User login
One-fifth of Medicaid kids receive mental health diagnoses
Twenty percent of children insured by Medicaid received a psychiatric diagnosis before 8 years of age, according to data from more than 35,000 Medicaid-insured children in a mid-Atlantic state.
Previous cross-sectional studies have addressed trends in psychiatric treatment of children. “However, little is known about the longitudinal patterns of pediatric use of psychiatric services,” wrote Dinci Pennap, MPH, of the University of Maryland, Baltimore, and her colleagues.
By the age of 8 years, 20% of the children had received a psychiatric diagnosis; 58% of these diagnoses were behavioral. The most common psychiatric diagnoses were ADHD (44%) and learning disorder (32%).
In addition, 10% (2,196) of children had received psychotropic medications. Of those receiving psychotropic medications, 81% received a single medication, 16% received two medications, and 4% received three medications for 60 days or more, the researchers said. Girls were significantly more likely than boys to be diagnosed with adjustment disorder (22% vs. 15%, respectively) or anxiety disorder (7% vs. 4%, respectively). Boys were significantly more likely than girls to be diagnosed with ADHD (30% vs. 22%).
the researchers said.
The study findings were limited by several factors, including the use of clinician-reported diagnoses rather than research-identified diagnoses and the possible lack of generalizability to Medicaid populations in other regions or to privately insured children, the researchers noted. However, the results captured long-term psychotropic use and “highlight the need for safety and outcomes research, particularly for health outcomes such as metabolic imbalance, weight gain, and sleep disturbances after initiation of psychotropic medication for very young children.”
Dr. Pennap had no financial conflicts to disclose. One of the study coauthors disclosed research grants from the National Institutes of Health.
SOURCE: Pennap D et al. JAMA Pediatr. 2018. doi: 10.1001/jamapediatrics.2018.0240.
Twenty percent of children insured by Medicaid received a psychiatric diagnosis before 8 years of age, according to data from more than 35,000 Medicaid-insured children in a mid-Atlantic state.
Previous cross-sectional studies have addressed trends in psychiatric treatment of children. “However, little is known about the longitudinal patterns of pediatric use of psychiatric services,” wrote Dinci Pennap, MPH, of the University of Maryland, Baltimore, and her colleagues.
By the age of 8 years, 20% of the children had received a psychiatric diagnosis; 58% of these diagnoses were behavioral. The most common psychiatric diagnoses were ADHD (44%) and learning disorder (32%).
In addition, 10% (2,196) of children had received psychotropic medications. Of those receiving psychotropic medications, 81% received a single medication, 16% received two medications, and 4% received three medications for 60 days or more, the researchers said. Girls were significantly more likely than boys to be diagnosed with adjustment disorder (22% vs. 15%, respectively) or anxiety disorder (7% vs. 4%, respectively). Boys were significantly more likely than girls to be diagnosed with ADHD (30% vs. 22%).
the researchers said.
The study findings were limited by several factors, including the use of clinician-reported diagnoses rather than research-identified diagnoses and the possible lack of generalizability to Medicaid populations in other regions or to privately insured children, the researchers noted. However, the results captured long-term psychotropic use and “highlight the need for safety and outcomes research, particularly for health outcomes such as metabolic imbalance, weight gain, and sleep disturbances after initiation of psychotropic medication for very young children.”
Dr. Pennap had no financial conflicts to disclose. One of the study coauthors disclosed research grants from the National Institutes of Health.
SOURCE: Pennap D et al. JAMA Pediatr. 2018. doi: 10.1001/jamapediatrics.2018.0240.
Twenty percent of children insured by Medicaid received a psychiatric diagnosis before 8 years of age, according to data from more than 35,000 Medicaid-insured children in a mid-Atlantic state.
Previous cross-sectional studies have addressed trends in psychiatric treatment of children. “However, little is known about the longitudinal patterns of pediatric use of psychiatric services,” wrote Dinci Pennap, MPH, of the University of Maryland, Baltimore, and her colleagues.
By the age of 8 years, 20% of the children had received a psychiatric diagnosis; 58% of these diagnoses were behavioral. The most common psychiatric diagnoses were ADHD (44%) and learning disorder (32%).
In addition, 10% (2,196) of children had received psychotropic medications. Of those receiving psychotropic medications, 81% received a single medication, 16% received two medications, and 4% received three medications for 60 days or more, the researchers said. Girls were significantly more likely than boys to be diagnosed with adjustment disorder (22% vs. 15%, respectively) or anxiety disorder (7% vs. 4%, respectively). Boys were significantly more likely than girls to be diagnosed with ADHD (30% vs. 22%).
the researchers said.
The study findings were limited by several factors, including the use of clinician-reported diagnoses rather than research-identified diagnoses and the possible lack of generalizability to Medicaid populations in other regions or to privately insured children, the researchers noted. However, the results captured long-term psychotropic use and “highlight the need for safety and outcomes research, particularly for health outcomes such as metabolic imbalance, weight gain, and sleep disturbances after initiation of psychotropic medication for very young children.”
Dr. Pennap had no financial conflicts to disclose. One of the study coauthors disclosed research grants from the National Institutes of Health.
SOURCE: Pennap D et al. JAMA Pediatr. 2018. doi: 10.1001/jamapediatrics.2018.0240.
FROM JAMA PEDIATRICS
Key clinical point: More safety and outcome data are needed for young children receiving psychiatric medications.
Major finding: Twenty percent of Medicaid-insured children in a mid-Atlantic state were diagnosed with a psychiatric disorder before 8 years of age.
Study details: The data come from a longitudinal study of 35,244 children insured with Medicaid born in 2007 in a mid-Atlantic state.
Disclosures: Dr. Pennap had no financial conflicts to disclose. One of the study coauthors disclosed research grants from the National Institutes of Health.
Source: Pennap D et al. JAMA Pediatr. 2018. doi: 10.1001/jamapediatrics.2018.0240.
Adjunct treatments assist with persistent asthma
Asthma patients who struggle with poor control despite using inhaled corticosteroids can benefit from additional treatment with long-acting muscarinic antagonists (LAMAs) or single maintenance and reliever therapy, suggest data from a pair of systematic reviews and meta-analyses.
Asthma control remains a problem for many patients despite the daily use of inhaled corticosteroids. The current preferred adjunct therapy for patients aged 12 years and older is long-acting beta-agonists (LABAs), wrote Diana M. Sobieraj, PharmD, of the University of Connecticut School of Pharmacy, Storrs, and her colleagues in a study published in JAMA. The researchers examined the efficacy of other adjunct therapies and therapeutic regimes, including the use of a LAMA, in two studies of patients with persistent asthma.
Overall, patients who took a LAMA had a lower risk of asthma exacerbation requiring systemic corticosteroids and improved spirometry measures than did the patients who took a placebo or used another controller as an adjunct therapy.
In trials that compared LAMAs with placebo as an add-on to inhaled corticosteroids, LAMA patients experienced a significantly reduced risk of exacerbation requiring systemic corticosteroids (–1.8) and a significantly reduced risk of asthma worsening (–4.8). Another benefit seen in the patients who used a LAMA rather than those who used a placebo was improved spirometry measures, but the differences between these two patient groups’ numbers did not reach statistical significance.
The analysis also included studies that compared “triple therapy” – defined as use of a LAMA as add-on therapy to inhaled corticosteroids and LABAs – to LABA plus use of inhaled corticosteroids.
Triple therapy was significantly associated with a lower risk of asthma worsening, compared with inhaled corticosteroids and LABAs, but not with a reduced risk of exacerbation. In addition, no significant differences appeared in Asthma Control Questionnaire-7 scores or overall Asthma Quality of Life Questionnaire scores between the two patient groups.
“Triple therapy was not significantly associated with improvements in rescue medication use vs. combined inhaled corticosteroids and LABA therapy,” the researchers added.
The review of LAMAs used as add-on therapy was limited by several factors, including a primary focus on tiotropium, a lack of analysis of harms or the costs of the various therapies, the lack of data for children, and an inability to perform a subgroup analysis, the researchers said. Although LAMA use was associated with a lower risk of asthma exacerbation, compared with placebo use, the review could not adequately compare LAMA with controllers other than LABA, they added.
In the second analysis, which also was published in JAMA, the researchers evaluated the use of inhaled corticosteroids and LABAs as both a controller and quick-relief treatment, a strategy known as SMART, or Single Maintenance and Reliever Therapy. The SMART protocol, which is not approved in the United States, involved taking a combination of the corticosteroid budesonide and the LABA formoterol in a dry-powder inhaler in most of the studies reviewed.
Overall, in the analysis of 22,524 patients aged 12 years and older, an absolute risk difference of –2.8% for asthma exacerbations was seen in those who used the SMART protocol versus those who used a higher dose of inhaled corticosteroids and inhaled LABA as controller therapy.
In addition, data from 341 children aged 4-11 years showed a –12% absolute difference in risk of asthma exacerbation with the SMART therapy.
In trials that compared patients using the SMART protocol with those taking only the dose of inhaled corticosteroids called for by SMART, the protocol was associated with an improvement in forced expiratory volume in 1 second (FEV1) and a reduction in the need for rescue medication.
The SMART protocol also demonstrated advantages over taking the same dose of inhaled corticosteroid called for by SMART plus a LABA controller therapy or a higher dose of inhaled corticosteroids with a LABA controller therapy. Specifically, SMART patients experienced a –6.4% risk of asthma exacerbations, versus the first comparator group; and a –2.7% risk of asthma, compared with the group who took a higher dose of inhaled corticosteroids with LABA controller therapy.
No significant associations appeared in any of the studies between the SMART protocol and outcomes that included all-cause mortality or changes in FEV1, forced vital capacity, or the percentage of predicted FEV1, when compared with those for patients who used a LABA controller therapy plus inhaled corticosteroids at either dose.
The SMART protocol review was limited by factors that included a lack of data on adverse events, a lack of subgroup analysis, and the potential for bias, because of the open label nature of some of the studies, the researchers noted.
However, despite the limitations in both reviews, the results support the SMART strategy and LAMAs as alternatives for patients with persistent asthma, and highlight the need for further research, they noted.
The reviews were supported by the Agency for Healthcare Research and Quality. Dr. Sobieraj had no financial conflicts to disclose.
SOURCE: Sobieraj D et al. JAMA. 2018;319(14):1473-84. Sobieraj D et al. JAMA. 2018;319(14):1485-96.
