User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
Study shows significant progress toward elimination of polio
Case incidence of wild poliovirus was significantly reduced in 2015-2016, compared with 2014, according to a report by the Centers for Disease Control and Prevention published in Morbidity and Mortality Weekly Report.
In 2015, 74 cases of wild poliovirus (WPV) were reported in Pakistan and Afghanistan, a reduction of 79% from 2014, when 359 cases were reported in nine countries. Twelve cases of WPV were reported from Jan. 1 to May 4, 2016, down from 23 cases during Jan. 1 to May 4, 2015.
Further progress toward the elimination of polio was made in September 2015, when the World Health Organization removed Nigeria from the list of countries with endemic polio. In that same month, the Global Commission for the Certification of Poliomyelitis Eradication announced that WPV type 2, not seen since 1999, had been eradicated.
“With progress made during 2015-2016 toward interruption of WPV transmission in Afghanistan and Pakistan, the world is closer than ever to the eradication of polio. Continued cooperation between the two countries is needed for this goal to be reached,” the CDC investigators said.
Find the report in MMWR (doi: 10.15585/mmwr.mm6518a4)
Case incidence of wild poliovirus was significantly reduced in 2015-2016, compared with 2014, according to a report by the Centers for Disease Control and Prevention published in Morbidity and Mortality Weekly Report.
In 2015, 74 cases of wild poliovirus (WPV) were reported in Pakistan and Afghanistan, a reduction of 79% from 2014, when 359 cases were reported in nine countries. Twelve cases of WPV were reported from Jan. 1 to May 4, 2016, down from 23 cases during Jan. 1 to May 4, 2015.
Further progress toward the elimination of polio was made in September 2015, when the World Health Organization removed Nigeria from the list of countries with endemic polio. In that same month, the Global Commission for the Certification of Poliomyelitis Eradication announced that WPV type 2, not seen since 1999, had been eradicated.
“With progress made during 2015-2016 toward interruption of WPV transmission in Afghanistan and Pakistan, the world is closer than ever to the eradication of polio. Continued cooperation between the two countries is needed for this goal to be reached,” the CDC investigators said.
Find the report in MMWR (doi: 10.15585/mmwr.mm6518a4)
Case incidence of wild poliovirus was significantly reduced in 2015-2016, compared with 2014, according to a report by the Centers for Disease Control and Prevention published in Morbidity and Mortality Weekly Report.
In 2015, 74 cases of wild poliovirus (WPV) were reported in Pakistan and Afghanistan, a reduction of 79% from 2014, when 359 cases were reported in nine countries. Twelve cases of WPV were reported from Jan. 1 to May 4, 2016, down from 23 cases during Jan. 1 to May 4, 2015.
Further progress toward the elimination of polio was made in September 2015, when the World Health Organization removed Nigeria from the list of countries with endemic polio. In that same month, the Global Commission for the Certification of Poliomyelitis Eradication announced that WPV type 2, not seen since 1999, had been eradicated.
“With progress made during 2015-2016 toward interruption of WPV transmission in Afghanistan and Pakistan, the world is closer than ever to the eradication of polio. Continued cooperation between the two countries is needed for this goal to be reached,” the CDC investigators said.
Find the report in MMWR (doi: 10.15585/mmwr.mm6518a4)
FROM MMWR
Hepatitis A and B combo vaccinations remain effective after 15 years
Young adults who received a combined hepatitis A and B vaccination at age 12-15 years maintained immunity after 15 years, making a booster shot unnecessary, according to Dr. Jiri Beran of the Vaccination and Travel Medicine Centre, Hradec Kralove, Czech Republic, and associates.
Study participants received either a 2-dose adult formulation or a 3-dose pediatric formulation. Of the 162 participants included in the 15-year follow-up, all were seropositive for anti–hepatitis A vaccine antibodies, 81.1% of those who received the two-dose vaccination had anti–hepatitis B antibodies, and 81.8% of those who received the three-dose vaccination had anti–hepatitis B antibodies.
In a subsequent hepatitis B vaccine challenge, all of 8 participants who received the two-dose vaccination and 10 of 11 participants who received the three-dose vaccination developed an anamnastic response. No side effects inconsistent with previous experience were observed.
“The present study confirms that the combined hepatitis A and B vaccine is equally immunogenic and safe in adolescents when administered as the standard three-dose pediatric regimen or as two doses of the adult strength vacciwne,” the investigators said.
Find the full study in Vaccine (doi: 10.1016/j.vaccine.2016.04.033).
Young adults who received a combined hepatitis A and B vaccination at age 12-15 years maintained immunity after 15 years, making a booster shot unnecessary, according to Dr. Jiri Beran of the Vaccination and Travel Medicine Centre, Hradec Kralove, Czech Republic, and associates.
