User login
100 coauthored papers, 10 years: Cancer transplant pioneers model 'team science'
On July 29, 2021, Sergio Giralt, MD, deputy division head of the division of hematologic malignancies and Miguel-Angel Perales, MD, chief of the adult bone marrow transplant service at MSKCC, published their 100th peer-reviewed paper as coauthors. Listing hundreds of such articles on a CV is standard for top-tier physicians, but the pair had gone one better: 100 publications written together in 10 years.
Their centenary article hit scientific newsstands almost exactly a decade after their first joint paper, which appeared in September 2011, not long after they met.
Born in Cuba, Dr. Giralt grew up in Venezuela. From the age of 14, he knew that medicine was his path, and in 1984 he earned a medical degree from the Universidad Central de Venezuela, Caracas. Next came a research position at Harvard Medical School, a residency at the Good Samaritan Hospital, Cincinnati, and a fellowship at the University of Texas MD Anderson Cancer Center, Houston. Dr. Giralt arrived at MSKCC in 2010 as the new chief of the adult bone marrow transplant service. There he was introduced to a new colleague, Dr. Perales. They soon learned that in addition to expertise in hematology, they had second language in common: Spanish.
Dr. Giralt said: “We both have a Spanish background and in a certain sense, there was an affinity there. ... We both have shared experiences.”
Dr. Perales was brought up in Belgium, a European nation with three official languages: French, Dutch, and German. He speaks five tongues in all and learned Spanish from his father, who came from Spain.
Fluency in Spanish enables both physicians to take care of the many New Yorkers who are more comfortable in that language – especially when navigating cancer treatment. However, both Dr. Giralt and Dr. Perales said that a second language is more than a professional tool. They described the enjoyable change of persona that happens when they switch to Spanish.
“People who are multilingual have different roles [as much as] different languages,” said Dr. Perales. “When I’m in Spanish, part of my brain is [thinking back to] summer vacations and hanging out with my cousins.”
When it comes to clinical science, however, English is the language of choice.
Global leaders in HSCT
Dr. Giralt and Dr. Perales are known worldwide in the field of allogeneic HSCT, a potentially curative treatment for an elongating list of both malignant and nonmalignant diseases.
In 1973, MSKCC conducted the first bone-marrow transplant from an unrelated donor. Fifty years on, medical oncologists in the United States conduct approximately 8,500 allogeneic transplants each year, 72% to treat acute leukemias or myelodysplastic syndrome (MDS).
However, stripping the immune system with intensive chemotherapy ‘conditioning,’ then rebuilding it with non-diseased donor hematopoietic cells is a hazardous undertaking. Older patients are less likely to survive the intensive conditioning, so historically have missed out. Also, even with a good human leukocyte antigen (HLA) match, the recipient needs often brutal immunosuppression.
Since Dr. Giralt and Dr. Perales began their partnership in 2010, the goals of their work have not changed: to develop safer, lower-intensity transplantation suitable for older, more vulnerable patients and reduce fearsome posttransplant sequelae such as graft-versus-host disease (GVHD).
Dr. Giralt’s publication list spans more than 600 peer-reviewed papers, articles and book chapters, almost exclusively on HSCT. Dr. Perales has more than 300 publication credits on the topic.
The two paired up on their first paper just months after Dr. Giralt arrived at MSKCC. That article, published in Biology of Blood and Marrow Transplantation, compared umbilical cord blood for HSCT with donor blood in 367 people with a variety of hematologic malignancies, including acute and chronic leukemias, MDS, and lymphoma.
The MSKCC team found that transplant-related mortality in the first 180 days was higher for the cord blood (21%), but thereafter mortality and relapse were much lower than for donated blood, with the result that 2-year progression-free survival of 55% was similar. Dr. Perales, Dr. Giralt and their coauthors concluded that the data provided “strong support” for further work on cord blood as an alternative stem-cell source.
During their first decade of collaboration, Dr. Giralt and Dr. Perales worked on any promising avenue that could improve outcomes and the experience of HSCT recipients, including reduced-intensity conditioning regimens to allow older adults to benefit from curative HSCT and donor T-cell depletion by CD34 selection, to reduce graft-versus-host disease (GVHD).
The CD34 protein is typically found on the surface of early stage and highly active stem cell types. Selecting these cell types using a range of techniques can eliminate many other potentially interfering or inactive cells. This enriches the transplant population with the most effective cells and can lower the risk of GVHD.
The 100th paper on which Dr. Giralt and Dr. Perales were coauthors was published in Blood Advances on July 27, 2021. The retrospective study examined the fate of 58 MSKCC patients with a rare form of chronic lymphocytic leukemia, CLL with Richter’s transformation (CLL-RT). It was the largest such study to date of this rare disease.
M.D. Anderson Cancer Center had shown in 2006 that, despite chemotherapy, overall survival in patients with CLL-RT was approximately 8 months. HSCT improved survival dramatically (75% at 3 years; n = 7). However, with the advent of novel targeted drugs for CLL such as ibrutinib (Imbruvica), venetoclax (Venclexta), or idelalisib (Zydelig), the MSKCC team asked themselves: What was the role of reduced-intensive conditioning HSCT? Was it even safe? Among other findings, Dr. Giralt and Dr. Perales’ 100th paper showed that reduced-intensity HSCT remained a viable alternative after a CLL-RT patient progressed on a novel agent.
Impact of the pandemic
When COVID-19 hit, the team lost many research staff and developed a huge backlog, said Dr. Giralt. He and Dr. Perales realized that they needed to be “thoughtful and careful” about which studies to continue. “For example, the CD-34 selection trials we did not close because these are our workhorse trials,” Dr. Giralt said. “We have people we need to treat, and some of the patients that we need to treat can only be treated on trial.”
The team was also able to pivot some of their work into COVID 19 itself, and they collected crucial information on HSCT in recovered COVID-19 patients, as an example.
“We were living through a critical time, but that doesn’t mean we [aren’t] obligated to continue our mission, our research mission,” said Dr. Giralt. “It really is team science. The way we look at it ... there’s a common thread: We both like to do allogeneic transplant, and we both believe in trying to make CD-34 selection better. So we’re both very much [working on] how can we improve what we call ‘the Memorial way’ of doing transplants. Where we separate is, Miguel does primarily lymphoma. He doesn’t do myeloma [like me]. So in those two areas, we’re helping develop the junior faculty in a different way.”
Something more in common
Right from the start, Dr. Perales and Dr. Giralt also shared a commitment to mentoring. Since 2010, Dr. Perales has mentored 22 up-and-coming junior faculty, including 10 from Europe (8 from Spain) and 2 from Latin America.
“[It makes] the research enterprise much more productive but [these young scientists] really increase the visibility of the program,” said Dr. Giralt.
He cited Dr. Perales’ track record of mentoring as one of the reasons for his promotion to chief of the adult bone marrow transplant service. In March 2020, Dr. Perales seamlessly stepped into Dr. Giralt’s shoes, while Dr. Giralt moved on to his present role as deputy division head of the division of hematologic malignancies.
Dr. Perales said: “The key aspect [of these promotions] is the fantastic working relationship that we’ve had over the years. ... I consider Sergio my mentor, but also a good friend and colleague. And so I think it’s this ability that we’ve had to work together and that relationship of trust, which has been key.”
“Sergio is somebody who lifts people up,” Dr. Perales added. “Many people will tell you that Sergio has helped them in their career. ... And I think that’s a lesson I’ve learned from him: training the next generation. And [that’s] not just in the U.S., but outside. I think that’s a key role that we have. And our responsibility.”
Asked to comment on their 100th-paper milestone, Dr. Perales firmly turned the spotlight from himself and Dr. Giralt to the junior investigators who have passed through the doors of the bone-marrow transplant program: “This body of work represents not just our collaboration but also the many contributions of our team at MSK ... and beyond MSK.”
This article was updated 1/26/22.
On July 29, 2021, Sergio Giralt, MD, deputy division head of the division of hematologic malignancies and Miguel-Angel Perales, MD, chief of the adult bone marrow transplant service at MSKCC, published their 100th peer-reviewed paper as coauthors. Listing hundreds of such articles on a CV is standard for top-tier physicians, but the pair had gone one better: 100 publications written together in 10 years.
Their centenary article hit scientific newsstands almost exactly a decade after their first joint paper, which appeared in September 2011, not long after they met.
Born in Cuba, Dr. Giralt grew up in Venezuela. From the age of 14, he knew that medicine was his path, and in 1984 he earned a medical degree from the Universidad Central de Venezuela, Caracas. Next came a research position at Harvard Medical School, a residency at the Good Samaritan Hospital, Cincinnati, and a fellowship at the University of Texas MD Anderson Cancer Center, Houston. Dr. Giralt arrived at MSKCC in 2010 as the new chief of the adult bone marrow transplant service. There he was introduced to a new colleague, Dr. Perales. They soon learned that in addition to expertise in hematology, they had second language in common: Spanish.
Dr. Giralt said: “We both have a Spanish background and in a certain sense, there was an affinity there. ... We both have shared experiences.”
Dr. Perales was brought up in Belgium, a European nation with three official languages: French, Dutch, and German. He speaks five tongues in all and learned Spanish from his father, who came from Spain.
Fluency in Spanish enables both physicians to take care of the many New Yorkers who are more comfortable in that language – especially when navigating cancer treatment. However, both Dr. Giralt and Dr. Perales said that a second language is more than a professional tool. They described the enjoyable change of persona that happens when they switch to Spanish.
“People who are multilingual have different roles [as much as] different languages,” said Dr. Perales. “When I’m in Spanish, part of my brain is [thinking back to] summer vacations and hanging out with my cousins.”
When it comes to clinical science, however, English is the language of choice.
Global leaders in HSCT
Dr. Giralt and Dr. Perales are known worldwide in the field of allogeneic HSCT, a potentially curative treatment for an elongating list of both malignant and nonmalignant diseases.
In 1973, MSKCC conducted the first bone-marrow transplant from an unrelated donor. Fifty years on, medical oncologists in the United States conduct approximately 8,500 allogeneic transplants each year, 72% to treat acute leukemias or myelodysplastic syndrome (MDS).
However, stripping the immune system with intensive chemotherapy ‘conditioning,’ then rebuilding it with non-diseased donor hematopoietic cells is a hazardous undertaking. Older patients are less likely to survive the intensive conditioning, so historically have missed out. Also, even with a good human leukocyte antigen (HLA) match, the recipient needs often brutal immunosuppression.
Since Dr. Giralt and Dr. Perales began their partnership in 2010, the goals of their work have not changed: to develop safer, lower-intensity transplantation suitable for older, more vulnerable patients and reduce fearsome posttransplant sequelae such as graft-versus-host disease (GVHD).
Dr. Giralt’s publication list spans more than 600 peer-reviewed papers, articles and book chapters, almost exclusively on HSCT. Dr. Perales has more than 300 publication credits on the topic.
The two paired up on their first paper just months after Dr. Giralt arrived at MSKCC. That article, published in Biology of Blood and Marrow Transplantation, compared umbilical cord blood for HSCT with donor blood in 367 people with a variety of hematologic malignancies, including acute and chronic leukemias, MDS, and lymphoma.
The MSKCC team found that transplant-related mortality in the first 180 days was higher for the cord blood (21%), but thereafter mortality and relapse were much lower than for donated blood, with the result that 2-year progression-free survival of 55% was similar. Dr. Perales, Dr. Giralt and their coauthors concluded that the data provided “strong support” for further work on cord blood as an alternative stem-cell source.
During their first decade of collaboration, Dr. Giralt and Dr. Perales worked on any promising avenue that could improve outcomes and the experience of HSCT recipients, including reduced-intensity conditioning regimens to allow older adults to benefit from curative HSCT and donor T-cell depletion by CD34 selection, to reduce graft-versus-host disease (GVHD).
The CD34 protein is typically found on the surface of early stage and highly active stem cell types. Selecting these cell types using a range of techniques can eliminate many other potentially interfering or inactive cells. This enriches the transplant population with the most effective cells and can lower the risk of GVHD.
The 100th paper on which Dr. Giralt and Dr. Perales were coauthors was published in Blood Advances on July 27, 2021. The retrospective study examined the fate of 58 MSKCC patients with a rare form of chronic lymphocytic leukemia, CLL with Richter’s transformation (CLL-RT). It was the largest such study to date of this rare disease.
M.D. Anderson Cancer Center had shown in 2006 that, despite chemotherapy, overall survival in patients with CLL-RT was approximately 8 months. HSCT improved survival dramatically (75% at 3 years; n = 7). However, with the advent of novel targeted drugs for CLL such as ibrutinib (Imbruvica), venetoclax (Venclexta), or idelalisib (Zydelig), the MSKCC team asked themselves: What was the role of reduced-intensive conditioning HSCT? Was it even safe? Among other findings, Dr. Giralt and Dr. Perales’ 100th paper showed that reduced-intensity HSCT remained a viable alternative after a CLL-RT patient progressed on a novel agent.
Impact of the pandemic
When COVID-19 hit, the team lost many research staff and developed a huge backlog, said Dr. Giralt. He and Dr. Perales realized that they needed to be “thoughtful and careful” about which studies to continue. “For example, the CD-34 selection trials we did not close because these are our workhorse trials,” Dr. Giralt said. “We have people we need to treat, and some of the patients that we need to treat can only be treated on trial.”
The team was also able to pivot some of their work into COVID 19 itself, and they collected crucial information on HSCT in recovered COVID-19 patients, as an example.
“We were living through a critical time, but that doesn’t mean we [aren’t] obligated to continue our mission, our research mission,” said Dr. Giralt. “It really is team science. The way we look at it ... there’s a common thread: We both like to do allogeneic transplant, and we both believe in trying to make CD-34 selection better. So we’re both very much [working on] how can we improve what we call ‘the Memorial way’ of doing transplants. Where we separate is, Miguel does primarily lymphoma. He doesn’t do myeloma [like me]. So in those two areas, we’re helping develop the junior faculty in a different way.”
Something more in common
Right from the start, Dr. Perales and Dr. Giralt also shared a commitment to mentoring. Since 2010, Dr. Perales has mentored 22 up-and-coming junior faculty, including 10 from Europe (8 from Spain) and 2 from Latin America.
“[It makes] the research enterprise much more productive but [these young scientists] really increase the visibility of the program,” said Dr. Giralt.
He cited Dr. Perales’ track record of mentoring as one of the reasons for his promotion to chief of the adult bone marrow transplant service. In March 2020, Dr. Perales seamlessly stepped into Dr. Giralt’s shoes, while Dr. Giralt moved on to his present role as deputy division head of the division of hematologic malignancies.
Dr. Perales said: “The key aspect [of these promotions] is the fantastic working relationship that we’ve had over the years. ... I consider Sergio my mentor, but also a good friend and colleague. And so I think it’s this ability that we’ve had to work together and that relationship of trust, which has been key.”
“Sergio is somebody who lifts people up,” Dr. Perales added. “Many people will tell you that Sergio has helped them in their career. ... And I think that’s a lesson I’ve learned from him: training the next generation. And [that’s] not just in the U.S., but outside. I think that’s a key role that we have. And our responsibility.”
Asked to comment on their 100th-paper milestone, Dr. Perales firmly turned the spotlight from himself and Dr. Giralt to the junior investigators who have passed through the doors of the bone-marrow transplant program: “This body of work represents not just our collaboration but also the many contributions of our team at MSK ... and beyond MSK.”
This article was updated 1/26/22.
On July 29, 2021, Sergio Giralt, MD, deputy division head of the division of hematologic malignancies and Miguel-Angel Perales, MD, chief of the adult bone marrow transplant service at MSKCC, published their 100th peer-reviewed paper as coauthors. Listing hundreds of such articles on a CV is standard for top-tier physicians, but the pair had gone one better: 100 publications written together in 10 years.
Their centenary article hit scientific newsstands almost exactly a decade after their first joint paper, which appeared in September 2011, not long after they met.
Born in Cuba, Dr. Giralt grew up in Venezuela. From the age of 14, he knew that medicine was his path, and in 1984 he earned a medical degree from the Universidad Central de Venezuela, Caracas. Next came a research position at Harvard Medical School, a residency at the Good Samaritan Hospital, Cincinnati, and a fellowship at the University of Texas MD Anderson Cancer Center, Houston. Dr. Giralt arrived at MSKCC in 2010 as the new chief of the adult bone marrow transplant service. There he was introduced to a new colleague, Dr. Perales. They soon learned that in addition to expertise in hematology, they had second language in common: Spanish.
Dr. Giralt said: “We both have a Spanish background and in a certain sense, there was an affinity there. ... We both have shared experiences.”
Dr. Perales was brought up in Belgium, a European nation with three official languages: French, Dutch, and German. He speaks five tongues in all and learned Spanish from his father, who came from Spain.
Fluency in Spanish enables both physicians to take care of the many New Yorkers who are more comfortable in that language – especially when navigating cancer treatment. However, both Dr. Giralt and Dr. Perales said that a second language is more than a professional tool. They described the enjoyable change of persona that happens when they switch to Spanish.
“People who are multilingual have different roles [as much as] different languages,” said Dr. Perales. “When I’m in Spanish, part of my brain is [thinking back to] summer vacations and hanging out with my cousins.”
When it comes to clinical science, however, English is the language of choice.
Global leaders in HSCT
Dr. Giralt and Dr. Perales are known worldwide in the field of allogeneic HSCT, a potentially curative treatment for an elongating list of both malignant and nonmalignant diseases.
In 1973, MSKCC conducted the first bone-marrow transplant from an unrelated donor. Fifty years on, medical oncologists in the United States conduct approximately 8,500 allogeneic transplants each year, 72% to treat acute leukemias or myelodysplastic syndrome (MDS).
However, stripping the immune system with intensive chemotherapy ‘conditioning,’ then rebuilding it with non-diseased donor hematopoietic cells is a hazardous undertaking. Older patients are less likely to survive the intensive conditioning, so historically have missed out. Also, even with a good human leukocyte antigen (HLA) match, the recipient needs often brutal immunosuppression.
Since Dr. Giralt and Dr. Perales began their partnership in 2010, the goals of their work have not changed: to develop safer, lower-intensity transplantation suitable for older, more vulnerable patients and reduce fearsome posttransplant sequelae such as graft-versus-host disease (GVHD).
Dr. Giralt’s publication list spans more than 600 peer-reviewed papers, articles and book chapters, almost exclusively on HSCT. Dr. Perales has more than 300 publication credits on the topic.
The two paired up on their first paper just months after Dr. Giralt arrived at MSKCC. That article, published in Biology of Blood and Marrow Transplantation, compared umbilical cord blood for HSCT with donor blood in 367 people with a variety of hematologic malignancies, including acute and chronic leukemias, MDS, and lymphoma.
The MSKCC team found that transplant-related mortality in the first 180 days was higher for the cord blood (21%), but thereafter mortality and relapse were much lower than for donated blood, with the result that 2-year progression-free survival of 55% was similar. Dr. Perales, Dr. Giralt and their coauthors concluded that the data provided “strong support” for further work on cord blood as an alternative stem-cell source.
During their first decade of collaboration, Dr. Giralt and Dr. Perales worked on any promising avenue that could improve outcomes and the experience of HSCT recipients, including reduced-intensity conditioning regimens to allow older adults to benefit from curative HSCT and donor T-cell depletion by CD34 selection, to reduce graft-versus-host disease (GVHD).
The CD34 protein is typically found on the surface of early stage and highly active stem cell types. Selecting these cell types using a range of techniques can eliminate many other potentially interfering or inactive cells. This enriches the transplant population with the most effective cells and can lower the risk of GVHD.
The 100th paper on which Dr. Giralt and Dr. Perales were coauthors was published in Blood Advances on July 27, 2021. The retrospective study examined the fate of 58 MSKCC patients with a rare form of chronic lymphocytic leukemia, CLL with Richter’s transformation (CLL-RT). It was the largest such study to date of this rare disease.
M.D. Anderson Cancer Center had shown in 2006 that, despite chemotherapy, overall survival in patients with CLL-RT was approximately 8 months. HSCT improved survival dramatically (75% at 3 years; n = 7). However, with the advent of novel targeted drugs for CLL such as ibrutinib (Imbruvica), venetoclax (Venclexta), or idelalisib (Zydelig), the MSKCC team asked themselves: What was the role of reduced-intensive conditioning HSCT? Was it even safe? Among other findings, Dr. Giralt and Dr. Perales’ 100th paper showed that reduced-intensity HSCT remained a viable alternative after a CLL-RT patient progressed on a novel agent.
Impact of the pandemic
When COVID-19 hit, the team lost many research staff and developed a huge backlog, said Dr. Giralt. He and Dr. Perales realized that they needed to be “thoughtful and careful” about which studies to continue. “For example, the CD-34 selection trials we did not close because these are our workhorse trials,” Dr. Giralt said. “We have people we need to treat, and some of the patients that we need to treat can only be treated on trial.”
The team was also able to pivot some of their work into COVID 19 itself, and they collected crucial information on HSCT in recovered COVID-19 patients, as an example.
“We were living through a critical time, but that doesn’t mean we [aren’t] obligated to continue our mission, our research mission,” said Dr. Giralt. “It really is team science. The way we look at it ... there’s a common thread: We both like to do allogeneic transplant, and we both believe in trying to make CD-34 selection better. So we’re both very much [working on] how can we improve what we call ‘the Memorial way’ of doing transplants. Where we separate is, Miguel does primarily lymphoma. He doesn’t do myeloma [like me]. So in those two areas, we’re helping develop the junior faculty in a different way.”
Something more in common
Right from the start, Dr. Perales and Dr. Giralt also shared a commitment to mentoring. Since 2010, Dr. Perales has mentored 22 up-and-coming junior faculty, including 10 from Europe (8 from Spain) and 2 from Latin America.
“[It makes] the research enterprise much more productive but [these young scientists] really increase the visibility of the program,” said Dr. Giralt.
He cited Dr. Perales’ track record of mentoring as one of the reasons for his promotion to chief of the adult bone marrow transplant service. In March 2020, Dr. Perales seamlessly stepped into Dr. Giralt’s shoes, while Dr. Giralt moved on to his present role as deputy division head of the division of hematologic malignancies.
Dr. Perales said: “The key aspect [of these promotions] is the fantastic working relationship that we’ve had over the years. ... I consider Sergio my mentor, but also a good friend and colleague. And so I think it’s this ability that we’ve had to work together and that relationship of trust, which has been key.”
“Sergio is somebody who lifts people up,” Dr. Perales added. “Many people will tell you that Sergio has helped them in their career. ... And I think that’s a lesson I’ve learned from him: training the next generation. And [that’s] not just in the U.S., but outside. I think that’s a key role that we have. And our responsibility.”
Asked to comment on their 100th-paper milestone, Dr. Perales firmly turned the spotlight from himself and Dr. Giralt to the junior investigators who have passed through the doors of the bone-marrow transplant program: “This body of work represents not just our collaboration but also the many contributions of our team at MSK ... and beyond MSK.”
This article was updated 1/26/22.
Peanut oral immunotherapy is safe and effective in toddlers in large placebo-controlled trial
In a large, blinded study of peanut-allergic toddlers published in The Lancet, 71% of treated participants could safely consume 5,000 mg of peanut protein – equivalent to nearly 17 peanuts – after 2½ years on oral immunotherapy. Even after stopping maintenance dosing for the next 6 months, more than 1 in 5 maintained that level of protection, and nearly 3 in 5 still met the 600-mg benchmark (about 2 peanuts) set by the phase 3 PALISADE trial of the FDA-approved peanut-flour product, Palforzia.
About 2% of children in the United States are allergic to peanuts, and most will not outgrow this allergy. In addition, other research suggests that the immune system is more malleable during early childhood.
Consistent with this idea, prior research showed that toddlers can succeed with peanut oral immunotherapy (OIT) – a regimen that builds tolerance through small amounts of the allergen consumed daily for months. However, that trial (DEVIL) was small, was conducted at a single site, and had no placebo group.
In contrast, the Peanut Oral Immunotherapy in Children Trial (IMPACT) enrolled 146 children aged 1-3 years at five academic medical centers in the United States – the first placebo-controlled study of OIT in this younger age group.
“This is a well done study,” Jaclyn Bjelac, MD, associate director of the Food Allergy Center of Excellence at the Cleveland Clinic, told this news organization. “We have seen improved outcomes in OIT, both in our own experience and other published studies, so while this is no surprise, the outcomes and large number of participants contribute to this being a really exciting publication.”
The trial was long and demanding for families. Toddlers who reacted to 500 mg or less of peanut protein in an entry food challenge were randomized in a 2:1 ratio to receive daily peanut flour or oat flour placebo. After initial dose escalation (from 0.1 mg to 6 mg) and biweekly buildup to a 2,000-mg target dose by week 30, participants continued with 20,00-mg daily maintenance dosing through week 134 – at which point they underwent a food challenge. They then went off treatment for 26 weeks and had another food challenge (week 160). In addition, participants came in for skin-prick and blood tests at baseline and at weeks 30, 82, 134, and 160.
In the placebo group, only 23 of 50 participants (46%) completed the study. “If you did 2½ years of this and then bombed the food challenge, you probably can guess that you were not on the real thing. And they were still asked to come back in 6 months and do it again. So, sure enough, a big chunk of those people chose not to continue, and you can’t blame them,” said Lancet co-author Edwin Kim, MD, in an interview. Dr. Kim directs the UNC Food Allergy Initiative at the University of North Carolina School of Medicine, Chapel Hill.
There was attrition in the treatment group as well. Among 96 children initially assigned to this arm, 68 (71%) passed the 5,000-mg peanut challenge at week 134 – but 11 withdrew in the study’s off-treatment phase. “It was a very tough decision. How much do you give toward science?” said Dr. Kim. “When push came to shove, some of the families couldn’t pull the trigger to potentially give up what they worked so hard for.”
In the intention-to-treat analysis, 20 of 96 treated participants (21%) could still tolerate 5,000 mg of peanut protein after going off therapy for 6 months. That translates to a 29% remission rate in the per-protocol subset (n = 70) who completed the study. Forty (57%) of these completers safely consumed at least 1,755 mg of peanut (cumulative dose). By comparison, the PALISADE trial of Palforzia used a 10,430-mg cumulative peanut dose to measure treatment efficacy.
On safety, 98% of treated participants – but also 80% of the placebo group – reported reactions, of which 35 were treated with epinephrine in 21 children receiving peanut OIT.
While some have noted that epinephrine use seemed high, Dr. Kim said, “we’re actually OK with that, because we’d much rather they overtreat and make sure that 1-year-old is safe than take any chances.” Overall, the safety profile looks similar to prior OIT studies of older children. “I think it suggests that, yeah, side effects will happen, [but] they’re all manageable, and people are not anaphylaxing left and right.”
On remission and immunologic parameters, benefits seemed stronger in the youngest subset (12 to 24 months), particularly those with lower peanut-specific IgE at baseline. These trends require further analyses, though, given the limited number of participants under 24 months.
Another noteworthy observation from longitudinal peanut-specific IgE trends in the placebo group: “Avoidance may not be benign,” Dr. Kim said. “If you look at their labs, they don’t stay flat. They actually go up.” The results jibe with the long-held idea of an early window of opportunity while a child’s immune system is maturing. “If you can grab this kid when his IgE is 10, versus next year when it might be 50, maybe you’ll get a different treatment effect,” Dr. Kim said. “We don’t know that for sure, but the placebo labs kind of point toward that.”
