User login
Richard Franki is the associate editor who writes and creates graphs. He started with the company in 1987, when it was known as the International Medical News Group. In his years as a journalist, Richard has worked for Cap Cities/ABC, Disney, Harcourt, Elsevier, Quadrant, Frontline, and Internet Brands. In the 1990s, he was a contributor to the ill-fated Indications column, predecessor of Livin' on the MDedge.
Flu activity levels down, but outpatient visits highest since 1998-99
Influenza activity measures declined for a third consecutive week, but levels are higher than usual at this point in the flu season, according to the Centers for Disease Control and Prevention.
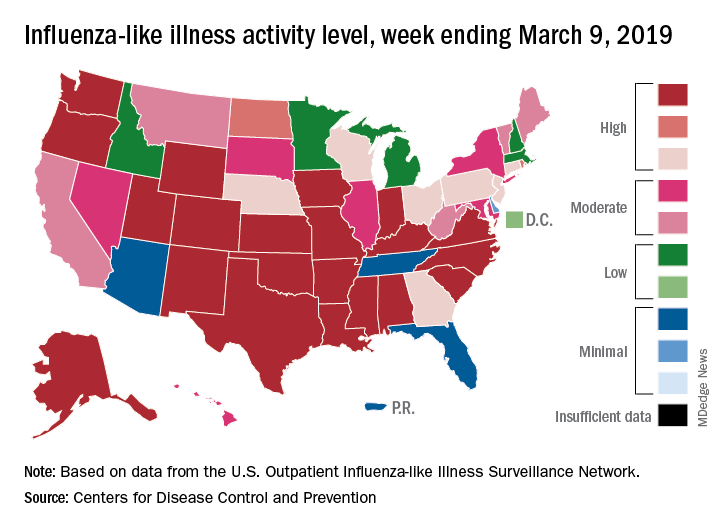
For the week ending March 9, an estimated 4.5% of outpatient visits were for influenza-like illness (ILI), which was down from 4.6% the previous week, the CDC’s influenza division reported March 15, but that is higher than the comparable week for any year since 1998-1999. During last year’s very severe flu season, the outpatient visit rate was just under 3.2% for the week ending March 10.
Although the number of states at level 10 on the CDC’s 1-10 scale remained at 21, the activity map actually looks more red than last week since Rhode Island and West Virgina were replaced by the much larger states of Iowa and Washington. The number of states in the high range (8-10), did go down from 32 to 30, data from the CDC’s Outpatient ILI Surveillance Network show.
Of those four deaths, only one occurred during the most recent reporting week, the CDC said.
Influenza activity measures declined for a third consecutive week, but levels are higher than usual at this point in the flu season, according to the Centers for Disease Control and Prevention.

For the week ending March 9, an estimated 4.5% of outpatient visits were for influenza-like illness (ILI), which was down from 4.6% the previous week, the CDC’s influenza division reported March 15, but that is higher than the comparable week for any year since 1998-1999. During last year’s very severe flu season, the outpatient visit rate was just under 3.2% for the week ending March 10.
Although the number of states at level 10 on the CDC’s 1-10 scale remained at 21, the activity map actually looks more red than last week since Rhode Island and West Virgina were replaced by the much larger states of Iowa and Washington. The number of states in the high range (8-10), did go down from 32 to 30, data from the CDC’s Outpatient ILI Surveillance Network show.
Of those four deaths, only one occurred during the most recent reporting week, the CDC said.
Influenza activity measures declined for a third consecutive week, but levels are higher than usual at this point in the flu season, according to the Centers for Disease Control and Prevention.

For the week ending March 9, an estimated 4.5% of outpatient visits were for influenza-like illness (ILI), which was down from 4.6% the previous week, the CDC’s influenza division reported March 15, but that is higher than the comparable week for any year since 1998-1999. During last year’s very severe flu season, the outpatient visit rate was just under 3.2% for the week ending March 10.
Although the number of states at level 10 on the CDC’s 1-10 scale remained at 21, the activity map actually looks more red than last week since Rhode Island and West Virgina were replaced by the much larger states of Iowa and Washington. The number of states in the high range (8-10), did go down from 32 to 30, data from the CDC’s Outpatient ILI Surveillance Network show.
Of those four deaths, only one occurred during the most recent reporting week, the CDC said.
Friendly gut bugs, MCI-battling mushrooms, and remembering to forget
Friend or foe, how do we know?
That’s the question immune cells ask all the time, especially about gut bacteria. A study published March 7 seeks to explain how immune systems can distinguish between happy-go-lucky gut microbes and deadly pathogens. Turns out, the friendly microbes simply high five!
Well, not really. But they do have a hook-like arm, called a holdfast, which latches onto the gut lining. The holdfast is lined with vesicles that carry antigens into the gut. While antigens normally cause immune cells to attack, something about these antigens are telling T cells to hold their fire.
The authors of the study hypothesized that the packaging of the antigens – the vesicles – might be the reason for the friendliness between microbes and T cells. It’s like the immune system expects a cannonball, but is pleasantly surprised by an Amazon Prime package full of goodies showing up on their doorstep instead. Yay for presents!
Don’t skimp on the ’shrooms
While you’re piling onions onto your plate to reduce cancer and cheese for your heart, make sure you add mushrooms for extra brain power. Researchers conducting a 6-year study in Singapore observed cognitive decline in 600 Chinese people aged at least 60 years, and they found that those who eat more than two portions of cooked mushrooms per week have up to 50% reduced odds of mild cognitive impairment.
Researchers here at the LOTME Lab have harnessed the power of these food studies to determine that a Philly cheesesteak with mushrooms and onions is the healthiest meal out there. Chow down!
As far as we know, all the mushrooms were standard edible fungi, and none were magic mushrooms (although, that might help, too; try that on your own time). Researchers believe that the compound ergothioneine, an antioxidant and anti-inflammatory that cannot be synthesized by humans, might be reason for the reduced risk of mild cognitive impairment Maybe it’s time to add a cup of cooked shiitake mushrooms to your morning routine.
Fuggedaboutit!
We all have unwanted memories that we’d rather forget about. An embarrassing incident, a painful experience – everyone has moments they’d rather not think about. So, the question is: How do you get rid of these bad memories?
The obvious solution is to stop thinking about it. But if you’re a regular reader of Livin’ on the MDedge, you can probably guess that the answer isn’t that simple.
And, in fact, it isn’t! A group of researchers at the University of Texas at Austin, has performed a study on intentional forgetting, and they found that the best way to forget something is ... to think about it. Study subjects were shown a series of images and told to either remember or forget those images while their ventral temporal cortex was monitored for activity. Not only were participants successfully able to forget images by thinking about it, but activity in the brain was higher when forgetting than while remembering.
Obviously, this research would be helpful for anyone dealing with trauma, and we hope doctors who have to treat such patients keep it in mind. Just don’t think about it too much, or you’ll forget about it.
The Golden Lobbyist
If you need health care in your neighborhood
Who you gonna call? Jack Nicklaus!
You need 20 mill to make it good
Who you gonna call? Jack Nicklaus!
Health care in general didn’t do very well in President Trump’s 2020 budget proposal; Medicare, Medicaid, and the National Cancer Institute were all targeted for cuts. But it did include one particular $20-million initiative for a mobile children’s hospital.
Politico reports that the nation’s golfer in chief “personally directed the Department of Health and Human Services to earmark the funds” after playing a couple of rounds with the Golden Bear himself, Jack Nicklaus. The mobile unit would be part of the Nicklaus Children’s Hospital in Miami. The golf legend turned lobbyist also had meetings off the course with HHS Secretary Alex Azar and then-OMB Director Mick Mulvaney.
Are health care ideas running through your head?
Who you gonna call? Jack Nicklaus!
He’ll golf with the prez, and get your bread
Who you gonna call? Jack Nicklaus!
He ain’t afraid of no tweets

