User login
CECCY: Carvedilol didn’t curb cardiotoxicity in breast cancer patients
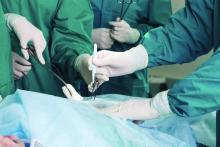
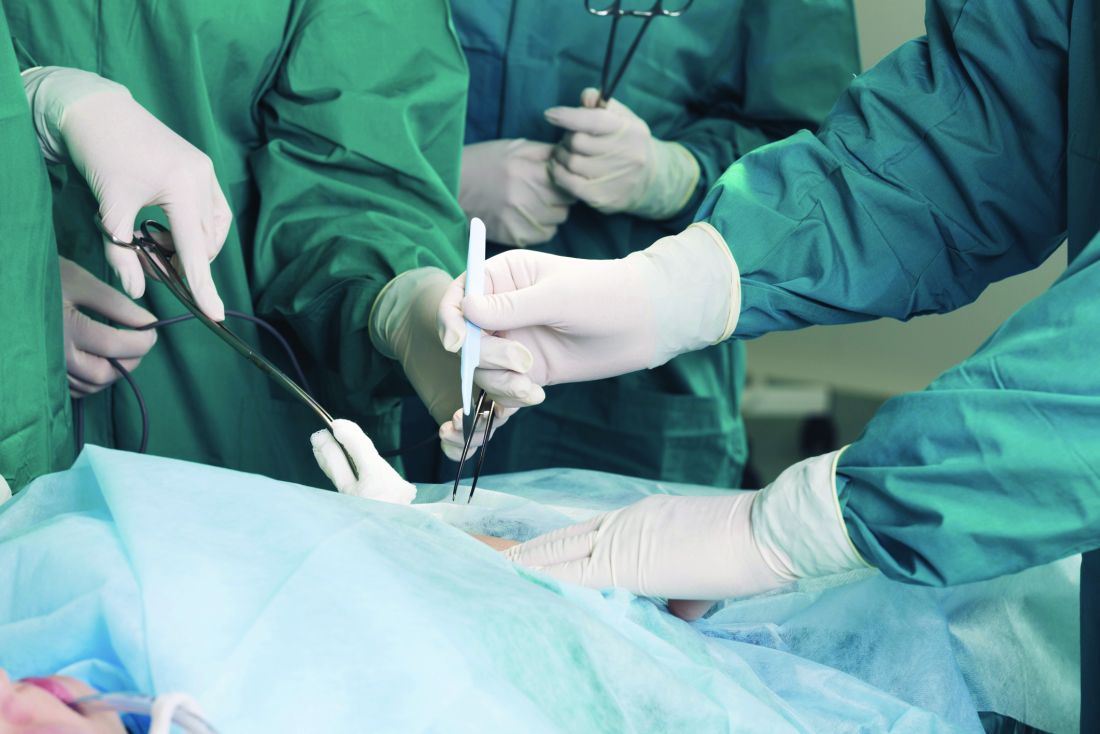
ORLANDO – Anthracycline chemotherapy was associated with a cardiotoxicity incidence of roughly 14% of breast cancer patients regardless of treatment with carvedilol, based on data from a randomized trial of 200 patients.
“Cardio-oncology has been neglected,” Monica Samuel Avila, MD, of Hospital das Clínicas da Faculdade de Medicina da Universidade in São Paulo, Brazil, said in a video interview at the annual meeting of the American College of Cardiology. “We have seen improvement of survival in patients with cancer, but with that comes complications related to treatment. I think that the interactions between cardiologists and oncologists are increasing in a more important way,” she said.
In the Carvedilol for Prevention of Chemotherapy-Induced Cardiotoxicity (CECCY) Trial, Dr. Avila and colleagues evaluated primary prevention of cardiotoxicity in women with normal hearts who were undergoing chemotherapy for breast cancer.
Patients in the treatment group received a median carvedilol dose of 18.4 mg/day. The primary endpoint of cardiotoxicity, defined as a decrease in left ventricular ejection fraction (LVEF) of at least 10% at 6 months, occurred in 15% of carvedilol patients and 14% placebo patients, a nonsignificant difference. No significant differences occurred in diastolic dysfunction or in B-type natriuretic peptide (BNP) levels at 6 weeks, 12 weeks, or 24 weeks between the groups.
However, carvedilol patients showed significantly reduced troponin 1 levels compared with placebo, which suggests protection against myocardial injury, Dr. Avila said.
“In short follow up, we can see cardiotoxicity appearing, and we know we have to treat it promptly to prevent cardiac events,” she said.
Dr. Avila and colleagues identified 200 women older than 18 years with HER2-negative breast cancer tumor status and normal left ventricular ejection fraction. The patients were undergoing chemotherapy with 240 mg/m2 of anthracycline and were randomized to treatment with carvedilol or a placebo. Baseline characteristics were similar between the two groups.
Adverse effects were not significantly different between the groups, and the most common events in each group included dizziness, dry mouth, symptomatic hypertension, stomachache, and nausea. Although the results suggest that carvedilol can reduce the risk of myocardial injury, more research is needed to address the question of the increase in troponin without change in the LVEF, Dr. Avila noted. The study is ongoing and the research team intends to follow the low-risk patient population for a total of 2 years. “For high-risk patients, I am already giving carvedilol,” she said. “We believe if we find a difference in LVEF or clinical events, we could encourage cardiologists to give carvedilol in a low-risk population,” she said.
“This study highlights that there is no safe dose of anthracycline,” commented Bonnie Ky, MD of the University of Pennsylvania, Philadelphia, at a press briefing. She emphasized the value of carvedilol for a high-risk population, and stressed the importance of following long-term changes in heart injury markers after 1-2 years for low-risk patients.
Dr. Avila had no financial conflicts to disclose. Dr. Ky disclosed relationships with multiple companies including Bioinvent and Bristol Myers.
The findings were published simultaneously in the Journal of the American College of Cardiology.
SOURCE: Avila, M. ACC 18
ORLANDO – Anthracycline chemotherapy was associated with a cardiotoxicity incidence of roughly 14% of breast cancer patients regardless of treatment with carvedilol, based on data from a randomized trial of 200 patients.
“Cardio-oncology has been neglected,” Monica Samuel Avila, MD, of Hospital das Clínicas da Faculdade de Medicina da Universidade in São Paulo, Brazil, said in a video interview at the annual meeting of the American College of Cardiology. “We have seen improvement of survival in patients with cancer, but with that comes complications related to treatment. I think that the interactions between cardiologists and oncologists are increasing in a more important way,” she said.
In the Carvedilol for Prevention of Chemotherapy-Induced Cardiotoxicity (CECCY) Trial, Dr. Avila and colleagues evaluated primary prevention of cardiotoxicity in women with normal hearts who were undergoing chemotherapy for breast cancer.
Patients in the treatment group received a median carvedilol dose of 18.4 mg/day. The primary endpoint of cardiotoxicity, defined as a decrease in left ventricular ejection fraction (LVEF) of at least 10% at 6 months, occurred in 15% of carvedilol patients and 14% placebo patients, a nonsignificant difference. No significant differences occurred in diastolic dysfunction or in B-type natriuretic peptide (BNP) levels at 6 weeks, 12 weeks, or 24 weeks between the groups.
However, carvedilol patients showed significantly reduced troponin 1 levels compared with placebo, which suggests protection against myocardial injury, Dr. Avila said.
“In short follow up, we can see cardiotoxicity appearing, and we know we have to treat it promptly to prevent cardiac events,” she said.
Dr. Avila and colleagues identified 200 women older than 18 years with HER2-negative breast cancer tumor status and normal left ventricular ejection fraction. The patients were undergoing chemotherapy with 240 mg/m2 of anthracycline and were randomized to treatment with carvedilol or a placebo. Baseline characteristics were similar between the two groups.
Adverse effects were not significantly different between the groups, and the most common events in each group included dizziness, dry mouth, symptomatic hypertension, stomachache, and nausea. Although the results suggest that carvedilol can reduce the risk of myocardial injury, more research is needed to address the question of the increase in troponin without change in the LVEF, Dr. Avila noted. The study is ongoing and the research team intends to follow the low-risk patient population for a total of 2 years. “For high-risk patients, I am already giving carvedilol,” she said. “We believe if we find a difference in LVEF or clinical events, we could encourage cardiologists to give carvedilol in a low-risk population,” she said.
“This study highlights that there is no safe dose of anthracycline,” commented Bonnie Ky, MD of the University of Pennsylvania, Philadelphia, at a press briefing. She emphasized the value of carvedilol for a high-risk population, and stressed the importance of following long-term changes in heart injury markers after 1-2 years for low-risk patients.
Dr. Avila had no financial conflicts to disclose. Dr. Ky disclosed relationships with multiple companies including Bioinvent and Bristol Myers.
The findings were published simultaneously in the Journal of the American College of Cardiology.
SOURCE: Avila, M. ACC 18
ORLANDO – Anthracycline chemotherapy was associated with a cardiotoxicity incidence of roughly 14% of breast cancer patients regardless of treatment with carvedilol, based on data from a randomized trial of 200 patients.
“Cardio-oncology has been neglected,” Monica Samuel Avila, MD, of Hospital das Clínicas da Faculdade de Medicina da Universidade in São Paulo, Brazil, said in a video interview at the annual meeting of the American College of Cardiology. “We have seen improvement of survival in patients with cancer, but with that comes complications related to treatment. I think that the interactions between cardiologists and oncologists are increasing in a more important way,” she said.
In the Carvedilol for Prevention of Chemotherapy-Induced Cardiotoxicity (CECCY) Trial, Dr. Avila and colleagues evaluated primary prevention of cardiotoxicity in women with normal hearts who were undergoing chemotherapy for breast cancer.
Patients in the treatment group received a median carvedilol dose of 18.4 mg/day. The primary endpoint of cardiotoxicity, defined as a decrease in left ventricular ejection fraction (LVEF) of at least 10% at 6 months, occurred in 15% of carvedilol patients and 14% placebo patients, a nonsignificant difference. No significant differences occurred in diastolic dysfunction or in B-type natriuretic peptide (BNP) levels at 6 weeks, 12 weeks, or 24 weeks between the groups.
However, carvedilol patients showed significantly reduced troponin 1 levels compared with placebo, which suggests protection against myocardial injury, Dr. Avila said.
“In short follow up, we can see cardiotoxicity appearing, and we know we have to treat it promptly to prevent cardiac events,” she said.
Dr. Avila and colleagues identified 200 women older than 18 years with HER2-negative breast cancer tumor status and normal left ventricular ejection fraction. The patients were undergoing chemotherapy with 240 mg/m2 of anthracycline and were randomized to treatment with carvedilol or a placebo. Baseline characteristics were similar between the two groups.
Adverse effects were not significantly different between the groups, and the most common events in each group included dizziness, dry mouth, symptomatic hypertension, stomachache, and nausea. Although the results suggest that carvedilol can reduce the risk of myocardial injury, more research is needed to address the question of the increase in troponin without change in the LVEF, Dr. Avila noted. The study is ongoing and the research team intends to follow the low-risk patient population for a total of 2 years. “For high-risk patients, I am already giving carvedilol,” she said. “We believe if we find a difference in LVEF or clinical events, we could encourage cardiologists to give carvedilol in a low-risk population,” she said.
