User login
Experts endorse metabolic surgery for diabetes intervention
Metabolic surgery should be recommended for obese patients with type 2 diabetes mellitus, according to an international consensus statement from 48 clinicians and scholars issued after the Second Diabetes Surgery Summit held as part of the World Congress on Interventional Therapies for Type 2 Diabetes in London in 2015.
Current treatment plans for patients with type 2 diabetes do no include bariatric/metabolic surgery, despite increasing evidence of improved glycemic control and reduced cardiovascular risk factors in surgically treated patients, wrote Dr. Francesco Rubino and colleagues on behalf of members of the Second Diabetes Surgery Summit (DSS-II). The guidelines were endorsed by 45 global medical and scientific societies at the time of publication. The statement was published in a special edition of Diabetes Care (Diabetes Care. 2016;39:861-77. doi:10.2337/dc16-0236).
The guidelines recommend metabolic surgery for patients with type 2 diabetes who have class III obesity (defined as a body mass index of at least 40 kg/m2) or class II obesity (defined as a BMI of 35 kg/m2-39.9 kg/m2). In addition, metabolic surgery should be considered as a option for those patients with type 2 diabetes whose BMI falls within the 30 kg/m2-34.9 kg/m2 range if hyperglycemia remains uncontrolled after treatment attempts with oral or injectable medications. For Asian patients, the BMI thresholds for surgery should be reduced by 2.5 kg/m2, the researchers noted.
The conclusions are based on a review of published evidence on metabolic surgery and type 2 diabetes from January 1, 2005, through September 30, 2015.
The researchers assessed the evidence based on factors including long-term effects of surgery on glycemic control, effectiveness of surgery compared with nonsurgical interventions, comparisons of surgical procedures, and effects of surgery on diabetes complications, cardiovascular risk factors, and mortality. They also considered the short- and long-term safety of different procedures. The recommendations offer guidance on patient selection, pre- and postoperative workups, choice of procedure, and defining goals and success of surgery.
“The success of metabolic surgery needs to be defined in the larger context of comprehensive diabetes care plans,” the researchers noted. “Metabolic surgery should be considered a means to achieve the glycemic control necessary to reduce risk of microvascular complications and CVD.”
The researchers acknowledged that complications from metabolic surgery may require reoperations and rehospitalizations. Other limitations include a lack of evidence in several areas including: cost-effectiveness, optimal nutrition management after surgery, postoperative lifestyle interventions, and long-term effects of surgery, and further research is needed.
However, “there is now sufficient clinical and mechanistic evidence to support inclusion of GI surgery among antidiabetes interventions for people with type 2 diabetes and obesity,” the researchers said. They called for collaboration between clinicians and regulators to recognize the potential value of metabolic surgery for type 2 diabetes and develop appropriate reimbursement plans.
The DSS-II and WCITD 2015 were sponsored by the International Diabetes Society Task Force, King’s College London, King’s College Hospital, Johnson & Johnson, Medtronic, Medimmune, Fractyl, DIAMOND MetaCure, Gore, Novo Nordisk, and NGM Biopharmaceuticals. The researchers reported no relevant conflicts.
“The new guidelines provide much needed guidance for general practitioners, endocrinologists, and diabetes specialists about the use of metabolic surgery in the treatment of obese patients with type 2 diabetes,” wrote Dr. William T. Cefalu and colleagues in an accompanying editorial.
However, “one of the many issues that remains unanswered for metabolic surgery pertains to the exact mechanism of action. Specifically, we now recognize that postoperative improvements in metabolic control occur rapidly and out of proportion to weight loss, yet the physiological and molecular mechanisms underlying these beneficial glycemic effects remain incompletely elucidated,” they wrote. In addition, “before we can fully appreciate the role of metabolic surgery in becoming a readily available, viable option in our treatment algorithm and expand the appropriate candidate pool, we need to fully understand the efficacy, complications, long-term clinical outcomes, and costs. In particular, it will be important to clarify the financial implications to patients, providers, and insurers (both private and government sectors) and to appreciate that these barriers may be hard to overcome in resource poor areas of the world,” they said.
“It is an exciting time for those of us in diabetes research, and the ability to be part of a paradigm change in the understanding, approach, and management of the disease will keep us focused on the next steps to address the larger issue of prevention,” they noted (Diabetes Care. 2016;39:857-60. doi:10.2337/dc16-0686) .
Dr. Cefalu is affiliated with the Pennington Biomedical Research Center at Louisiana State University in Baton Rouge, La. He disclosed financial relationships with multiple companies including AstraZeneca, Janssen, MannKind Corp., Intarcia Therapeutics, and Sanofi.
“The new guidelines provide much needed guidance for general practitioners, endocrinologists, and diabetes specialists about the use of metabolic surgery in the treatment of obese patients with type 2 diabetes,” wrote Dr. William T. Cefalu and colleagues in an accompanying editorial.
However, “one of the many issues that remains unanswered for metabolic surgery pertains to the exact mechanism of action. Specifically, we now recognize that postoperative improvements in metabolic control occur rapidly and out of proportion to weight loss, yet the physiological and molecular mechanisms underlying these beneficial glycemic effects remain incompletely elucidated,” they wrote. In addition, “before we can fully appreciate the role of metabolic surgery in becoming a readily available, viable option in our treatment algorithm and expand the appropriate candidate pool, we need to fully understand the efficacy, complications, long-term clinical outcomes, and costs. In particular, it will be important to clarify the financial implications to patients, providers, and insurers (both private and government sectors) and to appreciate that these barriers may be hard to overcome in resource poor areas of the world,” they said.
“It is an exciting time for those of us in diabetes research, and the ability to be part of a paradigm change in the understanding, approach, and management of the disease will keep us focused on the next steps to address the larger issue of prevention,” they noted (Diabetes Care. 2016;39:857-60. doi:10.2337/dc16-0686) .
Dr. Cefalu is affiliated with the Pennington Biomedical Research Center at Louisiana State University in Baton Rouge, La. He disclosed financial relationships with multiple companies including AstraZeneca, Janssen, MannKind Corp., Intarcia Therapeutics, and Sanofi.
“The new guidelines provide much needed guidance for general practitioners, endocrinologists, and diabetes specialists about the use of metabolic surgery in the treatment of obese patients with type 2 diabetes,” wrote Dr. William T. Cefalu and colleagues in an accompanying editorial.
However, “one of the many issues that remains unanswered for metabolic surgery pertains to the exact mechanism of action. Specifically, we now recognize that postoperative improvements in metabolic control occur rapidly and out of proportion to weight loss, yet the physiological and molecular mechanisms underlying these beneficial glycemic effects remain incompletely elucidated,” they wrote. In addition, “before we can fully appreciate the role of metabolic surgery in becoming a readily available, viable option in our treatment algorithm and expand the appropriate candidate pool, we need to fully understand the efficacy, complications, long-term clinical outcomes, and costs. In particular, it will be important to clarify the financial implications to patients, providers, and insurers (both private and government sectors) and to appreciate that these barriers may be hard to overcome in resource poor areas of the world,” they said.
“It is an exciting time for those of us in diabetes research, and the ability to be part of a paradigm change in the understanding, approach, and management of the disease will keep us focused on the next steps to address the larger issue of prevention,” they noted (Diabetes Care. 2016;39:857-60. doi:10.2337/dc16-0686) .
Dr. Cefalu is affiliated with the Pennington Biomedical Research Center at Louisiana State University in Baton Rouge, La. He disclosed financial relationships with multiple companies including AstraZeneca, Janssen, MannKind Corp., Intarcia Therapeutics, and Sanofi.
Metabolic surgery should be recommended for obese patients with type 2 diabetes mellitus, according to an international consensus statement from 48 clinicians and scholars issued after the Second Diabetes Surgery Summit held as part of the World Congress on Interventional Therapies for Type 2 Diabetes in London in 2015.
Current treatment plans for patients with type 2 diabetes do no include bariatric/metabolic surgery, despite increasing evidence of improved glycemic control and reduced cardiovascular risk factors in surgically treated patients, wrote Dr. Francesco Rubino and colleagues on behalf of members of the Second Diabetes Surgery Summit (DSS-II). The guidelines were endorsed by 45 global medical and scientific societies at the time of publication. The statement was published in a special edition of Diabetes Care (Diabetes Care. 2016;39:861-77. doi:10.2337/dc16-0236).
The guidelines recommend metabolic surgery for patients with type 2 diabetes who have class III obesity (defined as a body mass index of at least 40 kg/m2) or class II obesity (defined as a BMI of 35 kg/m2-39.9 kg/m2). In addition, metabolic surgery should be considered as a option for those patients with type 2 diabetes whose BMI falls within the 30 kg/m2-34.9 kg/m2 range if hyperglycemia remains uncontrolled after treatment attempts with oral or injectable medications. For Asian patients, the BMI thresholds for surgery should be reduced by 2.5 kg/m2, the researchers noted.
The conclusions are based on a review of published evidence on metabolic surgery and type 2 diabetes from January 1, 2005, through September 30, 2015.
