User login
Adalimumab May Be Best Anti-TNF for Psoriasis in Obesity
NEWPORT BEACH, CALIF. – Monoclonal tumor necrosis factor inhibitors such as adalimumab are the go-to treatments for management of psoriasis in obese patients.
Some anti–tumor necrosis factor inhibitors (anti-TNFs) are good treatments for patients with a healthy weight whose psoriasis requires systemic treatment, according to Dr. Jennifer Cather, medical director of the Modern Dermatology-Aesthetics Center in Dallas.
"It would be great to be able to do a cream and light therapy, but for a lot of people that’s just not going to work. The TNF antagonists are my treatment of choice" in those cases, said Dr. Cather, also codirector of the Cutaneous Lymphoma Clinic at Baylor University Medical Center in Dallas.
But obese psoriasis patients "can have success with adalimumab even after failing or partially responding to etanercept," she said at Perspectives in Rheumatic Diseases 2012, held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
Etanercept is her go-to, however, for people who aren’t overweight and "for my peripregnancy people. It seems like they can come on and off it multiple times [as needed and still] do okay." TNF inhibitors are pregnancy category B agents, but "people are reticent to use them" during pregnancy, Dr. Cather noted.
Infliximab is an option as well, but "I have all my infliximab administered by infectious disease [specialists so that patients can be tested for infection with hepatitis B or hepatitis C virus and tuberculosis], and rheumatologists assume care," she said.
Concomitant use of methotrexate can boost the efficacy of TNF inhibitors in the management of psoriasis. In addition, to find the drug that best suits the patient, various anti-TNF agents can be given a trial and stopped if there is no response, and another drug can be initiated. Dr. Cather said that she draws the line at two anti-TNF agents. If a patient has not responded to two of these agents, "usually I’m not going to do a third," she said.
"You want to make sure people are healthy when you put them on [these biologics]. I want to make sure they don’t have [infections or] cancer," both possible risks with treatment. "You have to ask women about cervical dysplasia," because immunosuppression may add fuel to a simmering neoplastic fire, she said.
New-onset, treatment-induced psoriasis is also a possibility. "Nobody really knows what to do with this. Everybody tries to treat through, but if they are getting localized palmoplantar pustular psoriasis, usually you are not going to be able to." Rotating between agents might help, as might adding methotrexate. The retinoid "acitretin works well for pustular psoriasis," Dr. Cather said.
"Remember," she added, "you’ve got to stop the picking in psoriasis." Shiny lesions are a hint that patients have picked off the scales. When they do that, "their plaques actually get thicker. A little bit of [the pain drug gabapentin], 100-300 mg at night, really helps people with this," she said.
Primary care providers may not know that psoriasis is a risk factor for cardiovascular disease and may not routinely screen psoriasis patients for other risk factors. So "when I have a new psoriasis patient, I will write their primary care doctor" and suggest they do so, she said.
Dr. Cather is a consultant, speaker, or researcher for Abbott, Amgen, Calgene, Centocor, Leo Pharma, Novartis, and Pfizer. SDEF and this news organization are owned by Frontline Medical Communications.
NEWPORT BEACH, CALIF. – Monoclonal tumor necrosis factor inhibitors such as adalimumab are the go-to treatments for management of psoriasis in obese patients.
Some anti–tumor necrosis factor inhibitors (anti-TNFs) are good treatments for patients with a healthy weight whose psoriasis requires systemic treatment, according to Dr. Jennifer Cather, medical director of the Modern Dermatology-Aesthetics Center in Dallas.
"It would be great to be able to do a cream and light therapy, but for a lot of people that’s just not going to work. The TNF antagonists are my treatment of choice" in those cases, said Dr. Cather, also codirector of the Cutaneous Lymphoma Clinic at Baylor University Medical Center in Dallas.
But obese psoriasis patients "can have success with adalimumab even after failing or partially responding to etanercept," she said at Perspectives in Rheumatic Diseases 2012, held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
Etanercept is her go-to, however, for people who aren’t overweight and "for my peripregnancy people. It seems like they can come on and off it multiple times [as needed and still] do okay." TNF inhibitors are pregnancy category B agents, but "people are reticent to use them" during pregnancy, Dr. Cather noted.
Infliximab is an option as well, but "I have all my infliximab administered by infectious disease [specialists so that patients can be tested for infection with hepatitis B or hepatitis C virus and tuberculosis], and rheumatologists assume care," she said.
Concomitant use of methotrexate can boost the efficacy of TNF inhibitors in the management of psoriasis. In addition, to find the drug that best suits the patient, various anti-TNF agents can be given a trial and stopped if there is no response, and another drug can be initiated. Dr. Cather said that she draws the line at two anti-TNF agents. If a patient has not responded to two of these agents, "usually I’m not going to do a third," she said.
"You want to make sure people are healthy when you put them on [these biologics]. I want to make sure they don’t have [infections or] cancer," both possible risks with treatment. "You have to ask women about cervical dysplasia," because immunosuppression may add fuel to a simmering neoplastic fire, she said.
New-onset, treatment-induced psoriasis is also a possibility. "Nobody really knows what to do with this. Everybody tries to treat through, but if they are getting localized palmoplantar pustular psoriasis, usually you are not going to be able to." Rotating between agents might help, as might adding methotrexate. The retinoid "acitretin works well for pustular psoriasis," Dr. Cather said.
"Remember," she added, "you’ve got to stop the picking in psoriasis." Shiny lesions are a hint that patients have picked off the scales. When they do that, "their plaques actually get thicker. A little bit of [the pain drug gabapentin], 100-300 mg at night, really helps people with this," she said.
Primary care providers may not know that psoriasis is a risk factor for cardiovascular disease and may not routinely screen psoriasis patients for other risk factors. So "when I have a new psoriasis patient, I will write their primary care doctor" and suggest they do so, she said.
Dr. Cather is a consultant, speaker, or researcher for Abbott, Amgen, Calgene, Centocor, Leo Pharma, Novartis, and Pfizer. SDEF and this news organization are owned by Frontline Medical Communications.
NEWPORT BEACH, CALIF. – Monoclonal tumor necrosis factor inhibitors such as adalimumab are the go-to treatments for management of psoriasis in obese patients.
Some anti–tumor necrosis factor inhibitors (anti-TNFs) are good treatments for patients with a healthy weight whose psoriasis requires systemic treatment, according to Dr. Jennifer Cather, medical director of the Modern Dermatology-Aesthetics Center in Dallas.
"It would be great to be able to do a cream and light therapy, but for a lot of people that’s just not going to work. The TNF antagonists are my treatment of choice" in those cases, said Dr. Cather, also codirector of the Cutaneous Lymphoma Clinic at Baylor University Medical Center in Dallas.
But obese psoriasis patients "can have success with adalimumab even after failing or partially responding to etanercept," she said at Perspectives in Rheumatic Diseases 2012, held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
Etanercept is her go-to, however, for people who aren’t overweight and "for my peripregnancy people. It seems like they can come on and off it multiple times [as needed and still] do okay." TNF inhibitors are pregnancy category B agents, but "people are reticent to use them" during pregnancy, Dr. Cather noted.
Infliximab is an option as well, but "I have all my infliximab administered by infectious disease [specialists so that patients can be tested for infection with hepatitis B or hepatitis C virus and tuberculosis], and rheumatologists assume care," she said.
Concomitant use of methotrexate can boost the efficacy of TNF inhibitors in the management of psoriasis. In addition, to find the drug that best suits the patient, various anti-TNF agents can be given a trial and stopped if there is no response, and another drug can be initiated. Dr. Cather said that she draws the line at two anti-TNF agents. If a patient has not responded to two of these agents, "usually I’m not going to do a third," she said.
"You want to make sure people are healthy when you put them on [these biologics]. I want to make sure they don’t have [infections or] cancer," both possible risks with treatment. "You have to ask women about cervical dysplasia," because immunosuppression may add fuel to a simmering neoplastic fire, she said.
New-onset, treatment-induced psoriasis is also a possibility. "Nobody really knows what to do with this. Everybody tries to treat through, but if they are getting localized palmoplantar pustular psoriasis, usually you are not going to be able to." Rotating between agents might help, as might adding methotrexate. The retinoid "acitretin works well for pustular psoriasis," Dr. Cather said.
"Remember," she added, "you’ve got to stop the picking in psoriasis." Shiny lesions are a hint that patients have picked off the scales. When they do that, "their plaques actually get thicker. A little bit of [the pain drug gabapentin], 100-300 mg at night, really helps people with this," she said.
Primary care providers may not know that psoriasis is a risk factor for cardiovascular disease and may not routinely screen psoriasis patients for other risk factors. So "when I have a new psoriasis patient, I will write their primary care doctor" and suggest they do so, she said.
Dr. Cather is a consultant, speaker, or researcher for Abbott, Amgen, Calgene, Centocor, Leo Pharma, Novartis, and Pfizer. SDEF and this news organization are owned by Frontline Medical Communications.
EXPERT ANALYSIS FROM PERSPECTIVES IN RHEUMATIC DISEASES 2012
Brodalumab Knocks Psoriasis Out of Park
PRAGUE – In a 48-week, phase-II study of brodalumab – a novel selective interleukin-17 inhibitor – 60% of psoriasis patients achieved a Psoriasis Area and Severity Index score of 100, reported Dr. Kim A. Papp.
There were 181 patients with moderate to severe plaque psoriasis in the multicenter, open-label study, and nearly 100% achieved at least a PASI 75 response, 80% achieved at least a PASI 90 response, and 60% achieved a PASI 100, Dr. Papp said at the annual congress of the European Academy of Dermatology and Venereology. Equally important, responses were maintained through week 48, essentially undiminished, he said.
Dr. Papp, director of research at Probity Medical Research, Waterloo, Ont., presented the results of the open-label extension of a previously published phase II, 12-week study (N. Engl. J. Med. 2012;366:1181-9). At the end of the 12-week study, participants were observed off therapy until their psoriasis relapsed, defined as a 50% loss of therapeutic benefit. At that point, they were treated with 210 mg of brodalumab administered subcutaneously every 2 weeks for 48 weeks. The peak response was achieved between weeks 8 and 12 or 16; few study dropouts occurred.
"The side effect profile was varied and included a mix of serious infections and development of atrial fibrillation and other cardiac disorders. Certainly, there were no obvious signals to suggest that we should have undue concerns going into the planned phase III program," said Dr. Papp.
Session cochair Dr. Peter van de Kerkhof was enthusiastic about the brodalumab data. "These are absolutely fabulous results. It’s really very impressive. This study gives us a lead as to where we’re going: to a new phase in biologic therapy where we get an efficacy which we couldn’t have dreamed of 10 years ago. A new bar is set," said Dr. van de Kerkhof, professor and chairman of the department of dermatology at Radboud University in Nijmegen, the Netherlands.
Brodalumab (Amgen) is a human monoclonal antibody directed against the interleukin-17A receptor as a means of quelling inflammatory cytokines. Another humanized monoclonal antibody that neutralizes interleukin-17, ixekizumab (Eli Lilly), was also the subject of a recently published, encouraging phase II study (N. Engl. J. Med. 2012;366:1190-9). Secukinumab (Novartis) is another fully-human monoclonal antibody directed against IL-17A, which has completed several successful phase II studies. These anti-IL-17 biologics are being considered as possible new therapies for other inflammatory diseases, including psoriatic arthritis and rheumatoid arthritis.
Dr. van de Kerkhof cautioned that from a safety standpoint, it will be important to scrutinize the upcoming large, definitive phase III clinical trials of these agents for evidence of an increase in infections, particularly Staphylococcus aureus and Candida albicans.
Interleukin-17A and IL-17F play roles in the normal host-immune defenses against microorganisms. Patients with genetic defects in IL-17 tend to have problems with recurrent chronic mucocutaneous candidiasis. Moreover, individuals with chronic mucocutaneous candidiasis have been shown to have antibodies to IL-17A, IL-17F, and IL-22, he noted.
