User login
American College of Rheumatology (ACR): Annual Scientific Meeting
Flare risk lower in early-gout patients treated with urate-lowering therapy
WASHINGTON – Putting patients on urate-lowering therapy after their first flare of gout and treating urate levels to target appeared to reduce risk for additional disease flares over a 2-year period, based on results from 314 patients in a randomized, double-blind, placebo-controlled trial.
Among patients with early gout – those experiencing their first gout flare or a second flare that occurred more than 1 year after their first flare – the risk for one or more gout flares during the course of the study was 41% in the placebo group and 29% in the group of patients given febuxostat, a statistically significant difference (P = .033).
The significant advantage for active therapy to prevent flares was seen at 6-12 months, 12-18 months, and 18-24 months.
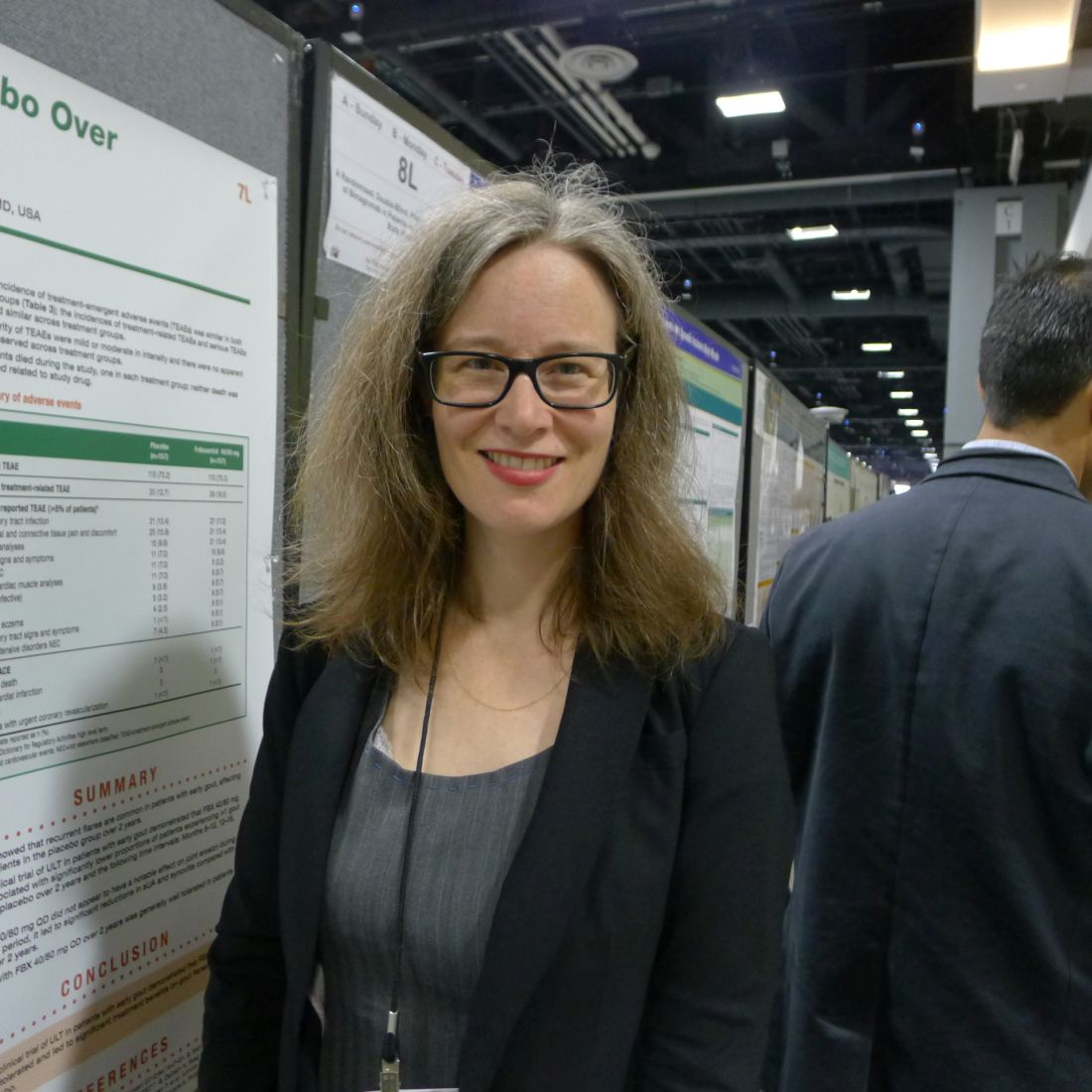
“The reduction in flares with febuxostat is clinically important and statistically significant,” said lead author Nicola Dalbeth, MD, of the University of Auckland (New Zealand). “This is the first clinical trial of [urate-lowering therapy] in patients with early gout. These are patients who would not be treated under current [American College of Rheumatology] guidelines,” which call for urate-lowering therapy if patients are symptomatic and have experienced two or more flares per year.
Dr. Dalbeth presented the study results at a late-breaker session during the annual meeting of the American College of Rheumatology.
The 314 patients were initially randomized to febuxostat 40 mg or placebo. The febuxostat dosage was increased to 80 mg if serum uric acid levels were above target on day 14, and 60 patients had their febuxostat doses increased.
The study was completed by 57% of placebo patients and 59% of febuxostat patients. Baseline characteristics were similar across treatment arms. Mean baseline serum uric acid was about 8.7 mg/dL, mean age was around 50 years, and more than three-quarters of study participants were white. Mean body-mass index was about 32.5, and mild renal impairment was present in 73% of placebo patients and 67% of febuxostat-treated patients.
Based on imaging studies, febuxostat had no significant effect on joint erosion during the observation period, but it reduced synovitis, compared with placebo, she said.
Dr. Dalbeth disclosed relationships with a variety of drug companies, including serving as a consultant for Takeda, the maker of febuxostat (Uloric).
WASHINGTON – Putting patients on urate-lowering therapy after their first flare of gout and treating urate levels to target appeared to reduce risk for additional disease flares over a 2-year period, based on results from 314 patients in a randomized, double-blind, placebo-controlled trial.
Among patients with early gout – those experiencing their first gout flare or a second flare that occurred more than 1 year after their first flare – the risk for one or more gout flares during the course of the study was 41% in the placebo group and 29% in the group of patients given febuxostat, a statistically significant difference (P = .033).
The significant advantage for active therapy to prevent flares was seen at 6-12 months, 12-18 months, and 18-24 months.
“The reduction in flares with febuxostat is clinically important and statistically significant,” said lead author Nicola Dalbeth, MD, of the University of Auckland (New Zealand). “This is the first clinical trial of [urate-lowering therapy] in patients with early gout. These are patients who would not be treated under current [American College of Rheumatology] guidelines,” which call for urate-lowering therapy if patients are symptomatic and have experienced two or more flares per year.
Dr. Dalbeth presented the study results at a late-breaker session during the annual meeting of the American College of Rheumatology.
The 314 patients were initially randomized to febuxostat 40 mg or placebo. The febuxostat dosage was increased to 80 mg if serum uric acid levels were above target on day 14, and 60 patients had their febuxostat doses increased.
The study was completed by 57% of placebo patients and 59% of febuxostat patients. Baseline characteristics were similar across treatment arms. Mean baseline serum uric acid was about 8.7 mg/dL, mean age was around 50 years, and more than three-quarters of study participants were white. Mean body-mass index was about 32.5, and mild renal impairment was present in 73% of placebo patients and 67% of febuxostat-treated patients.
Based on imaging studies, febuxostat had no significant effect on joint erosion during the observation period, but it reduced synovitis, compared with placebo, she said.
Dr. Dalbeth disclosed relationships with a variety of drug companies, including serving as a consultant for Takeda, the maker of febuxostat (Uloric).
WASHINGTON – Putting patients on urate-lowering therapy after their first flare of gout and treating urate levels to target appeared to reduce risk for additional disease flares over a 2-year period, based on results from 314 patients in a randomized, double-blind, placebo-controlled trial.
Among patients with early gout – those experiencing their first gout flare or a second flare that occurred more than 1 year after their first flare – the risk for one or more gout flares during the course of the study was 41% in the placebo group and 29% in the group of patients given febuxostat, a statistically significant difference (P = .033).
The significant advantage for active therapy to prevent flares was seen at 6-12 months, 12-18 months, and 18-24 months.
“The reduction in flares with febuxostat is clinically important and statistically significant,” said lead author Nicola Dalbeth, MD, of the University of Auckland (New Zealand). “This is the first clinical trial of [urate-lowering therapy] in patients with early gout. These are patients who would not be treated under current [American College of Rheumatology] guidelines,” which call for urate-lowering therapy if patients are symptomatic and have experienced two or more flares per year.
Dr. Dalbeth presented the study results at a late-breaker session during the annual meeting of the American College of Rheumatology.
The 314 patients were initially randomized to febuxostat 40 mg or placebo. The febuxostat dosage was increased to 80 mg if serum uric acid levels were above target on day 14, and 60 patients had their febuxostat doses increased.
The study was completed by 57% of placebo patients and 59% of febuxostat patients. Baseline characteristics were similar across treatment arms. Mean baseline serum uric acid was about 8.7 mg/dL, mean age was around 50 years, and more than three-quarters of study participants were white. Mean body-mass index was about 32.5, and mild renal impairment was present in 73% of placebo patients and 67% of febuxostat-treated patients.
Based on imaging studies, febuxostat had no significant effect on joint erosion during the observation period, but it reduced synovitis, compared with placebo, she said.
Dr. Dalbeth disclosed relationships with a variety of drug companies, including serving as a consultant for Takeda, the maker of febuxostat (Uloric).
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: Early-gout patients given febuxostat had a 29% risk of a flare and placebo-treated patients had a 41% risk of a flare over 2 years, a significant difference.
Data source: Randomized, double-blind, placebo-controlled, phase II study of 314 patients with early gout.
Disclosures: Dr. Dalbeth disclosed relationships with a variety of drug companies, including serving as a consultant for Takeda, the maker of febuxostat (Uloric).
AURA-LV study: Rapid remission with voclosporin for lupus nephritis
WASHINGTON – The investigational calcineurin inhibitor voclosporin, given in addition to mycophenolate mofetil and low-dose steroids, was associated with rapid and complete remissions in lupus nephritis patients in the randomized, controlled AURA-LV study.
Aurinia Urinary Protein Reduction Active – Lupus With Voclosporin (AURA-LV) included 265 subjects in over 20 countries with active lupus nephritis. Trial participants received low-dose voclosporin (23.7 mg b.i.d.) or high-dose voclosporin (39.5 mg b.i.d.) in addition to mycophenolate mofetil (2 g/day) and low-dose steroids. Patients began on 20-25 mg of a steroid with a taper to 5 mg at week 8 and 2.5 mg at week 16-24.
Complete remission occurred at 24 weeks in 32.6% of 89 subjects who received 23.7 mg of voclosporin twice daily and standard of care therapy and in 19.3% of 88 control subjects who received placebo and standard of care therapy (odds ratio, 2.03), Mary Anne Dooley, MD, reported at the annual meeting of the American College of Rheumatology.
The complete remission rate was 27.3% in the 88 subjects who received the higher dose (39.5 mg b.i.d.) of voclosporin. The difference between the high-dose voclosporin group and the control group was not statistically significant.
The “very exciting findings” of this study – the first lupus nephritis study to meet its primary endpoint of complete remission – are important, because “partial remission is insufficient for our patients,” she said.
“Clinical trials over the past 10 years have really shown that we’re not reaching a large group of patients. ... more than 40% of patients are complete nonresponders at 6 months,” she said. While attainment of partial remission has improved, half of those who achieve partial remission have been shown to have a 50% increase in the risk of end-stage renal disease in 10 years.
Complete remission was defined as urine protein/creatinine ratio of no more than 0.5 mg/mg using first morning void with an estimated glomerular filtration rate of at least 60 mL/min without a decrease of 20% or more, sustained low-dose steroids (at or below 10 mg/day) and no use of rescue medications.
Partial remission was a composite of reduction in protein/creatinine ratio of at least 50%, no use of rescue medication, and stability of renal function. Both the low- and high-dose voclosporin groups had outcomes that were superior to standard-of-care therapy, with 69.7% partial remission with low-dose voclosporin, 65.9% partial remission with high-dose voclosporin, and 49.4% partial remission with placebo, said Dr. Dooley, a rheumatologist in Chapel Hill, N.C.
“Patients began responding literally within weeks [to voclosporin] ... and we saw significant responses by 7-8 weeks. This was during the time period when the steroids rapidly decreased,” she said, noting that the steroid dosing at baseline was a median of 25 mg vs. 2.5 mg at 16 weeks.
Study subjects met ACR criteria for lupus and had biopsy-proven lupus nephritis, including proliferative nephritis class III/IV or class V alone or in combination with proliferative disease. All were treated with 2 g/day of mycophenolate mofetil, and the steroid taper “was such that by 10 weeks, patients were down to 5 mg, and that by 24 weeks the median dose was 2.5 mg,” she said.
Adverse events, most commonly infection and gastrointestinal disorders, occurred in 90% of study subjects. Infections occurred in 56.2% of those in the low-dose group, 63.6% of those in the high-dose group, and 50% of controls. GI disorders occurred in 41.6%, 52.3%, and 36.4% of patients in the groups, respectively.
Serious adverse events were more common in the voclosporin groups, occurring in 25.8% and 25% of patients in the low- and high-dose groups, respectively, compared with 15.8% of patients in the control group.
Ten of the 13 deaths occurred in the low-dose voclosporin group (3 due to infection, 3 due to thromboembolism, and 4 due to “other” causes); 2 occurred in the high-dose voclosporin group (1 each due to infection and thromboembolism); and 1 death due to thromboembolism occurred in the control group. As most of the deaths were clustered in the low-dose arm, and 11 of the 13 deaths occurred in areas with “compromised access to standard of care,” the deaths were not considered to be directly related to voclosporin therapy.
Patients who died had “a statistically different clinical baseline picture with higher levels of proteinuria or difficulty with comorbid conditions and some signs of poor nutrition,” Dr. Dooley said.
The findings of the study will be used as the basis for planned subsequent studies of the use of voclosporin in lupus nephritis, she said.
Voclosporin is an analogue of cyclosporin A that may allow flat dosing and a potentially improved safety profile compared with other calcineurin inhibitors.
Aurinia Pharmaceuticals, the maker of voclosporin, announced in early November 2016 that the twice-daily 23.7 mg voclosporin dose will advance to a global 52-week double-blind, placebo-controlled phase III study in the second quarter of 2017. Voclosporin has already received fast track designation from the Food and Drug Administration.
Dr. Dooley reported a financial relationship with Aurinia, which sponsored the study.
WASHINGTON – The investigational calcineurin inhibitor voclosporin, given in addition to mycophenolate mofetil and low-dose steroids, was associated with rapid and complete remissions in lupus nephritis patients in the randomized, controlled AURA-LV study.
Aurinia Urinary Protein Reduction Active – Lupus With Voclosporin (AURA-LV) included 265 subjects in over 20 countries with active lupus nephritis. Trial participants received low-dose voclosporin (23.7 mg b.i.d.) or high-dose voclosporin (39.5 mg b.i.d.) in addition to mycophenolate mofetil (2 g/day) and low-dose steroids. Patients began on 20-25 mg of a steroid with a taper to 5 mg at week 8 and 2.5 mg at week 16-24.
Complete remission occurred at 24 weeks in 32.6% of 89 subjects who received 23.7 mg of voclosporin twice daily and standard of care therapy and in 19.3% of 88 control subjects who received placebo and standard of care therapy (odds ratio, 2.03), Mary Anne Dooley, MD, reported at the annual meeting of the American College of Rheumatology.
The complete remission rate was 27.3% in the 88 subjects who received the higher dose (39.5 mg b.i.d.) of voclosporin. The difference between the high-dose voclosporin group and the control group was not statistically significant.
The “very exciting findings” of this study – the first lupus nephritis study to meet its primary endpoint of complete remission – are important, because “partial remission is insufficient for our patients,” she said.
“Clinical trials over the past 10 years have really shown that we’re not reaching a large group of patients. ... more than 40% of patients are complete nonresponders at 6 months,” she said. While attainment of partial remission has improved, half of those who achieve partial remission have been shown to have a 50% increase in the risk of end-stage renal disease in 10 years.
Complete remission was defined as urine protein/creatinine ratio of no more than 0.5 mg/mg using first morning void with an estimated glomerular filtration rate of at least 60 mL/min without a decrease of 20% or more, sustained low-dose steroids (at or below 10 mg/day) and no use of rescue medications.
Partial remission was a composite of reduction in protein/creatinine ratio of at least 50%, no use of rescue medication, and stability of renal function. Both the low- and high-dose voclosporin groups had outcomes that were superior to standard-of-care therapy, with 69.7% partial remission with low-dose voclosporin, 65.9% partial remission with high-dose voclosporin, and 49.4% partial remission with placebo, said Dr. Dooley, a rheumatologist in Chapel Hill, N.C.
“Patients began responding literally within weeks [to voclosporin] ... and we saw significant responses by 7-8 weeks. This was during the time period when the steroids rapidly decreased,” she said, noting that the steroid dosing at baseline was a median of 25 mg vs. 2.5 mg at 16 weeks.
