User login
Asthma exacerbation in pregnancy impacts mothers, infants
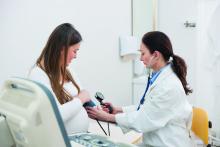
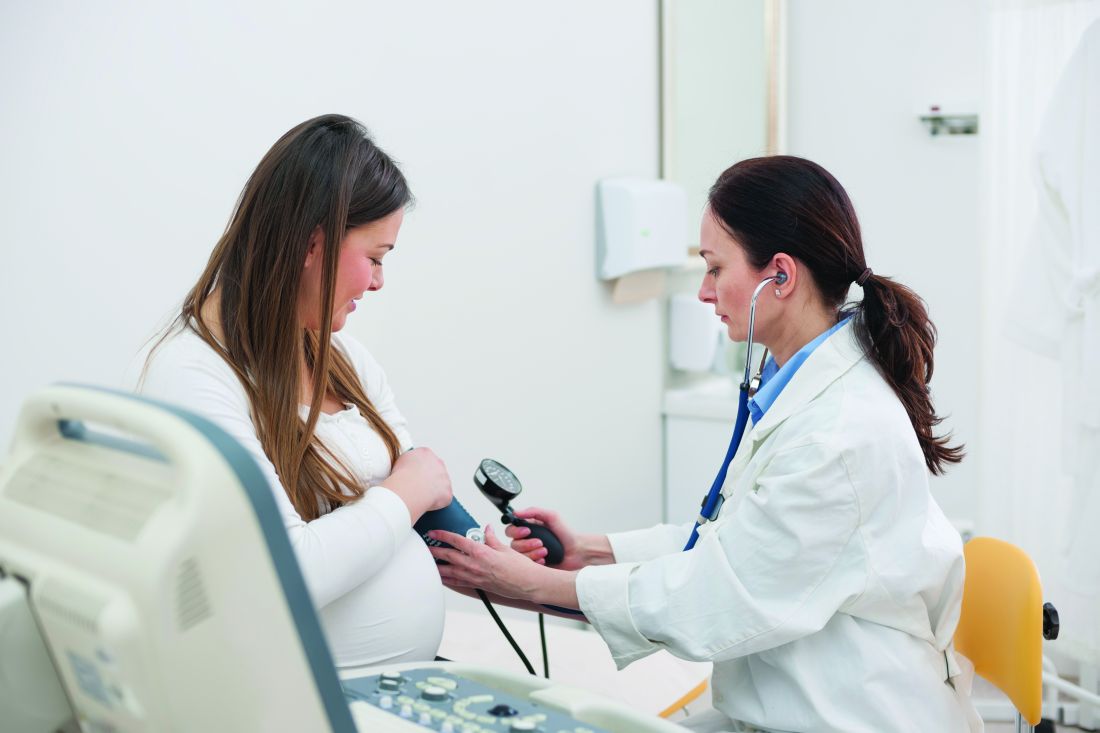
Women with asthma who suffer asthma exacerbation while pregnant are at increased risk for complications during pregnancy and delivery, and their infants are at increased risk for respiratory problems, according to data from a longitudinal study of 58,524 women with asthma.
“Asthma exacerbation during pregnancy has been found to be associated with adverse perinatal and pregnancy outcomes such as low birth weight, small for gestational age, preterm delivery, congenital malformation, preeclampsia, and perinatal mortality,” but previous studies have been small and limited to comparisons of asthmatic and nonasthmatic women, wrote Kawsari Abdullah, PhD, of Children’s Hospital of Eastern Ontario, Ottawa, and colleagues.
To determine the impact of asthma exacerbation on maternal and fetal outcomes, the researchers analyzed data from the Ontario Asthma Surveillance Information System to identify women with asthma who had at least one pregnancy resulting in a live or still birth between 2006 and 2012.
Overall, significantly more women with exacerbated asthma had preeclampsia or pregnancy-induced hypertension, compared with asthmatic women who had no exacerbations, at 5% vs. 4% and 7% vs. 5%, respectively (P less than .001), according to the study published in the European Respiratory Journal.
Adverse perinatal outcomes were significantly more likely among babies of mothers with exacerbated asthma, compared with those who had no exacerbations, including low birth weight (7% vs. 5%), small for gestational age (3% vs. 2%), preterm birth (8% vs. 7%), and congenital malformation (6% vs. 5%). All P values were less than .001, except for small for gestational age, which was P = .008.
In addition, significantly more babies of asthmatic women with exacerbated asthma during pregnancy had respiratory problems including asthma and pneumonia, compared with those of asthmatic women who had no exacerbations during pregnancy, at 38% vs. 31% and 24% vs. 22% (P less than .001 for both). The researchers found no significant interactions between maternal age and smoking and asthma exacerbations.
The findings were limited by several factors, including the lack of a validated algorithm for asthma exacerbation, which the researchers defined as five or more visits to a general practice clinician for asthma during pregnancy. Other limitations included the lack of categorizing asthma exacerbation by severity, and the inability to include the potential effects of asthma medication on maternal and fetal outcomes, Dr. Abdullah and colleagues noted.
However, the results were strengthened by the large sample size and ability to follow babies from birth until 5 years of age, they said.
“Targeting women with asthma during pregnancy and ensuring appropriate asthma management and postpartum follow-up may help to reduce the risk of pregnancy complications, adverse perinatal outcomes, and early childhood respiratory disorders,” they concluded.
This study is important because asthma is a common, potentially serious medical condition that complicates approximately 4%-8% of pregnancies, and one in three women with asthma experience an exacerbation during pregnancy, Iris Krishna, MD, a specialist in maternal/fetal medicine at Emory University, Atlanta, said in an interview.
“This study is unique in that it uses population-level data to assess the association between an asthma exacerbation during pregnancy and adverse perinatal outcomes,” Dr. Krishna said. “After adjusting for confounders, and consistent with previous studies, study findings suggest an increased risk for women with asthma who have an asthma exacerbation during pregnancy for preeclampsia [odds ratio, 1.3; P less than .001], pregnancy-induced hypertension [OR, 1.17; P less than .05], low-birth-weight infant [OR, 1.14; P less than .05], preterm birth [OR, 1.14; P less than .05], and congenital malformations [OR, 1.21; P less than .001].”
Dr. Krishna also noted the impact on early childhood outcomes. “In this study, children born to women who had an asthma exacerbation during pregnancy had a 23% higher risk of developing asthma before 5 years of age, which is consistent with previous studies. [The] investigators also reported a 12% higher risk of having pneumonia during the first 5 years of life for children born to women who had an asthma exacerbation during pregnancy.”
“Previous studies have suggested children born to mothers with uncontrolled asthma have an increased risk for respiratory infections, but this study is the first to report an association with pneumonia,” she said. This increased risk for childhood respiratory disorders warrants further study.
Consequently, “Women with asthma during pregnancy should have appropriate management to ensure good control to optimize pregnancy outcome,” Dr. Krishna emphasized. “Women who experience asthma exacerbations in pregnancy are at increased risk for preeclampsia, [pregnancy-induced hypertension], low birth weight, and preterm delivery and may require closer monitoring.”
The study was supported by the Institute for Clinical Evaluative Sciences. The researchers and Dr. Krishna had no financial conflicts to disclose.
SOURCE: Abdullah K et al. Eur Respir J. 2019 Nov 26. doi: 10.1183/13993003.01335-2019.
Women with asthma who suffer asthma exacerbation while pregnant are at increased risk for complications during pregnancy and delivery, and their infants are at increased risk for respiratory problems, according to data from a longitudinal study of 58,524 women with asthma.
“Asthma exacerbation during pregnancy has been found to be associated with adverse perinatal and pregnancy outcomes such as low birth weight, small for gestational age, preterm delivery, congenital malformation, preeclampsia, and perinatal mortality,” but previous studies have been small and limited to comparisons of asthmatic and nonasthmatic women, wrote Kawsari Abdullah, PhD, of Children’s Hospital of Eastern Ontario, Ottawa, and colleagues.
To determine the impact of asthma exacerbation on maternal and fetal outcomes, the researchers analyzed data from the Ontario Asthma Surveillance Information System to identify women with asthma who had at least one pregnancy resulting in a live or still birth between 2006 and 2012.
Overall, significantly more women with exacerbated asthma had preeclampsia or pregnancy-induced hypertension, compared with asthmatic women who had no exacerbations, at 5% vs. 4% and 7% vs. 5%, respectively (P less than .001), according to the study published in the European Respiratory Journal.
Adverse perinatal outcomes were significantly more likely among babies of mothers with exacerbated asthma, compared with those who had no exacerbations, including low birth weight (7% vs. 5%), small for gestational age (3% vs. 2%), preterm birth (8% vs. 7%), and congenital malformation (6% vs. 5%). All P values were less than .001, except for small for gestational age, which was P = .008.
In addition, significantly more babies of asthmatic women with exacerbated asthma during pregnancy had respiratory problems including asthma and pneumonia, compared with those of asthmatic women who had no exacerbations during pregnancy, at 38% vs. 31% and 24% vs. 22% (P less than .001 for both). The researchers found no significant interactions between maternal age and smoking and asthma exacerbations.
The findings were limited by several factors, including the lack of a validated algorithm for asthma exacerbation, which the researchers defined as five or more visits to a general practice clinician for asthma during pregnancy. Other limitations included the lack of categorizing asthma exacerbation by severity, and the inability to include the potential effects of asthma medication on maternal and fetal outcomes, Dr. Abdullah and colleagues noted.
However, the results were strengthened by the large sample size and ability to follow babies from birth until 5 years of age, they said.
“Targeting women with asthma during pregnancy and ensuring appropriate asthma management and postpartum follow-up may help to reduce the risk of pregnancy complications, adverse perinatal outcomes, and early childhood respiratory disorders,” they concluded.
This study is important because asthma is a common, potentially serious medical condition that complicates approximately 4%-8% of pregnancies, and one in three women with asthma experience an exacerbation during pregnancy, Iris Krishna, MD, a specialist in maternal/fetal medicine at Emory University, Atlanta, said in an interview.
“This study is unique in that it uses population-level data to assess the association between an asthma exacerbation during pregnancy and adverse perinatal outcomes,” Dr. Krishna said. “After adjusting for confounders, and consistent with previous studies, study findings suggest an increased risk for women with asthma who have an asthma exacerbation during pregnancy for preeclampsia [odds ratio, 1.3; P less than .001], pregnancy-induced hypertension [OR, 1.17; P less than .05], low-birth-weight infant [OR, 1.14; P less than .05], preterm birth [OR, 1.14; P less than .05], and congenital malformations [OR, 1.21; P less than .001].”
Dr. Krishna also noted the impact on early childhood outcomes. “In this study, children born to women who had an asthma exacerbation during pregnancy had a 23% higher risk of developing asthma before 5 years of age, which is consistent with previous studies. [The] investigators also reported a 12% higher risk of having pneumonia during the first 5 years of life for children born to women who had an asthma exacerbation during pregnancy.”
“Previous studies have suggested children born to mothers with uncontrolled asthma have an increased risk for respiratory infections, but this study is the first to report an association with pneumonia,” she said. This increased risk for childhood respiratory disorders warrants further study.
Consequently, “Women with asthma during pregnancy should have appropriate management to ensure good control to optimize pregnancy outcome,” Dr. Krishna emphasized. “Women who experience asthma exacerbations in pregnancy are at increased risk for preeclampsia, [pregnancy-induced hypertension], low birth weight, and preterm delivery and may require closer monitoring.”
The study was supported by the Institute for Clinical Evaluative Sciences. The researchers and Dr. Krishna had no financial conflicts to disclose.
SOURCE: Abdullah K et al. Eur Respir J. 2019 Nov 26. doi: 10.1183/13993003.01335-2019.
Women with asthma who suffer asthma exacerbation while pregnant are at increased risk for complications during pregnancy and delivery, and their infants are at increased risk for respiratory problems, according to data from a longitudinal study of 58,524 women with asthma.
“Asthma exacerbation during pregnancy has been found to be associated with adverse perinatal and pregnancy outcomes such as low birth weight, small for gestational age, preterm delivery, congenital malformation, preeclampsia, and perinatal mortality,” but previous studies have been small and limited to comparisons of asthmatic and nonasthmatic women, wrote Kawsari Abdullah, PhD, of Children’s Hospital of Eastern Ontario, Ottawa, and colleagues.
To determine the impact of asthma exacerbation on maternal and fetal outcomes, the researchers analyzed data from the Ontario Asthma Surveillance Information System to identify women with asthma who had at least one pregnancy resulting in a live or still birth between 2006 and 2012.
Overall, significantly more women with exacerbated asthma had preeclampsia or pregnancy-induced hypertension, compared with asthmatic women who had no exacerbations, at 5% vs. 4% and 7% vs. 5%, respectively (P less than .001), according to the study published in the European Respiratory Journal.
Adverse perinatal outcomes were significantly more likely among babies of mothers with exacerbated asthma, compared with those who had no exacerbations, including low birth weight (7% vs. 5%), small for gestational age (3% vs. 2%), preterm birth (8% vs. 7%), and congenital malformation (6% vs. 5%). All P values were less than .001, except for small for gestational age, which was P = .008.
