User login
EASI, Other Instruments Recommended to Evaluate Patients With Atopic Dermatitis
recommended.
These include the Eczema Area and Severity Index (EASI), the Validated Investigator Global Assessment for AD (vIGAAD), and the Investigator’s Global Assessment (IGA) multiplied by or measured concurrently with a body surface area (BSA) assessment.
The recommendations are part of a consensus statement based on an updated systematic review conducted by the Harmonizing Outcome Measures for Eczema Clinical Practice (HOME-CP) initiative, whose goal is to identify validated, feasible outcome instruments designed to measure AD in the clinical setting. In the statement, which was published in JAMA Dermatology on May 22, 2024, corresponding author Eric L. Simpson, MD, MCR, professor of dermatology at Oregon Health & Science University, Portland, and coauthors described HOME-CP as “a ‘pick-and-choose’ list of valid and feasible OMIs [outcome measure instruments] that can be incorporated into the practice setting depending on the particular need of that clinic or health system.”
For the effort, the authors implemented a mixed methods design and incorporated systematic reviews and qualitative consensus methods modeled after the HOME core outcome set initiative, which developed a set of consensus-based core outcome sets for clinical trials and clinical practice. In October of 2022, a daylong in-person consensus exercise was held in Montreal, Canada, where attendees met to reach consensus on recommended instruments to measure AD clinical signs in clinical practice, based on an updated systematic review evaluating the validity of clinical signs instruments.
The review included 22 studies describing 16 instruments that assessed AD clinical signs and an additional 12 variants of instruments. The meeting was attended by 34 individuals from 13 countries, including patient and patient advocate research partners, health care professionals, researchers, methodologists, and industry representatives. Consensus was defined as less than 30% disagreement.
Following their daylong consensus exercise, the stakeholders reached consensus on recommendations to use the EASI, the vIGAAD, and an IGA multiplied or measured alongside a BSA measurement to measure the domain of clinical signs of AD in the clinical practice setting. “The use of multiple IGAs, most with insufficient validation, and the diverse methods used to assess BSA prevented participants from making specific recommendations for the exact IGA/BSA instrument,” the authors wrote. “We recommend that clinicians include at least one of the recommended instruments in their clinical practices and in documentation.”
They explained that the ideal method of measuring BSA was difficult to assess “because multiple techniques exist for its measurement, including regional percentages, the Rule of Nines, or the handprint method. Most studies did not report which method was performed, and to our knowledge, no studies have been performed in patients with AD that have formally compared them.”
During the consensus exercise, the authors noted, several clinicians “expressed concern whether the EASI was feasible for universal use in clinical practice given its complexity, long completion time, and documentation/calculation requirements.” But clinicians who commonly perform the EASI in clinical practice said that the time it takes to complete this measure “has dropped substantially and now is not a considerable burden,” they wrote, adding that, “studies have shown that with trained investigators, EASI completion times can be as low as nearly 2 minutes.”
The authors acknowledged certain limitations of their recommendations, including the lack of input from primary care clinicians. “It is unknown whether ClinROMs [clinician-reported outcome measures] for AD clinical signs are used in the primary care setting, especially given the large amount of conditions that are managed simultaneously and the ever-increasing number of primary care documentation requirements,” they wrote.
Robert Sidbury, MD, MPH, chief of the division of dermatology at Seattle Children’s Hospital, who was asked to comment on the consensus statement, said that with the advent of new, improved, and more expensive medications for AD, “it is ever more important that [the clinical] assessment is reliable and reproducible.”
Insurers “are understandably less willing to rubber-stamp approval of more expensive medications without a reliable standard by which to justify such decisions,” he added. “This is even more important in a disease state like atopic dermatitis that lacks a reliable biomarker. Therefore, one or several practical, reliable, validated severity metrics will help standardize and improve AD care.”
Dr. Sidbury, who cochaired the 2023 American Academy of Dermatology guidelines of care for the management of AD in adults with phototherapy and systemic therapies, added that the instruments evaluated in the review “can be challenging for anyone,” not just primary care providers. “The EASI isn’t that easy, and while there is a learning curve and it ultimately does, like anything, become more efficient in the gathering, it is unclear if non-AD researchers will be willing to invest the time” to routinely use it, he said.
Dr. Simpson and several coauthors reported receiving grants and personal fees from multiple pharmaceutical companies. Dr. Sidbury reported that he serves as an investigator for Regeneron, Galderma, UCB, Castle, and Pfizer; is a consultant for LEO, Lilly, Arcutis, Dermavant, and Pierre Fabre; and a speaker for Beiersdorf.
A version of this article appeared on Medscape.com .
recommended.
These include the Eczema Area and Severity Index (EASI), the Validated Investigator Global Assessment for AD (vIGAAD), and the Investigator’s Global Assessment (IGA) multiplied by or measured concurrently with a body surface area (BSA) assessment.
The recommendations are part of a consensus statement based on an updated systematic review conducted by the Harmonizing Outcome Measures for Eczema Clinical Practice (HOME-CP) initiative, whose goal is to identify validated, feasible outcome instruments designed to measure AD in the clinical setting. In the statement, which was published in JAMA Dermatology on May 22, 2024, corresponding author Eric L. Simpson, MD, MCR, professor of dermatology at Oregon Health & Science University, Portland, and coauthors described HOME-CP as “a ‘pick-and-choose’ list of valid and feasible OMIs [outcome measure instruments] that can be incorporated into the practice setting depending on the particular need of that clinic or health system.”
For the effort, the authors implemented a mixed methods design and incorporated systematic reviews and qualitative consensus methods modeled after the HOME core outcome set initiative, which developed a set of consensus-based core outcome sets for clinical trials and clinical practice. In October of 2022, a daylong in-person consensus exercise was held in Montreal, Canada, where attendees met to reach consensus on recommended instruments to measure AD clinical signs in clinical practice, based on an updated systematic review evaluating the validity of clinical signs instruments.
The review included 22 studies describing 16 instruments that assessed AD clinical signs and an additional 12 variants of instruments. The meeting was attended by 34 individuals from 13 countries, including patient and patient advocate research partners, health care professionals, researchers, methodologists, and industry representatives. Consensus was defined as less than 30% disagreement.
Following their daylong consensus exercise, the stakeholders reached consensus on recommendations to use the EASI, the vIGAAD, and an IGA multiplied or measured alongside a BSA measurement to measure the domain of clinical signs of AD in the clinical practice setting. “The use of multiple IGAs, most with insufficient validation, and the diverse methods used to assess BSA prevented participants from making specific recommendations for the exact IGA/BSA instrument,” the authors wrote. “We recommend that clinicians include at least one of the recommended instruments in their clinical practices and in documentation.”
They explained that the ideal method of measuring BSA was difficult to assess “because multiple techniques exist for its measurement, including regional percentages, the Rule of Nines, or the handprint method. Most studies did not report which method was performed, and to our knowledge, no studies have been performed in patients with AD that have formally compared them.”
During the consensus exercise, the authors noted, several clinicians “expressed concern whether the EASI was feasible for universal use in clinical practice given its complexity, long completion time, and documentation/calculation requirements.” But clinicians who commonly perform the EASI in clinical practice said that the time it takes to complete this measure “has dropped substantially and now is not a considerable burden,” they wrote, adding that, “studies have shown that with trained investigators, EASI completion times can be as low as nearly 2 minutes.”
The authors acknowledged certain limitations of their recommendations, including the lack of input from primary care clinicians. “It is unknown whether ClinROMs [clinician-reported outcome measures] for AD clinical signs are used in the primary care setting, especially given the large amount of conditions that are managed simultaneously and the ever-increasing number of primary care documentation requirements,” they wrote.
Robert Sidbury, MD, MPH, chief of the division of dermatology at Seattle Children’s Hospital, who was asked to comment on the consensus statement, said that with the advent of new, improved, and more expensive medications for AD, “it is ever more important that [the clinical] assessment is reliable and reproducible.”
Insurers “are understandably less willing to rubber-stamp approval of more expensive medications without a reliable standard by which to justify such decisions,” he added. “This is even more important in a disease state like atopic dermatitis that lacks a reliable biomarker. Therefore, one or several practical, reliable, validated severity metrics will help standardize and improve AD care.”
Dr. Sidbury, who cochaired the 2023 American Academy of Dermatology guidelines of care for the management of AD in adults with phototherapy and systemic therapies, added that the instruments evaluated in the review “can be challenging for anyone,” not just primary care providers. “The EASI isn’t that easy, and while there is a learning curve and it ultimately does, like anything, become more efficient in the gathering, it is unclear if non-AD researchers will be willing to invest the time” to routinely use it, he said.
Dr. Simpson and several coauthors reported receiving grants and personal fees from multiple pharmaceutical companies. Dr. Sidbury reported that he serves as an investigator for Regeneron, Galderma, UCB, Castle, and Pfizer; is a consultant for LEO, Lilly, Arcutis, Dermavant, and Pierre Fabre; and a speaker for Beiersdorf.
A version of this article appeared on Medscape.com .
recommended.
These include the Eczema Area and Severity Index (EASI), the Validated Investigator Global Assessment for AD (vIGAAD), and the Investigator’s Global Assessment (IGA) multiplied by or measured concurrently with a body surface area (BSA) assessment.
