User login
Cannabis abuse and use
Cannabis abuse and THC content are on the rise
The authors of the July 2014 Residents’ Voices article (What we ought to talk about when we’re talking about decriminalizing Cannabis, Current Psychiatry, July 2014, p. 45-46 [http://bit.ly/1uAb7iK]) highlight the mental health complications of Cannabis and mention that, when Cannabis is juxtaposed with other illicit substances, it appears innocuous.
On the contrary: Data from the 2011 Drug Abuse Warning Network highlighted the rising involvement of Cannabis in emergency department (ED) visits. The report indicated that of the 1,252,500 ED visits involving illicit drugs in 2011, the most common illicit drug involved was cocaine, which accounted for 505,224 ED visits, with Cannabis a close second at 455,668 visits—not including synthetic cannabinoids, which came in fifth, with 28,531 ED visits.1
Another useful point to buttress the concerns raised by the authors is that the potency of delta-9-tetrahydrocannabinol (THC), the primary psychoactive ingredient in Cannabis, has increased gradually over the years. The University of Mississippi Potency Monitoring Project, a National Institute on Drug Abuse–funded landmark project that studied samples of Cannabis confiscated by law enforcement in the United States between 1993 and 2008, revealed that the mean THC content increased from 3.4% in 1993, to 8.8% in 2008.2 The THC content of Cannabis is responsible for most of its psychoactive effects, so that the higher the THC content, the greater the adverse effects on mental health.
A major phytocannabinoid, cannabidiol (CBD), also present in Cannabis, appears to counteract the adverse effects of THC, particularly by means of its antipsychotic property. Compared with the rising mean THC content of Cannabis from 1993 to 2008, CBD content has remained relatively the same: a mean of 0.3% in 1993 and 0.4% in 2008.3,4
Several factors have been postulated for the trend toward a high THC–low CBD profile in recent years: cultivation methods, the preference for cultivating seedless female plants (sinsemilla) that tend to have a high THC content, and global availability of seeds over the Internet. The high THC–low CBD profile has been linked to an increased risk of Cannabis dependence and increased treatment-seeking for Cannabis-related problems.3
Adegboyega Oyemade
Addiction Psychiatrist
Maryland Treatment Centers, Inc.
Attending Psychiatrist
Sinai Hospital
Baltimore, Maryland
-------------------------------------------------------------------
Research for 'Rx: Cannabis' is needed
Regarding the essay by Drs. Gershan and Gangahar on decriminalization of Cannabis, I want to comment on issues surrounding prescription Cannabis.
It is clear that Cannabis can exacerbate psychosis, among other risks, but its potential benefits remain relatively unexplored. The authors correctly point out that, among indications for Cannabis, none are FDA-approved. Yet, off-label prescribing is pervasive and accepted in psychiatry, lack of FDA approval of indications for Cannabis is not an especially compelling argument against such prescribing.*
Lack of research and funding hampers efforts to conduct trials of the therapeutic value of Cannabis, as does its Schedule I status (ie, “no currently accepted medical use and a high potential for abuse” [language of the Controlled Substances Act]). There are reports of benefit in intractable epilepsy and posttraumatic stress disorder (PTSD) that merit further investigation; however, such research is hampered, I believe, by bureaucracy.
For example, an approved study at the University of Arizona of the use of Cannabis to treat PTSD has remained in regulatory limbo for longer than 4 years because of the immense hurdles involved in performing research on this substance—despite how pressing such research is, given the large number of veterans returning from active duty with this diagnosis and the paucity of treatment options.
Perhaps, there also is something “missing” in the debate about research into Cannabis.
Wesley Ryan, MD
PGY-5 Addiction Psychiatry Fellow
University of Washington
Seattle, Washington
*Editor's Note: An earlier version of this article stated, "Yet, off-labeling prescribing of Cannabis is pervasive, and I've found, accepted in psychiatry," which does not reflect the author's opinion or intended meaning. The sentence has been corrected to read, "Yet, because off-label prescribing is pervasive and accepted in psychiatry, lack of FDA approval of indications for Cannabis is not an especially compelling argument against such prescribing."
1. U.S. Department of Health and Human Services. Drug Abuse Warning Network, 2011: National estimates of drug-related emergency department visits. http://www.samhsa.gov/data/2k13/ DAWN2k11ED/DAWN2k11ED.htm. Published May 2013. Accessed on July 26, 2014.
2. Mehmedic Z, Chandra S, Slade D, et al. Potency trends of Δ9-THC and other cannabinoids in confiscated cannabis preparations from 1993 to 2008. J Forensic Sci. 2010;55(5):1209-1217.
3. Swift W, Wong A, Li KM, et al. Analysis of cannabis seizures in NSW, Australia: cannabis potency and cannabinoid profile. PLos One. 2013;8(7):e70052. doi: 10.1371/journal.pone.0070052.
4. Morrison P. It’s the lack of balance in cannabis that does the harm. http://www.beckleyfoundation. org/2010/10/its-the-lack-of-balance-in-cannabis-that-does-the-harm. Published October 21, 2010. Accessed July 26, 2014.
Cannabis abuse and THC content are on the rise
The authors of the July 2014 Residents’ Voices article (What we ought to talk about when we’re talking about decriminalizing Cannabis, Current Psychiatry, July 2014, p. 45-46 [http://bit.ly/1uAb7iK]) highlight the mental health complications of Cannabis and mention that, when Cannabis is juxtaposed with other illicit substances, it appears innocuous.
On the contrary: Data from the 2011 Drug Abuse Warning Network highlighted the rising involvement of Cannabis in emergency department (ED) visits. The report indicated that of the 1,252,500 ED visits involving illicit drugs in 2011, the most common illicit drug involved was cocaine, which accounted for 505,224 ED visits, with Cannabis a close second at 455,668 visits—not including synthetic cannabinoids, which came in fifth, with 28,531 ED visits.1
Another useful point to buttress the concerns raised by the authors is that the potency of delta-9-tetrahydrocannabinol (THC), the primary psychoactive ingredient in Cannabis, has increased gradually over the years. The University of Mississippi Potency Monitoring Project, a National Institute on Drug Abuse–funded landmark project that studied samples of Cannabis confiscated by law enforcement in the United States between 1993 and 2008, revealed that the mean THC content increased from 3.4% in 1993, to 8.8% in 2008.2 The THC content of Cannabis is responsible for most of its psychoactive effects, so that the higher the THC content, the greater the adverse effects on mental health.
A major phytocannabinoid, cannabidiol (CBD), also present in Cannabis, appears to counteract the adverse effects of THC, particularly by means of its antipsychotic property. Compared with the rising mean THC content of Cannabis from 1993 to 2008, CBD content has remained relatively the same: a mean of 0.3% in 1993 and 0.4% in 2008.3,4
Several factors have been postulated for the trend toward a high THC–low CBD profile in recent years: cultivation methods, the preference for cultivating seedless female plants (sinsemilla) that tend to have a high THC content, and global availability of seeds over the Internet. The high THC–low CBD profile has been linked to an increased risk of Cannabis dependence and increased treatment-seeking for Cannabis-related problems.3
Adegboyega Oyemade
Addiction Psychiatrist
Maryland Treatment Centers, Inc.
Attending Psychiatrist
Sinai Hospital
Baltimore, Maryland
-------------------------------------------------------------------
Research for 'Rx: Cannabis' is needed
Regarding the essay by Drs. Gershan and Gangahar on decriminalization of Cannabis, I want to comment on issues surrounding prescription Cannabis.
It is clear that Cannabis can exacerbate psychosis, among other risks, but its potential benefits remain relatively unexplored. The authors correctly point out that, among indications for Cannabis, none are FDA-approved. Yet, off-label prescribing is pervasive and accepted in psychiatry, lack of FDA approval of indications for Cannabis is not an especially compelling argument against such prescribing.*
Lack of research and funding hampers efforts to conduct trials of the therapeutic value of Cannabis, as does its Schedule I status (ie, “no currently accepted medical use and a high potential for abuse” [language of the Controlled Substances Act]). There are reports of benefit in intractable epilepsy and posttraumatic stress disorder (PTSD) that merit further investigation; however, such research is hampered, I believe, by bureaucracy.
For example, an approved study at the University of Arizona of the use of Cannabis to treat PTSD has remained in regulatory limbo for longer than 4 years because of the immense hurdles involved in performing research on this substance—despite how pressing such research is, given the large number of veterans returning from active duty with this diagnosis and the paucity of treatment options.
Perhaps, there also is something “missing” in the debate about research into Cannabis.
Wesley Ryan, MD
PGY-5 Addiction Psychiatry Fellow
University of Washington
Seattle, Washington
*Editor's Note: An earlier version of this article stated, "Yet, off-labeling prescribing of Cannabis is pervasive, and I've found, accepted in psychiatry," which does not reflect the author's opinion or intended meaning. The sentence has been corrected to read, "Yet, because off-label prescribing is pervasive and accepted in psychiatry, lack of FDA approval of indications for Cannabis is not an especially compelling argument against such prescribing."
Cannabis abuse and THC content are on the rise
The authors of the July 2014 Residents’ Voices article (What we ought to talk about when we’re talking about decriminalizing Cannabis, Current Psychiatry, July 2014, p. 45-46 [http://bit.ly/1uAb7iK]) highlight the mental health complications of Cannabis and mention that, when Cannabis is juxtaposed with other illicit substances, it appears innocuous.
On the contrary: Data from the 2011 Drug Abuse Warning Network highlighted the rising involvement of Cannabis in emergency department (ED) visits. The report indicated that of the 1,252,500 ED visits involving illicit drugs in 2011, the most common illicit drug involved was cocaine, which accounted for 505,224 ED visits, with Cannabis a close second at 455,668 visits—not including synthetic cannabinoids, which came in fifth, with 28,531 ED visits.1
Another useful point to buttress the concerns raised by the authors is that the potency of delta-9-tetrahydrocannabinol (THC), the primary psychoactive ingredient in Cannabis, has increased gradually over the years. The University of Mississippi Potency Monitoring Project, a National Institute on Drug Abuse–funded landmark project that studied samples of Cannabis confiscated by law enforcement in the United States between 1993 and 2008, revealed that the mean THC content increased from 3.4% in 1993, to 8.8% in 2008.2 The THC content of Cannabis is responsible for most of its psychoactive effects, so that the higher the THC content, the greater the adverse effects on mental health.
A major phytocannabinoid, cannabidiol (CBD), also present in Cannabis, appears to counteract the adverse effects of THC, particularly by means of its antipsychotic property. Compared with the rising mean THC content of Cannabis from 1993 to 2008, CBD content has remained relatively the same: a mean of 0.3% in 1993 and 0.4% in 2008.3,4
Several factors have been postulated for the trend toward a high THC–low CBD profile in recent years: cultivation methods, the preference for cultivating seedless female plants (sinsemilla) that tend to have a high THC content, and global availability of seeds over the Internet. The high THC–low CBD profile has been linked to an increased risk of Cannabis dependence and increased treatment-seeking for Cannabis-related problems.3
Adegboyega Oyemade
Addiction Psychiatrist
Maryland Treatment Centers, Inc.
Attending Psychiatrist
Sinai Hospital
Baltimore, Maryland
-------------------------------------------------------------------
Research for 'Rx: Cannabis' is needed
Regarding the essay by Drs. Gershan and Gangahar on decriminalization of Cannabis, I want to comment on issues surrounding prescription Cannabis.
It is clear that Cannabis can exacerbate psychosis, among other risks, but its potential benefits remain relatively unexplored. The authors correctly point out that, among indications for Cannabis, none are FDA-approved. Yet, off-label prescribing is pervasive and accepted in psychiatry, lack of FDA approval of indications for Cannabis is not an especially compelling argument against such prescribing.*
Lack of research and funding hampers efforts to conduct trials of the therapeutic value of Cannabis, as does its Schedule I status (ie, “no currently accepted medical use and a high potential for abuse” [language of the Controlled Substances Act]). There are reports of benefit in intractable epilepsy and posttraumatic stress disorder (PTSD) that merit further investigation; however, such research is hampered, I believe, by bureaucracy.
For example, an approved study at the University of Arizona of the use of Cannabis to treat PTSD has remained in regulatory limbo for longer than 4 years because of the immense hurdles involved in performing research on this substance—despite how pressing such research is, given the large number of veterans returning from active duty with this diagnosis and the paucity of treatment options.
Perhaps, there also is something “missing” in the debate about research into Cannabis.
Wesley Ryan, MD
PGY-5 Addiction Psychiatry Fellow
University of Washington
Seattle, Washington
*Editor's Note: An earlier version of this article stated, "Yet, off-labeling prescribing of Cannabis is pervasive, and I've found, accepted in psychiatry," which does not reflect the author's opinion or intended meaning. The sentence has been corrected to read, "Yet, because off-label prescribing is pervasive and accepted in psychiatry, lack of FDA approval of indications for Cannabis is not an especially compelling argument against such prescribing."
1. U.S. Department of Health and Human Services. Drug Abuse Warning Network, 2011: National estimates of drug-related emergency department visits. http://www.samhsa.gov/data/2k13/ DAWN2k11ED/DAWN2k11ED.htm. Published May 2013. Accessed on July 26, 2014.
