60. Results at day 180 are pending.
The 1,444-nm pulsed Nd:YAG laser targets apocrine sweat glands in the deep dermis and subcutaneous fat layer. Pulse energy was 175 mJ, pulse rate was 40 Hz, power was 7 watts, and the energy density ranged from 20 J/cm2 to 30 J/cm2.
Other treatments for axillary bromhidrosis and hyperhidrosis include local topical medications, botulinum toxin injections, ultrasonic therapy, and liposuction curettage. However, this laser is one of the best modalities to treat these disorders, said Dr. Yi, of the department of dermatology, Korea University, Ansan Hospital, South Korea.
Most adverse events were temporary and mild. Bullae, mild ecchymoses, and bruises on the operative sites all resolved within 30 days, Dr. Yi said. "The most severe and unwanted complication was skin necrosis." This occurred in two patients. Necrosis is preventable if the tip of the probe is held properly and delivery of excess energy to any unit area is avoided, he noted.
Dr. Yi received research funding from Lutronic, which also funded the study.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
Major Finding: Patients rated 61% of axillary bromhidrosis and 86% of hyperhidrosis results as excellent or good.
Data Source: 18 patients with axillary bromhidrosis or hyperhidrosis.
Disclosures: Dr. Yi received research funding from Lutronic, which also funded the study.
Health Care Reform Law May Bolster Addiction Treatment
BOCA RATON, Fla. – Pharmacologic strategies are underused for alcohol use disorders, Dr. Charles P. O’Brien said, despite backing from evidence-based medicine. "This is terrible that we have such a divorce in this field between evidence-based medicine and treatment."
However, use of medication is expected to get a big boost from the recent health care reform legislation. "There is an understanding they [insurers] will pay for medication, including monthly depot injections," Dr. O’Brien, chair of the DSM-5 Substance Use Disorders Committee, said at the meeting.
Overall treatment of substance use is mandated in the legislation, including coverage for screening and brief interventions done in primary care settings.
"We need to identify these patients, treat them earlier, and intervene before they need really expensive [interventions] like liver transplants, said Dr. O’Brien, director of the Center for the Study of Addiction at the University of Pennsylvania in Philadelphia. "This is big news, [and is] going to impact your practice and the training programs."
Treatment of all addictions is going to be an integral part of health care reform, Dr. O’Brien said. "Economists in the Obama administration agree that treating addiction saves money. Doctors will be mandated to look for problems. Most of the people involved in substance abuse are not at the level that they [initially] come to the attention of the primary care provider. The health care system is going to have to look for the early signs of substance use problems and treat that."
Meanwhile, Dr. O’Brien confirmed that the next revision of the Diagnostic and Statistical Manual on Mental Disorders (the DSM-5) probably will feature several important changes in terminology for alcohol and other substance use disorders.
"’Dependence’ is no longer there in DSM-5," Dr. O’Brien said to a round of applause at the meeting. "We got rid of it ... everyone agrees dependence is not addiction."
He explained that physical dependence might be normal with a whole range of prescription pain medications, Dr. O’Brien said. Some patients become tolerant after a few days and "we don’t want it to count if that is the only symptom, because it’s normal."
"I insisted in the DSM-5 that they don’t count this as a symptom of addiction as it has [been] in the past. So we are excluding physical dependence from DSM-5 criteria for substance use disorder," Dr. O’Brien said.
In contrast, compulsive, out-of-control drug seeking is distinct and will most likely be part of the definition for a moderate or severe substance use disorder.
The abuse category will be eliminated as well from the DSM-5. A meeting attendee commented that he liked the word "abuse." Dr. O’Brien replied, "The proposal is that they would have a substance use disorder; for example, a patient could have a cocaine use disorder. It is not that the word abuse cannot be used; it’s just not part of the definition."
The legal components of substance use in DSM-IV-TR will be removed as well. The definitions vary worldwide, depending on the country in which you practice, Dr. O’Brien explained.
It remains unclear whether the term "addiction" will appear in the DSM-5 despite its widespread use in the English language. "It was avoided in DSM IIIR and DSM-IV," Dr. O’Brien said. "Addiction is a perfectly good word, and it’s useless to oppose it. It’s everywhere. We cannot change the language." However, some resistance to its inclusion exists among other members of his DSM-5 committee.
What is clear is that "craving" will be added to the next manual. "Craving is not in DSM-IV, but it will be in DSM-5, and that is a good thing," Dr. O’Brien said.
Diagnosis of craving might be based on a question such as: Have you ever in your life had such severe craving for a drug that you could not think of anything else?
Craving is useful because clinical trial researchers have measured it as an outcome for years, Dr. O’Brien said. In addition, a reduction in craving often reflects the efficacy of pharmacologic treatment. "The evidence about medications that reduce craving is very interesting. It turned out to be pretty consistent. In the latest studies out of Russia with depot naltrexone [Vivitrol, Alkermes] the biggest change they see is reduction in craving versus placebo [Curr. Opin. Psychiatry 2010 (Epub ahead of print)].
In addition to depot naltrexone, the Food and Drug Administration has cleared oral naltrexone (generic), disulfiram (Antabuse, Odyssey Pharmaceuticals), and acamprosate (Campral, Forest Labs) for treatment of alcohol use disorders in the United States.
Dr. O’Brien disclosed that he is a consultant and researcher for Embera NeuroTherapeutics and a consultant for Alkermes, Gilead, and Reckitt Benckiser
BOCA RATON, Fla. – Pharmacologic strategies are underused for alcohol use disorders, Dr. Charles P. O’Brien said, despite backing from evidence-based medicine. "This is terrible that we have such a divorce in this field between evidence-based medicine and treatment."
However, use of medication is expected to get a big boost from the recent health care reform legislation. "There is an understanding they [insurers] will pay for medication, including monthly depot injections," Dr. O’Brien, chair of the DSM-5 Substance Use Disorders Committee, said at the meeting.
Overall treatment of substance use is mandated in the legislation, including coverage for screening and brief interventions done in primary care settings.
"We need to identify these patients, treat them earlier, and intervene before they need really expensive [interventions] like liver transplants, said Dr. O’Brien, director of the Center for the Study of Addiction at the University of Pennsylvania in Philadelphia. "This is big news, [and is] going to impact your practice and the training programs."
Treatment of all addictions is going to be an integral part of health care reform, Dr. O’Brien said. "Economists in the Obama administration agree that treating addiction saves money. Doctors will be mandated to look for problems. Most of the people involved in substance abuse are not at the level that they [initially] come to the attention of the primary care provider. The health care system is going to have to look for the early signs of substance use problems and treat that."
Meanwhile, Dr. O’Brien confirmed that the next revision of the Diagnostic and Statistical Manual on Mental Disorders (the DSM-5) probably will feature several important changes in terminology for alcohol and other substance use disorders.
"’Dependence’ is no longer there in DSM-5," Dr. O’Brien said to a round of applause at the meeting. "We got rid of it ... everyone agrees dependence is not addiction."
He explained that physical dependence might be normal with a whole range of prescription pain medications, Dr. O’Brien said. Some patients become tolerant after a few days and "we don’t want it to count if that is the only symptom, because it’s normal."
"I insisted in the DSM-5 that they don’t count this as a symptom of addiction as it has [been] in the past. So we are excluding physical dependence from DSM-5 criteria for substance use disorder," Dr. O’Brien said.
In contrast, compulsive, out-of-control drug seeking is distinct and will most likely be part of the definition for a moderate or severe substance use disorder.
The abuse category will be eliminated as well from the DSM-5. A meeting attendee commented that he liked the word "abuse." Dr. O’Brien replied, "The proposal is that they would have a substance use disorder; for example, a patient could have a cocaine use disorder. It is not that the word abuse cannot be used; it’s just not part of the definition."
The legal components of substance use in DSM-IV-TR will be removed as well. The definitions vary worldwide, depending on the country in which you practice, Dr. O’Brien explained.
It remains unclear whether the term "addiction" will appear in the DSM-5 despite its widespread use in the English language. "It was avoided in DSM IIIR and DSM-IV," Dr. O’Brien said. "Addiction is a perfectly good word, and it’s useless to oppose it. It’s everywhere. We cannot change the language." However, some resistance to its inclusion exists among other members of his DSM-5 committee.
What is clear is that "craving" will be added to the next manual. "Craving is not in DSM-IV, but it will be in DSM-5, and that is a good thing," Dr. O’Brien said.
Diagnosis of craving might be based on a question such as: Have you ever in your life had such severe craving for a drug that you could not think of anything else?
Craving is useful because clinical trial researchers have measured it as an outcome for years, Dr. O’Brien said. In addition, a reduction in craving often reflects the efficacy of pharmacologic treatment. "The evidence about medications that reduce craving is very interesting. It turned out to be pretty consistent. In the latest studies out of Russia with depot naltrexone [Vivitrol, Alkermes] the biggest change they see is reduction in craving versus placebo [Curr. Opin. Psychiatry 2010 (Epub ahead of print)].
In addition to depot naltrexone, the Food and Drug Administration has cleared oral naltrexone (generic), disulfiram (Antabuse, Odyssey Pharmaceuticals), and acamprosate (Campral, Forest Labs) for treatment of alcohol use disorders in the United States.
Dr. O’Brien disclosed that he is a consultant and researcher for Embera NeuroTherapeutics and a consultant for Alkermes, Gilead, and Reckitt Benckiser
BOCA RATON, Fla. – Pharmacologic strategies are underused for alcohol use disorders, Dr. Charles P. O’Brien said, despite backing from evidence-based medicine. "This is terrible that we have such a divorce in this field between evidence-based medicine and treatment."
However, use of medication is expected to get a big boost from the recent health care reform legislation. "There is an understanding they [insurers] will pay for medication, including monthly depot injections," Dr. O’Brien, chair of the DSM-5 Substance Use Disorders Committee, said at the meeting.
Overall treatment of substance use is mandated in the legislation, including coverage for screening and brief interventions done in primary care settings.
"We need to identify these patients, treat them earlier, and intervene before they need really expensive [interventions] like liver transplants, said Dr. O’Brien, director of the Center for the Study of Addiction at the University of Pennsylvania in Philadelphia. "This is big news, [and is] going to impact your practice and the training programs."
Treatment of all addictions is going to be an integral part of health care reform, Dr. O’Brien said. "Economists in the Obama administration agree that treating addiction saves money. Doctors will be mandated to look for problems. Most of the people involved in substance abuse are not at the level that they [initially] come to the attention of the primary care provider. The health care system is going to have to look for the early signs of substance use problems and treat that."
Meanwhile, Dr. O’Brien confirmed that the next revision of the Diagnostic and Statistical Manual on Mental Disorders (the DSM-5) probably will feature several important changes in terminology for alcohol and other substance use disorders.
"’Dependence’ is no longer there in DSM-5," Dr. O’Brien said to a round of applause at the meeting. "We got rid of it ... everyone agrees dependence is not addiction."
He explained that physical dependence might be normal with a whole range of prescription pain medications, Dr. O’Brien said. Some patients become tolerant after a few days and "we don’t want it to count if that is the only symptom, because it’s normal."
"I insisted in the DSM-5 that they don’t count this as a symptom of addiction as it has [been] in the past. So we are excluding physical dependence from DSM-5 criteria for substance use disorder," Dr. O’Brien said.
In contrast, compulsive, out-of-control drug seeking is distinct and will most likely be part of the definition for a moderate or severe substance use disorder.
The abuse category will be eliminated as well from the DSM-5. A meeting attendee commented that he liked the word "abuse." Dr. O’Brien replied, "The proposal is that they would have a substance use disorder; for example, a patient could have a cocaine use disorder. It is not that the word abuse cannot be used; it’s just not part of the definition."
The legal components of substance use in DSM-IV-TR will be removed as well. The definitions vary worldwide, depending on the country in which you practice, Dr. O’Brien explained.
It remains unclear whether the term "addiction" will appear in the DSM-5 despite its widespread use in the English language. "It was avoided in DSM IIIR and DSM-IV," Dr. O’Brien said. "Addiction is a perfectly good word, and it’s useless to oppose it. It’s everywhere. We cannot change the language." However, some resistance to its inclusion exists among other members of his DSM-5 committee.
What is clear is that "craving" will be added to the next manual. "Craving is not in DSM-IV, but it will be in DSM-5, and that is a good thing," Dr. O’Brien said.