Friend or foe, how do we know?
That’s the question immune cells ask all the time, especially about gut bacteria. A study published March 7 seeks to explain how immune systems can distinguish between happy-go-lucky gut microbes and deadly pathogens. Turns out, the friendly microbes simply high five!
Well, not really. But they do have a hook-like arm, called a holdfast, which latches onto the gut lining. The holdfast is lined with vesicles that carry antigens into the gut. While antigens normally cause immune cells to attack, something about these antigens are telling T cells to hold their fire.
The authors of the study hypothesized that the packaging of the antigens – the vesicles – might be the reason for the friendliness between microbes and T cells. It’s like the immune system expects a cannonball, but is pleasantly surprised by an Amazon Prime package full of goodies showing up on their doorstep instead. Yay for presents!
Don’t skimp on the ’shrooms
While you’re piling onions onto your plate to reduce cancer and cheese for your heart, make sure you add mushrooms for extra brain power. Researchers conducting a 6-year study in Singapore observed cognitive decline in 600 Chinese people aged at least 60 years, and they found that those who eat more than two portions of cooked mushrooms per week have up to 50% reduced odds of mild cognitive impairment.
Researchers here at the LOTME Lab have harnessed the power of these food studies to determine that a Philly cheesesteak with mushrooms and onions is the healthiest meal out there. Chow down!
As far as we know, all the mushrooms were standard edible fungi, and none were magic mushrooms (although, that might help, too; try that on your own time). Researchers believe that the compound ergothioneine, an antioxidant and anti-inflammatory that cannot be synthesized by humans, might be reason for the reduced risk of mild cognitive impairment Maybe it’s time to add a cup of cooked shiitake mushrooms to your morning routine.
Fuggedaboutit!
We all have unwanted memories that we’d rather forget about. An embarrassing incident, a painful experience – everyone has moments they’d rather not think about. So, the question is: How do you get rid of these bad memories?
The obvious solution is to stop thinking about it. But if you’re a regular reader of Livin’ on the MDedge, you can probably guess that the answer isn’t that simple.
And, in fact, it isn’t! A group of researchers at the University of Texas at Austin, has performed a study on intentional forgetting, and they found that the best way to forget something is ... to think about it. Study subjects were shown a series of images and told to either remember or forget those images while their ventral temporal cortex was monitored for activity. Not only were participants successfully able to forget images by thinking about it, but activity in the brain was higher when forgetting than while remembering.
Obviously, this research would be helpful for anyone dealing with trauma, and we hope doctors who have to treat such patients keep it in mind. Just don’t think about it too much, or you’ll forget about it.
The Golden Lobbyist
If you need health care in your neighborhood
Who you gonna call? Jack Nicklaus!
You need 20 mill to make it good
Who you gonna call? Jack Nicklaus!
Health care in general didn’t do very well in President Trump’s 2020 budget proposal; Medicare, Medicaid, and the National Cancer Institute were all targeted for cuts. But it did include one particular $20-million initiative for a mobile children’s hospital.
Politico reports that the nation’s golfer in chief “personally directed the Department of Health and Human Services to earmark the funds” after playing a couple of rounds with the Golden Bear himself, Jack Nicklaus. The mobile unit would be part of the Nicklaus Children’s Hospital in Miami. The golf legend turned lobbyist also had meetings off the course with HHS Secretary Alex Azar and then-OMB Director Mick Mulvaney.
Are health care ideas running through your head?
Who you gonna call? Jack Nicklaus!
He’ll golf with the prez, and get your bread
Who you gonna call? Jack Nicklaus!
He ain’t afraid of no tweets

Friend or foe, how do we know?
That’s the question immune cells ask all the time, especially about gut bacteria. A study published March 7 seeks to explain how immune systems can distinguish between happy-go-lucky gut microbes and deadly pathogens. Turns out, the friendly microbes simply high five!
Well, not really. But they do have a hook-like arm, called a holdfast, which latches onto the gut lining. The holdfast is lined with vesicles that carry antigens into the gut. While antigens normally cause immune cells to attack, something about these antigens are telling T cells to hold their fire.
The authors of the study hypothesized that the packaging of the antigens – the vesicles – might be the reason for the friendliness between microbes and T cells. It’s like the immune system expects a cannonball, but is pleasantly surprised by an Amazon Prime package full of goodies showing up on their doorstep instead. Yay for presents!
Don’t skimp on the ’shrooms
While you’re piling onions onto your plate to reduce cancer and cheese for your heart, make sure you add mushrooms for extra brain power. Researchers conducting a 6-year study in Singapore observed cognitive decline in 600 Chinese people aged at least 60 years, and they found that those who eat more than two portions of cooked mushrooms per week have up to 50% reduced odds of mild cognitive impairment.
Researchers here at the LOTME Lab have harnessed the power of these food studies to determine that a Philly cheesesteak with mushrooms and onions is the healthiest meal out there. Chow down!
As far as we know, all the mushrooms were standard edible fungi, and none were magic mushrooms (although, that might help, too; try that on your own time). Researchers believe that the compound ergothioneine, an antioxidant and anti-inflammatory that cannot be synthesized by humans, might be reason for the reduced risk of mild cognitive impairment Maybe it’s time to add a cup of cooked shiitake mushrooms to your morning routine.
Fuggedaboutit!
We all have unwanted memories that we’d rather forget about. An embarrassing incident, a painful experience – everyone has moments they’d rather not think about. So, the question is: How do you get rid of these bad memories?
The obvious solution is to stop thinking about it. But if you’re a regular reader of Livin’ on the MDedge, you can probably guess that the answer isn’t that simple.
And, in fact, it isn’t! A group of researchers at the University of Texas at Austin, has performed a study on intentional forgetting, and they found that the best way to forget something is ... to think about it. Study subjects were shown a series of images and told to either remember or forget those images while their ventral temporal cortex was monitored for activity. Not only were participants successfully able to forget images by thinking about it, but activity in the brain was higher when forgetting than while remembering.
Obviously, this research would be helpful for anyone dealing with trauma, and we hope doctors who have to treat such patients keep it in mind. Just don’t think about it too much, or you’ll forget about it.
The Golden Lobbyist
If you need health care in your neighborhood
Who you gonna call? Jack Nicklaus!
You need 20 mill to make it good
Who you gonna call? Jack Nicklaus!
Health care in general didn’t do very well in President Trump’s 2020 budget proposal; Medicare, Medicaid, and the National Cancer Institute were all targeted for cuts. But it did include one particular $20-million initiative for a mobile children’s hospital.
Politico reports that the nation’s golfer in chief “personally directed the Department of Health and Human Services to earmark the funds” after playing a couple of rounds with the Golden Bear himself, Jack Nicklaus. The mobile unit would be part of the Nicklaus Children’s Hospital in Miami. The golf legend turned lobbyist also had meetings off the course with HHS Secretary Alex Azar and then-OMB Director Mick Mulvaney.
Are health care ideas running through your head?
Who you gonna call? Jack Nicklaus!
He’ll golf with the prez, and get your bread
Who you gonna call? Jack Nicklaus!
He ain’t afraid of no tweets

