User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'main-prefix')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
div[contains(@class, 'view-medstat-quiz-listing-panes')]
div[contains(@class, 'pane-article-sidebar-latest-news')]
div[contains(@class, 'medstat-accordion-set article-series')]
Concomitant methotrexate has no effect on ustekinumab immunogenicity in PsA
Key clinical point: Concomitant methotrexate had no effect on ustekimumab immunogenicity in patients with psoriatic arthritis (PsA), with the formation of antidrug antibody (ADA) not being associated with reductions in ustekinumab safety or efficacy.
Major finding: The prevalence of ADA at week 52 was not significantly different between the ustekinumab+methotrexate and ustekinumab+placebo groups, with disease activity, treatment response, dropout rates, effect of pretreatment with methotrexate, and safety outcomes not being significantly different in patients with vs without ADA (all P > .05).
Study details: This post hoc analysis of the MUST trial included 112 patients with active PsA who were naive to ustekimumab and were randomly assigned to receive ustekinumab with concomitant methotrexate or placebo.
Disclosures: This study was funded by Innovative Medicines Initiative 2 Joint Undertaking, which received support from the European Union’s Horizon 2020 Research and Innovation Program and others. F Behrens, M Koehm, and H Burkhardt declared receiving research grants from Janssen Cilag. The other authors reported no conflicts of interest.
Source: Poor SM et al. The role of antidrug antibodies in ustekinumab therapy and the impact of methotrexate. Rheumatology (Oxford). 2023 (Apr 20). Doi: 10.1093/rheumatology/kead177
Key clinical point: Concomitant methotrexate had no effect on ustekimumab immunogenicity in patients with psoriatic arthritis (PsA), with the formation of antidrug antibody (ADA) not being associated with reductions in ustekinumab safety or efficacy.
Major finding: The prevalence of ADA at week 52 was not significantly different between the ustekinumab+methotrexate and ustekinumab+placebo groups, with disease activity, treatment response, dropout rates, effect of pretreatment with methotrexate, and safety outcomes not being significantly different in patients with vs without ADA (all P > .05).
Study details: This post hoc analysis of the MUST trial included 112 patients with active PsA who were naive to ustekimumab and were randomly assigned to receive ustekinumab with concomitant methotrexate or placebo.
Disclosures: This study was funded by Innovative Medicines Initiative 2 Joint Undertaking, which received support from the European Union’s Horizon 2020 Research and Innovation Program and others. F Behrens, M Koehm, and H Burkhardt declared receiving research grants from Janssen Cilag. The other authors reported no conflicts of interest.
Source: Poor SM et al. The role of antidrug antibodies in ustekinumab therapy and the impact of methotrexate. Rheumatology (Oxford). 2023 (Apr 20). Doi: 10.1093/rheumatology/kead177
Key clinical point: Concomitant methotrexate had no effect on ustekimumab immunogenicity in patients with psoriatic arthritis (PsA), with the formation of antidrug antibody (ADA) not being associated with reductions in ustekinumab safety or efficacy.
Major finding: The prevalence of ADA at week 52 was not significantly different between the ustekinumab+methotrexate and ustekinumab+placebo groups, with disease activity, treatment response, dropout rates, effect of pretreatment with methotrexate, and safety outcomes not being significantly different in patients with vs without ADA (all P > .05).
Study details: This post hoc analysis of the MUST trial included 112 patients with active PsA who were naive to ustekimumab and were randomly assigned to receive ustekinumab with concomitant methotrexate or placebo.
Disclosures: This study was funded by Innovative Medicines Initiative 2 Joint Undertaking, which received support from the European Union’s Horizon 2020 Research and Innovation Program and others. F Behrens, M Koehm, and H Burkhardt declared receiving research grants from Janssen Cilag. The other authors reported no conflicts of interest.
Source: Poor SM et al. The role of antidrug antibodies in ustekinumab therapy and the impact of methotrexate. Rheumatology (Oxford). 2023 (Apr 20). Doi: 10.1093/rheumatology/kead177
Concomitant methotrexate has no effect on ustekinumab immunogenicity in PsA
Key clinical point: Concomitant methotrexate had no effect on ustekimumab immunogenicity in patients with psoriatic arthritis (PsA), with the formation of antidrug antibody (ADA) not being associated with reductions in ustekinumab safety or efficacy.
Major finding: The prevalence of ADA at week 52 was not significantly different between the ustekinumab+methotrexate and ustekinumab+placebo groups, with disease activity, treatment response, dropout rates, effect of pretreatment with methotrexate, and safety outcomes not being significantly different in patients with vs without ADA (all P > .05).
Study details: This post hoc analysis of the MUST trial included 112 patients with active PsA who were naive to ustekimumab and were randomly assigned to receive ustekinumab with concomitant methotrexate or placebo.
Disclosures: This study was funded by Innovative Medicines Initiative 2 Joint Undertaking, which received support from the European Union’s Horizon 2020 Research and Innovation Program and others. F Behrens, M Koehm, and H Burkhardt declared receiving research grants from Janssen Cilag. The other authors reported no conflicts of interest.
Source: Poor SM et al. The role of antidrug antibodies in ustekinumab therapy and the impact of methotrexate. Rheumatology (Oxford). 2023 (Apr 20). Doi: 10.1093/rheumatology/kead177
Key clinical point: Concomitant methotrexate had no effect on ustekimumab immunogenicity in patients with psoriatic arthritis (PsA), with the formation of antidrug antibody (ADA) not being associated with reductions in ustekinumab safety or efficacy.
Major finding: The prevalence of ADA at week 52 was not significantly different between the ustekinumab+methotrexate and ustekinumab+placebo groups, with disease activity, treatment response, dropout rates, effect of pretreatment with methotrexate, and safety outcomes not being significantly different in patients with vs without ADA (all P > .05).
Study details: This post hoc analysis of the MUST trial included 112 patients with active PsA who were naive to ustekimumab and were randomly assigned to receive ustekinumab with concomitant methotrexate or placebo.
Disclosures: This study was funded by Innovative Medicines Initiative 2 Joint Undertaking, which received support from the European Union’s Horizon 2020 Research and Innovation Program and others. F Behrens, M Koehm, and H Burkhardt declared receiving research grants from Janssen Cilag. The other authors reported no conflicts of interest.
Source: Poor SM et al. The role of antidrug antibodies in ustekinumab therapy and the impact of methotrexate. Rheumatology (Oxford). 2023 (Apr 20). Doi: 10.1093/rheumatology/kead177
Key clinical point: Concomitant methotrexate had no effect on ustekimumab immunogenicity in patients with psoriatic arthritis (PsA), with the formation of antidrug antibody (ADA) not being associated with reductions in ustekinumab safety or efficacy.
Major finding: The prevalence of ADA at week 52 was not significantly different between the ustekinumab+methotrexate and ustekinumab+placebo groups, with disease activity, treatment response, dropout rates, effect of pretreatment with methotrexate, and safety outcomes not being significantly different in patients with vs without ADA (all P > .05).
Study details: This post hoc analysis of the MUST trial included 112 patients with active PsA who were naive to ustekimumab and were randomly assigned to receive ustekinumab with concomitant methotrexate or placebo.