The researchers assessed the evidence based on factors including long-term effects of surgery on glycemic control, effectiveness of surgery compared with nonsurgical interventions, comparisons of surgical procedures, and effects of surgery on diabetes complications, cardiovascular risk factors, and mortality. They also considered the short- and long-term safety of different procedures. The recommendations offer guidance on patient selection, pre- and postoperative workups, choice of procedure, and defining goals and success of surgery.
“The success of metabolic surgery needs to be defined in the larger context of comprehensive diabetes care plans,” the researchers noted. “Metabolic surgery should be considered a means to achieve the glycemic control necessary to reduce risk of microvascular complications and CVD.”
The researchers acknowledged that complications from metabolic surgery may require reoperations and rehospitalizations. Other limitations include a lack of evidence in several areas including: cost-effectiveness, optimal nutrition management after surgery, postoperative lifestyle interventions, and long-term effects of surgery, and further research is needed.
However, “there is now sufficient clinical and mechanistic evidence to support inclusion of GI surgery among antidiabetes interventions for people with type 2 diabetes and obesity,” the researchers said. They called for collaboration between clinicians and regulators to recognize the potential value of metabolic surgery for type 2 diabetes and develop appropriate reimbursement plans.
The DSS-II and WCITD 2015 were sponsored by the International Diabetes Society Task Force, King’s College London, King’s College Hospital, Johnson & Johnson, Medtronic, Medimmune, Fractyl, DIAMOND MetaCure, Gore, Novo Nordisk, and NGM Biopharmaceuticals. The researchers reported no relevant conflicts.
Metabolic surgery should be recommended for obese patients with type 2 diabetes mellitus, according to an international consensus statement from 48 clinicians and scholars issued after the Second Diabetes Surgery Summit held as part of the World Congress on Interventional Therapies for Type 2 Diabetes in London in 2015.
Current treatment plans for patients with type 2 diabetes do no include bariatric/metabolic surgery, despite increasing evidence of improved glycemic control and reduced cardiovascular risk factors in surgically treated patients, wrote Dr. Francesco Rubino and colleagues on behalf of members of the Second Diabetes Surgery Summit (DSS-II). The guidelines were endorsed by 45 global medical and scientific societies at the time of publication. The statement was published in a special edition of Diabetes Care (Diabetes Care. 2016;39:861-77. doi:10.2337/dc16-0236).
The guidelines recommend metabolic surgery for patients with type 2 diabetes who have class III obesity (defined as a body mass index of at least 40 kg/m2) or class II obesity (defined as a BMI of 35 kg/m2-39.9 kg/m2). In addition, metabolic surgery should be considered as a option for those patients with type 2 diabetes whose BMI falls within the 30 kg/m2-34.9 kg/m2 range if hyperglycemia remains uncontrolled after treatment attempts with oral or injectable medications. For Asian patients, the BMI thresholds for surgery should be reduced by 2.5 kg/m2, the researchers noted.
The conclusions are based on a review of published evidence on metabolic surgery and type 2 diabetes from January 1, 2005, through September 30, 2015.
The researchers assessed the evidence based on factors including long-term effects of surgery on glycemic control, effectiveness of surgery compared with nonsurgical interventions, comparisons of surgical procedures, and effects of surgery on diabetes complications, cardiovascular risk factors, and mortality. They also considered the short- and long-term safety of different procedures. The recommendations offer guidance on patient selection, pre- and postoperative workups, choice of procedure, and defining goals and success of surgery.
“The success of metabolic surgery needs to be defined in the larger context of comprehensive diabetes care plans,” the researchers noted. “Metabolic surgery should be considered a means to achieve the glycemic control necessary to reduce risk of microvascular complications and CVD.”
The researchers acknowledged that complications from metabolic surgery may require reoperations and rehospitalizations. Other limitations include a lack of evidence in several areas including: cost-effectiveness, optimal nutrition management after surgery, postoperative lifestyle interventions, and long-term effects of surgery, and further research is needed.
However, “there is now sufficient clinical and mechanistic evidence to support inclusion of GI surgery among antidiabetes interventions for people with type 2 diabetes and obesity,” the researchers said. They called for collaboration between clinicians and regulators to recognize the potential value of metabolic surgery for type 2 diabetes and develop appropriate reimbursement plans.
The DSS-II and WCITD 2015 were sponsored by the International Diabetes Society Task Force, King’s College London, King’s College Hospital, Johnson & Johnson, Medtronic, Medimmune, Fractyl, DIAMOND MetaCure, Gore, Novo Nordisk, and NGM Biopharmaceuticals. The researchers reported no relevant conflicts.
FROM DIABETES CARE
Key clinical point: Metabolic surgery should be recommended for obese patients with type 2 diabetes mellitus.
Major finding: Surgery is recommended for patients with type 2 diabetes who have a BMI of 35 kg/m2 or higher and should be considered for patients with a BMI of 30 kg/m2-34.9 kg/m2 with uncontrolled hyperglycemia.
Data source: Published evidence on metabolic surgery and type 2 diabetes identified on Medline between January 1, 2005 and September 30, 2015.
Disclosures: The DSS-II and WCITD 2015 were sponsored by the International Diabetes Society Task Force, King’s College London, King’s College Hospital, Johnson & Johnson, Medtronic, Medimmune, Fractyl, DIAMOND MetaCure, Gore, Novo Nordisk, and NGM Biopharmaceuticals. The researchers reported no relevant conflicts.
Early HIV testing tempers transmission
Early and aggressive HIV testing may reduce HIV incidence, according to a data analysis of new HIV diagnoses in San Diego.
From 2006 to 2012, an average of 471 new HIV diagnoses were made in San Diego County annually. Given the increased risk of HIV transmission from recently infected individuals, the San Diego Department of Public Health designed an early testing program to screen those persons at high risk of HIV, wrote Dr. Sanjay R. Mehta of the University of California, San Diego, and colleagues, in Clinical Infectious Diseases (Clin Infect Dis. 2016 May 11. doi:10.1093/cid/ciw161).
HIV testing in San Diego between 1998 and 2012 was relatively stable, and ranged from approximately 9,236 tests in 2006 to approximately 16,797 in 1999. However, the expanded testing program – implemented in late 2011 – resulted in 39,688 tests performed in 2012, and the Early Test identified an average of 17 acute HIV infections (20% of Early Test diagnoses) and 21 early infections (24% of Early Test diagnoses) per year between 2008 and 2012.
Two zip codes in the central region of San Diego County associated with the gay community had the highest prevalence of HIV infection. Zip codes 92103 and 92104 had the highest net HIV importation of all the county zip codes, and several neighboring zip codes had the highest net exportation. “This suggested increased HIV transmission chain termination in the 92103 and 92104 zip codes, areas targeted by the Early Test program,” the researchers said.
“Our analysis demonstrated that the observed decrease in incident diagnoses was associated with the steady increase in testing by the Early Test program and not with an appreciable increase in ART uptake or effectiveness or a decrease in other STIs in the community,” Dr. Mehta and his colleagues added.
The study was supported in part by a grant from the National Institutes of Health. Dr. Mehta had no financial conflicts to disclose.
Early and aggressive HIV testing may reduce HIV incidence, according to a data analysis of new HIV diagnoses in San Diego.
From 2006 to 2012, an average of 471 new HIV diagnoses were made in San Diego County annually. Given the increased risk of HIV transmission from recently infected individuals, the San Diego Department of Public Health designed an early testing program to screen those persons at high risk of HIV, wrote Dr. Sanjay R. Mehta of the University of California, San Diego, and colleagues, in Clinical Infectious Diseases (Clin Infect Dis. 2016 May 11. doi:10.1093/cid/ciw161).
HIV testing in San Diego between 1998 and 2012 was relatively stable, and ranged from approximately 9,236 tests in 2006 to approximately 16,797 in 1999. However, the expanded testing program – implemented in late 2011 – resulted in 39,688 tests performed in 2012, and the Early Test identified an average of 17 acute HIV infections (20% of Early Test diagnoses) and 21 early infections (24% of Early Test diagnoses) per year between 2008 and 2012.
Two zip codes in the central region of San Diego County associated with the gay community had the highest prevalence of HIV infection. Zip codes 92103 and 92104 had the highest net HIV importation of all the county zip codes, and several neighboring zip codes had the highest net exportation. “This suggested increased HIV transmission chain termination in the 92103 and 92104 zip codes, areas targeted by the Early Test program,” the researchers said.
“Our analysis demonstrated that the observed decrease in incident diagnoses was associated with the steady increase in testing by the Early Test program and not with an appreciable increase in ART uptake or effectiveness or a decrease in other STIs in the community,” Dr. Mehta and his colleagues added.
The study was supported in part by a grant from the National Institutes of Health. Dr. Mehta had no financial conflicts to disclose.
Early and aggressive HIV testing may reduce HIV incidence, according to a data analysis of new HIV diagnoses in San Diego.
From 2006 to 2012, an average of 471 new HIV diagnoses were made in San Diego County annually. Given the increased risk of HIV transmission from recently infected individuals, the San Diego Department of Public Health designed an early testing program to screen those persons at high risk of HIV, wrote Dr. Sanjay R. Mehta of the University of California, San Diego, and colleagues, in Clinical Infectious Diseases (Clin Infect Dis. 2016 May 11. doi:10.1093/cid/ciw161).