Diagnosis of craving might be based on a question such as: Have you ever in your life had such severe craving for a drug that you could not think of anything else?
Craving is useful because clinical trial researchers have measured it as an outcome for years, Dr. O’Brien said. In addition, a reduction in craving often reflects the efficacy of pharmacologic treatment. "The evidence about medications that reduce craving is very interesting. It turned out to be pretty consistent. In the latest studies out of Russia with depot naltrexone [Vivitrol, Alkermes] the biggest change they see is reduction in craving versus placebo [Curr. Opin. Psychiatry 2010 (Epub ahead of print)].
In addition to depot naltrexone, the Food and Drug Administration has cleared oral naltrexone (generic), disulfiram (Antabuse, Odyssey Pharmaceuticals), and acamprosate (Campral, Forest Labs) for treatment of alcohol use disorders in the United States.
Dr. O’Brien disclosed that he is a consultant and researcher for Embera NeuroTherapeutics and a consultant for Alkermes, Gilead, and Reckitt Benckiser
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ADDICTION PSYCHIATRY
Risk of Delirium, DTs Greater in Older Inpatients With Alcohol Withdrawal
BOCA RATON, Fla. – Older patients hospitalized with acute alcohol withdrawal experience significantly more delirium tremens and delirium than do inpatients younger than 65 years, according to a retrospective study.
Screen older patients for alcohol consumption and consider medications other than benzodiazepines to treat withdrawal in this population, advised Dr. Jeremy Doniger, a resident at Harvard Longwood Psychiatry in Boston.
"Older people are drinking more than we realize. Be consistent about screening for it," Dr. Doniger said. In fact, with the aging of the population, the number of older adults with an alcohol use disorder is expected to double by 2020 (Brit. Med. J. 2003;327:664-7). A likely outcome is that more older patients will be admitted to hospitals for severe alcohol withdrawal in the future.
"Benzodiazepines can cause delirium, and older patients may be more susceptible [to these effects]," said Dr. Doniger. N-methyl-d-aspartate antagonists, for example, alone or in combination with benzodiazepines, are an effective alternative strategy, he added.
Reports in the literature are mixed as to whether older age predicts worse withdrawal, said Dr. Joji Suzuki, lead study investigator, and director of the Addiction Recovery Program at Brigham and Women’s Hospital and Harvard Medical School, Boston.
To find a more definitive answer, the investigators reviewed the charts of all medical inpatients at Brigham and Women’s Hospital for whom a psychiatry consultation was requested from 2008 to 2010. They identified 141 patients diagnosed and treated for alcohol withdrawal during hospital admission.
They compared 31 older patients to 110 younger ones. "We wanted to know if older patients, those 65 and older, have worse or the same outcomes as younger folks," said Dr. Suzuki. "We found something very striking: that DTs [delirium tremens] or delirium from any cause approaches 50% in older patients," Dr. Suzuki said. "Delirium is very serious, and can be a predictor for death."
Delirium from any cause affected 52% of the older group versus 30% of the younger patients, a statistically significant difference. In addition, 44% of older patients experienced DTs while hospitalized, compared with 20% of younger patients. This disparity also was significantly different.
"Part of it might be severity of comorbidities," Dr. Doniger said. The presence of more severe comorbidities was significantly associated with development of any delirium (odds ratio, 1.2), but not with DTs (OR, 1.13) or withdrawal seizures (OR, 1.02).
Prevalence of withdrawal seizures did not differ significantly between older patients (10%) and younger patients (6%). Nor did hospital length of stay differ significantly. Older patients stayed at Brigham and Women’s Hospital a mean 12.5 days compared with 8.6 days for the younger group.
The take-home message is that "younger patients going through withdrawal will fare about the same or a little worse than someone in a detox setting. But older patients are at greater risk for adverse outcomes, and the longer they stay in the hospital, the higher their risk for not doing well [because of nosocomial infections, falls, and other risk factors]," Dr. Suzuki said.
Inpatients who experienced DTs received significantly higher doses of benzodiazepines than did those who did not. In terms of lorazepam equivalents, the mean dose was 64.6 mg versus 30.5 mg in the non-DT group.
Dr. Doniger said differences in body composition and metabolism could contribute to greater benzodiazepine delirium in older patients because they typically have less water and more fat, which holds medications, and they have slower liver metabolism, he said.
The study was supported in part by the Department of Psychiatry at Harvard Medical School. Dr. Suzuki and Dr. Doniger had no relevant financial disclosures.
BOCA RATON, Fla. – Older patients hospitalized with acute alcohol withdrawal experience significantly more delirium tremens and delirium than do inpatients younger than 65 years, according to a retrospective study.
Screen older patients for alcohol consumption and consider medications other than benzodiazepines to treat withdrawal in this population, advised Dr. Jeremy Doniger, a resident at Harvard Longwood Psychiatry in Boston.
"Older people are drinking more than we realize. Be consistent about screening for it," Dr. Doniger said. In fact, with the aging of the population, the number of older adults with an alcohol use disorder is expected to double by 2020 (Brit. Med. J. 2003;327:664-7). A likely outcome is that more older patients will be admitted to hospitals for severe alcohol withdrawal in the future.
"Benzodiazepines can cause delirium, and older patients may be more susceptible [to these effects]," said Dr. Doniger. N-methyl-d-aspartate antagonists, for example, alone or in combination with benzodiazepines, are an effective alternative strategy, he added.
Reports in the literature are mixed as to whether older age predicts worse withdrawal, said Dr. Joji Suzuki, lead study investigator, and director of the Addiction Recovery Program at Brigham and Women’s Hospital and Harvard Medical School, Boston.
To find a more definitive answer, the investigators reviewed the charts of all medical inpatients at Brigham and Women’s Hospital for whom a psychiatry consultation was requested from 2008 to 2010. They identified 141 patients diagnosed and treated for alcohol withdrawal during hospital admission.
They compared 31 older patients to 110 younger ones. "We wanted to know if older patients, those 65 and older, have worse or the same outcomes as younger folks," said Dr. Suzuki. "We found something very striking: that DTs [delirium tremens] or delirium from any cause approaches 50% in older patients," Dr. Suzuki said. "Delirium is very serious, and can be a predictor for death."
Delirium from any cause affected 52% of the older group versus 30% of the younger patients, a statistically significant difference. In addition, 44% of older patients experienced DTs while hospitalized, compared with 20% of younger patients. This disparity also was significantly different.
"Part of it might be severity of comorbidities," Dr. Doniger said. The presence of more severe comorbidities was significantly associated with development of any delirium (odds ratio, 1.2), but not with DTs (OR, 1.13) or withdrawal seizures (OR, 1.02).
Prevalence of withdrawal seizures did not differ significantly between older patients (10%) and younger patients (6%). Nor did hospital length of stay differ significantly. Older patients stayed at Brigham and Women’s Hospital a mean 12.5 days compared with 8.6 days for the younger group.
The take-home message is that "younger patients going through withdrawal will fare about the same or a little worse than someone in a detox setting. But older patients are at greater risk for adverse outcomes, and the longer they stay in the hospital, the higher their risk for not doing well [because of nosocomial infections, falls, and other risk factors]," Dr. Suzuki said.
Inpatients who experienced DTs received significantly higher doses of benzodiazepines than did those who did not. In terms of lorazepam equivalents, the mean dose was 64.6 mg versus 30.5 mg in the non-DT group.
Dr. Doniger said differences in body composition and metabolism could contribute to greater benzodiazepine delirium in older patients because they typically have less water and more fat, which holds medications, and they have slower liver metabolism, he said.
The study was supported in part by the Department of Psychiatry at Harvard Medical School. Dr. Suzuki and Dr. Doniger had no relevant financial disclosures.
BOCA RATON, Fla. – Older patients hospitalized with acute alcohol withdrawal experience significantly more delirium tremens and delirium than do inpatients younger than 65 years, according to a retrospective study.
Screen older patients for alcohol consumption and consider medications other than benzodiazepines to treat withdrawal in this population, advised Dr. Jeremy Doniger, a resident at Harvard Longwood Psychiatry in Boston.
"Older people are drinking more than we realize. Be consistent about screening for it," Dr. Doniger said. In fact, with the aging of the population, the number of older adults with an alcohol use disorder is expected to double by 2020 (Brit. Med. J. 2003;327:664-7). A likely outcome is that more older patients will be admitted to hospitals for severe alcohol withdrawal in the future.
"Benzodiazepines can cause delirium, and older patients may be more susceptible [to these effects]," said Dr. Doniger. N-methyl-d-aspartate antagonists, for example, alone or in combination with benzodiazepines, are an effective alternative strategy, he added.
Reports in the literature are mixed as to whether older age predicts worse withdrawal, said Dr. Joji Suzuki, lead study investigator, and director of the Addiction Recovery Program at Brigham and Women’s Hospital and Harvard Medical School, Boston.
To find a more definitive answer, the investigators reviewed the charts of all medical inpatients at Brigham and Women’s Hospital for whom a psychiatry consultation was requested from 2008 to 2010. They identified 141 patients diagnosed and treated for alcohol withdrawal during hospital admission.
They compared 31 older patients to 110 younger ones. "We wanted to know if older patients, those 65 and older, have worse or the same outcomes as younger folks," said Dr. Suzuki. "We found something very striking: that DTs [delirium tremens] or delirium from any cause approaches 50% in older patients," Dr. Suzuki said. "Delirium is very serious, and can be a predictor for death."
Delirium from any cause affected 52% of the older group versus 30% of the younger patients, a statistically significant difference. In addition, 44% of older patients experienced DTs while hospitalized, compared with 20% of younger patients. This disparity also was significantly different.
"Part of it might be severity of comorbidities," Dr. Doniger said. The presence of more severe comorbidities was significantly associated with development of any delirium (odds ratio, 1.2), but not with DTs (OR, 1.13) or withdrawal seizures (OR, 1.02).
Prevalence of withdrawal seizures did not differ significantly between older patients (10%) and younger patients (6%). Nor did hospital length of stay differ significantly. Older patients stayed at Brigham and Women’s Hospital a mean 12.5 days compared with 8.6 days for the younger group.
The take-home message is that "younger patients going through withdrawal will fare about the same or a little worse than someone in a detox setting. But older patients are at greater risk for adverse outcomes, and the longer they stay in the hospital, the higher their risk for not doing well [because of nosocomial infections, falls, and other risk factors]," Dr. Suzuki said.
Inpatients who experienced DTs received significantly higher doses of benzodiazepines than did those who did not. In terms of lorazepam equivalents, the mean dose was 64.6 mg versus 30.5 mg in the non-DT group.
Dr. Doniger said differences in body composition and metabolism could contribute to greater benzodiazepine delirium in older patients because they typically have less water and more fat, which holds medications, and they have slower liver metabolism, he said.
The study was supported in part by the Department of Psychiatry at Harvard Medical School. Dr. Suzuki and Dr. Doniger had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ADDICTION PSYCHIATRY
Major Finding: A greater percentage of hospitalized patients 65 and older with alcohol withdrawal experience delirium, 52%, compared with 30% among younger patients.
Data Source: Review of 141 patient charts involving a psychiatry consultation from 2008 to 2010.
Disclosures: Dr. Joji Suzuki and Dr. Jeremy Doniger had no relevant disclosures.
New Data Support Safety of Dermatologic Office-Based Surgery
CHICAGO – Office-based surgery is safe when performed by dermatologists, according to a study of 10 years of complication and death reports from Florida and 6 years of data from Alabama.
Dermatologic surgeons could use the findings to combat any legislative attempts to curtail office procedures, including liposuction, Dr. Brett Coldiron said.
Some plastic surgeons, for example, are trying to restrict what types of office surgeries dermatologists can legally perform, said Dr. Coldiron, a private practice dermatologic surgeon and member of the dermatology faculty at the University of Cincinnati.
The study indicates procedures performed by plastic surgeons actually carry a greater risk for adverse events and death, compared with dermatologic surgeries, Dr. Coldiron said.
A plastic surgeon contacted for comment, Dr. Michael McGuire, said the comparison is unfair given the differing complexity of surgeries done by the two specialties. "It’s a total misrepresentation of the statistics. There is no question that the incidence and even the deaths are smaller with dermatology than with any other specialty."