Asthma remains a major public health problem in the United States, but 11 years have passed since the last update to treatment guidelines, and an update to the current guidelines for asthma treatment is needed, wrote Jerry A. Krishnan, MD, and David H. Au, MD, in an accompanying editorial (JAMA. 2018;319[14]:1441-3). “It is time to connect the efforts of the FDA, the evidence presented by Sobieraj et al., and the support from the National Education and Prevention Program to update the 2007 [Expert Panel Report 3] guidelines on asthma.”
Both reviews showed effectiveness for the treatments being assessed, compared with placebo, but each had limitations, the editorialists noted.
The study findings in the report on the efficacy of inhaled long-acting muscarinic antagonists (LAMAs) in adolescents and adults with uncontrolled asthma were limited by several factors including a focus primarily on tiotropium, absence of data on potential harms and relative costs of treatment, and a lack of data on children younger than 12 years, they noted. The findings in the analysis of the strategy known as Single Maintenance and Reliever Therapy (SMART) containing formoterol, a long-acting beta2-agonist, were similarly limited by a lack of assessment of potential harm and a data on children within the same age group, they said.
However, the effectiveness of the treatments seen in both reviews suggest that the forthcoming revision of the Expert Panel Report 3 guidelines on asthma from the National Asthma Education and Prevention Program should include the option for inhaled tiotropium, a LAMA, and for the formoterol-based SMART protocol, the editorialists wrote.
“For patients and clinicians, the results from these meta-analyses suggest that dual therapy with scheduled doses of inhaled corticosteroids and LABA or inhaled corticosteroids and LAMA should help reduce the risk of future asthma exacerbations in patients with inadequate asthma control while using inhaled corticosteroids alone,” they said. The new guidelines should include evidence for the SMART therapy as well, but “studies assessing the efficacy of SMART using combination formoterol and budesonide via a metered-dose inhaler are needed,” they concluded.
Dr. Krishnan is affiliated with the division of pulmonary, critical care, sleep, and allergy at the University of Illinois, Chicago, and disclosed having received compensation from Sanofi for participation on an independent data-monitoring committee. Dr. Au is affiliated with the division of pulmonary, critical care, and sleep medicine at the University of Washington, Seattle, and disclosed having received compensation from Novartis for participation on a data-monitoring committee and for serving as a consultant to Gilead Sciences.
Asthma remains a major public health problem in the United States, but 11 years have passed since the last update to treatment guidelines, and an update to the current guidelines for asthma treatment is needed, wrote Jerry A. Krishnan, MD, and David H. Au, MD, in an accompanying editorial (JAMA. 2018;319[14]:1441-3). “It is time to connect the efforts of the FDA, the evidence presented by Sobieraj et al., and the support from the National Education and Prevention Program to update the 2007 [Expert Panel Report 3] guidelines on asthma.”
Both reviews showed effectiveness for the treatments being assessed, compared with placebo, but each had limitations, the editorialists noted.
The study findings in the report on the efficacy of inhaled long-acting muscarinic antagonists (LAMAs) in adolescents and adults with uncontrolled asthma were limited by several factors including a focus primarily on tiotropium, absence of data on potential harms and relative costs of treatment, and a lack of data on children younger than 12 years, they noted. The findings in the analysis of the strategy known as Single Maintenance and Reliever Therapy (SMART) containing formoterol, a long-acting beta2-agonist, were similarly limited by a lack of assessment of potential harm and a data on children within the same age group, they said.
However, the effectiveness of the treatments seen in both reviews suggest that the forthcoming revision of the Expert Panel Report 3 guidelines on asthma from the National Asthma Education and Prevention Program should include the option for inhaled tiotropium, a LAMA, and for the formoterol-based SMART protocol, the editorialists wrote.
“For patients and clinicians, the results from these meta-analyses suggest that dual therapy with scheduled doses of inhaled corticosteroids and LABA or inhaled corticosteroids and LAMA should help reduce the risk of future asthma exacerbations in patients with inadequate asthma control while using inhaled corticosteroids alone,” they said. The new guidelines should include evidence for the SMART therapy as well, but “studies assessing the efficacy of SMART using combination formoterol and budesonide via a metered-dose inhaler are needed,” they concluded.
Dr. Krishnan is affiliated with the division of pulmonary, critical care, sleep, and allergy at the University of Illinois, Chicago, and disclosed having received compensation from Sanofi for participation on an independent data-monitoring committee. Dr. Au is affiliated with the division of pulmonary, critical care, and sleep medicine at the University of Washington, Seattle, and disclosed having received compensation from Novartis for participation on a data-monitoring committee and for serving as a consultant to Gilead Sciences.
Asthma remains a major public health problem in the United States, but 11 years have passed since the last update to treatment guidelines, and an update to the current guidelines for asthma treatment is needed, wrote Jerry A. Krishnan, MD, and David H. Au, MD, in an accompanying editorial (JAMA. 2018;319[14]:1441-3). “It is time to connect the efforts of the FDA, the evidence presented by Sobieraj et al., and the support from the National Education and Prevention Program to update the 2007 [Expert Panel Report 3] guidelines on asthma.”
Both reviews showed effectiveness for the treatments being assessed, compared with placebo, but each had limitations, the editorialists noted.
The study findings in the report on the efficacy of inhaled long-acting muscarinic antagonists (LAMAs) in adolescents and adults with uncontrolled asthma were limited by several factors including a focus primarily on tiotropium, absence of data on potential harms and relative costs of treatment, and a lack of data on children younger than 12 years, they noted. The findings in the analysis of the strategy known as Single Maintenance and Reliever Therapy (SMART) containing formoterol, a long-acting beta2-agonist, were similarly limited by a lack of assessment of potential harm and a data on children within the same age group, they said.
However, the effectiveness of the treatments seen in both reviews suggest that the forthcoming revision of the Expert Panel Report 3 guidelines on asthma from the National Asthma Education and Prevention Program should include the option for inhaled tiotropium, a LAMA, and for the formoterol-based SMART protocol, the editorialists wrote.
“For patients and clinicians, the results from these meta-analyses suggest that dual therapy with scheduled doses of inhaled corticosteroids and LABA or inhaled corticosteroids and LAMA should help reduce the risk of future asthma exacerbations in patients with inadequate asthma control while using inhaled corticosteroids alone,” they said. The new guidelines should include evidence for the SMART therapy as well, but “studies assessing the efficacy of SMART using combination formoterol and budesonide via a metered-dose inhaler are needed,” they concluded.
Dr. Krishnan is affiliated with the division of pulmonary, critical care, sleep, and allergy at the University of Illinois, Chicago, and disclosed having received compensation from Sanofi for participation on an independent data-monitoring committee. Dr. Au is affiliated with the division of pulmonary, critical care, and sleep medicine at the University of Washington, Seattle, and disclosed having received compensation from Novartis for participation on a data-monitoring committee and for serving as a consultant to Gilead Sciences.
Asthma patients who struggle with poor control despite using inhaled corticosteroids can benefit from additional treatment with long-acting muscarinic antagonists (LAMAs) or single maintenance and reliever therapy, suggest data from a pair of systematic reviews and meta-analyses.
Asthma control remains a problem for many patients despite the daily use of inhaled corticosteroids. The current preferred adjunct therapy for patients aged 12 years and older is long-acting beta-agonists (LABAs), wrote Diana M. Sobieraj, PharmD, of the University of Connecticut School of Pharmacy, Storrs, and her colleagues in a study published in JAMA. The researchers examined the efficacy of other adjunct therapies and therapeutic regimes, including the use of a LAMA, in two studies of patients with persistent asthma.
Overall, patients who took a LAMA had a lower risk of asthma exacerbation requiring systemic corticosteroids and improved spirometry measures than did the patients who took a placebo or used another controller as an adjunct therapy.
In trials that compared LAMAs with placebo as an add-on to inhaled corticosteroids, LAMA patients experienced a significantly reduced risk of exacerbation requiring systemic corticosteroids (–1.8) and a significantly reduced risk of asthma worsening (–4.8). Another benefit seen in the patients who used a LAMA rather than those who used a placebo was improved spirometry measures, but the differences between these two patient groups’ numbers did not reach statistical significance.
The analysis also included studies that compared “triple therapy” – defined as use of a LAMA as add-on therapy to inhaled corticosteroids and LABAs – to LABA plus use of inhaled corticosteroids.
Triple therapy was significantly associated with a lower risk of asthma worsening, compared with inhaled corticosteroids and LABAs, but not with a reduced risk of exacerbation. In addition, no significant differences appeared in Asthma Control Questionnaire-7 scores or overall Asthma Quality of Life Questionnaire scores between the two patient groups.
“Triple therapy was not significantly associated with improvements in rescue medication use vs. combined inhaled corticosteroids and LABA therapy,” the researchers added.
The review of LAMAs used as add-on therapy was limited by several factors, including a primary focus on tiotropium, a lack of analysis of harms or the costs of the various therapies, the lack of data for children, and an inability to perform a subgroup analysis, the researchers said. Although LAMA use was associated with a lower risk of asthma exacerbation, compared with placebo use, the review could not adequately compare LAMA with controllers other than LABA, they added.
In the second analysis, which also was published in JAMA, the researchers evaluated the use of inhaled corticosteroids and LABAs as both a controller and quick-relief treatment, a strategy known as SMART, or Single Maintenance and Reliever Therapy. The SMART protocol, which is not approved in the United States, involved taking a combination of the corticosteroid budesonide and the LABA formoterol in a dry-powder inhaler in most of the studies reviewed.
Overall, in the analysis of 22,524 patients aged 12 years and older, an absolute risk difference of –2.8% for asthma exacerbations was seen in those who used the SMART protocol versus those who used a higher dose of inhaled corticosteroids and inhaled LABA as controller therapy.
In addition, data from 341 children aged 4-11 years showed a –12% absolute difference in risk of asthma exacerbation with the SMART therapy.
In trials that compared patients using the SMART protocol with those taking only the dose of inhaled corticosteroids called for by SMART, the protocol was associated with an improvement in forced expiratory volume in 1 second (FEV1) and a reduction in the need for rescue medication.
The SMART protocol also demonstrated advantages over taking the same dose of inhaled corticosteroid called for by SMART plus a LABA controller therapy or a higher dose of inhaled corticosteroids with a LABA controller therapy. Specifically, SMART patients experienced a –6.4% risk of asthma exacerbations, versus the first comparator group; and a –2.7% risk of asthma, compared with the group who took a higher dose of inhaled corticosteroids with LABA controller therapy.
