User login
Official Newspaper of the American College of Surgeons
Topical Fluorocarbon Speeds Tattoo Removal Process
ATLANTA – Applying the topical fluorocarbon perfluorodecalin prior to Q-switched laser treatment for tattoo removal allows for immediate retreatment of the tattoo, thereby improving results while decreasing overall treatment time, according to Dr. Roy Geronemus.
The findings have important implications for improving outcomes and patient satisfaction, given that tattoo removal can require 10-20 sessions, depending on factors such as the age and colors of the tattoo, and that tattoos – and thus tattoo removal – continue to increase in popularity, he said. "For a busy practice or impatient patients like we have in New York, this has been a nice advance," Dr. Geronemus said at the annual meeting of the American Society for Dermatologic Surgery.
The approach builds on the "R20 technique" described earlier this year in a study published in the Journal of the American Academy of Dermatology. R20 involves the use of multiple treatment passes that are made at 20-minute intervals.
Typically, after an initial pass, tiny white bubbles form in the superficial papillary dermis, appearing as a whitening of the skin. Retreatment while these bubbles are present elicits a limited reaction.
The R20 technique was developed when investigators found that the bubbles disappear after 20 minutes, and, thus, tested the technique in a study of 12 adults. The patients were randomized to a single treatment pass with a Q-switched alexandrite laser (5.5 J/cm2, 755 nm, 100-nanosecond pulse duration, 3-mm spot size) or to four passes at 20 minute intervals.
The first treatment caused an immediate whitening reaction, but little or no whitening occurred after subsequent passes at 20-minute intervals. However, at 90-day follow-up, significant improvement was seen in the R20 group, compared with the single-treatment group, and light microscopy demonstrated greater dispersion of tattoo ink with the R20 approach. (J. Am. Acad. Dermatol. 2012;66:271-7).
Despite the increased efficacy using this approach, the time required to complete four passes at 20-minute intervals makes it impractical in the clinical setting, said Dr. Geronemus, a dermatologist in private practice in New York.
"So with this idea in mind, we began to look at a concept that would allow us to re-treat tattoos immediately without waiting 20 minutes," he said, explaining that topical perfluorodecalin helps dissolve the gas seen after the application of the Q-switched laser and speeds the resolution of the whitening.
"Rather than waiting 20 minutes, the gas dissolves almost immediately, allowing you to re-treat, and we’re now re-treating three or four times in a matter of minutes rather than waiting the 80 minutes that the R20 technique would take for a four-time treatment session," he said.
In his experience, results with perfluorodecalin are comparable to those seen with the R20 technique – but with greater convenience for the patient.
His observations were confirmed on optical coherence tomography scanning, which demonstrated that cavitation levels are indeed reduced by the use of perfluorodecalin.
Dr. Geronemus is an investigator for Cutera, Cynosure, Palomar, Solta Medical, and Syneron. He is also on the medical advisory board for Cynosure, Lumenis, Photomedex, Syneron, and Zeltiq. He reported that he is a Zeltiq shareholder.
ATLANTA – Applying the topical fluorocarbon perfluorodecalin prior to Q-switched laser treatment for tattoo removal allows for immediate retreatment of the tattoo, thereby improving results while decreasing overall treatment time, according to Dr. Roy Geronemus.
The findings have important implications for improving outcomes and patient satisfaction, given that tattoo removal can require 10-20 sessions, depending on factors such as the age and colors of the tattoo, and that tattoos – and thus tattoo removal – continue to increase in popularity, he said. "For a busy practice or impatient patients like we have in New York, this has been a nice advance," Dr. Geronemus said at the annual meeting of the American Society for Dermatologic Surgery.
The approach builds on the "R20 technique" described earlier this year in a study published in the Journal of the American Academy of Dermatology. R20 involves the use of multiple treatment passes that are made at 20-minute intervals.
Typically, after an initial pass, tiny white bubbles form in the superficial papillary dermis, appearing as a whitening of the skin. Retreatment while these bubbles are present elicits a limited reaction.
The R20 technique was developed when investigators found that the bubbles disappear after 20 minutes, and, thus, tested the technique in a study of 12 adults. The patients were randomized to a single treatment pass with a Q-switched alexandrite laser (5.5 J/cm2, 755 nm, 100-nanosecond pulse duration, 3-mm spot size) or to four passes at 20 minute intervals.
The first treatment caused an immediate whitening reaction, but little or no whitening occurred after subsequent passes at 20-minute intervals. However, at 90-day follow-up, significant improvement was seen in the R20 group, compared with the single-treatment group, and light microscopy demonstrated greater dispersion of tattoo ink with the R20 approach. (J. Am. Acad. Dermatol. 2012;66:271-7).
Despite the increased efficacy using this approach, the time required to complete four passes at 20-minute intervals makes it impractical in the clinical setting, said Dr. Geronemus, a dermatologist in private practice in New York.
"So with this idea in mind, we began to look at a concept that would allow us to re-treat tattoos immediately without waiting 20 minutes," he said, explaining that topical perfluorodecalin helps dissolve the gas seen after the application of the Q-switched laser and speeds the resolution of the whitening.
"Rather than waiting 20 minutes, the gas dissolves almost immediately, allowing you to re-treat, and we’re now re-treating three or four times in a matter of minutes rather than waiting the 80 minutes that the R20 technique would take for a four-time treatment session," he said.
In his experience, results with perfluorodecalin are comparable to those seen with the R20 technique – but with greater convenience for the patient.
His observations were confirmed on optical coherence tomography scanning, which demonstrated that cavitation levels are indeed reduced by the use of perfluorodecalin.
Dr. Geronemus is an investigator for Cutera, Cynosure, Palomar, Solta Medical, and Syneron. He is also on the medical advisory board for Cynosure, Lumenis, Photomedex, Syneron, and Zeltiq. He reported that he is a Zeltiq shareholder.
ATLANTA – Applying the topical fluorocarbon perfluorodecalin prior to Q-switched laser treatment for tattoo removal allows for immediate retreatment of the tattoo, thereby improving results while decreasing overall treatment time, according to Dr. Roy Geronemus.
The findings have important implications for improving outcomes and patient satisfaction, given that tattoo removal can require 10-20 sessions, depending on factors such as the age and colors of the tattoo, and that tattoos – and thus tattoo removal – continue to increase in popularity, he said. "For a busy practice or impatient patients like we have in New York, this has been a nice advance," Dr. Geronemus said at the annual meeting of the American Society for Dermatologic Surgery.
The approach builds on the "R20 technique" described earlier this year in a study published in the Journal of the American Academy of Dermatology. R20 involves the use of multiple treatment passes that are made at 20-minute intervals.
Typically, after an initial pass, tiny white bubbles form in the superficial papillary dermis, appearing as a whitening of the skin. Retreatment while these bubbles are present elicits a limited reaction.
The R20 technique was developed when investigators found that the bubbles disappear after 20 minutes, and, thus, tested the technique in a study of 12 adults. The patients were randomized to a single treatment pass with a Q-switched alexandrite laser (5.5 J/cm2, 755 nm, 100-nanosecond pulse duration, 3-mm spot size) or to four passes at 20 minute intervals.
The first treatment caused an immediate whitening reaction, but little or no whitening occurred after subsequent passes at 20-minute intervals. However, at 90-day follow-up, significant improvement was seen in the R20 group, compared with the single-treatment group, and light microscopy demonstrated greater dispersion of tattoo ink with the R20 approach. (J. Am. Acad. Dermatol. 2012;66:271-7).
Despite the increased efficacy using this approach, the time required to complete four passes at 20-minute intervals makes it impractical in the clinical setting, said Dr. Geronemus, a dermatologist in private practice in New York.
"So with this idea in mind, we began to look at a concept that would allow us to re-treat tattoos immediately without waiting 20 minutes," he said, explaining that topical perfluorodecalin helps dissolve the gas seen after the application of the Q-switched laser and speeds the resolution of the whitening.
"Rather than waiting 20 minutes, the gas dissolves almost immediately, allowing you to re-treat, and we’re now re-treating three or four times in a matter of minutes rather than waiting the 80 minutes that the R20 technique would take for a four-time treatment session," he said.
In his experience, results with perfluorodecalin are comparable to those seen with the R20 technique – but with greater convenience for the patient.
His observations were confirmed on optical coherence tomography scanning, which demonstrated that cavitation levels are indeed reduced by the use of perfluorodecalin.
Dr. Geronemus is an investigator for Cutera, Cynosure, Palomar, Solta Medical, and Syneron. He is also on the medical advisory board for Cynosure, Lumenis, Photomedex, Syneron, and Zeltiq. He reported that he is a Zeltiq shareholder.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
Bariatric Surgery May Benefit Extremely Obese Adolescents
SAN ANTONIO – Earlier may be better when it comes to bariatric surgery for obesity.
Data increasingly suggest that surgery for extreme obesity during adolescence is associated with prevention or reversal of obesity-related health problems, including diabetes, frequently seen in those who remain obese into adulthood, Dr. Thomas Inge said at the annual meeting of the Obesity Society.
Currently, an estimated 4%-7% of adolescents are extremely obese, and a number of researchers have noted significant detrimental effects decades down the road and even early in adulthood for those affected by obesity and diabetes, he said.
"Bariatric surgery earlier in life may be better than waiting until many more decades have eroded the important metabolic systems in the body."
These effects include years of life lost and "typical adult life complications of diabetes," such as amputation and renal disease, said Dr. Inge, a surgeon and director of the Center for Bariatric Research and Innovation at Cincinnati Children’s Hospital Medical Center.
Particularly disturbing is the fact that as many as 50% of children in some racial subgroups – including very young children – may develop diabetes in their lifetime, he added, noting that managing diabetes and obesity in this age group is quite challenging and that outcomes are often suboptimal.
Further, school-based studies suggest that morbidly obese children and teens tend to continue to gain weight over time, adding about 1 point of body mass index and 1 inch of waist circumference each year.
In a retrospective study designed to assess the association between adolescent weight status and adult health status, Dr. Inge found that obesity at age 18 based on participant recall increased the risk of diabetes and related comorbidities in adulthood by 37%, and increased the risk of renal disease fivefold.
The study, which involved nearly 1,500 adults who were part of the Longitudinal Assessment of Bariatric Surgery (LABS) 2 study, was reported in a poster at the meeting.
"By having been severely obese as an adolescent, they really did face quite significant problems later in life," he said.
The dilemma when it comes to treating obese adolescents is that medical treatment often fails. In one study, adolescents were found to have a greater risk of failure on metformin monotherapy at every time point compared with adults. Similar, but less striking, findings have been reported with rosiglitazone.
"One might propose, then, that adolescent diabetes is a more virulent condition, and if that’s the case, shouldn’t we really be thinking about more aggressive treatment – particularly today, in light of the fact that we do have surgical therapies with very high-powered evidence of demonstrated effectiveness?" he said.
Not only have studies in adults shown that gastric bypass surgery, for example, is highly effective for reducing fat mass and improving insulin resistance and beta-cell function, but adolescent data also show a benefit.
In a small retrospective study of 11 adolescent teens with type 2 diabetes and a preoperative BMI of about 50 kg/m2, Dr. Inge found that BMI and weight decreased by 34% at 1 year follow-up.
Additionally, all participants were using medication at baseline, including one who was on insulin, and all but that one patient were off their medications at follow-up, he said, noting that the patient on insulin had successfully reduced medication dosages by 50% at follow-up. Mean glucose levels in the participants fell from 140 to 84 mmol/L, mean insulin values normalized, and insulin sensitivity measures improved dramatically. Glycosylated hemoglobin normalized, on average, and cardiovascular measures also improved.
"So this leads to the question: What could be responsible for the reduced efficacy of medical treatment in adolescents?" Dr. Inge said.
Because compliance has been good in the studies looking at this, it is possible that biological factors are involved that affect insulin resistance, and this suggests there may be an even greater role for surgery in adolescents. In both adults and adolescents, surgery has been found to dramatically improve insulin resistance.
In fact, in one study gastric bypass seemed to restore a more normal relationship between insulin sensitivity and the first-phase response – even though participants still had "impressive obesity," with a BMI of nearly 40 on average after surgery, he said.