In addition, significantly more babies of asthmatic women with exacerbated asthma during pregnancy had respiratory problems including asthma and pneumonia, compared with those of asthmatic women who had no exacerbations during pregnancy, at 38% vs. 31% and 24% vs. 22% (P less than .001 for both). The researchers found no significant interactions between maternal age and smoking and asthma exacerbations.
The findings were limited by several factors, including the lack of a validated algorithm for asthma exacerbation, which the researchers defined as five or more visits to a general practice clinician for asthma during pregnancy. Other limitations included the lack of categorizing asthma exacerbation by severity, and the inability to include the potential effects of asthma medication on maternal and fetal outcomes, Dr. Abdullah and colleagues noted.
However, the results were strengthened by the large sample size and ability to follow babies from birth until 5 years of age, they said.
“Targeting women with asthma during pregnancy and ensuring appropriate asthma management and postpartum follow-up may help to reduce the risk of pregnancy complications, adverse perinatal outcomes, and early childhood respiratory disorders,” they concluded.
This study is important because asthma is a common, potentially serious medical condition that complicates approximately 4%-8% of pregnancies, and one in three women with asthma experience an exacerbation during pregnancy, Iris Krishna, MD, a specialist in maternal/fetal medicine at Emory University, Atlanta, said in an interview.
“This study is unique in that it uses population-level data to assess the association between an asthma exacerbation during pregnancy and adverse perinatal outcomes,” Dr. Krishna said. “After adjusting for confounders, and consistent with previous studies, study findings suggest an increased risk for women with asthma who have an asthma exacerbation during pregnancy for preeclampsia [odds ratio, 1.3; P less than .001], pregnancy-induced hypertension [OR, 1.17; P less than .05], low-birth-weight infant [OR, 1.14; P less than .05], preterm birth [OR, 1.14; P less than .05], and congenital malformations [OR, 1.21; P less than .001].”
Dr. Krishna also noted the impact on early childhood outcomes. “In this study, children born to women who had an asthma exacerbation during pregnancy had a 23% higher risk of developing asthma before 5 years of age, which is consistent with previous studies. [The] investigators also reported a 12% higher risk of having pneumonia during the first 5 years of life for children born to women who had an asthma exacerbation during pregnancy.”
“Previous studies have suggested children born to mothers with uncontrolled asthma have an increased risk for respiratory infections, but this study is the first to report an association with pneumonia,” she said. This increased risk for childhood respiratory disorders warrants further study.
Consequently, “Women with asthma during pregnancy should have appropriate management to ensure good control to optimize pregnancy outcome,” Dr. Krishna emphasized. “Women who experience asthma exacerbations in pregnancy are at increased risk for preeclampsia, [pregnancy-induced hypertension], low birth weight, and preterm delivery and may require closer monitoring.”
The study was supported by the Institute for Clinical Evaluative Sciences. The researchers and Dr. Krishna had no financial conflicts to disclose.
SOURCE: Abdullah K et al. Eur Respir J. 2019 Nov 26. doi: 10.1183/13993003.01335-2019.
FROM THE EUROPEAN RESPIRATORY JOURNAL
Task force advocates selective screening for abdominal aortic aneurysms
Men aged 65-75 years with a history of smoking should undergo one-time screening for abdominal aortic aneurysms (AAA), but clinicians can selectively screen men in this age group who don’t smoke, according to updated recommendations from the U.S. Preventive Services Task Force published in JAMA.
The task force issued a B recommendation for screening men aged 65-75 years with a smoking history and a C recommendation for selectively screening male never smokers in this age group in an update to the previous recommendations issued in 2014.
The task force also recommended against screening for AAA in women with no history of smoking (D recommendation) and cited insufficient evidence to make recommendations about AAA screening for women with a history of smoking or a family history of AAA (I statement).
The current prevalence of AAA in the United States is unclear because of the low rate of screening, but data from countries including the United Kingdom, Sweden, Denmark, and New Zealand have shown a decline in AAA among screened men aged 65 years and older, according to the USPSTF report.
Risk factors for AAA include smoking, male gender, older age, and having a first-degree relative with AAA, the task force noted.
In an evidence review accompanying the recommendations, Janelle M. Guirguis-Blake, MD, of the University of Washington, Tacoma, and colleagues analyzed data from 33 studies. They found a significant reduction in AAA-related mortality over 12-15 years’ follow-up among men aged 65 years and older who underwent AAA screening, compared with unscreened controls (odds ratio, 0.65). In addition, the risk of ruptures related to AAA was significantly lower over 12-15 years among men who underwent screening, compared with unscreened controls (OR, 0.62). However, no significant difference was noted in all-cause mortality over 12-15 years between screened and unscreened groups (relative risk, 0.99; 95% confidence interval, 0.98-1.00).
Data from four studies of early surgery to treat small aneurysms showed no significant difference in AAA-related mortality or all-cause mortality.
“Screening for AAA entails a simple, noninvasive, and focused ultrasonography examination that costs roughly $50. The only potential harms are the psychologic burden of knowing of the presence of an aneurysm and the risk of elective surgery,” wrote Marc Schermerhorn, MD, of Beth Israel Deaconess Medical Center, Boston, in an accompanying editorial published in JAMA Surgery (doi: 10.1001/jamasurg.2019.5234).
“The latter can be calculated for each patient, weighed against the risk of rupture, and together with the estimated life expectancy, should be factored into the decision to screen and the decision to operate. We as a country can do better to detect and treat this disease cost effectively for all appropriate patients including women and elderly individuals,” he said.
Dr. Schermerhorn noted that overall the recommendations are reasonable, but he expressed concern for three populations excluded from the guidelines that warrant additional consideration: nonsmokers with equivalent risk factors, patients older than 75 years, and women. “In the meantime, we should work to ensure that patients determined appropriate by the USPSTF are actually screened,” he said.
The USPSTF is supported by the Agency for Healthcare Research and Quality. The researchers had no financial conflicts to disclose. Dr. Schermerhorn disclosed relationships with Abbott, Cook Medical, Endologix, Medtronic, and Philips.
SOURCE: Guirguis-Blake JM et al. JAMA. 2019. doi: 10.1001/jama.2019.17021.
Men aged 65-75 years with a history of smoking should undergo one-time screening for abdominal aortic aneurysms (AAA), but clinicians can selectively screen men in this age group who don’t smoke, according to updated recommendations from the U.S. Preventive Services Task Force published in JAMA.
The task force issued a B recommendation for screening men aged 65-75 years with a smoking history and a C recommendation for selectively screening male never smokers in this age group in an update to the previous recommendations issued in 2014.
The task force also recommended against screening for AAA in women with no history of smoking (D recommendation) and cited insufficient evidence to make recommendations about AAA screening for women with a history of smoking or a family history of AAA (I statement).
The current prevalence of AAA in the United States is unclear because of the low rate of screening, but data from countries including the United Kingdom, Sweden, Denmark, and New Zealand have shown a decline in AAA among screened men aged 65 years and older, according to the USPSTF report.
Risk factors for AAA include smoking, male gender, older age, and having a first-degree relative with AAA, the task force noted.
In an evidence review accompanying the recommendations, Janelle M. Guirguis-Blake, MD, of the University of Washington, Tacoma, and colleagues analyzed data from 33 studies. They found a significant reduction in AAA-related mortality over 12-15 years’ follow-up among men aged 65 years and older who underwent AAA screening, compared with unscreened controls (odds ratio, 0.65). In addition, the risk of ruptures related to AAA was significantly lower over 12-15 years among men who underwent screening, compared with unscreened controls (OR, 0.62). However, no significant difference was noted in all-cause mortality over 12-15 years between screened and unscreened groups (relative risk, 0.99; 95% confidence interval, 0.98-1.00).
Data from four studies of early surgery to treat small aneurysms showed no significant difference in AAA-related mortality or all-cause mortality.
“Screening for AAA entails a simple, noninvasive, and focused ultrasonography examination that costs roughly $50. The only potential harms are the psychologic burden of knowing of the presence of an aneurysm and the risk of elective surgery,” wrote Marc Schermerhorn, MD, of Beth Israel Deaconess Medical Center, Boston, in an accompanying editorial published in JAMA Surgery (doi: 10.1001/jamasurg.2019.5234).
“The latter can be calculated for each patient, weighed against the risk of rupture, and together with the estimated life expectancy, should be factored into the decision to screen and the decision to operate. We as a country can do better to detect and treat this disease cost effectively for all appropriate patients including women and elderly individuals,” he said.
Dr. Schermerhorn noted that overall the recommendations are reasonable, but he expressed concern for three populations excluded from the guidelines that warrant additional consideration: nonsmokers with equivalent risk factors, patients older than 75 years, and women. “In the meantime, we should work to ensure that patients determined appropriate by the USPSTF are actually screened,” he said.
The USPSTF is supported by the Agency for Healthcare Research and Quality. The researchers had no financial conflicts to disclose. Dr. Schermerhorn disclosed relationships with Abbott, Cook Medical, Endologix, Medtronic, and Philips.
SOURCE: Guirguis-Blake JM et al. JAMA. 2019. doi: 10.1001/jama.2019.17021.
Men aged 65-75 years with a history of smoking should undergo one-time screening for abdominal aortic aneurysms (AAA), but clinicians can selectively screen men in this age group who don’t smoke, according to updated recommendations from the U.S. Preventive Services Task Force published in JAMA.
The task force issued a B recommendation for screening men aged 65-75 years with a smoking history and a C recommendation for selectively screening male never smokers in this age group in an update to the previous recommendations issued in 2014.
The task force also recommended against screening for AAA in women with no history of smoking (D recommendation) and cited insufficient evidence to make recommendations about AAA screening for women with a history of smoking or a family history of AAA (I statement).
The current prevalence of AAA in the United States is unclear because of the low rate of screening, but data from countries including the United Kingdom, Sweden, Denmark, and New Zealand have shown a decline in AAA among screened men aged 65 years and older, according to the USPSTF report.
Risk factors for AAA include smoking, male gender, older age, and having a first-degree relative with AAA, the task force noted.
In an evidence review accompanying the recommendations, Janelle M. Guirguis-Blake, MD, of the University of Washington, Tacoma, and colleagues analyzed data from 33 studies. They found a significant reduction in AAA-related mortality over 12-15 years’ follow-up among men aged 65 years and older who underwent AAA screening, compared with unscreened controls (odds ratio, 0.65). In addition, the risk of ruptures related to AAA was significantly lower over 12-15 years among men who underwent screening, compared with unscreened controls (OR, 0.62). However, no significant difference was noted in all-cause mortality over 12-15 years between screened and unscreened groups (relative risk, 0.99; 95% confidence interval, 0.98-1.00).
Data from four studies of early surgery to treat small aneurysms showed no significant difference in AAA-related mortality or all-cause mortality.
“Screening for AAA entails a simple, noninvasive, and focused ultrasonography examination that costs roughly $50. The only potential harms are the psychologic burden of knowing of the presence of an aneurysm and the risk of elective surgery,” wrote Marc Schermerhorn, MD, of Beth Israel Deaconess Medical Center, Boston, in an accompanying editorial published in JAMA Surgery (doi: 10.1001/jamasurg.2019.5234).
“The latter can be calculated for each patient, weighed against the risk of rupture, and together with the estimated life expectancy, should be factored into the decision to screen and the decision to operate. We as a country can do better to detect and treat this disease cost effectively for all appropriate patients including women and elderly individuals,” he said.
Dr. Schermerhorn noted that overall the recommendations are reasonable, but he expressed concern for three populations excluded from the guidelines that warrant additional consideration: nonsmokers with equivalent risk factors, patients older than 75 years, and women. “In the meantime, we should work to ensure that patients determined appropriate by the USPSTF are actually screened,” he said.
The USPSTF is supported by the Agency for Healthcare Research and Quality. The researchers had no financial conflicts to disclose. Dr. Schermerhorn disclosed relationships with Abbott, Cook Medical, Endologix, Medtronic, and Philips.
SOURCE: Guirguis-Blake JM et al. JAMA. 2019. doi: 10.1001/jama.2019.17021.
FROM JAMA
FDA fast-tracks psilocybin for major depressive disorder
Psilocybin, a short-acting compound that is the psychoactive ingredient in “magic mushrooms,” has received a Breakthrough Therapy designation from the Food and Drug Administration for the treatment of adults with major depressive disorder.
The designation was given to the Usona Institute, a nonprofit medical research organization, and comes in the wake of Usona’s launch of a phase 2 clinical trial that will include about 80 participants at seven study sites across the United States, according to a press release. Two sites are currently recruiting patients, and the others are expected to begin recruiting in 2020.
Breakthrough Therapy designation as defined by the FDA means that, based on preliminary research, “the drug may demonstrate substantial improvement over available therapy on a clinically significant endpoint.” In this case, Usona is working with the University of Wisconsin’s University Hospital in Madison, and other collaborators, according to a presentation by Malynn Utzinger, MD, director of integrative medicine and cofounder of the organization.
