User login
How does pentoxifylline affect survival of patients with alcoholic hepatitis?
Pentoxifylline improves short-term survival in patients admitted to the hospital with severe alcoholic hepatitis (strength of recommendation [SOR]: B, a single published randomized controlled trial [RCT]). Pentoxifylline does not improve survival when it is substituted for steroids in hospitalized patients who aren’t responding to steroids (SOR: C, case series).
Evidence summary
Patients with severe acute alcoholic hepatitis have elevated levels of serum tumor necrosis factor (TNF), suggesting that TNF release may play a role in liver inflammation.1 Because pentoxifylline inhibits TNF synthesis, it has been evaluated as a potential therapy for alcoholic hepatitis.
Decreases in mortality and hepatorenal syndrome
In a hospital-based clinical trial, 101 patients admitted with severe alcoholic hepatitis (mean age 42 years, 74% men) were randomized to oral pentoxifylline 400 mg twice a day or placebo (vitamin B12 tablets) for 4 weeks.1 The main outcome measures were short-term survival and progression to hepatorenal syndrome. Severe alcoholic hepatitis was defined as a Maddrey discriminant factor (DF) >32, jaundice, and at least one of the following: tender hepatomegaly, fever, leukocytosis, hepatic encephalopathy, or hepatic systolic bruit. The DF is calculated as follows: 4.6 × [prothrombin time in seconds – control time] + bilirubin (mg/dL). Medical management was “individualized according to each patient’s condition.”
Pentoxifylline therapy was associated with decreased mortality during the index hospitalization (relative risk [RR]=0.59; 95% confidence interval [CI], 0.35-0.97; number needed to treat [NNT]=5). Hepatorenal syndrome also decreased (RR=0.29; 95% CI, 0.13-0.65; NNT=4). Patients in the pentoxifylline group tended to have more headaches and gastrointestinal side effects, but no other serious health hazards were observed.
In a recently published abstract, 50 patients with severe alcoholic hepatitis (defined as DF >32) were enrolled in a randomized, double-blind, placebo-controlled trial of oral pentoxifylline, 400 mg twice a day or placebo for 4 weeks.2 Short-term survival and changes in laboratory values (TNF, creatinine, and DF) were the primary outcome measures.
Survival was 76% in the pentoxifylline group compared with 60% in the placebo group (P not given). In the sub-group of patients who died, however, hepatorenal syndrome was the cause of death in 83% of the pentoxifylline group and 60% of the placebo group (P not given).
In a 1991 pilot study, also published only in abstract form, 22 patients admitted to the hospital with severe alcoholic hepatitis were randomized to receive oral pentoxifylline (1200 mg daily) or placebo for 10 days. Serum creatinine dropped 0.3 mg/dL in the treatment group and rose 2.1 mg/dL in the control group (P<.05). At 30 days, 3 patients in the control group had died compared with 1 in the treatment group (P=not significant).3
It’s not effective for patients who don’t respond to steroids
A cohort study evaluated the effect of switching to pentoxifylline in hospitalized patients with severe alcoholic hepatitis who didn’t respond to initial therapy with steroids. Researchers identified 121 patients who were treated initially with 40 mg oral prednisolone daily. The 36 patients who failed to show a drop in bilirubin levels within 7 days were switched to oral pentoxifylline, 400 mg twice a day.
In the pentoxifylline group, 69% of patients died within 2 months, 27.6% of whom had some form of renal insufficiency. This outcome wasn’t statistically different from that of 58 matched historical controls with severe alcoholic hepatitis who were maintained on oral prednisolone despite failure to respond within the first week of therapy (65% mortality, 20% with renal insufficiency).4
Recommendations
The American College of Gastroenterology doesn’t recommend giving pentoxifylline to patients with severe alcoholic hepatitis, citing lack of evidence for improvement of patient-oriented outcomes.5 However, a group of French hepatologists consider pentoxifylline a reasonable alternative to corticosteroids for severe acute alcoholic hepatitis based on the studies cited here.6
1. Akriviadis E, Botla R, Briggs W, et al. Pentoxifylline improves short-term survival in severe acute alcoholic hepatitis: a double-blind, placebo-controlled trial. Gastroenterology. 2000;119:1637-1648.
2. Sidhu S, Singla M, Bhatia K, et al. Pentoxifylline reduces disease severity and prevents renal impairment in severe acute alcoholic hepatitis: a double-blind, placebo-controlled trial. Hepatology. 2006;44(suppl 1A):373A-374A.
3. McHutchison JG, Runyon BA, Draguesku JO, et al. Pentoxifylline may prevent renal impairment in severe alcoholic hepatitis. Hepatology. 1991;14:96A.-
4. Louvet A, Diaz E, Dharancy S, et al. Early switch to pentoxifylline in patients with severe alcoholic hepatitis is inefficient in non-responders to corticosteroids. J Hepatol. 2008;48:465-470.
5. McCullough AJ, O’Connor JF. Alcoholic liver disease: proposed recommendations for the American College of Gastroenterology. Am J Gastroenterol. 1998;93:2022-2036.
6. Mathurin P, Louvet A, Dharancy S. Treatment of severe forms of alcoholic hepatitis: where are we going? J Gastroenterol Hepatol. 2008;23(suppl 1):S60-S62.
Pentoxifylline improves short-term survival in patients admitted to the hospital with severe alcoholic hepatitis (strength of recommendation [SOR]: B, a single published randomized controlled trial [RCT]). Pentoxifylline does not improve survival when it is substituted for steroids in hospitalized patients who aren’t responding to steroids (SOR: C, case series).
Evidence summary
Patients with severe acute alcoholic hepatitis have elevated levels of serum tumor necrosis factor (TNF), suggesting that TNF release may play a role in liver inflammation.1 Because pentoxifylline inhibits TNF synthesis, it has been evaluated as a potential therapy for alcoholic hepatitis.
Decreases in mortality and hepatorenal syndrome
In a hospital-based clinical trial, 101 patients admitted with severe alcoholic hepatitis (mean age 42 years, 74% men) were randomized to oral pentoxifylline 400 mg twice a day or placebo (vitamin B12 tablets) for 4 weeks.1 The main outcome measures were short-term survival and progression to hepatorenal syndrome. Severe alcoholic hepatitis was defined as a Maddrey discriminant factor (DF) >32, jaundice, and at least one of the following: tender hepatomegaly, fever, leukocytosis, hepatic encephalopathy, or hepatic systolic bruit. The DF is calculated as follows: 4.6 × [prothrombin time in seconds – control time] + bilirubin (mg/dL). Medical management was “individualized according to each patient’s condition.”
Pentoxifylline therapy was associated with decreased mortality during the index hospitalization (relative risk [RR]=0.59; 95% confidence interval [CI], 0.35-0.97; number needed to treat [NNT]=5). Hepatorenal syndrome also decreased (RR=0.29; 95% CI, 0.13-0.65; NNT=4). Patients in the pentoxifylline group tended to have more headaches and gastrointestinal side effects, but no other serious health hazards were observed.
In a recently published abstract, 50 patients with severe alcoholic hepatitis (defined as DF >32) were enrolled in a randomized, double-blind, placebo-controlled trial of oral pentoxifylline, 400 mg twice a day or placebo for 4 weeks.2 Short-term survival and changes in laboratory values (TNF, creatinine, and DF) were the primary outcome measures.
Survival was 76% in the pentoxifylline group compared with 60% in the placebo group (P not given). In the sub-group of patients who died, however, hepatorenal syndrome was the cause of death in 83% of the pentoxifylline group and 60% of the placebo group (P not given).
In a 1991 pilot study, also published only in abstract form, 22 patients admitted to the hospital with severe alcoholic hepatitis were randomized to receive oral pentoxifylline (1200 mg daily) or placebo for 10 days. Serum creatinine dropped 0.3 mg/dL in the treatment group and rose 2.1 mg/dL in the control group (P<.05). At 30 days, 3 patients in the control group had died compared with 1 in the treatment group (P=not significant).3
It’s not effective for patients who don’t respond to steroids
A cohort study evaluated the effect of switching to pentoxifylline in hospitalized patients with severe alcoholic hepatitis who didn’t respond to initial therapy with steroids. Researchers identified 121 patients who were treated initially with 40 mg oral prednisolone daily. The 36 patients who failed to show a drop in bilirubin levels within 7 days were switched to oral pentoxifylline, 400 mg twice a day.
In the pentoxifylline group, 69% of patients died within 2 months, 27.6% of whom had some form of renal insufficiency. This outcome wasn’t statistically different from that of 58 matched historical controls with severe alcoholic hepatitis who were maintained on oral prednisolone despite failure to respond within the first week of therapy (65% mortality, 20% with renal insufficiency).4
Recommendations
The American College of Gastroenterology doesn’t recommend giving pentoxifylline to patients with severe alcoholic hepatitis, citing lack of evidence for improvement of patient-oriented outcomes.5 However, a group of French hepatologists consider pentoxifylline a reasonable alternative to corticosteroids for severe acute alcoholic hepatitis based on the studies cited here.6
Pentoxifylline improves short-term survival in patients admitted to the hospital with severe alcoholic hepatitis (strength of recommendation [SOR]: B, a single published randomized controlled trial [RCT]). Pentoxifylline does not improve survival when it is substituted for steroids in hospitalized patients who aren’t responding to steroids (SOR: C, case series).
Evidence summary
Patients with severe acute alcoholic hepatitis have elevated levels of serum tumor necrosis factor (TNF), suggesting that TNF release may play a role in liver inflammation.1 Because pentoxifylline inhibits TNF synthesis, it has been evaluated as a potential therapy for alcoholic hepatitis.
Decreases in mortality and hepatorenal syndrome
In a hospital-based clinical trial, 101 patients admitted with severe alcoholic hepatitis (mean age 42 years, 74% men) were randomized to oral pentoxifylline 400 mg twice a day or placebo (vitamin B12 tablets) for 4 weeks.1 The main outcome measures were short-term survival and progression to hepatorenal syndrome. Severe alcoholic hepatitis was defined as a Maddrey discriminant factor (DF) >32, jaundice, and at least one of the following: tender hepatomegaly, fever, leukocytosis, hepatic encephalopathy, or hepatic systolic bruit. The DF is calculated as follows: 4.6 × [prothrombin time in seconds – control time] + bilirubin (mg/dL). Medical management was “individualized according to each patient’s condition.”
Pentoxifylline therapy was associated with decreased mortality during the index hospitalization (relative risk [RR]=0.59; 95% confidence interval [CI], 0.35-0.97; number needed to treat [NNT]=5). Hepatorenal syndrome also decreased (RR=0.29; 95% CI, 0.13-0.65; NNT=4). Patients in the pentoxifylline group tended to have more headaches and gastrointestinal side effects, but no other serious health hazards were observed.
In a recently published abstract, 50 patients with severe alcoholic hepatitis (defined as DF >32) were enrolled in a randomized, double-blind, placebo-controlled trial of oral pentoxifylline, 400 mg twice a day or placebo for 4 weeks.2 Short-term survival and changes in laboratory values (TNF, creatinine, and DF) were the primary outcome measures.
Survival was 76% in the pentoxifylline group compared with 60% in the placebo group (P not given). In the sub-group of patients who died, however, hepatorenal syndrome was the cause of death in 83% of the pentoxifylline group and 60% of the placebo group (P not given).
In a 1991 pilot study, also published only in abstract form, 22 patients admitted to the hospital with severe alcoholic hepatitis were randomized to receive oral pentoxifylline (1200 mg daily) or placebo for 10 days. Serum creatinine dropped 0.3 mg/dL in the treatment group and rose 2.1 mg/dL in the control group (P<.05). At 30 days, 3 patients in the control group had died compared with 1 in the treatment group (P=not significant).3
It’s not effective for patients who don’t respond to steroids
A cohort study evaluated the effect of switching to pentoxifylline in hospitalized patients with severe alcoholic hepatitis who didn’t respond to initial therapy with steroids. Researchers identified 121 patients who were treated initially with 40 mg oral prednisolone daily. The 36 patients who failed to show a drop in bilirubin levels within 7 days were switched to oral pentoxifylline, 400 mg twice a day.
In the pentoxifylline group, 69% of patients died within 2 months, 27.6% of whom had some form of renal insufficiency. This outcome wasn’t statistically different from that of 58 matched historical controls with severe alcoholic hepatitis who were maintained on oral prednisolone despite failure to respond within the first week of therapy (65% mortality, 20% with renal insufficiency).4
Recommendations
The American College of Gastroenterology doesn’t recommend giving pentoxifylline to patients with severe alcoholic hepatitis, citing lack of evidence for improvement of patient-oriented outcomes.5 However, a group of French hepatologists consider pentoxifylline a reasonable alternative to corticosteroids for severe acute alcoholic hepatitis based on the studies cited here.6
1. Akriviadis E, Botla R, Briggs W, et al. Pentoxifylline improves short-term survival in severe acute alcoholic hepatitis: a double-blind, placebo-controlled trial. Gastroenterology. 2000;119:1637-1648.
2. Sidhu S, Singla M, Bhatia K, et al. Pentoxifylline reduces disease severity and prevents renal impairment in severe acute alcoholic hepatitis: a double-blind, placebo-controlled trial. Hepatology. 2006;44(suppl 1A):373A-374A.
3. McHutchison JG, Runyon BA, Draguesku JO, et al. Pentoxifylline may prevent renal impairment in severe alcoholic hepatitis. Hepatology. 1991;14:96A.-
4. Louvet A, Diaz E, Dharancy S, et al. Early switch to pentoxifylline in patients with severe alcoholic hepatitis is inefficient in non-responders to corticosteroids. J Hepatol. 2008;48:465-470.
5. McCullough AJ, O’Connor JF. Alcoholic liver disease: proposed recommendations for the American College of Gastroenterology. Am J Gastroenterol. 1998;93:2022-2036.
6. Mathurin P, Louvet A, Dharancy S. Treatment of severe forms of alcoholic hepatitis: where are we going? J Gastroenterol Hepatol. 2008;23(suppl 1):S60-S62.
1. Akriviadis E, Botla R, Briggs W, et al. Pentoxifylline improves short-term survival in severe acute alcoholic hepatitis: a double-blind, placebo-controlled trial. Gastroenterology. 2000;119:1637-1648.
2. Sidhu S, Singla M, Bhatia K, et al. Pentoxifylline reduces disease severity and prevents renal impairment in severe acute alcoholic hepatitis: a double-blind, placebo-controlled trial. Hepatology. 2006;44(suppl 1A):373A-374A.
3. McHutchison JG, Runyon BA, Draguesku JO, et al. Pentoxifylline may prevent renal impairment in severe alcoholic hepatitis. Hepatology. 1991;14:96A.-
4. Louvet A, Diaz E, Dharancy S, et al. Early switch to pentoxifylline in patients with severe alcoholic hepatitis is inefficient in non-responders to corticosteroids. J Hepatol. 2008;48:465-470.
5. McCullough AJ, O’Connor JF. Alcoholic liver disease: proposed recommendations for the American College of Gastroenterology. Am J Gastroenterol. 1998;93:2022-2036.
6. Mathurin P, Louvet A, Dharancy S. Treatment of severe forms of alcoholic hepatitis: where are we going? J Gastroenterol Hepatol. 2008;23(suppl 1):S60-S62.
Evidence-based answers from the Family Physicians Inquiries Network
Is osteopathic manipulation effective for headaches?
It can be. Spinal manipulative therapy (SMT), a component of osteopathy, has been shown to be variably effective for the treatment of headaches. For the prophylactic treatment of cervicogenic headaches and for acute tension headaches, SMT is superior to placebo.
For tension headache prophylaxis, research shows a trend toward better outcomes with amitriptyline than with SMT. For migraine prophylaxis, SMT has an effect similar to amitriptyline (strength of recommendation: B, based on a systematic review of various quality studies).
3 osteopathic techniques that work for my patients
Charles Webb, DO
Oregon Health and Science University, Portland
Headaches often have more than one cause—physical, psychological, and pharmacological—and each requires treatment. I start by systematically eliminating specific headache triggers. Meanwhile, I find osteopathic manipulative treatment to be an easy and timely intervention to abort headache symptoms and improve patient well-being. I use a variety of manipulation techniques, including cervical soft tissue massage, occipital decompression, and myofascial unwinding.
- Cervical soft tissue massage of the paraspinal tissues helps relieve the spasms of tension headaches.
- Occipital decompression involves using the fingertips to manually stretch the paraspinal tissues at the base of the occiput; it works well in my experience to abort migraine headaches. I teach patients to use a rolled up hand towel behind their neck to do occipital decompression at home, which helps prevent further headaches.
- Myofascial unwinding is a technique that literally unwinds the tissues encasing muscles in spasm.
Evidence summary
For cervicogenic headaches: Spinal manipulative therapy reduces pain
Three studies1 evaluated SMT for treatment of recurrent cervicogenic headaches). A multicenter trial2 randomized 200 patients with cervicogenic headaches to either SMT (8–12 sessions over 6 weeks) or placebo. The SMT group had significantly reduced pain (at 1 week, effect size [ES]=0.7; 95% confidence interval [CI], 0.3–1.2; and at 12 months, ES=0.4; 95% CI, 0.0–0.8) and fewer headaches (ES=0.7; 95% CI, 0.3–1.1 at both time points) than placebo.
Another RCT3 with 105 patients compared SMT (3 times a week for 3 weeks) with placebo. The SMT group reported significantly less pain after 3 weeks (ES=2.2; 95% CI, 1.7–2.7).
A third trial4 randomized 30 patients to either SMT, mobilization (small oscillatory movements to a joint within its normal range), or wait-list placement. At the end of treatment, there was a nonsignificant trend toward greater pain reduction in patients receiving SMT than either those receiving mobilization (ES=0.4; 95% CI, –0.5 to 1.4) or those on the wait list (ES=0.6; 95% CI, –0.4 to 1.5).
For tension-type headaches: Results are mixed
Two trials5 investigated the efficacy of SMT on tension-type headaches. The first, an RCT with 150 patients with recurrent headaches, compared SMT (2 sessions per week) with amitriptyline (10 mg daily week 1, 20 mg daily week 2, then 30 mg daily) for 6 weeks. At the end of 6 weeks, the SMT group reported a nonsignificant trend toward more headache pain (ES for SMT vs amitriptyline= –0.4; 95% CI, –0.8 to 0.0), but fewer side effects. They had similar headache frequency and medication use.
Another study6 of 22 patients compared SMT with 2 different controls (palpation and rest) for acute tension-type headache. The SMT group was significantly more likely to experience immediate improvement (ES=1.8; 95% CI, 0.4–3.2).
For migraine: Spinal manipulative therapy is similar to amitriptyline
In 1 trial7 of migraine prophylaxis, 218 patients were randomized to either 14 sessions of SMT for 2 months or oral amitriptyline (titrated up weekly during the first month and continued at 100 mg daily over the second month). The headache index (a measure of daily pain intensity) was equivalent in both groups in the last 4 weeks of treatment (ES for SMT vs amitriptyline= –0.1; 95% CI, –0.5 to 0.3).
A month after both therapies were stopped, there was a nonsignificant trend toward a lower headache index in the group that had received SMT than the group that had received amitriptyline (ES=0.4; 95% CI, 0.0–0.8). Ten percent of the medication group withdrew from this study due to side effects; no side effects were reported from SMT.7
Another RCT8 of migraine prophylaxis with 88 patients compared SMT twice weekly for 8 weeks with mobilization techniques. At 8 weeks post-treatment, there was a nonsignificant trend favoring SMT over mobilization in decreasing pain (ES=0.4; 95% CI, –0.2 to 1.0).
Recommendations from others
The National Headache Foundation9 states that “the value and cost-effectiveness of chiropractic, osteopathic medicine, and physical therapy in migraine have not been proven in clinical trials. Conflicting results and poor clinical trial design limit the ability to judge the effectiveness of manipulative treatments. Physical therapy, although limited in its study, has proven more effective than manipulative treatment in selective cases.”
1. Biondi DM. Cervicogenic headache: a review of diagnostic and treatment strategies. J Am Osteopath Assoc 2005;105(4 Suppl 2):16S-22S.
2. Jull G, Trott P, Potter H, et al. A randomized controlled trial of exercise and manipulative therapy for cervicogenic headache. Spine 2002;27:1835-1843.
3. Whittingham W. The efficacy of cervical adjustments (toggle recoil) for chronic cervicogenic headaches [PhD dissertation]. Melbourne, Australia: Royal Melbourne Institute of Technology; 1997.
4. Bronfort G, Nilsson N, Hass M, et al. Non-invasive physical treatments for chronic/recurrent headache. Cochrane Database Syst Rev 2004;(3):CD001878.-
5. Boline PD, Kassak K, Bronfort G, Nelson C, Anderson AV. Spinal manipulation vs. Amitriptyline for the treatment of chronic tension-type headaches: a randomized clinical trial. J Manipulative Physiol Ther. 1995;18:148-154.
6. Hoyt WH, Shaffer F, Bard DA, et al. Osteopathic manipulation in the treatment of muscle-contraction headache. J Am Osteopath Assoc 1979;78:322-325.
7. Nelson CF, Bronfort G, Evans R, Boline P, Goldsmith C, Anderson AV. The efficacy of spinal manipulation, amitriptyline and the combination of both therapies for the prophylaxis of migraine headache. J Manipulative Physiol Ther 1998;21:511-519.
8. Parker GB, Pryor DS, Tupling H. Why does migraine improve during a clinical trial? Further results from a trial of cervical manipulation for migraine. Aust N Z J Med 1980;10:192-198.
9. Mauskop A, Graff-Radford S. Special treatment situations: alternative headache treatments. In: Standards of Care for Headache Diagnosis and Treatment. Chicago, IL: National Headache Foundation; 2004;115-122.
It can be. Spinal manipulative therapy (SMT), a component of osteopathy, has been shown to be variably effective for the treatment of headaches. For the prophylactic treatment of cervicogenic headaches and for acute tension headaches, SMT is superior to placebo.
For tension headache prophylaxis, research shows a trend toward better outcomes with amitriptyline than with SMT. For migraine prophylaxis, SMT has an effect similar to amitriptyline (strength of recommendation: B, based on a systematic review of various quality studies).
3 osteopathic techniques that work for my patients
Charles Webb, DO
Oregon Health and Science University, Portland
Headaches often have more than one cause—physical, psychological, and pharmacological—and each requires treatment. I start by systematically eliminating specific headache triggers. Meanwhile, I find osteopathic manipulative treatment to be an easy and timely intervention to abort headache symptoms and improve patient well-being. I use a variety of manipulation techniques, including cervical soft tissue massage, occipital decompression, and myofascial unwinding.
