User login
Richard Franki is the associate editor who writes and creates graphs. He started with the company in 1987, when it was known as the International Medical News Group. In his years as a journalist, Richard has worked for Cap Cities/ABC, Disney, Harcourt, Elsevier, Quadrant, Frontline, and Internet Brands. In the 1990s, he was a contributor to the ill-fated Indications column, predecessor of Livin' on the MDedge.
Darwin’s diet of species, umbrellas’ searing SPF, and trypophobia terror
Forks out for science
True scientists should have no limits to what they’ll do for their research. Charles Darwin proved that greatly during his life – he spent years discovering and cataloging new species.
But did you know he also chowed down on nearly every animal he found?
His taste for unusual fare began at Cambridge as a member of the “Glutton Club.” He and his fellow gluttons were dedicated to sampling “birds and beasts which were before unknown to human palate,” as reported in an article on NPR. His eating adventures only grew while on the famed Beagle voyage, where he tried puma, iguanas, armadillos, giant tortoises, and even a 20-pound rodent that he declared “the very best meat I ever tasted.”
The noble tradition of tasting your test subjects continues today. The author of the article referenced above asked scientists on social media for stories of eating what they are supposed to be studying, and the answers came pouring in.
From tasting tadpoles to nibbling on 30,000-year-old bison meat, scientists all over the world have found they can’t resist the call to just have a tiny taste.
The umbrella’s just not cutting it
Bad news for everyone who hates melanoma but also hates sunscreen: That Tommy Bahama beach umbrella isn’t doing much to shield your skin.
A team lead by researcher Hao Ou-Yang conducted a study comparing the effects of harmful UV rays on subjects who used sunscreen with subjects who only used the shade of an umbrella.
In the battle of Sun vs. Umbrella, the humble parasol had no chance. While neither sun protection method completely prevented sunburn, 78% of the umbrella-only group experienced sunburn, compared with 25% of the sunscreen wearers.
The researchers determined that umbrella shade alone is not sufficient to protect against sunburn during extended exposure to the sun (in the case of this experiment, exposure was 3.5 hours). Sunscreen, despite being smelly and sticky and gloopy, is definitely needed to protect skin from those UV rays. So, suck it up and pile on that Coppertone this summer.
Oh no, there goes Tokyo (again)
Godzilla. The king of the monsters. For 65 years, the big green guy has been the scourge (mostly) of Japan and the entire world. He arrives, he destroys, and there is very nearly nothing we can do about him.
If you’re an astute fan of the Godzilla series (and we love a good Godzilla movie at MDedge headquarters), you’ll have noticed that Godzilla is a lot bigger than he used to be. In the first movie, he stood at a relatively meager 50 meters. Nowadays, he’s scraping 120 meters, more than double his original size.
What’s going on?
In an actual study published in Science, a team at Dartmouth College in Hanover, N.H., determined that Godzilla is evolving 30 times faster than any other organism on Earth. It’s enough to make even the influenza virus jealous.
So, what is going on? Why is Godzilla evolving so quickly? The scientists assumed that Godzilla is a ceratosaurid dinosaur and ran through the usual suspects. No other dinosaur of that family got so big. Genetic drift and natural selection can’t explain it either.
The truth may be more unsettling: Our own anxiety is fueling his growth. Godzilla was born because of nuclear testing and the fear stemming from it. And the Dartmouth team even found a correlation between Godzilla’s size and American military spending from 1954 to 2019, a neat barometer of the world’s collective anxiety.
Or, you know, people just want to see a 400-foot-tall lizard destroying things. But that’s hardly worthy of a study in an elite research journal.
Hole lotta trypophobia goin’ on
We didn’t know this was even a thing, but Twitter doesn’t like pictures of woodpeckers … digging little holes in tree trunks … and then stuffing the holes with acorns.
A recent tweet of such a photo caused a minor pandemic of virality when users reacted with revulsion and panic caused by trypophobia, which is a fear of irregular patterns of small holes or bumps. You won’t find trypophobia in the DSM-5 – the term was first used in an Internet forum in 2005 – but it is a source of some debate among academics, according to Live Science.
One group says the patterns look like some poisonous animals, and that people are programmed by evolution to fear such creatures. Others suggest that the reaction is not fear but disgust, because the patterns of holes look like the lesions and pustules caused by infectious diseases such as smallpox.
We’re not scientists, so we’ll stay out of the debate on causality. But we do think we’ve uncovered the first documented case, and it goes back to the 1960s TV series “Batman.” The hero’s trusted sidekick, Robin (coincidentally, another type of bird), must have been the first person with trypophobia:
“Holy tintinnabulation!”
“Holy uncanny photographic mental processes!”
“Holy priceless collection of Etruscan snoods!”
Holy patterns of woodpecker acorns! There can be no diagnostic doubt: For Robin, it was all about the holes.

Forks out for science
True scientists should have no limits to what they’ll do for their research. Charles Darwin proved that greatly during his life – he spent years discovering and cataloging new species.
But did you know he also chowed down on nearly every animal he found?
His taste for unusual fare began at Cambridge as a member of the “Glutton Club.” He and his fellow gluttons were dedicated to sampling “birds and beasts which were before unknown to human palate,” as reported in an article on NPR. His eating adventures only grew while on the famed Beagle voyage, where he tried puma, iguanas, armadillos, giant tortoises, and even a 20-pound rodent that he declared “the very best meat I ever tasted.”
The noble tradition of tasting your test subjects continues today. The author of the article referenced above asked scientists on social media for stories of eating what they are supposed to be studying, and the answers came pouring in.
From tasting tadpoles to nibbling on 30,000-year-old bison meat, scientists all over the world have found they can’t resist the call to just have a tiny taste.
The umbrella’s just not cutting it
Bad news for everyone who hates melanoma but also hates sunscreen: That Tommy Bahama beach umbrella isn’t doing much to shield your skin.
A team lead by researcher Hao Ou-Yang conducted a study comparing the effects of harmful UV rays on subjects who used sunscreen with subjects who only used the shade of an umbrella.
In the battle of Sun vs. Umbrella, the humble parasol had no chance. While neither sun protection method completely prevented sunburn, 78% of the umbrella-only group experienced sunburn, compared with 25% of the sunscreen wearers.
The researchers determined that umbrella shade alone is not sufficient to protect against sunburn during extended exposure to the sun (in the case of this experiment, exposure was 3.5 hours). Sunscreen, despite being smelly and sticky and gloopy, is definitely needed to protect skin from those UV rays. So, suck it up and pile on that Coppertone this summer.
Oh no, there goes Tokyo (again)
Godzilla. The king of the monsters. For 65 years, the big green guy has been the scourge (mostly) of Japan and the entire world. He arrives, he destroys, and there is very nearly nothing we can do about him.
If you’re an astute fan of the Godzilla series (and we love a good Godzilla movie at MDedge headquarters), you’ll have noticed that Godzilla is a lot bigger than he used to be. In the first movie, he stood at a relatively meager 50 meters. Nowadays, he’s scraping 120 meters, more than double his original size.
What’s going on?
In an actual study published in Science, a team at Dartmouth College in Hanover, N.H., determined that Godzilla is evolving 30 times faster than any other organism on Earth. It’s enough to make even the influenza virus jealous.
So, what is going on? Why is Godzilla evolving so quickly? The scientists assumed that Godzilla is a ceratosaurid dinosaur and ran through the usual suspects. No other dinosaur of that family got so big. Genetic drift and natural selection can’t explain it either.
The truth may be more unsettling: Our own anxiety is fueling his growth. Godzilla was born because of nuclear testing and the fear stemming from it. And the Dartmouth team even found a correlation between Godzilla’s size and American military spending from 1954 to 2019, a neat barometer of the world’s collective anxiety.
Or, you know, people just want to see a 400-foot-tall lizard destroying things. But that’s hardly worthy of a study in an elite research journal.
Hole lotta trypophobia goin’ on
We didn’t know this was even a thing, but Twitter doesn’t like pictures of woodpeckers … digging little holes in tree trunks … and then stuffing the holes with acorns.
A recent tweet of such a photo caused a minor pandemic of virality when users reacted with revulsion and panic caused by trypophobia, which is a fear of irregular patterns of small holes or bumps. You won’t find trypophobia in the DSM-5 – the term was first used in an Internet forum in 2005 – but it is a source of some debate among academics, according to Live Science.
One group says the patterns look like some poisonous animals, and that people are programmed by evolution to fear such creatures. Others suggest that the reaction is not fear but disgust, because the patterns of holes look like the lesions and pustules caused by infectious diseases such as smallpox.
We’re not scientists, so we’ll stay out of the debate on causality. But we do think we’ve uncovered the first documented case, and it goes back to the 1960s TV series “Batman.” The hero’s trusted sidekick, Robin (coincidentally, another type of bird), must have been the first person with trypophobia:
“Holy tintinnabulation!”
“Holy uncanny photographic mental processes!”
“Holy priceless collection of Etruscan snoods!”
Holy patterns of woodpecker acorns! There can be no diagnostic doubt: For Robin, it was all about the holes.