"Comparing an abdominoplasty – a tummy tuck – with a skin cancer excision or even a small volume of liposuction is ridiculous. To compare that with doing tummy tucks, and 4- or 5-hour facelifts, or major breast reconstructive surgery, all of which are done in outpatient surgery centers, is apples and oranges. They are totally different procedures," said Dr. McGuire, who is in private practice in Santa Monica, Calif., and director of The American Board of Plastic Surgeons.
The prospectively collected data show "that any claims by plastic surgeons or anesthesiologists that dermatologists are doing unsafe things and injuring patients in the office is unfounded," Dr. Coldiron said. "And ... if they are going to make such claims, they should have some data to back them up."
Both Alabama and Florida require notification when an outpatient experiences serious injury, transfer to a hospital, or death related to surgery. These mandatory reports are part of public record in the state of Florida, for example.
Dr. Coldiron found 46 deaths and 263 complications that required hospital transfers in Florida. Cosmetic (nonmedically necessary) procedures were associated with 57% of these deaths and almost 50% of such transfers in the state. Liposuction or liposuction with another cosmetic procedure (abdominoplasty, for example) resulted in death for 10 patients and hospital transfer in another 34 cases.
The majority of cosmetic procedure deaths (67%) and hospital transfers (74%) in Florida were performed under general anesthesia, said Dr. Coldiron.
This is relevant because some physicians who perform liposuction under general anesthesia are trying to restrict liposuction under local or tumescent anesthesia, he said. "There have been legislative attempts to prohibit this. The state of New York recently passed a law restricting liposuction in offices, under local anesthesia to 500 cc, which paradoxically will increase the number of injuries and deaths."
"When you try to restrict the use of local anesthesia or tumescent anesthesia ... you will force more people into using general anesthesia, which has more complications. Hospital transfers or deaths with the use of local anesthesia are incredibly rare," Dr. Coldiron said in an interview. "In fact, I’m only aware of a couple that occurred after anaphylactic reactions."
"They [dermatologists] like to blame the general anesthesia," Dr. McGuire said. "It’s not the general anesthesia that is the difference; it’s the magnitude of the surgery. Clearly there are going to be more risks and complications with major surgery compared to minor surgery under any kind of anesthesia." Plastic surgeons in Florida reported the most adverse events (45% of the total), compared with 1.3% reported by dermatologists.
A meeting attendee questioned a direct comparison between specialties, citing the higher complexity of cases typically performed by plastic surgeons. "Yes, the plastic surgeons do more big, multiple procedures and have more problems," Dr. Coldiron replied. "That does not give them the right to try and restrict our practices under the guise of patient safety at the level of the state medical boards and legislatures that is preposterous."
The current study is in press, and represents an update of Dr. Coldiron’s previously reported 7-year Florida data (Dermatol. Surg. 2008;34:285-91).
Additional information is available on the website for Dr. Coldiron's practice, including real adverse event incident reports.
Alabama reports support and validate the Florida data, Dr. Coldiron said. There were three deaths and 52 adverse events that required an office-to-hospital transfer in Alabama. Cosmetic procedures were associated with zero deaths and 42% of hospital transfers during the 6 years. The Alabama medical board provided Dr. Coldiron with the data upon request.
A majority of cosmetic procedure adverse events (86%) were from cases performed under general anesthesia.
Plastic surgery was the specialty most often involved in adverse event reports (42% of all complications), compared with 1.9% for dermatologists in that state (one report associated with tumescent anesthesia).
"Certainly we are not a major contributor in any sense. Dermatologic surgery is extremely safe," Dr. Coldiron said at the meeting, which was jointly sponsored by the American Society of Cosmetic Dermatology and Aesthetic Surgery.
Dr. McGuire said that office-based surgery is safe when performed at centers accredited by the American Association for Accreditation of Ambulatory Surgery Facilities (AAAASF). Studies cited on the organization's website reported 23 deaths of 1,141,418 outpatient procedures in the United States over 5.5 years.
Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
CHICAGO – Office-based surgery is safe when performed by dermatologists, according to a study of 10 years of complication and death reports from Florida and 6 years of data from Alabama.
Dermatologic surgeons could use the findings to combat any legislative attempts to curtail office procedures, including liposuction, Dr. Brett Coldiron said.
Some plastic surgeons, for example, are trying to restrict what types of office surgeries dermatologists can legally perform, said Dr. Coldiron, a private practice dermatologic surgeon and member of the dermatology faculty at the University of Cincinnati.
The study indicates procedures performed by plastic surgeons actually carry a greater risk for adverse events and death, compared with dermatologic surgeries, Dr. Coldiron said.
A plastic surgeon contacted for comment, Dr. Michael McGuire, said the comparison is unfair given the differing complexity of surgeries done by the two specialties. "It’s a total misrepresentation of the statistics. There is no question that the incidence and even the deaths are smaller with dermatology than with any other specialty."
"Comparing an abdominoplasty – a tummy tuck – with a skin cancer excision or even a small volume of liposuction is ridiculous. To compare that with doing tummy tucks, and 4- or 5-hour facelifts, or major breast reconstructive surgery, all of which are done in outpatient surgery centers, is apples and oranges. They are totally different procedures," said Dr. McGuire, who is in private practice in Santa Monica, Calif., and director of The American Board of Plastic Surgeons.
The prospectively collected data show "that any claims by plastic surgeons or anesthesiologists that dermatologists are doing unsafe things and injuring patients in the office is unfounded," Dr. Coldiron said. "And ... if they are going to make such claims, they should have some data to back them up."
Both Alabama and Florida require notification when an outpatient experiences serious injury, transfer to a hospital, or death related to surgery. These mandatory reports are part of public record in the state of Florida, for example.
Dr. Coldiron found 46 deaths and 263 complications that required hospital transfers in Florida. Cosmetic (nonmedically necessary) procedures were associated with 57% of these deaths and almost 50% of such transfers in the state. Liposuction or liposuction with another cosmetic procedure (abdominoplasty, for example) resulted in death for 10 patients and hospital transfer in another 34 cases.
The majority of cosmetic procedure deaths (67%) and hospital transfers (74%) in Florida were performed under general anesthesia, said Dr. Coldiron.
This is relevant because some physicians who perform liposuction under general anesthesia are trying to restrict liposuction under local or tumescent anesthesia, he said. "There have been legislative attempts to prohibit this. The state of New York recently passed a law restricting liposuction in offices, under local anesthesia to 500 cc, which paradoxically will increase the number of injuries and deaths."
"When you try to restrict the use of local anesthesia or tumescent anesthesia ... you will force more people into using general anesthesia, which has more complications. Hospital transfers or deaths with the use of local anesthesia are incredibly rare," Dr. Coldiron said in an interview. "In fact, I’m only aware of a couple that occurred after anaphylactic reactions."
"They [dermatologists] like to blame the general anesthesia," Dr. McGuire said. "It’s not the general anesthesia that is the difference; it’s the magnitude of the surgery. Clearly there are going to be more risks and complications with major surgery compared to minor surgery under any kind of anesthesia." Plastic surgeons in Florida reported the most adverse events (45% of the total), compared with 1.3% reported by dermatologists.
A meeting attendee questioned a direct comparison between specialties, citing the higher complexity of cases typically performed by plastic surgeons. "Yes, the plastic surgeons do more big, multiple procedures and have more problems," Dr. Coldiron replied. "That does not give them the right to try and restrict our practices under the guise of patient safety at the level of the state medical boards and legislatures that is preposterous."
The current study is in press, and represents an update of Dr. Coldiron’s previously reported 7-year Florida data (Dermatol. Surg. 2008;34:285-91).
Additional information is available on the website for Dr. Coldiron's practice, including real adverse event incident reports.
Alabama reports support and validate the Florida data, Dr. Coldiron said. There were three deaths and 52 adverse events that required an office-to-hospital transfer in Alabama. Cosmetic procedures were associated with zero deaths and 42% of hospital transfers during the 6 years. The Alabama medical board provided Dr. Coldiron with the data upon request.
A majority of cosmetic procedure adverse events (86%) were from cases performed under general anesthesia.
Plastic surgery was the specialty most often involved in adverse event reports (42% of all complications), compared with 1.9% for dermatologists in that state (one report associated with tumescent anesthesia).
"Certainly we are not a major contributor in any sense. Dermatologic surgery is extremely safe," Dr. Coldiron said at the meeting, which was jointly sponsored by the American Society of Cosmetic Dermatology and Aesthetic Surgery.
Dr. McGuire said that office-based surgery is safe when performed at centers accredited by the American Association for Accreditation of Ambulatory Surgery Facilities (AAAASF). Studies cited on the organization's website reported 23 deaths of 1,141,418 outpatient procedures in the United States over 5.5 years.
Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
CHICAGO – Office-based surgery is safe when performed by dermatologists, according to a study of 10 years of complication and death reports from Florida and 6 years of data from Alabama.
Dermatologic surgeons could use the findings to combat any legislative attempts to curtail office procedures, including liposuction, Dr. Brett Coldiron said.
Some plastic surgeons, for example, are trying to restrict what types of office surgeries dermatologists can legally perform, said Dr. Coldiron, a private practice dermatologic surgeon and member of the dermatology faculty at the University of Cincinnati.
The study indicates procedures performed by plastic surgeons actually carry a greater risk for adverse events and death, compared with dermatologic surgeries, Dr. Coldiron said.
A plastic surgeon contacted for comment, Dr. Michael McGuire, said the comparison is unfair given the differing complexity of surgeries done by the two specialties. "It’s a total misrepresentation of the statistics. There is no question that the incidence and even the deaths are smaller with dermatology than with any other specialty."
"Comparing an abdominoplasty – a tummy tuck – with a skin cancer excision or even a small volume of liposuction is ridiculous. To compare that with doing tummy tucks, and 4- or 5-hour facelifts, or major breast reconstructive surgery, all of which are done in outpatient surgery centers, is apples and oranges. They are totally different procedures," said Dr. McGuire, who is in private practice in Santa Monica, Calif., and director of The American Board of Plastic Surgeons.
The prospectively collected data show "that any claims by plastic surgeons or anesthesiologists that dermatologists are doing unsafe things and injuring patients in the office is unfounded," Dr. Coldiron said. "And ... if they are going to make such claims, they should have some data to back them up."
Both Alabama and Florida require notification when an outpatient experiences serious injury, transfer to a hospital, or death related to surgery. These mandatory reports are part of public record in the state of Florida, for example.
Dr. Coldiron found 46 deaths and 263 complications that required hospital transfers in Florida. Cosmetic (nonmedically necessary) procedures were associated with 57% of these deaths and almost 50% of such transfers in the state. Liposuction or liposuction with another cosmetic procedure (abdominoplasty, for example) resulted in death for 10 patients and hospital transfer in another 34 cases.
The majority of cosmetic procedure deaths (67%) and hospital transfers (74%) in Florida were performed under general anesthesia, said Dr. Coldiron.
This is relevant because some physicians who perform liposuction under general anesthesia are trying to restrict liposuction under local or tumescent anesthesia, he said. "There have been legislative attempts to prohibit this. The state of New York recently passed a law restricting liposuction in offices, under local anesthesia to 500 cc, which paradoxically will increase the number of injuries and deaths."
"When you try to restrict the use of local anesthesia or tumescent anesthesia ... you will force more people into using general anesthesia, which has more complications. Hospital transfers or deaths with the use of local anesthesia are incredibly rare," Dr. Coldiron said in an interview. "In fact, I’m only aware of a couple that occurred after anaphylactic reactions."
"They [dermatologists] like to blame the general anesthesia," Dr. McGuire said. "It’s not the general anesthesia that is the difference; it’s the magnitude of the surgery. Clearly there are going to be more risks and complications with major surgery compared to minor surgery under any kind of anesthesia." Plastic surgeons in Florida reported the most adverse events (45% of the total), compared with 1.3% reported by dermatologists.
A meeting attendee questioned a direct comparison between specialties, citing the higher complexity of cases typically performed by plastic surgeons. "Yes, the plastic surgeons do more big, multiple procedures and have more problems," Dr. Coldiron replied. "That does not give them the right to try and restrict our practices under the guise of patient safety at the level of the state medical boards and legislatures that is preposterous."
The current study is in press, and represents an update of Dr. Coldiron’s previously reported 7-year Florida data (Dermatol. Surg. 2008;34:285-91).
Additional information is available on the website for Dr. Coldiron's practice, including real adverse event incident reports.