- Cervical soft tissue massage of the paraspinal tissues helps relieve the spasms of tension headaches.
- Occipital decompression involves using the fingertips to manually stretch the paraspinal tissues at the base of the occiput; it works well in my experience to abort migraine headaches. I teach patients to use a rolled up hand towel behind their neck to do occipital decompression at home, which helps prevent further headaches.
- Myofascial unwinding is a technique that literally unwinds the tissues encasing muscles in spasm.
Evidence summary
For cervicogenic headaches: Spinal manipulative therapy reduces pain
Three studies1 evaluated SMT for treatment of recurrent cervicogenic headaches). A multicenter trial2 randomized 200 patients with cervicogenic headaches to either SMT (8–12 sessions over 6 weeks) or placebo. The SMT group had significantly reduced pain (at 1 week, effect size [ES]=0.7; 95% confidence interval [CI], 0.3–1.2; and at 12 months, ES=0.4; 95% CI, 0.0–0.8) and fewer headaches (ES=0.7; 95% CI, 0.3–1.1 at both time points) than placebo.
Another RCT3 with 105 patients compared SMT (3 times a week for 3 weeks) with placebo. The SMT group reported significantly less pain after 3 weeks (ES=2.2; 95% CI, 1.7–2.7).
A third trial4 randomized 30 patients to either SMT, mobilization (small oscillatory movements to a joint within its normal range), or wait-list placement. At the end of treatment, there was a nonsignificant trend toward greater pain reduction in patients receiving SMT than either those receiving mobilization (ES=0.4; 95% CI, –0.5 to 1.4) or those on the wait list (ES=0.6; 95% CI, –0.4 to 1.5).
For tension-type headaches: Results are mixed
Two trials5 investigated the efficacy of SMT on tension-type headaches. The first, an RCT with 150 patients with recurrent headaches, compared SMT (2 sessions per week) with amitriptyline (10 mg daily week 1, 20 mg daily week 2, then 30 mg daily) for 6 weeks. At the end of 6 weeks, the SMT group reported a nonsignificant trend toward more headache pain (ES for SMT vs amitriptyline= –0.4; 95% CI, –0.8 to 0.0), but fewer side effects. They had similar headache frequency and medication use.
Another study6 of 22 patients compared SMT with 2 different controls (palpation and rest) for acute tension-type headache. The SMT group was significantly more likely to experience immediate improvement (ES=1.8; 95% CI, 0.4–3.2).
For migraine: Spinal manipulative therapy is similar to amitriptyline
In 1 trial7 of migraine prophylaxis, 218 patients were randomized to either 14 sessions of SMT for 2 months or oral amitriptyline (titrated up weekly during the first month and continued at 100 mg daily over the second month). The headache index (a measure of daily pain intensity) was equivalent in both groups in the last 4 weeks of treatment (ES for SMT vs amitriptyline= –0.1; 95% CI, –0.5 to 0.3).
A month after both therapies were stopped, there was a nonsignificant trend toward a lower headache index in the group that had received SMT than the group that had received amitriptyline (ES=0.4; 95% CI, 0.0–0.8). Ten percent of the medication group withdrew from this study due to side effects; no side effects were reported from SMT.7
Another RCT8 of migraine prophylaxis with 88 patients compared SMT twice weekly for 8 weeks with mobilization techniques. At 8 weeks post-treatment, there was a nonsignificant trend favoring SMT over mobilization in decreasing pain (ES=0.4; 95% CI, –0.2 to 1.0).
Recommendations from others
The National Headache Foundation9 states that “the value and cost-effectiveness of chiropractic, osteopathic medicine, and physical therapy in migraine have not been proven in clinical trials. Conflicting results and poor clinical trial design limit the ability to judge the effectiveness of manipulative treatments. Physical therapy, although limited in its study, has proven more effective than manipulative treatment in selective cases.”
It can be. Spinal manipulative therapy (SMT), a component of osteopathy, has been shown to be variably effective for the treatment of headaches. For the prophylactic treatment of cervicogenic headaches and for acute tension headaches, SMT is superior to placebo.
For tension headache prophylaxis, research shows a trend toward better outcomes with amitriptyline than with SMT. For migraine prophylaxis, SMT has an effect similar to amitriptyline (strength of recommendation: B, based on a systematic review of various quality studies).
3 osteopathic techniques that work for my patients
Charles Webb, DO
Oregon Health and Science University, Portland
Headaches often have more than one cause—physical, psychological, and pharmacological—and each requires treatment. I start by systematically eliminating specific headache triggers. Meanwhile, I find osteopathic manipulative treatment to be an easy and timely intervention to abort headache symptoms and improve patient well-being. I use a variety of manipulation techniques, including cervical soft tissue massage, occipital decompression, and myofascial unwinding.
- Cervical soft tissue massage of the paraspinal tissues helps relieve the spasms of tension headaches.
- Occipital decompression involves using the fingertips to manually stretch the paraspinal tissues at the base of the occiput; it works well in my experience to abort migraine headaches. I teach patients to use a rolled up hand towel behind their neck to do occipital decompression at home, which helps prevent further headaches.
- Myofascial unwinding is a technique that literally unwinds the tissues encasing muscles in spasm.
Evidence summary
For cervicogenic headaches: Spinal manipulative therapy reduces pain
Three studies1 evaluated SMT for treatment of recurrent cervicogenic headaches). A multicenter trial2 randomized 200 patients with cervicogenic headaches to either SMT (8–12 sessions over 6 weeks) or placebo. The SMT group had significantly reduced pain (at 1 week, effect size [ES]=0.7; 95% confidence interval [CI], 0.3–1.2; and at 12 months, ES=0.4; 95% CI, 0.0–0.8) and fewer headaches (ES=0.7; 95% CI, 0.3–1.1 at both time points) than placebo.
Another RCT3 with 105 patients compared SMT (3 times a week for 3 weeks) with placebo. The SMT group reported significantly less pain after 3 weeks (ES=2.2; 95% CI, 1.7–2.7).
A third trial4 randomized 30 patients to either SMT, mobilization (small oscillatory movements to a joint within its normal range), or wait-list placement. At the end of treatment, there was a nonsignificant trend toward greater pain reduction in patients receiving SMT than either those receiving mobilization (ES=0.4; 95% CI, –0.5 to 1.4) or those on the wait list (ES=0.6; 95% CI, –0.4 to 1.5).
For tension-type headaches: Results are mixed
Two trials5 investigated the efficacy of SMT on tension-type headaches. The first, an RCT with 150 patients with recurrent headaches, compared SMT (2 sessions per week) with amitriptyline (10 mg daily week 1, 20 mg daily week 2, then 30 mg daily) for 6 weeks. At the end of 6 weeks, the SMT group reported a nonsignificant trend toward more headache pain (ES for SMT vs amitriptyline= –0.4; 95% CI, –0.8 to 0.0), but fewer side effects. They had similar headache frequency and medication use.
Another study6 of 22 patients compared SMT with 2 different controls (palpation and rest) for acute tension-type headache. The SMT group was significantly more likely to experience immediate improvement (ES=1.8; 95% CI, 0.4–3.2).
For migraine: Spinal manipulative therapy is similar to amitriptyline
In 1 trial7 of migraine prophylaxis, 218 patients were randomized to either 14 sessions of SMT for 2 months or oral amitriptyline (titrated up weekly during the first month and continued at 100 mg daily over the second month). The headache index (a measure of daily pain intensity) was equivalent in both groups in the last 4 weeks of treatment (ES for SMT vs amitriptyline= –0.1; 95% CI, –0.5 to 0.3).
A month after both therapies were stopped, there was a nonsignificant trend toward a lower headache index in the group that had received SMT than the group that had received amitriptyline (ES=0.4; 95% CI, 0.0–0.8). Ten percent of the medication group withdrew from this study due to side effects; no side effects were reported from SMT.7
Another RCT8 of migraine prophylaxis with 88 patients compared SMT twice weekly for 8 weeks with mobilization techniques. At 8 weeks post-treatment, there was a nonsignificant trend favoring SMT over mobilization in decreasing pain (ES=0.4; 95% CI, –0.2 to 1.0).
Recommendations from others
The National Headache Foundation9 states that “the value and cost-effectiveness of chiropractic, osteopathic medicine, and physical therapy in migraine have not been proven in clinical trials. Conflicting results and poor clinical trial design limit the ability to judge the effectiveness of manipulative treatments. Physical therapy, although limited in its study, has proven more effective than manipulative treatment in selective cases.”
1. Biondi DM. Cervicogenic headache: a review of diagnostic and treatment strategies. J Am Osteopath Assoc 2005;105(4 Suppl 2):16S-22S.
2. Jull G, Trott P, Potter H, et al. A randomized controlled trial of exercise and manipulative therapy for cervicogenic headache. Spine 2002;27:1835-1843.
3. Whittingham W. The efficacy of cervical adjustments (toggle recoil) for chronic cervicogenic headaches [PhD dissertation]. Melbourne, Australia: Royal Melbourne Institute of Technology; 1997.
4. Bronfort G, Nilsson N, Hass M, et al. Non-invasive physical treatments for chronic/recurrent headache. Cochrane Database Syst Rev 2004;(3):CD001878.-
5. Boline PD, Kassak K, Bronfort G, Nelson C, Anderson AV. Spinal manipulation vs. Amitriptyline for the treatment of chronic tension-type headaches: a randomized clinical trial. J Manipulative Physiol Ther. 1995;18:148-154.
6. Hoyt WH, Shaffer F, Bard DA, et al. Osteopathic manipulation in the treatment of muscle-contraction headache. J Am Osteopath Assoc 1979;78:322-325.
7. Nelson CF, Bronfort G, Evans R, Boline P, Goldsmith C, Anderson AV. The efficacy of spinal manipulation, amitriptyline and the combination of both therapies for the prophylaxis of migraine headache. J Manipulative Physiol Ther 1998;21:511-519.
8. Parker GB, Pryor DS, Tupling H. Why does migraine improve during a clinical trial? Further results from a trial of cervical manipulation for migraine. Aust N Z J Med 1980;10:192-198.
9. Mauskop A, Graff-Radford S. Special treatment situations: alternative headache treatments. In: Standards of Care for Headache Diagnosis and Treatment. Chicago, IL: National Headache Foundation; 2004;115-122.
1. Biondi DM. Cervicogenic headache: a review of diagnostic and treatment strategies. J Am Osteopath Assoc 2005;105(4 Suppl 2):16S-22S.
2. Jull G, Trott P, Potter H, et al. A randomized controlled trial of exercise and manipulative therapy for cervicogenic headache. Spine 2002;27:1835-1843.
3. Whittingham W. The efficacy of cervical adjustments (toggle recoil) for chronic cervicogenic headaches [PhD dissertation]. Melbourne, Australia: Royal Melbourne Institute of Technology; 1997.
4. Bronfort G, Nilsson N, Hass M, et al. Non-invasive physical treatments for chronic/recurrent headache. Cochrane Database Syst Rev 2004;(3):CD001878.-
5. Boline PD, Kassak K, Bronfort G, Nelson C, Anderson AV. Spinal manipulation vs. Amitriptyline for the treatment of chronic tension-type headaches: a randomized clinical trial. J Manipulative Physiol Ther. 1995;18:148-154.
6. Hoyt WH, Shaffer F, Bard DA, et al. Osteopathic manipulation in the treatment of muscle-contraction headache. J Am Osteopath Assoc 1979;78:322-325.
7. Nelson CF, Bronfort G, Evans R, Boline P, Goldsmith C, Anderson AV. The efficacy of spinal manipulation, amitriptyline and the combination of both therapies for the prophylaxis of migraine headache. J Manipulative Physiol Ther 1998;21:511-519.
8. Parker GB, Pryor DS, Tupling H. Why does migraine improve during a clinical trial? Further results from a trial of cervical manipulation for migraine. Aust N Z J Med 1980;10:192-198.
9. Mauskop A, Graff-Radford S. Special treatment situations: alternative headache treatments. In: Standards of Care for Headache Diagnosis and Treatment. Chicago, IL: National Headache Foundation; 2004;115-122.
Evidence-based answers from the Family Physicians Inquiries Network
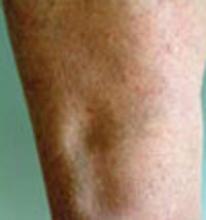
What is the differential diagnosis of chronic leg edema in primary care?
The differential diagnosis, in descending order, includes: elevated pulmonary artery pressure (often due to obstructive sleep apnea), congestive heart failure, idiopathic causes, venous insufficiency, use of nonsteroidal anti-inflammatory drugs (NSAIDs), and proteinuria (>1 g daily) (strength of recommendation: B, based on a nonconsecutive diagnostic cohort study with good reference standards).
Test for DVT in those with unilateral leg edema
Marcia Lu, MD
Department of Family and Community Medicine, University of Nevada School of Medicine, Reno
Based on presented evidence, it is premature to make the initial diagnosis of venous insufficiency without further evaluation through cardiovascular testing in patients >45 years of age.
Though this Clinical Inquiry is very convincing, I recommend cautious interpretation of this data due to the relatively small sample size, type of study, and demographics of the study population. A final note: remember to exclude pregnancy in women of reproductive age, and consider tests to exclude deep venous thrombosis in patients presenting with unilateral leg edema.
Evidence summary
Chronic leg edema is defined as palpable swelling caused by an increase in interstitial fluid volume lasting at least 72 hours.1
We were able to find only 1 moderate-quality study regarding the diagnosis of bilateral lower extremity edema that included a thorough cardiovascular evaluation.
Single study in bilateral leg edema: What the FPs thought…
A nonconsecutive cohort study2 evaluated the causes of bilateral leg edema among 58 ambulatory adults (between 29 and 83 years of age) enrolled from an inner-city family medicine clinic in Cleveland. Edema was present for >3 months in 78% of patients, and 84% were obese. Patients were excluded if the edema was known to be due to nifedipine, intra-abdominal malignancy, hypothyroidism, or idiopathic cyclic edema.
Family physicians obtained a history and performed a physical exam on all patients and recorded a clinical diagnosis for the edema. Initial clinical impressions included: venous insufficiency (71%), congestive heart failure (18%), nephrotic syndrome (13%), uncertain (7%), and other causes (2% each). Other causes included lymphedema, pulmonary hypertension, cor pulmonale, hypoalbuminemia, NSAID or corticosteroid use, sleep apnea, and obesity. (Total percentages exceed 100% because some patients had multiple conditions.)
All patients were then evaluated with a serum albumin, a 24-hour urine protein collection, echocardiogram, and lower extremity duplex venous ultrasound (13 of 58 patients did not complete the echocardiogram and venous duplex ultrasound). Investigators developed a final diagnosis using the results of this evaluation in conjunction with the clinical information obtained by the physician.
…and what the testing revealed
Final diagnoses included pulmonary hypertension/borderline pulmonary hyper-tension (>30 mm Hg) (42%), congestive heart failure (29%), idiopathic edema (27%), venous insufficiency (22%), medication use (15%, primarily corticosteroids and NSAIDs), proteinuria >1 g/day (15%), and other causes (2% each). These other causes included transient renal disease, hypoalbuminemia, lymphedema, and stenosis of the inferior vena cava. (Total percentages again exceed 100% because some patients had multiple diagnoses.)
All 15 patients with cardiac conditions and 17 of 19 patients with pulmonary hypertension were over 45 years of age. Of the 19 patients with pulmonary hypertension, 6 had CHF, 4 had chronic obstructive pulmonary disease, 4 had sleep apnea diagnosed in subsequent testing, 1 had an atrial septal defect, and 4 appeared to have primary pulmonary hypertension.
Investigators recommend 3 steps
The investigators recommended 3 steps to evaluate chronic leg edema.
- Stop any potentially causative medicines, such as NSAIDs or calcium-channel blockers.
- Obtain an echocardiogram if the patient is 45 years of age or older.
- Obtain a sleep study if the echo-cardiogram reveals pulmonary hypertension without an apparent cause.
Recommendations from others
The authors of a recent narrative systematic review1 stated that “most patients with chronic leg edema can be assumed to have venous insufficiency, CHF, or cyclic edema, unless another cause is suspected after a history and physical examination.” They also stated that: “pulmonary hypertension and early CHF can both cause leg edema before they become clinically obvious” and reiterate that patients over 45 years of age with edema of unclear cause should have an echocardiogram to rule out pulmonary hypertension.
The differential diagnosis, in descending order, includes: elevated pulmonary artery pressure (often due to obstructive sleep apnea), congestive heart failure, idiopathic causes, venous insufficiency, use of nonsteroidal anti-inflammatory drugs (NSAIDs), and proteinuria (>1 g daily) (strength of recommendation: B, based on a nonconsecutive diagnostic cohort study with good reference standards).
Test for DVT in those with unilateral leg edema
Marcia Lu, MD
Department of Family and Community Medicine, University of Nevada School of Medicine, Reno
Based on presented evidence, it is premature to make the initial diagnosis of venous insufficiency without further evaluation through cardiovascular testing in patients >45 years of age.
Though this Clinical Inquiry is very convincing, I recommend cautious interpretation of this data due to the relatively small sample size, type of study, and demographics of the study population. A final note: remember to exclude pregnancy in women of reproductive age, and consider tests to exclude deep venous thrombosis in patients presenting with unilateral leg edema.
Evidence summary
Chronic leg edema is defined as palpable swelling caused by an increase in interstitial fluid volume lasting at least 72 hours.1
We were able to find only 1 moderate-quality study regarding the diagnosis of bilateral lower extremity edema that included a thorough cardiovascular evaluation.
Single study in bilateral leg edema: What the FPs thought…
A nonconsecutive cohort study2 evaluated the causes of bilateral leg edema among 58 ambulatory adults (between 29 and 83 years of age) enrolled from an inner-city family medicine clinic in Cleveland. Edema was present for >3 months in 78% of patients, and 84% were obese. Patients were excluded if the edema was known to be due to nifedipine, intra-abdominal malignancy, hypothyroidism, or idiopathic cyclic edema.
Family physicians obtained a history and performed a physical exam on all patients and recorded a clinical diagnosis for the edema. Initial clinical impressions included: venous insufficiency (71%), congestive heart failure (18%), nephrotic syndrome (13%), uncertain (7%), and other causes (2% each). Other causes included lymphedema, pulmonary hypertension, cor pulmonale, hypoalbuminemia, NSAID or corticosteroid use, sleep apnea, and obesity. (Total percentages exceed 100% because some patients had multiple conditions.)
All patients were then evaluated with a serum albumin, a 24-hour urine protein collection, echocardiogram, and lower extremity duplex venous ultrasound (13 of 58 patients did not complete the echocardiogram and venous duplex ultrasound). Investigators developed a final diagnosis using the results of this evaluation in conjunction with the clinical information obtained by the physician.
…and what the testing revealed
Final diagnoses included pulmonary hypertension/borderline pulmonary hyper-tension (>30 mm Hg) (42%), congestive heart failure (29%), idiopathic edema (27%), venous insufficiency (22%), medication use (15%, primarily corticosteroids and NSAIDs), proteinuria >1 g/day (15%), and other causes (2% each). These other causes included transient renal disease, hypoalbuminemia, lymphedema, and stenosis of the inferior vena cava. (Total percentages again exceed 100% because some patients had multiple diagnoses.)
All 15 patients with cardiac conditions and 17 of 19 patients with pulmonary hypertension were over 45 years of age. Of the 19 patients with pulmonary hypertension, 6 had CHF, 4 had chronic obstructive pulmonary disease, 4 had sleep apnea diagnosed in subsequent testing, 1 had an atrial septal defect, and 4 appeared to have primary pulmonary hypertension.
Investigators recommend 3 steps
The investigators recommended 3 steps to evaluate chronic leg edema.
- Stop any potentially causative medicines, such as NSAIDs or calcium-channel blockers.
- Obtain an echocardiogram if the patient is 45 years of age or older.
- Obtain a sleep study if the echo-cardiogram reveals pulmonary hypertension without an apparent cause.
Recommendations from others
The authors of a recent narrative systematic review1 stated that “most patients with chronic leg edema can be assumed to have venous insufficiency, CHF, or cyclic edema, unless another cause is suspected after a history and physical examination.” They also stated that: “pulmonary hypertension and early CHF can both cause leg edema before they become clinically obvious” and reiterate that patients over 45 years of age with edema of unclear cause should have an echocardiogram to rule out pulmonary hypertension.
The differential diagnosis, in descending order, includes: elevated pulmonary artery pressure (often due to obstructive sleep apnea), congestive heart failure, idiopathic causes, venous insufficiency, use of nonsteroidal anti-inflammatory drugs (NSAIDs), and proteinuria (>1 g daily) (strength of recommendation: B, based on a nonconsecutive diagnostic cohort study with good reference standards).
Test for DVT in those with unilateral leg edema
Marcia Lu, MD
Department of Family and Community Medicine, University of Nevada School of Medicine, Reno
Based on presented evidence, it is premature to make the initial diagnosis of venous insufficiency without further evaluation through cardiovascular testing in patients >45 years of age.
Though this Clinical Inquiry is very convincing, I recommend cautious interpretation of this data due to the relatively small sample size, type of study, and demographics of the study population. A final note: remember to exclude pregnancy in women of reproductive age, and consider tests to exclude deep venous thrombosis in patients presenting with unilateral leg edema.
Evidence summary
Chronic leg edema is defined as palpable swelling caused by an increase in interstitial fluid volume lasting at least 72 hours.1
We were able to find only 1 moderate-quality study regarding the diagnosis of bilateral lower extremity edema that included a thorough cardiovascular evaluation.
Single study in bilateral leg edema: What the FPs thought…
A nonconsecutive cohort study2 evaluated the causes of bilateral leg edema among 58 ambulatory adults (between 29 and 83 years of age) enrolled from an inner-city family medicine clinic in Cleveland. Edema was present for >3 months in 78% of patients, and 84% were obese. Patients were excluded if the edema was known to be due to nifedipine, intra-abdominal malignancy, hypothyroidism, or idiopathic cyclic edema.
Family physicians obtained a history and performed a physical exam on all patients and recorded a clinical diagnosis for the edema. Initial clinical impressions included: venous insufficiency (71%), congestive heart failure (18%), nephrotic syndrome (13%), uncertain (7%), and other causes (2% each). Other causes included lymphedema, pulmonary hypertension, cor pulmonale, hypoalbuminemia, NSAID or corticosteroid use, sleep apnea, and obesity. (Total percentages exceed 100% because some patients had multiple conditions.)
