User login
Sharp blood pressure rise spikes stroke risk
Individuals whose blood pressure rose sharply over time had a significantly increased risk of stroke and death from nonstroke causes, compared with other blood pressure trajectories in a study of more than 6,000 adults published online May 9 in Hypertension.
The current association of blood pressure with stroke does not account for variations in blood pressure trajectories over the long term, wrote Dr. M. Arfan Ikram of Erasmus University, Rotterdam, the Netherlands, and his colleagues.
The researchers reviewed data from 6,745 adults aged 55-106 years participating in the population-based Rotterdam Study, and identified four blood pressure trajectories over 5 decades. Class 1 included individuals whose blood pressure increased from 120 to 160 mm Hg; class 2 increased from 120 to 200 mm Hg; class 3 included those with moderate midlife blood pressure averaging 140 mm Hg; class 4 included those with a high midlife blood pressure averaging 160 mm Hg.
After controlling for confounding variables, class 3 had the highest overall risk of stroke, but the lowest risk of dying from a nonstroke event. Class 2 and class 4 individuals were at the greatest risk of stroke and of dying from nonstroke disease before 80 years of age. Class 1 individuals (with a normal baseline blood pressure and gradual increase) were least likely to suffer a stroke or die from a nonstroke event (Hypertension. 2016 May 9).
Although the study was limited by its homogenous nature (small geographical region, mostly white population), the findings show the importance of regular blood pressure measurement, the researchers noted.
“Identifying the patterns described in our study is an important step, since they evoke new causal and treatment questions that can motivate future studies to explore the etiologic significance and predictive value of associations,” they said. The researchers had no financial conflicts to disclose.
Individuals whose blood pressure rose sharply over time had a significantly increased risk of stroke and death from nonstroke causes, compared with other blood pressure trajectories in a study of more than 6,000 adults published online May 9 in Hypertension.
The current association of blood pressure with stroke does not account for variations in blood pressure trajectories over the long term, wrote Dr. M. Arfan Ikram of Erasmus University, Rotterdam, the Netherlands, and his colleagues.
The researchers reviewed data from 6,745 adults aged 55-106 years participating in the population-based Rotterdam Study, and identified four blood pressure trajectories over 5 decades. Class 1 included individuals whose blood pressure increased from 120 to 160 mm Hg; class 2 increased from 120 to 200 mm Hg; class 3 included those with moderate midlife blood pressure averaging 140 mm Hg; class 4 included those with a high midlife blood pressure averaging 160 mm Hg.
After controlling for confounding variables, class 3 had the highest overall risk of stroke, but the lowest risk of dying from a nonstroke event. Class 2 and class 4 individuals were at the greatest risk of stroke and of dying from nonstroke disease before 80 years of age. Class 1 individuals (with a normal baseline blood pressure and gradual increase) were least likely to suffer a stroke or die from a nonstroke event (Hypertension. 2016 May 9).
Although the study was limited by its homogenous nature (small geographical region, mostly white population), the findings show the importance of regular blood pressure measurement, the researchers noted.
“Identifying the patterns described in our study is an important step, since they evoke new causal and treatment questions that can motivate future studies to explore the etiologic significance and predictive value of associations,” they said. The researchers had no financial conflicts to disclose.
Individuals whose blood pressure rose sharply over time had a significantly increased risk of stroke and death from nonstroke causes, compared with other blood pressure trajectories in a study of more than 6,000 adults published online May 9 in Hypertension.
The current association of blood pressure with stroke does not account for variations in blood pressure trajectories over the long term, wrote Dr. M. Arfan Ikram of Erasmus University, Rotterdam, the Netherlands, and his colleagues.
The researchers reviewed data from 6,745 adults aged 55-106 years participating in the population-based Rotterdam Study, and identified four blood pressure trajectories over 5 decades. Class 1 included individuals whose blood pressure increased from 120 to 160 mm Hg; class 2 increased from 120 to 200 mm Hg; class 3 included those with moderate midlife blood pressure averaging 140 mm Hg; class 4 included those with a high midlife blood pressure averaging 160 mm Hg.
After controlling for confounding variables, class 3 had the highest overall risk of stroke, but the lowest risk of dying from a nonstroke event. Class 2 and class 4 individuals were at the greatest risk of stroke and of dying from nonstroke disease before 80 years of age. Class 1 individuals (with a normal baseline blood pressure and gradual increase) were least likely to suffer a stroke or die from a nonstroke event (Hypertension. 2016 May 9).
Although the study was limited by its homogenous nature (small geographical region, mostly white population), the findings show the importance of regular blood pressure measurement, the researchers noted.
“Identifying the patterns described in our study is an important step, since they evoke new causal and treatment questions that can motivate future studies to explore the etiologic significance and predictive value of associations,” they said. The researchers had no financial conflicts to disclose.
FROM HYPERTENSION
Key clinical point: Blood pressure trajectories can help develop prevention strategies.
Major finding: The risk of stroke was significantly higher in classes 2-4 (4.7%-13.6%) vs. 0.7% for class 1.
Data source: A review of 6,745 community-dwelling adults aged 55-106 years participating in a population-based study (the Rotterdam Study).
Disclosures: The researchers had no financial conflicts to disclose.
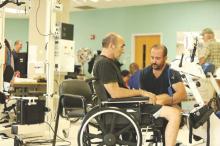
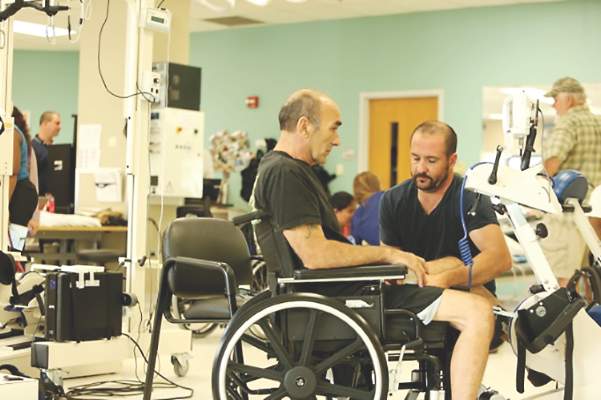
New stroke rehabilitation recommendations recognize role of interprofessional team
New guidelines issued jointly by the American Heart Association and American Stroke Association are the first to define multidisciplinary terms for stroke rehabilitation in adults. The guidelines were published online May 4 in the journal Stroke.
Previous guidelines have focused on medical issues related to stroke and its immediate aftermath, but the new document recognizes the importance of rehabilitation to quality of life, according to lead author Carolee J. Winstein, Ph.D., of the University of Southern California, Los Angeles, and colleagues (Stroke. 2016 May 4. doi: 10.1161/STR.0000000000000098).
In response to health care reform, the temptation remains to pare down postacute care and rehabilitation, “but without recognition of their clinical impact and ability to reduce the risk of downstream medical morbidity resulting from immobility, depression, loss of autonomy, and reduced functional independence,” the researchers wrote.
Considering the importance of early rehabilitation after stroke, the guidelines emphasize that initial rehabilitation occur in an inpatient facility rather than a nursing home setting, and that patients and caregivers be educated about fall prevention to reduce the risk of accidents once the patient arrives at home.
The guidelines consist of five sections: The Rehabilitation Program, Prevention and Medical Management of Comorbidities, Assessment, Sensorimotor Impairments and Activities, and Transitions in Care and Community Rehabilitation.
• The Rehabilitation Program. Options for poststroke rehabilitation should start with inpatient care, the researchers said. “It is recommended that stroke patients who are candidates for postacute rehabilitation receive organized, coordinated, interprofessional care,” they noted. Evidence suggests that such care reduces mortality and improves recovery and independence.
• Prevention and Medical Management of Comorbidities. Stroke is associated with a range of comorbid conditions, and the recommendations highlight several areas for which stroke patients should be evaluated regularly during rehabilitation, including skin breakdowns, hemiplegic limbs, urinary retention, and deep vein thrombosis.
• Assessment. Assessment of stroke patients should include communication abilities, motor ability, and ability to perform activities of daily living, the researchers wrote. “Evaluation of a stroke survivor’s rehabilitation needs is best performed by an interprofessional team that can include a physician with expertise in rehabilitation, nursing, PT, OT, speech therapy, case management, psychology, and orthotics,” they said.
• Sensorimotor Impairments and Activities. The researchers identified evidence to support management of dysphagia, which occurs in 42%-67% of stroke patients within 3 days after stroke. Screening and attention to cognitive impairment, limb apraxia, and hemispatial neglect should be part of stroke rehabilitation, they noted. Additional recommendations include tailored exercise programs; eye, speech, and balance therapy; mobility training; and a cognitively enriching environment that may include books, music, computer, and virtual reality games.
• Transitions in Care and Community Rehabilitation. The transition process should involve individualized discharge plans depending on the patient’s need for additional services, the researchers noted. Alternative communication methods such as telemedicine, web-based support, are reasonable options, especially for patients in rural areas, they noted. Resuming a previous lifestyle including work, driving, and recreational activities is recommended based on a tailored assessment of the individual’s needs and abilities for a particular job or activity.
Successful stroke rehabilitation is a team effort across medical specialties, the researchers emphasized. Communication and coordination “are paramount in maximizing the effectiveness and efficiency of rehabilitation and underlie this entire guideline,” they said.
Future directions for research in stroke rehabilitation include exploring models of care that view stroke as a chronic condition, developing more effective predictor models, and using new technology for personalized interventions, the researchers added.
The statement is the eighth and last in a set of stroke guidelines that completes the ASA recommendations on the continuum of care for stroke patients and families. The authors based the recommendations on a review of the relevant medical literature through 2014.
The guidelines are endorsed by the American Academy of Physical Medicine and Rehabilitation, the American Physical Therapy Association, the American Occupational Therapy Association, the American Society of Neurorehabilitation, and the American Congress of Rehabilitation Medicine. The American Academy of Neurology affirmed the value of the guidelines as an educational tool for neurologists.
Dr. Winstein has received research grants from the National Institutes of Health and serves as a consultant to St. Jude Medical Business Services. Some of the other authors reported receiving grants from the National Institutes of Health and/or industry, as well as serving as consultants or on an advisory board for various companies.