Disclosures: This study was funded by Innovative Medicines Initiative 2 Joint Undertaking, which received support from the European Union’s Horizon 2020 Research and Innovation Program and others. F Behrens, M Koehm, and H Burkhardt declared receiving research grants from Janssen Cilag. The other authors reported no conflicts of interest.
Source: Poor SM et al. The role of antidrug antibodies in ustekinumab therapy and the impact of methotrexate. Rheumatology (Oxford). 2023 (Apr 20). Doi: 10.1093/rheumatology/kead177
Entheseal fibrocartilage abnormalities: A potential imaging biomarker of PsA
Key clinical point: The entheseal fibrocartilage (EF) thickness assessed during power Doppler ultrasound evaluation was significantly different among patients with psoriatic arthritis (PsA) and control individuals and can be explored as an imaging biomarker for PsA.
Major finding: The median EF thickness was significantly greater in patients with PsA and athletes vs control individuals (0.035 and 0.036 vs 0.030 cm, respectively; P = .05 and P = .008, respectively), with the intra- and inter-reader reliability of the evaluation of EF thickness being excellent (intraclass correlation coefficient [ICC] 0.91) and good (ICC 0.80; both P < .001), respectively.
Study details: This cross-sectional study included patients with PsA (n = 30), athletes (n = 40), and control individuals (n = 20) who underwent power Doppler ultrasound evaluation during bilateral Achilles tendon insertions.
Disclosures: This study did not receive any external funding. The authors declared no conflicts of interest.
Source: Perrotta FM et al. Ultrasonographic evaluation of entheseal fibrocartilage in patients with psoriatic arthritis, athletes and healthy controls: A comparison study. Diagnostics (Basel). 2023;13(8):1446 (Apr 17). Doi: 10.3390/diagnostics13081446
Key clinical point: The entheseal fibrocartilage (EF) thickness assessed during power Doppler ultrasound evaluation was significantly different among patients with psoriatic arthritis (PsA) and control individuals and can be explored as an imaging biomarker for PsA.
Major finding: The median EF thickness was significantly greater in patients with PsA and athletes vs control individuals (0.035 and 0.036 vs 0.030 cm, respectively; P = .05 and P = .008, respectively), with the intra- and inter-reader reliability of the evaluation of EF thickness being excellent (intraclass correlation coefficient [ICC] 0.91) and good (ICC 0.80; both P < .001), respectively.
Study details: This cross-sectional study included patients with PsA (n = 30), athletes (n = 40), and control individuals (n = 20) who underwent power Doppler ultrasound evaluation during bilateral Achilles tendon insertions.
Disclosures: This study did not receive any external funding. The authors declared no conflicts of interest.
Source: Perrotta FM et al. Ultrasonographic evaluation of entheseal fibrocartilage in patients with psoriatic arthritis, athletes and healthy controls: A comparison study. Diagnostics (Basel). 2023;13(8):1446 (Apr 17). Doi: 10.3390/diagnostics13081446
Key clinical point: The entheseal fibrocartilage (EF) thickness assessed during power Doppler ultrasound evaluation was significantly different among patients with psoriatic arthritis (PsA) and control individuals and can be explored as an imaging biomarker for PsA.
Major finding: The median EF thickness was significantly greater in patients with PsA and athletes vs control individuals (0.035 and 0.036 vs 0.030 cm, respectively; P = .05 and P = .008, respectively), with the intra- and inter-reader reliability of the evaluation of EF thickness being excellent (intraclass correlation coefficient [ICC] 0.91) and good (ICC 0.80; both P < .001), respectively.
Study details: This cross-sectional study included patients with PsA (n = 30), athletes (n = 40), and control individuals (n = 20) who underwent power Doppler ultrasound evaluation during bilateral Achilles tendon insertions.
Disclosures: This study did not receive any external funding. The authors declared no conflicts of interest.
Source: Perrotta FM et al. Ultrasonographic evaluation of entheseal fibrocartilage in patients with psoriatic arthritis, athletes and healthy controls: A comparison study. Diagnostics (Basel). 2023;13(8):1446 (Apr 17). Doi: 10.3390/diagnostics13081446
Upadacitinib safe and effective in PsA patients with axial involvement
Key clinical point: Compared with placebo, 15 mg upadacitinib led to a greater improvement in axial symptoms with a consistent safety profile in patients with psoriatic arthritis (PsA).
Major finding: The improvement in overall Bath Ankylosing Spondylitis Disease Activity Index score at week 24 was significantly higher with 15 mg upadacitinib vs placebo in both SELECT-PsA 1 (−3.12 vs −1.70; P < .0001) and SELECT PsA 2 (−2.06 vs −0.21; P < .0001) trials. Treatment-emergent adverse events were generally similar among the sub-groups.
Study details: This post hoc analysis included patients with active PsA (n = 1,281 and n = 423, respectively) from the SELECT-PsA 1 and SELECT-PsA 2 trials who were randomly assigned to receive either 15 mg upadacitinib, placebo, or adalimumab and were categorized as those with or without axial involvement.
Disclosures: This study was funded by AbbVie. Five authors declared being employees or stockholders of AbbVie, and some authors reported ties with various sources, including AbbVie.
Source: Baraliakos X et al. Efficacy and safety of upadacitinib in patients with active psoriatic arthritis and axial involvement: Results from two phase 3 studies. Arthritis Res Ther. 2023;25:56 (Apr 10). Doi: 10.1186/s13075-023-03027-5
Key clinical point: Compared with placebo, 15 mg upadacitinib led to a greater improvement in axial symptoms with a consistent safety profile in patients with psoriatic arthritis (PsA).
Major finding: The improvement in overall Bath Ankylosing Spondylitis Disease Activity Index score at week 24 was significantly higher with 15 mg upadacitinib vs placebo in both SELECT-PsA 1 (−3.12 vs −1.70; P < .0001) and SELECT PsA 2 (−2.06 vs −0.21; P < .0001) trials. Treatment-emergent adverse events were generally similar among the sub-groups.
Study details: This post hoc analysis included patients with active PsA (n = 1,281 and n = 423, respectively) from the SELECT-PsA 1 and SELECT-PsA 2 trials who were randomly assigned to receive either 15 mg upadacitinib, placebo, or adalimumab and were categorized as those with or without axial involvement.
Disclosures: This study was funded by AbbVie. Five authors declared being employees or stockholders of AbbVie, and some authors reported ties with various sources, including AbbVie.
Source: Baraliakos X et al. Efficacy and safety of upadacitinib in patients with active psoriatic arthritis and axial involvement: Results from two phase 3 studies. Arthritis Res Ther. 2023;25:56 (Apr 10). Doi: 10.1186/s13075-023-03027-5
Key clinical point: Compared with placebo, 15 mg upadacitinib led to a greater improvement in axial symptoms with a consistent safety profile in patients with psoriatic arthritis (PsA).
Major finding: The improvement in overall Bath Ankylosing Spondylitis Disease Activity Index score at week 24 was significantly higher with 15 mg upadacitinib vs placebo in both SELECT-PsA 1 (−3.12 vs −1.70; P < .0001) and SELECT PsA 2 (−2.06 vs −0.21; P < .0001) trials. Treatment-emergent adverse events were generally similar among the sub-groups.
Study details: This post hoc analysis included patients with active PsA (n = 1,281 and n = 423, respectively) from the SELECT-PsA 1 and SELECT-PsA 2 trials who were randomly assigned to receive either 15 mg upadacitinib, placebo, or adalimumab and were categorized as those with or without axial involvement.
