User login
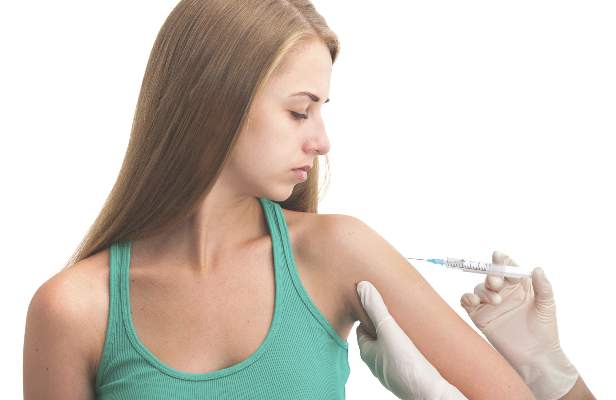
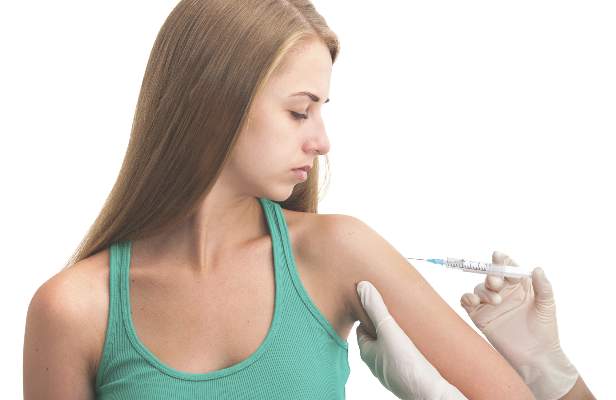
HPV Vaccination Protects High-risk Girls From Cervical Cancer
Full or partial vaccination with the quadrivalent human papillomavirus vaccine reduced the overall risk of abnormal cervical pathology by 36%, based on data from a retrospective cohort study of just over 4,000 high-risk girls and young adult women.
Early vaccination (ages 11-14 years) was the most protective, with reductions in risk of abnormal cervical pathology of 64% with at least one dose and 73% for three doses (JAMA Pediatr. 2016 March 14. doi: 10.1001/jamapediatrics.2015.3926).
“This study provides crucial information about the HPV vaccine in minority populations and females engaging in high-risk sexual behaviors who arguably were underrepresented in the HPV vaccine clinical trials and postlicensure studies, yet are at increased risk for cervical cancer,” wrote Dr. Annika M. Hofstetter of the University of Washington, Seattle, and her colleagues.
The researchers reviewed data from 4,127 girls and young women aged 11-20 years who were seen at 16 locations in New York City. Most (92%) of the patients were publicly insured, and 58% were Spanish speakers.
Overall, the risk for abnormal cervical pathology was lower in vaccinated vs. unvaccinated individuals, (hazard ratio 0.64) and even lower in those who received all three recommended doses (HR 0.48). Detection rates were 58 per 1,000 person-years in those vaccinated vs. 126 per 1,000 person-years among the unvaccinated.
The next steps for research should include a larger sample and a longer follow-up period after greater uptake of the nonavalent HPV vaccine, the researchers added.
Dr. Hofstetter has received funding for a separate investigator-initiated study from the Pfizer Medical Education Group, and the study was funded in part by a grant from the Merck Investigator-Initiated Studies Program.
Full or partial vaccination with the quadrivalent human papillomavirus vaccine reduced the overall risk of abnormal cervical pathology by 36%, based on data from a retrospective cohort study of just over 4,000 high-risk girls and young adult women.
Early vaccination (ages 11-14 years) was the most protective, with reductions in risk of abnormal cervical pathology of 64% with at least one dose and 73% for three doses (JAMA Pediatr. 2016 March 14. doi: 10.1001/jamapediatrics.2015.3926).
“This study provides crucial information about the HPV vaccine in minority populations and females engaging in high-risk sexual behaviors who arguably were underrepresented in the HPV vaccine clinical trials and postlicensure studies, yet are at increased risk for cervical cancer,” wrote Dr. Annika M. Hofstetter of the University of Washington, Seattle, and her colleagues.
The researchers reviewed data from 4,127 girls and young women aged 11-20 years who were seen at 16 locations in New York City. Most (92%) of the patients were publicly insured, and 58% were Spanish speakers.
Overall, the risk for abnormal cervical pathology was lower in vaccinated vs. unvaccinated individuals, (hazard ratio 0.64) and even lower in those who received all three recommended doses (HR 0.48). Detection rates were 58 per 1,000 person-years in those vaccinated vs. 126 per 1,000 person-years among the unvaccinated.
The next steps for research should include a larger sample and a longer follow-up period after greater uptake of the nonavalent HPV vaccine, the researchers added.
Dr. Hofstetter has received funding for a separate investigator-initiated study from the Pfizer Medical Education Group, and the study was funded in part by a grant from the Merck Investigator-Initiated Studies Program.
Full or partial vaccination with the quadrivalent human papillomavirus vaccine reduced the overall risk of abnormal cervical pathology by 36%, based on data from a retrospective cohort study of just over 4,000 high-risk girls and young adult women.
Early vaccination (ages 11-14 years) was the most protective, with reductions in risk of abnormal cervical pathology of 64% with at least one dose and 73% for three doses (JAMA Pediatr. 2016 March 14. doi: 10.1001/jamapediatrics.2015.3926).
“This study provides crucial information about the HPV vaccine in minority populations and females engaging in high-risk sexual behaviors who arguably were underrepresented in the HPV vaccine clinical trials and postlicensure studies, yet are at increased risk for cervical cancer,” wrote Dr. Annika M. Hofstetter of the University of Washington, Seattle, and her colleagues.
The researchers reviewed data from 4,127 girls and young women aged 11-20 years who were seen at 16 locations in New York City. Most (92%) of the patients were publicly insured, and 58% were Spanish speakers.
Overall, the risk for abnormal cervical pathology was lower in vaccinated vs. unvaccinated individuals, (hazard ratio 0.64) and even lower in those who received all three recommended doses (HR 0.48). Detection rates were 58 per 1,000 person-years in those vaccinated vs. 126 per 1,000 person-years among the unvaccinated.
The next steps for research should include a larger sample and a longer follow-up period after greater uptake of the nonavalent HPV vaccine, the researchers added.
Dr. Hofstetter has received funding for a separate investigator-initiated study from the Pfizer Medical Education Group, and the study was funded in part by a grant from the Merck Investigator-Initiated Studies Program.
FROM JAMA PEDIATRICS
HPV vaccination protects high-risk girls from cervical cancer
Full or partial vaccination with the quadrivalent human papillomavirus vaccine reduced the overall risk of abnormal cervical pathology by 36%, based on data from a retrospective cohort study of just over 4,000 high-risk girls and young adult women.
Early vaccination (ages 11-14 years) was the most protective, with reductions in risk of abnormal cervical pathology of 64% with at least one dose and 73% for three doses (JAMA Pediatr. 2016 March 14. doi: 10.1001/jamapediatrics.2015.3926).
“This study provides crucial information about the HPV vaccine in minority populations and females engaging in high-risk sexual behaviors who arguably were underrepresented in the HPV vaccine clinical trials and postlicensure studies, yet are at increased risk for cervical cancer,” wrote Dr. Annika M. Hofstetter of the University of Washington, Seattle, and her colleagues.
The researchers reviewed data from 4,127 girls and young women aged 11-20 years who were seen at 16 locations in New York City. Most (92%) of the patients were publicly insured, and 58% were Spanish speakers.
Overall, the risk for abnormal cervical pathology was lower in vaccinated vs. unvaccinated individuals, (hazard ratio 0.64) and even lower in those who received all three recommended doses (HR 0.48). Detection rates were 58 per 1,000 person-years in those vaccinated vs. 126 per 1,000 person-years among the unvaccinated.
The next steps for research should include a larger sample and a longer follow-up period after greater uptake of the nonavalent HPV vaccine, the researchers added.
Dr. Hofstetter has received funding for a separate investigator-initiated study from the Pfizer Medical Education Group, and the study was funded in part by a grant from the Merck Investigator-Initiated Studies Program.
Full or partial vaccination with the quadrivalent human papillomavirus vaccine reduced the overall risk of abnormal cervical pathology by 36%, based on data from a retrospective cohort study of just over 4,000 high-risk girls and young adult women.
Early vaccination (ages 11-14 years) was the most protective, with reductions in risk of abnormal cervical pathology of 64% with at least one dose and 73% for three doses (JAMA Pediatr. 2016 March 14. doi: 10.1001/jamapediatrics.2015.3926).
“This study provides crucial information about the HPV vaccine in minority populations and females engaging in high-risk sexual behaviors who arguably were underrepresented in the HPV vaccine clinical trials and postlicensure studies, yet are at increased risk for cervical cancer,” wrote Dr. Annika M. Hofstetter of the University of Washington, Seattle, and her colleagues.
The researchers reviewed data from 4,127 girls and young women aged 11-20 years who were seen at 16 locations in New York City. Most (92%) of the patients were publicly insured, and 58% were Spanish speakers.
Overall, the risk for abnormal cervical pathology was lower in vaccinated vs. unvaccinated individuals, (hazard ratio 0.64) and even lower in those who received all three recommended doses (HR 0.48). Detection rates were 58 per 1,000 person-years in those vaccinated vs. 126 per 1,000 person-years among the unvaccinated.
The next steps for research should include a larger sample and a longer follow-up period after greater uptake of the nonavalent HPV vaccine, the researchers added.
Dr. Hofstetter has received funding for a separate investigator-initiated study from the Pfizer Medical Education Group, and the study was funded in part by a grant from the Merck Investigator-Initiated Studies Program.
Full or partial vaccination with the quadrivalent human papillomavirus vaccine reduced the overall risk of abnormal cervical pathology by 36%, based on data from a retrospective cohort study of just over 4,000 high-risk girls and young adult women.