The guidelines are important to establish some form of common understanding or baseline of currently known best practices to treat and deliver rehabilitation to patients with stroke. Given recent health system studies suggesting significant variation in practices and cost across the United States, it is appropriate to describe guidelines that can set up standard practice. In addition, changes in the health care system toward population health make the creation of guidelines important, keeping in mind the current practices and frequent problems encountered when delivering rehabilitation to this patient population.
I think these guidelines might have a small chance to change clinical practice. On one side, it will provoke current providers to discuss what they are doing for this patient population, and what potential changes they need to do relative to the guidelines. However, it is also likely that current providers will not be compelled to change their habits for delivering care based on these guidelines.

|
Dr. Pablo Celnik |
On the other hand, while regulatory organization and insurance companies will likely look into this document to justify their practices, it is difficult to believe that they will change their policies based on this document. Nevertheless, this document, together with others, has the potential to create some momentum to advocate for best practices in stroke rehabilitation in a more homogeneous manner across the entire United States.
Rehabilitation has traditionally focused on improving the health and function of the individual. This is typically accomplished by training stroke survivors to deal with their deficits. However, many of the rehabilitation interventions have not been designed with a focus on restoring neurologic deficits. This may stem from a limited understanding of the mechanisms by which the brain recovers after stroke. However, recent studies have shown some of these mechanisms, and suggest potential approaches to augment restoration of neurologic function. Thus, more studies have tackled this problem by testing novel interventions such as high-intensity rehabilitation training using robots and games soon after the stroke (i.e., increasing the dose of training beyond that reported in the guidelines); carefully pairing noninvasive brain stimulation with training; or using exercises that take advantage of spared neurologic areas. Although these techniques have shown benefits in the laboratory setting, clinical trials are needed to determine whether they can be efficacious for broader stroke patient populations.
In sum, interventions specifically designed to restore neurologic deficits during stroke rehabilitation represent an important area of research that will need to be translated to the clinical setting and become part of best practices if proven effective. If we can reduce the amount of neurologic deficits after a stroke, it should result in a dramatic improvement of function at the individual level.
Dr. Pablo Celnik is a professor of physical medicine and rehabilitation at Johns Hopkins University in Baltimore, and medical director of the university’s outpatient neurorehabilitation program. He has received research funding from the National Institutes of Health. He was not involved in the drafting of the guidelines.
The guidelines are important to establish some form of common understanding or baseline of currently known best practices to treat and deliver rehabilitation to patients with stroke. Given recent health system studies suggesting significant variation in practices and cost across the United States, it is appropriate to describe guidelines that can set up standard practice. In addition, changes in the health care system toward population health make the creation of guidelines important, keeping in mind the current practices and frequent problems encountered when delivering rehabilitation to this patient population.
I think these guidelines might have a small chance to change clinical practice. On one side, it will provoke current providers to discuss what they are doing for this patient population, and what potential changes they need to do relative to the guidelines. However, it is also likely that current providers will not be compelled to change their habits for delivering care based on these guidelines.

|
Dr. Pablo Celnik |
On the other hand, while regulatory organization and insurance companies will likely look into this document to justify their practices, it is difficult to believe that they will change their policies based on this document. Nevertheless, this document, together with others, has the potential to create some momentum to advocate for best practices in stroke rehabilitation in a more homogeneous manner across the entire United States.
Rehabilitation has traditionally focused on improving the health and function of the individual. This is typically accomplished by training stroke survivors to deal with their deficits. However, many of the rehabilitation interventions have not been designed with a focus on restoring neurologic deficits. This may stem from a limited understanding of the mechanisms by which the brain recovers after stroke. However, recent studies have shown some of these mechanisms, and suggest potential approaches to augment restoration of neurologic function. Thus, more studies have tackled this problem by testing novel interventions such as high-intensity rehabilitation training using robots and games soon after the stroke (i.e., increasing the dose of training beyond that reported in the guidelines); carefully pairing noninvasive brain stimulation with training; or using exercises that take advantage of spared neurologic areas. Although these techniques have shown benefits in the laboratory setting, clinical trials are needed to determine whether they can be efficacious for broader stroke patient populations.
In sum, interventions specifically designed to restore neurologic deficits during stroke rehabilitation represent an important area of research that will need to be translated to the clinical setting and become part of best practices if proven effective. If we can reduce the amount of neurologic deficits after a stroke, it should result in a dramatic improvement of function at the individual level.
Dr. Pablo Celnik is a professor of physical medicine and rehabilitation at Johns Hopkins University in Baltimore, and medical director of the university’s outpatient neurorehabilitation program. He has received research funding from the National Institutes of Health. He was not involved in the drafting of the guidelines.
The guidelines are important to establish some form of common understanding or baseline of currently known best practices to treat and deliver rehabilitation to patients with stroke. Given recent health system studies suggesting significant variation in practices and cost across the United States, it is appropriate to describe guidelines that can set up standard practice. In addition, changes in the health care system toward population health make the creation of guidelines important, keeping in mind the current practices and frequent problems encountered when delivering rehabilitation to this patient population.
I think these guidelines might have a small chance to change clinical practice. On one side, it will provoke current providers to discuss what they are doing for this patient population, and what potential changes they need to do relative to the guidelines. However, it is also likely that current providers will not be compelled to change their habits for delivering care based on these guidelines.

|
Dr. Pablo Celnik |
On the other hand, while regulatory organization and insurance companies will likely look into this document to justify their practices, it is difficult to believe that they will change their policies based on this document. Nevertheless, this document, together with others, has the potential to create some momentum to advocate for best practices in stroke rehabilitation in a more homogeneous manner across the entire United States.
Rehabilitation has traditionally focused on improving the health and function of the individual. This is typically accomplished by training stroke survivors to deal with their deficits. However, many of the rehabilitation interventions have not been designed with a focus on restoring neurologic deficits. This may stem from a limited understanding of the mechanisms by which the brain recovers after stroke. However, recent studies have shown some of these mechanisms, and suggest potential approaches to augment restoration of neurologic function. Thus, more studies have tackled this problem by testing novel interventions such as high-intensity rehabilitation training using robots and games soon after the stroke (i.e., increasing the dose of training beyond that reported in the guidelines); carefully pairing noninvasive brain stimulation with training; or using exercises that take advantage of spared neurologic areas. Although these techniques have shown benefits in the laboratory setting, clinical trials are needed to determine whether they can be efficacious for broader stroke patient populations.
In sum, interventions specifically designed to restore neurologic deficits during stroke rehabilitation represent an important area of research that will need to be translated to the clinical setting and become part of best practices if proven effective. If we can reduce the amount of neurologic deficits after a stroke, it should result in a dramatic improvement of function at the individual level.
Dr. Pablo Celnik is a professor of physical medicine and rehabilitation at Johns Hopkins University in Baltimore, and medical director of the university’s outpatient neurorehabilitation program. He has received research funding from the National Institutes of Health. He was not involved in the drafting of the guidelines.
New guidelines issued jointly by the American Heart Association and American Stroke Association are the first to define multidisciplinary terms for stroke rehabilitation in adults. The guidelines were published online May 4 in the journal Stroke.
Previous guidelines have focused on medical issues related to stroke and its immediate aftermath, but the new document recognizes the importance of rehabilitation to quality of life, according to lead author Carolee J. Winstein, Ph.D., of the University of Southern California, Los Angeles, and colleagues (Stroke. 2016 May 4. doi: 10.1161/STR.0000000000000098).
In response to health care reform, the temptation remains to pare down postacute care and rehabilitation, “but without recognition of their clinical impact and ability to reduce the risk of downstream medical morbidity resulting from immobility, depression, loss of autonomy, and reduced functional independence,” the researchers wrote.
Considering the importance of early rehabilitation after stroke, the guidelines emphasize that initial rehabilitation occur in an inpatient facility rather than a nursing home setting, and that patients and caregivers be educated about fall prevention to reduce the risk of accidents once the patient arrives at home.
The guidelines consist of five sections: The Rehabilitation Program, Prevention and Medical Management of Comorbidities, Assessment, Sensorimotor Impairments and Activities, and Transitions in Care and Community Rehabilitation.
• The Rehabilitation Program. Options for poststroke rehabilitation should start with inpatient care, the researchers said. “It is recommended that stroke patients who are candidates for postacute rehabilitation receive organized, coordinated, interprofessional care,” they noted. Evidence suggests that such care reduces mortality and improves recovery and independence.
• Prevention and Medical Management of Comorbidities. Stroke is associated with a range of comorbid conditions, and the recommendations highlight several areas for which stroke patients should be evaluated regularly during rehabilitation, including skin breakdowns, hemiplegic limbs, urinary retention, and deep vein thrombosis.
• Assessment. Assessment of stroke patients should include communication abilities, motor ability, and ability to perform activities of daily living, the researchers wrote. “Evaluation of a stroke survivor’s rehabilitation needs is best performed by an interprofessional team that can include a physician with expertise in rehabilitation, nursing, PT, OT, speech therapy, case management, psychology, and orthotics,” they said.
• Sensorimotor Impairments and Activities. The researchers identified evidence to support management of dysphagia, which occurs in 42%-67% of stroke patients within 3 days after stroke. Screening and attention to cognitive impairment, limb apraxia, and hemispatial neglect should be part of stroke rehabilitation, they noted. Additional recommendations include tailored exercise programs; eye, speech, and balance therapy; mobility training; and a cognitively enriching environment that may include books, music, computer, and virtual reality games.
• Transitions in Care and Community Rehabilitation. The transition process should involve individualized discharge plans depending on the patient’s need for additional services, the researchers noted. Alternative communication methods such as telemedicine, web-based support, are reasonable options, especially for patients in rural areas, they noted. Resuming a previous lifestyle including work, driving, and recreational activities is recommended based on a tailored assessment of the individual’s needs and abilities for a particular job or activity.
Successful stroke rehabilitation is a team effort across medical specialties, the researchers emphasized. Communication and coordination “are paramount in maximizing the effectiveness and efficiency of rehabilitation and underlie this entire guideline,” they said.
Future directions for research in stroke rehabilitation include exploring models of care that view stroke as a chronic condition, developing more effective predictor models, and using new technology for personalized interventions, the researchers added.
The statement is the eighth and last in a set of stroke guidelines that completes the ASA recommendations on the continuum of care for stroke patients and families. The authors based the recommendations on a review of the relevant medical literature through 2014.