Forks out for science
True scientists should have no limits to what they’ll do for their research. Charles Darwin proved that greatly during his life – he spent years discovering and cataloging new species.
But did you know he also chowed down on nearly every animal he found?
His taste for unusual fare began at Cambridge as a member of the “Glutton Club.” He and his fellow gluttons were dedicated to sampling “birds and beasts which were before unknown to human palate,” as reported in an article on NPR. His eating adventures only grew while on the famed Beagle voyage, where he tried puma, iguanas, armadillos, giant tortoises, and even a 20-pound rodent that he declared “the very best meat I ever tasted.”
The noble tradition of tasting your test subjects continues today. The author of the article referenced above asked scientists on social media for stories of eating what they are supposed to be studying, and the answers came pouring in.
From tasting tadpoles to nibbling on 30,000-year-old bison meat, scientists all over the world have found they can’t resist the call to just have a tiny taste.
The umbrella’s just not cutting it
Bad news for everyone who hates melanoma but also hates sunscreen: That Tommy Bahama beach umbrella isn’t doing much to shield your skin.
A team lead by researcher Hao Ou-Yang conducted a study comparing the effects of harmful UV rays on subjects who used sunscreen with subjects who only used the shade of an umbrella.
In the battle of Sun vs. Umbrella, the humble parasol had no chance. While neither sun protection method completely prevented sunburn, 78% of the umbrella-only group experienced sunburn, compared with 25% of the sunscreen wearers.
The researchers determined that umbrella shade alone is not sufficient to protect against sunburn during extended exposure to the sun (in the case of this experiment, exposure was 3.5 hours). Sunscreen, despite being smelly and sticky and gloopy, is definitely needed to protect skin from those UV rays. So, suck it up and pile on that Coppertone this summer.
Oh no, there goes Tokyo (again)
Godzilla. The king of the monsters. For 65 years, the big green guy has been the scourge (mostly) of Japan and the entire world. He arrives, he destroys, and there is very nearly nothing we can do about him.
If you’re an astute fan of the Godzilla series (and we love a good Godzilla movie at MDedge headquarters), you’ll have noticed that Godzilla is a lot bigger than he used to be. In the first movie, he stood at a relatively meager 50 meters. Nowadays, he’s scraping 120 meters, more than double his original size.
What’s going on?
In an actual study published in Science, a team at Dartmouth College in Hanover, N.H., determined that Godzilla is evolving 30 times faster than any other organism on Earth. It’s enough to make even the influenza virus jealous.
So, what is going on? Why is Godzilla evolving so quickly? The scientists assumed that Godzilla is a ceratosaurid dinosaur and ran through the usual suspects. No other dinosaur of that family got so big. Genetic drift and natural selection can’t explain it either.
The truth may be more unsettling: Our own anxiety is fueling his growth. Godzilla was born because of nuclear testing and the fear stemming from it. And the Dartmouth team even found a correlation between Godzilla’s size and American military spending from 1954 to 2019, a neat barometer of the world’s collective anxiety.
Or, you know, people just want to see a 400-foot-tall lizard destroying things. But that’s hardly worthy of a study in an elite research journal.
Hole lotta trypophobia goin’ on
We didn’t know this was even a thing, but Twitter doesn’t like pictures of woodpeckers … digging little holes in tree trunks … and then stuffing the holes with acorns.
A recent tweet of such a photo caused a minor pandemic of virality when users reacted with revulsion and panic caused by trypophobia, which is a fear of irregular patterns of small holes or bumps. You won’t find trypophobia in the DSM-5 – the term was first used in an Internet forum in 2005 – but it is a source of some debate among academics, according to Live Science.
One group says the patterns look like some poisonous animals, and that people are programmed by evolution to fear such creatures. Others suggest that the reaction is not fear but disgust, because the patterns of holes look like the lesions and pustules caused by infectious diseases such as smallpox.
We’re not scientists, so we’ll stay out of the debate on causality. But we do think we’ve uncovered the first documented case, and it goes back to the 1960s TV series “Batman.” The hero’s trusted sidekick, Robin (coincidentally, another type of bird), must have been the first person with trypophobia:
“Holy tintinnabulation!”
“Holy uncanny photographic mental processes!”
“Holy priceless collection of Etruscan snoods!”
Holy patterns of woodpecker acorns! There can be no diagnostic doubt: For Robin, it was all about the holes.

United States now over 1,000 measles cases this year
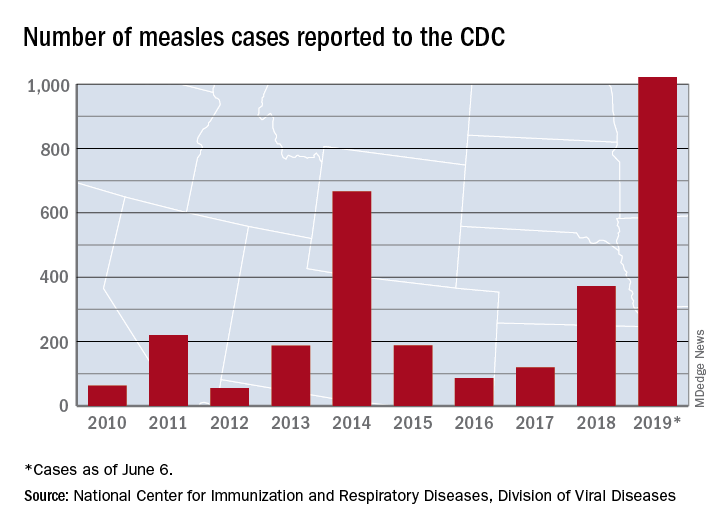
The 41 new cases reported for the week ending June 6 bring the total for the year to 1,022, the CDC reported June 10, and that is more than any year since 1992, when there were 2,237 cases.
Idaho and Virginia reported their first cases of 2019, which makes a total of 28 states with measles cases this year. The Idaho case was reported in Latah County and is the state’s first since 2001. In Virginia, health officials are investigating possible contacts with an infected individual at Dulles International Airport and two other locations on June 2 and 4.
Outbreaks in Georgia, Maryland, and Michigan have ended, while seven others continue in California (Butte, Los Angeles, and Sacramento Counties), New York (Rockland County and New York City), Pennsylvania, and Washington, the CDC said. New York City has the largest outbreak this year with 509 cases through June 3, most of them occurring in Brooklyn.

The 41 new cases reported for the week ending June 6 bring the total for the year to 1,022, the CDC reported June 10, and that is more than any year since 1992, when there were 2,237 cases.
Idaho and Virginia reported their first cases of 2019, which makes a total of 28 states with measles cases this year. The Idaho case was reported in Latah County and is the state’s first since 2001. In Virginia, health officials are investigating possible contacts with an infected individual at Dulles International Airport and two other locations on June 2 and 4.
Outbreaks in Georgia, Maryland, and Michigan have ended, while seven others continue in California (Butte, Los Angeles, and Sacramento Counties), New York (Rockland County and New York City), Pennsylvania, and Washington, the CDC said. New York City has the largest outbreak this year with 509 cases through June 3, most of them occurring in Brooklyn.

The 41 new cases reported for the week ending June 6 bring the total for the year to 1,022, the CDC reported June 10, and that is more than any year since 1992, when there were 2,237 cases.
Idaho and Virginia reported their first cases of 2019, which makes a total of 28 states with measles cases this year. The Idaho case was reported in Latah County and is the state’s first since 2001. In Virginia, health officials are investigating possible contacts with an infected individual at Dulles International Airport and two other locations on June 2 and 4.
Outbreaks in Georgia, Maryland, and Michigan have ended, while seven others continue in California (Butte, Los Angeles, and Sacramento Counties), New York (Rockland County and New York City), Pennsylvania, and Washington, the CDC said. New York City has the largest outbreak this year with 509 cases through June 3, most of them occurring in Brooklyn.
The costs of surviving cancer
Cancer survivors have significantly higher out-of-pocket medical costs than those with no history of cancer, and a quarter of those survivors have some type of material hardship related to their diagnosis, according to the Centers for Disease Control and Prevention.
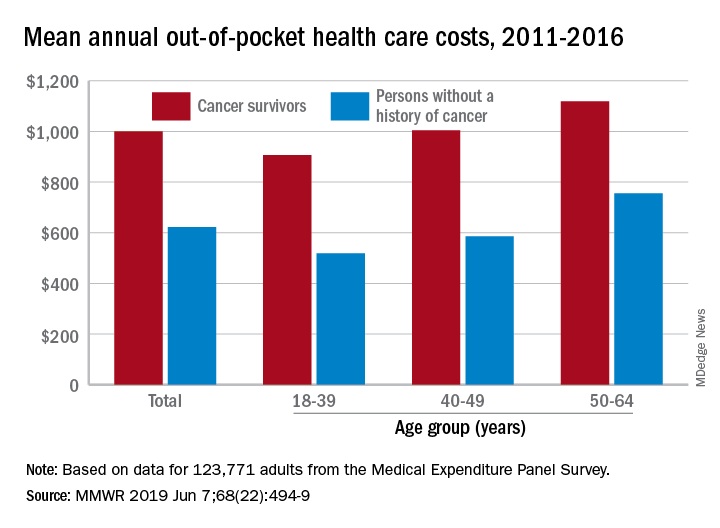
Along with those material financial hardships – the need to borrow money, go into debt, or declare bankruptcy – more than 34% of cancer survivors aged 18-64 years experienced psychological financial hardship, defined as worry about large medical bills, in 2011 and 2016, Donatus U. Ekwueme, PhD, and his associates reported in the Morbidity and Mortality Weekly Report.
Cancer survivors spend 60% more out of pocket than those with no cancer history: $1,000 a year from 2011 to 2016, compared with $622 for adults without a history of cancer. Spending was lowest among younger people (18-39 years) and increased with age, but the prevalence of both material and psychological hardships was highest in the middle age group (40-49 years) and lowest in the oldest group (50-64 years), they said.
Women had higher out-of-pocket costs than men, although the difference was smaller for those with cancer ($1,023 vs. $976) than for those without ($721 vs. $519). Material and psychological hardships were both more common among women, said Dr. Ekwueme of the CDC’s National Center for Chronic Disease Prevention and Health Promotion, Atlanta, and his associates.
Mean out-of-pocket spending was much higher for cancer survivors with private health insurance ($1,114) than for survivors with public insurance ($471), but material hardship was much more prevalent among those with public insurance (33.1% vs. 21.9%). Rates of psychological hardship, however, were much closer: 35.9% for those with public insurance and 32.5% for those with private insurance, the investigators said.
“The number of Americans with a history of cancer is projected to increase in the next decade, and the economic burden associated with living with a cancer diagnosis will likely increase as well,” they wrote, and interventions such as “systematic screening for financial hardship at cancer diagnosis and throughout the cancer care trajectory [are needed] to minimize financial hardship for cancer survivors.”
The analysis was based on data for 123,771 adults aged 18-64 years from the Medical Expenditure Panel Survey. Out-of-pocket costs were calculated using data from 2011 to 2016, with all costs adjusted to 2016 dollars, but the hardship calculations involved data from only 2011 and 2016.
SOURCE: Ekwueme DU et al. MMWR 2019 Jun 7;68(22):494-9.
Cancer survivors have significantly higher out-of-pocket medical costs than those with no history of cancer, and a quarter of those survivors have some type of material hardship related to their diagnosis, according to the Centers for Disease Control and Prevention.