2. Mehmedic Z, Chandra S, Slade D, et al. Potency trends of Δ9-THC and other cannabinoids in confiscated cannabis preparations from 1993 to 2008. J Forensic Sci. 2010;55(5):1209-1217.
3. Swift W, Wong A, Li KM, et al. Analysis of cannabis seizures in NSW, Australia: cannabis potency and cannabinoid profile. PLos One. 2013;8(7):e70052. doi: 10.1371/journal.pone.0070052.
4. Morrison P. It’s the lack of balance in cannabis that does the harm. http://www.beckleyfoundation. org/2010/10/its-the-lack-of-balance-in-cannabis-that-does-the-harm. Published October 21, 2010. Accessed July 26, 2014.
1. U.S. Department of Health and Human Services. Drug Abuse Warning Network, 2011: National estimates of drug-related emergency department visits. http://www.samhsa.gov/data/2k13/ DAWN2k11ED/DAWN2k11ED.htm. Published May 2013. Accessed on July 26, 2014.
2. Mehmedic Z, Chandra S, Slade D, et al. Potency trends of Δ9-THC and other cannabinoids in confiscated cannabis preparations from 1993 to 2008. J Forensic Sci. 2010;55(5):1209-1217.
3. Swift W, Wong A, Li KM, et al. Analysis of cannabis seizures in NSW, Australia: cannabis potency and cannabinoid profile. PLos One. 2013;8(7):e70052. doi: 10.1371/journal.pone.0070052.
4. Morrison P. It’s the lack of balance in cannabis that does the harm. http://www.beckleyfoundation. org/2010/10/its-the-lack-of-balance-in-cannabis-that-does-the-harm. Published October 21, 2010. Accessed July 26, 2014.
Tailored messages will defeat Ebola
The more we learn about Ebola, the more it is becoming apparent that overcoming the psychosocial reactions to this deadly virus comes down to one word: education.
Education that is tailored to the audience has been most successful, as has maintaining a focus on the psychosocial impact of the disease on patients (here and abroad), their families, and their health care workers. Take the case of Nigeria, which the World Health Organization (WHO) declared free of Ebola virus transmission on Oct. 20. Nigeria used contact tracing to physically monitor all identified contacts daily for 21 days. In addition to allocating government funds and disbursing that money quickly, the private sector reportedly contributed resources aimed at scaling up control measures.
Perhaps most importantly, according to the WHO, “house-to-house information campaigns and messages on local radio stations, in local dialects, were used to explain the level of risk, effective personal preventive measures, and the actions being taken for control. The full range of media opportunities was exploited – from social media to televised facts about the disease delivered by well-known ‘Nollywood’ movie stars.”
I cannot overemphasize the importance of tailoring our educational messages about the virus to specific audiences. The sort of information needed to help allay the anxiety of an administrative assistant who asks, “Why didn’t the vaccine those nurses took before treating the patient work?”) is different from the information required of a front-line nurse at a public sector hospital, who might ask “Will our gowns protect us if we have a patient?” or a hospitalist at a tertiary care pediatrics hospital who might wonder “Is our isolation unit appropriate for treating this disorder?”
Regarding the disease’s potential victims – patients, family, health care workers – we should be mindful of the psychosocial impact that even the possibility of contact with the virus has. Potential contacts with the virus face destruction of all of their belongings, an inability to work while bills mount, and even the stress of the unwelcome spotlight.
Indeed, while there is a dearth of information available on mental health aspects of Ebola, specifically, there are powerful stories out there (here and here, for example) on the persistent stigma associated with this terrible disease.
Several other community mental health perspectives need to be considered, as well:
• What if a potential victim is a transient homeless man known to the community mental health system who is not inclined to accept a voluntary quarantine?
• What if he slept the night before at a homeless shelter for 300 people, all of whom are required to leave the shelter each morning?
• What if the potential victim is an intravenous drug abuser not inclined to accept an offer of methadone as a substitute while in quarantine?
• What if the potential victim is actively psychotic, not committable under your particular state’s law, but refusing all assistance because of paranoia?
• What if a call comes from a school principal stating that an elementary student, the child of a health care worker involved in an Ebola case, is distraught over marginalization in class and in the cafeteria by fellow students?
• What if a community of first-generation immigrants, historically dependent upon the psychosocial support of a robust group of community volunteers, suddenly finds itself without those supports when one member of the community is diagnosed with the disease?
• What if some members of the community also have the challenge of a severe mental illness?
As physicians and mental health experts, we can take the lead in tamping down anxiety tied to Ebola. How do we do it? By fostering education and preparedness, advocating for minimizing the risk of more victims of this disease, and supporting efforts to end its spread in West Africa.
Here in the United States, we must help our communities maintain their empathy for the suffering of Ebola’s victims and their families, as well as the suffering of the health care workers (and their families, too) who bravely care for these unfortunate patients.
Dr. Baker is medical director for behavioral health in the Texas Department of State Health Services, Austin.
The more we learn about Ebola, the more it is becoming apparent that overcoming the psychosocial reactions to this deadly virus comes down to one word: education.
Education that is tailored to the audience has been most successful, as has maintaining a focus on the psychosocial impact of the disease on patients (here and abroad), their families, and their health care workers. Take the case of Nigeria, which the World Health Organization (WHO) declared free of Ebola virus transmission on Oct. 20. Nigeria used contact tracing to physically monitor all identified contacts daily for 21 days. In addition to allocating government funds and disbursing that money quickly, the private sector reportedly contributed resources aimed at scaling up control measures.
Perhaps most importantly, according to the WHO, “house-to-house information campaigns and messages on local radio stations, in local dialects, were used to explain the level of risk, effective personal preventive measures, and the actions being taken for control. The full range of media opportunities was exploited – from social media to televised facts about the disease delivered by well-known ‘Nollywood’ movie stars.”
I cannot overemphasize the importance of tailoring our educational messages about the virus to specific audiences. The sort of information needed to help allay the anxiety of an administrative assistant who asks, “Why didn’t the vaccine those nurses took before treating the patient work?”) is different from the information required of a front-line nurse at a public sector hospital, who might ask “Will our gowns protect us if we have a patient?” or a hospitalist at a tertiary care pediatrics hospital who might wonder “Is our isolation unit appropriate for treating this disorder?”
Regarding the disease’s potential victims – patients, family, health care workers – we should be mindful of the psychosocial impact that even the possibility of contact with the virus has. Potential contacts with the virus face destruction of all of their belongings, an inability to work while bills mount, and even the stress of the unwelcome spotlight.
Indeed, while there is a dearth of information available on mental health aspects of Ebola, specifically, there are powerful stories out there (here and here, for example) on the persistent stigma associated with this terrible disease.
Several other community mental health perspectives need to be considered, as well:
• What if a potential victim is a transient homeless man known to the community mental health system who is not inclined to accept a voluntary quarantine?
• What if he slept the night before at a homeless shelter for 300 people, all of whom are required to leave the shelter each morning?
• What if the potential victim is an intravenous drug abuser not inclined to accept an offer of methadone as a substitute while in quarantine?
• What if the potential victim is actively psychotic, not committable under your particular state’s law, but refusing all assistance because of paranoia?
• What if a call comes from a school principal stating that an elementary student, the child of a health care worker involved in an Ebola case, is distraught over marginalization in class and in the cafeteria by fellow students?
• What if a community of first-generation immigrants, historically dependent upon the psychosocial support of a robust group of community volunteers, suddenly finds itself without those supports when one member of the community is diagnosed with the disease?
• What if some members of the community also have the challenge of a severe mental illness?
As physicians and mental health experts, we can take the lead in tamping down anxiety tied to Ebola. How do we do it? By fostering education and preparedness, advocating for minimizing the risk of more victims of this disease, and supporting efforts to end its spread in West Africa.
Here in the United States, we must help our communities maintain their empathy for the suffering of Ebola’s victims and their families, as well as the suffering of the health care workers (and their families, too) who bravely care for these unfortunate patients.
Dr. Baker is medical director for behavioral health in the Texas Department of State Health Services, Austin.
The more we learn about Ebola, the more it is becoming apparent that overcoming the psychosocial reactions to this deadly virus comes down to one word: education.
Education that is tailored to the audience has been most successful, as has maintaining a focus on the psychosocial impact of the disease on patients (here and abroad), their families, and their health care workers. Take the case of Nigeria, which the World Health Organization (WHO) declared free of Ebola virus transmission on Oct. 20. Nigeria used contact tracing to physically monitor all identified contacts daily for 21 days. In addition to allocating government funds and disbursing that money quickly, the private sector reportedly contributed resources aimed at scaling up control measures.
Perhaps most importantly, according to the WHO, “house-to-house information campaigns and messages on local radio stations, in local dialects, were used to explain the level of risk, effective personal preventive measures, and the actions being taken for control. The full range of media opportunities was exploited – from social media to televised facts about the disease delivered by well-known ‘Nollywood’ movie stars.”
I cannot overemphasize the importance of tailoring our educational messages about the virus to specific audiences. The sort of information needed to help allay the anxiety of an administrative assistant who asks, “Why didn’t the vaccine those nurses took before treating the patient work?”) is different from the information required of a front-line nurse at a public sector hospital, who might ask “Will our gowns protect us if we have a patient?” or a hospitalist at a tertiary care pediatrics hospital who might wonder “Is our isolation unit appropriate for treating this disorder?”
Regarding the disease’s potential victims – patients, family, health care workers – we should be mindful of the psychosocial impact that even the possibility of contact with the virus has. Potential contacts with the virus face destruction of all of their belongings, an inability to work while bills mount, and even the stress of the unwelcome spotlight.
Indeed, while there is a dearth of information available on mental health aspects of Ebola, specifically, there are powerful stories out there (here and here, for example) on the persistent stigma associated with this terrible disease.
Several other community mental health perspectives need to be considered, as well:
• What if a potential victim is a transient homeless man known to the community mental health system who is not inclined to accept a voluntary quarantine?
• What if he slept the night before at a homeless shelter for 300 people, all of whom are required to leave the shelter each morning?
• What if the potential victim is an intravenous drug abuser not inclined to accept an offer of methadone as a substitute while in quarantine?
• What if the potential victim is actively psychotic, not committable under your particular state’s law, but refusing all assistance because of paranoia?
• What if a call comes from a school principal stating that an elementary student, the child of a health care worker involved in an Ebola case, is distraught over marginalization in class and in the cafeteria by fellow students?
• What if a community of first-generation immigrants, historically dependent upon the psychosocial support of a robust group of community volunteers, suddenly finds itself without those supports when one member of the community is diagnosed with the disease?
• What if some members of the community also have the challenge of a severe mental illness?
As physicians and mental health experts, we can take the lead in tamping down anxiety tied to Ebola. How do we do it? By fostering education and preparedness, advocating for minimizing the risk of more victims of this disease, and supporting efforts to end its spread in West Africa.
Here in the United States, we must help our communities maintain their empathy for the suffering of Ebola’s victims and their families, as well as the suffering of the health care workers (and their families, too) who bravely care for these unfortunate patients.
Dr. Baker is medical director for behavioral health in the Texas Department of State Health Services, Austin.
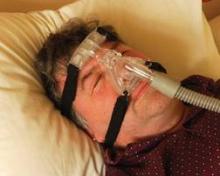
Clinical Guidelines: Obstructive sleep apnea
The Greek word apnea literally translates to “without breath.” More than 18 million American adults experience several moments “without breath” every night, according to the National Sleep Foundation. These pauses in breathing can last from a few seconds to minutes and can occur up to 30 times per hour or more. There are three types of apnea: obstructive, central, and mixed. Of the three, obstructive sleep apnea (OSA) is the most common. If left untreated, sleep apnea can have serious or life-threatening consequences, such as high blood pressure, heart disease, and day-time sleepiness that can lead to car accidents, depression, and headaches.
The significance of this condition has led the American College of Physicians (ACP) to publish guidelines regarding the management of OSA in adults. These guidelines are intended to provide clinicians with evidence-based recommendations that will have positive, long-term effects on patients’ cardiovascular risk, as well overall health and quality of life.
Recommendation 1: Encourage weight loss in all overweight and obese patients diagnosed with OSA.
There is strong evidence that shows how weight loss interventions can reduce the apnea/hypopnea index (AHI) and improve symptoms. The apnea/hypopnea index is a measure of the number of apnea and hypopnea episodes per hour of monitored sleep. According to the American Academy of Sleep Medicine, an OSA diagnosis is defined by ≥ 15 events/hr (with or without OSA symptoms) or ≥ 5 events/hr with OSA symptoms. Severity of OSA is classified as:
• Mild: 5-14 events/hr
• Moderate: 15-30 events/hr
• Severe: >30 events/hr
In patients with mild OSA, weight loss alone can be sufficient to normalize the apnea/hypopnea index, thereby reducing the need for continuous positive airway pressure (CPAP). In those with persistent OSA, weight loss can reduce the amount of PAP pressure required, which can increase tolerance of and adherence to CPAP. However, weight loss alone may not be sufficient to reduce OSA in all patients. In obese patients, weight loss must be encouraged with another primary treatment. In a meta-analysis of 342 patients in 12 published trials, weight loss produced substantial reductions in apnea/hypopnea index; however, the majority of patients continued to have persistent OSA after significant weight reduction. So, while weight loss should always be encouraged in patients with OSA, it should not be assumed that this intervention alone will be sufficient; patients need to be reassessed to determine whether OSA persists and if so, CPAP should be continued.
