User login
Official news magazine of the Society of Hospital Medicine
Copyright by Society of Hospital Medicine or related companies. All rights reserved. ISSN 1553-085X
nav[contains(@class, 'nav-ce-stack nav-ce-stack__large-screen')]
header[@id='header']
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'main-prefix')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
div[contains(@class, 'view-medstat-quiz-listing-panes')]
div[contains(@class, 'pane-article-sidebar-latest-news')]
div[contains(@class, 'pane-pub-article-hospitalist')]


Discontinuing Inhaled Corticosteroids in COPD Reduces Risk of Pneumonia
Clinical question: Is discontinuation of inhaled corticosteroids (ICSs) in patients with COPD associated with a decreased risk of pneumonia?
Background: ICSs are used in up to 85% of patients treated for COPD but may be associated with adverse systemic side effects including pneumonia. Trials looking at weaning patients off ICSs and replacing with long-acting bronchodilators have found few adverse outcomes; however, the benefits of discontinuation on adverse events, including pneumonia, have been unclear.
Study design: Case-control study.
Setting: Quebec health systems.
Synopsis: Using the Quebec health insurance databases, a study cohort of 103,386 patients with COPD on ICSs was created. Patients were followed for a mean of 4.9 years; 14,020 patients who were hospitalized for pneumonia or died from pneumonia outside the hospital were matched to control subjects. Discontinuation of ICSs was associated with a 37% decrease in serious pneumonia (relative risk [RR] 0.63; 95% CI, 0.60–0.66). The risk reduction occurred as early as one month after discontinuation of ICSs. Risk reduction was greater with fluticasone (RR 0.58; 95% CI, 0.54–0.61) than with budesonide (RR 0.87; 95% CI, 0.7–0.97).
Population size and follow-up may contribute to why risk reduction in pneumonia was seen in this study but not in other recent randomized trials on discontinuation of ICSs. A limitation of this study was its observational design; however, its results suggest that use of ICSs in COPD patients should be highly selective, as indiscriminate use can subject patients to elevated risk of hospitalization or death from pneumonia.
Bottom line: Discontinuation of ICSs in patients with COPD is associated with a decreased risk of contracting serious pneumonia. This reduction appears greatest with fluticasone.
Citation: Suissa S, Coulombe J, Ernst P. Discontinuation of inhaled corticosteroids in COPD and the risk reduction of pneumonia. Chest. 2015;148(5):1177-1183.
Short Take
Increase in Rates of Prescription Drug Use and Polypharmacy Seen
The percentage of Americans who reported taking prescription medications increased substantially from 1999 to 2012 (51% to 59%), as did the percentage who reported taking at least five prescription medications.
Citation: Kantor ED, Rehm CD, Haas JS, Chan AT, Giovannucci EL. Trends in prescription drug use among adults in the United States from 1999-2012. JAMA. 2015;314(17):1818-1830.
Clinical question: Is discontinuation of inhaled corticosteroids (ICSs) in patients with COPD associated with a decreased risk of pneumonia?
Background: ICSs are used in up to 85% of patients treated for COPD but may be associated with adverse systemic side effects including pneumonia. Trials looking at weaning patients off ICSs and replacing with long-acting bronchodilators have found few adverse outcomes; however, the benefits of discontinuation on adverse events, including pneumonia, have been unclear.
Study design: Case-control study.
Setting: Quebec health systems.
Synopsis: Using the Quebec health insurance databases, a study cohort of 103,386 patients with COPD on ICSs was created. Patients were followed for a mean of 4.9 years; 14,020 patients who were hospitalized for pneumonia or died from pneumonia outside the hospital were matched to control subjects. Discontinuation of ICSs was associated with a 37% decrease in serious pneumonia (relative risk [RR] 0.63; 95% CI, 0.60–0.66). The risk reduction occurred as early as one month after discontinuation of ICSs. Risk reduction was greater with fluticasone (RR 0.58; 95% CI, 0.54–0.61) than with budesonide (RR 0.87; 95% CI, 0.7–0.97).
Population size and follow-up may contribute to why risk reduction in pneumonia was seen in this study but not in other recent randomized trials on discontinuation of ICSs. A limitation of this study was its observational design; however, its results suggest that use of ICSs in COPD patients should be highly selective, as indiscriminate use can subject patients to elevated risk of hospitalization or death from pneumonia.
Bottom line: Discontinuation of ICSs in patients with COPD is associated with a decreased risk of contracting serious pneumonia. This reduction appears greatest with fluticasone.
Citation: Suissa S, Coulombe J, Ernst P. Discontinuation of inhaled corticosteroids in COPD and the risk reduction of pneumonia. Chest. 2015;148(5):1177-1183.
Short Take
Increase in Rates of Prescription Drug Use and Polypharmacy Seen
The percentage of Americans who reported taking prescription medications increased substantially from 1999 to 2012 (51% to 59%), as did the percentage who reported taking at least five prescription medications.
Citation: Kantor ED, Rehm CD, Haas JS, Chan AT, Giovannucci EL. Trends in prescription drug use among adults in the United States from 1999-2012. JAMA. 2015;314(17):1818-1830.
Clinical question: Is discontinuation of inhaled corticosteroids (ICSs) in patients with COPD associated with a decreased risk of pneumonia?
Background: ICSs are used in up to 85% of patients treated for COPD but may be associated with adverse systemic side effects including pneumonia. Trials looking at weaning patients off ICSs and replacing with long-acting bronchodilators have found few adverse outcomes; however, the benefits of discontinuation on adverse events, including pneumonia, have been unclear.
Study design: Case-control study.
Setting: Quebec health systems.
Synopsis: Using the Quebec health insurance databases, a study cohort of 103,386 patients with COPD on ICSs was created. Patients were followed for a mean of 4.9 years; 14,020 patients who were hospitalized for pneumonia or died from pneumonia outside the hospital were matched to control subjects. Discontinuation of ICSs was associated with a 37% decrease in serious pneumonia (relative risk [RR] 0.63; 95% CI, 0.60–0.66). The risk reduction occurred as early as one month after discontinuation of ICSs. Risk reduction was greater with fluticasone (RR 0.58; 95% CI, 0.54–0.61) than with budesonide (RR 0.87; 95% CI, 0.7–0.97).
Population size and follow-up may contribute to why risk reduction in pneumonia was seen in this study but not in other recent randomized trials on discontinuation of ICSs. A limitation of this study was its observational design; however, its results suggest that use of ICSs in COPD patients should be highly selective, as indiscriminate use can subject patients to elevated risk of hospitalization or death from pneumonia.
Bottom line: Discontinuation of ICSs in patients with COPD is associated with a decreased risk of contracting serious pneumonia. This reduction appears greatest with fluticasone.
Citation: Suissa S, Coulombe J, Ernst P. Discontinuation of inhaled corticosteroids in COPD and the risk reduction of pneumonia. Chest. 2015;148(5):1177-1183.
Short Take
Increase in Rates of Prescription Drug Use and Polypharmacy Seen
The percentage of Americans who reported taking prescription medications increased substantially from 1999 to 2012 (51% to 59%), as did the percentage who reported taking at least five prescription medications.
Citation: Kantor ED, Rehm CD, Haas JS, Chan AT, Giovannucci EL. Trends in prescription drug use among adults in the United States from 1999-2012. JAMA. 2015;314(17):1818-1830.
MEDS Score for Sepsis Might Best Predict ED Mortality
Clinical question: Which illness severity score best predicts outcomes in emergency department (ED) patients presenting with infection?
Background: Several scoring models have been developed to predict illness severity and mortality in patients with infection. Some scores were developed specifically for patients with sepsis and others for patients in a general critical care setting. These different scoring models have not been specifically compared and validated in the ED setting in patients with infection of various severities.
Study design: Prospective, observational study.
Setting: Adult ED in a metropolitan tertiary, university-affiliated hospital.
Synopsis: Investigators prospectively identified 8,871 adult inpatients with infection from a single-center ED. Data to calculate five prediction models were collected. The models were:
- Mortality in Emergency Department Sepsis (MEDS) score;
- Acute Physiology and Chronic Health Evaluation II (APACHE II);
- Simplified Acute Physiology Score II (SAPS II);
- Sequential Organ Failure Assessment (SOFA); and
- Severe Sepsis Score (SSS).
Severity score performance was assessed for the overall cohort and for subgroups, including infection without systemic inflammatory response syndrome, sepsis, severe sepsis, and septic shock. The MEDS score best predicted mortality in the cohort, with an area under the receiver operating characteristics curve of 0.92. However, older scoring models such as the APACHE II and SAPS II still discriminated well, especially in patients who were admitted to the ICU. All scores tended to overestimate mortality.
