User login
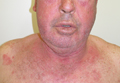
Pityriasis Rubra Pilaris Triggered by Photodynamic Therapy With Response to Tumor Necrosis Factor α–Blocking Agents and Acitretin
Comorbidities: The List Grows
There is a growing amount of literature demonstrating that psoriasis is a chronic and debilitating inflammatory disease associated with serious comorbidities. Emerging comorbidities of psoriasis include cardiovascular disease and metabolic syndrome. Psoriasis patients have an increased prevalence of the core components of metabolic syndrome, including obesity, dyslipidemia, and insulin resistance.
According to van der Voort et al (J Am Acad Dermatol. 2014;70:517-524), prior case-controlled studies observed an increased prevalence of nonalcoholic fatty liver disease (NAFLD) in patients with psoriasis, which they noted as a relevant factor in selecting optimal psoriasis treatment. Their study sought to compare the prevalence of NAFLD in participants with psoriasis and those without psoriasis. They conducted a large prospective population-based cohort study that enrolled elderly participants (>55 years). Nonalcoholic fatty liver disease was diagnosed as fatty liver on ultrasonography in the absence of other liver diseases. A multivariable logistic regression model was used to assess if psoriasis was associated with NAFLD after adjusting for demographic and lifestyle characteristics as well as laboratory findings.
In total, 2292 participants were included in the study; 118 (5.1%) participants had psoriasis. The prevalence of NAFLD was 46.2% in participants with psoriasis compared to 33.3% in those without psoriasis (P=.005); psoriasis was significantly associated with NAFLD. After the authors adjusted for alcohol consumption, pack-years and smoking status, presence of metabolic syndrome, and alanine aminotransferase levels, psoriasis remained a significant predictor of NAFLD (adjusted odds ratio, 1.7; 95% confidence interval, 1.1-2.6). The authors concluded that elderly participants with psoriasis were 70% more likely to have NAFLD than those without psoriasis independent of common NAFLD risk factors.
What’s the issue?
This study gives us a new comorbidity to be aware of and monitor. In considering therapy in this population, it also is important to consider the risk for NAFLD when selecting treatments that may have hepatic toxicity or are metabolized by the liver. How will this study change your approach to patients with psoriasis?
There is a growing amount of literature demonstrating that psoriasis is a chronic and debilitating inflammatory disease associated with serious comorbidities. Emerging comorbidities of psoriasis include cardiovascular disease and metabolic syndrome. Psoriasis patients have an increased prevalence of the core components of metabolic syndrome, including obesity, dyslipidemia, and insulin resistance.
According to van der Voort et al (J Am Acad Dermatol. 2014;70:517-524), prior case-controlled studies observed an increased prevalence of nonalcoholic fatty liver disease (NAFLD) in patients with psoriasis, which they noted as a relevant factor in selecting optimal psoriasis treatment. Their study sought to compare the prevalence of NAFLD in participants with psoriasis and those without psoriasis. They conducted a large prospective population-based cohort study that enrolled elderly participants (>55 years). Nonalcoholic fatty liver disease was diagnosed as fatty liver on ultrasonography in the absence of other liver diseases. A multivariable logistic regression model was used to assess if psoriasis was associated with NAFLD after adjusting for demographic and lifestyle characteristics as well as laboratory findings.
In total, 2292 participants were included in the study; 118 (5.1%) participants had psoriasis. The prevalence of NAFLD was 46.2% in participants with psoriasis compared to 33.3% in those without psoriasis (P=.005); psoriasis was significantly associated with NAFLD. After the authors adjusted for alcohol consumption, pack-years and smoking status, presence of metabolic syndrome, and alanine aminotransferase levels, psoriasis remained a significant predictor of NAFLD (adjusted odds ratio, 1.7; 95% confidence interval, 1.1-2.6). The authors concluded that elderly participants with psoriasis were 70% more likely to have NAFLD than those without psoriasis independent of common NAFLD risk factors.
What’s the issue?
This study gives us a new comorbidity to be aware of and monitor. In considering therapy in this population, it also is important to consider the risk for NAFLD when selecting treatments that may have hepatic toxicity or are metabolized by the liver. How will this study change your approach to patients with psoriasis?
There is a growing amount of literature demonstrating that psoriasis is a chronic and debilitating inflammatory disease associated with serious comorbidities. Emerging comorbidities of psoriasis include cardiovascular disease and metabolic syndrome. Psoriasis patients have an increased prevalence of the core components of metabolic syndrome, including obesity, dyslipidemia, and insulin resistance.
According to van der Voort et al (J Am Acad Dermatol. 2014;70:517-524), prior case-controlled studies observed an increased prevalence of nonalcoholic fatty liver disease (NAFLD) in patients with psoriasis, which they noted as a relevant factor in selecting optimal psoriasis treatment. Their study sought to compare the prevalence of NAFLD in participants with psoriasis and those without psoriasis. They conducted a large prospective population-based cohort study that enrolled elderly participants (>55 years). Nonalcoholic fatty liver disease was diagnosed as fatty liver on ultrasonography in the absence of other liver diseases. A multivariable logistic regression model was used to assess if psoriasis was associated with NAFLD after adjusting for demographic and lifestyle characteristics as well as laboratory findings.