More information on the Usona Institute and Usona’s clinical trials is available at https://usonaclinicaltrials.org/.
Psilocybin, a short-acting compound that is the psychoactive ingredient in “magic mushrooms,” has received a Breakthrough Therapy designation from the Food and Drug Administration for the treatment of adults with major depressive disorder.
The designation was given to the Usona Institute, a nonprofit medical research organization, and comes in the wake of Usona’s launch of a phase 2 clinical trial that will include about 80 participants at seven study sites across the United States, according to a press release. Two sites are currently recruiting patients, and the others are expected to begin recruiting in 2020.
Breakthrough Therapy designation as defined by the FDA means that, based on preliminary research, “the drug may demonstrate substantial improvement over available therapy on a clinically significant endpoint.” In this case, Usona is working with the University of Wisconsin’s University Hospital in Madison, and other collaborators, according to a presentation by Malynn Utzinger, MD, director of integrative medicine and cofounder of the organization.
More information on the Usona Institute and Usona’s clinical trials is available at https://usonaclinicaltrials.org/.
Psilocybin, a short-acting compound that is the psychoactive ingredient in “magic mushrooms,” has received a Breakthrough Therapy designation from the Food and Drug Administration for the treatment of adults with major depressive disorder.
The designation was given to the Usona Institute, a nonprofit medical research organization, and comes in the wake of Usona’s launch of a phase 2 clinical trial that will include about 80 participants at seven study sites across the United States, according to a press release. Two sites are currently recruiting patients, and the others are expected to begin recruiting in 2020.
Breakthrough Therapy designation as defined by the FDA means that, based on preliminary research, “the drug may demonstrate substantial improvement over available therapy on a clinically significant endpoint.” In this case, Usona is working with the University of Wisconsin’s University Hospital in Madison, and other collaborators, according to a presentation by Malynn Utzinger, MD, director of integrative medicine and cofounder of the organization.
More information on the Usona Institute and Usona’s clinical trials is available at https://usonaclinicaltrials.org/.
Researchers describe first cases of episodic visual snow associated with migraine
Episodic visual snow was tied to migraine attacks in a case series of three adults who denied any visual snow outside of the migraines, based on data collected at an outpatient headache center.
Visual snow, a condition in which patients experience visual distortion of tiny, flickering dots resembling analog television static, is often a comorbid condition in migraine patients with and without aura. However, “to our knowledge, this is the first report of patients with an episodic form of visual snow strictly occurring with migraine attacks,” wrote Julius Hodak, MD, of the University of Bern (Switzerland) and colleagues.
In a research letter published in JAMA Neurology, the investigators described 3 adults with histories of migraine but no aura who presented to a tertiary headache center between January 2016 and December 2017, in addition to 1,934 adults with migraine but no visual snow. The three patients initially presented with headaches, and neurologic and MRI results were normal.
Two patients experienced black and white episodic visual snow and one experienced black and yellow visual snow. In one patient, visual snow occurred for less than 2 minutes before and during a migraine attack. The other two patients experienced visual snow during the entire migraine attack.
Based on these patients, the researchers proposed distinguishing episodic visual snow from the distinct disorder of visual snow syndrome, in which patients experience continuous visual snow and other visual symptoms.
In addition, the cases were notable because of the lack of aura in the patients, the researchers wrote.
“In clinical practice, a detailed history in patients reporting visual flickering is therefore necessary to differentiate aura from [episodic visual snow],” they added, because an aura diagnosis would affect patient guidance on contraception use or the timing of triptans.
Dr. Hodak had no financial conflicts to disclose. The study was supported by Deutsche Migräne-und Kopfschmerzgesellschaft, Eye on Vision Foundation, and Baasch-Medicus Foundation.
SOURCE: Hodak J et al. JAMA Neurol. 2019 Nov 25. doi: 10.1001/jamaneurol.2019.4050.
Episodic visual snow was tied to migraine attacks in a case series of three adults who denied any visual snow outside of the migraines, based on data collected at an outpatient headache center.
Visual snow, a condition in which patients experience visual distortion of tiny, flickering dots resembling analog television static, is often a comorbid condition in migraine patients with and without aura. However, “to our knowledge, this is the first report of patients with an episodic form of visual snow strictly occurring with migraine attacks,” wrote Julius Hodak, MD, of the University of Bern (Switzerland) and colleagues.
In a research letter published in JAMA Neurology, the investigators described 3 adults with histories of migraine but no aura who presented to a tertiary headache center between January 2016 and December 2017, in addition to 1,934 adults with migraine but no visual snow. The three patients initially presented with headaches, and neurologic and MRI results were normal.
Two patients experienced black and white episodic visual snow and one experienced black and yellow visual snow. In one patient, visual snow occurred for less than 2 minutes before and during a migraine attack. The other two patients experienced visual snow during the entire migraine attack.
Based on these patients, the researchers proposed distinguishing episodic visual snow from the distinct disorder of visual snow syndrome, in which patients experience continuous visual snow and other visual symptoms.
In addition, the cases were notable because of the lack of aura in the patients, the researchers wrote.
“In clinical practice, a detailed history in patients reporting visual flickering is therefore necessary to differentiate aura from [episodic visual snow],” they added, because an aura diagnosis would affect patient guidance on contraception use or the timing of triptans.
Dr. Hodak had no financial conflicts to disclose. The study was supported by Deutsche Migräne-und Kopfschmerzgesellschaft, Eye on Vision Foundation, and Baasch-Medicus Foundation.
SOURCE: Hodak J et al. JAMA Neurol. 2019 Nov 25. doi: 10.1001/jamaneurol.2019.4050.
Episodic visual snow was tied to migraine attacks in a case series of three adults who denied any visual snow outside of the migraines, based on data collected at an outpatient headache center.
Visual snow, a condition in which patients experience visual distortion of tiny, flickering dots resembling analog television static, is often a comorbid condition in migraine patients with and without aura. However, “to our knowledge, this is the first report of patients with an episodic form of visual snow strictly occurring with migraine attacks,” wrote Julius Hodak, MD, of the University of Bern (Switzerland) and colleagues.
In a research letter published in JAMA Neurology, the investigators described 3 adults with histories of migraine but no aura who presented to a tertiary headache center between January 2016 and December 2017, in addition to 1,934 adults with migraine but no visual snow. The three patients initially presented with headaches, and neurologic and MRI results were normal.
Two patients experienced black and white episodic visual snow and one experienced black and yellow visual snow. In one patient, visual snow occurred for less than 2 minutes before and during a migraine attack. The other two patients experienced visual snow during the entire migraine attack.
Based on these patients, the researchers proposed distinguishing episodic visual snow from the distinct disorder of visual snow syndrome, in which patients experience continuous visual snow and other visual symptoms.
In addition, the cases were notable because of the lack of aura in the patients, the researchers wrote.
“In clinical practice, a detailed history in patients reporting visual flickering is therefore necessary to differentiate aura from [episodic visual snow],” they added, because an aura diagnosis would affect patient guidance on contraception use or the timing of triptans.
Dr. Hodak had no financial conflicts to disclose. The study was supported by Deutsche Migräne-und Kopfschmerzgesellschaft, Eye on Vision Foundation, and Baasch-Medicus Foundation.
SOURCE: Hodak J et al. JAMA Neurol. 2019 Nov 25. doi: 10.1001/jamaneurol.2019.4050.
FROM JAMA NEUROLOGY
Key clinical point: Episodic visual snow in patients with migraines appears to be distinct from an aura.
Major finding: Three patients with histories of migraine without aura reported episodic visual snow that occurred only at the onset or during a migraine attack.
Study details: The data come from a case series of 3 adults with episodic visual snow and migraine and 1,934 patients with migraine only seen at an outpatient headache center.
Disclosures: Dr. Hodak had no financial conflicts to disclose. The study was supported by Deutsche Migräne-und Kopfschmerzgesellschaft, Eye on Vision Foundation, and Baasch-Medicus Foundation.
Source: Hodak J et al. JAMA Neurol. 2019 Nov 25. doi: 10.1001/jamaneurol.2019.4050.
Naturopaths emphasize role of diet in atopic dermatitis
, based on data from a small survey of the two.
Data from previous studies show that more than half of patients with AD have used complementary and alternative medicine in addition to allopathic care, but providers may be unaware of each other’s treatment approaches and confuse patients, wrote Julie Dhossche, MD, of Oregon Health & Science University, Portland, and her colleagues.
In a study published in Pediatric Dermatology, the researchers assessed results of an 11-question, free-text survey of 30 allopathic providers and 21 naturopathic providers about AD. The survey included questions on patient education and evaluation, skin care, and treatment.
Overall, both allopathic and naturopathic providers recommended skin care protocols involving moisturization and “soak and seal” bathing. However, allopathic providers were more likely to prescribe topical corticosteroids for mild to moderate disease (100% vs. 19%), followed by phototherapy and systemic treatments in more severe cases. Naturopathic providers were more likely than allopathic providers to choose topical botanicals, oils, or probiotics (52% vs. 0%) for mild to moderate disease, as well stress relief and acupuncture. Naturopathic providers favored topical corticosteroids and referrals to dermatologists for second- or third-line treatment.
Of note, 85% of naturopathic providers said they thought diet had a probable or definite role in AD, compared with 3% of allopathic providers.
In addition, naturopathic providers differed in their response to an optional question on the use of additional education about food and diet. A total of 11 of 19 naturopathic providers (58%) recommended dietary changes, including “remove potential food allergens/reduce sugar” and “emphasize anti-inflammatory diet,” the researchers said.
“Confusion regarding the role of food in AD management is a common source of frustration for patients, and perhaps a consensus statement from both fields regarding the role of food allergy in AD management could be aspired toward in the name of reducing patient confusion,” they wrote.
The study findings were limited by several factors, including the small sample size and self-selection bias, as well as the subjective nature of an open-ended survey, the researchers noted. However, the results provide evidence of differences in treatment approaches between allopathic and naturopathic providers and suggest that “respectful collaboration between allopathic and naturopathic providers will help practitioners find common ground, decrease patient confusion, and improve patient outcomes,” they concluded.
The researchers had no financial conflicts to disclose.
SOURCE: Dhossche J et al. Ped Dermatol. 2019 Nov 19. doi: 10.1111/pde.14036.
, based on data from a small survey of the two.
Data from previous studies show that more than half of patients with AD have used complementary and alternative medicine in addition to allopathic care, but providers may be unaware of each other’s treatment approaches and confuse patients, wrote Julie Dhossche, MD, of Oregon Health & Science University, Portland, and her colleagues.
In a study published in Pediatric Dermatology, the researchers assessed results of an 11-question, free-text survey of 30 allopathic providers and 21 naturopathic providers about AD. The survey included questions on patient education and evaluation, skin care, and treatment.
Overall, both allopathic and naturopathic providers recommended skin care protocols involving moisturization and “soak and seal” bathing. However, allopathic providers were more likely to prescribe topical corticosteroids for mild to moderate disease (100% vs. 19%), followed by phototherapy and systemic treatments in more severe cases. Naturopathic providers were more likely than allopathic providers to choose topical botanicals, oils, or probiotics (52% vs. 0%) for mild to moderate disease, as well stress relief and acupuncture. Naturopathic providers favored topical corticosteroids and referrals to dermatologists for second- or third-line treatment.
Of note, 85% of naturopathic providers said they thought diet had a probable or definite role in AD, compared with 3% of allopathic providers.
In addition, naturopathic providers differed in their response to an optional question on the use of additional education about food and diet. A total of 11 of 19 naturopathic providers (58%) recommended dietary changes, including “remove potential food allergens/reduce sugar” and “emphasize anti-inflammatory diet,” the researchers said.
“Confusion regarding the role of food in AD management is a common source of frustration for patients, and perhaps a consensus statement from both fields regarding the role of food allergy in AD management could be aspired toward in the name of reducing patient confusion,” they wrote.
The study findings were limited by several factors, including the small sample size and self-selection bias, as well as the subjective nature of an open-ended survey, the researchers noted. However, the results provide evidence of differences in treatment approaches between allopathic and naturopathic providers and suggest that “respectful collaboration between allopathic and naturopathic providers will help practitioners find common ground, decrease patient confusion, and improve patient outcomes,” they concluded.
The researchers had no financial conflicts to disclose.
SOURCE: Dhossche J et al. Ped Dermatol. 2019 Nov 19. doi: 10.1111/pde.14036.
, based on data from a small survey of the two.
Data from previous studies show that more than half of patients with AD have used complementary and alternative medicine in addition to allopathic care, but providers may be unaware of each other’s treatment approaches and confuse patients, wrote Julie Dhossche, MD, of Oregon Health & Science University, Portland, and her colleagues.
In a study published in Pediatric Dermatology, the researchers assessed results of an 11-question, free-text survey of 30 allopathic providers and 21 naturopathic providers about AD. The survey included questions on patient education and evaluation, skin care, and treatment.