This suggests that in adolescents something more happens as a result of bariatric surgery than just weight loss or "a change in the plumbing."
"It’s changing, perhaps, something more fundamentally important. I think it’s true that these operations are doing something fundamentally metabolic to improve the patient’s response to whatever this pathologic obesity milieu is," Dr. Inge said, noting that additional study via the Teen-LABS multisite consortium and registry is underway.
Teen-LABS, which aims to facilitate coordinated clinical, epidemiological, and behavioral research in the field of adolescent bariatric surgery, recently finished recruitment.
"We’re really testing the hypothesis that bariatric surgery earlier in life may be better than waiting until many more decades have eroded the important metabolic systems in the body," Dr. Inge said, concluding that the future health of obese and severely obese children is of great concern, and that aggressive intervention will be increasingly needed and warranted.
"We need to build upon the evidence base for this, and really describe in detail the risks and benefits to be expected. After gastric bypass, I’m becoming more and more convinced that metabolic defects can dramatically improve. We don’t know exactly why ... but for now, it is fairly clear that this is metabolic surgery," he said, adding that he expects surgical models will provide important clues to mechanisms which can be exploited to expand the armamentarium for fighting pediatric obesity.
Dr. Inge’s research is supported by the National Institutes of Health. He had no other disclosures to report.
SAN ANTONIO – Earlier may be better when it comes to bariatric surgery for obesity.
Data increasingly suggest that surgery for extreme obesity during adolescence is associated with prevention or reversal of obesity-related health problems, including diabetes, frequently seen in those who remain obese into adulthood, Dr. Thomas Inge said at the annual meeting of the Obesity Society.
Currently, an estimated 4%-7% of adolescents are extremely obese, and a number of researchers have noted significant detrimental effects decades down the road and even early in adulthood for those affected by obesity and diabetes, he said.
"Bariatric surgery earlier in life may be better than waiting until many more decades have eroded the important metabolic systems in the body."
These effects include years of life lost and "typical adult life complications of diabetes," such as amputation and renal disease, said Dr. Inge, a surgeon and director of the Center for Bariatric Research and Innovation at Cincinnati Children’s Hospital Medical Center.
Particularly disturbing is the fact that as many as 50% of children in some racial subgroups – including very young children – may develop diabetes in their lifetime, he added, noting that managing diabetes and obesity in this age group is quite challenging and that outcomes are often suboptimal.
Further, school-based studies suggest that morbidly obese children and teens tend to continue to gain weight over time, adding about 1 point of body mass index and 1 inch of waist circumference each year.
In a retrospective study designed to assess the association between adolescent weight status and adult health status, Dr. Inge found that obesity at age 18 based on participant recall increased the risk of diabetes and related comorbidities in adulthood by 37%, and increased the risk of renal disease fivefold.
The study, which involved nearly 1,500 adults who were part of the Longitudinal Assessment of Bariatric Surgery (LABS) 2 study, was reported in a poster at the meeting.
"By having been severely obese as an adolescent, they really did face quite significant problems later in life," he said.
The dilemma when it comes to treating obese adolescents is that medical treatment often fails. In one study, adolescents were found to have a greater risk of failure on metformin monotherapy at every time point compared with adults. Similar, but less striking, findings have been reported with rosiglitazone.
"One might propose, then, that adolescent diabetes is a more virulent condition, and if that’s the case, shouldn’t we really be thinking about more aggressive treatment – particularly today, in light of the fact that we do have surgical therapies with very high-powered evidence of demonstrated effectiveness?" he said.
Not only have studies in adults shown that gastric bypass surgery, for example, is highly effective for reducing fat mass and improving insulin resistance and beta-cell function, but adolescent data also show a benefit.
In a small retrospective study of 11 adolescent teens with type 2 diabetes and a preoperative BMI of about 50 kg/m2, Dr. Inge found that BMI and weight decreased by 34% at 1 year follow-up.
Additionally, all participants were using medication at baseline, including one who was on insulin, and all but that one patient were off their medications at follow-up, he said, noting that the patient on insulin had successfully reduced medication dosages by 50% at follow-up. Mean glucose levels in the participants fell from 140 to 84 mmol/L, mean insulin values normalized, and insulin sensitivity measures improved dramatically. Glycosylated hemoglobin normalized, on average, and cardiovascular measures also improved.
"So this leads to the question: What could be responsible for the reduced efficacy of medical treatment in adolescents?" Dr. Inge said.
Because compliance has been good in the studies looking at this, it is possible that biological factors are involved that affect insulin resistance, and this suggests there may be an even greater role for surgery in adolescents. In both adults and adolescents, surgery has been found to dramatically improve insulin resistance.
In fact, in one study gastric bypass seemed to restore a more normal relationship between insulin sensitivity and the first-phase response – even though participants still had "impressive obesity," with a BMI of nearly 40 on average after surgery, he said.
This suggests that in adolescents something more happens as a result of bariatric surgery than just weight loss or "a change in the plumbing."
"It’s changing, perhaps, something more fundamentally important. I think it’s true that these operations are doing something fundamentally metabolic to improve the patient’s response to whatever this pathologic obesity milieu is," Dr. Inge said, noting that additional study via the Teen-LABS multisite consortium and registry is underway.
Teen-LABS, which aims to facilitate coordinated clinical, epidemiological, and behavioral research in the field of adolescent bariatric surgery, recently finished recruitment.
"We’re really testing the hypothesis that bariatric surgery earlier in life may be better than waiting until many more decades have eroded the important metabolic systems in the body," Dr. Inge said, concluding that the future health of obese and severely obese children is of great concern, and that aggressive intervention will be increasingly needed and warranted.
"We need to build upon the evidence base for this, and really describe in detail the risks and benefits to be expected. After gastric bypass, I’m becoming more and more convinced that metabolic defects can dramatically improve. We don’t know exactly why ... but for now, it is fairly clear that this is metabolic surgery," he said, adding that he expects surgical models will provide important clues to mechanisms which can be exploited to expand the armamentarium for fighting pediatric obesity.
Dr. Inge’s research is supported by the National Institutes of Health. He had no other disclosures to report.
SAN ANTONIO – Earlier may be better when it comes to bariatric surgery for obesity.
Data increasingly suggest that surgery for extreme obesity during adolescence is associated with prevention or reversal of obesity-related health problems, including diabetes, frequently seen in those who remain obese into adulthood, Dr. Thomas Inge said at the annual meeting of the Obesity Society.
Currently, an estimated 4%-7% of adolescents are extremely obese, and a number of researchers have noted significant detrimental effects decades down the road and even early in adulthood for those affected by obesity and diabetes, he said.
"Bariatric surgery earlier in life may be better than waiting until many more decades have eroded the important metabolic systems in the body."
These effects include years of life lost and "typical adult life complications of diabetes," such as amputation and renal disease, said Dr. Inge, a surgeon and director of the Center for Bariatric Research and Innovation at Cincinnati Children’s Hospital Medical Center.
Particularly disturbing is the fact that as many as 50% of children in some racial subgroups – including very young children – may develop diabetes in their lifetime, he added, noting that managing diabetes and obesity in this age group is quite challenging and that outcomes are often suboptimal.
Further, school-based studies suggest that morbidly obese children and teens tend to continue to gain weight over time, adding about 1 point of body mass index and 1 inch of waist circumference each year.
In a retrospective study designed to assess the association between adolescent weight status and adult health status, Dr. Inge found that obesity at age 18 based on participant recall increased the risk of diabetes and related comorbidities in adulthood by 37%, and increased the risk of renal disease fivefold.
The study, which involved nearly 1,500 adults who were part of the Longitudinal Assessment of Bariatric Surgery (LABS) 2 study, was reported in a poster at the meeting.
"By having been severely obese as an adolescent, they really did face quite significant problems later in life," he said.
The dilemma when it comes to treating obese adolescents is that medical treatment often fails. In one study, adolescents were found to have a greater risk of failure on metformin monotherapy at every time point compared with adults. Similar, but less striking, findings have been reported with rosiglitazone.
"One might propose, then, that adolescent diabetes is a more virulent condition, and if that’s the case, shouldn’t we really be thinking about more aggressive treatment – particularly today, in light of the fact that we do have surgical therapies with very high-powered evidence of demonstrated effectiveness?" he said.
Not only have studies in adults shown that gastric bypass surgery, for example, is highly effective for reducing fat mass and improving insulin resistance and beta-cell function, but adolescent data also show a benefit.
In a small retrospective study of 11 adolescent teens with type 2 diabetes and a preoperative BMI of about 50 kg/m2, Dr. Inge found that BMI and weight decreased by 34% at 1 year follow-up.
Additionally, all participants were using medication at baseline, including one who was on insulin, and all but that one patient were off their medications at follow-up, he said, noting that the patient on insulin had successfully reduced medication dosages by 50% at follow-up. Mean glucose levels in the participants fell from 140 to 84 mmol/L, mean insulin values normalized, and insulin sensitivity measures improved dramatically. Glycosylated hemoglobin normalized, on average, and cardiovascular measures also improved.
"So this leads to the question: What could be responsible for the reduced efficacy of medical treatment in adolescents?" Dr. Inge said.
Because compliance has been good in the studies looking at this, it is possible that biological factors are involved that affect insulin resistance, and this suggests there may be an even greater role for surgery in adolescents. In both adults and adolescents, surgery has been found to dramatically improve insulin resistance.
In fact, in one study gastric bypass seemed to restore a more normal relationship between insulin sensitivity and the first-phase response – even though participants still had "impressive obesity," with a BMI of nearly 40 on average after surgery, he said.
This suggests that in adolescents something more happens as a result of bariatric surgery than just weight loss or "a change in the plumbing."
"It’s changing, perhaps, something more fundamentally important. I think it’s true that these operations are doing something fundamentally metabolic to improve the patient’s response to whatever this pathologic obesity milieu is," Dr. Inge said, noting that additional study via the Teen-LABS multisite consortium and registry is underway.
Teen-LABS, which aims to facilitate coordinated clinical, epidemiological, and behavioral research in the field of adolescent bariatric surgery, recently finished recruitment.
"We’re really testing the hypothesis that bariatric surgery earlier in life may be better than waiting until many more decades have eroded the important metabolic systems in the body," Dr. Inge said, concluding that the future health of obese and severely obese children is of great concern, and that aggressive intervention will be increasingly needed and warranted.
"We need to build upon the evidence base for this, and really describe in detail the risks and benefits to be expected. After gastric bypass, I’m becoming more and more convinced that metabolic defects can dramatically improve. We don’t know exactly why ... but for now, it is fairly clear that this is metabolic surgery," he said, adding that he expects surgical models will provide important clues to mechanisms which can be exploited to expand the armamentarium for fighting pediatric obesity.
Dr. Inge’s research is supported by the National Institutes of Health. He had no other disclosures to report.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE OBESITY SOCIETY
Maggots Prove Wound-Cleaning Worth
PRAGUE – Maggot debridement of wounds proved significantly faster, less painful, and less labor intensive than surgical debridement and conventional dressings in a randomized, multicenter clinical trial.
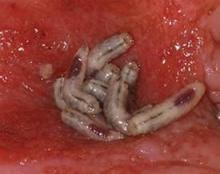
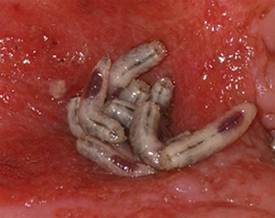
"There was quite an amazing debridement after 7 days of maggot therapy," Dr. Kristina Opletalova said of the phase III study findings presented at the annual congress of the European Academy of Dermatology and Venereology.
She reported on 119 patients hospitalized for 2 weeks for treatment of nonhealing sloughy wounds, most of which were venous ulcers on the lower limbs. Participants were randomized to maggot therapy or to thrice-weekly surgical debridement with topical anesthesia and conventional dressings.
The maggot therapy was administered via a novel delivery system: 80 maggots of Lucilia sericata were bagged in a special two-layer dressing, known as a Vitapad (BioMonde Laboratories), which allowed the critters to move and feed on the wound surface and kept them from escaping. The dressing was changed twice weekly.