In total, 2292 participants were included in the study; 118 (5.1%) participants had psoriasis. The prevalence of NAFLD was 46.2% in participants with psoriasis compared to 33.3% in those without psoriasis (P=.005); psoriasis was significantly associated with NAFLD. After the authors adjusted for alcohol consumption, pack-years and smoking status, presence of metabolic syndrome, and alanine aminotransferase levels, psoriasis remained a significant predictor of NAFLD (adjusted odds ratio, 1.7; 95% confidence interval, 1.1-2.6). The authors concluded that elderly participants with psoriasis were 70% more likely to have NAFLD than those without psoriasis independent of common NAFLD risk factors.
What’s the issue?
This study gives us a new comorbidity to be aware of and monitor. In considering therapy in this population, it also is important to consider the risk for NAFLD when selecting treatments that may have hepatic toxicity or are metabolized by the liver. How will this study change your approach to patients with psoriasis?
Gut-joint connection promising in psoriatic arthritis
SNOWMASS, COLO. – Mounting circumstantial evidence points to perturbation of bacterial communities in the gut and skin as important environmental triggers for psoriasis and psoriatic arthritis.
A distinctive pattern of alterations in the skin microbiota, termed bacterial "cutaneotypes," has recently been documented in lesional and uninvolved skin of psoriasis patients. Similarly, psoriatic arthritis patients show decreased diversity of their intestinal bacterial community in a pattern similar to patients with inflammatory bowel disease, Dr. Jose U. Scher said at the Winter Rheumatology Symposium sponsored by the American College of Rheumatology.
The current working hypothesis of disease pathogenesis is that, in individuals genetically predisposed to psoriasis or psoriatic arthritis, this microbial dysbiosis at the cutaneous and gut levels provides an environmental trigger for overt expression of clinical disease.
"This dysbiosis is potentially relevant as a diagnostic and/or therapeutic target in psoriasis and psoriatic arthritis. For example, it may eventually become possible to assess the gut microbiota to predict which psoriasis patients will later develop psoriatic arthritis. And reconstituting the gut flora may turn out to have therapeutic benefit. But much more work is needed," explained Dr. Scher, director of the Microbiome Center for Rheumatology and Autoimmunity at New York University.
About 25%-30% of psoriasis patients develop inflammatory psoriatic arthritis, most often roughly 7 years after onset of their skin disease. Genetics clearly plays a role, as shown in a classic Danish twin registry study with more than 21,000 subjects. Fifty-five percent of the siblings of monozygotic twins with psoriatic arthritis had skin psoriasis, but only 10% of the siblings had psoriatic arthritis, as did 3.8% of siblings of dizygotic twins with psoriatic arthritis. The lesser concordance rate seen for psoriatic arthritis hinted at the importance of environmental factors in disease genesis (Ann. Rheum. Dis. 2008;67:1417-21).
Subclinical gut inflammation is common in psoriatic arthritis. In one early study, histologic evidence of mild or moderate gut mucosal inflammation was detected in 45% of a group of psoriatic arthritis patients, compared with 15% of patients with rheumatoid arthritis and 0% of controls (Scand. J. Rheumatol. 1997;26:92-8).
Also, psoriasis patients are at a roughly 3.5-fold increased risk of developing Crohn’s disease. Among patients with established psoriatic arthritis, this risk climbs to 6.5-fold greater than in nonpsoriatic controls (Ann. Rheum. Dis. 2013;72:1200-5).
In a soon-to-be-published study, Dr. Scher and his coworkers have taken the field a step further, employing high-throughput gene sequencing to analyze the gut bacterial communities of psoriatic arthritis patients and controls. These were all new-onset psoriatic arthritis patients who had never been exposed to systemic corticosteroids, biologic agents, or conventional disease-modifying antirheumatic drugs.
Compared with the stool samples of healthy controls, several major bacterial species were underrepresented or absent in the gut microbiota of psoriatic arthritis patients. These included Akkermansia, the most common mucolytic bacterium in healthy subjects. Intriguingly, Akkermansia counts are decreased 15-fold in Crohn’s disease and 92-fold in ulcerative colitis, according to the rheumatologist.
Other bacterial species markedly less abundant in the psoriatic arthritis patients’ gut flora were Ruminoccocus, Alistipes, and Roseburia. Like Akkermansia, these are mucin-degrading bacteria that promote a healthy gut environment, and they, too, are reduced in inflammatory bowel disease, Dr. Scher said.
He theorized that these disruptions of the bacterial ecosystem might arise from a course of antibiotics, a change in diet, or other insults. The result is activation of dendritic cells to produce interleukin-23, which triggers a proinflammatory cascade including tumor necrosis factor-alpha, interleukin-22, and antimicrobial peptides.
As shown by other investigators (Mucosal Immunol. 2013;6:666-77), these proinflammatory cytokines inhibit RANK ligand, which is the critical factor for differentiation of microfold cells in the gut. These microfold cells, or M cells, are specialized epithelial cells that transport antigens across the gut epithelium and play an important role in maintenance of an efficient immune response. It’s plausible that, when these M cells are defective, the resultant loss of tolerance and chronic inflammatory state can result in psoriatic arthritis, he explained.
Dr. Scher’s colleagues at New York University have used high-throughput gene sequencing to analyze the cutaneous microbiota of lesional and nonlesional skin in psoriasis patients, as well as skin samples from the same sites in healthy controls. The impetus for this study was a hypothesis that psoriasis might represent an inappropriate cutaneous immune response directed against offending bacteria in the skin microbiota.