Early vaccination (ages 11-14 years) was the most protective, with reductions in risk of abnormal cervical pathology of 64% with at least one dose and 73% for three doses (JAMA Pediatr. 2016 March 14. doi: 10.1001/jamapediatrics.2015.3926).
“This study provides crucial information about the HPV vaccine in minority populations and females engaging in high-risk sexual behaviors who arguably were underrepresented in the HPV vaccine clinical trials and postlicensure studies, yet are at increased risk for cervical cancer,” wrote Dr. Annika M. Hofstetter of the University of Washington, Seattle, and her colleagues.
The researchers reviewed data from 4,127 girls and young women aged 11-20 years who were seen at 16 locations in New York City. Most (92%) of the patients were publicly insured, and 58% were Spanish speakers.
Overall, the risk for abnormal cervical pathology was lower in vaccinated vs. unvaccinated individuals, (hazard ratio 0.64) and even lower in those who received all three recommended doses (HR 0.48). Detection rates were 58 per 1,000 person-years in those vaccinated vs. 126 per 1,000 person-years among the unvaccinated.
The next steps for research should include a larger sample and a longer follow-up period after greater uptake of the nonavalent HPV vaccine, the researchers added.
Dr. Hofstetter has received funding for a separate investigator-initiated study from the Pfizer Medical Education Group, and the study was funded in part by a grant from the Merck Investigator-Initiated Studies Program.
FROM JAMA PEDIATRICS
Key clinical point: HPV vaccination, even partial vaccination, was protective against cervical cancer in minority girls at increased risk for infection.
Major finding: Abnormal cervical cytology was 36% lower in girls and young women who received any amount of HPV vaccine and 73% lower in those who were fully vaccinated, compared with those who were unvaccinated.
Data source: A retrospective cohort study including data from 4,127 females aged 11-20 years.
Disclosures: Dr. Hofstetter has received funding for a separate investigator-initiated study from the Pfizer Medical Education Group, and the study was funded in part by a grant from the Merck Investigator-Initiated Studies Program.
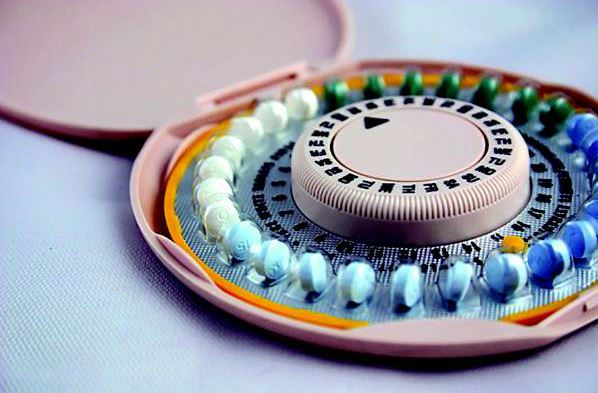
Obesity, oral contraceptive use are risk factors for cerebral venous thrombosis in women
Obese women taking oral contraceptives had a 30-fold increased odds for cerebral venous thrombosis (CVT), compared with normal-weight women, in an unmatched case-control study of 186 CVT cases and 6,134 controls.
The association between a body-mass index of 30 kg/m2 or higher and increased odds of CVT “appears to be fully attributable to a strongly increased risk in women who use oral contraceptives [OCs],” said Dr. Susanna M. Zuurbier of the Academic Medical Centre in Amsterdam, and her colleagues.
“Although the relative risks are increased substantially, the absolute risks of CVT are still small,” the researchers said. “Moreover, withholding oral contraceptives may lead to an increase in unintended pregnancies and thus the number of pregnancy-related thrombosis cases.”
After controlling for multiple variables, CVT was 2.63 times more likely to occur in obese individuals, compared with those of normal weight. When the findings were stratified by sex, a BMI greater than 30 kg/m2 had no significant impact on CVT in men, but the odds rose 3.5-fold in women, the investigators reported online March 14 in JAMA Neurology (JAMA Neurol. 2016 Mar 14. doi: 10.1001/jamaneurol.2016.000100).
On further analysis, overweight and obesity had a dose-dependent impact on the odds of CVT among women who used OCs. Adjusted odds ratios were 11.87 for those with BMIs ranging from 25 kg/m2 to 29 kg/m2, and 29.26 for those with BMIs of 30 kg/m2 or higher when compared against normal-weight women who did not use OCs. No association was found between obesity and CVT risk in women who did not use OCs, the researchers noted.
Patients with CVT were recruited in 2006-2014 from two medical centers, one in the Netherlands and the other in Switzerland. The controls were part of the Dutch Multiple Environmental and Genetic Assessment of Risk Factors for Venous Thrombosis (MEGA) study. Overall, patients with CVT were more likely to be younger than controls (median age 40 years vs. 48 years). They also were more likely than controls to be female (72% vs. 53%), users of oral contraceptives (73% vs. 24%) and have a history of cancer (9% vs. 4%).
The study was limited by several factors, including the small number of CVT cases, the lack of complete BMI data for the study population, and time difference in recruitment of cases and controls, the researchers noted, but they advised clinicians to keep the risk in mind when counseling obese women about OC use.
“Alternative methods of contraception that are not associated with thrombosis, such as an intrauterine device, might be offered to these women,” they wrote.
The study was funded by grants from the Netherlands Organisation for Scientific Research, the Dutch Thrombosis Society, the Remmert Adriaan Laan Foundation, and the Swiss Heart Foundation. Study coauthor Dr. Marcel Arnold disclosed receiving honoraria for giving lectures and serving on advisory boards for Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Pfizer, and Covidien.
“The discovery of increased rates of asymptomatic atherosclerosis in patients with VTE led to the systematic study of cardiovascular risk factors, such as obesity, in VTE,” but the possible association between obesity and CVT has not been explored, Dr. Chirantan Banerjee wrote in an accompanying editorial.
The current study results are “novel and in concordance with prior studies on obesity and OC use as risk factors for VTE,” Dr. Banerjee noted. The study’s strengths lie in the inclusion of appropriate subgroups, controls, and confounding variables. In addition to further research to validate the findings, “studies investigating the effect of inherited thrombophilia on the association between obesity and CVT would also be important because the current study did not have this data,” he noted. “Other potential confounders, such as obstructive sleep apnea and anemia, should be included in future studies.
In the meantime, “the authors correctly point out that despite the manifold increased relative risk, the absolute risk of CVT in obese women taking OCs still remains low and should not preclude OC use among them,” Dr. Banerjee said.
Dr. Banerjee is a member of the department of neurology at the Medical University of Charleston, S.C., and had no financial conflicts to disclose. These comments were taken from his editorial accompanying Dr. Zuurbier and colleagues’ report (JAMA Neurol. 2016 Mar 14. doi: 10.1001/jamaneurol.2015.5107).
“The discovery of increased rates of asymptomatic atherosclerosis in patients with VTE led to the systematic study of cardiovascular risk factors, such as obesity, in VTE,” but the possible association between obesity and CVT has not been explored, Dr. Chirantan Banerjee wrote in an accompanying editorial.
The current study results are “novel and in concordance with prior studies on obesity and OC use as risk factors for VTE,” Dr. Banerjee noted. The study’s strengths lie in the inclusion of appropriate subgroups, controls, and confounding variables. In addition to further research to validate the findings, “studies investigating the effect of inherited thrombophilia on the association between obesity and CVT would also be important because the current study did not have this data,” he noted. “Other potential confounders, such as obstructive sleep apnea and anemia, should be included in future studies.
In the meantime, “the authors correctly point out that despite the manifold increased relative risk, the absolute risk of CVT in obese women taking OCs still remains low and should not preclude OC use among them,” Dr. Banerjee said.
Dr. Banerjee is a member of the department of neurology at the Medical University of Charleston, S.C., and had no financial conflicts to disclose. These comments were taken from his editorial accompanying Dr. Zuurbier and colleagues’ report (JAMA Neurol. 2016 Mar 14. doi: 10.1001/jamaneurol.2015.5107).
“The discovery of increased rates of asymptomatic atherosclerosis in patients with VTE led to the systematic study of cardiovascular risk factors, such as obesity, in VTE,” but the possible association between obesity and CVT has not been explored, Dr. Chirantan Banerjee wrote in an accompanying editorial.
The current study results are “novel and in concordance with prior studies on obesity and OC use as risk factors for VTE,” Dr. Banerjee noted. The study’s strengths lie in the inclusion of appropriate subgroups, controls, and confounding variables. In addition to further research to validate the findings, “studies investigating the effect of inherited thrombophilia on the association between obesity and CVT would also be important because the current study did not have this data,” he noted. “Other potential confounders, such as obstructive sleep apnea and anemia, should be included in future studies.
In the meantime, “the authors correctly point out that despite the manifold increased relative risk, the absolute risk of CVT in obese women taking OCs still remains low and should not preclude OC use among them,” Dr. Banerjee said.
Dr. Banerjee is a member of the department of neurology at the Medical University of Charleston, S.C., and had no financial conflicts to disclose. These comments were taken from his editorial accompanying Dr. Zuurbier and colleagues’ report (JAMA Neurol. 2016 Mar 14. doi: 10.1001/jamaneurol.2015.5107).
Obese women taking oral contraceptives had a 30-fold increased odds for cerebral venous thrombosis (CVT), compared with normal-weight women, in an unmatched case-control study of 186 CVT cases and 6,134 controls.
The association between a body-mass index of 30 kg/m2 or higher and increased odds of CVT “appears to be fully attributable to a strongly increased risk in women who use oral contraceptives [OCs],” said Dr. Susanna M. Zuurbier of the Academic Medical Centre in Amsterdam, and her colleagues.
“Although the relative risks are increased substantially, the absolute risks of CVT are still small,” the researchers said. “Moreover, withholding oral contraceptives may lead to an increase in unintended pregnancies and thus the number of pregnancy-related thrombosis cases.”
