User login
Invasive approaches ‘overused’ for evaluating pulmonary nodules
One in four intermediate-sized (8-20 mm) pulmonary nodules were found to be malignant, based on results from a retrospective study of 377 patients seen in 18 community pulmonology practices.
Malignant nodules were more likely to be found in current or former smokers and to be larger than the benign nodules.
Further, despite guideline recommendations for surveillance of pulmonary nodules with less than a 5% pretest probability of malignancy, 44% of 36 patients with low-risk pulmonary nodules underwent at least one invasive procedure.
“To our knowledge, this is the first study that documents the prevalence of cancer (25%) in patients with intermediate-sized nodules referred to community-based pulmonologists,” wrote Dr. Nichole T. Tanner of the Medical University of South Carolina, Charleston, and her coauthors in the study published online (Chest 2015 June 18 [doi:10.1378/chest.15-0630]). “This finding has implications for managing pulmonary nodules in the community; because the risk of cancer is substantial, patients should be managed based on their individualized risk for malignancy.”
Biopsy – either by transthoracic needle aspiration or bronchoscopy – was performed in 33% (125) of patients, of whom 35% were found to have a malignancy and 57% had a specific benign diagnosis; biopsies in 8% were nondiagnostic and those patients were followed for 2 years.
Referrals for surgery were given to 20% (77) of patients; 19 had previously undergone a biopsy, with 11 having a nondiagnostic biopsy and eight having a received a benign result. Of patients who underwent surgery, 65% were diagnosed with a malignancy, and 35% had benign disease. However, the rate of surgical resection was similar regardless of patients’ pretest probability of malignancy.
PET scanning, performed in 37% of patients, was more likely in those who had a biopsy or surgery. The overall accuracy of PET was 74%, and the false-negative rate decreased slightly as the size of the nodule increased.
“Guidelines recommend surgery if the pretest probability of cancer is high (pCA > 65%) because a negative biopsy would not dissuade the clinician from pursuing a definitive diagnosis and a positive biopsy would lead to surgery anyway.”
The researchers pointed out that there are a range of noninvasive options now available to determine the likelihood that a nodule is malignant, such as CT scanning with the use of volumetric software to measure diameter and volume-doubling time of a nodule in between scans.
The study was supported by Integrated Diagnostics. All but one study author declared consulting fees, grant funding, stock options, or employment with Integrated Diagnostics.
One in four intermediate-sized (8-20 mm) pulmonary nodules were found to be malignant, based on results from a retrospective study of 377 patients seen in 18 community pulmonology practices.
Malignant nodules were more likely to be found in current or former smokers and to be larger than the benign nodules.
Further, despite guideline recommendations for surveillance of pulmonary nodules with less than a 5% pretest probability of malignancy, 44% of 36 patients with low-risk pulmonary nodules underwent at least one invasive procedure.
“To our knowledge, this is the first study that documents the prevalence of cancer (25%) in patients with intermediate-sized nodules referred to community-based pulmonologists,” wrote Dr. Nichole T. Tanner of the Medical University of South Carolina, Charleston, and her coauthors in the study published online (Chest 2015 June 18 [doi:10.1378/chest.15-0630]). “This finding has implications for managing pulmonary nodules in the community; because the risk of cancer is substantial, patients should be managed based on their individualized risk for malignancy.”
Biopsy – either by transthoracic needle aspiration or bronchoscopy – was performed in 33% (125) of patients, of whom 35% were found to have a malignancy and 57% had a specific benign diagnosis; biopsies in 8% were nondiagnostic and those patients were followed for 2 years.
Referrals for surgery were given to 20% (77) of patients; 19 had previously undergone a biopsy, with 11 having a nondiagnostic biopsy and eight having a received a benign result. Of patients who underwent surgery, 65% were diagnosed with a malignancy, and 35% had benign disease. However, the rate of surgical resection was similar regardless of patients’ pretest probability of malignancy.
PET scanning, performed in 37% of patients, was more likely in those who had a biopsy or surgery. The overall accuracy of PET was 74%, and the false-negative rate decreased slightly as the size of the nodule increased.
“Guidelines recommend surgery if the pretest probability of cancer is high (pCA > 65%) because a negative biopsy would not dissuade the clinician from pursuing a definitive diagnosis and a positive biopsy would lead to surgery anyway.”
The researchers pointed out that there are a range of noninvasive options now available to determine the likelihood that a nodule is malignant, such as CT scanning with the use of volumetric software to measure diameter and volume-doubling time of a nodule in between scans.
The study was supported by Integrated Diagnostics. All but one study author declared consulting fees, grant funding, stock options, or employment with Integrated Diagnostics.
One in four intermediate-sized (8-20 mm) pulmonary nodules were found to be malignant, based on results from a retrospective study of 377 patients seen in 18 community pulmonology practices.
Malignant nodules were more likely to be found in current or former smokers and to be larger than the benign nodules.
Further, despite guideline recommendations for surveillance of pulmonary nodules with less than a 5% pretest probability of malignancy, 44% of 36 patients with low-risk pulmonary nodules underwent at least one invasive procedure.
“To our knowledge, this is the first study that documents the prevalence of cancer (25%) in patients with intermediate-sized nodules referred to community-based pulmonologists,” wrote Dr. Nichole T. Tanner of the Medical University of South Carolina, Charleston, and her coauthors in the study published online (Chest 2015 June 18 [doi:10.1378/chest.15-0630]). “This finding has implications for managing pulmonary nodules in the community; because the risk of cancer is substantial, patients should be managed based on their individualized risk for malignancy.”
Biopsy – either by transthoracic needle aspiration or bronchoscopy – was performed in 33% (125) of patients, of whom 35% were found to have a malignancy and 57% had a specific benign diagnosis; biopsies in 8% were nondiagnostic and those patients were followed for 2 years.
Referrals for surgery were given to 20% (77) of patients; 19 had previously undergone a biopsy, with 11 having a nondiagnostic biopsy and eight having a received a benign result. Of patients who underwent surgery, 65% were diagnosed with a malignancy, and 35% had benign disease. However, the rate of surgical resection was similar regardless of patients’ pretest probability of malignancy.
PET scanning, performed in 37% of patients, was more likely in those who had a biopsy or surgery. The overall accuracy of PET was 74%, and the false-negative rate decreased slightly as the size of the nodule increased.
“Guidelines recommend surgery if the pretest probability of cancer is high (pCA > 65%) because a negative biopsy would not dissuade the clinician from pursuing a definitive diagnosis and a positive biopsy would lead to surgery anyway.”
The researchers pointed out that there are a range of noninvasive options now available to determine the likelihood that a nodule is malignant, such as CT scanning with the use of volumetric software to measure diameter and volume-doubling time of a nodule in between scans.
The study was supported by Integrated Diagnostics. All but one study author declared consulting fees, grant funding, stock options, or employment with Integrated Diagnostics.
FROM CHEST
Key clinical point: One in four pulmonary nodules 8-20 mm in size are malignant, and invasive tests are being overused in low-risk patients in community settings.
Major finding: Despite guidelines recommending pulmonary nodes with a less than 5% pretest probability of malignancy be managed with surveillance only, 44% of low-risk patients in the study underwent at least one invasive procedure for what proved to be a benign nodule.
Data source: A multicenter, retrospective study in 377 patients.
Disclosures: The study was supported by Integrated Diagnostics. All but one author declared consulting fees, grant funding, stock options, or employment with Integrated Diagnostics.
Recommendations for diabetes management during Ramadan
Individuals with diabetes who fast for Ramadan need regular glucose monitoring and may need to adjust their treatment regimen, according to updated recommendations from the International Group for Diabetes and Ramadan.
