User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
HIV vaccine could prevent 30 million cases by 2035
Global cases of HIV from 2015 to 2035 would be reduced by over 50% if the Joint United Nations Program on HIV/AIDS 95/95/95 target is met and a moderately effective HIV vaccine is introduced by 2020, according to new research published in Proceedings of the National Academy of Sciences.
A custom model based on current rates of diagnosis and treatment in 127 countries predicts that a total of 49 million new cases of HIV would occur globally from 2015 to 2035, investigators said. Achieving the UNAIDS goal of 95% disease diagnosis, 95% antiretroviral coverage, and 95% viral suppression by 2030 would avert 25 million cases by 2035. Achieving the more modest 90/90/90 target would avert 22 million cases within the same time period.
“Recent results from the HVTN 100 vaccine trial have bolstered optimism for the development and deployment of an HIV vaccine in the near term,” the investigators said. “HIV vaccination would enable a strategic shift from reactive to proactive control, as suggested by our finding that an HIV vaccine with even moderate efficacy rolled out in 2020 could avert 17 million new infections by 2035 relative to expectations under status quo interventions.”
Find the full study in PNAS (doi: 10.1073/pnas.1620788114)
[email protected]
On Twitter @IDPractitioner
Global cases of HIV from 2015 to 2035 would be reduced by over 50% if the Joint United Nations Program on HIV/AIDS 95/95/95 target is met and a moderately effective HIV vaccine is introduced by 2020, according to new research published in Proceedings of the National Academy of Sciences.
A custom model based on current rates of diagnosis and treatment in 127 countries predicts that a total of 49 million new cases of HIV would occur globally from 2015 to 2035, investigators said. Achieving the UNAIDS goal of 95% disease diagnosis, 95% antiretroviral coverage, and 95% viral suppression by 2030 would avert 25 million cases by 2035. Achieving the more modest 90/90/90 target would avert 22 million cases within the same time period.
“Recent results from the HVTN 100 vaccine trial have bolstered optimism for the development and deployment of an HIV vaccine in the near term,” the investigators said. “HIV vaccination would enable a strategic shift from reactive to proactive control, as suggested by our finding that an HIV vaccine with even moderate efficacy rolled out in 2020 could avert 17 million new infections by 2035 relative to expectations under status quo interventions.”
Find the full study in PNAS (doi: 10.1073/pnas.1620788114)
[email protected]
On Twitter @IDPractitioner
Global cases of HIV from 2015 to 2035 would be reduced by over 50% if the Joint United Nations Program on HIV/AIDS 95/95/95 target is met and a moderately effective HIV vaccine is introduced by 2020, according to new research published in Proceedings of the National Academy of Sciences.
A custom model based on current rates of diagnosis and treatment in 127 countries predicts that a total of 49 million new cases of HIV would occur globally from 2015 to 2035, investigators said. Achieving the UNAIDS goal of 95% disease diagnosis, 95% antiretroviral coverage, and 95% viral suppression by 2030 would avert 25 million cases by 2035. Achieving the more modest 90/90/90 target would avert 22 million cases within the same time period.
“Recent results from the HVTN 100 vaccine trial have bolstered optimism for the development and deployment of an HIV vaccine in the near term,” the investigators said. “HIV vaccination would enable a strategic shift from reactive to proactive control, as suggested by our finding that an HIV vaccine with even moderate efficacy rolled out in 2020 could avert 17 million new infections by 2035 relative to expectations under status quo interventions.”
Find the full study in PNAS (doi: 10.1073/pnas.1620788114)
[email protected]
On Twitter @IDPractitioner
Children with chronic conditions have poor influenza vaccination coverage
Poor influenza vaccination rates in children with chronic diseases is primarily due to poor parental understanding of influenza risk and vaccination benefits, according to Janita Pak Chun Chau, PhD, of the Chinese University of Hong Kong, and associates.
Studies show that children with chronic conditions “are at a disproportionately higher risk for severe influenza-associated complications, causing increased visits to outpatient or emergency departments, longer hospital stays, and higher mortality,” the researchers said.
A total of 623 parents of children with chronic conditions in Hong Kong were included in the study. The most common chronic condition was asthma, followed by chronic respiratory disease and cardiomyopathy. Only 33% of children had received an influenza vaccination in the previous 12 months, and 57% of children had ever received one.
