User login
COVID-19 cases highlight longstanding racial disparities in health care
African Americans are overrepresented among patients who have died as a result of the COVID-19 pandemic, but the current crisis puts a spotlight on long-standing racial disparities in health care and health access in the United States, according to David R. Williams, PhD, a professor of public health at the Harvard T.H. Chan School of Public Health in Boston.
Dr. Williams, a social scientist specializing in the link between race and health, is a professor of African and African American Studies and of Sociology at Harvard. He spoke on the topic of racial disparities amid the COVID-19 pandemic in a teleconference sponsored by the Robert Wood Johnson Foundation.
“Many Americans are shocked” by the higher mortality rates among African American COVID-19 patients, said Dr. Williams. However, data from decades of research show that “black people in America live sicker and shorter lives,” he said.
Keys to the increased mortality among African Americans include an increased prevalence of risk factors, increased risk for exposure to the virus because of socioeconomic factors, and less access to health care if they do become ill, he said.
Many minority individuals work outside the home in areas deemed essential during the pandemic, such as transit, delivery, maintenance, cleaning, and in businesses such as grocery stores, although in general “race continues to matter for health at every level of income and education,” Dr. Williams said.
In addition, social distance guidelines are not realistic for many people in high-density, low-income areas, who often live in shared, multigenerational housing, he said.
Data show that individuals with chronic conditions such as diabetes and cardiovascular disease are more likely to die as a result of COVID-19, and minority populations are more likely to develop these conditions at younger ages, Dr. Williams noted. Access to health care also plays a role. Many minority individuals of lower socioeconomic status are less likely to have health insurance, or if they do, may have Medicaid, which is not consistently accepted, he said. Also, some low-income neighborhoods lack convenient access to primary care and thus to screening services, he noted.
Dr. Williams said the COVID-19 pandemic could serve as an opportunity to examine and improve health care services for underserved communities. In the short term, “we need to collect data so we can see patterns” and address pressing needs, he said, but long-term goals should “prioritize investments that would create healthy homes and communities,” he emphasized.
A recent study from the Centers for Disease Control and Prevention’s Morbidity and Mortality Weekly Report cited COVID-NET (the COVID-19 Associated Hospitalization Surveillance Network) as showing that, in their catchment population, “approximately 59% of residents are white, 18% are black, and 14% are Hispanic; however, among 580 hospitalized COVID-19 patients with race/ethnicity data, approximately 45% were white, 33% were black, and 8% were Hispanic, suggesting that black populations might be disproportionately affected by COVID-19,” the researchers said.
“These findings, including the potential impact of both sex and race on COVID-19–associated hospitalization rates, need to be confirmed with additional data,” according to the report.
Collecting racial/ethnic information is not always feasible on the front lines, and many areas still face shortages of ventilators and protective equipment, said Dr. Williams.
“I want to salute the providers on the front lines of this pandemic, many putting their own lives at risk, I want to acknowledge the good that they are doing,” Dr. Williams emphasized. He noted that all of us, himself included, may have conscious or unconscious stereotypes, but the key is to acknowledge the potential for these thoughts and feelings and continue to provide the best care.
Clyde W. Yancy, MD, of Northwestern University in Chicago, expressed similar concerns about disparity in COVID-19 cases in an editorial published on April 15 in JAMA.
“Researchers have emphasized older age, male sex, hypertension, diabetes, obesity, concomitant cardiovascular diseases (including coronary artery disease and heart failure), and myocardial injury as important risk factors associated with worse outcomes,” wrote Dr. Yancy. However, evidence also suggests that “persons who are African American or black are contracting SARS-CoV-2 at higher rates and are more likely to die,” he said.
“Why is this uniquely important to me? I am an academic cardiologist; I study health care disparities; and I am a black man,” he wrote.
“Even though these data are preliminary and further study is warranted, the pattern is irrefutable: Underrepresented minorities are developing COVID-19 infection more frequently and dying disproportionately,” said Dr. Yancy.
Dr. Williams’ and Dr. Yancy’s comments were supported by an analysis of COVID-19 patient data from several areas of the country conducted by the Washington Post. In that analysis, data showed that several counties with a majority black population showed three times the rate of COVID-19 infections and approximately six times as many deaths compared with counties with a majority of white residents.
“The U.S. has needed a trigger to fully address health care disparities; COVID-19 may be that bellwether event,” said Dr. Yancy. “Certainly, within the broad and powerful economic and legislative engines of the US, there is room to definitively address a scourge even worse than COVID-19: health care disparities. It only takes will. It is time to end the refrain,” he said.
Dr. Williams had no financial conflicts to disclose. Dr. Yancy had no financial conflicts to disclose.
SOURCES: Yancy CW. JAMA 2020 Apr 15. doi: 10.1001/jama.2020.6548Garg S et al. MMWR Morb Mortal Wkly Rep 2020 Apr 8;69:458-64.
Thebault R et al. The coronavirus is infecting and killing black Americans at an alarmingly high rate. Washington Post. 2020 Apr 7.
African Americans are overrepresented among patients who have died as a result of the COVID-19 pandemic, but the current crisis puts a spotlight on long-standing racial disparities in health care and health access in the United States, according to David R. Williams, PhD, a professor of public health at the Harvard T.H. Chan School of Public Health in Boston.
Dr. Williams, a social scientist specializing in the link between race and health, is a professor of African and African American Studies and of Sociology at Harvard. He spoke on the topic of racial disparities amid the COVID-19 pandemic in a teleconference sponsored by the Robert Wood Johnson Foundation.
“Many Americans are shocked” by the higher mortality rates among African American COVID-19 patients, said Dr. Williams. However, data from decades of research show that “black people in America live sicker and shorter lives,” he said.
Keys to the increased mortality among African Americans include an increased prevalence of risk factors, increased risk for exposure to the virus because of socioeconomic factors, and less access to health care if they do become ill, he said.
Many minority individuals work outside the home in areas deemed essential during the pandemic, such as transit, delivery, maintenance, cleaning, and in businesses such as grocery stores, although in general “race continues to matter for health at every level of income and education,” Dr. Williams said.
In addition, social distance guidelines are not realistic for many people in high-density, low-income areas, who often live in shared, multigenerational housing, he said.
Data show that individuals with chronic conditions such as diabetes and cardiovascular disease are more likely to die as a result of COVID-19, and minority populations are more likely to develop these conditions at younger ages, Dr. Williams noted. Access to health care also plays a role. Many minority individuals of lower socioeconomic status are less likely to have health insurance, or if they do, may have Medicaid, which is not consistently accepted, he said. Also, some low-income neighborhoods lack convenient access to primary care and thus to screening services, he noted.
Dr. Williams said the COVID-19 pandemic could serve as an opportunity to examine and improve health care services for underserved communities. In the short term, “we need to collect data so we can see patterns” and address pressing needs, he said, but long-term goals should “prioritize investments that would create healthy homes and communities,” he emphasized.
A recent study from the Centers for Disease Control and Prevention’s Morbidity and Mortality Weekly Report cited COVID-NET (the COVID-19 Associated Hospitalization Surveillance Network) as showing that, in their catchment population, “approximately 59% of residents are white, 18% are black, and 14% are Hispanic; however, among 580 hospitalized COVID-19 patients with race/ethnicity data, approximately 45% were white, 33% were black, and 8% were Hispanic, suggesting that black populations might be disproportionately affected by COVID-19,” the researchers said.
“These findings, including the potential impact of both sex and race on COVID-19–associated hospitalization rates, need to be confirmed with additional data,” according to the report.
Collecting racial/ethnic information is not always feasible on the front lines, and many areas still face shortages of ventilators and protective equipment, said Dr. Williams.
“I want to salute the providers on the front lines of this pandemic, many putting their own lives at risk, I want to acknowledge the good that they are doing,” Dr. Williams emphasized. He noted that all of us, himself included, may have conscious or unconscious stereotypes, but the key is to acknowledge the potential for these thoughts and feelings and continue to provide the best care.
Clyde W. Yancy, MD, of Northwestern University in Chicago, expressed similar concerns about disparity in COVID-19 cases in an editorial published on April 15 in JAMA.
“Researchers have emphasized older age, male sex, hypertension, diabetes, obesity, concomitant cardiovascular diseases (including coronary artery disease and heart failure), and myocardial injury as important risk factors associated with worse outcomes,” wrote Dr. Yancy. However, evidence also suggests that “persons who are African American or black are contracting SARS-CoV-2 at higher rates and are more likely to die,” he said.
“Why is this uniquely important to me? I am an academic cardiologist; I study health care disparities; and I am a black man,” he wrote.
“Even though these data are preliminary and further study is warranted, the pattern is irrefutable: Underrepresented minorities are developing COVID-19 infection more frequently and dying disproportionately,” said Dr. Yancy.
Dr. Williams’ and Dr. Yancy’s comments were supported by an analysis of COVID-19 patient data from several areas of the country conducted by the Washington Post. In that analysis, data showed that several counties with a majority black population showed three times the rate of COVID-19 infections and approximately six times as many deaths compared with counties with a majority of white residents.
“The U.S. has needed a trigger to fully address health care disparities; COVID-19 may be that bellwether event,” said Dr. Yancy. “Certainly, within the broad and powerful economic and legislative engines of the US, there is room to definitively address a scourge even worse than COVID-19: health care disparities. It only takes will. It is time to end the refrain,” he said.
Dr. Williams had no financial conflicts to disclose. Dr. Yancy had no financial conflicts to disclose.
SOURCES: Yancy CW. JAMA 2020 Apr 15. doi: 10.1001/jama.2020.6548Garg S et al. MMWR Morb Mortal Wkly Rep 2020 Apr 8;69:458-64.
Thebault R et al. The coronavirus is infecting and killing black Americans at an alarmingly high rate. Washington Post. 2020 Apr 7.
African Americans are overrepresented among patients who have died as a result of the COVID-19 pandemic, but the current crisis puts a spotlight on long-standing racial disparities in health care and health access in the United States, according to David R. Williams, PhD, a professor of public health at the Harvard T.H. Chan School of Public Health in Boston.
Dr. Williams, a social scientist specializing in the link between race and health, is a professor of African and African American Studies and of Sociology at Harvard. He spoke on the topic of racial disparities amid the COVID-19 pandemic in a teleconference sponsored by the Robert Wood Johnson Foundation.
“Many Americans are shocked” by the higher mortality rates among African American COVID-19 patients, said Dr. Williams. However, data from decades of research show that “black people in America live sicker and shorter lives,” he said.
Keys to the increased mortality among African Americans include an increased prevalence of risk factors, increased risk for exposure to the virus because of socioeconomic factors, and less access to health care if they do become ill, he said.
Many minority individuals work outside the home in areas deemed essential during the pandemic, such as transit, delivery, maintenance, cleaning, and in businesses such as grocery stores, although in general “race continues to matter for health at every level of income and education,” Dr. Williams said.
In addition, social distance guidelines are not realistic for many people in high-density, low-income areas, who often live in shared, multigenerational housing, he said.
Data show that individuals with chronic conditions such as diabetes and cardiovascular disease are more likely to die as a result of COVID-19, and minority populations are more likely to develop these conditions at younger ages, Dr. Williams noted. Access to health care also plays a role. Many minority individuals of lower socioeconomic status are less likely to have health insurance, or if they do, may have Medicaid, which is not consistently accepted, he said. Also, some low-income neighborhoods lack convenient access to primary care and thus to screening services, he noted.
Dr. Williams said the COVID-19 pandemic could serve as an opportunity to examine and improve health care services for underserved communities. In the short term, “we need to collect data so we can see patterns” and address pressing needs, he said, but long-term goals should “prioritize investments that would create healthy homes and communities,” he emphasized.
A recent study from the Centers for Disease Control and Prevention’s Morbidity and Mortality Weekly Report cited COVID-NET (the COVID-19 Associated Hospitalization Surveillance Network) as showing that, in their catchment population, “approximately 59% of residents are white, 18% are black, and 14% are Hispanic; however, among 580 hospitalized COVID-19 patients with race/ethnicity data, approximately 45% were white, 33% were black, and 8% were Hispanic, suggesting that black populations might be disproportionately affected by COVID-19,” the researchers said.
“These findings, including the potential impact of both sex and race on COVID-19–associated hospitalization rates, need to be confirmed with additional data,” according to the report.
Collecting racial/ethnic information is not always feasible on the front lines, and many areas still face shortages of ventilators and protective equipment, said Dr. Williams.
“I want to salute the providers on the front lines of this pandemic, many putting their own lives at risk, I want to acknowledge the good that they are doing,” Dr. Williams emphasized. He noted that all of us, himself included, may have conscious or unconscious stereotypes, but the key is to acknowledge the potential for these thoughts and feelings and continue to provide the best care.
