User login
Nasogastric drainage may be unnecessary post PD
Fewer than 10% of pancreaticoduodenectomy patients required postoperative nasogastric drainage, the current postoperative standard of care for pancreaticoduodenectomy, the results of a longitudinal observational cohort study have shown.
Dr. John W. Kunstman and his colleagues in the surgery department of Yale University, New Haven, Conn., observed two consecutive cohorts of 125 pancreaticoduodenectomy (PD) patients. The first cohort had nasogastric tubes (NGTs) maintained postoperatively until clinically indicated, while the second cohort had NGTs maintained postoperatively "only in rare circumstances, such as inability to extubate the patient postoperatively," the authors said. All patients were treated by the same surgeon between July 2003 and February 2012, most commonly for pancreatic neoplasm.
There were no statistically significant differences between the two groups in patient demographics, including indications for surgery. The routine NGT group was 51% male with an average age of 63 years, while the selective NGT group was 46% male with an average age of 67 years. Bias was reduced in that both cohorts were analyzed in an intent-to-treat manner.
Pylorus-preserving pancreaticoduodenectomy (PPPD) was performed in the absence of oncologic or other disease-specific considerations; otherwise, a classic (Kausch-Whipple) PD was performed. The most common comorbidity overall was hypertension, although the routine NGT group had a higher incidence of coronary artery disease than the selective NGT group (20.8% vs. 8.8%) and a higher mean creatinine level (0.97 vs. 0.88 mg/dL) (J. Am. Coll. Surgeons 2013;217:481-8).
Primary outcomes included postoperative NGT insertion and reinsertion, delayed gastric emptying (DGE) incidence, time to dietary tolerance, and length of stay.
In the selective NGT cohort, only 9 patients required continued NGT, 5 of them for postoperative endotracheal intubation and 4 for surgical considerations.
Neither the incidence of NGT insertion and reinsertion, nor the duration of NGT replacement, differed significantly between groups. Overall complication rates were also similar, although patients in the selective NGT group were less likely to have DGE. Compared with the routine NGT cohort, the selective cohort had a shorter mean length of stay (10 vs. 7 days) and mean time to dietary tolerance.
Additionally, multivariate analysis of all outcome variables indicated that DGE, the most common adverse event associated with PD, was independently correlated with the routine use of NGT.
"This is of particular interest given the role that gastric decompression plays in treatment of DGE. However, this finding must be interpreted with care, as incidence of DGE varies from 10% to 50% of PD cases, depending on the reporting group," the authors wrote.
In terms of the study’s limitations, the higher number of PPPD and retrocolic gastroenteric anastomoses performed in the routine cohort may have been a factor in the differing DGE incidence rates, since pylorus preservation and anastomotic positioning are considered historically correlated to DGE, the authors said.
Among individually examined adverse events, routine NGT patients were more likely than selective patients to be reintubated (11.2% vs. 3.2%), require a postoperative blood transfusion (16.0% vs. 6.4%), and be diagnosed with DGE (18.4% vs. 8.0%).
There were a total of four deaths in the 30-day postoperative period, all occurring in patients over age 80. There were eight octogenarians in each cohort; three of the deaths occurred in the routine group.
Improvements in perioperative care and the surgeon’s increased skill over time may also have affected the results. However, the authors concluded, "based on these data, persistent concerns, such as fear of increased anastomotic leak or DGE, which have mandated customary nasogastric decompression after PD, can be safely reevaluated."
Dr. Kunstman and his coauthors reported no relevant disclosures.
Fewer than 10% of pancreaticoduodenectomy patients required postoperative nasogastric drainage, the current postoperative standard of care for pancreaticoduodenectomy, the results of a longitudinal observational cohort study have shown.
Dr. John W. Kunstman and his colleagues in the surgery department of Yale University, New Haven, Conn., observed two consecutive cohorts of 125 pancreaticoduodenectomy (PD) patients. The first cohort had nasogastric tubes (NGTs) maintained postoperatively until clinically indicated, while the second cohort had NGTs maintained postoperatively "only in rare circumstances, such as inability to extubate the patient postoperatively," the authors said. All patients were treated by the same surgeon between July 2003 and February 2012, most commonly for pancreatic neoplasm.
There were no statistically significant differences between the two groups in patient demographics, including indications for surgery. The routine NGT group was 51% male with an average age of 63 years, while the selective NGT group was 46% male with an average age of 67 years. Bias was reduced in that both cohorts were analyzed in an intent-to-treat manner.
Pylorus-preserving pancreaticoduodenectomy (PPPD) was performed in the absence of oncologic or other disease-specific considerations; otherwise, a classic (Kausch-Whipple) PD was performed. The most common comorbidity overall was hypertension, although the routine NGT group had a higher incidence of coronary artery disease than the selective NGT group (20.8% vs. 8.8%) and a higher mean creatinine level (0.97 vs. 0.88 mg/dL) (J. Am. Coll. Surgeons 2013;217:481-8).
Primary outcomes included postoperative NGT insertion and reinsertion, delayed gastric emptying (DGE) incidence, time to dietary tolerance, and length of stay.
In the selective NGT cohort, only 9 patients required continued NGT, 5 of them for postoperative endotracheal intubation and 4 for surgical considerations.
Neither the incidence of NGT insertion and reinsertion, nor the duration of NGT replacement, differed significantly between groups. Overall complication rates were also similar, although patients in the selective NGT group were less likely to have DGE. Compared with the routine NGT cohort, the selective cohort had a shorter mean length of stay (10 vs. 7 days) and mean time to dietary tolerance.
Additionally, multivariate analysis of all outcome variables indicated that DGE, the most common adverse event associated with PD, was independently correlated with the routine use of NGT.
"This is of particular interest given the role that gastric decompression plays in treatment of DGE. However, this finding must be interpreted with care, as incidence of DGE varies from 10% to 50% of PD cases, depending on the reporting group," the authors wrote.
In terms of the study’s limitations, the higher number of PPPD and retrocolic gastroenteric anastomoses performed in the routine cohort may have been a factor in the differing DGE incidence rates, since pylorus preservation and anastomotic positioning are considered historically correlated to DGE, the authors said.
Among individually examined adverse events, routine NGT patients were more likely than selective patients to be reintubated (11.2% vs. 3.2%), require a postoperative blood transfusion (16.0% vs. 6.4%), and be diagnosed with DGE (18.4% vs. 8.0%).
There were a total of four deaths in the 30-day postoperative period, all occurring in patients over age 80. There were eight octogenarians in each cohort; three of the deaths occurred in the routine group.
Improvements in perioperative care and the surgeon’s increased skill over time may also have affected the results. However, the authors concluded, "based on these data, persistent concerns, such as fear of increased anastomotic leak or DGE, which have mandated customary nasogastric decompression after PD, can be safely reevaluated."
Dr. Kunstman and his coauthors reported no relevant disclosures.
Fewer than 10% of pancreaticoduodenectomy patients required postoperative nasogastric drainage, the current postoperative standard of care for pancreaticoduodenectomy, the results of a longitudinal observational cohort study have shown.
Dr. John W. Kunstman and his colleagues in the surgery department of Yale University, New Haven, Conn., observed two consecutive cohorts of 125 pancreaticoduodenectomy (PD) patients. The first cohort had nasogastric tubes (NGTs) maintained postoperatively until clinically indicated, while the second cohort had NGTs maintained postoperatively "only in rare circumstances, such as inability to extubate the patient postoperatively," the authors said. All patients were treated by the same surgeon between July 2003 and February 2012, most commonly for pancreatic neoplasm.
There were no statistically significant differences between the two groups in patient demographics, including indications for surgery. The routine NGT group was 51% male with an average age of 63 years, while the selective NGT group was 46% male with an average age of 67 years. Bias was reduced in that both cohorts were analyzed in an intent-to-treat manner.
Pylorus-preserving pancreaticoduodenectomy (PPPD) was performed in the absence of oncologic or other disease-specific considerations; otherwise, a classic (Kausch-Whipple) PD was performed. The most common comorbidity overall was hypertension, although the routine NGT group had a higher incidence of coronary artery disease than the selective NGT group (20.8% vs. 8.8%) and a higher mean creatinine level (0.97 vs. 0.88 mg/dL) (J. Am. Coll. Surgeons 2013;217:481-8).
Primary outcomes included postoperative NGT insertion and reinsertion, delayed gastric emptying (DGE) incidence, time to dietary tolerance, and length of stay.
In the selective NGT cohort, only 9 patients required continued NGT, 5 of them for postoperative endotracheal intubation and 4 for surgical considerations.
Neither the incidence of NGT insertion and reinsertion, nor the duration of NGT replacement, differed significantly between groups. Overall complication rates were also similar, although patients in the selective NGT group were less likely to have DGE. Compared with the routine NGT cohort, the selective cohort had a shorter mean length of stay (10 vs. 7 days) and mean time to dietary tolerance.
Additionally, multivariate analysis of all outcome variables indicated that DGE, the most common adverse event associated with PD, was independently correlated with the routine use of NGT.
"This is of particular interest given the role that gastric decompression plays in treatment of DGE. However, this finding must be interpreted with care, as incidence of DGE varies from 10% to 50% of PD cases, depending on the reporting group," the authors wrote.
In terms of the study’s limitations, the higher number of PPPD and retrocolic gastroenteric anastomoses performed in the routine cohort may have been a factor in the differing DGE incidence rates, since pylorus preservation and anastomotic positioning are considered historically correlated to DGE, the authors said.
Among individually examined adverse events, routine NGT patients were more likely than selective patients to be reintubated (11.2% vs. 3.2%), require a postoperative blood transfusion (16.0% vs. 6.4%), and be diagnosed with DGE (18.4% vs. 8.0%).
There were a total of four deaths in the 30-day postoperative period, all occurring in patients over age 80. There were eight octogenarians in each cohort; three of the deaths occurred in the routine group.
Improvements in perioperative care and the surgeon’s increased skill over time may also have affected the results. However, the authors concluded, "based on these data, persistent concerns, such as fear of increased anastomotic leak or DGE, which have mandated customary nasogastric decompression after PD, can be safely reevaluated."
Dr. Kunstman and his coauthors reported no relevant disclosures.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF SURGEONS
Major finding: Selective use of nasogastric decompression is shown to be an effective treatment strategy post pancreaticoduodenectomy.
Data source: An observational cohort study of 250 PD patients, via a retrospective study of prospectively collected data.
Disclosures: Dr. Kunstman and his coauthors reported no relevant disclosures.
No inverse link found between H. pylori and gastroesophageal reflux disease
Helicobacter pylori was found to have a strong inverse link with Barrett’s esophagus, but not with symptoms of gastroesophageal reflux disease. Erosive esophagitis also was seen to trend toward an inverse association with H. pylori.
Previous reports have attributed a protective effect against gastroesophageal reflux disease (GERD), esophageal adenocarcinoma, and Barrett’s esophagus to H. pylori infection, particularly the cytotoxin-associated gene A (cagA+) strain. Having determined the studies associating H. pylori with GERD either yielded weak support for an inverse relationship, were prone to bias, or were otherwise flawed, a team led by Dr. Joel Rubenstein of the Veterans Affairs Center for Clinical Management Research, Washington, and the University of Michigan Medical School in Ann Arbor analyzed the associations of the three disease outcomes occurring in the same populations with the bacterium.