Overall, both allopathic and naturopathic providers recommended skin care protocols involving moisturization and “soak and seal” bathing. However, allopathic providers were more likely to prescribe topical corticosteroids for mild to moderate disease (100% vs. 19%), followed by phototherapy and systemic treatments in more severe cases. Naturopathic providers were more likely than allopathic providers to choose topical botanicals, oils, or probiotics (52% vs. 0%) for mild to moderate disease, as well stress relief and acupuncture. Naturopathic providers favored topical corticosteroids and referrals to dermatologists for second- or third-line treatment.
Of note, 85% of naturopathic providers said they thought diet had a probable or definite role in AD, compared with 3% of allopathic providers.
In addition, naturopathic providers differed in their response to an optional question on the use of additional education about food and diet. A total of 11 of 19 naturopathic providers (58%) recommended dietary changes, including “remove potential food allergens/reduce sugar” and “emphasize anti-inflammatory diet,” the researchers said.
“Confusion regarding the role of food in AD management is a common source of frustration for patients, and perhaps a consensus statement from both fields regarding the role of food allergy in AD management could be aspired toward in the name of reducing patient confusion,” they wrote.
The study findings were limited by several factors, including the small sample size and self-selection bias, as well as the subjective nature of an open-ended survey, the researchers noted. However, the results provide evidence of differences in treatment approaches between allopathic and naturopathic providers and suggest that “respectful collaboration between allopathic and naturopathic providers will help practitioners find common ground, decrease patient confusion, and improve patient outcomes,” they concluded.
The researchers had no financial conflicts to disclose.
SOURCE: Dhossche J et al. Ped Dermatol. 2019 Nov 19. doi: 10.1111/pde.14036.
FROM PEDIATRIC DERMATOLOGY
Melanoma incidence drops in younger age groups
, according to results of a population-based registry study of 988,103 cases of invasive melanoma.
These data are observational, “and thus cannot conclusively determine the cause of this statistically and clinically significant decrease,” wrote Kelly G. Paulson, MD, PhD, of the Fred Hutchinson Cancer Research Center, Seattle, and colleagues. However, they added, “a likely explanation for the reduced melanoma incidence in adolescents and young adults is success at increased UV exposure protection. These data provide an impetus to further improve multimodal efforts aimed at reducing the burden of melanoma and encourage ongoing UV exposure protection efforts throughout the lifetime of individuals.”
Public health measures to promote sun-protective behaviors including sunscreen use, protective clothing, and seeking shade were initiated in the United States in the late 1990s and early 2000s, but the public health impact remains unknown, they noted in the study, published in JAMA Dermatology.
For the study, they reviewed data from the National Program of Cancer Registries – Surveillance Epidemiology and End Results combined database for the years 2001-2015. Overall, the incidence of invasive melanoma among people of all ages in the United States increased from 50,272 cases in 2001 to 83,362 in 2015. However, in 2015 only 67 cases were reported in children younger than 10 years, 251 in adolescents aged 10-19 years, and 1,973 in young adults (aged 20-29 years).
Between 2006 and 2015, the annual percentage change in melanoma incidence decreased by 4.4% for male adolescents, 5.4% for female adolescents, 3.7% for male young adults, and 3.6% for female young adults; these changes were statistically significant. The trends in incidence was similar when the population was limited to non-Hispanic whites, considered a high-risk group for melanoma.
By contrast, melanoma incidence increased by an annual percentage change of 1.8% for both men and women aged 40 years and older during the same period of time. Young adult women had a greater incidence of melanoma compared with young adult men (about twofold greater), but older men had a greater incidence of melanoma compared with older women, the researchers said.
The findings were limited by a lack of data about potential confounders, such as skin pigmentation, UV light exposure, sunburn history, sunscreen use, sun avoidance, protective clothing, and tanning bed use; and the absence of information kept the researchers from estimating an association between increased sun-protective behaviors and decreased incidence of melanoma.
“However, this change in behavior remains a plausible explanation for decreased melanoma rates in adolescent and young adult populations,” and the data support continued strategies to promote UV protection throughout life, they said.
The study was supported in part by the National Institutes of Health, the Fred Hutchinson Cancer Research Center Integrated Immunotherapy Research Core, and a Society for Immunotherapy of Cancer–Merck fellowship. Dr. Paulson disclosed grants from the Society for Immunotherapy of Cancer–Merck, bluebird biosciences, EMD Serono; she also disclosed an issued and licensed patent for a Merkel cell carcinoma T cell receptor.
SOURCE: Paulson KG et al. JAMA Dermatol. 2019. Nov 13. doi: 10.1001/jamadermatol.2019.3353.
, according to results of a population-based registry study of 988,103 cases of invasive melanoma.
These data are observational, “and thus cannot conclusively determine the cause of this statistically and clinically significant decrease,” wrote Kelly G. Paulson, MD, PhD, of the Fred Hutchinson Cancer Research Center, Seattle, and colleagues. However, they added, “a likely explanation for the reduced melanoma incidence in adolescents and young adults is success at increased UV exposure protection. These data provide an impetus to further improve multimodal efforts aimed at reducing the burden of melanoma and encourage ongoing UV exposure protection efforts throughout the lifetime of individuals.”
Public health measures to promote sun-protective behaviors including sunscreen use, protective clothing, and seeking shade were initiated in the United States in the late 1990s and early 2000s, but the public health impact remains unknown, they noted in the study, published in JAMA Dermatology.
For the study, they reviewed data from the National Program of Cancer Registries – Surveillance Epidemiology and End Results combined database for the years 2001-2015. Overall, the incidence of invasive melanoma among people of all ages in the United States increased from 50,272 cases in 2001 to 83,362 in 2015. However, in 2015 only 67 cases were reported in children younger than 10 years, 251 in adolescents aged 10-19 years, and 1,973 in young adults (aged 20-29 years).
Between 2006 and 2015, the annual percentage change in melanoma incidence decreased by 4.4% for male adolescents, 5.4% for female adolescents, 3.7% for male young adults, and 3.6% for female young adults; these changes were statistically significant. The trends in incidence was similar when the population was limited to non-Hispanic whites, considered a high-risk group for melanoma.
By contrast, melanoma incidence increased by an annual percentage change of 1.8% for both men and women aged 40 years and older during the same period of time. Young adult women had a greater incidence of melanoma compared with young adult men (about twofold greater), but older men had a greater incidence of melanoma compared with older women, the researchers said.
The findings were limited by a lack of data about potential confounders, such as skin pigmentation, UV light exposure, sunburn history, sunscreen use, sun avoidance, protective clothing, and tanning bed use; and the absence of information kept the researchers from estimating an association between increased sun-protective behaviors and decreased incidence of melanoma.
“However, this change in behavior remains a plausible explanation for decreased melanoma rates in adolescent and young adult populations,” and the data support continued strategies to promote UV protection throughout life, they said.
The study was supported in part by the National Institutes of Health, the Fred Hutchinson Cancer Research Center Integrated Immunotherapy Research Core, and a Society for Immunotherapy of Cancer–Merck fellowship. Dr. Paulson disclosed grants from the Society for Immunotherapy of Cancer–Merck, bluebird biosciences, EMD Serono; she also disclosed an issued and licensed patent for a Merkel cell carcinoma T cell receptor.
SOURCE: Paulson KG et al. JAMA Dermatol. 2019. Nov 13. doi: 10.1001/jamadermatol.2019.3353.
, according to results of a population-based registry study of 988,103 cases of invasive melanoma.
These data are observational, “and thus cannot conclusively determine the cause of this statistically and clinically significant decrease,” wrote Kelly G. Paulson, MD, PhD, of the Fred Hutchinson Cancer Research Center, Seattle, and colleagues. However, they added, “a likely explanation for the reduced melanoma incidence in adolescents and young adults is success at increased UV exposure protection. These data provide an impetus to further improve multimodal efforts aimed at reducing the burden of melanoma and encourage ongoing UV exposure protection efforts throughout the lifetime of individuals.”
Public health measures to promote sun-protective behaviors including sunscreen use, protective clothing, and seeking shade were initiated in the United States in the late 1990s and early 2000s, but the public health impact remains unknown, they noted in the study, published in JAMA Dermatology.
For the study, they reviewed data from the National Program of Cancer Registries – Surveillance Epidemiology and End Results combined database for the years 2001-2015. Overall, the incidence of invasive melanoma among people of all ages in the United States increased from 50,272 cases in 2001 to 83,362 in 2015. However, in 2015 only 67 cases were reported in children younger than 10 years, 251 in adolescents aged 10-19 years, and 1,973 in young adults (aged 20-29 years).
Between 2006 and 2015, the annual percentage change in melanoma incidence decreased by 4.4% for male adolescents, 5.4% for female adolescents, 3.7% for male young adults, and 3.6% for female young adults; these changes were statistically significant. The trends in incidence was similar when the population was limited to non-Hispanic whites, considered a high-risk group for melanoma.
By contrast, melanoma incidence increased by an annual percentage change of 1.8% for both men and women aged 40 years and older during the same period of time. Young adult women had a greater incidence of melanoma compared with young adult men (about twofold greater), but older men had a greater incidence of melanoma compared with older women, the researchers said.
The findings were limited by a lack of data about potential confounders, such as skin pigmentation, UV light exposure, sunburn history, sunscreen use, sun avoidance, protective clothing, and tanning bed use; and the absence of information kept the researchers from estimating an association between increased sun-protective behaviors and decreased incidence of melanoma.
“However, this change in behavior remains a plausible explanation for decreased melanoma rates in adolescent and young adult populations,” and the data support continued strategies to promote UV protection throughout life, they said.
The study was supported in part by the National Institutes of Health, the Fred Hutchinson Cancer Research Center Integrated Immunotherapy Research Core, and a Society for Immunotherapy of Cancer–Merck fellowship. Dr. Paulson disclosed grants from the Society for Immunotherapy of Cancer–Merck, bluebird biosciences, EMD Serono; she also disclosed an issued and licensed patent for a Merkel cell carcinoma T cell receptor.
SOURCE: Paulson KG et al. JAMA Dermatol. 2019. Nov 13. doi: 10.1001/jamadermatol.2019.3353.
FROM JAMA DERMATOLOGY
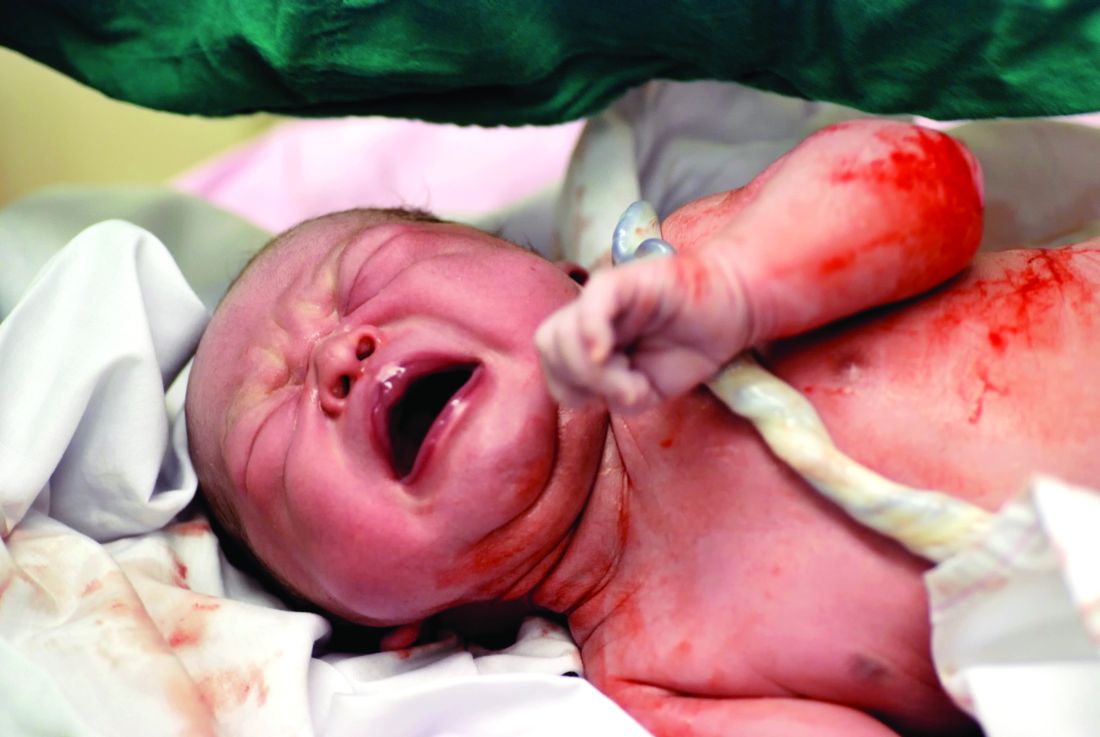
Umbilical cord management matters less for mothers than for infants
Immediate umbilical cord milking or delayed clamping of the umbilical cord had no significant impact on maternal outcomes, but infants were significantly more likely to experience severe intraventricular hemorrhage with umbilical cord milking, according to results of two studies published in JAMA.
“While the evidence for neonatal benefit with delayed cord clamping at term is strong, data related to maternal outcomes, particularly after cesarean delivery, are largely lacking,” wrote Stephanie E. Purisch, MD, of Columbia University Irving Medical Center, New York, and colleagues.