Beyond the science, there are practical advantages to starting OIT early. “Trying to convince a 9-year-old who’s been petrified of peanuts for their whole life to start doing this every day is not an easy task,” whereas with a 1- or 2-year-old, “you build it into their routine,” Dr. Kim said.
Plus, some say there’s no need for families to wait for regulatory approval of additional commercial products for very young children. Though some have advocated against the use of “grocery store” products, most peanut OIT research “has used the same 12% light roast defatted peanut flour used in IMPACT,” noted Marcus S. Shaker, MD, professor of pediatrics and of medicine at the Dartmouth Geisel School of Medicine and a physician at the Dartmouth-Hitchcock Medical Center, Lebanon, New Hampshire. The commercial product (Palforzia) and grocery-store products “come from the exact same source in the U.S.,” he said in an interview. “Both are an option for parents to consider, but a commercial product is not, nor has [it] ever been, a necessity.”
Dr. Bjelac reports no relevant financial relationships. Dr. Kim reports consultancy with Aimmune Therapeutics, Allako, AllerGenis, Belhaven Pharma, DBV Technologies, Duke Clinical Research Institute, and Nutricia; advisory board membership with ALK, DBV Technologies, Kenota Health, and Ukko; and grant support from the NIH’s National Institute of Allergy and Infectious Diseases, National Center for Complementary and Integrative Health and Immune Tolerance Network, Food Allergy Research and Education, and the Wallace Research Foundation. Dr. Shaker has participated in research funded by DBV, is cochair of the AAAAI/ACAAI Joint Task Force on Practice Parameters, is an associate editor at the Annals of Allergy, Asthma, and Immunology, and is an editorial board member of the Journal of Allergy and Clinical Immunology in Practice.
A version of this article first appeared on Medscape.com.
In a large, blinded study of peanut-allergic toddlers published in The Lancet, 71% of treated participants could safely consume 5,000 mg of peanut protein – equivalent to nearly 17 peanuts – after 2½ years on oral immunotherapy. Even after stopping maintenance dosing for the next 6 months, more than 1 in 5 maintained that level of protection, and nearly 3 in 5 still met the 600-mg benchmark (about 2 peanuts) set by the phase 3 PALISADE trial of the FDA-approved peanut-flour product, Palforzia.
About 2% of children in the United States are allergic to peanuts, and most will not outgrow this allergy. In addition, other research suggests that the immune system is more malleable during early childhood.
Consistent with this idea, prior research showed that toddlers can succeed with peanut oral immunotherapy (OIT) – a regimen that builds tolerance through small amounts of the allergen consumed daily for months. However, that trial (DEVIL) was small, was conducted at a single site, and had no placebo group.
In contrast, the Peanut Oral Immunotherapy in Children Trial (IMPACT) enrolled 146 children aged 1-3 years at five academic medical centers in the United States – the first placebo-controlled study of OIT in this younger age group.
“This is a well done study,” Jaclyn Bjelac, MD, associate director of the Food Allergy Center of Excellence at the Cleveland Clinic, told this news organization. “We have seen improved outcomes in OIT, both in our own experience and other published studies, so while this is no surprise, the outcomes and large number of participants contribute to this being a really exciting publication.”
The trial was long and demanding for families. Toddlers who reacted to 500 mg or less of peanut protein in an entry food challenge were randomized in a 2:1 ratio to receive daily peanut flour or oat flour placebo. After initial dose escalation (from 0.1 mg to 6 mg) and biweekly buildup to a 2,000-mg target dose by week 30, participants continued with 20,00-mg daily maintenance dosing through week 134 – at which point they underwent a food challenge. They then went off treatment for 26 weeks and had another food challenge (week 160). In addition, participants came in for skin-prick and blood tests at baseline and at weeks 30, 82, 134, and 160.
In the placebo group, only 23 of 50 participants (46%) completed the study. “If you did 2½ years of this and then bombed the food challenge, you probably can guess that you were not on the real thing. And they were still asked to come back in 6 months and do it again. So, sure enough, a big chunk of those people chose not to continue, and you can’t blame them,” said Lancet co-author Edwin Kim, MD, in an interview. Dr. Kim directs the UNC Food Allergy Initiative at the University of North Carolina School of Medicine, Chapel Hill.
There was attrition in the treatment group as well. Among 96 children initially assigned to this arm, 68 (71%) passed the 5,000-mg peanut challenge at week 134 – but 11 withdrew in the study’s off-treatment phase. “It was a very tough decision. How much do you give toward science?” said Dr. Kim. “When push came to shove, some of the families couldn’t pull the trigger to potentially give up what they worked so hard for.”
In the intention-to-treat analysis, 20 of 96 treated participants (21%) could still tolerate 5,000 mg of peanut protein after going off therapy for 6 months. That translates to a 29% remission rate in the per-protocol subset (n = 70) who completed the study. Forty (57%) of these completers safely consumed at least 1,755 mg of peanut (cumulative dose). By comparison, the PALISADE trial of Palforzia used a 10,430-mg cumulative peanut dose to measure treatment efficacy.
On safety, 98% of treated participants – but also 80% of the placebo group – reported reactions, of which 35 were treated with epinephrine in 21 children receiving peanut OIT.
While some have noted that epinephrine use seemed high, Dr. Kim said, “we’re actually OK with that, because we’d much rather they overtreat and make sure that 1-year-old is safe than take any chances.” Overall, the safety profile looks similar to prior OIT studies of older children. “I think it suggests that, yeah, side effects will happen, [but] they’re all manageable, and people are not anaphylaxing left and right.”
On remission and immunologic parameters, benefits seemed stronger in the youngest subset (12 to 24 months), particularly those with lower peanut-specific IgE at baseline. These trends require further analyses, though, given the limited number of participants under 24 months.
Another noteworthy observation from longitudinal peanut-specific IgE trends in the placebo group: “Avoidance may not be benign,” Dr. Kim said. “If you look at their labs, they don’t stay flat. They actually go up.” The results jibe with the long-held idea of an early window of opportunity while a child’s immune system is maturing. “If you can grab this kid when his IgE is 10, versus next year when it might be 50, maybe you’ll get a different treatment effect,” Dr. Kim said. “We don’t know that for sure, but the placebo labs kind of point toward that.”
Beyond the science, there are practical advantages to starting OIT early. “Trying to convince a 9-year-old who’s been petrified of peanuts for their whole life to start doing this every day is not an easy task,” whereas with a 1- or 2-year-old, “you build it into their routine,” Dr. Kim said.
Plus, some say there’s no need for families to wait for regulatory approval of additional commercial products for very young children. Though some have advocated against the use of “grocery store” products, most peanut OIT research “has used the same 12% light roast defatted peanut flour used in IMPACT,” noted Marcus S. Shaker, MD, professor of pediatrics and of medicine at the Dartmouth Geisel School of Medicine and a physician at the Dartmouth-Hitchcock Medical Center, Lebanon, New Hampshire. The commercial product (Palforzia) and grocery-store products “come from the exact same source in the U.S.,” he said in an interview. “Both are an option for parents to consider, but a commercial product is not, nor has [it] ever been, a necessity.”
Dr. Bjelac reports no relevant financial relationships. Dr. Kim reports consultancy with Aimmune Therapeutics, Allako, AllerGenis, Belhaven Pharma, DBV Technologies, Duke Clinical Research Institute, and Nutricia; advisory board membership with ALK, DBV Technologies, Kenota Health, and Ukko; and grant support from the NIH’s National Institute of Allergy and Infectious Diseases, National Center for Complementary and Integrative Health and Immune Tolerance Network, Food Allergy Research and Education, and the Wallace Research Foundation. Dr. Shaker has participated in research funded by DBV, is cochair of the AAAAI/ACAAI Joint Task Force on Practice Parameters, is an associate editor at the Annals of Allergy, Asthma, and Immunology, and is an editorial board member of the Journal of Allergy and Clinical Immunology in Practice.
A version of this article first appeared on Medscape.com.
In a large, blinded study of peanut-allergic toddlers published in The Lancet, 71% of treated participants could safely consume 5,000 mg of peanut protein – equivalent to nearly 17 peanuts – after 2½ years on oral immunotherapy. Even after stopping maintenance dosing for the next 6 months, more than 1 in 5 maintained that level of protection, and nearly 3 in 5 still met the 600-mg benchmark (about 2 peanuts) set by the phase 3 PALISADE trial of the FDA-approved peanut-flour product, Palforzia.
About 2% of children in the United States are allergic to peanuts, and most will not outgrow this allergy. In addition, other research suggests that the immune system is more malleable during early childhood.
Consistent with this idea, prior research showed that toddlers can succeed with peanut oral immunotherapy (OIT) – a regimen that builds tolerance through small amounts of the allergen consumed daily for months. However, that trial (DEVIL) was small, was conducted at a single site, and had no placebo group.
In contrast, the Peanut Oral Immunotherapy in Children Trial (IMPACT) enrolled 146 children aged 1-3 years at five academic medical centers in the United States – the first placebo-controlled study of OIT in this younger age group.
“This is a well done study,” Jaclyn Bjelac, MD, associate director of the Food Allergy Center of Excellence at the Cleveland Clinic, told this news organization. “We have seen improved outcomes in OIT, both in our own experience and other published studies, so while this is no surprise, the outcomes and large number of participants contribute to this being a really exciting publication.”
The trial was long and demanding for families. Toddlers who reacted to 500 mg or less of peanut protein in an entry food challenge were randomized in a 2:1 ratio to receive daily peanut flour or oat flour placebo. After initial dose escalation (from 0.1 mg to 6 mg) and biweekly buildup to a 2,000-mg target dose by week 30, participants continued with 20,00-mg daily maintenance dosing through week 134 – at which point they underwent a food challenge. They then went off treatment for 26 weeks and had another food challenge (week 160). In addition, participants came in for skin-prick and blood tests at baseline and at weeks 30, 82, 134, and 160.
In the placebo group, only 23 of 50 participants (46%) completed the study. “If you did 2½ years of this and then bombed the food challenge, you probably can guess that you were not on the real thing. And they were still asked to come back in 6 months and do it again. So, sure enough, a big chunk of those people chose not to continue, and you can’t blame them,” said Lancet co-author Edwin Kim, MD, in an interview. Dr. Kim directs the UNC Food Allergy Initiative at the University of North Carolina School of Medicine, Chapel Hill.
There was attrition in the treatment group as well. Among 96 children initially assigned to this arm, 68 (71%) passed the 5,000-mg peanut challenge at week 134 – but 11 withdrew in the study’s off-treatment phase. “It was a very tough decision. How much do you give toward science?” said Dr. Kim. “When push came to shove, some of the families couldn’t pull the trigger to potentially give up what they worked so hard for.”
In the intention-to-treat analysis, 20 of 96 treated participants (21%) could still tolerate 5,000 mg of peanut protein after going off therapy for 6 months. That translates to a 29% remission rate in the per-protocol subset (n = 70) who completed the study. Forty (57%) of these completers safely consumed at least 1,755 mg of peanut (cumulative dose). By comparison, the PALISADE trial of Palforzia used a 10,430-mg cumulative peanut dose to measure treatment efficacy.
On safety, 98% of treated participants – but also 80% of the placebo group – reported reactions, of which 35 were treated with epinephrine in 21 children receiving peanut OIT.
While some have noted that epinephrine use seemed high, Dr. Kim said, “we’re actually OK with that, because we’d much rather they overtreat and make sure that 1-year-old is safe than take any chances.” Overall, the safety profile looks similar to prior OIT studies of older children. “I think it suggests that, yeah, side effects will happen, [but] they’re all manageable, and people are not anaphylaxing left and right.”
On remission and immunologic parameters, benefits seemed stronger in the youngest subset (12 to 24 months), particularly those with lower peanut-specific IgE at baseline. These trends require further analyses, though, given the limited number of participants under 24 months.
Another noteworthy observation from longitudinal peanut-specific IgE trends in the placebo group: “Avoidance may not be benign,” Dr. Kim said. “If you look at their labs, they don’t stay flat. They actually go up.” The results jibe with the long-held idea of an early window of opportunity while a child’s immune system is maturing. “If you can grab this kid when his IgE is 10, versus next year when it might be 50, maybe you’ll get a different treatment effect,” Dr. Kim said. “We don’t know that for sure, but the placebo labs kind of point toward that.”
Beyond the science, there are practical advantages to starting OIT early. “Trying to convince a 9-year-old who’s been petrified of peanuts for their whole life to start doing this every day is not an easy task,” whereas with a 1- or 2-year-old, “you build it into their routine,” Dr. Kim said.
Plus, some say there’s no need for families to wait for regulatory approval of additional commercial products for very young children. Though some have advocated against the use of “grocery store” products, most peanut OIT research “has used the same 12% light roast defatted peanut flour used in IMPACT,” noted Marcus S. Shaker, MD, professor of pediatrics and of medicine at the Dartmouth Geisel School of Medicine and a physician at the Dartmouth-Hitchcock Medical Center, Lebanon, New Hampshire. The commercial product (Palforzia) and grocery-store products “come from the exact same source in the U.S.,” he said in an interview. “Both are an option for parents to consider, but a commercial product is not, nor has [it] ever been, a necessity.”
Dr. Bjelac reports no relevant financial relationships. Dr. Kim reports consultancy with Aimmune Therapeutics, Allako, AllerGenis, Belhaven Pharma, DBV Technologies, Duke Clinical Research Institute, and Nutricia; advisory board membership with ALK, DBV Technologies, Kenota Health, and Ukko; and grant support from the NIH’s National Institute of Allergy and Infectious Diseases, National Center for Complementary and Integrative Health and Immune Tolerance Network, Food Allergy Research and Education, and the Wallace Research Foundation. Dr. Shaker has participated in research funded by DBV, is cochair of the AAAAI/ACAAI Joint Task Force on Practice Parameters, is an associate editor at the Annals of Allergy, Asthma, and Immunology, and is an editorial board member of the Journal of Allergy and Clinical Immunology in Practice.
A version of this article first appeared on Medscape.com.
Things reproductive psychiatrists might ‘always’ or ‘never’ do in 2022
The experience of practicing reproductive psychiatry in the context of the pandemic has highlighted unique situations I’ve written about in previous columns that have affected pregnant and postpartum women during the pandemic, such as the management of anxiety and insomnia.
The pandemic has also seen a shift to telemedicine and an opportunity to use virtual platforms to engage with colleagues in our subspecialty across the country. These forums of engagement, which we realize virtually with so many of our colleagues, has prompted me to refine and galvanize what I consider to be some principles that guide frequently encountered clinical scenarios in reproductive psychiatry.
To open 2022, I wanted to revisit the practices I nearly “always” (or conversely, “never”) follow as a reproductive psychiatrist across the numerous clinical situations and variations on the associated clinical themes encountered as we see patients during pregnancy and the postpartum period.
Things we ‘always’ do
1. I continue to make maternal euthymia the North Star of treatment before, during, and after pregnancy.
Before pregnancy, maternal euthymia may be realized through optimization of pharmacologic and nonpharmacologic treatments and waiting to conceive until patients are emotionally well. Sustaining euthymia during pregnancy is a critical issue because of the extent to which euthymia during pregnancy predicts postpartum course. According to many studies, postpartum euthymia is the strongest predictor of long-term neurobehavioral outcome and risk for later child psychopathology. At the end of the day, there are few things I would not do with respect to treatment of maternal psychiatric disorder if the upside afforded maternal euthymia.
2. I almost always treat with consistency of medication across the peripartum period.
Although there have been discussions about the wisdom of changing medications, such as antidepressants, benzodiazepines, and mood stabilizers, that have afforded euthymia during pregnancy as patients approach their delivery date, the evidence base supporting switching medications at that time is exceedingly sparse. The time to adjust or to modify is typically not just prior to delivery unless it is to prevent postpartum psychiatric disorder (see below).
3. I simplify regimens before pregnancy if it’s unclear which medications have afforded patients euthymia.
We have a growing appreciation that polypharmacy is the rule in treatment of affective disorder for both unipolar and bipolar illness. Consultation before pregnancy is the ideal time to take a particularly careful history and think about simplifying regimens where adding medicines hasn’t clearly provided enhanced clinical benefit to the patient.
4. When making a treatment plan for psychiatric disorder during pregnancy, I consider the impact of untreated psychiatric disorder (even if not absolutely quantifiable) on fetal, neonatal, and maternal well-being.
Perhaps now more than even 5-10 years ago, we have better data describing the adverse effects of untreated psychiatric illness on fetal, neonatal, and maternal well-being.
We always try to deliberately consider the effect of a specific treatment on fetal well-being. Less attention (and science) has focused on the effect on pregnancy of deferring treatment; historically, this has not been adequately quantified in the risk-benefit decision. Yet, there is growing evidence of the increased adverse effects of activating the stress axis on everything from intrauterine fetal programming in the brain to effects on obstetrical outcomes such as preterm labor and delivery.
5. I appreciate the value of postpartum prophylaxis for pregnant women with bipolar disorder to mitigate risk of relapse.
We have spoken over the last 20 months of the pandemic, particularly in reproductive psychiatry circles, about the importance of keeping reproductive-age women with bipolar disorder emotionally well as they plan to conceive, during pregnancy, and in the postpartum period. The management of bipolar disorder during this time can be a humbling experience. Clinical roughening can be quick and severe, and so we do everything that we can for these women.
The area in which we have the strongest evidence base for mitigating risk with bipolar women is the value of postpartum prophylaxis during the peripartum period, regardless of what patients have done with their mood-stabilizing medications during pregnancy. Given the risk for postpartum disease, even though there are varying amounts of evidence on prophylactic benefit of specific mood stabilizers (i.e., lithium vs. atypical antipsychotics), the value of prophylaxis against worsening of bipolar disorder postpartum is widely accepted.
The importance of this has been particularly underscored during the pandemic where postpartum support, although available, has been more tenuous given the fluctuations in COVID-19 status around the country. The availability of friends and loved ones as support during the postpartum period has become less reliable in certain circumstances during the pandemic. In some cases, COVID-19 surges have wreaked havoc on travel plans and support persons have contracted the virus, rendering on-site support nonviable given safety concerns. Last-minute shifts of support plans have been responsible for disruption of care plans for new moms and by extension, have affected the ability to protect the sleep of bipolar women, which is critical. Keeping bipolar women well during the postpartum period with plans and backup plans for management remains critical.
Things we ‘never’ do
1. I never taper antidepressants (just prior to delivery), I never check plasma levels of selective serotonin reuptake inhibitors (across pregnancy, or just prior to labor and delivery), and I never use sodium valproate (during pregnancy).
Although there has been some discussion about the potential to mitigate risk for maternal or neonatal toxicity with lowering of agents such as lithium or lamotrigine during pregnancy, I do not routinely check plasma levels or arbitrarily change the dose of antidepressants, lithium, or lamotrigine during pregnancy in the absence of clinical symptoms.
We know full well that plasma levels of medications decline during pregnancy because of hemodilution with lithium and antidepressants and, in the case of lamotrigine, the effects of rising estrogen concentration during pregnancy on the metabolism of lamotrigine. While several studies have shown the decrease of SSRI concentration during pregnancy absent a change in dose of medication, these data have not correlated changes in plasma concentration of SSRI with a frank change in clinical status across pregnancy. Unlike what we see in conditions like epilepsy, where doses are increased to maintain therapeutic plasma levels to mitigate risk for seizure, those therapeutic plasma levels do not clearly exist for the psychiatric medications most widely used to treat psychiatric disorders.
We also almost never use sodium valproate in reproductive-age women despite its efficacy in both the acute and maintenance treatment of bipolar disorder given the risk of both major malformations associated with first-trimester fetal exposure to valproate and the data suggesting longer-term adverse neurobehavioral effects associated with its use during pregnancy.
2. We never suggest patients defer pregnancy based on their underlying psychiatric disorder.
Our role is to provide the best information regarding reproductive safety of psychiatric medications and risks of untreated psychiatric disorder to patients as they and relevant parties weigh the risks of pursuing one treatment or another. Those are private choices, and women and their partners make private decisions applying their own calculus with respect to moving forward with plans to conceive.
3. We never switch antidepressants once a woman has become pregnant.
Although we continue to see patients switched to older SSRIs such as sertraline with documentation of pregnancy, a patient’s road to getting well is sometimes very lengthy. In the absence of indicting reproductive safety data for any particular antidepressant, for patients who have gotten well on an antidepressant, even one for which we have less information, we stay the course and do not switch arbitrarily to an older SSRI for which we may have more reproductive safety data.
If we have the luxury prior to pregnancy to switch a patient to an untried and better studied antidepressant with more data supporting safety, we do so. But this is rarely the case. More often, we see women presenting with a newly documented pregnancy (frequently unplanned, with half of pregnancies across the country still being unplanned across sociodemographic lines) on an antidepressant with varying amounts of reproductive safety information available for the medicine being taken, and frequently after failed previous trials of other antidepressants. In this scenario, we rarely see the time of a newly documented pregnancy as an opportunity to pursue a new trial of an antidepressant without known efficacy for that patient; we stay the course and hope for sustained euthymia on the drug which has afforded euthymia to date.
Final thoughts
Dos and don’ts are relative in reproductive psychiatry. We tend to apply available data and clinical experience as we guide patients on a case-by-case basis, considering the most currently available rigorous reproductive safety data, as well as the individual patient’s clinical status and her personal wishes.
Dr. Cohen is the director of the Ammon-Pinizzotto Center for Women’s Mental Health at Massachusetts General Hospital (MGH) in Boston, which provides information resources and conducts clinical care and research in reproductive mental health. He has been a consultant to manufacturers of psychiatric medications. Email Dr. Cohen at [email protected].
The experience of practicing reproductive psychiatry in the context of the pandemic has highlighted unique situations I’ve written about in previous columns that have affected pregnant and postpartum women during the pandemic, such as the management of anxiety and insomnia.
The pandemic has also seen a shift to telemedicine and an opportunity to use virtual platforms to engage with colleagues in our subspecialty across the country. These forums of engagement, which we realize virtually with so many of our colleagues, has prompted me to refine and galvanize what I consider to be some principles that guide frequently encountered clinical scenarios in reproductive psychiatry.
To open 2022, I wanted to revisit the practices I nearly “always” (or conversely, “never”) follow as a reproductive psychiatrist across the numerous clinical situations and variations on the associated clinical themes encountered as we see patients during pregnancy and the postpartum period.
Things we ‘always’ do
1. I continue to make maternal euthymia the North Star of treatment before, during, and after pregnancy.
Before pregnancy, maternal euthymia may be realized through optimization of pharmacologic and nonpharmacologic treatments and waiting to conceive until patients are emotionally well. Sustaining euthymia during pregnancy is a critical issue because of the extent to which euthymia during pregnancy predicts postpartum course. According to many studies, postpartum euthymia is the strongest predictor of long-term neurobehavioral outcome and risk for later child psychopathology. At the end of the day, there are few things I would not do with respect to treatment of maternal psychiatric disorder if the upside afforded maternal euthymia.
2. I almost always treat with consistency of medication across the peripartum period.
Although there have been discussions about the wisdom of changing medications, such as antidepressants, benzodiazepines, and mood stabilizers, that have afforded euthymia during pregnancy as patients approach their delivery date, the evidence base supporting switching medications at that time is exceedingly sparse. The time to adjust or to modify is typically not just prior to delivery unless it is to prevent postpartum psychiatric disorder (see below).
3. I simplify regimens before pregnancy if it’s unclear which medications have afforded patients euthymia.
We have a growing appreciation that polypharmacy is the rule in treatment of affective disorder for both unipolar and bipolar illness. Consultation before pregnancy is the ideal time to take a particularly careful history and think about simplifying regimens where adding medicines hasn’t clearly provided enhanced clinical benefit to the patient.
4. When making a treatment plan for psychiatric disorder during pregnancy, I consider the impact of untreated psychiatric disorder (even if not absolutely quantifiable) on fetal, neonatal, and maternal well-being.
Perhaps now more than even 5-10 years ago, we have better data describing the adverse effects of untreated psychiatric illness on fetal, neonatal, and maternal well-being.
We always try to deliberately consider the effect of a specific treatment on fetal well-being. Less attention (and science) has focused on the effect on pregnancy of deferring treatment; historically, this has not been adequately quantified in the risk-benefit decision. Yet, there is growing evidence of the increased adverse effects of activating the stress axis on everything from intrauterine fetal programming in the brain to effects on obstetrical outcomes such as preterm labor and delivery.
5. I appreciate the value of postpartum prophylaxis for pregnant women with bipolar disorder to mitigate risk of relapse.
We have spoken over the last 20 months of the pandemic, particularly in reproductive psychiatry circles, about the importance of keeping reproductive-age women with bipolar disorder emotionally well as they plan to conceive, during pregnancy, and in the postpartum period. The management of bipolar disorder during this time can be a humbling experience. Clinical roughening can be quick and severe, and so we do everything that we can for these women.
The area in which we have the strongest evidence base for mitigating risk with bipolar women is the value of postpartum prophylaxis during the peripartum period, regardless of what patients have done with their mood-stabilizing medications during pregnancy. Given the risk for postpartum disease, even though there are varying amounts of evidence on prophylactic benefit of specific mood stabilizers (i.e., lithium vs. atypical antipsychotics), the value of prophylaxis against worsening of bipolar disorder postpartum is widely accepted.
The importance of this has been particularly underscored during the pandemic where postpartum support, although available, has been more tenuous given the fluctuations in COVID-19 status around the country. The availability of friends and loved ones as support during the postpartum period has become less reliable in certain circumstances during the pandemic. In some cases, COVID-19 surges have wreaked havoc on travel plans and support persons have contracted the virus, rendering on-site support nonviable given safety concerns. Last-minute shifts of support plans have been responsible for disruption of care plans for new moms and by extension, have affected the ability to protect the sleep of bipolar women, which is critical. Keeping bipolar women well during the postpartum period with plans and backup plans for management remains critical.
Things we ‘never’ do
1. I never taper antidepressants (just prior to delivery), I never check plasma levels of selective serotonin reuptake inhibitors (across pregnancy, or just prior to labor and delivery), and I never use sodium valproate (during pregnancy).
Although there has been some discussion about the potential to mitigate risk for maternal or neonatal toxicity with lowering of agents such as lithium or lamotrigine during pregnancy, I do not routinely check plasma levels or arbitrarily change the dose of antidepressants, lithium, or lamotrigine during pregnancy in the absence of clinical symptoms.
We know full well that plasma levels of medications decline during pregnancy because of hemodilution with lithium and antidepressants and, in the case of lamotrigine, the effects of rising estrogen concentration during pregnancy on the metabolism of lamotrigine. While several studies have shown the decrease of SSRI concentration during pregnancy absent a change in dose of medication, these data have not correlated changes in plasma concentration of SSRI with a frank change in clinical status across pregnancy. Unlike what we see in conditions like epilepsy, where doses are increased to maintain therapeutic plasma levels to mitigate risk for seizure, those therapeutic plasma levels do not clearly exist for the psychiatric medications most widely used to treat psychiatric disorders.
We also almost never use sodium valproate in reproductive-age women despite its efficacy in both the acute and maintenance treatment of bipolar disorder given the risk of both major malformations associated with first-trimester fetal exposure to valproate and the data suggesting longer-term adverse neurobehavioral effects associated with its use during pregnancy.