“This study highlights that there is no safe dose of anthracycline,” commented Bonnie Ky, MD of the University of Pennsylvania, Philadelphia, at a press briefing. She emphasized the value of carvedilol for a high-risk population, and stressed the importance of following long-term changes in heart injury markers after 1-2 years for low-risk patients.
Dr. Avila had no financial conflicts to disclose. Dr. Ky disclosed relationships with multiple companies including Bioinvent and Bristol Myers.
The findings were published simultaneously in the Journal of the American College of Cardiology.
SOURCE: Avila, M. ACC 18
REPORTING FROM ACC 18
Key clinical point:
Major finding: Cardiotoxicity was roughly 14% in breast cancer patients treated with anthracycline whether they received carvedilol or placebo.
Study details: CECCY was a randomized, placebo-controlled trial of 200 patients with HER2-negative breast cancer tumor status.
Disclosures: Dr. Avila had no financial conflicts to disclose.
Source: Avila M. ACC 2018.
Postmenopausal women: Walk farther and faster to reduce heart failure risk
Brisk walking for at least 40 minutes two or three times a week reduced the risk of heart failure by approximately 25% in postmenopausal women, according to data from more that 89,000 participants in the Women’s Health Initiative.
The benefits of walking are well understood, said Somwail Rasla, MD, of Saint Vincent Hospital in Worcester, Mass., but he and his colleagues focused for the first time on how the speed, frequency, and duration of walking affected health in older women who may be less likely to visit a gym or engage in a formal exercise program.
The researchers followed the women, aged 50-79 years, for approximately 10 years.
Overall, the risk of heart failure was 20%-25% less for women who walked at least twice a week than it was for women who walked less frequently. In addition, women who walked for at least 40 minutes per walk had a 21%-25% lower heart failure risk than did those who walked less than 40 minutes per walk.
Pace mattered as well, Dr. Rasla pointed out. Women walking at an average pace and a fast pace had, respectively, 26% and 38% lower heart failure risk, compared with women who walked at a casual pace.
The researchers measured the women’s energy expenditure using the Metabolic Equivalent of Task (MET), a value calculated using the women’s self-reports of their walking frequency, duration, and speed. The results were similar across different age groups, ethnicities, and baseline body weight, which suggests the findings can be generalized to apply to most women. “I think we could give the same advice [about walking] to women up to age 79,” said Dr. Rasla.
The findings were limited by the use of self-reports, Dr. Rasla noted. However, the results suggest that walking can be a valuable and accessible form of exercise for older women, he said.
The Women’s Health Initiative is sponsored by the National Institutes of Health. The investigators reported no relevant conflicts of interest.
SOURCE: Rasla S et al. ACC 18, Poster 1315M-03.
Brisk walking for at least 40 minutes two or three times a week reduced the risk of heart failure by approximately 25% in postmenopausal women, according to data from more that 89,000 participants in the Women’s Health Initiative.
The benefits of walking are well understood, said Somwail Rasla, MD, of Saint Vincent Hospital in Worcester, Mass., but he and his colleagues focused for the first time on how the speed, frequency, and duration of walking affected health in older women who may be less likely to visit a gym or engage in a formal exercise program.
The researchers followed the women, aged 50-79 years, for approximately 10 years.
Overall, the risk of heart failure was 20%-25% less for women who walked at least twice a week than it was for women who walked less frequently. In addition, women who walked for at least 40 minutes per walk had a 21%-25% lower heart failure risk than did those who walked less than 40 minutes per walk.
Pace mattered as well, Dr. Rasla pointed out. Women walking at an average pace and a fast pace had, respectively, 26% and 38% lower heart failure risk, compared with women who walked at a casual pace.
The researchers measured the women’s energy expenditure using the Metabolic Equivalent of Task (MET), a value calculated using the women’s self-reports of their walking frequency, duration, and speed. The results were similar across different age groups, ethnicities, and baseline body weight, which suggests the findings can be generalized to apply to most women. “I think we could give the same advice [about walking] to women up to age 79,” said Dr. Rasla.
The findings were limited by the use of self-reports, Dr. Rasla noted. However, the results suggest that walking can be a valuable and accessible form of exercise for older women, he said.
The Women’s Health Initiative is sponsored by the National Institutes of Health. The investigators reported no relevant conflicts of interest.
SOURCE: Rasla S et al. ACC 18, Poster 1315M-03.
Brisk walking for at least 40 minutes two or three times a week reduced the risk of heart failure by approximately 25% in postmenopausal women, according to data from more that 89,000 participants in the Women’s Health Initiative.
The benefits of walking are well understood, said Somwail Rasla, MD, of Saint Vincent Hospital in Worcester, Mass., but he and his colleagues focused for the first time on how the speed, frequency, and duration of walking affected health in older women who may be less likely to visit a gym or engage in a formal exercise program.
The researchers followed the women, aged 50-79 years, for approximately 10 years.
Overall, the risk of heart failure was 20%-25% less for women who walked at least twice a week than it was for women who walked less frequently. In addition, women who walked for at least 40 minutes per walk had a 21%-25% lower heart failure risk than did those who walked less than 40 minutes per walk.
Pace mattered as well, Dr. Rasla pointed out. Women walking at an average pace and a fast pace had, respectively, 26% and 38% lower heart failure risk, compared with women who walked at a casual pace.
The researchers measured the women’s energy expenditure using the Metabolic Equivalent of Task (MET), a value calculated using the women’s self-reports of their walking frequency, duration, and speed. The results were similar across different age groups, ethnicities, and baseline body weight, which suggests the findings can be generalized to apply to most women. “I think we could give the same advice [about walking] to women up to age 79,” said Dr. Rasla.
The findings were limited by the use of self-reports, Dr. Rasla noted. However, the results suggest that walking can be a valuable and accessible form of exercise for older women, he said.
The Women’s Health Initiative is sponsored by the National Institutes of Health. The investigators reported no relevant conflicts of interest.
SOURCE: Rasla S et al. ACC 18, Poster 1315M-03.
FROM ACC18
Key clinical point: Urge older female patients to walk briskly at least twice a week.
Major finding: Patients with a fast pace had a 38% lower risk of heart failure.
Study details: A long-term, national observational study of 89,270 women.
Disclosures: The Women’s Health Initiative is sponsored by the National Institutes of Health. The investigators reported no relevant conflicts of interest.
Source: Rasla S et al. ACC 18, Poster 1315M-03.
Finding a groove helps patients move
Listening to uptempo music significantly improved patients’ compared with patients who didn’t listen to music, according to data from a randomized trial of 127 patients.
Exercise stress tests are frequently recommended to evaluate patients for heart disease, but many patients don’t work hard enough to reach a useful level of exertion, Waseem Shami, MD, of Texas Tech University in El Paso, said in a web briefing in advance of the annual meeting of the American College of Cardiology.
The group of patients that listened to lively music averaged 55 seconds longer exercise time, compared with the no-music control group, Dr. Shami said. The average exercise time was 505.8 seconds in the music group and 455.2 in the control group (P = .045).
Dr. Shami and his colleagues randomized 67 adults scheduled for cardiac stress tests to listen to music during the test and 60 controls to undergo the test without music. The average age of the patients was 53 years, and 61% and 67% of those in the music and control groups, respectively, were women. Demographic characteristics and variables, including resting heart rate and blood pressure, were similar between the music and control groups.
In a clinical setting, the use of music may help reduce unnecessary stress testing, which is deemed unsuccessful if the patient doesn’t exercise hard enough to achieve a target heart rate. “Perhaps this motivational tool can help us make stress testing more valuable,” said Dr. Shami. The results were limited by the relatively small study population and the fact that the researchers, not the patients, chose the music, Dr. Shami said.
More research is needed in a larger trial, and “allowing patients to choose their own music might make an even bigger difference,” he noted. Also, patients’ discomfort with exercising in general and exercising in public may have impacted the results, he said.
Moderator Martha Gulati, MD, of the University of Arizona, Phoenix, noted that an area for future research might be to do a cardiac stress test without and without music on the same person, with the patient serving as his or her own control.
Dr. Shami had no relevant financial conflicts to disclose.
Listening to uptempo music significantly improved patients’ compared with patients who didn’t listen to music, according to data from a randomized trial of 127 patients.
Exercise stress tests are frequently recommended to evaluate patients for heart disease, but many patients don’t work hard enough to reach a useful level of exertion, Waseem Shami, MD, of Texas Tech University in El Paso, said in a web briefing in advance of the annual meeting of the American College of Cardiology.
The group of patients that listened to lively music averaged 55 seconds longer exercise time, compared with the no-music control group, Dr. Shami said. The average exercise time was 505.8 seconds in the music group and 455.2 in the control group (P = .045).
Dr. Shami and his colleagues randomized 67 adults scheduled for cardiac stress tests to listen to music during the test and 60 controls to undergo the test without music. The average age of the patients was 53 years, and 61% and 67% of those in the music and control groups, respectively, were women. Demographic characteristics and variables, including resting heart rate and blood pressure, were similar between the music and control groups.
In a clinical setting, the use of music may help reduce unnecessary stress testing, which is deemed unsuccessful if the patient doesn’t exercise hard enough to achieve a target heart rate. “Perhaps this motivational tool can help us make stress testing more valuable,” said Dr. Shami. The results were limited by the relatively small study population and the fact that the researchers, not the patients, chose the music, Dr. Shami said.
More research is needed in a larger trial, and “allowing patients to choose their own music might make an even bigger difference,” he noted. Also, patients’ discomfort with exercising in general and exercising in public may have impacted the results, he said.
Moderator Martha Gulati, MD, of the University of Arizona, Phoenix, noted that an area for future research might be to do a cardiac stress test without and without music on the same person, with the patient serving as his or her own control.
Dr. Shami had no relevant financial conflicts to disclose.
Listening to uptempo music significantly improved patients’ compared with patients who didn’t listen to music, according to data from a randomized trial of 127 patients.
Exercise stress tests are frequently recommended to evaluate patients for heart disease, but many patients don’t work hard enough to reach a useful level of exertion, Waseem Shami, MD, of Texas Tech University in El Paso, said in a web briefing in advance of the annual meeting of the American College of Cardiology.
The group of patients that listened to lively music averaged 55 seconds longer exercise time, compared with the no-music control group, Dr. Shami said. The average exercise time was 505.8 seconds in the music group and 455.2 in the control group (P = .045).
Dr. Shami and his colleagues randomized 67 adults scheduled for cardiac stress tests to listen to music during the test and 60 controls to undergo the test without music. The average age of the patients was 53 years, and 61% and 67% of those in the music and control groups, respectively, were women. Demographic characteristics and variables, including resting heart rate and blood pressure, were similar between the music and control groups.
In a clinical setting, the use of music may help reduce unnecessary stress testing, which is deemed unsuccessful if the patient doesn’t exercise hard enough to achieve a target heart rate. “Perhaps this motivational tool can help us make stress testing more valuable,” said Dr. Shami. The results were limited by the relatively small study population and the fact that the researchers, not the patients, chose the music, Dr. Shami said.
More research is needed in a larger trial, and “allowing patients to choose their own music might make an even bigger difference,” he noted. Also, patients’ discomfort with exercising in general and exercising in public may have impacted the results, he said.