Disclosures: This study was funded by AbbVie. Five authors declared being employees or stockholders of AbbVie, and some authors reported ties with various sources, including AbbVie.
Source: Baraliakos X et al. Efficacy and safety of upadacitinib in patients with active psoriatic arthritis and axial involvement: Results from two phase 3 studies. Arthritis Res Ther. 2023;25:56 (Apr 10). Doi: 10.1186/s13075-023-03027-5
The antimicrobial peptide that even Pharma can love
Fastest peptide north, south, east, aaaaand west of the Pecos
Bacterial infections are supposed to be simple. You get infected, you get an antibiotic to treat it. Easy. Some bacteria, though, don’t play by the rules. Those antibiotics may kill 99.9% of germs, but what about the 0.1% that gets left behind? With their fallen comrades out of the way, the accidentally drug resistant species are free to inherit the Earth.
Antibiotic resistance is thus a major concern for the medical community. Naturally, anything that prevents doctors from successfully curing sick people is a priority. Unless you’re a major pharmaceutical company that has been loath to develop new drugs that can beat antibiotic-resistant bacteria. Blah blah, time and money, blah blah, long time between development and market application, blah blah, no profit. We all know the story with pharmaceutical companies.
Research from other sources has continued, however, and Brazilian scientists recently published research involving a peptide known as plantaricin 149. This peptide, derived from the bacterium Lactobacillus plantarum, has been known for nearly 30 years to have antibacterial properties. Pln149 in its natural state, though, is not particularly efficient at bacteria-killing. Fortunately, we have science and technology on our side.
The researchers synthesized 20 analogs of Pln149, of which Pln149-PEP20 had the best results. The elegantly named compound is less than half the size of the original peptide, less toxic, and far better at killing any and all drug-resistant bacteria the researchers threw at it. How much better? Pln149-PEP20 started killing bacteria less than an hour after being introduced in lab trials.
The research is just in its early days – just because something is less toxic doesn’t necessarily mean you want to go and help yourself to it – but we can only hope that those lovely pharmaceutical companies deign to look down upon us and actually develop a drug utilizing Pln149-PEP20 to, you know, actually help sick people, instead of trying to build monopolies or avoiding paying billions in taxes. Yeah, we couldn’t keep a straight face through that last sentence either.
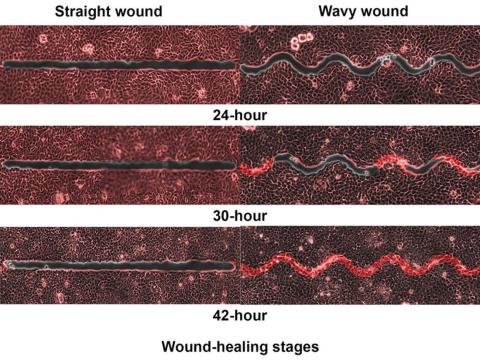
Speed healing: The wavy wound gets the swirl
Did you know that wavy wounds heal faster than straight wounds? Well, we didn’t, but apparently quite a few people did, because somebody has been trying to figure out why wavy wounds heal faster than straight ones. Do the surgeons know about this? How about you dermatologists? Wavy over straight? We’re the media. We’re supposed to report this kind of stuff. Maybe hit us with a tweet next time you do something important, or push a TikTok our way, okay?
You could be more like the investigators at Nanyang Technological University in Singapore, who figured out the why and then released a statement about it.
They created synthetic wounds – some straight, some wavy – in micropatterned hydrogel substrates that mimicked human skin. Then they used an advanced optical technique known as particle image velocimetry to measure fluid flow and learn how cells moved to close the wound gaps.
The wavy wounds “induced more complex collective cell movements, such as a swirly, vortex-like motion,” according to the written statement from NTU Singapore. In the straight wounds, cell movements paralleled the wound front, “moving in straight lines like a marching band,” they pointed out, unlike some researchers who never call us unless they need money.
Complex epithelial cell movements are better, it turns out. Over an observation period of 64 hours the NTU team found that the healing efficiency of wavy gaps – measured by the area covered by the cells over time – is nearly five times faster than straight gaps.
The complex motion “enabled cells to quickly connect with similar cells on the opposite site of the wound edge, forming a bridge and closing the wavy wound gaps faster than straight gaps,” explained lead author Xu Hongmei, a doctoral student at NTU’s School of Mechanical and Aerospace Engineering, who seems to have time to toss out a tumblr or two to keep the press informed.
As for the rest of you, would it kill you to pick up a phone once in a while? Maybe let a journalist know that you’re still alive? We have feelings too, you know, and we worry.
A little Jekyll, a little Hyde, and a little shop of horrors
More “Little Shop of Horrors” references are coming, so be prepared.
We begin with Triphyophyllum peltatum. This woody vine is of great interest to medical and pharmaceutical researchers because its constituents have shown promise against pancreatic cancer and leukemia cells, among others, along with the pathogens that cause malaria and other diseases. There is another side, however. T. peltatum also has a tendency to turn into a realistic Audrey II when deprived.
No, of course they’re not craving human flesh, but it does become … carnivorous in its appetite.
T. peltatum, native to the West African tropics and not found in a New York florist shop, has the unique ability to change its diet and development based on the environmental circumstances. For some unknown reason, the leaves would develop adhesive traps in the form of sticky drops that capture insect prey. The plant is notoriously hard to grow, however, so no one could study the transformation under lab conditions. Until now.
A group of German scientists “exposed the plant to different stress factors, including deficiencies of various nutrients, and studied how it responded to each,” said Dr. Traud Winkelmann of Leibniz University Hannover. “Only in one case were we able to observe the formation of traps: in the case of a lack of phosphorus.”
Well, there you have it: phosphorus. We need it for healthy bones and teeth, which this plant doesn’t have to worry about, unlike its Tony Award–nominated counterpart. The investigators hope that their findings could lead to “future molecular analyses that will help understand the origins of carnivory,” but we’re guessing that a certain singing alien species will be left out of that research.
Fastest peptide north, south, east, aaaaand west of the Pecos
Bacterial infections are supposed to be simple. You get infected, you get an antibiotic to treat it. Easy. Some bacteria, though, don’t play by the rules. Those antibiotics may kill 99.9% of germs, but what about the 0.1% that gets left behind? With their fallen comrades out of the way, the accidentally drug resistant species are free to inherit the Earth.
Antibiotic resistance is thus a major concern for the medical community. Naturally, anything that prevents doctors from successfully curing sick people is a priority. Unless you’re a major pharmaceutical company that has been loath to develop new drugs that can beat antibiotic-resistant bacteria. Blah blah, time and money, blah blah, long time between development and market application, blah blah, no profit. We all know the story with pharmaceutical companies.
Research from other sources has continued, however, and Brazilian scientists recently published research involving a peptide known as plantaricin 149. This peptide, derived from the bacterium Lactobacillus plantarum, has been known for nearly 30 years to have antibacterial properties. Pln149 in its natural state, though, is not particularly efficient at bacteria-killing. Fortunately, we have science and technology on our side.