Patients were blindfolded for all dressing changes so they didn’t know which study arm they were in. Wound sloughing was analyzed using computerized planimetry software, and other end points were assessed by an investigator blinded to treatment arm.
After 7 days of therapy, the wound status was significantly better in the maggot debridement group. The mean percentage of slough in wounds was 54.5%, compared with 66.5% in controls, but the significantly faster debridement didn’t boost the final healing rate. The day 15 percentage of slough in the wounds didn’t differ significantly between the two groups: 55.4% with maggot therapy and 53.8% in controls.
"So we think maggot debridement therapy should be stopped after 1 week and other types of dressings should then be used," said Dr. Opletalova, a dermatologist at the University of Caen (France).
Pain scores, which were assessed on a weekly basis, were similarly low in the two groups, but it must be noted that the control group received topical anesthetic and the maggot therapy group did not. Nursing time was four-fold greater in the control group. The study didn’t include a formal cost analysis, but the markedly reduced nursing time in the maggot therapy group is likely to spell cost savings, she said.
Maggot therapy was well tolerated. Patients expressed no reticence about it. A similar number of patients in both study arms reported a crawling sensation on their wounds.
Dr. Opletalova said that maggot therapy is likely to be particularly useful in patients with wounds that need rapid debridement, such as those with diabetes, or to prepare a wound for skin grafting or when there is an increased risk for infection.
Further details of the recently published randomized trial can be found in the Archives of Dermatology (2012;148:432-8).
The study was supported by university hospital research funding and by a grant from the French Society of Dermatology. Dr. Opletalova reported having no financial conflicts.
PRAGUE – Maggot debridement of wounds proved significantly faster, less painful, and less labor intensive than surgical debridement and conventional dressings in a randomized, multicenter clinical trial.
"There was quite an amazing debridement after 7 days of maggot therapy," Dr. Kristina Opletalova said of the phase III study findings presented at the annual congress of the European Academy of Dermatology and Venereology.
She reported on 119 patients hospitalized for 2 weeks for treatment of nonhealing sloughy wounds, most of which were venous ulcers on the lower limbs. Participants were randomized to maggot therapy or to thrice-weekly surgical debridement with topical anesthesia and conventional dressings.
The maggot therapy was administered via a novel delivery system: 80 maggots of Lucilia sericata were bagged in a special two-layer dressing, known as a Vitapad (BioMonde Laboratories), which allowed the critters to move and feed on the wound surface and kept them from escaping. The dressing was changed twice weekly.
Patients were blindfolded for all dressing changes so they didn’t know which study arm they were in. Wound sloughing was analyzed using computerized planimetry software, and other end points were assessed by an investigator blinded to treatment arm.
After 7 days of therapy, the wound status was significantly better in the maggot debridement group. The mean percentage of slough in wounds was 54.5%, compared with 66.5% in controls, but the significantly faster debridement didn’t boost the final healing rate. The day 15 percentage of slough in the wounds didn’t differ significantly between the two groups: 55.4% with maggot therapy and 53.8% in controls.
"So we think maggot debridement therapy should be stopped after 1 week and other types of dressings should then be used," said Dr. Opletalova, a dermatologist at the University of Caen (France).
Pain scores, which were assessed on a weekly basis, were similarly low in the two groups, but it must be noted that the control group received topical anesthetic and the maggot therapy group did not. Nursing time was four-fold greater in the control group. The study didn’t include a formal cost analysis, but the markedly reduced nursing time in the maggot therapy group is likely to spell cost savings, she said.
Maggot therapy was well tolerated. Patients expressed no reticence about it. A similar number of patients in both study arms reported a crawling sensation on their wounds.
Dr. Opletalova said that maggot therapy is likely to be particularly useful in patients with wounds that need rapid debridement, such as those with diabetes, or to prepare a wound for skin grafting or when there is an increased risk for infection.
Further details of the recently published randomized trial can be found in the Archives of Dermatology (2012;148:432-8).
The study was supported by university hospital research funding and by a grant from the French Society of Dermatology. Dr. Opletalova reported having no financial conflicts.
PRAGUE – Maggot debridement of wounds proved significantly faster, less painful, and less labor intensive than surgical debridement and conventional dressings in a randomized, multicenter clinical trial.
"There was quite an amazing debridement after 7 days of maggot therapy," Dr. Kristina Opletalova said of the phase III study findings presented at the annual congress of the European Academy of Dermatology and Venereology.
She reported on 119 patients hospitalized for 2 weeks for treatment of nonhealing sloughy wounds, most of which were venous ulcers on the lower limbs. Participants were randomized to maggot therapy or to thrice-weekly surgical debridement with topical anesthesia and conventional dressings.
The maggot therapy was administered via a novel delivery system: 80 maggots of Lucilia sericata were bagged in a special two-layer dressing, known as a Vitapad (BioMonde Laboratories), which allowed the critters to move and feed on the wound surface and kept them from escaping. The dressing was changed twice weekly.
Patients were blindfolded for all dressing changes so they didn’t know which study arm they were in. Wound sloughing was analyzed using computerized planimetry software, and other end points were assessed by an investigator blinded to treatment arm.
After 7 days of therapy, the wound status was significantly better in the maggot debridement group. The mean percentage of slough in wounds was 54.5%, compared with 66.5% in controls, but the significantly faster debridement didn’t boost the final healing rate. The day 15 percentage of slough in the wounds didn’t differ significantly between the two groups: 55.4% with maggot therapy and 53.8% in controls.
"So we think maggot debridement therapy should be stopped after 1 week and other types of dressings should then be used," said Dr. Opletalova, a dermatologist at the University of Caen (France).
Pain scores, which were assessed on a weekly basis, were similarly low in the two groups, but it must be noted that the control group received topical anesthetic and the maggot therapy group did not. Nursing time was four-fold greater in the control group. The study didn’t include a formal cost analysis, but the markedly reduced nursing time in the maggot therapy group is likely to spell cost savings, she said.
Maggot therapy was well tolerated. Patients expressed no reticence about it. A similar number of patients in both study arms reported a crawling sensation on their wounds.
Dr. Opletalova said that maggot therapy is likely to be particularly useful in patients with wounds that need rapid debridement, such as those with diabetes, or to prepare a wound for skin grafting or when there is an increased risk for infection.
Further details of the recently published randomized trial can be found in the Archives of Dermatology (2012;148:432-8).
The study was supported by university hospital research funding and by a grant from the French Society of Dermatology. Dr. Opletalova reported having no financial conflicts.
AT THE ANNUAL CONGRESS OF THE EUROPEAN ACADEMY OF DERMATOLOGY AND VENEREOLOGY
Major Finding: After 7 days of therapy, the mean percentage of slough in wounds was 54.5% in the maggot debridement group, compared with 66.5% in the control group.
Data Source: The phase-III findings come from a randomized, multicenter, blinded, prospective clinical trial involving 119 hospitalized patients.
Disclosures: The study was supported by university research funding and by a grant from the French Society of Dermatology. Dr. Opletalova reported having no financial conflicts.
Medicare at the VP Debate: The Policy & Practice Podcast
The vice presidential candidates sparred over Medicare’s future at their recent week’s debate. What one side calls “premium support,” the other calls “vouchers” and each has a very strong position on this potential change to the program. Vice President Joe Biden argued that vouchers would eliminate Medicare’s guaranteed benefit, while Congressman Paul Ryan shot back, saying the GOP plan will provide more coverage for the middle class and ensure the program’s solvency.
Meanwhile, lawmakers back in Washington engaged in a different debate, theirs over the Independent Payment Advisory Board. The 15-person panel was created under the Affordable Care Act to help regulate Medicare costs and has been a hot button topic. Interest groups from the left and right gave conflicting view on how the panel will directly affect physician pay.
For more details on that, and a recent poll on how doctors might vote on Nov. 6, listen to this week’s Policy & Practice Podcast.
The vice presidential candidates sparred over Medicare’s future at their recent week’s debate. What one side calls “premium support,” the other calls “vouchers” and each has a very strong position on this potential change to the program. Vice President Joe Biden argued that vouchers would eliminate Medicare’s guaranteed benefit, while Congressman Paul Ryan shot back, saying the GOP plan will provide more coverage for the middle class and ensure the program’s solvency.
Meanwhile, lawmakers back in Washington engaged in a different debate, theirs over the Independent Payment Advisory Board. The 15-person panel was created under the Affordable Care Act to help regulate Medicare costs and has been a hot button topic. Interest groups from the left and right gave conflicting view on how the panel will directly affect physician pay.
For more details on that, and a recent poll on how doctors might vote on Nov. 6, listen to this week’s Policy & Practice Podcast.
The vice presidential candidates sparred over Medicare’s future at their recent week’s debate. What one side calls “premium support,” the other calls “vouchers” and each has a very strong position on this potential change to the program. Vice President Joe Biden argued that vouchers would eliminate Medicare’s guaranteed benefit, while Congressman Paul Ryan shot back, saying the GOP plan will provide more coverage for the middle class and ensure the program’s solvency.
Meanwhile, lawmakers back in Washington engaged in a different debate, theirs over the Independent Payment Advisory Board. The 15-person panel was created under the Affordable Care Act to help regulate Medicare costs and has been a hot button topic. Interest groups from the left and right gave conflicting view on how the panel will directly affect physician pay.
For more details on that, and a recent poll on how doctors might vote on Nov. 6, listen to this week’s Policy & Practice Podcast.
Male Gender, Length of Stay Raise Readmission Risk
CHICAGO – Approximately half of hospital readmissions are surgery related and one-third of these are due to infections, data from nearly 3,000 Medicare patients indicated.
Risk factors for readmission included male gender, higher ASA (American Society of Anesthesiologists) class, and longer hospital stay, Dr. Shanu N. Kothari said at the annual clinical congress of the American College of Surgeons.
Recent health care reform initiatives include a proposal to reduce reimbursement for certain 30-day hospital readmissions among Medicare patients, he noted.
Dr. Kothari of Gundersen Lutheran Health System in La Crosse, Wis., and his colleagues reviewed data from 2,865 Medicare patients who had surgery at their institution between Jan. 1, 2010, and May 16, 2011. A readmission was defined as any patient who was readmitted within 30 days of initial surgery. Patients with incomplete follow-up data and those who died within 30 days were excluded.
The overall 30-day readmission rate was 7%. Readmitted patients were significantly more likely to be male compared with nonreadmitted patients (54% vs. 44%) and significantly more likely to have an ASA class of 3 or greater (84% vs. 66%). There were no significant differences in age or body mass index between readmitted and nonreadmitted patients.
In addition, the average length of stay and operative times were significantly longer for readmitted patients vs. nonreadmitted patients (4.8 days vs. 2.8 days and 123 minutes vs. 98 minutes).
A majority of the procedures were general and orthopedic, and 77% were elective.
Of the readmitted patients, "84% had at least one chronic condition, and patients with cardiac disease, renal disease, and diabetes had higher readmission rates," Dr. Kothari said.
The reasons for readmission were divided into four categories: surgery related (53%), not related to the surgical procedure (35%), planned (7%), and patient related (5%).
The most common surgery-related reasons for readmission were infections (32%), medication side effects (12%), or pulmonary complications (9%), Dr. Kothari noted.
Most of the readmissions unrelated to the index surgical procedure were exacerbations of underlying conditions, such as renal failure or heart failure. Patient-related reasons for readmission included noncompliance with discharge instructions or medications, as well as psychological issues.
"Further study is needed to address reasons for readmission on a multicenter level," said Dr. Kothari. "Decreased reimbursement should be discouraged for readmissions directly related to patient noncompliance."
Dr. Kothari said he had no relevant financial disclosures.
CHICAGO – Approximately half of hospital readmissions are surgery related and one-third of these are due to infections, data from nearly 3,000 Medicare patients indicated.
Risk factors for readmission included male gender, higher ASA (American Society of Anesthesiologists) class, and longer hospital stay, Dr. Shanu N. Kothari said at the annual clinical congress of the American College of Surgeons.
