User login
Richard Franki is the associate editor who writes and creates graphs. He started with the company in 1987, when it was known as the International Medical News Group. In his years as a journalist, Richard has worked for Cap Cities/ABC, Disney, Harcourt, Elsevier, Quadrant, Frontline, and Internet Brands. In the 1990s, he was a contributor to the ill-fated Indications column, predecessor of Livin' on the MDedge.
Tantrum-taming edibles, support gators, and chemo eggs
Chill out, kid
What do you do when your child has constant tantrums? A simple edible could do the trick, according to a Hollywood physician.
The natural medicine physician is in hot (bong) water after recommending marijuana cookies as treatment for a 4-year-old child’s ADHD and bipolar disorder. The icing on the cake (or cookie) is that both diagnoses weren’t even accurate. Perhaps the doctor was sampling his own treatments before the office visit?
The progressive physician has had his license revoked for the “grossly negligent” diagnosis, which he made in 30 minutes without consulting the child’s teachers, his father, or a psychiatrist. Probably not the best way to handle it, said the state medical board. Perhaps he should have suggested some CBD-infused Coke, instead?
Gator saver
Dogs, cats, peacocks – these are the animals that many people with anxiety, depression, and other mental health issues use for emotional support. But now, enter Wally, the emotional support alligator.
Spanning 5 feet long and sporting way too many teeth, Wally is the constant companion of a 65-year-old Pennsylvania man with depression. Wally’s owner decided to forgo pharmacologic treatment for something decidedly more reptilian.
Wally, who was rescued from Florida, loves chicken wings, hugs, and his adopted gator brother, Scrappy. He also has the potential to reach 16 feet long, which is … concerning. Something tells me you can’t take Wally on a plane as a service gator.
But don’t worry, Wally has been approved by a doctor. Rumors that Wally had the doctor’s arm in his jaws before approval are unsubstantiated.
Synergy is not always a good thing
Since it is generally agreed that two heads are better than one, three heads must be even better than two, right? But what if we’re not talking about heads? Suppose, instead, that the subject is global pandemics. Would it be better if three of the greatest threats to humanity’s existence on the planet decided to join forces?
The Lancet Global Syndemic Commission, a group of more than 40 international experts, said that obesity, undernutrition, and climate change “constitute a syndemic, or synergy of epidemics, because they co-occur in time and place, interact with each other to produce complex sequelae, and share common underlying societal drivers” (Lancet. 2019 Jan. 27. doi: 10.1016/S0140-6736[18]32822-8).
It gets better: The commission suggested that the “three interconnected health pandemics [have been] effectively orchestrated by the shadowy manipulations and influence of vested commercial interests – an entity collectively defined as ‘Big Food,’ ” according to Science Alert.
This all seems like a lot to overcome, but we here at LOTME have faith in science, and in the scientists who are working to solve these problems. After all, it’s not like anyone’s out there disregarding the science and saying that this stuff isn’t really happening. … Wait, what? … Climate change deniers? … Really? … The president tweeted what? … We’re doomed.
I prefer my medication sunny side up
Here’s a hypothetical question for you: If you were to have cancer, how would you prefer to be treated? Would you rather go through the rigors of chemotherapy? Or would you rather eat an omelet?
Okay, it probably wouldn’t work quite like that, but a group of physicians from the University of Edinburgh have successfully modified chickens to lay eggs containing a pair of human proteins within the egg white.
One of these proteins has antiviral and anticancer effects, and the other can help damaged tissue repair itself. The researchers added that the protein in the egg white could be modified to make the key ingredients for other protein-based drugs such as Avastin and Herceptin, which are used for treating cancer.
We know what you’re thinking: It’ll probably take a thousand eggs to make one dose – but no, it only takes three. Over the course of a year, one chicken could produce a hundred doses, and do it for far cheaper than is currently possible. We hate jumping on the social media bandwagon here, but frankly, this is an egg worth giving millions of Instagram likes.

Chill out, kid
What do you do when your child has constant tantrums? A simple edible could do the trick, according to a Hollywood physician.
The natural medicine physician is in hot (bong) water after recommending marijuana cookies as treatment for a 4-year-old child’s ADHD and bipolar disorder. The icing on the cake (or cookie) is that both diagnoses weren’t even accurate. Perhaps the doctor was sampling his own treatments before the office visit?
The progressive physician has had his license revoked for the “grossly negligent” diagnosis, which he made in 30 minutes without consulting the child’s teachers, his father, or a psychiatrist. Probably not the best way to handle it, said the state medical board. Perhaps he should have suggested some CBD-infused Coke, instead?
Gator saver
Dogs, cats, peacocks – these are the animals that many people with anxiety, depression, and other mental health issues use for emotional support. But now, enter Wally, the emotional support alligator.
Spanning 5 feet long and sporting way too many teeth, Wally is the constant companion of a 65-year-old Pennsylvania man with depression. Wally’s owner decided to forgo pharmacologic treatment for something decidedly more reptilian.
Wally, who was rescued from Florida, loves chicken wings, hugs, and his adopted gator brother, Scrappy. He also has the potential to reach 16 feet long, which is … concerning. Something tells me you can’t take Wally on a plane as a service gator.
But don’t worry, Wally has been approved by a doctor. Rumors that Wally had the doctor’s arm in his jaws before approval are unsubstantiated.
Synergy is not always a good thing
Since it is generally agreed that two heads are better than one, three heads must be even better than two, right? But what if we’re not talking about heads? Suppose, instead, that the subject is global pandemics. Would it be better if three of the greatest threats to humanity’s existence on the planet decided to join forces?
The Lancet Global Syndemic Commission, a group of more than 40 international experts, said that obesity, undernutrition, and climate change “constitute a syndemic, or synergy of epidemics, because they co-occur in time and place, interact with each other to produce complex sequelae, and share common underlying societal drivers” (Lancet. 2019 Jan. 27. doi: 10.1016/S0140-6736[18]32822-8).
It gets better: The commission suggested that the “three interconnected health pandemics [have been] effectively orchestrated by the shadowy manipulations and influence of vested commercial interests – an entity collectively defined as ‘Big Food,’ ” according to Science Alert.
This all seems like a lot to overcome, but we here at LOTME have faith in science, and in the scientists who are working to solve these problems. After all, it’s not like anyone’s out there disregarding the science and saying that this stuff isn’t really happening. … Wait, what? … Climate change deniers? … Really? … The president tweeted what? … We’re doomed.
I prefer my medication sunny side up
Here’s a hypothetical question for you: If you were to have cancer, how would you prefer to be treated? Would you rather go through the rigors of chemotherapy? Or would you rather eat an omelet?
Okay, it probably wouldn’t work quite like that, but a group of physicians from the University of Edinburgh have successfully modified chickens to lay eggs containing a pair of human proteins within the egg white.
One of these proteins has antiviral and anticancer effects, and the other can help damaged tissue repair itself. The researchers added that the protein in the egg white could be modified to make the key ingredients for other protein-based drugs such as Avastin and Herceptin, which are used for treating cancer.
We know what you’re thinking: It’ll probably take a thousand eggs to make one dose – but no, it only takes three. Over the course of a year, one chicken could produce a hundred doses, and do it for far cheaper than is currently possible. We hate jumping on the social media bandwagon here, but frankly, this is an egg worth giving millions of Instagram likes.

Chill out, kid
What do you do when your child has constant tantrums? A simple edible could do the trick, according to a Hollywood physician.
The natural medicine physician is in hot (bong) water after recommending marijuana cookies as treatment for a 4-year-old child’s ADHD and bipolar disorder. The icing on the cake (or cookie) is that both diagnoses weren’t even accurate. Perhaps the doctor was sampling his own treatments before the office visit?
The progressive physician has had his license revoked for the “grossly negligent” diagnosis, which he made in 30 minutes without consulting the child’s teachers, his father, or a psychiatrist. Probably not the best way to handle it, said the state medical board. Perhaps he should have suggested some CBD-infused Coke, instead?
Gator saver
Dogs, cats, peacocks – these are the animals that many people with anxiety, depression, and other mental health issues use for emotional support. But now, enter Wally, the emotional support alligator.
Spanning 5 feet long and sporting way too many teeth, Wally is the constant companion of a 65-year-old Pennsylvania man with depression. Wally’s owner decided to forgo pharmacologic treatment for something decidedly more reptilian.
Wally, who was rescued from Florida, loves chicken wings, hugs, and his adopted gator brother, Scrappy. He also has the potential to reach 16 feet long, which is … concerning. Something tells me you can’t take Wally on a plane as a service gator.
But don’t worry, Wally has been approved by a doctor. Rumors that Wally had the doctor’s arm in his jaws before approval are unsubstantiated.
Synergy is not always a good thing
Since it is generally agreed that two heads are better than one, three heads must be even better than two, right? But what if we’re not talking about heads? Suppose, instead, that the subject is global pandemics. Would it be better if three of the greatest threats to humanity’s existence on the planet decided to join forces?
The Lancet Global Syndemic Commission, a group of more than 40 international experts, said that obesity, undernutrition, and climate change “constitute a syndemic, or synergy of epidemics, because they co-occur in time and place, interact with each other to produce complex sequelae, and share common underlying societal drivers” (Lancet. 2019 Jan. 27. doi: 10.1016/S0140-6736[18]32822-8).
It gets better: The commission suggested that the “three interconnected health pandemics [have been] effectively orchestrated by the shadowy manipulations and influence of vested commercial interests – an entity collectively defined as ‘Big Food,’ ” according to Science Alert.
This all seems like a lot to overcome, but we here at LOTME have faith in science, and in the scientists who are working to solve these problems. After all, it’s not like anyone’s out there disregarding the science and saying that this stuff isn’t really happening. … Wait, what? … Climate change deniers? … Really? … The president tweeted what? … We’re doomed.
I prefer my medication sunny side up
Here’s a hypothetical question for you: If you were to have cancer, how would you prefer to be treated? Would you rather go through the rigors of chemotherapy? Or would you rather eat an omelet?
Okay, it probably wouldn’t work quite like that, but a group of physicians from the University of Edinburgh have successfully modified chickens to lay eggs containing a pair of human proteins within the egg white.
One of these proteins has antiviral and anticancer effects, and the other can help damaged tissue repair itself. The researchers added that the protein in the egg white could be modified to make the key ingredients for other protein-based drugs such as Avastin and Herceptin, which are used for treating cancer.
We know what you’re thinking: It’ll probably take a thousand eggs to make one dose – but no, it only takes three. Over the course of a year, one chicken could produce a hundred doses, and do it for far cheaper than is currently possible. We hate jumping on the social media bandwagon here, but frankly, this is an egg worth giving millions of Instagram likes.