Sure enough, the bacterial community present in psoriatic lesions displayed a markedly decreased diversity, compared with controls. This decreased diversity also was present, albeit to a lesser extent, in the psoriasis patients’ nonlesional skin. Both the lesional and nonlesional skin of psoriasis patients contained an increased abundance of Corynebacterium, Staphylococcus, and Streptococcus, compared with controls.
In addition, the skin microbiota could be classified into one of two characteristic patterns, which the investigators termed "cutaneotypes." Cutaneotype 1, which predominated in the skin of normal controls, contained an abundance of Proteobacteria. In contrast, cutaneotype 2, which was 3.5-fold more prevalent in psoriatic lesions than in controls, was enriched in Firmicutes and Actinobacteria. The psoriatic patients’ nonlesional skin contained a balance of cutaneotypes 1 and 2 (Microbiome 2013 Dec. 23 [doi:10.1186/2049-2618-1-31]).
Dr. Scher said that the next step in his own research is to learn whether the gut microbiota of psoriasis patients differs from that of psoriatic arthritis patients.
"That’s to me the most important piece of data. I think there’s a lot of work to do, and we’re doing it now, in prospective fashion. We’re following patients with psoriasis, and for those who later convert to psoriatic arthritis we’ll want to know if there’s alteration of their bacterial immunity, both in the gut and the skin," he explained.
Dr. Scher reported having no financial conflicts.
SNOWMASS, COLO. – Mounting circumstantial evidence points to perturbation of bacterial communities in the gut and skin as important environmental triggers for psoriasis and psoriatic arthritis.
A distinctive pattern of alterations in the skin microbiota, termed bacterial "cutaneotypes," has recently been documented in lesional and uninvolved skin of psoriasis patients. Similarly, psoriatic arthritis patients show decreased diversity of their intestinal bacterial community in a pattern similar to patients with inflammatory bowel disease, Dr. Jose U. Scher said at the Winter Rheumatology Symposium sponsored by the American College of Rheumatology.
The current working hypothesis of disease pathogenesis is that, in individuals genetically predisposed to psoriasis or psoriatic arthritis, this microbial dysbiosis at the cutaneous and gut levels provides an environmental trigger for overt expression of clinical disease.
"This dysbiosis is potentially relevant as a diagnostic and/or therapeutic target in psoriasis and psoriatic arthritis. For example, it may eventually become possible to assess the gut microbiota to predict which psoriasis patients will later develop psoriatic arthritis. And reconstituting the gut flora may turn out to have therapeutic benefit. But much more work is needed," explained Dr. Scher, director of the Microbiome Center for Rheumatology and Autoimmunity at New York University.
About 25%-30% of psoriasis patients develop inflammatory psoriatic arthritis, most often roughly 7 years after onset of their skin disease. Genetics clearly plays a role, as shown in a classic Danish twin registry study with more than 21,000 subjects. Fifty-five percent of the siblings of monozygotic twins with psoriatic arthritis had skin psoriasis, but only 10% of the siblings had psoriatic arthritis, as did 3.8% of siblings of dizygotic twins with psoriatic arthritis. The lesser concordance rate seen for psoriatic arthritis hinted at the importance of environmental factors in disease genesis (Ann. Rheum. Dis. 2008;67:1417-21).
Subclinical gut inflammation is common in psoriatic arthritis. In one early study, histologic evidence of mild or moderate gut mucosal inflammation was detected in 45% of a group of psoriatic arthritis patients, compared with 15% of patients with rheumatoid arthritis and 0% of controls (Scand. J. Rheumatol. 1997;26:92-8).
Also, psoriasis patients are at a roughly 3.5-fold increased risk of developing Crohn’s disease. Among patients with established psoriatic arthritis, this risk climbs to 6.5-fold greater than in nonpsoriatic controls (Ann. Rheum. Dis. 2013;72:1200-5).
In a soon-to-be-published study, Dr. Scher and his coworkers have taken the field a step further, employing high-throughput gene sequencing to analyze the gut bacterial communities of psoriatic arthritis patients and controls. These were all new-onset psoriatic arthritis patients who had never been exposed to systemic corticosteroids, biologic agents, or conventional disease-modifying antirheumatic drugs.
Compared with the stool samples of healthy controls, several major bacterial species were underrepresented or absent in the gut microbiota of psoriatic arthritis patients. These included Akkermansia, the most common mucolytic bacterium in healthy subjects. Intriguingly, Akkermansia counts are decreased 15-fold in Crohn’s disease and 92-fold in ulcerative colitis, according to the rheumatologist.
Other bacterial species markedly less abundant in the psoriatic arthritis patients’ gut flora were Ruminoccocus, Alistipes, and Roseburia. Like Akkermansia, these are mucin-degrading bacteria that promote a healthy gut environment, and they, too, are reduced in inflammatory bowel disease, Dr. Scher said.
He theorized that these disruptions of the bacterial ecosystem might arise from a course of antibiotics, a change in diet, or other insults. The result is activation of dendritic cells to produce interleukin-23, which triggers a proinflammatory cascade including tumor necrosis factor-alpha, interleukin-22, and antimicrobial peptides.