Bottom line: The MEDS score may best predict illness severity in septic patients presenting to the ED, but other scoring models may be better-suited for specific patient populations.
Citation: Williams JM, Greenslade JH, Chu K, Brown AF, Lipman J. Severity scores in emergency department patients with presumed infection: a prospective validation study. Crit Care Med. 2016;44(3):539-547.
Clinical question: Which illness severity score best predicts outcomes in emergency department (ED) patients presenting with infection?
Background: Several scoring models have been developed to predict illness severity and mortality in patients with infection. Some scores were developed specifically for patients with sepsis and others for patients in a general critical care setting. These different scoring models have not been specifically compared and validated in the ED setting in patients with infection of various severities.
Study design: Prospective, observational study.
Setting: Adult ED in a metropolitan tertiary, university-affiliated hospital.
Synopsis: Investigators prospectively identified 8,871 adult inpatients with infection from a single-center ED. Data to calculate five prediction models were collected. The models were:
- Mortality in Emergency Department Sepsis (MEDS) score;
- Acute Physiology and Chronic Health Evaluation II (APACHE II);
- Simplified Acute Physiology Score II (SAPS II);
- Sequential Organ Failure Assessment (SOFA); and
- Severe Sepsis Score (SSS).
Severity score performance was assessed for the overall cohort and for subgroups, including infection without systemic inflammatory response syndrome, sepsis, severe sepsis, and septic shock. The MEDS score best predicted mortality in the cohort, with an area under the receiver operating characteristics curve of 0.92. However, older scoring models such as the APACHE II and SAPS II still discriminated well, especially in patients who were admitted to the ICU. All scores tended to overestimate mortality.
Bottom line: The MEDS score may best predict illness severity in septic patients presenting to the ED, but other scoring models may be better-suited for specific patient populations.
Citation: Williams JM, Greenslade JH, Chu K, Brown AF, Lipman J. Severity scores in emergency department patients with presumed infection: a prospective validation study. Crit Care Med. 2016;44(3):539-547.
Clinical question: Which illness severity score best predicts outcomes in emergency department (ED) patients presenting with infection?
Background: Several scoring models have been developed to predict illness severity and mortality in patients with infection. Some scores were developed specifically for patients with sepsis and others for patients in a general critical care setting. These different scoring models have not been specifically compared and validated in the ED setting in patients with infection of various severities.
Study design: Prospective, observational study.
Setting: Adult ED in a metropolitan tertiary, university-affiliated hospital.
Synopsis: Investigators prospectively identified 8,871 adult inpatients with infection from a single-center ED. Data to calculate five prediction models were collected. The models were:
- Mortality in Emergency Department Sepsis (MEDS) score;
- Acute Physiology and Chronic Health Evaluation II (APACHE II);
- Simplified Acute Physiology Score II (SAPS II);
- Sequential Organ Failure Assessment (SOFA); and
- Severe Sepsis Score (SSS).
Severity score performance was assessed for the overall cohort and for subgroups, including infection without systemic inflammatory response syndrome, sepsis, severe sepsis, and septic shock. The MEDS score best predicted mortality in the cohort, with an area under the receiver operating characteristics curve of 0.92. However, older scoring models such as the APACHE II and SAPS II still discriminated well, especially in patients who were admitted to the ICU. All scores tended to overestimate mortality.
Bottom line: The MEDS score may best predict illness severity in septic patients presenting to the ED, but other scoring models may be better-suited for specific patient populations.
Citation: Williams JM, Greenslade JH, Chu K, Brown AF, Lipman J. Severity scores in emergency department patients with presumed infection: a prospective validation study. Crit Care Med. 2016;44(3):539-547.
Gum Disease is Linked to Faster Cognitive Decline for Alzhemier's Patients
(Reuters Health) - For people with Alzheimer's disease, having gum disease is tied to faster cognitive decline, according to a new study.
"What we have shown is that regardless of the severity of dementia (within this mild to moderate impaired group) that patients with more severe gum disease are declining more rapidly," said senior author Clive Holmes of the University of Southampton in the UK.
In other studies, Holmes and his coauthors have found that conditions such as chest infections, urinary tract infections, rheumatoid arthritis and diabetes are associated with faster disease progression in Alzheimer's, he said.
"We hadn't previously looked at gum disease because MDs tendto leave this in the hands of dentists but it is an important common low grade chronic infection," Holmes told Reuters Health by email.
The researchers observed 60 people with mild to moderate Alzheimer's disease living at home for six months. The participants did not smoke, had not been treated for gum disease within the previous six months, and had at least 10 teeth.
At the start, each participant completed a cognitive assessment, gave a blood sample, was examined by a dental hygienist and their main caregiver was interviewed to provide a medical and dental history. The same tests and interviews were repeated six months later.
Of the 60 people in the study, 22 had moderate to severe gum disease at the beginning of the study. By six months later, one participant had died, three had withdrawn from the study and three were lost to follow-up.
Cognitive score declined more for those who had periodontitis to begin with than for those who did not, the researchers reported February 24 in PLoS One.
According to one theory, cognitive impairment leads to adverse oral health due to inattention to routine oral hygiene and care, said Dr. James M. Noble of the Taub Institute for Research on Alzheimer's Disease and the Aging Brain at Columbia University Medical Center in New York City, who was not part of the new study.
"The second, and the one I'm most intrigued by, is whether or not periodontal disease has an influence on cognitive outcomes of aging, either as an independent risk factor for (new-onset) cognitive impairment including Alzheimer's disease, or more rapid decline once (Alzheimer's disease) has been diagnosed, as was suggested by this study," Noble told Reuters Health by email.
Gum disease may cause chronic low-grade inflammation in the rest of the body, and inflammation is associated with changes in the brain, he said.
"It is known that gum disease is associated with increased markers of inflammation," Holmes said.
But the new study indicates a connection between gum disease and cognitive decline, not necessarily that one causes the other, he said. Further studies need to assess whether treatingthe gum disease would also slow cognitive decline.
"Periodontitis has been associated with heart disease and stroke among other conditions," Noble said. Based on this and other studies, "it seems to be good advice to brush and floss," Noble said.
(Reuters Health) - For people with Alzheimer's disease, having gum disease is tied to faster cognitive decline, according to a new study.
"What we have shown is that regardless of the severity of dementia (within this mild to moderate impaired group) that patients with more severe gum disease are declining more rapidly," said senior author Clive Holmes of the University of Southampton in the UK.
In other studies, Holmes and his coauthors have found that conditions such as chest infections, urinary tract infections, rheumatoid arthritis and diabetes are associated with faster disease progression in Alzheimer's, he said.
"We hadn't previously looked at gum disease because MDs tendto leave this in the hands of dentists but it is an important common low grade chronic infection," Holmes told Reuters Health by email.
The researchers observed 60 people with mild to moderate Alzheimer's disease living at home for six months. The participants did not smoke, had not been treated for gum disease within the previous six months, and had at least 10 teeth.
At the start, each participant completed a cognitive assessment, gave a blood sample, was examined by a dental hygienist and their main caregiver was interviewed to provide a medical and dental history. The same tests and interviews were repeated six months later.
Of the 60 people in the study, 22 had moderate to severe gum disease at the beginning of the study. By six months later, one participant had died, three had withdrawn from the study and three were lost to follow-up.
Cognitive score declined more for those who had periodontitis to begin with than for those who did not, the researchers reported February 24 in PLoS One.
According to one theory, cognitive impairment leads to adverse oral health due to inattention to routine oral hygiene and care, said Dr. James M. Noble of the Taub Institute for Research on Alzheimer's Disease and the Aging Brain at Columbia University Medical Center in New York City, who was not part of the new study.
"The second, and the one I'm most intrigued by, is whether or not periodontal disease has an influence on cognitive outcomes of aging, either as an independent risk factor for (new-onset) cognitive impairment including Alzheimer's disease, or more rapid decline once (Alzheimer's disease) has been diagnosed, as was suggested by this study," Noble told Reuters Health by email.
Gum disease may cause chronic low-grade inflammation in the rest of the body, and inflammation is associated with changes in the brain, he said.
"It is known that gum disease is associated with increased markers of inflammation," Holmes said.
But the new study indicates a connection between gum disease and cognitive decline, not necessarily that one causes the other, he said. Further studies need to assess whether treatingthe gum disease would also slow cognitive decline.
"Periodontitis has been associated with heart disease and stroke among other conditions," Noble said. Based on this and other studies, "it seems to be good advice to brush and floss," Noble said.