Prior authorization an increasing burden
The use of prior authorization for prescriptions and medical services has continued to increase in recent years, despite the consequences to continuity of care, according to a survey by the American Medical Association.

and 41% said that PA for medical services has done the same. The corresponding numbers for 5-year decreases in PAs were 2% and 1%, the AMA reported March 12.
Results of the survey, conducted in December 2018, also show that 85% of physicians believe that prior authorization sometimes, often, or always has a negative effect on the continuity of patients’ care. Almost 70% of respondents said that it is somewhat or extremely difficult to determine when PA is required for a prescription or medical service, and only 8% reported contracting with a health plan that offers programs to exempt physicians from the PA process, the AMA said.
“Physicians follow insurance protocols for prior authorization that require faxing recurring paperwork, multiple phone calls, and hours spent on hold. At the same time, patients’ lives can hang in the balance until health plans decide if needed care will qualify for insurance coverage,” AMA President Barbara L. McAneny, MD, said in a statement.
In January 2018, two organizations representing insurers – America’s Health Insurance Plans and the Blue Cross Blue Shield Association – signed onto a joint consensus statement with the AMA and other health care groups that provided five areas for improvement of the PA process. The current survey results show that “most health plans are not making meaningful progress on reforming the cumbersome prior authorization process,” the AMA said.
The use of prior authorization for prescriptions and medical services has continued to increase in recent years, despite the consequences to continuity of care, according to a survey by the American Medical Association.

and 41% said that PA for medical services has done the same. The corresponding numbers for 5-year decreases in PAs were 2% and 1%, the AMA reported March 12.
Results of the survey, conducted in December 2018, also show that 85% of physicians believe that prior authorization sometimes, often, or always has a negative effect on the continuity of patients’ care. Almost 70% of respondents said that it is somewhat or extremely difficult to determine when PA is required for a prescription or medical service, and only 8% reported contracting with a health plan that offers programs to exempt physicians from the PA process, the AMA said.
“Physicians follow insurance protocols for prior authorization that require faxing recurring paperwork, multiple phone calls, and hours spent on hold. At the same time, patients’ lives can hang in the balance until health plans decide if needed care will qualify for insurance coverage,” AMA President Barbara L. McAneny, MD, said in a statement.
In January 2018, two organizations representing insurers – America’s Health Insurance Plans and the Blue Cross Blue Shield Association – signed onto a joint consensus statement with the AMA and other health care groups that provided five areas for improvement of the PA process. The current survey results show that “most health plans are not making meaningful progress on reforming the cumbersome prior authorization process,” the AMA said.
The use of prior authorization for prescriptions and medical services has continued to increase in recent years, despite the consequences to continuity of care, according to a survey by the American Medical Association.

and 41% said that PA for medical services has done the same. The corresponding numbers for 5-year decreases in PAs were 2% and 1%, the AMA reported March 12.
Results of the survey, conducted in December 2018, also show that 85% of physicians believe that prior authorization sometimes, often, or always has a negative effect on the continuity of patients’ care. Almost 70% of respondents said that it is somewhat or extremely difficult to determine when PA is required for a prescription or medical service, and only 8% reported contracting with a health plan that offers programs to exempt physicians from the PA process, the AMA said.
“Physicians follow insurance protocols for prior authorization that require faxing recurring paperwork, multiple phone calls, and hours spent on hold. At the same time, patients’ lives can hang in the balance until health plans decide if needed care will qualify for insurance coverage,” AMA President Barbara L. McAneny, MD, said in a statement.
In January 2018, two organizations representing insurers – America’s Health Insurance Plans and the Blue Cross Blue Shield Association – signed onto a joint consensus statement with the AMA and other health care groups that provided five areas for improvement of the PA process. The current survey results show that “most health plans are not making meaningful progress on reforming the cumbersome prior authorization process,” the AMA said.
Invasive cardiologists among top revenue-generating specialists
Physicians continue to be the major drivers of hospital revenue, and
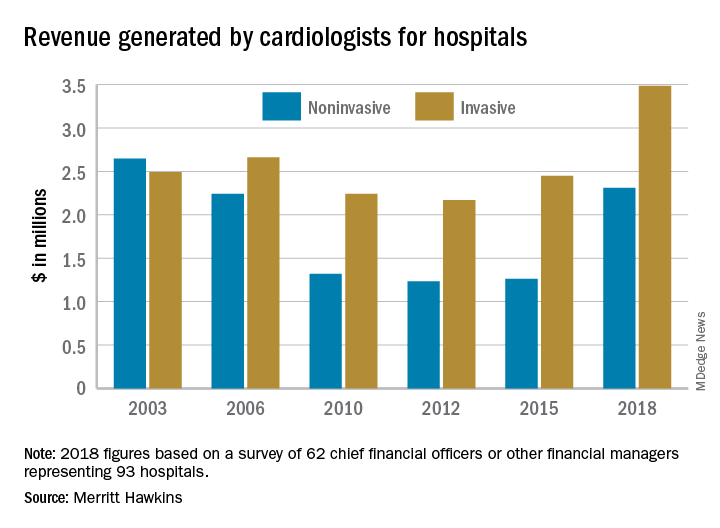
“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, wrote in a statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Invasive cardiologists generated an average of $3.48 million for their affiliated hospitals last year, second only to cardiovascular surgeons’ $3.70 million among the 19 specialties included in the survey. Average revenue generated by noninvasive cardiologists in 2018 came in at $2.31 million – that’s an 83% increase over the 3 years since the survey was last conducted, compared with the 42% rise seen by the invasive cardiologists over that time, Merritt Hawkins reported.
Specialist physicians as a group averaged over $2.45 million in revenue in 2018, compared with $2.13 million for primary care physicians, which “suggests that emerging value-based delivery models have yet to inhibit the revenue generating power of physician specialists,” the report said. Average revenue for all physicians in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The survey was conducted from October to December 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey” relative to their number nationwide, Merritt Hawkins said.
Physicians continue to be the major drivers of hospital revenue, and