They constructed a case-control study of men between the ages of 50 and 79 years (n = 533), who had colorectal cancer screening at one of two tertiary medical centers in Michigan between 2008 and 2011, and who were recruited to have upper endoscopy. The study served as a secondary analysis of the Newly Diagnosed Barrett’s Esophagus Study, and included three non–mutually exclusive case groups: Barrett’s esophagus, erosive esophagitis, and GERD symptoms. An additional group of men in the same age group (n = 80) found to have Barrett’s esophagus during clinically indicated upper endoscopy exams was also assessed.
Using logistic regression, the investigators estimated any associations between serum antibodies against H. pylori and cagA+ in the study group, and GERD symptoms, esophagitis, and Barrett’s esophagus. These results were compared with a control group of randomly selected men (n = 177) who did not have any of the three conditions and who were having colorectal screens.
Women were not studied, because of their typically low rates of Barrett’s esophagus. Also excluded were men with any history of upper endoscopy, Barrett’s esophagus, or esophagectomy; diagnostic indication for colonoscopy; inflammatory* bowel disease; known ascites or esophageal varices; any cancers other than melanoma in the previous 5 years; or notable coagulopathy.
The study did include consecutive men between the ages of 50 and 79 years, newly diagnosed at either of the two study sites with Barrett’s esophagus by way of a clinically indicated upper endoscopy.
To determine the presence of GERD, the study group was given a survey that was not formally validated, about their use of proton pump inhibitors (PPI) and histamine2 receptor agonists (HR2A) in relation to the frequency they experienced heartburn and regurgitation. Patients who reported weekly heartburn and regurgitation while not using medication were considered to have GERD. A validated survey, the Mayo Clinic’s Gastroesophageal Reflux Questionnaire (GERQ), was applied during the last quarter of the study, although because the GERQ does not address the role of acid-reducing medications, the investigators wrote that there is the chance that patients with GERD managed by medication could have been misclassified by the questionnaire as non-GERD controls.
The study group also underwent colonoscopy, followed by upper endoscopy. If Barrett’s esophagus was suspected, biopsies were obtained. Using the Los Angeles Classification scheme, if class C or D esophagitis was found, patients repeated the endoscopy while taking a PPI before investigators determined if the patient had Barrett’s esophagus. Patients who were not taking any acid-reducing medications at the time of the endoscopy who reported at least weekly symptoms of GERD and had a normal endoscopy without erosive esophagitis or Barrett’s esophagus were considered to have nonerosive reflux symptoms. Patients with Barrett’s esophagus identified on a clinically indicated upper endoscopy were included with the same as those identified among the the people screened for colorectal cancer. Blood samples were drawn from all subjects and assayed for H. pylori.
The results were that 822 of the colorectal cancer patients had upper endoscopy; 328 were randomly selected for descriptive analysis of assays, 22.3% of which were found to have antibodies against H. pylori, with 1.8% equivocal for H. pylori on two assays. Of those positive for H. pylori, nearly half (49.3%) were found to have antibodies against cagA while none of those who were equivocal for H. pylori were found to have antibodies against cagA. Compared with study group members who were seropositive for H. pylori, those who were seronegative were less likely to be smokers and to have higher education and income.
Noting that classification errors for GERD might have biased the estimated associations with H. pylori toward the null, the investigators discovered that while there was a strong inverse connection between H. pylori, especially the cagA+ strain, and erosive esophagus (H. pylori adjusted odds ratio, 0.63; 95% confidence interval: 0.37-1.08 and cagA+ OR, 0.47; 95% CI: 0.21-1.03) and Barrett’s esophagus (OR, 0.53; 95% CI: 0.29 -0.97), especially the cagA+ strain (OR, 0.36; 95% CI: 0.14-0.90), they could not make a decisive link between GERD symptoms and H. pylori infection (OR, 0.948; 95% CI: 0.548-1.64 and cagA+ OR, 0.967; 95% CI: 0.461-2.03) (Clin. Gastroenterol. Hepatol. 2013 [doi: 10.1016/j.cgh.2013.08.029]).
Dr. Rubenstein and his colleagues theorized that since the GERD link was not found, the mechanism of H. pylori’s negative association with Barrett’s esophagus might be from the direct impact of the bacteria on the inflammatory or mucosal response; its indirect effects on the production of leptin or ghrelin; or a confounding effect created by genetic regulation of cytokines or prior alterations in the esophageal and gastric microbiota.
The study was underwritten by the National Institutes of Health and by a senior marketing grant from the American Society for Gastrointestinal Endoscopy. Dr. Rubenstein and his associates reported no relevant disclosures.
*Correction, 9/20/2013: An earlier version of this story incorrectly identified inflammatory bowel disease.
Helicobacter pylori was found to have a strong inverse link with Barrett’s esophagus, but not with symptoms of gastroesophageal reflux disease. Erosive esophagitis also was seen to trend toward an inverse association with H. pylori.
Previous reports have attributed a protective effect against gastroesophageal reflux disease (GERD), esophageal adenocarcinoma, and Barrett’s esophagus to H. pylori infection, particularly the cytotoxin-associated gene A (cagA+) strain. Having determined the studies associating H. pylori with GERD either yielded weak support for an inverse relationship, were prone to bias, or were otherwise flawed, a team led by Dr. Joel Rubenstein of the Veterans Affairs Center for Clinical Management Research, Washington, and the University of Michigan Medical School in Ann Arbor analyzed the associations of the three disease outcomes occurring in the same populations with the bacterium.
They constructed a case-control study of men between the ages of 50 and 79 years (n = 533), who had colorectal cancer screening at one of two tertiary medical centers in Michigan between 2008 and 2011, and who were recruited to have upper endoscopy. The study served as a secondary analysis of the Newly Diagnosed Barrett’s Esophagus Study, and included three non–mutually exclusive case groups: Barrett’s esophagus, erosive esophagitis, and GERD symptoms. An additional group of men in the same age group (n = 80) found to have Barrett’s esophagus during clinically indicated upper endoscopy exams was also assessed.
Using logistic regression, the investigators estimated any associations between serum antibodies against H. pylori and cagA+ in the study group, and GERD symptoms, esophagitis, and Barrett’s esophagus. These results were compared with a control group of randomly selected men (n = 177) who did not have any of the three conditions and who were having colorectal screens.
Women were not studied, because of their typically low rates of Barrett’s esophagus. Also excluded were men with any history of upper endoscopy, Barrett’s esophagus, or esophagectomy; diagnostic indication for colonoscopy; inflammatory* bowel disease; known ascites or esophageal varices; any cancers other than melanoma in the previous 5 years; or notable coagulopathy.
The study did include consecutive men between the ages of 50 and 79 years, newly diagnosed at either of the two study sites with Barrett’s esophagus by way of a clinically indicated upper endoscopy.
To determine the presence of GERD, the study group was given a survey that was not formally validated, about their use of proton pump inhibitors (PPI) and histamine2 receptor agonists (HR2A) in relation to the frequency they experienced heartburn and regurgitation. Patients who reported weekly heartburn and regurgitation while not using medication were considered to have GERD. A validated survey, the Mayo Clinic’s Gastroesophageal Reflux Questionnaire (GERQ), was applied during the last quarter of the study, although because the GERQ does not address the role of acid-reducing medications, the investigators wrote that there is the chance that patients with GERD managed by medication could have been misclassified by the questionnaire as non-GERD controls.
The study group also underwent colonoscopy, followed by upper endoscopy. If Barrett’s esophagus was suspected, biopsies were obtained. Using the Los Angeles Classification scheme, if class C or D esophagitis was found, patients repeated the endoscopy while taking a PPI before investigators determined if the patient had Barrett’s esophagus. Patients who were not taking any acid-reducing medications at the time of the endoscopy who reported at least weekly symptoms of GERD and had a normal endoscopy without erosive esophagitis or Barrett’s esophagus were considered to have nonerosive reflux symptoms. Patients with Barrett’s esophagus identified on a clinically indicated upper endoscopy were included with the same as those identified among the the people screened for colorectal cancer. Blood samples were drawn from all subjects and assayed for H. pylori.
The results were that 822 of the colorectal cancer patients had upper endoscopy; 328 were randomly selected for descriptive analysis of assays, 22.3% of which were found to have antibodies against H. pylori, with 1.8% equivocal for H. pylori on two assays. Of those positive for H. pylori, nearly half (49.3%) were found to have antibodies against cagA while none of those who were equivocal for H. pylori were found to have antibodies against cagA. Compared with study group members who were seropositive for H. pylori, those who were seronegative were less likely to be smokers and to have higher education and income.
Noting that classification errors for GERD might have biased the estimated associations with H. pylori toward the null, the investigators discovered that while there was a strong inverse connection between H. pylori, especially the cagA+ strain, and erosive esophagus (H. pylori adjusted odds ratio, 0.63; 95% confidence interval: 0.37-1.08 and cagA+ OR, 0.47; 95% CI: 0.21-1.03) and Barrett’s esophagus (OR, 0.53; 95% CI: 0.29 -0.97), especially the cagA+ strain (OR, 0.36; 95% CI: 0.14-0.90), they could not make a decisive link between GERD symptoms and H. pylori infection (OR, 0.948; 95% CI: 0.548-1.64 and cagA+ OR, 0.967; 95% CI: 0.461-2.03) (Clin. Gastroenterol. Hepatol. 2013 [doi: 10.1016/j.cgh.2013.08.029]).
Dr. Rubenstein and his colleagues theorized that since the GERD link was not found, the mechanism of H. pylori’s negative association with Barrett’s esophagus might be from the direct impact of the bacteria on the inflammatory or mucosal response; its indirect effects on the production of leptin or ghrelin; or a confounding effect created by genetic regulation of cytokines or prior alterations in the esophageal and gastric microbiota.
The study was underwritten by the National Institutes of Health and by a senior marketing grant from the American Society for Gastrointestinal Endoscopy. Dr. Rubenstein and his associates reported no relevant disclosures.
*Correction, 9/20/2013: An earlier version of this story incorrectly identified inflammatory bowel disease.
Helicobacter pylori was found to have a strong inverse link with Barrett’s esophagus, but not with symptoms of gastroesophageal reflux disease. Erosive esophagitis also was seen to trend toward an inverse association with H. pylori.
Previous reports have attributed a protective effect against gastroesophageal reflux disease (GERD), esophageal adenocarcinoma, and Barrett’s esophagus to H. pylori infection, particularly the cytotoxin-associated gene A (cagA+) strain. Having determined the studies associating H. pylori with GERD either yielded weak support for an inverse relationship, were prone to bias, or were otherwise flawed, a team led by Dr. Joel Rubenstein of the Veterans Affairs Center for Clinical Management Research, Washington, and the University of Michigan Medical School in Ann Arbor analyzed the associations of the three disease outcomes occurring in the same populations with the bacterium.
They constructed a case-control study of men between the ages of 50 and 79 years (n = 533), who had colorectal cancer screening at one of two tertiary medical centers in Michigan between 2008 and 2011, and who were recruited to have upper endoscopy. The study served as a secondary analysis of the Newly Diagnosed Barrett’s Esophagus Study, and included three non–mutually exclusive case groups: Barrett’s esophagus, erosive esophagitis, and GERD symptoms. An additional group of men in the same age group (n = 80) found to have Barrett’s esophagus during clinically indicated upper endoscopy exams was also assessed.
