User login
What is seronegative rheumatoid arthritis, anyway?
MAUI, HAWAII – Viewing seronegative rheumatoid arthritis as something akin to RA-lite would be a big mistake, John J. Cush, MD, asserted at the 2020 Rheumatology Winter Clinical Symposium.
“It’s not a benign subtype of RA. And then again, it may not be RA,” Dr. Cush observed,
“Seronegative RA means that either you need to get serious about what is probably badass disease or you need to reevaluate whether this really is RA and your need for DMARDs [disease-modifying antirheumatic drugs] in an ongoing fashion,” the rheumatologist said. “Always reconsider whether they need less therapy or maybe no therapy at all. Maybe they had inflammation at one point and now they’re left with degenerative and mechanical changes that don’t require a DMARD or biologic.”
He highlighted a Finnish 10-year, prospective, observational study that sheds light on the subject. The study demonstrated that seronegative RA is seldom what it at first seems. The Finnish rheumatologists followed 435 consecutive patients initially diagnosed as having seronegative early RA. The structured follow-up entailed four or five interdisciplinary clinic visits within the first 2 years after diagnosis and again at 5 and 10 years.
By the 10-year mark only 4 of the 435 initially seronegative RA patients had been reclassified as having seropositive RA, while another 9 were reclassified as having erosive RA based upon the development of pathognomonic joint lesions. That’s a paltry 3% reclassification rate to classic RA.
Nearly two-thirds of patients were ultimately reclassified within 10 years as they evolved into diagnoses other than their original seronegative RA. The most common included nonerosive polymyalgia rheumatica in 16% of participants, psoriatic arthritis in 11%, osteoarthritis in 10%, spondyloarthritis in 8.7%, gout in 2.3%, and pseudogout in 3.9%.
“I think that’s sobering for you if you’re taking care of these patients, that maybe you need to rethink the diagnosis at every visit or at periodic intervals, especially if you’re going to change therapy,” advised Dr. Cush, who is professor of medicine and rheumatology at Baylor University Medical Center, Dallas, and director of clinical rheumatology at the Baylor Research Institute.
The Finnish rheumatologists observed that their findings have important implications both for clinical practice and for research, since RA clinical trials typically include a substantial proportion of seronegative patients.
“If seronegative patients are treated according to the treatment guidelines for progressive RA, a substantial proportion of patients is exposed to unnecessary long-term medication,” the investigators wrote, adding that their “results suggest that it may not be reasonable to study seronegative arthritis patients as a homogeneous entity in RA studies.”
The best recent data suggests about 15% of RA patients are seronegative, Dr. Cush said.
Delay in diagnosis is common in seronegative RA, as highlighted in a recent population-based study by Mayo Clinic rheumatologists. They reported that the median time from first joint swelling to diagnosis of seronegative RA using the 2010 American College of Rheumatology/European League Against Rheumatism criteria was 187 days, compared with a mere 11 days for seropositive RA. The median time to DMARD initiation was longer, too. Half of seropositive RA patients achieved remission within 5 years, as did 28% of seronegative patients, prompting the investigators to conclude “the window of opportunity for intervention may be more frequently missed in this group.”
Choosing the best treatment
Several medications appear to have greater efficacy in seropositive than seronegative RA patients. For example, a meta-analysis of four randomized trials including a collective 2,177 RA patients assigned 2:1 to rituximab (Rituxan) or placebo concluded that 75% of seropositive RA patients had a EULAR moderate or good response at week 24 on the biologic, compared with 44% of seronegative patients.
“Would you not use rituximab in someone who’s seronegative? No, I actually would use it. I may not rush to use it as much, maybe give it earlier in someone who’s seropositive, but I’ve used rituximab in seronegative patients who’ve done just fine,” according to Dr. Cush.
The published experience with abatacept (Orencia) is mixed, most of it coming from European observational datasets. On balance though, 80% of the articles addressing the issue have concluded that response rates to the biologic are better in seropositive RA, he continued.
Australian investigators who pooled data from five phase 3 randomized clinical trials of tofacitinib (Xeljanz) in RA concluded that double-positive patients – that is, those who were seropositive for both rheumatoid factor and anti–citrullinated protein antibody (ACPA) – were roughly twice as likely to achieve ACR20 and ACR50 responses to the oral Janus kinase inhibitor at either 5 or 10 mg twice daily than patients who were double negative.
“Double positivity is very important in prognosis and severity, compared to single positivity,” the rheumatologist observed. “I think you should worry most about the patients who have the highest titers of rheumatoid factor and ACPA.”
Asked about the merits of supplemental laboratory testing for serum 14-3-3 eta, a proposed novel biomarker in RA, as well as for anti–carbamylated protein antibodies (anti-CarP), Dr. Cush replied that it’s unclear that the additional testing is really worthwhile.
“Ordering more tests doesn’t make us smarter,” he commented. “Quite simply, with rheumatoid factor and ACPA, adding one on top of the other, you just gain maybe 10% more certainty in the diagnosis. Adding anti-CarP antibodies or serum 14-3-3 eta doesn’t add more than a few percentage points, but now you’ve quadrupled the cost of testing.”
Dr. Cush reported receiving research funding from and/or serving as a consultant to numerous pharmaceutical companies.
MAUI, HAWAII – Viewing seronegative rheumatoid arthritis as something akin to RA-lite would be a big mistake, John J. Cush, MD, asserted at the 2020 Rheumatology Winter Clinical Symposium.
“It’s not a benign subtype of RA. And then again, it may not be RA,” Dr. Cush observed,
“Seronegative RA means that either you need to get serious about what is probably badass disease or you need to reevaluate whether this really is RA and your need for DMARDs [disease-modifying antirheumatic drugs] in an ongoing fashion,” the rheumatologist said. “Always reconsider whether they need less therapy or maybe no therapy at all. Maybe they had inflammation at one point and now they’re left with degenerative and mechanical changes that don’t require a DMARD or biologic.”
He highlighted a Finnish 10-year, prospective, observational study that sheds light on the subject. The study demonstrated that seronegative RA is seldom what it at first seems. The Finnish rheumatologists followed 435 consecutive patients initially diagnosed as having seronegative early RA. The structured follow-up entailed four or five interdisciplinary clinic visits within the first 2 years after diagnosis and again at 5 and 10 years.
By the 10-year mark only 4 of the 435 initially seronegative RA patients had been reclassified as having seropositive RA, while another 9 were reclassified as having erosive RA based upon the development of pathognomonic joint lesions. That’s a paltry 3% reclassification rate to classic RA.
Nearly two-thirds of patients were ultimately reclassified within 10 years as they evolved into diagnoses other than their original seronegative RA. The most common included nonerosive polymyalgia rheumatica in 16% of participants, psoriatic arthritis in 11%, osteoarthritis in 10%, spondyloarthritis in 8.7%, gout in 2.3%, and pseudogout in 3.9%.
“I think that’s sobering for you if you’re taking care of these patients, that maybe you need to rethink the diagnosis at every visit or at periodic intervals, especially if you’re going to change therapy,” advised Dr. Cush, who is professor of medicine and rheumatology at Baylor University Medical Center, Dallas, and director of clinical rheumatology at the Baylor Research Institute.
The Finnish rheumatologists observed that their findings have important implications both for clinical practice and for research, since RA clinical trials typically include a substantial proportion of seronegative patients.
“If seronegative patients are treated according to the treatment guidelines for progressive RA, a substantial proportion of patients is exposed to unnecessary long-term medication,” the investigators wrote, adding that their “results suggest that it may not be reasonable to study seronegative arthritis patients as a homogeneous entity in RA studies.”
The best recent data suggests about 15% of RA patients are seronegative, Dr. Cush said.
Delay in diagnosis is common in seronegative RA, as highlighted in a recent population-based study by Mayo Clinic rheumatologists. They reported that the median time from first joint swelling to diagnosis of seronegative RA using the 2010 American College of Rheumatology/European League Against Rheumatism criteria was 187 days, compared with a mere 11 days for seropositive RA. The median time to DMARD initiation was longer, too. Half of seropositive RA patients achieved remission within 5 years, as did 28% of seronegative patients, prompting the investigators to conclude “the window of opportunity for intervention may be more frequently missed in this group.”
Choosing the best treatment
Several medications appear to have greater efficacy in seropositive than seronegative RA patients. For example, a meta-analysis of four randomized trials including a collective 2,177 RA patients assigned 2:1 to rituximab (Rituxan) or placebo concluded that 75% of seropositive RA patients had a EULAR moderate or good response at week 24 on the biologic, compared with 44% of seronegative patients.
“Would you not use rituximab in someone who’s seronegative? No, I actually would use it. I may not rush to use it as much, maybe give it earlier in someone who’s seropositive, but I’ve used rituximab in seronegative patients who’ve done just fine,” according to Dr. Cush.
The published experience with abatacept (Orencia) is mixed, most of it coming from European observational datasets. On balance though, 80% of the articles addressing the issue have concluded that response rates to the biologic are better in seropositive RA, he continued.
Australian investigators who pooled data from five phase 3 randomized clinical trials of tofacitinib (Xeljanz) in RA concluded that double-positive patients – that is, those who were seropositive for both rheumatoid factor and anti–citrullinated protein antibody (ACPA) – were roughly twice as likely to achieve ACR20 and ACR50 responses to the oral Janus kinase inhibitor at either 5 or 10 mg twice daily than patients who were double negative.
“Double positivity is very important in prognosis and severity, compared to single positivity,” the rheumatologist observed. “I think you should worry most about the patients who have the highest titers of rheumatoid factor and ACPA.”
Asked about the merits of supplemental laboratory testing for serum 14-3-3 eta, a proposed novel biomarker in RA, as well as for anti–carbamylated protein antibodies (anti-CarP), Dr. Cush replied that it’s unclear that the additional testing is really worthwhile.
“Ordering more tests doesn’t make us smarter,” he commented. “Quite simply, with rheumatoid factor and ACPA, adding one on top of the other, you just gain maybe 10% more certainty in the diagnosis. Adding anti-CarP antibodies or serum 14-3-3 eta doesn’t add more than a few percentage points, but now you’ve quadrupled the cost of testing.”
Dr. Cush reported receiving research funding from and/or serving as a consultant to numerous pharmaceutical companies.
MAUI, HAWAII – Viewing seronegative rheumatoid arthritis as something akin to RA-lite would be a big mistake, John J. Cush, MD, asserted at the 2020 Rheumatology Winter Clinical Symposium.
“It’s not a benign subtype of RA. And then again, it may not be RA,” Dr. Cush observed,
“Seronegative RA means that either you need to get serious about what is probably badass disease or you need to reevaluate whether this really is RA and your need for DMARDs [disease-modifying antirheumatic drugs] in an ongoing fashion,” the rheumatologist said. “Always reconsider whether they need less therapy or maybe no therapy at all. Maybe they had inflammation at one point and now they’re left with degenerative and mechanical changes that don’t require a DMARD or biologic.”
He highlighted a Finnish 10-year, prospective, observational study that sheds light on the subject. The study demonstrated that seronegative RA is seldom what it at first seems. The Finnish rheumatologists followed 435 consecutive patients initially diagnosed as having seronegative early RA. The structured follow-up entailed four or five interdisciplinary clinic visits within the first 2 years after diagnosis and again at 5 and 10 years.
By the 10-year mark only 4 of the 435 initially seronegative RA patients had been reclassified as having seropositive RA, while another 9 were reclassified as having erosive RA based upon the development of pathognomonic joint lesions. That’s a paltry 3% reclassification rate to classic RA.
Nearly two-thirds of patients were ultimately reclassified within 10 years as they evolved into diagnoses other than their original seronegative RA. The most common included nonerosive polymyalgia rheumatica in 16% of participants, psoriatic arthritis in 11%, osteoarthritis in 10%, spondyloarthritis in 8.7%, gout in 2.3%, and pseudogout in 3.9%.
“I think that’s sobering for you if you’re taking care of these patients, that maybe you need to rethink the diagnosis at every visit or at periodic intervals, especially if you’re going to change therapy,” advised Dr. Cush, who is professor of medicine and rheumatology at Baylor University Medical Center, Dallas, and director of clinical rheumatology at the Baylor Research Institute.
The Finnish rheumatologists observed that their findings have important implications both for clinical practice and for research, since RA clinical trials typically include a substantial proportion of seronegative patients.
“If seronegative patients are treated according to the treatment guidelines for progressive RA, a substantial proportion of patients is exposed to unnecessary long-term medication,” the investigators wrote, adding that their “results suggest that it may not be reasonable to study seronegative arthritis patients as a homogeneous entity in RA studies.”
The best recent data suggests about 15% of RA patients are seronegative, Dr. Cush said.
Delay in diagnosis is common in seronegative RA, as highlighted in a recent population-based study by Mayo Clinic rheumatologists. They reported that the median time from first joint swelling to diagnosis of seronegative RA using the 2010 American College of Rheumatology/European League Against Rheumatism criteria was 187 days, compared with a mere 11 days for seropositive RA. The median time to DMARD initiation was longer, too. Half of seropositive RA patients achieved remission within 5 years, as did 28% of seronegative patients, prompting the investigators to conclude “the window of opportunity for intervention may be more frequently missed in this group.”
Choosing the best treatment
Several medications appear to have greater efficacy in seropositive than seronegative RA patients. For example, a meta-analysis of four randomized trials including a collective 2,177 RA patients assigned 2:1 to rituximab (Rituxan) or placebo concluded that 75% of seropositive RA patients had a EULAR moderate or good response at week 24 on the biologic, compared with 44% of seronegative patients.
“Would you not use rituximab in someone who’s seronegative? No, I actually would use it. I may not rush to use it as much, maybe give it earlier in someone who’s seropositive, but I’ve used rituximab in seronegative patients who’ve done just fine,” according to Dr. Cush.
The published experience with abatacept (Orencia) is mixed, most of it coming from European observational datasets. On balance though, 80% of the articles addressing the issue have concluded that response rates to the biologic are better in seropositive RA, he continued.
Australian investigators who pooled data from five phase 3 randomized clinical trials of tofacitinib (Xeljanz) in RA concluded that double-positive patients – that is, those who were seropositive for both rheumatoid factor and anti–citrullinated protein antibody (ACPA) – were roughly twice as likely to achieve ACR20 and ACR50 responses to the oral Janus kinase inhibitor at either 5 or 10 mg twice daily than patients who were double negative.
“Double positivity is very important in prognosis and severity, compared to single positivity,” the rheumatologist observed. “I think you should worry most about the patients who have the highest titers of rheumatoid factor and ACPA.”
Asked about the merits of supplemental laboratory testing for serum 14-3-3 eta, a proposed novel biomarker in RA, as well as for anti–carbamylated protein antibodies (anti-CarP), Dr. Cush replied that it’s unclear that the additional testing is really worthwhile.
“Ordering more tests doesn’t make us smarter,” he commented. “Quite simply, with rheumatoid factor and ACPA, adding one on top of the other, you just gain maybe 10% more certainty in the diagnosis. Adding anti-CarP antibodies or serum 14-3-3 eta doesn’t add more than a few percentage points, but now you’ve quadrupled the cost of testing.”
Dr. Cush reported receiving research funding from and/or serving as a consultant to numerous pharmaceutical companies.
EXPERT ANALYSIS FROM RWCS 2020
Rheumatologists seek to reassure amid hydroxychloroquine shortage
Physicians and pharmacists are reporting shortages of hydroxychloroquine and chloroquine following President Trump’s promotion of the medications as potential COVID-19 treatments, leaving patients with rheumatic diseases wondering how it will impact their access.
The American Medical Association, the American Pharmacists Association, and the American Society of Health-System Pharmacists, issued a joint statement that strongly opposed prophylactic prescribing of these medications for COVID-19 or stockpiling them in anticipation of use for COVID-19. The concerns over shortages have also prompted the American College of Rheumatology, American Academy of Dermatology, Arthritis Foundation, and Lupus Foundation of America to send a joint statement to the Trump administration and the nation’s governors highlighting critical hydroxychloroquine access issues and asking policymakers to work together with health care providers and patient communities to ensure continued availability of these drugs.
Now
In a Q and A interview, NYU Langone Health rheumatology division director and Lupus Center director Jill P. Buyon, MD, and associate professor of rheumatology, Peter M. Izmirly, MD, noted that, while shortages have been reported across the United States because of large increases in off-label prescribing, many of the drugs’ manufacturers have committed to donating millions of doses and/or stepping up production to meet demand.
Later in this article, Michael H. Pillinger, MD, a rheumatologist and professor of medicine, biochemistry, and molecular pharmacology at NYU Langone Health, New York, answered questions about a new multicenter study called COLCORONA getting underway to test the anti-inflammatory drug colchicine. The answers in this Q&A have been edited for length and clarity.
Questions about hydroxychloroquine shortage
Q: What is the current situation with hydroxychloroquine in your practice?