Along with those material financial hardships – the need to borrow money, go into debt, or declare bankruptcy – more than 34% of cancer survivors aged 18-64 years experienced psychological financial hardship, defined as worry about large medical bills, in 2011 and 2016, Donatus U. Ekwueme, PhD, and his associates reported in the Morbidity and Mortality Weekly Report.
Cancer survivors spend 60% more out of pocket than those with no cancer history: $1,000 a year from 2011 to 2016, compared with $622 for adults without a history of cancer. Spending was lowest among younger people (18-39 years) and increased with age, but the prevalence of both material and psychological hardships was highest in the middle age group (40-49 years) and lowest in the oldest group (50-64 years), they said.
Women had higher out-of-pocket costs than men, although the difference was smaller for those with cancer ($1,023 vs. $976) than for those without ($721 vs. $519). Material and psychological hardships were both more common among women, said Dr. Ekwueme of the CDC’s National Center for Chronic Disease Prevention and Health Promotion, Atlanta, and his associates.
Mean out-of-pocket spending was much higher for cancer survivors with private health insurance ($1,114) than for survivors with public insurance ($471), but material hardship was much more prevalent among those with public insurance (33.1% vs. 21.9%). Rates of psychological hardship, however, were much closer: 35.9% for those with public insurance and 32.5% for those with private insurance, the investigators said.
“The number of Americans with a history of cancer is projected to increase in the next decade, and the economic burden associated with living with a cancer diagnosis will likely increase as well,” they wrote, and interventions such as “systematic screening for financial hardship at cancer diagnosis and throughout the cancer care trajectory [are needed] to minimize financial hardship for cancer survivors.”
The analysis was based on data for 123,771 adults aged 18-64 years from the Medical Expenditure Panel Survey. Out-of-pocket costs were calculated using data from 2011 to 2016, with all costs adjusted to 2016 dollars, but the hardship calculations involved data from only 2011 and 2016.
SOURCE: Ekwueme DU et al. MMWR 2019 Jun 7;68(22):494-9.
Cancer survivors have significantly higher out-of-pocket medical costs than those with no history of cancer, and a quarter of those survivors have some type of material hardship related to their diagnosis, according to the Centers for Disease Control and Prevention.

Along with those material financial hardships – the need to borrow money, go into debt, or declare bankruptcy – more than 34% of cancer survivors aged 18-64 years experienced psychological financial hardship, defined as worry about large medical bills, in 2011 and 2016, Donatus U. Ekwueme, PhD, and his associates reported in the Morbidity and Mortality Weekly Report.
Cancer survivors spend 60% more out of pocket than those with no cancer history: $1,000 a year from 2011 to 2016, compared with $622 for adults without a history of cancer. Spending was lowest among younger people (18-39 years) and increased with age, but the prevalence of both material and psychological hardships was highest in the middle age group (40-49 years) and lowest in the oldest group (50-64 years), they said.
Women had higher out-of-pocket costs than men, although the difference was smaller for those with cancer ($1,023 vs. $976) than for those without ($721 vs. $519). Material and psychological hardships were both more common among women, said Dr. Ekwueme of the CDC’s National Center for Chronic Disease Prevention and Health Promotion, Atlanta, and his associates.
Mean out-of-pocket spending was much higher for cancer survivors with private health insurance ($1,114) than for survivors with public insurance ($471), but material hardship was much more prevalent among those with public insurance (33.1% vs. 21.9%). Rates of psychological hardship, however, were much closer: 35.9% for those with public insurance and 32.5% for those with private insurance, the investigators said.
“The number of Americans with a history of cancer is projected to increase in the next decade, and the economic burden associated with living with a cancer diagnosis will likely increase as well,” they wrote, and interventions such as “systematic screening for financial hardship at cancer diagnosis and throughout the cancer care trajectory [are needed] to minimize financial hardship for cancer survivors.”
The analysis was based on data for 123,771 adults aged 18-64 years from the Medical Expenditure Panel Survey. Out-of-pocket costs were calculated using data from 2011 to 2016, with all costs adjusted to 2016 dollars, but the hardship calculations involved data from only 2011 and 2016.
SOURCE: Ekwueme DU et al. MMWR 2019 Jun 7;68(22):494-9.
FROM MMWR
Opposing cost trends seen for prescribed medications
according to the Agency for Healthcare Research and Quality.
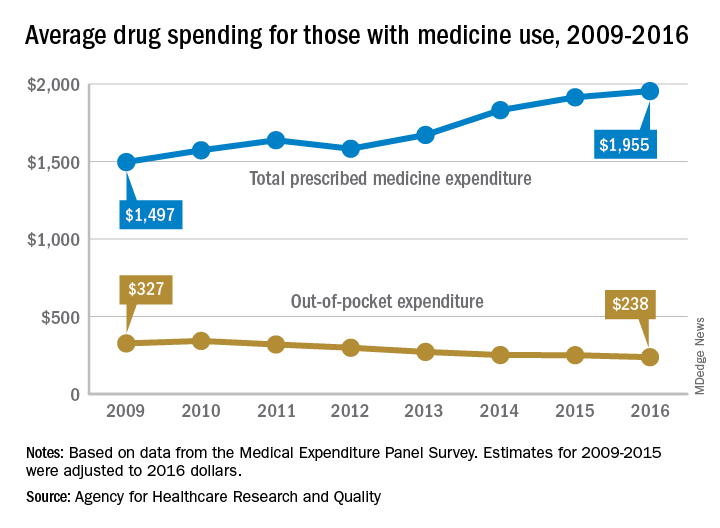
The average expenditure among persons who used at least one prescription drug went from $1,497 per individual in 2009 to $1,955 in 2016, for an increase of almost 31%. These cost figures cover medications obtained in outpatient settings only and “include the amount paid out of pocket plus any third-party payments from health insurance or other sources,” the AHRQ said.
When out-of-pocket spending for drugs obtained in outpatient settings was considered separately, the average per-person cost dropped by 27%, going from $327 per person with use in 2009 to $238 in 2016, the AHRQ researchers reported.
Over that time period, both total and out-of-pocket costs were considerably and consistently higher for those aged 65 years and older than for those under 65. In 2016, total spending was $3,288 each for elderly persons with at least one prescribed drug purchase and $1,539 for those under age 65, with respective out-of-pocket costs of $401 and $188, they said.
The AHRQ analysis was based on data from the Medical Expenditure Panel Survey, and expenditures for 2009-2015 were adjusted to 2016 dollars.
according to the Agency for Healthcare Research and Quality.

The average expenditure among persons who used at least one prescription drug went from $1,497 per individual in 2009 to $1,955 in 2016, for an increase of almost 31%. These cost figures cover medications obtained in outpatient settings only and “include the amount paid out of pocket plus any third-party payments from health insurance or other sources,” the AHRQ said.
When out-of-pocket spending for drugs obtained in outpatient settings was considered separately, the average per-person cost dropped by 27%, going from $327 per person with use in 2009 to $238 in 2016, the AHRQ researchers reported.
Over that time period, both total and out-of-pocket costs were considerably and consistently higher for those aged 65 years and older than for those under 65. In 2016, total spending was $3,288 each for elderly persons with at least one prescribed drug purchase and $1,539 for those under age 65, with respective out-of-pocket costs of $401 and $188, they said.
The AHRQ analysis was based on data from the Medical Expenditure Panel Survey, and expenditures for 2009-2015 were adjusted to 2016 dollars.
according to the Agency for Healthcare Research and Quality.