Study participants received either a 2-dose adult formulation or a 3-dose pediatric formulation. Of the 162 participants included in the 15-year follow-up, all were seropositive for anti–hepatitis A vaccine antibodies, 81.1% of those who received the two-dose vaccination had anti–hepatitis B antibodies, and 81.8% of those who received the three-dose vaccination had anti–hepatitis B antibodies.
In a subsequent hepatitis B vaccine challenge, all of 8 participants who received the two-dose vaccination and 10 of 11 participants who received the three-dose vaccination developed an anamnastic response. No side effects inconsistent with previous experience were observed.
“The present study confirms that the combined hepatitis A and B vaccine is equally immunogenic and safe in adolescents when administered as the standard three-dose pediatric regimen or as two doses of the adult strength vacciwne,” the investigators said.
Find the full study in Vaccine (doi: 10.1016/j.vaccine.2016.04.033).
Young adults who received a combined hepatitis A and B vaccination at age 12-15 years maintained immunity after 15 years, making a booster shot unnecessary, according to Dr. Jiri Beran of the Vaccination and Travel Medicine Centre, Hradec Kralove, Czech Republic, and associates.
Study participants received either a 2-dose adult formulation or a 3-dose pediatric formulation. Of the 162 participants included in the 15-year follow-up, all were seropositive for anti–hepatitis A vaccine antibodies, 81.1% of those who received the two-dose vaccination had anti–hepatitis B antibodies, and 81.8% of those who received the three-dose vaccination had anti–hepatitis B antibodies.
In a subsequent hepatitis B vaccine challenge, all of 8 participants who received the two-dose vaccination and 10 of 11 participants who received the three-dose vaccination developed an anamnastic response. No side effects inconsistent with previous experience were observed.
“The present study confirms that the combined hepatitis A and B vaccine is equally immunogenic and safe in adolescents when administered as the standard three-dose pediatric regimen or as two doses of the adult strength vacciwne,” the investigators said.
Find the full study in Vaccine (doi: 10.1016/j.vaccine.2016.04.033).
FROM VACCINE
Malaria vaccine provides long-term protection in phase I trial
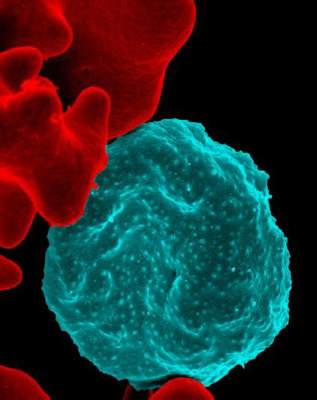
A new malaria vaccine successfully protected a group of healthy United States adults from malaria for more than a year, according to Dr. Andrew Ishizuka and his associates.
In a phase I trial, 57 malaria-naive people received the PfSPZ Vaccine, which contains live but weakened Plasmodium falciparum sporozoites. Participants received either three or four intravenous doses, or four intramuscular injections with a dosage strength 10 times that of the IV immunizations, and were exposed to malaria 3 weeks after completing immunization. Participants who received the four-dose IV immunization had the highest rate of protection at 78%.
To assess long-term effectiveness of the vaccine, a group of five participants who had previously been exposed to malaria at 3 and 21 weeks post-immunization were exposed again after 59 weeks. No P. falciparum was found in the blood of these participants, while a group of six unvaccinated controls who were exposed to the parasites developed malaria.
“Malaria remains one of the most devastating diseases in the world, especially among young children in Africa. A malaria vaccine that provides long-term protection is urgently needed to reduce mortality and eliminate transmission. This study is an encouraging step forward in our goal to control and ultimately eradicate malaria,” Dr. Anthony S. Fauci, director of the National Institute of Allergy and Infectious Diseases, said in a press release.
Find the study in Nature Medicine (2016 May. doi: 10.1038/nm.4110).
A new malaria vaccine successfully protected a group of healthy United States adults from malaria for more than a year, according to Dr. Andrew Ishizuka and his associates.
In a phase I trial, 57 malaria-naive people received the PfSPZ Vaccine, which contains live but weakened Plasmodium falciparum sporozoites. Participants received either three or four intravenous doses, or four intramuscular injections with a dosage strength 10 times that of the IV immunizations, and were exposed to malaria 3 weeks after completing immunization. Participants who received the four-dose IV immunization had the highest rate of protection at 78%.
To assess long-term effectiveness of the vaccine, a group of five participants who had previously been exposed to malaria at 3 and 21 weeks post-immunization were exposed again after 59 weeks. No P. falciparum was found in the blood of these participants, while a group of six unvaccinated controls who were exposed to the parasites developed malaria.
“Malaria remains one of the most devastating diseases in the world, especially among young children in Africa. A malaria vaccine that provides long-term protection is urgently needed to reduce mortality and eliminate transmission. This study is an encouraging step forward in our goal to control and ultimately eradicate malaria,” Dr. Anthony S. Fauci, director of the National Institute of Allergy and Infectious Diseases, said in a press release.