A: We have been getting calls from our patients asking about getting refills for hydroxychloroquine. Our group has been calling local pharmacies asking about the availability of hydroxychloroquine, and we are compiling a list of pharmacies in New York with current availabilities to share with patients. We are somewhat limited by our electronic health record system, Epic, which can only send a prescription to one pharmacy, so that has placed some limitations on knowing where it is available. Some pharmacies have not had hydroxychloroquine available, while others have. We have also been encouraging patients to check online and look for mail-order possibilities for 90-day supplies.
Nearly all prescriptions are for generic hydroxychloroquine. Branded hydroxychloroquine (Plaquenil) is much more expensive, and we can run into obstacles with getting it approved by insurers, too.
Q: What are you telling patients who seek to refill their prescription or call with concerns? Is it feasible for patients to stop hydroxychloroquine or cut their dosage if necessary?
A: If someone’s been on hydroxychloroquine and has benefited from its use there’s no reason to come off it at this time, and given the possibility that it may have an effect on COVID-19, that is all the better. But we want to reassure patients that they can get the drug and that it is not difficult to manufacture.
Given the significantly higher risk of disease flare that was first described in lupus patients who discontinued hydroxychloroquine in the Canadian Hydroxychloroquine Study Group’s 1991 randomized, controlled trial, it is not advisable for patients to stop the drug.
Some patients do split their dosage day-to-day if they are taking less than 400 mg daily, such that someone taking 300 mg daily may take two 200-mg tablets one day and just one 200-mg tablet the next day, and so on. To avoid eye toxicity that can occur after years of taking the drug, hydroxychloroquine is generally prescribed based on weight at 5 mg/kg.
The drug also stays in the body for quite a while [often up to 3 months and even longer], so that is helpful for patients to know.
Given the current situation and the possibility of its effectiveness against COVID-19, it is ironic that we are actually trying to recruit older lupus patients who have had long-term stable disease while on hydroxychloroquine to a trial of stopping the drug to reduce the risk of developing the side effect of retinopathy. We want to see if patients can safely withdraw hydroxychloroquine without flaring, so we hope to not run into enrollment difficulties based on the current situation with COVID-19.
Q: How do you view the balance between having enough hydroxychloroquine for patients with lupus or other rheumatic diseases and its use in COVID-19 patients?
A: We want to reassure patients that hydroxychloroquine will be available, and there is no reason to hoard the drug or to worry excessively about being unable to obtain it. Efforts to increase production by Mylan, Teva, Sanofi, Novartis, and other manufacturers of hydroxychloroquine should really help out.
Q: Are there pharmacy restrictions on prescription amounts?
A: This is not universal at this time, but some institutions are cutting back and offering only 1-month supplies.
Colchicine COVID-19 trial underway
Dr. Pillinger, of NYU Langone Health, explored the COLCORONA study of colchicine as a treatment for people infected with COVID-19 and the worry that shortage concerns may arise for it, too.
Q: What is the general availability of colchicine and its susceptibility to shortage?
A: There are two major manufacturers of colchicine in the United States, Takeda and Hikma, who together manufacture the majority of the drug.
The greatest use of colchicine in the United States is for gout, which affects approximately 4 million Americans, but the drug is not used chronically, so a much smaller number of patients are using colchicine at any one time. Colchicine is also used for other inflammatory conditions, primarily calcium pyrophosphate crystal disease and familial Mediterranean fever (FMF is rare in the United States). Cardiologists also regularly prescribe colchicine in pericarditis for short-term use. Physicians may use it off label for other purposes, too.
Overall, the number of patients using colchicine is much larger than that for the use of hydroxychloroquine, for example, suggesting that the immediate risk of shortage could be lower. However, if individuals started using it off label, or prescribing inappropriately for the COVID-19 indication, the supply would rapidly run short.
Q: What other points are there to consider regarding the use of colchicine to treat COVID-19?
A: There is no evidence – zero – that colchicine has any benefit for COVID-19, not even case reports. There is some rationale that it might be beneficial, but that is exactly why the COLCORONA trial would be logical to try.
The COLCORONA trial is exactly the kind of trial that would be needed for assessing colchicine, and it is big enough and happening quickly enough to get an answer. But if people start to use colchicine off label, we may never know the truth.
While colchicine can be used safely in most people, it can be very problematic and requires an experienced doctor’s supervision. Overdoses can be fatal, and colchicine interacts with many drugs, all of which require dose adjustment and some of which must be stopped in order to use colchicine – it isn’t candy. Some of the other drugs being looked at for COVID-19 in fact may interact with colchicine.
Colchicine must also be dose adjusted for kidney disease, and, in some of the COVID-19 patients, kidney function changes rapidly. So again, its use would require expert supervision even if there were evidence for its utility.
The side effects of colchicine, if mis-dosed, can be very unpleasant, including nausea, vomiting, and diarrhea. Even at the apparent right dose, some people will get these side effects, so colchicine has to be something that works to make the risk/benefit ratio worth it.
Some preparations of colchicine are made combined with probenecid, a gout drug. This is even more problematic because probenecid can raise the level of drugs excreted by the kidney and could affect other treatments.
So in sum, what may be a good idea in theory can turn out to be a disastrous idea in practice, and here we have nothing but theory. This is not an agent to use randomly; the studies will be rushed out quickly and hopefully will give us the knowledge to know what to do.
Dr. Izmirly and Dr. Buyon said they have research grants with the National Institutes of Health to study hydroxychloroquine in patients with lupus and in anti–SSA/Ro-positive pregnant women with a previous child with congenital heart block. Dr. Pillinger reports that he has an investigator-initiated grant from Hikma to study colchicine in osteoarthritis.
This article was reformatted on 3/30/2020 for clarity.
Physicians and pharmacists are reporting shortages of hydroxychloroquine and chloroquine following President Trump’s promotion of the medications as potential COVID-19 treatments, leaving patients with rheumatic diseases wondering how it will impact their access.
The American Medical Association, the American Pharmacists Association, and the American Society of Health-System Pharmacists, issued a joint statement that strongly opposed prophylactic prescribing of these medications for COVID-19 or stockpiling them in anticipation of use for COVID-19. The concerns over shortages have also prompted the American College of Rheumatology, American Academy of Dermatology, Arthritis Foundation, and Lupus Foundation of America to send a joint statement to the Trump administration and the nation’s governors highlighting critical hydroxychloroquine access issues and asking policymakers to work together with health care providers and patient communities to ensure continued availability of these drugs.
Now
In a Q and A interview, NYU Langone Health rheumatology division director and Lupus Center director Jill P. Buyon, MD, and associate professor of rheumatology, Peter M. Izmirly, MD, noted that, while shortages have been reported across the United States because of large increases in off-label prescribing, many of the drugs’ manufacturers have committed to donating millions of doses and/or stepping up production to meet demand.
Later in this article, Michael H. Pillinger, MD, a rheumatologist and professor of medicine, biochemistry, and molecular pharmacology at NYU Langone Health, New York, answered questions about a new multicenter study called COLCORONA getting underway to test the anti-inflammatory drug colchicine. The answers in this Q&A have been edited for length and clarity.
Questions about hydroxychloroquine shortage
Q: What is the current situation with hydroxychloroquine in your practice?
A: We have been getting calls from our patients asking about getting refills for hydroxychloroquine. Our group has been calling local pharmacies asking about the availability of hydroxychloroquine, and we are compiling a list of pharmacies in New York with current availabilities to share with patients. We are somewhat limited by our electronic health record system, Epic, which can only send a prescription to one pharmacy, so that has placed some limitations on knowing where it is available. Some pharmacies have not had hydroxychloroquine available, while others have. We have also been encouraging patients to check online and look for mail-order possibilities for 90-day supplies.
Nearly all prescriptions are for generic hydroxychloroquine. Branded hydroxychloroquine (Plaquenil) is much more expensive, and we can run into obstacles with getting it approved by insurers, too.
Q: What are you telling patients who seek to refill their prescription or call with concerns? Is it feasible for patients to stop hydroxychloroquine or cut their dosage if necessary?
A: If someone’s been on hydroxychloroquine and has benefited from its use there’s no reason to come off it at this time, and given the possibility that it may have an effect on COVID-19, that is all the better. But we want to reassure patients that they can get the drug and that it is not difficult to manufacture.
Given the significantly higher risk of disease flare that was first described in lupus patients who discontinued hydroxychloroquine in the Canadian Hydroxychloroquine Study Group’s 1991 randomized, controlled trial, it is not advisable for patients to stop the drug.
Some patients do split their dosage day-to-day if they are taking less than 400 mg daily, such that someone taking 300 mg daily may take two 200-mg tablets one day and just one 200-mg tablet the next day, and so on. To avoid eye toxicity that can occur after years of taking the drug, hydroxychloroquine is generally prescribed based on weight at 5 mg/kg.
The drug also stays in the body for quite a while [often up to 3 months and even longer], so that is helpful for patients to know.
Given the current situation and the possibility of its effectiveness against COVID-19, it is ironic that we are actually trying to recruit older lupus patients who have had long-term stable disease while on hydroxychloroquine to a trial of stopping the drug to reduce the risk of developing the side effect of retinopathy. We want to see if patients can safely withdraw hydroxychloroquine without flaring, so we hope to not run into enrollment difficulties based on the current situation with COVID-19.
Q: How do you view the balance between having enough hydroxychloroquine for patients with lupus or other rheumatic diseases and its use in COVID-19 patients?
A: We want to reassure patients that hydroxychloroquine will be available, and there is no reason to hoard the drug or to worry excessively about being unable to obtain it. Efforts to increase production by Mylan, Teva, Sanofi, Novartis, and other manufacturers of hydroxychloroquine should really help out.
Q: Are there pharmacy restrictions on prescription amounts?
A: This is not universal at this time, but some institutions are cutting back and offering only 1-month supplies.
Colchicine COVID-19 trial underway
Dr. Pillinger, of NYU Langone Health, explored the COLCORONA study of colchicine as a treatment for people infected with COVID-19 and the worry that shortage concerns may arise for it, too.
Q: What is the general availability of colchicine and its susceptibility to shortage?
A: There are two major manufacturers of colchicine in the United States, Takeda and Hikma, who together manufacture the majority of the drug.
The greatest use of colchicine in the United States is for gout, which affects approximately 4 million Americans, but the drug is not used chronically, so a much smaller number of patients are using colchicine at any one time. Colchicine is also used for other inflammatory conditions, primarily calcium pyrophosphate crystal disease and familial Mediterranean fever (FMF is rare in the United States). Cardiologists also regularly prescribe colchicine in pericarditis for short-term use. Physicians may use it off label for other purposes, too.
Overall, the number of patients using colchicine is much larger than that for the use of hydroxychloroquine, for example, suggesting that the immediate risk of shortage could be lower. However, if individuals started using it off label, or prescribing inappropriately for the COVID-19 indication, the supply would rapidly run short.
Q: What other points are there to consider regarding the use of colchicine to treat COVID-19?
A: There is no evidence – zero – that colchicine has any benefit for COVID-19, not even case reports. There is some rationale that it might be beneficial, but that is exactly why the COLCORONA trial would be logical to try.
The COLCORONA trial is exactly the kind of trial that would be needed for assessing colchicine, and it is big enough and happening quickly enough to get an answer. But if people start to use colchicine off label, we may never know the truth.
While colchicine can be used safely in most people, it can be very problematic and requires an experienced doctor’s supervision. Overdoses can be fatal, and colchicine interacts with many drugs, all of which require dose adjustment and some of which must be stopped in order to use colchicine – it isn’t candy. Some of the other drugs being looked at for COVID-19 in fact may interact with colchicine.
Colchicine must also be dose adjusted for kidney disease, and, in some of the COVID-19 patients, kidney function changes rapidly. So again, its use would require expert supervision even if there were evidence for its utility.
The side effects of colchicine, if mis-dosed, can be very unpleasant, including nausea, vomiting, and diarrhea. Even at the apparent right dose, some people will get these side effects, so colchicine has to be something that works to make the risk/benefit ratio worth it.
Some preparations of colchicine are made combined with probenecid, a gout drug. This is even more problematic because probenecid can raise the level of drugs excreted by the kidney and could affect other treatments.
So in sum, what may be a good idea in theory can turn out to be a disastrous idea in practice, and here we have nothing but theory. This is not an agent to use randomly; the studies will be rushed out quickly and hopefully will give us the knowledge to know what to do.
Dr. Izmirly and Dr. Buyon said they have research grants with the National Institutes of Health to study hydroxychloroquine in patients with lupus and in anti–SSA/Ro-positive pregnant women with a previous child with congenital heart block. Dr. Pillinger reports that he has an investigator-initiated grant from Hikma to study colchicine in osteoarthritis.
This article was reformatted on 3/30/2020 for clarity.
Physicians and pharmacists are reporting shortages of hydroxychloroquine and chloroquine following President Trump’s promotion of the medications as potential COVID-19 treatments, leaving patients with rheumatic diseases wondering how it will impact their access.
The American Medical Association, the American Pharmacists Association, and the American Society of Health-System Pharmacists, issued a joint statement that strongly opposed prophylactic prescribing of these medications for COVID-19 or stockpiling them in anticipation of use for COVID-19. The concerns over shortages have also prompted the American College of Rheumatology, American Academy of Dermatology, Arthritis Foundation, and Lupus Foundation of America to send a joint statement to the Trump administration and the nation’s governors highlighting critical hydroxychloroquine access issues and asking policymakers to work together with health care providers and patient communities to ensure continued availability of these drugs.
Now
In a Q and A interview, NYU Langone Health rheumatology division director and Lupus Center director Jill P. Buyon, MD, and associate professor of rheumatology, Peter M. Izmirly, MD, noted that, while shortages have been reported across the United States because of large increases in off-label prescribing, many of the drugs’ manufacturers have committed to donating millions of doses and/or stepping up production to meet demand.
Later in this article, Michael H. Pillinger, MD, a rheumatologist and professor of medicine, biochemistry, and molecular pharmacology at NYU Langone Health, New York, answered questions about a new multicenter study called COLCORONA getting underway to test the anti-inflammatory drug colchicine. The answers in this Q&A have been edited for length and clarity.
Questions about hydroxychloroquine shortage
Q: What is the current situation with hydroxychloroquine in your practice?
A: We have been getting calls from our patients asking about getting refills for hydroxychloroquine. Our group has been calling local pharmacies asking about the availability of hydroxychloroquine, and we are compiling a list of pharmacies in New York with current availabilities to share with patients. We are somewhat limited by our electronic health record system, Epic, which can only send a prescription to one pharmacy, so that has placed some limitations on knowing where it is available. Some pharmacies have not had hydroxychloroquine available, while others have. We have also been encouraging patients to check online and look for mail-order possibilities for 90-day supplies.
Nearly all prescriptions are for generic hydroxychloroquine. Branded hydroxychloroquine (Plaquenil) is much more expensive, and we can run into obstacles with getting it approved by insurers, too.
Q: What are you telling patients who seek to refill their prescription or call with concerns? Is it feasible for patients to stop hydroxychloroquine or cut their dosage if necessary?
A: If someone’s been on hydroxychloroquine and has benefited from its use there’s no reason to come off it at this time, and given the possibility that it may have an effect on COVID-19, that is all the better. But we want to reassure patients that they can get the drug and that it is not difficult to manufacture.
Given the significantly higher risk of disease flare that was first described in lupus patients who discontinued hydroxychloroquine in the Canadian Hydroxychloroquine Study Group’s 1991 randomized, controlled trial, it is not advisable for patients to stop the drug.
Some patients do split their dosage day-to-day if they are taking less than 400 mg daily, such that someone taking 300 mg daily may take two 200-mg tablets one day and just one 200-mg tablet the next day, and so on. To avoid eye toxicity that can occur after years of taking the drug, hydroxychloroquine is generally prescribed based on weight at 5 mg/kg.
The drug also stays in the body for quite a while [often up to 3 months and even longer], so that is helpful for patients to know.
Given the current situation and the possibility of its effectiveness against COVID-19, it is ironic that we are actually trying to recruit older lupus patients who have had long-term stable disease while on hydroxychloroquine to a trial of stopping the drug to reduce the risk of developing the side effect of retinopathy. We want to see if patients can safely withdraw hydroxychloroquine without flaring, so we hope to not run into enrollment difficulties based on the current situation with COVID-19.
Q: How do you view the balance between having enough hydroxychloroquine for patients with lupus or other rheumatic diseases and its use in COVID-19 patients?
A: We want to reassure patients that hydroxychloroquine will be available, and there is no reason to hoard the drug or to worry excessively about being unable to obtain it. Efforts to increase production by Mylan, Teva, Sanofi, Novartis, and other manufacturers of hydroxychloroquine should really help out.
Q: Are there pharmacy restrictions on prescription amounts?
A: This is not universal at this time, but some institutions are cutting back and offering only 1-month supplies.
Colchicine COVID-19 trial underway
Dr. Pillinger, of NYU Langone Health, explored the COLCORONA study of colchicine as a treatment for people infected with COVID-19 and the worry that shortage concerns may arise for it, too.