The study was sponsored by Amgen. Dr. Papp reported receiving research funds from and serving as a consultant to Amgen and numerous other pharmaceutical companies. Dr. van de Kerkhof has received research funding and consultancy fees from more than a dozen pharmaceutical companies.
PRAGUE – In a 48-week, phase-II study of brodalumab – a novel selective interleukin-17 inhibitor – 60% of psoriasis patients achieved a Psoriasis Area and Severity Index score of 100, reported Dr. Kim A. Papp.
There were 181 patients with moderate to severe plaque psoriasis in the multicenter, open-label study, and nearly 100% achieved at least a PASI 75 response, 80% achieved at least a PASI 90 response, and 60% achieved a PASI 100, Dr. Papp said at the annual congress of the European Academy of Dermatology and Venereology. Equally important, responses were maintained through week 48, essentially undiminished, he said.
Dr. Papp, director of research at Probity Medical Research, Waterloo, Ont., presented the results of the open-label extension of a previously published phase II, 12-week study (N. Engl. J. Med. 2012;366:1181-9). At the end of the 12-week study, participants were observed off therapy until their psoriasis relapsed, defined as a 50% loss of therapeutic benefit. At that point, they were treated with 210 mg of brodalumab administered subcutaneously every 2 weeks for 48 weeks. The peak response was achieved between weeks 8 and 12 or 16; few study dropouts occurred.
"The side effect profile was varied and included a mix of serious infections and development of atrial fibrillation and other cardiac disorders. Certainly, there were no obvious signals to suggest that we should have undue concerns going into the planned phase III program," said Dr. Papp.
Session cochair Dr. Peter van de Kerkhof was enthusiastic about the brodalumab data. "These are absolutely fabulous results. It’s really very impressive. This study gives us a lead as to where we’re going: to a new phase in biologic therapy where we get an efficacy which we couldn’t have dreamed of 10 years ago. A new bar is set," said Dr. van de Kerkhof, professor and chairman of the department of dermatology at Radboud University in Nijmegen, the Netherlands.
Brodalumab (Amgen) is a human monoclonal antibody directed against the interleukin-17A receptor as a means of quelling inflammatory cytokines. Another humanized monoclonal antibody that neutralizes interleukin-17, ixekizumab (Eli Lilly), was also the subject of a recently published, encouraging phase II study (N. Engl. J. Med. 2012;366:1190-9). Secukinumab (Novartis) is another fully-human monoclonal antibody directed against IL-17A, which has completed several successful phase II studies. These anti-IL-17 biologics are being considered as possible new therapies for other inflammatory diseases, including psoriatic arthritis and rheumatoid arthritis.
Dr. van de Kerkhof cautioned that from a safety standpoint, it will be important to scrutinize the upcoming large, definitive phase III clinical trials of these agents for evidence of an increase in infections, particularly Staphylococcus aureus and Candida albicans.
Interleukin-17A and IL-17F play roles in the normal host-immune defenses against microorganisms. Patients with genetic defects in IL-17 tend to have problems with recurrent chronic mucocutaneous candidiasis. Moreover, individuals with chronic mucocutaneous candidiasis have been shown to have antibodies to IL-17A, IL-17F, and IL-22, he noted.
The study was sponsored by Amgen. Dr. Papp reported receiving research funds from and serving as a consultant to Amgen and numerous other pharmaceutical companies. Dr. van de Kerkhof has received research funding and consultancy fees from more than a dozen pharmaceutical companies.
PRAGUE – In a 48-week, phase-II study of brodalumab – a novel selective interleukin-17 inhibitor – 60% of psoriasis patients achieved a Psoriasis Area and Severity Index score of 100, reported Dr. Kim A. Papp.
There were 181 patients with moderate to severe plaque psoriasis in the multicenter, open-label study, and nearly 100% achieved at least a PASI 75 response, 80% achieved at least a PASI 90 response, and 60% achieved a PASI 100, Dr. Papp said at the annual congress of the European Academy of Dermatology and Venereology. Equally important, responses were maintained through week 48, essentially undiminished, he said.
Dr. Papp, director of research at Probity Medical Research, Waterloo, Ont., presented the results of the open-label extension of a previously published phase II, 12-week study (N. Engl. J. Med. 2012;366:1181-9). At the end of the 12-week study, participants were observed off therapy until their psoriasis relapsed, defined as a 50% loss of therapeutic benefit. At that point, they were treated with 210 mg of brodalumab administered subcutaneously every 2 weeks for 48 weeks. The peak response was achieved between weeks 8 and 12 or 16; few study dropouts occurred.
"The side effect profile was varied and included a mix of serious infections and development of atrial fibrillation and other cardiac disorders. Certainly, there were no obvious signals to suggest that we should have undue concerns going into the planned phase III program," said Dr. Papp.
Session cochair Dr. Peter van de Kerkhof was enthusiastic about the brodalumab data. "These are absolutely fabulous results. It’s really very impressive. This study gives us a lead as to where we’re going: to a new phase in biologic therapy where we get an efficacy which we couldn’t have dreamed of 10 years ago. A new bar is set," said Dr. van de Kerkhof, professor and chairman of the department of dermatology at Radboud University in Nijmegen, the Netherlands.
Brodalumab (Amgen) is a human monoclonal antibody directed against the interleukin-17A receptor as a means of quelling inflammatory cytokines. Another humanized monoclonal antibody that neutralizes interleukin-17, ixekizumab (Eli Lilly), was also the subject of a recently published, encouraging phase II study (N. Engl. J. Med. 2012;366:1190-9). Secukinumab (Novartis) is another fully-human monoclonal antibody directed against IL-17A, which has completed several successful phase II studies. These anti-IL-17 biologics are being considered as possible new therapies for other inflammatory diseases, including psoriatic arthritis and rheumatoid arthritis.
Dr. van de Kerkhof cautioned that from a safety standpoint, it will be important to scrutinize the upcoming large, definitive phase III clinical trials of these agents for evidence of an increase in infections, particularly Staphylococcus aureus and Candida albicans.
Interleukin-17A and IL-17F play roles in the normal host-immune defenses against microorganisms. Patients with genetic defects in IL-17 tend to have problems with recurrent chronic mucocutaneous candidiasis. Moreover, individuals with chronic mucocutaneous candidiasis have been shown to have antibodies to IL-17A, IL-17F, and IL-22, he noted.
The study was sponsored by Amgen. Dr. Papp reported receiving research funds from and serving as a consultant to Amgen and numerous other pharmaceutical companies. Dr. van de Kerkhof has received research funding and consultancy fees from more than a dozen pharmaceutical companies.
AT THE ANNUAL CONGRESS OF THE EUROPEAN ACADEMY OF DERMATOLOGY AND VENEREOLOGY
Major Finding: After 48 weeks of treatment with brodalumab, 60% of patients with moderate to severe psoriasis displayed a PASI 100 response.
Data Source: This was a multicenter, open-label study involving 181 psoriasis patients who received 210 mg of brodalumab administered subcutaneously every 2 weeks.
Disclosures: This study was sponsored by Amgen. Dr. Papp reported receiving research funds from and serving as a consultant to Amgen and numerous other pharmaceutical companies. Dr. van de Kerkhof has received research funding and consultancy fees from more than a dozen pharmaceutical companies.
Thalidomide Remains a Good Choice for Refractory Cutaneous Lupus
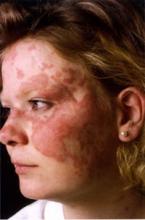
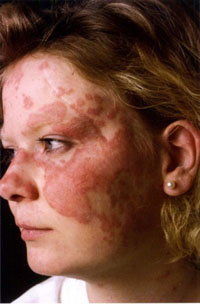
NEWPORT BEACH, CALIF. – Thalidomide remains a good therapeutic choice to control cutaneous lupus when steroid creams and antimalarials fail to do the job, according to Dr. Ruth Ann Vleugels.
Dr. Vleugels said that she sometimes turns to systemic therapy for cutaneous lupus to prevent the severe and disfiguring scarring the condition can cause. The presence of erythematous, scaling lesions suggest active disease amenable to treatment.
Hydroxychloroquine or chloroquine are her first choices for systemic therapy, with the option of adding quinacrine in cases when response is inadequate.
But what do you do "when patients fail to respond to antimalarials alone?" asked Dr. Vleugels, who is director of the connective tissue disease clinic at the Brigham and Women’s Hospital in Boston.
In those cases, she said she sometimes adds methotrexate, but "I keep them on their [hydroxychloroquine] because it has some photoprotective benefits and may lower the risk of developing more significant [disease] down the road."
"Our other favorite is thalidomide. We have good luck with thalidomide. It’s a really good drug to consider for patients who are quite refractory; 7 out of 10 will clear their rash," while on thalidomide, Dr. Vleugels said at the SDEF Perspectives in Rheumatic Diseases meeting, held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
As with isotretinoin, another teratogen, physicians have to enroll in a registry to prescribe thalidomide, and patients have to come back to the office every month for their next prescription because there are no refills.
In addition to being a teratogen, thalidomide is a sedative and so has to be dosed at night. The drug cannot be given to people at increased risk for clotting. About 30% of people on thalidomide develop peripheral neuropathies as well. Dr. Vleugels said that she tells her patients that "if they get bilateral pins and needles sensations, they need to let me know right away. Most the time, you just stop the medicine at that point," she said.
In general, the work-up for cutaneous lupus is like that for systemic lupus erythematosus, she said. "We do a full review of systems to hit all the [American College of Rheumatology] criteria but also ask about other things such as Reynaud’s, hair loss, miscarriages, history of clotting, etc. For labs, we get at least blood work, serology, and a urinalysis."
A medication and herbal review is also critical. "Probably at least 20% of SCLE [subacute cutaneous lupus erythematosus] patients have drug-induced disease. Hydrochlorothiazide is the classic cause, but also calcium channel blockers, and multiple other agents. We are seeing a lot of terbinafine-induced SCLE," she said.
St. John’s wort, ginkgo biloba, and Echinacea are photosensitizers. "If you have a patient with skin lupus, or SLE, who you are trying to photoprotect, you’re going to have a really hard time controlling their skin disease" if they are on any of these agents or supplements, Dr. Vleugels said.
Corticosteroid creams are an option for nonsystemic treatment. For body rashes, Dr. Vleugels said that she prefers a potent agent like clobetasol or a midpotency agent such as triamcinolone.
She said that she uses a low-potency agent such as desonide for the face "except when I really want to treat someone’s face aggressively. If patients have discoid lesions that I don’t want to scar or an impressive malar rash, I’ll give them a potent topical steroid for their face, but I make sure they use it one week on, one week off," she said.
"If you write for ‘one tube,’ a patient will get 15 g," which is insufficient for body rashes. "I’ll give most of my patients with body rashes a minimum of 120 g, but more likely 240 g. You really have to get away from writing for ‘one tube,’ " she said.
Up to 20% of patients with discoid lupus develop systemic disease, a higher proportion than once thought, and systemic disease can take almost a decade to manifest (Br. J. Dermatol. 2011;164:1335-41).
"[We used to think] that if we screened patients with skin-limited disease for the first few years, they’re over the hump. Now we realize we at least have to do careful reviews of systems and baseline labs for patients for longer than the first few years," Dr. Vleugels said.
SDEF and this news organization are owned by Frontline Medical Communications. Dr. Vleugels said she has no disclosures.
NEWPORT BEACH, CALIF. – Thalidomide remains a good therapeutic choice to control cutaneous lupus when steroid creams and antimalarials fail to do the job, according to Dr. Ruth Ann Vleugels.
