User login
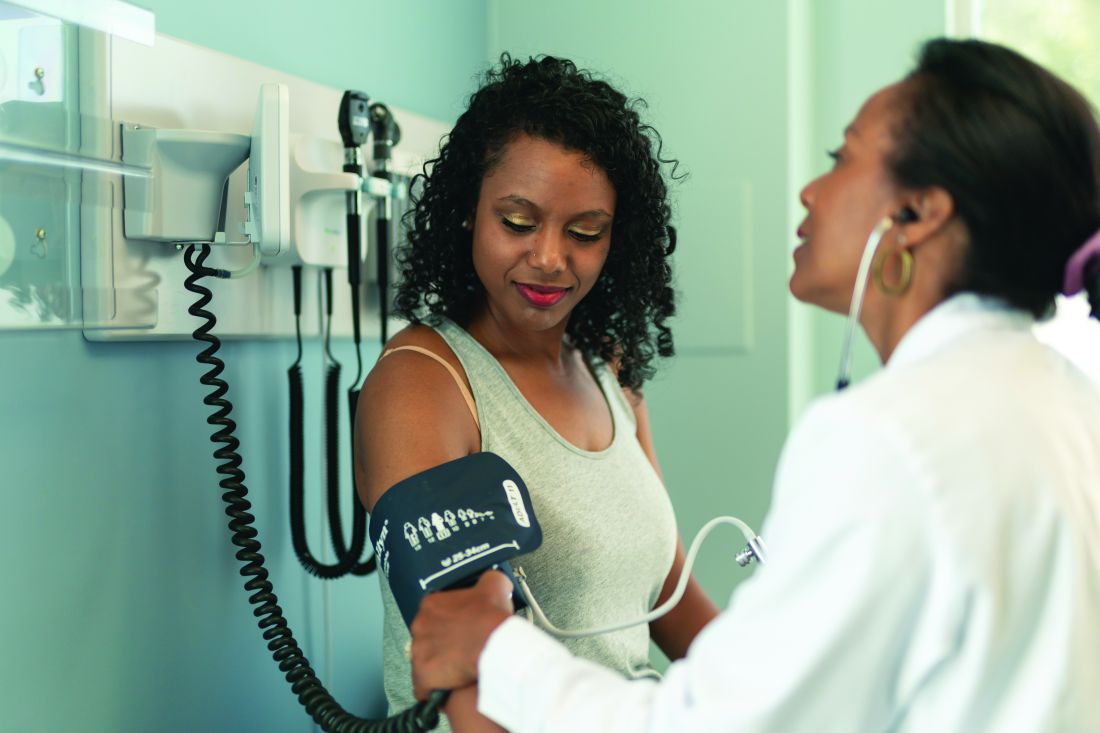
Treating COVID-19 in patients with diabetes
Patients with diabetes may be at extra risk for coronavirus disease (COVID-19) mortality, and doctors treating them need to keep up with the latest guidelines and expert advice.
Most health advisories about COVID-19 mention diabetes as one of the high-risk categories for the disease, likely because early data coming out of China, where the disease was first reported, indicated an elevated case-fatality rate for COVID-19 patients who also had diabetes.
In an article published in JAMA, Zunyou Wu, MD, and Jennifer M. McGoogan, PhD, summarized the findings from a February report on 44,672 confirmed cases of the disease from the Chinese Center for Disease Control and Prevention. The overall case-fatality rate (CFR) at that stage was 2.3% (1,023 deaths of the 44,672 confirmed cases). The data indicated that the CFR was elevated among COVID-19 patients with preexisting comorbid conditions, specifically, cardiovascular disease (CFR, 10.5%), diabetes (7.3%), chronic respiratory disease (6.3%), hypertension (6%), and cancer (5.6%).
The data also showed an aged-related trend in the CFR, with patients aged 80 years or older having a CFR of 14.8% and those aged 70-79 years, a rate of 8.0%, while there were no fatal cases reported in patients aged 9 years or younger (JAMA. 2020 Feb 24. doi: 10.1001/jama.2020.2648).
Those findings have been echoed by the U.S. Centers of Disease Control and Prevention. The American Diabetes Association and the American Association of Clinical Endocrinologists have in turn referenced the CDC in their COVID-19 guidance recommendations for patients with diabetes.
Guidelines were already in place for treatment of infections in patients with diabetes, and
In general, patients with diabetes – especially those whose disease is not controlled, or not well controlled – can be more susceptible to more common infections, such as influenza and pneumonia, possibly because hyperglycemia can subdue immunity by disrupting function of the white blood cells.
Glucose control is key
An important factor in any form of infection control in patients with diabetes seems to be whether or not a patient’s glucose levels are well controlled, according to comments from members of the editorial advisory board for Clinical Endocrinology News. Good glucose control, therefore, could be instrumental in reducing both the risk for and severity of infection.
Paul Jellinger, MD, of the Center for Diabetes & Endocrine Care, Hollywood, Fla., said that, over the years, he had not observed higher infection rates in general in patients with hemoglobin A1c levels below 7, or even higher. However, “a bigger question for me, given the broad category of ‘diabetes’ listed as a risk for serious coronavirus complications by the CDC, has been: Just which individuals with diabetes are really at risk? Are patients with well-controlled diabetes at increased risk as much as those with significant hyperglycemia and uncontrolled diabetes? In my view, not likely.”
Alan Jay Cohen, MD, agreed with Dr. Jellinger. “Many patients have called the office in the last 10 days to ask if there are special precautions they should take because they are reading that they are in the high-risk group because they have diabetes. Many of them are in superb, or at least pretty good, control. I have not seen where they have had a higher incidence of infection than the general population, and I have not seen data with COVID-19 that specifically demonstrates that a person with diabetes in good control has an increased risk,” he said.
“My recommendations to these patients have been the same as those given to the general population,” added Dr. Cohen, medical director at Baptist Medical Group: The Endocrine Clinic, Memphis.
Herbert I. Rettinger, MD, also conceded that poorly controlled blood sugars and confounding illnesses, such as renal and cardiac conditions, are common in patients with long-standing diabetes, but “there is a huge population of patients with type 1 diabetes, and very few seem to be more susceptible to infection. Perhaps I am missing those with poor diet and glucose control.”
Philip Levy, MD, picked up on that latter point, emphasizing that “endocrinologists take care of fewer patients with diabetes than do primary care physicians. Most patients with type 2 diabetes are not seen by us unless the PCP has problems [treating them],” so it could be that PCPs may see a higher number of patients who are at a greater risk for infections.
Ultimately, “good glucose control is very helpful in avoiding infections,” said Dr. Levy, of the Banner University Medical Group Endocrinology & Diabetes, Phoenix.
For sick patients
Guidelines for patients at the Joslin Diabetes Center in Boston advise patients who are feeling sick to continue taking their diabetes medications, unless instructed otherwise by their providers, and to monitor their glucose more frequently because it can spike suddenly.
Patients with type 1 diabetes should check for ketones if their glucose passes 250 mg/dL, according to the guidelines, and patients should remain hydrated at all times and get plenty of rest.
“Sick-day guidelines definitely apply, but patients should be advised to get tested if they have any symptoms they are concerned about,” said Dr. Rettinger, of the Endocrinology Medical Group of Orange County, Orange, Calif.
If patients with diabetes develop COVID-19, then home management may still be possible, according to Ritesh Gupta, MD, of Fortis C-DOC Hospital, New Delhi, and colleagues (Diabetes Metab Syndr. 2020 Mar 10;14[3]:211-2. doi: 10.1016/j.dsx.2020.03.002).
Dr. Rettinger agreed, noting that home management would be feasible as long as “everything is going well, that is, the patient is not experiencing respiratory problems or difficulties in controlling glucose levels. Consider patients with type 1 diabetes who have COVID-19 as you would a nursing home patient – ever vigilant.”
Dr. Gupta and coauthors also recommended basic treatment measures such as maintaining hydration and managing symptoms with acetaminophen and steam inhalation, and home isolation for 14 days or until the symptoms resolve. However, the ADA warns in its guidelines that patients should “be aware that some constant glucose monitoring sensors (Dexcom G5, Medtronic Enlite, and Guardian) are impacted by acetaminophen (Tylenol), and that patients should check with finger sticks to ensure accuracy [if they are taking acetaminophen].”
In the event of hyperglycemia with fever in patients with type 1 diabetes, blood glucose and urinary ketones should be monitored often, the authors wrote, cautioning that “frequent changes in dosage and correctional bolus may be required to maintain normoglycemia.” Dr Rettinger emphasized that “hyperglycemia, as always, is best treated with fluids and insulin and frequent checks of sugars to be sure the treatment regimen is successful.”
In regard to diabetic drug regimens, patients with type 1 or 2 disease should continue on their current medications, advised Yehuda Handelsman, MD. “Some, especially those on insulin, may require more of it. And the patient should increase fluid intake to prevent fluid depletion. We do not reduce antihyperglycemic medication to preserve fluids.
“As for hypoglycemia, we always aim for less to no hypoglycemia,” he continued. “Monitoring glucose and appropriate dosage is the way to go. In other words, do not reduce medications in sick patients who typically need more medication.”
Dr. Handelsman, medical director and principal investigator at Metabolic Institute of America, Tarzana, Calif., added that very sick patients who are hospitalized should be managed with insulin and that oral agents – particularly metformin and sodium-glucose transporter 2 inhibitors – should be stopped.
“Once the patient has recovered and stabilized, you can return to the prior regimen, and, even if the patient is still in hospital, noninsulin therapy can be reintroduced,” he said.
“This is standard procedure in very sick patients, especially those in critical care. Metformin may raise lactic acid levels, and the SGLT2 inhibitors cause volume contraction, fat metabolism, and acidosis,” he explained. “We also stop the glucagon-like peptide receptor–1 analogues, which can cause nausea and vomiting, and pioglitazone because it causes fluid overload.
“Only insulin can be used for acutely sick patients – those with sepsis, for example. The same would apply if they have severe breathing disorders, and definitely, if they are on a ventilator. This is also the time we stop aromatase inhibitor orals and we use insulin.”
Preventive measures
In the interest of maintaining good glucose control, patients also should monitor their glucose levels more frequently so that fluctuations can be detected early and quickly addressed with the appropriate medication adjustments, according to guidelines from the ADA and AACE. They should continue to follow a healthy diet that includes adequate protein and they should exercise regularly.
Patients should ensure that they have enough medication and testing supplies – for at least 14 days, and longer, if costs permit – in case they have to go into quarantine.
General preventive measures, such as frequent hand washing with soap and water, practicing good respiratory hygiene by sneezing or coughing into a facial tissue or bent elbow, also apply for reducing the risk of infection. Touching of the face should be avoided, as should nonessential travel and contact with infected individuals.
Patients with diabetes should always be current with their influenza and pneumonia shots.
Dr. Rettinger said that he always recommends the following preventative measures to his patients and he is using the current health crisis to reinforce them:
- Eat lots of multicolored fruits and vegetables.
- Eat yogurt and take probiotics to keep the intestinal biome strong and functional.
- Be extra vigilant regarding sugars and sugar control to avoid peaks and valleys wherever possible.
- Keep the immune system strong with at least 7-8 hours sleep and reduce stress levels whenever possible.
- Avoid crowds and handshaking.
- Wash hands regularly.
Possible therapies
There are currently no drugs that have been approved specifically for the treatment of COVID-19, although a vaccine against the disease is currently under development.
Dr. Gupta and his colleagues noted in their article that there have been reports of the anecdotal use of antiviral drugs such as lopinavir, ritonavir, interferon-beta, the RNA polymerase inhibitor remdesivir, and chloroquine.
However, Dr. Handelsman said that, as far as he knows, none of these drugs has been shown to be beneficial for COVID-19. “Some [providers] have tried Tamiflu, but with no clear outcomes, and for severely sick patients, they tried medications for anti-HIV, hepatitis C, and malaria, but so far, there has been no breakthrough.”
Dr. Cohen, Dr. Handelsman, Dr. Jellinger, Dr. Levy, and Dr. Rettinger are members of the editorial advisory board of Clinical Endocrinology News. Dr. Gupta and Dr. Wu, and their colleagues, reported no conflicts of interest.
Patients with diabetes may be at extra risk for coronavirus disease (COVID-19) mortality, and doctors treating them need to keep up with the latest guidelines and expert advice.
Most health advisories about COVID-19 mention diabetes as one of the high-risk categories for the disease, likely because early data coming out of China, where the disease was first reported, indicated an elevated case-fatality rate for COVID-19 patients who also had diabetes.
In an article published in JAMA, Zunyou Wu, MD, and Jennifer M. McGoogan, PhD, summarized the findings from a February report on 44,672 confirmed cases of the disease from the Chinese Center for Disease Control and Prevention. The overall case-fatality rate (CFR) at that stage was 2.3% (1,023 deaths of the 44,672 confirmed cases). The data indicated that the CFR was elevated among COVID-19 patients with preexisting comorbid conditions, specifically, cardiovascular disease (CFR, 10.5%), diabetes (7.3%), chronic respiratory disease (6.3%), hypertension (6%), and cancer (5.6%).
The data also showed an aged-related trend in the CFR, with patients aged 80 years or older having a CFR of 14.8% and those aged 70-79 years, a rate of 8.0%, while there were no fatal cases reported in patients aged 9 years or younger (JAMA. 2020 Feb 24. doi: 10.1001/jama.2020.2648).
Those findings have been echoed by the U.S. Centers of Disease Control and Prevention. The American Diabetes Association and the American Association of Clinical Endocrinologists have in turn referenced the CDC in their COVID-19 guidance recommendations for patients with diabetes.
Guidelines were already in place for treatment of infections in patients with diabetes, and
In general, patients with diabetes – especially those whose disease is not controlled, or not well controlled – can be more susceptible to more common infections, such as influenza and pneumonia, possibly because hyperglycemia can subdue immunity by disrupting function of the white blood cells.
Glucose control is key
An important factor in any form of infection control in patients with diabetes seems to be whether or not a patient’s glucose levels are well controlled, according to comments from members of the editorial advisory board for Clinical Endocrinology News. Good glucose control, therefore, could be instrumental in reducing both the risk for and severity of infection.
Paul Jellinger, MD, of the Center for Diabetes & Endocrine Care, Hollywood, Fla., said that, over the years, he had not observed higher infection rates in general in patients with hemoglobin A1c levels below 7, or even higher. However, “a bigger question for me, given the broad category of ‘diabetes’ listed as a risk for serious coronavirus complications by the CDC, has been: Just which individuals with diabetes are really at risk? Are patients with well-controlled diabetes at increased risk as much as those with significant hyperglycemia and uncontrolled diabetes? In my view, not likely.”
Alan Jay Cohen, MD, agreed with Dr. Jellinger. “Many patients have called the office in the last 10 days to ask if there are special precautions they should take because they are reading that they are in the high-risk group because they have diabetes. Many of them are in superb, or at least pretty good, control. I have not seen where they have had a higher incidence of infection than the general population, and I have not seen data with COVID-19 that specifically demonstrates that a person with diabetes in good control has an increased risk,” he said.
“My recommendations to these patients have been the same as those given to the general population,” added Dr. Cohen, medical director at Baptist Medical Group: The Endocrine Clinic, Memphis.
Herbert I. Rettinger, MD, also conceded that poorly controlled blood sugars and confounding illnesses, such as renal and cardiac conditions, are common in patients with long-standing diabetes, but “there is a huge population of patients with type 1 diabetes, and very few seem to be more susceptible to infection. Perhaps I am missing those with poor diet and glucose control.”
Philip Levy, MD, picked up on that latter point, emphasizing that “endocrinologists take care of fewer patients with diabetes than do primary care physicians. Most patients with type 2 diabetes are not seen by us unless the PCP has problems [treating them],” so it could be that PCPs may see a higher number of patients who are at a greater risk for infections.
Ultimately, “good glucose control is very helpful in avoiding infections,” said Dr. Levy, of the Banner University Medical Group Endocrinology & Diabetes, Phoenix.
For sick patients
Guidelines for patients at the Joslin Diabetes Center in Boston advise patients who are feeling sick to continue taking their diabetes medications, unless instructed otherwise by their providers, and to monitor their glucose more frequently because it can spike suddenly.
Patients with type 1 diabetes should check for ketones if their glucose passes 250 mg/dL, according to the guidelines, and patients should remain hydrated at all times and get plenty of rest.
“Sick-day guidelines definitely apply, but patients should be advised to get tested if they have any symptoms they are concerned about,” said Dr. Rettinger, of the Endocrinology Medical Group of Orange County, Orange, Calif.
If patients with diabetes develop COVID-19, then home management may still be possible, according to Ritesh Gupta, MD, of Fortis C-DOC Hospital, New Delhi, and colleagues (Diabetes Metab Syndr. 2020 Mar 10;14[3]:211-2. doi: 10.1016/j.dsx.2020.03.002).
Dr. Rettinger agreed, noting that home management would be feasible as long as “everything is going well, that is, the patient is not experiencing respiratory problems or difficulties in controlling glucose levels. Consider patients with type 1 diabetes who have COVID-19 as you would a nursing home patient – ever vigilant.”
Dr. Gupta and coauthors also recommended basic treatment measures such as maintaining hydration and managing symptoms with acetaminophen and steam inhalation, and home isolation for 14 days or until the symptoms resolve. However, the ADA warns in its guidelines that patients should “be aware that some constant glucose monitoring sensors (Dexcom G5, Medtronic Enlite, and Guardian) are impacted by acetaminophen (Tylenol), and that patients should check with finger sticks to ensure accuracy [if they are taking acetaminophen].”
In the event of hyperglycemia with fever in patients with type 1 diabetes, blood glucose and urinary ketones should be monitored often, the authors wrote, cautioning that “frequent changes in dosage and correctional bolus may be required to maintain normoglycemia.” Dr Rettinger emphasized that “hyperglycemia, as always, is best treated with fluids and insulin and frequent checks of sugars to be sure the treatment regimen is successful.”
In regard to diabetic drug regimens, patients with type 1 or 2 disease should continue on their current medications, advised Yehuda Handelsman, MD. “Some, especially those on insulin, may require more of it. And the patient should increase fluid intake to prevent fluid depletion. We do not reduce antihyperglycemic medication to preserve fluids.
“As for hypoglycemia, we always aim for less to no hypoglycemia,” he continued. “Monitoring glucose and appropriate dosage is the way to go. In other words, do not reduce medications in sick patients who typically need more medication.”
Dr. Handelsman, medical director and principal investigator at Metabolic Institute of America, Tarzana, Calif., added that very sick patients who are hospitalized should be managed with insulin and that oral agents – particularly metformin and sodium-glucose transporter 2 inhibitors – should be stopped.
“Once the patient has recovered and stabilized, you can return to the prior regimen, and, even if the patient is still in hospital, noninsulin therapy can be reintroduced,” he said.
“This is standard procedure in very sick patients, especially those in critical care. Metformin may raise lactic acid levels, and the SGLT2 inhibitors cause volume contraction, fat metabolism, and acidosis,” he explained. “We also stop the glucagon-like peptide receptor–1 analogues, which can cause nausea and vomiting, and pioglitazone because it causes fluid overload.
“Only insulin can be used for acutely sick patients – those with sepsis, for example. The same would apply if they have severe breathing disorders, and definitely, if they are on a ventilator. This is also the time we stop aromatase inhibitor orals and we use insulin.”