Q: What is the general availability of colchicine and its susceptibility to shortage?
A: There are two major manufacturers of colchicine in the United States, Takeda and Hikma, who together manufacture the majority of the drug.
The greatest use of colchicine in the United States is for gout, which affects approximately 4 million Americans, but the drug is not used chronically, so a much smaller number of patients are using colchicine at any one time. Colchicine is also used for other inflammatory conditions, primarily calcium pyrophosphate crystal disease and familial Mediterranean fever (FMF is rare in the United States). Cardiologists also regularly prescribe colchicine in pericarditis for short-term use. Physicians may use it off label for other purposes, too.
Overall, the number of patients using colchicine is much larger than that for the use of hydroxychloroquine, for example, suggesting that the immediate risk of shortage could be lower. However, if individuals started using it off label, or prescribing inappropriately for the COVID-19 indication, the supply would rapidly run short.
Q: What other points are there to consider regarding the use of colchicine to treat COVID-19?
A: There is no evidence – zero – that colchicine has any benefit for COVID-19, not even case reports. There is some rationale that it might be beneficial, but that is exactly why the COLCORONA trial would be logical to try.
The COLCORONA trial is exactly the kind of trial that would be needed for assessing colchicine, and it is big enough and happening quickly enough to get an answer. But if people start to use colchicine off label, we may never know the truth.
While colchicine can be used safely in most people, it can be very problematic and requires an experienced doctor’s supervision. Overdoses can be fatal, and colchicine interacts with many drugs, all of which require dose adjustment and some of which must be stopped in order to use colchicine – it isn’t candy. Some of the other drugs being looked at for COVID-19 in fact may interact with colchicine.
Colchicine must also be dose adjusted for kidney disease, and, in some of the COVID-19 patients, kidney function changes rapidly. So again, its use would require expert supervision even if there were evidence for its utility.
The side effects of colchicine, if mis-dosed, can be very unpleasant, including nausea, vomiting, and diarrhea. Even at the apparent right dose, some people will get these side effects, so colchicine has to be something that works to make the risk/benefit ratio worth it.
Some preparations of colchicine are made combined with probenecid, a gout drug. This is even more problematic because probenecid can raise the level of drugs excreted by the kidney and could affect other treatments.
So in sum, what may be a good idea in theory can turn out to be a disastrous idea in practice, and here we have nothing but theory. This is not an agent to use randomly; the studies will be rushed out quickly and hopefully will give us the knowledge to know what to do.
Dr. Izmirly and Dr. Buyon said they have research grants with the National Institutes of Health to study hydroxychloroquine in patients with lupus and in anti–SSA/Ro-positive pregnant women with a previous child with congenital heart block. Dr. Pillinger reports that he has an investigator-initiated grant from Hikma to study colchicine in osteoarthritis.
This article was reformatted on 3/30/2020 for clarity.
Live zoster vaccine confers limited protection during tofacitinib therapy
The live attenuated zoster vaccine (Zostavax) does not provide adequate long-term protection in patients with rheumatoid arthritis (RA) starting tofacitinib, suggests the ORAL Sequel extension study.
The incidence of herpes zoster in patients with RA taking tofacitinib (Xeljanz), an oral Janus kinase inhibitor, is about double the rate seen with biologic disease-modifying antirheumatic drugs, noted the investigators, who were led by Kevin L. Winthrop, MD, professor of infectious diseases, ophthalmology, public health, and preventive medicine at Oregon Health & Science University, Portland. The American College of Rheumatology’s guideline for the treatment of RA recommends herpes zoster vaccination before patients aged 50 years or older initiate any of these agents.
The investigators studied 100 patients with RA from an index randomized, placebo-controlled trial of tofacitinib who started the long-term extension study 14 weeks after receiving the live attenuated zoster vaccine. All were given open-label tofacitinib, at 5 or 10 mg two times per day, along with background RA therapy as needed.
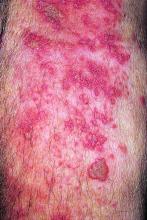
With a follow-up of 27 months, five patients (5%) developed herpes zoster, including two treated with the 5-mg dose and three treated with the 10-mg dose, according to results reported in Annals of the Rheumatic Diseases. Cases occurred between 218 and 741 days after vaccination.
Four of the patients had herpes zoster involving a single dermatome, while one had involvement of five dermatomes. All episodes were mild or moderate, and resolved with antiviral therapy.
Humoral and cell-mediated immunity to the varicella zoster virus were assessed with immunoglobulin G titer and an interferon-gamma enzyme-linked immunosorbent spot assay, respectively. Results showed that three of the patients developing herpes zoster had undetectable cell-mediated immunity to the virus at baseline and week 6 after vaccination. The other two patients had an adequate humoral and cell-mediated immune response to the vaccine, as assessed from changes from baseline, but had below-average immunoglobulin G titer at baseline and week 6.
“These results suggest that [live attenuated zoster vaccine] may not provide adequate long-term protection, as previously demonstrated in healthy individuals aged ≥60 years 3 years post-vaccination, in which [herpes zoster] risk was reduced by 51%,” Dr. Winthrop and colleagues wrote.
“While it is possible that [live attenuated zoster vaccine] booster vaccinations may improve vaccine efficacy, to date there is a lack of data on the use and timing of booster vaccinations, and no recommendations on the use of [live attenuated zoster vaccine] booster vaccinations currently exist,” they concluded. “This highlights the importance of evaluating the newly approved subunit non-live vaccine (Shingrix) in patients with RA receiving tofacitinib.”
The study was sponsored by Pfizer. Dr. Winthrop disclosed consulting for AbbVie, Bristol-Myers Squibb, Eli Lilly, Galapagos, Gilead, Pfizer, and UCB and receiving grant/research support from Bristol-Myers Squibb. Two coauthors disclosed financial relationships with Pfizer and other pharmaceutical companies, and the other seven coauthors were employees and shareholders of Pfizer.
SOURCE: Winthrop KL et al. Ann Rheum Dis. 2020 Mar 11. doi: 10.1136/annrheumdis-2019-216566.
The live attenuated zoster vaccine (Zostavax) does not provide adequate long-term protection in patients with rheumatoid arthritis (RA) starting tofacitinib, suggests the ORAL Sequel extension study.
The incidence of herpes zoster in patients with RA taking tofacitinib (Xeljanz), an oral Janus kinase inhibitor, is about double the rate seen with biologic disease-modifying antirheumatic drugs, noted the investigators, who were led by Kevin L. Winthrop, MD, professor of infectious diseases, ophthalmology, public health, and preventive medicine at Oregon Health & Science University, Portland. The American College of Rheumatology’s guideline for the treatment of RA recommends herpes zoster vaccination before patients aged 50 years or older initiate any of these agents.
The investigators studied 100 patients with RA from an index randomized, placebo-controlled trial of tofacitinib who started the long-term extension study 14 weeks after receiving the live attenuated zoster vaccine. All were given open-label tofacitinib, at 5 or 10 mg two times per day, along with background RA therapy as needed.
With a follow-up of 27 months, five patients (5%) developed herpes zoster, including two treated with the 5-mg dose and three treated with the 10-mg dose, according to results reported in Annals of the Rheumatic Diseases. Cases occurred between 218 and 741 days after vaccination.
Four of the patients had herpes zoster involving a single dermatome, while one had involvement of five dermatomes. All episodes were mild or moderate, and resolved with antiviral therapy.
Humoral and cell-mediated immunity to the varicella zoster virus were assessed with immunoglobulin G titer and an interferon-gamma enzyme-linked immunosorbent spot assay, respectively. Results showed that three of the patients developing herpes zoster had undetectable cell-mediated immunity to the virus at baseline and week 6 after vaccination. The other two patients had an adequate humoral and cell-mediated immune response to the vaccine, as assessed from changes from baseline, but had below-average immunoglobulin G titer at baseline and week 6.
“These results suggest that [live attenuated zoster vaccine] may not provide adequate long-term protection, as previously demonstrated in healthy individuals aged ≥60 years 3 years post-vaccination, in which [herpes zoster] risk was reduced by 51%,” Dr. Winthrop and colleagues wrote.
“While it is possible that [live attenuated zoster vaccine] booster vaccinations may improve vaccine efficacy, to date there is a lack of data on the use and timing of booster vaccinations, and no recommendations on the use of [live attenuated zoster vaccine] booster vaccinations currently exist,” they concluded. “This highlights the importance of evaluating the newly approved subunit non-live vaccine (Shingrix) in patients with RA receiving tofacitinib.”
The study was sponsored by Pfizer. Dr. Winthrop disclosed consulting for AbbVie, Bristol-Myers Squibb, Eli Lilly, Galapagos, Gilead, Pfizer, and UCB and receiving grant/research support from Bristol-Myers Squibb. Two coauthors disclosed financial relationships with Pfizer and other pharmaceutical companies, and the other seven coauthors were employees and shareholders of Pfizer.
SOURCE: Winthrop KL et al. Ann Rheum Dis. 2020 Mar 11. doi: 10.1136/annrheumdis-2019-216566.
The live attenuated zoster vaccine (Zostavax) does not provide adequate long-term protection in patients with rheumatoid arthritis (RA) starting tofacitinib, suggests the ORAL Sequel extension study.
The incidence of herpes zoster in patients with RA taking tofacitinib (Xeljanz), an oral Janus kinase inhibitor, is about double the rate seen with biologic disease-modifying antirheumatic drugs, noted the investigators, who were led by Kevin L. Winthrop, MD, professor of infectious diseases, ophthalmology, public health, and preventive medicine at Oregon Health & Science University, Portland. The American College of Rheumatology’s guideline for the treatment of RA recommends herpes zoster vaccination before patients aged 50 years or older initiate any of these agents.
The investigators studied 100 patients with RA from an index randomized, placebo-controlled trial of tofacitinib who started the long-term extension study 14 weeks after receiving the live attenuated zoster vaccine. All were given open-label tofacitinib, at 5 or 10 mg two times per day, along with background RA therapy as needed.
With a follow-up of 27 months, five patients (5%) developed herpes zoster, including two treated with the 5-mg dose and three treated with the 10-mg dose, according to results reported in Annals of the Rheumatic Diseases. Cases occurred between 218 and 741 days after vaccination.
Four of the patients had herpes zoster involving a single dermatome, while one had involvement of five dermatomes. All episodes were mild or moderate, and resolved with antiviral therapy.
Humoral and cell-mediated immunity to the varicella zoster virus were assessed with immunoglobulin G titer and an interferon-gamma enzyme-linked immunosorbent spot assay, respectively. Results showed that three of the patients developing herpes zoster had undetectable cell-mediated immunity to the virus at baseline and week 6 after vaccination. The other two patients had an adequate humoral and cell-mediated immune response to the vaccine, as assessed from changes from baseline, but had below-average immunoglobulin G titer at baseline and week 6.
“These results suggest that [live attenuated zoster vaccine] may not provide adequate long-term protection, as previously demonstrated in healthy individuals aged ≥60 years 3 years post-vaccination, in which [herpes zoster] risk was reduced by 51%,” Dr. Winthrop and colleagues wrote.
“While it is possible that [live attenuated zoster vaccine] booster vaccinations may improve vaccine efficacy, to date there is a lack of data on the use and timing of booster vaccinations, and no recommendations on the use of [live attenuated zoster vaccine] booster vaccinations currently exist,” they concluded. “This highlights the importance of evaluating the newly approved subunit non-live vaccine (Shingrix) in patients with RA receiving tofacitinib.”
The study was sponsored by Pfizer. Dr. Winthrop disclosed consulting for AbbVie, Bristol-Myers Squibb, Eli Lilly, Galapagos, Gilead, Pfizer, and UCB and receiving grant/research support from Bristol-Myers Squibb. Two coauthors disclosed financial relationships with Pfizer and other pharmaceutical companies, and the other seven coauthors were employees and shareholders of Pfizer.
SOURCE: Winthrop KL et al. Ann Rheum Dis. 2020 Mar 11. doi: 10.1136/annrheumdis-2019-216566.
FROM ANNALS OF THE RHEUMATIC DISEASES
Stronger links forged between RA and asthma, COPD
Asthma and chronic obstructive pulmonary disease were both linked to an increased risk of rheumatoid arthritis in a recent large, prospective cohort study, researchers have reported, which adds to a growing body of evidence that airway inflammation is implicated in the development of this disease.
RA risk was increased by about 50% among asthma patients, even when excluding those who had ever smoked, according to the study’s results, which were based on more than 200,000 women in the Nurses’ Health Study I and II.
Risk of RA nearly doubled among those with chronic obstructive pulmonary disease (COPD), with an even stronger association seen in older ever-smokers, according to authors of the study.
The findings not only strengthen the case for the potential role of obstructive lung diseases in RA development, according to the study’s authors, but also suggest that health care providers need to lower the bar for evaluation of patients with lung diseases and inflammatory joint symptoms.
“If these patients develop arthralgias, then the clinicians taking care of them should have a low threshold to consider RA, and perhaps refer, or check these patients with a diagnostic test for RA,” said researcher Jeffrey A. Sparks, MD, of Brigham and Women’s Hospital and Harvard Medical School in Boston.
What’s perhaps not as clear now is whether screening obstructive lung disease patients in the absence of early RA signs would be warranted: “I don’t know if we’re quite at the point where we would need to screen these patients if they’re not symptomatic,” Dr. Sparks said in an interview.
The study by Dr. Sparks and colleagues is, by far, not the first study to implicate asthma or other lung conditions in RA development. However, most previous studies are retrospective, and interpretation of the findings has been subject to limitations such as inadequate power to detect an increased risk or lack of adjustment for important confounding factors, such as smoking.
As such, the study by Dr. Sparks and colleagues is believed to be the first-ever prospective study to evaluate asthma and COPD as risk factors for RA, study authors reported in Arthritis & Rheumatology.
Researchers were able to identify 1,060 incident RA cases that developed in 15,148 women with asthma and 3,573 with COPD in the study with more than 4 million person-years of follow-up.
The association between asthma and increased RA risk was seen not only for the asthma population as a whole (hazard ratio, 1.53; 95% confidence interval, 1.24-1.88), but also for the subset of women who had never smoked, to a similar degree (HR, 1.53; 95% CI, 1.14-2.05), the report shows.
COPD’s association with RA risk was apparent overall (HR, 1.89; 95% CI, 1.31-2.75) and even more so in the subgroup of ever-smokers 55 years of age and older (HR, 2.20; 95% CI, 1.38-3.51), the data further show.
Findings of studies looking at the inflammation of airways and other mucosal sites are “critically important to understand” when it comes to trying to prevent RA, said Kevin Deane, MD, of the University of Colorado at Denver at Aurora.
“If we indeed are trying to prevent rheumatoid arthritis in terms of the joint disease, we may need to look at these mucosal sites in individuals who don’t yet have joint disease as potential sites to target for prevention, or at least areas to study to understand how prevention may work,” said Dr. Deane, principal investigator on the National Institutes of Health–funded Strategy for the Prevention of RA (StopRA) trial.
With that in mind, it’s conceivable targeting a lung process might prevent joint disease in a patient with asthma or airway inflammation and blood markers that indicate a risk of RA, Dr. Deane said in an interview.
Blood markers of RA have been evaluated in some recent studies, with findings that provide further evidence of a link between lung diseases and RA, and vice versa.
In particular, anti–citrullinated protein antibodies (ACPA) are clearly central to RA pathogenesis. And while asthma is increasingly linked to RA risk, there have been relatively little data on any potential links between ACPA and asthma.
That research gap led to a case-control study of the Nurses’ Health Study I and II (on which Dr. Sparks was senior author) showing that asthma was strongly linked to elevated ACPA in blood drawn from patients prior to a diagnosis of RA.
Results, published last year in Arthritis Research & Therapy, showed a significant association between asthma and pre-RA ACPA elevation (odds ratio, 3.57; 95% CI, 1.58-8.04), after adjustment for smoking and other potentially confounding factors. Investigators said the findings provided evidence that chronic mucosal airway inflammation is a factor in the development of ACPA and in the pathogenesis of RA.
In a follow-up study published more recently in Arthritis Care & Research, investigators showed that, among women in the Nurses Health Study I and II, pre-RA ACPA elevation was linked to increased risk of COPD, compared with controls (HR, 3.04; 95% CI, 1.33-7.00), while the risk for development of asthma was similar in women with or without elevated pre-RA ACPA.
That study was in part an attempt to establish a “timeline” related to antibodies, lung diseases, and RA onset, Dr. Sparks said in the interview.
“We think that probably the asthma is more important in developing the antibody, but that once you have the antibody, if you didn’t have asthma by then, you’re unlikely to develop it,” he said. “So asthma seems to be something that could happen before the antibody production, whereas COPD seems to happen after – but ACPA seems to be the common link in both of these obstructive lung diseases.”
The study in Arthritis & Rheumatology linking asthma and COPD to risk of incident RA was supported by the National Institutes of Health. Dr. Sparks reported grant support from Amgen and Bristol Myers Squibb and consulting fees from Inova and Optum. Coauthors provided disclosures related to GlaxoSmithKline, AstraZeneca, Merck, Neutrolis, and Genentech.