The recommendations are part of a consensus statement based on an updated systematic review conducted by the Harmonizing Outcome Measures for Eczema Clinical Practice (HOME-CP) initiative, whose goal is to identify validated, feasible outcome instruments designed to measure AD in the clinical setting. In the statement, which was published in JAMA Dermatology on May 22, 2024, corresponding author Eric L. Simpson, MD, MCR, professor of dermatology at Oregon Health & Science University, Portland, and coauthors described HOME-CP as “a ‘pick-and-choose’ list of valid and feasible OMIs [outcome measure instruments] that can be incorporated into the practice setting depending on the particular need of that clinic or health system.”
For the effort, the authors implemented a mixed methods design and incorporated systematic reviews and qualitative consensus methods modeled after the HOME core outcome set initiative, which developed a set of consensus-based core outcome sets for clinical trials and clinical practice. In October of 2022, a daylong in-person consensus exercise was held in Montreal, Canada, where attendees met to reach consensus on recommended instruments to measure AD clinical signs in clinical practice, based on an updated systematic review evaluating the validity of clinical signs instruments.
The review included 22 studies describing 16 instruments that assessed AD clinical signs and an additional 12 variants of instruments. The meeting was attended by 34 individuals from 13 countries, including patient and patient advocate research partners, health care professionals, researchers, methodologists, and industry representatives. Consensus was defined as less than 30% disagreement.
Following their daylong consensus exercise, the stakeholders reached consensus on recommendations to use the EASI, the vIGAAD, and an IGA multiplied or measured alongside a BSA measurement to measure the domain of clinical signs of AD in the clinical practice setting. “The use of multiple IGAs, most with insufficient validation, and the diverse methods used to assess BSA prevented participants from making specific recommendations for the exact IGA/BSA instrument,” the authors wrote. “We recommend that clinicians include at least one of the recommended instruments in their clinical practices and in documentation.”
They explained that the ideal method of measuring BSA was difficult to assess “because multiple techniques exist for its measurement, including regional percentages, the Rule of Nines, or the handprint method. Most studies did not report which method was performed, and to our knowledge, no studies have been performed in patients with AD that have formally compared them.”
During the consensus exercise, the authors noted, several clinicians “expressed concern whether the EASI was feasible for universal use in clinical practice given its complexity, long completion time, and documentation/calculation requirements.” But clinicians who commonly perform the EASI in clinical practice said that the time it takes to complete this measure “has dropped substantially and now is not a considerable burden,” they wrote, adding that, “studies have shown that with trained investigators, EASI completion times can be as low as nearly 2 minutes.”
The authors acknowledged certain limitations of their recommendations, including the lack of input from primary care clinicians. “It is unknown whether ClinROMs [clinician-reported outcome measures] for AD clinical signs are used in the primary care setting, especially given the large amount of conditions that are managed simultaneously and the ever-increasing number of primary care documentation requirements,” they wrote.
Robert Sidbury, MD, MPH, chief of the division of dermatology at Seattle Children’s Hospital, who was asked to comment on the consensus statement, said that with the advent of new, improved, and more expensive medications for AD, “it is ever more important that [the clinical] assessment is reliable and reproducible.”
Insurers “are understandably less willing to rubber-stamp approval of more expensive medications without a reliable standard by which to justify such decisions,” he added. “This is even more important in a disease state like atopic dermatitis that lacks a reliable biomarker. Therefore, one or several practical, reliable, validated severity metrics will help standardize and improve AD care.”
Dr. Sidbury, who cochaired the 2023 American Academy of Dermatology guidelines of care for the management of AD in adults with phototherapy and systemic therapies, added that the instruments evaluated in the review “can be challenging for anyone,” not just primary care providers. “The EASI isn’t that easy, and while there is a learning curve and it ultimately does, like anything, become more efficient in the gathering, it is unclear if non-AD researchers will be willing to invest the time” to routinely use it, he said.
Dr. Simpson and several coauthors reported receiving grants and personal fees from multiple pharmaceutical companies. Dr. Sidbury reported that he serves as an investigator for Regeneron, Galderma, UCB, Castle, and Pfizer; is a consultant for LEO, Lilly, Arcutis, Dermavant, and Pierre Fabre; and a speaker for Beiersdorf.
A version of this article appeared on Medscape.com .
FROM JAMA DERMATOLOGY
Decision-Making Help for Kids With Disabilities Entering Adulthood
About one in six children (17%) between 3 and 17 years have a disability, which may affect their ability to make decisions when they transition to adulthood.
Typically, at age 18, a young adult assumes rights such as the legal right to make medical decisions (including reproductive decisions), and mental health, financial, and education decisions.
.
Several Options in the Continuum
The AAP describes a continuum of decision-making for youth with IDD from fully autonomous decisions to decisions made by an appointed guardian.
Highlighting an array of options is one way this paper is helpful, said Matthew Siegel, MD, chief of clinical enterprise with the Department of Psychiatry & Behavioral Sciences at Boston Children’s Hospital in Massachusetts. “I suspect that for a lot of practitioners what they’re aware of is guardianship or no guardianship.” These authors highlight that the options are more nuanced, he said.
Pediatricians have widely different ideas about what their role should be in facilitating decision-making in the transition period, he said, so this paper helps clarify what advocacy and discussion are needed.
The paper, written by first author Renee M. Turchi, MD, MPH, and colleagues on behalf of the Council on Children with Disabilities’ Committee on Medical Liability and Risk Management, states that, “The goal should always be the least restrictive decision-making that balances autonomy with safety and supports.”
One Alternative Is Supported Decision-Making
Supported decision-making is one alternative to guardianship. Authors explain that under that framework, a patient can choose a trusted support person and create an agreement with that person on what kinds of decisions the person needs help with and how much assistance is needed. The individual makes the final decision, not the support person.
Authors explain the benefits of that approach: “Individuals with IDD who use supported decision-making report increased confidence in themselves and their decision-making, improved decision-making skills, increased engagement with their community, and perceived more control of their lives,” the authors wrote.
Another option for people with IDD might be, rather than formally naming a substitute decision-maker, allowing a parent or caregiver access to their electronic health record or allowing that person to have independent discussions with their physician.
With guardianship, also called conservatorship in some states, a court requires clear and convincing evidence that the youth is not competent to make his or her own decisions. The court may order evaluations by many professionals, including pediatricians.
State-Specific Legal Information Is Available
Many states have recently enacted laws surrounding supported decision-making and guardianship. The authors reference a national resource center website that details the legislation for each state and points to resources and tools for pediatricians, families, and patients.
“Historically, pediatricians have rarely discussed the legal aspects of transition to adult-oriented services with the youth with IDD and subsequently, their families,” the authors wrote.
Discussions Should Start Early
Ideally, the authors wrote, the discussions about what level of supports might be necessary in the transition to adulthood should start at age 12-14 and include the youth, teachers, parents, and the medical team.
That’s earlier than some of the previous guidance, Dr. Siegel said, and it will be important to evaluate future evidence on the best age to start planning “both from a cognitive development standpoint and from a practicality standpoint.”
The authors point out that the needs for level of support may change and “pediatricians can reevaluate the decision-making arrangement as part of the annual physical/mental examinations to align with the youth’s desires, needs, and decision-making abilities over time.”
The authors and Dr. Siegel report no relevant financial relationships.
About one in six children (17%) between 3 and 17 years have a disability, which may affect their ability to make decisions when they transition to adulthood.
Typically, at age 18, a young adult assumes rights such as the legal right to make medical decisions (including reproductive decisions), and mental health, financial, and education decisions.
.
Several Options in the Continuum
The AAP describes a continuum of decision-making for youth with IDD from fully autonomous decisions to decisions made by an appointed guardian.
Highlighting an array of options is one way this paper is helpful, said Matthew Siegel, MD, chief of clinical enterprise with the Department of Psychiatry & Behavioral Sciences at Boston Children’s Hospital in Massachusetts. “I suspect that for a lot of practitioners what they’re aware of is guardianship or no guardianship.” These authors highlight that the options are more nuanced, he said.
Pediatricians have widely different ideas about what their role should be in facilitating decision-making in the transition period, he said, so this paper helps clarify what advocacy and discussion are needed.
The paper, written by first author Renee M. Turchi, MD, MPH, and colleagues on behalf of the Council on Children with Disabilities’ Committee on Medical Liability and Risk Management, states that, “The goal should always be the least restrictive decision-making that balances autonomy with safety and supports.”
One Alternative Is Supported Decision-Making
Supported decision-making is one alternative to guardianship. Authors explain that under that framework, a patient can choose a trusted support person and create an agreement with that person on what kinds of decisions the person needs help with and how much assistance is needed. The individual makes the final decision, not the support person.
Authors explain the benefits of that approach: “Individuals with IDD who use supported decision-making report increased confidence in themselves and their decision-making, improved decision-making skills, increased engagement with their community, and perceived more control of their lives,” the authors wrote.
Another option for people with IDD might be, rather than formally naming a substitute decision-maker, allowing a parent or caregiver access to their electronic health record or allowing that person to have independent discussions with their physician.
With guardianship, also called conservatorship in some states, a court requires clear and convincing evidence that the youth is not competent to make his or her own decisions. The court may order evaluations by many professionals, including pediatricians.
State-Specific Legal Information Is Available
Many states have recently enacted laws surrounding supported decision-making and guardianship. The authors reference a national resource center website that details the legislation for each state and points to resources and tools for pediatricians, families, and patients.
“Historically, pediatricians have rarely discussed the legal aspects of transition to adult-oriented services with the youth with IDD and subsequently, their families,” the authors wrote.
Discussions Should Start Early
Ideally, the authors wrote, the discussions about what level of supports might be necessary in the transition to adulthood should start at age 12-14 and include the youth, teachers, parents, and the medical team.