Recommendation 2: Prescribe CPAP as the initial therapy for patients diagnosed with OSA.
CPAP is as critical as it is effective not only in reducing the AHI but also in improving sleep continuity and architecture and decreasing the sleep hypoxia that is associated with OSA. Because of the lack of adherence to CPAP, many new features have been added including heated humidification, broad pressure adjustments, and expiratory pressure relief; while many of these features mildly improve patients’ preferences, there is no evidence to suggest that these changes improve efficacy or adherence. Again, it is critical that each patient’s needs be taken into consideration. Some patients, particularly those with mild forms of OSA, may not need CPAP and instead, may benefit from positional therapy or weight loss. Other therapy such as surgery or mandibular advancement devices (MADs) may be better suited for some patients despite their lessor effectiveness when compared with CPAP.
Recommendation 3: Consider MAD as an alternate therapy to CPAP for patients diagnosed with OSA who prefer MAD or for those with adverse effects associated with CPAP.
MADs have been recommended for patients with moderate to severe OSA, those with apnea/hypopnea index values between 18-40 events/hour, and for individuals who experienced adverse events on CPAP or who can’t tolerate using it. While CPAP still is considered to be primary therapy, for those who must use a mandibular advancement device, it can often be very effective. Patients may find it easier to be compliant with MAD than with CPAP. One group of researchers observed that MADs were able to provide appropriate decrease in obstructive events in 70% of patients with mild OSA, 48% of those with moderate OSA, and 42% of those with severe OSA (Chest 2011:139:1331-9). The ACP concluded that, without sufficient evidence, it is unclear which patients will benefit from MADs. Data from several studies show that patients who are younger and thinner, with less severe OSA, may benefit more from the use of MADs. Although the ACP does not recommend surgery or pharmaceutical therapy for OSA, the ACP does acknowledge that it may work for certain patients. However, the documented efficacy rate ranges from 20%-100%, thereby making it challenging to determine its true effect.
Bottom Line
The ACP recommends weight loss for all overweight patients with OSA. CPAP is first-line therapy, particularly if weight loss cannot be sustained or does not sufficiently lessen symptoms. For selected patients who are younger and thinner, with less severe OSA, or for those patients who are unable to tolerate CPAP, MADs can be used as an alternative first-line therapy with moderate success.
Reference
Qaseem A., Holty J.C., Owens D. et al. Diagnosis of obstructive sleep apnea in adults: a Clinical Practice Guideline from the American College of Physicians. Ann. Intern. Med. 2014;161:210-20.
Dr. Grover is a second-year resident in the family medicine residency program at Abington Memorial Hospital. Dr. Skolnik is associate director of the family medicine residency program at Abington Memorial Hospital and professor of family and community medicine at Temple University in Philadelphia.
The Greek word apnea literally translates to “without breath.” More than 18 million American adults experience several moments “without breath” every night, according to the National Sleep Foundation. These pauses in breathing can last from a few seconds to minutes and can occur up to 30 times per hour or more. There are three types of apnea: obstructive, central, and mixed. Of the three, obstructive sleep apnea (OSA) is the most common. If left untreated, sleep apnea can have serious or life-threatening consequences, such as high blood pressure, heart disease, and day-time sleepiness that can lead to car accidents, depression, and headaches.
The significance of this condition has led the American College of Physicians (ACP) to publish guidelines regarding the management of OSA in adults. These guidelines are intended to provide clinicians with evidence-based recommendations that will have positive, long-term effects on patients’ cardiovascular risk, as well overall health and quality of life.
Recommendation 1: Encourage weight loss in all overweight and obese patients diagnosed with OSA.
There is strong evidence that shows how weight loss interventions can reduce the apnea/hypopnea index (AHI) and improve symptoms. The apnea/hypopnea index is a measure of the number of apnea and hypopnea episodes per hour of monitored sleep. According to the American Academy of Sleep Medicine, an OSA diagnosis is defined by ≥ 15 events/hr (with or without OSA symptoms) or ≥ 5 events/hr with OSA symptoms. Severity of OSA is classified as:
• Mild: 5-14 events/hr
• Moderate: 15-30 events/hr
• Severe: >30 events/hr
In patients with mild OSA, weight loss alone can be sufficient to normalize the apnea/hypopnea index, thereby reducing the need for continuous positive airway pressure (CPAP). In those with persistent OSA, weight loss can reduce the amount of PAP pressure required, which can increase tolerance of and adherence to CPAP. However, weight loss alone may not be sufficient to reduce OSA in all patients. In obese patients, weight loss must be encouraged with another primary treatment. In a meta-analysis of 342 patients in 12 published trials, weight loss produced substantial reductions in apnea/hypopnea index; however, the majority of patients continued to have persistent OSA after significant weight reduction. So, while weight loss should always be encouraged in patients with OSA, it should not be assumed that this intervention alone will be sufficient; patients need to be reassessed to determine whether OSA persists and if so, CPAP should be continued.
Recommendation 2: Prescribe CPAP as the initial therapy for patients diagnosed with OSA.
CPAP is as critical as it is effective not only in reducing the AHI but also in improving sleep continuity and architecture and decreasing the sleep hypoxia that is associated with OSA. Because of the lack of adherence to CPAP, many new features have been added including heated humidification, broad pressure adjustments, and expiratory pressure relief; while many of these features mildly improve patients’ preferences, there is no evidence to suggest that these changes improve efficacy or adherence. Again, it is critical that each patient’s needs be taken into consideration. Some patients, particularly those with mild forms of OSA, may not need CPAP and instead, may benefit from positional therapy or weight loss. Other therapy such as surgery or mandibular advancement devices (MADs) may be better suited for some patients despite their lessor effectiveness when compared with CPAP.
Recommendation 3: Consider MAD as an alternate therapy to CPAP for patients diagnosed with OSA who prefer MAD or for those with adverse effects associated with CPAP.
MADs have been recommended for patients with moderate to severe OSA, those with apnea/hypopnea index values between 18-40 events/hour, and for individuals who experienced adverse events on CPAP or who can’t tolerate using it. While CPAP still is considered to be primary therapy, for those who must use a mandibular advancement device, it can often be very effective. Patients may find it easier to be compliant with MAD than with CPAP. One group of researchers observed that MADs were able to provide appropriate decrease in obstructive events in 70% of patients with mild OSA, 48% of those with moderate OSA, and 42% of those with severe OSA (Chest 2011:139:1331-9). The ACP concluded that, without sufficient evidence, it is unclear which patients will benefit from MADs. Data from several studies show that patients who are younger and thinner, with less severe OSA, may benefit more from the use of MADs. Although the ACP does not recommend surgery or pharmaceutical therapy for OSA, the ACP does acknowledge that it may work for certain patients. However, the documented efficacy rate ranges from 20%-100%, thereby making it challenging to determine its true effect.
Bottom Line
The ACP recommends weight loss for all overweight patients with OSA. CPAP is first-line therapy, particularly if weight loss cannot be sustained or does not sufficiently lessen symptoms. For selected patients who are younger and thinner, with less severe OSA, or for those patients who are unable to tolerate CPAP, MADs can be used as an alternative first-line therapy with moderate success.
Reference
Qaseem A., Holty J.C., Owens D. et al. Diagnosis of obstructive sleep apnea in adults: a Clinical Practice Guideline from the American College of Physicians. Ann. Intern. Med. 2014;161:210-20.
Dr. Grover is a second-year resident in the family medicine residency program at Abington Memorial Hospital. Dr. Skolnik is associate director of the family medicine residency program at Abington Memorial Hospital and professor of family and community medicine at Temple University in Philadelphia.
The Greek word apnea literally translates to “without breath.” More than 18 million American adults experience several moments “without breath” every night, according to the National Sleep Foundation. These pauses in breathing can last from a few seconds to minutes and can occur up to 30 times per hour or more. There are three types of apnea: obstructive, central, and mixed. Of the three, obstructive sleep apnea (OSA) is the most common. If left untreated, sleep apnea can have serious or life-threatening consequences, such as high blood pressure, heart disease, and day-time sleepiness that can lead to car accidents, depression, and headaches.
The significance of this condition has led the American College of Physicians (ACP) to publish guidelines regarding the management of OSA in adults. These guidelines are intended to provide clinicians with evidence-based recommendations that will have positive, long-term effects on patients’ cardiovascular risk, as well overall health and quality of life.
Recommendation 1: Encourage weight loss in all overweight and obese patients diagnosed with OSA.
There is strong evidence that shows how weight loss interventions can reduce the apnea/hypopnea index (AHI) and improve symptoms. The apnea/hypopnea index is a measure of the number of apnea and hypopnea episodes per hour of monitored sleep. According to the American Academy of Sleep Medicine, an OSA diagnosis is defined by ≥ 15 events/hr (with or without OSA symptoms) or ≥ 5 events/hr with OSA symptoms. Severity of OSA is classified as:
• Mild: 5-14 events/hr
• Moderate: 15-30 events/hr
• Severe: >30 events/hr
In patients with mild OSA, weight loss alone can be sufficient to normalize the apnea/hypopnea index, thereby reducing the need for continuous positive airway pressure (CPAP). In those with persistent OSA, weight loss can reduce the amount of PAP pressure required, which can increase tolerance of and adherence to CPAP. However, weight loss alone may not be sufficient to reduce OSA in all patients. In obese patients, weight loss must be encouraged with another primary treatment. In a meta-analysis of 342 patients in 12 published trials, weight loss produced substantial reductions in apnea/hypopnea index; however, the majority of patients continued to have persistent OSA after significant weight reduction. So, while weight loss should always be encouraged in patients with OSA, it should not be assumed that this intervention alone will be sufficient; patients need to be reassessed to determine whether OSA persists and if so, CPAP should be continued.
Recommendation 2: Prescribe CPAP as the initial therapy for patients diagnosed with OSA.
CPAP is as critical as it is effective not only in reducing the AHI but also in improving sleep continuity and architecture and decreasing the sleep hypoxia that is associated with OSA. Because of the lack of adherence to CPAP, many new features have been added including heated humidification, broad pressure adjustments, and expiratory pressure relief; while many of these features mildly improve patients’ preferences, there is no evidence to suggest that these changes improve efficacy or adherence. Again, it is critical that each patient’s needs be taken into consideration. Some patients, particularly those with mild forms of OSA, may not need CPAP and instead, may benefit from positional therapy or weight loss. Other therapy such as surgery or mandibular advancement devices (MADs) may be better suited for some patients despite their lessor effectiveness when compared with CPAP.
Recommendation 3: Consider MAD as an alternate therapy to CPAP for patients diagnosed with OSA who prefer MAD or for those with adverse effects associated with CPAP.
MADs have been recommended for patients with moderate to severe OSA, those with apnea/hypopnea index values between 18-40 events/hour, and for individuals who experienced adverse events on CPAP or who can’t tolerate using it. While CPAP still is considered to be primary therapy, for those who must use a mandibular advancement device, it can often be very effective. Patients may find it easier to be compliant with MAD than with CPAP. One group of researchers observed that MADs were able to provide appropriate decrease in obstructive events in 70% of patients with mild OSA, 48% of those with moderate OSA, and 42% of those with severe OSA (Chest 2011:139:1331-9). The ACP concluded that, without sufficient evidence, it is unclear which patients will benefit from MADs. Data from several studies show that patients who are younger and thinner, with less severe OSA, may benefit more from the use of MADs. Although the ACP does not recommend surgery or pharmaceutical therapy for OSA, the ACP does acknowledge that it may work for certain patients. However, the documented efficacy rate ranges from 20%-100%, thereby making it challenging to determine its true effect.
Bottom Line
The ACP recommends weight loss for all overweight patients with OSA. CPAP is first-line therapy, particularly if weight loss cannot be sustained or does not sufficiently lessen symptoms. For selected patients who are younger and thinner, with less severe OSA, or for those patients who are unable to tolerate CPAP, MADs can be used as an alternative first-line therapy with moderate success.
Reference
Qaseem A., Holty J.C., Owens D. et al. Diagnosis of obstructive sleep apnea in adults: a Clinical Practice Guideline from the American College of Physicians. Ann. Intern. Med. 2014;161:210-20.
Dr. Grover is a second-year resident in the family medicine residency program at Abington Memorial Hospital. Dr. Skolnik is associate director of the family medicine residency program at Abington Memorial Hospital and professor of family and community medicine at Temple University in Philadelphia.
Fillers for men
Idealized masculine facial features tend to include an overhanging, horizontal brow with minimal arch, deeper-set eyes that look closer together, a somewhat larger nose, a wider mouth, a squared lower face, and a beard or coarser texture to the lower facial skin. A major component of aesthetic disharmony in the aging face in both men and women, however, is the loss or redistribution of subcutaneous fat. Detailed studies by Rohrich and Pessa have demonstrated that facial fat (unlike fat elsewhere in the body) is partitioned into discrete compartments that may age independently of one another. Redistribution and loss of these fat pads contribute to formation of the nasojugal fold, malar crease, nasolabial fold, prejowl sulcus and marionette lines, as well as wasting of the temples, superior brow, and buccal fat. These changes can be visualized most strikingly in cases of cachexia and severe HIV-associated lipodystrophy.