All patients were then evaluated with a serum albumin, a 24-hour urine protein collection, echocardiogram, and lower extremity duplex venous ultrasound (13 of 58 patients did not complete the echocardiogram and venous duplex ultrasound). Investigators developed a final diagnosis using the results of this evaluation in conjunction with the clinical information obtained by the physician.
…and what the testing revealed
Final diagnoses included pulmonary hypertension/borderline pulmonary hyper-tension (>30 mm Hg) (42%), congestive heart failure (29%), idiopathic edema (27%), venous insufficiency (22%), medication use (15%, primarily corticosteroids and NSAIDs), proteinuria >1 g/day (15%), and other causes (2% each). These other causes included transient renal disease, hypoalbuminemia, lymphedema, and stenosis of the inferior vena cava. (Total percentages again exceed 100% because some patients had multiple diagnoses.)
All 15 patients with cardiac conditions and 17 of 19 patients with pulmonary hypertension were over 45 years of age. Of the 19 patients with pulmonary hypertension, 6 had CHF, 4 had chronic obstructive pulmonary disease, 4 had sleep apnea diagnosed in subsequent testing, 1 had an atrial septal defect, and 4 appeared to have primary pulmonary hypertension.
Investigators recommend 3 steps
The investigators recommended 3 steps to evaluate chronic leg edema.
- Stop any potentially causative medicines, such as NSAIDs or calcium-channel blockers.
- Obtain an echocardiogram if the patient is 45 years of age or older.
- Obtain a sleep study if the echo-cardiogram reveals pulmonary hypertension without an apparent cause.
Recommendations from others
The authors of a recent narrative systematic review1 stated that “most patients with chronic leg edema can be assumed to have venous insufficiency, CHF, or cyclic edema, unless another cause is suspected after a history and physical examination.” They also stated that: “pulmonary hypertension and early CHF can both cause leg edema before they become clinically obvious” and reiterate that patients over 45 years of age with edema of unclear cause should have an echocardiogram to rule out pulmonary hypertension.
Evidence-based answers from the Family Physicians Inquiries Network
Does screening reduce lung cancer mortality?
It’s not clear. Neither routine chest x-ray (with or without sputum cytology) nor low-dose computed tomography (CT) have been proven to reduce mortality when used for lung cancer screening, although low-dose CT screening does identify lung cancer at an early stage in high-risk patients (strength of recommendation: B, based on heterogeneous cohort studies). Large studies of both imaging approaches are ongoing.
Let’s prevent lung cancer so we don’t have to worry about screening
Tim Huber, MD
Oroville Hospital, Oroville, Calif
While some trials suggest possibly useful screening tools, and myriad other trials are underway, one point often gets short shrift: the importance of preventing cancer from occurring in the first place. Most family physicians already screen for smoking and offer counseling and pharmacologic assistance to smokers. We should also be aggressively counseling our adolescent and young adult patients against starting to smoke. Ideally, we would help people reduce their exposure to secondhand smoke, as well. When a teachable moment comes along, we should take the time to educate our patients about their specific risk factors and how they can be modified. Preventing the problem before it starts is our patients’ best defense against lung cancer.
Evidence summary
Chest x-ray and cytology: A trend toward reduced mortality
A Cochrane review1 identified 6 randomized controlled trials (RCTs) and 1 non-RCT (with a total of 245,610 patients) that screened patients with serial chest x-rays, with or without sputum cytology. Most patients were current or ex-smokers or had significant exposure to industrial smoke. No studies included an unscreened control group, and only 1 included women.
There was a trend toward reduced mortality with the combination of annual chest x-ray and sputum cytology compared with annual x-ray alone, but it was not statistically significant (relative risk [RR]=0.88; 95% confidence interval [CI], 0.74–1.03). However, more frequent screening with chest x-rays (2 or 3 times/ year) was associated with an 11% increase in mortality compared with less frequent x-rays (RR=1.11; 95% CI, 1.00–1.23). The authors concluded that there was insufficient evidence to support screening with chest x-ray or sputum cytology.
Low-dose CT: Studies reach different conclusions
A 2006 study followed a cohort of at-risk patients using low-dose CT screening.2 There were 31,567 patients evaluated initially, of which 27,456 had an annual repeat screening. Most patients were current or former smokers (83%); patients with exposure to occupational and secondhand smoke were also included. A positive initial screen was defined as a solid or partly solid noncalcified nodule ≥5 mm in diameter; a nonsolid, noncalcified nodule ≥8 mm in diameter; or a solid endobronchial nodule. A positive screen during follow-up was defined as any new noncalcified nodule, regardless of size.
Positive tests occurred in 13% of baseline screens and 5% of annual screens. Biopsies were performed according to a study protocol based on a nodule’s size and behavior over time. Out of a total of 5646 positive screens, there were 535 biopsies, and a diagnosis of cancer in 492 patients. Of those with cancer, 412 (84%) had clinical stage I lung cancer; the authors estimated their 10-year survival rate was 88% (95% CI, 84%–91%). If patients with stage I disease underwent surgical resection within 1 month of diagnosis, their estimated 10-year survival increased to 92% (95% CI, 88%–95%).
However, a cohort study using annual CT scanning to screen 3246 patients for lung cancer came to a different conclusion.3 The authors compared the observed number of lung cancer cases, resections, advanced lung cancer diagnoses, and deaths in screened patients with the expected rates based on validated prediction models. Lung cancer was diagnosed in 144 patients compared with 44 expected cases (RR=3.2; 95% CI, 2.7–3.8). Subsequently, 109 patients underwent lung resection compared with 11 expected (RR=10.0; 95% CI, 8.2–11.9). However, there was no decline in advanced cancers (42 actual vs 33 expected; P=.14) and no difference in deaths due to lung cancer (38 actual vs 38.8 expected; P=.9). The 81 patients diagnosed in this study with stage I disease who underwent surgical resection had 4-year estimated survival rates of 94% (95% CI, 85%–97%), matching the prior low-dose CT study.
Major studies of both methods are ongoing
Other major studies are in progress. There is an RCT involving 154,942 male and female patients using annual chest x-ray screening vs no screening that will involve 14 years of follow-up.4 Another RCT is evaluating annual low-dose CT vs annual chest x-ray for 3 years in 50,000 at-risk men and women.5 Finally, investigators are conducting an RCT with 4000 at-risk patients comparing annual CT screening with no screening.6
Recommendations from others
The US Preventive Services Task Force gives an “I” recommendation (data insufficient) to screening for lung cancer with cytology, chest x-ray, or CT scanning.7 The American College of Chest Physicians stated in 2003 that the early studies of low-dose CT appeared promising; however, they recommended that individuals should only be screened with low-dose CT in the context of well- designed clinical trials.8
1. Manser RL, Irving LB, Stone C, Byrnes G, Abramson M, Campbell D. Screening for lung cancer. Cochrane Database System Rev. 2004;(1):CD001991.-
2. The International Early Lung Cancer Action Program Investigators; Henschke CI Yankelevitz DF Libby DM Pasmantier MW Smith JP, Miettinen OS. Survival of patients with stage I lung cancer detected on CT Screening. N Engl J Med. 2006;355:1763–1771.-
3. Bach PB, Jett JR, Pastorino U, Tockman MS, Swensen SJ, Begg CB. Computed tomography screening and Lung cancer outcomes. JAMA. 2008;279:953-961.
4. Oken MM, Marcus PM, Hu P, et al. PLCO Project Team. Baseline chest radiograph for lung cancer detection in the randomized Prostate, lung, Colorectal, and ovarian Cancer screening Trial. J Natl Cancer Inst. 2005;97:1832-1839.
5. National Lung Screening Trial (NLST) National Cancer Institute Web site. Available at: www.cancer.gov/nlst. Accessed on December 7, 2008.
6. Van Iersel CA, de Koning HJ, Draisma G, et al. Risk-based selection from the general population in a screening trial: selection criteria, recruitment and power for the Dutch-Belgian randomised lung cancer multi-slice CT screening trial (nelson). Int J Cancer 2008;120:868-874.
7. Recommendation statement lung cancer screening. US Preventive services Task Force Web site. Available at: www.ahrq.gov/clinic/3rduspstf/lungcancer/lungcanrs.htm. Accessed on December 7, 2008.
8. Bach PB, Niewoehner, Black WC. Screening for lung cancer: the guidelines. Chest 2003;123:83-88.
It’s not clear. Neither routine chest x-ray (with or without sputum cytology) nor low-dose computed tomography (CT) have been proven to reduce mortality when used for lung cancer screening, although low-dose CT screening does identify lung cancer at an early stage in high-risk patients (strength of recommendation: B, based on heterogeneous cohort studies). Large studies of both imaging approaches are ongoing.
Let’s prevent lung cancer so we don’t have to worry about screening
Tim Huber, MD
Oroville Hospital, Oroville, Calif
While some trials suggest possibly useful screening tools, and myriad other trials are underway, one point often gets short shrift: the importance of preventing cancer from occurring in the first place. Most family physicians already screen for smoking and offer counseling and pharmacologic assistance to smokers. We should also be aggressively counseling our adolescent and young adult patients against starting to smoke. Ideally, we would help people reduce their exposure to secondhand smoke, as well. When a teachable moment comes along, we should take the time to educate our patients about their specific risk factors and how they can be modified. Preventing the problem before it starts is our patients’ best defense against lung cancer.
Evidence summary
Chest x-ray and cytology: A trend toward reduced mortality
A Cochrane review1 identified 6 randomized controlled trials (RCTs) and 1 non-RCT (with a total of 245,610 patients) that screened patients with serial chest x-rays, with or without sputum cytology. Most patients were current or ex-smokers or had significant exposure to industrial smoke. No studies included an unscreened control group, and only 1 included women.
There was a trend toward reduced mortality with the combination of annual chest x-ray and sputum cytology compared with annual x-ray alone, but it was not statistically significant (relative risk [RR]=0.88; 95% confidence interval [CI], 0.74–1.03). However, more frequent screening with chest x-rays (2 or 3 times/ year) was associated with an 11% increase in mortality compared with less frequent x-rays (RR=1.11; 95% CI, 1.00–1.23). The authors concluded that there was insufficient evidence to support screening with chest x-ray or sputum cytology.
Low-dose CT: Studies reach different conclusions
A 2006 study followed a cohort of at-risk patients using low-dose CT screening.2 There were 31,567 patients evaluated initially, of which 27,456 had an annual repeat screening. Most patients were current or former smokers (83%); patients with exposure to occupational and secondhand smoke were also included. A positive initial screen was defined as a solid or partly solid noncalcified nodule ≥5 mm in diameter; a nonsolid, noncalcified nodule ≥8 mm in diameter; or a solid endobronchial nodule. A positive screen during follow-up was defined as any new noncalcified nodule, regardless of size.
Positive tests occurred in 13% of baseline screens and 5% of annual screens. Biopsies were performed according to a study protocol based on a nodule’s size and behavior over time. Out of a total of 5646 positive screens, there were 535 biopsies, and a diagnosis of cancer in 492 patients. Of those with cancer, 412 (84%) had clinical stage I lung cancer; the authors estimated their 10-year survival rate was 88% (95% CI, 84%–91%). If patients with stage I disease underwent surgical resection within 1 month of diagnosis, their estimated 10-year survival increased to 92% (95% CI, 88%–95%).
However, a cohort study using annual CT scanning to screen 3246 patients for lung cancer came to a different conclusion.3 The authors compared the observed number of lung cancer cases, resections, advanced lung cancer diagnoses, and deaths in screened patients with the expected rates based on validated prediction models. Lung cancer was diagnosed in 144 patients compared with 44 expected cases (RR=3.2; 95% CI, 2.7–3.8). Subsequently, 109 patients underwent lung resection compared with 11 expected (RR=10.0; 95% CI, 8.2–11.9). However, there was no decline in advanced cancers (42 actual vs 33 expected; P=.14) and no difference in deaths due to lung cancer (38 actual vs 38.8 expected; P=.9). The 81 patients diagnosed in this study with stage I disease who underwent surgical resection had 4-year estimated survival rates of 94% (95% CI, 85%–97%), matching the prior low-dose CT study.
Major studies of both methods are ongoing
Other major studies are in progress. There is an RCT involving 154,942 male and female patients using annual chest x-ray screening vs no screening that will involve 14 years of follow-up.4 Another RCT is evaluating annual low-dose CT vs annual chest x-ray for 3 years in 50,000 at-risk men and women.5 Finally, investigators are conducting an RCT with 4000 at-risk patients comparing annual CT screening with no screening.6
Recommendations from others
The US Preventive Services Task Force gives an “I” recommendation (data insufficient) to screening for lung cancer with cytology, chest x-ray, or CT scanning.7 The American College of Chest Physicians stated in 2003 that the early studies of low-dose CT appeared promising; however, they recommended that individuals should only be screened with low-dose CT in the context of well- designed clinical trials.8
It’s not clear. Neither routine chest x-ray (with or without sputum cytology) nor low-dose computed tomography (CT) have been proven to reduce mortality when used for lung cancer screening, although low-dose CT screening does identify lung cancer at an early stage in high-risk patients (strength of recommendation: B, based on heterogeneous cohort studies). Large studies of both imaging approaches are ongoing.
Let’s prevent lung cancer so we don’t have to worry about screening
Tim Huber, MD
Oroville Hospital, Oroville, Calif
While some trials suggest possibly useful screening tools, and myriad other trials are underway, one point often gets short shrift: the importance of preventing cancer from occurring in the first place. Most family physicians already screen for smoking and offer counseling and pharmacologic assistance to smokers. We should also be aggressively counseling our adolescent and young adult patients against starting to smoke. Ideally, we would help people reduce their exposure to secondhand smoke, as well. When a teachable moment comes along, we should take the time to educate our patients about their specific risk factors and how they can be modified. Preventing the problem before it starts is our patients’ best defense against lung cancer.
Evidence summary
Chest x-ray and cytology: A trend toward reduced mortality
A Cochrane review1 identified 6 randomized controlled trials (RCTs) and 1 non-RCT (with a total of 245,610 patients) that screened patients with serial chest x-rays, with or without sputum cytology. Most patients were current or ex-smokers or had significant exposure to industrial smoke. No studies included an unscreened control group, and only 1 included women.
There was a trend toward reduced mortality with the combination of annual chest x-ray and sputum cytology compared with annual x-ray alone, but it was not statistically significant (relative risk [RR]=0.88; 95% confidence interval [CI], 0.74–1.03). However, more frequent screening with chest x-rays (2 or 3 times/ year) was associated with an 11% increase in mortality compared with less frequent x-rays (RR=1.11; 95% CI, 1.00–1.23). The authors concluded that there was insufficient evidence to support screening with chest x-ray or sputum cytology.
Low-dose CT: Studies reach different conclusions
A 2006 study followed a cohort of at-risk patients using low-dose CT screening.2 There were 31,567 patients evaluated initially, of which 27,456 had an annual repeat screening. Most patients were current or former smokers (83%); patients with exposure to occupational and secondhand smoke were also included. A positive initial screen was defined as a solid or partly solid noncalcified nodule ≥5 mm in diameter; a nonsolid, noncalcified nodule ≥8 mm in diameter; or a solid endobronchial nodule. A positive screen during follow-up was defined as any new noncalcified nodule, regardless of size.
Positive tests occurred in 13% of baseline screens and 5% of annual screens. Biopsies were performed according to a study protocol based on a nodule’s size and behavior over time. Out of a total of 5646 positive screens, there were 535 biopsies, and a diagnosis of cancer in 492 patients. Of those with cancer, 412 (84%) had clinical stage I lung cancer; the authors estimated their 10-year survival rate was 88% (95% CI, 84%–91%). If patients with stage I disease underwent surgical resection within 1 month of diagnosis, their estimated 10-year survival increased to 92% (95% CI, 88%–95%).
However, a cohort study using annual CT scanning to screen 3246 patients for lung cancer came to a different conclusion.3 The authors compared the observed number of lung cancer cases, resections, advanced lung cancer diagnoses, and deaths in screened patients with the expected rates based on validated prediction models. Lung cancer was diagnosed in 144 patients compared with 44 expected cases (RR=3.2; 95% CI, 2.7–3.8). Subsequently, 109 patients underwent lung resection compared with 11 expected (RR=10.0; 95% CI, 8.2–11.9). However, there was no decline in advanced cancers (42 actual vs 33 expected; P=.14) and no difference in deaths due to lung cancer (38 actual vs 38.8 expected; P=.9). The 81 patients diagnosed in this study with stage I disease who underwent surgical resection had 4-year estimated survival rates of 94% (95% CI, 85%–97%), matching the prior low-dose CT study.
Major studies of both methods are ongoing
Other major studies are in progress. There is an RCT involving 154,942 male and female patients using annual chest x-ray screening vs no screening that will involve 14 years of follow-up.4 Another RCT is evaluating annual low-dose CT vs annual chest x-ray for 3 years in 50,000 at-risk men and women.5 Finally, investigators are conducting an RCT with 4000 at-risk patients comparing annual CT screening with no screening.6
Recommendations from others
The US Preventive Services Task Force gives an “I” recommendation (data insufficient) to screening for lung cancer with cytology, chest x-ray, or CT scanning.7 The American College of Chest Physicians stated in 2003 that the early studies of low-dose CT appeared promising; however, they recommended that individuals should only be screened with low-dose CT in the context of well- designed clinical trials.8
1. Manser RL, Irving LB, Stone C, Byrnes G, Abramson M, Campbell D. Screening for lung cancer. Cochrane Database System Rev. 2004;(1):CD001991.-
2. The International Early Lung Cancer Action Program Investigators; Henschke CI Yankelevitz DF Libby DM Pasmantier MW Smith JP, Miettinen OS. Survival of patients with stage I lung cancer detected on CT Screening. N Engl J Med. 2006;355:1763–1771.-
3. Bach PB, Jett JR, Pastorino U, Tockman MS, Swensen SJ, Begg CB. Computed tomography screening and Lung cancer outcomes. JAMA. 2008;279:953-961.
4. Oken MM, Marcus PM, Hu P, et al. PLCO Project Team. Baseline chest radiograph for lung cancer detection in the randomized Prostate, lung, Colorectal, and ovarian Cancer screening Trial. J Natl Cancer Inst. 2005;97:1832-1839.
5. National Lung Screening Trial (NLST) National Cancer Institute Web site. Available at: www.cancer.gov/nlst. Accessed on December 7, 2008.
6. Van Iersel CA, de Koning HJ, Draisma G, et al. Risk-based selection from the general population in a screening trial: selection criteria, recruitment and power for the Dutch-Belgian randomised lung cancer multi-slice CT screening trial (nelson). Int J Cancer 2008;120:868-874.
7. Recommendation statement lung cancer screening. US Preventive services Task Force Web site. Available at: www.ahrq.gov/clinic/3rduspstf/lungcancer/lungcanrs.htm. Accessed on December 7, 2008.
8. Bach PB, Niewoehner, Black WC. Screening for lung cancer: the guidelines. Chest 2003;123:83-88.
1. Manser RL, Irving LB, Stone C, Byrnes G, Abramson M, Campbell D. Screening for lung cancer. Cochrane Database System Rev. 2004;(1):CD001991.-
2. The International Early Lung Cancer Action Program Investigators; Henschke CI Yankelevitz DF Libby DM Pasmantier MW Smith JP, Miettinen OS. Survival of patients with stage I lung cancer detected on CT Screening. N Engl J Med. 2006;355:1763–1771.-
3. Bach PB, Jett JR, Pastorino U, Tockman MS, Swensen SJ, Begg CB. Computed tomography screening and Lung cancer outcomes. JAMA. 2008;279:953-961.
4. Oken MM, Marcus PM, Hu P, et al. PLCO Project Team. Baseline chest radiograph for lung cancer detection in the randomized Prostate, lung, Colorectal, and ovarian Cancer screening Trial. J Natl Cancer Inst. 2005;97:1832-1839.
5. National Lung Screening Trial (NLST) National Cancer Institute Web site. Available at: www.cancer.gov/nlst. Accessed on December 7, 2008.
6. Van Iersel CA, de Koning HJ, Draisma G, et al. Risk-based selection from the general population in a screening trial: selection criteria, recruitment and power for the Dutch-Belgian randomised lung cancer multi-slice CT screening trial (nelson). Int J Cancer 2008;120:868-874.
7. Recommendation statement lung cancer screening. US Preventive services Task Force Web site. Available at: www.ahrq.gov/clinic/3rduspstf/lungcancer/lungcanrs.htm. Accessed on December 7, 2008.
8. Bach PB, Niewoehner, Black WC. Screening for lung cancer: the guidelines. Chest 2003;123:83-88.
Evidence-based answers from the Family Physicians Inquiries Network
When are antibiotics indicated for acute COPD exacerbations?
Antibiotics (including those given orally) reduce mortality and treatment failures for hospitalized patients with acute exacerbations of chronic obstructive pulmonary disease (COPD) (strength of recommendation [SOR]: A, based on systematic reviews). Antibiotics may be prescribed in the outpatient setting for those with severe exacerbations (SOR: C, based on expert opinion).
Antibiotics are indicated in COPD exacerbations requiring hospitalization
Julie Taraday, MD
University of Washington, Seattle
In an era when physicians aim to use antibiotics judiciously, this article clarifies that antibiotics are indicated in COPD exacerbations requiring hospitalization. In the outpatient setting, the correct action is less clear. Available guidelines, which recommend antibiotics for severe exacerbations, do not generally differentiate between the inpatient and outpatient setting. Antibiotics clearly have no role in mild exacerbations and so should be avoided in many outpatient cases.
Evidence summary
A recent Cochrane review identified 11 randomized controlled trials (RCTs) (with a total of 917 patients) addressing antibiotic therapy for COPD exacerbations characterized by 1 or more of the following: an increase in sputum purulence or volume, dyspnea, wheezing, chest tightness, or fluid retention.1 Eight trials were conducted on hospital wards, 1 was in a medical intensive care unit, and 2 trials were in the outpatient setting. Antibiotics were given orally in 9 of the 11 studies.
Overall, antibiotics reduced risk of short-term mortality by 77% (relative risk [RR]=0.23; 95% confidence interval [CI],0.10–0.52; number needed to treat [NNT]=8), treatment failure by 53% (RR=0.47; 95% CI, 0.36–0.62; NNT=3), and sputum purulence by 44% (RR=0.56; 95% CI, 0.41–0.77; NNT=8). A subgroup analysis that excluded the outpatient and intensive-care unit studies did not change the result. Another subgroup analysis of the 2 outpatient studies failed to find a significant effect, although the studies had very different designs.
