User login
Long-term PPI use linked to increased risk of dementia
Long-term use of proton pump inhibitors was significantly associated with later diagnoses of dementia in adults aged 75 years and older in a prospective cohort study of more than 73,000 individuals. The findings were published online Feb. 15 in JAMA Neurology.
Overall, the risk of incident dementia was 44% higher among the 2,950 patients who received regular proton pump inhibitors, compared with 70,729 who didn’t receive PPIs (hazard ratio of 1.44), according to Willy Gomm, Ph.D., of the German Center for Neurodegenerative Diseases in Bonn, and his colleagues.
To assess the potential link between PPIs and dementia, the researchers reviewed data from a German insurance database during 2004-2011. The study population included 73,679 community-dwelling adults aged 75 years and older who were free of dementia at the start of the study (JAMA Neurol. 2016 Feb 15. doi: 10.1001/jamaneurol.2015.4791). The patients taking PPIs were slightly but significantly older than those not taking PPIs and had a higher proportion of women (P less than .001 for both). PPI users were also significantly more likely than nonusers to have a history of depression, stroke, coronary disease, and use of polypharmacy (P less than .001 for each).
The risk of incident dementia decreased with age, from 69% for patients aged 75-79 years to 49% among those 80-84-years and 32% among those aged 85 years and older.
In addition, the risk of dementia was not significantly different based on specific drug in a subgroup analysis of the three most often prescribed PPIs, omeprazole, pantoprazole, and esomeprazole, for which the hazard ratios were 1.51, 1.58, and 2.12, respectively.
“If PPIs have adverse effects, it is important to be aware of them,” Dr. Daniel E. Freedberg of Columbia University, New York, said in an interview. “When PPIs are indicated, the preponderance of data indicate that their benefits outweigh their potential risks,” he added. “Clinicians should reassure patients that this was a single study and that previous studies have reached different conclusions. Clinicians should focus on whether or not PPIs are indicated rather than on PPI side effects.”
Dr. Freedberg also noted several key limitations of the study.
“First, the authors were unable to adjust for crucial variables that might explain a noncausal link between PPIs and dementia. For example, lower socioeconomic status is an established predictor of dementia and may also be associated with PPI use. However, the authors could not capture socioeconomic status.
“Second, patients who use PPIs have more frequent and more intensive health care interactions than patients who do not use PPIs. These patients are thus also more likely to be diagnosed with dementia. This is another source for bias that the authors were not able to capture. Third, clinicians should be aware that this study was designed to compare extremes of PPI use,” Dr. Freedberg emphasized.
In addition, “In the primary analysis, patients were classified as exposed to PPIs only if they received at least one PPI prescription every 3 months for an 18-month period. Patients who used occasional PPIs were excluded from the study,” said Dr. Freedberg.
“The present study can only provide a statistical association between PPI use and risk of dementia,” the researchers noted. “The possible underlying causal biological mechanism has to be explored in future studies,” they wrote.
The researchers had no financial conflicts to disclose.
Challenging research lies ahead
The researchers have provided an important and interesting challenge to evaluate the possible association of the use of PPIs and the risk of dementia.

|
Dr. Lewis H. Kuller |
Further determinants of whether PPIs are causal for dementia requires validation in large cohorts and probably in well-designed case-control studies with good measures of long-term PPI use, covariates, and especially methods to measure incidence of dementia.
Dr. Lewis H. Kuller is affiliated with the department of epidemiology at the University of Pittsburgh. He made his remarks in an accompanying editorial and had no financial conflicts to disclose.
PPIs and dementia: More of much ado about nothing?
This study has attracted considerable media attention. Unfortunately, this was somewhat unbalanced. One TV news program stated that there was a “44% increased risk of dementia.” Many of our patients would not be able to interpret that appropriately – let alone weigh the potential risks and benefits of PPI treatment.
The 44% increase is derived from the hazard ratio of 1.44 that the investigators reported. However, to quote Dr. David A. Grimes and Dr. Kenneth F. Schulz, “Any claim coming from an observational study is most likely to be wrong. Of the reported associations that are correct, most are exaggerated” (Obstet Gynecol. 2012;120:920-7).
In the German study, the patients who had been taking PPIs were more likely to have prior diagnoses of depression, stroke, and ischemic heart disease than those not on PPIs. They were also much more likely to be on multiple other medicines. These patients may have been more likely to be given a PPI because of their comorbidity. There may, therefore, be an element of channeling bias or confounding by indication to explain the findings.
However, let us assume that there had been a stronger suggestion of a causal association between PPI use and the risk of developing dementia. It would be important to consider what its underlying biological rationale might be. The investigators state that PPI use “has been shown to be potentially involved in cognitive decline.” The evidence offered in support of this claim comes from a case-control study that did not evaluate cognitive function but reported an increased incidence of vitamin B12 deficiency among adults taking PPIs for 2 or more years [very small odds ratio of 1.65 (JAMA 2013;310:2435-42)]. Low B12 levels were linked to “cognitive deficit” in a population-based study from Norway (Psychosom Med. 2013;75:20-9). So, the proposed biological rationale for any association between PPI use and dementia is tenuous at best.
For PPIs, long-term or indefinite use is appropriate for indications such as erosive esophagitis, esophageal stricture, or the prevention of upper GI tract ulcers and ulcer bleeding in patients taking aspirin or NSAIDs. Patients with a valid indication for PPI treatment should continue to receive it for as long as clinically indicated – and at the lowest effective dose. It would be unfortunate if patients with indications for PPI treatment discontinued it on the basis of this study.
Dr. Colin W. Howden, AGAF, is Hyman Professor of Medicine, chief of the division of gastroenterology, University of Tennessee Health Science Center, Memphis. He is a consultant for Takeda, Otsuka, Ironwood, Allergan, Aralez, and Pfizer Consumer Health.
Challenging research lies ahead
The researchers have provided an important and interesting challenge to evaluate the possible association of the use of PPIs and the risk of dementia.

|
Dr. Lewis H. Kuller |
Further determinants of whether PPIs are causal for dementia requires validation in large cohorts and probably in well-designed case-control studies with good measures of long-term PPI use, covariates, and especially methods to measure incidence of dementia.
Dr. Lewis H. Kuller is affiliated with the department of epidemiology at the University of Pittsburgh. He made his remarks in an accompanying editorial and had no financial conflicts to disclose.
PPIs and dementia: More of much ado about nothing?
This study has attracted considerable media attention. Unfortunately, this was somewhat unbalanced. One TV news program stated that there was a “44% increased risk of dementia.” Many of our patients would not be able to interpret that appropriately – let alone weigh the potential risks and benefits of PPI treatment.
The 44% increase is derived from the hazard ratio of 1.44 that the investigators reported. However, to quote Dr. David A. Grimes and Dr. Kenneth F. Schulz, “Any claim coming from an observational study is most likely to be wrong. Of the reported associations that are correct, most are exaggerated” (Obstet Gynecol. 2012;120:920-7).
In the German study, the patients who had been taking PPIs were more likely to have prior diagnoses of depression, stroke, and ischemic heart disease than those not on PPIs. They were also much more likely to be on multiple other medicines. These patients may have been more likely to be given a PPI because of their comorbidity. There may, therefore, be an element of channeling bias or confounding by indication to explain the findings.