“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, wrote in a statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Invasive cardiologists generated an average of $3.48 million for their affiliated hospitals last year, second only to cardiovascular surgeons’ $3.70 million among the 19 specialties included in the survey. Average revenue generated by noninvasive cardiologists in 2018 came in at $2.31 million – that’s an 83% increase over the 3 years since the survey was last conducted, compared with the 42% rise seen by the invasive cardiologists over that time, Merritt Hawkins reported.
Specialist physicians as a group averaged over $2.45 million in revenue in 2018, compared with $2.13 million for primary care physicians, which “suggests that emerging value-based delivery models have yet to inhibit the revenue generating power of physician specialists,” the report said. Average revenue for all physicians in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The survey was conducted from October to December 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey” relative to their number nationwide, Merritt Hawkins said.
Physicians continue to be the major drivers of hospital revenue, and

“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, wrote in a statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Invasive cardiologists generated an average of $3.48 million for their affiliated hospitals last year, second only to cardiovascular surgeons’ $3.70 million among the 19 specialties included in the survey. Average revenue generated by noninvasive cardiologists in 2018 came in at $2.31 million – that’s an 83% increase over the 3 years since the survey was last conducted, compared with the 42% rise seen by the invasive cardiologists over that time, Merritt Hawkins reported.
Specialist physicians as a group averaged over $2.45 million in revenue in 2018, compared with $2.13 million for primary care physicians, which “suggests that emerging value-based delivery models have yet to inhibit the revenue generating power of physician specialists,” the report said. Average revenue for all physicians in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The survey was conducted from October to December 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey” relative to their number nationwide, Merritt Hawkins said.
Measles now confirmed in 12 states
The number of new measles cases was down by more than half last week, but another state has been added to the list of those with reported cases in 2019, according to the Centers for Disease Control and Prevention.
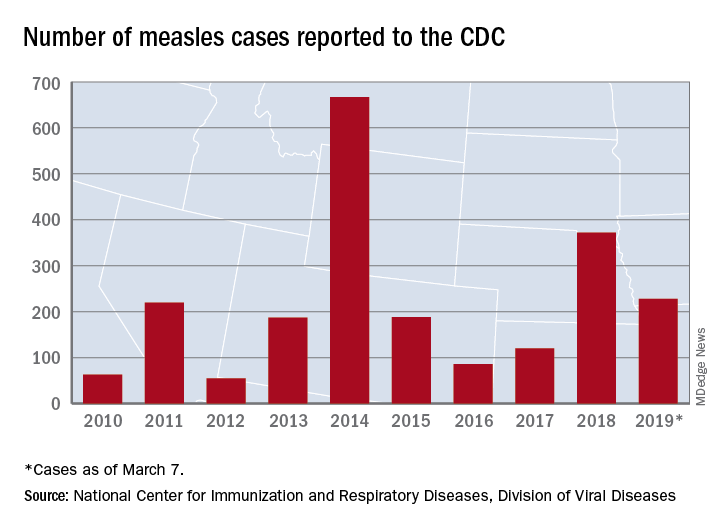
The total for the year is 228 cases, which moves 2019 ahead of 2011 for third place over the last decade, the CDC reported March 11. Going back even further in time, the 206 measles cases reported through January and February is the highest 2-month total in a quarter of a century, the Washington Post said.
New Hampshire became the 12th and latest state to report a case of measles this year, joining California, Colorado, Connecticut, Georgia, Illinois, Kentucky, New Jersey, New York, Oregon, Texas, and Washington. California’s situation is now considered an outbreak (defined as three or more cases), but one of the three outbreaks in New York has been taken off the list, so total outbreaks for 2019 remain at six, the CDC said.
For the third consecutive week, New York City produced the most measles cases, with Brooklyn’s Williamsburg neighborhood recording 11 of the U.S. total of 21. The outbreak in King County, Wash., – totaling 70 cases this year – may be winding down as only one new case was reported last week, and no new cases are being investigated, the county’s public health service reported.
The number of new measles cases was down by more than half last week, but another state has been added to the list of those with reported cases in 2019, according to the Centers for Disease Control and Prevention.

The total for the year is 228 cases, which moves 2019 ahead of 2011 for third place over the last decade, the CDC reported March 11. Going back even further in time, the 206 measles cases reported through January and February is the highest 2-month total in a quarter of a century, the Washington Post said.
New Hampshire became the 12th and latest state to report a case of measles this year, joining California, Colorado, Connecticut, Georgia, Illinois, Kentucky, New Jersey, New York, Oregon, Texas, and Washington. California’s situation is now considered an outbreak (defined as three or more cases), but one of the three outbreaks in New York has been taken off the list, so total outbreaks for 2019 remain at six, the CDC said.
For the third consecutive week, New York City produced the most measles cases, with Brooklyn’s Williamsburg neighborhood recording 11 of the U.S. total of 21. The outbreak in King County, Wash., – totaling 70 cases this year – may be winding down as only one new case was reported last week, and no new cases are being investigated, the county’s public health service reported.
The number of new measles cases was down by more than half last week, but another state has been added to the list of those with reported cases in 2019, according to the Centers for Disease Control and Prevention.