As shown by other investigators (Mucosal Immunol. 2013;6:666-77), these proinflammatory cytokines inhibit RANK ligand, which is the critical factor for differentiation of microfold cells in the gut. These microfold cells, or M cells, are specialized epithelial cells that transport antigens across the gut epithelium and play an important role in maintenance of an efficient immune response. It’s plausible that, when these M cells are defective, the resultant loss of tolerance and chronic inflammatory state can result in psoriatic arthritis, he explained.
Dr. Scher’s colleagues at New York University have used high-throughput gene sequencing to analyze the cutaneous microbiota of lesional and nonlesional skin in psoriasis patients, as well as skin samples from the same sites in healthy controls. The impetus for this study was a hypothesis that psoriasis might represent an inappropriate cutaneous immune response directed against offending bacteria in the skin microbiota.
Sure enough, the bacterial community present in psoriatic lesions displayed a markedly decreased diversity, compared with controls. This decreased diversity also was present, albeit to a lesser extent, in the psoriasis patients’ nonlesional skin. Both the lesional and nonlesional skin of psoriasis patients contained an increased abundance of Corynebacterium, Staphylococcus, and Streptococcus, compared with controls.
In addition, the skin microbiota could be classified into one of two characteristic patterns, which the investigators termed "cutaneotypes." Cutaneotype 1, which predominated in the skin of normal controls, contained an abundance of Proteobacteria. In contrast, cutaneotype 2, which was 3.5-fold more prevalent in psoriatic lesions than in controls, was enriched in Firmicutes and Actinobacteria. The psoriatic patients’ nonlesional skin contained a balance of cutaneotypes 1 and 2 (Microbiome 2013 Dec. 23 [doi:10.1186/2049-2618-1-31]).
Dr. Scher said that the next step in his own research is to learn whether the gut microbiota of psoriasis patients differs from that of psoriatic arthritis patients.
"That’s to me the most important piece of data. I think there’s a lot of work to do, and we’re doing it now, in prospective fashion. We’re following patients with psoriasis, and for those who later convert to psoriatic arthritis we’ll want to know if there’s alteration of their bacterial immunity, both in the gut and the skin," he explained.
Dr. Scher reported having no financial conflicts.
SNOWMASS, COLO. – Mounting circumstantial evidence points to perturbation of bacterial communities in the gut and skin as important environmental triggers for psoriasis and psoriatic arthritis.
A distinctive pattern of alterations in the skin microbiota, termed bacterial "cutaneotypes," has recently been documented in lesional and uninvolved skin of psoriasis patients. Similarly, psoriatic arthritis patients show decreased diversity of their intestinal bacterial community in a pattern similar to patients with inflammatory bowel disease, Dr. Jose U. Scher said at the Winter Rheumatology Symposium sponsored by the American College of Rheumatology.
The current working hypothesis of disease pathogenesis is that, in individuals genetically predisposed to psoriasis or psoriatic arthritis, this microbial dysbiosis at the cutaneous and gut levels provides an environmental trigger for overt expression of clinical disease.
"This dysbiosis is potentially relevant as a diagnostic and/or therapeutic target in psoriasis and psoriatic arthritis. For example, it may eventually become possible to assess the gut microbiota to predict which psoriasis patients will later develop psoriatic arthritis. And reconstituting the gut flora may turn out to have therapeutic benefit. But much more work is needed," explained Dr. Scher, director of the Microbiome Center for Rheumatology and Autoimmunity at New York University.
About 25%-30% of psoriasis patients develop inflammatory psoriatic arthritis, most often roughly 7 years after onset of their skin disease. Genetics clearly plays a role, as shown in a classic Danish twin registry study with more than 21,000 subjects. Fifty-five percent of the siblings of monozygotic twins with psoriatic arthritis had skin psoriasis, but only 10% of the siblings had psoriatic arthritis, as did 3.8% of siblings of dizygotic twins with psoriatic arthritis. The lesser concordance rate seen for psoriatic arthritis hinted at the importance of environmental factors in disease genesis (Ann. Rheum. Dis. 2008;67:1417-21).
Subclinical gut inflammation is common in psoriatic arthritis. In one early study, histologic evidence of mild or moderate gut mucosal inflammation was detected in 45% of a group of psoriatic arthritis patients, compared with 15% of patients with rheumatoid arthritis and 0% of controls (Scand. J. Rheumatol. 1997;26:92-8).
Also, psoriasis patients are at a roughly 3.5-fold increased risk of developing Crohn’s disease. Among patients with established psoriatic arthritis, this risk climbs to 6.5-fold greater than in nonpsoriatic controls (Ann. Rheum. Dis. 2013;72:1200-5).
In a soon-to-be-published study, Dr. Scher and his coworkers have taken the field a step further, employing high-throughput gene sequencing to analyze the gut bacterial communities of psoriatic arthritis patients and controls. These were all new-onset psoriatic arthritis patients who had never been exposed to systemic corticosteroids, biologic agents, or conventional disease-modifying antirheumatic drugs.
Compared with the stool samples of healthy controls, several major bacterial species were underrepresented or absent in the gut microbiota of psoriatic arthritis patients. These included Akkermansia, the most common mucolytic bacterium in healthy subjects. Intriguingly, Akkermansia counts are decreased 15-fold in Crohn’s disease and 92-fold in ulcerative colitis, according to the rheumatologist.