2. We never suggest patients defer pregnancy based on their underlying psychiatric disorder.
Our role is to provide the best information regarding reproductive safety of psychiatric medications and risks of untreated psychiatric disorder to patients as they and relevant parties weigh the risks of pursuing one treatment or another. Those are private choices, and women and their partners make private decisions applying their own calculus with respect to moving forward with plans to conceive.
3. We never switch antidepressants once a woman has become pregnant.
Although we continue to see patients switched to older SSRIs such as sertraline with documentation of pregnancy, a patient’s road to getting well is sometimes very lengthy. In the absence of indicting reproductive safety data for any particular antidepressant, for patients who have gotten well on an antidepressant, even one for which we have less information, we stay the course and do not switch arbitrarily to an older SSRI for which we may have more reproductive safety data.
If we have the luxury prior to pregnancy to switch a patient to an untried and better studied antidepressant with more data supporting safety, we do so. But this is rarely the case. More often, we see women presenting with a newly documented pregnancy (frequently unplanned, with half of pregnancies across the country still being unplanned across sociodemographic lines) on an antidepressant with varying amounts of reproductive safety information available for the medicine being taken, and frequently after failed previous trials of other antidepressants. In this scenario, we rarely see the time of a newly documented pregnancy as an opportunity to pursue a new trial of an antidepressant without known efficacy for that patient; we stay the course and hope for sustained euthymia on the drug which has afforded euthymia to date.
Final thoughts
Dos and don’ts are relative in reproductive psychiatry. We tend to apply available data and clinical experience as we guide patients on a case-by-case basis, considering the most currently available rigorous reproductive safety data, as well as the individual patient’s clinical status and her personal wishes.
Dr. Cohen is the director of the Ammon-Pinizzotto Center for Women’s Mental Health at Massachusetts General Hospital (MGH) in Boston, which provides information resources and conducts clinical care and research in reproductive mental health. He has been a consultant to manufacturers of psychiatric medications. Email Dr. Cohen at [email protected].
The experience of practicing reproductive psychiatry in the context of the pandemic has highlighted unique situations I’ve written about in previous columns that have affected pregnant and postpartum women during the pandemic, such as the management of anxiety and insomnia.
The pandemic has also seen a shift to telemedicine and an opportunity to use virtual platforms to engage with colleagues in our subspecialty across the country. These forums of engagement, which we realize virtually with so many of our colleagues, has prompted me to refine and galvanize what I consider to be some principles that guide frequently encountered clinical scenarios in reproductive psychiatry.
To open 2022, I wanted to revisit the practices I nearly “always” (or conversely, “never”) follow as a reproductive psychiatrist across the numerous clinical situations and variations on the associated clinical themes encountered as we see patients during pregnancy and the postpartum period.
Things we ‘always’ do
1. I continue to make maternal euthymia the North Star of treatment before, during, and after pregnancy.
Before pregnancy, maternal euthymia may be realized through optimization of pharmacologic and nonpharmacologic treatments and waiting to conceive until patients are emotionally well. Sustaining euthymia during pregnancy is a critical issue because of the extent to which euthymia during pregnancy predicts postpartum course. According to many studies, postpartum euthymia is the strongest predictor of long-term neurobehavioral outcome and risk for later child psychopathology. At the end of the day, there are few things I would not do with respect to treatment of maternal psychiatric disorder if the upside afforded maternal euthymia.
2. I almost always treat with consistency of medication across the peripartum period.
Although there have been discussions about the wisdom of changing medications, such as antidepressants, benzodiazepines, and mood stabilizers, that have afforded euthymia during pregnancy as patients approach their delivery date, the evidence base supporting switching medications at that time is exceedingly sparse. The time to adjust or to modify is typically not just prior to delivery unless it is to prevent postpartum psychiatric disorder (see below).
3. I simplify regimens before pregnancy if it’s unclear which medications have afforded patients euthymia.
We have a growing appreciation that polypharmacy is the rule in treatment of affective disorder for both unipolar and bipolar illness. Consultation before pregnancy is the ideal time to take a particularly careful history and think about simplifying regimens where adding medicines hasn’t clearly provided enhanced clinical benefit to the patient.
4. When making a treatment plan for psychiatric disorder during pregnancy, I consider the impact of untreated psychiatric disorder (even if not absolutely quantifiable) on fetal, neonatal, and maternal well-being.
Perhaps now more than even 5-10 years ago, we have better data describing the adverse effects of untreated psychiatric illness on fetal, neonatal, and maternal well-being.
We always try to deliberately consider the effect of a specific treatment on fetal well-being. Less attention (and science) has focused on the effect on pregnancy of deferring treatment; historically, this has not been adequately quantified in the risk-benefit decision. Yet, there is growing evidence of the increased adverse effects of activating the stress axis on everything from intrauterine fetal programming in the brain to effects on obstetrical outcomes such as preterm labor and delivery.
5. I appreciate the value of postpartum prophylaxis for pregnant women with bipolar disorder to mitigate risk of relapse.
We have spoken over the last 20 months of the pandemic, particularly in reproductive psychiatry circles, about the importance of keeping reproductive-age women with bipolar disorder emotionally well as they plan to conceive, during pregnancy, and in the postpartum period. The management of bipolar disorder during this time can be a humbling experience. Clinical roughening can be quick and severe, and so we do everything that we can for these women.
The area in which we have the strongest evidence base for mitigating risk with bipolar women is the value of postpartum prophylaxis during the peripartum period, regardless of what patients have done with their mood-stabilizing medications during pregnancy. Given the risk for postpartum disease, even though there are varying amounts of evidence on prophylactic benefit of specific mood stabilizers (i.e., lithium vs. atypical antipsychotics), the value of prophylaxis against worsening of bipolar disorder postpartum is widely accepted.
The importance of this has been particularly underscored during the pandemic where postpartum support, although available, has been more tenuous given the fluctuations in COVID-19 status around the country. The availability of friends and loved ones as support during the postpartum period has become less reliable in certain circumstances during the pandemic. In some cases, COVID-19 surges have wreaked havoc on travel plans and support persons have contracted the virus, rendering on-site support nonviable given safety concerns. Last-minute shifts of support plans have been responsible for disruption of care plans for new moms and by extension, have affected the ability to protect the sleep of bipolar women, which is critical. Keeping bipolar women well during the postpartum period with plans and backup plans for management remains critical.
Things we ‘never’ do
1. I never taper antidepressants (just prior to delivery), I never check plasma levels of selective serotonin reuptake inhibitors (across pregnancy, or just prior to labor and delivery), and I never use sodium valproate (during pregnancy).
Although there has been some discussion about the potential to mitigate risk for maternal or neonatal toxicity with lowering of agents such as lithium or lamotrigine during pregnancy, I do not routinely check plasma levels or arbitrarily change the dose of antidepressants, lithium, or lamotrigine during pregnancy in the absence of clinical symptoms.
We know full well that plasma levels of medications decline during pregnancy because of hemodilution with lithium and antidepressants and, in the case of lamotrigine, the effects of rising estrogen concentration during pregnancy on the metabolism of lamotrigine. While several studies have shown the decrease of SSRI concentration during pregnancy absent a change in dose of medication, these data have not correlated changes in plasma concentration of SSRI with a frank change in clinical status across pregnancy. Unlike what we see in conditions like epilepsy, where doses are increased to maintain therapeutic plasma levels to mitigate risk for seizure, those therapeutic plasma levels do not clearly exist for the psychiatric medications most widely used to treat psychiatric disorders.
We also almost never use sodium valproate in reproductive-age women despite its efficacy in both the acute and maintenance treatment of bipolar disorder given the risk of both major malformations associated with first-trimester fetal exposure to valproate and the data suggesting longer-term adverse neurobehavioral effects associated with its use during pregnancy.
2. We never suggest patients defer pregnancy based on their underlying psychiatric disorder.
Our role is to provide the best information regarding reproductive safety of psychiatric medications and risks of untreated psychiatric disorder to patients as they and relevant parties weigh the risks of pursuing one treatment or another. Those are private choices, and women and their partners make private decisions applying their own calculus with respect to moving forward with plans to conceive.
3. We never switch antidepressants once a woman has become pregnant.
Although we continue to see patients switched to older SSRIs such as sertraline with documentation of pregnancy, a patient’s road to getting well is sometimes very lengthy. In the absence of indicting reproductive safety data for any particular antidepressant, for patients who have gotten well on an antidepressant, even one for which we have less information, we stay the course and do not switch arbitrarily to an older SSRI for which we may have more reproductive safety data.
If we have the luxury prior to pregnancy to switch a patient to an untried and better studied antidepressant with more data supporting safety, we do so. But this is rarely the case. More often, we see women presenting with a newly documented pregnancy (frequently unplanned, with half of pregnancies across the country still being unplanned across sociodemographic lines) on an antidepressant with varying amounts of reproductive safety information available for the medicine being taken, and frequently after failed previous trials of other antidepressants. In this scenario, we rarely see the time of a newly documented pregnancy as an opportunity to pursue a new trial of an antidepressant without known efficacy for that patient; we stay the course and hope for sustained euthymia on the drug which has afforded euthymia to date.
Final thoughts
Dos and don’ts are relative in reproductive psychiatry. We tend to apply available data and clinical experience as we guide patients on a case-by-case basis, considering the most currently available rigorous reproductive safety data, as well as the individual patient’s clinical status and her personal wishes.
Dr. Cohen is the director of the Ammon-Pinizzotto Center for Women’s Mental Health at Massachusetts General Hospital (MGH) in Boston, which provides information resources and conducts clinical care and research in reproductive mental health. He has been a consultant to manufacturers of psychiatric medications. Email Dr. Cohen at [email protected].
Survey shows more women drinking during pregnancy
More pregnant Americans indulged – and overindulged – in alcohol from 2018 to 2020 than in previous years, but researchers found no sharp increase associated with the first wave of COVID-19 lockdowns, according to a new report from the Centers for Disease Control and Prevention.
The pandemic notwithstanding, health officials worry about a rising tide of pregnant women using alcohol and binge drinking since the CDC survey began in 2011. In the period ending in 2013, 1 in 10 women reported having had a drink in the previous 30 days; by 2017, that figure was 1 in 9; and in the latest survey, the number had risen to 1 in 7.
That mark is “the highest to date,” said Lucas Gosdin, PhD, MPH, an epidemic intelligence officer at the CDC’s National Center on Birth Defects and Developmental Disabilities, Atlanta, and first author of the report, which was published in Morbidity and Mortality Weekly Report.
“We’re concerned that this number has been slowly increasing,” Amanda Cohn, MD, director of the CDC’s Division of Birth Defects and Infant Disorders, told this news organization. “We need to be doing more outreach, both to pregnant persons as well as health care providers who are caring for them.”
Exposure to alcohol in the womb has been linked to a wide range of neurologic and physical problems in children, ranging from fetal alcohol syndrome to stunted learning abilities. Even if these problems are unlikely, experts insist there’s no known “safe” amount of alcohol a pregnant woman can have.
Dr. Cohn likened alcohol use to that of tobacco. “Lots of people smoke who don’t get lung cancer. Still, everyone is at an increased risk,” she said. “The safest way to not get lung cancer is to not smoke at all. It’s a behavior that can prevent additional harm.”
The report summarizes the results of a phone survey of 6,327 pregnant Americans between the ages of 18 and 49. The survey asked whether women had consumed an alcoholic beverage or had at least four drinks on one occasion – a common definition of binge drinking – in the past 30 days.
According to the report, 13.5% of women reported using alcohol, and 5.2% said they had binged on alcohol. Women who experienced frequent mental distress – describing their mental health as “not good” for 14 or more days in the past month – were twice as likely to drink and three times likelier to binge drink, the researchers found.
The increase within the 3-year period was roughly the same as in previous surveys.
“There was no evidence of increased alcohol consumption by pregnant adults in 2020 relative to 2019, despite possible increased alcohol sales and consumption among the general population during the first months of the COVID-19 pandemic,” the report states.
“That is one finding that was unexpected but that we were pleased to see,” Dr. Gosdin said.
Experts stressed that the survey covered only the first 9 months of the COVID-19 pandemic. “We’re still in the depths of it,” Samuel T. Bauer, MD, associate professor of obstetrics and gynecology at Duke University Medical Center, Durham, N.C., told this news organization. “People with alcohol use disorders certainly have been challenged during COVID. I think this is a preliminary answer.”
Dr. Gosdin said the effects of the pandemic on drinking habits bear watching. “We are concerned about the impacts of COVID-19,” he said. “We know it’s affected how people access regular care.”
Although virtual care has “exploded during COVID,” Dr. Bauer said, insurers have “turned off reimbursing” for doctor-patient visits via telephone, but not for visits by Internet-based video platforms like Zoom.
That split creates equity issues in many parts of the country, including his home state of North Carolina, where broadband is scarce, and patients may live 100 miles or more away from caregivers.
The “full-blown birth defect” of fetal alcohol syndrome is just the most visible hazard of drinking. Other medical and developmental issues include speech delays, slower learning and reading skills, attention-deficit and hyperactivity disorders, and problems with the heart and kidneys.
So, when Dr. Bauer encounters patients who believe that a few drinks will not harm their baby, he says he tells them: “’Why is this going to be where you put your flag?’ That leads to a different form of conversation.”
A version of this article first appeared on Medscape.com.
More pregnant Americans indulged – and overindulged – in alcohol from 2018 to 2020 than in previous years, but researchers found no sharp increase associated with the first wave of COVID-19 lockdowns, according to a new report from the Centers for Disease Control and Prevention.
The pandemic notwithstanding, health officials worry about a rising tide of pregnant women using alcohol and binge drinking since the CDC survey began in 2011. In the period ending in 2013, 1 in 10 women reported having had a drink in the previous 30 days; by 2017, that figure was 1 in 9; and in the latest survey, the number had risen to 1 in 7.
That mark is “the highest to date,” said Lucas Gosdin, PhD, MPH, an epidemic intelligence officer at the CDC’s National Center on Birth Defects and Developmental Disabilities, Atlanta, and first author of the report, which was published in Morbidity and Mortality Weekly Report.
“We’re concerned that this number has been slowly increasing,” Amanda Cohn, MD, director of the CDC’s Division of Birth Defects and Infant Disorders, told this news organization. “We need to be doing more outreach, both to pregnant persons as well as health care providers who are caring for them.”
Exposure to alcohol in the womb has been linked to a wide range of neurologic and physical problems in children, ranging from fetal alcohol syndrome to stunted learning abilities. Even if these problems are unlikely, experts insist there’s no known “safe” amount of alcohol a pregnant woman can have.
Dr. Cohn likened alcohol use to that of tobacco. “Lots of people smoke who don’t get lung cancer. Still, everyone is at an increased risk,” she said. “The safest way to not get lung cancer is to not smoke at all. It’s a behavior that can prevent additional harm.”
The report summarizes the results of a phone survey of 6,327 pregnant Americans between the ages of 18 and 49. The survey asked whether women had consumed an alcoholic beverage or had at least four drinks on one occasion – a common definition of binge drinking – in the past 30 days.
According to the report, 13.5% of women reported using alcohol, and 5.2% said they had binged on alcohol. Women who experienced frequent mental distress – describing their mental health as “not good” for 14 or more days in the past month – were twice as likely to drink and three times likelier to binge drink, the researchers found.
The increase within the 3-year period was roughly the same as in previous surveys.
“There was no evidence of increased alcohol consumption by pregnant adults in 2020 relative to 2019, despite possible increased alcohol sales and consumption among the general population during the first months of the COVID-19 pandemic,” the report states.
“That is one finding that was unexpected but that we were pleased to see,” Dr. Gosdin said.
Experts stressed that the survey covered only the first 9 months of the COVID-19 pandemic. “We’re still in the depths of it,” Samuel T. Bauer, MD, associate professor of obstetrics and gynecology at Duke University Medical Center, Durham, N.C., told this news organization. “People with alcohol use disorders certainly have been challenged during COVID. I think this is a preliminary answer.”
Dr. Gosdin said the effects of the pandemic on drinking habits bear watching. “We are concerned about the impacts of COVID-19,” he said. “We know it’s affected how people access regular care.”
Although virtual care has “exploded during COVID,” Dr. Bauer said, insurers have “turned off reimbursing” for doctor-patient visits via telephone, but not for visits by Internet-based video platforms like Zoom.
That split creates equity issues in many parts of the country, including his home state of North Carolina, where broadband is scarce, and patients may live 100 miles or more away from caregivers.
The “full-blown birth defect” of fetal alcohol syndrome is just the most visible hazard of drinking. Other medical and developmental issues include speech delays, slower learning and reading skills, attention-deficit and hyperactivity disorders, and problems with the heart and kidneys.
So, when Dr. Bauer encounters patients who believe that a few drinks will not harm their baby, he says he tells them: “’Why is this going to be where you put your flag?’ That leads to a different form of conversation.”
A version of this article first appeared on Medscape.com.
More pregnant Americans indulged – and overindulged – in alcohol from 2018 to 2020 than in previous years, but researchers found no sharp increase associated with the first wave of COVID-19 lockdowns, according to a new report from the Centers for Disease Control and Prevention.
The pandemic notwithstanding, health officials worry about a rising tide of pregnant women using alcohol and binge drinking since the CDC survey began in 2011. In the period ending in 2013, 1 in 10 women reported having had a drink in the previous 30 days; by 2017, that figure was 1 in 9; and in the latest survey, the number had risen to 1 in 7.
That mark is “the highest to date,” said Lucas Gosdin, PhD, MPH, an epidemic intelligence officer at the CDC’s National Center on Birth Defects and Developmental Disabilities, Atlanta, and first author of the report, which was published in Morbidity and Mortality Weekly Report.
“We’re concerned that this number has been slowly increasing,” Amanda Cohn, MD, director of the CDC’s Division of Birth Defects and Infant Disorders, told this news organization. “We need to be doing more outreach, both to pregnant persons as well as health care providers who are caring for them.”
Exposure to alcohol in the womb has been linked to a wide range of neurologic and physical problems in children, ranging from fetal alcohol syndrome to stunted learning abilities. Even if these problems are unlikely, experts insist there’s no known “safe” amount of alcohol a pregnant woman can have.
Dr. Cohn likened alcohol use to that of tobacco. “Lots of people smoke who don’t get lung cancer. Still, everyone is at an increased risk,” she said. “The safest way to not get lung cancer is to not smoke at all. It’s a behavior that can prevent additional harm.”
The report summarizes the results of a phone survey of 6,327 pregnant Americans between the ages of 18 and 49. The survey asked whether women had consumed an alcoholic beverage or had at least four drinks on one occasion – a common definition of binge drinking – in the past 30 days.
According to the report, 13.5% of women reported using alcohol, and 5.2% said they had binged on alcohol. Women who experienced frequent mental distress – describing their mental health as “not good” for 14 or more days in the past month – were twice as likely to drink and three times likelier to binge drink, the researchers found.
The increase within the 3-year period was roughly the same as in previous surveys.
“There was no evidence of increased alcohol consumption by pregnant adults in 2020 relative to 2019, despite possible increased alcohol sales and consumption among the general population during the first months of the COVID-19 pandemic,” the report states.
“That is one finding that was unexpected but that we were pleased to see,” Dr. Gosdin said.
Experts stressed that the survey covered only the first 9 months of the COVID-19 pandemic. “We’re still in the depths of it,” Samuel T. Bauer, MD, associate professor of obstetrics and gynecology at Duke University Medical Center, Durham, N.C., told this news organization. “People with alcohol use disorders certainly have been challenged during COVID. I think this is a preliminary answer.”
Dr. Gosdin said the effects of the pandemic on drinking habits bear watching. “We are concerned about the impacts of COVID-19,” he said. “We know it’s affected how people access regular care.”
Although virtual care has “exploded during COVID,” Dr. Bauer said, insurers have “turned off reimbursing” for doctor-patient visits via telephone, but not for visits by Internet-based video platforms like Zoom.
That split creates equity issues in many parts of the country, including his home state of North Carolina, where broadband is scarce, and patients may live 100 miles or more away from caregivers.
The “full-blown birth defect” of fetal alcohol syndrome is just the most visible hazard of drinking. Other medical and developmental issues include speech delays, slower learning and reading skills, attention-deficit and hyperactivity disorders, and problems with the heart and kidneys.
So, when Dr. Bauer encounters patients who believe that a few drinks will not harm their baby, he says he tells them: “’Why is this going to be where you put your flag?’ That leads to a different form of conversation.”
A version of this article first appeared on Medscape.com.
FROM MMWR
High-risk women–What breast screening is appropriate?
Text copyright DenseBreast-info.org.
Answer
B. For a 28-year-old woman, herself untested, with a known pathogenic BRCA1 or BRCA2 mutation in a first-degree relative (mother/ father, sister/brother, daughter/son), screening annual magnetic resonance imaging (MRI) alone is recommended until age 30, followed by screening annual MRI and mammography/tomosynthesis at age 30 and beyond. If MRI is not an option, ultrasonography or contrast-enhanced mammography should be considered.
Most medical societies in the United States recommend mammography screening beginning at age 40 if a woman is at average risk. If a woman is determined to be at high risk, breast cancer screening may be recommended to begin by age 30. Breast cancer risk assessment, with a risk model based largely on family history, should begin by age 30 for all women.
The American College of Radiology (ACR),1 National Comprehensive Cancer Network (NCCN),2,3 and American Society of Breast Surgeons recommend annual MRI screening for the following high-risk subgroups of women:
- Women with known disease-causing BRCA1 or BRCA2 mutations, or other disease-causing mutations, or their untested first-degree relatives. (Age to begin screening MRI and screening mammography/tomosynthesis varies by mutation).1,3 Women with known pathogenic BRCA1 or BRCA2 mutations, or their untested first-degree relatives, should begin annual screening with MRI only between ages 25-29, adding annual digital mammography/tomosynthesis at age 30 and beyond (unless the woman has had bilateral mastectomy). Note: There is emerging evidence that the benefit of mammography is relatively small in pathogenic BRCA1 carriers prior to the age of 40; therefore, the ACR suggests BRCA1 mutation carriers may consider delaying mammography until age 40 only if they receive contrast-enhanced MRI annually starting at age 25.1 Annual mammography is of benefit beginning at age 30 in those with BRCA2 or other disease-causing mutations.Age to begin annual MRI screening and mammography/tomosynthesis in women who are known to carry or are first-degree untested relatives of individuals with less common disease-causing mutations (such as those associated with Li-Fraumeni syndrome [TP53]; Bannayan-Riley-Ruvalcaba syndrome or Cowden syndrome [PTEN]; hereditary diffuse gastric cancer [CDH1]; Peutz-Jeghers syndrome [STK11]; neurofibromatosis type 1 [NF1]; PALB2; ATM; CHEK2; or BARD1) ranges from 20-40 years depending on the mutation and family history.3 (See https://densebreast-info.org/providers-faqs /what-is-the-screening-management-for -various-other-mutation-carriers/.)
- Women who received chest/mantle radiation therapy by age 30 (such as for Hodgkin disease) and at least 8 years prior. Women with prior chest radiation therapy (such as for Hodgkin disease) between ages 10 and 30 are at high risk for developing breast cancer,1,2,4,5 with risk similar in magnitude to BRCA1 or BRCA2 carriers, and are recommended for annual screening MRI starting at age 25 or 8 years after the chest radiation therapy, whichever is later.
- Women with a calculated lifetime risk of breast cancer of ≥20% are recommended to begin annual screening MRI by age 25-30.1,2,5 Any of the models that include detailed family history such as the Tyrer-Cuzick (IBIS, which now includes breast density as a risk factor); BRCAPRO; BOADICEA; Claus; or Penn II; but not the Gail or Breast Cancer Surveillance Consortium (BCSC) models, can be used to estimate lifetime risk for the purposes of screening MRI guidelines. (See https://densebreast -info.org/for-providers/risk-model-tutorial/ for a summary table with live links.)
- Women with a personal history of breast cancer and dense breasts or diagnosis by age 50, regardless of breast density. A personal history of breast cancer is not included in risk models, but all women diagnosed with breast cancer at or before age 50 and treated with breast-conserving therapy have a ≥20% lifetime risk for a new breast cancer.1,2 Annual MRI may be considered in addition to annual mammography or tomosynthesis in women with a personal history of breast cancer diagnosed after age 50 and without dense breasts, and/or a history of lobular carcinoma in situ (LCIS) or prior atypia (eg, atypical ductal hyperplasia (ADH), atypical lobular hyperplasia (ALH), or atypical papilloma).1,2
Supplemental MRI screening should continue until age 75, after which management should be considered on an individual basis. If MRI screening is not an option, ultrasound or contrast-enhanced mammography (where available) should be considered as an alternative.6-8 ●
For more information, visit medically sourced DenseBreastinfo.org. Comprehensive resources include a free CME opportunity, Dense Breasts and Supplemental Screening.
- Monticciolo DL, Newell MS, Moy L, et al. Breast cancer screening in women at higher-than-average risk: recommendations from the ACR. J Am Coll Radiol. 2018;15 (3 Pt A):408-414. doi: 10.1016/j.jacr.2017.11.034.
- National Comprehensive Cancer Network. Breast Cancer Screening and Diagnosis (Version 1.2021). https://www .nccn.org/professionals/physician_gls/pdf/breast-screening .pdf. Accessed November 18, 2021.
- National Comprehensive Cancer Network. Genetic/Familial High-Risk Assessment: Breast and Ovarian (Version 1.2020). https://www.nccn.org/professionals/physician_gls/pdf /genetics_bop.pdf. Accessed July 31, 2020.
- Oeffinger KC, Ford JS, Moskowitz CS, et al. Breast cancer surveillance practices among women previously treated with chest radiation for a childhood cancer. JAMA. 2009;301(4):404-414. DOI: 10.1001/jama.2008.1039.
- Saslow D, Boetes C, Burke W, et al. American Cancer Society guidelines for breast screening with MRI as an adjunct to mammography. CA Cancer J Clin. 2007;57:75-89. doi: 10.3322/canjclin.57.2.75.
- Sorin V, Yagil Y, Yosepovich A, et al. Contrast-enhanced spectral mammography in women with intermediate breast cancer risk and dense breasts. AJR Am J Roentgenol. 2018;211:W267-W274. doi: 10.2214/AJR.17.19355.
- Sung JS, Lebron L, Keating D, et al. Performance of dualenergy contrast-enhanced digital mammography for screening women at increased risk of breast cancer. Radiology. 2019;293:81-88. doi: 10.1148/radiol.2019182660.
- Xiang W, Rao H, Zhou L. A meta-analysis of contrastenhanced spectral mammography versus MRI in the diagnosis of breast cancer. Thorac Cancer. 2020;11:1423-1432. doi: 10.1111/1759-7714.13400.
Text copyright DenseBreast-info.org.
Answer
B. For a 28-year-old woman, herself untested, with a known pathogenic BRCA1 or BRCA2 mutation in a first-degree relative (mother/ father, sister/brother, daughter/son), screening annual magnetic resonance imaging (MRI) alone is recommended until age 30, followed by screening annual MRI and mammography/tomosynthesis at age 30 and beyond. If MRI is not an option, ultrasonography or contrast-enhanced mammography should be considered.