That’s earlier than some of the previous guidance, Dr. Siegel said, and it will be important to evaluate future evidence on the best age to start planning “both from a cognitive development standpoint and from a practicality standpoint.”
The authors point out that the needs for level of support may change and “pediatricians can reevaluate the decision-making arrangement as part of the annual physical/mental examinations to align with the youth’s desires, needs, and decision-making abilities over time.”
The authors and Dr. Siegel report no relevant financial relationships.
About one in six children (17%) between 3 and 17 years have a disability, which may affect their ability to make decisions when they transition to adulthood.
Typically, at age 18, a young adult assumes rights such as the legal right to make medical decisions (including reproductive decisions), and mental health, financial, and education decisions.
.
Several Options in the Continuum
The AAP describes a continuum of decision-making for youth with IDD from fully autonomous decisions to decisions made by an appointed guardian.
Highlighting an array of options is one way this paper is helpful, said Matthew Siegel, MD, chief of clinical enterprise with the Department of Psychiatry & Behavioral Sciences at Boston Children’s Hospital in Massachusetts. “I suspect that for a lot of practitioners what they’re aware of is guardianship or no guardianship.” These authors highlight that the options are more nuanced, he said.
Pediatricians have widely different ideas about what their role should be in facilitating decision-making in the transition period, he said, so this paper helps clarify what advocacy and discussion are needed.
The paper, written by first author Renee M. Turchi, MD, MPH, and colleagues on behalf of the Council on Children with Disabilities’ Committee on Medical Liability and Risk Management, states that, “The goal should always be the least restrictive decision-making that balances autonomy with safety and supports.”
One Alternative Is Supported Decision-Making
Supported decision-making is one alternative to guardianship. Authors explain that under that framework, a patient can choose a trusted support person and create an agreement with that person on what kinds of decisions the person needs help with and how much assistance is needed. The individual makes the final decision, not the support person.
Authors explain the benefits of that approach: “Individuals with IDD who use supported decision-making report increased confidence in themselves and their decision-making, improved decision-making skills, increased engagement with their community, and perceived more control of their lives,” the authors wrote.
Another option for people with IDD might be, rather than formally naming a substitute decision-maker, allowing a parent or caregiver access to their electronic health record or allowing that person to have independent discussions with their physician.
With guardianship, also called conservatorship in some states, a court requires clear and convincing evidence that the youth is not competent to make his or her own decisions. The court may order evaluations by many professionals, including pediatricians.
State-Specific Legal Information Is Available
Many states have recently enacted laws surrounding supported decision-making and guardianship. The authors reference a national resource center website that details the legislation for each state and points to resources and tools for pediatricians, families, and patients.
“Historically, pediatricians have rarely discussed the legal aspects of transition to adult-oriented services with the youth with IDD and subsequently, their families,” the authors wrote.
Discussions Should Start Early
Ideally, the authors wrote, the discussions about what level of supports might be necessary in the transition to adulthood should start at age 12-14 and include the youth, teachers, parents, and the medical team.
That’s earlier than some of the previous guidance, Dr. Siegel said, and it will be important to evaluate future evidence on the best age to start planning “both from a cognitive development standpoint and from a practicality standpoint.”
The authors point out that the needs for level of support may change and “pediatricians can reevaluate the decision-making arrangement as part of the annual physical/mental examinations to align with the youth’s desires, needs, and decision-making abilities over time.”
The authors and Dr. Siegel report no relevant financial relationships.
FROM PEDIATRICS
Treatments for Early HS Range From Topical Therapies to Laser Hair Removal
This can be challenging because to date, no Food and Drug Administration–approved treatments exist for early-stage HS and only two biologics exist for moderate to severe disease.
“For someone with occasional nodules and abscesses, we often use antibiotics and topical antiseptics,” Christopher Sayed, MD, a dermatologist at the HS and Follicular Disorders Clinic at the University of North Carolina, Chapel Hill, told this news organization. “We may use these daily for weeks or months or just provide them to use for 1-2 weeks at a time for intermittent flares if a patient doesn’t want to take a pill every day,” he said. “For women, hormonal options like oral contraceptive pills and spironolactone can be a great option” if they don’t mind taking a daily pill.
Topical options that Jennifer L. Hsiao, MD, reaches for in her role as director of the HS clinic at the University of Southern California, Los Angeles, include chlorhexidine wash, topical clindamycin, and topical resorcinol. Systemic medications include oral antibiotics such as doxycycline or clindamycin, while hormonal options include oral contraceptives and/or spironolactone for women and finasteride for men.
Laser hair removal for both men and women can also help treat lesions and abscesses in the groin and axillae, since reducing hair follicles tends to result in fewer follicles that become inflamed and form nodules and abscesses over time, “but it requires multiple visits and not all patients have access to it,” Dr. Sayed said. “Once patients start to develop tunnels or scars or fail to respond to some of these other treatments, I am quick to open the conversation on biologics to help avoid progression and long-term need for surgery.”
Metformin Among Options to Consider
According to Dr. Hsiao, other treatment options to consider trying in patients with mild HS include metformin, “especially in patients who also have prediabetes, PCOS, or obesity;” isotretinoin if the patient has concomitant severe acne; botulinum toxin injections; apremilast or topical roflumilast, and antihyperhidrosis medications such as prescription aluminum chloride topicals, glycopyrronium wipes, and glycopyrrolate.
Recommending lifestyle modifications such as smoking cessation and weight loss for patients diagnosed with early-stage HS is “challenging,” Dr. Sayed said, “because the evidence on different triggers and lifestyle modifications isn’t very strong. There can also be a lot of stigmas around weight and smoking in HS, and it can alienate patients to go straight to these topics in the first visit.”
Many patients also ask what dietary changes they can make to improve their HS. “The most common things patients tend to bring up are dairy avoidance and reducing carbohydrates,” he said. “Supplements like zinc and turmeric are also frequently brought up by patients and some find them helpful. Once rapport is built, I may discuss smoking cessation as potentially helping prevent as much activity over time or weight loss as possibly helping improve response to treatments, but I don’t promise that these things always help since modifying them doesn’t always lead to improvement.”
Dr. Hsiao noted that existing research suggests that following a Mediterranean diet may benefit HS symptoms.
Early Data on Ruxolitinib Cream Promising
At the 2024 annual meeting of the American Academy of Dermatology, researchers reported on the results of a phase 2 study, which found that topical 1.5% ruxolitinib, a Janus kinase (JAK) inhibitor (currently FDA-approved for atopic dermatitis) was effective in reducing abscess and inflammatory nodule count in patients with mild HS. “There is a major need for this kind of option, and the early results are promising,” said Dr. Sayed, who was not involved with the study. “It’s very difficult to get this covered for patients currently since it is off label for HS. We’ve gotten it for a few patients, and one has really liked it, but it’s unclear how consistent the others were with their use, and their level of improvement was not clear to me.”
For mild HS, he added, “the most important area in which we’ve seen growing evidence is around hair removal lasers such as Nd:YAG and alexandrite lasers. Improving access for patients is a major priority in the coming years.”
According to Dr. Hsiao, other approaches being studied for treating mild HS include a topical aryl hydrocarbon receptor agonist known as AT193, and oral medications, such as phosphodiesterase-4 inhibitors. Laser therapies are also being studied, “such as fractional ablative CO2 laser therapy combined with topical triamcinolone,” she said. “However, the majority of ongoing HS trials are for moderate to severe disease, so there is certainly a need for more investigation into mild HS treatment approaches.”
Dr. Sayed disclosed that he is secretary of the HS Foundation and a member of the European HS Foundation. He has served as a consultant for AbbVie, Alumis, AstraZeneca, Incyte, InflaRx, Novartis, Sanofi, Sonoma Biotherapeutics, and UCB; as a speaker for AbbVie, Novartis, and UCB; and as an investigator for Chemocentryx, Incyte, InflaRx, Novartis, and UCB. Dr. Hsiao disclosed that she is a member of the board of directors for the HS Foundation and has served as a consultant for AbbVie, Aclaris, Boehringer Ingelheim, Incyte, Novartis, and UCB; as a speaker for AbbVie, Novartis, Sanofi Regeneron, and UCB; and as an investigator for Amgen, Boehringer Ingelheim, and Incyte.
A version of this article first appeared on Medscape.com.
This can be challenging because to date, no Food and Drug Administration–approved treatments exist for early-stage HS and only two biologics exist for moderate to severe disease.
“For someone with occasional nodules and abscesses, we often use antibiotics and topical antiseptics,” Christopher Sayed, MD, a dermatologist at the HS and Follicular Disorders Clinic at the University of North Carolina, Chapel Hill, told this news organization. “We may use these daily for weeks or months or just provide them to use for 1-2 weeks at a time for intermittent flares if a patient doesn’t want to take a pill every day,” he said. “For women, hormonal options like oral contraceptive pills and spironolactone can be a great option” if they don’t mind taking a daily pill.
Topical options that Jennifer L. Hsiao, MD, reaches for in her role as director of the HS clinic at the University of Southern California, Los Angeles, include chlorhexidine wash, topical clindamycin, and topical resorcinol. Systemic medications include oral antibiotics such as doxycycline or clindamycin, while hormonal options include oral contraceptives and/or spironolactone for women and finasteride for men.
Laser hair removal for both men and women can also help treat lesions and abscesses in the groin and axillae, since reducing hair follicles tends to result in fewer follicles that become inflamed and form nodules and abscesses over time, “but it requires multiple visits and not all patients have access to it,” Dr. Sayed said. “Once patients start to develop tunnels or scars or fail to respond to some of these other treatments, I am quick to open the conversation on biologics to help avoid progression and long-term need for surgery.”