After controlling for multiple variables, CVT was 2.63 times more likely to occur in obese individuals, compared with those of normal weight. When the findings were stratified by sex, a BMI greater than 30 kg/m2 had no significant impact on CVT in men, but the odds rose 3.5-fold in women, the investigators reported online March 14 in JAMA Neurology (JAMA Neurol. 2016 Mar 14. doi: 10.1001/jamaneurol.2016.000100).
On further analysis, overweight and obesity had a dose-dependent impact on the odds of CVT among women who used OCs. Adjusted odds ratios were 11.87 for those with BMIs ranging from 25 kg/m2 to 29 kg/m2, and 29.26 for those with BMIs of 30 kg/m2 or higher when compared against normal-weight women who did not use OCs. No association was found between obesity and CVT risk in women who did not use OCs, the researchers noted.
Patients with CVT were recruited in 2006-2014 from two medical centers, one in the Netherlands and the other in Switzerland. The controls were part of the Dutch Multiple Environmental and Genetic Assessment of Risk Factors for Venous Thrombosis (MEGA) study. Overall, patients with CVT were more likely to be younger than controls (median age 40 years vs. 48 years). They also were more likely than controls to be female (72% vs. 53%), users of oral contraceptives (73% vs. 24%) and have a history of cancer (9% vs. 4%).
The study was limited by several factors, including the small number of CVT cases, the lack of complete BMI data for the study population, and time difference in recruitment of cases and controls, the researchers noted, but they advised clinicians to keep the risk in mind when counseling obese women about OC use.
“Alternative methods of contraception that are not associated with thrombosis, such as an intrauterine device, might be offered to these women,” they wrote.
The study was funded by grants from the Netherlands Organisation for Scientific Research, the Dutch Thrombosis Society, the Remmert Adriaan Laan Foundation, and the Swiss Heart Foundation. Study coauthor Dr. Marcel Arnold disclosed receiving honoraria for giving lectures and serving on advisory boards for Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Pfizer, and Covidien.
Obese women taking oral contraceptives had a 30-fold increased odds for cerebral venous thrombosis (CVT), compared with normal-weight women, in an unmatched case-control study of 186 CVT cases and 6,134 controls.
The association between a body-mass index of 30 kg/m2 or higher and increased odds of CVT “appears to be fully attributable to a strongly increased risk in women who use oral contraceptives [OCs],” said Dr. Susanna M. Zuurbier of the Academic Medical Centre in Amsterdam, and her colleagues.
“Although the relative risks are increased substantially, the absolute risks of CVT are still small,” the researchers said. “Moreover, withholding oral contraceptives may lead to an increase in unintended pregnancies and thus the number of pregnancy-related thrombosis cases.”
After controlling for multiple variables, CVT was 2.63 times more likely to occur in obese individuals, compared with those of normal weight. When the findings were stratified by sex, a BMI greater than 30 kg/m2 had no significant impact on CVT in men, but the odds rose 3.5-fold in women, the investigators reported online March 14 in JAMA Neurology (JAMA Neurol. 2016 Mar 14. doi: 10.1001/jamaneurol.2016.000100).
On further analysis, overweight and obesity had a dose-dependent impact on the odds of CVT among women who used OCs. Adjusted odds ratios were 11.87 for those with BMIs ranging from 25 kg/m2 to 29 kg/m2, and 29.26 for those with BMIs of 30 kg/m2 or higher when compared against normal-weight women who did not use OCs. No association was found between obesity and CVT risk in women who did not use OCs, the researchers noted.
Patients with CVT were recruited in 2006-2014 from two medical centers, one in the Netherlands and the other in Switzerland. The controls were part of the Dutch Multiple Environmental and Genetic Assessment of Risk Factors for Venous Thrombosis (MEGA) study. Overall, patients with CVT were more likely to be younger than controls (median age 40 years vs. 48 years). They also were more likely than controls to be female (72% vs. 53%), users of oral contraceptives (73% vs. 24%) and have a history of cancer (9% vs. 4%).
The study was limited by several factors, including the small number of CVT cases, the lack of complete BMI data for the study population, and time difference in recruitment of cases and controls, the researchers noted, but they advised clinicians to keep the risk in mind when counseling obese women about OC use.
“Alternative methods of contraception that are not associated with thrombosis, such as an intrauterine device, might be offered to these women,” they wrote.
The study was funded by grants from the Netherlands Organisation for Scientific Research, the Dutch Thrombosis Society, the Remmert Adriaan Laan Foundation, and the Swiss Heart Foundation. Study coauthor Dr. Marcel Arnold disclosed receiving honoraria for giving lectures and serving on advisory boards for Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Pfizer, and Covidien.
FROM JAMA NEUROLOGY
Key clinical point: Obesity and oral contraceptive use significantly increased the odds for cerebral venous thrombosis in adults.
Major finding: The risk of CVT was 2.63 times more likely among obese women compared to nonobese women, and nearly 30 times more likely in women taking oral contraceptives.
Data source: An unmatched, case-control study of 186 CVT patients and 6,134 healthy controls.
Disclosures: The study was funded by grants from the Netherlands Organisation for Scientific Research, the Dutch Thrombosis Society, the Remmert Adriaan Laan Foundation, and the Swiss Heart Foundation. Study coauthor Dr. Marcel Arnold disclosed receiving honoraria for giving lectures and serving on advisory boards for Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Pfizer, and Covidien.
AD patients start antidepressants before diagnosis
The incidence of antidepressant use was almost twice as high among adults later diagnosed with Alzheimer’s disease compared with adults who were not diagnosed with the illness, according to a study of 62,104 Alzheimer’s cases and 62,104 controls.
Using data from the Medication Use Among Persons with Alzheimer’s Disease (MEDALZ) study, Arto Puranen and colleagues found that 9 years before the Alzheimer’s diagnosis, the incidence of antidepressant use was higher among the cohort that developed disease than it was among those who did not. “The reason for this remains unknown but cannot be explained by burden of psychiatric disorders,” wrote Mr. Puranen of the University of Eastern Finland, Kuopio, Finland, and his colleagues.
The study period covered 9 years before and 4 years after diagnosis of Alzheimer’s. The mean ages of antidepressant users were comparable (77.7 years for those with AD and 78.2 years for those without). Selective serotonin reuptake inhibitors were the most often initiated antidepressant in patients with and without Alzheimer’s (88% and 73%, respectively).
The researchers found the high incidence of antidepressants in future Alzheimer’s patients 9 years prior to diagnosis “somewhat surprising.” However, they noted that AD takes hold several years before a diagnosis, and that depressive symptoms often occur in this early stage.
Careful monitoring of depressive symptoms in older patients may help identify cognitive decline earlier, they added.
Find the study here (Int J Geriatr Psychiatry. 2016. doi: 10.1002/gps.4450).
The incidence of antidepressant use was almost twice as high among adults later diagnosed with Alzheimer’s disease compared with adults who were not diagnosed with the illness, according to a study of 62,104 Alzheimer’s cases and 62,104 controls.
Using data from the Medication Use Among Persons with Alzheimer’s Disease (MEDALZ) study, Arto Puranen and colleagues found that 9 years before the Alzheimer’s diagnosis, the incidence of antidepressant use was higher among the cohort that developed disease than it was among those who did not. “The reason for this remains unknown but cannot be explained by burden of psychiatric disorders,” wrote Mr. Puranen of the University of Eastern Finland, Kuopio, Finland, and his colleagues.
The study period covered 9 years before and 4 years after diagnosis of Alzheimer’s. The mean ages of antidepressant users were comparable (77.7 years for those with AD and 78.2 years for those without). Selective serotonin reuptake inhibitors were the most often initiated antidepressant in patients with and without Alzheimer’s (88% and 73%, respectively).
The researchers found the high incidence of antidepressants in future Alzheimer’s patients 9 years prior to diagnosis “somewhat surprising.” However, they noted that AD takes hold several years before a diagnosis, and that depressive symptoms often occur in this early stage.
Careful monitoring of depressive symptoms in older patients may help identify cognitive decline earlier, they added.
Find the study here (Int J Geriatr Psychiatry. 2016. doi: 10.1002/gps.4450).
The incidence of antidepressant use was almost twice as high among adults later diagnosed with Alzheimer’s disease compared with adults who were not diagnosed with the illness, according to a study of 62,104 Alzheimer’s cases and 62,104 controls.
Using data from the Medication Use Among Persons with Alzheimer’s Disease (MEDALZ) study, Arto Puranen and colleagues found that 9 years before the Alzheimer’s diagnosis, the incidence of antidepressant use was higher among the cohort that developed disease than it was among those who did not. “The reason for this remains unknown but cannot be explained by burden of psychiatric disorders,” wrote Mr. Puranen of the University of Eastern Finland, Kuopio, Finland, and his colleagues.
The study period covered 9 years before and 4 years after diagnosis of Alzheimer’s. The mean ages of antidepressant users were comparable (77.7 years for those with AD and 78.2 years for those without). Selective serotonin reuptake inhibitors were the most often initiated antidepressant in patients with and without Alzheimer’s (88% and 73%, respectively).
The researchers found the high incidence of antidepressants in future Alzheimer’s patients 9 years prior to diagnosis “somewhat surprising.” However, they noted that AD takes hold several years before a diagnosis, and that depressive symptoms often occur in this early stage.
Careful monitoring of depressive symptoms in older patients may help identify cognitive decline earlier, they added.
Find the study here (Int J Geriatr Psychiatry. 2016. doi: 10.1002/gps.4450).