Dr. Vleugels said that she sometimes turns to systemic therapy for cutaneous lupus to prevent the severe and disfiguring scarring the condition can cause. The presence of erythematous, scaling lesions suggest active disease amenable to treatment.
Hydroxychloroquine or chloroquine are her first choices for systemic therapy, with the option of adding quinacrine in cases when response is inadequate.
But what do you do "when patients fail to respond to antimalarials alone?" asked Dr. Vleugels, who is director of the connective tissue disease clinic at the Brigham and Women’s Hospital in Boston.
In those cases, she said she sometimes adds methotrexate, but "I keep them on their [hydroxychloroquine] because it has some photoprotective benefits and may lower the risk of developing more significant [disease] down the road."
"Our other favorite is thalidomide. We have good luck with thalidomide. It’s a really good drug to consider for patients who are quite refractory; 7 out of 10 will clear their rash," while on thalidomide, Dr. Vleugels said at the SDEF Perspectives in Rheumatic Diseases meeting, held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
As with isotretinoin, another teratogen, physicians have to enroll in a registry to prescribe thalidomide, and patients have to come back to the office every month for their next prescription because there are no refills.
In addition to being a teratogen, thalidomide is a sedative and so has to be dosed at night. The drug cannot be given to people at increased risk for clotting. About 30% of people on thalidomide develop peripheral neuropathies as well. Dr. Vleugels said that she tells her patients that "if they get bilateral pins and needles sensations, they need to let me know right away. Most the time, you just stop the medicine at that point," she said.
In general, the work-up for cutaneous lupus is like that for systemic lupus erythematosus, she said. "We do a full review of systems to hit all the [American College of Rheumatology] criteria but also ask about other things such as Reynaud’s, hair loss, miscarriages, history of clotting, etc. For labs, we get at least blood work, serology, and a urinalysis."
A medication and herbal review is also critical. "Probably at least 20% of SCLE [subacute cutaneous lupus erythematosus] patients have drug-induced disease. Hydrochlorothiazide is the classic cause, but also calcium channel blockers, and multiple other agents. We are seeing a lot of terbinafine-induced SCLE," she said.
St. John’s wort, ginkgo biloba, and Echinacea are photosensitizers. "If you have a patient with skin lupus, or SLE, who you are trying to photoprotect, you’re going to have a really hard time controlling their skin disease" if they are on any of these agents or supplements, Dr. Vleugels said.
Corticosteroid creams are an option for nonsystemic treatment. For body rashes, Dr. Vleugels said that she prefers a potent agent like clobetasol or a midpotency agent such as triamcinolone.
She said that she uses a low-potency agent such as desonide for the face "except when I really want to treat someone’s face aggressively. If patients have discoid lesions that I don’t want to scar or an impressive malar rash, I’ll give them a potent topical steroid for their face, but I make sure they use it one week on, one week off," she said.
"If you write for ‘one tube,’ a patient will get 15 g," which is insufficient for body rashes. "I’ll give most of my patients with body rashes a minimum of 120 g, but more likely 240 g. You really have to get away from writing for ‘one tube,’ " she said.
Up to 20% of patients with discoid lupus develop systemic disease, a higher proportion than once thought, and systemic disease can take almost a decade to manifest (Br. J. Dermatol. 2011;164:1335-41).
"[We used to think] that if we screened patients with skin-limited disease for the first few years, they’re over the hump. Now we realize we at least have to do careful reviews of systems and baseline labs for patients for longer than the first few years," Dr. Vleugels said.
SDEF and this news organization are owned by Frontline Medical Communications. Dr. Vleugels said she has no disclosures.
NEWPORT BEACH, CALIF. – Thalidomide remains a good therapeutic choice to control cutaneous lupus when steroid creams and antimalarials fail to do the job, according to Dr. Ruth Ann Vleugels.
Dr. Vleugels said that she sometimes turns to systemic therapy for cutaneous lupus to prevent the severe and disfiguring scarring the condition can cause. The presence of erythematous, scaling lesions suggest active disease amenable to treatment.
Hydroxychloroquine or chloroquine are her first choices for systemic therapy, with the option of adding quinacrine in cases when response is inadequate.
But what do you do "when patients fail to respond to antimalarials alone?" asked Dr. Vleugels, who is director of the connective tissue disease clinic at the Brigham and Women’s Hospital in Boston.
In those cases, she said she sometimes adds methotrexate, but "I keep them on their [hydroxychloroquine] because it has some photoprotective benefits and may lower the risk of developing more significant [disease] down the road."
"Our other favorite is thalidomide. We have good luck with thalidomide. It’s a really good drug to consider for patients who are quite refractory; 7 out of 10 will clear their rash," while on thalidomide, Dr. Vleugels said at the SDEF Perspectives in Rheumatic Diseases meeting, held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
As with isotretinoin, another teratogen, physicians have to enroll in a registry to prescribe thalidomide, and patients have to come back to the office every month for their next prescription because there are no refills.
In addition to being a teratogen, thalidomide is a sedative and so has to be dosed at night. The drug cannot be given to people at increased risk for clotting. About 30% of people on thalidomide develop peripheral neuropathies as well. Dr. Vleugels said that she tells her patients that "if they get bilateral pins and needles sensations, they need to let me know right away. Most the time, you just stop the medicine at that point," she said.
In general, the work-up for cutaneous lupus is like that for systemic lupus erythematosus, she said. "We do a full review of systems to hit all the [American College of Rheumatology] criteria but also ask about other things such as Reynaud’s, hair loss, miscarriages, history of clotting, etc. For labs, we get at least blood work, serology, and a urinalysis."
A medication and herbal review is also critical. "Probably at least 20% of SCLE [subacute cutaneous lupus erythematosus] patients have drug-induced disease. Hydrochlorothiazide is the classic cause, but also calcium channel blockers, and multiple other agents. We are seeing a lot of terbinafine-induced SCLE," she said.
St. John’s wort, ginkgo biloba, and Echinacea are photosensitizers. "If you have a patient with skin lupus, or SLE, who you are trying to photoprotect, you’re going to have a really hard time controlling their skin disease" if they are on any of these agents or supplements, Dr. Vleugels said.
Corticosteroid creams are an option for nonsystemic treatment. For body rashes, Dr. Vleugels said that she prefers a potent agent like clobetasol or a midpotency agent such as triamcinolone.
She said that she uses a low-potency agent such as desonide for the face "except when I really want to treat someone’s face aggressively. If patients have discoid lesions that I don’t want to scar or an impressive malar rash, I’ll give them a potent topical steroid for their face, but I make sure they use it one week on, one week off," she said.
"If you write for ‘one tube,’ a patient will get 15 g," which is insufficient for body rashes. "I’ll give most of my patients with body rashes a minimum of 120 g, but more likely 240 g. You really have to get away from writing for ‘one tube,’ " she said.
Up to 20% of patients with discoid lupus develop systemic disease, a higher proportion than once thought, and systemic disease can take almost a decade to manifest (Br. J. Dermatol. 2011;164:1335-41).
"[We used to think] that if we screened patients with skin-limited disease for the first few years, they’re over the hump. Now we realize we at least have to do careful reviews of systems and baseline labs for patients for longer than the first few years," Dr. Vleugels said.
SDEF and this news organization are owned by Frontline Medical Communications. Dr. Vleugels said she has no disclosures.
EXPERT ANALYSIS FROM PERSPECTIVES IN RHEUMATIC DISEASES 2012
Antibiotics Helpful in Chlamydia-Induced Reactive Arthritis
Reactive arthritis that is due to Chlamydia trachomatis infection responds to antibiotic therapy. Other infectious causes of the condition do not.
So it is worth checking the synovial fluid of affected joints for evidence of chlamydia polymerase chain reaction (PCR), according to Dr. Atul Deodhar, professor of medicine at Oregon Health and Science University in Portland.
In a recent randomized trial, 6 months of rifampin plus either azithromycin or doxycycline significantly improved outcomes versus placebo in patients with chlamydia-induced reactive arthritis. Synovial fluid PCRs were positive for chlamydia in all 42 patients (Arthritis Rheum. 2010;62:1298-307).
The study "has changed my practice. I now send synovial fluid for PCR. I have found several patients" positive for chlamydia, "and we are treating them with antibiotics," Dr. Deodhar said; he also sends urine samples for chlamydia testing.
The primary end point in the study – an improvement of 20% or more in at least four of six variables such as swollen joint count – was achieved by 17 of 27 antibiotic patients (63%) but only 3 of 15 placebo patients (20%). Six patients treated with antibiotics but none of the patients in the placebo group went into complete remission during the trial. Patients on antibiotic were also more likely to clear chlamydia from their joints.
It’s a different story when reactive arthritis is triggered by gastrointestinal pathogens such as salmonella, shigella, campylobacter, and yersinia. In those cases, "avoid antibiotics," Dr. Deodhar said.
He and his colleagues found antibiotic therapy just didn’t help in a population study of 575 likely reactive arthritis cases among 6,379 people with culture-confirmed GI infections. His team confirmed reactive arthritis in 54 of the 82 (66%) subjects they were able to exam. Enthesitis was the most frequent finding; arthritis was less common (Ann. Rheum. Dis. 2008;67:1689-96).
Some patients had been given antibiotics for their GI infections, others not. It "didn’t really make any difference to patients developing or not developing reactive arthritis or the severity of it. [Antibiotics] are not going to prevent people [with dysentery] from developing reactive arthritis," Dr. Deodhar said.
They also found that the presence or absence of human leukocyte antigen B27 did not predict risk. In sporadic reactive arthritis cases, the presence of the antigen is "not actually that important in deciding if someone has or does not have reactive arthritis," he said.
Onset of reactive arthritis comes a few days to a maximum of several weeks following the inducing infection. Asymmetrical mono- or oligoarthritis of the lower extremity is the most common joint finding. Uveitis, dactylitis, and enthesitis are also possible.
Besides antibiotics for chlamydia-induced disease, sulfasalazine and tumor necrosis factor inhibitors may help with difficult cases.
Dr. Deodhar disclosed research and grant support from Abbott, Janssen, and UCB.
Reactive arthritis that is due to Chlamydia trachomatis infection responds to antibiotic therapy. Other infectious causes of the condition do not.
So it is worth checking the synovial fluid of affected joints for evidence of chlamydia polymerase chain reaction (PCR), according to Dr. Atul Deodhar, professor of medicine at Oregon Health and Science University in Portland.
In a recent randomized trial, 6 months of rifampin plus either azithromycin or doxycycline significantly improved outcomes versus placebo in patients with chlamydia-induced reactive arthritis. Synovial fluid PCRs were positive for chlamydia in all 42 patients (Arthritis Rheum. 2010;62:1298-307).
The study "has changed my practice. I now send synovial fluid for PCR. I have found several patients" positive for chlamydia, "and we are treating them with antibiotics," Dr. Deodhar said; he also sends urine samples for chlamydia testing.
The primary end point in the study – an improvement of 20% or more in at least four of six variables such as swollen joint count – was achieved by 17 of 27 antibiotic patients (63%) but only 3 of 15 placebo patients (20%). Six patients treated with antibiotics but none of the patients in the placebo group went into complete remission during the trial. Patients on antibiotic were also more likely to clear chlamydia from their joints.
It’s a different story when reactive arthritis is triggered by gastrointestinal pathogens such as salmonella, shigella, campylobacter, and yersinia. In those cases, "avoid antibiotics," Dr. Deodhar said.
He and his colleagues found antibiotic therapy just didn’t help in a population study of 575 likely reactive arthritis cases among 6,379 people with culture-confirmed GI infections. His team confirmed reactive arthritis in 54 of the 82 (66%) subjects they were able to exam. Enthesitis was the most frequent finding; arthritis was less common (Ann. Rheum. Dis. 2008;67:1689-96).