Other bacterial species markedly less abundant in the psoriatic arthritis patients’ gut flora were Ruminoccocus, Alistipes, and Roseburia. Like Akkermansia, these are mucin-degrading bacteria that promote a healthy gut environment, and they, too, are reduced in inflammatory bowel disease, Dr. Scher said.
He theorized that these disruptions of the bacterial ecosystem might arise from a course of antibiotics, a change in diet, or other insults. The result is activation of dendritic cells to produce interleukin-23, which triggers a proinflammatory cascade including tumor necrosis factor-alpha, interleukin-22, and antimicrobial peptides.
As shown by other investigators (Mucosal Immunol. 2013;6:666-77), these proinflammatory cytokines inhibit RANK ligand, which is the critical factor for differentiation of microfold cells in the gut. These microfold cells, or M cells, are specialized epithelial cells that transport antigens across the gut epithelium and play an important role in maintenance of an efficient immune response. It’s plausible that, when these M cells are defective, the resultant loss of tolerance and chronic inflammatory state can result in psoriatic arthritis, he explained.
Dr. Scher’s colleagues at New York University have used high-throughput gene sequencing to analyze the cutaneous microbiota of lesional and nonlesional skin in psoriasis patients, as well as skin samples from the same sites in healthy controls. The impetus for this study was a hypothesis that psoriasis might represent an inappropriate cutaneous immune response directed against offending bacteria in the skin microbiota.
Sure enough, the bacterial community present in psoriatic lesions displayed a markedly decreased diversity, compared with controls. This decreased diversity also was present, albeit to a lesser extent, in the psoriasis patients’ nonlesional skin. Both the lesional and nonlesional skin of psoriasis patients contained an increased abundance of Corynebacterium, Staphylococcus, and Streptococcus, compared with controls.
In addition, the skin microbiota could be classified into one of two characteristic patterns, which the investigators termed "cutaneotypes." Cutaneotype 1, which predominated in the skin of normal controls, contained an abundance of Proteobacteria. In contrast, cutaneotype 2, which was 3.5-fold more prevalent in psoriatic lesions than in controls, was enriched in Firmicutes and Actinobacteria. The psoriatic patients’ nonlesional skin contained a balance of cutaneotypes 1 and 2 (Microbiome 2013 Dec. 23 [doi:10.1186/2049-2618-1-31]).
Dr. Scher said that the next step in his own research is to learn whether the gut microbiota of psoriasis patients differs from that of psoriatic arthritis patients.
"That’s to me the most important piece of data. I think there’s a lot of work to do, and we’re doing it now, in prospective fashion. We’re following patients with psoriasis, and for those who later convert to psoriatic arthritis we’ll want to know if there’s alteration of their bacterial immunity, both in the gut and the skin," he explained.
Dr. Scher reported having no financial conflicts.
EXPERT ANALYSIS FROM THE WINTER RHEUMATOLOGY SYMPOSIUM
VIDEO: Don’t overlook the signs of psoriatic arthritis
PALM BEACH, ARUBA – When evaluating patients for psoriasis, don’t forget to ask them about potential symptoms of psoriatic arthritis, cautions Dr. Mark Jackson of the University of Louisville. In an interview at the Caribbean Dermatology Seminar, Dr. Jackson also discusses the need to have psoriasis patients without psoriatic arthritis be alert to the development of potential symptoms of the joint disease.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
PALM BEACH, ARUBA – When evaluating patients for psoriasis, don’t forget to ask them about potential symptoms of psoriatic arthritis, cautions Dr. Mark Jackson of the University of Louisville. In an interview at the Caribbean Dermatology Seminar, Dr. Jackson also discusses the need to have psoriasis patients without psoriatic arthritis be alert to the development of potential symptoms of the joint disease.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
PALM BEACH, ARUBA – When evaluating patients for psoriasis, don’t forget to ask them about potential symptoms of psoriatic arthritis, cautions Dr. Mark Jackson of the University of Louisville. In an interview at the Caribbean Dermatology Seminar, Dr. Jackson also discusses the need to have psoriasis patients without psoriatic arthritis be alert to the development of potential symptoms of the joint disease.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
FROM THE CARIBBEAN DERMATOLOGY SEMINAR
VIDEO: How to evaluate the need for systemic psoriasis therapy
PALM BEACH, ARUBA – When is it time to transition a patient with psoriasis from topical therapy to systemic therapy? Dr. Mark Jackson of the University of Louisville (Ky.) discusses how to evaluate the need for a new treatment approach, and how to help patients make the transition to systemic therapy. We caught up with Dr. Jackson in this video interview at the Caribbean Dermatology Seminar.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
PALM BEACH, ARUBA – When is it time to transition a patient with psoriasis from topical therapy to systemic therapy? Dr. Mark Jackson of the University of Louisville (Ky.) discusses how to evaluate the need for a new treatment approach, and how to help patients make the transition to systemic therapy. We caught up with Dr. Jackson in this video interview at the Caribbean Dermatology Seminar.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
PALM BEACH, ARUBA – When is it time to transition a patient with psoriasis from topical therapy to systemic therapy? Dr. Mark Jackson of the University of Louisville (Ky.) discusses how to evaluate the need for a new treatment approach, and how to help patients make the transition to systemic therapy. We caught up with Dr. Jackson in this video interview at the Caribbean Dermatology Seminar.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
EXPERT ANALYSIS FROM THE CARIBBEAN DERMATOLOGY SEMINAR
VIDEO: Take the ‘whole’ approach to treating psoriasis patients
PALM BEACH, ARUBA – Dr. Kenneth Gordon, professor of dermatology at Northwestern University, Chicago, explains why it’s important to treat not just the physical manifestations of psoriasis, but also to consider the condition’s emotional and practical aspects for patients. He made his comments in a video interview during the Caribbean Dermatology Symposium.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
PALM BEACH, ARUBA – Dr. Kenneth Gordon, professor of dermatology at Northwestern University, Chicago, explains why it’s important to treat not just the physical manifestations of psoriasis, but also to consider the condition’s emotional and practical aspects for patients. He made his comments in a video interview during the Caribbean Dermatology Symposium.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
PALM BEACH, ARUBA – Dr. Kenneth Gordon, professor of dermatology at Northwestern University, Chicago, explains why it’s important to treat not just the physical manifestations of psoriasis, but also to consider the condition’s emotional and practical aspects for patients. He made his comments in a video interview during the Caribbean Dermatology Symposium.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ANALYSIS FROM THE CARIBBEAN DERMATOLOGY SYMPOSIUM
VIDEO: Are those musculoskeletal symptoms psoriatic arthritis?