Preventive measures
In the interest of maintaining good glucose control, patients also should monitor their glucose levels more frequently so that fluctuations can be detected early and quickly addressed with the appropriate medication adjustments, according to guidelines from the ADA and AACE. They should continue to follow a healthy diet that includes adequate protein and they should exercise regularly.
Patients should ensure that they have enough medication and testing supplies – for at least 14 days, and longer, if costs permit – in case they have to go into quarantine.
General preventive measures, such as frequent hand washing with soap and water, practicing good respiratory hygiene by sneezing or coughing into a facial tissue or bent elbow, also apply for reducing the risk of infection. Touching of the face should be avoided, as should nonessential travel and contact with infected individuals.
Patients with diabetes should always be current with their influenza and pneumonia shots.
Dr. Rettinger said that he always recommends the following preventative measures to his patients and he is using the current health crisis to reinforce them:
- Eat lots of multicolored fruits and vegetables.
- Eat yogurt and take probiotics to keep the intestinal biome strong and functional.
- Be extra vigilant regarding sugars and sugar control to avoid peaks and valleys wherever possible.
- Keep the immune system strong with at least 7-8 hours sleep and reduce stress levels whenever possible.
- Avoid crowds and handshaking.
- Wash hands regularly.
Possible therapies
There are currently no drugs that have been approved specifically for the treatment of COVID-19, although a vaccine against the disease is currently under development.
Dr. Gupta and his colleagues noted in their article that there have been reports of the anecdotal use of antiviral drugs such as lopinavir, ritonavir, interferon-beta, the RNA polymerase inhibitor remdesivir, and chloroquine.
However, Dr. Handelsman said that, as far as he knows, none of these drugs has been shown to be beneficial for COVID-19. “Some [providers] have tried Tamiflu, but with no clear outcomes, and for severely sick patients, they tried medications for anti-HIV, hepatitis C, and malaria, but so far, there has been no breakthrough.”
Dr. Cohen, Dr. Handelsman, Dr. Jellinger, Dr. Levy, and Dr. Rettinger are members of the editorial advisory board of Clinical Endocrinology News. Dr. Gupta and Dr. Wu, and their colleagues, reported no conflicts of interest.
Patients with diabetes may be at extra risk for coronavirus disease (COVID-19) mortality, and doctors treating them need to keep up with the latest guidelines and expert advice.
Most health advisories about COVID-19 mention diabetes as one of the high-risk categories for the disease, likely because early data coming out of China, where the disease was first reported, indicated an elevated case-fatality rate for COVID-19 patients who also had diabetes.
In an article published in JAMA, Zunyou Wu, MD, and Jennifer M. McGoogan, PhD, summarized the findings from a February report on 44,672 confirmed cases of the disease from the Chinese Center for Disease Control and Prevention. The overall case-fatality rate (CFR) at that stage was 2.3% (1,023 deaths of the 44,672 confirmed cases). The data indicated that the CFR was elevated among COVID-19 patients with preexisting comorbid conditions, specifically, cardiovascular disease (CFR, 10.5%), diabetes (7.3%), chronic respiratory disease (6.3%), hypertension (6%), and cancer (5.6%).
The data also showed an aged-related trend in the CFR, with patients aged 80 years or older having a CFR of 14.8% and those aged 70-79 years, a rate of 8.0%, while there were no fatal cases reported in patients aged 9 years or younger (JAMA. 2020 Feb 24. doi: 10.1001/jama.2020.2648).
Those findings have been echoed by the U.S. Centers of Disease Control and Prevention. The American Diabetes Association and the American Association of Clinical Endocrinologists have in turn referenced the CDC in their COVID-19 guidance recommendations for patients with diabetes.
Guidelines were already in place for treatment of infections in patients with diabetes, and
In general, patients with diabetes – especially those whose disease is not controlled, or not well controlled – can be more susceptible to more common infections, such as influenza and pneumonia, possibly because hyperglycemia can subdue immunity by disrupting function of the white blood cells.
Glucose control is key
An important factor in any form of infection control in patients with diabetes seems to be whether or not a patient’s glucose levels are well controlled, according to comments from members of the editorial advisory board for Clinical Endocrinology News. Good glucose control, therefore, could be instrumental in reducing both the risk for and severity of infection.
Paul Jellinger, MD, of the Center for Diabetes & Endocrine Care, Hollywood, Fla., said that, over the years, he had not observed higher infection rates in general in patients with hemoglobin A1c levels below 7, or even higher. However, “a bigger question for me, given the broad category of ‘diabetes’ listed as a risk for serious coronavirus complications by the CDC, has been: Just which individuals with diabetes are really at risk? Are patients with well-controlled diabetes at increased risk as much as those with significant hyperglycemia and uncontrolled diabetes? In my view, not likely.”
Alan Jay Cohen, MD, agreed with Dr. Jellinger. “Many patients have called the office in the last 10 days to ask if there are special precautions they should take because they are reading that they are in the high-risk group because they have diabetes. Many of them are in superb, or at least pretty good, control. I have not seen where they have had a higher incidence of infection than the general population, and I have not seen data with COVID-19 that specifically demonstrates that a person with diabetes in good control has an increased risk,” he said.
“My recommendations to these patients have been the same as those given to the general population,” added Dr. Cohen, medical director at Baptist Medical Group: The Endocrine Clinic, Memphis.
Herbert I. Rettinger, MD, also conceded that poorly controlled blood sugars and confounding illnesses, such as renal and cardiac conditions, are common in patients with long-standing diabetes, but “there is a huge population of patients with type 1 diabetes, and very few seem to be more susceptible to infection. Perhaps I am missing those with poor diet and glucose control.”
Philip Levy, MD, picked up on that latter point, emphasizing that “endocrinologists take care of fewer patients with diabetes than do primary care physicians. Most patients with type 2 diabetes are not seen by us unless the PCP has problems [treating them],” so it could be that PCPs may see a higher number of patients who are at a greater risk for infections.
Ultimately, “good glucose control is very helpful in avoiding infections,” said Dr. Levy, of the Banner University Medical Group Endocrinology & Diabetes, Phoenix.
For sick patients
Guidelines for patients at the Joslin Diabetes Center in Boston advise patients who are feeling sick to continue taking their diabetes medications, unless instructed otherwise by their providers, and to monitor their glucose more frequently because it can spike suddenly.
Patients with type 1 diabetes should check for ketones if their glucose passes 250 mg/dL, according to the guidelines, and patients should remain hydrated at all times and get plenty of rest.
“Sick-day guidelines definitely apply, but patients should be advised to get tested if they have any symptoms they are concerned about,” said Dr. Rettinger, of the Endocrinology Medical Group of Orange County, Orange, Calif.
If patients with diabetes develop COVID-19, then home management may still be possible, according to Ritesh Gupta, MD, of Fortis C-DOC Hospital, New Delhi, and colleagues (Diabetes Metab Syndr. 2020 Mar 10;14[3]:211-2. doi: 10.1016/j.dsx.2020.03.002).
Dr. Rettinger agreed, noting that home management would be feasible as long as “everything is going well, that is, the patient is not experiencing respiratory problems or difficulties in controlling glucose levels. Consider patients with type 1 diabetes who have COVID-19 as you would a nursing home patient – ever vigilant.”
Dr. Gupta and coauthors also recommended basic treatment measures such as maintaining hydration and managing symptoms with acetaminophen and steam inhalation, and home isolation for 14 days or until the symptoms resolve. However, the ADA warns in its guidelines that patients should “be aware that some constant glucose monitoring sensors (Dexcom G5, Medtronic Enlite, and Guardian) are impacted by acetaminophen (Tylenol), and that patients should check with finger sticks to ensure accuracy [if they are taking acetaminophen].”
In the event of hyperglycemia with fever in patients with type 1 diabetes, blood glucose and urinary ketones should be monitored often, the authors wrote, cautioning that “frequent changes in dosage and correctional bolus may be required to maintain normoglycemia.” Dr Rettinger emphasized that “hyperglycemia, as always, is best treated with fluids and insulin and frequent checks of sugars to be sure the treatment regimen is successful.”
In regard to diabetic drug regimens, patients with type 1 or 2 disease should continue on their current medications, advised Yehuda Handelsman, MD. “Some, especially those on insulin, may require more of it. And the patient should increase fluid intake to prevent fluid depletion. We do not reduce antihyperglycemic medication to preserve fluids.
“As for hypoglycemia, we always aim for less to no hypoglycemia,” he continued. “Monitoring glucose and appropriate dosage is the way to go. In other words, do not reduce medications in sick patients who typically need more medication.”
Dr. Handelsman, medical director and principal investigator at Metabolic Institute of America, Tarzana, Calif., added that very sick patients who are hospitalized should be managed with insulin and that oral agents – particularly metformin and sodium-glucose transporter 2 inhibitors – should be stopped.
“Once the patient has recovered and stabilized, you can return to the prior regimen, and, even if the patient is still in hospital, noninsulin therapy can be reintroduced,” he said.
“This is standard procedure in very sick patients, especially those in critical care. Metformin may raise lactic acid levels, and the SGLT2 inhibitors cause volume contraction, fat metabolism, and acidosis,” he explained. “We also stop the glucagon-like peptide receptor–1 analogues, which can cause nausea and vomiting, and pioglitazone because it causes fluid overload.
“Only insulin can be used for acutely sick patients – those with sepsis, for example. The same would apply if they have severe breathing disorders, and definitely, if they are on a ventilator. This is also the time we stop aromatase inhibitor orals and we use insulin.”
Preventive measures
In the interest of maintaining good glucose control, patients also should monitor their glucose levels more frequently so that fluctuations can be detected early and quickly addressed with the appropriate medication adjustments, according to guidelines from the ADA and AACE. They should continue to follow a healthy diet that includes adequate protein and they should exercise regularly.
Patients should ensure that they have enough medication and testing supplies – for at least 14 days, and longer, if costs permit – in case they have to go into quarantine.
General preventive measures, such as frequent hand washing with soap and water, practicing good respiratory hygiene by sneezing or coughing into a facial tissue or bent elbow, also apply for reducing the risk of infection. Touching of the face should be avoided, as should nonessential travel and contact with infected individuals.
Patients with diabetes should always be current with their influenza and pneumonia shots.
Dr. Rettinger said that he always recommends the following preventative measures to his patients and he is using the current health crisis to reinforce them:
- Eat lots of multicolored fruits and vegetables.
- Eat yogurt and take probiotics to keep the intestinal biome strong and functional.
- Be extra vigilant regarding sugars and sugar control to avoid peaks and valleys wherever possible.
- Keep the immune system strong with at least 7-8 hours sleep and reduce stress levels whenever possible.
- Avoid crowds and handshaking.
- Wash hands regularly.
Possible therapies
There are currently no drugs that have been approved specifically for the treatment of COVID-19, although a vaccine against the disease is currently under development.
Dr. Gupta and his colleagues noted in their article that there have been reports of the anecdotal use of antiviral drugs such as lopinavir, ritonavir, interferon-beta, the RNA polymerase inhibitor remdesivir, and chloroquine.
However, Dr. Handelsman said that, as far as he knows, none of these drugs has been shown to be beneficial for COVID-19. “Some [providers] have tried Tamiflu, but with no clear outcomes, and for severely sick patients, they tried medications for anti-HIV, hepatitis C, and malaria, but so far, there has been no breakthrough.”
Dr. Cohen, Dr. Handelsman, Dr. Jellinger, Dr. Levy, and Dr. Rettinger are members of the editorial advisory board of Clinical Endocrinology News. Dr. Gupta and Dr. Wu, and their colleagues, reported no conflicts of interest.
Dupilumab approval sought for AD under age 12
LAHAINA, HAWAII – Reassuring evidence of the long-term effectiveness and safety of dupilumab in adolescents with moderate to severe atopic dermatitis comes from a phase 3 open-label extension study of the first teenagers in the world to have received the monoclonal antibody, Lawrence F. Eichenfield, MD, reported at the SDEF Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
Dupilumab (Dupixent), a monoclonal antibody directed against interleukins-4 and -13 initially approved in adults, received an expanded indication from the Food and Drug Administration in March 2019 for treatment of 12- to 17-year-olds with moderate to severe atopic dermatitis (AD) on the strength of a pivotal 251-patient, phase 3 randomized trial of 16 weeks’ duration (JAMA Dermatol. 2019 Nov 6. doi: 10.1001/jamadermatol.2019.3336). But since AD is a chronic disease, it was important to learn how dupilumab performs well beyond the 16-week mark in adolescents, observed Dr. Eichenfield, professor of dermatology and pediatrics at the University of California, San Diego, and chief of pediatric and adolescent dermatology at Rady Children’s Hospital.
In addition to highlighting some of the emerging fine points of dupilumab therapy in adolescents, Dr. Eichenfield discussed the clinical implications of a potential further expanded indication for treatment of 6- to 12-year-olds, an event he considers likely in the coming months. He also described early data from an ongoing dupilumab clinical trials program in the 2- to 5-year-olds.
Long-term dupilumab in teens
Dr. Eichenfield was a coauthor of the recently published phase 3 international long-term extension study. The 40 participants experienced a mean 85% decrease from baseline at 52 weeks in EASI (Eczema Area and Severity Index) scores on 2 mg/kg per week dosing and an 84% reduction on 4 mg/kg per week dosing. This represented a substantial further improvement from week 2, when the EASI reductions were 34% and 51%, respectively.
The mean trough serum dupilumab concentrations over the course of the year were markedly lower in the 2 mg/kg group: 74 mg/L, as compared to 161 mg/L with dosing at 4 mg/kg per week (Br J Dermatol. 2020 Jan;182[1]:85-96).
“It’ll be interesting to see how this works out over time,” the dermatologist commented. “The issue of dose by weight becomes important as we start to treat younger patients because the pharmacokinetics are very different at 4 and 2 mg/kg, and it may have an impact on efficacy.”
The extension study also established the safety and effectiveness of utilizing dupilumab in combination with standard topical corticosteroid therapy, which wasn’t allowed in the pivotal 16-week trial.
Some have commented that dupilumab may be less effective in adolescents than in adults. They point to the 24% rate of an Investigator Global Assessment (IGA) of 0 or 1 – that is, clear or almost clear – at week 16 in the pivotal adolescent trial, a substantially lower rate than in the adult trials. However, Dr. Eichenfield noted that the adolescent study population was heavily skewed to the severe end of the disease spectrum, the placebo response rate was very low, and the absolute placebo-subtracted benefit turned out to be quite similar to what was seen in the adult trials. Moreover, he added, in a post hoc analysis of the pivotal trial data which utilized a different measure of clinically meaningful response – a composite of either a 50% reduction in EASI score, a 3-point or greater improvement on a 10-point pruritus scale, or at least a 6-point improvement from baseline on the Children’s Dermatology Quality Life Index – that outcome was achieved by 74% of adolescents who didn’t achieve clear or almost clear.
What’s next for dupilumab in pediatric AD
Approval of dupilumab in children under aged 12 years is eagerly awaited, Dr. Eichenfield said. The Food and Drug Administration is now analyzing as-yet unreleased data from completed clinical trials of dupilumab in 6- to 12-year-olds with moderate to severe AD with an eye toward a possible further expanded indication. The side effect profile appears to be the same as in 12- to 18-year-olds.
“I assume it will be approved,” Dr. Eichenfield said. “We don’t know what’s going to happen in 6- to 12-year-olds in terms of the ultimate dosing recommendations that will be put out, but be aware that the pharmacokinetics vary by weight over time.”
Early data in children aged 2-5 years with severe AD from the phase 2, open-label, single ascending dose Liberty AD PRESCHOOL study showed that weight-based dosing in that age group made a big difference in terms of pharmacokinetics. In terms of efficacy, the mean reduction in EASI scores 4 weeks after a single dose of dupilumab was 27% with 3 mg/kg and 49% with 6 mg/kg.
Avoidance of live vaccines while on dupilumab becomes more of a consideration in the under-12 population. The second dose of varicella is supposed to be administered at 4 to 6 years of age, as is the second dose of MMR. The nasal influenza vaccine is a live virus vaccine, as is the yellow fever vaccine.
“We don’t know if live vaccines are dangerous for someone on dupilumab, it’s just that it’s listed that you shouldn’t use them and they haven’t been studied,” Dr. Eichenfield observed.
He reported receiving research grants from or serving as a consultant to several dozen pharmaceutical companies.
The SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
LAHAINA, HAWAII – Reassuring evidence of the long-term effectiveness and safety of dupilumab in adolescents with moderate to severe atopic dermatitis comes from a phase 3 open-label extension study of the first teenagers in the world to have received the monoclonal antibody, Lawrence F. Eichenfield, MD, reported at the SDEF Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
Dupilumab (Dupixent), a monoclonal antibody directed against interleukins-4 and -13 initially approved in adults, received an expanded indication from the Food and Drug Administration in March 2019 for treatment of 12- to 17-year-olds with moderate to severe atopic dermatitis (AD) on the strength of a pivotal 251-patient, phase 3 randomized trial of 16 weeks’ duration (JAMA Dermatol. 2019 Nov 6. doi: 10.1001/jamadermatol.2019.3336). But since AD is a chronic disease, it was important to learn how dupilumab performs well beyond the 16-week mark in adolescents, observed Dr. Eichenfield, professor of dermatology and pediatrics at the University of California, San Diego, and chief of pediatric and adolescent dermatology at Rady Children’s Hospital.
In addition to highlighting some of the emerging fine points of dupilumab therapy in adolescents, Dr. Eichenfield discussed the clinical implications of a potential further expanded indication for treatment of 6- to 12-year-olds, an event he considers likely in the coming months. He also described early data from an ongoing dupilumab clinical trials program in the 2- to 5-year-olds.
Long-term dupilumab in teens
Dr. Eichenfield was a coauthor of the recently published phase 3 international long-term extension study. The 40 participants experienced a mean 85% decrease from baseline at 52 weeks in EASI (Eczema Area and Severity Index) scores on 2 mg/kg per week dosing and an 84% reduction on 4 mg/kg per week dosing. This represented a substantial further improvement from week 2, when the EASI reductions were 34% and 51%, respectively.
The mean trough serum dupilumab concentrations over the course of the year were markedly lower in the 2 mg/kg group: 74 mg/L, as compared to 161 mg/L with dosing at 4 mg/kg per week (Br J Dermatol. 2020 Jan;182[1]:85-96).
“It’ll be interesting to see how this works out over time,” the dermatologist commented. “The issue of dose by weight becomes important as we start to treat younger patients because the pharmacokinetics are very different at 4 and 2 mg/kg, and it may have an impact on efficacy.”
The extension study also established the safety and effectiveness of utilizing dupilumab in combination with standard topical corticosteroid therapy, which wasn’t allowed in the pivotal 16-week trial.
Some have commented that dupilumab may be less effective in adolescents than in adults. They point to the 24% rate of an Investigator Global Assessment (IGA) of 0 or 1 – that is, clear or almost clear – at week 16 in the pivotal adolescent trial, a substantially lower rate than in the adult trials. However, Dr. Eichenfield noted that the adolescent study population was heavily skewed to the severe end of the disease spectrum, the placebo response rate was very low, and the absolute placebo-subtracted benefit turned out to be quite similar to what was seen in the adult trials. Moreover, he added, in a post hoc analysis of the pivotal trial data which utilized a different measure of clinically meaningful response – a composite of either a 50% reduction in EASI score, a 3-point or greater improvement on a 10-point pruritus scale, or at least a 6-point improvement from baseline on the Children’s Dermatology Quality Life Index – that outcome was achieved by 74% of adolescents who didn’t achieve clear or almost clear.