The average expenditure among persons who used at least one prescription drug went from $1,497 per individual in 2009 to $1,955 in 2016, for an increase of almost 31%. These cost figures cover medications obtained in outpatient settings only and “include the amount paid out of pocket plus any third-party payments from health insurance or other sources,” the AHRQ said.
When out-of-pocket spending for drugs obtained in outpatient settings was considered separately, the average per-person cost dropped by 27%, going from $327 per person with use in 2009 to $238 in 2016, the AHRQ researchers reported.
Over that time period, both total and out-of-pocket costs were considerably and consistently higher for those aged 65 years and older than for those under 65. In 2016, total spending was $3,288 each for elderly persons with at least one prescribed drug purchase and $1,539 for those under age 65, with respective out-of-pocket costs of $401 and $188, they said.
The AHRQ analysis was based on data from the Medical Expenditure Panel Survey, and expenditures for 2009-2015 were adjusted to 2016 dollars.
Air-conditioned cognition, brain worm, and six-fingered success
(Women’s) Winter is coming
Summer approaches and the Great Freeze begins to make its way through offices across the country.
Women everywhere start dragging out those cardigans stored in desks long ago. Blankets start appearing draped over the backs of chairs. “God, it’s freezing in here” becomes the oft-repeated refrain. It’s women’s winter … and a recent study has shown it has a marked effect on productivity.
Published last month in PlosOne, the study examined the effect of temperature on cognitive performance in both men and women. After studying participants’ performances on math and verbal tasks at various temperatures, researchers found that the women performed better at higher temps while the men performed worse. However, the performance increase for women was much larger than the decrease for men.
The authors concluded that workplaces with mixed genders might increase productivity (and overall office happiness) by cranking that thermostat a little higher than current standards. Perhaps this will be the beginning of the end of the thermostat war.
Need a hand – or finger?
Polydactyly. No, not the flying dinosaur – the congenital condition of having extra fingers or toes. One in every 2,000-3,000 babies is born with polydactyly, and while most doctors quickly remove the extra digits, a German study found that maybe they shouldn’t be so quick to the chopping block.
Researchers found that polydactyl people have more dexterity of movement, and the subjects’ brains showed a distinct representation of the extra digit. The subjects were able to carry out two-handed tasks with just one hand, and the study authors concluded that the subjects’ hand movements “had increased complexity relative to common five-fingered hands.”
Researchers also designed a special video game to test the six-fingered hand vs. using both hands. Video game results were the same with one hand or two, proving that more fingers equals more fun.
Cooking up controversy
If you had a giant spoon, what would you do with it?
Boston artist Domenic Esposito has just such a spoon – being an artist, he made it himself – and he’s been using it to draw attention to the opioid use disorder crisis by placing it “on the doorsteps of corporations and individuals whose recklessness and irresponsibility have fueled the epidemic,” according to the spoon’s website, The Opioid Spoon Project.
Since its creation, the 800-lb, 10.5-foot-long steel heroin spoon has visited Purdue Pharma headquarters in Stamford, Conn. – the spoon was hauled off by the city and taken to a police evidence lot – and Rhodes Pharmaceuticals in Coventry, R.I.
More recently, Mr. Esposito has taken the spoon on a 14-city “Honor Tour.” At each stop, individuals have the opportunity to sign the spoon in memory of “those who have lost their opioid addiction battles.”
The tour, which began in Marlborough, Mass., on May 11 and has been to such cities as Providence, R.I., and Boston, ends on June 7 in Rockville, Md., which happens to be the home of LOTME world headquarters. So, who doesn’t want to see a spoon over 10 feet long?
Worms on (or in) my mind
It sounds like a bad riddle: What looks like a brain tumor, acts like a brain tumor, but isn’t a brain tumor?
Rachel Palma, a 42-year-old woman from Middletown, N.Y., had the joy of finding out the answer.
For months, she’d been having strange symptoms: hallucinations, nightmares, trouble remembering words, memory blackouts, occasional loss of motor control. Her doctors were stumped, until they performed an MRI of her brain, discovering a marble-sized lesion in her brain. Another MRI, performed with contrast, caused the lesion to light up, a surefire sign of a malignant brain tumor. Treatment would require surgery, then chemo and radiation therapy.
But when the surgeons opened her head, they were greeted not with a tumor, but with something they described as looking “like a quail egg.” The object was removed and opened up, and to the delight of the doctors, a tapeworm popped out.
The condition – neurocysticercosis – is common in developing countries but rare in the United States. We won’t share all the details on how tapeworms end up in the brain, but needless to say, poor washing of hands is involved.
On the one hand, Mrs. Palma has made a full recovery with no need for chemo or radiation. On the other hand, she had a tapeworm in her brain. Somehow, she’s managed to make the brain tumor seem like the less unpleasant option. And for that, we salute her.

(Women’s) Winter is coming
Summer approaches and the Great Freeze begins to make its way through offices across the country.
Women everywhere start dragging out those cardigans stored in desks long ago. Blankets start appearing draped over the backs of chairs. “God, it’s freezing in here” becomes the oft-repeated refrain. It’s women’s winter … and a recent study has shown it has a marked effect on productivity.
Published last month in PlosOne, the study examined the effect of temperature on cognitive performance in both men and women. After studying participants’ performances on math and verbal tasks at various temperatures, researchers found that the women performed better at higher temps while the men performed worse. However, the performance increase for women was much larger than the decrease for men.
The authors concluded that workplaces with mixed genders might increase productivity (and overall office happiness) by cranking that thermostat a little higher than current standards. Perhaps this will be the beginning of the end of the thermostat war.
Need a hand – or finger?
Polydactyly. No, not the flying dinosaur – the congenital condition of having extra fingers or toes. One in every 2,000-3,000 babies is born with polydactyly, and while most doctors quickly remove the extra digits, a German study found that maybe they shouldn’t be so quick to the chopping block.
Researchers found that polydactyl people have more dexterity of movement, and the subjects’ brains showed a distinct representation of the extra digit. The subjects were able to carry out two-handed tasks with just one hand, and the study authors concluded that the subjects’ hand movements “had increased complexity relative to common five-fingered hands.”
Researchers also designed a special video game to test the six-fingered hand vs. using both hands. Video game results were the same with one hand or two, proving that more fingers equals more fun.
Cooking up controversy
If you had a giant spoon, what would you do with it?
Boston artist Domenic Esposito has just such a spoon – being an artist, he made it himself – and he’s been using it to draw attention to the opioid use disorder crisis by placing it “on the doorsteps of corporations and individuals whose recklessness and irresponsibility have fueled the epidemic,” according to the spoon’s website, The Opioid Spoon Project.
Since its creation, the 800-lb, 10.5-foot-long steel heroin spoon has visited Purdue Pharma headquarters in Stamford, Conn. – the spoon was hauled off by the city and taken to a police evidence lot – and Rhodes Pharmaceuticals in Coventry, R.I.
More recently, Mr. Esposito has taken the spoon on a 14-city “Honor Tour.” At each stop, individuals have the opportunity to sign the spoon in memory of “those who have lost their opioid addiction battles.”
The tour, which began in Marlborough, Mass., on May 11 and has been to such cities as Providence, R.I., and Boston, ends on June 7 in Rockville, Md., which happens to be the home of LOTME world headquarters. So, who doesn’t want to see a spoon over 10 feet long?
Worms on (or in) my mind
It sounds like a bad riddle: What looks like a brain tumor, acts like a brain tumor, but isn’t a brain tumor?
Rachel Palma, a 42-year-old woman from Middletown, N.Y., had the joy of finding out the answer.
For months, she’d been having strange symptoms: hallucinations, nightmares, trouble remembering words, memory blackouts, occasional loss of motor control. Her doctors were stumped, until they performed an MRI of her brain, discovering a marble-sized lesion in her brain. Another MRI, performed with contrast, caused the lesion to light up, a surefire sign of a malignant brain tumor. Treatment would require surgery, then chemo and radiation therapy.
But when the surgeons opened her head, they were greeted not with a tumor, but with something they described as looking “like a quail egg.” The object was removed and opened up, and to the delight of the doctors, a tapeworm popped out.
The condition – neurocysticercosis – is common in developing countries but rare in the United States. We won’t share all the details on how tapeworms end up in the brain, but needless to say, poor washing of hands is involved.
On the one hand, Mrs. Palma has made a full recovery with no need for chemo or radiation. On the other hand, she had a tapeworm in her brain. Somehow, she’s managed to make the brain tumor seem like the less unpleasant option. And for that, we salute her.

(Women’s) Winter is coming
Summer approaches and the Great Freeze begins to make its way through offices across the country.
Women everywhere start dragging out those cardigans stored in desks long ago. Blankets start appearing draped over the backs of chairs. “God, it’s freezing in here” becomes the oft-repeated refrain. It’s women’s winter … and a recent study has shown it has a marked effect on productivity.
Published last month in PlosOne, the study examined the effect of temperature on cognitive performance in both men and women. After studying participants’ performances on math and verbal tasks at various temperatures, researchers found that the women performed better at higher temps while the men performed worse. However, the performance increase for women was much larger than the decrease for men.
The authors concluded that workplaces with mixed genders might increase productivity (and overall office happiness) by cranking that thermostat a little higher than current standards. Perhaps this will be the beginning of the end of the thermostat war.
Need a hand – or finger?
Polydactyly. No, not the flying dinosaur – the congenital condition of having extra fingers or toes. One in every 2,000-3,000 babies is born with polydactyly, and while most doctors quickly remove the extra digits, a German study found that maybe they shouldn’t be so quick to the chopping block.
Researchers found that polydactyl people have more dexterity of movement, and the subjects’ brains showed a distinct representation of the extra digit. The subjects were able to carry out two-handed tasks with just one hand, and the study authors concluded that the subjects’ hand movements “had increased complexity relative to common five-fingered hands.”
Researchers also designed a special video game to test the six-fingered hand vs. using both hands. Video game results were the same with one hand or two, proving that more fingers equals more fun.
Cooking up controversy
If you had a giant spoon, what would you do with it?
Boston artist Domenic Esposito has just such a spoon – being an artist, he made it himself – and he’s been using it to draw attention to the opioid use disorder crisis by placing it “on the doorsteps of corporations and individuals whose recklessness and irresponsibility have fueled the epidemic,” according to the spoon’s website, The Opioid Spoon Project.
Since its creation, the 800-lb, 10.5-foot-long steel heroin spoon has visited Purdue Pharma headquarters in Stamford, Conn. – the spoon was hauled off by the city and taken to a police evidence lot – and Rhodes Pharmaceuticals in Coventry, R.I.
More recently, Mr. Esposito has taken the spoon on a 14-city “Honor Tour.” At each stop, individuals have the opportunity to sign the spoon in memory of “those who have lost their opioid addiction battles.”
The tour, which began in Marlborough, Mass., on May 11 and has been to such cities as Providence, R.I., and Boston, ends on June 7 in Rockville, Md., which happens to be the home of LOTME world headquarters. So, who doesn’t want to see a spoon over 10 feet long?
Worms on (or in) my mind
It sounds like a bad riddle: What looks like a brain tumor, acts like a brain tumor, but isn’t a brain tumor?
Rachel Palma, a 42-year-old woman from Middletown, N.Y., had the joy of finding out the answer.
For months, she’d been having strange symptoms: hallucinations, nightmares, trouble remembering words, memory blackouts, occasional loss of motor control. Her doctors were stumped, until they performed an MRI of her brain, discovering a marble-sized lesion in her brain. Another MRI, performed with contrast, caused the lesion to light up, a surefire sign of a malignant brain tumor. Treatment would require surgery, then chemo and radiation therapy.
But when the surgeons opened her head, they were greeted not with a tumor, but with something they described as looking “like a quail egg.” The object was removed and opened up, and to the delight of the doctors, a tapeworm popped out.
The condition – neurocysticercosis – is common in developing countries but rare in the United States. We won’t share all the details on how tapeworms end up in the brain, but needless to say, poor washing of hands is involved.
On the one hand, Mrs. Palma has made a full recovery with no need for chemo or radiation. On the other hand, she had a tapeworm in her brain. Somehow, she’s managed to make the brain tumor seem like the less unpleasant option. And for that, we salute her.