Find the study in Nature Medicine (2016 May. doi: 10.1038/nm.4110).
A new malaria vaccine successfully protected a group of healthy United States adults from malaria for more than a year, according to Dr. Andrew Ishizuka and his associates.
In a phase I trial, 57 malaria-naive people received the PfSPZ Vaccine, which contains live but weakened Plasmodium falciparum sporozoites. Participants received either three or four intravenous doses, or four intramuscular injections with a dosage strength 10 times that of the IV immunizations, and were exposed to malaria 3 weeks after completing immunization. Participants who received the four-dose IV immunization had the highest rate of protection at 78%.
To assess long-term effectiveness of the vaccine, a group of five participants who had previously been exposed to malaria at 3 and 21 weeks post-immunization were exposed again after 59 weeks. No P. falciparum was found in the blood of these participants, while a group of six unvaccinated controls who were exposed to the parasites developed malaria.
“Malaria remains one of the most devastating diseases in the world, especially among young children in Africa. A malaria vaccine that provides long-term protection is urgently needed to reduce mortality and eliminate transmission. This study is an encouraging step forward in our goal to control and ultimately eradicate malaria,” Dr. Anthony S. Fauci, director of the National Institute of Allergy and Infectious Diseases, said in a press release.
Find the study in Nature Medicine (2016 May. doi: 10.1038/nm.4110).
FROM NATURE MEDICINE
Patient-centered medical homes boost likelihood of preventive care in teens
Adolescents and young adults enrolled in patient-centered medical homes were more likely to receive most kinds of preventive care, according to Dr. Diego Garcia-Huidobro of the University of Minnesota, Minneapolis, and his associates.
Compared with patients of the same age who were not enrolled in PCMHs, patients aged 10-24 years enrolled in PCMHs were most likely to receive long-acting reversible contraceptive (LARC) prescriptions, with an adjusted odds ratio (aOR) of 2.66. PCMH enrollees were more likely to receive preventative visits (aOR, 1.10), meningococcal vaccines (aOR, 1.53) and HPV vaccines (aOR, 1.53), sexually transmitted disease screening (aOR, 1.68), any kind of contraceptive prescription (aOR, 2.18), and cervical cancer screening (aOR, 1.14), but were slightly less likely to receive influenza vaccinations (aOR, 0.89).
The average age of PCMH patients was 19 years, and nearly 60% were female. Nearly 65% were Hispanic/Latino, and 26% were non-Hispanic blacks. Just under 58% of patients were publicly insured, and 3% had private insurance. Non-PCMH patients tended to be older (21 years), and 56% were female. Forty-two percent were Hispanic/Latino, and 33% were non-Hispanic blacks. About 47% had public insurance and 11% had private insurance.
“This finding highlights the value of this model of care at addressing not only the specific needs of patients but also improving their preventive care,” the investigators concluded.
Find the full study in Pediatrics (2016. doi: 10.1542/peds.2015-3813).
Adolescents and young adults enrolled in patient-centered medical homes were more likely to receive most kinds of preventive care, according to Dr. Diego Garcia-Huidobro of the University of Minnesota, Minneapolis, and his associates.
Compared with patients of the same age who were not enrolled in PCMHs, patients aged 10-24 years enrolled in PCMHs were most likely to receive long-acting reversible contraceptive (LARC) prescriptions, with an adjusted odds ratio (aOR) of 2.66. PCMH enrollees were more likely to receive preventative visits (aOR, 1.10), meningococcal vaccines (aOR, 1.53) and HPV vaccines (aOR, 1.53), sexually transmitted disease screening (aOR, 1.68), any kind of contraceptive prescription (aOR, 2.18), and cervical cancer screening (aOR, 1.14), but were slightly less likely to receive influenza vaccinations (aOR, 0.89).
The average age of PCMH patients was 19 years, and nearly 60% were female. Nearly 65% were Hispanic/Latino, and 26% were non-Hispanic blacks. Just under 58% of patients were publicly insured, and 3% had private insurance. Non-PCMH patients tended to be older (21 years), and 56% were female. Forty-two percent were Hispanic/Latino, and 33% were non-Hispanic blacks. About 47% had public insurance and 11% had private insurance.
“This finding highlights the value of this model of care at addressing not only the specific needs of patients but also improving their preventive care,” the investigators concluded.
Find the full study in Pediatrics (2016. doi: 10.1542/peds.2015-3813).
Adolescents and young adults enrolled in patient-centered medical homes were more likely to receive most kinds of preventive care, according to Dr. Diego Garcia-Huidobro of the University of Minnesota, Minneapolis, and his associates.