These findings are more robust than those of an earlier, lower-quality meta-analysis of 9 randomized controlled trials (RCTs) with 1101 patients with presumed COPD, which also compared antibiotic therapy with placebo for acute exacerbations.2 Specific diagnostic criteria were not stated for the diagnosis of either COPD or an acute exacerbation. No single outcome measure was common to all studies. The authors found a summary beneficial effect size of antibiotic therapy of 0.22 (95% CI, 0.10–0.34), which is generally interpreted as small. One clinical parameter, peak expiratory flow rate (PEFR), was reported in 6 of the studies. Antibiotic therapy resulted in an average 10.75 L/min improvement in PEFR compared with placebo (95% CI, 4.96–16.54 L/min).
Two RCTs addressing antibiotic use in the outpatient setting were identified in the Cochrane review. One double-blind crossover trial performed in Canada compared antibiotic with placebo therapy for 173 outpatients with 362 exacerbations classified according to severity.3 The protocol used oral trimethoprim-sulfamethoxazole, amoxicillin, or doxycycline (according to the attending physician’s preference) or a look-alike placebo. Symptom resolution was seen by 21 days in 68% of antibiotic users vs 55% of those on placebo (P<.01, NNT=8). Ten percent of patients taking antibiotics deteriorated to the point where hospitalization or unblinding of the therapy was necessary, compared with 19% in the placebo group (P<.05, NNT=11).
For patients with all 3 cardinal COPD symptoms (increased dyspnea, sputum production, and sputum purulence) at enrollment, there was resolution at 21 days in 63% with antibiotics vs 43% for placebo (P value not given). Antibiotics did not benefit patients with 1 cardinal symptom (74% success with antibiotics vs 70% on placebo; P value not given).
The Cochrane review also identified a Danish RCT that studied 278 patients presenting to their general practitioners with subjective acute worsening of their COPD. Patients were randomized to 7 days of oral amoxicillin or placebo. There was no difference between the groups in terms of symptom resolution at 1 week (odds ratio=1.03, favoring placebo; 95% CI, 0.75–1.41) or in changes in PEFR (weighted mean difference=–0.89, favoring placebo; 95% CI, –29 to 27 L/min).
Recommendations from others
The Veterans Health Administration recommends antibiotics if a patient with COPD has changes in sputum volume or quality as well as increased dyspnea, cough, or fever; infiltrate on x-ray suggesting pneumonia should be treated as such.4
The American College of Chest Physicians recommends that with severe COPD exacerbations, narrow spectrum antibiotics are reasonable first-line agents.5 They also note that the superiority of newer, more broad-spectrum antibiotics has not been established.
1. Ram FSF, Rodriguez-Roisin R, Granados-Navarrete A, Garcia-Aymerich J, Barnes NC. Antibiotics for exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2006;(2):CD004403.-
2. Saint S, Bent S, Vittinghoff E, Grady D. Antibiotics in chronic obstructive pulmonary disease exacerbations. JAMA 1995;273:957-60.
3. Anthonisen NR, Manfreda J, Warren CP, Hershfield ES, Harding GK, Nelson NA. Antibiotic therapy in exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 1987;106:196-204.
4. Medical advisory panel for the pharmacy benefits management strategic healthcare group The pharmacologic management of chronic obstructive pulmonary disease. Washington, DC: Veterans Health Administration, Department of Veterans Affairs; 2002.
5. Snow V, Lascher S. Mottur-Pilson C, and the Joint Expert Panel on Chronic Obstructive Pulmonary Disease of the American College of Chest Physicians and the American College of Physicians-American Society of Internal Medicine Evidence base for management of acute exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 2001;134:595-599.
Antibiotics (including those given orally) reduce mortality and treatment failures for hospitalized patients with acute exacerbations of chronic obstructive pulmonary disease (COPD) (strength of recommendation [SOR]: A, based on systematic reviews). Antibiotics may be prescribed in the outpatient setting for those with severe exacerbations (SOR: C, based on expert opinion).
Antibiotics are indicated in COPD exacerbations requiring hospitalization
Julie Taraday, MD
University of Washington, Seattle
In an era when physicians aim to use antibiotics judiciously, this article clarifies that antibiotics are indicated in COPD exacerbations requiring hospitalization. In the outpatient setting, the correct action is less clear. Available guidelines, which recommend antibiotics for severe exacerbations, do not generally differentiate between the inpatient and outpatient setting. Antibiotics clearly have no role in mild exacerbations and so should be avoided in many outpatient cases.
Evidence summary
A recent Cochrane review identified 11 randomized controlled trials (RCTs) (with a total of 917 patients) addressing antibiotic therapy for COPD exacerbations characterized by 1 or more of the following: an increase in sputum purulence or volume, dyspnea, wheezing, chest tightness, or fluid retention.1 Eight trials were conducted on hospital wards, 1 was in a medical intensive care unit, and 2 trials were in the outpatient setting. Antibiotics were given orally in 9 of the 11 studies.
Overall, antibiotics reduced risk of short-term mortality by 77% (relative risk [RR]=0.23; 95% confidence interval [CI],0.10–0.52; number needed to treat [NNT]=8), treatment failure by 53% (RR=0.47; 95% CI, 0.36–0.62; NNT=3), and sputum purulence by 44% (RR=0.56; 95% CI, 0.41–0.77; NNT=8). A subgroup analysis that excluded the outpatient and intensive-care unit studies did not change the result. Another subgroup analysis of the 2 outpatient studies failed to find a significant effect, although the studies had very different designs.
These findings are more robust than those of an earlier, lower-quality meta-analysis of 9 randomized controlled trials (RCTs) with 1101 patients with presumed COPD, which also compared antibiotic therapy with placebo for acute exacerbations.2 Specific diagnostic criteria were not stated for the diagnosis of either COPD or an acute exacerbation. No single outcome measure was common to all studies. The authors found a summary beneficial effect size of antibiotic therapy of 0.22 (95% CI, 0.10–0.34), which is generally interpreted as small. One clinical parameter, peak expiratory flow rate (PEFR), was reported in 6 of the studies. Antibiotic therapy resulted in an average 10.75 L/min improvement in PEFR compared with placebo (95% CI, 4.96–16.54 L/min).
Two RCTs addressing antibiotic use in the outpatient setting were identified in the Cochrane review. One double-blind crossover trial performed in Canada compared antibiotic with placebo therapy for 173 outpatients with 362 exacerbations classified according to severity.3 The protocol used oral trimethoprim-sulfamethoxazole, amoxicillin, or doxycycline (according to the attending physician’s preference) or a look-alike placebo. Symptom resolution was seen by 21 days in 68% of antibiotic users vs 55% of those on placebo (P<.01, NNT=8). Ten percent of patients taking antibiotics deteriorated to the point where hospitalization or unblinding of the therapy was necessary, compared with 19% in the placebo group (P<.05, NNT=11).
For patients with all 3 cardinal COPD symptoms (increased dyspnea, sputum production, and sputum purulence) at enrollment, there was resolution at 21 days in 63% with antibiotics vs 43% for placebo (P value not given). Antibiotics did not benefit patients with 1 cardinal symptom (74% success with antibiotics vs 70% on placebo; P value not given).
The Cochrane review also identified a Danish RCT that studied 278 patients presenting to their general practitioners with subjective acute worsening of their COPD. Patients were randomized to 7 days of oral amoxicillin or placebo. There was no difference between the groups in terms of symptom resolution at 1 week (odds ratio=1.03, favoring placebo; 95% CI, 0.75–1.41) or in changes in PEFR (weighted mean difference=–0.89, favoring placebo; 95% CI, –29 to 27 L/min).
Recommendations from others
The Veterans Health Administration recommends antibiotics if a patient with COPD has changes in sputum volume or quality as well as increased dyspnea, cough, or fever; infiltrate on x-ray suggesting pneumonia should be treated as such.4
The American College of Chest Physicians recommends that with severe COPD exacerbations, narrow spectrum antibiotics are reasonable first-line agents.5 They also note that the superiority of newer, more broad-spectrum antibiotics has not been established.
Antibiotics (including those given orally) reduce mortality and treatment failures for hospitalized patients with acute exacerbations of chronic obstructive pulmonary disease (COPD) (strength of recommendation [SOR]: A, based on systematic reviews). Antibiotics may be prescribed in the outpatient setting for those with severe exacerbations (SOR: C, based on expert opinion).
Antibiotics are indicated in COPD exacerbations requiring hospitalization
Julie Taraday, MD
University of Washington, Seattle
In an era when physicians aim to use antibiotics judiciously, this article clarifies that antibiotics are indicated in COPD exacerbations requiring hospitalization. In the outpatient setting, the correct action is less clear. Available guidelines, which recommend antibiotics for severe exacerbations, do not generally differentiate between the inpatient and outpatient setting. Antibiotics clearly have no role in mild exacerbations and so should be avoided in many outpatient cases.
Evidence summary
A recent Cochrane review identified 11 randomized controlled trials (RCTs) (with a total of 917 patients) addressing antibiotic therapy for COPD exacerbations characterized by 1 or more of the following: an increase in sputum purulence or volume, dyspnea, wheezing, chest tightness, or fluid retention.1 Eight trials were conducted on hospital wards, 1 was in a medical intensive care unit, and 2 trials were in the outpatient setting. Antibiotics were given orally in 9 of the 11 studies.
Overall, antibiotics reduced risk of short-term mortality by 77% (relative risk [RR]=0.23; 95% confidence interval [CI],0.10–0.52; number needed to treat [NNT]=8), treatment failure by 53% (RR=0.47; 95% CI, 0.36–0.62; NNT=3), and sputum purulence by 44% (RR=0.56; 95% CI, 0.41–0.77; NNT=8). A subgroup analysis that excluded the outpatient and intensive-care unit studies did not change the result. Another subgroup analysis of the 2 outpatient studies failed to find a significant effect, although the studies had very different designs.
These findings are more robust than those of an earlier, lower-quality meta-analysis of 9 randomized controlled trials (RCTs) with 1101 patients with presumed COPD, which also compared antibiotic therapy with placebo for acute exacerbations.2 Specific diagnostic criteria were not stated for the diagnosis of either COPD or an acute exacerbation. No single outcome measure was common to all studies. The authors found a summary beneficial effect size of antibiotic therapy of 0.22 (95% CI, 0.10–0.34), which is generally interpreted as small. One clinical parameter, peak expiratory flow rate (PEFR), was reported in 6 of the studies. Antibiotic therapy resulted in an average 10.75 L/min improvement in PEFR compared with placebo (95% CI, 4.96–16.54 L/min).
Two RCTs addressing antibiotic use in the outpatient setting were identified in the Cochrane review. One double-blind crossover trial performed in Canada compared antibiotic with placebo therapy for 173 outpatients with 362 exacerbations classified according to severity.3 The protocol used oral trimethoprim-sulfamethoxazole, amoxicillin, or doxycycline (according to the attending physician’s preference) or a look-alike placebo. Symptom resolution was seen by 21 days in 68% of antibiotic users vs 55% of those on placebo (P<.01, NNT=8). Ten percent of patients taking antibiotics deteriorated to the point where hospitalization or unblinding of the therapy was necessary, compared with 19% in the placebo group (P<.05, NNT=11).
For patients with all 3 cardinal COPD symptoms (increased dyspnea, sputum production, and sputum purulence) at enrollment, there was resolution at 21 days in 63% with antibiotics vs 43% for placebo (P value not given). Antibiotics did not benefit patients with 1 cardinal symptom (74% success with antibiotics vs 70% on placebo; P value not given).
The Cochrane review also identified a Danish RCT that studied 278 patients presenting to their general practitioners with subjective acute worsening of their COPD. Patients were randomized to 7 days of oral amoxicillin or placebo. There was no difference between the groups in terms of symptom resolution at 1 week (odds ratio=1.03, favoring placebo; 95% CI, 0.75–1.41) or in changes in PEFR (weighted mean difference=–0.89, favoring placebo; 95% CI, –29 to 27 L/min).
Recommendations from others
The Veterans Health Administration recommends antibiotics if a patient with COPD has changes in sputum volume or quality as well as increased dyspnea, cough, or fever; infiltrate on x-ray suggesting pneumonia should be treated as such.4
The American College of Chest Physicians recommends that with severe COPD exacerbations, narrow spectrum antibiotics are reasonable first-line agents.5 They also note that the superiority of newer, more broad-spectrum antibiotics has not been established.
1. Ram FSF, Rodriguez-Roisin R, Granados-Navarrete A, Garcia-Aymerich J, Barnes NC. Antibiotics for exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2006;(2):CD004403.-
2. Saint S, Bent S, Vittinghoff E, Grady D. Antibiotics in chronic obstructive pulmonary disease exacerbations. JAMA 1995;273:957-60.
3. Anthonisen NR, Manfreda J, Warren CP, Hershfield ES, Harding GK, Nelson NA. Antibiotic therapy in exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 1987;106:196-204.
4. Medical advisory panel for the pharmacy benefits management strategic healthcare group The pharmacologic management of chronic obstructive pulmonary disease. Washington, DC: Veterans Health Administration, Department of Veterans Affairs; 2002.
5. Snow V, Lascher S. Mottur-Pilson C, and the Joint Expert Panel on Chronic Obstructive Pulmonary Disease of the American College of Chest Physicians and the American College of Physicians-American Society of Internal Medicine Evidence base for management of acute exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 2001;134:595-599.
1. Ram FSF, Rodriguez-Roisin R, Granados-Navarrete A, Garcia-Aymerich J, Barnes NC. Antibiotics for exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2006;(2):CD004403.-
2. Saint S, Bent S, Vittinghoff E, Grady D. Antibiotics in chronic obstructive pulmonary disease exacerbations. JAMA 1995;273:957-60.
3. Anthonisen NR, Manfreda J, Warren CP, Hershfield ES, Harding GK, Nelson NA. Antibiotic therapy in exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 1987;106:196-204.
4. Medical advisory panel for the pharmacy benefits management strategic healthcare group The pharmacologic management of chronic obstructive pulmonary disease. Washington, DC: Veterans Health Administration, Department of Veterans Affairs; 2002.
5. Snow V, Lascher S. Mottur-Pilson C, and the Joint Expert Panel on Chronic Obstructive Pulmonary Disease of the American College of Chest Physicians and the American College of Physicians-American Society of Internal Medicine Evidence base for management of acute exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 2001;134:595-599.
Evidence-based answers from the Family Physicians Inquiries Network
How can we best treat and monitor VTE during pregnancy?
Unfractionated heparin and low-molecular-weight heparin are equally effective for the treatment of acute venous thromboembolism (VTE) in pregnancy (strength of recommendation [SOR]: C; based on expert opinion and 1 low-power cohort study). Low-molecular-weight heparin may be associated with fewer bleeding events than unfractionated heparin (SOR: B; extrapolated from a randomized controlled trial of thromboprophylaxis in pregnancy).
Unfractionated heparin for treatment of VTE should be given by IV bolus followed by continuous infusion, maintaining the activated partial thromboplastin time (aPTT) in therapeutic range for at least 5 days, followed by subcutaneous heparin 2 or 3 times daily to maintain aPTT levels 1.5 to 2.5 times normal for at least 3 months (SOR: C, expert opinion). Low-molecular-weight heparin should be initially dosed based on weight as for nonpregnant patients, then adjusted to goal peak antifactor Xa levels of 0.5–1.2 IU/mL (SOR: C; expert opinion). The US Food and Drug Administration has labeled warfarin as category X, indicating that it is contraindicated during pregnancy due to fetal loss and probable teratogenicity.
Safety is most important when treating pregnant women
Linda French, MD, FAAFP
Michigan State University, East Lansing
We have enough evidence to conclude that unfractionated heparin and low-molecular-weight heparin are both effective treatments for acute VTE in pregnant women. Unfortunately, we don’t know whether 1 treatment is safer or more effective than the other. The safety issue is the most important consideration in treating pregnant women. A large number of patients would need to be studied to identify a small but significant difference between the 2. We as clinicians would want to know if 1 therapy had even a slightly increased risk of a catastrophic harm. Clinical experience is not enough to tell us that; we need more research.
Evidence summary
Pulmonary embolism remains one of the leading causes of maternal mortality in developed nations. For nonpregnant populations, low-molecular-weight heparin has equal efficacy as unfractionated heparin with a lower overall mortality.1,2
The only direct comparison of unfractionated with low-molecular-weight heparin for treatment of VTE in pregnancy was a prospective cohort study of 31 patients.3 For the initial week of treatment, the unfractionated heparin group received an IV bolus followed by infusion titrated to aPTT levels (goal 70–100s), while lowmolecular-weight heparin group received subcutaneous dalteparin 115 IU/kg twice daily adjusted to target antifactor Xa levels of 1 to 1.5 IU/mL 3 hours after injection. After 7 days, both groups received prophylactic doses of dalteparin throughout the remainder of pregnancy. There were no significant differences in outcome including bleeding or fetal effects. No cases of thrombocytopenia or pulmonary embolus were seen. There was 1 case of progressive thrombosis for a patient on low-molecular-weight heparin.
One randomized controlled trial compared unfractionated with low-molecular-weight heparin for VTE prophylaxis among 107 high-risk pregnant patients.4 The unfractionated heparin group received 7500 IU subcutaneously twice daily adjusted to aPTT levels, while the dalteparin group received weight-adjusted doses to target antifactor Xa levels >0.2 IU/mL at 3 hours. No thromboembolic complications occurred in either group (95% confidence interval, 0 to 2 in both groups). Minor bleeding complications were significantly more common with unfractionated heparin than with low-molecular-weight heparin. Two bleeds requiring transfusion and 2 lumbosacral compression fractures were also observed in the unfractionated heparin group, compared with none in the dalteparin group (difference not statistically significant).
Heparinoid metabolism appears to significantly alter in pregnancy. Several studies of low-molecular-weight heparin for the treatment of VTE in pregnancy used target antifactor Xa levels of 0.5 to 1.5 at 3 hours and found patients often need doses greater than those used for nonpregnant patients.3,5-7 The only study of unfractionated heparin for the treatment of VTE in pregnancy used aPTT levels extrapolated from nonpregnant patients, with a mean heparin dose of 25,430 IU/d, similar to mean doses for nonpregnant patients.3
There are no studies of repeat lower extremity ultrasounds for pregnant patients; however, 1 study of nonpregnant patients revealed proximal extension of deep venous thrombosis despite anticoagulation predicted increased risk of pulmonary embolism.8
Recommendations from others
Both the American College of Obstetrics and Gynecologists9 and the American College of Chest Physicians10 recommends treating acute VTE in pregnancy with either weight-adjusted-dose low-molecular-weight heparin (goal antifactor Xa levels, 0.5–1.2) throughout pregnancy or full-dose intravenous unfractionated heparin, followed by adjusted-dose unfractionated or low-molecular-weight heparin, for the remainder of the pregnancy and at least 6 weeks postpartum.
1 Dolovich LR, Ginsberg JS, Douketis JD, Holbrook AM, Cheah G. A meta-analysis comparing low-molecular-weight heparins with unfractionated heparin in the treatment of venous thromboembolism: examining some unanswered questions regarding location of treatment, product type, and dosing frequency. Arch Intern Med 2000;160:181-188.
2. Gould MK, Dembitzer AD, Doyle RL, Hastie TJ, Garber AM. Low-molecular-weight heparins compared with unfractionated heparin for treatment of acute deep venous thrombosis. A meta-analysis of randomized, controlled trials. Ann Intern Med 1999;130:800-809.
3. Ulander VM, Stenqvist P, Kaaja R. Treatment of deep venous thrombosis with low-molecular-weight heparin during pregnancy. Thromb Res 2002;106:13-17.
4. Pettila V, Kaaja R, Leinonen P, Ekblad U, Kataja M, Ikkala E. Thromboprophylaxis with low molecular weight heparin (dalteparin) in pregnancy. Thromb Res 1999;96:275-282.
5. Jacobsen AF, Qvigstad E, Sandset PM. Low molecular weight heparin (dalteparin) for the treatment of venous thromboembolism in pregnancy. BJOG 2003;110:139-144.
6. Rodie VA, Thomson AJ, Stewart FM, Quinn AJ, Walker ID, Greer IA. Low molecular weight heparin for the treatment of venous thromboembolism in pregnancy: a case series. BJOG 2002;109:1020-1024.
7. Rowan JA, McLintock C, Taylor RS, North RA. Prophylactic and therapeutic enoxaparin during pregnancy: indications, outcomes and monitoring. Aust N Z J Obstet Gynaecol 2003;43:123-128.
8. Ascher E, Depippo PS, Hingorani A, Yorkovich W, Salles-Cunha S. Does repeat duplex ultrasound for lower extremity deep vein thrombosis influence patient management? Vasc Endovascular Surg 2004;38:525-531.
9. American College of Obstetricians and Gynecologists Committee on Practice Bulletins-Obstetrics. ACOG Practice Bulletin. Thromboembolism in pregnancy. Int J Gynaecol Obstet 2001;75:203-212.
10. Bates SM, Greer IA, Hirsh J, Ginsberg JS. Use of antithrombotic agents during pregnancy: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 2004;126:627S-644S.
Unfractionated heparin and low-molecular-weight heparin are equally effective for the treatment of acute venous thromboembolism (VTE) in pregnancy (strength of recommendation [SOR]: C; based on expert opinion and 1 low-power cohort study). Low-molecular-weight heparin may be associated with fewer bleeding events than unfractionated heparin (SOR: B; extrapolated from a randomized controlled trial of thromboprophylaxis in pregnancy).
Unfractionated heparin for treatment of VTE should be given by IV bolus followed by continuous infusion, maintaining the activated partial thromboplastin time (aPTT) in therapeutic range for at least 5 days, followed by subcutaneous heparin 2 or 3 times daily to maintain aPTT levels 1.5 to 2.5 times normal for at least 3 months (SOR: C, expert opinion). Low-molecular-weight heparin should be initially dosed based on weight as for nonpregnant patients, then adjusted to goal peak antifactor Xa levels of 0.5–1.2 IU/mL (SOR: C; expert opinion). The US Food and Drug Administration has labeled warfarin as category X, indicating that it is contraindicated during pregnancy due to fetal loss and probable teratogenicity.
