User login
Medical malpractice: Its evolution to today’s risk of the “big verdict”
Medical malpractice (more formally, professional liability, but we will use the term malpractice) has been of concern to ObGyns for many years, and for good reasons. This specialty has some of the highest incidents of malpractice claims, some of the largest verdicts, and some of the highest malpractice insurance rates. We look more closely at ObGyn malpractice issues in a 3-part “What’s the Verdict” series over the next few months.
In part 1, we discuss the background on malpractice and reasons why malpractice rates have been so high—including large verdicts and lawsuit-prone physicians. In the second part we will look at recent experience and developments in malpractice exposure—who is sued and why. Finally, in the third part we will consider suggestions for reducing the likelihood of a malpractice lawsuit, with a special focus on recent research regarding apologies.
Two reports of recent trials involving ObGyn care illustrate the risk of “the big verdict.”1,2 (Note that the following vignettes are drawn from actual cases but are outlines of those cases and not complete descriptions of the claims. Because the information does not come from formal court records, the facts may be inaccurate and are incomplete; they should be viewed as illustrations only.)
CASE 1 Delayed delivery, $19M verdict
At 39 weeks’ gestation, a woman was admitted to the hospital in spontaneous labor. Artificial rupture of membranes with clear amniotic fluid was noted. Active contractions occurred for 11 hours. Oxytocin was then initiated, and 17 minutes later, profound fetal bradycardia was detected. There was recurrent evidence of fetal distress with meconium. After a nursing staff change a second nurse restarted oxytocin for a prolonged period. The physician allowed labor to continue despite fetal distress, and performed a cesarean delivery (CD) 4.5 hours later. Five hours postdelivery the neonate was noted to have a pneumothorax, lung damage, and respiratory failure. The infant died at 18 days of age.
The jury felt that there was negligence—failure to timely diagnose fetal distress and failure to timely perform CD, all of which resulted in a verdict for the plaintiff. The jury awarded in excess of $19 million.1
CASE 2 An undiagnosed tumor, $20M verdict
A patient underwent bilateral mastectomy. Following surgery, she reported pain and swelling at the surgical site for 2 years, and the defendant physician “dismissed” her complaint, refusing to evaluate it as the provider felt it was related to scar tissue. Three years after the mastectomies, the patient underwent surgical exploration and removal of 3 ribs and sternum secondary to a desmoid tumor. Surgical mesh and chest reconstruction was required, necessitating long-term opioids and sleeping medications that “will slow her wits, dull her senses and limit activities of daily living.” Of note, discrepancies were found in the medical records maintained by the defendant. (There was, for example, no report in the record of the plaintiff’s pain until late in the process.) The plaintiff based her claim on the fact that her pain and lump were neither evaluated nor discovered until it was too late.
The jury awarded $20 million. The verdict was reduced to $2 million by the court based on state statutory limits on malpractice damages.2,3

Continue to: Medical malpractice: Evolution of a standard of care...
Medical malpractice: Evolution of a standard of care
Medical malpractice is not a modern invention. Some historians trace malpractice to the Code of Hammurabi (2030 BC), through Roman law,4 into English common law.5 It was sufficiently established by 1765 that the classic legal treatise of the century referred to medical malpractice.6,7 Although medical malpractice existed for a long time, actual malpractice cases were relatively rare before the last half of the 20th century.8
Defensive medicine born out of necessity. The number of malpractice cases increased substantially—described as a “geometric increase”—after 1960, with a 300% rise between 1965 and 1970.7,9 This “malpractice maelstrom of the 70s”7 resulted in dramatic increases in malpractice insurance costs and invited the practice of defensive medicine—medically unnecessary or unjustified tests and services.10Although there is controversy about what is defensive medicine and what is reasonably cautious medicine, the practice may account for 3% of total health care spending.11 Mello and others have estimated that there may be a $55 billion annual cost related to the medical malpractice system.12
Several malpractice crises and waves of malpractice or tort reform ensued,13 beginning in the 1970s and extending into the 2000s.11 Malpractice law is primarily a matter of state law, so reform essentially has been at the state level—as we will see in the second part in this series.
Defining a standard of care
Medical malpractice is the application of standard legal principles to medical practice. Those principles generally are torts (intentional torts and negligence), and sometimes contracts.14 Eventually, medical malpractice came to focus primarily on negligence. The legal purposes of imposing negligence liability are compensation (to repay the plaintiff the costs of the harm caused by the defendant) and deterrence (to discourage careless conduct that can harm others.)
Negligence is essentially carelessness that falls below the acceptable standard of care. Negligence may arise, for example, from15:
- doing something (giving a drug to a patient with a known allergy to it)
- not doing something (failing to test for a possible tumor, as in the second case above)
- not giving appropriate informed consent
- failing to conduct an adequate examination
- abandoning a patient
- failing to refer a patient to a specialist (or conduct a consultation).
(In recent years, law reforms directed specifically at medical malpractice have somewhat separated medical malpractice from other tort law.)
In malpractice cases, the core question is whether the provider did (or did not) do something that a reasonably careful physician would have done. It is axiomatic that not all bad outcomes are negligent. Indeed, not all mistakes are negligent—only the mistakes that were unreasonable given all of the circumstances. In the first case above, for example, given all of the facts that preceded it, the delay of the physician for 4.5 hours after the fetal distress started was, as seen by the jury, not just a mistake but an unreasonable mistake. Hence, it was negligent. In the second case, the failure to investigate the pain and swelling in the surgical site for 2 years (or failure to refer the patient to another physician) was seen by the jury as an unreasonable mistake—one that would not have been made by a reasonably careful practitioner.
Continue to: The big verdict...
The big verdict
Everyone—every professional providing service, every manufacturer, every driver—eventually will make an unreasonable mistake (ie, commit negligence). If that negligence results in harming someone else, our standard legal response is that the negligent person should be financially responsible for the harm to the other. So, a driver who fails to stop at a red light and hits another car is responsible for those damages. But the damages may vary—perhaps a banged-up fender, or, in another instance, with the same negligence, perhaps terrible personal injuries that will disable the other driver for life. Thus, the damages can vary for the same level of carelessness. The “big verdict” may therefore fall on someone who was not especially careless.
Big verdicts often involve long-term care. The opening case vignettes illustrate a concern of medical malpractice generally—especially for ObGyn practice—the very high verdict. Very high verdicts generally reflect catastrophic damages that will continue for a long time. Bixenstine and colleagues found, for example, that catastrophic payouts often involved “patient age less than 1 year, quadriplegia, brain damage, or lifelong care.”16 In the case of serious injuries during delivery, for example, the harm to the child may last a lifetime and require years and years of intensive medical services.
Million-dollar-plus payouts are on the rise. The percentage of paid claims (through settlement or trial) that are above $1 million is increasing. These million-dollar cases represent 36% of the total dollars paid in ObGyn malpractice claims, even though they represent only 8% of the number of claims paid.16 The increase in the big verdict cases (above $1 million) suggests that ObGyn practitioners should consider their malpractice policy limits—a million dollars may not be enough.
In big verdict cases, the great harm to the plaintiff is often combined with facts that produce extraordinary sympathy for the plaintiff. Sometimes there is decidedly unsympathetic conduct by the defendant as well. In the second case, for example, the problems with the medical record may have suggested to the jury that the doctor was either trying to hide something or did not care enough about the patient even to note a serious complaint. In a case we reviewed in an earlier “What’s the Verdict” column, a physician left the room for several minutes during a critical time—to take a call from a stockbroker.16-18
The big verdict does not necessarily suggest that the defendant was especially or grossly negligent.16 It was a bad injury that occurred, for instance. On the other hand, the physician with several malpractice judgments may suggest that this is a problem physician.
Physicians facing multiple lawsuits are the exceptions
A number of studies have demonstrated that only a small proportion of physicians are responsible for a disproportionate number of paid medical malpractice claims. (“Paid claims” are those in which the plaintiff receives money from the doctor’s insurance. “Filed claims” are all malpractice lawsuits filed. Many claims are filed, but few are paid.)
ObGyn has high number of paid claims and high risk of claim payment recurrence. Studdert and colleagues found that the probability of future paid malpractice climbed with each past paid claim.19 They also found that 1% of physicians accounted for 32% of all paid claims. The number of paid claims varied by specialty—obstetrics and gynecology accounted for the second largest number of paid claims (13%). The risk of recurrence (more than one paid claim) was highest among 4 surgical specialties and ObGyns (about double the recurrence rate in these specialties compared with internal medicine).19
A minority of physicians responsible for lion share of paid claims. Black and colleagues followed up the Studdert study. Although there were some differences in what they found, the results were very similar.20 For example, they found that having even a single prior paid claim strongly predicted future claims over the next 5 years. They also found that some “outlier” physicians with multiple paid claims “are responsible for a significant share of paid claims.” They specifically found that, even for physicians in high-risk specialties in high-risk states, “bad luck is highly unlikely to explain” multiple claims within 5 years.
Continue to: Both of the studies just mentioned relied on...
Both of the studies just mentioned relied on the National Practitioner Data Bank for information about paid claims. This source has some limitations in capturing claims or payments made by hospitals or other institutions for the actions of its agent-physicians. Some of these limitations were resolved in another recent study that looked at Indiana state insurance and licensing discipline records (over a 41-year period).21 Not surprisingly, this study found that claims paid increase with more severe licensure discipline. On the other hand, although, the “frequent fliers” in terms of malpractice claims made and paid could be identified as a “small number of repeat defendants,” these physicians were not routinely disciplined by the state medical board. This was only a single state study, of course, but it also found that a few physicians accounted for a significant number of the claims. The state board was not taking licensing action against this small group, however.
Should the few bad apples be picked from the orchard?
Collectively, these studies are fairly overwhelming in demonstrating that there are some physicians who are “prone” to malpractice claims (for whom all physicians in the specialty are probably paying higher malpractice rates), but who do not attract the attention of licensing agencies for careful examination. In addition to its self-interest in eliminating physicians prone to malpractice claims and payments, the obligation of professions to protect the public interest suggests that state boards should be more aggressive in pursuing those physicians practicing risky medicine.
This medical malpractice series will continue next month with a look at how to reduce malpractice exposure.
- Delivery delay blamed for baby’s death days later—$19.2 million Illinois verdict. Medical Malpractice: Verdicts, Settlements & Experts. 2019;35:17.
- Failure to identify signs of a growing tumor—$20 million Virginia verdict. Medical Malpractice: Verdicts, Settlements & Experts. 2019;35:18.
- Hellinger FJ, Encinosa WE. The impact of state laws limiting malpractice damage awards on health care expenditures. Am J Public Health. 2006;96:1375-1381.
- Bal BS. An introduction to medical malpractice in the United States. Clin Orthop Relat Res. 2009;467:339–347.
- Everad v. Hopkins, 80 English Reports 1164 (1615).
- Blackstone W. Commentaries on the laws of England. Oxford, England: Clarendon Press; 1768:122.
- Berlin L. Medical errors, malpractice, and defensive medicine: an ill-fated triad. Diagnosis (Berl). 2017;4:133-139.
- DeVille KA. Medical Malpractice in Nineteenth-Century America: Origins and Legacy. New York, NY: NYU Press; 1990.
- Hershey N. The defensive practice of medicine. Myth or reality. Milbank Mem Fund Q. 1972;50:69-98.
- Agarwal R, Gupta A, Gupta S. The impact of tort reform on defensive medicine, quality of care, and physician supply: a systematic review. Health Serv Res. 2019;54:851-859.
- Gerlach J, Abodunde B, Sollosy M, et al. Rethinking the obvious: time for new ideas on medical malpractice tort reform. Health Care Manag (Frederick). 2019;38:109-115.
- Mello MM, Chandra A, Gawande AA, et al. National costs of the medical liability system. Health Aff. 2010;29:1569-1577.
- Bovbjerg RR. Malpractice crisis and reform. Clin Perinatol. 2005;32:203-233, viii-ix.
- Hawkins v. McGee, 84 N.H. 114, 146 A. 641 (1929).
- Gittler GJ, Goldstein EJ. The elements of medical malpractice: an overview. Clin Infect Dis. 1996;23:1152–1155.
- Bixenstine PJ, Shore AD, Mehtsun WT, et al. Catastrophic medical malpractice payouts in the United States. J Healthc Quality. 2014;36:43-53.
- Sanfilippo JS, Smith SR. Lessons from a daunting malpractice event. OBG Manag. 2018;30:41-47.
- Chang D. Miami doctor hit with $33 million judgment in brain-damaged baby suit. Miami Herald. April 28, 2017. http://www.miamiherald.com/news/health-care/ article147506019.html. Accessed December 12, 2019.
- Studdert DM, Bismark MM, Mello MM, et al. Prevalence and characteristics of physicians prone to malpractice claims. N Engl J Med. 2016;374:354-362.
- Black B, Hyman DA, Lerner JY. Physicians with multiple paid medical malpractice claims: Are they outliers or just unlucky? Int Rev Law Econ. 2019;59:146-157.
- Liu J, Hyman DA. Targeting bad doctors: lessons from Indiana, 1975–2015. J Empirical Legal Studies. 2019;16: 248-328.
Medical malpractice (more formally, professional liability, but we will use the term malpractice) has been of concern to ObGyns for many years, and for good reasons. This specialty has some of the highest incidents of malpractice claims, some of the largest verdicts, and some of the highest malpractice insurance rates. We look more closely at ObGyn malpractice issues in a 3-part “What’s the Verdict” series over the next few months.
In part 1, we discuss the background on malpractice and reasons why malpractice rates have been so high—including large verdicts and lawsuit-prone physicians. In the second part we will look at recent experience and developments in malpractice exposure—who is sued and why. Finally, in the third part we will consider suggestions for reducing the likelihood of a malpractice lawsuit, with a special focus on recent research regarding apologies.
Two reports of recent trials involving ObGyn care illustrate the risk of “the big verdict.”1,2 (Note that the following vignettes are drawn from actual cases but are outlines of those cases and not complete descriptions of the claims. Because the information does not come from formal court records, the facts may be inaccurate and are incomplete; they should be viewed as illustrations only.)
CASE 1 Delayed delivery, $19M verdict
At 39 weeks’ gestation, a woman was admitted to the hospital in spontaneous labor. Artificial rupture of membranes with clear amniotic fluid was noted. Active contractions occurred for 11 hours. Oxytocin was then initiated, and 17 minutes later, profound fetal bradycardia was detected. There was recurrent evidence of fetal distress with meconium. After a nursing staff change a second nurse restarted oxytocin for a prolonged period. The physician allowed labor to continue despite fetal distress, and performed a cesarean delivery (CD) 4.5 hours later. Five hours postdelivery the neonate was noted to have a pneumothorax, lung damage, and respiratory failure. The infant died at 18 days of age.
The jury felt that there was negligence—failure to timely diagnose fetal distress and failure to timely perform CD, all of which resulted in a verdict for the plaintiff. The jury awarded in excess of $19 million.1
CASE 2 An undiagnosed tumor, $20M verdict
A patient underwent bilateral mastectomy. Following surgery, she reported pain and swelling at the surgical site for 2 years, and the defendant physician “dismissed” her complaint, refusing to evaluate it as the provider felt it was related to scar tissue. Three years after the mastectomies, the patient underwent surgical exploration and removal of 3 ribs and sternum secondary to a desmoid tumor. Surgical mesh and chest reconstruction was required, necessitating long-term opioids and sleeping medications that “will slow her wits, dull her senses and limit activities of daily living.” Of note, discrepancies were found in the medical records maintained by the defendant. (There was, for example, no report in the record of the plaintiff’s pain until late in the process.) The plaintiff based her claim on the fact that her pain and lump were neither evaluated nor discovered until it was too late.
The jury awarded $20 million. The verdict was reduced to $2 million by the court based on state statutory limits on malpractice damages.2,3

Continue to: Medical malpractice: Evolution of a standard of care...
Medical malpractice: Evolution of a standard of care
Medical malpractice is not a modern invention. Some historians trace malpractice to the Code of Hammurabi (2030 BC), through Roman law,4 into English common law.5 It was sufficiently established by 1765 that the classic legal treatise of the century referred to medical malpractice.6,7 Although medical malpractice existed for a long time, actual malpractice cases were relatively rare before the last half of the 20th century.8
Defensive medicine born out of necessity. The number of malpractice cases increased substantially—described as a “geometric increase”—after 1960, with a 300% rise between 1965 and 1970.7,9 This “malpractice maelstrom of the 70s”7 resulted in dramatic increases in malpractice insurance costs and invited the practice of defensive medicine—medically unnecessary or unjustified tests and services.10Although there is controversy about what is defensive medicine and what is reasonably cautious medicine, the practice may account for 3% of total health care spending.11 Mello and others have estimated that there may be a $55 billion annual cost related to the medical malpractice system.12
Several malpractice crises and waves of malpractice or tort reform ensued,13 beginning in the 1970s and extending into the 2000s.11 Malpractice law is primarily a matter of state law, so reform essentially has been at the state level—as we will see in the second part in this series.
Defining a standard of care
Medical malpractice is the application of standard legal principles to medical practice. Those principles generally are torts (intentional torts and negligence), and sometimes contracts.14 Eventually, medical malpractice came to focus primarily on negligence. The legal purposes of imposing negligence liability are compensation (to repay the plaintiff the costs of the harm caused by the defendant) and deterrence (to discourage careless conduct that can harm others.)
Negligence is essentially carelessness that falls below the acceptable standard of care. Negligence may arise, for example, from15:
- doing something (giving a drug to a patient with a known allergy to it)
- not doing something (failing to test for a possible tumor, as in the second case above)
- not giving appropriate informed consent
- failing to conduct an adequate examination
- abandoning a patient
- failing to refer a patient to a specialist (or conduct a consultation).
(In recent years, law reforms directed specifically at medical malpractice have somewhat separated medical malpractice from other tort law.)
In malpractice cases, the core question is whether the provider did (or did not) do something that a reasonably careful physician would have done. It is axiomatic that not all bad outcomes are negligent. Indeed, not all mistakes are negligent—only the mistakes that were unreasonable given all of the circumstances. In the first case above, for example, given all of the facts that preceded it, the delay of the physician for 4.5 hours after the fetal distress started was, as seen by the jury, not just a mistake but an unreasonable mistake. Hence, it was negligent. In the second case, the failure to investigate the pain and swelling in the surgical site for 2 years (or failure to refer the patient to another physician) was seen by the jury as an unreasonable mistake—one that would not have been made by a reasonably careful practitioner.
Continue to: The big verdict...
The big verdict
Everyone—every professional providing service, every manufacturer, every driver—eventually will make an unreasonable mistake (ie, commit negligence). If that negligence results in harming someone else, our standard legal response is that the negligent person should be financially responsible for the harm to the other. So, a driver who fails to stop at a red light and hits another car is responsible for those damages. But the damages may vary—perhaps a banged-up fender, or, in another instance, with the same negligence, perhaps terrible personal injuries that will disable the other driver for life. Thus, the damages can vary for the same level of carelessness. The “big verdict” may therefore fall on someone who was not especially careless.
Big verdicts often involve long-term care. The opening case vignettes illustrate a concern of medical malpractice generally—especially for ObGyn practice—the very high verdict. Very high verdicts generally reflect catastrophic damages that will continue for a long time. Bixenstine and colleagues found, for example, that catastrophic payouts often involved “patient age less than 1 year, quadriplegia, brain damage, or lifelong care.”16 In the case of serious injuries during delivery, for example, the harm to the child may last a lifetime and require years and years of intensive medical services.
Million-dollar-plus payouts are on the rise. The percentage of paid claims (through settlement or trial) that are above $1 million is increasing. These million-dollar cases represent 36% of the total dollars paid in ObGyn malpractice claims, even though they represent only 8% of the number of claims paid.16 The increase in the big verdict cases (above $1 million) suggests that ObGyn practitioners should consider their malpractice policy limits—a million dollars may not be enough.
In big verdict cases, the great harm to the plaintiff is often combined with facts that produce extraordinary sympathy for the plaintiff. Sometimes there is decidedly unsympathetic conduct by the defendant as well. In the second case, for example, the problems with the medical record may have suggested to the jury that the doctor was either trying to hide something or did not care enough about the patient even to note a serious complaint. In a case we reviewed in an earlier “What’s the Verdict” column, a physician left the room for several minutes during a critical time—to take a call from a stockbroker.16-18
The big verdict does not necessarily suggest that the defendant was especially or grossly negligent.16 It was a bad injury that occurred, for instance. On the other hand, the physician with several malpractice judgments may suggest that this is a problem physician.
Physicians facing multiple lawsuits are the exceptions
A number of studies have demonstrated that only a small proportion of physicians are responsible for a disproportionate number of paid medical malpractice claims. (“Paid claims” are those in which the plaintiff receives money from the doctor’s insurance. “Filed claims” are all malpractice lawsuits filed. Many claims are filed, but few are paid.)
ObGyn has high number of paid claims and high risk of claim payment recurrence. Studdert and colleagues found that the probability of future paid malpractice climbed with each past paid claim.19 They also found that 1% of physicians accounted for 32% of all paid claims. The number of paid claims varied by specialty—obstetrics and gynecology accounted for the second largest number of paid claims (13%). The risk of recurrence (more than one paid claim) was highest among 4 surgical specialties and ObGyns (about double the recurrence rate in these specialties compared with internal medicine).19
A minority of physicians responsible for lion share of paid claims. Black and colleagues followed up the Studdert study. Although there were some differences in what they found, the results were very similar.20 For example, they found that having even a single prior paid claim strongly predicted future claims over the next 5 years. They also found that some “outlier” physicians with multiple paid claims “are responsible for a significant share of paid claims.” They specifically found that, even for physicians in high-risk specialties in high-risk states, “bad luck is highly unlikely to explain” multiple claims within 5 years.
Continue to: Both of the studies just mentioned relied on...
Both of the studies just mentioned relied on the National Practitioner Data Bank for information about paid claims. This source has some limitations in capturing claims or payments made by hospitals or other institutions for the actions of its agent-physicians. Some of these limitations were resolved in another recent study that looked at Indiana state insurance and licensing discipline records (over a 41-year period).21 Not surprisingly, this study found that claims paid increase with more severe licensure discipline. On the other hand, although, the “frequent fliers” in terms of malpractice claims made and paid could be identified as a “small number of repeat defendants,” these physicians were not routinely disciplined by the state medical board. This was only a single state study, of course, but it also found that a few physicians accounted for a significant number of the claims. The state board was not taking licensing action against this small group, however.
Should the few bad apples be picked from the orchard?
Collectively, these studies are fairly overwhelming in demonstrating that there are some physicians who are “prone” to malpractice claims (for whom all physicians in the specialty are probably paying higher malpractice rates), but who do not attract the attention of licensing agencies for careful examination. In addition to its self-interest in eliminating physicians prone to malpractice claims and payments, the obligation of professions to protect the public interest suggests that state boards should be more aggressive in pursuing those physicians practicing risky medicine.
This medical malpractice series will continue next month with a look at how to reduce malpractice exposure.
Medical malpractice (more formally, professional liability, but we will use the term malpractice) has been of concern to ObGyns for many years, and for good reasons. This specialty has some of the highest incidents of malpractice claims, some of the largest verdicts, and some of the highest malpractice insurance rates. We look more closely at ObGyn malpractice issues in a 3-part “What’s the Verdict” series over the next few months.
In part 1, we discuss the background on malpractice and reasons why malpractice rates have been so high—including large verdicts and lawsuit-prone physicians. In the second part we will look at recent experience and developments in malpractice exposure—who is sued and why. Finally, in the third part we will consider suggestions for reducing the likelihood of a malpractice lawsuit, with a special focus on recent research regarding apologies.
Two reports of recent trials involving ObGyn care illustrate the risk of “the big verdict.”1,2 (Note that the following vignettes are drawn from actual cases but are outlines of those cases and not complete descriptions of the claims. Because the information does not come from formal court records, the facts may be inaccurate and are incomplete; they should be viewed as illustrations only.)
CASE 1 Delayed delivery, $19M verdict
At 39 weeks’ gestation, a woman was admitted to the hospital in spontaneous labor. Artificial rupture of membranes with clear amniotic fluid was noted. Active contractions occurred for 11 hours. Oxytocin was then initiated, and 17 minutes later, profound fetal bradycardia was detected. There was recurrent evidence of fetal distress with meconium. After a nursing staff change a second nurse restarted oxytocin for a prolonged period. The physician allowed labor to continue despite fetal distress, and performed a cesarean delivery (CD) 4.5 hours later. Five hours postdelivery the neonate was noted to have a pneumothorax, lung damage, and respiratory failure. The infant died at 18 days of age.
The jury felt that there was negligence—failure to timely diagnose fetal distress and failure to timely perform CD, all of which resulted in a verdict for the plaintiff. The jury awarded in excess of $19 million.1
CASE 2 An undiagnosed tumor, $20M verdict
A patient underwent bilateral mastectomy. Following surgery, she reported pain and swelling at the surgical site for 2 years, and the defendant physician “dismissed” her complaint, refusing to evaluate it as the provider felt it was related to scar tissue. Three years after the mastectomies, the patient underwent surgical exploration and removal of 3 ribs and sternum secondary to a desmoid tumor. Surgical mesh and chest reconstruction was required, necessitating long-term opioids and sleeping medications that “will slow her wits, dull her senses and limit activities of daily living.” Of note, discrepancies were found in the medical records maintained by the defendant. (There was, for example, no report in the record of the plaintiff’s pain until late in the process.) The plaintiff based her claim on the fact that her pain and lump were neither evaluated nor discovered until it was too late.
The jury awarded $20 million. The verdict was reduced to $2 million by the court based on state statutory limits on malpractice damages.2,3

Continue to: Medical malpractice: Evolution of a standard of care...
Medical malpractice: Evolution of a standard of care
Medical malpractice is not a modern invention. Some historians trace malpractice to the Code of Hammurabi (2030 BC), through Roman law,4 into English common law.5 It was sufficiently established by 1765 that the classic legal treatise of the century referred to medical malpractice.6,7 Although medical malpractice existed for a long time, actual malpractice cases were relatively rare before the last half of the 20th century.8
Defensive medicine born out of necessity. The number of malpractice cases increased substantially—described as a “geometric increase”—after 1960, with a 300% rise between 1965 and 1970.7,9 This “malpractice maelstrom of the 70s”7 resulted in dramatic increases in malpractice insurance costs and invited the practice of defensive medicine—medically unnecessary or unjustified tests and services.10Although there is controversy about what is defensive medicine and what is reasonably cautious medicine, the practice may account for 3% of total health care spending.11 Mello and others have estimated that there may be a $55 billion annual cost related to the medical malpractice system.12
Several malpractice crises and waves of malpractice or tort reform ensued,13 beginning in the 1970s and extending into the 2000s.11 Malpractice law is primarily a matter of state law, so reform essentially has been at the state level—as we will see in the second part in this series.
Defining a standard of care
Medical malpractice is the application of standard legal principles to medical practice. Those principles generally are torts (intentional torts and negligence), and sometimes contracts.14 Eventually, medical malpractice came to focus primarily on negligence. The legal purposes of imposing negligence liability are compensation (to repay the plaintiff the costs of the harm caused by the defendant) and deterrence (to discourage careless conduct that can harm others.)
Negligence is essentially carelessness that falls below the acceptable standard of care. Negligence may arise, for example, from15:
- doing something (giving a drug to a patient with a known allergy to it)
- not doing something (failing to test for a possible tumor, as in the second case above)
- not giving appropriate informed consent
- failing to conduct an adequate examination
- abandoning a patient
- failing to refer a patient to a specialist (or conduct a consultation).
(In recent years, law reforms directed specifically at medical malpractice have somewhat separated medical malpractice from other tort law.)
In malpractice cases, the core question is whether the provider did (or did not) do something that a reasonably careful physician would have done. It is axiomatic that not all bad outcomes are negligent. Indeed, not all mistakes are negligent—only the mistakes that were unreasonable given all of the circumstances. In the first case above, for example, given all of the facts that preceded it, the delay of the physician for 4.5 hours after the fetal distress started was, as seen by the jury, not just a mistake but an unreasonable mistake. Hence, it was negligent. In the second case, the failure to investigate the pain and swelling in the surgical site for 2 years (or failure to refer the patient to another physician) was seen by the jury as an unreasonable mistake—one that would not have been made by a reasonably careful practitioner.
Continue to: The big verdict...