Clyde W. Yancy, MD, of Northwestern University in Chicago, expressed similar concerns about disparity in COVID-19 cases in an editorial published on April 15 in JAMA.
“Researchers have emphasized older age, male sex, hypertension, diabetes, obesity, concomitant cardiovascular diseases (including coronary artery disease and heart failure), and myocardial injury as important risk factors associated with worse outcomes,” wrote Dr. Yancy. However, evidence also suggests that “persons who are African American or black are contracting SARS-CoV-2 at higher rates and are more likely to die,” he said.
“Why is this uniquely important to me? I am an academic cardiologist; I study health care disparities; and I am a black man,” he wrote.
“Even though these data are preliminary and further study is warranted, the pattern is irrefutable: Underrepresented minorities are developing COVID-19 infection more frequently and dying disproportionately,” said Dr. Yancy.
Dr. Williams’ and Dr. Yancy’s comments were supported by an analysis of COVID-19 patient data from several areas of the country conducted by the Washington Post. In that analysis, data showed that several counties with a majority black population showed three times the rate of COVID-19 infections and approximately six times as many deaths compared with counties with a majority of white residents.
“The U.S. has needed a trigger to fully address health care disparities; COVID-19 may be that bellwether event,” said Dr. Yancy. “Certainly, within the broad and powerful economic and legislative engines of the US, there is room to definitively address a scourge even worse than COVID-19: health care disparities. It only takes will. It is time to end the refrain,” he said.
Dr. Williams had no financial conflicts to disclose. Dr. Yancy had no financial conflicts to disclose.
SOURCES: Yancy CW. JAMA 2020 Apr 15. doi: 10.1001/jama.2020.6548Garg S et al. MMWR Morb Mortal Wkly Rep 2020 Apr 8;69:458-64.
Thebault R et al. The coronavirus is infecting and killing black Americans at an alarmingly high rate. Washington Post. 2020 Apr 7.
FROM A TELECONFERENCE SPONSORED BY THE ROBERT WOOD JOHNSON FOUNDATION
Preschoolers with higher BMI have elevated risk for fracture
Children with overweight or obese body mass index measures at preschool age were significantly more likely than were normal weight children to suffer upper- and lower-limb fractures before age 15 years, according to data from almost 470,000 children.
Previous studies of adults have shown associations between obesity and fractures, but the impact of higher BMI at preschool age on fracture incidence later in childhood has not been explored, according to Jennifer C.E. Lane, MD, of the University of Oxford (England), and colleagues. “A focused study of the association between preschool obesity and fracture risk offers the opportunity to better understand the impact of obesity in early life,” they wrote in the Journal of Bone and Mineral Research.
The researchers reviewed data from 466,997 children at 296 primary care centers using the Information System for Research in Primary Care, a Spanish national database, for the years 2003-2013. The children were assessed starting at age 4 years and followed until age 15 years or until they left the region or died, or until the study period ended, on Dec. 31, 2016. The average follow-up time was 4.9 years, and 49% of the children were girls. BMI categories were determined via the World Health Organization growth standards for calculating age- and sex-specific BMI z scores, and the categories were defined as underweight (< −2 BMI z score), normal weight (−2 to +2 BMI z score), overweight (> +2 BMI z score), and obese (> +3 BMI z score).
Overall, children with a BMI in the overweight or obese ranges at first assessment were significantly more likely than were their normal weight counterparts to suffer lower-limb fractures (adjusted hazard ratios, 1.42 and 1.74, respectively) and upper-limb fractures (aHRs, 1.10 and 1.19, respectively) during the follow-up period.
The total incidence of fractures during childhood for those in the study who were underweight, normal weight, overweight, or obese, was 9.20%, 10.06%, 11.28%, and 13.05% respectively.
In a secondary analysis, fracture risk varied by anatomic location and reflected previous findings showing an increased risk of distal limb fractures associated with high BMI, the researchers said.
The findings were limited by several factors, including the smaller-than-average proportion of children with overweight or obese BMI measures, the imprecise nature of the BMI z score as a predictor of obesity in children, and the lack of data on sports, medical issues, and general activity levels, the researchers noted.
However, the results were strengthened by the population-based sample and long-term follow-up, and the work “suggests that interventions to treat obesity in early childhood could have benefits for the primary or secondary prevention of fractures later in childhood, especially in the prevention of fractures within the forearm and hand or foot and ankle,” the authors concluded.
The study was supported in part by the NIHR Biomedical Research Centre, Oxford, and La Marató de TV3 Foundation. Dr. Lane disclosed funding from a Versus Arthritis Clinical Research Fellowship but had no financial conflicts to disclose. Some authors reported relationships with numerous pharmaceutical firms.
SOURCE: Lane JCE et al. J Bone Miner Res. 2020 Apr 7. doi: 10.1002/jbmr.3984
Children with overweight or obese body mass index measures at preschool age were significantly more likely than were normal weight children to suffer upper- and lower-limb fractures before age 15 years, according to data from almost 470,000 children.
Previous studies of adults have shown associations between obesity and fractures, but the impact of higher BMI at preschool age on fracture incidence later in childhood has not been explored, according to Jennifer C.E. Lane, MD, of the University of Oxford (England), and colleagues. “A focused study of the association between preschool obesity and fracture risk offers the opportunity to better understand the impact of obesity in early life,” they wrote in the Journal of Bone and Mineral Research.
The researchers reviewed data from 466,997 children at 296 primary care centers using the Information System for Research in Primary Care, a Spanish national database, for the years 2003-2013. The children were assessed starting at age 4 years and followed until age 15 years or until they left the region or died, or until the study period ended, on Dec. 31, 2016. The average follow-up time was 4.9 years, and 49% of the children were girls. BMI categories were determined via the World Health Organization growth standards for calculating age- and sex-specific BMI z scores, and the categories were defined as underweight (< −2 BMI z score), normal weight (−2 to +2 BMI z score), overweight (> +2 BMI z score), and obese (> +3 BMI z score).
Overall, children with a BMI in the overweight or obese ranges at first assessment were significantly more likely than were their normal weight counterparts to suffer lower-limb fractures (adjusted hazard ratios, 1.42 and 1.74, respectively) and upper-limb fractures (aHRs, 1.10 and 1.19, respectively) during the follow-up period.
The total incidence of fractures during childhood for those in the study who were underweight, normal weight, overweight, or obese, was 9.20%, 10.06%, 11.28%, and 13.05% respectively.
In a secondary analysis, fracture risk varied by anatomic location and reflected previous findings showing an increased risk of distal limb fractures associated with high BMI, the researchers said.
The findings were limited by several factors, including the smaller-than-average proportion of children with overweight or obese BMI measures, the imprecise nature of the BMI z score as a predictor of obesity in children, and the lack of data on sports, medical issues, and general activity levels, the researchers noted.
However, the results were strengthened by the population-based sample and long-term follow-up, and the work “suggests that interventions to treat obesity in early childhood could have benefits for the primary or secondary prevention of fractures later in childhood, especially in the prevention of fractures within the forearm and hand or foot and ankle,” the authors concluded.
The study was supported in part by the NIHR Biomedical Research Centre, Oxford, and La Marató de TV3 Foundation. Dr. Lane disclosed funding from a Versus Arthritis Clinical Research Fellowship but had no financial conflicts to disclose. Some authors reported relationships with numerous pharmaceutical firms.
SOURCE: Lane JCE et al. J Bone Miner Res. 2020 Apr 7. doi: 10.1002/jbmr.3984
Children with overweight or obese body mass index measures at preschool age were significantly more likely than were normal weight children to suffer upper- and lower-limb fractures before age 15 years, according to data from almost 470,000 children.
Previous studies of adults have shown associations between obesity and fractures, but the impact of higher BMI at preschool age on fracture incidence later in childhood has not been explored, according to Jennifer C.E. Lane, MD, of the University of Oxford (England), and colleagues. “A focused study of the association between preschool obesity and fracture risk offers the opportunity to better understand the impact of obesity in early life,” they wrote in the Journal of Bone and Mineral Research.
The researchers reviewed data from 466,997 children at 296 primary care centers using the Information System for Research in Primary Care, a Spanish national database, for the years 2003-2013. The children were assessed starting at age 4 years and followed until age 15 years or until they left the region or died, or until the study period ended, on Dec. 31, 2016. The average follow-up time was 4.9 years, and 49% of the children were girls. BMI categories were determined via the World Health Organization growth standards for calculating age- and sex-specific BMI z scores, and the categories were defined as underweight (< −2 BMI z score), normal weight (−2 to +2 BMI z score), overweight (> +2 BMI z score), and obese (> +3 BMI z score).
Overall, children with a BMI in the overweight or obese ranges at first assessment were significantly more likely than were their normal weight counterparts to suffer lower-limb fractures (adjusted hazard ratios, 1.42 and 1.74, respectively) and upper-limb fractures (aHRs, 1.10 and 1.19, respectively) during the follow-up period.
The total incidence of fractures during childhood for those in the study who were underweight, normal weight, overweight, or obese, was 9.20%, 10.06%, 11.28%, and 13.05% respectively.
In a secondary analysis, fracture risk varied by anatomic location and reflected previous findings showing an increased risk of distal limb fractures associated with high BMI, the researchers said.
The findings were limited by several factors, including the smaller-than-average proportion of children with overweight or obese BMI measures, the imprecise nature of the BMI z score as a predictor of obesity in children, and the lack of data on sports, medical issues, and general activity levels, the researchers noted.
However, the results were strengthened by the population-based sample and long-term follow-up, and the work “suggests that interventions to treat obesity in early childhood could have benefits for the primary or secondary prevention of fractures later in childhood, especially in the prevention of fractures within the forearm and hand or foot and ankle,” the authors concluded.
The study was supported in part by the NIHR Biomedical Research Centre, Oxford, and La Marató de TV3 Foundation. Dr. Lane disclosed funding from a Versus Arthritis Clinical Research Fellowship but had no financial conflicts to disclose. Some authors reported relationships with numerous pharmaceutical firms.
SOURCE: Lane JCE et al. J Bone Miner Res. 2020 Apr 7. doi: 10.1002/jbmr.3984
FROM THE JOURNAL OF BONE AND MINERAL RESEARCH
History of smoking gives higher risk for ANCA-associated vasculitis
according to data from a large case-control study.
Although smokers have shown an increased risk for ANCA-associated vasculitis (AAV), compared with nonsmokers, previous studies of the association between smoking and AAV risk have been small and the results have been inconsistent, Greg McDermott, MD, and colleagues at Massachusetts General Hospital, Boston, wrote in JAMA Internal Medicine.
The researchers reviewed data from 473 adults diagnosed with AAV between 2002 and 2017 and compared them with 1,419 matched controls without AAV who had completed a smoking history questionnaire.
Overall, the odds of having a diagnosis of AAV were significantly higher among former smokers or current smokers, compared with never smokers (odds ratios, 1.58 and 2.70, respectively). In addition, the researchers found a significant dose-response relationship between pack-years of exposure and risk of AAV. The average age of the cases and controls was 59 years, 59% were women, and 84% were white.
The association between AAV risk and former or current smoking was greater among the 147 former and 29 current smokers with AAV positive for myeloperoxidase (MPO) (OR, 1.73 and 3.54, respectively). “Proteinase 3-ANCA– and MPO-ANCA–positive AAV are increasingly recognized as distinct conditions characterized by differences in genetic risk, pathogenesis, disease manifestations, and response to treatment,” the researchers said. No stronger association was noted in patients with proteinase 3-ANCA–positive AAV, they said. However, the overall associations remained strong after adjustment for demographics and disease manifestations, they noted.
The study findings were limited by several factors including the observational design, homogeneous study population at a single center, and use of self-reports, the researchers wrote. However, the results were strengthened by the large sample size and number of patients who were MPO-ANCA positive, and the data associating smoking with AAV “expand the list of potential risk factors for AAV, including genetics and silica exposure,” they said. “Further studies to confirm these results and investigate a potential pathogenic mechanism are needed,” they concluded.
The study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The researchers had no financial conflicts to disclose.
SOURCE: McDermott G et al. JAMA Intern Med. 2020 Apr 13. doi: 10.1001/jamainternmed.2020.0675.
according to data from a large case-control study.
Although smokers have shown an increased risk for ANCA-associated vasculitis (AAV), compared with nonsmokers, previous studies of the association between smoking and AAV risk have been small and the results have been inconsistent, Greg McDermott, MD, and colleagues at Massachusetts General Hospital, Boston, wrote in JAMA Internal Medicine.
The researchers reviewed data from 473 adults diagnosed with AAV between 2002 and 2017 and compared them with 1,419 matched controls without AAV who had completed a smoking history questionnaire.