Alabama reports support and validate the Florida data, Dr. Coldiron said. There were three deaths and 52 adverse events that required an office-to-hospital transfer in Alabama. Cosmetic procedures were associated with zero deaths and 42% of hospital transfers during the 6 years. The Alabama medical board provided Dr. Coldiron with the data upon request.
A majority of cosmetic procedure adverse events (86%) were from cases performed under general anesthesia.
Plastic surgery was the specialty most often involved in adverse event reports (42% of all complications), compared with 1.9% for dermatologists in that state (one report associated with tumescent anesthesia).
"Certainly we are not a major contributor in any sense. Dermatologic surgery is extremely safe," Dr. Coldiron said at the meeting, which was jointly sponsored by the American Society of Cosmetic Dermatology and Aesthetic Surgery.
Dr. McGuire said that office-based surgery is safe when performed at centers accredited by the American Association for Accreditation of Ambulatory Surgery Facilities (AAAASF). Studies cited on the organization's website reported 23 deaths of 1,141,418 outpatient procedures in the United States over 5.5 years.
Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
Major Finding: Forty-six deaths and 263 complications required hospital transfers in Florida. Cosmetic procedures were associated with 57% of these deaths and almost 50% of such transfers in the state.
Data Source: Ten years of complication and death reports from Florida and 6 years of data from Alabama
Disclosures: Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
New Data Support Safety of Dermatologic Office-Based Surgery
CHICAGO – Office-based surgery is safe when performed by dermatologists, according to a study of 10 years of complication and death reports from Florida and 6 years of data from Alabama.
Dermatologic surgeons could use the findings to combat any legislative attempts to curtail office procedures, including liposuction, Dr. Brett Coldiron said.
Some plastic surgeons, for example, are trying to restrict what types of office surgeries dermatologists can legally perform, said Dr. Coldiron, a private practice dermatologic surgeon and member of the dermatology faculty at the University of Cincinnati.
The study indicates procedures performed by plastic surgeons actually carry a greater risk for adverse events and death, compared with dermatologic surgeries, Dr. Coldiron said.
A plastic surgeon contacted for comment, Dr. Michael McGuire, said the comparison is unfair given the differing complexity of surgeries done by the two specialties. "It’s a total misrepresentation of the statistics. There is no question that the incidence and even the deaths are smaller with dermatology than with any other specialty."
"Comparing an abdominoplasty – a tummy tuck – with a skin cancer excision or even a small volume of liposuction is ridiculous. To compare that with doing tummy tucks, and 4- or 5-hour facelifts, or major breast reconstructive surgery, all of which are done in outpatient surgery centers, is apples and oranges. They are totally different procedures," said Dr. McGuire, who is in private practice in Santa Monica, Calif., and director of The American Board of Plastic Surgeons.
The prospectively collected data show "that any claims by plastic surgeons or anesthesiologists that dermatologists are doing unsafe things and injuring patients in the office is unfounded," Dr. Coldiron said. "And ... if they are going to make such claims, they should have some data to back them up."
Both Alabama and Florida require notification when an outpatient experiences serious injury, transfer to a hospital, or death related to surgery. These mandatory reports are part of public record in the state of Florida, for example.
Dr. Coldiron found 46 deaths and 263 complications that required hospital transfers in Florida. Cosmetic (nonmedically necessary) procedures were associated with 57% of these deaths and almost 50% of such transfers in the state. Liposuction or liposuction with another cosmetic procedure (abdominoplasty, for example) resulted in death for 10 patients and hospital transfer in another 34 cases.
The majority of cosmetic procedure deaths (67%) and hospital transfers (74%) in Florida were performed under general anesthesia, said Dr. Coldiron.
This is relevant because some physicians who perform liposuction under general anesthesia are trying to restrict liposuction under local or tumescent anesthesia, he said. "There have been legislative attempts to prohibit this. The state of New York recently passed a law restricting liposuction in offices, under local anesthesia to 500 cc, which paradoxically will increase the number of injuries and deaths."
"When you try to restrict the use of local anesthesia or tumescent anesthesia ... you will force more people into using general anesthesia, which has more complications. Hospital transfers or deaths with the use of local anesthesia are incredibly rare," Dr. Coldiron said in an interview. "In fact, I’m only aware of a couple that occurred after anaphylactic reactions."
"They [dermatologists] like to blame the general anesthesia," Dr. McGuire said. "It’s not the general anesthesia that is the difference; it’s the magnitude of the surgery. Clearly there are going to be more risks and complications with major surgery compared to minor surgery under any kind of anesthesia." Plastic surgeons in Florida reported the most adverse events (45% of the total), compared with 1.3% reported by dermatologists.
A meeting attendee questioned a direct comparison between specialties, citing the higher complexity of cases typically performed by plastic surgeons. "Yes, the plastic surgeons do more big, multiple procedures and have more problems," Dr. Coldiron replied. "That does not give them the right to try and restrict our practices under the guise of patient safety at the level of the state medical boards and legislatures that is preposterous."
The current study is in press, and represents an update of Dr. Coldiron’s previously reported 7-year Florida data (Dermatol. Surg. 2008;34:285-91).
Additional information is available on the website for Dr. Coldiron's practice, including real adverse event incident reports.
Alabama reports support and validate the Florida data, Dr. Coldiron said. There were three deaths and 52 adverse events that required an office-to-hospital transfer in Alabama. Cosmetic procedures were associated with zero deaths and 42% of hospital transfers during the 6 years. The Alabama medical board provided Dr. Coldiron with the data upon request.
A majority of cosmetic procedure adverse events (86%) were from cases performed under general anesthesia.
Plastic surgery was the specialty most often involved in adverse event reports (42% of all complications), compared with 1.9% for dermatologists in that state (one report associated with tumescent anesthesia).
"Certainly we are not a major contributor in any sense. Dermatologic surgery is extremely safe," Dr. Coldiron said at the meeting, which was jointly sponsored by the American Society of Cosmetic Dermatology and Aesthetic Surgery.
Dr. McGuire said that office-based surgery is safe when performed at centers accredited by the American Association for Accreditation of Ambulatory Surgery Facilities (AAAASF). Studies cited on the organization's website reported 23 deaths of 1,141,418 outpatient procedures in the United States over 5.5 years.
Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
CHICAGO – Office-based surgery is safe when performed by dermatologists, according to a study of 10 years of complication and death reports from Florida and 6 years of data from Alabama.
Dermatologic surgeons could use the findings to combat any legislative attempts to curtail office procedures, including liposuction, Dr. Brett Coldiron said.
Some plastic surgeons, for example, are trying to restrict what types of office surgeries dermatologists can legally perform, said Dr. Coldiron, a private practice dermatologic surgeon and member of the dermatology faculty at the University of Cincinnati.
The study indicates procedures performed by plastic surgeons actually carry a greater risk for adverse events and death, compared with dermatologic surgeries, Dr. Coldiron said.
A plastic surgeon contacted for comment, Dr. Michael McGuire, said the comparison is unfair given the differing complexity of surgeries done by the two specialties. "It’s a total misrepresentation of the statistics. There is no question that the incidence and even the deaths are smaller with dermatology than with any other specialty."
"Comparing an abdominoplasty – a tummy tuck – with a skin cancer excision or even a small volume of liposuction is ridiculous. To compare that with doing tummy tucks, and 4- or 5-hour facelifts, or major breast reconstructive surgery, all of which are done in outpatient surgery centers, is apples and oranges. They are totally different procedures," said Dr. McGuire, who is in private practice in Santa Monica, Calif., and director of The American Board of Plastic Surgeons.
The prospectively collected data show "that any claims by plastic surgeons or anesthesiologists that dermatologists are doing unsafe things and injuring patients in the office is unfounded," Dr. Coldiron said. "And ... if they are going to make such claims, they should have some data to back them up."
Both Alabama and Florida require notification when an outpatient experiences serious injury, transfer to a hospital, or death related to surgery. These mandatory reports are part of public record in the state of Florida, for example.
Dr. Coldiron found 46 deaths and 263 complications that required hospital transfers in Florida. Cosmetic (nonmedically necessary) procedures were associated with 57% of these deaths and almost 50% of such transfers in the state. Liposuction or liposuction with another cosmetic procedure (abdominoplasty, for example) resulted in death for 10 patients and hospital transfer in another 34 cases.
The majority of cosmetic procedure deaths (67%) and hospital transfers (74%) in Florida were performed under general anesthesia, said Dr. Coldiron.
This is relevant because some physicians who perform liposuction under general anesthesia are trying to restrict liposuction under local or tumescent anesthesia, he said. "There have been legislative attempts to prohibit this. The state of New York recently passed a law restricting liposuction in offices, under local anesthesia to 500 cc, which paradoxically will increase the number of injuries and deaths."
"When you try to restrict the use of local anesthesia or tumescent anesthesia ... you will force more people into using general anesthesia, which has more complications. Hospital transfers or deaths with the use of local anesthesia are incredibly rare," Dr. Coldiron said in an interview. "In fact, I’m only aware of a couple that occurred after anaphylactic reactions."
"They [dermatologists] like to blame the general anesthesia," Dr. McGuire said. "It’s not the general anesthesia that is the difference; it’s the magnitude of the surgery. Clearly there are going to be more risks and complications with major surgery compared to minor surgery under any kind of anesthesia." Plastic surgeons in Florida reported the most adverse events (45% of the total), compared with 1.3% reported by dermatologists.
A meeting attendee questioned a direct comparison between specialties, citing the higher complexity of cases typically performed by plastic surgeons. "Yes, the plastic surgeons do more big, multiple procedures and have more problems," Dr. Coldiron replied. "That does not give them the right to try and restrict our practices under the guise of patient safety at the level of the state medical boards and legislatures that is preposterous."
The current study is in press, and represents an update of Dr. Coldiron’s previously reported 7-year Florida data (Dermatol. Surg. 2008;34:285-91).
Additional information is available on the website for Dr. Coldiron's practice, including real adverse event incident reports.
Alabama reports support and validate the Florida data, Dr. Coldiron said. There were three deaths and 52 adverse events that required an office-to-hospital transfer in Alabama. Cosmetic procedures were associated with zero deaths and 42% of hospital transfers during the 6 years. The Alabama medical board provided Dr. Coldiron with the data upon request.
A majority of cosmetic procedure adverse events (86%) were from cases performed under general anesthesia.
Plastic surgery was the specialty most often involved in adverse event reports (42% of all complications), compared with 1.9% for dermatologists in that state (one report associated with tumescent anesthesia).
"Certainly we are not a major contributor in any sense. Dermatologic surgery is extremely safe," Dr. Coldiron said at the meeting, which was jointly sponsored by the American Society of Cosmetic Dermatology and Aesthetic Surgery.
Dr. McGuire said that office-based surgery is safe when performed at centers accredited by the American Association for Accreditation of Ambulatory Surgery Facilities (AAAASF). Studies cited on the organization's website reported 23 deaths of 1,141,418 outpatient procedures in the United States over 5.5 years.
Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
CHICAGO – Office-based surgery is safe when performed by dermatologists, according to a study of 10 years of complication and death reports from Florida and 6 years of data from Alabama.
Dermatologic surgeons could use the findings to combat any legislative attempts to curtail office procedures, including liposuction, Dr. Brett Coldiron said.
Some plastic surgeons, for example, are trying to restrict what types of office surgeries dermatologists can legally perform, said Dr. Coldiron, a private practice dermatologic surgeon and member of the dermatology faculty at the University of Cincinnati.
The study indicates procedures performed by plastic surgeons actually carry a greater risk for adverse events and death, compared with dermatologic surgeries, Dr. Coldiron said.
A plastic surgeon contacted for comment, Dr. Michael McGuire, said the comparison is unfair given the differing complexity of surgeries done by the two specialties. "It’s a total misrepresentation of the statistics. There is no question that the incidence and even the deaths are smaller with dermatology than with any other specialty."
"Comparing an abdominoplasty – a tummy tuck – with a skin cancer excision or even a small volume of liposuction is ridiculous. To compare that with doing tummy tucks, and 4- or 5-hour facelifts, or major breast reconstructive surgery, all of which are done in outpatient surgery centers, is apples and oranges. They are totally different procedures," said Dr. McGuire, who is in private practice in Santa Monica, Calif., and director of The American Board of Plastic Surgeons.
The prospectively collected data show "that any claims by plastic surgeons or anesthesiologists that dermatologists are doing unsafe things and injuring patients in the office is unfounded," Dr. Coldiron said. "And ... if they are going to make such claims, they should have some data to back them up."