However, let us assume that there had been a stronger suggestion of a causal association between PPI use and the risk of developing dementia. It would be important to consider what its underlying biological rationale might be. The investigators state that PPI use “has been shown to be potentially involved in cognitive decline.” The evidence offered in support of this claim comes from a case-control study that did not evaluate cognitive function but reported an increased incidence of vitamin B12 deficiency among adults taking PPIs for 2 or more years [very small odds ratio of 1.65 (JAMA 2013;310:2435-42)]. Low B12 levels were linked to “cognitive deficit” in a population-based study from Norway (Psychosom Med. 2013;75:20-9). So, the proposed biological rationale for any association between PPI use and dementia is tenuous at best.
For PPIs, long-term or indefinite use is appropriate for indications such as erosive esophagitis, esophageal stricture, or the prevention of upper GI tract ulcers and ulcer bleeding in patients taking aspirin or NSAIDs. Patients with a valid indication for PPI treatment should continue to receive it for as long as clinically indicated – and at the lowest effective dose. It would be unfortunate if patients with indications for PPI treatment discontinued it on the basis of this study.
Dr. Colin W. Howden, AGAF, is Hyman Professor of Medicine, chief of the division of gastroenterology, University of Tennessee Health Science Center, Memphis. He is a consultant for Takeda, Otsuka, Ironwood, Allergan, Aralez, and Pfizer Consumer Health.
Challenging research lies ahead
The researchers have provided an important and interesting challenge to evaluate the possible association of the use of PPIs and the risk of dementia.

|
Dr. Lewis H. Kuller |
Further determinants of whether PPIs are causal for dementia requires validation in large cohorts and probably in well-designed case-control studies with good measures of long-term PPI use, covariates, and especially methods to measure incidence of dementia.
Dr. Lewis H. Kuller is affiliated with the department of epidemiology at the University of Pittsburgh. He made his remarks in an accompanying editorial and had no financial conflicts to disclose.
PPIs and dementia: More of much ado about nothing?
This study has attracted considerable media attention. Unfortunately, this was somewhat unbalanced. One TV news program stated that there was a “44% increased risk of dementia.” Many of our patients would not be able to interpret that appropriately – let alone weigh the potential risks and benefits of PPI treatment.
The 44% increase is derived from the hazard ratio of 1.44 that the investigators reported. However, to quote Dr. David A. Grimes and Dr. Kenneth F. Schulz, “Any claim coming from an observational study is most likely to be wrong. Of the reported associations that are correct, most are exaggerated” (Obstet Gynecol. 2012;120:920-7).
In the German study, the patients who had been taking PPIs were more likely to have prior diagnoses of depression, stroke, and ischemic heart disease than those not on PPIs. They were also much more likely to be on multiple other medicines. These patients may have been more likely to be given a PPI because of their comorbidity. There may, therefore, be an element of channeling bias or confounding by indication to explain the findings.
However, let us assume that there had been a stronger suggestion of a causal association between PPI use and the risk of developing dementia. It would be important to consider what its underlying biological rationale might be. The investigators state that PPI use “has been shown to be potentially involved in cognitive decline.” The evidence offered in support of this claim comes from a case-control study that did not evaluate cognitive function but reported an increased incidence of vitamin B12 deficiency among adults taking PPIs for 2 or more years [very small odds ratio of 1.65 (JAMA 2013;310:2435-42)]. Low B12 levels were linked to “cognitive deficit” in a population-based study from Norway (Psychosom Med. 2013;75:20-9). So, the proposed biological rationale for any association between PPI use and dementia is tenuous at best.
For PPIs, long-term or indefinite use is appropriate for indications such as erosive esophagitis, esophageal stricture, or the prevention of upper GI tract ulcers and ulcer bleeding in patients taking aspirin or NSAIDs. Patients with a valid indication for PPI treatment should continue to receive it for as long as clinically indicated – and at the lowest effective dose. It would be unfortunate if patients with indications for PPI treatment discontinued it on the basis of this study.
Dr. Colin W. Howden, AGAF, is Hyman Professor of Medicine, chief of the division of gastroenterology, University of Tennessee Health Science Center, Memphis. He is a consultant for Takeda, Otsuka, Ironwood, Allergan, Aralez, and Pfizer Consumer Health.
Long-term use of proton pump inhibitors was significantly associated with later diagnoses of dementia in adults aged 75 years and older in a prospective cohort study of more than 73,000 individuals. The findings were published online Feb. 15 in JAMA Neurology.
Overall, the risk of incident dementia was 44% higher among the 2,950 patients who received regular proton pump inhibitors, compared with 70,729 who didn’t receive PPIs (hazard ratio of 1.44), according to Willy Gomm, Ph.D., of the German Center for Neurodegenerative Diseases in Bonn, and his colleagues.
To assess the potential link between PPIs and dementia, the researchers reviewed data from a German insurance database during 2004-2011. The study population included 73,679 community-dwelling adults aged 75 years and older who were free of dementia at the start of the study (JAMA Neurol. 2016 Feb 15. doi: 10.1001/jamaneurol.2015.4791). The patients taking PPIs were slightly but significantly older than those not taking PPIs and had a higher proportion of women (P less than .001 for both). PPI users were also significantly more likely than nonusers to have a history of depression, stroke, coronary disease, and use of polypharmacy (P less than .001 for each).
The risk of incident dementia decreased with age, from 69% for patients aged 75-79 years to 49% among those 80-84-years and 32% among those aged 85 years and older.
In addition, the risk of dementia was not significantly different based on specific drug in a subgroup analysis of the three most often prescribed PPIs, omeprazole, pantoprazole, and esomeprazole, for which the hazard ratios were 1.51, 1.58, and 2.12, respectively.
“If PPIs have adverse effects, it is important to be aware of them,” Dr. Daniel E. Freedberg of Columbia University, New York, said in an interview. “When PPIs are indicated, the preponderance of data indicate that their benefits outweigh their potential risks,” he added. “Clinicians should reassure patients that this was a single study and that previous studies have reached different conclusions. Clinicians should focus on whether or not PPIs are indicated rather than on PPI side effects.”
Dr. Freedberg also noted several key limitations of the study.
“First, the authors were unable to adjust for crucial variables that might explain a noncausal link between PPIs and dementia. For example, lower socioeconomic status is an established predictor of dementia and may also be associated with PPI use. However, the authors could not capture socioeconomic status.
“Second, patients who use PPIs have more frequent and more intensive health care interactions than patients who do not use PPIs. These patients are thus also more likely to be diagnosed with dementia. This is another source for bias that the authors were not able to capture. Third, clinicians should be aware that this study was designed to compare extremes of PPI use,” Dr. Freedberg emphasized.
In addition, “In the primary analysis, patients were classified as exposed to PPIs only if they received at least one PPI prescription every 3 months for an 18-month period. Patients who used occasional PPIs were excluded from the study,” said Dr. Freedberg.
“The present study can only provide a statistical association between PPI use and risk of dementia,” the researchers noted. “The possible underlying causal biological mechanism has to be explored in future studies,” they wrote.
The researchers had no financial conflicts to disclose.
Long-term use of proton pump inhibitors was significantly associated with later diagnoses of dementia in adults aged 75 years and older in a prospective cohort study of more than 73,000 individuals. The findings were published online Feb. 15 in JAMA Neurology.
Overall, the risk of incident dementia was 44% higher among the 2,950 patients who received regular proton pump inhibitors, compared with 70,729 who didn’t receive PPIs (hazard ratio of 1.44), according to Willy Gomm, Ph.D., of the German Center for Neurodegenerative Diseases in Bonn, and his colleagues.