FROM THE INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY
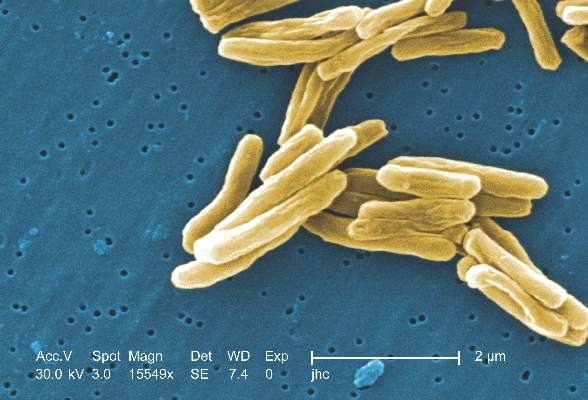
Urine test use to guide treatment reduced TB mortality in HIV patients
Use of a low-cost urine test to guide tuberculosis treatment significantly improved mortality in HIV-positive patients, based on data from a randomized, multicenter trial including 2,528 adults at 10 locations in Africa.
The test involved a urine-based, lateral flow, point-of-care, lipoarabinomannan assay (LAM), and no associated adverse events were reported in this study.
Mortality at 8 weeks after LAM was significantly lower among patients who received LAM-guided antituberculosis treatment (21%), compared with control patients (25%). The relative risk reduction with LAM was 17%, and use of LAM improved the time to treatment initiation at all study locations, the researchers noted.
“The implementation of LAM testing is likely to offer the greatest benefit in hospitals where diagnostic resources are most limited, and where patients often present with severe illness, advanced immunosuppression, and an inability to self-expectorate sputum,” wrote Jonny G. Peter, Ph.D., of the University of Cape Town, South Africa, and colleagues.
Read the full study in the Lancet (2016 Mar 9. doi: 10.1016/S0140-6736(15)01092-2).
Use of a low-cost urine test to guide tuberculosis treatment significantly improved mortality in HIV-positive patients, based on data from a randomized, multicenter trial including 2,528 adults at 10 locations in Africa.
The test involved a urine-based, lateral flow, point-of-care, lipoarabinomannan assay (LAM), and no associated adverse events were reported in this study.
Mortality at 8 weeks after LAM was significantly lower among patients who received LAM-guided antituberculosis treatment (21%), compared with control patients (25%). The relative risk reduction with LAM was 17%, and use of LAM improved the time to treatment initiation at all study locations, the researchers noted.
“The implementation of LAM testing is likely to offer the greatest benefit in hospitals where diagnostic resources are most limited, and where patients often present with severe illness, advanced immunosuppression, and an inability to self-expectorate sputum,” wrote Jonny G. Peter, Ph.D., of the University of Cape Town, South Africa, and colleagues.
Read the full study in the Lancet (2016 Mar 9. doi: 10.1016/S0140-6736(15)01092-2).
Use of a low-cost urine test to guide tuberculosis treatment significantly improved mortality in HIV-positive patients, based on data from a randomized, multicenter trial including 2,528 adults at 10 locations in Africa.
The test involved a urine-based, lateral flow, point-of-care, lipoarabinomannan assay (LAM), and no associated adverse events were reported in this study.
Mortality at 8 weeks after LAM was significantly lower among patients who received LAM-guided antituberculosis treatment (21%), compared with control patients (25%). The relative risk reduction with LAM was 17%, and use of LAM improved the time to treatment initiation at all study locations, the researchers noted.
“The implementation of LAM testing is likely to offer the greatest benefit in hospitals where diagnostic resources are most limited, and where patients often present with severe illness, advanced immunosuppression, and an inability to self-expectorate sputum,” wrote Jonny G. Peter, Ph.D., of the University of Cape Town, South Africa, and colleagues.
Read the full study in the Lancet (2016 Mar 9. doi: 10.1016/S0140-6736(15)01092-2).
FROM THE LANCET
Low incidence, mortality described for mixed connective tissue disease
Mixed connective tissue disease (MCTD) occurred with an annual incidence of 1.9 cases per 100,000 individuals in a population-based study of adults conducted during 1985-2014 in Olmsted County, Minnesota.
The study also is the first to report a standardized mortality ratio for MCTD, at 1.1 (95% confidence interval, 0.4-2.6), which was not different from the general population, according to Dr. Patompong Ungprasert and other researchers from the Mayo Clinic, Rochester, Minn. They identified Raynaud’s phenomenon as the most common initial symptom of MCTD (in 50% of patients), followed by arthralgia (30%) and swollen hands (16%).
The proportion of patients whose MCTD evolved to other diagnoses was relatively low, occurring in only 10% of the cohort (4% to systemic sclerosis and 6% to systemic lupus erythematosus), corresponding to 10-year rates of 6.3% and 8.5%, respectively. The findings serve as additional “evidence to support the existence of MCTD as distinct entity, not just a transitional stage to other connective tissue diseases,” wrote the investigators, who reviewed data from 50 patients who met criteria for MCTD.
Read the full study in Arthritis Care & Research.
Mixed connective tissue disease (MCTD) occurred with an annual incidence of 1.9 cases per 100,000 individuals in a population-based study of adults conducted during 1985-2014 in Olmsted County, Minnesota.
The study also is the first to report a standardized mortality ratio for MCTD, at 1.1 (95% confidence interval, 0.4-2.6), which was not different from the general population, according to Dr. Patompong Ungprasert and other researchers from the Mayo Clinic, Rochester, Minn. They identified Raynaud’s phenomenon as the most common initial symptom of MCTD (in 50% of patients), followed by arthralgia (30%) and swollen hands (16%).
The proportion of patients whose MCTD evolved to other diagnoses was relatively low, occurring in only 10% of the cohort (4% to systemic sclerosis and 6% to systemic lupus erythematosus), corresponding to 10-year rates of 6.3% and 8.5%, respectively. The findings serve as additional “evidence to support the existence of MCTD as distinct entity, not just a transitional stage to other connective tissue diseases,” wrote the investigators, who reviewed data from 50 patients who met criteria for MCTD.
Read the full study in Arthritis Care & Research.
Mixed connective tissue disease (MCTD) occurred with an annual incidence of 1.9 cases per 100,000 individuals in a population-based study of adults conducted during 1985-2014 in Olmsted County, Minnesota.
The study also is the first to report a standardized mortality ratio for MCTD, at 1.1 (95% confidence interval, 0.4-2.6), which was not different from the general population, according to Dr. Patompong Ungprasert and other researchers from the Mayo Clinic, Rochester, Minn. They identified Raynaud’s phenomenon as the most common initial symptom of MCTD (in 50% of patients), followed by arthralgia (30%) and swollen hands (16%).
The proportion of patients whose MCTD evolved to other diagnoses was relatively low, occurring in only 10% of the cohort (4% to systemic sclerosis and 6% to systemic lupus erythematosus), corresponding to 10-year rates of 6.3% and 8.5%, respectively. The findings serve as additional “evidence to support the existence of MCTD as distinct entity, not just a transitional stage to other connective tissue diseases,” wrote the investigators, who reviewed data from 50 patients who met criteria for MCTD.
Read the full study in Arthritis Care & Research.
FROM ARTHRITIS CARE & RESEARCH
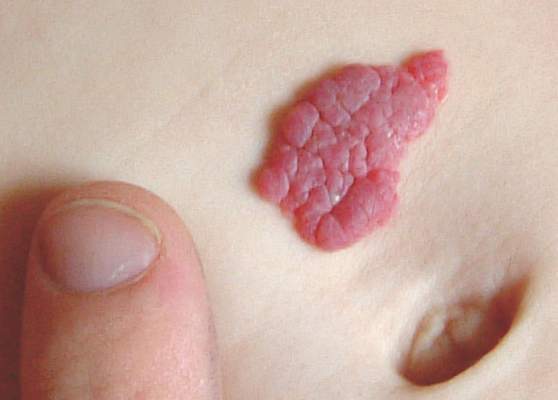
Hemangiomas Recur in 25% of Infants After Propranolol Stopped
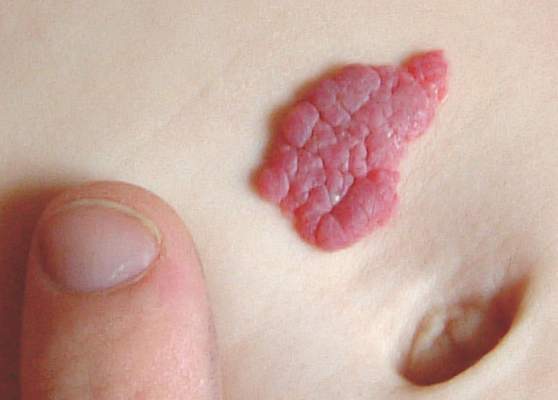
Infantile hemangiomas treated with propranolol recurred in 25% of children after discontinuation of propranolol in a retrospective study of nearly 1,000 patients, according to findings published online March 7 in Pediatrics.
“Identifying risk factors for rebound growth could affect treatment strategies, particularly duration of therapy,” wrote Dr. Sonal D. Shah of the University of California, San Francisco, and colleagues.
The study population was the largest to date, the researchers noted, and included 980 children seen at 10 academic centers between 2008 and 2013. Most were term (82%) and female (77%). The average age at the start of treatment was 6 months, and a visual analog scale was used to determine the children’s response to treatment (Pediatrics. 2016. doi: 10.1542/peds.2015-1754). Overall, hemangiomas rebounded in 231 patients (25%). Of these, 191 (83%) required treatment modification. The mean age before initial hemangioma rebound was 17 months, after a mean treatment duration of 11 months.
“The most potent risk factor for rebound was the presence of a deep infantile hemangioma component (i.e., deep or mixed morphology), which was also noted in other studies,” the researchers wrote.
In a multivariate analysis, deep hemangiomas and mixed hemangiomas were significantly more likely (odds ratio, 3.3 and 2.4, respectively) to rebound than superficial hemangiomas, and rebounds were significantly more likely among girls than boys (OR, 1.7).
“The exact reasons for this are uncertain, but it appears that girls are intrinsically more predisposed not only to hemangioma development but also to growth,” Dr. Shah and associates said.