No significant associations appeared in any of the studies between the SMART protocol and outcomes that included all-cause mortality or changes in FEV1, forced vital capacity, or the percentage of predicted FEV1, when compared with those for patients who used a LABA controller therapy plus inhaled corticosteroids at either dose.
The SMART protocol review was limited by factors that included a lack of data on adverse events, a lack of subgroup analysis, and the potential for bias, because of the open label nature of some of the studies, the researchers noted.
However, despite the limitations in both reviews, the results support the SMART strategy and LAMAs as alternatives for patients with persistent asthma, and highlight the need for further research, they noted.
The reviews were supported by the Agency for Healthcare Research and Quality. Dr. Sobieraj had no financial conflicts to disclose.
SOURCE: Sobieraj D et al. JAMA. 2018;319(14):1473-84. Sobieraj D et al. JAMA. 2018;319(14):1485-96.
Asthma patients who struggle with poor control despite using inhaled corticosteroids can benefit from additional treatment with long-acting muscarinic antagonists (LAMAs) or single maintenance and reliever therapy, suggest data from a pair of systematic reviews and meta-analyses.
Asthma control remains a problem for many patients despite the daily use of inhaled corticosteroids. The current preferred adjunct therapy for patients aged 12 years and older is long-acting beta-agonists (LABAs), wrote Diana M. Sobieraj, PharmD, of the University of Connecticut School of Pharmacy, Storrs, and her colleagues in a study published in JAMA. The researchers examined the efficacy of other adjunct therapies and therapeutic regimes, including the use of a LAMA, in two studies of patients with persistent asthma.
Overall, patients who took a LAMA had a lower risk of asthma exacerbation requiring systemic corticosteroids and improved spirometry measures than did the patients who took a placebo or used another controller as an adjunct therapy.
In trials that compared LAMAs with placebo as an add-on to inhaled corticosteroids, LAMA patients experienced a significantly reduced risk of exacerbation requiring systemic corticosteroids (–1.8) and a significantly reduced risk of asthma worsening (–4.8). Another benefit seen in the patients who used a LAMA rather than those who used a placebo was improved spirometry measures, but the differences between these two patient groups’ numbers did not reach statistical significance.
The analysis also included studies that compared “triple therapy” – defined as use of a LAMA as add-on therapy to inhaled corticosteroids and LABAs – to LABA plus use of inhaled corticosteroids.
Triple therapy was significantly associated with a lower risk of asthma worsening, compared with inhaled corticosteroids and LABAs, but not with a reduced risk of exacerbation. In addition, no significant differences appeared in Asthma Control Questionnaire-7 scores or overall Asthma Quality of Life Questionnaire scores between the two patient groups.
“Triple therapy was not significantly associated with improvements in rescue medication use vs. combined inhaled corticosteroids and LABA therapy,” the researchers added.
The review of LAMAs used as add-on therapy was limited by several factors, including a primary focus on tiotropium, a lack of analysis of harms or the costs of the various therapies, the lack of data for children, and an inability to perform a subgroup analysis, the researchers said. Although LAMA use was associated with a lower risk of asthma exacerbation, compared with placebo use, the review could not adequately compare LAMA with controllers other than LABA, they added.
In the second analysis, which also was published in JAMA, the researchers evaluated the use of inhaled corticosteroids and LABAs as both a controller and quick-relief treatment, a strategy known as SMART, or Single Maintenance and Reliever Therapy. The SMART protocol, which is not approved in the United States, involved taking a combination of the corticosteroid budesonide and the LABA formoterol in a dry-powder inhaler in most of the studies reviewed.
Overall, in the analysis of 22,524 patients aged 12 years and older, an absolute risk difference of –2.8% for asthma exacerbations was seen in those who used the SMART protocol versus those who used a higher dose of inhaled corticosteroids and inhaled LABA as controller therapy.
In addition, data from 341 children aged 4-11 years showed a –12% absolute difference in risk of asthma exacerbation with the SMART therapy.
In trials that compared patients using the SMART protocol with those taking only the dose of inhaled corticosteroids called for by SMART, the protocol was associated with an improvement in forced expiratory volume in 1 second (FEV1) and a reduction in the need for rescue medication.
The SMART protocol also demonstrated advantages over taking the same dose of inhaled corticosteroid called for by SMART plus a LABA controller therapy or a higher dose of inhaled corticosteroids with a LABA controller therapy. Specifically, SMART patients experienced a –6.4% risk of asthma exacerbations, versus the first comparator group; and a –2.7% risk of asthma, compared with the group who took a higher dose of inhaled corticosteroids with LABA controller therapy.
No significant associations appeared in any of the studies between the SMART protocol and outcomes that included all-cause mortality or changes in FEV1, forced vital capacity, or the percentage of predicted FEV1, when compared with those for patients who used a LABA controller therapy plus inhaled corticosteroids at either dose.
The SMART protocol review was limited by factors that included a lack of data on adverse events, a lack of subgroup analysis, and the potential for bias, because of the open label nature of some of the studies, the researchers noted.
However, despite the limitations in both reviews, the results support the SMART strategy and LAMAs as alternatives for patients with persistent asthma, and highlight the need for further research, they noted.
The reviews were supported by the Agency for Healthcare Research and Quality. Dr. Sobieraj had no financial conflicts to disclose.
SOURCE: Sobieraj D et al. JAMA. 2018;319(14):1473-84. Sobieraj D et al. JAMA. 2018;319(14):1485-96.
FROM JAMA
Key clinical point:
Major finding: LAMA patients had a risk difference of –1.8 for asthma exacerbations, compared with placebo users, while patients using the SMART protocol had an absolute risk difference of –2.8%, compared with those taking a higher dose of inhaled corticosteroids plus LABAs as a controller.
Study details: The data came from two reviews of randomized clinical trials; the first included 7,122 patients and the second included 22,524 patients.
Disclosures: The reviews were supported in part by the Agency for Healthcare Research and Quality. Dr. Sobieraj had no financial conflicts to disclose.
Source: Sobieraj D et al. JAMA. 2018;319(14):1473-84. Sobieraj D et al. JAMA. 2018;319(14):1485-96.
Don’t discount rare pityriasis rosea for kids with persistent itch
Persistent cases of small erythematous lesions could be the rare condition of relapsing pityriasis rosea, based on data from a case report of an 11-year-old girl.
Unlike standard pityriasis rosea (PR), relapsing cases tend to present with fewer, smaller lesions, Ilka Engelmann, MD, of the Centre P Boulanger Hôpital A Calmette in Lille, France, and colleagues wrote in Pediatrics.
“A viral etiology of PR is strongly suspected because human herpesvirus 7 (HHV-7) DNA is frequently detected in blood and saliva of patients with PR,” they said. Infection with the HHV-7 virus generally occurs in childhood and remains a lifelong latent condition with the potential for multiple recurrences, they added.
The authors described the case of an 11-year-old white girl who presented with pruritic, erythematous, oval-shaped lesions that began on the right side of her trunk and spread across the trunk over the next few days. The patient had no other symptoms or physical abnormalities on examination and was not taking any medications, although she reported some trouble sleeping.
The treating clinicians identified HHV-7 in a blood sample and diagnosed PR. The lesions resolved in approximately 2 months with no treatment, but, 2 years after the initial presentation, the patient developed similar lesions on her legs, which also resolved without treatment. Over the next 5 years, she presented with similar lesions in different locations approximately three times per year, and these episodes were usually associated with times of stress, such as school examinations. Some saliva specimens taken during the episodes tested positive for HHV-7. The lesions persisted for 4-8 weeks and resolved without treatment, but they were reduced in size and number after the third recurrence. The change in size and location are characteristic of relapsing PR, the authors said, but more than three relapses is rare. “To our knowledge, this is the first report of a case with frequently relapsing PR for 7 years, with several episodes per year,” they said.
The occurrence of the relapses during stressful periods “is consistent with the hypothesis of viral reactivation because stress has been described as a stimulus inducing the reactivation of Herpesviridae from latency,” they noted.
A differential diagnosis of PR includes other infectious diseases and medication-induced skin reactions, but a medication history and virologic tests can help make or rule out a relapsing PR diagnosis, the authors said.
The authors had no financial conflicts to disclose.
SOURCE: Engelmann I et al. Pediatrics. 2018 Apr 19; doi: 10.1542/peds.2017-3179.
Persistent cases of small erythematous lesions could be the rare condition of relapsing pityriasis rosea, based on data from a case report of an 11-year-old girl.
Unlike standard pityriasis rosea (PR), relapsing cases tend to present with fewer, smaller lesions, Ilka Engelmann, MD, of the Centre P Boulanger Hôpital A Calmette in Lille, France, and colleagues wrote in Pediatrics.
“A viral etiology of PR is strongly suspected because human herpesvirus 7 (HHV-7) DNA is frequently detected in blood and saliva of patients with PR,” they said. Infection with the HHV-7 virus generally occurs in childhood and remains a lifelong latent condition with the potential for multiple recurrences, they added.
The authors described the case of an 11-year-old white girl who presented with pruritic, erythematous, oval-shaped lesions that began on the right side of her trunk and spread across the trunk over the next few days. The patient had no other symptoms or physical abnormalities on examination and was not taking any medications, although she reported some trouble sleeping.
The treating clinicians identified HHV-7 in a blood sample and diagnosed PR. The lesions resolved in approximately 2 months with no treatment, but, 2 years after the initial presentation, the patient developed similar lesions on her legs, which also resolved without treatment. Over the next 5 years, she presented with similar lesions in different locations approximately three times per year, and these episodes were usually associated with times of stress, such as school examinations. Some saliva specimens taken during the episodes tested positive for HHV-7. The lesions persisted for 4-8 weeks and resolved without treatment, but they were reduced in size and number after the third recurrence. The change in size and location are characteristic of relapsing PR, the authors said, but more than three relapses is rare. “To our knowledge, this is the first report of a case with frequently relapsing PR for 7 years, with several episodes per year,” they said.
The occurrence of the relapses during stressful periods “is consistent with the hypothesis of viral reactivation because stress has been described as a stimulus inducing the reactivation of Herpesviridae from latency,” they noted.