What’s next for dupilumab in pediatric AD
Approval of dupilumab in children under aged 12 years is eagerly awaited, Dr. Eichenfield said. The Food and Drug Administration is now analyzing as-yet unreleased data from completed clinical trials of dupilumab in 6- to 12-year-olds with moderate to severe AD with an eye toward a possible further expanded indication. The side effect profile appears to be the same as in 12- to 18-year-olds.
“I assume it will be approved,” Dr. Eichenfield said. “We don’t know what’s going to happen in 6- to 12-year-olds in terms of the ultimate dosing recommendations that will be put out, but be aware that the pharmacokinetics vary by weight over time.”
Early data in children aged 2-5 years with severe AD from the phase 2, open-label, single ascending dose Liberty AD PRESCHOOL study showed that weight-based dosing in that age group made a big difference in terms of pharmacokinetics. In terms of efficacy, the mean reduction in EASI scores 4 weeks after a single dose of dupilumab was 27% with 3 mg/kg and 49% with 6 mg/kg.
Avoidance of live vaccines while on dupilumab becomes more of a consideration in the under-12 population. The second dose of varicella is supposed to be administered at 4 to 6 years of age, as is the second dose of MMR. The nasal influenza vaccine is a live virus vaccine, as is the yellow fever vaccine.
“We don’t know if live vaccines are dangerous for someone on dupilumab, it’s just that it’s listed that you shouldn’t use them and they haven’t been studied,” Dr. Eichenfield observed.
He reported receiving research grants from or serving as a consultant to several dozen pharmaceutical companies.
The SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
LAHAINA, HAWAII – Reassuring evidence of the long-term effectiveness and safety of dupilumab in adolescents with moderate to severe atopic dermatitis comes from a phase 3 open-label extension study of the first teenagers in the world to have received the monoclonal antibody, Lawrence F. Eichenfield, MD, reported at the SDEF Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
Dupilumab (Dupixent), a monoclonal antibody directed against interleukins-4 and -13 initially approved in adults, received an expanded indication from the Food and Drug Administration in March 2019 for treatment of 12- to 17-year-olds with moderate to severe atopic dermatitis (AD) on the strength of a pivotal 251-patient, phase 3 randomized trial of 16 weeks’ duration (JAMA Dermatol. 2019 Nov 6. doi: 10.1001/jamadermatol.2019.3336). But since AD is a chronic disease, it was important to learn how dupilumab performs well beyond the 16-week mark in adolescents, observed Dr. Eichenfield, professor of dermatology and pediatrics at the University of California, San Diego, and chief of pediatric and adolescent dermatology at Rady Children’s Hospital.
In addition to highlighting some of the emerging fine points of dupilumab therapy in adolescents, Dr. Eichenfield discussed the clinical implications of a potential further expanded indication for treatment of 6- to 12-year-olds, an event he considers likely in the coming months. He also described early data from an ongoing dupilumab clinical trials program in the 2- to 5-year-olds.
Long-term dupilumab in teens
Dr. Eichenfield was a coauthor of the recently published phase 3 international long-term extension study. The 40 participants experienced a mean 85% decrease from baseline at 52 weeks in EASI (Eczema Area and Severity Index) scores on 2 mg/kg per week dosing and an 84% reduction on 4 mg/kg per week dosing. This represented a substantial further improvement from week 2, when the EASI reductions were 34% and 51%, respectively.
The mean trough serum dupilumab concentrations over the course of the year were markedly lower in the 2 mg/kg group: 74 mg/L, as compared to 161 mg/L with dosing at 4 mg/kg per week (Br J Dermatol. 2020 Jan;182[1]:85-96).
“It’ll be interesting to see how this works out over time,” the dermatologist commented. “The issue of dose by weight becomes important as we start to treat younger patients because the pharmacokinetics are very different at 4 and 2 mg/kg, and it may have an impact on efficacy.”
The extension study also established the safety and effectiveness of utilizing dupilumab in combination with standard topical corticosteroid therapy, which wasn’t allowed in the pivotal 16-week trial.
Some have commented that dupilumab may be less effective in adolescents than in adults. They point to the 24% rate of an Investigator Global Assessment (IGA) of 0 or 1 – that is, clear or almost clear – at week 16 in the pivotal adolescent trial, a substantially lower rate than in the adult trials. However, Dr. Eichenfield noted that the adolescent study population was heavily skewed to the severe end of the disease spectrum, the placebo response rate was very low, and the absolute placebo-subtracted benefit turned out to be quite similar to what was seen in the adult trials. Moreover, he added, in a post hoc analysis of the pivotal trial data which utilized a different measure of clinically meaningful response – a composite of either a 50% reduction in EASI score, a 3-point or greater improvement on a 10-point pruritus scale, or at least a 6-point improvement from baseline on the Children’s Dermatology Quality Life Index – that outcome was achieved by 74% of adolescents who didn’t achieve clear or almost clear.
What’s next for dupilumab in pediatric AD
Approval of dupilumab in children under aged 12 years is eagerly awaited, Dr. Eichenfield said. The Food and Drug Administration is now analyzing as-yet unreleased data from completed clinical trials of dupilumab in 6- to 12-year-olds with moderate to severe AD with an eye toward a possible further expanded indication. The side effect profile appears to be the same as in 12- to 18-year-olds.
“I assume it will be approved,” Dr. Eichenfield said. “We don’t know what’s going to happen in 6- to 12-year-olds in terms of the ultimate dosing recommendations that will be put out, but be aware that the pharmacokinetics vary by weight over time.”
Early data in children aged 2-5 years with severe AD from the phase 2, open-label, single ascending dose Liberty AD PRESCHOOL study showed that weight-based dosing in that age group made a big difference in terms of pharmacokinetics. In terms of efficacy, the mean reduction in EASI scores 4 weeks after a single dose of dupilumab was 27% with 3 mg/kg and 49% with 6 mg/kg.
Avoidance of live vaccines while on dupilumab becomes more of a consideration in the under-12 population. The second dose of varicella is supposed to be administered at 4 to 6 years of age, as is the second dose of MMR. The nasal influenza vaccine is a live virus vaccine, as is the yellow fever vaccine.
“We don’t know if live vaccines are dangerous for someone on dupilumab, it’s just that it’s listed that you shouldn’t use them and they haven’t been studied,” Dr. Eichenfield observed.
He reported receiving research grants from or serving as a consultant to several dozen pharmaceutical companies.
The SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
REPORTING FROM SDEF HAWAII DERMATOLOGY SEMINAR
COVID-19: Extra caution needed for patients with diabetes
Patients with diabetes may have an increased risk of developing coronavirus infection (COVID-19), along with increased risks of morbidity and mortality, according to researchers writing in Diabetes & Metabolic Syndrome.
Although relevant clinical data remain scarce, patients with diabetes should take extra precautions to avoid infection and, if infected, may require special care, reported Ritesh Gupta, MD, of Fortis C-DOC Hospital, New Delhi, and colleagues.
“The disease severity [with COVID-19] has varied from mild, self-limiting, flu-like illness to fulminant pneumonia, respiratory failure, and death,” the authors wrote.
As of March 16, 2020, the World Health Organization reported 167,515 confirmed cases of COVID-19 and 6,606 deaths from around the world, with a mortality rate of 3.9%. But the actual mortality rate may be lower, the authors suggested, because a study involving more than 1,000 confirmed cases reported a mortality rate of 1.4%.
“Considering that the number of unreported and unconfirmed cases is likely to be much higher than the reported cases, the actual mortality may be less than 1%, which is similar to that of severe seasonal influenza,” the authors said, in reference to an editorial by Anthony S. Fauci, MD, and colleagues in the New England Journal of Medicine. In addition, they noted, mortality rates may vary by region.
The largest study relevant to patients with diabetes, which involved 72,314 cases of COVID-19, showed that patients with diabetes had a threefold higher mortality rate than did those without diabetes (7.3% vs. 2.3%, respectively). These figures were reported by the Chinese Centre for Disease Control and Prevention.
However, data from smaller cohorts with diabetes and COVID-19 have yielded mixed results. For instance, one study, involving 140 patients from Wuhan, suggested that diabetes was not a risk factor for severe disease, and in an analysis of 11 studies reporting on laboratory abnormalities in patients with a diagnosis of COVID-19, raised blood sugar levels or diabetes were not mentioned among the predictors of severe disease.
“Our knowledge about the prevalence of COVID-19 and disease course in people with diabetes will evolve as more detailed analyses are carried out,” the authors wrote. “For now, it is reasonable to assume that people with diabetes are at increased risk of developing infection. Coexisting heart disease, kidney disease, advanced age, and frailty are likely to further increase the severity of disease.”
Prevention first
“It is important that people with diabetes maintain good glycemic control, because it might help in reducing the risk of infection and the severity,” the authors wrote.
In addition to more frequent monitoring of blood glucose levels, they recommended other preventive measures, such as getting adequate nutrition, exercising, and being current with vaccinations for influenza and pneumonia. The latter, they said, may also reduce the risk of secondary bacterial pneumonia after a respiratory viral infection.
In regard to nutrition, adequate protein intake is important and “any deficiencies of minerals and vitamins need to be taken care of,” they advised. Likewise, exercise is known to improve immunity and should continue, but they suggest avoiding gyms and swimming pools.
For patients with coexisting heart and/or kidney disease, they also recommended efforts to stabilize cardiac/renal status.
In addition, the general preventive measures, such as regular and thorough hand washing with soap and water, practicing good respiratory hygiene by sneezing and coughing into a bent elbow or a facial tissue, and avoiding contact with anyone who is infected, should be observed.
As with other patients with chronic diseases that are managed long-term medications, patients with diabetes should always ensure that they have a sufficient supply of their medications and refills, if possible.
After a diagnosis
If patients with diabetes develop COVID-19, then home management may still be possible, wrote the authors, who recommended basic treatment measures such as maintaining hydration and managing symptoms with acetaminophen and steam inhalation, and home isolation for 14 days or until the symptoms resolve.
In the event of hyperglycemia with fever in patients with type 1 diabetes, blood glucose and urinary ketones should be monitored often. “Frequent changes in dosage and correctional bolus may be required to maintain normoglycemia,” they cautioned.
Concerning diabetic drug regimens, they suggest patients avoid antihyperglycemic agents that can cause volume depletion or hypoglycemia and, if necessary, that they reduce oral antidiabetic drugs and follow sick-day guidelines.
For hospitalized patients, the investigators strengthened that statement, advising that oral agents need to be stopped, particularly sodium-glucose cotransporter 2 inhibitors and metformin. “Insulin is the preferred agent for control of hyperglycemia in hospitalized sick patients,” they wrote.
Untested therapies
The authors also discussed a range of untested therapies that may help fight COVID-19, such as antiviral drugs (such as lopinavir and ritonavir), zinc nanoparticles, and vitamin C. Supplementing those recommendations, Dr. Gupta and colleagues provided a concise review of COVID-19 epidemiology and extant data relevant to patients with diabetes.
The investigators reported no conflicts of interest.
SOURCE: Gupta et al. Diabetes Metab Syndr. 2020;14(3):211-12.
Patients with diabetes may have an increased risk of developing coronavirus infection (COVID-19), along with increased risks of morbidity and mortality, according to researchers writing in Diabetes & Metabolic Syndrome.
Although relevant clinical data remain scarce, patients with diabetes should take extra precautions to avoid infection and, if infected, may require special care, reported Ritesh Gupta, MD, of Fortis C-DOC Hospital, New Delhi, and colleagues.
“The disease severity [with COVID-19] has varied from mild, self-limiting, flu-like illness to fulminant pneumonia, respiratory failure, and death,” the authors wrote.
As of March 16, 2020, the World Health Organization reported 167,515 confirmed cases of COVID-19 and 6,606 deaths from around the world, with a mortality rate of 3.9%. But the actual mortality rate may be lower, the authors suggested, because a study involving more than 1,000 confirmed cases reported a mortality rate of 1.4%.
“Considering that the number of unreported and unconfirmed cases is likely to be much higher than the reported cases, the actual mortality may be less than 1%, which is similar to that of severe seasonal influenza,” the authors said, in reference to an editorial by Anthony S. Fauci, MD, and colleagues in the New England Journal of Medicine. In addition, they noted, mortality rates may vary by region.
The largest study relevant to patients with diabetes, which involved 72,314 cases of COVID-19, showed that patients with diabetes had a threefold higher mortality rate than did those without diabetes (7.3% vs. 2.3%, respectively). These figures were reported by the Chinese Centre for Disease Control and Prevention.
However, data from smaller cohorts with diabetes and COVID-19 have yielded mixed results. For instance, one study, involving 140 patients from Wuhan, suggested that diabetes was not a risk factor for severe disease, and in an analysis of 11 studies reporting on laboratory abnormalities in patients with a diagnosis of COVID-19, raised blood sugar levels or diabetes were not mentioned among the predictors of severe disease.
“Our knowledge about the prevalence of COVID-19 and disease course in people with diabetes will evolve as more detailed analyses are carried out,” the authors wrote. “For now, it is reasonable to assume that people with diabetes are at increased risk of developing infection. Coexisting heart disease, kidney disease, advanced age, and frailty are likely to further increase the severity of disease.”
Prevention first
“It is important that people with diabetes maintain good glycemic control, because it might help in reducing the risk of infection and the severity,” the authors wrote.
In addition to more frequent monitoring of blood glucose levels, they recommended other preventive measures, such as getting adequate nutrition, exercising, and being current with vaccinations for influenza and pneumonia. The latter, they said, may also reduce the risk of secondary bacterial pneumonia after a respiratory viral infection.
In regard to nutrition, adequate protein intake is important and “any deficiencies of minerals and vitamins need to be taken care of,” they advised. Likewise, exercise is known to improve immunity and should continue, but they suggest avoiding gyms and swimming pools.
For patients with coexisting heart and/or kidney disease, they also recommended efforts to stabilize cardiac/renal status.
In addition, the general preventive measures, such as regular and thorough hand washing with soap and water, practicing good respiratory hygiene by sneezing and coughing into a bent elbow or a facial tissue, and avoiding contact with anyone who is infected, should be observed.
As with other patients with chronic diseases that are managed long-term medications, patients with diabetes should always ensure that they have a sufficient supply of their medications and refills, if possible.
After a diagnosis
If patients with diabetes develop COVID-19, then home management may still be possible, wrote the authors, who recommended basic treatment measures such as maintaining hydration and managing symptoms with acetaminophen and steam inhalation, and home isolation for 14 days or until the symptoms resolve.
In the event of hyperglycemia with fever in patients with type 1 diabetes, blood glucose and urinary ketones should be monitored often. “Frequent changes in dosage and correctional bolus may be required to maintain normoglycemia,” they cautioned.
Concerning diabetic drug regimens, they suggest patients avoid antihyperglycemic agents that can cause volume depletion or hypoglycemia and, if necessary, that they reduce oral antidiabetic drugs and follow sick-day guidelines.
For hospitalized patients, the investigators strengthened that statement, advising that oral agents need to be stopped, particularly sodium-glucose cotransporter 2 inhibitors and metformin. “Insulin is the preferred agent for control of hyperglycemia in hospitalized sick patients,” they wrote.
Untested therapies
The authors also discussed a range of untested therapies that may help fight COVID-19, such as antiviral drugs (such as lopinavir and ritonavir), zinc nanoparticles, and vitamin C. Supplementing those recommendations, Dr. Gupta and colleagues provided a concise review of COVID-19 epidemiology and extant data relevant to patients with diabetes.
The investigators reported no conflicts of interest.
SOURCE: Gupta et al. Diabetes Metab Syndr. 2020;14(3):211-12.
Patients with diabetes may have an increased risk of developing coronavirus infection (COVID-19), along with increased risks of morbidity and mortality, according to researchers writing in Diabetes & Metabolic Syndrome.
Although relevant clinical data remain scarce, patients with diabetes should take extra precautions to avoid infection and, if infected, may require special care, reported Ritesh Gupta, MD, of Fortis C-DOC Hospital, New Delhi, and colleagues.
“The disease severity [with COVID-19] has varied from mild, self-limiting, flu-like illness to fulminant pneumonia, respiratory failure, and death,” the authors wrote.
As of March 16, 2020, the World Health Organization reported 167,515 confirmed cases of COVID-19 and 6,606 deaths from around the world, with a mortality rate of 3.9%. But the actual mortality rate may be lower, the authors suggested, because a study involving more than 1,000 confirmed cases reported a mortality rate of 1.4%.
“Considering that the number of unreported and unconfirmed cases is likely to be much higher than the reported cases, the actual mortality may be less than 1%, which is similar to that of severe seasonal influenza,” the authors said, in reference to an editorial by Anthony S. Fauci, MD, and colleagues in the New England Journal of Medicine. In addition, they noted, mortality rates may vary by region.
The largest study relevant to patients with diabetes, which involved 72,314 cases of COVID-19, showed that patients with diabetes had a threefold higher mortality rate than did those without diabetes (7.3% vs. 2.3%, respectively). These figures were reported by the Chinese Centre for Disease Control and Prevention.
However, data from smaller cohorts with diabetes and COVID-19 have yielded mixed results. For instance, one study, involving 140 patients from Wuhan, suggested that diabetes was not a risk factor for severe disease, and in an analysis of 11 studies reporting on laboratory abnormalities in patients with a diagnosis of COVID-19, raised blood sugar levels or diabetes were not mentioned among the predictors of severe disease.
“Our knowledge about the prevalence of COVID-19 and disease course in people with diabetes will evolve as more detailed analyses are carried out,” the authors wrote. “For now, it is reasonable to assume that people with diabetes are at increased risk of developing infection. Coexisting heart disease, kidney disease, advanced age, and frailty are likely to further increase the severity of disease.”
Prevention first
“It is important that people with diabetes maintain good glycemic control, because it might help in reducing the risk of infection and the severity,” the authors wrote.
In addition to more frequent monitoring of blood glucose levels, they recommended other preventive measures, such as getting adequate nutrition, exercising, and being current with vaccinations for influenza and pneumonia. The latter, they said, may also reduce the risk of secondary bacterial pneumonia after a respiratory viral infection.
In regard to nutrition, adequate protein intake is important and “any deficiencies of minerals and vitamins need to be taken care of,” they advised. Likewise, exercise is known to improve immunity and should continue, but they suggest avoiding gyms and swimming pools.
For patients with coexisting heart and/or kidney disease, they also recommended efforts to stabilize cardiac/renal status.
In addition, the general preventive measures, such as regular and thorough hand washing with soap and water, practicing good respiratory hygiene by sneezing and coughing into a bent elbow or a facial tissue, and avoiding contact with anyone who is infected, should be observed.
As with other patients with chronic diseases that are managed long-term medications, patients with diabetes should always ensure that they have a sufficient supply of their medications and refills, if possible.
After a diagnosis
If patients with diabetes develop COVID-19, then home management may still be possible, wrote the authors, who recommended basic treatment measures such as maintaining hydration and managing symptoms with acetaminophen and steam inhalation, and home isolation for 14 days or until the symptoms resolve.