The total for the year is 228 cases, which moves 2019 ahead of 2011 for third place over the last decade, the CDC reported March 11. Going back even further in time, the 206 measles cases reported through January and February is the highest 2-month total in a quarter of a century, the Washington Post said.
New Hampshire became the 12th and latest state to report a case of measles this year, joining California, Colorado, Connecticut, Georgia, Illinois, Kentucky, New Jersey, New York, Oregon, Texas, and Washington. California’s situation is now considered an outbreak (defined as three or more cases), but one of the three outbreaks in New York has been taken off the list, so total outbreaks for 2019 remain at six, the CDC said.
For the third consecutive week, New York City produced the most measles cases, with Brooklyn’s Williamsburg neighborhood recording 11 of the U.S. total of 21. The outbreak in King County, Wash., – totaling 70 cases this year – may be winding down as only one new case was reported last week, and no new cases are being investigated, the county’s public health service reported.
For FPs, 2018 was a big year for generating hospital revenue
Physicians continue to be the major drivers of hospital revenue, and according to a new survey by physician search firm Merritt Hawkins.
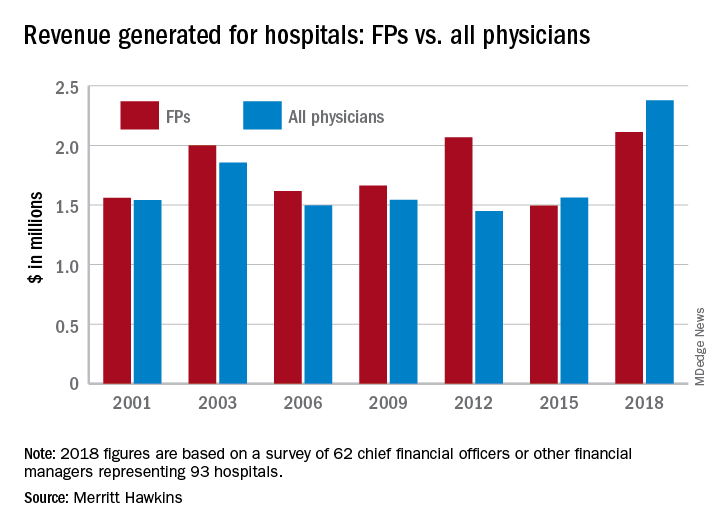
“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, said in a written statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Family physicians generated an average of $2.11 million for their affiliated hospitals last year, which was up by 41% over 2015 (the survey is conducted every 3 years) and even managed to top the previous FP high of $2.07 million in 2012, Merritt Hawkins reported.
Primary care physicians as a group averaged just over $2.13 million in revenue in 2018, compared with almost $2.45 million for specialists, which “suggests that emerging value-based delivery models have yet to inhibit the revenue generating power of physician specialists,” the report said. The average revenue for physicians in all 19 specialties in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The current survey was conducted from October to December 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey” relative to their number nationwide, Merritt Hawkins said.
Physicians continue to be the major drivers of hospital revenue, and according to a new survey by physician search firm Merritt Hawkins.

“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, said in a written statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Family physicians generated an average of $2.11 million for their affiliated hospitals last year, which was up by 41% over 2015 (the survey is conducted every 3 years) and even managed to top the previous FP high of $2.07 million in 2012, Merritt Hawkins reported.
Primary care physicians as a group averaged just over $2.13 million in revenue in 2018, compared with almost $2.45 million for specialists, which “suggests that emerging value-based delivery models have yet to inhibit the revenue generating power of physician specialists,” the report said. The average revenue for physicians in all 19 specialties in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The current survey was conducted from October to December 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey” relative to their number nationwide, Merritt Hawkins said.
Physicians continue to be the major drivers of hospital revenue, and according to a new survey by physician search firm Merritt Hawkins.

“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, said in a written statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Family physicians generated an average of $2.11 million for their affiliated hospitals last year, which was up by 41% over 2015 (the survey is conducted every 3 years) and even managed to top the previous FP high of $2.07 million in 2012, Merritt Hawkins reported.
Primary care physicians as a group averaged just over $2.13 million in revenue in 2018, compared with almost $2.45 million for specialists, which “suggests that emerging value-based delivery models have yet to inhibit the revenue generating power of physician specialists,” the report said. The average revenue for physicians in all 19 specialties in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The current survey was conducted from October to December 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey” relative to their number nationwide, Merritt Hawkins said.
Flu activity down for a second straight week
A second straight week of reduced influenza activity suggests that the 2018-2019 flu season is on the decline, according to the most recent data from the Centers for Disease Control and Prevention.
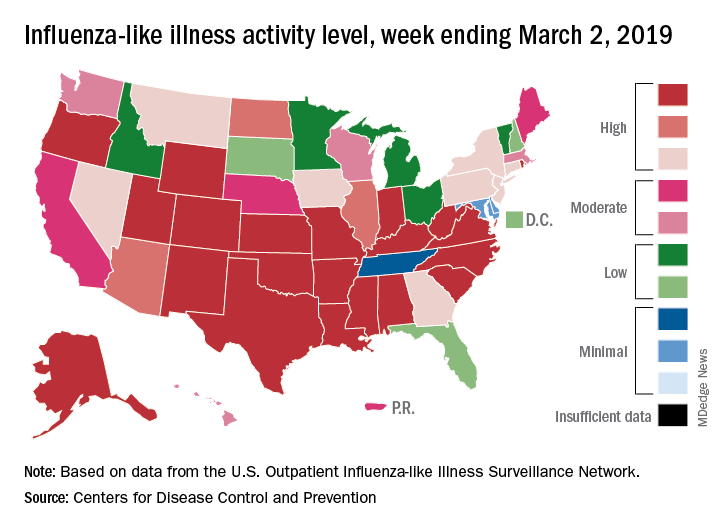
The proportion of outpatient visits for influenza-like illness (ILI) was 4.7% during the week ending March 2, which means that, thanks to a revision of the number for the previous week (Feb. 23) from 5.0% down to 4.9%, there have been two straight weeks of declines since outpatient visits reached a season-high 5.0% for the week ending Feb. 16, the CDC’s influenza division said March 8. The national baseline level is 2.2%.
This marks the second 2-week drop in ILI visits for the 2018-2019 season, as there was similar dip in the beginning of January before activity started rising again.
This compares with 24 the week before; 32 states were in the high range of 8-10, compared with the 33 reported last week, based on data from the Outpatient ILI Surveillance Network.
There were nine flu-related pediatric deaths reported during the week, with three occurring in the week ending March 2. To underscore the preliminary nature of these data, one of the deaths reported this week occurred in 2016. A total of 64 deaths in children have been associated with influenza so far for the 2018-2019 season, and the total for the 2015-2016 season is now 95, the CDC said.
A second straight week of reduced influenza activity suggests that the 2018-2019 flu season is on the decline, according to the most recent data from the Centers for Disease Control and Prevention.

The proportion of outpatient visits for influenza-like illness (ILI) was 4.7% during the week ending March 2, which means that, thanks to a revision of the number for the previous week (Feb. 23) from 5.0% down to 4.9%, there have been two straight weeks of declines since outpatient visits reached a season-high 5.0% for the week ending Feb. 16, the CDC’s influenza division said March 8. The national baseline level is 2.2%.
This marks the second 2-week drop in ILI visits for the 2018-2019 season, as there was similar dip in the beginning of January before activity started rising again.
This compares with 24 the week before; 32 states were in the high range of 8-10, compared with the 33 reported last week, based on data from the Outpatient ILI Surveillance Network.
There were nine flu-related pediatric deaths reported during the week, with three occurring in the week ending March 2. To underscore the preliminary nature of these data, one of the deaths reported this week occurred in 2016. A total of 64 deaths in children have been associated with influenza so far for the 2018-2019 season, and the total for the 2015-2016 season is now 95, the CDC said.
A second straight week of reduced influenza activity suggests that the 2018-2019 flu season is on the decline, according to the most recent data from the Centers for Disease Control and Prevention.