In a randomized trial of 113 women who underwent cesarean deliveries of singleton infants, the researchers hypothesized that maternal blood loss would be greater with delayed cord clamping (JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.15995).
However, maternal blood loss, based on mean hemoglobin levels 1 day after delivery, was not significantly different between the delayed group (10.1 g/dL) and the immediate group (98 g/dL). The median time to cord clamping was 63 seconds in the delayed group and 6 seconds in the immediate group.
In addition, no significant differences occurred in 15 of 19 prespecified secondary outcomes. However, for whom data were available (18.1 g/dL vs. 16.4 g/dL; P less than .001).
The results were limited by factors including lack of generalizability to other situations such as emergency or preterm deliveries and by the lack of a definition of a “clinically important postoperative hemoglobin change,” the researchers noted. However, the results show no significant impact of umbilical cord management on maternal hemoglobin in the study population.
In another study published in JAMA, Anup Katheria, MD, of Sharp Mary Birch Hospital for Women & Newborns, San Diego, and colleagues found no significant difference in rates of a composite outcome of death or severe intraventricular hemorrhage among infants randomized to umbilical cord milking (12%) vs. delayed umbilical cord clamping (8%). However, immediate umbilical cord milking was significantly associated with a higher rate of intraventricular hemorrhage alone, compared with delayed clamping (8% vs. 3%), and this signal of risk prompted the researchers to terminate the study earlier than intended.
The researchers randomized 474 infants born at less than 32 weeks’ gestation to umbilical cord milking or delayed umbilical cord clamping (JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.16004). The study was conducted at six sites in the United States and one site each in Ireland, Germany, and Canada between June 2017 and September 2018. “Because of the importance of long-term neurodevelopment, all surviving infants will be followed up to determine developmental outcomes at 22 to 26 months’ corrected gestational age,” they said.
The study was terminated early, which prevents definitive conclusions, the researchers noted, but a new study has been approved to compare umbilical cord milking with delayed umbilical cord clamping in infants of 30-32 weeks’ gestational age, they said.
“Although the safety of placental transfusion for the mother seems well established, it remains unclear which method of providing placental transfusion is best for the infant: delayed clamping and cutting the cord or milking the intact cord. The latter provides a transfusion more rapidly, which may facilitate initiation of resuscitation when needed,” Heike Rabe, MD, of the University of Sussex, Brighton, and Ola Andersson, PhD, of Lund (Sweden) University, wrote in an editorial accompanying the two studies (JAMA. 2019 Nov 19;322:1864-5. doi: 10.1001/jama.2019.16003).
The 8% incidence of severe intraventricular hemorrhage in the umbilical milking group in the study by Katheria and colleagues was higher than the 5.2% in a recent Cochrane review, but the 3% incidence of severe intraventricular hemorrhage in the delayed group was lower than the 4.5% in the Cochrane review, they said.
“Umbilical cord milking has been used in many hospitals without an increase in intraventricular hemorrhage being observed,” they noted.
“The study by Purisch et al. demonstrated the safety of delayed cord clamping for mothers delivering by cesarean at term,” the editorialists wrote. Studies are underway to identify the best techniques for cord clamping, they said.
“In the meantime, clinicians should follow the World Health Organization recommendation to delay cord clamping and cutting for 1 to 3 minutes for term infants and for at least 60 seconds for preterm infants to prevent iron deficiency and potentially enable more premature infants to survive,” they concluded.
Dr. Purisch received funding from the Maternal-Fetal Medicine Fellow Research Fund for the first study. Coauthor Cynthia Gyamfi-Bannerman, MD, reported receiving grants from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the Society for Maternal-Fetal Medicine/AMAG Pharmaceuticals, and personal fees from Sera Prognostics outside the submitted work. The second study was supported by NICHD in a grant to Dr. Katheria, who had no financial conflicts to disclose. Coauthor Gary Cutter, PhD, had numerous ties to pharmaceutical companies. The editorialists had no financial conflicts to disclose.
SOURCES: Purisch SE et al. JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.15995; Katheria A et al. JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.16004; Rabe H and Andersson O. JAMA. 2019 Nov 19; 322:1864-5.
Immediate umbilical cord milking or delayed clamping of the umbilical cord had no significant impact on maternal outcomes, but infants were significantly more likely to experience severe intraventricular hemorrhage with umbilical cord milking, according to results of two studies published in JAMA.
“While the evidence for neonatal benefit with delayed cord clamping at term is strong, data related to maternal outcomes, particularly after cesarean delivery, are largely lacking,” wrote Stephanie E. Purisch, MD, of Columbia University Irving Medical Center, New York, and colleagues.
In a randomized trial of 113 women who underwent cesarean deliveries of singleton infants, the researchers hypothesized that maternal blood loss would be greater with delayed cord clamping (JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.15995).
However, maternal blood loss, based on mean hemoglobin levels 1 day after delivery, was not significantly different between the delayed group (10.1 g/dL) and the immediate group (98 g/dL). The median time to cord clamping was 63 seconds in the delayed group and 6 seconds in the immediate group.
In addition, no significant differences occurred in 15 of 19 prespecified secondary outcomes. However, for whom data were available (18.1 g/dL vs. 16.4 g/dL; P less than .001).
The results were limited by factors including lack of generalizability to other situations such as emergency or preterm deliveries and by the lack of a definition of a “clinically important postoperative hemoglobin change,” the researchers noted. However, the results show no significant impact of umbilical cord management on maternal hemoglobin in the study population.
In another study published in JAMA, Anup Katheria, MD, of Sharp Mary Birch Hospital for Women & Newborns, San Diego, and colleagues found no significant difference in rates of a composite outcome of death or severe intraventricular hemorrhage among infants randomized to umbilical cord milking (12%) vs. delayed umbilical cord clamping (8%). However, immediate umbilical cord milking was significantly associated with a higher rate of intraventricular hemorrhage alone, compared with delayed clamping (8% vs. 3%), and this signal of risk prompted the researchers to terminate the study earlier than intended.
The researchers randomized 474 infants born at less than 32 weeks’ gestation to umbilical cord milking or delayed umbilical cord clamping (JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.16004). The study was conducted at six sites in the United States and one site each in Ireland, Germany, and Canada between June 2017 and September 2018. “Because of the importance of long-term neurodevelopment, all surviving infants will be followed up to determine developmental outcomes at 22 to 26 months’ corrected gestational age,” they said.
The study was terminated early, which prevents definitive conclusions, the researchers noted, but a new study has been approved to compare umbilical cord milking with delayed umbilical cord clamping in infants of 30-32 weeks’ gestational age, they said.
“Although the safety of placental transfusion for the mother seems well established, it remains unclear which method of providing placental transfusion is best for the infant: delayed clamping and cutting the cord or milking the intact cord. The latter provides a transfusion more rapidly, which may facilitate initiation of resuscitation when needed,” Heike Rabe, MD, of the University of Sussex, Brighton, and Ola Andersson, PhD, of Lund (Sweden) University, wrote in an editorial accompanying the two studies (JAMA. 2019 Nov 19;322:1864-5. doi: 10.1001/jama.2019.16003).
The 8% incidence of severe intraventricular hemorrhage in the umbilical milking group in the study by Katheria and colleagues was higher than the 5.2% in a recent Cochrane review, but the 3% incidence of severe intraventricular hemorrhage in the delayed group was lower than the 4.5% in the Cochrane review, they said.
“Umbilical cord milking has been used in many hospitals without an increase in intraventricular hemorrhage being observed,” they noted.
“The study by Purisch et al. demonstrated the safety of delayed cord clamping for mothers delivering by cesarean at term,” the editorialists wrote. Studies are underway to identify the best techniques for cord clamping, they said.
“In the meantime, clinicians should follow the World Health Organization recommendation to delay cord clamping and cutting for 1 to 3 minutes for term infants and for at least 60 seconds for preterm infants to prevent iron deficiency and potentially enable more premature infants to survive,” they concluded.
Dr. Purisch received funding from the Maternal-Fetal Medicine Fellow Research Fund for the first study. Coauthor Cynthia Gyamfi-Bannerman, MD, reported receiving grants from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the Society for Maternal-Fetal Medicine/AMAG Pharmaceuticals, and personal fees from Sera Prognostics outside the submitted work. The second study was supported by NICHD in a grant to Dr. Katheria, who had no financial conflicts to disclose. Coauthor Gary Cutter, PhD, had numerous ties to pharmaceutical companies. The editorialists had no financial conflicts to disclose.
SOURCES: Purisch SE et al. JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.15995; Katheria A et al. JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.16004; Rabe H and Andersson O. JAMA. 2019 Nov 19; 322:1864-5.
Immediate umbilical cord milking or delayed clamping of the umbilical cord had no significant impact on maternal outcomes, but infants were significantly more likely to experience severe intraventricular hemorrhage with umbilical cord milking, according to results of two studies published in JAMA.
“While the evidence for neonatal benefit with delayed cord clamping at term is strong, data related to maternal outcomes, particularly after cesarean delivery, are largely lacking,” wrote Stephanie E. Purisch, MD, of Columbia University Irving Medical Center, New York, and colleagues.
In a randomized trial of 113 women who underwent cesarean deliveries of singleton infants, the researchers hypothesized that maternal blood loss would be greater with delayed cord clamping (JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.15995).
However, maternal blood loss, based on mean hemoglobin levels 1 day after delivery, was not significantly different between the delayed group (10.1 g/dL) and the immediate group (98 g/dL). The median time to cord clamping was 63 seconds in the delayed group and 6 seconds in the immediate group.
In addition, no significant differences occurred in 15 of 19 prespecified secondary outcomes. However, for whom data were available (18.1 g/dL vs. 16.4 g/dL; P less than .001).
The results were limited by factors including lack of generalizability to other situations such as emergency or preterm deliveries and by the lack of a definition of a “clinically important postoperative hemoglobin change,” the researchers noted. However, the results show no significant impact of umbilical cord management on maternal hemoglobin in the study population.
In another study published in JAMA, Anup Katheria, MD, of Sharp Mary Birch Hospital for Women & Newborns, San Diego, and colleagues found no significant difference in rates of a composite outcome of death or severe intraventricular hemorrhage among infants randomized to umbilical cord milking (12%) vs. delayed umbilical cord clamping (8%). However, immediate umbilical cord milking was significantly associated with a higher rate of intraventricular hemorrhage alone, compared with delayed clamping (8% vs. 3%), and this signal of risk prompted the researchers to terminate the study earlier than intended.
The researchers randomized 474 infants born at less than 32 weeks’ gestation to umbilical cord milking or delayed umbilical cord clamping (JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.16004). The study was conducted at six sites in the United States and one site each in Ireland, Germany, and Canada between June 2017 and September 2018. “Because of the importance of long-term neurodevelopment, all surviving infants will be followed up to determine developmental outcomes at 22 to 26 months’ corrected gestational age,” they said.
The study was terminated early, which prevents definitive conclusions, the researchers noted, but a new study has been approved to compare umbilical cord milking with delayed umbilical cord clamping in infants of 30-32 weeks’ gestational age, they said.
“Although the safety of placental transfusion for the mother seems well established, it remains unclear which method of providing placental transfusion is best for the infant: delayed clamping and cutting the cord or milking the intact cord. The latter provides a transfusion more rapidly, which may facilitate initiation of resuscitation when needed,” Heike Rabe, MD, of the University of Sussex, Brighton, and Ola Andersson, PhD, of Lund (Sweden) University, wrote in an editorial accompanying the two studies (JAMA. 2019 Nov 19;322:1864-5. doi: 10.1001/jama.2019.16003).
The 8% incidence of severe intraventricular hemorrhage in the umbilical milking group in the study by Katheria and colleagues was higher than the 5.2% in a recent Cochrane review, but the 3% incidence of severe intraventricular hemorrhage in the delayed group was lower than the 4.5% in the Cochrane review, they said.
“Umbilical cord milking has been used in many hospitals without an increase in intraventricular hemorrhage being observed,” they noted.
“The study by Purisch et al. demonstrated the safety of delayed cord clamping for mothers delivering by cesarean at term,” the editorialists wrote. Studies are underway to identify the best techniques for cord clamping, they said.
“In the meantime, clinicians should follow the World Health Organization recommendation to delay cord clamping and cutting for 1 to 3 minutes for term infants and for at least 60 seconds for preterm infants to prevent iron deficiency and potentially enable more premature infants to survive,” they concluded.
Dr. Purisch received funding from the Maternal-Fetal Medicine Fellow Research Fund for the first study. Coauthor Cynthia Gyamfi-Bannerman, MD, reported receiving grants from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the Society for Maternal-Fetal Medicine/AMAG Pharmaceuticals, and personal fees from Sera Prognostics outside the submitted work. The second study was supported by NICHD in a grant to Dr. Katheria, who had no financial conflicts to disclose. Coauthor Gary Cutter, PhD, had numerous ties to pharmaceutical companies. The editorialists had no financial conflicts to disclose.