Some patients had been given antibiotics for their GI infections, others not. It "didn’t really make any difference to patients developing or not developing reactive arthritis or the severity of it. [Antibiotics] are not going to prevent people [with dysentery] from developing reactive arthritis," Dr. Deodhar said.
They also found that the presence or absence of human leukocyte antigen B27 did not predict risk. In sporadic reactive arthritis cases, the presence of the antigen is "not actually that important in deciding if someone has or does not have reactive arthritis," he said.
Onset of reactive arthritis comes a few days to a maximum of several weeks following the inducing infection. Asymmetrical mono- or oligoarthritis of the lower extremity is the most common joint finding. Uveitis, dactylitis, and enthesitis are also possible.
Besides antibiotics for chlamydia-induced disease, sulfasalazine and tumor necrosis factor inhibitors may help with difficult cases.
Dr. Deodhar disclosed research and grant support from Abbott, Janssen, and UCB.
Reactive arthritis that is due to Chlamydia trachomatis infection responds to antibiotic therapy. Other infectious causes of the condition do not.
So it is worth checking the synovial fluid of affected joints for evidence of chlamydia polymerase chain reaction (PCR), according to Dr. Atul Deodhar, professor of medicine at Oregon Health and Science University in Portland.
In a recent randomized trial, 6 months of rifampin plus either azithromycin or doxycycline significantly improved outcomes versus placebo in patients with chlamydia-induced reactive arthritis. Synovial fluid PCRs were positive for chlamydia in all 42 patients (Arthritis Rheum. 2010;62:1298-307).
The study "has changed my practice. I now send synovial fluid for PCR. I have found several patients" positive for chlamydia, "and we are treating them with antibiotics," Dr. Deodhar said; he also sends urine samples for chlamydia testing.
The primary end point in the study – an improvement of 20% or more in at least four of six variables such as swollen joint count – was achieved by 17 of 27 antibiotic patients (63%) but only 3 of 15 placebo patients (20%). Six patients treated with antibiotics but none of the patients in the placebo group went into complete remission during the trial. Patients on antibiotic were also more likely to clear chlamydia from their joints.
It’s a different story when reactive arthritis is triggered by gastrointestinal pathogens such as salmonella, shigella, campylobacter, and yersinia. In those cases, "avoid antibiotics," Dr. Deodhar said.
He and his colleagues found antibiotic therapy just didn’t help in a population study of 575 likely reactive arthritis cases among 6,379 people with culture-confirmed GI infections. His team confirmed reactive arthritis in 54 of the 82 (66%) subjects they were able to exam. Enthesitis was the most frequent finding; arthritis was less common (Ann. Rheum. Dis. 2008;67:1689-96).
Some patients had been given antibiotics for their GI infections, others not. It "didn’t really make any difference to patients developing or not developing reactive arthritis or the severity of it. [Antibiotics] are not going to prevent people [with dysentery] from developing reactive arthritis," Dr. Deodhar said.
They also found that the presence or absence of human leukocyte antigen B27 did not predict risk. In sporadic reactive arthritis cases, the presence of the antigen is "not actually that important in deciding if someone has or does not have reactive arthritis," he said.
Onset of reactive arthritis comes a few days to a maximum of several weeks following the inducing infection. Asymmetrical mono- or oligoarthritis of the lower extremity is the most common joint finding. Uveitis, dactylitis, and enthesitis are also possible.
Besides antibiotics for chlamydia-induced disease, sulfasalazine and tumor necrosis factor inhibitors may help with difficult cases.
Dr. Deodhar disclosed research and grant support from Abbott, Janssen, and UCB.
EXPERT ANALYSIS FROM PERSPECTIVES IN RHEUMATOLOGY
Using CORRONA Registry Data to Treat Rheumatic Diseases
The Consortium of Rheumatology Researchers of North America (or CORRONA) primarily manages a database, and data analysis, of rheumatic diseases. Dr. Joel Kremer, CORRONA president and CEO, offered an update on the group's work at the 2012 Perspectives of Rheumatic Diseases in Newport Beach, Calif., held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
The Consortium of Rheumatology Researchers of North America (or CORRONA) primarily manages a database, and data analysis, of rheumatic diseases. Dr. Joel Kremer, CORRONA president and CEO, offered an update on the group's work at the 2012 Perspectives of Rheumatic Diseases in Newport Beach, Calif., held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
The Consortium of Rheumatology Researchers of North America (or CORRONA) primarily manages a database, and data analysis, of rheumatic diseases. Dr. Joel Kremer, CORRONA president and CEO, offered an update on the group's work at the 2012 Perspectives of Rheumatic Diseases in Newport Beach, Calif., held by Global Academy for Medical Education. GAME and this news organization are owned by Frontline Medical Communications.
Severe Psoriasis Linked to Doubled Diabetes Risk
MUNICH – Patients with severe psoriasis have a twofold increased risk of developing new-onset diabetes based on a review of more than 4 million Danish children and adults, the first nationwide cohort to be evaluated for a link between the two diseases.
"Our results underline the importance of considering psoriatic patients as a high-risk population in terms of diabetes and cardiovascular risk," Mr. Usman Khalid said at the Annual Congress of the European Society of Cardiology. "Screening for diabetes and cardiovascular risk factors in patients with psoriasis is warranted," and follows existing guidelines for managing patients with psoriasis, said Mr. Khalid, a researcher in the cardiovascular research unit of Gentofte Hospital in Copenhagen.
The likely mechanism underlying the association is the inflammatory state of patients with psoriasis, he added.
"These observations are new, interesting, and important," commented Dr. Lars Rydén, professor of cardiology at the Karolinska Institute in Stockholm. Physicians should add "carefully looking for diabetes" to their existing routine screening in psoriasis patients, he said.
The study used Danish national population and patient records for more than 4.6 million Danish citizens aged 10 years or older from 1997 through the end of 2009. The researchers excluded the 97,000 people who had diabetes, psoriasis, or both at entry into the database, which left just more than 4.5 million people, of whom 52,613 developed new-onset psoriasis during follow-up, and 4,465,643 people without psoriasis who served as the reference population. The researchers defined severe psoriasis as a case that required hospitalization at least three times, or patients diagnosed with psoriatic arthritis. The cohort of children and adults with incidence psoriasis included 45,829 mild cases, and 6,784 severe cases.
The researchers tallied the number of people who developed new-onset diabetes, both among those who never had psoriasis during the study period, and among those who developed psoriasis. They identified new diabetes cases based on initiation of treatment with one or more glucose-lowering drugs. During follow-up, the number of new cases of diabetes was 3.67/1,000 person-years among those with no psoriasis, 6.93/1,000 patient-years among patients with mild psoriasis, and 9.65/1,000 patient-years among patients with severe psoriasis. The vast majority of the diabetes that developed was type 2.
Using adjustments that controlled for potential confounders at baseline, including age, sex, comorbidities, medications, and socioeconomic status, the researchers found that, compared with the people without psoriasis, those with mild psoriasis had a statistically significant 47% increased incidence of diabetes, and severe psoriasis linked with a statistically significant twofold increased risk for diabetes, Mr. Khalid reported. The median time from onset of psoriasis to the first treatment for diabetes was about 6 years.
The analysis notably focused on patients who developed diabetes following initial development of psoriasis, which provided insight into the sequence of the two diseases that had not been available in previously-reported studies, noted Dr. Ole Ahlehoff, a cardiology researcher at Gentofte Hospital and collaborator on the study.
"I suggest screening patients with psoriasis once a year for cardiovascular risk factors, including hypertension, dyslipidemia, lifestyle factors, and diabetes based on their glucose level," said Dr. Ahlehoff, who spoke about the research at a press conference. Medical groups have released guidelines that recommend annual risk assessment for patients with severe psoriasis, such as psoriatic arthritis, including the European League Against Arthritis (Ann. Rheum. Dis. 2010;69:325-31), and the Scottish Intercollegiate Guidelines Network.
Mr. Khalid and Dr. Ahlehoff said that they had no disclosures. Dr. Rydén had no relevant disclosures.
MUNICH – Patients with severe psoriasis have a twofold increased risk of developing new-onset diabetes based on a review of more than 4 million Danish children and adults, the first nationwide cohort to be evaluated for a link between the two diseases.
"Our results underline the importance of considering psoriatic patients as a high-risk population in terms of diabetes and cardiovascular risk," Mr. Usman Khalid said at the Annual Congress of the European Society of Cardiology. "Screening for diabetes and cardiovascular risk factors in patients with psoriasis is warranted," and follows existing guidelines for managing patients with psoriasis, said Mr. Khalid, a researcher in the cardiovascular research unit of Gentofte Hospital in Copenhagen.
The likely mechanism underlying the association is the inflammatory state of patients with psoriasis, he added.
"These observations are new, interesting, and important," commented Dr. Lars Rydén, professor of cardiology at the Karolinska Institute in Stockholm. Physicians should add "carefully looking for diabetes" to their existing routine screening in psoriasis patients, he said.
The study used Danish national population and patient records for more than 4.6 million Danish citizens aged 10 years or older from 1997 through the end of 2009. The researchers excluded the 97,000 people who had diabetes, psoriasis, or both at entry into the database, which left just more than 4.5 million people, of whom 52,613 developed new-onset psoriasis during follow-up, and 4,465,643 people without psoriasis who served as the reference population. The researchers defined severe psoriasis as a case that required hospitalization at least three times, or patients diagnosed with psoriatic arthritis. The cohort of children and adults with incidence psoriasis included 45,829 mild cases, and 6,784 severe cases.
The researchers tallied the number of people who developed new-onset diabetes, both among those who never had psoriasis during the study period, and among those who developed psoriasis. They identified new diabetes cases based on initiation of treatment with one or more glucose-lowering drugs. During follow-up, the number of new cases of diabetes was 3.67/1,000 person-years among those with no psoriasis, 6.93/1,000 patient-years among patients with mild psoriasis, and 9.65/1,000 patient-years among patients with severe psoriasis. The vast majority of the diabetes that developed was type 2.
Using adjustments that controlled for potential confounders at baseline, including age, sex, comorbidities, medications, and socioeconomic status, the researchers found that, compared with the people without psoriasis, those with mild psoriasis had a statistically significant 47% increased incidence of diabetes, and severe psoriasis linked with a statistically significant twofold increased risk for diabetes, Mr. Khalid reported. The median time from onset of psoriasis to the first treatment for diabetes was about 6 years.
The analysis notably focused on patients who developed diabetes following initial development of psoriasis, which provided insight into the sequence of the two diseases that had not been available in previously-reported studies, noted Dr. Ole Ahlehoff, a cardiology researcher at Gentofte Hospital and collaborator on the study.
"I suggest screening patients with psoriasis once a year for cardiovascular risk factors, including hypertension, dyslipidemia, lifestyle factors, and diabetes based on their glucose level," said Dr. Ahlehoff, who spoke about the research at a press conference. Medical groups have released guidelines that recommend annual risk assessment for patients with severe psoriasis, such as psoriatic arthritis, including the European League Against Arthritis (Ann. Rheum. Dis. 2010;69:325-31), and the Scottish Intercollegiate Guidelines Network.
Mr. Khalid and Dr. Ahlehoff said that they had no disclosures. Dr. Rydén had no relevant disclosures.
MUNICH – Patients with severe psoriasis have a twofold increased risk of developing new-onset diabetes based on a review of more than 4 million Danish children and adults, the first nationwide cohort to be evaluated for a link between the two diseases.
"Our results underline the importance of considering psoriatic patients as a high-risk population in terms of diabetes and cardiovascular risk," Mr. Usman Khalid said at the Annual Congress of the European Society of Cardiology. "Screening for diabetes and cardiovascular risk factors in patients with psoriasis is warranted," and follows existing guidelines for managing patients with psoriasis, said Mr. Khalid, a researcher in the cardiovascular research unit of Gentofte Hospital in Copenhagen.
The likely mechanism underlying the association is the inflammatory state of patients with psoriasis, he added.
