User login
M. Alexander Otto began his reporting career early in 1999 covering the pharmaceutical industry for a national pharmacists' magazine and freelancing for the Washington Post and other newspapers. He then joined BNA, now part of Bloomberg News, covering health law and the protection of people and animals in medical research. Alex next worked for the McClatchy Company. Based on his work, Alex won a year-long Knight Science Journalism Fellowship to MIT in 2008-2009. He joined the company shortly thereafter. Alex has a newspaper journalism degree from Syracuse (N.Y.) University and a master's degree in medical science -- a physician assistant degree -- from George Washington University. Alex is based in Seattle.
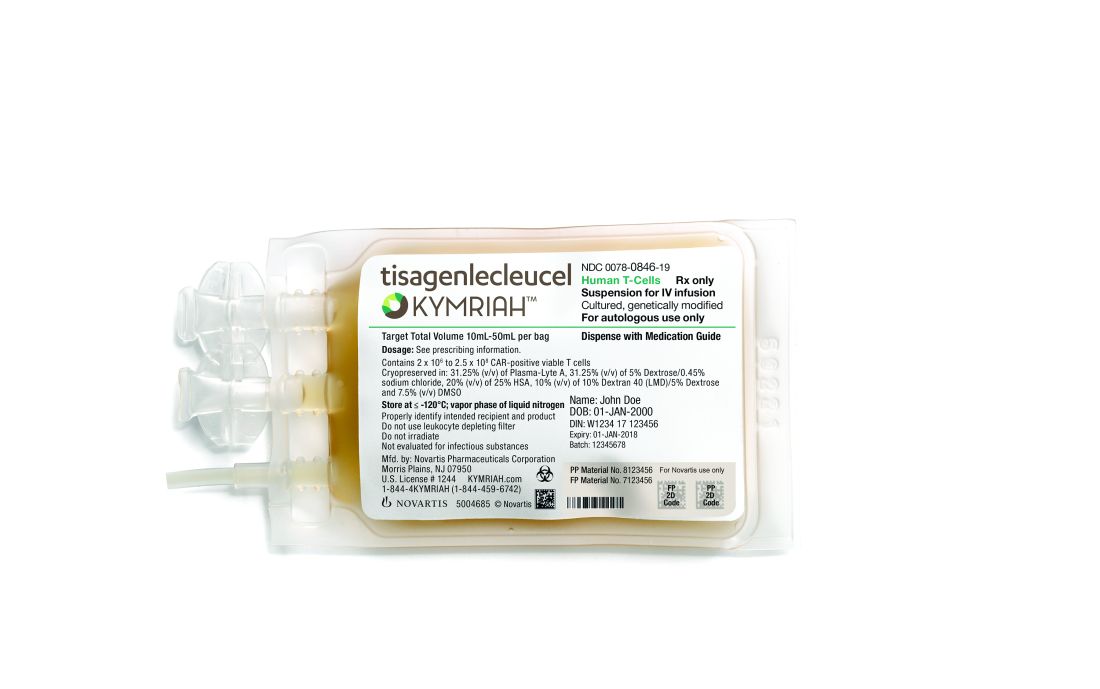
Novartis CAR T-cell therapy adds a lymphoma indication
Novartis’s after failure of two or more lines of systemic therapy.
The Food and Drug Administration approved the expanded indication on May 1. The chimeric antigen receptor (CAR) T-cell therapy was initially approved in Aug. 2017 for refractory or relapsed B-cell precursor acute lymphoblastic leukemia (ALL) in patients up to 25 years old. The new approval brings tisagenlecleucel into direct competition with Gilead Science’s CAR T-cell therapy axicabtagene ciloleucel (Yescarta), which was approved in Oct. 2017 for B-cell lymphoma.
Besides matching the competition, she said the lower price is because tisagenlecleucel takes longer to work for lymphoma, and the response isn’t as potent as for childhood ALL. Novartis is looking into chronic lymphocytic leukemia, multiple myeloma, and solid tumor indications for tisagenlecleucel and other CAR T-cell agents, she added.
The Centers for Medicare & Medicaid Services recently committed to covering outpatient administration of both agents for their initial indications; Novartis is working with CMS for coverage of the new lymphoma indication.
With both products, T cells are collected then shipped off to a company facility where a CAR gene is spliced into their DNA, essentially programming the T cells to attack the targeted cancer. The cells are then infused back into the patient.
In the phase 2 JULIET trial, tisagenlecleucel showed an overall response rate of 50% among 68 B-cell lymphoma patients, with 32% achieving complete response (CR) and 18% achieving partial response (PR). The median duration of response was not reached.
Axicabtagene ciloleucel’s label reports an objective response rate of 72% among 101 patients, with CR in 51% and PR in 21%. Median duration of response was 9.2 months but was also not reached among complete responders.
“Different trials. Different CARTs. Different levels of disease. Our drug is cryopreserved and theirs is not. No way to compare them,” the Novartis spokeswoman said when asked about the response differences.
T-cell reprogramming isn’t clean at this point in medical history; both agents carry black box warnings of potentially fatal cytokine release syndrome and neurologic toxicity, and both are subject to Risk Evaluation and Mitigation Strategy programs.
The B-cell lymphoma indication for both therapies includes diffuse large B-cell lymphoma (DLBCL), high grade B-cell lymphoma, and DLBCL arising from follicular lymphoma. The Gilead product carries an additional indication for primary mediastinal large B-cell lymphoma. Neither agent is indicated for primary central nervous system lymphoma. Both labels say that patients should not donate blood, organs, or tissues after treatment. Tisagenlecleucel labeling also notes that some commercial HIV nucleic acid tests may yield false positives after treatment.
Novartis said in a press release that T cells are treated at the company’s Morris Plains, N.J., facility with a turnaround time of about 22 days. Cryopreservation of the harvested cells gives providers some flexibility in treatment timing.
Novartis’s after failure of two or more lines of systemic therapy.
The Food and Drug Administration approved the expanded indication on May 1. The chimeric antigen receptor (CAR) T-cell therapy was initially approved in Aug. 2017 for refractory or relapsed B-cell precursor acute lymphoblastic leukemia (ALL) in patients up to 25 years old. The new approval brings tisagenlecleucel into direct competition with Gilead Science’s CAR T-cell therapy axicabtagene ciloleucel (Yescarta), which was approved in Oct. 2017 for B-cell lymphoma.
Besides matching the competition, she said the lower price is because tisagenlecleucel takes longer to work for lymphoma, and the response isn’t as potent as for childhood ALL. Novartis is looking into chronic lymphocytic leukemia, multiple myeloma, and solid tumor indications for tisagenlecleucel and other CAR T-cell agents, she added.
The Centers for Medicare & Medicaid Services recently committed to covering outpatient administration of both agents for their initial indications; Novartis is working with CMS for coverage of the new lymphoma indication.
With both products, T cells are collected then shipped off to a company facility where a CAR gene is spliced into their DNA, essentially programming the T cells to attack the targeted cancer. The cells are then infused back into the patient.
In the phase 2 JULIET trial, tisagenlecleucel showed an overall response rate of 50% among 68 B-cell lymphoma patients, with 32% achieving complete response (CR) and 18% achieving partial response (PR). The median duration of response was not reached.
Axicabtagene ciloleucel’s label reports an objective response rate of 72% among 101 patients, with CR in 51% and PR in 21%. Median duration of response was 9.2 months but was also not reached among complete responders.
“Different trials. Different CARTs. Different levels of disease. Our drug is cryopreserved and theirs is not. No way to compare them,” the Novartis spokeswoman said when asked about the response differences.
T-cell reprogramming isn’t clean at this point in medical history; both agents carry black box warnings of potentially fatal cytokine release syndrome and neurologic toxicity, and both are subject to Risk Evaluation and Mitigation Strategy programs.
The B-cell lymphoma indication for both therapies includes diffuse large B-cell lymphoma (DLBCL), high grade B-cell lymphoma, and DLBCL arising from follicular lymphoma. The Gilead product carries an additional indication for primary mediastinal large B-cell lymphoma. Neither agent is indicated for primary central nervous system lymphoma. Both labels say that patients should not donate blood, organs, or tissues after treatment. Tisagenlecleucel labeling also notes that some commercial HIV nucleic acid tests may yield false positives after treatment.
Novartis said in a press release that T cells are treated at the company’s Morris Plains, N.J., facility with a turnaround time of about 22 days. Cryopreservation of the harvested cells gives providers some flexibility in treatment timing.
Novartis’s after failure of two or more lines of systemic therapy.
The Food and Drug Administration approved the expanded indication on May 1. The chimeric antigen receptor (CAR) T-cell therapy was initially approved in Aug. 2017 for refractory or relapsed B-cell precursor acute lymphoblastic leukemia (ALL) in patients up to 25 years old. The new approval brings tisagenlecleucel into direct competition with Gilead Science’s CAR T-cell therapy axicabtagene ciloleucel (Yescarta), which was approved in Oct. 2017 for B-cell lymphoma.
Besides matching the competition, she said the lower price is because tisagenlecleucel takes longer to work for lymphoma, and the response isn’t as potent as for childhood ALL. Novartis is looking into chronic lymphocytic leukemia, multiple myeloma, and solid tumor indications for tisagenlecleucel and other CAR T-cell agents, she added.
The Centers for Medicare & Medicaid Services recently committed to covering outpatient administration of both agents for their initial indications; Novartis is working with CMS for coverage of the new lymphoma indication.
With both products, T cells are collected then shipped off to a company facility where a CAR gene is spliced into their DNA, essentially programming the T cells to attack the targeted cancer. The cells are then infused back into the patient.
In the phase 2 JULIET trial, tisagenlecleucel showed an overall response rate of 50% among 68 B-cell lymphoma patients, with 32% achieving complete response (CR) and 18% achieving partial response (PR). The median duration of response was not reached.
Axicabtagene ciloleucel’s label reports an objective response rate of 72% among 101 patients, with CR in 51% and PR in 21%. Median duration of response was 9.2 months but was also not reached among complete responders.
“Different trials. Different CARTs. Different levels of disease. Our drug is cryopreserved and theirs is not. No way to compare them,” the Novartis spokeswoman said when asked about the response differences.
T-cell reprogramming isn’t clean at this point in medical history; both agents carry black box warnings of potentially fatal cytokine release syndrome and neurologic toxicity, and both are subject to Risk Evaluation and Mitigation Strategy programs.
The B-cell lymphoma indication for both therapies includes diffuse large B-cell lymphoma (DLBCL), high grade B-cell lymphoma, and DLBCL arising from follicular lymphoma. The Gilead product carries an additional indication for primary mediastinal large B-cell lymphoma. Neither agent is indicated for primary central nervous system lymphoma. Both labels say that patients should not donate blood, organs, or tissues after treatment. Tisagenlecleucel labeling also notes that some commercial HIV nucleic acid tests may yield false positives after treatment.
Novartis said in a press release that T cells are treated at the company’s Morris Plains, N.J., facility with a turnaround time of about 22 days. Cryopreservation of the harvested cells gives providers some flexibility in treatment timing.
REM sleep behavior disorder predicts impending synucleinopathy
LOS ANGELES – , according to a years-long, multicenter investigation of 1,280 patients – the largest study of the issue to date.
REM sleep behavior disorder (RBD) has been known for years to increase the risk for synucleinopathies, namely Parkinson’s disease, dementia with Lewy bodies, and multiple system atrophy. However, previous studies have mostly been conducted at single institutions, so the exact extent to which RBD increases the risk wasn’t clear.