In the event of hyperglycemia with fever in patients with type 1 diabetes, blood glucose and urinary ketones should be monitored often. “Frequent changes in dosage and correctional bolus may be required to maintain normoglycemia,” they cautioned.
Concerning diabetic drug regimens, they suggest patients avoid antihyperglycemic agents that can cause volume depletion or hypoglycemia and, if necessary, that they reduce oral antidiabetic drugs and follow sick-day guidelines.
For hospitalized patients, the investigators strengthened that statement, advising that oral agents need to be stopped, particularly sodium-glucose cotransporter 2 inhibitors and metformin. “Insulin is the preferred agent for control of hyperglycemia in hospitalized sick patients,” they wrote.
Untested therapies
The authors also discussed a range of untested therapies that may help fight COVID-19, such as antiviral drugs (such as lopinavir and ritonavir), zinc nanoparticles, and vitamin C. Supplementing those recommendations, Dr. Gupta and colleagues provided a concise review of COVID-19 epidemiology and extant data relevant to patients with diabetes.
The investigators reported no conflicts of interest.
SOURCE: Gupta et al. Diabetes Metab Syndr. 2020;14(3):211-12.
FROM DIABETES & METABOLIC SYNDROME
The role of oleuropein, the primary phenol in olives, in skin health
Olives and olive oil have long been known to confer salutary effects to the skin.1 Leaves and fruits of the olive plant (Olea europaea) have been used as external emollients to treat skin ulcers and inflammatory wounds.2 The phenolic compound oleuropein, the most abundant phenolic found in olive leaves and oil, has been shown to exhibit antioxidant and free radical–scavenging activities.3,4 Also present in the stems and flowers of the plant, oleuropein, an ester of elenolic acid and 3,4-dihydroxyphenyl ethanol and the primary glycoside in olives,5 is thought to be the major contributor to its antioxidant and antimelanogenesis activities.6 Notably, olive leaves, which contain a copious supply of oleuropein, are thought to exert significantly more antioxidant activity than olive fruit.7
Hydroxytyrosol is an ortho-diphenolic substance and essential constituent of oleuropein that has been shown in vitro to prevent apoptotic cell death caused by UVB in HaCaT cells.8,9 Both oleuropein and hydroxytyrosol impart various anticancer properties at the initiation, promotion, and metastasis stages and yield protection against multiple cancers, including skin tumors.10 The antioxidant activity of both compounds, which has been found to be more potent than that of vitamin E, is attributed to their phenolic content.11,12 In addition, oleuropein and lipophilic olive mill wastewater derivatives have been useful as active ingredients for stabilizing cosmetic formulations.13 This column revisits oleuropein after 10 years to focus on its dermatologic potential.
Protection against UV damage
A hairless mouse study by Kimura and Sumiyoshi in 2009 revealed that olive leaf extract and its primary constituent oleuropein exert a skin-protective effect against chronic UVB-induced skin damage and carcinogenesis, as well as tumor growth. This is likely caused by reducing cutaneous cyclooxygenase (COX)-2 levels, thus suppressing the expression of vascular endothelial growth factor (VEGF) and various matrix metalloproteinases, specifically MMP-2, MMP-9, and MMP-13.14
A year later, the same researchers examined the potential protective effects of olive leaf extract and oleuropein on acute damage induced by UVB exposure in C57BL/6J mice. Both oral extract (300 mg/kg or 1,000 mg/kg) and oral oleuropein (25mg/kg or 85 mg/kg) hindered skin thickness increases engendered by daily doses of UVB (120 mJ/cm2 for 5 days, then every other day for 9 days). Olive leaf extract and oleuropein also suppressed increases in Ki-67- and 8-hydroxy-2’-deoxyguanosine–positive cell numbers, melanin granule area, and MMP-13 expression, the investigators noted.15 Preinitiation with oleuropein also appears to have prevented skin tumor formation in a two-stage carcinogenesis model in mice, which the investigators ascribed to the antioxidant and antiapoptotic properties of the olive protein.16
The cosmetic characteristics of oleuropein against UVB-induced erythema in healthy volunteers were assessed by Perugini et al. in 2008. Using an emulsion and emulgel containing oleuropein and vitamin E as a reference compound, the investigators found that the botanical ingredient was responsible for decreases in erythema (22%), transepidermal water loss (35%), and blood flow (30%). They suggested that the use of oleuropein in cosmetic formulations warrants further investigation for its potential to help mitigate UV damage.3
Wound healing
Koca et al. assessed the wound healing activity of O. europaea leaf extracts using in vivo wound models and the reference ointment Madecassol (Bayer; Istanbul) for comparison, in 2011. The results showed that the aqueous extract exhibited wound healing properties, with secoiridoid oleuropein (4.6059%) found to be the primary active constituent.2
In a 2014 skin wound–healing investigation in aged male Balb/c mice, Mehraein et al. divided 24 mice, 16 months of age, into control and experimental groups. On days 3 and 7 after incision, collagen fiber deposition was significantly increased and reepithelialization more advanced in the oleuropein group (administered via an intradermal injection once a day), which also experienced decreased cell infiltration. The investigators concluded that oleuropein speeds cutaneous wound healing in mice and may have potential for clinical applications in human would healing from surgery.17
Later that year, the same team investigated the therapeutic effects of oleuropein on the wounded skin of young male Balb/c mice, finding similar results, with the phenolic compound again accelerating reepithelialization, improving collagen fiber synthesis, and augmenting blood flow to wound areas via up-regulating VEGF protein expression.4
Hair growth
In 2015, Tong et al. reported that topically applied oleuropein spurred the anagen hair growth phase in telogenic C57BL/6N mouse skin.18 An O. europaea subcutaneous immunotherapy has also demonstrated reductions in cutaneous reactivity, safety, and tolerability in patients with rhinoconjunctivitis.19
Conclusion
The benefits of consuming olives and olive oil are well established and continue to be studied. backed by many years of anecdotal reporting and use in traditional medicine. While the emerging data on the dermatologic uses of the olive phenolic constituent oleuropein are encouraging, much more information, particularly derived from randomized, controlled trials in humans, is necessary to establish the full potential of oleuropein for indications such as wound healing and protection against UV damage.
Dr. Baumann is a private practice dermatologist, researcher, author, and entrepreneur who practices in Miami. She founded the Cosmetic Dermatology Center at the University of Miami in 1997. Dr. Baumann wrote two textbooks: “Cosmetic Dermatology: Principles and Practice” (New York: McGraw-Hill, 2002), and “Cosmeceuticals and Cosmetic Ingredients” (New York: McGraw-Hill, 2014), and a New York Times Best Sellers book for consumers, “The Skin Type Solution” (New York: Bantam Dell, 2006). Dr. Baumann has received funding for advisory boards and/or clinical research trials from Allergan, Evolus, Galderma, and Revance. She is the founder and CEO of Skin Type Solutions Franchise Systems. Write to her at [email protected].
References
1. Baumann LS, Weisberg EM. “Olive oil in botanical cosmeceuticals.” Olives and Olive Oil in Health and Disease Prevention. New York: Academic Press, 2010.
2. Koca U et al. J Med Food. 2011 Jan-Feb;14(1-2):140-6.
3. Perugini P et al. Int J Cosmet Sci. 2008 Apr;30(2):113-20.
4. Mehraein F et al. Wounds. 2014 Mar;26(3):83-8.
5. Imran M et al. J Food Sci. 2018 Jul;83(7):1781-91.
6. Kishikawa A et al. Phytother Res. 2015 Jun;29(6):877-86.
7. Zheng J et al. Zhongguo Zhong Yao Za Zhi. 2016 Feb;41(4):613-8.
8. Salucci S et al. J Dermatol Sci. 2015 Oct;80(1):61-8.
9. Jeon S, Choi M. Biomed Dermatol. 2018;2:21.
10. Imran M et al. J Food Sci. 2018 Jul;83(7):1781-91.
11. Visioli F et al. Biochem Biophys Res Commun. 1998 Jun 9;247(1):60-4.
12. Polišak N et al. Phytother Res. 2019 Oct 27. doi: 10.1002/ptr.6524.
13. Aissa I et al. Biotechnol Appl Biochem. 2017 Jul;64(4):579-89.
14. Kimura Y, Sumiyoshi M. J Nutr. 2009 Nov;139(11):2079-86.
15. Sumiyoshi M, Kimura Y. Phytother Res. 2010 Jul;24(7):995-1003.
16. John DNS et al. JKIMSU. 2019 Jan-Mar;8(1):43-51.
17. Mehraein F et al. Cell J. 2014 Feb 3;16(1):25-30.
18. Tong T et al. PLoS One. 2015 Jun 10;10(6):e0129578.
19. Saenza De San Pedro B et al. Eur All Allergy Clin Immunol. 2019 Nov 27. doi: 10.23822/EurAnnACI.1764-1489.124.
Olives and olive oil have long been known to confer salutary effects to the skin.1 Leaves and fruits of the olive plant (Olea europaea) have been used as external emollients to treat skin ulcers and inflammatory wounds.2 The phenolic compound oleuropein, the most abundant phenolic found in olive leaves and oil, has been shown to exhibit antioxidant and free radical–scavenging activities.3,4 Also present in the stems and flowers of the plant, oleuropein, an ester of elenolic acid and 3,4-dihydroxyphenyl ethanol and the primary glycoside in olives,5 is thought to be the major contributor to its antioxidant and antimelanogenesis activities.6 Notably, olive leaves, which contain a copious supply of oleuropein, are thought to exert significantly more antioxidant activity than olive fruit.7
Hydroxytyrosol is an ortho-diphenolic substance and essential constituent of oleuropein that has been shown in vitro to prevent apoptotic cell death caused by UVB in HaCaT cells.8,9 Both oleuropein and hydroxytyrosol impart various anticancer properties at the initiation, promotion, and metastasis stages and yield protection against multiple cancers, including skin tumors.10 The antioxidant activity of both compounds, which has been found to be more potent than that of vitamin E, is attributed to their phenolic content.11,12 In addition, oleuropein and lipophilic olive mill wastewater derivatives have been useful as active ingredients for stabilizing cosmetic formulations.13 This column revisits oleuropein after 10 years to focus on its dermatologic potential.
Protection against UV damage
A hairless mouse study by Kimura and Sumiyoshi in 2009 revealed that olive leaf extract and its primary constituent oleuropein exert a skin-protective effect against chronic UVB-induced skin damage and carcinogenesis, as well as tumor growth. This is likely caused by reducing cutaneous cyclooxygenase (COX)-2 levels, thus suppressing the expression of vascular endothelial growth factor (VEGF) and various matrix metalloproteinases, specifically MMP-2, MMP-9, and MMP-13.14
A year later, the same researchers examined the potential protective effects of olive leaf extract and oleuropein on acute damage induced by UVB exposure in C57BL/6J mice. Both oral extract (300 mg/kg or 1,000 mg/kg) and oral oleuropein (25mg/kg or 85 mg/kg) hindered skin thickness increases engendered by daily doses of UVB (120 mJ/cm2 for 5 days, then every other day for 9 days). Olive leaf extract and oleuropein also suppressed increases in Ki-67- and 8-hydroxy-2’-deoxyguanosine–positive cell numbers, melanin granule area, and MMP-13 expression, the investigators noted.15 Preinitiation with oleuropein also appears to have prevented skin tumor formation in a two-stage carcinogenesis model in mice, which the investigators ascribed to the antioxidant and antiapoptotic properties of the olive protein.16
The cosmetic characteristics of oleuropein against UVB-induced erythema in healthy volunteers were assessed by Perugini et al. in 2008. Using an emulsion and emulgel containing oleuropein and vitamin E as a reference compound, the investigators found that the botanical ingredient was responsible for decreases in erythema (22%), transepidermal water loss (35%), and blood flow (30%). They suggested that the use of oleuropein in cosmetic formulations warrants further investigation for its potential to help mitigate UV damage.3
Wound healing
Koca et al. assessed the wound healing activity of O. europaea leaf extracts using in vivo wound models and the reference ointment Madecassol (Bayer; Istanbul) for comparison, in 2011. The results showed that the aqueous extract exhibited wound healing properties, with secoiridoid oleuropein (4.6059%) found to be the primary active constituent.2
In a 2014 skin wound–healing investigation in aged male Balb/c mice, Mehraein et al. divided 24 mice, 16 months of age, into control and experimental groups. On days 3 and 7 after incision, collagen fiber deposition was significantly increased and reepithelialization more advanced in the oleuropein group (administered via an intradermal injection once a day), which also experienced decreased cell infiltration. The investigators concluded that oleuropein speeds cutaneous wound healing in mice and may have potential for clinical applications in human would healing from surgery.17
Later that year, the same team investigated the therapeutic effects of oleuropein on the wounded skin of young male Balb/c mice, finding similar results, with the phenolic compound again accelerating reepithelialization, improving collagen fiber synthesis, and augmenting blood flow to wound areas via up-regulating VEGF protein expression.4
Hair growth
In 2015, Tong et al. reported that topically applied oleuropein spurred the anagen hair growth phase in telogenic C57BL/6N mouse skin.18 An O. europaea subcutaneous immunotherapy has also demonstrated reductions in cutaneous reactivity, safety, and tolerability in patients with rhinoconjunctivitis.19
Conclusion
The benefits of consuming olives and olive oil are well established and continue to be studied. backed by many years of anecdotal reporting and use in traditional medicine. While the emerging data on the dermatologic uses of the olive phenolic constituent oleuropein are encouraging, much more information, particularly derived from randomized, controlled trials in humans, is necessary to establish the full potential of oleuropein for indications such as wound healing and protection against UV damage.
Dr. Baumann is a private practice dermatologist, researcher, author, and entrepreneur who practices in Miami. She founded the Cosmetic Dermatology Center at the University of Miami in 1997. Dr. Baumann wrote two textbooks: “Cosmetic Dermatology: Principles and Practice” (New York: McGraw-Hill, 2002), and “Cosmeceuticals and Cosmetic Ingredients” (New York: McGraw-Hill, 2014), and a New York Times Best Sellers book for consumers, “The Skin Type Solution” (New York: Bantam Dell, 2006). Dr. Baumann has received funding for advisory boards and/or clinical research trials from Allergan, Evolus, Galderma, and Revance. She is the founder and CEO of Skin Type Solutions Franchise Systems. Write to her at [email protected].
References
1. Baumann LS, Weisberg EM. “Olive oil in botanical cosmeceuticals.” Olives and Olive Oil in Health and Disease Prevention. New York: Academic Press, 2010.
2. Koca U et al. J Med Food. 2011 Jan-Feb;14(1-2):140-6.
3. Perugini P et al. Int J Cosmet Sci. 2008 Apr;30(2):113-20.
4. Mehraein F et al. Wounds. 2014 Mar;26(3):83-8.
5. Imran M et al. J Food Sci. 2018 Jul;83(7):1781-91.
6. Kishikawa A et al. Phytother Res. 2015 Jun;29(6):877-86.
7. Zheng J et al. Zhongguo Zhong Yao Za Zhi. 2016 Feb;41(4):613-8.
8. Salucci S et al. J Dermatol Sci. 2015 Oct;80(1):61-8.
9. Jeon S, Choi M. Biomed Dermatol. 2018;2:21.
10. Imran M et al. J Food Sci. 2018 Jul;83(7):1781-91.
11. Visioli F et al. Biochem Biophys Res Commun. 1998 Jun 9;247(1):60-4.
12. Polišak N et al. Phytother Res. 2019 Oct 27. doi: 10.1002/ptr.6524.
13. Aissa I et al. Biotechnol Appl Biochem. 2017 Jul;64(4):579-89.
14. Kimura Y, Sumiyoshi M. J Nutr. 2009 Nov;139(11):2079-86.
15. Sumiyoshi M, Kimura Y. Phytother Res. 2010 Jul;24(7):995-1003.
16. John DNS et al. JKIMSU. 2019 Jan-Mar;8(1):43-51.
17. Mehraein F et al. Cell J. 2014 Feb 3;16(1):25-30.
18. Tong T et al. PLoS One. 2015 Jun 10;10(6):e0129578.
19. Saenza De San Pedro B et al. Eur All Allergy Clin Immunol. 2019 Nov 27. doi: 10.23822/EurAnnACI.1764-1489.124.
Olives and olive oil have long been known to confer salutary effects to the skin.1 Leaves and fruits of the olive plant (Olea europaea) have been used as external emollients to treat skin ulcers and inflammatory wounds.2 The phenolic compound oleuropein, the most abundant phenolic found in olive leaves and oil, has been shown to exhibit antioxidant and free radical–scavenging activities.3,4 Also present in the stems and flowers of the plant, oleuropein, an ester of elenolic acid and 3,4-dihydroxyphenyl ethanol and the primary glycoside in olives,5 is thought to be the major contributor to its antioxidant and antimelanogenesis activities.6 Notably, olive leaves, which contain a copious supply of oleuropein, are thought to exert significantly more antioxidant activity than olive fruit.7
Hydroxytyrosol is an ortho-diphenolic substance and essential constituent of oleuropein that has been shown in vitro to prevent apoptotic cell death caused by UVB in HaCaT cells.8,9 Both oleuropein and hydroxytyrosol impart various anticancer properties at the initiation, promotion, and metastasis stages and yield protection against multiple cancers, including skin tumors.10 The antioxidant activity of both compounds, which has been found to be more potent than that of vitamin E, is attributed to their phenolic content.11,12 In addition, oleuropein and lipophilic olive mill wastewater derivatives have been useful as active ingredients for stabilizing cosmetic formulations.13 This column revisits oleuropein after 10 years to focus on its dermatologic potential.