Just under 40% of parents indicated intent to have their children vaccinated in the next 12 months. Parents who had their children vaccinated were more aware of vaccination benefits and considered vaccination a social norm, compared with parents who had not had their children vaccinated. Television was by far the most common source of information about influenza, followed by health professionals, and newspapers and magazines.
“Development of community-based influenza vaccination programs by health care professionals targeted to promote awareness and communicate the benefits and effectiveness of the vaccines in children with chronic conditions, as well as clarifying safety issues concerning the vaccination, may be able to promote the uptake of influenza vaccination,” the investigators wrote.
Find the study in the Pediatric Infectious Disease Journal (doi: INF.0000000000001550).
Poor influenza vaccination rates in children with chronic diseases is primarily due to poor parental understanding of influenza risk and vaccination benefits, according to Janita Pak Chun Chau, PhD, of the Chinese University of Hong Kong, and associates.
Studies show that children with chronic conditions “are at a disproportionately higher risk for severe influenza-associated complications, causing increased visits to outpatient or emergency departments, longer hospital stays, and higher mortality,” the researchers said.
A total of 623 parents of children with chronic conditions in Hong Kong were included in the study. The most common chronic condition was asthma, followed by chronic respiratory disease and cardiomyopathy. Only 33% of children had received an influenza vaccination in the previous 12 months, and 57% of children had ever received one.
Just under 40% of parents indicated intent to have their children vaccinated in the next 12 months. Parents who had their children vaccinated were more aware of vaccination benefits and considered vaccination a social norm, compared with parents who had not had their children vaccinated. Television was by far the most common source of information about influenza, followed by health professionals, and newspapers and magazines.
“Development of community-based influenza vaccination programs by health care professionals targeted to promote awareness and communicate the benefits and effectiveness of the vaccines in children with chronic conditions, as well as clarifying safety issues concerning the vaccination, may be able to promote the uptake of influenza vaccination,” the investigators wrote.
Find the study in the Pediatric Infectious Disease Journal (doi: INF.0000000000001550).
Poor influenza vaccination rates in children with chronic diseases is primarily due to poor parental understanding of influenza risk and vaccination benefits, according to Janita Pak Chun Chau, PhD, of the Chinese University of Hong Kong, and associates.
Studies show that children with chronic conditions “are at a disproportionately higher risk for severe influenza-associated complications, causing increased visits to outpatient or emergency departments, longer hospital stays, and higher mortality,” the researchers said.
A total of 623 parents of children with chronic conditions in Hong Kong were included in the study. The most common chronic condition was asthma, followed by chronic respiratory disease and cardiomyopathy. Only 33% of children had received an influenza vaccination in the previous 12 months, and 57% of children had ever received one.
Just under 40% of parents indicated intent to have their children vaccinated in the next 12 months. Parents who had their children vaccinated were more aware of vaccination benefits and considered vaccination a social norm, compared with parents who had not had their children vaccinated. Television was by far the most common source of information about influenza, followed by health professionals, and newspapers and magazines.
“Development of community-based influenza vaccination programs by health care professionals targeted to promote awareness and communicate the benefits and effectiveness of the vaccines in children with chronic conditions, as well as clarifying safety issues concerning the vaccination, may be able to promote the uptake of influenza vaccination,” the investigators wrote.
Find the study in the Pediatric Infectious Disease Journal (doi: INF.0000000000001550).
FROM THE PEDIATRIC INFECTIOUS DISEASE JOURNAL
In Oregon pertussis outbreak, unvaccinated children were affected earlier
were, according to Steve G. Robison, MPH, and Juventila Liko, MD, MPH, from the Immunization Program, Oregon Health Authority, Portland.
A total of 351 pertussis cases in children aged 2 months to 10 years were reported in Portland and the upper Willamette Valley from Jan. 1 to Nov. 1, 2012. Children who were unvaccinated accounted for 76 (22%) of the reported cases, and children who were poorly vaccinated accounted for 50 of the 275 (18%) cases in vaccinated children.
“Children who are not immunized represent a dynamic risk of spreading disease in an outbreak and have an impact that is greater than simply lessening overall community immunity levels. Diseases such as pertussis may spread across areas through the choice of parents to not immunize or to limit immunizations. Once locally present, pertussis will spread to the unimmunized and vulnerable, who in turn through the weight of exposure, may then ignite a wider outbreak in vaccinated populations,” the investigators noted.