The proportion of outpatient visits for influenza-like illness (ILI) was 4.7% during the week ending March 2, which means that, thanks to a revision of the number for the previous week (Feb. 23) from 5.0% down to 4.9%, there have been two straight weeks of declines since outpatient visits reached a season-high 5.0% for the week ending Feb. 16, the CDC’s influenza division said March 8. The national baseline level is 2.2%.
This marks the second 2-week drop in ILI visits for the 2018-2019 season, as there was similar dip in the beginning of January before activity started rising again.
This compares with 24 the week before; 32 states were in the high range of 8-10, compared with the 33 reported last week, based on data from the Outpatient ILI Surveillance Network.
There were nine flu-related pediatric deaths reported during the week, with three occurring in the week ending March 2. To underscore the preliminary nature of these data, one of the deaths reported this week occurred in 2016. A total of 64 deaths in children have been associated with influenza so far for the 2018-2019 season, and the total for the 2015-2016 season is now 95, the CDC said.
Internists’ hospital revenue up 46% since 2015
and the average internist generated more revenue for hospitals in 2018 than ever before, according to a new survey by physician search firm Merritt Hawkins.
“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, said in a written statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”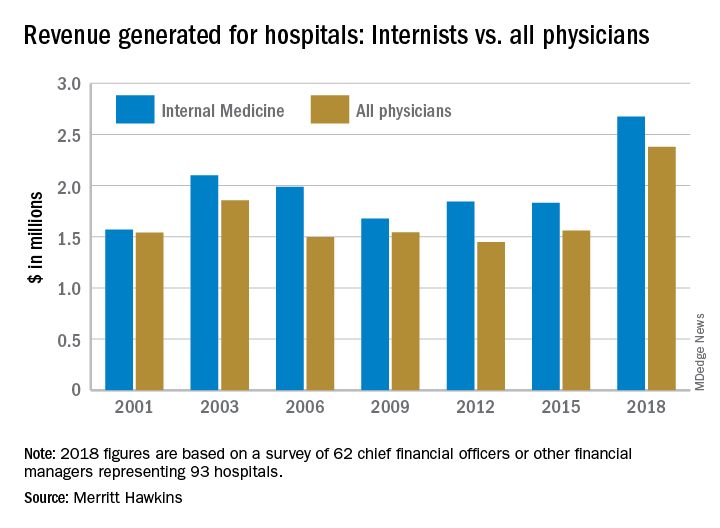
Internists generated an average of nearly $2.68 million for their affiliated hospitals last year, which was up by 46% over 2015 (the survey is conducted every 3 years) and exceeded the previous high of $2.1 million in 2003, Merritt Hawkins reported.
Primary care physicians as a group averaged just over $2.13 million in revenue in 2018, compared with almost $2.45 million for specialists, which “suggests that emerging value-based delivery models have yet to inhibit the revenue-generating power of physician specialists,” the report said. Average revenue for all physicians in all 19 specialties in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The current survey was conducted from October through December of 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey,” relative to their number nationwide, Merritt Hawkins said.
and the average internist generated more revenue for hospitals in 2018 than ever before, according to a new survey by physician search firm Merritt Hawkins.
“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, said in a written statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Internists generated an average of nearly $2.68 million for their affiliated hospitals last year, which was up by 46% over 2015 (the survey is conducted every 3 years) and exceeded the previous high of $2.1 million in 2003, Merritt Hawkins reported.
Primary care physicians as a group averaged just over $2.13 million in revenue in 2018, compared with almost $2.45 million for specialists, which “suggests that emerging value-based delivery models have yet to inhibit the revenue-generating power of physician specialists,” the report said. Average revenue for all physicians in all 19 specialties in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The current survey was conducted from October through December of 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey,” relative to their number nationwide, Merritt Hawkins said.
and the average internist generated more revenue for hospitals in 2018 than ever before, according to a new survey by physician search firm Merritt Hawkins.
“The value of physician care is not only related to the quality of patient outcomes,” Travis Singleton, the company’s executive vice president, said in a written statement. “Physicians continue to drive the financial health and viability of hospitals, even in a health care system that is evolving towards value-based payments.”
Internists generated an average of nearly $2.68 million for their affiliated hospitals last year, which was up by 46% over 2015 (the survey is conducted every 3 years) and exceeded the previous high of $2.1 million in 2003, Merritt Hawkins reported.
Primary care physicians as a group averaged just over $2.13 million in revenue in 2018, compared with almost $2.45 million for specialists, which “suggests that emerging value-based delivery models have yet to inhibit the revenue-generating power of physician specialists,” the report said. Average revenue for all physicians in all 19 specialties in the survey was almost $2.38 million, an increase of 52% since Merritt Hawkins’ last survey.
The current survey was conducted from October through December of 2018 and is based on responses from 62 chief financial officers or other financial managers who represented 93 hospitals. Responses from smaller hospitals (0-99 beds) were “somewhat overrepresented in the survey,” relative to their number nationwide, Merritt Hawkins said.
Severe maternal morbidity increasing in California
The according to a study covering almost 8.3 million births in California.
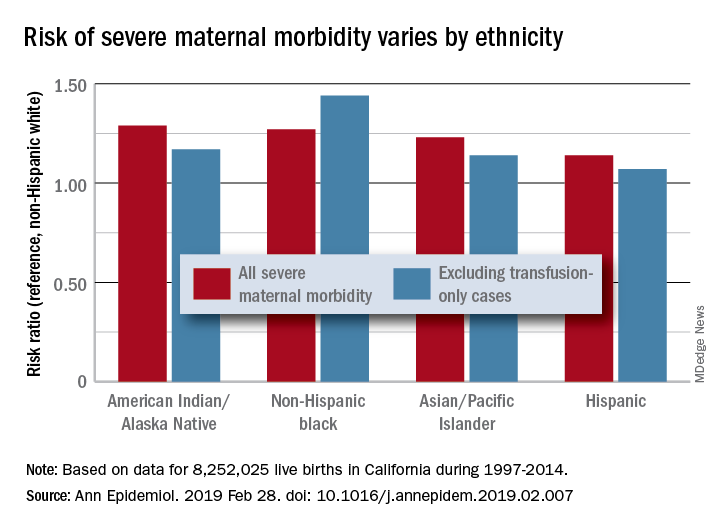
Changes in severe maternal morbidity (SMM) prevalence from 1997 to 2014 were fairly consistent by race/ethnicity, although increases for black (179%), Asian/Pacific Islander (175%), and Hispanic (173%) women were somewhat larger than for whites (163%), Stephanie A. Leonard, PhD, of Stanford (Calif.) University, and her associates reported in Annals of Epidemiology.
Differences between races/ethnicities over the entire study period were seen for SMM with and without transfusion-only cases. Individual-level factors such as cesarean birth, comorbidities, and anemia “contribute to, but do not fully explain, these disparities. Additionally, changes in the characteristics of pregnant women – including increases in comorbidities – have not affected racial/ethnic differences in severe maternal morbidity over time,” the investigators wrote.
The cohort study used data for 8,252,025 live births with birth certificates that were previously linked to delivery discharge records. SMM was measured using the Severe Maternity Morbidity Index. Because “blood transfusion is the only qualifying indicator for approximately half of SMM cases … we also studied a subset of SMM that excluded those cases for which the only indication was a blood transfusion,” they noted.
SOURCE: Leonard SA et al. Ann Epidemiol. 2019 Feb 28. doi: 10.1016/j.annepidem.2019.02.007.
The according to a study covering almost 8.3 million births in California.