Protection against UV damage
A hairless mouse study by Kimura and Sumiyoshi in 2009 revealed that olive leaf extract and its primary constituent oleuropein exert a skin-protective effect against chronic UVB-induced skin damage and carcinogenesis, as well as tumor growth. This is likely caused by reducing cutaneous cyclooxygenase (COX)-2 levels, thus suppressing the expression of vascular endothelial growth factor (VEGF) and various matrix metalloproteinases, specifically MMP-2, MMP-9, and MMP-13.14
A year later, the same researchers examined the potential protective effects of olive leaf extract and oleuropein on acute damage induced by UVB exposure in C57BL/6J mice. Both oral extract (300 mg/kg or 1,000 mg/kg) and oral oleuropein (25mg/kg or 85 mg/kg) hindered skin thickness increases engendered by daily doses of UVB (120 mJ/cm2 for 5 days, then every other day for 9 days). Olive leaf extract and oleuropein also suppressed increases in Ki-67- and 8-hydroxy-2’-deoxyguanosine–positive cell numbers, melanin granule area, and MMP-13 expression, the investigators noted.15 Preinitiation with oleuropein also appears to have prevented skin tumor formation in a two-stage carcinogenesis model in mice, which the investigators ascribed to the antioxidant and antiapoptotic properties of the olive protein.16
The cosmetic characteristics of oleuropein against UVB-induced erythema in healthy volunteers were assessed by Perugini et al. in 2008. Using an emulsion and emulgel containing oleuropein and vitamin E as a reference compound, the investigators found that the botanical ingredient was responsible for decreases in erythema (22%), transepidermal water loss (35%), and blood flow (30%). They suggested that the use of oleuropein in cosmetic formulations warrants further investigation for its potential to help mitigate UV damage.3
Wound healing
Koca et al. assessed the wound healing activity of O. europaea leaf extracts using in vivo wound models and the reference ointment Madecassol (Bayer; Istanbul) for comparison, in 2011. The results showed that the aqueous extract exhibited wound healing properties, with secoiridoid oleuropein (4.6059%) found to be the primary active constituent.2
In a 2014 skin wound–healing investigation in aged male Balb/c mice, Mehraein et al. divided 24 mice, 16 months of age, into control and experimental groups. On days 3 and 7 after incision, collagen fiber deposition was significantly increased and reepithelialization more advanced in the oleuropein group (administered via an intradermal injection once a day), which also experienced decreased cell infiltration. The investigators concluded that oleuropein speeds cutaneous wound healing in mice and may have potential for clinical applications in human would healing from surgery.17
Later that year, the same team investigated the therapeutic effects of oleuropein on the wounded skin of young male Balb/c mice, finding similar results, with the phenolic compound again accelerating reepithelialization, improving collagen fiber synthesis, and augmenting blood flow to wound areas via up-regulating VEGF protein expression.4
Hair growth
In 2015, Tong et al. reported that topically applied oleuropein spurred the anagen hair growth phase in telogenic C57BL/6N mouse skin.18 An O. europaea subcutaneous immunotherapy has also demonstrated reductions in cutaneous reactivity, safety, and tolerability in patients with rhinoconjunctivitis.19
Conclusion
The benefits of consuming olives and olive oil are well established and continue to be studied. backed by many years of anecdotal reporting and use in traditional medicine. While the emerging data on the dermatologic uses of the olive phenolic constituent oleuropein are encouraging, much more information, particularly derived from randomized, controlled trials in humans, is necessary to establish the full potential of oleuropein for indications such as wound healing and protection against UV damage.
Dr. Baumann is a private practice dermatologist, researcher, author, and entrepreneur who practices in Miami. She founded the Cosmetic Dermatology Center at the University of Miami in 1997. Dr. Baumann wrote two textbooks: “Cosmetic Dermatology: Principles and Practice” (New York: McGraw-Hill, 2002), and “Cosmeceuticals and Cosmetic Ingredients” (New York: McGraw-Hill, 2014), and a New York Times Best Sellers book for consumers, “The Skin Type Solution” (New York: Bantam Dell, 2006). Dr. Baumann has received funding for advisory boards and/or clinical research trials from Allergan, Evolus, Galderma, and Revance. She is the founder and CEO of Skin Type Solutions Franchise Systems. Write to her at [email protected].
References
1. Baumann LS, Weisberg EM. “Olive oil in botanical cosmeceuticals.” Olives and Olive Oil in Health and Disease Prevention. New York: Academic Press, 2010.
2. Koca U et al. J Med Food. 2011 Jan-Feb;14(1-2):140-6.
3. Perugini P et al. Int J Cosmet Sci. 2008 Apr;30(2):113-20.
4. Mehraein F et al. Wounds. 2014 Mar;26(3):83-8.
5. Imran M et al. J Food Sci. 2018 Jul;83(7):1781-91.
6. Kishikawa A et al. Phytother Res. 2015 Jun;29(6):877-86.
7. Zheng J et al. Zhongguo Zhong Yao Za Zhi. 2016 Feb;41(4):613-8.
8. Salucci S et al. J Dermatol Sci. 2015 Oct;80(1):61-8.
9. Jeon S, Choi M. Biomed Dermatol. 2018;2:21.
10. Imran M et al. J Food Sci. 2018 Jul;83(7):1781-91.
11. Visioli F et al. Biochem Biophys Res Commun. 1998 Jun 9;247(1):60-4.
12. Polišak N et al. Phytother Res. 2019 Oct 27. doi: 10.1002/ptr.6524.
13. Aissa I et al. Biotechnol Appl Biochem. 2017 Jul;64(4):579-89.
14. Kimura Y, Sumiyoshi M. J Nutr. 2009 Nov;139(11):2079-86.
15. Sumiyoshi M, Kimura Y. Phytother Res. 2010 Jul;24(7):995-1003.
16. John DNS et al. JKIMSU. 2019 Jan-Mar;8(1):43-51.
17. Mehraein F et al. Cell J. 2014 Feb 3;16(1):25-30.
18. Tong T et al. PLoS One. 2015 Jun 10;10(6):e0129578.
19. Saenza De San Pedro B et al. Eur All Allergy Clin Immunol. 2019 Nov 27. doi: 10.23822/EurAnnACI.1764-1489.124.
High CV event risk seen in SLE patients with ACC/AHA-defined hypertension
, results of a retrospective, single-center investigation suggest.
Risk of atherosclerotic vascular events was increased by 73% for patients with systemic lupus erythematosus (SLE) who sustained a mean blood pressure of 130/80 to 139/89 mm Hg over 2 years in the study, which included 1,532 patients treated at a clinic in Toronto.
Management of hypertension in SLE patients should start early, and should aim to achieve levels below 130/80 mm Hg, according to the investigators, led by Konstantinos Tselios, MD, PhD, of the Centre for Prognosis Studies in the Rheumatic Diseases at the University of Toronto.
“The findings of the present study support that the target BP should be less than 130/80 mm Hg in all patients with lupus in order to minimize their cardiovascular risk,” Dr. Tselios and coauthors said in their study, which appears in Annals of the Rheumatic Diseases.
Despite the limitations inherent in a retrospective, observational study, this work by Dr. Tselios and colleagues may help inform the care of patients with SLE, according to C. Michael Stein, MBChB, professor of medicine at Vanderbilt University in Nashville, Tenn.
“It’s really interesting data that’s important and helps us think in terms of figuring out what may be reasonable to do for a particular patient,” Dr. Stein said in an interview.
Starting antihypertensive management early and aiming at levels below 130/80 mm Hg is a strategy that should be “reasonable” for most patients with SLE, said Dr. Stein, adding that the approach specified in the 2017 American College of Cardiology/American Heart Association (ACC/AHA) hypertension guidelines are appropriate to follow. In those guidelines, the threshold for diagnosis of hypertension was lowered to 130/80 mm Hg.
“You can start with risk factor modification, in terms of losing weight, exercising, stopping alcohol, and decreasing salt in the diet to see if you can get the blood pressure down, though it may come down to drug therapy for many patients, I believe,” Dr. Stein said.
Authors of those 2017 ACC/AHA guidelines made no recommendations for patients with SLE or other connective tissue diseases, despite including a section devoted to specific patient subgroups and comorbidities of interest, Dr. Tselios and coauthors noted in their report.
Management of hypertension in patients with lupus may be “delayed” in patients with blood pressures reaching the current hypertension threshold, according to Dr. Tselios and colleagues, due in part to difficulties in cardiovascular risk calculation in SLE patients, as well as current risk considerations outlined in the guidelines.
“On the basis of the recent guidelines, the patient with typical lupus (young female with no traditional atherosclerotic risk factors) would be considered as a low-risk individual and not offered treatment for a BP of 130-139/80-89 mm Hg,” they said in their report.
Accordingly, Dr. Tselios and colleagues sought to determine whether the new hypertension definition predicted atherosclerotic vascular events, including new-onset angina, acute myocardial infarction, cerebrovascular events, revascularization procedures, heart failure, or peripheral vascular disease requiring angioplasty, in patients with SLE treated at a Canadian clinic.
Their analysis comprised 1,532 patients with SLE who had at least 2 years of follow-up and had no prior atherosclerotic events on record. Over a mean follow-up of nearly 11 years, there were 124 such events documented in those patients.
With a mean follow-up of nearly 11 years, the incidence of atherosclerotic events was 18.9 per 1,000 patient-years for patients with blood pressure ≥ 140/90 mm Hg, 11.5 per 1,000 patient-years for the 130-139/80-89 mm Hg group, and 4.5 per 1,000 patient-years for those with blood pressures of 130/80 mm Hg or lower, with differences that were statistically significant between groups, according to the report.
An adjusted blood pressure of 130-139/80-89 mm Hg over the first 2 years since enrollment in the clinic was independently associated with the occurrence of an atherosclerotic event, with a hazard ratio of 1.73 (95% confidence interval, 1.13-2.69, P = 0.011), according to results of a multivariable analysis.
Those findings support targeting a blood pressure below 130/80 mm Hg in all patients with lupus, according to Dr. Tselios and coauthors.
“It seems reasonable that clinicians should not rely on CV risk calculators in SLE and commence treatment as soon as possible in cases of sustained BP elevation above the threshold of 130/80 mm Hg,” they wrote in their report.
How low to go remains unclear, however, as targeting lower levels of blood pressure might be unsafe in certain groups, such as those SLE patients with prior heart disease or heart failure; nevertheless, recent observational data from non-SLE populations suggest that effective treatment to levels lower than 130/80 mm Hg would “further reduce the incidence of atherosclerotic events in SLE,” the authors said in a discussion of their results.
Dr. Tselios and coauthors said they had no competing interests relative to the study. They reported funding for the University of Toronto Lupus Clinic from the University Health Network, Lou & Marissa Rocca, Mark & Diana Bozzo, and the Lupus Foundation of Ontario.
SOURCE: Tselios K et al. Ann Rheum Dis. 2020 Mar 10. doi: 10.1136/annrheumdis-2019-216764
, results of a retrospective, single-center investigation suggest.
Risk of atherosclerotic vascular events was increased by 73% for patients with systemic lupus erythematosus (SLE) who sustained a mean blood pressure of 130/80 to 139/89 mm Hg over 2 years in the study, which included 1,532 patients treated at a clinic in Toronto.
Management of hypertension in SLE patients should start early, and should aim to achieve levels below 130/80 mm Hg, according to the investigators, led by Konstantinos Tselios, MD, PhD, of the Centre for Prognosis Studies in the Rheumatic Diseases at the University of Toronto.
“The findings of the present study support that the target BP should be less than 130/80 mm Hg in all patients with lupus in order to minimize their cardiovascular risk,” Dr. Tselios and coauthors said in their study, which appears in Annals of the Rheumatic Diseases.
Despite the limitations inherent in a retrospective, observational study, this work by Dr. Tselios and colleagues may help inform the care of patients with SLE, according to C. Michael Stein, MBChB, professor of medicine at Vanderbilt University in Nashville, Tenn.
“It’s really interesting data that’s important and helps us think in terms of figuring out what may be reasonable to do for a particular patient,” Dr. Stein said in an interview.
Starting antihypertensive management early and aiming at levels below 130/80 mm Hg is a strategy that should be “reasonable” for most patients with SLE, said Dr. Stein, adding that the approach specified in the 2017 American College of Cardiology/American Heart Association (ACC/AHA) hypertension guidelines are appropriate to follow. In those guidelines, the threshold for diagnosis of hypertension was lowered to 130/80 mm Hg.
“You can start with risk factor modification, in terms of losing weight, exercising, stopping alcohol, and decreasing salt in the diet to see if you can get the blood pressure down, though it may come down to drug therapy for many patients, I believe,” Dr. Stein said.
Authors of those 2017 ACC/AHA guidelines made no recommendations for patients with SLE or other connective tissue diseases, despite including a section devoted to specific patient subgroups and comorbidities of interest, Dr. Tselios and coauthors noted in their report.
Management of hypertension in patients with lupus may be “delayed” in patients with blood pressures reaching the current hypertension threshold, according to Dr. Tselios and colleagues, due in part to difficulties in cardiovascular risk calculation in SLE patients, as well as current risk considerations outlined in the guidelines.
“On the basis of the recent guidelines, the patient with typical lupus (young female with no traditional atherosclerotic risk factors) would be considered as a low-risk individual and not offered treatment for a BP of 130-139/80-89 mm Hg,” they said in their report.
Accordingly, Dr. Tselios and colleagues sought to determine whether the new hypertension definition predicted atherosclerotic vascular events, including new-onset angina, acute myocardial infarction, cerebrovascular events, revascularization procedures, heart failure, or peripheral vascular disease requiring angioplasty, in patients with SLE treated at a Canadian clinic.
Their analysis comprised 1,532 patients with SLE who had at least 2 years of follow-up and had no prior atherosclerotic events on record. Over a mean follow-up of nearly 11 years, there were 124 such events documented in those patients.
With a mean follow-up of nearly 11 years, the incidence of atherosclerotic events was 18.9 per 1,000 patient-years for patients with blood pressure ≥ 140/90 mm Hg, 11.5 per 1,000 patient-years for the 130-139/80-89 mm Hg group, and 4.5 per 1,000 patient-years for those with blood pressures of 130/80 mm Hg or lower, with differences that were statistically significant between groups, according to the report.
An adjusted blood pressure of 130-139/80-89 mm Hg over the first 2 years since enrollment in the clinic was independently associated with the occurrence of an atherosclerotic event, with a hazard ratio of 1.73 (95% confidence interval, 1.13-2.69, P = 0.011), according to results of a multivariable analysis.
Those findings support targeting a blood pressure below 130/80 mm Hg in all patients with lupus, according to Dr. Tselios and coauthors.
“It seems reasonable that clinicians should not rely on CV risk calculators in SLE and commence treatment as soon as possible in cases of sustained BP elevation above the threshold of 130/80 mm Hg,” they wrote in their report.
How low to go remains unclear, however, as targeting lower levels of blood pressure might be unsafe in certain groups, such as those SLE patients with prior heart disease or heart failure; nevertheless, recent observational data from non-SLE populations suggest that effective treatment to levels lower than 130/80 mm Hg would “further reduce the incidence of atherosclerotic events in SLE,” the authors said in a discussion of their results.
Dr. Tselios and coauthors said they had no competing interests relative to the study. They reported funding for the University of Toronto Lupus Clinic from the University Health Network, Lou & Marissa Rocca, Mark & Diana Bozzo, and the Lupus Foundation of Ontario.
SOURCE: Tselios K et al. Ann Rheum Dis. 2020 Mar 10. doi: 10.1136/annrheumdis-2019-216764
, results of a retrospective, single-center investigation suggest.
Risk of atherosclerotic vascular events was increased by 73% for patients with systemic lupus erythematosus (SLE) who sustained a mean blood pressure of 130/80 to 139/89 mm Hg over 2 years in the study, which included 1,532 patients treated at a clinic in Toronto.
Management of hypertension in SLE patients should start early, and should aim to achieve levels below 130/80 mm Hg, according to the investigators, led by Konstantinos Tselios, MD, PhD, of the Centre for Prognosis Studies in the Rheumatic Diseases at the University of Toronto.
“The findings of the present study support that the target BP should be less than 130/80 mm Hg in all patients with lupus in order to minimize their cardiovascular risk,” Dr. Tselios and coauthors said in their study, which appears in Annals of the Rheumatic Diseases.
Despite the limitations inherent in a retrospective, observational study, this work by Dr. Tselios and colleagues may help inform the care of patients with SLE, according to C. Michael Stein, MBChB, professor of medicine at Vanderbilt University in Nashville, Tenn.
“It’s really interesting data that’s important and helps us think in terms of figuring out what may be reasonable to do for a particular patient,” Dr. Stein said in an interview.
Starting antihypertensive management early and aiming at levels below 130/80 mm Hg is a strategy that should be “reasonable” for most patients with SLE, said Dr. Stein, adding that the approach specified in the 2017 American College of Cardiology/American Heart Association (ACC/AHA) hypertension guidelines are appropriate to follow. In those guidelines, the threshold for diagnosis of hypertension was lowered to 130/80 mm Hg.
“You can start with risk factor modification, in terms of losing weight, exercising, stopping alcohol, and decreasing salt in the diet to see if you can get the blood pressure down, though it may come down to drug therapy for many patients, I believe,” Dr. Stein said.
Authors of those 2017 ACC/AHA guidelines made no recommendations for patients with SLE or other connective tissue diseases, despite including a section devoted to specific patient subgroups and comorbidities of interest, Dr. Tselios and coauthors noted in their report.
Management of hypertension in patients with lupus may be “delayed” in patients with blood pressures reaching the current hypertension threshold, according to Dr. Tselios and colleagues, due in part to difficulties in cardiovascular risk calculation in SLE patients, as well as current risk considerations outlined in the guidelines.
“On the basis of the recent guidelines, the patient with typical lupus (young female with no traditional atherosclerotic risk factors) would be considered as a low-risk individual and not offered treatment for a BP of 130-139/80-89 mm Hg,” they said in their report.
Accordingly, Dr. Tselios and colleagues sought to determine whether the new hypertension definition predicted atherosclerotic vascular events, including new-onset angina, acute myocardial infarction, cerebrovascular events, revascularization procedures, heart failure, or peripheral vascular disease requiring angioplasty, in patients with SLE treated at a Canadian clinic.
Their analysis comprised 1,532 patients with SLE who had at least 2 years of follow-up and had no prior atherosclerotic events on record. Over a mean follow-up of nearly 11 years, there were 124 such events documented in those patients.
With a mean follow-up of nearly 11 years, the incidence of atherosclerotic events was 18.9 per 1,000 patient-years for patients with blood pressure ≥ 140/90 mm Hg, 11.5 per 1,000 patient-years for the 130-139/80-89 mm Hg group, and 4.5 per 1,000 patient-years for those with blood pressures of 130/80 mm Hg or lower, with differences that were statistically significant between groups, according to the report.
An adjusted blood pressure of 130-139/80-89 mm Hg over the first 2 years since enrollment in the clinic was independently associated with the occurrence of an atherosclerotic event, with a hazard ratio of 1.73 (95% confidence interval, 1.13-2.69, P = 0.011), according to results of a multivariable analysis.
Those findings support targeting a blood pressure below 130/80 mm Hg in all patients with lupus, according to Dr. Tselios and coauthors.
“It seems reasonable that clinicians should not rely on CV risk calculators in SLE and commence treatment as soon as possible in cases of sustained BP elevation above the threshold of 130/80 mm Hg,” they wrote in their report.
How low to go remains unclear, however, as targeting lower levels of blood pressure might be unsafe in certain groups, such as those SLE patients with prior heart disease or heart failure; nevertheless, recent observational data from non-SLE populations suggest that effective treatment to levels lower than 130/80 mm Hg would “further reduce the incidence of atherosclerotic events in SLE,” the authors said in a discussion of their results.
Dr. Tselios and coauthors said they had no competing interests relative to the study. They reported funding for the University of Toronto Lupus Clinic from the University Health Network, Lou & Marissa Rocca, Mark & Diana Bozzo, and the Lupus Foundation of Ontario.
SOURCE: Tselios K et al. Ann Rheum Dis. 2020 Mar 10. doi: 10.1136/annrheumdis-2019-216764
FROM ANNALS OF THE RHEUMATIC DISEASES
FDA provides flexibility to improve COVID-19 test availability
First, the FDA is giving states more flexibility to approve and implement testing for COVID-19.
“States can set up a system in which they take responsibility for authorizing such tests and the laboratories will not engage with the FDA,” agency Commissioner Stephen Hahn, MD, said in a March 16 statement announcing the policy updates. “Laboratories developing tests in these states can engage directly with the appropriate state authorities, instead of with the FDA.”
A copy of the updated guidance document can be found here.
Dr. Hahn added that laboratories working within this authority granted to states will not have to pursue an emergency use authorization (EUA). New York state was previously granted a waiver to allow for more state oversight over the introduction of diagnostic testing.