To assess the potential link between PPIs and dementia, the researchers reviewed data from a German insurance database during 2004-2011. The study population included 73,679 community-dwelling adults aged 75 years and older who were free of dementia at the start of the study (JAMA Neurol. 2016 Feb 15. doi: 10.1001/jamaneurol.2015.4791). The patients taking PPIs were slightly but significantly older than those not taking PPIs and had a higher proportion of women (P less than .001 for both). PPI users were also significantly more likely than nonusers to have a history of depression, stroke, coronary disease, and use of polypharmacy (P less than .001 for each).
The risk of incident dementia decreased with age, from 69% for patients aged 75-79 years to 49% among those 80-84-years and 32% among those aged 85 years and older.
In addition, the risk of dementia was not significantly different based on specific drug in a subgroup analysis of the three most often prescribed PPIs, omeprazole, pantoprazole, and esomeprazole, for which the hazard ratios were 1.51, 1.58, and 2.12, respectively.
“If PPIs have adverse effects, it is important to be aware of them,” Dr. Daniel E. Freedberg of Columbia University, New York, said in an interview. “When PPIs are indicated, the preponderance of data indicate that their benefits outweigh their potential risks,” he added. “Clinicians should reassure patients that this was a single study and that previous studies have reached different conclusions. Clinicians should focus on whether or not PPIs are indicated rather than on PPI side effects.”
Dr. Freedberg also noted several key limitations of the study.
“First, the authors were unable to adjust for crucial variables that might explain a noncausal link between PPIs and dementia. For example, lower socioeconomic status is an established predictor of dementia and may also be associated with PPI use. However, the authors could not capture socioeconomic status.
“Second, patients who use PPIs have more frequent and more intensive health care interactions than patients who do not use PPIs. These patients are thus also more likely to be diagnosed with dementia. This is another source for bias that the authors were not able to capture. Third, clinicians should be aware that this study was designed to compare extremes of PPI use,” Dr. Freedberg emphasized.
In addition, “In the primary analysis, patients were classified as exposed to PPIs only if they received at least one PPI prescription every 3 months for an 18-month period. Patients who used occasional PPIs were excluded from the study,” said Dr. Freedberg.
“The present study can only provide a statistical association between PPI use and risk of dementia,” the researchers noted. “The possible underlying causal biological mechanism has to be explored in future studies,” they wrote.
The researchers had no financial conflicts to disclose.
FROM JAMA NEUROLOGY
Key clinical point: Proton pump inhibitors may add to the risk of dementia in older adults.
Major finding: The risk of incident dementia was 44% higher in adults who used PPIs long term, compared with those who did not.
Data source: The prospective cohort study included 73,679 adults aged 75 years and older.
Disclosures: The researchers had no financial conflicts to disclose.
Rheumatic problems plague chikungunya patients
Approximately one-third of chikungunya patients who acquired the disease during Caribbean travel reported postchikungunya muscle pain, joint pain, and joint swelling, according to data for 28 patients seen at a single center in 2014. The findings were published in Travel Medicine and Infectious Disease (2016. doi: 10.1016/j.tmaid.2016.01.009).
The researchers contacted 19 of the patients approximately 13 months after their original diagnoses. Of these, 37% described ongoing rheumatic problems; 32% reported joint pain, 32% reported joint swelling, and 26% reported muscle pain.
Dr. Cosmina Zeana of Bronx-Lebanon Hospital Center, New York, and colleagues initially identified 28 adult patients with a median age of 52 years. Most were Hispanic (96%) and half were women (54%). The average length of stay in the Caribbean was 30 days, and 82% had visited the Dominican Republic. The follow-up data were collected via a telephone questionnaire.
Chikungunya has become endemic in Latin America, the researchers noted. “Of increasing concern is the occurrence of persistent rheumatic and general disabling symptoms that can last for several years following acute infection,” they wrote. Transmission of chikungunya has been documented throughout the Caribbean, but this study is the first known assessment of postchikungunya rheumatologic disorders among individuals diagnosed with acute chikungunya after traveling to the Caribbean in particular, they added.
At follow-up, three patients without preexisting rheumatic disease met criteria for diffuse postchikungunya (pCHIK) musculoskeletal disorders. In addition, four patients with preexisting rheumatic disease reported an increase in symptom severity including worsening knee osteoarthritis in both knees (one patient) and increased joint involvement (three patients).
Significantly more patients with preexisting disease reported using pain medication, compared with those without preexisting disease. However, no significant differences appeared in the percentage of patients in each group reporting other symptoms including joint pain, muscle pain, and joint swelling.
Nearly all the patients presented for acute care with fever (99%), joint pain (89%), myalgia (70%), and joint swelling (68%). The median pain level was 8 on a scale of 1-10.
Other symptoms reported at the time of acute diagnosis included gastrointestinal problems (59%), headache (48%), and rash (48%). Almost half the patients (46%) required inpatient care, with complications including hypotensive episodes, syncope, electrolyte imbalance, and thrombocytopenia.
“Patients seeking pretravel health care in preparation for a trip to the Caribbean – as to any other CHIK-endemic 185 region – need to be comprehensively counseled about the health risks related to the acute stage of the infection as well as related to the risk for developing a potentially long-lasting rheumatic disorder,” the researchers said.
“An integrated care plan for patients with acute CHIK consisting of follow-up appointments with the primary care provider and a rheumatologist with the aim of reducing the time to identify patients with pCHIK rheumatic disorders and initiation of optimal disease management may be useful and need further study,” they added.
The findings were limited by several factors including small sample size, use of self-reports, and narrow geographic range. The researchers had no financial conflicts to disclose.
Approximately one-third of chikungunya patients who acquired the disease during Caribbean travel reported postchikungunya muscle pain, joint pain, and joint swelling, according to data for 28 patients seen at a single center in 2014. The findings were published in Travel Medicine and Infectious Disease (2016. doi: 10.1016/j.tmaid.2016.01.009).
The researchers contacted 19 of the patients approximately 13 months after their original diagnoses. Of these, 37% described ongoing rheumatic problems; 32% reported joint pain, 32% reported joint swelling, and 26% reported muscle pain.
Dr. Cosmina Zeana of Bronx-Lebanon Hospital Center, New York, and colleagues initially identified 28 adult patients with a median age of 52 years. Most were Hispanic (96%) and half were women (54%). The average length of stay in the Caribbean was 30 days, and 82% had visited the Dominican Republic. The follow-up data were collected via a telephone questionnaire.
Chikungunya has become endemic in Latin America, the researchers noted. “Of increasing concern is the occurrence of persistent rheumatic and general disabling symptoms that can last for several years following acute infection,” they wrote. Transmission of chikungunya has been documented throughout the Caribbean, but this study is the first known assessment of postchikungunya rheumatologic disorders among individuals diagnosed with acute chikungunya after traveling to the Caribbean in particular, they added.
At follow-up, three patients without preexisting rheumatic disease met criteria for diffuse postchikungunya (pCHIK) musculoskeletal disorders. In addition, four patients with preexisting rheumatic disease reported an increase in symptom severity including worsening knee osteoarthritis in both knees (one patient) and increased joint involvement (three patients).
Significantly more patients with preexisting disease reported using pain medication, compared with those without preexisting disease. However, no significant differences appeared in the percentage of patients in each group reporting other symptoms including joint pain, muscle pain, and joint swelling.
Nearly all the patients presented for acute care with fever (99%), joint pain (89%), myalgia (70%), and joint swelling (68%). The median pain level was 8 on a scale of 1-10.
Other symptoms reported at the time of acute diagnosis included gastrointestinal problems (59%), headache (48%), and rash (48%). Almost half the patients (46%) required inpatient care, with complications including hypotensive episodes, syncope, electrolyte imbalance, and thrombocytopenia.