(Reuters Health) - For people with Alzheimer's disease, having gum disease is tied to faster cognitive decline, according to a new study.
"What we have shown is that regardless of the severity of dementia (within this mild to moderate impaired group) that patients with more severe gum disease are declining more rapidly," said senior author Clive Holmes of the University of Southampton in the UK.
In other studies, Holmes and his coauthors have found that conditions such as chest infections, urinary tract infections, rheumatoid arthritis and diabetes are associated with faster disease progression in Alzheimer's, he said.
"We hadn't previously looked at gum disease because MDs tendto leave this in the hands of dentists but it is an important common low grade chronic infection," Holmes told Reuters Health by email.
The researchers observed 60 people with mild to moderate Alzheimer's disease living at home for six months. The participants did not smoke, had not been treated for gum disease within the previous six months, and had at least 10 teeth.
At the start, each participant completed a cognitive assessment, gave a blood sample, was examined by a dental hygienist and their main caregiver was interviewed to provide a medical and dental history. The same tests and interviews were repeated six months later.
Of the 60 people in the study, 22 had moderate to severe gum disease at the beginning of the study. By six months later, one participant had died, three had withdrawn from the study and three were lost to follow-up.
Cognitive score declined more for those who had periodontitis to begin with than for those who did not, the researchers reported February 24 in PLoS One.
According to one theory, cognitive impairment leads to adverse oral health due to inattention to routine oral hygiene and care, said Dr. James M. Noble of the Taub Institute for Research on Alzheimer's Disease and the Aging Brain at Columbia University Medical Center in New York City, who was not part of the new study.
"The second, and the one I'm most intrigued by, is whether or not periodontal disease has an influence on cognitive outcomes of aging, either as an independent risk factor for (new-onset) cognitive impairment including Alzheimer's disease, or more rapid decline once (Alzheimer's disease) has been diagnosed, as was suggested by this study," Noble told Reuters Health by email.
Gum disease may cause chronic low-grade inflammation in the rest of the body, and inflammation is associated with changes in the brain, he said.
"It is known that gum disease is associated with increased markers of inflammation," Holmes said.
But the new study indicates a connection between gum disease and cognitive decline, not necessarily that one causes the other, he said. Further studies need to assess whether treatingthe gum disease would also slow cognitive decline.
"Periodontitis has been associated with heart disease and stroke among other conditions," Noble said. Based on this and other studies, "it seems to be good advice to brush and floss," Noble said.
Key Communication Tactics Highlighted in 'Everything We Say and Do'
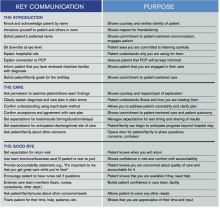
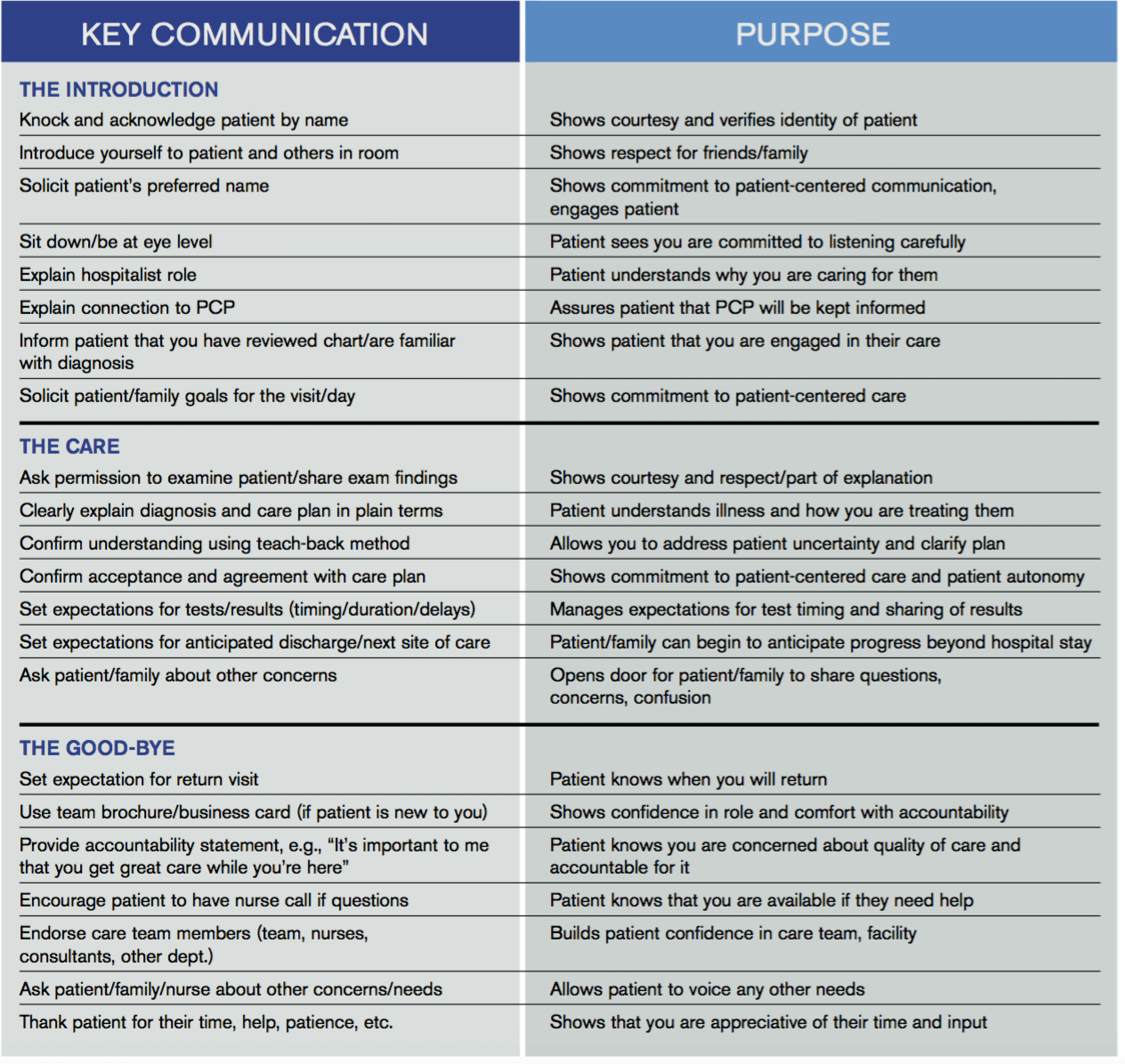
“Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Below is a chart of the “key communication” tactics.
“Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Below is a chart of the “key communication” tactics.
“Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Below is a chart of the “key communication” tactics.
CDC Released Voluntary Guidelines to Help Lower Opioid and Abuse of Painkillers
(Reuters) - Addressing a growing "epidemic" of opioid overdoses and abuse of the prescribed painkillers in the United States, the Centers for Disease Control and Prevention on Tuesday released voluntary guidelines that instruct primary care doctors to sharply deter use of the medicines for chronic pain.
"Overprescribing opioids, largely for chronic pain, is a key driver of America's drug-overdose epidemic," said CDC Director Tom Frieden. Sales of the prescription therapies have quadrupled since 1999, causing 165,000 fatal overdoses over the same period and now growing at more than 40 per day, according to the agency.
Primary care doctors who treat adults for chronic pain in outpatient settings account for nearly half of all opioid prescriptions, the CDC said. It defined chronic pain as lasting longer than three months, or past the typical time it takes for normal tissue healing.
The new guidelines recommend non-opioids, including acetaminophen and ibuprofen, as preferred therapy for chronic pain unless patients have active cancer or are receiving palliative or end-of-life care.
When opioids are used, the lowest possible dose should be prescribed to reduce risks of opioid abuse and overdose and patients should then be closely monitored, according to the CDC guidelines. The drugs should also be combined with non-drug approaches to controlling pain, like physical therapy and exercise, the agency said.
Moreover, when starting opioid therapy for chronic pain, doctors should prescribe immediate-release formulations instead of long-acting versions, the guidelines say. They recommend doctors avoid prescribing opioids with sedatives called benzodiazepines.
When prescribed for acute, or short-term pain, doctors should prescribe the lowest effective dose of immediate release opioids.
"Three days or less will often be sufficient; more than seven days will rarely be needed," the guidelines say.
Some studies suggest only 5 percent of patients prescribed opioids receive them for chronic pain, but they account for 70 percent of overall opioid prescriptions and the majority of overdoses.
For the vast majority of patients taking opioids for chronic pain, risks from the drugs will outweigh benefits, Frieden said. "The prescription overdose epidemic is doctor-driven," Frieden said, adding it can be reversed if doctors rein in their prescriptions of the painkillers.
