User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
Internet-based CBT may be effective treatment for chronic insomnia
Internet-delivered cognitive-behavioral therapy is effective at overcoming chronic insomnia, a randomized controlled trial of 303 adults showed.
In the trial, patients who were randomized to receive cognitive-behavioral therapy for insomnia (CBT-I) used a Web-based program called Sleep Healthy Using the Internet (SHUTi), which “incorporates the primary tenets of face-to-face CBT-I, including sleep restriction, stimulus control, cognitive restructuring, sleep hygiene, and relapse prevention,” wrote Lee M. Ritterband, PhD, and his associates. Meanwhile, patients in the control group received online, nonspecific patient education.
After a 9-week study period, the investigators found that sleep-onset latency, wake after sleep onset, and ratings on the Insomnia Severity Index all were significantly reduced in the SHUTi group, compared with the control group. The effect remained after the 6-month and 1-year follow-ups, reported Dr. Ritterband of the Center for Behavioral Health and Technology at the University of Virginia, Charlottesville, and his associates.
No significant difference was found in total sleep time between the SHUTi group and the control group, but sleep efficiency and sleep quality did improve. In addition, the number of awakenings dropped in the SHUTi group. Both groups reported a decrease in the use of sleep aids, such as medication. After completing the post assessment and 6-month follow-up, participants received online gift certificates of $50 each, and after completing the assessment at the 1-year follow-up, they received $100 gift certificates.
“Internet-delivered CBT-I provides a less expensive, scalable treatment option that could reach previously unimaginable numbers of people,” the investigators said. “Future studies are necessary to determine who may be best served by this type of intervention and how the next steps of dissemination should occur. Ensuring that these interventions work with different patient populations, whether tailored or not for those groups, should also be examined,” they noted.
Find the full study in JAMA Psychiatry (2016 Nov 30. doi: 10.1001/jamapsychiatry.2016.3249)
Internet-delivered cognitive-behavioral therapy is effective at overcoming chronic insomnia, a randomized controlled trial of 303 adults showed.
In the trial, patients who were randomized to receive cognitive-behavioral therapy for insomnia (CBT-I) used a Web-based program called Sleep Healthy Using the Internet (SHUTi), which “incorporates the primary tenets of face-to-face CBT-I, including sleep restriction, stimulus control, cognitive restructuring, sleep hygiene, and relapse prevention,” wrote Lee M. Ritterband, PhD, and his associates. Meanwhile, patients in the control group received online, nonspecific patient education.
After a 9-week study period, the investigators found that sleep-onset latency, wake after sleep onset, and ratings on the Insomnia Severity Index all were significantly reduced in the SHUTi group, compared with the control group. The effect remained after the 6-month and 1-year follow-ups, reported Dr. Ritterband of the Center for Behavioral Health and Technology at the University of Virginia, Charlottesville, and his associates.
No significant difference was found in total sleep time between the SHUTi group and the control group, but sleep efficiency and sleep quality did improve. In addition, the number of awakenings dropped in the SHUTi group. Both groups reported a decrease in the use of sleep aids, such as medication. After completing the post assessment and 6-month follow-up, participants received online gift certificates of $50 each, and after completing the assessment at the 1-year follow-up, they received $100 gift certificates.
“Internet-delivered CBT-I provides a less expensive, scalable treatment option that could reach previously unimaginable numbers of people,” the investigators said. “Future studies are necessary to determine who may be best served by this type of intervention and how the next steps of dissemination should occur. Ensuring that these interventions work with different patient populations, whether tailored or not for those groups, should also be examined,” they noted.
Find the full study in JAMA Psychiatry (2016 Nov 30. doi: 10.1001/jamapsychiatry.2016.3249)
Internet-delivered cognitive-behavioral therapy is effective at overcoming chronic insomnia, a randomized controlled trial of 303 adults showed.
In the trial, patients who were randomized to receive cognitive-behavioral therapy for insomnia (CBT-I) used a Web-based program called Sleep Healthy Using the Internet (SHUTi), which “incorporates the primary tenets of face-to-face CBT-I, including sleep restriction, stimulus control, cognitive restructuring, sleep hygiene, and relapse prevention,” wrote Lee M. Ritterband, PhD, and his associates. Meanwhile, patients in the control group received online, nonspecific patient education.
After a 9-week study period, the investigators found that sleep-onset latency, wake after sleep onset, and ratings on the Insomnia Severity Index all were significantly reduced in the SHUTi group, compared with the control group. The effect remained after the 6-month and 1-year follow-ups, reported Dr. Ritterband of the Center for Behavioral Health and Technology at the University of Virginia, Charlottesville, and his associates.
No significant difference was found in total sleep time between the SHUTi group and the control group, but sleep efficiency and sleep quality did improve. In addition, the number of awakenings dropped in the SHUTi group. Both groups reported a decrease in the use of sleep aids, such as medication. After completing the post assessment and 6-month follow-up, participants received online gift certificates of $50 each, and after completing the assessment at the 1-year follow-up, they received $100 gift certificates.
“Internet-delivered CBT-I provides a less expensive, scalable treatment option that could reach previously unimaginable numbers of people,” the investigators said. “Future studies are necessary to determine who may be best served by this type of intervention and how the next steps of dissemination should occur. Ensuring that these interventions work with different patient populations, whether tailored or not for those groups, should also be examined,” they noted.
Find the full study in JAMA Psychiatry (2016 Nov 30. doi: 10.1001/jamapsychiatry.2016.3249)
FROM JAMA PSYCHIATRY
Many premature infants receive reflux medication after NICU discharge
Three-quarters of premature infants who receive gastroesophageal reflux medications get those drugs after being discharged from neonatal intensive care units, despite questions about the safety and efficacy of the medications in premature infants.
In a retrospective study of 2,217 premature infants treated within the Children’s Hospital of Philadelphia primary care network from 2005 to 2009, 812 were treated with gastroesophageal reflux (GER) medications. Of this group, 77% were started on GER medication after neonatal intensive care unit (NICU) discharge, according to Jo Ann D’Agostino, DNP, CRNP, and her associates (Pediatrics. 2016 Nov 23. doi: 10.1542/peds.2016-1977).
Histamine-2 receptor antagonists were the most commonly prescribed GER medication, received by 90% of infants. Proton pump inhibitors were prescribed to 37% of infants, 22% received prokinetics, and 2% received cholinergics. During the first year of life, 40% of treated infants received multiple GER medications, with 73% of these infants receiving at least two medications simultaneously.
Risk factors associated with the use of multiple GER medications include a gestation period less than 32 weeks, feeding difficulty, tube feeding, a need for supplemental oxygen, and asthma.
“Because premature infants are a medically fragile group, the need for 1 acid suppression medication, let alone 2 or more in combination, should be given careful consideration. The potential impact of acid suppression on community-acquired illnesses has yet to be explored for this vulnerable population,” said Dr. D’Agostino of the department of pediatrics at the Children’s Hospital of Philadelphia, and her coauthors.
Infants who received GER treatment after NICU discharge were started on medication at a mean chronological age of 95 days and received medication for a mean of 294 days. Infants who started GER treatment while in the NICU received medication for a mean of 375 days.
A total of 743 infants were started on GER medications before the age of 6 months, and of this group, 43% were still being treated at the age of 1 year. Extended medication usage was associated with a gestational age under 32 weeks, chronic lung disease, airway malacia, and reactive airways disease.
A gestation period of less than 32 weeks was associated with a 31% increase in GER medication duration, compared with infants with a gestation period of 34-35 weeks, and a gestation period of less than 28 weeks was associated with a 50% increase in medication duration.