HIV testing in San Diego between 1998 and 2012 was relatively stable, and ranged from approximately 9,236 tests in 2006 to approximately 16,797 in 1999. However, the expanded testing program – implemented in late 2011 – resulted in 39,688 tests performed in 2012, and the Early Test identified an average of 17 acute HIV infections (20% of Early Test diagnoses) and 21 early infections (24% of Early Test diagnoses) per year between 2008 and 2012.
Two zip codes in the central region of San Diego County associated with the gay community had the highest prevalence of HIV infection. Zip codes 92103 and 92104 had the highest net HIV importation of all the county zip codes, and several neighboring zip codes had the highest net exportation. “This suggested increased HIV transmission chain termination in the 92103 and 92104 zip codes, areas targeted by the Early Test program,” the researchers said.
“Our analysis demonstrated that the observed decrease in incident diagnoses was associated with the steady increase in testing by the Early Test program and not with an appreciable increase in ART uptake or effectiveness or a decrease in other STIs in the community,” Dr. Mehta and his colleagues added.
The study was supported in part by a grant from the National Institutes of Health. Dr. Mehta had no financial conflicts to disclose.
FROM CLINICAL INFECTIOUS DISEASES
Key clinical point: Early HIV diagnosis via a primary infection screening reduced new HIV diagnoses overall in San Diego County.
Major finding: Early HIV testing identified an annual average of 17 acute and 21 early infections.
Data source: A regression analysis of new HIV diagnoses in San Diego County from 2006 to 2012.
Disclosures: The study was supported in part by a grant from the National Institutes of Health. Dr. Mehta had no financial conflicts to disclose.
Less education tied to more anxiety
Adults with less than a high school education are more than twice as likely as are those with high school degrees to have reported an anxiety disorder in the past year, according to the National Survey on Drug Use and Health’s 2008 to 2012 Mental Health Surveillance Study (MHSS), published June 2.
The data identified anxiety disorders in 13% of non–high school graduates vs. 5% of high school graduates. Adults with at least a college degree had the lowest rates of past year anxiety (4.3%). The MHSS estimated that approximately 13 million adults in the United States had at least one anxiety disorder within the past year.
“Although the MHSS results cannot be used to determine whether anxiety stopped people from finishing high school, having an anxiety disorder can lower the odds of graduating from high school and the odds of attending college,” the researchers wrote. The findings emphasize the need to support people with anxiety to help them remain in school and succeed, they added.
The findings were published in the Center for Behavioral Health Statistics and Quality Report. Read the full study here.
Adults with less than a high school education are more than twice as likely as are those with high school degrees to have reported an anxiety disorder in the past year, according to the National Survey on Drug Use and Health’s 2008 to 2012 Mental Health Surveillance Study (MHSS), published June 2.
The data identified anxiety disorders in 13% of non–high school graduates vs. 5% of high school graduates. Adults with at least a college degree had the lowest rates of past year anxiety (4.3%). The MHSS estimated that approximately 13 million adults in the United States had at least one anxiety disorder within the past year.
“Although the MHSS results cannot be used to determine whether anxiety stopped people from finishing high school, having an anxiety disorder can lower the odds of graduating from high school and the odds of attending college,” the researchers wrote. The findings emphasize the need to support people with anxiety to help them remain in school and succeed, they added.
The findings were published in the Center for Behavioral Health Statistics and Quality Report. Read the full study here.
Adults with less than a high school education are more than twice as likely as are those with high school degrees to have reported an anxiety disorder in the past year, according to the National Survey on Drug Use and Health’s 2008 to 2012 Mental Health Surveillance Study (MHSS), published June 2.
The data identified anxiety disorders in 13% of non–high school graduates vs. 5% of high school graduates. Adults with at least a college degree had the lowest rates of past year anxiety (4.3%). The MHSS estimated that approximately 13 million adults in the United States had at least one anxiety disorder within the past year.
“Although the MHSS results cannot be used to determine whether anxiety stopped people from finishing high school, having an anxiety disorder can lower the odds of graduating from high school and the odds of attending college,” the researchers wrote. The findings emphasize the need to support people with anxiety to help them remain in school and succeed, they added.
The findings were published in the Center for Behavioral Health Statistics and Quality Report. Read the full study here.
FROM THE CBHSQ REPORT
Antiretroviral therapy inadequate against arterial inflammation
Combined antiretroviral therapy (ART) significantly reduced viral load from 4.3 copies/mL to 1.3 copies/mL in a study of a dozen treatment-naive HIV-infected adults after 6 months. However, arterial inflammation, as measured by aortic target-background ratio (TBR), did not improve significantly, wrote Dr. Markella V. Zanni of Harvard Medical School, Boston, and colleagues.
The patients received a combination regimen including elvitegravir, cobicistat, emtricitabine, and tenofovir disoproxil fumarate. Arterial inflammation was assessed via fludeoxyglucose F 18 positron emission tomography.
The findings affirm the overall benefits of ART, but suggest that ART alone may not be enough to prevent cardiovascular disease in HIV patients in the short term, the researchers wrote.
“Complementary strategies to further improve immune activation indices and arterial inflammation – including statins and other immunomodulatory strategies – may be needed in addition to ART,” the researchers noted. “Future studies are needed to elucidate the relationship between arterial inflammation, atherogenesis, and myocardial infarction in HIV,” they added (JAMA Cardiol. 2016 May 25. doi: 10.1001/jamacardio.2016.0846). Read the study here.
Combined antiretroviral therapy (ART) significantly reduced viral load from 4.3 copies/mL to 1.3 copies/mL in a study of a dozen treatment-naive HIV-infected adults after 6 months. However, arterial inflammation, as measured by aortic target-background ratio (TBR), did not improve significantly, wrote Dr. Markella V. Zanni of Harvard Medical School, Boston, and colleagues.
The patients received a combination regimen including elvitegravir, cobicistat, emtricitabine, and tenofovir disoproxil fumarate. Arterial inflammation was assessed via fludeoxyglucose F 18 positron emission tomography.
The findings affirm the overall benefits of ART, but suggest that ART alone may not be enough to prevent cardiovascular disease in HIV patients in the short term, the researchers wrote.
“Complementary strategies to further improve immune activation indices and arterial inflammation – including statins and other immunomodulatory strategies – may be needed in addition to ART,” the researchers noted. “Future studies are needed to elucidate the relationship between arterial inflammation, atherogenesis, and myocardial infarction in HIV,” they added (JAMA Cardiol. 2016 May 25. doi: 10.1001/jamacardio.2016.0846). Read the study here.
Combined antiretroviral therapy (ART) significantly reduced viral load from 4.3 copies/mL to 1.3 copies/mL in a study of a dozen treatment-naive HIV-infected adults after 6 months. However, arterial inflammation, as measured by aortic target-background ratio (TBR), did not improve significantly, wrote Dr. Markella V. Zanni of Harvard Medical School, Boston, and colleagues.
The patients received a combination regimen including elvitegravir, cobicistat, emtricitabine, and tenofovir disoproxil fumarate. Arterial inflammation was assessed via fludeoxyglucose F 18 positron emission tomography.
The findings affirm the overall benefits of ART, but suggest that ART alone may not be enough to prevent cardiovascular disease in HIV patients in the short term, the researchers wrote.
“Complementary strategies to further improve immune activation indices and arterial inflammation – including statins and other immunomodulatory strategies – may be needed in addition to ART,” the researchers noted. “Future studies are needed to elucidate the relationship between arterial inflammation, atherogenesis, and myocardial infarction in HIV,” they added (JAMA Cardiol. 2016 May 25. doi: 10.1001/jamacardio.2016.0846). Read the study here.
FROM JAMA CARDIOLOGY
Rooming in cuts costs and improves care for neonatal abstinence syndrome
A neonatal abstinence syndrome program that focused on rooming in significantly decreased hospital costs, drug use, and length of hospital stay, based on data from a program in a single hospital in a rural academic tertiary care center.
“The aim of this project was to improve the care of opioid-exposed newborns by involving families, standardizing assessment and treatment, and transitioning to rooming-in for the full hospital stay,” reported Dr. Alison Volpe Holmes of the Geisel School of Medicine at Dartmouth, Hanover, N.H., and colleagues.
The researchers reviewed data from 163 newborns with neonatal abstinence syndrome (NAS) treated at Children’s Hospital at Dartmouth-Hitchcock between March 2012 and February 2015. Between the preintervention period and the study’s end, cumulative morphine exposure per infant dropped from 13.7 mg to 6.6 mg, length of hospital stay for newborns needing pharmacologic care dropped from 16.9 days to 12.3 days, and the average cost for newborns needing pharmacologic care dropped from $19,737 to $8,755. No adverse events were reported during the study period.
“We reduced system costs by more than half by caring for infants with prenatal opioid exposure and NAS in a rooming-in model, safely eliminating the use of critical care beds for this condition,” they noted.