When using fillers to restore volume loss and wrinkles in men, care must be taken to not overfeminize the male face. Filler placement in the anteromedial cheek, submalar cheek, temples, tear trough area, nasolabial folds, and marionette areas are often similar to filler placement in women if the patient has an issue with volume loss in those areas. The main difference is placement in the zygomaticomalar region of the cheek (or the point where the maximal light reflection is off of the highest point of the zygoma, or cheek bone) and the lips. Care must be taken not to overvolumize this region in men.
Also, even within ethnic groups, the male lip is typically not as tall and curvy as the female lip; it often appears less full, with more of a shadow cast by the lower lip.
Men tend to prefer treatments with less downtime and more natural results and are less risk tolerant than women are. Keeping these points in mind can increase patient satisfaction when offering fillers to male patients.
Source: Rohrich R., Pessa J. The fat compartments of the face: anatomy and clinical implications for cosmetic surgery. J. Plast. Reconstr. Surg. 2007;119:2219-27.
Dr. Talakoub and Dr. Wesley are co-contributors to a monthly Aesthetic Dermatology column in Skin & Allergy News. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Wesley.
Idealized masculine facial features tend to include an overhanging, horizontal brow with minimal arch, deeper-set eyes that look closer together, a somewhat larger nose, a wider mouth, a squared lower face, and a beard or coarser texture to the lower facial skin. A major component of aesthetic disharmony in the aging face in both men and women, however, is the loss or redistribution of subcutaneous fat. Detailed studies by Rohrich and Pessa have demonstrated that facial fat (unlike fat elsewhere in the body) is partitioned into discrete compartments that may age independently of one another. Redistribution and loss of these fat pads contribute to formation of the nasojugal fold, malar crease, nasolabial fold, prejowl sulcus and marionette lines, as well as wasting of the temples, superior brow, and buccal fat. These changes can be visualized most strikingly in cases of cachexia and severe HIV-associated lipodystrophy.
When using fillers to restore volume loss and wrinkles in men, care must be taken to not overfeminize the male face. Filler placement in the anteromedial cheek, submalar cheek, temples, tear trough area, nasolabial folds, and marionette areas are often similar to filler placement in women if the patient has an issue with volume loss in those areas. The main difference is placement in the zygomaticomalar region of the cheek (or the point where the maximal light reflection is off of the highest point of the zygoma, or cheek bone) and the lips. Care must be taken not to overvolumize this region in men.
Also, even within ethnic groups, the male lip is typically not as tall and curvy as the female lip; it often appears less full, with more of a shadow cast by the lower lip.
Men tend to prefer treatments with less downtime and more natural results and are less risk tolerant than women are. Keeping these points in mind can increase patient satisfaction when offering fillers to male patients.
Source: Rohrich R., Pessa J. The fat compartments of the face: anatomy and clinical implications for cosmetic surgery. J. Plast. Reconstr. Surg. 2007;119:2219-27.
Dr. Talakoub and Dr. Wesley are co-contributors to a monthly Aesthetic Dermatology column in Skin & Allergy News. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Wesley.
Idealized masculine facial features tend to include an overhanging, horizontal brow with minimal arch, deeper-set eyes that look closer together, a somewhat larger nose, a wider mouth, a squared lower face, and a beard or coarser texture to the lower facial skin. A major component of aesthetic disharmony in the aging face in both men and women, however, is the loss or redistribution of subcutaneous fat. Detailed studies by Rohrich and Pessa have demonstrated that facial fat (unlike fat elsewhere in the body) is partitioned into discrete compartments that may age independently of one another. Redistribution and loss of these fat pads contribute to formation of the nasojugal fold, malar crease, nasolabial fold, prejowl sulcus and marionette lines, as well as wasting of the temples, superior brow, and buccal fat. These changes can be visualized most strikingly in cases of cachexia and severe HIV-associated lipodystrophy.
When using fillers to restore volume loss and wrinkles in men, care must be taken to not overfeminize the male face. Filler placement in the anteromedial cheek, submalar cheek, temples, tear trough area, nasolabial folds, and marionette areas are often similar to filler placement in women if the patient has an issue with volume loss in those areas. The main difference is placement in the zygomaticomalar region of the cheek (or the point where the maximal light reflection is off of the highest point of the zygoma, or cheek bone) and the lips. Care must be taken not to overvolumize this region in men.
Also, even within ethnic groups, the male lip is typically not as tall and curvy as the female lip; it often appears less full, with more of a shadow cast by the lower lip.
Men tend to prefer treatments with less downtime and more natural results and are less risk tolerant than women are. Keeping these points in mind can increase patient satisfaction when offering fillers to male patients.
Source: Rohrich R., Pessa J. The fat compartments of the face: anatomy and clinical implications for cosmetic surgery. J. Plast. Reconstr. Surg. 2007;119:2219-27.
Dr. Talakoub and Dr. Wesley are co-contributors to a monthly Aesthetic Dermatology column in Skin & Allergy News. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Wesley.
The Joys of a Life in Surgery
I have been privileged to spend over one half of my 70 years on this planet as a surgeon. Even considering the innumerable highly stressful moments and the occasional failures in patient care that continue to haunt me, I cannot conceive of a more satisfying and enjoyable vocation. It saddens me to know that a significant percentage of those in our profession have not been able to gain a similar level of fulfillment from their lives in surgery as I have.
There is no doubt that a pall of negativity has descended upon the medical profession in recent years. The factors that have caused it are real – declining compensation in face of an increased workload, less autonomy in practice with a steadily increasing number of physicians and surgeons being employees rather than independent practitioners, an oppressive regulatory environment necessitating a seemingly endless amount of paperwork, and finally the uncertainty of what our profession will look like once health care reform settles into its final form.
These issues – along with the always-present stresses that accompany caring for sick patients and the challenge of balancing a too-busy professional life with a meaningful personal existence – have led to a shocking number of our colleagues experiencing the symptoms of burnout; emotional exhaustion, depersonalization, and a sense of low personal accomplishment.
It would be inappropriate for me to in any way minimize the effect that burnout is having on medical professionals. It is now a greater threat to surgeon wellness than any other dynamic, including alcoholism and drug abuse. I will deal with it in some detail in a future editorial. But here I would like to consider some of the unique and positive features that, in my opinion, still make surgery the most noble of professions and a career that we can highly recommend to our children and grandchildren. I sincerely hope that emphasizing the more upbeat and constructive aspects of our profession, most of which are obvious but are unfortunately obscured by the cloud of negativity, will provide at least a small beacon of light for those having difficulty seeing their way forward.
I feel compelled to admit to some important disclaimers. While I do not consider myself a Pollyanna, ever since reading a Dutch study (Giltay et al., Arch. Gen. Psychiatry 2004;61:1126-35) that showed an impressive difference in longevity between optimists and pessimists, I have solidly placed myself in the optimist camp. Additionally, I have spent my entire surgical career within the ivy-covered walls of academe. Finally, I fully realize that what brings joy to one person may not do so to another.
My basic assertion is that, while many aspects of our profession have changed, the basic core – the opportunity to make positive changes in the lives of others – remains solidly intact. As a surgical academician, this was not limited to just patients, but extended to medical students, surgical residents, and surgical faculty. I suspect in the private setting there are also numerous opportunities to mentor young colleagues and lend support to surgeons who are experiencing burnout or other issues that compromise the quality of their lives and their effectiveness as surgeons.
The most satisfying aspect of my practice was the nonmonetary rewards I received from grateful patients. The patient-doctor relationship that surgeons enjoy with their patients is particularly special. We alone among medical professionals have the opportunity to suddenly and dramatically alter the course of patients’ pain, suffering, and prognosis. We alone invade the sacred spaces of their bodies. Although what we do is based on science and anatomy, to many patients, it is almost in the realm of the supernatural. I have always thought that the designing and construction of a complex building is a more challenging feat than removing a diseased gallbladder, but patients don’t see it that way. If we are willing to simply maintain meaningful and kind communication with them, they freely and liberally express their gratitude for even minimal surgical achievements. When a life-threatening situation has been suddenly erased by a surgical operation, many consider it in the domain of the heroic.
Especially amazing to me is the generosity of patients and their families even when complications or death compromise the outcome. Occasionally, gratitude comes in the guise of a gift. The most memorable for me was an envelope labeled “Pennies from Heaven” that contained $2.83 designated for bile duct cancer research given to me by the grandchildren of a woman with that dread disease on whom I had operated. The sum may have been insufficient to have any scientific impact but was more than enough to brighten my day after I observed this lovely woman enduring a long, difficult, and eventually unsuccessful postoperative course (“Pennies from Heaven,” ACS Surgery News, December 2011, p. 18).
Aside from the privilege of caring for patients, the most rewarding element of my professional life has been the opportunity to mentor others. Nearly all of us who have had success in our profession have had one or more valuable mentors. Performing this function for others is not only appropriate, but, in a sense, represents a giving back for what others have done for us. An effective mentor provides a nurturing environment in which the mentee can reach his/her full potential. Whether you are helping a resident or junior associate better adjust to life as a surgeon or find their best career path, assisting them in achieving their goals is nearly as satisfying as successfully seeing a patient through a challenging operation and complicated postoperative course.
As difficult as life in surgery can often be, focusing on the unique positives – the appreciative patient cured of a life-threatening tumor, the skilled and accomplished senior resident who you helped train, the young associate who seeks your wisdom on difficult cases and becomes a better surgeon because of it – rather than the negative background of uncertainty and loss of control may help to confirm that what you are doing is worthwhile and most likely making the world a better place.
Dr. Rikkers is the editor in chief of ACS Surgery News.
I have been privileged to spend over one half of my 70 years on this planet as a surgeon. Even considering the innumerable highly stressful moments and the occasional failures in patient care that continue to haunt me, I cannot conceive of a more satisfying and enjoyable vocation. It saddens me to know that a significant percentage of those in our profession have not been able to gain a similar level of fulfillment from their lives in surgery as I have.
There is no doubt that a pall of negativity has descended upon the medical profession in recent years. The factors that have caused it are real – declining compensation in face of an increased workload, less autonomy in practice with a steadily increasing number of physicians and surgeons being employees rather than independent practitioners, an oppressive regulatory environment necessitating a seemingly endless amount of paperwork, and finally the uncertainty of what our profession will look like once health care reform settles into its final form.
These issues – along with the always-present stresses that accompany caring for sick patients and the challenge of balancing a too-busy professional life with a meaningful personal existence – have led to a shocking number of our colleagues experiencing the symptoms of burnout; emotional exhaustion, depersonalization, and a sense of low personal accomplishment.
It would be inappropriate for me to in any way minimize the effect that burnout is having on medical professionals. It is now a greater threat to surgeon wellness than any other dynamic, including alcoholism and drug abuse. I will deal with it in some detail in a future editorial. But here I would like to consider some of the unique and positive features that, in my opinion, still make surgery the most noble of professions and a career that we can highly recommend to our children and grandchildren. I sincerely hope that emphasizing the more upbeat and constructive aspects of our profession, most of which are obvious but are unfortunately obscured by the cloud of negativity, will provide at least a small beacon of light for those having difficulty seeing their way forward.
I feel compelled to admit to some important disclaimers. While I do not consider myself a Pollyanna, ever since reading a Dutch study (Giltay et al., Arch. Gen. Psychiatry 2004;61:1126-35) that showed an impressive difference in longevity between optimists and pessimists, I have solidly placed myself in the optimist camp. Additionally, I have spent my entire surgical career within the ivy-covered walls of academe. Finally, I fully realize that what brings joy to one person may not do so to another.
My basic assertion is that, while many aspects of our profession have changed, the basic core – the opportunity to make positive changes in the lives of others – remains solidly intact. As a surgical academician, this was not limited to just patients, but extended to medical students, surgical residents, and surgical faculty. I suspect in the private setting there are also numerous opportunities to mentor young colleagues and lend support to surgeons who are experiencing burnout or other issues that compromise the quality of their lives and their effectiveness as surgeons.
The most satisfying aspect of my practice was the nonmonetary rewards I received from grateful patients. The patient-doctor relationship that surgeons enjoy with their patients is particularly special. We alone among medical professionals have the opportunity to suddenly and dramatically alter the course of patients’ pain, suffering, and prognosis. We alone invade the sacred spaces of their bodies. Although what we do is based on science and anatomy, to many patients, it is almost in the realm of the supernatural. I have always thought that the designing and construction of a complex building is a more challenging feat than removing a diseased gallbladder, but patients don’t see it that way. If we are willing to simply maintain meaningful and kind communication with them, they freely and liberally express their gratitude for even minimal surgical achievements. When a life-threatening situation has been suddenly erased by a surgical operation, many consider it in the domain of the heroic.
Especially amazing to me is the generosity of patients and their families even when complications or death compromise the outcome. Occasionally, gratitude comes in the guise of a gift. The most memorable for me was an envelope labeled “Pennies from Heaven” that contained $2.83 designated for bile duct cancer research given to me by the grandchildren of a woman with that dread disease on whom I had operated. The sum may have been insufficient to have any scientific impact but was more than enough to brighten my day after I observed this lovely woman enduring a long, difficult, and eventually unsuccessful postoperative course (“Pennies from Heaven,” ACS Surgery News, December 2011, p. 18).