Recent health care reform initiatives include a proposal to reduce reimbursement for certain 30-day hospital readmissions among Medicare patients, he noted.
Dr. Kothari of Gundersen Lutheran Health System in La Crosse, Wis., and his colleagues reviewed data from 2,865 Medicare patients who had surgery at their institution between Jan. 1, 2010, and May 16, 2011. A readmission was defined as any patient who was readmitted within 30 days of initial surgery. Patients with incomplete follow-up data and those who died within 30 days were excluded.
The overall 30-day readmission rate was 7%. Readmitted patients were significantly more likely to be male compared with nonreadmitted patients (54% vs. 44%) and significantly more likely to have an ASA class of 3 or greater (84% vs. 66%). There were no significant differences in age or body mass index between readmitted and nonreadmitted patients.
In addition, the average length of stay and operative times were significantly longer for readmitted patients vs. nonreadmitted patients (4.8 days vs. 2.8 days and 123 minutes vs. 98 minutes).
A majority of the procedures were general and orthopedic, and 77% were elective.
Of the readmitted patients, "84% had at least one chronic condition, and patients with cardiac disease, renal disease, and diabetes had higher readmission rates," Dr. Kothari said.
The reasons for readmission were divided into four categories: surgery related (53%), not related to the surgical procedure (35%), planned (7%), and patient related (5%).
The most common surgery-related reasons for readmission were infections (32%), medication side effects (12%), or pulmonary complications (9%), Dr. Kothari noted.
Most of the readmissions unrelated to the index surgical procedure were exacerbations of underlying conditions, such as renal failure or heart failure. Patient-related reasons for readmission included noncompliance with discharge instructions or medications, as well as psychological issues.
"Further study is needed to address reasons for readmission on a multicenter level," said Dr. Kothari. "Decreased reimbursement should be discouraged for readmissions directly related to patient noncompliance."
Dr. Kothari said he had no relevant financial disclosures.
CHICAGO – Approximately half of hospital readmissions are surgery related and one-third of these are due to infections, data from nearly 3,000 Medicare patients indicated.
Risk factors for readmission included male gender, higher ASA (American Society of Anesthesiologists) class, and longer hospital stay, Dr. Shanu N. Kothari said at the annual clinical congress of the American College of Surgeons.
Recent health care reform initiatives include a proposal to reduce reimbursement for certain 30-day hospital readmissions among Medicare patients, he noted.
Dr. Kothari of Gundersen Lutheran Health System in La Crosse, Wis., and his colleagues reviewed data from 2,865 Medicare patients who had surgery at their institution between Jan. 1, 2010, and May 16, 2011. A readmission was defined as any patient who was readmitted within 30 days of initial surgery. Patients with incomplete follow-up data and those who died within 30 days were excluded.
The overall 30-day readmission rate was 7%. Readmitted patients were significantly more likely to be male compared with nonreadmitted patients (54% vs. 44%) and significantly more likely to have an ASA class of 3 or greater (84% vs. 66%). There were no significant differences in age or body mass index between readmitted and nonreadmitted patients.
In addition, the average length of stay and operative times were significantly longer for readmitted patients vs. nonreadmitted patients (4.8 days vs. 2.8 days and 123 minutes vs. 98 minutes).
A majority of the procedures were general and orthopedic, and 77% were elective.
Of the readmitted patients, "84% had at least one chronic condition, and patients with cardiac disease, renal disease, and diabetes had higher readmission rates," Dr. Kothari said.
The reasons for readmission were divided into four categories: surgery related (53%), not related to the surgical procedure (35%), planned (7%), and patient related (5%).
The most common surgery-related reasons for readmission were infections (32%), medication side effects (12%), or pulmonary complications (9%), Dr. Kothari noted.
Most of the readmissions unrelated to the index surgical procedure were exacerbations of underlying conditions, such as renal failure or heart failure. Patient-related reasons for readmission included noncompliance with discharge instructions or medications, as well as psychological issues.
"Further study is needed to address reasons for readmission on a multicenter level," said Dr. Kothari. "Decreased reimbursement should be discouraged for readmissions directly related to patient noncompliance."
Dr. Kothari said he had no relevant financial disclosures.
AT THE ANNUAL CLINICAL CONGRESS OF THE AMERICAN COLLEGE OF SURGEONS
Major Finding: A total of 53% of 30-day readmissions at a single institution were surgically related, and 32% of these were due to infections.
Data Source: The data come from a retrospective study of 2,865 Medicare patients who underwent surgery at a single institution between Jan. 1, 2010, and May 16, 2011.
Disclosures: Dr. Kothari said he had no relevant financial disclosures.
One-Third of Postop Problems Arise After Discharge
CHICAGO – Approximately one-third of surgical complications were diagnosed after patients left the hospital, based on data from nearly 60,000 procedures performed at 112 hospitals.
Reporting postoperative complications, including surgical site infections, has become a mandatory quality reporting initiative for hospitals, and the Affordable Care Act requires reporting of readmissions, said Dr. Melanie Morris of the University of Alabama at Birmingham.
"Some postoperative complications may lead to readmissions, but this may not tell the whole story," she noted at the annual clinical congress of the American College of Surgeons.
To determine the timing of postoperative complications and the nature of readmissions, Dr. Morris and her colleagues reviewed Veterans Affairs data from the noncardiac Surgical Care Improvement Project (SCIP) cohort from 2005 to 2009 for 59,464 surgical procedures in which there was at least one complication.
"It’s very important that patients are accurately educated on the signs and symptoms of complications so they know to seek timely care after discharge."
Surgical cases were classified by specialty into gastrointestinal, gynecologic, orthopedic, and vascular. Complications were grouped into organ-based systems. For example, urinary complications included renal failure, renal insufficiency, and urinary tract infections; respiratory complications included failure to wean, pneumonia, and reintubation; and surgical site infections (SSIs) included both deep and superficial wounds.
The overall complication rate was approximately 15%, and 32% of complications were diagnosed after hospital discharge, Dr. Morris said. More than half (56%) of all SSIs were diagnosed after discharge, she added.
A statistically significant difference appeared in postdischarge complications by surgical specialty. The SSI rate was 5.4%, followed by respiratory complications (5.0%), urinary tract infection (4.9%), cardiac complications (3.2%), and venous thromboembolism (1.2%).
"Our GI surgical patients had the highest overall complication rate," Dr. Morris noted. Among GI patients, colectomy patients had the highest SSI rate (11%), and 23% of the GI complications were diagnosed after hospital discharge.
In addition, 78% of SSIs in orthopedic patients were diagnosed after discharge, as were 39% of SSIs in GI patients, 77% of SSIs in vascular surgery patients, and 95% of SSIs in gynecologic patients, said Dr. Morris.
There were no significant differences in length of hospital stay based on complications, Dr. Morris said.
The overall readmission rate was 11.9%, and 70% of these patients had no identifiable postoperative complication. Of those who did have an identifiable postop complication, 72% were diagnosed before discharge from the hospital.
The probability of being readmitted to the hospital over time was highest in patients with a postdischarge diagnosis of a complication. The overall length of stay was 5 days, and the average length of stay for patients with any complication was 9 days.
Patient-specific factors associated with an increased risk of readmission included a history of heart failure, renal failure, diabetes, weight loss, and smoking. Procedure-specific factors associated with an increased risk of readmission included a longer operating time, a more contaminated wound, and a higher ASA (American Society of Anesthesiologists) class.
Length of stay was slightly protective for readmission, and the presence of any complication was associated with a high risk of readmission.
"It’s very important that patients are accurately educated on the signs and symptoms of complications so they know to seek timely care after discharge," said Dr. Morris. "Postoperative complications must be measured beyond hospital discharge to capture the whole story.
"Systematic collection of postoperative complications must include postdischarge data as well as readmissions to accurately measure quality," she said.
Dr. Morris said she had no relevant financial disclosures.
CHICAGO – Approximately one-third of surgical complications were diagnosed after patients left the hospital, based on data from nearly 60,000 procedures performed at 112 hospitals.
Reporting postoperative complications, including surgical site infections, has become a mandatory quality reporting initiative for hospitals, and the Affordable Care Act requires reporting of readmissions, said Dr. Melanie Morris of the University of Alabama at Birmingham.
"Some postoperative complications may lead to readmissions, but this may not tell the whole story," she noted at the annual clinical congress of the American College of Surgeons.
To determine the timing of postoperative complications and the nature of readmissions, Dr. Morris and her colleagues reviewed Veterans Affairs data from the noncardiac Surgical Care Improvement Project (SCIP) cohort from 2005 to 2009 for 59,464 surgical procedures in which there was at least one complication.
"It’s very important that patients are accurately educated on the signs and symptoms of complications so they know to seek timely care after discharge."
Surgical cases were classified by specialty into gastrointestinal, gynecologic, orthopedic, and vascular. Complications were grouped into organ-based systems. For example, urinary complications included renal failure, renal insufficiency, and urinary tract infections; respiratory complications included failure to wean, pneumonia, and reintubation; and surgical site infections (SSIs) included both deep and superficial wounds.
The overall complication rate was approximately 15%, and 32% of complications were diagnosed after hospital discharge, Dr. Morris said. More than half (56%) of all SSIs were diagnosed after discharge, she added.
A statistically significant difference appeared in postdischarge complications by surgical specialty. The SSI rate was 5.4%, followed by respiratory complications (5.0%), urinary tract infection (4.9%), cardiac complications (3.2%), and venous thromboembolism (1.2%).
"Our GI surgical patients had the highest overall complication rate," Dr. Morris noted. Among GI patients, colectomy patients had the highest SSI rate (11%), and 23% of the GI complications were diagnosed after hospital discharge.
In addition, 78% of SSIs in orthopedic patients were diagnosed after discharge, as were 39% of SSIs in GI patients, 77% of SSIs in vascular surgery patients, and 95% of SSIs in gynecologic patients, said Dr. Morris.
There were no significant differences in length of hospital stay based on complications, Dr. Morris said.
The overall readmission rate was 11.9%, and 70% of these patients had no identifiable postoperative complication. Of those who did have an identifiable postop complication, 72% were diagnosed before discharge from the hospital.
The probability of being readmitted to the hospital over time was highest in patients with a postdischarge diagnosis of a complication. The overall length of stay was 5 days, and the average length of stay for patients with any complication was 9 days.
Patient-specific factors associated with an increased risk of readmission included a history of heart failure, renal failure, diabetes, weight loss, and smoking. Procedure-specific factors associated with an increased risk of readmission included a longer operating time, a more contaminated wound, and a higher ASA (American Society of Anesthesiologists) class.
Length of stay was slightly protective for readmission, and the presence of any complication was associated with a high risk of readmission.
"It’s very important that patients are accurately educated on the signs and symptoms of complications so they know to seek timely care after discharge," said Dr. Morris. "Postoperative complications must be measured beyond hospital discharge to capture the whole story.
"Systematic collection of postoperative complications must include postdischarge data as well as readmissions to accurately measure quality," she said.
Dr. Morris said she had no relevant financial disclosures.
CHICAGO – Approximately one-third of surgical complications were diagnosed after patients left the hospital, based on data from nearly 60,000 procedures performed at 112 hospitals.
Reporting postoperative complications, including surgical site infections, has become a mandatory quality reporting initiative for hospitals, and the Affordable Care Act requires reporting of readmissions, said Dr. Melanie Morris of the University of Alabama at Birmingham.
"Some postoperative complications may lead to readmissions, but this may not tell the whole story," she noted at the annual clinical congress of the American College of Surgeons.
To determine the timing of postoperative complications and the nature of readmissions, Dr. Morris and her colleagues reviewed Veterans Affairs data from the noncardiac Surgical Care Improvement Project (SCIP) cohort from 2005 to 2009 for 59,464 surgical procedures in which there was at least one complication.
"It’s very important that patients are accurately educated on the signs and symptoms of complications so they know to seek timely care after discharge."
Surgical cases were classified by specialty into gastrointestinal, gynecologic, orthopedic, and vascular. Complications were grouped into organ-based systems. For example, urinary complications included renal failure, renal insufficiency, and urinary tract infections; respiratory complications included failure to wean, pneumonia, and reintubation; and surgical site infections (SSIs) included both deep and superficial wounds.