Moderator Martha Gulati, MD, of the University of Arizona, Phoenix, noted that an area for future research might be to do a cardiac stress test without and without music on the same person, with the patient serving as his or her own control.
Dr. Shami had no relevant financial conflicts to disclose.
FROM ACC 18
Heart attacks soar in young IBD patients
Inflammatory bowel disease significantly increases the risk of a heart attack in adults, but especially young adults aged 18-24 years, and in women compared with men across all age groups, according to data from about 200,000 IBD patients.
The odds ratio for heart attack in IBD patients vs. controls remained a significant 1.2 after adjustment for traditional cardiovascular risk factors, Muhammad S. Panhwar, MD, said in a media briefing in advance of the annual meeting of the American College of Cardiology.
“Chronic inflammation has been recognized as having an important role in the development of heart disease,” he noted.
Although other chronic inflammatory conditions are associated with increased heart attack risk, the link between heart attacks and IBD has not been well studied, despite its high prevalence in the United States (about 3 million adults, according to the Centers for Disease Control and Prevention), said Dr. Panhwar, an internal medicine resident at Case Western Reserve University in Cleveland. He and his colleagues reviewed a nationwide medical records database of 17.5 million adults aged 18-65 years for diagnoses of IBD between 2013 and 2017. Overall, 1.2% of the patients (211,870) had IBD, and most of the patients in the IBD group were younger, female, and white, Dr. Panhwar noted.
The relative risk of myocardial infarction was roughly twice as high in IBD patients as that of controls without IBD (5.9% vs. 3.5%), Dr. Panhwar said. That risk was highest in patients aged 20-25 years, with a relative risk of 20.5, occurring mostly in women, and decreased to 1.8 by age 60-64 (both P less than .001).
In addition, IBD patients tended to have a higher prevalence of common cardiovascular risk factors such as high blood pressure, obesity, and smoking.
The IBD patients’ higher prevalence of smoking – 21%, vs. 12% of the controls – is not a surprise, said Martha Gulati, MD, who moderated the briefing. Many people with IBD smoke, particularly those with Crohn’s disease, because it seems to reduce the number of flares, said Dr. Gulati, chief of cardiology at the University of Arizona, Phoenix.
The findings may be affected by the increased inflammation often observed in younger individuals with IBD and younger women with IBD, who may not present with traditional cardiovascular risk factors, the researchers noted.
“Clinicians who care for patients with traditional cardiovascular risk factors who also have IBD should recognize IBD as an independent risk factor as well, and treat appropriately,” Dr. Panhwar said.
Dr. Panhwar had no relevant financial conflicts to disclose.
SOURCE: Panhwar M. ACC 18.
Inflammatory bowel disease significantly increases the risk of a heart attack in adults, but especially young adults aged 18-24 years, and in women compared with men across all age groups, according to data from about 200,000 IBD patients.
The odds ratio for heart attack in IBD patients vs. controls remained a significant 1.2 after adjustment for traditional cardiovascular risk factors, Muhammad S. Panhwar, MD, said in a media briefing in advance of the annual meeting of the American College of Cardiology.
“Chronic inflammation has been recognized as having an important role in the development of heart disease,” he noted.
Although other chronic inflammatory conditions are associated with increased heart attack risk, the link between heart attacks and IBD has not been well studied, despite its high prevalence in the United States (about 3 million adults, according to the Centers for Disease Control and Prevention), said Dr. Panhwar, an internal medicine resident at Case Western Reserve University in Cleveland. He and his colleagues reviewed a nationwide medical records database of 17.5 million adults aged 18-65 years for diagnoses of IBD between 2013 and 2017. Overall, 1.2% of the patients (211,870) had IBD, and most of the patients in the IBD group were younger, female, and white, Dr. Panhwar noted.
The relative risk of myocardial infarction was roughly twice as high in IBD patients as that of controls without IBD (5.9% vs. 3.5%), Dr. Panhwar said. That risk was highest in patients aged 20-25 years, with a relative risk of 20.5, occurring mostly in women, and decreased to 1.8 by age 60-64 (both P less than .001).
In addition, IBD patients tended to have a higher prevalence of common cardiovascular risk factors such as high blood pressure, obesity, and smoking.
The IBD patients’ higher prevalence of smoking – 21%, vs. 12% of the controls – is not a surprise, said Martha Gulati, MD, who moderated the briefing. Many people with IBD smoke, particularly those with Crohn’s disease, because it seems to reduce the number of flares, said Dr. Gulati, chief of cardiology at the University of Arizona, Phoenix.
The findings may be affected by the increased inflammation often observed in younger individuals with IBD and younger women with IBD, who may not present with traditional cardiovascular risk factors, the researchers noted.
“Clinicians who care for patients with traditional cardiovascular risk factors who also have IBD should recognize IBD as an independent risk factor as well, and treat appropriately,” Dr. Panhwar said.
Dr. Panhwar had no relevant financial conflicts to disclose.
SOURCE: Panhwar M. ACC 18.
Inflammatory bowel disease significantly increases the risk of a heart attack in adults, but especially young adults aged 18-24 years, and in women compared with men across all age groups, according to data from about 200,000 IBD patients.
The odds ratio for heart attack in IBD patients vs. controls remained a significant 1.2 after adjustment for traditional cardiovascular risk factors, Muhammad S. Panhwar, MD, said in a media briefing in advance of the annual meeting of the American College of Cardiology.
“Chronic inflammation has been recognized as having an important role in the development of heart disease,” he noted.
Although other chronic inflammatory conditions are associated with increased heart attack risk, the link between heart attacks and IBD has not been well studied, despite its high prevalence in the United States (about 3 million adults, according to the Centers for Disease Control and Prevention), said Dr. Panhwar, an internal medicine resident at Case Western Reserve University in Cleveland. He and his colleagues reviewed a nationwide medical records database of 17.5 million adults aged 18-65 years for diagnoses of IBD between 2013 and 2017. Overall, 1.2% of the patients (211,870) had IBD, and most of the patients in the IBD group were younger, female, and white, Dr. Panhwar noted.
The relative risk of myocardial infarction was roughly twice as high in IBD patients as that of controls without IBD (5.9% vs. 3.5%), Dr. Panhwar said. That risk was highest in patients aged 20-25 years, with a relative risk of 20.5, occurring mostly in women, and decreased to 1.8 by age 60-64 (both P less than .001).
In addition, IBD patients tended to have a higher prevalence of common cardiovascular risk factors such as high blood pressure, obesity, and smoking.
The IBD patients’ higher prevalence of smoking – 21%, vs. 12% of the controls – is not a surprise, said Martha Gulati, MD, who moderated the briefing. Many people with IBD smoke, particularly those with Crohn’s disease, because it seems to reduce the number of flares, said Dr. Gulati, chief of cardiology at the University of Arizona, Phoenix.
The findings may be affected by the increased inflammation often observed in younger individuals with IBD and younger women with IBD, who may not present with traditional cardiovascular risk factors, the researchers noted.
“Clinicians who care for patients with traditional cardiovascular risk factors who also have IBD should recognize IBD as an independent risk factor as well, and treat appropriately,” Dr. Panhwar said.
Dr. Panhwar had no relevant financial conflicts to disclose.
SOURCE: Panhwar M. ACC 18.
FROM ACC 18
Key clinical point:
Major finding: The relative risk of MI was roughly twice as high in IBD patients compared with controls without IBD (5.9% vs. 3.5%).
Study details: Review of a nationwide medical records database of 17.5 million adults aged 18-65 years.
Disclosures: Dr. Panhwar had no relevant financial conflicts to disclose.
Source: Panhwar M. ACC 18.
Collaboration, consultation part of AAP teen depression guidelines update
The updated information includes recommendations on collaborative care, practice preparation, establishing networks of referrals, and much more.
“These guidelines were developed for PC clinicians who are in a position to identify and assist youth with depression in their practice settings,” they said. The guidelines apply to individuals aged 10-21 years, and support universal depression screening for those aged 12 and older.
Known as the Guidelines for Adolescent Depression in Primary Care (GLAD-PC), they consist of two parts: Practice Preparation, Identification, Assessment, and Initial Management, with Dr. Zuckerbrot as the lead author, and Treatment and Ongoing Management, led by Amy H. Cheung, MD, of the University of Toronto. They were published online in Pediatrics.
“It has been over 10 years since the [last] guidelines were published and they are supposed to be updated every 5,” Dr. Zuckerbrot said in an interview. “Given the new evidence on screening, psychopharmacology, and collaborative care, the guidelines needed to be revised. The USPSTF [United States Preventive Services Task Force ] and the AAP had already supported universal adolescent depression screening, and these guidelines are finally aligned with those positions.
“Different parts of the guidelines will be the go-to for different pediatricians, depending on where they are in their delivery of mental health care,” she explained. “Some may need help with practice preparation while others may need advice on screening; others may already be prescribing and may need advice on ongoing treatment and follow-up. I think there is something for everyone.”
Implementation of the guidelines is difficult in a short visit, Dr. Zuckerbrot acknowledged. “In addition, pediatricians may not have been well trained in the management of adolescent depression during their residencies.” However, the guidelines discuss both “real teams to support the pediatricians in their efforts, as well as virtual teams when staffing is limited.
“The guidelines advise that pediatricians learn about child psychiatry primary care consultation programs in their state and make use of those free telephone consultation programs.” The guidelines also discuss strategies for collaborative or integrative care, she said.
Part I
Part I of the guidelines, “Practice Preparation, Identification, Assessment, and Initial Management,” includes several recommendations for each topic.
For practice preparation, the guidelines recommend that clinicians seek training in the assessment, diagnosis, and treatment of depression, and that they establish a network of referrals and mental health resources in their communities. This network may include not only health professionals, but also current patients and families who are managing teen depression. If available, state-wide or regional child and adolescent psychiatry consultation programs can be included.
The identification and surveillance section of the guidelines calls for screening all patients aged 12 years and older for depression each year, using a formal screening tool on paper or online. The screening could occur at an annual wellness visit or any other medical visit, such as a sports physical. A second recommendation calls for identifying patients at increased risk for depression because of factors such as personal history, family history, substance use, other psychiatric disorders, frequent somatic complaints, or trauma, and monitoring these individuals regularly for signs of depression using a formal screening tool.
The assessment and diagnosis section states that assessment should include interviews with the patients alone as well as with their families or caregivers, and should include screening teens for functional impairment.
Primary care physicians should evaluate for depression not only if an adolescent tests positive on a screening tool, but also in children who present with any emotional problem as the chief complaint, and in those in whom depression is highly suspected even if they test negative on a formal screening tool, the guidelines state.
The three recommendations for initial management of depression in the primary care setting are educating patients and families about depression; developing a treatment plan (if the primary care clinician has had appropriate training) and setting specific treatment goals in areas of functioning such as at home, with peers, and at school; and developing a safety plan that includes restricting access to weapons or other means of self-harm, according to the guidelines.
Part II
Part II of the recommendations, “Treatment and Ongoing Management,” discusses options for managing depression in the primary care setting and utilizing outside resources.