“Physiologic reflux symptoms are reported to peak at 4 months of age. Feeding issues are also common for premature infants. Whether this combination of issues is influencing the decision to start treatment, as opposed to actual GER disease, is an important distinction for providers to consider before starting medication,” Dr. D’Agostino and her associates noted.
“With uncertain evidence of efficacy, the rationale for using these medications in this high-risk population should be carefully evaluated,” they concluded.
The study was funded by the National Institutes of Health. The authors had no relevant financial disclosures.
“Medications are frequently used to treat gastroesophageal reflux in premature infants,” wrote P. Brian Smith, MD, but “a number of these medications have been associated with significant harm” and the “short- or long-term benefits of GER medications in this population are undocumented.”
Histamine-2 receptor blockers, the most common GER medications, induce alterations to the fecal microbiota of premature infants by lowering microbial diversity and promoting overgrowth of Proteobacteria. “These alterations weaken the gastrointestinal tract’s protective barrier and render very low birth weight infants, already predisposed to [necrotizing enterocolitis] and other infections, even more vulnerable,” he noted.
“Infants receiving antacid therapy are also at increased risk of bacteremia, lower respiratory tract infections, aspiration pneumonia, and death,” he added.
“Pediatrics has a long history of widespread use of medications for which the risks did not outweigh the benefits. All drugs should be shown to be both safe and effective before use. [This study] has documented widespread, long-term use of medications that are likely neither,” he said.
Dr. Smith is with Duke University Medical Center, Durham, N.C. These comments are taken from an accompanying editorial (Pediatrics. 2016 Nov 23. doi: 10.1542/peds.2016-2849). Dr. Smith is a consultant for Astellas Pharma and Abbvie and receives grant support from Cempra Pharmaceuticals and Shionogi. Dr Smith receives salary support from the National Institutes of Health and the U.S. Food and Drug Administration.
“Medications are frequently used to treat gastroesophageal reflux in premature infants,” wrote P. Brian Smith, MD, but “a number of these medications have been associated with significant harm” and the “short- or long-term benefits of GER medications in this population are undocumented.”
Histamine-2 receptor blockers, the most common GER medications, induce alterations to the fecal microbiota of premature infants by lowering microbial diversity and promoting overgrowth of Proteobacteria. “These alterations weaken the gastrointestinal tract’s protective barrier and render very low birth weight infants, already predisposed to [necrotizing enterocolitis] and other infections, even more vulnerable,” he noted.
“Infants receiving antacid therapy are also at increased risk of bacteremia, lower respiratory tract infections, aspiration pneumonia, and death,” he added.
“Pediatrics has a long history of widespread use of medications for which the risks did not outweigh the benefits. All drugs should be shown to be both safe and effective before use. [This study] has documented widespread, long-term use of medications that are likely neither,” he said.
Dr. Smith is with Duke University Medical Center, Durham, N.C. These comments are taken from an accompanying editorial (Pediatrics. 2016 Nov 23. doi: 10.1542/peds.2016-2849). Dr. Smith is a consultant for Astellas Pharma and Abbvie and receives grant support from Cempra Pharmaceuticals and Shionogi. Dr Smith receives salary support from the National Institutes of Health and the U.S. Food and Drug Administration.
“Medications are frequently used to treat gastroesophageal reflux in premature infants,” wrote P. Brian Smith, MD, but “a number of these medications have been associated with significant harm” and the “short- or long-term benefits of GER medications in this population are undocumented.”
Histamine-2 receptor blockers, the most common GER medications, induce alterations to the fecal microbiota of premature infants by lowering microbial diversity and promoting overgrowth of Proteobacteria. “These alterations weaken the gastrointestinal tract’s protective barrier and render very low birth weight infants, already predisposed to [necrotizing enterocolitis] and other infections, even more vulnerable,” he noted.
“Infants receiving antacid therapy are also at increased risk of bacteremia, lower respiratory tract infections, aspiration pneumonia, and death,” he added.
“Pediatrics has a long history of widespread use of medications for which the risks did not outweigh the benefits. All drugs should be shown to be both safe and effective before use. [This study] has documented widespread, long-term use of medications that are likely neither,” he said.
Dr. Smith is with Duke University Medical Center, Durham, N.C. These comments are taken from an accompanying editorial (Pediatrics. 2016 Nov 23. doi: 10.1542/peds.2016-2849). Dr. Smith is a consultant for Astellas Pharma and Abbvie and receives grant support from Cempra Pharmaceuticals and Shionogi. Dr Smith receives salary support from the National Institutes of Health and the U.S. Food and Drug Administration.
Three-quarters of premature infants who receive gastroesophageal reflux medications get those drugs after being discharged from neonatal intensive care units, despite questions about the safety and efficacy of the medications in premature infants.
In a retrospective study of 2,217 premature infants treated within the Children’s Hospital of Philadelphia primary care network from 2005 to 2009, 812 were treated with gastroesophageal reflux (GER) medications. Of this group, 77% were started on GER medication after neonatal intensive care unit (NICU) discharge, according to Jo Ann D’Agostino, DNP, CRNP, and her associates (Pediatrics. 2016 Nov 23. doi: 10.1542/peds.2016-1977).
Histamine-2 receptor antagonists were the most commonly prescribed GER medication, received by 90% of infants. Proton pump inhibitors were prescribed to 37% of infants, 22% received prokinetics, and 2% received cholinergics. During the first year of life, 40% of treated infants received multiple GER medications, with 73% of these infants receiving at least two medications simultaneously.
Risk factors associated with the use of multiple GER medications include a gestation period less than 32 weeks, feeding difficulty, tube feeding, a need for supplemental oxygen, and asthma.
“Because premature infants are a medically fragile group, the need for 1 acid suppression medication, let alone 2 or more in combination, should be given careful consideration. The potential impact of acid suppression on community-acquired illnesses has yet to be explored for this vulnerable population,” said Dr. D’Agostino of the department of pediatrics at the Children’s Hospital of Philadelphia, and her coauthors.
Infants who received GER treatment after NICU discharge were started on medication at a mean chronological age of 95 days and received medication for a mean of 294 days. Infants who started GER treatment while in the NICU received medication for a mean of 375 days.
A total of 743 infants were started on GER medications before the age of 6 months, and of this group, 43% were still being treated at the age of 1 year. Extended medication usage was associated with a gestational age under 32 weeks, chronic lung disease, airway malacia, and reactive airways disease.
A gestation period of less than 32 weeks was associated with a 31% increase in GER medication duration, compared with infants with a gestation period of 34-35 weeks, and a gestation period of less than 28 weeks was associated with a 50% increase in medication duration.
“Physiologic reflux symptoms are reported to peak at 4 months of age. Feeding issues are also common for premature infants. Whether this combination of issues is influencing the decision to start treatment, as opposed to actual GER disease, is an important distinction for providers to consider before starting medication,” Dr. D’Agostino and her associates noted.
“With uncertain evidence of efficacy, the rationale for using these medications in this high-risk population should be carefully evaluated,” they concluded.
The study was funded by the National Institutes of Health. The authors had no relevant financial disclosures.
Three-quarters of premature infants who receive gastroesophageal reflux medications get those drugs after being discharged from neonatal intensive care units, despite questions about the safety and efficacy of the medications in premature infants.