SOURCE: Ford JA et al. Arthritis Rheumatol. 2020 Mar 4. doi: 10.1002/art.41194.
Asthma and chronic obstructive pulmonary disease were both linked to an increased risk of rheumatoid arthritis in a recent large, prospective cohort study, researchers have reported, which adds to a growing body of evidence that airway inflammation is implicated in the development of this disease.
RA risk was increased by about 50% among asthma patients, even when excluding those who had ever smoked, according to the study’s results, which were based on more than 200,000 women in the Nurses’ Health Study I and II.
Risk of RA nearly doubled among those with chronic obstructive pulmonary disease (COPD), with an even stronger association seen in older ever-smokers, according to authors of the study.
The findings not only strengthen the case for the potential role of obstructive lung diseases in RA development, according to the study’s authors, but also suggest that health care providers need to lower the bar for evaluation of patients with lung diseases and inflammatory joint symptoms.
“If these patients develop arthralgias, then the clinicians taking care of them should have a low threshold to consider RA, and perhaps refer, or check these patients with a diagnostic test for RA,” said researcher Jeffrey A. Sparks, MD, of Brigham and Women’s Hospital and Harvard Medical School in Boston.
What’s perhaps not as clear now is whether screening obstructive lung disease patients in the absence of early RA signs would be warranted: “I don’t know if we’re quite at the point where we would need to screen these patients if they’re not symptomatic,” Dr. Sparks said in an interview.
The study by Dr. Sparks and colleagues is, by far, not the first study to implicate asthma or other lung conditions in RA development. However, most previous studies are retrospective, and interpretation of the findings has been subject to limitations such as inadequate power to detect an increased risk or lack of adjustment for important confounding factors, such as smoking.
As such, the study by Dr. Sparks and colleagues is believed to be the first-ever prospective study to evaluate asthma and COPD as risk factors for RA, study authors reported in Arthritis & Rheumatology.
Researchers were able to identify 1,060 incident RA cases that developed in 15,148 women with asthma and 3,573 with COPD in the study with more than 4 million person-years of follow-up.
The association between asthma and increased RA risk was seen not only for the asthma population as a whole (hazard ratio, 1.53; 95% confidence interval, 1.24-1.88), but also for the subset of women who had never smoked, to a similar degree (HR, 1.53; 95% CI, 1.14-2.05), the report shows.
COPD’s association with RA risk was apparent overall (HR, 1.89; 95% CI, 1.31-2.75) and even more so in the subgroup of ever-smokers 55 years of age and older (HR, 2.20; 95% CI, 1.38-3.51), the data further show.
Findings of studies looking at the inflammation of airways and other mucosal sites are “critically important to understand” when it comes to trying to prevent RA, said Kevin Deane, MD, of the University of Colorado at Denver at Aurora.
“If we indeed are trying to prevent rheumatoid arthritis in terms of the joint disease, we may need to look at these mucosal sites in individuals who don’t yet have joint disease as potential sites to target for prevention, or at least areas to study to understand how prevention may work,” said Dr. Deane, principal investigator on the National Institutes of Health–funded Strategy for the Prevention of RA (StopRA) trial.
With that in mind, it’s conceivable targeting a lung process might prevent joint disease in a patient with asthma or airway inflammation and blood markers that indicate a risk of RA, Dr. Deane said in an interview.
Blood markers of RA have been evaluated in some recent studies, with findings that provide further evidence of a link between lung diseases and RA, and vice versa.
In particular, anti–citrullinated protein antibodies (ACPA) are clearly central to RA pathogenesis. And while asthma is increasingly linked to RA risk, there have been relatively little data on any potential links between ACPA and asthma.
That research gap led to a case-control study of the Nurses’ Health Study I and II (on which Dr. Sparks was senior author) showing that asthma was strongly linked to elevated ACPA in blood drawn from patients prior to a diagnosis of RA.
Results, published last year in Arthritis Research & Therapy, showed a significant association between asthma and pre-RA ACPA elevation (odds ratio, 3.57; 95% CI, 1.58-8.04), after adjustment for smoking and other potentially confounding factors. Investigators said the findings provided evidence that chronic mucosal airway inflammation is a factor in the development of ACPA and in the pathogenesis of RA.
In a follow-up study published more recently in Arthritis Care & Research, investigators showed that, among women in the Nurses Health Study I and II, pre-RA ACPA elevation was linked to increased risk of COPD, compared with controls (HR, 3.04; 95% CI, 1.33-7.00), while the risk for development of asthma was similar in women with or without elevated pre-RA ACPA.
That study was in part an attempt to establish a “timeline” related to antibodies, lung diseases, and RA onset, Dr. Sparks said in the interview.
“We think that probably the asthma is more important in developing the antibody, but that once you have the antibody, if you didn’t have asthma by then, you’re unlikely to develop it,” he said. “So asthma seems to be something that could happen before the antibody production, whereas COPD seems to happen after – but ACPA seems to be the common link in both of these obstructive lung diseases.”
The study in Arthritis & Rheumatology linking asthma and COPD to risk of incident RA was supported by the National Institutes of Health. Dr. Sparks reported grant support from Amgen and Bristol Myers Squibb and consulting fees from Inova and Optum. Coauthors provided disclosures related to GlaxoSmithKline, AstraZeneca, Merck, Neutrolis, and Genentech.
SOURCE: Ford JA et al. Arthritis Rheumatol. 2020 Mar 4. doi: 10.1002/art.41194.
Asthma and chronic obstructive pulmonary disease were both linked to an increased risk of rheumatoid arthritis in a recent large, prospective cohort study, researchers have reported, which adds to a growing body of evidence that airway inflammation is implicated in the development of this disease.
RA risk was increased by about 50% among asthma patients, even when excluding those who had ever smoked, according to the study’s results, which were based on more than 200,000 women in the Nurses’ Health Study I and II.
Risk of RA nearly doubled among those with chronic obstructive pulmonary disease (COPD), with an even stronger association seen in older ever-smokers, according to authors of the study.
The findings not only strengthen the case for the potential role of obstructive lung diseases in RA development, according to the study’s authors, but also suggest that health care providers need to lower the bar for evaluation of patients with lung diseases and inflammatory joint symptoms.
“If these patients develop arthralgias, then the clinicians taking care of them should have a low threshold to consider RA, and perhaps refer, or check these patients with a diagnostic test for RA,” said researcher Jeffrey A. Sparks, MD, of Brigham and Women’s Hospital and Harvard Medical School in Boston.
What’s perhaps not as clear now is whether screening obstructive lung disease patients in the absence of early RA signs would be warranted: “I don’t know if we’re quite at the point where we would need to screen these patients if they’re not symptomatic,” Dr. Sparks said in an interview.
The study by Dr. Sparks and colleagues is, by far, not the first study to implicate asthma or other lung conditions in RA development. However, most previous studies are retrospective, and interpretation of the findings has been subject to limitations such as inadequate power to detect an increased risk or lack of adjustment for important confounding factors, such as smoking.
As such, the study by Dr. Sparks and colleagues is believed to be the first-ever prospective study to evaluate asthma and COPD as risk factors for RA, study authors reported in Arthritis & Rheumatology.
Researchers were able to identify 1,060 incident RA cases that developed in 15,148 women with asthma and 3,573 with COPD in the study with more than 4 million person-years of follow-up.
The association between asthma and increased RA risk was seen not only for the asthma population as a whole (hazard ratio, 1.53; 95% confidence interval, 1.24-1.88), but also for the subset of women who had never smoked, to a similar degree (HR, 1.53; 95% CI, 1.14-2.05), the report shows.
COPD’s association with RA risk was apparent overall (HR, 1.89; 95% CI, 1.31-2.75) and even more so in the subgroup of ever-smokers 55 years of age and older (HR, 2.20; 95% CI, 1.38-3.51), the data further show.
Findings of studies looking at the inflammation of airways and other mucosal sites are “critically important to understand” when it comes to trying to prevent RA, said Kevin Deane, MD, of the University of Colorado at Denver at Aurora.
“If we indeed are trying to prevent rheumatoid arthritis in terms of the joint disease, we may need to look at these mucosal sites in individuals who don’t yet have joint disease as potential sites to target for prevention, or at least areas to study to understand how prevention may work,” said Dr. Deane, principal investigator on the National Institutes of Health–funded Strategy for the Prevention of RA (StopRA) trial.
With that in mind, it’s conceivable targeting a lung process might prevent joint disease in a patient with asthma or airway inflammation and blood markers that indicate a risk of RA, Dr. Deane said in an interview.
Blood markers of RA have been evaluated in some recent studies, with findings that provide further evidence of a link between lung diseases and RA, and vice versa.
In particular, anti–citrullinated protein antibodies (ACPA) are clearly central to RA pathogenesis. And while asthma is increasingly linked to RA risk, there have been relatively little data on any potential links between ACPA and asthma.
That research gap led to a case-control study of the Nurses’ Health Study I and II (on which Dr. Sparks was senior author) showing that asthma was strongly linked to elevated ACPA in blood drawn from patients prior to a diagnosis of RA.
Results, published last year in Arthritis Research & Therapy, showed a significant association between asthma and pre-RA ACPA elevation (odds ratio, 3.57; 95% CI, 1.58-8.04), after adjustment for smoking and other potentially confounding factors. Investigators said the findings provided evidence that chronic mucosal airway inflammation is a factor in the development of ACPA and in the pathogenesis of RA.
In a follow-up study published more recently in Arthritis Care & Research, investigators showed that, among women in the Nurses Health Study I and II, pre-RA ACPA elevation was linked to increased risk of COPD, compared with controls (HR, 3.04; 95% CI, 1.33-7.00), while the risk for development of asthma was similar in women with or without elevated pre-RA ACPA.
That study was in part an attempt to establish a “timeline” related to antibodies, lung diseases, and RA onset, Dr. Sparks said in the interview.
“We think that probably the asthma is more important in developing the antibody, but that once you have the antibody, if you didn’t have asthma by then, you’re unlikely to develop it,” he said. “So asthma seems to be something that could happen before the antibody production, whereas COPD seems to happen after – but ACPA seems to be the common link in both of these obstructive lung diseases.”
The study in Arthritis & Rheumatology linking asthma and COPD to risk of incident RA was supported by the National Institutes of Health. Dr. Sparks reported grant support from Amgen and Bristol Myers Squibb and consulting fees from Inova and Optum. Coauthors provided disclosures related to GlaxoSmithKline, AstraZeneca, Merck, Neutrolis, and Genentech.
SOURCE: Ford JA et al. Arthritis Rheumatol. 2020 Mar 4. doi: 10.1002/art.41194.
FROM ARTHRITIS & RHEUMATOLOGY
Are CRMO and SAPHO syndrome one and the same?
MAUI, HAWAII – Chronic recurrent multifocal osteomyelitis (CRMO) in children and SAPHO syndrome in adults may well be a single clinical syndrome.
That contention, recently put forth by Austrian investigators, resonates with Anne M. Stevens, MD, PhD, a pediatric rheumatologist at the University of Washington, Seattle, and senior director for the adaptive immunity research program at Janssen Pharmaceuticals.
“Is CRMO just for kids? No,” she asserted at the 2020 Rheumatology Winter Clinical Symposium.
First off, she noted that the nomenclature is shifting: The more familiar acronym CRMO is giving way to CNO (chronic nonbacterial osteomyelitis) in light of evidence that roughly 30% of patients with CRMO start out with a single characteristic bone lesion, with the disease turning multifocal in the subsequent 4 years in the great majority of cases.
SAPHO syndrome – an acronym for synovitis, acne, pustulosis, hyperostosis, and osteitis – a formerly obscure disease entity first described in 1987 in France, has suddenly become a trendy research topic, with three small studies presented at the 2019 annual meeting of the American College of Rheumatology.
CNO is a pediatric autoinflammatory bone disease characterized by sterile bone lesions, most often on the clavicle, spine, mandible, and lower extremities. It is marked by prominent focal bone and/or joint pain, worse at night, with or without swelling. With no agreed-upon diagnostic criteria or biomarkers, CNO is a diagnosis of exclusion. Two-thirds of the time the condition is initially misdiagnosed as bacterial osteomyelitis or a malignant tumor.
Austrian investigators at the University of Graz recently conducted a retrospective comparison of 24 pediatric patients diagnosed with CNO and 10 adults with SAPHO syndrome. The median age at diagnosis of CNO was 12.3 years versus 32.5 years for SAPHO syndrome. The two groups shared compelling similarities in mean number of bone lesions, prevalence of skin involvement, and other aspects of initial clinical presentation, as well as laboratory and histopathologic findings on bone biopsy.
There were, however, several notable clinical differences in this small dataset: CNO bone lesions affected mainly the lower extremities, clavicle, spine, and mandible, while SAPHO syndrome more commonly involved the sternum (50% vs. 8%) and vertebrae (50% vs. 21%). Also, the most frequent cutaneous manifestation was palmoplantar pustulosis in adults with SAPHO syndrome, while severe acne predominated in children with CNO. In both children and adults, the skin lesions most often arose after the bone symptoms, making early diagnosis a challenge.
Another similarity: Although there have been no randomized treatment trials in either CNO or SAPHO syndrome, case series suggest the same treatments are effective for both, with NSAIDs as first line, followed by nonbiologic disease-modifying antirheumatic drugs, tumor necrosis factor (TNF) inhibitors, or bisphosphonates.
CNO diagnosis, treatment, and follow-up
Various investigators have pegged the sensitivity of physical examination for diagnosis of CNO at 31%, radiographs at a lowly 13%, and bone scintigraphy at 74%, all in comparison with MRI.
“Our go-to now is MRI with STIR [short tau inversion recovery],” according to Dr. Stevens. “There’s no contrast – so no IV – no radiation, and it’s fast, 20 minutes for a whole body MRI in a little kid, 45 minutes in a big one.”
Insurers are reluctant to pay for serial whole-body MRIs for patient follow-up, so it’s often necessary to order a series of images covering different body parts.
Her University of Washington colleague Dan Zhao, MD, PhD, is developing infrared thermal imaging as an inexpensive, convenient alternative to MRI which could theoretically be done at home. In a pilot study in 30 children with CNO and 31 controls, inflamed leg segments showed significantly higher temperatures. Larger studies are planned.
Dr. Stevens advised leaning towards a diagnosis of CNO with avoidance of bone biopsy in a patient with multifocal osteomyelitis at the typical sites, a normal CBC, the typical extraosseous manifestations, and normal or only mildly elevated erythrocyte sedimentation rate and C-reactive protein in an otherwise well-appearing child. In contrast, strongly consider a bone biopsy to rule out malignancy or infection if the child has unexplained highly elevated C-reactive protein and erythrocyte sedimentation rate, cytopenia, high fever, excessive pain, lymphadenopathy, hepatosplenomegaly, or suspicious imaging findings.
German rheumatologists have developed a clinical score for diagnosis of CNO. A normal blood cell count gets 13 points; symmetric bone lesions 10; lesions with marginal sclerosis 10; a normal body temperature 9; two or more radiologically proven lesions 7; a C-reactive protein of 1 mg/dL or greater 6; and vertebral, clavicular, or sternal lesions 8. A score of 39 points or more out of a possible 63 had a 97% positive predictive value for CNO in a retrospective study of 224 children with CNO, proven bacterial osteomyelitis, or malignant bone tumors. A score of 28 points or less had a 97% negative predictive value for CNO. An indeterminate score of 29-38 warrants close monitoring.
The scoring system hasn’t been validated, but most pediatric rheumatologists agree that it’s useful, according to Dr. Stevens.
The Childhood Arthritis and Rheumatology Research Alliance (CARRA) is in the process of developing standardized diagnostic and classification criteria and treatment plans for CNO. Dr. Zhao was first author of a CARRA consensus treatment plan for CNO refractory to NSAID monotherapy. The plan for the first 12 months includes three options: methotrexate or sulfasalazine, TNF inhibitors with or without methotrexate, and bisphosphonates.
“The main point of this is you try a medicine and then wait 3 months. If they’re not responding then, switch medicines or add another drug. Monitor every 3 months based upon pain,” she said.
Dr. Stevens reported research collaborations with Kineta and Seattle Genetics in addition to her employment at Janssen Pharmaceuticals.
MAUI, HAWAII – Chronic recurrent multifocal osteomyelitis (CRMO) in children and SAPHO syndrome in adults may well be a single clinical syndrome.
That contention, recently put forth by Austrian investigators, resonates with Anne M. Stevens, MD, PhD, a pediatric rheumatologist at the University of Washington, Seattle, and senior director for the adaptive immunity research program at Janssen Pharmaceuticals.
“Is CRMO just for kids? No,” she asserted at the 2020 Rheumatology Winter Clinical Symposium.