The guidelines are endorsed by the American Academy of Physical Medicine and Rehabilitation, the American Physical Therapy Association, the American Occupational Therapy Association, the American Society of Neurorehabilitation, and the American Congress of Rehabilitation Medicine. The American Academy of Neurology affirmed the value of the guidelines as an educational tool for neurologists.
Dr. Winstein has received research grants from the National Institutes of Health and serves as a consultant to St. Jude Medical Business Services. Some of the other authors reported receiving grants from the National Institutes of Health and/or industry, as well as serving as consultants or on an advisory board for various companies.
New guidelines issued jointly by the American Heart Association and American Stroke Association are the first to define multidisciplinary terms for stroke rehabilitation in adults. The guidelines were published online May 4 in the journal Stroke.
Previous guidelines have focused on medical issues related to stroke and its immediate aftermath, but the new document recognizes the importance of rehabilitation to quality of life, according to lead author Carolee J. Winstein, Ph.D., of the University of Southern California, Los Angeles, and colleagues (Stroke. 2016 May 4. doi: 10.1161/STR.0000000000000098).
In response to health care reform, the temptation remains to pare down postacute care and rehabilitation, “but without recognition of their clinical impact and ability to reduce the risk of downstream medical morbidity resulting from immobility, depression, loss of autonomy, and reduced functional independence,” the researchers wrote.
Considering the importance of early rehabilitation after stroke, the guidelines emphasize that initial rehabilitation occur in an inpatient facility rather than a nursing home setting, and that patients and caregivers be educated about fall prevention to reduce the risk of accidents once the patient arrives at home.
The guidelines consist of five sections: The Rehabilitation Program, Prevention and Medical Management of Comorbidities, Assessment, Sensorimotor Impairments and Activities, and Transitions in Care and Community Rehabilitation.
• The Rehabilitation Program. Options for poststroke rehabilitation should start with inpatient care, the researchers said. “It is recommended that stroke patients who are candidates for postacute rehabilitation receive organized, coordinated, interprofessional care,” they noted. Evidence suggests that such care reduces mortality and improves recovery and independence.
• Prevention and Medical Management of Comorbidities. Stroke is associated with a range of comorbid conditions, and the recommendations highlight several areas for which stroke patients should be evaluated regularly during rehabilitation, including skin breakdowns, hemiplegic limbs, urinary retention, and deep vein thrombosis.
• Assessment. Assessment of stroke patients should include communication abilities, motor ability, and ability to perform activities of daily living, the researchers wrote. “Evaluation of a stroke survivor’s rehabilitation needs is best performed by an interprofessional team that can include a physician with expertise in rehabilitation, nursing, PT, OT, speech therapy, case management, psychology, and orthotics,” they said.
• Sensorimotor Impairments and Activities. The researchers identified evidence to support management of dysphagia, which occurs in 42%-67% of stroke patients within 3 days after stroke. Screening and attention to cognitive impairment, limb apraxia, and hemispatial neglect should be part of stroke rehabilitation, they noted. Additional recommendations include tailored exercise programs; eye, speech, and balance therapy; mobility training; and a cognitively enriching environment that may include books, music, computer, and virtual reality games.
• Transitions in Care and Community Rehabilitation. The transition process should involve individualized discharge plans depending on the patient’s need for additional services, the researchers noted. Alternative communication methods such as telemedicine, web-based support, are reasonable options, especially for patients in rural areas, they noted. Resuming a previous lifestyle including work, driving, and recreational activities is recommended based on a tailored assessment of the individual’s needs and abilities for a particular job or activity.
Successful stroke rehabilitation is a team effort across medical specialties, the researchers emphasized. Communication and coordination “are paramount in maximizing the effectiveness and efficiency of rehabilitation and underlie this entire guideline,” they said.
Future directions for research in stroke rehabilitation include exploring models of care that view stroke as a chronic condition, developing more effective predictor models, and using new technology for personalized interventions, the researchers added.
The statement is the eighth and last in a set of stroke guidelines that completes the ASA recommendations on the continuum of care for stroke patients and families. The authors based the recommendations on a review of the relevant medical literature through 2014.
The guidelines are endorsed by the American Academy of Physical Medicine and Rehabilitation, the American Physical Therapy Association, the American Occupational Therapy Association, the American Society of Neurorehabilitation, and the American Congress of Rehabilitation Medicine. The American Academy of Neurology affirmed the value of the guidelines as an educational tool for neurologists.
Dr. Winstein has received research grants from the National Institutes of Health and serves as a consultant to St. Jude Medical Business Services. Some of the other authors reported receiving grants from the National Institutes of Health and/or industry, as well as serving as consultants or on an advisory board for various companies.
FROM STROKE
Autism screening rises after process-based training
A 3- to 6-month learning program for pediatric and family medicine providers significantly improved their screening for autism spectrum disorders (ASD) at 18- and 24-month well child visits, based on data from 26 primary care practices that participated in the program and from 43 physicians who completed surveys before and after the program, according to findings published online May 5 in Pediatrics.
“Unlike traditional continuing medical education, the LC [learning collaborative] focused on improvement of processes of care at the practice level,” wrote Dr. Paul S. Carbone and his colleagues of the University of Utah, Salt Lake City. The first signs of ASD can be present as early as 2 years of age, but often remain undiagnosed for lack of screening at 18- and 24-month visits, they noted.
Rates of documented ASD screening among toddlers increased from 16% before starting the program to 91% during the last month of the program, and 70% of the practices sustained the 91% screening rate 4 years later.
Physician self-efficacy improved significantly from baseline to after the program on the nine autism conditions (such as sleep problems, constipation, and attention deficit/hyperactivity disorder [ADHD]) and seven autism needs (such as making referrals, addressing developmental concerns, and identifying community support services) included in the survey. On a scale of 1 to 10, the average physician’s progress rating was 6.5 after completing the program.
“A LC using the methods we describe is a successful approach to improving the early identification and ongoing care of children with ASD in primary care practices,” they researchers said.
Read the whole article at Pediatrics (2016 May. doi: 10.1542/peds.2015-1850).
A 3- to 6-month learning program for pediatric and family medicine providers significantly improved their screening for autism spectrum disorders (ASD) at 18- and 24-month well child visits, based on data from 26 primary care practices that participated in the program and from 43 physicians who completed surveys before and after the program, according to findings published online May 5 in Pediatrics.
“Unlike traditional continuing medical education, the LC [learning collaborative] focused on improvement of processes of care at the practice level,” wrote Dr. Paul S. Carbone and his colleagues of the University of Utah, Salt Lake City. The first signs of ASD can be present as early as 2 years of age, but often remain undiagnosed for lack of screening at 18- and 24-month visits, they noted.
Rates of documented ASD screening among toddlers increased from 16% before starting the program to 91% during the last month of the program, and 70% of the practices sustained the 91% screening rate 4 years later.
Physician self-efficacy improved significantly from baseline to after the program on the nine autism conditions (such as sleep problems, constipation, and attention deficit/hyperactivity disorder [ADHD]) and seven autism needs (such as making referrals, addressing developmental concerns, and identifying community support services) included in the survey. On a scale of 1 to 10, the average physician’s progress rating was 6.5 after completing the program.
“A LC using the methods we describe is a successful approach to improving the early identification and ongoing care of children with ASD in primary care practices,” they researchers said.
Read the whole article at Pediatrics (2016 May. doi: 10.1542/peds.2015-1850).
A 3- to 6-month learning program for pediatric and family medicine providers significantly improved their screening for autism spectrum disorders (ASD) at 18- and 24-month well child visits, based on data from 26 primary care practices that participated in the program and from 43 physicians who completed surveys before and after the program, according to findings published online May 5 in Pediatrics.
“Unlike traditional continuing medical education, the LC [learning collaborative] focused on improvement of processes of care at the practice level,” wrote Dr. Paul S. Carbone and his colleagues of the University of Utah, Salt Lake City. The first signs of ASD can be present as early as 2 years of age, but often remain undiagnosed for lack of screening at 18- and 24-month visits, they noted.
Rates of documented ASD screening among toddlers increased from 16% before starting the program to 91% during the last month of the program, and 70% of the practices sustained the 91% screening rate 4 years later.
Physician self-efficacy improved significantly from baseline to after the program on the nine autism conditions (such as sleep problems, constipation, and attention deficit/hyperactivity disorder [ADHD]) and seven autism needs (such as making referrals, addressing developmental concerns, and identifying community support services) included in the survey. On a scale of 1 to 10, the average physician’s progress rating was 6.5 after completing the program.
“A LC using the methods we describe is a successful approach to improving the early identification and ongoing care of children with ASD in primary care practices,” they researchers said.
Read the whole article at Pediatrics (2016 May. doi: 10.1542/peds.2015-1850).
FROM PEDIATRICS
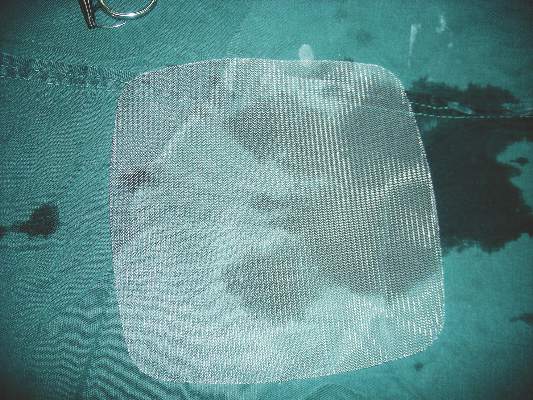
Light mesh doesn’t outweigh heavy mesh for hernia repair
Lightweight mesh has no significant benefit over heavyweight mesh for inguinal hernia repair and was associated with greater pain and higher risk of recurrence, based on data from a randomized trial of 950 patients published in the May issue of the Annals of Surgery.
Although the use of mesh for hernia surgery has been associated with lower recurrence rates and less chronic pain in open hernia repair procedures, the benefits of lightweight vs. heavyweight mesh for laparoscopic procedures has not been well studied, “and there is no consensus which type of mesh is optimal in these procedures,” wrote Dr. Josephina P.J. Burgmans of Diakonessenhuis Utrecht/Zeist (the Netherlands) and colleagues (Ann. Surg. 2016;263[5]:862-6).