The treatment recommendations emphasize the use of integrated models, if possible. “There is a growing recognition that complex chronic conditions, such as depression, are most successfully managed with proactive, multidisciplinary, patient-centered care teams,” Dr. Cheung and her associates said.
The recommendation for cases of mild depression calls for a period of “active support and monitoring” for 6-8 weeks before reassessing if the teen shows no improvement. By contrast, for cases of moderate to severe depression or cases with evidence of substance abuse or other psychoses, the recommendation calls for potential consultation with a mental health specialist and a discussion of the roles primary and specialty care will play in treatment. The guidelines include a flow chart for PC physicians to follow.
The guidelines suggest that PC clinicians recommend “scientifically tested and proven treatments,” such as psychotherapies, cognitive behavioral therapy (CBT) or interpersonal psychotherapy for adolescents, and/or antidepressant treatment, such as SSRIs, whenever possible and appropriate. It is important to monitor teens on antidepressants regularly to identify adverse events.
Recommendations for the ongoing management of teens with depression in the primary care setting include regular tracking of progress, reassessment if the teen shows no improvement in 6-8 weeks, and consultation with a mental health professional for those who show only partial improvement after exhausting primary care diagnostic and treatment options. Assessment of depressive symptoms is not the only thing to track. Functioning at home, school, and among peers also is important.
The final treatment recommendation is for active support of a depressed teen’s referral to mental health if necessary for best management and sharing care if possible, with an understanding of the roles of the primary and specialty clinicians, the guidelines state.
The guidelines project was funded by the Resource for Advancing Children’s Health Institute and the Bell Canada Chair in Adolescent Mood and Anxiety Disorders.
Dr. Cheung and Dr. Zuckerbrot receive book royalties. Dr Zuckerbrot works for child and adolescent psychiatry for primary care (CAP-PC), now a regional provider for Project TEACH in New York State, and she is on the steering committee as well as faculty for the REACH Institute; both of these institutions are described in the guidelines. Peter S. Jensen, MD, has received royalties from Random House, Oxford University Press, and APPI Inc. He is a part owner of a consulting company, CATCH Services LLC. He is the chief executive officer and president of a nonprofit organization, the Resource for Advancing Children’s Health Institute, but receives no compensation. The other authors indicated they have no financial relationships relevant to the guidelines.
“Mental health disorders have become one of the new morbidities in pediatric care,” Karalyn Kinsella, MD, said in an interview. “With one in five patients having depression, it is an illness that must be within our domain to identify and treat. I think the guidelines will make providers feel more confident in making a diagnosis and providing initial treatment. For those that do not feel comfortable, hopefully the guidelines will encourage them to seek training.
The take-home message for general pediatricians is that a standardized screening tool makes identifying depression relatively easy. “We have been using the PHQ-9 [Patient Health Questionnaire-9] in my office for several years, and it is very easy to administer and score, and is billable,” said Dr. Kinsella. “It can take some practice to tease out some typical teen behaviors, especially on the sleep and fatigue questions, but it provides an opportunity to open up discussion with the teen.
“Treatment [of depression] can be more complicated and time consuming, but rewarding and invaluable to the patient,” she emphasized. “Many states now have psychiatrists available by phone consultation to aid in management of medication. The key is establishing a list of quality counselors for referrals. With those supports and frequent follow-up, pediatricians can play a key role in the treatment of this prevalent and important illness that affects our patients.”
Dr. Kinsella is a pediatrician in Cheshire, Conn., and a member of the Pediatric News editorial advisory board. She was asked to comment on the new AAP teen depression guidelines.
“Mental health disorders have become one of the new morbidities in pediatric care,” Karalyn Kinsella, MD, said in an interview. “With one in five patients having depression, it is an illness that must be within our domain to identify and treat. I think the guidelines will make providers feel more confident in making a diagnosis and providing initial treatment. For those that do not feel comfortable, hopefully the guidelines will encourage them to seek training.
The take-home message for general pediatricians is that a standardized screening tool makes identifying depression relatively easy. “We have been using the PHQ-9 [Patient Health Questionnaire-9] in my office for several years, and it is very easy to administer and score, and is billable,” said Dr. Kinsella. “It can take some practice to tease out some typical teen behaviors, especially on the sleep and fatigue questions, but it provides an opportunity to open up discussion with the teen.
“Treatment [of depression] can be more complicated and time consuming, but rewarding and invaluable to the patient,” she emphasized. “Many states now have psychiatrists available by phone consultation to aid in management of medication. The key is establishing a list of quality counselors for referrals. With those supports and frequent follow-up, pediatricians can play a key role in the treatment of this prevalent and important illness that affects our patients.”
Dr. Kinsella is a pediatrician in Cheshire, Conn., and a member of the Pediatric News editorial advisory board. She was asked to comment on the new AAP teen depression guidelines.
“Mental health disorders have become one of the new morbidities in pediatric care,” Karalyn Kinsella, MD, said in an interview. “With one in five patients having depression, it is an illness that must be within our domain to identify and treat. I think the guidelines will make providers feel more confident in making a diagnosis and providing initial treatment. For those that do not feel comfortable, hopefully the guidelines will encourage them to seek training.
The take-home message for general pediatricians is that a standardized screening tool makes identifying depression relatively easy. “We have been using the PHQ-9 [Patient Health Questionnaire-9] in my office for several years, and it is very easy to administer and score, and is billable,” said Dr. Kinsella. “It can take some practice to tease out some typical teen behaviors, especially on the sleep and fatigue questions, but it provides an opportunity to open up discussion with the teen.
“Treatment [of depression] can be more complicated and time consuming, but rewarding and invaluable to the patient,” she emphasized. “Many states now have psychiatrists available by phone consultation to aid in management of medication. The key is establishing a list of quality counselors for referrals. With those supports and frequent follow-up, pediatricians can play a key role in the treatment of this prevalent and important illness that affects our patients.”
Dr. Kinsella is a pediatrician in Cheshire, Conn., and a member of the Pediatric News editorial advisory board. She was asked to comment on the new AAP teen depression guidelines.
The updated information includes recommendations on collaborative care, practice preparation, establishing networks of referrals, and much more.
“These guidelines were developed for PC clinicians who are in a position to identify and assist youth with depression in their practice settings,” they said. The guidelines apply to individuals aged 10-21 years, and support universal depression screening for those aged 12 and older.
Known as the Guidelines for Adolescent Depression in Primary Care (GLAD-PC), they consist of two parts: Practice Preparation, Identification, Assessment, and Initial Management, with Dr. Zuckerbrot as the lead author, and Treatment and Ongoing Management, led by Amy H. Cheung, MD, of the University of Toronto. They were published online in Pediatrics.
“It has been over 10 years since the [last] guidelines were published and they are supposed to be updated every 5,” Dr. Zuckerbrot said in an interview. “Given the new evidence on screening, psychopharmacology, and collaborative care, the guidelines needed to be revised. The USPSTF [United States Preventive Services Task Force ] and the AAP had already supported universal adolescent depression screening, and these guidelines are finally aligned with those positions.
“Different parts of the guidelines will be the go-to for different pediatricians, depending on where they are in their delivery of mental health care,” she explained. “Some may need help with practice preparation while others may need advice on screening; others may already be prescribing and may need advice on ongoing treatment and follow-up. I think there is something for everyone.”
Implementation of the guidelines is difficult in a short visit, Dr. Zuckerbrot acknowledged. “In addition, pediatricians may not have been well trained in the management of adolescent depression during their residencies.” However, the guidelines discuss both “real teams to support the pediatricians in their efforts, as well as virtual teams when staffing is limited.
“The guidelines advise that pediatricians learn about child psychiatry primary care consultation programs in their state and make use of those free telephone consultation programs.” The guidelines also discuss strategies for collaborative or integrative care, she said.
Part I
Part I of the guidelines, “Practice Preparation, Identification, Assessment, and Initial Management,” includes several recommendations for each topic.
For practice preparation, the guidelines recommend that clinicians seek training in the assessment, diagnosis, and treatment of depression, and that they establish a network of referrals and mental health resources in their communities. This network may include not only health professionals, but also current patients and families who are managing teen depression. If available, state-wide or regional child and adolescent psychiatry consultation programs can be included.
The identification and surveillance section of the guidelines calls for screening all patients aged 12 years and older for depression each year, using a formal screening tool on paper or online. The screening could occur at an annual wellness visit or any other medical visit, such as a sports physical. A second recommendation calls for identifying patients at increased risk for depression because of factors such as personal history, family history, substance use, other psychiatric disorders, frequent somatic complaints, or trauma, and monitoring these individuals regularly for signs of depression using a formal screening tool.
The assessment and diagnosis section states that assessment should include interviews with the patients alone as well as with their families or caregivers, and should include screening teens for functional impairment.
Primary care physicians should evaluate for depression not only if an adolescent tests positive on a screening tool, but also in children who present with any emotional problem as the chief complaint, and in those in whom depression is highly suspected even if they test negative on a formal screening tool, the guidelines state.
The three recommendations for initial management of depression in the primary care setting are educating patients and families about depression; developing a treatment plan (if the primary care clinician has had appropriate training) and setting specific treatment goals in areas of functioning such as at home, with peers, and at school; and developing a safety plan that includes restricting access to weapons or other means of self-harm, according to the guidelines.
Part II
Part II of the recommendations, “Treatment and Ongoing Management,” discusses options for managing depression in the primary care setting and utilizing outside resources.
The treatment recommendations emphasize the use of integrated models, if possible. “There is a growing recognition that complex chronic conditions, such as depression, are most successfully managed with proactive, multidisciplinary, patient-centered care teams,” Dr. Cheung and her associates said.
The recommendation for cases of mild depression calls for a period of “active support and monitoring” for 6-8 weeks before reassessing if the teen shows no improvement. By contrast, for cases of moderate to severe depression or cases with evidence of substance abuse or other psychoses, the recommendation calls for potential consultation with a mental health specialist and a discussion of the roles primary and specialty care will play in treatment. The guidelines include a flow chart for PC physicians to follow.
The guidelines suggest that PC clinicians recommend “scientifically tested and proven treatments,” such as psychotherapies, cognitive behavioral therapy (CBT) or interpersonal psychotherapy for adolescents, and/or antidepressant treatment, such as SSRIs, whenever possible and appropriate. It is important to monitor teens on antidepressants regularly to identify adverse events.
Recommendations for the ongoing management of teens with depression in the primary care setting include regular tracking of progress, reassessment if the teen shows no improvement in 6-8 weeks, and consultation with a mental health professional for those who show only partial improvement after exhausting primary care diagnostic and treatment options. Assessment of depressive symptoms is not the only thing to track. Functioning at home, school, and among peers also is important.
The final treatment recommendation is for active support of a depressed teen’s referral to mental health if necessary for best management and sharing care if possible, with an understanding of the roles of the primary and specialty clinicians, the guidelines state.
The guidelines project was funded by the Resource for Advancing Children’s Health Institute and the Bell Canada Chair in Adolescent Mood and Anxiety Disorders.