Read the full study in Pediatrics (2016;137[6]:e20152929).
A neonatal abstinence syndrome program that focused on rooming in significantly decreased hospital costs, drug use, and length of hospital stay, based on data from a program in a single hospital in a rural academic tertiary care center.
“The aim of this project was to improve the care of opioid-exposed newborns by involving families, standardizing assessment and treatment, and transitioning to rooming-in for the full hospital stay,” reported Dr. Alison Volpe Holmes of the Geisel School of Medicine at Dartmouth, Hanover, N.H., and colleagues.
The researchers reviewed data from 163 newborns with neonatal abstinence syndrome (NAS) treated at Children’s Hospital at Dartmouth-Hitchcock between March 2012 and February 2015. Between the preintervention period and the study’s end, cumulative morphine exposure per infant dropped from 13.7 mg to 6.6 mg, length of hospital stay for newborns needing pharmacologic care dropped from 16.9 days to 12.3 days, and the average cost for newborns needing pharmacologic care dropped from $19,737 to $8,755. No adverse events were reported during the study period.
“We reduced system costs by more than half by caring for infants with prenatal opioid exposure and NAS in a rooming-in model, safely eliminating the use of critical care beds for this condition,” they noted.
Read the full study in Pediatrics (2016;137[6]:e20152929).
A neonatal abstinence syndrome program that focused on rooming in significantly decreased hospital costs, drug use, and length of hospital stay, based on data from a program in a single hospital in a rural academic tertiary care center.
“The aim of this project was to improve the care of opioid-exposed newborns by involving families, standardizing assessment and treatment, and transitioning to rooming-in for the full hospital stay,” reported Dr. Alison Volpe Holmes of the Geisel School of Medicine at Dartmouth, Hanover, N.H., and colleagues.
The researchers reviewed data from 163 newborns with neonatal abstinence syndrome (NAS) treated at Children’s Hospital at Dartmouth-Hitchcock between March 2012 and February 2015. Between the preintervention period and the study’s end, cumulative morphine exposure per infant dropped from 13.7 mg to 6.6 mg, length of hospital stay for newborns needing pharmacologic care dropped from 16.9 days to 12.3 days, and the average cost for newborns needing pharmacologic care dropped from $19,737 to $8,755. No adverse events were reported during the study period.
“We reduced system costs by more than half by caring for infants with prenatal opioid exposure and NAS in a rooming-in model, safely eliminating the use of critical care beds for this condition,” they noted.
Read the full study in Pediatrics (2016;137[6]:e20152929).
FROM PEDIATRICS
Competitive surgical outcomes observed at critical access hospitals
Thirty-day mortality rates for several common operations were not significantly different for patients seen at “critical access” hospitals, compared with larger high-volume facilities, according to a study using a large, national Medicare database.
The findings suggest that such procedures can be performed safely in smaller, rural hospitals. The Medicare Provider Analysis and Review (MEDPAR) file was used by investigators to examine data from 2009 through 2013 on more than 1 million patients at both types of facilities. The findings were published in JAMA on May 17.
The study was important to conduct for two reasons, coauthors Dr. Andrew Ibrahim and Dr. Justin Dimick of the University of Michigan, Ann Arbor, said in an interview.
“First, this study helps inform important policy decision making regarding rural access to surgery. Critical access hospitals receive more than $9 billion dollars annually from Medicare under payment provisions established in the Medicare Rural Hospital Flexibility Program to help keep them financially viable,” they said. “Plans to modify and even eliminate this program have been proposed largely based on studies demonstrating lower quality of care for common medical conditions (such as heart failure, pneumonia, or heart attack.) This study provides important information about common surgical procedures done in these same hospitals,” they stated.
“Second, this study gives us a better understanding of how to ensure safe surgical care without limiting access for common procedures. We have years of research demonstrating that relatively rare, complex operations (such as open heart operations and cancer resections) should be centralized to high-volume centers where patients travel to obtain their care,” the researchers said. “On the other end of the spectrum, this paper describes common, less complex operations where it is safe for patients to stay at their local hospital without the burden of traveling. This is particularly important now as large health case systems are consolidating and developing strategies to regionalize procedures within their network,” they noted.
The researchers and their colleagues reviewed data from 28,512 patients treated at critical access hospitals and 1,603,392 seen at non–critical access hospitals (JAMA 2016;315:2095-2103. doi:10.1001/jama.2016.5618). The patients underwent one of four surgeries: appendectomy, cholecystectomy, colectomy, or hernia repair.
After the researchers controlled for confounding variables, 30-day mortality rates were not significantly different among patients at critical access and non–critical access hospitals (5.4% vs. 5.6%), although the rates of serious complications were significantly lower in critical access vs. non–critical access hospitals (6.5 vs. 14%). In addition, Medicare expenses were significantly lower at critical access vs. non–critical access hospitals after factoring in risk-adjustment and price standardization ($14,450 vs. $15,845).
Overall, patients treated at critical access hospitals were significantly less likely than were those seen at non–critical access hospitals to have chronic medical problems including heart failure (8% vs. 10%), diabetes (20% vs. 22%), obesity (7% vs. 11%), and two or more comorbidities (60% vs. 70%). The average age of the patients was 77 years, and approximately half were women.

The findings on 30-day mortality and Medicare expenses contradict previous studies of nonsurgical admissions in critical access and non–critical access settings, the researchers noted. However, patients were less likely to proceed to post–acute care facilities from critical access hospitals compared with non–critical access hospitals.
“Based on information about admissions for common medical problems to these hospitals having higher mortality rates and decreased compliance with process measures, we thought this might be the same for surgical admissions,” the researchers said in the interview. “Our findings, however, show that critical access hospitals perform well for common surgical admissions with no difference in their risk-adjusted 30-day mortality rates.”
The results were limited by the use of administrative data, the potential overestimation of complication rates, and the lack of data on younger patients. The data illustrate how new payment models might impact critical care facilities, but several areas of research should be explored, the investigators said.
“First, we need a better understanding of how these small rural hospitals appear to be providing safe care at lower costs. Our data suggest it may be related to patient-selection, but even when we accounted for that in our models they still perform well,” they explained.
“Second, as many of these hospitals may in fact close in the next year, studies will be needed to inform how this might impact cost and access to rural surgical care. Finally, there are many other operations that we do not yet understand if they should be centralized to a large urban hospital, of if they are safe to be done in small hospital settings. As large health care systems continue to consolidate, each one will need a ‘health care systems architect’ to help organize how surgical services should be centralized or decentralized across their network to optimize both quality and access,” they added.
Dr. Ibrahim has received funding from the Robert Wood Johnson Foundation and the U.S. Department of Veterans Affairs. Dr. Justin Dimick has a financial interest in ArborMetrix Inc. and has received funds from the Agency for Healthcare Research and Quality and the National Institutes of Health, as well as honoraria from Stanford University, Emory University, and the University of Texas.
Thirty-day mortality rates for several common operations were not significantly different for patients seen at “critical access” hospitals, compared with larger high-volume facilities, according to a study using a large, national Medicare database.
The findings suggest that such procedures can be performed safely in smaller, rural hospitals. The Medicare Provider Analysis and Review (MEDPAR) file was used by investigators to examine data from 2009 through 2013 on more than 1 million patients at both types of facilities. The findings were published in JAMA on May 17.
The study was important to conduct for two reasons, coauthors Dr. Andrew Ibrahim and Dr. Justin Dimick of the University of Michigan, Ann Arbor, said in an interview.
“First, this study helps inform important policy decision making regarding rural access to surgery. Critical access hospitals receive more than $9 billion dollars annually from Medicare under payment provisions established in the Medicare Rural Hospital Flexibility Program to help keep them financially viable,” they said. “Plans to modify and even eliminate this program have been proposed largely based on studies demonstrating lower quality of care for common medical conditions (such as heart failure, pneumonia, or heart attack.) This study provides important information about common surgical procedures done in these same hospitals,” they stated.
“Second, this study gives us a better understanding of how to ensure safe surgical care without limiting access for common procedures. We have years of research demonstrating that relatively rare, complex operations (such as open heart operations and cancer resections) should be centralized to high-volume centers where patients travel to obtain their care,” the researchers said. “On the other end of the spectrum, this paper describes common, less complex operations where it is safe for patients to stay at their local hospital without the burden of traveling. This is particularly important now as large health case systems are consolidating and developing strategies to regionalize procedures within their network,” they noted.
The researchers and their colleagues reviewed data from 28,512 patients treated at critical access hospitals and 1,603,392 seen at non–critical access hospitals (JAMA 2016;315:2095-2103. doi:10.1001/jama.2016.5618). The patients underwent one of four surgeries: appendectomy, cholecystectomy, colectomy, or hernia repair.
After the researchers controlled for confounding variables, 30-day mortality rates were not significantly different among patients at critical access and non–critical access hospitals (5.4% vs. 5.6%), although the rates of serious complications were significantly lower in critical access vs. non–critical access hospitals (6.5 vs. 14%). In addition, Medicare expenses were significantly lower at critical access vs. non–critical access hospitals after factoring in risk-adjustment and price standardization ($14,450 vs. $15,845).