Compared with patients of the same age who were not enrolled in PCMHs, patients aged 10-24 years enrolled in PCMHs were most likely to receive long-acting reversible contraceptive (LARC) prescriptions, with an adjusted odds ratio (aOR) of 2.66. PCMH enrollees were more likely to receive preventative visits (aOR, 1.10), meningococcal vaccines (aOR, 1.53) and HPV vaccines (aOR, 1.53), sexually transmitted disease screening (aOR, 1.68), any kind of contraceptive prescription (aOR, 2.18), and cervical cancer screening (aOR, 1.14), but were slightly less likely to receive influenza vaccinations (aOR, 0.89).
The average age of PCMH patients was 19 years, and nearly 60% were female. Nearly 65% were Hispanic/Latino, and 26% were non-Hispanic blacks. Just under 58% of patients were publicly insured, and 3% had private insurance. Non-PCMH patients tended to be older (21 years), and 56% were female. Forty-two percent were Hispanic/Latino, and 33% were non-Hispanic blacks. About 47% had public insurance and 11% had private insurance.
“This finding highlights the value of this model of care at addressing not only the specific needs of patients but also improving their preventive care,” the investigators concluded.
Find the full study in Pediatrics (2016. doi: 10.1542/peds.2015-3813).
FROM PEDIATRICS
Astrovirus MLB2 may cause CNS infection in immunocompromised patients
The astrovirus MLB2, normally prevalent in feces, can spread outside the digestive system and cause central nervous system infection in immunocompromised patients, according to Dr. Samuel Cordey and his associates.
The initial case-patient was a 21-year-old woman who was admitted because of an unusually severe headache and a fever. She was diagnosed with acute meningitis. Next-generation sequencing (NGS) identified 155 reads of astrovirus MLB2 in the patient’s cerebrospinal fluid, 9,340 in an anal swab, 18 in the patient’s plasma, and 16 in the urine. NGS did not identify any other RNA viruses, and no viral or bacterial pathogens were found in DNA sequencing.
In a subsequent pilot study, 943 stool samples from 615 patients and 424 CSF samples from 404 patients were tested for astrovirus MLB2 via reverse transcription PCR. Stool samples were positive for MLB2 in six patients, five of whom were severely immunocompromised. CSF samples were positive for MLB2 in one patient, a recipient of a hematopoietic stem cell transplant.
The study findings “could place astrovirus MLB2 in the differential diagnosis not only of diarrhea but also of aseptic meningitis and protracted infection in highly immunocompromised hosts. Potential determinants of extraintestinal dissemination, such as viral load kinetic, immune response, and host and viral genetic factors, require further characterization,” the investigators said.
Find the study in Emerging Infectious Diseases (doi: 10.3201/eid2205.151807).
The astrovirus MLB2, normally prevalent in feces, can spread outside the digestive system and cause central nervous system infection in immunocompromised patients, according to Dr. Samuel Cordey and his associates.
The initial case-patient was a 21-year-old woman who was admitted because of an unusually severe headache and a fever. She was diagnosed with acute meningitis. Next-generation sequencing (NGS) identified 155 reads of astrovirus MLB2 in the patient’s cerebrospinal fluid, 9,340 in an anal swab, 18 in the patient’s plasma, and 16 in the urine. NGS did not identify any other RNA viruses, and no viral or bacterial pathogens were found in DNA sequencing.
In a subsequent pilot study, 943 stool samples from 615 patients and 424 CSF samples from 404 patients were tested for astrovirus MLB2 via reverse transcription PCR. Stool samples were positive for MLB2 in six patients, five of whom were severely immunocompromised. CSF samples were positive for MLB2 in one patient, a recipient of a hematopoietic stem cell transplant.
The study findings “could place astrovirus MLB2 in the differential diagnosis not only of diarrhea but also of aseptic meningitis and protracted infection in highly immunocompromised hosts. Potential determinants of extraintestinal dissemination, such as viral load kinetic, immune response, and host and viral genetic factors, require further characterization,” the investigators said.
Find the study in Emerging Infectious Diseases (doi: 10.3201/eid2205.151807).
The astrovirus MLB2, normally prevalent in feces, can spread outside the digestive system and cause central nervous system infection in immunocompromised patients, according to Dr. Samuel Cordey and his associates.
The initial case-patient was a 21-year-old woman who was admitted because of an unusually severe headache and a fever. She was diagnosed with acute meningitis. Next-generation sequencing (NGS) identified 155 reads of astrovirus MLB2 in the patient’s cerebrospinal fluid, 9,340 in an anal swab, 18 in the patient’s plasma, and 16 in the urine. NGS did not identify any other RNA viruses, and no viral or bacterial pathogens were found in DNA sequencing.
In a subsequent pilot study, 943 stool samples from 615 patients and 424 CSF samples from 404 patients were tested for astrovirus MLB2 via reverse transcription PCR. Stool samples were positive for MLB2 in six patients, five of whom were severely immunocompromised. CSF samples were positive for MLB2 in one patient, a recipient of a hematopoietic stem cell transplant.