A differential diagnosis of PR includes other infectious diseases and medication-induced skin reactions, but a medication history and virologic tests can help make or rule out a relapsing PR diagnosis, the authors said.
The authors had no financial conflicts to disclose.
SOURCE: Engelmann I et al. Pediatrics. 2018 Apr 19; doi: 10.1542/peds.2017-3179.
Persistent cases of small erythematous lesions could be the rare condition of relapsing pityriasis rosea, based on data from a case report of an 11-year-old girl.
Unlike standard pityriasis rosea (PR), relapsing cases tend to present with fewer, smaller lesions, Ilka Engelmann, MD, of the Centre P Boulanger Hôpital A Calmette in Lille, France, and colleagues wrote in Pediatrics.
“A viral etiology of PR is strongly suspected because human herpesvirus 7 (HHV-7) DNA is frequently detected in blood and saliva of patients with PR,” they said. Infection with the HHV-7 virus generally occurs in childhood and remains a lifelong latent condition with the potential for multiple recurrences, they added.
The authors described the case of an 11-year-old white girl who presented with pruritic, erythematous, oval-shaped lesions that began on the right side of her trunk and spread across the trunk over the next few days. The patient had no other symptoms or physical abnormalities on examination and was not taking any medications, although she reported some trouble sleeping.
The treating clinicians identified HHV-7 in a blood sample and diagnosed PR. The lesions resolved in approximately 2 months with no treatment, but, 2 years after the initial presentation, the patient developed similar lesions on her legs, which also resolved without treatment. Over the next 5 years, she presented with similar lesions in different locations approximately three times per year, and these episodes were usually associated with times of stress, such as school examinations. Some saliva specimens taken during the episodes tested positive for HHV-7. The lesions persisted for 4-8 weeks and resolved without treatment, but they were reduced in size and number after the third recurrence. The change in size and location are characteristic of relapsing PR, the authors said, but more than three relapses is rare. “To our knowledge, this is the first report of a case with frequently relapsing PR for 7 years, with several episodes per year,” they said.
The occurrence of the relapses during stressful periods “is consistent with the hypothesis of viral reactivation because stress has been described as a stimulus inducing the reactivation of Herpesviridae from latency,” they noted.
A differential diagnosis of PR includes other infectious diseases and medication-induced skin reactions, but a medication history and virologic tests can help make or rule out a relapsing PR diagnosis, the authors said.
The authors had no financial conflicts to disclose.
SOURCE: Engelmann I et al. Pediatrics. 2018 Apr 19; doi: 10.1542/peds.2017-3179.
FROM PEDIATRICS
Key clinical point: Check children with persistent erythematous lesions for human herpesvirus and possible pityriasis rosea.
Major finding: A presentation of erythematous lesions in an 11-year-old girl recurred over 7 years.
Study details: The data come from a case report of rare relapsing pityriasis rosea.
Disclosures: The authors presenting the case had no financial conflicts to disclose.
Source: Engelmann I et al. Pediatrics. 2018 Apr 19; doi: 10.1542/peds.2017-3179.
Eating disorders put teens at risk for depression, bullying
Disordered eating behavior may put adolescents at greater risk for both depression and peer bullying, data from a longitudinal study of 612 teens show.
“Questions remain as to whether clinically significant disordered eating behavior is an antecedent or consequent of bullying by peers among adolescent girls and boys,” wrote Kirsty S. Lee, PhD, and Tracy Vaillancourt, PhD, of the University of Ottawa.
In a study published online April 11 in JAMA Psychiatry, the researchers reviewed data on adolescents aged 13-17 years who were enrolled in the McMaster Teen Study, a longitudinal study of Canadian teens examining bullying, academic achievement, and mental health. The average age of the study participants was 13 years; 54% were girls, and 71% were white.
At each annual follow-up during the 5-year study period, bullying was significantly concurrently associated with both disordered eating behavior (such as vomiting after eating) and depressive symptoms (P less than .01). In addition, disordered eating was significantly longitudinally associated with depression at every time point (P less than .02) and with peer bullying at two points (P less than .04) during the 5-year study (grades 8-9 and grades 10-11). However, no longitudinal association appeared between peer bullying and depression.
The participants completed a questionnaire each year between grades 7 and 11. The researchers assessed eating disordered behavior using the Short Screen for Eating Disorders; bullying was assessed by providing the teens with a standard definition of bullying to accompany questions about their experiences. Depression was assessed via the Behavior Assessment System for Children, second edition. A cascade model was used to show the relationships among the factors over time.
“At every time point, adolescent girls reported greater bullying by peers, depressive symptoms, and disordered eating behavior than adolescent boys, except in grade 7 when there were no sex differences in disordered eating behavior,” the researchers noted.
The results were consistent with data from previous cross-sectional studies with regard to the stronger associations in girls vs. boys, the researchers said. However, contrary to previous research, they found no mediating effect of depression on the association between peer bullying and disordered eating behavior, and no longitudinal associations between peer bullying and depression.
The findings were limited by several factors, including the inability to analyze different types of eating disorders and the use of self-reports to assess bullying, the researchers said. However, the results support the value of targeting disordered eating behavior to help reduce the risk of other mental health problems, they noted.
, which can reduce symptoms of disordered eating and other psychopathologic symptoms,” they wrote.
The researchers had no financial conflicts to disclose. The study was supported in part by the Ontario Mental Health Foundation, the Canadian Institute of Health Research, and the Social Sciences and Humanities Research Council of Canada.
SOURCE: Lee KS and Vaillancourt T. JAMA Psychiatry 2018 Apr 11. doi: 10.1001/jamapsychiatry.2018.0284.
Disordered eating behavior may put adolescents at greater risk for both depression and peer bullying, data from a longitudinal study of 612 teens show.
“Questions remain as to whether clinically significant disordered eating behavior is an antecedent or consequent of bullying by peers among adolescent girls and boys,” wrote Kirsty S. Lee, PhD, and Tracy Vaillancourt, PhD, of the University of Ottawa.
In a study published online April 11 in JAMA Psychiatry, the researchers reviewed data on adolescents aged 13-17 years who were enrolled in the McMaster Teen Study, a longitudinal study of Canadian teens examining bullying, academic achievement, and mental health. The average age of the study participants was 13 years; 54% were girls, and 71% were white.
At each annual follow-up during the 5-year study period, bullying was significantly concurrently associated with both disordered eating behavior (such as vomiting after eating) and depressive symptoms (P less than .01). In addition, disordered eating was significantly longitudinally associated with depression at every time point (P less than .02) and with peer bullying at two points (P less than .04) during the 5-year study (grades 8-9 and grades 10-11). However, no longitudinal association appeared between peer bullying and depression.
The participants completed a questionnaire each year between grades 7 and 11. The researchers assessed eating disordered behavior using the Short Screen for Eating Disorders; bullying was assessed by providing the teens with a standard definition of bullying to accompany questions about their experiences. Depression was assessed via the Behavior Assessment System for Children, second edition. A cascade model was used to show the relationships among the factors over time.
“At every time point, adolescent girls reported greater bullying by peers, depressive symptoms, and disordered eating behavior than adolescent boys, except in grade 7 when there were no sex differences in disordered eating behavior,” the researchers noted.
The results were consistent with data from previous cross-sectional studies with regard to the stronger associations in girls vs. boys, the researchers said. However, contrary to previous research, they found no mediating effect of depression on the association between peer bullying and disordered eating behavior, and no longitudinal associations between peer bullying and depression.
The findings were limited by several factors, including the inability to analyze different types of eating disorders and the use of self-reports to assess bullying, the researchers said. However, the results support the value of targeting disordered eating behavior to help reduce the risk of other mental health problems, they noted.
, which can reduce symptoms of disordered eating and other psychopathologic symptoms,” they wrote.
The researchers had no financial conflicts to disclose. The study was supported in part by the Ontario Mental Health Foundation, the Canadian Institute of Health Research, and the Social Sciences and Humanities Research Council of Canada.
SOURCE: Lee KS and Vaillancourt T. JAMA Psychiatry 2018 Apr 11. doi: 10.1001/jamapsychiatry.2018.0284.
Disordered eating behavior may put adolescents at greater risk for both depression and peer bullying, data from a longitudinal study of 612 teens show.
“Questions remain as to whether clinically significant disordered eating behavior is an antecedent or consequent of bullying by peers among adolescent girls and boys,” wrote Kirsty S. Lee, PhD, and Tracy Vaillancourt, PhD, of the University of Ottawa.
In a study published online April 11 in JAMA Psychiatry, the researchers reviewed data on adolescents aged 13-17 years who were enrolled in the McMaster Teen Study, a longitudinal study of Canadian teens examining bullying, academic achievement, and mental health. The average age of the study participants was 13 years; 54% were girls, and 71% were white.
At each annual follow-up during the 5-year study period, bullying was significantly concurrently associated with both disordered eating behavior (such as vomiting after eating) and depressive symptoms (P less than .01). In addition, disordered eating was significantly longitudinally associated with depression at every time point (P less than .02) and with peer bullying at two points (P less than .04) during the 5-year study (grades 8-9 and grades 10-11). However, no longitudinal association appeared between peer bullying and depression.
The participants completed a questionnaire each year between grades 7 and 11. The researchers assessed eating disordered behavior using the Short Screen for Eating Disorders; bullying was assessed by providing the teens with a standard definition of bullying to accompany questions about their experiences. Depression was assessed via the Behavior Assessment System for Children, second edition. A cascade model was used to show the relationships among the factors over time.
“At every time point, adolescent girls reported greater bullying by peers, depressive symptoms, and disordered eating behavior than adolescent boys, except in grade 7 when there were no sex differences in disordered eating behavior,” the researchers noted.
The results were consistent with data from previous cross-sectional studies with regard to the stronger associations in girls vs. boys, the researchers said. However, contrary to previous research, they found no mediating effect of depression on the association between peer bullying and disordered eating behavior, and no longitudinal associations between peer bullying and depression.
The findings were limited by several factors, including the inability to analyze different types of eating disorders and the use of self-reports to assess bullying, the researchers said. However, the results support the value of targeting disordered eating behavior to help reduce the risk of other mental health problems, they noted.
, which can reduce symptoms of disordered eating and other psychopathologic symptoms,” they wrote.
The researchers had no financial conflicts to disclose. The study was supported in part by the Ontario Mental Health Foundation, the Canadian Institute of Health Research, and the Social Sciences and Humanities Research Council of Canada.