Overall, patients treated at critical access hospitals were significantly less likely than were those seen at non–critical access hospitals to have chronic medical problems including heart failure (8% vs. 10%), diabetes (20% vs. 22%), obesity (7% vs. 11%), and two or more comorbidities (60% vs. 70%). The average age of the patients was 77 years, and approximately half were women.

The findings on 30-day mortality and Medicare expenses contradict previous studies of nonsurgical admissions in critical access and non–critical access settings, the researchers noted. However, patients were less likely to proceed to post–acute care facilities from critical access hospitals compared with non–critical access hospitals.
“Based on information about admissions for common medical problems to these hospitals having higher mortality rates and decreased compliance with process measures, we thought this might be the same for surgical admissions,” the researchers said in the interview. “Our findings, however, show that critical access hospitals perform well for common surgical admissions with no difference in their risk-adjusted 30-day mortality rates.”
The results were limited by the use of administrative data, the potential overestimation of complication rates, and the lack of data on younger patients. The data illustrate how new payment models might impact critical care facilities, but several areas of research should be explored, the investigators said.
“First, we need a better understanding of how these small rural hospitals appear to be providing safe care at lower costs. Our data suggest it may be related to patient-selection, but even when we accounted for that in our models they still perform well,” they explained.
“Second, as many of these hospitals may in fact close in the next year, studies will be needed to inform how this might impact cost and access to rural surgical care. Finally, there are many other operations that we do not yet understand if they should be centralized to a large urban hospital, of if they are safe to be done in small hospital settings. As large health care systems continue to consolidate, each one will need a ‘health care systems architect’ to help organize how surgical services should be centralized or decentralized across their network to optimize both quality and access,” they added.
Dr. Ibrahim has received funding from the Robert Wood Johnson Foundation and the U.S. Department of Veterans Affairs. Dr. Justin Dimick has a financial interest in ArborMetrix Inc. and has received funds from the Agency for Healthcare Research and Quality and the National Institutes of Health, as well as honoraria from Stanford University, Emory University, and the University of Texas.
Thirty-day mortality rates for several common operations were not significantly different for patients seen at “critical access” hospitals, compared with larger high-volume facilities, according to a study using a large, national Medicare database.
The findings suggest that such procedures can be performed safely in smaller, rural hospitals. The Medicare Provider Analysis and Review (MEDPAR) file was used by investigators to examine data from 2009 through 2013 on more than 1 million patients at both types of facilities. The findings were published in JAMA on May 17.
The study was important to conduct for two reasons, coauthors Dr. Andrew Ibrahim and Dr. Justin Dimick of the University of Michigan, Ann Arbor, said in an interview.
“First, this study helps inform important policy decision making regarding rural access to surgery. Critical access hospitals receive more than $9 billion dollars annually from Medicare under payment provisions established in the Medicare Rural Hospital Flexibility Program to help keep them financially viable,” they said. “Plans to modify and even eliminate this program have been proposed largely based on studies demonstrating lower quality of care for common medical conditions (such as heart failure, pneumonia, or heart attack.) This study provides important information about common surgical procedures done in these same hospitals,” they stated.
“Second, this study gives us a better understanding of how to ensure safe surgical care without limiting access for common procedures. We have years of research demonstrating that relatively rare, complex operations (such as open heart operations and cancer resections) should be centralized to high-volume centers where patients travel to obtain their care,” the researchers said. “On the other end of the spectrum, this paper describes common, less complex operations where it is safe for patients to stay at their local hospital without the burden of traveling. This is particularly important now as large health case systems are consolidating and developing strategies to regionalize procedures within their network,” they noted.
The researchers and their colleagues reviewed data from 28,512 patients treated at critical access hospitals and 1,603,392 seen at non–critical access hospitals (JAMA 2016;315:2095-2103. doi:10.1001/jama.2016.5618). The patients underwent one of four surgeries: appendectomy, cholecystectomy, colectomy, or hernia repair.
After the researchers controlled for confounding variables, 30-day mortality rates were not significantly different among patients at critical access and non–critical access hospitals (5.4% vs. 5.6%), although the rates of serious complications were significantly lower in critical access vs. non–critical access hospitals (6.5 vs. 14%). In addition, Medicare expenses were significantly lower at critical access vs. non–critical access hospitals after factoring in risk-adjustment and price standardization ($14,450 vs. $15,845).
Overall, patients treated at critical access hospitals were significantly less likely than were those seen at non–critical access hospitals to have chronic medical problems including heart failure (8% vs. 10%), diabetes (20% vs. 22%), obesity (7% vs. 11%), and two or more comorbidities (60% vs. 70%). The average age of the patients was 77 years, and approximately half were women.

The findings on 30-day mortality and Medicare expenses contradict previous studies of nonsurgical admissions in critical access and non–critical access settings, the researchers noted. However, patients were less likely to proceed to post–acute care facilities from critical access hospitals compared with non–critical access hospitals.
“Based on information about admissions for common medical problems to these hospitals having higher mortality rates and decreased compliance with process measures, we thought this might be the same for surgical admissions,” the researchers said in the interview. “Our findings, however, show that critical access hospitals perform well for common surgical admissions with no difference in their risk-adjusted 30-day mortality rates.”
The results were limited by the use of administrative data, the potential overestimation of complication rates, and the lack of data on younger patients. The data illustrate how new payment models might impact critical care facilities, but several areas of research should be explored, the investigators said.
“First, we need a better understanding of how these small rural hospitals appear to be providing safe care at lower costs. Our data suggest it may be related to patient-selection, but even when we accounted for that in our models they still perform well,” they explained.
“Second, as many of these hospitals may in fact close in the next year, studies will be needed to inform how this might impact cost and access to rural surgical care. Finally, there are many other operations that we do not yet understand if they should be centralized to a large urban hospital, of if they are safe to be done in small hospital settings. As large health care systems continue to consolidate, each one will need a ‘health care systems architect’ to help organize how surgical services should be centralized or decentralized across their network to optimize both quality and access,” they added.
Dr. Ibrahim has received funding from the Robert Wood Johnson Foundation and the U.S. Department of Veterans Affairs. Dr. Justin Dimick has a financial interest in ArborMetrix Inc. and has received funds from the Agency for Healthcare Research and Quality and the National Institutes of Health, as well as honoraria from Stanford University, Emory University, and the University of Texas.
FROM JAMA
Key clinical point: Common surgical procedures can be performed at smaller hospitals safety and cost-effectively for appropriate patients.
Major finding: Thirty-day mortality rates were similar among patients at critical access and non–critical access hospitals (5.4% vs. 5.6%).
Data source: A cross-sectional, retrospective review of 1,631,904 Medicare beneficiary admissions for appendectomy, cholecystectomy, colectomy, or hernia repair.
Disclosures: Dr. Ibrahim has received funding from the Robert Wood Johnson Foundation and the U.S. Department of Veterans Affairs; coauthor Dr. Dennis Dimick has a financial interest in ArborMetrix Inc. and has received funds from the Agency for Healthcare Research and Quality and the National Institutes of Health, as well as honoraria from Stanford University, Emory University, and the University of Texas.
FDG-PET/CT leads pack for small-cell lung cancer staging
For pretreatment staging of small-cell lung cancer (SCLC) the use of positron-emission tomography combined with CT was more sensitive compared with several other tests, according to a new report on a review of studies.
Overall, positron emission tomography using [F]-fluorodeoxyglucose as a radiotracer combined with CT (FDG-PET/CT) had greater sensitivity to detect osseous metastases than did bone scintigraphy or CT alone, according to Dr. Jonathan R. Treadwell, Ph.D., of ECRI Institute–Penn Medicine’s Evidence-based Practice Center in Plymouth Meeting, Pa., and colleagues. In addition, the researchers concluded that adding FDG-PET/CT to the protocol for patients who have undergone standard staging increased the sensitivity for detecting additional metastases. Data on endobronchial ultrasound were insufficient to draw any conclusions.
The findings generally line up with recent guidelines from the American College of Radiology (ACR) and American College of Chest Physicians (ACCP). In 2014, the ACR gave the highest rating of “usually appropriate” (with regard to staging SCLC) to FDG-PET/CT from skull base to mid-thigh, while bone scintigraphy was rated as “may be appropriate” and not necessary if PET/CT had been done, the researchers wrote. The 2013 ACCP guideline “suggested” FDG PET instead of bone scintigraphy for patients with limited disease, they added.
The researchers reviewed data from seven studies to assess the accuracy and effectiveness of several imaging modalities for the pretreatment staging of SCLC. The report was generated for the Agency for Healthcare Research and Quality (AHRQ) as part of its Comparative Effectiveness Review series, and is not an official AHRQ position, the researchers noted.
Combining FDG-PET with CT scanning has demonstrated even greater effectiveness at identifying malignant tumors and metabolically active metastases than has PET alone, because the CT allows for more localized anatomic detail, the researchers explained. “False negative scans usually result from non–metabolically active sites of tumor or from suboptimal quality studies,” they said, while false positives using FDG-PET are usually attributed to inflammation or metabolically active infection.