Children least likely to rebound were those who discontinued or tapered propranolol between ages 12 and 18 months, and this group was used as a reference group. By comparison, the odds of rebound were notably high among children who discontinued when they were younger than 9 months (OR, 2.4). The odds ratios for rebound when propranolol was discontinued at ages 18-21 months, 21-24 months, and older than 24 months were 2.0, 1.7, and 2.5, respectively.
The results were limited by the fact that most patients represented more severe cases that were referred for additional treatment, Dr. Shah and associates said. However, the findings suggest that recognizing the risk factors for rebound could aid clinicians when planning therapy.
Lead author Dr. Shah had no relevant financial conflicts to disclose. Several coauthors reported serving as investigators or consultants for Pfizer and for Pierre Fabre Dermatology, which manufactures the propranolol product used in the study. The study was supported by the University of California, San Francisco, Pediatric Dermatology research fund.
“Understanding the phenomenon of postpropranolol rebound, and being able to predict or (better yet) prevent it, will increase clinical success and parental satisfaction with oral propranolol therapy and, in some instances, help prevent morbidity (such as airway blockage resulting from subglottic infantile hemangioma rebound),” Dr. Anthony J. Mancini of Northwestern University in Chicago commented.
The rebound risk factor data in this study expand on and support findings from previous studies, Dr. Mancini noted. Many research questions remain regarding the propranolol dose and duration to manage infantile hemangiomas most effectively. However, “the results of this large cohort review by Shah et al. will help guide clinicians in optimizing oral propranolol therapy and minimizing rebound growth in select higher-risk lesions,” he said.
Dr. Mancini, who commented in an accompanying editorial (Pediatrics. 2016. doi: 10.1542/peds.2015-3739), is a consultant, grant recipient, and speaker for Pierre Fabre Dermatology, and is a member of the Hemangioma Investigator Group, a research consortium that includes several of the study’s coauthors.
“Understanding the phenomenon of postpropranolol rebound, and being able to predict or (better yet) prevent it, will increase clinical success and parental satisfaction with oral propranolol therapy and, in some instances, help prevent morbidity (such as airway blockage resulting from subglottic infantile hemangioma rebound),” Dr. Anthony J. Mancini of Northwestern University in Chicago commented.
The rebound risk factor data in this study expand on and support findings from previous studies, Dr. Mancini noted. Many research questions remain regarding the propranolol dose and duration to manage infantile hemangiomas most effectively. However, “the results of this large cohort review by Shah et al. will help guide clinicians in optimizing oral propranolol therapy and minimizing rebound growth in select higher-risk lesions,” he said.
Dr. Mancini, who commented in an accompanying editorial (Pediatrics. 2016. doi: 10.1542/peds.2015-3739), is a consultant, grant recipient, and speaker for Pierre Fabre Dermatology, and is a member of the Hemangioma Investigator Group, a research consortium that includes several of the study’s coauthors.
“Understanding the phenomenon of postpropranolol rebound, and being able to predict or (better yet) prevent it, will increase clinical success and parental satisfaction with oral propranolol therapy and, in some instances, help prevent morbidity (such as airway blockage resulting from subglottic infantile hemangioma rebound),” Dr. Anthony J. Mancini of Northwestern University in Chicago commented.
The rebound risk factor data in this study expand on and support findings from previous studies, Dr. Mancini noted. Many research questions remain regarding the propranolol dose and duration to manage infantile hemangiomas most effectively. However, “the results of this large cohort review by Shah et al. will help guide clinicians in optimizing oral propranolol therapy and minimizing rebound growth in select higher-risk lesions,” he said.
Dr. Mancini, who commented in an accompanying editorial (Pediatrics. 2016. doi: 10.1542/peds.2015-3739), is a consultant, grant recipient, and speaker for Pierre Fabre Dermatology, and is a member of the Hemangioma Investigator Group, a research consortium that includes several of the study’s coauthors.
Infantile hemangiomas treated with propranolol recurred in 25% of children after discontinuation of propranolol in a retrospective study of nearly 1,000 patients, according to findings published online March 7 in Pediatrics.
“Identifying risk factors for rebound growth could affect treatment strategies, particularly duration of therapy,” wrote Dr. Sonal D. Shah of the University of California, San Francisco, and colleagues.
The study population was the largest to date, the researchers noted, and included 980 children seen at 10 academic centers between 2008 and 2013. Most were term (82%) and female (77%). The average age at the start of treatment was 6 months, and a visual analog scale was used to determine the children’s response to treatment (Pediatrics. 2016. doi: 10.1542/peds.2015-1754). Overall, hemangiomas rebounded in 231 patients (25%). Of these, 191 (83%) required treatment modification. The mean age before initial hemangioma rebound was 17 months, after a mean treatment duration of 11 months.
“The most potent risk factor for rebound was the presence of a deep infantile hemangioma component (i.e., deep or mixed morphology), which was also noted in other studies,” the researchers wrote.
In a multivariate analysis, deep hemangiomas and mixed hemangiomas were significantly more likely (odds ratio, 3.3 and 2.4, respectively) to rebound than superficial hemangiomas, and rebounds were significantly more likely among girls than boys (OR, 1.7).
“The exact reasons for this are uncertain, but it appears that girls are intrinsically more predisposed not only to hemangioma development but also to growth,” Dr. Shah and associates said.
Children least likely to rebound were those who discontinued or tapered propranolol between ages 12 and 18 months, and this group was used as a reference group. By comparison, the odds of rebound were notably high among children who discontinued when they were younger than 9 months (OR, 2.4). The odds ratios for rebound when propranolol was discontinued at ages 18-21 months, 21-24 months, and older than 24 months were 2.0, 1.7, and 2.5, respectively.
The results were limited by the fact that most patients represented more severe cases that were referred for additional treatment, Dr. Shah and associates said. However, the findings suggest that recognizing the risk factors for rebound could aid clinicians when planning therapy.
Lead author Dr. Shah had no relevant financial conflicts to disclose. Several coauthors reported serving as investigators or consultants for Pfizer and for Pierre Fabre Dermatology, which manufactures the propranolol product used in the study. The study was supported by the University of California, San Francisco, Pediatric Dermatology research fund.
Infantile hemangiomas treated with propranolol recurred in 25% of children after discontinuation of propranolol in a retrospective study of nearly 1,000 patients, according to findings published online March 7 in Pediatrics.
“Identifying risk factors for rebound growth could affect treatment strategies, particularly duration of therapy,” wrote Dr. Sonal D. Shah of the University of California, San Francisco, and colleagues.
The study population was the largest to date, the researchers noted, and included 980 children seen at 10 academic centers between 2008 and 2013. Most were term (82%) and female (77%). The average age at the start of treatment was 6 months, and a visual analog scale was used to determine the children’s response to treatment (Pediatrics. 2016. doi: 10.1542/peds.2015-1754). Overall, hemangiomas rebounded in 231 patients (25%). Of these, 191 (83%) required treatment modification. The mean age before initial hemangioma rebound was 17 months, after a mean treatment duration of 11 months.
“The most potent risk factor for rebound was the presence of a deep infantile hemangioma component (i.e., deep or mixed morphology), which was also noted in other studies,” the researchers wrote.
In a multivariate analysis, deep hemangiomas and mixed hemangiomas were significantly more likely (odds ratio, 3.3 and 2.4, respectively) to rebound than superficial hemangiomas, and rebounds were significantly more likely among girls than boys (OR, 1.7).
“The exact reasons for this are uncertain, but it appears that girls are intrinsically more predisposed not only to hemangioma development but also to growth,” Dr. Shah and associates said.
Children least likely to rebound were those who discontinued or tapered propranolol between ages 12 and 18 months, and this group was used as a reference group. By comparison, the odds of rebound were notably high among children who discontinued when they were younger than 9 months (OR, 2.4). The odds ratios for rebound when propranolol was discontinued at ages 18-21 months, 21-24 months, and older than 24 months were 2.0, 1.7, and 2.5, respectively.
The results were limited by the fact that most patients represented more severe cases that were referred for additional treatment, Dr. Shah and associates said. However, the findings suggest that recognizing the risk factors for rebound could aid clinicians when planning therapy.
Lead author Dr. Shah had no relevant financial conflicts to disclose. Several coauthors reported serving as investigators or consultants for Pfizer and for Pierre Fabre Dermatology, which manufactures the propranolol product used in the study. The study was supported by the University of California, San Francisco, Pediatric Dermatology research fund.
FROM PEDIATRICS
Hemangiomas recur in 25% of infants after propranolol stopped
Infantile hemangiomas treated with propranolol recurred in 25% of children after discontinuation of propranolol in a retrospective study of nearly 1,000 patients, according to findings published online March 7 in Pediatrics.
“Identifying risk factors for rebound growth could affect treatment strategies, particularly duration of therapy,” wrote Dr. Sonal D. Shah of the University of California, San Francisco, and colleagues.
The study population was the largest to date, the researchers noted, and included 980 children seen at 10 academic centers between 2008 and 2013. Most were term (82%) and female (77%). The average age at the start of treatment was 6 months, and a visual analog scale was used to determine the children’s response to treatment (Pediatrics. 2016. doi: 10.1542/peds.2015-1754). Overall, hemangiomas rebounded in 231 patients (25%). Of these, 191 (83%) required treatment modification. The mean age before initial hemangioma rebound was 17 months, after a mean treatment duration of 11 months.
“The most potent risk factor for rebound was the presence of a deep infantile hemangioma component (i.e., deep or mixed morphology), which was also noted in other studies,” the researchers wrote.
In a multivariate analysis, deep hemangiomas and mixed hemangiomas were significantly more likely (odds ratio, 3.3 and 2.4, respectively) to rebound than superficial hemangiomas, and rebounds were significantly more likely among girls than boys (OR, 1.7).
“The exact reasons for this are uncertain, but it appears that girls are intrinsically more predisposed not only to hemangioma development but also to growth,” Dr. Shah and associates said.