Using logistic regression, the investigators estimated any associations between serum antibodies against H. pylori and cagA+ in the study group, and GERD symptoms, esophagitis, and Barrett’s esophagus. These results were compared with a control group of randomly selected men (n = 177) who did not have any of the three conditions and who were having colorectal screens.
Women were not studied, because of their typically low rates of Barrett’s esophagus. Also excluded were men with any history of upper endoscopy, Barrett’s esophagus, or esophagectomy; diagnostic indication for colonoscopy; inflammatory* bowel disease; known ascites or esophageal varices; any cancers other than melanoma in the previous 5 years; or notable coagulopathy.
The study did include consecutive men between the ages of 50 and 79 years, newly diagnosed at either of the two study sites with Barrett’s esophagus by way of a clinically indicated upper endoscopy.
To determine the presence of GERD, the study group was given a survey that was not formally validated, about their use of proton pump inhibitors (PPI) and histamine2 receptor agonists (HR2A) in relation to the frequency they experienced heartburn and regurgitation. Patients who reported weekly heartburn and regurgitation while not using medication were considered to have GERD. A validated survey, the Mayo Clinic’s Gastroesophageal Reflux Questionnaire (GERQ), was applied during the last quarter of the study, although because the GERQ does not address the role of acid-reducing medications, the investigators wrote that there is the chance that patients with GERD managed by medication could have been misclassified by the questionnaire as non-GERD controls.
The study group also underwent colonoscopy, followed by upper endoscopy. If Barrett’s esophagus was suspected, biopsies were obtained. Using the Los Angeles Classification scheme, if class C or D esophagitis was found, patients repeated the endoscopy while taking a PPI before investigators determined if the patient had Barrett’s esophagus. Patients who were not taking any acid-reducing medications at the time of the endoscopy who reported at least weekly symptoms of GERD and had a normal endoscopy without erosive esophagitis or Barrett’s esophagus were considered to have nonerosive reflux symptoms. Patients with Barrett’s esophagus identified on a clinically indicated upper endoscopy were included with the same as those identified among the the people screened for colorectal cancer. Blood samples were drawn from all subjects and assayed for H. pylori.
The results were that 822 of the colorectal cancer patients had upper endoscopy; 328 were randomly selected for descriptive analysis of assays, 22.3% of which were found to have antibodies against H. pylori, with 1.8% equivocal for H. pylori on two assays. Of those positive for H. pylori, nearly half (49.3%) were found to have antibodies against cagA while none of those who were equivocal for H. pylori were found to have antibodies against cagA. Compared with study group members who were seropositive for H. pylori, those who were seronegative were less likely to be smokers and to have higher education and income.
Noting that classification errors for GERD might have biased the estimated associations with H. pylori toward the null, the investigators discovered that while there was a strong inverse connection between H. pylori, especially the cagA+ strain, and erosive esophagus (H. pylori adjusted odds ratio, 0.63; 95% confidence interval: 0.37-1.08 and cagA+ OR, 0.47; 95% CI: 0.21-1.03) and Barrett’s esophagus (OR, 0.53; 95% CI: 0.29 -0.97), especially the cagA+ strain (OR, 0.36; 95% CI: 0.14-0.90), they could not make a decisive link between GERD symptoms and H. pylori infection (OR, 0.948; 95% CI: 0.548-1.64 and cagA+ OR, 0.967; 95% CI: 0.461-2.03) (Clin. Gastroenterol. Hepatol. 2013 [doi: 10.1016/j.cgh.2013.08.029]).
Dr. Rubenstein and his colleagues theorized that since the GERD link was not found, the mechanism of H. pylori’s negative association with Barrett’s esophagus might be from the direct impact of the bacteria on the inflammatory or mucosal response; its indirect effects on the production of leptin or ghrelin; or a confounding effect created by genetic regulation of cytokines or prior alterations in the esophageal and gastric microbiota.
The study was underwritten by the National Institutes of Health and by a senior marketing grant from the American Society for Gastrointestinal Endoscopy. Dr. Rubenstein and his associates reported no relevant disclosures.
*Correction, 9/20/2013: An earlier version of this story incorrectly identified inflammatory bowel disease.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Major finding: An inverse relationship exists between H. pylori infection and Barrett’s esophagus, but not GERD.
Data source: Large case-controlled study of men (aged 50-79 years) undergoing colorectal screenings and upper endoscopy at two tertiary medical centers, with no previous diagnoses of Barrett’s esophagus.
Disclosures: The study was underwritten by the National Institutes of Health and by a senior marketing grant from the American Society for Gastrointestinal Endoscopy. Dr. Rubenstein and his associates reported no relevant disclosures.
FDA announces classwide label changes to extended-release/long-acting opioids
The U.S. Food and Drug Administration has announced that it is making classwide label changes to extended-release and long-acting opioid analgesics for treatment of chronic pain. In addition, drug manufacturers will now be required to conduct postmarket studies to help the agency determine whether further actions are merited.
"The FDA is invoking its authority to require safety labeling changes and postmarket studies to combat the crisis of misuse, abuse, addiction, overdose, and death from these potent drugs that have harmed too many patients and devastated too many families and communities," Dr. Margaret A. Hamburg, FDA commissioner, said Sept. 10 in a press briefing. "Today’s action demonstrates the FDA’s resolve to reduce the serious risks of long-acting and extended release opioids while still seeking to preserve appropriate access for those patients who rely on these medications to manage their pain."
Extended-release and long-acting opioids include hydromorphone, morphine, oxycodone, oxymorphone, and tapentadol. Changes to labels will include updated information about dosage and administration, warnings and precautions, drug interactions, use in specific populations, patient counseling information, and the medication guide. Modifications also will be made to the extended-release/long-acting opioid analgesics Risk Evaluation and Mitigation Strategy (REMS), to reflect the updated information.
The key change centers on moving prescribers away from the assessment of a patient’s pain based solely on a pain scale to a more "comprehensive one," according to Dr. Douglas Throckmorton, deputy director for regulatory programs in the FDA’s Center for Drug Evaluation and Research. "The updated indication states that extended-release, long-acting opioids are indicated for the management of pain severe enough to require daily, around-the-clock, long-term opioid treatment and for which alternative treatment options are inadequate," Dr. Throckmorton stated in the briefing. Alternative pain medications noted in an agency statement released prior to the briefing include immediate-release opioids, which are currently unaffected by the agency’s labeling changes.
Dr. Throckmorton said he hopes the FDA’s action is part of a "broader effort to encourage people to consider how best to use these medications." When asked whether prescribers and their patients weren’t already addressing the risks and benefits involved in the use of these opioids, the current labeling for which indicates their use in patients experiencing "moderate to severe pain," rather than "round-the-clock" pain, Dr. Throckmorton said the labeling changes "will help reinforce the importance of the conversation in a busy practice."
The agency’s announcement comes amid growing data about the inherent risks of opioid use reported in the medical literature and the filing with the FDA of two citizen petitions to change how opioids are prescribed, including one by the Physicians for Responsible Opioid Prescribing. Also part of the focus on opioid use is the 19 to 10 vote by the FDA’s Drug Safety and Risk Management Advisory Committee in January to reschedule hydrocodone drug combinations from schedule III under the Controlled Substances Act (CSA) to schedule II. The vote was prompted by the U.S. Drug Enforcement Administration’s call for the FDA to react to evidence that the medications are overprescribed, diverted, and abused. Statistics cited by FDA officials in the briefing included nearly 16,000 opioid-related deaths in the United States in 2009, reflecting a 300% increase in the last 20 years.
Speaking about the importance of the dosage and duration of the medications, Dr. Throckmorton said the agency did not have enough information at this time to make changes to how these drugs are prescribed, but that the postmarket studies such as clinical trials, and other studies of at least 12 weeks’ duration, would play a role in providing this data. "We expect some of those studies will provide information for us to use in 2 years. So, by end of 2015, we will have more," Dr. Throckmorton said.
Also announced in the briefing was the addition of a boxed warning on extended-release/long-acting opioid analgesics to warn expectant mothers of neonatal opioid withdrawal syndrome (NOWS), which might be life-threatening and require management according to protocols developed by neonatology experts. NOWS can occur in a newborn exposed to opioid drugs while in the mother’s womb. Symptoms may include poor feeding, rapid breathing, trembling, and excessive or high-pitched crying.
The U.S. Food and Drug Administration has announced that it is making classwide label changes to extended-release and long-acting opioid analgesics for treatment of chronic pain. In addition, drug manufacturers will now be required to conduct postmarket studies to help the agency determine whether further actions are merited.
"The FDA is invoking its authority to require safety labeling changes and postmarket studies to combat the crisis of misuse, abuse, addiction, overdose, and death from these potent drugs that have harmed too many patients and devastated too many families and communities," Dr. Margaret A. Hamburg, FDA commissioner, said Sept. 10 in a press briefing. "Today’s action demonstrates the FDA’s resolve to reduce the serious risks of long-acting and extended release opioids while still seeking to preserve appropriate access for those patients who rely on these medications to manage their pain."
Extended-release and long-acting opioids include hydromorphone, morphine, oxycodone, oxymorphone, and tapentadol. Changes to labels will include updated information about dosage and administration, warnings and precautions, drug interactions, use in specific populations, patient counseling information, and the medication guide. Modifications also will be made to the extended-release/long-acting opioid analgesics Risk Evaluation and Mitigation Strategy (REMS), to reflect the updated information.
The key change centers on moving prescribers away from the assessment of a patient’s pain based solely on a pain scale to a more "comprehensive one," according to Dr. Douglas Throckmorton, deputy director for regulatory programs in the FDA’s Center for Drug Evaluation and Research. "The updated indication states that extended-release, long-acting opioids are indicated for the management of pain severe enough to require daily, around-the-clock, long-term opioid treatment and for which alternative treatment options are inadequate," Dr. Throckmorton stated in the briefing. Alternative pain medications noted in an agency statement released prior to the briefing include immediate-release opioids, which are currently unaffected by the agency’s labeling changes.
Dr. Throckmorton said he hopes the FDA’s action is part of a "broader effort to encourage people to consider how best to use these medications." When asked whether prescribers and their patients weren’t already addressing the risks and benefits involved in the use of these opioids, the current labeling for which indicates their use in patients experiencing "moderate to severe pain," rather than "round-the-clock" pain, Dr. Throckmorton said the labeling changes "will help reinforce the importance of the conversation in a busy practice."
The agency’s announcement comes amid growing data about the inherent risks of opioid use reported in the medical literature and the filing with the FDA of two citizen petitions to change how opioids are prescribed, including one by the Physicians for Responsible Opioid Prescribing. Also part of the focus on opioid use is the 19 to 10 vote by the FDA’s Drug Safety and Risk Management Advisory Committee in January to reschedule hydrocodone drug combinations from schedule III under the Controlled Substances Act (CSA) to schedule II. The vote was prompted by the U.S. Drug Enforcement Administration’s call for the FDA to react to evidence that the medications are overprescribed, diverted, and abused. Statistics cited by FDA officials in the briefing included nearly 16,000 opioid-related deaths in the United States in 2009, reflecting a 300% increase in the last 20 years.