In a retrospective study of 2,217 premature infants treated within the Children’s Hospital of Philadelphia primary care network from 2005 to 2009, 812 were treated with gastroesophageal reflux (GER) medications. Of this group, 77% were started on GER medication after neonatal intensive care unit (NICU) discharge, according to Jo Ann D’Agostino, DNP, CRNP, and her associates (Pediatrics. 2016 Nov 23. doi: 10.1542/peds.2016-1977).
Histamine-2 receptor antagonists were the most commonly prescribed GER medication, received by 90% of infants. Proton pump inhibitors were prescribed to 37% of infants, 22% received prokinetics, and 2% received cholinergics. During the first year of life, 40% of treated infants received multiple GER medications, with 73% of these infants receiving at least two medications simultaneously.
Risk factors associated with the use of multiple GER medications include a gestation period less than 32 weeks, feeding difficulty, tube feeding, a need for supplemental oxygen, and asthma.
“Because premature infants are a medically fragile group, the need for 1 acid suppression medication, let alone 2 or more in combination, should be given careful consideration. The potential impact of acid suppression on community-acquired illnesses has yet to be explored for this vulnerable population,” said Dr. D’Agostino of the department of pediatrics at the Children’s Hospital of Philadelphia, and her coauthors.
Infants who received GER treatment after NICU discharge were started on medication at a mean chronological age of 95 days and received medication for a mean of 294 days. Infants who started GER treatment while in the NICU received medication for a mean of 375 days.
A total of 743 infants were started on GER medications before the age of 6 months, and of this group, 43% were still being treated at the age of 1 year. Extended medication usage was associated with a gestational age under 32 weeks, chronic lung disease, airway malacia, and reactive airways disease.
A gestation period of less than 32 weeks was associated with a 31% increase in GER medication duration, compared with infants with a gestation period of 34-35 weeks, and a gestation period of less than 28 weeks was associated with a 50% increase in medication duration.
“Physiologic reflux symptoms are reported to peak at 4 months of age. Feeding issues are also common for premature infants. Whether this combination of issues is influencing the decision to start treatment, as opposed to actual GER disease, is an important distinction for providers to consider before starting medication,” Dr. D’Agostino and her associates noted.
“With uncertain evidence of efficacy, the rationale for using these medications in this high-risk population should be carefully evaluated,” they concluded.
The study was funded by the National Institutes of Health. The authors had no relevant financial disclosures.
FROM PEDIATRICS
Key clinical point:
Major finding: 37% of infants in the study received GER medication, with 77% of prescriptions occurring after NICU discharge.
Data source: Retrospective study of 2,217 preterm infants in the primary care network of the Children’s Hospital of Philadelphia.
Disclosures: The study was funded by the National Institutes of Health. The authors have no relevant financial disclosures.
Mastoid stimulation significantly reduces episodic migraine frequency
Episodic migraines were safely and effectively treated using percutaneous mastoid electrical stimulators in a randomized, double-blind, sham-controlled, multicenter trial.
Yang Juan of the department of neurology at the Second People’s Hospital of Chengdu (China), and associates reported that a group of 39 migraine patients who received percutaneous mastoid electrical stimulation (PMES) experienced significantly fewer migraine days, compared with a control group of 37 patients who received sham electrical treatment. After 3 months, migraine days were reduced by 71.3% from baseline, compared with a 14.4% reduction in the control group. About a third of PMES patients experienced no migraines in the third month, whereas no patients in the control group had more than a 75% reduction in migraine incidence.
There were no adverse reactions reported either in the PMES group or in the control group during the treatment period.
“The best treatment mode including current intensity and duration is unclear. Whether extension of the time interval (e.g., once or twice a week) of PMES treatment may also have preventive effect remains to be determined. In addition, as the patients recruited in this study were not highly disabled, the preventive effect of PMES treatment in patients with more frequent migraine episodes and in patients with chronic migraine needs further study,” the investigators wrote.
Read the full study in Cephalalgia (2016 Nov 7. doi: 10.1177/0333102416678623).
Episodic migraines were safely and effectively treated using percutaneous mastoid electrical stimulators in a randomized, double-blind, sham-controlled, multicenter trial.
Yang Juan of the department of neurology at the Second People’s Hospital of Chengdu (China), and associates reported that a group of 39 migraine patients who received percutaneous mastoid electrical stimulation (PMES) experienced significantly fewer migraine days, compared with a control group of 37 patients who received sham electrical treatment. After 3 months, migraine days were reduced by 71.3% from baseline, compared with a 14.4% reduction in the control group. About a third of PMES patients experienced no migraines in the third month, whereas no patients in the control group had more than a 75% reduction in migraine incidence.
There were no adverse reactions reported either in the PMES group or in the control group during the treatment period.
“The best treatment mode including current intensity and duration is unclear. Whether extension of the time interval (e.g., once or twice a week) of PMES treatment may also have preventive effect remains to be determined. In addition, as the patients recruited in this study were not highly disabled, the preventive effect of PMES treatment in patients with more frequent migraine episodes and in patients with chronic migraine needs further study,” the investigators wrote.
Read the full study in Cephalalgia (2016 Nov 7. doi: 10.1177/0333102416678623).
Episodic migraines were safely and effectively treated using percutaneous mastoid electrical stimulators in a randomized, double-blind, sham-controlled, multicenter trial.
Yang Juan of the department of neurology at the Second People’s Hospital of Chengdu (China), and associates reported that a group of 39 migraine patients who received percutaneous mastoid electrical stimulation (PMES) experienced significantly fewer migraine days, compared with a control group of 37 patients who received sham electrical treatment. After 3 months, migraine days were reduced by 71.3% from baseline, compared with a 14.4% reduction in the control group. About a third of PMES patients experienced no migraines in the third month, whereas no patients in the control group had more than a 75% reduction in migraine incidence.
There were no adverse reactions reported either in the PMES group or in the control group during the treatment period.
“The best treatment mode including current intensity and duration is unclear. Whether extension of the time interval (e.g., once or twice a week) of PMES treatment may also have preventive effect remains to be determined. In addition, as the patients recruited in this study were not highly disabled, the preventive effect of PMES treatment in patients with more frequent migraine episodes and in patients with chronic migraine needs further study,” the investigators wrote.
Read the full study in Cephalalgia (2016 Nov 7. doi: 10.1177/0333102416678623).