Tick-borne disease has become a national issue
Pennsylvania had more reported cases of tick-borne disease from 2004 to 2016 than any other state, but these diseases are becoming a national threat, according to the Centers for Disease Control and Prevention.
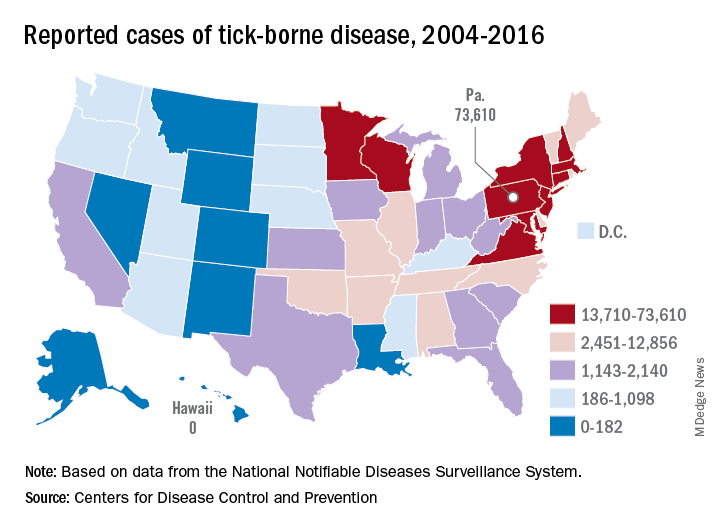
There were 73,000 cases reported in Pennsylvania over that period, and tick-borne diseases, including Lyme disease, anaplasmosis/ehrlichiosis, spotted fever rickettsiosis, babesiosis, tularemia, and Powassan virus, among others, affected almost 492,000 people nationwide, with Lyme disease representing the majority of cases, the CDC said in a Vital Signs report.
Although it’s no surprise that Pennsylvania, New York, and Connecticut were tick-borne disease hot spots, non-Northeastern states like Virginia, Wisconsin, and Minnesota also were among the top 10 in cases. States even further away from the Northeast can be found in the next 10: Arkansas had more than 7,000 cases in 13 years, and Oklahoma had over 4,600 cases, data from the National Notifiable Diseases Surveillance System show.
Nationally, the number of cases more than doubled from 23,000 in 2004 to 49,000 in 2016, and tick-borne disease hit every state except Hawaii. Over that same time, seven new tick-borne pathogens were discovered or introduced into the United States, the CDC reported.
“Local and state health departments and vector control organizations face increasing demands to respond to these threats,” the CDC said, but “more than 80% of vector control organizations report needing improvement in one or more of five core competencies, such as testing for pesticide resistance [and using] data to drive local decisions about vector control.”
Pennsylvania had more reported cases of tick-borne disease from 2004 to 2016 than any other state, but these diseases are becoming a national threat, according to the Centers for Disease Control and Prevention.

There were 73,000 cases reported in Pennsylvania over that period, and tick-borne diseases, including Lyme disease, anaplasmosis/ehrlichiosis, spotted fever rickettsiosis, babesiosis, tularemia, and Powassan virus, among others, affected almost 492,000 people nationwide, with Lyme disease representing the majority of cases, the CDC said in a Vital Signs report.
Although it’s no surprise that Pennsylvania, New York, and Connecticut were tick-borne disease hot spots, non-Northeastern states like Virginia, Wisconsin, and Minnesota also were among the top 10 in cases. States even further away from the Northeast can be found in the next 10: Arkansas had more than 7,000 cases in 13 years, and Oklahoma had over 4,600 cases, data from the National Notifiable Diseases Surveillance System show.
Nationally, the number of cases more than doubled from 23,000 in 2004 to 49,000 in 2016, and tick-borne disease hit every state except Hawaii. Over that same time, seven new tick-borne pathogens were discovered or introduced into the United States, the CDC reported.
“Local and state health departments and vector control organizations face increasing demands to respond to these threats,” the CDC said, but “more than 80% of vector control organizations report needing improvement in one or more of five core competencies, such as testing for pesticide resistance [and using] data to drive local decisions about vector control.”
Pennsylvania had more reported cases of tick-borne disease from 2004 to 2016 than any other state, but these diseases are becoming a national threat, according to the Centers for Disease Control and Prevention.

There were 73,000 cases reported in Pennsylvania over that period, and tick-borne diseases, including Lyme disease, anaplasmosis/ehrlichiosis, spotted fever rickettsiosis, babesiosis, tularemia, and Powassan virus, among others, affected almost 492,000 people nationwide, with Lyme disease representing the majority of cases, the CDC said in a Vital Signs report.
Although it’s no surprise that Pennsylvania, New York, and Connecticut were tick-borne disease hot spots, non-Northeastern states like Virginia, Wisconsin, and Minnesota also were among the top 10 in cases. States even further away from the Northeast can be found in the next 10: Arkansas had more than 7,000 cases in 13 years, and Oklahoma had over 4,600 cases, data from the National Notifiable Diseases Surveillance System show.
Nationally, the number of cases more than doubled from 23,000 in 2004 to 49,000 in 2016, and tick-borne disease hit every state except Hawaii. Over that same time, seven new tick-borne pathogens were discovered or introduced into the United States, the CDC reported.
“Local and state health departments and vector control organizations face increasing demands to respond to these threats,” the CDC said, but “more than 80% of vector control organizations report needing improvement in one or more of five core competencies, such as testing for pesticide resistance [and using] data to drive local decisions about vector control.”
Cost of physician burnout estimated at $4.6 billion a year
Physician burnout costs the U.S. health care system approximately $4.6 billion a year in physician turnover and reduced productivity, according to the results of a cost-consequence analysis.
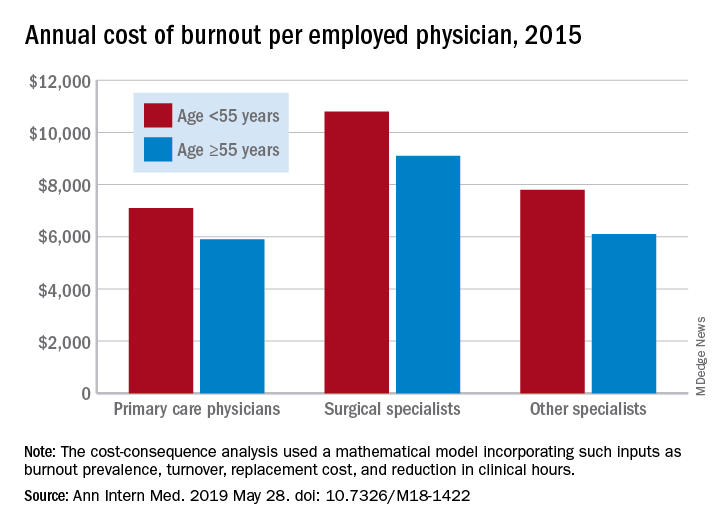
In 2015, the burnout-attributable cost per physician was $7,600 – an estimate occupying the conservative middle ground between the $3,700 and $11,000 extremes produced by the study’s mathematical model.
“Traditionally, the case for ameliorating physician burnout has been made primarily on ethical grounds.” This study, believed to be the first to look at the system-wide costs of burnout, “provides tools to evaluate the economic dimension of this problem,” wrote Shasha Han, MS, of the National University of Singapore and her associates in Annals of Internal Medicine.
Individual burnout-attributable costs were higher for physicians in the younger age group (less than 55 years) in all three specialty categories: $7,100 versus $5,900 for those aged at least 55 years among primary care physicians, $10,800 versus $9,100 for surgical specialists, and $7,800 versus $6,100 for other specialists, the investigators reported.
The mathematical model used in the study focused on two productivity metrics related to burnout – cost associated with physician replacement and lost income from unfilled physician positions. “Estimated turnover costs were generally higher than costs of reduced productivity across all” the various segments of age and specialty, Ms. Han and associates wrote.
“Burnout is a problem that extends beyond physicians to nurses and other health care staff. Future work holistically investigating the costs associated with burnout in health care organizations would be valuable. Studies focusing on differences in burnout-attributable costs across provider segments other than the ones investigated in this study, including academic versus private settings, or across a finer segmentation of physician specialties also might be fruitful,” they wrote.
One investigator has received grants from the American Medical Association Accelerating Change in Medical Education Consortium, the Physicians Foundation, and the National Institutes of Health. Another received a startup grant from the National University of Singapore. Ms. Han said that she had no financial conflicts to disclose. All of the investigators’ disclosures are available online.
Learn practical tips to avoid physician burnout presented during an AGA symposium at DDW® at https://www.ddwnews.org/news/aga-symposium-provides-practical-tips-to-avoid-physician-burnout/.
SOURCE: Han S et al. Ann Intern Med. 2019 May 28. doi: 10.7326/M18-1422.
Physician burnout costs the U.S. health care system approximately $4.6 billion a year in physician turnover and reduced productivity, according to the results of a cost-consequence analysis.