Speaking about the importance of the dosage and duration of the medications, Dr. Throckmorton said the agency did not have enough information at this time to make changes to how these drugs are prescribed, but that the postmarket studies such as clinical trials, and other studies of at least 12 weeks’ duration, would play a role in providing this data. "We expect some of those studies will provide information for us to use in 2 years. So, by end of 2015, we will have more," Dr. Throckmorton said.
Also announced in the briefing was the addition of a boxed warning on extended-release/long-acting opioid analgesics to warn expectant mothers of neonatal opioid withdrawal syndrome (NOWS), which might be life-threatening and require management according to protocols developed by neonatology experts. NOWS can occur in a newborn exposed to opioid drugs while in the mother’s womb. Symptoms may include poor feeding, rapid breathing, trembling, and excessive or high-pitched crying.
The U.S. Food and Drug Administration has announced that it is making classwide label changes to extended-release and long-acting opioid analgesics for treatment of chronic pain. In addition, drug manufacturers will now be required to conduct postmarket studies to help the agency determine whether further actions are merited.
"The FDA is invoking its authority to require safety labeling changes and postmarket studies to combat the crisis of misuse, abuse, addiction, overdose, and death from these potent drugs that have harmed too many patients and devastated too many families and communities," Dr. Margaret A. Hamburg, FDA commissioner, said Sept. 10 in a press briefing. "Today’s action demonstrates the FDA’s resolve to reduce the serious risks of long-acting and extended release opioids while still seeking to preserve appropriate access for those patients who rely on these medications to manage their pain."
Extended-release and long-acting opioids include hydromorphone, morphine, oxycodone, oxymorphone, and tapentadol. Changes to labels will include updated information about dosage and administration, warnings and precautions, drug interactions, use in specific populations, patient counseling information, and the medication guide. Modifications also will be made to the extended-release/long-acting opioid analgesics Risk Evaluation and Mitigation Strategy (REMS), to reflect the updated information.
The key change centers on moving prescribers away from the assessment of a patient’s pain based solely on a pain scale to a more "comprehensive one," according to Dr. Douglas Throckmorton, deputy director for regulatory programs in the FDA’s Center for Drug Evaluation and Research. "The updated indication states that extended-release, long-acting opioids are indicated for the management of pain severe enough to require daily, around-the-clock, long-term opioid treatment and for which alternative treatment options are inadequate," Dr. Throckmorton stated in the briefing. Alternative pain medications noted in an agency statement released prior to the briefing include immediate-release opioids, which are currently unaffected by the agency’s labeling changes.
Dr. Throckmorton said he hopes the FDA’s action is part of a "broader effort to encourage people to consider how best to use these medications." When asked whether prescribers and their patients weren’t already addressing the risks and benefits involved in the use of these opioids, the current labeling for which indicates their use in patients experiencing "moderate to severe pain," rather than "round-the-clock" pain, Dr. Throckmorton said the labeling changes "will help reinforce the importance of the conversation in a busy practice."
The agency’s announcement comes amid growing data about the inherent risks of opioid use reported in the medical literature and the filing with the FDA of two citizen petitions to change how opioids are prescribed, including one by the Physicians for Responsible Opioid Prescribing. Also part of the focus on opioid use is the 19 to 10 vote by the FDA’s Drug Safety and Risk Management Advisory Committee in January to reschedule hydrocodone drug combinations from schedule III under the Controlled Substances Act (CSA) to schedule II. The vote was prompted by the U.S. Drug Enforcement Administration’s call for the FDA to react to evidence that the medications are overprescribed, diverted, and abused. Statistics cited by FDA officials in the briefing included nearly 16,000 opioid-related deaths in the United States in 2009, reflecting a 300% increase in the last 20 years.
Speaking about the importance of the dosage and duration of the medications, Dr. Throckmorton said the agency did not have enough information at this time to make changes to how these drugs are prescribed, but that the postmarket studies such as clinical trials, and other studies of at least 12 weeks’ duration, would play a role in providing this data. "We expect some of those studies will provide information for us to use in 2 years. So, by end of 2015, we will have more," Dr. Throckmorton said.
Also announced in the briefing was the addition of a boxed warning on extended-release/long-acting opioid analgesics to warn expectant mothers of neonatal opioid withdrawal syndrome (NOWS), which might be life-threatening and require management according to protocols developed by neonatology experts. NOWS can occur in a newborn exposed to opioid drugs while in the mother’s womb. Symptoms may include poor feeding, rapid breathing, trembling, and excessive or high-pitched crying.
Vascular risk factors increased likelihood of restless legs syndrome in women
Vascular risk factors such as diabetes, hypercholesterolemia, body mass index, smoking status, and exercise were associated with the prevalence of restless legs syndrome in 12% of women aged older than 45 years, although a link was not found with cardiovascular events such as stroke or myocardial infarction, according to a study.
Previous studies have indicated that an unhealthy vascular profile might be the mechanism linking restless legs syndrome with cardiovascular disease (CVD) in women, but the data are inconsistent.
Dr. Tobias Kurth of Inserm Research Center for Epidemiology and Biostatistics and the University of Bordeaux, France, and his colleagues, sought a more definitive connection in a cross-sectional study of 30,262 women who participated in the Women’s Health Study (WHS). In the 9th year of the study, validated criteria from the International Restless Legs Study Group were added to the follow-up survey.
Dr. Kurth and his investigators applied age-adjusted and multivariable-adjusted logistic regression models to the complete data provided by 30,262 respondents (mean age 63.6 years) to evaluate the association between restless legs syndrome and independent vascular risk factors such as diabetes, hypertension, hypercholesterolemia, BMI, alcohol, smoking, exercise, and family history of MI. They adjusted for age, aspirin use, postmenopausal status, postmenopausal hormone use, and history of oral contraceptive use (Am. J. Med. 2013;126:220-7 [doi:10.1016/j.amjmed.2012.06.040]).
Patient-reported data on cardiovascular events were confirmed by medical record review.
A total of 3,634 (12%) of the women had restless legs syndrome. Women with several vascular risk factors were at greater odds of having restless legs syndrome, BMI greater than 35 (OR 1.35), diabetes (OR 1.19), hypercholesterolemia (OR 1.17), smoking 15 or more cigarettes per day (OR 1.41), and exercise less than four times per week (OR 0.84). Those who underwent coronary revascularization had a multivariable-adjusted OR of 1.39 for restless legs syndrome.
Noting that genetics, endocrine disturbances, and lifestyle-related comorbidities such as smoking have been theorized as mechanisms of restless legs syndrome, the authors wrote that "the cross-sectional design of our study and previous reports does not allow drawing conclusions regarding direction and causality of the association."
Furthermore, while reports cited by the investigators found similar prevalence rates between restless legs syndrome and vascular risk, the authors concluded they "could not confirm results from previous studies indicating an association between prevalent cardiovascular disease and restless legs syndrome."
The study was funded by the National Heart, Lung, and Blood Institute. The Women’s Health Study was underwritten by NHBLI and the National Cancer Institute. The investigators listed multiple financial conflicts of interest regarding restless legs syndrome research and treatments.
Vascular risk factors such as diabetes, hypercholesterolemia, body mass index, smoking status, and exercise were associated with the prevalence of restless legs syndrome in 12% of women aged older than 45 years, although a link was not found with cardiovascular events such as stroke or myocardial infarction, according to a study.
Previous studies have indicated that an unhealthy vascular profile might be the mechanism linking restless legs syndrome with cardiovascular disease (CVD) in women, but the data are inconsistent.
Dr. Tobias Kurth of Inserm Research Center for Epidemiology and Biostatistics and the University of Bordeaux, France, and his colleagues, sought a more definitive connection in a cross-sectional study of 30,262 women who participated in the Women’s Health Study (WHS). In the 9th year of the study, validated criteria from the International Restless Legs Study Group were added to the follow-up survey.
Dr. Kurth and his investigators applied age-adjusted and multivariable-adjusted logistic regression models to the complete data provided by 30,262 respondents (mean age 63.6 years) to evaluate the association between restless legs syndrome and independent vascular risk factors such as diabetes, hypertension, hypercholesterolemia, BMI, alcohol, smoking, exercise, and family history of MI. They adjusted for age, aspirin use, postmenopausal status, postmenopausal hormone use, and history of oral contraceptive use (Am. J. Med. 2013;126:220-7 [doi:10.1016/j.amjmed.2012.06.040]).
Patient-reported data on cardiovascular events were confirmed by medical record review.
A total of 3,634 (12%) of the women had restless legs syndrome. Women with several vascular risk factors were at greater odds of having restless legs syndrome, BMI greater than 35 (OR 1.35), diabetes (OR 1.19), hypercholesterolemia (OR 1.17), smoking 15 or more cigarettes per day (OR 1.41), and exercise less than four times per week (OR 0.84). Those who underwent coronary revascularization had a multivariable-adjusted OR of 1.39 for restless legs syndrome.
Noting that genetics, endocrine disturbances, and lifestyle-related comorbidities such as smoking have been theorized as mechanisms of restless legs syndrome, the authors wrote that "the cross-sectional design of our study and previous reports does not allow drawing conclusions regarding direction and causality of the association."
Furthermore, while reports cited by the investigators found similar prevalence rates between restless legs syndrome and vascular risk, the authors concluded they "could not confirm results from previous studies indicating an association between prevalent cardiovascular disease and restless legs syndrome."
The study was funded by the National Heart, Lung, and Blood Institute. The Women’s Health Study was underwritten by NHBLI and the National Cancer Institute. The investigators listed multiple financial conflicts of interest regarding restless legs syndrome research and treatments.
Vascular risk factors such as diabetes, hypercholesterolemia, body mass index, smoking status, and exercise were associated with the prevalence of restless legs syndrome in 12% of women aged older than 45 years, although a link was not found with cardiovascular events such as stroke or myocardial infarction, according to a study.
Previous studies have indicated that an unhealthy vascular profile might be the mechanism linking restless legs syndrome with cardiovascular disease (CVD) in women, but the data are inconsistent.
Dr. Tobias Kurth of Inserm Research Center for Epidemiology and Biostatistics and the University of Bordeaux, France, and his colleagues, sought a more definitive connection in a cross-sectional study of 30,262 women who participated in the Women’s Health Study (WHS). In the 9th year of the study, validated criteria from the International Restless Legs Study Group were added to the follow-up survey.
Dr. Kurth and his investigators applied age-adjusted and multivariable-adjusted logistic regression models to the complete data provided by 30,262 respondents (mean age 63.6 years) to evaluate the association between restless legs syndrome and independent vascular risk factors such as diabetes, hypertension, hypercholesterolemia, BMI, alcohol, smoking, exercise, and family history of MI. They adjusted for age, aspirin use, postmenopausal status, postmenopausal hormone use, and history of oral contraceptive use (Am. J. Med. 2013;126:220-7 [doi:10.1016/j.amjmed.2012.06.040]).
Patient-reported data on cardiovascular events were confirmed by medical record review.
A total of 3,634 (12%) of the women had restless legs syndrome. Women with several vascular risk factors were at greater odds of having restless legs syndrome, BMI greater than 35 (OR 1.35), diabetes (OR 1.19), hypercholesterolemia (OR 1.17), smoking 15 or more cigarettes per day (OR 1.41), and exercise less than four times per week (OR 0.84). Those who underwent coronary revascularization had a multivariable-adjusted OR of 1.39 for restless legs syndrome.