“Patients seeking pretravel health care in preparation for a trip to the Caribbean – as to any other CHIK-endemic 185 region – need to be comprehensively counseled about the health risks related to the acute stage of the infection as well as related to the risk for developing a potentially long-lasting rheumatic disorder,” the researchers said.
“An integrated care plan for patients with acute CHIK consisting of follow-up appointments with the primary care provider and a rheumatologist with the aim of reducing the time to identify patients with pCHIK rheumatic disorders and initiation of optimal disease management may be useful and need further study,” they added.
The findings were limited by several factors including small sample size, use of self-reports, and narrow geographic range. The researchers had no financial conflicts to disclose.
Approximately one-third of chikungunya patients who acquired the disease during Caribbean travel reported postchikungunya muscle pain, joint pain, and joint swelling, according to data for 28 patients seen at a single center in 2014. The findings were published in Travel Medicine and Infectious Disease (2016. doi: 10.1016/j.tmaid.2016.01.009).
The researchers contacted 19 of the patients approximately 13 months after their original diagnoses. Of these, 37% described ongoing rheumatic problems; 32% reported joint pain, 32% reported joint swelling, and 26% reported muscle pain.
Dr. Cosmina Zeana of Bronx-Lebanon Hospital Center, New York, and colleagues initially identified 28 adult patients with a median age of 52 years. Most were Hispanic (96%) and half were women (54%). The average length of stay in the Caribbean was 30 days, and 82% had visited the Dominican Republic. The follow-up data were collected via a telephone questionnaire.
Chikungunya has become endemic in Latin America, the researchers noted. “Of increasing concern is the occurrence of persistent rheumatic and general disabling symptoms that can last for several years following acute infection,” they wrote. Transmission of chikungunya has been documented throughout the Caribbean, but this study is the first known assessment of postchikungunya rheumatologic disorders among individuals diagnosed with acute chikungunya after traveling to the Caribbean in particular, they added.
At follow-up, three patients without preexisting rheumatic disease met criteria for diffuse postchikungunya (pCHIK) musculoskeletal disorders. In addition, four patients with preexisting rheumatic disease reported an increase in symptom severity including worsening knee osteoarthritis in both knees (one patient) and increased joint involvement (three patients).
Significantly more patients with preexisting disease reported using pain medication, compared with those without preexisting disease. However, no significant differences appeared in the percentage of patients in each group reporting other symptoms including joint pain, muscle pain, and joint swelling.
Nearly all the patients presented for acute care with fever (99%), joint pain (89%), myalgia (70%), and joint swelling (68%). The median pain level was 8 on a scale of 1-10.
Other symptoms reported at the time of acute diagnosis included gastrointestinal problems (59%), headache (48%), and rash (48%). Almost half the patients (46%) required inpatient care, with complications including hypotensive episodes, syncope, electrolyte imbalance, and thrombocytopenia.
“Patients seeking pretravel health care in preparation for a trip to the Caribbean – as to any other CHIK-endemic 185 region – need to be comprehensively counseled about the health risks related to the acute stage of the infection as well as related to the risk for developing a potentially long-lasting rheumatic disorder,” the researchers said.
“An integrated care plan for patients with acute CHIK consisting of follow-up appointments with the primary care provider and a rheumatologist with the aim of reducing the time to identify patients with pCHIK rheumatic disorders and initiation of optimal disease management may be useful and need further study,” they added.
The findings were limited by several factors including small sample size, use of self-reports, and narrow geographic range. The researchers had no financial conflicts to disclose.
FROM TRAVEL MEDICINE AND INFECTIOUS DISEASE
Key clinical point: Individuals traveling to the Caribbean should be counseled about the possible acute and long-term health risks associated with chikungunya infections.
Major finding: Approximately 37% of Caribbean travelers who developed chikungunya infections reported ongoing rheumatic problems an average of 13 months later.
Data source: Data from 28 adults treated for acute chikungunya infection at a single center.
Disclosures: The researchers had no financial conflicts to disclose.
Poverty promotes flu hospitalizations
Influenza-related hospitalizations were approximately twice as high among residents of areas where at least 20% of the population lived below the federal poverty level, compared with areas of less poverty, based on data from more than 27 million individuals in the United States.
Census and hospitalization data included 14 states and spanned two flu seasons (2010-2011 and 2011-2012). Overall, the incidence of flu-related hospitalizations was approximately 21 per 100,000 person-years in high-poverty areas, compared with approximately 11 per 100,000 person-years in census areas where less than 5% of the population lived below the poverty level. The data were consistent across all age groups and ethnicities.
Flu vaccination rates were inversely associated with poverty level, ranging from a high of 48% in high-income areas to a low of 35% in areas with the most poverty. This finding, however, was probably caused by lower vaccination rates among adults aged 65 years and older in higher-poverty areas, compared with high-income areas (80% vs. 94%) noted Dr. James L. Hadler of the Yale School of Public Health in New Haven, Conn., and colleagues.
“Enhanced influenza outreach to improve influenza vaccination coverage for persons living in poorer neighborhoods and efforts to increase use of antivirals by clinicians serving these neighborhoods could reduce poverty-related disparities in severe influenza outcomes,” the researchers noted.
The findings were published in the Morbidity and Mortality Weekly Report (MMWR 2016;65[5]:101-5). Read the full article here.
Influenza-related hospitalizations were approximately twice as high among residents of areas where at least 20% of the population lived below the federal poverty level, compared with areas of less poverty, based on data from more than 27 million individuals in the United States.
Census and hospitalization data included 14 states and spanned two flu seasons (2010-2011 and 2011-2012). Overall, the incidence of flu-related hospitalizations was approximately 21 per 100,000 person-years in high-poverty areas, compared with approximately 11 per 100,000 person-years in census areas where less than 5% of the population lived below the poverty level. The data were consistent across all age groups and ethnicities.
Flu vaccination rates were inversely associated with poverty level, ranging from a high of 48% in high-income areas to a low of 35% in areas with the most poverty. This finding, however, was probably caused by lower vaccination rates among adults aged 65 years and older in higher-poverty areas, compared with high-income areas (80% vs. 94%) noted Dr. James L. Hadler of the Yale School of Public Health in New Haven, Conn., and colleagues.
“Enhanced influenza outreach to improve influenza vaccination coverage for persons living in poorer neighborhoods and efforts to increase use of antivirals by clinicians serving these neighborhoods could reduce poverty-related disparities in severe influenza outcomes,” the researchers noted.
The findings were published in the Morbidity and Mortality Weekly Report (MMWR 2016;65[5]:101-5). Read the full article here.
Influenza-related hospitalizations were approximately twice as high among residents of areas where at least 20% of the population lived below the federal poverty level, compared with areas of less poverty, based on data from more than 27 million individuals in the United States.
Census and hospitalization data included 14 states and spanned two flu seasons (2010-2011 and 2011-2012). Overall, the incidence of flu-related hospitalizations was approximately 21 per 100,000 person-years in high-poverty areas, compared with approximately 11 per 100,000 person-years in census areas where less than 5% of the population lived below the poverty level. The data were consistent across all age groups and ethnicities.
Flu vaccination rates were inversely associated with poverty level, ranging from a high of 48% in high-income areas to a low of 35% in areas with the most poverty. This finding, however, was probably caused by lower vaccination rates among adults aged 65 years and older in higher-poverty areas, compared with high-income areas (80% vs. 94%) noted Dr. James L. Hadler of the Yale School of Public Health in New Haven, Conn., and colleagues.