SOURCES: Purisch SE et al. JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.15995; Katheria A et al. JAMA. 2019 Nov 19. doi: 10.1001/jama.2019.16004; Rabe H and Andersson O. JAMA. 2019 Nov 19; 322:1864-5.
FROM JAMA
AAP advises pediatricians to support emergency contraception for all teenagers
Educating pediatricians to inform their teenage patients about emergency contraception is an important step toward reducing adolescent pregnancy in the United States, according to a policy statement issued by the American Academy of Pediatrics.
“Improved use of contraception, not declines in sexual activity, has been the most significant contributor to the decline in pregnancy risk among U.S. teenagers over the past decade,” wrote Krishna K. Upadhya, MD, MPH, and colleagues on the AAP’s Committee on Adolescence.
; however, many pediatricians do not routinely counsel adolescents about emergency contraception, they noted.
In the statement published Nov. 18 in Pediatrics, the committee listed indications for emergency contraception as unprotected or underprotected intercourse for reasons including sexual assault, lack of contraception use, or ineffective contraception use. The committee recommended that pediatricians provide emergency contraception in the form of oral pills (levonorgestrel or ulipristal acetate) or copper IUDs to adolescents in immediate need of emergency contraception, and ideally, to make those products available in advance so teens have them on hand.
The committee recommended the use of combined contraceptive pills known as the Yuzpe method, if dedicated emergency contraceptive pills or IUDs are not available, and emphasized the possible impact of overweight and obesity on the effectiveness of emergency contraceptive pills.
The recommendations also include advising adolescents about proper use of emergency contraception, and the need for follow-up visits to address ongoing contraception and testing for sexually transmitted diseases. The committee noted that adolescents using emergency contraceptive pills must be counseled to abstain or use additional contraception (such as condoms) because of the delay in ovulation associated with these products.
The committee recommended that all adolescents receive counseling on emergency contraception as part of a general discussion on sexual health, regardless of current sexual activity or lack of it. “In addition, it is important that information about EC be included in all contraceptive and STI counseling for adolescents wherever these visits occur, including emergency departments, clinics, and hospitals,” and that pediatricians provide this information to teens with physical and cognitive disabilities and their parents as well, they wrote.
The committee concluded the recommendations by asking clinicians to advocate for free or inexpensive nonprescription access to emergency contraceptive pills for adolescents regardless of age and insurance status.
M. Susan Jay, MD, program director of adolescent health and medicine at the Children’s Hospital of Wisconsin, Milwaukee, commented in an interview, “Forty years ago, as I completed my training, I don’t believe it would have been possible to contemplate the growth of adolescent health care, including reproductive health care that current pediatric practitioners are asked to provide to the adolescents under their care.”
“Today we are asked to be a resource from topics related to vaping and trafficking as well as psychosocial concerns from anxiety to eating disorders. This policy statement from the AAP addresses how best to approach and counsel both young women and young men as they traverse the issues of sexual engagement and responsibility. I have been privileged to work with pediatric residents who are far more sophisticated and knowledgeable than I have ever been, but they call and ask the very questions so adroitly presented in this policy statement. Most of my pediatric colleagues have had a limited adolescent medicine experience, and yet they are asked to care for youth in sensitive situations and want the tools necessary to provide the very best and safest care to their patients. Most of us will not be skilled in the placement of copper IUDs as outlined as an option for emergency contraception, but knowledge of the medications reviewed is of importance and relevant to everyday practice.
"This policy statement is a resource and educational update rolled into one, and Dr. Upadhya and her colleagues on the AAP’s Committee on Adolescence should be commended for assisting providers to offer the best and safest care,” said Dr. Jay, who was not involved in writing the AAP policy statement, and is a member of the Pediatric News Editorial Advisory Board who was asked to comment on the new policy statement.
The American College of Pediatricians (ACPeds), a conservative-leaning pediatric organization opposes the AAP’s recent opinion and the provision of emergency contraception to youth, Michelle Cretella, MD, executive director for the group, said in an interview. In its own position statement, ACPeds wrote that preprescribing EC to adolescent patients, or making them available without prescription, “carries significant medical risk and is counterproductive to the parent-adolescent and patient-physician relationships.”
“Increased access to [EC] does not result in lower pregnancy rates among adolescents and young adults,” said Dr. Cretella, a board-certified pediatrician who is not currently in practice. The ACPeds position statement cites a 2012 study that examined a Washington state program that allowed patients to access EC through pharmacies without a prescription. The analysis found the increased access to EC resulted in a statistically significant rise in gonorrhea for women and overall for both genders. The increased access to EC did not impact birth rates or abortion rates, according to the study (Economic Inquiry. 2013 Jul;51[3]:1682-95).
The ACPeds statement also notes a report by the Heritage Foundation that found sexually active teenagers were less likely to be happy and more likely to be depressed than were youth who were not having sex. The 2003 report, which examined responses from 6,500 adolescents through the 1996 National Longitudinal Survey of Adolescent Health, also found that sexually active teenagers were significantly more likely to attempt suicide, compared with teens who were not sexually active.
Dr. Upadhya disclosed having no financial conflicts.
SOURCE: Upadhya KK et al. Pediatrics. 2019 Nov 18. doi: 10.1542/peds.2019-3149.
This article was updated on 11/19/19 and 12/16/19.
Despite declining teen birth rates, the United States has the highest rate of teen pregnancy among developed nations outside the former Soviet Bloc, according to the Guttmacher Institute. This high rate remains in part because of the significant barriers that prevent access to reproductive health services for adolescents. Teen pregnancy prevention remains an important adolescent health issue because of the high risk of poor health outcomes facing teen parents and their children. As advocates for children, pediatricians should educate, advocate for, and provide contraception to their patients. To this end, the AAP’s policy statement on emergency contraception (EC) provides practical guidance to increase access for EC for adolescents.
Simply put, EC provides contraception for “emergencies” such as unprotected sex, sexual assault, missed birth control pills, and condom failure. While EC is not meant to be the sole form of contraception used by adolescents, it is an important stop-gap measure – and the only one that can be used after sex. The “gold standard” for contraception in teens remains long-acting reversible contraception (LARC) methods such as the intrauterine device and the hormonal implant. These methods are recommended first line by the AAP because of their high efficacy.
Despite these recommendations, LARC use remains low, with only 6% of sexually active U.S. teens using these methods. While pediatricians should continue to encourage LARC methods, they should not neglect counseling on other contraceptive methods, including on EC.
In fact, studies demonstrate that pediatricians often omit counseling about EC, and most do not prescribe these medications routinely. Despite several available over-the-counter formulations, there still are significant barriers to teens in accessing these medications. In my practice, I have experienced teens who miss the opportunity to use this medication because of its cost and nonavailability when it is needed – from either inadequate stock at the pharmacy or from pharmacists’ conscientious objections. Ideally, counseling on EC should be part of the routine anticipatory guidance provided to all adolescents, and routine prescriptions should be given to adolescent women. When I prescribe EC to teens preventively, I tell them to fill the prescription and have it “on hand” at home in case it is ever needed, given the time-sensitive nature of most formulations. This policy also saliently addresses counseling for adolescent men – who often are overlooked in conversations about EC as they cannot use these methods. However, increasing their awareness and knowledge of this method can increase its use in their partners.
This policy provides excellent technical information on different formulations of EC, side effects, contraindications, and anticipatory guidance to give patients about the use of these medications. Additionally, it highlights the copper IUD – the often forgotten, but most effective form of EC that provides lasting pregnancy prevention. Overall, this policy provides great information to “demystify” EC and encourages pediatricians to engage in improving reproductive health access for adolescents.*
Kelly Curran, MD, specializes in adolescent medicine at the University of Oklahoma Health Sciences Center, Oklahoma City. She was asked to comment on the AAP policy statement on emergency contraception. Dr. Curran is a member of the Pediatric News Editorial Advisory Board. Email her at [email protected].
Despite declining teen birth rates, the United States has the highest rate of teen pregnancy among developed nations outside the former Soviet Bloc, according to the Guttmacher Institute. This high rate remains in part because of the significant barriers that prevent access to reproductive health services for adolescents. Teen pregnancy prevention remains an important adolescent health issue because of the high risk of poor health outcomes facing teen parents and their children. As advocates for children, pediatricians should educate, advocate for, and provide contraception to their patients. To this end, the AAP’s policy statement on emergency contraception (EC) provides practical guidance to increase access for EC for adolescents.
Simply put, EC provides contraception for “emergencies” such as unprotected sex, sexual assault, missed birth control pills, and condom failure. While EC is not meant to be the sole form of contraception used by adolescents, it is an important stop-gap measure – and the only one that can be used after sex. The “gold standard” for contraception in teens remains long-acting reversible contraception (LARC) methods such as the intrauterine device and the hormonal implant. These methods are recommended first line by the AAP because of their high efficacy.
Despite these recommendations, LARC use remains low, with only 6% of sexually active U.S. teens using these methods. While pediatricians should continue to encourage LARC methods, they should not neglect counseling on other contraceptive methods, including on EC.
In fact, studies demonstrate that pediatricians often omit counseling about EC, and most do not prescribe these medications routinely. Despite several available over-the-counter formulations, there still are significant barriers to teens in accessing these medications. In my practice, I have experienced teens who miss the opportunity to use this medication because of its cost and nonavailability when it is needed – from either inadequate stock at the pharmacy or from pharmacists’ conscientious objections. Ideally, counseling on EC should be part of the routine anticipatory guidance provided to all adolescents, and routine prescriptions should be given to adolescent women. When I prescribe EC to teens preventively, I tell them to fill the prescription and have it “on hand” at home in case it is ever needed, given the time-sensitive nature of most formulations. This policy also saliently addresses counseling for adolescent men – who often are overlooked in conversations about EC as they cannot use these methods. However, increasing their awareness and knowledge of this method can increase its use in their partners.
This policy provides excellent technical information on different formulations of EC, side effects, contraindications, and anticipatory guidance to give patients about the use of these medications. Additionally, it highlights the copper IUD – the often forgotten, but most effective form of EC that provides lasting pregnancy prevention. Overall, this policy provides great information to “demystify” EC and encourages pediatricians to engage in improving reproductive health access for adolescents.*
Kelly Curran, MD, specializes in adolescent medicine at the University of Oklahoma Health Sciences Center, Oklahoma City. She was asked to comment on the AAP policy statement on emergency contraception. Dr. Curran is a member of the Pediatric News Editorial Advisory Board. Email her at [email protected].
Despite declining teen birth rates, the United States has the highest rate of teen pregnancy among developed nations outside the former Soviet Bloc, according to the Guttmacher Institute. This high rate remains in part because of the significant barriers that prevent access to reproductive health services for adolescents. Teen pregnancy prevention remains an important adolescent health issue because of the high risk of poor health outcomes facing teen parents and their children. As advocates for children, pediatricians should educate, advocate for, and provide contraception to their patients. To this end, the AAP’s policy statement on emergency contraception (EC) provides practical guidance to increase access for EC for adolescents.
Simply put, EC provides contraception for “emergencies” such as unprotected sex, sexual assault, missed birth control pills, and condom failure. While EC is not meant to be the sole form of contraception used by adolescents, it is an important stop-gap measure – and the only one that can be used after sex. The “gold standard” for contraception in teens remains long-acting reversible contraception (LARC) methods such as the intrauterine device and the hormonal implant. These methods are recommended first line by the AAP because of their high efficacy.
Despite these recommendations, LARC use remains low, with only 6% of sexually active U.S. teens using these methods. While pediatricians should continue to encourage LARC methods, they should not neglect counseling on other contraceptive methods, including on EC.
In fact, studies demonstrate that pediatricians often omit counseling about EC, and most do not prescribe these medications routinely. Despite several available over-the-counter formulations, there still are significant barriers to teens in accessing these medications. In my practice, I have experienced teens who miss the opportunity to use this medication because of its cost and nonavailability when it is needed – from either inadequate stock at the pharmacy or from pharmacists’ conscientious objections. Ideally, counseling on EC should be part of the routine anticipatory guidance provided to all adolescents, and routine prescriptions should be given to adolescent women. When I prescribe EC to teens preventively, I tell them to fill the prescription and have it “on hand” at home in case it is ever needed, given the time-sensitive nature of most formulations. This policy also saliently addresses counseling for adolescent men – who often are overlooked in conversations about EC as they cannot use these methods. However, increasing their awareness and knowledge of this method can increase its use in their partners.
This policy provides excellent technical information on different formulations of EC, side effects, contraindications, and anticipatory guidance to give patients about the use of these medications. Additionally, it highlights the copper IUD – the often forgotten, but most effective form of EC that provides lasting pregnancy prevention. Overall, this policy provides great information to “demystify” EC and encourages pediatricians to engage in improving reproductive health access for adolescents.*
Kelly Curran, MD, specializes in adolescent medicine at the University of Oklahoma Health Sciences Center, Oklahoma City. She was asked to comment on the AAP policy statement on emergency contraception. Dr. Curran is a member of the Pediatric News Editorial Advisory Board. Email her at [email protected].
Educating pediatricians to inform their teenage patients about emergency contraception is an important step toward reducing adolescent pregnancy in the United States, according to a policy statement issued by the American Academy of Pediatrics.