Dr. Cheung and Dr. Zuckerbrot receive book royalties. Dr Zuckerbrot works for child and adolescent psychiatry for primary care (CAP-PC), now a regional provider for Project TEACH in New York State, and she is on the steering committee as well as faculty for the REACH Institute; both of these institutions are described in the guidelines. Peter S. Jensen, MD, has received royalties from Random House, Oxford University Press, and APPI Inc. He is a part owner of a consulting company, CATCH Services LLC. He is the chief executive officer and president of a nonprofit organization, the Resource for Advancing Children’s Health Institute, but receives no compensation. The other authors indicated they have no financial relationships relevant to the guidelines.
The updated information includes recommendations on collaborative care, practice preparation, establishing networks of referrals, and much more.
“These guidelines were developed for PC clinicians who are in a position to identify and assist youth with depression in their practice settings,” they said. The guidelines apply to individuals aged 10-21 years, and support universal depression screening for those aged 12 and older.
Known as the Guidelines for Adolescent Depression in Primary Care (GLAD-PC), they consist of two parts: Practice Preparation, Identification, Assessment, and Initial Management, with Dr. Zuckerbrot as the lead author, and Treatment and Ongoing Management, led by Amy H. Cheung, MD, of the University of Toronto. They were published online in Pediatrics.
“It has been over 10 years since the [last] guidelines were published and they are supposed to be updated every 5,” Dr. Zuckerbrot said in an interview. “Given the new evidence on screening, psychopharmacology, and collaborative care, the guidelines needed to be revised. The USPSTF [United States Preventive Services Task Force ] and the AAP had already supported universal adolescent depression screening, and these guidelines are finally aligned with those positions.
“Different parts of the guidelines will be the go-to for different pediatricians, depending on where they are in their delivery of mental health care,” she explained. “Some may need help with practice preparation while others may need advice on screening; others may already be prescribing and may need advice on ongoing treatment and follow-up. I think there is something for everyone.”
Implementation of the guidelines is difficult in a short visit, Dr. Zuckerbrot acknowledged. “In addition, pediatricians may not have been well trained in the management of adolescent depression during their residencies.” However, the guidelines discuss both “real teams to support the pediatricians in their efforts, as well as virtual teams when staffing is limited.
“The guidelines advise that pediatricians learn about child psychiatry primary care consultation programs in their state and make use of those free telephone consultation programs.” The guidelines also discuss strategies for collaborative or integrative care, she said.
Part I
Part I of the guidelines, “Practice Preparation, Identification, Assessment, and Initial Management,” includes several recommendations for each topic.
For practice preparation, the guidelines recommend that clinicians seek training in the assessment, diagnosis, and treatment of depression, and that they establish a network of referrals and mental health resources in their communities. This network may include not only health professionals, but also current patients and families who are managing teen depression. If available, state-wide or regional child and adolescent psychiatry consultation programs can be included.
The identification and surveillance section of the guidelines calls for screening all patients aged 12 years and older for depression each year, using a formal screening tool on paper or online. The screening could occur at an annual wellness visit or any other medical visit, such as a sports physical. A second recommendation calls for identifying patients at increased risk for depression because of factors such as personal history, family history, substance use, other psychiatric disorders, frequent somatic complaints, or trauma, and monitoring these individuals regularly for signs of depression using a formal screening tool.
The assessment and diagnosis section states that assessment should include interviews with the patients alone as well as with their families or caregivers, and should include screening teens for functional impairment.
Primary care physicians should evaluate for depression not only if an adolescent tests positive on a screening tool, but also in children who present with any emotional problem as the chief complaint, and in those in whom depression is highly suspected even if they test negative on a formal screening tool, the guidelines state.
The three recommendations for initial management of depression in the primary care setting are educating patients and families about depression; developing a treatment plan (if the primary care clinician has had appropriate training) and setting specific treatment goals in areas of functioning such as at home, with peers, and at school; and developing a safety plan that includes restricting access to weapons or other means of self-harm, according to the guidelines.
Part II
Part II of the recommendations, “Treatment and Ongoing Management,” discusses options for managing depression in the primary care setting and utilizing outside resources.
The treatment recommendations emphasize the use of integrated models, if possible. “There is a growing recognition that complex chronic conditions, such as depression, are most successfully managed with proactive, multidisciplinary, patient-centered care teams,” Dr. Cheung and her associates said.
The recommendation for cases of mild depression calls for a period of “active support and monitoring” for 6-8 weeks before reassessing if the teen shows no improvement. By contrast, for cases of moderate to severe depression or cases with evidence of substance abuse or other psychoses, the recommendation calls for potential consultation with a mental health specialist and a discussion of the roles primary and specialty care will play in treatment. The guidelines include a flow chart for PC physicians to follow.
The guidelines suggest that PC clinicians recommend “scientifically tested and proven treatments,” such as psychotherapies, cognitive behavioral therapy (CBT) or interpersonal psychotherapy for adolescents, and/or antidepressant treatment, such as SSRIs, whenever possible and appropriate. It is important to monitor teens on antidepressants regularly to identify adverse events.
Recommendations for the ongoing management of teens with depression in the primary care setting include regular tracking of progress, reassessment if the teen shows no improvement in 6-8 weeks, and consultation with a mental health professional for those who show only partial improvement after exhausting primary care diagnostic and treatment options. Assessment of depressive symptoms is not the only thing to track. Functioning at home, school, and among peers also is important.
The final treatment recommendation is for active support of a depressed teen’s referral to mental health if necessary for best management and sharing care if possible, with an understanding of the roles of the primary and specialty clinicians, the guidelines state.
The guidelines project was funded by the Resource for Advancing Children’s Health Institute and the Bell Canada Chair in Adolescent Mood and Anxiety Disorders.
Dr. Cheung and Dr. Zuckerbrot receive book royalties. Dr Zuckerbrot works for child and adolescent psychiatry for primary care (CAP-PC), now a regional provider for Project TEACH in New York State, and she is on the steering committee as well as faculty for the REACH Institute; both of these institutions are described in the guidelines. Peter S. Jensen, MD, has received royalties from Random House, Oxford University Press, and APPI Inc. He is a part owner of a consulting company, CATCH Services LLC. He is the chief executive officer and president of a nonprofit organization, the Resource for Advancing Children’s Health Institute, but receives no compensation. The other authors indicated they have no financial relationships relevant to the guidelines.
FROM PEDIATRICS
Aesthetic procedures becoming more popular in skin of color patients
in a presentation at the Caribbean Dermatology Symposium.
In 2015, ethnic minority patients accounted for 25% of aesthetic procedures in the United States, up from 20% in 2010, according to data from the American Society for Aesthetic Plastic Surgery, said Dr. Alexis, chair of dermatology and director of the Skin of Color Center at Mount Sinai St. Luke’s and Mount Sinai West hospitals in New York.
Chemical peels can be used successfully to treat a range of conditions in skin of color patients, including postinflammatory hyperpigmentation, acne, melasma, textural irregularities, and pseudofolliculitis barbae. They also can be used for skin brightening, said Dr. Alexis, who recommended a chemical peel protocol of salicylic acid, glycolic acid, or Jessner’s every 2-4 weeks. “Consider hydroquinone 4% concurrently to enhance efficacy for treating hyperpigmentation and to prevent postinflammatory hyperpigmentation,” he said. Patients on retinoids should discontinue them for 1 week prior to a chemical peel, he added.
Dr. Alexis shared several treatment pearls to promote successful peels in skin of color patients:
- Salicylic acid: Resist the urge to overapply and “titrate according to patient tolerability.” The endpoint of a salicylic acid peel is white precipitate, not frost; cool compresses can be used for patient comfort and for later removal of the white precipitate.
- Glycolic acid: Stick to a contact time of 2-4 minutes to avoid epidermolysis. “Completely neutralize all areas of application to avoid overpeeling.”
- Trichloroacetic acid (TCA): TCA carries a greater risk of dyspigmentation, and should be reserved for patients who have not been successfully treated with salicylic or glycolic acid; a 10%-15% concentration of TCA, applied conservatively, is recommended.
Regardless of the type of chemical, potential pitfalls of peels in patients of color include using too much product, allowing too long of an application time, and applying the chemical to an inflamed or excoriated area, Dr. Alexis said. Patients who don’t discontinue retinoids before a peel are at increased risk of developing erosions or crusting, he added.
Dr. Alexis disclosed relationships with Allergan, BioPharmX, Dermira, Galderma, Novan, Novartis, RXi, Unilever, and Valeant.
Global Academy and this news organization are owned by the same parent company.
in a presentation at the Caribbean Dermatology Symposium.
In 2015, ethnic minority patients accounted for 25% of aesthetic procedures in the United States, up from 20% in 2010, according to data from the American Society for Aesthetic Plastic Surgery, said Dr. Alexis, chair of dermatology and director of the Skin of Color Center at Mount Sinai St. Luke’s and Mount Sinai West hospitals in New York.
Chemical peels can be used successfully to treat a range of conditions in skin of color patients, including postinflammatory hyperpigmentation, acne, melasma, textural irregularities, and pseudofolliculitis barbae. They also can be used for skin brightening, said Dr. Alexis, who recommended a chemical peel protocol of salicylic acid, glycolic acid, or Jessner’s every 2-4 weeks. “Consider hydroquinone 4% concurrently to enhance efficacy for treating hyperpigmentation and to prevent postinflammatory hyperpigmentation,” he said. Patients on retinoids should discontinue them for 1 week prior to a chemical peel, he added.
Dr. Alexis shared several treatment pearls to promote successful peels in skin of color patients:
- Salicylic acid: Resist the urge to overapply and “titrate according to patient tolerability.” The endpoint of a salicylic acid peel is white precipitate, not frost; cool compresses can be used for patient comfort and for later removal of the white precipitate.
- Glycolic acid: Stick to a contact time of 2-4 minutes to avoid epidermolysis. “Completely neutralize all areas of application to avoid overpeeling.”
- Trichloroacetic acid (TCA): TCA carries a greater risk of dyspigmentation, and should be reserved for patients who have not been successfully treated with salicylic or glycolic acid; a 10%-15% concentration of TCA, applied conservatively, is recommended.
Regardless of the type of chemical, potential pitfalls of peels in patients of color include using too much product, allowing too long of an application time, and applying the chemical to an inflamed or excoriated area, Dr. Alexis said. Patients who don’t discontinue retinoids before a peel are at increased risk of developing erosions or crusting, he added.
Dr. Alexis disclosed relationships with Allergan, BioPharmX, Dermira, Galderma, Novan, Novartis, RXi, Unilever, and Valeant.
Global Academy and this news organization are owned by the same parent company.
in a presentation at the Caribbean Dermatology Symposium.
In 2015, ethnic minority patients accounted for 25% of aesthetic procedures in the United States, up from 20% in 2010, according to data from the American Society for Aesthetic Plastic Surgery, said Dr. Alexis, chair of dermatology and director of the Skin of Color Center at Mount Sinai St. Luke’s and Mount Sinai West hospitals in New York.
Chemical peels can be used successfully to treat a range of conditions in skin of color patients, including postinflammatory hyperpigmentation, acne, melasma, textural irregularities, and pseudofolliculitis barbae. They also can be used for skin brightening, said Dr. Alexis, who recommended a chemical peel protocol of salicylic acid, glycolic acid, or Jessner’s every 2-4 weeks. “Consider hydroquinone 4% concurrently to enhance efficacy for treating hyperpigmentation and to prevent postinflammatory hyperpigmentation,” he said. Patients on retinoids should discontinue them for 1 week prior to a chemical peel, he added.