Metformin Among Options to Consider
According to Dr. Hsiao, other treatment options to consider trying in patients with mild HS include metformin, “especially in patients who also have prediabetes, PCOS, or obesity;” isotretinoin if the patient has concomitant severe acne; botulinum toxin injections; apremilast or topical roflumilast, and antihyperhidrosis medications such as prescription aluminum chloride topicals, glycopyrronium wipes, and glycopyrrolate.
Recommending lifestyle modifications such as smoking cessation and weight loss for patients diagnosed with early-stage HS is “challenging,” Dr. Sayed said, “because the evidence on different triggers and lifestyle modifications isn’t very strong. There can also be a lot of stigmas around weight and smoking in HS, and it can alienate patients to go straight to these topics in the first visit.”
Many patients also ask what dietary changes they can make to improve their HS. “The most common things patients tend to bring up are dairy avoidance and reducing carbohydrates,” he said. “Supplements like zinc and turmeric are also frequently brought up by patients and some find them helpful. Once rapport is built, I may discuss smoking cessation as potentially helping prevent as much activity over time or weight loss as possibly helping improve response to treatments, but I don’t promise that these things always help since modifying them doesn’t always lead to improvement.”
Dr. Hsiao noted that existing research suggests that following a Mediterranean diet may benefit HS symptoms.
Early Data on Ruxolitinib Cream Promising
At the 2024 annual meeting of the American Academy of Dermatology, researchers reported on the results of a phase 2 study, which found that topical 1.5% ruxolitinib, a Janus kinase (JAK) inhibitor (currently FDA-approved for atopic dermatitis) was effective in reducing abscess and inflammatory nodule count in patients with mild HS. “There is a major need for this kind of option, and the early results are promising,” said Dr. Sayed, who was not involved with the study. “It’s very difficult to get this covered for patients currently since it is off label for HS. We’ve gotten it for a few patients, and one has really liked it, but it’s unclear how consistent the others were with their use, and their level of improvement was not clear to me.”
For mild HS, he added, “the most important area in which we’ve seen growing evidence is around hair removal lasers such as Nd:YAG and alexandrite lasers. Improving access for patients is a major priority in the coming years.”
According to Dr. Hsiao, other approaches being studied for treating mild HS include a topical aryl hydrocarbon receptor agonist known as AT193, and oral medications, such as phosphodiesterase-4 inhibitors. Laser therapies are also being studied, “such as fractional ablative CO2 laser therapy combined with topical triamcinolone,” she said. “However, the majority of ongoing HS trials are for moderate to severe disease, so there is certainly a need for more investigation into mild HS treatment approaches.”
Dr. Sayed disclosed that he is secretary of the HS Foundation and a member of the European HS Foundation. He has served as a consultant for AbbVie, Alumis, AstraZeneca, Incyte, InflaRx, Novartis, Sanofi, Sonoma Biotherapeutics, and UCB; as a speaker for AbbVie, Novartis, and UCB; and as an investigator for Chemocentryx, Incyte, InflaRx, Novartis, and UCB. Dr. Hsiao disclosed that she is a member of the board of directors for the HS Foundation and has served as a consultant for AbbVie, Aclaris, Boehringer Ingelheim, Incyte, Novartis, and UCB; as a speaker for AbbVie, Novartis, Sanofi Regeneron, and UCB; and as an investigator for Amgen, Boehringer Ingelheim, and Incyte.
A version of this article first appeared on Medscape.com.
This can be challenging because to date, no Food and Drug Administration–approved treatments exist for early-stage HS and only two biologics exist for moderate to severe disease.
“For someone with occasional nodules and abscesses, we often use antibiotics and topical antiseptics,” Christopher Sayed, MD, a dermatologist at the HS and Follicular Disorders Clinic at the University of North Carolina, Chapel Hill, told this news organization. “We may use these daily for weeks or months or just provide them to use for 1-2 weeks at a time for intermittent flares if a patient doesn’t want to take a pill every day,” he said. “For women, hormonal options like oral contraceptive pills and spironolactone can be a great option” if they don’t mind taking a daily pill.
Topical options that Jennifer L. Hsiao, MD, reaches for in her role as director of the HS clinic at the University of Southern California, Los Angeles, include chlorhexidine wash, topical clindamycin, and topical resorcinol. Systemic medications include oral antibiotics such as doxycycline or clindamycin, while hormonal options include oral contraceptives and/or spironolactone for women and finasteride for men.
Laser hair removal for both men and women can also help treat lesions and abscesses in the groin and axillae, since reducing hair follicles tends to result in fewer follicles that become inflamed and form nodules and abscesses over time, “but it requires multiple visits and not all patients have access to it,” Dr. Sayed said. “Once patients start to develop tunnels or scars or fail to respond to some of these other treatments, I am quick to open the conversation on biologics to help avoid progression and long-term need for surgery.”
Metformin Among Options to Consider
According to Dr. Hsiao, other treatment options to consider trying in patients with mild HS include metformin, “especially in patients who also have prediabetes, PCOS, or obesity;” isotretinoin if the patient has concomitant severe acne; botulinum toxin injections; apremilast or topical roflumilast, and antihyperhidrosis medications such as prescription aluminum chloride topicals, glycopyrronium wipes, and glycopyrrolate.
Recommending lifestyle modifications such as smoking cessation and weight loss for patients diagnosed with early-stage HS is “challenging,” Dr. Sayed said, “because the evidence on different triggers and lifestyle modifications isn’t very strong. There can also be a lot of stigmas around weight and smoking in HS, and it can alienate patients to go straight to these topics in the first visit.”
Many patients also ask what dietary changes they can make to improve their HS. “The most common things patients tend to bring up are dairy avoidance and reducing carbohydrates,” he said. “Supplements like zinc and turmeric are also frequently brought up by patients and some find them helpful. Once rapport is built, I may discuss smoking cessation as potentially helping prevent as much activity over time or weight loss as possibly helping improve response to treatments, but I don’t promise that these things always help since modifying them doesn’t always lead to improvement.”
Dr. Hsiao noted that existing research suggests that following a Mediterranean diet may benefit HS symptoms.
Early Data on Ruxolitinib Cream Promising
At the 2024 annual meeting of the American Academy of Dermatology, researchers reported on the results of a phase 2 study, which found that topical 1.5% ruxolitinib, a Janus kinase (JAK) inhibitor (currently FDA-approved for atopic dermatitis) was effective in reducing abscess and inflammatory nodule count in patients with mild HS. “There is a major need for this kind of option, and the early results are promising,” said Dr. Sayed, who was not involved with the study. “It’s very difficult to get this covered for patients currently since it is off label for HS. We’ve gotten it for a few patients, and one has really liked it, but it’s unclear how consistent the others were with their use, and their level of improvement was not clear to me.”
For mild HS, he added, “the most important area in which we’ve seen growing evidence is around hair removal lasers such as Nd:YAG and alexandrite lasers. Improving access for patients is a major priority in the coming years.”
According to Dr. Hsiao, other approaches being studied for treating mild HS include a topical aryl hydrocarbon receptor agonist known as AT193, and oral medications, such as phosphodiesterase-4 inhibitors. Laser therapies are also being studied, “such as fractional ablative CO2 laser therapy combined with topical triamcinolone,” she said. “However, the majority of ongoing HS trials are for moderate to severe disease, so there is certainly a need for more investigation into mild HS treatment approaches.”
Dr. Sayed disclosed that he is secretary of the HS Foundation and a member of the European HS Foundation. He has served as a consultant for AbbVie, Alumis, AstraZeneca, Incyte, InflaRx, Novartis, Sanofi, Sonoma Biotherapeutics, and UCB; as a speaker for AbbVie, Novartis, and UCB; and as an investigator for Chemocentryx, Incyte, InflaRx, Novartis, and UCB. Dr. Hsiao disclosed that she is a member of the board of directors for the HS Foundation and has served as a consultant for AbbVie, Aclaris, Boehringer Ingelheim, Incyte, Novartis, and UCB; as a speaker for AbbVie, Novartis, Sanofi Regeneron, and UCB; and as an investigator for Amgen, Boehringer Ingelheim, and Incyte.
A version of this article first appeared on Medscape.com.
Diagnosing Mild Hidradenitis Suppurativa: Early Stage Can Mimic Other Diseases
, such as an infection, folliculitis, and acne.
According to 2019 guidelines from the United States and Canadian hidradenitis suppurativa foundations, the diagnostic criteria for HS in general are the presence of typical lesions such as abscesses, nodules, and tunnels in classic locations such as underarms, groins, and buttocks that recur over the course of at least 6 months. “There is no need for additional testing or imaging to make the diagnosis,” said Dr. Sayed, co-chair of the 2019 guidelines work group, who sees patients at the HS and Follicular Disorders Clinic at the University of North Carolina, Chapel Hill. “In many ways, the diagnosis should be very simple since the presentation is classic in most cases, though it can be confusing in the first 6 months or so.”