Both Alabama and Florida require notification when an outpatient experiences serious injury, transfer to a hospital, or death related to surgery. These mandatory reports are part of public record in the state of Florida, for example.
Dr. Coldiron found 46 deaths and 263 complications that required hospital transfers in Florida. Cosmetic (nonmedically necessary) procedures were associated with 57% of these deaths and almost 50% of such transfers in the state. Liposuction or liposuction with another cosmetic procedure (abdominoplasty, for example) resulted in death for 10 patients and hospital transfer in another 34 cases.
The majority of cosmetic procedure deaths (67%) and hospital transfers (74%) in Florida were performed under general anesthesia, said Dr. Coldiron.
This is relevant because some physicians who perform liposuction under general anesthesia are trying to restrict liposuction under local or tumescent anesthesia, he said. "There have been legislative attempts to prohibit this. The state of New York recently passed a law restricting liposuction in offices, under local anesthesia to 500 cc, which paradoxically will increase the number of injuries and deaths."
"When you try to restrict the use of local anesthesia or tumescent anesthesia ... you will force more people into using general anesthesia, which has more complications. Hospital transfers or deaths with the use of local anesthesia are incredibly rare," Dr. Coldiron said in an interview. "In fact, I’m only aware of a couple that occurred after anaphylactic reactions."
"They [dermatologists] like to blame the general anesthesia," Dr. McGuire said. "It’s not the general anesthesia that is the difference; it’s the magnitude of the surgery. Clearly there are going to be more risks and complications with major surgery compared to minor surgery under any kind of anesthesia." Plastic surgeons in Florida reported the most adverse events (45% of the total), compared with 1.3% reported by dermatologists.
A meeting attendee questioned a direct comparison between specialties, citing the higher complexity of cases typically performed by plastic surgeons. "Yes, the plastic surgeons do more big, multiple procedures and have more problems," Dr. Coldiron replied. "That does not give them the right to try and restrict our practices under the guise of patient safety at the level of the state medical boards and legislatures that is preposterous."
The current study is in press, and represents an update of Dr. Coldiron’s previously reported 7-year Florida data (Dermatol. Surg. 2008;34:285-91).
Additional information is available on the website for Dr. Coldiron's practice, including real adverse event incident reports.
Alabama reports support and validate the Florida data, Dr. Coldiron said. There were three deaths and 52 adverse events that required an office-to-hospital transfer in Alabama. Cosmetic procedures were associated with zero deaths and 42% of hospital transfers during the 6 years. The Alabama medical board provided Dr. Coldiron with the data upon request.
A majority of cosmetic procedure adverse events (86%) were from cases performed under general anesthesia.
Plastic surgery was the specialty most often involved in adverse event reports (42% of all complications), compared with 1.9% for dermatologists in that state (one report associated with tumescent anesthesia).
"Certainly we are not a major contributor in any sense. Dermatologic surgery is extremely safe," Dr. Coldiron said at the meeting, which was jointly sponsored by the American Society of Cosmetic Dermatology and Aesthetic Surgery.
Dr. McGuire said that office-based surgery is safe when performed at centers accredited by the American Association for Accreditation of Ambulatory Surgery Facilities (AAAASF). Studies cited on the organization's website reported 23 deaths of 1,141,418 outpatient procedures in the United States over 5.5 years.
Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
Major Finding: Forty-six deaths and 263 complications required hospital transfers in Florida. Cosmetic procedures were associated with 57% of these deaths and almost 50% of such transfers in the state.
Data Source: Ten years of complication and death reports from Florida and 6 years of data from Alabama
Disclosures: Dr. McGuire is past president of the AAASF. Dr. Coldiron said he had no disclosures.
Atopic Children at Increased Risk of Contact Dermatitis
SAN FRANCISCO — What do you consider when one of your atopic pediatric patients has recalcitrant dermatitis? Or a new-onset dermatitis that lasts longer than 2 months? It might be time to expand your differential diagnosis to consider contact dermatitis, said Dr. Sharon Jacob.
There is a high prevalence of allergic contact dermatitis in moderate to severe atopic patients. Also, think systemic allergic contact dermatitis in highly sensitized children. Although more commonly reported in adults, systemic allergies can affect pediatric patients, Dr. Jacob said at a meeting sponsored by Skin Disease Education Foundation (SDEF).
Exposure to nickel, cobalt, fragrances, formaldehyde and balsam of Peru – including from dietary sources – can trigger a systemic reaction. System allergy “should be considered in children with a positive patch test who fail to improve with skin contact avoidance,” she said.
A diet devoid of the suspected trigger(s) for 6 weeks or more can make a difference for some recalcitrant children, said Dr. Jacob, an assistant clinical professor of medicine (dermatology) and pediatrics at the University of California, San Diego, and at Rady Children's Hospital. Such an avoidance diet improved the outcome for eight pediatric patients with systemic allergies, according to a recent report from Dr. Jacob and Dr. C. Matiz (Pediatr. Dermatol. 2010 Aug 27 [doi: 10.1111/j.1525-1470.2010.01130.x]).
An avoidance diet is particularly challenging for children with allergy to balsam of Peru. This allergen is found in many foods, including tomatoes, citrus, and certain spices, according to a study in adults (J. Am. Acad. Dermatol. 2001;45:377-81).
“The food we have the most problem with is ketchup. Ketchup and pizza are the bane of my existence,” Dr. Jacob said. Keep the diet simple if possible and encourage adherence with incentives for the child, such as a points and rewards system, she added.
Be careful how you counsel these children, Dr. Jacob said. “Start off with the fact they cannot have asparagus – 'Yes!' – or spinach - 'Yay!' Then mention ketchup, chocolate, and soda, and you become the evil contact derm pediatrician.”
Sometimes an affected anatomic site is an important clinical clue. For example, Dr. Jacob described a 10-month-old child with generalized dermatitis who also presented with specific perioral dermatitis. “When we see this we think balsam of Peru.” Involvement of the eyelids is another clinical clue.
Another interesting case Dr. Jacob presented was a toddler with a fragrance contact allergy that triggered a systemic reaction. Initially, however, she had to figure out how a toddler could have an allergy to fragrance. She discovered that the toddler became sensitized from “connubial contact” – or a physical transfer – of fragrance from the mother's neck. Following this discovery, the child was doing well until a flare associated with vanilla teething wafers. “It's amazing how much vanilla is everywhere.”
When an allergen or chemical is transferred by the patient to another site on their body, it is called “ectopic dermatitis.” Dr. Jacob cited the case of a 3-year-old whose older sister lacquered her fingernails, for example. The younger child scratched other areas and reacted to the tosylamide formaldehyde resin on her nails.
If you have a child whose controlled condition suddenly worsens in their atopic areas, consider these potential culprits: lanolin, neomycin, and bacitracin, Dr. Jacob said.
Lanolin is derived from the sebaceous gland in sheep. Although removed from most wool clothing during processing, it remains in cashmere clothing to keep it soft. “Lanolin is a top offender in children – because it is used in emollients,” Dr. Jacob said.
Also assess these patients for exposure to plants in the Compositae family – including feverfew and chamomile.
Keep in mind some components may be found in preparations you prescribe for their atopic dermatitis, such as bisabolol, an alcohol compound derived from chamomile and found in Aquaphor ointment (Beiersdorf Inc.) and sometimes prescribed for atopic dermatitis in children (Pediatr. Dermatol. 2010;27:103-4)
Also watch out for emulsifiers used in diaper creams and topical steroids, including sorbitan sesquioleate. Reports of contact dermatitis to this sorbitan are increasing (Dermatitis. 2008:19:339-41).
Dr. Jacob noted that patch testing of children for contact allergies is “off-label” – not approved by the Food and Drug Administration.
A meeting attendee asked Dr. Jacob about the youngest age patient that she will patch test. “I have patch tested a patient as young as 10 months old. But I generally do not patch test children under 5 years old unless absolutely indicated,” she replied.
She first tries “preemptive avoidance” of suspected allergens in these young children before patch testing.
SDEF and this news organization are owned by Elsevier. Dr. Jacob is a speaker for Coria Laboratories, Astellas Pharma, and Shire. She is also an independent investigator for Allerderm, maker of the T.R.U.E. test.
Nickel, cobalt, formaldehyde, and balsam of Peru can trigger a systemic reaction in atopic children.
Source DR. JACOB
SAN FRANCISCO — What do you consider when one of your atopic pediatric patients has recalcitrant dermatitis? Or a new-onset dermatitis that lasts longer than 2 months? It might be time to expand your differential diagnosis to consider contact dermatitis, said Dr. Sharon Jacob.
There is a high prevalence of allergic contact dermatitis in moderate to severe atopic patients. Also, think systemic allergic contact dermatitis in highly sensitized children. Although more commonly reported in adults, systemic allergies can affect pediatric patients, Dr. Jacob said at a meeting sponsored by Skin Disease Education Foundation (SDEF).
Exposure to nickel, cobalt, fragrances, formaldehyde and balsam of Peru – including from dietary sources – can trigger a systemic reaction. System allergy “should be considered in children with a positive patch test who fail to improve with skin contact avoidance,” she said.
A diet devoid of the suspected trigger(s) for 6 weeks or more can make a difference for some recalcitrant children, said Dr. Jacob, an assistant clinical professor of medicine (dermatology) and pediatrics at the University of California, San Diego, and at Rady Children's Hospital. Such an avoidance diet improved the outcome for eight pediatric patients with systemic allergies, according to a recent report from Dr. Jacob and Dr. C. Matiz (Pediatr. Dermatol. 2010 Aug 27 [doi: 10.1111/j.1525-1470.2010.01130.x]).
An avoidance diet is particularly challenging for children with allergy to balsam of Peru. This allergen is found in many foods, including tomatoes, citrus, and certain spices, according to a study in adults (J. Am. Acad. Dermatol. 2001;45:377-81).
“The food we have the most problem with is ketchup. Ketchup and pizza are the bane of my existence,” Dr. Jacob said. Keep the diet simple if possible and encourage adherence with incentives for the child, such as a points and rewards system, she added.
Be careful how you counsel these children, Dr. Jacob said. “Start off with the fact they cannot have asparagus – 'Yes!' – or spinach - 'Yay!' Then mention ketchup, chocolate, and soda, and you become the evil contact derm pediatrician.”
Sometimes an affected anatomic site is an important clinical clue. For example, Dr. Jacob described a 10-month-old child with generalized dermatitis who also presented with specific perioral dermatitis. “When we see this we think balsam of Peru.” Involvement of the eyelids is another clinical clue.
Another interesting case Dr. Jacob presented was a toddler with a fragrance contact allergy that triggered a systemic reaction. Initially, however, she had to figure out how a toddler could have an allergy to fragrance. She discovered that the toddler became sensitized from “connubial contact” – or a physical transfer – of fragrance from the mother's neck. Following this discovery, the child was doing well until a flare associated with vanilla teething wafers. “It's amazing how much vanilla is everywhere.”
When an allergen or chemical is transferred by the patient to another site on their body, it is called “ectopic dermatitis.” Dr. Jacob cited the case of a 3-year-old whose older sister lacquered her fingernails, for example. The younger child scratched other areas and reacted to the tosylamide formaldehyde resin on her nails.
If you have a child whose controlled condition suddenly worsens in their atopic areas, consider these potential culprits: lanolin, neomycin, and bacitracin, Dr. Jacob said.
Lanolin is derived from the sebaceous gland in sheep. Although removed from most wool clothing during processing, it remains in cashmere clothing to keep it soft. “Lanolin is a top offender in children – because it is used in emollients,” Dr. Jacob said.
Also assess these patients for exposure to plants in the Compositae family – including feverfew and chamomile.
Keep in mind some components may be found in preparations you prescribe for their atopic dermatitis, such as bisabolol, an alcohol compound derived from chamomile and found in Aquaphor ointment (Beiersdorf Inc.) and sometimes prescribed for atopic dermatitis in children (Pediatr. Dermatol. 2010;27:103-4)
Also watch out for emulsifiers used in diaper creams and topical steroids, including sorbitan sesquioleate. Reports of contact dermatitis to this sorbitan are increasing (Dermatitis. 2008:19:339-41).
Dr. Jacob noted that patch testing of children for contact allergies is “off-label” – not approved by the Food and Drug Administration.