Overall, the odds of having a diagnosis of AAV were significantly higher among former smokers or current smokers, compared with never smokers (odds ratios, 1.58 and 2.70, respectively). In addition, the researchers found a significant dose-response relationship between pack-years of exposure and risk of AAV. The average age of the cases and controls was 59 years, 59% were women, and 84% were white.
The association between AAV risk and former or current smoking was greater among the 147 former and 29 current smokers with AAV positive for myeloperoxidase (MPO) (OR, 1.73 and 3.54, respectively). “Proteinase 3-ANCA– and MPO-ANCA–positive AAV are increasingly recognized as distinct conditions characterized by differences in genetic risk, pathogenesis, disease manifestations, and response to treatment,” the researchers said. No stronger association was noted in patients with proteinase 3-ANCA–positive AAV, they said. However, the overall associations remained strong after adjustment for demographics and disease manifestations, they noted.
The study findings were limited by several factors including the observational design, homogeneous study population at a single center, and use of self-reports, the researchers wrote. However, the results were strengthened by the large sample size and number of patients who were MPO-ANCA positive, and the data associating smoking with AAV “expand the list of potential risk factors for AAV, including genetics and silica exposure,” they said. “Further studies to confirm these results and investigate a potential pathogenic mechanism are needed,” they concluded.
The study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The researchers had no financial conflicts to disclose.
SOURCE: McDermott G et al. JAMA Intern Med. 2020 Apr 13. doi: 10.1001/jamainternmed.2020.0675.
according to data from a large case-control study.
Although smokers have shown an increased risk for ANCA-associated vasculitis (AAV), compared with nonsmokers, previous studies of the association between smoking and AAV risk have been small and the results have been inconsistent, Greg McDermott, MD, and colleagues at Massachusetts General Hospital, Boston, wrote in JAMA Internal Medicine.
The researchers reviewed data from 473 adults diagnosed with AAV between 2002 and 2017 and compared them with 1,419 matched controls without AAV who had completed a smoking history questionnaire.
Overall, the odds of having a diagnosis of AAV were significantly higher among former smokers or current smokers, compared with never smokers (odds ratios, 1.58 and 2.70, respectively). In addition, the researchers found a significant dose-response relationship between pack-years of exposure and risk of AAV. The average age of the cases and controls was 59 years, 59% were women, and 84% were white.
The association between AAV risk and former or current smoking was greater among the 147 former and 29 current smokers with AAV positive for myeloperoxidase (MPO) (OR, 1.73 and 3.54, respectively). “Proteinase 3-ANCA– and MPO-ANCA–positive AAV are increasingly recognized as distinct conditions characterized by differences in genetic risk, pathogenesis, disease manifestations, and response to treatment,” the researchers said. No stronger association was noted in patients with proteinase 3-ANCA–positive AAV, they said. However, the overall associations remained strong after adjustment for demographics and disease manifestations, they noted.
The study findings were limited by several factors including the observational design, homogeneous study population at a single center, and use of self-reports, the researchers wrote. However, the results were strengthened by the large sample size and number of patients who were MPO-ANCA positive, and the data associating smoking with AAV “expand the list of potential risk factors for AAV, including genetics and silica exposure,” they said. “Further studies to confirm these results and investigate a potential pathogenic mechanism are needed,” they concluded.
The study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The researchers had no financial conflicts to disclose.
SOURCE: McDermott G et al. JAMA Intern Med. 2020 Apr 13. doi: 10.1001/jamainternmed.2020.0675.
FROM JAMA INTERNAL MEDICINE
Klotho allele lowers APOE4-associated risk of Alzheimer’s
Cognitively normal carriers of the apolipoprotein E epsilon-4 (APOE4) allele aged 60 years and older who also showed heterozygosity for the Klotho-VS allele had a significantly reduced risk of developing Alzheimer’s disease, according to data from 22 research groups including more than 20,000 adults.
The transmembrane protein known as klotho (KL) is part of a functional haplotype known as KL-VS. “Specifically, heterozygosity for KL-VS (KL-VSHET+ status) has been shown to increase serum levels of KL and exert protective effects on healthy aging and longevity when compared with individuals who are homozygotes for the major or minor alleles (KL-VSHET−),” wrote Michael E. Belloy, PhD, of Stanford (Calif.) University and colleagues. However, the possible role of KL-VS in protecting against neurodegenerative disorders such as Alzheimer’s disease (AD) remains unclear, they said.
In a study published in JAMA Neurology, the researchers reviewed data from 20,928 participants in case-control studies, as well as 3,008 participants in conversion studies, 556 in amyloid-beta (a-beta) cerebrospinal fluid regression analyses, and 251 in brain amyloid PET regression analyses. The participants were aged 60-80 years, and of non-Hispanic northern European ancestry and were identified as cognitively normal or having mild cognitive impairment (MCI) or AD.
Overall, individuals with the APOE4 allele who were cognitively normal and heterozygous for KL-VS had a significantly reduced risk for developing AD (odds ratio, 0.75).
In addition, cognitively normal carriers of APOE4 with KL-VS heterozygosity had significantly lower risk of developing either MCI or AD (hazard ratio, 0.64). Also, those persons with APOE4 and positive KL-VS heterozygosity had higher a-beta in cerebrospinal fluid (P = .03) and lower a-beta on PET scans (P = .04). However, no association with cognitive outcomes were noted among APOE4 noncarriers, the researchers noted.
“This suggests that KL-VS interacts with aspects of AD pathology that are more pronounced in those who carry APOE4, such as a-beta accumulation during the presymptomatic phases of the disease,” they said.
The study findings were limited by the variable age and diagnoses across the multiple cohorts, but strengthened by the meta- and mega-analyses and sensitivity analyses that yielded consistent results, the researchers noted.
“Our work paves the way for biological validation studies to elucidate the molecular pathways by which KL-VS and APOE interact,” they said.
“The specificity of KL-VS benefits on AD in individuals who carry APOE4 is striking and suggests a yet-unstudied interaction between biological pathways of the klotho and APOE4 proteins,” wrote Dena B. Dubal, MD, and Jennifer S. Yokoyama, PhD, of the University of California, San Francisco, in an accompanying editorial. Despite limitations, the study findings have implications for clinical neurology, as well as clinical and translational research, they said.
“For personalized genomics, KL-VS status should integrate into knowledge that both lifestyle and genetics can negate or at least mitigate harmful influences of APOE4,” they noted. “In light of this, we might consider an individual’s KLOTHO genotype when counseling individuals who carry APOE4 about their prognosis for AD. In clinical trials using APOE4 for trial enrichment, further selection of individuals who carry APOE4 without KL-VS could define a population more likely to convert to AD and thus increase detection of a therapeutic benefit. In translational research, understanding how klotho itself or its biological pathways may counter APOE4 could lead to monumental progress in the future treatment of AD,” they added.
“Applying our growing knowledge of klotho to APOE4 and AD could ultimately pave the path to novel therapeutics for individuals who carry APOE4,” they concluded.
The study was supported by the Iqbal Farrukh & Asad Jamal Center for Cognitive Health in Aging, the South Palm Beach County Foundation, and the National Institutes of Health. The researchers had no financial conflicts to disclose. Dr. Dubal disclosed holding a patent for Methods for Improving Cognition that includes klotho, as well as consulting for Unity Biotechnology and receiving research funding from the National Institutes of Health, the American Federation for Aging Research, Glenn Medical Foundation, Unity Biotechnology, and other philanthropic support for translational research. Dr. Yokoyama disclosed research funding from the National Institutes of Health, the Department of Defense, and other foundations and philanthropic donors.
SOURCE: Belloy ME et al. JAMA Neurol. 2020 Apr 13. doi: 10.1001/jamaneurol.2020.0414.
Cognitively normal carriers of the apolipoprotein E epsilon-4 (APOE4) allele aged 60 years and older who also showed heterozygosity for the Klotho-VS allele had a significantly reduced risk of developing Alzheimer’s disease, according to data from 22 research groups including more than 20,000 adults.
The transmembrane protein known as klotho (KL) is part of a functional haplotype known as KL-VS. “Specifically, heterozygosity for KL-VS (KL-VSHET+ status) has been shown to increase serum levels of KL and exert protective effects on healthy aging and longevity when compared with individuals who are homozygotes for the major or minor alleles (KL-VSHET−),” wrote Michael E. Belloy, PhD, of Stanford (Calif.) University and colleagues. However, the possible role of KL-VS in protecting against neurodegenerative disorders such as Alzheimer’s disease (AD) remains unclear, they said.
In a study published in JAMA Neurology, the researchers reviewed data from 20,928 participants in case-control studies, as well as 3,008 participants in conversion studies, 556 in amyloid-beta (a-beta) cerebrospinal fluid regression analyses, and 251 in brain amyloid PET regression analyses. The participants were aged 60-80 years, and of non-Hispanic northern European ancestry and were identified as cognitively normal or having mild cognitive impairment (MCI) or AD.
Overall, individuals with the APOE4 allele who were cognitively normal and heterozygous for KL-VS had a significantly reduced risk for developing AD (odds ratio, 0.75).
In addition, cognitively normal carriers of APOE4 with KL-VS heterozygosity had significantly lower risk of developing either MCI or AD (hazard ratio, 0.64). Also, those persons with APOE4 and positive KL-VS heterozygosity had higher a-beta in cerebrospinal fluid (P = .03) and lower a-beta on PET scans (P = .04). However, no association with cognitive outcomes were noted among APOE4 noncarriers, the researchers noted.
“This suggests that KL-VS interacts with aspects of AD pathology that are more pronounced in those who carry APOE4, such as a-beta accumulation during the presymptomatic phases of the disease,” they said.
The study findings were limited by the variable age and diagnoses across the multiple cohorts, but strengthened by the meta- and mega-analyses and sensitivity analyses that yielded consistent results, the researchers noted.
“Our work paves the way for biological validation studies to elucidate the molecular pathways by which KL-VS and APOE interact,” they said.
“The specificity of KL-VS benefits on AD in individuals who carry APOE4 is striking and suggests a yet-unstudied interaction between biological pathways of the klotho and APOE4 proteins,” wrote Dena B. Dubal, MD, and Jennifer S. Yokoyama, PhD, of the University of California, San Francisco, in an accompanying editorial. Despite limitations, the study findings have implications for clinical neurology, as well as clinical and translational research, they said.
“For personalized genomics, KL-VS status should integrate into knowledge that both lifestyle and genetics can negate or at least mitigate harmful influences of APOE4,” they noted. “In light of this, we might consider an individual’s KLOTHO genotype when counseling individuals who carry APOE4 about their prognosis for AD. In clinical trials using APOE4 for trial enrichment, further selection of individuals who carry APOE4 without KL-VS could define a population more likely to convert to AD and thus increase detection of a therapeutic benefit. In translational research, understanding how klotho itself or its biological pathways may counter APOE4 could lead to monumental progress in the future treatment of AD,” they added.
“Applying our growing knowledge of klotho to APOE4 and AD could ultimately pave the path to novel therapeutics for individuals who carry APOE4,” they concluded.
The study was supported by the Iqbal Farrukh & Asad Jamal Center for Cognitive Health in Aging, the South Palm Beach County Foundation, and the National Institutes of Health. The researchers had no financial conflicts to disclose. Dr. Dubal disclosed holding a patent for Methods for Improving Cognition that includes klotho, as well as consulting for Unity Biotechnology and receiving research funding from the National Institutes of Health, the American Federation for Aging Research, Glenn Medical Foundation, Unity Biotechnology, and other philanthropic support for translational research. Dr. Yokoyama disclosed research funding from the National Institutes of Health, the Department of Defense, and other foundations and philanthropic donors.
SOURCE: Belloy ME et al. JAMA Neurol. 2020 Apr 13. doi: 10.1001/jamaneurol.2020.0414.
Cognitively normal carriers of the apolipoprotein E epsilon-4 (APOE4) allele aged 60 years and older who also showed heterozygosity for the Klotho-VS allele had a significantly reduced risk of developing Alzheimer’s disease, according to data from 22 research groups including more than 20,000 adults.
The transmembrane protein known as klotho (KL) is part of a functional haplotype known as KL-VS. “Specifically, heterozygosity for KL-VS (KL-VSHET+ status) has been shown to increase serum levels of KL and exert protective effects on healthy aging and longevity when compared with individuals who are homozygotes for the major or minor alleles (KL-VSHET−),” wrote Michael E. Belloy, PhD, of Stanford (Calif.) University and colleagues. However, the possible role of KL-VS in protecting against neurodegenerative disorders such as Alzheimer’s disease (AD) remains unclear, they said.