Second, the FDA is expanding guidance issued on Feb. 29 on who can develop diagnostic tests. Originally, the Feb. 29 guidance was aimed at labs certified to perform high-complexity testing consistent with requirements outlined in the Clinical Laboratory Improvement Amendments.
“Under the update published today, the agency does not intend to object to commercial manufacturers distributing and labs using new commercially developed tests prior to the FDA granting an EUA, under certain circumstances,” Commissioner Hahn said, adding that a number of commercial manufacturers are developing tests for the coronavirus with the intent of submitting an EUA request.
“During this public health emergency, the FDA does not intend to object to the distribution and use of these tests for specimen testing for a reasonable period of time after the manufacturer’s validation of the test while the manufacturer is preparing its EUA request,” he added.
The updated guidance also provides recommendations for test developers working on serologic tests for COVID-19.
During a March 16 conference call with reporters, Commissioner Hahn said the flexibility would add a “significant number of tests and we believe this will be a surge to meet the demand that we expect to see, although it is somewhat difficult” to quantify the number of tests this new flexibility will bring to the market.
First, the FDA is giving states more flexibility to approve and implement testing for COVID-19.
“States can set up a system in which they take responsibility for authorizing such tests and the laboratories will not engage with the FDA,” agency Commissioner Stephen Hahn, MD, said in a March 16 statement announcing the policy updates. “Laboratories developing tests in these states can engage directly with the appropriate state authorities, instead of with the FDA.”
A copy of the updated guidance document can be found here.
Dr. Hahn added that laboratories working within this authority granted to states will not have to pursue an emergency use authorization (EUA). New York state was previously granted a waiver to allow for more state oversight over the introduction of diagnostic testing.
Second, the FDA is expanding guidance issued on Feb. 29 on who can develop diagnostic tests. Originally, the Feb. 29 guidance was aimed at labs certified to perform high-complexity testing consistent with requirements outlined in the Clinical Laboratory Improvement Amendments.
“Under the update published today, the agency does not intend to object to commercial manufacturers distributing and labs using new commercially developed tests prior to the FDA granting an EUA, under certain circumstances,” Commissioner Hahn said, adding that a number of commercial manufacturers are developing tests for the coronavirus with the intent of submitting an EUA request.
“During this public health emergency, the FDA does not intend to object to the distribution and use of these tests for specimen testing for a reasonable period of time after the manufacturer’s validation of the test while the manufacturer is preparing its EUA request,” he added.
The updated guidance also provides recommendations for test developers working on serologic tests for COVID-19.
During a March 16 conference call with reporters, Commissioner Hahn said the flexibility would add a “significant number of tests and we believe this will be a surge to meet the demand that we expect to see, although it is somewhat difficult” to quantify the number of tests this new flexibility will bring to the market.
First, the FDA is giving states more flexibility to approve and implement testing for COVID-19.
“States can set up a system in which they take responsibility for authorizing such tests and the laboratories will not engage with the FDA,” agency Commissioner Stephen Hahn, MD, said in a March 16 statement announcing the policy updates. “Laboratories developing tests in these states can engage directly with the appropriate state authorities, instead of with the FDA.”
A copy of the updated guidance document can be found here.
Dr. Hahn added that laboratories working within this authority granted to states will not have to pursue an emergency use authorization (EUA). New York state was previously granted a waiver to allow for more state oversight over the introduction of diagnostic testing.
Second, the FDA is expanding guidance issued on Feb. 29 on who can develop diagnostic tests. Originally, the Feb. 29 guidance was aimed at labs certified to perform high-complexity testing consistent with requirements outlined in the Clinical Laboratory Improvement Amendments.
“Under the update published today, the agency does not intend to object to commercial manufacturers distributing and labs using new commercially developed tests prior to the FDA granting an EUA, under certain circumstances,” Commissioner Hahn said, adding that a number of commercial manufacturers are developing tests for the coronavirus with the intent of submitting an EUA request.
“During this public health emergency, the FDA does not intend to object to the distribution and use of these tests for specimen testing for a reasonable period of time after the manufacturer’s validation of the test while the manufacturer is preparing its EUA request,” he added.
The updated guidance also provides recommendations for test developers working on serologic tests for COVID-19.
During a March 16 conference call with reporters, Commissioner Hahn said the flexibility would add a “significant number of tests and we believe this will be a surge to meet the demand that we expect to see, although it is somewhat difficult” to quantify the number of tests this new flexibility will bring to the market.
Vision symptoms are common and often life-altering for patients with Parkinson’s disease
according to the results of a multicenter, cross-sectional cohort study.
“Ophthalmologic symptoms are underreported by patients with Parkinson’s disease and often overlooked by their treating physicians,” noted the investigators, who were led by Carlijn D.J.M. Borm, MD, Parkinson Centre Nijmegen (the Netherlands), Department of Neurology, Donders Institute for Brain, Cognition and Behaviour at Radboud University Medical Centre. “Importantly, intact vision is especially vital for patients with Parkinson’s disease to compensate (through visual guidance) for their common loss of motor automaticity that is caused by basal ganglia dysfunction.”
The investigators studied 848 patients with Parkinson’s disease in the Netherlands and Austria who were recruited by e-mail or in outpatient clinics and 250 age-matched healthy controls drawn from partners and acquaintances, comparing the groups on symptoms assessed with the Visual Impairment in Parkinson’s Disease Questionnaire (VIPD-Q).
Results reported in Neurology showed that 82% of patients with Parkinson’s disease reported at least one ophthalmologic symptom, compared with 48% of age-matched healthy controls (P < .001). Symptoms related to the ocular surface – blurry near vision, a burning or gritty sensation, mucus or particles, and watering of the eyes – were the most common.
Moreover, 68% of patients reported having ophthalmologic symptoms that interfered with daily activities, compared with 35% of healthy controls (P < .001).
The study’s findings suggest “that either Parkinson’s disease itself or its treatment has an effect on ophthalmologic functions beyond the normal aging process,” Dr. Borm and coinvestigators wrote. “The high prevalence of ophthalmologic symptoms and their effect on daily life is striking, and emphasizes the need to address this subject in both research and clinical practice.”
“Patients who report ophthalmologic symptoms need a referral for further evaluation. For those patients who do not volunteer problems themselves, a screening questionnaire such as the VIPD-Q may help with identifying ophthalmologic symptoms in patients with Parkinson’s disease that might otherwise be missed, thereby enabling timely referral and treatment,” they noted.
Study details
The study participants were 70 years old, on average, and the patients with Parkinson’s disease had had the disease for a median duration of 7 years. Compared with the healthy control group, the patient group more often reported that they used visual aids (95% vs. 88%; P = .001) and had visited an ophthalmologist (35% vs. 19%; P < .001). The median score on the VIPD-Q, out of a possible 51 points, was 10 among the patients with Parkinson’s disease, compared with 2 among the healthy controls (P < .001).
Patients most commonly reported symptoms related to the ocular surface (63% vs. 24% among controls; P < .001). But they also often reported symptoms in the intraocular domain (54% vs. 25%; P < .001), the oculomotor domain (44% vs. 10%; P < .001), and the optic nerve domain (44% vs. 19%; P < .001). Fully 22% of the patients reported visual hallucinations, compared with just 2% of the healthy controls (P < .001).
As VIPD-Q score increased, so did the likelihood of falls (odds ratio, 1.043; P < .001). In addition, patients with Parkinson’s disease more often reported that ophthalmologic symptoms had a moderate or severe impact on their quality of life (53% vs. 16%; P < .001).
Dr. Borm disclosed no relevant conflicts of interest. The study was funded by the Stichting Parkinson Fonds.
Awareness is key to spotting these treatable symptoms
“This study confirms a lot of what we already knew about Parkinson’s disease, but it gives more numbers to it and also the patient’s perspective rather than the doctor’s perspective,” Andrew G. Lee, MD, commented in an interview. “We know that patients with Parkinson’s disease have a lot of ophthalmologic symptoms – probably more than we recognize or ask about in the clinic – and their symptoms predominantly are out of proportion to what we see on exam,” said Dr. Lee, who is chairman of the Department of Ophthalmology at Blanton Eye Institute, Houston Methodist Hospital.
In fact, patients may have normal acuity, normal visual fields, and a normal structural eye exam, yet still report vision problems because of the central neurodegeneration occurring, he noted. “Ophthalmologists cannot rely on just the eye exam when examining patients with Parkinson’s disease. They have to take symptoms into consideration. It’s really important to be aware of how brain disease can affect the eyes symptom-wise, even though the eye exam is normal.”
Administering the questionnaire used in the study is not very difficult but is somewhat time consuming, so most ophthalmologists and neurologists are unlikely to use it, according to Dr. Lee. But knowing common symptoms and asking about them can ensure they are promptly recognized, the first step in addressing them.
“None of the visual complaints in patients with Parkinson’s disease are curable because Parkinson’s disease is not curable and the disease is the underlying major etiology for the problems. However, all of the symptoms have treatments,” he said.
For example, dry eye, caused by decreased blinking, can be treated with drops. Convergence insufficiency, which generates double vision when focusing on nearby objects, can be managed with prisms, exercises, and if needed, eye muscle surgery. Impaired eye movement is best treated with different sets of glasses specific to tasks, such as one pair for reading and one pair for distance. And visual hallucinations can be addressed with changes to existing medications or new medication, or simple reassurance that the hallucinations aren’t harmful.
“It’s important that this kind of study increases awareness in the medical community,” concluded Dr. Lee, who disclosed no relevant conflicts of interest. “The take-home messages are that eye doctors know that these are real complaints, that the eye exam is not going to give the answer, and that all of the symptoms have treatments even though there is no cure.”
SOURCE: Borm CDJM et al. Neurology. 2020 Mar 11. doi: 10.1212/WNL.0000000000009214.
according to the results of a multicenter, cross-sectional cohort study.
“Ophthalmologic symptoms are underreported by patients with Parkinson’s disease and often overlooked by their treating physicians,” noted the investigators, who were led by Carlijn D.J.M. Borm, MD, Parkinson Centre Nijmegen (the Netherlands), Department of Neurology, Donders Institute for Brain, Cognition and Behaviour at Radboud University Medical Centre. “Importantly, intact vision is especially vital for patients with Parkinson’s disease to compensate (through visual guidance) for their common loss of motor automaticity that is caused by basal ganglia dysfunction.”
The investigators studied 848 patients with Parkinson’s disease in the Netherlands and Austria who were recruited by e-mail or in outpatient clinics and 250 age-matched healthy controls drawn from partners and acquaintances, comparing the groups on symptoms assessed with the Visual Impairment in Parkinson’s Disease Questionnaire (VIPD-Q).
Results reported in Neurology showed that 82% of patients with Parkinson’s disease reported at least one ophthalmologic symptom, compared with 48% of age-matched healthy controls (P < .001). Symptoms related to the ocular surface – blurry near vision, a burning or gritty sensation, mucus or particles, and watering of the eyes – were the most common.
Moreover, 68% of patients reported having ophthalmologic symptoms that interfered with daily activities, compared with 35% of healthy controls (P < .001).
The study’s findings suggest “that either Parkinson’s disease itself or its treatment has an effect on ophthalmologic functions beyond the normal aging process,” Dr. Borm and coinvestigators wrote. “The high prevalence of ophthalmologic symptoms and their effect on daily life is striking, and emphasizes the need to address this subject in both research and clinical practice.”
“Patients who report ophthalmologic symptoms need a referral for further evaluation. For those patients who do not volunteer problems themselves, a screening questionnaire such as the VIPD-Q may help with identifying ophthalmologic symptoms in patients with Parkinson’s disease that might otherwise be missed, thereby enabling timely referral and treatment,” they noted.
Study details
The study participants were 70 years old, on average, and the patients with Parkinson’s disease had had the disease for a median duration of 7 years. Compared with the healthy control group, the patient group more often reported that they used visual aids (95% vs. 88%; P = .001) and had visited an ophthalmologist (35% vs. 19%; P < .001). The median score on the VIPD-Q, out of a possible 51 points, was 10 among the patients with Parkinson’s disease, compared with 2 among the healthy controls (P < .001).
Patients most commonly reported symptoms related to the ocular surface (63% vs. 24% among controls; P < .001). But they also often reported symptoms in the intraocular domain (54% vs. 25%; P < .001), the oculomotor domain (44% vs. 10%; P < .001), and the optic nerve domain (44% vs. 19%; P < .001). Fully 22% of the patients reported visual hallucinations, compared with just 2% of the healthy controls (P < .001).
As VIPD-Q score increased, so did the likelihood of falls (odds ratio, 1.043; P < .001). In addition, patients with Parkinson’s disease more often reported that ophthalmologic symptoms had a moderate or severe impact on their quality of life (53% vs. 16%; P < .001).
Dr. Borm disclosed no relevant conflicts of interest. The study was funded by the Stichting Parkinson Fonds.
Awareness is key to spotting these treatable symptoms
“This study confirms a lot of what we already knew about Parkinson’s disease, but it gives more numbers to it and also the patient’s perspective rather than the doctor’s perspective,” Andrew G. Lee, MD, commented in an interview. “We know that patients with Parkinson’s disease have a lot of ophthalmologic symptoms – probably more than we recognize or ask about in the clinic – and their symptoms predominantly are out of proportion to what we see on exam,” said Dr. Lee, who is chairman of the Department of Ophthalmology at Blanton Eye Institute, Houston Methodist Hospital.
In fact, patients may have normal acuity, normal visual fields, and a normal structural eye exam, yet still report vision problems because of the central neurodegeneration occurring, he noted. “Ophthalmologists cannot rely on just the eye exam when examining patients with Parkinson’s disease. They have to take symptoms into consideration. It’s really important to be aware of how brain disease can affect the eyes symptom-wise, even though the eye exam is normal.”
Administering the questionnaire used in the study is not very difficult but is somewhat time consuming, so most ophthalmologists and neurologists are unlikely to use it, according to Dr. Lee. But knowing common symptoms and asking about them can ensure they are promptly recognized, the first step in addressing them.
“None of the visual complaints in patients with Parkinson’s disease are curable because Parkinson’s disease is not curable and the disease is the underlying major etiology for the problems. However, all of the symptoms have treatments,” he said.
For example, dry eye, caused by decreased blinking, can be treated with drops. Convergence insufficiency, which generates double vision when focusing on nearby objects, can be managed with prisms, exercises, and if needed, eye muscle surgery. Impaired eye movement is best treated with different sets of glasses specific to tasks, such as one pair for reading and one pair for distance. And visual hallucinations can be addressed with changes to existing medications or new medication, or simple reassurance that the hallucinations aren’t harmful.
“It’s important that this kind of study increases awareness in the medical community,” concluded Dr. Lee, who disclosed no relevant conflicts of interest. “The take-home messages are that eye doctors know that these are real complaints, that the eye exam is not going to give the answer, and that all of the symptoms have treatments even though there is no cure.”
SOURCE: Borm CDJM et al. Neurology. 2020 Mar 11. doi: 10.1212/WNL.0000000000009214.
according to the results of a multicenter, cross-sectional cohort study.
“Ophthalmologic symptoms are underreported by patients with Parkinson’s disease and often overlooked by their treating physicians,” noted the investigators, who were led by Carlijn D.J.M. Borm, MD, Parkinson Centre Nijmegen (the Netherlands), Department of Neurology, Donders Institute for Brain, Cognition and Behaviour at Radboud University Medical Centre. “Importantly, intact vision is especially vital for patients with Parkinson’s disease to compensate (through visual guidance) for their common loss of motor automaticity that is caused by basal ganglia dysfunction.”
The investigators studied 848 patients with Parkinson’s disease in the Netherlands and Austria who were recruited by e-mail or in outpatient clinics and 250 age-matched healthy controls drawn from partners and acquaintances, comparing the groups on symptoms assessed with the Visual Impairment in Parkinson’s Disease Questionnaire (VIPD-Q).
Results reported in Neurology showed that 82% of patients with Parkinson’s disease reported at least one ophthalmologic symptom, compared with 48% of age-matched healthy controls (P < .001). Symptoms related to the ocular surface – blurry near vision, a burning or gritty sensation, mucus or particles, and watering of the eyes – were the most common.
Moreover, 68% of patients reported having ophthalmologic symptoms that interfered with daily activities, compared with 35% of healthy controls (P < .001).
The study’s findings suggest “that either Parkinson’s disease itself or its treatment has an effect on ophthalmologic functions beyond the normal aging process,” Dr. Borm and coinvestigators wrote. “The high prevalence of ophthalmologic symptoms and their effect on daily life is striking, and emphasizes the need to address this subject in both research and clinical practice.”
“Patients who report ophthalmologic symptoms need a referral for further evaluation. For those patients who do not volunteer problems themselves, a screening questionnaire such as the VIPD-Q may help with identifying ophthalmologic symptoms in patients with Parkinson’s disease that might otherwise be missed, thereby enabling timely referral and treatment,” they noted.
Study details
The study participants were 70 years old, on average, and the patients with Parkinson’s disease had had the disease for a median duration of 7 years. Compared with the healthy control group, the patient group more often reported that they used visual aids (95% vs. 88%; P = .001) and had visited an ophthalmologist (35% vs. 19%; P < .001). The median score on the VIPD-Q, out of a possible 51 points, was 10 among the patients with Parkinson’s disease, compared with 2 among the healthy controls (P < .001).
Patients most commonly reported symptoms related to the ocular surface (63% vs. 24% among controls; P < .001). But they also often reported symptoms in the intraocular domain (54% vs. 25%; P < .001), the oculomotor domain (44% vs. 10%; P < .001), and the optic nerve domain (44% vs. 19%; P < .001). Fully 22% of the patients reported visual hallucinations, compared with just 2% of the healthy controls (P < .001).
As VIPD-Q score increased, so did the likelihood of falls (odds ratio, 1.043; P < .001). In addition, patients with Parkinson’s disease more often reported that ophthalmologic symptoms had a moderate or severe impact on their quality of life (53% vs. 16%; P < .001).
Dr. Borm disclosed no relevant conflicts of interest. The study was funded by the Stichting Parkinson Fonds.
Awareness is key to spotting these treatable symptoms
“This study confirms a lot of what we already knew about Parkinson’s disease, but it gives more numbers to it and also the patient’s perspective rather than the doctor’s perspective,” Andrew G. Lee, MD, commented in an interview. “We know that patients with Parkinson’s disease have a lot of ophthalmologic symptoms – probably more than we recognize or ask about in the clinic – and their symptoms predominantly are out of proportion to what we see on exam,” said Dr. Lee, who is chairman of the Department of Ophthalmology at Blanton Eye Institute, Houston Methodist Hospital.
In fact, patients may have normal acuity, normal visual fields, and a normal structural eye exam, yet still report vision problems because of the central neurodegeneration occurring, he noted. “Ophthalmologists cannot rely on just the eye exam when examining patients with Parkinson’s disease. They have to take symptoms into consideration. It’s really important to be aware of how brain disease can affect the eyes symptom-wise, even though the eye exam is normal.”
Administering the questionnaire used in the study is not very difficult but is somewhat time consuming, so most ophthalmologists and neurologists are unlikely to use it, according to Dr. Lee. But knowing common symptoms and asking about them can ensure they are promptly recognized, the first step in addressing them.
“None of the visual complaints in patients with Parkinson’s disease are curable because Parkinson’s disease is not curable and the disease is the underlying major etiology for the problems. However, all of the symptoms have treatments,” he said.