"These observations are new, interesting, and important," commented Dr. Lars Rydén, professor of cardiology at the Karolinska Institute in Stockholm. Physicians should add "carefully looking for diabetes" to their existing routine screening in psoriasis patients, he said.
The study used Danish national population and patient records for more than 4.6 million Danish citizens aged 10 years or older from 1997 through the end of 2009. The researchers excluded the 97,000 people who had diabetes, psoriasis, or both at entry into the database, which left just more than 4.5 million people, of whom 52,613 developed new-onset psoriasis during follow-up, and 4,465,643 people without psoriasis who served as the reference population. The researchers defined severe psoriasis as a case that required hospitalization at least three times, or patients diagnosed with psoriatic arthritis. The cohort of children and adults with incidence psoriasis included 45,829 mild cases, and 6,784 severe cases.
The researchers tallied the number of people who developed new-onset diabetes, both among those who never had psoriasis during the study period, and among those who developed psoriasis. They identified new diabetes cases based on initiation of treatment with one or more glucose-lowering drugs. During follow-up, the number of new cases of diabetes was 3.67/1,000 person-years among those with no psoriasis, 6.93/1,000 patient-years among patients with mild psoriasis, and 9.65/1,000 patient-years among patients with severe psoriasis. The vast majority of the diabetes that developed was type 2.
Using adjustments that controlled for potential confounders at baseline, including age, sex, comorbidities, medications, and socioeconomic status, the researchers found that, compared with the people without psoriasis, those with mild psoriasis had a statistically significant 47% increased incidence of diabetes, and severe psoriasis linked with a statistically significant twofold increased risk for diabetes, Mr. Khalid reported. The median time from onset of psoriasis to the first treatment for diabetes was about 6 years.
The analysis notably focused on patients who developed diabetes following initial development of psoriasis, which provided insight into the sequence of the two diseases that had not been available in previously-reported studies, noted Dr. Ole Ahlehoff, a cardiology researcher at Gentofte Hospital and collaborator on the study.
"I suggest screening patients with psoriasis once a year for cardiovascular risk factors, including hypertension, dyslipidemia, lifestyle factors, and diabetes based on their glucose level," said Dr. Ahlehoff, who spoke about the research at a press conference. Medical groups have released guidelines that recommend annual risk assessment for patients with severe psoriasis, such as psoriatic arthritis, including the European League Against Arthritis (Ann. Rheum. Dis. 2010;69:325-31), and the Scottish Intercollegiate Guidelines Network.
Mr. Khalid and Dr. Ahlehoff said that they had no disclosures. Dr. Rydén had no relevant disclosures.
AT THE ANNUAL CONGRESS OF THE EUROPEAN SOCIETY OF CARDIOLOGY
Major Finding: New-onset, severe psoriasis doubled the risk for incident diabetes during a median of 6 years compared with people without psoriasis.
Data Source: Data came from an analysis of 4.5 million Danish children and adults followed during 1997-2009.
Disclosures: Mr. Khalid and Dr. Ahlehoff said that they had no disclosures. Dr. Rydén had no relevant disclosures.
Antimalarial Response in CLE Takes Time
BOSTON – The use of adjunctive therapy and a lot of patience may go a long way to improving the response of cutaneous lupus erythematosus to antimalarial agents, according to Dr. Jennie T. Clarke.
Antimalarials are the go-to treatment for cutaneous lupus erythematosus (CLE), yet roughly a third of patients do not respond, said Dr. Clarke, who spoke at the American Academy of Dermatology’s Summer Academy Meeting.
Findings from some recent studies shed light on how to improve that dismal response rate. In one of these trials involving 128 patients with CLE, researchers found that slightly more than half of patients who initiated treatment with hydroxychloroquine monotherapy were responders (55%) (Arch. Dermatol. 2011;147:1261-7). When quinacrine was added to the treatment regimen of the nonresponders, two-thirds experienced a lessening of their disease. Improvement continued beyond 2 months in 43%.
"With antimalarials remember that patience is important. [These agents] have a slow onset. You have to give the drugs for 2-3 months before assessing for efficacy. Patients need to know this because otherwise they’re going to become frustrated and noncompliant," said Dr. Clarke of the department of dermatology at Pennsylvania State University, Hershey.
The other important lesson from the study is about combination antimalarial therapy. Quinacrine can be added to either hydroxychloroquine or chloroquine to achieve improvement in patients who don’t respond to a single antimalarial agent.
However, roughly a third of patients don’t respond to a combination of antimalarials. Some research in the last 18 months has tried to identify which patients fail antimalarial treatment and why, in order to improve subsequent treatment. Three possible reasons have been identified: dosing and compliance, disease severity, and smoking status.
Bioavailability and clearance of hydroxychloroquine seems to vary by individual, she said. In addition, noncompliance is estimated to be about 10%. In a study of 300 CLE patients, French researchers found that the median blood concentration of hydroxychloroquine correlated with response (Arch. Dermatol. 2012;148:479-84). Specifically, the median blood hydroxychloroquine concentration was significantly higher in patients with complete remission compared with those with either partial remission or treatment failure. Findings from the multivariate analysis showed that complete remission was associated with higher blood hydroxychloroquine concentrations and the absence of discoid lesions.
Concentration and response were correlated with actual rather than ideal body weight dosing. Smoking was not found to be related to concentration, and the subset of 170 patients with discoid lupus erythematosus (DLE) was less responsive to hydroxychloroquine.
Thirty patients (10%) had very low blood hydroxychloroquine concentrations (less than 200 ng/mL) and may be considered nonadherent to the treatment regimen, Dr. Clarke noted. However, additional study is needed to determine the optimal blood concentration of hydroxychloroquine and the impact of toxicity with actual weight-based dosing rather than ideal body weight dosing.
In another study, researchers assessed the clinical and pharmacogenic influences of disease severity on response to blood concentration of hydroxychloroquine (J. Invest. Dermatol. 2011;131:1981-6). They assessed 200 patients with DLE. Slightly more than a third (35%) of patients had not responded to hydroxychloroquine at 6 months. Poor response was associated with disease severity and concomitant systemic lupus erythematosus (SLE). However, response was not associated with the presence of cytochrome P450 genotype or smoking.
It has been long held medical dogma that smoking lessens patients’ response to antimalarial drugs. The impact of smoking in patients with CLE was assessed directly in another paper (Arch. Dermatol. 2012;148:317-22). The researchers included 218 patients with CLE or SLE with skin disease. They found that current smokers had more severe disease and poorer disease-related quality of life. Smokers were also more likely to receive combination antimalarial therapy. Current smokers responded better to antimalarials than past or never smokers. However, smokers responded worse than nonsmokers if antimalarials and immunomodulator/suppressives were required.
"This tells us that antimalarials can be effective for smokers, particularly in those with more mild disease. But we need to remember that smokers who don’t respond are likely going to have poorer outcomes than nonsmokers who don’t respond to antimalarials."
Dr. Clarke reported having no relevant financial conflicts.
BOSTON – The use of adjunctive therapy and a lot of patience may go a long way to improving the response of cutaneous lupus erythematosus to antimalarial agents, according to Dr. Jennie T. Clarke.
Antimalarials are the go-to treatment for cutaneous lupus erythematosus (CLE), yet roughly a third of patients do not respond, said Dr. Clarke, who spoke at the American Academy of Dermatology’s Summer Academy Meeting.
Findings from some recent studies shed light on how to improve that dismal response rate. In one of these trials involving 128 patients with CLE, researchers found that slightly more than half of patients who initiated treatment with hydroxychloroquine monotherapy were responders (55%) (Arch. Dermatol. 2011;147:1261-7). When quinacrine was added to the treatment regimen of the nonresponders, two-thirds experienced a lessening of their disease. Improvement continued beyond 2 months in 43%.
"With antimalarials remember that patience is important. [These agents] have a slow onset. You have to give the drugs for 2-3 months before assessing for efficacy. Patients need to know this because otherwise they’re going to become frustrated and noncompliant," said Dr. Clarke of the department of dermatology at Pennsylvania State University, Hershey.
The other important lesson from the study is about combination antimalarial therapy. Quinacrine can be added to either hydroxychloroquine or chloroquine to achieve improvement in patients who don’t respond to a single antimalarial agent.
However, roughly a third of patients don’t respond to a combination of antimalarials. Some research in the last 18 months has tried to identify which patients fail antimalarial treatment and why, in order to improve subsequent treatment. Three possible reasons have been identified: dosing and compliance, disease severity, and smoking status.
Bioavailability and clearance of hydroxychloroquine seems to vary by individual, she said. In addition, noncompliance is estimated to be about 10%. In a study of 300 CLE patients, French researchers found that the median blood concentration of hydroxychloroquine correlated with response (Arch. Dermatol. 2012;148:479-84). Specifically, the median blood hydroxychloroquine concentration was significantly higher in patients with complete remission compared with those with either partial remission or treatment failure. Findings from the multivariate analysis showed that complete remission was associated with higher blood hydroxychloroquine concentrations and the absence of discoid lesions.
Concentration and response were correlated with actual rather than ideal body weight dosing. Smoking was not found to be related to concentration, and the subset of 170 patients with discoid lupus erythematosus (DLE) was less responsive to hydroxychloroquine.
Thirty patients (10%) had very low blood hydroxychloroquine concentrations (less than 200 ng/mL) and may be considered nonadherent to the treatment regimen, Dr. Clarke noted. However, additional study is needed to determine the optimal blood concentration of hydroxychloroquine and the impact of toxicity with actual weight-based dosing rather than ideal body weight dosing.
In another study, researchers assessed the clinical and pharmacogenic influences of disease severity on response to blood concentration of hydroxychloroquine (J. Invest. Dermatol. 2011;131:1981-6). They assessed 200 patients with DLE. Slightly more than a third (35%) of patients had not responded to hydroxychloroquine at 6 months. Poor response was associated with disease severity and concomitant systemic lupus erythematosus (SLE). However, response was not associated with the presence of cytochrome P450 genotype or smoking.
It has been long held medical dogma that smoking lessens patients’ response to antimalarial drugs. The impact of smoking in patients with CLE was assessed directly in another paper (Arch. Dermatol. 2012;148:317-22). The researchers included 218 patients with CLE or SLE with skin disease. They found that current smokers had more severe disease and poorer disease-related quality of life. Smokers were also more likely to receive combination antimalarial therapy. Current smokers responded better to antimalarials than past or never smokers. However, smokers responded worse than nonsmokers if antimalarials and immunomodulator/suppressives were required.
"This tells us that antimalarials can be effective for smokers, particularly in those with more mild disease. But we need to remember that smokers who don’t respond are likely going to have poorer outcomes than nonsmokers who don’t respond to antimalarials."
Dr. Clarke reported having no relevant financial conflicts.
BOSTON – The use of adjunctive therapy and a lot of patience may go a long way to improving the response of cutaneous lupus erythematosus to antimalarial agents, according to Dr. Jennie T. Clarke.
Antimalarials are the go-to treatment for cutaneous lupus erythematosus (CLE), yet roughly a third of patients do not respond, said Dr. Clarke, who spoke at the American Academy of Dermatology’s Summer Academy Meeting.
Findings from some recent studies shed light on how to improve that dismal response rate. In one of these trials involving 128 patients with CLE, researchers found that slightly more than half of patients who initiated treatment with hydroxychloroquine monotherapy were responders (55%) (Arch. Dermatol. 2011;147:1261-7). When quinacrine was added to the treatment regimen of the nonresponders, two-thirds experienced a lessening of their disease. Improvement continued beyond 2 months in 43%.
"With antimalarials remember that patience is important. [These agents] have a slow onset. You have to give the drugs for 2-3 months before assessing for efficacy. Patients need to know this because otherwise they’re going to become frustrated and noncompliant," said Dr. Clarke of the department of dermatology at Pennsylvania State University, Hershey.