The study findings “could place astrovirus MLB2 in the differential diagnosis not only of diarrhea but also of aseptic meningitis and protracted infection in highly immunocompromised hosts. Potential determinants of extraintestinal dissemination, such as viral load kinetic, immune response, and host and viral genetic factors, require further characterization,” the investigators said.
Find the study in Emerging Infectious Diseases (doi: 10.3201/eid2205.151807).
FROM EMERGING INFECTIOUS DISEASES
SIDS most likely in swaddled infants placed on front or side
Sudden infant death syndrome is significantly more likely in infants who are swaddled and placed on the front or side, according to a meta-analysis by Anna S. Pease of the University of Bristol (England), and her associates.
They looked at four studies covering 760 cases of SIDS and 1,759 controls. The odds ratio for swaddling when infant death occurred was 1.58. Risk was highest when swaddled infants were placed on their stomachs, with an OR of 12.99, though risk was also high for children placed on their sides, with an OR of 3.16. Swaddled infants placed on their backs had the lowest risk, with an OR of 1.93.
Some evidence suggested that swaddling risk increased as the infant got older, with an odds ratio of 2.53 in children older than 6 months; however, cases were uncommon and the relationship is not definitive.
“Given the marked increase in infants swaddled and found prone (rather than placed prone), coupled with an increased risk of swaddling with increased age regardless of sleeping position, health professionals and current guidelines should consider an appropriate age limit at which swaddling should be discouraged,” the investigators concluded.
Find the full study in Pediatrics (2016. doi: 10.1542/peds.2015-3275).
Sudden infant death syndrome is significantly more likely in infants who are swaddled and placed on the front or side, according to a meta-analysis by Anna S. Pease of the University of Bristol (England), and her associates.
They looked at four studies covering 760 cases of SIDS and 1,759 controls. The odds ratio for swaddling when infant death occurred was 1.58. Risk was highest when swaddled infants were placed on their stomachs, with an OR of 12.99, though risk was also high for children placed on their sides, with an OR of 3.16. Swaddled infants placed on their backs had the lowest risk, with an OR of 1.93.
Some evidence suggested that swaddling risk increased as the infant got older, with an odds ratio of 2.53 in children older than 6 months; however, cases were uncommon and the relationship is not definitive.
“Given the marked increase in infants swaddled and found prone (rather than placed prone), coupled with an increased risk of swaddling with increased age regardless of sleeping position, health professionals and current guidelines should consider an appropriate age limit at which swaddling should be discouraged,” the investigators concluded.
Find the full study in Pediatrics (2016. doi: 10.1542/peds.2015-3275).
Sudden infant death syndrome is significantly more likely in infants who are swaddled and placed on the front or side, according to a meta-analysis by Anna S. Pease of the University of Bristol (England), and her associates.
They looked at four studies covering 760 cases of SIDS and 1,759 controls. The odds ratio for swaddling when infant death occurred was 1.58. Risk was highest when swaddled infants were placed on their stomachs, with an OR of 12.99, though risk was also high for children placed on their sides, with an OR of 3.16. Swaddled infants placed on their backs had the lowest risk, with an OR of 1.93.
Some evidence suggested that swaddling risk increased as the infant got older, with an odds ratio of 2.53 in children older than 6 months; however, cases were uncommon and the relationship is not definitive.
“Given the marked increase in infants swaddled and found prone (rather than placed prone), coupled with an increased risk of swaddling with increased age regardless of sleeping position, health professionals and current guidelines should consider an appropriate age limit at which swaddling should be discouraged,” the investigators concluded.
Find the full study in Pediatrics (2016. doi: 10.1542/peds.2015-3275).
FROM PEDIATRICS
E-cigarettes fuel increase in nicotine exposures in young children
The incidence of exposure to nicotine and tobacco products in children less than 6 years old increased significantly from 2012 to 2015, according to Alisha Kamboj and her associates.
From January 2012 to April 2015, the National Poison Data System received 29,141 reports of nicotine and tobacco product exposure in children under 6 years of age, averaging 729 children per month. The annual rate of exposure increased from 3.0/100,000 children in 2012 to 4.2/100,000 in 2014. A dramatic increase in exposure to e-cigarettes drove the overall increase, with monthly reports of e-cigarette use rising nearly 1,500% from January 2012 to April 2015.
Nearly 80% of children exposed were younger than 2 years old, and the median age of exposed children was 1.1 years. Children younger than 2 accounted for 44.1% of e-cigarette exposures, 91.6% of cigarette exposures, and 75.4% of exposures to other tobacco products, the investigators noted.