“Improved use of contraception, not declines in sexual activity, has been the most significant contributor to the decline in pregnancy risk among U.S. teenagers over the past decade,” wrote Krishna K. Upadhya, MD, MPH, and colleagues on the AAP’s Committee on Adolescence.
; however, many pediatricians do not routinely counsel adolescents about emergency contraception, they noted.
In the statement published Nov. 18 in Pediatrics, the committee listed indications for emergency contraception as unprotected or underprotected intercourse for reasons including sexual assault, lack of contraception use, or ineffective contraception use. The committee recommended that pediatricians provide emergency contraception in the form of oral pills (levonorgestrel or ulipristal acetate) or copper IUDs to adolescents in immediate need of emergency contraception, and ideally, to make those products available in advance so teens have them on hand.
The committee recommended the use of combined contraceptive pills known as the Yuzpe method, if dedicated emergency contraceptive pills or IUDs are not available, and emphasized the possible impact of overweight and obesity on the effectiveness of emergency contraceptive pills.
The recommendations also include advising adolescents about proper use of emergency contraception, and the need for follow-up visits to address ongoing contraception and testing for sexually transmitted diseases. The committee noted that adolescents using emergency contraceptive pills must be counseled to abstain or use additional contraception (such as condoms) because of the delay in ovulation associated with these products.
The committee recommended that all adolescents receive counseling on emergency contraception as part of a general discussion on sexual health, regardless of current sexual activity or lack of it. “In addition, it is important that information about EC be included in all contraceptive and STI counseling for adolescents wherever these visits occur, including emergency departments, clinics, and hospitals,” and that pediatricians provide this information to teens with physical and cognitive disabilities and their parents as well, they wrote.
The committee concluded the recommendations by asking clinicians to advocate for free or inexpensive nonprescription access to emergency contraceptive pills for adolescents regardless of age and insurance status.
M. Susan Jay, MD, program director of adolescent health and medicine at the Children’s Hospital of Wisconsin, Milwaukee, commented in an interview, “Forty years ago, as I completed my training, I don’t believe it would have been possible to contemplate the growth of adolescent health care, including reproductive health care that current pediatric practitioners are asked to provide to the adolescents under their care.”
“Today we are asked to be a resource from topics related to vaping and trafficking as well as psychosocial concerns from anxiety to eating disorders. This policy statement from the AAP addresses how best to approach and counsel both young women and young men as they traverse the issues of sexual engagement and responsibility. I have been privileged to work with pediatric residents who are far more sophisticated and knowledgeable than I have ever been, but they call and ask the very questions so adroitly presented in this policy statement. Most of my pediatric colleagues have had a limited adolescent medicine experience, and yet they are asked to care for youth in sensitive situations and want the tools necessary to provide the very best and safest care to their patients. Most of us will not be skilled in the placement of copper IUDs as outlined as an option for emergency contraception, but knowledge of the medications reviewed is of importance and relevant to everyday practice.
"This policy statement is a resource and educational update rolled into one, and Dr. Upadhya and her colleagues on the AAP’s Committee on Adolescence should be commended for assisting providers to offer the best and safest care,” said Dr. Jay, who was not involved in writing the AAP policy statement, and is a member of the Pediatric News Editorial Advisory Board who was asked to comment on the new policy statement.
The American College of Pediatricians (ACPeds), a conservative-leaning pediatric organization opposes the AAP’s recent opinion and the provision of emergency contraception to youth, Michelle Cretella, MD, executive director for the group, said in an interview. In its own position statement, ACPeds wrote that preprescribing EC to adolescent patients, or making them available without prescription, “carries significant medical risk and is counterproductive to the parent-adolescent and patient-physician relationships.”
“Increased access to [EC] does not result in lower pregnancy rates among adolescents and young adults,” said Dr. Cretella, a board-certified pediatrician who is not currently in practice. The ACPeds position statement cites a 2012 study that examined a Washington state program that allowed patients to access EC through pharmacies without a prescription. The analysis found the increased access to EC resulted in a statistically significant rise in gonorrhea for women and overall for both genders. The increased access to EC did not impact birth rates or abortion rates, according to the study (Economic Inquiry. 2013 Jul;51[3]:1682-95).
The ACPeds statement also notes a report by the Heritage Foundation that found sexually active teenagers were less likely to be happy and more likely to be depressed than were youth who were not having sex. The 2003 report, which examined responses from 6,500 adolescents through the 1996 National Longitudinal Survey of Adolescent Health, also found that sexually active teenagers were significantly more likely to attempt suicide, compared with teens who were not sexually active.
Dr. Upadhya disclosed having no financial conflicts.
SOURCE: Upadhya KK et al. Pediatrics. 2019 Nov 18. doi: 10.1542/peds.2019-3149.
This article was updated on 11/19/19 and 12/16/19.
Educating pediatricians to inform their teenage patients about emergency contraception is an important step toward reducing adolescent pregnancy in the United States, according to a policy statement issued by the American Academy of Pediatrics.
“Improved use of contraception, not declines in sexual activity, has been the most significant contributor to the decline in pregnancy risk among U.S. teenagers over the past decade,” wrote Krishna K. Upadhya, MD, MPH, and colleagues on the AAP’s Committee on Adolescence.
; however, many pediatricians do not routinely counsel adolescents about emergency contraception, they noted.
In the statement published Nov. 18 in Pediatrics, the committee listed indications for emergency contraception as unprotected or underprotected intercourse for reasons including sexual assault, lack of contraception use, or ineffective contraception use. The committee recommended that pediatricians provide emergency contraception in the form of oral pills (levonorgestrel or ulipristal acetate) or copper IUDs to adolescents in immediate need of emergency contraception, and ideally, to make those products available in advance so teens have them on hand.
The committee recommended the use of combined contraceptive pills known as the Yuzpe method, if dedicated emergency contraceptive pills or IUDs are not available, and emphasized the possible impact of overweight and obesity on the effectiveness of emergency contraceptive pills.
The recommendations also include advising adolescents about proper use of emergency contraception, and the need for follow-up visits to address ongoing contraception and testing for sexually transmitted diseases. The committee noted that adolescents using emergency contraceptive pills must be counseled to abstain or use additional contraception (such as condoms) because of the delay in ovulation associated with these products.
The committee recommended that all adolescents receive counseling on emergency contraception as part of a general discussion on sexual health, regardless of current sexual activity or lack of it. “In addition, it is important that information about EC be included in all contraceptive and STI counseling for adolescents wherever these visits occur, including emergency departments, clinics, and hospitals,” and that pediatricians provide this information to teens with physical and cognitive disabilities and their parents as well, they wrote.
The committee concluded the recommendations by asking clinicians to advocate for free or inexpensive nonprescription access to emergency contraceptive pills for adolescents regardless of age and insurance status.
M. Susan Jay, MD, program director of adolescent health and medicine at the Children’s Hospital of Wisconsin, Milwaukee, commented in an interview, “Forty years ago, as I completed my training, I don’t believe it would have been possible to contemplate the growth of adolescent health care, including reproductive health care that current pediatric practitioners are asked to provide to the adolescents under their care.”
“Today we are asked to be a resource from topics related to vaping and trafficking as well as psychosocial concerns from anxiety to eating disorders. This policy statement from the AAP addresses how best to approach and counsel both young women and young men as they traverse the issues of sexual engagement and responsibility. I have been privileged to work with pediatric residents who are far more sophisticated and knowledgeable than I have ever been, but they call and ask the very questions so adroitly presented in this policy statement. Most of my pediatric colleagues have had a limited adolescent medicine experience, and yet they are asked to care for youth in sensitive situations and want the tools necessary to provide the very best and safest care to their patients. Most of us will not be skilled in the placement of copper IUDs as outlined as an option for emergency contraception, but knowledge of the medications reviewed is of importance and relevant to everyday practice.
"This policy statement is a resource and educational update rolled into one, and Dr. Upadhya and her colleagues on the AAP’s Committee on Adolescence should be commended for assisting providers to offer the best and safest care,” said Dr. Jay, who was not involved in writing the AAP policy statement, and is a member of the Pediatric News Editorial Advisory Board who was asked to comment on the new policy statement.
The American College of Pediatricians (ACPeds), a conservative-leaning pediatric organization opposes the AAP’s recent opinion and the provision of emergency contraception to youth, Michelle Cretella, MD, executive director for the group, said in an interview. In its own position statement, ACPeds wrote that preprescribing EC to adolescent patients, or making them available without prescription, “carries significant medical risk and is counterproductive to the parent-adolescent and patient-physician relationships.”
“Increased access to [EC] does not result in lower pregnancy rates among adolescents and young adults,” said Dr. Cretella, a board-certified pediatrician who is not currently in practice. The ACPeds position statement cites a 2012 study that examined a Washington state program that allowed patients to access EC through pharmacies without a prescription. The analysis found the increased access to EC resulted in a statistically significant rise in gonorrhea for women and overall for both genders. The increased access to EC did not impact birth rates or abortion rates, according to the study (Economic Inquiry. 2013 Jul;51[3]:1682-95).
The ACPeds statement also notes a report by the Heritage Foundation that found sexually active teenagers were less likely to be happy and more likely to be depressed than were youth who were not having sex. The 2003 report, which examined responses from 6,500 adolescents through the 1996 National Longitudinal Survey of Adolescent Health, also found that sexually active teenagers were significantly more likely to attempt suicide, compared with teens who were not sexually active.
Dr. Upadhya disclosed having no financial conflicts.
SOURCE: Upadhya KK et al. Pediatrics. 2019 Nov 18. doi: 10.1542/peds.2019-3149.
This article was updated on 11/19/19 and 12/16/19.
FROM PEDIATRICS
Early use of ustekinumab levels could predict psoriasis outcomes
Early ustekinumab levels are significantly associated with a 75% reduction in Psoriasis Area and Severity Index scores from baseline, according to data from 491 adults with psoriasis.
“Evidence suggests that ustekinumab dosing is suboptimal in some patients,” because of factors including weight-based dosing and dosing intervals; therefore “individualized dose optimization and therapeutic drug monitoring (TDM) of ustekinumab may have clinical utility,” Teresa Tsakok, MRCP, of King’s College London, and colleagues wrote in JAMA Dermatology.
The researchers identified 491 adults with psoriasis who were part of the BSTOP (Biomarkers of Systemic Treatment Outcomes in Psoriasis) cohort study in the United Kingdom. Blood samples were collected during clinical reviews to assess ustekinumab levels, and primary treatment response was 75% reduction in Psoriasis Area and Severity Index (PASI 75) scores.
Ustekinumab levels measured from 1-12 weeks after the start of treatment were significantly associated with PASI 75 after 6 months (odds ratio, 1.38) after controlling for factors including baseline PASI scores, age, and ustekinumab dose. The association, however, did not hold for other PASI outcomes, including PASI 90 and PASI scores of 1.5 or less.
The participants had at least one serum sample collected at 0-56 weeks from the start of treatment and at least one PSAI score measured within the first year of treatment. The average baseline PASI score was 13.3, the average body mass index was 32 kg/m2, and 65% of the patients were male.
Antidrug antibodies were detected in 17 patients (3.5% of the study population), compared with a rate of 37.5% in patients from the same study cohort who were taking adalimumab, the researchers noted.
The study findings were limited by several factors, including a dropoff in patient numbers over the study period and the difficulty in accounting for the association between drug level and treatment response in a logistic regression model, the researchers said.
The results, however, suggest “that adequate drug exposure early in the treatment cycle may be particularly important in determining clinical outcome with ustekinumab,” and that “future work should focus on pharmacokinetic-pharmacodynamic modeling of the whole time course of response to ustekinumab” as a key step toward personalized treatment regimens, they concluded.
The study was supported by several entities, including the Medical Research Council (MRC), the National Institute for Health Research Biomedical Research Center and the Psoriasis Association. Dr. Tsakok had no financial conflicts to disclose and was supported by an MRC Clinical Research Training Fellowship.
SOURCE: Tsakok T et al. JAMA Dermatol. 2019 Sep 18. doi: 10.1001/jamadermatol.2019.1783.
Early ustekinumab levels are significantly associated with a 75% reduction in Psoriasis Area and Severity Index scores from baseline, according to data from 491 adults with psoriasis.
“Evidence suggests that ustekinumab dosing is suboptimal in some patients,” because of factors including weight-based dosing and dosing intervals; therefore “individualized dose optimization and therapeutic drug monitoring (TDM) of ustekinumab may have clinical utility,” Teresa Tsakok, MRCP, of King’s College London, and colleagues wrote in JAMA Dermatology.
The researchers identified 491 adults with psoriasis who were part of the BSTOP (Biomarkers of Systemic Treatment Outcomes in Psoriasis) cohort study in the United Kingdom. Blood samples were collected during clinical reviews to assess ustekinumab levels, and primary treatment response was 75% reduction in Psoriasis Area and Severity Index (PASI 75) scores.