A meeting attendee asked Dr. Jacob about the youngest age patient that she will patch test. “I have patch tested a patient as young as 10 months old. But I generally do not patch test children under 5 years old unless absolutely indicated,” she replied.
She first tries “preemptive avoidance” of suspected allergens in these young children before patch testing.
SDEF and this news organization are owned by Elsevier. Dr. Jacob is a speaker for Coria Laboratories, Astellas Pharma, and Shire. She is also an independent investigator for Allerderm, maker of the T.R.U.E. test.
Nickel, cobalt, formaldehyde, and balsam of Peru can trigger a systemic reaction in atopic children.
Source DR. JACOB
SAN FRANCISCO — What do you consider when one of your atopic pediatric patients has recalcitrant dermatitis? Or a new-onset dermatitis that lasts longer than 2 months? It might be time to expand your differential diagnosis to consider contact dermatitis, said Dr. Sharon Jacob.
There is a high prevalence of allergic contact dermatitis in moderate to severe atopic patients. Also, think systemic allergic contact dermatitis in highly sensitized children. Although more commonly reported in adults, systemic allergies can affect pediatric patients, Dr. Jacob said at a meeting sponsored by Skin Disease Education Foundation (SDEF).
Exposure to nickel, cobalt, fragrances, formaldehyde and balsam of Peru – including from dietary sources – can trigger a systemic reaction. System allergy “should be considered in children with a positive patch test who fail to improve with skin contact avoidance,” she said.
A diet devoid of the suspected trigger(s) for 6 weeks or more can make a difference for some recalcitrant children, said Dr. Jacob, an assistant clinical professor of medicine (dermatology) and pediatrics at the University of California, San Diego, and at Rady Children's Hospital. Such an avoidance diet improved the outcome for eight pediatric patients with systemic allergies, according to a recent report from Dr. Jacob and Dr. C. Matiz (Pediatr. Dermatol. 2010 Aug 27 [doi: 10.1111/j.1525-1470.2010.01130.x]).
An avoidance diet is particularly challenging for children with allergy to balsam of Peru. This allergen is found in many foods, including tomatoes, citrus, and certain spices, according to a study in adults (J. Am. Acad. Dermatol. 2001;45:377-81).
“The food we have the most problem with is ketchup. Ketchup and pizza are the bane of my existence,” Dr. Jacob said. Keep the diet simple if possible and encourage adherence with incentives for the child, such as a points and rewards system, she added.
Be careful how you counsel these children, Dr. Jacob said. “Start off with the fact they cannot have asparagus – 'Yes!' – or spinach - 'Yay!' Then mention ketchup, chocolate, and soda, and you become the evil contact derm pediatrician.”
Sometimes an affected anatomic site is an important clinical clue. For example, Dr. Jacob described a 10-month-old child with generalized dermatitis who also presented with specific perioral dermatitis. “When we see this we think balsam of Peru.” Involvement of the eyelids is another clinical clue.
Another interesting case Dr. Jacob presented was a toddler with a fragrance contact allergy that triggered a systemic reaction. Initially, however, she had to figure out how a toddler could have an allergy to fragrance. She discovered that the toddler became sensitized from “connubial contact” – or a physical transfer – of fragrance from the mother's neck. Following this discovery, the child was doing well until a flare associated with vanilla teething wafers. “It's amazing how much vanilla is everywhere.”
When an allergen or chemical is transferred by the patient to another site on their body, it is called “ectopic dermatitis.” Dr. Jacob cited the case of a 3-year-old whose older sister lacquered her fingernails, for example. The younger child scratched other areas and reacted to the tosylamide formaldehyde resin on her nails.
If you have a child whose controlled condition suddenly worsens in their atopic areas, consider these potential culprits: lanolin, neomycin, and bacitracin, Dr. Jacob said.
Lanolin is derived from the sebaceous gland in sheep. Although removed from most wool clothing during processing, it remains in cashmere clothing to keep it soft. “Lanolin is a top offender in children – because it is used in emollients,” Dr. Jacob said.
Also assess these patients for exposure to plants in the Compositae family – including feverfew and chamomile.
Keep in mind some components may be found in preparations you prescribe for their atopic dermatitis, such as bisabolol, an alcohol compound derived from chamomile and found in Aquaphor ointment (Beiersdorf Inc.) and sometimes prescribed for atopic dermatitis in children (Pediatr. Dermatol. 2010;27:103-4)
Also watch out for emulsifiers used in diaper creams and topical steroids, including sorbitan sesquioleate. Reports of contact dermatitis to this sorbitan are increasing (Dermatitis. 2008:19:339-41).
Dr. Jacob noted that patch testing of children for contact allergies is “off-label” – not approved by the Food and Drug Administration.
A meeting attendee asked Dr. Jacob about the youngest age patient that she will patch test. “I have patch tested a patient as young as 10 months old. But I generally do not patch test children under 5 years old unless absolutely indicated,” she replied.
She first tries “preemptive avoidance” of suspected allergens in these young children before patch testing.
SDEF and this news organization are owned by Elsevier. Dr. Jacob is a speaker for Coria Laboratories, Astellas Pharma, and Shire. She is also an independent investigator for Allerderm, maker of the T.R.U.E. test.
Nickel, cobalt, formaldehyde, and balsam of Peru can trigger a systemic reaction in atopic children.
Source DR. JACOB
Heart Rate Changes After Stimulants Negligible
BOCA RATON, FLA. – The use of methylphenidate or mixed amphetamine salts for attention-deficit/hyperactivity disorder can increase heart rate, blood pressure, and the QT interval in children, adolescents, and adults, according to a review of placebo-controlled and open-label extension trials published since 2000.
The magnitude of the effects appears small for most patients, which points to the importance of screening for preexisting cardiovascular disease and asking about any relevant family or patient history, Dr. Raul R. Silva said.
Despite long-term use and the effectiveness of these stimulant medications to reduce core symptoms of ADHD, concerns arose about increased potential for cardiovascular events. The American Heart Association released guidelines for cardiac monitoring of all children with ADHD before treatment (Circulation 2008;117:2407–23). “Some of what they came out with was severe,” said Dr. Silva, vice chair of the department of child and adolescent psychiatry at New York University. For example, he pointed out, the American Academy of Pediatrics said it had to temper its recommendations (Pediatrics 2008;122:451–3).
Ultimately, the two organizations released a clarification statement that recognizes the need for responsible cardiovascular monitoring while not withholding these medications to treat ADHD, Dr. Silva said (J. Dev. Behav. Pediatr. 2008;29:335. Despite the joint clarification, confusion about the actual risks remains, Dr. Silva said.
To determine more, Dr. Silva and his colleagues identified and reviewed five double-blind, placebo-controlled studies and six open-label studies that reported relevant cardiovascular data.
“We looked at 10 years' worth of studies in children and adults that reported heart rate, blood pressure, and EKG changes,” Dr. Silva said in an interview at his poster presentation during the meeting, which was sponsored by the National Institute of Mental Health.
Both types of studies were included because double-blind, placebo-controlled studies “are so short, there is not always a clear picture” and because “long-term studies tend to be open label,” said Dr. Silva, who also has a private practice in Cresskill, N.J.
In the double-blind studies, mean heart rate increased by 1–8.5 beats per minute after 3–6 weeks of treatment. The percentages of patients who experienced predefined, “clinically notable” heart rate events were similar among groups who received methylphenidate (MPH), mixed amphetamine salts (MAS), or placebo. Significant increases of 1.5–4.4 bpm in mean heart rate were reported by most of the long-term, open-label extension studies. A comparison of the short-term and long-term studies does not suggest an accumulative risk, Dr. Silva said. He added that it is unclear whether long-term increases in heart rate associated with these stimulants could increase the risk for stroke, heart attacks, or dysrhythmias.
“It may be reasonable to assume that increases in heart rate with therapeutic doses of stimulants are relatively safe in patients without predisposing or preexisting cardiac risk factors; however, further research and data are required to confirm any potential increased risk for cardiovascular events later in life,” the authors wrote.
In terms of blood pressure changes, most of the double-blind studies demonstrated no significant increases with stimulant treatment, compared with baseline. Again, the percentages of patients who experienced clinically notable increases in blood pressure were similar among groups that received MPH, MAS, or placebo.
In contrast, most of the open-label studies found significant increases in systolic blood pressure (0.6–3.5 mm Hg) and diastolic blood pressure (0.7–2.6 mm Hg), compared with baseline. Despite the disparity in significance, numerically, the changes in blood pressure in both study types were similar, suggesting no accumulative effect.
Researchers have not demonstrated a relationship between such small increases in blood pressure and increased morbidity, Dr. Silva said. It is also unclear whether these increases translate to an increased risk for cardiovascular events in patients with preexisting hypertension.
“In essence, you end up seeing [that] there aren't that many serious changes that occur, and there are some you see in the placebo group as well,” Dr. Silva said. Even so, he added, the rate for these heart rate and blood pressure changes “tends to be a little higher for stimulant drugs, and that is what you want to be most concerned about.”
Acute consequences in children with preexisting cardiac disease and the unknown potential for long-term adverse effects in all children who are exposed to these stimulants are two major concerns. “Personally, I always follow up [with patients]. I take a family history, for example, of arrhythmias, and personal history for syncope and chest pain,” Dr. Silva said.
These are among the recommendations in the 12-item screening recommendations from the American Heart Association (Circulation 2008;117:2407–23 and Circulation 2007;115:1643–55). Also, pay attention to symptoms such as palpitations, near syncope, or syncope that could indicate a cardiac condition. Family history should include hypertrophic cardiomyopathy, long QT syndrome, Wolff-Parkinson-White syndrome, and Marfan syndrome.
Novartis Pharmaceuticals Corp. supported the study. Dr. Silva disclosed that he is a consultant and on the speakers bureau for Novartis.
'I take a family history … of arrhythmias, and personal history for syncope and chest pain.'
Source DR. SILVA
BOCA RATON, FLA. – The use of methylphenidate or mixed amphetamine salts for attention-deficit/hyperactivity disorder can increase heart rate, blood pressure, and the QT interval in children, adolescents, and adults, according to a review of placebo-controlled and open-label extension trials published since 2000.
The magnitude of the effects appears small for most patients, which points to the importance of screening for preexisting cardiovascular disease and asking about any relevant family or patient history, Dr. Raul R. Silva said.
Despite long-term use and the effectiveness of these stimulant medications to reduce core symptoms of ADHD, concerns arose about increased potential for cardiovascular events. The American Heart Association released guidelines for cardiac monitoring of all children with ADHD before treatment (Circulation 2008;117:2407–23). “Some of what they came out with was severe,” said Dr. Silva, vice chair of the department of child and adolescent psychiatry at New York University. For example, he pointed out, the American Academy of Pediatrics said it had to temper its recommendations (Pediatrics 2008;122:451–3).
Ultimately, the two organizations released a clarification statement that recognizes the need for responsible cardiovascular monitoring while not withholding these medications to treat ADHD, Dr. Silva said (J. Dev. Behav. Pediatr. 2008;29:335. Despite the joint clarification, confusion about the actual risks remains, Dr. Silva said.
To determine more, Dr. Silva and his colleagues identified and reviewed five double-blind, placebo-controlled studies and six open-label studies that reported relevant cardiovascular data.
“We looked at 10 years' worth of studies in children and adults that reported heart rate, blood pressure, and EKG changes,” Dr. Silva said in an interview at his poster presentation during the meeting, which was sponsored by the National Institute of Mental Health.
Both types of studies were included because double-blind, placebo-controlled studies “are so short, there is not always a clear picture” and because “long-term studies tend to be open label,” said Dr. Silva, who also has a private practice in Cresskill, N.J.
In the double-blind studies, mean heart rate increased by 1–8.5 beats per minute after 3–6 weeks of treatment. The percentages of patients who experienced predefined, “clinically notable” heart rate events were similar among groups who received methylphenidate (MPH), mixed amphetamine salts (MAS), or placebo. Significant increases of 1.5–4.4 bpm in mean heart rate were reported by most of the long-term, open-label extension studies. A comparison of the short-term and long-term studies does not suggest an accumulative risk, Dr. Silva said. He added that it is unclear whether long-term increases in heart rate associated with these stimulants could increase the risk for stroke, heart attacks, or dysrhythmias.