Aside from the privilege of caring for patients, the most rewarding element of my professional life has been the opportunity to mentor others. Nearly all of us who have had success in our profession have had one or more valuable mentors. Performing this function for others is not only appropriate, but, in a sense, represents a giving back for what others have done for us. An effective mentor provides a nurturing environment in which the mentee can reach his/her full potential. Whether you are helping a resident or junior associate better adjust to life as a surgeon or find their best career path, assisting them in achieving their goals is nearly as satisfying as successfully seeing a patient through a challenging operation and complicated postoperative course.
As difficult as life in surgery can often be, focusing on the unique positives – the appreciative patient cured of a life-threatening tumor, the skilled and accomplished senior resident who you helped train, the young associate who seeks your wisdom on difficult cases and becomes a better surgeon because of it – rather than the negative background of uncertainty and loss of control may help to confirm that what you are doing is worthwhile and most likely making the world a better place.
Dr. Rikkers is the editor in chief of ACS Surgery News.
I have been privileged to spend over one half of my 70 years on this planet as a surgeon. Even considering the innumerable highly stressful moments and the occasional failures in patient care that continue to haunt me, I cannot conceive of a more satisfying and enjoyable vocation. It saddens me to know that a significant percentage of those in our profession have not been able to gain a similar level of fulfillment from their lives in surgery as I have.
There is no doubt that a pall of negativity has descended upon the medical profession in recent years. The factors that have caused it are real – declining compensation in face of an increased workload, less autonomy in practice with a steadily increasing number of physicians and surgeons being employees rather than independent practitioners, an oppressive regulatory environment necessitating a seemingly endless amount of paperwork, and finally the uncertainty of what our profession will look like once health care reform settles into its final form.
These issues – along with the always-present stresses that accompany caring for sick patients and the challenge of balancing a too-busy professional life with a meaningful personal existence – have led to a shocking number of our colleagues experiencing the symptoms of burnout; emotional exhaustion, depersonalization, and a sense of low personal accomplishment.
It would be inappropriate for me to in any way minimize the effect that burnout is having on medical professionals. It is now a greater threat to surgeon wellness than any other dynamic, including alcoholism and drug abuse. I will deal with it in some detail in a future editorial. But here I would like to consider some of the unique and positive features that, in my opinion, still make surgery the most noble of professions and a career that we can highly recommend to our children and grandchildren. I sincerely hope that emphasizing the more upbeat and constructive aspects of our profession, most of which are obvious but are unfortunately obscured by the cloud of negativity, will provide at least a small beacon of light for those having difficulty seeing their way forward.
I feel compelled to admit to some important disclaimers. While I do not consider myself a Pollyanna, ever since reading a Dutch study (Giltay et al., Arch. Gen. Psychiatry 2004;61:1126-35) that showed an impressive difference in longevity between optimists and pessimists, I have solidly placed myself in the optimist camp. Additionally, I have spent my entire surgical career within the ivy-covered walls of academe. Finally, I fully realize that what brings joy to one person may not do so to another.
My basic assertion is that, while many aspects of our profession have changed, the basic core – the opportunity to make positive changes in the lives of others – remains solidly intact. As a surgical academician, this was not limited to just patients, but extended to medical students, surgical residents, and surgical faculty. I suspect in the private setting there are also numerous opportunities to mentor young colleagues and lend support to surgeons who are experiencing burnout or other issues that compromise the quality of their lives and their effectiveness as surgeons.
The most satisfying aspect of my practice was the nonmonetary rewards I received from grateful patients. The patient-doctor relationship that surgeons enjoy with their patients is particularly special. We alone among medical professionals have the opportunity to suddenly and dramatically alter the course of patients’ pain, suffering, and prognosis. We alone invade the sacred spaces of their bodies. Although what we do is based on science and anatomy, to many patients, it is almost in the realm of the supernatural. I have always thought that the designing and construction of a complex building is a more challenging feat than removing a diseased gallbladder, but patients don’t see it that way. If we are willing to simply maintain meaningful and kind communication with them, they freely and liberally express their gratitude for even minimal surgical achievements. When a life-threatening situation has been suddenly erased by a surgical operation, many consider it in the domain of the heroic.
Especially amazing to me is the generosity of patients and their families even when complications or death compromise the outcome. Occasionally, gratitude comes in the guise of a gift. The most memorable for me was an envelope labeled “Pennies from Heaven” that contained $2.83 designated for bile duct cancer research given to me by the grandchildren of a woman with that dread disease on whom I had operated. The sum may have been insufficient to have any scientific impact but was more than enough to brighten my day after I observed this lovely woman enduring a long, difficult, and eventually unsuccessful postoperative course (“Pennies from Heaven,” ACS Surgery News, December 2011, p. 18).
Aside from the privilege of caring for patients, the most rewarding element of my professional life has been the opportunity to mentor others. Nearly all of us who have had success in our profession have had one or more valuable mentors. Performing this function for others is not only appropriate, but, in a sense, represents a giving back for what others have done for us. An effective mentor provides a nurturing environment in which the mentee can reach his/her full potential. Whether you are helping a resident or junior associate better adjust to life as a surgeon or find their best career path, assisting them in achieving their goals is nearly as satisfying as successfully seeing a patient through a challenging operation and complicated postoperative course.
As difficult as life in surgery can often be, focusing on the unique positives – the appreciative patient cured of a life-threatening tumor, the skilled and accomplished senior resident who you helped train, the young associate who seeks your wisdom on difficult cases and becomes a better surgeon because of it – rather than the negative background of uncertainty and loss of control may help to confirm that what you are doing is worthwhile and most likely making the world a better place.
Dr. Rikkers is the editor in chief of ACS Surgery News.
Advanced practice registered nurses in cardiology
In case you didn’t notice, our clinical practice has been reinforced by a entirely new class of performers who have become essential to our daily activities.
They are Advanced Practice Registered Nurses, whose role has evolved over the last 50 years from the Coronary Care Unit nurse with special training in coronary care to an array of well-trained women and men who have received both Bachelor’s and Master’s degrees in Nursing.
As a further extension of their training, many are now going on to achieve a further doctorate degree in nursing after 90 hours of postgraduate classes at certified academic centers and additional clinical experience in a variety of fields, including cardiology. The nurses completing those programs will be certified and licensed as APRNs. They come to our practice with remarkable experience and expertise in arrhythmia and heart failure management, as well as interventional skills, on top of wide experience in the management of patients in critical care units. Their integration into comprehensive and collaborative cardiac care raises challenges to and opportunities for the cardiologist.
A recent survey of large cardiology clinics initiated by the Summit Medical Group assessed the role of the APRN in the care of patients both in hospitals and in clinics. It reported that in many of cardiology clinics surveyed, APRNs provide an expanding role in patient care leading to variable relationships between the patient and the cardiologist. In some settings, the APRNs often function independent of physician interaction, initiating the patients’ entrance into the clinic and managing their follow-up. In other situations, they may be supervised by a cardiologist and their future laboratory studies and therapy are completely managed by the APRN, who functions as a professional associate of a physician. However, in many situations the cardiologist may have little or no contact with the patient.
While the APRN is seeing the patient, the cardiologists often are seeing their own patients or, more likely, are involved with maintaining the electronic medical record or performing or interpreting tests that are usually reimbursed at a fee that is a multiple of that received for a patient visit alone. Much of this is carried out under the heading of “coordinated care” and is managed in a multidisciplinary matrix in which many specialists and APRNs play a role in the care of the patient. In this setting, the doctor has become manager of a diverse group of support staff, including APRNs, and may be increasingly remote from direct patient care. My medical colleagues find the process as a way to increase the patient “pass through.” Many patients presume that the APRN is a reasonable alternative to a busy cardiologist or are interacting with their cardiologist.
As doctors, we are divesting ourselves from the one thing that sets us apart and makes us unique in the health care system; the ability to interact with patients in a comprehensive way. We seem to be on the slippery slope to medical obsolescence, soon to be replaced by staff who can triage our patients to the next appropriate test. Both the patient and doctor seem to have slipped into a Walmart-like world where expedience dominates over skill and shortcuts are the alternative to thoughtful personal physician-patient interaction.
Dr. Goldstein, medical editor of Cardiology News, is professor of medicine at Wayne State University and division head emeritus of cardiovascular medicine at Henry Ford Hospital, both in Detroit. He is on data safety monitoring committees for the National Institutes of Health and several pharmaceutical companies.
In case you didn’t notice, our clinical practice has been reinforced by a entirely new class of performers who have become essential to our daily activities.
They are Advanced Practice Registered Nurses, whose role has evolved over the last 50 years from the Coronary Care Unit nurse with special training in coronary care to an array of well-trained women and men who have received both Bachelor’s and Master’s degrees in Nursing.
As a further extension of their training, many are now going on to achieve a further doctorate degree in nursing after 90 hours of postgraduate classes at certified academic centers and additional clinical experience in a variety of fields, including cardiology. The nurses completing those programs will be certified and licensed as APRNs. They come to our practice with remarkable experience and expertise in arrhythmia and heart failure management, as well as interventional skills, on top of wide experience in the management of patients in critical care units. Their integration into comprehensive and collaborative cardiac care raises challenges to and opportunities for the cardiologist.
A recent survey of large cardiology clinics initiated by the Summit Medical Group assessed the role of the APRN in the care of patients both in hospitals and in clinics. It reported that in many of cardiology clinics surveyed, APRNs provide an expanding role in patient care leading to variable relationships between the patient and the cardiologist. In some settings, the APRNs often function independent of physician interaction, initiating the patients’ entrance into the clinic and managing their follow-up. In other situations, they may be supervised by a cardiologist and their future laboratory studies and therapy are completely managed by the APRN, who functions as a professional associate of a physician. However, in many situations the cardiologist may have little or no contact with the patient.
While the APRN is seeing the patient, the cardiologists often are seeing their own patients or, more likely, are involved with maintaining the electronic medical record or performing or interpreting tests that are usually reimbursed at a fee that is a multiple of that received for a patient visit alone. Much of this is carried out under the heading of “coordinated care” and is managed in a multidisciplinary matrix in which many specialists and APRNs play a role in the care of the patient. In this setting, the doctor has become manager of a diverse group of support staff, including APRNs, and may be increasingly remote from direct patient care. My medical colleagues find the process as a way to increase the patient “pass through.” Many patients presume that the APRN is a reasonable alternative to a busy cardiologist or are interacting with their cardiologist.
As doctors, we are divesting ourselves from the one thing that sets us apart and makes us unique in the health care system; the ability to interact with patients in a comprehensive way. We seem to be on the slippery slope to medical obsolescence, soon to be replaced by staff who can triage our patients to the next appropriate test. Both the patient and doctor seem to have slipped into a Walmart-like world where expedience dominates over skill and shortcuts are the alternative to thoughtful personal physician-patient interaction.
Dr. Goldstein, medical editor of Cardiology News, is professor of medicine at Wayne State University and division head emeritus of cardiovascular medicine at Henry Ford Hospital, both in Detroit. He is on data safety monitoring committees for the National Institutes of Health and several pharmaceutical companies.
In case you didn’t notice, our clinical practice has been reinforced by a entirely new class of performers who have become essential to our daily activities.
They are Advanced Practice Registered Nurses, whose role has evolved over the last 50 years from the Coronary Care Unit nurse with special training in coronary care to an array of well-trained women and men who have received both Bachelor’s and Master’s degrees in Nursing.
As a further extension of their training, many are now going on to achieve a further doctorate degree in nursing after 90 hours of postgraduate classes at certified academic centers and additional clinical experience in a variety of fields, including cardiology. The nurses completing those programs will be certified and licensed as APRNs. They come to our practice with remarkable experience and expertise in arrhythmia and heart failure management, as well as interventional skills, on top of wide experience in the management of patients in critical care units. Their integration into comprehensive and collaborative cardiac care raises challenges to and opportunities for the cardiologist.
A recent survey of large cardiology clinics initiated by the Summit Medical Group assessed the role of the APRN in the care of patients both in hospitals and in clinics. It reported that in many of cardiology clinics surveyed, APRNs provide an expanding role in patient care leading to variable relationships between the patient and the cardiologist. In some settings, the APRNs often function independent of physician interaction, initiating the patients’ entrance into the clinic and managing their follow-up. In other situations, they may be supervised by a cardiologist and their future laboratory studies and therapy are completely managed by the APRN, who functions as a professional associate of a physician. However, in many situations the cardiologist may have little or no contact with the patient.
While the APRN is seeing the patient, the cardiologists often are seeing their own patients or, more likely, are involved with maintaining the electronic medical record or performing or interpreting tests that are usually reimbursed at a fee that is a multiple of that received for a patient visit alone. Much of this is carried out under the heading of “coordinated care” and is managed in a multidisciplinary matrix in which many specialists and APRNs play a role in the care of the patient. In this setting, the doctor has become manager of a diverse group of support staff, including APRNs, and may be increasingly remote from direct patient care. My medical colleagues find the process as a way to increase the patient “pass through.” Many patients presume that the APRN is a reasonable alternative to a busy cardiologist or are interacting with their cardiologist.