The American College of Physicians on Tuesday said the new guidelines provide important guidance "at a time when many communities are being devastated by the adverse impact of opioid misuse."
The most widely used opioids include hydrocodone, which is the main active ingredient of Vicodin, and oxycodone, an active ingredient of OxyContin and Percocet. They are synthetic narcotics which work by binding to opioid receptors in the brain and are mostly available in pill form.
Nearly two million Americans aged 12 or older either abused or were dependent on prescription opioids in 2014, the CDC said.
Opioids also include heroin, an illegal injectable drug which has become a far cheaper alternative to oral opioids on the streets of many U.S. communities, causing many overdoses.
Other U.S. health officials on Tuesday said first responders should have wider access to naloxone, a drug that can reverse opioid overdoses.
SHM offers a safe opioid prescribing implementation guideline. The Implementation Toolkit, Reducing Adverse Drug Events related to Opioids, or RADEO, provides step-by step instructions for hospitals to implement a successful QI program to make opioid prescribing safer, with fewer adverse events, and much less likely to result in dangerous sedation, respiratory depression and death. Its scope is for hospitalized patients.
(Reuters) - Addressing a growing "epidemic" of opioid overdoses and abuse of the prescribed painkillers in the United States, the Centers for Disease Control and Prevention on Tuesday released voluntary guidelines that instruct primary care doctors to sharply deter use of the medicines for chronic pain.
"Overprescribing opioids, largely for chronic pain, is a key driver of America's drug-overdose epidemic," said CDC Director Tom Frieden. Sales of the prescription therapies have quadrupled since 1999, causing 165,000 fatal overdoses over the same period and now growing at more than 40 per day, according to the agency.
Primary care doctors who treat adults for chronic pain in outpatient settings account for nearly half of all opioid prescriptions, the CDC said. It defined chronic pain as lasting longer than three months, or past the typical time it takes for normal tissue healing.
The new guidelines recommend non-opioids, including acetaminophen and ibuprofen, as preferred therapy for chronic pain unless patients have active cancer or are receiving palliative or end-of-life care.
When opioids are used, the lowest possible dose should be prescribed to reduce risks of opioid abuse and overdose and patients should then be closely monitored, according to the CDC guidelines. The drugs should also be combined with non-drug approaches to controlling pain, like physical therapy and exercise, the agency said.
Moreover, when starting opioid therapy for chronic pain, doctors should prescribe immediate-release formulations instead of long-acting versions, the guidelines say. They recommend doctors avoid prescribing opioids with sedatives called benzodiazepines.
When prescribed for acute, or short-term pain, doctors should prescribe the lowest effective dose of immediate release opioids.
"Three days or less will often be sufficient; more than seven days will rarely be needed," the guidelines say.
Some studies suggest only 5 percent of patients prescribed opioids receive them for chronic pain, but they account for 70 percent of overall opioid prescriptions and the majority of overdoses.
For the vast majority of patients taking opioids for chronic pain, risks from the drugs will outweigh benefits, Frieden said. "The prescription overdose epidemic is doctor-driven," Frieden said, adding it can be reversed if doctors rein in their prescriptions of the painkillers.
The American College of Physicians on Tuesday said the new guidelines provide important guidance "at a time when many communities are being devastated by the adverse impact of opioid misuse."
The most widely used opioids include hydrocodone, which is the main active ingredient of Vicodin, and oxycodone, an active ingredient of OxyContin and Percocet. They are synthetic narcotics which work by binding to opioid receptors in the brain and are mostly available in pill form.
Nearly two million Americans aged 12 or older either abused or were dependent on prescription opioids in 2014, the CDC said.
Opioids also include heroin, an illegal injectable drug which has become a far cheaper alternative to oral opioids on the streets of many U.S. communities, causing many overdoses.
Other U.S. health officials on Tuesday said first responders should have wider access to naloxone, a drug that can reverse opioid overdoses.
SHM offers a safe opioid prescribing implementation guideline. The Implementation Toolkit, Reducing Adverse Drug Events related to Opioids, or RADEO, provides step-by step instructions for hospitals to implement a successful QI program to make opioid prescribing safer, with fewer adverse events, and much less likely to result in dangerous sedation, respiratory depression and death. Its scope is for hospitalized patients.
(Reuters) - Addressing a growing "epidemic" of opioid overdoses and abuse of the prescribed painkillers in the United States, the Centers for Disease Control and Prevention on Tuesday released voluntary guidelines that instruct primary care doctors to sharply deter use of the medicines for chronic pain.
"Overprescribing opioids, largely for chronic pain, is a key driver of America's drug-overdose epidemic," said CDC Director Tom Frieden. Sales of the prescription therapies have quadrupled since 1999, causing 165,000 fatal overdoses over the same period and now growing at more than 40 per day, according to the agency.
Primary care doctors who treat adults for chronic pain in outpatient settings account for nearly half of all opioid prescriptions, the CDC said. It defined chronic pain as lasting longer than three months, or past the typical time it takes for normal tissue healing.
The new guidelines recommend non-opioids, including acetaminophen and ibuprofen, as preferred therapy for chronic pain unless patients have active cancer or are receiving palliative or end-of-life care.
When opioids are used, the lowest possible dose should be prescribed to reduce risks of opioid abuse and overdose and patients should then be closely monitored, according to the CDC guidelines. The drugs should also be combined with non-drug approaches to controlling pain, like physical therapy and exercise, the agency said.
Moreover, when starting opioid therapy for chronic pain, doctors should prescribe immediate-release formulations instead of long-acting versions, the guidelines say. They recommend doctors avoid prescribing opioids with sedatives called benzodiazepines.
When prescribed for acute, or short-term pain, doctors should prescribe the lowest effective dose of immediate release opioids.
"Three days or less will often be sufficient; more than seven days will rarely be needed," the guidelines say.
Some studies suggest only 5 percent of patients prescribed opioids receive them for chronic pain, but they account for 70 percent of overall opioid prescriptions and the majority of overdoses.
For the vast majority of patients taking opioids for chronic pain, risks from the drugs will outweigh benefits, Frieden said. "The prescription overdose epidemic is doctor-driven," Frieden said, adding it can be reversed if doctors rein in their prescriptions of the painkillers.
The American College of Physicians on Tuesday said the new guidelines provide important guidance "at a time when many communities are being devastated by the adverse impact of opioid misuse."
The most widely used opioids include hydrocodone, which is the main active ingredient of Vicodin, and oxycodone, an active ingredient of OxyContin and Percocet. They are synthetic narcotics which work by binding to opioid receptors in the brain and are mostly available in pill form.
Nearly two million Americans aged 12 or older either abused or were dependent on prescription opioids in 2014, the CDC said.
Opioids also include heroin, an illegal injectable drug which has become a far cheaper alternative to oral opioids on the streets of many U.S. communities, causing many overdoses.
Other U.S. health officials on Tuesday said first responders should have wider access to naloxone, a drug that can reverse opioid overdoses.
SHM offers a safe opioid prescribing implementation guideline. The Implementation Toolkit, Reducing Adverse Drug Events related to Opioids, or RADEO, provides step-by step instructions for hospitals to implement a successful QI program to make opioid prescribing safer, with fewer adverse events, and much less likely to result in dangerous sedation, respiratory depression and death. Its scope is for hospitalized patients.
Hospital Medicine 2016 Brims with Lively Talks, Record Crowds in San Diego
Yes, it rained some in dry San Diego—for the first time in a month, according to locals. But that was the extent of the disappointment at HM16—SHM’s annual meeting highlighted by inspiring words from the U.S. surgeon general, a fellow hospitalist.
Read more about the speakers at HM16.
HM16 featured fascinating perspectives from giants in the field, vigorous panel discussions, lively workshops, streamlined how-to’s, encouraging work-life talks, and practical presentations on management.
And a record-breaking crowd continued the field’s trajectory of expansion.
“You were 4,000 strong this year,” said assistant course director Leonard Feldman, MD, SFHM. “Next year, let’s try for five.”
Yes, it rained some in dry San Diego—for the first time in a month, according to locals. But that was the extent of the disappointment at HM16—SHM’s annual meeting highlighted by inspiring words from the U.S. surgeon general, a fellow hospitalist.
Read more about the speakers at HM16.
HM16 featured fascinating perspectives from giants in the field, vigorous panel discussions, lively workshops, streamlined how-to’s, encouraging work-life talks, and practical presentations on management.
And a record-breaking crowd continued the field’s trajectory of expansion.
“You were 4,000 strong this year,” said assistant course director Leonard Feldman, MD, SFHM. “Next year, let’s try for five.”