Dr. Alexis shared several treatment pearls to promote successful peels in skin of color patients:
- Salicylic acid: Resist the urge to overapply and “titrate according to patient tolerability.” The endpoint of a salicylic acid peel is white precipitate, not frost; cool compresses can be used for patient comfort and for later removal of the white precipitate.
- Glycolic acid: Stick to a contact time of 2-4 minutes to avoid epidermolysis. “Completely neutralize all areas of application to avoid overpeeling.”
- Trichloroacetic acid (TCA): TCA carries a greater risk of dyspigmentation, and should be reserved for patients who have not been successfully treated with salicylic or glycolic acid; a 10%-15% concentration of TCA, applied conservatively, is recommended.
Regardless of the type of chemical, potential pitfalls of peels in patients of color include using too much product, allowing too long of an application time, and applying the chemical to an inflamed or excoriated area, Dr. Alexis said. Patients who don’t discontinue retinoids before a peel are at increased risk of developing erosions or crusting, he added.
Dr. Alexis disclosed relationships with Allergan, BioPharmX, Dermira, Galderma, Novan, Novartis, RXi, Unilever, and Valeant.
Global Academy and this news organization are owned by the same parent company.
EXPERT ANALYSIS FROM THE CARIBBEAN DERMATOLOGY SYMPOSIUM
Teens are all about the sexting
More teenagers are sending and receiving sexts than in previous years, based on data from a meta-analysis of 39 studies including 110,380 individuals younger than 18 years.
Published rates of sexting in teens range from 1% to 60%, wrote Sheri Madigan, PhD, of the University of Calgary, Alberta, Canada, and her colleagues. “However, the true public health importance of youth sexting is unclear at present because the field is handicapped by inconsistent information regarding its prevalence.”
“Higher prevalence rates were found in more recent studies, with older youth, and with youth using a mobile device to sext,” the researchers said.
The increase in sexting among teens should inform sexting legislation, the researchers noted. However, given the increasing use of smartphones among children and the possibility that sexting may be a normal part of sexual behavior in the smartphone era, “efforts and resources to criminalize sexts should be redirected to educational programs on digital citizenship and healthy relationships,” they said. “Given that the mean age of first smartphone acquisition is 10.3 years, it is important for middle school educators, pediatricians, and parents to have ongoing conversations with tweens regarding sexting and digital citizenship.”
The meta-analysis’s results were limited by several factors, such as the focus on frequency of sexting alone and not on elements that might influence sexting behavior, as well as inclusion of relatively few studies on nonconsensual sexting.
The mean age was 15 years (range, 12-17 years). More than half of the studies were from the United States, followed by 12 from Europe, 2 from Australia, 1 from Canada, 1 from South Africa , and 1 study from South Korea.
The researchers had no relevant financial disclosures. The study was supported by the Alberta Children’s Hospital Foundation and the Canada Research Chairs Program.
SOURCE: Madigan S et al. JAMA Pediatr. 2018 Feb 26. doi: 10.1001/jamapediatrics.2017.5314.
“Sexting is a new behavior that is evolving rapidly, as technology changes and awareness increases,” Elizabeth Englander, PhD, and Meghan McCoy, EdD, wrote.
The current study adds to the limited knowledge about sexting in children and teens and also identifies areas in need of additional study, including the lack of a consistent definition of sexting and differences in sexting activity between males and females. Another challenge is determining the context of sexting, with the recognition that sexting within relationships is different than sexting between unattached individuals, they said. In addition, the study by Madigan et al. emphasized the concern for sexting behaviors among children younger than 12 years of age because children this age are increasingly likely to own cell phones.
Dr. Englander and Dr. McCoy concluded that the current study represents “an important step forward in understanding prevalence, including the prevalence of unauthorized distribution of sexts.”
Dr. Englander and Dr. McCoy are affiliated with the Massachusetts Aggression Reduction Center at Bridgewater (Mass.) State University. They commented in an editorial accompanying the meta-analysis by Madigan et al. (JAMA Pediatr. 2018 Feb 26. doi: 10.1001/jamapediatrics.2017.5682). They had no relevant financial disclosures.
“Sexting is a new behavior that is evolving rapidly, as technology changes and awareness increases,” Elizabeth Englander, PhD, and Meghan McCoy, EdD, wrote.
The current study adds to the limited knowledge about sexting in children and teens and also identifies areas in need of additional study, including the lack of a consistent definition of sexting and differences in sexting activity between males and females. Another challenge is determining the context of sexting, with the recognition that sexting within relationships is different than sexting between unattached individuals, they said. In addition, the study by Madigan et al. emphasized the concern for sexting behaviors among children younger than 12 years of age because children this age are increasingly likely to own cell phones.
Dr. Englander and Dr. McCoy concluded that the current study represents “an important step forward in understanding prevalence, including the prevalence of unauthorized distribution of sexts.”
Dr. Englander and Dr. McCoy are affiliated with the Massachusetts Aggression Reduction Center at Bridgewater (Mass.) State University. They commented in an editorial accompanying the meta-analysis by Madigan et al. (JAMA Pediatr. 2018 Feb 26. doi: 10.1001/jamapediatrics.2017.5682). They had no relevant financial disclosures.
“Sexting is a new behavior that is evolving rapidly, as technology changes and awareness increases,” Elizabeth Englander, PhD, and Meghan McCoy, EdD, wrote.
The current study adds to the limited knowledge about sexting in children and teens and also identifies areas in need of additional study, including the lack of a consistent definition of sexting and differences in sexting activity between males and females. Another challenge is determining the context of sexting, with the recognition that sexting within relationships is different than sexting between unattached individuals, they said. In addition, the study by Madigan et al. emphasized the concern for sexting behaviors among children younger than 12 years of age because children this age are increasingly likely to own cell phones.
Dr. Englander and Dr. McCoy concluded that the current study represents “an important step forward in understanding prevalence, including the prevalence of unauthorized distribution of sexts.”
Dr. Englander and Dr. McCoy are affiliated with the Massachusetts Aggression Reduction Center at Bridgewater (Mass.) State University. They commented in an editorial accompanying the meta-analysis by Madigan et al. (JAMA Pediatr. 2018 Feb 26. doi: 10.1001/jamapediatrics.2017.5682). They had no relevant financial disclosures.
More teenagers are sending and receiving sexts than in previous years, based on data from a meta-analysis of 39 studies including 110,380 individuals younger than 18 years.
Published rates of sexting in teens range from 1% to 60%, wrote Sheri Madigan, PhD, of the University of Calgary, Alberta, Canada, and her colleagues. “However, the true public health importance of youth sexting is unclear at present because the field is handicapped by inconsistent information regarding its prevalence.”
“Higher prevalence rates were found in more recent studies, with older youth, and with youth using a mobile device to sext,” the researchers said.
The increase in sexting among teens should inform sexting legislation, the researchers noted. However, given the increasing use of smartphones among children and the possibility that sexting may be a normal part of sexual behavior in the smartphone era, “efforts and resources to criminalize sexts should be redirected to educational programs on digital citizenship and healthy relationships,” they said. “Given that the mean age of first smartphone acquisition is 10.3 years, it is important for middle school educators, pediatricians, and parents to have ongoing conversations with tweens regarding sexting and digital citizenship.”
The meta-analysis’s results were limited by several factors, such as the focus on frequency of sexting alone and not on elements that might influence sexting behavior, as well as inclusion of relatively few studies on nonconsensual sexting.
The mean age was 15 years (range, 12-17 years). More than half of the studies were from the United States, followed by 12 from Europe, 2 from Australia, 1 from Canada, 1 from South Africa , and 1 study from South Korea.
The researchers had no relevant financial disclosures. The study was supported by the Alberta Children’s Hospital Foundation and the Canada Research Chairs Program.
SOURCE: Madigan S et al. JAMA Pediatr. 2018 Feb 26. doi: 10.1001/jamapediatrics.2017.5314.
More teenagers are sending and receiving sexts than in previous years, based on data from a meta-analysis of 39 studies including 110,380 individuals younger than 18 years.
Published rates of sexting in teens range from 1% to 60%, wrote Sheri Madigan, PhD, of the University of Calgary, Alberta, Canada, and her colleagues. “However, the true public health importance of youth sexting is unclear at present because the field is handicapped by inconsistent information regarding its prevalence.”
“Higher prevalence rates were found in more recent studies, with older youth, and with youth using a mobile device to sext,” the researchers said.
The increase in sexting among teens should inform sexting legislation, the researchers noted. However, given the increasing use of smartphones among children and the possibility that sexting may be a normal part of sexual behavior in the smartphone era, “efforts and resources to criminalize sexts should be redirected to educational programs on digital citizenship and healthy relationships,” they said. “Given that the mean age of first smartphone acquisition is 10.3 years, it is important for middle school educators, pediatricians, and parents to have ongoing conversations with tweens regarding sexting and digital citizenship.”
The meta-analysis’s results were limited by several factors, such as the focus on frequency of sexting alone and not on elements that might influence sexting behavior, as well as inclusion of relatively few studies on nonconsensual sexting.
The mean age was 15 years (range, 12-17 years). More than half of the studies were from the United States, followed by 12 from Europe, 2 from Australia, 1 from Canada, 1 from South Africa , and 1 study from South Korea.
The researchers had no relevant financial disclosures. The study was supported by the Alberta Children’s Hospital Foundation and the Canada Research Chairs Program.
SOURCE: Madigan S et al. JAMA Pediatr. 2018 Feb 26. doi: 10.1001/jamapediatrics.2017.5314.
FROM JAMA PEDIATRICS
Key clinical point: Sexting frequency has increased among teens in recent years, and this frequency increases with age.
Major finding:
Study details: The data come from a meta-analysis of 39 studies with 110,380 participants.
Disclosures: The researchers had no financial conflicts to disclose. The study was supported by the Alberta Children’s Hospital Foundation and the Canada Research Chairs Program.
Source: Madigan S et al. JAMA Pediatr. 2018 Feb 26. doi: 10.1001/jamapediatrics.2017.5314.
Guidelines update best practices for hemorrhoid treatment
Each year, more than 2.2 million patients in the United States undergo evaluations for symptoms of hemorrhoids, according to updated guidelines on the management of hemorrhoids issued by the American Society of Colon and Rectal Surgeons.
“As a result, it is important to identify symptomatic hemorrhoids as the underlying source of the anorectal symptom and to have a clear understanding of the evaluation and management of this disease process,” wrote Bradley R. Davis, MD, FACS, chief of colon and rectal surgery at the Carolinas Medical Center, Charlotte, N.C., and the fellow members of the Clinical Practice Guidelines Committee of the ASCRS.
The guidelines are based on the ASCRS Practice Parameters for the Management of Hemorrhoids published in 2011. The 2018 update was published in the Diseases of the Colon & Rectum.
The guidelines recommend evaluation of hemorrhoids based on a disease-specific history, and a physical that emphasizes the degree and duration of symptoms and identifies risk factors. But the guideline writers note that the recommendation is a grade 1C because the supporting data mainly come from observational or case studies.