As doctors, we are divesting ourselves from the one thing that sets us apart and makes us unique in the health care system; the ability to interact with patients in a comprehensive way. We seem to be on the slippery slope to medical obsolescence, soon to be replaced by staff who can triage our patients to the next appropriate test. Both the patient and doctor seem to have slipped into a Walmart-like world where expedience dominates over skill and shortcuts are the alternative to thoughtful personal physician-patient interaction.
Dr. Goldstein, medical editor of Cardiology News, is professor of medicine at Wayne State University and division head emeritus of cardiovascular medicine at Henry Ford Hospital, both in Detroit. He is on data safety monitoring committees for the National Institutes of Health and several pharmaceutical companies.
VIDEO: Winning health apps link patients, researchers
SANTA CLARA, CALIF. – The federal Patient-Centered Outcomes Research Institute picked three apps for $150,000 in award funding to help patients and researchers connect and collaborate.
The Institute’s Dr. Karen Odom Walker moderated a Hospital Innovation Roundtable session at the Health 2.0 fall conference. In a video interview at the meeting, she described the work of the Patient-Centered Outcomes Research Institute (PCORI), which was part of the Affordable Care Act and is based in Washington, D.C.
So far, PCORI has awarded more than $500 million to 300 projects for patient-centered research, and it plans to distribute another $3.5 billion by 2019, she said.
The winners of PCORI’s 2014 Matchmaking App Challenge, announced at the conference, developed ready-to-use Web-based or smartphone apps to link patients, caregivers, clinicians, and researchers in various ways.
First-place winner PatientPowered.us of San Francisco received $100,000 for its mobile network connecting patients with researchers and healthcare professionals to share ideas for solving their medical conditions, such as Crohn’s disease, sleep apnea, migraines, or others, and to connect patients with clinical trials.
Second-place winner WellSpringboard, from the University of Michigan, Ann Arbor, received $35,000 for its software platform to enable crowdfunding of patient-focused research. CareHubs of Beaverton, Ore. received $15,000 in third-place prize money for a platform for patient engagement in health systems.
Dr. Walker’s spouse works for MedImmune. She reported having no other financial disclosures.
On Twitter @sherryboschert
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
SANTA CLARA, CALIF. – The federal Patient-Centered Outcomes Research Institute picked three apps for $150,000 in award funding to help patients and researchers connect and collaborate.
The Institute’s Dr. Karen Odom Walker moderated a Hospital Innovation Roundtable session at the Health 2.0 fall conference. In a video interview at the meeting, she described the work of the Patient-Centered Outcomes Research Institute (PCORI), which was part of the Affordable Care Act and is based in Washington, D.C.
So far, PCORI has awarded more than $500 million to 300 projects for patient-centered research, and it plans to distribute another $3.5 billion by 2019, she said.
The winners of PCORI’s 2014 Matchmaking App Challenge, announced at the conference, developed ready-to-use Web-based or smartphone apps to link patients, caregivers, clinicians, and researchers in various ways.
First-place winner PatientPowered.us of San Francisco received $100,000 for its mobile network connecting patients with researchers and healthcare professionals to share ideas for solving their medical conditions, such as Crohn’s disease, sleep apnea, migraines, or others, and to connect patients with clinical trials.
Second-place winner WellSpringboard, from the University of Michigan, Ann Arbor, received $35,000 for its software platform to enable crowdfunding of patient-focused research. CareHubs of Beaverton, Ore. received $15,000 in third-place prize money for a platform for patient engagement in health systems.
Dr. Walker’s spouse works for MedImmune. She reported having no other financial disclosures.
On Twitter @sherryboschert
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
SANTA CLARA, CALIF. – The federal Patient-Centered Outcomes Research Institute picked three apps for $150,000 in award funding to help patients and researchers connect and collaborate.
The Institute’s Dr. Karen Odom Walker moderated a Hospital Innovation Roundtable session at the Health 2.0 fall conference. In a video interview at the meeting, she described the work of the Patient-Centered Outcomes Research Institute (PCORI), which was part of the Affordable Care Act and is based in Washington, D.C.
So far, PCORI has awarded more than $500 million to 300 projects for patient-centered research, and it plans to distribute another $3.5 billion by 2019, she said.
The winners of PCORI’s 2014 Matchmaking App Challenge, announced at the conference, developed ready-to-use Web-based or smartphone apps to link patients, caregivers, clinicians, and researchers in various ways.
First-place winner PatientPowered.us of San Francisco received $100,000 for its mobile network connecting patients with researchers and healthcare professionals to share ideas for solving their medical conditions, such as Crohn’s disease, sleep apnea, migraines, or others, and to connect patients with clinical trials.
Second-place winner WellSpringboard, from the University of Michigan, Ann Arbor, received $35,000 for its software platform to enable crowdfunding of patient-focused research. CareHubs of Beaverton, Ore. received $15,000 in third-place prize money for a platform for patient engagement in health systems.
Dr. Walker’s spouse works for MedImmune. She reported having no other financial disclosures.
On Twitter @sherryboschert
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT THE HEALTH 2.0 FALL CONFERENCE 2014
VIDEO: Software platform may improve care efficiency
SANTA CLARA, CALIF. – Electronic health records are everywhere, but how can a health system best use all the data that it collects?
Software platforms are emerging to organize and analyze the data for population health management. One new system from the company Acupera has been implemented in St. Vincent Health, an 18-hospital system in Indiana that’s part of Ascension Health, based in St. Louis.
The computerized platform led to a sixfold improvement in the efficiency of care managers, increasing their case loads from 14 patients to more than 85 patients per week, says Dr. Ronald Razmi, a former cardiologist who founded and serves as chief executive officer of San Francisco-based Acupera.
In a video interview at the Health 2.0 fall conference 2014, he described the platform, how it works, and how it could improve health outcomes.
On Twitter @sherryboschert
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
SANTA CLARA, CALIF. – Electronic health records are everywhere, but how can a health system best use all the data that it collects?
Software platforms are emerging to organize and analyze the data for population health management. One new system from the company Acupera has been implemented in St. Vincent Health, an 18-hospital system in Indiana that’s part of Ascension Health, based in St. Louis.
The computerized platform led to a sixfold improvement in the efficiency of care managers, increasing their case loads from 14 patients to more than 85 patients per week, says Dr. Ronald Razmi, a former cardiologist who founded and serves as chief executive officer of San Francisco-based Acupera.
In a video interview at the Health 2.0 fall conference 2014, he described the platform, how it works, and how it could improve health outcomes.
On Twitter @sherryboschert
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
SANTA CLARA, CALIF. – Electronic health records are everywhere, but how can a health system best use all the data that it collects?
Software platforms are emerging to organize and analyze the data for population health management. One new system from the company Acupera has been implemented in St. Vincent Health, an 18-hospital system in Indiana that’s part of Ascension Health, based in St. Louis.
The computerized platform led to a sixfold improvement in the efficiency of care managers, increasing their case loads from 14 patients to more than 85 patients per week, says Dr. Ronald Razmi, a former cardiologist who founded and serves as chief executive officer of San Francisco-based Acupera.
In a video interview at the Health 2.0 fall conference 2014, he described the platform, how it works, and how it could improve health outcomes.
On Twitter @sherryboschert
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT THE HEALTH 2.0 FALL CONFERENCE 2014
Should ductal carcinoma in situ be treated?
Remarks given during a session of the ASCO Breast Cancer Symposium titled Ductal Carcinoma in Situ Debate: Treatment vs. Observation
Dr. Kuerer comments: There has been a marked increase ductal carcinoma in situ (DCIS) in what is being called overdiagnosis, and this is leading to concerns of overtreatment, which has been in the news now for several years. We have more than 60,000 cases of DCIS diagnosed per year in the United States. We’re trying to prevent invasive breast cancer and distant metastases. The problem is identifying which patients will go on to develop invasive disease. That’s really unknown.
At M.D. Anderson, looking at 10-year follow-up of 2,449 patients, the rate of developing distant metastases was 0.1%. The problem with this is that no prominent variables were associated with the development of invasive metastatic disease. Overall, we are doing a good job at preventing death from breast cancer when we treat DCIS, with less than 1% of patients dying of breast cancer (Ann. Surg. Onc. 2011;18:2873-8).
Dr. Shelley E. Hwang and her group very elegantly started exploring preoperative systemic therapy as a way to get a clue about which patients might be safely observed alone (that is, a core biopsy diagnosis of DCIS and then just follow-up without surgery or other treatments). At M.D. Anderson, we studied whether or not we could eradicate DCIS in patients with human epidermal growth factor receptor 2 (HER2) overexpression by treatment with trastuzumab prior to surgery, under the hypothesis that if we could eradicate the DCIS, we might eventually use this drug potentially to prevent HER2-positive invasive breast cancers. We saw very dramatic responses in their immune response with antibody-dependent cellular cytotoxicity mediated by natural killer cells, which is exciting, but there were no histopathologic changes. The most important finding was that 42% of our patients who we thought only had DCIS actually had occult invasive breast cancer (Cancer 2011;117:39-47). This is concerning because without surgery, we may be missing or leaving untreated invasive breast cancers in some patients.
So, we have an underestimation of invasive breast cancer at DCIS diagnosis. A very elegant meta-analysis of 7,350 patients reported that even if we take patients with non–high-grade, very-small DCIS, we’re still looking at an upgrade to invasive cancer of about 20% (Radiology 2011;260:119-28). The best and most recent studies of MRI and DCIS again found a diagnostic upgrade of about 27%. There were no MRI features correlating with invasive breast cancer, and this resulted in a 31% increase in procedures and more biopsies with the use of MRI.
So where are we? In active surveillance of 14 patients with DCIS at the University of California, San Francisco, 8 went on to surgery at a median follow-up of 28 months, and 5 of the 8 (62%) had invasive breast cancer (The Breast 2011;20:529-33).
What’s the cost to the health care system of surveillance if we biopsy only the DCIS and follow it without surgery or other adjuvant therapies? The psychological cost to our patients? What is the natural history of DCIS if left in place? What will be the result of microcalcifications? How are we going to follow this? What are the criteria that we will use for repeat biopsy? This really is not known.
Which are the patients that we’re going to select for observation alone? There are trials in Europe that have begun or will begin to address the safety of just observing DCIS without surgery and other therapies.
The United Kingdom Low-Risk DCIS Trial is randomizing patients with low and intermediate grade DCIS of any size to biopsy alone without surgical intervention (active monitoring) or standard therapy. Another trial, a joint Dutch Breast Cancer Research Group and European Organization for the Research and Treatment of Cancer trial is randomizing women with low-risk, low-grade DCIS to active surveillance or standard treatment. If we look at M.D. Anderson’s data and our National Cancer Database, only about 10%-15% of patients would be eligible for the latter study. I don’t think with these numbers we’d have a great impact, but it is a start.
I submit that the best U.S. patients to study will be patients with a diagnosis of atypical ductal hyperplasia (generally the smallest lesions and perhaps the earliest form of DCIS) because we have about 100,000 cases each year.
What’s the patient’s perspective? What about the need for continued repeat biopsies, and how this will affect their overall quality of life? Do patients in the United States really want to observe the DCIS in an era when our patients are requesting more and more mastectomy with reconstruction and contralateral mastectomy at diagnosis of DCIS? I seriously doubt that our patients in the United States would agree to be randomized in DCIS trials to no treatment at all. I really don’t know.
Dr. Kuerer is a professor of surgery at the University of Texas M.D. Anderson Cancer Center, Houston. He reported financial associations with Gerson Lehrman Group and McGraw-Hill Publishing.
Dr. Hwang comments: Today, about 1/1,300 screening mammograms result in a diagnosis of DCIS. There are two important considerations when we talk about active surveillance or doing less aggressive treatment. First, what is the rate at which progression to invasive cancer can occur, either with or without treatment? Second, what is the fate of these DCIS lesions? These are issues for which we currently don’t have good answers.
We’re treating all disease detected at an early stage, and for the sake of argument, I’ll include DCIS, as if it likely will cause harm if we did absolutely nothing when, in fact, there could be many cancers that progress so slowly and have such a low propensity for developing metastatic disease that they would not likely cause any symptoms or harm during a patient’s lifetime.
In autopsy series, the disease reservoir of unrecognized DCIS is about 9% and the disease reservoir of invasive cancer is about 1%. It’s not that different from prostate cancer, although at a much lower rate. These data show that there certainly are women who die with DCIS rather than of it.
We really don’t have a very solid understanding of the natural history of DCIS. If we do nothing, but maybe surgically biopsy it, what happens to these patients in the long term? In a meta-analysis, the world’s literature included only 151 cases of women who had surgical biopsy of DCIS that initially was misdiagnosed as a benign lesion and therefore didn’t undergo any further therapy, some with up to 31 years of follow-up. The long-term risk of invasive cancer in this cohort is only 22% (Breast Cancer Res. Treat. 2006;97:135-44). The annual risk of breast cancer in women with atypia is 1% per year, so this ends up looking very similar to the risk of progression that you see for atypical ductal hyperplasia or lobular carcinoma in situ.