A theory of relativity for rosacea patients
Rosacea has several known comorbidities, but the widespread use of their relative, rather than absolute, risks “may result in overestimation of the clinical importance of exposures,” Leonardo A. Tjahjono and his associates wrote.
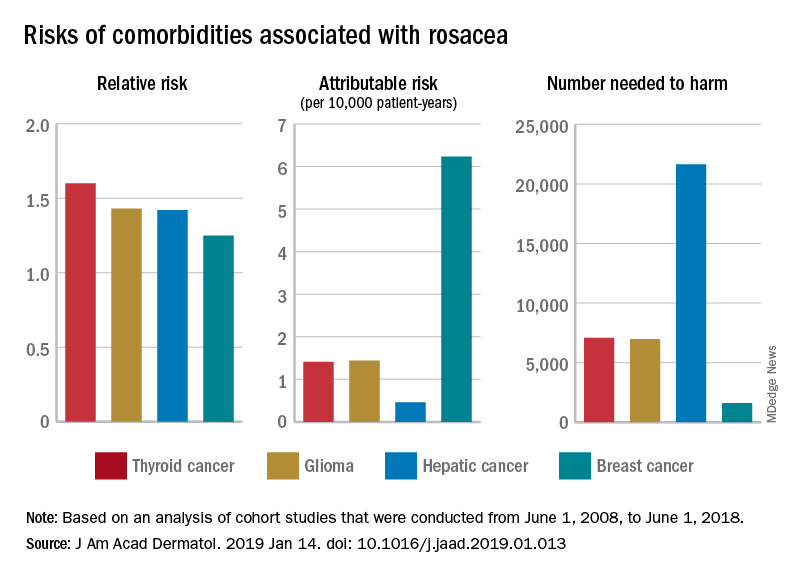
For a patient with rosacea, the relative risk of hepatic cancer is 1.42, but the attributable risk and the number needed to harm (NNH), which provide “a clearer, absolute picture regarding the association” with rosacea, are 0.46 per 10,000 patient-years and 21,645, respectively. The relative risk of comorbid breast cancer is 1.25, compared with an attributable risk of 6.23 per 10,000 patient-years and an NNH of 1,606, Mr. Tjahjono of Wake Forest University in Winston-Salem, N.C., and his associates reported in the Journal of the American Academy of Dermatology.
Physician misconceptions based on patients’ relative risks of comorbidities may lead to increased cancer screenings, which “can provide great benefit in a proper context; however, they are not without consequences. For example, 0.7 % of liver biopsies result in severe intraperitoneal hematoma,” the investigators said.
The absolute risks – calculated by the investigators using cohort studies that were conducted from June 1, 2008, to June 1, 2018 – present “a better understanding regarding rosacea’s impact on public health and clinical settings, “ they wrote.
SOURCE: Tjahjono LA et al. J Am Acad Dermatol. 2019 Jan 14. doi: 10.1016/j.jaad.2019.01.013.
Rosacea has several known comorbidities, but the widespread use of their relative, rather than absolute, risks “may result in overestimation of the clinical importance of exposures,” Leonardo A. Tjahjono and his associates wrote.

For a patient with rosacea, the relative risk of hepatic cancer is 1.42, but the attributable risk and the number needed to harm (NNH), which provide “a clearer, absolute picture regarding the association” with rosacea, are 0.46 per 10,000 patient-years and 21,645, respectively. The relative risk of comorbid breast cancer is 1.25, compared with an attributable risk of 6.23 per 10,000 patient-years and an NNH of 1,606, Mr. Tjahjono of Wake Forest University in Winston-Salem, N.C., and his associates reported in the Journal of the American Academy of Dermatology.
Physician misconceptions based on patients’ relative risks of comorbidities may lead to increased cancer screenings, which “can provide great benefit in a proper context; however, they are not without consequences. For example, 0.7 % of liver biopsies result in severe intraperitoneal hematoma,” the investigators said.
The absolute risks – calculated by the investigators using cohort studies that were conducted from June 1, 2008, to June 1, 2018 – present “a better understanding regarding rosacea’s impact on public health and clinical settings, “ they wrote.
SOURCE: Tjahjono LA et al. J Am Acad Dermatol. 2019 Jan 14. doi: 10.1016/j.jaad.2019.01.013.
Rosacea has several known comorbidities, but the widespread use of their relative, rather than absolute, risks “may result in overestimation of the clinical importance of exposures,” Leonardo A. Tjahjono and his associates wrote.

For a patient with rosacea, the relative risk of hepatic cancer is 1.42, but the attributable risk and the number needed to harm (NNH), which provide “a clearer, absolute picture regarding the association” with rosacea, are 0.46 per 10,000 patient-years and 21,645, respectively. The relative risk of comorbid breast cancer is 1.25, compared with an attributable risk of 6.23 per 10,000 patient-years and an NNH of 1,606, Mr. Tjahjono of Wake Forest University in Winston-Salem, N.C., and his associates reported in the Journal of the American Academy of Dermatology.
Physician misconceptions based on patients’ relative risks of comorbidities may lead to increased cancer screenings, which “can provide great benefit in a proper context; however, they are not without consequences. For example, 0.7 % of liver biopsies result in severe intraperitoneal hematoma,” the investigators said.
The absolute risks – calculated by the investigators using cohort studies that were conducted from June 1, 2008, to June 1, 2018 – present “a better understanding regarding rosacea’s impact on public health and clinical settings, “ they wrote.
SOURCE: Tjahjono LA et al. J Am Acad Dermatol. 2019 Jan 14. doi: 10.1016/j.jaad.2019.01.013.
FROM THE JOURNAL OF THE AMERICAN ACADEMY OF DERMATOLOGY
Flu activity increases after 2 weeks of declines
according to the Centers for Disease Control and Prevention.
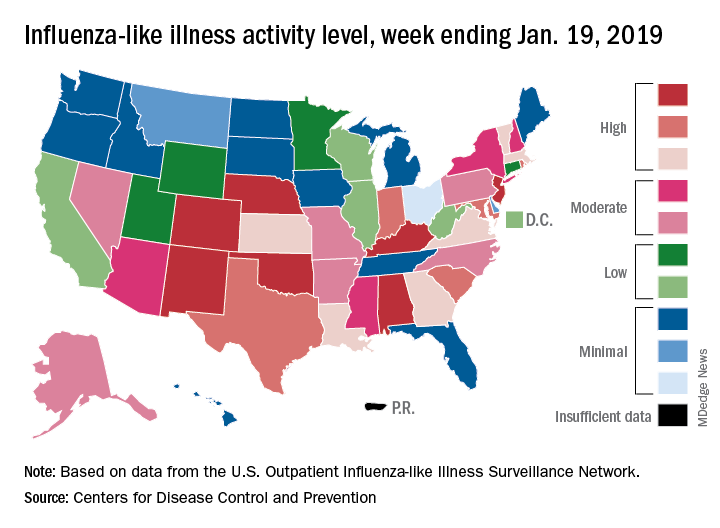
The proportion of outpatient visits for influenza-like illness (ILI) was 3.3% for the most recent measurement period, the CDC’s influenza division reported Jan 25. The previous 2-week decline had seen ILI visits dip down to 3.1% for the week ending Jan. 12 after hitting a season high of 4%.
To go along with the national increase in visits, more states reported high levels of flu activity. For the week ending Jan. 19, seven states were at level 10 on the CDC’s 1-10 scale, compared with four the previous week, and there were 18 states in the high range (levels 8-10), compared with 9 the week before, the CDC said.
Three flu-related pediatric deaths were reported in the week ending Jan. 19, although all three occurred during earlier weeks. The total number of pediatric deaths for the 2018-2019 season is now up to 22. Deaths among all ages, which are reported a week later, totaled 118 for the week ending Jan. 12, with 63% of reporting complete. There were 144 deaths during the week ending Jan. 5, with reporting 86% complete. During the second full week of 2018, in the middle of the very severe 2017-2018 season, there were 1,537 flu-related deaths, CDC data show.
according to the Centers for Disease Control and Prevention.