These findings have important implications for the field. Now that it’s known who’s at risk, “we have a chance to do neuroprotective therapy. It’s time to move forward and start preventing disease,” Dr. Postuma said at the American Academy of Neurology annual meeting. He estimated that it would take only a few hundred patients to do a 2-year trial of neuroprotective therapy.
The 1,280 study subjects were culled from 24 sleep centers on four continents, all participants in the international RBD study group. The patients needed for a trial “are sitting right now” in the study group, “so maybe we can get on with this,” he said.
REM sleep – the dream state – normally paralyzes people, but something breaks down in RBD, and people act out their dreams, sometimes to disturbing effects. It occurs in about 1% of the population, usually in older people and in slightly more men than women.
The risk of neurodegenerative disease in RBD increases even more if patients test positive at baseline for movement declines, cognitive issues, olfactory problems, constipation, color vision loss, erectile dysfunction, or abnormal dopamine transporter scans. Dr. Postuma and his team found no predictive value for somnolence, insomnia, urinary problems, depression, or anxiety. These negative findings were surprising, he said, because mood disorders and sleep troubles are known to increase the risk in the general population.
The subjects all had polysomnographic-proven RBD at baseline, without neurodegenerative disease. Most of them were men and were about 70 years old, on average. Subjects were tested for synucleinopathies and risk variables annually. The mean disease-free follow-up was about 4 years, but ranged out to 19 years. Risks were adjusted for age, sex, and study center.
Cognition deficits were the only thing that distinguished future dementia patients from those destined for movement disorders. “Everything [else] is really the same between who gets dementia and who gets Parkinsonism,” Dr. Postuma said.
The study was funded by the Canadian Institute of Health Research and the Fonds de la Recherche Sante Quebec. Dr. Postuma disclosed consulting, speaking, and other fees from Biotie, Roche/Prothena, Teva Neurosciences, Novartis Canada, Theranexus, Jazz Pharmaceuticals, and GE HealthCare.
SOURCE: Postuma R et al. AAN 2018, plenary session.
LOS ANGELES – , according to a years-long, multicenter investigation of 1,280 patients – the largest study of the issue to date.
REM sleep behavior disorder (RBD) has been known for years to increase the risk for synucleinopathies, namely Parkinson’s disease, dementia with Lewy bodies, and multiple system atrophy. However, previous studies have mostly been conducted at single institutions, so the exact extent to which RBD increases the risk wasn’t clear.
These findings have important implications for the field. Now that it’s known who’s at risk, “we have a chance to do neuroprotective therapy. It’s time to move forward and start preventing disease,” Dr. Postuma said at the American Academy of Neurology annual meeting. He estimated that it would take only a few hundred patients to do a 2-year trial of neuroprotective therapy.
The 1,280 study subjects were culled from 24 sleep centers on four continents, all participants in the international RBD study group. The patients needed for a trial “are sitting right now” in the study group, “so maybe we can get on with this,” he said.
REM sleep – the dream state – normally paralyzes people, but something breaks down in RBD, and people act out their dreams, sometimes to disturbing effects. It occurs in about 1% of the population, usually in older people and in slightly more men than women.
The risk of neurodegenerative disease in RBD increases even more if patients test positive at baseline for movement declines, cognitive issues, olfactory problems, constipation, color vision loss, erectile dysfunction, or abnormal dopamine transporter scans. Dr. Postuma and his team found no predictive value for somnolence, insomnia, urinary problems, depression, or anxiety. These negative findings were surprising, he said, because mood disorders and sleep troubles are known to increase the risk in the general population.
The subjects all had polysomnographic-proven RBD at baseline, without neurodegenerative disease. Most of them were men and were about 70 years old, on average. Subjects were tested for synucleinopathies and risk variables annually. The mean disease-free follow-up was about 4 years, but ranged out to 19 years. Risks were adjusted for age, sex, and study center.
Cognition deficits were the only thing that distinguished future dementia patients from those destined for movement disorders. “Everything [else] is really the same between who gets dementia and who gets Parkinsonism,” Dr. Postuma said.
The study was funded by the Canadian Institute of Health Research and the Fonds de la Recherche Sante Quebec. Dr. Postuma disclosed consulting, speaking, and other fees from Biotie, Roche/Prothena, Teva Neurosciences, Novartis Canada, Theranexus, Jazz Pharmaceuticals, and GE HealthCare.
SOURCE: Postuma R et al. AAN 2018, plenary session.
LOS ANGELES – , according to a years-long, multicenter investigation of 1,280 patients – the largest study of the issue to date.
REM sleep behavior disorder (RBD) has been known for years to increase the risk for synucleinopathies, namely Parkinson’s disease, dementia with Lewy bodies, and multiple system atrophy. However, previous studies have mostly been conducted at single institutions, so the exact extent to which RBD increases the risk wasn’t clear.
These findings have important implications for the field. Now that it’s known who’s at risk, “we have a chance to do neuroprotective therapy. It’s time to move forward and start preventing disease,” Dr. Postuma said at the American Academy of Neurology annual meeting. He estimated that it would take only a few hundred patients to do a 2-year trial of neuroprotective therapy.
The 1,280 study subjects were culled from 24 sleep centers on four continents, all participants in the international RBD study group. The patients needed for a trial “are sitting right now” in the study group, “so maybe we can get on with this,” he said.
REM sleep – the dream state – normally paralyzes people, but something breaks down in RBD, and people act out their dreams, sometimes to disturbing effects. It occurs in about 1% of the population, usually in older people and in slightly more men than women.
The risk of neurodegenerative disease in RBD increases even more if patients test positive at baseline for movement declines, cognitive issues, olfactory problems, constipation, color vision loss, erectile dysfunction, or abnormal dopamine transporter scans. Dr. Postuma and his team found no predictive value for somnolence, insomnia, urinary problems, depression, or anxiety. These negative findings were surprising, he said, because mood disorders and sleep troubles are known to increase the risk in the general population.
The subjects all had polysomnographic-proven RBD at baseline, without neurodegenerative disease. Most of them were men and were about 70 years old, on average. Subjects were tested for synucleinopathies and risk variables annually. The mean disease-free follow-up was about 4 years, but ranged out to 19 years. Risks were adjusted for age, sex, and study center.
Cognition deficits were the only thing that distinguished future dementia patients from those destined for movement disorders. “Everything [else] is really the same between who gets dementia and who gets Parkinsonism,” Dr. Postuma said.
The study was funded by the Canadian Institute of Health Research and the Fonds de la Recherche Sante Quebec. Dr. Postuma disclosed consulting, speaking, and other fees from Biotie, Roche/Prothena, Teva Neurosciences, Novartis Canada, Theranexus, Jazz Pharmaceuticals, and GE HealthCare.
SOURCE: Postuma R et al. AAN 2018, plenary session.
REPORTING FROM AAN 2018
Key clinical point: Idiopathic REM sleep behavior disorder patients need neuroprotection.
Major finding: At least 70% of patients with idiopathic REM sleep behavior disorder (RBD) will develop a neurodegenerative disease within about a decade.
Study details: An observational study of 1,280 RBD patients from 24 asleep centers on four continents.
Disclosures: The study was funded by the Canadian Institute of Health Research and the Fonds de la Recherche Sante Quebec. Dr. Postuma disclosed consulting, speaking, and other fees from Biotie, Roche/Prothena, Teva Neurosciences, Novartis Canada, Theranexus, Jazz Pharmaceuticals, and GE HealthCare.
Source: Postuma R et al. AAN 2018, plenary session.
Intraventricular enzyme replacement slows CLN2 disease progression
LOS ANGELES – Intraventricular administration of cerliponase alfa seemed to slow the rate of motor and language decline in an open-label trial of 23 children with neuronal ceroid lipofuscinosis type 2 disease.
Neuronal ceroid lipofuscinosis type 2 disease (CLN2), a form of Batten’s disease, is a rare lysosomal storage disorder that causes progressive dementia in children. Patients have pathogenic variants in the gene encoding lysosomal enzyme tripeptidyl peptidase 1 (TPP1). Without functioning enzyme, lysosomal storage material accumulates in neurons throughout the CNS and retina.
Symptoms start at 2-4 years with seizures and language delays, followed by rapid motor, language, and cognitive declines, and blindness. Children die in early adolescence. Treatment is symptomatic; there are no approved therapies.
The idea of the study was to replace the enzyme in the CNS with cerliponase alfa, a recombinant form of TPP1. Twenty-four children aged 3-16 years received 30 mg, 100 mg, or 300 mg intraventricular infusions every 2 weeks during the dose-finding phase of the open-label trial; they were then switched to 300 mg infused over 4 hours every 14 days for at least 96 weeks. One child dropped out after the first dose in the study, but the others continued.
The investigators used Ommaya or Rickham ventricular reservoirs to deliver the enzyme, which were more convenient than intrathecal administration, said investigator Emily de Los Reyes, MD, a pediatric neurologist at Nationwide Children’s Hospital, Columbus, Ohio.
The primary outcome was the time until a 2-point decline on the motor and language scores of the CLN2 Clinical Rating Scale, with 0 representing no function and 6 representing normal function in both domains. The mean unadjusted rate of decline in the motor-language score per 48-week period was 0.27 points in treated patients, versus 2.12 points in 42 historical controls (P less than .001). The treatment difference at 96 weeks was about 3.3 points. There was also a decrease in seizure severity and frequency.
All but one child experienced convulsions, over two-thirds pyrexia, and almost two-thirds vomiting and hypersensitivity. About half developed upper respiratory tract infections, and about half had increased CSF white-cell counts. There were also cases of device leakage, and two children developed infections detected by CSF monitoring, without symptoms of meningitis. Both continued treatment after removal of the intraventricular device, followed by antibiotics, and device replacement.
Fourteen patients (58%) had at least one grade 3 adverse event, and there was one grade 4 event: status epilepticus deemed unrelated to the study. Side effects resolved on their own or responded to medical management. There were no deaths, study discontinuations, or dose reductions.
The mean age in the study was 60 months, about two-thirds of the patients were girls, and CLN2 diagnosis was confirmed by genotyping. Almost all the children had seizure histories. The majority were moderately advanced at baseline, with motor-language scores of 3 out of 6 in 11 patients.
An audience member asked Dr. de Los Reyes if there would be even more benefit by starting treatment before children became symptomatic. “I think all the neurologists in this group, we know that the earlier the treatment for rare diseases, the better the response,” she said.
The results were published simultaneously in the New England Journal of Medicine.
BioMarin Pharmaceutical funded the work, along with grants from the German Federal Ministry of Education and Research, the European Union’s Horizon 2020 Research and Innovation Program, and the National Institute for Health Research. Several authors were BioMarin employees. Dr. de Los Reyes is a consultant and reported a grant from the company.
SOURCE: Schulz A et al. N Engl J Med. 2018 Apr 24. doi: 10.1056/NEJMoa1712649.
LOS ANGELES – Intraventricular administration of cerliponase alfa seemed to slow the rate of motor and language decline in an open-label trial of 23 children with neuronal ceroid lipofuscinosis type 2 disease.
Neuronal ceroid lipofuscinosis type 2 disease (CLN2), a form of Batten’s disease, is a rare lysosomal storage disorder that causes progressive dementia in children. Patients have pathogenic variants in the gene encoding lysosomal enzyme tripeptidyl peptidase 1 (TPP1). Without functioning enzyme, lysosomal storage material accumulates in neurons throughout the CNS and retina.
Symptoms start at 2-4 years with seizures and language delays, followed by rapid motor, language, and cognitive declines, and blindness. Children die in early adolescence. Treatment is symptomatic; there are no approved therapies.