Safety is most important when treating pregnant women
Linda French, MD, FAAFP
Michigan State University, East Lansing
We have enough evidence to conclude that unfractionated heparin and low-molecular-weight heparin are both effective treatments for acute VTE in pregnant women. Unfortunately, we don’t know whether 1 treatment is safer or more effective than the other. The safety issue is the most important consideration in treating pregnant women. A large number of patients would need to be studied to identify a small but significant difference between the 2. We as clinicians would want to know if 1 therapy had even a slightly increased risk of a catastrophic harm. Clinical experience is not enough to tell us that; we need more research.
Evidence summary
Pulmonary embolism remains one of the leading causes of maternal mortality in developed nations. For nonpregnant populations, low-molecular-weight heparin has equal efficacy as unfractionated heparin with a lower overall mortality.1,2
The only direct comparison of unfractionated with low-molecular-weight heparin for treatment of VTE in pregnancy was a prospective cohort study of 31 patients.3 For the initial week of treatment, the unfractionated heparin group received an IV bolus followed by infusion titrated to aPTT levels (goal 70–100s), while lowmolecular-weight heparin group received subcutaneous dalteparin 115 IU/kg twice daily adjusted to target antifactor Xa levels of 1 to 1.5 IU/mL 3 hours after injection. After 7 days, both groups received prophylactic doses of dalteparin throughout the remainder of pregnancy. There were no significant differences in outcome including bleeding or fetal effects. No cases of thrombocytopenia or pulmonary embolus were seen. There was 1 case of progressive thrombosis for a patient on low-molecular-weight heparin.
One randomized controlled trial compared unfractionated with low-molecular-weight heparin for VTE prophylaxis among 107 high-risk pregnant patients.4 The unfractionated heparin group received 7500 IU subcutaneously twice daily adjusted to aPTT levels, while the dalteparin group received weight-adjusted doses to target antifactor Xa levels >0.2 IU/mL at 3 hours. No thromboembolic complications occurred in either group (95% confidence interval, 0 to 2 in both groups). Minor bleeding complications were significantly more common with unfractionated heparin than with low-molecular-weight heparin. Two bleeds requiring transfusion and 2 lumbosacral compression fractures were also observed in the unfractionated heparin group, compared with none in the dalteparin group (difference not statistically significant).
Heparinoid metabolism appears to significantly alter in pregnancy. Several studies of low-molecular-weight heparin for the treatment of VTE in pregnancy used target antifactor Xa levels of 0.5 to 1.5 at 3 hours and found patients often need doses greater than those used for nonpregnant patients.3,5-7 The only study of unfractionated heparin for the treatment of VTE in pregnancy used aPTT levels extrapolated from nonpregnant patients, with a mean heparin dose of 25,430 IU/d, similar to mean doses for nonpregnant patients.3
There are no studies of repeat lower extremity ultrasounds for pregnant patients; however, 1 study of nonpregnant patients revealed proximal extension of deep venous thrombosis despite anticoagulation predicted increased risk of pulmonary embolism.8
Recommendations from others
Both the American College of Obstetrics and Gynecologists9 and the American College of Chest Physicians10 recommends treating acute VTE in pregnancy with either weight-adjusted-dose low-molecular-weight heparin (goal antifactor Xa levels, 0.5–1.2) throughout pregnancy or full-dose intravenous unfractionated heparin, followed by adjusted-dose unfractionated or low-molecular-weight heparin, for the remainder of the pregnancy and at least 6 weeks postpartum.
Unfractionated heparin and low-molecular-weight heparin are equally effective for the treatment of acute venous thromboembolism (VTE) in pregnancy (strength of recommendation [SOR]: C; based on expert opinion and 1 low-power cohort study). Low-molecular-weight heparin may be associated with fewer bleeding events than unfractionated heparin (SOR: B; extrapolated from a randomized controlled trial of thromboprophylaxis in pregnancy).
Unfractionated heparin for treatment of VTE should be given by IV bolus followed by continuous infusion, maintaining the activated partial thromboplastin time (aPTT) in therapeutic range for at least 5 days, followed by subcutaneous heparin 2 or 3 times daily to maintain aPTT levels 1.5 to 2.5 times normal for at least 3 months (SOR: C, expert opinion). Low-molecular-weight heparin should be initially dosed based on weight as for nonpregnant patients, then adjusted to goal peak antifactor Xa levels of 0.5–1.2 IU/mL (SOR: C; expert opinion). The US Food and Drug Administration has labeled warfarin as category X, indicating that it is contraindicated during pregnancy due to fetal loss and probable teratogenicity.
Safety is most important when treating pregnant women
Linda French, MD, FAAFP
Michigan State University, East Lansing
We have enough evidence to conclude that unfractionated heparin and low-molecular-weight heparin are both effective treatments for acute VTE in pregnant women. Unfortunately, we don’t know whether 1 treatment is safer or more effective than the other. The safety issue is the most important consideration in treating pregnant women. A large number of patients would need to be studied to identify a small but significant difference between the 2. We as clinicians would want to know if 1 therapy had even a slightly increased risk of a catastrophic harm. Clinical experience is not enough to tell us that; we need more research.
Evidence summary
Pulmonary embolism remains one of the leading causes of maternal mortality in developed nations. For nonpregnant populations, low-molecular-weight heparin has equal efficacy as unfractionated heparin with a lower overall mortality.1,2
The only direct comparison of unfractionated with low-molecular-weight heparin for treatment of VTE in pregnancy was a prospective cohort study of 31 patients.3 For the initial week of treatment, the unfractionated heparin group received an IV bolus followed by infusion titrated to aPTT levels (goal 70–100s), while lowmolecular-weight heparin group received subcutaneous dalteparin 115 IU/kg twice daily adjusted to target antifactor Xa levels of 1 to 1.5 IU/mL 3 hours after injection. After 7 days, both groups received prophylactic doses of dalteparin throughout the remainder of pregnancy. There were no significant differences in outcome including bleeding or fetal effects. No cases of thrombocytopenia or pulmonary embolus were seen. There was 1 case of progressive thrombosis for a patient on low-molecular-weight heparin.
One randomized controlled trial compared unfractionated with low-molecular-weight heparin for VTE prophylaxis among 107 high-risk pregnant patients.4 The unfractionated heparin group received 7500 IU subcutaneously twice daily adjusted to aPTT levels, while the dalteparin group received weight-adjusted doses to target antifactor Xa levels >0.2 IU/mL at 3 hours. No thromboembolic complications occurred in either group (95% confidence interval, 0 to 2 in both groups). Minor bleeding complications were significantly more common with unfractionated heparin than with low-molecular-weight heparin. Two bleeds requiring transfusion and 2 lumbosacral compression fractures were also observed in the unfractionated heparin group, compared with none in the dalteparin group (difference not statistically significant).
Heparinoid metabolism appears to significantly alter in pregnancy. Several studies of low-molecular-weight heparin for the treatment of VTE in pregnancy used target antifactor Xa levels of 0.5 to 1.5 at 3 hours and found patients often need doses greater than those used for nonpregnant patients.3,5-7 The only study of unfractionated heparin for the treatment of VTE in pregnancy used aPTT levels extrapolated from nonpregnant patients, with a mean heparin dose of 25,430 IU/d, similar to mean doses for nonpregnant patients.3
There are no studies of repeat lower extremity ultrasounds for pregnant patients; however, 1 study of nonpregnant patients revealed proximal extension of deep venous thrombosis despite anticoagulation predicted increased risk of pulmonary embolism.8
Recommendations from others
Both the American College of Obstetrics and Gynecologists9 and the American College of Chest Physicians10 recommends treating acute VTE in pregnancy with either weight-adjusted-dose low-molecular-weight heparin (goal antifactor Xa levels, 0.5–1.2) throughout pregnancy or full-dose intravenous unfractionated heparin, followed by adjusted-dose unfractionated or low-molecular-weight heparin, for the remainder of the pregnancy and at least 6 weeks postpartum.
1 Dolovich LR, Ginsberg JS, Douketis JD, Holbrook AM, Cheah G. A meta-analysis comparing low-molecular-weight heparins with unfractionated heparin in the treatment of venous thromboembolism: examining some unanswered questions regarding location of treatment, product type, and dosing frequency. Arch Intern Med 2000;160:181-188.
2. Gould MK, Dembitzer AD, Doyle RL, Hastie TJ, Garber AM. Low-molecular-weight heparins compared with unfractionated heparin for treatment of acute deep venous thrombosis. A meta-analysis of randomized, controlled trials. Ann Intern Med 1999;130:800-809.
3. Ulander VM, Stenqvist P, Kaaja R. Treatment of deep venous thrombosis with low-molecular-weight heparin during pregnancy. Thromb Res 2002;106:13-17.
4. Pettila V, Kaaja R, Leinonen P, Ekblad U, Kataja M, Ikkala E. Thromboprophylaxis with low molecular weight heparin (dalteparin) in pregnancy. Thromb Res 1999;96:275-282.
5. Jacobsen AF, Qvigstad E, Sandset PM. Low molecular weight heparin (dalteparin) for the treatment of venous thromboembolism in pregnancy. BJOG 2003;110:139-144.
6. Rodie VA, Thomson AJ, Stewart FM, Quinn AJ, Walker ID, Greer IA. Low molecular weight heparin for the treatment of venous thromboembolism in pregnancy: a case series. BJOG 2002;109:1020-1024.
7. Rowan JA, McLintock C, Taylor RS, North RA. Prophylactic and therapeutic enoxaparin during pregnancy: indications, outcomes and monitoring. Aust N Z J Obstet Gynaecol 2003;43:123-128.
8. Ascher E, Depippo PS, Hingorani A, Yorkovich W, Salles-Cunha S. Does repeat duplex ultrasound for lower extremity deep vein thrombosis influence patient management? Vasc Endovascular Surg 2004;38:525-531.
9. American College of Obstetricians and Gynecologists Committee on Practice Bulletins-Obstetrics. ACOG Practice Bulletin. Thromboembolism in pregnancy. Int J Gynaecol Obstet 2001;75:203-212.
10. Bates SM, Greer IA, Hirsh J, Ginsberg JS. Use of antithrombotic agents during pregnancy: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 2004;126:627S-644S.
1 Dolovich LR, Ginsberg JS, Douketis JD, Holbrook AM, Cheah G. A meta-analysis comparing low-molecular-weight heparins with unfractionated heparin in the treatment of venous thromboembolism: examining some unanswered questions regarding location of treatment, product type, and dosing frequency. Arch Intern Med 2000;160:181-188.
2. Gould MK, Dembitzer AD, Doyle RL, Hastie TJ, Garber AM. Low-molecular-weight heparins compared with unfractionated heparin for treatment of acute deep venous thrombosis. A meta-analysis of randomized, controlled trials. Ann Intern Med 1999;130:800-809.
3. Ulander VM, Stenqvist P, Kaaja R. Treatment of deep venous thrombosis with low-molecular-weight heparin during pregnancy. Thromb Res 2002;106:13-17.
4. Pettila V, Kaaja R, Leinonen P, Ekblad U, Kataja M, Ikkala E. Thromboprophylaxis with low molecular weight heparin (dalteparin) in pregnancy. Thromb Res 1999;96:275-282.
5. Jacobsen AF, Qvigstad E, Sandset PM. Low molecular weight heparin (dalteparin) for the treatment of venous thromboembolism in pregnancy. BJOG 2003;110:139-144.
6. Rodie VA, Thomson AJ, Stewart FM, Quinn AJ, Walker ID, Greer IA. Low molecular weight heparin for the treatment of venous thromboembolism in pregnancy: a case series. BJOG 2002;109:1020-1024.
7. Rowan JA, McLintock C, Taylor RS, North RA. Prophylactic and therapeutic enoxaparin during pregnancy: indications, outcomes and monitoring. Aust N Z J Obstet Gynaecol 2003;43:123-128.
8. Ascher E, Depippo PS, Hingorani A, Yorkovich W, Salles-Cunha S. Does repeat duplex ultrasound for lower extremity deep vein thrombosis influence patient management? Vasc Endovascular Surg 2004;38:525-531.
9. American College of Obstetricians and Gynecologists Committee on Practice Bulletins-Obstetrics. ACOG Practice Bulletin. Thromboembolism in pregnancy. Int J Gynaecol Obstet 2001;75:203-212.
10. Bates SM, Greer IA, Hirsh J, Ginsberg JS. Use of antithrombotic agents during pregnancy: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 2004;126:627S-644S.
Evidence-based answers from the Family Physicians Inquiries Network
When is neuroimaging warranted for headache?
Neuroimaging is warranted to evaluate headaches when patients present to an emergency department with signs or symptoms of an intracranial lesion. These signs or symptoms include abrupt onset of headache, focal neurological abnormalities (strength of recommendation [SOR]: B, based on a validating cohort study), decreased level of consciousness (SOR: B, based on a retrospective, nonconsecutive case study), occipitonuchal location, multiple associated symptoms, and age older than 55 years (SOR: B, based on a case-control study).
Neuroimaging is also recommended in the ambulatory setting for patients with headaches of migraine type and abnormal findings on neurological exam; that are accompanied by signs or symptoms of increased intracranial pressure; or that are new for a patient who is HIV-positive (SOR: C, based on expert opinion).
There are no studies or consistent opinions on the need for neuroimaging with headaches of tension type, described as the “worst ever,” increasing in frequency, that awaken the patient, or are associated with nausea, dizziness, or syncope.
Careful clinical judgment is important in decision for neuroimaging
Zahida Siddiqi, MD
Baylor College of Medicine, Houston, Tex
Determining the utility of neuroimaging for headache is a taxing question for clinicians working in the emergency room or an outpatient clinic. In the county health system where I work, I find it increasingly difficult to get neuroimaging studies done within an appropriate time frame. Thus I must rely heavily on clinical judgment to determine how urgently they must be done. I also feel an ethical obligation to avoid unnecessary demands on this limited resource.
I have found the criteria recommended in this Clinical Inquiry to be most helpful in prioritizing the need for neuroimaging. These include focal neurological deficit, alteration in the character of headache, persistence of headache despite analgesics, abrupt onset, and increasing frequency and intensity of headache. In addition, I have found the persistence of the patient in returning for reevaluation to be a helpful indicator of pathology.
Evidence summary
A validating cohort study looked at 5 clinical warning criteria (TABLE) for patients seen in an emergency department for headache; 70 adults with acute headache as the chief complaint were included. All patients received computed tomography (CT) scanning as part of their evaluation. Abrupt onset and focal neurologic findings most strongly predicted intracranial lesions. Overall, 36% of the patients (25/70) had significant pathology.1
A retrospective study reviewed records of 111 patients seen in an emergency department with headache and who had undergone neuroimaging (CT or magnetic resonance imaging [MRI]). Three symptoms predicted a lesion: decreased level of consciousness (sensitivity=23%; positive likelihood ratio [LR+]=3.8), paralysis (sensitivity=25%; LR+=3.5), and papilledema (numbers not reported). In this study, 35% (39/111) of those receiving neuroimaging had intracranial pathology.2
A case-control study reviewed hospital records of 468 patients evaluated in the emergency department for nontraumatic headache. Neuroimaging (CT scan or cerebral angiogram) was performed for 160 of these patients. Final diagnosis and outcome was obtained at 6 months. The symptoms and their ability to predict intracranial pathology are as follows: abnormal neurologic examination (sensitivity=39%; LR+=19.5), location of headache (sensitivity=78%; LR+=4.87), age of patient (sensitivity=61%; LR+=2.26), multiple associated symptoms (sensitivity=61%; LR+=2.26), mode of onset of headache (sensitivity=78%; LR+=2.23), and presence of associated symptoms (sensitivity=89%; LR+=1.41). Again, abnormal neurologic examination was the most significant indicator for imaging. This study did not define associated symptoms nor did it specify what determined which patients were imaged.3
Information concerning the workup of headache in the ambulatory setting is limited. In actual practice, only about 3% of patients who present with a new headache in the office setting have neuroimaging ordered.4 When neuroimaging is performed, about 4% of CT scans find a significant and treatable lesion (in one sample of 293 CT scans, there were 12 true-positive scans and 2 false-positive scans).5 Expert guidelines regarding headaches among ambulatory patients recommend neuroimaging for migraine patients only in the presence of persistent focal abnormal neurological findings. They note insufficient evidence for recommendations concerning neuroimaging for patients with tension-type headaches. They also note insufficient evidence for or against neuroimaging when headache occurs in the presence or absence of nonfocal symptoms: dizziness, syncope, nausea, lack of coordination, the “worst headache ever,” headache that awakens the patient from sleep, and increasing frequency of headaches.6
TABLE
Five clinical warning criteria for headache
| CLINICAL FEATURE | SENSITIVITY | SPECIFICITY | LR+ | LR– |
|---|---|---|---|---|
| FOR INTRACRANICAL PATHOLOGY | ||||
| Presence of focal neurological symptoms or findings | 1.0 | 0.76 | 4.21 | 0 |
| Abrupt onset | 0.55 | 0.79 | 2.5 | 0.57 |
| Alteration of characteristics | 0.67 | 0.67 | 2.0 | 0.49 |
| Increased intensity and frequency | 0.39 | 0.73 | 1.44 | 0.83 |
| Persistence despite analgesics | 0.60 | 0.56 | 1.36 | 0.71 |
| LR+, positive likelihood ratio; LR–, negative likelihood ratio. | ||||
| Source: Aygun and Bildik, Eur J Neurol 2003.1 | ||||
Recommendations from others
Rosen’s Emergency Medicine and Mettler: Essentials of Radiology add the following indications for imaging in headache: signs and symptoms of elevated intracranial pressure (eg, papilledema); meningismus; partial seizure; nocturnal headaches that awaken the patient from sleep; increase in pain with coughing, sneezing or change in body position; sudden onset headaches that reach maximum intensity in 2 to 3 minutes; headache associated with mental status changes or decreased alertness; any new headache in an HIV-positive patient.7,8
1. Aygun D, Bildik F. Clinical warning criteria in evaluation by computed tomography the secondary neurological headaches in adults. Eur J Neurol 2003;10:437-442.
2. Sobri M, Lamont AC, Alias NA, Win MN. Red flags in patients presenting with headache: clinical indications for neuroimaging. Br J Radiol 2003;76:532-535.
3. Ramirez-Lassepas M, Espinosa C, Cicero JJ, Johnston KL, Cipolle RJ, Barber DL. Predictors of intracranial pathologic findings in patients who see emergency care because of headache. Arch Neurol 1997;54:1506-1509.
4. Becker L, Iverson DC, Reed FM, Calonge N, Miller RS, Freeman WL. Patients with a new headache in primary care: a report from ASPN. J Fam Pract 1988;27:41-47.
5. Becker LA, Green LA, Beaufait D, Kirk J, Froom J, Freeman WL. Use of CT scans for the investigation of headache: a report from ASPN, part 1. J Fam Pract 1993;37:129-134.
6. Morey SS. Headache Consortium releases guidelines for use of CT or MRI in migraine work-up. Am Fam Physician 2000;62:1699-1701.
7. Mettler FA, Jr. Essentials of Radiology. 2nd ed. Philadelphia, Pa: Saunders; 2005.
8. Marx JA, Hockberger RS, Walls JM. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 5th ed. St. Louis, Mo: Mosby; 2002.
Neuroimaging is warranted to evaluate headaches when patients present to an emergency department with signs or symptoms of an intracranial lesion. These signs or symptoms include abrupt onset of headache, focal neurological abnormalities (strength of recommendation [SOR]: B, based on a validating cohort study), decreased level of consciousness (SOR: B, based on a retrospective, nonconsecutive case study), occipitonuchal location, multiple associated symptoms, and age older than 55 years (SOR: B, based on a case-control study).
Neuroimaging is also recommended in the ambulatory setting for patients with headaches of migraine type and abnormal findings on neurological exam; that are accompanied by signs or symptoms of increased intracranial pressure; or that are new for a patient who is HIV-positive (SOR: C, based on expert opinion).
There are no studies or consistent opinions on the need for neuroimaging with headaches of tension type, described as the “worst ever,” increasing in frequency, that awaken the patient, or are associated with nausea, dizziness, or syncope.
Careful clinical judgment is important in decision for neuroimaging
Zahida Siddiqi, MD
Baylor College of Medicine, Houston, Tex
Determining the utility of neuroimaging for headache is a taxing question for clinicians working in the emergency room or an outpatient clinic. In the county health system where I work, I find it increasingly difficult to get neuroimaging studies done within an appropriate time frame. Thus I must rely heavily on clinical judgment to determine how urgently they must be done. I also feel an ethical obligation to avoid unnecessary demands on this limited resource.
I have found the criteria recommended in this Clinical Inquiry to be most helpful in prioritizing the need for neuroimaging. These include focal neurological deficit, alteration in the character of headache, persistence of headache despite analgesics, abrupt onset, and increasing frequency and intensity of headache. In addition, I have found the persistence of the patient in returning for reevaluation to be a helpful indicator of pathology.