The overall complication rate was approximately 15%, and 32% of complications were diagnosed after hospital discharge, Dr. Morris said. More than half (56%) of all SSIs were diagnosed after discharge, she added.
A statistically significant difference appeared in postdischarge complications by surgical specialty. The SSI rate was 5.4%, followed by respiratory complications (5.0%), urinary tract infection (4.9%), cardiac complications (3.2%), and venous thromboembolism (1.2%).
"Our GI surgical patients had the highest overall complication rate," Dr. Morris noted. Among GI patients, colectomy patients had the highest SSI rate (11%), and 23% of the GI complications were diagnosed after hospital discharge.
In addition, 78% of SSIs in orthopedic patients were diagnosed after discharge, as were 39% of SSIs in GI patients, 77% of SSIs in vascular surgery patients, and 95% of SSIs in gynecologic patients, said Dr. Morris.
There were no significant differences in length of hospital stay based on complications, Dr. Morris said.
The overall readmission rate was 11.9%, and 70% of these patients had no identifiable postoperative complication. Of those who did have an identifiable postop complication, 72% were diagnosed before discharge from the hospital.
The probability of being readmitted to the hospital over time was highest in patients with a postdischarge diagnosis of a complication. The overall length of stay was 5 days, and the average length of stay for patients with any complication was 9 days.
Patient-specific factors associated with an increased risk of readmission included a history of heart failure, renal failure, diabetes, weight loss, and smoking. Procedure-specific factors associated with an increased risk of readmission included a longer operating time, a more contaminated wound, and a higher ASA (American Society of Anesthesiologists) class.
Length of stay was slightly protective for readmission, and the presence of any complication was associated with a high risk of readmission.
"It’s very important that patients are accurately educated on the signs and symptoms of complications so they know to seek timely care after discharge," said Dr. Morris. "Postoperative complications must be measured beyond hospital discharge to capture the whole story.
"Systematic collection of postoperative complications must include postdischarge data as well as readmissions to accurately measure quality," she said.
Dr. Morris said she had no relevant financial disclosures.
AT THE ANNUAL CLINICAL CONGRESS OF THE AMERICAN COLLEGE OF SURGEONS
Major Finding: Approximately 32% of surgical complications, including 56% of surgical site infections, were diagnosed after patients were discharged from the hospital.
Data Source: The data come from a review of 59,464 surgical procedures performed at 112 VA hospitals.
Disclosures: Dr. Morris said she had no relevant financial disclosures.
Nonpayment Fails to Improve Hospital Infection Rates
The 2008 Medicare policy to withhold payment for treating certain hospital-acquired infections failed to decrease infection rates in U.S. hospitals, according to a report published online Oct. 10 in the New England Journal of Medicine.
In a study involving 398 hospitals or medical systems across the country, implementing a Centers for Medicare and Medicaid Services policy of nonpayment for the treatment of preventable catheter-associated bloodstream infections and catheter-associated urinary tract infections appeared to have no impact at all on the acquisition of those infections, according to Dr. Ashish K. Jha of the department of health policy and management, Harvard School of Public Health, Boston, and his associates.
"As CMS continues to expand this policy to cover Medicaid through the Affordable Care Act, require public reporting of National Healthcare Safety Network [NHSN] data through the Hospital Compare website, and impose greater financial penalties on hospitals that perform poorly on these measures, careful evaluation is needed to determine when these programs work, when they have unintended consequences, and what might be done to improve patient outcomes," Dr. Jha noted.
Dr. Jha and his colleagues assessed data from the NHSN, a public health surveillance program for monitoring health care–associated infections across the country. A total of 1,166 nonfederal acute-care hospitals report their infection rates to this Centers for Disease Control and Prevention–sponsored network every month.
Dr. Jha and his colleagues assessed NHSN data on three types of infection at 398 of those hospitals in 41 states. They examined central catheter–associated bloodstream and catheter-associated urinary tract infections because these are the two hospital-acquired infections for which CMS currently does not pay. They also looked at ventilator-associated pneumonia, which is not targeted by the CMS policy, as a control.
Rates of central catheter–associated bloodstream infections were already decreasing at the time the CMS policy was implemented, likely because the federal government, national organizations, and accrediting agencies had already focused attention on preventing these nosocomial infections. The rate of these infections was 4.8% per quarter before the policy was implemented and 4.7% afterward, a nonsignificant difference, the investigators said (N. Engl. J. Med. 2012 [doi:10.1056/NEJMsa1202419]).
This pattern also was seen with catheter-associated UTIs, in which there was a small, nonsignificant increase in the infection rate after implementation of the CMS policy. For the control condition of ventilator-associated pneumonia, the infection rate was 7.3% before implementation and 8.2% after implementation of the policy, also showing no significant impact on infection rates.
These findings were consistent across all hospital types, regardless of size, regional location, type of ownership, or teaching status.
To assess whether any benefit of the nonpayment policy may have been offset by strategies to lower infection rates, such as mandatory reporting, the researchers performed a separate analysis involving only the hospital units located in states that didn’t have mandatory reporting. Again, no demonstrable effect on infection rates was seen.
To allow more time for hospitals to adapt to the policy change, the investigators performed a sensitivity analysis comparing infection rates 2 years after implementation with those before implementation. Again, they found no further decreases in the rates of any infections.
A possible explanation for these findings is that the amount of this financial disincentive was quite small. "Reductions in payment may have been equivalent to as little as 0.6% of Medicare revenue for the average hospital," Dr. Jha and his associates said. "Greater financial penalties might induce a greater change in hospital responsiveness to the CMS policy."
The study results are particularly important given the increasing use of financial disincentives to improve the quality of healthcare. There is very little evidence that this strategy, or other pay-for-performance strategies, actually improves patient outcomes, they said.
This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
The 2008 Medicare policy to withhold payment for treating certain hospital-acquired infections failed to decrease infection rates in U.S. hospitals, according to a report published online Oct. 10 in the New England Journal of Medicine.
In a study involving 398 hospitals or medical systems across the country, implementing a Centers for Medicare and Medicaid Services policy of nonpayment for the treatment of preventable catheter-associated bloodstream infections and catheter-associated urinary tract infections appeared to have no impact at all on the acquisition of those infections, according to Dr. Ashish K. Jha of the department of health policy and management, Harvard School of Public Health, Boston, and his associates.
"As CMS continues to expand this policy to cover Medicaid through the Affordable Care Act, require public reporting of National Healthcare Safety Network [NHSN] data through the Hospital Compare website, and impose greater financial penalties on hospitals that perform poorly on these measures, careful evaluation is needed to determine when these programs work, when they have unintended consequences, and what might be done to improve patient outcomes," Dr. Jha noted.
Dr. Jha and his colleagues assessed data from the NHSN, a public health surveillance program for monitoring health care–associated infections across the country. A total of 1,166 nonfederal acute-care hospitals report their infection rates to this Centers for Disease Control and Prevention–sponsored network every month.
Dr. Jha and his colleagues assessed NHSN data on three types of infection at 398 of those hospitals in 41 states. They examined central catheter–associated bloodstream and catheter-associated urinary tract infections because these are the two hospital-acquired infections for which CMS currently does not pay. They also looked at ventilator-associated pneumonia, which is not targeted by the CMS policy, as a control.
Rates of central catheter–associated bloodstream infections were already decreasing at the time the CMS policy was implemented, likely because the federal government, national organizations, and accrediting agencies had already focused attention on preventing these nosocomial infections. The rate of these infections was 4.8% per quarter before the policy was implemented and 4.7% afterward, a nonsignificant difference, the investigators said (N. Engl. J. Med. 2012 [doi:10.1056/NEJMsa1202419]).
This pattern also was seen with catheter-associated UTIs, in which there was a small, nonsignificant increase in the infection rate after implementation of the CMS policy. For the control condition of ventilator-associated pneumonia, the infection rate was 7.3% before implementation and 8.2% after implementation of the policy, also showing no significant impact on infection rates.
These findings were consistent across all hospital types, regardless of size, regional location, type of ownership, or teaching status.
To assess whether any benefit of the nonpayment policy may have been offset by strategies to lower infection rates, such as mandatory reporting, the researchers performed a separate analysis involving only the hospital units located in states that didn’t have mandatory reporting. Again, no demonstrable effect on infection rates was seen.
To allow more time for hospitals to adapt to the policy change, the investigators performed a sensitivity analysis comparing infection rates 2 years after implementation with those before implementation. Again, they found no further decreases in the rates of any infections.
A possible explanation for these findings is that the amount of this financial disincentive was quite small. "Reductions in payment may have been equivalent to as little as 0.6% of Medicare revenue for the average hospital," Dr. Jha and his associates said. "Greater financial penalties might induce a greater change in hospital responsiveness to the CMS policy."
The study results are particularly important given the increasing use of financial disincentives to improve the quality of healthcare. There is very little evidence that this strategy, or other pay-for-performance strategies, actually improves patient outcomes, they said.
This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
The 2008 Medicare policy to withhold payment for treating certain hospital-acquired infections failed to decrease infection rates in U.S. hospitals, according to a report published online Oct. 10 in the New England Journal of Medicine.
In a study involving 398 hospitals or medical systems across the country, implementing a Centers for Medicare and Medicaid Services policy of nonpayment for the treatment of preventable catheter-associated bloodstream infections and catheter-associated urinary tract infections appeared to have no impact at all on the acquisition of those infections, according to Dr. Ashish K. Jha of the department of health policy and management, Harvard School of Public Health, Boston, and his associates.
"As CMS continues to expand this policy to cover Medicaid through the Affordable Care Act, require public reporting of National Healthcare Safety Network [NHSN] data through the Hospital Compare website, and impose greater financial penalties on hospitals that perform poorly on these measures, careful evaluation is needed to determine when these programs work, when they have unintended consequences, and what might be done to improve patient outcomes," Dr. Jha noted.
Dr. Jha and his colleagues assessed data from the NHSN, a public health surveillance program for monitoring health care–associated infections across the country. A total of 1,166 nonfederal acute-care hospitals report their infection rates to this Centers for Disease Control and Prevention–sponsored network every month.
Dr. Jha and his colleagues assessed NHSN data on three types of infection at 398 of those hospitals in 41 states. They examined central catheter–associated bloodstream and catheter-associated urinary tract infections because these are the two hospital-acquired infections for which CMS currently does not pay. They also looked at ventilator-associated pneumonia, which is not targeted by the CMS policy, as a control.
Rates of central catheter–associated bloodstream infections were already decreasing at the time the CMS policy was implemented, likely because the federal government, national organizations, and accrediting agencies had already focused attention on preventing these nosocomial infections. The rate of these infections was 4.8% per quarter before the policy was implemented and 4.7% afterward, a nonsignificant difference, the investigators said (N. Engl. J. Med. 2012 [doi:10.1056/NEJMsa1202419]).
This pattern also was seen with catheter-associated UTIs, in which there was a small, nonsignificant increase in the infection rate after implementation of the CMS policy. For the control condition of ventilator-associated pneumonia, the infection rate was 7.3% before implementation and 8.2% after implementation of the policy, also showing no significant impact on infection rates.
These findings were consistent across all hospital types, regardless of size, regional location, type of ownership, or teaching status.
To assess whether any benefit of the nonpayment policy may have been offset by strategies to lower infection rates, such as mandatory reporting, the researchers performed a separate analysis involving only the hospital units located in states that didn’t have mandatory reporting. Again, no demonstrable effect on infection rates was seen.
To allow more time for hospitals to adapt to the policy change, the investigators performed a sensitivity analysis comparing infection rates 2 years after implementation with those before implementation. Again, they found no further decreases in the rates of any infections.
A possible explanation for these findings is that the amount of this financial disincentive was quite small. "Reductions in payment may have been equivalent to as little as 0.6% of Medicare revenue for the average hospital," Dr. Jha and his associates said. "Greater financial penalties might induce a greater change in hospital responsiveness to the CMS policy."