The meta-analysis included data on endobronchial ultrasound, which involves ultrasound to view structures inside and adjacent to the airway; bone scintigraphy, a less expensive planar molecular imaging technique; and CT alone.
Comparative evidence on pretreatment staging for SCLC is limited, according to the researchers. The data did not allow them to determine how FDG-PET/CT compared to other imaging in terms of specificity, and any type of imaging can yield false positives, they said. However, higher sensitivity alone can benefit patients in terms of improving patient selection for optimal therapy, sparing patients chemotherapy if not needed, and improving the prediction value of ongoing research, they noted.
“Although high-quality evidence may not be voluminous, I think most physicians would agree with the conclusion that a bone scan is not mandatory in the work-up of possible SCLC, if a PET/CT has been done,” Dr. W. Michael Alberts of the Moffitt Cancer Center in Tampa, Fla., said in an interview.
Cost might play a role in why the guidelines are being issued at this time, he noted, because “the initial work-up of the patient with suspected SCLC may prove to be quite expensive, and the elimination of a superfluous test may be a fiscal winner.” However, more research is needed in this area, particularly in the areas of including the order of pretreatment testing and the incorporation of new procedures and imaging modalities, he added. “Perhaps more intellectually challenging, however, might be the question of why SCLC is becoming less common, or why has improvement in treatment been so slow compared to NSCLC,” he added.
The researchers had no financial conflicts to disclose.
For pretreatment staging of small-cell lung cancer (SCLC) the use of positron-emission tomography combined with CT was more sensitive compared with several other tests, according to a new report on a review of studies.
Overall, positron emission tomography using [F]-fluorodeoxyglucose as a radiotracer combined with CT (FDG-PET/CT) had greater sensitivity to detect osseous metastases than did bone scintigraphy or CT alone, according to Dr. Jonathan R. Treadwell, Ph.D., of ECRI Institute–Penn Medicine’s Evidence-based Practice Center in Plymouth Meeting, Pa., and colleagues. In addition, the researchers concluded that adding FDG-PET/CT to the protocol for patients who have undergone standard staging increased the sensitivity for detecting additional metastases. Data on endobronchial ultrasound were insufficient to draw any conclusions.
The findings generally line up with recent guidelines from the American College of Radiology (ACR) and American College of Chest Physicians (ACCP). In 2014, the ACR gave the highest rating of “usually appropriate” (with regard to staging SCLC) to FDG-PET/CT from skull base to mid-thigh, while bone scintigraphy was rated as “may be appropriate” and not necessary if PET/CT had been done, the researchers wrote. The 2013 ACCP guideline “suggested” FDG PET instead of bone scintigraphy for patients with limited disease, they added.
The researchers reviewed data from seven studies to assess the accuracy and effectiveness of several imaging modalities for the pretreatment staging of SCLC. The report was generated for the Agency for Healthcare Research and Quality (AHRQ) as part of its Comparative Effectiveness Review series, and is not an official AHRQ position, the researchers noted.
Combining FDG-PET with CT scanning has demonstrated even greater effectiveness at identifying malignant tumors and metabolically active metastases than has PET alone, because the CT allows for more localized anatomic detail, the researchers explained. “False negative scans usually result from non–metabolically active sites of tumor or from suboptimal quality studies,” they said, while false positives using FDG-PET are usually attributed to inflammation or metabolically active infection.
The meta-analysis included data on endobronchial ultrasound, which involves ultrasound to view structures inside and adjacent to the airway; bone scintigraphy, a less expensive planar molecular imaging technique; and CT alone.
Comparative evidence on pretreatment staging for SCLC is limited, according to the researchers. The data did not allow them to determine how FDG-PET/CT compared to other imaging in terms of specificity, and any type of imaging can yield false positives, they said. However, higher sensitivity alone can benefit patients in terms of improving patient selection for optimal therapy, sparing patients chemotherapy if not needed, and improving the prediction value of ongoing research, they noted.
“Although high-quality evidence may not be voluminous, I think most physicians would agree with the conclusion that a bone scan is not mandatory in the work-up of possible SCLC, if a PET/CT has been done,” Dr. W. Michael Alberts of the Moffitt Cancer Center in Tampa, Fla., said in an interview.
Cost might play a role in why the guidelines are being issued at this time, he noted, because “the initial work-up of the patient with suspected SCLC may prove to be quite expensive, and the elimination of a superfluous test may be a fiscal winner.” However, more research is needed in this area, particularly in the areas of including the order of pretreatment testing and the incorporation of new procedures and imaging modalities, he added. “Perhaps more intellectually challenging, however, might be the question of why SCLC is becoming less common, or why has improvement in treatment been so slow compared to NSCLC,” he added.
The researchers had no financial conflicts to disclose.
For pretreatment staging of small-cell lung cancer (SCLC) the use of positron-emission tomography combined with CT was more sensitive compared with several other tests, according to a new report on a review of studies.
Overall, positron emission tomography using [F]-fluorodeoxyglucose as a radiotracer combined with CT (FDG-PET/CT) had greater sensitivity to detect osseous metastases than did bone scintigraphy or CT alone, according to Dr. Jonathan R. Treadwell, Ph.D., of ECRI Institute–Penn Medicine’s Evidence-based Practice Center in Plymouth Meeting, Pa., and colleagues. In addition, the researchers concluded that adding FDG-PET/CT to the protocol for patients who have undergone standard staging increased the sensitivity for detecting additional metastases. Data on endobronchial ultrasound were insufficient to draw any conclusions.
The findings generally line up with recent guidelines from the American College of Radiology (ACR) and American College of Chest Physicians (ACCP). In 2014, the ACR gave the highest rating of “usually appropriate” (with regard to staging SCLC) to FDG-PET/CT from skull base to mid-thigh, while bone scintigraphy was rated as “may be appropriate” and not necessary if PET/CT had been done, the researchers wrote. The 2013 ACCP guideline “suggested” FDG PET instead of bone scintigraphy for patients with limited disease, they added.
The researchers reviewed data from seven studies to assess the accuracy and effectiveness of several imaging modalities for the pretreatment staging of SCLC. The report was generated for the Agency for Healthcare Research and Quality (AHRQ) as part of its Comparative Effectiveness Review series, and is not an official AHRQ position, the researchers noted.
Combining FDG-PET with CT scanning has demonstrated even greater effectiveness at identifying malignant tumors and metabolically active metastases than has PET alone, because the CT allows for more localized anatomic detail, the researchers explained. “False negative scans usually result from non–metabolically active sites of tumor or from suboptimal quality studies,” they said, while false positives using FDG-PET are usually attributed to inflammation or metabolically active infection.
The meta-analysis included data on endobronchial ultrasound, which involves ultrasound to view structures inside and adjacent to the airway; bone scintigraphy, a less expensive planar molecular imaging technique; and CT alone.
Comparative evidence on pretreatment staging for SCLC is limited, according to the researchers. The data did not allow them to determine how FDG-PET/CT compared to other imaging in terms of specificity, and any type of imaging can yield false positives, they said. However, higher sensitivity alone can benefit patients in terms of improving patient selection for optimal therapy, sparing patients chemotherapy if not needed, and improving the prediction value of ongoing research, they noted.
“Although high-quality evidence may not be voluminous, I think most physicians would agree with the conclusion that a bone scan is not mandatory in the work-up of possible SCLC, if a PET/CT has been done,” Dr. W. Michael Alberts of the Moffitt Cancer Center in Tampa, Fla., said in an interview.
Cost might play a role in why the guidelines are being issued at this time, he noted, because “the initial work-up of the patient with suspected SCLC may prove to be quite expensive, and the elimination of a superfluous test may be a fiscal winner.” However, more research is needed in this area, particularly in the areas of including the order of pretreatment testing and the incorporation of new procedures and imaging modalities, he added. “Perhaps more intellectually challenging, however, might be the question of why SCLC is becoming less common, or why has improvement in treatment been so slow compared to NSCLC,” he added.
The researchers had no financial conflicts to disclose.
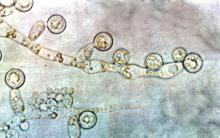
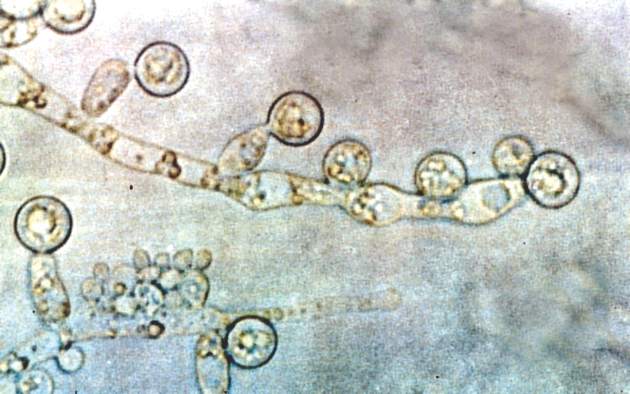
Candida linked to sex-specific schizophrenia symptoms
Exposure to Candida albicans significantly increased the odds of a schizophrenia diagnosis in men, according to case-control data from two cohorts of 947 adults.