Most medical societies in the United States recommend mammography screening beginning at age 40 if a woman is at average risk. If a woman is determined to be at high risk, breast cancer screening may be recommended to begin by age 30. Breast cancer risk assessment, with a risk model based largely on family history, should begin by age 30 for all women.
The American College of Radiology (ACR),1 National Comprehensive Cancer Network (NCCN),2,3 and American Society of Breast Surgeons recommend annual MRI screening for the following high-risk subgroups of women:
- Women with known disease-causing BRCA1 or BRCA2 mutations, or other disease-causing mutations, or their untested first-degree relatives. (Age to begin screening MRI and screening mammography/tomosynthesis varies by mutation).1,3 Women with known pathogenic BRCA1 or BRCA2 mutations, or their untested first-degree relatives, should begin annual screening with MRI only between ages 25-29, adding annual digital mammography/tomosynthesis at age 30 and beyond (unless the woman has had bilateral mastectomy). Note: There is emerging evidence that the benefit of mammography is relatively small in pathogenic BRCA1 carriers prior to the age of 40; therefore, the ACR suggests BRCA1 mutation carriers may consider delaying mammography until age 40 only if they receive contrast-enhanced MRI annually starting at age 25.1 Annual mammography is of benefit beginning at age 30 in those with BRCA2 or other disease-causing mutations.Age to begin annual MRI screening and mammography/tomosynthesis in women who are known to carry or are first-degree untested relatives of individuals with less common disease-causing mutations (such as those associated with Li-Fraumeni syndrome [TP53]; Bannayan-Riley-Ruvalcaba syndrome or Cowden syndrome [PTEN]; hereditary diffuse gastric cancer [CDH1]; Peutz-Jeghers syndrome [STK11]; neurofibromatosis type 1 [NF1]; PALB2; ATM; CHEK2; or BARD1) ranges from 20-40 years depending on the mutation and family history.3 (See https://densebreast-info.org/providers-faqs /what-is-the-screening-management-for -various-other-mutation-carriers/.)
- Women who received chest/mantle radiation therapy by age 30 (such as for Hodgkin disease) and at least 8 years prior. Women with prior chest radiation therapy (such as for Hodgkin disease) between ages 10 and 30 are at high risk for developing breast cancer,1,2,4,5 with risk similar in magnitude to BRCA1 or BRCA2 carriers, and are recommended for annual screening MRI starting at age 25 or 8 years after the chest radiation therapy, whichever is later.
- Women with a calculated lifetime risk of breast cancer of ≥20% are recommended to begin annual screening MRI by age 25-30.1,2,5 Any of the models that include detailed family history such as the Tyrer-Cuzick (IBIS, which now includes breast density as a risk factor); BRCAPRO; BOADICEA; Claus; or Penn II; but not the Gail or Breast Cancer Surveillance Consortium (BCSC) models, can be used to estimate lifetime risk for the purposes of screening MRI guidelines. (See https://densebreast -info.org/for-providers/risk-model-tutorial/ for a summary table with live links.)
- Women with a personal history of breast cancer and dense breasts or diagnosis by age 50, regardless of breast density. A personal history of breast cancer is not included in risk models, but all women diagnosed with breast cancer at or before age 50 and treated with breast-conserving therapy have a ≥20% lifetime risk for a new breast cancer.1,2 Annual MRI may be considered in addition to annual mammography or tomosynthesis in women with a personal history of breast cancer diagnosed after age 50 and without dense breasts, and/or a history of lobular carcinoma in situ (LCIS) or prior atypia (eg, atypical ductal hyperplasia (ADH), atypical lobular hyperplasia (ALH), or atypical papilloma).1,2
Supplemental MRI screening should continue until age 75, after which management should be considered on an individual basis. If MRI screening is not an option, ultrasound or contrast-enhanced mammography (where available) should be considered as an alternative.6-8 ●
For more information, visit medically sourced DenseBreastinfo.org. Comprehensive resources include a free CME opportunity, Dense Breasts and Supplemental Screening.
Text copyright DenseBreast-info.org.
Answer
B. For a 28-year-old woman, herself untested, with a known pathogenic BRCA1 or BRCA2 mutation in a first-degree relative (mother/ father, sister/brother, daughter/son), screening annual magnetic resonance imaging (MRI) alone is recommended until age 30, followed by screening annual MRI and mammography/tomosynthesis at age 30 and beyond. If MRI is not an option, ultrasonography or contrast-enhanced mammography should be considered.
Most medical societies in the United States recommend mammography screening beginning at age 40 if a woman is at average risk. If a woman is determined to be at high risk, breast cancer screening may be recommended to begin by age 30. Breast cancer risk assessment, with a risk model based largely on family history, should begin by age 30 for all women.
The American College of Radiology (ACR),1 National Comprehensive Cancer Network (NCCN),2,3 and American Society of Breast Surgeons recommend annual MRI screening for the following high-risk subgroups of women:
- Women with known disease-causing BRCA1 or BRCA2 mutations, or other disease-causing mutations, or their untested first-degree relatives. (Age to begin screening MRI and screening mammography/tomosynthesis varies by mutation).1,3 Women with known pathogenic BRCA1 or BRCA2 mutations, or their untested first-degree relatives, should begin annual screening with MRI only between ages 25-29, adding annual digital mammography/tomosynthesis at age 30 and beyond (unless the woman has had bilateral mastectomy). Note: There is emerging evidence that the benefit of mammography is relatively small in pathogenic BRCA1 carriers prior to the age of 40; therefore, the ACR suggests BRCA1 mutation carriers may consider delaying mammography until age 40 only if they receive contrast-enhanced MRI annually starting at age 25.1 Annual mammography is of benefit beginning at age 30 in those with BRCA2 or other disease-causing mutations.Age to begin annual MRI screening and mammography/tomosynthesis in women who are known to carry or are first-degree untested relatives of individuals with less common disease-causing mutations (such as those associated with Li-Fraumeni syndrome [TP53]; Bannayan-Riley-Ruvalcaba syndrome or Cowden syndrome [PTEN]; hereditary diffuse gastric cancer [CDH1]; Peutz-Jeghers syndrome [STK11]; neurofibromatosis type 1 [NF1]; PALB2; ATM; CHEK2; or BARD1) ranges from 20-40 years depending on the mutation and family history.3 (See https://densebreast-info.org/providers-faqs /what-is-the-screening-management-for -various-other-mutation-carriers/.)
- Women who received chest/mantle radiation therapy by age 30 (such as for Hodgkin disease) and at least 8 years prior. Women with prior chest radiation therapy (such as for Hodgkin disease) between ages 10 and 30 are at high risk for developing breast cancer,1,2,4,5 with risk similar in magnitude to BRCA1 or BRCA2 carriers, and are recommended for annual screening MRI starting at age 25 or 8 years after the chest radiation therapy, whichever is later.
- Women with a calculated lifetime risk of breast cancer of ≥20% are recommended to begin annual screening MRI by age 25-30.1,2,5 Any of the models that include detailed family history such as the Tyrer-Cuzick (IBIS, which now includes breast density as a risk factor); BRCAPRO; BOADICEA; Claus; or Penn II; but not the Gail or Breast Cancer Surveillance Consortium (BCSC) models, can be used to estimate lifetime risk for the purposes of screening MRI guidelines. (See https://densebreast -info.org/for-providers/risk-model-tutorial/ for a summary table with live links.)
- Women with a personal history of breast cancer and dense breasts or diagnosis by age 50, regardless of breast density. A personal history of breast cancer is not included in risk models, but all women diagnosed with breast cancer at or before age 50 and treated with breast-conserving therapy have a ≥20% lifetime risk for a new breast cancer.1,2 Annual MRI may be considered in addition to annual mammography or tomosynthesis in women with a personal history of breast cancer diagnosed after age 50 and without dense breasts, and/or a history of lobular carcinoma in situ (LCIS) or prior atypia (eg, atypical ductal hyperplasia (ADH), atypical lobular hyperplasia (ALH), or atypical papilloma).1,2
Supplemental MRI screening should continue until age 75, after which management should be considered on an individual basis. If MRI screening is not an option, ultrasound or contrast-enhanced mammography (where available) should be considered as an alternative.6-8 ●
For more information, visit medically sourced DenseBreastinfo.org. Comprehensive resources include a free CME opportunity, Dense Breasts and Supplemental Screening.
- Monticciolo DL, Newell MS, Moy L, et al. Breast cancer screening in women at higher-than-average risk: recommendations from the ACR. J Am Coll Radiol. 2018;15 (3 Pt A):408-414. doi: 10.1016/j.jacr.2017.11.034.
- National Comprehensive Cancer Network. Breast Cancer Screening and Diagnosis (Version 1.2021). https://www .nccn.org/professionals/physician_gls/pdf/breast-screening .pdf. Accessed November 18, 2021.
- National Comprehensive Cancer Network. Genetic/Familial High-Risk Assessment: Breast and Ovarian (Version 1.2020). https://www.nccn.org/professionals/physician_gls/pdf /genetics_bop.pdf. Accessed July 31, 2020.
- Oeffinger KC, Ford JS, Moskowitz CS, et al. Breast cancer surveillance practices among women previously treated with chest radiation for a childhood cancer. JAMA. 2009;301(4):404-414. DOI: 10.1001/jama.2008.1039.
- Saslow D, Boetes C, Burke W, et al. American Cancer Society guidelines for breast screening with MRI as an adjunct to mammography. CA Cancer J Clin. 2007;57:75-89. doi: 10.3322/canjclin.57.2.75.
- Sorin V, Yagil Y, Yosepovich A, et al. Contrast-enhanced spectral mammography in women with intermediate breast cancer risk and dense breasts. AJR Am J Roentgenol. 2018;211:W267-W274. doi: 10.2214/AJR.17.19355.
- Sung JS, Lebron L, Keating D, et al. Performance of dualenergy contrast-enhanced digital mammography for screening women at increased risk of breast cancer. Radiology. 2019;293:81-88. doi: 10.1148/radiol.2019182660.
- Xiang W, Rao H, Zhou L. A meta-analysis of contrastenhanced spectral mammography versus MRI in the diagnosis of breast cancer. Thorac Cancer. 2020;11:1423-1432. doi: 10.1111/1759-7714.13400.
- Monticciolo DL, Newell MS, Moy L, et al. Breast cancer screening in women at higher-than-average risk: recommendations from the ACR. J Am Coll Radiol. 2018;15 (3 Pt A):408-414. doi: 10.1016/j.jacr.2017.11.034.
- National Comprehensive Cancer Network. Breast Cancer Screening and Diagnosis (Version 1.2021). https://www .nccn.org/professionals/physician_gls/pdf/breast-screening .pdf. Accessed November 18, 2021.
- National Comprehensive Cancer Network. Genetic/Familial High-Risk Assessment: Breast and Ovarian (Version 1.2020). https://www.nccn.org/professionals/physician_gls/pdf /genetics_bop.pdf. Accessed July 31, 2020.
- Oeffinger KC, Ford JS, Moskowitz CS, et al. Breast cancer surveillance practices among women previously treated with chest radiation for a childhood cancer. JAMA. 2009;301(4):404-414. DOI: 10.1001/jama.2008.1039.
- Saslow D, Boetes C, Burke W, et al. American Cancer Society guidelines for breast screening with MRI as an adjunct to mammography. CA Cancer J Clin. 2007;57:75-89. doi: 10.3322/canjclin.57.2.75.
- Sorin V, Yagil Y, Yosepovich A, et al. Contrast-enhanced spectral mammography in women with intermediate breast cancer risk and dense breasts. AJR Am J Roentgenol. 2018;211:W267-W274. doi: 10.2214/AJR.17.19355.
- Sung JS, Lebron L, Keating D, et al. Performance of dualenergy contrast-enhanced digital mammography for screening women at increased risk of breast cancer. Radiology. 2019;293:81-88. doi: 10.1148/radiol.2019182660.
- Xiang W, Rao H, Zhou L. A meta-analysis of contrastenhanced spectral mammography versus MRI in the diagnosis of breast cancer. Thorac Cancer. 2020;11:1423-1432. doi: 10.1111/1759-7714.13400.
Infectious disease pop quiz: Clinical challenge #11 for the ObGyn
In a pregnant woman with a history of recurrent herpes simplex virus infection, what is the best way to prevent an outbreak of lesions near term?
Continue to the answer...
Obstetric patients with a history of recurrent herpes simplex infection should be treated with acyclovir 400 mg orally 3 times daily from 36 weeks until delivery. This regimen significantly reduces the likelihood of a recurrent outbreak near the time of delivery, which if it occurred, would necessitate a cesarean delivery. In patients at increased risk for preterm delivery, the prophylactic regimen should be started earlier.
Valacyclovir, 500 mg orally twice daily, is an acceptable alternative but is significantly more expensive.
- Duff P. Maternal and perinatal infections: bacterial. In: Landon MB, Galan HL, Jauniaux ERM, et al. Gabbe’s Obstetrics: Normal and Problem Pregnancies. 8th ed. Elsevier; 2021:1124-1146.
- Duff P. Maternal and fetal infections. In: Resnik R, Lockwood CJ, Moore TJ, et al. Creasy & Resnik’s Maternal-Fetal Medicine: Principles and Practice. 8th ed. Elsevier; 2019:862-919.
In a pregnant woman with a history of recurrent herpes simplex virus infection, what is the best way to prevent an outbreak of lesions near term?
Continue to the answer...
Obstetric patients with a history of recurrent herpes simplex infection should be treated with acyclovir 400 mg orally 3 times daily from 36 weeks until delivery. This regimen significantly reduces the likelihood of a recurrent outbreak near the time of delivery, which if it occurred, would necessitate a cesarean delivery. In patients at increased risk for preterm delivery, the prophylactic regimen should be started earlier.
Valacyclovir, 500 mg orally twice daily, is an acceptable alternative but is significantly more expensive.
In a pregnant woman with a history of recurrent herpes simplex virus infection, what is the best way to prevent an outbreak of lesions near term?
Continue to the answer...
Obstetric patients with a history of recurrent herpes simplex infection should be treated with acyclovir 400 mg orally 3 times daily from 36 weeks until delivery. This regimen significantly reduces the likelihood of a recurrent outbreak near the time of delivery, which if it occurred, would necessitate a cesarean delivery. In patients at increased risk for preterm delivery, the prophylactic regimen should be started earlier.
Valacyclovir, 500 mg orally twice daily, is an acceptable alternative but is significantly more expensive.
- Duff P. Maternal and perinatal infections: bacterial. In: Landon MB, Galan HL, Jauniaux ERM, et al. Gabbe’s Obstetrics: Normal and Problem Pregnancies. 8th ed. Elsevier; 2021:1124-1146.
- Duff P. Maternal and fetal infections. In: Resnik R, Lockwood CJ, Moore TJ, et al. Creasy & Resnik’s Maternal-Fetal Medicine: Principles and Practice. 8th ed. Elsevier; 2019:862-919.
- Duff P. Maternal and perinatal infections: bacterial. In: Landon MB, Galan HL, Jauniaux ERM, et al. Gabbe’s Obstetrics: Normal and Problem Pregnancies. 8th ed. Elsevier; 2021:1124-1146.
- Duff P. Maternal and fetal infections. In: Resnik R, Lockwood CJ, Moore TJ, et al. Creasy & Resnik’s Maternal-Fetal Medicine: Principles and Practice. 8th ed. Elsevier; 2019:862-919.
Are SERMs safe and effective for the treatment of hypogonadism in men?
Evidence summary
Alone or in combination with hCG, clomiphene citrate is effective
A 2018 multicenter prospective RCT (n = 283) compared the serum testosterone response in men (mean age, 41.8 ± 10.4 years) with hypogonadism before and after treatment with either CC, human chorionic gonadotropin (hCG), or a combination of both therapies.1 All patients wanted to maintain fertility, had normal follicle-stimulating hormone (FSH) and luteinizing hormone (LH) levels, had no history of testosterone therapy, had low (< 300 ng/dL) serum testosterone levels on at least 2 samples, and had at least 3 positive symptoms from the quantitative Androgen Deficiency in the Aging Male questionnaire (qADAM; a 10-item, graded-response tool measuring symptom severity from 1 to 5).
Patients were randomized into either the CC group (50 mg oral; n = 95), the hCG group (5000 IU injections twice weekly; n = 94), or the CC + hCG group (n = 94). Testosterone levels were measured at baseline and at 1 and 3 months after therapy initiation; qADAM questionnaire scores were also recorded but ultimately not used due to concerns with baseline heterogeneity among groups.
Average baseline serum testosterone levels for the CC, hCG, and CC + hCG groups were 243 ng/dL, 222 ng/dL, and 226 ng/dL, respectively. By 3 months, these levels had increased to 548 ng/dL (95% CI, 505-591) in the CC group, 467 ng/dL (95% CI, 440-494) in the hCG group, and 531 ng/dL (95% CI, 492-570) in the CC + hCG group. While there was not a significant difference between the CC and CC + hCG groups at 3 months (P = .579), both groups were superior to the hCG-only group (P = .002 for each).
CC and testosterone gel are comparable; testosterone injection is better
In a 2014 retrospective study, researchers reviewed the charts of 1150 men taking any form of testosterone supplementation therapy (TST). They compared treatment efficacy and qADAM satisfaction scores in 93 age-matched men with symptomatic hypogonadism who were treated with either CC (n = 31), testosterone injections (n = 31), or testosterone topical gel (n = 31).2 Eugonadal men not taking TST (n = 31) served as controls.
Inclusion criteria were based on treatment regimens of CC and TST. Participants in the treatment groups had a baseline total testosterone level < 300 ng/dL and had reported ≤ 3 positive symptoms on the qADAM questionnaire. Treatment regimens included CC (25 mg orally once daily), testosterone injections (testosterone cypionate 100 to 200 mg intramuscularly once weekly), and testosterone gel (Testim 1% or AndroGel 1.62%, 2 to 4 pumps/d).
The study results demonstrated an increase in median testosterone from baseline levels in all treatment groups when compared to placebo: CC (from 247 to 504 ng/dL), testosterone injections (from 224 to 1104 ng/dL), and testosterone gels (from 230 to 412 ng/dL) (P < .05). Men receiving testosterone injections had the highest increase in serum testosterone levels (956 ng/dL).
While the final mean serum total testosterone was highest in the testosterone injection group (1014 ng/dL; P < .01), the mean levels for those using CC and those using testosterone gels were comparable (525 ng/dL vs 412 ng/dL). Serum estradiol levels were also higher in men receiving testosterone injections, compared to men using CC, those using testosterone gels, and those not receiving TST (6.0 vs 2.0, 2.0, and 2.0 ng/dL, respectively; each P < .01).
Continue to: The qADAM scores...
The qADAM scores for hypogonadal symptoms showed no significant difference in men treated with CC, testosterone injections, and testosterone gels and those not receiving TST (35, 39, 36, and 34, respectively). Men receiving testosterone injections reported greater libido (range, 1-5) than men using CC, those using testosterone gels, and those not on TST (4 vs 3, 3, and 3; P = .047, .04, and < .01, respectively), but it is uncertain if this is clinically meaningful.
Enclomiphene citrate demonstrates improvement in hormone levels
A 2014 Phase II RCT investigated the effects of oral EC—a trans-isomer of CC—compared to topical testosterone 1% gel (T gel) in 124 men with secondary hypogonadism.3 Entry criteria included a baseline morning total testosterone level of < 250 ng/dL on 2 occasions. Participants were divided into 4 groups: 12.5-mg dose of EC, 25-mg dose of EC, T gel, and placebo.
The EC groups and the T gel group had comparable increases in testosterone levels after 3 months of treatment, without statistical significance. The 3-month change in serum testosterone level from baseline was 217 to 471 ng/dL (95% CI, 399-543) in the 12.5-mg dose group; 209 to 405 ng/dL (95% CI, 349-462) in the 25-mg dose group; and 210 to 462 ng/dL (95% CI, 359-565) in the T gel group. The placebo group had a decrease in serum testosterone levels, from 213 to 198 ng/dL (95% CI, 171-226).
Also, the EC groups demonstrated increases in LH and FSH levels from baseline to 3 months, while the T gel group showed a suppression (to low-normal range) in both levels: LH, 1.4 mIU/mL (decrease of 4.4 mIU/mL) and FSH, 2.4 mIU/mL (decrease of 2.4 mIU/mL). Among a subset of men (n = 67) who had at least 2 assessments at the end of 3 months, the researchers also analyzed changes in sperm concentration, using the lower limit of normal (15 million/mL). The number of men with a low sperm concentration increased significantly in the topical T gel group (16% to 53%) compared to the 12.5-mg EC group (decrease from 16% to 12%; P = .0008) and the 25-mg EC group (decrease from 5% to 0%; P = .0007), as well as compared to the placebo group (increase from 8% to 15%; P = .007).
With EC, testosterone remains elevated after treatment cessation
A 2016 2-center parallel, double-blind, placebo-controlled RCT evaluated the effect of 2 doses of EC (12.5 mg and 25 mg; n = 85) vs testosterone gel (1.62%; n = 85) vs placebo (n = 86) on serum testosterone, LH, FSH, and sperm counts in 256 overweight and obese men ages 18 to 60 years who had 2 morning testosterone measurements < 300 ng/dL and a low or inappropriately normal LH level for 16 weeks.4 All baseline characteristics, including age, BMI, sperm concentration, and serum total testosterone were statistically consistent within groups at both centers. For men receiving EC who did not achieve a testosterone level > 450 ng/dL, there was an up-titration from 12.5 mg to 25 mg at Week 4.
Continue to: All active treatment groups...
All active treatment groups showed increases in testosterone level during treatment (P < .001); however, FSH and LH levels increased in the EC group and decreased in the testosterone gel group (P < .001). Serum testosterone levels improved to 428.8 ng/dL (95% CI, 395-462) and 368.8 ng/dL (95% CI, 307-431), respectively, in the combined EC and testosterone gel groups at 16 weeks. Of note, total testosterone levels after cessation of treatment (off-drug point) rapidly decreased below baseline in the testosterone gel group compared to the pooled EC group, which remained elevated above baseline for at least 7 days.
Composite end-point analysis was performed, with success considered if men achieved both testosterone in normal range (300-1040 ng/dL) and sperm concentrations ≥ 10 × 106. The pooled data studies showed EC was more successful than testosterone gel in achieving both endpoints (63.5% vs 24.7%; P < .001). No difference in the incidence of treatment-related adverse effects between groups was noted.
There were no major adverse effects, even after 3+ years of treatment
A 2019 retrospective cohort study of 400 men treated for symptomatic hypogonadism with CC sought to determine if improvements in testosterone, hypogonadal symptoms, and adverse effects were similar for those treated for ≤ 3 years (n = 280) and those treated for > 3 years (n = 120).5 Outcomes included serum testosterone and estradiol levels, symptom improvement (by qADAM questionnaire), and adverse effects.
All participants had a baseline testosterone level < 300 ng/dL, and all participants received CC therapy. Men received 25 mg/d with titration to 50 mg/d when testosterone did not improve to ≥ 300 ng/dL after 4 weeks.
When comparing outcomes across the 2 groups, there were no significant differences. Serum testosterone levels improved to 579 ng/dL (95% CI, 554-605) and 542 ng/dL (95% CI, 504-580) in the ≤ 3 years and > 3 years groups, respectively. Meanwhile, 79% of men in the ≤ 3 years group reported symptom improvement (improvement in libido, erection, or 3 other of the 10 domains of the qADAM questionnaire), while 77% of those in the > 3 years group reported improvement (P = .60).
Continue to: Finally, the percentage of men reporting...
Finally, the percentage of men reporting adverse effects did not significantly differ between groups: 9% in the ≤ 3 years group and 8% in the > 3 years group (P = .85). The most common adverse effects reported in order of frequency were mood changes, blurred vision, breast tenderness, hypertension, hematocrit changes, and flushing. No major adverse events (eg, myocardial infarction, cerebrovascular accident, venous thromboembolism, suicidal behavior) were reported in any patients.
Of note, although measured estrogen levels at the end of treatment were similar for both groups (54.8 pg/mL in the ≤ 3 years group vs 54.6 pg/mL in the > 3 years group), 37% of patients treated for > 3 years did receive anastrozole treatment for hyperestrogenism compared to 15% in the ≤ 3 years group (P = .05). The authors caution, though, that due to only 20% of the cohort patients having data on pre- and post-treatment estradiol levels, the study was likely underpowered to detect true differences among subgroups.
Recommendations from others
Current American Urological Association and Canadian Urological Association Guidelines note that while greater study on nontraditional testosterone therapies is needed, both organizations support use of SERMs, especially in hypogonadal men who are interested in fertility preservation, as increases in endogenous serum testosterone production do not impact fertility potential, unlike exogenous hormonal replacement.6,7 Additionally, men with low or low-normal serum LH levels may also be good candidates for the use of SERMs for management of testosterone deficiency.
Editor’s takeaway
Laboratory data (disease oriented) consistently shows that SERMs effectively increase testosterone levels to those comparable with testosterone gels. SERMs resulted in higher semen counts and maintained LH and FSH levels, but there were instances of hyperestrogenism. Data on longer-term benefits and adverse effects of both SERMs and testosterone supplementation are still needed.
1. Habous M, Giona S, Tealab A, et al. Clomiphene citrate and human chorionic gonadotropin are both effective in restoring testosterone in hypogonadism: a short-course randomized study. BJU Int. 2018;122:889-897. doi: 10.1111/bju.14401
2. Ramasamy R, Scovell JM, Kovac JR, et al. Testosterone supplementation versus clomiphene citrate for hypogonadism: an age matched comparison of satisfaction and efficacy. J Urol. 2014;192:875-879. doi: 10.1016/j.juro.2014.03.089
3. Wiehle RD, Fontenot GK, Wike J, et al. Enclomiphene citrate stimulates testosterone production while preventing oligospermia: a randomized phase II clinical trial comparing topical testosterone. Fertil Steril. 2014;102:720-727. doi: 10.1016/j.fertnstert.2014.06.004
4. Kim ED, McCullough A, Kaminetsky J. Oral enclomiphene citrate raises testosterone and preserves sperm counts in obese hypogonadal men, unlike topical testosterone: restoration instead of replacement. BJU Int. 2016;117:677-685. doi: 10.1111/bju.13337
5. Krzastek SC, Sharma D, Abdullah N, et al. Long-term safety and efficacy of clomiphene citrate for the treatment of hypogonadism. J Urol. 2019;202:1029-1035. doi: 10.1097/JU.0000000000000396
6. Grober ED, Krakowsky Y, Khera M, et al. Canadian Urological Association clinical practice guideline on testosterone deficiency in men: evidence-based Q&A. Can Urol Assoc J. 2021;15:E234-E243. doi: 10.5489/cuaj.7252
7. Mulhall JP, Trost LW, Brannigan RE, et al. Evaluation and management of testosterone deficiency: AUA guideline. J Urol. 2018;200:423-432. doi: 10.1016/j.juro.2018.03.115
Evidence summary
Alone or in combination with hCG, clomiphene citrate is effective
A 2018 multicenter prospective RCT (n = 283) compared the serum testosterone response in men (mean age, 41.8 ± 10.4 years) with hypogonadism before and after treatment with either CC, human chorionic gonadotropin (hCG), or a combination of both therapies.1 All patients wanted to maintain fertility, had normal follicle-stimulating hormone (FSH) and luteinizing hormone (LH) levels, had no history of testosterone therapy, had low (< 300 ng/dL) serum testosterone levels on at least 2 samples, and had at least 3 positive symptoms from the quantitative Androgen Deficiency in the Aging Male questionnaire (qADAM; a 10-item, graded-response tool measuring symptom severity from 1 to 5).