In a study published in JAMA Neurology, the researchers reviewed data from 20,928 participants in case-control studies, as well as 3,008 participants in conversion studies, 556 in amyloid-beta (a-beta) cerebrospinal fluid regression analyses, and 251 in brain amyloid PET regression analyses. The participants were aged 60-80 years, and of non-Hispanic northern European ancestry and were identified as cognitively normal or having mild cognitive impairment (MCI) or AD.
Overall, individuals with the APOE4 allele who were cognitively normal and heterozygous for KL-VS had a significantly reduced risk for developing AD (odds ratio, 0.75).
In addition, cognitively normal carriers of APOE4 with KL-VS heterozygosity had significantly lower risk of developing either MCI or AD (hazard ratio, 0.64). Also, those persons with APOE4 and positive KL-VS heterozygosity had higher a-beta in cerebrospinal fluid (P = .03) and lower a-beta on PET scans (P = .04). However, no association with cognitive outcomes were noted among APOE4 noncarriers, the researchers noted.
“This suggests that KL-VS interacts with aspects of AD pathology that are more pronounced in those who carry APOE4, such as a-beta accumulation during the presymptomatic phases of the disease,” they said.
The study findings were limited by the variable age and diagnoses across the multiple cohorts, but strengthened by the meta- and mega-analyses and sensitivity analyses that yielded consistent results, the researchers noted.
“Our work paves the way for biological validation studies to elucidate the molecular pathways by which KL-VS and APOE interact,” they said.
“The specificity of KL-VS benefits on AD in individuals who carry APOE4 is striking and suggests a yet-unstudied interaction between biological pathways of the klotho and APOE4 proteins,” wrote Dena B. Dubal, MD, and Jennifer S. Yokoyama, PhD, of the University of California, San Francisco, in an accompanying editorial. Despite limitations, the study findings have implications for clinical neurology, as well as clinical and translational research, they said.
“For personalized genomics, KL-VS status should integrate into knowledge that both lifestyle and genetics can negate or at least mitigate harmful influences of APOE4,” they noted. “In light of this, we might consider an individual’s KLOTHO genotype when counseling individuals who carry APOE4 about their prognosis for AD. In clinical trials using APOE4 for trial enrichment, further selection of individuals who carry APOE4 without KL-VS could define a population more likely to convert to AD and thus increase detection of a therapeutic benefit. In translational research, understanding how klotho itself or its biological pathways may counter APOE4 could lead to monumental progress in the future treatment of AD,” they added.
“Applying our growing knowledge of klotho to APOE4 and AD could ultimately pave the path to novel therapeutics for individuals who carry APOE4,” they concluded.
The study was supported by the Iqbal Farrukh & Asad Jamal Center for Cognitive Health in Aging, the South Palm Beach County Foundation, and the National Institutes of Health. The researchers had no financial conflicts to disclose. Dr. Dubal disclosed holding a patent for Methods for Improving Cognition that includes klotho, as well as consulting for Unity Biotechnology and receiving research funding from the National Institutes of Health, the American Federation for Aging Research, Glenn Medical Foundation, Unity Biotechnology, and other philanthropic support for translational research. Dr. Yokoyama disclosed research funding from the National Institutes of Health, the Department of Defense, and other foundations and philanthropic donors.
SOURCE: Belloy ME et al. JAMA Neurol. 2020 Apr 13. doi: 10.1001/jamaneurol.2020.0414.
FROM JAMA NEUROLOGY
With mild or stable lupus, few patients flare during, after pregnancy
Approximately 26% of women with inactive or mild lupus at conception experienced flares at some point during pregnancy, based on data from 384 patients.
Active systemic lupus erythematosus (SLE) is a known predictor of poor pregnancy outcomes, including preterm birth, growth restriction, and fetal loss, but predictors of flares during and after pregnancy in women with SLE have not been well studied, wrote Julia Davis-Porada, MD, of the Hospital for Special Surgery, New York, and her colleagues.
In a study published in Arthritis Research & Therapy, the investigators reviewed data from the PROMISSE (Predictors of Pregnancy Outcome: Biomarkers in Antiphospholipid Antibody Syndrome and Systemic Lupus Erythematosus) study, a prospective study of pregnant women aged 18-45 years. The women were enrolled at less than 12 weeks’ gestation, and participants had a baseline hematocrit greater than 26%. Participants met criteria for inactive or mild/stable disease at the time of conception.
Overall, 20.8% of patients experienced at least one mild or moderate flare and 6.25% had one or more severe flares during pregnancy. Mild to moderate flares and severe flares occurred postpartum (2-6 months after the end of pregnancy) in 22.7% and 1.7% of patients, respectively.
Patients who were younger and those who had lower C4 at baseline and higher Physician Global Assessment scores at baseline were significantly more likely to have at least one flare during pregnancy (P = .003, P = .024, P = .0005, respectively).
In the analysis of postpartum flares, the incidence rates for mild to moderate and severe flares were 0.8 and 0.06 per person-year, respectively. “In contrast to the findings observed for flares that occurred during pregnancy, baseline patient characteristics were not correlated with postpartum flares,” the researchers wrote.
No medications were associated with flares during or after pregnancy.
The study findings were limited by several factors, including the exclusion of SLE patients with current nephritis and those who needed high-dose prednisone; the potential for missed flares; and the lack of postpartum data for approximately 10% of patients, the researchers noted. Also, “since many patients presented to this study only after conception, we have no data to review disease activity prior to pregnancy to determine whether pregnancy per se increased the risk for flare,” they said.
However, the results were strengthened by the large, multiethnic population and prospective study design, and support physicians in reassuring patients with SLE that pregnancy and postpartum flares are unlikely if they plan pregnancy during a time of mild or inactive disease, they concluded.
The study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The researchers had no financial conflicts to disclose.
SOURCE: Davis-Porada J et al. Arthritis Res Ther. 2020 Mar 19. doi: 10.1186/s13075-020-2139-9.
Approximately 26% of women with inactive or mild lupus at conception experienced flares at some point during pregnancy, based on data from 384 patients.
Active systemic lupus erythematosus (SLE) is a known predictor of poor pregnancy outcomes, including preterm birth, growth restriction, and fetal loss, but predictors of flares during and after pregnancy in women with SLE have not been well studied, wrote Julia Davis-Porada, MD, of the Hospital for Special Surgery, New York, and her colleagues.
In a study published in Arthritis Research & Therapy, the investigators reviewed data from the PROMISSE (Predictors of Pregnancy Outcome: Biomarkers in Antiphospholipid Antibody Syndrome and Systemic Lupus Erythematosus) study, a prospective study of pregnant women aged 18-45 years. The women were enrolled at less than 12 weeks’ gestation, and participants had a baseline hematocrit greater than 26%. Participants met criteria for inactive or mild/stable disease at the time of conception.
Overall, 20.8% of patients experienced at least one mild or moderate flare and 6.25% had one or more severe flares during pregnancy. Mild to moderate flares and severe flares occurred postpartum (2-6 months after the end of pregnancy) in 22.7% and 1.7% of patients, respectively.
Patients who were younger and those who had lower C4 at baseline and higher Physician Global Assessment scores at baseline were significantly more likely to have at least one flare during pregnancy (P = .003, P = .024, P = .0005, respectively).
In the analysis of postpartum flares, the incidence rates for mild to moderate and severe flares were 0.8 and 0.06 per person-year, respectively. “In contrast to the findings observed for flares that occurred during pregnancy, baseline patient characteristics were not correlated with postpartum flares,” the researchers wrote.
No medications were associated with flares during or after pregnancy.
The study findings were limited by several factors, including the exclusion of SLE patients with current nephritis and those who needed high-dose prednisone; the potential for missed flares; and the lack of postpartum data for approximately 10% of patients, the researchers noted. Also, “since many patients presented to this study only after conception, we have no data to review disease activity prior to pregnancy to determine whether pregnancy per se increased the risk for flare,” they said.
However, the results were strengthened by the large, multiethnic population and prospective study design, and support physicians in reassuring patients with SLE that pregnancy and postpartum flares are unlikely if they plan pregnancy during a time of mild or inactive disease, they concluded.
The study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The researchers had no financial conflicts to disclose.
SOURCE: Davis-Porada J et al. Arthritis Res Ther. 2020 Mar 19. doi: 10.1186/s13075-020-2139-9.
Approximately 26% of women with inactive or mild lupus at conception experienced flares at some point during pregnancy, based on data from 384 patients.
Active systemic lupus erythematosus (SLE) is a known predictor of poor pregnancy outcomes, including preterm birth, growth restriction, and fetal loss, but predictors of flares during and after pregnancy in women with SLE have not been well studied, wrote Julia Davis-Porada, MD, of the Hospital for Special Surgery, New York, and her colleagues.
In a study published in Arthritis Research & Therapy, the investigators reviewed data from the PROMISSE (Predictors of Pregnancy Outcome: Biomarkers in Antiphospholipid Antibody Syndrome and Systemic Lupus Erythematosus) study, a prospective study of pregnant women aged 18-45 years. The women were enrolled at less than 12 weeks’ gestation, and participants had a baseline hematocrit greater than 26%. Participants met criteria for inactive or mild/stable disease at the time of conception.
Overall, 20.8% of patients experienced at least one mild or moderate flare and 6.25% had one or more severe flares during pregnancy. Mild to moderate flares and severe flares occurred postpartum (2-6 months after the end of pregnancy) in 22.7% and 1.7% of patients, respectively.
Patients who were younger and those who had lower C4 at baseline and higher Physician Global Assessment scores at baseline were significantly more likely to have at least one flare during pregnancy (P = .003, P = .024, P = .0005, respectively).
In the analysis of postpartum flares, the incidence rates for mild to moderate and severe flares were 0.8 and 0.06 per person-year, respectively. “In contrast to the findings observed for flares that occurred during pregnancy, baseline patient characteristics were not correlated with postpartum flares,” the researchers wrote.
No medications were associated with flares during or after pregnancy.
The study findings were limited by several factors, including the exclusion of SLE patients with current nephritis and those who needed high-dose prednisone; the potential for missed flares; and the lack of postpartum data for approximately 10% of patients, the researchers noted. Also, “since many patients presented to this study only after conception, we have no data to review disease activity prior to pregnancy to determine whether pregnancy per se increased the risk for flare,” they said.
However, the results were strengthened by the large, multiethnic population and prospective study design, and support physicians in reassuring patients with SLE that pregnancy and postpartum flares are unlikely if they plan pregnancy during a time of mild or inactive disease, they concluded.
The study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The researchers had no financial conflicts to disclose.
SOURCE: Davis-Porada J et al. Arthritis Res Ther. 2020 Mar 19. doi: 10.1186/s13075-020-2139-9.
FROM ARTHRITIS RESEARCH & THERAPY
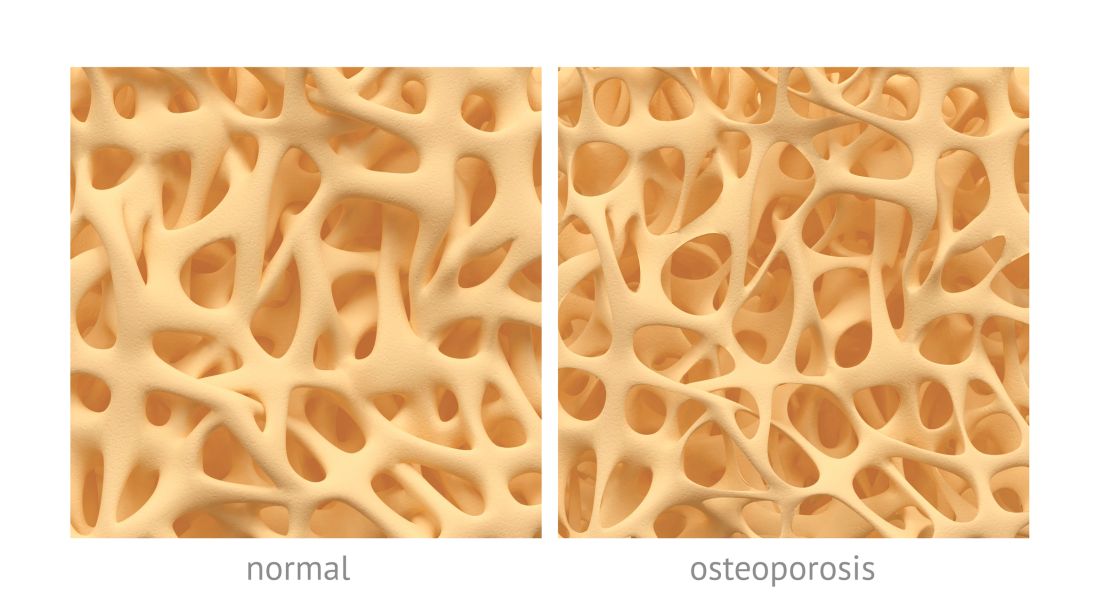
High and low trauma yield similar future osteoporotic fracture risk
Average measures of bone mineral density were similar for individuals with high-trauma and low-trauma fractures, and both were significantly distinct from those with no fracture history, based on data from a cohort study of adults aged 40 years and older.