The study results are particularly important given the increasing use of financial disincentives to improve the quality of healthcare. There is very little evidence that this strategy, or other pay-for-performance strategies, actually improves patient outcomes, they said.
This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The rate of central catheter–associated bloodstream infections was 4.8% before the nonpayment policy was implemented and 4.7% afterward, showing that the policy failed to decrease the infection rate.
Data Source: The data come from an analysis of trends in hospital-acquired infection rates before and after implementation of a federal policy to withhold payment for treating those infections, involving 398 hospitals in 41 states.
Disclosures: This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
High Remediation, Attrition Rates Among Surgery Residents
Almost one-third of general surgery residents required remediation over an 11-year period, most often because of a deficiency in medical knowledge, judging from findings in a retrospective study of remediation and attrition rates among general surgery residents at six academic surgical residency programs in California.
The high remediation rate identified in this study "begs the question of whether we are falling short in the education of surgical residents," said Dr. Arezou Yaghoubian of the department of surgery, Harbor-UCLA Medical Center, Los Angeles, and associates. The study was published in the September issue of Archives of Surgery (2012;147:829-33).
They conducted the study to determine which of the six Accreditation Council for Graduate Medical Education (ACGME) competencies (patient care, medical knowledge, practice-based learning, interpersonal and communication skills, professionalism, and system-based practice), most often require remediation and to identify predictors of remediation. There is a scarcity of data on how well surgical residency programs have been achieving these competencies, and this information may provide insight into how to modify the surgical curriculum more effectively in this new era of limited hours, they said.
In the study of 348 general surgery residents at the six training programs between 1999 and 2010, the most common reason for remediation was medical knowledge in 74%, followed by interpersonal and communication skills in 24%, patient care in 22%, professionalism in 18%, system-based practice in 14%, and practice-based learning in 8%. Of the 107 residents who required remediation, 27 required remediation more than once. Almost 16% of the residents left their programs, but most (53 of 55 residents) left voluntarily. The other two failed remediation and had to leave the program.
Monthly meetings with faculty was the most common form of remediation, in 79%, followed by specific reading assignments (72%), required attendance at review courses and/or conferences (27%), evaluation by a therapist, psychologist, or psychiatrist (12%), and having to repeat a clinical year (6.5%).
More than half of the remediations were initiated during the first 2 postgraduate years (25% in the first and 35% in the second year), followed by 21% during the third year, 16% during the fourth year, and 4% during the fifth year.
A predictor of remediation was having received honors during the third-year surgery clerkship (58% of those who were subject to remediation vs. 45% of those who were not remediated, a statistically significant difference), which, the authors noted, was counterintuitive.
United States Medical Licensing Examination (USMLE) step 1 and/or step 2 scores and American Board of Surgery In-Training Examination (ABSITE) scores at postgraduate years 1 through 4 were also predictive of remediation. The median USMLE step 1 and step 2 scores were 225 and 223 among the residents subject to remediation, vs. 232 for step 1 and step 2 scores among those who were not remediated, statistically significant differences. The ABSITE scores during postgraduate years 1 through 4 were significantly lower among those who were subject to remediation, but the differences in median scores in years 5 through 7 were not significantly different.
But remediation was not a predictor of attrition. The only predictor of attrition was the ABSITE score at the third postgraduate year, which was a median of 34 among those who left the program and 62 among those who stayed.
Possible explanations for the high remediation rate is that residents are not well prepared for the demands of a surgical residency, they need to be more efficient with their time because of the 80-hour work week, and they may not necessarily be spending their increased time outside of the hospital studying at home, the authors said. Possible reasons for the attrition rate among the residents, an "ongoing concern" in general surgery, may be marital, family, and personal issues and a need for a less stressful environment, they added.
Acknowledging the study’s limitations, including the retrospective design and lack of information on how many residents passed the American Board of Surgery boards, the authors concluded that the high remediation rate "should give surgical educators pause as we should closely examine the potential sources of these deficiencies." They called on surgical societies to "take the initiative to encourage the restructuring of medical school education, such that future surgeons are better prepared to enter surgical residencies," and for residency programs to "determine whether current educational methods are adequate to prepare future surgeons."
The authors had no financial disclosures.
The surgical residents in this study were intelligent high achievers and the mean USMLE step 1 score of the residents who were remediated was a "quite respectable 225," Dr. Karen Deveney said in an editorial.
"A substantial portion of our very bright residents who have a history of great success in everything they do may have difficulty keeping up with the fast pace and high workload demands," while some may opt for a less stressful career path, and others may need more help from faculty to meet expectations and will "persevere," she said. "It is incumbent on those of us in more senior positions to create educational systems that eliminate nonessential tasks so that residents can devote more attention during the compressed work hours to learning what they need to become competent surgeons," she wrote. "Only then can we have a better chance of training and retaining the best and the brightest" (Arch. Surg. 2012;147; 833).
Dr. Deveney is professor of surgery and vice chair of education and program director, department of surgery, Oregon Health and Science University, Portland. She had no financial disclosures to report.
The surgical residents in this study were intelligent high achievers and the mean USMLE step 1 score of the residents who were remediated was a "quite respectable 225," Dr. Karen Deveney said in an editorial.
"A substantial portion of our very bright residents who have a history of great success in everything they do may have difficulty keeping up with the fast pace and high workload demands," while some may opt for a less stressful career path, and others may need more help from faculty to meet expectations and will "persevere," she said. "It is incumbent on those of us in more senior positions to create educational systems that eliminate nonessential tasks so that residents can devote more attention during the compressed work hours to learning what they need to become competent surgeons," she wrote. "Only then can we have a better chance of training and retaining the best and the brightest" (Arch. Surg. 2012;147; 833).
Dr. Deveney is professor of surgery and vice chair of education and program director, department of surgery, Oregon Health and Science University, Portland. She had no financial disclosures to report.
The surgical residents in this study were intelligent high achievers and the mean USMLE step 1 score of the residents who were remediated was a "quite respectable 225," Dr. Karen Deveney said in an editorial.
"A substantial portion of our very bright residents who have a history of great success in everything they do may have difficulty keeping up with the fast pace and high workload demands," while some may opt for a less stressful career path, and others may need more help from faculty to meet expectations and will "persevere," she said. "It is incumbent on those of us in more senior positions to create educational systems that eliminate nonessential tasks so that residents can devote more attention during the compressed work hours to learning what they need to become competent surgeons," she wrote. "Only then can we have a better chance of training and retaining the best and the brightest" (Arch. Surg. 2012;147; 833).
Dr. Deveney is professor of surgery and vice chair of education and program director, department of surgery, Oregon Health and Science University, Portland. She had no financial disclosures to report.
Almost one-third of general surgery residents required remediation over an 11-year period, most often because of a deficiency in medical knowledge, judging from findings in a retrospective study of remediation and attrition rates among general surgery residents at six academic surgical residency programs in California.
The high remediation rate identified in this study "begs the question of whether we are falling short in the education of surgical residents," said Dr. Arezou Yaghoubian of the department of surgery, Harbor-UCLA Medical Center, Los Angeles, and associates. The study was published in the September issue of Archives of Surgery (2012;147:829-33).
They conducted the study to determine which of the six Accreditation Council for Graduate Medical Education (ACGME) competencies (patient care, medical knowledge, practice-based learning, interpersonal and communication skills, professionalism, and system-based practice), most often require remediation and to identify predictors of remediation. There is a scarcity of data on how well surgical residency programs have been achieving these competencies, and this information may provide insight into how to modify the surgical curriculum more effectively in this new era of limited hours, they said.
In the study of 348 general surgery residents at the six training programs between 1999 and 2010, the most common reason for remediation was medical knowledge in 74%, followed by interpersonal and communication skills in 24%, patient care in 22%, professionalism in 18%, system-based practice in 14%, and practice-based learning in 8%. Of the 107 residents who required remediation, 27 required remediation more than once. Almost 16% of the residents left their programs, but most (53 of 55 residents) left voluntarily. The other two failed remediation and had to leave the program.
Monthly meetings with faculty was the most common form of remediation, in 79%, followed by specific reading assignments (72%), required attendance at review courses and/or conferences (27%), evaluation by a therapist, psychologist, or psychiatrist (12%), and having to repeat a clinical year (6.5%).
More than half of the remediations were initiated during the first 2 postgraduate years (25% in the first and 35% in the second year), followed by 21% during the third year, 16% during the fourth year, and 4% during the fifth year.
A predictor of remediation was having received honors during the third-year surgery clerkship (58% of those who were subject to remediation vs. 45% of those who were not remediated, a statistically significant difference), which, the authors noted, was counterintuitive.
United States Medical Licensing Examination (USMLE) step 1 and/or step 2 scores and American Board of Surgery In-Training Examination (ABSITE) scores at postgraduate years 1 through 4 were also predictive of remediation. The median USMLE step 1 and step 2 scores were 225 and 223 among the residents subject to remediation, vs. 232 for step 1 and step 2 scores among those who were not remediated, statistically significant differences. The ABSITE scores during postgraduate years 1 through 4 were significantly lower among those who were subject to remediation, but the differences in median scores in years 5 through 7 were not significantly different.
But remediation was not a predictor of attrition. The only predictor of attrition was the ABSITE score at the third postgraduate year, which was a median of 34 among those who left the program and 62 among those who stayed.
Possible explanations for the high remediation rate is that residents are not well prepared for the demands of a surgical residency, they need to be more efficient with their time because of the 80-hour work week, and they may not necessarily be spending their increased time outside of the hospital studying at home, the authors said. Possible reasons for the attrition rate among the residents, an "ongoing concern" in general surgery, may be marital, family, and personal issues and a need for a less stressful environment, they added.
Acknowledging the study’s limitations, including the retrospective design and lack of information on how many residents passed the American Board of Surgery boards, the authors concluded that the high remediation rate "should give surgical educators pause as we should closely examine the potential sources of these deficiencies." They called on surgical societies to "take the initiative to encourage the restructuring of medical school education, such that future surgeons are better prepared to enter surgical residencies," and for residency programs to "determine whether current educational methods are adequate to prepare future surgeons."
The authors had no financial disclosures.
Almost one-third of general surgery residents required remediation over an 11-year period, most often because of a deficiency in medical knowledge, judging from findings in a retrospective study of remediation and attrition rates among general surgery residents at six academic surgical residency programs in California.
The high remediation rate identified in this study "begs the question of whether we are falling short in the education of surgical residents," said Dr. Arezou Yaghoubian of the department of surgery, Harbor-UCLA Medical Center, Los Angeles, and associates. The study was published in the September issue of Archives of Surgery (2012;147:829-33).
They conducted the study to determine which of the six Accreditation Council for Graduate Medical Education (ACGME) competencies (patient care, medical knowledge, practice-based learning, interpersonal and communication skills, professionalism, and system-based practice), most often require remediation and to identify predictors of remediation. There is a scarcity of data on how well surgical residency programs have been achieving these competencies, and this information may provide insight into how to modify the surgical curriculum more effectively in this new era of limited hours, they said.
In the study of 348 general surgery residents at the six training programs between 1999 and 2010, the most common reason for remediation was medical knowledge in 74%, followed by interpersonal and communication skills in 24%, patient care in 22%, professionalism in 18%, system-based practice in 14%, and practice-based learning in 8%. Of the 107 residents who required remediation, 27 required remediation more than once. Almost 16% of the residents left their programs, but most (53 of 55 residents) left voluntarily. The other two failed remediation and had to leave the program.
Monthly meetings with faculty was the most common form of remediation, in 79%, followed by specific reading assignments (72%), required attendance at review courses and/or conferences (27%), evaluation by a therapist, psychologist, or psychiatrist (12%), and having to repeat a clinical year (6.5%).
More than half of the remediations were initiated during the first 2 postgraduate years (25% in the first and 35% in the second year), followed by 21% during the third year, 16% during the fourth year, and 4% during the fifth year.
A predictor of remediation was having received honors during the third-year surgery clerkship (58% of those who were subject to remediation vs. 45% of those who were not remediated, a statistically significant difference), which, the authors noted, was counterintuitive.