The big verdict
Everyone—every professional providing service, every manufacturer, every driver—eventually will make an unreasonable mistake (ie, commit negligence). If that negligence results in harming someone else, our standard legal response is that the negligent person should be financially responsible for the harm to the other. So, a driver who fails to stop at a red light and hits another car is responsible for those damages. But the damages may vary—perhaps a banged-up fender, or, in another instance, with the same negligence, perhaps terrible personal injuries that will disable the other driver for life. Thus, the damages can vary for the same level of carelessness. The “big verdict” may therefore fall on someone who was not especially careless.
Big verdicts often involve long-term care. The opening case vignettes illustrate a concern of medical malpractice generally—especially for ObGyn practice—the very high verdict. Very high verdicts generally reflect catastrophic damages that will continue for a long time. Bixenstine and colleagues found, for example, that catastrophic payouts often involved “patient age less than 1 year, quadriplegia, brain damage, or lifelong care.”16 In the case of serious injuries during delivery, for example, the harm to the child may last a lifetime and require years and years of intensive medical services.
Million-dollar-plus payouts are on the rise. The percentage of paid claims (through settlement or trial) that are above $1 million is increasing. These million-dollar cases represent 36% of the total dollars paid in ObGyn malpractice claims, even though they represent only 8% of the number of claims paid.16 The increase in the big verdict cases (above $1 million) suggests that ObGyn practitioners should consider their malpractice policy limits—a million dollars may not be enough.
In big verdict cases, the great harm to the plaintiff is often combined with facts that produce extraordinary sympathy for the plaintiff. Sometimes there is decidedly unsympathetic conduct by the defendant as well. In the second case, for example, the problems with the medical record may have suggested to the jury that the doctor was either trying to hide something or did not care enough about the patient even to note a serious complaint. In a case we reviewed in an earlier “What’s the Verdict” column, a physician left the room for several minutes during a critical time—to take a call from a stockbroker.16-18
The big verdict does not necessarily suggest that the defendant was especially or grossly negligent.16 It was a bad injury that occurred, for instance. On the other hand, the physician with several malpractice judgments may suggest that this is a problem physician.
Physicians facing multiple lawsuits are the exceptions
A number of studies have demonstrated that only a small proportion of physicians are responsible for a disproportionate number of paid medical malpractice claims. (“Paid claims” are those in which the plaintiff receives money from the doctor’s insurance. “Filed claims” are all malpractice lawsuits filed. Many claims are filed, but few are paid.)
ObGyn has high number of paid claims and high risk of claim payment recurrence. Studdert and colleagues found that the probability of future paid malpractice climbed with each past paid claim.19 They also found that 1% of physicians accounted for 32% of all paid claims. The number of paid claims varied by specialty—obstetrics and gynecology accounted for the second largest number of paid claims (13%). The risk of recurrence (more than one paid claim) was highest among 4 surgical specialties and ObGyns (about double the recurrence rate in these specialties compared with internal medicine).19
A minority of physicians responsible for lion share of paid claims. Black and colleagues followed up the Studdert study. Although there were some differences in what they found, the results were very similar.20 For example, they found that having even a single prior paid claim strongly predicted future claims over the next 5 years. They also found that some “outlier” physicians with multiple paid claims “are responsible for a significant share of paid claims.” They specifically found that, even for physicians in high-risk specialties in high-risk states, “bad luck is highly unlikely to explain” multiple claims within 5 years.
Continue to: Both of the studies just mentioned relied on...
Both of the studies just mentioned relied on the National Practitioner Data Bank for information about paid claims. This source has some limitations in capturing claims or payments made by hospitals or other institutions for the actions of its agent-physicians. Some of these limitations were resolved in another recent study that looked at Indiana state insurance and licensing discipline records (over a 41-year period).21 Not surprisingly, this study found that claims paid increase with more severe licensure discipline. On the other hand, although, the “frequent fliers” in terms of malpractice claims made and paid could be identified as a “small number of repeat defendants,” these physicians were not routinely disciplined by the state medical board. This was only a single state study, of course, but it also found that a few physicians accounted for a significant number of the claims. The state board was not taking licensing action against this small group, however.
Should the few bad apples be picked from the orchard?
Collectively, these studies are fairly overwhelming in demonstrating that there are some physicians who are “prone” to malpractice claims (for whom all physicians in the specialty are probably paying higher malpractice rates), but who do not attract the attention of licensing agencies for careful examination. In addition to its self-interest in eliminating physicians prone to malpractice claims and payments, the obligation of professions to protect the public interest suggests that state boards should be more aggressive in pursuing those physicians practicing risky medicine.
This medical malpractice series will continue next month with a look at how to reduce malpractice exposure.
- Delivery delay blamed for baby’s death days later—$19.2 million Illinois verdict. Medical Malpractice: Verdicts, Settlements & Experts. 2019;35:17.
- Failure to identify signs of a growing tumor—$20 million Virginia verdict. Medical Malpractice: Verdicts, Settlements & Experts. 2019;35:18.
- Hellinger FJ, Encinosa WE. The impact of state laws limiting malpractice damage awards on health care expenditures. Am J Public Health. 2006;96:1375-1381.
- Bal BS. An introduction to medical malpractice in the United States. Clin Orthop Relat Res. 2009;467:339–347.
- Everad v. Hopkins, 80 English Reports 1164 (1615).
- Blackstone W. Commentaries on the laws of England. Oxford, England: Clarendon Press; 1768:122.
- Berlin L. Medical errors, malpractice, and defensive medicine: an ill-fated triad. Diagnosis (Berl). 2017;4:133-139.
- DeVille KA. Medical Malpractice in Nineteenth-Century America: Origins and Legacy. New York, NY: NYU Press; 1990.
- Hershey N. The defensive practice of medicine. Myth or reality. Milbank Mem Fund Q. 1972;50:69-98.
- Agarwal R, Gupta A, Gupta S. The impact of tort reform on defensive medicine, quality of care, and physician supply: a systematic review. Health Serv Res. 2019;54:851-859.
- Gerlach J, Abodunde B, Sollosy M, et al. Rethinking the obvious: time for new ideas on medical malpractice tort reform. Health Care Manag (Frederick). 2019;38:109-115.
- Mello MM, Chandra A, Gawande AA, et al. National costs of the medical liability system. Health Aff. 2010;29:1569-1577.
- Bovbjerg RR. Malpractice crisis and reform. Clin Perinatol. 2005;32:203-233, viii-ix.
- Hawkins v. McGee, 84 N.H. 114, 146 A. 641 (1929).
- Gittler GJ, Goldstein EJ. The elements of medical malpractice: an overview. Clin Infect Dis. 1996;23:1152–1155.
- Bixenstine PJ, Shore AD, Mehtsun WT, et al. Catastrophic medical malpractice payouts in the United States. J Healthc Quality. 2014;36:43-53.
- Sanfilippo JS, Smith SR. Lessons from a daunting malpractice event. OBG Manag. 2018;30:41-47.
- Chang D. Miami doctor hit with $33 million judgment in brain-damaged baby suit. Miami Herald. April 28, 2017. http://www.miamiherald.com/news/health-care/ article147506019.html. Accessed December 12, 2019.
- Studdert DM, Bismark MM, Mello MM, et al. Prevalence and characteristics of physicians prone to malpractice claims. N Engl J Med. 2016;374:354-362.
- Black B, Hyman DA, Lerner JY. Physicians with multiple paid medical malpractice claims: Are they outliers or just unlucky? Int Rev Law Econ. 2019;59:146-157.
- Liu J, Hyman DA. Targeting bad doctors: lessons from Indiana, 1975–2015. J Empirical Legal Studies. 2019;16: 248-328.
- Delivery delay blamed for baby’s death days later—$19.2 million Illinois verdict. Medical Malpractice: Verdicts, Settlements & Experts. 2019;35:17.
- Failure to identify signs of a growing tumor—$20 million Virginia verdict. Medical Malpractice: Verdicts, Settlements & Experts. 2019;35:18.
- Hellinger FJ, Encinosa WE. The impact of state laws limiting malpractice damage awards on health care expenditures. Am J Public Health. 2006;96:1375-1381.
- Bal BS. An introduction to medical malpractice in the United States. Clin Orthop Relat Res. 2009;467:339–347.
- Everad v. Hopkins, 80 English Reports 1164 (1615).
- Blackstone W. Commentaries on the laws of England. Oxford, England: Clarendon Press; 1768:122.
- Berlin L. Medical errors, malpractice, and defensive medicine: an ill-fated triad. Diagnosis (Berl). 2017;4:133-139.
- DeVille KA. Medical Malpractice in Nineteenth-Century America: Origins and Legacy. New York, NY: NYU Press; 1990.
- Hershey N. The defensive practice of medicine. Myth or reality. Milbank Mem Fund Q. 1972;50:69-98.
- Agarwal R, Gupta A, Gupta S. The impact of tort reform on defensive medicine, quality of care, and physician supply: a systematic review. Health Serv Res. 2019;54:851-859.
- Gerlach J, Abodunde B, Sollosy M, et al. Rethinking the obvious: time for new ideas on medical malpractice tort reform. Health Care Manag (Frederick). 2019;38:109-115.
- Mello MM, Chandra A, Gawande AA, et al. National costs of the medical liability system. Health Aff. 2010;29:1569-1577.
- Bovbjerg RR. Malpractice crisis and reform. Clin Perinatol. 2005;32:203-233, viii-ix.
- Hawkins v. McGee, 84 N.H. 114, 146 A. 641 (1929).
- Gittler GJ, Goldstein EJ. The elements of medical malpractice: an overview. Clin Infect Dis. 1996;23:1152–1155.
- Bixenstine PJ, Shore AD, Mehtsun WT, et al. Catastrophic medical malpractice payouts in the United States. J Healthc Quality. 2014;36:43-53.
- Sanfilippo JS, Smith SR. Lessons from a daunting malpractice event. OBG Manag. 2018;30:41-47.
- Chang D. Miami doctor hit with $33 million judgment in brain-damaged baby suit. Miami Herald. April 28, 2017. http://www.miamiherald.com/news/health-care/ article147506019.html. Accessed December 12, 2019.
- Studdert DM, Bismark MM, Mello MM, et al. Prevalence and characteristics of physicians prone to malpractice claims. N Engl J Med. 2016;374:354-362.
- Black B, Hyman DA, Lerner JY. Physicians with multiple paid medical malpractice claims: Are they outliers or just unlucky? Int Rev Law Econ. 2019;59:146-157.
- Liu J, Hyman DA. Targeting bad doctors: lessons from Indiana, 1975–2015. J Empirical Legal Studies. 2019;16: 248-328.
Called to court? Tips for testifying
As a psychiatrist, you could be called to court to testify as a fact witness in a hearing or trial. Your role as a fact witness would differ from that of an expert witness in that you would likely testify about the information that you have gathered through direct observation of patients or others. Fact witnesses are generally not asked to give expert opinions regarding forensic issues, and treating psychiatrists should not do so about their patients. As a fact witness, depending on the form of litigation, you might be in one of the following 4 roles1:
- Observer. As the term implies, you have observed an event. For example, you are asked to testify about a fight that you witnessed between another clinician’s patient and a nurse while you were making your rounds on an inpatient unit.
- Non-defendant treater. You are the treating psychiatrist for a patient who is involved in litigation to recover damages for injuries sustained from a third party. For example, you are asked to testify about your patient’s premorbid functioning before a claimed injury that spurred the lawsuit.
- Plaintiff. You are suing someone else and may be claiming your own damages. For example, in your attempt to claim damages as a plaintiff, you use your clinical knowledge to testify about your own mental health symptoms and the adverse impact these have had on you.
- Defendant treater. You are being sued by one of your patients. For example, a patient brings a malpractice case against you for allegations of not meeting the standard of care. You testify about your direct observations of the patient, the diagnoses you provided, and your rationale for the implemented treatment plan.
Preparing yourself as a fact witness
For many psychiatrists, testifying can be an intimidating process. Although there are similarities between testifying in a courtroom and giving a deposition, there are also significant differences. For guidelines on providing depositions, see Knoll and Resnick’s “Deposition dos and don’ts: How to answer 8 tricky questions” (
Don’t panic. Although your first reaction may be to panic upon receiving a subpoena or court order, you should “keep your cool” and remember that the observations you made or treatment provided have already taken place.1 Your role as a fact witness is to inform the judge and jury about what you saw and did.1
Continue to: Refresh your memory and practice
Refresh your memory and practice. Gather all required information (eg, medical records, your notes, etc.) and review it before testifying. This will help you to recall the facts more accurately when you are asked a question. Consider practicing your testimony with the attorney who requested you to get feedback on how you present yourself.1 However, do not try to memorize what you are going to say because this could make your testimony sound rehearsed and unconvincing.
Plan ahead, and have a pretrial conference. Because court proceedings are unpredictable, you should clear your schedule to allow enough time to appear in court. Before your court appearance, meet with the attorney who requested you to discuss any new facts or issues as well as learn what the attorney aims to accomplish with your testimony.1
Speak clearly in your own words, and avoid jargon. Courtroom officials are unlikely to understand psychiatric jargon. Therefore, you should explain psychiatric terms in language that laypeople would comprehend. Because the court stenographer will require you to use actual words for the court transcripts, you should answer clearly and verbally or respond with a definitive “yes” or “no” (and not by nodding or shaking your head).
Testimony is also not a time for guessing. If you don’t know the answer, you should say “I don’t know.”
1. Gutheil TG. The psychiatrist in court: a survival guide. Washington, DC: American Psychiatric Press, Inc.; 1998.
2. Knoll JL, Resnick PJ. Deposition dos and don’ts: how to answer 8 tricky questions. Current Psychiatry. 2008;7(3):25-28,36,39-40.
As a psychiatrist, you could be called to court to testify as a fact witness in a hearing or trial. Your role as a fact witness would differ from that of an expert witness in that you would likely testify about the information that you have gathered through direct observation of patients or others. Fact witnesses are generally not asked to give expert opinions regarding forensic issues, and treating psychiatrists should not do so about their patients. As a fact witness, depending on the form of litigation, you might be in one of the following 4 roles1:
- Observer. As the term implies, you have observed an event. For example, you are asked to testify about a fight that you witnessed between another clinician’s patient and a nurse while you were making your rounds on an inpatient unit.
- Non-defendant treater. You are the treating psychiatrist for a patient who is involved in litigation to recover damages for injuries sustained from a third party. For example, you are asked to testify about your patient’s premorbid functioning before a claimed injury that spurred the lawsuit.
- Plaintiff. You are suing someone else and may be claiming your own damages. For example, in your attempt to claim damages as a plaintiff, you use your clinical knowledge to testify about your own mental health symptoms and the adverse impact these have had on you.
- Defendant treater. You are being sued by one of your patients. For example, a patient brings a malpractice case against you for allegations of not meeting the standard of care. You testify about your direct observations of the patient, the diagnoses you provided, and your rationale for the implemented treatment plan.
Preparing yourself as a fact witness
For many psychiatrists, testifying can be an intimidating process. Although there are similarities between testifying in a courtroom and giving a deposition, there are also significant differences. For guidelines on providing depositions, see Knoll and Resnick’s “Deposition dos and don’ts: How to answer 8 tricky questions” (
Don’t panic. Although your first reaction may be to panic upon receiving a subpoena or court order, you should “keep your cool” and remember that the observations you made or treatment provided have already taken place.1 Your role as a fact witness is to inform the judge and jury about what you saw and did.1
Continue to: Refresh your memory and practice
Refresh your memory and practice. Gather all required information (eg, medical records, your notes, etc.) and review it before testifying. This will help you to recall the facts more accurately when you are asked a question. Consider practicing your testimony with the attorney who requested you to get feedback on how you present yourself.1 However, do not try to memorize what you are going to say because this could make your testimony sound rehearsed and unconvincing.
Plan ahead, and have a pretrial conference. Because court proceedings are unpredictable, you should clear your schedule to allow enough time to appear in court. Before your court appearance, meet with the attorney who requested you to discuss any new facts or issues as well as learn what the attorney aims to accomplish with your testimony.1
Speak clearly in your own words, and avoid jargon. Courtroom officials are unlikely to understand psychiatric jargon. Therefore, you should explain psychiatric terms in language that laypeople would comprehend. Because the court stenographer will require you to use actual words for the court transcripts, you should answer clearly and verbally or respond with a definitive “yes” or “no” (and not by nodding or shaking your head).
Testimony is also not a time for guessing. If you don’t know the answer, you should say “I don’t know.”
As a psychiatrist, you could be called to court to testify as a fact witness in a hearing or trial. Your role as a fact witness would differ from that of an expert witness in that you would likely testify about the information that you have gathered through direct observation of patients or others. Fact witnesses are generally not asked to give expert opinions regarding forensic issues, and treating psychiatrists should not do so about their patients. As a fact witness, depending on the form of litigation, you might be in one of the following 4 roles1:
- Observer. As the term implies, you have observed an event. For example, you are asked to testify about a fight that you witnessed between another clinician’s patient and a nurse while you were making your rounds on an inpatient unit.
- Non-defendant treater. You are the treating psychiatrist for a patient who is involved in litigation to recover damages for injuries sustained from a third party. For example, you are asked to testify about your patient’s premorbid functioning before a claimed injury that spurred the lawsuit.
- Plaintiff. You are suing someone else and may be claiming your own damages. For example, in your attempt to claim damages as a plaintiff, you use your clinical knowledge to testify about your own mental health symptoms and the adverse impact these have had on you.
- Defendant treater. You are being sued by one of your patients. For example, a patient brings a malpractice case against you for allegations of not meeting the standard of care. You testify about your direct observations of the patient, the diagnoses you provided, and your rationale for the implemented treatment plan.
Preparing yourself as a fact witness
For many psychiatrists, testifying can be an intimidating process. Although there are similarities between testifying in a courtroom and giving a deposition, there are also significant differences. For guidelines on providing depositions, see Knoll and Resnick’s “Deposition dos and don’ts: How to answer 8 tricky questions” (
Don’t panic. Although your first reaction may be to panic upon receiving a subpoena or court order, you should “keep your cool” and remember that the observations you made or treatment provided have already taken place.1 Your role as a fact witness is to inform the judge and jury about what you saw and did.1
Continue to: Refresh your memory and practice
Refresh your memory and practice. Gather all required information (eg, medical records, your notes, etc.) and review it before testifying. This will help you to recall the facts more accurately when you are asked a question. Consider practicing your testimony with the attorney who requested you to get feedback on how you present yourself.1 However, do not try to memorize what you are going to say because this could make your testimony sound rehearsed and unconvincing.
Plan ahead, and have a pretrial conference. Because court proceedings are unpredictable, you should clear your schedule to allow enough time to appear in court. Before your court appearance, meet with the attorney who requested you to discuss any new facts or issues as well as learn what the attorney aims to accomplish with your testimony.1
Speak clearly in your own words, and avoid jargon. Courtroom officials are unlikely to understand psychiatric jargon. Therefore, you should explain psychiatric terms in language that laypeople would comprehend. Because the court stenographer will require you to use actual words for the court transcripts, you should answer clearly and verbally or respond with a definitive “yes” or “no” (and not by nodding or shaking your head).
Testimony is also not a time for guessing. If you don’t know the answer, you should say “I don’t know.”
1. Gutheil TG. The psychiatrist in court: a survival guide. Washington, DC: American Psychiatric Press, Inc.; 1998.
2. Knoll JL, Resnick PJ. Deposition dos and don’ts: how to answer 8 tricky questions. Current Psychiatry. 2008;7(3):25-28,36,39-40.
1. Gutheil TG. The psychiatrist in court: a survival guide. Washington, DC: American Psychiatric Press, Inc.; 1998.
2. Knoll JL, Resnick PJ. Deposition dos and don’ts: how to answer 8 tricky questions. Current Psychiatry. 2008;7(3):25-28,36,39-40.
Not All Stool Discussions Are Unproductive
On August 22, 2014, a baby girl was born healthy and at full term. She was discharged on August 24 after a routine hospital stay. A day later, the infant’s mother called the pediatrician’s emergency after-hours hotline, in distress. She was concerned because the infant had not had a bowel movement since August 23. She was also concerned that each feeding was lasting an hour. A nurse told the mother that her concerns would be discussed in a routine follow-up appointment scheduled for the next morning.
At the appointment, the pediatrician noted the infant was having feeding problems and had lost 11% of her at-birth weight. The pediatrician also noted a high respiratory rate and abnormal skin coloring. However, the pediatrician concluded that the infant’s feeding problems had resolved, reassured the parents she was healthy, and discharged her, telling her parents to return in 2 weeks.
On August 29, the mother again called the pediatrician’s office, this time with concerns over a decrease in the infant’s feeding. A nurse told her to bring the infant to the emergency department (ED). At the ED, the infant was found to have lost 12% of her weight since birth and to be severely dehydrated. Due to hypovolemia, health care providers could not complete lab tests on the infant until aggressive resuscitation had been performed for 4 hours. The infant’s lab values showed she had hypernatremia, which put her at risk for brain injury through a decrease in cellular hydration, increased vascular permeability, or elevated intracranial pressure.
The infant did sustain a permanent brain injury from the condition: right-side paralysis. Her multi-organ failure from dehydration also caused significant damage to her left kidney, which stopped functioning altogether in 2017.
The infant sued her pediatrician and his office. Plaintiff’s counsel stated that the infant’s early weight loss was a red flag and that the standard of care required the pediatrician to order in-office follow-up within 24 hours to confirm if the loss had been corrected. Plaintiff’s counsel also alleged the baby’s respiratory rate and poor coloring were also red flags for dehydration. He further alleged that if the infant had returned to the office, her weight loss would have prompted supplementation before the dehydration caused her brain injury.
VERDICT
The case was settled for $1,375,000.
COMMENTARY
This case merits discussion because it involves a type of patient many clinicians see in practice. Complaints of newborn and infant feeding problems are common. Most cases require reassurance and troubleshooting about common feeding problems—but the clinician must be on the lookout for serious issues. Thus, it is helpful to revisit expected newborn feeding, stooling, and weight status.
Continue to: With regard to feeding...
With regard to feeding, breastfed infants should receive between 8-12 feeds per day during the newborn hospitalization.1 Bottlefed infants should be fed 20 kcal per 30 mL of iron-containing formula. Infants are fed on demand, and the duration of the feeding should not exceed 4 hours. The volume of the feed for the first few days of life should be 15-30 mL per feed.
For breastfed infants, clinicians should be attentive to issues that can impact nutrition, including latching difficulties, pain, mastitis, blocked duct, and engorgement. These can limit nutrition and be extremely upsetting to the mother.
Stooling frequency for newborns varies and depends on whether the infant is bottle fed or breast fed. During the first week of life, infants pass a mean of 4 stools per day.2 Breastfed infants may have as few as one stool per day, increasing as mother’s milk production increases.2
With regard to weight loss, term infants may lose up to 10% of their birth weight in the first few days of life, which is typically regained in 10 to 14 days.1 Infants born via cesarean section lose more weight, with 25% of these babies losing more than 10% by 72 hours. Of them, 76% return to birth weight by 14 days and 92% by 21 days. By contrast, vaginally born infants regain weight faster, with 86% returning to their birth weight by 14 days and 95% by the 21st day.1
Here, the infant was term and healthy, but we are not told some important details. Was she breast fed or bottle fed? Was she born by cesarean section or vaginally? We do know she was discharged on August 24th, her mother called the hotline on the 25th, and she was seen by the pediatrician on the 26th—at which point the infant had not stooled in 3 days. The mother called the physician’s office again on August 29th and was sent to the ED. We are told only that each feeding lasted an hour and the infant hadn’t stooled.
Continue to: Regarding stool...
Regarding stool—we have all had discussions with patients regarding hypervigilant concerns about stool color. We know there are some big things to look for with stool color (eg, black tarry reveals upper GI bleeding, while clay-colored or pale may reveal the absence of bile). Yet, patients’ expectations of the color-coded diagnostic abilities of their stool knows no bounds. Patients are convinced that we have some color wheel in our jacket pocket corresponding to stool color—and that the nuances between shades have important medical implications. If you ask, “Would you say it is more marigold, butterscotch yellow, or Tuscan sun?” … your patient will have an answer.
Patients reveal stool color hesitantly, reservedly, with nervous expectation. They wait for your response in quivering anticipation that the coming reply will include words to the effect that a boysenberry-purple stool is equivalent to a Death tarot card. A subconjunctival hemorrhage is the only thing that approaches the anxiety level of the oddly hued stool (Oddly Hued Stool Anxiety). Woe be the patient with both. For a patient bearing a subconjunctival hemorrhage who has also passed a jungle-green stool in the past 24 hours fully expects to explode within the next 60 minutes.
I’ve been rather facetious for a reason. My purpose is to acknowledge and to help you recognize that most discussions regarding stooling will not be (forgive me) productive. They are not productive because most stool coloration issues are nonentities—yet they produce patient anxiety that takes some time to address, leaving a busy clinician prone to curtly dismiss such discussions out of hand. Because many patient-initiated stool discussions aren’t productive, there is the risk for stool tune-out. As gross and unproductive as they can be, don’t tune out all stool discussions.
In this case, the appropriate frequency of stooling should have been at least once per day. For newborns, a stool color question is helpful; stool should not be white, pale, or clay-colored, which is suggestive of acholic stools from biliary atresia. Here, despite the absence of stool over a 3-day period, the defendant concluded the feeding problem was resolved and set a return visit for 2 weeks later. The plaintiff’s expert contended that the weight loss and absence of stooling was evidence of inadequate intake and warranted a return check the next day. Rather than risk the case going to trial, the defendant settled for $1,375,000.
IN SUM
Newborn nutrition is important. Understand that parents will be anxious about newborn feeding, although often there is no major medical concern. However, do not be dismissive of feeding concerns because of this expected anxiety. Listen to the parents fully, paying particular attention to quantifying feeding difficulty and stooling frequency matters. Don’t let patients’ rainbow parade of needless stool concerns blind you to considering important information. In other words, don’t be a stool fool.
1. McKee-Garrett TM. Overview of the routine management of the healthy newborn infant. UpToDate. Updated July 12, 2019. www.uptodate.com/contents/overview-of-the-routine-management-of-the-healthy-newborn-infant. Accessed November 18, 2019.
2. Sood MR. Constipation in infants and children: evaluation. UpToDate. Updated August 1, 2019. www.uptodate.com/contents/constipation-in-infants-and-children-evaluation. Accessed November 18, 2019.
On August 22, 2014, a baby girl was born healthy and at full term. She was discharged on August 24 after a routine hospital stay. A day later, the infant’s mother called the pediatrician’s emergency after-hours hotline, in distress. She was concerned because the infant had not had a bowel movement since August 23. She was also concerned that each feeding was lasting an hour. A nurse told the mother that her concerns would be discussed in a routine follow-up appointment scheduled for the next morning.
At the appointment, the pediatrician noted the infant was having feeding problems and had lost 11% of her at-birth weight. The pediatrician also noted a high respiratory rate and abnormal skin coloring. However, the pediatrician concluded that the infant’s feeding problems had resolved, reassured the parents she was healthy, and discharged her, telling her parents to return in 2 weeks.
On August 29, the mother again called the pediatrician’s office, this time with concerns over a decrease in the infant’s feeding. A nurse told her to bring the infant to the emergency department (ED). At the ED, the infant was found to have lost 12% of her weight since birth and to be severely dehydrated. Due to hypovolemia, health care providers could not complete lab tests on the infant until aggressive resuscitation had been performed for 4 hours. The infant’s lab values showed she had hypernatremia, which put her at risk for brain injury through a decrease in cellular hydration, increased vascular permeability, or elevated intracranial pressure.
The infant did sustain a permanent brain injury from the condition: right-side paralysis. Her multi-organ failure from dehydration also caused significant damage to her left kidney, which stopped functioning altogether in 2017.
The infant sued her pediatrician and his office. Plaintiff’s counsel stated that the infant’s early weight loss was a red flag and that the standard of care required the pediatrician to order in-office follow-up within 24 hours to confirm if the loss had been corrected. Plaintiff’s counsel also alleged the baby’s respiratory rate and poor coloring were also red flags for dehydration. He further alleged that if the infant had returned to the office, her weight loss would have prompted supplementation before the dehydration caused her brain injury.
VERDICT
The case was settled for $1,375,000.
COMMENTARY
This case merits discussion because it involves a type of patient many clinicians see in practice. Complaints of newborn and infant feeding problems are common. Most cases require reassurance and troubleshooting about common feeding problems—but the clinician must be on the lookout for serious issues. Thus, it is helpful to revisit expected newborn feeding, stooling, and weight status.