“Enhanced influenza outreach to improve influenza vaccination coverage for persons living in poorer neighborhoods and efforts to increase use of antivirals by clinicians serving these neighborhoods could reduce poverty-related disparities in severe influenza outcomes,” the researchers noted.
The findings were published in the Morbidity and Mortality Weekly Report (MMWR 2016;65[5]:101-5). Read the full article here.
FROM MMWR
Picosecond pulses take on tattoos
Unwanted tattoos, beware: Picosecond pulse duration lasers shatter tattoo particles with lower fluence and fewer treatments than nanosecond pulses, according to Dr. Emil A. Tanghetti.
“Picosecond pulse duration lasers open a new mechanism for breaking up tattoo particles that is not currently accessible using nanosecond laser pulses,” he said at the meeting held by Global Academy for Medical Education.
The targets in tattoo removal treatment are the individual tattoo particles, which generally range from 40 to 100 nm and are loosely packed, said Dr. Tanghetti of the Center for Dermatology and Laser Surgery in Sacramento, Calif.
When using nanosecond pulses, “Graphite particles common in tattoo removal have a larger absorption at 755 nm vs. 1064 nm,” he noted. Although the fluence is greater for the 1064 nm, the energy absorbed in the target particles is greater (16%-40% higher) for 755 nm, combined with epidermal and dermal screening.
By contrast, the picosecond pulse provides a sufficiently powerful impact to shatter small tattoo particles, and the picosecond pulse duration is 7-10 times shorter than a Q-switched Nd:YAG and 70-100 times shorter than a Q-switched Alexandrite laser, Dr. Tanghetti explained. The greater photomechanical impact means that less fluence is required.
The picosecond laser allows for fewer treatments with “significantly better clearance,” including stubborn green and blue tattoos (with only the 755-nm devices) and previously treated but hard-to-clear tattoos, he said. Clinical data show effective treatment of tattoos with one-half to one-third of the fluence and one-half the number of treatments needed to achieve the same result with a nanosecond laser, he added.
“These devices work in different ways and have different powers,” he said in an interview. “The one strong point about Alexandrite technology is that it works much better for green and blue.”
Dr. Tanghetti noted that the picosecond Alexandrite nonablative laser with the fractional optic focus lens array can be useful because of the minimal downtime with no need for anesthesia, and the focus lens allows for targeting of pigment as well as acne scars. “This type of device can be an important asset in a practice with active working clients, as well as patients with darker skin, and those with acne scars and dyspigmentation where downtime and postinflammatory hyperpigmentation is a concern,” he said.
The picosecond devices, “add a new dimension to what we can do,” he remarked.
Dr. Tanghetti disclosed serving as an advisor for Cynosure and receiving discounts on equipment from the company.
Global Academy and this news organization are owned by the same company.
Unwanted tattoos, beware: Picosecond pulse duration lasers shatter tattoo particles with lower fluence and fewer treatments than nanosecond pulses, according to Dr. Emil A. Tanghetti.
“Picosecond pulse duration lasers open a new mechanism for breaking up tattoo particles that is not currently accessible using nanosecond laser pulses,” he said at the meeting held by Global Academy for Medical Education.
The targets in tattoo removal treatment are the individual tattoo particles, which generally range from 40 to 100 nm and are loosely packed, said Dr. Tanghetti of the Center for Dermatology and Laser Surgery in Sacramento, Calif.
When using nanosecond pulses, “Graphite particles common in tattoo removal have a larger absorption at 755 nm vs. 1064 nm,” he noted. Although the fluence is greater for the 1064 nm, the energy absorbed in the target particles is greater (16%-40% higher) for 755 nm, combined with epidermal and dermal screening.
By contrast, the picosecond pulse provides a sufficiently powerful impact to shatter small tattoo particles, and the picosecond pulse duration is 7-10 times shorter than a Q-switched Nd:YAG and 70-100 times shorter than a Q-switched Alexandrite laser, Dr. Tanghetti explained. The greater photomechanical impact means that less fluence is required.
The picosecond laser allows for fewer treatments with “significantly better clearance,” including stubborn green and blue tattoos (with only the 755-nm devices) and previously treated but hard-to-clear tattoos, he said. Clinical data show effective treatment of tattoos with one-half to one-third of the fluence and one-half the number of treatments needed to achieve the same result with a nanosecond laser, he added.
“These devices work in different ways and have different powers,” he said in an interview. “The one strong point about Alexandrite technology is that it works much better for green and blue.”
Dr. Tanghetti noted that the picosecond Alexandrite nonablative laser with the fractional optic focus lens array can be useful because of the minimal downtime with no need for anesthesia, and the focus lens allows for targeting of pigment as well as acne scars. “This type of device can be an important asset in a practice with active working clients, as well as patients with darker skin, and those with acne scars and dyspigmentation where downtime and postinflammatory hyperpigmentation is a concern,” he said.
The picosecond devices, “add a new dimension to what we can do,” he remarked.
Dr. Tanghetti disclosed serving as an advisor for Cynosure and receiving discounts on equipment from the company.
Global Academy and this news organization are owned by the same company.
Unwanted tattoos, beware: Picosecond pulse duration lasers shatter tattoo particles with lower fluence and fewer treatments than nanosecond pulses, according to Dr. Emil A. Tanghetti.
“Picosecond pulse duration lasers open a new mechanism for breaking up tattoo particles that is not currently accessible using nanosecond laser pulses,” he said at the meeting held by Global Academy for Medical Education.
The targets in tattoo removal treatment are the individual tattoo particles, which generally range from 40 to 100 nm and are loosely packed, said Dr. Tanghetti of the Center for Dermatology and Laser Surgery in Sacramento, Calif.
When using nanosecond pulses, “Graphite particles common in tattoo removal have a larger absorption at 755 nm vs. 1064 nm,” he noted. Although the fluence is greater for the 1064 nm, the energy absorbed in the target particles is greater (16%-40% higher) for 755 nm, combined with epidermal and dermal screening.
By contrast, the picosecond pulse provides a sufficiently powerful impact to shatter small tattoo particles, and the picosecond pulse duration is 7-10 times shorter than a Q-switched Nd:YAG and 70-100 times shorter than a Q-switched Alexandrite laser, Dr. Tanghetti explained. The greater photomechanical impact means that less fluence is required.
The picosecond laser allows for fewer treatments with “significantly better clearance,” including stubborn green and blue tattoos (with only the 755-nm devices) and previously treated but hard-to-clear tattoos, he said. Clinical data show effective treatment of tattoos with one-half to one-third of the fluence and one-half the number of treatments needed to achieve the same result with a nanosecond laser, he added.
“These devices work in different ways and have different powers,” he said in an interview. “The one strong point about Alexandrite technology is that it works much better for green and blue.”
Dr. Tanghetti noted that the picosecond Alexandrite nonablative laser with the fractional optic focus lens array can be useful because of the minimal downtime with no need for anesthesia, and the focus lens allows for targeting of pigment as well as acne scars. “This type of device can be an important asset in a practice with active working clients, as well as patients with darker skin, and those with acne scars and dyspigmentation where downtime and postinflammatory hyperpigmentation is a concern,” he said.
The picosecond devices, “add a new dimension to what we can do,” he remarked.
Dr. Tanghetti disclosed serving as an advisor for Cynosure and receiving discounts on equipment from the company.
Global Academy and this news organization are owned by the same company.