Persistence, Recurrence Major Clues
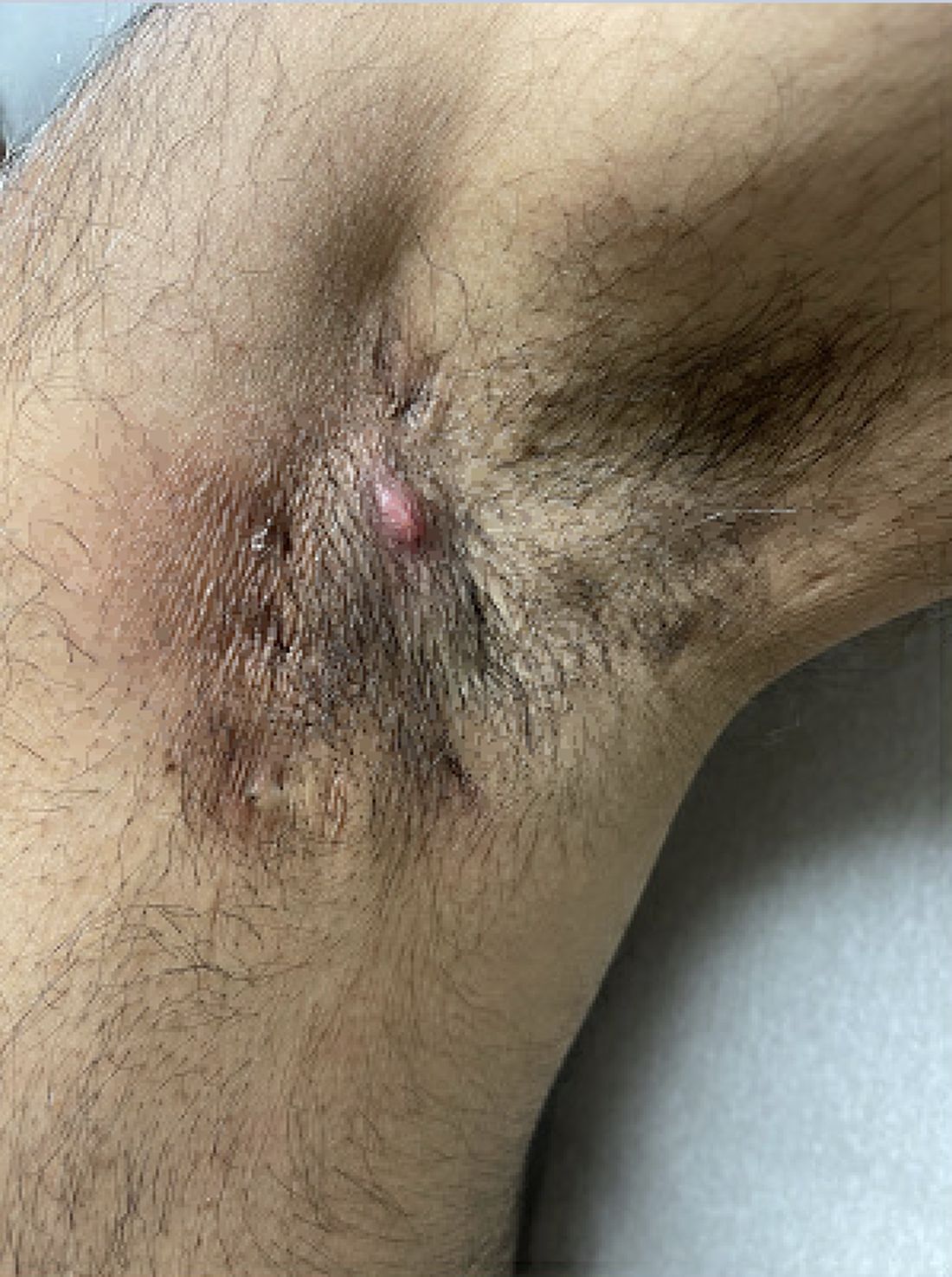
Prior to being diagnosed with Hurley stage I HS — characterized by recurrent nodules and abscesses with minimal scars, according to the guidelines — most people figure they’ve been getting recurrent Staphylococcus aureus infections or are having trouble with ingrown hairs from shaving, he continued. They may also say they get “boils” without an understanding of what has been causing them.
“Early HS can mimic an intense folliculitis or furuncles that can sometimes be caused by Staphylococcus infections, but the history of persistence or recurrence for months, despite treatment that should cover something like a Staph infection is a major clue,” Dr. Sayed said. “Thanks to improved resources on the internet, more patients, compared to several years ago, come in asking about HS after they’ve done their own research. As public awareness improves, hopefully this trend will grow, and patients will be diagnosed and treated earlier.” Family history is also a strong predictor of HS, since about half of patients have first-degree relatives who have a history of HS, he noted.
Clinicians can use the Hurley staging system to characterize the extent of disease and the Dermatology Life Quality Index to measure the impact of HS on quality of life. “We perform these assessments in our specialty clinic at each visit, but they are not necessary for diagnosis,” Dr. Sayed told this news organization.
The ‘2-2-6 Rule’
When she sees a patient who might have HS, Jennifer L. Hsiao, MD, a dermatologist who directs the HS clinic at the University of Southern California, Los Angeles, follows the “2-2-6 rule,” which involves asking patients if they have had 2 episodes of 2 or more abscesses in 6 months. “If the patient answers yes, there’s a high likelihood that person has HS,” she said.
Hurley stage I HS is defined as nodules and abscesses without sinus tracts (tunnels) or scarring. But in Dr. Hsiao’s opinion, the Hurley staging system “is not the best way to characterize disease activity” because some patients meet criteria for Hurley stage I disease, meaning they do not have any scars or sinus tracts/tunnels, “but they have high disease activity with several inflammatory nodules and large painful abscesses that are limiting their quality of life and ability to function.”
Most cases of early-stage HS can be diagnosed in a single clinic visit, but some patients may present with a limited history of disease. For example, they may report having only had one episode of an axillary abscess or one episode of a few folliculitis-like papules in the groin. “In the absence of other physical exam findings suggestive of HS, such as open or double-headed comedones in flexural regions, I tell the patient that it is too early to call their condition HS, and I recommend that if they have another episode to call the office for an appointment for evaluation,” Dr. Hsiao said in an interview.
“What sets HS apart from an isolated incidence of a Staphylococcus aureus furuncle is the history of recurrence,” she added. To better characterize HS disease severity, she uses the six-point HS Physician Global Assessment score, a scale from 0 to 5, which classifies a patient as having moderate HS if they have five or more inflammatory nodules, or one abscess and one or more inflammatory nodule(s), without the requirement of demonstrating a scar or tunnel on a physical exam.
To help guide management decisions, Dr. Hsiao also considers asking patients with early-stage HS the following questions:
- Do you have a primary care provider (PCP)? PCPs are important care partners for patients with HS doctor to help screen for the comorbidities associated with the condition.
- What seems to make your HS worse? This can help identify potential triggers to avoid.
- What other medical conditions do you have?
- How would you describe the impact HS has on your quality of life?
- For women: Does your HS get worse around your period? “This can help to identify a potential hormonal trigger,” she said. “If the patient answers ‘yes,’ I would strongly consider a combined oral contraceptive pill and/or spironolactone as part of the patient’s treatment regimen.”
‘Window of Opportunity’ to Intervene
According to Dr. Hsiao, there has been a paradigm shift in the approach to HS management that emphasizes a “window of opportunity,” where earlier initiation of appropriate long-term immunomodulator therapy is recommended to try to mitigate disease progression. The development of tunnels and scars is a telltale sign that permanent tissue destruction is occurring, and the patient’s HS is no longer mild.
Ideally, a conversation about adalimumab, a tumor necrosis factor inhibitor, and secukinumab, an interleukin-17A antagonist (the two currently Food and Drug Administration–approved medications for HS, for moderate to severe disease/Hurley stage II/III) will have already been started with patients prior to development of a high tunnel or scar burden, signs of later-stage disease.
“Medications like this have the potential to slow and prevent that progression and reduce the surgical burden patients face over time, which is a major priority,” Dr. Sayed said. He noted that while comfort level with managing HS can vary among clinicians, “I’d encourage dermatologists to stay engaged with these patients because our training in the medical and surgical management of complex diseases like this is unmatched among other specialties,” he said. “Education of colleagues in other specialties should also be a big priority, especially for those in urgent care, emergency medicine, surgery, and ob.gyn. who often encounter these patients and may be less familiar” with HS.
Besides the North American clinical management guidelines for HS, which are expected to be updated in the next 18-24 months, as well as comorbidity screening recommendations for HS published in 2022, another resource Dr. Sayed and Dr. Hsiao recommend is the HS Foundation website, which features a link to Continuing Medical Education video lectures. The foundation also hosts an annual Symposium on HS Advances. This year’s event is scheduled in November in Austin, Texas.
Dr. Sayed disclosed that he is secretary of the HS Foundation and a member of the European HS Foundation. He has served as a consultant for AbbVie, Alumis, AstraZeneca, Incyte, InflaRx, Novartis, Sanofi, Sonoma Biotherapeutics, and UCB; as a speaker for AbbVie, Novartis, and UCB; and as an investigator for Chemocentryx, Incyte, InflaRx, Novartis, and UCB. Dr. Hsiao disclosed that she is a member of the board of directors for the HS Foundation and has served as a consultant for AbbVie, Aclaris, Boehringer Ingelheim, Incyte, Novartis, and UCB; as a speaker for AbbVie, Novartis, Sanofi Regeneron, and UCB; and as an investigator for Amgen, Boehringer Ingelheim, and Incyte.
A version of this article first appeared on Medscape.com.
, such as an infection, folliculitis, and acne.
According to 2019 guidelines from the United States and Canadian hidradenitis suppurativa foundations, the diagnostic criteria for HS in general are the presence of typical lesions such as abscesses, nodules, and tunnels in classic locations such as underarms, groins, and buttocks that recur over the course of at least 6 months. “There is no need for additional testing or imaging to make the diagnosis,” said Dr. Sayed, co-chair of the 2019 guidelines work group, who sees patients at the HS and Follicular Disorders Clinic at the University of North Carolina, Chapel Hill. “In many ways, the diagnosis should be very simple since the presentation is classic in most cases, though it can be confusing in the first 6 months or so.”