The idea of the study was to replace the enzyme in the CNS with cerliponase alfa, a recombinant form of TPP1. Twenty-four children aged 3-16 years received 30 mg, 100 mg, or 300 mg intraventricular infusions every 2 weeks during the dose-finding phase of the open-label trial; they were then switched to 300 mg infused over 4 hours every 14 days for at least 96 weeks. One child dropped out after the first dose in the study, but the others continued.
The investigators used Ommaya or Rickham ventricular reservoirs to deliver the enzyme, which were more convenient than intrathecal administration, said investigator Emily de Los Reyes, MD, a pediatric neurologist at Nationwide Children’s Hospital, Columbus, Ohio.
The primary outcome was the time until a 2-point decline on the motor and language scores of the CLN2 Clinical Rating Scale, with 0 representing no function and 6 representing normal function in both domains. The mean unadjusted rate of decline in the motor-language score per 48-week period was 0.27 points in treated patients, versus 2.12 points in 42 historical controls (P less than .001). The treatment difference at 96 weeks was about 3.3 points. There was also a decrease in seizure severity and frequency.
All but one child experienced convulsions, over two-thirds pyrexia, and almost two-thirds vomiting and hypersensitivity. About half developed upper respiratory tract infections, and about half had increased CSF white-cell counts. There were also cases of device leakage, and two children developed infections detected by CSF monitoring, without symptoms of meningitis. Both continued treatment after removal of the intraventricular device, followed by antibiotics, and device replacement.
Fourteen patients (58%) had at least one grade 3 adverse event, and there was one grade 4 event: status epilepticus deemed unrelated to the study. Side effects resolved on their own or responded to medical management. There were no deaths, study discontinuations, or dose reductions.
The mean age in the study was 60 months, about two-thirds of the patients were girls, and CLN2 diagnosis was confirmed by genotyping. Almost all the children had seizure histories. The majority were moderately advanced at baseline, with motor-language scores of 3 out of 6 in 11 patients.
An audience member asked Dr. de Los Reyes if there would be even more benefit by starting treatment before children became symptomatic. “I think all the neurologists in this group, we know that the earlier the treatment for rare diseases, the better the response,” she said.
The results were published simultaneously in the New England Journal of Medicine.
BioMarin Pharmaceutical funded the work, along with grants from the German Federal Ministry of Education and Research, the European Union’s Horizon 2020 Research and Innovation Program, and the National Institute for Health Research. Several authors were BioMarin employees. Dr. de Los Reyes is a consultant and reported a grant from the company.
SOURCE: Schulz A et al. N Engl J Med. 2018 Apr 24. doi: 10.1056/NEJMoa1712649.
LOS ANGELES – Intraventricular administration of cerliponase alfa seemed to slow the rate of motor and language decline in an open-label trial of 23 children with neuronal ceroid lipofuscinosis type 2 disease.
Neuronal ceroid lipofuscinosis type 2 disease (CLN2), a form of Batten’s disease, is a rare lysosomal storage disorder that causes progressive dementia in children. Patients have pathogenic variants in the gene encoding lysosomal enzyme tripeptidyl peptidase 1 (TPP1). Without functioning enzyme, lysosomal storage material accumulates in neurons throughout the CNS and retina.
Symptoms start at 2-4 years with seizures and language delays, followed by rapid motor, language, and cognitive declines, and blindness. Children die in early adolescence. Treatment is symptomatic; there are no approved therapies.
The idea of the study was to replace the enzyme in the CNS with cerliponase alfa, a recombinant form of TPP1. Twenty-four children aged 3-16 years received 30 mg, 100 mg, or 300 mg intraventricular infusions every 2 weeks during the dose-finding phase of the open-label trial; they were then switched to 300 mg infused over 4 hours every 14 days for at least 96 weeks. One child dropped out after the first dose in the study, but the others continued.
The investigators used Ommaya or Rickham ventricular reservoirs to deliver the enzyme, which were more convenient than intrathecal administration, said investigator Emily de Los Reyes, MD, a pediatric neurologist at Nationwide Children’s Hospital, Columbus, Ohio.
The primary outcome was the time until a 2-point decline on the motor and language scores of the CLN2 Clinical Rating Scale, with 0 representing no function and 6 representing normal function in both domains. The mean unadjusted rate of decline in the motor-language score per 48-week period was 0.27 points in treated patients, versus 2.12 points in 42 historical controls (P less than .001). The treatment difference at 96 weeks was about 3.3 points. There was also a decrease in seizure severity and frequency.
All but one child experienced convulsions, over two-thirds pyrexia, and almost two-thirds vomiting and hypersensitivity. About half developed upper respiratory tract infections, and about half had increased CSF white-cell counts. There were also cases of device leakage, and two children developed infections detected by CSF monitoring, without symptoms of meningitis. Both continued treatment after removal of the intraventricular device, followed by antibiotics, and device replacement.
Fourteen patients (58%) had at least one grade 3 adverse event, and there was one grade 4 event: status epilepticus deemed unrelated to the study. Side effects resolved on their own or responded to medical management. There were no deaths, study discontinuations, or dose reductions.
The mean age in the study was 60 months, about two-thirds of the patients were girls, and CLN2 diagnosis was confirmed by genotyping. Almost all the children had seizure histories. The majority were moderately advanced at baseline, with motor-language scores of 3 out of 6 in 11 patients.
An audience member asked Dr. de Los Reyes if there would be even more benefit by starting treatment before children became symptomatic. “I think all the neurologists in this group, we know that the earlier the treatment for rare diseases, the better the response,” she said.
The results were published simultaneously in the New England Journal of Medicine.
BioMarin Pharmaceutical funded the work, along with grants from the German Federal Ministry of Education and Research, the European Union’s Horizon 2020 Research and Innovation Program, and the National Institute for Health Research. Several authors were BioMarin employees. Dr. de Los Reyes is a consultant and reported a grant from the company.
SOURCE: Schulz A et al. N Engl J Med. 2018 Apr 24. doi: 10.1056/NEJMoa1712649.
REPORTING FROM AAN 2018
Key clinical point: Intraventricular administration of cerliponase alfa seemed to slow the rate of motor and language decline in 23 children with neuronal ceroid lipofuscinosis type 2 disease.
Major finding: The mean unadjusted rate of decline in the motor-language score per 48-week period was 0.27 points in treated patients, versus 2.12 points in 42 historical controls (P less than .001).
Study details: Open-label trial of 23 children.
Disclosures: BioMarin Pharmaceutical funded the work, along with grants from the German Federal Ministry of Education and Research, the European Union’s Horizon 2020 Research and Innovation Program, and the National Institute for Health Research. Several authors were BioMarin employees. The presenter is a consultant to BioMarin and reported a grant from the company.
Source: Schulz A et al. N Engl J Med. 2018 Apr 24. doi: 10.1056/NEJMoa1712649.
DAAs open up organ donation from HCV patients
BOSTON – There was no sign of HCV infection more than a year after 10 patients at Johns Hopkins University, Baltimore, received kidneys from HCV-infected donors.
The patients were treated with prophylactic direct-acting antivirals (DAAs) before and after the procedure. Low levels of hepatitis C RNA were detected shortly after transplant in five patients, but it became undetectable within a week. None of the patients developed any clinical signs of chronic hepatitis C infection, and the transplanted kidneys functioned well.
The number of organs from HCV–infected people is on the rise because of the opioid epidemic. Organ donations from drug overdoses used to be rare, but about 10% of transplanted organs are now from an overdose death, and about 30% of people who overdose have HCV. “These are young people who could donate hearts, lungs, and kidneys, and their parents and families want them to be able to make that gift of life,” said lead investigator Christine Durand, MD, of Johns Hopkins University, Baltimore.
DAAs make that possible because they cure HCV. “If the success of these transplants continues, it could pave the way for other hepatitis C–positive organs, including hearts and livers, to be transplanted as well,” Dr. Durand and her colleagues said in a press release from Johns Hopkins.
The 10 patients were over age 50 years, with a mean age of 71 years, and had been on the kidney transplant list for an average of 4 months. The HCV-positive donors were 13-50 years old with no evidence of kidney disease (Ann Intern Med. 2018 Mar 6. doi: 10.7326/M17-2871)..
Each recipient received a dose of grazoprevir/elbasvir (Zepatier) before transplant and stayed on the medication daily for 12 weeks postop. Three patients also took a daily dose of sofosbuvir (Sovaldi) because of the strain of HCV in the donor kidney. Maybe 8 weeks of treatment, or even 4, is enough, Dr. Durand said at the Conference on Retroviruses and Opportunistic Infections.
“I am thrilled to report that at 1 year post transplant 10 out of 10 of these recipients are HCV free, and they are doing very well. Prophylactic treatment may mean that more individuals can receive transplants from hepatitis C–infected donors without transmission of infection. The use of organs from infected donors can help everyone on the transplant list by shortening wait times and shortening the wait list,” she said.
“I’m not surprised by the results of the study because these DAAs are highly effective, but I was surprised by how willing patients were to sign up for the study. They said it was a no-brainer. In our region, if you need a kidney, you are going to wait for up to 5 years, and you may die while you are waiting. If you can accept a hepatitis C–positive donor organ, you will get transplanted in a matter of weeks,” she said.
“I hope providers tell their patients with HCV that they can register as organ donors,” she said.
The work is being supported primarily by Merck Sharp & Dohme. Dr. Durand is an advisor to Bristol-Meyers Squibb, Gilead Sciences, and Merck Pharmaceuticals and has research funding from the companies.
SOURCE: Durand CM et al. Ann Intern Med. 2018 Mar 6. doi: 10.7326/M17-2871.
BOSTON – There was no sign of HCV infection more than a year after 10 patients at Johns Hopkins University, Baltimore, received kidneys from HCV-infected donors.
The patients were treated with prophylactic direct-acting antivirals (DAAs) before and after the procedure. Low levels of hepatitis C RNA were detected shortly after transplant in five patients, but it became undetectable within a week. None of the patients developed any clinical signs of chronic hepatitis C infection, and the transplanted kidneys functioned well.
The number of organs from HCV–infected people is on the rise because of the opioid epidemic. Organ donations from drug overdoses used to be rare, but about 10% of transplanted organs are now from an overdose death, and about 30% of people who overdose have HCV. “These are young people who could donate hearts, lungs, and kidneys, and their parents and families want them to be able to make that gift of life,” said lead investigator Christine Durand, MD, of Johns Hopkins University, Baltimore.
DAAs make that possible because they cure HCV. “If the success of these transplants continues, it could pave the way for other hepatitis C–positive organs, including hearts and livers, to be transplanted as well,” Dr. Durand and her colleagues said in a press release from Johns Hopkins.
The 10 patients were over age 50 years, with a mean age of 71 years, and had been on the kidney transplant list for an average of 4 months. The HCV-positive donors were 13-50 years old with no evidence of kidney disease (Ann Intern Med. 2018 Mar 6. doi: 10.7326/M17-2871)..
Each recipient received a dose of grazoprevir/elbasvir (Zepatier) before transplant and stayed on the medication daily for 12 weeks postop. Three patients also took a daily dose of sofosbuvir (Sovaldi) because of the strain of HCV in the donor kidney. Maybe 8 weeks of treatment, or even 4, is enough, Dr. Durand said at the Conference on Retroviruses and Opportunistic Infections.
“I am thrilled to report that at 1 year post transplant 10 out of 10 of these recipients are HCV free, and they are doing very well. Prophylactic treatment may mean that more individuals can receive transplants from hepatitis C–infected donors without transmission of infection. The use of organs from infected donors can help everyone on the transplant list by shortening wait times and shortening the wait list,” she said.