For example, dry eye, caused by decreased blinking, can be treated with drops. Convergence insufficiency, which generates double vision when focusing on nearby objects, can be managed with prisms, exercises, and if needed, eye muscle surgery. Impaired eye movement is best treated with different sets of glasses specific to tasks, such as one pair for reading and one pair for distance. And visual hallucinations can be addressed with changes to existing medications or new medication, or simple reassurance that the hallucinations aren’t harmful.
“It’s important that this kind of study increases awareness in the medical community,” concluded Dr. Lee, who disclosed no relevant conflicts of interest. “The take-home messages are that eye doctors know that these are real complaints, that the eye exam is not going to give the answer, and that all of the symptoms have treatments even though there is no cure.”
SOURCE: Borm CDJM et al. Neurology. 2020 Mar 11. doi: 10.1212/WNL.0000000000009214.
FROM NEUROLOGY
Combo maintenance boosts PFS, not OS, in advanced NSCLC
(NSCLC).
However, the addition of pemetrexed to bevacizumab maintenance improved OS for patients with wild-type EGFR, reported Takashi Seto, MD, of the National Kyushu Cancer Center, Japan, and colleagues. Their report was published in the Journal of Clinical Oncology.
The researchers conducted a phase 3 trial of 599 patients with previously untreated, advanced nonsquamous NSCLC. Patients were randomly allocated to receive maintenance with either pemetrexed (500 mg/m2) and bevacizumab (15 mg/kg) or bevacizumab alone (15 mg/kg once every 3 weeks).
Prior to starting maintenance, patients received induction with carboplatin, pemetrexed, and bevacizumab. Both interventions were maintained until unacceptable toxicity, disease progression, death, or withdrawal for other reasons.
The primary outcome was OS, measured from the time of randomization until death from any cause. Secondary outcomes included PFS and safety.
Survival
Overall, there was no significant difference in OS between the treatment arms. The median OS was 23.3 months in the pemetrexed-bevacizumab arm and 19.6 months in the bevacizumab arm (hazard ratio, 0.87; P = .069).
However, OS was significantly prolonged for patients with wild-type EGFR who received pemetrexed plus bevacizumab. The median OS was 23.3 months in the pemetrexed-bevacizumab arm and 18.8 months in the bevacizumab arm (HR, 0.82; P = .020).
For the entire cohort, PFS was significantly better in the pemetrexed-bevacizumab arm. The median PFS was 5.7 months in the pemetrexed-bevacizumab arm and 4.0 months in the bevacizumab arm (HR, 0.67; P < .001).
Safety
In the pemetrexed-bevacizumab arm, the most common grade 3 or higher adverse events were low neutrophil count (14.0%), hypertension (11.7%), and low white blood cell count (5.4%).
Treatment-related deaths occurred in four patients receiving pemetrexed-bevacizumab maintenance. The causes of death were interstitial pneumonitis (n = 2), alveolar hemorrhage, and lung infection.
“The safety profile obtained in this study was predictable and similar to previous reports,” the researchers wrote. They acknowledged that bevacizumab-induced hypertension was commonly observed but was not problematic from a clinical perspective.
Based on these results, the researchers concluded that pemetrexed plus bevacizumab maintenance is “useful” in patients with advanced nonsquamous NSCLC, especially in patients with wild-type EGFR.
This study was supported, in part, by Eli Lilly Japan KK. The authors disclosed financial affiliations with Eli Lilly and other companies.
SOURCE: Seto T et al. J Clin Oncol. 2020 Mar 10;38(8):793-803.
(NSCLC).
However, the addition of pemetrexed to bevacizumab maintenance improved OS for patients with wild-type EGFR, reported Takashi Seto, MD, of the National Kyushu Cancer Center, Japan, and colleagues. Their report was published in the Journal of Clinical Oncology.
The researchers conducted a phase 3 trial of 599 patients with previously untreated, advanced nonsquamous NSCLC. Patients were randomly allocated to receive maintenance with either pemetrexed (500 mg/m2) and bevacizumab (15 mg/kg) or bevacizumab alone (15 mg/kg once every 3 weeks).
Prior to starting maintenance, patients received induction with carboplatin, pemetrexed, and bevacizumab. Both interventions were maintained until unacceptable toxicity, disease progression, death, or withdrawal for other reasons.
The primary outcome was OS, measured from the time of randomization until death from any cause. Secondary outcomes included PFS and safety.
Survival
Overall, there was no significant difference in OS between the treatment arms. The median OS was 23.3 months in the pemetrexed-bevacizumab arm and 19.6 months in the bevacizumab arm (hazard ratio, 0.87; P = .069).
However, OS was significantly prolonged for patients with wild-type EGFR who received pemetrexed plus bevacizumab. The median OS was 23.3 months in the pemetrexed-bevacizumab arm and 18.8 months in the bevacizumab arm (HR, 0.82; P = .020).
For the entire cohort, PFS was significantly better in the pemetrexed-bevacizumab arm. The median PFS was 5.7 months in the pemetrexed-bevacizumab arm and 4.0 months in the bevacizumab arm (HR, 0.67; P < .001).
Safety
In the pemetrexed-bevacizumab arm, the most common grade 3 or higher adverse events were low neutrophil count (14.0%), hypertension (11.7%), and low white blood cell count (5.4%).
Treatment-related deaths occurred in four patients receiving pemetrexed-bevacizumab maintenance. The causes of death were interstitial pneumonitis (n = 2), alveolar hemorrhage, and lung infection.
“The safety profile obtained in this study was predictable and similar to previous reports,” the researchers wrote. They acknowledged that bevacizumab-induced hypertension was commonly observed but was not problematic from a clinical perspective.
Based on these results, the researchers concluded that pemetrexed plus bevacizumab maintenance is “useful” in patients with advanced nonsquamous NSCLC, especially in patients with wild-type EGFR.
This study was supported, in part, by Eli Lilly Japan KK. The authors disclosed financial affiliations with Eli Lilly and other companies.
SOURCE: Seto T et al. J Clin Oncol. 2020 Mar 10;38(8):793-803.
(NSCLC).
However, the addition of pemetrexed to bevacizumab maintenance improved OS for patients with wild-type EGFR, reported Takashi Seto, MD, of the National Kyushu Cancer Center, Japan, and colleagues. Their report was published in the Journal of Clinical Oncology.
The researchers conducted a phase 3 trial of 599 patients with previously untreated, advanced nonsquamous NSCLC. Patients were randomly allocated to receive maintenance with either pemetrexed (500 mg/m2) and bevacizumab (15 mg/kg) or bevacizumab alone (15 mg/kg once every 3 weeks).
Prior to starting maintenance, patients received induction with carboplatin, pemetrexed, and bevacizumab. Both interventions were maintained until unacceptable toxicity, disease progression, death, or withdrawal for other reasons.
The primary outcome was OS, measured from the time of randomization until death from any cause. Secondary outcomes included PFS and safety.
Survival
Overall, there was no significant difference in OS between the treatment arms. The median OS was 23.3 months in the pemetrexed-bevacizumab arm and 19.6 months in the bevacizumab arm (hazard ratio, 0.87; P = .069).
However, OS was significantly prolonged for patients with wild-type EGFR who received pemetrexed plus bevacizumab. The median OS was 23.3 months in the pemetrexed-bevacizumab arm and 18.8 months in the bevacizumab arm (HR, 0.82; P = .020).
For the entire cohort, PFS was significantly better in the pemetrexed-bevacizumab arm. The median PFS was 5.7 months in the pemetrexed-bevacizumab arm and 4.0 months in the bevacizumab arm (HR, 0.67; P < .001).
Safety
In the pemetrexed-bevacizumab arm, the most common grade 3 or higher adverse events were low neutrophil count (14.0%), hypertension (11.7%), and low white blood cell count (5.4%).
Treatment-related deaths occurred in four patients receiving pemetrexed-bevacizumab maintenance. The causes of death were interstitial pneumonitis (n = 2), alveolar hemorrhage, and lung infection.
“The safety profile obtained in this study was predictable and similar to previous reports,” the researchers wrote. They acknowledged that bevacizumab-induced hypertension was commonly observed but was not problematic from a clinical perspective.
Based on these results, the researchers concluded that pemetrexed plus bevacizumab maintenance is “useful” in patients with advanced nonsquamous NSCLC, especially in patients with wild-type EGFR.
This study was supported, in part, by Eli Lilly Japan KK. The authors disclosed financial affiliations with Eli Lilly and other companies.
SOURCE: Seto T et al. J Clin Oncol. 2020 Mar 10;38(8):793-803.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Fracture liaison services confer benefit on recurrent fracture risk
Implementation of fracture liaison services (FLS) at two Swedish hospitals was associated with an 18% reduction of recurrent fracture over a median follow-up of 2.2 years, results from an observational cohort study found.
“Patients receiving fracture care within an FLS have higher rates of [bone mineral density] testing, treatment initiation and better adherence,” first author Kristian F. Axelsson, MD, and colleagues wrote in a study published in the Journal of Bone and Mineral Research. “However, the evidence regarding FLS and association to reduced risk of recurrent fracture is insufficient, consisting of smaller studies, studies with short follow-up time, and studies with high risk of various biases.”
Dr. Axelsson, of the department of orthopedic surgery at Skaraborg Hospital, Skövde, Sweden, and colleagues used electronic patient records from four hospitals in Western Sweden to identify all patients aged 50 years or older with a major osteoporotic fracture – defined as a fracture of the wrist, upper arm, hip, vertebra, or pelvis – between 2012 and 2017. The study population consisted of 15,449 patients from two hospitals with FLS and 5,634 patients from two hospitals with no FLS. The researchers used multivariable Cox models to compare all patients with a major osteoporotic fracture during the FLS period with all patients with a major osteoporotic fracture prior to the FLS implementation. The FLS hospitals and non-FLS hospitals were analyzed separately using the same methodology.
The mean age of patients was 74 years, 76% were female, and the most common index fracture site was the wrist (42%). In the hospitals with FLS, the researchers observed 1,247 recurrent fractures during a median follow-up time of 2.2 years. In an unadjusted Cox model, the risk of recurrent fracture was 18% lower in the FLS period, compared with the control period (hazard ratio, 0.82; P = .001). This corresponded to a 3-year number needed to screen of 61, and did not change after adjustment for clinical risk factors. In the non-FLS hospitals, no change in recurrent fracture rate was observed.
Osteoporosis medication treatment rates after fracture did not differ between the FLS and non-FLS hospitals, prior to FLS implementation (14.7% vs. 13.3%, respectively; P = .10). However, following FLS implementation, a larger proportion of fracture patients were treated at the FLS hospitals, compared with those at the non-FLS hospitals (28% vs. 12.9%; P less than .001).
“Our study is the largest yet, including both historic controls and controls at nearby hospitals without implementations of fracture liaison services,” one of the study authors, Mattias Lorentzon, MD, said in an interview. “We were able to rule out temporal trends in refracture risk and show that, [in] patients who had an index fracture at a hospital with an FLS, the refracture rate was lower than for patients who had an index fracture before the FLS was started, indicating that FLS reduce the risk of recurrent fracture. No such trends were observed in hospitals without FLS during the same time period.”
Dr. Lorentzon, head of geriatric medicine at Sahlgrenska University Hospital, Mölndal, Sweden, said that FLS implementation “led to a large increase in the use of osteoporosis medication, which we believe is the reason for the reduction in recurrent fracture risk observed. We believe that our results provide solid evidence that FLS implementation can reduce the rate of recurrent fractures, suggesting that all hospitals treating fracture patients should have fracture liaison services.”
In an interview, Stuart L. Silverman, MD, said that the study adds to compelling data on the efficacy and need for patients with clinical fracture to have case management by a FLS. “We recognize that near term risk is substantial in the year following a fracture,” said Dr. Silverman, who is clinical professor of medicine at Cedars-Sinai Medical Center and the University of California, Los Angeles, and is not affiliated with the Swedish study. “For example, the risk of a subsequent fracture after hip fracture is 8.3%, which is similar to the risk of subsequent acute myocardial infarction after an initial acute MI. However, only 23% of patients receive osteoporosis medication after a hip fracture. Yet a fracture is to osteoporosis what an acute MI is to cardiovascular disease. We recognize that men and women age 65 years and older who have suffered a hip or vertebral fracture should be evaluated for treatment, as this subpopulation is at high risk for a second fracture and evidence supporting treatment efficacy is robust. We need a multidisciplinary clinical system which includes case management such as a fracture liaison service. We know FLS can reduce hip fracture rate in a closed system such as Kaiser by over 40%. This manuscript addresses the utility of a FLS in terms of reducing risk of future fracture.”
The researchers acknowledged certain limitations of the study, including its observational design and the fact that patients prior to the FLS period were fewer and had longer follow-up time, compared with patients during the FLS period.
The study was funded by the Swedish Research Council and by grants from the Sahlgrenska University Hospital. Dr. Axelsson reported that he has received lecture fees from Lilly, Meda/Mylan, and Amgen. Dr. Lorentzon has received lecture fees from Amgen, Lilly, UCB, Radius Health, Meda, GE-Lunar, and Santax Medico/Hologic. The other coauthors reported having no financial disclosures. Dr. Silverman reported that he is a member of the speakers’ bureaus for Amgen and Radius. He is also a consultant for Lilly, Pfizer, and Amgen and has received research grants from Radius and Amgen.
SOURCE: Axelsson K et al. J Bone Min Res. 2020 Feb 25. doi: 10.1002/jbmr.3990.
Implementation of fracture liaison services (FLS) at two Swedish hospitals was associated with an 18% reduction of recurrent fracture over a median follow-up of 2.2 years, results from an observational cohort study found.
“Patients receiving fracture care within an FLS have higher rates of [bone mineral density] testing, treatment initiation and better adherence,” first author Kristian F. Axelsson, MD, and colleagues wrote in a study published in the Journal of Bone and Mineral Research. “However, the evidence regarding FLS and association to reduced risk of recurrent fracture is insufficient, consisting of smaller studies, studies with short follow-up time, and studies with high risk of various biases.”
Dr. Axelsson, of the department of orthopedic surgery at Skaraborg Hospital, Skövde, Sweden, and colleagues used electronic patient records from four hospitals in Western Sweden to identify all patients aged 50 years or older with a major osteoporotic fracture – defined as a fracture of the wrist, upper arm, hip, vertebra, or pelvis – between 2012 and 2017. The study population consisted of 15,449 patients from two hospitals with FLS and 5,634 patients from two hospitals with no FLS. The researchers used multivariable Cox models to compare all patients with a major osteoporotic fracture during the FLS period with all patients with a major osteoporotic fracture prior to the FLS implementation. The FLS hospitals and non-FLS hospitals were analyzed separately using the same methodology.
The mean age of patients was 74 years, 76% were female, and the most common index fracture site was the wrist (42%). In the hospitals with FLS, the researchers observed 1,247 recurrent fractures during a median follow-up time of 2.2 years. In an unadjusted Cox model, the risk of recurrent fracture was 18% lower in the FLS period, compared with the control period (hazard ratio, 0.82; P = .001). This corresponded to a 3-year number needed to screen of 61, and did not change after adjustment for clinical risk factors. In the non-FLS hospitals, no change in recurrent fracture rate was observed.
Osteoporosis medication treatment rates after fracture did not differ between the FLS and non-FLS hospitals, prior to FLS implementation (14.7% vs. 13.3%, respectively; P = .10). However, following FLS implementation, a larger proportion of fracture patients were treated at the FLS hospitals, compared with those at the non-FLS hospitals (28% vs. 12.9%; P less than .001).
“Our study is the largest yet, including both historic controls and controls at nearby hospitals without implementations of fracture liaison services,” one of the study authors, Mattias Lorentzon, MD, said in an interview. “We were able to rule out temporal trends in refracture risk and show that, [in] patients who had an index fracture at a hospital with an FLS, the refracture rate was lower than for patients who had an index fracture before the FLS was started, indicating that FLS reduce the risk of recurrent fracture. No such trends were observed in hospitals without FLS during the same time period.”
Dr. Lorentzon, head of geriatric medicine at Sahlgrenska University Hospital, Mölndal, Sweden, said that FLS implementation “led to a large increase in the use of osteoporosis medication, which we believe is the reason for the reduction in recurrent fracture risk observed. We believe that our results provide solid evidence that FLS implementation can reduce the rate of recurrent fractures, suggesting that all hospitals treating fracture patients should have fracture liaison services.”
In an interview, Stuart L. Silverman, MD, said that the study adds to compelling data on the efficacy and need for patients with clinical fracture to have case management by a FLS. “We recognize that near term risk is substantial in the year following a fracture,” said Dr. Silverman, who is clinical professor of medicine at Cedars-Sinai Medical Center and the University of California, Los Angeles, and is not affiliated with the Swedish study. “For example, the risk of a subsequent fracture after hip fracture is 8.3%, which is similar to the risk of subsequent acute myocardial infarction after an initial acute MI. However, only 23% of patients receive osteoporosis medication after a hip fracture. Yet a fracture is to osteoporosis what an acute MI is to cardiovascular disease. We recognize that men and women age 65 years and older who have suffered a hip or vertebral fracture should be evaluated for treatment, as this subpopulation is at high risk for a second fracture and evidence supporting treatment efficacy is robust. We need a multidisciplinary clinical system which includes case management such as a fracture liaison service. We know FLS can reduce hip fracture rate in a closed system such as Kaiser by over 40%. This manuscript addresses the utility of a FLS in terms of reducing risk of future fracture.”
The researchers acknowledged certain limitations of the study, including its observational design and the fact that patients prior to the FLS period were fewer and had longer follow-up time, compared with patients during the FLS period.
The study was funded by the Swedish Research Council and by grants from the Sahlgrenska University Hospital. Dr. Axelsson reported that he has received lecture fees from Lilly, Meda/Mylan, and Amgen. Dr. Lorentzon has received lecture fees from Amgen, Lilly, UCB, Radius Health, Meda, GE-Lunar, and Santax Medico/Hologic. The other coauthors reported having no financial disclosures. Dr. Silverman reported that he is a member of the speakers’ bureaus for Amgen and Radius. He is also a consultant for Lilly, Pfizer, and Amgen and has received research grants from Radius and Amgen.
SOURCE: Axelsson K et al. J Bone Min Res. 2020 Feb 25. doi: 10.1002/jbmr.3990.
Implementation of fracture liaison services (FLS) at two Swedish hospitals was associated with an 18% reduction of recurrent fracture over a median follow-up of 2.2 years, results from an observational cohort study found.
“Patients receiving fracture care within an FLS have higher rates of [bone mineral density] testing, treatment initiation and better adherence,” first author Kristian F. Axelsson, MD, and colleagues wrote in a study published in the Journal of Bone and Mineral Research. “However, the evidence regarding FLS and association to reduced risk of recurrent fracture is insufficient, consisting of smaller studies, studies with short follow-up time, and studies with high risk of various biases.”
Dr. Axelsson, of the department of orthopedic surgery at Skaraborg Hospital, Skövde, Sweden, and colleagues used electronic patient records from four hospitals in Western Sweden to identify all patients aged 50 years or older with a major osteoporotic fracture – defined as a fracture of the wrist, upper arm, hip, vertebra, or pelvis – between 2012 and 2017. The study population consisted of 15,449 patients from two hospitals with FLS and 5,634 patients from two hospitals with no FLS. The researchers used multivariable Cox models to compare all patients with a major osteoporotic fracture during the FLS period with all patients with a major osteoporotic fracture prior to the FLS implementation. The FLS hospitals and non-FLS hospitals were analyzed separately using the same methodology.