The proportion of outpatient visits for influenza-like illness (ILI) was 3.3% for the most recent measurement period, the CDC’s influenza division reported Jan 25. The previous 2-week decline had seen ILI visits dip down to 3.1% for the week ending Jan. 12 after hitting a season high of 4%.
To go along with the national increase in visits, more states reported high levels of flu activity. For the week ending Jan. 19, seven states were at level 10 on the CDC’s 1-10 scale, compared with four the previous week, and there were 18 states in the high range (levels 8-10), compared with 9 the week before, the CDC said.
Three flu-related pediatric deaths were reported in the week ending Jan. 19, although all three occurred during earlier weeks. The total number of pediatric deaths for the 2018-2019 season is now up to 22. Deaths among all ages, which are reported a week later, totaled 118 for the week ending Jan. 12, with 63% of reporting complete. There were 144 deaths during the week ending Jan. 5, with reporting 86% complete. During the second full week of 2018, in the middle of the very severe 2017-2018 season, there were 1,537 flu-related deaths, CDC data show.
according to the Centers for Disease Control and Prevention.

The proportion of outpatient visits for influenza-like illness (ILI) was 3.3% for the most recent measurement period, the CDC’s influenza division reported Jan 25. The previous 2-week decline had seen ILI visits dip down to 3.1% for the week ending Jan. 12 after hitting a season high of 4%.
To go along with the national increase in visits, more states reported high levels of flu activity. For the week ending Jan. 19, seven states were at level 10 on the CDC’s 1-10 scale, compared with four the previous week, and there were 18 states in the high range (levels 8-10), compared with 9 the week before, the CDC said.
Three flu-related pediatric deaths were reported in the week ending Jan. 19, although all three occurred during earlier weeks. The total number of pediatric deaths for the 2018-2019 season is now up to 22. Deaths among all ages, which are reported a week later, totaled 118 for the week ending Jan. 12, with 63% of reporting complete. There were 144 deaths during the week ending Jan. 5, with reporting 86% complete. During the second full week of 2018, in the middle of the very severe 2017-2018 season, there were 1,537 flu-related deaths, CDC data show.
Survey: Americans support Medicare for all
A majority of Americans support the concept of Medicare for all, but “larger majorities favor more incremental changes to the health care system,” according to a new survey by the Kaiser Family Foundation.
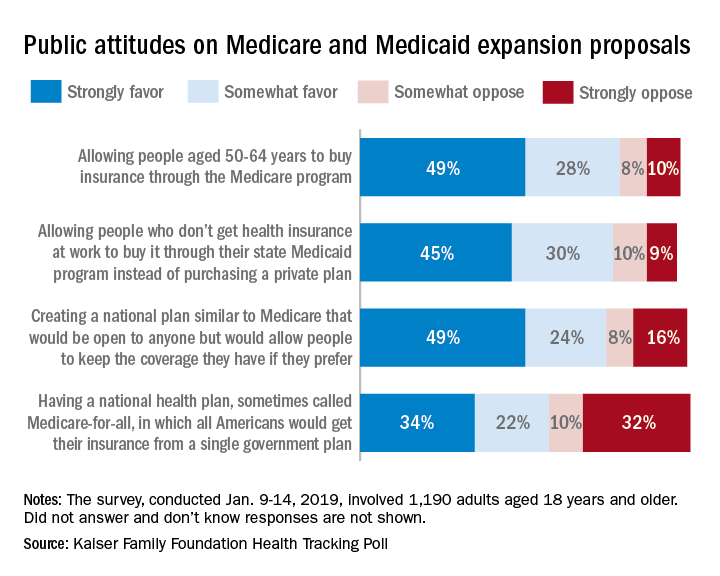
Support for a Medicare-for-all health care system came in at 56% (strongly favor, 34%; somewhat favor, 22%) among the 1,190 respondents to the latest KFF Health Tracking Poll, which was conducted Jan. 9-14, 2019. That support came largely from Democrats, 81% of whom favored the plan, compared with only 23% of Republicans, the Kaiser investigators said Jan. 23.
A Medicare buy-in plan for Americans aged 50-64 years also was highly popular, receiving support from 77% of all respondents – 85% of Democrats, 75% of Independents, and 69% of Republicans. Support by party identification was similar for a proposal to enable all those who don’t have employer-based insurance to get coverage through state Medicaid programs, which received 75% support overall, they reported.
Just behind those proposals at 74% support was a federally administered health plan that would be open to anyone but would allow people to keep the coverage they have. It was the most popular proposal among Democrats (91%) but did not garner a majority among Republicans (47%), the investigators said.
Support for the Medicare-for-all plan varied considerably, depending on number of arguments presented to respondents. When told that such a proposal would guarantee insurance as a right for all Americans, 71% favored it, and when they heard that it would eliminate health insurance premiums and reduce out-of-pockets costs, 67% of respondents expressed support. Favorable responses, however, were in the minority when people were told that Medicare-for-all would eliminate private health insurance companies (37%), threaten the current Medicare program (32%), and lead to some delayed medical tests and treatments (26%), according to the Kaiser report.
A majority of Americans support the concept of Medicare for all, but “larger majorities favor more incremental changes to the health care system,” according to a new survey by the Kaiser Family Foundation.

Support for a Medicare-for-all health care system came in at 56% (strongly favor, 34%; somewhat favor, 22%) among the 1,190 respondents to the latest KFF Health Tracking Poll, which was conducted Jan. 9-14, 2019. That support came largely from Democrats, 81% of whom favored the plan, compared with only 23% of Republicans, the Kaiser investigators said Jan. 23.
A Medicare buy-in plan for Americans aged 50-64 years also was highly popular, receiving support from 77% of all respondents – 85% of Democrats, 75% of Independents, and 69% of Republicans. Support by party identification was similar for a proposal to enable all those who don’t have employer-based insurance to get coverage through state Medicaid programs, which received 75% support overall, they reported.
Just behind those proposals at 74% support was a federally administered health plan that would be open to anyone but would allow people to keep the coverage they have. It was the most popular proposal among Democrats (91%) but did not garner a majority among Republicans (47%), the investigators said.
Support for the Medicare-for-all plan varied considerably, depending on number of arguments presented to respondents. When told that such a proposal would guarantee insurance as a right for all Americans, 71% favored it, and when they heard that it would eliminate health insurance premiums and reduce out-of-pockets costs, 67% of respondents expressed support. Favorable responses, however, were in the minority when people were told that Medicare-for-all would eliminate private health insurance companies (37%), threaten the current Medicare program (32%), and lead to some delayed medical tests and treatments (26%), according to the Kaiser report.
A majority of Americans support the concept of Medicare for all, but “larger majorities favor more incremental changes to the health care system,” according to a new survey by the Kaiser Family Foundation.