Evidence summary
A validating cohort study looked at 5 clinical warning criteria (TABLE) for patients seen in an emergency department for headache; 70 adults with acute headache as the chief complaint were included. All patients received computed tomography (CT) scanning as part of their evaluation. Abrupt onset and focal neurologic findings most strongly predicted intracranial lesions. Overall, 36% of the patients (25/70) had significant pathology.1
A retrospective study reviewed records of 111 patients seen in an emergency department with headache and who had undergone neuroimaging (CT or magnetic resonance imaging [MRI]). Three symptoms predicted a lesion: decreased level of consciousness (sensitivity=23%; positive likelihood ratio [LR+]=3.8), paralysis (sensitivity=25%; LR+=3.5), and papilledema (numbers not reported). In this study, 35% (39/111) of those receiving neuroimaging had intracranial pathology.2
A case-control study reviewed hospital records of 468 patients evaluated in the emergency department for nontraumatic headache. Neuroimaging (CT scan or cerebral angiogram) was performed for 160 of these patients. Final diagnosis and outcome was obtained at 6 months. The symptoms and their ability to predict intracranial pathology are as follows: abnormal neurologic examination (sensitivity=39%; LR+=19.5), location of headache (sensitivity=78%; LR+=4.87), age of patient (sensitivity=61%; LR+=2.26), multiple associated symptoms (sensitivity=61%; LR+=2.26), mode of onset of headache (sensitivity=78%; LR+=2.23), and presence of associated symptoms (sensitivity=89%; LR+=1.41). Again, abnormal neurologic examination was the most significant indicator for imaging. This study did not define associated symptoms nor did it specify what determined which patients were imaged.3
Information concerning the workup of headache in the ambulatory setting is limited. In actual practice, only about 3% of patients who present with a new headache in the office setting have neuroimaging ordered.4 When neuroimaging is performed, about 4% of CT scans find a significant and treatable lesion (in one sample of 293 CT scans, there were 12 true-positive scans and 2 false-positive scans).5 Expert guidelines regarding headaches among ambulatory patients recommend neuroimaging for migraine patients only in the presence of persistent focal abnormal neurological findings. They note insufficient evidence for recommendations concerning neuroimaging for patients with tension-type headaches. They also note insufficient evidence for or against neuroimaging when headache occurs in the presence or absence of nonfocal symptoms: dizziness, syncope, nausea, lack of coordination, the “worst headache ever,” headache that awakens the patient from sleep, and increasing frequency of headaches.6
TABLE
Five clinical warning criteria for headache
| CLINICAL FEATURE | SENSITIVITY | SPECIFICITY | LR+ | LR– |
|---|---|---|---|---|
| FOR INTRACRANICAL PATHOLOGY | ||||
| Presence of focal neurological symptoms or findings | 1.0 | 0.76 | 4.21 | 0 |
| Abrupt onset | 0.55 | 0.79 | 2.5 | 0.57 |
| Alteration of characteristics | 0.67 | 0.67 | 2.0 | 0.49 |
| Increased intensity and frequency | 0.39 | 0.73 | 1.44 | 0.83 |
| Persistence despite analgesics | 0.60 | 0.56 | 1.36 | 0.71 |
| LR+, positive likelihood ratio; LR–, negative likelihood ratio. | ||||
| Source: Aygun and Bildik, Eur J Neurol 2003.1 | ||||
Recommendations from others
Rosen’s Emergency Medicine and Mettler: Essentials of Radiology add the following indications for imaging in headache: signs and symptoms of elevated intracranial pressure (eg, papilledema); meningismus; partial seizure; nocturnal headaches that awaken the patient from sleep; increase in pain with coughing, sneezing or change in body position; sudden onset headaches that reach maximum intensity in 2 to 3 minutes; headache associated with mental status changes or decreased alertness; any new headache in an HIV-positive patient.7,8
Neuroimaging is warranted to evaluate headaches when patients present to an emergency department with signs or symptoms of an intracranial lesion. These signs or symptoms include abrupt onset of headache, focal neurological abnormalities (strength of recommendation [SOR]: B, based on a validating cohort study), decreased level of consciousness (SOR: B, based on a retrospective, nonconsecutive case study), occipitonuchal location, multiple associated symptoms, and age older than 55 years (SOR: B, based on a case-control study).
Neuroimaging is also recommended in the ambulatory setting for patients with headaches of migraine type and abnormal findings on neurological exam; that are accompanied by signs or symptoms of increased intracranial pressure; or that are new for a patient who is HIV-positive (SOR: C, based on expert opinion).
There are no studies or consistent opinions on the need for neuroimaging with headaches of tension type, described as the “worst ever,” increasing in frequency, that awaken the patient, or are associated with nausea, dizziness, or syncope.
Careful clinical judgment is important in decision for neuroimaging
Zahida Siddiqi, MD
Baylor College of Medicine, Houston, Tex
Determining the utility of neuroimaging for headache is a taxing question for clinicians working in the emergency room or an outpatient clinic. In the county health system where I work, I find it increasingly difficult to get neuroimaging studies done within an appropriate time frame. Thus I must rely heavily on clinical judgment to determine how urgently they must be done. I also feel an ethical obligation to avoid unnecessary demands on this limited resource.
I have found the criteria recommended in this Clinical Inquiry to be most helpful in prioritizing the need for neuroimaging. These include focal neurological deficit, alteration in the character of headache, persistence of headache despite analgesics, abrupt onset, and increasing frequency and intensity of headache. In addition, I have found the persistence of the patient in returning for reevaluation to be a helpful indicator of pathology.
Evidence summary
A validating cohort study looked at 5 clinical warning criteria (TABLE) for patients seen in an emergency department for headache; 70 adults with acute headache as the chief complaint were included. All patients received computed tomography (CT) scanning as part of their evaluation. Abrupt onset and focal neurologic findings most strongly predicted intracranial lesions. Overall, 36% of the patients (25/70) had significant pathology.1
A retrospective study reviewed records of 111 patients seen in an emergency department with headache and who had undergone neuroimaging (CT or magnetic resonance imaging [MRI]). Three symptoms predicted a lesion: decreased level of consciousness (sensitivity=23%; positive likelihood ratio [LR+]=3.8), paralysis (sensitivity=25%; LR+=3.5), and papilledema (numbers not reported). In this study, 35% (39/111) of those receiving neuroimaging had intracranial pathology.2
A case-control study reviewed hospital records of 468 patients evaluated in the emergency department for nontraumatic headache. Neuroimaging (CT scan or cerebral angiogram) was performed for 160 of these patients. Final diagnosis and outcome was obtained at 6 months. The symptoms and their ability to predict intracranial pathology are as follows: abnormal neurologic examination (sensitivity=39%; LR+=19.5), location of headache (sensitivity=78%; LR+=4.87), age of patient (sensitivity=61%; LR+=2.26), multiple associated symptoms (sensitivity=61%; LR+=2.26), mode of onset of headache (sensitivity=78%; LR+=2.23), and presence of associated symptoms (sensitivity=89%; LR+=1.41). Again, abnormal neurologic examination was the most significant indicator for imaging. This study did not define associated symptoms nor did it specify what determined which patients were imaged.3
Information concerning the workup of headache in the ambulatory setting is limited. In actual practice, only about 3% of patients who present with a new headache in the office setting have neuroimaging ordered.4 When neuroimaging is performed, about 4% of CT scans find a significant and treatable lesion (in one sample of 293 CT scans, there were 12 true-positive scans and 2 false-positive scans).5 Expert guidelines regarding headaches among ambulatory patients recommend neuroimaging for migraine patients only in the presence of persistent focal abnormal neurological findings. They note insufficient evidence for recommendations concerning neuroimaging for patients with tension-type headaches. They also note insufficient evidence for or against neuroimaging when headache occurs in the presence or absence of nonfocal symptoms: dizziness, syncope, nausea, lack of coordination, the “worst headache ever,” headache that awakens the patient from sleep, and increasing frequency of headaches.6
TABLE
Five clinical warning criteria for headache
| CLINICAL FEATURE | SENSITIVITY | SPECIFICITY | LR+ | LR– |
|---|---|---|---|---|
| FOR INTRACRANICAL PATHOLOGY | ||||
| Presence of focal neurological symptoms or findings | 1.0 | 0.76 | 4.21 | 0 |
| Abrupt onset | 0.55 | 0.79 | 2.5 | 0.57 |
| Alteration of characteristics | 0.67 | 0.67 | 2.0 | 0.49 |
| Increased intensity and frequency | 0.39 | 0.73 | 1.44 | 0.83 |
| Persistence despite analgesics | 0.60 | 0.56 | 1.36 | 0.71 |
| LR+, positive likelihood ratio; LR–, negative likelihood ratio. | ||||
| Source: Aygun and Bildik, Eur J Neurol 2003.1 | ||||
Recommendations from others
Rosen’s Emergency Medicine and Mettler: Essentials of Radiology add the following indications for imaging in headache: signs and symptoms of elevated intracranial pressure (eg, papilledema); meningismus; partial seizure; nocturnal headaches that awaken the patient from sleep; increase in pain with coughing, sneezing or change in body position; sudden onset headaches that reach maximum intensity in 2 to 3 minutes; headache associated with mental status changes or decreased alertness; any new headache in an HIV-positive patient.7,8
1. Aygun D, Bildik F. Clinical warning criteria in evaluation by computed tomography the secondary neurological headaches in adults. Eur J Neurol 2003;10:437-442.
2. Sobri M, Lamont AC, Alias NA, Win MN. Red flags in patients presenting with headache: clinical indications for neuroimaging. Br J Radiol 2003;76:532-535.
3. Ramirez-Lassepas M, Espinosa C, Cicero JJ, Johnston KL, Cipolle RJ, Barber DL. Predictors of intracranial pathologic findings in patients who see emergency care because of headache. Arch Neurol 1997;54:1506-1509.
4. Becker L, Iverson DC, Reed FM, Calonge N, Miller RS, Freeman WL. Patients with a new headache in primary care: a report from ASPN. J Fam Pract 1988;27:41-47.
5. Becker LA, Green LA, Beaufait D, Kirk J, Froom J, Freeman WL. Use of CT scans for the investigation of headache: a report from ASPN, part 1. J Fam Pract 1993;37:129-134.
6. Morey SS. Headache Consortium releases guidelines for use of CT or MRI in migraine work-up. Am Fam Physician 2000;62:1699-1701.
7. Mettler FA, Jr. Essentials of Radiology. 2nd ed. Philadelphia, Pa: Saunders; 2005.
8. Marx JA, Hockberger RS, Walls JM. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 5th ed. St. Louis, Mo: Mosby; 2002.
1. Aygun D, Bildik F. Clinical warning criteria in evaluation by computed tomography the secondary neurological headaches in adults. Eur J Neurol 2003;10:437-442.
2. Sobri M, Lamont AC, Alias NA, Win MN. Red flags in patients presenting with headache: clinical indications for neuroimaging. Br J Radiol 2003;76:532-535.
3. Ramirez-Lassepas M, Espinosa C, Cicero JJ, Johnston KL, Cipolle RJ, Barber DL. Predictors of intracranial pathologic findings in patients who see emergency care because of headache. Arch Neurol 1997;54:1506-1509.
4. Becker L, Iverson DC, Reed FM, Calonge N, Miller RS, Freeman WL. Patients with a new headache in primary care: a report from ASPN. J Fam Pract 1988;27:41-47.
5. Becker LA, Green LA, Beaufait D, Kirk J, Froom J, Freeman WL. Use of CT scans for the investigation of headache: a report from ASPN, part 1. J Fam Pract 1993;37:129-134.
6. Morey SS. Headache Consortium releases guidelines for use of CT or MRI in migraine work-up. Am Fam Physician 2000;62:1699-1701.
7. Mettler FA, Jr. Essentials of Radiology. 2nd ed. Philadelphia, Pa: Saunders; 2005.
8. Marx JA, Hockberger RS, Walls JM. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 5th ed. St. Louis, Mo: Mosby; 2002.
Evidence-based answers from the Family Physicians Inquiries Network
Do TZDs increase the risk of heart failure for patients with diabetes?
Patients with diabetes who take thiazolidinediones (TZDs) have a higher incidence of congestive heart failure (CHF) than those who do not; the incidence of CHF is similar with the use of pioglitazone (Actos), troglitazone (Rezulin), or rosiglitazone (Avandia) (strength of recommendation [SOR]: B, based on a large retrospective cohort study). However, patients on regimens that include pioglitazone but not insulin have lower rates of CHF than those taking insulin but not pioglitazone (SOR: B, based on a retrospective cohort study). Still, patients starting any TZD should be warned of the possibility of CHF and should be monitored for its development. TZDs are contraindicated for patients with class III and IV CHF (SOR: C, based on expert opinion).
Consider stopping TZDs for patients developing edema or CHF
Richard Hoffman, MD
Chesterfield Family Practice, Richmond, Va
Improved glycemic control decreases the risk of end organ damage and heart failure in patients with diabetes. Thiazolidinediones are very useful drugs, particularly for patients with marked insulin resistance and hyperlipidemia. However, they do precipitate edema and heart failure. The edema can be severe enough to lead to discontinuation of the drug, and the risk of heart failure limits the population in which they can be used. They can be used safely in some cardiac patients but, as noted in the article, they should be avoided or used with caution in patients with CHF. Patients taking a TZD who subsequently develop edema should be carefully evaluated for CHF.
Evidence summary
A retrospective cohort study of health insurance claims compared the incidence of CHF among 5441 patients with diabetes who had taken TZDs (rosiglitazone, troglitazone, or pioglitazone) vs 28,103 who had not. Patients were allowed other oral agents and insulin, and they were followed for up to 6 years. The TZD group had more patients on insulin and with pre-existing comorbidities. Based on Kaplan-Meier estimates, which control for censored information, the incidence of new heart failure at 40 months was 8.2% in the TZD group and 5.3% in the non-TZD group (number needed to harm [NNH]=34.5). Using a multivariate analysis that controlled for the coadministration of insulin, the hazard ratio for TZD use was 1.76 (95% confidence interval [CI], 1.43–2.17).1 The incidence of CHF was 3.24% in the troglitazone group (n=1665), 2.39% in the rosiglitazone group (n=1882), and 1.63% in the pioglitazone group (n=1347). The difference in these rates is not statistically significant. Of the 28,103 patients not on a TZD, 1.41% developed heart failure. Individual agents were not compared with placebo.
A manufacturer-sponsored study that combined data from 4 separate unpublished randomized controlled trials compared the incidence of CHF at 1 year for patients treated with pioglitazone (as monotherapy and in combination with other oral agents) with those treated only with other oral agents. Cardiac failure was noted in 12 of 1857 in the pioglitazone group vs 10 of 1856 subjects in the non-pioglitazone groups (not statistically significant). The paper did not comment on how the patients were recruited, how outcomes were measured, or why the 4 original studies were not published.2
Another manufacturer-sponsored retrospective cohort study of pioglitazone analyzed insurance claims data to compare the incidence of CHF among 1668 adult patients taking pioglitazone (and possibly other medications, but not insulin) vs 1668 adult patients taking insulin (and possibly other medications, but not a TZD). The 2 groups were matched in terms of comorbid conditions, but statistical analysis did not take disease severity into account. The incidence of CHF was 2% of pioglitazone users compared with 4% of patients using insulin (NNH for insulin=50). In addition, CHF-related hospitalizations were 0.7% for CHF in the pioglitazone group vs 2.5% in the insulin group (NNH for insulin=55). Both of these findings are statistically significant.3
Recommendations from others
The American Diabetes Association/American Heart Association recommends that patients be evaluated for heart disease or heart failure before starting TZD therapy and monitored for symptoms thereafter. Patients who are at risk for developing CHF, who already have New York Heart Association class I or II CHF, or who take insulin should begin TZD therapy with low doses that are titrated up gradually. The US Food and Drug Administration has not approved TZDs for patients with class III or IV CHF, as there are no studies in these populations.4
1. Delea TE, Edelsberg JS, Hagiwara M, Oster G, Phillips LS. Use of thiazolidinediones and risk of heart failure in people with type 2 diabetes: a retrospective cohort study. Diabetes Care 2003;26:2983-2989.
2. Belcher G, Lambert C, Goh KL, Edwards G, Valbuena M. Cardiovascular effects of treatment of type 2 diabetes with pioglitazone, metformin and gliclazide. Int J Clin Pract 2004;58:833-837.
3. Rajagopalan R, Rosenson RS, Fernandes AW, Khan M, Murray FT. Association between congestive heart failure and hospitalization in patients with type 2 diabetes mellitus receiving treatment with insulin or pioglitazone: a retrospective data analysis. Clin Ther 2004;26:1400-1410.
4. Nesto RW, Bell D, Bonow RO, et al. Thiazolidinedione use, fluid retention, and congestive heart failure: a consensus statement from the American Heart Association and American Diabetes Association, October 7, 2003. Circulation 2003;108:2941-2948.
Patients with diabetes who take thiazolidinediones (TZDs) have a higher incidence of congestive heart failure (CHF) than those who do not; the incidence of CHF is similar with the use of pioglitazone (Actos), troglitazone (Rezulin), or rosiglitazone (Avandia) (strength of recommendation [SOR]: B, based on a large retrospective cohort study). However, patients on regimens that include pioglitazone but not insulin have lower rates of CHF than those taking insulin but not pioglitazone (SOR: B, based on a retrospective cohort study). Still, patients starting any TZD should be warned of the possibility of CHF and should be monitored for its development. TZDs are contraindicated for patients with class III and IV CHF (SOR: C, based on expert opinion).
Consider stopping TZDs for patients developing edema or CHF
Richard Hoffman, MD
Chesterfield Family Practice, Richmond, Va
Improved glycemic control decreases the risk of end organ damage and heart failure in patients with diabetes. Thiazolidinediones are very useful drugs, particularly for patients with marked insulin resistance and hyperlipidemia. However, they do precipitate edema and heart failure. The edema can be severe enough to lead to discontinuation of the drug, and the risk of heart failure limits the population in which they can be used. They can be used safely in some cardiac patients but, as noted in the article, they should be avoided or used with caution in patients with CHF. Patients taking a TZD who subsequently develop edema should be carefully evaluated for CHF.
Evidence summary
A retrospective cohort study of health insurance claims compared the incidence of CHF among 5441 patients with diabetes who had taken TZDs (rosiglitazone, troglitazone, or pioglitazone) vs 28,103 who had not. Patients were allowed other oral agents and insulin, and they were followed for up to 6 years. The TZD group had more patients on insulin and with pre-existing comorbidities. Based on Kaplan-Meier estimates, which control for censored information, the incidence of new heart failure at 40 months was 8.2% in the TZD group and 5.3% in the non-TZD group (number needed to harm [NNH]=34.5). Using a multivariate analysis that controlled for the coadministration of insulin, the hazard ratio for TZD use was 1.76 (95% confidence interval [CI], 1.43–2.17).1 The incidence of CHF was 3.24% in the troglitazone group (n=1665), 2.39% in the rosiglitazone group (n=1882), and 1.63% in the pioglitazone group (n=1347). The difference in these rates is not statistically significant. Of the 28,103 patients not on a TZD, 1.41% developed heart failure. Individual agents were not compared with placebo.
A manufacturer-sponsored study that combined data from 4 separate unpublished randomized controlled trials compared the incidence of CHF at 1 year for patients treated with pioglitazone (as monotherapy and in combination with other oral agents) with those treated only with other oral agents. Cardiac failure was noted in 12 of 1857 in the pioglitazone group vs 10 of 1856 subjects in the non-pioglitazone groups (not statistically significant). The paper did not comment on how the patients were recruited, how outcomes were measured, or why the 4 original studies were not published.2
Another manufacturer-sponsored retrospective cohort study of pioglitazone analyzed insurance claims data to compare the incidence of CHF among 1668 adult patients taking pioglitazone (and possibly other medications, but not insulin) vs 1668 adult patients taking insulin (and possibly other medications, but not a TZD). The 2 groups were matched in terms of comorbid conditions, but statistical analysis did not take disease severity into account. The incidence of CHF was 2% of pioglitazone users compared with 4% of patients using insulin (NNH for insulin=50). In addition, CHF-related hospitalizations were 0.7% for CHF in the pioglitazone group vs 2.5% in the insulin group (NNH for insulin=55). Both of these findings are statistically significant.3
Recommendations from others
The American Diabetes Association/American Heart Association recommends that patients be evaluated for heart disease or heart failure before starting TZD therapy and monitored for symptoms thereafter. Patients who are at risk for developing CHF, who already have New York Heart Association class I or II CHF, or who take insulin should begin TZD therapy with low doses that are titrated up gradually. The US Food and Drug Administration has not approved TZDs for patients with class III or IV CHF, as there are no studies in these populations.4
Patients with diabetes who take thiazolidinediones (TZDs) have a higher incidence of congestive heart failure (CHF) than those who do not; the incidence of CHF is similar with the use of pioglitazone (Actos), troglitazone (Rezulin), or rosiglitazone (Avandia) (strength of recommendation [SOR]: B, based on a large retrospective cohort study). However, patients on regimens that include pioglitazone but not insulin have lower rates of CHF than those taking insulin but not pioglitazone (SOR: B, based on a retrospective cohort study). Still, patients starting any TZD should be warned of the possibility of CHF and should be monitored for its development. TZDs are contraindicated for patients with class III and IV CHF (SOR: C, based on expert opinion).
Consider stopping TZDs for patients developing edema or CHF
Richard Hoffman, MD
Chesterfield Family Practice, Richmond, Va
Improved glycemic control decreases the risk of end organ damage and heart failure in patients with diabetes. Thiazolidinediones are very useful drugs, particularly for patients with marked insulin resistance and hyperlipidemia. However, they do precipitate edema and heart failure. The edema can be severe enough to lead to discontinuation of the drug, and the risk of heart failure limits the population in which they can be used. They can be used safely in some cardiac patients but, as noted in the article, they should be avoided or used with caution in patients with CHF. Patients taking a TZD who subsequently develop edema should be carefully evaluated for CHF.
Evidence summary
A retrospective cohort study of health insurance claims compared the incidence of CHF among 5441 patients with diabetes who had taken TZDs (rosiglitazone, troglitazone, or pioglitazone) vs 28,103 who had not. Patients were allowed other oral agents and insulin, and they were followed for up to 6 years. The TZD group had more patients on insulin and with pre-existing comorbidities. Based on Kaplan-Meier estimates, which control for censored information, the incidence of new heart failure at 40 months was 8.2% in the TZD group and 5.3% in the non-TZD group (number needed to harm [NNH]=34.5). Using a multivariate analysis that controlled for the coadministration of insulin, the hazard ratio for TZD use was 1.76 (95% confidence interval [CI], 1.43–2.17).1 The incidence of CHF was 3.24% in the troglitazone group (n=1665), 2.39% in the rosiglitazone group (n=1882), and 1.63% in the pioglitazone group (n=1347). The difference in these rates is not statistically significant. Of the 28,103 patients not on a TZD, 1.41% developed heart failure. Individual agents were not compared with placebo.
A manufacturer-sponsored study that combined data from 4 separate unpublished randomized controlled trials compared the incidence of CHF at 1 year for patients treated with pioglitazone (as monotherapy and in combination with other oral agents) with those treated only with other oral agents. Cardiac failure was noted in 12 of 1857 in the pioglitazone group vs 10 of 1856 subjects in the non-pioglitazone groups (not statistically significant). The paper did not comment on how the patients were recruited, how outcomes were measured, or why the 4 original studies were not published.2
Another manufacturer-sponsored retrospective cohort study of pioglitazone analyzed insurance claims data to compare the incidence of CHF among 1668 adult patients taking pioglitazone (and possibly other medications, but not insulin) vs 1668 adult patients taking insulin (and possibly other medications, but not a TZD). The 2 groups were matched in terms of comorbid conditions, but statistical analysis did not take disease severity into account. The incidence of CHF was 2% of pioglitazone users compared with 4% of patients using insulin (NNH for insulin=50). In addition, CHF-related hospitalizations were 0.7% for CHF in the pioglitazone group vs 2.5% in the insulin group (NNH for insulin=55). Both of these findings are statistically significant.3
Recommendations from others
The American Diabetes Association/American Heart Association recommends that patients be evaluated for heart disease or heart failure before starting TZD therapy and monitored for symptoms thereafter. Patients who are at risk for developing CHF, who already have New York Heart Association class I or II CHF, or who take insulin should begin TZD therapy with low doses that are titrated up gradually. The US Food and Drug Administration has not approved TZDs for patients with class III or IV CHF, as there are no studies in these populations.4
1. Delea TE, Edelsberg JS, Hagiwara M, Oster G, Phillips LS. Use of thiazolidinediones and risk of heart failure in people with type 2 diabetes: a retrospective cohort study. Diabetes Care 2003;26:2983-2989.