To compare the clinical outcomes for patients who received lightweight vs. heavyweight mesh in hernia repairs, the researchers randomized 478 patients to a lightweight-mesh group and 471 to a heavyweight-mesh group. One patient was excluded because the type of mesh was unknown. The study population included men older than 18 years with a primary, reducible, unilateral inguinal hernia who underwent surgery at a single center with one of four surgeons between March 2010 and October 2012. Demographic characteristics were similar between the two groups, as were preoperation pain, operation time, and complications during and after surgery.
At 1 year post surgery, the prevalence of reported relevant pain was significantly higher in the lightweight group, compared with the heavyweight group (2.9% vs. 0.7%). The difference remained statistically significant at 2 years’ follow-up, with relevant pain reported in 3.0% of the lightweight group and 0.9% of the heavyweight group; the difference also remained significant after controlling for factors including age, body mass index, hernia type, severe preoperative pain, recurrence, and surgeon).
Recurrence rates were similar between the two groups at 3 months (two cases in each group), but recurrences became more common in the lightweight group, compared with the heavyweight group, at 1 year (1.7% vs. 0.6%) and significantly more common at 2 years (2.7% vs. 0.8%). The difference remained significant after controlling for multiple variables including hernia type, operating time, surgeon, and body mass index.
No significant differences in foreign body feeling, testicular pain, or sexual-related pain or discomfort were reported between the two groups at the 1-year and 2-year follow-ups.
The study’s strengths include the large patient population and prospective data collection, the researchers noted. The findings were limited by the small number of patients with relevant pain at 1 and 2 years; the homogenous, male-only study population; and the use of questionnaires, which might affect the accuracy of recurrence-rate reports. The results, however, suggest that “there is no benefit for lightweight [meshes] and a conventional heavyweight standard polypropylene 10 cm × 15 cm mesh is recommended for laparoscopic inguinal hernia repair,” Dr. Burgmans and associates wrote
The study was sponsored in part by a grant to the Hernia Centre Zeist from Johnson & Johnston. The researchers had no other relevant financial conflicts to disclose.
Lightweight mesh has no significant benefit over heavyweight mesh for inguinal hernia repair and was associated with greater pain and higher risk of recurrence, based on data from a randomized trial of 950 patients published in the May issue of the Annals of Surgery.
Although the use of mesh for hernia surgery has been associated with lower recurrence rates and less chronic pain in open hernia repair procedures, the benefits of lightweight vs. heavyweight mesh for laparoscopic procedures has not been well studied, “and there is no consensus which type of mesh is optimal in these procedures,” wrote Dr. Josephina P.J. Burgmans of Diakonessenhuis Utrecht/Zeist (the Netherlands) and colleagues (Ann. Surg. 2016;263[5]:862-6).
To compare the clinical outcomes for patients who received lightweight vs. heavyweight mesh in hernia repairs, the researchers randomized 478 patients to a lightweight-mesh group and 471 to a heavyweight-mesh group. One patient was excluded because the type of mesh was unknown. The study population included men older than 18 years with a primary, reducible, unilateral inguinal hernia who underwent surgery at a single center with one of four surgeons between March 2010 and October 2012. Demographic characteristics were similar between the two groups, as were preoperation pain, operation time, and complications during and after surgery.
At 1 year post surgery, the prevalence of reported relevant pain was significantly higher in the lightweight group, compared with the heavyweight group (2.9% vs. 0.7%). The difference remained statistically significant at 2 years’ follow-up, with relevant pain reported in 3.0% of the lightweight group and 0.9% of the heavyweight group; the difference also remained significant after controlling for factors including age, body mass index, hernia type, severe preoperative pain, recurrence, and surgeon).
Recurrence rates were similar between the two groups at 3 months (two cases in each group), but recurrences became more common in the lightweight group, compared with the heavyweight group, at 1 year (1.7% vs. 0.6%) and significantly more common at 2 years (2.7% vs. 0.8%). The difference remained significant after controlling for multiple variables including hernia type, operating time, surgeon, and body mass index.
No significant differences in foreign body feeling, testicular pain, or sexual-related pain or discomfort were reported between the two groups at the 1-year and 2-year follow-ups.
The study’s strengths include the large patient population and prospective data collection, the researchers noted. The findings were limited by the small number of patients with relevant pain at 1 and 2 years; the homogenous, male-only study population; and the use of questionnaires, which might affect the accuracy of recurrence-rate reports. The results, however, suggest that “there is no benefit for lightweight [meshes] and a conventional heavyweight standard polypropylene 10 cm × 15 cm mesh is recommended for laparoscopic inguinal hernia repair,” Dr. Burgmans and associates wrote
The study was sponsored in part by a grant to the Hernia Centre Zeist from Johnson & Johnston. The researchers had no other relevant financial conflicts to disclose.
Lightweight mesh has no significant benefit over heavyweight mesh for inguinal hernia repair and was associated with greater pain and higher risk of recurrence, based on data from a randomized trial of 950 patients published in the May issue of the Annals of Surgery.
Although the use of mesh for hernia surgery has been associated with lower recurrence rates and less chronic pain in open hernia repair procedures, the benefits of lightweight vs. heavyweight mesh for laparoscopic procedures has not been well studied, “and there is no consensus which type of mesh is optimal in these procedures,” wrote Dr. Josephina P.J. Burgmans of Diakonessenhuis Utrecht/Zeist (the Netherlands) and colleagues (Ann. Surg. 2016;263[5]:862-6).
To compare the clinical outcomes for patients who received lightweight vs. heavyweight mesh in hernia repairs, the researchers randomized 478 patients to a lightweight-mesh group and 471 to a heavyweight-mesh group. One patient was excluded because the type of mesh was unknown. The study population included men older than 18 years with a primary, reducible, unilateral inguinal hernia who underwent surgery at a single center with one of four surgeons between March 2010 and October 2012. Demographic characteristics were similar between the two groups, as were preoperation pain, operation time, and complications during and after surgery.
At 1 year post surgery, the prevalence of reported relevant pain was significantly higher in the lightweight group, compared with the heavyweight group (2.9% vs. 0.7%). The difference remained statistically significant at 2 years’ follow-up, with relevant pain reported in 3.0% of the lightweight group and 0.9% of the heavyweight group; the difference also remained significant after controlling for factors including age, body mass index, hernia type, severe preoperative pain, recurrence, and surgeon).
Recurrence rates were similar between the two groups at 3 months (two cases in each group), but recurrences became more common in the lightweight group, compared with the heavyweight group, at 1 year (1.7% vs. 0.6%) and significantly more common at 2 years (2.7% vs. 0.8%). The difference remained significant after controlling for multiple variables including hernia type, operating time, surgeon, and body mass index.
No significant differences in foreign body feeling, testicular pain, or sexual-related pain or discomfort were reported between the two groups at the 1-year and 2-year follow-ups.
The study’s strengths include the large patient population and prospective data collection, the researchers noted. The findings were limited by the small number of patients with relevant pain at 1 and 2 years; the homogenous, male-only study population; and the use of questionnaires, which might affect the accuracy of recurrence-rate reports. The results, however, suggest that “there is no benefit for lightweight [meshes] and a conventional heavyweight standard polypropylene 10 cm × 15 cm mesh is recommended for laparoscopic inguinal hernia repair,” Dr. Burgmans and associates wrote
The study was sponsored in part by a grant to the Hernia Centre Zeist from Johnson & Johnston. The researchers had no other relevant financial conflicts to disclose.
FROM ANNALS OF SURGERY
Key clinical point: Lightweight mesh was associated with more pain and higher recurrence risk 1 and 2 years after surgery.
Major finding: Two years after surgery, relevant pain was reported in 3.0% of the lightweight-mesh patients vs. 0.9% of heavyweight-mesh patients.
Data source: A randomized trial including 950 adult men with inguinal hernias.
Disclosures: The study was sponsored in part by a grant to the Hernia Centre Zeist from Johnson & Johnston. The researchers had no other relevant financial conflicts to disclose.
Cell-based strategy curbs constipation
Treatment at the nanomolecular level may become an alternative for various types of constipation, in particular for the opioid-induced constipation that is common after surgery, based on data from a proof of concept study involving mice and a small-molecule activator.
“Activation of the cystic fibrosis transmembrane conductance regulator (CFTR) chloride channel is the primary pathway that drives fluid secretion in the intestine, which maintains lubrication of luminal contents,” wrote Dr. Onur Cil of the University of California, San Francisco, and colleagues. The researchers examined whether direct activation of the CFTR would prompt fluid secretion and reverse stool dehydration when applied to constipated mice. The findings were published online in the May issue of the journal Cellular and Molecular Gastroenterology and Hepatology (2016. doi: 10.1016/j.jcmgh.2015.12.010).
The researchers identified a promising activator, the phenylquinoxalinone CFTRact-J027. Mice received up to 10 mg/kg CFTRact-J027 either orally or intraperitoneally (IP), with doses including 0.1 mg/kg, 0.3 mg/kg, 1 mg/kg, 3 mg/kg, and 10 mg/kg.
Overall, IP doses of CFTRact-J027 at 10 mg/kg normalized stool in the constipated mice, and dose-response studies showed a 50% effective dose of 2 mg/kg in these mice.
When given orally, CFTRact-J027 “normalized stool output and water content in a loperamide-induced mouse model of constipation with a 50% effective dose of approximately 0.5 mg/kg,” that was significantly lower than the IP administration, the researchers noted. An oral dose of 10 mg/kg CFTRact-J027 1 hour before inducing constipation also was effective in normalizing stool output and water content in loperamide-treated mice, with no effect in control nonconstipated mice.
The activator was not effective against constipation in cystic fibrosis mice that were missing a functional CFTR, they added.
The researchers used an in vivo closed loop model to specifically test the effects of CFTRact-J027 on intestinal fluid secretion and absorption and found that CFTRact-J027 caused “a 140% increase in loop weight/length ratio, indicating fluid secretion into the intestinal lumen in wild-type mice.” However, there was no effect in cystic fibrosis mice, further supporting the CFTR-selective mechanism of action, the researchers said.
As for potential toxic effects of the treatment, CFTRact-J027 showed no impact on the major serum chemistry and blood parameters of the mice after 7 days, and had no apparent impact on body weight. No accumulation of fluid (the most significant potential adverse effect) was noted in the airway or lungs of the treated mice.