WAIKOLOA, HAWAII – Dermatologists are in a unique position to identify psoriatic arthritis in patients with psoriasis whose musculoskeletal symptoms may be too subtle for them to mention to an internist or seek out a rheumatologist, according to Dr. Brian Mandell of the Cleveland Clinic.
Dr. Mandell spoke with us in a video interview at the Hawaii Dermatology Seminar about the key questions to ask patients.
WAIKOLOA, HAWAII – Dermatologists are in a unique position to identify psoriatic arthritis in patients with psoriasis whose musculoskeletal symptoms may be too subtle for them to mention to an internist or seek out a rheumatologist, according to Dr. Brian Mandell of the Cleveland Clinic.
Dr. Mandell spoke with us in a video interview at the Hawaii Dermatology Seminar about the key questions to ask patients.
WAIKOLOA, HAWAII – Dermatologists are in a unique position to identify psoriatic arthritis in patients with psoriasis whose musculoskeletal symptoms may be too subtle for them to mention to an internist or seek out a rheumatologist, according to Dr. Brian Mandell of the Cleveland Clinic.
Dr. Mandell spoke with us in a video interview at the Hawaii Dermatology Seminar about the key questions to ask patients.
ANALYSIS FROM SDEF HAWAII DERMATOLOGY SEMINAR
VIDEO: Coffee Break 2: What did you learn at the meeting?
WAIKOLOA, HAWAII – Our editor, Heidi Splete, catches up with attendees at the Hawaii Dermatology Seminar to find out what they learned at the meeting that they will take back to their practices.
During a coffee break video interview, doctors said they enjoyed presentations on tips to treat fine lines around the eyes and mouth, the link between psoriasis and increased cardiovascular risks, and the "two Cs" of potential leather allergies.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAIKOLOA, HAWAII – Our editor, Heidi Splete, catches up with attendees at the Hawaii Dermatology Seminar to find out what they learned at the meeting that they will take back to their practices.
During a coffee break video interview, doctors said they enjoyed presentations on tips to treat fine lines around the eyes and mouth, the link between psoriasis and increased cardiovascular risks, and the "two Cs" of potential leather allergies.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAIKOLOA, HAWAII – Our editor, Heidi Splete, catches up with attendees at the Hawaii Dermatology Seminar to find out what they learned at the meeting that they will take back to their practices.
During a coffee break video interview, doctors said they enjoyed presentations on tips to treat fine lines around the eyes and mouth, the link between psoriasis and increased cardiovascular risks, and the "two Cs" of potential leather allergies.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
FROM SDEF HAWAII DERMATOLOGY SYMPOSIUM
Psoriasis: The Story Worsens

We have already come a long way from thinking that psoriasis is merely a cutaneous disease caused by a defect in cellular replication; we now recognize that psoriasis is a systemic inflammatory process that has broad health implications. This association is manifested by comorbidities such as the occurrence of the metabolic syndrome and an increased risk for myocardial infarction. An increased incidence of chronic obstructive pulmonary disease also has been demonstrated in patients with psoriasis, especially those who smoke. Unfortunately, recent publications have highlighted investigative work that expands the scope of psoriatic comorbidity into new realms.
Li and colleagues (Ann Rheum Dis. 2013;72:1200-1205) performed a retrospective analysis of 174,476 women enrolled in several large national health studies. They found an increased risk for incident Crohn disease (relative risk [RR], 4.00; 95% confidence interval [CI], 1.72-9.27) among women with psoriasis. This increased risk rose (RR, 6.43; 95% CI, 2.04-20.32) if both psoriasis and psoriatic arthritis were present. Although the risk for those who already have Crohn disease to develop psoriasis has been previously noted, this study provides the first convincing clinical evidence that the converse association also is true, which is is not totally surprising when one considers common genetic and aberrant cytokine profiles between Crohn disease and psoriasis to suggest an overlap in pathogenic mechanisms.