The recommendations were published online June 16 in BMJ Open Diabetes Research & Care.
“In general, patients should be instructed on the use of glucose monitoring and frequency of glucose testing [and] patients receiving insulin or insulin secretagogues should be monitored two to four times daily before, during, and after the fasting period,” wrote Dr. Mahmoud Ibrahim of the Center for Diabetes Education, McDonough, Ga., and his associates.
Metformin was the ideal agent for managing patients with type 2 diabetes who are undergoing prolonged fasting, as it carries a low risk of hypoglycemia and is associated with a 1%-2% reduction in hemoglobin A1c (BMJ Open Diab. Res. Care 2015, June 16 [doi:10.1136/bmjdrc-2015-000108]).
Similarly, thiazolidinediones are considered a useful agent for use during Ramadan because of the low risk of hypoglycemia and the effectiveness in improving glucose control.
Thiazolidinedione therapy should be initiated well before the start of the fast as these agents may take up to 10-12 weeks to reach maximum effectiveness, the researchers noted.
Dipeptidyl peptidase-4 (DPP4) inhibitors are another option for Ramadan fasting, as there is a low risk of hypoglycemia, and studies suggest that they are effective at improving glycemic control during fasting.
However, insulin secretagogues and most sulfonylureas should be avoided or should be used with extreme caution during Ramadan fasting, the authors said, pointing to recent studies showing an increased risk of hypoglycemia during fasting with these agents.
“The risk of hypoglycemia increases exponentially in elderly patients and patients with renal failure and medical illnesses treated with sulfonylureas,” wrote the authors.
There were few studies examining the safety and efficacy of glucagon-like peptide 1 receptor agonists in patients with diabetes during Ramadan, they noted.
For patients with type 1 or type 2 diabetes who receive insulin injections, their total insulin dose will likely require frequent adjustment during Ramadan.
“The use of basal (glargine or detemir) and rapid-acting insulin analogs (lispro, aspart, and glulisine) has been shown to be superior to human insulin formulations (NPH and regular) during Ramadan by reducing the risk of hypoglycemia,” the authors wrote.
Insulin pump therapy is effective during fasting, providing a continuous basal rate of insulin, but is able to rapidly cover for the meal intake when the fast is broken.
Premixed insulin formulations are among the most frequently prescribed in many Muslim countries, but data from some studies suggest a higher risk of hypoglycemia than with basal insulin analogs, and their safety and efficacy during Ramadan fasting is not known.
Practical outlines on adjusting insulin levels during fasting are available, but the authors recommended a trial fast for 3 consecutive days before Ramadan to guide self-titration of the premix insulin dosage.
The authors also suggested structured diabetes education as an essential tool for managing diabetes during fasting and after breaking the fast, citing a retrospective study showing that patients who received diabetes education prior to Ramadan had less weight gain and fewer episodes of hypoglycemia compared to those who did not.
One author was supported by the American Diabetes Association and National Institutes of Health, and declared unrestricted research support, consulting fees, honoraria, and advisory board memberships from pharmaceutical companies.
Individuals with diabetes who fast for Ramadan need regular glucose monitoring and may need to adjust their treatment regimen, according to updated recommendations from the International Group for Diabetes and Ramadan.
The recommendations were published online June 16 in BMJ Open Diabetes Research & Care.
“In general, patients should be instructed on the use of glucose monitoring and frequency of glucose testing [and] patients receiving insulin or insulin secretagogues should be monitored two to four times daily before, during, and after the fasting period,” wrote Dr. Mahmoud Ibrahim of the Center for Diabetes Education, McDonough, Ga., and his associates.
Metformin was the ideal agent for managing patients with type 2 diabetes who are undergoing prolonged fasting, as it carries a low risk of hypoglycemia and is associated with a 1%-2% reduction in hemoglobin A1c (BMJ Open Diab. Res. Care 2015, June 16 [doi:10.1136/bmjdrc-2015-000108]).
Similarly, thiazolidinediones are considered a useful agent for use during Ramadan because of the low risk of hypoglycemia and the effectiveness in improving glucose control.
Thiazolidinedione therapy should be initiated well before the start of the fast as these agents may take up to 10-12 weeks to reach maximum effectiveness, the researchers noted.
Dipeptidyl peptidase-4 (DPP4) inhibitors are another option for Ramadan fasting, as there is a low risk of hypoglycemia, and studies suggest that they are effective at improving glycemic control during fasting.
However, insulin secretagogues and most sulfonylureas should be avoided or should be used with extreme caution during Ramadan fasting, the authors said, pointing to recent studies showing an increased risk of hypoglycemia during fasting with these agents.
“The risk of hypoglycemia increases exponentially in elderly patients and patients with renal failure and medical illnesses treated with sulfonylureas,” wrote the authors.
There were few studies examining the safety and efficacy of glucagon-like peptide 1 receptor agonists in patients with diabetes during Ramadan, they noted.
For patients with type 1 or type 2 diabetes who receive insulin injections, their total insulin dose will likely require frequent adjustment during Ramadan.
“The use of basal (glargine or detemir) and rapid-acting insulin analogs (lispro, aspart, and glulisine) has been shown to be superior to human insulin formulations (NPH and regular) during Ramadan by reducing the risk of hypoglycemia,” the authors wrote.
Insulin pump therapy is effective during fasting, providing a continuous basal rate of insulin, but is able to rapidly cover for the meal intake when the fast is broken.
Premixed insulin formulations are among the most frequently prescribed in many Muslim countries, but data from some studies suggest a higher risk of hypoglycemia than with basal insulin analogs, and their safety and efficacy during Ramadan fasting is not known.
Practical outlines on adjusting insulin levels during fasting are available, but the authors recommended a trial fast for 3 consecutive days before Ramadan to guide self-titration of the premix insulin dosage.
The authors also suggested structured diabetes education as an essential tool for managing diabetes during fasting and after breaking the fast, citing a retrospective study showing that patients who received diabetes education prior to Ramadan had less weight gain and fewer episodes of hypoglycemia compared to those who did not.
One author was supported by the American Diabetes Association and National Institutes of Health, and declared unrestricted research support, consulting fees, honoraria, and advisory board memberships from pharmaceutical companies.
Individuals with diabetes who fast for Ramadan need regular glucose monitoring and may need to adjust their treatment regimen, according to updated recommendations from the International Group for Diabetes and Ramadan.
The recommendations were published online June 16 in BMJ Open Diabetes Research & Care.
“In general, patients should be instructed on the use of glucose monitoring and frequency of glucose testing [and] patients receiving insulin or insulin secretagogues should be monitored two to four times daily before, during, and after the fasting period,” wrote Dr. Mahmoud Ibrahim of the Center for Diabetes Education, McDonough, Ga., and his associates.
Metformin was the ideal agent for managing patients with type 2 diabetes who are undergoing prolonged fasting, as it carries a low risk of hypoglycemia and is associated with a 1%-2% reduction in hemoglobin A1c (BMJ Open Diab. Res. Care 2015, June 16 [doi:10.1136/bmjdrc-2015-000108]).
Similarly, thiazolidinediones are considered a useful agent for use during Ramadan because of the low risk of hypoglycemia and the effectiveness in improving glucose control.
Thiazolidinedione therapy should be initiated well before the start of the fast as these agents may take up to 10-12 weeks to reach maximum effectiveness, the researchers noted.
Dipeptidyl peptidase-4 (DPP4) inhibitors are another option for Ramadan fasting, as there is a low risk of hypoglycemia, and studies suggest that they are effective at improving glycemic control during fasting.