“I’m not surprised by the results of the study because these DAAs are highly effective, but I was surprised by how willing patients were to sign up for the study. They said it was a no-brainer. In our region, if you need a kidney, you are going to wait for up to 5 years, and you may die while you are waiting. If you can accept a hepatitis C–positive donor organ, you will get transplanted in a matter of weeks,” she said.
“I hope providers tell their patients with HCV that they can register as organ donors,” she said.
The work is being supported primarily by Merck Sharp & Dohme. Dr. Durand is an advisor to Bristol-Meyers Squibb, Gilead Sciences, and Merck Pharmaceuticals and has research funding from the companies.
SOURCE: Durand CM et al. Ann Intern Med. 2018 Mar 6. doi: 10.7326/M17-2871.
BOSTON – There was no sign of HCV infection more than a year after 10 patients at Johns Hopkins University, Baltimore, received kidneys from HCV-infected donors.
The patients were treated with prophylactic direct-acting antivirals (DAAs) before and after the procedure. Low levels of hepatitis C RNA were detected shortly after transplant in five patients, but it became undetectable within a week. None of the patients developed any clinical signs of chronic hepatitis C infection, and the transplanted kidneys functioned well.
The number of organs from HCV–infected people is on the rise because of the opioid epidemic. Organ donations from drug overdoses used to be rare, but about 10% of transplanted organs are now from an overdose death, and about 30% of people who overdose have HCV. “These are young people who could donate hearts, lungs, and kidneys, and their parents and families want them to be able to make that gift of life,” said lead investigator Christine Durand, MD, of Johns Hopkins University, Baltimore.
DAAs make that possible because they cure HCV. “If the success of these transplants continues, it could pave the way for other hepatitis C–positive organs, including hearts and livers, to be transplanted as well,” Dr. Durand and her colleagues said in a press release from Johns Hopkins.
The 10 patients were over age 50 years, with a mean age of 71 years, and had been on the kidney transplant list for an average of 4 months. The HCV-positive donors were 13-50 years old with no evidence of kidney disease (Ann Intern Med. 2018 Mar 6. doi: 10.7326/M17-2871)..
Each recipient received a dose of grazoprevir/elbasvir (Zepatier) before transplant and stayed on the medication daily for 12 weeks postop. Three patients also took a daily dose of sofosbuvir (Sovaldi) because of the strain of HCV in the donor kidney. Maybe 8 weeks of treatment, or even 4, is enough, Dr. Durand said at the Conference on Retroviruses and Opportunistic Infections.
“I am thrilled to report that at 1 year post transplant 10 out of 10 of these recipients are HCV free, and they are doing very well. Prophylactic treatment may mean that more individuals can receive transplants from hepatitis C–infected donors without transmission of infection. The use of organs from infected donors can help everyone on the transplant list by shortening wait times and shortening the wait list,” she said.
“I’m not surprised by the results of the study because these DAAs are highly effective, but I was surprised by how willing patients were to sign up for the study. They said it was a no-brainer. In our region, if you need a kidney, you are going to wait for up to 5 years, and you may die while you are waiting. If you can accept a hepatitis C–positive donor organ, you will get transplanted in a matter of weeks,” she said.
“I hope providers tell their patients with HCV that they can register as organ donors,” she said.
The work is being supported primarily by Merck Sharp & Dohme. Dr. Durand is an advisor to Bristol-Meyers Squibb, Gilead Sciences, and Merck Pharmaceuticals and has research funding from the companies.
SOURCE: Durand CM et al. Ann Intern Med. 2018 Mar 6. doi: 10.7326/M17-2871.
REPORTING FROM CROI
Key clinical point: HCV may soon no longer bar organ donation.
Major finding: There was no sign of HCV infection more than a year after 10 patients at Johns Hopkins University, Baltimore, received kidneys from HCV-infected donors.
Study details: Open-label nonrandomized trial.
Disclosures: The work is being supported primarily by Merck Sharp & Dohme. The study lead is an advisor to Bristol-Meyers Squibb, Gilead Sciences, and Merck Pharmaceuticals, and has research funding from the companies.
Source: Durand CM et al. Ann Intern Med. 2018 Mar 6. doi: 10.7326/M17-2871.
VTE risk after bariatric surgery should be assessed
SEATTLE – Preop thromboelastometry can identify patients who need extra according to a prospective investigation of 40 patients at Conemaugh Memorial Medical Center in Johnstown, Pa.
Enoxaparin 40 mg twice daily just wasn’t enough for people who were hypercoagulable before surgery. The goal of the study was to find the best way to prevent venous thromboembolism (VTE) after weight loss surgery. At present, there’s no consensus on prophylaxis dosing, timing, duration, or even what agent to use for these patients. Conemaugh uses postop enoxaparin, a low-molecular-weight heparin. Among many other options, some hospitals opt for preop dosing with traditional heparin, which is less expensive.
The Conemaugh team turned to thromboelastometry (TEM) to look at the question of VTE risk in bariatric surgery patients. The test gauges coagulation status by measuring elasticity as a small blood sample clots over a few minutes. The investigators found that patients who were hypercoagulable before surgery were likely to be hypercoagulable afterwards. The finding argues for baseline TEM testing to guide postop anticoagulation.
The problem is that bariatric services don’t often have access to TEM equipment, and insurance doesn’t cover the $60 test. In this instance, the Lake Erie College of Osteopathic Medicine in Erie, Pa., had the equipment and covered the testing for the study.
The patients had TEM at baseline and then received 40 mg of enoxaparin about 4 hours after surgery – mostly laparoscopic gastric bypasses – and a second dose about 12 hours after the first. TEM was repeated about 2 hours after the second dose.
At baseline, 2 (5%) of the patients were hypocoagulable, 15 (37.5%) were normal, and 23 (57.5%) were hypercoagulable. On postop TEM, 17 patients (42.5%) were normal and 23 (57.5%) were hypercoagulable: “These 23 were inadequately anticoagulated,” said lead investigator Daniel Urias, MD, a general surgery resident at the medical center.
“There was an association between being normal at baseline and being normal postop, and being hypercoagulable at baseline and hypercoagulable postop. We didn’t anticipate finding such similarity between the numbers. Our suspicion that baseline status plays a major role is holding true,” Dr. Urias said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
When patients test hypercoagulable at baseline, “we are [now] leaning towards [enoxaparin] 60 mg twice daily,” he said.
Ultimately, anticoagulation TEM could be used to titrate patients into the normal range. For best outcomes, it’s likely that “obese patients require goal-directed therapy instead of weight-based or fixed dosing,” he said, but nothing is going to happen until insurance steps up.
The patients did not have underlying coagulopathies, and 33 (82.5%) were women; the average age was 44 years and average body mass index was 43.6 kg/m2. The mean preop Caprini score was 4, indicating moderate VTE risk. Surgery lasted about 200 minutes. Patients were out of bed and walking on postop day 0.
The investigators had no relevant disclosures.
SOURCE: Urias D et al. World Congress of Endoscopic Surgery hosted by SAGES & CAGS abstract S023.
SEATTLE – Preop thromboelastometry can identify patients who need extra according to a prospective investigation of 40 patients at Conemaugh Memorial Medical Center in Johnstown, Pa.
Enoxaparin 40 mg twice daily just wasn’t enough for people who were hypercoagulable before surgery. The goal of the study was to find the best way to prevent venous thromboembolism (VTE) after weight loss surgery. At present, there’s no consensus on prophylaxis dosing, timing, duration, or even what agent to use for these patients. Conemaugh uses postop enoxaparin, a low-molecular-weight heparin. Among many other options, some hospitals opt for preop dosing with traditional heparin, which is less expensive.
The Conemaugh team turned to thromboelastometry (TEM) to look at the question of VTE risk in bariatric surgery patients. The test gauges coagulation status by measuring elasticity as a small blood sample clots over a few minutes. The investigators found that patients who were hypercoagulable before surgery were likely to be hypercoagulable afterwards. The finding argues for baseline TEM testing to guide postop anticoagulation.
The problem is that bariatric services don’t often have access to TEM equipment, and insurance doesn’t cover the $60 test. In this instance, the Lake Erie College of Osteopathic Medicine in Erie, Pa., had the equipment and covered the testing for the study.
The patients had TEM at baseline and then received 40 mg of enoxaparin about 4 hours after surgery – mostly laparoscopic gastric bypasses – and a second dose about 12 hours after the first. TEM was repeated about 2 hours after the second dose.
At baseline, 2 (5%) of the patients were hypocoagulable, 15 (37.5%) were normal, and 23 (57.5%) were hypercoagulable. On postop TEM, 17 patients (42.5%) were normal and 23 (57.5%) were hypercoagulable: “These 23 were inadequately anticoagulated,” said lead investigator Daniel Urias, MD, a general surgery resident at the medical center.
“There was an association between being normal at baseline and being normal postop, and being hypercoagulable at baseline and hypercoagulable postop. We didn’t anticipate finding such similarity between the numbers. Our suspicion that baseline status plays a major role is holding true,” Dr. Urias said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
When patients test hypercoagulable at baseline, “we are [now] leaning towards [enoxaparin] 60 mg twice daily,” he said.
Ultimately, anticoagulation TEM could be used to titrate patients into the normal range. For best outcomes, it’s likely that “obese patients require goal-directed therapy instead of weight-based or fixed dosing,” he said, but nothing is going to happen until insurance steps up.
The patients did not have underlying coagulopathies, and 33 (82.5%) were women; the average age was 44 years and average body mass index was 43.6 kg/m2. The mean preop Caprini score was 4, indicating moderate VTE risk. Surgery lasted about 200 minutes. Patients were out of bed and walking on postop day 0.
The investigators had no relevant disclosures.
SOURCE: Urias D et al. World Congress of Endoscopic Surgery hosted by SAGES & CAGS abstract S023.
SEATTLE – Preop thromboelastometry can identify patients who need extra according to a prospective investigation of 40 patients at Conemaugh Memorial Medical Center in Johnstown, Pa.
Enoxaparin 40 mg twice daily just wasn’t enough for people who were hypercoagulable before surgery. The goal of the study was to find the best way to prevent venous thromboembolism (VTE) after weight loss surgery. At present, there’s no consensus on prophylaxis dosing, timing, duration, or even what agent to use for these patients. Conemaugh uses postop enoxaparin, a low-molecular-weight heparin. Among many other options, some hospitals opt for preop dosing with traditional heparin, which is less expensive.
The Conemaugh team turned to thromboelastometry (TEM) to look at the question of VTE risk in bariatric surgery patients. The test gauges coagulation status by measuring elasticity as a small blood sample clots over a few minutes. The investigators found that patients who were hypercoagulable before surgery were likely to be hypercoagulable afterwards. The finding argues for baseline TEM testing to guide postop anticoagulation.
The problem is that bariatric services don’t often have access to TEM equipment, and insurance doesn’t cover the $60 test. In this instance, the Lake Erie College of Osteopathic Medicine in Erie, Pa., had the equipment and covered the testing for the study.
The patients had TEM at baseline and then received 40 mg of enoxaparin about 4 hours after surgery – mostly laparoscopic gastric bypasses – and a second dose about 12 hours after the first. TEM was repeated about 2 hours after the second dose.
At baseline, 2 (5%) of the patients were hypocoagulable, 15 (37.5%) were normal, and 23 (57.5%) were hypercoagulable. On postop TEM, 17 patients (42.5%) were normal and 23 (57.5%) were hypercoagulable: “These 23 were inadequately anticoagulated,” said lead investigator Daniel Urias, MD, a general surgery resident at the medical center.