Study subjects met ACR criteria for lupus and had biopsy-proven lupus nephritis, including proliferative nephritis class III/IV or class V alone or in combination with proliferative disease. All were treated with 2 g/day of mycophenolate mofetil, and the steroid taper “was such that by 10 weeks, patients were down to 5 mg, and that by 24 weeks the median dose was 2.5 mg,” she said.
Adverse events, most commonly infection and gastrointestinal disorders, occurred in 90% of study subjects. Infections occurred in 56.2% of those in the low-dose group, 63.6% of those in the high-dose group, and 50% of controls. GI disorders occurred in 41.6%, 52.3%, and 36.4% of patients in the groups, respectively.
Serious adverse events were more common in the voclosporin groups, occurring in 25.8% and 25% of patients in the low- and high-dose groups, respectively, compared with 15.8% of patients in the control group.
Ten of the 13 deaths occurred in the low-dose voclosporin group (3 due to infection, 3 due to thromboembolism, and 4 due to “other” causes); 2 occurred in the high-dose voclosporin group (1 each due to infection and thromboembolism); and 1 death due to thromboembolism occurred in the control group. As most of the deaths were clustered in the low-dose arm, and 11 of the 13 deaths occurred in areas with “compromised access to standard of care,” the deaths were not considered to be directly related to voclosporin therapy.
Patients who died had “a statistically different clinical baseline picture with higher levels of proteinuria or difficulty with comorbid conditions and some signs of poor nutrition,” Dr. Dooley said.
The findings of the study will be used as the basis for planned subsequent studies of the use of voclosporin in lupus nephritis, she said.
Voclosporin is an analogue of cyclosporin A that may allow flat dosing and a potentially improved safety profile compared with other calcineurin inhibitors.
Aurinia Pharmaceuticals, the maker of voclosporin, announced in early November 2016 that the twice-daily 23.7 mg voclosporin dose will advance to a global 52-week double-blind, placebo-controlled phase III study in the second quarter of 2017. Voclosporin has already received fast track designation from the Food and Drug Administration.
Dr. Dooley reported a financial relationship with Aurinia, which sponsored the study.
WASHINGTON – The investigational calcineurin inhibitor voclosporin, given in addition to mycophenolate mofetil and low-dose steroids, was associated with rapid and complete remissions in lupus nephritis patients in the randomized, controlled AURA-LV study.
Aurinia Urinary Protein Reduction Active – Lupus With Voclosporin (AURA-LV) included 265 subjects in over 20 countries with active lupus nephritis. Trial participants received low-dose voclosporin (23.7 mg b.i.d.) or high-dose voclosporin (39.5 mg b.i.d.) in addition to mycophenolate mofetil (2 g/day) and low-dose steroids. Patients began on 20-25 mg of a steroid with a taper to 5 mg at week 8 and 2.5 mg at week 16-24.
Complete remission occurred at 24 weeks in 32.6% of 89 subjects who received 23.7 mg of voclosporin twice daily and standard of care therapy and in 19.3% of 88 control subjects who received placebo and standard of care therapy (odds ratio, 2.03), Mary Anne Dooley, MD, reported at the annual meeting of the American College of Rheumatology.
The complete remission rate was 27.3% in the 88 subjects who received the higher dose (39.5 mg b.i.d.) of voclosporin. The difference between the high-dose voclosporin group and the control group was not statistically significant.
The “very exciting findings” of this study – the first lupus nephritis study to meet its primary endpoint of complete remission – are important, because “partial remission is insufficient for our patients,” she said.
“Clinical trials over the past 10 years have really shown that we’re not reaching a large group of patients. ... more than 40% of patients are complete nonresponders at 6 months,” she said. While attainment of partial remission has improved, half of those who achieve partial remission have been shown to have a 50% increase in the risk of end-stage renal disease in 10 years.
Complete remission was defined as urine protein/creatinine ratio of no more than 0.5 mg/mg using first morning void with an estimated glomerular filtration rate of at least 60 mL/min without a decrease of 20% or more, sustained low-dose steroids (at or below 10 mg/day) and no use of rescue medications.
Partial remission was a composite of reduction in protein/creatinine ratio of at least 50%, no use of rescue medication, and stability of renal function. Both the low- and high-dose voclosporin groups had outcomes that were superior to standard-of-care therapy, with 69.7% partial remission with low-dose voclosporin, 65.9% partial remission with high-dose voclosporin, and 49.4% partial remission with placebo, said Dr. Dooley, a rheumatologist in Chapel Hill, N.C.
“Patients began responding literally within weeks [to voclosporin] ... and we saw significant responses by 7-8 weeks. This was during the time period when the steroids rapidly decreased,” she said, noting that the steroid dosing at baseline was a median of 25 mg vs. 2.5 mg at 16 weeks.
Study subjects met ACR criteria for lupus and had biopsy-proven lupus nephritis, including proliferative nephritis class III/IV or class V alone or in combination with proliferative disease. All were treated with 2 g/day of mycophenolate mofetil, and the steroid taper “was such that by 10 weeks, patients were down to 5 mg, and that by 24 weeks the median dose was 2.5 mg,” she said.
Adverse events, most commonly infection and gastrointestinal disorders, occurred in 90% of study subjects. Infections occurred in 56.2% of those in the low-dose group, 63.6% of those in the high-dose group, and 50% of controls. GI disorders occurred in 41.6%, 52.3%, and 36.4% of patients in the groups, respectively.
Serious adverse events were more common in the voclosporin groups, occurring in 25.8% and 25% of patients in the low- and high-dose groups, respectively, compared with 15.8% of patients in the control group.
Ten of the 13 deaths occurred in the low-dose voclosporin group (3 due to infection, 3 due to thromboembolism, and 4 due to “other” causes); 2 occurred in the high-dose voclosporin group (1 each due to infection and thromboembolism); and 1 death due to thromboembolism occurred in the control group. As most of the deaths were clustered in the low-dose arm, and 11 of the 13 deaths occurred in areas with “compromised access to standard of care,” the deaths were not considered to be directly related to voclosporin therapy.
Patients who died had “a statistically different clinical baseline picture with higher levels of proteinuria or difficulty with comorbid conditions and some signs of poor nutrition,” Dr. Dooley said.
The findings of the study will be used as the basis for planned subsequent studies of the use of voclosporin in lupus nephritis, she said.
Voclosporin is an analogue of cyclosporin A that may allow flat dosing and a potentially improved safety profile compared with other calcineurin inhibitors.
Aurinia Pharmaceuticals, the maker of voclosporin, announced in early November 2016 that the twice-daily 23.7 mg voclosporin dose will advance to a global 52-week double-blind, placebo-controlled phase III study in the second quarter of 2017. Voclosporin has already received fast track designation from the Food and Drug Administration.
Dr. Dooley reported a financial relationship with Aurinia, which sponsored the study.
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: The complete remission rate at 24 weeks was 32.6% vs. 19.3% in patients receiving low-dose voclosporin vs. controls (odds ratio, 2.03).
Data source: The randomized, controlled AURA-LV study of 265 lupus nephritis patients.
Disclosures: Dr. Dooley reported a financial relationship with Aurinia Pharmaceuticals, which sponsored the study.
Breast milk doesn’t contain meaningful levels of certolizumab pegol
WASHINGTON – Certolizumab pegol is not transmitted into human breast milk in any clinically meaningful level, a postmarketing pharmacokinetic study has determined.
While there were individual differences in how much of the TNF inhibitor did cross into milk, none of the 17 women in the study transmitted more than 0.076 mcg/mL in any sample, Megan Clowse, MD, said at the annual meeting of the American College of Rheumatology.
“This is well below even 1% of the expected plasma concentration of a therapeutic dose,” said Dr. Clowse, a rheumatologist and director of the Duke Autoimmunity in Pregnancy Registry at Duke University, Durham, N.C. “Additionally, the mean relative infant dose was 0.125% – also far below the cutoff of less than 10% of the adult dose, the level generally thought to be of little concern for infant well-being.”
The transmission potential, however, has always been assumed to be low. “It’s a protein that would largely be degraded in the gastrointestinal tract of the baby, so there would be low bioavailability. But also CZP has no Fc portion, so it is not pulled across the intestinal lumina by the neonatal Fc receptor.”
Despite those assumptions and the positive – although limited – data, UCB conducted a 4-week postmarketing study to fully determine transmission levels. The CRADLE study enrolled 17 women taking CZP while breastfeeding healthy, full-term infants. Breast milk samples were taken at days 0, 2, 4, 6, 8, 10, 12, and 14 across one dosing period (14 days for those taking 200 mg every 2 weeks; and 28 days for those taking 400 mg every 4 weeks).
In addition to being the first study to estimate the average daily infant dose, CRADLE used a specially created ELISA to measure the drug. “This was a very carefully thought-out measure designed to be 10 times more sensitive than any assay ever used to identify this drug,” Dr. Clowse said. “It had a very high specificity, having to attach to both the TNF portion and the PEG component.”
All the women had a healthy term infant who was exclusively breastfed. Mothers had to be in steady-state dosing with at least three prior doses before the first sample and could not have taken any other biologics within five half-lives of those medications.
The mean age of the 17 women in the analysis was 34 years. Rheumatoid arthritis was the most common diagnosis (7); other conditions were Crohn’s disease (5), psoriatic arthritis (3), and ankylosing spondylitis (2). The majority of the infants (13) were younger than 6 months at the time of the study.
Most of the women (13) had some measurable CZP in at least one sample, and four had measurable CZP in almost every sample. But of the entire 137 samples tested, 77 (56%) came back below the limit of quantification, which was less than 0.032 mcg/mL. Another 52 samples came back as less than twice the lower limit of quantification (less than 0.064 mcg/mL). Among these, though, most were less than 0.050 mcg/mL. Only eight samples approached the level of less than three times the lower limit of quantification (less than 0.096 mcg/mL); of these, the highest level was 0.076 mcg/mL.
There were some strong individual trends, Dr. Clowse noted. Only two women showed the highest levels: Out of seven samples, one had two such readings, and the other had five. In four women, all of the samples were below the lower limit of quantification. The rest of the women had mixed results, which tended to cluster in the middle of their treatment cycle and then go down.
The median maximum concentration in breast milk was 0.04285 mcg/mL, which translated to an average daily infant dose of 0.0035 mg/kg/day. This was an infant dose of 0.125% of the mother’s dose, Dr. Clowse said.
A 5-week safety study followed the breast milk sampling phase. During this time, nine infants had some sort of event. These were mild and not different from that normally seen in breastfed infants. Several events were paired with maternal events, Dr. Clowse said. Two pairs had upper respiratory tract infections, and one mother developed a Candida skin infection while her infant developed oral candidiasis.
UCB sponsored the CRADLE study. Dr. Clowse is a consultant for the company.
[email protected]
On Twitter @alz_gal
WASHINGTON – Certolizumab pegol is not transmitted into human breast milk in any clinically meaningful level, a postmarketing pharmacokinetic study has determined.
While there were individual differences in how much of the TNF inhibitor did cross into milk, none of the 17 women in the study transmitted more than 0.076 mcg/mL in any sample, Megan Clowse, MD, said at the annual meeting of the American College of Rheumatology.
“This is well below even 1% of the expected plasma concentration of a therapeutic dose,” said Dr. Clowse, a rheumatologist and director of the Duke Autoimmunity in Pregnancy Registry at Duke University, Durham, N.C. “Additionally, the mean relative infant dose was 0.125% – also far below the cutoff of less than 10% of the adult dose, the level generally thought to be of little concern for infant well-being.”
The transmission potential, however, has always been assumed to be low. “It’s a protein that would largely be degraded in the gastrointestinal tract of the baby, so there would be low bioavailability. But also CZP has no Fc portion, so it is not pulled across the intestinal lumina by the neonatal Fc receptor.”
Despite those assumptions and the positive – although limited – data, UCB conducted a 4-week postmarketing study to fully determine transmission levels. The CRADLE study enrolled 17 women taking CZP while breastfeeding healthy, full-term infants. Breast milk samples were taken at days 0, 2, 4, 6, 8, 10, 12, and 14 across one dosing period (14 days for those taking 200 mg every 2 weeks; and 28 days for those taking 400 mg every 4 weeks).
In addition to being the first study to estimate the average daily infant dose, CRADLE used a specially created ELISA to measure the drug. “This was a very carefully thought-out measure designed to be 10 times more sensitive than any assay ever used to identify this drug,” Dr. Clowse said. “It had a very high specificity, having to attach to both the TNF portion and the PEG component.”
All the women had a healthy term infant who was exclusively breastfed. Mothers had to be in steady-state dosing with at least three prior doses before the first sample and could not have taken any other biologics within five half-lives of those medications.
The mean age of the 17 women in the analysis was 34 years. Rheumatoid arthritis was the most common diagnosis (7); other conditions were Crohn’s disease (5), psoriatic arthritis (3), and ankylosing spondylitis (2). The majority of the infants (13) were younger than 6 months at the time of the study.
Most of the women (13) had some measurable CZP in at least one sample, and four had measurable CZP in almost every sample. But of the entire 137 samples tested, 77 (56%) came back below the limit of quantification, which was less than 0.032 mcg/mL. Another 52 samples came back as less than twice the lower limit of quantification (less than 0.064 mcg/mL). Among these, though, most were less than 0.050 mcg/mL. Only eight samples approached the level of less than three times the lower limit of quantification (less than 0.096 mcg/mL); of these, the highest level was 0.076 mcg/mL.
There were some strong individual trends, Dr. Clowse noted. Only two women showed the highest levels: Out of seven samples, one had two such readings, and the other had five. In four women, all of the samples were below the lower limit of quantification. The rest of the women had mixed results, which tended to cluster in the middle of their treatment cycle and then go down.
The median maximum concentration in breast milk was 0.04285 mcg/mL, which translated to an average daily infant dose of 0.0035 mg/kg/day. This was an infant dose of 0.125% of the mother’s dose, Dr. Clowse said.
A 5-week safety study followed the breast milk sampling phase. During this time, nine infants had some sort of event. These were mild and not different from that normally seen in breastfed infants. Several events were paired with maternal events, Dr. Clowse said. Two pairs had upper respiratory tract infections, and one mother developed a Candida skin infection while her infant developed oral candidiasis.
UCB sponsored the CRADLE study. Dr. Clowse is a consultant for the company.
[email protected]
On Twitter @alz_gal
WASHINGTON – Certolizumab pegol is not transmitted into human breast milk in any clinically meaningful level, a postmarketing pharmacokinetic study has determined.
While there were individual differences in how much of the TNF inhibitor did cross into milk, none of the 17 women in the study transmitted more than 0.076 mcg/mL in any sample, Megan Clowse, MD, said at the annual meeting of the American College of Rheumatology.
“This is well below even 1% of the expected plasma concentration of a therapeutic dose,” said Dr. Clowse, a rheumatologist and director of the Duke Autoimmunity in Pregnancy Registry at Duke University, Durham, N.C. “Additionally, the mean relative infant dose was 0.125% – also far below the cutoff of less than 10% of the adult dose, the level generally thought to be of little concern for infant well-being.”
The transmission potential, however, has always been assumed to be low. “It’s a protein that would largely be degraded in the gastrointestinal tract of the baby, so there would be low bioavailability. But also CZP has no Fc portion, so it is not pulled across the intestinal lumina by the neonatal Fc receptor.”
Despite those assumptions and the positive – although limited – data, UCB conducted a 4-week postmarketing study to fully determine transmission levels. The CRADLE study enrolled 17 women taking CZP while breastfeeding healthy, full-term infants. Breast milk samples were taken at days 0, 2, 4, 6, 8, 10, 12, and 14 across one dosing period (14 days for those taking 200 mg every 2 weeks; and 28 days for those taking 400 mg every 4 weeks).
In addition to being the first study to estimate the average daily infant dose, CRADLE used a specially created ELISA to measure the drug. “This was a very carefully thought-out measure designed to be 10 times more sensitive than any assay ever used to identify this drug,” Dr. Clowse said. “It had a very high specificity, having to attach to both the TNF portion and the PEG component.”
All the women had a healthy term infant who was exclusively breastfed. Mothers had to be in steady-state dosing with at least three prior doses before the first sample and could not have taken any other biologics within five half-lives of those medications.
The mean age of the 17 women in the analysis was 34 years. Rheumatoid arthritis was the most common diagnosis (7); other conditions were Crohn’s disease (5), psoriatic arthritis (3), and ankylosing spondylitis (2). The majority of the infants (13) were younger than 6 months at the time of the study.
Most of the women (13) had some measurable CZP in at least one sample, and four had measurable CZP in almost every sample. But of the entire 137 samples tested, 77 (56%) came back below the limit of quantification, which was less than 0.032 mcg/mL. Another 52 samples came back as less than twice the lower limit of quantification (less than 0.064 mcg/mL). Among these, though, most were less than 0.050 mcg/mL. Only eight samples approached the level of less than three times the lower limit of quantification (less than 0.096 mcg/mL); of these, the highest level was 0.076 mcg/mL.
There were some strong individual trends, Dr. Clowse noted. Only two women showed the highest levels: Out of seven samples, one had two such readings, and the other had five. In four women, all of the samples were below the lower limit of quantification. The rest of the women had mixed results, which tended to cluster in the middle of their treatment cycle and then go down.