EXPERT ANALYSIS FROM THE SUMMIT IN AESTHETIC MEDICINE
Consider combining therapies for atopic dermatitis
Cyclosporine and oral antihistamine therapy showed inconsistent effects on clinical and laboratory markers of atopic dermatitis in older children and adults, based on data from a study of 48 patients.
A total of 25 patients aged 16-42 years received oral cyclosporine and 23 patients aged 15-32 years received oral antihistamine therapy. The patients’ laboratory findings were reviewed, including high-sensitivity C-reactive protein (CRP) and thymus and activation-regulated chemokine (TARC).
Overall, TARC levels were significantly lower after oral cyclosporine therapy, compared with before therapy. Basophil counts in peripheral blood, however, were significantly higher after the therapy than before. After antihistamine therapy, serum high-sensitivity CRP levels and basophil counts in peripheral blood were significantly decreased, compared with before therapy.
“A combination of these two therapies may be more effective for the treatment of AD in adults,” noted study author Dr. Tsutomu Ohtsuka of International University of Health and Welfare Hospital in Nasushiobara, Japan.
The study was published in the June issue of the International Journal of Dermatology (Int. J. Dermatol. 2015;54:648-55 [doi:10.1111/ijd.12374]).
Find the full article online here.
Cyclosporine and oral antihistamine therapy showed inconsistent effects on clinical and laboratory markers of atopic dermatitis in older children and adults, based on data from a study of 48 patients.
A total of 25 patients aged 16-42 years received oral cyclosporine and 23 patients aged 15-32 years received oral antihistamine therapy. The patients’ laboratory findings were reviewed, including high-sensitivity C-reactive protein (CRP) and thymus and activation-regulated chemokine (TARC).
Overall, TARC levels were significantly lower after oral cyclosporine therapy, compared with before therapy. Basophil counts in peripheral blood, however, were significantly higher after the therapy than before. After antihistamine therapy, serum high-sensitivity CRP levels and basophil counts in peripheral blood were significantly decreased, compared with before therapy.
“A combination of these two therapies may be more effective for the treatment of AD in adults,” noted study author Dr. Tsutomu Ohtsuka of International University of Health and Welfare Hospital in Nasushiobara, Japan.
The study was published in the June issue of the International Journal of Dermatology (Int. J. Dermatol. 2015;54:648-55 [doi:10.1111/ijd.12374]).
Find the full article online here.
Cyclosporine and oral antihistamine therapy showed inconsistent effects on clinical and laboratory markers of atopic dermatitis in older children and adults, based on data from a study of 48 patients.
A total of 25 patients aged 16-42 years received oral cyclosporine and 23 patients aged 15-32 years received oral antihistamine therapy. The patients’ laboratory findings were reviewed, including high-sensitivity C-reactive protein (CRP) and thymus and activation-regulated chemokine (TARC).
Overall, TARC levels were significantly lower after oral cyclosporine therapy, compared with before therapy. Basophil counts in peripheral blood, however, were significantly higher after the therapy than before. After antihistamine therapy, serum high-sensitivity CRP levels and basophil counts in peripheral blood were significantly decreased, compared with before therapy.
“A combination of these two therapies may be more effective for the treatment of AD in adults,” noted study author Dr. Tsutomu Ohtsuka of International University of Health and Welfare Hospital in Nasushiobara, Japan.
The study was published in the June issue of the International Journal of Dermatology (Int. J. Dermatol. 2015;54:648-55 [doi:10.1111/ijd.12374]).
Find the full article online here.
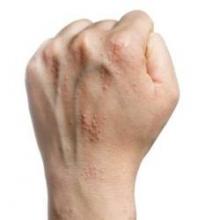
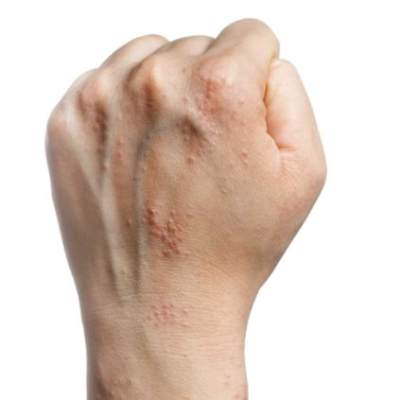
Hand eczema linked to anxiety, not depression
Adults with chronic hand eczema showed significantly higher levels of anxiety but no difference in depression, compared with healthy controls, based on data from a review of 71 patients. The patients were assessed for anxiety and depression with the Hospital Anxiety and Depression Scale (HADS), and also for compulsive behavior with the Leyton Trait Scale.
Overall quality of life was evaluated according to the Dermatology Life Quality Index (DLQI), and the average score in the patient population was 11.11.
Patients with hand dermatitis had significantly higher scores on the HADS-Anxiety subscale compared to healthy controls, but there was no significant difference in HADS-Depression subscale scores between the groups, noted lead author Dr. Anargyros Kouris of Andreas Sygros Hospital, Athens, and colleagues.
“Hand eczema treatment should address the severity of skin lesions as well as the psychological impact of hand eczema,” the researchers concluded (Contact Dermatitis 2015 June [doi: 10.1111/cod.12366]).
Find the full article online here.
Adults with chronic hand eczema showed significantly higher levels of anxiety but no difference in depression, compared with healthy controls, based on data from a review of 71 patients. The patients were assessed for anxiety and depression with the Hospital Anxiety and Depression Scale (HADS), and also for compulsive behavior with the Leyton Trait Scale.
Overall quality of life was evaluated according to the Dermatology Life Quality Index (DLQI), and the average score in the patient population was 11.11.
Patients with hand dermatitis had significantly higher scores on the HADS-Anxiety subscale compared to healthy controls, but there was no significant difference in HADS-Depression subscale scores between the groups, noted lead author Dr. Anargyros Kouris of Andreas Sygros Hospital, Athens, and colleagues.
“Hand eczema treatment should address the severity of skin lesions as well as the psychological impact of hand eczema,” the researchers concluded (Contact Dermatitis 2015 June [doi: 10.1111/cod.12366]).
Find the full article online here.
Adults with chronic hand eczema showed significantly higher levels of anxiety but no difference in depression, compared with healthy controls, based on data from a review of 71 patients. The patients were assessed for anxiety and depression with the Hospital Anxiety and Depression Scale (HADS), and also for compulsive behavior with the Leyton Trait Scale.
Overall quality of life was evaluated according to the Dermatology Life Quality Index (DLQI), and the average score in the patient population was 11.11.
Patients with hand dermatitis had significantly higher scores on the HADS-Anxiety subscale compared to healthy controls, but there was no significant difference in HADS-Depression subscale scores between the groups, noted lead author Dr. Anargyros Kouris of Andreas Sygros Hospital, Athens, and colleagues.
“Hand eczema treatment should address the severity of skin lesions as well as the psychological impact of hand eczema,” the researchers concluded (Contact Dermatitis 2015 June [doi: 10.1111/cod.12366]).
Find the full article online here.