PBC patients show brain abnormalities before cirrhosis occurs
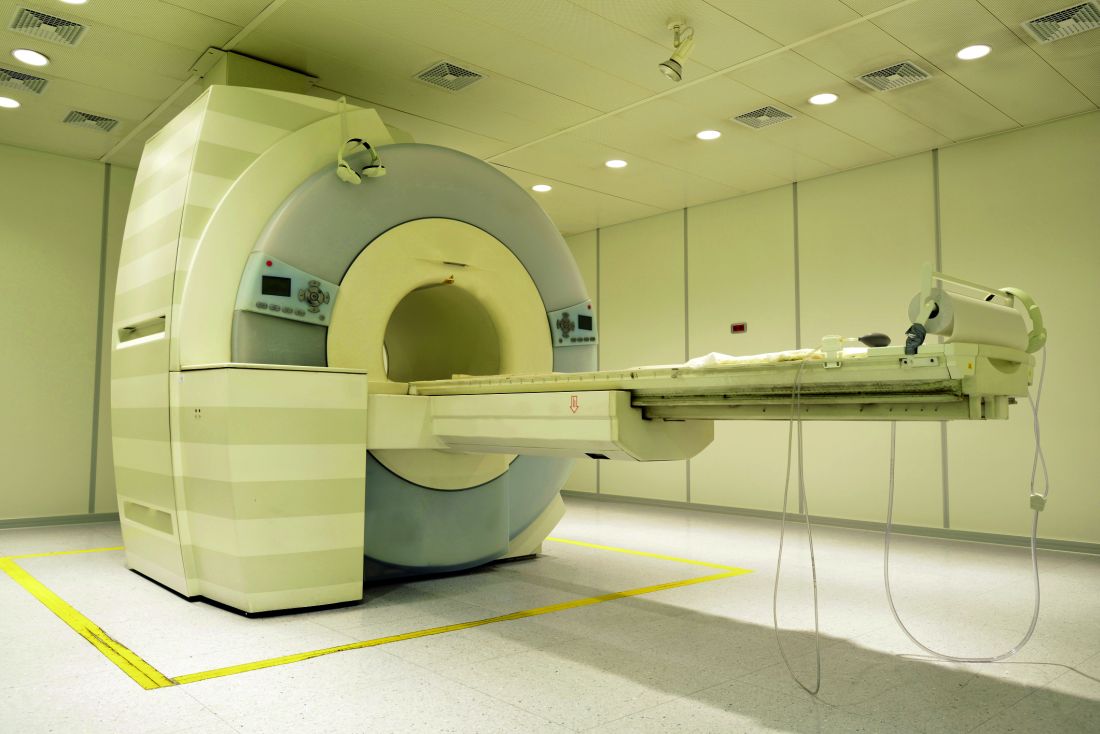
Brain abnormalities associated with primary biliary cholangitis (PBC) can be observed via magnetic resonance imaging before significant liver damage occurs, according to V.B.P. Grover, MD, and associates at the Liver Unit and Robert Steiner MRI Unit, MRC Clinical Sciences Centre, Imperial College London.
In a study of 13 newly diagnosed precirrhotic PBC patients and 17 healthy volunteers, mean magnetization transfer ratios (MTR) were lower in the thalamus, putamen, and head of caudate in PBC patients, compared with the control group, with the greatest difference seen in the thalamus. Severity of PBC symptoms did not have any significant effect on MTR.
An increase in the apparent diffusion coefficient was seen in the thalamus of PBC patients; however, no significant difference in cerebral metabolite ratios or pallidal index was observed. No correlation between neuroimaging data, lab data, symptom severity scores, or age was observed.
“Larger scale, and in particular linear studies, will be needed to explore the relationship of this change to symptoms and its response to therapies such as UDCA [ursodeoxycholic acid] and OCA [obeticholic acid]. The presence of brain change so early in the disease process would, however, suggest that the current step-up approach to therapy in which treatment change follows failure of a therapy type may allow the progressive accumulation of brain injury whilst waiting for adequate therapeutic response,” the investigators concluded.
Find the full study in Alimentary Pharmacology & Therapeutics (doi: 10.1111/apt.13797).
Brain abnormalities associated with primary biliary cholangitis (PBC) can be observed via magnetic resonance imaging before significant liver damage occurs, according to V.B.P. Grover, MD, and associates at the Liver Unit and Robert Steiner MRI Unit, MRC Clinical Sciences Centre, Imperial College London.
In a study of 13 newly diagnosed precirrhotic PBC patients and 17 healthy volunteers, mean magnetization transfer ratios (MTR) were lower in the thalamus, putamen, and head of caudate in PBC patients, compared with the control group, with the greatest difference seen in the thalamus. Severity of PBC symptoms did not have any significant effect on MTR.
An increase in the apparent diffusion coefficient was seen in the thalamus of PBC patients; however, no significant difference in cerebral metabolite ratios or pallidal index was observed. No correlation between neuroimaging data, lab data, symptom severity scores, or age was observed.
“Larger scale, and in particular linear studies, will be needed to explore the relationship of this change to symptoms and its response to therapies such as UDCA [ursodeoxycholic acid] and OCA [obeticholic acid]. The presence of brain change so early in the disease process would, however, suggest that the current step-up approach to therapy in which treatment change follows failure of a therapy type may allow the progressive accumulation of brain injury whilst waiting for adequate therapeutic response,” the investigators concluded.
Find the full study in Alimentary Pharmacology & Therapeutics (doi: 10.1111/apt.13797).
Brain abnormalities associated with primary biliary cholangitis (PBC) can be observed via magnetic resonance imaging before significant liver damage occurs, according to V.B.P. Grover, MD, and associates at the Liver Unit and Robert Steiner MRI Unit, MRC Clinical Sciences Centre, Imperial College London.
In a study of 13 newly diagnosed precirrhotic PBC patients and 17 healthy volunteers, mean magnetization transfer ratios (MTR) were lower in the thalamus, putamen, and head of caudate in PBC patients, compared with the control group, with the greatest difference seen in the thalamus. Severity of PBC symptoms did not have any significant effect on MTR.
An increase in the apparent diffusion coefficient was seen in the thalamus of PBC patients; however, no significant difference in cerebral metabolite ratios or pallidal index was observed. No correlation between neuroimaging data, lab data, symptom severity scores, or age was observed.
“Larger scale, and in particular linear studies, will be needed to explore the relationship of this change to symptoms and its response to therapies such as UDCA [ursodeoxycholic acid] and OCA [obeticholic acid]. The presence of brain change so early in the disease process would, however, suggest that the current step-up approach to therapy in which treatment change follows failure of a therapy type may allow the progressive accumulation of brain injury whilst waiting for adequate therapeutic response,” the investigators concluded.
Find the full study in Alimentary Pharmacology & Therapeutics (doi: 10.1111/apt.13797).
FROM ALIMENTARY PHARMACOLOGY & THERAPEUTICS
NRS awards grants for rosacea studies
The National Rosacea Society (NRS) is awarding funding to three new studies and continuing funding for two ongoing studies on topics that include the impact of epigenetics on rosacea, the society announced.
The first study, by Dr. Luis Garza at John Hopkins University, Baltimore, will examine epigenetic lesions in rosacea. Epigenetics, the study of how DNA can be modified to act in certain ways, “may be responsible for why rosacea persists even though keratinocytes … slough off and are replaced every 2 months,” the NRS said in a written statement.
The second study, by Dr. Wenqing Li of Brown University, Providence, R.I., will use data from the Nurses’ Health Study II to examine how hormone use and hormone levels during menopause and pregnancy affect the risk of developing rosacea.
The third study, by Dr. Anna Di Nardo of the University of California, San Diego, and her associates, is looking at “whether the release of cathelicidin antimicrobial peptides, key players in the body’s normal innate immune system response, is central to the connection between the nervous system and skin inflammation through the activation of mast cells in rosacea,” the NRS statement noted.
Ongoing studies that also are receiving funding include work by Dr. Gideon Smith of Massachusetts General Hospital, Boston, and his associates, who are examining the risk of vascular disorders in people with rosacea, and a study by Dr. Lori Lee Stohl of Cornell University, New York, who is researching how stress-related biochemicals can increase mast-cell count.
“Research supported by the NRS has led to important insights into the physiology of the disorder, providing an essential foundation for developing new and better treatments. In addition, our growing knowledge is now pointing toward potentially meaningful connections between rosacea and other systemic illnesses,” Dr. Martin Steinhoff, chairman of dermatology and director of the Charles Institute of Dermatology, University College, Dublin, and a member of the NRS Medical Advisory Board, said in the statement.
Find the full NRS statement on the society’s website.
The National Rosacea Society (NRS) is awarding funding to three new studies and continuing funding for two ongoing studies on topics that include the impact of epigenetics on rosacea, the society announced.