Continue to: With regard to feeding...
With regard to feeding, breastfed infants should receive between 8-12 feeds per day during the newborn hospitalization.1 Bottlefed infants should be fed 20 kcal per 30 mL of iron-containing formula. Infants are fed on demand, and the duration of the feeding should not exceed 4 hours. The volume of the feed for the first few days of life should be 15-30 mL per feed.
For breastfed infants, clinicians should be attentive to issues that can impact nutrition, including latching difficulties, pain, mastitis, blocked duct, and engorgement. These can limit nutrition and be extremely upsetting to the mother.
Stooling frequency for newborns varies and depends on whether the infant is bottle fed or breast fed. During the first week of life, infants pass a mean of 4 stools per day.2 Breastfed infants may have as few as one stool per day, increasing as mother’s milk production increases.2
With regard to weight loss, term infants may lose up to 10% of their birth weight in the first few days of life, which is typically regained in 10 to 14 days.1 Infants born via cesarean section lose more weight, with 25% of these babies losing more than 10% by 72 hours. Of them, 76% return to birth weight by 14 days and 92% by 21 days. By contrast, vaginally born infants regain weight faster, with 86% returning to their birth weight by 14 days and 95% by the 21st day.1
Here, the infant was term and healthy, but we are not told some important details. Was she breast fed or bottle fed? Was she born by cesarean section or vaginally? We do know she was discharged on August 24th, her mother called the hotline on the 25th, and she was seen by the pediatrician on the 26th—at which point the infant had not stooled in 3 days. The mother called the physician’s office again on August 29th and was sent to the ED. We are told only that each feeding lasted an hour and the infant hadn’t stooled.
Continue to: Regarding stool...
Regarding stool—we have all had discussions with patients regarding hypervigilant concerns about stool color. We know there are some big things to look for with stool color (eg, black tarry reveals upper GI bleeding, while clay-colored or pale may reveal the absence of bile). Yet, patients’ expectations of the color-coded diagnostic abilities of their stool knows no bounds. Patients are convinced that we have some color wheel in our jacket pocket corresponding to stool color—and that the nuances between shades have important medical implications. If you ask, “Would you say it is more marigold, butterscotch yellow, or Tuscan sun?” … your patient will have an answer.
Patients reveal stool color hesitantly, reservedly, with nervous expectation. They wait for your response in quivering anticipation that the coming reply will include words to the effect that a boysenberry-purple stool is equivalent to a Death tarot card. A subconjunctival hemorrhage is the only thing that approaches the anxiety level of the oddly hued stool (Oddly Hued Stool Anxiety). Woe be the patient with both. For a patient bearing a subconjunctival hemorrhage who has also passed a jungle-green stool in the past 24 hours fully expects to explode within the next 60 minutes.
I’ve been rather facetious for a reason. My purpose is to acknowledge and to help you recognize that most discussions regarding stooling will not be (forgive me) productive. They are not productive because most stool coloration issues are nonentities—yet they produce patient anxiety that takes some time to address, leaving a busy clinician prone to curtly dismiss such discussions out of hand. Because many patient-initiated stool discussions aren’t productive, there is the risk for stool tune-out. As gross and unproductive as they can be, don’t tune out all stool discussions.
In this case, the appropriate frequency of stooling should have been at least once per day. For newborns, a stool color question is helpful; stool should not be white, pale, or clay-colored, which is suggestive of acholic stools from biliary atresia. Here, despite the absence of stool over a 3-day period, the defendant concluded the feeding problem was resolved and set a return visit for 2 weeks later. The plaintiff’s expert contended that the weight loss and absence of stooling was evidence of inadequate intake and warranted a return check the next day. Rather than risk the case going to trial, the defendant settled for $1,375,000.
IN SUM
Newborn nutrition is important. Understand that parents will be anxious about newborn feeding, although often there is no major medical concern. However, do not be dismissive of feeding concerns because of this expected anxiety. Listen to the parents fully, paying particular attention to quantifying feeding difficulty and stooling frequency matters. Don’t let patients’ rainbow parade of needless stool concerns blind you to considering important information. In other words, don’t be a stool fool.
On August 22, 2014, a baby girl was born healthy and at full term. She was discharged on August 24 after a routine hospital stay. A day later, the infant’s mother called the pediatrician’s emergency after-hours hotline, in distress. She was concerned because the infant had not had a bowel movement since August 23. She was also concerned that each feeding was lasting an hour. A nurse told the mother that her concerns would be discussed in a routine follow-up appointment scheduled for the next morning.
At the appointment, the pediatrician noted the infant was having feeding problems and had lost 11% of her at-birth weight. The pediatrician also noted a high respiratory rate and abnormal skin coloring. However, the pediatrician concluded that the infant’s feeding problems had resolved, reassured the parents she was healthy, and discharged her, telling her parents to return in 2 weeks.
On August 29, the mother again called the pediatrician’s office, this time with concerns over a decrease in the infant’s feeding. A nurse told her to bring the infant to the emergency department (ED). At the ED, the infant was found to have lost 12% of her weight since birth and to be severely dehydrated. Due to hypovolemia, health care providers could not complete lab tests on the infant until aggressive resuscitation had been performed for 4 hours. The infant’s lab values showed she had hypernatremia, which put her at risk for brain injury through a decrease in cellular hydration, increased vascular permeability, or elevated intracranial pressure.
The infant did sustain a permanent brain injury from the condition: right-side paralysis. Her multi-organ failure from dehydration also caused significant damage to her left kidney, which stopped functioning altogether in 2017.
The infant sued her pediatrician and his office. Plaintiff’s counsel stated that the infant’s early weight loss was a red flag and that the standard of care required the pediatrician to order in-office follow-up within 24 hours to confirm if the loss had been corrected. Plaintiff’s counsel also alleged the baby’s respiratory rate and poor coloring were also red flags for dehydration. He further alleged that if the infant had returned to the office, her weight loss would have prompted supplementation before the dehydration caused her brain injury.
VERDICT
The case was settled for $1,375,000.
COMMENTARY
This case merits discussion because it involves a type of patient many clinicians see in practice. Complaints of newborn and infant feeding problems are common. Most cases require reassurance and troubleshooting about common feeding problems—but the clinician must be on the lookout for serious issues. Thus, it is helpful to revisit expected newborn feeding, stooling, and weight status.
Continue to: With regard to feeding...
With regard to feeding, breastfed infants should receive between 8-12 feeds per day during the newborn hospitalization.1 Bottlefed infants should be fed 20 kcal per 30 mL of iron-containing formula. Infants are fed on demand, and the duration of the feeding should not exceed 4 hours. The volume of the feed for the first few days of life should be 15-30 mL per feed.
For breastfed infants, clinicians should be attentive to issues that can impact nutrition, including latching difficulties, pain, mastitis, blocked duct, and engorgement. These can limit nutrition and be extremely upsetting to the mother.
Stooling frequency for newborns varies and depends on whether the infant is bottle fed or breast fed. During the first week of life, infants pass a mean of 4 stools per day.2 Breastfed infants may have as few as one stool per day, increasing as mother’s milk production increases.2
With regard to weight loss, term infants may lose up to 10% of their birth weight in the first few days of life, which is typically regained in 10 to 14 days.1 Infants born via cesarean section lose more weight, with 25% of these babies losing more than 10% by 72 hours. Of them, 76% return to birth weight by 14 days and 92% by 21 days. By contrast, vaginally born infants regain weight faster, with 86% returning to their birth weight by 14 days and 95% by the 21st day.1
Here, the infant was term and healthy, but we are not told some important details. Was she breast fed or bottle fed? Was she born by cesarean section or vaginally? We do know she was discharged on August 24th, her mother called the hotline on the 25th, and she was seen by the pediatrician on the 26th—at which point the infant had not stooled in 3 days. The mother called the physician’s office again on August 29th and was sent to the ED. We are told only that each feeding lasted an hour and the infant hadn’t stooled.
Continue to: Regarding stool...
Regarding stool—we have all had discussions with patients regarding hypervigilant concerns about stool color. We know there are some big things to look for with stool color (eg, black tarry reveals upper GI bleeding, while clay-colored or pale may reveal the absence of bile). Yet, patients’ expectations of the color-coded diagnostic abilities of their stool knows no bounds. Patients are convinced that we have some color wheel in our jacket pocket corresponding to stool color—and that the nuances between shades have important medical implications. If you ask, “Would you say it is more marigold, butterscotch yellow, or Tuscan sun?” … your patient will have an answer.
Patients reveal stool color hesitantly, reservedly, with nervous expectation. They wait for your response in quivering anticipation that the coming reply will include words to the effect that a boysenberry-purple stool is equivalent to a Death tarot card. A subconjunctival hemorrhage is the only thing that approaches the anxiety level of the oddly hued stool (Oddly Hued Stool Anxiety). Woe be the patient with both. For a patient bearing a subconjunctival hemorrhage who has also passed a jungle-green stool in the past 24 hours fully expects to explode within the next 60 minutes.
I’ve been rather facetious for a reason. My purpose is to acknowledge and to help you recognize that most discussions regarding stooling will not be (forgive me) productive. They are not productive because most stool coloration issues are nonentities—yet they produce patient anxiety that takes some time to address, leaving a busy clinician prone to curtly dismiss such discussions out of hand. Because many patient-initiated stool discussions aren’t productive, there is the risk for stool tune-out. As gross and unproductive as they can be, don’t tune out all stool discussions.
In this case, the appropriate frequency of stooling should have been at least once per day. For newborns, a stool color question is helpful; stool should not be white, pale, or clay-colored, which is suggestive of acholic stools from biliary atresia. Here, despite the absence of stool over a 3-day period, the defendant concluded the feeding problem was resolved and set a return visit for 2 weeks later. The plaintiff’s expert contended that the weight loss and absence of stooling was evidence of inadequate intake and warranted a return check the next day. Rather than risk the case going to trial, the defendant settled for $1,375,000.
IN SUM
Newborn nutrition is important. Understand that parents will be anxious about newborn feeding, although often there is no major medical concern. However, do not be dismissive of feeding concerns because of this expected anxiety. Listen to the parents fully, paying particular attention to quantifying feeding difficulty and stooling frequency matters. Don’t let patients’ rainbow parade of needless stool concerns blind you to considering important information. In other words, don’t be a stool fool.
1. McKee-Garrett TM. Overview of the routine management of the healthy newborn infant. UpToDate. Updated July 12, 2019. www.uptodate.com/contents/overview-of-the-routine-management-of-the-healthy-newborn-infant. Accessed November 18, 2019.
2. Sood MR. Constipation in infants and children: evaluation. UpToDate. Updated August 1, 2019. www.uptodate.com/contents/constipation-in-infants-and-children-evaluation. Accessed November 18, 2019.
1. McKee-Garrett TM. Overview of the routine management of the healthy newborn infant. UpToDate. Updated July 12, 2019. www.uptodate.com/contents/overview-of-the-routine-management-of-the-healthy-newborn-infant. Accessed November 18, 2019.
2. Sood MR. Constipation in infants and children: evaluation. UpToDate. Updated August 1, 2019. www.uptodate.com/contents/constipation-in-infants-and-children-evaluation. Accessed November 18, 2019.
What every ObGyn should know about Supreme Court rulings in the recent term
The most recently concluded term of the US Supreme Court, which began on October 1, 2018, yielded a number of decisions of interest to health care professionals and to ObGyns in particular. Although the term was viewed by some observers as less consequential than other recent terms, a review of the cases decided paints a picture of a more important term than some commentators expected.
When the term began, the Court had only 8 justices—1 short of a full bench: Judge Brett Kavanaugh had not yet been confirmed by the Senate. He was confirmed on October 6, by a 50-48 vote, and Justice Kavanaugh immediately joined the Court and began to hear and decide cases.
Increasingly, important decisions affect medical practice
From the nature of practice (abortion), to payment for service (Medicare reimbursement), resolution of disputes (arbitration), and fraud and abuse (the federal False Claims Act), the decisions of the Court will have an impact on many areas of medical practice. Organized medicine increasingly has recognized the significance of the work of the Court; nowhere has this been more clearly demonstrated than with amicus curiae (friend of the court) briefs filed by medical organizations.
Amicus curiae briefs. These briefs are filed by persons or organizations not a party to a case the Court is hearing. Their legitimate purpose is to inform the Court of 1) special information within the expertise of the amicus (or amici, plural) or 2) consequences of the decision that might not be apparent from arguments made by the parties to the case. Sometimes, the Court cites amicus briefs for having provided important information about the case.
Filing amicus briefs is time-consuming and expensive; organizations do not file them for trivial reasons. Organizations frequently join together to file a joint brief, to share expenses and express to the Court a stronger position.
Three categories of health professionals file amicus briefs in ObGyn-related cases:
- Major national organizations, often representing broad interests of health care professions or institutions (the American Medical Association [AMA], the Association of American Medical Colleges, and the American Hospital Association [AHA]), have filed a number of amicus briefs over the years.
- Specialty boards increasingly file amicus briefs. For example, the American College of Obstetricians and Gynecologists (ACOG) and the American Society for Reproductive Medicine have filed briefs related to abortion issues.
- In reproductive issues, the American Association of Pro-Life Obstetricians and Gynecologists, the American College of Pediatricians, and the Christian Medical & Dental Associations have been active amicus filers—frequently taking positions different than, even inconsistent with, amicus briefs filed by major specialty boards.
Amicus briefs filed by medical associations provide strong clues to what is important to clinicians. We have looked at such briefs to help us identify topics and cases from the just-concluded term that can be of particular interest to you.
Continue to: Surveying the shadow docket...
Surveying the shadow docket. As part of our review of the past term, we also looked at the so-called shadow docket, which includes decisions regarding writs of certiorari (which cases it agrees to hear); stays (usually delaying implementation of a law); or denials of stays. (Persuading the Court to hear a case is not easy: It hears approximately 70 cases per year out of as many as 7,000 applications to be heard.)
Abortion ruling
At stake. A number of states recently enacted a variety of provisions that might make an abortion more difficult to obtain. Some of the cases challenging these restrictions are making their way through lower courts, and one day might be argued before the Supreme Court. However, the Court has not (yet) agreed to hear the substance of many new abortion-related provisions.
Box v Planned Parenthood of Indiana and Kentucky, Inc.
The Court decided only 1 abortion restriction case this term.1 The Indiana law in question included 2 provisions that the Court considered:
Disposal of remains. The law regulated the manner in which abortion providers can dispose of fetal remains (ie, they cannot be treated as “infectious and pathologic waste”).
Motivation for seeking abortion. The Indiana law makes it illegal for an abortion provider to perform an abortion when the provider knows that the mother is seeking that abortion “solely” because of the fetus’s race, sex, diagnosis of Down syndrome, disability, or related characteristics.
Final rulings. The Court held that the disposal-of-remains provision is constitutional. The provision is “rationally related to the state’s interest in proper disposal of fetal remains.”2 Planned Parenthood had not raised the issue of whether the law might impose an undue burden on a woman’s right to obtain an abortion, so the Court did not decide that issue.
The Court did not consider the constitutionality of the part of the law proscribing certain reasons for seeking an otherwise legal abortion; instead, it awaits lower courts’ review of the issue. Justice Clarence Thomas wrote an extensive concurring opinion suggesting that this law is intended to avoid abortion to achieve eugenic goals.3
Key developments from the shadow docket
The Court issued a stay preventing a Louisiana statute that requires physicians who perform abortions to have admitting privileges at a nearby hospital from going into effect, pending the outcome of litigation about that law.4 Four dissenters noted that all 4 physicians who perform abortions in Louisiana have such privileges. Chief Justice Roberts was the fifth vote to grant the stay. This case likely will make its way back to the Court, as will a number of other state laws being adopted. The issue may be back as soon as the term just starting.
The Court is also considering whether to take another Indiana case, Box v Planned Parenthood of Indiana and Kentucky, Inc. (Box II). This case involves an Indiana ultrasonography viewing option as part of the abortion consent process.5
The Court declined to hear cases from Louisiana and Kansas in which the states had cut off Medicaid funding to Planned Parenthood. Lower courts had stopped the implementation of those laws.6 The legal issue was whether private parties, as opposed to the federal government, had standing to bring the case. For now, the decision of the lower courts to stop implementation of the funding cutoff is in effect. There is a split in the Circuit Courts on the issue, however, making it likely that the Supreme Court will have to resolve it sooner or later.
Health care organizations have filed a number of amicus briefs in these and other cases involving new abortion regulations. ACOG and others filed a brief opposing a Louisiana law that requires abortion providers to have admitting privileges at a nearby facility,7 and a brief opposing a similar Oklahoma law.8 The Association of Pro-Life Obstetricians and Gynecologists and others filed amicus curiae briefs in Box II9 and in an Alabama case involving so-called dismemberment abortion.10
Continue to: Medicare payments...
Medicare payments
Azar, Secretary of Health and Human Services v Allina Health Services, et al11
This case drew interest—and many amicus briefs—from health care providers, including the AMA and the AHA.12,13 There was good reason for their interest: First, the case involved more than $3 billion in reimbursements; second, it represented a potentially important precedent about the rights of providers and patients to comment on Medicare reimbursement changes. The question involved the technical calculation of additional payments made to institutions that serve a disproportionate number of low-income patients (known as Medicare Fractions).
At stake. The issue was a statutory requirement for a 60-day public notice and comment period for rules that “change a substantive legal standard” governing the scope of benefits, eligibility, or payment for services.14 In 2014, the Secretary of the Department of Health and Human Services (HHS) in the Obama administration posted a spreadsheet announcing Medicare fractions rates for hospitals (for 2012)—without formal notice or comment regarding the formula used. (The spreadsheet listed what each qualifying institution would receive, but it was based on a formula that, as noted, had not been subject to public notice and comment.) The AMA and AHA briefs emphasized the importance of a notice and comment period, especially when Medicare reimbursement is involved.
Final ruling. The Court held that the HHS process violated the notice and comment provision, thereby invalidating the policy underlying the so-called spreadsheet reimbursement. The decision was significant: This was a careful statutory interpretation of the 60-day notice and comment period, not the reimbursement policy itself. Presumably, had the HHS Secretary provided for sufficient notice and comment, the formula used would have met the requirements for issuing reimbursement formulas.
Key points. Hospitals will collectively receive $3 or $4 billion as a consequence of the ruling. Perhaps more importantly, the decision signals that HHS is going to have to take seriously the requirement that it publish Medicare-related reimbursement policies for the 60-day period.
A number of diverse cases ruled on by the Supreme Court are worth mentioning. The Court:
- allowed the President to move various funds from the US Department of Defense into accounts from which the money could be used to build a portion of a wall along the southern US border.1
- essentially killed the "citizenship question" on the census form. Technically, the Court sent the issue back to the Commerce Department for better justification for including the question (the announced reasons appeared to be pretextual).2
- changed, perhaps substantially, the deference that courts give to federal agencies in interpreting regulations.3
- upheld, in 2 cases, treaty rights of Native Americans to special treatment on Indian Lands4,5; the Court held that treaties ordinarily should be interpreted as the tribe understood them at the time they were signed. (These were 5 to 4 decisions; the split in the Court leaves many unanswered questions.)
- made it easier for landowners to file suit in federal court when they claim that the state has "taken" their property without just compensation.6
- held that a refusal of the US Patent and Trademark Office to register "immoral" or "scandalous" trademarks infringes on the First Amendment. (The petitioner sought to register "FUCT" as a trademark for a line of clothing.)7
- allowed an antitrust case by iPhone users against Apple to go forward. At issue: the claim that Apple monopolizes the retail market for apps by requiring buyers to obtain apps from Apple.8
- held that, if a drunk-driving suspect who has been taken into custody is, or becomes, unconscious, the "reasonable search" provision of the Fourth Amendment generally does not prevent a state from taking a blood specimen without a warrant. (Wisconsin had a specific "implied consent" law, by which someone receiving a driving license consents to a blood draw.9)
- decided numerous capital punishment cases. In many ways, this term seemed to be a "capital term." Issues involved in these cases have split the Court; it is reasonable to expect that the divide will endure through upcoming terms.
References
- Donald J. Trump, President of the United States, et al. v Sierra Club, et al. 588 US 19A60 (2019).
- Department of Commerce et al. v New York et al. 18 996 (2018).
- Kisor v Wilkie, Secretary of Veterans Affairs. 18 15 (2018).
- Washington State Department of Licensing v Cougar Den, Inc. 16 1498 (2018).
- Herrera v Wyoming. 17 532 (2018).
- Knick v Township of Scott, Pennsylvania, et al. 17 647 (2018).
- Iancu, Under Secretary of Commerce for Intellectual Property and Director, Patent and Trademark Office v Brunetti. 18 302 (2018).
- Apple Inc. v Pepper et al. 17 204 (2018).
- Mitchell v Wisconsin. 18 6210 (2018).
Liability under the False Claims Act
The False Claims Act (FCA) protects the federal government from fraudulent claims for payment and for shoddy goods and services. It incentivizes (by a percentage of recovery) private parties to bring cases to enforce the law.15 (Of course, the federal government also enforces the Act.)
At stake. The FCA has been of considerable concern to the AHA, the Association of American Medical Colleges, and other health care organizations—understandably so.16 As the AHA informed the Court in an amicus brief, “The prevalence of [FCA] cases has ballooned over the past three decades.... These suits disproportionately target healthcare entities.... Of the 767 new FCA cases filed in 2018, for example, 506 involved healthcare defendants.”17
Final ruling. The Court considered an ambiguity in the statute of limitations for these actions and the Court unanimously ruled to permit an extended time in which qui tam actions (private actions under the law) can be filed.18
Key points. As long a period as 10 years can pass between the time an FCA violation occurs and an action is brought. This decision is likely to increase the number of FCA actions against health care providers because the case can be filed many years after the conduct that gave rise to the complaint.
Continue to: Registering sex offenders...
Registering sex offenders
The Court upheld the constitutionality of the federal Sex Offender Registration and Notification Act (SORNA).19 Sex offenders must register and periodically report, in person, to law enforcement in every state in which the offender works, studies, or resides.
At stake. The case involved the applicability of SORNA registration obligations to those convicted of sex offenses before SORNA was adopted (pre-Act offenders).20 The court upheld registration requirements for pre-Act offenders.
Former Justice Stevens, the longest-living and third-longest-serving Supreme Court justice, died in July 2019 at 99 years of age. He was appointed to the Court in 1975 by President Ford and served until his retirement in 2010, when he was 90. Stevens had recently published a memoir, The Making of a Justice: Reflections on My First 94 Years.
Stevens's judicial philosophy generally is described as having changed over the course of his 35 years of service: He was viewed as becoming more liberal. He was a justice of enduring kindness and integrity. It is possible to find people who disagree with him, but almost impossible to find anyone who disliked him. He was continuously committed to the law and justice in the United States.
Arbitration
The Court continued its practice of deciding at least one case each term that emphasizes that federal law requires that courts rather strictly enforce agreements to arbitrate (instead of to litigate) future disputes.21 In another case, the Court ruled that there can be “class” or “joint” arbitration only if the agreement to arbitrate a dispute clearly permits such class arbitration.22
Pharma’s liability regarding product risk
The Court somewhat limited the liability of pharmaceutical companies for failing to provide adequate warning about the risk that their products pose. The case against Merck involved 500 patients who took denosumab (Fosamax) and suffered atypical femoral fractures.23
At stake. Because prescribing information (in which warnings are provided) must be approved by the US Food and Drug Administration (FDA), the legal test is: Would the FDA have refused to approve a change in the warning if Merck had “fully informed the FDA of the justifications for the warning” required by state law to avoid liability?24,25 Lower-court judges (not juries) will be expected to apply this test in the future.
The doctor and the death penalty
The Court has established a rule that, when a prisoner facing capital punishment objects to a form of execution because it is too painful, he has to propose an alternative that is reasonably available. In one case,26 a physician, an expert witness for the prisoner, did not answer some essential relative-pain questions (ie, would one procedure be more painful than another?).
At stake. The AMA filed an amicus brief in this case, indicating that it is unethical for physicians to participate in an execution. The brief noted that “testimony used to determine which method of execution would reduce physical suffering would constitute physician participation in capital punishment and would be unethical.”27
The expert witness’s failure to answer the question on relative pain had the unfortunate result of reducing the likelihood that the prisoner would prevail in his request for an alternative method of execution.
Analysis
Despite obvious disagreements about big issues (notably, abortion and the death penalty) the Court maintained a courteous and civil demeanor—something not always seen nowadays in other branches of government. Here are facts about the Court’s term just concluded:
- The Court issued 72 merits opinions (about average).
- Only 39% of decisions were unanimous (compared with the average of 49% in recent terms).
- On the other hand, 26% of decisions were split 5 to 4 (compared with a 10% recent average).
- In those 5 to 4 decisions, Justices were in the majority as follows28: Justice Gorsuch, 65%; Justice Kavanaugh, 61%; Justice Thomas, 60%; Chief Justice Roberts and Justices Ginsburg and Alito, each 55%; Justice Breyer, 50%; and Justices Sotomayor and Kagan each at 45%.
- There were 57 dissenting opinions—up from 48 in the previous term.
- What is referred to as “the liberal-conservative split” might seem more profound than it really is: “Every conservative member of the court at some point voted to form a majority with the liberal justices. And every liberal at least once left behind all of his or her usual voting partners to join the conservatives.”29
Continue to: Last, it was a year of personal health issues for...
Last, it was a year of personal health issues for the Court: Justice Ginsburg had a diagnosis of lung cancer and was absent, following surgery, in January. Of retired Justices, Sandra Day O’Connor suffers from dementia and former Justice John Paul Stevens died.
In closing
The Court has accepted approximately 50 cases for the current term, which began on October 7. The first 2 days of the term were spent on arguments about, first, whether a state can abolish the insanity defense and, second, whether nondiscrimination laws (“based on sex”) prohibit discrimination based on sexual orientation or transgender status. Cases also will deal with Patient Protection and Affordable Care Act payments to providers; the Deferred Action for Childhood Arrivals, or DACA; the death penalty; and international child custody disputes. The Court will be accepting more cases for several months. It promises to be a very interesting term.
- Box v Planned Parenthood of Indiana and Kentucky, Inc. 587 US 18 483 (2019).
- Box v Planned Parenthood of Indiana and Kentucky, Inc., at 2.
- Box v Planned Parenthood of Indiana and Kentucky, Inc., Justice Thomas concurring.
- June Medical Services, LLC, et al. v Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals. 586 US 18A774 (2019).
- Box v Planned Parenthood of Indiana and Kentucky, Inc. Docket 18-1019.
- Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals v Planned Parenthood of Gulf Coast, Inc., et al. 586 US 17 1492 (2018).
- June Medical Services L.L.C., et al., Petitioners, v Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals. No. 18-1323. Brief of Amici Curiae American College of Obstetricians and Gynecologists, American Academy of Family Physicians, American Academy of Pediatrics, American College of Nurse-Midwives, American College of Osteopathic Obstetricians and Gynecologists, American College of Physicians, American Society for Reproductive Medicine, National Association of Nurse Practitioners in Women's Health, North American Society for Pediatric and Adolescent Gynecology, and Society For Maternal-Fetal Medicine, Amicus Curiae in Support of Petitioners. May 2019.
- Planned Parenthood of Kansas & Eastern Oklahoma, et al., Petitioners, v Larry Jegley, et al., Respondents. No. 17-935. Brief Amici Curiae of American College of Obstetricians and Gynecologists and American Public Health Association as Amici Curiae in Support of Petitioners. February 1, 2018.
- Box v Planned Parenthood of Indiana & Kentucky. No. 18-1019. Brief Amici Curiae of American Association of Pro-Life Obstetricians & Gynecologists, American College of Pediatricians, Care Net, Christian Medical Association, Heartbeat International, Inc., and National Institute Of Family & Life Advocates in Support of Petitioners. March 6, 2019.
- Steven T. Marshall, et al., Petitioners, v West Alabama Women's Center, et al., Respondents. No. 18-837. Brief of Amici Curiae American Association of Pro-Life Obstetricians & Gynecologists and American College of Pediatricians, in Support of Petitioners. January 18, 2019.
- Azar, Secretary of Health and Human Services v Allina Health Services, et al. 17 1484 (2018).
- Alex M. Azar, II, Secretary of Health and Human Services, Petitioner, v Allina Health Services, et al., Respondents. Brief of the American Hospital Association, Federation of American Hospitals, and Association of American Medical Colleges as Amici Curiae in Support of Respondents. December 2018.