Patients were randomized into either the CC group (50 mg oral; n = 95), the hCG group (5000 IU injections twice weekly; n = 94), or the CC + hCG group (n = 94). Testosterone levels were measured at baseline and at 1 and 3 months after therapy initiation; qADAM questionnaire scores were also recorded but ultimately not used due to concerns with baseline heterogeneity among groups.
Average baseline serum testosterone levels for the CC, hCG, and CC + hCG groups were 243 ng/dL, 222 ng/dL, and 226 ng/dL, respectively. By 3 months, these levels had increased to 548 ng/dL (95% CI, 505-591) in the CC group, 467 ng/dL (95% CI, 440-494) in the hCG group, and 531 ng/dL (95% CI, 492-570) in the CC + hCG group. While there was not a significant difference between the CC and CC + hCG groups at 3 months (P = .579), both groups were superior to the hCG-only group (P = .002 for each).
CC and testosterone gel are comparable; testosterone injection is better
In a 2014 retrospective study, researchers reviewed the charts of 1150 men taking any form of testosterone supplementation therapy (TST). They compared treatment efficacy and qADAM satisfaction scores in 93 age-matched men with symptomatic hypogonadism who were treated with either CC (n = 31), testosterone injections (n = 31), or testosterone topical gel (n = 31).2 Eugonadal men not taking TST (n = 31) served as controls.
Inclusion criteria were based on treatment regimens of CC and TST. Participants in the treatment groups had a baseline total testosterone level < 300 ng/dL and had reported ≤ 3 positive symptoms on the qADAM questionnaire. Treatment regimens included CC (25 mg orally once daily), testosterone injections (testosterone cypionate 100 to 200 mg intramuscularly once weekly), and testosterone gel (Testim 1% or AndroGel 1.62%, 2 to 4 pumps/d).
The study results demonstrated an increase in median testosterone from baseline levels in all treatment groups when compared to placebo: CC (from 247 to 504 ng/dL), testosterone injections (from 224 to 1104 ng/dL), and testosterone gels (from 230 to 412 ng/dL) (P < .05). Men receiving testosterone injections had the highest increase in serum testosterone levels (956 ng/dL).
While the final mean serum total testosterone was highest in the testosterone injection group (1014 ng/dL; P < .01), the mean levels for those using CC and those using testosterone gels were comparable (525 ng/dL vs 412 ng/dL). Serum estradiol levels were also higher in men receiving testosterone injections, compared to men using CC, those using testosterone gels, and those not receiving TST (6.0 vs 2.0, 2.0, and 2.0 ng/dL, respectively; each P < .01).
Continue to: The qADAM scores...
The qADAM scores for hypogonadal symptoms showed no significant difference in men treated with CC, testosterone injections, and testosterone gels and those not receiving TST (35, 39, 36, and 34, respectively). Men receiving testosterone injections reported greater libido (range, 1-5) than men using CC, those using testosterone gels, and those not on TST (4 vs 3, 3, and 3; P = .047, .04, and < .01, respectively), but it is uncertain if this is clinically meaningful.
Enclomiphene citrate demonstrates improvement in hormone levels
A 2014 Phase II RCT investigated the effects of oral EC—a trans-isomer of CC—compared to topical testosterone 1% gel (T gel) in 124 men with secondary hypogonadism.3 Entry criteria included a baseline morning total testosterone level of < 250 ng/dL on 2 occasions. Participants were divided into 4 groups: 12.5-mg dose of EC, 25-mg dose of EC, T gel, and placebo.
The EC groups and the T gel group had comparable increases in testosterone levels after 3 months of treatment, without statistical significance. The 3-month change in serum testosterone level from baseline was 217 to 471 ng/dL (95% CI, 399-543) in the 12.5-mg dose group; 209 to 405 ng/dL (95% CI, 349-462) in the 25-mg dose group; and 210 to 462 ng/dL (95% CI, 359-565) in the T gel group. The placebo group had a decrease in serum testosterone levels, from 213 to 198 ng/dL (95% CI, 171-226).
Also, the EC groups demonstrated increases in LH and FSH levels from baseline to 3 months, while the T gel group showed a suppression (to low-normal range) in both levels: LH, 1.4 mIU/mL (decrease of 4.4 mIU/mL) and FSH, 2.4 mIU/mL (decrease of 2.4 mIU/mL). Among a subset of men (n = 67) who had at least 2 assessments at the end of 3 months, the researchers also analyzed changes in sperm concentration, using the lower limit of normal (15 million/mL). The number of men with a low sperm concentration increased significantly in the topical T gel group (16% to 53%) compared to the 12.5-mg EC group (decrease from 16% to 12%; P = .0008) and the 25-mg EC group (decrease from 5% to 0%; P = .0007), as well as compared to the placebo group (increase from 8% to 15%; P = .007).
With EC, testosterone remains elevated after treatment cessation
A 2016 2-center parallel, double-blind, placebo-controlled RCT evaluated the effect of 2 doses of EC (12.5 mg and 25 mg; n = 85) vs testosterone gel (1.62%; n = 85) vs placebo (n = 86) on serum testosterone, LH, FSH, and sperm counts in 256 overweight and obese men ages 18 to 60 years who had 2 morning testosterone measurements < 300 ng/dL and a low or inappropriately normal LH level for 16 weeks.4 All baseline characteristics, including age, BMI, sperm concentration, and serum total testosterone were statistically consistent within groups at both centers. For men receiving EC who did not achieve a testosterone level > 450 ng/dL, there was an up-titration from 12.5 mg to 25 mg at Week 4.
Continue to: All active treatment groups...
All active treatment groups showed increases in testosterone level during treatment (P < .001); however, FSH and LH levels increased in the EC group and decreased in the testosterone gel group (P < .001). Serum testosterone levels improved to 428.8 ng/dL (95% CI, 395-462) and 368.8 ng/dL (95% CI, 307-431), respectively, in the combined EC and testosterone gel groups at 16 weeks. Of note, total testosterone levels after cessation of treatment (off-drug point) rapidly decreased below baseline in the testosterone gel group compared to the pooled EC group, which remained elevated above baseline for at least 7 days.
Composite end-point analysis was performed, with success considered if men achieved both testosterone in normal range (300-1040 ng/dL) and sperm concentrations ≥ 10 × 106. The pooled data studies showed EC was more successful than testosterone gel in achieving both endpoints (63.5% vs 24.7%; P < .001). No difference in the incidence of treatment-related adverse effects between groups was noted.
There were no major adverse effects, even after 3+ years of treatment
A 2019 retrospective cohort study of 400 men treated for symptomatic hypogonadism with CC sought to determine if improvements in testosterone, hypogonadal symptoms, and adverse effects were similar for those treated for ≤ 3 years (n = 280) and those treated for > 3 years (n = 120).5 Outcomes included serum testosterone and estradiol levels, symptom improvement (by qADAM questionnaire), and adverse effects.
All participants had a baseline testosterone level < 300 ng/dL, and all participants received CC therapy. Men received 25 mg/d with titration to 50 mg/d when testosterone did not improve to ≥ 300 ng/dL after 4 weeks.
When comparing outcomes across the 2 groups, there were no significant differences. Serum testosterone levels improved to 579 ng/dL (95% CI, 554-605) and 542 ng/dL (95% CI, 504-580) in the ≤ 3 years and > 3 years groups, respectively. Meanwhile, 79% of men in the ≤ 3 years group reported symptom improvement (improvement in libido, erection, or 3 other of the 10 domains of the qADAM questionnaire), while 77% of those in the > 3 years group reported improvement (P = .60).
Continue to: Finally, the percentage of men reporting...
Finally, the percentage of men reporting adverse effects did not significantly differ between groups: 9% in the ≤ 3 years group and 8% in the > 3 years group (P = .85). The most common adverse effects reported in order of frequency were mood changes, blurred vision, breast tenderness, hypertension, hematocrit changes, and flushing. No major adverse events (eg, myocardial infarction, cerebrovascular accident, venous thromboembolism, suicidal behavior) were reported in any patients.
Of note, although measured estrogen levels at the end of treatment were similar for both groups (54.8 pg/mL in the ≤ 3 years group vs 54.6 pg/mL in the > 3 years group), 37% of patients treated for > 3 years did receive anastrozole treatment for hyperestrogenism compared to 15% in the ≤ 3 years group (P = .05). The authors caution, though, that due to only 20% of the cohort patients having data on pre- and post-treatment estradiol levels, the study was likely underpowered to detect true differences among subgroups.
Recommendations from others
Current American Urological Association and Canadian Urological Association Guidelines note that while greater study on nontraditional testosterone therapies is needed, both organizations support use of SERMs, especially in hypogonadal men who are interested in fertility preservation, as increases in endogenous serum testosterone production do not impact fertility potential, unlike exogenous hormonal replacement.6,7 Additionally, men with low or low-normal serum LH levels may also be good candidates for the use of SERMs for management of testosterone deficiency.
Editor’s takeaway
Laboratory data (disease oriented) consistently shows that SERMs effectively increase testosterone levels to those comparable with testosterone gels. SERMs resulted in higher semen counts and maintained LH and FSH levels, but there were instances of hyperestrogenism. Data on longer-term benefits and adverse effects of both SERMs and testosterone supplementation are still needed.
Evidence summary
Alone or in combination with hCG, clomiphene citrate is effective
A 2018 multicenter prospective RCT (n = 283) compared the serum testosterone response in men (mean age, 41.8 ± 10.4 years) with hypogonadism before and after treatment with either CC, human chorionic gonadotropin (hCG), or a combination of both therapies.1 All patients wanted to maintain fertility, had normal follicle-stimulating hormone (FSH) and luteinizing hormone (LH) levels, had no history of testosterone therapy, had low (< 300 ng/dL) serum testosterone levels on at least 2 samples, and had at least 3 positive symptoms from the quantitative Androgen Deficiency in the Aging Male questionnaire (qADAM; a 10-item, graded-response tool measuring symptom severity from 1 to 5).
Patients were randomized into either the CC group (50 mg oral; n = 95), the hCG group (5000 IU injections twice weekly; n = 94), or the CC + hCG group (n = 94). Testosterone levels were measured at baseline and at 1 and 3 months after therapy initiation; qADAM questionnaire scores were also recorded but ultimately not used due to concerns with baseline heterogeneity among groups.
Average baseline serum testosterone levels for the CC, hCG, and CC + hCG groups were 243 ng/dL, 222 ng/dL, and 226 ng/dL, respectively. By 3 months, these levels had increased to 548 ng/dL (95% CI, 505-591) in the CC group, 467 ng/dL (95% CI, 440-494) in the hCG group, and 531 ng/dL (95% CI, 492-570) in the CC + hCG group. While there was not a significant difference between the CC and CC + hCG groups at 3 months (P = .579), both groups were superior to the hCG-only group (P = .002 for each).
CC and testosterone gel are comparable; testosterone injection is better
In a 2014 retrospective study, researchers reviewed the charts of 1150 men taking any form of testosterone supplementation therapy (TST). They compared treatment efficacy and qADAM satisfaction scores in 93 age-matched men with symptomatic hypogonadism who were treated with either CC (n = 31), testosterone injections (n = 31), or testosterone topical gel (n = 31).2 Eugonadal men not taking TST (n = 31) served as controls.
Inclusion criteria were based on treatment regimens of CC and TST. Participants in the treatment groups had a baseline total testosterone level < 300 ng/dL and had reported ≤ 3 positive symptoms on the qADAM questionnaire. Treatment regimens included CC (25 mg orally once daily), testosterone injections (testosterone cypionate 100 to 200 mg intramuscularly once weekly), and testosterone gel (Testim 1% or AndroGel 1.62%, 2 to 4 pumps/d).
The study results demonstrated an increase in median testosterone from baseline levels in all treatment groups when compared to placebo: CC (from 247 to 504 ng/dL), testosterone injections (from 224 to 1104 ng/dL), and testosterone gels (from 230 to 412 ng/dL) (P < .05). Men receiving testosterone injections had the highest increase in serum testosterone levels (956 ng/dL).
While the final mean serum total testosterone was highest in the testosterone injection group (1014 ng/dL; P < .01), the mean levels for those using CC and those using testosterone gels were comparable (525 ng/dL vs 412 ng/dL). Serum estradiol levels were also higher in men receiving testosterone injections, compared to men using CC, those using testosterone gels, and those not receiving TST (6.0 vs 2.0, 2.0, and 2.0 ng/dL, respectively; each P < .01).
Continue to: The qADAM scores...
The qADAM scores for hypogonadal symptoms showed no significant difference in men treated with CC, testosterone injections, and testosterone gels and those not receiving TST (35, 39, 36, and 34, respectively). Men receiving testosterone injections reported greater libido (range, 1-5) than men using CC, those using testosterone gels, and those not on TST (4 vs 3, 3, and 3; P = .047, .04, and < .01, respectively), but it is uncertain if this is clinically meaningful.
Enclomiphene citrate demonstrates improvement in hormone levels
A 2014 Phase II RCT investigated the effects of oral EC—a trans-isomer of CC—compared to topical testosterone 1% gel (T gel) in 124 men with secondary hypogonadism.3 Entry criteria included a baseline morning total testosterone level of < 250 ng/dL on 2 occasions. Participants were divided into 4 groups: 12.5-mg dose of EC, 25-mg dose of EC, T gel, and placebo.
The EC groups and the T gel group had comparable increases in testosterone levels after 3 months of treatment, without statistical significance. The 3-month change in serum testosterone level from baseline was 217 to 471 ng/dL (95% CI, 399-543) in the 12.5-mg dose group; 209 to 405 ng/dL (95% CI, 349-462) in the 25-mg dose group; and 210 to 462 ng/dL (95% CI, 359-565) in the T gel group. The placebo group had a decrease in serum testosterone levels, from 213 to 198 ng/dL (95% CI, 171-226).
Also, the EC groups demonstrated increases in LH and FSH levels from baseline to 3 months, while the T gel group showed a suppression (to low-normal range) in both levels: LH, 1.4 mIU/mL (decrease of 4.4 mIU/mL) and FSH, 2.4 mIU/mL (decrease of 2.4 mIU/mL). Among a subset of men (n = 67) who had at least 2 assessments at the end of 3 months, the researchers also analyzed changes in sperm concentration, using the lower limit of normal (15 million/mL). The number of men with a low sperm concentration increased significantly in the topical T gel group (16% to 53%) compared to the 12.5-mg EC group (decrease from 16% to 12%; P = .0008) and the 25-mg EC group (decrease from 5% to 0%; P = .0007), as well as compared to the placebo group (increase from 8% to 15%; P = .007).
With EC, testosterone remains elevated after treatment cessation
A 2016 2-center parallel, double-blind, placebo-controlled RCT evaluated the effect of 2 doses of EC (12.5 mg and 25 mg; n = 85) vs testosterone gel (1.62%; n = 85) vs placebo (n = 86) on serum testosterone, LH, FSH, and sperm counts in 256 overweight and obese men ages 18 to 60 years who had 2 morning testosterone measurements < 300 ng/dL and a low or inappropriately normal LH level for 16 weeks.4 All baseline characteristics, including age, BMI, sperm concentration, and serum total testosterone were statistically consistent within groups at both centers. For men receiving EC who did not achieve a testosterone level > 450 ng/dL, there was an up-titration from 12.5 mg to 25 mg at Week 4.
Continue to: All active treatment groups...
All active treatment groups showed increases in testosterone level during treatment (P < .001); however, FSH and LH levels increased in the EC group and decreased in the testosterone gel group (P < .001). Serum testosterone levels improved to 428.8 ng/dL (95% CI, 395-462) and 368.8 ng/dL (95% CI, 307-431), respectively, in the combined EC and testosterone gel groups at 16 weeks. Of note, total testosterone levels after cessation of treatment (off-drug point) rapidly decreased below baseline in the testosterone gel group compared to the pooled EC group, which remained elevated above baseline for at least 7 days.
Composite end-point analysis was performed, with success considered if men achieved both testosterone in normal range (300-1040 ng/dL) and sperm concentrations ≥ 10 × 106. The pooled data studies showed EC was more successful than testosterone gel in achieving both endpoints (63.5% vs 24.7%; P < .001). No difference in the incidence of treatment-related adverse effects between groups was noted.
There were no major adverse effects, even after 3+ years of treatment
A 2019 retrospective cohort study of 400 men treated for symptomatic hypogonadism with CC sought to determine if improvements in testosterone, hypogonadal symptoms, and adverse effects were similar for those treated for ≤ 3 years (n = 280) and those treated for > 3 years (n = 120).5 Outcomes included serum testosterone and estradiol levels, symptom improvement (by qADAM questionnaire), and adverse effects.
All participants had a baseline testosterone level < 300 ng/dL, and all participants received CC therapy. Men received 25 mg/d with titration to 50 mg/d when testosterone did not improve to ≥ 300 ng/dL after 4 weeks.
When comparing outcomes across the 2 groups, there were no significant differences. Serum testosterone levels improved to 579 ng/dL (95% CI, 554-605) and 542 ng/dL (95% CI, 504-580) in the ≤ 3 years and > 3 years groups, respectively. Meanwhile, 79% of men in the ≤ 3 years group reported symptom improvement (improvement in libido, erection, or 3 other of the 10 domains of the qADAM questionnaire), while 77% of those in the > 3 years group reported improvement (P = .60).
Continue to: Finally, the percentage of men reporting...
Finally, the percentage of men reporting adverse effects did not significantly differ between groups: 9% in the ≤ 3 years group and 8% in the > 3 years group (P = .85). The most common adverse effects reported in order of frequency were mood changes, blurred vision, breast tenderness, hypertension, hematocrit changes, and flushing. No major adverse events (eg, myocardial infarction, cerebrovascular accident, venous thromboembolism, suicidal behavior) were reported in any patients.
Of note, although measured estrogen levels at the end of treatment were similar for both groups (54.8 pg/mL in the ≤ 3 years group vs 54.6 pg/mL in the > 3 years group), 37% of patients treated for > 3 years did receive anastrozole treatment for hyperestrogenism compared to 15% in the ≤ 3 years group (P = .05). The authors caution, though, that due to only 20% of the cohort patients having data on pre- and post-treatment estradiol levels, the study was likely underpowered to detect true differences among subgroups.
Recommendations from others
Current American Urological Association and Canadian Urological Association Guidelines note that while greater study on nontraditional testosterone therapies is needed, both organizations support use of SERMs, especially in hypogonadal men who are interested in fertility preservation, as increases in endogenous serum testosterone production do not impact fertility potential, unlike exogenous hormonal replacement.6,7 Additionally, men with low or low-normal serum LH levels may also be good candidates for the use of SERMs for management of testosterone deficiency.
Editor’s takeaway
Laboratory data (disease oriented) consistently shows that SERMs effectively increase testosterone levels to those comparable with testosterone gels. SERMs resulted in higher semen counts and maintained LH and FSH levels, but there were instances of hyperestrogenism. Data on longer-term benefits and adverse effects of both SERMs and testosterone supplementation are still needed.
1. Habous M, Giona S, Tealab A, et al. Clomiphene citrate and human chorionic gonadotropin are both effective in restoring testosterone in hypogonadism: a short-course randomized study. BJU Int. 2018;122:889-897. doi: 10.1111/bju.14401
2. Ramasamy R, Scovell JM, Kovac JR, et al. Testosterone supplementation versus clomiphene citrate for hypogonadism: an age matched comparison of satisfaction and efficacy. J Urol. 2014;192:875-879. doi: 10.1016/j.juro.2014.03.089
3. Wiehle RD, Fontenot GK, Wike J, et al. Enclomiphene citrate stimulates testosterone production while preventing oligospermia: a randomized phase II clinical trial comparing topical testosterone. Fertil Steril. 2014;102:720-727. doi: 10.1016/j.fertnstert.2014.06.004
4. Kim ED, McCullough A, Kaminetsky J. Oral enclomiphene citrate raises testosterone and preserves sperm counts in obese hypogonadal men, unlike topical testosterone: restoration instead of replacement. BJU Int. 2016;117:677-685. doi: 10.1111/bju.13337
5. Krzastek SC, Sharma D, Abdullah N, et al. Long-term safety and efficacy of clomiphene citrate for the treatment of hypogonadism. J Urol. 2019;202:1029-1035. doi: 10.1097/JU.0000000000000396
6. Grober ED, Krakowsky Y, Khera M, et al. Canadian Urological Association clinical practice guideline on testosterone deficiency in men: evidence-based Q&A. Can Urol Assoc J. 2021;15:E234-E243. doi: 10.5489/cuaj.7252
7. Mulhall JP, Trost LW, Brannigan RE, et al. Evaluation and management of testosterone deficiency: AUA guideline. J Urol. 2018;200:423-432. doi: 10.1016/j.juro.2018.03.115
1. Habous M, Giona S, Tealab A, et al. Clomiphene citrate and human chorionic gonadotropin are both effective in restoring testosterone in hypogonadism: a short-course randomized study. BJU Int. 2018;122:889-897. doi: 10.1111/bju.14401
2. Ramasamy R, Scovell JM, Kovac JR, et al. Testosterone supplementation versus clomiphene citrate for hypogonadism: an age matched comparison of satisfaction and efficacy. J Urol. 2014;192:875-879. doi: 10.1016/j.juro.2014.03.089
3. Wiehle RD, Fontenot GK, Wike J, et al. Enclomiphene citrate stimulates testosterone production while preventing oligospermia: a randomized phase II clinical trial comparing topical testosterone. Fertil Steril. 2014;102:720-727. doi: 10.1016/j.fertnstert.2014.06.004
4. Kim ED, McCullough A, Kaminetsky J. Oral enclomiphene citrate raises testosterone and preserves sperm counts in obese hypogonadal men, unlike topical testosterone: restoration instead of replacement. BJU Int. 2016;117:677-685. doi: 10.1111/bju.13337
5. Krzastek SC, Sharma D, Abdullah N, et al. Long-term safety and efficacy of clomiphene citrate for the treatment of hypogonadism. J Urol. 2019;202:1029-1035. doi: 10.1097/JU.0000000000000396
6. Grober ED, Krakowsky Y, Khera M, et al. Canadian Urological Association clinical practice guideline on testosterone deficiency in men: evidence-based Q&A. Can Urol Assoc J. 2021;15:E234-E243. doi: 10.5489/cuaj.7252
7. Mulhall JP, Trost LW, Brannigan RE, et al. Evaluation and management of testosterone deficiency: AUA guideline. J Urol. 2018;200:423-432. doi: 10.1016/j.juro.2018.03.115
EVIDENCE-BASED ANSWER:
YES. For both normal-weight and obese men with low testosterone levels and hypogonadal symptoms, selective estrogen receptor modulators (SERMs), such as clomiphene citrate (CC) and enclomiphene citrate (EC), appear to be effective and safe for improving serum testosterone levels (strength of recommendation [SOR]: C, disease-oriented outcomes from randomized controlled trials [RCTs] and cohort studies). Studies also show that symptom improvement is comparable to that with exogenous testosterone replacement and similar to eugonadal men (SOR: B, patient-oriented outcomes from retrospective cohort studies).
Should we stop prescribing IM progesterone to women with a history of preterm labor?
Evidence summary
Early evidence suggested benefit from IM progesterone
A 2003 RCT compared weekly IM progesterone (n = 310) and placebo (n = 153) injections in women with a history of spontaneous preterm delivery. Participants were at 15w0d to 20w3d of a singleton pregnancy with no fetal abnormality. The 17-OHP group, compared to the placebo group, had significantly fewer deliveries at < 37 weeks (36.3% vs 54.9%; relative risk [RR] = 0.66; 95% CI, 0.54 to 0.81; number needed to treat [NNT] = 6), at < 35 weeks (20.6% vs 30.7%; RR = 0.67; 95% CI, 0.48 to 0.93; NNT = 10), and at < 32 weeks (11.4% vs 19.6%; RR = 0.58; 95% CI, 0.37 to 0.91; NNT = 13).1 There were significantly lower rates of necrotizing enterocolitis, intraventricular hemorrhage, and need for supplemental oxygen in infants of women in the treatment group.1 The study was underpowered to detect neonatal morbidity.
A 2013 Cochrane Review (5 studies including the 2003 RCT; 602 women) found that 17-OHP led to a decreased risk of birth at < 34 weeks (RR = 0.31; 95% CI, 0.14-0.69). It also led to a significant reduction in perinatal and neonatal mortality, birth at < 37 weeks, birthweight < 2500 g, use of assisted ventilation, incidence of necrotizing enterocolitis, and admission to the neonatal ICU.2
In a large follow-up study, progesterone did not demonstrate benefit
The PROLONG study was a double-blind, placebo-controlled international RCT of women with a previous singleton spontaneous preterm birth. The study involved 93 clinical centers in 9 countries: 41 in the United States and 52 outside the United States. The PROLONG study was much larger than the 2003 study: 1139 active treatment (vs 310) and 578 placebo (vs 153) participants. Women were randomized 2:1 to receive either 250 mg 17-OHP or inert oil placebo weekly from 16w0d-20w6d until 36 weeks. The outcome measures were: (1) delivery at < 35 weeks and (2) a neonatal morbidity composite index. This composite index included any of the following: neonatal death, grade 3 or 4 intraventricular hemorrhage, respiratory distress syndrome, bronchopulmonary dysplasia, necrotizing enterocolitis, and proven sepsis.3
Progesterone did not improve any of the studied outcomes: there were no significant differences in the frequency of birth at < 35 weeks (17-OHP 11% vs placebo 11.5%; RR = 0.95; 95% CI, 0.71-1.26), in neonatal morbidity index (17-OHP 5.6% vs placebo 5%; RR = 1.12; 95% CI, 0.68-1.61), and in frequency of fetal/early infant death (17-OHP 1.7% vs placebo 1.9%; RR = 0.87; 95% CI, 0.4-1.81).3 In the United States subgroup (n = 391; 23% of all patients), there was no significant difference in rate of birth at < 35 weeks (17-OHP 15.6% vs placebo 17.6%; RR = 0.88; 95% CI, 0.55-1.40).3
However, PROLONG had some limitations. Importantly, the 2003 RCT included 183 (59%) non-Hispanic Black women in the experimental group and 90 (58.5%) in the control group, whereas the 2020 PROLONG study had only 6.6% non-Hispanic Black participants. The neonatal outcome data for the PROLONG study only included 6 Black women in the experimental arm and 3 in the control arm.3,4 Black women have prematurity rates that are 2 to 3 times higher than those in White women.5
Additionally, the PROLONG study had fewer smokers and more women who were married/living with a partner. Compared with prior studies, the PROLONG study had a lower proportion of women with > 1 spontaneous preterm birth and fewer with a shortened cervix (< 2%).3 As a result of having lower risk participants, PROLONG may have been underpowered to detect improvements in outcome.3
A subsequent meta-analysis suggests some benefit for high-risk women
The 2021 Evaluating Progestogens for Preventing Preterm birth International Collaborative (EPPPIC) meta-analysis of individual data from 31 RCTs—involving 11,644 women and 16,185 babies—found that, compared with placebo, 17-OHP for women with a history of preterm delivery or short cervix did not significantly decrease the number of babies born before 34 weeks (5 trials [including the 2003 RCT and PROLONG studies]; 3053 women; RR = 0.83; 95% CI, 0.68–1.01).6 However, it found that vaginal progesterone significantly decreased birth prior to 34 weeks (9 trials; 3769 women; RR = 0.78, 95% CI, 0.68-0.90).6 The authors concluded that both IM and vaginal progesterone decreased preterm delivery in high-risk women. The effect was stronger for women with a short cervix than for women with a history of preterm delivery.6
Continue to: Recommendations from others
Recommendations from others
In 2008, a joint ACOG/SMFM statement said, “Progesterone supplementation for the prevention of recurrent preterm birth should be offered to women with a singleton pregnancy and prior spontaneous preterm birth.”7 A 2012 ACOG Practice Bulletin stated that, “A woman with a singleton gestation and a prior spontaneous preterm singleton birth should be offered progesterone supplementation starting at 16 to 24 weeks of gestation, regardless of transvaginal ultrasound cervical length, to reduce the risk of recurrent spontaneous preterm birth.”8
In 2011, Makena (hydroxyprogesterone caproate injection) received accelerated approval from the FDA. In October 2020, the FDA Advisory Committee recommended that Makena be withdrawn from the market (9 to 7 vote).9 On October 5, 2020, the FDA’s Center for Drug Evaluation and Research (CDER) proposed that Makena be withdrawn from the market “because the required postmarket study failed to verify clinical benefit and we have concluded that the available evidence does not show Makena is effective for its approved use.”10 A subgroup analysis by CDER did not find benefit for any subgroup, including high-risk women.10 However, Makena will remain on the market unless its manufacturer withdraws it or the FDA Commissioner mandates its removal.