The other important lesson from the study is about combination antimalarial therapy. Quinacrine can be added to either hydroxychloroquine or chloroquine to achieve improvement in patients who don’t respond to a single antimalarial agent.
However, roughly a third of patients don’t respond to a combination of antimalarials. Some research in the last 18 months has tried to identify which patients fail antimalarial treatment and why, in order to improve subsequent treatment. Three possible reasons have been identified: dosing and compliance, disease severity, and smoking status.
Bioavailability and clearance of hydroxychloroquine seems to vary by individual, she said. In addition, noncompliance is estimated to be about 10%. In a study of 300 CLE patients, French researchers found that the median blood concentration of hydroxychloroquine correlated with response (Arch. Dermatol. 2012;148:479-84). Specifically, the median blood hydroxychloroquine concentration was significantly higher in patients with complete remission compared with those with either partial remission or treatment failure. Findings from the multivariate analysis showed that complete remission was associated with higher blood hydroxychloroquine concentrations and the absence of discoid lesions.
Concentration and response were correlated with actual rather than ideal body weight dosing. Smoking was not found to be related to concentration, and the subset of 170 patients with discoid lupus erythematosus (DLE) was less responsive to hydroxychloroquine.
Thirty patients (10%) had very low blood hydroxychloroquine concentrations (less than 200 ng/mL) and may be considered nonadherent to the treatment regimen, Dr. Clarke noted. However, additional study is needed to determine the optimal blood concentration of hydroxychloroquine and the impact of toxicity with actual weight-based dosing rather than ideal body weight dosing.
In another study, researchers assessed the clinical and pharmacogenic influences of disease severity on response to blood concentration of hydroxychloroquine (J. Invest. Dermatol. 2011;131:1981-6). They assessed 200 patients with DLE. Slightly more than a third (35%) of patients had not responded to hydroxychloroquine at 6 months. Poor response was associated with disease severity and concomitant systemic lupus erythematosus (SLE). However, response was not associated with the presence of cytochrome P450 genotype or smoking.
It has been long held medical dogma that smoking lessens patients’ response to antimalarial drugs. The impact of smoking in patients with CLE was assessed directly in another paper (Arch. Dermatol. 2012;148:317-22). The researchers included 218 patients with CLE or SLE with skin disease. They found that current smokers had more severe disease and poorer disease-related quality of life. Smokers were also more likely to receive combination antimalarial therapy. Current smokers responded better to antimalarials than past or never smokers. However, smokers responded worse than nonsmokers if antimalarials and immunomodulator/suppressives were required.
"This tells us that antimalarials can be effective for smokers, particularly in those with more mild disease. But we need to remember that smokers who don’t respond are likely going to have poorer outcomes than nonsmokers who don’t respond to antimalarials."
Dr. Clarke reported having no relevant financial conflicts.
EXPERT ANALYSIS FROM THE AMERICAN ACADEMY OF DERMATOLOGY'S SUMMER ACADEMY MEETING
Psoriasis Severity Linked to Tonsil Size
BOSTON – Patients with psoriasis are almost nine times more likely to have enlarged tonsils, compared with patients without psoriasis, according to the results of a small study.
"Our findings suggest that hypertrophic tonsils may be associated with a pathogenic role in psoriasis," Dr. Marianna Shvartsbeyn and her coinvestigators reported in a poster presented at the American Academy of Dermatology’s Summer Academy Meeting. But it is still too soon to know the clinical implications.
In all, 32 patients with psoriasis and 14 patients with noninflammatory skin conditions (common warts, melanoma, and nonmelanoma skin diseases) were recruited. Patients who previously underwent tonsillectomy were excluded.
Tonsils were examined by one investigator, using a 5-point standardized tonsillar hypertrophy grading scale (adopted from Am. Fam. Physician 2004;69:1147-55).
Tonsils that were entirely within the tonsillar fossa received a grade of 0. Tonsils occupying less than 25% of the lateral dimension of the oropharynx, as measured between the anterior tonsillar pillars, received a grade of 1; tonsils occupying less than 50% of the lateral dimension of the oropharynx were a 2; tonsils occupying less than 75% of the lateral dimension of the oropharynx were a 3; and tonsils occupying 75 % or more of the lateral dimension of the oropharynx received a grade of 4.
Chart reviews were conducted to collect information on patient age, sex, race, social history (tobacco, alcohol, and drug use), diagnosis of skin condition, and the duration/severity of disease, noted Dr. Shvartsbeyn and her colleague of the departments of pathology and dermatology at the New York University.
Patients with psoriasis were found to have had an odds ratio of 8.77 for having enlarged tonsils (grade 2 or greater), compared with healthy controls. Tonsillar size also was significantly larger in patients with psoriasis (mean tonsil grade, 1.78), than in control patients (mean tonsil grade, 0.86); the severity of psoriasis was positively associated with tonsil size, Dr. Shvartsbeyn and her colleagues reported.
Limited clinical data have suggested that there is an association between hypertrophic tonsils and inflammatory skin disease. Small studies have shown that among patients with psoriasis, the cutaneous lesions disappeared or improved after tonsillectomy. It is suspected that there may be a genetic predisposition that makes certain patient populations more susceptible, the researchers noted.
Histopathologic studies also point to the possible link between the robust immune response that takes place in the tonsils and the changes in the skin of patients with pustulosis palmaris et plantaris (PPP).
Histologic evaluation of tonsils obtained from patients with PPP has revealed enlargement of the secondary T nodules and atrophy of the lymph follicles, with a decrease in the number of the germinal center cells and fibrosis – changes typically seen in older tonsils. This finding provides indirect evidence of the intensely advanced stage of the immune response within the tonsils.
"Our hypothesis is that in chronic tonsillar hypertrophy, bacterial species that reside in the tonsils are released into the circulation and cause stimulation of T cells. As a result of this constant chronic stimulation, an autoreactive clone may be formed. The auto-clone may produce an antibody attacking the skin and drive inflammatory response. In some individuals, this exaggerated immune response may manifest as psoriasis," the investigators wrote.
And although there is empirical evidence "that tonsillectomy improved skin lesions in patients with psoriasis and pustulosis palmaris et plantaris in small retrospective studies, further studies are needed. ... The observed association needs validation and interventional study is needed to prove causation/contribution," Dr. Shvartsbeyn noted in an interview.
The study was supported by grants from the National Cancer Institute, the National Institute for Allergy and Infectious Diseases, and the National Institute of Dental and Craniofacial Research. The investigators did not report having any conflicts of interest.
BOSTON – Patients with psoriasis are almost nine times more likely to have enlarged tonsils, compared with patients without psoriasis, according to the results of a small study.
"Our findings suggest that hypertrophic tonsils may be associated with a pathogenic role in psoriasis," Dr. Marianna Shvartsbeyn and her coinvestigators reported in a poster presented at the American Academy of Dermatology’s Summer Academy Meeting. But it is still too soon to know the clinical implications.
In all, 32 patients with psoriasis and 14 patients with noninflammatory skin conditions (common warts, melanoma, and nonmelanoma skin diseases) were recruited. Patients who previously underwent tonsillectomy were excluded.
Tonsils were examined by one investigator, using a 5-point standardized tonsillar hypertrophy grading scale (adopted from Am. Fam. Physician 2004;69:1147-55).
Tonsils that were entirely within the tonsillar fossa received a grade of 0. Tonsils occupying less than 25% of the lateral dimension of the oropharynx, as measured between the anterior tonsillar pillars, received a grade of 1; tonsils occupying less than 50% of the lateral dimension of the oropharynx were a 2; tonsils occupying less than 75% of the lateral dimension of the oropharynx were a 3; and tonsils occupying 75 % or more of the lateral dimension of the oropharynx received a grade of 4.
Chart reviews were conducted to collect information on patient age, sex, race, social history (tobacco, alcohol, and drug use), diagnosis of skin condition, and the duration/severity of disease, noted Dr. Shvartsbeyn and her colleague of the departments of pathology and dermatology at the New York University.
Patients with psoriasis were found to have had an odds ratio of 8.77 for having enlarged tonsils (grade 2 or greater), compared with healthy controls. Tonsillar size also was significantly larger in patients with psoriasis (mean tonsil grade, 1.78), than in control patients (mean tonsil grade, 0.86); the severity of psoriasis was positively associated with tonsil size, Dr. Shvartsbeyn and her colleagues reported.
Limited clinical data have suggested that there is an association between hypertrophic tonsils and inflammatory skin disease. Small studies have shown that among patients with psoriasis, the cutaneous lesions disappeared or improved after tonsillectomy. It is suspected that there may be a genetic predisposition that makes certain patient populations more susceptible, the researchers noted.
Histopathologic studies also point to the possible link between the robust immune response that takes place in the tonsils and the changes in the skin of patients with pustulosis palmaris et plantaris (PPP).
Histologic evaluation of tonsils obtained from patients with PPP has revealed enlargement of the secondary T nodules and atrophy of the lymph follicles, with a decrease in the number of the germinal center cells and fibrosis – changes typically seen in older tonsils. This finding provides indirect evidence of the intensely advanced stage of the immune response within the tonsils.
"Our hypothesis is that in chronic tonsillar hypertrophy, bacterial species that reside in the tonsils are released into the circulation and cause stimulation of T cells. As a result of this constant chronic stimulation, an autoreactive clone may be formed. The auto-clone may produce an antibody attacking the skin and drive inflammatory response. In some individuals, this exaggerated immune response may manifest as psoriasis," the investigators wrote.
And although there is empirical evidence "that tonsillectomy improved skin lesions in patients with psoriasis and pustulosis palmaris et plantaris in small retrospective studies, further studies are needed. ... The observed association needs validation and interventional study is needed to prove causation/contribution," Dr. Shvartsbeyn noted in an interview.
The study was supported by grants from the National Cancer Institute, the National Institute for Allergy and Infectious Diseases, and the National Institute of Dental and Craniofacial Research. The investigators did not report having any conflicts of interest.
BOSTON – Patients with psoriasis are almost nine times more likely to have enlarged tonsils, compared with patients without psoriasis, according to the results of a small study.
"Our findings suggest that hypertrophic tonsils may be associated with a pathogenic role in psoriasis," Dr. Marianna Shvartsbeyn and her coinvestigators reported in a poster presented at the American Academy of Dermatology’s Summer Academy Meeting. But it is still too soon to know the clinical implications.
In all, 32 patients with psoriasis and 14 patients with noninflammatory skin conditions (common warts, melanoma, and nonmelanoma skin diseases) were recruited. Patients who previously underwent tonsillectomy were excluded.
Tonsils were examined by one investigator, using a 5-point standardized tonsillar hypertrophy grading scale (adopted from Am. Fam. Physician 2004;69:1147-55).
Tonsils that were entirely within the tonsillar fossa received a grade of 0. Tonsils occupying less than 25% of the lateral dimension of the oropharynx, as measured between the anterior tonsillar pillars, received a grade of 1; tonsils occupying less than 50% of the lateral dimension of the oropharynx were a 2; tonsils occupying less than 75% of the lateral dimension of the oropharynx were a 3; and tonsils occupying 75 % or more of the lateral dimension of the oropharynx received a grade of 4.
Chart reviews were conducted to collect information on patient age, sex, race, social history (tobacco, alcohol, and drug use), diagnosis of skin condition, and the duration/severity of disease, noted Dr. Shvartsbeyn and her colleague of the departments of pathology and dermatology at the New York University.
Patients with psoriasis were found to have had an odds ratio of 8.77 for having enlarged tonsils (grade 2 or greater), compared with healthy controls. Tonsillar size also was significantly larger in patients with psoriasis (mean tonsil grade, 1.78), than in control patients (mean tonsil grade, 0.86); the severity of psoriasis was positively associated with tonsil size, Dr. Shvartsbeyn and her colleagues reported.