The median maximum concentration in breast milk was 0.04285 mcg/mL, which translated to an average daily infant dose of 0.0035 mg/kg/day. This was an infant dose of 0.125% of the mother’s dose, Dr. Clowse said.
A 5-week safety study followed the breast milk sampling phase. During this time, nine infants had some sort of event. These were mild and not different from that normally seen in breastfed infants. Several events were paired with maternal events, Dr. Clowse said. Two pairs had upper respiratory tract infections, and one mother developed a Candida skin infection while her infant developed oral candidiasis.
UCB sponsored the CRADLE study. Dr. Clowse is a consultant for the company.
[email protected]
On Twitter @alz_gal
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: None of the 137 samples contained more than 0.076 mcg/mL of the drug.
Data source: The 4-week postmarketing study comprised 17 breastfeeding women.
Disclosures: UCB sponsored the study. Dr. Clowse is a consultant for the company.
Infliximab biosimilar posts mostly reassuring data in Norway’s NOR-SWITCH study
WASHINGTON – Data from the first randomized trial of switching from an originator biologic to a biosimilar of the originator indicate that the infliximab biosimilar Remsima is no different from the infliximab originator Remicade in the rate of disease worsening over 1 year across a combination of all its approved indications.
The outcomes of the Norwegian, double-blind, noninferiority trial, called NOR-SWITCH, indicate similar rates of disease worsening across patients switched to Remsima and those who stayed on Remicade. However, exploratory group analyses conducted on the different disease subgroups in the trial (Crohn’s disease, ulcerative colitis, spondyloarthritis, rheumatoid arthritis, psoriasis, and psoriatic arthritis) showed a potentially concerning level of disease worsening among Crohn’s disease patients on Remsima with a confidence interval that nearly fell entirely within the range favoring Remicade.
In the United States, Remsima, also known as CT-P13, is marketed by Pfizer as Inflectra.
The trial randomized 482 patients who were on stable treatment with Remicade for at least 6 months for any of the six indications for which Remicade and Remsima are approved to either stay on Remicade or switch to Remsima with the same dosing regimen for 52 weeks. Overall, patients had a mean age of about 48 years and 36%-41% were female. They had a mean disease duration of about 17 years and had been taking Remicade for a mean of nearly 7 years.
The primary endpoint was disease worsening during follow-up, according to worsening in disease-specific composite measures and/or a consensus between an investigator and a patient that led to a major change in treatment. The investigators made an assumption of 30% disease worsening across all the indications for the trial’s power calculation, based on available literature and observational data.
Disease worsening occurred in 26.2% of patients who stayed on Remicade and 29.6% of patients who switched to Remsima, based on a per-protocol analysis of 202 Remicade and 206 Remsima patients. The 95% confidence interval of the adjusted treatment difference of –4.4% was –12.7% to 3.9%, which was within the pre-specified noninferiority margin of 15%.
Exploratory subgroup analyses of the different disease subgroups showed no statistically significant differences between the two treatments in disease worsening. However, in Crohn’s disease patients, who formed the largest subgroup in the study at 155 patients, the adjusted treatment difference was –14.3% (21.2% with disease worsening for Remicade and 36.5% for Remsima) with a 95% CI of –29.3% to 0.7%.
It’s difficult to discern whether the 95% confidence interval seen in the Crohn’s disease subgroup is a part of the natural variation one would expect to see in a subgroup analysis of different diseases or if there might be a true signal for disease worsening in the Crohn’s disease patients who took Remsima. “The problem is that it’s in the largest subgroup that has no other data. If this had been in rheumatoid arthritis, that would be different,” coauthor Inge C. Olsen, PhD, a biostatistician at Diakonhjemmet Hospital, said in an interview. “All the registry trials were done in RA and spondyloarthritis patients. ... That’s an issue, but with regards to the [NOR-SWITCH] study, it’s very clear that you have no power to show anything in the subgroup analysis, and they are exploratory analyses and are not answering any hypothesis.” Currently, there are no plans to follow up on these results in another study, he said.
Other issues that the NOR-SWITCH study does not answer are the outcomes of switching back and forth between Remicade and Remsima, switching from one infliximab biosimilar to another infliximab biosimilar, and switching from other originator biologics to their biosimilars.
“Is that feasible? Is that safe? Will it retain efficacy? We don’t know. There’s a real need for those studies to be done,” Dr. Goll said.
In Norway, the remaining patients who had not switched yet from Remicade to Remsima are now doing so based on the trial’s results, Dr. Goll said. The cost of Remsima in Norway was about 75% less than Remicade in 2015 and about 60% less in 2016, she noted.
It’s still an open question what the results of the NOR-SWITCH trial might indicate for how clinicians in the United States will use Inflectra and other biosimilars, according to John J. Cush, MD, professor of medicine and rheumatology at Baylor University, Dallas.
“I think the real problem here is that it’s nice to know that [CT-P13] wasn’t inferior, but when you get into the weeds and you look at the details, those of us who may not have a lot of certainty about this might worry about this, especially when there are three new biosimilars approved in the United States: Amjevita, which is an adalimumab biosimilar; Erelzi, which is an etanercept biosimilar; and Inflectra’s about to be launched as an infliximab biosimilar,” Dr. Cush said during a session reviewing selected abstracts from the meeting. “When this NOR-SWITCH study was done in Norway, it’s a 70% savings over the original product. The new ones being introduced over here [in the United States] start at about 15%. I’m less motivated with that degree of savings to want to take some chances on my patients. So we need a little bit more certainty; we need to feel better about the cost savings to patients and health care overall. Confidence in biosimilars is what’s going to sell biosimilars. We’re a long way from confidence still.”
NOR-SWITCH was funded by the Norwegian government. Some of the investigators disclosed relationships with Pfizer and/or Celltrion, which separately market CT-P13 in different parts of the world.
[email protected]
WASHINGTON – Data from the first randomized trial of switching from an originator biologic to a biosimilar of the originator indicate that the infliximab biosimilar Remsima is no different from the infliximab originator Remicade in the rate of disease worsening over 1 year across a combination of all its approved indications.
The outcomes of the Norwegian, double-blind, noninferiority trial, called NOR-SWITCH, indicate similar rates of disease worsening across patients switched to Remsima and those who stayed on Remicade. However, exploratory group analyses conducted on the different disease subgroups in the trial (Crohn’s disease, ulcerative colitis, spondyloarthritis, rheumatoid arthritis, psoriasis, and psoriatic arthritis) showed a potentially concerning level of disease worsening among Crohn’s disease patients on Remsima with a confidence interval that nearly fell entirely within the range favoring Remicade.
In the United States, Remsima, also known as CT-P13, is marketed by Pfizer as Inflectra.
The trial randomized 482 patients who were on stable treatment with Remicade for at least 6 months for any of the six indications for which Remicade and Remsima are approved to either stay on Remicade or switch to Remsima with the same dosing regimen for 52 weeks. Overall, patients had a mean age of about 48 years and 36%-41% were female. They had a mean disease duration of about 17 years and had been taking Remicade for a mean of nearly 7 years.
The primary endpoint was disease worsening during follow-up, according to worsening in disease-specific composite measures and/or a consensus between an investigator and a patient that led to a major change in treatment. The investigators made an assumption of 30% disease worsening across all the indications for the trial’s power calculation, based on available literature and observational data.
Disease worsening occurred in 26.2% of patients who stayed on Remicade and 29.6% of patients who switched to Remsima, based on a per-protocol analysis of 202 Remicade and 206 Remsima patients. The 95% confidence interval of the adjusted treatment difference of –4.4% was –12.7% to 3.9%, which was within the pre-specified noninferiority margin of 15%.
Exploratory subgroup analyses of the different disease subgroups showed no statistically significant differences between the two treatments in disease worsening. However, in Crohn’s disease patients, who formed the largest subgroup in the study at 155 patients, the adjusted treatment difference was –14.3% (21.2% with disease worsening for Remicade and 36.5% for Remsima) with a 95% CI of –29.3% to 0.7%.
It’s difficult to discern whether the 95% confidence interval seen in the Crohn’s disease subgroup is a part of the natural variation one would expect to see in a subgroup analysis of different diseases or if there might be a true signal for disease worsening in the Crohn’s disease patients who took Remsima. “The problem is that it’s in the largest subgroup that has no other data. If this had been in rheumatoid arthritis, that would be different,” coauthor Inge C. Olsen, PhD, a biostatistician at Diakonhjemmet Hospital, said in an interview. “All the registry trials were done in RA and spondyloarthritis patients. ... That’s an issue, but with regards to the [NOR-SWITCH] study, it’s very clear that you have no power to show anything in the subgroup analysis, and they are exploratory analyses and are not answering any hypothesis.” Currently, there are no plans to follow up on these results in another study, he said.
Other issues that the NOR-SWITCH study does not answer are the outcomes of switching back and forth between Remicade and Remsima, switching from one infliximab biosimilar to another infliximab biosimilar, and switching from other originator biologics to their biosimilars.
“Is that feasible? Is that safe? Will it retain efficacy? We don’t know. There’s a real need for those studies to be done,” Dr. Goll said.
In Norway, the remaining patients who had not switched yet from Remicade to Remsima are now doing so based on the trial’s results, Dr. Goll said. The cost of Remsima in Norway was about 75% less than Remicade in 2015 and about 60% less in 2016, she noted.
It’s still an open question what the results of the NOR-SWITCH trial might indicate for how clinicians in the United States will use Inflectra and other biosimilars, according to John J. Cush, MD, professor of medicine and rheumatology at Baylor University, Dallas.
“I think the real problem here is that it’s nice to know that [CT-P13] wasn’t inferior, but when you get into the weeds and you look at the details, those of us who may not have a lot of certainty about this might worry about this, especially when there are three new biosimilars approved in the United States: Amjevita, which is an adalimumab biosimilar; Erelzi, which is an etanercept biosimilar; and Inflectra’s about to be launched as an infliximab biosimilar,” Dr. Cush said during a session reviewing selected abstracts from the meeting. “When this NOR-SWITCH study was done in Norway, it’s a 70% savings over the original product. The new ones being introduced over here [in the United States] start at about 15%. I’m less motivated with that degree of savings to want to take some chances on my patients. So we need a little bit more certainty; we need to feel better about the cost savings to patients and health care overall. Confidence in biosimilars is what’s going to sell biosimilars. We’re a long way from confidence still.”
NOR-SWITCH was funded by the Norwegian government. Some of the investigators disclosed relationships with Pfizer and/or Celltrion, which separately market CT-P13 in different parts of the world.
[email protected]
WASHINGTON – Data from the first randomized trial of switching from an originator biologic to a biosimilar of the originator indicate that the infliximab biosimilar Remsima is no different from the infliximab originator Remicade in the rate of disease worsening over 1 year across a combination of all its approved indications.
The outcomes of the Norwegian, double-blind, noninferiority trial, called NOR-SWITCH, indicate similar rates of disease worsening across patients switched to Remsima and those who stayed on Remicade. However, exploratory group analyses conducted on the different disease subgroups in the trial (Crohn’s disease, ulcerative colitis, spondyloarthritis, rheumatoid arthritis, psoriasis, and psoriatic arthritis) showed a potentially concerning level of disease worsening among Crohn’s disease patients on Remsima with a confidence interval that nearly fell entirely within the range favoring Remicade.
In the United States, Remsima, also known as CT-P13, is marketed by Pfizer as Inflectra.
The trial randomized 482 patients who were on stable treatment with Remicade for at least 6 months for any of the six indications for which Remicade and Remsima are approved to either stay on Remicade or switch to Remsima with the same dosing regimen for 52 weeks. Overall, patients had a mean age of about 48 years and 36%-41% were female. They had a mean disease duration of about 17 years and had been taking Remicade for a mean of nearly 7 years.
The primary endpoint was disease worsening during follow-up, according to worsening in disease-specific composite measures and/or a consensus between an investigator and a patient that led to a major change in treatment. The investigators made an assumption of 30% disease worsening across all the indications for the trial’s power calculation, based on available literature and observational data.
Disease worsening occurred in 26.2% of patients who stayed on Remicade and 29.6% of patients who switched to Remsima, based on a per-protocol analysis of 202 Remicade and 206 Remsima patients. The 95% confidence interval of the adjusted treatment difference of –4.4% was –12.7% to 3.9%, which was within the pre-specified noninferiority margin of 15%.
Exploratory subgroup analyses of the different disease subgroups showed no statistically significant differences between the two treatments in disease worsening. However, in Crohn’s disease patients, who formed the largest subgroup in the study at 155 patients, the adjusted treatment difference was –14.3% (21.2% with disease worsening for Remicade and 36.5% for Remsima) with a 95% CI of –29.3% to 0.7%.
It’s difficult to discern whether the 95% confidence interval seen in the Crohn’s disease subgroup is a part of the natural variation one would expect to see in a subgroup analysis of different diseases or if there might be a true signal for disease worsening in the Crohn’s disease patients who took Remsima. “The problem is that it’s in the largest subgroup that has no other data. If this had been in rheumatoid arthritis, that would be different,” coauthor Inge C. Olsen, PhD, a biostatistician at Diakonhjemmet Hospital, said in an interview. “All the registry trials were done in RA and spondyloarthritis patients. ... That’s an issue, but with regards to the [NOR-SWITCH] study, it’s very clear that you have no power to show anything in the subgroup analysis, and they are exploratory analyses and are not answering any hypothesis.” Currently, there are no plans to follow up on these results in another study, he said.
Other issues that the NOR-SWITCH study does not answer are the outcomes of switching back and forth between Remicade and Remsima, switching from one infliximab biosimilar to another infliximab biosimilar, and switching from other originator biologics to their biosimilars.
“Is that feasible? Is that safe? Will it retain efficacy? We don’t know. There’s a real need for those studies to be done,” Dr. Goll said.
In Norway, the remaining patients who had not switched yet from Remicade to Remsima are now doing so based on the trial’s results, Dr. Goll said. The cost of Remsima in Norway was about 75% less than Remicade in 2015 and about 60% less in 2016, she noted.
It’s still an open question what the results of the NOR-SWITCH trial might indicate for how clinicians in the United States will use Inflectra and other biosimilars, according to John J. Cush, MD, professor of medicine and rheumatology at Baylor University, Dallas.
“I think the real problem here is that it’s nice to know that [CT-P13] wasn’t inferior, but when you get into the weeds and you look at the details, those of us who may not have a lot of certainty about this might worry about this, especially when there are three new biosimilars approved in the United States: Amjevita, which is an adalimumab biosimilar; Erelzi, which is an etanercept biosimilar; and Inflectra’s about to be launched as an infliximab biosimilar,” Dr. Cush said during a session reviewing selected abstracts from the meeting. “When this NOR-SWITCH study was done in Norway, it’s a 70% savings over the original product. The new ones being introduced over here [in the United States] start at about 15%. I’m less motivated with that degree of savings to want to take some chances on my patients. So we need a little bit more certainty; we need to feel better about the cost savings to patients and health care overall. Confidence in biosimilars is what’s going to sell biosimilars. We’re a long way from confidence still.”
NOR-SWITCH was funded by the Norwegian government. Some of the investigators disclosed relationships with Pfizer and/or Celltrion, which separately market CT-P13 in different parts of the world.
[email protected]
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: Disease worsening occurred in 26.2% of patients who stayed on Remicade and 29.6% of patients who switched to Remsima, based on a per-protocol analysis.
Data source: The multicenter, double-blind, randomized NOR-SWITCH trial of 482 patients.
Disclosures: The trial was funded by the Norwegian government. Some of the investigators disclosed relationships with Pfizer and/or Celltrion, which separately market CT-P13 in different parts of the world.
First JAK inhibitor in psoriatic arthritis achieves results similar to adalimumab
WASHINGTON – Tofacitinib demonstrated efficacy comparable to adalimumab in patients with active psoriatic arthritis (PsA) and an inadequate response to conventional disease-modifying antirheumatic drugs in the phase III OPAL Broaden study.
“This is the first study to demonstrate efficacy of a JAK [Janus kinase] inhibitor in PsA,” said lead author Philip J. Mease, MD, of Swedish Medical Center, Seattle. “The primary endpoints were achieved with tofacitinib [Xeljanz] versus placebo. Onset of efficacy of tofacitinib on the ACR20 [the American College of Rheumatology 20% improvement criteria] was observed as early as week 2. Radiographic non-progression rates were low and similar to placebo. Improvement was seen in enthesitis and dactylitis as well as in joint and skin symptoms, and efficacy was maintained through month 12. Tofacitinib is a potential future option for the treatment of PsA.”
The study enrolled 422 patients with active PsA diagnosed within the last 6 months or longer, and all also had plaque psoriasis at screening. The primary endpoint was ACR20 response at 3 months.
Patients were randomized to receive tofacitinib 5 mg twice daily, tofacitinib 10 mg twice daily, adalimumab (Humira) 40 mg subcutaneously every 2 weeks, or placebo. At 3 months, placebo patients were re-randomized to tofacitinib 5 mg or 10 mg twice daily. The trial was completed by 372 patients (88.4%).
At baseline, groups had similar demographic and disease characteristics. Patients had a median age just under 50 years, tended to be overweight, and had disease duration that ranged from 5 to 7 years. The majority of patients had enthesitis and dactylitis, and all were on background disease-modifying antirheumatic drugs.