First off, she noted that the nomenclature is shifting: The more familiar acronym CRMO is giving way to CNO (chronic nonbacterial osteomyelitis) in light of evidence that roughly 30% of patients with CRMO start out with a single characteristic bone lesion, with the disease turning multifocal in the subsequent 4 years in the great majority of cases.
SAPHO syndrome – an acronym for synovitis, acne, pustulosis, hyperostosis, and osteitis – a formerly obscure disease entity first described in 1987 in France, has suddenly become a trendy research topic, with three small studies presented at the 2019 annual meeting of the American College of Rheumatology.
CNO is a pediatric autoinflammatory bone disease characterized by sterile bone lesions, most often on the clavicle, spine, mandible, and lower extremities. It is marked by prominent focal bone and/or joint pain, worse at night, with or without swelling. With no agreed-upon diagnostic criteria or biomarkers, CNO is a diagnosis of exclusion. Two-thirds of the time the condition is initially misdiagnosed as bacterial osteomyelitis or a malignant tumor.
Austrian investigators at the University of Graz recently conducted a retrospective comparison of 24 pediatric patients diagnosed with CNO and 10 adults with SAPHO syndrome. The median age at diagnosis of CNO was 12.3 years versus 32.5 years for SAPHO syndrome. The two groups shared compelling similarities in mean number of bone lesions, prevalence of skin involvement, and other aspects of initial clinical presentation, as well as laboratory and histopathologic findings on bone biopsy.
There were, however, several notable clinical differences in this small dataset: CNO bone lesions affected mainly the lower extremities, clavicle, spine, and mandible, while SAPHO syndrome more commonly involved the sternum (50% vs. 8%) and vertebrae (50% vs. 21%). Also, the most frequent cutaneous manifestation was palmoplantar pustulosis in adults with SAPHO syndrome, while severe acne predominated in children with CNO. In both children and adults, the skin lesions most often arose after the bone symptoms, making early diagnosis a challenge.
Another similarity: Although there have been no randomized treatment trials in either CNO or SAPHO syndrome, case series suggest the same treatments are effective for both, with NSAIDs as first line, followed by nonbiologic disease-modifying antirheumatic drugs, tumor necrosis factor (TNF) inhibitors, or bisphosphonates.
CNO diagnosis, treatment, and follow-up
Various investigators have pegged the sensitivity of physical examination for diagnosis of CNO at 31%, radiographs at a lowly 13%, and bone scintigraphy at 74%, all in comparison with MRI.
“Our go-to now is MRI with STIR [short tau inversion recovery],” according to Dr. Stevens. “There’s no contrast – so no IV – no radiation, and it’s fast, 20 minutes for a whole body MRI in a little kid, 45 minutes in a big one.”
Insurers are reluctant to pay for serial whole-body MRIs for patient follow-up, so it’s often necessary to order a series of images covering different body parts.
Her University of Washington colleague Dan Zhao, MD, PhD, is developing infrared thermal imaging as an inexpensive, convenient alternative to MRI which could theoretically be done at home. In a pilot study in 30 children with CNO and 31 controls, inflamed leg segments showed significantly higher temperatures. Larger studies are planned.
Dr. Stevens advised leaning towards a diagnosis of CNO with avoidance of bone biopsy in a patient with multifocal osteomyelitis at the typical sites, a normal CBC, the typical extraosseous manifestations, and normal or only mildly elevated erythrocyte sedimentation rate and C-reactive protein in an otherwise well-appearing child. In contrast, strongly consider a bone biopsy to rule out malignancy or infection if the child has unexplained highly elevated C-reactive protein and erythrocyte sedimentation rate, cytopenia, high fever, excessive pain, lymphadenopathy, hepatosplenomegaly, or suspicious imaging findings.
German rheumatologists have developed a clinical score for diagnosis of CNO. A normal blood cell count gets 13 points; symmetric bone lesions 10; lesions with marginal sclerosis 10; a normal body temperature 9; two or more radiologically proven lesions 7; a C-reactive protein of 1 mg/dL or greater 6; and vertebral, clavicular, or sternal lesions 8. A score of 39 points or more out of a possible 63 had a 97% positive predictive value for CNO in a retrospective study of 224 children with CNO, proven bacterial osteomyelitis, or malignant bone tumors. A score of 28 points or less had a 97% negative predictive value for CNO. An indeterminate score of 29-38 warrants close monitoring.
The scoring system hasn’t been validated, but most pediatric rheumatologists agree that it’s useful, according to Dr. Stevens.
The Childhood Arthritis and Rheumatology Research Alliance (CARRA) is in the process of developing standardized diagnostic and classification criteria and treatment plans for CNO. Dr. Zhao was first author of a CARRA consensus treatment plan for CNO refractory to NSAID monotherapy. The plan for the first 12 months includes three options: methotrexate or sulfasalazine, TNF inhibitors with or without methotrexate, and bisphosphonates.
“The main point of this is you try a medicine and then wait 3 months. If they’re not responding then, switch medicines or add another drug. Monitor every 3 months based upon pain,” she said.
Dr. Stevens reported research collaborations with Kineta and Seattle Genetics in addition to her employment at Janssen Pharmaceuticals.
MAUI, HAWAII – Chronic recurrent multifocal osteomyelitis (CRMO) in children and SAPHO syndrome in adults may well be a single clinical syndrome.
That contention, recently put forth by Austrian investigators, resonates with Anne M. Stevens, MD, PhD, a pediatric rheumatologist at the University of Washington, Seattle, and senior director for the adaptive immunity research program at Janssen Pharmaceuticals.
“Is CRMO just for kids? No,” she asserted at the 2020 Rheumatology Winter Clinical Symposium.
First off, she noted that the nomenclature is shifting: The more familiar acronym CRMO is giving way to CNO (chronic nonbacterial osteomyelitis) in light of evidence that roughly 30% of patients with CRMO start out with a single characteristic bone lesion, with the disease turning multifocal in the subsequent 4 years in the great majority of cases.
SAPHO syndrome – an acronym for synovitis, acne, pustulosis, hyperostosis, and osteitis – a formerly obscure disease entity first described in 1987 in France, has suddenly become a trendy research topic, with three small studies presented at the 2019 annual meeting of the American College of Rheumatology.
CNO is a pediatric autoinflammatory bone disease characterized by sterile bone lesions, most often on the clavicle, spine, mandible, and lower extremities. It is marked by prominent focal bone and/or joint pain, worse at night, with or without swelling. With no agreed-upon diagnostic criteria or biomarkers, CNO is a diagnosis of exclusion. Two-thirds of the time the condition is initially misdiagnosed as bacterial osteomyelitis or a malignant tumor.
Austrian investigators at the University of Graz recently conducted a retrospective comparison of 24 pediatric patients diagnosed with CNO and 10 adults with SAPHO syndrome. The median age at diagnosis of CNO was 12.3 years versus 32.5 years for SAPHO syndrome. The two groups shared compelling similarities in mean number of bone lesions, prevalence of skin involvement, and other aspects of initial clinical presentation, as well as laboratory and histopathologic findings on bone biopsy.
There were, however, several notable clinical differences in this small dataset: CNO bone lesions affected mainly the lower extremities, clavicle, spine, and mandible, while SAPHO syndrome more commonly involved the sternum (50% vs. 8%) and vertebrae (50% vs. 21%). Also, the most frequent cutaneous manifestation was palmoplantar pustulosis in adults with SAPHO syndrome, while severe acne predominated in children with CNO. In both children and adults, the skin lesions most often arose after the bone symptoms, making early diagnosis a challenge.
Another similarity: Although there have been no randomized treatment trials in either CNO or SAPHO syndrome, case series suggest the same treatments are effective for both, with NSAIDs as first line, followed by nonbiologic disease-modifying antirheumatic drugs, tumor necrosis factor (TNF) inhibitors, or bisphosphonates.
CNO diagnosis, treatment, and follow-up
Various investigators have pegged the sensitivity of physical examination for diagnosis of CNO at 31%, radiographs at a lowly 13%, and bone scintigraphy at 74%, all in comparison with MRI.
“Our go-to now is MRI with STIR [short tau inversion recovery],” according to Dr. Stevens. “There’s no contrast – so no IV – no radiation, and it’s fast, 20 minutes for a whole body MRI in a little kid, 45 minutes in a big one.”
Insurers are reluctant to pay for serial whole-body MRIs for patient follow-up, so it’s often necessary to order a series of images covering different body parts.
Her University of Washington colleague Dan Zhao, MD, PhD, is developing infrared thermal imaging as an inexpensive, convenient alternative to MRI which could theoretically be done at home. In a pilot study in 30 children with CNO and 31 controls, inflamed leg segments showed significantly higher temperatures. Larger studies are planned.
Dr. Stevens advised leaning towards a diagnosis of CNO with avoidance of bone biopsy in a patient with multifocal osteomyelitis at the typical sites, a normal CBC, the typical extraosseous manifestations, and normal or only mildly elevated erythrocyte sedimentation rate and C-reactive protein in an otherwise well-appearing child. In contrast, strongly consider a bone biopsy to rule out malignancy or infection if the child has unexplained highly elevated C-reactive protein and erythrocyte sedimentation rate, cytopenia, high fever, excessive pain, lymphadenopathy, hepatosplenomegaly, or suspicious imaging findings.
German rheumatologists have developed a clinical score for diagnosis of CNO. A normal blood cell count gets 13 points; symmetric bone lesions 10; lesions with marginal sclerosis 10; a normal body temperature 9; two or more radiologically proven lesions 7; a C-reactive protein of 1 mg/dL or greater 6; and vertebral, clavicular, or sternal lesions 8. A score of 39 points or more out of a possible 63 had a 97% positive predictive value for CNO in a retrospective study of 224 children with CNO, proven bacterial osteomyelitis, or malignant bone tumors. A score of 28 points or less had a 97% negative predictive value for CNO. An indeterminate score of 29-38 warrants close monitoring.
The scoring system hasn’t been validated, but most pediatric rheumatologists agree that it’s useful, according to Dr. Stevens.
The Childhood Arthritis and Rheumatology Research Alliance (CARRA) is in the process of developing standardized diagnostic and classification criteria and treatment plans for CNO. Dr. Zhao was first author of a CARRA consensus treatment plan for CNO refractory to NSAID monotherapy. The plan for the first 12 months includes three options: methotrexate or sulfasalazine, TNF inhibitors with or without methotrexate, and bisphosphonates.
“The main point of this is you try a medicine and then wait 3 months. If they’re not responding then, switch medicines or add another drug. Monitor every 3 months based upon pain,” she said.
Dr. Stevens reported research collaborations with Kineta and Seattle Genetics in addition to her employment at Janssen Pharmaceuticals.
EXPERT ANALYSIS FROM RWCS 2020
Rheumatologists to share knowledge in COVID-19 patient-centered registry
Rheumatologists the world over are joining forces to create a COVID-19 rheumatology registry designed to help both patients and providers learn from each other regarding management of rheumatologic diseases and risk of infection among patients who are commonly on chronic immunosuppressive medications.
The COVID-19 Global Rheumatology Alliance, a consortium supported by more than 50 major clinical societies and foundations, quickly grew from messages on social media platforms to a multinational group focused on the common goal of helping to “guide rheumatology clinicians in assessing and treating patients with rheumatologic disease and in evaluating the risk of infection in patients on immunosuppression.”
As of this writing, the rheumatology registry is still being assembled, and organizers are currently seeking approvals from various authorities. As of March 17, 2020, the Institutional Review Board (IRB) at the University of California, San Francisco, has determined that the registry is exempt from IRB approval requirements, a finding that should apply elsewhere in the United States, according to the registry website.
When it is fully up and running, clinicians will be able to report to the secure website on any and all cases of patients with rheumatologic disorders who present with COVID-19 of any severity, including patients with mild disease or asymptomatic patients who test positive.
“We are aiming for 5 to 10 minutes to input the data. We don’t want to drag them away from their clinical duties too much, but if clinicians are able to spare a few minutes to put in details about a patient, then that’s going to help build our knowledge and it’s going to help them with other patients,” said Philip Robinson, MBChB, associate professor of medicine at the University of Queensland in Brisbane, Australia, and the chief architect of the registry.
The data will be deindentified, with no protected health care information required or included, and made available to the global rheumatology community, but the registry will not offer clinical advice, Dr. Robinson said in an interview.
“This is observational data, it’s not randomized, but our approach is that some data is better than no data,” he said.
He also cautioned that the data will need careful interpretation, because information about patients with mild symptoms may offer false reassurances about the severity or extent of infection.
“For example, the patients with severe cases may be in the ICU, and can’t tell their doctors that they’re on methotrexate, so you can see how we need to be really careful about the messages from that data and not misinterpret it,” he said.
The COVID-19 rheumatology registry was inspired by a similar effort in the gastroenterology community, the Surveillance Epidemiology of Coronavirus Under Research Exclusion (SECURE-IBD) registry. Patients with inflammatory bowel disease are often treated with immunosuppressive biologic agents familiar to the rheumatology community, such as infliximab (Remicade and biosimilars) and adalimumab (Humira and biosimilars), and methotrexate.
Rheumatologists the world over are joining forces to create a COVID-19 rheumatology registry designed to help both patients and providers learn from each other regarding management of rheumatologic diseases and risk of infection among patients who are commonly on chronic immunosuppressive medications.
The COVID-19 Global Rheumatology Alliance, a consortium supported by more than 50 major clinical societies and foundations, quickly grew from messages on social media platforms to a multinational group focused on the common goal of helping to “guide rheumatology clinicians in assessing and treating patients with rheumatologic disease and in evaluating the risk of infection in patients on immunosuppression.”
As of this writing, the rheumatology registry is still being assembled, and organizers are currently seeking approvals from various authorities. As of March 17, 2020, the Institutional Review Board (IRB) at the University of California, San Francisco, has determined that the registry is exempt from IRB approval requirements, a finding that should apply elsewhere in the United States, according to the registry website.
When it is fully up and running, clinicians will be able to report to the secure website on any and all cases of patients with rheumatologic disorders who present with COVID-19 of any severity, including patients with mild disease or asymptomatic patients who test positive.
“We are aiming for 5 to 10 minutes to input the data. We don’t want to drag them away from their clinical duties too much, but if clinicians are able to spare a few minutes to put in details about a patient, then that’s going to help build our knowledge and it’s going to help them with other patients,” said Philip Robinson, MBChB, associate professor of medicine at the University of Queensland in Brisbane, Australia, and the chief architect of the registry.
The data will be deindentified, with no protected health care information required or included, and made available to the global rheumatology community, but the registry will not offer clinical advice, Dr. Robinson said in an interview.
“This is observational data, it’s not randomized, but our approach is that some data is better than no data,” he said.
He also cautioned that the data will need careful interpretation, because information about patients with mild symptoms may offer false reassurances about the severity or extent of infection.
“For example, the patients with severe cases may be in the ICU, and can’t tell their doctors that they’re on methotrexate, so you can see how we need to be really careful about the messages from that data and not misinterpret it,” he said.
The COVID-19 rheumatology registry was inspired by a similar effort in the gastroenterology community, the Surveillance Epidemiology of Coronavirus Under Research Exclusion (SECURE-IBD) registry. Patients with inflammatory bowel disease are often treated with immunosuppressive biologic agents familiar to the rheumatology community, such as infliximab (Remicade and biosimilars) and adalimumab (Humira and biosimilars), and methotrexate.
Rheumatologists the world over are joining forces to create a COVID-19 rheumatology registry designed to help both patients and providers learn from each other regarding management of rheumatologic diseases and risk of infection among patients who are commonly on chronic immunosuppressive medications.
The COVID-19 Global Rheumatology Alliance, a consortium supported by more than 50 major clinical societies and foundations, quickly grew from messages on social media platforms to a multinational group focused on the common goal of helping to “guide rheumatology clinicians in assessing and treating patients with rheumatologic disease and in evaluating the risk of infection in patients on immunosuppression.”
As of this writing, the rheumatology registry is still being assembled, and organizers are currently seeking approvals from various authorities. As of March 17, 2020, the Institutional Review Board (IRB) at the University of California, San Francisco, has determined that the registry is exempt from IRB approval requirements, a finding that should apply elsewhere in the United States, according to the registry website.
When it is fully up and running, clinicians will be able to report to the secure website on any and all cases of patients with rheumatologic disorders who present with COVID-19 of any severity, including patients with mild disease or asymptomatic patients who test positive.
“We are aiming for 5 to 10 minutes to input the data. We don’t want to drag them away from their clinical duties too much, but if clinicians are able to spare a few minutes to put in details about a patient, then that’s going to help build our knowledge and it’s going to help them with other patients,” said Philip Robinson, MBChB, associate professor of medicine at the University of Queensland in Brisbane, Australia, and the chief architect of the registry.
The data will be deindentified, with no protected health care information required or included, and made available to the global rheumatology community, but the registry will not offer clinical advice, Dr. Robinson said in an interview.
“This is observational data, it’s not randomized, but our approach is that some data is better than no data,” he said.
He also cautioned that the data will need careful interpretation, because information about patients with mild symptoms may offer false reassurances about the severity or extent of infection.