Children least likely to rebound were those who discontinued or tapered propranolol between ages 12 and 18 months, and this group was used as a reference group. By comparison, the odds of rebound were notably high among children who discontinued when they were younger than 9 months (OR, 2.4). The odds ratios for rebound when propranolol was discontinued at ages 18-21 months, 21-24 months, and older than 24 months were 2.0, 1.7, and 2.5, respectively.
The results were limited by the fact that most patients represented more severe cases that were referred for additional treatment, Dr. Shah and associates said. However, the findings suggest that recognizing the risk factors for rebound could aid clinicians when planning therapy.
Lead author Dr. Shah had no relevant financial conflicts to disclose. Several coauthors reported serving as investigators or consultants for Pfizer and for Pierre Fabre Dermatology, which manufactures the propranolol product used in the study. The study was supported by the University of California, San Francisco, Pediatric Dermatology research fund.
“Understanding the phenomenon of postpropranolol rebound, and being able to predict or (better yet) prevent it, will increase clinical success and parental satisfaction with oral propranolol therapy and, in some instances, help prevent morbidity (such as airway blockage resulting from subglottic infantile hemangioma rebound),” Dr. Anthony J. Mancini of Northwestern University in Chicago commented.
The rebound risk factor data in this study expand on and support findings from previous studies, Dr. Mancini noted. Many research questions remain regarding the propranolol dose and duration to manage infantile hemangiomas most effectively. However, “the results of this large cohort review by Shah et al. will help guide clinicians in optimizing oral propranolol therapy and minimizing rebound growth in select higher-risk lesions,” he said.
Dr. Mancini, who commented in an accompanying editorial (Pediatrics. 2016. doi: 10.1542/peds.2015-3739), is a consultant, grant recipient, and speaker for Pierre Fabre Dermatology, and is a member of the Hemangioma Investigator Group, a research consortium that includes several of the study’s coauthors.
“Understanding the phenomenon of postpropranolol rebound, and being able to predict or (better yet) prevent it, will increase clinical success and parental satisfaction with oral propranolol therapy and, in some instances, help prevent morbidity (such as airway blockage resulting from subglottic infantile hemangioma rebound),” Dr. Anthony J. Mancini of Northwestern University in Chicago commented.
The rebound risk factor data in this study expand on and support findings from previous studies, Dr. Mancini noted. Many research questions remain regarding the propranolol dose and duration to manage infantile hemangiomas most effectively. However, “the results of this large cohort review by Shah et al. will help guide clinicians in optimizing oral propranolol therapy and minimizing rebound growth in select higher-risk lesions,” he said.
Dr. Mancini, who commented in an accompanying editorial (Pediatrics. 2016. doi: 10.1542/peds.2015-3739), is a consultant, grant recipient, and speaker for Pierre Fabre Dermatology, and is a member of the Hemangioma Investigator Group, a research consortium that includes several of the study’s coauthors.
“Understanding the phenomenon of postpropranolol rebound, and being able to predict or (better yet) prevent it, will increase clinical success and parental satisfaction with oral propranolol therapy and, in some instances, help prevent morbidity (such as airway blockage resulting from subglottic infantile hemangioma rebound),” Dr. Anthony J. Mancini of Northwestern University in Chicago commented.
The rebound risk factor data in this study expand on and support findings from previous studies, Dr. Mancini noted. Many research questions remain regarding the propranolol dose and duration to manage infantile hemangiomas most effectively. However, “the results of this large cohort review by Shah et al. will help guide clinicians in optimizing oral propranolol therapy and minimizing rebound growth in select higher-risk lesions,” he said.
Dr. Mancini, who commented in an accompanying editorial (Pediatrics. 2016. doi: 10.1542/peds.2015-3739), is a consultant, grant recipient, and speaker for Pierre Fabre Dermatology, and is a member of the Hemangioma Investigator Group, a research consortium that includes several of the study’s coauthors.
Infantile hemangiomas treated with propranolol recurred in 25% of children after discontinuation of propranolol in a retrospective study of nearly 1,000 patients, according to findings published online March 7 in Pediatrics.
“Identifying risk factors for rebound growth could affect treatment strategies, particularly duration of therapy,” wrote Dr. Sonal D. Shah of the University of California, San Francisco, and colleagues.
The study population was the largest to date, the researchers noted, and included 980 children seen at 10 academic centers between 2008 and 2013. Most were term (82%) and female (77%). The average age at the start of treatment was 6 months, and a visual analog scale was used to determine the children’s response to treatment (Pediatrics. 2016. doi: 10.1542/peds.2015-1754). Overall, hemangiomas rebounded in 231 patients (25%). Of these, 191 (83%) required treatment modification. The mean age before initial hemangioma rebound was 17 months, after a mean treatment duration of 11 months.
“The most potent risk factor for rebound was the presence of a deep infantile hemangioma component (i.e., deep or mixed morphology), which was also noted in other studies,” the researchers wrote.
In a multivariate analysis, deep hemangiomas and mixed hemangiomas were significantly more likely (odds ratio, 3.3 and 2.4, respectively) to rebound than superficial hemangiomas, and rebounds were significantly more likely among girls than boys (OR, 1.7).
“The exact reasons for this are uncertain, but it appears that girls are intrinsically more predisposed not only to hemangioma development but also to growth,” Dr. Shah and associates said.
Children least likely to rebound were those who discontinued or tapered propranolol between ages 12 and 18 months, and this group was used as a reference group. By comparison, the odds of rebound were notably high among children who discontinued when they were younger than 9 months (OR, 2.4). The odds ratios for rebound when propranolol was discontinued at ages 18-21 months, 21-24 months, and older than 24 months were 2.0, 1.7, and 2.5, respectively.
The results were limited by the fact that most patients represented more severe cases that were referred for additional treatment, Dr. Shah and associates said. However, the findings suggest that recognizing the risk factors for rebound could aid clinicians when planning therapy.
Lead author Dr. Shah had no relevant financial conflicts to disclose. Several coauthors reported serving as investigators or consultants for Pfizer and for Pierre Fabre Dermatology, which manufactures the propranolol product used in the study. The study was supported by the University of California, San Francisco, Pediatric Dermatology research fund.
Infantile hemangiomas treated with propranolol recurred in 25% of children after discontinuation of propranolol in a retrospective study of nearly 1,000 patients, according to findings published online March 7 in Pediatrics.
“Identifying risk factors for rebound growth could affect treatment strategies, particularly duration of therapy,” wrote Dr. Sonal D. Shah of the University of California, San Francisco, and colleagues.
The study population was the largest to date, the researchers noted, and included 980 children seen at 10 academic centers between 2008 and 2013. Most were term (82%) and female (77%). The average age at the start of treatment was 6 months, and a visual analog scale was used to determine the children’s response to treatment (Pediatrics. 2016. doi: 10.1542/peds.2015-1754). Overall, hemangiomas rebounded in 231 patients (25%). Of these, 191 (83%) required treatment modification. The mean age before initial hemangioma rebound was 17 months, after a mean treatment duration of 11 months.
“The most potent risk factor for rebound was the presence of a deep infantile hemangioma component (i.e., deep or mixed morphology), which was also noted in other studies,” the researchers wrote.
In a multivariate analysis, deep hemangiomas and mixed hemangiomas were significantly more likely (odds ratio, 3.3 and 2.4, respectively) to rebound than superficial hemangiomas, and rebounds were significantly more likely among girls than boys (OR, 1.7).
“The exact reasons for this are uncertain, but it appears that girls are intrinsically more predisposed not only to hemangioma development but also to growth,” Dr. Shah and associates said.
Children least likely to rebound were those who discontinued or tapered propranolol between ages 12 and 18 months, and this group was used as a reference group. By comparison, the odds of rebound were notably high among children who discontinued when they were younger than 9 months (OR, 2.4). The odds ratios for rebound when propranolol was discontinued at ages 18-21 months, 21-24 months, and older than 24 months were 2.0, 1.7, and 2.5, respectively.
The results were limited by the fact that most patients represented more severe cases that were referred for additional treatment, Dr. Shah and associates said. However, the findings suggest that recognizing the risk factors for rebound could aid clinicians when planning therapy.
Lead author Dr. Shah had no relevant financial conflicts to disclose. Several coauthors reported serving as investigators or consultants for Pfizer and for Pierre Fabre Dermatology, which manufactures the propranolol product used in the study. The study was supported by the University of California, San Francisco, Pediatric Dermatology research fund.
FROM PEDIATRICS
Key clinical point: This large study of nearly 1,000 patients identifies risk factors for hemangioma rebound that may help guide oral propranolol treatment decisions.
Major finding: Infantile hemangiomas recurred in 25% of children after discontinuation of oral propranolol therapy.
Data source: A retrospective study including 980 children seen at 10 academic centers in the United States.
Disclosures: Lead author Dr. Shah had no relevant financial conflicts to disclose. Several coauthors reported serving as investigators or consultants for Pfizer and for Pierre Fabre Dermatology, which manufactures the propranolol product used in the study. The study was supported by the University of California, San Francisco, Pediatric Dermatology research fund.
Childhood Emotional Abuse Fuels Odds for Migraine in Adulthood
Emotionally abused children are 52% more likely to develop migraine in young adulthood than are those who were never abused, based on longitudinal survey data from nearly 15,000 individuals.
“Childhood maltreatment, and especially emotional abuse, is a common, likely under-recognized occurrence, which has enduring consequences for health throughout life. The association of emotional abuse with migraine has not heretofore been well studied, being the subject of only population-based study,” lead author Dr. Gretchen E. Tietjen of the University of Toledo (Ohio) said in an interview in advance of the presentation of the study at the annual meeting of the American Academy of Neurology in Vancouver in April.