Changes in severe maternal morbidity (SMM) prevalence from 1997 to 2014 were fairly consistent by race/ethnicity, although increases for black (179%), Asian/Pacific Islander (175%), and Hispanic (173%) women were somewhat larger than for whites (163%), Stephanie A. Leonard, PhD, of Stanford (Calif.) University, and her associates reported in Annals of Epidemiology.
Differences between races/ethnicities over the entire study period were seen for SMM with and without transfusion-only cases. Individual-level factors such as cesarean birth, comorbidities, and anemia “contribute to, but do not fully explain, these disparities. Additionally, changes in the characteristics of pregnant women – including increases in comorbidities – have not affected racial/ethnic differences in severe maternal morbidity over time,” the investigators wrote.
The cohort study used data for 8,252,025 live births with birth certificates that were previously linked to delivery discharge records. SMM was measured using the Severe Maternity Morbidity Index. Because “blood transfusion is the only qualifying indicator for approximately half of SMM cases … we also studied a subset of SMM that excluded those cases for which the only indication was a blood transfusion,” they noted.
SOURCE: Leonard SA et al. Ann Epidemiol. 2019 Feb 28. doi: 10.1016/j.annepidem.2019.02.007.
The according to a study covering almost 8.3 million births in California.

Changes in severe maternal morbidity (SMM) prevalence from 1997 to 2014 were fairly consistent by race/ethnicity, although increases for black (179%), Asian/Pacific Islander (175%), and Hispanic (173%) women were somewhat larger than for whites (163%), Stephanie A. Leonard, PhD, of Stanford (Calif.) University, and her associates reported in Annals of Epidemiology.
Differences between races/ethnicities over the entire study period were seen for SMM with and without transfusion-only cases. Individual-level factors such as cesarean birth, comorbidities, and anemia “contribute to, but do not fully explain, these disparities. Additionally, changes in the characteristics of pregnant women – including increases in comorbidities – have not affected racial/ethnic differences in severe maternal morbidity over time,” the investigators wrote.
The cohort study used data for 8,252,025 live births with birth certificates that were previously linked to delivery discharge records. SMM was measured using the Severe Maternity Morbidity Index. Because “blood transfusion is the only qualifying indicator for approximately half of SMM cases … we also studied a subset of SMM that excluded those cases for which the only indication was a blood transfusion,” they noted.
SOURCE: Leonard SA et al. Ann Epidemiol. 2019 Feb 28. doi: 10.1016/j.annepidem.2019.02.007.
FROM ANNALS OF EPIDEMIOLOGY
Poppy-seeking parrots, harmonious mice, and feline-fueled hospital bills
Polly want another hit?
Once again, the animals are getting high.
Parrots in India are giving opium farmers a huge and expensive headache. The birds have become addicted to the poppy crop and are taking a huge bite out of the seasonal yields. According to an opium specialist, the birds get a jolt of instant energy from the poppy flower, similar to drinking a cup of coffee. No wonder the birds keep coming back for more.
This roving (flying?) gang of parrot menaces are feeding 30-40 times a day on the plants. Farmers have tried in vain to use firecrackers to scare off the birds, but nothing will stop Polly from getting her next fix. Opium dens might be long gone, but opium nests might be the next big thing.
Sing your little mouse heart out
In addition to being a big star on American Idol: Rodent Edition, the Alston’s singing mouse could also be a key player in understanding how mammalian brains control conversations.
These musical mice, native to Central America, do something unique: They take turns singing, rather than all belting it out at once. Researchers at New York University are using these mouse powerhouses as a model to study how conversation is regulated.
Unsurprisingly, this superstar is reportedly the mouse version of Mariah Carey, requiring a very specific environment: a palatial terrarium, a highly specialized diet, a microphone-shaped swimming pool, no brown M&Ms … you get the picture.
Researchers believe the demands are worth it, however. They’ve discovered that the mice time their songs very precisely to avoid any overlap with a singing neighbor. This could lead to insight on how humans delay conversation in order to not talk over one another (except for that one annoying coworker – you know who you are).
Reason No. 48,512 to hate cats
It really is true that no good deed goes unpunished. Jeannette Parker was nice to a cat, and she ended up with a hospital bill of $48,512.
We will elaborate. Ms. Parker, a wildlife biologist in Florida, offered a stray kitten some tuna and got bitten in the process. (Reason No. 48,513: Cats will bite the hand that feeds them.) There had been rabies warnings recently and the bite did break the skin, so she decided to go to the emergency department at Mariners Hospital in Tavernier, Fla., according to Kaiser Health News. She was there 2 hours and never spoke with a physician, but she did get the first in a series of rabies shots and 12 mL of rabies immune globulin.
The next thing she received from the hospital was a bill for – you guessed it – $48,512, of which $46,422 was for the immune globulin. “My funeral would have been cheaper,” she told Kaiser.
Her husband’s insurance covered most of the bill, but Ms. Parker ended up paying the rest of her deductible and 10% of the charges accepted by her insurer, almost $4,200.
All because she tried to help a cat. Way to go, cat.
And the best doctor award goes to ...
Normally, it requires a lot of time and money to become a respected physician. Medical school, residencies – it’s tough just becoming a doctor, let alone reaching the top of your field.
However, if you’re a reporter at ProPublica who specializes in health care, you can receive the prestigious Top Doctor award for just $289 – or only $99 if you act right now. For your money, you get a customized plaque made of either cherry wood with gold trim or black with chrome trim. That’s an offer too good to pass up.
A reasonable question to ask at this point would probably be, Why is a reporter receiving an award presumably meant for an actual doctor? Well, according to the company selling the award, the reporter’s peers had nominated him and his patients had given him stellar reviews. He was without a doubt one of America’s Top Doctors. His lack of medical degree was absolutely not a problem.
Okay, the award is probably a scam. But we’re also health care reporters here at Livin’ on the MDedge, so if the Top Doctor people are reading, we’ll have the cherry wood with gold trim.