“For example, the patients with severe cases may be in the ICU, and can’t tell their doctors that they’re on methotrexate, so you can see how we need to be really careful about the messages from that data and not misinterpret it,” he said.
The COVID-19 rheumatology registry was inspired by a similar effort in the gastroenterology community, the Surveillance Epidemiology of Coronavirus Under Research Exclusion (SECURE-IBD) registry. Patients with inflammatory bowel disease are often treated with immunosuppressive biologic agents familiar to the rheumatology community, such as infliximab (Remicade and biosimilars) and adalimumab (Humira and biosimilars), and methotrexate.
Inactivated flu vaccine succeeds among autoimmune rheumatic disease patients
Use of the inactivated influenza vaccine by adults with autoimmune rheumatic diseases significantly reduced their risk of influenza-like illness, hospitalization for pneumonia and chronic obstructive pulmonary disease, and death from pneumonia, according to findings from an observational study of more than 30,000 patients in the U.K. Clinical Practice Research Datalink.
Although the inactivated vaccine has been recommended for patients with autoimmune rheumatic diseases (AIRDs), including rheumatoid arthritis and spondyloarthritis, the vaccine’s impact on patient outcomes including pneumonia, hospitalization, and death has not been well studied, wrote Georgina Nakafero, PhD, of the University of Nottingham, England, and colleagues.
In a study published in Rheumatology, the researchers identified 30,788 adults with AIRDs from the longitudinal Clinical Practice Research Datalink database in the United Kingdom. Of these, 66% were women, 76% had rheumatoid arthritis, and 61% had been prescribed methotrexate. The study included a total of 125,034 flu cycles between 2006 and 2009 and between 2010 and 2015.
Overall, vaccination with the inactivated influenza vaccine (IIV) reduced the risk of primary care consultation for influenza-like illness (adjusted odds ratio, 0.70), hospitalization for pneumonia (aOR, 0.61), exacerbation of chronic obstructive pulmonary disease (aOR, 0.67), and death caused by pneumonia (aOR, 0.48) in the study population. In a propensity score–adjusted analysis, only protection from influenza-like illness lost statistical significance.
In addition, vaccination was associated with a reduction in all-cause mortality among AIRDs patients, but restricting the outcomes to the active influenza periods may have confounded this result, the researchers said.
The study findings were limited by several factors including observational design, the use of a single vaccine efficacy estimate for each outcome, potential missed vaccination cycles, and potential confounding by indication and healthy user bias that could inflate the vaccine effectiveness, the researchers noted. However, the results were strengthened by the large sample size, including a range of AIRDs, and the use of both diagnostic and prescription codes, they said.
“The findings of this study, together with the results of our previous study demonstrating the safety of IIV in people with AIRDs, provides evidence to promote seasonal flu vaccination in this population,” they concluded. They still emphasized that randomized, controlled trials are needed for an assessment of vaccine efficacy.
The study was supported by Versus Arthritis and the National Institute of Health Research. Lead author Dr. Nakafero had no financial conflicts to disclose. Several coauthors disclosed relationships with companies, including AstraZeneca, Roche, and Pfizer.
SOURCE: Nakafero G et al. Rheumatology. 2020 Mar 11. doi: 10.1093/rheumatology/keaa078.
Use of the inactivated influenza vaccine by adults with autoimmune rheumatic diseases significantly reduced their risk of influenza-like illness, hospitalization for pneumonia and chronic obstructive pulmonary disease, and death from pneumonia, according to findings from an observational study of more than 30,000 patients in the U.K. Clinical Practice Research Datalink.
Although the inactivated vaccine has been recommended for patients with autoimmune rheumatic diseases (AIRDs), including rheumatoid arthritis and spondyloarthritis, the vaccine’s impact on patient outcomes including pneumonia, hospitalization, and death has not been well studied, wrote Georgina Nakafero, PhD, of the University of Nottingham, England, and colleagues.
In a study published in Rheumatology, the researchers identified 30,788 adults with AIRDs from the longitudinal Clinical Practice Research Datalink database in the United Kingdom. Of these, 66% were women, 76% had rheumatoid arthritis, and 61% had been prescribed methotrexate. The study included a total of 125,034 flu cycles between 2006 and 2009 and between 2010 and 2015.
Overall, vaccination with the inactivated influenza vaccine (IIV) reduced the risk of primary care consultation for influenza-like illness (adjusted odds ratio, 0.70), hospitalization for pneumonia (aOR, 0.61), exacerbation of chronic obstructive pulmonary disease (aOR, 0.67), and death caused by pneumonia (aOR, 0.48) in the study population. In a propensity score–adjusted analysis, only protection from influenza-like illness lost statistical significance.
In addition, vaccination was associated with a reduction in all-cause mortality among AIRDs patients, but restricting the outcomes to the active influenza periods may have confounded this result, the researchers said.
The study findings were limited by several factors including observational design, the use of a single vaccine efficacy estimate for each outcome, potential missed vaccination cycles, and potential confounding by indication and healthy user bias that could inflate the vaccine effectiveness, the researchers noted. However, the results were strengthened by the large sample size, including a range of AIRDs, and the use of both diagnostic and prescription codes, they said.
“The findings of this study, together with the results of our previous study demonstrating the safety of IIV in people with AIRDs, provides evidence to promote seasonal flu vaccination in this population,” they concluded. They still emphasized that randomized, controlled trials are needed for an assessment of vaccine efficacy.
The study was supported by Versus Arthritis and the National Institute of Health Research. Lead author Dr. Nakafero had no financial conflicts to disclose. Several coauthors disclosed relationships with companies, including AstraZeneca, Roche, and Pfizer.
SOURCE: Nakafero G et al. Rheumatology. 2020 Mar 11. doi: 10.1093/rheumatology/keaa078.
Use of the inactivated influenza vaccine by adults with autoimmune rheumatic diseases significantly reduced their risk of influenza-like illness, hospitalization for pneumonia and chronic obstructive pulmonary disease, and death from pneumonia, according to findings from an observational study of more than 30,000 patients in the U.K. Clinical Practice Research Datalink.
Although the inactivated vaccine has been recommended for patients with autoimmune rheumatic diseases (AIRDs), including rheumatoid arthritis and spondyloarthritis, the vaccine’s impact on patient outcomes including pneumonia, hospitalization, and death has not been well studied, wrote Georgina Nakafero, PhD, of the University of Nottingham, England, and colleagues.
In a study published in Rheumatology, the researchers identified 30,788 adults with AIRDs from the longitudinal Clinical Practice Research Datalink database in the United Kingdom. Of these, 66% were women, 76% had rheumatoid arthritis, and 61% had been prescribed methotrexate. The study included a total of 125,034 flu cycles between 2006 and 2009 and between 2010 and 2015.
Overall, vaccination with the inactivated influenza vaccine (IIV) reduced the risk of primary care consultation for influenza-like illness (adjusted odds ratio, 0.70), hospitalization for pneumonia (aOR, 0.61), exacerbation of chronic obstructive pulmonary disease (aOR, 0.67), and death caused by pneumonia (aOR, 0.48) in the study population. In a propensity score–adjusted analysis, only protection from influenza-like illness lost statistical significance.
In addition, vaccination was associated with a reduction in all-cause mortality among AIRDs patients, but restricting the outcomes to the active influenza periods may have confounded this result, the researchers said.
The study findings were limited by several factors including observational design, the use of a single vaccine efficacy estimate for each outcome, potential missed vaccination cycles, and potential confounding by indication and healthy user bias that could inflate the vaccine effectiveness, the researchers noted. However, the results were strengthened by the large sample size, including a range of AIRDs, and the use of both diagnostic and prescription codes, they said.
“The findings of this study, together with the results of our previous study demonstrating the safety of IIV in people with AIRDs, provides evidence to promote seasonal flu vaccination in this population,” they concluded. They still emphasized that randomized, controlled trials are needed for an assessment of vaccine efficacy.
The study was supported by Versus Arthritis and the National Institute of Health Research. Lead author Dr. Nakafero had no financial conflicts to disclose. Several coauthors disclosed relationships with companies, including AstraZeneca, Roche, and Pfizer.
SOURCE: Nakafero G et al. Rheumatology. 2020 Mar 11. doi: 10.1093/rheumatology/keaa078.
FROM RHEUMATOLOGY
Key clinical point: Adults with autoimmune rheumatic diseases who received the inactivated flu vaccine had lower rates of flu-like illness, hospitalization, and death than did those not vaccinated.
Major finding: Vaccination significantly reduced the risk of flu-like illness, hospitalization for pneumonia or COPD exacerbation, and death from pneumonia by 30%, 39%, 33%, and 52%, respectively.
Study details: The data come from 30,788 adults with AIRD and included 125,034 influenza cycles.
Disclosures: The study was supported by Versus Arthritis and the National Institute of Health Research. Lead author Dr. Nakafero had no financial conflicts to disclose. Several coauthors disclosed relationships with companies, including AstraZeneca, Roche, and Pfizer.
Source: Nakafero G et al. Rheumatology. 2020 Mar 11. doi: 10.1093/rheumatology/keaa078.
African Americans with SLE face increased risk of CVD hospitalizations
PHOENIX – African Americans with systemic lupus erythematosus are more likely to experience recurrent hospitalizations for cardiovascular disease, compared with other racial/ethnic groups, results from a single-state registry study found.
“SLE is an autoimmune disease that causes inflammation affecting multiple organ systems including the cardiovascular system,” Meghan Angley, MPH, said at the Epidemiology and Prevention/Lifestyle and Cardiometabolic Health meeting. “Therefore, individuals with SLE are at risk for early CVD. African Americans represent the racial group at greatest risk for SLE.”
According to Ms. Angley, with the department of epidemiology at Emory University, Atlanta, white women with SLE have CVD associated mortality 12 years earlier than their non-SLE counterparts, while African American women with SLE have CVD-associated mortality 19 years earlier than their non-SLE counterparts. “We know that recurrent hospitalizations for CVD are associated with mortality,” she said. “These represent potential points of identification of high-risk individuals and also points of interventions.”
In order to study racial disparities across recurrent hospitalizations for cardiovascular disease in an SLE population, Ms. Angley and her colleagues drew from the Georgia Lupus Registry, which is a population-based registry of patients with validated SLE in two Georgia counties. They included all cases diagnosed between 2000 and 2004. The registry was linked to records of all inpatient hospitalizations in Georgia between 2000 and 2013. The researchers used ICD-9 codes to identify hospitalizations for coronary heart disease, peripheral artery disease, cerebrovascular disease, and heart failure and used the Prentice-Williams-Peterson model for recurrent time-to-event analysis. Specifically, they looked at the total time scale from the point of diagnosis to each of the subsequent CVD hospitalizations and truncated the number of hospitalizations at three to maintain stable modeling estimates. The analysis was censored at the time of patient death or at the end of 2013 and adjusted for sex and age at diagnosis.
The sample included 417 African Americans with SLE and 149 non–African Americans with the disease. Most (86%) were female, and the non–African American group was slightly more likely to have been diagnosed with SLE after the age of 45 years, compared with the African American group (36% vs. 30%, respectively).
Ms. Angley and her colleagues found that 24% of African Americans had at least one CVD hospitalization, and 14% had at least two, while 13% of non–African Americans had at least one CVD hospitalization, and 5% had at least two. Among those in the African American group, reasons for hospitalizations were congestive heart failure, (58%), cerebrovascular disease (27%), coronary heart disease (18%), and peripheral artery disease (2%). Among those in the non–African American group, reasons for hospitalizations were congestive heart failure (38%), coronary heart disease (38%), cerebrovascular disease (25%), and peripheral artery disease (6%).
Overall, African American race was associated with recurrent hospitalizations (adjusted hazard ratio, 1.9). In an event-specific stratified analysis, the association between African American race and the hazard of recurrence became even more pronounced with each event (hospitalization 1 aHR, 1.2; hospitalization 2 aHR, 1.5; hospitalization 3 aHR, 1.9). The researchers also observed that African Americans were hospitalized sooner, compared with non–African Americans: a median of 3.68 versus 4.61 years for hospitalization 1, 3.73 years versus 5.98 years for hospitalization 2, and 4.84 years versus 8.14 years for hospitalization 3.
“African Americans with SLE are more likely to experience recurrent hospitalizations for CVD,” Ms. Angley concluded at the meeting, which was sponsored by the American Heart Association. “The events occur sooner after diagnosis than in non–African Americans, suggesting that African Americans may be more vulnerable to the cardiovascular complications of SLE. Our next steps include examining potential reasons for these disparities, such as looking at primary care patterns over time, SLE severity over time, and treatment at CVD hospitalizations.”
In an interview, one of the meeting session’s moderators, Sherry-Ann Brown, MD, called for additional research to determine the reasons for disparities that were observed between African Americans with SLE and their non–African American counterparts. “We need to figure out why and address it,” said Dr. Brown, who is a cardiologist and physician-scientist at Mayo Clinic, Rochester, Minn. “We recognize that social determinants of health, such as insurance, socioeconomic factors, and psychosocial factors, can contribute. We need to figure out the additional steps we need to take in order to close that gap.”
Ms. Angley reported having no disclosures. The study was funded by grants from the Centers for Disease Control and Prevention and by the National Institutes of Health.
SOURCE: Angley M et al. Epi/Lifestyle 2020, Abstract 5.
PHOENIX – African Americans with systemic lupus erythematosus are more likely to experience recurrent hospitalizations for cardiovascular disease, compared with other racial/ethnic groups, results from a single-state registry study found.
“SLE is an autoimmune disease that causes inflammation affecting multiple organ systems including the cardiovascular system,” Meghan Angley, MPH, said at the Epidemiology and Prevention/Lifestyle and Cardiometabolic Health meeting. “Therefore, individuals with SLE are at risk for early CVD. African Americans represent the racial group at greatest risk for SLE.”
According to Ms. Angley, with the department of epidemiology at Emory University, Atlanta, white women with SLE have CVD associated mortality 12 years earlier than their non-SLE counterparts, while African American women with SLE have CVD-associated mortality 19 years earlier than their non-SLE counterparts. “We know that recurrent hospitalizations for CVD are associated with mortality,” she said. “These represent potential points of identification of high-risk individuals and also points of interventions.”
In order to study racial disparities across recurrent hospitalizations for cardiovascular disease in an SLE population, Ms. Angley and her colleagues drew from the Georgia Lupus Registry, which is a population-based registry of patients with validated SLE in two Georgia counties. They included all cases diagnosed between 2000 and 2004. The registry was linked to records of all inpatient hospitalizations in Georgia between 2000 and 2013. The researchers used ICD-9 codes to identify hospitalizations for coronary heart disease, peripheral artery disease, cerebrovascular disease, and heart failure and used the Prentice-Williams-Peterson model for recurrent time-to-event analysis. Specifically, they looked at the total time scale from the point of diagnosis to each of the subsequent CVD hospitalizations and truncated the number of hospitalizations at three to maintain stable modeling estimates. The analysis was censored at the time of patient death or at the end of 2013 and adjusted for sex and age at diagnosis.
The sample included 417 African Americans with SLE and 149 non–African Americans with the disease. Most (86%) were female, and the non–African American group was slightly more likely to have been diagnosed with SLE after the age of 45 years, compared with the African American group (36% vs. 30%, respectively).
Ms. Angley and her colleagues found that 24% of African Americans had at least one CVD hospitalization, and 14% had at least two, while 13% of non–African Americans had at least one CVD hospitalization, and 5% had at least two. Among those in the African American group, reasons for hospitalizations were congestive heart failure, (58%), cerebrovascular disease (27%), coronary heart disease (18%), and peripheral artery disease (2%). Among those in the non–African American group, reasons for hospitalizations were congestive heart failure (38%), coronary heart disease (38%), cerebrovascular disease (25%), and peripheral artery disease (6%).
Overall, African American race was associated with recurrent hospitalizations (adjusted hazard ratio, 1.9). In an event-specific stratified analysis, the association between African American race and the hazard of recurrence became even more pronounced with each event (hospitalization 1 aHR, 1.2; hospitalization 2 aHR, 1.5; hospitalization 3 aHR, 1.9). The researchers also observed that African Americans were hospitalized sooner, compared with non–African Americans: a median of 3.68 versus 4.61 years for hospitalization 1, 3.73 years versus 5.98 years for hospitalization 2, and 4.84 years versus 8.14 years for hospitalization 3.
“African Americans with SLE are more likely to experience recurrent hospitalizations for CVD,” Ms. Angley concluded at the meeting, which was sponsored by the American Heart Association. “The events occur sooner after diagnosis than in non–African Americans, suggesting that African Americans may be more vulnerable to the cardiovascular complications of SLE. Our next steps include examining potential reasons for these disparities, such as looking at primary care patterns over time, SLE severity over time, and treatment at CVD hospitalizations.”