Dr. Tietjen and her colleagues assessed data from 14,484 adults aged 24-32 years who took part in wave four of the National Longitudinal Study of Adolescent to Adult Health. Of these, 2,061 (14%) reported a migraine diagnosis, and 1,246 (60%) of those diagnosed with migraines reported some type of childhood abuse. A total of 6,088 (49%) individuals without migraine reported some type of childhood abuse.
Overall, the odds of migraine in adulthood was 55% higher in children who reported emotional abuse, physical abuse, or sexual abuse, compared with those who reported no childhood abuse, after controlling for age, race, sex, and income (odds ratio, 1.55; 95% confidence interval, 1.35-1.77). However, only emotional abuse remained significantly associated with increased odds for migraine after controlling for other types of abuse (OR, 1.52; 95% CI, 1.34-1.73).
Emotional abuse was assessed by asking, “How often did a parent or other adult caregiver say things that really hurt your feelings or made you feel like you were not wanted or loved?” Physical abuse was defined as being hit with a fist, kicked, or thrown down on the floor, into a wall, or down stairs. Sexual abuse included forced sexual touching or sexual relations.
Controlling for depression and anxiety weakened the associations between childhood abuse overall and likelihood of migraine in young adulthood, as well as for emotional abuse in particular, but the relationships remained statistically significant (OR, 1.32 and 1.33, respectively).
Dr. Tietjen said she was surprised by the absence of an association between migraine and physical and sexual abuse after controlling for other types of abuse.
“Sexual and physical abuse may be less frequent, occur over a briefer duration, and if limited, lead in some cases to resilience,” Dr. Tietjen noted. “Emotional abuse is likely more insidious, being ingrained in the fabric of the family dynamic. It may occur over years without recognition or intervention,” she said. “This type of abuse may cause more cumulative stress, with subsequent dysregulation of the HPA axis, immune, autonomic, and metabolic systems,” she added.
The study does not show cause and effect, the researchers noted, and more research is needed. But the findings suggest that clinicians might consider childhood abuse when counseling adult migraine patients.
“In migraineurs, childhood abuse, particularly emotional abuse, is common and possibly causally related,” Dr. Tietjen said. “Knowledge of adverse childhood experiences allows physicians to identify migraineurs at higher risk for psychiatric disease, pain comorbidities, and conditions associated with inflammation. These patients would likely benefit from exposure to cognitive behavioral therapy strategies, in order to decrease neurophysiological responses to stress,” she noted.
“There are currently therapies which reverse stress-induced epigenetic changes, which might be particularly useful in the subset of migraineurs who have been abused,” said Dr. Tietjen. Her next steps for research involve studying the effect of early life stress on factors such as pain sensitivity, anxiety, and depression.
The University of Toledo and the Clair Martig Endowment funded the study.
Emotionally abused children are 52% more likely to develop migraine in young adulthood than are those who were never abused, based on longitudinal survey data from nearly 15,000 individuals.
“Childhood maltreatment, and especially emotional abuse, is a common, likely under-recognized occurrence, which has enduring consequences for health throughout life. The association of emotional abuse with migraine has not heretofore been well studied, being the subject of only population-based study,” lead author Dr. Gretchen E. Tietjen of the University of Toledo (Ohio) said in an interview in advance of the presentation of the study at the annual meeting of the American Academy of Neurology in Vancouver in April.
Dr. Tietjen and her colleagues assessed data from 14,484 adults aged 24-32 years who took part in wave four of the National Longitudinal Study of Adolescent to Adult Health. Of these, 2,061 (14%) reported a migraine diagnosis, and 1,246 (60%) of those diagnosed with migraines reported some type of childhood abuse. A total of 6,088 (49%) individuals without migraine reported some type of childhood abuse.
Overall, the odds of migraine in adulthood was 55% higher in children who reported emotional abuse, physical abuse, or sexual abuse, compared with those who reported no childhood abuse, after controlling for age, race, sex, and income (odds ratio, 1.55; 95% confidence interval, 1.35-1.77). However, only emotional abuse remained significantly associated with increased odds for migraine after controlling for other types of abuse (OR, 1.52; 95% CI, 1.34-1.73).
Emotional abuse was assessed by asking, “How often did a parent or other adult caregiver say things that really hurt your feelings or made you feel like you were not wanted or loved?” Physical abuse was defined as being hit with a fist, kicked, or thrown down on the floor, into a wall, or down stairs. Sexual abuse included forced sexual touching or sexual relations.
Controlling for depression and anxiety weakened the associations between childhood abuse overall and likelihood of migraine in young adulthood, as well as for emotional abuse in particular, but the relationships remained statistically significant (OR, 1.32 and 1.33, respectively).
Dr. Tietjen said she was surprised by the absence of an association between migraine and physical and sexual abuse after controlling for other types of abuse.
“Sexual and physical abuse may be less frequent, occur over a briefer duration, and if limited, lead in some cases to resilience,” Dr. Tietjen noted. “Emotional abuse is likely more insidious, being ingrained in the fabric of the family dynamic. It may occur over years without recognition or intervention,” she said. “This type of abuse may cause more cumulative stress, with subsequent dysregulation of the HPA axis, immune, autonomic, and metabolic systems,” she added.
The study does not show cause and effect, the researchers noted, and more research is needed. But the findings suggest that clinicians might consider childhood abuse when counseling adult migraine patients.
“In migraineurs, childhood abuse, particularly emotional abuse, is common and possibly causally related,” Dr. Tietjen said. “Knowledge of adverse childhood experiences allows physicians to identify migraineurs at higher risk for psychiatric disease, pain comorbidities, and conditions associated with inflammation. These patients would likely benefit from exposure to cognitive behavioral therapy strategies, in order to decrease neurophysiological responses to stress,” she noted.
“There are currently therapies which reverse stress-induced epigenetic changes, which might be particularly useful in the subset of migraineurs who have been abused,” said Dr. Tietjen. Her next steps for research involve studying the effect of early life stress on factors such as pain sensitivity, anxiety, and depression.
The University of Toledo and the Clair Martig Endowment funded the study.
Emotionally abused children are 52% more likely to develop migraine in young adulthood than are those who were never abused, based on longitudinal survey data from nearly 15,000 individuals.
“Childhood maltreatment, and especially emotional abuse, is a common, likely under-recognized occurrence, which has enduring consequences for health throughout life. The association of emotional abuse with migraine has not heretofore been well studied, being the subject of only population-based study,” lead author Dr. Gretchen E. Tietjen of the University of Toledo (Ohio) said in an interview in advance of the presentation of the study at the annual meeting of the American Academy of Neurology in Vancouver in April.
Dr. Tietjen and her colleagues assessed data from 14,484 adults aged 24-32 years who took part in wave four of the National Longitudinal Study of Adolescent to Adult Health. Of these, 2,061 (14%) reported a migraine diagnosis, and 1,246 (60%) of those diagnosed with migraines reported some type of childhood abuse. A total of 6,088 (49%) individuals without migraine reported some type of childhood abuse.
Overall, the odds of migraine in adulthood was 55% higher in children who reported emotional abuse, physical abuse, or sexual abuse, compared with those who reported no childhood abuse, after controlling for age, race, sex, and income (odds ratio, 1.55; 95% confidence interval, 1.35-1.77). However, only emotional abuse remained significantly associated with increased odds for migraine after controlling for other types of abuse (OR, 1.52; 95% CI, 1.34-1.73).
Emotional abuse was assessed by asking, “How often did a parent or other adult caregiver say things that really hurt your feelings or made you feel like you were not wanted or loved?” Physical abuse was defined as being hit with a fist, kicked, or thrown down on the floor, into a wall, or down stairs. Sexual abuse included forced sexual touching or sexual relations.
Controlling for depression and anxiety weakened the associations between childhood abuse overall and likelihood of migraine in young adulthood, as well as for emotional abuse in particular, but the relationships remained statistically significant (OR, 1.32 and 1.33, respectively).
Dr. Tietjen said she was surprised by the absence of an association between migraine and physical and sexual abuse after controlling for other types of abuse.
“Sexual and physical abuse may be less frequent, occur over a briefer duration, and if limited, lead in some cases to resilience,” Dr. Tietjen noted. “Emotional abuse is likely more insidious, being ingrained in the fabric of the family dynamic. It may occur over years without recognition or intervention,” she said. “This type of abuse may cause more cumulative stress, with subsequent dysregulation of the HPA axis, immune, autonomic, and metabolic systems,” she added.
The study does not show cause and effect, the researchers noted, and more research is needed. But the findings suggest that clinicians might consider childhood abuse when counseling adult migraine patients.
“In migraineurs, childhood abuse, particularly emotional abuse, is common and possibly causally related,” Dr. Tietjen said. “Knowledge of adverse childhood experiences allows physicians to identify migraineurs at higher risk for psychiatric disease, pain comorbidities, and conditions associated with inflammation. These patients would likely benefit from exposure to cognitive behavioral therapy strategies, in order to decrease neurophysiological responses to stress,” she noted.
“There are currently therapies which reverse stress-induced epigenetic changes, which might be particularly useful in the subset of migraineurs who have been abused,” said Dr. Tietjen. Her next steps for research involve studying the effect of early life stress on factors such as pain sensitivity, anxiety, and depression.
The University of Toledo and the Clair Martig Endowment funded the study.
FROM THE AAN 2016 ANNUAL MEETING
Childhood emotional abuse fuels odds for migraine in adulthood
Emotionally abused children are 52% more likely to develop migraine in young adulthood than are those who were never abused, based on longitudinal survey data from nearly 15,000 individuals.
“Childhood maltreatment, and especially emotional abuse, is a common, likely under-recognized occurrence, which has enduring consequences for health throughout life. The association of emotional abuse with migraine has not heretofore been well studied, being the subject of only population-based study,” lead author Dr. Gretchen E. Tietjen of the University of Toledo (Ohio) said in an interview in advance of the presentation of the study at the annual meeting of the American Academy of Neurology in Vancouver in April.