Persistence, Recurrence Major Clues
Prior to being diagnosed with Hurley stage I HS — characterized by recurrent nodules and abscesses with minimal scars, according to the guidelines — most people figure they’ve been getting recurrent Staphylococcus aureus infections or are having trouble with ingrown hairs from shaving, he continued. They may also say they get “boils” without an understanding of what has been causing them.
“Early HS can mimic an intense folliculitis or furuncles that can sometimes be caused by Staphylococcus infections, but the history of persistence or recurrence for months, despite treatment that should cover something like a Staph infection is a major clue,” Dr. Sayed said. “Thanks to improved resources on the internet, more patients, compared to several years ago, come in asking about HS after they’ve done their own research. As public awareness improves, hopefully this trend will grow, and patients will be diagnosed and treated earlier.” Family history is also a strong predictor of HS, since about half of patients have first-degree relatives who have a history of HS, he noted.
Clinicians can use the Hurley staging system to characterize the extent of disease and the Dermatology Life Quality Index to measure the impact of HS on quality of life. “We perform these assessments in our specialty clinic at each visit, but they are not necessary for diagnosis,” Dr. Sayed told this news organization.
The ‘2-2-6 Rule’
When she sees a patient who might have HS, Jennifer L. Hsiao, MD, a dermatologist who directs the HS clinic at the University of Southern California, Los Angeles, follows the “2-2-6 rule,” which involves asking patients if they have had 2 episodes of 2 or more abscesses in 6 months. “If the patient answers yes, there’s a high likelihood that person has HS,” she said.
Hurley stage I HS is defined as nodules and abscesses without sinus tracts (tunnels) or scarring. But in Dr. Hsiao’s opinion, the Hurley staging system “is not the best way to characterize disease activity” because some patients meet criteria for Hurley stage I disease, meaning they do not have any scars or sinus tracts/tunnels, “but they have high disease activity with several inflammatory nodules and large painful abscesses that are limiting their quality of life and ability to function.”
Most cases of early-stage HS can be diagnosed in a single clinic visit, but some patients may present with a limited history of disease. For example, they may report having only had one episode of an axillary abscess or one episode of a few folliculitis-like papules in the groin. “In the absence of other physical exam findings suggestive of HS, such as open or double-headed comedones in flexural regions, I tell the patient that it is too early to call their condition HS, and I recommend that if they have another episode to call the office for an appointment for evaluation,” Dr. Hsiao said in an interview.
“What sets HS apart from an isolated incidence of a Staphylococcus aureus furuncle is the history of recurrence,” she added. To better characterize HS disease severity, she uses the six-point HS Physician Global Assessment score, a scale from 0 to 5, which classifies a patient as having moderate HS if they have five or more inflammatory nodules, or one abscess and one or more inflammatory nodule(s), without the requirement of demonstrating a scar or tunnel on a physical exam.
To help guide management decisions, Dr. Hsiao also considers asking patients with early-stage HS the following questions:
- Do you have a primary care provider (PCP)? PCPs are important care partners for patients with HS doctor to help screen for the comorbidities associated with the condition.
- What seems to make your HS worse? This can help identify potential triggers to avoid.
- What other medical conditions do you have?
- How would you describe the impact HS has on your quality of life?
- For women: Does your HS get worse around your period? “This can help to identify a potential hormonal trigger,” she said. “If the patient answers ‘yes,’ I would strongly consider a combined oral contraceptive pill and/or spironolactone as part of the patient’s treatment regimen.”
‘Window of Opportunity’ to Intervene
According to Dr. Hsiao, there has been a paradigm shift in the approach to HS management that emphasizes a “window of opportunity,” where earlier initiation of appropriate long-term immunomodulator therapy is recommended to try to mitigate disease progression. The development of tunnels and scars is a telltale sign that permanent tissue destruction is occurring, and the patient’s HS is no longer mild.
Ideally, a conversation about adalimumab, a tumor necrosis factor inhibitor, and secukinumab, an interleukin-17A antagonist (the two currently Food and Drug Administration–approved medications for HS, for moderate to severe disease/Hurley stage II/III) will have already been started with patients prior to development of a high tunnel or scar burden, signs of later-stage disease.
“Medications like this have the potential to slow and prevent that progression and reduce the surgical burden patients face over time, which is a major priority,” Dr. Sayed said. He noted that while comfort level with managing HS can vary among clinicians, “I’d encourage dermatologists to stay engaged with these patients because our training in the medical and surgical management of complex diseases like this is unmatched among other specialties,” he said. “Education of colleagues in other specialties should also be a big priority, especially for those in urgent care, emergency medicine, surgery, and ob.gyn. who often encounter these patients and may be less familiar” with HS.
Besides the North American clinical management guidelines for HS, which are expected to be updated in the next 18-24 months, as well as comorbidity screening recommendations for HS published in 2022, another resource Dr. Sayed and Dr. Hsiao recommend is the HS Foundation website, which features a link to Continuing Medical Education video lectures. The foundation also hosts an annual Symposium on HS Advances. This year’s event is scheduled in November in Austin, Texas.
Dr. Sayed disclosed that he is secretary of the HS Foundation and a member of the European HS Foundation. He has served as a consultant for AbbVie, Alumis, AstraZeneca, Incyte, InflaRx, Novartis, Sanofi, Sonoma Biotherapeutics, and UCB; as a speaker for AbbVie, Novartis, and UCB; and as an investigator for Chemocentryx, Incyte, InflaRx, Novartis, and UCB. Dr. Hsiao disclosed that she is a member of the board of directors for the HS Foundation and has served as a consultant for AbbVie, Aclaris, Boehringer Ingelheim, Incyte, Novartis, and UCB; as a speaker for AbbVie, Novartis, Sanofi Regeneron, and UCB; and as an investigator for Amgen, Boehringer Ingelheim, and Incyte.
A version of this article first appeared on Medscape.com.
, such as an infection, folliculitis, and acne.
According to 2019 guidelines from the United States and Canadian hidradenitis suppurativa foundations, the diagnostic criteria for HS in general are the presence of typical lesions such as abscesses, nodules, and tunnels in classic locations such as underarms, groins, and buttocks that recur over the course of at least 6 months. “There is no need for additional testing or imaging to make the diagnosis,” said Dr. Sayed, co-chair of the 2019 guidelines work group, who sees patients at the HS and Follicular Disorders Clinic at the University of North Carolina, Chapel Hill. “In many ways, the diagnosis should be very simple since the presentation is classic in most cases, though it can be confusing in the first 6 months or so.”
Persistence, Recurrence Major Clues
Prior to being diagnosed with Hurley stage I HS — characterized by recurrent nodules and abscesses with minimal scars, according to the guidelines — most people figure they’ve been getting recurrent Staphylococcus aureus infections or are having trouble with ingrown hairs from shaving, he continued. They may also say they get “boils” without an understanding of what has been causing them.
“Early HS can mimic an intense folliculitis or furuncles that can sometimes be caused by Staphylococcus infections, but the history of persistence or recurrence for months, despite treatment that should cover something like a Staph infection is a major clue,” Dr. Sayed said. “Thanks to improved resources on the internet, more patients, compared to several years ago, come in asking about HS after they’ve done their own research. As public awareness improves, hopefully this trend will grow, and patients will be diagnosed and treated earlier.” Family history is also a strong predictor of HS, since about half of patients have first-degree relatives who have a history of HS, he noted.
Clinicians can use the Hurley staging system to characterize the extent of disease and the Dermatology Life Quality Index to measure the impact of HS on quality of life. “We perform these assessments in our specialty clinic at each visit, but they are not necessary for diagnosis,” Dr. Sayed told this news organization.
The ‘2-2-6 Rule’
When she sees a patient who might have HS, Jennifer L. Hsiao, MD, a dermatologist who directs the HS clinic at the University of Southern California, Los Angeles, follows the “2-2-6 rule,” which involves asking patients if they have had 2 episodes of 2 or more abscesses in 6 months. “If the patient answers yes, there’s a high likelihood that person has HS,” she said.
Hurley stage I HS is defined as nodules and abscesses without sinus tracts (tunnels) or scarring. But in Dr. Hsiao’s opinion, the Hurley staging system “is not the best way to characterize disease activity” because some patients meet criteria for Hurley stage I disease, meaning they do not have any scars or sinus tracts/tunnels, “but they have high disease activity with several inflammatory nodules and large painful abscesses that are limiting their quality of life and ability to function.”
Most cases of early-stage HS can be diagnosed in a single clinic visit, but some patients may present with a limited history of disease. For example, they may report having only had one episode of an axillary abscess or one episode of a few folliculitis-like papules in the groin. “In the absence of other physical exam findings suggestive of HS, such as open or double-headed comedones in flexural regions, I tell the patient that it is too early to call their condition HS, and I recommend that if they have another episode to call the office for an appointment for evaluation,” Dr. Hsiao said in an interview.
“What sets HS apart from an isolated incidence of a Staphylococcus aureus furuncle is the history of recurrence,” she added. To better characterize HS disease severity, she uses the six-point HS Physician Global Assessment score, a scale from 0 to 5, which classifies a patient as having moderate HS if they have five or more inflammatory nodules, or one abscess and one or more inflammatory nodule(s), without the requirement of demonstrating a scar or tunnel on a physical exam.
To help guide management decisions, Dr. Hsiao also considers asking patients with early-stage HS the following questions:
- Do you have a primary care provider (PCP)? PCPs are important care partners for patients with HS doctor to help screen for the comorbidities associated with the condition.