In the past, low-trauma fractures have typically been associated with osteoporosis, wrote William D. Leslie, MD, of the University of Manitoba, Canada, and his colleagues. However, features distinguishing between low- and high-trauma fractures are often arbitrary and “empirical data have questioned whether distinguishing low-trauma from high-trauma fractures is clinically useful for purposes of risk assessment and treatment,” they wrote.
In a study published in Osteoporosis International, the researchers reviewed data from 64,626 individuals with no prior fracture, 858 with high-trauma fractures, and 14,758 with low-trauma fractures. Overall, the average BMD Z-scores for individuals with no previous fracture were slightly positive, while those with either a high-trauma or low-trauma fracture were negative. The scores for individuals with high-trauma fractures or major osteoporotic fractures were similar to those with low-trauma fractures, and significantly lower (P less than .001) than among individuals with no prior fractures.
The study population included adults aged 40 years and older with baseline DXA scans between Jan. 1, 1996, and Mar. 31, 2016. Those with high-trauma fractures were younger than those with low-trauma fractures (65 years vs. 67 years), and fewer individuals with high-trauma fractures were women (77% vs. 87%).
Both high-trauma and low-trauma fractures were similarly and significantly associated with increased risk for incident major osteoporotic fractures (adjusted hazard ratios 1.31 and 1.55, respectively).
The study findings were limited by several factors including incomplete data on external injury codes, the retrospective study design, and the lack of analysis of the time since prior fractures, the researchers noted. However, the results were strengthened by the large sample size, long-term follow-up, and large numbers of incident fractures, they wrote.
The results support data from previous studies and support “the inclusion of high-trauma clinical fractures in clinical assessment for underlying osteoporosis and in the evaluation for intervention to reduce future fracture risk,” they wrote.
In an accompanying editorial, Steven R. Cummings, MD, of California Pacific Medical Center Research Institute, San Francisco, and Richard Eastell, MD, of the University of Sheffield, England, wrote that the practice of rating fractures according to degree of trauma should be eliminated.
“The study adds evidence to the case that it is time to abandon the mistaken beliefs that fractures rated as high trauma are not associated with decreased BMD, indicate no higher risk of subsequent fracture, or are less likely to be prevented by treatments for osteoporosis,” they wrote.
Describing some fractures as due to trauma reinforces the mistaken belief that the fractures are simply due to the trauma, not decreased bone strength, they noted.
“Indeed, we recommend that people stop attempting to rate or record degree of trauma because such ratings are at best inaccurate and would promote the continued neglect of those patients who are misclassified as having fractures that do not warrant evaluation and treatment,” they concluded.
The study received no outside funding. Dr. Leslie, the study’s first author, reported having no financial conflicts to disclose.
Dr. Cummings disclosed consultancy and grant funding from Amgen and Radius. Dr. Eastell disclosed consultancy funding from IDS, Roche Diagnostics, GSK Nutrition, FNIH, Mereo, Lilly, Sandoz, Nittobo, Abbvie, Samsung, and Haoma Medica and grant funding from Nittobo, IDS, Roche, Amgen, and Alexion.
SOURCE: Leslie WD et al. Osteroporos Int. 2020 Mar 16. doi: 10.1007/s00198-019-05274-2.
Average measures of bone mineral density were similar for individuals with high-trauma and low-trauma fractures, and both were significantly distinct from those with no fracture history, based on data from a cohort study of adults aged 40 years and older.
In the past, low-trauma fractures have typically been associated with osteoporosis, wrote William D. Leslie, MD, of the University of Manitoba, Canada, and his colleagues. However, features distinguishing between low- and high-trauma fractures are often arbitrary and “empirical data have questioned whether distinguishing low-trauma from high-trauma fractures is clinically useful for purposes of risk assessment and treatment,” they wrote.
In a study published in Osteoporosis International, the researchers reviewed data from 64,626 individuals with no prior fracture, 858 with high-trauma fractures, and 14,758 with low-trauma fractures. Overall, the average BMD Z-scores for individuals with no previous fracture were slightly positive, while those with either a high-trauma or low-trauma fracture were negative. The scores for individuals with high-trauma fractures or major osteoporotic fractures were similar to those with low-trauma fractures, and significantly lower (P less than .001) than among individuals with no prior fractures.
The study population included adults aged 40 years and older with baseline DXA scans between Jan. 1, 1996, and Mar. 31, 2016. Those with high-trauma fractures were younger than those with low-trauma fractures (65 years vs. 67 years), and fewer individuals with high-trauma fractures were women (77% vs. 87%).
Both high-trauma and low-trauma fractures were similarly and significantly associated with increased risk for incident major osteoporotic fractures (adjusted hazard ratios 1.31 and 1.55, respectively).
The study findings were limited by several factors including incomplete data on external injury codes, the retrospective study design, and the lack of analysis of the time since prior fractures, the researchers noted. However, the results were strengthened by the large sample size, long-term follow-up, and large numbers of incident fractures, they wrote.
The results support data from previous studies and support “the inclusion of high-trauma clinical fractures in clinical assessment for underlying osteoporosis and in the evaluation for intervention to reduce future fracture risk,” they wrote.
In an accompanying editorial, Steven R. Cummings, MD, of California Pacific Medical Center Research Institute, San Francisco, and Richard Eastell, MD, of the University of Sheffield, England, wrote that the practice of rating fractures according to degree of trauma should be eliminated.
“The study adds evidence to the case that it is time to abandon the mistaken beliefs that fractures rated as high trauma are not associated with decreased BMD, indicate no higher risk of subsequent fracture, or are less likely to be prevented by treatments for osteoporosis,” they wrote.
Describing some fractures as due to trauma reinforces the mistaken belief that the fractures are simply due to the trauma, not decreased bone strength, they noted.
“Indeed, we recommend that people stop attempting to rate or record degree of trauma because such ratings are at best inaccurate and would promote the continued neglect of those patients who are misclassified as having fractures that do not warrant evaluation and treatment,” they concluded.
The study received no outside funding. Dr. Leslie, the study’s first author, reported having no financial conflicts to disclose.
Dr. Cummings disclosed consultancy and grant funding from Amgen and Radius. Dr. Eastell disclosed consultancy funding from IDS, Roche Diagnostics, GSK Nutrition, FNIH, Mereo, Lilly, Sandoz, Nittobo, Abbvie, Samsung, and Haoma Medica and grant funding from Nittobo, IDS, Roche, Amgen, and Alexion.
SOURCE: Leslie WD et al. Osteroporos Int. 2020 Mar 16. doi: 10.1007/s00198-019-05274-2.
Average measures of bone mineral density were similar for individuals with high-trauma and low-trauma fractures, and both were significantly distinct from those with no fracture history, based on data from a cohort study of adults aged 40 years and older.
In the past, low-trauma fractures have typically been associated with osteoporosis, wrote William D. Leslie, MD, of the University of Manitoba, Canada, and his colleagues. However, features distinguishing between low- and high-trauma fractures are often arbitrary and “empirical data have questioned whether distinguishing low-trauma from high-trauma fractures is clinically useful for purposes of risk assessment and treatment,” they wrote.
In a study published in Osteoporosis International, the researchers reviewed data from 64,626 individuals with no prior fracture, 858 with high-trauma fractures, and 14,758 with low-trauma fractures. Overall, the average BMD Z-scores for individuals with no previous fracture were slightly positive, while those with either a high-trauma or low-trauma fracture were negative. The scores for individuals with high-trauma fractures or major osteoporotic fractures were similar to those with low-trauma fractures, and significantly lower (P less than .001) than among individuals with no prior fractures.
The study population included adults aged 40 years and older with baseline DXA scans between Jan. 1, 1996, and Mar. 31, 2016. Those with high-trauma fractures were younger than those with low-trauma fractures (65 years vs. 67 years), and fewer individuals with high-trauma fractures were women (77% vs. 87%).
Both high-trauma and low-trauma fractures were similarly and significantly associated with increased risk for incident major osteoporotic fractures (adjusted hazard ratios 1.31 and 1.55, respectively).
The study findings were limited by several factors including incomplete data on external injury codes, the retrospective study design, and the lack of analysis of the time since prior fractures, the researchers noted. However, the results were strengthened by the large sample size, long-term follow-up, and large numbers of incident fractures, they wrote.
The results support data from previous studies and support “the inclusion of high-trauma clinical fractures in clinical assessment for underlying osteoporosis and in the evaluation for intervention to reduce future fracture risk,” they wrote.
In an accompanying editorial, Steven R. Cummings, MD, of California Pacific Medical Center Research Institute, San Francisco, and Richard Eastell, MD, of the University of Sheffield, England, wrote that the practice of rating fractures according to degree of trauma should be eliminated.
“The study adds evidence to the case that it is time to abandon the mistaken beliefs that fractures rated as high trauma are not associated with decreased BMD, indicate no higher risk of subsequent fracture, or are less likely to be prevented by treatments for osteoporosis,” they wrote.
Describing some fractures as due to trauma reinforces the mistaken belief that the fractures are simply due to the trauma, not decreased bone strength, they noted.
“Indeed, we recommend that people stop attempting to rate or record degree of trauma because such ratings are at best inaccurate and would promote the continued neglect of those patients who are misclassified as having fractures that do not warrant evaluation and treatment,” they concluded.
The study received no outside funding. Dr. Leslie, the study’s first author, reported having no financial conflicts to disclose.
Dr. Cummings disclosed consultancy and grant funding from Amgen and Radius. Dr. Eastell disclosed consultancy funding from IDS, Roche Diagnostics, GSK Nutrition, FNIH, Mereo, Lilly, Sandoz, Nittobo, Abbvie, Samsung, and Haoma Medica and grant funding from Nittobo, IDS, Roche, Amgen, and Alexion.
SOURCE: Leslie WD et al. Osteroporos Int. 2020 Mar 16. doi: 10.1007/s00198-019-05274-2.
FROM OSTEOPOROSIS INTERNATIONAL
Behavior, family traits impact kids’ vulnerability as bullying targets
according to data from a large, cohort study of 1,760 children in Canada.
“Peer victimization is characterized by substantial individual variability in its timing, duration, and intensity,” but the specific variations in victimization patterns have not been well studied, wrote Sinziana I. Oncioiu, MPH, of the University of Bordeaux (France) and colleagues.
To better describe the trajectories of peer victimization and identify factors associated with them, the researchers used data from the Quebec Longitudinal Study of Child Development of children born in Quebec in 1997-1998 and followed from 5 months to 17 years of age. Participants reported being the target of a bully at least once in ages 6-17 years. The study included 862 boys and 898 girls; 59% provided data on being bullied seven or eight times out of a possible eight assessments in the study published in Pediatrics.
The researchers identified four trajectories of peer victimization for ages 6-17 years: low (33%), moderate emerging (30%), childhood limited (26%), and high chronic (11%). Low victimization was defined as low victimization throughout the follow-up period. Moderate-emerging victimization was defined as steady levels from 6-12 years, followed by adolescent victimization. Childhood-limited peer victimization was defined as a high level of bullying at 6 years of age, followed by a sharp decline from 6 to 17 years. High-chronic victimization was defined as persistently high victimization compared, with the other groups, although levels declined from 6 to 17 years.
Overall, in a multivariate analysis, children in the moderate-emerging, childhood-limited, and high-chronic groups were more likely than those in the low victimization group to demonstrate externalizing behavior problems in early childhood. In addition, children with a paternal history of antisocial behavior were significantly more likely to be in moderate-emerging and high-chronic groups, compared with the low group (odds ratios 1.54 and 1.93, respectively). Children living in a nonintact family in early childhood were significantly more likely to fall into the childhood-limited and high-chronic groups, compared with the low group.
The study findings were limited by several factors including lack of assessment of power imbalances between bullies and victims and a lack of differentiation between children who were both bullies and victims and those who were victims only, the researchers noted. The use of self-reports and some attrition of the study population also limited the results, they said.
However, the study’s large size and long-term follow-up strengthen the results, which support the need for targeted interventions to address individual and family vulnerabilities and prevent persistent victimization during children’s school years, the researchers concluded.
Pediatricians have an important role to play in reducing potential vulnerability to being bullied among their patients, Stephen S. Leff, PhD; Brooke S. Paskewich, PsyD; and Nathan J. Blum, MD, of Children’s Hospital of Philadelphia, wrote in an accompanying editorial.