- Alex M. Azar, II, Secretary of Health and Human Services, Petitioner, v Allina Health Services, et al., Respondents. Brief of Amici Curiae American Medical Association and Medical Society of the District of Columbia Amici Curiae in Support of Respondents. December 2018.
- 42 U. S. C. §1395hh. https://uscode.house.gov/view.xhtml?req=(title:42%20section:1395hh%20edition:prelim). Accessed October 22, 2019.
- The False Claims Act: a primer. Washington DC: US Department of Justice. www.justice.gov/sites/default/files/civil/legacy/2011/04/22/C-FRAUDS_FCA_Primer.pdf. Accessed October 18, 2019.
- Universal Health Services, Inc., v United States and Commonwealth of Massachusetts ex rel. Julio Escobar and Carmen Correa. Brief of the American Hospital Association, Federation of American Hospitals, and Association of American Medical Colleges Amici Curiae in Support of Petitioner. No. 15-7. January 2016.
- Intermountain Health Care, Inc., et al., Petitioners, v United States ex rel. Gerald Polukoff, et al., Respondents. No. 18-911. Brief of the American Hospital Association and Federation of American Hospitals as Amici Curiae in Support of Petitioners. February 13, 2019.
- Cochise Consultancy, Inc., et al., v United States ex rel. Hunt. 18 315 (2018).
- 34 U.S.C. §20901 et seq. [Chapter 209--Child Protection and Safety.] https://uscode.house.gov/view.xhtml?path=/prelim@title34/subtitle2/chapter209&edition=prelim. Accessed October 17, 2019.
- Gundy v United States. 17 6086 (2018).
- Henry Schein, Inc., et al., v Archer & White Sales, Inc. 17 1272 (2018).
- Lamps Plus, Inc., et al., v Varela. 17 988 (2018).
- Merck Sharp & Dohme Corp. v Albrecht et al. 17 290 (2018).
- Merck Sharp & Dohme Corp. v Albrecht et al. 17 290 (2018) at 13-14.
- Wyeth v Levine, 555 US 555, 571 (2009).
- Russell Bucklew, Petitioner, v Anne L. Precythe, Director, Missouri Department of Corrections, et al., Respondents. 17 8151 (2018).
- Russell Bucklew, Petitioner, v Anne L. Precythe, Director, Missouri Department of Corrections, et al., Respondents. 17 8151 (2018). American Medical Association, Amicus Curiae Brief, in Support of Neither Party. July 23, 2018.
- Final stat pack for October term 2018. SCOTUSblog.com. June 28, 2019. https://www.scotusblog.com/wp-content/uploads/2019/07/StatPack_OT18-7_8_19.pdf. Accessed October 17, 2019.
- Barnes R. They're not 'wonder twins': Gorsuch, Kavanaugh shift the Supreme Court, but their differences are striking. Washington Post, June 28, 2019.
The most recently concluded term of the US Supreme Court, which began on October 1, 2018, yielded a number of decisions of interest to health care professionals and to ObGyns in particular. Although the term was viewed by some observers as less consequential than other recent terms, a review of the cases decided paints a picture of a more important term than some commentators expected.
When the term began, the Court had only 8 justices—1 short of a full bench: Judge Brett Kavanaugh had not yet been confirmed by the Senate. He was confirmed on October 6, by a 50-48 vote, and Justice Kavanaugh immediately joined the Court and began to hear and decide cases.
Increasingly, important decisions affect medical practice
From the nature of practice (abortion), to payment for service (Medicare reimbursement), resolution of disputes (arbitration), and fraud and abuse (the federal False Claims Act), the decisions of the Court will have an impact on many areas of medical practice. Organized medicine increasingly has recognized the significance of the work of the Court; nowhere has this been more clearly demonstrated than with amicus curiae (friend of the court) briefs filed by medical organizations.
Amicus curiae briefs. These briefs are filed by persons or organizations not a party to a case the Court is hearing. Their legitimate purpose is to inform the Court of 1) special information within the expertise of the amicus (or amici, plural) or 2) consequences of the decision that might not be apparent from arguments made by the parties to the case. Sometimes, the Court cites amicus briefs for having provided important information about the case.
Filing amicus briefs is time-consuming and expensive; organizations do not file them for trivial reasons. Organizations frequently join together to file a joint brief, to share expenses and express to the Court a stronger position.
Three categories of health professionals file amicus briefs in ObGyn-related cases:
- Major national organizations, often representing broad interests of health care professions or institutions (the American Medical Association [AMA], the Association of American Medical Colleges, and the American Hospital Association [AHA]), have filed a number of amicus briefs over the years.
- Specialty boards increasingly file amicus briefs. For example, the American College of Obstetricians and Gynecologists (ACOG) and the American Society for Reproductive Medicine have filed briefs related to abortion issues.
- In reproductive issues, the American Association of Pro-Life Obstetricians and Gynecologists, the American College of Pediatricians, and the Christian Medical & Dental Associations have been active amicus filers—frequently taking positions different than, even inconsistent with, amicus briefs filed by major specialty boards.
Amicus briefs filed by medical associations provide strong clues to what is important to clinicians. We have looked at such briefs to help us identify topics and cases from the just-concluded term that can be of particular interest to you.
Continue to: Surveying the shadow docket...
Surveying the shadow docket. As part of our review of the past term, we also looked at the so-called shadow docket, which includes decisions regarding writs of certiorari (which cases it agrees to hear); stays (usually delaying implementation of a law); or denials of stays. (Persuading the Court to hear a case is not easy: It hears approximately 70 cases per year out of as many as 7,000 applications to be heard.)
Abortion ruling
At stake. A number of states recently enacted a variety of provisions that might make an abortion more difficult to obtain. Some of the cases challenging these restrictions are making their way through lower courts, and one day might be argued before the Supreme Court. However, the Court has not (yet) agreed to hear the substance of many new abortion-related provisions.
Box v Planned Parenthood of Indiana and Kentucky, Inc.
The Court decided only 1 abortion restriction case this term.1 The Indiana law in question included 2 provisions that the Court considered:
Disposal of remains. The law regulated the manner in which abortion providers can dispose of fetal remains (ie, they cannot be treated as “infectious and pathologic waste”).
Motivation for seeking abortion. The Indiana law makes it illegal for an abortion provider to perform an abortion when the provider knows that the mother is seeking that abortion “solely” because of the fetus’s race, sex, diagnosis of Down syndrome, disability, or related characteristics.
Final rulings. The Court held that the disposal-of-remains provision is constitutional. The provision is “rationally related to the state’s interest in proper disposal of fetal remains.”2 Planned Parenthood had not raised the issue of whether the law might impose an undue burden on a woman’s right to obtain an abortion, so the Court did not decide that issue.
The Court did not consider the constitutionality of the part of the law proscribing certain reasons for seeking an otherwise legal abortion; instead, it awaits lower courts’ review of the issue. Justice Clarence Thomas wrote an extensive concurring opinion suggesting that this law is intended to avoid abortion to achieve eugenic goals.3
Key developments from the shadow docket
The Court issued a stay preventing a Louisiana statute that requires physicians who perform abortions to have admitting privileges at a nearby hospital from going into effect, pending the outcome of litigation about that law.4 Four dissenters noted that all 4 physicians who perform abortions in Louisiana have such privileges. Chief Justice Roberts was the fifth vote to grant the stay. This case likely will make its way back to the Court, as will a number of other state laws being adopted. The issue may be back as soon as the term just starting.
The Court is also considering whether to take another Indiana case, Box v Planned Parenthood of Indiana and Kentucky, Inc. (Box II). This case involves an Indiana ultrasonography viewing option as part of the abortion consent process.5
The Court declined to hear cases from Louisiana and Kansas in which the states had cut off Medicaid funding to Planned Parenthood. Lower courts had stopped the implementation of those laws.6 The legal issue was whether private parties, as opposed to the federal government, had standing to bring the case. For now, the decision of the lower courts to stop implementation of the funding cutoff is in effect. There is a split in the Circuit Courts on the issue, however, making it likely that the Supreme Court will have to resolve it sooner or later.
Health care organizations have filed a number of amicus briefs in these and other cases involving new abortion regulations. ACOG and others filed a brief opposing a Louisiana law that requires abortion providers to have admitting privileges at a nearby facility,7 and a brief opposing a similar Oklahoma law.8 The Association of Pro-Life Obstetricians and Gynecologists and others filed amicus curiae briefs in Box II9 and in an Alabama case involving so-called dismemberment abortion.10
Continue to: Medicare payments...
Medicare payments
Azar, Secretary of Health and Human Services v Allina Health Services, et al11
This case drew interest—and many amicus briefs—from health care providers, including the AMA and the AHA.12,13 There was good reason for their interest: First, the case involved more than $3 billion in reimbursements; second, it represented a potentially important precedent about the rights of providers and patients to comment on Medicare reimbursement changes. The question involved the technical calculation of additional payments made to institutions that serve a disproportionate number of low-income patients (known as Medicare Fractions).
At stake. The issue was a statutory requirement for a 60-day public notice and comment period for rules that “change a substantive legal standard” governing the scope of benefits, eligibility, or payment for services.14 In 2014, the Secretary of the Department of Health and Human Services (HHS) in the Obama administration posted a spreadsheet announcing Medicare fractions rates for hospitals (for 2012)—without formal notice or comment regarding the formula used. (The spreadsheet listed what each qualifying institution would receive, but it was based on a formula that, as noted, had not been subject to public notice and comment.) The AMA and AHA briefs emphasized the importance of a notice and comment period, especially when Medicare reimbursement is involved.
Final ruling. The Court held that the HHS process violated the notice and comment provision, thereby invalidating the policy underlying the so-called spreadsheet reimbursement. The decision was significant: This was a careful statutory interpretation of the 60-day notice and comment period, not the reimbursement policy itself. Presumably, had the HHS Secretary provided for sufficient notice and comment, the formula used would have met the requirements for issuing reimbursement formulas.
Key points. Hospitals will collectively receive $3 or $4 billion as a consequence of the ruling. Perhaps more importantly, the decision signals that HHS is going to have to take seriously the requirement that it publish Medicare-related reimbursement policies for the 60-day period.
A number of diverse cases ruled on by the Supreme Court are worth mentioning. The Court:
- allowed the President to move various funds from the US Department of Defense into accounts from which the money could be used to build a portion of a wall along the southern US border.1
- essentially killed the "citizenship question" on the census form. Technically, the Court sent the issue back to the Commerce Department for better justification for including the question (the announced reasons appeared to be pretextual).2
- changed, perhaps substantially, the deference that courts give to federal agencies in interpreting regulations.3
- upheld, in 2 cases, treaty rights of Native Americans to special treatment on Indian Lands4,5; the Court held that treaties ordinarily should be interpreted as the tribe understood them at the time they were signed. (These were 5 to 4 decisions; the split in the Court leaves many unanswered questions.)
- made it easier for landowners to file suit in federal court when they claim that the state has "taken" their property without just compensation.6
- held that a refusal of the US Patent and Trademark Office to register "immoral" or "scandalous" trademarks infringes on the First Amendment. (The petitioner sought to register "FUCT" as a trademark for a line of clothing.)7
- allowed an antitrust case by iPhone users against Apple to go forward. At issue: the claim that Apple monopolizes the retail market for apps by requiring buyers to obtain apps from Apple.8
- held that, if a drunk-driving suspect who has been taken into custody is, or becomes, unconscious, the "reasonable search" provision of the Fourth Amendment generally does not prevent a state from taking a blood specimen without a warrant. (Wisconsin had a specific "implied consent" law, by which someone receiving a driving license consents to a blood draw.9)
- decided numerous capital punishment cases. In many ways, this term seemed to be a "capital term." Issues involved in these cases have split the Court; it is reasonable to expect that the divide will endure through upcoming terms.
References
- Donald J. Trump, President of the United States, et al. v Sierra Club, et al. 588 US 19A60 (2019).
- Department of Commerce et al. v New York et al. 18 996 (2018).
- Kisor v Wilkie, Secretary of Veterans Affairs. 18 15 (2018).
- Washington State Department of Licensing v Cougar Den, Inc. 16 1498 (2018).
- Herrera v Wyoming. 17 532 (2018).
- Knick v Township of Scott, Pennsylvania, et al. 17 647 (2018).
- Iancu, Under Secretary of Commerce for Intellectual Property and Director, Patent and Trademark Office v Brunetti. 18 302 (2018).
- Apple Inc. v Pepper et al. 17 204 (2018).
- Mitchell v Wisconsin. 18 6210 (2018).
Liability under the False Claims Act
The False Claims Act (FCA) protects the federal government from fraudulent claims for payment and for shoddy goods and services. It incentivizes (by a percentage of recovery) private parties to bring cases to enforce the law.15 (Of course, the federal government also enforces the Act.)
At stake. The FCA has been of considerable concern to the AHA, the Association of American Medical Colleges, and other health care organizations—understandably so.16 As the AHA informed the Court in an amicus brief, “The prevalence of [FCA] cases has ballooned over the past three decades.... These suits disproportionately target healthcare entities.... Of the 767 new FCA cases filed in 2018, for example, 506 involved healthcare defendants.”17
Final ruling. The Court considered an ambiguity in the statute of limitations for these actions and the Court unanimously ruled to permit an extended time in which qui tam actions (private actions under the law) can be filed.18
Key points. As long a period as 10 years can pass between the time an FCA violation occurs and an action is brought. This decision is likely to increase the number of FCA actions against health care providers because the case can be filed many years after the conduct that gave rise to the complaint.
Continue to: Registering sex offenders...
Registering sex offenders
The Court upheld the constitutionality of the federal Sex Offender Registration and Notification Act (SORNA).19 Sex offenders must register and periodically report, in person, to law enforcement in every state in which the offender works, studies, or resides.
At stake. The case involved the applicability of SORNA registration obligations to those convicted of sex offenses before SORNA was adopted (pre-Act offenders).20 The court upheld registration requirements for pre-Act offenders.
Former Justice Stevens, the longest-living and third-longest-serving Supreme Court justice, died in July 2019 at 99 years of age. He was appointed to the Court in 1975 by President Ford and served until his retirement in 2010, when he was 90. Stevens had recently published a memoir, The Making of a Justice: Reflections on My First 94 Years.
Stevens's judicial philosophy generally is described as having changed over the course of his 35 years of service: He was viewed as becoming more liberal. He was a justice of enduring kindness and integrity. It is possible to find people who disagree with him, but almost impossible to find anyone who disliked him. He was continuously committed to the law and justice in the United States.
Arbitration
The Court continued its practice of deciding at least one case each term that emphasizes that federal law requires that courts rather strictly enforce agreements to arbitrate (instead of to litigate) future disputes.21 In another case, the Court ruled that there can be “class” or “joint” arbitration only if the agreement to arbitrate a dispute clearly permits such class arbitration.22
Pharma’s liability regarding product risk
The Court somewhat limited the liability of pharmaceutical companies for failing to provide adequate warning about the risk that their products pose. The case against Merck involved 500 patients who took denosumab (Fosamax) and suffered atypical femoral fractures.23
At stake. Because prescribing information (in which warnings are provided) must be approved by the US Food and Drug Administration (FDA), the legal test is: Would the FDA have refused to approve a change in the warning if Merck had “fully informed the FDA of the justifications for the warning” required by state law to avoid liability?24,25 Lower-court judges (not juries) will be expected to apply this test in the future.
The doctor and the death penalty
The Court has established a rule that, when a prisoner facing capital punishment objects to a form of execution because it is too painful, he has to propose an alternative that is reasonably available. In one case,26 a physician, an expert witness for the prisoner, did not answer some essential relative-pain questions (ie, would one procedure be more painful than another?).
At stake. The AMA filed an amicus brief in this case, indicating that it is unethical for physicians to participate in an execution. The brief noted that “testimony used to determine which method of execution would reduce physical suffering would constitute physician participation in capital punishment and would be unethical.”27
The expert witness’s failure to answer the question on relative pain had the unfortunate result of reducing the likelihood that the prisoner would prevail in his request for an alternative method of execution.
Analysis
Despite obvious disagreements about big issues (notably, abortion and the death penalty) the Court maintained a courteous and civil demeanor—something not always seen nowadays in other branches of government. Here are facts about the Court’s term just concluded:
- The Court issued 72 merits opinions (about average).
- Only 39% of decisions were unanimous (compared with the average of 49% in recent terms).
- On the other hand, 26% of decisions were split 5 to 4 (compared with a 10% recent average).
- In those 5 to 4 decisions, Justices were in the majority as follows28: Justice Gorsuch, 65%; Justice Kavanaugh, 61%; Justice Thomas, 60%; Chief Justice Roberts and Justices Ginsburg and Alito, each 55%; Justice Breyer, 50%; and Justices Sotomayor and Kagan each at 45%.
- There were 57 dissenting opinions—up from 48 in the previous term.
- What is referred to as “the liberal-conservative split” might seem more profound than it really is: “Every conservative member of the court at some point voted to form a majority with the liberal justices. And every liberal at least once left behind all of his or her usual voting partners to join the conservatives.”29
Continue to: Last, it was a year of personal health issues for...
Last, it was a year of personal health issues for the Court: Justice Ginsburg had a diagnosis of lung cancer and was absent, following surgery, in January. Of retired Justices, Sandra Day O’Connor suffers from dementia and former Justice John Paul Stevens died.
In closing
The Court has accepted approximately 50 cases for the current term, which began on October 7. The first 2 days of the term were spent on arguments about, first, whether a state can abolish the insanity defense and, second, whether nondiscrimination laws (“based on sex”) prohibit discrimination based on sexual orientation or transgender status. Cases also will deal with Patient Protection and Affordable Care Act payments to providers; the Deferred Action for Childhood Arrivals, or DACA; the death penalty; and international child custody disputes. The Court will be accepting more cases for several months. It promises to be a very interesting term.
The most recently concluded term of the US Supreme Court, which began on October 1, 2018, yielded a number of decisions of interest to health care professionals and to ObGyns in particular. Although the term was viewed by some observers as less consequential than other recent terms, a review of the cases decided paints a picture of a more important term than some commentators expected.
When the term began, the Court had only 8 justices—1 short of a full bench: Judge Brett Kavanaugh had not yet been confirmed by the Senate. He was confirmed on October 6, by a 50-48 vote, and Justice Kavanaugh immediately joined the Court and began to hear and decide cases.
Increasingly, important decisions affect medical practice
From the nature of practice (abortion), to payment for service (Medicare reimbursement), resolution of disputes (arbitration), and fraud and abuse (the federal False Claims Act), the decisions of the Court will have an impact on many areas of medical practice. Organized medicine increasingly has recognized the significance of the work of the Court; nowhere has this been more clearly demonstrated than with amicus curiae (friend of the court) briefs filed by medical organizations.
Amicus curiae briefs. These briefs are filed by persons or organizations not a party to a case the Court is hearing. Their legitimate purpose is to inform the Court of 1) special information within the expertise of the amicus (or amici, plural) or 2) consequences of the decision that might not be apparent from arguments made by the parties to the case. Sometimes, the Court cites amicus briefs for having provided important information about the case.
Filing amicus briefs is time-consuming and expensive; organizations do not file them for trivial reasons. Organizations frequently join together to file a joint brief, to share expenses and express to the Court a stronger position.
Three categories of health professionals file amicus briefs in ObGyn-related cases:
- Major national organizations, often representing broad interests of health care professions or institutions (the American Medical Association [AMA], the Association of American Medical Colleges, and the American Hospital Association [AHA]), have filed a number of amicus briefs over the years.
- Specialty boards increasingly file amicus briefs. For example, the American College of Obstetricians and Gynecologists (ACOG) and the American Society for Reproductive Medicine have filed briefs related to abortion issues.
- In reproductive issues, the American Association of Pro-Life Obstetricians and Gynecologists, the American College of Pediatricians, and the Christian Medical & Dental Associations have been active amicus filers—frequently taking positions different than, even inconsistent with, amicus briefs filed by major specialty boards.
Amicus briefs filed by medical associations provide strong clues to what is important to clinicians. We have looked at such briefs to help us identify topics and cases from the just-concluded term that can be of particular interest to you.
Continue to: Surveying the shadow docket...
Surveying the shadow docket. As part of our review of the past term, we also looked at the so-called shadow docket, which includes decisions regarding writs of certiorari (which cases it agrees to hear); stays (usually delaying implementation of a law); or denials of stays. (Persuading the Court to hear a case is not easy: It hears approximately 70 cases per year out of as many as 7,000 applications to be heard.)
Abortion ruling
At stake. A number of states recently enacted a variety of provisions that might make an abortion more difficult to obtain. Some of the cases challenging these restrictions are making their way through lower courts, and one day might be argued before the Supreme Court. However, the Court has not (yet) agreed to hear the substance of many new abortion-related provisions.
Box v Planned Parenthood of Indiana and Kentucky, Inc.
The Court decided only 1 abortion restriction case this term.1 The Indiana law in question included 2 provisions that the Court considered:
Disposal of remains. The law regulated the manner in which abortion providers can dispose of fetal remains (ie, they cannot be treated as “infectious and pathologic waste”).
Motivation for seeking abortion. The Indiana law makes it illegal for an abortion provider to perform an abortion when the provider knows that the mother is seeking that abortion “solely” because of the fetus’s race, sex, diagnosis of Down syndrome, disability, or related characteristics.
Final rulings. The Court held that the disposal-of-remains provision is constitutional. The provision is “rationally related to the state’s interest in proper disposal of fetal remains.”2 Planned Parenthood had not raised the issue of whether the law might impose an undue burden on a woman’s right to obtain an abortion, so the Court did not decide that issue.
The Court did not consider the constitutionality of the part of the law proscribing certain reasons for seeking an otherwise legal abortion; instead, it awaits lower courts’ review of the issue. Justice Clarence Thomas wrote an extensive concurring opinion suggesting that this law is intended to avoid abortion to achieve eugenic goals.3
Key developments from the shadow docket
The Court issued a stay preventing a Louisiana statute that requires physicians who perform abortions to have admitting privileges at a nearby hospital from going into effect, pending the outcome of litigation about that law.4 Four dissenters noted that all 4 physicians who perform abortions in Louisiana have such privileges. Chief Justice Roberts was the fifth vote to grant the stay. This case likely will make its way back to the Court, as will a number of other state laws being adopted. The issue may be back as soon as the term just starting.
The Court is also considering whether to take another Indiana case, Box v Planned Parenthood of Indiana and Kentucky, Inc. (Box II). This case involves an Indiana ultrasonography viewing option as part of the abortion consent process.5
The Court declined to hear cases from Louisiana and Kansas in which the states had cut off Medicaid funding to Planned Parenthood. Lower courts had stopped the implementation of those laws.6 The legal issue was whether private parties, as opposed to the federal government, had standing to bring the case. For now, the decision of the lower courts to stop implementation of the funding cutoff is in effect. There is a split in the Circuit Courts on the issue, however, making it likely that the Supreme Court will have to resolve it sooner or later.
Health care organizations have filed a number of amicus briefs in these and other cases involving new abortion regulations. ACOG and others filed a brief opposing a Louisiana law that requires abortion providers to have admitting privileges at a nearby facility,7 and a brief opposing a similar Oklahoma law.8 The Association of Pro-Life Obstetricians and Gynecologists and others filed amicus curiae briefs in Box II9 and in an Alabama case involving so-called dismemberment abortion.10
Continue to: Medicare payments...
Medicare payments
Azar, Secretary of Health and Human Services v Allina Health Services, et al11
This case drew interest—and many amicus briefs—from health care providers, including the AMA and the AHA.12,13 There was good reason for their interest: First, the case involved more than $3 billion in reimbursements; second, it represented a potentially important precedent about the rights of providers and patients to comment on Medicare reimbursement changes. The question involved the technical calculation of additional payments made to institutions that serve a disproportionate number of low-income patients (known as Medicare Fractions).
At stake. The issue was a statutory requirement for a 60-day public notice and comment period for rules that “change a substantive legal standard” governing the scope of benefits, eligibility, or payment for services.14 In 2014, the Secretary of the Department of Health and Human Services (HHS) in the Obama administration posted a spreadsheet announcing Medicare fractions rates for hospitals (for 2012)—without formal notice or comment regarding the formula used. (The spreadsheet listed what each qualifying institution would receive, but it was based on a formula that, as noted, had not been subject to public notice and comment.) The AMA and AHA briefs emphasized the importance of a notice and comment period, especially when Medicare reimbursement is involved.
Final ruling. The Court held that the HHS process violated the notice and comment provision, thereby invalidating the policy underlying the so-called spreadsheet reimbursement. The decision was significant: This was a careful statutory interpretation of the 60-day notice and comment period, not the reimbursement policy itself. Presumably, had the HHS Secretary provided for sufficient notice and comment, the formula used would have met the requirements for issuing reimbursement formulas.
Key points. Hospitals will collectively receive $3 or $4 billion as a consequence of the ruling. Perhaps more importantly, the decision signals that HHS is going to have to take seriously the requirement that it publish Medicare-related reimbursement policies for the 60-day period.
A number of diverse cases ruled on by the Supreme Court are worth mentioning. The Court:
- allowed the President to move various funds from the US Department of Defense into accounts from which the money could be used to build a portion of a wall along the southern US border.1
- essentially killed the "citizenship question" on the census form. Technically, the Court sent the issue back to the Commerce Department for better justification for including the question (the announced reasons appeared to be pretextual).2
- changed, perhaps substantially, the deference that courts give to federal agencies in interpreting regulations.3
- upheld, in 2 cases, treaty rights of Native Americans to special treatment on Indian Lands4,5; the Court held that treaties ordinarily should be interpreted as the tribe understood them at the time they were signed. (These were 5 to 4 decisions; the split in the Court leaves many unanswered questions.)
- made it easier for landowners to file suit in federal court when they claim that the state has "taken" their property without just compensation.6
- held that a refusal of the US Patent and Trademark Office to register "immoral" or "scandalous" trademarks infringes on the First Amendment. (The petitioner sought to register "FUCT" as a trademark for a line of clothing.)7
- allowed an antitrust case by iPhone users against Apple to go forward. At issue: the claim that Apple monopolizes the retail market for apps by requiring buyers to obtain apps from Apple.8
- held that, if a drunk-driving suspect who has been taken into custody is, or becomes, unconscious, the "reasonable search" provision of the Fourth Amendment generally does not prevent a state from taking a blood specimen without a warrant. (Wisconsin had a specific "implied consent" law, by which someone receiving a driving license consents to a blood draw.9)
- decided numerous capital punishment cases. In many ways, this term seemed to be a "capital term." Issues involved in these cases have split the Court; it is reasonable to expect that the divide will endure through upcoming terms.
References
- Donald J. Trump, President of the United States, et al. v Sierra Club, et al. 588 US 19A60 (2019).
- Department of Commerce et al. v New York et al. 18 996 (2018).
- Kisor v Wilkie, Secretary of Veterans Affairs. 18 15 (2018).
- Washington State Department of Licensing v Cougar Den, Inc. 16 1498 (2018).
- Herrera v Wyoming. 17 532 (2018).
- Knick v Township of Scott, Pennsylvania, et al. 17 647 (2018).
- Iancu, Under Secretary of Commerce for Intellectual Property and Director, Patent and Trademark Office v Brunetti. 18 302 (2018).
- Apple Inc. v Pepper et al. 17 204 (2018).
- Mitchell v Wisconsin. 18 6210 (2018).
Liability under the False Claims Act
The False Claims Act (FCA) protects the federal government from fraudulent claims for payment and for shoddy goods and services. It incentivizes (by a percentage of recovery) private parties to bring cases to enforce the law.15 (Of course, the federal government also enforces the Act.)
At stake. The FCA has been of considerable concern to the AHA, the Association of American Medical Colleges, and other health care organizations—understandably so.16 As the AHA informed the Court in an amicus brief, “The prevalence of [FCA] cases has ballooned over the past three decades.... These suits disproportionately target healthcare entities.... Of the 767 new FCA cases filed in 2018, for example, 506 involved healthcare defendants.”17
Final ruling. The Court considered an ambiguity in the statute of limitations for these actions and the Court unanimously ruled to permit an extended time in which qui tam actions (private actions under the law) can be filed.18
Key points. As long a period as 10 years can pass between the time an FCA violation occurs and an action is brought. This decision is likely to increase the number of FCA actions against health care providers because the case can be filed many years after the conduct that gave rise to the complaint.
Continue to: Registering sex offenders...
Registering sex offenders
The Court upheld the constitutionality of the federal Sex Offender Registration and Notification Act (SORNA).19 Sex offenders must register and periodically report, in person, to law enforcement in every state in which the offender works, studies, or resides.