Ustekinumab levels measured from 1-12 weeks after the start of treatment were significantly associated with PASI 75 after 6 months (odds ratio, 1.38) after controlling for factors including baseline PASI scores, age, and ustekinumab dose. The association, however, did not hold for other PASI outcomes, including PASI 90 and PASI scores of 1.5 or less.
The participants had at least one serum sample collected at 0-56 weeks from the start of treatment and at least one PSAI score measured within the first year of treatment. The average baseline PASI score was 13.3, the average body mass index was 32 kg/m2, and 65% of the patients were male.
Antidrug antibodies were detected in 17 patients (3.5% of the study population), compared with a rate of 37.5% in patients from the same study cohort who were taking adalimumab, the researchers noted.
The study findings were limited by several factors, including a dropoff in patient numbers over the study period and the difficulty in accounting for the association between drug level and treatment response in a logistic regression model, the researchers said.
The results, however, suggest “that adequate drug exposure early in the treatment cycle may be particularly important in determining clinical outcome with ustekinumab,” and that “future work should focus on pharmacokinetic-pharmacodynamic modeling of the whole time course of response to ustekinumab” as a key step toward personalized treatment regimens, they concluded.
The study was supported by several entities, including the Medical Research Council (MRC), the National Institute for Health Research Biomedical Research Center and the Psoriasis Association. Dr. Tsakok had no financial conflicts to disclose and was supported by an MRC Clinical Research Training Fellowship.
SOURCE: Tsakok T et al. JAMA Dermatol. 2019 Sep 18. doi: 10.1001/jamadermatol.2019.1783.
Early ustekinumab levels are significantly associated with a 75% reduction in Psoriasis Area and Severity Index scores from baseline, according to data from 491 adults with psoriasis.
“Evidence suggests that ustekinumab dosing is suboptimal in some patients,” because of factors including weight-based dosing and dosing intervals; therefore “individualized dose optimization and therapeutic drug monitoring (TDM) of ustekinumab may have clinical utility,” Teresa Tsakok, MRCP, of King’s College London, and colleagues wrote in JAMA Dermatology.
The researchers identified 491 adults with psoriasis who were part of the BSTOP (Biomarkers of Systemic Treatment Outcomes in Psoriasis) cohort study in the United Kingdom. Blood samples were collected during clinical reviews to assess ustekinumab levels, and primary treatment response was 75% reduction in Psoriasis Area and Severity Index (PASI 75) scores.
Ustekinumab levels measured from 1-12 weeks after the start of treatment were significantly associated with PASI 75 after 6 months (odds ratio, 1.38) after controlling for factors including baseline PASI scores, age, and ustekinumab dose. The association, however, did not hold for other PASI outcomes, including PASI 90 and PASI scores of 1.5 or less.
The participants had at least one serum sample collected at 0-56 weeks from the start of treatment and at least one PSAI score measured within the first year of treatment. The average baseline PASI score was 13.3, the average body mass index was 32 kg/m2, and 65% of the patients were male.
Antidrug antibodies were detected in 17 patients (3.5% of the study population), compared with a rate of 37.5% in patients from the same study cohort who were taking adalimumab, the researchers noted.
The study findings were limited by several factors, including a dropoff in patient numbers over the study period and the difficulty in accounting for the association between drug level and treatment response in a logistic regression model, the researchers said.
The results, however, suggest “that adequate drug exposure early in the treatment cycle may be particularly important in determining clinical outcome with ustekinumab,” and that “future work should focus on pharmacokinetic-pharmacodynamic modeling of the whole time course of response to ustekinumab” as a key step toward personalized treatment regimens, they concluded.
The study was supported by several entities, including the Medical Research Council (MRC), the National Institute for Health Research Biomedical Research Center and the Psoriasis Association. Dr. Tsakok had no financial conflicts to disclose and was supported by an MRC Clinical Research Training Fellowship.
SOURCE: Tsakok T et al. JAMA Dermatol. 2019 Sep 18. doi: 10.1001/jamadermatol.2019.1783.
FROM JAMA DERMATOLOGY
Key clinical point: Measurement of ustekinumab levels early in treatment could help direct strategies and ensure correct dosage in psoriasis patients.
Major finding: Early serum ustekinumab levels 1-12 weeks after starting treatment were associated with a 75% reduction in PASI scores from baseline at 6 months.
Study details: The prospective, observational study involved 491 adults with psoriasis.
Disclosures: The study was supported by several entities, including the Medical Research Council (MRC), the National Institute for Health Research Biomedical Research Center, and the Psoriasis Association. Dr. Tsakok disclosed financial conflicts and was supported by an MRC Clinical Research Training Fellowship.
Source: Tsakok T et al. JAMA Dermatol. 2019 Sep 18. doi: 10.1001/jamadermatol.2019.1783.
Worse air quality linked to premature deaths
, according to a working paper issued by the National Bureau of Economic Research.
The increase in air pollution, defined as the amount of fine particulate matter (PM2.5) in the air, was associated with an additional 9,700 premature deaths from 2016 to 2018, representing damages totaling $89 billion, wrote Karen Clay and Nicholas C. Miller of Carnegie Mellon University, Pittsburgh. The increase may reflect in part the impact of the a major wildfire that occurred in the fall of 2018.
“These increases are worrisome, because previous studies have shown that PM2.5 increases premature mortality risk,” the researchers wrote. To assess the changes in air quality, they reviewed data from the Air Quality System (AQS) database including total PM2.5 and three PM2.5 species: ammonium nitrate, sulfate, and elemental carbon.
To examine the impact of pollution on public health, the researchers used data from the damage function approach used in the Environmental Protection Agency’s Benefit-Cost Analysis of the Clean Air Act, the Regulatory Impact Analysis for PM2.5, and multiple academic studies.
The number of premature deaths linked to PM2.5 increased by approximately 4,900 between 2016 and 2017 and by 9,700 from 2016 to 2018 in U.S. counties with monitors.
Elderly individuals are especially vulnerable to particulate matter exposure and experience approximately 80% of the burden of disease related to pollution, the researchers said.
“While some deaths among the elderly are shifted by days or weeks, recent research suggests that the burden is ‘concentrated among the elderly with 5-10 years of remaining life expectancy, followed by those with 2-5 years remaining, because these groups represent a large fraction of the Medicare population and are also vulnerable to acute particulate matter exposure,’” they said.
Overall, pollution levels across the United States stopped declining in 2016. When broken down by four Census regions, no change in PM2.5 levels occurred in the Northeast and South between 2016 and 2018; the Midwest and West showed increases in PM2.5 of 9.3% and 11.5%, respectively.
The researchers suggested three possible factors affecting the increase in pollution: economic activity, wildfires, and air quality enforcement. They noted that increases in PM2.5 were especially high in California, and that California accounted for 43% of the increase in pollution-related premature deaths nationwide between 2016 and 2018. When the researchers examined PM2.5 month by month, “November 2018 had an outsized effect on our mortality calculations,” largely because the devastating Camp Fire occurred in California at that time, they said.
With regard to the impact of economic activity on pollution, the researchers reviewed data from the National Highway Administration and Energy Information Administration that showed increased use of natural gas and increased vehicle travel as contributing to higher levels of nitrate and elemental carbon in the air.
Finally, the researchers reported that enforcement of the Clean Air Act appeared to have declined since 2013, and this decline, although it might reflect increased compliance in some areas “is concerning in light of the increases in air pollution in both attainment and nonattainment counties after 2016,” they said.
The researchers had no financial conflicts to disclose.
SOURCE: Clay K, Miller NZ. NBER 2019. Working Paper 26381. doi: 10.3386/w26381.
, according to a working paper issued by the National Bureau of Economic Research.
The increase in air pollution, defined as the amount of fine particulate matter (PM2.5) in the air, was associated with an additional 9,700 premature deaths from 2016 to 2018, representing damages totaling $89 billion, wrote Karen Clay and Nicholas C. Miller of Carnegie Mellon University, Pittsburgh. The increase may reflect in part the impact of the a major wildfire that occurred in the fall of 2018.
“These increases are worrisome, because previous studies have shown that PM2.5 increases premature mortality risk,” the researchers wrote. To assess the changes in air quality, they reviewed data from the Air Quality System (AQS) database including total PM2.5 and three PM2.5 species: ammonium nitrate, sulfate, and elemental carbon.
To examine the impact of pollution on public health, the researchers used data from the damage function approach used in the Environmental Protection Agency’s Benefit-Cost Analysis of the Clean Air Act, the Regulatory Impact Analysis for PM2.5, and multiple academic studies.
The number of premature deaths linked to PM2.5 increased by approximately 4,900 between 2016 and 2017 and by 9,700 from 2016 to 2018 in U.S. counties with monitors.
Elderly individuals are especially vulnerable to particulate matter exposure and experience approximately 80% of the burden of disease related to pollution, the researchers said.
“While some deaths among the elderly are shifted by days or weeks, recent research suggests that the burden is ‘concentrated among the elderly with 5-10 years of remaining life expectancy, followed by those with 2-5 years remaining, because these groups represent a large fraction of the Medicare population and are also vulnerable to acute particulate matter exposure,’” they said.
Overall, pollution levels across the United States stopped declining in 2016. When broken down by four Census regions, no change in PM2.5 levels occurred in the Northeast and South between 2016 and 2018; the Midwest and West showed increases in PM2.5 of 9.3% and 11.5%, respectively.
The researchers suggested three possible factors affecting the increase in pollution: economic activity, wildfires, and air quality enforcement. They noted that increases in PM2.5 were especially high in California, and that California accounted for 43% of the increase in pollution-related premature deaths nationwide between 2016 and 2018. When the researchers examined PM2.5 month by month, “November 2018 had an outsized effect on our mortality calculations,” largely because the devastating Camp Fire occurred in California at that time, they said.
With regard to the impact of economic activity on pollution, the researchers reviewed data from the National Highway Administration and Energy Information Administration that showed increased use of natural gas and increased vehicle travel as contributing to higher levels of nitrate and elemental carbon in the air.
Finally, the researchers reported that enforcement of the Clean Air Act appeared to have declined since 2013, and this decline, although it might reflect increased compliance in some areas “is concerning in light of the increases in air pollution in both attainment and nonattainment counties after 2016,” they said.
The researchers had no financial conflicts to disclose.
SOURCE: Clay K, Miller NZ. NBER 2019. Working Paper 26381. doi: 10.3386/w26381.
, according to a working paper issued by the National Bureau of Economic Research.
The increase in air pollution, defined as the amount of fine particulate matter (PM2.5) in the air, was associated with an additional 9,700 premature deaths from 2016 to 2018, representing damages totaling $89 billion, wrote Karen Clay and Nicholas C. Miller of Carnegie Mellon University, Pittsburgh. The increase may reflect in part the impact of the a major wildfire that occurred in the fall of 2018.
“These increases are worrisome, because previous studies have shown that PM2.5 increases premature mortality risk,” the researchers wrote. To assess the changes in air quality, they reviewed data from the Air Quality System (AQS) database including total PM2.5 and three PM2.5 species: ammonium nitrate, sulfate, and elemental carbon.
To examine the impact of pollution on public health, the researchers used data from the damage function approach used in the Environmental Protection Agency’s Benefit-Cost Analysis of the Clean Air Act, the Regulatory Impact Analysis for PM2.5, and multiple academic studies.
The number of premature deaths linked to PM2.5 increased by approximately 4,900 between 2016 and 2017 and by 9,700 from 2016 to 2018 in U.S. counties with monitors.
Elderly individuals are especially vulnerable to particulate matter exposure and experience approximately 80% of the burden of disease related to pollution, the researchers said.
“While some deaths among the elderly are shifted by days or weeks, recent research suggests that the burden is ‘concentrated among the elderly with 5-10 years of remaining life expectancy, followed by those with 2-5 years remaining, because these groups represent a large fraction of the Medicare population and are also vulnerable to acute particulate matter exposure,’” they said.
Overall, pollution levels across the United States stopped declining in 2016. When broken down by four Census regions, no change in PM2.5 levels occurred in the Northeast and South between 2016 and 2018; the Midwest and West showed increases in PM2.5 of 9.3% and 11.5%, respectively.
The researchers suggested three possible factors affecting the increase in pollution: economic activity, wildfires, and air quality enforcement. They noted that increases in PM2.5 were especially high in California, and that California accounted for 43% of the increase in pollution-related premature deaths nationwide between 2016 and 2018. When the researchers examined PM2.5 month by month, “November 2018 had an outsized effect on our mortality calculations,” largely because the devastating Camp Fire occurred in California at that time, they said.
With regard to the impact of economic activity on pollution, the researchers reviewed data from the National Highway Administration and Energy Information Administration that showed increased use of natural gas and increased vehicle travel as contributing to higher levels of nitrate and elemental carbon in the air.
Finally, the researchers reported that enforcement of the Clean Air Act appeared to have declined since 2013, and this decline, although it might reflect increased compliance in some areas “is concerning in light of the increases in air pollution in both attainment and nonattainment counties after 2016,” they said.
The researchers had no financial conflicts to disclose.
SOURCE: Clay K, Miller NZ. NBER 2019. Working Paper 26381. doi: 10.3386/w26381.
FROM AN NBER AIR QUALITY STUDY