Yes, it rained some in dry San Diego—for the first time in a month, according to locals. But that was the extent of the disappointment at HM16—SHM’s annual meeting highlighted by inspiring words from the U.S. surgeon general, a fellow hospitalist.
Read more about the speakers at HM16.
HM16 featured fascinating perspectives from giants in the field, vigorous panel discussions, lively workshops, streamlined how-to’s, encouraging work-life talks, and practical presentations on management.
And a record-breaking crowd continued the field’s trajectory of expansion.
“You were 4,000 strong this year,” said assistant course director Leonard Feldman, MD, SFHM. “Next year, let’s try for five.”
Community Partnerships, Data Key to Readmission Reduction in Diverse Populations
“We found it wasn’t on a bus route,” says Janice Finder, RN, MSN, director of the hospital’s Transitions in Care program and a part of SHM’s Project BOOST, which focuses on successful discharge outcomes. So in collaboration with the Texas Department of Aging and Disability Services, the hospital provided cab vouchers for these patients to travel to and from appointments.
The hospital also realized that to improve the chances its large Hispanic diabetic population remained healthy, it would need to tailor its disease management efforts to their culture, particularly when it came to diet.
“Their eating habits are very different, and we want to ensure they have meals based on what they actually eat,” Finder says.
These are exactly the kinds of approaches a new guide developed for the Centers for Medicare & Medicaid Services (CMS) by the Disparities Solutions Center (DSC), based at Massachusetts General Hospital (MGH) in Boston, is looking to promote in an effort to reduce unnecessary hospital readmissions.1 CMS recently made the Guide to Preventing Readmissions among Racially and Ethnically Diverse Medicare Beneficiaries available on its website.
“We know readmissions is an issue for diverse populations, that they are more likely than their white counterparts to be admitted within 30 days of discharge,” says Aswita Tan-McGrory, MBA, MSPH, deputy director of DSC within the Mongan Institute for Health Policy at MGH. “So there was a good business case for creating this guide.”
Keys to Success
Within the guide is a collection of evidence-based information, case studies, and seven recommendations the DSC team assembled to assist hospital leaders looking to reduce readmissions among some of the nation’s highest-risk populations.
While Tan-McGrory acknowledges it may be impractical for hospitals to adopt each recommendation, she says they can pick and choose which they can most effectively adopt.
“We put together these seven steps and looked for who does this really well, and the honest truth is not very many are,” she says. “It’s a complicated process, but it’s some guidance because there really wasn’t anything out there.”
Included in the recommendations: Create a “strong radar” (engage in robust data collection), identify root causes, begin to think about discharge at admission, deploy a team, consider systems and social determinants, focus on culturally competent communication, and foster community partnerships.
“It’s not just medication reconciliation or discharge instructions in a different language,” Tan-McGrory says. “What happens when a patient gets home?”
These types of questions are important because CMS now penalizes hospitals for what it deems excessive avoidable readmissions within 30 days of discharge. In 2016, hospitals can lose up to 3% of their Medicare payments under the Hospital Readmissions Reduction Program.
In 2014, nearly 18% of Medicare patients were admitted within a month of discharge at a cost of $26 billion.2 According to the new guide, Agency for Healthcare Research and Quality data indicate African-American and Hispanic patients make up a higher share of these readmissions, in part because they are disproportionately affected by chronic high-readmission-risk diseases like congestive heart failure.
Social Determinants
Though it’s challenging for healthcare providers, one way to reduce readmissions is to address the social determinants of health, Tan-McGrory says.
“Hospitals have felt in the past that it’s not their domain, but their patients are coming back,” she says. “How do you address people’s isolation at home? How can you send them from the hospital when no one is there to follow up or take care of them?”
The answers may lie in part on building community partnerships, something in which Finder’s hospital has successfully engaged. For example, the hospital has teamed with its local United Way to work with Asian patients on issues related to pain management and palliative care.
At Berkshire Medical Center, a 300-bed community teaching hospital in western Massachusetts, electronic health software helps staff flag patients at admission for potential readmission risks. Looking briefly at the new guide, William DeMarco, DO, SFHM, chief of hospital medicine (and also part of Project BOOST), noticed several new areas they may be able to incorporate into the system.
But adequate data collection and interpretation to help understand these disparities is not always possible, particularly for readmissions, Dr. DeMarco says.
However, as in one of the case studies examined in the DCS guide, Berkshire recently began to identify its high utilizers, pairing multidisciplinary teams with individual primary care providers in order to help meet these patients’ needs.
“It can take several hours for one patient, coordinating and getting a lot of people together,” Dr. DeMarco says. “It’s the only way to accomplish that goal, but it’s very resource intensive.”
Although hospitals traditionally focus on what they can do within their four walls, providers are becoming increasingly aware that the social determinants of health—like transportation, dietary choices, and language barriers—deeply impact some racial and ethnically diverse populations. Now, CMS thinks it’s worth paying closer attention. TH
Kelly April Tyrrell is a freelance writer in Madison, Wis.
References
- Betancourt JR, Tan-McGrory A, Kenst KS. Guide to preventing readmissions among racially and ethnically diverse medicare beneficiaries. Prepared by the Disparities Solutions Center, Mongan Institute for Health Policy at Massachusetts General Hospital. Baltimore, MD: Centers for Medicare & Medicaid Services Office of Minority Health; September 2015.
- Rau J. Medicare fines 2,610 hospitals in third round of readmission penalties. Kaiser Health News. Available at: http://kaiserhealthnews.org/news/medicare-readmissions-penalties-2015/. Accessed February 15, 2016.
“We found it wasn’t on a bus route,” says Janice Finder, RN, MSN, director of the hospital’s Transitions in Care program and a part of SHM’s Project BOOST, which focuses on successful discharge outcomes. So in collaboration with the Texas Department of Aging and Disability Services, the hospital provided cab vouchers for these patients to travel to and from appointments.
The hospital also realized that to improve the chances its large Hispanic diabetic population remained healthy, it would need to tailor its disease management efforts to their culture, particularly when it came to diet.
“Their eating habits are very different, and we want to ensure they have meals based on what they actually eat,” Finder says.
These are exactly the kinds of approaches a new guide developed for the Centers for Medicare & Medicaid Services (CMS) by the Disparities Solutions Center (DSC), based at Massachusetts General Hospital (MGH) in Boston, is looking to promote in an effort to reduce unnecessary hospital readmissions.1 CMS recently made the Guide to Preventing Readmissions among Racially and Ethnically Diverse Medicare Beneficiaries available on its website.
“We know readmissions is an issue for diverse populations, that they are more likely than their white counterparts to be admitted within 30 days of discharge,” says Aswita Tan-McGrory, MBA, MSPH, deputy director of DSC within the Mongan Institute for Health Policy at MGH. “So there was a good business case for creating this guide.”
Keys to Success
Within the guide is a collection of evidence-based information, case studies, and seven recommendations the DSC team assembled to assist hospital leaders looking to reduce readmissions among some of the nation’s highest-risk populations.
While Tan-McGrory acknowledges it may be impractical for hospitals to adopt each recommendation, she says they can pick and choose which they can most effectively adopt.
“We put together these seven steps and looked for who does this really well, and the honest truth is not very many are,” she says. “It’s a complicated process, but it’s some guidance because there really wasn’t anything out there.”
Included in the recommendations: Create a “strong radar” (engage in robust data collection), identify root causes, begin to think about discharge at admission, deploy a team, consider systems and social determinants, focus on culturally competent communication, and foster community partnerships.
“It’s not just medication reconciliation or discharge instructions in a different language,” Tan-McGrory says. “What happens when a patient gets home?”
These types of questions are important because CMS now penalizes hospitals for what it deems excessive avoidable readmissions within 30 days of discharge. In 2016, hospitals can lose up to 3% of their Medicare payments under the Hospital Readmissions Reduction Program.
In 2014, nearly 18% of Medicare patients were admitted within a month of discharge at a cost of $26 billion.2 According to the new guide, Agency for Healthcare Research and Quality data indicate African-American and Hispanic patients make up a higher share of these readmissions, in part because they are disproportionately affected by chronic high-readmission-risk diseases like congestive heart failure.
Social Determinants
Though it’s challenging for healthcare providers, one way to reduce readmissions is to address the social determinants of health, Tan-McGrory says.
“Hospitals have felt in the past that it’s not their domain, but their patients are coming back,” she says. “How do you address people’s isolation at home? How can you send them from the hospital when no one is there to follow up or take care of them?”
The answers may lie in part on building community partnerships, something in which Finder’s hospital has successfully engaged. For example, the hospital has teamed with its local United Way to work with Asian patients on issues related to pain management and palliative care.