- What seems to make your HS worse? This can help identify potential triggers to avoid.
- What other medical conditions do you have?
- How would you describe the impact HS has on your quality of life?
- For women: Does your HS get worse around your period? “This can help to identify a potential hormonal trigger,” she said. “If the patient answers ‘yes,’ I would strongly consider a combined oral contraceptive pill and/or spironolactone as part of the patient’s treatment regimen.”
‘Window of Opportunity’ to Intervene
According to Dr. Hsiao, there has been a paradigm shift in the approach to HS management that emphasizes a “window of opportunity,” where earlier initiation of appropriate long-term immunomodulator therapy is recommended to try to mitigate disease progression. The development of tunnels and scars is a telltale sign that permanent tissue destruction is occurring, and the patient’s HS is no longer mild.
Ideally, a conversation about adalimumab, a tumor necrosis factor inhibitor, and secukinumab, an interleukin-17A antagonist (the two currently Food and Drug Administration–approved medications for HS, for moderate to severe disease/Hurley stage II/III) will have already been started with patients prior to development of a high tunnel or scar burden, signs of later-stage disease.
“Medications like this have the potential to slow and prevent that progression and reduce the surgical burden patients face over time, which is a major priority,” Dr. Sayed said. He noted that while comfort level with managing HS can vary among clinicians, “I’d encourage dermatologists to stay engaged with these patients because our training in the medical and surgical management of complex diseases like this is unmatched among other specialties,” he said. “Education of colleagues in other specialties should also be a big priority, especially for those in urgent care, emergency medicine, surgery, and ob.gyn. who often encounter these patients and may be less familiar” with HS.
Besides the North American clinical management guidelines for HS, which are expected to be updated in the next 18-24 months, as well as comorbidity screening recommendations for HS published in 2022, another resource Dr. Sayed and Dr. Hsiao recommend is the HS Foundation website, which features a link to Continuing Medical Education video lectures. The foundation also hosts an annual Symposium on HS Advances. This year’s event is scheduled in November in Austin, Texas.
Dr. Sayed disclosed that he is secretary of the HS Foundation and a member of the European HS Foundation. He has served as a consultant for AbbVie, Alumis, AstraZeneca, Incyte, InflaRx, Novartis, Sanofi, Sonoma Biotherapeutics, and UCB; as a speaker for AbbVie, Novartis, and UCB; and as an investigator for Chemocentryx, Incyte, InflaRx, Novartis, and UCB. Dr. Hsiao disclosed that she is a member of the board of directors for the HS Foundation and has served as a consultant for AbbVie, Aclaris, Boehringer Ingelheim, Incyte, Novartis, and UCB; as a speaker for AbbVie, Novartis, Sanofi Regeneron, and UCB; and as an investigator for Amgen, Boehringer Ingelheim, and Incyte.
A version of this article first appeared on Medscape.com.
Psychiatric Comorbidity Prevalent in Eating Disorders
NEW YORK — Psychiatric comorbidities are highly prevalent in patients with eating disorders (EDs), a large study showed.
In a propensity-matched cohort of young adults with and without EDs, a wide variety of psychiatric disorders including depression and anxiety, as well as cannabis and alcohol use disorders, were more common in those with EDs, investigators found.
Comorbid psychiatric disorders should be “top of mind when working with someone with an eating disorder. If you are able to treat the comorbid psychiatric conditions, they might have a better recovery from the eating disorder,” study investigator Angela Liu, MD, with Northwell Health at Zucker Hillside Hospital, Glen Oaks, New York, told this news organization.
The findings were presented at the annual meeting of the American Psychiatric Association.
Data Gap
As previously reported by this news organization, more than one in five children worldwide are at risk for an ED and US medical admissions for adolescents with restrictive EDs more than doubled during the pandemic.
Yet there remains a “gap in the literature” about the prevalence of comorbid psychiatric conditions in people with EDs, specifically in young people, Dr. Liu explained.
“To our knowledge, this is the first study using a real-world, multistate administrative dataset to estimate the prevalence of psychiatric comorbidities in young people diagnosed with an eating disorder,” Dr. Liu said.
Using the TriNetX database, the researchers identified through ICD-10 codes 14,524 individuals with EDs (mean age, 15.9 years; 79% women) and 110,051 without EDs who were receiving antidepressants (mean age, 17.8 years; 65% women).
“There was a much higher prevalence of almost all other psychiatric conditions in those with an eating disorder compared to the general psychiatry population,” coinvestigator Binx Y. Lin, MD, MSc, with Virginia Tech Carilion School of Medicine in Roanoke, Virginia, told this news organization.
In the baseline comparison (before matching), psychiatric disorders seen more often in adults with than in those without EDs included (but were not limited to) mood disorders (51% vs 23%), generalized anxiety disorder (GAD; 30% vs 8%), posttraumatic stress disorder (PTSD; 10% vs 2%), obsessive-compulsive disorder (OCD; 8% vs 1%), panic disorder (6% vs 2%), substance use disorder (8% vs 5%), and adjustment disorders (5% vs 2%).
The results held after propensity score matching, with numerous psychiatric conditions significantly (P < .001) more prevalent in the ED cohort.
Understanding the burden of comorbid psychiatric disorders in young people with EDs is important to design comprehensive, evidence-based interventions, the researchers said.
Providing perspective on this topic, Petros Levounis, MD, professor and chair, Department of Psychiatry, Rutgers New Jersey Medical School, Newark, New Jersey, noted that “comorbidity between substance use disorders and other psychiatric disorders has both been grossly underestimated and grossly overestimated.
“I go around the country and see rehab programs, and there are people that very strongly believe that if you stop using the drugs, you won’t have problems with depression or anxiety or whatever,” Dr. Levounis, immediate past president of the APA, shared with this news organization.
“Others say they have never seen somebody who’s addicted to something that doesn’t also have some other psychiatric disorders and if you just scratch the surface, you always find some other psychological or psychiatric problem lying behind. Neither of them are true,” he cautioned.
Dr. Levounis said it’s important to recognize that “some people with addiction will also have another psychiatric disorder. But clearly there are people who just have a mental illness without addiction, and there are clearly people who will just have addiction without other mental illness.”
This research had no commercial funding and was supported in part by the American Psychiatric Association Research Fellowship. Dr. Liu, Dr. Lin, and Dr. Levounis had no relevant disclosures.
A version of this article appeared on Medscape.com .
NEW YORK — Psychiatric comorbidities are highly prevalent in patients with eating disorders (EDs), a large study showed.
In a propensity-matched cohort of young adults with and without EDs, a wide variety of psychiatric disorders including depression and anxiety, as well as cannabis and alcohol use disorders, were more common in those with EDs, investigators found.
Comorbid psychiatric disorders should be “top of mind when working with someone with an eating disorder. If you are able to treat the comorbid psychiatric conditions, they might have a better recovery from the eating disorder,” study investigator Angela Liu, MD, with Northwell Health at Zucker Hillside Hospital, Glen Oaks, New York, told this news organization.
The findings were presented at the annual meeting of the American Psychiatric Association.
Data Gap
As previously reported by this news organization, more than one in five children worldwide are at risk for an ED and US medical admissions for adolescents with restrictive EDs more than doubled during the pandemic.
Yet there remains a “gap in the literature” about the prevalence of comorbid psychiatric conditions in people with EDs, specifically in young people, Dr. Liu explained.
“To our knowledge, this is the first study using a real-world, multistate administrative dataset to estimate the prevalence of psychiatric comorbidities in young people diagnosed with an eating disorder,” Dr. Liu said.
Using the TriNetX database, the researchers identified through ICD-10 codes 14,524 individuals with EDs (mean age, 15.9 years; 79% women) and 110,051 without EDs who were receiving antidepressants (mean age, 17.8 years; 65% women).
“There was a much higher prevalence of almost all other psychiatric conditions in those with an eating disorder compared to the general psychiatry population,” coinvestigator Binx Y. Lin, MD, MSc, with Virginia Tech Carilion School of Medicine in Roanoke, Virginia, told this news organization.
In the baseline comparison (before matching), psychiatric disorders seen more often in adults with than in those without EDs included (but were not limited to) mood disorders (51% vs 23%), generalized anxiety disorder (GAD; 30% vs 8%), posttraumatic stress disorder (PTSD; 10% vs 2%), obsessive-compulsive disorder (OCD; 8% vs 1%), panic disorder (6% vs 2%), substance use disorder (8% vs 5%), and adjustment disorders (5% vs 2%).
The results held after propensity score matching, with numerous psychiatric conditions significantly (P < .001) more prevalent in the ED cohort.
Understanding the burden of comorbid psychiatric disorders in young people with EDs is important to design comprehensive, evidence-based interventions, the researchers said.
Providing perspective on this topic, Petros Levounis, MD, professor and chair, Department of Psychiatry, Rutgers New Jersey Medical School, Newark, New Jersey, noted that “comorbidity between substance use disorders and other psychiatric disorders has both been grossly underestimated and grossly overestimated.
“I go around the country and see rehab programs, and there are people that very strongly believe that if you stop using the drugs, you won’t have problems with depression or anxiety or whatever,” Dr. Levounis, immediate past president of the APA, shared with this news organization.
“Others say they have never seen somebody who’s addicted to something that doesn’t also have some other psychiatric disorders and if you just scratch the surface, you always find some other psychological or psychiatric problem lying behind. Neither of them are true,” he cautioned.