The first study, by Dr. Luis Garza at John Hopkins University, Baltimore, will examine epigenetic lesions in rosacea. Epigenetics, the study of how DNA can be modified to act in certain ways, “may be responsible for why rosacea persists even though keratinocytes … slough off and are replaced every 2 months,” the NRS said in a written statement.
The second study, by Dr. Wenqing Li of Brown University, Providence, R.I., will use data from the Nurses’ Health Study II to examine how hormone use and hormone levels during menopause and pregnancy affect the risk of developing rosacea.
The third study, by Dr. Anna Di Nardo of the University of California, San Diego, and her associates, is looking at “whether the release of cathelicidin antimicrobial peptides, key players in the body’s normal innate immune system response, is central to the connection between the nervous system and skin inflammation through the activation of mast cells in rosacea,” the NRS statement noted.
Ongoing studies that also are receiving funding include work by Dr. Gideon Smith of Massachusetts General Hospital, Boston, and his associates, who are examining the risk of vascular disorders in people with rosacea, and a study by Dr. Lori Lee Stohl of Cornell University, New York, who is researching how stress-related biochemicals can increase mast-cell count.
“Research supported by the NRS has led to important insights into the physiology of the disorder, providing an essential foundation for developing new and better treatments. In addition, our growing knowledge is now pointing toward potentially meaningful connections between rosacea and other systemic illnesses,” Dr. Martin Steinhoff, chairman of dermatology and director of the Charles Institute of Dermatology, University College, Dublin, and a member of the NRS Medical Advisory Board, said in the statement.
Find the full NRS statement on the society’s website.
The National Rosacea Society (NRS) is awarding funding to three new studies and continuing funding for two ongoing studies on topics that include the impact of epigenetics on rosacea, the society announced.
The first study, by Dr. Luis Garza at John Hopkins University, Baltimore, will examine epigenetic lesions in rosacea. Epigenetics, the study of how DNA can be modified to act in certain ways, “may be responsible for why rosacea persists even though keratinocytes … slough off and are replaced every 2 months,” the NRS said in a written statement.
The second study, by Dr. Wenqing Li of Brown University, Providence, R.I., will use data from the Nurses’ Health Study II to examine how hormone use and hormone levels during menopause and pregnancy affect the risk of developing rosacea.
The third study, by Dr. Anna Di Nardo of the University of California, San Diego, and her associates, is looking at “whether the release of cathelicidin antimicrobial peptides, key players in the body’s normal innate immune system response, is central to the connection between the nervous system and skin inflammation through the activation of mast cells in rosacea,” the NRS statement noted.
Ongoing studies that also are receiving funding include work by Dr. Gideon Smith of Massachusetts General Hospital, Boston, and his associates, who are examining the risk of vascular disorders in people with rosacea, and a study by Dr. Lori Lee Stohl of Cornell University, New York, who is researching how stress-related biochemicals can increase mast-cell count.
“Research supported by the NRS has led to important insights into the physiology of the disorder, providing an essential foundation for developing new and better treatments. In addition, our growing knowledge is now pointing toward potentially meaningful connections between rosacea and other systemic illnesses,” Dr. Martin Steinhoff, chairman of dermatology and director of the Charles Institute of Dermatology, University College, Dublin, and a member of the NRS Medical Advisory Board, said in the statement.
Find the full NRS statement on the society’s website.
Absolute humidity most important environmental factor in global influenza
Absolute humidity and temperature are the most important environmental drivers of global influenza, despite differences in outbreak patterns between tropical and temperate countries, according to a new analysis by U.S.-based researchers.
Using convergent cross-mapping and an empirical dynamic modeling approach on data collected by the World Health Organization, investigators led by George Sugihara, PhD, of the Scripps Institution of Oceanography at the University of California, San Diego, confirmed a hypothetical U-shaped relationship between influenza outbreaks and absolute humidity. At low latitudes in the tropics, absolute humidity has a positive effect, increasing the likelihood of influenza as humidity rises but at higher latitudes in temperate countries, absolute humidity has a negative effect, making influenza more likely when absolute humidity is low.
While absolute humidity was the most important factor in the likelihood of influenza outbreaks, the U-shaped relationship was dictated by average temperature. An average temperature below 70 °F had little effect on the negative relationship between absolute humidity and influenza at that range of temperatures, but if the temperature was between 75 °F and 85 °F, the effect was positive. Above 85 °F, aerosol transmission of influenza is blocked, the investigators noted.
“Augmented with further laboratory testing, these population-level results could help set the stage for public health initiatives such as placing humidifiers in schools and hospitals during cold, dry, temperate winter, and in the tropics, perhaps using dehumidifiers or air conditioners set above 75 °F to dry air in public buildings,” Dr. Sugihara and his colleagues wrote.
Find the full study in Proceedings of the National Academy of Sciences of the United States of America (doi: 10.1073/pnas.1607747113).
Absolute humidity and temperature are the most important environmental drivers of global influenza, despite differences in outbreak patterns between tropical and temperate countries, according to a new analysis by U.S.-based researchers.
Using convergent cross-mapping and an empirical dynamic modeling approach on data collected by the World Health Organization, investigators led by George Sugihara, PhD, of the Scripps Institution of Oceanography at the University of California, San Diego, confirmed a hypothetical U-shaped relationship between influenza outbreaks and absolute humidity. At low latitudes in the tropics, absolute humidity has a positive effect, increasing the likelihood of influenza as humidity rises but at higher latitudes in temperate countries, absolute humidity has a negative effect, making influenza more likely when absolute humidity is low.
While absolute humidity was the most important factor in the likelihood of influenza outbreaks, the U-shaped relationship was dictated by average temperature. An average temperature below 70 °F had little effect on the negative relationship between absolute humidity and influenza at that range of temperatures, but if the temperature was between 75 °F and 85 °F, the effect was positive. Above 85 °F, aerosol transmission of influenza is blocked, the investigators noted.
“Augmented with further laboratory testing, these population-level results could help set the stage for public health initiatives such as placing humidifiers in schools and hospitals during cold, dry, temperate winter, and in the tropics, perhaps using dehumidifiers or air conditioners set above 75 °F to dry air in public buildings,” Dr. Sugihara and his colleagues wrote.
Find the full study in Proceedings of the National Academy of Sciences of the United States of America (doi: 10.1073/pnas.1607747113).
Absolute humidity and temperature are the most important environmental drivers of global influenza, despite differences in outbreak patterns between tropical and temperate countries, according to a new analysis by U.S.-based researchers.
Using convergent cross-mapping and an empirical dynamic modeling approach on data collected by the World Health Organization, investigators led by George Sugihara, PhD, of the Scripps Institution of Oceanography at the University of California, San Diego, confirmed a hypothetical U-shaped relationship between influenza outbreaks and absolute humidity. At low latitudes in the tropics, absolute humidity has a positive effect, increasing the likelihood of influenza as humidity rises but at higher latitudes in temperate countries, absolute humidity has a negative effect, making influenza more likely when absolute humidity is low.
While absolute humidity was the most important factor in the likelihood of influenza outbreaks, the U-shaped relationship was dictated by average temperature. An average temperature below 70 °F had little effect on the negative relationship between absolute humidity and influenza at that range of temperatures, but if the temperature was between 75 °F and 85 °F, the effect was positive. Above 85 °F, aerosol transmission of influenza is blocked, the investigators noted.
“Augmented with further laboratory testing, these population-level results could help set the stage for public health initiatives such as placing humidifiers in schools and hospitals during cold, dry, temperate winter, and in the tropics, perhaps using dehumidifiers or air conditioners set above 75 °F to dry air in public buildings,” Dr. Sugihara and his colleagues wrote.