All of the active treatment arms achieved statistically significant rates versus placebo on the primary endpoint of ACR20 response at 3 months: 50% in the tofacitinib 5-mg group, 61% in the tofacitinib 10-mg group, and 52% in the adalimumab group, compared with 33% of placebo-treated patients. ACR20 responses increased out to 12 months in 68%, 70%, and 60%, respectively in the three active treatment arms. At 3 months, ACR50 responses in the three active treatment arms were 28%, 40%, and 33%, respectively, and for ACR70 were 17%, 14%, and 19%.
Health Assessment Questionnaire Disability Index (HAQ-DI) responses were statistically significant for all three active dosing arms, compared with placebo.
“Placebo patients re-randomized to tofacitinib also had good ACR responses at month 12,” Dr. Mease said.
The rate of radiographic non-progression at month 12 was similar in all treatment arms at about 95%, including former placebo patients who switched to tofacitinib.
Skin responses, according to Psoriasis Area and Severity Index (PASI) 75, were 43% for tofacitinib 5 mg twice daily, 44% for tofacitinib 10 mg twice daily, and 39% for adalimumab. At 12 months, the percentage of patients achieving PASI 75 increased for all three treatment arms.
The same pattern was observed for enthesitis and dactylitis.
Minimal disease activity was seen at 3 months in about 25% of all the active treatment arms, and the rates improved at month 12.
There were few discontinuations due to adverse events in any group. Adverse event rates were similar across all treatment arms at month 3, including the placebo arm. The rate of serious adverse events reported at month 12 was 5% for tofacitinib 5 mg twice daily, 2.9% for tofacitinib 10 mg twice daily, 7.8% for adalimumab, and 6% in placebo patients switched to either dose of tofacitinib at month 3.
Laboratory changes were similar to those reported with tofacitinib monotherapy in rheumatoid arthritis.
The study was sponsored by Pfizer. Dr. Mease’s financial disclosures included Pfizer as well as a long list of companies that make conventional and biologic disease-modifying antirheumatic drugs. Another four authors disclosed financial ties to Pfizer and other pharmaceutical companies. Five coauthors were employees of Pfizer.
WASHINGTON – Tofacitinib demonstrated efficacy comparable to adalimumab in patients with active psoriatic arthritis (PsA) and an inadequate response to conventional disease-modifying antirheumatic drugs in the phase III OPAL Broaden study.
“This is the first study to demonstrate efficacy of a JAK [Janus kinase] inhibitor in PsA,” said lead author Philip J. Mease, MD, of Swedish Medical Center, Seattle. “The primary endpoints were achieved with tofacitinib [Xeljanz] versus placebo. Onset of efficacy of tofacitinib on the ACR20 [the American College of Rheumatology 20% improvement criteria] was observed as early as week 2. Radiographic non-progression rates were low and similar to placebo. Improvement was seen in enthesitis and dactylitis as well as in joint and skin symptoms, and efficacy was maintained through month 12. Tofacitinib is a potential future option for the treatment of PsA.”
The study enrolled 422 patients with active PsA diagnosed within the last 6 months or longer, and all also had plaque psoriasis at screening. The primary endpoint was ACR20 response at 3 months.
Patients were randomized to receive tofacitinib 5 mg twice daily, tofacitinib 10 mg twice daily, adalimumab (Humira) 40 mg subcutaneously every 2 weeks, or placebo. At 3 months, placebo patients were re-randomized to tofacitinib 5 mg or 10 mg twice daily. The trial was completed by 372 patients (88.4%).
At baseline, groups had similar demographic and disease characteristics. Patients had a median age just under 50 years, tended to be overweight, and had disease duration that ranged from 5 to 7 years. The majority of patients had enthesitis and dactylitis, and all were on background disease-modifying antirheumatic drugs.
All of the active treatment arms achieved statistically significant rates versus placebo on the primary endpoint of ACR20 response at 3 months: 50% in the tofacitinib 5-mg group, 61% in the tofacitinib 10-mg group, and 52% in the adalimumab group, compared with 33% of placebo-treated patients. ACR20 responses increased out to 12 months in 68%, 70%, and 60%, respectively in the three active treatment arms. At 3 months, ACR50 responses in the three active treatment arms were 28%, 40%, and 33%, respectively, and for ACR70 were 17%, 14%, and 19%.
Health Assessment Questionnaire Disability Index (HAQ-DI) responses were statistically significant for all three active dosing arms, compared with placebo.
“Placebo patients re-randomized to tofacitinib also had good ACR responses at month 12,” Dr. Mease said.
The rate of radiographic non-progression at month 12 was similar in all treatment arms at about 95%, including former placebo patients who switched to tofacitinib.
Skin responses, according to Psoriasis Area and Severity Index (PASI) 75, were 43% for tofacitinib 5 mg twice daily, 44% for tofacitinib 10 mg twice daily, and 39% for adalimumab. At 12 months, the percentage of patients achieving PASI 75 increased for all three treatment arms.
The same pattern was observed for enthesitis and dactylitis.
Minimal disease activity was seen at 3 months in about 25% of all the active treatment arms, and the rates improved at month 12.
There were few discontinuations due to adverse events in any group. Adverse event rates were similar across all treatment arms at month 3, including the placebo arm. The rate of serious adverse events reported at month 12 was 5% for tofacitinib 5 mg twice daily, 2.9% for tofacitinib 10 mg twice daily, 7.8% for adalimumab, and 6% in placebo patients switched to either dose of tofacitinib at month 3.
Laboratory changes were similar to those reported with tofacitinib monotherapy in rheumatoid arthritis.
The study was sponsored by Pfizer. Dr. Mease’s financial disclosures included Pfizer as well as a long list of companies that make conventional and biologic disease-modifying antirheumatic drugs. Another four authors disclosed financial ties to Pfizer and other pharmaceutical companies. Five coauthors were employees of Pfizer.
WASHINGTON – Tofacitinib demonstrated efficacy comparable to adalimumab in patients with active psoriatic arthritis (PsA) and an inadequate response to conventional disease-modifying antirheumatic drugs in the phase III OPAL Broaden study.
“This is the first study to demonstrate efficacy of a JAK [Janus kinase] inhibitor in PsA,” said lead author Philip J. Mease, MD, of Swedish Medical Center, Seattle. “The primary endpoints were achieved with tofacitinib [Xeljanz] versus placebo. Onset of efficacy of tofacitinib on the ACR20 [the American College of Rheumatology 20% improvement criteria] was observed as early as week 2. Radiographic non-progression rates were low and similar to placebo. Improvement was seen in enthesitis and dactylitis as well as in joint and skin symptoms, and efficacy was maintained through month 12. Tofacitinib is a potential future option for the treatment of PsA.”
The study enrolled 422 patients with active PsA diagnosed within the last 6 months or longer, and all also had plaque psoriasis at screening. The primary endpoint was ACR20 response at 3 months.
Patients were randomized to receive tofacitinib 5 mg twice daily, tofacitinib 10 mg twice daily, adalimumab (Humira) 40 mg subcutaneously every 2 weeks, or placebo. At 3 months, placebo patients were re-randomized to tofacitinib 5 mg or 10 mg twice daily. The trial was completed by 372 patients (88.4%).
At baseline, groups had similar demographic and disease characteristics. Patients had a median age just under 50 years, tended to be overweight, and had disease duration that ranged from 5 to 7 years. The majority of patients had enthesitis and dactylitis, and all were on background disease-modifying antirheumatic drugs.
All of the active treatment arms achieved statistically significant rates versus placebo on the primary endpoint of ACR20 response at 3 months: 50% in the tofacitinib 5-mg group, 61% in the tofacitinib 10-mg group, and 52% in the adalimumab group, compared with 33% of placebo-treated patients. ACR20 responses increased out to 12 months in 68%, 70%, and 60%, respectively in the three active treatment arms. At 3 months, ACR50 responses in the three active treatment arms were 28%, 40%, and 33%, respectively, and for ACR70 were 17%, 14%, and 19%.
Health Assessment Questionnaire Disability Index (HAQ-DI) responses were statistically significant for all three active dosing arms, compared with placebo.
“Placebo patients re-randomized to tofacitinib also had good ACR responses at month 12,” Dr. Mease said.
The rate of radiographic non-progression at month 12 was similar in all treatment arms at about 95%, including former placebo patients who switched to tofacitinib.
Skin responses, according to Psoriasis Area and Severity Index (PASI) 75, were 43% for tofacitinib 5 mg twice daily, 44% for tofacitinib 10 mg twice daily, and 39% for adalimumab. At 12 months, the percentage of patients achieving PASI 75 increased for all three treatment arms.
The same pattern was observed for enthesitis and dactylitis.
Minimal disease activity was seen at 3 months in about 25% of all the active treatment arms, and the rates improved at month 12.
There were few discontinuations due to adverse events in any group. Adverse event rates were similar across all treatment arms at month 3, including the placebo arm. The rate of serious adverse events reported at month 12 was 5% for tofacitinib 5 mg twice daily, 2.9% for tofacitinib 10 mg twice daily, 7.8% for adalimumab, and 6% in placebo patients switched to either dose of tofacitinib at month 3.
Laboratory changes were similar to those reported with tofacitinib monotherapy in rheumatoid arthritis.
The study was sponsored by Pfizer. Dr. Mease’s financial disclosures included Pfizer as well as a long list of companies that make conventional and biologic disease-modifying antirheumatic drugs. Another four authors disclosed financial ties to Pfizer and other pharmaceutical companies. Five coauthors were employees of Pfizer.
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: ACR20 was achieved at 3 months by 50% in the tofacitinib 5 mg group, 61% in the tofacitinib 10 mg group, and 52% of the adalimumab group versus 33% of placebo patients, and responses persisted out to Month 12.
Data source: OPAL Broaden was a Phase III trial that included 422 patients with active psoriatic arthritis in both joints and skin.
Disclosures: The study was sponsored by Pfizer. Dr. Mease’s financial disclosures included Pfizer as well as a long list of companies that make conventional and biologic disease-modifying antirheumatic drugs. Another four authors disclosed financial ties to Pfizer and other pharmaceutical companies. Five coauthors were employees of Pfizer.
Tofacitinib effective after TNFi failure
WASHINGTON – The oral Janus kinase inhibitor tofacitinib is safe and effective in patients with active psoriatic arthritis and an inadequate response to tumor necrosis factor inhibitors, according to findings from the phase III OPAL Beyond trial.
Both the American College of Rheumatology 20% improvement criteria (ACR20) response rate and change from baseline in Health Assessment Questionnaire Disability Index (HAQ-DI) scores at month 3 – the primary endpoints of the study – were superior with tofacitinib (Xeljanz) versus placebo in the 6-month, double-blind, randomized, multicenter trial, Dafna D. Gladman, MD, reported in a late-breaking poster at the annual meeting of the American College of Rheumatology.
The superiority of tofacitinib over placebo in achieving an ACR20 response was evident as early as 2 weeks when the response rates were 13% in 131 patients who received placebo, 26.7% in 131 patients who received 5 mg of tofacitinib twice daily, and 28.8% in 132 patients who received 10 mg of tofacitinib twice daily, Dr. Gladman said. Later on at 3 months, the ACR20 response rates were 23.7% for placebo, 49.6% for 5 mg of tofacitinib twice daily, and 47% for 10 mg of tofacitinib twice daily.
The change from baseline in HAQ-DI scores was –0.14 with placebo, –0.39 with 5 mg tofacitinib, and –0.35 with 10 mg tofacitinib.
Study subjects had a 6-month or greater psoriatic arthritis diagnosis, fulfilled classification criteria for psoriatic arthritis, had active arthritis at screening and baseline and active plaque psoriasis at screening, and inadequate response to TNF inhibitors, which was defined as discontinuation for inadequate efficacy or due to an adverse event. All had ongoing treatment with a conventional synthetic disease-modifying antirheumatic agent, and those in the placebo group were advanced after 3 months to receive either 5 mg or 10 mg of tofacitinib twice daily (66 and 65 patients, respectively).
The effects of treatment on secondary efficacy endpoints were generally consistent with the findings with respect to the primary endpoints, Dr. Gladman said.
As for safety endpoints, serious adverse events and drug discontinuations due to adverse events were rare. Serious adverse event rates at 6 months were 3% in the placebo group who advanced to 5 mg tofacitinib, 1.5% in those who advanced to 10 mg tofacitinib, 3.8% in the original 5 mg tofacitinib group, and 6.1% in the original 10 mg tofacitinib group. Corresponding rates for all adverse events were 60.6%, 58.5%, 71%, and 72.7%. The most common adverse events were upper respiratory tract infections, nasopharyngitis, and headache.
OPAL Beyond was sponsored by Pfizer. Dr. Gladman disclosed financial relationships with AbbVie, Amgen, Bristol-Myers Squibb, Celgene, Janssen, Novartis, Pfizer, and UCB. Several other authors disclosed financial relationships with pharmaceutical companies, including Pfizer. Five of the 11 authors were employees of Pfizer.
[email protected]
WASHINGTON – The oral Janus kinase inhibitor tofacitinib is safe and effective in patients with active psoriatic arthritis and an inadequate response to tumor necrosis factor inhibitors, according to findings from the phase III OPAL Beyond trial.
Both the American College of Rheumatology 20% improvement criteria (ACR20) response rate and change from baseline in Health Assessment Questionnaire Disability Index (HAQ-DI) scores at month 3 – the primary endpoints of the study – were superior with tofacitinib (Xeljanz) versus placebo in the 6-month, double-blind, randomized, multicenter trial, Dafna D. Gladman, MD, reported in a late-breaking poster at the annual meeting of the American College of Rheumatology.
The superiority of tofacitinib over placebo in achieving an ACR20 response was evident as early as 2 weeks when the response rates were 13% in 131 patients who received placebo, 26.7% in 131 patients who received 5 mg of tofacitinib twice daily, and 28.8% in 132 patients who received 10 mg of tofacitinib twice daily, Dr. Gladman said. Later on at 3 months, the ACR20 response rates were 23.7% for placebo, 49.6% for 5 mg of tofacitinib twice daily, and 47% for 10 mg of tofacitinib twice daily.
The change from baseline in HAQ-DI scores was –0.14 with placebo, –0.39 with 5 mg tofacitinib, and –0.35 with 10 mg tofacitinib.
Study subjects had a 6-month or greater psoriatic arthritis diagnosis, fulfilled classification criteria for psoriatic arthritis, had active arthritis at screening and baseline and active plaque psoriasis at screening, and inadequate response to TNF inhibitors, which was defined as discontinuation for inadequate efficacy or due to an adverse event. All had ongoing treatment with a conventional synthetic disease-modifying antirheumatic agent, and those in the placebo group were advanced after 3 months to receive either 5 mg or 10 mg of tofacitinib twice daily (66 and 65 patients, respectively).
The effects of treatment on secondary efficacy endpoints were generally consistent with the findings with respect to the primary endpoints, Dr. Gladman said.
As for safety endpoints, serious adverse events and drug discontinuations due to adverse events were rare. Serious adverse event rates at 6 months were 3% in the placebo group who advanced to 5 mg tofacitinib, 1.5% in those who advanced to 10 mg tofacitinib, 3.8% in the original 5 mg tofacitinib group, and 6.1% in the original 10 mg tofacitinib group. Corresponding rates for all adverse events were 60.6%, 58.5%, 71%, and 72.7%. The most common adverse events were upper respiratory tract infections, nasopharyngitis, and headache.
OPAL Beyond was sponsored by Pfizer. Dr. Gladman disclosed financial relationships with AbbVie, Amgen, Bristol-Myers Squibb, Celgene, Janssen, Novartis, Pfizer, and UCB. Several other authors disclosed financial relationships with pharmaceutical companies, including Pfizer. Five of the 11 authors were employees of Pfizer.
[email protected]
WASHINGTON – The oral Janus kinase inhibitor tofacitinib is safe and effective in patients with active psoriatic arthritis and an inadequate response to tumor necrosis factor inhibitors, according to findings from the phase III OPAL Beyond trial.
Both the American College of Rheumatology 20% improvement criteria (ACR20) response rate and change from baseline in Health Assessment Questionnaire Disability Index (HAQ-DI) scores at month 3 – the primary endpoints of the study – were superior with tofacitinib (Xeljanz) versus placebo in the 6-month, double-blind, randomized, multicenter trial, Dafna D. Gladman, MD, reported in a late-breaking poster at the annual meeting of the American College of Rheumatology.
The superiority of tofacitinib over placebo in achieving an ACR20 response was evident as early as 2 weeks when the response rates were 13% in 131 patients who received placebo, 26.7% in 131 patients who received 5 mg of tofacitinib twice daily, and 28.8% in 132 patients who received 10 mg of tofacitinib twice daily, Dr. Gladman said. Later on at 3 months, the ACR20 response rates were 23.7% for placebo, 49.6% for 5 mg of tofacitinib twice daily, and 47% for 10 mg of tofacitinib twice daily.
The change from baseline in HAQ-DI scores was –0.14 with placebo, –0.39 with 5 mg tofacitinib, and –0.35 with 10 mg tofacitinib.