SOURCE: Lee KS and Vaillancourt T. JAMA Psychiatry 2018 Apr 11. doi: 10.1001/jamapsychiatry.2018.0284.
FROM JAMA PSYCHIATRY
Key clinical point: Teens who demonstrate disordered eating behavior may be at increased risk for depression and peer bullying.
Major finding: Disordered eating was longitudinally linked to depression and peer bullying (P less than .02).
Study details: A 5-year longitudinal study of 612 adolescents.
Disclosures: The researchers had no financial conflicts to disclose. The study was supported in part by the Ontario Mental Health Foundation, the Canadian Institute of Health Research, and the Social Sciences and Humanities Research Council of Canada.
Source: Lee KS and Vaillancourt T. JAMA Psychiatry 2018 Apr 11. doi: 10.1001/jamapsychiatry.2018.0284.
New developments in critical care and sepsis
Sepsis and critical care issues are in the spotlight at HM18, and these hot topics were the focus of the Monday education session, “He-Who-Shall-Not-Be-Named: Updates in Sepsis and Critical Care.”
Patricia Kritek, MD, EdM, of the University of Washington, Seattle, led an interactive and engaging session, educating attendees about the current research in sepsis and critical care areas so they would feel comfortable implementing the latest evidence into practice in the ICU.
The session focused on “what’s new” in critical care and sepsis from the literature published in the past year.
According to the National Center for Health Statistics at the Centers for Disease Control and Prevention, sepsis or septicemia patients averaged a 75% longer length of stay and were more than eight times likely to die, compared with patients hospitalized for other conditions.
“There has been a lot of discussion about steroids in sepsis that is potentially practice changing,” Dr. Kritek said in an interview. To tackle the always-tricky topic of steroids and sepsis, Dr. Kritek selected a trio of studies for review and discussion. In the first, vitamin C was potentially as effective as hydrocortisone and thiamine for the treatment of severe sepsis and septic shock (CHEST. 2017;151[6]:1229‐38). Another study addressed adjunctive glucocorticoid therapy for septic shock patients, and a third examined the use of hydrocortisone plus fludrocortisone for adults with septic shock.
The trials not involving vitamin C were published in the New England Journal of Medicine this year, conducted in Australia (2018;378:797‐808) and France (2018;378:809‐18), and included 3,658 and 1,241 adult sepsis patients, respectively. The studies were similar in size and design. Based on these two studies, hydrocortisone appears to shorten septic shock duration, and treatment with hydrocortisone and possibly fludrocortisone could be helpful for the more seriously ill patients, said Dr. Kritek. As for the value of vitamin C and thiamine, “the jury is still out,” she noted.
Sepsis and critical care issues are in the spotlight at HM18, and these hot topics were the focus of the Monday education session, “He-Who-Shall-Not-Be-Named: Updates in Sepsis and Critical Care.”
Patricia Kritek, MD, EdM, of the University of Washington, Seattle, led an interactive and engaging session, educating attendees about the current research in sepsis and critical care areas so they would feel comfortable implementing the latest evidence into practice in the ICU.
The session focused on “what’s new” in critical care and sepsis from the literature published in the past year.
According to the National Center for Health Statistics at the Centers for Disease Control and Prevention, sepsis or septicemia patients averaged a 75% longer length of stay and were more than eight times likely to die, compared with patients hospitalized for other conditions.
“There has been a lot of discussion about steroids in sepsis that is potentially practice changing,” Dr. Kritek said in an interview. To tackle the always-tricky topic of steroids and sepsis, Dr. Kritek selected a trio of studies for review and discussion. In the first, vitamin C was potentially as effective as hydrocortisone and thiamine for the treatment of severe sepsis and septic shock (CHEST. 2017;151[6]:1229‐38). Another study addressed adjunctive glucocorticoid therapy for septic shock patients, and a third examined the use of hydrocortisone plus fludrocortisone for adults with septic shock.
The trials not involving vitamin C were published in the New England Journal of Medicine this year, conducted in Australia (2018;378:797‐808) and France (2018;378:809‐18), and included 3,658 and 1,241 adult sepsis patients, respectively. The studies were similar in size and design. Based on these two studies, hydrocortisone appears to shorten septic shock duration, and treatment with hydrocortisone and possibly fludrocortisone could be helpful for the more seriously ill patients, said Dr. Kritek. As for the value of vitamin C and thiamine, “the jury is still out,” she noted.
Sepsis and critical care issues are in the spotlight at HM18, and these hot topics were the focus of the Monday education session, “He-Who-Shall-Not-Be-Named: Updates in Sepsis and Critical Care.”
Patricia Kritek, MD, EdM, of the University of Washington, Seattle, led an interactive and engaging session, educating attendees about the current research in sepsis and critical care areas so they would feel comfortable implementing the latest evidence into practice in the ICU.
The session focused on “what’s new” in critical care and sepsis from the literature published in the past year.
According to the National Center for Health Statistics at the Centers for Disease Control and Prevention, sepsis or septicemia patients averaged a 75% longer length of stay and were more than eight times likely to die, compared with patients hospitalized for other conditions.
“There has been a lot of discussion about steroids in sepsis that is potentially practice changing,” Dr. Kritek said in an interview. To tackle the always-tricky topic of steroids and sepsis, Dr. Kritek selected a trio of studies for review and discussion. In the first, vitamin C was potentially as effective as hydrocortisone and thiamine for the treatment of severe sepsis and septic shock (CHEST. 2017;151[6]:1229‐38). Another study addressed adjunctive glucocorticoid therapy for septic shock patients, and a third examined the use of hydrocortisone plus fludrocortisone for adults with septic shock.
The trials not involving vitamin C were published in the New England Journal of Medicine this year, conducted in Australia (2018;378:797‐808) and France (2018;378:809‐18), and included 3,658 and 1,241 adult sepsis patients, respectively. The studies were similar in size and design. Based on these two studies, hydrocortisone appears to shorten septic shock duration, and treatment with hydrocortisone and possibly fludrocortisone could be helpful for the more seriously ill patients, said Dr. Kritek. As for the value of vitamin C and thiamine, “the jury is still out,” she noted.
Antibiotic awareness tops ID agenda
Antibiotic resistance is “one of the greatest problems we face,” according to Jennifer A. Hanrahan, DO, MSc, of MetroHealth Medical Center in Cleveland. Dr. Hanrahan led the education session, “A Bug’s Life: Infectious Disease Pearls,” and she called the topic “timely and timeless.”
Antibiotic resistance stems from several problems, Dr. Hanrahan said in her Monday presentation. “One of these is overuse of antibiotics, specifically overuse of broad-spectrum antibiotics, and the other problem is overuse of testing.”
Data from the Centers for Disease Control and Prevention show that at least 2 million people in the United States develop antibiotic-resistant bacterial infections each year. At least 23,000 of these patients die each year because of these infections.
In 2013, the CDC published a report on drug-resistant threats in the United States. The three offenders deemed most serious – Clostridium difficile, Carbapenem-resistant Enterobacteriaceae, and Neisseria gonorrhoeae, continue to challenge clinicians.
Clinicians can help curb antibiotic resistance by practicing good stewardship, said Dr. Hanrahan. “Antimicrobial stewardship and laboratory stewardship are two things that can greatly improve patient care and outcomes for patients,” she said.
“Testing stewardship means ordering tests that are necessary based on signs and symptoms,” said Dr. Hanrahan. “For example, people often order urine cultures when there are no symptoms of urinary tract infection, and then end up treating positive cultures with antibiotics even when there are no symptoms of infection. This leads to unnecessary antibiotic exposure,” she noted.
The CDC’s core plans to fight antimicrobial resistance include:
- Preventing infections in the first place: The CDC emphasizes the importance of prevention through hand washing, safe food handling practices, and immunizations.
- Tracking data: The CDC collects and uses data on resistant infections to identify risk factors for resistance and develop strategies to prevent the spread of resistant bacteria.
- Practicing antibiotic stewardship: As Dr. Hanrahan noted, judicious use of antibiotics can help cut down on resistant bacteria.
- Developing alternatives: The CDC supports the development of new antibiotics and new tests to track antibacterial resistance.
Dr. Hanrahan discussed the Top 10 things hospitalists can do to improve lab testing and antimicrobial use.
“Hospitalists must recognize the need to decrease antibiotic use, utilize laboratory testing appropriately, and improve patient safety,” she said.
“There are a wide range of resources available on the Internet that can help you delve further into this topic and to find the appropriate balance for testing and treatment,” Dr. Hanrahan concluded.
Antibiotic resistance is “one of the greatest problems we face,” according to Jennifer A. Hanrahan, DO, MSc, of MetroHealth Medical Center in Cleveland. Dr. Hanrahan led the education session, “A Bug’s Life: Infectious Disease Pearls,” and she called the topic “timely and timeless.”
Antibiotic resistance stems from several problems, Dr. Hanrahan said in her Monday presentation. “One of these is overuse of antibiotics, specifically overuse of broad-spectrum antibiotics, and the other problem is overuse of testing.”
Data from the Centers for Disease Control and Prevention show that at least 2 million people in the United States develop antibiotic-resistant bacterial infections each year. At least 23,000 of these patients die each year because of these infections.
In 2013, the CDC published a report on drug-resistant threats in the United States. The three offenders deemed most serious – Clostridium difficile, Carbapenem-resistant Enterobacteriaceae, and Neisseria gonorrhoeae, continue to challenge clinicians.
Clinicians can help curb antibiotic resistance by practicing good stewardship, said Dr. Hanrahan. “Antimicrobial stewardship and laboratory stewardship are two things that can greatly improve patient care and outcomes for patients,” she said.
“Testing stewardship means ordering tests that are necessary based on signs and symptoms,” said Dr. Hanrahan. “For example, people often order urine cultures when there are no symptoms of urinary tract infection, and then end up treating positive cultures with antibiotics even when there are no symptoms of infection. This leads to unnecessary antibiotic exposure,” she noted.
The CDC’s core plans to fight antimicrobial resistance include:
- Preventing infections in the first place: The CDC emphasizes the importance of prevention through hand washing, safe food handling practices, and immunizations.
- Tracking data: The CDC collects and uses data on resistant infections to identify risk factors for resistance and develop strategies to prevent the spread of resistant bacteria.
- Practicing antibiotic stewardship: As Dr. Hanrahan noted, judicious use of antibiotics can help cut down on resistant bacteria.