In response to the FDA’s proposal, both ACOG and SMFM recommended that “obstetric health care professionals discuss Makena’s benefits, risks, and uncertainties with their patients”11 as part of “a shared decision-making approach, taking into account the lack of short-term safety concerns but uncertainty regarding benefit.”12 Both organizations reiterated their position on shared decision-making after the EPPPIC meta-analysis was published.13
Studies comparing the 2 routes of administration (vaginal and IM) are underway.13
Editor’s takeaway
Our best evidence does not support routine IM progesterone use to prevent preterm delivery. However, therapeutic inertia, uncertainty, and defensive medicine may slow down adoption of this newer evidence. Shared decision-making can assist treatment decisions, but it is not a substitute for following the best evidence.
1. Meis P, Klebanoff M, Thom E, et al; National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. Prevention of recurrent preterm delivery by 17 alpha-hydroxyprogesterone caproate. N Engl J Med. 2003;348:2379-2385. doi: 10.1056/NEJMoa035140
2. Dodd J, Jones L, Flenady V, et al. Prenatal administration of progesterone for preventing preterm birth in women considered to be at risk of preterm birth. Cochrane Database Syst Rev. 2013;(7):CD004947. doi: 10.1002/14651858.CD004947.pub3
3. Blackell S, Gyamfi-Bannerman C, Biggio JJ, et al. 17-OHPC to Prevent Recurrent Preterm Birth in Singleton Gestations (PROLONG study): a multicenter, international, randomized double-blind trial. Am J Perinatol. 2020;37:127-136. doi: 10.1055/s-0039-3400227
4. Greene M, Klebanoff M, Harrington D. Preterm birth and 17OHP—why the FDA should not withdraw approval. N Engl J Med. 2020;383:e130. doi: 10.1056/NEJMp2031727
5. Schlenker T, Dresang L, Ndiaye M, et al. The effect of prenatal support on birth outcomes in an urban Midwestern county. WMJ. 2012;111:267-273.
6. EPPPIC Group. Evaluating Progestogens for Preventing Preterm birth International Collaborative (EPPPIC): meta-analysis of individual participant data from randomised controlled trials. Lancet. 2021;397:1183-1194. doi: 10.1016/S0140-6736(21)00217-8
7. Society for Maternal Fetal Medicine Publications Committee. ACOG Committee Opinion number 419 October 2008 (replaces no. 291, November 2003). Use of progesterone to reduce preterm birth. Obstet Gynecol. 2008;112:963-965. doi: 10.1097/AOG.0b013e31818b1ff6
8. Committee on Practice Bulletins—Obstetrics, The American College of Obstetricians and Gynecologists. Practice Bulletin no. 130: prediction and prevention of preterm birth. Obstet Gynecol. 2012;120:964-973. doi: 10.1097/AOG.0b013e3182723b1b
9. Chang C, Nguyen C, Wesley B, et al. Withdrawing approval of Makena—a proposal from the FDA Center for Drug Evaluation and Research. N Engl J Med. 2020;383:e131. doi: 10.1056/NEJMp2031055
10. US Food and Drug Administration. CDER proposes withdrawal of approval for Makena. Published October 5, 2020. Accessed December 10, 2021. www.fda.gov/drugs/drug-safety-and-availability/cder-proposes-withdrawal-approval-makena
11. Zahn CM. ACOG statement on FDA proposal to withdraw 17p hydroxyprogesterone caproate. Published October 7, 2020. Accessed December 10, 2021. www.acog.org/en/News/News%20Releases/2020/10/ACOG%20Statement%20on%20FDA%20Proposal%20to%20Withdraw%2017p%20Hydroxyprogesterone%20Caproate
12. Society for Maternal-Fetal Medicine Publications Committee. SMFM Statement: Use of 17-alpha hydroxyprogesterone caproate for prevention of recurrent preterm birth. Published October 5, 2021. Accessed December 10, 2021. https://s3.amazonaws.com/cdn.smfm.org/media/2543/Makena,_10.5.pdf
13. Society for Maternal-Fetal Medicine. SMFM Statement: Response to EPPPIC and considerations of the use of progestogens for the prevention of preterm birth. Published March 2021. Accessed December 10, 2021. www.smfm.org/publications/383-smfm-statement-response-to-epppic-and-considerations-of-the-use-of-progestogens-for-the-prevention-of-preterm-birth
Evidence summary
Early evidence suggested benefit from IM progesterone
A 2003 RCT compared weekly IM progesterone (n = 310) and placebo (n = 153) injections in women with a history of spontaneous preterm delivery. Participants were at 15w0d to 20w3d of a singleton pregnancy with no fetal abnormality. The 17-OHP group, compared to the placebo group, had significantly fewer deliveries at < 37 weeks (36.3% vs 54.9%; relative risk [RR] = 0.66; 95% CI, 0.54 to 0.81; number needed to treat [NNT] = 6), at < 35 weeks (20.6% vs 30.7%; RR = 0.67; 95% CI, 0.48 to 0.93; NNT = 10), and at < 32 weeks (11.4% vs 19.6%; RR = 0.58; 95% CI, 0.37 to 0.91; NNT = 13).1 There were significantly lower rates of necrotizing enterocolitis, intraventricular hemorrhage, and need for supplemental oxygen in infants of women in the treatment group.1 The study was underpowered to detect neonatal morbidity.
A 2013 Cochrane Review (5 studies including the 2003 RCT; 602 women) found that 17-OHP led to a decreased risk of birth at < 34 weeks (RR = 0.31; 95% CI, 0.14-0.69). It also led to a significant reduction in perinatal and neonatal mortality, birth at < 37 weeks, birthweight < 2500 g, use of assisted ventilation, incidence of necrotizing enterocolitis, and admission to the neonatal ICU.2
In a large follow-up study, progesterone did not demonstrate benefit
The PROLONG study was a double-blind, placebo-controlled international RCT of women with a previous singleton spontaneous preterm birth. The study involved 93 clinical centers in 9 countries: 41 in the United States and 52 outside the United States. The PROLONG study was much larger than the 2003 study: 1139 active treatment (vs 310) and 578 placebo (vs 153) participants. Women were randomized 2:1 to receive either 250 mg 17-OHP or inert oil placebo weekly from 16w0d-20w6d until 36 weeks. The outcome measures were: (1) delivery at < 35 weeks and (2) a neonatal morbidity composite index. This composite index included any of the following: neonatal death, grade 3 or 4 intraventricular hemorrhage, respiratory distress syndrome, bronchopulmonary dysplasia, necrotizing enterocolitis, and proven sepsis.3
Progesterone did not improve any of the studied outcomes: there were no significant differences in the frequency of birth at < 35 weeks (17-OHP 11% vs placebo 11.5%; RR = 0.95; 95% CI, 0.71-1.26), in neonatal morbidity index (17-OHP 5.6% vs placebo 5%; RR = 1.12; 95% CI, 0.68-1.61), and in frequency of fetal/early infant death (17-OHP 1.7% vs placebo 1.9%; RR = 0.87; 95% CI, 0.4-1.81).3 In the United States subgroup (n = 391; 23% of all patients), there was no significant difference in rate of birth at < 35 weeks (17-OHP 15.6% vs placebo 17.6%; RR = 0.88; 95% CI, 0.55-1.40).3
However, PROLONG had some limitations. Importantly, the 2003 RCT included 183 (59%) non-Hispanic Black women in the experimental group and 90 (58.5%) in the control group, whereas the 2020 PROLONG study had only 6.6% non-Hispanic Black participants. The neonatal outcome data for the PROLONG study only included 6 Black women in the experimental arm and 3 in the control arm.3,4 Black women have prematurity rates that are 2 to 3 times higher than those in White women.5
Additionally, the PROLONG study had fewer smokers and more women who were married/living with a partner. Compared with prior studies, the PROLONG study had a lower proportion of women with > 1 spontaneous preterm birth and fewer with a shortened cervix (< 2%).3 As a result of having lower risk participants, PROLONG may have been underpowered to detect improvements in outcome.3
A subsequent meta-analysis suggests some benefit for high-risk women
The 2021 Evaluating Progestogens for Preventing Preterm birth International Collaborative (EPPPIC) meta-analysis of individual data from 31 RCTs—involving 11,644 women and 16,185 babies—found that, compared with placebo, 17-OHP for women with a history of preterm delivery or short cervix did not significantly decrease the number of babies born before 34 weeks (5 trials [including the 2003 RCT and PROLONG studies]; 3053 women; RR = 0.83; 95% CI, 0.68–1.01).6 However, it found that vaginal progesterone significantly decreased birth prior to 34 weeks (9 trials; 3769 women; RR = 0.78, 95% CI, 0.68-0.90).6 The authors concluded that both IM and vaginal progesterone decreased preterm delivery in high-risk women. The effect was stronger for women with a short cervix than for women with a history of preterm delivery.6
Continue to: Recommendations from others
Recommendations from others
In 2008, a joint ACOG/SMFM statement said, “Progesterone supplementation for the prevention of recurrent preterm birth should be offered to women with a singleton pregnancy and prior spontaneous preterm birth.”7 A 2012 ACOG Practice Bulletin stated that, “A woman with a singleton gestation and a prior spontaneous preterm singleton birth should be offered progesterone supplementation starting at 16 to 24 weeks of gestation, regardless of transvaginal ultrasound cervical length, to reduce the risk of recurrent spontaneous preterm birth.”8
In 2011, Makena (hydroxyprogesterone caproate injection) received accelerated approval from the FDA. In October 2020, the FDA Advisory Committee recommended that Makena be withdrawn from the market (9 to 7 vote).9 On October 5, 2020, the FDA’s Center for Drug Evaluation and Research (CDER) proposed that Makena be withdrawn from the market “because the required postmarket study failed to verify clinical benefit and we have concluded that the available evidence does not show Makena is effective for its approved use.”10 A subgroup analysis by CDER did not find benefit for any subgroup, including high-risk women.10 However, Makena will remain on the market unless its manufacturer withdraws it or the FDA Commissioner mandates its removal.
In response to the FDA’s proposal, both ACOG and SMFM recommended that “obstetric health care professionals discuss Makena’s benefits, risks, and uncertainties with their patients”11 as part of “a shared decision-making approach, taking into account the lack of short-term safety concerns but uncertainty regarding benefit.”12 Both organizations reiterated their position on shared decision-making after the EPPPIC meta-analysis was published.13
Studies comparing the 2 routes of administration (vaginal and IM) are underway.13
Editor’s takeaway
Our best evidence does not support routine IM progesterone use to prevent preterm delivery. However, therapeutic inertia, uncertainty, and defensive medicine may slow down adoption of this newer evidence. Shared decision-making can assist treatment decisions, but it is not a substitute for following the best evidence.
Evidence summary
Early evidence suggested benefit from IM progesterone
A 2003 RCT compared weekly IM progesterone (n = 310) and placebo (n = 153) injections in women with a history of spontaneous preterm delivery. Participants were at 15w0d to 20w3d of a singleton pregnancy with no fetal abnormality. The 17-OHP group, compared to the placebo group, had significantly fewer deliveries at < 37 weeks (36.3% vs 54.9%; relative risk [RR] = 0.66; 95% CI, 0.54 to 0.81; number needed to treat [NNT] = 6), at < 35 weeks (20.6% vs 30.7%; RR = 0.67; 95% CI, 0.48 to 0.93; NNT = 10), and at < 32 weeks (11.4% vs 19.6%; RR = 0.58; 95% CI, 0.37 to 0.91; NNT = 13).1 There were significantly lower rates of necrotizing enterocolitis, intraventricular hemorrhage, and need for supplemental oxygen in infants of women in the treatment group.1 The study was underpowered to detect neonatal morbidity.
A 2013 Cochrane Review (5 studies including the 2003 RCT; 602 women) found that 17-OHP led to a decreased risk of birth at < 34 weeks (RR = 0.31; 95% CI, 0.14-0.69). It also led to a significant reduction in perinatal and neonatal mortality, birth at < 37 weeks, birthweight < 2500 g, use of assisted ventilation, incidence of necrotizing enterocolitis, and admission to the neonatal ICU.2
In a large follow-up study, progesterone did not demonstrate benefit
The PROLONG study was a double-blind, placebo-controlled international RCT of women with a previous singleton spontaneous preterm birth. The study involved 93 clinical centers in 9 countries: 41 in the United States and 52 outside the United States. The PROLONG study was much larger than the 2003 study: 1139 active treatment (vs 310) and 578 placebo (vs 153) participants. Women were randomized 2:1 to receive either 250 mg 17-OHP or inert oil placebo weekly from 16w0d-20w6d until 36 weeks. The outcome measures were: (1) delivery at < 35 weeks and (2) a neonatal morbidity composite index. This composite index included any of the following: neonatal death, grade 3 or 4 intraventricular hemorrhage, respiratory distress syndrome, bronchopulmonary dysplasia, necrotizing enterocolitis, and proven sepsis.3
Progesterone did not improve any of the studied outcomes: there were no significant differences in the frequency of birth at < 35 weeks (17-OHP 11% vs placebo 11.5%; RR = 0.95; 95% CI, 0.71-1.26), in neonatal morbidity index (17-OHP 5.6% vs placebo 5%; RR = 1.12; 95% CI, 0.68-1.61), and in frequency of fetal/early infant death (17-OHP 1.7% vs placebo 1.9%; RR = 0.87; 95% CI, 0.4-1.81).3 In the United States subgroup (n = 391; 23% of all patients), there was no significant difference in rate of birth at < 35 weeks (17-OHP 15.6% vs placebo 17.6%; RR = 0.88; 95% CI, 0.55-1.40).3
However, PROLONG had some limitations. Importantly, the 2003 RCT included 183 (59%) non-Hispanic Black women in the experimental group and 90 (58.5%) in the control group, whereas the 2020 PROLONG study had only 6.6% non-Hispanic Black participants. The neonatal outcome data for the PROLONG study only included 6 Black women in the experimental arm and 3 in the control arm.3,4 Black women have prematurity rates that are 2 to 3 times higher than those in White women.5
Additionally, the PROLONG study had fewer smokers and more women who were married/living with a partner. Compared with prior studies, the PROLONG study had a lower proportion of women with > 1 spontaneous preterm birth and fewer with a shortened cervix (< 2%).3 As a result of having lower risk participants, PROLONG may have been underpowered to detect improvements in outcome.3
A subsequent meta-analysis suggests some benefit for high-risk women
The 2021 Evaluating Progestogens for Preventing Preterm birth International Collaborative (EPPPIC) meta-analysis of individual data from 31 RCTs—involving 11,644 women and 16,185 babies—found that, compared with placebo, 17-OHP for women with a history of preterm delivery or short cervix did not significantly decrease the number of babies born before 34 weeks (5 trials [including the 2003 RCT and PROLONG studies]; 3053 women; RR = 0.83; 95% CI, 0.68–1.01).6 However, it found that vaginal progesterone significantly decreased birth prior to 34 weeks (9 trials; 3769 women; RR = 0.78, 95% CI, 0.68-0.90).6 The authors concluded that both IM and vaginal progesterone decreased preterm delivery in high-risk women. The effect was stronger for women with a short cervix than for women with a history of preterm delivery.6
Continue to: Recommendations from others
Recommendations from others
In 2008, a joint ACOG/SMFM statement said, “Progesterone supplementation for the prevention of recurrent preterm birth should be offered to women with a singleton pregnancy and prior spontaneous preterm birth.”7 A 2012 ACOG Practice Bulletin stated that, “A woman with a singleton gestation and a prior spontaneous preterm singleton birth should be offered progesterone supplementation starting at 16 to 24 weeks of gestation, regardless of transvaginal ultrasound cervical length, to reduce the risk of recurrent spontaneous preterm birth.”8
In 2011, Makena (hydroxyprogesterone caproate injection) received accelerated approval from the FDA. In October 2020, the FDA Advisory Committee recommended that Makena be withdrawn from the market (9 to 7 vote).9 On October 5, 2020, the FDA’s Center for Drug Evaluation and Research (CDER) proposed that Makena be withdrawn from the market “because the required postmarket study failed to verify clinical benefit and we have concluded that the available evidence does not show Makena is effective for its approved use.”10 A subgroup analysis by CDER did not find benefit for any subgroup, including high-risk women.10 However, Makena will remain on the market unless its manufacturer withdraws it or the FDA Commissioner mandates its removal.
In response to the FDA’s proposal, both ACOG and SMFM recommended that “obstetric health care professionals discuss Makena’s benefits, risks, and uncertainties with their patients”11 as part of “a shared decision-making approach, taking into account the lack of short-term safety concerns but uncertainty regarding benefit.”12 Both organizations reiterated their position on shared decision-making after the EPPPIC meta-analysis was published.13
Studies comparing the 2 routes of administration (vaginal and IM) are underway.13
Editor’s takeaway
Our best evidence does not support routine IM progesterone use to prevent preterm delivery. However, therapeutic inertia, uncertainty, and defensive medicine may slow down adoption of this newer evidence. Shared decision-making can assist treatment decisions, but it is not a substitute for following the best evidence.
1. Meis P, Klebanoff M, Thom E, et al; National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. Prevention of recurrent preterm delivery by 17 alpha-hydroxyprogesterone caproate. N Engl J Med. 2003;348:2379-2385. doi: 10.1056/NEJMoa035140
2. Dodd J, Jones L, Flenady V, et al. Prenatal administration of progesterone for preventing preterm birth in women considered to be at risk of preterm birth. Cochrane Database Syst Rev. 2013;(7):CD004947. doi: 10.1002/14651858.CD004947.pub3
3. Blackell S, Gyamfi-Bannerman C, Biggio JJ, et al. 17-OHPC to Prevent Recurrent Preterm Birth in Singleton Gestations (PROLONG study): a multicenter, international, randomized double-blind trial. Am J Perinatol. 2020;37:127-136. doi: 10.1055/s-0039-3400227
4. Greene M, Klebanoff M, Harrington D. Preterm birth and 17OHP—why the FDA should not withdraw approval. N Engl J Med. 2020;383:e130. doi: 10.1056/NEJMp2031727
5. Schlenker T, Dresang L, Ndiaye M, et al. The effect of prenatal support on birth outcomes in an urban Midwestern county. WMJ. 2012;111:267-273.
6. EPPPIC Group. Evaluating Progestogens for Preventing Preterm birth International Collaborative (EPPPIC): meta-analysis of individual participant data from randomised controlled trials. Lancet. 2021;397:1183-1194. doi: 10.1016/S0140-6736(21)00217-8
7. Society for Maternal Fetal Medicine Publications Committee. ACOG Committee Opinion number 419 October 2008 (replaces no. 291, November 2003). Use of progesterone to reduce preterm birth. Obstet Gynecol. 2008;112:963-965. doi: 10.1097/AOG.0b013e31818b1ff6
8. Committee on Practice Bulletins—Obstetrics, The American College of Obstetricians and Gynecologists. Practice Bulletin no. 130: prediction and prevention of preterm birth. Obstet Gynecol. 2012;120:964-973. doi: 10.1097/AOG.0b013e3182723b1b
9. Chang C, Nguyen C, Wesley B, et al. Withdrawing approval of Makena—a proposal from the FDA Center for Drug Evaluation and Research. N Engl J Med. 2020;383:e131. doi: 10.1056/NEJMp2031055
10. US Food and Drug Administration. CDER proposes withdrawal of approval for Makena. Published October 5, 2020. Accessed December 10, 2021. www.fda.gov/drugs/drug-safety-and-availability/cder-proposes-withdrawal-approval-makena
11. Zahn CM. ACOG statement on FDA proposal to withdraw 17p hydroxyprogesterone caproate. Published October 7, 2020. Accessed December 10, 2021. www.acog.org/en/News/News%20Releases/2020/10/ACOG%20Statement%20on%20FDA%20Proposal%20to%20Withdraw%2017p%20Hydroxyprogesterone%20Caproate
12. Society for Maternal-Fetal Medicine Publications Committee. SMFM Statement: Use of 17-alpha hydroxyprogesterone caproate for prevention of recurrent preterm birth. Published October 5, 2021. Accessed December 10, 2021. https://s3.amazonaws.com/cdn.smfm.org/media/2543/Makena,_10.5.pdf
13. Society for Maternal-Fetal Medicine. SMFM Statement: Response to EPPPIC and considerations of the use of progestogens for the prevention of preterm birth. Published March 2021. Accessed December 10, 2021. www.smfm.org/publications/383-smfm-statement-response-to-epppic-and-considerations-of-the-use-of-progestogens-for-the-prevention-of-preterm-birth
1. Meis P, Klebanoff M, Thom E, et al; National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. Prevention of recurrent preterm delivery by 17 alpha-hydroxyprogesterone caproate. N Engl J Med. 2003;348:2379-2385. doi: 10.1056/NEJMoa035140
2. Dodd J, Jones L, Flenady V, et al. Prenatal administration of progesterone for preventing preterm birth in women considered to be at risk of preterm birth. Cochrane Database Syst Rev. 2013;(7):CD004947. doi: 10.1002/14651858.CD004947.pub3
3. Blackell S, Gyamfi-Bannerman C, Biggio JJ, et al. 17-OHPC to Prevent Recurrent Preterm Birth in Singleton Gestations (PROLONG study): a multicenter, international, randomized double-blind trial. Am J Perinatol. 2020;37:127-136. doi: 10.1055/s-0039-3400227
4. Greene M, Klebanoff M, Harrington D. Preterm birth and 17OHP—why the FDA should not withdraw approval. N Engl J Med. 2020;383:e130. doi: 10.1056/NEJMp2031727
5. Schlenker T, Dresang L, Ndiaye M, et al. The effect of prenatal support on birth outcomes in an urban Midwestern county. WMJ. 2012;111:267-273.
6. EPPPIC Group. Evaluating Progestogens for Preventing Preterm birth International Collaborative (EPPPIC): meta-analysis of individual participant data from randomised controlled trials. Lancet. 2021;397:1183-1194. doi: 10.1016/S0140-6736(21)00217-8
7. Society for Maternal Fetal Medicine Publications Committee. ACOG Committee Opinion number 419 October 2008 (replaces no. 291, November 2003). Use of progesterone to reduce preterm birth. Obstet Gynecol. 2008;112:963-965. doi: 10.1097/AOG.0b013e31818b1ff6
8. Committee on Practice Bulletins—Obstetrics, The American College of Obstetricians and Gynecologists. Practice Bulletin no. 130: prediction and prevention of preterm birth. Obstet Gynecol. 2012;120:964-973. doi: 10.1097/AOG.0b013e3182723b1b
9. Chang C, Nguyen C, Wesley B, et al. Withdrawing approval of Makena—a proposal from the FDA Center for Drug Evaluation and Research. N Engl J Med. 2020;383:e131. doi: 10.1056/NEJMp2031055
10. US Food and Drug Administration. CDER proposes withdrawal of approval for Makena. Published October 5, 2020. Accessed December 10, 2021. www.fda.gov/drugs/drug-safety-and-availability/cder-proposes-withdrawal-approval-makena
11. Zahn CM. ACOG statement on FDA proposal to withdraw 17p hydroxyprogesterone caproate. Published October 7, 2020. Accessed December 10, 2021. www.acog.org/en/News/News%20Releases/2020/10/ACOG%20Statement%20on%20FDA%20Proposal%20to%20Withdraw%2017p%20Hydroxyprogesterone%20Caproate
12. Society for Maternal-Fetal Medicine Publications Committee. SMFM Statement: Use of 17-alpha hydroxyprogesterone caproate for prevention of recurrent preterm birth. Published October 5, 2021. Accessed December 10, 2021. https://s3.amazonaws.com/cdn.smfm.org/media/2543/Makena,_10.5.pdf
13. Society for Maternal-Fetal Medicine. SMFM Statement: Response to EPPPIC and considerations of the use of progestogens for the prevention of preterm birth. Published March 2021. Accessed December 10, 2021. www.smfm.org/publications/383-smfm-statement-response-to-epppic-and-considerations-of-the-use-of-progestogens-for-the-prevention-of-preterm-birth
EVIDENCE-BASED REVIEW:
YES, we should stop the routine prescribin
The US Food and Drug Administration (FDA) has recommended withdrawing 17-OHP from the market. The American College of Obstetricians and Gynecologists (ACOG) and the Society for Maternal-Fetal Medicine (SMFM) have released statements supporting shared decision-making with women regarding the prescribing of 17-OHP for preterm delivery prevention (SOR: C, expert opinion).
58-year-old man • bilateral shoulder pain • history of prostate cancer • limited shoulder range of motion • Dx?
THE CASE
A 58-year-old African American man with a past medical history of prostate cancer, hypertension, hyperlipidemia, osteoarthritis, and gastroesophageal reflux disease presented to our office to establish care with a new provider. He complained of bilateral shoulder pain, that was worse on the right side, for the past year. He denied any previous falls, trauma, or injury. He reported that lifting his grandkids was becoming increasingly difficult due to the pain but denied any weakness or neurologic symptoms. He had been using over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), which provided minimal relief.
On physical examination, the overlying skin was normal and there was no tenderness to palpation. His shoulder range of motion was limited with complete flexion, but otherwise intact. Muscle strength was 5 out of 5 bilaterally, and neurovascular and sensory examinations were normal. On the right side, the Empty Can Test was positive, but the Neer and Apley tests were negative. All testing was negative on the left side.
The patient was referred for 10 sessions of physical therapy, which he completed. His pain persisted, and an x-ray of his right shoulder was performed. The x-ray indicated a high-riding humeral head, and magnetic resonance imaging (MRI) of the right shoulder was recommended due to possible rotator cuff tendinopathy.