Study subjects had a 6-month or greater psoriatic arthritis diagnosis, fulfilled classification criteria for psoriatic arthritis, had active arthritis at screening and baseline and active plaque psoriasis at screening, and inadequate response to TNF inhibitors, which was defined as discontinuation for inadequate efficacy or due to an adverse event. All had ongoing treatment with a conventional synthetic disease-modifying antirheumatic agent, and those in the placebo group were advanced after 3 months to receive either 5 mg or 10 mg of tofacitinib twice daily (66 and 65 patients, respectively).
The effects of treatment on secondary efficacy endpoints were generally consistent with the findings with respect to the primary endpoints, Dr. Gladman said.
As for safety endpoints, serious adverse events and drug discontinuations due to adverse events were rare. Serious adverse event rates at 6 months were 3% in the placebo group who advanced to 5 mg tofacitinib, 1.5% in those who advanced to 10 mg tofacitinib, 3.8% in the original 5 mg tofacitinib group, and 6.1% in the original 10 mg tofacitinib group. Corresponding rates for all adverse events were 60.6%, 58.5%, 71%, and 72.7%. The most common adverse events were upper respiratory tract infections, nasopharyngitis, and headache.
OPAL Beyond was sponsored by Pfizer. Dr. Gladman disclosed financial relationships with AbbVie, Amgen, Bristol-Myers Squibb, Celgene, Janssen, Novartis, Pfizer, and UCB. Several other authors disclosed financial relationships with pharmaceutical companies, including Pfizer. Five of the 11 authors were employees of Pfizer.
[email protected]
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: ACR20 response rates at 3 months were 23.7%, 49.6%, and 47% with placebo, 5 mg, and 10 mg of tofacitinib twice daily, respectively.
Data source: The phase III, double-blind, randomized, placebo-controlled OPAL Beyond trial.
Disclosures: OPAL Beyond was sponsored by Pfizer. Dr. Gladman disclosed financial relationships with AbbVie, Amgen, Bristol-Myers Squibb, Celgene, Janssen, Novartis, Pfizer, and UCB. Several other authors disclosed financial relationships with pharmaceutical companies, including Pfizer. Five of the 11 authors were employees of Pfizer.
Guselkumab appears safe, effective for psoriatic arthritis
WASHINGTON – The investigational anti-interleukin-23 monoclonal antibody guselkumab was safe and well tolerated, and demonstrated significant improvement on a variety of measures in patients with active psoriatic arthritis in a randomized, placebo-controlled phase IIa study.
The primary endpoint of ACR20 at 24 weeks was achieved in 58% of 100 patients randomized to receive treatment with guselkumab versus 18.4% of 49 patients who received placebo, Atul A. Deodhar, MD, reported in a late-breaking abstract presentation at the annual meeting of the American College of Rheumatology.
For example, PASI75 response at 24 weeks was 78.6% for guselkumab and 12.5% for placebo, and the ACR50 response at 24 weeks was 34% vs. 10.2%, respectively. The HAQ-DI score mean change from baseline was –0.42 vs. –0.06, respectively.
Further, ACR20 response was seen as early as week 4 (21% vs. 0% for placebo), and the effect increased over time, reaching the maximum effect by week 16 (60% vs. 16.3%), Dr. Deodhar said.
Subjects in the double-blind, multicenter study had active psoriatic arthritis and at least 3% body surface area of plaque psoriasis despite treatment with standard-of-care therapies. Patients with prior exposure to anti–tumor necrosis factor–alpha agents were included. They received either 100 mg guselkumab delivered subcutaneously or placebo at week 0 and 4, then every 8 weeks thereafter through week 44.
Patients with less than 5% improvement in swollen and tender joint count at week 16 were allowed early escape to open-label ustekinumab (Stelara), and at week 24 all remaining patients crossed over to receive guselkumab, which was repeated at week 28 and every 8 weeks thereafter through week 44.
Treatment was well tolerated; the proportion of patients with one or more adverse events was similar in the treatment and placebo groups (36% and 32.7%, respectively), with infections being the most common adverse event, occurring in 17% and 20.4% of patients in the groups, respectively.
“And even though 10% and 14% of the patients received systemic treatment, no patient received [intravenous] antibiotics,” he said.
Severe adverse events occurred in two patients – one in each group – and included a knee injury and myocardial infarction. Specific information about which group these occurred in is not available as the study is ongoing and investigators remain blinded, Dr. Deodhar noted.
No serious infections, malignancies, or deaths occurred through week 24, he said.
“Guselkumab is the first anti-IL23 biologic to demonstrate efficacy in psoriatic arthritis. In patients with active psoriatic arthritis ... treatment with guselkumab shows significant improvements in joint symptoms, physical function, psoriasis, enthesitis, dactylitis, and quality of life,” he concluded, adding that there were no unexpected safety findings in this population.
On Nov. 17, Janssen Biotech, Inc. announced the submission of a Biologics License Application to the Food and Drug Administration seeking approval of guselkumab for the treatment of adults with moderate to severe plaque psoriasis based on findings from prior studies for that indication.
The current study was sponsored by Janssen Research & Development. Dr. Deodhar reported financial relationships with AbbVie, Amgen, Boehringer Ingelheim, Janssen, Novartis, Pfizer, and UCB. Two other authors also reported financial ties to industry, including Janssen. Four of the seven authors of the abstract were employees of Janssen.
WASHINGTON – The investigational anti-interleukin-23 monoclonal antibody guselkumab was safe and well tolerated, and demonstrated significant improvement on a variety of measures in patients with active psoriatic arthritis in a randomized, placebo-controlled phase IIa study.
The primary endpoint of ACR20 at 24 weeks was achieved in 58% of 100 patients randomized to receive treatment with guselkumab versus 18.4% of 49 patients who received placebo, Atul A. Deodhar, MD, reported in a late-breaking abstract presentation at the annual meeting of the American College of Rheumatology.
For example, PASI75 response at 24 weeks was 78.6% for guselkumab and 12.5% for placebo, and the ACR50 response at 24 weeks was 34% vs. 10.2%, respectively. The HAQ-DI score mean change from baseline was –0.42 vs. –0.06, respectively.
Further, ACR20 response was seen as early as week 4 (21% vs. 0% for placebo), and the effect increased over time, reaching the maximum effect by week 16 (60% vs. 16.3%), Dr. Deodhar said.
Subjects in the double-blind, multicenter study had active psoriatic arthritis and at least 3% body surface area of plaque psoriasis despite treatment with standard-of-care therapies. Patients with prior exposure to anti–tumor necrosis factor–alpha agents were included. They received either 100 mg guselkumab delivered subcutaneously or placebo at week 0 and 4, then every 8 weeks thereafter through week 44.
Patients with less than 5% improvement in swollen and tender joint count at week 16 were allowed early escape to open-label ustekinumab (Stelara), and at week 24 all remaining patients crossed over to receive guselkumab, which was repeated at week 28 and every 8 weeks thereafter through week 44.
Treatment was well tolerated; the proportion of patients with one or more adverse events was similar in the treatment and placebo groups (36% and 32.7%, respectively), with infections being the most common adverse event, occurring in 17% and 20.4% of patients in the groups, respectively.
“And even though 10% and 14% of the patients received systemic treatment, no patient received [intravenous] antibiotics,” he said.
Severe adverse events occurred in two patients – one in each group – and included a knee injury and myocardial infarction. Specific information about which group these occurred in is not available as the study is ongoing and investigators remain blinded, Dr. Deodhar noted.
No serious infections, malignancies, or deaths occurred through week 24, he said.
“Guselkumab is the first anti-IL23 biologic to demonstrate efficacy in psoriatic arthritis. In patients with active psoriatic arthritis ... treatment with guselkumab shows significant improvements in joint symptoms, physical function, psoriasis, enthesitis, dactylitis, and quality of life,” he concluded, adding that there were no unexpected safety findings in this population.
On Nov. 17, Janssen Biotech, Inc. announced the submission of a Biologics License Application to the Food and Drug Administration seeking approval of guselkumab for the treatment of adults with moderate to severe plaque psoriasis based on findings from prior studies for that indication.
The current study was sponsored by Janssen Research & Development. Dr. Deodhar reported financial relationships with AbbVie, Amgen, Boehringer Ingelheim, Janssen, Novartis, Pfizer, and UCB. Two other authors also reported financial ties to industry, including Janssen. Four of the seven authors of the abstract were employees of Janssen.
WASHINGTON – The investigational anti-interleukin-23 monoclonal antibody guselkumab was safe and well tolerated, and demonstrated significant improvement on a variety of measures in patients with active psoriatic arthritis in a randomized, placebo-controlled phase IIa study.
The primary endpoint of ACR20 at 24 weeks was achieved in 58% of 100 patients randomized to receive treatment with guselkumab versus 18.4% of 49 patients who received placebo, Atul A. Deodhar, MD, reported in a late-breaking abstract presentation at the annual meeting of the American College of Rheumatology.
For example, PASI75 response at 24 weeks was 78.6% for guselkumab and 12.5% for placebo, and the ACR50 response at 24 weeks was 34% vs. 10.2%, respectively. The HAQ-DI score mean change from baseline was –0.42 vs. –0.06, respectively.
Further, ACR20 response was seen as early as week 4 (21% vs. 0% for placebo), and the effect increased over time, reaching the maximum effect by week 16 (60% vs. 16.3%), Dr. Deodhar said.
Subjects in the double-blind, multicenter study had active psoriatic arthritis and at least 3% body surface area of plaque psoriasis despite treatment with standard-of-care therapies. Patients with prior exposure to anti–tumor necrosis factor–alpha agents were included. They received either 100 mg guselkumab delivered subcutaneously or placebo at week 0 and 4, then every 8 weeks thereafter through week 44.
Patients with less than 5% improvement in swollen and tender joint count at week 16 were allowed early escape to open-label ustekinumab (Stelara), and at week 24 all remaining patients crossed over to receive guselkumab, which was repeated at week 28 and every 8 weeks thereafter through week 44.
Treatment was well tolerated; the proportion of patients with one or more adverse events was similar in the treatment and placebo groups (36% and 32.7%, respectively), with infections being the most common adverse event, occurring in 17% and 20.4% of patients in the groups, respectively.
“And even though 10% and 14% of the patients received systemic treatment, no patient received [intravenous] antibiotics,” he said.
Severe adverse events occurred in two patients – one in each group – and included a knee injury and myocardial infarction. Specific information about which group these occurred in is not available as the study is ongoing and investigators remain blinded, Dr. Deodhar noted.
No serious infections, malignancies, or deaths occurred through week 24, he said.
“Guselkumab is the first anti-IL23 biologic to demonstrate efficacy in psoriatic arthritis. In patients with active psoriatic arthritis ... treatment with guselkumab shows significant improvements in joint symptoms, physical function, psoriasis, enthesitis, dactylitis, and quality of life,” he concluded, adding that there were no unexpected safety findings in this population.
On Nov. 17, Janssen Biotech, Inc. announced the submission of a Biologics License Application to the Food and Drug Administration seeking approval of guselkumab for the treatment of adults with moderate to severe plaque psoriasis based on findings from prior studies for that indication.
The current study was sponsored by Janssen Research & Development. Dr. Deodhar reported financial relationships with AbbVie, Amgen, Boehringer Ingelheim, Janssen, Novartis, Pfizer, and UCB. Two other authors also reported financial ties to industry, including Janssen. Four of the seven authors of the abstract were employees of Janssen.
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: ACR20 at 24 weeks was achieved in 58% of 100 patients randomized to receive treatment with guselkumab vs. 18.4% of 49 patients who received placebo.
Data source: A randomized, placebo-controlled phase IIa study of 149 patients.
Disclosures: The current study was sponsored by Janssen Research & Development. Dr. Deodhar reported financial relationships with AbbVie, Amgen, Boehringer Ingelheim, Janssen, Novartis, Pfizer, and UCB. Two other authors also reported financial ties to industry, including Janssen. Four of the seven authors of the abstract were employees of Janssen.
ACR 2015 Workforce Study: Fewer rheumatologists, more patients, and the struggle to bridge the gap
WASHINGTON – The mass retirement of Baby Boomer workhorses, the changing face of a Millennial workforce, and the graying of America will deliver a triple-whammy to rheumatology over the next 15 years: By 2030, the United States will be short 4,700 full-time rheumatologists – just about as many as are currently in practice.
“This is drastic,” Marcy Bolster, MD, said at the annual meeting of the American College of Rheumatology. “We need to take action now or we will not be able to meet the expected increases in patient demand.”
Dr. Bolster, director of the rheumatology fellowship training program at Massachusetts General Hospital, Boston, was one of 10 clinicians who discussed the ACR’s massive new project, “The 2015 Workforce Study of Rheumatology Specialists in the United States,” a comprehensive assessment of the current supply of rheumatologists in this country, and a sobering prediction of how many will be needed in the future.
Released at the ACR meeting in Washington, the 2015 survey is the first that ACR has conducted since 2005. The project drew on a number of sources: questionnaires sent out to the entire ACR membership; published research, position papers, and government reports; the Institute of Medicine; and state licensure and National Resident Matching Program data. Four online questionnaires surveyed not only rheumatology clinicians and fellows, but other health professionals, adult and young patients with rheumatic diseases, and the parents of pediatric patients.
The survey response rate of 31% among practicing rheumatologists was not as high as the Committee on Rheumatology Training and Workforce Issues would have liked, said Daniel Battafarano, DO, a study cochair. But fellows had a 95% response rate, offering the study a very solid look at the near future of the specialty.
The 2015 results were a striking contrast to the 2005 report, which examined supply and demand up to 2025. It came to a brighter conclusion: that a relative balance would be maintained. Not so now.
The reasons for this projected imbalance are not overly complicated, and are actually recapitulated in other areas of medicine, said Dr. Battafarano, chief of rheumatology at San Antonio (Tex.) Military Medical Center. Baby Boomer senior physicians are tired of working 70 hours a week, and moving toward retirement in unprecedented numbers. In fact, according to the report, 50% of today’s full-time rheumatologists will retire within the next 15 years, and 80% of those plan to cut back their workload by about 25%.
It’s not that new blood isn’t coming into the profession. In fact, Dr. Bolster said during her presentation, the percentage of internal medicine residents moving into rheumatology will stay stable, at about 4%. But the number isn’t projected to increase as patient demand does, and these new doctors will look and practice very differently than the new doctors of 30 or 40 years ago.
“The majority of medical school graduates now – about 60% – are women,” Dr. Battafarano said. “And they are entering the workforce at a very challenging time of life, simultaneously building careers and families.”
Studies have also demonstrated that women have different practice patterns than men. They tend to spend more time with patients, so they sometimes see fewer in a day. In fact, in its supply assessment, the ACR study characterized women rheumatologists as 0.7 of a full-time equivalent position – an important factor in the projected supply gap.
But the projected workforce shortage does not hinge on the practice patterns of women rheumatologists, Dr. Battafarano cautioned. Part of it is based on his own generation of work-a-holism. In general, young physicians now place more importance on a healthy work-life balance than did his generation, and this he sees as a healthy way to approach a new career.
“I’ll admit it: Baby Boomers are dysfunctionally working too hard, and they miss the importance of a health work/life balance. That’s changing, and that’s a good thing.”
His protégé, Katrina Lawrence-Wolff, DO, agrees. A second-year rheumatology fellow, Dr. Lawrence-Wolff is also expecting her first child. She presented the breakout results focusing on the adult rheumatologist supply/demand picture.
“None of us think working 80 hours a week is a good idea for us personally, or a good way to give good medical care to patients,” she said in an interview. “We would rather have more time with family, more time for volunteering in our community, or to do advocacy work. We want to be flexible, and we do understand that this attitude may change the level of our reimbursement. But we are willing to forgo some salary to become a happier, better-balanced person.”
International medical graduates also affect this snapshot of the future, Dr. Bolster said during her lecture. More than half of new medical graduates are international students, and 17% of those intend to leave the United States after their education is complete.
Shortages will affect all regions, but some more than others
All of these issues are now converging at a time when patient demand is expected to soar. In the United States, about 22.5 million adults and 300,000 children have a rheumatic disease. According to the study, that number will increase by 61% by 2030.
Dr. Lawrence-Wolff used population statistics to really put the numbers needed to care for these patients into perspective. Studies in the United States, Canada, and Europe generally agree that the ideal rheumatologist:patient ratio is somewhere around 2 per 100,000 adults. “In 2005, when we were felt to be balanced in this way, our ratio was 1.67/100,000 patients.”
This ratio will look very different by 2025, she said, and the regional imbalances already seen will be magnified. These regional differences aren’t a surprise, Dr. Lawrence-Wolff noted. They directly reflect the density of academic rheumatology training centers. “Most practicing rheumatologists tend to stay in the region where they received their training,” she said, “so we have more clinicians in areas with more academic centers.”
For example, the Northeast U.S. hosts a highly enriched rheumatologist population, with a rheumatologist:patient ratio of 3.7/100,000. By 2025, this will be reduced to 1.6/100,000 – still acceptable, but more than a 50% decrease.
That same decrease will be much more drastically felt in regions that already have a paucity of rheumatologists. In the Southwest, the current ratio is 1.2/100,000; in 10 years, this will be 0.64/100,000. Even areas that are moderately well supplied now will suffer. Both the Northwest and North Central regions have a ratio of about 1.6/100,000. Both those regions will sink into the range of 0.6-0.5/100,000.