Children exposed to e-cigarettes were significantly more likely to be admitted to a health care facility and to have severe outcomes than were children exposed to cigarettes, with odds ratios of 5.19 and 2.6, respectively. One death – of a 1-year-old child – was associated with nicotine liquid.
“Educating child caregivers about potential clinical effects and outcomes associated with nicotine exposure may help motivate adoption of safety behaviors and aid in identification of symptoms in the event of an exposure. Adults in households with children [younger than] 6 years should be counseled on vaping cessation and strongly encouraged not to use or store e-cigarettes, e-liquid, and related products in the home,” the investigators recommended.
Find the full study in Pediatrics (doi: 10.1542/peds.2016-0041).
The incidence of exposure to nicotine and tobacco products in children less than 6 years old increased significantly from 2012 to 2015, according to Alisha Kamboj and her associates.
From January 2012 to April 2015, the National Poison Data System received 29,141 reports of nicotine and tobacco product exposure in children under 6 years of age, averaging 729 children per month. The annual rate of exposure increased from 3.0/100,000 children in 2012 to 4.2/100,000 in 2014. A dramatic increase in exposure to e-cigarettes drove the overall increase, with monthly reports of e-cigarette use rising nearly 1,500% from January 2012 to April 2015.
Nearly 80% of children exposed were younger than 2 years old, and the median age of exposed children was 1.1 years. Children younger than 2 accounted for 44.1% of e-cigarette exposures, 91.6% of cigarette exposures, and 75.4% of exposures to other tobacco products, the investigators noted.
Children exposed to e-cigarettes were significantly more likely to be admitted to a health care facility and to have severe outcomes than were children exposed to cigarettes, with odds ratios of 5.19 and 2.6, respectively. One death – of a 1-year-old child – was associated with nicotine liquid.
“Educating child caregivers about potential clinical effects and outcomes associated with nicotine exposure may help motivate adoption of safety behaviors and aid in identification of symptoms in the event of an exposure. Adults in households with children [younger than] 6 years should be counseled on vaping cessation and strongly encouraged not to use or store e-cigarettes, e-liquid, and related products in the home,” the investigators recommended.
Find the full study in Pediatrics (doi: 10.1542/peds.2016-0041).
The incidence of exposure to nicotine and tobacco products in children less than 6 years old increased significantly from 2012 to 2015, according to Alisha Kamboj and her associates.
From January 2012 to April 2015, the National Poison Data System received 29,141 reports of nicotine and tobacco product exposure in children under 6 years of age, averaging 729 children per month. The annual rate of exposure increased from 3.0/100,000 children in 2012 to 4.2/100,000 in 2014. A dramatic increase in exposure to e-cigarettes drove the overall increase, with monthly reports of e-cigarette use rising nearly 1,500% from January 2012 to April 2015.
Nearly 80% of children exposed were younger than 2 years old, and the median age of exposed children was 1.1 years. Children younger than 2 accounted for 44.1% of e-cigarette exposures, 91.6% of cigarette exposures, and 75.4% of exposures to other tobacco products, the investigators noted.
Children exposed to e-cigarettes were significantly more likely to be admitted to a health care facility and to have severe outcomes than were children exposed to cigarettes, with odds ratios of 5.19 and 2.6, respectively. One death – of a 1-year-old child – was associated with nicotine liquid.
“Educating child caregivers about potential clinical effects and outcomes associated with nicotine exposure may help motivate adoption of safety behaviors and aid in identification of symptoms in the event of an exposure. Adults in households with children [younger than] 6 years should be counseled on vaping cessation and strongly encouraged not to use or store e-cigarettes, e-liquid, and related products in the home,” the investigators recommended.
Find the full study in Pediatrics (doi: 10.1542/peds.2016-0041).
FROM PEDIATRICS
Opioid-based therapies reduce TKA needs for OA patients, but not costs
Treatment with opioids is not cost effective in osteoarthritis patients without comorbidities, according to Savannah R. Smith and her associates.
When a 10% reduction in total knee arthroplasty (TKA) effectiveness from opioid-based therapies was assumed, tramadol therapy delayed TKA by 7 years and tramadol plus oxycodone therapy delayed TKA by 9 years. Opioid-based therapy reduced primary TKA utilization by 4% for tramadol and by 10% for tramadol plus oxycodone, and reduced revision TKA use by 23% and 39%, respectively.
While both opioid-based therapies reduced dependence on TKA, treatment was more expensive and it reduced quality of life, compared with an opioid-sparing therapy. For a 60-year-old OA patient for whom TKA was not an option, the incremental cost-effectiveness ratio for tramadol was $39,600 per quality-adjusted life-year, compared with a therapy without opioids, and the incremental cost-effectiveness ratio for tramadol plus oxycodone was $116,800 per quality-adjusted life-year.