At stake. The case involved the applicability of SORNA registration obligations to those convicted of sex offenses before SORNA was adopted (pre-Act offenders).20 The court upheld registration requirements for pre-Act offenders.
Former Justice Stevens, the longest-living and third-longest-serving Supreme Court justice, died in July 2019 at 99 years of age. He was appointed to the Court in 1975 by President Ford and served until his retirement in 2010, when he was 90. Stevens had recently published a memoir, The Making of a Justice: Reflections on My First 94 Years.
Stevens's judicial philosophy generally is described as having changed over the course of his 35 years of service: He was viewed as becoming more liberal. He was a justice of enduring kindness and integrity. It is possible to find people who disagree with him, but almost impossible to find anyone who disliked him. He was continuously committed to the law and justice in the United States.
Arbitration
The Court continued its practice of deciding at least one case each term that emphasizes that federal law requires that courts rather strictly enforce agreements to arbitrate (instead of to litigate) future disputes.21 In another case, the Court ruled that there can be “class” or “joint” arbitration only if the agreement to arbitrate a dispute clearly permits such class arbitration.22
Pharma’s liability regarding product risk
The Court somewhat limited the liability of pharmaceutical companies for failing to provide adequate warning about the risk that their products pose. The case against Merck involved 500 patients who took denosumab (Fosamax) and suffered atypical femoral fractures.23
At stake. Because prescribing information (in which warnings are provided) must be approved by the US Food and Drug Administration (FDA), the legal test is: Would the FDA have refused to approve a change in the warning if Merck had “fully informed the FDA of the justifications for the warning” required by state law to avoid liability?24,25 Lower-court judges (not juries) will be expected to apply this test in the future.
The doctor and the death penalty
The Court has established a rule that, when a prisoner facing capital punishment objects to a form of execution because it is too painful, he has to propose an alternative that is reasonably available. In one case,26 a physician, an expert witness for the prisoner, did not answer some essential relative-pain questions (ie, would one procedure be more painful than another?).
At stake. The AMA filed an amicus brief in this case, indicating that it is unethical for physicians to participate in an execution. The brief noted that “testimony used to determine which method of execution would reduce physical suffering would constitute physician participation in capital punishment and would be unethical.”27
The expert witness’s failure to answer the question on relative pain had the unfortunate result of reducing the likelihood that the prisoner would prevail in his request for an alternative method of execution.
Analysis
Despite obvious disagreements about big issues (notably, abortion and the death penalty) the Court maintained a courteous and civil demeanor—something not always seen nowadays in other branches of government. Here are facts about the Court’s term just concluded:
- The Court issued 72 merits opinions (about average).
- Only 39% of decisions were unanimous (compared with the average of 49% in recent terms).
- On the other hand, 26% of decisions were split 5 to 4 (compared with a 10% recent average).
- In those 5 to 4 decisions, Justices were in the majority as follows28: Justice Gorsuch, 65%; Justice Kavanaugh, 61%; Justice Thomas, 60%; Chief Justice Roberts and Justices Ginsburg and Alito, each 55%; Justice Breyer, 50%; and Justices Sotomayor and Kagan each at 45%.
- There were 57 dissenting opinions—up from 48 in the previous term.
- What is referred to as “the liberal-conservative split” might seem more profound than it really is: “Every conservative member of the court at some point voted to form a majority with the liberal justices. And every liberal at least once left behind all of his or her usual voting partners to join the conservatives.”29
Continue to: Last, it was a year of personal health issues for...
Last, it was a year of personal health issues for the Court: Justice Ginsburg had a diagnosis of lung cancer and was absent, following surgery, in January. Of retired Justices, Sandra Day O’Connor suffers from dementia and former Justice John Paul Stevens died.
In closing
The Court has accepted approximately 50 cases for the current term, which began on October 7. The first 2 days of the term were spent on arguments about, first, whether a state can abolish the insanity defense and, second, whether nondiscrimination laws (“based on sex”) prohibit discrimination based on sexual orientation or transgender status. Cases also will deal with Patient Protection and Affordable Care Act payments to providers; the Deferred Action for Childhood Arrivals, or DACA; the death penalty; and international child custody disputes. The Court will be accepting more cases for several months. It promises to be a very interesting term.
- Box v Planned Parenthood of Indiana and Kentucky, Inc. 587 US 18 483 (2019).
- Box v Planned Parenthood of Indiana and Kentucky, Inc., at 2.
- Box v Planned Parenthood of Indiana and Kentucky, Inc., Justice Thomas concurring.
- June Medical Services, LLC, et al. v Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals. 586 US 18A774 (2019).
- Box v Planned Parenthood of Indiana and Kentucky, Inc. Docket 18-1019.
- Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals v Planned Parenthood of Gulf Coast, Inc., et al. 586 US 17 1492 (2018).
- June Medical Services L.L.C., et al., Petitioners, v Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals. No. 18-1323. Brief of Amici Curiae American College of Obstetricians and Gynecologists, American Academy of Family Physicians, American Academy of Pediatrics, American College of Nurse-Midwives, American College of Osteopathic Obstetricians and Gynecologists, American College of Physicians, American Society for Reproductive Medicine, National Association of Nurse Practitioners in Women's Health, North American Society for Pediatric and Adolescent Gynecology, and Society For Maternal-Fetal Medicine, Amicus Curiae in Support of Petitioners. May 2019.
- Planned Parenthood of Kansas & Eastern Oklahoma, et al., Petitioners, v Larry Jegley, et al., Respondents. No. 17-935. Brief Amici Curiae of American College of Obstetricians and Gynecologists and American Public Health Association as Amici Curiae in Support of Petitioners. February 1, 2018.
- Box v Planned Parenthood of Indiana & Kentucky. No. 18-1019. Brief Amici Curiae of American Association of Pro-Life Obstetricians & Gynecologists, American College of Pediatricians, Care Net, Christian Medical Association, Heartbeat International, Inc., and National Institute Of Family & Life Advocates in Support of Petitioners. March 6, 2019.
- Steven T. Marshall, et al., Petitioners, v West Alabama Women's Center, et al., Respondents. No. 18-837. Brief of Amici Curiae American Association of Pro-Life Obstetricians & Gynecologists and American College of Pediatricians, in Support of Petitioners. January 18, 2019.
- Azar, Secretary of Health and Human Services v Allina Health Services, et al. 17 1484 (2018).
- Alex M. Azar, II, Secretary of Health and Human Services, Petitioner, v Allina Health Services, et al., Respondents. Brief of the American Hospital Association, Federation of American Hospitals, and Association of American Medical Colleges as Amici Curiae in Support of Respondents. December 2018.
- Alex M. Azar, II, Secretary of Health and Human Services, Petitioner, v Allina Health Services, et al., Respondents. Brief of Amici Curiae American Medical Association and Medical Society of the District of Columbia Amici Curiae in Support of Respondents. December 2018.
- 42 U. S. C. §1395hh. https://uscode.house.gov/view.xhtml?req=(title:42%20section:1395hh%20edition:prelim). Accessed October 22, 2019.
- The False Claims Act: a primer. Washington DC: US Department of Justice. www.justice.gov/sites/default/files/civil/legacy/2011/04/22/C-FRAUDS_FCA_Primer.pdf. Accessed October 18, 2019.
- Universal Health Services, Inc., v United States and Commonwealth of Massachusetts ex rel. Julio Escobar and Carmen Correa. Brief of the American Hospital Association, Federation of American Hospitals, and Association of American Medical Colleges Amici Curiae in Support of Petitioner. No. 15-7. January 2016.
- Intermountain Health Care, Inc., et al., Petitioners, v United States ex rel. Gerald Polukoff, et al., Respondents. No. 18-911. Brief of the American Hospital Association and Federation of American Hospitals as Amici Curiae in Support of Petitioners. February 13, 2019.
- Cochise Consultancy, Inc., et al., v United States ex rel. Hunt. 18 315 (2018).
- 34 U.S.C. §20901 et seq. [Chapter 209--Child Protection and Safety.] https://uscode.house.gov/view.xhtml?path=/prelim@title34/subtitle2/chapter209&edition=prelim. Accessed October 17, 2019.
- Gundy v United States. 17 6086 (2018).
- Henry Schein, Inc., et al., v Archer & White Sales, Inc. 17 1272 (2018).
- Lamps Plus, Inc., et al., v Varela. 17 988 (2018).
- Merck Sharp & Dohme Corp. v Albrecht et al. 17 290 (2018).
- Merck Sharp & Dohme Corp. v Albrecht et al. 17 290 (2018) at 13-14.
- Wyeth v Levine, 555 US 555, 571 (2009).
- Russell Bucklew, Petitioner, v Anne L. Precythe, Director, Missouri Department of Corrections, et al., Respondents. 17 8151 (2018).
- Russell Bucklew, Petitioner, v Anne L. Precythe, Director, Missouri Department of Corrections, et al., Respondents. 17 8151 (2018). American Medical Association, Amicus Curiae Brief, in Support of Neither Party. July 23, 2018.
- Final stat pack for October term 2018. SCOTUSblog.com. June 28, 2019. https://www.scotusblog.com/wp-content/uploads/2019/07/StatPack_OT18-7_8_19.pdf. Accessed October 17, 2019.
- Barnes R. They're not 'wonder twins': Gorsuch, Kavanaugh shift the Supreme Court, but their differences are striking. Washington Post, June 28, 2019.
- Box v Planned Parenthood of Indiana and Kentucky, Inc. 587 US 18 483 (2019).
- Box v Planned Parenthood of Indiana and Kentucky, Inc., at 2.
- Box v Planned Parenthood of Indiana and Kentucky, Inc., Justice Thomas concurring.
- June Medical Services, LLC, et al. v Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals. 586 US 18A774 (2019).
- Box v Planned Parenthood of Indiana and Kentucky, Inc. Docket 18-1019.
- Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals v Planned Parenthood of Gulf Coast, Inc., et al. 586 US 17 1492 (2018).
- June Medical Services L.L.C., et al., Petitioners, v Rebekah Gee, Secretary, Louisiana Department of Health and Hospitals. No. 18-1323. Brief of Amici Curiae American College of Obstetricians and Gynecologists, American Academy of Family Physicians, American Academy of Pediatrics, American College of Nurse-Midwives, American College of Osteopathic Obstetricians and Gynecologists, American College of Physicians, American Society for Reproductive Medicine, National Association of Nurse Practitioners in Women's Health, North American Society for Pediatric and Adolescent Gynecology, and Society For Maternal-Fetal Medicine, Amicus Curiae in Support of Petitioners. May 2019.
- Planned Parenthood of Kansas & Eastern Oklahoma, et al., Petitioners, v Larry Jegley, et al., Respondents. No. 17-935. Brief Amici Curiae of American College of Obstetricians and Gynecologists and American Public Health Association as Amici Curiae in Support of Petitioners. February 1, 2018.
- Box v Planned Parenthood of Indiana & Kentucky. No. 18-1019. Brief Amici Curiae of American Association of Pro-Life Obstetricians & Gynecologists, American College of Pediatricians, Care Net, Christian Medical Association, Heartbeat International, Inc., and National Institute Of Family & Life Advocates in Support of Petitioners. March 6, 2019.
- Steven T. Marshall, et al., Petitioners, v West Alabama Women's Center, et al., Respondents. No. 18-837. Brief of Amici Curiae American Association of Pro-Life Obstetricians & Gynecologists and American College of Pediatricians, in Support of Petitioners. January 18, 2019.
- Azar, Secretary of Health and Human Services v Allina Health Services, et al. 17 1484 (2018).
- Alex M. Azar, II, Secretary of Health and Human Services, Petitioner, v Allina Health Services, et al., Respondents. Brief of the American Hospital Association, Federation of American Hospitals, and Association of American Medical Colleges as Amici Curiae in Support of Respondents. December 2018.
- Alex M. Azar, II, Secretary of Health and Human Services, Petitioner, v Allina Health Services, et al., Respondents. Brief of Amici Curiae American Medical Association and Medical Society of the District of Columbia Amici Curiae in Support of Respondents. December 2018.
- 42 U. S. C. §1395hh. https://uscode.house.gov/view.xhtml?req=(title:42%20section:1395hh%20edition:prelim). Accessed October 22, 2019.
- The False Claims Act: a primer. Washington DC: US Department of Justice. www.justice.gov/sites/default/files/civil/legacy/2011/04/22/C-FRAUDS_FCA_Primer.pdf. Accessed October 18, 2019.
- Universal Health Services, Inc., v United States and Commonwealth of Massachusetts ex rel. Julio Escobar and Carmen Correa. Brief of the American Hospital Association, Federation of American Hospitals, and Association of American Medical Colleges Amici Curiae in Support of Petitioner. No. 15-7. January 2016.
- Intermountain Health Care, Inc., et al., Petitioners, v United States ex rel. Gerald Polukoff, et al., Respondents. No. 18-911. Brief of the American Hospital Association and Federation of American Hospitals as Amici Curiae in Support of Petitioners. February 13, 2019.
- Cochise Consultancy, Inc., et al., v United States ex rel. Hunt. 18 315 (2018).
- 34 U.S.C. §20901 et seq. [Chapter 209--Child Protection and Safety.] https://uscode.house.gov/view.xhtml?path=/prelim@title34/subtitle2/chapter209&edition=prelim. Accessed October 17, 2019.
- Gundy v United States. 17 6086 (2018).
- Henry Schein, Inc., et al., v Archer & White Sales, Inc. 17 1272 (2018).
- Lamps Plus, Inc., et al., v Varela. 17 988 (2018).
- Merck Sharp & Dohme Corp. v Albrecht et al. 17 290 (2018).
- Merck Sharp & Dohme Corp. v Albrecht et al. 17 290 (2018) at 13-14.
- Wyeth v Levine, 555 US 555, 571 (2009).
- Russell Bucklew, Petitioner, v Anne L. Precythe, Director, Missouri Department of Corrections, et al., Respondents. 17 8151 (2018).
- Russell Bucklew, Petitioner, v Anne L. Precythe, Director, Missouri Department of Corrections, et al., Respondents. 17 8151 (2018). American Medical Association, Amicus Curiae Brief, in Support of Neither Party. July 23, 2018.
- Final stat pack for October term 2018. SCOTUSblog.com. June 28, 2019. https://www.scotusblog.com/wp-content/uploads/2019/07/StatPack_OT18-7_8_19.pdf. Accessed October 17, 2019.
- Barnes R. They're not 'wonder twins': Gorsuch, Kavanaugh shift the Supreme Court, but their differences are striking. Washington Post, June 28, 2019.
Stay Informed About Informed Consent
On May 24, 2011, a 53-year-old woman presented to a Wisconsin hospital emergency department (ED) with complaints of severe abdominal pain, a rapid heartbeat, and a fever of 101.3°F. During her 9-hour visit, she was treated by a PA and his supervising physician. She was seen by the physician for a total of 6 minutes; the rest of her care was provided by the PA. The patient was discharged around midnight with instructions to contact her gynecologist in the morning for management of uterine fibroids. At the time of discharge, her temperature was 102.9°F.
The following day, May 25, the patient collapsed in her home and was transported to another hospital. She was treated for septic shock from a group A streptococcus infection. Although the infection was halted, the patient sustained ischemic damage to her extremities and a month later required amputation of her 4 limbs.The plaintiff claimed that the supervising physician was negligent in failing to diagnose the strep A infection, which, left undetected, led to septic shock. She also alleged that the PA should have recognized the potential for her condition’s severity to quickly escalate. She maintained that the supervising physician should have been more involved in her case because of its complexity.
Plaintiff’s counsel also argued that the PA should have provided “alternative medical diagnoses,” which would have prompted consideration of other treatment options. The plaintiff contended that under Wisconsin’s informed consent law, both the PA and the physician failed to disclose enough information about her condition and failed to inform her of any choices for treatment.
The defense argued that the plaintiff received proper treatment based on the information available to the providers at the time.
VERDICT
The jury found for the plaintiff and apportioned 65% liability to the physician and 35% liability to the PA. A total of $25,342,096 was awarded to the plaintiff.
COMMENTARY
This is a huge verdict. Cases involving group A strep or necrotizing fasciitis frequently give rise to large medical malpractice verdicts, because everything about them is difficult to defend: Although there is typically trivial to no trauma involved, the wounds from these infections provide explicit images of damage, intraoperatively and postoperatively. Vasopressors required for hemodynamic support or sepsis itself frequently result in limb ischemia, gangrene, and amputation. In this case, the plaintiff, as a quadruple amputee, was a sympathetic and impressive courtroom presence—the personal toll was evident to anyone in the room.
Two providers—a PA and a physician—saw the patient. We are told only that she complained of severe abdominal pain, rapid heartbeat, and fever, which increased at some point during her ED stay. We aren’t given specifics on the rest of the patient’s vital signs or examination details. However, we can infer that the exam and lab findings were not impressive, because they weren’t mentioned in the case report. But as a result of the failure to catch the group A strep infection, the plaintiff suffered what one judge hearing the case described as a harrowing and unimaginable ordeal: the life-changing amputation of 4 limbs.1 While the jury did not find the PA or physician negligent, they still found the clinicians liable and awarded a staggering verdict.
Continue to: How could this happen?
How could this happen? The answer is the theory of recovery: The jury found that the physician and the PA failed to provide the patient with informed consent in the form of “alternative medical diagnoses.”2 The plaintiff’s attorney argued that the patient was never told a life-threatening bacterial infection was one possible diagnosis and claimed that if she had known, the patient would have pursued other treatment.
As in many malpractice cases, the plaintiff alleged failure to diagnose and failure to provide informed consent. Depending on state law, there are 3 standards for informed consent: subjective patient, reasonable patient, and reasonable physician.3 About half of the states have a physician-focused standard, while the other half have a patient-focused standard.3
Under the subjective patient standard, we would ask, “What would this patient need to know and understand to make an informed decision?”4 The subjective standard requires the clinician to essentially “get in the head” of a specific patient to determine what he or she would want to know when making a medical decision. This standard is problematic because it requires the clinician to have an intimate familiarity with the patient’s belief system and medical decision-making process—a daunting requirement for many clinicians, particularly in the absence of a longstanding clinician-patient relationship, as is the case in most emergency settings. Thankfully, the subjective patient standard is not followed by most states that have a patient-focused standard.
Under the objective reasonable patient standard, we would ask “What would the average patient need to know to be an informed participant in the decision?”4 One could argue that this standard more adequately allows the patient to be an active participant in shared decision-making. However, the drawback is that what is “reasonable” often falls on a spectrum, which would require the clinician to gauge the volume and type of information a patient cohort would want to have when making a medical decision. Under this standard, the plaintiff must prove that the clinician omitted information that a reasonable patient would want to know. Therefore, these standards are more friendly to the plaintiff, whereas the reasonable physician standard is more defendant friendly.
To meet the standard of care under a reasonable physician standard, information must be provided to the patient that a “reasonably prudent practitioner in the same field of practice or specialty” would provide to a patient.5 For a plaintiff to successfully sue under this standard, the plaintiff’s expert must testify that a reasonably prudent physician would have disclosed the omitted information.6 The reasonable physician standard is obviously better for malpractice defendants.
Continue to: While reasonable clinicians...
While reasonable clinicians can disagree (as can reasonable patients), clinicians are more likely to be closer in opinion. Clinicians are a smaller group whose opinions are underpinned by similar education, training, and experience. By contrast, among the general population, beliefs held by one hypothetical “reasonable person” are much less settled, and in some cases, wildly divergent from another’s. For example, vaccine skepticism would probably be considered unreasonable in the majority of jury pools but absolutely reasonable in some. The large size of the general population, coupled with opinions untethered to any definable discipline, make the reasonable patient standard hard to predict.
Additionally, the reasonable physician standard forces the plaintiff to prove his or her case by producing an expert witness (clinician) to specifically testify that the standard of care required the defendant clinician to disclose certain specific information, and that disclosure was lacking. That is an important requirement. Under patient-focused standards, the plaintiff doesn’t need a medical expert on this point and can simply argue to the jury that a reasonable patient would require an exhaustive discussion of each possibility in the differential diagnosis. Therefore, I would argue that the reasonable physician standard is more predictable and workable and should be followed.
At the time of this case, Wisconsin’s informed consent law was based on the reasonable patient standard. As a result of this case, Wisconsin lawmakers changed the law to a “reasonable physician standard,” which states “any physician who treats a patient shall inform the patient about the availability of reasonable alternate medical modes of treatment and about the benefits and risks of these treatments.”7 However, the law stipulates that this duty to inform does not require disclosure of (among others):
- Detailed technical information that in all probability a patient would not understand
- Risks apparent or known to the patient
- Extremely remote possibilities that might falsely or detrimentally alarm the patient
- Information about alternate medical modes of treatment for any condition the physician has not included in his or her diagnosis at the time the physician informs the patient.7
Finally, this case involved an extremely high verdict of more than $25 million. It may surprise you to learn that many states have caps for medical malpractice awards for noneconomic damages, such as pain and suffering. If you’re having a holiday dinner with friends or family members who are plaintiff’s attorneys and you’re itching for a good argument, skip current politics and go all-in: How about liability caps, Uncle Jim? Get ready for a lively debate.
Of the $25 million verdict, $16.5 million was awarded for pain and suffering—the jury was obviously shocked by the extent of the life-changing nature of the plaintiff’s injuries. At the time of this case, Wisconsin had a cap of $750,000 for noneconomic damages.8 However, plaintiffs may challenge state constitutionality of these caps when they feel they have the right case, which the plaintiff and her attorney felt they did. Two lower courts found the state cap unconstitutional and gave the plaintiff the full award. But the state Supreme Court later reversed that decision, upholding the cap.1 The court decided that the legislature had a rational basis for making the law and changes to it should occur through the legislature, not the courts. The dissenting justices argued that there was no rational basis for the $750,000 cap, because there was no evidence that clinicians would flee the state fearing malpractice liability, or practice more defensive medicine, or suffer runaway malpractice insurance premiums without the cap. As a result of this case, the cap was upheld, and there was a “lively debate” on this issue at the highest levels of government.
Continue to: IN SUM
IN SUM
Become familiar with your state’s informed consent laws. Involve patients in decision-making, and convey information related to reasonable treatment options and risks. Document all of these discussions. Lastly, state-level political discussions on issues of tort reform, caps, and malpractice matters are ongoing—so take n
1. Mayo v Wisconsin Injured Patients & Families Compensation Fund. WI 78 (2018).
2. Spivak C. Jury awards Milwaukee woman $25.3 million in medical malpractice case. Milwaukee Journal Sentinel. July 7, 2014.
3. Moore GP, Matlock AG, Kiley JL, et al. Emergency physicians: beware of the consent standard of care. Clin Pract Cases Emerg Med. 2018; 2(2):109-111.
4. Gossman W, Thornton I, Hipskind JE. Informed Consent. StatPearls. www.ncbi.nlm.nih.gov/books/NBK430827/. Updated July 10, 2019. Accessed October 25, 2019.
5. King JS, Moulton BW. Rethinking informed consent: the case for shared medical decision-making. Am J Law Med. 2006;32:429-501.
6. Tashman v Gibbs, 556 SE 2d 772 (263 Va 2002).
7. Wis Stat subchapter 2, §448.30.
8. Wis Stat §893.55.
On May 24, 2011, a 53-year-old woman presented to a Wisconsin hospital emergency department (ED) with complaints of severe abdominal pain, a rapid heartbeat, and a fever of 101.3°F. During her 9-hour visit, she was treated by a PA and his supervising physician. She was seen by the physician for a total of 6 minutes; the rest of her care was provided by the PA. The patient was discharged around midnight with instructions to contact her gynecologist in the morning for management of uterine fibroids. At the time of discharge, her temperature was 102.9°F.
The following day, May 25, the patient collapsed in her home and was transported to another hospital. She was treated for septic shock from a group A streptococcus infection. Although the infection was halted, the patient sustained ischemic damage to her extremities and a month later required amputation of her 4 limbs.The plaintiff claimed that the supervising physician was negligent in failing to diagnose the strep A infection, which, left undetected, led to septic shock. She also alleged that the PA should have recognized the potential for her condition’s severity to quickly escalate. She maintained that the supervising physician should have been more involved in her case because of its complexity.
Plaintiff’s counsel also argued that the PA should have provided “alternative medical diagnoses,” which would have prompted consideration of other treatment options. The plaintiff contended that under Wisconsin’s informed consent law, both the PA and the physician failed to disclose enough information about her condition and failed to inform her of any choices for treatment.
The defense argued that the plaintiff received proper treatment based on the information available to the providers at the time.
VERDICT
The jury found for the plaintiff and apportioned 65% liability to the physician and 35% liability to the PA. A total of $25,342,096 was awarded to the plaintiff.
COMMENTARY
This is a huge verdict. Cases involving group A strep or necrotizing fasciitis frequently give rise to large medical malpractice verdicts, because everything about them is difficult to defend: Although there is typically trivial to no trauma involved, the wounds from these infections provide explicit images of damage, intraoperatively and postoperatively. Vasopressors required for hemodynamic support or sepsis itself frequently result in limb ischemia, gangrene, and amputation. In this case, the plaintiff, as a quadruple amputee, was a sympathetic and impressive courtroom presence—the personal toll was evident to anyone in the room.
Two providers—a PA and a physician—saw the patient. We are told only that she complained of severe abdominal pain, rapid heartbeat, and fever, which increased at some point during her ED stay. We aren’t given specifics on the rest of the patient’s vital signs or examination details. However, we can infer that the exam and lab findings were not impressive, because they weren’t mentioned in the case report. But as a result of the failure to catch the group A strep infection, the plaintiff suffered what one judge hearing the case described as a harrowing and unimaginable ordeal: the life-changing amputation of 4 limbs.1 While the jury did not find the PA or physician negligent, they still found the clinicians liable and awarded a staggering verdict.
Continue to: How could this happen?
How could this happen? The answer is the theory of recovery: The jury found that the physician and the PA failed to provide the patient with informed consent in the form of “alternative medical diagnoses.”2 The plaintiff’s attorney argued that the patient was never told a life-threatening bacterial infection was one possible diagnosis and claimed that if she had known, the patient would have pursued other treatment.
As in many malpractice cases, the plaintiff alleged failure to diagnose and failure to provide informed consent. Depending on state law, there are 3 standards for informed consent: subjective patient, reasonable patient, and reasonable physician.3 About half of the states have a physician-focused standard, while the other half have a patient-focused standard.3
Under the subjective patient standard, we would ask, “What would this patient need to know and understand to make an informed decision?”4 The subjective standard requires the clinician to essentially “get in the head” of a specific patient to determine what he or she would want to know when making a medical decision. This standard is problematic because it requires the clinician to have an intimate familiarity with the patient’s belief system and medical decision-making process—a daunting requirement for many clinicians, particularly in the absence of a longstanding clinician-patient relationship, as is the case in most emergency settings. Thankfully, the subjective patient standard is not followed by most states that have a patient-focused standard.
Under the objective reasonable patient standard, we would ask “What would the average patient need to know to be an informed participant in the decision?”4 One could argue that this standard more adequately allows the patient to be an active participant in shared decision-making. However, the drawback is that what is “reasonable” often falls on a spectrum, which would require the clinician to gauge the volume and type of information a patient cohort would want to have when making a medical decision. Under this standard, the plaintiff must prove that the clinician omitted information that a reasonable patient would want to know. Therefore, these standards are more friendly to the plaintiff, whereas the reasonable physician standard is more defendant friendly.
To meet the standard of care under a reasonable physician standard, information must be provided to the patient that a “reasonably prudent practitioner in the same field of practice or specialty” would provide to a patient.5 For a plaintiff to successfully sue under this standard, the plaintiff’s expert must testify that a reasonably prudent physician would have disclosed the omitted information.6 The reasonable physician standard is obviously better for malpractice defendants.
Continue to: While reasonable clinicians...
While reasonable clinicians can disagree (as can reasonable patients), clinicians are more likely to be closer in opinion. Clinicians are a smaller group whose opinions are underpinned by similar education, training, and experience. By contrast, among the general population, beliefs held by one hypothetical “reasonable person” are much less settled, and in some cases, wildly divergent from another’s. For example, vaccine skepticism would probably be considered unreasonable in the majority of jury pools but absolutely reasonable in some. The large size of the general population, coupled with opinions untethered to any definable discipline, make the reasonable patient standard hard to predict.