In an interview, one of the meeting session’s moderators, Sherry-Ann Brown, MD, called for additional research to determine the reasons for disparities that were observed between African Americans with SLE and their non–African American counterparts. “We need to figure out why and address it,” said Dr. Brown, who is a cardiologist and physician-scientist at Mayo Clinic, Rochester, Minn. “We recognize that social determinants of health, such as insurance, socioeconomic factors, and psychosocial factors, can contribute. We need to figure out the additional steps we need to take in order to close that gap.”
Ms. Angley reported having no disclosures. The study was funded by grants from the Centers for Disease Control and Prevention and by the National Institutes of Health.
SOURCE: Angley M et al. Epi/Lifestyle 2020, Abstract 5.
PHOENIX – African Americans with systemic lupus erythematosus are more likely to experience recurrent hospitalizations for cardiovascular disease, compared with other racial/ethnic groups, results from a single-state registry study found.
“SLE is an autoimmune disease that causes inflammation affecting multiple organ systems including the cardiovascular system,” Meghan Angley, MPH, said at the Epidemiology and Prevention/Lifestyle and Cardiometabolic Health meeting. “Therefore, individuals with SLE are at risk for early CVD. African Americans represent the racial group at greatest risk for SLE.”
According to Ms. Angley, with the department of epidemiology at Emory University, Atlanta, white women with SLE have CVD associated mortality 12 years earlier than their non-SLE counterparts, while African American women with SLE have CVD-associated mortality 19 years earlier than their non-SLE counterparts. “We know that recurrent hospitalizations for CVD are associated with mortality,” she said. “These represent potential points of identification of high-risk individuals and also points of interventions.”
In order to study racial disparities across recurrent hospitalizations for cardiovascular disease in an SLE population, Ms. Angley and her colleagues drew from the Georgia Lupus Registry, which is a population-based registry of patients with validated SLE in two Georgia counties. They included all cases diagnosed between 2000 and 2004. The registry was linked to records of all inpatient hospitalizations in Georgia between 2000 and 2013. The researchers used ICD-9 codes to identify hospitalizations for coronary heart disease, peripheral artery disease, cerebrovascular disease, and heart failure and used the Prentice-Williams-Peterson model for recurrent time-to-event analysis. Specifically, they looked at the total time scale from the point of diagnosis to each of the subsequent CVD hospitalizations and truncated the number of hospitalizations at three to maintain stable modeling estimates. The analysis was censored at the time of patient death or at the end of 2013 and adjusted for sex and age at diagnosis.
The sample included 417 African Americans with SLE and 149 non–African Americans with the disease. Most (86%) were female, and the non–African American group was slightly more likely to have been diagnosed with SLE after the age of 45 years, compared with the African American group (36% vs. 30%, respectively).
Ms. Angley and her colleagues found that 24% of African Americans had at least one CVD hospitalization, and 14% had at least two, while 13% of non–African Americans had at least one CVD hospitalization, and 5% had at least two. Among those in the African American group, reasons for hospitalizations were congestive heart failure, (58%), cerebrovascular disease (27%), coronary heart disease (18%), and peripheral artery disease (2%). Among those in the non–African American group, reasons for hospitalizations were congestive heart failure (38%), coronary heart disease (38%), cerebrovascular disease (25%), and peripheral artery disease (6%).
Overall, African American race was associated with recurrent hospitalizations (adjusted hazard ratio, 1.9). In an event-specific stratified analysis, the association between African American race and the hazard of recurrence became even more pronounced with each event (hospitalization 1 aHR, 1.2; hospitalization 2 aHR, 1.5; hospitalization 3 aHR, 1.9). The researchers also observed that African Americans were hospitalized sooner, compared with non–African Americans: a median of 3.68 versus 4.61 years for hospitalization 1, 3.73 years versus 5.98 years for hospitalization 2, and 4.84 years versus 8.14 years for hospitalization 3.
“African Americans with SLE are more likely to experience recurrent hospitalizations for CVD,” Ms. Angley concluded at the meeting, which was sponsored by the American Heart Association. “The events occur sooner after diagnosis than in non–African Americans, suggesting that African Americans may be more vulnerable to the cardiovascular complications of SLE. Our next steps include examining potential reasons for these disparities, such as looking at primary care patterns over time, SLE severity over time, and treatment at CVD hospitalizations.”
In an interview, one of the meeting session’s moderators, Sherry-Ann Brown, MD, called for additional research to determine the reasons for disparities that were observed between African Americans with SLE and their non–African American counterparts. “We need to figure out why and address it,” said Dr. Brown, who is a cardiologist and physician-scientist at Mayo Clinic, Rochester, Minn. “We recognize that social determinants of health, such as insurance, socioeconomic factors, and psychosocial factors, can contribute. We need to figure out the additional steps we need to take in order to close that gap.”
Ms. Angley reported having no disclosures. The study was funded by grants from the Centers for Disease Control and Prevention and by the National Institutes of Health.
SOURCE: Angley M et al. Epi/Lifestyle 2020, Abstract 5.
REPORTING FROM EPI/LIFESTYLE 2020
High CV event risk seen in SLE patients with ACC/AHA-defined hypertension
, results of a retrospective, single-center investigation suggest.
Risk of atherosclerotic vascular events was increased by 73% for patients with systemic lupus erythematosus (SLE) who sustained a mean blood pressure of 130/80 to 139/89 mm Hg over 2 years in the study, which included 1,532 patients treated at a clinic in Toronto.
Management of hypertension in SLE patients should start early, and should aim to achieve levels below 130/80 mm Hg, according to the investigators, led by Konstantinos Tselios, MD, PhD, of the Centre for Prognosis Studies in the Rheumatic Diseases at the University of Toronto.
“The findings of the present study support that the target BP should be less than 130/80 mm Hg in all patients with lupus in order to minimize their cardiovascular risk,” Dr. Tselios and coauthors said in their study, which appears in Annals of the Rheumatic Diseases.
Despite the limitations inherent in a retrospective, observational study, this work by Dr. Tselios and colleagues may help inform the care of patients with SLE, according to C. Michael Stein, MBChB, professor of medicine at Vanderbilt University in Nashville, Tenn.
“It’s really interesting data that’s important and helps us think in terms of figuring out what may be reasonable to do for a particular patient,” Dr. Stein said in an interview.
Starting antihypertensive management early and aiming at levels below 130/80 mm Hg is a strategy that should be “reasonable” for most patients with SLE, said Dr. Stein, adding that the approach specified in the 2017 American College of Cardiology/American Heart Association (ACC/AHA) hypertension guidelines are appropriate to follow. In those guidelines, the threshold for diagnosis of hypertension was lowered to 130/80 mm Hg.
“You can start with risk factor modification, in terms of losing weight, exercising, stopping alcohol, and decreasing salt in the diet to see if you can get the blood pressure down, though it may come down to drug therapy for many patients, I believe,” Dr. Stein said.
Authors of those 2017 ACC/AHA guidelines made no recommendations for patients with SLE or other connective tissue diseases, despite including a section devoted to specific patient subgroups and comorbidities of interest, Dr. Tselios and coauthors noted in their report.
Management of hypertension in patients with lupus may be “delayed” in patients with blood pressures reaching the current hypertension threshold, according to Dr. Tselios and colleagues, due in part to difficulties in cardiovascular risk calculation in SLE patients, as well as current risk considerations outlined in the guidelines.
“On the basis of the recent guidelines, the patient with typical lupus (young female with no traditional atherosclerotic risk factors) would be considered as a low-risk individual and not offered treatment for a BP of 130-139/80-89 mm Hg,” they said in their report.
Accordingly, Dr. Tselios and colleagues sought to determine whether the new hypertension definition predicted atherosclerotic vascular events, including new-onset angina, acute myocardial infarction, cerebrovascular events, revascularization procedures, heart failure, or peripheral vascular disease requiring angioplasty, in patients with SLE treated at a Canadian clinic.
Their analysis comprised 1,532 patients with SLE who had at least 2 years of follow-up and had no prior atherosclerotic events on record. Over a mean follow-up of nearly 11 years, there were 124 such events documented in those patients.
With a mean follow-up of nearly 11 years, the incidence of atherosclerotic events was 18.9 per 1,000 patient-years for patients with blood pressure ≥ 140/90 mm Hg, 11.5 per 1,000 patient-years for the 130-139/80-89 mm Hg group, and 4.5 per 1,000 patient-years for those with blood pressures of 130/80 mm Hg or lower, with differences that were statistically significant between groups, according to the report.
An adjusted blood pressure of 130-139/80-89 mm Hg over the first 2 years since enrollment in the clinic was independently associated with the occurrence of an atherosclerotic event, with a hazard ratio of 1.73 (95% confidence interval, 1.13-2.69, P = 0.011), according to results of a multivariable analysis.
Those findings support targeting a blood pressure below 130/80 mm Hg in all patients with lupus, according to Dr. Tselios and coauthors.
“It seems reasonable that clinicians should not rely on CV risk calculators in SLE and commence treatment as soon as possible in cases of sustained BP elevation above the threshold of 130/80 mm Hg,” they wrote in their report.
How low to go remains unclear, however, as targeting lower levels of blood pressure might be unsafe in certain groups, such as those SLE patients with prior heart disease or heart failure; nevertheless, recent observational data from non-SLE populations suggest that effective treatment to levels lower than 130/80 mm Hg would “further reduce the incidence of atherosclerotic events in SLE,” the authors said in a discussion of their results.
Dr. Tselios and coauthors said they had no competing interests relative to the study. They reported funding for the University of Toronto Lupus Clinic from the University Health Network, Lou & Marissa Rocca, Mark & Diana Bozzo, and the Lupus Foundation of Ontario.
SOURCE: Tselios K et al. Ann Rheum Dis. 2020 Mar 10. doi: 10.1136/annrheumdis-2019-216764
, results of a retrospective, single-center investigation suggest.
Risk of atherosclerotic vascular events was increased by 73% for patients with systemic lupus erythematosus (SLE) who sustained a mean blood pressure of 130/80 to 139/89 mm Hg over 2 years in the study, which included 1,532 patients treated at a clinic in Toronto.
Management of hypertension in SLE patients should start early, and should aim to achieve levels below 130/80 mm Hg, according to the investigators, led by Konstantinos Tselios, MD, PhD, of the Centre for Prognosis Studies in the Rheumatic Diseases at the University of Toronto.
“The findings of the present study support that the target BP should be less than 130/80 mm Hg in all patients with lupus in order to minimize their cardiovascular risk,” Dr. Tselios and coauthors said in their study, which appears in Annals of the Rheumatic Diseases.
Despite the limitations inherent in a retrospective, observational study, this work by Dr. Tselios and colleagues may help inform the care of patients with SLE, according to C. Michael Stein, MBChB, professor of medicine at Vanderbilt University in Nashville, Tenn.
“It’s really interesting data that’s important and helps us think in terms of figuring out what may be reasonable to do for a particular patient,” Dr. Stein said in an interview.
Starting antihypertensive management early and aiming at levels below 130/80 mm Hg is a strategy that should be “reasonable” for most patients with SLE, said Dr. Stein, adding that the approach specified in the 2017 American College of Cardiology/American Heart Association (ACC/AHA) hypertension guidelines are appropriate to follow. In those guidelines, the threshold for diagnosis of hypertension was lowered to 130/80 mm Hg.
“You can start with risk factor modification, in terms of losing weight, exercising, stopping alcohol, and decreasing salt in the diet to see if you can get the blood pressure down, though it may come down to drug therapy for many patients, I believe,” Dr. Stein said.
Authors of those 2017 ACC/AHA guidelines made no recommendations for patients with SLE or other connective tissue diseases, despite including a section devoted to specific patient subgroups and comorbidities of interest, Dr. Tselios and coauthors noted in their report.
Management of hypertension in patients with lupus may be “delayed” in patients with blood pressures reaching the current hypertension threshold, according to Dr. Tselios and colleagues, due in part to difficulties in cardiovascular risk calculation in SLE patients, as well as current risk considerations outlined in the guidelines.
“On the basis of the recent guidelines, the patient with typical lupus (young female with no traditional atherosclerotic risk factors) would be considered as a low-risk individual and not offered treatment for a BP of 130-139/80-89 mm Hg,” they said in their report.
Accordingly, Dr. Tselios and colleagues sought to determine whether the new hypertension definition predicted atherosclerotic vascular events, including new-onset angina, acute myocardial infarction, cerebrovascular events, revascularization procedures, heart failure, or peripheral vascular disease requiring angioplasty, in patients with SLE treated at a Canadian clinic.
Their analysis comprised 1,532 patients with SLE who had at least 2 years of follow-up and had no prior atherosclerotic events on record. Over a mean follow-up of nearly 11 years, there were 124 such events documented in those patients.
With a mean follow-up of nearly 11 years, the incidence of atherosclerotic events was 18.9 per 1,000 patient-years for patients with blood pressure ≥ 140/90 mm Hg, 11.5 per 1,000 patient-years for the 130-139/80-89 mm Hg group, and 4.5 per 1,000 patient-years for those with blood pressures of 130/80 mm Hg or lower, with differences that were statistically significant between groups, according to the report.
An adjusted blood pressure of 130-139/80-89 mm Hg over the first 2 years since enrollment in the clinic was independently associated with the occurrence of an atherosclerotic event, with a hazard ratio of 1.73 (95% confidence interval, 1.13-2.69, P = 0.011), according to results of a multivariable analysis.
Those findings support targeting a blood pressure below 130/80 mm Hg in all patients with lupus, according to Dr. Tselios and coauthors.
“It seems reasonable that clinicians should not rely on CV risk calculators in SLE and commence treatment as soon as possible in cases of sustained BP elevation above the threshold of 130/80 mm Hg,” they wrote in their report.
How low to go remains unclear, however, as targeting lower levels of blood pressure might be unsafe in certain groups, such as those SLE patients with prior heart disease or heart failure; nevertheless, recent observational data from non-SLE populations suggest that effective treatment to levels lower than 130/80 mm Hg would “further reduce the incidence of atherosclerotic events in SLE,” the authors said in a discussion of their results.
Dr. Tselios and coauthors said they had no competing interests relative to the study. They reported funding for the University of Toronto Lupus Clinic from the University Health Network, Lou & Marissa Rocca, Mark & Diana Bozzo, and the Lupus Foundation of Ontario.
SOURCE: Tselios K et al. Ann Rheum Dis. 2020 Mar 10. doi: 10.1136/annrheumdis-2019-216764
, results of a retrospective, single-center investigation suggest.
Risk of atherosclerotic vascular events was increased by 73% for patients with systemic lupus erythematosus (SLE) who sustained a mean blood pressure of 130/80 to 139/89 mm Hg over 2 years in the study, which included 1,532 patients treated at a clinic in Toronto.
Management of hypertension in SLE patients should start early, and should aim to achieve levels below 130/80 mm Hg, according to the investigators, led by Konstantinos Tselios, MD, PhD, of the Centre for Prognosis Studies in the Rheumatic Diseases at the University of Toronto.
“The findings of the present study support that the target BP should be less than 130/80 mm Hg in all patients with lupus in order to minimize their cardiovascular risk,” Dr. Tselios and coauthors said in their study, which appears in Annals of the Rheumatic Diseases.
Despite the limitations inherent in a retrospective, observational study, this work by Dr. Tselios and colleagues may help inform the care of patients with SLE, according to C. Michael Stein, MBChB, professor of medicine at Vanderbilt University in Nashville, Tenn.
“It’s really interesting data that’s important and helps us think in terms of figuring out what may be reasonable to do for a particular patient,” Dr. Stein said in an interview.
Starting antihypertensive management early and aiming at levels below 130/80 mm Hg is a strategy that should be “reasonable” for most patients with SLE, said Dr. Stein, adding that the approach specified in the 2017 American College of Cardiology/American Heart Association (ACC/AHA) hypertension guidelines are appropriate to follow. In those guidelines, the threshold for diagnosis of hypertension was lowered to 130/80 mm Hg.
“You can start with risk factor modification, in terms of losing weight, exercising, stopping alcohol, and decreasing salt in the diet to see if you can get the blood pressure down, though it may come down to drug therapy for many patients, I believe,” Dr. Stein said.
Authors of those 2017 ACC/AHA guidelines made no recommendations for patients with SLE or other connective tissue diseases, despite including a section devoted to specific patient subgroups and comorbidities of interest, Dr. Tselios and coauthors noted in their report.
Management of hypertension in patients with lupus may be “delayed” in patients with blood pressures reaching the current hypertension threshold, according to Dr. Tselios and colleagues, due in part to difficulties in cardiovascular risk calculation in SLE patients, as well as current risk considerations outlined in the guidelines.
“On the basis of the recent guidelines, the patient with typical lupus (young female with no traditional atherosclerotic risk factors) would be considered as a low-risk individual and not offered treatment for a BP of 130-139/80-89 mm Hg,” they said in their report.
Accordingly, Dr. Tselios and colleagues sought to determine whether the new hypertension definition predicted atherosclerotic vascular events, including new-onset angina, acute myocardial infarction, cerebrovascular events, revascularization procedures, heart failure, or peripheral vascular disease requiring angioplasty, in patients with SLE treated at a Canadian clinic.