Support for a Medicare-for-all health care system came in at 56% (strongly favor, 34%; somewhat favor, 22%) among the 1,190 respondents to the latest KFF Health Tracking Poll, which was conducted Jan. 9-14, 2019. That support came largely from Democrats, 81% of whom favored the plan, compared with only 23% of Republicans, the Kaiser investigators said Jan. 23.
A Medicare buy-in plan for Americans aged 50-64 years also was highly popular, receiving support from 77% of all respondents – 85% of Democrats, 75% of Independents, and 69% of Republicans. Support by party identification was similar for a proposal to enable all those who don’t have employer-based insurance to get coverage through state Medicaid programs, which received 75% support overall, they reported.
Just behind those proposals at 74% support was a federally administered health plan that would be open to anyone but would allow people to keep the coverage they have. It was the most popular proposal among Democrats (91%) but did not garner a majority among Republicans (47%), the investigators said.
Support for the Medicare-for-all plan varied considerably, depending on number of arguments presented to respondents. When told that such a proposal would guarantee insurance as a right for all Americans, 71% favored it, and when they heard that it would eliminate health insurance premiums and reduce out-of-pockets costs, 67% of respondents expressed support. Favorable responses, however, were in the minority when people were told that Medicare-for-all would eliminate private health insurance companies (37%), threaten the current Medicare program (32%), and lead to some delayed medical tests and treatments (26%), according to the Kaiser report.
Gametes for back pain, Alice in Wonderland syndrome, and liver-saving beer
A case of emission and injection
In what might win “Most Bizarre Attempt at Home Medicine” of 2019, a 33-year-old Irish man was hospitalized after injecting himself with his own semen … in his arm … multiple times … to reduce back pain. Whew. Does this count as holistic medicine?
This at-home remedy did not cure his back pain, shockingly enough. The patient instead developed a subcutaneous abscess after a year and a half of monthly intramuscular and intravenous injections, during which the semen has leaked into the soft tissues. He reported to a Dublin hospital after suffering severe back pain and a swollen arm, and eventually revealed to doctors his miracle cure.
The doctors did some Googling and found studies where rats and rabbits were injected with semen – possibly the research that inspired this trailblazer. Or, possibly, this was just an extreme case of reduce, reuse, and recycle.
In case you’re concerned, the man was given a course of more traditional medicine, and his back pain improved greatly. The patient chose to discharge himself before doctors could drain the “local collection” – perhaps he was proud of his work.
Down the rabbit hole
Imagine sitting at your computer when suddenly the icons begin to move off the screen and hover directly in front of your eyes. Your first thought might be that someone spiked your morning coffee with acid – and you’re not far off.
This curious occurrence happened to a 54-year-old man who was diagnosed with the rare perceptual disorder Alice in Wonderland syndrome (AIWS). AIWS causes people to develop a misperception of their body or surrounding space, and can be caused by a number of things, including migraine.
In this case, the man’s LSD-like visions were caused by a glioblastoma in the left temporal-occipital region of the brain. Tumors there can interfere with spatial perception, hence the temporary trip down the rabbit hole for this patient. After chemotherapy and radiation, the tumor was defeated, and the patient is back to feeling happier than the Mad Hatter at a tea party.
Must have been some party
On Dec. 25 in the Vietnamese province of Quang Tri, a 48-year-old man was taken to a hospital with a case of alcohol poisoning. Specifically, his body contained more than 1,000 times the recommended limit of methanol.
While the two types of alcohol, ethanol and methanol, are both toxic to the human body to some degree, the liver processes methanol differently and more slowly, making it far more dangerous than ethanol, the key ingredient in commercially available alcoholic beverages. Methanol is found in bootleg liquor and in such products as gasoline, paint, ink, and cleaning products. It can cause blindness, nervous system depression, and death.
However, there is a happy ending to this story. To save their patient’s life, his doctors hit upon an ingenious solution – one that would make Homer Simpson proud.
They administered cans of beer.
When the man was admitted, the doctors immediately gave him 3 cans’ worth, and then transfused an additional 12 at the rate of 1 can per hour. The liver will always prioritize processing ethanol over methanol. By feeding the patient a steady stream of relatively friendly and ethanol-rich beer, the doctors had enough time to perform dialysis and remove the methanol from the man’s system.
So, as Homer himself might declare, here’s to alcohol – truly the cause of, and solution to, all of life’s problems.
A mistake of the bloody type
Nurse: Mr. Smeggins, I need to clear up some of the answers on your new-patient information form.
Patient: I filled the whole thing out, didn’t I?
Nurse: You did, but a couple of your responses are less than helpful. You do realize that “Helvetica” is not a blood type, right?
Patient: I took a stab at it.
Nurse: You’re not the only one. It turns out that 43% of adults don’t know their blood type, and 62% don’t know their cholesterol level, according to a recent survey by Quest Diagnostics. The 1,004 respondents were more likely to know their bank account balances (75%) or their wifi passwords (74%).
Patient: Hey, that’s right! Mine is Earwiglover122.
Nurse: Great. And can I assume that you’re one of the 30% or so supposedly Web-savvy millennials (ages 20-37 years) who keep lab results in a filing cabinet at home?
Patient: Actually, I have a pile for stuff like that.
Nurse: Fine. Now about your other answers. When we asked about sex, we were not looking for “just last night.”

A case of emission and injection
In what might win “Most Bizarre Attempt at Home Medicine” of 2019, a 33-year-old Irish man was hospitalized after injecting himself with his own semen … in his arm … multiple times … to reduce back pain. Whew. Does this count as holistic medicine?
This at-home remedy did not cure his back pain, shockingly enough. The patient instead developed a subcutaneous abscess after a year and a half of monthly intramuscular and intravenous injections, during which the semen has leaked into the soft tissues. He reported to a Dublin hospital after suffering severe back pain and a swollen arm, and eventually revealed to doctors his miracle cure.
The doctors did some Googling and found studies where rats and rabbits were injected with semen – possibly the research that inspired this trailblazer. Or, possibly, this was just an extreme case of reduce, reuse, and recycle.
In case you’re concerned, the man was given a course of more traditional medicine, and his back pain improved greatly. The patient chose to discharge himself before doctors could drain the “local collection” – perhaps he was proud of his work.
Down the rabbit hole
Imagine sitting at your computer when suddenly the icons begin to move off the screen and hover directly in front of your eyes. Your first thought might be that someone spiked your morning coffee with acid – and you’re not far off.
This curious occurrence happened to a 54-year-old man who was diagnosed with the rare perceptual disorder Alice in Wonderland syndrome (AIWS). AIWS causes people to develop a misperception of their body or surrounding space, and can be caused by a number of things, including migraine.
In this case, the man’s LSD-like visions were caused by a glioblastoma in the left temporal-occipital region of the brain. Tumors there can interfere with spatial perception, hence the temporary trip down the rabbit hole for this patient. After chemotherapy and radiation, the tumor was defeated, and the patient is back to feeling happier than the Mad Hatter at a tea party.
Must have been some party
On Dec. 25 in the Vietnamese province of Quang Tri, a 48-year-old man was taken to a hospital with a case of alcohol poisoning. Specifically, his body contained more than 1,000 times the recommended limit of methanol.
While the two types of alcohol, ethanol and methanol, are both toxic to the human body to some degree, the liver processes methanol differently and more slowly, making it far more dangerous than ethanol, the key ingredient in commercially available alcoholic beverages. Methanol is found in bootleg liquor and in such products as gasoline, paint, ink, and cleaning products. It can cause blindness, nervous system depression, and death.
However, there is a happy ending to this story. To save their patient’s life, his doctors hit upon an ingenious solution – one that would make Homer Simpson proud.
They administered cans of beer.
When the man was admitted, the doctors immediately gave him 3 cans’ worth, and then transfused an additional 12 at the rate of 1 can per hour. The liver will always prioritize processing ethanol over methanol. By feeding the patient a steady stream of relatively friendly and ethanol-rich beer, the doctors had enough time to perform dialysis and remove the methanol from the man’s system.
So, as Homer himself might declare, here’s to alcohol – truly the cause of, and solution to, all of life’s problems.
A mistake of the bloody type
Nurse: Mr. Smeggins, I need to clear up some of the answers on your new-patient information form.
Patient: I filled the whole thing out, didn’t I?
Nurse: You did, but a couple of your responses are less than helpful. You do realize that “Helvetica” is not a blood type, right?
Patient: I took a stab at it.
Nurse: You’re not the only one. It turns out that 43% of adults don’t know their blood type, and 62% don’t know their cholesterol level, according to a recent survey by Quest Diagnostics. The 1,004 respondents were more likely to know their bank account balances (75%) or their wifi passwords (74%).
Patient: Hey, that’s right! Mine is Earwiglover122.
Nurse: Great. And can I assume that you’re one of the 30% or so supposedly Web-savvy millennials (ages 20-37 years) who keep lab results in a filing cabinet at home?
Patient: Actually, I have a pile for stuff like that.
Nurse: Fine. Now about your other answers. When we asked about sex, we were not looking for “just last night.”