“Given the risk of diversion and its associated cost for potent opioids, policy makers may consider limiting the use of potent opioids in knee OA patients. From a cost-effectiveness standpoint, both opioid-based strategies led to higher costs without providing additional benefits, unless patients were unwilling or unable to undergo TKA later,” the investigators noted.
Find the full study in Arthritis Care and Research (doi: 10.1002/acr.22916).
Treatment with opioids is not cost effective in osteoarthritis patients without comorbidities, according to Savannah R. Smith and her associates.
When a 10% reduction in total knee arthroplasty (TKA) effectiveness from opioid-based therapies was assumed, tramadol therapy delayed TKA by 7 years and tramadol plus oxycodone therapy delayed TKA by 9 years. Opioid-based therapy reduced primary TKA utilization by 4% for tramadol and by 10% for tramadol plus oxycodone, and reduced revision TKA use by 23% and 39%, respectively.
While both opioid-based therapies reduced dependence on TKA, treatment was more expensive and it reduced quality of life, compared with an opioid-sparing therapy. For a 60-year-old OA patient for whom TKA was not an option, the incremental cost-effectiveness ratio for tramadol was $39,600 per quality-adjusted life-year, compared with a therapy without opioids, and the incremental cost-effectiveness ratio for tramadol plus oxycodone was $116,800 per quality-adjusted life-year.
“Given the risk of diversion and its associated cost for potent opioids, policy makers may consider limiting the use of potent opioids in knee OA patients. From a cost-effectiveness standpoint, both opioid-based strategies led to higher costs without providing additional benefits, unless patients were unwilling or unable to undergo TKA later,” the investigators noted.
Find the full study in Arthritis Care and Research (doi: 10.1002/acr.22916).
Treatment with opioids is not cost effective in osteoarthritis patients without comorbidities, according to Savannah R. Smith and her associates.
When a 10% reduction in total knee arthroplasty (TKA) effectiveness from opioid-based therapies was assumed, tramadol therapy delayed TKA by 7 years and tramadol plus oxycodone therapy delayed TKA by 9 years. Opioid-based therapy reduced primary TKA utilization by 4% for tramadol and by 10% for tramadol plus oxycodone, and reduced revision TKA use by 23% and 39%, respectively.
While both opioid-based therapies reduced dependence on TKA, treatment was more expensive and it reduced quality of life, compared with an opioid-sparing therapy. For a 60-year-old OA patient for whom TKA was not an option, the incremental cost-effectiveness ratio for tramadol was $39,600 per quality-adjusted life-year, compared with a therapy without opioids, and the incremental cost-effectiveness ratio for tramadol plus oxycodone was $116,800 per quality-adjusted life-year.
“Given the risk of diversion and its associated cost for potent opioids, policy makers may consider limiting the use of potent opioids in knee OA patients. From a cost-effectiveness standpoint, both opioid-based strategies led to higher costs without providing additional benefits, unless patients were unwilling or unable to undergo TKA later,” the investigators noted.
Find the full study in Arthritis Care and Research (doi: 10.1002/acr.22916).
FROM ARTHRITIS CARE AND RESEARCH
Survey: Teens view e-cigarettes as less harmful than traditional tobacco products
New and emerging tobacco products such as hookah and e-cigarettes are perceived as being less harmful and more socially acceptable than traditional cigarettes, according to Maria Roditis, Ph.D., and her associates.
In a survey of 722 students aged 13-19, cigarettes were perceived as being most harmful to one’s health, to the health of friends, and to the environment. Perceived harm to one’s own health was similar for cigars and chewing tobacco, but chewing tobacco was seen as significantly less harmful to friends and to the environment. E-cigarettes were seen as least harmful overall, followed by hookah.
E-cigarettes were seen to have the least social risk, while cigarettes and cigars had the greatest social risk. Chewing tobacco had the smallest perceived social benefit, while hookah had the greatest social benefit. All tobacco products were seen as having significant long-term health risks, though the effect was smaller in older adolescents and for e-cigarettes.
“There is a clear need to expand messaging campaigns to discuss the risks related to all tobacco products and not focus solely on the risk of cigarettes alone. Although such messaging campaigns should continually be updated to reflect the current body of research, the public health community needs to actively start messaging on known risks related to all tobacco products now,” the investigators noted.
Find the full study in the Journal of Adolescent Health (doi: 10.1016/j.jadohealth.2016.01.012).
New and emerging tobacco products such as hookah and e-cigarettes are perceived as being less harmful and more socially acceptable than traditional cigarettes, according to Maria Roditis, Ph.D., and her associates.
In a survey of 722 students aged 13-19, cigarettes were perceived as being most harmful to one’s health, to the health of friends, and to the environment. Perceived harm to one’s own health was similar for cigars and chewing tobacco, but chewing tobacco was seen as significantly less harmful to friends and to the environment. E-cigarettes were seen as least harmful overall, followed by hookah.