In 2015, the burnout-attributable cost per physician was $7,600 – an estimate occupying the conservative middle ground between the $3,700 and $11,000 extremes produced by the study’s mathematical model.
“Traditionally, the case for ameliorating physician burnout has been made primarily on ethical grounds.” This study, believed to be the first to look at the system-wide costs of burnout, “provides tools to evaluate the economic dimension of this problem,” wrote Shasha Han, MS, of the National University of Singapore and her associates in Annals of Internal Medicine.
Individual burnout-attributable costs were higher for physicians in the younger age group (less than 55 years) in all three specialty categories: $7,100 versus $5,900 for those aged at least 55 years among primary care physicians, $10,800 versus $9,100 for surgical specialists, and $7,800 versus $6,100 for other specialists, the investigators reported.
The mathematical model used in the study focused on two productivity metrics related to burnout – cost associated with physician replacement and lost income from unfilled physician positions. “Estimated turnover costs were generally higher than costs of reduced productivity across all” the various segments of age and specialty, Ms. Han and associates wrote.
“Burnout is a problem that extends beyond physicians to nurses and other health care staff. Future work holistically investigating the costs associated with burnout in health care organizations would be valuable. Studies focusing on differences in burnout-attributable costs across provider segments other than the ones investigated in this study, including academic versus private settings, or across a finer segmentation of physician specialties also might be fruitful,” they wrote.
One investigator has received grants from the American Medical Association Accelerating Change in Medical Education Consortium, the Physicians Foundation, and the National Institutes of Health. Another received a startup grant from the National University of Singapore. Ms. Han said that she had no financial conflicts to disclose. All of the investigators’ disclosures are available online.
Learn practical tips to avoid physician burnout presented during an AGA symposium at DDW® at https://www.ddwnews.org/news/aga-symposium-provides-practical-tips-to-avoid-physician-burnout/.
SOURCE: Han S et al. Ann Intern Med. 2019 May 28. doi: 10.7326/M18-1422.
Physician burnout costs the U.S. health care system approximately $4.6 billion a year in physician turnover and reduced productivity, according to the results of a cost-consequence analysis.