The researchers synthesized 20 analogs of Pln149, of which Pln149-PEP20 had the best results. The elegantly named compound is less than half the size of the original peptide, less toxic, and far better at killing any and all drug-resistant bacteria the researchers threw at it. How much better? Pln149-PEP20 started killing bacteria less than an hour after being introduced in lab trials.
The research is just in its early days – just because something is less toxic doesn’t necessarily mean you want to go and help yourself to it – but we can only hope that those lovely pharmaceutical companies deign to look down upon us and actually develop a drug utilizing Pln149-PEP20 to, you know, actually help sick people, instead of trying to build monopolies or avoiding paying billions in taxes. Yeah, we couldn’t keep a straight face through that last sentence either.
Speed healing: The wavy wound gets the swirl
Did you know that wavy wounds heal faster than straight wounds? Well, we didn’t, but apparently quite a few people did, because somebody has been trying to figure out why wavy wounds heal faster than straight ones. Do the surgeons know about this? How about you dermatologists? Wavy over straight? We’re the media. We’re supposed to report this kind of stuff. Maybe hit us with a tweet next time you do something important, or push a TikTok our way, okay?
You could be more like the investigators at Nanyang Technological University in Singapore, who figured out the why and then released a statement about it.
They created synthetic wounds – some straight, some wavy – in micropatterned hydrogel substrates that mimicked human skin. Then they used an advanced optical technique known as particle image velocimetry to measure fluid flow and learn how cells moved to close the wound gaps.
The wavy wounds “induced more complex collective cell movements, such as a swirly, vortex-like motion,” according to the written statement from NTU Singapore. In the straight wounds, cell movements paralleled the wound front, “moving in straight lines like a marching band,” they pointed out, unlike some researchers who never call us unless they need money.
Complex epithelial cell movements are better, it turns out. Over an observation period of 64 hours the NTU team found that the healing efficiency of wavy gaps – measured by the area covered by the cells over time – is nearly five times faster than straight gaps.
The complex motion “enabled cells to quickly connect with similar cells on the opposite site of the wound edge, forming a bridge and closing the wavy wound gaps faster than straight gaps,” explained lead author Xu Hongmei, a doctoral student at NTU’s School of Mechanical and Aerospace Engineering, who seems to have time to toss out a tumblr or two to keep the press informed.
As for the rest of you, would it kill you to pick up a phone once in a while? Maybe let a journalist know that you’re still alive? We have feelings too, you know, and we worry.
A little Jekyll, a little Hyde, and a little shop of horrors
More “Little Shop of Horrors” references are coming, so be prepared.
We begin with Triphyophyllum peltatum. This woody vine is of great interest to medical and pharmaceutical researchers because its constituents have shown promise against pancreatic cancer and leukemia cells, among others, along with the pathogens that cause malaria and other diseases. There is another side, however. T. peltatum also has a tendency to turn into a realistic Audrey II when deprived.
No, of course they’re not craving human flesh, but it does become … carnivorous in its appetite.
T. peltatum, native to the West African tropics and not found in a New York florist shop, has the unique ability to change its diet and development based on the environmental circumstances. For some unknown reason, the leaves would develop adhesive traps in the form of sticky drops that capture insect prey. The plant is notoriously hard to grow, however, so no one could study the transformation under lab conditions. Until now.
A group of German scientists “exposed the plant to different stress factors, including deficiencies of various nutrients, and studied how it responded to each,” said Dr. Traud Winkelmann of Leibniz University Hannover. “Only in one case were we able to observe the formation of traps: in the case of a lack of phosphorus.”
Well, there you have it: phosphorus. We need it for healthy bones and teeth, which this plant doesn’t have to worry about, unlike its Tony Award–nominated counterpart. The investigators hope that their findings could lead to “future molecular analyses that will help understand the origins of carnivory,” but we’re guessing that a certain singing alien species will be left out of that research.
Fastest peptide north, south, east, aaaaand west of the Pecos
Bacterial infections are supposed to be simple. You get infected, you get an antibiotic to treat it. Easy. Some bacteria, though, don’t play by the rules. Those antibiotics may kill 99.9% of germs, but what about the 0.1% that gets left behind? With their fallen comrades out of the way, the accidentally drug resistant species are free to inherit the Earth.
Antibiotic resistance is thus a major concern for the medical community. Naturally, anything that prevents doctors from successfully curing sick people is a priority. Unless you’re a major pharmaceutical company that has been loath to develop new drugs that can beat antibiotic-resistant bacteria. Blah blah, time and money, blah blah, long time between development and market application, blah blah, no profit. We all know the story with pharmaceutical companies.
Research from other sources has continued, however, and Brazilian scientists recently published research involving a peptide known as plantaricin 149. This peptide, derived from the bacterium Lactobacillus plantarum, has been known for nearly 30 years to have antibacterial properties. Pln149 in its natural state, though, is not particularly efficient at bacteria-killing. Fortunately, we have science and technology on our side.
The researchers synthesized 20 analogs of Pln149, of which Pln149-PEP20 had the best results. The elegantly named compound is less than half the size of the original peptide, less toxic, and far better at killing any and all drug-resistant bacteria the researchers threw at it. How much better? Pln149-PEP20 started killing bacteria less than an hour after being introduced in lab trials.
The research is just in its early days – just because something is less toxic doesn’t necessarily mean you want to go and help yourself to it – but we can only hope that those lovely pharmaceutical companies deign to look down upon us and actually develop a drug utilizing Pln149-PEP20 to, you know, actually help sick people, instead of trying to build monopolies or avoiding paying billions in taxes. Yeah, we couldn’t keep a straight face through that last sentence either.
Speed healing: The wavy wound gets the swirl
Did you know that wavy wounds heal faster than straight wounds? Well, we didn’t, but apparently quite a few people did, because somebody has been trying to figure out why wavy wounds heal faster than straight ones. Do the surgeons know about this? How about you dermatologists? Wavy over straight? We’re the media. We’re supposed to report this kind of stuff. Maybe hit us with a tweet next time you do something important, or push a TikTok our way, okay?
You could be more like the investigators at Nanyang Technological University in Singapore, who figured out the why and then released a statement about it.
They created synthetic wounds – some straight, some wavy – in micropatterned hydrogel substrates that mimicked human skin. Then they used an advanced optical technique known as particle image velocimetry to measure fluid flow and learn how cells moved to close the wound gaps.
The wavy wounds “induced more complex collective cell movements, such as a swirly, vortex-like motion,” according to the written statement from NTU Singapore. In the straight wounds, cell movements paralleled the wound front, “moving in straight lines like a marching band,” they pointed out, unlike some researchers who never call us unless they need money.
Complex epithelial cell movements are better, it turns out. Over an observation period of 64 hours the NTU team found that the healing efficiency of wavy gaps – measured by the area covered by the cells over time – is nearly five times faster than straight gaps.
The complex motion “enabled cells to quickly connect with similar cells on the opposite site of the wound edge, forming a bridge and closing the wavy wound gaps faster than straight gaps,” explained lead author Xu Hongmei, a doctoral student at NTU’s School of Mechanical and Aerospace Engineering, who seems to have time to toss out a tumblr or two to keep the press informed.
As for the rest of you, would it kill you to pick up a phone once in a while? Maybe let a journalist know that you’re still alive? We have feelings too, you know, and we worry.
A little Jekyll, a little Hyde, and a little shop of horrors
More “Little Shop of Horrors” references are coming, so be prepared.