“All regions are going to decline below the 1.67 threshold by 2030,” she said. “Every single one.”
Troubles for pediatric rheumatology workforce
If things are concerning in the world of adult rheumatology, they’re downright alarming in the world of pediatric rheumatology, said Dr. Battafarano, who broke out the pediatric subspecialty results.
These clinicians are already scarce, with only 287 currently practicing full-time in 2015. By 2030, 461 will be needed, but the supply is expected to drop to 231.
The pediatric supply problem starts much earlier in the academic process, he said. For years, about 50% of the slots of pediatric rheumatology fellows have gone unfilled. In this world, recruitment woes will drive supply problems more than retirement. “As a whole, pediatric rheumatologists are younger,” Dr. Battafarano said, with only 32% planning to retire by 2030.
“Recruitment into adult rheumatology isn’t a problem, but on the pediatric side, it’s been very hard to recruit. This isn’t unique to rheumatology; it’s being seen in other pediatric subspecialties as well.”
Reimbursement and work overload are at the root of it, he believes.
“It translates pretty well to income. Reimbursement for chronic diseases, like what we see, is predominately Medicaid. The reimbursement rate and income for subspecialty pediatrics is definitely lower than it is in other academic subspecialties. And I have to think that time spent observing an exhausted, overworked physician isn’t helpful either.”
The mandatory 3-year pediatric rheumatology fellowship may also be a deal killer for some potential recruits, Dr. Battafarano said. The prevailing thought has always been to include a year of academic research in the pediatric track, which extends it beyond the 2-year fellowship that adult rheumatologists experience.
“So you marry the 3-year fellowship with workload, quality of life, student debt, and income and you get a combination that’s just less appealing than some other areas.”
Adjusting that fellowship track is one way to potentially improve the pediatric supply picture, he said. “One of the things I recommended is adding a 2-year clinical track. There are ways to do research that can be folded into a clinical setting that wouldn’t require an entire year. The majority of adult fellowships are 2 years with concurrent research, so there is already a precedent.”
In fact, Dr. Lawrence-Wolff is doing just that, he said. “She will do clinical research that’s integrated into her practice, but her primary role is to learn to be a clinical rheumatologist.”
Ideas for stretching rheumatologic care
Dr. Battafarano had some other practical suggestions for improving recruitment into the field. “We have to offer some incentives. I’d like to see us exploring the potential of loan repayment and visa programs.”
Overall, expanding the musculoskeletal expertise of primary care providers should also be on the table, Dr. Lawrence-Wolff said. “It’s possible that we can help our primary care colleagues extend rheumatology care by treating things like osteoarthritis and gout.”
Rheumatologists also can’t afford to ignore the expanding-role of mid-level providers, she said. “We would like to recruit more nurse practitioners and physician assistants into the specialty. The numbers we hope will go up, even if the percentage remains the same as it is, about 2%-5%.”
Skillfully leveraging these clinicians’ strengths will be the key to successfully employing them.
“We see different ways to utilize them to stretch our care. One suggestion is having them in the clinic to see more patients per day, but also to use them to see lower-level patients so the rheumatologist can take care of the more complex cases.”
They could also serve patients who have multiple regularly scheduled checkups for chronic illness. “If you have a patient who needs to be seen four times a year, the NP or PA can see that person, check the labs and determine if the patent is stable, and doesn’t really need to see the rheumatologist.”
Technology will invariably come into play as well, Dr. Battafarano said.
“We envision this as a multipronged approach that includes telehealth and ‘E-consults,’ although we don’t precisely know what that will look like. But other specialties – and primary care as well – are going through very similar trends here. We are all talking about working with other providers to reach more patients, and telemedicine is a key area of investigation. We really are all in the same boat.”
Finally, Dr. Battafarano urges his fellow senior clinicians to consider severing professional ties gradually. “It’s not just a dearth of bodies we’re facing, but a sudden depletion of valuable experience and clinical wisdom. In my practice, for example, the three of us each have more than 30 years’ experience. That’s close to a century of experience, and two of them want to retire. It’s such a brain-drain on a terrific practice to lose our colleagues overnight.”
For some reason, he said, the locum tenens model has never really caught on in rheumatology, and he’d like to see that idea explored and embraced. It’s a perfect way to keep experienced hands in the mix, both seeing patients and mentoring young rheumatologists, he added.
“Even if we’re in our 60s and 70s, we’re not brain-dead yet. A lot of us want to keep contributing, just not full-time.”
None of the clinicians quoted in this article had any relevant financial disclosures.
[email protected]
On Twitter @alz_gal
WASHINGTON – The mass retirement of Baby Boomer workhorses, the changing face of a Millennial workforce, and the graying of America will deliver a triple-whammy to rheumatology over the next 15 years: By 2030, the United States will be short 4,700 full-time rheumatologists – just about as many as are currently in practice.
“This is drastic,” Marcy Bolster, MD, said at the annual meeting of the American College of Rheumatology. “We need to take action now or we will not be able to meet the expected increases in patient demand.”
Dr. Bolster, director of the rheumatology fellowship training program at Massachusetts General Hospital, Boston, was one of 10 clinicians who discussed the ACR’s massive new project, “The 2015 Workforce Study of Rheumatology Specialists in the United States,” a comprehensive assessment of the current supply of rheumatologists in this country, and a sobering prediction of how many will be needed in the future.
Released at the ACR meeting in Washington, the 2015 survey is the first that ACR has conducted since 2005. The project drew on a number of sources: questionnaires sent out to the entire ACR membership; published research, position papers, and government reports; the Institute of Medicine; and state licensure and National Resident Matching Program data. Four online questionnaires surveyed not only rheumatology clinicians and fellows, but other health professionals, adult and young patients with rheumatic diseases, and the parents of pediatric patients.
The survey response rate of 31% among practicing rheumatologists was not as high as the Committee on Rheumatology Training and Workforce Issues would have liked, said Daniel Battafarano, DO, a study cochair. But fellows had a 95% response rate, offering the study a very solid look at the near future of the specialty.
The 2015 results were a striking contrast to the 2005 report, which examined supply and demand up to 2025. It came to a brighter conclusion: that a relative balance would be maintained. Not so now.
The reasons for this projected imbalance are not overly complicated, and are actually recapitulated in other areas of medicine, said Dr. Battafarano, chief of rheumatology at San Antonio (Tex.) Military Medical Center. Baby Boomer senior physicians are tired of working 70 hours a week, and moving toward retirement in unprecedented numbers. In fact, according to the report, 50% of today’s full-time rheumatologists will retire within the next 15 years, and 80% of those plan to cut back their workload by about 25%.
It’s not that new blood isn’t coming into the profession. In fact, Dr. Bolster said during her presentation, the percentage of internal medicine residents moving into rheumatology will stay stable, at about 4%. But the number isn’t projected to increase as patient demand does, and these new doctors will look and practice very differently than the new doctors of 30 or 40 years ago.
“The majority of medical school graduates now – about 60% – are women,” Dr. Battafarano said. “And they are entering the workforce at a very challenging time of life, simultaneously building careers and families.”
Studies have also demonstrated that women have different practice patterns than men. They tend to spend more time with patients, so they sometimes see fewer in a day. In fact, in its supply assessment, the ACR study characterized women rheumatologists as 0.7 of a full-time equivalent position – an important factor in the projected supply gap.
But the projected workforce shortage does not hinge on the practice patterns of women rheumatologists, Dr. Battafarano cautioned. Part of it is based on his own generation of work-a-holism. In general, young physicians now place more importance on a healthy work-life balance than did his generation, and this he sees as a healthy way to approach a new career.
“I’ll admit it: Baby Boomers are dysfunctionally working too hard, and they miss the importance of a health work/life balance. That’s changing, and that’s a good thing.”
His protégé, Katrina Lawrence-Wolff, DO, agrees. A second-year rheumatology fellow, Dr. Lawrence-Wolff is also expecting her first child. She presented the breakout results focusing on the adult rheumatologist supply/demand picture.
“None of us think working 80 hours a week is a good idea for us personally, or a good way to give good medical care to patients,” she said in an interview. “We would rather have more time with family, more time for volunteering in our community, or to do advocacy work. We want to be flexible, and we do understand that this attitude may change the level of our reimbursement. But we are willing to forgo some salary to become a happier, better-balanced person.”
International medical graduates also affect this snapshot of the future, Dr. Bolster said during her lecture. More than half of new medical graduates are international students, and 17% of those intend to leave the United States after their education is complete.
Shortages will affect all regions, but some more than others
All of these issues are now converging at a time when patient demand is expected to soar. In the United States, about 22.5 million adults and 300,000 children have a rheumatic disease. According to the study, that number will increase by 61% by 2030.
Dr. Lawrence-Wolff used population statistics to really put the numbers needed to care for these patients into perspective. Studies in the United States, Canada, and Europe generally agree that the ideal rheumatologist:patient ratio is somewhere around 2 per 100,000 adults. “In 2005, when we were felt to be balanced in this way, our ratio was 1.67/100,000 patients.”
This ratio will look very different by 2025, she said, and the regional imbalances already seen will be magnified. These regional differences aren’t a surprise, Dr. Lawrence-Wolff noted. They directly reflect the density of academic rheumatology training centers. “Most practicing rheumatologists tend to stay in the region where they received their training,” she said, “so we have more clinicians in areas with more academic centers.”
For example, the Northeast U.S. hosts a highly enriched rheumatologist population, with a rheumatologist:patient ratio of 3.7/100,000. By 2025, this will be reduced to 1.6/100,000 – still acceptable, but more than a 50% decrease.
That same decrease will be much more drastically felt in regions that already have a paucity of rheumatologists. In the Southwest, the current ratio is 1.2/100,000; in 10 years, this will be 0.64/100,000. Even areas that are moderately well supplied now will suffer. Both the Northwest and North Central regions have a ratio of about 1.6/100,000. Both those regions will sink into the range of 0.6-0.5/100,000.
“All regions are going to decline below the 1.67 threshold by 2030,” she said. “Every single one.”
Troubles for pediatric rheumatology workforce
If things are concerning in the world of adult rheumatology, they’re downright alarming in the world of pediatric rheumatology, said Dr. Battafarano, who broke out the pediatric subspecialty results.
These clinicians are already scarce, with only 287 currently practicing full-time in 2015. By 2030, 461 will be needed, but the supply is expected to drop to 231.
The pediatric supply problem starts much earlier in the academic process, he said. For years, about 50% of the slots of pediatric rheumatology fellows have gone unfilled. In this world, recruitment woes will drive supply problems more than retirement. “As a whole, pediatric rheumatologists are younger,” Dr. Battafarano said, with only 32% planning to retire by 2030.
“Recruitment into adult rheumatology isn’t a problem, but on the pediatric side, it’s been very hard to recruit. This isn’t unique to rheumatology; it’s being seen in other pediatric subspecialties as well.”
Reimbursement and work overload are at the root of it, he believes.
“It translates pretty well to income. Reimbursement for chronic diseases, like what we see, is predominately Medicaid. The reimbursement rate and income for subspecialty pediatrics is definitely lower than it is in other academic subspecialties. And I have to think that time spent observing an exhausted, overworked physician isn’t helpful either.”
The mandatory 3-year pediatric rheumatology fellowship may also be a deal killer for some potential recruits, Dr. Battafarano said. The prevailing thought has always been to include a year of academic research in the pediatric track, which extends it beyond the 2-year fellowship that adult rheumatologists experience.
“So you marry the 3-year fellowship with workload, quality of life, student debt, and income and you get a combination that’s just less appealing than some other areas.”
Adjusting that fellowship track is one way to potentially improve the pediatric supply picture, he said. “One of the things I recommended is adding a 2-year clinical track. There are ways to do research that can be folded into a clinical setting that wouldn’t require an entire year. The majority of adult fellowships are 2 years with concurrent research, so there is already a precedent.”
In fact, Dr. Lawrence-Wolff is doing just that, he said. “She will do clinical research that’s integrated into her practice, but her primary role is to learn to be a clinical rheumatologist.”
Ideas for stretching rheumatologic care
Dr. Battafarano had some other practical suggestions for improving recruitment into the field. “We have to offer some incentives. I’d like to see us exploring the potential of loan repayment and visa programs.”
Overall, expanding the musculoskeletal expertise of primary care providers should also be on the table, Dr. Lawrence-Wolff said. “It’s possible that we can help our primary care colleagues extend rheumatology care by treating things like osteoarthritis and gout.”
Rheumatologists also can’t afford to ignore the expanding-role of mid-level providers, she said. “We would like to recruit more nurse practitioners and physician assistants into the specialty. The numbers we hope will go up, even if the percentage remains the same as it is, about 2%-5%.”
Skillfully leveraging these clinicians’ strengths will be the key to successfully employing them.
“We see different ways to utilize them to stretch our care. One suggestion is having them in the clinic to see more patients per day, but also to use them to see lower-level patients so the rheumatologist can take care of the more complex cases.”
They could also serve patients who have multiple regularly scheduled checkups for chronic illness. “If you have a patient who needs to be seen four times a year, the NP or PA can see that person, check the labs and determine if the patent is stable, and doesn’t really need to see the rheumatologist.”
Technology will invariably come into play as well, Dr. Battafarano said.
“We envision this as a multipronged approach that includes telehealth and ‘E-consults,’ although we don’t precisely know what that will look like. But other specialties – and primary care as well – are going through very similar trends here. We are all talking about working with other providers to reach more patients, and telemedicine is a key area of investigation. We really are all in the same boat.”
Finally, Dr. Battafarano urges his fellow senior clinicians to consider severing professional ties gradually. “It’s not just a dearth of bodies we’re facing, but a sudden depletion of valuable experience and clinical wisdom. In my practice, for example, the three of us each have more than 30 years’ experience. That’s close to a century of experience, and two of them want to retire. It’s such a brain-drain on a terrific practice to lose our colleagues overnight.”
For some reason, he said, the locum tenens model has never really caught on in rheumatology, and he’d like to see that idea explored and embraced. It’s a perfect way to keep experienced hands in the mix, both seeing patients and mentoring young rheumatologists, he added.
“Even if we’re in our 60s and 70s, we’re not brain-dead yet. A lot of us want to keep contributing, just not full-time.”
None of the clinicians quoted in this article had any relevant financial disclosures.
[email protected]
On Twitter @alz_gal
WASHINGTON – The mass retirement of Baby Boomer workhorses, the changing face of a Millennial workforce, and the graying of America will deliver a triple-whammy to rheumatology over the next 15 years: By 2030, the United States will be short 4,700 full-time rheumatologists – just about as many as are currently in practice.
“This is drastic,” Marcy Bolster, MD, said at the annual meeting of the American College of Rheumatology. “We need to take action now or we will not be able to meet the expected increases in patient demand.”
Dr. Bolster, director of the rheumatology fellowship training program at Massachusetts General Hospital, Boston, was one of 10 clinicians who discussed the ACR’s massive new project, “The 2015 Workforce Study of Rheumatology Specialists in the United States,” a comprehensive assessment of the current supply of rheumatologists in this country, and a sobering prediction of how many will be needed in the future.
Released at the ACR meeting in Washington, the 2015 survey is the first that ACR has conducted since 2005. The project drew on a number of sources: questionnaires sent out to the entire ACR membership; published research, position papers, and government reports; the Institute of Medicine; and state licensure and National Resident Matching Program data. Four online questionnaires surveyed not only rheumatology clinicians and fellows, but other health professionals, adult and young patients with rheumatic diseases, and the parents of pediatric patients.
The survey response rate of 31% among practicing rheumatologists was not as high as the Committee on Rheumatology Training and Workforce Issues would have liked, said Daniel Battafarano, DO, a study cochair. But fellows had a 95% response rate, offering the study a very solid look at the near future of the specialty.
The 2015 results were a striking contrast to the 2005 report, which examined supply and demand up to 2025. It came to a brighter conclusion: that a relative balance would be maintained. Not so now.
The reasons for this projected imbalance are not overly complicated, and are actually recapitulated in other areas of medicine, said Dr. Battafarano, chief of rheumatology at San Antonio (Tex.) Military Medical Center. Baby Boomer senior physicians are tired of working 70 hours a week, and moving toward retirement in unprecedented numbers. In fact, according to the report, 50% of today’s full-time rheumatologists will retire within the next 15 years, and 80% of those plan to cut back their workload by about 25%.
It’s not that new blood isn’t coming into the profession. In fact, Dr. Bolster said during her presentation, the percentage of internal medicine residents moving into rheumatology will stay stable, at about 4%. But the number isn’t projected to increase as patient demand does, and these new doctors will look and practice very differently than the new doctors of 30 or 40 years ago.
“The majority of medical school graduates now – about 60% – are women,” Dr. Battafarano said. “And they are entering the workforce at a very challenging time of life, simultaneously building careers and families.”
Studies have also demonstrated that women have different practice patterns than men. They tend to spend more time with patients, so they sometimes see fewer in a day. In fact, in its supply assessment, the ACR study characterized women rheumatologists as 0.7 of a full-time equivalent position – an important factor in the projected supply gap.
But the projected workforce shortage does not hinge on the practice patterns of women rheumatologists, Dr. Battafarano cautioned. Part of it is based on his own generation of work-a-holism. In general, young physicians now place more importance on a healthy work-life balance than did his generation, and this he sees as a healthy way to approach a new career.