Limited clinical data have suggested that there is an association between hypertrophic tonsils and inflammatory skin disease. Small studies have shown that among patients with psoriasis, the cutaneous lesions disappeared or improved after tonsillectomy. It is suspected that there may be a genetic predisposition that makes certain patient populations more susceptible, the researchers noted.
Histopathologic studies also point to the possible link between the robust immune response that takes place in the tonsils and the changes in the skin of patients with pustulosis palmaris et plantaris (PPP).
Histologic evaluation of tonsils obtained from patients with PPP has revealed enlargement of the secondary T nodules and atrophy of the lymph follicles, with a decrease in the number of the germinal center cells and fibrosis – changes typically seen in older tonsils. This finding provides indirect evidence of the intensely advanced stage of the immune response within the tonsils.
"Our hypothesis is that in chronic tonsillar hypertrophy, bacterial species that reside in the tonsils are released into the circulation and cause stimulation of T cells. As a result of this constant chronic stimulation, an autoreactive clone may be formed. The auto-clone may produce an antibody attacking the skin and drive inflammatory response. In some individuals, this exaggerated immune response may manifest as psoriasis," the investigators wrote.
And although there is empirical evidence "that tonsillectomy improved skin lesions in patients with psoriasis and pustulosis palmaris et plantaris in small retrospective studies, further studies are needed. ... The observed association needs validation and interventional study is needed to prove causation/contribution," Dr. Shvartsbeyn noted in an interview.
The study was supported by grants from the National Cancer Institute, the National Institute for Allergy and Infectious Diseases, and the National Institute of Dental and Craniofacial Research. The investigators did not report having any conflicts of interest.
AT THE AMERICAN ACADEMY OF DERMATOLOGY'S SUMMER ACADEMY MEETING
Major Finding: Patients with psoriasis had an odds ratio of 8.77 for having enlarged tonsils (grade 2 or greater), compared with healthy controls.
Data Source: The findings come from a prospective study of 32 patients with psoriasis and 14 patients with noninflammatory skin conditions, who served as controls.
Disclosures: The study was supported by grants from the National Cancer Institute, the National Institute for Allergy and Infectious Diseases, and the National Institute of Dental and Craniofacial Research. The investigators did not report having any conflicts of interest.
Anti-TNF Use Linked to Cardiovascular-Disease Drop in RA
Evidence continues to accumulate that the potent anti-inflammatory effect of drugs that block tumor necrosis factor can significantly dampen cardiovascular-disease risk in patients with rheumatoid arthritis, even though definitive proof from a prospective trial is still lacking.
Two recent pieces of suggestive evidence came from a meta-analysis of four placebo-controlled trials of adalimumab (Humira) that together included nearly 2,500 patients with rheumatoid arthritis, and from two prospective cohort studies of 828 RA patients that compared the outcomes of those treated with either adalimumab or etanercept (Enbrel) to the outcomes of similar patients who did not receive an anti–tumor necrosis factor drug.
In both studies, treatment with an anti-TNF agent was linked to a statistically significant cut in cardiovascular (CV) events of about 50%.
These results support another recent, similar finding reported in June at the Annual European Congress of Rheumatology in London. In that study, analysis of medical records from more than 109,000 U.S. patients with RA showed that every 6 months of treatment with an anti-TNF drug reduced the rate of CV events by 13%, compared with RA patients who did not receive a TNF blocker.
The meta-analysis of four trials included data collected in the ARMADA (Arthritis Rheum. 2003;48:35-45), DEO19 (Arthritis Rheum. 2004;50:1400-11), PREMIER (Arthritis Rheum. 2006;54:26-37), and OPTIMA (Ann. Rheum. Dis. 2012 May [doi: 10.1136/annrheumdis-2011-201247]) trials. Collectively, these four studies included 1,411 RA patients treated with both adalimumab and methotrexate, and 1,036 patients who received methotrexate but no anti-TNF drug. At baseline, patients in these two treatment groups had similar demographic and CV disease risk profiles.
During study periods that ranged from 16 to 104 weeks, the incidence of major adverse CV events was 1.3% in patients who received adalimumab, and 2% in those who didn’t. This difference represents a statistically significant, 2/3 drop in the risk for a major CV event in a proportional-hazard model, said Dr. Gerd Burmester, lead investigator for the analysis and a rheumatologist and professor of medicine at Charité Hospital in Berlin. His analysis also showed a statistically significant risk reduction with adalimumab in the rate of nonfatal myocardial infarction, but no significant effect of adalimumab on the rates of nonfatal myocardial infarction or nonfatal stroke compared with patients not receiving adalimumab.
A limitation of the analysis was that none of the four trials was powered to assess CV outcomes, Dr. Burmester said.
The second study used data collected from two cohorts: the CARRÉ (Cardiovascular Research and Rheumatoid Arthritis) study, a prospective Dutch cohort study of 309 randomly selected RA patients who were not treated with a TNF blocker; and the Biologics cohort, which involves 519 Dutch RA patients who have been followed since they began treatment with an anti-TNF drug for the first time, either adalimumab or etanercept.
During follow-up, there were 8 CV events per 1,000 patient-years in the cohort receiving an anti-TNF drug, compared with 23 events per 1,000 patient-years in patients not on an anti-TNF agent, a statistically significant reduction. In a proportional hazards model that adjusted for baseline differences in age and gender, treatment with an anti-TNF agent reduced the rate of CV events by about half, a statistically significant effect, said Dr. Alper M. van Sijl, a researcher at the Reade Centre for Rehabilitation and Rheumatology at the VU Medical Center in Amsterdam.
"Our observations confirm the association between strong suppression of inflammation [with an anti-TNF drug] and curbing the cardiovascular risk in RA," said Dr. van Sijl and his colleagues. But they cautioned that because of the design of the study it remains unclear whether this was a real effect of the anti-TNF drugs, or a bias to treat patients with lower CV disease risk with a TNF blocker.
Dr. Burmester said that he has been a consultant to, served as a speaker for, and received research support from Abbott, the company that markets adalimumab. Dr. van Silj said that he had no disclosures.
Evidence continues to accumulate that the potent anti-inflammatory effect of drugs that block tumor necrosis factor can significantly dampen cardiovascular-disease risk in patients with rheumatoid arthritis, even though definitive proof from a prospective trial is still lacking.
Two recent pieces of suggestive evidence came from a meta-analysis of four placebo-controlled trials of adalimumab (Humira) that together included nearly 2,500 patients with rheumatoid arthritis, and from two prospective cohort studies of 828 RA patients that compared the outcomes of those treated with either adalimumab or etanercept (Enbrel) to the outcomes of similar patients who did not receive an anti–tumor necrosis factor drug.
In both studies, treatment with an anti-TNF agent was linked to a statistically significant cut in cardiovascular (CV) events of about 50%.
These results support another recent, similar finding reported in June at the Annual European Congress of Rheumatology in London. In that study, analysis of medical records from more than 109,000 U.S. patients with RA showed that every 6 months of treatment with an anti-TNF drug reduced the rate of CV events by 13%, compared with RA patients who did not receive a TNF blocker.
The meta-analysis of four trials included data collected in the ARMADA (Arthritis Rheum. 2003;48:35-45), DEO19 (Arthritis Rheum. 2004;50:1400-11), PREMIER (Arthritis Rheum. 2006;54:26-37), and OPTIMA (Ann. Rheum. Dis. 2012 May [doi: 10.1136/annrheumdis-2011-201247]) trials. Collectively, these four studies included 1,411 RA patients treated with both adalimumab and methotrexate, and 1,036 patients who received methotrexate but no anti-TNF drug. At baseline, patients in these two treatment groups had similar demographic and CV disease risk profiles.
During study periods that ranged from 16 to 104 weeks, the incidence of major adverse CV events was 1.3% in patients who received adalimumab, and 2% in those who didn’t. This difference represents a statistically significant, 2/3 drop in the risk for a major CV event in a proportional-hazard model, said Dr. Gerd Burmester, lead investigator for the analysis and a rheumatologist and professor of medicine at Charité Hospital in Berlin. His analysis also showed a statistically significant risk reduction with adalimumab in the rate of nonfatal myocardial infarction, but no significant effect of adalimumab on the rates of nonfatal myocardial infarction or nonfatal stroke compared with patients not receiving adalimumab.
A limitation of the analysis was that none of the four trials was powered to assess CV outcomes, Dr. Burmester said.
The second study used data collected from two cohorts: the CARRÉ (Cardiovascular Research and Rheumatoid Arthritis) study, a prospective Dutch cohort study of 309 randomly selected RA patients who were not treated with a TNF blocker; and the Biologics cohort, which involves 519 Dutch RA patients who have been followed since they began treatment with an anti-TNF drug for the first time, either adalimumab or etanercept.
During follow-up, there were 8 CV events per 1,000 patient-years in the cohort receiving an anti-TNF drug, compared with 23 events per 1,000 patient-years in patients not on an anti-TNF agent, a statistically significant reduction. In a proportional hazards model that adjusted for baseline differences in age and gender, treatment with an anti-TNF agent reduced the rate of CV events by about half, a statistically significant effect, said Dr. Alper M. van Sijl, a researcher at the Reade Centre for Rehabilitation and Rheumatology at the VU Medical Center in Amsterdam.
"Our observations confirm the association between strong suppression of inflammation [with an anti-TNF drug] and curbing the cardiovascular risk in RA," said Dr. van Sijl and his colleagues. But they cautioned that because of the design of the study it remains unclear whether this was a real effect of the anti-TNF drugs, or a bias to treat patients with lower CV disease risk with a TNF blocker.
Dr. Burmester said that he has been a consultant to, served as a speaker for, and received research support from Abbott, the company that markets adalimumab. Dr. van Silj said that he had no disclosures.
Evidence continues to accumulate that the potent anti-inflammatory effect of drugs that block tumor necrosis factor can significantly dampen cardiovascular-disease risk in patients with rheumatoid arthritis, even though definitive proof from a prospective trial is still lacking.
Two recent pieces of suggestive evidence came from a meta-analysis of four placebo-controlled trials of adalimumab (Humira) that together included nearly 2,500 patients with rheumatoid arthritis, and from two prospective cohort studies of 828 RA patients that compared the outcomes of those treated with either adalimumab or etanercept (Enbrel) to the outcomes of similar patients who did not receive an anti–tumor necrosis factor drug.
In both studies, treatment with an anti-TNF agent was linked to a statistically significant cut in cardiovascular (CV) events of about 50%.
These results support another recent, similar finding reported in June at the Annual European Congress of Rheumatology in London. In that study, analysis of medical records from more than 109,000 U.S. patients with RA showed that every 6 months of treatment with an anti-TNF drug reduced the rate of CV events by 13%, compared with RA patients who did not receive a TNF blocker.
The meta-analysis of four trials included data collected in the ARMADA (Arthritis Rheum. 2003;48:35-45), DEO19 (Arthritis Rheum. 2004;50:1400-11), PREMIER (Arthritis Rheum. 2006;54:26-37), and OPTIMA (Ann. Rheum. Dis. 2012 May [doi: 10.1136/annrheumdis-2011-201247]) trials. Collectively, these four studies included 1,411 RA patients treated with both adalimumab and methotrexate, and 1,036 patients who received methotrexate but no anti-TNF drug. At baseline, patients in these two treatment groups had similar demographic and CV disease risk profiles.
During study periods that ranged from 16 to 104 weeks, the incidence of major adverse CV events was 1.3% in patients who received adalimumab, and 2% in those who didn’t. This difference represents a statistically significant, 2/3 drop in the risk for a major CV event in a proportional-hazard model, said Dr. Gerd Burmester, lead investigator for the analysis and a rheumatologist and professor of medicine at Charité Hospital in Berlin. His analysis also showed a statistically significant risk reduction with adalimumab in the rate of nonfatal myocardial infarction, but no significant effect of adalimumab on the rates of nonfatal myocardial infarction or nonfatal stroke compared with patients not receiving adalimumab.