Find the full study in the Journal of Pediatrics (doi: 10.1016/j.jpeds.2016.12.047).
were, according to Steve G. Robison, MPH, and Juventila Liko, MD, MPH, from the Immunization Program, Oregon Health Authority, Portland.
A total of 351 pertussis cases in children aged 2 months to 10 years were reported in Portland and the upper Willamette Valley from Jan. 1 to Nov. 1, 2012. Children who were unvaccinated accounted for 76 (22%) of the reported cases, and children who were poorly vaccinated accounted for 50 of the 275 (18%) cases in vaccinated children.
“Children who are not immunized represent a dynamic risk of spreading disease in an outbreak and have an impact that is greater than simply lessening overall community immunity levels. Diseases such as pertussis may spread across areas through the choice of parents to not immunize or to limit immunizations. Once locally present, pertussis will spread to the unimmunized and vulnerable, who in turn through the weight of exposure, may then ignite a wider outbreak in vaccinated populations,” the investigators noted.
Find the full study in the Journal of Pediatrics (doi: 10.1016/j.jpeds.2016.12.047).
were, according to Steve G. Robison, MPH, and Juventila Liko, MD, MPH, from the Immunization Program, Oregon Health Authority, Portland.
A total of 351 pertussis cases in children aged 2 months to 10 years were reported in Portland and the upper Willamette Valley from Jan. 1 to Nov. 1, 2012. Children who were unvaccinated accounted for 76 (22%) of the reported cases, and children who were poorly vaccinated accounted for 50 of the 275 (18%) cases in vaccinated children.
“Children who are not immunized represent a dynamic risk of spreading disease in an outbreak and have an impact that is greater than simply lessening overall community immunity levels. Diseases such as pertussis may spread across areas through the choice of parents to not immunize or to limit immunizations. Once locally present, pertussis will spread to the unimmunized and vulnerable, who in turn through the weight of exposure, may then ignite a wider outbreak in vaccinated populations,” the investigators noted.
Find the full study in the Journal of Pediatrics (doi: 10.1016/j.jpeds.2016.12.047).
FROM THE JOURNAL OF PEDIATRICS
Sirolimus shows promise for pediatric refractory IBD treatment
Sirolimus may be an effective rescue treatment option for children with refractory inflammatory bowel disease, according to Dr. Mohamed Mutalib and his associates.
In a retrospective analysis of 11 ulcerative colitis (UC) and 3 Crohn’s disease patients treated with sirolimus, 5 of the UC patients and all of the Crohn’s disease patients achieved clinical remission. An additional 2 UC patients achieved clinical response. The remaining 4 UC patients did not respond to sirolimus treatment.
Mucosal healing was achieved in 5 of 11 UC patients and 2 of 3 Crohn’s patients. Clinical response to treatment occurred at least 2 weeks after treatment was started. The only significant side effect reported was minor gastrointestinal distress.
“Our data provide compelling evidence that sirolimus is effective as rescue therapy in a subgroup of children with severe [inflammatory bowel disease] refractory to conventional therapies by inducing both clinical remission and mucosal healing. However, randomized placebo-controlled studies are warranted to extend our encouraging initial findings,” the investigators concluded.
Find the full study in the Journal of Crohn’s and Colitis (doi: 10.1016/j.crohns.2014.08.014).
Sirolimus may be an effective rescue treatment option for children with refractory inflammatory bowel disease, according to Dr. Mohamed Mutalib and his associates.
In a retrospective analysis of 11 ulcerative colitis (UC) and 3 Crohn’s disease patients treated with sirolimus, 5 of the UC patients and all of the Crohn’s disease patients achieved clinical remission. An additional 2 UC patients achieved clinical response. The remaining 4 UC patients did not respond to sirolimus treatment.
Mucosal healing was achieved in 5 of 11 UC patients and 2 of 3 Crohn’s patients. Clinical response to treatment occurred at least 2 weeks after treatment was started. The only significant side effect reported was minor gastrointestinal distress.
“Our data provide compelling evidence that sirolimus is effective as rescue therapy in a subgroup of children with severe [inflammatory bowel disease] refractory to conventional therapies by inducing both clinical remission and mucosal healing. However, randomized placebo-controlled studies are warranted to extend our encouraging initial findings,” the investigators concluded.
Find the full study in the Journal of Crohn’s and Colitis (doi: 10.1016/j.crohns.2014.08.014).
Sirolimus may be an effective rescue treatment option for children with refractory inflammatory bowel disease, according to Dr. Mohamed Mutalib and his associates.