United States Medical Licensing Examination (USMLE) step 1 and/or step 2 scores and American Board of Surgery In-Training Examination (ABSITE) scores at postgraduate years 1 through 4 were also predictive of remediation. The median USMLE step 1 and step 2 scores were 225 and 223 among the residents subject to remediation, vs. 232 for step 1 and step 2 scores among those who were not remediated, statistically significant differences. The ABSITE scores during postgraduate years 1 through 4 were significantly lower among those who were subject to remediation, but the differences in median scores in years 5 through 7 were not significantly different.
But remediation was not a predictor of attrition. The only predictor of attrition was the ABSITE score at the third postgraduate year, which was a median of 34 among those who left the program and 62 among those who stayed.
Possible explanations for the high remediation rate is that residents are not well prepared for the demands of a surgical residency, they need to be more efficient with their time because of the 80-hour work week, and they may not necessarily be spending their increased time outside of the hospital studying at home, the authors said. Possible reasons for the attrition rate among the residents, an "ongoing concern" in general surgery, may be marital, family, and personal issues and a need for a less stressful environment, they added.
Acknowledging the study’s limitations, including the retrospective design and lack of information on how many residents passed the American Board of Surgery boards, the authors concluded that the high remediation rate "should give surgical educators pause as we should closely examine the potential sources of these deficiencies." They called on surgical societies to "take the initiative to encourage the restructuring of medical school education, such that future surgeons are better prepared to enter surgical residencies," and for residency programs to "determine whether current educational methods are adequate to prepare future surgeons."
The authors had no financial disclosures.
FROM ARCHIVES OF SURGERY
Post-EVAR Survival for Women on Par with Men
MILWAUKEE – Although female gender is associated with a higher rate of complications, women did not have significantly lower long-term survival after endovascular abdominal aortic aneurysm repair in a review of the Mayo Clinic AAA Registry.
At 30 days, 24% of women experienced complications after EVAR, compared with 15% of men (P value = .003).
On the other hand, death at 30 days was similar (2.5% vs. 1.5%; P = .41), as was combined early or late death (hazard ratio 1.1 vs. 1.0; P = .36), Dr. Peter Gloviczki reported at the meeting.
He highlighted a recent prospective analysis from Albany (N.Y.) Medical College showing that women had significantly higher mortality than did men (3.2% vs. 0.96%, P less than .005) and more frequent colon ischemia, native arterial rupture, and type 1 endoleaks after elective EVAR. There were no gender differences, however, for any of these outcomes following elective open repair or emergency EVAR or surgery (Vasc. Surg. 2012;55:906-13. Epub 2012 Feb. 8).
In the Mayo Clinic analysis, urgent presentation, age over 70 years, and high comorbidity scores were all significantly associated with complications and higher mortality, said Dr. Gloviczki, president of the Society for Vascular Surgery (SVS) and chair emeritus vascular and endovascular surgery, Mayo Clinic, Rochester, Minn.
The retrospective analysis included 1,002 consecutive patients with abdominal aortic aneurysm (AAA) treated with EVAR at Mayo Clinic from January 1997 to June 30, 2011. Of these, 871 were male (87%) and 131 female (13%). The majority (919) of cases were elective (92%), 43 symptomatic (4%), and 40 ruptured AAA (4%). Patients’ average age was 76 years (range 51-99 years).
Thirty-day mortality was 1% in the elective group, compared with 2.3% in the symptomatic AAA group and 12.5% in the ruptured AAA group (both P less than .0001), he said.
In contrast to the Albany analysis, early mortality after elective repair was similar between men and women (0.75% vs. 2.61%; P = .09). This was further confirmed by multivariate analysis (hazard ratio for all-cause death 1.16; P = .40), despite an increased risk in women for complications (HR 1.67; P = .001) and reinterventions (HR 1.96; P = .002), Dr. Gloviczki said.
High-risk patients, defined by an SVS comorbidity score of more than 10, however, had significantly higher 30-day mortality after elective EVAR than did low-risk patients (2.33% vs. 0.18%; P = .004).
This was driven by a significantly higher rate of early complications in the high-risk group (19.3% vs. 11.4%), particularly myocardial infarction (1.6% vs. 0.18%) and acute renal failure requiring temporary dialysis (3.26% vs. 1.09%; P less than .05 for all), Dr. Gloviczki observed.
At an average follow-up of 3.2 years, overall survival was significantly higher in patients undergoing elective EVAR vs. symptomatic or ruptured repair (64% vs. 50% and 56%; P less than .001), and in low-risk vs. high-risk elective patients (72% vs. 51%; P less than .001).
Both 30-day mortality and complications significantly increased with age after elective repair, he said.
Overall, there were five late ruptures and nine late conversions, for a complication-free 5-year survival of 64% in the elective group.
Dr. Gloviczki noted that access-related difficulties are driving the higher early complication rate in women, but that other factors like age and comorbidities may be at play.
He noted that Mayo Clinic performed its first EVAR in 1996, and that today, 63% of patients with an aneurysm undergo endovascular repair.
When asked what’s changed in his patient selection and aneurysm size cutoff, Dr. Gloviczki said that in younger patients, surgeons may want to intervene earlier if the aneurysm appears likely to increase in size and is suitable for an endograft, but that overall, age alone should not drive patient selection.
"What this study showed me is that characterizing patients as high risk vs. low risk is important, in addition to age," he said. "As you could see, there was an increased mortality in age, but when we looked at high-risk and low-risk criteria, we only lost one patient in the low-risk group. So age alone does not put you into a high-risk category, it is your additional cardiac, pulmonary and renal disease that does."
Dr. Gloviczki and his coauthors reported no relevant conflicts of interest.
MILWAUKEE – Although female gender is associated with a higher rate of complications, women did not have significantly lower long-term survival after endovascular abdominal aortic aneurysm repair in a review of the Mayo Clinic AAA Registry.
At 30 days, 24% of women experienced complications after EVAR, compared with 15% of men (P value = .003).
On the other hand, death at 30 days was similar (2.5% vs. 1.5%; P = .41), as was combined early or late death (hazard ratio 1.1 vs. 1.0; P = .36), Dr. Peter Gloviczki reported at the meeting.
He highlighted a recent prospective analysis from Albany (N.Y.) Medical College showing that women had significantly higher mortality than did men (3.2% vs. 0.96%, P less than .005) and more frequent colon ischemia, native arterial rupture, and type 1 endoleaks after elective EVAR. There were no gender differences, however, for any of these outcomes following elective open repair or emergency EVAR or surgery (Vasc. Surg. 2012;55:906-13. Epub 2012 Feb. 8).
In the Mayo Clinic analysis, urgent presentation, age over 70 years, and high comorbidity scores were all significantly associated with complications and higher mortality, said Dr. Gloviczki, president of the Society for Vascular Surgery (SVS) and chair emeritus vascular and endovascular surgery, Mayo Clinic, Rochester, Minn.
The retrospective analysis included 1,002 consecutive patients with abdominal aortic aneurysm (AAA) treated with EVAR at Mayo Clinic from January 1997 to June 30, 2011. Of these, 871 were male (87%) and 131 female (13%). The majority (919) of cases were elective (92%), 43 symptomatic (4%), and 40 ruptured AAA (4%). Patients’ average age was 76 years (range 51-99 years).
Thirty-day mortality was 1% in the elective group, compared with 2.3% in the symptomatic AAA group and 12.5% in the ruptured AAA group (both P less than .0001), he said.
In contrast to the Albany analysis, early mortality after elective repair was similar between men and women (0.75% vs. 2.61%; P = .09). This was further confirmed by multivariate analysis (hazard ratio for all-cause death 1.16; P = .40), despite an increased risk in women for complications (HR 1.67; P = .001) and reinterventions (HR 1.96; P = .002), Dr. Gloviczki said.
High-risk patients, defined by an SVS comorbidity score of more than 10, however, had significantly higher 30-day mortality after elective EVAR than did low-risk patients (2.33% vs. 0.18%; P = .004).
This was driven by a significantly higher rate of early complications in the high-risk group (19.3% vs. 11.4%), particularly myocardial infarction (1.6% vs. 0.18%) and acute renal failure requiring temporary dialysis (3.26% vs. 1.09%; P less than .05 for all), Dr. Gloviczki observed.
At an average follow-up of 3.2 years, overall survival was significantly higher in patients undergoing elective EVAR vs. symptomatic or ruptured repair (64% vs. 50% and 56%; P less than .001), and in low-risk vs. high-risk elective patients (72% vs. 51%; P less than .001).
Both 30-day mortality and complications significantly increased with age after elective repair, he said.
Overall, there were five late ruptures and nine late conversions, for a complication-free 5-year survival of 64% in the elective group.
Dr. Gloviczki noted that access-related difficulties are driving the higher early complication rate in women, but that other factors like age and comorbidities may be at play.
He noted that Mayo Clinic performed its first EVAR in 1996, and that today, 63% of patients with an aneurysm undergo endovascular repair.
When asked what’s changed in his patient selection and aneurysm size cutoff, Dr. Gloviczki said that in younger patients, surgeons may want to intervene earlier if the aneurysm appears likely to increase in size and is suitable for an endograft, but that overall, age alone should not drive patient selection.
"What this study showed me is that characterizing patients as high risk vs. low risk is important, in addition to age," he said. "As you could see, there was an increased mortality in age, but when we looked at high-risk and low-risk criteria, we only lost one patient in the low-risk group. So age alone does not put you into a high-risk category, it is your additional cardiac, pulmonary and renal disease that does."
Dr. Gloviczki and his coauthors reported no relevant conflicts of interest.
MILWAUKEE – Although female gender is associated with a higher rate of complications, women did not have significantly lower long-term survival after endovascular abdominal aortic aneurysm repair in a review of the Mayo Clinic AAA Registry.
At 30 days, 24% of women experienced complications after EVAR, compared with 15% of men (P value = .003).
On the other hand, death at 30 days was similar (2.5% vs. 1.5%; P = .41), as was combined early or late death (hazard ratio 1.1 vs. 1.0; P = .36), Dr. Peter Gloviczki reported at the meeting.
He highlighted a recent prospective analysis from Albany (N.Y.) Medical College showing that women had significantly higher mortality than did men (3.2% vs. 0.96%, P less than .005) and more frequent colon ischemia, native arterial rupture, and type 1 endoleaks after elective EVAR. There were no gender differences, however, for any of these outcomes following elective open repair or emergency EVAR or surgery (Vasc. Surg. 2012;55:906-13. Epub 2012 Feb. 8).
In the Mayo Clinic analysis, urgent presentation, age over 70 years, and high comorbidity scores were all significantly associated with complications and higher mortality, said Dr. Gloviczki, president of the Society for Vascular Surgery (SVS) and chair emeritus vascular and endovascular surgery, Mayo Clinic, Rochester, Minn.
The retrospective analysis included 1,002 consecutive patients with abdominal aortic aneurysm (AAA) treated with EVAR at Mayo Clinic from January 1997 to June 30, 2011. Of these, 871 were male (87%) and 131 female (13%). The majority (919) of cases were elective (92%), 43 symptomatic (4%), and 40 ruptured AAA (4%). Patients’ average age was 76 years (range 51-99 years).
Thirty-day mortality was 1% in the elective group, compared with 2.3% in the symptomatic AAA group and 12.5% in the ruptured AAA group (both P less than .0001), he said.
In contrast to the Albany analysis, early mortality after elective repair was similar between men and women (0.75% vs. 2.61%; P = .09). This was further confirmed by multivariate analysis (hazard ratio for all-cause death 1.16; P = .40), despite an increased risk in women for complications (HR 1.67; P = .001) and reinterventions (HR 1.96; P = .002), Dr. Gloviczki said.
High-risk patients, defined by an SVS comorbidity score of more than 10, however, had significantly higher 30-day mortality after elective EVAR than did low-risk patients (2.33% vs. 0.18%; P = .004).
This was driven by a significantly higher rate of early complications in the high-risk group (19.3% vs. 11.4%), particularly myocardial infarction (1.6% vs. 0.18%) and acute renal failure requiring temporary dialysis (3.26% vs. 1.09%; P less than .05 for all), Dr. Gloviczki observed.