FROM CONTACT DERMATITIS
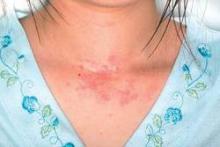
Severe Acne Erupts During Transgender Transition
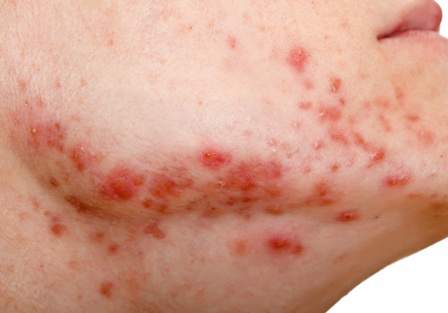
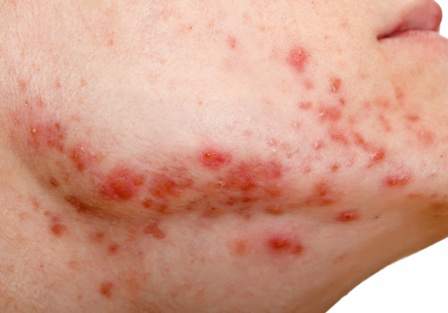
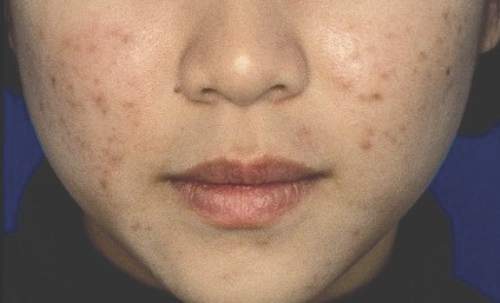
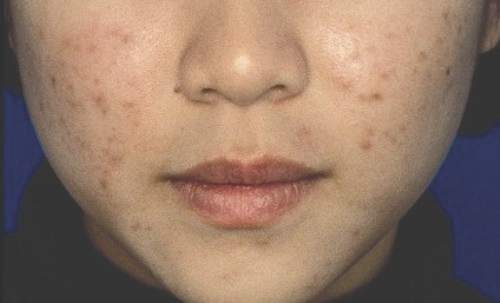
Individuals undergoing a transition from female to male (trans men) may be prone to severe acne in response to the testosterone therapy associated with that process, according to data from case reports presented in a research letter in JAMA Dermatology.
Data on the impact of testosterone therapy on the skin of trans men are limited, and previous studies suggested that the therapy did not promote acne, but Dr. Lucia Turrion-Merino of Ramón y Cajal Hospital, Madrid, and colleagues reported otherwise.
“Our 2 patients developed severe inflammatory acne with scarring, even with physiological male T [testosterone] levels,” they said.
Both patients were in their 20s, with no history of severe acne, but they presented with, in one case, inflammatory acne and scarring on the face and chest, and in the second case, seborrhea and severe acne on the face and trunk. In both cases, the acne arose within 6 months of starting testosterone therapy. Both patients improved on isotretinoin but have required ongoing treatment, as the acne returned when the isotretinoin was discontinued.
“In our opinion, it is reasonable to think that if the patient keeps receiving masculinizing doses of T, virilizing characteristics such as acne will persist,” the researchers wrote.
The findings were published online May 20 (JAMA Dermatol. 2015 [doi:10.1001/jamadermatol.2015.0761]). Find the full study here.
Individuals undergoing a transition from female to male (trans men) may be prone to severe acne in response to the testosterone therapy associated with that process, according to data from case reports presented in a research letter in JAMA Dermatology.
Data on the impact of testosterone therapy on the skin of trans men are limited, and previous studies suggested that the therapy did not promote acne, but Dr. Lucia Turrion-Merino of Ramón y Cajal Hospital, Madrid, and colleagues reported otherwise.
“Our 2 patients developed severe inflammatory acne with scarring, even with physiological male T [testosterone] levels,” they said.
Both patients were in their 20s, with no history of severe acne, but they presented with, in one case, inflammatory acne and scarring on the face and chest, and in the second case, seborrhea and severe acne on the face and trunk. In both cases, the acne arose within 6 months of starting testosterone therapy. Both patients improved on isotretinoin but have required ongoing treatment, as the acne returned when the isotretinoin was discontinued.
“In our opinion, it is reasonable to think that if the patient keeps receiving masculinizing doses of T, virilizing characteristics such as acne will persist,” the researchers wrote.
The findings were published online May 20 (JAMA Dermatol. 2015 [doi:10.1001/jamadermatol.2015.0761]). Find the full study here.
Individuals undergoing a transition from female to male (trans men) may be prone to severe acne in response to the testosterone therapy associated with that process, according to data from case reports presented in a research letter in JAMA Dermatology.
Data on the impact of testosterone therapy on the skin of trans men are limited, and previous studies suggested that the therapy did not promote acne, but Dr. Lucia Turrion-Merino of Ramón y Cajal Hospital, Madrid, and colleagues reported otherwise.
“Our 2 patients developed severe inflammatory acne with scarring, even with physiological male T [testosterone] levels,” they said.
Both patients were in their 20s, with no history of severe acne, but they presented with, in one case, inflammatory acne and scarring on the face and chest, and in the second case, seborrhea and severe acne on the face and trunk. In both cases, the acne arose within 6 months of starting testosterone therapy. Both patients improved on isotretinoin but have required ongoing treatment, as the acne returned when the isotretinoin was discontinued.
“In our opinion, it is reasonable to think that if the patient keeps receiving masculinizing doses of T, virilizing characteristics such as acne will persist,” the researchers wrote.
The findings were published online May 20 (JAMA Dermatol. 2015 [doi:10.1001/jamadermatol.2015.0761]). Find the full study here.
FROM JAMA DERMATOLOGY
Severe acne erupts during transgender transition
Individuals undergoing a transition from female to male (trans men) may be prone to severe acne in response to the testosterone therapy associated with that process, according to data from case reports presented in a research letter in JAMA Dermatology.
Data on the impact of testosterone therapy on the skin of trans men are limited, and previous studies suggested that the therapy did not promote acne, but Dr. Lucia Turrion-Merino of Ramón y Cajal Hospital, Madrid, and colleagues reported otherwise.
“Our 2 patients developed severe inflammatory acne with scarring, even with physiological male T [testosterone] levels,” they said.
Both patients were in their 20s, with no history of severe acne, but they presented with, in one case, inflammatory acne and scarring on the face and chest, and in the second case, seborrhea and severe acne on the face and trunk. In both cases, the acne arose within 6 months of starting testosterone therapy. Both patients improved on isotretinoin but have required ongoing treatment, as the acne returned when the isotretinoin was discontinued.
“In our opinion, it is reasonable to think that if the patient keeps receiving masculinizing doses of T, virilizing characteristics such as acne will persist,” the researchers wrote.
The findings were published online May 20 (JAMA Dermatol. 2015 [doi:10.1001/jamadermatol.2015.0761]). Find the full study here.
Individuals undergoing a transition from female to male (trans men) may be prone to severe acne in response to the testosterone therapy associated with that process, according to data from case reports presented in a research letter in JAMA Dermatology.
Data on the impact of testosterone therapy on the skin of trans men are limited, and previous studies suggested that the therapy did not promote acne, but Dr. Lucia Turrion-Merino of Ramón y Cajal Hospital, Madrid, and colleagues reported otherwise.
“Our 2 patients developed severe inflammatory acne with scarring, even with physiological male T [testosterone] levels,” they said.
Both patients were in their 20s, with no history of severe acne, but they presented with, in one case, inflammatory acne and scarring on the face and chest, and in the second case, seborrhea and severe acne on the face and trunk. In both cases, the acne arose within 6 months of starting testosterone therapy. Both patients improved on isotretinoin but have required ongoing treatment, as the acne returned when the isotretinoin was discontinued.
“In our opinion, it is reasonable to think that if the patient keeps receiving masculinizing doses of T, virilizing characteristics such as acne will persist,” the researchers wrote.
The findings were published online May 20 (JAMA Dermatol. 2015 [doi:10.1001/jamadermatol.2015.0761]). Find the full study here.