In a retrospective analysis of 11 ulcerative colitis (UC) and 3 Crohn’s disease patients treated with sirolimus, 5 of the UC patients and all of the Crohn’s disease patients achieved clinical remission. An additional 2 UC patients achieved clinical response. The remaining 4 UC patients did not respond to sirolimus treatment.
Mucosal healing was achieved in 5 of 11 UC patients and 2 of 3 Crohn’s patients. Clinical response to treatment occurred at least 2 weeks after treatment was started. The only significant side effect reported was minor gastrointestinal distress.
“Our data provide compelling evidence that sirolimus is effective as rescue therapy in a subgroup of children with severe [inflammatory bowel disease] refractory to conventional therapies by inducing both clinical remission and mucosal healing. However, randomized placebo-controlled studies are warranted to extend our encouraging initial findings,” the investigators concluded.
Find the full study in the Journal of Crohn’s and Colitis (doi: 10.1016/j.crohns.2014.08.014).
FROM THE JOURNAL OF CROHN'S AND COLITIS
Daptomycin safe, effective for pediatric cSSSI treatment
, according to Dr. John Bradley of the University of California, San Diego, and his associates.
A total of 389 cSSSI patients were included in the study, with 257 receiving daptomycin and 132 receiving standard-of-care (SOC) treatment (mostly vancomycin or clindamycin). Clinical success rates were similar for both groups, at 91% in the daptomycin group and 87% in the SOC group. Therapeutic success rates also were similar, at 97% in the daptomycin group and 99% in the SOC group.
“Daptomycin is a suitable once-daily alternative to vancomycin or clindamycin in the pediatric setting, particularly for suspected or confirmed MRSA [methicillin-resistant Staphylococcus aureus] infections,” the investigators concluded.
Find the full study in Pediatrics (doi: 10.1542/peds.2016-2477).
, according to Dr. John Bradley of the University of California, San Diego, and his associates.
A total of 389 cSSSI patients were included in the study, with 257 receiving daptomycin and 132 receiving standard-of-care (SOC) treatment (mostly vancomycin or clindamycin). Clinical success rates were similar for both groups, at 91% in the daptomycin group and 87% in the SOC group. Therapeutic success rates also were similar, at 97% in the daptomycin group and 99% in the SOC group.
“Daptomycin is a suitable once-daily alternative to vancomycin or clindamycin in the pediatric setting, particularly for suspected or confirmed MRSA [methicillin-resistant Staphylococcus aureus] infections,” the investigators concluded.
Find the full study in Pediatrics (doi: 10.1542/peds.2016-2477).
, according to Dr. John Bradley of the University of California, San Diego, and his associates.
A total of 389 cSSSI patients were included in the study, with 257 receiving daptomycin and 132 receiving standard-of-care (SOC) treatment (mostly vancomycin or clindamycin). Clinical success rates were similar for both groups, at 91% in the daptomycin group and 87% in the SOC group. Therapeutic success rates also were similar, at 97% in the daptomycin group and 99% in the SOC group.
“Daptomycin is a suitable once-daily alternative to vancomycin or clindamycin in the pediatric setting, particularly for suspected or confirmed MRSA [methicillin-resistant Staphylococcus aureus] infections,” the investigators concluded.
Find the full study in Pediatrics (doi: 10.1542/peds.2016-2477).
FROM PEDIATRICS
History of child abuse worsens depression course in elderly adults
Older adults with depression who reported experiencing child abuse were more likely to have persistent disease at follow-up than those who did not, according to a study carried out by Ilse Wielaard and associates at the VU University Medical Centre, Amsterdam, the Netherlands.
The mean age of the 282 study participants included in the 2-year study was 70.6 years, and of this group, 152 patients reported a history of child abuse. Patients with a history of child abuse were significantly more likely to be depressed at the end of the 2-year follow-up period.
“In the treatment of late-life depression it is important to detect childhood abuse and to consider mediating characteristics that influence its course negatively,” the investigators concluded.
Find the full study in the American Journal of Geriatric Psychiatry (doi: 10.1016/j.jagp.2017.01.014).
Older adults with depression who reported experiencing child abuse were more likely to have persistent disease at follow-up than those who did not, according to a study carried out by Ilse Wielaard and associates at the VU University Medical Centre, Amsterdam, the Netherlands.