At Berkshire Medical Center, a 300-bed community teaching hospital in western Massachusetts, electronic health software helps staff flag patients at admission for potential readmission risks. Looking briefly at the new guide, William DeMarco, DO, SFHM, chief of hospital medicine (and also part of Project BOOST), noticed several new areas they may be able to incorporate into the system.
But adequate data collection and interpretation to help understand these disparities is not always possible, particularly for readmissions, Dr. DeMarco says.
However, as in one of the case studies examined in the DCS guide, Berkshire recently began to identify its high utilizers, pairing multidisciplinary teams with individual primary care providers in order to help meet these patients’ needs.
“It can take several hours for one patient, coordinating and getting a lot of people together,” Dr. DeMarco says. “It’s the only way to accomplish that goal, but it’s very resource intensive.”
Although hospitals traditionally focus on what they can do within their four walls, providers are becoming increasingly aware that the social determinants of health—like transportation, dietary choices, and language barriers—deeply impact some racial and ethnically diverse populations. Now, CMS thinks it’s worth paying closer attention. TH
Kelly April Tyrrell is a freelance writer in Madison, Wis.
References
- Betancourt JR, Tan-McGrory A, Kenst KS. Guide to preventing readmissions among racially and ethnically diverse medicare beneficiaries. Prepared by the Disparities Solutions Center, Mongan Institute for Health Policy at Massachusetts General Hospital. Baltimore, MD: Centers for Medicare & Medicaid Services Office of Minority Health; September 2015.
- Rau J. Medicare fines 2,610 hospitals in third round of readmission penalties. Kaiser Health News. Available at: http://kaiserhealthnews.org/news/medicare-readmissions-penalties-2015/. Accessed February 15, 2016.
“We found it wasn’t on a bus route,” says Janice Finder, RN, MSN, director of the hospital’s Transitions in Care program and a part of SHM’s Project BOOST, which focuses on successful discharge outcomes. So in collaboration with the Texas Department of Aging and Disability Services, the hospital provided cab vouchers for these patients to travel to and from appointments.
The hospital also realized that to improve the chances its large Hispanic diabetic population remained healthy, it would need to tailor its disease management efforts to their culture, particularly when it came to diet.
“Their eating habits are very different, and we want to ensure they have meals based on what they actually eat,” Finder says.
These are exactly the kinds of approaches a new guide developed for the Centers for Medicare & Medicaid Services (CMS) by the Disparities Solutions Center (DSC), based at Massachusetts General Hospital (MGH) in Boston, is looking to promote in an effort to reduce unnecessary hospital readmissions.1 CMS recently made the Guide to Preventing Readmissions among Racially and Ethnically Diverse Medicare Beneficiaries available on its website.
“We know readmissions is an issue for diverse populations, that they are more likely than their white counterparts to be admitted within 30 days of discharge,” says Aswita Tan-McGrory, MBA, MSPH, deputy director of DSC within the Mongan Institute for Health Policy at MGH. “So there was a good business case for creating this guide.”
Keys to Success
Within the guide is a collection of evidence-based information, case studies, and seven recommendations the DSC team assembled to assist hospital leaders looking to reduce readmissions among some of the nation’s highest-risk populations.
While Tan-McGrory acknowledges it may be impractical for hospitals to adopt each recommendation, she says they can pick and choose which they can most effectively adopt.
“We put together these seven steps and looked for who does this really well, and the honest truth is not very many are,” she says. “It’s a complicated process, but it’s some guidance because there really wasn’t anything out there.”
Included in the recommendations: Create a “strong radar” (engage in robust data collection), identify root causes, begin to think about discharge at admission, deploy a team, consider systems and social determinants, focus on culturally competent communication, and foster community partnerships.
“It’s not just medication reconciliation or discharge instructions in a different language,” Tan-McGrory says. “What happens when a patient gets home?”
These types of questions are important because CMS now penalizes hospitals for what it deems excessive avoidable readmissions within 30 days of discharge. In 2016, hospitals can lose up to 3% of their Medicare payments under the Hospital Readmissions Reduction Program.
In 2014, nearly 18% of Medicare patients were admitted within a month of discharge at a cost of $26 billion.2 According to the new guide, Agency for Healthcare Research and Quality data indicate African-American and Hispanic patients make up a higher share of these readmissions, in part because they are disproportionately affected by chronic high-readmission-risk diseases like congestive heart failure.
Social Determinants
Though it’s challenging for healthcare providers, one way to reduce readmissions is to address the social determinants of health, Tan-McGrory says.
“Hospitals have felt in the past that it’s not their domain, but their patients are coming back,” she says. “How do you address people’s isolation at home? How can you send them from the hospital when no one is there to follow up or take care of them?”
The answers may lie in part on building community partnerships, something in which Finder’s hospital has successfully engaged. For example, the hospital has teamed with its local United Way to work with Asian patients on issues related to pain management and palliative care.
At Berkshire Medical Center, a 300-bed community teaching hospital in western Massachusetts, electronic health software helps staff flag patients at admission for potential readmission risks. Looking briefly at the new guide, William DeMarco, DO, SFHM, chief of hospital medicine (and also part of Project BOOST), noticed several new areas they may be able to incorporate into the system.
But adequate data collection and interpretation to help understand these disparities is not always possible, particularly for readmissions, Dr. DeMarco says.
However, as in one of the case studies examined in the DCS guide, Berkshire recently began to identify its high utilizers, pairing multidisciplinary teams with individual primary care providers in order to help meet these patients’ needs.
“It can take several hours for one patient, coordinating and getting a lot of people together,” Dr. DeMarco says. “It’s the only way to accomplish that goal, but it’s very resource intensive.”
Although hospitals traditionally focus on what they can do within their four walls, providers are becoming increasingly aware that the social determinants of health—like transportation, dietary choices, and language barriers—deeply impact some racial and ethnically diverse populations. Now, CMS thinks it’s worth paying closer attention. TH
Kelly April Tyrrell is a freelance writer in Madison, Wis.
References
- Betancourt JR, Tan-McGrory A, Kenst KS. Guide to preventing readmissions among racially and ethnically diverse medicare beneficiaries. Prepared by the Disparities Solutions Center, Mongan Institute for Health Policy at Massachusetts General Hospital. Baltimore, MD: Centers for Medicare & Medicaid Services Office of Minority Health; September 2015.
- Rau J. Medicare fines 2,610 hospitals in third round of readmission penalties. Kaiser Health News. Available at: http://kaiserhealthnews.org/news/medicare-readmissions-penalties-2015/. Accessed February 15, 2016.
'Everything We Say and Do': Soliciting Goals from Our Patients and Their Families
Editor’s note: “Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Each article will focus on how the contributor applies one ormore of the “key communication” tactics in practice to maintain provider accountability for “Everything we say and do that affects our patients’ thoughts, feelings and well-being.”
Read more from the “Everything We Say and Do” series.
What I Say and Do
Why I Do It
The literature shows that, in most cases, doctors interrupt within 18 to 23 seconds and that when we interrupt, patients often never get back to what they were saying, the course of their story changes, and our diagnostic accuracy decreases. I also do it because I learn things that I wouldn’t otherwise know, and my patients feel heard and treated with respect. Listening has a healing effect, and in medicine, it can be equally if not more therapeutic than the medicines and clinical care we provide. I find that it helps me to be a more effective doctor, one who is helping my patient in the way that is most meaningful and helpful to them. It is very easy to navigate an encounter from the physician point of view and to make assumptions about what people want and need from me, but in reality, what is most important to me is not always what is most important to them.
Allowing patients to tell me what is important shows them respect and also sets me up for success as I am more likely to know and meet their needs. Doing this up front saves time by preventing the “doorknob” questions on the way out. The human connection that follows keeps me connected to my purpose as a doctor. People often worry that listening will take too much time, but we know from the literature that most patients will talk for no more than 90 seconds. It’s really a very short amount of time for a gold mine of information.
How I Do It
Before I jump into my agenda, I make sure to know what is on the patient’s and family’s mind. What is most important to them to address? Once we have agreed on what we will be discussing or doing with our time in a way that includes both what I and the patient/family find important, I start by asking the patient to tell me everything about the first item at hand. I do not interrupt by asking questions, making comments, or “fixing.” I approach them with authentic curiosity, encouraging more without directing what they say.
I start with, “I’m here to talk to you about _____, but first, can you tell me what you’d like to make sure we talk about today?” Or, “Tell me a list of things that you’d like to make sure we talk about today.”