Their analysis comprised 1,532 patients with SLE who had at least 2 years of follow-up and had no prior atherosclerotic events on record. Over a mean follow-up of nearly 11 years, there were 124 such events documented in those patients.
With a mean follow-up of nearly 11 years, the incidence of atherosclerotic events was 18.9 per 1,000 patient-years for patients with blood pressure ≥ 140/90 mm Hg, 11.5 per 1,000 patient-years for the 130-139/80-89 mm Hg group, and 4.5 per 1,000 patient-years for those with blood pressures of 130/80 mm Hg or lower, with differences that were statistically significant between groups, according to the report.
An adjusted blood pressure of 130-139/80-89 mm Hg over the first 2 years since enrollment in the clinic was independently associated with the occurrence of an atherosclerotic event, with a hazard ratio of 1.73 (95% confidence interval, 1.13-2.69, P = 0.011), according to results of a multivariable analysis.
Those findings support targeting a blood pressure below 130/80 mm Hg in all patients with lupus, according to Dr. Tselios and coauthors.
“It seems reasonable that clinicians should not rely on CV risk calculators in SLE and commence treatment as soon as possible in cases of sustained BP elevation above the threshold of 130/80 mm Hg,” they wrote in their report.
How low to go remains unclear, however, as targeting lower levels of blood pressure might be unsafe in certain groups, such as those SLE patients with prior heart disease or heart failure; nevertheless, recent observational data from non-SLE populations suggest that effective treatment to levels lower than 130/80 mm Hg would “further reduce the incidence of atherosclerotic events in SLE,” the authors said in a discussion of their results.
Dr. Tselios and coauthors said they had no competing interests relative to the study. They reported funding for the University of Toronto Lupus Clinic from the University Health Network, Lou & Marissa Rocca, Mark & Diana Bozzo, and the Lupus Foundation of Ontario.
SOURCE: Tselios K et al. Ann Rheum Dis. 2020 Mar 10. doi: 10.1136/annrheumdis-2019-216764
FROM ANNALS OF THE RHEUMATIC DISEASES
Fracture liaison services confer benefit on recurrent fracture risk
Implementation of fracture liaison services (FLS) at two Swedish hospitals was associated with an 18% reduction of recurrent fracture over a median follow-up of 2.2 years, results from an observational cohort study found.
“Patients receiving fracture care within an FLS have higher rates of [bone mineral density] testing, treatment initiation and better adherence,” first author Kristian F. Axelsson, MD, and colleagues wrote in a study published in the Journal of Bone and Mineral Research. “However, the evidence regarding FLS and association to reduced risk of recurrent fracture is insufficient, consisting of smaller studies, studies with short follow-up time, and studies with high risk of various biases.”
Dr. Axelsson, of the department of orthopedic surgery at Skaraborg Hospital, Skövde, Sweden, and colleagues used electronic patient records from four hospitals in Western Sweden to identify all patients aged 50 years or older with a major osteoporotic fracture – defined as a fracture of the wrist, upper arm, hip, vertebra, or pelvis – between 2012 and 2017. The study population consisted of 15,449 patients from two hospitals with FLS and 5,634 patients from two hospitals with no FLS. The researchers used multivariable Cox models to compare all patients with a major osteoporotic fracture during the FLS period with all patients with a major osteoporotic fracture prior to the FLS implementation. The FLS hospitals and non-FLS hospitals were analyzed separately using the same methodology.
The mean age of patients was 74 years, 76% were female, and the most common index fracture site was the wrist (42%). In the hospitals with FLS, the researchers observed 1,247 recurrent fractures during a median follow-up time of 2.2 years. In an unadjusted Cox model, the risk of recurrent fracture was 18% lower in the FLS period, compared with the control period (hazard ratio, 0.82; P = .001). This corresponded to a 3-year number needed to screen of 61, and did not change after adjustment for clinical risk factors. In the non-FLS hospitals, no change in recurrent fracture rate was observed.
Osteoporosis medication treatment rates after fracture did not differ between the FLS and non-FLS hospitals, prior to FLS implementation (14.7% vs. 13.3%, respectively; P = .10). However, following FLS implementation, a larger proportion of fracture patients were treated at the FLS hospitals, compared with those at the non-FLS hospitals (28% vs. 12.9%; P less than .001).
“Our study is the largest yet, including both historic controls and controls at nearby hospitals without implementations of fracture liaison services,” one of the study authors, Mattias Lorentzon, MD, said in an interview. “We were able to rule out temporal trends in refracture risk and show that, [in] patients who had an index fracture at a hospital with an FLS, the refracture rate was lower than for patients who had an index fracture before the FLS was started, indicating that FLS reduce the risk of recurrent fracture. No such trends were observed in hospitals without FLS during the same time period.”
Dr. Lorentzon, head of geriatric medicine at Sahlgrenska University Hospital, Mölndal, Sweden, said that FLS implementation “led to a large increase in the use of osteoporosis medication, which we believe is the reason for the reduction in recurrent fracture risk observed. We believe that our results provide solid evidence that FLS implementation can reduce the rate of recurrent fractures, suggesting that all hospitals treating fracture patients should have fracture liaison services.”
In an interview, Stuart L. Silverman, MD, said that the study adds to compelling data on the efficacy and need for patients with clinical fracture to have case management by a FLS. “We recognize that near term risk is substantial in the year following a fracture,” said Dr. Silverman, who is clinical professor of medicine at Cedars-Sinai Medical Center and the University of California, Los Angeles, and is not affiliated with the Swedish study. “For example, the risk of a subsequent fracture after hip fracture is 8.3%, which is similar to the risk of subsequent acute myocardial infarction after an initial acute MI. However, only 23% of patients receive osteoporosis medication after a hip fracture. Yet a fracture is to osteoporosis what an acute MI is to cardiovascular disease. We recognize that men and women age 65 years and older who have suffered a hip or vertebral fracture should be evaluated for treatment, as this subpopulation is at high risk for a second fracture and evidence supporting treatment efficacy is robust. We need a multidisciplinary clinical system which includes case management such as a fracture liaison service. We know FLS can reduce hip fracture rate in a closed system such as Kaiser by over 40%. This manuscript addresses the utility of a FLS in terms of reducing risk of future fracture.”
The researchers acknowledged certain limitations of the study, including its observational design and the fact that patients prior to the FLS period were fewer and had longer follow-up time, compared with patients during the FLS period.
The study was funded by the Swedish Research Council and by grants from the Sahlgrenska University Hospital. Dr. Axelsson reported that he has received lecture fees from Lilly, Meda/Mylan, and Amgen. Dr. Lorentzon has received lecture fees from Amgen, Lilly, UCB, Radius Health, Meda, GE-Lunar, and Santax Medico/Hologic. The other coauthors reported having no financial disclosures. Dr. Silverman reported that he is a member of the speakers’ bureaus for Amgen and Radius. He is also a consultant for Lilly, Pfizer, and Amgen and has received research grants from Radius and Amgen.
SOURCE: Axelsson K et al. J Bone Min Res. 2020 Feb 25. doi: 10.1002/jbmr.3990.
Implementation of fracture liaison services (FLS) at two Swedish hospitals was associated with an 18% reduction of recurrent fracture over a median follow-up of 2.2 years, results from an observational cohort study found.
“Patients receiving fracture care within an FLS have higher rates of [bone mineral density] testing, treatment initiation and better adherence,” first author Kristian F. Axelsson, MD, and colleagues wrote in a study published in the Journal of Bone and Mineral Research. “However, the evidence regarding FLS and association to reduced risk of recurrent fracture is insufficient, consisting of smaller studies, studies with short follow-up time, and studies with high risk of various biases.”
Dr. Axelsson, of the department of orthopedic surgery at Skaraborg Hospital, Skövde, Sweden, and colleagues used electronic patient records from four hospitals in Western Sweden to identify all patients aged 50 years or older with a major osteoporotic fracture – defined as a fracture of the wrist, upper arm, hip, vertebra, or pelvis – between 2012 and 2017. The study population consisted of 15,449 patients from two hospitals with FLS and 5,634 patients from two hospitals with no FLS. The researchers used multivariable Cox models to compare all patients with a major osteoporotic fracture during the FLS period with all patients with a major osteoporotic fracture prior to the FLS implementation. The FLS hospitals and non-FLS hospitals were analyzed separately using the same methodology.
The mean age of patients was 74 years, 76% were female, and the most common index fracture site was the wrist (42%). In the hospitals with FLS, the researchers observed 1,247 recurrent fractures during a median follow-up time of 2.2 years. In an unadjusted Cox model, the risk of recurrent fracture was 18% lower in the FLS period, compared with the control period (hazard ratio, 0.82; P = .001). This corresponded to a 3-year number needed to screen of 61, and did not change after adjustment for clinical risk factors. In the non-FLS hospitals, no change in recurrent fracture rate was observed.
Osteoporosis medication treatment rates after fracture did not differ between the FLS and non-FLS hospitals, prior to FLS implementation (14.7% vs. 13.3%, respectively; P = .10). However, following FLS implementation, a larger proportion of fracture patients were treated at the FLS hospitals, compared with those at the non-FLS hospitals (28% vs. 12.9%; P less than .001).
“Our study is the largest yet, including both historic controls and controls at nearby hospitals without implementations of fracture liaison services,” one of the study authors, Mattias Lorentzon, MD, said in an interview. “We were able to rule out temporal trends in refracture risk and show that, [in] patients who had an index fracture at a hospital with an FLS, the refracture rate was lower than for patients who had an index fracture before the FLS was started, indicating that FLS reduce the risk of recurrent fracture. No such trends were observed in hospitals without FLS during the same time period.”
Dr. Lorentzon, head of geriatric medicine at Sahlgrenska University Hospital, Mölndal, Sweden, said that FLS implementation “led to a large increase in the use of osteoporosis medication, which we believe is the reason for the reduction in recurrent fracture risk observed. We believe that our results provide solid evidence that FLS implementation can reduce the rate of recurrent fractures, suggesting that all hospitals treating fracture patients should have fracture liaison services.”
In an interview, Stuart L. Silverman, MD, said that the study adds to compelling data on the efficacy and need for patients with clinical fracture to have case management by a FLS. “We recognize that near term risk is substantial in the year following a fracture,” said Dr. Silverman, who is clinical professor of medicine at Cedars-Sinai Medical Center and the University of California, Los Angeles, and is not affiliated with the Swedish study. “For example, the risk of a subsequent fracture after hip fracture is 8.3%, which is similar to the risk of subsequent acute myocardial infarction after an initial acute MI. However, only 23% of patients receive osteoporosis medication after a hip fracture. Yet a fracture is to osteoporosis what an acute MI is to cardiovascular disease. We recognize that men and women age 65 years and older who have suffered a hip or vertebral fracture should be evaluated for treatment, as this subpopulation is at high risk for a second fracture and evidence supporting treatment efficacy is robust. We need a multidisciplinary clinical system which includes case management such as a fracture liaison service. We know FLS can reduce hip fracture rate in a closed system such as Kaiser by over 40%. This manuscript addresses the utility of a FLS in terms of reducing risk of future fracture.”
The researchers acknowledged certain limitations of the study, including its observational design and the fact that patients prior to the FLS period were fewer and had longer follow-up time, compared with patients during the FLS period.
The study was funded by the Swedish Research Council and by grants from the Sahlgrenska University Hospital. Dr. Axelsson reported that he has received lecture fees from Lilly, Meda/Mylan, and Amgen. Dr. Lorentzon has received lecture fees from Amgen, Lilly, UCB, Radius Health, Meda, GE-Lunar, and Santax Medico/Hologic. The other coauthors reported having no financial disclosures. Dr. Silverman reported that he is a member of the speakers’ bureaus for Amgen and Radius. He is also a consultant for Lilly, Pfizer, and Amgen and has received research grants from Radius and Amgen.
SOURCE: Axelsson K et al. J Bone Min Res. 2020 Feb 25. doi: 10.1002/jbmr.3990.
Implementation of fracture liaison services (FLS) at two Swedish hospitals was associated with an 18% reduction of recurrent fracture over a median follow-up of 2.2 years, results from an observational cohort study found.
“Patients receiving fracture care within an FLS have higher rates of [bone mineral density] testing, treatment initiation and better adherence,” first author Kristian F. Axelsson, MD, and colleagues wrote in a study published in the Journal of Bone and Mineral Research. “However, the evidence regarding FLS and association to reduced risk of recurrent fracture is insufficient, consisting of smaller studies, studies with short follow-up time, and studies with high risk of various biases.”
Dr. Axelsson, of the department of orthopedic surgery at Skaraborg Hospital, Skövde, Sweden, and colleagues used electronic patient records from four hospitals in Western Sweden to identify all patients aged 50 years or older with a major osteoporotic fracture – defined as a fracture of the wrist, upper arm, hip, vertebra, or pelvis – between 2012 and 2017. The study population consisted of 15,449 patients from two hospitals with FLS and 5,634 patients from two hospitals with no FLS. The researchers used multivariable Cox models to compare all patients with a major osteoporotic fracture during the FLS period with all patients with a major osteoporotic fracture prior to the FLS implementation. The FLS hospitals and non-FLS hospitals were analyzed separately using the same methodology.
The mean age of patients was 74 years, 76% were female, and the most common index fracture site was the wrist (42%). In the hospitals with FLS, the researchers observed 1,247 recurrent fractures during a median follow-up time of 2.2 years. In an unadjusted Cox model, the risk of recurrent fracture was 18% lower in the FLS period, compared with the control period (hazard ratio, 0.82; P = .001). This corresponded to a 3-year number needed to screen of 61, and did not change after adjustment for clinical risk factors. In the non-FLS hospitals, no change in recurrent fracture rate was observed.
Osteoporosis medication treatment rates after fracture did not differ between the FLS and non-FLS hospitals, prior to FLS implementation (14.7% vs. 13.3%, respectively; P = .10). However, following FLS implementation, a larger proportion of fracture patients were treated at the FLS hospitals, compared with those at the non-FLS hospitals (28% vs. 12.9%; P less than .001).
“Our study is the largest yet, including both historic controls and controls at nearby hospitals without implementations of fracture liaison services,” one of the study authors, Mattias Lorentzon, MD, said in an interview. “We were able to rule out temporal trends in refracture risk and show that, [in] patients who had an index fracture at a hospital with an FLS, the refracture rate was lower than for patients who had an index fracture before the FLS was started, indicating that FLS reduce the risk of recurrent fracture. No such trends were observed in hospitals without FLS during the same time period.”
Dr. Lorentzon, head of geriatric medicine at Sahlgrenska University Hospital, Mölndal, Sweden, said that FLS implementation “led to a large increase in the use of osteoporosis medication, which we believe is the reason for the reduction in recurrent fracture risk observed. We believe that our results provide solid evidence that FLS implementation can reduce the rate of recurrent fractures, suggesting that all hospitals treating fracture patients should have fracture liaison services.”
In an interview, Stuart L. Silverman, MD, said that the study adds to compelling data on the efficacy and need for patients with clinical fracture to have case management by a FLS. “We recognize that near term risk is substantial in the year following a fracture,” said Dr. Silverman, who is clinical professor of medicine at Cedars-Sinai Medical Center and the University of California, Los Angeles, and is not affiliated with the Swedish study. “For example, the risk of a subsequent fracture after hip fracture is 8.3%, which is similar to the risk of subsequent acute myocardial infarction after an initial acute MI. However, only 23% of patients receive osteoporosis medication after a hip fracture. Yet a fracture is to osteoporosis what an acute MI is to cardiovascular disease. We recognize that men and women age 65 years and older who have suffered a hip or vertebral fracture should be evaluated for treatment, as this subpopulation is at high risk for a second fracture and evidence supporting treatment efficacy is robust. We need a multidisciplinary clinical system which includes case management such as a fracture liaison service. We know FLS can reduce hip fracture rate in a closed system such as Kaiser by over 40%. This manuscript addresses the utility of a FLS in terms of reducing risk of future fracture.”
The researchers acknowledged certain limitations of the study, including its observational design and the fact that patients prior to the FLS period were fewer and had longer follow-up time, compared with patients during the FLS period.
The study was funded by the Swedish Research Council and by grants from the Sahlgrenska University Hospital. Dr. Axelsson reported that he has received lecture fees from Lilly, Meda/Mylan, and Amgen. Dr. Lorentzon has received lecture fees from Amgen, Lilly, UCB, Radius Health, Meda, GE-Lunar, and Santax Medico/Hologic. The other coauthors reported having no financial disclosures. Dr. Silverman reported that he is a member of the speakers’ bureaus for Amgen and Radius. He is also a consultant for Lilly, Pfizer, and Amgen and has received research grants from Radius and Amgen.
SOURCE: Axelsson K et al. J Bone Min Res. 2020 Feb 25. doi: 10.1002/jbmr.3990.
FROM THE JOURNAL OF BONE AND MINERAL RESEARCH