Dr. Tietjen and her colleagues assessed data from 14,484 adults aged 24-32 years who took part in wave four of the National Longitudinal Study of Adolescent to Adult Health. Of these, 2,061 (14%) reported a migraine diagnosis, and 1,246 (60%) of those diagnosed with migraines reported some type of childhood abuse. A total of 6,088 (49%) individuals without migraine reported some type of childhood abuse.
Overall, the odds of migraine in adulthood was 55% higher in children who reported emotional abuse, physical abuse, or sexual abuse, compared with those who reported no childhood abuse, after controlling for age, race, sex, and income (odds ratio, 1.55; 95% confidence interval, 1.35-1.77). However, only emotional abuse remained significantly associated with increased odds for migraine after controlling for other types of abuse (OR, 1.52; 95% CI, 1.34-1.73).
Emotional abuse was assessed by asking, “How often did a parent or other adult caregiver say things that really hurt your feelings or made you feel like you were not wanted or loved?” Physical abuse was defined as being hit with a fist, kicked, or thrown down on the floor, into a wall, or down stairs. Sexual abuse included forced sexual touching or sexual relations.
Controlling for depression and anxiety weakened the associations between childhood abuse overall and likelihood of migraine in young adulthood, as well as for emotional abuse in particular, but the relationships remained statistically significant (OR, 1.32 and 1.33, respectively).
Dr. Tietjen said she was surprised by the absence of an association between migraine and physical and sexual abuse after controlling for other types of abuse.
“Sexual and physical abuse may be less frequent, occur over a briefer duration, and if limited, lead in some cases to resilience,” Dr. Tietjen noted. “Emotional abuse is likely more insidious, being ingrained in the fabric of the family dynamic. It may occur over years without recognition or intervention,” she said. “This type of abuse may cause more cumulative stress, with subsequent dysregulation of the HPA axis, immune, autonomic, and metabolic systems,” she added.
The study does not show cause and effect, the researchers noted, and more research is needed. But the findings suggest that clinicians might consider childhood abuse when counseling adult migraine patients.
“In migraineurs, childhood abuse, particularly emotional abuse, is common and possibly causally related,” Dr. Tietjen said. “Knowledge of adverse childhood experiences allows physicians to identify migraineurs at higher risk for psychiatric disease, pain comorbidities, and conditions associated with inflammation. These patients would likely benefit from exposure to cognitive behavioral therapy strategies, in order to decrease neurophysiological responses to stress,” she noted.
“There are currently therapies which reverse stress-induced epigenetic changes, which might be particularly useful in the subset of migraineurs who have been abused,” said Dr. Tietjen. Her next steps for research involve studying the effect of early life stress on factors such as pain sensitivity, anxiety, and depression.
The University of Toledo and the Clair Martig Endowment funded the study.
Emotionally abused children are 52% more likely to develop migraine in young adulthood than are those who were never abused, based on longitudinal survey data from nearly 15,000 individuals.
“Childhood maltreatment, and especially emotional abuse, is a common, likely under-recognized occurrence, which has enduring consequences for health throughout life. The association of emotional abuse with migraine has not heretofore been well studied, being the subject of only population-based study,” lead author Dr. Gretchen E. Tietjen of the University of Toledo (Ohio) said in an interview in advance of the presentation of the study at the annual meeting of the American Academy of Neurology in Vancouver in April.
Dr. Tietjen and her colleagues assessed data from 14,484 adults aged 24-32 years who took part in wave four of the National Longitudinal Study of Adolescent to Adult Health. Of these, 2,061 (14%) reported a migraine diagnosis, and 1,246 (60%) of those diagnosed with migraines reported some type of childhood abuse. A total of 6,088 (49%) individuals without migraine reported some type of childhood abuse.
Overall, the odds of migraine in adulthood was 55% higher in children who reported emotional abuse, physical abuse, or sexual abuse, compared with those who reported no childhood abuse, after controlling for age, race, sex, and income (odds ratio, 1.55; 95% confidence interval, 1.35-1.77). However, only emotional abuse remained significantly associated with increased odds for migraine after controlling for other types of abuse (OR, 1.52; 95% CI, 1.34-1.73).
Emotional abuse was assessed by asking, “How often did a parent or other adult caregiver say things that really hurt your feelings or made you feel like you were not wanted or loved?” Physical abuse was defined as being hit with a fist, kicked, or thrown down on the floor, into a wall, or down stairs. Sexual abuse included forced sexual touching or sexual relations.
Controlling for depression and anxiety weakened the associations between childhood abuse overall and likelihood of migraine in young adulthood, as well as for emotional abuse in particular, but the relationships remained statistically significant (OR, 1.32 and 1.33, respectively).
Dr. Tietjen said she was surprised by the absence of an association between migraine and physical and sexual abuse after controlling for other types of abuse.
“Sexual and physical abuse may be less frequent, occur over a briefer duration, and if limited, lead in some cases to resilience,” Dr. Tietjen noted. “Emotional abuse is likely more insidious, being ingrained in the fabric of the family dynamic. It may occur over years without recognition or intervention,” she said. “This type of abuse may cause more cumulative stress, with subsequent dysregulation of the HPA axis, immune, autonomic, and metabolic systems,” she added.
The study does not show cause and effect, the researchers noted, and more research is needed. But the findings suggest that clinicians might consider childhood abuse when counseling adult migraine patients.
“In migraineurs, childhood abuse, particularly emotional abuse, is common and possibly causally related,” Dr. Tietjen said. “Knowledge of adverse childhood experiences allows physicians to identify migraineurs at higher risk for psychiatric disease, pain comorbidities, and conditions associated with inflammation. These patients would likely benefit from exposure to cognitive behavioral therapy strategies, in order to decrease neurophysiological responses to stress,” she noted.
“There are currently therapies which reverse stress-induced epigenetic changes, which might be particularly useful in the subset of migraineurs who have been abused,” said Dr. Tietjen. Her next steps for research involve studying the effect of early life stress on factors such as pain sensitivity, anxiety, and depression.
The University of Toledo and the Clair Martig Endowment funded the study.
Emotionally abused children are 52% more likely to develop migraine in young adulthood than are those who were never abused, based on longitudinal survey data from nearly 15,000 individuals.
“Childhood maltreatment, and especially emotional abuse, is a common, likely under-recognized occurrence, which has enduring consequences for health throughout life. The association of emotional abuse with migraine has not heretofore been well studied, being the subject of only population-based study,” lead author Dr. Gretchen E. Tietjen of the University of Toledo (Ohio) said in an interview in advance of the presentation of the study at the annual meeting of the American Academy of Neurology in Vancouver in April.
Dr. Tietjen and her colleagues assessed data from 14,484 adults aged 24-32 years who took part in wave four of the National Longitudinal Study of Adolescent to Adult Health. Of these, 2,061 (14%) reported a migraine diagnosis, and 1,246 (60%) of those diagnosed with migraines reported some type of childhood abuse. A total of 6,088 (49%) individuals without migraine reported some type of childhood abuse.
Overall, the odds of migraine in adulthood was 55% higher in children who reported emotional abuse, physical abuse, or sexual abuse, compared with those who reported no childhood abuse, after controlling for age, race, sex, and income (odds ratio, 1.55; 95% confidence interval, 1.35-1.77). However, only emotional abuse remained significantly associated with increased odds for migraine after controlling for other types of abuse (OR, 1.52; 95% CI, 1.34-1.73).
Emotional abuse was assessed by asking, “How often did a parent or other adult caregiver say things that really hurt your feelings or made you feel like you were not wanted or loved?” Physical abuse was defined as being hit with a fist, kicked, or thrown down on the floor, into a wall, or down stairs. Sexual abuse included forced sexual touching or sexual relations.
Controlling for depression and anxiety weakened the associations between childhood abuse overall and likelihood of migraine in young adulthood, as well as for emotional abuse in particular, but the relationships remained statistically significant (OR, 1.32 and 1.33, respectively).
Dr. Tietjen said she was surprised by the absence of an association between migraine and physical and sexual abuse after controlling for other types of abuse.
“Sexual and physical abuse may be less frequent, occur over a briefer duration, and if limited, lead in some cases to resilience,” Dr. Tietjen noted. “Emotional abuse is likely more insidious, being ingrained in the fabric of the family dynamic. It may occur over years without recognition or intervention,” she said. “This type of abuse may cause more cumulative stress, with subsequent dysregulation of the HPA axis, immune, autonomic, and metabolic systems,” she added.
The study does not show cause and effect, the researchers noted, and more research is needed. But the findings suggest that clinicians might consider childhood abuse when counseling adult migraine patients.
“In migraineurs, childhood abuse, particularly emotional abuse, is common and possibly causally related,” Dr. Tietjen said. “Knowledge of adverse childhood experiences allows physicians to identify migraineurs at higher risk for psychiatric disease, pain comorbidities, and conditions associated with inflammation. These patients would likely benefit from exposure to cognitive behavioral therapy strategies, in order to decrease neurophysiological responses to stress,” she noted.
“There are currently therapies which reverse stress-induced epigenetic changes, which might be particularly useful in the subset of migraineurs who have been abused,” said Dr. Tietjen. Her next steps for research involve studying the effect of early life stress on factors such as pain sensitivity, anxiety, and depression.
The University of Toledo and the Clair Martig Endowment funded the study.
FROM THE AAN 2016 ANNUAL MEETING
Key clinical point: Childhood abuse had a significant effect on the likelihood of developing migraine in young adulthood, and emotional abuse was a stronger factor than physical or sexual abuse.
Major finding: Childhood abuse increased the odds of a migraine diagnosis in young adulthood by 55%; emotional abuse was associated with a 52% increased likelihood of migraine.
Data source: The data were taken from 14,484 adults aged 24-32 years in wave four of the National Longitudinal Study of Adolescent to Adult Health.
Disclosures: The University of Toledo and the Clair Martig Endowment funded the study.