A limitation of the analysis was that none of the four trials was powered to assess CV outcomes, Dr. Burmester said.
The second study used data collected from two cohorts: the CARRÉ (Cardiovascular Research and Rheumatoid Arthritis) study, a prospective Dutch cohort study of 309 randomly selected RA patients who were not treated with a TNF blocker; and the Biologics cohort, which involves 519 Dutch RA patients who have been followed since they began treatment with an anti-TNF drug for the first time, either adalimumab or etanercept.
During follow-up, there were 8 CV events per 1,000 patient-years in the cohort receiving an anti-TNF drug, compared with 23 events per 1,000 patient-years in patients not on an anti-TNF agent, a statistically significant reduction. In a proportional hazards model that adjusted for baseline differences in age and gender, treatment with an anti-TNF agent reduced the rate of CV events by about half, a statistically significant effect, said Dr. Alper M. van Sijl, a researcher at the Reade Centre for Rehabilitation and Rheumatology at the VU Medical Center in Amsterdam.
"Our observations confirm the association between strong suppression of inflammation [with an anti-TNF drug] and curbing the cardiovascular risk in RA," said Dr. van Sijl and his colleagues. But they cautioned that because of the design of the study it remains unclear whether this was a real effect of the anti-TNF drugs, or a bias to treat patients with lower CV disease risk with a TNF blocker.
Dr. Burmester said that he has been a consultant to, served as a speaker for, and received research support from Abbott, the company that markets adalimumab. Dr. van Silj said that he had no disclosures.
Psoriasis Patients Still Going Unscreened for Heart Disease
BOSTON – Despite the growing body of literature linking psoriasis to poor cardiovascular outcomes, most psoriasis patients are not being regularly screened for the major CV risk factors, according to the results of a new analysis.
"Screening for high blood pressure, diabetes, hypercholesterolemia, and obesity are not performed at most outpatient visits for psoriasis," wrote clinical research fellow Amir Al-Dabagh and colleagues at the center for dermatology research at Wake Forest University, Winston-Salem, N.C.
To determine whether and to what degree CV screening is taking place during outpatient psoriasis visits in the ambulatory care setting, the investigators reviewed data from the NAMCS (National Ambulatory Medical Care Survey) from 2005 to 2009. They calculated the probability of a patient’s being screened for at least one of four CV risk factors (blood pressure, glucose, cholesterol, and body mass index). They also compared screening rates by physician specialty, patient demographics, and clinical practice characteristics.
Approximately 11.4 million psoriasis patient visits were recorded during the study period. Age was found to be the only demographic factor that was significantly associated with all CV risk screens, Mr. Al-Dabagh reported in a poster presented at the American Academy of Dermatology’s Summer Academy Meeting. "Psoriasis had a statistically significant negative association on overall screening rates for blood pressure and BMI screening, but not for glucose or cholesterol."
A comparison of screening rates among patients with and without psoriasis showed that only 41.2% of the psoriasis patients were screened for at least one of the four risk factors, compared with 66.3% of patients without psoriasis. When looking at psoriasis patients only, the researchers found that screening for each of the risk factors occurred more frequently during nondermatology vs. dermatology visits, regardless of disease severity.
Specifically, among patients with severe and nonsevere psoriasis, respectively, 100% and 89.9% of psoriasis visits to nondermatology offices included screening for at least one risk factor, compared with 28.9% and 12.3% of psoriasis visits to dermatology offices, according to the analysis. In both settings, screening rates were higher among male patients, as well as among black and non-Hispanic patients, Mr. Al-Dabagh noted.
The majority of nondermatologist visits for patients with severe and nonsevere psoriasis included screening for blood pressure (100% for severe; 87.9% for not severe) and BMI (88.3% for severe; 54.4% for not severe). By comparison, during dermatology visits, 3.8% of patients with severe disease and 2.4% of those with mild to moderate disease had blood pressure screens, and 14.8% and 8.5%, respectively, had BMI recorded. Relatively few visits in either setting included glucose or cholesterol measurement, regardless of disease severity.
In 2008, the National Psoriasis Foundation issued a clinical consensus report recommending that screening psoriasis patients for cardiovascular risk factors begin as early as 20 years of age. The recommendation was based on mounting evidence from population-based studies that found psoriasis to be a risk factor for developing atherosclerosis and myocardial infarction (J. Amer. Acad. Derm. 2008;58:1031-42).
In addition to early, routine screening, psoriasis patients should be counseled to modify cholesterol levels when necessary, to take measures to control depression, to quit smoking, to moderate their alcohol intake, to eat a healthy diet, and to exercise at least three times a week, according to the consensus report.
The center for dermatology research at Wake Forest University is supported by an educational grant from Galderma. The study investigators reported financial relationships with multiple pharmaceutical companies, including Galderma.
BOSTON – Despite the growing body of literature linking psoriasis to poor cardiovascular outcomes, most psoriasis patients are not being regularly screened for the major CV risk factors, according to the results of a new analysis.
"Screening for high blood pressure, diabetes, hypercholesterolemia, and obesity are not performed at most outpatient visits for psoriasis," wrote clinical research fellow Amir Al-Dabagh and colleagues at the center for dermatology research at Wake Forest University, Winston-Salem, N.C.
To determine whether and to what degree CV screening is taking place during outpatient psoriasis visits in the ambulatory care setting, the investigators reviewed data from the NAMCS (National Ambulatory Medical Care Survey) from 2005 to 2009. They calculated the probability of a patient’s being screened for at least one of four CV risk factors (blood pressure, glucose, cholesterol, and body mass index). They also compared screening rates by physician specialty, patient demographics, and clinical practice characteristics.
Approximately 11.4 million psoriasis patient visits were recorded during the study period. Age was found to be the only demographic factor that was significantly associated with all CV risk screens, Mr. Al-Dabagh reported in a poster presented at the American Academy of Dermatology’s Summer Academy Meeting. "Psoriasis had a statistically significant negative association on overall screening rates for blood pressure and BMI screening, but not for glucose or cholesterol."
A comparison of screening rates among patients with and without psoriasis showed that only 41.2% of the psoriasis patients were screened for at least one of the four risk factors, compared with 66.3% of patients without psoriasis. When looking at psoriasis patients only, the researchers found that screening for each of the risk factors occurred more frequently during nondermatology vs. dermatology visits, regardless of disease severity.
Specifically, among patients with severe and nonsevere psoriasis, respectively, 100% and 89.9% of psoriasis visits to nondermatology offices included screening for at least one risk factor, compared with 28.9% and 12.3% of psoriasis visits to dermatology offices, according to the analysis. In both settings, screening rates were higher among male patients, as well as among black and non-Hispanic patients, Mr. Al-Dabagh noted.
The majority of nondermatologist visits for patients with severe and nonsevere psoriasis included screening for blood pressure (100% for severe; 87.9% for not severe) and BMI (88.3% for severe; 54.4% for not severe). By comparison, during dermatology visits, 3.8% of patients with severe disease and 2.4% of those with mild to moderate disease had blood pressure screens, and 14.8% and 8.5%, respectively, had BMI recorded. Relatively few visits in either setting included glucose or cholesterol measurement, regardless of disease severity.
In 2008, the National Psoriasis Foundation issued a clinical consensus report recommending that screening psoriasis patients for cardiovascular risk factors begin as early as 20 years of age. The recommendation was based on mounting evidence from population-based studies that found psoriasis to be a risk factor for developing atherosclerosis and myocardial infarction (J. Amer. Acad. Derm. 2008;58:1031-42).
In addition to early, routine screening, psoriasis patients should be counseled to modify cholesterol levels when necessary, to take measures to control depression, to quit smoking, to moderate their alcohol intake, to eat a healthy diet, and to exercise at least three times a week, according to the consensus report.
The center for dermatology research at Wake Forest University is supported by an educational grant from Galderma. The study investigators reported financial relationships with multiple pharmaceutical companies, including Galderma.
BOSTON – Despite the growing body of literature linking psoriasis to poor cardiovascular outcomes, most psoriasis patients are not being regularly screened for the major CV risk factors, according to the results of a new analysis.
"Screening for high blood pressure, diabetes, hypercholesterolemia, and obesity are not performed at most outpatient visits for psoriasis," wrote clinical research fellow Amir Al-Dabagh and colleagues at the center for dermatology research at Wake Forest University, Winston-Salem, N.C.
To determine whether and to what degree CV screening is taking place during outpatient psoriasis visits in the ambulatory care setting, the investigators reviewed data from the NAMCS (National Ambulatory Medical Care Survey) from 2005 to 2009. They calculated the probability of a patient’s being screened for at least one of four CV risk factors (blood pressure, glucose, cholesterol, and body mass index). They also compared screening rates by physician specialty, patient demographics, and clinical practice characteristics.
Approximately 11.4 million psoriasis patient visits were recorded during the study period. Age was found to be the only demographic factor that was significantly associated with all CV risk screens, Mr. Al-Dabagh reported in a poster presented at the American Academy of Dermatology’s Summer Academy Meeting. "Psoriasis had a statistically significant negative association on overall screening rates for blood pressure and BMI screening, but not for glucose or cholesterol."
A comparison of screening rates among patients with and without psoriasis showed that only 41.2% of the psoriasis patients were screened for at least one of the four risk factors, compared with 66.3% of patients without psoriasis. When looking at psoriasis patients only, the researchers found that screening for each of the risk factors occurred more frequently during nondermatology vs. dermatology visits, regardless of disease severity.
Specifically, among patients with severe and nonsevere psoriasis, respectively, 100% and 89.9% of psoriasis visits to nondermatology offices included screening for at least one risk factor, compared with 28.9% and 12.3% of psoriasis visits to dermatology offices, according to the analysis. In both settings, screening rates were higher among male patients, as well as among black and non-Hispanic patients, Mr. Al-Dabagh noted.
The majority of nondermatologist visits for patients with severe and nonsevere psoriasis included screening for blood pressure (100% for severe; 87.9% for not severe) and BMI (88.3% for severe; 54.4% for not severe). By comparison, during dermatology visits, 3.8% of patients with severe disease and 2.4% of those with mild to moderate disease had blood pressure screens, and 14.8% and 8.5%, respectively, had BMI recorded. Relatively few visits in either setting included glucose or cholesterol measurement, regardless of disease severity.
In 2008, the National Psoriasis Foundation issued a clinical consensus report recommending that screening psoriasis patients for cardiovascular risk factors begin as early as 20 years of age. The recommendation was based on mounting evidence from population-based studies that found psoriasis to be a risk factor for developing atherosclerosis and myocardial infarction (J. Amer. Acad. Derm. 2008;58:1031-42).
In addition to early, routine screening, psoriasis patients should be counseled to modify cholesterol levels when necessary, to take measures to control depression, to quit smoking, to moderate their alcohol intake, to eat a healthy diet, and to exercise at least three times a week, according to the consensus report.
The center for dermatology research at Wake Forest University is supported by an educational grant from Galderma. The study investigators reported financial relationships with multiple pharmaceutical companies, including Galderma.
AT THE AMERICAN ACADEMY OF DERMATOLOGY'S SUMMER ACADEMY MEETING
Major Finding: Approximately 41% of psoriasis patients were screened for at least one of four risk factors for cardiovascular disease during outpatient visits, compared with 66.3% of patients without the chronic inflammatory disease.
Data Source: Analysis of data from the National Ambulatory Medical Care Survey on outpatient psoriasis visits from 2005-2009.
Disclosures: The Center for Dermatology Research at Wake Forest University is supported by an educational grant from Galderma. The study investigators reported financial relationships with multiple pharmaceutical companies, including Galderma.