Additional toxicity data are needed to continue preclinical development, the researchers said. However, “our data provide evidence for the prosecretory action of a CFTR activator in mouse intestine and proof of concept for its use in the treatment of various types of constipation, which could include opioid-induced constipation, chronic idiopathic constipation, and irritable bowel syndrome with constipation predominance,” they wrote. In addition, a CFTR activator similar to that used in this study may have clinical applications for other conditions including asthma, dry eye, cholestatic liver disease, chronic obstructive pulmonary disease and bronchitis, and cigarette smoke–induced lung dysfunction, they added.
Dr. Cil and two coauthors are inventors on a provisional patent filing, with rights owned by the University of California, San Francisco. The study was funded in part by several grants from organizations including the National Institutes of Health and the Cystic Fibrosis Foundation.
Treatment at the nanomolecular level may become an alternative for various types of constipation, in particular for the opioid-induced constipation that is common after surgery, based on data from a proof of concept study involving mice and a small-molecule activator.
“Activation of the cystic fibrosis transmembrane conductance regulator (CFTR) chloride channel is the primary pathway that drives fluid secretion in the intestine, which maintains lubrication of luminal contents,” wrote Dr. Onur Cil of the University of California, San Francisco, and colleagues. The researchers examined whether direct activation of the CFTR would prompt fluid secretion and reverse stool dehydration when applied to constipated mice. The findings were published online in the May issue of the journal Cellular and Molecular Gastroenterology and Hepatology (2016. doi: 10.1016/j.jcmgh.2015.12.010).
The researchers identified a promising activator, the phenylquinoxalinone CFTRact-J027. Mice received up to 10 mg/kg CFTRact-J027 either orally or intraperitoneally (IP), with doses including 0.1 mg/kg, 0.3 mg/kg, 1 mg/kg, 3 mg/kg, and 10 mg/kg.
Overall, IP doses of CFTRact-J027 at 10 mg/kg normalized stool in the constipated mice, and dose-response studies showed a 50% effective dose of 2 mg/kg in these mice.
When given orally, CFTRact-J027 “normalized stool output and water content in a loperamide-induced mouse model of constipation with a 50% effective dose of approximately 0.5 mg/kg,” that was significantly lower than the IP administration, the researchers noted. An oral dose of 10 mg/kg CFTRact-J027 1 hour before inducing constipation also was effective in normalizing stool output and water content in loperamide-treated mice, with no effect in control nonconstipated mice.
The activator was not effective against constipation in cystic fibrosis mice that were missing a functional CFTR, they added.
The researchers used an in vivo closed loop model to specifically test the effects of CFTRact-J027 on intestinal fluid secretion and absorption and found that CFTRact-J027 caused “a 140% increase in loop weight/length ratio, indicating fluid secretion into the intestinal lumen in wild-type mice.” However, there was no effect in cystic fibrosis mice, further supporting the CFTR-selective mechanism of action, the researchers said.
As for potential toxic effects of the treatment, CFTRact-J027 showed no impact on the major serum chemistry and blood parameters of the mice after 7 days, and had no apparent impact on body weight. No accumulation of fluid (the most significant potential adverse effect) was noted in the airway or lungs of the treated mice.
Additional toxicity data are needed to continue preclinical development, the researchers said. However, “our data provide evidence for the prosecretory action of a CFTR activator in mouse intestine and proof of concept for its use in the treatment of various types of constipation, which could include opioid-induced constipation, chronic idiopathic constipation, and irritable bowel syndrome with constipation predominance,” they wrote. In addition, a CFTR activator similar to that used in this study may have clinical applications for other conditions including asthma, dry eye, cholestatic liver disease, chronic obstructive pulmonary disease and bronchitis, and cigarette smoke–induced lung dysfunction, they added.
Dr. Cil and two coauthors are inventors on a provisional patent filing, with rights owned by the University of California, San Francisco. The study was funded in part by several grants from organizations including the National Institutes of Health and the Cystic Fibrosis Foundation.
Treatment at the nanomolecular level may become an alternative for various types of constipation, in particular for the opioid-induced constipation that is common after surgery, based on data from a proof of concept study involving mice and a small-molecule activator.
“Activation of the cystic fibrosis transmembrane conductance regulator (CFTR) chloride channel is the primary pathway that drives fluid secretion in the intestine, which maintains lubrication of luminal contents,” wrote Dr. Onur Cil of the University of California, San Francisco, and colleagues. The researchers examined whether direct activation of the CFTR would prompt fluid secretion and reverse stool dehydration when applied to constipated mice. The findings were published online in the May issue of the journal Cellular and Molecular Gastroenterology and Hepatology (2016. doi: 10.1016/j.jcmgh.2015.12.010).
The researchers identified a promising activator, the phenylquinoxalinone CFTRact-J027. Mice received up to 10 mg/kg CFTRact-J027 either orally or intraperitoneally (IP), with doses including 0.1 mg/kg, 0.3 mg/kg, 1 mg/kg, 3 mg/kg, and 10 mg/kg.
Overall, IP doses of CFTRact-J027 at 10 mg/kg normalized stool in the constipated mice, and dose-response studies showed a 50% effective dose of 2 mg/kg in these mice.
When given orally, CFTRact-J027 “normalized stool output and water content in a loperamide-induced mouse model of constipation with a 50% effective dose of approximately 0.5 mg/kg,” that was significantly lower than the IP administration, the researchers noted. An oral dose of 10 mg/kg CFTRact-J027 1 hour before inducing constipation also was effective in normalizing stool output and water content in loperamide-treated mice, with no effect in control nonconstipated mice.
The activator was not effective against constipation in cystic fibrosis mice that were missing a functional CFTR, they added.
The researchers used an in vivo closed loop model to specifically test the effects of CFTRact-J027 on intestinal fluid secretion and absorption and found that CFTRact-J027 caused “a 140% increase in loop weight/length ratio, indicating fluid secretion into the intestinal lumen in wild-type mice.” However, there was no effect in cystic fibrosis mice, further supporting the CFTR-selective mechanism of action, the researchers said.
As for potential toxic effects of the treatment, CFTRact-J027 showed no impact on the major serum chemistry and blood parameters of the mice after 7 days, and had no apparent impact on body weight. No accumulation of fluid (the most significant potential adverse effect) was noted in the airway or lungs of the treated mice.
Additional toxicity data are needed to continue preclinical development, the researchers said. However, “our data provide evidence for the prosecretory action of a CFTR activator in mouse intestine and proof of concept for its use in the treatment of various types of constipation, which could include opioid-induced constipation, chronic idiopathic constipation, and irritable bowel syndrome with constipation predominance,” they wrote. In addition, a CFTR activator similar to that used in this study may have clinical applications for other conditions including asthma, dry eye, cholestatic liver disease, chronic obstructive pulmonary disease and bronchitis, and cigarette smoke–induced lung dysfunction, they added.
Dr. Cil and two coauthors are inventors on a provisional patent filing, with rights owned by the University of California, San Francisco. The study was funded in part by several grants from organizations including the National Institutes of Health and the Cystic Fibrosis Foundation.
FROM CELLULAR AND MOLECULAR GASTROENTEROLOGY AND HEPATOLOGY
Key clinical point: Treatment at the nanomolecular level may become an alternative for various types of constipation.
Major finding: Oral doses of CFTRact-J027 normalized stool output and water content in a loperamide-induced mouse model of constipation with a 50% effective dose of approximately 0.5 mg/kg.
Data source: A proof-of-concept study in which a cell-based screen was performed for 120,000 druglike, synthetic small molecules that were then tested in constipation-induced mice and control mice.
Disclosures: Dr. Cil and two coauthors are inventors on a provisional patent filing, with rights owned by the University of California, San Francisco. The study was funded in part by several grants from organizations including the National Institutes of Health and the Cystic Fibrosis Foundation.
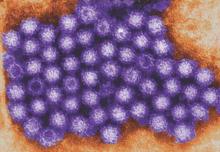
Norovirus costs $60 billion worldwide, making inroads in U.S.
The global economic impact of norovirus is roughly $60 billion in societal costs and $4 billion in direct health care costs per year, according to an simulation model analysis.
Most of the costs (84%-99%, varying by region) resulted from lost productivity. The total societal cost was highest in children younger than 5 years, nearly $40 billion, compared with $20 billion for all other age groups combined, but the cost per illness was highest among adults aged 55 years and older.
Disease incidence was similar across all countries in the simulation model that included 233 countries stratified by World Health Organization region and globally but high-income countries accounted for 62% of the global health system costs, wrote Sarah M. Bartsch of Johns Hopkins University, Baltimore, and colleagues (PLoS ONE 2016. doi: 10.1371/journal.pone.0151219).
In the United States, norovirus was the most common pathogen identified in cases of acute gastroenteritis (AGE, 6%), followed by rotavirus and sapovirus (2% for both) and astrovirus (1%), according to data from a population-based study, including 1,099 stool specimens collected between August 2012 and September 2013. These findings were published in a separate study (PLoS ONE 2016. doi: 10.1371/journal.pone.0148395).
Overall, U.S. children younger than 5 years of age had the highest prevalence of norovirus; outpatient incidence and community incidences were 25.6 and 152.2 per 1,000 person-years, respectively. The next highest norovirus prevalence occurred in adults older than 65 years; outpatient and community incidence were 7.8 and 7.8 per 1,000 person-years, respectively. The study provides “the first U.S. laboratory-based age-specific norovirus AGE incidence rates in both community and outpatient settings,” wrote Scott P. Grytdal of the Centers for Disease Control and Prevention in Atlanta, and colleagues.
The global economic impact of norovirus is roughly $60 billion in societal costs and $4 billion in direct health care costs per year, according to an simulation model analysis.
Most of the costs (84%-99%, varying by region) resulted from lost productivity. The total societal cost was highest in children younger than 5 years, nearly $40 billion, compared with $20 billion for all other age groups combined, but the cost per illness was highest among adults aged 55 years and older.
Disease incidence was similar across all countries in the simulation model that included 233 countries stratified by World Health Organization region and globally but high-income countries accounted for 62% of the global health system costs, wrote Sarah M. Bartsch of Johns Hopkins University, Baltimore, and colleagues (PLoS ONE 2016. doi: 10.1371/journal.pone.0151219).