However, insulin secretagogues and most sulfonylureas should be avoided or should be used with extreme caution during Ramadan fasting, the authors said, pointing to recent studies showing an increased risk of hypoglycemia during fasting with these agents.
“The risk of hypoglycemia increases exponentially in elderly patients and patients with renal failure and medical illnesses treated with sulfonylureas,” wrote the authors.
There were few studies examining the safety and efficacy of glucagon-like peptide 1 receptor agonists in patients with diabetes during Ramadan, they noted.
For patients with type 1 or type 2 diabetes who receive insulin injections, their total insulin dose will likely require frequent adjustment during Ramadan.
“The use of basal (glargine or detemir) and rapid-acting insulin analogs (lispro, aspart, and glulisine) has been shown to be superior to human insulin formulations (NPH and regular) during Ramadan by reducing the risk of hypoglycemia,” the authors wrote.
Insulin pump therapy is effective during fasting, providing a continuous basal rate of insulin, but is able to rapidly cover for the meal intake when the fast is broken.
Premixed insulin formulations are among the most frequently prescribed in many Muslim countries, but data from some studies suggest a higher risk of hypoglycemia than with basal insulin analogs, and their safety and efficacy during Ramadan fasting is not known.
Practical outlines on adjusting insulin levels during fasting are available, but the authors recommended a trial fast for 3 consecutive days before Ramadan to guide self-titration of the premix insulin dosage.
The authors also suggested structured diabetes education as an essential tool for managing diabetes during fasting and after breaking the fast, citing a retrospective study showing that patients who received diabetes education prior to Ramadan had less weight gain and fewer episodes of hypoglycemia compared to those who did not.
One author was supported by the American Diabetes Association and National Institutes of Health, and declared unrestricted research support, consulting fees, honoraria, and advisory board memberships from pharmaceutical companies.
FROM BMJ OPEN DIABETES RESEARCH & CARE
Key clinical point: Individuals with diabetes who fast for Ramadan need regular glucose monitoring and may need to adjust their treatment regimen.
Major finding: Metformin is the ideal agent for managing patients with type 2 diabetes who are undergoing prolonged fasting for Ramadan.
Data source: International Group for Diabetes and Ramadan.
Disclosures: One author was supported by the American Diabetes Association and National Institutes of Health, and declared unrestricted research support, consulting fees, honoraria, and advisory board memberships from pharmaceutical companies.
Alisertib shows activity in non-Hodgkin lymphoma
The novel Aurora A kinase inhibitor alisertib has shown significant antitumor activity in patients with relapsed or refractory peripheral T-cell non-Hodgkin lymphoma but not transformed mycosis fungoides, according to data from a phase II trial.
The study in 37 patients showed the overall treatment response rate among peripheral T-cell non-Hodgkin lymphoma (PTCL) was 30%, with two (7%) complete responses, seven (23%) partial responses, and five patients (17%) achieving stable disease, although there was no response from patients with transformed mycosis fungoides.
Grade 3 and 4 adverse events were observed in less than 5% of patients, the most common being neutropenia (32%), followed by anemia, thrombocytopenia, and febrile neutropenia; around half of all patients experienced fatigue, according to a study published online in the Journal of Clinical Oncology (J. Clin. Oncol. 2015 June 15 [doi:10.1200/JCO.2014.60.6327]).
“Frequent drug resistance and overall poor outcomes complicate the management of relapsed and refractory PTCL; the need for effective new agents with favorable toxicity profiles is clear,” wrote Dr. Paul M. Barr of the University of Rochester (N.Y.) and his coauthors.
The study was supported by the National Institutes of Health and the National Cancer Institute. Dr. Barr reported consulting or advisory roles with Millennium, Pharmacyclics, Gilead Sciences, and TG Therapeutics and research funding from Pharmacyclics.
The novel Aurora A kinase inhibitor alisertib has shown significant antitumor activity in patients with relapsed or refractory peripheral T-cell non-Hodgkin lymphoma but not transformed mycosis fungoides, according to data from a phase II trial.
The study in 37 patients showed the overall treatment response rate among peripheral T-cell non-Hodgkin lymphoma (PTCL) was 30%, with two (7%) complete responses, seven (23%) partial responses, and five patients (17%) achieving stable disease, although there was no response from patients with transformed mycosis fungoides.
Grade 3 and 4 adverse events were observed in less than 5% of patients, the most common being neutropenia (32%), followed by anemia, thrombocytopenia, and febrile neutropenia; around half of all patients experienced fatigue, according to a study published online in the Journal of Clinical Oncology (J. Clin. Oncol. 2015 June 15 [doi:10.1200/JCO.2014.60.6327]).
“Frequent drug resistance and overall poor outcomes complicate the management of relapsed and refractory PTCL; the need for effective new agents with favorable toxicity profiles is clear,” wrote Dr. Paul M. Barr of the University of Rochester (N.Y.) and his coauthors.
The study was supported by the National Institutes of Health and the National Cancer Institute. Dr. Barr reported consulting or advisory roles with Millennium, Pharmacyclics, Gilead Sciences, and TG Therapeutics and research funding from Pharmacyclics.
The novel Aurora A kinase inhibitor alisertib has shown significant antitumor activity in patients with relapsed or refractory peripheral T-cell non-Hodgkin lymphoma but not transformed mycosis fungoides, according to data from a phase II trial.
The study in 37 patients showed the overall treatment response rate among peripheral T-cell non-Hodgkin lymphoma (PTCL) was 30%, with two (7%) complete responses, seven (23%) partial responses, and five patients (17%) achieving stable disease, although there was no response from patients with transformed mycosis fungoides.
Grade 3 and 4 adverse events were observed in less than 5% of patients, the most common being neutropenia (32%), followed by anemia, thrombocytopenia, and febrile neutropenia; around half of all patients experienced fatigue, according to a study published online in the Journal of Clinical Oncology (J. Clin. Oncol. 2015 June 15 [doi:10.1200/JCO.2014.60.6327]).
“Frequent drug resistance and overall poor outcomes complicate the management of relapsed and refractory PTCL; the need for effective new agents with favorable toxicity profiles is clear,” wrote Dr. Paul M. Barr of the University of Rochester (N.Y.) and his coauthors.
The study was supported by the National Institutes of Health and the National Cancer Institute. Dr. Barr reported consulting or advisory roles with Millennium, Pharmacyclics, Gilead Sciences, and TG Therapeutics and research funding from Pharmacyclics.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Alisertib has shown significant antitumor activity in patients with relapsed or refractory peripheral T-cell non-Hodgkin lymphoma.
Major finding: Alisertib showed an overall response rate of 30% among patients with peripheral T-cell non-Hodgkin lymphoma.
Data source: A prospective phase II clinical trial in 37 patients with peripheral T-cell non-Hodgkin lymphoma or transformed mycosis fungoides.
Disclosures: The study was supported by the National Institutes of Health and the National Cancer Institute. Dr. Barr reported consulting or advisory roles with Millennium, Pharmacyclics, Gilead Sciences, and TG Therapeutics and research funding from Pharmacyclics.
To sleep, perchance to reprogram behaviors?
Could auditory cues during slow-wave sleep help one to quit smoking or alter other undesired behaviors?
Social biases based on gender and race were “unlearned,” according to researchers who used auditory cues to implement counterbias training in sleeping subjects, based on the results of a study by Xiaoqing Hu, Ph.D., of Northwestern University, Evanston, Ill., and his associates.
The researchers studied 40 white university students found to hold implicit bias against women or black people. The study subjects were engaged in a training program that used image and word associations, combined with an auditory cue, to challenge their biases.