Polly want another hit?
Once again, the animals are getting high.
Parrots in India are giving opium farmers a huge and expensive headache. The birds have become addicted to the poppy crop and are taking a huge bite out of the seasonal yields. According to an opium specialist, the birds get a jolt of instant energy from the poppy flower, similar to drinking a cup of coffee. No wonder the birds keep coming back for more.
This roving (flying?) gang of parrot menaces are feeding 30-40 times a day on the plants. Farmers have tried in vain to use firecrackers to scare off the birds, but nothing will stop Polly from getting her next fix. Opium dens might be long gone, but opium nests might be the next big thing.
Sing your little mouse heart out
In addition to being a big star on American Idol: Rodent Edition, the Alston’s singing mouse could also be a key player in understanding how mammalian brains control conversations.
These musical mice, native to Central America, do something unique: They take turns singing, rather than all belting it out at once. Researchers at New York University are using these mouse powerhouses as a model to study how conversation is regulated.
Unsurprisingly, this superstar is reportedly the mouse version of Mariah Carey, requiring a very specific environment: a palatial terrarium, a highly specialized diet, a microphone-shaped swimming pool, no brown M&Ms … you get the picture.
Researchers believe the demands are worth it, however. They’ve discovered that the mice time their songs very precisely to avoid any overlap with a singing neighbor. This could lead to insight on how humans delay conversation in order to not talk over one another (except for that one annoying coworker – you know who you are).
Reason No. 48,512 to hate cats
It really is true that no good deed goes unpunished. Jeannette Parker was nice to a cat, and she ended up with a hospital bill of $48,512.
We will elaborate. Ms. Parker, a wildlife biologist in Florida, offered a stray kitten some tuna and got bitten in the process. (Reason No. 48,513: Cats will bite the hand that feeds them.) There had been rabies warnings recently and the bite did break the skin, so she decided to go to the emergency department at Mariners Hospital in Tavernier, Fla., according to Kaiser Health News. She was there 2 hours and never spoke with a physician, but she did get the first in a series of rabies shots and 12 mL of rabies immune globulin.
The next thing she received from the hospital was a bill for – you guessed it – $48,512, of which $46,422 was for the immune globulin. “My funeral would have been cheaper,” she told Kaiser.
Her husband’s insurance covered most of the bill, but Ms. Parker ended up paying the rest of her deductible and 10% of the charges accepted by her insurer, almost $4,200.
All because she tried to help a cat. Way to go, cat.
And the best doctor award goes to ...
Normally, it requires a lot of time and money to become a respected physician. Medical school, residencies – it’s tough just becoming a doctor, let alone reaching the top of your field.
However, if you’re a reporter at ProPublica who specializes in health care, you can receive the prestigious Top Doctor award for just $289 – or only $99 if you act right now. For your money, you get a customized plaque made of either cherry wood with gold trim or black with chrome trim. That’s an offer too good to pass up.
A reasonable question to ask at this point would probably be, Why is a reporter receiving an award presumably meant for an actual doctor? Well, according to the company selling the award, the reporter’s peers had nominated him and his patients had given him stellar reviews. He was without a doubt one of America’s Top Doctors. His lack of medical degree was absolutely not a problem.
Okay, the award is probably a scam. But we’re also health care reporters here at Livin’ on the MDedge, so if the Top Doctor people are reading, we’ll have the cherry wood with gold trim.

Polly want another hit?
Once again, the animals are getting high.
Parrots in India are giving opium farmers a huge and expensive headache. The birds have become addicted to the poppy crop and are taking a huge bite out of the seasonal yields. According to an opium specialist, the birds get a jolt of instant energy from the poppy flower, similar to drinking a cup of coffee. No wonder the birds keep coming back for more.
This roving (flying?) gang of parrot menaces are feeding 30-40 times a day on the plants. Farmers have tried in vain to use firecrackers to scare off the birds, but nothing will stop Polly from getting her next fix. Opium dens might be long gone, but opium nests might be the next big thing.
Sing your little mouse heart out
In addition to being a big star on American Idol: Rodent Edition, the Alston’s singing mouse could also be a key player in understanding how mammalian brains control conversations.
These musical mice, native to Central America, do something unique: They take turns singing, rather than all belting it out at once. Researchers at New York University are using these mouse powerhouses as a model to study how conversation is regulated.
Unsurprisingly, this superstar is reportedly the mouse version of Mariah Carey, requiring a very specific environment: a palatial terrarium, a highly specialized diet, a microphone-shaped swimming pool, no brown M&Ms … you get the picture.
Researchers believe the demands are worth it, however. They’ve discovered that the mice time their songs very precisely to avoid any overlap with a singing neighbor. This could lead to insight on how humans delay conversation in order to not talk over one another (except for that one annoying coworker – you know who you are).
Reason No. 48,512 to hate cats
It really is true that no good deed goes unpunished. Jeannette Parker was nice to a cat, and she ended up with a hospital bill of $48,512.
We will elaborate. Ms. Parker, a wildlife biologist in Florida, offered a stray kitten some tuna and got bitten in the process. (Reason No. 48,513: Cats will bite the hand that feeds them.) There had been rabies warnings recently and the bite did break the skin, so she decided to go to the emergency department at Mariners Hospital in Tavernier, Fla., according to Kaiser Health News. She was there 2 hours and never spoke with a physician, but she did get the first in a series of rabies shots and 12 mL of rabies immune globulin.
The next thing she received from the hospital was a bill for – you guessed it – $48,512, of which $46,422 was for the immune globulin. “My funeral would have been cheaper,” she told Kaiser.
Her husband’s insurance covered most of the bill, but Ms. Parker ended up paying the rest of her deductible and 10% of the charges accepted by her insurer, almost $4,200.
All because she tried to help a cat. Way to go, cat.
And the best doctor award goes to ...
Normally, it requires a lot of time and money to become a respected physician. Medical school, residencies – it’s tough just becoming a doctor, let alone reaching the top of your field.
However, if you’re a reporter at ProPublica who specializes in health care, you can receive the prestigious Top Doctor award for just $289 – or only $99 if you act right now. For your money, you get a customized plaque made of either cherry wood with gold trim or black with chrome trim. That’s an offer too good to pass up.
A reasonable question to ask at this point would probably be, Why is a reporter receiving an award presumably meant for an actual doctor? Well, according to the company selling the award, the reporter’s peers had nominated him and his patients had given him stellar reviews. He was without a doubt one of America’s Top Doctors. His lack of medical degree was absolutely not a problem.
Okay, the award is probably a scam. But we’re also health care reporters here at Livin’ on the MDedge, so if the Top Doctor people are reading, we’ll have the cherry wood with gold trim.