A case of emission and injection
In what might win “Most Bizarre Attempt at Home Medicine” of 2019, a 33-year-old Irish man was hospitalized after injecting himself with his own semen … in his arm … multiple times … to reduce back pain. Whew. Does this count as holistic medicine?
This at-home remedy did not cure his back pain, shockingly enough. The patient instead developed a subcutaneous abscess after a year and a half of monthly intramuscular and intravenous injections, during which the semen has leaked into the soft tissues. He reported to a Dublin hospital after suffering severe back pain and a swollen arm, and eventually revealed to doctors his miracle cure.
The doctors did some Googling and found studies where rats and rabbits were injected with semen – possibly the research that inspired this trailblazer. Or, possibly, this was just an extreme case of reduce, reuse, and recycle.
In case you’re concerned, the man was given a course of more traditional medicine, and his back pain improved greatly. The patient chose to discharge himself before doctors could drain the “local collection” – perhaps he was proud of his work.
Down the rabbit hole
Imagine sitting at your computer when suddenly the icons begin to move off the screen and hover directly in front of your eyes. Your first thought might be that someone spiked your morning coffee with acid – and you’re not far off.
This curious occurrence happened to a 54-year-old man who was diagnosed with the rare perceptual disorder Alice in Wonderland syndrome (AIWS). AIWS causes people to develop a misperception of their body or surrounding space, and can be caused by a number of things, including migraine.
In this case, the man’s LSD-like visions were caused by a glioblastoma in the left temporal-occipital region of the brain. Tumors there can interfere with spatial perception, hence the temporary trip down the rabbit hole for this patient. After chemotherapy and radiation, the tumor was defeated, and the patient is back to feeling happier than the Mad Hatter at a tea party.
Must have been some party
On Dec. 25 in the Vietnamese province of Quang Tri, a 48-year-old man was taken to a hospital with a case of alcohol poisoning. Specifically, his body contained more than 1,000 times the recommended limit of methanol.
While the two types of alcohol, ethanol and methanol, are both toxic to the human body to some degree, the liver processes methanol differently and more slowly, making it far more dangerous than ethanol, the key ingredient in commercially available alcoholic beverages. Methanol is found in bootleg liquor and in such products as gasoline, paint, ink, and cleaning products. It can cause blindness, nervous system depression, and death.
However, there is a happy ending to this story. To save their patient’s life, his doctors hit upon an ingenious solution – one that would make Homer Simpson proud.
They administered cans of beer.
When the man was admitted, the doctors immediately gave him 3 cans’ worth, and then transfused an additional 12 at the rate of 1 can per hour. The liver will always prioritize processing ethanol over methanol. By feeding the patient a steady stream of relatively friendly and ethanol-rich beer, the doctors had enough time to perform dialysis and remove the methanol from the man’s system.
So, as Homer himself might declare, here’s to alcohol – truly the cause of, and solution to, all of life’s problems.
A mistake of the bloody type
Nurse: Mr. Smeggins, I need to clear up some of the answers on your new-patient information form.
Patient: I filled the whole thing out, didn’t I?
Nurse: You did, but a couple of your responses are less than helpful. You do realize that “Helvetica” is not a blood type, right?
Patient: I took a stab at it.
Nurse: You’re not the only one. It turns out that 43% of adults don’t know their blood type, and 62% don’t know their cholesterol level, according to a recent survey by Quest Diagnostics. The 1,004 respondents were more likely to know their bank account balances (75%) or their wifi passwords (74%).
Patient: Hey, that’s right! Mine is Earwiglover122.
Nurse: Great. And can I assume that you’re one of the 30% or so supposedly Web-savvy millennials (ages 20-37 years) who keep lab results in a filing cabinet at home?
Patient: Actually, I have a pile for stuff like that.
Nurse: Fine. Now about your other answers. When we asked about sex, we were not looking for “just last night.”

Flu activity down for second consecutive week
The second week of the new year brought a second straight week of declining activity for the 2018-2019 flu season, according to the Centers for Disease Control and Prevention.
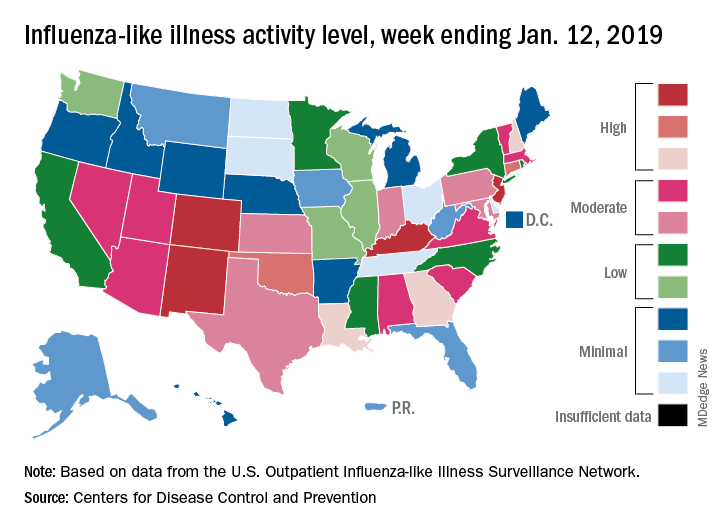
The proportion of outpatient visits for influenza-like illness (ILI) was 3.1% for the week ending Jan. 12, 2019, down from 3.5% the previous week but still above the national baseline level of 2.2%, the CDC’s influenza division reported Jan. 18.
Activity was also down at the state level. There were 4 states – Colorado, Kentucky, New Jersey, and New Mexico – at level 10 on the CDC’s 1-10 scale for ILI activity, compared with 10 the week before, and a total of 9 were in the high range from 8 to 10, compared with 15 the previous week, data from the influenza division show.
Reports of total influenza deaths, which lag a week behind other measures, continue to rise: 111 for the week ending Jan. 5, although reporting is only 72% complete. There were 89 deaths during the previous week, with reporting 82% complete so far. Total flu-related deaths among children are up to 19 for the 2018-2019 season after three more were reported during the week ending Jan. 12, the CDC said. Influenza deaths from the comparable weeks of the much more severe 2017-2018 season were 1,163 for all ages and 10 for children.
The second week of the new year brought a second straight week of declining activity for the 2018-2019 flu season, according to the Centers for Disease Control and Prevention.

The proportion of outpatient visits for influenza-like illness (ILI) was 3.1% for the week ending Jan. 12, 2019, down from 3.5% the previous week but still above the national baseline level of 2.2%, the CDC’s influenza division reported Jan. 18.
Activity was also down at the state level. There were 4 states – Colorado, Kentucky, New Jersey, and New Mexico – at level 10 on the CDC’s 1-10 scale for ILI activity, compared with 10 the week before, and a total of 9 were in the high range from 8 to 10, compared with 15 the previous week, data from the influenza division show.
Reports of total influenza deaths, which lag a week behind other measures, continue to rise: 111 for the week ending Jan. 5, although reporting is only 72% complete. There were 89 deaths during the previous week, with reporting 82% complete so far. Total flu-related deaths among children are up to 19 for the 2018-2019 season after three more were reported during the week ending Jan. 12, the CDC said. Influenza deaths from the comparable weeks of the much more severe 2017-2018 season were 1,163 for all ages and 10 for children.
The second week of the new year brought a second straight week of declining activity for the 2018-2019 flu season, according to the Centers for Disease Control and Prevention.

The proportion of outpatient visits for influenza-like illness (ILI) was 3.1% for the week ending Jan. 12, 2019, down from 3.5% the previous week but still above the national baseline level of 2.2%, the CDC’s influenza division reported Jan. 18.
Activity was also down at the state level. There were 4 states – Colorado, Kentucky, New Jersey, and New Mexico – at level 10 on the CDC’s 1-10 scale for ILI activity, compared with 10 the week before, and a total of 9 were in the high range from 8 to 10, compared with 15 the previous week, data from the influenza division show.
Reports of total influenza deaths, which lag a week behind other measures, continue to rise: 111 for the week ending Jan. 5, although reporting is only 72% complete. There were 89 deaths during the previous week, with reporting 82% complete so far. Total flu-related deaths among children are up to 19 for the 2018-2019 season after three more were reported during the week ending Jan. 12, the CDC said. Influenza deaths from the comparable weeks of the much more severe 2017-2018 season were 1,163 for all ages and 10 for children.
Survey: Government shutdown is affecting patient health
A majority of U.S. health care professionals report that their patients have been negatively affected by the federal government’s partial shutdown, according to a survey conducted Jan. 11 by health care market research company InCrowd.
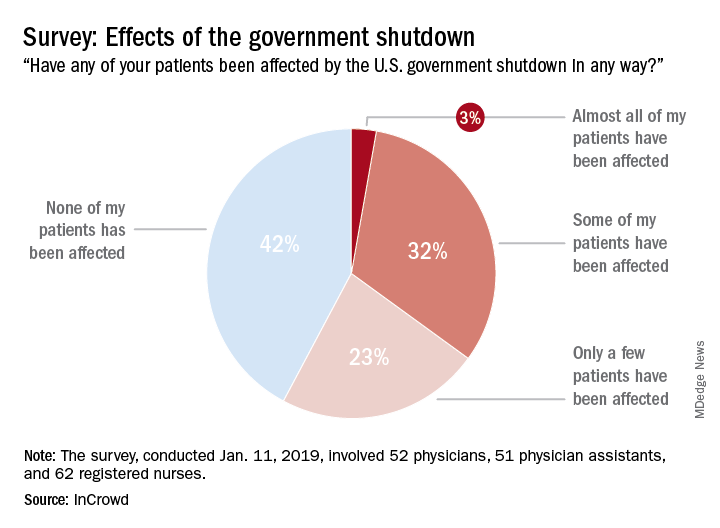
The results showed that 58% of the 165 respondents (52 primary care physicians, 51 physician assistants, and 63 registered nurses) surveyed believe that their patents have been affected in some way by the shutdown: Three percent said that almost all of their patients have been affected, 32% said that some have been affected, and 23% said that only a few patients have been affected. The largest share of clinicians (42%), however, believes that none of their patients have experienced any effects from the shutdown, InCrowd reported Jan. 17.
That distribution changes considerably, however, when looking at the physicians only: 4% (almost all), 39% (some), 31% (a few), and 26% (none). Registered nurses (50%) and physician assistants (45%) were much more likely to say that none of their patients had been affected, InCrowd reported.
“Patient access to care and compliance issues due to financial concerns and loss of benefits are already being observed by respondents. Forty percent of respondents reported a high degree of both issues with patients affording medicine and incidences where patient avoided treatments and appointments all together,” the InCrowd investigators said.
This article was updated 1/18/19.
A majority of U.S. health care professionals report that their patients have been negatively affected by the federal government’s partial shutdown, according to a survey conducted Jan. 11 by health care market research company InCrowd.