Perhaps more ominous was the recently published work of Wan and associates (BMJ. 2013;347:f5961). In this massive retrospective analysis utilizing detailed British electronic medical records, 136,529 patients with mild psoriasis and 7354 patients with severe psoriasis based on treatment patterns were matched to 689,702 unaffected patients. The investigators found a clear increased risk for chronic renal disease (RR, 1.93; 95% CI, 1.79-2.08) among those with severe psoriasis. The risk was higher in younger patients; for example, among those aged 30 years, the RR rose to 3.82 (95% CI, 3.15-4.64). The risk for developing renal disease was independent of well-known predisposing factors, such as diabetes mellitus and hypertension. The association between severe psoriasis and renal disease also appeared to be independent of medications administered for psoriasis (eg, cyclosporine).
Also alarming was a recently published systematic review and meta-analysis of 1080 publications concerning the potential association between psoriasis and cancer (J Eur Acad Dermatol Venereol. 2013;27[suppl 3]:36-46). Pouplard et al found that there may be an increased risk for the following solid cancers in psoriasis patients: respiratory tract cancer (RR, 1.52; 95% CI, 1.35-1.71), upper aerodigestive tract cancer (RR, 3.05; 95% CI, 1.74-5.32), urinary tract cancer (RR, 1.31; 95% CI, 1.11-1.55), and liver cancer (RR, 1.90; 95% CI, 1.48-2.44). To the authors, the association seemed particularly strong with these neoplasms, which are associated with excessive alcohol ingestion and smoking.
What’s the issue?
Why might these comorbidities occur? Perhaps chronic inflammation due to abnormal cytokine production and/or deviant immune defenses may promote these new (or better documented) psoriatic comorbidities. Why are they of importance to dermatologists? Because we are the primary source of care for patients with psoriasis, especially those with severe disease. We cannot stop our historical reviews and physical examination with the skin and joints; rather, we must consider the whole patient. We probably should at least perform a comprehensive history at each visit, being carefully attune to any new concerns that suggest gastrointestinal, pulmonary, and renal disease or internal neoplasia, which places an extra (and perhaps unwanted) burden of care on the dermatologist. However, the way I see it is that our role in early detection of an ever-expanding list of serious psoriatic comorbidities may be crucial to the ultimate long-term health of our patients. Are you ready to accept that intensified and enhanced medical responsibility?

We have already come a long way from thinking that psoriasis is merely a cutaneous disease caused by a defect in cellular replication; we now recognize that psoriasis is a systemic inflammatory process that has broad health implications. This association is manifested by comorbidities such as the occurrence of the metabolic syndrome and an increased risk for myocardial infarction. An increased incidence of chronic obstructive pulmonary disease also has been demonstrated in patients with psoriasis, especially those who smoke. Unfortunately, recent publications have highlighted investigative work that expands the scope of psoriatic comorbidity into new realms.
Li and colleagues (Ann Rheum Dis. 2013;72:1200-1205) performed a retrospective analysis of 174,476 women enrolled in several large national health studies. They found an increased risk for incident Crohn disease (relative risk [RR], 4.00; 95% confidence interval [CI], 1.72-9.27) among women with psoriasis. This increased risk rose (RR, 6.43; 95% CI, 2.04-20.32) if both psoriasis and psoriatic arthritis were present. Although the risk for those who already have Crohn disease to develop psoriasis has been previously noted, this study provides the first convincing clinical evidence that the converse association also is true, which is is not totally surprising when one considers common genetic and aberrant cytokine profiles between Crohn disease and psoriasis to suggest an overlap in pathogenic mechanisms.
Perhaps more ominous was the recently published work of Wan and associates (BMJ. 2013;347:f5961). In this massive retrospective analysis utilizing detailed British electronic medical records, 136,529 patients with mild psoriasis and 7354 patients with severe psoriasis based on treatment patterns were matched to 689,702 unaffected patients. The investigators found a clear increased risk for chronic renal disease (RR, 1.93; 95% CI, 1.79-2.08) among those with severe psoriasis. The risk was higher in younger patients; for example, among those aged 30 years, the RR rose to 3.82 (95% CI, 3.15-4.64). The risk for developing renal disease was independent of well-known predisposing factors, such as diabetes mellitus and hypertension. The association between severe psoriasis and renal disease also appeared to be independent of medications administered for psoriasis (eg, cyclosporine).
Also alarming was a recently published systematic review and meta-analysis of 1080 publications concerning the potential association between psoriasis and cancer (J Eur Acad Dermatol Venereol. 2013;27[suppl 3]:36-46). Pouplard et al found that there may be an increased risk for the following solid cancers in psoriasis patients: respiratory tract cancer (RR, 1.52; 95% CI, 1.35-1.71), upper aerodigestive tract cancer (RR, 3.05; 95% CI, 1.74-5.32), urinary tract cancer (RR, 1.31; 95% CI, 1.11-1.55), and liver cancer (RR, 1.90; 95% CI, 1.48-2.44). To the authors, the association seemed particularly strong with these neoplasms, which are associated with excessive alcohol ingestion and smoking.
What’s the issue?
Why might these comorbidities occur? Perhaps chronic inflammation due to abnormal cytokine production and/or deviant immune defenses may promote these new (or better documented) psoriatic comorbidities. Why are they of importance to dermatologists? Because we are the primary source of care for patients with psoriasis, especially those with severe disease. We cannot stop our historical reviews and physical examination with the skin and joints; rather, we must consider the whole patient. We probably should at least perform a comprehensive history at each visit, being carefully attune to any new concerns that suggest gastrointestinal, pulmonary, and renal disease or internal neoplasia, which places an extra (and perhaps unwanted) burden of care on the dermatologist. However, the way I see it is that our role in early detection of an ever-expanding list of serious psoriatic comorbidities may be crucial to the ultimate long-term health of our patients. Are you ready to accept that intensified and enhanced medical responsibility?