Additionally, the reasonable physician standard forces the plaintiff to prove his or her case by producing an expert witness (clinician) to specifically testify that the standard of care required the defendant clinician to disclose certain specific information, and that disclosure was lacking. That is an important requirement. Under patient-focused standards, the plaintiff doesn’t need a medical expert on this point and can simply argue to the jury that a reasonable patient would require an exhaustive discussion of each possibility in the differential diagnosis. Therefore, I would argue that the reasonable physician standard is more predictable and workable and should be followed.
At the time of this case, Wisconsin’s informed consent law was based on the reasonable patient standard. As a result of this case, Wisconsin lawmakers changed the law to a “reasonable physician standard,” which states “any physician who treats a patient shall inform the patient about the availability of reasonable alternate medical modes of treatment and about the benefits and risks of these treatments.”7 However, the law stipulates that this duty to inform does not require disclosure of (among others):
- Detailed technical information that in all probability a patient would not understand
- Risks apparent or known to the patient
- Extremely remote possibilities that might falsely or detrimentally alarm the patient
- Information about alternate medical modes of treatment for any condition the physician has not included in his or her diagnosis at the time the physician informs the patient.7
Finally, this case involved an extremely high verdict of more than $25 million. It may surprise you to learn that many states have caps for medical malpractice awards for noneconomic damages, such as pain and suffering. If you’re having a holiday dinner with friends or family members who are plaintiff’s attorneys and you’re itching for a good argument, skip current politics and go all-in: How about liability caps, Uncle Jim? Get ready for a lively debate.
Of the $25 million verdict, $16.5 million was awarded for pain and suffering—the jury was obviously shocked by the extent of the life-changing nature of the plaintiff’s injuries. At the time of this case, Wisconsin had a cap of $750,000 for noneconomic damages.8 However, plaintiffs may challenge state constitutionality of these caps when they feel they have the right case, which the plaintiff and her attorney felt they did. Two lower courts found the state cap unconstitutional and gave the plaintiff the full award. But the state Supreme Court later reversed that decision, upholding the cap.1 The court decided that the legislature had a rational basis for making the law and changes to it should occur through the legislature, not the courts. The dissenting justices argued that there was no rational basis for the $750,000 cap, because there was no evidence that clinicians would flee the state fearing malpractice liability, or practice more defensive medicine, or suffer runaway malpractice insurance premiums without the cap. As a result of this case, the cap was upheld, and there was a “lively debate” on this issue at the highest levels of government.
Continue to: IN SUM
IN SUM
Become familiar with your state’s informed consent laws. Involve patients in decision-making, and convey information related to reasonable treatment options and risks. Document all of these discussions. Lastly, state-level political discussions on issues of tort reform, caps, and malpractice matters are ongoing—so take n
On May 24, 2011, a 53-year-old woman presented to a Wisconsin hospital emergency department (ED) with complaints of severe abdominal pain, a rapid heartbeat, and a fever of 101.3°F. During her 9-hour visit, she was treated by a PA and his supervising physician. She was seen by the physician for a total of 6 minutes; the rest of her care was provided by the PA. The patient was discharged around midnight with instructions to contact her gynecologist in the morning for management of uterine fibroids. At the time of discharge, her temperature was 102.9°F.
The following day, May 25, the patient collapsed in her home and was transported to another hospital. She was treated for septic shock from a group A streptococcus infection. Although the infection was halted, the patient sustained ischemic damage to her extremities and a month later required amputation of her 4 limbs.The plaintiff claimed that the supervising physician was negligent in failing to diagnose the strep A infection, which, left undetected, led to septic shock. She also alleged that the PA should have recognized the potential for her condition’s severity to quickly escalate. She maintained that the supervising physician should have been more involved in her case because of its complexity.
Plaintiff’s counsel also argued that the PA should have provided “alternative medical diagnoses,” which would have prompted consideration of other treatment options. The plaintiff contended that under Wisconsin’s informed consent law, both the PA and the physician failed to disclose enough information about her condition and failed to inform her of any choices for treatment.
The defense argued that the plaintiff received proper treatment based on the information available to the providers at the time.
VERDICT
The jury found for the plaintiff and apportioned 65% liability to the physician and 35% liability to the PA. A total of $25,342,096 was awarded to the plaintiff.
COMMENTARY
This is a huge verdict. Cases involving group A strep or necrotizing fasciitis frequently give rise to large medical malpractice verdicts, because everything about them is difficult to defend: Although there is typically trivial to no trauma involved, the wounds from these infections provide explicit images of damage, intraoperatively and postoperatively. Vasopressors required for hemodynamic support or sepsis itself frequently result in limb ischemia, gangrene, and amputation. In this case, the plaintiff, as a quadruple amputee, was a sympathetic and impressive courtroom presence—the personal toll was evident to anyone in the room.
Two providers—a PA and a physician—saw the patient. We are told only that she complained of severe abdominal pain, rapid heartbeat, and fever, which increased at some point during her ED stay. We aren’t given specifics on the rest of the patient’s vital signs or examination details. However, we can infer that the exam and lab findings were not impressive, because they weren’t mentioned in the case report. But as a result of the failure to catch the group A strep infection, the plaintiff suffered what one judge hearing the case described as a harrowing and unimaginable ordeal: the life-changing amputation of 4 limbs.1 While the jury did not find the PA or physician negligent, they still found the clinicians liable and awarded a staggering verdict.
Continue to: How could this happen?
How could this happen? The answer is the theory of recovery: The jury found that the physician and the PA failed to provide the patient with informed consent in the form of “alternative medical diagnoses.”2 The plaintiff’s attorney argued that the patient was never told a life-threatening bacterial infection was one possible diagnosis and claimed that if she had known, the patient would have pursued other treatment.
As in many malpractice cases, the plaintiff alleged failure to diagnose and failure to provide informed consent. Depending on state law, there are 3 standards for informed consent: subjective patient, reasonable patient, and reasonable physician.3 About half of the states have a physician-focused standard, while the other half have a patient-focused standard.3
Under the subjective patient standard, we would ask, “What would this patient need to know and understand to make an informed decision?”4 The subjective standard requires the clinician to essentially “get in the head” of a specific patient to determine what he or she would want to know when making a medical decision. This standard is problematic because it requires the clinician to have an intimate familiarity with the patient’s belief system and medical decision-making process—a daunting requirement for many clinicians, particularly in the absence of a longstanding clinician-patient relationship, as is the case in most emergency settings. Thankfully, the subjective patient standard is not followed by most states that have a patient-focused standard.
Under the objective reasonable patient standard, we would ask “What would the average patient need to know to be an informed participant in the decision?”4 One could argue that this standard more adequately allows the patient to be an active participant in shared decision-making. However, the drawback is that what is “reasonable” often falls on a spectrum, which would require the clinician to gauge the volume and type of information a patient cohort would want to have when making a medical decision. Under this standard, the plaintiff must prove that the clinician omitted information that a reasonable patient would want to know. Therefore, these standards are more friendly to the plaintiff, whereas the reasonable physician standard is more defendant friendly.
To meet the standard of care under a reasonable physician standard, information must be provided to the patient that a “reasonably prudent practitioner in the same field of practice or specialty” would provide to a patient.5 For a plaintiff to successfully sue under this standard, the plaintiff’s expert must testify that a reasonably prudent physician would have disclosed the omitted information.6 The reasonable physician standard is obviously better for malpractice defendants.
Continue to: While reasonable clinicians...
While reasonable clinicians can disagree (as can reasonable patients), clinicians are more likely to be closer in opinion. Clinicians are a smaller group whose opinions are underpinned by similar education, training, and experience. By contrast, among the general population, beliefs held by one hypothetical “reasonable person” are much less settled, and in some cases, wildly divergent from another’s. For example, vaccine skepticism would probably be considered unreasonable in the majority of jury pools but absolutely reasonable in some. The large size of the general population, coupled with opinions untethered to any definable discipline, make the reasonable patient standard hard to predict.
Additionally, the reasonable physician standard forces the plaintiff to prove his or her case by producing an expert witness (clinician) to specifically testify that the standard of care required the defendant clinician to disclose certain specific information, and that disclosure was lacking. That is an important requirement. Under patient-focused standards, the plaintiff doesn’t need a medical expert on this point and can simply argue to the jury that a reasonable patient would require an exhaustive discussion of each possibility in the differential diagnosis. Therefore, I would argue that the reasonable physician standard is more predictable and workable and should be followed.
At the time of this case, Wisconsin’s informed consent law was based on the reasonable patient standard. As a result of this case, Wisconsin lawmakers changed the law to a “reasonable physician standard,” which states “any physician who treats a patient shall inform the patient about the availability of reasonable alternate medical modes of treatment and about the benefits and risks of these treatments.”7 However, the law stipulates that this duty to inform does not require disclosure of (among others):
- Detailed technical information that in all probability a patient would not understand
- Risks apparent or known to the patient
- Extremely remote possibilities that might falsely or detrimentally alarm the patient
- Information about alternate medical modes of treatment for any condition the physician has not included in his or her diagnosis at the time the physician informs the patient.7
Finally, this case involved an extremely high verdict of more than $25 million. It may surprise you to learn that many states have caps for medical malpractice awards for noneconomic damages, such as pain and suffering. If you’re having a holiday dinner with friends or family members who are plaintiff’s attorneys and you’re itching for a good argument, skip current politics and go all-in: How about liability caps, Uncle Jim? Get ready for a lively debate.
Of the $25 million verdict, $16.5 million was awarded for pain and suffering—the jury was obviously shocked by the extent of the life-changing nature of the plaintiff’s injuries. At the time of this case, Wisconsin had a cap of $750,000 for noneconomic damages.8 However, plaintiffs may challenge state constitutionality of these caps when they feel they have the right case, which the plaintiff and her attorney felt they did. Two lower courts found the state cap unconstitutional and gave the plaintiff the full award. But the state Supreme Court later reversed that decision, upholding the cap.1 The court decided that the legislature had a rational basis for making the law and changes to it should occur through the legislature, not the courts. The dissenting justices argued that there was no rational basis for the $750,000 cap, because there was no evidence that clinicians would flee the state fearing malpractice liability, or practice more defensive medicine, or suffer runaway malpractice insurance premiums without the cap. As a result of this case, the cap was upheld, and there was a “lively debate” on this issue at the highest levels of government.
Continue to: IN SUM
IN SUM
Become familiar with your state’s informed consent laws. Involve patients in decision-making, and convey information related to reasonable treatment options and risks. Document all of these discussions. Lastly, state-level political discussions on issues of tort reform, caps, and malpractice matters are ongoing—so take n
1. Mayo v Wisconsin Injured Patients & Families Compensation Fund. WI 78 (2018).
2. Spivak C. Jury awards Milwaukee woman $25.3 million in medical malpractice case. Milwaukee Journal Sentinel. July 7, 2014.
3. Moore GP, Matlock AG, Kiley JL, et al. Emergency physicians: beware of the consent standard of care. Clin Pract Cases Emerg Med. 2018; 2(2):109-111.
4. Gossman W, Thornton I, Hipskind JE. Informed Consent. StatPearls. www.ncbi.nlm.nih.gov/books/NBK430827/. Updated July 10, 2019. Accessed October 25, 2019.
5. King JS, Moulton BW. Rethinking informed consent: the case for shared medical decision-making. Am J Law Med. 2006;32:429-501.
6. Tashman v Gibbs, 556 SE 2d 772 (263 Va 2002).
7. Wis Stat subchapter 2, §448.30.
8. Wis Stat §893.55.
1. Mayo v Wisconsin Injured Patients & Families Compensation Fund. WI 78 (2018).
2. Spivak C. Jury awards Milwaukee woman $25.3 million in medical malpractice case. Milwaukee Journal Sentinel. July 7, 2014.
3. Moore GP, Matlock AG, Kiley JL, et al. Emergency physicians: beware of the consent standard of care. Clin Pract Cases Emerg Med. 2018; 2(2):109-111.
4. Gossman W, Thornton I, Hipskind JE. Informed Consent. StatPearls. www.ncbi.nlm.nih.gov/books/NBK430827/. Updated July 10, 2019. Accessed October 25, 2019.
5. King JS, Moulton BW. Rethinking informed consent: the case for shared medical decision-making. Am J Law Med. 2006;32:429-501.
6. Tashman v Gibbs, 556 SE 2d 772 (263 Va 2002).
7. Wis Stat subchapter 2, §448.30.
8. Wis Stat §893.55.
Don’t Take the Fall With Head Injuries
In the early morning hours of June 10, 2009, a 77-year-old man who had been undergoing chemotherapy for multiple myeloma took sleep medication. He then fell down a flight of stairs in his split-level home.
The patient sustained a laceration to his scalp but returned to bed and waited until later that morning to call his internist for an appointment. Later that day, the physician placed 11 sutures for the scalp laceration and performed a neurologic examination; he did not note any abnormalities. The patient complained of back pain, so the physician ordered a back x-ray, which revealed a TI2 fracture that had occurred from the fall. No further treatment was provided for the scalp injury, except removal of the stitches about a week later.
Six days after the fall and doctor visit, the patient’s condition began to deteriorate rapidly, with noted slurred speech and loss of consciousness. He was transported to an emergency department, where CT revealed a massive subdural hematoma. An immediate craniotomy was performed. However, on June 27, 2009, the patient died as a result of the brain bleed.
His estate filed suit against the physician and his practice, alleging medical malpractice and violations in the standard of care. The estate alleged that the standard of care required the physician to obtain a CT scan and that, had one been performed, it would have revealed a small subdural hematoma in time for it to have been successfully treated (ie, before the massive second related bleed). The estate’s theory of the case did not rest on the presentation of clinical symptoms. A medical expert who testified for the estate stated that the subdural hematoma began at the time of the fall.
The defense denied any violations in the standard of care. The physician contended that the patient had presented with no symptoms other than a head laceration, and there were no criteria for ordering CT. Further, the defense asserted that the patient was symptom free for 6 days post-fall. According to the defense, the patient experienced a sudden arterial bleed that was not caused by the fall and would not have been revealed on CT ordered at the time of initial presentation, because it did not occur until 6 days later.
VERDICT
After a 10-day trial and 25 minutes’ deliberation, the jury returned a defense verdict.
COMMENTARY
The 25-minute deliberation suggests that terms such as “bridging veins” and “shearing injury” were unlikely bandied about in the jury room. The jury was likely dismissive of the plaintiff’s claim owing to his cancer diagnosis, and perhaps rightly so. But if we eliminate the multiple myeloma diagnosis, the jury might have decided differently.
Continue to: The defendant physician...
The defendant physician did a good job of documenting a negative neurologic exam, which helped him convince the jury that the patient did not have any signs or symptoms when first evaluated. But in this patient, was imaging to rule out intracranial bleeding indicated?
As an oversimplification, we tend to think of intracranial hemorrhage in 2 varieties: the insidious and the bold. Subdural hematomas are stealthy, they are sneaky, and they prey on the old. They step out of the shadows to cause symptoms. They are the ninjas of intracranial hemorrhage. Beware.
Epidural hematomas and subarachnoid hemorrhage (SAH) are the opposite. They classically present with a sudden and severe symptom complex: with epidural hematoma, the loss of consciousness, lucid interval, and final loss of consciousness; with SAH, the “worst in your life” thunder-clap headache, which may be heralded by a sentinel headache.1 When manifesting this way, they are brash, direct, and unsubtle to the point of being obnoxious—the Steven Stifler of intracranial bleeding.
This generalization is made to highlight the potentially sneaky nature of subdural hemorrhage. There are circumstances in which the clinical presentation of epidural hematoma and SAH will be more challenging. The question here is whether a negative initial neurologic exam can adequately screen for a potentially stealthy subdural hematoma.
Subdural hemorrhage is caused by rapidly changing velocity that may stretch and tear small bridging veins.2,3 Subdural hematoma is more common in the elderly, those who abuse alcohol, and those with a prior history of head trauma.4 As the brain shrinks with age or atrophy, the subdural space enlarges and traversing veins are stretched to cover a wider distance—rendering them vulnerable to rupture.5 These structures may also weaken as a result of low cerebrospinal fluid (intracranial hypotension); as pressure decreases (eg, from a leak), the brain’s buoyancy is reduced, causing traction on anchoring and supporting structures (eg, bridging veins).5 Injury to bridging veins can even occur as a result of a coup-contrecoup mechanism in the absence of direct physical impact.6,7 Bottom line: the injury itself may be subtle, requiring an index of suspicion to make the diagnosis.
Continue to: The case patient was...
The case patient was elderly. He had a chronic malignancy and sustained a fall down the stairs. He was taking sleeping pills, which may have slowed reflexive protective mechanisms after he started to fall (resulting in greater force imparted to his head). Multiple myeloma can predispose a patient to coagulopathy, and we don’t know in this case if this patient’s multiple myeloma made him more susceptible to bleeding—but it certainly didn’t help.8 The patient’s age, the mechanism of injury, and the history of malignancy made this a setup for hemorrhage.
Interestingly, we are not given details about how the patient looked during his suture removal. We are told the time between the initial fall and deterioration was 6 days. Scalp sutures were removed “about a week later,” which was after the deterioration—so this can’t be correct. Removing scalp sutures after 5 days seems premature, but that is the only possibility if 6 days elapsed between the fall and the deterioration.
In short, these are difficult cases. If intracranial bleeding can be subtle and delayed, how can we be sure a patient is not experiencing a bleed? We can only apply the relevant standard of care using all the clinical information we have. The Canadian CT Head Rule and New Orleans Criteria are clinical tools designed to help providers determine when to image (see Table for details).9
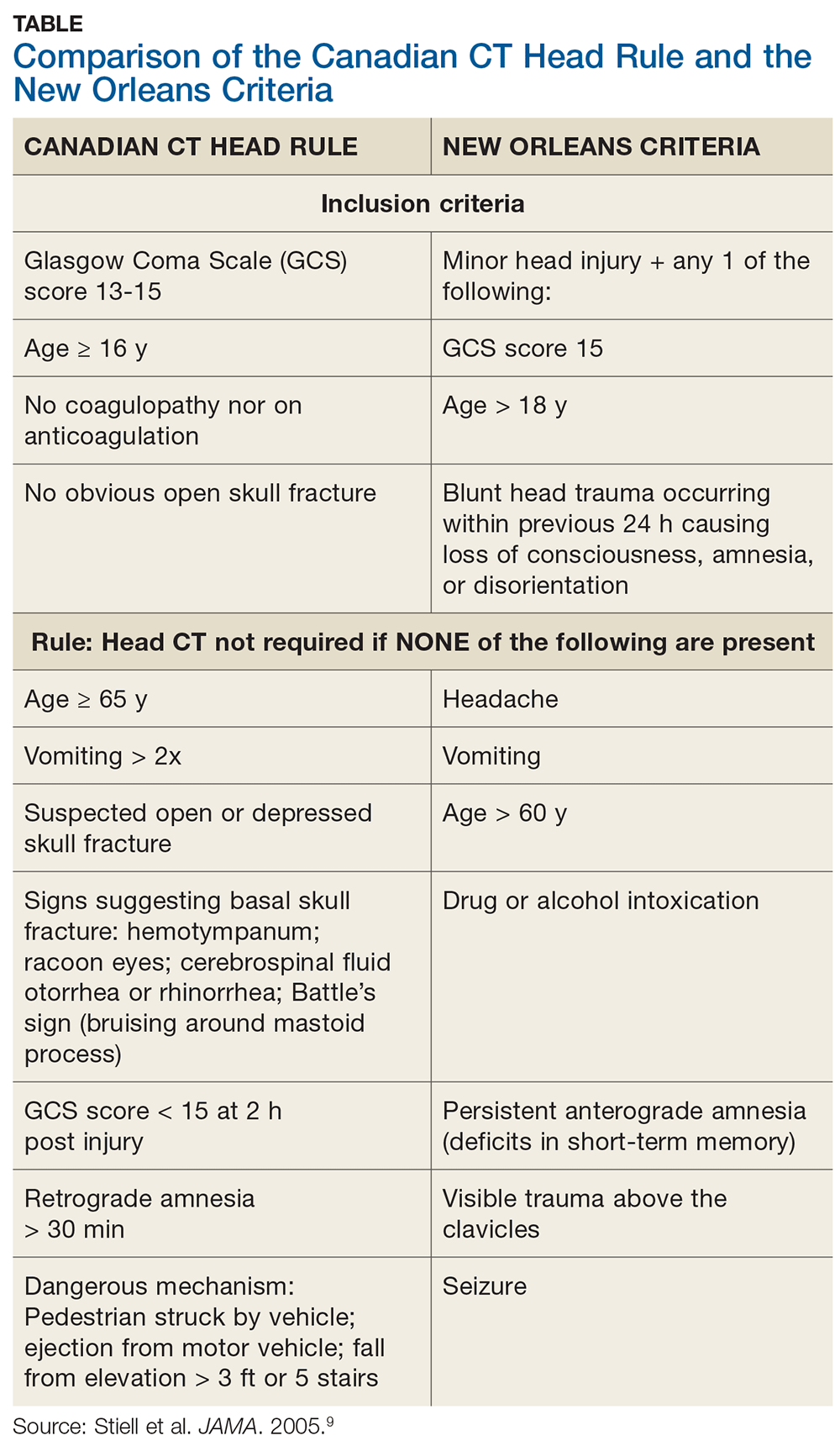
Applying the Canadian CT Head Rule to the facts of this case, we would image the patient because he fell down a “flight” of stairs (which is > 5 stairs) and he is 77 years old (older than 65). The New Orleans Criteria require head CT for minor injury with any positive findings.9 Because the patient is older than 60, he would be scanned according this rule.
In this case, the tools indicate scanning would have been appropriate. The patient’s multiple myeloma might have further impelled a decision to image. However, the jury was persuaded that the defendant’s negative neurologic exam was reasonable under the circumstances. This was likely made possible by the physician’s good recordkeeping and demonstrated genuine concern for the patient’s well-being—as well as a differing viewpoint of the patient’s age and health status.
Continue to: Finally, a word about...
Finally, a word about falls and the elderly: We’ve all heard the 80s advertising catchphrase (which lives on as a present-day meme) “I’ve fallen, and I can’t get up!” The problem is, many don’t. It would be more clinically accurate to say, “I’ve fallen, and I’ll be hospitalized for an extended period of time, then transferred to a skilled nursing facility, but I won’t survive to discharge.” The reality is that falls kill, and the severity is underestimated.10 If it were a “brain-eating amoeba,” the media would be all over it. With falls, not so much. We tend to pay less attention.
Risk factors for a fall include postural hypotension; use of benzodiazepines or other sedative-hypnotic drugs; use of ≥ 4 medications; environmental hazards for tripping; impairment in balance and transfer skills; and gait impairment.11 Home setup also contributes—loose throw rugs, uneven carpet edges, cracked sidewalks, clutter and furniture, cables and wires and cords, oh my.
Do your older patients a favor by reinforcing fall risk. Instruct them to rise slowly from seated or recumbent positions; always consider central nervous system sedation and/or the coordination-hampering properties of medications, particularly in combination. Raise the issue of home safety. A brief 10-second comment from you may plant a seed in a family member’s head to do what you cannot: scan and make safe the patient’s living environment.
1. de Falco FA. Sentinel headache. Neurol Sci. 2004;25(suppl 3):S215-S217.
2. Miller JD, Nader R. Acute subdural hematoma from bridging vein rupture: a potential mechanism for growth. J Neurosurg. 2014;120(6):1378-1384.
3. Victor M, Ropper A. Craniocerebral trauma. In: Victor M, Ropper A, eds. Adams and Victor’s Principles of Neurology. 7th ed. New York, NY: McGraw-Hill; 2001:925.
4. McBridde W. Subdural hematoma in adults: etiology, clinical features, and diagnosis. UpToDate website. www.uptodate.com/contents/subdural-hematoma-in-adults-etiology-clinical-features-and-diagnosis? search=subdural%20hematoma. Published December 10, 2018. Accessed September 23, 2019.
5. US National Library of Medicine. Subdural hematoma. Medline Plus website. https://medlineplus.gov/ency/article/000713.htm. Accessed September 23, 2019.
6. Besenski N. Traumatic injuries: imaging of head injuries. Eur Radiol. 2002;12(6):1237-1252.
7. Mayer S, Rowland L. Head injury. In: Rowland L, ed. Merritt’s Neurology. Philadelphia, PA: Lippincott Williams & Wilkins; 2000:401.
8. Saif MW, Allegra CJ, Greenberg B. Bleeding diathesis in multiple myeloma. J Hematother Stem Cell Res. 2001;10(5):657-660.
9. Stiell IG, Clement CM, Rowe BH, et al. Comparison of the Canadian CT Head Rule and the New Orleans Criteria in patients with minor head injury. JAMA. 2005;294(12):1511-1518.
10. Abdelrahman H, Almadani A, El-Menyar A, et al. Home-related falls: an underestimated mechanism of injury. J Family Community Med. 2018; 25(1):48-51.
11. Fuller GF. Falls in the elderly. Am Fam Physician. 2000;61(7):2159-2168.
In the early morning hours of June 10, 2009, a 77-year-old man who had been undergoing chemotherapy for multiple myeloma took sleep medication. He then fell down a flight of stairs in his split-level home.
The patient sustained a laceration to his scalp but returned to bed and waited until later that morning to call his internist for an appointment. Later that day, the physician placed 11 sutures for the scalp laceration and performed a neurologic examination; he did not note any abnormalities. The patient complained of back pain, so the physician ordered a back x-ray, which revealed a TI2 fracture that had occurred from the fall. No further treatment was provided for the scalp injury, except removal of the stitches about a week later.
Six days after the fall and doctor visit, the patient’s condition began to deteriorate rapidly, with noted slurred speech and loss of consciousness. He was transported to an emergency department, where CT revealed a massive subdural hematoma. An immediate craniotomy was performed. However, on June 27, 2009, the patient died as a result of the brain bleed.
His estate filed suit against the physician and his practice, alleging medical malpractice and violations in the standard of care. The estate alleged that the standard of care required the physician to obtain a CT scan and that, had one been performed, it would have revealed a small subdural hematoma in time for it to have been successfully treated (ie, before the massive second related bleed). The estate’s theory of the case did not rest on the presentation of clinical symptoms. A medical expert who testified for the estate stated that the subdural hematoma began at the time of the fall.
The defense denied any violations in the standard of care. The physician contended that the patient had presented with no symptoms other than a head laceration, and there were no criteria for ordering CT. Further, the defense asserted that the patient was symptom free for 6 days post-fall. According to the defense, the patient experienced a sudden arterial bleed that was not caused by the fall and would not have been revealed on CT ordered at the time of initial presentation, because it did not occur until 6 days later.
VERDICT
After a 10-day trial and 25 minutes’ deliberation, the jury returned a defense verdict.
COMMENTARY
The 25-minute deliberation suggests that terms such as “bridging veins” and “shearing injury” were unlikely bandied about in the jury room. The jury was likely dismissive of the plaintiff’s claim owing to his cancer diagnosis, and perhaps rightly so. But if we eliminate the multiple myeloma diagnosis, the jury might have decided differently.
Continue to: The defendant physician...
The defendant physician did a good job of documenting a negative neurologic exam, which helped him convince the jury that the patient did not have any signs or symptoms when first evaluated. But in this patient, was imaging to rule out intracranial bleeding indicated?
As an oversimplification, we tend to think of intracranial hemorrhage in 2 varieties: the insidious and the bold. Subdural hematomas are stealthy, they are sneaky, and they prey on the old. They step out of the shadows to cause symptoms. They are the ninjas of intracranial hemorrhage. Beware.
Epidural hematomas and subarachnoid hemorrhage (SAH) are the opposite. They classically present with a sudden and severe symptom complex: with epidural hematoma, the loss of consciousness, lucid interval, and final loss of consciousness; with SAH, the “worst in your life” thunder-clap headache, which may be heralded by a sentinel headache.1 When manifesting this way, they are brash, direct, and unsubtle to the point of being obnoxious—the Steven Stifler of intracranial bleeding.
This generalization is made to highlight the potentially sneaky nature of subdural hemorrhage. There are circumstances in which the clinical presentation of epidural hematoma and SAH will be more challenging. The question here is whether a negative initial neurologic exam can adequately screen for a potentially stealthy subdural hematoma.