Noting that genetics, endocrine disturbances, and lifestyle-related comorbidities such as smoking have been theorized as mechanisms of restless legs syndrome, the authors wrote that "the cross-sectional design of our study and previous reports does not allow drawing conclusions regarding direction and causality of the association."
Furthermore, while reports cited by the investigators found similar prevalence rates between restless legs syndrome and vascular risk, the authors concluded they "could not confirm results from previous studies indicating an association between prevalent cardiovascular disease and restless legs syndrome."
The study was funded by the National Heart, Lung, and Blood Institute. The Women’s Health Study was underwritten by NHBLI and the National Cancer Institute. The investigators listed multiple financial conflicts of interest regarding restless legs syndrome research and treatments.
FROM THE JOURNAL OF AMERICAN MEDICINE
Major finding: Diabetes, hypercholesterolemia, BMI, smoking, and lack of exercise were linked to restless legs syndrome in 12% of women aged 45 years and over.
Data source: Logistic regression analysis of cross-sectional, cohort study of 30,262 participants in the Women’s Health Study.
Disclosures: The study was underwritten by a grant from the National Heart, Lung, and Blood Institute. The Women’s Health Study was underwritten by NHBLI and the National Cancer Institute. The investigators listed multiple financial conflicts of interest regarding restless legs syndrome research and treatments.
Communicating with chronic pain patients about opioids: Three patterns found
Reassurance, agreeing to avoid opioids, and information gathering were the three most common communication strategies used by physicians and their patients with chronic pain. Those are the findings from a small pilot study conducted to determine how doctors and patients approach the inherent uncertainty of opioid use, given the absence of long-term data about opioids’ efficacy in noncancer or end-of-life pain treatment.
To conduct the study, a team led by Marianne S. Matthias, Ph.D., of the Veterans Health Administration in Indianapolis, audio-recorded the primary care visits of 30 patients with chronic musculoskeletal pain between August 2010 and March 2011.
Study participants had a score of 4 or greater on a pain scale of 0 (no pain) to 10 (worst pain imaginable); were already a patient of one of the five doctors participating in the study (three doctors were women); and had an appointment scheduled within the study’s duration. Patients were excluded if they had terminal cancer or poorly controlled psychiatric comorbidities, such as paranoia (Patient Educ. Couns. 2013 Aug. 5 (doi: 10.1016/j.pec.2013.06.021).
The age range of the patients was 27-70 years (mean age, 57 years). Back pain was the most common complaint (17 patients), and 13 patients were being treated for arthritis. In all, 20 patients were taking prescription opioids, wrote Dr. Matthias and her colleagues, who are affiliated with the VA Health Services Research and Development Center of Excellence on Implementing Evidence-Based Practice.
To help with appropriate patient recruitment, doctors in the study were told that researchers were studying communication strategies for pain management; patients were told only that the study would collect data about doctor-patient communications, in order to avoid affecting any discussions that might emerge about pain. Although discussions specifically addressing opioid use occurred in 19 visits, all patients were interviewed immediately after each recorded visit about their relationship with their doctor, and their pain and treatment.
The researchers used emergent thematic analysis to determine which communication strategies prevailed in all transcriptions of the recorded physician-patient encounters and follow-up interviews. They then independently listed the categories they believed were most persistent before all agreed upon a set of predominant themes. All transcriptions were then divided among the analysts and reevaluated according to the established categories. Every fourth set of transcriptions was analyzed by the entire team to ensure consistency.
Although researchers noted that side effects of opioid use, appropriateness of opioids, and correct titration were topics of concern for some patients, the chief concern was the risk of opioid misuse or addiction, particularly in patients with histories of substance use disorder. Using problematic integration theory, a framework of coping with uncertainty through communication, Dr. Matthias and her colleagues determined that the physicians and their patients confronted the unknowns about opioids through either reassurance, agreeing to avoid opioids in treatment, or gathering additional information.
The researchers noted that the strategies often overlapped, but all of them hinged on the quality and quantity of information available to the individual, and on the person’s probability judgment, both of which are central tenets of problematic integration theory.
In visits where reassurance occurred, particularly in patients with a history of substance abuse, uncertainty was met by candid discussions about the possibility of misuse or addiction. The researchers noted as an example of reassurance the case of a physician who reassured her patient that she was not concerned that he would become addicted to hydrocodone. Dr. Matthias and her associates wrote that this type of strategy was intended to change the other person’s probability judgment that misuse or addiction was unlikely. This strategy was reinforced by the doctor offering the patient information about hydrocodone, the investigators wrote.
Agreeing to avoid opioids entirely was a second pattern investigators observed doctors and patients using as a means of eliminating the uncertainties in opioid use. The third discrete pattern was for the doctor or patient to gather more information, such as by offering the patient more facts about hydrocodone, asking questions, or performing tests such as a urinalysis for drug use.
Dr. Matthias and her colleagues reported that uncertainty in problematic integration theory exists in relation to what an individual values. For example, the premium placed on pain relief by those prescribed opioids, motivated these patients to reassure their physicians that they were not abusing their prescriptions. The investigators hypothesized that the value placed on pain relief from opioids contributed to the lack of confrontation observed in the patient-doctor conversations.
"Regardless of whether uncertainties originated with the doctor or patient, both parties often employed partnership language ... collaboratively seeking to cope with the uncertainty of opioid treatment," Dr. Matthias and her colleagues wrote. "Many of the communication behaviors documented in this study might serve as a model for training patients and physicians to communicate effectively about opioids," the authors concluded.
Limitations of the study included its small size, which might have precluded observation of a fuller range of communication strategies, the investigators noted. In addition, clinical considerations about opioid use such as dosage, type, and treatment duration were not assessed, nor were the preexisting beliefs and knowledge about opioids held by the individual physicians and patients. The study also did not include the physicians’ perspectives on their interactions with patients.
This study was supported by the Veterans Health Administration’s Health Services Research and Development Service and an Indiana Institute for Medical Research Young Investigator Award. Dr. Matthias and her colleagues declared that they had no conflicts of interest.
Reassurance, agreeing to avoid opioids, and information gathering were the three most common communication strategies used by physicians and their patients with chronic pain. Those are the findings from a small pilot study conducted to determine how doctors and patients approach the inherent uncertainty of opioid use, given the absence of long-term data about opioids’ efficacy in noncancer or end-of-life pain treatment.
To conduct the study, a team led by Marianne S. Matthias, Ph.D., of the Veterans Health Administration in Indianapolis, audio-recorded the primary care visits of 30 patients with chronic musculoskeletal pain between August 2010 and March 2011.
Study participants had a score of 4 or greater on a pain scale of 0 (no pain) to 10 (worst pain imaginable); were already a patient of one of the five doctors participating in the study (three doctors were women); and had an appointment scheduled within the study’s duration. Patients were excluded if they had terminal cancer or poorly controlled psychiatric comorbidities, such as paranoia (Patient Educ. Couns. 2013 Aug. 5 (doi: 10.1016/j.pec.2013.06.021).
The age range of the patients was 27-70 years (mean age, 57 years). Back pain was the most common complaint (17 patients), and 13 patients were being treated for arthritis. In all, 20 patients were taking prescription opioids, wrote Dr. Matthias and her colleagues, who are affiliated with the VA Health Services Research and Development Center of Excellence on Implementing Evidence-Based Practice.
To help with appropriate patient recruitment, doctors in the study were told that researchers were studying communication strategies for pain management; patients were told only that the study would collect data about doctor-patient communications, in order to avoid affecting any discussions that might emerge about pain. Although discussions specifically addressing opioid use occurred in 19 visits, all patients were interviewed immediately after each recorded visit about their relationship with their doctor, and their pain and treatment.
The researchers used emergent thematic analysis to determine which communication strategies prevailed in all transcriptions of the recorded physician-patient encounters and follow-up interviews. They then independently listed the categories they believed were most persistent before all agreed upon a set of predominant themes. All transcriptions were then divided among the analysts and reevaluated according to the established categories. Every fourth set of transcriptions was analyzed by the entire team to ensure consistency.
Although researchers noted that side effects of opioid use, appropriateness of opioids, and correct titration were topics of concern for some patients, the chief concern was the risk of opioid misuse or addiction, particularly in patients with histories of substance use disorder. Using problematic integration theory, a framework of coping with uncertainty through communication, Dr. Matthias and her colleagues determined that the physicians and their patients confronted the unknowns about opioids through either reassurance, agreeing to avoid opioids in treatment, or gathering additional information.
The researchers noted that the strategies often overlapped, but all of them hinged on the quality and quantity of information available to the individual, and on the person’s probability judgment, both of which are central tenets of problematic integration theory.
In visits where reassurance occurred, particularly in patients with a history of substance abuse, uncertainty was met by candid discussions about the possibility of misuse or addiction. The researchers noted as an example of reassurance the case of a physician who reassured her patient that she was not concerned that he would become addicted to hydrocodone. Dr. Matthias and her associates wrote that this type of strategy was intended to change the other person’s probability judgment that misuse or addiction was unlikely. This strategy was reinforced by the doctor offering the patient information about hydrocodone, the investigators wrote.
Agreeing to avoid opioids entirely was a second pattern investigators observed doctors and patients using as a means of eliminating the uncertainties in opioid use. The third discrete pattern was for the doctor or patient to gather more information, such as by offering the patient more facts about hydrocodone, asking questions, or performing tests such as a urinalysis for drug use.
Dr. Matthias and her colleagues reported that uncertainty in problematic integration theory exists in relation to what an individual values. For example, the premium placed on pain relief by those prescribed opioids, motivated these patients to reassure their physicians that they were not abusing their prescriptions. The investigators hypothesized that the value placed on pain relief from opioids contributed to the lack of confrontation observed in the patient-doctor conversations.
"Regardless of whether uncertainties originated with the doctor or patient, both parties often employed partnership language ... collaboratively seeking to cope with the uncertainty of opioid treatment," Dr. Matthias and her colleagues wrote. "Many of the communication behaviors documented in this study might serve as a model for training patients and physicians to communicate effectively about opioids," the authors concluded.
Limitations of the study included its small size, which might have precluded observation of a fuller range of communication strategies, the investigators noted. In addition, clinical considerations about opioid use such as dosage, type, and treatment duration were not assessed, nor were the preexisting beliefs and knowledge about opioids held by the individual physicians and patients. The study also did not include the physicians’ perspectives on their interactions with patients.
This study was supported by the Veterans Health Administration’s Health Services Research and Development Service and an Indiana Institute for Medical Research Young Investigator Award. Dr. Matthias and her colleagues declared that they had no conflicts of interest.
Reassurance, agreeing to avoid opioids, and information gathering were the three most common communication strategies used by physicians and their patients with chronic pain. Those are the findings from a small pilot study conducted to determine how doctors and patients approach the inherent uncertainty of opioid use, given the absence of long-term data about opioids’ efficacy in noncancer or end-of-life pain treatment.
To conduct the study, a team led by Marianne S. Matthias, Ph.D., of the Veterans Health Administration in Indianapolis, audio-recorded the primary care visits of 30 patients with chronic musculoskeletal pain between August 2010 and March 2011.
Study participants had a score of 4 or greater on a pain scale of 0 (no pain) to 10 (worst pain imaginable); were already a patient of one of the five doctors participating in the study (three doctors were women); and had an appointment scheduled within the study’s duration. Patients were excluded if they had terminal cancer or poorly controlled psychiatric comorbidities, such as paranoia (Patient Educ. Couns. 2013 Aug. 5 (doi: 10.1016/j.pec.2013.06.021).