The results showed that 58% of the 165 respondents (52 primary care physicians, 51 physician assistants, and 63 registered nurses) surveyed believe that their patents have been affected in some way by the shutdown: Three percent said that almost all of their patients have been affected, 32% said that some have been affected, and 23% said that only a few patients have been affected. The largest share of clinicians (42%), however, believes that none of their patients have experienced any effects from the shutdown, InCrowd reported Jan. 17.
That distribution changes considerably, however, when looking at the physicians only: 4% (almost all), 39% (some), 31% (a few), and 26% (none). Registered nurses (50%) and physician assistants (45%) were much more likely to say that none of their patients had been affected, InCrowd reported.
“Patient access to care and compliance issues due to financial concerns and loss of benefits are already being observed by respondents. Forty percent of respondents reported a high degree of both issues with patients affording medicine and incidences where patient avoided treatments and appointments all together,” the InCrowd investigators said.
This article was updated 1/18/19.
A majority of U.S. health care professionals report that their patients have been negatively affected by the federal government’s partial shutdown, according to a survey conducted Jan. 11 by health care market research company InCrowd.

The results showed that 58% of the 165 respondents (52 primary care physicians, 51 physician assistants, and 63 registered nurses) surveyed believe that their patents have been affected in some way by the shutdown: Three percent said that almost all of their patients have been affected, 32% said that some have been affected, and 23% said that only a few patients have been affected. The largest share of clinicians (42%), however, believes that none of their patients have experienced any effects from the shutdown, InCrowd reported Jan. 17.
That distribution changes considerably, however, when looking at the physicians only: 4% (almost all), 39% (some), 31% (a few), and 26% (none). Registered nurses (50%) and physician assistants (45%) were much more likely to say that none of their patients had been affected, InCrowd reported.
“Patient access to care and compliance issues due to financial concerns and loss of benefits are already being observed by respondents. Forty percent of respondents reported a high degree of both issues with patients affording medicine and incidences where patient avoided treatments and appointments all together,” the InCrowd investigators said.
This article was updated 1/18/19.
More than 23% of antibiotic fills deemed unnecessary
More than 23% of all antibiotic prescriptions filled in 2016 were medically unnecessary, and another 36% were questionable, according to an analysis of prescribing data for 19.2 million children and nonelderly adults.
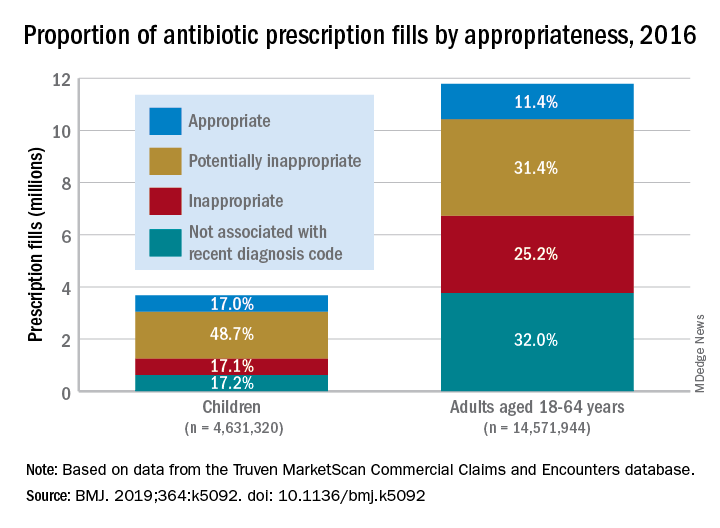
Based on the diagnosis codes for 15.5 million prescriptions filled that year, at least 3.6 million (23.2%) were “inappropriate” – prescribed for conditions for which an antibiotic is almost never recommended, such as acute upper respiratory conditions – and 5.5 million (35.5%) were “potentially inappropriate” – conditions such as acute sinusitis or otitis media, for which an antibiotic is only sometimes recommended, Kao-Ping Chua, MD, PhD, of the University of Michigan, Ann Arbor, and his associates reported in the BMJ.
Only 12.8% of filled prescriptions for the 39 oral antibiotics assessed were classified as “appropriate” under the investigators’ scheme, which assigned an antibiotic appropriateness level to all 91,738 diagnostic codes in the 2016 ICD-10-CM. Finally, 28.5% of antibiotic fills were not associated with a recent diagnosis code, suggesting that they involved phone consultations that did not result in claims or visits that were paid out of pocket and did not make it into the Truven MarketScan Commercial Claims and Encounters database used in the study, the investigators said.
The three highest levels of inappropriate fills were 70.7% in office-based settings, 6.2% in urgent care centers, and 4.7% in emergency departments.
“The unacceptable scale of inappropriate antibiotic prescribing in the United States ... underscores the need to learn more about prescriptions that aren’t justified by a diagnosis – or are written after no diagnosis at all,” coinvestigator Jeffrey Linder, MD, of Northwestern University, Chicago, said in a written statement.
Prescriptions for children, who represented almost a quarter of all antibiotic fills, were less likely to be inappropriate than those for adults aged 18-64 years. Proportions for children were 17.1% inappropriate, 48.7% potentially inappropriate, and 17.0% appropriate, compared with 25.2%, 31.4%, and 11.4%, respectively, for adults, Dr. Chua and his associates said.
“This study shows how data and analytics can help us identify and understand important challenges facing the American health care system,” said Gopal Khanna, director of the Agency for Healthcare Research and Quality, which funded the study. “We now need to use these data to spur change in the prescribing of these very common medications.”
SOURCE: Chua K-P et al. BMJ. 2019;364:k5092. doi: 10.1136/bmj.k5092.
More than 23% of all antibiotic prescriptions filled in 2016 were medically unnecessary, and another 36% were questionable, according to an analysis of prescribing data for 19.2 million children and nonelderly adults.

Based on the diagnosis codes for 15.5 million prescriptions filled that year, at least 3.6 million (23.2%) were “inappropriate” – prescribed for conditions for which an antibiotic is almost never recommended, such as acute upper respiratory conditions – and 5.5 million (35.5%) were “potentially inappropriate” – conditions such as acute sinusitis or otitis media, for which an antibiotic is only sometimes recommended, Kao-Ping Chua, MD, PhD, of the University of Michigan, Ann Arbor, and his associates reported in the BMJ.
Only 12.8% of filled prescriptions for the 39 oral antibiotics assessed were classified as “appropriate” under the investigators’ scheme, which assigned an antibiotic appropriateness level to all 91,738 diagnostic codes in the 2016 ICD-10-CM. Finally, 28.5% of antibiotic fills were not associated with a recent diagnosis code, suggesting that they involved phone consultations that did not result in claims or visits that were paid out of pocket and did not make it into the Truven MarketScan Commercial Claims and Encounters database used in the study, the investigators said.
The three highest levels of inappropriate fills were 70.7% in office-based settings, 6.2% in urgent care centers, and 4.7% in emergency departments.
“The unacceptable scale of inappropriate antibiotic prescribing in the United States ... underscores the need to learn more about prescriptions that aren’t justified by a diagnosis – or are written after no diagnosis at all,” coinvestigator Jeffrey Linder, MD, of Northwestern University, Chicago, said in a written statement.
Prescriptions for children, who represented almost a quarter of all antibiotic fills, were less likely to be inappropriate than those for adults aged 18-64 years. Proportions for children were 17.1% inappropriate, 48.7% potentially inappropriate, and 17.0% appropriate, compared with 25.2%, 31.4%, and 11.4%, respectively, for adults, Dr. Chua and his associates said.
“This study shows how data and analytics can help us identify and understand important challenges facing the American health care system,” said Gopal Khanna, director of the Agency for Healthcare Research and Quality, which funded the study. “We now need to use these data to spur change in the prescribing of these very common medications.”
SOURCE: Chua K-P et al. BMJ. 2019;364:k5092. doi: 10.1136/bmj.k5092.
More than 23% of all antibiotic prescriptions filled in 2016 were medically unnecessary, and another 36% were questionable, according to an analysis of prescribing data for 19.2 million children and nonelderly adults.