The mean age of the 282 study participants included in the 2-year study was 70.6 years, and of this group, 152 patients reported a history of child abuse. Patients with a history of child abuse were significantly more likely to be depressed at the end of the 2-year follow-up period.
“In the treatment of late-life depression it is important to detect childhood abuse and to consider mediating characteristics that influence its course negatively,” the investigators concluded.
Find the full study in the American Journal of Geriatric Psychiatry (doi: 10.1016/j.jagp.2017.01.014).
Older adults with depression who reported experiencing child abuse were more likely to have persistent disease at follow-up than those who did not, according to a study carried out by Ilse Wielaard and associates at the VU University Medical Centre, Amsterdam, the Netherlands.
The mean age of the 282 study participants included in the 2-year study was 70.6 years, and of this group, 152 patients reported a history of child abuse. Patients with a history of child abuse were significantly more likely to be depressed at the end of the 2-year follow-up period.
“In the treatment of late-life depression it is important to detect childhood abuse and to consider mediating characteristics that influence its course negatively,” the investigators concluded.
Find the full study in the American Journal of Geriatric Psychiatry (doi: 10.1016/j.jagp.2017.01.014).
FROM THE AMERICAN JOURNAL OF GERIATRIC PSYCHIATRY
Initial HCV test results are false positive in almost half of general population
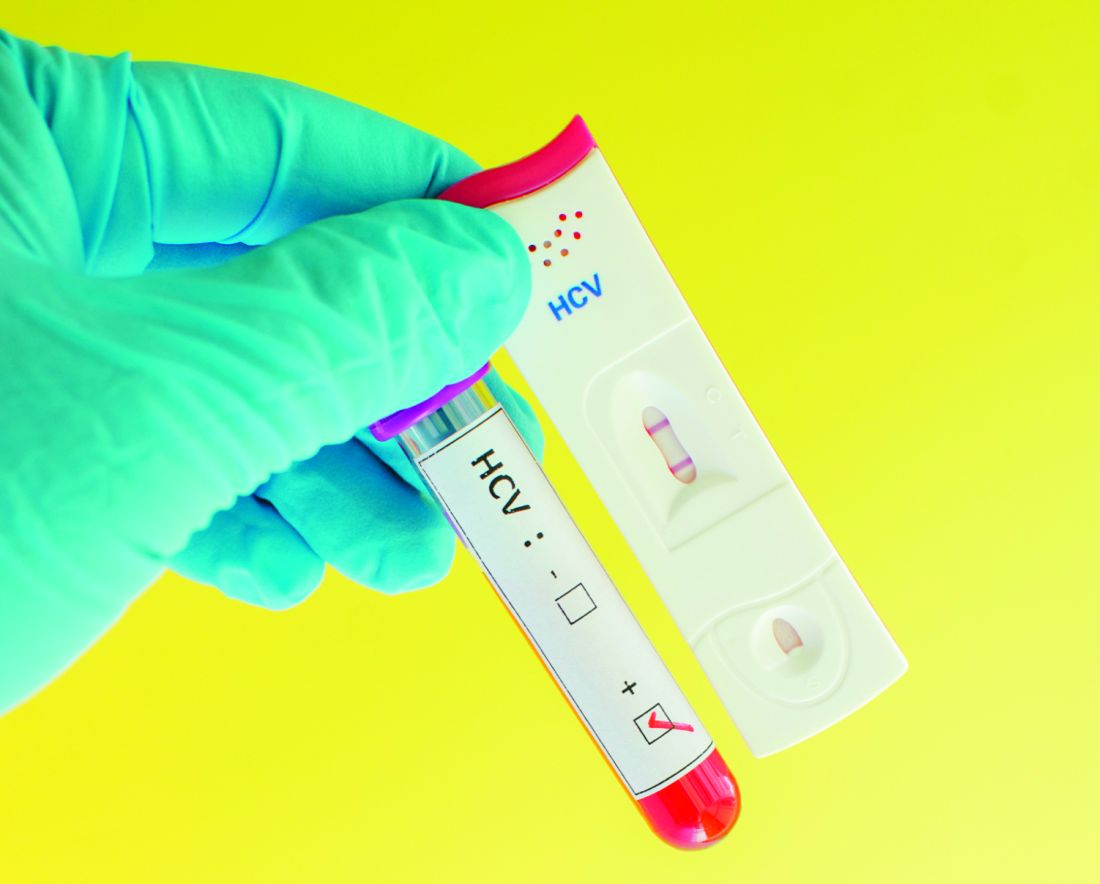
Nearly half of patients in the general population who test positive for hepatitis C virus (HCV) do not have the disease, according to Dr. Anne Moorman and her associates.