In 2015, the burnout-attributable cost per physician was $7,600 – an estimate occupying the conservative middle ground between the $3,700 and $11,000 extremes produced by the study’s mathematical model.
“Traditionally, the case for ameliorating physician burnout has been made primarily on ethical grounds.” This study, believed to be the first to look at the system-wide costs of burnout, “provides tools to evaluate the economic dimension of this problem,” wrote Shasha Han, MS, of the National University of Singapore and her associates in Annals of Internal Medicine.
Individual burnout-attributable costs were higher for physicians in the younger age group (less than 55 years) in all three specialty categories: $7,100 versus $5,900 for those aged at least 55 years among primary care physicians, $10,800 versus $9,100 for surgical specialists, and $7,800 versus $6,100 for other specialists, the investigators reported.
The mathematical model used in the study focused on two productivity metrics related to burnout – cost associated with physician replacement and lost income from unfilled physician positions. “Estimated turnover costs were generally higher than costs of reduced productivity across all” the various segments of age and specialty, Ms. Han and associates wrote.
“Burnout is a problem that extends beyond physicians to nurses and other health care staff. Future work holistically investigating the costs associated with burnout in health care organizations would be valuable. Studies focusing on differences in burnout-attributable costs across provider segments other than the ones investigated in this study, including academic versus private settings, or across a finer segmentation of physician specialties also might be fruitful,” they wrote.
One investigator has received grants from the American Medical Association Accelerating Change in Medical Education Consortium, the Physicians Foundation, and the National Institutes of Health. Another received a startup grant from the National University of Singapore. Ms. Han said that she had no financial conflicts to disclose. All of the investigators’ disclosures are available online.
Learn practical tips to avoid physician burnout presented during an AGA symposium at DDW® at https://www.ddwnews.org/news/aga-symposium-provides-practical-tips-to-avoid-physician-burnout/.
SOURCE: Han S et al. Ann Intern Med. 2019 May 28. doi: 10.7326/M18-1422.
FROM ANNALS OF INTERNAL MEDICINE
Key clinical point: Burnout-attributable costs were higher for younger physicians.
Major finding: Physician burnout costs the U.S. health care system approximately $4.6 billion a year.
Study details: A cost-consequence analysis focusing on physician turnover and lost clinical hours.
Disclosures: One investigator has received grants from the American Medical Association Accelerating Change in Medical Education Consortium, the Physicians Foundation, and the National Institutes of Health. Another received a startup grant from the National University of Singapore. Ms. Han said that she had no financial conflicts.
Source: Han S et al. Ann Intern Med. 2019 May 28. doi: 10.7326/M18-1422.
Measles cases now at highest level since 1992
With 971 cases of measles reported after just 5 months of 2019, the United States has hit another dubious milestone by surpassing the 963 cases reported in the preelimination year of 1994, according to the Centers for Disease Control and Prevention.
That leaves 1992, when there were 2,237 cases reported, as the next big obstacle on measles’ current path of distinction, the CDC data show. Only 312 cases were reported in 1993.
“Outbreaks in New York City and Rockland County, New York have continued for nearly 8 months. That loss would be a huge blow for the nation and erase the hard work done by all levels of public health,” the CDC said May 30.
The CDC defines measles elimination as “the absence of continuous disease transmission for 12 months or more in a specific geographic area” and notes that “measles is no longer endemic [constantly present] in the United States.”
“Measles is preventable and the way to end this outbreak is to ensure that all children and adults who can get vaccinated, do get vaccinated. Again, I want to reassure parents that vaccines are safe, they do not cause autism. The greater danger is the disease that vaccination prevents,” CDC director Robert Redfield, MD, said in a statement.
With 971 cases of measles reported after just 5 months of 2019, the United States has hit another dubious milestone by surpassing the 963 cases reported in the preelimination year of 1994, according to the Centers for Disease Control and Prevention.
That leaves 1992, when there were 2,237 cases reported, as the next big obstacle on measles’ current path of distinction, the CDC data show. Only 312 cases were reported in 1993.
“Outbreaks in New York City and Rockland County, New York have continued for nearly 8 months. That loss would be a huge blow for the nation and erase the hard work done by all levels of public health,” the CDC said May 30.
The CDC defines measles elimination as “the absence of continuous disease transmission for 12 months or more in a specific geographic area” and notes that “measles is no longer endemic [constantly present] in the United States.”
“Measles is preventable and the way to end this outbreak is to ensure that all children and adults who can get vaccinated, do get vaccinated. Again, I want to reassure parents that vaccines are safe, they do not cause autism. The greater danger is the disease that vaccination prevents,” CDC director Robert Redfield, MD, said in a statement.
With 971 cases of measles reported after just 5 months of 2019, the United States has hit another dubious milestone by surpassing the 963 cases reported in the preelimination year of 1994, according to the Centers for Disease Control and Prevention.
That leaves 1992, when there were 2,237 cases reported, as the next big obstacle on measles’ current path of distinction, the CDC data show. Only 312 cases were reported in 1993.
“Outbreaks in New York City and Rockland County, New York have continued for nearly 8 months. That loss would be a huge blow for the nation and erase the hard work done by all levels of public health,” the CDC said May 30.
The CDC defines measles elimination as “the absence of continuous disease transmission for 12 months or more in a specific geographic area” and notes that “measles is no longer endemic [constantly present] in the United States.”
“Measles is preventable and the way to end this outbreak is to ensure that all children and adults who can get vaccinated, do get vaccinated. Again, I want to reassure parents that vaccines are safe, they do not cause autism. The greater danger is the disease that vaccination prevents,” CDC director Robert Redfield, MD, said in a statement.
Human cheddar, bacteria-bashing berries, and constipation amnesia
No celeb cheese, please
You don’t mess with cheese. Cheese is love, cheese is life. But now, science has gone too far by bridging the gap between man and cheese.
In a new London art exhibit, a biologist and an artist teamed up to create different types of cheese made from … British celebs? Look, we love the Spice Girls as much as the next person, but that doesn’t mean we want Baby Spice Brie.
Bacteria taken from their face, armpits, ears, and even bellybuttons were used to create cheddar, Cheshire, and Stilton cheeses, among others. Yum. The goal of the (possibly blasphemous) exhibit is to change people’s view of microbes and demonstrate how they are essential to human existence. The cheesy contributors included Ruby Tandoh from the Great British Bake Off, chef Heston Blumenthal, and Blur bassist Alex James.
The artists and scientists involved did not yet determine if the cheese was safe for human consumption – not that anyone would eat them, anyway.
A poop oops
I’m sure we’ve all been in the position – you’re on your porcelain throne, things aren’t going your way. You’re praying to any and every deity under the sun to get things moving. Maybe you start bargaining … but would you give up a decade’s worth of memories to jump-start your intestines?
One woman in China seems to have made this deal with the devil. After straining a bit too hard during a nasty bout of constipation, the Hong Kong woman emerged from the bathroom displaying signs of amnesia. Her family quickly discovered she could not remember anything from the past 10 years and took her to the hospital, where she was diagnosed with transient global amnesia. The temporary amnesia was caused by an increase in abdominal and intracerebral pressure that limited oxygen flow to her brain.
The woman regained her memories after about 8 hours and had no recollection of the unfortunate series of events. Or so she claims. We imagine she might remember a bit and is going to start stocking up on prune juice from now on.
Juicy, red, and ready to save the world
The Avengers may have finally stopped Thanos, but what could they do against Escherichia coli? And Superman may be more powerful than a locomotive, but could he take on Pseudomonas aeruginosa?
In this week’s episode of Bacteria vs. the World, we meet the superhero the world really needs.
The humble cranberry doesn’t have super speed or an armored flying exoskeleton, but it does have the power to help antibiotics fight the bacterial menace, as researchers at McGill University and Institut National de la Recherche Scientifique, both in Montreal, discovered.
They found that bacteria exposed to a cranberry extract known as proanthocyanidin had increased sensitivity to antibiotics. The extract, it appears, makes bacterial cell walls more permeable to antibiotics and interferes with the pump mechanism that bacteria use to rid themselves of the drugs. “The antibiotic penetrates more easily, and the bacteria have a harder time getting rid of it,” so the drug is effective at a lower dose, they explained.
But wait, there’s more! “When we simultaneously treated the bacteria with an antibiotic and the cranberry extract, no resistance developed. We were very surprised by this,” lead author Nathalie Tufenkji, PhD, said in a written statement.
This is all great news, of course, but we’re a little surprised by their surprise. Here’s why: The scientific name of the American cranberry is Vaccinium macrocarpon. Vaccinium? Coincidence? We think not.
Who needs oncologists anyway?
We’re no strangers to gross-out stories here at Livin’ on the MDedge, but fair warning: This is really up there on the gross-ometer. You may want to brace yourselves.
As with so many good stories, our tale begins with a drunk man vomiting. The 63-year-old man from China had been feeling some discomfort in his throat for some time, especially when eating, but had, up to that point, ignored it. But as the man voided the evening’s mistakes back up to where they came from, something in his throat came loose. Specifically, a meatball-like mass that the man would later describe as a “long, forked tongue.”
Thinking as only a drunk man could, our intrepid friend decided that this object was an integral part of his body and that the best course of action would be to find a glass of water and swallow the mass. However, he did follow this flash of brilliance with an actual good decision, checking himself into the nearest hospital.
As the doctors were examining the man, they discovered the cherry on top of this disgusting story: He’d actually barfed up a tumor. Specifically, a large fibroma, measuring 15 cm by 4 cm, that had taken up residence in the man’s throat. If it hadn’t come out, the fibroma could have continued to grow, potentially obstructing the man’s ability to breathe.
While we’re glad things worked out for our inebriated friend, we’d like to recommend a trip to the doctor for anyone currently having mysterious difficulty swallowing. Don’t make us read about more people throwing up parts of their body. Please.
No celeb cheese, please
You don’t mess with cheese. Cheese is love, cheese is life. But now, science has gone too far by bridging the gap between man and cheese.
In a new London art exhibit, a biologist and an artist teamed up to create different types of cheese made from … British celebs? Look, we love the Spice Girls as much as the next person, but that doesn’t mean we want Baby Spice Brie.
Bacteria taken from their face, armpits, ears, and even bellybuttons were used to create cheddar, Cheshire, and Stilton cheeses, among others. Yum. The goal of the (possibly blasphemous) exhibit is to change people’s view of microbes and demonstrate how they are essential to human existence. The cheesy contributors included Ruby Tandoh from the Great British Bake Off, chef Heston Blumenthal, and Blur bassist Alex James.
The artists and scientists involved did not yet determine if the cheese was safe for human consumption – not that anyone would eat them, anyway.
A poop oops
I’m sure we’ve all been in the position – you’re on your porcelain throne, things aren’t going your way. You’re praying to any and every deity under the sun to get things moving. Maybe you start bargaining … but would you give up a decade’s worth of memories to jump-start your intestines?
One woman in China seems to have made this deal with the devil. After straining a bit too hard during a nasty bout of constipation, the Hong Kong woman emerged from the bathroom displaying signs of amnesia. Her family quickly discovered she could not remember anything from the past 10 years and took her to the hospital, where she was diagnosed with transient global amnesia. The temporary amnesia was caused by an increase in abdominal and intracerebral pressure that limited oxygen flow to her brain.
The woman regained her memories after about 8 hours and had no recollection of the unfortunate series of events. Or so she claims. We imagine she might remember a bit and is going to start stocking up on prune juice from now on.
Juicy, red, and ready to save the world
The Avengers may have finally stopped Thanos, but what could they do against Escherichia coli? And Superman may be more powerful than a locomotive, but could he take on Pseudomonas aeruginosa?
In this week’s episode of Bacteria vs. the World, we meet the superhero the world really needs.
The humble cranberry doesn’t have super speed or an armored flying exoskeleton, but it does have the power to help antibiotics fight the bacterial menace, as researchers at McGill University and Institut National de la Recherche Scientifique, both in Montreal, discovered.
They found that bacteria exposed to a cranberry extract known as proanthocyanidin had increased sensitivity to antibiotics. The extract, it appears, makes bacterial cell walls more permeable to antibiotics and interferes with the pump mechanism that bacteria use to rid themselves of the drugs. “The antibiotic penetrates more easily, and the bacteria have a harder time getting rid of it,” so the drug is effective at a lower dose, they explained.
But wait, there’s more! “When we simultaneously treated the bacteria with an antibiotic and the cranberry extract, no resistance developed. We were very surprised by this,” lead author Nathalie Tufenkji, PhD, said in a written statement.
This is all great news, of course, but we’re a little surprised by their surprise. Here’s why: The scientific name of the American cranberry is Vaccinium macrocarpon. Vaccinium? Coincidence? We think not.
Who needs oncologists anyway?
We’re no strangers to gross-out stories here at Livin’ on the MDedge, but fair warning: This is really up there on the gross-ometer. You may want to brace yourselves.
As with so many good stories, our tale begins with a drunk man vomiting. The 63-year-old man from China had been feeling some discomfort in his throat for some time, especially when eating, but had, up to that point, ignored it. But as the man voided the evening’s mistakes back up to where they came from, something in his throat came loose. Specifically, a meatball-like mass that the man would later describe as a “long, forked tongue.”
Thinking as only a drunk man could, our intrepid friend decided that this object was an integral part of his body and that the best course of action would be to find a glass of water and swallow the mass. However, he did follow this flash of brilliance with an actual good decision, checking himself into the nearest hospital.
As the doctors were examining the man, they discovered the cherry on top of this disgusting story: He’d actually barfed up a tumor. Specifically, a large fibroma, measuring 15 cm by 4 cm, that had taken up residence in the man’s throat. If it hadn’t come out, the fibroma could have continued to grow, potentially obstructing the man’s ability to breathe.
While we’re glad things worked out for our inebriated friend, we’d like to recommend a trip to the doctor for anyone currently having mysterious difficulty swallowing. Don’t make us read about more people throwing up parts of their body. Please.

No celeb cheese, please
You don’t mess with cheese. Cheese is love, cheese is life. But now, science has gone too far by bridging the gap between man and cheese.
In a new London art exhibit, a biologist and an artist teamed up to create different types of cheese made from … British celebs? Look, we love the Spice Girls as much as the next person, but that doesn’t mean we want Baby Spice Brie.
Bacteria taken from their face, armpits, ears, and even bellybuttons were used to create cheddar, Cheshire, and Stilton cheeses, among others. Yum. The goal of the (possibly blasphemous) exhibit is to change people’s view of microbes and demonstrate how they are essential to human existence. The cheesy contributors included Ruby Tandoh from the Great British Bake Off, chef Heston Blumenthal, and Blur bassist Alex James.
The artists and scientists involved did not yet determine if the cheese was safe for human consumption – not that anyone would eat them, anyway.
A poop oops
I’m sure we’ve all been in the position – you’re on your porcelain throne, things aren’t going your way. You’re praying to any and every deity under the sun to get things moving. Maybe you start bargaining … but would you give up a decade’s worth of memories to jump-start your intestines?
One woman in China seems to have made this deal with the devil. After straining a bit too hard during a nasty bout of constipation, the Hong Kong woman emerged from the bathroom displaying signs of amnesia. Her family quickly discovered she could not remember anything from the past 10 years and took her to the hospital, where she was diagnosed with transient global amnesia. The temporary amnesia was caused by an increase in abdominal and intracerebral pressure that limited oxygen flow to her brain.
The woman regained her memories after about 8 hours and had no recollection of the unfortunate series of events. Or so she claims. We imagine she might remember a bit and is going to start stocking up on prune juice from now on.
Juicy, red, and ready to save the world
The Avengers may have finally stopped Thanos, but what could they do against Escherichia coli? And Superman may be more powerful than a locomotive, but could he take on Pseudomonas aeruginosa?
In this week’s episode of Bacteria vs. the World, we meet the superhero the world really needs.
The humble cranberry doesn’t have super speed or an armored flying exoskeleton, but it does have the power to help antibiotics fight the bacterial menace, as researchers at McGill University and Institut National de la Recherche Scientifique, both in Montreal, discovered.
They found that bacteria exposed to a cranberry extract known as proanthocyanidin had increased sensitivity to antibiotics. The extract, it appears, makes bacterial cell walls more permeable to antibiotics and interferes with the pump mechanism that bacteria use to rid themselves of the drugs. “The antibiotic penetrates more easily, and the bacteria have a harder time getting rid of it,” so the drug is effective at a lower dose, they explained.
But wait, there’s more! “When we simultaneously treated the bacteria with an antibiotic and the cranberry extract, no resistance developed. We were very surprised by this,” lead author Nathalie Tufenkji, PhD, said in a written statement.
This is all great news, of course, but we’re a little surprised by their surprise. Here’s why: The scientific name of the American cranberry is Vaccinium macrocarpon. Vaccinium? Coincidence? We think not.
Who needs oncologists anyway?
We’re no strangers to gross-out stories here at Livin’ on the MDedge, but fair warning: This is really up there on the gross-ometer. You may want to brace yourselves.
As with so many good stories, our tale begins with a drunk man vomiting. The 63-year-old man from China had been feeling some discomfort in his throat for some time, especially when eating, but had, up to that point, ignored it. But as the man voided the evening’s mistakes back up to where they came from, something in his throat came loose. Specifically, a meatball-like mass that the man would later describe as a “long, forked tongue.”
Thinking as only a drunk man could, our intrepid friend decided that this object was an integral part of his body and that the best course of action would be to find a glass of water and swallow the mass. However, he did follow this flash of brilliance with an actual good decision, checking himself into the nearest hospital.
As the doctors were examining the man, they discovered the cherry on top of this disgusting story: He’d actually barfed up a tumor. Specifically, a large fibroma, measuring 15 cm by 4 cm, that had taken up residence in the man’s throat. If it hadn’t come out, the fibroma could have continued to grow, potentially obstructing the man’s ability to breathe.
While we’re glad things worked out for our inebriated friend, we’d like to recommend a trip to the doctor for anyone currently having mysterious difficulty swallowing. Don’t make us read about more people throwing up parts of their body. Please.