“Given that nearly two-thirds of school-aged youth in the current study report peer victimization during elementary and/or middle school, this is an important period in which pediatricians can screen for victimization during well-child visits,” they said. It also is important to have resources and referral information available, whether it is in the practice, the community, or online. Anticipatory guidance also is valuable by defining bullying (“aggressive or mean behavior that happens repeatedly in the context of a power imbalance,”) forms of bullying (physical, verbal, using gossip, and social exclusion in real time or online), and the impact of bullying on children and families.
In addition, pediatricians should “recognize externalizing behaviors as risk factors for adverse outcomes and assist families in accessing evidence-based interventions such as family behavioral counseling or parent training,” the editorialists said. “There may also be value in pediatricians being more attuned to indicators of parental psychopathology so that they can make recommendations to address the parents’ mental health needs and better prepare parents to support their child’s social-emotional development.”
The study was supported by the Quebec Government Ministry of Health, Canadian Institute of Health Research, Quebec’s Health Research Fund, and other Canadian organizations and universities. The editorial was supported in part by the National Institutes of Health and the Department of Health and Human Services. The researchers and editorialists had no financial conflicts to disclose.
SOURCEs: Oncioiu SI et al. Pediatrics. 2020. doi: 10.1542/peds.2019-2654.
according to data from a large, cohort study of 1,760 children in Canada.
“Peer victimization is characterized by substantial individual variability in its timing, duration, and intensity,” but the specific variations in victimization patterns have not been well studied, wrote Sinziana I. Oncioiu, MPH, of the University of Bordeaux (France) and colleagues.
To better describe the trajectories of peer victimization and identify factors associated with them, the researchers used data from the Quebec Longitudinal Study of Child Development of children born in Quebec in 1997-1998 and followed from 5 months to 17 years of age. Participants reported being the target of a bully at least once in ages 6-17 years. The study included 862 boys and 898 girls; 59% provided data on being bullied seven or eight times out of a possible eight assessments in the study published in Pediatrics.
The researchers identified four trajectories of peer victimization for ages 6-17 years: low (33%), moderate emerging (30%), childhood limited (26%), and high chronic (11%). Low victimization was defined as low victimization throughout the follow-up period. Moderate-emerging victimization was defined as steady levels from 6-12 years, followed by adolescent victimization. Childhood-limited peer victimization was defined as a high level of bullying at 6 years of age, followed by a sharp decline from 6 to 17 years. High-chronic victimization was defined as persistently high victimization compared, with the other groups, although levels declined from 6 to 17 years.
Overall, in a multivariate analysis, children in the moderate-emerging, childhood-limited, and high-chronic groups were more likely than those in the low victimization group to demonstrate externalizing behavior problems in early childhood. In addition, children with a paternal history of antisocial behavior were significantly more likely to be in moderate-emerging and high-chronic groups, compared with the low group (odds ratios 1.54 and 1.93, respectively). Children living in a nonintact family in early childhood were significantly more likely to fall into the childhood-limited and high-chronic groups, compared with the low group.
The study findings were limited by several factors including lack of assessment of power imbalances between bullies and victims and a lack of differentiation between children who were both bullies and victims and those who were victims only, the researchers noted. The use of self-reports and some attrition of the study population also limited the results, they said.
However, the study’s large size and long-term follow-up strengthen the results, which support the need for targeted interventions to address individual and family vulnerabilities and prevent persistent victimization during children’s school years, the researchers concluded.
Pediatricians have an important role to play in reducing potential vulnerability to being bullied among their patients, Stephen S. Leff, PhD; Brooke S. Paskewich, PsyD; and Nathan J. Blum, MD, of Children’s Hospital of Philadelphia, wrote in an accompanying editorial.
“Given that nearly two-thirds of school-aged youth in the current study report peer victimization during elementary and/or middle school, this is an important period in which pediatricians can screen for victimization during well-child visits,” they said. It also is important to have resources and referral information available, whether it is in the practice, the community, or online. Anticipatory guidance also is valuable by defining bullying (“aggressive or mean behavior that happens repeatedly in the context of a power imbalance,”) forms of bullying (physical, verbal, using gossip, and social exclusion in real time or online), and the impact of bullying on children and families.
In addition, pediatricians should “recognize externalizing behaviors as risk factors for adverse outcomes and assist families in accessing evidence-based interventions such as family behavioral counseling or parent training,” the editorialists said. “There may also be value in pediatricians being more attuned to indicators of parental psychopathology so that they can make recommendations to address the parents’ mental health needs and better prepare parents to support their child’s social-emotional development.”
The study was supported by the Quebec Government Ministry of Health, Canadian Institute of Health Research, Quebec’s Health Research Fund, and other Canadian organizations and universities. The editorial was supported in part by the National Institutes of Health and the Department of Health and Human Services. The researchers and editorialists had no financial conflicts to disclose.
SOURCEs: Oncioiu SI et al. Pediatrics. 2020. doi: 10.1542/peds.2019-2654.
according to data from a large, cohort study of 1,760 children in Canada.
“Peer victimization is characterized by substantial individual variability in its timing, duration, and intensity,” but the specific variations in victimization patterns have not been well studied, wrote Sinziana I. Oncioiu, MPH, of the University of Bordeaux (France) and colleagues.
To better describe the trajectories of peer victimization and identify factors associated with them, the researchers used data from the Quebec Longitudinal Study of Child Development of children born in Quebec in 1997-1998 and followed from 5 months to 17 years of age. Participants reported being the target of a bully at least once in ages 6-17 years. The study included 862 boys and 898 girls; 59% provided data on being bullied seven or eight times out of a possible eight assessments in the study published in Pediatrics.
The researchers identified four trajectories of peer victimization for ages 6-17 years: low (33%), moderate emerging (30%), childhood limited (26%), and high chronic (11%). Low victimization was defined as low victimization throughout the follow-up period. Moderate-emerging victimization was defined as steady levels from 6-12 years, followed by adolescent victimization. Childhood-limited peer victimization was defined as a high level of bullying at 6 years of age, followed by a sharp decline from 6 to 17 years. High-chronic victimization was defined as persistently high victimization compared, with the other groups, although levels declined from 6 to 17 years.
Overall, in a multivariate analysis, children in the moderate-emerging, childhood-limited, and high-chronic groups were more likely than those in the low victimization group to demonstrate externalizing behavior problems in early childhood. In addition, children with a paternal history of antisocial behavior were significantly more likely to be in moderate-emerging and high-chronic groups, compared with the low group (odds ratios 1.54 and 1.93, respectively). Children living in a nonintact family in early childhood were significantly more likely to fall into the childhood-limited and high-chronic groups, compared with the low group.
The study findings were limited by several factors including lack of assessment of power imbalances between bullies and victims and a lack of differentiation between children who were both bullies and victims and those who were victims only, the researchers noted. The use of self-reports and some attrition of the study population also limited the results, they said.
However, the study’s large size and long-term follow-up strengthen the results, which support the need for targeted interventions to address individual and family vulnerabilities and prevent persistent victimization during children’s school years, the researchers concluded.
Pediatricians have an important role to play in reducing potential vulnerability to being bullied among their patients, Stephen S. Leff, PhD; Brooke S. Paskewich, PsyD; and Nathan J. Blum, MD, of Children’s Hospital of Philadelphia, wrote in an accompanying editorial.
“Given that nearly two-thirds of school-aged youth in the current study report peer victimization during elementary and/or middle school, this is an important period in which pediatricians can screen for victimization during well-child visits,” they said. It also is important to have resources and referral information available, whether it is in the practice, the community, or online. Anticipatory guidance also is valuable by defining bullying (“aggressive or mean behavior that happens repeatedly in the context of a power imbalance,”) forms of bullying (physical, verbal, using gossip, and social exclusion in real time or online), and the impact of bullying on children and families.
In addition, pediatricians should “recognize externalizing behaviors as risk factors for adverse outcomes and assist families in accessing evidence-based interventions such as family behavioral counseling or parent training,” the editorialists said. “There may also be value in pediatricians being more attuned to indicators of parental psychopathology so that they can make recommendations to address the parents’ mental health needs and better prepare parents to support their child’s social-emotional development.”
The study was supported by the Quebec Government Ministry of Health, Canadian Institute of Health Research, Quebec’s Health Research Fund, and other Canadian organizations and universities. The editorial was supported in part by the National Institutes of Health and the Department of Health and Human Services. The researchers and editorialists had no financial conflicts to disclose.
SOURCEs: Oncioiu SI et al. Pediatrics. 2020. doi: 10.1542/peds.2019-2654.
FROM PEDIATRICS
Key clinical point: Being targeted by bullies as children and adolescents may be affected in part by early childhood externalizing behavior and family vulnerability
Major finding: The researchers identified four distinct trajectories of peer victimization in the study population: low (33%), moderate emerging (30%), childhood limited (26%), and high chronic (11%).
Study details: The data come from a population-based cohort study of 1,760 Canadian children.
Disclosures: The study was supported by the Quebec Government Ministry of Health, Canadian Institute of Health Research, Quebec’s Health Research Fund, and other Canadian organizations and universities. The researchers had no financial conflicts to disclose.
Sources: Oncioiu SI et al. Pediatrics. 2020. doi: 10.1542/peds.2019-2654.
AI algorithm predicts treatment success in lung cancer patients
Radiomics signatures developed by artificial intelligence can predict sensitivity to treatment in adults with non–small cell lung cancer (NSCLC), according to a study published in Clinical Cancer Research.
“Radiomics features are calculated by algorithmic analysis of tumor images and have been linked to characteristics of NSCLC,” wrote Laurent Dercle, MD, of Columbia University, New York, and colleagues.
With their study, the researchers found that “radiomic signatures, derived from quantitative, artificial intelligence–based analysis of standard-of-care CT images, offer the potential to enhance clinical decision-making as on-treatment markers of efficacy.”
The researchers identified 188 adults with NSCLC: 92 receiving nivolumab, 50 receiving docetaxel, and 46 receiving gefitinib.
The team extracted 1,160 radiomics features from the largest measurable lung lesion in each patient. The researchers used CT images from baseline and the patients’ first treatment assessment (3 weeks for gefitinib and 8 weeks for nivolumab and docetaxel) to develop a model that would predict treatment sensitivity based on changes to the largest lung lesion.
In validation sets following training sets, the prediction models for nivolumab, docetaxel, and gefitinib yielded area under the curve results of 0.77, 0.67, and 0.82, respectively.
“Machine-learning techniques successfully performed a specific complex task: identifying a pattern of baseline and treatment-induced changes on CT images associated with sensitivity to systemic nivolumab, docetaxel, and gefitinib therapy in patients with a diagnosis of NSCLC,” the researchers wrote.
They noted that this study was limited by several factors, including the small sample size and the inability to evaluate the impact of various time intervals on feature selection and classification.
However, the researchers concluded that “this study is a proof of concept that AI [artificial intelligence] support could provide clinicians an early indication of the likelihood of success of treatment with the new generation of systemic anticancer therapies using conventional imaging techniques.”
This study was supported by Bristol-Myers Squibb, the National Institutes of Health, Fondation Philanthropia, and Fondation Nuovo-Soldati. The authors disclosed relationships, including employment, with Bristol-Myers Squibb. They also disclosed relationships with Roche, Novartis, Merck, and Boehringer Ingelheim.
SOURCE: Dercle L et al. Clin Cancer Res. 2020 Mar 20. doi: 10.1158/1078-0432.CCR-19-2942.
Radiomics signatures developed by artificial intelligence can predict sensitivity to treatment in adults with non–small cell lung cancer (NSCLC), according to a study published in Clinical Cancer Research.
“Radiomics features are calculated by algorithmic analysis of tumor images and have been linked to characteristics of NSCLC,” wrote Laurent Dercle, MD, of Columbia University, New York, and colleagues.
With their study, the researchers found that “radiomic signatures, derived from quantitative, artificial intelligence–based analysis of standard-of-care CT images, offer the potential to enhance clinical decision-making as on-treatment markers of efficacy.”
The researchers identified 188 adults with NSCLC: 92 receiving nivolumab, 50 receiving docetaxel, and 46 receiving gefitinib.
The team extracted 1,160 radiomics features from the largest measurable lung lesion in each patient. The researchers used CT images from baseline and the patients’ first treatment assessment (3 weeks for gefitinib and 8 weeks for nivolumab and docetaxel) to develop a model that would predict treatment sensitivity based on changes to the largest lung lesion.
In validation sets following training sets, the prediction models for nivolumab, docetaxel, and gefitinib yielded area under the curve results of 0.77, 0.67, and 0.82, respectively.