From a sample of 22,359 National Health and Nutrition Examination Study participants, 479 people received positive HCV antibody test results from 2007 to 2012. Of this group, 477 participants underwent further follow-up testing using a recombinant immunoblot assay. RIBA testing confirmed positive test results for 323 participants, while 105 patients received negative test results and 49 received indeterminate test results.
“False-positive antibody assays may occur with great frequency, emphasizing the need for “reflex” HCV RNA testing to ascertain current infection status,” the investigators noted.
Find the full study in the Journal of Clinical Virology (doi: 10.1016/j.jcv.2017.01.007).
Nearly half of patients in the general population who test positive for hepatitis C virus (HCV) do not have the disease, according to Dr. Anne Moorman and her associates.
From a sample of 22,359 National Health and Nutrition Examination Study participants, 479 people received positive HCV antibody test results from 2007 to 2012. Of this group, 477 participants underwent further follow-up testing using a recombinant immunoblot assay. RIBA testing confirmed positive test results for 323 participants, while 105 patients received negative test results and 49 received indeterminate test results.
“False-positive antibody assays may occur with great frequency, emphasizing the need for “reflex” HCV RNA testing to ascertain current infection status,” the investigators noted.
Find the full study in the Journal of Clinical Virology (doi: 10.1016/j.jcv.2017.01.007).
Nearly half of patients in the general population who test positive for hepatitis C virus (HCV) do not have the disease, according to Dr. Anne Moorman and her associates.
From a sample of 22,359 National Health and Nutrition Examination Study participants, 479 people received positive HCV antibody test results from 2007 to 2012. Of this group, 477 participants underwent further follow-up testing using a recombinant immunoblot assay. RIBA testing confirmed positive test results for 323 participants, while 105 patients received negative test results and 49 received indeterminate test results.
“False-positive antibody assays may occur with great frequency, emphasizing the need for “reflex” HCV RNA testing to ascertain current infection status,” the investigators noted.
Find the full study in the Journal of Clinical Virology (doi: 10.1016/j.jcv.2017.01.007).
FROM JOURNAL OF CLINICAL VIROLOGY
Adverse event reporting in second-dose varicella vaccination shows no surprises
No new or unexpected adverse events were reported in association with second-dose varicella vaccination in children age 4-18 years during 2006-2014.
During the study period of 2006-2014, 14,641 reports regarding second-dose varicella vaccinations were made to the Vaccine Adverse Event Reporting System, according to John Su, MD, PhD, and his associates. Of these reports, only 3% were serious adverse events (AE), with the most common nonserious AE being injection-site reaction, which occurred in 48% of patients age 4-6 years reporting AEs, and in 38% of patients age 7-18 years reporting AEs.
Of the 494 serious AEs reported, pyrexia was the most common in children age 4-6 years, and headache and vomiting were the most common in children age 7-18 years. A total of seven deaths from various causes were reported, though no causal relation to vaccination was seen, and significant chronic medical problems were common in these children.
“The safety data on second-dose varicella vaccination are reassuring,” the investigators noted. “Reported AEs after second-dose varicella vaccination were mild, self limiting, and similar in reported frequency to AEs after first-dose vaccination, with no new or unexpected safety concerns.”
Find the full study in Pediatrics (2017 Feb 7. doi: 1542/peds.2016-2536).
No new or unexpected adverse events were reported in association with second-dose varicella vaccination in children age 4-18 years during 2006-2014.
During the study period of 2006-2014, 14,641 reports regarding second-dose varicella vaccinations were made to the Vaccine Adverse Event Reporting System, according to John Su, MD, PhD, and his associates. Of these reports, only 3% were serious adverse events (AE), with the most common nonserious AE being injection-site reaction, which occurred in 48% of patients age 4-6 years reporting AEs, and in 38% of patients age 7-18 years reporting AEs.
Of the 494 serious AEs reported, pyrexia was the most common in children age 4-6 years, and headache and vomiting were the most common in children age 7-18 years. A total of seven deaths from various causes were reported, though no causal relation to vaccination was seen, and significant chronic medical problems were common in these children.
“The safety data on second-dose varicella vaccination are reassuring,” the investigators noted. “Reported AEs after second-dose varicella vaccination were mild, self limiting, and similar in reported frequency to AEs after first-dose vaccination, with no new or unexpected safety concerns.”