“It may be reasonable to assume that increases in heart rate with therapeutic doses of stimulants are relatively safe in patients without predisposing or preexisting cardiac risk factors; however, further research and data are required to confirm any potential increased risk for cardiovascular events later in life,” the authors wrote.
In terms of blood pressure changes, most of the double-blind studies demonstrated no significant increases with stimulant treatment, compared with baseline. Again, the percentages of patients who experienced clinically notable increases in blood pressure were similar among groups that received MPH, MAS, or placebo.
In contrast, most of the open-label studies found significant increases in systolic blood pressure (0.6–3.5 mm Hg) and diastolic blood pressure (0.7–2.6 mm Hg), compared with baseline. Despite the disparity in significance, numerically, the changes in blood pressure in both study types were similar, suggesting no accumulative effect.
Researchers have not demonstrated a relationship between such small increases in blood pressure and increased morbidity, Dr. Silva said. It is also unclear whether these increases translate to an increased risk for cardiovascular events in patients with preexisting hypertension.
“In essence, you end up seeing [that] there aren't that many serious changes that occur, and there are some you see in the placebo group as well,” Dr. Silva said. Even so, he added, the rate for these heart rate and blood pressure changes “tends to be a little higher for stimulant drugs, and that is what you want to be most concerned about.”
Acute consequences in children with preexisting cardiac disease and the unknown potential for long-term adverse effects in all children who are exposed to these stimulants are two major concerns. “Personally, I always follow up [with patients]. I take a family history, for example, of arrhythmias, and personal history for syncope and chest pain,” Dr. Silva said.
These are among the recommendations in the 12-item screening recommendations from the American Heart Association (Circulation 2008;117:2407–23 and Circulation 2007;115:1643–55). Also, pay attention to symptoms such as palpitations, near syncope, or syncope that could indicate a cardiac condition. Family history should include hypertrophic cardiomyopathy, long QT syndrome, Wolff-Parkinson-White syndrome, and Marfan syndrome.
Novartis Pharmaceuticals Corp. supported the study. Dr. Silva disclosed that he is a consultant and on the speakers bureau for Novartis.
'I take a family history … of arrhythmias, and personal history for syncope and chest pain.'
Source DR. SILVA
BOCA RATON, FLA. – The use of methylphenidate or mixed amphetamine salts for attention-deficit/hyperactivity disorder can increase heart rate, blood pressure, and the QT interval in children, adolescents, and adults, according to a review of placebo-controlled and open-label extension trials published since 2000.
The magnitude of the effects appears small for most patients, which points to the importance of screening for preexisting cardiovascular disease and asking about any relevant family or patient history, Dr. Raul R. Silva said.
Despite long-term use and the effectiveness of these stimulant medications to reduce core symptoms of ADHD, concerns arose about increased potential for cardiovascular events. The American Heart Association released guidelines for cardiac monitoring of all children with ADHD before treatment (Circulation 2008;117:2407–23). “Some of what they came out with was severe,” said Dr. Silva, vice chair of the department of child and adolescent psychiatry at New York University. For example, he pointed out, the American Academy of Pediatrics said it had to temper its recommendations (Pediatrics 2008;122:451–3).
Ultimately, the two organizations released a clarification statement that recognizes the need for responsible cardiovascular monitoring while not withholding these medications to treat ADHD, Dr. Silva said (J. Dev. Behav. Pediatr. 2008;29:335. Despite the joint clarification, confusion about the actual risks remains, Dr. Silva said.
To determine more, Dr. Silva and his colleagues identified and reviewed five double-blind, placebo-controlled studies and six open-label studies that reported relevant cardiovascular data.
“We looked at 10 years' worth of studies in children and adults that reported heart rate, blood pressure, and EKG changes,” Dr. Silva said in an interview at his poster presentation during the meeting, which was sponsored by the National Institute of Mental Health.
Both types of studies were included because double-blind, placebo-controlled studies “are so short, there is not always a clear picture” and because “long-term studies tend to be open label,” said Dr. Silva, who also has a private practice in Cresskill, N.J.
In the double-blind studies, mean heart rate increased by 1–8.5 beats per minute after 3–6 weeks of treatment. The percentages of patients who experienced predefined, “clinically notable” heart rate events were similar among groups who received methylphenidate (MPH), mixed amphetamine salts (MAS), or placebo. Significant increases of 1.5–4.4 bpm in mean heart rate were reported by most of the long-term, open-label extension studies. A comparison of the short-term and long-term studies does not suggest an accumulative risk, Dr. Silva said. He added that it is unclear whether long-term increases in heart rate associated with these stimulants could increase the risk for stroke, heart attacks, or dysrhythmias.
“It may be reasonable to assume that increases in heart rate with therapeutic doses of stimulants are relatively safe in patients without predisposing or preexisting cardiac risk factors; however, further research and data are required to confirm any potential increased risk for cardiovascular events later in life,” the authors wrote.
In terms of blood pressure changes, most of the double-blind studies demonstrated no significant increases with stimulant treatment, compared with baseline. Again, the percentages of patients who experienced clinically notable increases in blood pressure were similar among groups that received MPH, MAS, or placebo.
In contrast, most of the open-label studies found significant increases in systolic blood pressure (0.6–3.5 mm Hg) and diastolic blood pressure (0.7–2.6 mm Hg), compared with baseline. Despite the disparity in significance, numerically, the changes in blood pressure in both study types were similar, suggesting no accumulative effect.
Researchers have not demonstrated a relationship between such small increases in blood pressure and increased morbidity, Dr. Silva said. It is also unclear whether these increases translate to an increased risk for cardiovascular events in patients with preexisting hypertension.
“In essence, you end up seeing [that] there aren't that many serious changes that occur, and there are some you see in the placebo group as well,” Dr. Silva said. Even so, he added, the rate for these heart rate and blood pressure changes “tends to be a little higher for stimulant drugs, and that is what you want to be most concerned about.”
Acute consequences in children with preexisting cardiac disease and the unknown potential for long-term adverse effects in all children who are exposed to these stimulants are two major concerns. “Personally, I always follow up [with patients]. I take a family history, for example, of arrhythmias, and personal history for syncope and chest pain,” Dr. Silva said.
These are among the recommendations in the 12-item screening recommendations from the American Heart Association (Circulation 2008;117:2407–23 and Circulation 2007;115:1643–55). Also, pay attention to symptoms such as palpitations, near syncope, or syncope that could indicate a cardiac condition. Family history should include hypertrophic cardiomyopathy, long QT syndrome, Wolff-Parkinson-White syndrome, and Marfan syndrome.
Novartis Pharmaceuticals Corp. supported the study. Dr. Silva disclosed that he is a consultant and on the speakers bureau for Novartis.
'I take a family history … of arrhythmias, and personal history for syncope and chest pain.'
Source DR. SILVA
International Dermatologic Surgery Exchange Fund Established
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field's donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, the program has about 70 mentors from 19 nations.* The program continues to expand and is actively seeking host institutions around the world to work with the faculty. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I'll go home, and I'll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Saudi Arabia.** As a consultant to the DermaClinic, Dr. Field shared his expertise to transfer fat from a patient's abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also
hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. To apply or find out more, visit www.asds.net/InternationalEd/.
Dr. Field said that he has no relevant disclosures.
*CORRECTION 1/10/11: The article originally stated that the program had 29 U.S. dermatologic mentors and the program is active in 18 countries. The statement was corrected to: 70 mentors from 19 countries.
**CORRECTION 1/10/11: The article originally stated that Dr. Field has taught and learned about...fat transfer in Iran. That statement was revised to state: fat transfer in Saudi Arabia.
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field's donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, the program has about 70 mentors from 19 nations.* The program continues to expand and is actively seeking host institutions around the world to work with the faculty. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I'll go home, and I'll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Saudi Arabia.** As a consultant to the DermaClinic, Dr. Field shared his expertise to transfer fat from a patient's abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also
hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. To apply or find out more, visit www.asds.net/InternationalEd/.
Dr. Field said that he has no relevant disclosures.
*CORRECTION 1/10/11: The article originally stated that the program had 29 U.S. dermatologic mentors and the program is active in 18 countries. The statement was corrected to: 70 mentors from 19 countries.
**CORRECTION 1/10/11: The article originally stated that Dr. Field has taught and learned about...fat transfer in Iran. That statement was revised to state: fat transfer in Saudi Arabia.
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field's donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, the program has about 70 mentors from 19 nations.* The program continues to expand and is actively seeking host institutions around the world to work with the faculty. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I'll go home, and I'll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Saudi Arabia.** As a consultant to the DermaClinic, Dr. Field shared his expertise to transfer fat from a patient's abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also
hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. To apply or find out more, visit www.asds.net/InternationalEd/.
Dr. Field said that he has no relevant disclosures.
*CORRECTION 1/10/11: The article originally stated that the program had 29 U.S. dermatologic mentors and the program is active in 18 countries. The statement was corrected to: 70 mentors from 19 countries.
**CORRECTION 1/10/11: The article originally stated that Dr. Field has taught and learned about...fat transfer in Iran. That statement was revised to state: fat transfer in Saudi Arabia.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
International Dermatologic Surgery Educational Exchange Fund Is Established
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field’s donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, 29 U.S. dermatologic surgeons are mentors and the program is active in 18 countries. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I’ll go home, and I’ll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Iran. As a consultant to the DermaClinic in Tehran, Dr. Field shared his expertise to transfer fat from a patient’s abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. The International Educational Exchange Program's website offers more information.
Dr. Field said that he has no relevant disclosures.
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field’s donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, 29 U.S. dermatologic surgeons are mentors and the program is active in 18 countries. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I’ll go home, and I’ll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Iran. As a consultant to the DermaClinic in Tehran, Dr. Field shared his expertise to transfer fat from a patient’s abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. The International Educational Exchange Program's website offers more information.
Dr. Field said that he has no relevant disclosures.
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field’s donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, 29 U.S. dermatologic surgeons are mentors and the program is active in 18 countries. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I’ll go home, and I’ll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Iran. As a consultant to the DermaClinic in Tehran, Dr. Field shared his expertise to transfer fat from a patient’s abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. The International Educational Exchange Program's website offers more information.
Dr. Field said that he has no relevant disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
Recommended Approaches to the Adult Woman With Acne
SAN FRANCISCO – Dermatologists are seeing an increasing incidence of adult women with acne in their offices and they are a clear challenge to treat, Dr. Hilary E. Baldwin said.
Compared to teenagers, women in their 30s, 40s and 50s and their acne lesions can be more resistant to treatment, Dr. Baldwin said at a seminar on women’s and pediatric dermatology sponsored by the Skin Disease Education Foundation (SDEF).
"One of the problems of treating moderate-to-severe acne in the adult woman is that topical medications may not work particularly well. It may be that she is a little harder to treat, but also she has acne on the neck and the jaw, which is more sensitive skin, and the topical products tend to be quite irritating," Dr. Baldwin said.
Acne after adolescence also can be more psychosocially devastating. Unlike a teenage girl, an affected woman may have no one else in her social group who has acne. And "because teenagers are supposed to have acne," Dr. Baldwin said, "people will question: What is she doing wrong? Is she not eating right?"
Acne can have a detrimental effect on sexuality, motherhood, and/or returning to the workplace, and can deepen a midlife crisis, said Dr. Baldwin, vice chair of the Department of Dermatology at SUNY-Downstate in Brooklyn, N.Y.
With fewer topical agents in their armamentarium for the adult woman with acne, dermatologists tend to prescribe oral medication, Dr. Baldwin said.
Oral antibiotics are an example, such as anti-inflammatory dose doxycycline (acne is an off-label indication). This agent does not kill Propionibacterium acnes, but can improve acne through an anti-inflammatory effect similar to full-dose doxycycline, Dr. Baldwin said.
One caveat: if you prescribe an oral antibiotic, you may experience pushback from some patients, Dr. Baldwin said. "I have women who say that they get a yeast infection every time they get an antibiotic." Strategies include antibiotic treatment through a yeast infection; a simultaneous prescription to prevent yeast growth; and/or selection of an antibiotic less likely to cause this effect. For example, extended-release minocycline may be less likely to spur yeast growth than traditional minocycline, she said.
Non-antibiotic alternatives for moderate-to-severe acne are limited, especially in women of child-bearing potential.