Individuals undergoing a transition from female to male (trans men) may be prone to severe acne in response to the testosterone therapy associated with that process, according to data from case reports presented in a research letter in JAMA Dermatology.
Data on the impact of testosterone therapy on the skin of trans men are limited, and previous studies suggested that the therapy did not promote acne, but Dr. Lucia Turrion-Merino of Ramón y Cajal Hospital, Madrid, and colleagues reported otherwise.
“Our 2 patients developed severe inflammatory acne with scarring, even with physiological male T [testosterone] levels,” they said.
Both patients were in their 20s, with no history of severe acne, but they presented with, in one case, inflammatory acne and scarring on the face and chest, and in the second case, seborrhea and severe acne on the face and trunk. In both cases, the acne arose within 6 months of starting testosterone therapy. Both patients improved on isotretinoin but have required ongoing treatment, as the acne returned when the isotretinoin was discontinued.
“In our opinion, it is reasonable to think that if the patient keeps receiving masculinizing doses of T, virilizing characteristics such as acne will persist,” the researchers wrote.
The findings were published online May 20 (JAMA Dermatol. 2015 [doi:10.1001/jamadermatol.2015.0761]). Find the full study here.
FROM JAMA DERMATOLOGY
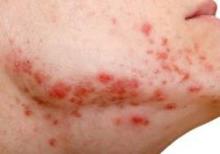
Women’s Acne Mirrors Teen Acne
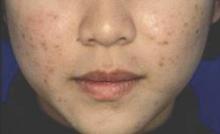
The distribution of acne lesions in adults is similar to that in adolescents, based on data from a prospective study of 374 women aged 25 years and older.
“The stereotype of adult female acne being due to hormonal disturbances presenting as inflammatory acne localized only to the mandibular area was not found in the majority of this large group,” noted Dr. Brigitte Dreno of Nantes (France) University and colleagues.
Approximately 90% of the women demonstrated facial acne severity typical to that seen in adolescents, with involvement of the cheeks, forehead, temples, and mandibular area, the researchers noted. The most common presentation was mixed facial acne, with both inflammatory and noninflammatory lesions. A total of 6% of women had inflammatory acne only, with no reported noninflammatory lesions, and 17% had comedonal acne and no reported inflammatory lesions.
“We recommend that the general treatment approach for adult acne should include agents that target each of the acne lesion subtypes,” the researchers wrote.
The findings were published in the Journal of the European Academy of Dermatology and Venereology (2015;29:1096-106 [doi:10.1111/jdv.12757]).
The distribution of acne lesions in adults is similar to that in adolescents, based on data from a prospective study of 374 women aged 25 years and older.
“The stereotype of adult female acne being due to hormonal disturbances presenting as inflammatory acne localized only to the mandibular area was not found in the majority of this large group,” noted Dr. Brigitte Dreno of Nantes (France) University and colleagues.
Approximately 90% of the women demonstrated facial acne severity typical to that seen in adolescents, with involvement of the cheeks, forehead, temples, and mandibular area, the researchers noted. The most common presentation was mixed facial acne, with both inflammatory and noninflammatory lesions. A total of 6% of women had inflammatory acne only, with no reported noninflammatory lesions, and 17% had comedonal acne and no reported inflammatory lesions.
“We recommend that the general treatment approach for adult acne should include agents that target each of the acne lesion subtypes,” the researchers wrote.
The findings were published in the Journal of the European Academy of Dermatology and Venereology (2015;29:1096-106 [doi:10.1111/jdv.12757]).
The distribution of acne lesions in adults is similar to that in adolescents, based on data from a prospective study of 374 women aged 25 years and older.
“The stereotype of adult female acne being due to hormonal disturbances presenting as inflammatory acne localized only to the mandibular area was not found in the majority of this large group,” noted Dr. Brigitte Dreno of Nantes (France) University and colleagues.
Approximately 90% of the women demonstrated facial acne severity typical to that seen in adolescents, with involvement of the cheeks, forehead, temples, and mandibular area, the researchers noted. The most common presentation was mixed facial acne, with both inflammatory and noninflammatory lesions. A total of 6% of women had inflammatory acne only, with no reported noninflammatory lesions, and 17% had comedonal acne and no reported inflammatory lesions.
“We recommend that the general treatment approach for adult acne should include agents that target each of the acne lesion subtypes,” the researchers wrote.
The findings were published in the Journal of the European Academy of Dermatology and Venereology (2015;29:1096-106 [doi:10.1111/jdv.12757]).
FROM JEADV
Women’s acne mirrors teen acne
The distribution of acne lesions in adults is similar to that in adolescents, based on data from a prospective study of 374 women aged 25 years and older.
“The stereotype of adult female acne being due to hormonal disturbances presenting as inflammatory acne localized only to the mandibular area was not found in the majority of this large group,” noted Dr. Brigitte Dreno of Nantes (France) University and colleagues.
Approximately 90% of the women demonstrated facial acne severity typical to that seen in adolescents, with involvement of the cheeks, forehead, temples, and mandibular area, the researchers noted. The most common presentation was mixed facial acne, with both inflammatory and noninflammatory lesions. A total of 6% of women had inflammatory acne only, with no reported noninflammatory lesions, and 17% had comedonal acne and no reported inflammatory lesions.
“We recommend that the general treatment approach for adult acne should include agents that target each of the acne lesion subtypes,” the researchers wrote.
The findings were published in the Journal of the European Academy of Dermatology and Venereology (2015;29:1096-106 [doi:10.1111/jdv.12757]).
The distribution of acne lesions in adults is similar to that in adolescents, based on data from a prospective study of 374 women aged 25 years and older.
“The stereotype of adult female acne being due to hormonal disturbances presenting as inflammatory acne localized only to the mandibular area was not found in the majority of this large group,” noted Dr. Brigitte Dreno of Nantes (France) University and colleagues.
Approximately 90% of the women demonstrated facial acne severity typical to that seen in adolescents, with involvement of the cheeks, forehead, temples, and mandibular area, the researchers noted. The most common presentation was mixed facial acne, with both inflammatory and noninflammatory lesions. A total of 6% of women had inflammatory acne only, with no reported noninflammatory lesions, and 17% had comedonal acne and no reported inflammatory lesions.
“We recommend that the general treatment approach for adult acne should include agents that target each of the acne lesion subtypes,” the researchers wrote.
The findings were published in the Journal of the European Academy of Dermatology and Venereology (2015;29:1096-106 [doi:10.1111/jdv.12757]).
The distribution of acne lesions in adults is similar to that in adolescents, based on data from a prospective study of 374 women aged 25 years and older.
“The stereotype of adult female acne being due to hormonal disturbances presenting as inflammatory acne localized only to the mandibular area was not found in the majority of this large group,” noted Dr. Brigitte Dreno of Nantes (France) University and colleagues.
Approximately 90% of the women demonstrated facial acne severity typical to that seen in adolescents, with involvement of the cheeks, forehead, temples, and mandibular area, the researchers noted. The most common presentation was mixed facial acne, with both inflammatory and noninflammatory lesions. A total of 6% of women had inflammatory acne only, with no reported noninflammatory lesions, and 17% had comedonal acne and no reported inflammatory lesions.
“We recommend that the general treatment approach for adult acne should include agents that target each of the acne lesion subtypes,” the researchers wrote.
The findings were published in the Journal of the European Academy of Dermatology and Venereology (2015;29:1096-106 [doi:10.1111/jdv.12757]).
FROM JEADV