In the United States, norovirus was the most common pathogen identified in cases of acute gastroenteritis (AGE, 6%), followed by rotavirus and sapovirus (2% for both) and astrovirus (1%), according to data from a population-based study, including 1,099 stool specimens collected between August 2012 and September 2013. These findings were published in a separate study (PLoS ONE 2016. doi: 10.1371/journal.pone.0148395).
Overall, U.S. children younger than 5 years of age had the highest prevalence of norovirus; outpatient incidence and community incidences were 25.6 and 152.2 per 1,000 person-years, respectively. The next highest norovirus prevalence occurred in adults older than 65 years; outpatient and community incidence were 7.8 and 7.8 per 1,000 person-years, respectively. The study provides “the first U.S. laboratory-based age-specific norovirus AGE incidence rates in both community and outpatient settings,” wrote Scott P. Grytdal of the Centers for Disease Control and Prevention in Atlanta, and colleagues.
The global economic impact of norovirus is roughly $60 billion in societal costs and $4 billion in direct health care costs per year, according to an simulation model analysis.
Most of the costs (84%-99%, varying by region) resulted from lost productivity. The total societal cost was highest in children younger than 5 years, nearly $40 billion, compared with $20 billion for all other age groups combined, but the cost per illness was highest among adults aged 55 years and older.
Disease incidence was similar across all countries in the simulation model that included 233 countries stratified by World Health Organization region and globally but high-income countries accounted for 62% of the global health system costs, wrote Sarah M. Bartsch of Johns Hopkins University, Baltimore, and colleagues (PLoS ONE 2016. doi: 10.1371/journal.pone.0151219).
In the United States, norovirus was the most common pathogen identified in cases of acute gastroenteritis (AGE, 6%), followed by rotavirus and sapovirus (2% for both) and astrovirus (1%), according to data from a population-based study, including 1,099 stool specimens collected between August 2012 and September 2013. These findings were published in a separate study (PLoS ONE 2016. doi: 10.1371/journal.pone.0148395).
Overall, U.S. children younger than 5 years of age had the highest prevalence of norovirus; outpatient incidence and community incidences were 25.6 and 152.2 per 1,000 person-years, respectively. The next highest norovirus prevalence occurred in adults older than 65 years; outpatient and community incidence were 7.8 and 7.8 per 1,000 person-years, respectively. The study provides “the first U.S. laboratory-based age-specific norovirus AGE incidence rates in both community and outpatient settings,” wrote Scott P. Grytdal of the Centers for Disease Control and Prevention in Atlanta, and colleagues.
FROM PLOS ONE
Hepatitis B test identifies active carriers
A one-time test combining hepatitis B virus (HBV) surface antigen and HBV DNA measurement accurately distinguished inactive carriers from active cases of chronic HBV, based on data from 1,529 patients published online in the journal Hepatology.
Correct identification of active chronic HBV patients vs. inactive cases “is a crucial step in identifying patients in need of less stringent follow-up, as well as patients who may benefit from additional follow-up and earlier initiation of antiviral therapy,” wrote Dr. Jessica Liu of the Genomics Research Center, Academia Sinica, in Taipei, Taiwan, and her colleagues (Hepatology. 2016. doi: 10.1002/hep.28552).
The investigators reviewed data from patients in the REVEAL-HBV cohort, which included individuals aged 30-65 years with chronic HBV who were recruited between 1991 and 1992. All patients were free of liver cirrhosis and were seronegative for anti–hepatitis C virus and hepatitis B surface antigen (HBsAg) at baseline, and were characterized as inactive carriers or active cases based on their serologic profiles at 18 months’ follow-up. Blood was collected at study entry and every 6-12 months.
At 18 months’ follow-up, the combined test distinguished inactive carriers from active cases with a sensitivity of 71% and a specificity of 85%. The positive and negative predictive values were 83% and 74%, respectively, and the diagnostic accuracy was 78%. In addition, the one-time combination measurement predicted cirrhosis, hepatocelluar carcinoma, and HBsAg seroclearance with areas under the receiver operating characteristic curves of 0.72, 0.79, and 0.78, respectively. The combination test also yielded information about the predictability of inactive carrier status, showing that inactive carriers had a significantly lower risk of cirrhosis and hepatocelluar carcinoma; adjusted hazard ratios were 0.43 and 0.13, respectively.
“To our knowledge, this is the first study to externally validate the usage of a one-time measurement of serum HBsAg less than 1,000 IU/mL and HBV DNA less than 2,000 IU/mL,” the researchers wrote.
The study was limited by a relatively short follow-up period, but the results suggest that “this single-point strategy may provide new and complementary information useful for simplifying or tailoring management of patients with chronic hepatitis B infection,” they said.
The study was supported by the Taiwan Department of Health, Bristol-Myers Squibb, Roche Diagnostics, and Academia Sinica. One of the coauthors is employed by Roche Diagnostics.
A one-time test combining hepatitis B virus (HBV) surface antigen and HBV DNA measurement accurately distinguished inactive carriers from active cases of chronic HBV, based on data from 1,529 patients published online in the journal Hepatology.
Correct identification of active chronic HBV patients vs. inactive cases “is a crucial step in identifying patients in need of less stringent follow-up, as well as patients who may benefit from additional follow-up and earlier initiation of antiviral therapy,” wrote Dr. Jessica Liu of the Genomics Research Center, Academia Sinica, in Taipei, Taiwan, and her colleagues (Hepatology. 2016. doi: 10.1002/hep.28552).
The investigators reviewed data from patients in the REVEAL-HBV cohort, which included individuals aged 30-65 years with chronic HBV who were recruited between 1991 and 1992. All patients were free of liver cirrhosis and were seronegative for anti–hepatitis C virus and hepatitis B surface antigen (HBsAg) at baseline, and were characterized as inactive carriers or active cases based on their serologic profiles at 18 months’ follow-up. Blood was collected at study entry and every 6-12 months.
At 18 months’ follow-up, the combined test distinguished inactive carriers from active cases with a sensitivity of 71% and a specificity of 85%. The positive and negative predictive values were 83% and 74%, respectively, and the diagnostic accuracy was 78%. In addition, the one-time combination measurement predicted cirrhosis, hepatocelluar carcinoma, and HBsAg seroclearance with areas under the receiver operating characteristic curves of 0.72, 0.79, and 0.78, respectively. The combination test also yielded information about the predictability of inactive carrier status, showing that inactive carriers had a significantly lower risk of cirrhosis and hepatocelluar carcinoma; adjusted hazard ratios were 0.43 and 0.13, respectively.
“To our knowledge, this is the first study to externally validate the usage of a one-time measurement of serum HBsAg less than 1,000 IU/mL and HBV DNA less than 2,000 IU/mL,” the researchers wrote.
The study was limited by a relatively short follow-up period, but the results suggest that “this single-point strategy may provide new and complementary information useful for simplifying or tailoring management of patients with chronic hepatitis B infection,” they said.
The study was supported by the Taiwan Department of Health, Bristol-Myers Squibb, Roche Diagnostics, and Academia Sinica. One of the coauthors is employed by Roche Diagnostics.
A one-time test combining hepatitis B virus (HBV) surface antigen and HBV DNA measurement accurately distinguished inactive carriers from active cases of chronic HBV, based on data from 1,529 patients published online in the journal Hepatology.
Correct identification of active chronic HBV patients vs. inactive cases “is a crucial step in identifying patients in need of less stringent follow-up, as well as patients who may benefit from additional follow-up and earlier initiation of antiviral therapy,” wrote Dr. Jessica Liu of the Genomics Research Center, Academia Sinica, in Taipei, Taiwan, and her colleagues (Hepatology. 2016. doi: 10.1002/hep.28552).
The investigators reviewed data from patients in the REVEAL-HBV cohort, which included individuals aged 30-65 years with chronic HBV who were recruited between 1991 and 1992. All patients were free of liver cirrhosis and were seronegative for anti–hepatitis C virus and hepatitis B surface antigen (HBsAg) at baseline, and were characterized as inactive carriers or active cases based on their serologic profiles at 18 months’ follow-up. Blood was collected at study entry and every 6-12 months.
At 18 months’ follow-up, the combined test distinguished inactive carriers from active cases with a sensitivity of 71% and a specificity of 85%. The positive and negative predictive values were 83% and 74%, respectively, and the diagnostic accuracy was 78%. In addition, the one-time combination measurement predicted cirrhosis, hepatocelluar carcinoma, and HBsAg seroclearance with areas under the receiver operating characteristic curves of 0.72, 0.79, and 0.78, respectively. The combination test also yielded information about the predictability of inactive carrier status, showing that inactive carriers had a significantly lower risk of cirrhosis and hepatocelluar carcinoma; adjusted hazard ratios were 0.43 and 0.13, respectively.
“To our knowledge, this is the first study to externally validate the usage of a one-time measurement of serum HBsAg less than 1,000 IU/mL and HBV DNA less than 2,000 IU/mL,” the researchers wrote.
The study was limited by a relatively short follow-up period, but the results suggest that “this single-point strategy may provide new and complementary information useful for simplifying or tailoring management of patients with chronic hepatitis B infection,” they said.
The study was supported by the Taiwan Department of Health, Bristol-Myers Squibb, Roche Diagnostics, and Academia Sinica. One of the coauthors is employed by Roche Diagnostics.
FROM HEPATOLOGY
Key clinical point: The data confirm the predictability of a one-time test for chronic hepatitis B progression that combines hepatitis B surface antigen and hepatitis B DNA measurement.
Major finding: The one-time combined test distinguished inactive carriers from active cases with a sensitivity of 71% and specificity of 85%.
Data source: A study of 1,529 adults aged 30-65 years with chronic hepatitis B.
Disclosures: The study was supported by the Taiwan Department of Health, Bristol-Myers Squibb, Roche Diagnostics, and Academia Sinica. One of the coauthors is employed by Roche Diagnostics.
Laser treatment effective for nongenital warts
Laser treatment is effective against nongenital cutaneous warts, based on data from a review of 35 studies comprising 2,149 adult patients.
“No monotherapy has achieved completed remission [of nongenital cutaneous warts] in every case,” wrote Jannett Nguyen, a medical student at the University of California, Irvine, and colleagues (JAMA Dermatol. 2016 April 27. doi: 10.1001/jamadermatol.2016.0826).