The auditory cue was then later used when the subject reached slow-wave sleep during a nap, with the results suggesting that intervention resulted in a significant and sustained reduction in implicit bias.
“Given that training to reduce implicit bias can be conceptualized as a type of habit learning, perhaps novel sleep manipulations could be adapted to aid people in changing various unwanted or maladaptive habits, such as smoking, unhealthy eating, catastrophizing, or selfishness,” wrote Dr. Hu and his coauthors (Science 2015;348:1013-15.
The study was supported by Northwestern University, the National Science Foundation, and the National Institutes of Health. One author declared serving as an advisor to a company developing educational technologies relating to sleep.
Could auditory cues during slow-wave sleep help one to quit smoking or alter other undesired behaviors?
Social biases based on gender and race were “unlearned,” according to researchers who used auditory cues to implement counterbias training in sleeping subjects, based on the results of a study by Xiaoqing Hu, Ph.D., of Northwestern University, Evanston, Ill., and his associates.
The researchers studied 40 white university students found to hold implicit bias against women or black people. The study subjects were engaged in a training program that used image and word associations, combined with an auditory cue, to challenge their biases.
The auditory cue was then later used when the subject reached slow-wave sleep during a nap, with the results suggesting that intervention resulted in a significant and sustained reduction in implicit bias.
“Given that training to reduce implicit bias can be conceptualized as a type of habit learning, perhaps novel sleep manipulations could be adapted to aid people in changing various unwanted or maladaptive habits, such as smoking, unhealthy eating, catastrophizing, or selfishness,” wrote Dr. Hu and his coauthors (Science 2015;348:1013-15.
The study was supported by Northwestern University, the National Science Foundation, and the National Institutes of Health. One author declared serving as an advisor to a company developing educational technologies relating to sleep.
Could auditory cues during slow-wave sleep help one to quit smoking or alter other undesired behaviors?
Social biases based on gender and race were “unlearned,” according to researchers who used auditory cues to implement counterbias training in sleeping subjects, based on the results of a study by Xiaoqing Hu, Ph.D., of Northwestern University, Evanston, Ill., and his associates.
The researchers studied 40 white university students found to hold implicit bias against women or black people. The study subjects were engaged in a training program that used image and word associations, combined with an auditory cue, to challenge their biases.
The auditory cue was then later used when the subject reached slow-wave sleep during a nap, with the results suggesting that intervention resulted in a significant and sustained reduction in implicit bias.
“Given that training to reduce implicit bias can be conceptualized as a type of habit learning, perhaps novel sleep manipulations could be adapted to aid people in changing various unwanted or maladaptive habits, such as smoking, unhealthy eating, catastrophizing, or selfishness,” wrote Dr. Hu and his coauthors (Science 2015;348:1013-15.
The study was supported by Northwestern University, the National Science Foundation, and the National Institutes of Health. One author declared serving as an advisor to a company developing educational technologies relating to sleep.
FROM SCIENCE
Insurance, location, income drive breast cancer surgery choices
The rates of breast-conserving surgery have increased over the last 2 decades among women with early-stage breast cancers in the United States, but disparities persist, based on an analysis of data from the National Cancer Data Base.
The rate of breast-conserving surgery has risen from approximately 54% in 1998 to 60% in 2011, but this rate may have been affected by “technical advances and changes in societal norms [that] include genetic testing for BRCA1 and BRCA2 mutation, advances in reconstruction techniques, breast magnetic resonance imaging, and increased patient interest in contralateral prophylactic mastectomy,” Dr. Meeghan Lautner and her colleagues at University of Texas MD Anderson Cancer Care Center, Houston, wrote.
“Among the most encouraging findings from our analysis is the considerable improvement of disparities based on facility type and the options afforded to older populations … however, insurance, income, and travel distance to treatment facilities persist as key barriers to [breast-conserving therapy] use,” the researchers said.
Their analysis of a cohort of 727,927 women, published online June 17 in JAMA Surgery, showed that women with early breast cancer were less likely to receive breast-conserving surgery if they had a low educational level, public or no health insurance, and low income.
Women aged 52-61 years were 14% more likely to be treated with breast-conserving surgery, compared with younger women. White race, fewer comorbidities, and living closer to a treatment facility were all positively associated with being treated with breast-conserving surgery.
Those in southern regions of the United States were significantly less likely to receive breast-conserving surgery, compared with those in the Northeast. The researchers said their data suggest the lower rates are because of the greater travel distances to treatment facilities in the South.
Women with no insurance were 25% less likely than those with private insurance to have breast-conserving therapy (JAMA Surgery 2015 June 17 [doi:10.1001/jamasurg.2015.1102]).
The researchers declared no conflicts of interest.
Optimal breast-conserving surgery for most lumpectomy-eligible patients requires a commitment to whole-breast radiation, which also requires access to a radiation oncologist and specialized treatment facility. This is an often insurmountable barrier for patients who lack transportation, have job or family responsibilities, or who live a considerable distance from a radiation facility.
Document
|
Dr. Lisa A. Newman |
Socioeconomically disadvantaged patients are typically the ones who face these obstacles, and these burdens of financial deprivation are disproportionately faced by minority racial/ethnic groups and rural communities.
Tragically, disadvantage will continue to breed more disadvantage.
Dr. Lisa A. Newman is director of the Breast Care Center at the University of Michigan Comprehensive Cancer Care Center, Ann Arbor, Mich. These comments are taken from an accompanying editorial (JAMA Surgery 2015 June 17 [doi:10.1001/jamasurg.2015.1114]). Dr. Newman declared no conflicts of interest.
Optimal breast-conserving surgery for most lumpectomy-eligible patients requires a commitment to whole-breast radiation, which also requires access to a radiation oncologist and specialized treatment facility. This is an often insurmountable barrier for patients who lack transportation, have job or family responsibilities, or who live a considerable distance from a radiation facility.
Document
|
Dr. Lisa A. Newman |
Socioeconomically disadvantaged patients are typically the ones who face these obstacles, and these burdens of financial deprivation are disproportionately faced by minority racial/ethnic groups and rural communities.
Tragically, disadvantage will continue to breed more disadvantage.
Dr. Lisa A. Newman is director of the Breast Care Center at the University of Michigan Comprehensive Cancer Care Center, Ann Arbor, Mich. These comments are taken from an accompanying editorial (JAMA Surgery 2015 June 17 [doi:10.1001/jamasurg.2015.1114]). Dr. Newman declared no conflicts of interest.
Optimal breast-conserving surgery for most lumpectomy-eligible patients requires a commitment to whole-breast radiation, which also requires access to a radiation oncologist and specialized treatment facility. This is an often insurmountable barrier for patients who lack transportation, have job or family responsibilities, or who live a considerable distance from a radiation facility.
Document
|
Dr. Lisa A. Newman |
Socioeconomically disadvantaged patients are typically the ones who face these obstacles, and these burdens of financial deprivation are disproportionately faced by minority racial/ethnic groups and rural communities.
Tragically, disadvantage will continue to breed more disadvantage.
Dr. Lisa A. Newman is director of the Breast Care Center at the University of Michigan Comprehensive Cancer Care Center, Ann Arbor, Mich. These comments are taken from an accompanying editorial (JAMA Surgery 2015 June 17 [doi:10.1001/jamasurg.2015.1114]). Dr. Newman declared no conflicts of interest.
The rates of breast-conserving surgery have increased over the last 2 decades among women with early-stage breast cancers in the United States, but disparities persist, based on an analysis of data from the National Cancer Data Base.