“The cardinal signs of internal hemorrhoids are painless bleeding with bowel movements with intermittent protrusion,” the committee said, also emphasizing that patients should be evaluated for fecal incontinence, which could inform surgical decision making.
In addition, the guidelines call for a complete endoscopic evaluation of the colon for patients who present with symptomatic hemorrhoids and rectal bleeding; this recommendation is based on moderately strong evidence, and presented with a grade of 1B.
Medical management of hemorrhoids may include office-based procedures or surgery, according to the guidelines.
“Most patients with grade I and II and select patients with grade III internal hemorrhoidal disease who fail medical treatment can be effectively treated with office-based procedures, such as banding, sclerotherapy, and infrared coagulation,” the committee wrote, and medical office treatment received a strong grade 1A recommendation based on high-quality evidence. Although office procedures are generally well tolerated, the condition can recur. Bleeding is the most common complication, and it is more likely after rubber-band ligation than other office-based options, the guidelines state.
The guidelines offer a weak recommendation of 2C, based on the lack of quality evidence, for the use of early surgical excision to treat patients with thrombosed external hemorrhoids. “Although most patients treated nonoperatively will experience eventual resolution of their symptoms, excision of thrombosed external hemorrhoids may result in more rapid symptom resolution, lower incidence of recurrence, and longer remission intervals,” the committee noted.
Surgical hemorrhoidectomy received the strongest possible recommendation (1A, based on high-quality evidence) for the treatment of patients with external hemorrhoids or a combination of internal and external hemorrhoids with prolapse.
Surgical options described in the recommendations include surgical excision (hemorrhoidectomy), hemorrhoidopexy, and Doppler-guided hemorrhoidectomy, with citations of studies on each procedure. Data from a meta-analysis of 18 randomized prospective studies comparing hemorrhoidectomy with office-based procedures showed that hemorrhoidectomy was “the most effective treatment for patients with grade III hemorrhoids,” but it was associated with greater pain and complication rates, according to the guidelines.
However, complications in general are low after surgical hemorrhoidectomy, with reported complication rates of 1%-2% for the most common complication of postprocedure hemorrhage, the guidelines state. After surgery, the guidelines recommend with a 1B grade (moderate quality evidence) that patients use “a multimodality pain regimen to reduce narcotic usage and promote a faster recovery.”
The committee members had no financial conflicts to disclose.
AGA offers information for your patients about hemorrhoids at http://www.gastro.org/patient-care/conditions-diseases/hemorrhoids.
SOURCE: Davis BR et al. Dis Colon Rectum. 2018; 61:284-92.
Each year, more than 2.2 million patients in the United States undergo evaluations for symptoms of hemorrhoids, according to updated guidelines on the management of hemorrhoids issued by the American Society of Colon and Rectal Surgeons.
“As a result, it is important to identify symptomatic hemorrhoids as the underlying source of the anorectal symptom and to have a clear understanding of the evaluation and management of this disease process,” wrote Bradley R. Davis, MD, FACS, chief of colon and rectal surgery at the Carolinas Medical Center, Charlotte, N.C., and the fellow members of the Clinical Practice Guidelines Committee of the ASCRS.
The guidelines are based on the ASCRS Practice Parameters for the Management of Hemorrhoids published in 2011. The 2018 update was published in the Diseases of the Colon & Rectum.
The guidelines recommend evaluation of hemorrhoids based on a disease-specific history, and a physical that emphasizes the degree and duration of symptoms and identifies risk factors. But the guideline writers note that the recommendation is a grade 1C because the supporting data mainly come from observational or case studies.
“The cardinal signs of internal hemorrhoids are painless bleeding with bowel movements with intermittent protrusion,” the committee said, also emphasizing that patients should be evaluated for fecal incontinence, which could inform surgical decision making.
In addition, the guidelines call for a complete endoscopic evaluation of the colon for patients who present with symptomatic hemorrhoids and rectal bleeding; this recommendation is based on moderately strong evidence, and presented with a grade of 1B.
Medical management of hemorrhoids may include office-based procedures or surgery, according to the guidelines.
“Most patients with grade I and II and select patients with grade III internal hemorrhoidal disease who fail medical treatment can be effectively treated with office-based procedures, such as banding, sclerotherapy, and infrared coagulation,” the committee wrote, and medical office treatment received a strong grade 1A recommendation based on high-quality evidence. Although office procedures are generally well tolerated, the condition can recur. Bleeding is the most common complication, and it is more likely after rubber-band ligation than other office-based options, the guidelines state.
The guidelines offer a weak recommendation of 2C, based on the lack of quality evidence, for the use of early surgical excision to treat patients with thrombosed external hemorrhoids. “Although most patients treated nonoperatively will experience eventual resolution of their symptoms, excision of thrombosed external hemorrhoids may result in more rapid symptom resolution, lower incidence of recurrence, and longer remission intervals,” the committee noted.
Surgical hemorrhoidectomy received the strongest possible recommendation (1A, based on high-quality evidence) for the treatment of patients with external hemorrhoids or a combination of internal and external hemorrhoids with prolapse.
Surgical options described in the recommendations include surgical excision (hemorrhoidectomy), hemorrhoidopexy, and Doppler-guided hemorrhoidectomy, with citations of studies on each procedure. Data from a meta-analysis of 18 randomized prospective studies comparing hemorrhoidectomy with office-based procedures showed that hemorrhoidectomy was “the most effective treatment for patients with grade III hemorrhoids,” but it was associated with greater pain and complication rates, according to the guidelines.
However, complications in general are low after surgical hemorrhoidectomy, with reported complication rates of 1%-2% for the most common complication of postprocedure hemorrhage, the guidelines state. After surgery, the guidelines recommend with a 1B grade (moderate quality evidence) that patients use “a multimodality pain regimen to reduce narcotic usage and promote a faster recovery.”
The committee members had no financial conflicts to disclose.
AGA offers information for your patients about hemorrhoids at http://www.gastro.org/patient-care/conditions-diseases/hemorrhoids.
SOURCE: Davis BR et al. Dis Colon Rectum. 2018; 61:284-92.
Each year, more than 2.2 million patients in the United States undergo evaluations for symptoms of hemorrhoids, according to updated guidelines on the management of hemorrhoids issued by the American Society of Colon and Rectal Surgeons.
“As a result, it is important to identify symptomatic hemorrhoids as the underlying source of the anorectal symptom and to have a clear understanding of the evaluation and management of this disease process,” wrote Bradley R. Davis, MD, FACS, chief of colon and rectal surgery at the Carolinas Medical Center, Charlotte, N.C., and the fellow members of the Clinical Practice Guidelines Committee of the ASCRS.
The guidelines are based on the ASCRS Practice Parameters for the Management of Hemorrhoids published in 2011. The 2018 update was published in the Diseases of the Colon & Rectum.
The guidelines recommend evaluation of hemorrhoids based on a disease-specific history, and a physical that emphasizes the degree and duration of symptoms and identifies risk factors. But the guideline writers note that the recommendation is a grade 1C because the supporting data mainly come from observational or case studies.
“The cardinal signs of internal hemorrhoids are painless bleeding with bowel movements with intermittent protrusion,” the committee said, also emphasizing that patients should be evaluated for fecal incontinence, which could inform surgical decision making.
In addition, the guidelines call for a complete endoscopic evaluation of the colon for patients who present with symptomatic hemorrhoids and rectal bleeding; this recommendation is based on moderately strong evidence, and presented with a grade of 1B.
Medical management of hemorrhoids may include office-based procedures or surgery, according to the guidelines.
“Most patients with grade I and II and select patients with grade III internal hemorrhoidal disease who fail medical treatment can be effectively treated with office-based procedures, such as banding, sclerotherapy, and infrared coagulation,” the committee wrote, and medical office treatment received a strong grade 1A recommendation based on high-quality evidence. Although office procedures are generally well tolerated, the condition can recur. Bleeding is the most common complication, and it is more likely after rubber-band ligation than other office-based options, the guidelines state.
The guidelines offer a weak recommendation of 2C, based on the lack of quality evidence, for the use of early surgical excision to treat patients with thrombosed external hemorrhoids. “Although most patients treated nonoperatively will experience eventual resolution of their symptoms, excision of thrombosed external hemorrhoids may result in more rapid symptom resolution, lower incidence of recurrence, and longer remission intervals,” the committee noted.
Surgical hemorrhoidectomy received the strongest possible recommendation (1A, based on high-quality evidence) for the treatment of patients with external hemorrhoids or a combination of internal and external hemorrhoids with prolapse.
Surgical options described in the recommendations include surgical excision (hemorrhoidectomy), hemorrhoidopexy, and Doppler-guided hemorrhoidectomy, with citations of studies on each procedure. Data from a meta-analysis of 18 randomized prospective studies comparing hemorrhoidectomy with office-based procedures showed that hemorrhoidectomy was “the most effective treatment for patients with grade III hemorrhoids,” but it was associated with greater pain and complication rates, according to the guidelines.
However, complications in general are low after surgical hemorrhoidectomy, with reported complication rates of 1%-2% for the most common complication of postprocedure hemorrhage, the guidelines state. After surgery, the guidelines recommend with a 1B grade (moderate quality evidence) that patients use “a multimodality pain regimen to reduce narcotic usage and promote a faster recovery.”
The committee members had no financial conflicts to disclose.
AGA offers information for your patients about hemorrhoids at http://www.gastro.org/patient-care/conditions-diseases/hemorrhoids.
SOURCE: Davis BR et al. Dis Colon Rectum. 2018; 61:284-92.
FROM DISEASES OF THE COLON & RECTUM
Combo therapy does not improve outcomes for A. Baumannii
, based on data from 406 patients.
In a study published online in The Lancet Infectious Diseases, Mical Paul, MD, of Rambam Health Care Campus, Haifa, Israel, and colleagues randomized 198 patients to colistin alone and 208 to colistin plus meropenem (Lancet Infect Dis. 2018 Feb 15. doi: 10.1016/S1473-3099[18]30099-9).
The demographics were similar between the groups and approximately 77% of patients in each group were infected with A. baumannii.
The results highlight “the necessity of assessing combination therapy in randomized trials before adopting it into clinical use,” the researchers said.
The study was not designed to examine the effect of the two types of therapy on bacteria other than A. baumannii, the researchers noted. However, based on the findings, “we recommend against the routine use of carbapenems for the treatment of carbapenem-resistant A. baumannii infections,” they said.
The study was supported by EU AIDA grant Health-F3-2011-278348. Dr. Paul had no financial conflicts to disclose.
SOURCE: Paul M et al. Lancet Infect Dis. 2018 Feb 15. doi: 10.1016/S1473-3099(18)30099-9.
, based on data from 406 patients.
In a study published online in The Lancet Infectious Diseases, Mical Paul, MD, of Rambam Health Care Campus, Haifa, Israel, and colleagues randomized 198 patients to colistin alone and 208 to colistin plus meropenem (Lancet Infect Dis. 2018 Feb 15. doi: 10.1016/S1473-3099[18]30099-9).
The demographics were similar between the groups and approximately 77% of patients in each group were infected with A. baumannii.
The results highlight “the necessity of assessing combination therapy in randomized trials before adopting it into clinical use,” the researchers said.