“There was an association between being normal at baseline and being normal postop, and being hypercoagulable at baseline and hypercoagulable postop. We didn’t anticipate finding such similarity between the numbers. Our suspicion that baseline status plays a major role is holding true,” Dr. Urias said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
When patients test hypercoagulable at baseline, “we are [now] leaning towards [enoxaparin] 60 mg twice daily,” he said.
Ultimately, anticoagulation TEM could be used to titrate patients into the normal range. For best outcomes, it’s likely that “obese patients require goal-directed therapy instead of weight-based or fixed dosing,” he said, but nothing is going to happen until insurance steps up.
The patients did not have underlying coagulopathies, and 33 (82.5%) were women; the average age was 44 years and average body mass index was 43.6 kg/m2. The mean preop Caprini score was 4, indicating moderate VTE risk. Surgery lasted about 200 minutes. Patients were out of bed and walking on postop day 0.
The investigators had no relevant disclosures.
SOURCE: Urias D et al. World Congress of Endoscopic Surgery hosted by SAGES & CAGS abstract S023.
REPORTING FROM SAGES 2018
Key clinical point: Preoperative thromboelastometry identifies patients who need extra anticoagulation against venous thromboembolism following bariatric surgery.
Major finding: Baseline and postop coagulation were similar: 37.5% vs. 42.5% were normal and 57.5% vs 57.5% were hypercoagulable.
Study details: Prospective study of 40 bariatric surgery patients.
Disclosures: The investigators did not have any relevant disclosures. The Lake Erie College of Osteopathic Medicine paid for the testing.
Source: Urias D et al. World Congress of Endoscopic Surgery hosted by SAGES & CAGS abstract S023.
Dexamethasone lowered risk of urinary retention in laparoscopic hernia repair
SEATTLE – Intraoperative in 955 men at the NorthShore University HealthSystem, Chicago.
Urinary retention occurs in up to a third of hernia repair patients. Men are at far higher risk than women; benign prostatic hypertrophy (BPH) and older age also increase the risk.
Intraoperative dexamethasone is a common antiemetic. The investigators had a hunch that it also reduces urinary retention by calming overstimulation of the bladder neck and prostate during the operation. “We believe this overstimulation” causes urinary retention, lead investigator Merritt Denham, BS, said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
She and her team went back in the records about 8 years to compare 617 laparoscopic inguinal hernia repair patients who received intraoperative dexamethasone with 338 who did not. They were all men: women were excluded from the review. The men voided before surgery. Those who received dexamethasone received more fluids during the operation than those who did not, a mean of 973 mL versus 878 mL (P = .0019).
Even so, urinary retention was far less likely in the dexamethasone group (3.7% vs. 9.8%; P = .0001). Controlling for age and BPH, the corticosteroid was highly protective (odds ratio, 0.48; 95% confidence interval, 0.26-0.87; P = .0147). The benefit was the same regardless of the intraoperative dexamethasone dosage, which ranged from 4 mg to 8 mg.
Dexamethasone patients had a shorter length of stay, and, counterintuitively, fewer surgical site infections (0.2% vs. 1.7%; P = .0109). They were also less likely to have BPH (16.7% vs. 22.5%; P = 0.026). The urinary retention odds ratio controlled for the difference in BPH.
The results are “interesting, but I don’t think the conclusion is there yet; there are a lot of variables to consider. We need more data,” said moderator Eduardo Parra-Davila, MD, FACS, director of minimally invasive and colorectal surgery at Florida Hospital Celebration Health in Celebration, Fla.
In both groups, mean body mass index was about 26 kg/m2, mean age about 57 years, and mean operative time about 40 minutes. Four general surgeons performed the repairs.
There was no external funding for the work, and the investigators had no disclosures.
SOURCE: Denham M. et al. SAGES 2018, Abstract S006.
SEATTLE – Intraoperative in 955 men at the NorthShore University HealthSystem, Chicago.
Urinary retention occurs in up to a third of hernia repair patients. Men are at far higher risk than women; benign prostatic hypertrophy (BPH) and older age also increase the risk.
Intraoperative dexamethasone is a common antiemetic. The investigators had a hunch that it also reduces urinary retention by calming overstimulation of the bladder neck and prostate during the operation. “We believe this overstimulation” causes urinary retention, lead investigator Merritt Denham, BS, said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
She and her team went back in the records about 8 years to compare 617 laparoscopic inguinal hernia repair patients who received intraoperative dexamethasone with 338 who did not. They were all men: women were excluded from the review. The men voided before surgery. Those who received dexamethasone received more fluids during the operation than those who did not, a mean of 973 mL versus 878 mL (P = .0019).
Even so, urinary retention was far less likely in the dexamethasone group (3.7% vs. 9.8%; P = .0001). Controlling for age and BPH, the corticosteroid was highly protective (odds ratio, 0.48; 95% confidence interval, 0.26-0.87; P = .0147). The benefit was the same regardless of the intraoperative dexamethasone dosage, which ranged from 4 mg to 8 mg.
Dexamethasone patients had a shorter length of stay, and, counterintuitively, fewer surgical site infections (0.2% vs. 1.7%; P = .0109). They were also less likely to have BPH (16.7% vs. 22.5%; P = 0.026). The urinary retention odds ratio controlled for the difference in BPH.
The results are “interesting, but I don’t think the conclusion is there yet; there are a lot of variables to consider. We need more data,” said moderator Eduardo Parra-Davila, MD, FACS, director of minimally invasive and colorectal surgery at Florida Hospital Celebration Health in Celebration, Fla.
In both groups, mean body mass index was about 26 kg/m2, mean age about 57 years, and mean operative time about 40 minutes. Four general surgeons performed the repairs.
There was no external funding for the work, and the investigators had no disclosures.
SOURCE: Denham M. et al. SAGES 2018, Abstract S006.
SEATTLE – Intraoperative in 955 men at the NorthShore University HealthSystem, Chicago.
Urinary retention occurs in up to a third of hernia repair patients. Men are at far higher risk than women; benign prostatic hypertrophy (BPH) and older age also increase the risk.
Intraoperative dexamethasone is a common antiemetic. The investigators had a hunch that it also reduces urinary retention by calming overstimulation of the bladder neck and prostate during the operation. “We believe this overstimulation” causes urinary retention, lead investigator Merritt Denham, BS, said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
She and her team went back in the records about 8 years to compare 617 laparoscopic inguinal hernia repair patients who received intraoperative dexamethasone with 338 who did not. They were all men: women were excluded from the review. The men voided before surgery. Those who received dexamethasone received more fluids during the operation than those who did not, a mean of 973 mL versus 878 mL (P = .0019).
Even so, urinary retention was far less likely in the dexamethasone group (3.7% vs. 9.8%; P = .0001). Controlling for age and BPH, the corticosteroid was highly protective (odds ratio, 0.48; 95% confidence interval, 0.26-0.87; P = .0147). The benefit was the same regardless of the intraoperative dexamethasone dosage, which ranged from 4 mg to 8 mg.
Dexamethasone patients had a shorter length of stay, and, counterintuitively, fewer surgical site infections (0.2% vs. 1.7%; P = .0109). They were also less likely to have BPH (16.7% vs. 22.5%; P = 0.026). The urinary retention odds ratio controlled for the difference in BPH.
The results are “interesting, but I don’t think the conclusion is there yet; there are a lot of variables to consider. We need more data,” said moderator Eduardo Parra-Davila, MD, FACS, director of minimally invasive and colorectal surgery at Florida Hospital Celebration Health in Celebration, Fla.
In both groups, mean body mass index was about 26 kg/m2, mean age about 57 years, and mean operative time about 40 minutes. Four general surgeons performed the repairs.
There was no external funding for the work, and the investigators had no disclosures.
SOURCE: Denham M. et al. SAGES 2018, Abstract S006.
REPORTING FROM SAGES 2018
Key clinical point: Patients given dexamethasone intraoperatively were less likely to have urinary retention.
Major finding: The dexamethasone group was less likely to have urinary retention, 3.7% versus 9.8% (P = 0.0001).
Study details: A review of 955 laparoscopic inguinal hernia repairs.
Disclosures: There was no external funding for the work, and the investigators had no disclosures.
Source: Denham M et al. SAGES 2018, Abstract S006.
Robotic approach falls short for sleeve gastrectomy
SEATTLE – according to a review of 86,953 cases in the 2015 Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program database.
“Robotic sleeve gastrectomy increases [use of] hospital resources. ... These findings may explain the low utilization rate of the robotic approach to sleeve gastrectomy,” said lead investigator Reza Alizadeh, MD, a surgery resident at the University of California, Irvine.
Sleeve gastrectomy has eclipsed gastric bypass as the most common weight loss surgery in United States. While most are done laparoscopically, the use of robots is becoming more common, so the investigators wanted to compare outcomes in a large number of cases. They turned to the metabolic and bariatric surgery database, which is jointly maintained by the American College of Surgeons and the American Society for Metabolic and Bariatric Surgery. Emergent, converted, and revision cases were excluded from the analysis to avoid confounding.
Almost 94% of the cases were done laparoscopically, with the rest done robotically. Mean operative time was 101 min in the robotic arm, and 1.5% of patients developed anastomotic leaks. Mean operative time in the laparoscopic group was 74 minutes, and 0.5% of patients developed leaks. After adjustment for potential confounders, leaks were 3.4 times more likely with the robotic approach (95% confidence interval, 2.47-4.0; P less than .01). It wasn’t possible to determine whether there were any differences in the type of stapling done in the two groups.
Meanwhile, 0.8% of robotic surgery patients developed surgical site infections versus 0.6% of the laparoscopic cases. After adjustment, infections were 38% more likely with the robot (95% CI, 1.01-1.89; P = 0.03). Dr. Alizadeh noted that the database only goes out to 30 days, so “the true complication rates may be underestimated.”
The findings are consistent with previous investigations. It’s unclear whether there’s something inherently riskier about robotic sleeve gastrectomy itself or whether surgeons haven’t quite got the knack of it yet. The higher leak rate with robotic surgery, “I believe, is mostly related to the small number of [robotic] cases being done. We are still in the beginning stages of utilizing the robotic approach. Maybe there’s a learning curve, and we need more experience and more practice,” Dr. Alizadeh said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
Indeed, others have reported that it takes more than two dozen cases to become proficient in another procedure, robotic esophagectomy.
The mean length of stay in the study was slightly, but not statistically significantly, longer in the robotic arm (1.8 vs. 1.7 days; P = 0.17). There was no statistically significant difference in in-hospital mortality.
The laparoscopic group had more men than did the robotic group (21.4% vs. 19.7%, respectively) and more chronic steroid use (1.7% vs. 1.3%), plus more patients were dependent on oxygen (0.7% vs. 0.3%). The robotic group had more obstructive sleep apnea than did the laparoscopic group (37.3% vs. 36% of cases) and a higher incidence of hypoalbuminemia (8.4% vs. 7%). The analysis adjusted for the differences.
The findings were pretty much the same when the team repeated their analysis with the 2016 database numbers, which were released while the SAGES presentation was being prepared. The only big difference was an increase in the number of robotic cases, up from 6.1% in 2015 to 6.6% of cases in 2016.
The was no external funding for the work, and the investigators had no relevant disclosures.
SOURCE: Alizadeh RF et al. SAGES 2018, Abstract S024.
SEATTLE – according to a review of 86,953 cases in the 2015 Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program database.
“Robotic sleeve gastrectomy increases [use of] hospital resources. ... These findings may explain the low utilization rate of the robotic approach to sleeve gastrectomy,” said lead investigator Reza Alizadeh, MD, a surgery resident at the University of California, Irvine.