The rate of breast-conserving surgery has risen from approximately 54% in 1998 to 60% in 2011, but this rate may have been affected by “technical advances and changes in societal norms [that] include genetic testing for BRCA1 and BRCA2 mutation, advances in reconstruction techniques, breast magnetic resonance imaging, and increased patient interest in contralateral prophylactic mastectomy,” Dr. Meeghan Lautner and her colleagues at University of Texas MD Anderson Cancer Care Center, Houston, wrote.
“Among the most encouraging findings from our analysis is the considerable improvement of disparities based on facility type and the options afforded to older populations … however, insurance, income, and travel distance to treatment facilities persist as key barriers to [breast-conserving therapy] use,” the researchers said.
Their analysis of a cohort of 727,927 women, published online June 17 in JAMA Surgery, showed that women with early breast cancer were less likely to receive breast-conserving surgery if they had a low educational level, public or no health insurance, and low income.
Women aged 52-61 years were 14% more likely to be treated with breast-conserving surgery, compared with younger women. White race, fewer comorbidities, and living closer to a treatment facility were all positively associated with being treated with breast-conserving surgery.
Those in southern regions of the United States were significantly less likely to receive breast-conserving surgery, compared with those in the Northeast. The researchers said their data suggest the lower rates are because of the greater travel distances to treatment facilities in the South.
Women with no insurance were 25% less likely than those with private insurance to have breast-conserving therapy (JAMA Surgery 2015 June 17 [doi:10.1001/jamasurg.2015.1102]).
The researchers declared no conflicts of interest.
The rates of breast-conserving surgery have increased over the last 2 decades among women with early-stage breast cancers in the United States, but disparities persist, based on an analysis of data from the National Cancer Data Base.
The rate of breast-conserving surgery has risen from approximately 54% in 1998 to 60% in 2011, but this rate may have been affected by “technical advances and changes in societal norms [that] include genetic testing for BRCA1 and BRCA2 mutation, advances in reconstruction techniques, breast magnetic resonance imaging, and increased patient interest in contralateral prophylactic mastectomy,” Dr. Meeghan Lautner and her colleagues at University of Texas MD Anderson Cancer Care Center, Houston, wrote.
“Among the most encouraging findings from our analysis is the considerable improvement of disparities based on facility type and the options afforded to older populations … however, insurance, income, and travel distance to treatment facilities persist as key barriers to [breast-conserving therapy] use,” the researchers said.
Their analysis of a cohort of 727,927 women, published online June 17 in JAMA Surgery, showed that women with early breast cancer were less likely to receive breast-conserving surgery if they had a low educational level, public or no health insurance, and low income.
Women aged 52-61 years were 14% more likely to be treated with breast-conserving surgery, compared with younger women. White race, fewer comorbidities, and living closer to a treatment facility were all positively associated with being treated with breast-conserving surgery.
Those in southern regions of the United States were significantly less likely to receive breast-conserving surgery, compared with those in the Northeast. The researchers said their data suggest the lower rates are because of the greater travel distances to treatment facilities in the South.
Women with no insurance were 25% less likely than those with private insurance to have breast-conserving therapy (JAMA Surgery 2015 June 17 [doi:10.1001/jamasurg.2015.1102]).
The researchers declared no conflicts of interest.
FROM JAMA SURGERY
Key clinical point: Insurance status, income, and travel distance to treatment facilities are associated with the likelihood of having breast-conserving surgery.
Major finding: Women with no health insurance were 25% less likely than those with private insurance to receive breast-conserving surgery.
Data source: Analysis of data from 727,927 women in the National Cancer Data Base.
Disclosures: The researchers declared no conflicts of interest.
Cortical volume linked to IQ changes in schizophrenia
Changes in cortical volume and thickness are significantly associated with IQ changes in individuals with schizophrenia, according to a case-control longitudinal study in 84 patients with schizophrenia and 116 age-matched healthy controls.
Researchers compared magnetic resonance imaging at baseline and the 3-year follow-up with patients’ IQ scores. They found that a decrease in IQ was associated with a decrease in cortical volume and less cortical thickening, but increased lateral ventricular volume, in patients with schizophrenia but not controls.
The study, published online June 17 in JAMA Psychiatry, showed significant relationships between IQ changes and brain tissue changes in patients with schizophrenia across the frontal, temporal, parietal, and cingulate cortices, and in the cortical surface areas of the frontal pole, right temporal, left postcentral, left precuneus, and left occipital regions.
“The effect might be explained by a subgroup characterized by both cognitive deterioration and brain tissue loss, which could well be clinically and genetically distinct with implications for diagnosis, treatment, and drug development,” wrote Dr. Manubu Kubota and colleagues from the University Medical Center Utrecht, the Netherlands (JAMA Psychiatry 2015 June 17 [doi:10.1001/jamapsychiatry.2015.0712]).
The study was supported by the Dutch Health Research Council and the Uehara Memorial Foundation. There were no conflicts of interest declared.
Changes in cortical volume and thickness are significantly associated with IQ changes in individuals with schizophrenia, according to a case-control longitudinal study in 84 patients with schizophrenia and 116 age-matched healthy controls.
Researchers compared magnetic resonance imaging at baseline and the 3-year follow-up with patients’ IQ scores. They found that a decrease in IQ was associated with a decrease in cortical volume and less cortical thickening, but increased lateral ventricular volume, in patients with schizophrenia but not controls.
The study, published online June 17 in JAMA Psychiatry, showed significant relationships between IQ changes and brain tissue changes in patients with schizophrenia across the frontal, temporal, parietal, and cingulate cortices, and in the cortical surface areas of the frontal pole, right temporal, left postcentral, left precuneus, and left occipital regions.
“The effect might be explained by a subgroup characterized by both cognitive deterioration and brain tissue loss, which could well be clinically and genetically distinct with implications for diagnosis, treatment, and drug development,” wrote Dr. Manubu Kubota and colleagues from the University Medical Center Utrecht, the Netherlands (JAMA Psychiatry 2015 June 17 [doi:10.1001/jamapsychiatry.2015.0712]).
The study was supported by the Dutch Health Research Council and the Uehara Memorial Foundation. There were no conflicts of interest declared.
Changes in cortical volume and thickness are significantly associated with IQ changes in individuals with schizophrenia, according to a case-control longitudinal study in 84 patients with schizophrenia and 116 age-matched healthy controls.
Researchers compared magnetic resonance imaging at baseline and the 3-year follow-up with patients’ IQ scores. They found that a decrease in IQ was associated with a decrease in cortical volume and less cortical thickening, but increased lateral ventricular volume, in patients with schizophrenia but not controls.
The study, published online June 17 in JAMA Psychiatry, showed significant relationships between IQ changes and brain tissue changes in patients with schizophrenia across the frontal, temporal, parietal, and cingulate cortices, and in the cortical surface areas of the frontal pole, right temporal, left postcentral, left precuneus, and left occipital regions.
“The effect might be explained by a subgroup characterized by both cognitive deterioration and brain tissue loss, which could well be clinically and genetically distinct with implications for diagnosis, treatment, and drug development,” wrote Dr. Manubu Kubota and colleagues from the University Medical Center Utrecht, the Netherlands (JAMA Psychiatry 2015 June 17 [doi:10.1001/jamapsychiatry.2015.0712]).
The study was supported by the Dutch Health Research Council and the Uehara Memorial Foundation. There were no conflicts of interest declared.
FROM JAMA PSYCHIATRY
Key clinical point: Changes in cortical volume and thickness are significantly associated with IQ changes in individuals with schizophrenia.
Major finding: A decrease in IQ among patients with schizophrenia was associated with a decrease in cortical volume and less cortical thickening, but increased lateral ventricular volume.