“Machine-learning techniques successfully performed a specific complex task: identifying a pattern of baseline and treatment-induced changes on CT images associated with sensitivity to systemic nivolumab, docetaxel, and gefitinib therapy in patients with a diagnosis of NSCLC,” the researchers wrote.
They noted that this study was limited by several factors, including the small sample size and the inability to evaluate the impact of various time intervals on feature selection and classification.
However, the researchers concluded that “this study is a proof of concept that AI [artificial intelligence] support could provide clinicians an early indication of the likelihood of success of treatment with the new generation of systemic anticancer therapies using conventional imaging techniques.”
This study was supported by Bristol-Myers Squibb, the National Institutes of Health, Fondation Philanthropia, and Fondation Nuovo-Soldati. The authors disclosed relationships, including employment, with Bristol-Myers Squibb. They also disclosed relationships with Roche, Novartis, Merck, and Boehringer Ingelheim.
SOURCE: Dercle L et al. Clin Cancer Res. 2020 Mar 20. doi: 10.1158/1078-0432.CCR-19-2942.
Radiomics signatures developed by artificial intelligence can predict sensitivity to treatment in adults with non–small cell lung cancer (NSCLC), according to a study published in Clinical Cancer Research.
“Radiomics features are calculated by algorithmic analysis of tumor images and have been linked to characteristics of NSCLC,” wrote Laurent Dercle, MD, of Columbia University, New York, and colleagues.
With their study, the researchers found that “radiomic signatures, derived from quantitative, artificial intelligence–based analysis of standard-of-care CT images, offer the potential to enhance clinical decision-making as on-treatment markers of efficacy.”
The researchers identified 188 adults with NSCLC: 92 receiving nivolumab, 50 receiving docetaxel, and 46 receiving gefitinib.
The team extracted 1,160 radiomics features from the largest measurable lung lesion in each patient. The researchers used CT images from baseline and the patients’ first treatment assessment (3 weeks for gefitinib and 8 weeks for nivolumab and docetaxel) to develop a model that would predict treatment sensitivity based on changes to the largest lung lesion.
In validation sets following training sets, the prediction models for nivolumab, docetaxel, and gefitinib yielded area under the curve results of 0.77, 0.67, and 0.82, respectively.
“Machine-learning techniques successfully performed a specific complex task: identifying a pattern of baseline and treatment-induced changes on CT images associated with sensitivity to systemic nivolumab, docetaxel, and gefitinib therapy in patients with a diagnosis of NSCLC,” the researchers wrote.
They noted that this study was limited by several factors, including the small sample size and the inability to evaluate the impact of various time intervals on feature selection and classification.
However, the researchers concluded that “this study is a proof of concept that AI [artificial intelligence] support could provide clinicians an early indication of the likelihood of success of treatment with the new generation of systemic anticancer therapies using conventional imaging techniques.”
This study was supported by Bristol-Myers Squibb, the National Institutes of Health, Fondation Philanthropia, and Fondation Nuovo-Soldati. The authors disclosed relationships, including employment, with Bristol-Myers Squibb. They also disclosed relationships with Roche, Novartis, Merck, and Boehringer Ingelheim.
SOURCE: Dercle L et al. Clin Cancer Res. 2020 Mar 20. doi: 10.1158/1078-0432.CCR-19-2942.
FROM CLINICAL CANCER RESEARCH
Hormone therapy boosts body image in transgender youth
based on data from 148 individuals.
“Understanding the impact of gender-affirming hormone therapy on the mental health of transgender youth is critical given the health disparities documented in this population,” wrote Laura E. Kuper, PhD, of Children’s Health Systems of Texas, Dallas, and colleagues.
In a study published in Pediatrics, the researchers reviewed data from 148 youth aged 9-18 years who underwent gender-affirming hormone therapy in a multidisciplinary program. The average age of the patients was 15 years; 25 were receiving puberty suppression hormones only, 93 were receiving just feminizing or masculinizing hormones, and 30 were receiving both treatments.
At baseline and at approximately 1 year follow-up, all patients completed the Body Image Scale, Quick Inventory of Depressive Symptoms, and Screen for Child Anxiety Related Emotional Disorders. In addition, clinicians collected information on patients’ suicidal ideation, suicide attempts, and nonsuicidal self-injury.
Overall, the average scores on the Body Image Scale on body dissatisfaction decreased from 70 to 52, and average scores on the Quick Inventory of Depressive Symptoms decreased from 9 to 7; both were statistically significant (P less than .001), as were changes from baseline on the anxiety subscale of the Screen for Child Anxiety Related Emotional Disorders, which decreased from 32 to 29 (P less than .01). No change occurred in the average overall clinician-reported depressive symptoms.
During the follow-up period, the rates of suicidal ideation, suicide attempts, and nonsuicidal self-injury were 38%, 5%, and 17%, respectively. Of patients who reported these experiences, the lifetime histories of suicidal ideation, suicide attempts, and nonsuicidal self-injury were 81%, 15%, and 52%, respectively.
The findings were limited by several factors including some missing data and the relatively small sample size, the researchers noted.
Nonetheless, the results suggest “that youth receiving gender-affirming hormone therapy experience meaningful short-term improvements in body dissatisfaction, and no participants discontinued feminizing or masculinizing hormone therapy.” These results support the use of such therapy, Dr. Kuper and associates wrote.
The study is important because of the need for evidence that hormones actually improve patient outcomes, said Shauna M. Lawlis, MD, of the University of Oklahoma Medical Center, Oklahoma City.
“Especially given the rash of legislation across the country aimed at blocking care for transgender youth, it is helpful to show that these treatments really do decrease patients’ anxiety and depressive symptoms,” she said in an interview. “In addition, previous research has been focused on those who have undergone puberty suppression followed by gender-affirming hormone therapy, but many patients are too far along in puberty for puberty suppression to be effective and providers often go straight to gender-affirming hormones in those cases.”
Dr. Lawlis said she was not at all surprised by the study findings. “In my own practice, I have seen patients improve greatly on gender-affirming hormones with overall improvement in anxiety and depression. As a patient’s outward appearance more closely matches their gender identity, they feel more comfortable in their own bodies and their interactions with the world around them, thus improving these symptoms.”
Dr. Lawlis added that the message for pediatricians who treat transgender youth is simple: Gender-affirming hormones improve patient outcomes. “They are essential for the mental health of this vulnerable population.”
She noted that long-term follow-up studies would be useful. “There is still a lot of concern about regret and detransitioning among health care providers and the general population – showing that patients maintain satisfaction in the long-term would be helpful.
“In addition, long-term studies about other health outcomes (cardiovascular disease, cancer risk, etc.) would also be helpful,” said Dr. Lawlis, who was asked to comment on this study, with which she had no involvement.
The study was supported in part by Children’s Health. The researchers had no financial conflicts to disclose. Dr. Lawlis had no relevant financial disclosures.
SOURCE: Kuper LE et al. Pediatrics. 2020 Mar 27. doi: 10.1542/peds.2019-3006.
based on data from 148 individuals.
“Understanding the impact of gender-affirming hormone therapy on the mental health of transgender youth is critical given the health disparities documented in this population,” wrote Laura E. Kuper, PhD, of Children’s Health Systems of Texas, Dallas, and colleagues.
In a study published in Pediatrics, the researchers reviewed data from 148 youth aged 9-18 years who underwent gender-affirming hormone therapy in a multidisciplinary program. The average age of the patients was 15 years; 25 were receiving puberty suppression hormones only, 93 were receiving just feminizing or masculinizing hormones, and 30 were receiving both treatments.
At baseline and at approximately 1 year follow-up, all patients completed the Body Image Scale, Quick Inventory of Depressive Symptoms, and Screen for Child Anxiety Related Emotional Disorders. In addition, clinicians collected information on patients’ suicidal ideation, suicide attempts, and nonsuicidal self-injury.
Overall, the average scores on the Body Image Scale on body dissatisfaction decreased from 70 to 52, and average scores on the Quick Inventory of Depressive Symptoms decreased from 9 to 7; both were statistically significant (P less than .001), as were changes from baseline on the anxiety subscale of the Screen for Child Anxiety Related Emotional Disorders, which decreased from 32 to 29 (P less than .01). No change occurred in the average overall clinician-reported depressive symptoms.
During the follow-up period, the rates of suicidal ideation, suicide attempts, and nonsuicidal self-injury were 38%, 5%, and 17%, respectively. Of patients who reported these experiences, the lifetime histories of suicidal ideation, suicide attempts, and nonsuicidal self-injury were 81%, 15%, and 52%, respectively.
The findings were limited by several factors including some missing data and the relatively small sample size, the researchers noted.
Nonetheless, the results suggest “that youth receiving gender-affirming hormone therapy experience meaningful short-term improvements in body dissatisfaction, and no participants discontinued feminizing or masculinizing hormone therapy.” These results support the use of such therapy, Dr. Kuper and associates wrote.
The study is important because of the need for evidence that hormones actually improve patient outcomes, said Shauna M. Lawlis, MD, of the University of Oklahoma Medical Center, Oklahoma City.
“Especially given the rash of legislation across the country aimed at blocking care for transgender youth, it is helpful to show that these treatments really do decrease patients’ anxiety and depressive symptoms,” she said in an interview. “In addition, previous research has been focused on those who have undergone puberty suppression followed by gender-affirming hormone therapy, but many patients are too far along in puberty for puberty suppression to be effective and providers often go straight to gender-affirming hormones in those cases.”
Dr. Lawlis said she was not at all surprised by the study findings. “In my own practice, I have seen patients improve greatly on gender-affirming hormones with overall improvement in anxiety and depression. As a patient’s outward appearance more closely matches their gender identity, they feel more comfortable in their own bodies and their interactions with the world around them, thus improving these symptoms.”
Dr. Lawlis added that the message for pediatricians who treat transgender youth is simple: Gender-affirming hormones improve patient outcomes. “They are essential for the mental health of this vulnerable population.”
She noted that long-term follow-up studies would be useful. “There is still a lot of concern about regret and detransitioning among health care providers and the general population – showing that patients maintain satisfaction in the long-term would be helpful.
“In addition, long-term studies about other health outcomes (cardiovascular disease, cancer risk, etc.) would also be helpful,” said Dr. Lawlis, who was asked to comment on this study, with which she had no involvement.
The study was supported in part by Children’s Health. The researchers had no financial conflicts to disclose. Dr. Lawlis had no relevant financial disclosures.
SOURCE: Kuper LE et al. Pediatrics. 2020 Mar 27. doi: 10.1542/peds.2019-3006.
based on data from 148 individuals.
“Understanding the impact of gender-affirming hormone therapy on the mental health of transgender youth is critical given the health disparities documented in this population,” wrote Laura E. Kuper, PhD, of Children’s Health Systems of Texas, Dallas, and colleagues.
In a study published in Pediatrics, the researchers reviewed data from 148 youth aged 9-18 years who underwent gender-affirming hormone therapy in a multidisciplinary program. The average age of the patients was 15 years; 25 were receiving puberty suppression hormones only, 93 were receiving just feminizing or masculinizing hormones, and 30 were receiving both treatments.
At baseline and at approximately 1 year follow-up, all patients completed the Body Image Scale, Quick Inventory of Depressive Symptoms, and Screen for Child Anxiety Related Emotional Disorders. In addition, clinicians collected information on patients’ suicidal ideation, suicide attempts, and nonsuicidal self-injury.
Overall, the average scores on the Body Image Scale on body dissatisfaction decreased from 70 to 52, and average scores on the Quick Inventory of Depressive Symptoms decreased from 9 to 7; both were statistically significant (P less than .001), as were changes from baseline on the anxiety subscale of the Screen for Child Anxiety Related Emotional Disorders, which decreased from 32 to 29 (P less than .01). No change occurred in the average overall clinician-reported depressive symptoms.
During the follow-up period, the rates of suicidal ideation, suicide attempts, and nonsuicidal self-injury were 38%, 5%, and 17%, respectively. Of patients who reported these experiences, the lifetime histories of suicidal ideation, suicide attempts, and nonsuicidal self-injury were 81%, 15%, and 52%, respectively.
The findings were limited by several factors including some missing data and the relatively small sample size, the researchers noted.
Nonetheless, the results suggest “that youth receiving gender-affirming hormone therapy experience meaningful short-term improvements in body dissatisfaction, and no participants discontinued feminizing or masculinizing hormone therapy.” These results support the use of such therapy, Dr. Kuper and associates wrote.
The study is important because of the need for evidence that hormones actually improve patient outcomes, said Shauna M. Lawlis, MD, of the University of Oklahoma Medical Center, Oklahoma City.