E-cigarettes were seen to have the least social risk, while cigarettes and cigars had the greatest social risk. Chewing tobacco had the smallest perceived social benefit, while hookah had the greatest social benefit. All tobacco products were seen as having significant long-term health risks, though the effect was smaller in older adolescents and for e-cigarettes.
“There is a clear need to expand messaging campaigns to discuss the risks related to all tobacco products and not focus solely on the risk of cigarettes alone. Although such messaging campaigns should continually be updated to reflect the current body of research, the public health community needs to actively start messaging on known risks related to all tobacco products now,” the investigators noted.
Find the full study in the Journal of Adolescent Health (doi: 10.1016/j.jadohealth.2016.01.012).
New and emerging tobacco products such as hookah and e-cigarettes are perceived as being less harmful and more socially acceptable than traditional cigarettes, according to Maria Roditis, Ph.D., and her associates.
In a survey of 722 students aged 13-19, cigarettes were perceived as being most harmful to one’s health, to the health of friends, and to the environment. Perceived harm to one’s own health was similar for cigars and chewing tobacco, but chewing tobacco was seen as significantly less harmful to friends and to the environment. E-cigarettes were seen as least harmful overall, followed by hookah.
E-cigarettes were seen to have the least social risk, while cigarettes and cigars had the greatest social risk. Chewing tobacco had the smallest perceived social benefit, while hookah had the greatest social benefit. All tobacco products were seen as having significant long-term health risks, though the effect was smaller in older adolescents and for e-cigarettes.
“There is a clear need to expand messaging campaigns to discuss the risks related to all tobacco products and not focus solely on the risk of cigarettes alone. Although such messaging campaigns should continually be updated to reflect the current body of research, the public health community needs to actively start messaging on known risks related to all tobacco products now,” the investigators noted.
Find the full study in the Journal of Adolescent Health (doi: 10.1016/j.jadohealth.2016.01.012).
FROM THE JOURNAL OF ADOLESCENT HEALTH
Aripiprazole linked to rare but serious compulsion problems
Rare but serious instances of impulse control problems have been reported in people taking the antipsychotic drug aripiprazole, according to a May 3 press release from the Food and Drug Administration.
Pathological gambling is listed as a side effect of aripiprazole (Abilify, Abilify Maintena, Aristada, and generics). Additional side effects seen in patients include compulsive eating, shopping, and sexual actions. The symptoms are rare but can affect anyone taking the medication and can result in serious harm to the patient.
All compulsive symptoms stopped when patients stopped taking aripiprazole or reduced their dosage. The FDA will add new warnings about the symptoms to all drug labels and patient medication guides.
“Health care professionals should make patients and caregivers aware of the risk of these uncontrollable urges when prescribing aripiprazole, and specifically ask patients about any new or increasing urges while they are being treated with aripiprazole. Closely monitor for new or worsening uncontrollable urges in patients at higher risk for impulse control problems,” the FDA said in the press release.
Find the full press release on the FDA website.
Rare but serious instances of impulse control problems have been reported in people taking the antipsychotic drug aripiprazole, according to a May 3 press release from the Food and Drug Administration.
Pathological gambling is listed as a side effect of aripiprazole (Abilify, Abilify Maintena, Aristada, and generics). Additional side effects seen in patients include compulsive eating, shopping, and sexual actions. The symptoms are rare but can affect anyone taking the medication and can result in serious harm to the patient.
All compulsive symptoms stopped when patients stopped taking aripiprazole or reduced their dosage. The FDA will add new warnings about the symptoms to all drug labels and patient medication guides.
“Health care professionals should make patients and caregivers aware of the risk of these uncontrollable urges when prescribing aripiprazole, and specifically ask patients about any new or increasing urges while they are being treated with aripiprazole. Closely monitor for new or worsening uncontrollable urges in patients at higher risk for impulse control problems,” the FDA said in the press release.
Find the full press release on the FDA website.
Rare but serious instances of impulse control problems have been reported in people taking the antipsychotic drug aripiprazole, according to a May 3 press release from the Food and Drug Administration.
Pathological gambling is listed as a side effect of aripiprazole (Abilify, Abilify Maintena, Aristada, and generics). Additional side effects seen in patients include compulsive eating, shopping, and sexual actions. The symptoms are rare but can affect anyone taking the medication and can result in serious harm to the patient.
All compulsive symptoms stopped when patients stopped taking aripiprazole or reduced their dosage. The FDA will add new warnings about the symptoms to all drug labels and patient medication guides.
“Health care professionals should make patients and caregivers aware of the risk of these uncontrollable urges when prescribing aripiprazole, and specifically ask patients about any new or increasing urges while they are being treated with aripiprazole. Closely monitor for new or worsening uncontrollable urges in patients at higher risk for impulse control problems,” the FDA said in the press release.
Find the full press release on the FDA website.