I follow that with, “What else?” until there is nothing else. Once we have negotiated what we will discuss, I say, “Tell me all about _______.” I do not interrupt or think about my response while I am listening. My only response is to use nonverbal continuers (“Uh huh,” “mmmm”), reflections (“That sounds really hard”), verbal continuers (“Tell me more”), empathic statements (“I can see why you would feel that way”), and body language that shows I am with them (sitting at eye level, facing them, looking at them rather than at my phone, pager or a computer screen.)
All of this happens before I jump into any of my own focused or clarifying questions.
Dr. Sliwka is medical director of patient and provider experience, medical director of the Goldman Medical Service, and associate clinical professor of medicine in the Division of Hospital Medicine at the UCSF Medical Center in San Francisco.
Table 1.
Editor’s note: “Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Each article will focus on how the contributor applies one ormore of the “key communication” tactics in practice to maintain provider accountability for “Everything we say and do that affects our patients’ thoughts, feelings and well-being.”
Read more from the “Everything We Say and Do” series.
What I Say and Do
Why I Do It
The literature shows that, in most cases, doctors interrupt within 18 to 23 seconds and that when we interrupt, patients often never get back to what they were saying, the course of their story changes, and our diagnostic accuracy decreases. I also do it because I learn things that I wouldn’t otherwise know, and my patients feel heard and treated with respect. Listening has a healing effect, and in medicine, it can be equally if not more therapeutic than the medicines and clinical care we provide. I find that it helps me to be a more effective doctor, one who is helping my patient in the way that is most meaningful and helpful to them. It is very easy to navigate an encounter from the physician point of view and to make assumptions about what people want and need from me, but in reality, what is most important to me is not always what is most important to them.
Allowing patients to tell me what is important shows them respect and also sets me up for success as I am more likely to know and meet their needs. Doing this up front saves time by preventing the “doorknob” questions on the way out. The human connection that follows keeps me connected to my purpose as a doctor. People often worry that listening will take too much time, but we know from the literature that most patients will talk for no more than 90 seconds. It’s really a very short amount of time for a gold mine of information.
How I Do It
Before I jump into my agenda, I make sure to know what is on the patient’s and family’s mind. What is most important to them to address? Once we have agreed on what we will be discussing or doing with our time in a way that includes both what I and the patient/family find important, I start by asking the patient to tell me everything about the first item at hand. I do not interrupt by asking questions, making comments, or “fixing.” I approach them with authentic curiosity, encouraging more without directing what they say.
I start with, “I’m here to talk to you about _____, but first, can you tell me what you’d like to make sure we talk about today?” Or, “Tell me a list of things that you’d like to make sure we talk about today.”
I follow that with, “What else?” until there is nothing else. Once we have negotiated what we will discuss, I say, “Tell me all about _______.” I do not interrupt or think about my response while I am listening. My only response is to use nonverbal continuers (“Uh huh,” “mmmm”), reflections (“That sounds really hard”), verbal continuers (“Tell me more”), empathic statements (“I can see why you would feel that way”), and body language that shows I am with them (sitting at eye level, facing them, looking at them rather than at my phone, pager or a computer screen.)
All of this happens before I jump into any of my own focused or clarifying questions.
Dr. Sliwka is medical director of patient and provider experience, medical director of the Goldman Medical Service, and associate clinical professor of medicine in the Division of Hospital Medicine at the UCSF Medical Center in San Francisco.
Table 1.
Editor’s note: “Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Each article will focus on how the contributor applies one ormore of the “key communication” tactics in practice to maintain provider accountability for “Everything we say and do that affects our patients’ thoughts, feelings and well-being.”
Read more from the “Everything We Say and Do” series.
What I Say and Do
Why I Do It
The literature shows that, in most cases, doctors interrupt within 18 to 23 seconds and that when we interrupt, patients often never get back to what they were saying, the course of their story changes, and our diagnostic accuracy decreases. I also do it because I learn things that I wouldn’t otherwise know, and my patients feel heard and treated with respect. Listening has a healing effect, and in medicine, it can be equally if not more therapeutic than the medicines and clinical care we provide. I find that it helps me to be a more effective doctor, one who is helping my patient in the way that is most meaningful and helpful to them. It is very easy to navigate an encounter from the physician point of view and to make assumptions about what people want and need from me, but in reality, what is most important to me is not always what is most important to them.
Allowing patients to tell me what is important shows them respect and also sets me up for success as I am more likely to know and meet their needs. Doing this up front saves time by preventing the “doorknob” questions on the way out. The human connection that follows keeps me connected to my purpose as a doctor. People often worry that listening will take too much time, but we know from the literature that most patients will talk for no more than 90 seconds. It’s really a very short amount of time for a gold mine of information.
How I Do It
Before I jump into my agenda, I make sure to know what is on the patient’s and family’s mind. What is most important to them to address? Once we have agreed on what we will be discussing or doing with our time in a way that includes both what I and the patient/family find important, I start by asking the patient to tell me everything about the first item at hand. I do not interrupt by asking questions, making comments, or “fixing.” I approach them with authentic curiosity, encouraging more without directing what they say.
I start with, “I’m here to talk to you about _____, but first, can you tell me what you’d like to make sure we talk about today?” Or, “Tell me a list of things that you’d like to make sure we talk about today.”
I follow that with, “What else?” until there is nothing else. Once we have negotiated what we will discuss, I say, “Tell me all about _______.” I do not interrupt or think about my response while I am listening. My only response is to use nonverbal continuers (“Uh huh,” “mmmm”), reflections (“That sounds really hard”), verbal continuers (“Tell me more”), empathic statements (“I can see why you would feel that way”), and body language that shows I am with them (sitting at eye level, facing them, looking at them rather than at my phone, pager or a computer screen.)
All of this happens before I jump into any of my own focused or clarifying questions.
Dr. Sliwka is medical director of patient and provider experience, medical director of the Goldman Medical Service, and associate clinical professor of medicine in the Division of Hospital Medicine at the UCSF Medical Center in San Francisco.
Table 1.
Study Suggests Growing Up in a Stress-Free Environment Lowers your Risk of Heart Attacks
(Reuters Health) - Kids who live in a stress-free environment may grow up to be adults with a lower risk of heart attacks than their peers who experience social, emotional or financial difficulties during childhood, a Finnish study suggests.
Researchers assessed psychosocial factors in 311 kids at age 12 and 18. Then, at age 28, they looked for coronary artery calcification.
The adults who had high psychosocial wellbeing as kids were 15% less likely to have calcium deposits clogging their arteries as adults, the study found.
"This study suggests that childhood psychosocial factors may have long-term consequences on cardiovascular health," lead study author Dr. Markus Juonala of the University of Turku in Finland said by email.
To understand the connection between how kids feel growing up and how their arteries look decades later, Juonala and colleagues analyzed data gathered from 1980 to 2008 as part of the Cardiovascular Risk in Young Finns Study.
Among other things, this study measured psychosocial wellbeing by looking at family income and education levels, parents' job status, parents' mental health and history of smoking or substance abuse, parents' weight and exercise habits, stressful events such as divorce, death or moves, as well as the child's level of aggressive or anti-social behaviors and ability to interact with other people.
In addition, researchers analyzed results from computed tomography (CT) scans assessing coronary artery calcification. Overall, 55 participants, or about 18%, had at least some calcification in their arteries, researchers report in JAMA Pediatrics, March 14.
Among this group with calcification, 28 participants had low levels of buildup, 20 had moderate amounts of calcium and 7 had substantial deposits, the study found.
Even after accounting for adult circumstances like psychosocial factors and risk factors for heart disease like obesity, smoking, hypertension and elevated cholesterol, the research team still found well-being during childhood was associated with reduced coronary artery calcification in adulthood.
The study is observational and doesn't prove childhood stress causes clogged arteries or heart attacks, only that the two things are related, the authors note.
It's possible, however, that stress during childhood might trigger changes in metabolic functioning and inflammation that later contribute to calcium deposits in the arteries, the researchers point out.
It's also possible that happier kids may develop healthier habits like better diets and more rigorous exercise routines that help keep arteries unclogged and lower their risk of heart disease later in life.
"The take-home message for parents is to understand that stress in childhood may have many adverse effects and that they should help their children avoid stress," said Dr. Stephen Daniels, a researcher at the University of Colorado School of Medicine and pediatrician-in-chief at Children's Hospital Colorado.
Parents may not always be able to eliminate stress, however, particularly the stress that can come from environmental factors like lower socioeconomic status, Daniels, who wasn't involved in the study, added by email.
When children grow up with stress, they can still take charge of their health as adults to lower their risk of heart disease, Daniels noted.