Sleeve gastrectomy has eclipsed gastric bypass as the most common weight loss surgery in United States. While most are done laparoscopically, the use of robots is becoming more common, so the investigators wanted to compare outcomes in a large number of cases. They turned to the metabolic and bariatric surgery database, which is jointly maintained by the American College of Surgeons and the American Society for Metabolic and Bariatric Surgery. Emergent, converted, and revision cases were excluded from the analysis to avoid confounding.
Almost 94% of the cases were done laparoscopically, with the rest done robotically. Mean operative time was 101 min in the robotic arm, and 1.5% of patients developed anastomotic leaks. Mean operative time in the laparoscopic group was 74 minutes, and 0.5% of patients developed leaks. After adjustment for potential confounders, leaks were 3.4 times more likely with the robotic approach (95% confidence interval, 2.47-4.0; P less than .01). It wasn’t possible to determine whether there were any differences in the type of stapling done in the two groups.
Meanwhile, 0.8% of robotic surgery patients developed surgical site infections versus 0.6% of the laparoscopic cases. After adjustment, infections were 38% more likely with the robot (95% CI, 1.01-1.89; P = 0.03). Dr. Alizadeh noted that the database only goes out to 30 days, so “the true complication rates may be underestimated.”
The findings are consistent with previous investigations. It’s unclear whether there’s something inherently riskier about robotic sleeve gastrectomy itself or whether surgeons haven’t quite got the knack of it yet. The higher leak rate with robotic surgery, “I believe, is mostly related to the small number of [robotic] cases being done. We are still in the beginning stages of utilizing the robotic approach. Maybe there’s a learning curve, and we need more experience and more practice,” Dr. Alizadeh said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
Indeed, others have reported that it takes more than two dozen cases to become proficient in another procedure, robotic esophagectomy.
The mean length of stay in the study was slightly, but not statistically significantly, longer in the robotic arm (1.8 vs. 1.7 days; P = 0.17). There was no statistically significant difference in in-hospital mortality.
The laparoscopic group had more men than did the robotic group (21.4% vs. 19.7%, respectively) and more chronic steroid use (1.7% vs. 1.3%), plus more patients were dependent on oxygen (0.7% vs. 0.3%). The robotic group had more obstructive sleep apnea than did the laparoscopic group (37.3% vs. 36% of cases) and a higher incidence of hypoalbuminemia (8.4% vs. 7%). The analysis adjusted for the differences.
The findings were pretty much the same when the team repeated their analysis with the 2016 database numbers, which were released while the SAGES presentation was being prepared. The only big difference was an increase in the number of robotic cases, up from 6.1% in 2015 to 6.6% of cases in 2016.
The was no external funding for the work, and the investigators had no relevant disclosures.
SOURCE: Alizadeh RF et al. SAGES 2018, Abstract S024.
SEATTLE – according to a review of 86,953 cases in the 2015 Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program database.
“Robotic sleeve gastrectomy increases [use of] hospital resources. ... These findings may explain the low utilization rate of the robotic approach to sleeve gastrectomy,” said lead investigator Reza Alizadeh, MD, a surgery resident at the University of California, Irvine.
Sleeve gastrectomy has eclipsed gastric bypass as the most common weight loss surgery in United States. While most are done laparoscopically, the use of robots is becoming more common, so the investigators wanted to compare outcomes in a large number of cases. They turned to the metabolic and bariatric surgery database, which is jointly maintained by the American College of Surgeons and the American Society for Metabolic and Bariatric Surgery. Emergent, converted, and revision cases were excluded from the analysis to avoid confounding.
Almost 94% of the cases were done laparoscopically, with the rest done robotically. Mean operative time was 101 min in the robotic arm, and 1.5% of patients developed anastomotic leaks. Mean operative time in the laparoscopic group was 74 minutes, and 0.5% of patients developed leaks. After adjustment for potential confounders, leaks were 3.4 times more likely with the robotic approach (95% confidence interval, 2.47-4.0; P less than .01). It wasn’t possible to determine whether there were any differences in the type of stapling done in the two groups.
Meanwhile, 0.8% of robotic surgery patients developed surgical site infections versus 0.6% of the laparoscopic cases. After adjustment, infections were 38% more likely with the robot (95% CI, 1.01-1.89; P = 0.03). Dr. Alizadeh noted that the database only goes out to 30 days, so “the true complication rates may be underestimated.”
The findings are consistent with previous investigations. It’s unclear whether there’s something inherently riskier about robotic sleeve gastrectomy itself or whether surgeons haven’t quite got the knack of it yet. The higher leak rate with robotic surgery, “I believe, is mostly related to the small number of [robotic] cases being done. We are still in the beginning stages of utilizing the robotic approach. Maybe there’s a learning curve, and we need more experience and more practice,” Dr. Alizadeh said at the World Congress of Endoscopic Surgery hosted by SAGES & CAGS.
Indeed, others have reported that it takes more than two dozen cases to become proficient in another procedure, robotic esophagectomy.
The mean length of stay in the study was slightly, but not statistically significantly, longer in the robotic arm (1.8 vs. 1.7 days; P = 0.17). There was no statistically significant difference in in-hospital mortality.
The laparoscopic group had more men than did the robotic group (21.4% vs. 19.7%, respectively) and more chronic steroid use (1.7% vs. 1.3%), plus more patients were dependent on oxygen (0.7% vs. 0.3%). The robotic group had more obstructive sleep apnea than did the laparoscopic group (37.3% vs. 36% of cases) and a higher incidence of hypoalbuminemia (8.4% vs. 7%). The analysis adjusted for the differences.
The findings were pretty much the same when the team repeated their analysis with the 2016 database numbers, which were released while the SAGES presentation was being prepared. The only big difference was an increase in the number of robotic cases, up from 6.1% in 2015 to 6.6% of cases in 2016.
The was no external funding for the work, and the investigators had no relevant disclosures.
SOURCE: Alizadeh RF et al. SAGES 2018, Abstract S024.
REPORTING FROM SAGES 2018
Key clinical point: Operative times are longer, and leaks and surgical site infections more common, when surgeons opt for robotic instead of laparoscopic sleeve gastrectomy.
Major finding: Anastomotic leaks were 3.4 times more likely with the robotic approach (95% CI 2.47-4.0; P less than .01).
Study details: Review of 86,953 cases in the 2015 Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program database
Disclosures: The was no external funding for the project, and the investigators had no relevant disclosures.
Source: Alizadeh RF et al. SAGES 2018, Abstract S024
Estrogen patch counters eating disorders in women athletes
CHICAGO – It’s a good idea to look for eating disorders in young, athletic women who present with oligomenorrhea; they are at high risk for them and can be helped with estrogen replacement, especially with a patch, according to investigators from Massachusetts General Hospital, Boston.
Estrogen replacement will also help with stress fractures and other bone problems, but young, athletic women might resist the idea. They worry that it might hurt their performance and are often proud that they work out hard enough to stop their periods, according to investigator Vibha Singhal, MD, a pediatric endocrinologist and eating disorder specialist at the hospital.
Earlier research done at Massachusetts General had shown that replacing estrogen to physiological levels helped reduce anxiety and body dissatisfaction in anorexia nervosa. Both are key drivers of the condition, along with the drive for thinness, lead investigator Franziska Plessow, PhD, a neuroendocrine researcher at the hospital, said at the Endocrine Society’s annual meeting.
But the researchers wondered whether estrogen also helps healthy weight women with nascent eating disorders, so the investigators turned to female athletes aged 14-25 years who had stopped menstruating or were about to.
The 117 oligomenorrheic athletes (OA) they investigated – none of whom had formally diagnosed eating disorders – scored significantly higher on measures of body dissatisfaction, drive for thinness, perfectionism, and “cognitive restraint of eating,” compared with 50 female athletes and 41 nonathletic women, both with normal periods. For instance, OA women scored a mean of 4.21 on the drive for thinness scale of the Eating Disorder Inventory–2, a low score, but still significantly higher than the 1.66 points in eumenorrheic athletes and 1.61 points in nonathletes (P = .0005).
Oligomenorrheic female athletes “show more disordered eating behavior and psychopathology at the subclinical level,” Dr. Plessow said.
Seventy OA women were then randomized to three groups: 25 to physiological estrogen replacement with an estradiol patch and cyclic progesterone for 12 days/month; 19 to replacement with contraceptive pills on the standard monthly schedule; and 26 to no replacement.
Over 12 months, women on the patch dropped their drive for thinness, body dissatisfaction, and uncontrolled eating scores. Body dissatisfaction scores on the Eating Disorder Inventory–2, for example, fell about two points, compared with staying about the same in the pill group and increasing by about two points in the no-estrogen group.
The pill seemed to help a bit on some measures, too, but the benefit of the pill versus that of no estrogen wasn’t generally statistically significant. Meanwhile, symptoms worsened in women who didn’t get estrogen. “The practice right now is the pill. We are shifting our practice with these data to the patch,” Dr. Singhal said.
Overall, “these findings emphasize the importance of normalizing estrogen levels in this population,” she and her colleagues concluded.
It’s a mystery why estrogen helps with eating disorders. Maybe it has something to do with the estrogen receptors in the appetite centers of the brain. Maybe the patch works better than the pill because there’s no first-pass through the liver, Dr. Singhal said.
Subjects were aged about 20 years, on average. OA women had a mean body mass index of 20.6 kg/m2 and a mean estradiol level of 45 pg/mL. Subjects with regular periods had mean BMIs of about 22 kg/m2; mean estradiol levels were 70.2 pg/mL in eumenorrheic athletes and 83.6 pg/mL in nonathletic women.
The work was funded by the National Institutes of Health. The investigators didn’t have any relevant disclosures.
SOURCE: Plessow F et al. ENDO 2018, Abstract SAT-290.
CHICAGO – It’s a good idea to look for eating disorders in young, athletic women who present with oligomenorrhea; they are at high risk for them and can be helped with estrogen replacement, especially with a patch, according to investigators from Massachusetts General Hospital, Boston.
Estrogen replacement will also help with stress fractures and other bone problems, but young, athletic women might resist the idea. They worry that it might hurt their performance and are often proud that they work out hard enough to stop their periods, according to investigator Vibha Singhal, MD, a pediatric endocrinologist and eating disorder specialist at the hospital.
Earlier research done at Massachusetts General had shown that replacing estrogen to physiological levels helped reduce anxiety and body dissatisfaction in anorexia nervosa. Both are key drivers of the condition, along with the drive for thinness, lead investigator Franziska Plessow, PhD, a neuroendocrine researcher at the hospital, said at the Endocrine Society’s annual meeting.
But the researchers wondered whether estrogen also helps healthy weight women with nascent eating disorders, so the investigators turned to female athletes aged 14-25 years who had stopped menstruating or were about to.
The 117 oligomenorrheic athletes (OA) they investigated – none of whom had formally diagnosed eating disorders – scored significantly higher on measures of body dissatisfaction, drive for thinness, perfectionism, and “cognitive restraint of eating,” compared with 50 female athletes and 41 nonathletic women, both with normal periods. For instance, OA women scored a mean of 4.21 on the drive for thinness scale of the Eating Disorder Inventory–2, a low score, but still significantly higher than the 1.66 points in eumenorrheic athletes and 1.61 points in nonathletes (P = .0005).
Oligomenorrheic female athletes “show more disordered eating behavior and psychopathology at the subclinical level,” Dr. Plessow said.