Find the full study in Proceedings of the National Academy of Sciences of the United States of America (doi: 10.1073/pnas.1607747113).
ZMapp shows promise for Ebola treatment, but misses efficacy goal
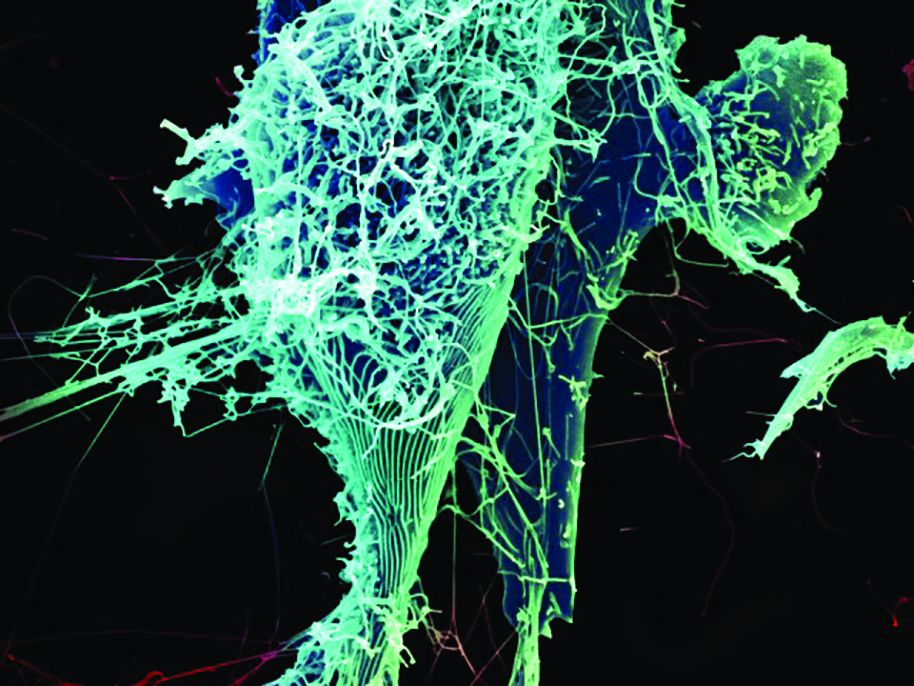
ZMapp, a potential monoclonal antibody treatment for Ebola virus disease, did not meet its efficacy goal in a clinical trial of patients in Liberia, Sierra Leone, and Guinea, according to a report in the New England Journal of Medicine.
ZMapp, developed by Mapp Biopharmaceutical, comprises three different laboratory-generated monoclonal antibodies. The drug targets the main surface protein of the Ebola virus. Earlier studies in nonhuman primates demonstrated that ZMapp had strong antiviral activity and prevented death when administered as late as 5 days after experimental infection with the Zaire Ebola virus strain.
The process of ZMapp infusion was generally safe, with only one serious adverse event – hypertension – attributed to the infusion itself. Of the 93 infusions attempted in the ZMapp group, 8 were stopped because of adverse events, and 9 were slowed down to accommodate for side effects.
While ZMapp did not meet its goal, the relative risk of death was 40% lower in the ZMapp group then in the control group. Treatment with ZMapp was delayed for a week after patients became symptomatic, exceeding the 5-day window where ZMapp has been shown to have at least 90% effectiveness. In addition, of the eight patients who died in the ZMapp group, seven died before the second of the three planned ZMapp infusions were delivered.
The abrupt end to the Ebola epidemic prevented the ZMapp trial from being adequately completed. A goal of 100 patients in both groups was desired but could not be reached.
“Despite the concerted efforts of many dedicated researchers domestically and internationally who participated in this and other trials, the outbreak appears to have ended with no incontrovertible evidence that any single treatment intervention, or combination of interventions, was unequivocally superior to the types of supportive medical care typically provided,” the investigators said.
Find the full study in the New England Journal of Medicine (doi: 10.1056/NEJMoa1604330).
ZMapp, a potential monoclonal antibody treatment for Ebola virus disease, did not meet its efficacy goal in a clinical trial of patients in Liberia, Sierra Leone, and Guinea, according to a report in the New England Journal of Medicine.
ZMapp, developed by Mapp Biopharmaceutical, comprises three different laboratory-generated monoclonal antibodies. The drug targets the main surface protein of the Ebola virus. Earlier studies in nonhuman primates demonstrated that ZMapp had strong antiviral activity and prevented death when administered as late as 5 days after experimental infection with the Zaire Ebola virus strain.
The process of ZMapp infusion was generally safe, with only one serious adverse event – hypertension – attributed to the infusion itself. Of the 93 infusions attempted in the ZMapp group, 8 were stopped because of adverse events, and 9 were slowed down to accommodate for side effects.
While ZMapp did not meet its goal, the relative risk of death was 40% lower in the ZMapp group then in the control group. Treatment with ZMapp was delayed for a week after patients became symptomatic, exceeding the 5-day window where ZMapp has been shown to have at least 90% effectiveness. In addition, of the eight patients who died in the ZMapp group, seven died before the second of the three planned ZMapp infusions were delivered.
The abrupt end to the Ebola epidemic prevented the ZMapp trial from being adequately completed. A goal of 100 patients in both groups was desired but could not be reached.
“Despite the concerted efforts of many dedicated researchers domestically and internationally who participated in this and other trials, the outbreak appears to have ended with no incontrovertible evidence that any single treatment intervention, or combination of interventions, was unequivocally superior to the types of supportive medical care typically provided,” the investigators said.
Find the full study in the New England Journal of Medicine (doi: 10.1056/NEJMoa1604330).
ZMapp, a potential monoclonal antibody treatment for Ebola virus disease, did not meet its efficacy goal in a clinical trial of patients in Liberia, Sierra Leone, and Guinea, according to a report in the New England Journal of Medicine.
ZMapp, developed by Mapp Biopharmaceutical, comprises three different laboratory-generated monoclonal antibodies. The drug targets the main surface protein of the Ebola virus. Earlier studies in nonhuman primates demonstrated that ZMapp had strong antiviral activity and prevented death when administered as late as 5 days after experimental infection with the Zaire Ebola virus strain.
The process of ZMapp infusion was generally safe, with only one serious adverse event – hypertension – attributed to the infusion itself. Of the 93 infusions attempted in the ZMapp group, 8 were stopped because of adverse events, and 9 were slowed down to accommodate for side effects.
While ZMapp did not meet its goal, the relative risk of death was 40% lower in the ZMapp group then in the control group. Treatment with ZMapp was delayed for a week after patients became symptomatic, exceeding the 5-day window where ZMapp has been shown to have at least 90% effectiveness. In addition, of the eight patients who died in the ZMapp group, seven died before the second of the three planned ZMapp infusions were delivered.
The abrupt end to the Ebola epidemic prevented the ZMapp trial from being adequately completed. A goal of 100 patients in both groups was desired but could not be reached.
“Despite the concerted efforts of many dedicated researchers domestically and internationally who participated in this and other trials, the outbreak appears to have ended with no incontrovertible evidence that any single treatment intervention, or combination of interventions, was unequivocally superior to the types of supportive medical care typically provided,” the investigators said.
Find the full study in the New England Journal of Medicine (doi: 10.1056/NEJMoa1604330).