Find the full study in Pediatrics (2017 Feb 7. doi: 1542/peds.2016-2536).
No new or unexpected adverse events were reported in association with second-dose varicella vaccination in children age 4-18 years during 2006-2014.
During the study period of 2006-2014, 14,641 reports regarding second-dose varicella vaccinations were made to the Vaccine Adverse Event Reporting System, according to John Su, MD, PhD, and his associates. Of these reports, only 3% were serious adverse events (AE), with the most common nonserious AE being injection-site reaction, which occurred in 48% of patients age 4-6 years reporting AEs, and in 38% of patients age 7-18 years reporting AEs.
Of the 494 serious AEs reported, pyrexia was the most common in children age 4-6 years, and headache and vomiting were the most common in children age 7-18 years. A total of seven deaths from various causes were reported, though no causal relation to vaccination was seen, and significant chronic medical problems were common in these children.
“The safety data on second-dose varicella vaccination are reassuring,” the investigators noted. “Reported AEs after second-dose varicella vaccination were mild, self limiting, and similar in reported frequency to AEs after first-dose vaccination, with no new or unexpected safety concerns.”
Find the full study in Pediatrics (2017 Feb 7. doi: 1542/peds.2016-2536).
Latuda receives FDA approval for adolescent schizophrenia treatment
Lurasidone HCl, marketed as Latuda, has received approval from the Food and Drug Administration for the treatment of schizophrenia in adolescents aged 13-17 years old, according to a press release from Sunovion Pharmaceuticals.
FDA approval of Latuda is based on results of a 6-week study in which adolescents with schizophrenia received either 40 mg of lurasidone per day, 80 mg per day, or a placebo. Patients who received lurasidone HCI showed statistical and clinical improvements in schizophrenia symptoms, compared with the placebo group. The drug was well tolerated with no significant adverse events reported.
“The impact on development and poor prognosis frequently associated with schizophrenia that begins in adolescence underscores the need for treatment that is both well tolerated and effective,” Robert L. Findling, MD, study investigator, and director of child and adolescent psychiatry at Johns Hopkins University, Baltimore, said in the press release. “The availability of Latuda provides health care providers with an important new option for helping adolescents with this illness that is chronic and severely disabling,” said Dr. Findling, also vice president of psychiatric services and research at the Kennedy Krieger Institute, Baltimore.
Find the full press release on the Sunovion Pharmaceuticals website.
Lurasidone HCl, marketed as Latuda, has received approval from the Food and Drug Administration for the treatment of schizophrenia in adolescents aged 13-17 years old, according to a press release from Sunovion Pharmaceuticals.
FDA approval of Latuda is based on results of a 6-week study in which adolescents with schizophrenia received either 40 mg of lurasidone per day, 80 mg per day, or a placebo. Patients who received lurasidone HCI showed statistical and clinical improvements in schizophrenia symptoms, compared with the placebo group. The drug was well tolerated with no significant adverse events reported.
“The impact on development and poor prognosis frequently associated with schizophrenia that begins in adolescence underscores the need for treatment that is both well tolerated and effective,” Robert L. Findling, MD, study investigator, and director of child and adolescent psychiatry at Johns Hopkins University, Baltimore, said in the press release. “The availability of Latuda provides health care providers with an important new option for helping adolescents with this illness that is chronic and severely disabling,” said Dr. Findling, also vice president of psychiatric services and research at the Kennedy Krieger Institute, Baltimore.
Find the full press release on the Sunovion Pharmaceuticals website.
Lurasidone HCl, marketed as Latuda, has received approval from the Food and Drug Administration for the treatment of schizophrenia in adolescents aged 13-17 years old, according to a press release from Sunovion Pharmaceuticals.
FDA approval of Latuda is based on results of a 6-week study in which adolescents with schizophrenia received either 40 mg of lurasidone per day, 80 mg per day, or a placebo. Patients who received lurasidone HCI showed statistical and clinical improvements in schizophrenia symptoms, compared with the placebo group. The drug was well tolerated with no significant adverse events reported.
“The impact on development and poor prognosis frequently associated with schizophrenia that begins in adolescence underscores the need for treatment that is both well tolerated and effective,” Robert L. Findling, MD, study investigator, and director of child and adolescent psychiatry at Johns Hopkins University, Baltimore, said in the press release. “The availability of Latuda provides health care providers with an important new option for helping adolescents with this illness that is chronic and severely disabling,” said Dr. Findling, also vice president of psychiatric services and research at the Kennedy Krieger Institute, Baltimore.