Seventy OA women were then randomized to three groups: 25 to physiological estrogen replacement with an estradiol patch and cyclic progesterone for 12 days/month; 19 to replacement with contraceptive pills on the standard monthly schedule; and 26 to no replacement.
Over 12 months, women on the patch dropped their drive for thinness, body dissatisfaction, and uncontrolled eating scores. Body dissatisfaction scores on the Eating Disorder Inventory–2, for example, fell about two points, compared with staying about the same in the pill group and increasing by about two points in the no-estrogen group.
The pill seemed to help a bit on some measures, too, but the benefit of the pill versus that of no estrogen wasn’t generally statistically significant. Meanwhile, symptoms worsened in women who didn’t get estrogen. “The practice right now is the pill. We are shifting our practice with these data to the patch,” Dr. Singhal said.
Overall, “these findings emphasize the importance of normalizing estrogen levels in this population,” she and her colleagues concluded.
It’s a mystery why estrogen helps with eating disorders. Maybe it has something to do with the estrogen receptors in the appetite centers of the brain. Maybe the patch works better than the pill because there’s no first-pass through the liver, Dr. Singhal said.
Subjects were aged about 20 years, on average. OA women had a mean body mass index of 20.6 kg/m2 and a mean estradiol level of 45 pg/mL. Subjects with regular periods had mean BMIs of about 22 kg/m2; mean estradiol levels were 70.2 pg/mL in eumenorrheic athletes and 83.6 pg/mL in nonathletic women.
The work was funded by the National Institutes of Health. The investigators didn’t have any relevant disclosures.
SOURCE: Plessow F et al. ENDO 2018, Abstract SAT-290.
CHICAGO – It’s a good idea to look for eating disorders in young, athletic women who present with oligomenorrhea; they are at high risk for them and can be helped with estrogen replacement, especially with a patch, according to investigators from Massachusetts General Hospital, Boston.
Estrogen replacement will also help with stress fractures and other bone problems, but young, athletic women might resist the idea. They worry that it might hurt their performance and are often proud that they work out hard enough to stop their periods, according to investigator Vibha Singhal, MD, a pediatric endocrinologist and eating disorder specialist at the hospital.
Earlier research done at Massachusetts General had shown that replacing estrogen to physiological levels helped reduce anxiety and body dissatisfaction in anorexia nervosa. Both are key drivers of the condition, along with the drive for thinness, lead investigator Franziska Plessow, PhD, a neuroendocrine researcher at the hospital, said at the Endocrine Society’s annual meeting.
But the researchers wondered whether estrogen also helps healthy weight women with nascent eating disorders, so the investigators turned to female athletes aged 14-25 years who had stopped menstruating or were about to.
The 117 oligomenorrheic athletes (OA) they investigated – none of whom had formally diagnosed eating disorders – scored significantly higher on measures of body dissatisfaction, drive for thinness, perfectionism, and “cognitive restraint of eating,” compared with 50 female athletes and 41 nonathletic women, both with normal periods. For instance, OA women scored a mean of 4.21 on the drive for thinness scale of the Eating Disorder Inventory–2, a low score, but still significantly higher than the 1.66 points in eumenorrheic athletes and 1.61 points in nonathletes (P = .0005).
Oligomenorrheic female athletes “show more disordered eating behavior and psychopathology at the subclinical level,” Dr. Plessow said.
Seventy OA women were then randomized to three groups: 25 to physiological estrogen replacement with an estradiol patch and cyclic progesterone for 12 days/month; 19 to replacement with contraceptive pills on the standard monthly schedule; and 26 to no replacement.
Over 12 months, women on the patch dropped their drive for thinness, body dissatisfaction, and uncontrolled eating scores. Body dissatisfaction scores on the Eating Disorder Inventory–2, for example, fell about two points, compared with staying about the same in the pill group and increasing by about two points in the no-estrogen group.
The pill seemed to help a bit on some measures, too, but the benefit of the pill versus that of no estrogen wasn’t generally statistically significant. Meanwhile, symptoms worsened in women who didn’t get estrogen. “The practice right now is the pill. We are shifting our practice with these data to the patch,” Dr. Singhal said.
Overall, “these findings emphasize the importance of normalizing estrogen levels in this population,” she and her colleagues concluded.
It’s a mystery why estrogen helps with eating disorders. Maybe it has something to do with the estrogen receptors in the appetite centers of the brain. Maybe the patch works better than the pill because there’s no first-pass through the liver, Dr. Singhal said.
Subjects were aged about 20 years, on average. OA women had a mean body mass index of 20.6 kg/m2 and a mean estradiol level of 45 pg/mL. Subjects with regular periods had mean BMIs of about 22 kg/m2; mean estradiol levels were 70.2 pg/mL in eumenorrheic athletes and 83.6 pg/mL in nonathletic women.
The work was funded by the National Institutes of Health. The investigators didn’t have any relevant disclosures.
SOURCE: Plessow F et al. ENDO 2018, Abstract SAT-290.
REPORTING FROM ENDO 2018
Key clinical point: It’s a good idea to look for eating disorders in young, athletic women who present with oligo-amenorrhea; they’re at high risk for them and can be helped with estrogen replacement, especially with a patch.
Major finding: Over 12 months, body dissatisfaction scores fell about 2 points among women on the patch, versus staying about the same in the pill group, and increasing about 2 points in the no-estrogen group.
Study details: Combined cross-sectional and randomized investigation
Disclosures: The work was supported by the National Institutes of Health. The investigators didn’t have any disclosures.
Source: Plessow F et al. ENDO 2018 abstract SAT-290
Empiric fluid restriction cuts transsphenoidal surgery readmissions
CHICAGO – A 70% drop in 30-day was achieved at the University of Colorado, Aurora, after endocrinologists there restricted fluid for the first 2 weeks postop, according to a report at the Endocrine Society annual meeting.
The antidiuretic hormone (ADH) rebound following pituitary adenoma resection often leads to fluid retention, and potentially dangerous hyponatremia, in about 25% of patients. It’s the leading cause of readmission for this procedure, occurring in up to 15% of patients.
To counter the problem, endocrinology fellow Kelsi Deaver, MD, and her colleagues limited patients to 1.5 L of fluid for 2 weeks after discharge, with a serum sodium check at day 7. If the sodium level was normal, patients remained on 1.5 L until the 2-week postop visit. If levels trended upward – a sign of dehydration – restrictions were eased to 2 or even 3 L, which is about the normal daily intake. If sodium levels trended downward, fluids were tightened to 1-1.2 L, or patients were brought in for further workup. The discharge packet included a 1.5-L cup so patients could track their intake.
Among 118 patients studied before the protocol was implemented in September 2015, 9 (7.6%) were readmitted for symptomatic hyponatremia within 30 days. Among 169 studied after the implementation of the fluid restriction protocol, just 4 (2.4%) were readmitted for hyponatremia (P = .044).
At present, there are no widely accepted postop fluid management guidelines for transsphenoidal surgery, but some hospitals have taken similar steps, she said.
It was the fluid restriction, not the 7-day sodium check, that drove the results. Among the four readmissions after the protocol took effect, two patients had their sodium checked, and two did not because their sodium drop was so precipitous that they were back in the hospital before the week was out. Overall, only about 70% of patients got their sodium checked as instructed.
Fluid restriction isn’t easy for patients. “The last day before discharge, we try to coach them through it,” with tips about sucking on ice chips and other strategies; “anything really to help them through it,” Dr. Deaver said.
Readmitted patients were no different from others in terms of pituitary tumor subtype, tumor size, gender, and other factors. “We couldn’t find any predictors,” she said. There were a higher percentage of macroadenomas in the preimplementation patients (91.5% versus 81.7%), but they were otherwise similar to postimplementation patients.
Those with evidence of diabetes insipidus at discharge were excluded from the study.
The National Institutes of Health funded the study. The investigators did not have any disclosures.
SOURCE: Deaver KE et al. Endocrine Society 2018 annual meeting abstract SUN-572.
CHICAGO – A 70% drop in 30-day was achieved at the University of Colorado, Aurora, after endocrinologists there restricted fluid for the first 2 weeks postop, according to a report at the Endocrine Society annual meeting.
The antidiuretic hormone (ADH) rebound following pituitary adenoma resection often leads to fluid retention, and potentially dangerous hyponatremia, in about 25% of patients. It’s the leading cause of readmission for this procedure, occurring in up to 15% of patients.
To counter the problem, endocrinology fellow Kelsi Deaver, MD, and her colleagues limited patients to 1.5 L of fluid for 2 weeks after discharge, with a serum sodium check at day 7. If the sodium level was normal, patients remained on 1.5 L until the 2-week postop visit. If levels trended upward – a sign of dehydration – restrictions were eased to 2 or even 3 L, which is about the normal daily intake. If sodium levels trended downward, fluids were tightened to 1-1.2 L, or patients were brought in for further workup. The discharge packet included a 1.5-L cup so patients could track their intake.
Among 118 patients studied before the protocol was implemented in September 2015, 9 (7.6%) were readmitted for symptomatic hyponatremia within 30 days. Among 169 studied after the implementation of the fluid restriction protocol, just 4 (2.4%) were readmitted for hyponatremia (P = .044).
At present, there are no widely accepted postop fluid management guidelines for transsphenoidal surgery, but some hospitals have taken similar steps, she said.
It was the fluid restriction, not the 7-day sodium check, that drove the results. Among the four readmissions after the protocol took effect, two patients had their sodium checked, and two did not because their sodium drop was so precipitous that they were back in the hospital before the week was out. Overall, only about 70% of patients got their sodium checked as instructed.
Fluid restriction isn’t easy for patients. “The last day before discharge, we try to coach them through it,” with tips about sucking on ice chips and other strategies; “anything really to help them through it,” Dr. Deaver said.
Readmitted patients were no different from others in terms of pituitary tumor subtype, tumor size, gender, and other factors. “We couldn’t find any predictors,” she said. There were a higher percentage of macroadenomas in the preimplementation patients (91.5% versus 81.7%), but they were otherwise similar to postimplementation patients.
Those with evidence of diabetes insipidus at discharge were excluded from the study.
The National Institutes of Health funded the study. The investigators did not have any disclosures.
SOURCE: Deaver KE et al. Endocrine Society 2018 annual meeting abstract SUN-572.
CHICAGO – A 70% drop in 30-day was achieved at the University of Colorado, Aurora, after endocrinologists there restricted fluid for the first 2 weeks postop, according to a report at the Endocrine Society annual meeting.
The antidiuretic hormone (ADH) rebound following pituitary adenoma resection often leads to fluid retention, and potentially dangerous hyponatremia, in about 25% of patients. It’s the leading cause of readmission for this procedure, occurring in up to 15% of patients.
To counter the problem, endocrinology fellow Kelsi Deaver, MD, and her colleagues limited patients to 1.5 L of fluid for 2 weeks after discharge, with a serum sodium check at day 7. If the sodium level was normal, patients remained on 1.5 L until the 2-week postop visit. If levels trended upward – a sign of dehydration – restrictions were eased to 2 or even 3 L, which is about the normal daily intake. If sodium levels trended downward, fluids were tightened to 1-1.2 L, or patients were brought in for further workup. The discharge packet included a 1.5-L cup so patients could track their intake.
Among 118 patients studied before the protocol was implemented in September 2015, 9 (7.6%) were readmitted for symptomatic hyponatremia within 30 days. Among 169 studied after the implementation of the fluid restriction protocol, just 4 (2.4%) were readmitted for hyponatremia (P = .044).
At present, there are no widely accepted postop fluid management guidelines for transsphenoidal surgery, but some hospitals have taken similar steps, she said.