The MRI demonstrated a full-thickness tear of the distal supraspinatus tendon along with “metastatic lesions” (FIGURE). As a result, a bone scan was obtained and revealed activity in the proximal right humerus; however, it was nonconclusive for osteoblastic metastasis. A positron emission tomography (PET) scan was ordered, which revealed findings suggestive of bony metastasis in the proximal left tibia, distal shaft of the right tibia, and the right and left humeral heads. The patient was then scheduled for a bone biopsy; a chest, abdomen, and pelvis computed tomography (CT) scan with IV and oral contrast was also ordered.
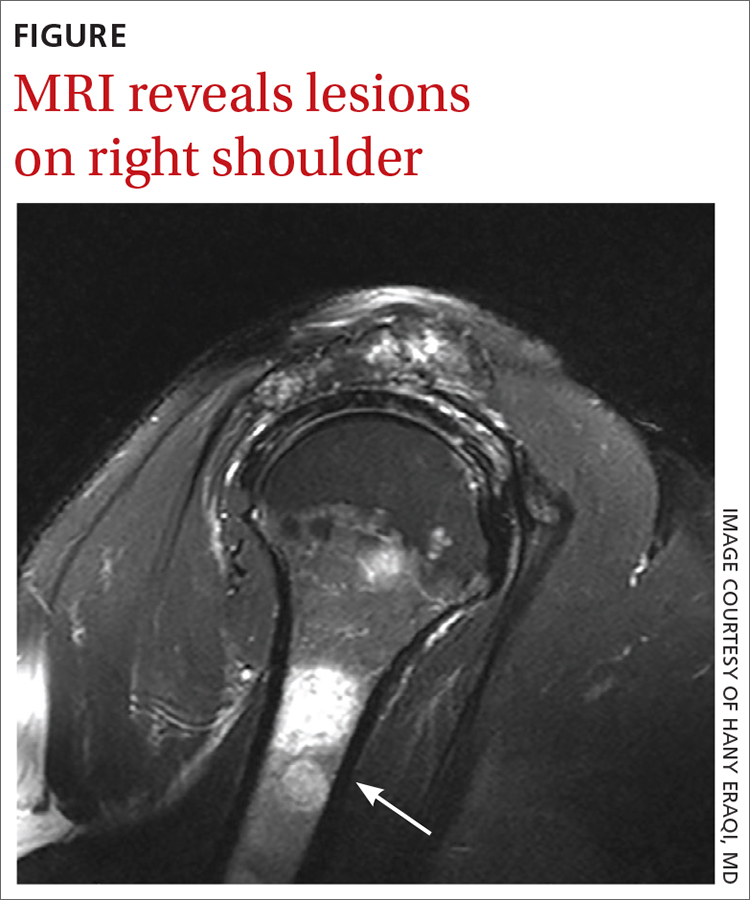
THE DIAGNOSIS
A bone biopsy of the left tibia indicated prominent non-necrotizing granulomatous inflammation and stains were negative for microorganisms. The CT scan demonstrated peribronchial vascular reticulonodular opacities in the upper lung zones compatible with sarcoidosis; no metastatic lesions were identified. Laboratory studies were obtained and demonstrated an elevated angiotensin-converting enzyme (ACE) level consistent with sarcoidosis. The cumulative test results pointed to a diagnosis of osseous sarcoidosis.
DISCUSSION
Osseous sarcoidosis is a rare manifestation of larger systemic disease. It is estimated that bony lesions occur in only 3% to 13% of patients with sarcoidosis.1 Bone involvement is most common in African Americans and occurs primarily in the hands and feet.1-3
Osseous lesions are comprised of noncaseating granulomatous inflammation.4,5 They are often asymptomatic but can be painful and associated with overlying skin disease and soft-tissue swelling.1,4 Although it’s not typical, patients may present with symptoms such as pain, stiffness, or fractures. On CT imaging and MRI (as in this case), osseous lesions can be confused with metastatic bone disease, and biopsy may be required for diagnosis.4
Continue to: There are multiple patterns of bone involvement
There are multiple patterns of bone involvement in osseous sarcoidosis, ranging from large cystic lesions that can lead to stress fractures to “tunnels” or “lace-like” reticulated patterns found in the bones of the hands and feet. 2,3,5,6 Long bone involvement is typically limited to the proximal and distal thirds of the bone.6 Sarcoidosis is also known to involve the axial skeleton, and less commonly, the cranial vault.6 Although multiple variations may manifest over time, skin changes usually precede bone lesions3,6; however, that was not the case with this patient.
Treatment entails pain management
Up to 50% of patients with bone lesions are symptomatic and may require treatment.3,5 Treatment is reserved for these symptomatic patients, with the goal of pain reduction.2,3,7
Low- to moderate-dose corticosteroids have been shown to relieve soft-tissue swelling and decrease pain.2,3,7 A prolonged course of steroids is not recommended, due to the risk of osteoporosis and fractures, and does not normalize bone structure.3,7
Other options. NSAIDs, such as colchicine and indomethacin, have also been found to be effective in pain management.7 Treatments such as methotrexate and hydroxychloroquine may be considered for those cases that are refractory to steroids.2
Given the extent of our patient’s disease, he was referred to multiple specialists to rule out further organ involvement. He was found to have neurosarcoidosis on brain imaging and was subsequently treated with prednisone 10 mg/d. The patient is being routinely monitored for active disease at various intervals or as symptoms arise.
THE TAKEAWAY
Consideration for systemic diseases (eg, sarcoidosis) should be given to patients presenting with musculoskeletal complaints without a significant history of trauma or injury. In those with risk factors associated with a higher incidence of sarcoidosis, such as age and race, a work-up should include imaging and biopsy. Treatment (eg, corticosteroids, NSAIDs) is provided to those patients who are symptomatic, with the goal of symptom relief.3
1. Rao DA, Dellaripa PF. Extrapulmonary manifestations of sarcoidosis. Rheum Dis Clin North Am. 2013;39:277-297. doi: 10.1016/j.rdc.2013.02.007
2. Kobak S. Sarcoidosis: a rheumatologist’s perspective. Ther Adv Musculoskelet Dis. 2015;7:196-205. doi: 10.1177/1759720X15591310
3. Bechman K, Christidis D, Walsh S, et al. A review of the musculoskeletal manifestations of sarcoidosis. Rheumatology (Oxford). 2018;57:777-783. doi: 10.1093/rheumatology/kex317
4. Iannuzzi MC, Rybicki BA, Teirstein AS. Sarcoidosis. N Engl J Med. 2007;357:2153-2165. doi: 10.1056/NEJMra071714
5. Yachoui R, Parker BJ, Nguyen TT. Bone and bone marrow involvement in sarcoidosis. Rheumatol Int. 2015;35:1917-1924. doi: 10.1007/s00296-015-3341-y
6. Aptel S, Lecocq-Teixeira S, Olivier P, et al. Multimodality evaluation of musculoskeletal sarcoidosis: Imaging findings and literature review. Diagn Interv Imaging. 2016;97:5-18. doi: 10.1016/j.diii.2014.11.038
7. Wilcox A, Bharadwaj P, Sharma OP. Bone sarcoidosis. Curr Opin Rheumatol. 2000;12:321-330. doi: 10.1097/00002281-200007000-00016
THE CASE
A 58-year-old African American man with a past medical history of prostate cancer, hypertension, hyperlipidemia, osteoarthritis, and gastroesophageal reflux disease presented to our office to establish care with a new provider. He complained of bilateral shoulder pain, that was worse on the right side, for the past year. He denied any previous falls, trauma, or injury. He reported that lifting his grandkids was becoming increasingly difficult due to the pain but denied any weakness or neurologic symptoms. He had been using over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), which provided minimal relief.
On physical examination, the overlying skin was normal and there was no tenderness to palpation. His shoulder range of motion was limited with complete flexion, but otherwise intact. Muscle strength was 5 out of 5 bilaterally, and neurovascular and sensory examinations were normal. On the right side, the Empty Can Test was positive, but the Neer and Apley tests were negative. All testing was negative on the left side.
The patient was referred for 10 sessions of physical therapy, which he completed. His pain persisted, and an x-ray of his right shoulder was performed. The x-ray indicated a high-riding humeral head, and magnetic resonance imaging (MRI) of the right shoulder was recommended due to possible rotator cuff tendinopathy.
The MRI demonstrated a full-thickness tear of the distal supraspinatus tendon along with “metastatic lesions” (FIGURE). As a result, a bone scan was obtained and revealed activity in the proximal right humerus; however, it was nonconclusive for osteoblastic metastasis. A positron emission tomography (PET) scan was ordered, which revealed findings suggestive of bony metastasis in the proximal left tibia, distal shaft of the right tibia, and the right and left humeral heads. The patient was then scheduled for a bone biopsy; a chest, abdomen, and pelvis computed tomography (CT) scan with IV and oral contrast was also ordered.

THE DIAGNOSIS
A bone biopsy of the left tibia indicated prominent non-necrotizing granulomatous inflammation and stains were negative for microorganisms. The CT scan demonstrated peribronchial vascular reticulonodular opacities in the upper lung zones compatible with sarcoidosis; no metastatic lesions were identified. Laboratory studies were obtained and demonstrated an elevated angiotensin-converting enzyme (ACE) level consistent with sarcoidosis. The cumulative test results pointed to a diagnosis of osseous sarcoidosis.
DISCUSSION
Osseous sarcoidosis is a rare manifestation of larger systemic disease. It is estimated that bony lesions occur in only 3% to 13% of patients with sarcoidosis.1 Bone involvement is most common in African Americans and occurs primarily in the hands and feet.1-3
Osseous lesions are comprised of noncaseating granulomatous inflammation.4,5 They are often asymptomatic but can be painful and associated with overlying skin disease and soft-tissue swelling.1,4 Although it’s not typical, patients may present with symptoms such as pain, stiffness, or fractures. On CT imaging and MRI (as in this case), osseous lesions can be confused with metastatic bone disease, and biopsy may be required for diagnosis.4
Continue to: There are multiple patterns of bone involvement
There are multiple patterns of bone involvement in osseous sarcoidosis, ranging from large cystic lesions that can lead to stress fractures to “tunnels” or “lace-like” reticulated patterns found in the bones of the hands and feet. 2,3,5,6 Long bone involvement is typically limited to the proximal and distal thirds of the bone.6 Sarcoidosis is also known to involve the axial skeleton, and less commonly, the cranial vault.6 Although multiple variations may manifest over time, skin changes usually precede bone lesions3,6; however, that was not the case with this patient.
Treatment entails pain management
Up to 50% of patients with bone lesions are symptomatic and may require treatment.3,5 Treatment is reserved for these symptomatic patients, with the goal of pain reduction.2,3,7
Low- to moderate-dose corticosteroids have been shown to relieve soft-tissue swelling and decrease pain.2,3,7 A prolonged course of steroids is not recommended, due to the risk of osteoporosis and fractures, and does not normalize bone structure.3,7
Other options. NSAIDs, such as colchicine and indomethacin, have also been found to be effective in pain management.7 Treatments such as methotrexate and hydroxychloroquine may be considered for those cases that are refractory to steroids.2
Given the extent of our patient’s disease, he was referred to multiple specialists to rule out further organ involvement. He was found to have neurosarcoidosis on brain imaging and was subsequently treated with prednisone 10 mg/d. The patient is being routinely monitored for active disease at various intervals or as symptoms arise.
THE TAKEAWAY
Consideration for systemic diseases (eg, sarcoidosis) should be given to patients presenting with musculoskeletal complaints without a significant history of trauma or injury. In those with risk factors associated with a higher incidence of sarcoidosis, such as age and race, a work-up should include imaging and biopsy. Treatment (eg, corticosteroids, NSAIDs) is provided to those patients who are symptomatic, with the goal of symptom relief.3
THE CASE
A 58-year-old African American man with a past medical history of prostate cancer, hypertension, hyperlipidemia, osteoarthritis, and gastroesophageal reflux disease presented to our office to establish care with a new provider. He complained of bilateral shoulder pain, that was worse on the right side, for the past year. He denied any previous falls, trauma, or injury. He reported that lifting his grandkids was becoming increasingly difficult due to the pain but denied any weakness or neurologic symptoms. He had been using over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), which provided minimal relief.
On physical examination, the overlying skin was normal and there was no tenderness to palpation. His shoulder range of motion was limited with complete flexion, but otherwise intact. Muscle strength was 5 out of 5 bilaterally, and neurovascular and sensory examinations were normal. On the right side, the Empty Can Test was positive, but the Neer and Apley tests were negative. All testing was negative on the left side.
The patient was referred for 10 sessions of physical therapy, which he completed. His pain persisted, and an x-ray of his right shoulder was performed. The x-ray indicated a high-riding humeral head, and magnetic resonance imaging (MRI) of the right shoulder was recommended due to possible rotator cuff tendinopathy.
The MRI demonstrated a full-thickness tear of the distal supraspinatus tendon along with “metastatic lesions” (FIGURE). As a result, a bone scan was obtained and revealed activity in the proximal right humerus; however, it was nonconclusive for osteoblastic metastasis. A positron emission tomography (PET) scan was ordered, which revealed findings suggestive of bony metastasis in the proximal left tibia, distal shaft of the right tibia, and the right and left humeral heads. The patient was then scheduled for a bone biopsy; a chest, abdomen, and pelvis computed tomography (CT) scan with IV and oral contrast was also ordered.

THE DIAGNOSIS
A bone biopsy of the left tibia indicated prominent non-necrotizing granulomatous inflammation and stains were negative for microorganisms. The CT scan demonstrated peribronchial vascular reticulonodular opacities in the upper lung zones compatible with sarcoidosis; no metastatic lesions were identified. Laboratory studies were obtained and demonstrated an elevated angiotensin-converting enzyme (ACE) level consistent with sarcoidosis. The cumulative test results pointed to a diagnosis of osseous sarcoidosis.
DISCUSSION
Osseous sarcoidosis is a rare manifestation of larger systemic disease. It is estimated that bony lesions occur in only 3% to 13% of patients with sarcoidosis.1 Bone involvement is most common in African Americans and occurs primarily in the hands and feet.1-3
Osseous lesions are comprised of noncaseating granulomatous inflammation.4,5 They are often asymptomatic but can be painful and associated with overlying skin disease and soft-tissue swelling.1,4 Although it’s not typical, patients may present with symptoms such as pain, stiffness, or fractures. On CT imaging and MRI (as in this case), osseous lesions can be confused with metastatic bone disease, and biopsy may be required for diagnosis.4
Continue to: There are multiple patterns of bone involvement
There are multiple patterns of bone involvement in osseous sarcoidosis, ranging from large cystic lesions that can lead to stress fractures to “tunnels” or “lace-like” reticulated patterns found in the bones of the hands and feet. 2,3,5,6 Long bone involvement is typically limited to the proximal and distal thirds of the bone.6 Sarcoidosis is also known to involve the axial skeleton, and less commonly, the cranial vault.6 Although multiple variations may manifest over time, skin changes usually precede bone lesions3,6; however, that was not the case with this patient.
Treatment entails pain management
Up to 50% of patients with bone lesions are symptomatic and may require treatment.3,5 Treatment is reserved for these symptomatic patients, with the goal of pain reduction.2,3,7
Low- to moderate-dose corticosteroids have been shown to relieve soft-tissue swelling and decrease pain.2,3,7 A prolonged course of steroids is not recommended, due to the risk of osteoporosis and fractures, and does not normalize bone structure.3,7
Other options. NSAIDs, such as colchicine and indomethacin, have also been found to be effective in pain management.7 Treatments such as methotrexate and hydroxychloroquine may be considered for those cases that are refractory to steroids.2
Given the extent of our patient’s disease, he was referred to multiple specialists to rule out further organ involvement. He was found to have neurosarcoidosis on brain imaging and was subsequently treated with prednisone 10 mg/d. The patient is being routinely monitored for active disease at various intervals or as symptoms arise.
THE TAKEAWAY
Consideration for systemic diseases (eg, sarcoidosis) should be given to patients presenting with musculoskeletal complaints without a significant history of trauma or injury. In those with risk factors associated with a higher incidence of sarcoidosis, such as age and race, a work-up should include imaging and biopsy. Treatment (eg, corticosteroids, NSAIDs) is provided to those patients who are symptomatic, with the goal of symptom relief.3
1. Rao DA, Dellaripa PF. Extrapulmonary manifestations of sarcoidosis. Rheum Dis Clin North Am. 2013;39:277-297. doi: 10.1016/j.rdc.2013.02.007
2. Kobak S. Sarcoidosis: a rheumatologist’s perspective. Ther Adv Musculoskelet Dis. 2015;7:196-205. doi: 10.1177/1759720X15591310
3. Bechman K, Christidis D, Walsh S, et al. A review of the musculoskeletal manifestations of sarcoidosis. Rheumatology (Oxford). 2018;57:777-783. doi: 10.1093/rheumatology/kex317
4. Iannuzzi MC, Rybicki BA, Teirstein AS. Sarcoidosis. N Engl J Med. 2007;357:2153-2165. doi: 10.1056/NEJMra071714
5. Yachoui R, Parker BJ, Nguyen TT. Bone and bone marrow involvement in sarcoidosis. Rheumatol Int. 2015;35:1917-1924. doi: 10.1007/s00296-015-3341-y
6. Aptel S, Lecocq-Teixeira S, Olivier P, et al. Multimodality evaluation of musculoskeletal sarcoidosis: Imaging findings and literature review. Diagn Interv Imaging. 2016;97:5-18. doi: 10.1016/j.diii.2014.11.038
7. Wilcox A, Bharadwaj P, Sharma OP. Bone sarcoidosis. Curr Opin Rheumatol. 2000;12:321-330. doi: 10.1097/00002281-200007000-00016
1. Rao DA, Dellaripa PF. Extrapulmonary manifestations of sarcoidosis. Rheum Dis Clin North Am. 2013;39:277-297. doi: 10.1016/j.rdc.2013.02.007
2. Kobak S. Sarcoidosis: a rheumatologist’s perspective. Ther Adv Musculoskelet Dis. 2015;7:196-205. doi: 10.1177/1759720X15591310
3. Bechman K, Christidis D, Walsh S, et al. A review of the musculoskeletal manifestations of sarcoidosis. Rheumatology (Oxford). 2018;57:777-783. doi: 10.1093/rheumatology/kex317
4. Iannuzzi MC, Rybicki BA, Teirstein AS. Sarcoidosis. N Engl J Med. 2007;357:2153-2165. doi: 10.1056/NEJMra071714
5. Yachoui R, Parker BJ, Nguyen TT. Bone and bone marrow involvement in sarcoidosis. Rheumatol Int. 2015;35:1917-1924. doi: 10.1007/s00296-015-3341-y
6. Aptel S, Lecocq-Teixeira S, Olivier P, et al. Multimodality evaluation of musculoskeletal sarcoidosis: Imaging findings and literature review. Diagn Interv Imaging. 2016;97:5-18. doi: 10.1016/j.diii.2014.11.038
7. Wilcox A, Bharadwaj P, Sharma OP. Bone sarcoidosis. Curr Opin Rheumatol. 2000;12:321-330. doi: 10.1097/00002281-200007000-00016
Rituximab and COVID-19 vaccines: Studies begin to answer key questions
Rituximab has presented something of a conundrum for patients taking the monoclonal antibody during the COVID-19 pandemic.
Used to manage a variety of autoimmune diseases and cancers, rituximab acts against CD20 proteins expressed on the surface of B cells, causing B-cell depletion. However, it is this B-cell depletion that may put these patients at greater risk of COVID-19 development, progression to more severe disease, and in-hospital mortality. Evidence for this appears to be mixed, with studies showing both that patients using rituximab to manage various diseases are and are not at increased risk for SARS-CoV-2 infection, COVID-19 progression, and mortality.
As COVID-19 vaccine rollouts take place across the world, more questions have been raised about the relationship between B-cell depletion from anti-CD20 therapies and COVID-19 vaccines. Do rituximab and other anti-CD20 therapies affect a patient’s response to COVID-19 vaccines? If this is the case, does the timing of anti-CD20 treatment matter to maximize B-cell levels and improve the vaccine’s effectiveness? And how do COVID-19 vaccine booster doses factor into the equation?
Humoral and cell-mediated responses following COVID-19 vaccination
First, the bad news: The vaccine is unquestionably safe to administer in patients taking rituximab, but one thing that has been well established is that antibody response to COVID-19 vaccination in these individuals does is reduced. This isn’t entirely unprecedented, as previous studies have shown a weakened immune response to pneumococcal polysaccharide and keyhole limpet hemocyanin vaccines among patients taking rituximab.
“Compromised immunogenicity to the SARS-CoV-2 vaccines has been demonstrated in rituximab-treated patients, which is of particular concern given the observation that B-cell–depleting therapies may be associated with worse COVID outcomes,” Robert F. Spiera, MD, director of the Scleroderma, Vasculitis, and Myositis Center at the Hospital for Special Surgery in New York, said in an interview.
For example, in a recent study from the Medical University of Vienna, 29 (39%) of 74 patients receiving rituximab (43% as monotherapy, 57% with conventional-synthetic disease-modifying antirheumatic drugs) who were vaccinated with either the Comirnaty (Pfizer-BioNTech) or Spikevax (Moderna) COVID-19 vaccine achieved seroconversion, compared with 100% of patients in a healthy control group, and all but 1 patient without detectable CD19+ peripheral B cells did not develop anti–SARS-CoV-2 receptor-binding domain antibodies.
“There is an increasing number of studies in this field, and they confirm that patients treated with rituximab and other anti-CD20 agents have severely reduced serological responses to COVID-19 vaccines,” Ingrid Jyssum, MD, of the division of rheumatology and research at Diakonhjemmet Hospital in Oslo, said in an interview.
One silver lining is that patients treated with anti-CD20 therapies appear to have a cell-mediated response following vaccination even if they don’t develop SARS-CoV-2 antibodies. “Studies that also investigate T-cell responses are starting to emerge, and so far, they show that, even if the patients do not have antibodies, they may have T-cell responses,” Dr. Jyssum said.
One study of 24 patients with autoimmune diseases taking rituximab that evaluated humoral and T-cell responses following vaccination with the Comirnaty vaccine found that none had a humoral response to the vaccine, but the T-cell response from that group did not significantly differ from 35 patients receiving other immunosuppressants and 26 patients in a healthy control group. In another study of rituximab- or ocrelizumab-treated patients who received mRNA-based COVID-19 vaccines, 69.4% developed SARS-CoV-2–specific antibodies, compared with a control group, but 96.2% of patients taking ocrelizumab and 81.8% of patients taking rituximab mounted a spike-specific CD8+ T-cell response, compared with 66.7% in the control group, and there were comparable rates (85%-90%) of spike-specific CD4+ T cells in all groups. In the study from the Medical University of Vienna, T-cell response was detected in rituximab-treated patients who both did and did not mount an antibody response.
The clinical relevance of how a blunted humoral immune response but a respectable T-cell response to COVID-19 vaccines affects patients treated with anti-CD20 therapies isn’t currently known, Dr. Jyssum said.
While these data are reassuring, they’re also incomplete, Dr. Spiera noted. “The ultimate outcome of relevance to assess vaccine efficacy is protection from COVID and from severe outcomes of COVID infection (i.e., hospitalization, mechanical ventilation, death). That data will require assessment of very large numbers of rituximab-treated vaccinated patients to be compared with rituximab-treated unvaccinated patients, and is unlikely to be forthcoming in the very near future.
“In the meantime, however, achieving serologic positivity, meaning having evidence of serologic as well as cellular immunity following vaccination, is a desired outcome, and likely implies more robust immunity.”
Does treatment timing impact COVID-19 vaccine response?
Given enough time, B-cell reconstitution will occur in patients taking rituximab. With that in mind, is it beneficial to wait a certain amount of time after a patient has stopped rituximab therapy or time since their last dose before giving them a COVID-19 vaccine? In their guidance on COVID-19 vaccines for patients with rheumatic and musculoskeletal diseases, the American College of Rheumatology said there is moderate evidence to consider “optimal timing of dosing and vaccination with the rheumatology provider before proceeding.”
“Guidelines and preliminary studies of serologic response to COVID vaccine in rituximab-treated patients have suggested that longer time from last rituximab exposure is associated with a greater likelihood of a serologic response,” Dr. Spiera said.
In a brief report published in Arthritis & Rheumatology, Dr. Spiera and colleagues performed a retrospective chart review of 56 patients with varying levels of last exposure to rituximab who received a COVID-19 vaccine. Their results showed that, when patients were vaccinated 6-12 months after the last rituximab dose, 55% were seronegative, and when this was more than 12 months, only 13% were seronegative, compared with seronegativity in 86% who were vaccinated less than 6 months after their last rituximab dose.
The RituxiVac trial, conducted by researchers in Switzerland, also examined vaccine responses of 96 rituximab-treated patients who received Comirnaty or Spikevax; results recently published in The Lancet Rheumatology showed findings similar to other studies, with reduced humoral and cell-mediated responses. In the RituxiVac trial, the median time to last anti-CD20 treatment was 1.07 years.
“The typical interval between rituximab doses [for treatment of rheumatoid arthritis, as well as for remission maintenance in antineutrophil cytoplasmic antibody–associated vasculitis] is typically 6 months, and this has become widely used as the interval from last rituximab to time of COVID vaccination, with a recommendation to wait 4 weeks (if possible) from time of vaccination until the next rituximab administration,” Dr. Spiera explained. However, this window seems to vary depending on the study.
Recent research published in Arthritis & Rheumatology indicates B-cell levels could be a relevant indicator for humoral and cell-mediated response in patients with rheumatic diseases treated with rituximab, with a level of 10 B cells/mcL (0.4% of lymphocytes) identified as one potential marker for likely seroconversion following COVID-19 vaccination.
“In some smaller case series, it has been further recognized that rituximab-treated patients who were beginning to reconstitute peripheral B cells were most likely to respond serologically. Our present study confirmed those findings, demonstrating that the presence of detectable B cells was strongly associated with vaccine responsiveness, and affords complementary information to time from last [rituximab dose] in informing the likelihood of a vaccine response,” Dr. Spiera said.
However, the literature is limited in this area, and an exact cutoff for B-cell counts in these patients isn’t currently known, Dr. Jyssum said. A better metric is time away from anti-CD20 therapies, with CD19 cell count being highly correlated with last infusion.
Dr. Spiera agreed that there is no consistent B-cell percentage that works as a cutoff. “In our study, we looked at it as a binary variable, although we did find that a higher percentage of B cells in the peripheral lymphocyte population was associated with a higher likelihood of seroconversion. We did not, however, identify a ‘threshold’ for vaccine serologic responsiveness.”
Should clinicians measure antibodies?
The Food and Drug Administration and the Centers for Disease Control and Prevention have recommended that health care providers and the public not use COVID-19 antibody tests as a way to gauge immunity after exposure to SARS-CoV-2 and after receiving a COVID-19 vaccination. The ACR’s guidance on COVID-19 vaccination for patients with rheumatic and musculoskeletal diseases strongly recommends against ordering antibody tests for patients with autoimmune inflammatory rheumatic diseases as a way to measure immunity.
“Generally, such measurements are not recommended as the clinical correlate of various antibody levels are not known,” Dr. Jyssum said. “With regular infusions of rituximab or other anti-CD20 agents, one cannot expect that these patients will develop significant levels of antibodies.”