2. Belcher G, Lambert C, Goh KL, Edwards G, Valbuena M. Cardiovascular effects of treatment of type 2 diabetes with pioglitazone, metformin and gliclazide. Int J Clin Pract 2004;58:833-837.
3. Rajagopalan R, Rosenson RS, Fernandes AW, Khan M, Murray FT. Association between congestive heart failure and hospitalization in patients with type 2 diabetes mellitus receiving treatment with insulin or pioglitazone: a retrospective data analysis. Clin Ther 2004;26:1400-1410.
4. Nesto RW, Bell D, Bonow RO, et al. Thiazolidinedione use, fluid retention, and congestive heart failure: a consensus statement from the American Heart Association and American Diabetes Association, October 7, 2003. Circulation 2003;108:2941-2948.
1. Delea TE, Edelsberg JS, Hagiwara M, Oster G, Phillips LS. Use of thiazolidinediones and risk of heart failure in people with type 2 diabetes: a retrospective cohort study. Diabetes Care 2003;26:2983-2989.
2. Belcher G, Lambert C, Goh KL, Edwards G, Valbuena M. Cardiovascular effects of treatment of type 2 diabetes with pioglitazone, metformin and gliclazide. Int J Clin Pract 2004;58:833-837.
3. Rajagopalan R, Rosenson RS, Fernandes AW, Khan M, Murray FT. Association between congestive heart failure and hospitalization in patients with type 2 diabetes mellitus receiving treatment with insulin or pioglitazone: a retrospective data analysis. Clin Ther 2004;26:1400-1410.
4. Nesto RW, Bell D, Bonow RO, et al. Thiazolidinedione use, fluid retention, and congestive heart failure: a consensus statement from the American Heart Association and American Diabetes Association, October 7, 2003. Circulation 2003;108:2941-2948.
Evidence-based answers from the Family Physicians Inquiries Network
What is the best therapy for superficial thrombophlebitis?
For proximal saphenous vein thrombosis, anticoagulation is more effective than venous ligation (with or without stripping) in preventing deep venous thrombosis (DVT) and pulmonary embolus (PE) (strength of recommendation [SOR]: C, qualitative systematic review of primarily case series).
For patients with superficial venous thrombophlebitis (SVTP) distal to the saphenous vein of the thigh, tenoxicam (a nonsteroidal anti-inflammatory agent [NSAID]) and low-molecular-weight heparin are similarly effective for reducing extension and subsequent DVT when administered along with compression therapy (SOR: B, 1 randomized controlled trial). Oral or topical NSAIDs, topical heparin, and topical nitroglycerin all alleviate symptoms and speed resolution of SVTP caused by infusion catheters (SOR: B, smaller, occasionally conflicting randomized trials).
Evidence summary
Superficial thrombophlebitis refers to erythema, pain, induration, and other findings of inflammation in superficial veins, usually due to infection or thrombosis. Typically, SVTP is localized problem, but some lower-extremity SVTP is associated with increased risk of DVT and PE, particularly the long saphenous vein. This review will not address thrombosis in the superficial femoral vein, a portion of the deep venous system, which requires full DVT therapy.1
Since saphenous vein thrombosis above the knee is associated with DVT and PE, 1 systematic review looked at papers comparing anticoagulation (IV heparin followed by 6 weeks to 6 months of warfarin) with surgical ligation of the saphenous vein (either alone or combined with vein stripping or with vein stripping and perforator ligation).1 The review included primarily case series with widely varying protocols. According to the authors, the data “suggests that medical management with anticoagulants is somewhat superior” to surgery for preventing DVT and PE. However, the fewest extensions of SVTP occurred when vein ligation was combined with stripping of the thrombosed vein and interruption of perforators.
In a more recent trial, patients randomized to subcutaneous heparin at 12,500 units twice daily for a week followed by 10,000 units twice daily had fewer vascular complications of proximal saphenous vein thrombosis than those receiving heparin at 5000 units twice daily (6/30 in the low-dose group and 1/30 in the high-dose group; P<.05; number needed to treat [NNT]=6).2 There were no bleeding complications in either group.
One large double-blind randomized controlled trial compared tenoxicam (an NSAID available in Canada, similar to piroxicam), enoxaparin (Lovenox), and placebo for 8 to 12 days in 427 patients with SVTP of the leg measuring 5 cm or more.3 Patients were also treated with compression hose. Patients who required immediate anticoagulation or venous ligation were excluded. Within 3 months, 35% of patients taking placebo developed an extension or recurrence of their SVTP or a DVT, compared with 16% to 17% of treated patients (NNT=6). There was no significant difference in outcome between subcutaneous enoxaparin at fixed (40 mg/d) or adjusted doses (1.5 mg/kg), or 20 mg/d oral tenoxicam. In a small randomized trial (n=40), intramuscular defibrotide provided better symptom resolution than low-dose heparin for patients with uncomplicated SVTP of the leg.4
For infusion-related SVTP, a randomized controlled trial of 120 patients found both oral and topical diclofenac effective in reducing symptoms (NNT=3), although oral diclofenac had significantly more gastrointestinal side effects (number needed to harm=3 for dyspepsia).5 Two double-blind trials of topical heparin showed it to be superior to placebo in reducing symptoms and speeding healing.6,7
In the larger study (n=126), 44% of patients treated with 1000 IU/g heparin gel 3 times a day were symptom-free at 1 week, compared with 26% on placebo (NNT=6).7 A randomized trial of infusion-related SVTP (n=100) found that 2% nitroglycerin gel eliminated pain in 50 hours vs 72 hours with topical heparin (P<.05).8 A smaller, underpowered double-blind trial of topical heparin, piroxicam gel, and placebo (22 to 24 patients in each treatment arm) failed to find efficacy with either therapy.9
Recommendation from others
For SVTP of the leg that does not include the proximal saphenous vein, Up To Date recommends compression and oral NSAIDs, noting that NSAIDs are inexpensive, help with symptom control, and appear comparable to low-molecular-weight heparin in limiting complications.10
Those with symptoms in the thigh need closer follow-up, more aggressive therapy
James L. Greenwald, MD
SUNY Upstate Medical University, Syracuse, NY
Patients with a red, swollen, painful extremity are commonly encountered in my practice. I see this among patients with venous stasis due to obesity, aging, and varicosities. I find ready access to a D-dimer blood test and a venous Doppler can help me rule out DVT. I end up treating many of these patients with both an NSAID and an antistaphylococcal antibiotic, because of the lack of certainty in differentiating superficial phlebitis from cellulitis.
Upper extremity phlebitis is less common. It can occur in a delayed fashion several days after a patient has received intravenous therapy. The characteristic on exam is a knotty, red, ropey painful structure correlating to the course of the basilic or cephalic vein.
This review is helpful to me; it reinforces that the patients I see with symptoms in the thigh need closer follow-up and more aggressive therapy with anticoagulation, no matter what the Doppler shows. I usually hold off on anticoagulating other patients until they show no improvement with a trial of the NSAIDs and compression. Topical heparin and nitroglycerin gel are therapies new to me and appear worth looking into for the patient who is not improving. In a quick search for topical heparin, I could not find a US source, and it is not used locally.
1. Sullivan V, Denk PM, Sonnad SS, Eagleton MJ, Wakefield TW. Ligation versus anticoagulation: treatment of aboveknee superficial thrombophlebitis not involving the deep venous system. J Am Coll Surg 2001;193:556-562.
2. Marchiori A, Verlato F, Sabbion P, et al. High versus low doses of unfractionated heparin for the treatment of superficial thrombophlebitis of the leg. A prospective, controlled, randomized study. Haematologica 2002;87:523-527.
3. Superficial Thrombophlebitis Treated by Enoxaparin Study Group. A pilot randomized double-blind comparison of a low-molecular-weight heparin, a nonsteroidal anti-inflammatory agent, and placebo in the treatment of superficial vein thrombosis. Arch Intern Med 2003;163:1657-1663.
4. Belcaro G. Evolution of superficial vein thrombosis treated with defibrotide: comparison with low dose subcutaneous heparin. Int J Tissue React 1990;12:319-324.
5. Becherucci A, Bagilet D, Marenghini J, Diab M, Biancardi H. [Effect of topical and oral diclofenac on superficial thrombophlebitis caused by intravenous infusion]. Med Clin (Barc) 2000;114:371-373.
6. Mehta PP, Sagar S, Kakkar VV. Treatment of superficial thrombophlebitis: a randomized, double-blind trial of heparinoid cream. Br Med J 1975;3:614-616.
7. Vilardell M, Sabat D, Arnaiz JA, et al. Topical heparin for the treatment of acute superficial phlebitis secondary to indwelling intravenous catheter. A double-blind, randomized, placebo-controlled trial. Eur J Clin Pharmacol 1999;54:917-921.
8. Almenar L, Hernandez M, Gimeno JV, Palencia M, Algarra F. [Heparionoids versus nitroglycerin in the treatment of superficial phlebitis]. Rev Clin Esp 1993;193:229-231.
9. Bergqvist D, Brunkwall J, Jensen N, Persson NH. Treatment of superficial thrombophlebitis. A comparative trial between placebo, Hirudoid cream, and piroxicam gel. Ann Chir Gynaecol 1990;79:92-96.
10. Fernandez L. Superficial phlebitis. UpToDate [online database]. Last updated September 2, 2003. Available at: www.uptodateonline.com.
For proximal saphenous vein thrombosis, anticoagulation is more effective than venous ligation (with or without stripping) in preventing deep venous thrombosis (DVT) and pulmonary embolus (PE) (strength of recommendation [SOR]: C, qualitative systematic review of primarily case series).
For patients with superficial venous thrombophlebitis (SVTP) distal to the saphenous vein of the thigh, tenoxicam (a nonsteroidal anti-inflammatory agent [NSAID]) and low-molecular-weight heparin are similarly effective for reducing extension and subsequent DVT when administered along with compression therapy (SOR: B, 1 randomized controlled trial). Oral or topical NSAIDs, topical heparin, and topical nitroglycerin all alleviate symptoms and speed resolution of SVTP caused by infusion catheters (SOR: B, smaller, occasionally conflicting randomized trials).
Evidence summary
Superficial thrombophlebitis refers to erythema, pain, induration, and other findings of inflammation in superficial veins, usually due to infection or thrombosis. Typically, SVTP is localized problem, but some lower-extremity SVTP is associated with increased risk of DVT and PE, particularly the long saphenous vein. This review will not address thrombosis in the superficial femoral vein, a portion of the deep venous system, which requires full DVT therapy.1
Since saphenous vein thrombosis above the knee is associated with DVT and PE, 1 systematic review looked at papers comparing anticoagulation (IV heparin followed by 6 weeks to 6 months of warfarin) with surgical ligation of the saphenous vein (either alone or combined with vein stripping or with vein stripping and perforator ligation).1 The review included primarily case series with widely varying protocols. According to the authors, the data “suggests that medical management with anticoagulants is somewhat superior” to surgery for preventing DVT and PE. However, the fewest extensions of SVTP occurred when vein ligation was combined with stripping of the thrombosed vein and interruption of perforators.
In a more recent trial, patients randomized to subcutaneous heparin at 12,500 units twice daily for a week followed by 10,000 units twice daily had fewer vascular complications of proximal saphenous vein thrombosis than those receiving heparin at 5000 units twice daily (6/30 in the low-dose group and 1/30 in the high-dose group; P<.05; number needed to treat [NNT]=6).2 There were no bleeding complications in either group.
One large double-blind randomized controlled trial compared tenoxicam (an NSAID available in Canada, similar to piroxicam), enoxaparin (Lovenox), and placebo for 8 to 12 days in 427 patients with SVTP of the leg measuring 5 cm or more.3 Patients were also treated with compression hose. Patients who required immediate anticoagulation or venous ligation were excluded. Within 3 months, 35% of patients taking placebo developed an extension or recurrence of their SVTP or a DVT, compared with 16% to 17% of treated patients (NNT=6). There was no significant difference in outcome between subcutaneous enoxaparin at fixed (40 mg/d) or adjusted doses (1.5 mg/kg), or 20 mg/d oral tenoxicam. In a small randomized trial (n=40), intramuscular defibrotide provided better symptom resolution than low-dose heparin for patients with uncomplicated SVTP of the leg.4
For infusion-related SVTP, a randomized controlled trial of 120 patients found both oral and topical diclofenac effective in reducing symptoms (NNT=3), although oral diclofenac had significantly more gastrointestinal side effects (number needed to harm=3 for dyspepsia).5 Two double-blind trials of topical heparin showed it to be superior to placebo in reducing symptoms and speeding healing.6,7
In the larger study (n=126), 44% of patients treated with 1000 IU/g heparin gel 3 times a day were symptom-free at 1 week, compared with 26% on placebo (NNT=6).7 A randomized trial of infusion-related SVTP (n=100) found that 2% nitroglycerin gel eliminated pain in 50 hours vs 72 hours with topical heparin (P<.05).8 A smaller, underpowered double-blind trial of topical heparin, piroxicam gel, and placebo (22 to 24 patients in each treatment arm) failed to find efficacy with either therapy.9
Recommendation from others
For SVTP of the leg that does not include the proximal saphenous vein, Up To Date recommends compression and oral NSAIDs, noting that NSAIDs are inexpensive, help with symptom control, and appear comparable to low-molecular-weight heparin in limiting complications.10
Those with symptoms in the thigh need closer follow-up, more aggressive therapy
James L. Greenwald, MD
SUNY Upstate Medical University, Syracuse, NY
Patients with a red, swollen, painful extremity are commonly encountered in my practice. I see this among patients with venous stasis due to obesity, aging, and varicosities. I find ready access to a D-dimer blood test and a venous Doppler can help me rule out DVT. I end up treating many of these patients with both an NSAID and an antistaphylococcal antibiotic, because of the lack of certainty in differentiating superficial phlebitis from cellulitis.
Upper extremity phlebitis is less common. It can occur in a delayed fashion several days after a patient has received intravenous therapy. The characteristic on exam is a knotty, red, ropey painful structure correlating to the course of the basilic or cephalic vein.
This review is helpful to me; it reinforces that the patients I see with symptoms in the thigh need closer follow-up and more aggressive therapy with anticoagulation, no matter what the Doppler shows. I usually hold off on anticoagulating other patients until they show no improvement with a trial of the NSAIDs and compression. Topical heparin and nitroglycerin gel are therapies new to me and appear worth looking into for the patient who is not improving. In a quick search for topical heparin, I could not find a US source, and it is not used locally.
For proximal saphenous vein thrombosis, anticoagulation is more effective than venous ligation (with or without stripping) in preventing deep venous thrombosis (DVT) and pulmonary embolus (PE) (strength of recommendation [SOR]: C, qualitative systematic review of primarily case series).
For patients with superficial venous thrombophlebitis (SVTP) distal to the saphenous vein of the thigh, tenoxicam (a nonsteroidal anti-inflammatory agent [NSAID]) and low-molecular-weight heparin are similarly effective for reducing extension and subsequent DVT when administered along with compression therapy (SOR: B, 1 randomized controlled trial). Oral or topical NSAIDs, topical heparin, and topical nitroglycerin all alleviate symptoms and speed resolution of SVTP caused by infusion catheters (SOR: B, smaller, occasionally conflicting randomized trials).
Evidence summary
Superficial thrombophlebitis refers to erythema, pain, induration, and other findings of inflammation in superficial veins, usually due to infection or thrombosis. Typically, SVTP is localized problem, but some lower-extremity SVTP is associated with increased risk of DVT and PE, particularly the long saphenous vein. This review will not address thrombosis in the superficial femoral vein, a portion of the deep venous system, which requires full DVT therapy.1
Since saphenous vein thrombosis above the knee is associated with DVT and PE, 1 systematic review looked at papers comparing anticoagulation (IV heparin followed by 6 weeks to 6 months of warfarin) with surgical ligation of the saphenous vein (either alone or combined with vein stripping or with vein stripping and perforator ligation).1 The review included primarily case series with widely varying protocols. According to the authors, the data “suggests that medical management with anticoagulants is somewhat superior” to surgery for preventing DVT and PE. However, the fewest extensions of SVTP occurred when vein ligation was combined with stripping of the thrombosed vein and interruption of perforators.
In a more recent trial, patients randomized to subcutaneous heparin at 12,500 units twice daily for a week followed by 10,000 units twice daily had fewer vascular complications of proximal saphenous vein thrombosis than those receiving heparin at 5000 units twice daily (6/30 in the low-dose group and 1/30 in the high-dose group; P<.05; number needed to treat [NNT]=6).2 There were no bleeding complications in either group.
One large double-blind randomized controlled trial compared tenoxicam (an NSAID available in Canada, similar to piroxicam), enoxaparin (Lovenox), and placebo for 8 to 12 days in 427 patients with SVTP of the leg measuring 5 cm or more.3 Patients were also treated with compression hose. Patients who required immediate anticoagulation or venous ligation were excluded. Within 3 months, 35% of patients taking placebo developed an extension or recurrence of their SVTP or a DVT, compared with 16% to 17% of treated patients (NNT=6). There was no significant difference in outcome between subcutaneous enoxaparin at fixed (40 mg/d) or adjusted doses (1.5 mg/kg), or 20 mg/d oral tenoxicam. In a small randomized trial (n=40), intramuscular defibrotide provided better symptom resolution than low-dose heparin for patients with uncomplicated SVTP of the leg.4
For infusion-related SVTP, a randomized controlled trial of 120 patients found both oral and topical diclofenac effective in reducing symptoms (NNT=3), although oral diclofenac had significantly more gastrointestinal side effects (number needed to harm=3 for dyspepsia).5 Two double-blind trials of topical heparin showed it to be superior to placebo in reducing symptoms and speeding healing.6,7
In the larger study (n=126), 44% of patients treated with 1000 IU/g heparin gel 3 times a day were symptom-free at 1 week, compared with 26% on placebo (NNT=6).7 A randomized trial of infusion-related SVTP (n=100) found that 2% nitroglycerin gel eliminated pain in 50 hours vs 72 hours with topical heparin (P<.05).8 A smaller, underpowered double-blind trial of topical heparin, piroxicam gel, and placebo (22 to 24 patients in each treatment arm) failed to find efficacy with either therapy.9
Recommendation from others
For SVTP of the leg that does not include the proximal saphenous vein, Up To Date recommends compression and oral NSAIDs, noting that NSAIDs are inexpensive, help with symptom control, and appear comparable to low-molecular-weight heparin in limiting complications.10
Those with symptoms in the thigh need closer follow-up, more aggressive therapy
James L. Greenwald, MD
SUNY Upstate Medical University, Syracuse, NY
Patients with a red, swollen, painful extremity are commonly encountered in my practice. I see this among patients with venous stasis due to obesity, aging, and varicosities. I find ready access to a D-dimer blood test and a venous Doppler can help me rule out DVT. I end up treating many of these patients with both an NSAID and an antistaphylococcal antibiotic, because of the lack of certainty in differentiating superficial phlebitis from cellulitis.
Upper extremity phlebitis is less common. It can occur in a delayed fashion several days after a patient has received intravenous therapy. The characteristic on exam is a knotty, red, ropey painful structure correlating to the course of the basilic or cephalic vein.
This review is helpful to me; it reinforces that the patients I see with symptoms in the thigh need closer follow-up and more aggressive therapy with anticoagulation, no matter what the Doppler shows. I usually hold off on anticoagulating other patients until they show no improvement with a trial of the NSAIDs and compression. Topical heparin and nitroglycerin gel are therapies new to me and appear worth looking into for the patient who is not improving. In a quick search for topical heparin, I could not find a US source, and it is not used locally.
1. Sullivan V, Denk PM, Sonnad SS, Eagleton MJ, Wakefield TW. Ligation versus anticoagulation: treatment of aboveknee superficial thrombophlebitis not involving the deep venous system. J Am Coll Surg 2001;193:556-562.
2. Marchiori A, Verlato F, Sabbion P, et al. High versus low doses of unfractionated heparin for the treatment of superficial thrombophlebitis of the leg. A prospective, controlled, randomized study. Haematologica 2002;87:523-527.
3. Superficial Thrombophlebitis Treated by Enoxaparin Study Group. A pilot randomized double-blind comparison of a low-molecular-weight heparin, a nonsteroidal anti-inflammatory agent, and placebo in the treatment of superficial vein thrombosis. Arch Intern Med 2003;163:1657-1663.
4. Belcaro G. Evolution of superficial vein thrombosis treated with defibrotide: comparison with low dose subcutaneous heparin. Int J Tissue React 1990;12:319-324.
5. Becherucci A, Bagilet D, Marenghini J, Diab M, Biancardi H. [Effect of topical and oral diclofenac on superficial thrombophlebitis caused by intravenous infusion]. Med Clin (Barc) 2000;114:371-373.
6. Mehta PP, Sagar S, Kakkar VV. Treatment of superficial thrombophlebitis: a randomized, double-blind trial of heparinoid cream. Br Med J 1975;3:614-616.
7. Vilardell M, Sabat D, Arnaiz JA, et al. Topical heparin for the treatment of acute superficial phlebitis secondary to indwelling intravenous catheter. A double-blind, randomized, placebo-controlled trial. Eur J Clin Pharmacol 1999;54:917-921.
8. Almenar L, Hernandez M, Gimeno JV, Palencia M, Algarra F. [Heparionoids versus nitroglycerin in the treatment of superficial phlebitis]. Rev Clin Esp 1993;193:229-231.
9. Bergqvist D, Brunkwall J, Jensen N, Persson NH. Treatment of superficial thrombophlebitis. A comparative trial between placebo, Hirudoid cream, and piroxicam gel. Ann Chir Gynaecol 1990;79:92-96.
10. Fernandez L. Superficial phlebitis. UpToDate [online database]. Last updated September 2, 2003. Available at: www.uptodateonline.com.
1. Sullivan V, Denk PM, Sonnad SS, Eagleton MJ, Wakefield TW. Ligation versus anticoagulation: treatment of aboveknee superficial thrombophlebitis not involving the deep venous system. J Am Coll Surg 2001;193:556-562.