“Fungal pathogens have not been extensively evaluated in studies of psychiatric disorders,” wrote Dr. Emily G. Severance of Johns Hopkins University in Baltimore, and her colleagues, in njp (Nature Partner Journals) Schizophrenia.
The researchers compared C. albicans IgG levels of individuals with schizophrenia and bipolar disorder with controls and found no diagnostic differences. However, stratification by sex showed a significantly increased risk of schizophrenia in men with elevated C. albicans IgG levels, with a ninefold increase in risk at the highest of three levels of seropositivity (odds ratio, 9.53). Elevated C. albicans levels in males with bipolar disorder were attributed to a history of homelessness.
C. albicans antibodies in women were not significantly different between groups. However, C. albicans was significantly associated with cognitive impairment in women with schizophrenia vs. control women (OR, 1.12), but no such difference was noted in men.
High levels of C. albicans antibodies were associated with comorbid gastrointestinal, genitourinary, and neoplastic conditions among individuals with psychiatric disorders overall.
“It may be premature to list this pathogen as a risk factor for disease causation, but its status as a comorbidity requires clinical attention,” the researchers wrote. “In the long term, more research is required to understand the mechanisms that trigger pathogenicity of fungal commensals and how this might impact brain function in psychiatric disorders.”
The findings were published in npj Schizophrenia. Read the full study here (npj Schizophrenia 2016 May 4. doi: 10.1038/npjschz.2016.18).
Exposure to Candida albicans significantly increased the odds of a schizophrenia diagnosis in men, according to case-control data from two cohorts of 947 adults.
“Fungal pathogens have not been extensively evaluated in studies of psychiatric disorders,” wrote Dr. Emily G. Severance of Johns Hopkins University in Baltimore, and her colleagues, in njp (Nature Partner Journals) Schizophrenia.
The researchers compared C. albicans IgG levels of individuals with schizophrenia and bipolar disorder with controls and found no diagnostic differences. However, stratification by sex showed a significantly increased risk of schizophrenia in men with elevated C. albicans IgG levels, with a ninefold increase in risk at the highest of three levels of seropositivity (odds ratio, 9.53). Elevated C. albicans levels in males with bipolar disorder were attributed to a history of homelessness.
C. albicans antibodies in women were not significantly different between groups. However, C. albicans was significantly associated with cognitive impairment in women with schizophrenia vs. control women (OR, 1.12), but no such difference was noted in men.
High levels of C. albicans antibodies were associated with comorbid gastrointestinal, genitourinary, and neoplastic conditions among individuals with psychiatric disorders overall.
“It may be premature to list this pathogen as a risk factor for disease causation, but its status as a comorbidity requires clinical attention,” the researchers wrote. “In the long term, more research is required to understand the mechanisms that trigger pathogenicity of fungal commensals and how this might impact brain function in psychiatric disorders.”
The findings were published in npj Schizophrenia. Read the full study here (npj Schizophrenia 2016 May 4. doi: 10.1038/npjschz.2016.18).
Exposure to Candida albicans significantly increased the odds of a schizophrenia diagnosis in men, according to case-control data from two cohorts of 947 adults.
“Fungal pathogens have not been extensively evaluated in studies of psychiatric disorders,” wrote Dr. Emily G. Severance of Johns Hopkins University in Baltimore, and her colleagues, in njp (Nature Partner Journals) Schizophrenia.
The researchers compared C. albicans IgG levels of individuals with schizophrenia and bipolar disorder with controls and found no diagnostic differences. However, stratification by sex showed a significantly increased risk of schizophrenia in men with elevated C. albicans IgG levels, with a ninefold increase in risk at the highest of three levels of seropositivity (odds ratio, 9.53). Elevated C. albicans levels in males with bipolar disorder were attributed to a history of homelessness.
C. albicans antibodies in women were not significantly different between groups. However, C. albicans was significantly associated with cognitive impairment in women with schizophrenia vs. control women (OR, 1.12), but no such difference was noted in men.
High levels of C. albicans antibodies were associated with comorbid gastrointestinal, genitourinary, and neoplastic conditions among individuals with psychiatric disorders overall.
“It may be premature to list this pathogen as a risk factor for disease causation, but its status as a comorbidity requires clinical attention,” the researchers wrote. “In the long term, more research is required to understand the mechanisms that trigger pathogenicity of fungal commensals and how this might impact brain function in psychiatric disorders.”
The findings were published in npj Schizophrenia. Read the full study here (npj Schizophrenia 2016 May 4. doi: 10.1038/npjschz.2016.18).
FROM NPJ SCHIZOPHRENIA
Extended PPI use accelerates cell aging
Long-term exposure to common nonprescription heartburn medication caused cells in blood vessels to age faster in a laboratory setting, compared with exposure to placebo, according to data published online May 10 in the American Heart Association’s journal, Circulation Research.
Proton pump inhibitors (PPIs) are routinely sold over the counter, mainly for gastroesophageal reflux disease, but data suggest that as much as 70% of PPI use is inappropriate, according to Gautham Yepuri, Ph.D., a postdoctoral research fellow at Houston Methodist Research Institute, and his associates.
The researchers examined how long-term use of PPIs might increase the risk of serious illnesses by studying cultured human microvascular endothelial cells (Circulation Research 2016 [doi: 10.1161/circresaha.116.308807]). They hypothesized that PPIs contribute to endothelial dysfunction, which in turn is associated with the development of conditions including heart disease, kidney disease, and dementia. They compared endothelial cells exposed to a PPI with those exposed to placebo.
Endothelial cells exposed to the PPI esomeprazole (ESO) showed reduced fluorescence “consistent with an increase in lysosomal pH,” the researchers wrote. In addition, endothelial cells treated with ESO demonstrated increased cell senescence and impaired endothelial function. PPI exposure also was associated with significant telomere shortening.
“This adverse effect appears to be due to an inhibition of lysosomal acidification and subsequent impairment of proteostasis,” the researchers noted. “In the presence of consistent epidemiological evidence of harm and a unifying mechanism for the disparate disorders linked to PPI use, and with the knowledge that PPIs are being used by millions of people for indications and durations that were never tested or approved, it is time for the pharmaceutical industry and regulatory agencies to revisit the specificity and the safety of these agents,” they stated. However, clinical studies are needed to determine whether the damage seen in the laboratory occurs in the body as well.
The study was funded in part by the National Institutes of Health and the Swiss National Science Foundation. The researchers reported having no financial conflicts to disclose.
Long-term exposure to common nonprescription heartburn medication caused cells in blood vessels to age faster in a laboratory setting, compared with exposure to placebo, according to data published online May 10 in the American Heart Association’s journal, Circulation Research.
Proton pump inhibitors (PPIs) are routinely sold over the counter, mainly for gastroesophageal reflux disease, but data suggest that as much as 70% of PPI use is inappropriate, according to Gautham Yepuri, Ph.D., a postdoctoral research fellow at Houston Methodist Research Institute, and his associates.
The researchers examined how long-term use of PPIs might increase the risk of serious illnesses by studying cultured human microvascular endothelial cells (Circulation Research 2016 [doi: 10.1161/circresaha.116.308807]). They hypothesized that PPIs contribute to endothelial dysfunction, which in turn is associated with the development of conditions including heart disease, kidney disease, and dementia. They compared endothelial cells exposed to a PPI with those exposed to placebo.
Endothelial cells exposed to the PPI esomeprazole (ESO) showed reduced fluorescence “consistent with an increase in lysosomal pH,” the researchers wrote. In addition, endothelial cells treated with ESO demonstrated increased cell senescence and impaired endothelial function. PPI exposure also was associated with significant telomere shortening.
“This adverse effect appears to be due to an inhibition of lysosomal acidification and subsequent impairment of proteostasis,” the researchers noted. “In the presence of consistent epidemiological evidence of harm and a unifying mechanism for the disparate disorders linked to PPI use, and with the knowledge that PPIs are being used by millions of people for indications and durations that were never tested or approved, it is time for the pharmaceutical industry and regulatory agencies to revisit the specificity and the safety of these agents,” they stated. However, clinical studies are needed to determine whether the damage seen in the laboratory occurs in the body as well.
The study was funded in part by the National Institutes of Health and the Swiss National Science Foundation. The researchers reported having no financial conflicts to disclose.
Long-term exposure to common nonprescription heartburn medication caused cells in blood vessels to age faster in a laboratory setting, compared with exposure to placebo, according to data published online May 10 in the American Heart Association’s journal, Circulation Research.
Proton pump inhibitors (PPIs) are routinely sold over the counter, mainly for gastroesophageal reflux disease, but data suggest that as much as 70% of PPI use is inappropriate, according to Gautham Yepuri, Ph.D., a postdoctoral research fellow at Houston Methodist Research Institute, and his associates.
The researchers examined how long-term use of PPIs might increase the risk of serious illnesses by studying cultured human microvascular endothelial cells (Circulation Research 2016 [doi: 10.1161/circresaha.116.308807]). They hypothesized that PPIs contribute to endothelial dysfunction, which in turn is associated with the development of conditions including heart disease, kidney disease, and dementia. They compared endothelial cells exposed to a PPI with those exposed to placebo.