The age range of the patients was 27-70 years (mean age, 57 years). Back pain was the most common complaint (17 patients), and 13 patients were being treated for arthritis. In all, 20 patients were taking prescription opioids, wrote Dr. Matthias and her colleagues, who are affiliated with the VA Health Services Research and Development Center of Excellence on Implementing Evidence-Based Practice.
To help with appropriate patient recruitment, doctors in the study were told that researchers were studying communication strategies for pain management; patients were told only that the study would collect data about doctor-patient communications, in order to avoid affecting any discussions that might emerge about pain. Although discussions specifically addressing opioid use occurred in 19 visits, all patients were interviewed immediately after each recorded visit about their relationship with their doctor, and their pain and treatment.
The researchers used emergent thematic analysis to determine which communication strategies prevailed in all transcriptions of the recorded physician-patient encounters and follow-up interviews. They then independently listed the categories they believed were most persistent before all agreed upon a set of predominant themes. All transcriptions were then divided among the analysts and reevaluated according to the established categories. Every fourth set of transcriptions was analyzed by the entire team to ensure consistency.
Although researchers noted that side effects of opioid use, appropriateness of opioids, and correct titration were topics of concern for some patients, the chief concern was the risk of opioid misuse or addiction, particularly in patients with histories of substance use disorder. Using problematic integration theory, a framework of coping with uncertainty through communication, Dr. Matthias and her colleagues determined that the physicians and their patients confronted the unknowns about opioids through either reassurance, agreeing to avoid opioids in treatment, or gathering additional information.
The researchers noted that the strategies often overlapped, but all of them hinged on the quality and quantity of information available to the individual, and on the person’s probability judgment, both of which are central tenets of problematic integration theory.
In visits where reassurance occurred, particularly in patients with a history of substance abuse, uncertainty was met by candid discussions about the possibility of misuse or addiction. The researchers noted as an example of reassurance the case of a physician who reassured her patient that she was not concerned that he would become addicted to hydrocodone. Dr. Matthias and her associates wrote that this type of strategy was intended to change the other person’s probability judgment that misuse or addiction was unlikely. This strategy was reinforced by the doctor offering the patient information about hydrocodone, the investigators wrote.
Agreeing to avoid opioids entirely was a second pattern investigators observed doctors and patients using as a means of eliminating the uncertainties in opioid use. The third discrete pattern was for the doctor or patient to gather more information, such as by offering the patient more facts about hydrocodone, asking questions, or performing tests such as a urinalysis for drug use.
Dr. Matthias and her colleagues reported that uncertainty in problematic integration theory exists in relation to what an individual values. For example, the premium placed on pain relief by those prescribed opioids, motivated these patients to reassure their physicians that they were not abusing their prescriptions. The investigators hypothesized that the value placed on pain relief from opioids contributed to the lack of confrontation observed in the patient-doctor conversations.
"Regardless of whether uncertainties originated with the doctor or patient, both parties often employed partnership language ... collaboratively seeking to cope with the uncertainty of opioid treatment," Dr. Matthias and her colleagues wrote. "Many of the communication behaviors documented in this study might serve as a model for training patients and physicians to communicate effectively about opioids," the authors concluded.
Limitations of the study included its small size, which might have precluded observation of a fuller range of communication strategies, the investigators noted. In addition, clinical considerations about opioid use such as dosage, type, and treatment duration were not assessed, nor were the preexisting beliefs and knowledge about opioids held by the individual physicians and patients. The study also did not include the physicians’ perspectives on their interactions with patients.
This study was supported by the Veterans Health Administration’s Health Services Research and Development Service and an Indiana Institute for Medical Research Young Investigator Award. Dr. Matthias and her colleagues declared that they had no conflicts of interest.
FROM PATIENT EDUCATION AND COUNSELING
Major finding: The uncertainty of opioid treatment leads physicians and patients to work collaboratively by using three patterns of responses: reassurance, deciding to avoid opioids, and gathering additional information.
Data source: Pilot study of 30 patients with chronic musculoskeletal pain who were taking prescription opioids.
Disclosures: This study was supported by the Veterans Health Administration’s Health Services Research and Development Service and an Indiana Institute for Medical Research Young Investigator Award. Dr. Matthias and her colleagues declared that they had no conflicts of interest.
Perceived stigma linked to depression in female SLE patients
Depression in women with systemic lupus erythematosus has been linked by a cross-sectional study to their perceptions of being stigmatized by their illness.
The findings indicate that when overt central nervous system manifestations of SLE are not present, depression in this patient population is attributable to nonorganic causes and not the disease, according to the study investigators.
"Dealing with this stigma may be important in promoting optimal coping for these women," wrote Dr. Mohammad G. Sehlo and his associates. Dr. Sehlo is a psychiatrist and professor of medicine at King Adbulaziz University in Jeddah, Saudi Arabia.
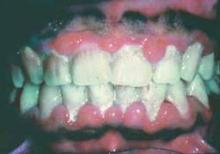
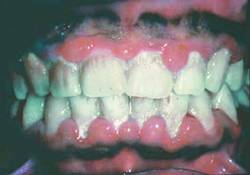
The investigators noted that between 10.8% and 39.6% of women with SLE also have depression, making it one of the most common psychiatric comorbidities in SLE. The authors referenced several studies showing that while depression can result in SLE from brain damage directly related to the disease, as well as the high doses of corticosteroids often used in treatment, SLE’s prototypical skin rash, uneven pigmentation, vitiligo, scars, tooth loss, alopecia, increased facial hair, and other physical manifestations "may contribute to higher levels of perceived illness stigma that subsequently may be associated with depression in these patients" (J. Psychosomatic Res. 2013;74:248-51).
Fifteen of the 80 patients randomly selected by Dr. Sehlo and his colleagues were found to have depression according to the Structured Clinical Interview for DSM-IV Axis 1 Disorders, Clinician Version (SCID-1-CV). The women, whose average age was 34.8 years, were regular attendees of a rheumatology outpatient clinic in Jeddah between March 2011 and March 2012. Patients with neuropsychiatric lupus-related neurologic syndrome, as well as those with any other serious medical comorbidities, were excluded, as were those who demonstrated a language barrier.
"...adequate coping strategies, social support, and the ability to deal with stress can reduce the perceived illness stigma and its serious consequences for patients with SLE."
Depression severity was measured in the study group by the Hospital Anxiety and Depression Scale-Depression Subscale (HADS-D), a self-assessment composed of seven questions. Illness stigma was measured using a 4-point Likert-type scale by the Stigma Impact Scale (SIS), covering perceived stigma from social rejection, financial insecurity, internalized shame, and social isolation.
Dr. Sehlo and his associates recorded significantly higher mean scores on HADS-D and SIS in the patients with depression, compared with patients who were not found to have depression (P less than .001). Other differences between the two groups such as age, duration of illness, daily prednisone dosage, and physical damage as measured by the SLEDAI (Systemic Lupus Erythematosus Disease Activity Index) and the SLICC/ACR (Systemic Lupus International Collaborating Clinics/American College of Rheumatology) Damage Index were not found to be significant.
The investigators noted a significant positive relationship between SIS and HADS-D scores (P = .002) and between perceived illness stigma and a diagnosis of depression (odds ratio, 3.2; P = .002), leading to an increase in the severity of depressive symptoms (P less than .001).
Although the cross-sectional design of the study did not allow for causal conclusions or for the measurement of a third causative variable such as neuroticism, the authors concluded that their data were important, because "adequate coping strategies, social support, and the ability to deal with stress can reduce the perceived illness stigma and its serious consequences for patients with SLE."
Dr. Sehlo and his colleagues said they had no conflicts of interest to disclose.
Depression in women with systemic lupus erythematosus has been linked by a cross-sectional study to their perceptions of being stigmatized by their illness.
The findings indicate that when overt central nervous system manifestations of SLE are not present, depression in this patient population is attributable to nonorganic causes and not the disease, according to the study investigators.
"Dealing with this stigma may be important in promoting optimal coping for these women," wrote Dr. Mohammad G. Sehlo and his associates. Dr. Sehlo is a psychiatrist and professor of medicine at King Adbulaziz University in Jeddah, Saudi Arabia.
The investigators noted that between 10.8% and 39.6% of women with SLE also have depression, making it one of the most common psychiatric comorbidities in SLE. The authors referenced several studies showing that while depression can result in SLE from brain damage directly related to the disease, as well as the high doses of corticosteroids often used in treatment, SLE’s prototypical skin rash, uneven pigmentation, vitiligo, scars, tooth loss, alopecia, increased facial hair, and other physical manifestations "may contribute to higher levels of perceived illness stigma that subsequently may be associated with depression in these patients" (J. Psychosomatic Res. 2013;74:248-51).
Fifteen of the 80 patients randomly selected by Dr. Sehlo and his colleagues were found to have depression according to the Structured Clinical Interview for DSM-IV Axis 1 Disorders, Clinician Version (SCID-1-CV). The women, whose average age was 34.8 years, were regular attendees of a rheumatology outpatient clinic in Jeddah between March 2011 and March 2012. Patients with neuropsychiatric lupus-related neurologic syndrome, as well as those with any other serious medical comorbidities, were excluded, as were those who demonstrated a language barrier.
"...adequate coping strategies, social support, and the ability to deal with stress can reduce the perceived illness stigma and its serious consequences for patients with SLE."
Depression severity was measured in the study group by the Hospital Anxiety and Depression Scale-Depression Subscale (HADS-D), a self-assessment composed of seven questions. Illness stigma was measured using a 4-point Likert-type scale by the Stigma Impact Scale (SIS), covering perceived stigma from social rejection, financial insecurity, internalized shame, and social isolation.
Dr. Sehlo and his associates recorded significantly higher mean scores on HADS-D and SIS in the patients with depression, compared with patients who were not found to have depression (P less than .001). Other differences between the two groups such as age, duration of illness, daily prednisone dosage, and physical damage as measured by the SLEDAI (Systemic Lupus Erythematosus Disease Activity Index) and the SLICC/ACR (Systemic Lupus International Collaborating Clinics/American College of Rheumatology) Damage Index were not found to be significant.
The investigators noted a significant positive relationship between SIS and HADS-D scores (P = .002) and between perceived illness stigma and a diagnosis of depression (odds ratio, 3.2; P = .002), leading to an increase in the severity of depressive symptoms (P less than .001).
Although the cross-sectional design of the study did not allow for causal conclusions or for the measurement of a third causative variable such as neuroticism, the authors concluded that their data were important, because "adequate coping strategies, social support, and the ability to deal with stress can reduce the perceived illness stigma and its serious consequences for patients with SLE."
Dr. Sehlo and his colleagues said they had no conflicts of interest to disclose.
Depression in women with systemic lupus erythematosus has been linked by a cross-sectional study to their perceptions of being stigmatized by their illness.
The findings indicate that when overt central nervous system manifestations of SLE are not present, depression in this patient population is attributable to nonorganic causes and not the disease, according to the study investigators.
"Dealing with this stigma may be important in promoting optimal coping for these women," wrote Dr. Mohammad G. Sehlo and his associates. Dr. Sehlo is a psychiatrist and professor of medicine at King Adbulaziz University in Jeddah, Saudi Arabia.