At an average follow-up of 3.2 years, overall survival was significantly higher in patients undergoing elective EVAR vs. symptomatic or ruptured repair (64% vs. 50% and 56%; P less than .001), and in low-risk vs. high-risk elective patients (72% vs. 51%; P less than .001).
Both 30-day mortality and complications significantly increased with age after elective repair, he said.
Overall, there were five late ruptures and nine late conversions, for a complication-free 5-year survival of 64% in the elective group.
Dr. Gloviczki noted that access-related difficulties are driving the higher early complication rate in women, but that other factors like age and comorbidities may be at play.
He noted that Mayo Clinic performed its first EVAR in 1996, and that today, 63% of patients with an aneurysm undergo endovascular repair.
When asked what’s changed in his patient selection and aneurysm size cutoff, Dr. Gloviczki said that in younger patients, surgeons may want to intervene earlier if the aneurysm appears likely to increase in size and is suitable for an endograft, but that overall, age alone should not drive patient selection.
"What this study showed me is that characterizing patients as high risk vs. low risk is important, in addition to age," he said. "As you could see, there was an increased mortality in age, but when we looked at high-risk and low-risk criteria, we only lost one patient in the low-risk group. So age alone does not put you into a high-risk category, it is your additional cardiac, pulmonary and renal disease that does."
Dr. Gloviczki and his coauthors reported no relevant conflicts of interest.
AT THE ANNUAL MEETING OF THE MIDWESTERN VASCULAR SURGICAL SOCIETY
Major Finding: Death rates were similar between women and men at 30 days (2.5% vs. 1.5%) as were rates for combined early or late death (hazard ratio 1.1 vs. 1.0).
Data Source: The study is a database review of 1,002 consecutive patients in the Mayo Clinic AAA Registry.
Disclosures: Dr. Gloviczki and his coauthors reported no relevant conflicts of interest.
General Surgery Residents Seeing Far Fewer Open Aortic Surgeries
MILWAUKEE – General surgery residents in a community-based residency program experienced a significant 49% decline in open aortic surgeries over the last decade, an analysis showed.
In 2000-2001, residents were exposed to 20-25 open aortic cases per year, but now get in on 8-15 cases per year, said Dr. Adam Rothermel, a third-year general surgery resident at Mount Carmel Hospital in Columbus, Ohio, where the analysis was conducted.
"Open aortic cases are difficult to find, and our residents, as a whole, would agree that we’re not coming out with good enough experience with these cases," he said at the annual meeting of the Midwestern Vascular Surgical Society.
The results reflect the exponential shift from open vascular surgery to endovascular procedures over the last decade, as well as the more recent implementation of the 80-hour resident work week.
The total number of carotid endarterectomy, infrainguinal bypass, and open aortic cases for the entire hospital decreased by 55%, 30%, and 71%, respectively, over the study period of 2000 to 2011.
Total resident cases over the same period were unchanged for carotid endarterectomy (77 vs. 84 cases), trended downward for infrainguinal bypass (62 vs. 52 cases), and were significantly lower for open aortic cases (43 vs. 8 cases) according to a review of resident case logs, Dr. Rothermel said.
He pointed out that a significant portion of vascular surgery in the United States is still performed by general surgeons, citing surveys showing that general surgeons performed 59% of the vascular procedures in the United States in 1985 (J. Vasc. Surg. 1987;6:611-21) and 49% in 1992 (J. Vasc. Surg. 1996:23:172-81).
Session moderator Dr. Jean E. Starr, medical director of endovascular services at Ohio State University Medical Center in Columbus, said the current results parallel what’s found nationally. She went on to ask what the findings imply for general surgery residents when they’ve finished training, and how this will reflect on patient practice in light of general surgeons performing half of vascular surgeries in the United States.
"When you get out of your general surgery training from a community based program and are expected then, going into say a rural center, to perform these operations, you have to give pause," Dr. Rothermel replied. "I don’t think I have a good way to fix the problem at this point, but I think we need to be aware of the trend."
Audience member Dr. Joseph Giglia, principal investigator for the laparoscopic aortic surgery program at the University of Cincinnati Medical Center, countered by asking whether the findings really matter given that open aortic cases are decreasing significantly across the country. He pointed out that the latest survey data were 20 years old, and submitted that general surgeons no longer perform 50% of vascular surgeries in the United States.
"I think these cases are important for our primary vascular residents to participate in," Dr. Giglia said. "I think there has to be a sea change, a real shift in the paradigm about who’s doing these cases and what we’re going to do in the future."
Dr. Rothermel agreed that another survey should be conducted to better reflect current practice trends.
If vascular surgeons are to pick up the bulk of the caseload, however, efforts to recruit medical students to the specialty may need to be enhanced. A recent survey of 338 medical students showed that 236 first- and second-year students had no clinical exposure to vascular surgery, while only 38 of the 102 third-year students had been exposed to vascular surgery after completing a general surgery rotation (Ann. Vasc. Surg. 2012 July 25 [doi:10.1016/j.avsg.2012.02.012]). Nearly half (49%) of first- and second-year students said that they would consider vascular surgery, however, with another 19% willing to do so if the length of training were reduced.
Dr. Rothermel and Dr. Starr reported no conflicts of interest.
MILWAUKEE – General surgery residents in a community-based residency program experienced a significant 49% decline in open aortic surgeries over the last decade, an analysis showed.
In 2000-2001, residents were exposed to 20-25 open aortic cases per year, but now get in on 8-15 cases per year, said Dr. Adam Rothermel, a third-year general surgery resident at Mount Carmel Hospital in Columbus, Ohio, where the analysis was conducted.
"Open aortic cases are difficult to find, and our residents, as a whole, would agree that we’re not coming out with good enough experience with these cases," he said at the annual meeting of the Midwestern Vascular Surgical Society.
The results reflect the exponential shift from open vascular surgery to endovascular procedures over the last decade, as well as the more recent implementation of the 80-hour resident work week.
The total number of carotid endarterectomy, infrainguinal bypass, and open aortic cases for the entire hospital decreased by 55%, 30%, and 71%, respectively, over the study period of 2000 to 2011.
Total resident cases over the same period were unchanged for carotid endarterectomy (77 vs. 84 cases), trended downward for infrainguinal bypass (62 vs. 52 cases), and were significantly lower for open aortic cases (43 vs. 8 cases) according to a review of resident case logs, Dr. Rothermel said.
He pointed out that a significant portion of vascular surgery in the United States is still performed by general surgeons, citing surveys showing that general surgeons performed 59% of the vascular procedures in the United States in 1985 (J. Vasc. Surg. 1987;6:611-21) and 49% in 1992 (J. Vasc. Surg. 1996:23:172-81).
Session moderator Dr. Jean E. Starr, medical director of endovascular services at Ohio State University Medical Center in Columbus, said the current results parallel what’s found nationally. She went on to ask what the findings imply for general surgery residents when they’ve finished training, and how this will reflect on patient practice in light of general surgeons performing half of vascular surgeries in the United States.
"When you get out of your general surgery training from a community based program and are expected then, going into say a rural center, to perform these operations, you have to give pause," Dr. Rothermel replied. "I don’t think I have a good way to fix the problem at this point, but I think we need to be aware of the trend."
Audience member Dr. Joseph Giglia, principal investigator for the laparoscopic aortic surgery program at the University of Cincinnati Medical Center, countered by asking whether the findings really matter given that open aortic cases are decreasing significantly across the country. He pointed out that the latest survey data were 20 years old, and submitted that general surgeons no longer perform 50% of vascular surgeries in the United States.
"I think these cases are important for our primary vascular residents to participate in," Dr. Giglia said. "I think there has to be a sea change, a real shift in the paradigm about who’s doing these cases and what we’re going to do in the future."
Dr. Rothermel agreed that another survey should be conducted to better reflect current practice trends.
If vascular surgeons are to pick up the bulk of the caseload, however, efforts to recruit medical students to the specialty may need to be enhanced. A recent survey of 338 medical students showed that 236 first- and second-year students had no clinical exposure to vascular surgery, while only 38 of the 102 third-year students had been exposed to vascular surgery after completing a general surgery rotation (Ann. Vasc. Surg. 2012 July 25 [doi:10.1016/j.avsg.2012.02.012]). Nearly half (49%) of first- and second-year students said that they would consider vascular surgery, however, with another 19% willing to do so if the length of training were reduced.
Dr. Rothermel and Dr. Starr reported no conflicts of interest.
MILWAUKEE – General surgery residents in a community-based residency program experienced a significant 49% decline in open aortic surgeries over the last decade, an analysis showed.
In 2000-2001, residents were exposed to 20-25 open aortic cases per year, but now get in on 8-15 cases per year, said Dr. Adam Rothermel, a third-year general surgery resident at Mount Carmel Hospital in Columbus, Ohio, where the analysis was conducted.
"Open aortic cases are difficult to find, and our residents, as a whole, would agree that we’re not coming out with good enough experience with these cases," he said at the annual meeting of the Midwestern Vascular Surgical Society.
The results reflect the exponential shift from open vascular surgery to endovascular procedures over the last decade, as well as the more recent implementation of the 80-hour resident work week.
The total number of carotid endarterectomy, infrainguinal bypass, and open aortic cases for the entire hospital decreased by 55%, 30%, and 71%, respectively, over the study period of 2000 to 2011.
Total resident cases over the same period were unchanged for carotid endarterectomy (77 vs. 84 cases), trended downward for infrainguinal bypass (62 vs. 52 cases), and were significantly lower for open aortic cases (43 vs. 8 cases) according to a review of resident case logs, Dr. Rothermel said.
He pointed out that a significant portion of vascular surgery in the United States is still performed by general surgeons, citing surveys showing that general surgeons performed 59% of the vascular procedures in the United States in 1985 (J. Vasc. Surg. 1987;6:611-21) and 49% in 1992 (J. Vasc. Surg. 1996:23:172-81).
Session moderator Dr. Jean E. Starr, medical director of endovascular services at Ohio State University Medical Center in Columbus, said the current results parallel what’s found nationally. She went on to ask what the findings imply for general surgery residents when they’ve finished training, and how this will reflect on patient practice in light of general surgeons performing half of vascular surgeries in the United States.
"When you get out of your general surgery training from a community based program and are expected then, going into say a rural center, to perform these operations, you have to give pause," Dr. Rothermel replied. "I don’t think I have a good way to fix the problem at this point, but I think we need to be aware of the trend."
Audience member Dr. Joseph Giglia, principal investigator for the laparoscopic aortic surgery program at the University of Cincinnati Medical Center, countered by asking whether the findings really matter given that open aortic cases are decreasing significantly across the country. He pointed out that the latest survey data were 20 years old, and submitted that general surgeons no longer perform 50% of vascular surgeries in the United States.
"I think these cases are important for our primary vascular residents to participate in," Dr. Giglia said. "I think there has to be a sea change, a real shift in the paradigm about who’s doing these cases and what we’re going to do in the future."
Dr. Rothermel agreed that another survey should be conducted to better reflect current practice trends.
If vascular surgeons are to pick up the bulk of the caseload, however, efforts to recruit medical students to the specialty may need to be enhanced. A recent survey of 338 medical students showed that 236 first- and second-year students had no clinical exposure to vascular surgery, while only 38 of the 102 third-year students had been exposed to vascular surgery after completing a general surgery rotation (Ann. Vasc. Surg. 2012 July 25 [doi:10.1016/j.avsg.2012.02.012]). Nearly half (49%) of first- and second-year students said that they would consider vascular surgery, however, with another 19% willing to do so if the length of training were reduced.
Dr. Rothermel and Dr. Starr reported no conflicts of interest.
AT THE ANNUAL MEETING OF THE MIDWESTERN VASCULAR SURGICAL SOCIETY
Major Finding: General surgery residents in a community-based program experienced a significant 49% decline in open aortic surgeries from 2000 to 2011.
Data Source: Review of all carotid endarterectomy, femoro-popliteal bypass, and open aortic surgeries performed at a community hospital and by residents from 2000 to 2011.
Disclosures: Dr. Rothermel and Dr. Starr reported no conflicts of interest.