“I’ll admit it: Baby Boomers are dysfunctionally working too hard, and they miss the importance of a health work/life balance. That’s changing, and that’s a good thing.”
His protégé, Katrina Lawrence-Wolff, DO, agrees. A second-year rheumatology fellow, Dr. Lawrence-Wolff is also expecting her first child. She presented the breakout results focusing on the adult rheumatologist supply/demand picture.
“None of us think working 80 hours a week is a good idea for us personally, or a good way to give good medical care to patients,” she said in an interview. “We would rather have more time with family, more time for volunteering in our community, or to do advocacy work. We want to be flexible, and we do understand that this attitude may change the level of our reimbursement. But we are willing to forgo some salary to become a happier, better-balanced person.”
International medical graduates also affect this snapshot of the future, Dr. Bolster said during her lecture. More than half of new medical graduates are international students, and 17% of those intend to leave the United States after their education is complete.
Shortages will affect all regions, but some more than others
All of these issues are now converging at a time when patient demand is expected to soar. In the United States, about 22.5 million adults and 300,000 children have a rheumatic disease. According to the study, that number will increase by 61% by 2030.
Dr. Lawrence-Wolff used population statistics to really put the numbers needed to care for these patients into perspective. Studies in the United States, Canada, and Europe generally agree that the ideal rheumatologist:patient ratio is somewhere around 2 per 100,000 adults. “In 2005, when we were felt to be balanced in this way, our ratio was 1.67/100,000 patients.”
This ratio will look very different by 2025, she said, and the regional imbalances already seen will be magnified. These regional differences aren’t a surprise, Dr. Lawrence-Wolff noted. They directly reflect the density of academic rheumatology training centers. “Most practicing rheumatologists tend to stay in the region where they received their training,” she said, “so we have more clinicians in areas with more academic centers.”
For example, the Northeast U.S. hosts a highly enriched rheumatologist population, with a rheumatologist:patient ratio of 3.7/100,000. By 2025, this will be reduced to 1.6/100,000 – still acceptable, but more than a 50% decrease.
That same decrease will be much more drastically felt in regions that already have a paucity of rheumatologists. In the Southwest, the current ratio is 1.2/100,000; in 10 years, this will be 0.64/100,000. Even areas that are moderately well supplied now will suffer. Both the Northwest and North Central regions have a ratio of about 1.6/100,000. Both those regions will sink into the range of 0.6-0.5/100,000.
“All regions are going to decline below the 1.67 threshold by 2030,” she said. “Every single one.”
Troubles for pediatric rheumatology workforce
If things are concerning in the world of adult rheumatology, they’re downright alarming in the world of pediatric rheumatology, said Dr. Battafarano, who broke out the pediatric subspecialty results.
These clinicians are already scarce, with only 287 currently practicing full-time in 2015. By 2030, 461 will be needed, but the supply is expected to drop to 231.
The pediatric supply problem starts much earlier in the academic process, he said. For years, about 50% of the slots of pediatric rheumatology fellows have gone unfilled. In this world, recruitment woes will drive supply problems more than retirement. “As a whole, pediatric rheumatologists are younger,” Dr. Battafarano said, with only 32% planning to retire by 2030.
“Recruitment into adult rheumatology isn’t a problem, but on the pediatric side, it’s been very hard to recruit. This isn’t unique to rheumatology; it’s being seen in other pediatric subspecialties as well.”
Reimbursement and work overload are at the root of it, he believes.
“It translates pretty well to income. Reimbursement for chronic diseases, like what we see, is predominately Medicaid. The reimbursement rate and income for subspecialty pediatrics is definitely lower than it is in other academic subspecialties. And I have to think that time spent observing an exhausted, overworked physician isn’t helpful either.”
The mandatory 3-year pediatric rheumatology fellowship may also be a deal killer for some potential recruits, Dr. Battafarano said. The prevailing thought has always been to include a year of academic research in the pediatric track, which extends it beyond the 2-year fellowship that adult rheumatologists experience.
“So you marry the 3-year fellowship with workload, quality of life, student debt, and income and you get a combination that’s just less appealing than some other areas.”
Adjusting that fellowship track is one way to potentially improve the pediatric supply picture, he said. “One of the things I recommended is adding a 2-year clinical track. There are ways to do research that can be folded into a clinical setting that wouldn’t require an entire year. The majority of adult fellowships are 2 years with concurrent research, so there is already a precedent.”
In fact, Dr. Lawrence-Wolff is doing just that, he said. “She will do clinical research that’s integrated into her practice, but her primary role is to learn to be a clinical rheumatologist.”
Ideas for stretching rheumatologic care
Dr. Battafarano had some other practical suggestions for improving recruitment into the field. “We have to offer some incentives. I’d like to see us exploring the potential of loan repayment and visa programs.”
Overall, expanding the musculoskeletal expertise of primary care providers should also be on the table, Dr. Lawrence-Wolff said. “It’s possible that we can help our primary care colleagues extend rheumatology care by treating things like osteoarthritis and gout.”
Rheumatologists also can’t afford to ignore the expanding-role of mid-level providers, she said. “We would like to recruit more nurse practitioners and physician assistants into the specialty. The numbers we hope will go up, even if the percentage remains the same as it is, about 2%-5%.”
Skillfully leveraging these clinicians’ strengths will be the key to successfully employing them.
“We see different ways to utilize them to stretch our care. One suggestion is having them in the clinic to see more patients per day, but also to use them to see lower-level patients so the rheumatologist can take care of the more complex cases.”
They could also serve patients who have multiple regularly scheduled checkups for chronic illness. “If you have a patient who needs to be seen four times a year, the NP or PA can see that person, check the labs and determine if the patent is stable, and doesn’t really need to see the rheumatologist.”
Technology will invariably come into play as well, Dr. Battafarano said.
“We envision this as a multipronged approach that includes telehealth and ‘E-consults,’ although we don’t precisely know what that will look like. But other specialties – and primary care as well – are going through very similar trends here. We are all talking about working with other providers to reach more patients, and telemedicine is a key area of investigation. We really are all in the same boat.”
Finally, Dr. Battafarano urges his fellow senior clinicians to consider severing professional ties gradually. “It’s not just a dearth of bodies we’re facing, but a sudden depletion of valuable experience and clinical wisdom. In my practice, for example, the three of us each have more than 30 years’ experience. That’s close to a century of experience, and two of them want to retire. It’s such a brain-drain on a terrific practice to lose our colleagues overnight.”
For some reason, he said, the locum tenens model has never really caught on in rheumatology, and he’d like to see that idea explored and embraced. It’s a perfect way to keep experienced hands in the mix, both seeing patients and mentoring young rheumatologists, he added.
“Even if we’re in our 60s and 70s, we’re not brain-dead yet. A lot of us want to keep contributing, just not full-time.”
None of the clinicians quoted in this article had any relevant financial disclosures.
[email protected]
On Twitter @alz_gal
AT THE ACR ANNUAL MEETING
VIDEO: ACR recommendations for glucocorticoid-induced osteoporosis unveiled
WASHINGTON – New American College of Rheumatology recommendations for glucocorticoid-induced osteoporosis prevention and treatment include refinements in risk assessment and treatment.
“These are draft recommendations not yet accepted by ACR,” said Lenore M. Buckley, MD, of Yale University, New Haven, Conn. “They are intended to be dynamic, because risk factors change for patients over time,” she added.
The draft recommendations build upon the 2010 ACR recommendations.
“About 1% of the United States population is on glucocorticoid treatment. Fracture is the most common adverse event, and trabecular bone in the spine is the most vulnerable,” Dr. Buckley explained in her presentation of the recommendations at the annual meeting of the American College of Rheumatology. “The risk of glucocorticoid (GC)-induced fracture is related to dose level and cumulative dose.”
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The draft recommendations were developed via GRADE (Grading of Assessment, Development, and Evaluation) methodology by a core team of internists, rheumatologists, a GRADE expert, a voting panel, and an expert panel.
Recommendations for risk assessment
Risk assessment for GC-induced osteoporosis is individualized. “You need to know the patient in front of you. Fracture risk is not just related to GC use, but also to bone mass, age, and race. Older age, female gender, Caucasian race all increase risk, and these factors need to be brought in to assessment,” Dr. Buckley explained.
For men and women over age 40, the Fracture Risk Assessment Tool (FRAX), which calculates the 10-year fracture risk in adults over age 40, should be used for risk assessment, incorporating GC use as a risk factor, she said.
“Adjust risk of FRAX according to dose of glucocorticoid. For 2.5-7.5 mg/day, the FRAX risk is fine, but if the patient is on higher doses, adjust the FRAX accordingly,” she said.
FRAX is not valid for women and men under age 40, she continued. A new recommendation is the inclusion of a moderate risk group based on very low bone mass score (Z score less than –3 below the standard deviation of the mean) and/or rapid bone loss (greater than 10% in 1 year). Patients who had prior GC-associated fracture under 40 years are considered high risk.
A thorough history and physical exam are necessary for all patients, and risk assessment should be done within 6 months of GC initiation. Physical exam should be repeated annually, and bone mineral density (BMD) should be assessed every 2-3 years for patients who continue on GC.
Treatment
The proposed treatment recommendations were not age dependent. Patients with moderate to high risk should be treated, in descending order, with oral bisphosphonates, intravenous bisphosphonates, teriparatide (Forteo), and denosumab (Prolia). The order of preference for these treatments was based on cost, efficacy, toxicity, and patient preference.
All patients should take calcium and vitamin D, regardless of risk level.
The proposed recommendations also addressed four special groups considered at significant risk: women of childbearing potential, organ transplant recipients, children, and people on very high doses of GC (greater than 30 mg/day, cumulative dose of 5 g/year).
“For women of childbearing potential, there are emerging data suggesting that bisphosphonates are safe. For this group, consider oral bisphosphonate and teriparatide as a second choice. Animal data suggest that IV bisphosphonates and denosumab are harmful to the fetus,” Dr. Buckley said.
For organ transplant recipients, general recommendations can be followed with two provisions: Kidney transplant recipients should have a work-up for metabolic bone disease, and denosumab should not be used in people on multiple immunosuppressants.
Optimize calcium and vitamin D for children, and treat with oral bisphosphonate, Dr. Buckley continued. If oral bisphosphonates are contraindicated, IV bisphosphonates can be used.
Patients on very high GC dose should be treated with oral bisphosphonates if they are age 30 or older.
Osteoporosis medications can be discontinued in low-risk patients who stop taking GC, but should be continued for those at moderate to high risk.
Patients who benefit from osteoporosis medications but remain at moderate to high risk at the end of 3 years should continue GC treatment.
The authors and sponsors had no relevant financial disclosures.
WASHINGTON – New American College of Rheumatology recommendations for glucocorticoid-induced osteoporosis prevention and treatment include refinements in risk assessment and treatment.
“These are draft recommendations not yet accepted by ACR,” said Lenore M. Buckley, MD, of Yale University, New Haven, Conn. “They are intended to be dynamic, because risk factors change for patients over time,” she added.
The draft recommendations build upon the 2010 ACR recommendations.
“About 1% of the United States population is on glucocorticoid treatment. Fracture is the most common adverse event, and trabecular bone in the spine is the most vulnerable,” Dr. Buckley explained in her presentation of the recommendations at the annual meeting of the American College of Rheumatology. “The risk of glucocorticoid (GC)-induced fracture is related to dose level and cumulative dose.”
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The draft recommendations were developed via GRADE (Grading of Assessment, Development, and Evaluation) methodology by a core team of internists, rheumatologists, a GRADE expert, a voting panel, and an expert panel.
Recommendations for risk assessment
Risk assessment for GC-induced osteoporosis is individualized. “You need to know the patient in front of you. Fracture risk is not just related to GC use, but also to bone mass, age, and race. Older age, female gender, Caucasian race all increase risk, and these factors need to be brought in to assessment,” Dr. Buckley explained.
For men and women over age 40, the Fracture Risk Assessment Tool (FRAX), which calculates the 10-year fracture risk in adults over age 40, should be used for risk assessment, incorporating GC use as a risk factor, she said.
“Adjust risk of FRAX according to dose of glucocorticoid. For 2.5-7.5 mg/day, the FRAX risk is fine, but if the patient is on higher doses, adjust the FRAX accordingly,” she said.
FRAX is not valid for women and men under age 40, she continued. A new recommendation is the inclusion of a moderate risk group based on very low bone mass score (Z score less than –3 below the standard deviation of the mean) and/or rapid bone loss (greater than 10% in 1 year). Patients who had prior GC-associated fracture under 40 years are considered high risk.
A thorough history and physical exam are necessary for all patients, and risk assessment should be done within 6 months of GC initiation. Physical exam should be repeated annually, and bone mineral density (BMD) should be assessed every 2-3 years for patients who continue on GC.
Treatment
The proposed treatment recommendations were not age dependent. Patients with moderate to high risk should be treated, in descending order, with oral bisphosphonates, intravenous bisphosphonates, teriparatide (Forteo), and denosumab (Prolia). The order of preference for these treatments was based on cost, efficacy, toxicity, and patient preference.
All patients should take calcium and vitamin D, regardless of risk level.
The proposed recommendations also addressed four special groups considered at significant risk: women of childbearing potential, organ transplant recipients, children, and people on very high doses of GC (greater than 30 mg/day, cumulative dose of 5 g/year).
“For women of childbearing potential, there are emerging data suggesting that bisphosphonates are safe. For this group, consider oral bisphosphonate and teriparatide as a second choice. Animal data suggest that IV bisphosphonates and denosumab are harmful to the fetus,” Dr. Buckley said.
For organ transplant recipients, general recommendations can be followed with two provisions: Kidney transplant recipients should have a work-up for metabolic bone disease, and denosumab should not be used in people on multiple immunosuppressants.
Optimize calcium and vitamin D for children, and treat with oral bisphosphonate, Dr. Buckley continued. If oral bisphosphonates are contraindicated, IV bisphosphonates can be used.
Patients on very high GC dose should be treated with oral bisphosphonates if they are age 30 or older.
Osteoporosis medications can be discontinued in low-risk patients who stop taking GC, but should be continued for those at moderate to high risk.
Patients who benefit from osteoporosis medications but remain at moderate to high risk at the end of 3 years should continue GC treatment.
The authors and sponsors had no relevant financial disclosures.
WASHINGTON – New American College of Rheumatology recommendations for glucocorticoid-induced osteoporosis prevention and treatment include refinements in risk assessment and treatment.
“These are draft recommendations not yet accepted by ACR,” said Lenore M. Buckley, MD, of Yale University, New Haven, Conn. “They are intended to be dynamic, because risk factors change for patients over time,” she added.
The draft recommendations build upon the 2010 ACR recommendations.
“About 1% of the United States population is on glucocorticoid treatment. Fracture is the most common adverse event, and trabecular bone in the spine is the most vulnerable,” Dr. Buckley explained in her presentation of the recommendations at the annual meeting of the American College of Rheumatology. “The risk of glucocorticoid (GC)-induced fracture is related to dose level and cumulative dose.”
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The draft recommendations were developed via GRADE (Grading of Assessment, Development, and Evaluation) methodology by a core team of internists, rheumatologists, a GRADE expert, a voting panel, and an expert panel.
Recommendations for risk assessment
Risk assessment for GC-induced osteoporosis is individualized. “You need to know the patient in front of you. Fracture risk is not just related to GC use, but also to bone mass, age, and race. Older age, female gender, Caucasian race all increase risk, and these factors need to be brought in to assessment,” Dr. Buckley explained.
For men and women over age 40, the Fracture Risk Assessment Tool (FRAX), which calculates the 10-year fracture risk in adults over age 40, should be used for risk assessment, incorporating GC use as a risk factor, she said.
“Adjust risk of FRAX according to dose of glucocorticoid. For 2.5-7.5 mg/day, the FRAX risk is fine, but if the patient is on higher doses, adjust the FRAX accordingly,” she said.
FRAX is not valid for women and men under age 40, she continued. A new recommendation is the inclusion of a moderate risk group based on very low bone mass score (Z score less than –3 below the standard deviation of the mean) and/or rapid bone loss (greater than 10% in 1 year). Patients who had prior GC-associated fracture under 40 years are considered high risk.
A thorough history and physical exam are necessary for all patients, and risk assessment should be done within 6 months of GC initiation. Physical exam should be repeated annually, and bone mineral density (BMD) should be assessed every 2-3 years for patients who continue on GC.
Treatment
The proposed treatment recommendations were not age dependent. Patients with moderate to high risk should be treated, in descending order, with oral bisphosphonates, intravenous bisphosphonates, teriparatide (Forteo), and denosumab (Prolia). The order of preference for these treatments was based on cost, efficacy, toxicity, and patient preference.
All patients should take calcium and vitamin D, regardless of risk level.
The proposed recommendations also addressed four special groups considered at significant risk: women of childbearing potential, organ transplant recipients, children, and people on very high doses of GC (greater than 30 mg/day, cumulative dose of 5 g/year).
“For women of childbearing potential, there are emerging data suggesting that bisphosphonates are safe. For this group, consider oral bisphosphonate and teriparatide as a second choice. Animal data suggest that IV bisphosphonates and denosumab are harmful to the fetus,” Dr. Buckley said.