“Especially given the rash of legislation across the country aimed at blocking care for transgender youth, it is helpful to show that these treatments really do decrease patients’ anxiety and depressive symptoms,” she said in an interview. “In addition, previous research has been focused on those who have undergone puberty suppression followed by gender-affirming hormone therapy, but many patients are too far along in puberty for puberty suppression to be effective and providers often go straight to gender-affirming hormones in those cases.”
Dr. Lawlis said she was not at all surprised by the study findings. “In my own practice, I have seen patients improve greatly on gender-affirming hormones with overall improvement in anxiety and depression. As a patient’s outward appearance more closely matches their gender identity, they feel more comfortable in their own bodies and their interactions with the world around them, thus improving these symptoms.”
Dr. Lawlis added that the message for pediatricians who treat transgender youth is simple: Gender-affirming hormones improve patient outcomes. “They are essential for the mental health of this vulnerable population.”
She noted that long-term follow-up studies would be useful. “There is still a lot of concern about regret and detransitioning among health care providers and the general population – showing that patients maintain satisfaction in the long-term would be helpful.
“In addition, long-term studies about other health outcomes (cardiovascular disease, cancer risk, etc.) would also be helpful,” said Dr. Lawlis, who was asked to comment on this study, with which she had no involvement.
The study was supported in part by Children’s Health. The researchers had no financial conflicts to disclose. Dr. Lawlis had no relevant financial disclosures.
SOURCE: Kuper LE et al. Pediatrics. 2020 Mar 27. doi: 10.1542/peds.2019-3006.
FROM PEDIATRICS
HCV screening risk factors in pregnant women need updating
“Because risk-factor screening has obvious limitations, universal screening in pregnancy has been suggested to allow for linkage to postpartum care and identification of children for future testing and treatment,” wrote Mona Prasad, DO, of Ohio State University, Columbus, and colleagues.
In a study published in Obstetrics & Gynecology, the researchers reviewed data from women with singleton pregnancies presenting for prenatal care prior to 23 weeks’ gestation during 2012-2015. Of these, 254 tested positive for the hepatitis C virus (HCV) antibody, for a seroprevalence rate of 2.4 cases per 1,000 women.
The researchers conducted a case-control analysis of 131 women who tested positive and 251 controls to identify HCV infection risk factors based on interviews and chart reviews. They found that risk factors significantly associated with positive HCV antibodies included injection drug use (adjusted odds ratio, 22.9), a history of blood transfusion (aOR, 3.7), having an HCV-infected partner (aOR, 6.3), having had more than three sexual partners (aOR, 5.3), and smoking during pregnancy (aOR, 2.4).
In an unadjusted analysis, the researchers confirmed two of the risk factors currently recommended by the Centers for Disease Control and Prevention for screening for HCV: injection drug use and being born to a mother with HCV infection, but not dialysis, organ transplantation, or HIV infection.
“Our results demonstrate that current risk factors could be contemporized,” Dr. Prasad and colleagues noted. “The currently accepted risk factors such as exposure to clotting factors, dialysis, and organ transplants are unlikely to be found. A thorough assessment of injection drug use history, smoking, transfusions, number of sexual partners, and partners with HCV infection is more sensitive in an obstetric population.”
The study findings were limited by several factors including possible selection bias and inclusion of only 65% of eligible women who were HCV positive, as well as a lack of screening data from 2016 to the present, which may not reflect the impact of the recent opioid epidemic, the researchers noted. However, the results were strengthened by the large sample size, and the generalizability of the study population.
“Our results regarding prevalence rates and risk factors of HCV antibody among pregnant women in the United States will be valuable to policymakers as they weigh the costs and benefits of universal screening,” Dr. Prasad and associates concluded.
Although universal screening has the potential to be more cost effective, given the small population of pregnant women eligible for treatment and lack of an available treatment, “the rationale is weaker for unique universal HCV screening recommendations for pregnant women,” they said.
By contrast, Sammy Saab, MD, MPH, of the University of California, Los Angeles; Ravina Kullar, PharmD, MPH, of Gilead Sciences, Foster City, Calif.; and Prabhu Gounder, MD, MPH, of the Los Angeles Department of Public Health, wrote an accompanying commentary in favor of universal HCV screening for pregnant women, in part because of the increase in HCV in the younger population overall.
“For many women of reproductive age, pregnancy is one of their few points of contact with their health care provider; therefore, pregnancy could provide a crucial time for targeting this population,” they noted.
Risk-based screening is of limited effectiveness because patients are not identified by way of current screening tools or they decline to reveal risk factors that providers might miss, the editorialists said. Pregnancy has not been shown to affect the accuracy of HCV tests, and identifying infections in mothers allows for screening in children as well.
“The perinatal hepatitis B virus infection program, which has been implemented in several state and local public health departments, could serve as an example for how to conduct surveillance for mothers with HCV infection and to ensure that HCV-exposed children receive appropriate follow-up testing and linkage to care,” the editorialists concluded.
The study was supported in part by multiple grants from the National Institute of Child Health and Human Development. Dr. Prasad disclosed funding from Ohio State University and from Gilead. Coauthors had links with pharmaceutical companies, associations, and organizations – most unrelated to this study. The editorialists had no financial conflicts to disclose.
SOURCES: Prasad M et al. Obstet Gynecol. 2020;135:778-88; Saab S et al. Obstet Gynecol. 2020;135:773-7.
“Because risk-factor screening has obvious limitations, universal screening in pregnancy has been suggested to allow for linkage to postpartum care and identification of children for future testing and treatment,” wrote Mona Prasad, DO, of Ohio State University, Columbus, and colleagues.
In a study published in Obstetrics & Gynecology, the researchers reviewed data from women with singleton pregnancies presenting for prenatal care prior to 23 weeks’ gestation during 2012-2015. Of these, 254 tested positive for the hepatitis C virus (HCV) antibody, for a seroprevalence rate of 2.4 cases per 1,000 women.
The researchers conducted a case-control analysis of 131 women who tested positive and 251 controls to identify HCV infection risk factors based on interviews and chart reviews. They found that risk factors significantly associated with positive HCV antibodies included injection drug use (adjusted odds ratio, 22.9), a history of blood transfusion (aOR, 3.7), having an HCV-infected partner (aOR, 6.3), having had more than three sexual partners (aOR, 5.3), and smoking during pregnancy (aOR, 2.4).
In an unadjusted analysis, the researchers confirmed two of the risk factors currently recommended by the Centers for Disease Control and Prevention for screening for HCV: injection drug use and being born to a mother with HCV infection, but not dialysis, organ transplantation, or HIV infection.
“Our results demonstrate that current risk factors could be contemporized,” Dr. Prasad and colleagues noted. “The currently accepted risk factors such as exposure to clotting factors, dialysis, and organ transplants are unlikely to be found. A thorough assessment of injection drug use history, smoking, transfusions, number of sexual partners, and partners with HCV infection is more sensitive in an obstetric population.”
The study findings were limited by several factors including possible selection bias and inclusion of only 65% of eligible women who were HCV positive, as well as a lack of screening data from 2016 to the present, which may not reflect the impact of the recent opioid epidemic, the researchers noted. However, the results were strengthened by the large sample size, and the generalizability of the study population.
“Our results regarding prevalence rates and risk factors of HCV antibody among pregnant women in the United States will be valuable to policymakers as they weigh the costs and benefits of universal screening,” Dr. Prasad and associates concluded.
Although universal screening has the potential to be more cost effective, given the small population of pregnant women eligible for treatment and lack of an available treatment, “the rationale is weaker for unique universal HCV screening recommendations for pregnant women,” they said.
By contrast, Sammy Saab, MD, MPH, of the University of California, Los Angeles; Ravina Kullar, PharmD, MPH, of Gilead Sciences, Foster City, Calif.; and Prabhu Gounder, MD, MPH, of the Los Angeles Department of Public Health, wrote an accompanying commentary in favor of universal HCV screening for pregnant women, in part because of the increase in HCV in the younger population overall.
“For many women of reproductive age, pregnancy is one of their few points of contact with their health care provider; therefore, pregnancy could provide a crucial time for targeting this population,” they noted.
Risk-based screening is of limited effectiveness because patients are not identified by way of current screening tools or they decline to reveal risk factors that providers might miss, the editorialists said. Pregnancy has not been shown to affect the accuracy of HCV tests, and identifying infections in mothers allows for screening in children as well.
“The perinatal hepatitis B virus infection program, which has been implemented in several state and local public health departments, could serve as an example for how to conduct surveillance for mothers with HCV infection and to ensure that HCV-exposed children receive appropriate follow-up testing and linkage to care,” the editorialists concluded.
The study was supported in part by multiple grants from the National Institute of Child Health and Human Development. Dr. Prasad disclosed funding from Ohio State University and from Gilead. Coauthors had links with pharmaceutical companies, associations, and organizations – most unrelated to this study. The editorialists had no financial conflicts to disclose.
SOURCES: Prasad M et al. Obstet Gynecol. 2020;135:778-88; Saab S et al. Obstet Gynecol. 2020;135:773-7.
“Because risk-factor screening has obvious limitations, universal screening in pregnancy has been suggested to allow for linkage to postpartum care and identification of children for future testing and treatment,” wrote Mona Prasad, DO, of Ohio State University, Columbus, and colleagues.
In a study published in Obstetrics & Gynecology, the researchers reviewed data from women with singleton pregnancies presenting for prenatal care prior to 23 weeks’ gestation during 2012-2015. Of these, 254 tested positive for the hepatitis C virus (HCV) antibody, for a seroprevalence rate of 2.4 cases per 1,000 women.
The researchers conducted a case-control analysis of 131 women who tested positive and 251 controls to identify HCV infection risk factors based on interviews and chart reviews. They found that risk factors significantly associated with positive HCV antibodies included injection drug use (adjusted odds ratio, 22.9), a history of blood transfusion (aOR, 3.7), having an HCV-infected partner (aOR, 6.3), having had more than three sexual partners (aOR, 5.3), and smoking during pregnancy (aOR, 2.4).
In an unadjusted analysis, the researchers confirmed two of the risk factors currently recommended by the Centers for Disease Control and Prevention for screening for HCV: injection drug use and being born to a mother with HCV infection, but not dialysis, organ transplantation, or HIV infection.
“Our results demonstrate that current risk factors could be contemporized,” Dr. Prasad and colleagues noted. “The currently accepted risk factors such as exposure to clotting factors, dialysis, and organ transplants are unlikely to be found. A thorough assessment of injection drug use history, smoking, transfusions, number of sexual partners, and partners with HCV infection is more sensitive in an obstetric population.”
The study findings were limited by several factors including possible selection bias and inclusion of only 65% of eligible women who were HCV positive, as well as a lack of screening data from 2016 to the present, which may not reflect the impact of the recent opioid epidemic, the researchers noted. However, the results were strengthened by the large sample size, and the generalizability of the study population.
“Our results regarding prevalence rates and risk factors of HCV antibody among pregnant women in the United States will be valuable to policymakers as they weigh the costs and benefits of universal screening,” Dr. Prasad and associates concluded.
Although universal screening has the potential to be more cost effective, given the small population of pregnant women eligible for treatment and lack of an available treatment, “the rationale is weaker for unique universal HCV screening recommendations for pregnant women,” they said.
By contrast, Sammy Saab, MD, MPH, of the University of California, Los Angeles; Ravina Kullar, PharmD, MPH, of Gilead Sciences, Foster City, Calif.; and Prabhu Gounder, MD, MPH, of the Los Angeles Department of Public Health, wrote an accompanying commentary in favor of universal HCV screening for pregnant women, in part because of the increase in HCV in the younger population overall.
“For many women of reproductive age, pregnancy is one of their few points of contact with their health care provider; therefore, pregnancy could provide a crucial time for targeting this population,” they noted.
Risk-based screening is of limited effectiveness because patients are not identified by way of current screening tools or they decline to reveal risk factors that providers might miss, the editorialists said. Pregnancy has not been shown to affect the accuracy of HCV tests, and identifying infections in mothers allows for screening in children as well.
“The perinatal hepatitis B virus infection program, which has been implemented in several state and local public health departments, could serve as an example for how to conduct surveillance for mothers with HCV infection and to ensure that HCV-exposed children receive appropriate follow-up testing and linkage to care,” the editorialists concluded.
The study was supported in part by multiple grants from the National Institute of Child Health and Human Development. Dr. Prasad disclosed funding from Ohio State University and from Gilead. Coauthors had links with pharmaceutical companies, associations, and organizations – most unrelated to this study. The editorialists had no financial conflicts to disclose.
SOURCES: Prasad M et al. Obstet Gynecol. 2020;135:778-88; Saab S et al. Obstet Gynecol. 2020;135:773-7.
FROM OBSTETRICS & GYNECOLOGY