We begin with Triphyophyllum peltatum. This woody vine is of great interest to medical and pharmaceutical researchers because its constituents have shown promise against pancreatic cancer and leukemia cells, among others, along with the pathogens that cause malaria and other diseases. There is another side, however. T. peltatum also has a tendency to turn into a realistic Audrey II when deprived.
No, of course they’re not craving human flesh, but it does become … carnivorous in its appetite.
T. peltatum, native to the West African tropics and not found in a New York florist shop, has the unique ability to change its diet and development based on the environmental circumstances. For some unknown reason, the leaves would develop adhesive traps in the form of sticky drops that capture insect prey. The plant is notoriously hard to grow, however, so no one could study the transformation under lab conditions. Until now.
A group of German scientists “exposed the plant to different stress factors, including deficiencies of various nutrients, and studied how it responded to each,” said Dr. Traud Winkelmann of Leibniz University Hannover. “Only in one case were we able to observe the formation of traps: in the case of a lack of phosphorus.”
Well, there you have it: phosphorus. We need it for healthy bones and teeth, which this plant doesn’t have to worry about, unlike its Tony Award–nominated counterpart. The investigators hope that their findings could lead to “future molecular analyses that will help understand the origins of carnivory,” but we’re guessing that a certain singing alien species will be left out of that research.
Sonographic enthesitis associated with sonographic synovitis and tenosynovitis in PsA
Key clinical point: Sonographic enthesitis showed strong association with sonographic synovitis and tenosynovitis in patients with psoriatic arthritis (PsA), suggesting the clinical significance of sonographic enthesitis as a potential marker for inflammation in other musculoskeletal domains.
Major finding: Sonographic enthesitis was significantly associated with sonographic synovitis (β 0.19; P = .004) and sonographic tenosynovitis (β 0.1; P = .003) and showed strong correlation with patient-reported outcomes, such as Health Assessment Questionnaire (P = .003), morning stiffness (P = .002), and others.
Study details: This study prospectively recruited 158 patients with PsA who underwent sonographic assessment of 52 joints, 40 tendons, and 14 entheses points along with clinical evaluation.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Balulu G et al. The association between sonographic enthesitis with sonographic synovitis and tenosynovitis in psoriatic arthritis patients. Rheumatology (Oxford). 2023 (May 11). Doi: 10.1093/rheumatology/kead202
Key clinical point: Sonographic enthesitis showed strong association with sonographic synovitis and tenosynovitis in patients with psoriatic arthritis (PsA), suggesting the clinical significance of sonographic enthesitis as a potential marker for inflammation in other musculoskeletal domains.
Major finding: Sonographic enthesitis was significantly associated with sonographic synovitis (β 0.19; P = .004) and sonographic tenosynovitis (β 0.1; P = .003) and showed strong correlation with patient-reported outcomes, such as Health Assessment Questionnaire (P = .003), morning stiffness (P = .002), and others.
Study details: This study prospectively recruited 158 patients with PsA who underwent sonographic assessment of 52 joints, 40 tendons, and 14 entheses points along with clinical evaluation.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Balulu G et al. The association between sonographic enthesitis with sonographic synovitis and tenosynovitis in psoriatic arthritis patients. Rheumatology (Oxford). 2023 (May 11). Doi: 10.1093/rheumatology/kead202
Key clinical point: Sonographic enthesitis showed strong association with sonographic synovitis and tenosynovitis in patients with psoriatic arthritis (PsA), suggesting the clinical significance of sonographic enthesitis as a potential marker for inflammation in other musculoskeletal domains.
Major finding: Sonographic enthesitis was significantly associated with sonographic synovitis (β 0.19; P = .004) and sonographic tenosynovitis (β 0.1; P = .003) and showed strong correlation with patient-reported outcomes, such as Health Assessment Questionnaire (P = .003), morning stiffness (P = .002), and others.
Study details: This study prospectively recruited 158 patients with PsA who underwent sonographic assessment of 52 joints, 40 tendons, and 14 entheses points along with clinical evaluation.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Balulu G et al. The association between sonographic enthesitis with sonographic synovitis and tenosynovitis in psoriatic arthritis patients. Rheumatology (Oxford). 2023 (May 11). Doi: 10.1093/rheumatology/kead202
Enthesitis resolution similar with secukinumab and adalimumab in PsA
Key clinical point: Patients with psoriatic arthritis (PsA) achieved enthesitis resolution over 52 weeks with secukinumab treatment, which was comparable to that with adalimumab treatment.
Major finding: At week 52, secukinumab vs adalimumab led to a similar proportion of patients achieving enthesitis resolution (53.2% vs 51.4%) along with site-specific resolution of lateral epicondyle enthesitis (84.6% vs 87.1%) and showing relapse after first resolution (21.0% vs 15.6%), as assessed by the Spondyloarthritis Research Consortium of Canada Enthesitis Index (SPARCC). Moreover, secukinumab vs adalimumab had a comparable response time to SPARCC enthesitis resolution (113 vs 88 days).
Study details: This post hoc analysis of the EXCEED study included 853 patients with PsA who received either secukinumab (300 mg) or adalimumab (40 mg) over 52 weeks.
Disclosures: This study was supported by Novartis Pharmaceuticals Corporation, USA. C Gaillez and B Parikh declared being current or former employees of Novartis Pharma or Novartis Pharmaceuticals Corporation, and several authors reported ties with various sources, including Novartis.
Source: Kaeley GS et al. Enthesitis in patients with psoriatic arthritis treated with secukinumab or adalimumab: A post hoc analysis of the EXCEED study. Rheumatology (Oxford). 2023 (Apr 25). Doi: 10.1093/rheumatology/kead181
Key clinical point: Patients with psoriatic arthritis (PsA) achieved enthesitis resolution over 52 weeks with secukinumab treatment, which was comparable to that with adalimumab treatment.
Major finding: At week 52, secukinumab vs adalimumab led to a similar proportion of patients achieving enthesitis resolution (53.2% vs 51.4%) along with site-specific resolution of lateral epicondyle enthesitis (84.6% vs 87.1%) and showing relapse after first resolution (21.0% vs 15.6%), as assessed by the Spondyloarthritis Research Consortium of Canada Enthesitis Index (SPARCC). Moreover, secukinumab vs adalimumab had a comparable response time to SPARCC enthesitis resolution (113 vs 88 days).
Study details: This post hoc analysis of the EXCEED study included 853 patients with PsA who received either secukinumab (300 mg) or adalimumab (40 mg) over 52 weeks.
Disclosures: This study was supported by Novartis Pharmaceuticals Corporation, USA. C Gaillez and B Parikh declared being current or former employees of Novartis Pharma or Novartis Pharmaceuticals Corporation, and several authors reported ties with various sources, including Novartis.
Source: Kaeley GS et al. Enthesitis in patients with psoriatic arthritis treated with secukinumab or adalimumab: A post hoc analysis of the EXCEED study. Rheumatology (Oxford). 2023 (Apr 25). Doi: 10.1093/rheumatology/kead181
Key clinical point: Patients with psoriatic arthritis (PsA) achieved enthesitis resolution over 52 weeks with secukinumab treatment, which was comparable to that with adalimumab treatment.