- Developing alternatives: The CDC supports the development of new antibiotics and new tests to track antibacterial resistance.
Dr. Hanrahan discussed the Top 10 things hospitalists can do to improve lab testing and antimicrobial use.
“Hospitalists must recognize the need to decrease antibiotic use, utilize laboratory testing appropriately, and improve patient safety,” she said.
“There are a wide range of resources available on the Internet that can help you delve further into this topic and to find the appropriate balance for testing and treatment,” Dr. Hanrahan concluded.
Antibiotic resistance is “one of the greatest problems we face,” according to Jennifer A. Hanrahan, DO, MSc, of MetroHealth Medical Center in Cleveland. Dr. Hanrahan led the education session, “A Bug’s Life: Infectious Disease Pearls,” and she called the topic “timely and timeless.”
Antibiotic resistance stems from several problems, Dr. Hanrahan said in her Monday presentation. “One of these is overuse of antibiotics, specifically overuse of broad-spectrum antibiotics, and the other problem is overuse of testing.”
Data from the Centers for Disease Control and Prevention show that at least 2 million people in the United States develop antibiotic-resistant bacterial infections each year. At least 23,000 of these patients die each year because of these infections.
In 2013, the CDC published a report on drug-resistant threats in the United States. The three offenders deemed most serious – Clostridium difficile, Carbapenem-resistant Enterobacteriaceae, and Neisseria gonorrhoeae, continue to challenge clinicians.
Clinicians can help curb antibiotic resistance by practicing good stewardship, said Dr. Hanrahan. “Antimicrobial stewardship and laboratory stewardship are two things that can greatly improve patient care and outcomes for patients,” she said.
“Testing stewardship means ordering tests that are necessary based on signs and symptoms,” said Dr. Hanrahan. “For example, people often order urine cultures when there are no symptoms of urinary tract infection, and then end up treating positive cultures with antibiotics even when there are no symptoms of infection. This leads to unnecessary antibiotic exposure,” she noted.
The CDC’s core plans to fight antimicrobial resistance include:
- Preventing infections in the first place: The CDC emphasizes the importance of prevention through hand washing, safe food handling practices, and immunizations.
- Tracking data: The CDC collects and uses data on resistant infections to identify risk factors for resistance and develop strategies to prevent the spread of resistant bacteria.
- Practicing antibiotic stewardship: As Dr. Hanrahan noted, judicious use of antibiotics can help cut down on resistant bacteria.
- Developing alternatives: The CDC supports the development of new antibiotics and new tests to track antibacterial resistance.
Dr. Hanrahan discussed the Top 10 things hospitalists can do to improve lab testing and antimicrobial use.
“Hospitalists must recognize the need to decrease antibiotic use, utilize laboratory testing appropriately, and improve patient safety,” she said.
“There are a wide range of resources available on the Internet that can help you delve further into this topic and to find the appropriate balance for testing and treatment,” Dr. Hanrahan concluded.
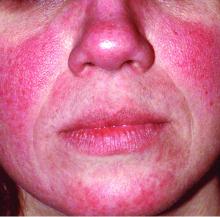
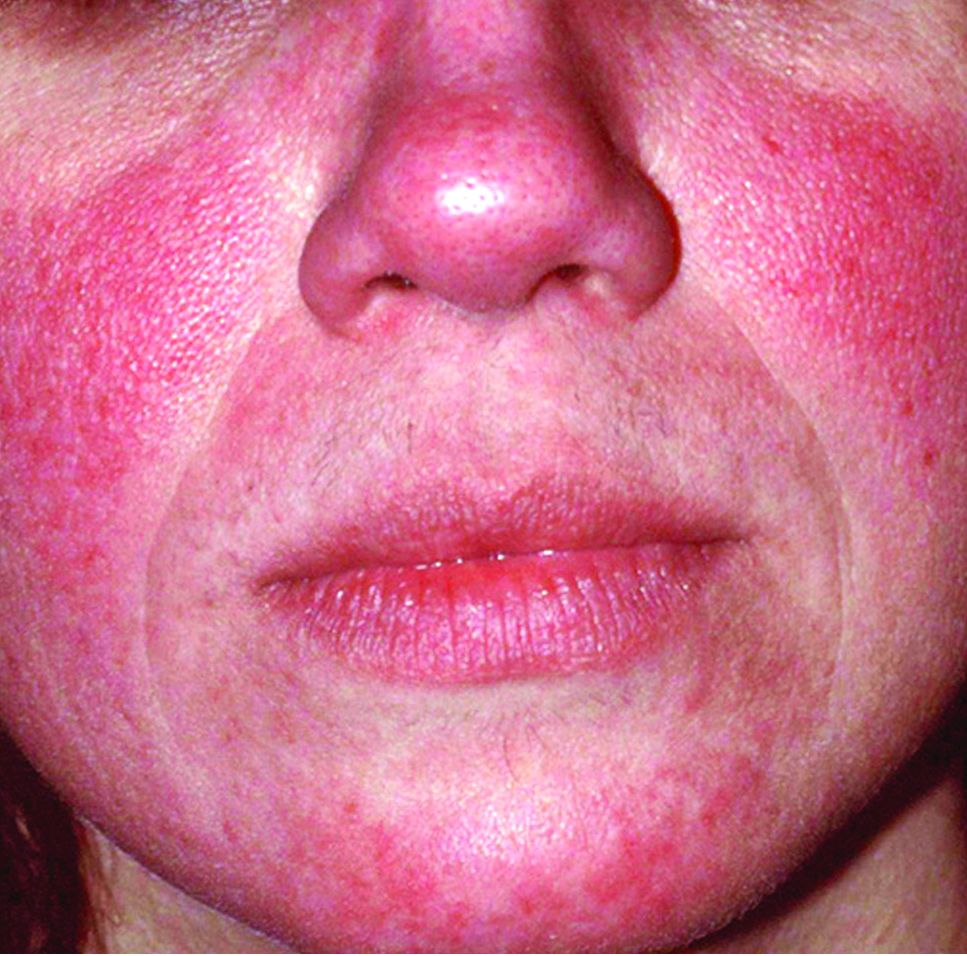
Rosacea tied to physical and psychological comorbidities
according to a review of 29 studies.
The recognition of rosacea as an inflammatory condition similar to psoriasis suggests that, as with psoriasis, rosacea may be associated with a range of systemic diseases, but data on such an association are limited, wrote Roger Haber, MD, from the department of dermatology at Saint George Hospital University Medical Center, Beirut, Lebanon.
“To the best of our knowledge, our study is the first review analyzing available data regarding the diseases associated with rosacea,” they said.
Overall, the most common comorbidities associated with rosacea were depression (reported in 117,848 patients), hypertension (18,176 patients), cardiovascular disease (9,739 patients), anxiety disorder (9,079 patients), dyslipidemia (7,004 patients), diabetes mellitus (6,306 patients), and migraine (6,136 patients). All associations were statistically significant.
Psychological problems significantly associated with rosacea include depression and anxiety, which may be related to similar inflammatory pathways among these conditions, the researchers noted.
Cardiovascular disease risk factors significantly associated with rosacea included coronary artery disease, cardiovascular disease, peripheral artery disease, heart failure, diabetes mellitus, hypertension, dyslipidemia, and metabolic syndrome. The association with coronary artery disease remained significant after adjusting for multiple variables, as has been shown with psoriasis, which supports consideration of rosacea as an independent risk factor for CAD, the researchers said.
In terms of gastrointestinal comorbidities, the studies reviewed found an association between rosacea and several GI disorders, including celiac disease, Crohn’s disease, and ulcerative colitis, and Helicobacter pylori infection, they wrote. Although the current data do not imply causality, clinicians should screen rosacea patients for GI disorders, they noted.
The link between rosacea and migraine may stem from the similar vascular abnormalities and triggers common to both conditions, such as stress and alcohol, the researchers added.
The review does not establish causality between rosacea and any of the comorbidities examined in part because of the inclusion of observational studies, the researchers noted. “It is also possible that the observed association with rosacea is explained by shared environmental or lifestyle factors rather than by a common genetic disposition or pathophysiologic pathways,” they said. Controlled and prospective studies are needed to better identify associations, but general physicians and dermatologists who recognize the potential risk of comorbidities in rosacea patients may be better able to manage and treat them, they added.
The researchers had no financial conflicts to disclose. There was no funding source for the study.
SOURCE: Haber R et al. J Am Acad Dermatol. 2018 April;78(4):786-92.
according to a review of 29 studies.
The recognition of rosacea as an inflammatory condition similar to psoriasis suggests that, as with psoriasis, rosacea may be associated with a range of systemic diseases, but data on such an association are limited, wrote Roger Haber, MD, from the department of dermatology at Saint George Hospital University Medical Center, Beirut, Lebanon.
“To the best of our knowledge, our study is the first review analyzing available data regarding the diseases associated with rosacea,” they said.
Overall, the most common comorbidities associated with rosacea were depression (reported in 117,848 patients), hypertension (18,176 patients), cardiovascular disease (9,739 patients), anxiety disorder (9,079 patients), dyslipidemia (7,004 patients), diabetes mellitus (6,306 patients), and migraine (6,136 patients). All associations were statistically significant.
Psychological problems significantly associated with rosacea include depression and anxiety, which may be related to similar inflammatory pathways among these conditions, the researchers noted.
Cardiovascular disease risk factors significantly associated with rosacea included coronary artery disease, cardiovascular disease, peripheral artery disease, heart failure, diabetes mellitus, hypertension, dyslipidemia, and metabolic syndrome. The association with coronary artery disease remained significant after adjusting for multiple variables, as has been shown with psoriasis, which supports consideration of rosacea as an independent risk factor for CAD, the researchers said.
In terms of gastrointestinal comorbidities, the studies reviewed found an association between rosacea and several GI disorders, including celiac disease, Crohn’s disease, and ulcerative colitis, and Helicobacter pylori infection, they wrote. Although the current data do not imply causality, clinicians should screen rosacea patients for GI disorders, they noted.
The link between rosacea and migraine may stem from the similar vascular abnormalities and triggers common to both conditions, such as stress and alcohol, the researchers added.
The review does not establish causality between rosacea and any of the comorbidities examined in part because of the inclusion of observational studies, the researchers noted. “It is also possible that the observed association with rosacea is explained by shared environmental or lifestyle factors rather than by a common genetic disposition or pathophysiologic pathways,” they said. Controlled and prospective studies are needed to better identify associations, but general physicians and dermatologists who recognize the potential risk of comorbidities in rosacea patients may be better able to manage and treat them, they added.