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Vaccination rates up in U.S. kindergartners in 2015, steady in 19- to 35-month-olds
Vaccination coverage for MMR and DTaP increased for children in kindergarten during the 2015-2016 school year, but remained steady for children aged 19-35 months in 2015, according to reports from the Centers for Disease Control and Prevention.
The median MMR vaccination rate for kindergartners in 2015 was 94.6%, up significantly from 92.6% in 2014. DTaP coverage also increased, rising from 92.4% to 94.2%. A total of 32 states saw an increase in MMR coverage in 2015, with 22 states reporting greater than 95% coverage. Only 3 states and the District of Columbia reported less than 90% coverage, down from 7 states and D.C. in 2014.
While the median vaccination rates were increased in 2015, the median exemption rate also increased by nearly 11% to 1.9% overall. This was caused in part by the addition of reports from Texas and Wyoming, neither of which reported the number of exemptions in 2014, the CDC investigators remarked.
In a second CDC report from Dr. Holly Hill and her associates based on data collected from the National Immunization Survey, the vaccination rate for children aged 19-35 months in 2015 did not increase significantly from the previous year (MMWR. 2016 Oct 6. doi: 10.15585/mmwr.mm639a4). The rate of children who received four or more doses of DTaP and at least one dose of MMR increased by 0.4 percentage points each from 84.2% to 84.6% and from 91.5% to 91.9%, respectively. The largest increase was seen in hepatitis A vaccine, where the rate of vaccination increased from 57.5% to 59.6%.
Healthy People 2020 goals for greater than 90% coverage for children aged 19-35 months were met for four vaccines in 2015: three or more doses of poliovirus vaccine, one or more doses of MMR, three or more doses of hepatitis B vaccine, and one or more doses of varicella vaccine. Vaccine coverage was lower in almost all cases for children living below the poverty level. The largest discrepancies were seen in rotavirus and varicella vaccines. The combined seven-vaccine series rate for children at or above the poverty line was 74.7%, and was 68.7% for children below the poverty line.
“Continued surveillance is needed to monitor coverage, locate pockets of susceptibility, and evaluate the impact of interventions designed to ensure that all children remain adequately protected against vaccine-preventable diseases,” Dr. Hill and her associates noted.
The CDC investigators had no relevant financial disclosures to report.
Vaccination coverage for MMR and DTaP increased for children in kindergarten during the 2015-2016 school year, but remained steady for children aged 19-35 months in 2015, according to reports from the Centers for Disease Control and Prevention.
The median MMR vaccination rate for kindergartners in 2015 was 94.6%, up significantly from 92.6% in 2014. DTaP coverage also increased, rising from 92.4% to 94.2%. A total of 32 states saw an increase in MMR coverage in 2015, with 22 states reporting greater than 95% coverage. Only 3 states and the District of Columbia reported less than 90% coverage, down from 7 states and D.C. in 2014.
While the median vaccination rates were increased in 2015, the median exemption rate also increased by nearly 11% to 1.9% overall. This was caused in part by the addition of reports from Texas and Wyoming, neither of which reported the number of exemptions in 2014, the CDC investigators remarked.
In a second CDC report from Dr. Holly Hill and her associates based on data collected from the National Immunization Survey, the vaccination rate for children aged 19-35 months in 2015 did not increase significantly from the previous year (MMWR. 2016 Oct 6. doi: 10.15585/mmwr.mm639a4). The rate of children who received four or more doses of DTaP and at least one dose of MMR increased by 0.4 percentage points each from 84.2% to 84.6% and from 91.5% to 91.9%, respectively. The largest increase was seen in hepatitis A vaccine, where the rate of vaccination increased from 57.5% to 59.6%.
Healthy People 2020 goals for greater than 90% coverage for children aged 19-35 months were met for four vaccines in 2015: three or more doses of poliovirus vaccine, one or more doses of MMR, three or more doses of hepatitis B vaccine, and one or more doses of varicella vaccine. Vaccine coverage was lower in almost all cases for children living below the poverty level. The largest discrepancies were seen in rotavirus and varicella vaccines. The combined seven-vaccine series rate for children at or above the poverty line was 74.7%, and was 68.7% for children below the poverty line.
“Continued surveillance is needed to monitor coverage, locate pockets of susceptibility, and evaluate the impact of interventions designed to ensure that all children remain adequately protected against vaccine-preventable diseases,” Dr. Hill and her associates noted.
The CDC investigators had no relevant financial disclosures to report.
Vaccination coverage for MMR and DTaP increased for children in kindergarten during the 2015-2016 school year, but remained steady for children aged 19-35 months in 2015, according to reports from the Centers for Disease Control and Prevention.
The median MMR vaccination rate for kindergartners in 2015 was 94.6%, up significantly from 92.6% in 2014. DTaP coverage also increased, rising from 92.4% to 94.2%. A total of 32 states saw an increase in MMR coverage in 2015, with 22 states reporting greater than 95% coverage. Only 3 states and the District of Columbia reported less than 90% coverage, down from 7 states and D.C. in 2014.
While the median vaccination rates were increased in 2015, the median exemption rate also increased by nearly 11% to 1.9% overall. This was caused in part by the addition of reports from Texas and Wyoming, neither of which reported the number of exemptions in 2014, the CDC investigators remarked.
In a second CDC report from Dr. Holly Hill and her associates based on data collected from the National Immunization Survey, the vaccination rate for children aged 19-35 months in 2015 did not increase significantly from the previous year (MMWR. 2016 Oct 6. doi: 10.15585/mmwr.mm639a4). The rate of children who received four or more doses of DTaP and at least one dose of MMR increased by 0.4 percentage points each from 84.2% to 84.6% and from 91.5% to 91.9%, respectively. The largest increase was seen in hepatitis A vaccine, where the rate of vaccination increased from 57.5% to 59.6%.
Healthy People 2020 goals for greater than 90% coverage for children aged 19-35 months were met for four vaccines in 2015: three or more doses of poliovirus vaccine, one or more doses of MMR, three or more doses of hepatitis B vaccine, and one or more doses of varicella vaccine. Vaccine coverage was lower in almost all cases for children living below the poverty level. The largest discrepancies were seen in rotavirus and varicella vaccines. The combined seven-vaccine series rate for children at or above the poverty line was 74.7%, and was 68.7% for children below the poverty line.
“Continued surveillance is needed to monitor coverage, locate pockets of susceptibility, and evaluate the impact of interventions designed to ensure that all children remain adequately protected against vaccine-preventable diseases,” Dr. Hill and her associates noted.
The CDC investigators had no relevant financial disclosures to report.
New chikungunya diagnostic assay proves quick, effective
A reverse transcription recombinase polymerase amplification (RT-RPA) assay was able to quickly and effectively identify chikungunya virus (CHIKV), according to a study published in PLOS Neglected Tropical Diseases.
Using chikungunya virus RNA samples, the RT-RPA assay detected down to 80 genome copies per reaction within 15 minutes, a time period four to six times faster than other molecular diagnostic techniques, such as reverse transcription-polymerase chain reaction (RT-PCR). In a sensitivity test involving all chikungunya serotypes and various alphaviruses, flaviviruses, and one phlebovirus, the RT-RPA assay identified all virus genotypes, with the only cross-reaction occurring with O’nyong’nyong virus.
In a test involving 58 plasma samples of suspected chikungunya fever from a trial in Thailand, two real-time RT-PCR tests identified 36 out of 58 samples (62%) as positive for chikungunya. The RT-RPA test successfully detected the virus in all 36 positive samples and did not detect the virus in any of the negative samples, giving a sensitivity and specificity of 100%.