Major finding: At week 52, secukinumab vs adalimumab led to a similar proportion of patients achieving enthesitis resolution (53.2% vs 51.4%) along with site-specific resolution of lateral epicondyle enthesitis (84.6% vs 87.1%) and showing relapse after first resolution (21.0% vs 15.6%), as assessed by the Spondyloarthritis Research Consortium of Canada Enthesitis Index (SPARCC). Moreover, secukinumab vs adalimumab had a comparable response time to SPARCC enthesitis resolution (113 vs 88 days).
Study details: This post hoc analysis of the EXCEED study included 853 patients with PsA who received either secukinumab (300 mg) or adalimumab (40 mg) over 52 weeks.
Disclosures: This study was supported by Novartis Pharmaceuticals Corporation, USA. C Gaillez and B Parikh declared being current or former employees of Novartis Pharma or Novartis Pharmaceuticals Corporation, and several authors reported ties with various sources, including Novartis.
Source: Kaeley GS et al. Enthesitis in patients with psoriatic arthritis treated with secukinumab or adalimumab: A post hoc analysis of the EXCEED study. Rheumatology (Oxford). 2023 (Apr 25). Doi: 10.1093/rheumatology/kead181
Secukinumab improves treatment outcomes and inhibits structural damage in PsA
Key clinical point: The achievement of stringent treatment goals with secukinumab led to clinically meaningful benefits in physical function in patients with psoriatic arthritis (PsA), with secukinumab showing a protective effect on radiographic progression.
Major finding: Overall, over 2 years, a relatively small percentage of patients receiving secukinumab achieved sustained remission (REM) according to very low disease activity (LDA; 19%-24%) or Disease Activity index for PsA (DAPSA) REM (30%-36%), with those achieving DAPSA LDA+REM or DAPSA REM showing numerically greater improvement in physical function. A higher proportion of secukinumab-treated patients were non-structural progressors at 2 years irrespective of achieving sustained LDA/REM.
Study details: This was a retrospective analysis from the FUTURE 5 study including 996 patients with active PsA who were randomly assigned to receive secukinumab or placebo.
Disclosures: This study was funded by Novartis Pharma AG. Two authors declared being employees of or owning stocks/shares in Novartis, and several authors reported ties with various sources, including Novartis.
Source: Coates LC et al. Secukinumab improves physical function and quality of life and inhibits structural damage in patients with PsA with sustained remission or low disease activity: Results from the 2-year phase 3 FUTURE 5 study. RMD Open. 2023;9(2):e002939 (Apr 24). Doi: 10.1136/rmdopen-2022-002939
Key clinical point: The achievement of stringent treatment goals with secukinumab led to clinically meaningful benefits in physical function in patients with psoriatic arthritis (PsA), with secukinumab showing a protective effect on radiographic progression.
Major finding: Overall, over 2 years, a relatively small percentage of patients receiving secukinumab achieved sustained remission (REM) according to very low disease activity (LDA; 19%-24%) or Disease Activity index for PsA (DAPSA) REM (30%-36%), with those achieving DAPSA LDA+REM or DAPSA REM showing numerically greater improvement in physical function. A higher proportion of secukinumab-treated patients were non-structural progressors at 2 years irrespective of achieving sustained LDA/REM.
Study details: This was a retrospective analysis from the FUTURE 5 study including 996 patients with active PsA who were randomly assigned to receive secukinumab or placebo.
Disclosures: This study was funded by Novartis Pharma AG. Two authors declared being employees of or owning stocks/shares in Novartis, and several authors reported ties with various sources, including Novartis.
Source: Coates LC et al. Secukinumab improves physical function and quality of life and inhibits structural damage in patients with PsA with sustained remission or low disease activity: Results from the 2-year phase 3 FUTURE 5 study. RMD Open. 2023;9(2):e002939 (Apr 24). Doi: 10.1136/rmdopen-2022-002939
Key clinical point: The achievement of stringent treatment goals with secukinumab led to clinically meaningful benefits in physical function in patients with psoriatic arthritis (PsA), with secukinumab showing a protective effect on radiographic progression.
Major finding: Overall, over 2 years, a relatively small percentage of patients receiving secukinumab achieved sustained remission (REM) according to very low disease activity (LDA; 19%-24%) or Disease Activity index for PsA (DAPSA) REM (30%-36%), with those achieving DAPSA LDA+REM or DAPSA REM showing numerically greater improvement in physical function. A higher proportion of secukinumab-treated patients were non-structural progressors at 2 years irrespective of achieving sustained LDA/REM.
Study details: This was a retrospective analysis from the FUTURE 5 study including 996 patients with active PsA who were randomly assigned to receive secukinumab or placebo.
Disclosures: This study was funded by Novartis Pharma AG. Two authors declared being employees of or owning stocks/shares in Novartis, and several authors reported ties with various sources, including Novartis.
Source: Coates LC et al. Secukinumab improves physical function and quality of life and inhibits structural damage in patients with PsA with sustained remission or low disease activity: Results from the 2-year phase 3 FUTURE 5 study. RMD Open. 2023;9(2):e002939 (Apr 24). Doi: 10.1136/rmdopen-2022-002939
Investigational drug peresolimab shows efficacy in patients with RA
(RA), according to results from a phase 2 clinical trial.
After 12 weeks, patients receiving peresolimab 700 mg saw a greater improvement in the primary endpoint of change in Disease Activity Score for 28 joints based on C-reactive protein (DAS28-CRP), compared with placebo.
“These results provide evidence that stimulation of the PD-1 receptor has potential efficacy in the treatment of rheumatoid arthritis,” said the authors, led by Jay Tuttle, PhD, of Eli Lilly and Company. The study was published in the New England Journal of Medicine.
A total of 98 patients with treatment-resistant, moderate to severe RA were enrolled in the double-blind, placebo-controlled trial. All patients had previously experienced treatment failure with biologic, targeted synthetic, or conventional synthetic disease-modifying antirheumatic drugs. Patients were randomized to receive 700 mg of peresolimab (49 patients), 300 mg of peresolimab (25 patients), or placebo (24 patients) intravenously once every 4 weeks.
Only patients taking peresolimab 700 mg had a significantly greater change in DAS28-CRP scores after 12 weeks, compared with placebo. In secondary outcomes, 71% of the 700-mg group experienced an improvement of at least 20% in American College of Rheumatology response criteria (ACR20), as compared with 42% in the placebo group. There was no difference between the placebo and peresolimab groups in ACR50 or ACR70 responses.
The safety profiles were similar across all three groups, although the 700-mg peresolimab group had numerically more adverse events (n = 14) than the 300-mg peresolimab group (n = 8) and the placebo group (n = 9). There were no severe adverse events reported during the study period. The authors noted that larger and longer studies are necessary to understand the safety of peresolimab.
“Careful evaluation of the effect of peresolimab on the risk of cancer will be important given the efficacy of PD-1 inhibitors in oncologic disease,” the authors wrote.
Eli Lilly funded the research. Researchers disclosed financial relationships with AbbVie, Eli Lilly, Janssen, Novartis, Pfizer, and several other pharmaceutical companies.
(RA), according to results from a phase 2 clinical trial.
After 12 weeks, patients receiving peresolimab 700 mg saw a greater improvement in the primary endpoint of change in Disease Activity Score for 28 joints based on C-reactive protein (DAS28-CRP), compared with placebo.