The researchers had no financial conflicts to disclose. There was no funding source for the study.
SOURCE: Haber R et al. J Am Acad Dermatol. 2018 April;78(4):786-92.
according to a review of 29 studies.
The recognition of rosacea as an inflammatory condition similar to psoriasis suggests that, as with psoriasis, rosacea may be associated with a range of systemic diseases, but data on such an association are limited, wrote Roger Haber, MD, from the department of dermatology at Saint George Hospital University Medical Center, Beirut, Lebanon.
“To the best of our knowledge, our study is the first review analyzing available data regarding the diseases associated with rosacea,” they said.
Overall, the most common comorbidities associated with rosacea were depression (reported in 117,848 patients), hypertension (18,176 patients), cardiovascular disease (9,739 patients), anxiety disorder (9,079 patients), dyslipidemia (7,004 patients), diabetes mellitus (6,306 patients), and migraine (6,136 patients). All associations were statistically significant.
Psychological problems significantly associated with rosacea include depression and anxiety, which may be related to similar inflammatory pathways among these conditions, the researchers noted.
Cardiovascular disease risk factors significantly associated with rosacea included coronary artery disease, cardiovascular disease, peripheral artery disease, heart failure, diabetes mellitus, hypertension, dyslipidemia, and metabolic syndrome. The association with coronary artery disease remained significant after adjusting for multiple variables, as has been shown with psoriasis, which supports consideration of rosacea as an independent risk factor for CAD, the researchers said.
In terms of gastrointestinal comorbidities, the studies reviewed found an association between rosacea and several GI disorders, including celiac disease, Crohn’s disease, and ulcerative colitis, and Helicobacter pylori infection, they wrote. Although the current data do not imply causality, clinicians should screen rosacea patients for GI disorders, they noted.
The link between rosacea and migraine may stem from the similar vascular abnormalities and triggers common to both conditions, such as stress and alcohol, the researchers added.
The review does not establish causality between rosacea and any of the comorbidities examined in part because of the inclusion of observational studies, the researchers noted. “It is also possible that the observed association with rosacea is explained by shared environmental or lifestyle factors rather than by a common genetic disposition or pathophysiologic pathways,” they said. Controlled and prospective studies are needed to better identify associations, but general physicians and dermatologists who recognize the potential risk of comorbidities in rosacea patients may be better able to manage and treat them, they added.
The researchers had no financial conflicts to disclose. There was no funding source for the study.
SOURCE: Haber R et al. J Am Acad Dermatol. 2018 April;78(4):786-92.
FROM JAAD
Key clinical point: Rosacea is significantly associated with several comorbidities, including depression, hypertension, cardiovascular disease, and anxiety.
Major finding: Approximately 75% of studies on depression and rosacea showed a positive correlation between these conditions.
Study details: A systematic review of 29 studies: 14 case-control, 8 cross-sectional, and 7 cohort.
Disclosures: The researchers had no financial conflicts to disclose.
Source: Haber R et al. J Am Acad Dermatol. 2018 April;78(4):786-92.
Chikungunya infection in children masquerades as SJS-TEN
Chikungunya infections in young children resemble skin symptoms characteristic of Stevens-Johnson syndrome and toxic epidermal necrolysis, (SJS-TEN), according to data from a case series of 21 children seen during a chikungunya outbreak in India in August and September 2016.
The researchers described their observations of 13 boys and eight girls aged 1-36 months in Pediatric Dermatology. All 21 children presented with vesiculobullous and necrotic lesions and mild to moderate fever; 16 children (76%) had large erosions, purpuric macules, and necrosis. Most of the lesions occurred on the extremities.
The time from the onset of illness to presentation ranged from 1 to 9 days, and the skin lesions resolved in 5-7 days. The lesions resolved with no sequelae in 11 patients, with hyperpigmentation in seven (33%) , and with hypopigmentation in three patients (14%).
In addition, three patients (14%) developed minor oral erosions, and four (19%) developed palmoplantar erythema, which also may be associated with SJS-TEN. However, none of the patients experienced the severe mucositis and ocular and genital involvement common to SJS-TEN, Dr. Garg and associates noted. A total of seven children tested positive for chikungunya based on enzyme-linked immunosorbent assay results.
Severity of illness can be helpful to distinguish chikungunya from SJS-TEN, the researchers said. Based on the Nelson severity index, 11 children in this series met the criteria for “not sick,” nine were “moderately sick,” and one was “very sick.”
It is key “to be aware of SJS-TEN–like presentation of chikungunya and not to misinterpret it as true SJS-TEN, which will lead to unnecessary intervention and management,” Dr. Garg and associates said.
The researchers had no financial conflicts to disclose.
SOURCE: Garg T et al. Pediatr Dermatol. 2018 Mar 24. doi: 10.1111/pde.13450.
Chikungunya infections in young children resemble skin symptoms characteristic of Stevens-Johnson syndrome and toxic epidermal necrolysis, (SJS-TEN), according to data from a case series of 21 children seen during a chikungunya outbreak in India in August and September 2016.
The researchers described their observations of 13 boys and eight girls aged 1-36 months in Pediatric Dermatology. All 21 children presented with vesiculobullous and necrotic lesions and mild to moderate fever; 16 children (76%) had large erosions, purpuric macules, and necrosis. Most of the lesions occurred on the extremities.
The time from the onset of illness to presentation ranged from 1 to 9 days, and the skin lesions resolved in 5-7 days. The lesions resolved with no sequelae in 11 patients, with hyperpigmentation in seven (33%) , and with hypopigmentation in three patients (14%).
In addition, three patients (14%) developed minor oral erosions, and four (19%) developed palmoplantar erythema, which also may be associated with SJS-TEN. However, none of the patients experienced the severe mucositis and ocular and genital involvement common to SJS-TEN, Dr. Garg and associates noted. A total of seven children tested positive for chikungunya based on enzyme-linked immunosorbent assay results.
Severity of illness can be helpful to distinguish chikungunya from SJS-TEN, the researchers said. Based on the Nelson severity index, 11 children in this series met the criteria for “not sick,” nine were “moderately sick,” and one was “very sick.”
It is key “to be aware of SJS-TEN–like presentation of chikungunya and not to misinterpret it as true SJS-TEN, which will lead to unnecessary intervention and management,” Dr. Garg and associates said.
The researchers had no financial conflicts to disclose.
SOURCE: Garg T et al. Pediatr Dermatol. 2018 Mar 24. doi: 10.1111/pde.13450.
Chikungunya infections in young children resemble skin symptoms characteristic of Stevens-Johnson syndrome and toxic epidermal necrolysis, (SJS-TEN), according to data from a case series of 21 children seen during a chikungunya outbreak in India in August and September 2016.
The researchers described their observations of 13 boys and eight girls aged 1-36 months in Pediatric Dermatology. All 21 children presented with vesiculobullous and necrotic lesions and mild to moderate fever; 16 children (76%) had large erosions, purpuric macules, and necrosis. Most of the lesions occurred on the extremities.
The time from the onset of illness to presentation ranged from 1 to 9 days, and the skin lesions resolved in 5-7 days. The lesions resolved with no sequelae in 11 patients, with hyperpigmentation in seven (33%) , and with hypopigmentation in three patients (14%).
In addition, three patients (14%) developed minor oral erosions, and four (19%) developed palmoplantar erythema, which also may be associated with SJS-TEN. However, none of the patients experienced the severe mucositis and ocular and genital involvement common to SJS-TEN, Dr. Garg and associates noted. A total of seven children tested positive for chikungunya based on enzyme-linked immunosorbent assay results.
Severity of illness can be helpful to distinguish chikungunya from SJS-TEN, the researchers said. Based on the Nelson severity index, 11 children in this series met the criteria for “not sick,” nine were “moderately sick,” and one was “very sick.”
It is key “to be aware of SJS-TEN–like presentation of chikungunya and not to misinterpret it as true SJS-TEN, which will lead to unnecessary intervention and management,” Dr. Garg and associates said.
The researchers had no financial conflicts to disclose.
SOURCE: Garg T et al. Pediatr Dermatol. 2018 Mar 24. doi: 10.1111/pde.13450.
FROM PEDIATRIC DERMATOLOGY
Key clinical point:
Major finding: Of 21 children with chikungunya, 76% had developed vesicles and bullae with purpuric macules and necrosis.
Study details: A case series of 21 children with chikungunya fever in India.
Disclosures: The researchers had no financial conflicts to disclose.
Source: Garg T et al. Pediatr Dermatol. 2018 Mar 24. doi: 10.1111/pde.13450.
Boosting bedside skills in hands-on session
A low faculty-to-learner ratio helped HM18 attendees get the most from their learning experience in the Sunday pre-conference course “Bedside Procedures for the Hospitalist.”
The pre-course blended live didactic teaching and hands-on training with simulators so participants could not only learn but also review and demonstrate techniques for many common invasive procedures hospitalists encounter in practice.
“Our goal is to make the entire bedside procedures pre-course a unique experience,” course codirector Alyssa Burkhart, MD, of the Billings (Mont.) Clinic, said in an interview before the session.
“We carefully select the curriculum to create a program most relevant to the participants and their day-to-day work in patient care,” said Dr. Burkhart.
“The low faculty-to-learner ratio coupled with ample time to practice under expert guidance separates us from others. ... It’s a privilege to share our love of procedures with this year’s SHM participants,” said Dr. Burkhart, who comoderated the session with Joshua Lenchus, DO, SFHM, of the University of Miami.
An interactive focus on bedside procedures benefits novices and experienced clinicians, said Dr. Lenchus.
The simulation experience involved practice with ultrasound as well as anatomically representative training equipment.
“Our hope is that many hospitalists may once again find that spark of interest in performing more of their own procedures. The interactive sessions embedded within the pre-course are vital to the success of our program. Many other training sessions are didactics based. We strive to keep lecture time to a minimum so that small groups can learn from the expert facilitators,” Dr. Burkhart added.
“Ample hands-on practice time, interactive experience, and direct supervision separate our pre-course from other commercially available offerings,” Dr. Lenchus said.
The agenda kicked off with vascular and intraosseous access in the morning, followed by paracentesis, thoracentesis, lumbar puncture, and basic airway management, including the use of supraglottic devices.