The investigators noted that between 10.8% and 39.6% of women with SLE also have depression, making it one of the most common psychiatric comorbidities in SLE. The authors referenced several studies showing that while depression can result in SLE from brain damage directly related to the disease, as well as the high doses of corticosteroids often used in treatment, SLE’s prototypical skin rash, uneven pigmentation, vitiligo, scars, tooth loss, alopecia, increased facial hair, and other physical manifestations "may contribute to higher levels of perceived illness stigma that subsequently may be associated with depression in these patients" (J. Psychosomatic Res. 2013;74:248-51).
Fifteen of the 80 patients randomly selected by Dr. Sehlo and his colleagues were found to have depression according to the Structured Clinical Interview for DSM-IV Axis 1 Disorders, Clinician Version (SCID-1-CV). The women, whose average age was 34.8 years, were regular attendees of a rheumatology outpatient clinic in Jeddah between March 2011 and March 2012. Patients with neuropsychiatric lupus-related neurologic syndrome, as well as those with any other serious medical comorbidities, were excluded, as were those who demonstrated a language barrier.
"...adequate coping strategies, social support, and the ability to deal with stress can reduce the perceived illness stigma and its serious consequences for patients with SLE."
Depression severity was measured in the study group by the Hospital Anxiety and Depression Scale-Depression Subscale (HADS-D), a self-assessment composed of seven questions. Illness stigma was measured using a 4-point Likert-type scale by the Stigma Impact Scale (SIS), covering perceived stigma from social rejection, financial insecurity, internalized shame, and social isolation.
Dr. Sehlo and his associates recorded significantly higher mean scores on HADS-D and SIS in the patients with depression, compared with patients who were not found to have depression (P less than .001). Other differences between the two groups such as age, duration of illness, daily prednisone dosage, and physical damage as measured by the SLEDAI (Systemic Lupus Erythematosus Disease Activity Index) and the SLICC/ACR (Systemic Lupus International Collaborating Clinics/American College of Rheumatology) Damage Index were not found to be significant.
The investigators noted a significant positive relationship between SIS and HADS-D scores (P = .002) and between perceived illness stigma and a diagnosis of depression (odds ratio, 3.2; P = .002), leading to an increase in the severity of depressive symptoms (P less than .001).
Although the cross-sectional design of the study did not allow for causal conclusions or for the measurement of a third causative variable such as neuroticism, the authors concluded that their data were important, because "adequate coping strategies, social support, and the ability to deal with stress can reduce the perceived illness stigma and its serious consequences for patients with SLE."
Dr. Sehlo and his colleagues said they had no conflicts of interest to disclose.
FROM THE JOURNAL OF PSYCHOSOMATIC RESEARCH
Major finding: Fifteen of the 80 randomly selected women with SLE were found to have depression, based on the Structured Clinical Interview for DSM-IV Axis 1 Disorders, Clinician Version. The depressed group also had significantly higher mean scores on the Stigma Impact Scale and the Hospital Anxiety and Depression Scale–Depression Subscale, compared with patients who were not found to have depression.
Data source: A cross-sectional group of 80 women with SLE who did not have neuropsychiatric lupus-related neurologic syndrome of any other serious medical comorbidities.
Disclosures: Dr. Sehlo and his colleagues said they had no conflicts of interest to disclose.
Poor oral health a risk factor in oncogenic HPV infection
Poor oral health is an independent risk factor of oral human papillomavirus infection regardless of smoking and oral sex practices, analysis of a large, nationally representative sample showed.
Poor oral health was associated with a 56% higher prevalence of oral HPV infection in 3,439 study participants aged 30-69 years, Thanh Cong Bui, Dr.P.H., of the University of Texas Health Sciences Center, Houston, and his colleagues wrote in Cancer Prevention Research.
For those with gum disease and dental problems, prevalence of oral HPV infection was 51% and 28% higher, respectively. More men (12%) than women (3%) were infected with oral HPV (Cancer Prev. Res. 2013 Aug. 21 [doi:10.1158/1940-6207.CAPR-13-008]).
Marijuana use also was linked to higher rates of infection: 5% in nonusers, 8% in former users, and 14% in current users.
The findings were derived from the 2009-2010 National Health and Nutrition Examination Survey (NHANES), a nationally representative sampling conducted by the Centers for Disease Control and Prevention. Oral health data were taken from participants’ self-assessments of overall oral health, presence of gum disease, use of mouthwash to treat dental problems within past 7 days of the survey, and number of teeth lost.
"The good news is, this risk factor is modifiable – by maintaining good oral hygiene and good oral health, one can prevent HPV infection and subsequent HPV-related cancers," Dr. Bui said in a statement.
Previous studies have linked oral sex, number of sex partners, and cigarettes smoked per day with infection with high-risk oral HPV. Because oral sex and smoking previously had been found to have similar predictive value, Dr. Bui and colleagues examined NHANES data for both low-risk and high-risk HPV type. Using multivariable logistic regression models, they determined oral HPV infection was significantly linked with self-rated overall poor oral health, independent of tobacco use and oral sex.
According to the researchers, the study was limited because the temporal relationship between variables could not be established because of the cross-sectional nature of the data; however, because oral HPV infection normally is asymptomatic, "it is unlikely to affect self-reported oral health." Still, they noted that the data, based on self-report, could be subject to recall bias or under-reporting.
"Public health interventions may aim to promote oral hygiene and oral health as additional preventative measures for HPV-related oral cancers," Dr. Bui and his colleagues said.
The study was supported by a grant from the University of Texas Health Innovation for Cancer Prevention Research. The authors reported no conflicts of interest.
Poor oral health is an independent risk factor of oral human papillomavirus infection regardless of smoking and oral sex practices, analysis of a large, nationally representative sample showed.
Poor oral health was associated with a 56% higher prevalence of oral HPV infection in 3,439 study participants aged 30-69 years, Thanh Cong Bui, Dr.P.H., of the University of Texas Health Sciences Center, Houston, and his colleagues wrote in Cancer Prevention Research.
For those with gum disease and dental problems, prevalence of oral HPV infection was 51% and 28% higher, respectively. More men (12%) than women (3%) were infected with oral HPV (Cancer Prev. Res. 2013 Aug. 21 [doi:10.1158/1940-6207.CAPR-13-008]).
Marijuana use also was linked to higher rates of infection: 5% in nonusers, 8% in former users, and 14% in current users.
The findings were derived from the 2009-2010 National Health and Nutrition Examination Survey (NHANES), a nationally representative sampling conducted by the Centers for Disease Control and Prevention. Oral health data were taken from participants’ self-assessments of overall oral health, presence of gum disease, use of mouthwash to treat dental problems within past 7 days of the survey, and number of teeth lost.
"The good news is, this risk factor is modifiable – by maintaining good oral hygiene and good oral health, one can prevent HPV infection and subsequent HPV-related cancers," Dr. Bui said in a statement.
Previous studies have linked oral sex, number of sex partners, and cigarettes smoked per day with infection with high-risk oral HPV. Because oral sex and smoking previously had been found to have similar predictive value, Dr. Bui and colleagues examined NHANES data for both low-risk and high-risk HPV type. Using multivariable logistic regression models, they determined oral HPV infection was significantly linked with self-rated overall poor oral health, independent of tobacco use and oral sex.
According to the researchers, the study was limited because the temporal relationship between variables could not be established because of the cross-sectional nature of the data; however, because oral HPV infection normally is asymptomatic, "it is unlikely to affect self-reported oral health." Still, they noted that the data, based on self-report, could be subject to recall bias or under-reporting.
"Public health interventions may aim to promote oral hygiene and oral health as additional preventative measures for HPV-related oral cancers," Dr. Bui and his colleagues said.
The study was supported by a grant from the University of Texas Health Innovation for Cancer Prevention Research. The authors reported no conflicts of interest.
Poor oral health is an independent risk factor of oral human papillomavirus infection regardless of smoking and oral sex practices, analysis of a large, nationally representative sample showed.
Poor oral health was associated with a 56% higher prevalence of oral HPV infection in 3,439 study participants aged 30-69 years, Thanh Cong Bui, Dr.P.H., of the University of Texas Health Sciences Center, Houston, and his colleagues wrote in Cancer Prevention Research.
For those with gum disease and dental problems, prevalence of oral HPV infection was 51% and 28% higher, respectively. More men (12%) than women (3%) were infected with oral HPV (Cancer Prev. Res. 2013 Aug. 21 [doi:10.1158/1940-6207.CAPR-13-008]).
Marijuana use also was linked to higher rates of infection: 5% in nonusers, 8% in former users, and 14% in current users.
The findings were derived from the 2009-2010 National Health and Nutrition Examination Survey (NHANES), a nationally representative sampling conducted by the Centers for Disease Control and Prevention. Oral health data were taken from participants’ self-assessments of overall oral health, presence of gum disease, use of mouthwash to treat dental problems within past 7 days of the survey, and number of teeth lost.
"The good news is, this risk factor is modifiable – by maintaining good oral hygiene and good oral health, one can prevent HPV infection and subsequent HPV-related cancers," Dr. Bui said in a statement.
Previous studies have linked oral sex, number of sex partners, and cigarettes smoked per day with infection with high-risk oral HPV. Because oral sex and smoking previously had been found to have similar predictive value, Dr. Bui and colleagues examined NHANES data for both low-risk and high-risk HPV type. Using multivariable logistic regression models, they determined oral HPV infection was significantly linked with self-rated overall poor oral health, independent of tobacco use and oral sex.
According to the researchers, the study was limited because the temporal relationship between variables could not be established because of the cross-sectional nature of the data; however, because oral HPV infection normally is asymptomatic, "it is unlikely to affect self-reported oral health." Still, they noted that the data, based on self-report, could be subject to recall bias or under-reporting.
"Public health interventions may aim to promote oral hygiene and oral health as additional preventative measures for HPV-related oral cancers," Dr. Bui and his colleagues said.
The study was supported by a grant from the University of Texas Health Innovation for Cancer Prevention Research. The authors reported no conflicts of interest.
FROM CANCER PREVENTION RESEARCH
Major finding: Poor oral health was associated with a 56% higher prevalence of oral infection with human papillomavirus.
Data source: A nationally representative sampling of 3,439 people aged 30-69 years for whom reliable oral health data were available.
Disclosures: The study was supported by a grant from the University of Texas. The researchers reported no relevant conflicts of interest.
Intermittent positive-pressure ventilation similar to continuous positive airway pressure in preventing lung injury in preemies
The incidence of severe lung injury in extremely premature neonates with bronchopulmonary dysplasia given nasal intermittent positive-pressure ventilation is not significantly different for those who receive nasal continuous positive airway pressure, a randomized study of more than 1,000 infants shows.
"Although somewhat discouraging, this research is significant, as it refutes the common assumption that the noninvasive therapies being used are reducing severe lung injury in these tiny babies," said lead author Dr. Haresh Kirpalani, attending neonatologist at the Children’s Hospital of Philadelphia, in a statement about the results. "The study alerts us that we still need to develop new therapies for babies to avoid lung injury and [bronchopulmonary dysplasia]."