“These results provide evidence that stimulation of the PD-1 receptor has potential efficacy in the treatment of rheumatoid arthritis,” said the authors, led by Jay Tuttle, PhD, of Eli Lilly and Company. The study was published in the New England Journal of Medicine.
A total of 98 patients with treatment-resistant, moderate to severe RA were enrolled in the double-blind, placebo-controlled trial. All patients had previously experienced treatment failure with biologic, targeted synthetic, or conventional synthetic disease-modifying antirheumatic drugs. Patients were randomized to receive 700 mg of peresolimab (49 patients), 300 mg of peresolimab (25 patients), or placebo (24 patients) intravenously once every 4 weeks.
Only patients taking peresolimab 700 mg had a significantly greater change in DAS28-CRP scores after 12 weeks, compared with placebo. In secondary outcomes, 71% of the 700-mg group experienced an improvement of at least 20% in American College of Rheumatology response criteria (ACR20), as compared with 42% in the placebo group. There was no difference between the placebo and peresolimab groups in ACR50 or ACR70 responses.
The safety profiles were similar across all three groups, although the 700-mg peresolimab group had numerically more adverse events (n = 14) than the 300-mg peresolimab group (n = 8) and the placebo group (n = 9). There were no severe adverse events reported during the study period. The authors noted that larger and longer studies are necessary to understand the safety of peresolimab.
“Careful evaluation of the effect of peresolimab on the risk of cancer will be important given the efficacy of PD-1 inhibitors in oncologic disease,” the authors wrote.
Eli Lilly funded the research. Researchers disclosed financial relationships with AbbVie, Eli Lilly, Janssen, Novartis, Pfizer, and several other pharmaceutical companies.
(RA), according to results from a phase 2 clinical trial.
After 12 weeks, patients receiving peresolimab 700 mg saw a greater improvement in the primary endpoint of change in Disease Activity Score for 28 joints based on C-reactive protein (DAS28-CRP), compared with placebo.
“These results provide evidence that stimulation of the PD-1 receptor has potential efficacy in the treatment of rheumatoid arthritis,” said the authors, led by Jay Tuttle, PhD, of Eli Lilly and Company. The study was published in the New England Journal of Medicine.
A total of 98 patients with treatment-resistant, moderate to severe RA were enrolled in the double-blind, placebo-controlled trial. All patients had previously experienced treatment failure with biologic, targeted synthetic, or conventional synthetic disease-modifying antirheumatic drugs. Patients were randomized to receive 700 mg of peresolimab (49 patients), 300 mg of peresolimab (25 patients), or placebo (24 patients) intravenously once every 4 weeks.
Only patients taking peresolimab 700 mg had a significantly greater change in DAS28-CRP scores after 12 weeks, compared with placebo. In secondary outcomes, 71% of the 700-mg group experienced an improvement of at least 20% in American College of Rheumatology response criteria (ACR20), as compared with 42% in the placebo group. There was no difference between the placebo and peresolimab groups in ACR50 or ACR70 responses.
The safety profiles were similar across all three groups, although the 700-mg peresolimab group had numerically more adverse events (n = 14) than the 300-mg peresolimab group (n = 8) and the placebo group (n = 9). There were no severe adverse events reported during the study period. The authors noted that larger and longer studies are necessary to understand the safety of peresolimab.
“Careful evaluation of the effect of peresolimab on the risk of cancer will be important given the efficacy of PD-1 inhibitors in oncologic disease,” the authors wrote.
Eli Lilly funded the research. Researchers disclosed financial relationships with AbbVie, Eli Lilly, Janssen, Novartis, Pfizer, and several other pharmaceutical companies.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Brepocitinib shows promise for psoriatic arthritis patients
The investigational drug brepocitinib showed superior symptom reduction in adults with moderate to severe active psoriatic arthritis (PsA), compared with placebo, by meeting primary and secondary endpoints of a phase 2b trial at 16 weeks, which persisted out to 1 year, according to data from 218 individuals.
Brepocitinib, a combination tyrosine kinase 2 and Janus kinase 1 inhibitor, is being studied for the treatment of several immunologic diseases including PsA, wrote Philip Mease, MD, of the Swedish Medical Center/Providence St. Joseph Health and the University of Washington, both in Seattle.
Previous studies in patients with PsA support the use of Janus kinase inhibitors and demonstrate the efficacy of tyrosine kinase 2 inhibitors, but more data are needed in patients with active PsA, the researchers noted.
In a study published in Arthritis & Rheumatology, the researchers randomized adults aged 18-75 years with moderate to severe PsA to once-daily oral doses of brepocitinib at 10 mg, 30 mg, or 60 mg, or a placebo for 16 weeks to assess safety, efficacy, and dose response. Placebo-treated patients were advanced to 30 mg or 60 mg of brepocitinib at week 16. Baseline demographics and disease characteristics were similar among the treatment groups. The mean Psoriatic Arthritis Disease Activity Score (PASDAS) and Disease Activity Index for PsA scores were 5.6 and 38.2, respectively, for the overall study population. Approximately two-thirds (64.7%) had a baseline Psoriasis Area and Severity Index (PASI) score greater than 0 and 3% or more of their body surface area affected by psoriasis.
The primary endpoint was the proportion of patients achieving 20% improvement in American College of Rheumatology response criteria (ACR 20) at week 16. Secondary endpoints included rates of patients meeting ACR 50 and ACR 70 response criteria, the proportion of patients achieving 75% and 90% improvement in PASI scores (PASI 70 and 90), as well as the rates of patients meeting Minimal Disease Activity (MDA) criteria at 16 and 52 weeks.
At week 16, ACR 20 response rates were significantly higher in the brepocitinib 30-mg and 60-mg groups, compared with the placebo group (66.7% and 74.6%, respectively, vs. 43.3%), but not for those who received brepocitinib 10 mg (64.5%).
Response rates for ACR 50, ACR 70, PASI 75, PASI 90, and MDA were similarly higher in the 30-mg and 60-mg brepocitinib groups, compared with placebo, and these responses persisted at week 52. Notably, significant differences in PASI 75 and PASI 90 were observed in patients taking 30 mg and 60 mg brepocitinib, compared with placebo, as early as weeks 4 and 8, respectively, the researchers said.
In addition, disease activity based on PASDAS improved significantly more from baseline to week 16 in all brepocitinib groups, compared with placebo.
The overall safety data were consistent with previous brepocitinib studies, and most of the adverse events were mild or moderate, the researchers said. A total of 12 participants (5.5%) experienced a total of 15 serious adverse events, including 6 infections with brepocitinib 30 mg or 60 mg. No major adverse cardiovascular events or deaths occurred during the study period.
The findings were limited by several factors, including the use of clinics in a limited geographic area (11 countries in Europe), small sample size, and mainly White population, the researchers noted. Other limitations included the large placebo effect and relatively short placebo-controlled period.
The study was supported by Pfizer. Dr. Mease disclosed relationships with Pfizer and other companies including AbbVie, Amgen, Bristol-Myers Squibb, Boehringer Ingelheim, Galapagos, Gilead, GlaxoSmithKline, Inmagene, Janssen, Lilly, Novartis, Sun, and UCB. Many coauthors were employees of Pfizer, and others reported financial relationships with Pfizer and other pharmaceutical companies.