The most common treatment for DCIS in the United States is lumpectomy with radiation. A meta-analysis by the European Breast Cancer Trialists’ Group found a 50% proportional reduction in local recurrence risk in women treated with lumpectomy and radiation vs. lumpectomy alone. The absolute magnitude of reduction was dependent on baseline recurrence risk. That’s a really important concept, because if your baseline risk is only 5%, then the 50% proportional reduction only translates into a 2.5% reduction in risk in 10 years.
The prospective, randomized Radiation Therapy Oncologists Group 9804 study randomized low-risk women with DCIS, unlike prior randomized trials that included broad eligibility criteria for DCIS. In 5 years of follow-up, the ipsilateral recurrence risk (which includes both invasive cancer and DCIS) was 3.2% in the lumpectomy-only group vs. 0.4% in the lumpectomy and radiation therapy group. The difference is highly statistically significant, however, given the small absolute difference between groups, the clinical significance certainly can be argued. There was no significant difference between groups in contralateral new primary lesions (Radiat. Oncol. 2012;84:S5).
We just presented a study this year looking at DCIS and competing causes of mortality in different age groups with different types of treatment. Among women with DCIS over 70 years of age, there was a significant difference in overall survival but none of the treatments conferred any benefit in disease-specific survival.
Active surveillance alone may be reasonable to consider in some patients. We can learn a lot from our colleagues who treat prostate cancer. They’re at least 10 years ahead of us in thinking about reducing the harms that have been introduced by screening for prostate cancer. When you look at breast cancer–specific and other-cause mortality in the setting of DCIS, the mortality curves look very similar to those with early-stage prostate cancer. Women with DCIS, regardless of what they are treated with, die of other causes and very rarely die of breast cancer.
When we compare such different options as mastectomy to active surveillance only, it’s really hard for a patient to feel that both of those approaches can offer them the same outcomes. But when you look at the actual data and evidence, the differences in recurrence or progression to invasive cancer don’t translate easily into a large difference in breast cancer mortality provided that patients are diagnosed at stage I or II, with more than a 90% survival from breast cancer.
We have an opportunity to take a big step back and redefine our goals of DCIS “treatment” from “curing” DCIS to trying to reduce breast cancer-specific mortality. This will help us reduce the harms that can result from screening and will reserve our aggressive treatments for those most likely to benefit from them.
Dr. Hwang is a professor of surgery at Duke University, Durham, N.C. She serves as a consultant for Genomic Health.
Remarks given during a session of the ASCO Breast Cancer Symposium titled Ductal Carcinoma in Situ Debate: Treatment vs. Observation
Dr. Kuerer comments: There has been a marked increase ductal carcinoma in situ (DCIS) in what is being called overdiagnosis, and this is leading to concerns of overtreatment, which has been in the news now for several years. We have more than 60,000 cases of DCIS diagnosed per year in the United States. We’re trying to prevent invasive breast cancer and distant metastases. The problem is identifying which patients will go on to develop invasive disease. That’s really unknown.
At M.D. Anderson, looking at 10-year follow-up of 2,449 patients, the rate of developing distant metastases was 0.1%. The problem with this is that no prominent variables were associated with the development of invasive metastatic disease. Overall, we are doing a good job at preventing death from breast cancer when we treat DCIS, with less than 1% of patients dying of breast cancer (Ann. Surg. Onc. 2011;18:2873-8).
Dr. Shelley E. Hwang and her group very elegantly started exploring preoperative systemic therapy as a way to get a clue about which patients might be safely observed alone (that is, a core biopsy diagnosis of DCIS and then just follow-up without surgery or other treatments). At M.D. Anderson, we studied whether or not we could eradicate DCIS in patients with human epidermal growth factor receptor 2 (HER2) overexpression by treatment with trastuzumab prior to surgery, under the hypothesis that if we could eradicate the DCIS, we might eventually use this drug potentially to prevent HER2-positive invasive breast cancers. We saw very dramatic responses in their immune response with antibody-dependent cellular cytotoxicity mediated by natural killer cells, which is exciting, but there were no histopathologic changes. The most important finding was that 42% of our patients who we thought only had DCIS actually had occult invasive breast cancer (Cancer 2011;117:39-47). This is concerning because without surgery, we may be missing or leaving untreated invasive breast cancers in some patients.
So, we have an underestimation of invasive breast cancer at DCIS diagnosis. A very elegant meta-analysis of 7,350 patients reported that even if we take patients with non–high-grade, very-small DCIS, we’re still looking at an upgrade to invasive cancer of about 20% (Radiology 2011;260:119-28). The best and most recent studies of MRI and DCIS again found a diagnostic upgrade of about 27%. There were no MRI features correlating with invasive breast cancer, and this resulted in a 31% increase in procedures and more biopsies with the use of MRI.
So where are we? In active surveillance of 14 patients with DCIS at the University of California, San Francisco, 8 went on to surgery at a median follow-up of 28 months, and 5 of the 8 (62%) had invasive breast cancer (The Breast 2011;20:529-33).
What’s the cost to the health care system of surveillance if we biopsy only the DCIS and follow it without surgery or other adjuvant therapies? The psychological cost to our patients? What is the natural history of DCIS if left in place? What will be the result of microcalcifications? How are we going to follow this? What are the criteria that we will use for repeat biopsy? This really is not known.
Which are the patients that we’re going to select for observation alone? There are trials in Europe that have begun or will begin to address the safety of just observing DCIS without surgery and other therapies.
The United Kingdom Low-Risk DCIS Trial is randomizing patients with low and intermediate grade DCIS of any size to biopsy alone without surgical intervention (active monitoring) or standard therapy. Another trial, a joint Dutch Breast Cancer Research Group and European Organization for the Research and Treatment of Cancer trial is randomizing women with low-risk, low-grade DCIS to active surveillance or standard treatment. If we look at M.D. Anderson’s data and our National Cancer Database, only about 10%-15% of patients would be eligible for the latter study. I don’t think with these numbers we’d have a great impact, but it is a start.
I submit that the best U.S. patients to study will be patients with a diagnosis of atypical ductal hyperplasia (generally the smallest lesions and perhaps the earliest form of DCIS) because we have about 100,000 cases each year.
What’s the patient’s perspective? What about the need for continued repeat biopsies, and how this will affect their overall quality of life? Do patients in the United States really want to observe the DCIS in an era when our patients are requesting more and more mastectomy with reconstruction and contralateral mastectomy at diagnosis of DCIS? I seriously doubt that our patients in the United States would agree to be randomized in DCIS trials to no treatment at all. I really don’t know.
Dr. Kuerer is a professor of surgery at the University of Texas M.D. Anderson Cancer Center, Houston. He reported financial associations with Gerson Lehrman Group and McGraw-Hill Publishing.
Dr. Hwang comments: Today, about 1/1,300 screening mammograms result in a diagnosis of DCIS. There are two important considerations when we talk about active surveillance or doing less aggressive treatment. First, what is the rate at which progression to invasive cancer can occur, either with or without treatment? Second, what is the fate of these DCIS lesions? These are issues for which we currently don’t have good answers.
We’re treating all disease detected at an early stage, and for the sake of argument, I’ll include DCIS, as if it likely will cause harm if we did absolutely nothing when, in fact, there could be many cancers that progress so slowly and have such a low propensity for developing metastatic disease that they would not likely cause any symptoms or harm during a patient’s lifetime.
In autopsy series, the disease reservoir of unrecognized DCIS is about 9% and the disease reservoir of invasive cancer is about 1%. It’s not that different from prostate cancer, although at a much lower rate. These data show that there certainly are women who die with DCIS rather than of it.
We really don’t have a very solid understanding of the natural history of DCIS. If we do nothing, but maybe surgically biopsy it, what happens to these patients in the long term? In a meta-analysis, the world’s literature included only 151 cases of women who had surgical biopsy of DCIS that initially was misdiagnosed as a benign lesion and therefore didn’t undergo any further therapy, some with up to 31 years of follow-up. The long-term risk of invasive cancer in this cohort is only 22% (Breast Cancer Res. Treat. 2006;97:135-44). The annual risk of breast cancer in women with atypia is 1% per year, so this ends up looking very similar to the risk of progression that you see for atypical ductal hyperplasia or lobular carcinoma in situ.
The most common treatment for DCIS in the United States is lumpectomy with radiation. A meta-analysis by the European Breast Cancer Trialists’ Group found a 50% proportional reduction in local recurrence risk in women treated with lumpectomy and radiation vs. lumpectomy alone. The absolute magnitude of reduction was dependent on baseline recurrence risk. That’s a really important concept, because if your baseline risk is only 5%, then the 50% proportional reduction only translates into a 2.5% reduction in risk in 10 years.
The prospective, randomized Radiation Therapy Oncologists Group 9804 study randomized low-risk women with DCIS, unlike prior randomized trials that included broad eligibility criteria for DCIS. In 5 years of follow-up, the ipsilateral recurrence risk (which includes both invasive cancer and DCIS) was 3.2% in the lumpectomy-only group vs. 0.4% in the lumpectomy and radiation therapy group. The difference is highly statistically significant, however, given the small absolute difference between groups, the clinical significance certainly can be argued. There was no significant difference between groups in contralateral new primary lesions (Radiat. Oncol. 2012;84:S5).
We just presented a study this year looking at DCIS and competing causes of mortality in different age groups with different types of treatment. Among women with DCIS over 70 years of age, there was a significant difference in overall survival but none of the treatments conferred any benefit in disease-specific survival.
Active surveillance alone may be reasonable to consider in some patients. We can learn a lot from our colleagues who treat prostate cancer. They’re at least 10 years ahead of us in thinking about reducing the harms that have been introduced by screening for prostate cancer. When you look at breast cancer–specific and other-cause mortality in the setting of DCIS, the mortality curves look very similar to those with early-stage prostate cancer. Women with DCIS, regardless of what they are treated with, die of other causes and very rarely die of breast cancer.
When we compare such different options as mastectomy to active surveillance only, it’s really hard for a patient to feel that both of those approaches can offer them the same outcomes. But when you look at the actual data and evidence, the differences in recurrence or progression to invasive cancer don’t translate easily into a large difference in breast cancer mortality provided that patients are diagnosed at stage I or II, with more than a 90% survival from breast cancer.
We have an opportunity to take a big step back and redefine our goals of DCIS “treatment” from “curing” DCIS to trying to reduce breast cancer-specific mortality. This will help us reduce the harms that can result from screening and will reserve our aggressive treatments for those most likely to benefit from them.
Dr. Hwang is a professor of surgery at Duke University, Durham, N.C. She serves as a consultant for Genomic Health.
Remarks given during a session of the ASCO Breast Cancer Symposium titled Ductal Carcinoma in Situ Debate: Treatment vs. Observation
Dr. Kuerer comments: There has been a marked increase ductal carcinoma in situ (DCIS) in what is being called overdiagnosis, and this is leading to concerns of overtreatment, which has been in the news now for several years. We have more than 60,000 cases of DCIS diagnosed per year in the United States. We’re trying to prevent invasive breast cancer and distant metastases. The problem is identifying which patients will go on to develop invasive disease. That’s really unknown.
At M.D. Anderson, looking at 10-year follow-up of 2,449 patients, the rate of developing distant metastases was 0.1%. The problem with this is that no prominent variables were associated with the development of invasive metastatic disease. Overall, we are doing a good job at preventing death from breast cancer when we treat DCIS, with less than 1% of patients dying of breast cancer (Ann. Surg. Onc. 2011;18:2873-8).
Dr. Shelley E. Hwang and her group very elegantly started exploring preoperative systemic therapy as a way to get a clue about which patients might be safely observed alone (that is, a core biopsy diagnosis of DCIS and then just follow-up without surgery or other treatments). At M.D. Anderson, we studied whether or not we could eradicate DCIS in patients with human epidermal growth factor receptor 2 (HER2) overexpression by treatment with trastuzumab prior to surgery, under the hypothesis that if we could eradicate the DCIS, we might eventually use this drug potentially to prevent HER2-positive invasive breast cancers. We saw very dramatic responses in their immune response with antibody-dependent cellular cytotoxicity mediated by natural killer cells, which is exciting, but there were no histopathologic changes. The most important finding was that 42% of our patients who we thought only had DCIS actually had occult invasive breast cancer (Cancer 2011;117:39-47). This is concerning because without surgery, we may be missing or leaving untreated invasive breast cancers in some patients.
So, we have an underestimation of invasive breast cancer at DCIS diagnosis. A very elegant meta-analysis of 7,350 patients reported that even if we take patients with non–high-grade, very-small DCIS, we’re still looking at an upgrade to invasive cancer of about 20% (Radiology 2011;260:119-28). The best and most recent studies of MRI and DCIS again found a diagnostic upgrade of about 27%. There were no MRI features correlating with invasive breast cancer, and this resulted in a 31% increase in procedures and more biopsies with the use of MRI.
So where are we? In active surveillance of 14 patients with DCIS at the University of California, San Francisco, 8 went on to surgery at a median follow-up of 28 months, and 5 of the 8 (62%) had invasive breast cancer (The Breast 2011;20:529-33).