Neonatologists often introduce the noninvasive therapies of nasal intermittent positive-pressure ventilation (IPPV) and nasal continuous positive airway pressure (CPAP) early in the lives of extremely low-birth-weight neonates. Their goal is to avoid potentially severe scarring and inflammation of the lungs that can result from the more invasive respiratory technique of endotracheal intubation and mechanical ventilation. Bronchopulmonary dysplasia (BPD) is a leading cause of neurological injury and death in this cohort.
Previously, a meta-analysis of trials of early nasal CPAP vs. intubation and ventilation showed that nasal CPAP is associated with a lower risk of BPD. Still, Dr. Kirpalani and his colleagues quoted several studies showing that 34%-83% of extremely low-birth-weight infants given nasal CPAP require subsequent intubation. Meanwhile, nasal IPPV has been associated with nasal trauma and necrotizing enterocolitis. Only small randomized trials have compared nasal CPAP with nasal IPPV, commonly used in extremely low-birth-weight infants in several countries.
Researchers in the current study enrolled infants in 10 countries between May 7, 2007, and June 29, 2011. Eligible infants weighed less than 1,000 grams, had a gestational age of less than 30 weeks, and were candidates for noninvasive respiratory support. Infants expected to die were excluded, as were those with congenital abnormalities, a need for surgery, or a neuromuscular disorder. Key baseline characteristics in the study were similar, although the proportion of male infants was higher in the nasal IPPV group (52.6%) than in the nasal CPAP group (46.1%).
Of the 497 infants assigned by researchers to nasal IPPV, 38.4% of those for whom sufficient data were available reached the primary outcome of death before 36 weeks of postmenstrual age or survival with BPD (N. Engl. J. Med. 2013;369:611-20). In a similar group of 490 infants given nasal CPAP, 36.7% reached the primary outcome (adjusted odds ratio, 1.09; 95% CI, 0.83-1.43; P = .56).
Dr. Kirpalani and his associates found no significant difference in rates of other neonatal complications between the two treatment groups.
Of the surviving infants, 58.3% in the nasal IPPV group needed postrandomization intubation, as did 59.1% in the nasal CPAP group. According to the researchers, the high number of reintubations in both groups indicates the difficulty in discontinuing respiratory support, despite the equally high use of caffeine at least once to mitigate the level of BDP in both groups (98.8% of the nasal IPPV group; 99.4% of the nasal CPAP group).
The researchers noted that despite guidelines for weaning, extubation, and reintubation, a potential for bias existed because their study did not permit blinding. However, the authors wrote that one strength of their study was their objective assessment of BPD in their study groups, determined by a standardized, blinded oxygen-reduction test. In the 20 infants for whom oxygen-reduction data were not available, similar data were obtained in a secondary analysis that used National Institutes of Health criteria for BPD.
They concluded that although the overall rates of the primary outcome of death or survival with BPD were similar in the two groups, "on the basis of the 95% confidence interval around the adjusted odds ratio, our results are compatible with an efficacy that ranges from a 21% reduction to a 35% increase in the risk of this outcome with the use of nasal IPPV versus nasal CPAP. These findings call into question the current widespread use of nasal IPPV."
The study was funded by the Canadian Institutes of Health Research. Dr. Kirpalani said he has no conflicts of interest related to this study.
The incidence of severe lung injury in extremely premature neonates with bronchopulmonary dysplasia given nasal intermittent positive-pressure ventilation is not significantly different for those who receive nasal continuous positive airway pressure, a randomized study of more than 1,000 infants shows.
"Although somewhat discouraging, this research is significant, as it refutes the common assumption that the noninvasive therapies being used are reducing severe lung injury in these tiny babies," said lead author Dr. Haresh Kirpalani, attending neonatologist at the Children’s Hospital of Philadelphia, in a statement about the results. "The study alerts us that we still need to develop new therapies for babies to avoid lung injury and [bronchopulmonary dysplasia]."
Neonatologists often introduce the noninvasive therapies of nasal intermittent positive-pressure ventilation (IPPV) and nasal continuous positive airway pressure (CPAP) early in the lives of extremely low-birth-weight neonates. Their goal is to avoid potentially severe scarring and inflammation of the lungs that can result from the more invasive respiratory technique of endotracheal intubation and mechanical ventilation. Bronchopulmonary dysplasia (BPD) is a leading cause of neurological injury and death in this cohort.
Previously, a meta-analysis of trials of early nasal CPAP vs. intubation and ventilation showed that nasal CPAP is associated with a lower risk of BPD. Still, Dr. Kirpalani and his colleagues quoted several studies showing that 34%-83% of extremely low-birth-weight infants given nasal CPAP require subsequent intubation. Meanwhile, nasal IPPV has been associated with nasal trauma and necrotizing enterocolitis. Only small randomized trials have compared nasal CPAP with nasal IPPV, commonly used in extremely low-birth-weight infants in several countries.
Researchers in the current study enrolled infants in 10 countries between May 7, 2007, and June 29, 2011. Eligible infants weighed less than 1,000 grams, had a gestational age of less than 30 weeks, and were candidates for noninvasive respiratory support. Infants expected to die were excluded, as were those with congenital abnormalities, a need for surgery, or a neuromuscular disorder. Key baseline characteristics in the study were similar, although the proportion of male infants was higher in the nasal IPPV group (52.6%) than in the nasal CPAP group (46.1%).
Of the 497 infants assigned by researchers to nasal IPPV, 38.4% of those for whom sufficient data were available reached the primary outcome of death before 36 weeks of postmenstrual age or survival with BPD (N. Engl. J. Med. 2013;369:611-20). In a similar group of 490 infants given nasal CPAP, 36.7% reached the primary outcome (adjusted odds ratio, 1.09; 95% CI, 0.83-1.43; P = .56).
Dr. Kirpalani and his associates found no significant difference in rates of other neonatal complications between the two treatment groups.
Of the surviving infants, 58.3% in the nasal IPPV group needed postrandomization intubation, as did 59.1% in the nasal CPAP group. According to the researchers, the high number of reintubations in both groups indicates the difficulty in discontinuing respiratory support, despite the equally high use of caffeine at least once to mitigate the level of BDP in both groups (98.8% of the nasal IPPV group; 99.4% of the nasal CPAP group).
The researchers noted that despite guidelines for weaning, extubation, and reintubation, a potential for bias existed because their study did not permit blinding. However, the authors wrote that one strength of their study was their objective assessment of BPD in their study groups, determined by a standardized, blinded oxygen-reduction test. In the 20 infants for whom oxygen-reduction data were not available, similar data were obtained in a secondary analysis that used National Institutes of Health criteria for BPD.
They concluded that although the overall rates of the primary outcome of death or survival with BPD were similar in the two groups, "on the basis of the 95% confidence interval around the adjusted odds ratio, our results are compatible with an efficacy that ranges from a 21% reduction to a 35% increase in the risk of this outcome with the use of nasal IPPV versus nasal CPAP. These findings call into question the current widespread use of nasal IPPV."
The study was funded by the Canadian Institutes of Health Research. Dr. Kirpalani said he has no conflicts of interest related to this study.
The incidence of severe lung injury in extremely premature neonates with bronchopulmonary dysplasia given nasal intermittent positive-pressure ventilation is not significantly different for those who receive nasal continuous positive airway pressure, a randomized study of more than 1,000 infants shows.
"Although somewhat discouraging, this research is significant, as it refutes the common assumption that the noninvasive therapies being used are reducing severe lung injury in these tiny babies," said lead author Dr. Haresh Kirpalani, attending neonatologist at the Children’s Hospital of Philadelphia, in a statement about the results. "The study alerts us that we still need to develop new therapies for babies to avoid lung injury and [bronchopulmonary dysplasia]."
Neonatologists often introduce the noninvasive therapies of nasal intermittent positive-pressure ventilation (IPPV) and nasal continuous positive airway pressure (CPAP) early in the lives of extremely low-birth-weight neonates. Their goal is to avoid potentially severe scarring and inflammation of the lungs that can result from the more invasive respiratory technique of endotracheal intubation and mechanical ventilation. Bronchopulmonary dysplasia (BPD) is a leading cause of neurological injury and death in this cohort.
Previously, a meta-analysis of trials of early nasal CPAP vs. intubation and ventilation showed that nasal CPAP is associated with a lower risk of BPD. Still, Dr. Kirpalani and his colleagues quoted several studies showing that 34%-83% of extremely low-birth-weight infants given nasal CPAP require subsequent intubation. Meanwhile, nasal IPPV has been associated with nasal trauma and necrotizing enterocolitis. Only small randomized trials have compared nasal CPAP with nasal IPPV, commonly used in extremely low-birth-weight infants in several countries.
Researchers in the current study enrolled infants in 10 countries between May 7, 2007, and June 29, 2011. Eligible infants weighed less than 1,000 grams, had a gestational age of less than 30 weeks, and were candidates for noninvasive respiratory support. Infants expected to die were excluded, as were those with congenital abnormalities, a need for surgery, or a neuromuscular disorder. Key baseline characteristics in the study were similar, although the proportion of male infants was higher in the nasal IPPV group (52.6%) than in the nasal CPAP group (46.1%).
Of the 497 infants assigned by researchers to nasal IPPV, 38.4% of those for whom sufficient data were available reached the primary outcome of death before 36 weeks of postmenstrual age or survival with BPD (N. Engl. J. Med. 2013;369:611-20). In a similar group of 490 infants given nasal CPAP, 36.7% reached the primary outcome (adjusted odds ratio, 1.09; 95% CI, 0.83-1.43; P = .56).
Dr. Kirpalani and his associates found no significant difference in rates of other neonatal complications between the two treatment groups.
Of the surviving infants, 58.3% in the nasal IPPV group needed postrandomization intubation, as did 59.1% in the nasal CPAP group. According to the researchers, the high number of reintubations in both groups indicates the difficulty in discontinuing respiratory support, despite the equally high use of caffeine at least once to mitigate the level of BDP in both groups (98.8% of the nasal IPPV group; 99.4% of the nasal CPAP group).
The researchers noted that despite guidelines for weaning, extubation, and reintubation, a potential for bias existed because their study did not permit blinding. However, the authors wrote that one strength of their study was their objective assessment of BPD in their study groups, determined by a standardized, blinded oxygen-reduction test. In the 20 infants for whom oxygen-reduction data were not available, similar data were obtained in a secondary analysis that used National Institutes of Health criteria for BPD.
They concluded that although the overall rates of the primary outcome of death or survival with BPD were similar in the two groups, "on the basis of the 95% confidence interval around the adjusted odds ratio, our results are compatible with an efficacy that ranges from a 21% reduction to a 35% increase in the risk of this outcome with the use of nasal IPPV versus nasal CPAP. These findings call into question the current widespread use of nasal IPPV."
The study was funded by the Canadian Institutes of Health Research. Dr. Kirpalani said he has no conflicts of interest related to this study.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: Of the 497 infants assigned to nasal IPPV, 38.4% reached the primary outcome of death before 36 weeks of postmenstrual age or survival with BPD. In a similar group of 490 infants given nasal CPAP, 36.7% reached the primary outcome (adjusted odds ratio, 1.09; 95% CI, 0.83-1.43; P = .56).
Data source: A randomized study of 1,009 infants who weighed less than 1,000 grams at birth, had a gestational age of less than 30 weeks, and were candidates for noninvasive respiratory support.
Disclosures: The study was funded by the Canadian Institutes of Health Research. Dr. Kirpalani said he has no conflicts of interest related to this study.