Data source: Case-control longitudinal study in 84 patients with schizophrenia and 116 age-matched healthy controls.
Disclosures: The study was supported by the Dutch Health Research Council and the Uehara Memorial Foundation. There were no conflicts of interest declared.
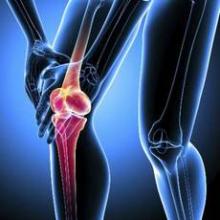
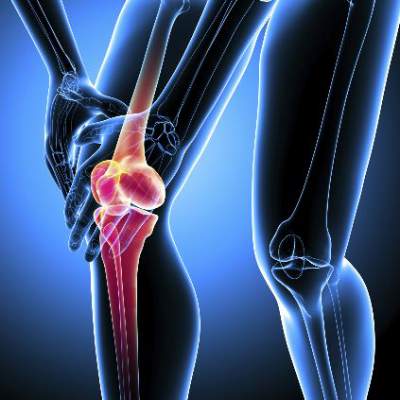
Arthroscopic knee surgery offers no lasting pain benefit
Arthroscopic knee surgery in middle-aged or older patients with knee pain is associated with greater harm than good, according to a meta-analysis.
The analysis of nine randomized, controlled trials in 1,270 patients of arthroscopic surgery involving partial meniscectomy, debridement, or both showed a small but statistically significant benefit from the procedure – comparable to the pain-relieving effects of paracetamol – but which falls below significance after 12 months.
However, there were no significant improvements in knee function, and there were significant increases in the risk of deep vein thrombosis (4.13 events per 1,000 procedures) as well as infection, pulmonary embolism, and death, according to the paper published online June 16 in BMJ.
“Thus, middle-aged patients with knee pain and meniscal tears should be considered as having early-stage osteoarthritis and be treated according to clinical guidelines for knee osteoarthritis, starting with information, exercise, and often weight loss,” wrote Dr. Jonas B. Thorlund of the University of Southern Denmark, Odense, and coauthors (BMJ 2015, June 16 [doi:10.1136/bmj.h2747]).
The study was supported by the Swedish Research Council. One author declared personal fees from several pharmaceutical and medical companies and relevant journal editorship, while another declared fees from lectureships and books.
While randomized trials, uncontrolled observational studies, and surgeons’ own observations suggest that patients improve after arthroscopy, robust and bias-free trials that use placebo controls show that active treatment works no better than control treatment.
We may be close to a tipping point where the weight of evidence against arthroscopic knee surgery for pain is enough to overcome concerns about the quality of the studies, confirmation bias, and vested interests. When that point is reached, we should anticipate a swift reversal of established practice.
Dr. Andy Carr is from the Oxford University Institute of Musculoskeletal Sciences at the NIHR Oxford Musculoskeletal Biomedical Research Unit, Oxford, England. These comments are taken from an accompanying editorial (BMJ 2015, June 16 [doi:10.1136/bmj.h2983]). He declared research grants from NIHR and Arthritis Research UK.
While randomized trials, uncontrolled observational studies, and surgeons’ own observations suggest that patients improve after arthroscopy, robust and bias-free trials that use placebo controls show that active treatment works no better than control treatment.
We may be close to a tipping point where the weight of evidence against arthroscopic knee surgery for pain is enough to overcome concerns about the quality of the studies, confirmation bias, and vested interests. When that point is reached, we should anticipate a swift reversal of established practice.
Dr. Andy Carr is from the Oxford University Institute of Musculoskeletal Sciences at the NIHR Oxford Musculoskeletal Biomedical Research Unit, Oxford, England. These comments are taken from an accompanying editorial (BMJ 2015, June 16 [doi:10.1136/bmj.h2983]). He declared research grants from NIHR and Arthritis Research UK.
While randomized trials, uncontrolled observational studies, and surgeons’ own observations suggest that patients improve after arthroscopy, robust and bias-free trials that use placebo controls show that active treatment works no better than control treatment.
We may be close to a tipping point where the weight of evidence against arthroscopic knee surgery for pain is enough to overcome concerns about the quality of the studies, confirmation bias, and vested interests. When that point is reached, we should anticipate a swift reversal of established practice.
Dr. Andy Carr is from the Oxford University Institute of Musculoskeletal Sciences at the NIHR Oxford Musculoskeletal Biomedical Research Unit, Oxford, England. These comments are taken from an accompanying editorial (BMJ 2015, June 16 [doi:10.1136/bmj.h2983]). He declared research grants from NIHR and Arthritis Research UK.
Arthroscopic knee surgery in middle-aged or older patients with knee pain is associated with greater harm than good, according to a meta-analysis.
The analysis of nine randomized, controlled trials in 1,270 patients of arthroscopic surgery involving partial meniscectomy, debridement, or both showed a small but statistically significant benefit from the procedure – comparable to the pain-relieving effects of paracetamol – but which falls below significance after 12 months.
However, there were no significant improvements in knee function, and there were significant increases in the risk of deep vein thrombosis (4.13 events per 1,000 procedures) as well as infection, pulmonary embolism, and death, according to the paper published online June 16 in BMJ.
“Thus, middle-aged patients with knee pain and meniscal tears should be considered as having early-stage osteoarthritis and be treated according to clinical guidelines for knee osteoarthritis, starting with information, exercise, and often weight loss,” wrote Dr. Jonas B. Thorlund of the University of Southern Denmark, Odense, and coauthors (BMJ 2015, June 16 [doi:10.1136/bmj.h2747]).
The study was supported by the Swedish Research Council. One author declared personal fees from several pharmaceutical and medical companies and relevant journal editorship, while another declared fees from lectureships and books.
Arthroscopic knee surgery in middle-aged or older patients with knee pain is associated with greater harm than good, according to a meta-analysis.
The analysis of nine randomized, controlled trials in 1,270 patients of arthroscopic surgery involving partial meniscectomy, debridement, or both showed a small but statistically significant benefit from the procedure – comparable to the pain-relieving effects of paracetamol – but which falls below significance after 12 months.
However, there were no significant improvements in knee function, and there were significant increases in the risk of deep vein thrombosis (4.13 events per 1,000 procedures) as well as infection, pulmonary embolism, and death, according to the paper published online June 16 in BMJ.
“Thus, middle-aged patients with knee pain and meniscal tears should be considered as having early-stage osteoarthritis and be treated according to clinical guidelines for knee osteoarthritis, starting with information, exercise, and often weight loss,” wrote Dr. Jonas B. Thorlund of the University of Southern Denmark, Odense, and coauthors (BMJ 2015, June 16 [doi:10.1136/bmj.h2747]).
The study was supported by the Swedish Research Council. One author declared personal fees from several pharmaceutical and medical companies and relevant journal editorship, while another declared fees from lectureships and books.
FROM BMJ
Key clinical point: The potential harms of arthroscopic knee surgery in middle-aged or older patients with knee pain outweigh the benefits.
Major finding: Arthroscopic knee surgery is associated with a small but significant improvement in symptoms that disappears after 12 months.
Data source: Meta-analysis of nine randomized, controlled trials in 1,270 patients.
Disclosures: The study was supported by the Swedish Research Council. One author declared personal fees from several pharmaceutical and medical companies and relevant journal editorship, while another declared fees from lectureships and books.
Significant worker productivity gains with newer hepatitis C drugs
Achieving a cure in hepatitis C infection could result in significant economic gains, with a study estimating that the beneficial effects in terms of improved worker productivity could total around $3.23 billion per year for the United States alone.