Cholesterol guideline: Risk assessment gets personal
according to the 2018 update to U.S. guidelines for cholesterol management from the American Heart Association and the American College of Cardiology.
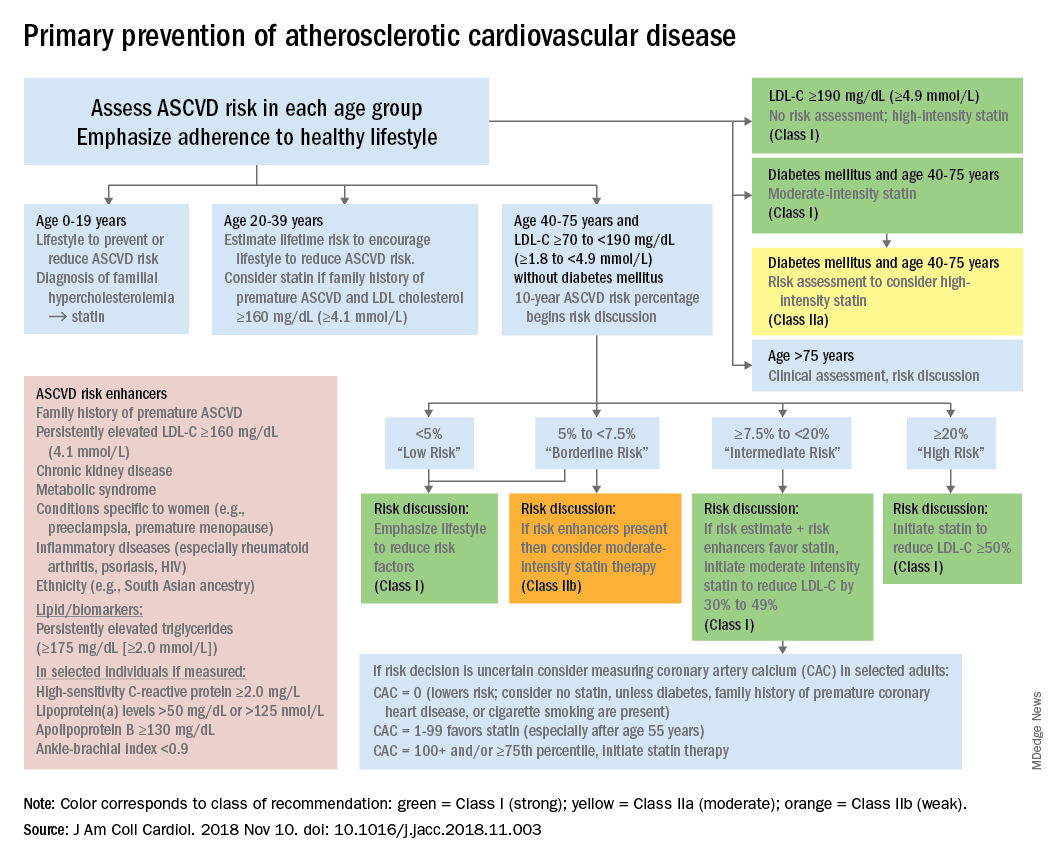
The guideline also emphasizes “careful adherence to lifestyle recommendations at an early age [to] reduce risk factor burden over the lifespan and decrease the need for preventive drug therapies later in life,” Scott M. Grundy, MD, PhD, and Neil J. Stone, MD, said in a synopsis of the document in the Annals of Internal Medicine.
For primary prevention in patients aged 40-75 years, estimation of 10-year ASCVD risk – introduced in the 2013 guidelines – and stratification into one of four categories should set the stage for clinician-patient discussion. A score of less than 5% indicates low risk and should prompt a risk discussion that emphasizes lifestyle recommendations. “Statins are clinically efficacious in the latter three categories, but the higher the risk, the stronger the statin indication,” said Dr. Grundy of the University of Texas, Dallas, and Dr. Stone of Northwestern University, Chicago.
When risk status is uncertain, measurement of coronary artery calcium should be considered in patients aged 40-75 years with LDL cholesterol levels of 70-189 mg/dL who do no not have diabetes, they noted.
The guideline emphasizes secondary prevention with “maximally tolerated doses of statins” and the use of nonstatin drugs such as ezetimibe and PCSK9 inhibitors for patients with very high ASCVD risk – defined as a history of multiple major events or one event and other high-risk conditions, Dr. Grundy and Dr. Stone wrote.
Financial support for the Guideline Writing Committee for the 2018 Cholesterol Guidelines came from the AHA and the ACC. Dr. Grundy and Dr. Stone said that they had no relevant conflicts of interest.
SOURCE: Grundy SM and Stone NJ. Ann Intern Med. 2019 May 28. doi: 10.7326/M19-0365.
according to the 2018 update to U.S. guidelines for cholesterol management from the American Heart Association and the American College of Cardiology.

The guideline also emphasizes “careful adherence to lifestyle recommendations at an early age [to] reduce risk factor burden over the lifespan and decrease the need for preventive drug therapies later in life,” Scott M. Grundy, MD, PhD, and Neil J. Stone, MD, said in a synopsis of the document in the Annals of Internal Medicine.
For primary prevention in patients aged 40-75 years, estimation of 10-year ASCVD risk – introduced in the 2013 guidelines – and stratification into one of four categories should set the stage for clinician-patient discussion. A score of less than 5% indicates low risk and should prompt a risk discussion that emphasizes lifestyle recommendations. “Statins are clinically efficacious in the latter three categories, but the higher the risk, the stronger the statin indication,” said Dr. Grundy of the University of Texas, Dallas, and Dr. Stone of Northwestern University, Chicago.
When risk status is uncertain, measurement of coronary artery calcium should be considered in patients aged 40-75 years with LDL cholesterol levels of 70-189 mg/dL who do no not have diabetes, they noted.
The guideline emphasizes secondary prevention with “maximally tolerated doses of statins” and the use of nonstatin drugs such as ezetimibe and PCSK9 inhibitors for patients with very high ASCVD risk – defined as a history of multiple major events or one event and other high-risk conditions, Dr. Grundy and Dr. Stone wrote.
Financial support for the Guideline Writing Committee for the 2018 Cholesterol Guidelines came from the AHA and the ACC. Dr. Grundy and Dr. Stone said that they had no relevant conflicts of interest.
SOURCE: Grundy SM and Stone NJ. Ann Intern Med. 2019 May 28. doi: 10.7326/M19-0365.
according to the 2018 update to U.S. guidelines for cholesterol management from the American Heart Association and the American College of Cardiology.

The guideline also emphasizes “careful adherence to lifestyle recommendations at an early age [to] reduce risk factor burden over the lifespan and decrease the need for preventive drug therapies later in life,” Scott M. Grundy, MD, PhD, and Neil J. Stone, MD, said in a synopsis of the document in the Annals of Internal Medicine.
For primary prevention in patients aged 40-75 years, estimation of 10-year ASCVD risk – introduced in the 2013 guidelines – and stratification into one of four categories should set the stage for clinician-patient discussion. A score of less than 5% indicates low risk and should prompt a risk discussion that emphasizes lifestyle recommendations. “Statins are clinically efficacious in the latter three categories, but the higher the risk, the stronger the statin indication,” said Dr. Grundy of the University of Texas, Dallas, and Dr. Stone of Northwestern University, Chicago.
When risk status is uncertain, measurement of coronary artery calcium should be considered in patients aged 40-75 years with LDL cholesterol levels of 70-189 mg/dL who do no not have diabetes, they noted.
The guideline emphasizes secondary prevention with “maximally tolerated doses of statins” and the use of nonstatin drugs such as ezetimibe and PCSK9 inhibitors for patients with very high ASCVD risk – defined as a history of multiple major events or one event and other high-risk conditions, Dr. Grundy and Dr. Stone wrote.
Financial support for the Guideline Writing Committee for the 2018 Cholesterol Guidelines came from the AHA and the ACC. Dr. Grundy and Dr. Stone said that they had no relevant conflicts of interest.
SOURCE: Grundy SM and Stone NJ. Ann Intern Med. 2019 May 28. doi: 10.7326/M19-0365.
FROM THE ANNALS OF INTERNAL MEDICINE