The mean age of patients was 74 years, 76% were female, and the most common index fracture site was the wrist (42%). In the hospitals with FLS, the researchers observed 1,247 recurrent fractures during a median follow-up time of 2.2 years. In an unadjusted Cox model, the risk of recurrent fracture was 18% lower in the FLS period, compared with the control period (hazard ratio, 0.82; P = .001). This corresponded to a 3-year number needed to screen of 61, and did not change after adjustment for clinical risk factors. In the non-FLS hospitals, no change in recurrent fracture rate was observed.
Osteoporosis medication treatment rates after fracture did not differ between the FLS and non-FLS hospitals, prior to FLS implementation (14.7% vs. 13.3%, respectively; P = .10). However, following FLS implementation, a larger proportion of fracture patients were treated at the FLS hospitals, compared with those at the non-FLS hospitals (28% vs. 12.9%; P less than .001).
“Our study is the largest yet, including both historic controls and controls at nearby hospitals without implementations of fracture liaison services,” one of the study authors, Mattias Lorentzon, MD, said in an interview. “We were able to rule out temporal trends in refracture risk and show that, [in] patients who had an index fracture at a hospital with an FLS, the refracture rate was lower than for patients who had an index fracture before the FLS was started, indicating that FLS reduce the risk of recurrent fracture. No such trends were observed in hospitals without FLS during the same time period.”
Dr. Lorentzon, head of geriatric medicine at Sahlgrenska University Hospital, Mölndal, Sweden, said that FLS implementation “led to a large increase in the use of osteoporosis medication, which we believe is the reason for the reduction in recurrent fracture risk observed. We believe that our results provide solid evidence that FLS implementation can reduce the rate of recurrent fractures, suggesting that all hospitals treating fracture patients should have fracture liaison services.”
In an interview, Stuart L. Silverman, MD, said that the study adds to compelling data on the efficacy and need for patients with clinical fracture to have case management by a FLS. “We recognize that near term risk is substantial in the year following a fracture,” said Dr. Silverman, who is clinical professor of medicine at Cedars-Sinai Medical Center and the University of California, Los Angeles, and is not affiliated with the Swedish study. “For example, the risk of a subsequent fracture after hip fracture is 8.3%, which is similar to the risk of subsequent acute myocardial infarction after an initial acute MI. However, only 23% of patients receive osteoporosis medication after a hip fracture. Yet a fracture is to osteoporosis what an acute MI is to cardiovascular disease. We recognize that men and women age 65 years and older who have suffered a hip or vertebral fracture should be evaluated for treatment, as this subpopulation is at high risk for a second fracture and evidence supporting treatment efficacy is robust. We need a multidisciplinary clinical system which includes case management such as a fracture liaison service. We know FLS can reduce hip fracture rate in a closed system such as Kaiser by over 40%. This manuscript addresses the utility of a FLS in terms of reducing risk of future fracture.”
The researchers acknowledged certain limitations of the study, including its observational design and the fact that patients prior to the FLS period were fewer and had longer follow-up time, compared with patients during the FLS period.
The study was funded by the Swedish Research Council and by grants from the Sahlgrenska University Hospital. Dr. Axelsson reported that he has received lecture fees from Lilly, Meda/Mylan, and Amgen. Dr. Lorentzon has received lecture fees from Amgen, Lilly, UCB, Radius Health, Meda, GE-Lunar, and Santax Medico/Hologic. The other coauthors reported having no financial disclosures. Dr. Silverman reported that he is a member of the speakers’ bureaus for Amgen and Radius. He is also a consultant for Lilly, Pfizer, and Amgen and has received research grants from Radius and Amgen.
SOURCE: Axelsson K et al. J Bone Min Res. 2020 Feb 25. doi: 10.1002/jbmr.3990.
FROM THE JOURNAL OF BONE AND MINERAL RESEARCH
CDC expert answers top COVID-19 questions
With new developments daily and lingering uncertainty about COVID-19, questions about testing and treatment for the coronavirus are at the forefront.
To address these top questions, Jay C. Butler, MD, deputy director for infectious diseases at the Centers for Disease Control and Prevention, sat down with JAMA editor Howard Bauchner, MD, to discuss the latest data on COVID-19 and to outline updated guidance from the agency. The following question-and-answer session was part of a live stream interview hosted by JAMA on March 16, 2020. The questions have been edited for length and clarity.
What test is being used to identify COVID-19?
In the United States, the most common and widely available test is the RT-polymerase chain reaction (rRT-PCR), which over the past few weeks has become available at public health labs across the country, Dr. Butler said during the JAMA interview. Capacity for the test is now possible in all 50 states and in Washington, D.C.
“More recently, there’s been a number of commercial labs that have come online to be able to do the testing,” Dr. Butler said. “Additionally, a number of academic centers are now able to run [Food and Drug Administration]–approved testing using slightly different PCR platforms.”
How accurate is the test?
Dr. Butler called PCR the “gold standard,” for testing COVID-19, and said it’s safe to say the test’s likelihood of identifying infection or past infection is extremely high. However, data on test sensitivity is limited.
“This may be frustrating to those of us who really like to know specifics of how to interpret the test results, but it’s important to keep in mind, we’re talking about a virus that we didn’t know existed 3 months ago,” he said.
At what point does a person with coronavirus test positive?
When exactly a test becomes positive is an unknown, Dr. Butler said. The assumption is that a patient who tests positive is more likely to be infectious, and data suggest the level of infectiousness is greatest after the onset of symptoms.
“There is at least some anecdotal reports that suggest that transmission could occur before onset of symptoms, but the data is still very limited,” he said. “Of course that has big implications in terms of how well we can really slow the spread of the virus.”
Who should get tested?
Dr. Butler said the focus should be individuals who are symptomatic with evidence of respiratory tract infection. People who are concerned about the virus and want a test are not the target.
“It’s important when talking to patients to help them to understand, this is different than a test for HIV or hepatitis C, where much of the message is: ‘Please get tested.’ ” he said. “This a situation where we’re trying to diagnose an acute infection. We do have a resource that may become limited again as some of the equipment required for running the test or collecting the specimen may come into short supply, so we want to focus on those people who are symptomatic and particularly on people who may be at higher risk of more severe illness.”
If a previously infected patient tests negative, can they still shed virus?
The CDC is currently analyzing how a negative PCR test relates to viral load, according to Dr. Butler. He added there have been situations in which a patient has twice tested negative for the virus, but a third swab resulted in a weakly positive result.
“It’s not clear if those are people who are actually infectious,” he said. “The PCR is detecting viral RNA, it doesn’t necessarily indicate there is viable virus present in the respiratory tract. So in general, I think it is safe to go back to work, but a positive test in a situation like that can be very difficult to interpret because we think it probably doesn’t reflect infectivity, but we don’t know for sure.”
Do we have an adequate supply of tests in the United States?
The CDC has addressed supply concerns by broadening the number of PCR platforms that can be used to run COVID-19 analyses, Dr. Butler said. Expansion of these platforms has been one way the government is furthering testing options and enabling consumer labs and academic centers to contribute to testing.
When can people who test positive go back to work?
The CDC is still researching that question and reviewing the data, Dr. Butler said. The current recommendation is that a patient who tests positive is considered clear to return to work after two negative tests at least 24 hours apart, following the resolution of symptoms. The CDC has not yet made an official recommendation on an exact time frame, but the CDC is considering a 14-day minimum of quarantine.
“The one caveat I’ll add is that someone who is a health care worker, even if they have resolved symptoms, it’s still a good idea to wear a surgical mask [when they return to work], just as an extra precaution.”
What do we know about immunity? Can patients get reinfected?
Long-term immunity after exposure and infection is virtually unknown, Dr. Butler said. Investigators know those with COVID-19 have an antibody response, but whether that is protective or not, is unclear. In regard to older coronaviruses, such as those that cause colds, patients generally develop an antibody response and may have a period of immunity, but that immunity eventually wanes and reinfection can occur.
What is the latest on therapies?
A number of trials are underway in China and in the United States to test possible therapies for COVID-19, Dr. Butler said. One of the candidate drugs is the broad spectrum antiviral drug remdesivir, which was developed for the treatment of the Ebola virus. Additionally, the National Institutes of Health is studying the potential for monoclonal antibodies to treat COVID-19.
“Of course these are drugs not yet FDA approved,” he said. “We all want to have them in our toolbox as soon as possible, but we want to make sure these drugs are going to benefit and not harm, and that they really do have the utility that we hope for.”
Is there specific guidance for healthcare workers about COVID-19?
Health care workers have a much higher likelihood of being exposed or exposing others who are at high risk of severe infection, Dr. Butler said. That’s why, if a health care worker becomes infected and recovers, it’s still important to take extra precautions when going back to work, such as wearing a mask.
“These are recommendations that are in-draft,” he said. “I want to be clear, I’m floating concepts out there that people can consider. ... I recognize as a former infection control medical director at a hospital that sometimes you have to adapt those guidelines based on your local conditions.”
With new developments daily and lingering uncertainty about COVID-19, questions about testing and treatment for the coronavirus are at the forefront.
To address these top questions, Jay C. Butler, MD, deputy director for infectious diseases at the Centers for Disease Control and Prevention, sat down with JAMA editor Howard Bauchner, MD, to discuss the latest data on COVID-19 and to outline updated guidance from the agency. The following question-and-answer session was part of a live stream interview hosted by JAMA on March 16, 2020. The questions have been edited for length and clarity.
What test is being used to identify COVID-19?
In the United States, the most common and widely available test is the RT-polymerase chain reaction (rRT-PCR), which over the past few weeks has become available at public health labs across the country, Dr. Butler said during the JAMA interview. Capacity for the test is now possible in all 50 states and in Washington, D.C.
“More recently, there’s been a number of commercial labs that have come online to be able to do the testing,” Dr. Butler said. “Additionally, a number of academic centers are now able to run [Food and Drug Administration]–approved testing using slightly different PCR platforms.”
How accurate is the test?
Dr. Butler called PCR the “gold standard,” for testing COVID-19, and said it’s safe to say the test’s likelihood of identifying infection or past infection is extremely high. However, data on test sensitivity is limited.
“This may be frustrating to those of us who really like to know specifics of how to interpret the test results, but it’s important to keep in mind, we’re talking about a virus that we didn’t know existed 3 months ago,” he said.
At what point does a person with coronavirus test positive?
When exactly a test becomes positive is an unknown, Dr. Butler said. The assumption is that a patient who tests positive is more likely to be infectious, and data suggest the level of infectiousness is greatest after the onset of symptoms.
“There is at least some anecdotal reports that suggest that transmission could occur before onset of symptoms, but the data is still very limited,” he said. “Of course that has big implications in terms of how well we can really slow the spread of the virus.”
Who should get tested?
Dr. Butler said the focus should be individuals who are symptomatic with evidence of respiratory tract infection. People who are concerned about the virus and want a test are not the target.
“It’s important when talking to patients to help them to understand, this is different than a test for HIV or hepatitis C, where much of the message is: ‘Please get tested.’ ” he said. “This a situation where we’re trying to diagnose an acute infection. We do have a resource that may become limited again as some of the equipment required for running the test or collecting the specimen may come into short supply, so we want to focus on those people who are symptomatic and particularly on people who may be at higher risk of more severe illness.”
If a previously infected patient tests negative, can they still shed virus?
The CDC is currently analyzing how a negative PCR test relates to viral load, according to Dr. Butler. He added there have been situations in which a patient has twice tested negative for the virus, but a third swab resulted in a weakly positive result.
“It’s not clear if those are people who are actually infectious,” he said. “The PCR is detecting viral RNA, it doesn’t necessarily indicate there is viable virus present in the respiratory tract. So in general, I think it is safe to go back to work, but a positive test in a situation like that can be very difficult to interpret because we think it probably doesn’t reflect infectivity, but we don’t know for sure.”
Do we have an adequate supply of tests in the United States?
The CDC has addressed supply concerns by broadening the number of PCR platforms that can be used to run COVID-19 analyses, Dr. Butler said. Expansion of these platforms has been one way the government is furthering testing options and enabling consumer labs and academic centers to contribute to testing.
When can people who test positive go back to work?
The CDC is still researching that question and reviewing the data, Dr. Butler said. The current recommendation is that a patient who tests positive is considered clear to return to work after two negative tests at least 24 hours apart, following the resolution of symptoms. The CDC has not yet made an official recommendation on an exact time frame, but the CDC is considering a 14-day minimum of quarantine.
“The one caveat I’ll add is that someone who is a health care worker, even if they have resolved symptoms, it’s still a good idea to wear a surgical mask [when they return to work], just as an extra precaution.”
What do we know about immunity? Can patients get reinfected?
Long-term immunity after exposure and infection is virtually unknown, Dr. Butler said. Investigators know those with COVID-19 have an antibody response, but whether that is protective or not, is unclear. In regard to older coronaviruses, such as those that cause colds, patients generally develop an antibody response and may have a period of immunity, but that immunity eventually wanes and reinfection can occur.
What is the latest on therapies?
A number of trials are underway in China and in the United States to test possible therapies for COVID-19, Dr. Butler said. One of the candidate drugs is the broad spectrum antiviral drug remdesivir, which was developed for the treatment of the Ebola virus. Additionally, the National Institutes of Health is studying the potential for monoclonal antibodies to treat COVID-19.
“Of course these are drugs not yet FDA approved,” he said. “We all want to have them in our toolbox as soon as possible, but we want to make sure these drugs are going to benefit and not harm, and that they really do have the utility that we hope for.”
Is there specific guidance for healthcare workers about COVID-19?
Health care workers have a much higher likelihood of being exposed or exposing others who are at high risk of severe infection, Dr. Butler said. That’s why, if a health care worker becomes infected and recovers, it’s still important to take extra precautions when going back to work, such as wearing a mask.
“These are recommendations that are in-draft,” he said. “I want to be clear, I’m floating concepts out there that people can consider. ... I recognize as a former infection control medical director at a hospital that sometimes you have to adapt those guidelines based on your local conditions.”
With new developments daily and lingering uncertainty about COVID-19, questions about testing and treatment for the coronavirus are at the forefront.
To address these top questions, Jay C. Butler, MD, deputy director for infectious diseases at the Centers for Disease Control and Prevention, sat down with JAMA editor Howard Bauchner, MD, to discuss the latest data on COVID-19 and to outline updated guidance from the agency. The following question-and-answer session was part of a live stream interview hosted by JAMA on March 16, 2020. The questions have been edited for length and clarity.
What test is being used to identify COVID-19?
In the United States, the most common and widely available test is the RT-polymerase chain reaction (rRT-PCR), which over the past few weeks has become available at public health labs across the country, Dr. Butler said during the JAMA interview. Capacity for the test is now possible in all 50 states and in Washington, D.C.
“More recently, there’s been a number of commercial labs that have come online to be able to do the testing,” Dr. Butler said. “Additionally, a number of academic centers are now able to run [Food and Drug Administration]–approved testing using slightly different PCR platforms.”
How accurate is the test?
Dr. Butler called PCR the “gold standard,” for testing COVID-19, and said it’s safe to say the test’s likelihood of identifying infection or past infection is extremely high. However, data on test sensitivity is limited.
“This may be frustrating to those of us who really like to know specifics of how to interpret the test results, but it’s important to keep in mind, we’re talking about a virus that we didn’t know existed 3 months ago,” he said.
At what point does a person with coronavirus test positive?
When exactly a test becomes positive is an unknown, Dr. Butler said. The assumption is that a patient who tests positive is more likely to be infectious, and data suggest the level of infectiousness is greatest after the onset of symptoms.
“There is at least some anecdotal reports that suggest that transmission could occur before onset of symptoms, but the data is still very limited,” he said. “Of course that has big implications in terms of how well we can really slow the spread of the virus.”
Who should get tested?
Dr. Butler said the focus should be individuals who are symptomatic with evidence of respiratory tract infection. People who are concerned about the virus and want a test are not the target.
“It’s important when talking to patients to help them to understand, this is different than a test for HIV or hepatitis C, where much of the message is: ‘Please get tested.’ ” he said. “This a situation where we’re trying to diagnose an acute infection. We do have a resource that may become limited again as some of the equipment required for running the test or collecting the specimen may come into short supply, so we want to focus on those people who are symptomatic and particularly on people who may be at higher risk of more severe illness.”
If a previously infected patient tests negative, can they still shed virus?
The CDC is currently analyzing how a negative PCR test relates to viral load, according to Dr. Butler. He added there have been situations in which a patient has twice tested negative for the virus, but a third swab resulted in a weakly positive result.
“It’s not clear if those are people who are actually infectious,” he said. “The PCR is detecting viral RNA, it doesn’t necessarily indicate there is viable virus present in the respiratory tract. So in general, I think it is safe to go back to work, but a positive test in a situation like that can be very difficult to interpret because we think it probably doesn’t reflect infectivity, but we don’t know for sure.”
Do we have an adequate supply of tests in the United States?
The CDC has addressed supply concerns by broadening the number of PCR platforms that can be used to run COVID-19 analyses, Dr. Butler said. Expansion of these platforms has been one way the government is furthering testing options and enabling consumer labs and academic centers to contribute to testing.
When can people who test positive go back to work?
The CDC is still researching that question and reviewing the data, Dr. Butler said. The current recommendation is that a patient who tests positive is considered clear to return to work after two negative tests at least 24 hours apart, following the resolution of symptoms. The CDC has not yet made an official recommendation on an exact time frame, but the CDC is considering a 14-day minimum of quarantine.
“The one caveat I’ll add is that someone who is a health care worker, even if they have resolved symptoms, it’s still a good idea to wear a surgical mask [when they return to work], just as an extra precaution.”
What do we know about immunity? Can patients get reinfected?
Long-term immunity after exposure and infection is virtually unknown, Dr. Butler said. Investigators know those with COVID-19 have an antibody response, but whether that is protective or not, is unclear. In regard to older coronaviruses, such as those that cause colds, patients generally develop an antibody response and may have a period of immunity, but that immunity eventually wanes and reinfection can occur.
What is the latest on therapies?
A number of trials are underway in China and in the United States to test possible therapies for COVID-19, Dr. Butler said. One of the candidate drugs is the broad spectrum antiviral drug remdesivir, which was developed for the treatment of the Ebola virus. Additionally, the National Institutes of Health is studying the potential for monoclonal antibodies to treat COVID-19.
“Of course these are drugs not yet FDA approved,” he said. “We all want to have them in our toolbox as soon as possible, but we want to make sure these drugs are going to benefit and not harm, and that they really do have the utility that we hope for.”
Is there specific guidance for healthcare workers about COVID-19?
Health care workers have a much higher likelihood of being exposed or exposing others who are at high risk of severe infection, Dr. Butler said. That’s why, if a health care worker becomes infected and recovers, it’s still important to take extra precautions when going back to work, such as wearing a mask.
“These are recommendations that are in-draft,” he said. “I want to be clear, I’m floating concepts out there that people can consider. ... I recognize as a former infection control medical director at a hospital that sometimes you have to adapt those guidelines based on your local conditions.”