The researchers reviewed data on warts treated with one of four types of lasers: Carbon dioxide (CO2), erbium:yttrium-aluminum-garnet (Er:YAG), pulsed dye laser (PDL), or neodymium-doped yttrium aluminum garnet (Nd:YAG).
The response rates for the different lasers were 50%-100% for CO2, 72%-100% for Er:YAG, 31%-100% for PDL, and 46%-100% for Nd:YAG. The studies included data on laser treatment of several types of nongenital warts including simple and recalcitrant common warts, periungual and subungual warts, and palmoplantar warts.
In general, side effects from laser treatment of warts were highest with CO2 lasers, and included scarring, hypopigmentation, postoperative pain, and prolonged wound healing. PDL was associated with the lowest risk of side effects, and was as effective as conventional therapies, including cryotherapy and cantharidin.
In Er:YAG treatments, the laser was used for direct ablation of the epidermis on the wart, repeating through layers until normal skin is revealed. Overall, patients treated with Er:YAG demonstrated a higher response and lower recurrence when treated in combination with podofilox. Nd:YAG treatment was similar to PDL, but with a longer wavelength that allows for deeper penetration.
Treatment is limited by a lack of evidence to guide selection of the most appropriate lasers for different warts and by a lack of recommendations for specific laser settings, the researchers noted. Additional studies are needed to establish treatment protocols by comparing lasers to each other and to nonlaser treatments.
However, laser treatment of warts can be “an additional therapeutic option and the studies reviewed here can provide a starting point in determining settings,” they said.
The researchers had no financial disclosures.
Laser treatment is effective against nongenital cutaneous warts, based on data from a review of 35 studies comprising 2,149 adult patients.
“No monotherapy has achieved completed remission [of nongenital cutaneous warts] in every case,” wrote Jannett Nguyen, a medical student at the University of California, Irvine, and colleagues (JAMA Dermatol. 2016 April 27. doi: 10.1001/jamadermatol.2016.0826).
The researchers reviewed data on warts treated with one of four types of lasers: Carbon dioxide (CO2), erbium:yttrium-aluminum-garnet (Er:YAG), pulsed dye laser (PDL), or neodymium-doped yttrium aluminum garnet (Nd:YAG).
The response rates for the different lasers were 50%-100% for CO2, 72%-100% for Er:YAG, 31%-100% for PDL, and 46%-100% for Nd:YAG. The studies included data on laser treatment of several types of nongenital warts including simple and recalcitrant common warts, periungual and subungual warts, and palmoplantar warts.
In general, side effects from laser treatment of warts were highest with CO2 lasers, and included scarring, hypopigmentation, postoperative pain, and prolonged wound healing. PDL was associated with the lowest risk of side effects, and was as effective as conventional therapies, including cryotherapy and cantharidin.
In Er:YAG treatments, the laser was used for direct ablation of the epidermis on the wart, repeating through layers until normal skin is revealed. Overall, patients treated with Er:YAG demonstrated a higher response and lower recurrence when treated in combination with podofilox. Nd:YAG treatment was similar to PDL, but with a longer wavelength that allows for deeper penetration.
Treatment is limited by a lack of evidence to guide selection of the most appropriate lasers for different warts and by a lack of recommendations for specific laser settings, the researchers noted. Additional studies are needed to establish treatment protocols by comparing lasers to each other and to nonlaser treatments.
However, laser treatment of warts can be “an additional therapeutic option and the studies reviewed here can provide a starting point in determining settings,” they said.
The researchers had no financial disclosures.
Laser treatment is effective against nongenital cutaneous warts, based on data from a review of 35 studies comprising 2,149 adult patients.
“No monotherapy has achieved completed remission [of nongenital cutaneous warts] in every case,” wrote Jannett Nguyen, a medical student at the University of California, Irvine, and colleagues (JAMA Dermatol. 2016 April 27. doi: 10.1001/jamadermatol.2016.0826).
The researchers reviewed data on warts treated with one of four types of lasers: Carbon dioxide (CO2), erbium:yttrium-aluminum-garnet (Er:YAG), pulsed dye laser (PDL), or neodymium-doped yttrium aluminum garnet (Nd:YAG).
The response rates for the different lasers were 50%-100% for CO2, 72%-100% for Er:YAG, 31%-100% for PDL, and 46%-100% for Nd:YAG. The studies included data on laser treatment of several types of nongenital warts including simple and recalcitrant common warts, periungual and subungual warts, and palmoplantar warts.
In general, side effects from laser treatment of warts were highest with CO2 lasers, and included scarring, hypopigmentation, postoperative pain, and prolonged wound healing. PDL was associated with the lowest risk of side effects, and was as effective as conventional therapies, including cryotherapy and cantharidin.
In Er:YAG treatments, the laser was used for direct ablation of the epidermis on the wart, repeating through layers until normal skin is revealed. Overall, patients treated with Er:YAG demonstrated a higher response and lower recurrence when treated in combination with podofilox. Nd:YAG treatment was similar to PDL, but with a longer wavelength that allows for deeper penetration.
Treatment is limited by a lack of evidence to guide selection of the most appropriate lasers for different warts and by a lack of recommendations for specific laser settings, the researchers noted. Additional studies are needed to establish treatment protocols by comparing lasers to each other and to nonlaser treatments.
However, laser treatment of warts can be “an additional therapeutic option and the studies reviewed here can provide a starting point in determining settings,” they said.
The researchers had no financial disclosures.
FROM JAMA DERMATOLOGY
Key clinical point: Lasers are an effective treatment for both simple and stubborn nongenital warts.
Major finding: The response rates ranged from 46% to 100% for lasers including CO2, Er:YAG, PDL, and Nd:YAG.
Data source: A review of 35 studies comprising 2,149 patients.
Disclosures: The researchers had no financial disclosures.
Adding tomosynthesis may benefit women with dense breasts
Women with dense breasts may benefit from additional screening at the time of digital mammography, but the messages notifying these women of potential risks and benefits of more screening are often poorly written and understood, according to a pair of studies published online in JAMA on April 26.
Adding tomosynthesis to screening digital mammography significantly increased cancer detection rates in women with dense and nondense breasts, based on data from a retrospective study of 452,320 examinations.
Dense breast tissue may be an independent risk factor for breast cancer, but the impact of additional treatment modalities on women with dense breasts has not been well studied, wrote Dr. Elizabeth A. Rafferty of L&M Radiology in West Acton, Mass., and associates. Dr. Rafferty conducted the study with colleagues while affiliated with Massachusetts General Hospital in Boston (JAMA 2016 Apr 26. doi: 10.1001/jama.2016.1708).
The researchers reviewed data from an earlier multicenter study involving 13 U.S. institutions, with data reported for 12 months that included 278,906 digital mammographies and 173,414 digital mammographies plus tomosynthesis. A total of 2,157 cancers were diagnosed. Cancer detection rates increased in both groups with the addition of tomosynthesis: Invasive cancer detection increased from 3.0 to 4.0 per 1,000 screens in nondense breasts and from 2.9 to 4.2 per 1,000 screens in dense breasts.
In addition, recall rates decreased from 90 to 79 per 1,000 screens in nondense breasts and from 127 to 109 per 1,000 screens in dense breasts.
Although the study was limited by its retrospective design, the results suggest that the “combined gains were largest for women with heterogeneously dense breasts, potentially addressing limitations in cancer detection seen with digital mammography alone in this group, but were not significant in women with extremely dense breasts,” the researchers noted.
The researchers had no financial conflicts to disclose, and the study was supported by a research grant from Hologic.
Meanwhile, a separate study published in JAMA found that most messages sent to notify women of breast density are poorly understood.
Nancy R. Kressin, Ph.D., of Veterans Affairs Boston Healthcare System and Boston University and colleagues examined the dense breast notifications sent to women following screening mammography in 23 of the 24 states that required such notifications as of January 2016. They assessed the messages for content, readability, and understandability (JAMA 2016 Apr 26. doi: 10.1001/jama.2016.1712).
Although all the notifications reviewed mentioned masking bias (how dense breasts can mask cancer on mammography), the researchers found considerable variation in other content: 74% of notifications mentioned increased cancer risk and 65% mentioned the option of additional screening. Of the 15 states that require supplemental screening to be mentioned, six state notifications explained that the women might benefit from such screening and four state notifications mentioned specific screening modalities.
Only three states’ notifications were written at grade 8 reading level or below, although approximately 20% of the U.S. population reads at grade 5 level or below, the researchers noted. All states’ notifications scored between 11% and 33% on a measure of readability.
“Many [dense breast notifications] appropriately encourage discussions and shared decision making between patients and physicians,” the researchers noted. However, “efforts should focus on enhancing the understandability of [dense breast notifications] so that all women are clearly and accurately informed about their density status, its effect on their breast cancer risk, and the harms and benefits of supplemental screening,” they wrote.
Dr. Kressin reported receiving a Research Career Scientist award from the Department of Veterans Affairs, and coauthor Dr. Tracy Battaglia is the chair elect of the American Cancer Society of New England.
Women with dense breasts may benefit from additional screening at the time of digital mammography, but the messages notifying these women of potential risks and benefits of more screening are often poorly written and understood, according to a pair of studies published online in JAMA on April 26.
Adding tomosynthesis to screening digital mammography significantly increased cancer detection rates in women with dense and nondense breasts, based on data from a retrospective study of 452,320 examinations.
Dense breast tissue may be an independent risk factor for breast cancer, but the impact of additional treatment modalities on women with dense breasts has not been well studied, wrote Dr. Elizabeth A. Rafferty of L&M Radiology in West Acton, Mass., and associates. Dr. Rafferty conducted the study with colleagues while affiliated with Massachusetts General Hospital in Boston (JAMA 2016 Apr 26. doi: 10.1001/jama.2016.1708).
The researchers reviewed data from an earlier multicenter study involving 13 U.S. institutions, with data reported for 12 months that included 278,906 digital mammographies and 173,414 digital mammographies plus tomosynthesis. A total of 2,157 cancers were diagnosed. Cancer detection rates increased in both groups with the addition of tomosynthesis: Invasive cancer detection increased from 3.0 to 4.0 per 1,000 screens in nondense breasts and from 2.9 to 4.2 per 1,000 screens in dense breasts.