We have already come a long way from thinking that psoriasis is merely a cutaneous disease caused by a defect in cellular replication; we now recognize that psoriasis is a systemic inflammatory process that has broad health implications. This association is manifested by comorbidities such as the occurrence of the metabolic syndrome and an increased risk for myocardial infarction. An increased incidence of chronic obstructive pulmonary disease also has been demonstrated in patients with psoriasis, especially those who smoke. Unfortunately, recent publications have highlighted investigative work that expands the scope of psoriatic comorbidity into new realms.
Li and colleagues (Ann Rheum Dis. 2013;72:1200-1205) performed a retrospective analysis of 174,476 women enrolled in several large national health studies. They found an increased risk for incident Crohn disease (relative risk [RR], 4.00; 95% confidence interval [CI], 1.72-9.27) among women with psoriasis. This increased risk rose (RR, 6.43; 95% CI, 2.04-20.32) if both psoriasis and psoriatic arthritis were present. Although the risk for those who already have Crohn disease to develop psoriasis has been previously noted, this study provides the first convincing clinical evidence that the converse association also is true, which is is not totally surprising when one considers common genetic and aberrant cytokine profiles between Crohn disease and psoriasis to suggest an overlap in pathogenic mechanisms.
Perhaps more ominous was the recently published work of Wan and associates (BMJ. 2013;347:f5961). In this massive retrospective analysis utilizing detailed British electronic medical records, 136,529 patients with mild psoriasis and 7354 patients with severe psoriasis based on treatment patterns were matched to 689,702 unaffected patients. The investigators found a clear increased risk for chronic renal disease (RR, 1.93; 95% CI, 1.79-2.08) among those with severe psoriasis. The risk was higher in younger patients; for example, among those aged 30 years, the RR rose to 3.82 (95% CI, 3.15-4.64). The risk for developing renal disease was independent of well-known predisposing factors, such as diabetes mellitus and hypertension. The association between severe psoriasis and renal disease also appeared to be independent of medications administered for psoriasis (eg, cyclosporine).
Also alarming was a recently published systematic review and meta-analysis of 1080 publications concerning the potential association between psoriasis and cancer (J Eur Acad Dermatol Venereol. 2013;27[suppl 3]:36-46). Pouplard et al found that there may be an increased risk for the following solid cancers in psoriasis patients: respiratory tract cancer (RR, 1.52; 95% CI, 1.35-1.71), upper aerodigestive tract cancer (RR, 3.05; 95% CI, 1.74-5.32), urinary tract cancer (RR, 1.31; 95% CI, 1.11-1.55), and liver cancer (RR, 1.90; 95% CI, 1.48-2.44). To the authors, the association seemed particularly strong with these neoplasms, which are associated with excessive alcohol ingestion and smoking.
What’s the issue?
Why might these comorbidities occur? Perhaps chronic inflammation due to abnormal cytokine production and/or deviant immune defenses may promote these new (or better documented) psoriatic comorbidities. Why are they of importance to dermatologists? Because we are the primary source of care for patients with psoriasis, especially those with severe disease. We cannot stop our historical reviews and physical examination with the skin and joints; rather, we must consider the whole patient. We probably should at least perform a comprehensive history at each visit, being carefully attune to any new concerns that suggest gastrointestinal, pulmonary, and renal disease or internal neoplasia, which places an extra (and perhaps unwanted) burden of care on the dermatologist. However, the way I see it is that our role in early detection of an ever-expanding list of serious psoriatic comorbidities may be crucial to the ultimate long-term health of our patients. Are you ready to accept that intensified and enhanced medical responsibility?
VIDEO: Coffee Break 1: What did you learn at the meeting?
WAIKOLOA, HAWAII – Our editor, Heidi Splete, catches up with attendees at the SDEF Hawaii Dermatology Seminar to find out what they learned at the meeting that they will take back to their practices.
During a coffee break video interview, doctors said they enjoyed presentations on the need to treat onychomycosis aggressively in patients with diabetes; diet and acne; and recent trends in the use of systemic biologic therapies for psoriasis.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAIKOLOA, HAWAII – Our editor, Heidi Splete, catches up with attendees at the SDEF Hawaii Dermatology Seminar to find out what they learned at the meeting that they will take back to their practices.
During a coffee break video interview, doctors said they enjoyed presentations on the need to treat onychomycosis aggressively in patients with diabetes; diet and acne; and recent trends in the use of systemic biologic therapies for psoriasis.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAIKOLOA, HAWAII – Our editor, Heidi Splete, catches up with attendees at the SDEF Hawaii Dermatology Seminar to find out what they learned at the meeting that they will take back to their practices.
During a coffee break video interview, doctors said they enjoyed presentations on the need to treat onychomycosis aggressively in patients with diabetes; diet and acne; and recent trends in the use of systemic biologic therapies for psoriasis.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
EXPERT ANALYSIS FROM SDEF HAWAII DERMATOLOGY SEMINAR