What’s the cost to the health care system of surveillance if we biopsy only the DCIS and follow it without surgery or other adjuvant therapies? The psychological cost to our patients? What is the natural history of DCIS if left in place? What will be the result of microcalcifications? How are we going to follow this? What are the criteria that we will use for repeat biopsy? This really is not known.
Which are the patients that we’re going to select for observation alone? There are trials in Europe that have begun or will begin to address the safety of just observing DCIS without surgery and other therapies.
The United Kingdom Low-Risk DCIS Trial is randomizing patients with low and intermediate grade DCIS of any size to biopsy alone without surgical intervention (active monitoring) or standard therapy. Another trial, a joint Dutch Breast Cancer Research Group and European Organization for the Research and Treatment of Cancer trial is randomizing women with low-risk, low-grade DCIS to active surveillance or standard treatment. If we look at M.D. Anderson’s data and our National Cancer Database, only about 10%-15% of patients would be eligible for the latter study. I don’t think with these numbers we’d have a great impact, but it is a start.
I submit that the best U.S. patients to study will be patients with a diagnosis of atypical ductal hyperplasia (generally the smallest lesions and perhaps the earliest form of DCIS) because we have about 100,000 cases each year.
What’s the patient’s perspective? What about the need for continued repeat biopsies, and how this will affect their overall quality of life? Do patients in the United States really want to observe the DCIS in an era when our patients are requesting more and more mastectomy with reconstruction and contralateral mastectomy at diagnosis of DCIS? I seriously doubt that our patients in the United States would agree to be randomized in DCIS trials to no treatment at all. I really don’t know.
Dr. Kuerer is a professor of surgery at the University of Texas M.D. Anderson Cancer Center, Houston. He reported financial associations with Gerson Lehrman Group and McGraw-Hill Publishing.
Dr. Hwang comments: Today, about 1/1,300 screening mammograms result in a diagnosis of DCIS. There are two important considerations when we talk about active surveillance or doing less aggressive treatment. First, what is the rate at which progression to invasive cancer can occur, either with or without treatment? Second, what is the fate of these DCIS lesions? These are issues for which we currently don’t have good answers.
We’re treating all disease detected at an early stage, and for the sake of argument, I’ll include DCIS, as if it likely will cause harm if we did absolutely nothing when, in fact, there could be many cancers that progress so slowly and have such a low propensity for developing metastatic disease that they would not likely cause any symptoms or harm during a patient’s lifetime.
In autopsy series, the disease reservoir of unrecognized DCIS is about 9% and the disease reservoir of invasive cancer is about 1%. It’s not that different from prostate cancer, although at a much lower rate. These data show that there certainly are women who die with DCIS rather than of it.
We really don’t have a very solid understanding of the natural history of DCIS. If we do nothing, but maybe surgically biopsy it, what happens to these patients in the long term? In a meta-analysis, the world’s literature included only 151 cases of women who had surgical biopsy of DCIS that initially was misdiagnosed as a benign lesion and therefore didn’t undergo any further therapy, some with up to 31 years of follow-up. The long-term risk of invasive cancer in this cohort is only 22% (Breast Cancer Res. Treat. 2006;97:135-44). The annual risk of breast cancer in women with atypia is 1% per year, so this ends up looking very similar to the risk of progression that you see for atypical ductal hyperplasia or lobular carcinoma in situ.
The most common treatment for DCIS in the United States is lumpectomy with radiation. A meta-analysis by the European Breast Cancer Trialists’ Group found a 50% proportional reduction in local recurrence risk in women treated with lumpectomy and radiation vs. lumpectomy alone. The absolute magnitude of reduction was dependent on baseline recurrence risk. That’s a really important concept, because if your baseline risk is only 5%, then the 50% proportional reduction only translates into a 2.5% reduction in risk in 10 years.
The prospective, randomized Radiation Therapy Oncologists Group 9804 study randomized low-risk women with DCIS, unlike prior randomized trials that included broad eligibility criteria for DCIS. In 5 years of follow-up, the ipsilateral recurrence risk (which includes both invasive cancer and DCIS) was 3.2% in the lumpectomy-only group vs. 0.4% in the lumpectomy and radiation therapy group. The difference is highly statistically significant, however, given the small absolute difference between groups, the clinical significance certainly can be argued. There was no significant difference between groups in contralateral new primary lesions (Radiat. Oncol. 2012;84:S5).
We just presented a study this year looking at DCIS and competing causes of mortality in different age groups with different types of treatment. Among women with DCIS over 70 years of age, there was a significant difference in overall survival but none of the treatments conferred any benefit in disease-specific survival.
Active surveillance alone may be reasonable to consider in some patients. We can learn a lot from our colleagues who treat prostate cancer. They’re at least 10 years ahead of us in thinking about reducing the harms that have been introduced by screening for prostate cancer. When you look at breast cancer–specific and other-cause mortality in the setting of DCIS, the mortality curves look very similar to those with early-stage prostate cancer. Women with DCIS, regardless of what they are treated with, die of other causes and very rarely die of breast cancer.
When we compare such different options as mastectomy to active surveillance only, it’s really hard for a patient to feel that both of those approaches can offer them the same outcomes. But when you look at the actual data and evidence, the differences in recurrence or progression to invasive cancer don’t translate easily into a large difference in breast cancer mortality provided that patients are diagnosed at stage I or II, with more than a 90% survival from breast cancer.
We have an opportunity to take a big step back and redefine our goals of DCIS “treatment” from “curing” DCIS to trying to reduce breast cancer-specific mortality. This will help us reduce the harms that can result from screening and will reserve our aggressive treatments for those most likely to benefit from them.
Dr. Hwang is a professor of surgery at Duke University, Durham, N.C. She serves as a consultant for Genomic Health.
Promoting recovery for patients with schizophrenia
This year’s theme for World Mental Health Day, “living with schizophrenia,” is a valuable message for those of us who treat patients with the illness and for the patients themselves.
After all, about 25% of people with schizophrenia reportedly recover fully, and 25%-35% improve considerably. This means that with effective treatment and interventions, up to 50% of people with schizophrenia can live productive and satisfying lives (Schizophr. Bull 2006;32:432-42).
The medications, awareness, and research needed to make schizophrenia a manageable disease must be combined with a supportive network for the patient. In addition, compliance in terms of strict adherence to medications is needed to keep the illness at bay, as are employment, nutrition, physical well-being, and avoidance of substance abuse.
Authors of the World Federation for Mental Health’s report on World Mental Health Day 2014 cited two examples of the kinds of services that can help patients with schizophrenia lead productive lives. Fountain House, a professional self-help program based in New York, assists people living with mental illness with securing jobs, schooling, housing, and wellness. Some suggest that these kinds of recovery centers might be an “emerging best practice” (Psychiatric Serv. 2012 [doi:10.1176/appi.ps.201200p10]).
The other example of a model cited by the authors describes the chain-free initiative in Mogadishu, Somalia. This model includes three phases. In phase 1, chains are literally removed from patients; in phase 2, professionals visit patients at home and provide family psychosocial education; and in phase 3, the focus is on “removing the ‘invisible chains’ of stigma and restrictions affecting the human rights of persons with mental illness.” Thanks to this initiative, more former patients reportedly are living in the community, and the community has greater awareness about the rights of people with severe mental illness.
Reducing stigma is critical, as this factor has the capacity to determine the prognosis of schizophrenia. Let’s toss out terms describing people with schizophrenia such as “crazy,” “dangerous,” “not manageable at home,” “unemployable,” and “unable to function in society.”
In 2012, the 5th Geneva Conference on Person-Centered Medicine made several recommendations that incorporate many of the principles promoted by Fountain House and the chain-free initiative. They include integrating health promotion and illness prevention; engaging health services in prevention, diagnosis, and treatment of diseases through multidisciplinary approaches; collaborating closely on clinical care and public health; engaging civil society in such efforts.
Health care workers across the globe face big challenges when it comes to managing schizophrenia. Those of us practicing medicine in developing and developed countries must educate, raise awareness, and mobilize resources in the fight against the illness.
Schizophrenia remains a major global mental health problem, but living with the illness has become possible. Perhaps 10 to 20 years down the road, we will be closer to identifying a cause, and this discovery, in turn, might lead to new horizons for treatment.
Dr. Gadit is a professor of psychiatry at the University of Toronto.
This year’s theme for World Mental Health Day, “living with schizophrenia,” is a valuable message for those of us who treat patients with the illness and for the patients themselves.
After all, about 25% of people with schizophrenia reportedly recover fully, and 25%-35% improve considerably. This means that with effective treatment and interventions, up to 50% of people with schizophrenia can live productive and satisfying lives (Schizophr. Bull 2006;32:432-42).
The medications, awareness, and research needed to make schizophrenia a manageable disease must be combined with a supportive network for the patient. In addition, compliance in terms of strict adherence to medications is needed to keep the illness at bay, as are employment, nutrition, physical well-being, and avoidance of substance abuse.
Authors of the World Federation for Mental Health’s report on World Mental Health Day 2014 cited two examples of the kinds of services that can help patients with schizophrenia lead productive lives. Fountain House, a professional self-help program based in New York, assists people living with mental illness with securing jobs, schooling, housing, and wellness. Some suggest that these kinds of recovery centers might be an “emerging best practice” (Psychiatric Serv. 2012 [doi:10.1176/appi.ps.201200p10]).
The other example of a model cited by the authors describes the chain-free initiative in Mogadishu, Somalia. This model includes three phases. In phase 1, chains are literally removed from patients; in phase 2, professionals visit patients at home and provide family psychosocial education; and in phase 3, the focus is on “removing the ‘invisible chains’ of stigma and restrictions affecting the human rights of persons with mental illness.” Thanks to this initiative, more former patients reportedly are living in the community, and the community has greater awareness about the rights of people with severe mental illness.
Reducing stigma is critical, as this factor has the capacity to determine the prognosis of schizophrenia. Let’s toss out terms describing people with schizophrenia such as “crazy,” “dangerous,” “not manageable at home,” “unemployable,” and “unable to function in society.”
In 2012, the 5th Geneva Conference on Person-Centered Medicine made several recommendations that incorporate many of the principles promoted by Fountain House and the chain-free initiative. They include integrating health promotion and illness prevention; engaging health services in prevention, diagnosis, and treatment of diseases through multidisciplinary approaches; collaborating closely on clinical care and public health; engaging civil society in such efforts.
Health care workers across the globe face big challenges when it comes to managing schizophrenia. Those of us practicing medicine in developing and developed countries must educate, raise awareness, and mobilize resources in the fight against the illness.
Schizophrenia remains a major global mental health problem, but living with the illness has become possible. Perhaps 10 to 20 years down the road, we will be closer to identifying a cause, and this discovery, in turn, might lead to new horizons for treatment.
Dr. Gadit is a professor of psychiatry at the University of Toronto.
This year’s theme for World Mental Health Day, “living with schizophrenia,” is a valuable message for those of us who treat patients with the illness and for the patients themselves.
After all, about 25% of people with schizophrenia reportedly recover fully, and 25%-35% improve considerably. This means that with effective treatment and interventions, up to 50% of people with schizophrenia can live productive and satisfying lives (Schizophr. Bull 2006;32:432-42).
The medications, awareness, and research needed to make schizophrenia a manageable disease must be combined with a supportive network for the patient. In addition, compliance in terms of strict adherence to medications is needed to keep the illness at bay, as are employment, nutrition, physical well-being, and avoidance of substance abuse.
Authors of the World Federation for Mental Health’s report on World Mental Health Day 2014 cited two examples of the kinds of services that can help patients with schizophrenia lead productive lives. Fountain House, a professional self-help program based in New York, assists people living with mental illness with securing jobs, schooling, housing, and wellness. Some suggest that these kinds of recovery centers might be an “emerging best practice” (Psychiatric Serv. 2012 [doi:10.1176/appi.ps.201200p10]).
The other example of a model cited by the authors describes the chain-free initiative in Mogadishu, Somalia. This model includes three phases. In phase 1, chains are literally removed from patients; in phase 2, professionals visit patients at home and provide family psychosocial education; and in phase 3, the focus is on “removing the ‘invisible chains’ of stigma and restrictions affecting the human rights of persons with mental illness.” Thanks to this initiative, more former patients reportedly are living in the community, and the community has greater awareness about the rights of people with severe mental illness.
Reducing stigma is critical, as this factor has the capacity to determine the prognosis of schizophrenia. Let’s toss out terms describing people with schizophrenia such as “crazy,” “dangerous,” “not manageable at home,” “unemployable,” and “unable to function in society.”
In 2012, the 5th Geneva Conference on Person-Centered Medicine made several recommendations that incorporate many of the principles promoted by Fountain House and the chain-free initiative. They include integrating health promotion and illness prevention; engaging health services in prevention, diagnosis, and treatment of diseases through multidisciplinary approaches; collaborating closely on clinical care and public health; engaging civil society in such efforts.
Health care workers across the globe face big challenges when it comes to managing schizophrenia. Those of us practicing medicine in developing and developed countries must educate, raise awareness, and mobilize resources in the fight against the illness.
Schizophrenia remains a major global mental health problem, but living with the illness has become possible. Perhaps 10 to 20 years down the road, we will be closer to identifying a cause, and this discovery, in turn, might lead to new horizons for treatment.
Dr. Gadit is a professor of psychiatry at the University of Toronto.