It was the fluid restriction, not the 7-day sodium check, that drove the results. Among the four readmissions after the protocol took effect, two patients had their sodium checked, and two did not because their sodium drop was so precipitous that they were back in the hospital before the week was out. Overall, only about 70% of patients got their sodium checked as instructed.
Fluid restriction isn’t easy for patients. “The last day before discharge, we try to coach them through it,” with tips about sucking on ice chips and other strategies; “anything really to help them through it,” Dr. Deaver said.
Readmitted patients were no different from others in terms of pituitary tumor subtype, tumor size, gender, and other factors. “We couldn’t find any predictors,” she said. There were a higher percentage of macroadenomas in the preimplementation patients (91.5% versus 81.7%), but they were otherwise similar to postimplementation patients.
Those with evidence of diabetes insipidus at discharge were excluded from the study.
The National Institutes of Health funded the study. The investigators did not have any disclosures.
SOURCE: Deaver KE et al. Endocrine Society 2018 annual meeting abstract SUN-572.
REPORTING FROM ENDO 2018
Key clinical point: A simple fluid restriction protocol cuts readmissions 70% following transsphenoidal surgery.
Major finding: The readmission rate among the transsphenoidal surgery patients was 7.6% before the fluid restriction protocol was implemented, compared with 2.4% (P = .044) afterward.
Study details: Review of 287 transsphenoidal surgery patients.
Disclosures: The National Institutes of Health supported the work. The investigators did not have any disclosures.
Source: Deaver KE et al. Abstract SUN-572
Diabetes from checkpoint inhibitors probably means lifelong insulin
CHICAGO – , according to Priyanka Iyer, MD, an endocrinology fellow at MD Anderson Cancer Center, Houston.
“As long as we get glycemic control, they can continue,” she said at the annual meeting of the Endocrine Society.
Diabetes is a known side effect of immune checkpoint inhibitors (ICIs) but it’s rare, occurring in maybe 0.17% of patients, and its natural history and risk factors are unknown.
ICIs are fairly new agents, and as their use expands beyond clinical trials, “we anticipate seeing larger numbers of cases. Patients should be educated about the symptoms of uncontrolled blood sugars while on ICIs,” and endocrinologists “have to get involved and recognize this entity sooner,” Dr. Iyer said.
In short, her team found that ICI-mediated diabetes can occur in patients with or without preexisting diabetes, and that most patients have evidence of beta-cell failure, likely T-cell mediated destruction due to immune activation. In all but one case, patients remained on insulin at a median follow-up of 44 weeks, even after stopping ICIs. For most, ICI-mediated diabetes likely means lifelong insulin.
They were all on the programmed cell death protein (PD-1) inhibitors nivolumab (Opdivo) or pembrolizumab (Keytruda), or the PD-1 ligand (PD-L) inhibitor durvalumab (Imfinzi). The agents are used for a range of cancers, including renal cell, melanoma, and Hodgkin lymphoma. There were no diabetes cases in patients on single-agent ipilimumab (Yervoy) or tremelimumab, which target cytotoxic T-lymphocyte associated antigen-4 and are used for melanoma and mesothelioma.
Median time to diabetes presentation after the start of ICI treatment was 12.3 weeks but ranged from 1 to 67.2 weeks. Half of the cases presented in diabetic ketoacidosis (DKA). Patients had upward trending hyperglycemia and most had diabetes symptoms for a while before diagnosis. They presented with a blood glucose above 250 mg/dL, and more than half above 500 mg/dL. Median hemoglobin A1c at presentation was 8%, but ranged up to 12.5%.
Every patient required insulin, including the six that discontinued ICIs after developing diabetes. Diabetes resolved in just one patient at 10.2 months; she presented with DKA.
There were no obvious predisposing factors. None of the patients had histories of type 1 diabetes or other autoimmune disease. Five patients had well-controlled type 2 diabetes prior to ICI initiation; four had prediabetes. Some had family members with type 2 diabetes, but not type 1. Four had prior ICI exposure. Just three patients were on concomitant steroids.
A few patients also developed thyroid or pituitary dysfunction, which are more common side effects of ICIs.
The median age at diabetes presentation was 61 years and ranged from 32 to 82 years. The majority of patients were men, which reflects MD Anderson demographics, not a predisposing risk factor, Dr. Iyer said.
Melanoma was the most common cancer, followed by renal cell and prostate; patients had stage 2-4 disease. About half the subjects were on single agent anti-PD-1 treatment, about a third on anti-PD-1 combination treatment, and the rest on anti-PD-L1 combination therapy. C-peptide levels were below 0.9 ng/mL at diabetes diagnosis in most of the patients. Eleven of the 20 tested (55%) were positive for the pancreatic islet cell antibody GAD65.
The investigators had no disclosures. A funding source was not reported.
SOURCE: Iyer PC et al. Abstract OR05-5.
CHICAGO – , according to Priyanka Iyer, MD, an endocrinology fellow at MD Anderson Cancer Center, Houston.
“As long as we get glycemic control, they can continue,” she said at the annual meeting of the Endocrine Society.
Diabetes is a known side effect of immune checkpoint inhibitors (ICIs) but it’s rare, occurring in maybe 0.17% of patients, and its natural history and risk factors are unknown.
ICIs are fairly new agents, and as their use expands beyond clinical trials, “we anticipate seeing larger numbers of cases. Patients should be educated about the symptoms of uncontrolled blood sugars while on ICIs,” and endocrinologists “have to get involved and recognize this entity sooner,” Dr. Iyer said.
In short, her team found that ICI-mediated diabetes can occur in patients with or without preexisting diabetes, and that most patients have evidence of beta-cell failure, likely T-cell mediated destruction due to immune activation. In all but one case, patients remained on insulin at a median follow-up of 44 weeks, even after stopping ICIs. For most, ICI-mediated diabetes likely means lifelong insulin.
They were all on the programmed cell death protein (PD-1) inhibitors nivolumab (Opdivo) or pembrolizumab (Keytruda), or the PD-1 ligand (PD-L) inhibitor durvalumab (Imfinzi). The agents are used for a range of cancers, including renal cell, melanoma, and Hodgkin lymphoma. There were no diabetes cases in patients on single-agent ipilimumab (Yervoy) or tremelimumab, which target cytotoxic T-lymphocyte associated antigen-4 and are used for melanoma and mesothelioma.
Median time to diabetes presentation after the start of ICI treatment was 12.3 weeks but ranged from 1 to 67.2 weeks. Half of the cases presented in diabetic ketoacidosis (DKA). Patients had upward trending hyperglycemia and most had diabetes symptoms for a while before diagnosis. They presented with a blood glucose above 250 mg/dL, and more than half above 500 mg/dL. Median hemoglobin A1c at presentation was 8%, but ranged up to 12.5%.
Every patient required insulin, including the six that discontinued ICIs after developing diabetes. Diabetes resolved in just one patient at 10.2 months; she presented with DKA.
There were no obvious predisposing factors. None of the patients had histories of type 1 diabetes or other autoimmune disease. Five patients had well-controlled type 2 diabetes prior to ICI initiation; four had prediabetes. Some had family members with type 2 diabetes, but not type 1. Four had prior ICI exposure. Just three patients were on concomitant steroids.
A few patients also developed thyroid or pituitary dysfunction, which are more common side effects of ICIs.
The median age at diabetes presentation was 61 years and ranged from 32 to 82 years. The majority of patients were men, which reflects MD Anderson demographics, not a predisposing risk factor, Dr. Iyer said.
Melanoma was the most common cancer, followed by renal cell and prostate; patients had stage 2-4 disease. About half the subjects were on single agent anti-PD-1 treatment, about a third on anti-PD-1 combination treatment, and the rest on anti-PD-L1 combination therapy. C-peptide levels were below 0.9 ng/mL at diabetes diagnosis in most of the patients. Eleven of the 20 tested (55%) were positive for the pancreatic islet cell antibody GAD65.
The investigators had no disclosures. A funding source was not reported.
SOURCE: Iyer PC et al. Abstract OR05-5.
CHICAGO – , according to Priyanka Iyer, MD, an endocrinology fellow at MD Anderson Cancer Center, Houston.
“As long as we get glycemic control, they can continue,” she said at the annual meeting of the Endocrine Society.
Diabetes is a known side effect of immune checkpoint inhibitors (ICIs) but it’s rare, occurring in maybe 0.17% of patients, and its natural history and risk factors are unknown.
ICIs are fairly new agents, and as their use expands beyond clinical trials, “we anticipate seeing larger numbers of cases. Patients should be educated about the symptoms of uncontrolled blood sugars while on ICIs,” and endocrinologists “have to get involved and recognize this entity sooner,” Dr. Iyer said.
In short, her team found that ICI-mediated diabetes can occur in patients with or without preexisting diabetes, and that most patients have evidence of beta-cell failure, likely T-cell mediated destruction due to immune activation. In all but one case, patients remained on insulin at a median follow-up of 44 weeks, even after stopping ICIs. For most, ICI-mediated diabetes likely means lifelong insulin.
They were all on the programmed cell death protein (PD-1) inhibitors nivolumab (Opdivo) or pembrolizumab (Keytruda), or the PD-1 ligand (PD-L) inhibitor durvalumab (Imfinzi). The agents are used for a range of cancers, including renal cell, melanoma, and Hodgkin lymphoma. There were no diabetes cases in patients on single-agent ipilimumab (Yervoy) or tremelimumab, which target cytotoxic T-lymphocyte associated antigen-4 and are used for melanoma and mesothelioma.
Median time to diabetes presentation after the start of ICI treatment was 12.3 weeks but ranged from 1 to 67.2 weeks. Half of the cases presented in diabetic ketoacidosis (DKA). Patients had upward trending hyperglycemia and most had diabetes symptoms for a while before diagnosis. They presented with a blood glucose above 250 mg/dL, and more than half above 500 mg/dL. Median hemoglobin A1c at presentation was 8%, but ranged up to 12.5%.
Every patient required insulin, including the six that discontinued ICIs after developing diabetes. Diabetes resolved in just one patient at 10.2 months; she presented with DKA.
There were no obvious predisposing factors. None of the patients had histories of type 1 diabetes or other autoimmune disease. Five patients had well-controlled type 2 diabetes prior to ICI initiation; four had prediabetes. Some had family members with type 2 diabetes, but not type 1. Four had prior ICI exposure. Just three patients were on concomitant steroids.
A few patients also developed thyroid or pituitary dysfunction, which are more common side effects of ICIs.
The median age at diabetes presentation was 61 years and ranged from 32 to 82 years. The majority of patients were men, which reflects MD Anderson demographics, not a predisposing risk factor, Dr. Iyer said.
Melanoma was the most common cancer, followed by renal cell and prostate; patients had stage 2-4 disease. About half the subjects were on single agent anti-PD-1 treatment, about a third on anti-PD-1 combination treatment, and the rest on anti-PD-L1 combination therapy. C-peptide levels were below 0.9 ng/mL at diabetes diagnosis in most of the patients. Eleven of the 20 tested (55%) were positive for the pancreatic islet cell antibody GAD65.
The investigators had no disclosures. A funding source was not reported.
SOURCE: Iyer PC et al. Abstract OR05-5.
REPORTING FROM ENDO 2018
Key clinical point: Be on the lookout for new-onset diabetes when patients start immune checkpoint inhibitors.
Major finding: In all but one case, patients remained on insulin at a median follow-up of 44 weeks, even after stopping ICIs.
Study details: Review of 24 cases.
Disclosures: The investigators had no disclosures. A funding source was not reported.
Source: Iyer PC et al. Abstract OR05-5.