However, she said there might be situations where it’s useful to know whether a patient has developed antibodies at all. “Assessing the significance of specific antibody levels is difficult, and the subject of scientific studies. Patients lacking a humoral vaccine response are left to rely on their T-cell responses and on infectious control measures to prevent disease.”
Dr. Spiera said he disagreed with guidelines recommending against checking antibody levels after vaccination, “particularly in patients treated with immunosuppressive medications that might be expected to blunt their serologic response to the vaccines.
“Although we cannot be sure what level of measurable antibodies offer what level of protection, most clinicians would agree that patients who demonstrate no detectable antibodies (which is a common finding in rituximab-treated patients) should be considered at higher risk,” he said. “Indeed, recommendations regarding booster vaccine administration in general was initially based on the observation of declining antibody levels with longer time from vaccination.”
Do COVID-19 vaccine boosters help patients on anti-CD20 therapy?
As of January 2022, the FDA and CDC have recommended a third primary series shot of COVID-19 vaccines for some moderately to severely immunocompromised patients as young as 5 years old (for Comirnaty vaccine) or a booster shot of either Comirnaty or Spikevax for everyone aged 12 years and older, including immunocompromised people, while the ACR goes into more detail and recommends clinicians time a patient’s booster shot with temporary treatment interruption.
In The Lancet Rheumatology, Dr. Jyssum and colleagues recently published results from the prospective Nor-vaC study examining the humoral and cell-mediated immune responses of 87 patients with RA being treated with rituximab who received the Comirnaty, Spikevax, or Vaxzevria (AstraZeneca) COVID-19 vaccines; of these, 49 patients received a booster dose at a median of 70 days after completing their primary series. The results showed 19 patients (28.1%) had a serologic response after their primary series, while 8 of 49 patients (16.3%) who received their booster dose had a serologic response.
All patients who received a third dose in the study had a T-cell response, Dr. Jyssum said. “This is reassuring for patients and clinicians. T cells have been found to be important in countering COVID-19 disease, but whether we can rely on the T-cell response alone in the absence of antibodies to protect patients from infection or from serious COVID disease is still not determined,” she said.
When asked if she would recommend COVID-19 vaccine booster doses for patients on rituximab, Dr. Jyssum replied: “Absolutely.”
Another study, recently published in Annals of the Rheumatic Diseases, examined heterologous and homologous booster doses for 60 patients receiving rituximab without seroconversion after their COVID-19 vaccine primary series. The results showed no significant difference in new seroconversion at 4 weeks based on whether the patient received a vector or mRNA vaccine (22% vs. 32%), but all patients who received a booster dose with a vector vaccine had specific T-cell responses, compared with 81% of patients who received an mRNA vaccine booster. There was a new humoral and/or cellular response in 9 of 11 patients (82%), and most patients with peripheral B cells (12 of 18 patients; 67%) achieved seroconversion.
“Our data show that a cellular and/or humoral immune response can be achieved on a third COVID-19 vaccination in most of the patients who initially developed neither a humoral nor a cellular immune response,” the researchers concluded. “The efficacy data together with the safety data seen in our trial provide a favorable risk/benefit ratio and support the implementation of a third vaccination for nonseroconverted high-risk autoimmune disease patients treated with B-cell–depleting agents.”
Dr. Spiera said booster doses are an important part of the equation, and “it is important to consider factors that would be associated with a greater likelihood of achieving a serologic response, particularly in those patients who did not demonstrate a serologic response to the initial vaccines series.
“Preliminary data shows that the beginnings of B-cell reconstitution is also associated with a positive serologic response following a booster of the COVID-19 vaccine,” he said.
The authors of the cited studies reported numerous relevant financial disclosures. Dr. Spiera and Dr. Jyssum reported no relevant financial disclosures.
Rituximab has presented something of a conundrum for patients taking the monoclonal antibody during the COVID-19 pandemic.
Used to manage a variety of autoimmune diseases and cancers, rituximab acts against CD20 proteins expressed on the surface of B cells, causing B-cell depletion. However, it is this B-cell depletion that may put these patients at greater risk of COVID-19 development, progression to more severe disease, and in-hospital mortality. Evidence for this appears to be mixed, with studies showing both that patients using rituximab to manage various diseases are and are not at increased risk for SARS-CoV-2 infection, COVID-19 progression, and mortality.
As COVID-19 vaccine rollouts take place across the world, more questions have been raised about the relationship between B-cell depletion from anti-CD20 therapies and COVID-19 vaccines. Do rituximab and other anti-CD20 therapies affect a patient’s response to COVID-19 vaccines? If this is the case, does the timing of anti-CD20 treatment matter to maximize B-cell levels and improve the vaccine’s effectiveness? And how do COVID-19 vaccine booster doses factor into the equation?
Humoral and cell-mediated responses following COVID-19 vaccination
First, the bad news: The vaccine is unquestionably safe to administer in patients taking rituximab, but one thing that has been well established is that antibody response to COVID-19 vaccination in these individuals does is reduced. This isn’t entirely unprecedented, as previous studies have shown a weakened immune response to pneumococcal polysaccharide and keyhole limpet hemocyanin vaccines among patients taking rituximab.
“Compromised immunogenicity to the SARS-CoV-2 vaccines has been demonstrated in rituximab-treated patients, which is of particular concern given the observation that B-cell–depleting therapies may be associated with worse COVID outcomes,” Robert F. Spiera, MD, director of the Scleroderma, Vasculitis, and Myositis Center at the Hospital for Special Surgery in New York, said in an interview.
For example, in a recent study from the Medical University of Vienna, 29 (39%) of 74 patients receiving rituximab (43% as monotherapy, 57% with conventional-synthetic disease-modifying antirheumatic drugs) who were vaccinated with either the Comirnaty (Pfizer-BioNTech) or Spikevax (Moderna) COVID-19 vaccine achieved seroconversion, compared with 100% of patients in a healthy control group, and all but 1 patient without detectable CD19+ peripheral B cells did not develop anti–SARS-CoV-2 receptor-binding domain antibodies.
“There is an increasing number of studies in this field, and they confirm that patients treated with rituximab and other anti-CD20 agents have severely reduced serological responses to COVID-19 vaccines,” Ingrid Jyssum, MD, of the division of rheumatology and research at Diakonhjemmet Hospital in Oslo, said in an interview.
One silver lining is that patients treated with anti-CD20 therapies appear to have a cell-mediated response following vaccination even if they don’t develop SARS-CoV-2 antibodies. “Studies that also investigate T-cell responses are starting to emerge, and so far, they show that, even if the patients do not have antibodies, they may have T-cell responses,” Dr. Jyssum said.
One study of 24 patients with autoimmune diseases taking rituximab that evaluated humoral and T-cell responses following vaccination with the Comirnaty vaccine found that none had a humoral response to the vaccine, but the T-cell response from that group did not significantly differ from 35 patients receiving other immunosuppressants and 26 patients in a healthy control group. In another study of rituximab- or ocrelizumab-treated patients who received mRNA-based COVID-19 vaccines, 69.4% developed SARS-CoV-2–specific antibodies, compared with a control group, but 96.2% of patients taking ocrelizumab and 81.8% of patients taking rituximab mounted a spike-specific CD8+ T-cell response, compared with 66.7% in the control group, and there were comparable rates (85%-90%) of spike-specific CD4+ T cells in all groups. In the study from the Medical University of Vienna, T-cell response was detected in rituximab-treated patients who both did and did not mount an antibody response.
The clinical relevance of how a blunted humoral immune response but a respectable T-cell response to COVID-19 vaccines affects patients treated with anti-CD20 therapies isn’t currently known, Dr. Jyssum said.
While these data are reassuring, they’re also incomplete, Dr. Spiera noted. “The ultimate outcome of relevance to assess vaccine efficacy is protection from COVID and from severe outcomes of COVID infection (i.e., hospitalization, mechanical ventilation, death). That data will require assessment of very large numbers of rituximab-treated vaccinated patients to be compared with rituximab-treated unvaccinated patients, and is unlikely to be forthcoming in the very near future.
“In the meantime, however, achieving serologic positivity, meaning having evidence of serologic as well as cellular immunity following vaccination, is a desired outcome, and likely implies more robust immunity.”
Does treatment timing impact COVID-19 vaccine response?
Given enough time, B-cell reconstitution will occur in patients taking rituximab. With that in mind, is it beneficial to wait a certain amount of time after a patient has stopped rituximab therapy or time since their last dose before giving them a COVID-19 vaccine? In their guidance on COVID-19 vaccines for patients with rheumatic and musculoskeletal diseases, the American College of Rheumatology said there is moderate evidence to consider “optimal timing of dosing and vaccination with the rheumatology provider before proceeding.”
“Guidelines and preliminary studies of serologic response to COVID vaccine in rituximab-treated patients have suggested that longer time from last rituximab exposure is associated with a greater likelihood of a serologic response,” Dr. Spiera said.
In a brief report published in Arthritis & Rheumatology, Dr. Spiera and colleagues performed a retrospective chart review of 56 patients with varying levels of last exposure to rituximab who received a COVID-19 vaccine. Their results showed that, when patients were vaccinated 6-12 months after the last rituximab dose, 55% were seronegative, and when this was more than 12 months, only 13% were seronegative, compared with seronegativity in 86% who were vaccinated less than 6 months after their last rituximab dose.
The RituxiVac trial, conducted by researchers in Switzerland, also examined vaccine responses of 96 rituximab-treated patients who received Comirnaty or Spikevax; results recently published in The Lancet Rheumatology showed findings similar to other studies, with reduced humoral and cell-mediated responses. In the RituxiVac trial, the median time to last anti-CD20 treatment was 1.07 years.
“The typical interval between rituximab doses [for treatment of rheumatoid arthritis, as well as for remission maintenance in antineutrophil cytoplasmic antibody–associated vasculitis] is typically 6 months, and this has become widely used as the interval from last rituximab to time of COVID vaccination, with a recommendation to wait 4 weeks (if possible) from time of vaccination until the next rituximab administration,” Dr. Spiera explained. However, this window seems to vary depending on the study.
Recent research published in Arthritis & Rheumatology indicates B-cell levels could be a relevant indicator for humoral and cell-mediated response in patients with rheumatic diseases treated with rituximab, with a level of 10 B cells/mcL (0.4% of lymphocytes) identified as one potential marker for likely seroconversion following COVID-19 vaccination.
“In some smaller case series, it has been further recognized that rituximab-treated patients who were beginning to reconstitute peripheral B cells were most likely to respond serologically. Our present study confirmed those findings, demonstrating that the presence of detectable B cells was strongly associated with vaccine responsiveness, and affords complementary information to time from last [rituximab dose] in informing the likelihood of a vaccine response,” Dr. Spiera said.
However, the literature is limited in this area, and an exact cutoff for B-cell counts in these patients isn’t currently known, Dr. Jyssum said. A better metric is time away from anti-CD20 therapies, with CD19 cell count being highly correlated with last infusion.
Dr. Spiera agreed that there is no consistent B-cell percentage that works as a cutoff. “In our study, we looked at it as a binary variable, although we did find that a higher percentage of B cells in the peripheral lymphocyte population was associated with a higher likelihood of seroconversion. We did not, however, identify a ‘threshold’ for vaccine serologic responsiveness.”
Should clinicians measure antibodies?
The Food and Drug Administration and the Centers for Disease Control and Prevention have recommended that health care providers and the public not use COVID-19 antibody tests as a way to gauge immunity after exposure to SARS-CoV-2 and after receiving a COVID-19 vaccination. The ACR’s guidance on COVID-19 vaccination for patients with rheumatic and musculoskeletal diseases strongly recommends against ordering antibody tests for patients with autoimmune inflammatory rheumatic diseases as a way to measure immunity.
“Generally, such measurements are not recommended as the clinical correlate of various antibody levels are not known,” Dr. Jyssum said. “With regular infusions of rituximab or other anti-CD20 agents, one cannot expect that these patients will develop significant levels of antibodies.”
However, she said there might be situations where it’s useful to know whether a patient has developed antibodies at all. “Assessing the significance of specific antibody levels is difficult, and the subject of scientific studies. Patients lacking a humoral vaccine response are left to rely on their T-cell responses and on infectious control measures to prevent disease.”
Dr. Spiera said he disagreed with guidelines recommending against checking antibody levels after vaccination, “particularly in patients treated with immunosuppressive medications that might be expected to blunt their serologic response to the vaccines.
“Although we cannot be sure what level of measurable antibodies offer what level of protection, most clinicians would agree that patients who demonstrate no detectable antibodies (which is a common finding in rituximab-treated patients) should be considered at higher risk,” he said. “Indeed, recommendations regarding booster vaccine administration in general was initially based on the observation of declining antibody levels with longer time from vaccination.”
Do COVID-19 vaccine boosters help patients on anti-CD20 therapy?
As of January 2022, the FDA and CDC have recommended a third primary series shot of COVID-19 vaccines for some moderately to severely immunocompromised patients as young as 5 years old (for Comirnaty vaccine) or a booster shot of either Comirnaty or Spikevax for everyone aged 12 years and older, including immunocompromised people, while the ACR goes into more detail and recommends clinicians time a patient’s booster shot with temporary treatment interruption.
In The Lancet Rheumatology, Dr. Jyssum and colleagues recently published results from the prospective Nor-vaC study examining the humoral and cell-mediated immune responses of 87 patients with RA being treated with rituximab who received the Comirnaty, Spikevax, or Vaxzevria (AstraZeneca) COVID-19 vaccines; of these, 49 patients received a booster dose at a median of 70 days after completing their primary series. The results showed 19 patients (28.1%) had a serologic response after their primary series, while 8 of 49 patients (16.3%) who received their booster dose had a serologic response.
All patients who received a third dose in the study had a T-cell response, Dr. Jyssum said. “This is reassuring for patients and clinicians. T cells have been found to be important in countering COVID-19 disease, but whether we can rely on the T-cell response alone in the absence of antibodies to protect patients from infection or from serious COVID disease is still not determined,” she said.
When asked if she would recommend COVID-19 vaccine booster doses for patients on rituximab, Dr. Jyssum replied: “Absolutely.”
Another study, recently published in Annals of the Rheumatic Diseases, examined heterologous and homologous booster doses for 60 patients receiving rituximab without seroconversion after their COVID-19 vaccine primary series. The results showed no significant difference in new seroconversion at 4 weeks based on whether the patient received a vector or mRNA vaccine (22% vs. 32%), but all patients who received a booster dose with a vector vaccine had specific T-cell responses, compared with 81% of patients who received an mRNA vaccine booster. There was a new humoral and/or cellular response in 9 of 11 patients (82%), and most patients with peripheral B cells (12 of 18 patients; 67%) achieved seroconversion.
“Our data show that a cellular and/or humoral immune response can be achieved on a third COVID-19 vaccination in most of the patients who initially developed neither a humoral nor a cellular immune response,” the researchers concluded. “The efficacy data together with the safety data seen in our trial provide a favorable risk/benefit ratio and support the implementation of a third vaccination for nonseroconverted high-risk autoimmune disease patients treated with B-cell–depleting agents.”
Dr. Spiera said booster doses are an important part of the equation, and “it is important to consider factors that would be associated with a greater likelihood of achieving a serologic response, particularly in those patients who did not demonstrate a serologic response to the initial vaccines series.
“Preliminary data shows that the beginnings of B-cell reconstitution is also associated with a positive serologic response following a booster of the COVID-19 vaccine,” he said.
The authors of the cited studies reported numerous relevant financial disclosures. Dr. Spiera and Dr. Jyssum reported no relevant financial disclosures.
Rituximab has presented something of a conundrum for patients taking the monoclonal antibody during the COVID-19 pandemic.
Used to manage a variety of autoimmune diseases and cancers, rituximab acts against CD20 proteins expressed on the surface of B cells, causing B-cell depletion. However, it is this B-cell depletion that may put these patients at greater risk of COVID-19 development, progression to more severe disease, and in-hospital mortality. Evidence for this appears to be mixed, with studies showing both that patients using rituximab to manage various diseases are and are not at increased risk for SARS-CoV-2 infection, COVID-19 progression, and mortality.
As COVID-19 vaccine rollouts take place across the world, more questions have been raised about the relationship between B-cell depletion from anti-CD20 therapies and COVID-19 vaccines. Do rituximab and other anti-CD20 therapies affect a patient’s response to COVID-19 vaccines? If this is the case, does the timing of anti-CD20 treatment matter to maximize B-cell levels and improve the vaccine’s effectiveness? And how do COVID-19 vaccine booster doses factor into the equation?
Humoral and cell-mediated responses following COVID-19 vaccination
First, the bad news: The vaccine is unquestionably safe to administer in patients taking rituximab, but one thing that has been well established is that antibody response to COVID-19 vaccination in these individuals does is reduced. This isn’t entirely unprecedented, as previous studies have shown a weakened immune response to pneumococcal polysaccharide and keyhole limpet hemocyanin vaccines among patients taking rituximab.
“Compromised immunogenicity to the SARS-CoV-2 vaccines has been demonstrated in rituximab-treated patients, which is of particular concern given the observation that B-cell–depleting therapies may be associated with worse COVID outcomes,” Robert F. Spiera, MD, director of the Scleroderma, Vasculitis, and Myositis Center at the Hospital for Special Surgery in New York, said in an interview.
For example, in a recent study from the Medical University of Vienna, 29 (39%) of 74 patients receiving rituximab (43% as monotherapy, 57% with conventional-synthetic disease-modifying antirheumatic drugs) who were vaccinated with either the Comirnaty (Pfizer-BioNTech) or Spikevax (Moderna) COVID-19 vaccine achieved seroconversion, compared with 100% of patients in a healthy control group, and all but 1 patient without detectable CD19+ peripheral B cells did not develop anti–SARS-CoV-2 receptor-binding domain antibodies.
“There is an increasing number of studies in this field, and they confirm that patients treated with rituximab and other anti-CD20 agents have severely reduced serological responses to COVID-19 vaccines,” Ingrid Jyssum, MD, of the division of rheumatology and research at Diakonhjemmet Hospital in Oslo, said in an interview.
One silver lining is that patients treated with anti-CD20 therapies appear to have a cell-mediated response following vaccination even if they don’t develop SARS-CoV-2 antibodies. “Studies that also investigate T-cell responses are starting to emerge, and so far, they show that, even if the patients do not have antibodies, they may have T-cell responses,” Dr. Jyssum said.
One study of 24 patients with autoimmune diseases taking rituximab that evaluated humoral and T-cell responses following vaccination with the Comirnaty vaccine found that none had a humoral response to the vaccine, but the T-cell response from that group did not significantly differ from 35 patients receiving other immunosuppressants and 26 patients in a healthy control group. In another study of rituximab- or ocrelizumab-treated patients who received mRNA-based COVID-19 vaccines, 69.4% developed SARS-CoV-2–specific antibodies, compared with a control group, but 96.2% of patients taking ocrelizumab and 81.8% of patients taking rituximab mounted a spike-specific CD8+ T-cell response, compared with 66.7% in the control group, and there were comparable rates (85%-90%) of spike-specific CD4+ T cells in all groups. In the study from the Medical University of Vienna, T-cell response was detected in rituximab-treated patients who both did and did not mount an antibody response.
The clinical relevance of how a blunted humoral immune response but a respectable T-cell response to COVID-19 vaccines affects patients treated with anti-CD20 therapies isn’t currently known, Dr. Jyssum said.
While these data are reassuring, they’re also incomplete, Dr. Spiera noted. “The ultimate outcome of relevance to assess vaccine efficacy is protection from COVID and from severe outcomes of COVID infection (i.e., hospitalization, mechanical ventilation, death). That data will require assessment of very large numbers of rituximab-treated vaccinated patients to be compared with rituximab-treated unvaccinated patients, and is unlikely to be forthcoming in the very near future.
“In the meantime, however, achieving serologic positivity, meaning having evidence of serologic as well as cellular immunity following vaccination, is a desired outcome, and likely implies more robust immunity.”
Does treatment timing impact COVID-19 vaccine response?
Given enough time, B-cell reconstitution will occur in patients taking rituximab. With that in mind, is it beneficial to wait a certain amount of time after a patient has stopped rituximab therapy or time since their last dose before giving them a COVID-19 vaccine? In their guidance on COVID-19 vaccines for patients with rheumatic and musculoskeletal diseases, the American College of Rheumatology said there is moderate evidence to consider “optimal timing of dosing and vaccination with the rheumatology provider before proceeding.”
“Guidelines and preliminary studies of serologic response to COVID vaccine in rituximab-treated patients have suggested that longer time from last rituximab exposure is associated with a greater likelihood of a serologic response,” Dr. Spiera said.
In a brief report published in Arthritis & Rheumatology, Dr. Spiera and colleagues performed a retrospective chart review of 56 patients with varying levels of last exposure to rituximab who received a COVID-19 vaccine. Their results showed that, when patients were vaccinated 6-12 months after the last rituximab dose, 55% were seronegative, and when this was more than 12 months, only 13% were seronegative, compared with seronegativity in 86% who were vaccinated less than 6 months after their last rituximab dose.
The RituxiVac trial, conducted by researchers in Switzerland, also examined vaccine responses of 96 rituximab-treated patients who received Comirnaty or Spikevax; results recently published in The Lancet Rheumatology showed findings similar to other studies, with reduced humoral and cell-mediated responses. In the RituxiVac trial, the median time to last anti-CD20 treatment was 1.07 years.
“The typical interval between rituximab doses [for treatment of rheumatoid arthritis, as well as for remission maintenance in antineutrophil cytoplasmic antibody–associated vasculitis] is typically 6 months, and this has become widely used as the interval from last rituximab to time of COVID vaccination, with a recommendation to wait 4 weeks (if possible) from time of vaccination until the next rituximab administration,” Dr. Spiera explained. However, this window seems to vary depending on the study.
Recent research published in Arthritis & Rheumatology indicates B-cell levels could be a relevant indicator for humoral and cell-mediated response in patients with rheumatic diseases treated with rituximab, with a level of 10 B cells/mcL (0.4% of lymphocytes) identified as one potential marker for likely seroconversion following COVID-19 vaccination.
“In some smaller case series, it has been further recognized that rituximab-treated patients who were beginning to reconstitute peripheral B cells were most likely to respond serologically. Our present study confirmed those findings, demonstrating that the presence of detectable B cells was strongly associated with vaccine responsiveness, and affords complementary information to time from last [rituximab dose] in informing the likelihood of a vaccine response,” Dr. Spiera said.
However, the literature is limited in this area, and an exact cutoff for B-cell counts in these patients isn’t currently known, Dr. Jyssum said. A better metric is time away from anti-CD20 therapies, with CD19 cell count being highly correlated with last infusion.
Dr. Spiera agreed that there is no consistent B-cell percentage that works as a cutoff. “In our study, we looked at it as a binary variable, although we did find that a higher percentage of B cells in the peripheral lymphocyte population was associated with a higher likelihood of seroconversion. We did not, however, identify a ‘threshold’ for vaccine serologic responsiveness.”
Should clinicians measure antibodies?
The Food and Drug Administration and the Centers for Disease Control and Prevention have recommended that health care providers and the public not use COVID-19 antibody tests as a way to gauge immunity after exposure to SARS-CoV-2 and after receiving a COVID-19 vaccination. The ACR’s guidance on COVID-19 vaccination for patients with rheumatic and musculoskeletal diseases strongly recommends against ordering antibody tests for patients with autoimmune inflammatory rheumatic diseases as a way to measure immunity.
“Generally, such measurements are not recommended as the clinical correlate of various antibody levels are not known,” Dr. Jyssum said. “With regular infusions of rituximab or other anti-CD20 agents, one cannot expect that these patients will develop significant levels of antibodies.”
However, she said there might be situations where it’s useful to know whether a patient has developed antibodies at all. “Assessing the significance of specific antibody levels is difficult, and the subject of scientific studies. Patients lacking a humoral vaccine response are left to rely on their T-cell responses and on infectious control measures to prevent disease.”
Dr. Spiera said he disagreed with guidelines recommending against checking antibody levels after vaccination, “particularly in patients treated with immunosuppressive medications that might be expected to blunt their serologic response to the vaccines.
“Although we cannot be sure what level of measurable antibodies offer what level of protection, most clinicians would agree that patients who demonstrate no detectable antibodies (which is a common finding in rituximab-treated patients) should be considered at higher risk,” he said. “Indeed, recommendations regarding booster vaccine administration in general was initially based on the observation of declining antibody levels with longer time from vaccination.”
Do COVID-19 vaccine boosters help patients on anti-CD20 therapy?
As of January 2022, the FDA and CDC have recommended a third primary series shot of COVID-19 vaccines for some moderately to severely immunocompromised patients as young as 5 years old (for Comirnaty vaccine) or a booster shot of either Comirnaty or Spikevax for everyone aged 12 years and older, including immunocompromised people, while the ACR goes into more detail and recommends clinicians time a patient’s booster shot with temporary treatment interruption.
In The Lancet Rheumatology, Dr. Jyssum and colleagues recently published results from the prospective Nor-vaC study examining the humoral and cell-mediated immune responses of 87 patients with RA being treated with rituximab who received the Comirnaty, Spikevax, or Vaxzevria (AstraZeneca) COVID-19 vaccines; of these, 49 patients received a booster dose at a median of 70 days after completing their primary series. The results showed 19 patients (28.1%) had a serologic response after their primary series, while 8 of 49 patients (16.3%) who received their booster dose had a serologic response.
All patients who received a third dose in the study had a T-cell response, Dr. Jyssum said. “This is reassuring for patients and clinicians. T cells have been found to be important in countering COVID-19 disease, but whether we can rely on the T-cell response alone in the absence of antibodies to protect patients from infection or from serious COVID disease is still not determined,” she said.
When asked if she would recommend COVID-19 vaccine booster doses for patients on rituximab, Dr. Jyssum replied: “Absolutely.”
Another study, recently published in Annals of the Rheumatic Diseases, examined heterologous and homologous booster doses for 60 patients receiving rituximab without seroconversion after their COVID-19 vaccine primary series. The results showed no significant difference in new seroconversion at 4 weeks based on whether the patient received a vector or mRNA vaccine (22% vs. 32%), but all patients who received a booster dose with a vector vaccine had specific T-cell responses, compared with 81% of patients who received an mRNA vaccine booster. There was a new humoral and/or cellular response in 9 of 11 patients (82%), and most patients with peripheral B cells (12 of 18 patients; 67%) achieved seroconversion.
“Our data show that a cellular and/or humoral immune response can be achieved on a third COVID-19 vaccination in most of the patients who initially developed neither a humoral nor a cellular immune response,” the researchers concluded. “The efficacy data together with the safety data seen in our trial provide a favorable risk/benefit ratio and support the implementation of a third vaccination for nonseroconverted high-risk autoimmune disease patients treated with B-cell–depleting agents.”
Dr. Spiera said booster doses are an important part of the equation, and “it is important to consider factors that would be associated with a greater likelihood of achieving a serologic response, particularly in those patients who did not demonstrate a serologic response to the initial vaccines series.
“Preliminary data shows that the beginnings of B-cell reconstitution is also associated with a positive serologic response following a booster of the COVID-19 vaccine,” he said.
The authors of the cited studies reported numerous relevant financial disclosures. Dr. Spiera and Dr. Jyssum reported no relevant financial disclosures.