Subdural hemorrhage is caused by rapidly changing velocity that may stretch and tear small bridging veins.2,3 Subdural hematoma is more common in the elderly, those who abuse alcohol, and those with a prior history of head trauma.4 As the brain shrinks with age or atrophy, the subdural space enlarges and traversing veins are stretched to cover a wider distance—rendering them vulnerable to rupture.5 These structures may also weaken as a result of low cerebrospinal fluid (intracranial hypotension); as pressure decreases (eg, from a leak), the brain’s buoyancy is reduced, causing traction on anchoring and supporting structures (eg, bridging veins).5 Injury to bridging veins can even occur as a result of a coup-contrecoup mechanism in the absence of direct physical impact.6,7 Bottom line: the injury itself may be subtle, requiring an index of suspicion to make the diagnosis.
Continue to: The case patient was...
The case patient was elderly. He had a chronic malignancy and sustained a fall down the stairs. He was taking sleeping pills, which may have slowed reflexive protective mechanisms after he started to fall (resulting in greater force imparted to his head). Multiple myeloma can predispose a patient to coagulopathy, and we don’t know in this case if this patient’s multiple myeloma made him more susceptible to bleeding—but it certainly didn’t help.8 The patient’s age, the mechanism of injury, and the history of malignancy made this a setup for hemorrhage.
Interestingly, we are not given details about how the patient looked during his suture removal. We are told the time between the initial fall and deterioration was 6 days. Scalp sutures were removed “about a week later,” which was after the deterioration—so this can’t be correct. Removing scalp sutures after 5 days seems premature, but that is the only possibility if 6 days elapsed between the fall and the deterioration.
In short, these are difficult cases. If intracranial bleeding can be subtle and delayed, how can we be sure a patient is not experiencing a bleed? We can only apply the relevant standard of care using all the clinical information we have. The Canadian CT Head Rule and New Orleans Criteria are clinical tools designed to help providers determine when to image (see Table for details).9

Applying the Canadian CT Head Rule to the facts of this case, we would image the patient because he fell down a “flight” of stairs (which is > 5 stairs) and he is 77 years old (older than 65). The New Orleans Criteria require head CT for minor injury with any positive findings.9 Because the patient is older than 60, he would be scanned according this rule.
In this case, the tools indicate scanning would have been appropriate. The patient’s multiple myeloma might have further impelled a decision to image. However, the jury was persuaded that the defendant’s negative neurologic exam was reasonable under the circumstances. This was likely made possible by the physician’s good recordkeeping and demonstrated genuine concern for the patient’s well-being—as well as a differing viewpoint of the patient’s age and health status.
Continue to: Finally, a word about...
Finally, a word about falls and the elderly: We’ve all heard the 80s advertising catchphrase (which lives on as a present-day meme) “I’ve fallen, and I can’t get up!” The problem is, many don’t. It would be more clinically accurate to say, “I’ve fallen, and I’ll be hospitalized for an extended period of time, then transferred to a skilled nursing facility, but I won’t survive to discharge.” The reality is that falls kill, and the severity is underestimated.10 If it were a “brain-eating amoeba,” the media would be all over it. With falls, not so much. We tend to pay less attention.
Risk factors for a fall include postural hypotension; use of benzodiazepines or other sedative-hypnotic drugs; use of ≥ 4 medications; environmental hazards for tripping; impairment in balance and transfer skills; and gait impairment.11 Home setup also contributes—loose throw rugs, uneven carpet edges, cracked sidewalks, clutter and furniture, cables and wires and cords, oh my.
Do your older patients a favor by reinforcing fall risk. Instruct them to rise slowly from seated or recumbent positions; always consider central nervous system sedation and/or the coordination-hampering properties of medications, particularly in combination. Raise the issue of home safety. A brief 10-second comment from you may plant a seed in a family member’s head to do what you cannot: scan and make safe the patient’s living environment.
In the early morning hours of June 10, 2009, a 77-year-old man who had been undergoing chemotherapy for multiple myeloma took sleep medication. He then fell down a flight of stairs in his split-level home.
The patient sustained a laceration to his scalp but returned to bed and waited until later that morning to call his internist for an appointment. Later that day, the physician placed 11 sutures for the scalp laceration and performed a neurologic examination; he did not note any abnormalities. The patient complained of back pain, so the physician ordered a back x-ray, which revealed a TI2 fracture that had occurred from the fall. No further treatment was provided for the scalp injury, except removal of the stitches about a week later.
Six days after the fall and doctor visit, the patient’s condition began to deteriorate rapidly, with noted slurred speech and loss of consciousness. He was transported to an emergency department, where CT revealed a massive subdural hematoma. An immediate craniotomy was performed. However, on June 27, 2009, the patient died as a result of the brain bleed.
His estate filed suit against the physician and his practice, alleging medical malpractice and violations in the standard of care. The estate alleged that the standard of care required the physician to obtain a CT scan and that, had one been performed, it would have revealed a small subdural hematoma in time for it to have been successfully treated (ie, before the massive second related bleed). The estate’s theory of the case did not rest on the presentation of clinical symptoms. A medical expert who testified for the estate stated that the subdural hematoma began at the time of the fall.
The defense denied any violations in the standard of care. The physician contended that the patient had presented with no symptoms other than a head laceration, and there were no criteria for ordering CT. Further, the defense asserted that the patient was symptom free for 6 days post-fall. According to the defense, the patient experienced a sudden arterial bleed that was not caused by the fall and would not have been revealed on CT ordered at the time of initial presentation, because it did not occur until 6 days later.
VERDICT
After a 10-day trial and 25 minutes’ deliberation, the jury returned a defense verdict.
COMMENTARY
The 25-minute deliberation suggests that terms such as “bridging veins” and “shearing injury” were unlikely bandied about in the jury room. The jury was likely dismissive of the plaintiff’s claim owing to his cancer diagnosis, and perhaps rightly so. But if we eliminate the multiple myeloma diagnosis, the jury might have decided differently.
Continue to: The defendant physician...
The defendant physician did a good job of documenting a negative neurologic exam, which helped him convince the jury that the patient did not have any signs or symptoms when first evaluated. But in this patient, was imaging to rule out intracranial bleeding indicated?
As an oversimplification, we tend to think of intracranial hemorrhage in 2 varieties: the insidious and the bold. Subdural hematomas are stealthy, they are sneaky, and they prey on the old. They step out of the shadows to cause symptoms. They are the ninjas of intracranial hemorrhage. Beware.
Epidural hematomas and subarachnoid hemorrhage (SAH) are the opposite. They classically present with a sudden and severe symptom complex: with epidural hematoma, the loss of consciousness, lucid interval, and final loss of consciousness; with SAH, the “worst in your life” thunder-clap headache, which may be heralded by a sentinel headache.1 When manifesting this way, they are brash, direct, and unsubtle to the point of being obnoxious—the Steven Stifler of intracranial bleeding.
This generalization is made to highlight the potentially sneaky nature of subdural hemorrhage. There are circumstances in which the clinical presentation of epidural hematoma and SAH will be more challenging. The question here is whether a negative initial neurologic exam can adequately screen for a potentially stealthy subdural hematoma.
Subdural hemorrhage is caused by rapidly changing velocity that may stretch and tear small bridging veins.2,3 Subdural hematoma is more common in the elderly, those who abuse alcohol, and those with a prior history of head trauma.4 As the brain shrinks with age or atrophy, the subdural space enlarges and traversing veins are stretched to cover a wider distance—rendering them vulnerable to rupture.5 These structures may also weaken as a result of low cerebrospinal fluid (intracranial hypotension); as pressure decreases (eg, from a leak), the brain’s buoyancy is reduced, causing traction on anchoring and supporting structures (eg, bridging veins).5 Injury to bridging veins can even occur as a result of a coup-contrecoup mechanism in the absence of direct physical impact.6,7 Bottom line: the injury itself may be subtle, requiring an index of suspicion to make the diagnosis.
Continue to: The case patient was...
The case patient was elderly. He had a chronic malignancy and sustained a fall down the stairs. He was taking sleeping pills, which may have slowed reflexive protective mechanisms after he started to fall (resulting in greater force imparted to his head). Multiple myeloma can predispose a patient to coagulopathy, and we don’t know in this case if this patient’s multiple myeloma made him more susceptible to bleeding—but it certainly didn’t help.8 The patient’s age, the mechanism of injury, and the history of malignancy made this a setup for hemorrhage.
Interestingly, we are not given details about how the patient looked during his suture removal. We are told the time between the initial fall and deterioration was 6 days. Scalp sutures were removed “about a week later,” which was after the deterioration—so this can’t be correct. Removing scalp sutures after 5 days seems premature, but that is the only possibility if 6 days elapsed between the fall and the deterioration.
In short, these are difficult cases. If intracranial bleeding can be subtle and delayed, how can we be sure a patient is not experiencing a bleed? We can only apply the relevant standard of care using all the clinical information we have. The Canadian CT Head Rule and New Orleans Criteria are clinical tools designed to help providers determine when to image (see Table for details).9

Applying the Canadian CT Head Rule to the facts of this case, we would image the patient because he fell down a “flight” of stairs (which is > 5 stairs) and he is 77 years old (older than 65). The New Orleans Criteria require head CT for minor injury with any positive findings.9 Because the patient is older than 60, he would be scanned according this rule.
In this case, the tools indicate scanning would have been appropriate. The patient’s multiple myeloma might have further impelled a decision to image. However, the jury was persuaded that the defendant’s negative neurologic exam was reasonable under the circumstances. This was likely made possible by the physician’s good recordkeeping and demonstrated genuine concern for the patient’s well-being—as well as a differing viewpoint of the patient’s age and health status.
Continue to: Finally, a word about...
Finally, a word about falls and the elderly: We’ve all heard the 80s advertising catchphrase (which lives on as a present-day meme) “I’ve fallen, and I can’t get up!” The problem is, many don’t. It would be more clinically accurate to say, “I’ve fallen, and I’ll be hospitalized for an extended period of time, then transferred to a skilled nursing facility, but I won’t survive to discharge.” The reality is that falls kill, and the severity is underestimated.10 If it were a “brain-eating amoeba,” the media would be all over it. With falls, not so much. We tend to pay less attention.
Risk factors for a fall include postural hypotension; use of benzodiazepines or other sedative-hypnotic drugs; use of ≥ 4 medications; environmental hazards for tripping; impairment in balance and transfer skills; and gait impairment.11 Home setup also contributes—loose throw rugs, uneven carpet edges, cracked sidewalks, clutter and furniture, cables and wires and cords, oh my.
Do your older patients a favor by reinforcing fall risk. Instruct them to rise slowly from seated or recumbent positions; always consider central nervous system sedation and/or the coordination-hampering properties of medications, particularly in combination. Raise the issue of home safety. A brief 10-second comment from you may plant a seed in a family member’s head to do what you cannot: scan and make safe the patient’s living environment.
1. de Falco FA. Sentinel headache. Neurol Sci. 2004;25(suppl 3):S215-S217.
2. Miller JD, Nader R. Acute subdural hematoma from bridging vein rupture: a potential mechanism for growth. J Neurosurg. 2014;120(6):1378-1384.
3. Victor M, Ropper A. Craniocerebral trauma. In: Victor M, Ropper A, eds. Adams and Victor’s Principles of Neurology. 7th ed. New York, NY: McGraw-Hill; 2001:925.
4. McBridde W. Subdural hematoma in adults: etiology, clinical features, and diagnosis. UpToDate website. www.uptodate.com/contents/subdural-hematoma-in-adults-etiology-clinical-features-and-diagnosis? search=subdural%20hematoma. Published December 10, 2018. Accessed September 23, 2019.
5. US National Library of Medicine. Subdural hematoma. Medline Plus website. https://medlineplus.gov/ency/article/000713.htm. Accessed September 23, 2019.
6. Besenski N. Traumatic injuries: imaging of head injuries. Eur Radiol. 2002;12(6):1237-1252.
7. Mayer S, Rowland L. Head injury. In: Rowland L, ed. Merritt’s Neurology. Philadelphia, PA: Lippincott Williams & Wilkins; 2000:401.
8. Saif MW, Allegra CJ, Greenberg B. Bleeding diathesis in multiple myeloma. J Hematother Stem Cell Res. 2001;10(5):657-660.
9. Stiell IG, Clement CM, Rowe BH, et al. Comparison of the Canadian CT Head Rule and the New Orleans Criteria in patients with minor head injury. JAMA. 2005;294(12):1511-1518.
10. Abdelrahman H, Almadani A, El-Menyar A, et al. Home-related falls: an underestimated mechanism of injury. J Family Community Med. 2018; 25(1):48-51.
11. Fuller GF. Falls in the elderly. Am Fam Physician. 2000;61(7):2159-2168.
1. de Falco FA. Sentinel headache. Neurol Sci. 2004;25(suppl 3):S215-S217.
2. Miller JD, Nader R. Acute subdural hematoma from bridging vein rupture: a potential mechanism for growth. J Neurosurg. 2014;120(6):1378-1384.
3. Victor M, Ropper A. Craniocerebral trauma. In: Victor M, Ropper A, eds. Adams and Victor’s Principles of Neurology. 7th ed. New York, NY: McGraw-Hill; 2001:925.
4. McBridde W. Subdural hematoma in adults: etiology, clinical features, and diagnosis. UpToDate website. www.uptodate.com/contents/subdural-hematoma-in-adults-etiology-clinical-features-and-diagnosis? search=subdural%20hematoma. Published December 10, 2018. Accessed September 23, 2019.
5. US National Library of Medicine. Subdural hematoma. Medline Plus website. https://medlineplus.gov/ency/article/000713.htm. Accessed September 23, 2019.
6. Besenski N. Traumatic injuries: imaging of head injuries. Eur Radiol. 2002;12(6):1237-1252.
7. Mayer S, Rowland L. Head injury. In: Rowland L, ed. Merritt’s Neurology. Philadelphia, PA: Lippincott Williams & Wilkins; 2000:401.
8. Saif MW, Allegra CJ, Greenberg B. Bleeding diathesis in multiple myeloma. J Hematother Stem Cell Res. 2001;10(5):657-660.
9. Stiell IG, Clement CM, Rowe BH, et al. Comparison of the Canadian CT Head Rule and the New Orleans Criteria in patients with minor head injury. JAMA. 2005;294(12):1511-1518.
10. Abdelrahman H, Almadani A, El-Menyar A, et al. Home-related falls: an underestimated mechanism of injury. J Family Community Med. 2018; 25(1):48-51.
11. Fuller GF. Falls in the elderly. Am Fam Physician. 2000;61(7):2159-2168.
Don’t Be a Maverick; Get a Wingman
A 39-year-old woman presented to an Arkansas cardiologist on February 12, 2010, with complaints of chest pain. The physician conducted an ankle-brachial index (ABI) test to measure the blood pressure in her lower extremity and interpreted it as less than 0.9%. He then ordered an echocardiogram to gauge the patient’s ejection fraction and interpreted the reading at 25%. Both measurements were below the normal average, which prompted the cardiologist to diagnose peripheral vascular disease and congestive heart failure.
The patient was eventually prescribed a course of cardiac medication and monitored over the ensuing months. On April 15, the cardiologist conducted a nuclear stress test; the computer-generated measurement of her ejection fraction was 50%, which the physician adjusted to 42%. In May, the patient underwent cardiac catheterization, which showed no lesions or blockages in the vessels. In the following months, the patient’s medication dosages were increased. On September 27, the cardiologist conducted another echocardiogram, which he read as 30%, and reaffirmed his diagnosis of congestive heart failure.
The physician continued to monitor the patient. On November 11, after being diagnosed with congestive heart failure, the patient was admitted to the hospital, where the cardiologist implanted an automated implantable cardioverter defibrillator (AICD).
On May 18, 2011, while running with her 2 daughters and a friend, the patient suddenly collapsed and experienced electrical currents coursing through her body (5 times). She was driven to a hospital, where it was determined that she did not go into cardiac arrest (which she suspected) but rather her defibrillator malfunctioned. The defibrillator was recalibrated to a higher setting, and she experienced no further issues.
In the ensuing years, the patient continued to follow up with her cardiologist. She eventually filed a lawsuit claiming that he had misdiagnosed congestive heart failure and unnecessarily implanted the AICD. Her experts in cardiology and cardiac electrophysiology testified that the defendant’s readings of the February 2010 ABI and echocardiogram results were incorrect; the ABIs were in fact .128 and .138 and the ejection fractions were 50% to 55% percent—in both instances, normal results. Furthermore, the September 2010 echocardiogram and another taken in February 2011, which showed little change from the first echocardiogram, were also normal, according to the experts.
The experts also opined that American College of Cardiology/American Heart Association guidelines state that a patient’s ejection fraction has to be less than 35% before a defibrillator is placed. Both experts concluded that the plaintiff did not have congestive heart failure and was therefore not a candidate for an AICD. The cardiac electrophysiology expert stated that to be a candidate, a patient must have an enlarged left ventricle—which plaintiff did not have. Moreover, none of the plaintiff’s physical findings were ever consistent with congestive heart failure: She did not have fluid in her lungs, as examinations always revealed clear lungs without congestion; there was no distention in her jugular veins; she did not experience sleep apnea; she did not lose consciousness; and she only experienced fatigue with exertion. The cardiology expert further faulted the defendant for failing to adjust the patient’s medication dosages to optimize her cardiac repair.
The defense maintained that the defendant’s treatment of the patient met the standard of care. According to the defense, the defendant’s judgment and interpretation of the patient’s ABI and echocardiogram results were medically sound and the defibrillator was necessary.
Continue to: VERDICT
VERDICT
After a 4-day trial and 3 hours of deliberation, the jury found that the defendant was liable and his actions were a factual cause of injury to plaintiff, who was awarded $1.75 million in damages.
COMMENTARY
In this case, the defendant cardiologist placed an AICD (also known as an implantable cardioverter defibrillator, or ICD). There was no allegation that the placement itself was negligent; rather, the claimed negligence was the decision to place it. But the plaintiff’s damages arise from the device’s malfunction—not the cardiologist’s decision to place it.
This case brings up an interesting issue of causation. As most of us know, medical malpractice plaintiffs must show (1) duty, (2) breach, (3) causation, and (4) harm. In law, there are 2 ways to think of causation: “but for” causation and “proximate” causation.
So-called “but for” causation is based on whether any causal relationship exists between an action and an outcome. For example, a drunk driver veers off the highway, through the breakdown lane, and strikes a tree, catching his car on fire. One minute later, a driver in the high-speed lane is captivated by the flaming vehicle, rubbernecks, fails to pay attention to traffic, and rear-ends the vehicle in front of him—injuring the driver of that car. Using “but for” causation, the drunk driver striking the tree “caused” the accident. If that had never happened, the second driver would never have been distracted, and if the driver wasn’t distracted, the second accident would not have occurred.
By contrast, “proximate” causation entails the immediate cause, which is foreseeable. Black’s Law defines proximate cause as “The result of a direct action and cause of loss to property that sets in motion a chain of events that is unbroken and causes damage, injury and destruction with no other interference” (emphasis added).1 Using a proximate causation analysis, the second driver’s negligent failure to pay attention to the road would be the proximate cause of the second crash.
Continue to: Generally, causation analysis...
Generally, causation analysis is limited to proximate cause on the basis that harm is reasonably foreseeable. A famous example is the case of Palsgraf v. Long Island Railroad.2
Mrs. Palsgraf was standing on a train platform. A man carrying an ordinary-looking package rushed to board a moving train, with help from 2 railroad employees (1 in the car and 1 on the platform). As the employees pushed and pulled the man aboard, the package fell onto the tracks. Unbeknownst to everyone but the package’s owner, it contained fireworks—which exploded when the rear wheels of the train ran over the package. The explosion caused a large standing scale to fall over and land on Mrs. Palsgraf, injuring her. This is what law professors live for.
Mrs. Palsgraf sued the railroad, arguing that if the employees had not negligently pushed and pulled the man, the package would not have fallen and would not have exploded, and the scale never would have fallen on her. Mrs. Palsgraf won her trial and won her first appeal. In a famous decision by a famous judge, the win was overturned on the basis that Mrs. Palsgraf’s injuries “were not a reasonably foreseeable consequence of any possible negligence by the railroad.” This case set a foundation of American law regarding reasonable foreseeability, both in terms of identifiable plaintiffs and expected danger.
What does a railroad accident have to do with medical malpractice? In the case described here, we had an arguably negligent medical decision to place the defibrillator. Then we had a malfunction of the device, which caused the plaintiff injury. Was it reasonably foreseeable that the device would malfunction and cause harm—and should the physician be on the hook for that?
Unlike the unforeseeable risk of knocking a simple package to the ground—which unexpectedly turned out to contain fireworks—the risk of device malfunction would be foreseeable. Why? Beyond the usual surgical risks of bleeding and infection, an ICD’s leads can dislodge, the device can fail, and devices can shock inappropriately (with younger patients at increased risk for inappropriate shocks).3,4 These risks are known, and it is highly likely the defendant cardiologist disclosed them on the consent form he asked the plaintiff to sign. The defense could not credibly argue that device malfunction was an unforeseeable risk. The malpractice here was the decision to place the ICD—and because placement wasn’t warranted in this patient, neither were the risks.
Continue to: This brings us to...
This brings us to the first malpractice trap: If you practice in a setting where a procedure is routinely offered, and that treatment has a billable cost, be cautious. Your decision-making can be made to appear driven by a profit motive. The lay public (including jurors) is suspicious of profit motive in medicine—a concept most clinicians find alien and repugnant.
Back in 2009, while outlining his rationale for the Affordable Care Act, President Obama made several statements that earned him swift rebuke from physician groups; I include them here not to incite political rants but to demonstrate the keen suspicion the public has for profit motives in clinical decision-making. On one occasion, he said, “Right now, doctors a lot of times are forced to make decisions based on the fee payment schedule. ... The doctor may look at the reimbursement system and say to himself, ‘You know what? I make a lot more money if I take this kid’s tonsils out.’”5 In another statement, while acknowledging that primary care providers offering preventive diabetes care make “a pittance,” Obama added, “But if that same [patient] ends up getting their foot amputated, that’s $30,000, $40,000, $50,000 immediately the surgeon is reimbursed.”6
For most clinicians, the idea of deciding on a course of treatment because it will be lucrative is an alien concept. Good clinicians base treatment on the accepted medical standard, and cost factors are a distant consideration if one at all.
However, if your practice involves a procedure or intervention that is a particularly lucrative billable event, do your part to play mental “devil’s advocate” and ensure that patients are genuinely in need of the treatment.
In some rare, bad (and usually highly publicized) cases, a procedure will be overused in a patently fraudulent way, which we all recognize is unethical and illegal. However, in other instances, a procedure may be overused because it is familiar and available. We’ve all heard the adage, “If all you have is a hammer, everything looks like a nail.” This “cute” expression holds some truth about the risk for cognitive bias based on the over-reliance on a familiar remedy.7 This particularly involves specialty practices that perform certain procedures frequently.
Continue to: In this case...
In this case, the plaintiff’s nuclear stress test showed an ejection fraction of 50%, which the defendant decreased to 42%. That is substantially different than the first ejection fraction of 25% and the second of 30% in a 39-year-old patient without any clinical signs of congestive heart failure. Did the defendant’s ability to offer an ICD color his appraisal of the patient’s cardiac function?
In closing arguments to the jury, the plaintiff’s attorney probably argued “this defendant behaved as if every human heart could be improved with a battery and wires.” Examine your practice to be sure you aren’t seeing nails where they don’t exist—because tomorrow, they will be the nails in the coffin of your career.
One thing missing from this case summary—but available via court records—is that the plaintiff claimed she had wanted a second opinion but was told she couldn’t have one: “I wanted a second opinion. And when I called [the defendant’s] office and asked ‘Could I have a second opinion,’ his nurse answered the phone and said that if I did get a second opinion, then I couldn’t come back.”8
There are a few aspects to discuss here, one of which is the second malpractice trap: viewing second opinions as an enemy. Most clinicians realize they are actually your friend. However, some providers are threatened by second opinions. It is as if they roll out of bed in the morning and consult the mirror to ask, “Who is the top cardiologist of them all?” and need the validation of that voice saying, “You, Dr. Smith—why of course, you!”
To that I say, forget the mirror, you egotistical so-and-so. Snow White will help protect you, your career, and most importantly, your patient. Allow the second opinion. In fact, integrate an expectation of the them into your practice style, to disarm any feelings of awkwardness, confrontation, or defensiveness. Think of the benefits: If Snow White validates your opinion, you have much stronger case that a course of treatment was indicated. Conversely, if Snow White arrives at a different opinion, she may have seen something you did not, and/or it may also relieve pressure from the patient to take an action with which you were only borderline comfortable.
Continue to: In cases I've worked on...
In cases I’ve worked on, I’ve seen some excellent surgeons who require a second opinion as a precondition to operating. This is particularly helpful when patient expectations are uncertain or there is a track record of unsuccessful interventions (eg, chronic back pain with multiple failed surgeries). Furthermore, a second opinion shows diligence, humility, and concern for the patient. It also gives you backup. As Top Gun taught us, there is no need to be a “maverick” when you can have a wingman.
As far as the alleged comment by the cardiologist’s nurse: We don’t know for certain if this actually happened—but if it did, it was unwarranted and foolish. Any jury would hear this and conclude the defendant (1) was an ass, (2) had something to hide, or (3) was guarding a profit source. Any way you slice it, this is bad for the patient and ultimately bad for the defendant. Make room in your practice for second opinions.
There was a legal fight regarding the admissibility of what the nurse had said. The defense filed a motion to prevent the plaintiff from telling the jury about the nurse’s statement, on the basis that the nurse’s statement was inadmissible hearsay. The court denied the motion, ruling that the cardiologist’s nurse was his agent and her words could be properly brought before the jury. The court found that the plaintiff relied on that statement in determining whether to have the ICD placed or obtain a second opinion.
This raises an interesting malpractice awareness point: If you are sued for malpractice, anything you had said to a patient, the patient’s family, or your coworkers will be admissible in court as a “party admission,” classified as either nonhearsay or a hearsay exception (assuming the statement was not made as part of a bona fide peer review, in which case it will likely be subject to peer review privilege). As seen in this case, this also applies to people acting as agents on your behalf. Be cautious of what you say and how you say it—and what your practice’s representatives are saying as well.
Interestingly, the jury found for the plaintiff in the amount of $1.75 million, but they declined to award punitive damages, which are designed to punish defendants rather than compensate the plaintiff. In Arkansas, the standard for punitive damages is tough; the plaintiff must “prove by clear and convincing evidence that the defendant knew or ought to have known, that their conduct would naturally and probably result in injury or damage and that they continued the conduct with malice or in reckless disregard of the consequences from which malice may be inferred.”9 A similar standard exists in most states. Because there were no punitive damages, we can infer the jury did not think the defendant implanted the ICD (for profit) knowing it wasn’t indicated.
Continue to: IN SUMMARY
IN SUMMARY
Consider foreseeable risks of practice interventions; be sure your practice is not on “autopilot,” recommending a common procedure or intervention too frequently. Don’t be threatened by second opinions; welcome them. And watch your words—as they say on every police procedural you’ve ever watched, they can be used against you.
1. The Law Dictionary. What is proximate cause? https://thelawdictionary.org/proximate-cause. Accessed August 21, 2019.
2. Palsgraf v Long Island R.R. Co (248 NY 339, 162 NE 99 [1928]).
3. Stanford Health Care. Risks: our approach for ICD. https://stanfordhealthcare.org/medical-treatments/i/icd/risks.html. Accessed August 21, 2019.
4. Hofer D, Steffel J, Hürlimann D, et al. Long-term incidence of inappropriate shocks in patients with implantable cardioverter defibrillators in clinical practice—an underestimated complication? J Interv Card Electrophysiol. 2017;50(3):219-226.
5. Transcript: Obama pleads health care case. CNN.com. July 22, 2009. www.cnn.com/2009/POLITICS/07/22/transcript.obama. Accessed August 21, 2019.
6. The White House Office of the Press Secretary. Remarks by the President at Town Hall on Health Insurance Reform in Portsmouth, New Hampshire [press release]. August 11, 2009. https://obamawhitehouse.archives.gov/the-press-office/remarks-president-town-hall-health-insurance-reform-portsmouth-new-hampshire. Accessed August 21, 2019.
7. Maslow AH. The Psychology of Science: a Reconnaissance. New York, NY: Harper & Row; 1966:15.
8. Thornton Dep. 55:3-55:7, March 16, 2014, AR Cir No. CV-2012-640-2.
9. Arkansas Code Title 16. Practice, procedure, and courts § 16-55-206: standards for award of punitive damages. https://codes.findlaw.com/ar/title-16-practice-procedure-and-courts/ar-code-sect-16-55-206.html. Accessed August 21, 2019.