Researchers used data on work productivity and activity scores from patients enrolled in clinical trials of the all-oral sofosbuvir and lepidasvir combo to estimate the impact of achieving sustained virologic response at 12 weeks (SVR-12) on workers’ productivity.
They calculated an average work productivity loss of $4,954 for each employed patient with chronic hepatitis C infection per year in the United States and $1,129 per year for the five European Union countries included in the mix.“These new all-oral combinations such as lepidasvir and sofosbuvir have cure rates between 95% and 99% with minimum side effects, [so] treating patients with these combinations results in improved work productivity, improved quality of life, and patient-reported outcomes that can translate into economic benefit,” Dr. Zobair M. Younossi of the Inova Fairfax Medical Campus, Falls Church, Va., said at the annual Digestive Disease Week.
No conflicts of interest were disclosed.
Achieving a cure in hepatitis C infection could result in significant economic gains, with a study estimating that the beneficial effects in terms of improved worker productivity could total around $3.23 billion per year for the United States alone.
Researchers used data on work productivity and activity scores from patients enrolled in clinical trials of the all-oral sofosbuvir and lepidasvir combo to estimate the impact of achieving sustained virologic response at 12 weeks (SVR-12) on workers’ productivity.
They calculated an average work productivity loss of $4,954 for each employed patient with chronic hepatitis C infection per year in the United States and $1,129 per year for the five European Union countries included in the mix.“These new all-oral combinations such as lepidasvir and sofosbuvir have cure rates between 95% and 99% with minimum side effects, [so] treating patients with these combinations results in improved work productivity, improved quality of life, and patient-reported outcomes that can translate into economic benefit,” Dr. Zobair M. Younossi of the Inova Fairfax Medical Campus, Falls Church, Va., said at the annual Digestive Disease Week.
No conflicts of interest were disclosed.
Achieving a cure in hepatitis C infection could result in significant economic gains, with a study estimating that the beneficial effects in terms of improved worker productivity could total around $3.23 billion per year for the United States alone.
Researchers used data on work productivity and activity scores from patients enrolled in clinical trials of the all-oral sofosbuvir and lepidasvir combo to estimate the impact of achieving sustained virologic response at 12 weeks (SVR-12) on workers’ productivity.
They calculated an average work productivity loss of $4,954 for each employed patient with chronic hepatitis C infection per year in the United States and $1,129 per year for the five European Union countries included in the mix.“These new all-oral combinations such as lepidasvir and sofosbuvir have cure rates between 95% and 99% with minimum side effects, [so] treating patients with these combinations results in improved work productivity, improved quality of life, and patient-reported outcomes that can translate into economic benefit,” Dr. Zobair M. Younossi of the Inova Fairfax Medical Campus, Falls Church, Va., said at the annual Digestive Disease Week.
No conflicts of interest were disclosed.
FROM DDW 2015
Key clinical point: Achieving a cure in hepatitis C infection could result in significant economic gains from improved worker productivity.
Major finding: The beneficial effects in terms of improved worker productivity could total around $3.23 billion per year for the United States alone.
Data source: Economic model using data from hepatitis C clinical trials in the United States and Europe.
Disclosures: No conflicts of interest were disclosed.
Obesity boosts postmenopausal breast cancer risk
Women who are overweight and obese have a significantly higher risk of invasive breast cancer after menopause compared with normal-weight women, according to secondary analysis of data from the Women’s Health Initiative.
An analysis of data from 67,142 postmenopausal women aged 50-79 years found that women with a body mass index greater than 35 had a 58% increased risk of invasive breast cancer, compared with women with a BMI lower than 25. Obese women with a BMI of greater than 35 were also at increased risk for estrogen- and progesterone-receptor–positive breast cancer compared to normal-weight women (hazard ratio, 1.86), but they were not at increased risk for hormone receptor–negative breast cancer.
This group also had a twofold increase in the risk of being diagnosed with a larger tumor, and significantly higher risk of having positive lymph nodes, regional and/or distant stage, and also of dying after breast cancer, according to an article published June 11 in JAMA Oncology.
“Well-designed clinical trials are needed to definitively test whether weight loss and body composition changes in overweight and obese women or obesity prevention in women of normal weight will reduce breast cancer risk,” wrote Marian L. Neuhouser, Ph.D., of the Fred Hutchinson Cancer Research Center in Seattle, and her colleagues (JAMA Oncol. 2015. June 11 [doi: 10.1001/jamaoncol. 2015.1546]).
The Women’s Health Initiative programs are supported by the National Heart, Lung, and Blood Institute, part of the National Institutes of Health. One of the researchers disclosed having financial relationships with Novartis, Novo Nordisk, Pfizer, Genetech, and Amgen. The other researchers reported having no financial disclosures.
This article makes an important contribution in extending and refining our understanding of one particular risk associated with overweight and obesity; namely the increase in postmenopausal, hormone receptor–positive breast cancer.
The researchers also made the frustrating observation that weight loss is not protective, which challenges the notion that patients who are overweight or obese should lose weight to reduce their cancer risk. The study highlights the need for clinical trials to explore whether weight loss or body composition changes in overweight and obesity can reduce breast cancer risk.
Dr. Clifford A. Hudis is from the Memorial Sloan Kettering Cancer Center in New York, and Dr. Andrew Dannenberg is from the Weill Cornell Medical College in New York. These comments are adapted from an editorial (JAMA Oncol. 2015 June 11 [doi: 10.1001/jamaoncol. 2015.1547]). The authors reported having no financial disclosures.
This article makes an important contribution in extending and refining our understanding of one particular risk associated with overweight and obesity; namely the increase in postmenopausal, hormone receptor–positive breast cancer.
The researchers also made the frustrating observation that weight loss is not protective, which challenges the notion that patients who are overweight or obese should lose weight to reduce their cancer risk. The study highlights the need for clinical trials to explore whether weight loss or body composition changes in overweight and obesity can reduce breast cancer risk.
Dr. Clifford A. Hudis is from the Memorial Sloan Kettering Cancer Center in New York, and Dr. Andrew Dannenberg is from the Weill Cornell Medical College in New York. These comments are adapted from an editorial (JAMA Oncol. 2015 June 11 [doi: 10.1001/jamaoncol. 2015.1547]). The authors reported having no financial disclosures.
This article makes an important contribution in extending and refining our understanding of one particular risk associated with overweight and obesity; namely the increase in postmenopausal, hormone receptor–positive breast cancer.
The researchers also made the frustrating observation that weight loss is not protective, which challenges the notion that patients who are overweight or obese should lose weight to reduce their cancer risk. The study highlights the need for clinical trials to explore whether weight loss or body composition changes in overweight and obesity can reduce breast cancer risk.
Dr. Clifford A. Hudis is from the Memorial Sloan Kettering Cancer Center in New York, and Dr. Andrew Dannenberg is from the Weill Cornell Medical College in New York. These comments are adapted from an editorial (JAMA Oncol. 2015 June 11 [doi: 10.1001/jamaoncol. 2015.1547]). The authors reported having no financial disclosures.
Women who are overweight and obese have a significantly higher risk of invasive breast cancer after menopause compared with normal-weight women, according to secondary analysis of data from the Women’s Health Initiative.
An analysis of data from 67,142 postmenopausal women aged 50-79 years found that women with a body mass index greater than 35 had a 58% increased risk of invasive breast cancer, compared with women with a BMI lower than 25. Obese women with a BMI of greater than 35 were also at increased risk for estrogen- and progesterone-receptor–positive breast cancer compared to normal-weight women (hazard ratio, 1.86), but they were not at increased risk for hormone receptor–negative breast cancer.