Dr. Burkhart noted that the course included two separate practice sessions for vascular access because of the number of technical steps and potential complications. “Attendees typically wish to spend a considerable amount of time on vascular access,” she said. “The intraosseous access station and its exceptional trainers always receive very positive feedback.”
Dr. Burkhart and Dr. Lenchus had no financial conflicts to disclose.
A low faculty-to-learner ratio helped HM18 attendees get the most from their learning experience in the Sunday pre-conference course “Bedside Procedures for the Hospitalist.”
The pre-course blended live didactic teaching and hands-on training with simulators so participants could not only learn but also review and demonstrate techniques for many common invasive procedures hospitalists encounter in practice.
“Our goal is to make the entire bedside procedures pre-course a unique experience,” course codirector Alyssa Burkhart, MD, of the Billings (Mont.) Clinic, said in an interview before the session.
“We carefully select the curriculum to create a program most relevant to the participants and their day-to-day work in patient care,” said Dr. Burkhart.
“The low faculty-to-learner ratio coupled with ample time to practice under expert guidance separates us from others. ... It’s a privilege to share our love of procedures with this year’s SHM participants,” said Dr. Burkhart, who comoderated the session with Joshua Lenchus, DO, SFHM, of the University of Miami.
An interactive focus on bedside procedures benefits novices and experienced clinicians, said Dr. Lenchus.
The simulation experience involved practice with ultrasound as well as anatomically representative training equipment.
“Our hope is that many hospitalists may once again find that spark of interest in performing more of their own procedures. The interactive sessions embedded within the pre-course are vital to the success of our program. Many other training sessions are didactics based. We strive to keep lecture time to a minimum so that small groups can learn from the expert facilitators,” Dr. Burkhart added.
“Ample hands-on practice time, interactive experience, and direct supervision separate our pre-course from other commercially available offerings,” Dr. Lenchus said.
The agenda kicked off with vascular and intraosseous access in the morning, followed by paracentesis, thoracentesis, lumbar puncture, and basic airway management, including the use of supraglottic devices.
Dr. Burkhart noted that the course included two separate practice sessions for vascular access because of the number of technical steps and potential complications. “Attendees typically wish to spend a considerable amount of time on vascular access,” she said. “The intraosseous access station and its exceptional trainers always receive very positive feedback.”
Dr. Burkhart and Dr. Lenchus had no financial conflicts to disclose.
A low faculty-to-learner ratio helped HM18 attendees get the most from their learning experience in the Sunday pre-conference course “Bedside Procedures for the Hospitalist.”
The pre-course blended live didactic teaching and hands-on training with simulators so participants could not only learn but also review and demonstrate techniques for many common invasive procedures hospitalists encounter in practice.
“Our goal is to make the entire bedside procedures pre-course a unique experience,” course codirector Alyssa Burkhart, MD, of the Billings (Mont.) Clinic, said in an interview before the session.
“We carefully select the curriculum to create a program most relevant to the participants and their day-to-day work in patient care,” said Dr. Burkhart.
“The low faculty-to-learner ratio coupled with ample time to practice under expert guidance separates us from others. ... It’s a privilege to share our love of procedures with this year’s SHM participants,” said Dr. Burkhart, who comoderated the session with Joshua Lenchus, DO, SFHM, of the University of Miami.
An interactive focus on bedside procedures benefits novices and experienced clinicians, said Dr. Lenchus.
The simulation experience involved practice with ultrasound as well as anatomically representative training equipment.
“Our hope is that many hospitalists may once again find that spark of interest in performing more of their own procedures. The interactive sessions embedded within the pre-course are vital to the success of our program. Many other training sessions are didactics based. We strive to keep lecture time to a minimum so that small groups can learn from the expert facilitators,” Dr. Burkhart added.
“Ample hands-on practice time, interactive experience, and direct supervision separate our pre-course from other commercially available offerings,” Dr. Lenchus said.
The agenda kicked off with vascular and intraosseous access in the morning, followed by paracentesis, thoracentesis, lumbar puncture, and basic airway management, including the use of supraglottic devices.
Dr. Burkhart noted that the course included two separate practice sessions for vascular access because of the number of technical steps and potential complications. “Attendees typically wish to spend a considerable amount of time on vascular access,” she said. “The intraosseous access station and its exceptional trainers always receive very positive feedback.”
Dr. Burkhart and Dr. Lenchus had no financial conflicts to disclose.
Melanoma in young children may be biologically distinct from that in teens
Pediatric melanomas appear to be more progressive in adolescents than in young children, based on data from a retrospective study of 32 cases.
Few young children with melanoma die, despite a greater likelihood of thicker tumors, lymph node metastasis, and later diagnosis, which suggests that melanoma in young children may be biologically distinct from melanoma in adolescents, wrote Diana W. Bartenstein, of Harvard University Medical School, Boston, and her colleagues.
Overall, significantly more children than adolescents had spitzoid melanoma (50% vs. 10%, P = .01). In addition, children were more likely than adolescents to present with stage 3 or 4 cancer (58% vs. 25%) and with Clark level IV and V tumors (42% vs. 35%), although these differences were not significant. The median Breslow thickness of lesions was greater in children than in adolescents (3.5 mm vs. 1.5 mm) as was the median mitotic index (5 mitotic figures per mm2 vs. 2 mitotic figures per mm2) and children were more likely than adolescents to have neural invasion, but these differences were not significant either.
During the study period of more than 20 years, none of the children younger than 11 years died, compared with four deaths in adolescents, a statistically significant difference (P = .04). The follow-up for surviving individuals ranged from 9-37 months with a median of 44 months.
The study findings were limited by several factors including the small sample size and difficulty in assessing spitzoid tumors, the researchers noted.
However, “these results support the hypothesis that melanoma in young children may be biologically distinct from melanoma in adults,” they said. “Alternatively, melanoma subtype may drive survival differences between children and adolescents.”
No conflicts of interest were reported. The study was supported by the Alpha Omega Alpha Carolyn L. Kuckein Student Research Fellowship and the Society for Pediatric Dermatology and Pediatric Dermatology Research Alliance.
SOURCE: Bartenstein DW et al. Pediatr Dermatol. 2018 Mar 23. doi: 10.1111/pde.13454.
Pediatric melanomas appear to be more progressive in adolescents than in young children, based on data from a retrospective study of 32 cases.
Few young children with melanoma die, despite a greater likelihood of thicker tumors, lymph node metastasis, and later diagnosis, which suggests that melanoma in young children may be biologically distinct from melanoma in adolescents, wrote Diana W. Bartenstein, of Harvard University Medical School, Boston, and her colleagues.
Overall, significantly more children than adolescents had spitzoid melanoma (50% vs. 10%, P = .01). In addition, children were more likely than adolescents to present with stage 3 or 4 cancer (58% vs. 25%) and with Clark level IV and V tumors (42% vs. 35%), although these differences were not significant. The median Breslow thickness of lesions was greater in children than in adolescents (3.5 mm vs. 1.5 mm) as was the median mitotic index (5 mitotic figures per mm2 vs. 2 mitotic figures per mm2) and children were more likely than adolescents to have neural invasion, but these differences were not significant either.
During the study period of more than 20 years, none of the children younger than 11 years died, compared with four deaths in adolescents, a statistically significant difference (P = .04). The follow-up for surviving individuals ranged from 9-37 months with a median of 44 months.
The study findings were limited by several factors including the small sample size and difficulty in assessing spitzoid tumors, the researchers noted.
However, “these results support the hypothesis that melanoma in young children may be biologically distinct from melanoma in adults,” they said. “Alternatively, melanoma subtype may drive survival differences between children and adolescents.”
No conflicts of interest were reported. The study was supported by the Alpha Omega Alpha Carolyn L. Kuckein Student Research Fellowship and the Society for Pediatric Dermatology and Pediatric Dermatology Research Alliance.
SOURCE: Bartenstein DW et al. Pediatr Dermatol. 2018 Mar 23. doi: 10.1111/pde.13454.
Pediatric melanomas appear to be more progressive in adolescents than in young children, based on data from a retrospective study of 32 cases.
Few young children with melanoma die, despite a greater likelihood of thicker tumors, lymph node metastasis, and later diagnosis, which suggests that melanoma in young children may be biologically distinct from melanoma in adolescents, wrote Diana W. Bartenstein, of Harvard University Medical School, Boston, and her colleagues.
Overall, significantly more children than adolescents had spitzoid melanoma (50% vs. 10%, P = .01). In addition, children were more likely than adolescents to present with stage 3 or 4 cancer (58% vs. 25%) and with Clark level IV and V tumors (42% vs. 35%), although these differences were not significant. The median Breslow thickness of lesions was greater in children than in adolescents (3.5 mm vs. 1.5 mm) as was the median mitotic index (5 mitotic figures per mm2 vs. 2 mitotic figures per mm2) and children were more likely than adolescents to have neural invasion, but these differences were not significant either.
During the study period of more than 20 years, none of the children younger than 11 years died, compared with four deaths in adolescents, a statistically significant difference (P = .04). The follow-up for surviving individuals ranged from 9-37 months with a median of 44 months.
The study findings were limited by several factors including the small sample size and difficulty in assessing spitzoid tumors, the researchers noted.
However, “these results support the hypothesis that melanoma in young children may be biologically distinct from melanoma in adults,” they said. “Alternatively, melanoma subtype may drive survival differences between children and adolescents.”
No conflicts of interest were reported. The study was supported by the Alpha Omega Alpha Carolyn L. Kuckein Student Research Fellowship and the Society for Pediatric Dermatology and Pediatric Dermatology Research Alliance.
SOURCE: Bartenstein DW et al. Pediatr Dermatol. 2018 Mar 23. doi: 10.1111/pde.13454.
FROM PEDIATRIC DERMATOLOGY
Key clinical point:
Major finding: Significantly more children than adolescents had spitzoid melanoma (50% vs. 10%, P = .01).
Study details: A retrospective cohort study of 32 children and adolescents with melanoma.
Disclosures: The study was supported by the Alpha Omega Alpha–Carolyn L. Kuckein Student Research Fellowship and the Society for Pediatric Dermatology and Pediatric Dermatology Research Alliance. No conflicts of interest were reported.
Source: Bartenstein DW et al. Pediatr Dermatol. 2018 Mar 23. doi: 10.1111/pde.13454.