Based on the diagnosis codes for 15.5 million prescriptions filled that year, at least 3.6 million (23.2%) were “inappropriate” – prescribed for conditions for which an antibiotic is almost never recommended, such as acute upper respiratory conditions – and 5.5 million (35.5%) were “potentially inappropriate” – conditions such as acute sinusitis or otitis media, for which an antibiotic is only sometimes recommended, Kao-Ping Chua, MD, PhD, of the University of Michigan, Ann Arbor, and his associates reported in the BMJ.
Only 12.8% of filled prescriptions for the 39 oral antibiotics assessed were classified as “appropriate” under the investigators’ scheme, which assigned an antibiotic appropriateness level to all 91,738 diagnostic codes in the 2016 ICD-10-CM. Finally, 28.5% of antibiotic fills were not associated with a recent diagnosis code, suggesting that they involved phone consultations that did not result in claims or visits that were paid out of pocket and did not make it into the Truven MarketScan Commercial Claims and Encounters database used in the study, the investigators said.
The three highest levels of inappropriate fills were 70.7% in office-based settings, 6.2% in urgent care centers, and 4.7% in emergency departments.
“The unacceptable scale of inappropriate antibiotic prescribing in the United States ... underscores the need to learn more about prescriptions that aren’t justified by a diagnosis – or are written after no diagnosis at all,” coinvestigator Jeffrey Linder, MD, of Northwestern University, Chicago, said in a written statement.
Prescriptions for children, who represented almost a quarter of all antibiotic fills, were less likely to be inappropriate than those for adults aged 18-64 years. Proportions for children were 17.1% inappropriate, 48.7% potentially inappropriate, and 17.0% appropriate, compared with 25.2%, 31.4%, and 11.4%, respectively, for adults, Dr. Chua and his associates said.
“This study shows how data and analytics can help us identify and understand important challenges facing the American health care system,” said Gopal Khanna, director of the Agency for Healthcare Research and Quality, which funded the study. “We now need to use these data to spur change in the prescribing of these very common medications.”
SOURCE: Chua K-P et al. BMJ. 2019;364:k5092. doi: 10.1136/bmj.k5092.
FROM THE BMJ
Prescription puppy, China’s commode hospital, Hall of Fame diuretics
Prescription puppies
I’d like a script for a golden retriever who loves fetch and has a super sniffer, please. Turns out, man’s best friend can be especially friendly for patients with type 1 diabetes mellitus.
Dogs have been trained to detect seizures, lead the blind, and even call 9-1-1, and now they are increasingly being used as glycemia monitors for people with diabetes. Obviously, people don’t get a prescription for their helpful furry friends, but one can dream about an all-puppy pharmacy, right?
A recently published study took a look at how glycemia-alert dogs improve the quality of life of people living with type 1 diabetes, and assessed the reliability of the dogs to respond to hypo- and hyperglycemic episodes.
Researchers concluded that, overall, a trained pup’s response to these episodes is more sensitive than previously thought. In addition, researchers also found that 100% of the study participants were extremely good dogs.
Really selective hearing loss
A woman in China is experiencing something straight out of a movie – she woke up one morning and couldn’t hear men’s voices anymore. Some might say this is a tragic loss. Others might contend that she is living the dream.
The woman was diagnosed with reverse-slope hearing loss, a very rare type of hearing loss that makes the patient unable able to hear low-frequency sounds, such as a man’s voice. Only 1 in every 12,000 people with hearing loss has this kind, and it is most often caused by genetics.
In this case, the woman’s stress and extreme fatigue appear to be contributing factors to her newfound superpower. Her doctor expects her to make a full recovery, but I’d milk it for as long as possible: “What’s that? Something about the dishes, honey? Sorry I can’t hear what you’re saying!”
The epitome of crappy design
Here at MDedge News, we approve of all scatologically related humor, and the Guangxi International Zhuangyi Hospital in Nanning, China, certainly fits the bill. In an ode to the digestive system, the Chinese have built a hospital that bears an undeniable resemblance to a toilet.
The building is huge, spread out over 42 acres. The patients are contained in the multistory tank, while the medical departments line the outside of the massive bowl.
According to a local citizen, the hospital was designed this way so patients could go from the main section to the departments without carrying an umbrella. We hope it’s because they have an excellent gastroenterology department they want to show off.
Leaking the news: Hall of Fame edition
Can you name the ultimate prize for a life-saving achievement in medicine? You’re right, it is induction into the National Inventors Hall of Fame!
And that’s just what’s about to happen to the inventors of thiazide diuretics. The NIHF just announced its class of 2019, and it includes pharmacologists John Baer and Karl H. Beyer Jr. and organic chemists Frederick Novello and James Sprague, who developed Diuril (chlorothiazide) while at Merck Sharp & Dohme in the 1950s. (Is it just us, or do you get the feeling that Don Draper and the rest of the Sterling Cooper crew must have handled the Diuril account?)
The honor is, unfortunately, posthumous for all four men, but they were around for the Lasker Foundation Special Public Health Award they received in 1975.
We here at LOTME can’t top either of these commendations, but there’s at least one hypertensive on the staff who will be thinking of these men and their achievement when he experiences his next forced diuresis.

Prescription puppies
I’d like a script for a golden retriever who loves fetch and has a super sniffer, please. Turns out, man’s best friend can be especially friendly for patients with type 1 diabetes mellitus.
Dogs have been trained to detect seizures, lead the blind, and even call 9-1-1, and now they are increasingly being used as glycemia monitors for people with diabetes. Obviously, people don’t get a prescription for their helpful furry friends, but one can dream about an all-puppy pharmacy, right?
A recently published study took a look at how glycemia-alert dogs improve the quality of life of people living with type 1 diabetes, and assessed the reliability of the dogs to respond to hypo- and hyperglycemic episodes.
Researchers concluded that, overall, a trained pup’s response to these episodes is more sensitive than previously thought. In addition, researchers also found that 100% of the study participants were extremely good dogs.
Really selective hearing loss
A woman in China is experiencing something straight out of a movie – she woke up one morning and couldn’t hear men’s voices anymore. Some might say this is a tragic loss. Others might contend that she is living the dream.
The woman was diagnosed with reverse-slope hearing loss, a very rare type of hearing loss that makes the patient unable able to hear low-frequency sounds, such as a man’s voice. Only 1 in every 12,000 people with hearing loss has this kind, and it is most often caused by genetics.
In this case, the woman’s stress and extreme fatigue appear to be contributing factors to her newfound superpower. Her doctor expects her to make a full recovery, but I’d milk it for as long as possible: “What’s that? Something about the dishes, honey? Sorry I can’t hear what you’re saying!”
The epitome of crappy design
Here at MDedge News, we approve of all scatologically related humor, and the Guangxi International Zhuangyi Hospital in Nanning, China, certainly fits the bill. In an ode to the digestive system, the Chinese have built a hospital that bears an undeniable resemblance to a toilet.
The building is huge, spread out over 42 acres. The patients are contained in the multistory tank, while the medical departments line the outside of the massive bowl.
According to a local citizen, the hospital was designed this way so patients could go from the main section to the departments without carrying an umbrella. We hope it’s because they have an excellent gastroenterology department they want to show off.
Leaking the news: Hall of Fame edition
Can you name the ultimate prize for a life-saving achievement in medicine? You’re right, it is induction into the National Inventors Hall of Fame!
And that’s just what’s about to happen to the inventors of thiazide diuretics. The NIHF just announced its class of 2019, and it includes pharmacologists John Baer and Karl H. Beyer Jr. and organic chemists Frederick Novello and James Sprague, who developed Diuril (chlorothiazide) while at Merck Sharp & Dohme in the 1950s. (Is it just us, or do you get the feeling that Don Draper and the rest of the Sterling Cooper crew must have handled the Diuril account?)
The honor is, unfortunately, posthumous for all four men, but they were around for the Lasker Foundation Special Public Health Award they received in 1975.
We here at LOTME can’t top either of these commendations, but there’s at least one hypertensive on the staff who will be thinking of these men and their achievement when he experiences his next forced diuresis.

Prescription puppies
I’d like a script for a golden retriever who loves fetch and has a super sniffer, please. Turns out, man’s best friend can be especially friendly for patients with type 1 diabetes mellitus.
Dogs have been trained to detect seizures, lead the blind, and even call 9-1-1, and now they are increasingly being used as glycemia monitors for people with diabetes. Obviously, people don’t get a prescription for their helpful furry friends, but one can dream about an all-puppy pharmacy, right?
A recently published study took a look at how glycemia-alert dogs improve the quality of life of people living with type 1 diabetes, and assessed the reliability of the dogs to respond to hypo- and hyperglycemic episodes.
Researchers concluded that, overall, a trained pup’s response to these episodes is more sensitive than previously thought. In addition, researchers also found that 100% of the study participants were extremely good dogs.
Really selective hearing loss
A woman in China is experiencing something straight out of a movie – she woke up one morning and couldn’t hear men’s voices anymore. Some might say this is a tragic loss. Others might contend that she is living the dream.
The woman was diagnosed with reverse-slope hearing loss, a very rare type of hearing loss that makes the patient unable able to hear low-frequency sounds, such as a man’s voice. Only 1 in every 12,000 people with hearing loss has this kind, and it is most often caused by genetics.
In this case, the woman’s stress and extreme fatigue appear to be contributing factors to her newfound superpower. Her doctor expects her to make a full recovery, but I’d milk it for as long as possible: “What’s that? Something about the dishes, honey? Sorry I can’t hear what you’re saying!”
The epitome of crappy design
Here at MDedge News, we approve of all scatologically related humor, and the Guangxi International Zhuangyi Hospital in Nanning, China, certainly fits the bill. In an ode to the digestive system, the Chinese have built a hospital that bears an undeniable resemblance to a toilet.
The building is huge, spread out over 42 acres. The patients are contained in the multistory tank, while the medical departments line the outside of the massive bowl.
According to a local citizen, the hospital was designed this way so patients could go from the main section to the departments without carrying an umbrella. We hope it’s because they have an excellent gastroenterology department they want to show off.
Leaking the news: Hall of Fame edition
Can you name the ultimate prize for a life-saving achievement in medicine? You’re right, it is induction into the National Inventors Hall of Fame!
And that’s just what’s about to happen to the inventors of thiazide diuretics. The NIHF just announced its class of 2019, and it includes pharmacologists John Baer and Karl H. Beyer Jr. and organic chemists Frederick Novello and James Sprague, who developed Diuril (chlorothiazide) while at Merck Sharp & Dohme in the 1950s. (Is it just us, or do you get the feeling that Don Draper and the rest of the Sterling Cooper crew must have handled the Diuril account?)
The honor is, unfortunately, posthumous for all four men, but they were around for the Lasker Foundation Special Public Health Award they received in 1975.
We here at LOTME can’t top either of these commendations, but there’s at least one hypertensive on the staff who will be thinking of these men and their achievement when he experiences his next forced diuresis.