This group also had a twofold increase in the risk of being diagnosed with a larger tumor, and significantly higher risk of having positive lymph nodes, regional and/or distant stage, and also of dying after breast cancer, according to an article published June 11 in JAMA Oncology.
“Well-designed clinical trials are needed to definitively test whether weight loss and body composition changes in overweight and obese women or obesity prevention in women of normal weight will reduce breast cancer risk,” wrote Marian L. Neuhouser, Ph.D., of the Fred Hutchinson Cancer Research Center in Seattle, and her colleagues (JAMA Oncol. 2015. June 11 [doi: 10.1001/jamaoncol. 2015.1546]).
The Women’s Health Initiative programs are supported by the National Heart, Lung, and Blood Institute, part of the National Institutes of Health. One of the researchers disclosed having financial relationships with Novartis, Novo Nordisk, Pfizer, Genetech, and Amgen. The other researchers reported having no financial disclosures.
Women who are overweight and obese have a significantly higher risk of invasive breast cancer after menopause compared with normal-weight women, according to secondary analysis of data from the Women’s Health Initiative.
An analysis of data from 67,142 postmenopausal women aged 50-79 years found that women with a body mass index greater than 35 had a 58% increased risk of invasive breast cancer, compared with women with a BMI lower than 25. Obese women with a BMI of greater than 35 were also at increased risk for estrogen- and progesterone-receptor–positive breast cancer compared to normal-weight women (hazard ratio, 1.86), but they were not at increased risk for hormone receptor–negative breast cancer.
This group also had a twofold increase in the risk of being diagnosed with a larger tumor, and significantly higher risk of having positive lymph nodes, regional and/or distant stage, and also of dying after breast cancer, according to an article published June 11 in JAMA Oncology.
“Well-designed clinical trials are needed to definitively test whether weight loss and body composition changes in overweight and obese women or obesity prevention in women of normal weight will reduce breast cancer risk,” wrote Marian L. Neuhouser, Ph.D., of the Fred Hutchinson Cancer Research Center in Seattle, and her colleagues (JAMA Oncol. 2015. June 11 [doi: 10.1001/jamaoncol. 2015.1546]).
The Women’s Health Initiative programs are supported by the National Heart, Lung, and Blood Institute, part of the National Institutes of Health. One of the researchers disclosed having financial relationships with Novartis, Novo Nordisk, Pfizer, Genetech, and Amgen. The other researchers reported having no financial disclosures.
FROM JAMA ONCOLOGY
Key clinical point: Women who are overweight and obese have a significantly higher risk of postmenopausal invasive breast cancer, particularly hormone receptor–positive cancer.
Major finding: Postmenopausal women with a body mass index of 35 or greater had an 86% increase in the risk of estrogen- and progesterone-receptor–positive breast cancer, compared to normal-weight women.
Data source: Analysis of data from 67,142 postmenopausal women enrolled in the Women’s Health Initiative clinical trials.
Disclosures: The Women’s Health Initiative programs are supported by the National Heart, Lung, and Blood Institute. One of the researchers disclosed ties with Novartis, Novo Nordisk, Pfizer, Genetech, and Amgen. The other researchers reported having no financial disclosures.
Communication failures behind many surgical ‘never events’
Poor communication remains at the heart of most surgical “never events” (i.e., preventable events), say the authors of a systematic review that estimates around 500 wrong-site surgeries and 5,000 retained surgical items incidents still happen each year in the United States.
The review of 138 empirical studies of wrong-site surgery, retained surgical items, and surgical fires, published between 2004 and 2014, found wrong-site surgery occurred roughly once per 100,000 surgical procedures, and retained surgical items incidents at a rate of 1.32 events per 10,000 procedures, with unknown data on the per-procedure incidence of surgical fire, according to data published online June 10 in JAMA Surgery.
“A frequently reported cause of wrong-site surgery across 28 identified analyses was communication problems, including miscommunications among staff, missing information that should have been available to the operating room staff, surgical team members not speaking up when they noticed that a procedure targeted the wrong side, and a surgeon ignoring surgical team members who questioned laterality,” wrote Susanne Hempel, PhD, of the Southern California Evidence-Based Practice Center, Santa Monica, and her coauthors.
They found that very few evaluations of interventions designed specifically to reduce the incidence of never events were conclusive, although they pointed out that given the rarity of these events, it was methodologically challenging to assess the effectiveness of these interventions (JAMA Surg. 2015 June 10 [doi:10.1001/jamasurg.2015.0301]).
The Department of Veterans Affairs supported the study. There were no conflicts of interest declared.
Poor communication remains at the heart of most surgical “never events” (i.e., preventable events), say the authors of a systematic review that estimates around 500 wrong-site surgeries and 5,000 retained surgical items incidents still happen each year in the United States.
The review of 138 empirical studies of wrong-site surgery, retained surgical items, and surgical fires, published between 2004 and 2014, found wrong-site surgery occurred roughly once per 100,000 surgical procedures, and retained surgical items incidents at a rate of 1.32 events per 10,000 procedures, with unknown data on the per-procedure incidence of surgical fire, according to data published online June 10 in JAMA Surgery.
“A frequently reported cause of wrong-site surgery across 28 identified analyses was communication problems, including miscommunications among staff, missing information that should have been available to the operating room staff, surgical team members not speaking up when they noticed that a procedure targeted the wrong side, and a surgeon ignoring surgical team members who questioned laterality,” wrote Susanne Hempel, PhD, of the Southern California Evidence-Based Practice Center, Santa Monica, and her coauthors.
They found that very few evaluations of interventions designed specifically to reduce the incidence of never events were conclusive, although they pointed out that given the rarity of these events, it was methodologically challenging to assess the effectiveness of these interventions (JAMA Surg. 2015 June 10 [doi:10.1001/jamasurg.2015.0301]).
The Department of Veterans Affairs supported the study. There were no conflicts of interest declared.
Poor communication remains at the heart of most surgical “never events” (i.e., preventable events), say the authors of a systematic review that estimates around 500 wrong-site surgeries and 5,000 retained surgical items incidents still happen each year in the United States.
The review of 138 empirical studies of wrong-site surgery, retained surgical items, and surgical fires, published between 2004 and 2014, found wrong-site surgery occurred roughly once per 100,000 surgical procedures, and retained surgical items incidents at a rate of 1.32 events per 10,000 procedures, with unknown data on the per-procedure incidence of surgical fire, according to data published online June 10 in JAMA Surgery.
“A frequently reported cause of wrong-site surgery across 28 identified analyses was communication problems, including miscommunications among staff, missing information that should have been available to the operating room staff, surgical team members not speaking up when they noticed that a procedure targeted the wrong side, and a surgeon ignoring surgical team members who questioned laterality,” wrote Susanne Hempel, PhD, of the Southern California Evidence-Based Practice Center, Santa Monica, and her coauthors.
They found that very few evaluations of interventions designed specifically to reduce the incidence of never events were conclusive, although they pointed out that given the rarity of these events, it was methodologically challenging to assess the effectiveness of these interventions (JAMA Surg. 2015 June 10 [doi:10.1001/jamasurg.2015.0301]).
The Department of Veterans Affairs supported the study. There were no conflicts of interest declared.
FROM JAMA SURGERY
Key clinical point: Around 500 wrong-site surgeries and 5,000 retained surgical items incidents still happen each year, many caused by inadequate communication.
Major finding: Wrong-site surgery occurs roughly once per 100,000 surgical procedures, and retained surgical items incidents occur at a rate of 1.32 events per 10,000 procedures.
Data source: Systematic review of 138 empirical studies.
Disclosures: The Department of Veterans Affairs supported the study. There were no conflicts of interest declared.