“The CHIKV RPA assay presented here is a promising tool for CHIKV diagnostics at the point of need,” the investigators wrote. “Integration into a multimer or multiplex assay for simultaneous and differential detection of CHIKV, Dengue virus, and Zika virus, as well as an internal positive control would improve outbreak investigations, since the three viruses induce the same clinical picture upon infection and increasingly cocirculate in many parts of the world.”
Find the full study in PLOS Neglected Tropical Diseases (doi: 10.1371/journal.pntd.0004953).
A reverse transcription recombinase polymerase amplification (RT-RPA) assay was able to quickly and effectively identify chikungunya virus (CHIKV), according to a study published in PLOS Neglected Tropical Diseases.
Using chikungunya virus RNA samples, the RT-RPA assay detected down to 80 genome copies per reaction within 15 minutes, a time period four to six times faster than other molecular diagnostic techniques, such as reverse transcription-polymerase chain reaction (RT-PCR). In a sensitivity test involving all chikungunya serotypes and various alphaviruses, flaviviruses, and one phlebovirus, the RT-RPA assay identified all virus genotypes, with the only cross-reaction occurring with O’nyong’nyong virus.
In a test involving 58 plasma samples of suspected chikungunya fever from a trial in Thailand, two real-time RT-PCR tests identified 36 out of 58 samples (62%) as positive for chikungunya. The RT-RPA test successfully detected the virus in all 36 positive samples and did not detect the virus in any of the negative samples, giving a sensitivity and specificity of 100%.
“The CHIKV RPA assay presented here is a promising tool for CHIKV diagnostics at the point of need,” the investigators wrote. “Integration into a multimer or multiplex assay for simultaneous and differential detection of CHIKV, Dengue virus, and Zika virus, as well as an internal positive control would improve outbreak investigations, since the three viruses induce the same clinical picture upon infection and increasingly cocirculate in many parts of the world.”
Find the full study in PLOS Neglected Tropical Diseases (doi: 10.1371/journal.pntd.0004953).
A reverse transcription recombinase polymerase amplification (RT-RPA) assay was able to quickly and effectively identify chikungunya virus (CHIKV), according to a study published in PLOS Neglected Tropical Diseases.
Using chikungunya virus RNA samples, the RT-RPA assay detected down to 80 genome copies per reaction within 15 minutes, a time period four to six times faster than other molecular diagnostic techniques, such as reverse transcription-polymerase chain reaction (RT-PCR). In a sensitivity test involving all chikungunya serotypes and various alphaviruses, flaviviruses, and one phlebovirus, the RT-RPA assay identified all virus genotypes, with the only cross-reaction occurring with O’nyong’nyong virus.
In a test involving 58 plasma samples of suspected chikungunya fever from a trial in Thailand, two real-time RT-PCR tests identified 36 out of 58 samples (62%) as positive for chikungunya. The RT-RPA test successfully detected the virus in all 36 positive samples and did not detect the virus in any of the negative samples, giving a sensitivity and specificity of 100%.
“The CHIKV RPA assay presented here is a promising tool for CHIKV diagnostics at the point of need,” the investigators wrote. “Integration into a multimer or multiplex assay for simultaneous and differential detection of CHIKV, Dengue virus, and Zika virus, as well as an internal positive control would improve outbreak investigations, since the three viruses induce the same clinical picture upon infection and increasingly cocirculate in many parts of the world.”
Find the full study in PLOS Neglected Tropical Diseases (doi: 10.1371/journal.pntd.0004953).
FROM PLOS NEGLECTED TROPICAL DISEASES
Tetravalent dengue vaccine shows efficacy against asymptomatic dengue
A tetravalent dengue vaccine reduced symptomatic and asymptomatic dengue infection in Asian and Latin American children aged 2-16 years, according to Gustavo Olivera-Botello, PhD, and his associates at Sanofi Pasteur.
They analyzed data from 3,736 individuals in two phase III clinical trials. Patients received either the dengue vaccine CYD-TDV or placebo at month 0, month 6, and month 12, and had immunologic results from months 13 to 25. The seroconversion rate in individuals with virologically confirmed dengue between 13 and 25 months after vaccination was 88% in the vaccine group, and 98% in the placebo group.
In individuals without virologically confirmed dengue, 219 of 2,485 participants in the vaccine group and 157 of 1,184 in the placebo group seroconverted during months 13-25. Total vaccine efficacy against asymptomatic dengue was 33.5%, and was higher in children aged 9-16, with vaccine efficacy at 38.6%.
“Since about 80% of DENV [dengue virus] infections are asymptomatic, it is likely that they contribute significantly to viral transmission to mosquitoes and thus to other human hosts. Consequently, providing simultaneous protection against both asymptomatic and symptomatic infections could contribute to reduced transmission and thus to indirect protection if the vaccine coverage rates are sufficient,” the investigators wrote.
Find the full study in the Journal of Infectious Disease (doi: 10.1093/infdis/jiw297)
A tetravalent dengue vaccine reduced symptomatic and asymptomatic dengue infection in Asian and Latin American children aged 2-16 years, according to Gustavo Olivera-Botello, PhD, and his associates at Sanofi Pasteur.
They analyzed data from 3,736 individuals in two phase III clinical trials. Patients received either the dengue vaccine CYD-TDV or placebo at month 0, month 6, and month 12, and had immunologic results from months 13 to 25. The seroconversion rate in individuals with virologically confirmed dengue between 13 and 25 months after vaccination was 88% in the vaccine group, and 98% in the placebo group.
In individuals without virologically confirmed dengue, 219 of 2,485 participants in the vaccine group and 157 of 1,184 in the placebo group seroconverted during months 13-25. Total vaccine efficacy against asymptomatic dengue was 33.5%, and was higher in children aged 9-16, with vaccine efficacy at 38.6%.
“Since about 80% of DENV [dengue virus] infections are asymptomatic, it is likely that they contribute significantly to viral transmission to mosquitoes and thus to other human hosts. Consequently, providing simultaneous protection against both asymptomatic and symptomatic infections could contribute to reduced transmission and thus to indirect protection if the vaccine coverage rates are sufficient,” the investigators wrote.
Find the full study in the Journal of Infectious Disease (doi: 10.1093/infdis/jiw297)
A tetravalent dengue vaccine reduced symptomatic and asymptomatic dengue infection in Asian and Latin American children aged 2-16 years, according to Gustavo Olivera-Botello, PhD, and his associates at Sanofi Pasteur.
They analyzed data from 3,736 individuals in two phase III clinical trials. Patients received either the dengue vaccine CYD-TDV or placebo at month 0, month 6, and month 12, and had immunologic results from months 13 to 25. The seroconversion rate in individuals with virologically confirmed dengue between 13 and 25 months after vaccination was 88% in the vaccine group, and 98% in the placebo group.
In individuals without virologically confirmed dengue, 219 of 2,485 participants in the vaccine group and 157 of 1,184 in the placebo group seroconverted during months 13-25. Total vaccine efficacy against asymptomatic dengue was 33.5%, and was higher in children aged 9-16, with vaccine efficacy at 38.6%.
“Since about 80% of DENV [dengue virus] infections are asymptomatic, it is likely that they contribute significantly to viral transmission to mosquitoes and thus to other human hosts. Consequently, providing simultaneous protection against both asymptomatic and symptomatic infections could contribute to reduced transmission and thus to indirect protection if the vaccine coverage rates are sufficient,” the investigators wrote.
Find the full study in the Journal of Infectious Disease (doi: 10.1093/infdis/jiw297)
FROM THE JOURNAL OF INFECTIOUS DISEASES