The investigational drug brepocitinib showed superior symptom reduction in adults with moderate to severe active psoriatic arthritis (PsA), compared with placebo, by meeting primary and secondary endpoints of a phase 2b trial at 16 weeks, which persisted out to 1 year, according to data from 218 individuals.
Brepocitinib, a combination tyrosine kinase 2 and Janus kinase 1 inhibitor, is being studied for the treatment of several immunologic diseases including PsA, wrote Philip Mease, MD, of the Swedish Medical Center/Providence St. Joseph Health and the University of Washington, both in Seattle.
Previous studies in patients with PsA support the use of Janus kinase inhibitors and demonstrate the efficacy of tyrosine kinase 2 inhibitors, but more data are needed in patients with active PsA, the researchers noted.
In a study published in Arthritis & Rheumatology, the researchers randomized adults aged 18-75 years with moderate to severe PsA to once-daily oral doses of brepocitinib at 10 mg, 30 mg, or 60 mg, or a placebo for 16 weeks to assess safety, efficacy, and dose response. Placebo-treated patients were advanced to 30 mg or 60 mg of brepocitinib at week 16. Baseline demographics and disease characteristics were similar among the treatment groups. The mean Psoriatic Arthritis Disease Activity Score (PASDAS) and Disease Activity Index for PsA scores were 5.6 and 38.2, respectively, for the overall study population. Approximately two-thirds (64.7%) had a baseline Psoriasis Area and Severity Index (PASI) score greater than 0 and 3% or more of their body surface area affected by psoriasis.
The primary endpoint was the proportion of patients achieving 20% improvement in American College of Rheumatology response criteria (ACR 20) at week 16. Secondary endpoints included rates of patients meeting ACR 50 and ACR 70 response criteria, the proportion of patients achieving 75% and 90% improvement in PASI scores (PASI 70 and 90), as well as the rates of patients meeting Minimal Disease Activity (MDA) criteria at 16 and 52 weeks.
At week 16, ACR 20 response rates were significantly higher in the brepocitinib 30-mg and 60-mg groups, compared with the placebo group (66.7% and 74.6%, respectively, vs. 43.3%), but not for those who received brepocitinib 10 mg (64.5%).
Response rates for ACR 50, ACR 70, PASI 75, PASI 90, and MDA were similarly higher in the 30-mg and 60-mg brepocitinib groups, compared with placebo, and these responses persisted at week 52. Notably, significant differences in PASI 75 and PASI 90 were observed in patients taking 30 mg and 60 mg brepocitinib, compared with placebo, as early as weeks 4 and 8, respectively, the researchers said.
In addition, disease activity based on PASDAS improved significantly more from baseline to week 16 in all brepocitinib groups, compared with placebo.
The overall safety data were consistent with previous brepocitinib studies, and most of the adverse events were mild or moderate, the researchers said. A total of 12 participants (5.5%) experienced a total of 15 serious adverse events, including 6 infections with brepocitinib 30 mg or 60 mg. No major adverse cardiovascular events or deaths occurred during the study period.
The findings were limited by several factors, including the use of clinics in a limited geographic area (11 countries in Europe), small sample size, and mainly White population, the researchers noted. Other limitations included the large placebo effect and relatively short placebo-controlled period.
The study was supported by Pfizer. Dr. Mease disclosed relationships with Pfizer and other companies including AbbVie, Amgen, Bristol-Myers Squibb, Boehringer Ingelheim, Galapagos, Gilead, GlaxoSmithKline, Inmagene, Janssen, Lilly, Novartis, Sun, and UCB. Many coauthors were employees of Pfizer, and others reported financial relationships with Pfizer and other pharmaceutical companies.
The investigational drug brepocitinib showed superior symptom reduction in adults with moderate to severe active psoriatic arthritis (PsA), compared with placebo, by meeting primary and secondary endpoints of a phase 2b trial at 16 weeks, which persisted out to 1 year, according to data from 218 individuals.
Brepocitinib, a combination tyrosine kinase 2 and Janus kinase 1 inhibitor, is being studied for the treatment of several immunologic diseases including PsA, wrote Philip Mease, MD, of the Swedish Medical Center/Providence St. Joseph Health and the University of Washington, both in Seattle.
Previous studies in patients with PsA support the use of Janus kinase inhibitors and demonstrate the efficacy of tyrosine kinase 2 inhibitors, but more data are needed in patients with active PsA, the researchers noted.
In a study published in Arthritis & Rheumatology, the researchers randomized adults aged 18-75 years with moderate to severe PsA to once-daily oral doses of brepocitinib at 10 mg, 30 mg, or 60 mg, or a placebo for 16 weeks to assess safety, efficacy, and dose response. Placebo-treated patients were advanced to 30 mg or 60 mg of brepocitinib at week 16. Baseline demographics and disease characteristics were similar among the treatment groups. The mean Psoriatic Arthritis Disease Activity Score (PASDAS) and Disease Activity Index for PsA scores were 5.6 and 38.2, respectively, for the overall study population. Approximately two-thirds (64.7%) had a baseline Psoriasis Area and Severity Index (PASI) score greater than 0 and 3% or more of their body surface area affected by psoriasis.
The primary endpoint was the proportion of patients achieving 20% improvement in American College of Rheumatology response criteria (ACR 20) at week 16. Secondary endpoints included rates of patients meeting ACR 50 and ACR 70 response criteria, the proportion of patients achieving 75% and 90% improvement in PASI scores (PASI 70 and 90), as well as the rates of patients meeting Minimal Disease Activity (MDA) criteria at 16 and 52 weeks.
At week 16, ACR 20 response rates were significantly higher in the brepocitinib 30-mg and 60-mg groups, compared with the placebo group (66.7% and 74.6%, respectively, vs. 43.3%), but not for those who received brepocitinib 10 mg (64.5%).
Response rates for ACR 50, ACR 70, PASI 75, PASI 90, and MDA were similarly higher in the 30-mg and 60-mg brepocitinib groups, compared with placebo, and these responses persisted at week 52. Notably, significant differences in PASI 75 and PASI 90 were observed in patients taking 30 mg and 60 mg brepocitinib, compared with placebo, as early as weeks 4 and 8, respectively, the researchers said.
In addition, disease activity based on PASDAS improved significantly more from baseline to week 16 in all brepocitinib groups, compared with placebo.
The overall safety data were consistent with previous brepocitinib studies, and most of the adverse events were mild or moderate, the researchers said. A total of 12 participants (5.5%) experienced a total of 15 serious adverse events, including 6 infections with brepocitinib 30 mg or 60 mg. No major adverse cardiovascular events or deaths occurred during the study period.
The findings were limited by several factors, including the use of clinics in a limited geographic area (11 countries in Europe), small sample size, and mainly White population, the researchers noted. Other limitations included the large placebo effect and relatively short placebo-controlled period.
The study was supported by Pfizer. Dr. Mease disclosed relationships with Pfizer and other companies including AbbVie, Amgen, Bristol-Myers Squibb, Boehringer Ingelheim, Galapagos, Gilead, GlaxoSmithKline, Inmagene, Janssen, Lilly, Novartis, Sun, and UCB. Many coauthors were employees of Pfizer, and others reported financial relationships with Pfizer and other pharmaceutical companies.
FROM ARTHRITIS & RHEUMATOLOGY