No drop in gout prevalence, but no increase either
according to data from an ongoing, nationally representative survey.
Findings from the National Health and Nutrition Examination Survey (NHANES) also show that only about one-third of gout patients were using urate-lowering therapies, Michael Chen-Xu, MBChB, MPH, of the Harvard T.H. Chan School of Public Health, Boston, and his associates wrote in Arthritis & Rheumatology.
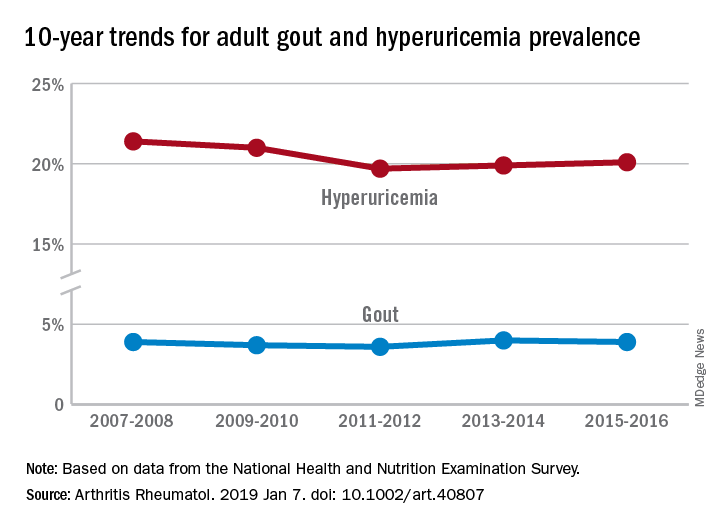
“The prevalence of gout and hyperuricemia in the United States more than doubled between the 1960s and the 1990s and continued to increase steadily afterwards,” they wrote. By 2007-2008, the earliest 2-year NHANES cycle in the study, gout prevalence among adults stood at 3.9%, but after a slight dip and a rise it was 3.9% again in 2015-2016, the last cycle in the study, the investigators reported.
The prevalence of hyperuricemia – defined as a serum urate level of more than 7.0 mg/dL in males and more than 5.7 mg/dL in females – did drop from 21.4% in 2007-2008 to 20.1% in 2015-16, but the change was not significant, Dr. Chen-Xu and his associates said.
Overall use of urate-lowering therapy (ULT) among patients with gout was 32.8% over the study period, with use showing a nonsignificant increase from 33.0% in 2007-2008 to 35.5% in 2013-2014, with a dip down to 29.4% in 2011-2012. (Data on ULT use were not available for the 2015-2016 NHANES cycle.) Current ULT use among male gout patients was 35.5% in 2013-2014 and 15.5% among women, and nearly all ULT use (95.3%) consisted of allopurinol, they said.
“Although we did not find a significant change in the trends of gout or hyperuricemia prevalence from 2007 to 2016,” Dr. Chen-Xu and his associates wrote, “10 years may not be long enough to detect what might actually be a significant trend(s) over a longer period.”
The study was supported by Ironwood and Horizon. Dr. Chen-Xu had no conflicts to disclose. One of his associates has served on advisory boards for Takeda, Ironwood, Horizon, Kowa, and Selecta. Another has served on advisory boards for Pfizer, Horizon, SOBI, and Ironwood and as a study site investigator for Takeda.
SOURCE: Chen-Xu M et al. Arthritis Rheumatol. 2019 Jan 7. doi: 10.1002/art.40807.
according to data from an ongoing, nationally representative survey.

Findings from the National Health and Nutrition Examination Survey (NHANES) also show that only about one-third of gout patients were using urate-lowering therapies, Michael Chen-Xu, MBChB, MPH, of the Harvard T.H. Chan School of Public Health, Boston, and his associates wrote in Arthritis & Rheumatology.
“The prevalence of gout and hyperuricemia in the United States more than doubled between the 1960s and the 1990s and continued to increase steadily afterwards,” they wrote. By 2007-2008, the earliest 2-year NHANES cycle in the study, gout prevalence among adults stood at 3.9%, but after a slight dip and a rise it was 3.9% again in 2015-2016, the last cycle in the study, the investigators reported.
The prevalence of hyperuricemia – defined as a serum urate level of more than 7.0 mg/dL in males and more than 5.7 mg/dL in females – did drop from 21.4% in 2007-2008 to 20.1% in 2015-16, but the change was not significant, Dr. Chen-Xu and his associates said.
Overall use of urate-lowering therapy (ULT) among patients with gout was 32.8% over the study period, with use showing a nonsignificant increase from 33.0% in 2007-2008 to 35.5% in 2013-2014, with a dip down to 29.4% in 2011-2012. (Data on ULT use were not available for the 2015-2016 NHANES cycle.) Current ULT use among male gout patients was 35.5% in 2013-2014 and 15.5% among women, and nearly all ULT use (95.3%) consisted of allopurinol, they said.
“Although we did not find a significant change in the trends of gout or hyperuricemia prevalence from 2007 to 2016,” Dr. Chen-Xu and his associates wrote, “10 years may not be long enough to detect what might actually be a significant trend(s) over a longer period.”
The study was supported by Ironwood and Horizon. Dr. Chen-Xu had no conflicts to disclose. One of his associates has served on advisory boards for Takeda, Ironwood, Horizon, Kowa, and Selecta. Another has served on advisory boards for Pfizer, Horizon, SOBI, and Ironwood and as a study site investigator for Takeda.
SOURCE: Chen-Xu M et al. Arthritis Rheumatol. 2019 Jan 7. doi: 10.1002/art.40807.
according to data from an ongoing, nationally representative survey.

Findings from the National Health and Nutrition Examination Survey (NHANES) also show that only about one-third of gout patients were using urate-lowering therapies, Michael Chen-Xu, MBChB, MPH, of the Harvard T.H. Chan School of Public Health, Boston, and his associates wrote in Arthritis & Rheumatology.
“The prevalence of gout and hyperuricemia in the United States more than doubled between the 1960s and the 1990s and continued to increase steadily afterwards,” they wrote. By 2007-2008, the earliest 2-year NHANES cycle in the study, gout prevalence among adults stood at 3.9%, but after a slight dip and a rise it was 3.9% again in 2015-2016, the last cycle in the study, the investigators reported.
The prevalence of hyperuricemia – defined as a serum urate level of more than 7.0 mg/dL in males and more than 5.7 mg/dL in females – did drop from 21.4% in 2007-2008 to 20.1% in 2015-16, but the change was not significant, Dr. Chen-Xu and his associates said.
Overall use of urate-lowering therapy (ULT) among patients with gout was 32.8% over the study period, with use showing a nonsignificant increase from 33.0% in 2007-2008 to 35.5% in 2013-2014, with a dip down to 29.4% in 2011-2012. (Data on ULT use were not available for the 2015-2016 NHANES cycle.) Current ULT use among male gout patients was 35.5% in 2013-2014 and 15.5% among women, and nearly all ULT use (95.3%) consisted of allopurinol, they said.
“Although we did not find a significant change in the trends of gout or hyperuricemia prevalence from 2007 to 2016,” Dr. Chen-Xu and his associates wrote, “10 years may not be long enough to detect what might actually be a significant trend(s) over a longer period.”
The study was supported by Ironwood and Horizon. Dr. Chen-Xu had no conflicts to disclose. One of his associates has served on advisory boards for Takeda, Ironwood, Horizon, Kowa, and Selecta. Another has served on advisory boards for Pfizer, Horizon, SOBI, and Ironwood and as a study site investigator for Takeda.
SOURCE: Chen-Xu M et al. Arthritis Rheumatol. 2019 Jan 7. doi: 10.1002/art.40807.
FROM ARTHRITIS & RHEUMATOLOGY