Oral hormonal contraceptives also can improve acne in adult women, Dr. Baldwin said. In the United States, ethinyl estradiol/norethindrone acetate (Estrostep, Warner Chilcott); drospirenone/ethinyl estradiol (Yaz, Bayer); and ethinyl estradiol/norgestimate (Ortho Tri-Cyclen, Ortho McNeil Janssen) are FDA-approved for acne treatment "and others with estrogen may be effective."
Because their full acne-fighting effects can take up to six months, Dr. Baldwin recommended prescription of oral contraceptives in combination with a quicker onset agent. "For me it’s a medication on top of a medication that is going to give more immediate improvement, one I can take them off when I start to see the oral contraceptive kick in."
"The difference becomes significant with Yaz at about 6 months," Dr. Baldwin said. "But waiting for six months for this to happen is not something most of our patients will do."
Keep potential adverse effects of oral contraceptives in mind. Evidence in the literatures suggests there is no increased cardiovascular risk among non-smokers, Dr. Baldwin said. In addition, studies indicate no increase risk of breast cancer. An increased likelihood for a thrombolic event is elevated during the first year then becomes normalized, she said.
The FDA added a black box warning to labeling for spironolactone (Aldactone, GD Searle, plus generics) in 2008 that cites an increased risk for tumors based on animal studies. The warning recommends use only for approved indications, "which acne is not," Dr. Baldwin said. There have been five cases of breast cancer reported in women taking spironolactone and other medications, but there was "no clear link to the medication." Also, a review article found no evidence of risk (J. Clin. Aesthet. Dermatol 2009;2:16-22). Still you "need to discuss this risk with your patients," Dr. Baldwin said.
"A recent Cochrane review on spironolactone which concluded that, although it was very helpful for hirsutism and for alopecia, that it had no evidence-based medicine to support its use in the treatment of acne," Dr. Baldwin said in an interview (Cochrane Database Syst. Rev. 2009;(2):CD000194). "Now that flies in the face of numerous small studies which have demonstrated clearly over the years that spironolactone in doses from 50 to 200 mg per day are very helpful in the treatment of acne, especially in the adult woman."
The number of participants in these studies was "so small that it didn’t pass muster for the Cochrane review," Dr. Baldwin said. "I still believe spironolactone is an incredibly useful drug in the treatment of acne."
An estimated 13% to 15% of women in the United States have acne. The number has been increasing in recent past. Dr. Baldwin said, however, it is unclear if the increase is due to greater awareness of quality acne therapy and/or a true increase in prevalence.
Dr. Baldwin recommended the American Acne and Rosacea Society's website for more information.
Dr. Baldwin is a consultant and has received honoraria from Ortho, Galderma, Allergan, Coria, Graceway, GlaxoSmithKline, and L’Oreal. The SDEF and this news organization are owned by Elsevier.
SAN FRANCISCO – Dermatologists are seeing an increasing incidence of adult women with acne in their offices and they are a clear challenge to treat, Dr. Hilary E. Baldwin said.
Compared to teenagers, women in their 30s, 40s and 50s and their acne lesions can be more resistant to treatment, Dr. Baldwin said at a seminar on women’s and pediatric dermatology sponsored by the Skin Disease Education Foundation (SDEF).
"One of the problems of treating moderate-to-severe acne in the adult woman is that topical medications may not work particularly well. It may be that she is a little harder to treat, but also she has acne on the neck and the jaw, which is more sensitive skin, and the topical products tend to be quite irritating," Dr. Baldwin said.
Acne after adolescence also can be more psychosocially devastating. Unlike a teenage girl, an affected woman may have no one else in her social group who has acne. And "because teenagers are supposed to have acne," Dr. Baldwin said, "people will question: What is she doing wrong? Is she not eating right?"
Acne can have a detrimental effect on sexuality, motherhood, and/or returning to the workplace, and can deepen a midlife crisis, said Dr. Baldwin, vice chair of the Department of Dermatology at SUNY-Downstate in Brooklyn, N.Y.
With fewer topical agents in their armamentarium for the adult woman with acne, dermatologists tend to prescribe oral medication, Dr. Baldwin said.
Oral antibiotics are an example, such as anti-inflammatory dose doxycycline (acne is an off-label indication). This agent does not kill Propionibacterium acnes, but can improve acne through an anti-inflammatory effect similar to full-dose doxycycline, Dr. Baldwin said.
One caveat: if you prescribe an oral antibiotic, you may experience pushback from some patients, Dr. Baldwin said. "I have women who say that they get a yeast infection every time they get an antibiotic." Strategies include antibiotic treatment through a yeast infection; a simultaneous prescription to prevent yeast growth; and/or selection of an antibiotic less likely to cause this effect. For example, extended-release minocycline may be less likely to spur yeast growth than traditional minocycline, she said.
Non-antibiotic alternatives for moderate-to-severe acne are limited, especially in women of child-bearing potential.
Oral hormonal contraceptives also can improve acne in adult women, Dr. Baldwin said. In the United States, ethinyl estradiol/norethindrone acetate (Estrostep, Warner Chilcott); drospirenone/ethinyl estradiol (Yaz, Bayer); and ethinyl estradiol/norgestimate (Ortho Tri-Cyclen, Ortho McNeil Janssen) are FDA-approved for acne treatment "and others with estrogen may be effective."
Because their full acne-fighting effects can take up to six months, Dr. Baldwin recommended prescription of oral contraceptives in combination with a quicker onset agent. "For me it’s a medication on top of a medication that is going to give more immediate improvement, one I can take them off when I start to see the oral contraceptive kick in."
"The difference becomes significant with Yaz at about 6 months," Dr. Baldwin said. "But waiting for six months for this to happen is not something most of our patients will do."
Keep potential adverse effects of oral contraceptives in mind. Evidence in the literatures suggests there is no increased cardiovascular risk among non-smokers, Dr. Baldwin said. In addition, studies indicate no increase risk of breast cancer. An increased likelihood for a thrombolic event is elevated during the first year then becomes normalized, she said.
The FDA added a black box warning to labeling for spironolactone (Aldactone, GD Searle, plus generics) in 2008 that cites an increased risk for tumors based on animal studies. The warning recommends use only for approved indications, "which acne is not," Dr. Baldwin said. There have been five cases of breast cancer reported in women taking spironolactone and other medications, but there was "no clear link to the medication." Also, a review article found no evidence of risk (J. Clin. Aesthet. Dermatol 2009;2:16-22). Still you "need to discuss this risk with your patients," Dr. Baldwin said.
"A recent Cochrane review on spironolactone which concluded that, although it was very helpful for hirsutism and for alopecia, that it had no evidence-based medicine to support its use in the treatment of acne," Dr. Baldwin said in an interview (Cochrane Database Syst. Rev. 2009;(2):CD000194). "Now that flies in the face of numerous small studies which have demonstrated clearly over the years that spironolactone in doses from 50 to 200 mg per day are very helpful in the treatment of acne, especially in the adult woman."
The number of participants in these studies was "so small that it didn’t pass muster for the Cochrane review," Dr. Baldwin said. "I still believe spironolactone is an incredibly useful drug in the treatment of acne."
An estimated 13% to 15% of women in the United States have acne. The number has been increasing in recent past. Dr. Baldwin said, however, it is unclear if the increase is due to greater awareness of quality acne therapy and/or a true increase in prevalence.
Dr. Baldwin recommended the American Acne and Rosacea Society's website for more information.
Dr. Baldwin is a consultant and has received honoraria from Ortho, Galderma, Allergan, Coria, Graceway, GlaxoSmithKline, and L’Oreal. The SDEF and this news organization are owned by Elsevier.
SAN FRANCISCO – Dermatologists are seeing an increasing incidence of adult women with acne in their offices and they are a clear challenge to treat, Dr. Hilary E. Baldwin said.
Compared to teenagers, women in their 30s, 40s and 50s and their acne lesions can be more resistant to treatment, Dr. Baldwin said at a seminar on women’s and pediatric dermatology sponsored by the Skin Disease Education Foundation (SDEF).
"One of the problems of treating moderate-to-severe acne in the adult woman is that topical medications may not work particularly well. It may be that she is a little harder to treat, but also she has acne on the neck and the jaw, which is more sensitive skin, and the topical products tend to be quite irritating," Dr. Baldwin said.
Acne after adolescence also can be more psychosocially devastating. Unlike a teenage girl, an affected woman may have no one else in her social group who has acne. And "because teenagers are supposed to have acne," Dr. Baldwin said, "people will question: What is she doing wrong? Is she not eating right?"
Acne can have a detrimental effect on sexuality, motherhood, and/or returning to the workplace, and can deepen a midlife crisis, said Dr. Baldwin, vice chair of the Department of Dermatology at SUNY-Downstate in Brooklyn, N.Y.
With fewer topical agents in their armamentarium for the adult woman with acne, dermatologists tend to prescribe oral medication, Dr. Baldwin said.
Oral antibiotics are an example, such as anti-inflammatory dose doxycycline (acne is an off-label indication). This agent does not kill Propionibacterium acnes, but can improve acne through an anti-inflammatory effect similar to full-dose doxycycline, Dr. Baldwin said.
One caveat: if you prescribe an oral antibiotic, you may experience pushback from some patients, Dr. Baldwin said. "I have women who say that they get a yeast infection every time they get an antibiotic." Strategies include antibiotic treatment through a yeast infection; a simultaneous prescription to prevent yeast growth; and/or selection of an antibiotic less likely to cause this effect. For example, extended-release minocycline may be less likely to spur yeast growth than traditional minocycline, she said.
Non-antibiotic alternatives for moderate-to-severe acne are limited, especially in women of child-bearing potential.
Oral hormonal contraceptives also can improve acne in adult women, Dr. Baldwin said. In the United States, ethinyl estradiol/norethindrone acetate (Estrostep, Warner Chilcott); drospirenone/ethinyl estradiol (Yaz, Bayer); and ethinyl estradiol/norgestimate (Ortho Tri-Cyclen, Ortho McNeil Janssen) are FDA-approved for acne treatment "and others with estrogen may be effective."
Because their full acne-fighting effects can take up to six months, Dr. Baldwin recommended prescription of oral contraceptives in combination with a quicker onset agent. "For me it’s a medication on top of a medication that is going to give more immediate improvement, one I can take them off when I start to see the oral contraceptive kick in."
"The difference becomes significant with Yaz at about 6 months," Dr. Baldwin said. "But waiting for six months for this to happen is not something most of our patients will do."
Keep potential adverse effects of oral contraceptives in mind. Evidence in the literatures suggests there is no increased cardiovascular risk among non-smokers, Dr. Baldwin said. In addition, studies indicate no increase risk of breast cancer. An increased likelihood for a thrombolic event is elevated during the first year then becomes normalized, she said.
The FDA added a black box warning to labeling for spironolactone (Aldactone, GD Searle, plus generics) in 2008 that cites an increased risk for tumors based on animal studies. The warning recommends use only for approved indications, "which acne is not," Dr. Baldwin said. There have been five cases of breast cancer reported in women taking spironolactone and other medications, but there was "no clear link to the medication." Also, a review article found no evidence of risk (J. Clin. Aesthet. Dermatol 2009;2:16-22). Still you "need to discuss this risk with your patients," Dr. Baldwin said.
"A recent Cochrane review on spironolactone which concluded that, although it was very helpful for hirsutism and for alopecia, that it had no evidence-based medicine to support its use in the treatment of acne," Dr. Baldwin said in an interview (Cochrane Database Syst. Rev. 2009;(2):CD000194). "Now that flies in the face of numerous small studies which have demonstrated clearly over the years that spironolactone in doses from 50 to 200 mg per day are very helpful in the treatment of acne, especially in the adult woman."
The number of participants in these studies was "so small that it didn’t pass muster for the Cochrane review," Dr. Baldwin said. "I still believe spironolactone is an incredibly useful drug in the treatment of acne."
An estimated 13% to 15% of women in the United States have acne. The number has been increasing in recent past. Dr. Baldwin said, however, it is unclear if the increase is due to greater awareness of quality acne therapy and/or a true increase in prevalence.
Dr. Baldwin recommended the American Acne and Rosacea Society's website for more information.
Dr. Baldwin is a consultant and has received honoraria from Ortho, Galderma, Allergan, Coria, Graceway, GlaxoSmithKline, and L’Oreal. The SDEF and this news organization are owned by Elsevier.
FROM A SEMINAR ON WOMEN’S AND PEDIATRIC DERMATOLOGY SPONSORED BY THE SKIN DISEASE EDUCATION FOUNDATION