For organ transplant recipients, general recommendations can be followed with two provisions: Kidney transplant recipients should have a work-up for metabolic bone disease, and denosumab should not be used in people on multiple immunosuppressants.
Optimize calcium and vitamin D for children, and treat with oral bisphosphonate, Dr. Buckley continued. If oral bisphosphonates are contraindicated, IV bisphosphonates can be used.
Patients on very high GC dose should be treated with oral bisphosphonates if they are age 30 or older.
Osteoporosis medications can be discontinued in low-risk patients who stop taking GC, but should be continued for those at moderate to high risk.
Patients who benefit from osteoporosis medications but remain at moderate to high risk at the end of 3 years should continue GC treatment.
The authors and sponsors had no relevant financial disclosures.
AT THE ACR ANNUAL MEETING
VIDEO: TNF inhibitors don’t boost cancer risk in JIA
WASHINGTON – Tumor necrosis factor inhibitors don’t appear to confer any additional cancer risk upon children with juvenile idiopathic arthritis above the increased incidence of cancer that comes hand in hand with the disease itself.
In 2009, the drugs came under suspicion of boosting the already-known increased cancer risk in these patients, Timothy G. Beukelman, MD, said at the annual meeting of the American College of Rheumatology. But the large database review that he conducted with his colleagues doesn’t validate those fears.
“I feel fairly confident now that I can stand in front of parents and say that we can treat their child effectively without putting that child at an even higher risk of a malignancy,” he said in a video interview.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Thomas J.A. Lehman, MD, chief of pediatric rheumatology at the Hospital for Special Surgery, New York, and professor of clinical pediatrics at Weill Cornell Medical College in New York, agreed.
“This study again indicates that anti-TNF therapy does not increase the risk of cancer for children with arthritis,” he said in an interview. “Although children with rheumatic diseases have a small increased background risk of malignancies, this is independent of the use of anti-TNF therapies. For physicians who have cared for children in the era when we did not have anti-TNF therapies available, it is clear that any minor risks associated with these medications are far outweighed by their dramatic benefits.”
In the last few years, five large studies have found that children with juvenile idiopathic arthritis (JIA) have a two- to sixfold increased malignancy risk, compared with the general pediatric population. However, only two of those studies included children taking TNF inhibitors, who comprised just 2% and 9% of those study populations.
In 2009, based on voluntary adverse event reporting, the Food and Drug Administration issued a black box warning on TNF inhibitors, citing a possibly increased risk of cancer in children and adolescents who received the drugs for JIA, inflammatory bowel diseases, and other inflammatory diseases.
Shortly thereafter, a report identified a fivefold increase in the risk of childhood lymphoma associated with the medications (Arthritis Rheum. 2010 Aug;62[8]:2517-24). Other studies have not borne this out, but the boxed warning stands.
To further explore the association, Dr. Beukelman of the University of Alabama, Birmingham, and his associates examined billing data from two large national billing databases: the National U.S. Truven MarketScan claims database and Medicaid billing records. Together, the databases contained information on 27,000 children with JIA who received a prescription for a TNF inhibitor any time during 2000-2014. Cancer rates in this population were compared with those seen in a cohort of 2.64 million children with attention-deficit/hyperactivity disorder who were included in the national Surveillance, Epidemiology, and End Results (SEER) database. The investigators chose individuals with ADHD as a control group because of ADHD’s chronicity and lack of any association with cancer risk.
Dr. Beukelman also performed a within-group analysis on the JIA patients, comparing cancer rates among those treated with a TNF inhibitor and with methotrexate. The mean follow-up for patients who took TNF inhibitors was 4 years (median of 1.4 years), but there were a full 14 years of data for some patients.
Among the controls, with more than 4 million person-years of follow-up, there were 727 cases of any malignancy – a standardized incident rate (SIR) of 1.03. Among all children with JIA, with more than 52,000 person-years of follow-up, there were 20 malignancies. The SEER database predicted eight among a sex- and age-matched cohort of healthy children. This translated to an SIR of 2.4. This represents the baseline increased risk of cancer conferred by JIA alone.
Nine malignancies occurred in the subgroup of children with JIA who took no medications. The SEER expectation among this group was 3.8 cancers, also translating to an SIR of 2.4
One malignancy occurred in the group treated with methotrexate only. Among these children, the SEER expected number was 1.9; the SIR in this group was 0.53.
Seven malignancies occurred among children who took TNF inhibitors, translating to an SIR of 2.9. Six occurred in children who took a TNF inhibitor in combination with or without methotrexate – an SIR of 3.0.
A final group consisted of children who took a wide range of other medications used in JIA (abatacept, anakinra, canakinumab, rilonacept, rituximab, tocilizumab, ustekinumab, tofacitinib, azathioprine, cyclosporine, gold, leflunomide, mycophenolate mofetil, tacrolimus, thalidomide, lenalidomide). This group also included patients who may or may not have taken methotrexate or a TNF inhibitor. Among these, there were four cancers when the SEER expected number was 0.7. This translated to an SIR of almost 6 – a surprising finding, Dr. Beukelman said. But since there were only four cancers and the group was exposed to so many different medications, it’s tough to know what that means, if anything, Dr. Beukelman said.
“There’s a lot to unpack here. The treatment paradigm for JIA is methotrexate followed by a TNF inhibitor if that’s ineffective. So these kids were on all of these more uncommon drugs,” suggesting that neither TNF inhibition nor methotrexate worked. “Some of these patients might actually have had systemic arthritis, Still’s disease, which is a completely separate thing, and we don’t know anything about the risk of malignancy in that. They might have an even higher rate of malignancies at baseline due to having worse disease, or uncontrolled inflammation. It is concerning, but I think it probably speaks to the fact that these patients are difficult to treat and probably at higher risk.”
Dr. Beukelman didn’t specifically break out the types and numbers of cancer, except to say that 3 of the 20 were lymphomas. The rest were leukemias and brain cancers – a finding that reflects the general pattern of childhood malignancies.
“Unfortunately, the most common childhood cancers are lymphomas, leukemias, and brain cancers, and that is what we saw in this study as well,” he said.
The study was supported by the U.S. Agency for Healthcare Research and Quality. Dr. Beukelman noted that he has received consulting fees from Novartis, Genetech/Roche, and UCB.
[email protected]
On Twitter @alz_gal
WASHINGTON – Tumor necrosis factor inhibitors don’t appear to confer any additional cancer risk upon children with juvenile idiopathic arthritis above the increased incidence of cancer that comes hand in hand with the disease itself.
In 2009, the drugs came under suspicion of boosting the already-known increased cancer risk in these patients, Timothy G. Beukelman, MD, said at the annual meeting of the American College of Rheumatology. But the large database review that he conducted with his colleagues doesn’t validate those fears.
“I feel fairly confident now that I can stand in front of parents and say that we can treat their child effectively without putting that child at an even higher risk of a malignancy,” he said in a video interview.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Thomas J.A. Lehman, MD, chief of pediatric rheumatology at the Hospital for Special Surgery, New York, and professor of clinical pediatrics at Weill Cornell Medical College in New York, agreed.
“This study again indicates that anti-TNF therapy does not increase the risk of cancer for children with arthritis,” he said in an interview. “Although children with rheumatic diseases have a small increased background risk of malignancies, this is independent of the use of anti-TNF therapies. For physicians who have cared for children in the era when we did not have anti-TNF therapies available, it is clear that any minor risks associated with these medications are far outweighed by their dramatic benefits.”
In the last few years, five large studies have found that children with juvenile idiopathic arthritis (JIA) have a two- to sixfold increased malignancy risk, compared with the general pediatric population. However, only two of those studies included children taking TNF inhibitors, who comprised just 2% and 9% of those study populations.
In 2009, based on voluntary adverse event reporting, the Food and Drug Administration issued a black box warning on TNF inhibitors, citing a possibly increased risk of cancer in children and adolescents who received the drugs for JIA, inflammatory bowel diseases, and other inflammatory diseases.
Shortly thereafter, a report identified a fivefold increase in the risk of childhood lymphoma associated with the medications (Arthritis Rheum. 2010 Aug;62[8]:2517-24). Other studies have not borne this out, but the boxed warning stands.
To further explore the association, Dr. Beukelman of the University of Alabama, Birmingham, and his associates examined billing data from two large national billing databases: the National U.S. Truven MarketScan claims database and Medicaid billing records. Together, the databases contained information on 27,000 children with JIA who received a prescription for a TNF inhibitor any time during 2000-2014. Cancer rates in this population were compared with those seen in a cohort of 2.64 million children with attention-deficit/hyperactivity disorder who were included in the national Surveillance, Epidemiology, and End Results (SEER) database. The investigators chose individuals with ADHD as a control group because of ADHD’s chronicity and lack of any association with cancer risk.
Dr. Beukelman also performed a within-group analysis on the JIA patients, comparing cancer rates among those treated with a TNF inhibitor and with methotrexate. The mean follow-up for patients who took TNF inhibitors was 4 years (median of 1.4 years), but there were a full 14 years of data for some patients.
Among the controls, with more than 4 million person-years of follow-up, there were 727 cases of any malignancy – a standardized incident rate (SIR) of 1.03. Among all children with JIA, with more than 52,000 person-years of follow-up, there were 20 malignancies. The SEER database predicted eight among a sex- and age-matched cohort of healthy children. This translated to an SIR of 2.4. This represents the baseline increased risk of cancer conferred by JIA alone.
Nine malignancies occurred in the subgroup of children with JIA who took no medications. The SEER expectation among this group was 3.8 cancers, also translating to an SIR of 2.4
One malignancy occurred in the group treated with methotrexate only. Among these children, the SEER expected number was 1.9; the SIR in this group was 0.53.
Seven malignancies occurred among children who took TNF inhibitors, translating to an SIR of 2.9. Six occurred in children who took a TNF inhibitor in combination with or without methotrexate – an SIR of 3.0.
A final group consisted of children who took a wide range of other medications used in JIA (abatacept, anakinra, canakinumab, rilonacept, rituximab, tocilizumab, ustekinumab, tofacitinib, azathioprine, cyclosporine, gold, leflunomide, mycophenolate mofetil, tacrolimus, thalidomide, lenalidomide). This group also included patients who may or may not have taken methotrexate or a TNF inhibitor. Among these, there were four cancers when the SEER expected number was 0.7. This translated to an SIR of almost 6 – a surprising finding, Dr. Beukelman said. But since there were only four cancers and the group was exposed to so many different medications, it’s tough to know what that means, if anything, Dr. Beukelman said.
“There’s a lot to unpack here. The treatment paradigm for JIA is methotrexate followed by a TNF inhibitor if that’s ineffective. So these kids were on all of these more uncommon drugs,” suggesting that neither TNF inhibition nor methotrexate worked. “Some of these patients might actually have had systemic arthritis, Still’s disease, which is a completely separate thing, and we don’t know anything about the risk of malignancy in that. They might have an even higher rate of malignancies at baseline due to having worse disease, or uncontrolled inflammation. It is concerning, but I think it probably speaks to the fact that these patients are difficult to treat and probably at higher risk.”
Dr. Beukelman didn’t specifically break out the types and numbers of cancer, except to say that 3 of the 20 were lymphomas. The rest were leukemias and brain cancers – a finding that reflects the general pattern of childhood malignancies.
“Unfortunately, the most common childhood cancers are lymphomas, leukemias, and brain cancers, and that is what we saw in this study as well,” he said.
The study was supported by the U.S. Agency for Healthcare Research and Quality. Dr. Beukelman noted that he has received consulting fees from Novartis, Genetech/Roche, and UCB.
[email protected]
On Twitter @alz_gal
WASHINGTON – Tumor necrosis factor inhibitors don’t appear to confer any additional cancer risk upon children with juvenile idiopathic arthritis above the increased incidence of cancer that comes hand in hand with the disease itself.
In 2009, the drugs came under suspicion of boosting the already-known increased cancer risk in these patients, Timothy G. Beukelman, MD, said at the annual meeting of the American College of Rheumatology. But the large database review that he conducted with his colleagues doesn’t validate those fears.
“I feel fairly confident now that I can stand in front of parents and say that we can treat their child effectively without putting that child at an even higher risk of a malignancy,” he said in a video interview.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Thomas J.A. Lehman, MD, chief of pediatric rheumatology at the Hospital for Special Surgery, New York, and professor of clinical pediatrics at Weill Cornell Medical College in New York, agreed.
“This study again indicates that anti-TNF therapy does not increase the risk of cancer for children with arthritis,” he said in an interview. “Although children with rheumatic diseases have a small increased background risk of malignancies, this is independent of the use of anti-TNF therapies. For physicians who have cared for children in the era when we did not have anti-TNF therapies available, it is clear that any minor risks associated with these medications are far outweighed by their dramatic benefits.”
In the last few years, five large studies have found that children with juvenile idiopathic arthritis (JIA) have a two- to sixfold increased malignancy risk, compared with the general pediatric population. However, only two of those studies included children taking TNF inhibitors, who comprised just 2% and 9% of those study populations.
In 2009, based on voluntary adverse event reporting, the Food and Drug Administration issued a black box warning on TNF inhibitors, citing a possibly increased risk of cancer in children and adolescents who received the drugs for JIA, inflammatory bowel diseases, and other inflammatory diseases.
Shortly thereafter, a report identified a fivefold increase in the risk of childhood lymphoma associated with the medications (Arthritis Rheum. 2010 Aug;62[8]:2517-24). Other studies have not borne this out, but the boxed warning stands.
To further explore the association, Dr. Beukelman of the University of Alabama, Birmingham, and his associates examined billing data from two large national billing databases: the National U.S. Truven MarketScan claims database and Medicaid billing records. Together, the databases contained information on 27,000 children with JIA who received a prescription for a TNF inhibitor any time during 2000-2014. Cancer rates in this population were compared with those seen in a cohort of 2.64 million children with attention-deficit/hyperactivity disorder who were included in the national Surveillance, Epidemiology, and End Results (SEER) database. The investigators chose individuals with ADHD as a control group because of ADHD’s chronicity and lack of any association with cancer risk.
Dr. Beukelman also performed a within-group analysis on the JIA patients, comparing cancer rates among those treated with a TNF inhibitor and with methotrexate. The mean follow-up for patients who took TNF inhibitors was 4 years (median of 1.4 years), but there were a full 14 years of data for some patients.
Among the controls, with more than 4 million person-years of follow-up, there were 727 cases of any malignancy – a standardized incident rate (SIR) of 1.03. Among all children with JIA, with more than 52,000 person-years of follow-up, there were 20 malignancies. The SEER database predicted eight among a sex- and age-matched cohort of healthy children. This translated to an SIR of 2.4. This represents the baseline increased risk of cancer conferred by JIA alone.
Nine malignancies occurred in the subgroup of children with JIA who took no medications. The SEER expectation among this group was 3.8 cancers, also translating to an SIR of 2.4
One malignancy occurred in the group treated with methotrexate only. Among these children, the SEER expected number was 1.9; the SIR in this group was 0.53.
Seven malignancies occurred among children who took TNF inhibitors, translating to an SIR of 2.9. Six occurred in children who took a TNF inhibitor in combination with or without methotrexate – an SIR of 3.0.
A final group consisted of children who took a wide range of other medications used in JIA (abatacept, anakinra, canakinumab, rilonacept, rituximab, tocilizumab, ustekinumab, tofacitinib, azathioprine, cyclosporine, gold, leflunomide, mycophenolate mofetil, tacrolimus, thalidomide, lenalidomide). This group also included patients who may or may not have taken methotrexate or a TNF inhibitor. Among these, there were four cancers when the SEER expected number was 0.7. This translated to an SIR of almost 6 – a surprising finding, Dr. Beukelman said. But since there were only four cancers and the group was exposed to so many different medications, it’s tough to know what that means, if anything, Dr. Beukelman said.
“There’s a lot to unpack here. The treatment paradigm for JIA is methotrexate followed by a TNF inhibitor if that’s ineffective. So these kids were on all of these more uncommon drugs,” suggesting that neither TNF inhibition nor methotrexate worked. “Some of these patients might actually have had systemic arthritis, Still’s disease, which is a completely separate thing, and we don’t know anything about the risk of malignancy in that. They might have an even higher rate of malignancies at baseline due to having worse disease, or uncontrolled inflammation. It is concerning, but I think it probably speaks to the fact that these patients are difficult to treat and probably at higher risk.”
Dr. Beukelman didn’t specifically break out the types and numbers of cancer, except to say that 3 of the 20 were lymphomas. The rest were leukemias and brain cancers – a finding that reflects the general pattern of childhood malignancies.
“Unfortunately, the most common childhood cancers are lymphomas, leukemias, and brain cancers, and that is what we saw in this study as well,” he said.
The study was supported by the U.S. Agency for Healthcare Research and Quality. Dr. Beukelman noted that he has received consulting fees from Novartis, Genetech/Roche, and UCB.
[email protected]
On Twitter @alz_gal
AT THE ACR ANNUAL MEETING
Key clinical point:
Major finding: Children with JIA were about twice as likely to get cancer as the general population, regardless of whether they took a TNF inhibitor.
Data source: A database review comprising 27,000 patients and 2.5 million controls.
Disclosures: The study was supported by the U.S. Agency for Healthcare Research and Quality. Dr. Beukelman noted that he has received consulting fees from Novartis, Genetech/Roche, and UCB.