In addition, recall rates decreased from 90 to 79 per 1,000 screens in nondense breasts and from 127 to 109 per 1,000 screens in dense breasts.
Although the study was limited by its retrospective design, the results suggest that the “combined gains were largest for women with heterogeneously dense breasts, potentially addressing limitations in cancer detection seen with digital mammography alone in this group, but were not significant in women with extremely dense breasts,” the researchers noted.
The researchers had no financial conflicts to disclose, and the study was supported by a research grant from Hologic.
Meanwhile, a separate study published in JAMA found that most messages sent to notify women of breast density are poorly understood.
Nancy R. Kressin, Ph.D., of Veterans Affairs Boston Healthcare System and Boston University and colleagues examined the dense breast notifications sent to women following screening mammography in 23 of the 24 states that required such notifications as of January 2016. They assessed the messages for content, readability, and understandability (JAMA 2016 Apr 26. doi: 10.1001/jama.2016.1712).
Although all the notifications reviewed mentioned masking bias (how dense breasts can mask cancer on mammography), the researchers found considerable variation in other content: 74% of notifications mentioned increased cancer risk and 65% mentioned the option of additional screening. Of the 15 states that require supplemental screening to be mentioned, six state notifications explained that the women might benefit from such screening and four state notifications mentioned specific screening modalities.
Only three states’ notifications were written at grade 8 reading level or below, although approximately 20% of the U.S. population reads at grade 5 level or below, the researchers noted. All states’ notifications scored between 11% and 33% on a measure of readability.
“Many [dense breast notifications] appropriately encourage discussions and shared decision making between patients and physicians,” the researchers noted. However, “efforts should focus on enhancing the understandability of [dense breast notifications] so that all women are clearly and accurately informed about their density status, its effect on their breast cancer risk, and the harms and benefits of supplemental screening,” they wrote.
Dr. Kressin reported receiving a Research Career Scientist award from the Department of Veterans Affairs, and coauthor Dr. Tracy Battaglia is the chair elect of the American Cancer Society of New England.
Women with dense breasts may benefit from additional screening at the time of digital mammography, but the messages notifying these women of potential risks and benefits of more screening are often poorly written and understood, according to a pair of studies published online in JAMA on April 26.
Adding tomosynthesis to screening digital mammography significantly increased cancer detection rates in women with dense and nondense breasts, based on data from a retrospective study of 452,320 examinations.
Dense breast tissue may be an independent risk factor for breast cancer, but the impact of additional treatment modalities on women with dense breasts has not been well studied, wrote Dr. Elizabeth A. Rafferty of L&M Radiology in West Acton, Mass., and associates. Dr. Rafferty conducted the study with colleagues while affiliated with Massachusetts General Hospital in Boston (JAMA 2016 Apr 26. doi: 10.1001/jama.2016.1708).
The researchers reviewed data from an earlier multicenter study involving 13 U.S. institutions, with data reported for 12 months that included 278,906 digital mammographies and 173,414 digital mammographies plus tomosynthesis. A total of 2,157 cancers were diagnosed. Cancer detection rates increased in both groups with the addition of tomosynthesis: Invasive cancer detection increased from 3.0 to 4.0 per 1,000 screens in nondense breasts and from 2.9 to 4.2 per 1,000 screens in dense breasts.
In addition, recall rates decreased from 90 to 79 per 1,000 screens in nondense breasts and from 127 to 109 per 1,000 screens in dense breasts.
Although the study was limited by its retrospective design, the results suggest that the “combined gains were largest for women with heterogeneously dense breasts, potentially addressing limitations in cancer detection seen with digital mammography alone in this group, but were not significant in women with extremely dense breasts,” the researchers noted.
The researchers had no financial conflicts to disclose, and the study was supported by a research grant from Hologic.
Meanwhile, a separate study published in JAMA found that most messages sent to notify women of breast density are poorly understood.
Nancy R. Kressin, Ph.D., of Veterans Affairs Boston Healthcare System and Boston University and colleagues examined the dense breast notifications sent to women following screening mammography in 23 of the 24 states that required such notifications as of January 2016. They assessed the messages for content, readability, and understandability (JAMA 2016 Apr 26. doi: 10.1001/jama.2016.1712).
Although all the notifications reviewed mentioned masking bias (how dense breasts can mask cancer on mammography), the researchers found considerable variation in other content: 74% of notifications mentioned increased cancer risk and 65% mentioned the option of additional screening. Of the 15 states that require supplemental screening to be mentioned, six state notifications explained that the women might benefit from such screening and four state notifications mentioned specific screening modalities.
Only three states’ notifications were written at grade 8 reading level or below, although approximately 20% of the U.S. population reads at grade 5 level or below, the researchers noted. All states’ notifications scored between 11% and 33% on a measure of readability.
“Many [dense breast notifications] appropriately encourage discussions and shared decision making between patients and physicians,” the researchers noted. However, “efforts should focus on enhancing the understandability of [dense breast notifications] so that all women are clearly and accurately informed about their density status, its effect on their breast cancer risk, and the harms and benefits of supplemental screening,” they wrote.
Dr. Kressin reported receiving a Research Career Scientist award from the Department of Veterans Affairs, and coauthor Dr. Tracy Battaglia is the chair elect of the American Cancer Society of New England.
FROM JAMA
Key clinical point: Women with dense breasts may benefit from additional screening, but state-mandated density notification messages are often hard for them to understand.
Major finding: Invasive cancer detection increased from 3.0 to 4.0 per 1,000 screens in nondense breasts, and from 2.9 to 4.2 per 1,000 screens in dense breasts, with the addition of tomosynthesis to digital screening mammography. In another study, 65% of dense breast notifications mentioned the option of additional screening.
Data source: A retrospective study of 452,320 breast cancer screening examinations, and a review of dense breast notifications sent to women in 23 states as of January 2016.
Disclosures: Dr. Rafferty had no financial conflicts to disclose, and the study was supported by a research grant from Hologic. Dr. Kressin disclosed support from a Research Career Scientist award from the Department of Veterans Affairs, and coauthor Dr. Tracy Battaglia is the chair elect of the American Cancer Society of New England.
Breastfeeding reduces infants’ respiratory symptoms early on
Breastfeeding during the first 27 weeks of life had a risk-specific effect on reducing respiratory symptoms in healthy term infants, based on data from a prospective cohort study of 436 children in Switzerland.
“Breastfeeding is generally accepted to be protective against respiratory symptoms in early life,” but most published studies on this topic are cross-sectional and more likely biased, wrote Dr. Olga Gorlanova of the University of Basel (Switzerland) and her colleagues.
The researchers studied infants enrolled in the Bern-Basel Infant Lung Development cohort via weekly telephone interviews during the first year of life. In addition, weekly measurements of environmental particulate matter were collected from local monitoring stations. Risk factors included maternal history of atopy, vaginal vs. cesarean delivery, parents’ level of education, smoking during and after pregnancy, number of older siblings, child care attendance, and housing conditions.
Overall, infants breastfed during the first 27 weeks of life had significantly reduced respiratory symptoms, compared with nonbreastfed infants (risk ratio, .70)
The study “suggests that breastfeeding attenuates the effects of risk factors such as sex, age, gestational age, cesarean delivery, and prenatal maternal tobacco smoking in healthy term infants,” Dr. Gorlanova and her associates wrote. No significant interaction was noted between breastfeeding and child care attendance, number of older siblings, maternal atopy, or environmental particulate matter.
Read the full study here (J Pediatr. 2016. doi: 10.1016/j.jpeds.2016.03.041).
Breastfeeding during the first 27 weeks of life had a risk-specific effect on reducing respiratory symptoms in healthy term infants, based on data from a prospective cohort study of 436 children in Switzerland.
“Breastfeeding is generally accepted to be protective against respiratory symptoms in early life,” but most published studies on this topic are cross-sectional and more likely biased, wrote Dr. Olga Gorlanova of the University of Basel (Switzerland) and her colleagues.
The researchers studied infants enrolled in the Bern-Basel Infant Lung Development cohort via weekly telephone interviews during the first year of life. In addition, weekly measurements of environmental particulate matter were collected from local monitoring stations. Risk factors included maternal history of atopy, vaginal vs. cesarean delivery, parents’ level of education, smoking during and after pregnancy, number of older siblings, child care attendance, and housing conditions.
Overall, infants breastfed during the first 27 weeks of life had significantly reduced respiratory symptoms, compared with nonbreastfed infants (risk ratio, .70)
The study “suggests that breastfeeding attenuates the effects of risk factors such as sex, age, gestational age, cesarean delivery, and prenatal maternal tobacco smoking in healthy term infants,” Dr. Gorlanova and her associates wrote. No significant interaction was noted between breastfeeding and child care attendance, number of older siblings, maternal atopy, or environmental particulate matter.
Read the full study here (J Pediatr. 2016. doi: 10.1016/j.jpeds.2016.03.041).
Breastfeeding during the first 27 weeks of life had a risk-specific effect on reducing respiratory symptoms in healthy term infants, based on data from a prospective cohort study of 436 children in Switzerland.
“Breastfeeding is generally accepted to be protective against respiratory symptoms in early life,” but most published studies on this topic are cross-sectional and more likely biased, wrote Dr. Olga Gorlanova of the University of Basel (Switzerland) and her colleagues.
The researchers studied infants enrolled in the Bern-Basel Infant Lung Development cohort via weekly telephone interviews during the first year of life. In addition, weekly measurements of environmental particulate matter were collected from local monitoring stations. Risk factors included maternal history of atopy, vaginal vs. cesarean delivery, parents’ level of education, smoking during and after pregnancy, number of older siblings, child care attendance, and housing conditions.
Overall, infants breastfed during the first 27 weeks of life had significantly reduced respiratory symptoms, compared with nonbreastfed infants (risk ratio, .70)
The study “suggests that breastfeeding attenuates the effects of risk factors such as sex, age, gestational age, cesarean delivery, and prenatal maternal tobacco smoking in healthy term infants,” Dr. Gorlanova and her associates wrote. No significant interaction was noted between breastfeeding and child care attendance, number of older siblings, maternal atopy, or environmental particulate matter.
Read the full study here (J Pediatr. 2016. doi: 10.1016/j.jpeds.2016.03.041).
FROM THE JOURNAL OF PEDIATRICS