"For an adult who had a stressful childhood, the best approach is to be aware of their cardiovascular risk status and to reduce their risk by improving diet and physical activity and avoiding cigarette smoking," Daniels added. "Where risk factors exist, such as high blood pressure, they should be appropriately treated."
(Reuters Health) - Kids who live in a stress-free environment may grow up to be adults with a lower risk of heart attacks than their peers who experience social, emotional or financial difficulties during childhood, a Finnish study suggests.
Researchers assessed psychosocial factors in 311 kids at age 12 and 18. Then, at age 28, they looked for coronary artery calcification.
The adults who had high psychosocial wellbeing as kids were 15% less likely to have calcium deposits clogging their arteries as adults, the study found.
"This study suggests that childhood psychosocial factors may have long-term consequences on cardiovascular health," lead study author Dr. Markus Juonala of the University of Turku in Finland said by email.
To understand the connection between how kids feel growing up and how their arteries look decades later, Juonala and colleagues analyzed data gathered from 1980 to 2008 as part of the Cardiovascular Risk in Young Finns Study.
Among other things, this study measured psychosocial wellbeing by looking at family income and education levels, parents' job status, parents' mental health and history of smoking or substance abuse, parents' weight and exercise habits, stressful events such as divorce, death or moves, as well as the child's level of aggressive or anti-social behaviors and ability to interact with other people.
In addition, researchers analyzed results from computed tomography (CT) scans assessing coronary artery calcification. Overall, 55 participants, or about 18%, had at least some calcification in their arteries, researchers report in JAMA Pediatrics, March 14.
Among this group with calcification, 28 participants had low levels of buildup, 20 had moderate amounts of calcium and 7 had substantial deposits, the study found.
Even after accounting for adult circumstances like psychosocial factors and risk factors for heart disease like obesity, smoking, hypertension and elevated cholesterol, the research team still found well-being during childhood was associated with reduced coronary artery calcification in adulthood.
The study is observational and doesn't prove childhood stress causes clogged arteries or heart attacks, only that the two things are related, the authors note.
It's possible, however, that stress during childhood might trigger changes in metabolic functioning and inflammation that later contribute to calcium deposits in the arteries, the researchers point out.
It's also possible that happier kids may develop healthier habits like better diets and more rigorous exercise routines that help keep arteries unclogged and lower their risk of heart disease later in life.
"The take-home message for parents is to understand that stress in childhood may have many adverse effects and that they should help their children avoid stress," said Dr. Stephen Daniels, a researcher at the University of Colorado School of Medicine and pediatrician-in-chief at Children's Hospital Colorado.
Parents may not always be able to eliminate stress, however, particularly the stress that can come from environmental factors like lower socioeconomic status, Daniels, who wasn't involved in the study, added by email.
When children grow up with stress, they can still take charge of their health as adults to lower their risk of heart disease, Daniels noted.
"For an adult who had a stressful childhood, the best approach is to be aware of their cardiovascular risk status and to reduce their risk by improving diet and physical activity and avoiding cigarette smoking," Daniels added. "Where risk factors exist, such as high blood pressure, they should be appropriately treated."
(Reuters Health) - Kids who live in a stress-free environment may grow up to be adults with a lower risk of heart attacks than their peers who experience social, emotional or financial difficulties during childhood, a Finnish study suggests.
Researchers assessed psychosocial factors in 311 kids at age 12 and 18. Then, at age 28, they looked for coronary artery calcification.
The adults who had high psychosocial wellbeing as kids were 15% less likely to have calcium deposits clogging their arteries as adults, the study found.
"This study suggests that childhood psychosocial factors may have long-term consequences on cardiovascular health," lead study author Dr. Markus Juonala of the University of Turku in Finland said by email.
To understand the connection between how kids feel growing up and how their arteries look decades later, Juonala and colleagues analyzed data gathered from 1980 to 2008 as part of the Cardiovascular Risk in Young Finns Study.
Among other things, this study measured psychosocial wellbeing by looking at family income and education levels, parents' job status, parents' mental health and history of smoking or substance abuse, parents' weight and exercise habits, stressful events such as divorce, death or moves, as well as the child's level of aggressive or anti-social behaviors and ability to interact with other people.
In addition, researchers analyzed results from computed tomography (CT) scans assessing coronary artery calcification. Overall, 55 participants, or about 18%, had at least some calcification in their arteries, researchers report in JAMA Pediatrics, March 14.
Among this group with calcification, 28 participants had low levels of buildup, 20 had moderate amounts of calcium and 7 had substantial deposits, the study found.
Even after accounting for adult circumstances like psychosocial factors and risk factors for heart disease like obesity, smoking, hypertension and elevated cholesterol, the research team still found well-being during childhood was associated with reduced coronary artery calcification in adulthood.
The study is observational and doesn't prove childhood stress causes clogged arteries or heart attacks, only that the two things are related, the authors note.
It's possible, however, that stress during childhood might trigger changes in metabolic functioning and inflammation that later contribute to calcium deposits in the arteries, the researchers point out.
It's also possible that happier kids may develop healthier habits like better diets and more rigorous exercise routines that help keep arteries unclogged and lower their risk of heart disease later in life.
"The take-home message for parents is to understand that stress in childhood may have many adverse effects and that they should help their children avoid stress," said Dr. Stephen Daniels, a researcher at the University of Colorado School of Medicine and pediatrician-in-chief at Children's Hospital Colorado.
Parents may not always be able to eliminate stress, however, particularly the stress that can come from environmental factors like lower socioeconomic status, Daniels, who wasn't involved in the study, added by email.
When children grow up with stress, they can still take charge of their health as adults to lower their risk of heart disease, Daniels noted.
"For an adult who had a stressful childhood, the best approach is to be aware of their cardiovascular risk status and to reduce their risk by improving diet and physical activity and avoiding cigarette smoking," Daniels added. "Where risk factors exist, such as high blood pressure, they should be appropriately treated."
Hospitalist Engagement Benchmarking Service Returns for 2016
Engaged hospitalists drive quality care, and SHM has the tools to help you assess the level of engagement of hospitalists in your hospital medicine group. SHM offered a Hospitalist Engagement Benchmarking Service in 2015 and analyzed engagement of approximately 1,500 hospitalists. Organizational climate, care quality, autonomy, effective motivation, and burnout risk are just a few of the domains that were benchmarked.
“The engagement survey opened conversations about everything from how we relate to the C-suite to what we can do to sustain teamwork,” says Erin Stucky Fisher, MD, MHM, pediatric hospitalist at Rady Children’s Hospital-San Diego. “[It] highlighted what was working well and identified what needs work.”
More than 80% of respondents indicated that they will utilize the service again and plan to recommend it to a colleague. Help ensure hospitalists are engaged in your hospital medicine group by registering now for the next cohort at www.hospitalmedicine.org/engage. TH
Brett Radler is SHM’s communications coordinator.
Engaged hospitalists drive quality care, and SHM has the tools to help you assess the level of engagement of hospitalists in your hospital medicine group. SHM offered a Hospitalist Engagement Benchmarking Service in 2015 and analyzed engagement of approximately 1,500 hospitalists. Organizational climate, care quality, autonomy, effective motivation, and burnout risk are just a few of the domains that were benchmarked.
“The engagement survey opened conversations about everything from how we relate to the C-suite to what we can do to sustain teamwork,” says Erin Stucky Fisher, MD, MHM, pediatric hospitalist at Rady Children’s Hospital-San Diego. “[It] highlighted what was working well and identified what needs work.”
More than 80% of respondents indicated that they will utilize the service again and plan to recommend it to a colleague. Help ensure hospitalists are engaged in your hospital medicine group by registering now for the next cohort at www.hospitalmedicine.org/engage. TH
Brett Radler is SHM’s communications coordinator.
Engaged hospitalists drive quality care, and SHM has the tools to help you assess the level of engagement of hospitalists in your hospital medicine group. SHM offered a Hospitalist Engagement Benchmarking Service in 2015 and analyzed engagement of approximately 1,500 hospitalists. Organizational climate, care quality, autonomy, effective motivation, and burnout risk are just a few of the domains that were benchmarked.
“The engagement survey opened conversations about everything from how we relate to the C-suite to what we can do to sustain teamwork,” says Erin Stucky Fisher, MD, MHM, pediatric hospitalist at Rady Children’s Hospital-San Diego. “[It] highlighted what was working well and identified what needs work.”
More than 80% of respondents indicated that they will utilize the service again and plan to recommend it to a colleague. Help ensure hospitalists are engaged in your hospital medicine group by registering now for the next cohort at www.hospitalmedicine.org/engage. TH
Brett Radler is SHM’s communications coordinator.