The study was not designed to examine the effect of the two types of therapy on bacteria other than A. baumannii, the researchers noted. However, based on the findings, “we recommend against the routine use of carbapenems for the treatment of carbapenem-resistant A. baumannii infections,” they said.
The study was supported by EU AIDA grant Health-F3-2011-278348. Dr. Paul had no financial conflicts to disclose.
SOURCE: Paul M et al. Lancet Infect Dis. 2018 Feb 15. doi: 10.1016/S1473-3099(18)30099-9.
, based on data from 406 patients.
In a study published online in The Lancet Infectious Diseases, Mical Paul, MD, of Rambam Health Care Campus, Haifa, Israel, and colleagues randomized 198 patients to colistin alone and 208 to colistin plus meropenem (Lancet Infect Dis. 2018 Feb 15. doi: 10.1016/S1473-3099[18]30099-9).
The demographics were similar between the groups and approximately 77% of patients in each group were infected with A. baumannii.
The results highlight “the necessity of assessing combination therapy in randomized trials before adopting it into clinical use,” the researchers said.
The study was not designed to examine the effect of the two types of therapy on bacteria other than A. baumannii, the researchers noted. However, based on the findings, “we recommend against the routine use of carbapenems for the treatment of carbapenem-resistant A. baumannii infections,” they said.
The study was supported by EU AIDA grant Health-F3-2011-278348. Dr. Paul had no financial conflicts to disclose.
SOURCE: Paul M et al. Lancet Infect Dis. 2018 Feb 15. doi: 10.1016/S1473-3099(18)30099-9.
FROM THE LANCET INFECTIOUS DISEASES
Guidelines update best practices for hemorrhoid treatment
Each year, more than 2.2 million patients in the United States undergo evaluations for symptoms of hemorrhoids, according to updated guidelines on the management of hemorrhoids issued by the American Society of Colon and Rectal Surgeons.
“As a result, it is important to identify symptomatic hemorrhoids as the underlying source of the anorectal symptom and to have a clear understanding of the evaluation and management of this disease process,” wrote Bradley R. Davis, MD, FACS, chief of colon and rectal surgery at the Carolinas Medical Center, Charlotte, N.C., and the fellow members of the Clinical Practice Guidelines Committee of the ASCRS.
The guidelines recommend evaluation of hemorrhoids based on a disease-specific history, and a physical that emphasizes the degree and duration of symptoms and identifies risk factors. But the guideline writers note that the recommendation is a grade 1C because the supporting data mainly come from observational or case studies.
“The cardinal signs of internal hemorrhoids are painless bleeding with bowel movements with intermittent protrusion,” the committee said, also emphasizing that patients should be evaluated for fecal incontinence, which could inform surgical decision making.
In addition, the guidelines call for a complete endoscopic evaluation of the colon for patients who present with symptomatic hemorrhoids and rectal bleeding; this recommendation is based on moderately strong evidence, and presented with a grade of 1B.
Medical management of hemorrhoids may include office-based procedures or surgery, according to the guidelines.
“Most patients with grade I and II and select patients with grade III internal hemorrhoidal disease who fail medical treatment can be effectively treated with office-based procedures, such as banding, sclerotherapy, and infrared coagulation,” the committee wrote, and medical office treatment received a strong grade 1A recommendation based on high-quality evidence. Although office procedures are generally well tolerated, the condition can recur. Bleeding is the most common complication, and it is more likely after rubber-band ligation than other office-based options, the guidelines state.
The guidelines offer a weak recommendation of 2C, based on the lack of quality evidence, for the use of early surgical excision to treat patients with thrombosed external hemorrhoids. “Although most patients treated nonoperatively will experience eventual resolution of their symptoms, excision of thrombosed external hemorrhoids may result in more rapid symptom resolution, lower incidence of recurrence, and longer remission intervals,” the committee noted.
Surgical hemorrhoidectomy received the strongest possible recommendation (1A, based on high-quality evidence) for the treatment of patients with external hemorrhoids or a combination of internal and external hemorrhoids with prolapse.
Surgical options described in the recommendations include surgical excision (hemorrhoidectomy), hemorrhoidopexy, and Doppler-guided hemorrhoidectomy, with citations of studies on each procedure. Data from a meta-analysis of 18 randomized prospective studies comparing hemorrhoidectomy with office-based procedures showed that hemorrhoidectomy was “the most effective treatment for patients with grade III hemorrhoids,” but it was associated with greater pain and complication rates, according to the guidelines.
However, complications in general are low after surgical hemorrhoidectomy, with reported complication rates of 1%-2% for the most common complication of postprocedure hemorrhage, the guidelines state. After surgery, the guidelines recommend with a 1B grade (moderate quality evidence) that patients use “a multimodality pain regimen to reduce narcotic usage and promote a faster recovery.”
The committee members had no financial conflicts to disclose.
SOURCE: Davis BR et al. Dis Colon Rectum. 2018; 61:284-92.
Each year, more than 2.2 million patients in the United States undergo evaluations for symptoms of hemorrhoids, according to updated guidelines on the management of hemorrhoids issued by the American Society of Colon and Rectal Surgeons.
“As a result, it is important to identify symptomatic hemorrhoids as the underlying source of the anorectal symptom and to have a clear understanding of the evaluation and management of this disease process,” wrote Bradley R. Davis, MD, FACS, chief of colon and rectal surgery at the Carolinas Medical Center, Charlotte, N.C., and the fellow members of the Clinical Practice Guidelines Committee of the ASCRS.
The guidelines recommend evaluation of hemorrhoids based on a disease-specific history, and a physical that emphasizes the degree and duration of symptoms and identifies risk factors. But the guideline writers note that the recommendation is a grade 1C because the supporting data mainly come from observational or case studies.
“The cardinal signs of internal hemorrhoids are painless bleeding with bowel movements with intermittent protrusion,” the committee said, also emphasizing that patients should be evaluated for fecal incontinence, which could inform surgical decision making.
In addition, the guidelines call for a complete endoscopic evaluation of the colon for patients who present with symptomatic hemorrhoids and rectal bleeding; this recommendation is based on moderately strong evidence, and presented with a grade of 1B.
Medical management of hemorrhoids may include office-based procedures or surgery, according to the guidelines.
“Most patients with grade I and II and select patients with grade III internal hemorrhoidal disease who fail medical treatment can be effectively treated with office-based procedures, such as banding, sclerotherapy, and infrared coagulation,” the committee wrote, and medical office treatment received a strong grade 1A recommendation based on high-quality evidence. Although office procedures are generally well tolerated, the condition can recur. Bleeding is the most common complication, and it is more likely after rubber-band ligation than other office-based options, the guidelines state.
The guidelines offer a weak recommendation of 2C, based on the lack of quality evidence, for the use of early surgical excision to treat patients with thrombosed external hemorrhoids. “Although most patients treated nonoperatively will experience eventual resolution of their symptoms, excision of thrombosed external hemorrhoids may result in more rapid symptom resolution, lower incidence of recurrence, and longer remission intervals,” the committee noted.
Surgical hemorrhoidectomy received the strongest possible recommendation (1A, based on high-quality evidence) for the treatment of patients with external hemorrhoids or a combination of internal and external hemorrhoids with prolapse.
Surgical options described in the recommendations include surgical excision (hemorrhoidectomy), hemorrhoidopexy, and Doppler-guided hemorrhoidectomy, with citations of studies on each procedure. Data from a meta-analysis of 18 randomized prospective studies comparing hemorrhoidectomy with office-based procedures showed that hemorrhoidectomy was “the most effective treatment for patients with grade III hemorrhoids,” but it was associated with greater pain and complication rates, according to the guidelines.
However, complications in general are low after surgical hemorrhoidectomy, with reported complication rates of 1%-2% for the most common complication of postprocedure hemorrhage, the guidelines state. After surgery, the guidelines recommend with a 1B grade (moderate quality evidence) that patients use “a multimodality pain regimen to reduce narcotic usage and promote a faster recovery.”
The committee members had no financial conflicts to disclose.
SOURCE: Davis BR et al. Dis Colon Rectum. 2018; 61:284-92.
Each year, more than 2.2 million patients in the United States undergo evaluations for symptoms of hemorrhoids, according to updated guidelines on the management of hemorrhoids issued by the American Society of Colon and Rectal Surgeons.
“As a result, it is important to identify symptomatic hemorrhoids as the underlying source of the anorectal symptom and to have a clear understanding of the evaluation and management of this disease process,” wrote Bradley R. Davis, MD, FACS, chief of colon and rectal surgery at the Carolinas Medical Center, Charlotte, N.C., and the fellow members of the Clinical Practice Guidelines Committee of the ASCRS.
The guidelines recommend evaluation of hemorrhoids based on a disease-specific history, and a physical that emphasizes the degree and duration of symptoms and identifies risk factors. But the guideline writers note that the recommendation is a grade 1C because the supporting data mainly come from observational or case studies.
“The cardinal signs of internal hemorrhoids are painless bleeding with bowel movements with intermittent protrusion,” the committee said, also emphasizing that patients should be evaluated for fecal incontinence, which could inform surgical decision making.
In addition, the guidelines call for a complete endoscopic evaluation of the colon for patients who present with symptomatic hemorrhoids and rectal bleeding; this recommendation is based on moderately strong evidence, and presented with a grade of 1B.
Medical management of hemorrhoids may include office-based procedures or surgery, according to the guidelines.
“Most patients with grade I and II and select patients with grade III internal hemorrhoidal disease who fail medical treatment can be effectively treated with office-based procedures, such as banding, sclerotherapy, and infrared coagulation,” the committee wrote, and medical office treatment received a strong grade 1A recommendation based on high-quality evidence. Although office procedures are generally well tolerated, the condition can recur. Bleeding is the most common complication, and it is more likely after rubber-band ligation than other office-based options, the guidelines state.
The guidelines offer a weak recommendation of 2C, based on the lack of quality evidence, for the use of early surgical excision to treat patients with thrombosed external hemorrhoids. “Although most patients treated nonoperatively will experience eventual resolution of their symptoms, excision of thrombosed external hemorrhoids may result in more rapid symptom resolution, lower incidence of recurrence, and longer remission intervals,” the committee noted.
Surgical hemorrhoidectomy received the strongest possible recommendation (1A, based on high-quality evidence) for the treatment of patients with external hemorrhoids or a combination of internal and external hemorrhoids with prolapse.
Surgical options described in the recommendations include surgical excision (hemorrhoidectomy), hemorrhoidopexy, and Doppler-guided hemorrhoidectomy, with citations of studies on each procedure. Data from a meta-analysis of 18 randomized prospective studies comparing hemorrhoidectomy with office-based procedures showed that hemorrhoidectomy was “the most effective treatment for patients with grade III hemorrhoids,” but it was associated with greater pain and complication rates, according to the guidelines.
However, complications in general are low after surgical hemorrhoidectomy, with reported complication rates of 1%-2% for the most common complication of postprocedure hemorrhage, the guidelines state. After surgery, the guidelines recommend with a 1B grade (moderate quality evidence) that patients use “a multimodality pain regimen to reduce narcotic usage and promote a faster recovery.”
The committee members had no financial conflicts to disclose.
SOURCE: Davis BR et al. Dis Colon Rectum. 2018; 61:284-92.
FROM DISEASES OF THE COLON & RECTUM