A 39-year-old woman presented to an Arkansas cardiologist on February 12, 2010, with complaints of chest pain. The physician conducted an ankle-brachial index (ABI) test to measure the blood pressure in her lower extremity and interpreted it as less than 0.9%. He then ordered an echocardiogram to gauge the patient’s ejection fraction and interpreted the reading at 25%. Both measurements were below the normal average, which prompted the cardiologist to diagnose peripheral vascular disease and congestive heart failure.
The patient was eventually prescribed a course of cardiac medication and monitored over the ensuing months. On April 15, the cardiologist conducted a nuclear stress test; the computer-generated measurement of her ejection fraction was 50%, which the physician adjusted to 42%. In May, the patient underwent cardiac catheterization, which showed no lesions or blockages in the vessels. In the following months, the patient’s medication dosages were increased. On September 27, the cardiologist conducted another echocardiogram, which he read as 30%, and reaffirmed his diagnosis of congestive heart failure.
The physician continued to monitor the patient. On November 11, after being diagnosed with congestive heart failure, the patient was admitted to the hospital, where the cardiologist implanted an automated implantable cardioverter defibrillator (AICD).
On May 18, 2011, while running with her 2 daughters and a friend, the patient suddenly collapsed and experienced electrical currents coursing through her body (5 times). She was driven to a hospital, where it was determined that she did not go into cardiac arrest (which she suspected) but rather her defibrillator malfunctioned. The defibrillator was recalibrated to a higher setting, and she experienced no further issues.
In the ensuing years, the patient continued to follow up with her cardiologist. She eventually filed a lawsuit claiming that he had misdiagnosed congestive heart failure and unnecessarily implanted the AICD. Her experts in cardiology and cardiac electrophysiology testified that the defendant’s readings of the February 2010 ABI and echocardiogram results were incorrect; the ABIs were in fact .128 and .138 and the ejection fractions were 50% to 55% percent—in both instances, normal results. Furthermore, the September 2010 echocardiogram and another taken in February 2011, which showed little change from the first echocardiogram, were also normal, according to the experts.
The experts also opined that American College of Cardiology/American Heart Association guidelines state that a patient’s ejection fraction has to be less than 35% before a defibrillator is placed. Both experts concluded that the plaintiff did not have congestive heart failure and was therefore not a candidate for an AICD. The cardiac electrophysiology expert stated that to be a candidate, a patient must have an enlarged left ventricle—which plaintiff did not have. Moreover, none of the plaintiff’s physical findings were ever consistent with congestive heart failure: She did not have fluid in her lungs, as examinations always revealed clear lungs without congestion; there was no distention in her jugular veins; she did not experience sleep apnea; she did not lose consciousness; and she only experienced fatigue with exertion. The cardiology expert further faulted the defendant for failing to adjust the patient’s medication dosages to optimize her cardiac repair.
The defense maintained that the defendant’s treatment of the patient met the standard of care. According to the defense, the defendant’s judgment and interpretation of the patient’s ABI and echocardiogram results were medically sound and the defibrillator was necessary.
Continue to: VERDICT
VERDICT
After a 4-day trial and 3 hours of deliberation, the jury found that the defendant was liable and his actions were a factual cause of injury to plaintiff, who was awarded $1.75 million in damages.
COMMENTARY
In this case, the defendant cardiologist placed an AICD (also known as an implantable cardioverter defibrillator, or ICD). There was no allegation that the placement itself was negligent; rather, the claimed negligence was the decision to place it. But the plaintiff’s damages arise from the device’s malfunction—not the cardiologist’s decision to place it.
This case brings up an interesting issue of causation. As most of us know, medical malpractice plaintiffs must show (1) duty, (2) breach, (3) causation, and (4) harm. In law, there are 2 ways to think of causation: “but for” causation and “proximate” causation.
So-called “but for” causation is based on whether any causal relationship exists between an action and an outcome. For example, a drunk driver veers off the highway, through the breakdown lane, and strikes a tree, catching his car on fire. One minute later, a driver in the high-speed lane is captivated by the flaming vehicle, rubbernecks, fails to pay attention to traffic, and rear-ends the vehicle in front of him—injuring the driver of that car. Using “but for” causation, the drunk driver striking the tree “caused” the accident. If that had never happened, the second driver would never have been distracted, and if the driver wasn’t distracted, the second accident would not have occurred.
By contrast, “proximate” causation entails the immediate cause, which is foreseeable. Black’s Law defines proximate cause as “The result of a direct action and cause of loss to property that sets in motion a chain of events that is unbroken and causes damage, injury and destruction with no other interference” (emphasis added).1 Using a proximate causation analysis, the second driver’s negligent failure to pay attention to the road would be the proximate cause of the second crash.
Continue to: Generally, causation analysis...
Generally, causation analysis is limited to proximate cause on the basis that harm is reasonably foreseeable. A famous example is the case of Palsgraf v. Long Island Railroad.2
Mrs. Palsgraf was standing on a train platform. A man carrying an ordinary-looking package rushed to board a moving train, with help from 2 railroad employees (1 in the car and 1 on the platform). As the employees pushed and pulled the man aboard, the package fell onto the tracks. Unbeknownst to everyone but the package’s owner, it contained fireworks—which exploded when the rear wheels of the train ran over the package. The explosion caused a large standing scale to fall over and land on Mrs. Palsgraf, injuring her. This is what law professors live for.
Mrs. Palsgraf sued the railroad, arguing that if the employees had not negligently pushed and pulled the man, the package would not have fallen and would not have exploded, and the scale never would have fallen on her. Mrs. Palsgraf won her trial and won her first appeal. In a famous decision by a famous judge, the win was overturned on the basis that Mrs. Palsgraf’s injuries “were not a reasonably foreseeable consequence of any possible negligence by the railroad.” This case set a foundation of American law regarding reasonable foreseeability, both in terms of identifiable plaintiffs and expected danger.
What does a railroad accident have to do with medical malpractice? In the case described here, we had an arguably negligent medical decision to place the defibrillator. Then we had a malfunction of the device, which caused the plaintiff injury. Was it reasonably foreseeable that the device would malfunction and cause harm—and should the physician be on the hook for that?
Unlike the unforeseeable risk of knocking a simple package to the ground—which unexpectedly turned out to contain fireworks—the risk of device malfunction would be foreseeable. Why? Beyond the usual surgical risks of bleeding and infection, an ICD’s leads can dislodge, the device can fail, and devices can shock inappropriately (with younger patients at increased risk for inappropriate shocks).3,4 These risks are known, and it is highly likely the defendant cardiologist disclosed them on the consent form he asked the plaintiff to sign. The defense could not credibly argue that device malfunction was an unforeseeable risk. The malpractice here was the decision to place the ICD—and because placement wasn’t warranted in this patient, neither were the risks.
Continue to: This brings us to...
This brings us to the first malpractice trap: If you practice in a setting where a procedure is routinely offered, and that treatment has a billable cost, be cautious. Your decision-making can be made to appear driven by a profit motive. The lay public (including jurors) is suspicious of profit motive in medicine—a concept most clinicians find alien and repugnant.
Back in 2009, while outlining his rationale for the Affordable Care Act, President Obama made several statements that earned him swift rebuke from physician groups; I include them here not to incite political rants but to demonstrate the keen suspicion the public has for profit motives in clinical decision-making. On one occasion, he said, “Right now, doctors a lot of times are forced to make decisions based on the fee payment schedule. ... The doctor may look at the reimbursement system and say to himself, ‘You know what? I make a lot more money if I take this kid’s tonsils out.’”5 In another statement, while acknowledging that primary care providers offering preventive diabetes care make “a pittance,” Obama added, “But if that same [patient] ends up getting their foot amputated, that’s $30,000, $40,000, $50,000 immediately the surgeon is reimbursed.”6
For most clinicians, the idea of deciding on a course of treatment because it will be lucrative is an alien concept. Good clinicians base treatment on the accepted medical standard, and cost factors are a distant consideration if one at all.
However, if your practice involves a procedure or intervention that is a particularly lucrative billable event, do your part to play mental “devil’s advocate” and ensure that patients are genuinely in need of the treatment.
In some rare, bad (and usually highly publicized) cases, a procedure will be overused in a patently fraudulent way, which we all recognize is unethical and illegal. However, in other instances, a procedure may be overused because it is familiar and available. We’ve all heard the adage, “If all you have is a hammer, everything looks like a nail.” This “cute” expression holds some truth about the risk for cognitive bias based on the over-reliance on a familiar remedy.7 This particularly involves specialty practices that perform certain procedures frequently.
Continue to: In this case...
In this case, the plaintiff’s nuclear stress test showed an ejection fraction of 50%, which the defendant decreased to 42%. That is substantially different than the first ejection fraction of 25% and the second of 30% in a 39-year-old patient without any clinical signs of congestive heart failure. Did the defendant’s ability to offer an ICD color his appraisal of the patient’s cardiac function?
In closing arguments to the jury, the plaintiff’s attorney probably argued “this defendant behaved as if every human heart could be improved with a battery and wires.” Examine your practice to be sure you aren’t seeing nails where they don’t exist—because tomorrow, they will be the nails in the coffin of your career.
One thing missing from this case summary—but available via court records—is that the plaintiff claimed she had wanted a second opinion but was told she couldn’t have one: “I wanted a second opinion. And when I called [the defendant’s] office and asked ‘Could I have a second opinion,’ his nurse answered the phone and said that if I did get a second opinion, then I couldn’t come back.”8
There are a few aspects to discuss here, one of which is the second malpractice trap: viewing second opinions as an enemy. Most clinicians realize they are actually your friend. However, some providers are threatened by second opinions. It is as if they roll out of bed in the morning and consult the mirror to ask, “Who is the top cardiologist of them all?” and need the validation of that voice saying, “You, Dr. Smith—why of course, you!”
To that I say, forget the mirror, you egotistical so-and-so. Snow White will help protect you, your career, and most importantly, your patient. Allow the second opinion. In fact, integrate an expectation of the them into your practice style, to disarm any feelings of awkwardness, confrontation, or defensiveness. Think of the benefits: If Snow White validates your opinion, you have much stronger case that a course of treatment was indicated. Conversely, if Snow White arrives at a different opinion, she may have seen something you did not, and/or it may also relieve pressure from the patient to take an action with which you were only borderline comfortable.
Continue to: In cases I've worked on...
In cases I’ve worked on, I’ve seen some excellent surgeons who require a second opinion as a precondition to operating. This is particularly helpful when patient expectations are uncertain or there is a track record of unsuccessful interventions (eg, chronic back pain with multiple failed surgeries). Furthermore, a second opinion shows diligence, humility, and concern for the patient. It also gives you backup. As Top Gun taught us, there is no need to be a “maverick” when you can have a wingman.
As far as the alleged comment by the cardiologist’s nurse: We don’t know for certain if this actually happened—but if it did, it was unwarranted and foolish. Any jury would hear this and conclude the defendant (1) was an ass, (2) had something to hide, or (3) was guarding a profit source. Any way you slice it, this is bad for the patient and ultimately bad for the defendant. Make room in your practice for second opinions.
There was a legal fight regarding the admissibility of what the nurse had said. The defense filed a motion to prevent the plaintiff from telling the jury about the nurse’s statement, on the basis that the nurse’s statement was inadmissible hearsay. The court denied the motion, ruling that the cardiologist’s nurse was his agent and her words could be properly brought before the jury. The court found that the plaintiff relied on that statement in determining whether to have the ICD placed or obtain a second opinion.
This raises an interesting malpractice awareness point: If you are sued for malpractice, anything you had said to a patient, the patient’s family, or your coworkers will be admissible in court as a “party admission,” classified as either nonhearsay or a hearsay exception (assuming the statement was not made as part of a bona fide peer review, in which case it will likely be subject to peer review privilege). As seen in this case, this also applies to people acting as agents on your behalf. Be cautious of what you say and how you say it—and what your practice’s representatives are saying as well.
Interestingly, the jury found for the plaintiff in the amount of $1.75 million, but they declined to award punitive damages, which are designed to punish defendants rather than compensate the plaintiff. In Arkansas, the standard for punitive damages is tough; the plaintiff must “prove by clear and convincing evidence that the defendant knew or ought to have known, that their conduct would naturally and probably result in injury or damage and that they continued the conduct with malice or in reckless disregard of the consequences from which malice may be inferred.”9 A similar standard exists in most states. Because there were no punitive damages, we can infer the jury did not think the defendant implanted the ICD (for profit) knowing it wasn’t indicated.
Continue to: IN SUMMARY
IN SUMMARY
Consider foreseeable risks of practice interventions; be sure your practice is not on “autopilot,” recommending a common procedure or intervention too frequently. Don’t be threatened by second opinions; welcome them. And watch your words—as they say on every police procedural you’ve ever watched, they can be used against you.
A 39-year-old woman presented to an Arkansas cardiologist on February 12, 2010, with complaints of chest pain. The physician conducted an ankle-brachial index (ABI) test to measure the blood pressure in her lower extremity and interpreted it as less than 0.9%. He then ordered an echocardiogram to gauge the patient’s ejection fraction and interpreted the reading at 25%. Both measurements were below the normal average, which prompted the cardiologist to diagnose peripheral vascular disease and congestive heart failure.
The patient was eventually prescribed a course of cardiac medication and monitored over the ensuing months. On April 15, the cardiologist conducted a nuclear stress test; the computer-generated measurement of her ejection fraction was 50%, which the physician adjusted to 42%. In May, the patient underwent cardiac catheterization, which showed no lesions or blockages in the vessels. In the following months, the patient’s medication dosages were increased. On September 27, the cardiologist conducted another echocardiogram, which he read as 30%, and reaffirmed his diagnosis of congestive heart failure.
The physician continued to monitor the patient. On November 11, after being diagnosed with congestive heart failure, the patient was admitted to the hospital, where the cardiologist implanted an automated implantable cardioverter defibrillator (AICD).
On May 18, 2011, while running with her 2 daughters and a friend, the patient suddenly collapsed and experienced electrical currents coursing through her body (5 times). She was driven to a hospital, where it was determined that she did not go into cardiac arrest (which she suspected) but rather her defibrillator malfunctioned. The defibrillator was recalibrated to a higher setting, and she experienced no further issues.
In the ensuing years, the patient continued to follow up with her cardiologist. She eventually filed a lawsuit claiming that he had misdiagnosed congestive heart failure and unnecessarily implanted the AICD. Her experts in cardiology and cardiac electrophysiology testified that the defendant’s readings of the February 2010 ABI and echocardiogram results were incorrect; the ABIs were in fact .128 and .138 and the ejection fractions were 50% to 55% percent—in both instances, normal results. Furthermore, the September 2010 echocardiogram and another taken in February 2011, which showed little change from the first echocardiogram, were also normal, according to the experts.
The experts also opined that American College of Cardiology/American Heart Association guidelines state that a patient’s ejection fraction has to be less than 35% before a defibrillator is placed. Both experts concluded that the plaintiff did not have congestive heart failure and was therefore not a candidate for an AICD. The cardiac electrophysiology expert stated that to be a candidate, a patient must have an enlarged left ventricle—which plaintiff did not have. Moreover, none of the plaintiff’s physical findings were ever consistent with congestive heart failure: She did not have fluid in her lungs, as examinations always revealed clear lungs without congestion; there was no distention in her jugular veins; she did not experience sleep apnea; she did not lose consciousness; and she only experienced fatigue with exertion. The cardiology expert further faulted the defendant for failing to adjust the patient’s medication dosages to optimize her cardiac repair.
The defense maintained that the defendant’s treatment of the patient met the standard of care. According to the defense, the defendant’s judgment and interpretation of the patient’s ABI and echocardiogram results were medically sound and the defibrillator was necessary.
Continue to: VERDICT
VERDICT
After a 4-day trial and 3 hours of deliberation, the jury found that the defendant was liable and his actions were a factual cause of injury to plaintiff, who was awarded $1.75 million in damages.
COMMENTARY
In this case, the defendant cardiologist placed an AICD (also known as an implantable cardioverter defibrillator, or ICD). There was no allegation that the placement itself was negligent; rather, the claimed negligence was the decision to place it. But the plaintiff’s damages arise from the device’s malfunction—not the cardiologist’s decision to place it.
This case brings up an interesting issue of causation. As most of us know, medical malpractice plaintiffs must show (1) duty, (2) breach, (3) causation, and (4) harm. In law, there are 2 ways to think of causation: “but for” causation and “proximate” causation.
So-called “but for” causation is based on whether any causal relationship exists between an action and an outcome. For example, a drunk driver veers off the highway, through the breakdown lane, and strikes a tree, catching his car on fire. One minute later, a driver in the high-speed lane is captivated by the flaming vehicle, rubbernecks, fails to pay attention to traffic, and rear-ends the vehicle in front of him—injuring the driver of that car. Using “but for” causation, the drunk driver striking the tree “caused” the accident. If that had never happened, the second driver would never have been distracted, and if the driver wasn’t distracted, the second accident would not have occurred.
By contrast, “proximate” causation entails the immediate cause, which is foreseeable. Black’s Law defines proximate cause as “The result of a direct action and cause of loss to property that sets in motion a chain of events that is unbroken and causes damage, injury and destruction with no other interference” (emphasis added).1 Using a proximate causation analysis, the second driver’s negligent failure to pay attention to the road would be the proximate cause of the second crash.
Continue to: Generally, causation analysis...
Generally, causation analysis is limited to proximate cause on the basis that harm is reasonably foreseeable. A famous example is the case of Palsgraf v. Long Island Railroad.2
Mrs. Palsgraf was standing on a train platform. A man carrying an ordinary-looking package rushed to board a moving train, with help from 2 railroad employees (1 in the car and 1 on the platform). As the employees pushed and pulled the man aboard, the package fell onto the tracks. Unbeknownst to everyone but the package’s owner, it contained fireworks—which exploded when the rear wheels of the train ran over the package. The explosion caused a large standing scale to fall over and land on Mrs. Palsgraf, injuring her. This is what law professors live for.
Mrs. Palsgraf sued the railroad, arguing that if the employees had not negligently pushed and pulled the man, the package would not have fallen and would not have exploded, and the scale never would have fallen on her. Mrs. Palsgraf won her trial and won her first appeal. In a famous decision by a famous judge, the win was overturned on the basis that Mrs. Palsgraf’s injuries “were not a reasonably foreseeable consequence of any possible negligence by the railroad.” This case set a foundation of American law regarding reasonable foreseeability, both in terms of identifiable plaintiffs and expected danger.
What does a railroad accident have to do with medical malpractice? In the case described here, we had an arguably negligent medical decision to place the defibrillator. Then we had a malfunction of the device, which caused the plaintiff injury. Was it reasonably foreseeable that the device would malfunction and cause harm—and should the physician be on the hook for that?
Unlike the unforeseeable risk of knocking a simple package to the ground—which unexpectedly turned out to contain fireworks—the risk of device malfunction would be foreseeable. Why? Beyond the usual surgical risks of bleeding and infection, an ICD’s leads can dislodge, the device can fail, and devices can shock inappropriately (with younger patients at increased risk for inappropriate shocks).3,4 These risks are known, and it is highly likely the defendant cardiologist disclosed them on the consent form he asked the plaintiff to sign. The defense could not credibly argue that device malfunction was an unforeseeable risk. The malpractice here was the decision to place the ICD—and because placement wasn’t warranted in this patient, neither were the risks.
Continue to: This brings us to...
This brings us to the first malpractice trap: If you practice in a setting where a procedure is routinely offered, and that treatment has a billable cost, be cautious. Your decision-making can be made to appear driven by a profit motive. The lay public (including jurors) is suspicious of profit motive in medicine—a concept most clinicians find alien and repugnant.
Back in 2009, while outlining his rationale for the Affordable Care Act, President Obama made several statements that earned him swift rebuke from physician groups; I include them here not to incite political rants but to demonstrate the keen suspicion the public has for profit motives in clinical decision-making. On one occasion, he said, “Right now, doctors a lot of times are forced to make decisions based on the fee payment schedule. ... The doctor may look at the reimbursement system and say to himself, ‘You know what? I make a lot more money if I take this kid’s tonsils out.’”5 In another statement, while acknowledging that primary care providers offering preventive diabetes care make “a pittance,” Obama added, “But if that same [patient] ends up getting their foot amputated, that’s $30,000, $40,000, $50,000 immediately the surgeon is reimbursed.”6
For most clinicians, the idea of deciding on a course of treatment because it will be lucrative is an alien concept. Good clinicians base treatment on the accepted medical standard, and cost factors are a distant consideration if one at all.
However, if your practice involves a procedure or intervention that is a particularly lucrative billable event, do your part to play mental “devil’s advocate” and ensure that patients are genuinely in need of the treatment.
In some rare, bad (and usually highly publicized) cases, a procedure will be overused in a patently fraudulent way, which we all recognize is unethical and illegal. However, in other instances, a procedure may be overused because it is familiar and available. We’ve all heard the adage, “If all you have is a hammer, everything looks like a nail.” This “cute” expression holds some truth about the risk for cognitive bias based on the over-reliance on a familiar remedy.7 This particularly involves specialty practices that perform certain procedures frequently.
Continue to: In this case...
In this case, the plaintiff’s nuclear stress test showed an ejection fraction of 50%, which the defendant decreased to 42%. That is substantially different than the first ejection fraction of 25% and the second of 30% in a 39-year-old patient without any clinical signs of congestive heart failure. Did the defendant’s ability to offer an ICD color his appraisal of the patient’s cardiac function?
In closing arguments to the jury, the plaintiff’s attorney probably argued “this defendant behaved as if every human heart could be improved with a battery and wires.” Examine your practice to be sure you aren’t seeing nails where they don’t exist—because tomorrow, they will be the nails in the coffin of your career.
One thing missing from this case summary—but available via court records—is that the plaintiff claimed she had wanted a second opinion but was told she couldn’t have one: “I wanted a second opinion. And when I called [the defendant’s] office and asked ‘Could I have a second opinion,’ his nurse answered the phone and said that if I did get a second opinion, then I couldn’t come back.”8
There are a few aspects to discuss here, one of which is the second malpractice trap: viewing second opinions as an enemy. Most clinicians realize they are actually your friend. However, some providers are threatened by second opinions. It is as if they roll out of bed in the morning and consult the mirror to ask, “Who is the top cardiologist of them all?” and need the validation of that voice saying, “You, Dr. Smith—why of course, you!”
To that I say, forget the mirror, you egotistical so-and-so. Snow White will help protect you, your career, and most importantly, your patient. Allow the second opinion. In fact, integrate an expectation of the them into your practice style, to disarm any feelings of awkwardness, confrontation, or defensiveness. Think of the benefits: If Snow White validates your opinion, you have much stronger case that a course of treatment was indicated. Conversely, if Snow White arrives at a different opinion, she may have seen something you did not, and/or it may also relieve pressure from the patient to take an action with which you were only borderline comfortable.
Continue to: In cases I've worked on...
In cases I’ve worked on, I’ve seen some excellent surgeons who require a second opinion as a precondition to operating. This is particularly helpful when patient expectations are uncertain or there is a track record of unsuccessful interventions (eg, chronic back pain with multiple failed surgeries). Furthermore, a second opinion shows diligence, humility, and concern for the patient. It also gives you backup. As Top Gun taught us, there is no need to be a “maverick” when you can have a wingman.
As far as the alleged comment by the cardiologist’s nurse: We don’t know for certain if this actually happened—but if it did, it was unwarranted and foolish. Any jury would hear this and conclude the defendant (1) was an ass, (2) had something to hide, or (3) was guarding a profit source. Any way you slice it, this is bad for the patient and ultimately bad for the defendant. Make room in your practice for second opinions.
There was a legal fight regarding the admissibility of what the nurse had said. The defense filed a motion to prevent the plaintiff from telling the jury about the nurse’s statement, on the basis that the nurse’s statement was inadmissible hearsay. The court denied the motion, ruling that the cardiologist’s nurse was his agent and her words could be properly brought before the jury. The court found that the plaintiff relied on that statement in determining whether to have the ICD placed or obtain a second opinion.
This raises an interesting malpractice awareness point: If you are sued for malpractice, anything you had said to a patient, the patient’s family, or your coworkers will be admissible in court as a “party admission,” classified as either nonhearsay or a hearsay exception (assuming the statement was not made as part of a bona fide peer review, in which case it will likely be subject to peer review privilege). As seen in this case, this also applies to people acting as agents on your behalf. Be cautious of what you say and how you say it—and what your practice’s representatives are saying as well.
Interestingly, the jury found for the plaintiff in the amount of $1.75 million, but they declined to award punitive damages, which are designed to punish defendants rather than compensate the plaintiff. In Arkansas, the standard for punitive damages is tough; the plaintiff must “prove by clear and convincing evidence that the defendant knew or ought to have known, that their conduct would naturally and probably result in injury or damage and that they continued the conduct with malice or in reckless disregard of the consequences from which malice may be inferred.”9 A similar standard exists in most states. Because there were no punitive damages, we can infer the jury did not think the defendant implanted the ICD (for profit) knowing it wasn’t indicated.
Continue to: IN SUMMARY
IN SUMMARY
Consider foreseeable risks of practice interventions; be sure your practice is not on “autopilot,” recommending a common procedure or intervention too frequently. Don’t be threatened by second opinions; welcome them. And watch your words—as they say on every police procedural you’ve ever watched, they can be used against you.
1. The Law Dictionary. What is proximate cause? https://thelawdictionary.org/proximate-cause. Accessed August 21, 2019.
2. Palsgraf v Long Island R.R. Co (248 NY 339, 162 NE 99 [1928]).
3. Stanford Health Care. Risks: our approach for ICD. https://stanfordhealthcare.org/medical-treatments/i/icd/risks.html. Accessed August 21, 2019.
4. Hofer D, Steffel J, Hürlimann D, et al. Long-term incidence of inappropriate shocks in patients with implantable cardioverter defibrillators in clinical practice—an underestimated complication? J Interv Card Electrophysiol. 2017;50(3):219-226.
5. Transcript: Obama pleads health care case. CNN.com. July 22, 2009. www.cnn.com/2009/POLITICS/07/22/transcript.obama. Accessed August 21, 2019.
6. The White House Office of the Press Secretary. Remarks by the President at Town Hall on Health Insurance Reform in Portsmouth, New Hampshire [press release]. August 11, 2009. https://obamawhitehouse.archives.gov/the-press-office/remarks-president-town-hall-health-insurance-reform-portsmouth-new-hampshire. Accessed August 21, 2019.
7. Maslow AH. The Psychology of Science: a Reconnaissance. New York, NY: Harper & Row; 1966:15.
8. Thornton Dep. 55:3-55:7, March 16, 2014, AR Cir No. CV-2012-640-2.
9. Arkansas Code Title 16. Practice, procedure, and courts § 16-55-206: standards for award of punitive damages. https://codes.findlaw.com/ar/title-16-practice-procedure-and-courts/ar-code-sect-16-55-206.html. Accessed August 21, 2019.
1. The Law Dictionary. What is proximate cause? https://thelawdictionary.org/proximate-cause. Accessed August 21, 2019.
2. Palsgraf v Long Island R.R. Co (248 NY 339, 162 NE 99 [1928]).
3. Stanford Health Care. Risks: our approach for ICD. https://stanfordhealthcare.org/medical-treatments/i/icd/risks.html. Accessed August 21, 2019.
4. Hofer D, Steffel J, Hürlimann D, et al. Long-term incidence of inappropriate shocks in patients with implantable cardioverter defibrillators in clinical practice—an underestimated complication? J Interv Card Electrophysiol. 2017;50(3):219-226.
5. Transcript: Obama pleads health care case. CNN.com. July 22, 2009. www.cnn.com/2009/POLITICS/07/22/transcript.obama. Accessed August 21, 2019.
6. The White House Office of the Press Secretary. Remarks by the President at Town Hall on Health Insurance Reform in Portsmouth, New Hampshire [press release]. August 11, 2009. https://obamawhitehouse.archives.gov/the-press-office/remarks-president-town-hall-health-insurance-reform-portsmouth-new-hampshire. Accessed August 21, 2019.
7. Maslow AH. The Psychology of Science: a Reconnaissance. New York, NY: Harper & Row; 1966:15.
8. Thornton Dep. 55:3-55:7, March 16, 2014, AR Cir No. CV-2012-640-2.
9. Arkansas Code Title 16. Practice, procedure, and courts § 16-55-206: standards for award of punitive damages. https://codes.findlaw.com/ar/title-16-practice-procedure-and-courts/ar-code-sect-16-55-206.html. Accessed August 21, 2019.