2. Marchiori A, Verlato F, Sabbion P, et al. High versus low doses of unfractionated heparin for the treatment of superficial thrombophlebitis of the leg. A prospective, controlled, randomized study. Haematologica 2002;87:523-527.
3. Superficial Thrombophlebitis Treated by Enoxaparin Study Group. A pilot randomized double-blind comparison of a low-molecular-weight heparin, a nonsteroidal anti-inflammatory agent, and placebo in the treatment of superficial vein thrombosis. Arch Intern Med 2003;163:1657-1663.
4. Belcaro G. Evolution of superficial vein thrombosis treated with defibrotide: comparison with low dose subcutaneous heparin. Int J Tissue React 1990;12:319-324.
5. Becherucci A, Bagilet D, Marenghini J, Diab M, Biancardi H. [Effect of topical and oral diclofenac on superficial thrombophlebitis caused by intravenous infusion]. Med Clin (Barc) 2000;114:371-373.
6. Mehta PP, Sagar S, Kakkar VV. Treatment of superficial thrombophlebitis: a randomized, double-blind trial of heparinoid cream. Br Med J 1975;3:614-616.
7. Vilardell M, Sabat D, Arnaiz JA, et al. Topical heparin for the treatment of acute superficial phlebitis secondary to indwelling intravenous catheter. A double-blind, randomized, placebo-controlled trial. Eur J Clin Pharmacol 1999;54:917-921.
8. Almenar L, Hernandez M, Gimeno JV, Palencia M, Algarra F. [Heparionoids versus nitroglycerin in the treatment of superficial phlebitis]. Rev Clin Esp 1993;193:229-231.
9. Bergqvist D, Brunkwall J, Jensen N, Persson NH. Treatment of superficial thrombophlebitis. A comparative trial between placebo, Hirudoid cream, and piroxicam gel. Ann Chir Gynaecol 1990;79:92-96.
10. Fernandez L. Superficial phlebitis. UpToDate [online database]. Last updated September 2, 2003. Available at: www.uptodateonline.com.
Evidence-based answers from the Family Physicians Inquiries Network
What is the best macrolide for atypical pneumonia?
Erythromycin, clarithromycin, and azithromycin are equally effective in treating pneumonia caused by Mycoplasma pneumoniae or Chlamydophila (formerly Chlamydia) pneumoniae (strength of recommendation [SOR]: B, small head-to-head trials). Macrolide choice can be based on other considerations—cost, side effects, and effectiveness against other suspected pathogens (SOR: C, expert opinion).
Evidence summary
M pneumoniae and C pneumoniae account for about 30% of community-acquired pneumonia (CAP), making them the most common “atypicals.” Clinically they are indistinguishable from other causes of pneumonia; most studies use cultures to identify cases among populations with CAP.
Azithromycin and erythromycin were compared in 3 studies of children with CAP.1-3 Together, they identified 69 cases due to M pneumoniae or C pneumoniae. Only 3 patients did not respond to either antibiotic. In the largest of the 3 studies,3 side effects were noted in 10% of CAP patients on azithromycin and 20% on erythromycin (P<.05).
Another study looked at patients aged 12 to 80 years with pneumonia due to M pneumoniae (75 cases) or Chlamydophila psittaci (formerly Chlamydia psittaci, 16 cases).4 All patients responded to treatment. Clarithromycin and erythromycin were compared in children aged 3 to 12 years with CAP.5 M pneumoniae or C pneumoniae was identified in 42 cases. Two of 18 patients did not respond to erythromycin; 3 of 27 patients did not respond to clarithromycin.
Another study compared these antibiotics for patients with CAP aged 12 to 93 years.6 Subgroup analysis of those with M pneumoniae or C pneumoniae (n=27) showed similar efficacy. Pooling all 268 patients with CAP, side effects were seen in 31% of patients on clarithromycin and 59% on erythromycin (P<.001).
A comparison study of newer macrolides in 40 adults with CAP identified 13 with M pneumoniae or C pneumoniae (Table).7 One patient did not respond of the 8 treated with clarithromycin; none among the 5 treated with azithromycin. There was 1 adverse event (from clarithromycin).
TABLE
Macrolides: comparison studies
| Antibiotic | Response rates* (%) | Side-effect rates †(%) | Cost for course of therapy in adult ‡ |
|---|---|---|---|
| Erythromycin1-4 | 77-100 | 10-59 | $11 (500 mg #40) |
| Clarithromycin5 7 | 88-94 | 5-31 | $76 (250 mg #20) |
| Azithromycin1 4,7 | 87-100 | 0-14 | $57 (250 mg #6) |
| *Response rates of pneumonia due to M pneumoniae and C pneumoniae. | |||
| † In community-acquired pneumonia treated with macrolide as single agent. | |||
| ‡ Prices from www.drugstore.com. | |||
Recommendations from others
The Infectious Diseases Society of America8 recommends a macrolide for adults with pneumonia caused by M pneumoniae or C pneumoniae, and does not promote one over another. The British Thoracic Society9 recommends any of the macrolides for pneumonia caused by these pathogens in children.
Since CAP is often caused by “atypical organisms,” macrolides are sometimes recommended as empiric outpatient therapy. In this setting, the American Thoracic Society10 discourages using erythromycin, citing a higher side-effect rate and poorer effectiveness against Haemophilus influenza. However, the Canadian Infectious Disease Society11 supports the use of any of the 3 macrolides in mild CAP except for patients with chronic obstructive pulmonary disease, who are more likely to harbor H influenza.
Lower respiratory infections—a number of problematic decisions
David Mouw, MD
Mountain Area AHEC, Asheville, NC
You face several problematic decisions when treating a patient with a lower respiratory infection. First, is this pneumonia or just bronchitis? Clinical findings can be confusing, and a chest film is helpful.12 If pneumonia is likely, you consider hospitalization, and prescribe antibiotics, usually without knowing the pathogen.
Because they cover both typical and atypical pathogens, macrolides (or doxycycline) are generally recommended, with cephalosporins to be added for higher-risk patients. (Quinolones are an alternative to this combination.) Finally, if you choose a macrolide, you face yet another decision without a clear answer: which one to use? All macrolides appear to be equally effective, so the choice depends on cost balanced against convenience and side effects.
1. Wubbel L, Muniz L, Ahmed A, et al. Etiology and treatment of community-acquired pneumonia in ambulatory children. Pediatr Infect Dis J 1999;18:98-104.
2. Harris JS, Kolokathis A, Campbell M, Cassell GH, Hammerschlag MR. Safety and efficacy of azithromycin in the treatment of community-acquired pneumonia. Pediatr Infect Dis J 1998;17:865-871.
3. Manfredi R, Jannuzzi C, Mantero E, et al. Clinical comparative study of azithromycin versus erythromycin in the treatment of acute respiratory tract infections in children. J Chemother 1992;4:364-370.
4. Schonwald S, Gunjaca M, Kolacny-Babic L, Car V, Gosev M. Comparison of azithromycin and erythromycin in the treatment of atypical pneumonias. J Antimicrob Chemother 1990;25(Suppl A):123-126.
5. Block S, Hedrick J, Hammerschlag MR, Cassell GH, Craft JC. Mycoplasma pneumoniae and Chlamydia pneumoniae in pediatric community-acquired pneumonia: comparative efficacy and safety of clarithromycin vs. erythromycin ethylsuccinate. Pediatr Infect Dis J 1995;14:471-477.
6. Chien M, Pichotta P, Siepman N, Chan CK. Treatment of community-acquired pneumonia: a multicenter, double-blind, randomized study comparing clarithromycin with erythromycin. Canada-Sweden Clarithromycin-Pneumonia Study Group. Chest 1993;103-697-701.
7. Rizzato G, Montemurro L, Fraioli P, et al. Efficacy of a three day course of azithromycin in moderately severe community-acquired pneumonia. Eur Respir J 1995;8:398-402.
8. Bartlett JG, Dowell SF, Mandell LA, File TM, Jr, Musher DM, Fine M. Practice guidelines for the management of community-acquired pneumonia in adults. Infectious Diseases Society of America. Clin Infect Dis 2000;31:347-382.
9. British. Thoracic Society Standards of Care Committee. British Thoracic Society Guidelines for the Management of Community Acquired Pneumonia in Childhood. Thorax 2002;57(Suppl 1):i1-i24.
10. American. Thoracic Society. Guidelines for the management of adults with community-acquired pneumonia: diagnosis, assessment of severity, antimicrobial therapy, and prevention. Am J Respir Crit Care Med 2001;163:1730-1754.
11. Mandell LA, Marrie TJ, Grossman RF, Chow AW, Hyland RH. Canadian guidelines for the initial management of community-acquired pneumonia: an evidence-based update by the Canadian Infectious Diseases Society and the Canadian Thoracic Society. The Canadian Community-Acquired Pneumonia Working Group. Clin Infect Dis 2000;31:383-421.
12. Kelsberg G, Safranek S. How accurate is the clinical diagnosis of pneumonia? J Fam Pract 2003;52:63-64.
Erythromycin, clarithromycin, and azithromycin are equally effective in treating pneumonia caused by Mycoplasma pneumoniae or Chlamydophila (formerly Chlamydia) pneumoniae (strength of recommendation [SOR]: B, small head-to-head trials). Macrolide choice can be based on other considerations—cost, side effects, and effectiveness against other suspected pathogens (SOR: C, expert opinion).
Evidence summary
M pneumoniae and C pneumoniae account for about 30% of community-acquired pneumonia (CAP), making them the most common “atypicals.” Clinically they are indistinguishable from other causes of pneumonia; most studies use cultures to identify cases among populations with CAP.
Azithromycin and erythromycin were compared in 3 studies of children with CAP.1-3 Together, they identified 69 cases due to M pneumoniae or C pneumoniae. Only 3 patients did not respond to either antibiotic. In the largest of the 3 studies,3 side effects were noted in 10% of CAP patients on azithromycin and 20% on erythromycin (P<.05).
Another study looked at patients aged 12 to 80 years with pneumonia due to M pneumoniae (75 cases) or Chlamydophila psittaci (formerly Chlamydia psittaci, 16 cases).4 All patients responded to treatment. Clarithromycin and erythromycin were compared in children aged 3 to 12 years with CAP.5 M pneumoniae or C pneumoniae was identified in 42 cases. Two of 18 patients did not respond to erythromycin; 3 of 27 patients did not respond to clarithromycin.
Another study compared these antibiotics for patients with CAP aged 12 to 93 years.6 Subgroup analysis of those with M pneumoniae or C pneumoniae (n=27) showed similar efficacy. Pooling all 268 patients with CAP, side effects were seen in 31% of patients on clarithromycin and 59% on erythromycin (P<.001).
A comparison study of newer macrolides in 40 adults with CAP identified 13 with M pneumoniae or C pneumoniae (Table).7 One patient did not respond of the 8 treated with clarithromycin; none among the 5 treated with azithromycin. There was 1 adverse event (from clarithromycin).
TABLE
Macrolides: comparison studies
| Antibiotic | Response rates* (%) | Side-effect rates †(%) | Cost for course of therapy in adult ‡ |
|---|---|---|---|
| Erythromycin1-4 | 77-100 | 10-59 | $11 (500 mg #40) |
| Clarithromycin5 7 | 88-94 | 5-31 | $76 (250 mg #20) |
| Azithromycin1 4,7 | 87-100 | 0-14 | $57 (250 mg #6) |
| *Response rates of pneumonia due to M pneumoniae and C pneumoniae. | |||
| † In community-acquired pneumonia treated with macrolide as single agent. | |||
| ‡ Prices from www.drugstore.com. | |||
Recommendations from others
The Infectious Diseases Society of America8 recommends a macrolide for adults with pneumonia caused by M pneumoniae or C pneumoniae, and does not promote one over another. The British Thoracic Society9 recommends any of the macrolides for pneumonia caused by these pathogens in children.
Since CAP is often caused by “atypical organisms,” macrolides are sometimes recommended as empiric outpatient therapy. In this setting, the American Thoracic Society10 discourages using erythromycin, citing a higher side-effect rate and poorer effectiveness against Haemophilus influenza. However, the Canadian Infectious Disease Society11 supports the use of any of the 3 macrolides in mild CAP except for patients with chronic obstructive pulmonary disease, who are more likely to harbor H influenza.
Lower respiratory infections—a number of problematic decisions
David Mouw, MD
Mountain Area AHEC, Asheville, NC
You face several problematic decisions when treating a patient with a lower respiratory infection. First, is this pneumonia or just bronchitis? Clinical findings can be confusing, and a chest film is helpful.12 If pneumonia is likely, you consider hospitalization, and prescribe antibiotics, usually without knowing the pathogen.
Because they cover both typical and atypical pathogens, macrolides (or doxycycline) are generally recommended, with cephalosporins to be added for higher-risk patients. (Quinolones are an alternative to this combination.) Finally, if you choose a macrolide, you face yet another decision without a clear answer: which one to use? All macrolides appear to be equally effective, so the choice depends on cost balanced against convenience and side effects.
Erythromycin, clarithromycin, and azithromycin are equally effective in treating pneumonia caused by Mycoplasma pneumoniae or Chlamydophila (formerly Chlamydia) pneumoniae (strength of recommendation [SOR]: B, small head-to-head trials). Macrolide choice can be based on other considerations—cost, side effects, and effectiveness against other suspected pathogens (SOR: C, expert opinion).
Evidence summary
M pneumoniae and C pneumoniae account for about 30% of community-acquired pneumonia (CAP), making them the most common “atypicals.” Clinically they are indistinguishable from other causes of pneumonia; most studies use cultures to identify cases among populations with CAP.
Azithromycin and erythromycin were compared in 3 studies of children with CAP.1-3 Together, they identified 69 cases due to M pneumoniae or C pneumoniae. Only 3 patients did not respond to either antibiotic. In the largest of the 3 studies,3 side effects were noted in 10% of CAP patients on azithromycin and 20% on erythromycin (P<.05).
Another study looked at patients aged 12 to 80 years with pneumonia due to M pneumoniae (75 cases) or Chlamydophila psittaci (formerly Chlamydia psittaci, 16 cases).4 All patients responded to treatment. Clarithromycin and erythromycin were compared in children aged 3 to 12 years with CAP.5 M pneumoniae or C pneumoniae was identified in 42 cases. Two of 18 patients did not respond to erythromycin; 3 of 27 patients did not respond to clarithromycin.
Another study compared these antibiotics for patients with CAP aged 12 to 93 years.6 Subgroup analysis of those with M pneumoniae or C pneumoniae (n=27) showed similar efficacy. Pooling all 268 patients with CAP, side effects were seen in 31% of patients on clarithromycin and 59% on erythromycin (P<.001).
A comparison study of newer macrolides in 40 adults with CAP identified 13 with M pneumoniae or C pneumoniae (Table).7 One patient did not respond of the 8 treated with clarithromycin; none among the 5 treated with azithromycin. There was 1 adverse event (from clarithromycin).
TABLE
Macrolides: comparison studies
| Antibiotic | Response rates* (%) | Side-effect rates †(%) | Cost for course of therapy in adult ‡ |
|---|---|---|---|
| Erythromycin1-4 | 77-100 | 10-59 | $11 (500 mg #40) |
| Clarithromycin5 7 | 88-94 | 5-31 | $76 (250 mg #20) |
| Azithromycin1 4,7 | 87-100 | 0-14 | $57 (250 mg #6) |
| *Response rates of pneumonia due to M pneumoniae and C pneumoniae. | |||
| † In community-acquired pneumonia treated with macrolide as single agent. | |||
| ‡ Prices from www.drugstore.com. | |||
Recommendations from others
The Infectious Diseases Society of America8 recommends a macrolide for adults with pneumonia caused by M pneumoniae or C pneumoniae, and does not promote one over another. The British Thoracic Society9 recommends any of the macrolides for pneumonia caused by these pathogens in children.
Since CAP is often caused by “atypical organisms,” macrolides are sometimes recommended as empiric outpatient therapy. In this setting, the American Thoracic Society10 discourages using erythromycin, citing a higher side-effect rate and poorer effectiveness against Haemophilus influenza. However, the Canadian Infectious Disease Society11 supports the use of any of the 3 macrolides in mild CAP except for patients with chronic obstructive pulmonary disease, who are more likely to harbor H influenza.
Lower respiratory infections—a number of problematic decisions
David Mouw, MD
Mountain Area AHEC, Asheville, NC
You face several problematic decisions when treating a patient with a lower respiratory infection. First, is this pneumonia or just bronchitis? Clinical findings can be confusing, and a chest film is helpful.12 If pneumonia is likely, you consider hospitalization, and prescribe antibiotics, usually without knowing the pathogen.
Because they cover both typical and atypical pathogens, macrolides (or doxycycline) are generally recommended, with cephalosporins to be added for higher-risk patients. (Quinolones are an alternative to this combination.) Finally, if you choose a macrolide, you face yet another decision without a clear answer: which one to use? All macrolides appear to be equally effective, so the choice depends on cost balanced against convenience and side effects.
1. Wubbel L, Muniz L, Ahmed A, et al. Etiology and treatment of community-acquired pneumonia in ambulatory children. Pediatr Infect Dis J 1999;18:98-104.
2. Harris JS, Kolokathis A, Campbell M, Cassell GH, Hammerschlag MR. Safety and efficacy of azithromycin in the treatment of community-acquired pneumonia. Pediatr Infect Dis J 1998;17:865-871.
3. Manfredi R, Jannuzzi C, Mantero E, et al. Clinical comparative study of azithromycin versus erythromycin in the treatment of acute respiratory tract infections in children. J Chemother 1992;4:364-370.
4. Schonwald S, Gunjaca M, Kolacny-Babic L, Car V, Gosev M. Comparison of azithromycin and erythromycin in the treatment of atypical pneumonias. J Antimicrob Chemother 1990;25(Suppl A):123-126.
5. Block S, Hedrick J, Hammerschlag MR, Cassell GH, Craft JC. Mycoplasma pneumoniae and Chlamydia pneumoniae in pediatric community-acquired pneumonia: comparative efficacy and safety of clarithromycin vs. erythromycin ethylsuccinate. Pediatr Infect Dis J 1995;14:471-477.
6. Chien M, Pichotta P, Siepman N, Chan CK. Treatment of community-acquired pneumonia: a multicenter, double-blind, randomized study comparing clarithromycin with erythromycin. Canada-Sweden Clarithromycin-Pneumonia Study Group. Chest 1993;103-697-701.
7. Rizzato G, Montemurro L, Fraioli P, et al. Efficacy of a three day course of azithromycin in moderately severe community-acquired pneumonia. Eur Respir J 1995;8:398-402.
8. Bartlett JG, Dowell SF, Mandell LA, File TM, Jr, Musher DM, Fine M. Practice guidelines for the management of community-acquired pneumonia in adults. Infectious Diseases Society of America. Clin Infect Dis 2000;31:347-382.
9. British. Thoracic Society Standards of Care Committee. British Thoracic Society Guidelines for the Management of Community Acquired Pneumonia in Childhood. Thorax 2002;57(Suppl 1):i1-i24.
10. American. Thoracic Society. Guidelines for the management of adults with community-acquired pneumonia: diagnosis, assessment of severity, antimicrobial therapy, and prevention. Am J Respir Crit Care Med 2001;163:1730-1754.
11. Mandell LA, Marrie TJ, Grossman RF, Chow AW, Hyland RH. Canadian guidelines for the initial management of community-acquired pneumonia: an evidence-based update by the Canadian Infectious Diseases Society and the Canadian Thoracic Society. The Canadian Community-Acquired Pneumonia Working Group. Clin Infect Dis 2000;31:383-421.
12. Kelsberg G, Safranek S. How accurate is the clinical diagnosis of pneumonia? J Fam Pract 2003;52:63-64.
1. Wubbel L, Muniz L, Ahmed A, et al. Etiology and treatment of community-acquired pneumonia in ambulatory children. Pediatr Infect Dis J 1999;18:98-104.
2. Harris JS, Kolokathis A, Campbell M, Cassell GH, Hammerschlag MR. Safety and efficacy of azithromycin in the treatment of community-acquired pneumonia. Pediatr Infect Dis J 1998;17:865-871.
3. Manfredi R, Jannuzzi C, Mantero E, et al. Clinical comparative study of azithromycin versus erythromycin in the treatment of acute respiratory tract infections in children. J Chemother 1992;4:364-370.
4. Schonwald S, Gunjaca M, Kolacny-Babic L, Car V, Gosev M. Comparison of azithromycin and erythromycin in the treatment of atypical pneumonias. J Antimicrob Chemother 1990;25(Suppl A):123-126.
5. Block S, Hedrick J, Hammerschlag MR, Cassell GH, Craft JC. Mycoplasma pneumoniae and Chlamydia pneumoniae in pediatric community-acquired pneumonia: comparative efficacy and safety of clarithromycin vs. erythromycin ethylsuccinate. Pediatr Infect Dis J 1995;14:471-477.
6. Chien M, Pichotta P, Siepman N, Chan CK. Treatment of community-acquired pneumonia: a multicenter, double-blind, randomized study comparing clarithromycin with erythromycin. Canada-Sweden Clarithromycin-Pneumonia Study Group. Chest 1993;103-697-701.
7. Rizzato G, Montemurro L, Fraioli P, et al. Efficacy of a three day course of azithromycin in moderately severe community-acquired pneumonia. Eur Respir J 1995;8:398-402.
8. Bartlett JG, Dowell SF, Mandell LA, File TM, Jr, Musher DM, Fine M. Practice guidelines for the management of community-acquired pneumonia in adults. Infectious Diseases Society of America. Clin Infect Dis 2000;31:347-382.
9. British. Thoracic Society Standards of Care Committee. British Thoracic Society Guidelines for the Management of Community Acquired Pneumonia in Childhood. Thorax 2002;57(Suppl 1):i1-i24.
10. American. Thoracic Society. Guidelines for the management of adults with community-acquired pneumonia: diagnosis, assessment of severity, antimicrobial therapy, and prevention. Am J Respir Crit Care Med 2001;163:1730-1754.
11. Mandell LA, Marrie TJ, Grossman RF, Chow AW, Hyland RH. Canadian guidelines for the initial management of community-acquired pneumonia: an evidence-based update by the Canadian Infectious Diseases Society and the Canadian Thoracic Society. The Canadian Community-Acquired Pneumonia Working Group. Clin Infect Dis 2000;31:383-421.
12. Kelsberg G, Safranek S. How accurate is the clinical diagnosis of pneumonia? J Fam Pract 2003;52:63-64.
Evidence-based answers from the Family Physicians Inquiries Network