Endothelial cells exposed to the PPI esomeprazole (ESO) showed reduced fluorescence “consistent with an increase in lysosomal pH,” the researchers wrote. In addition, endothelial cells treated with ESO demonstrated increased cell senescence and impaired endothelial function. PPI exposure also was associated with significant telomere shortening.
“This adverse effect appears to be due to an inhibition of lysosomal acidification and subsequent impairment of proteostasis,” the researchers noted. “In the presence of consistent epidemiological evidence of harm and a unifying mechanism for the disparate disorders linked to PPI use, and with the knowledge that PPIs are being used by millions of people for indications and durations that were never tested or approved, it is time for the pharmaceutical industry and regulatory agencies to revisit the specificity and the safety of these agents,” they stated. However, clinical studies are needed to determine whether the damage seen in the laboratory occurs in the body as well.
The study was funded in part by the National Institutes of Health and the Swiss National Science Foundation. The researchers reported having no financial conflicts to disclose.
FROM CIRCULATION RESEARCH
Key clinical point: PPIs impair endothelial lysosomal acidification, thereby contributing to cell aging.
Major finding: Telomere length, a sign of endothelial senescence, was significantly reduced in the cells exposed to PPIs, compared with placebo.
Data source: An examination comparing human endothelial cells exposed to PPIs with those exposed to placebo.
Disclosures: The study was funded in part by the National Institutes of Health and the Swiss National Science Foundation. The researchers had no financial conflicts to disclose.
Macitentan falls short to stop digital ulcers in systemic sclerosis
Macitentan failed to reduce digital ulcers in systemic sclerosis patients in a pair of randomized trials including approximately 500 adults. The findings were published online May 10 in JAMA.
Digital ulcers occur in 35%-68% of systemic sclerosis patients, and endothelin-1 (ET-1) has demonstrated overexpression in the plasma of these patients, wrote Dr. Dinesh Khanna of the University of Michigan, Ann Arbor, and colleagues (JAMA. 2016;315:1975-88. doi: 10.1001/jama.2016.5258).
To determine whether macitentan (Opsumit), a dual ET-receptor antagonist, reduced the number of new digital ulcers and their related disabilities, the researchers randomized adults aged 18 years and older with physician-diagnosed systemic sclerosis to oral macitentan doses of 3 mg or 10 mg or to placebo for 16 weeks. The first study, DUAL-1, enrolled 289 patients at a total of 70 centers in 17 countries; the second study, DUAL-2, included 265 patients from 73 centers in 20 countries. Macitentan is approved by the Food and Drug Administration for the treatment of pulmonary arterial hypertension.
A total of 226 patients completed DUAL-1 and 216 completed DUAL-2. Patients averaged 0.94 ulcers on 3 mg of oral macitentan, 1.08 ulcers on 10 mg of macitentan, and 0.85 ulcers on placebo in DUAL-1. The results were similar in DUAL-2, which was halted prematurely because the odds of benefits to the patients were deemed small.
No treatment effects were associated with either macitentan dose or placebo with regard to other endpoints, including complete healing of digital ulcers, hand function, and outcomes reported by physicians or patients. Serious adverse events occurred in 18% of the 3-mg macitentan group, 14% of the 10-mg group, and 13% of the placebo group in DUAL-1.
The results were limited by the lack of a standard classification system for digital ulcers, the researchers noted. However, “differences in physician attitudes and standard practices, and the lower than expected number of new digital ulcers after 16 weeks may have ultimately influenced the ability to demonstrate any treatment effect in the DUAL trials,” they said.
The study was funded by Actelion Pharmaceuticals, the manufacturer of macitentan. Dr. Khanna disclosed receiving grants from multiple organizations and companies and has received consulting fees from Actelion. Several coauthors are Actelion employees and stockholders.
Macitentan failed to reduce digital ulcers in systemic sclerosis patients in a pair of randomized trials including approximately 500 adults. The findings were published online May 10 in JAMA.
Digital ulcers occur in 35%-68% of systemic sclerosis patients, and endothelin-1 (ET-1) has demonstrated overexpression in the plasma of these patients, wrote Dr. Dinesh Khanna of the University of Michigan, Ann Arbor, and colleagues (JAMA. 2016;315:1975-88. doi: 10.1001/jama.2016.5258).
To determine whether macitentan (Opsumit), a dual ET-receptor antagonist, reduced the number of new digital ulcers and their related disabilities, the researchers randomized adults aged 18 years and older with physician-diagnosed systemic sclerosis to oral macitentan doses of 3 mg or 10 mg or to placebo for 16 weeks. The first study, DUAL-1, enrolled 289 patients at a total of 70 centers in 17 countries; the second study, DUAL-2, included 265 patients from 73 centers in 20 countries. Macitentan is approved by the Food and Drug Administration for the treatment of pulmonary arterial hypertension.
A total of 226 patients completed DUAL-1 and 216 completed DUAL-2. Patients averaged 0.94 ulcers on 3 mg of oral macitentan, 1.08 ulcers on 10 mg of macitentan, and 0.85 ulcers on placebo in DUAL-1. The results were similar in DUAL-2, which was halted prematurely because the odds of benefits to the patients were deemed small.
No treatment effects were associated with either macitentan dose or placebo with regard to other endpoints, including complete healing of digital ulcers, hand function, and outcomes reported by physicians or patients. Serious adverse events occurred in 18% of the 3-mg macitentan group, 14% of the 10-mg group, and 13% of the placebo group in DUAL-1.
The results were limited by the lack of a standard classification system for digital ulcers, the researchers noted. However, “differences in physician attitudes and standard practices, and the lower than expected number of new digital ulcers after 16 weeks may have ultimately influenced the ability to demonstrate any treatment effect in the DUAL trials,” they said.
The study was funded by Actelion Pharmaceuticals, the manufacturer of macitentan. Dr. Khanna disclosed receiving grants from multiple organizations and companies and has received consulting fees from Actelion. Several coauthors are Actelion employees and stockholders.
Macitentan failed to reduce digital ulcers in systemic sclerosis patients in a pair of randomized trials including approximately 500 adults. The findings were published online May 10 in JAMA.
Digital ulcers occur in 35%-68% of systemic sclerosis patients, and endothelin-1 (ET-1) has demonstrated overexpression in the plasma of these patients, wrote Dr. Dinesh Khanna of the University of Michigan, Ann Arbor, and colleagues (JAMA. 2016;315:1975-88. doi: 10.1001/jama.2016.5258).
To determine whether macitentan (Opsumit), a dual ET-receptor antagonist, reduced the number of new digital ulcers and their related disabilities, the researchers randomized adults aged 18 years and older with physician-diagnosed systemic sclerosis to oral macitentan doses of 3 mg or 10 mg or to placebo for 16 weeks. The first study, DUAL-1, enrolled 289 patients at a total of 70 centers in 17 countries; the second study, DUAL-2, included 265 patients from 73 centers in 20 countries. Macitentan is approved by the Food and Drug Administration for the treatment of pulmonary arterial hypertension.
A total of 226 patients completed DUAL-1 and 216 completed DUAL-2. Patients averaged 0.94 ulcers on 3 mg of oral macitentan, 1.08 ulcers on 10 mg of macitentan, and 0.85 ulcers on placebo in DUAL-1. The results were similar in DUAL-2, which was halted prematurely because the odds of benefits to the patients were deemed small.
No treatment effects were associated with either macitentan dose or placebo with regard to other endpoints, including complete healing of digital ulcers, hand function, and outcomes reported by physicians or patients. Serious adverse events occurred in 18% of the 3-mg macitentan group, 14% of the 10-mg group, and 13% of the placebo group in DUAL-1.
The results were limited by the lack of a standard classification system for digital ulcers, the researchers noted. However, “differences in physician attitudes and standard practices, and the lower than expected number of new digital ulcers after 16 weeks may have ultimately influenced the ability to demonstrate any treatment effect in the DUAL trials,” they said.
The study was funded by Actelion Pharmaceuticals, the manufacturer of macitentan. Dr. Khanna disclosed receiving grants from multiple organizations and companies and has received consulting fees from Actelion. Several coauthors are Actelion employees and stockholders.
FROM JAMA
Key clinical point: Macitentan did not reduce the number of new digital ulcers in systemic sclerosis patients in two 16-week studies.
Major finding: Patients averaged 0.94 ulcers on 3 mg of oral macitentan, 1.08 ulcers on 10 mg of macitentan, and 0.85 ulcers on placebo in DUAL-1; results were similar in DUAL-2.
Data source: A pair of randomized, double-blind, placebo-controlled trials (DUAL-1 and DUAL-2) including 289 and 265 patients, respectively, with systemic sclerosis and digital ulcers.
Disclosures: The study was funded by Actelion Pharmaceuticals, the manufacturer of macitentan. Dr. Khanna disclosed receiving grants from multiple organizations and companies and has received consulting fees from Actelion. Several coauthors are Actelion employees and stockholders.