Find the full press release on the Sunovion Pharmaceuticals website.
Carbapenem-resistant K. pneumoniae occurs in 25% of long-term acute care hospital cultures
Nearly one-quarter of Klebsiella pneumoniae cultures in a network of U.S. long-term acute care hospitals are resistant to carbapenem, according to Jennifer H. Han, MD, and her associates.
From a sample of 3,846 K. pneumoniae cultures taken from 64 long-term acute care hospitals in 16 states, 946, or 24.6%, of the cultures were carbapenem-resistant, and were taken from 821 patients. Just under 54% of CRKP isolates were taken from a respiratory source, with 37% coming from urine and the remaining 9.4% coming from blood. Nearly all CRKP isolates were resistant to fluoroquinolones, and 59.2% were resistant to amikacin.
Of the 16 states where cultures were taken from, California had the highest rate of carbapenem resistance, with 45.5% of K. pneumoniae cultures showing resistance. Other states with high rates of CRKP included South Carolina, Kentucky, and Indiana.
“Given the chronically, critically ill population, with convergence of at-risk patients from multiple facilities, future studies of optimal infection prevention strategies are urgently needed for this setting. In addition, expansion of national surveillance efforts and improved communication between [long-term acute care hospitals] and acute care hospitals will be critical for reducing the continued emergence and dissemination of CRKP across the health care continuum,” Dr. Han and her associates concluded.
Find the full study in Clinical Infectious Diseases (doi: 10.1 LTACHs 093/cid/ciw856)
Nearly one-quarter of Klebsiella pneumoniae cultures in a network of U.S. long-term acute care hospitals are resistant to carbapenem, according to Jennifer H. Han, MD, and her associates.
From a sample of 3,846 K. pneumoniae cultures taken from 64 long-term acute care hospitals in 16 states, 946, or 24.6%, of the cultures were carbapenem-resistant, and were taken from 821 patients. Just under 54% of CRKP isolates were taken from a respiratory source, with 37% coming from urine and the remaining 9.4% coming from blood. Nearly all CRKP isolates were resistant to fluoroquinolones, and 59.2% were resistant to amikacin.
Of the 16 states where cultures were taken from, California had the highest rate of carbapenem resistance, with 45.5% of K. pneumoniae cultures showing resistance. Other states with high rates of CRKP included South Carolina, Kentucky, and Indiana.
“Given the chronically, critically ill population, with convergence of at-risk patients from multiple facilities, future studies of optimal infection prevention strategies are urgently needed for this setting. In addition, expansion of national surveillance efforts and improved communication between [long-term acute care hospitals] and acute care hospitals will be critical for reducing the continued emergence and dissemination of CRKP across the health care continuum,” Dr. Han and her associates concluded.
Find the full study in Clinical Infectious Diseases (doi: 10.1 LTACHs 093/cid/ciw856)
Nearly one-quarter of Klebsiella pneumoniae cultures in a network of U.S. long-term acute care hospitals are resistant to carbapenem, according to Jennifer H. Han, MD, and her associates.
From a sample of 3,846 K. pneumoniae cultures taken from 64 long-term acute care hospitals in 16 states, 946, or 24.6%, of the cultures were carbapenem-resistant, and were taken from 821 patients. Just under 54% of CRKP isolates were taken from a respiratory source, with 37% coming from urine and the remaining 9.4% coming from blood. Nearly all CRKP isolates were resistant to fluoroquinolones, and 59.2% were resistant to amikacin.
Of the 16 states where cultures were taken from, California had the highest rate of carbapenem resistance, with 45.5% of K. pneumoniae cultures showing resistance. Other states with high rates of CRKP included South Carolina, Kentucky, and Indiana.
“Given the chronically, critically ill population, with convergence of at-risk patients from multiple facilities, future studies of optimal infection prevention strategies are urgently needed for this setting. In addition, expansion of national surveillance efforts and improved communication between [long-term acute care hospitals] and acute care hospitals will be critical for reducing the continued emergence and dissemination of CRKP across the health care continuum,” Dr. Han and her associates concluded.
Find the full study in Clinical Infectious Diseases (doi: 10.1 LTACHs 093/cid/ciw856)
FROM CLINICAL INFECTIOUS DISEASES