Dr. Levounis said it’s important to recognize that “some people with addiction will also have another psychiatric disorder. But clearly there are people who just have a mental illness without addiction, and there are clearly people who will just have addiction without other mental illness.”
This research had no commercial funding and was supported in part by the American Psychiatric Association Research Fellowship. Dr. Liu, Dr. Lin, and Dr. Levounis had no relevant disclosures.
A version of this article appeared on Medscape.com .
NEW YORK — Psychiatric comorbidities are highly prevalent in patients with eating disorders (EDs), a large study showed.
In a propensity-matched cohort of young adults with and without EDs, a wide variety of psychiatric disorders including depression and anxiety, as well as cannabis and alcohol use disorders, were more common in those with EDs, investigators found.
Comorbid psychiatric disorders should be “top of mind when working with someone with an eating disorder. If you are able to treat the comorbid psychiatric conditions, they might have a better recovery from the eating disorder,” study investigator Angela Liu, MD, with Northwell Health at Zucker Hillside Hospital, Glen Oaks, New York, told this news organization.
The findings were presented at the annual meeting of the American Psychiatric Association.
Data Gap
As previously reported by this news organization, more than one in five children worldwide are at risk for an ED and US medical admissions for adolescents with restrictive EDs more than doubled during the pandemic.
Yet there remains a “gap in the literature” about the prevalence of comorbid psychiatric conditions in people with EDs, specifically in young people, Dr. Liu explained.
“To our knowledge, this is the first study using a real-world, multistate administrative dataset to estimate the prevalence of psychiatric comorbidities in young people diagnosed with an eating disorder,” Dr. Liu said.
Using the TriNetX database, the researchers identified through ICD-10 codes 14,524 individuals with EDs (mean age, 15.9 years; 79% women) and 110,051 without EDs who were receiving antidepressants (mean age, 17.8 years; 65% women).
“There was a much higher prevalence of almost all other psychiatric conditions in those with an eating disorder compared to the general psychiatry population,” coinvestigator Binx Y. Lin, MD, MSc, with Virginia Tech Carilion School of Medicine in Roanoke, Virginia, told this news organization.
In the baseline comparison (before matching), psychiatric disorders seen more often in adults with than in those without EDs included (but were not limited to) mood disorders (51% vs 23%), generalized anxiety disorder (GAD; 30% vs 8%), posttraumatic stress disorder (PTSD; 10% vs 2%), obsessive-compulsive disorder (OCD; 8% vs 1%), panic disorder (6% vs 2%), substance use disorder (8% vs 5%), and adjustment disorders (5% vs 2%).
The results held after propensity score matching, with numerous psychiatric conditions significantly (P < .001) more prevalent in the ED cohort.
Understanding the burden of comorbid psychiatric disorders in young people with EDs is important to design comprehensive, evidence-based interventions, the researchers said.
Providing perspective on this topic, Petros Levounis, MD, professor and chair, Department of Psychiatry, Rutgers New Jersey Medical School, Newark, New Jersey, noted that “comorbidity between substance use disorders and other psychiatric disorders has both been grossly underestimated and grossly overestimated.
“I go around the country and see rehab programs, and there are people that very strongly believe that if you stop using the drugs, you won’t have problems with depression or anxiety or whatever,” Dr. Levounis, immediate past president of the APA, shared with this news organization.
“Others say they have never seen somebody who’s addicted to something that doesn’t also have some other psychiatric disorders and if you just scratch the surface, you always find some other psychological or psychiatric problem lying behind. Neither of them are true,” he cautioned.
Dr. Levounis said it’s important to recognize that “some people with addiction will also have another psychiatric disorder. But clearly there are people who just have a mental illness without addiction, and there are clearly people who will just have addiction without other mental illness.”
This research had no commercial funding and was supported in part by the American Psychiatric Association Research Fellowship. Dr. Liu, Dr. Lin, and Dr. Levounis had no relevant disclosures.
A version of this article appeared on Medscape.com .
More Rapid Confirmation of an Autism Diagnosis Is Coming to Primary Care
TORONTO — , according to a series of studies presented at the Pediatric Academic Societies annual meeting.
Accelerated Diagnosis
In one study, 80% of the evaluations were conducted within 6 weeks of patient enrollment, according to Corinna Rea, MD, a clinician in the primary care center at Boston Children’s Hospital as well as an assistant professor at Harvard Medical School, Boston, Massachusetts.
This outcome was drawn from a pilot study with 179 children suspected of autism spectrum disorder (ASD) by clinicians in a pediatric clinic. All were under the age of 3 years. In the first step, families completed the Bayley-4 Social-Emotional and Adaptive Behavior Scale.
The next step was a virtual assessment by a trained clinician using the TELE-ADS-PEDs (TAP) tool developed by Vanderbilt University, Nashville, Tennessee. Patients and families participated from their homes. The diagnosis of ASD was made by a psychologist using the patient’s history and data provided by the two assessment tools.
Through this approach, the median time to diagnosis was 30 days, according to Dr. Rea. Relative to a median time of 168 days to diagnosis among patients considered likely to have ASD at Dr. Rea’s center in the year prior to this pilot study, the time was reduced significantly (P < .001).
All patients in the study were subsequently evaluated by traditional methods. One hundred percent of the ASD diagnoses were confirmed with traditional assessment.
On the basis of these data, the accelerated approach “seems efficient and quite accurate,” Dr. Rea reported. When family members were surveyed at the end of the pilot study, 60% were satisfied and 28% were moderately satisfied. Although 59% reported that they would have preferred an in-person assessment, approximately 90% agreed the child’s development was mostly or completely captured in the accelerated assessment.
Dr. Rea pointed out that the psychologists participating in this study offered the opinion that home-based assessments are in their experience better than in-person evaluations due to the more natural behavior of the child in their own environment. However, she said that the diagnostic approach in the pilot study is still being modified, and one of the goals is to make virtual assessment more acceptable to the families.
A Commercialized Diagnostic Approach
A similar approach has been commercialized by a firm called As You Are, according to Steven D. Hicks, MD, PhD, who is an associate professor of pediatrics at Pennsylvania State University College of Medicine, Hershey, Pennsylvania. Dr. Hicks is a principal in the enterprise, which is also assessing ASD virtually.
Trained pediatricians are evaluating patients with multiple tools in addition to TAP, including the Childhood Autism Rating Scale (CARS) and the Diagnostic and Statistical Manual (DSM-V) checklist for ASD. The company, which began offering this diagnostic service in 2022, now employs more than 30 pediatricians who participated in a 1-month training program.
At the 2024 PAS meeting, quality assurance data were presented on 215 (2.2%) of the 9632 children evaluated between February 2023 and March 2024. The diagnostic assessments of these randomly selected children were reviewed by one of three randomly assigned experts (a developmental pediatrician, a child psychologist, or a pediatrician with 7 years’ diagnostic experience) blinded to the initial scoring.
The diagnostic agreement was 94%, according to the data presented, providing a specificity of 90% and a sensitivity of 90% for ASD. The commercialized diagnostic approach is providing a diagnosis in a mean time of 29 days from initial contact, compared with delays that typically exceed 1 year for many children with suspected ASD, according to Dr. Hicks.
Additional Studies Aim at Streamlining Diagnosis
Two additional studies also evaluated strategies to streamline the diagnosis of ASD. Both were positive. In one, the accuracy and time to diagnosis among pediatricians trained in TAP and CARS were compared with those of ASD specialists in a dedicated autism clinic. Both were located at Nemours Children’s Health Center, Wilmington, Delaware.
In this study, presented by Meghan Harrison, DO, an attending pediatrician at Nemours Children’s Health, time to diagnosis among the 39 patients evaluated by pediatricians relative to the 349 patients evaluated at the dedicated ASD center (2.0 vs 5.1 months; P = .001) was significantly shorter. The age at diagnosis in the pediatrician-assessed population (27.5 vs 36.5 months; P < .001) was also significantly younger.
In another study, led by Ashely L. Early, MSW, a clinical social worker at the Medical University of South Carolina, Charleston, South Carolina, switching to a screening tool called the Rapid Interactive Screening Test for Autism in Toddlers (RITA-1) reduced the wait time to evaluation by approximately 5 months relative to previous practice with a more cumbersome screening method.
An ‘Urgent Need’ to Accelerate Diagnosis
In most places in the United States, children suspected of ASD are referred to specialists for confirmation of the diagnosis, which is needed to quality for ASD services, according to Katherine Zuckerman, MD, a professor of pediatrics the Oregon Health and Science University, Portland, Oregon. Dr. Zuckerman, who was moderator of the session in which all four of these abstracts were presented, explained that there is an urgent need to accelerate the time to diagnosis, which involves long delays for many if not most children with ASD. This is important because treatment and supportive services for ASD are almost always dependent on a diagnosis.
“There are tons of data to show that earlier access to ASD services has important patient benefits, including higher IQs,” she said. Other benefits she listed include a better quality of life for the child and the family.
“It can provide a huge reduction in family stress,” she added, suggesting that early interventions favorably modify the trajectory of the disability over time with accruing benefits.
“The lifetime costs of ASD exceed cancer and most other disease, so there are major implications for the cumulative cost of ASD management,” Dr. Zuckerman said. She suggested that the studies presented at the meeting reflect a likely evolution in who evaluates children for ASD and how quickly the evaluation is performed.
Dr. Rea, Dr. Harrison, Dr. Zuckerman, and Ms. Early reported no potential conflicts of interest. In addition to his executive role in As You Are, Dr. Hicks has financial relationships with Quadrant Biosciences and Spectrum Solutions.
TORONTO — , according to a series of studies presented at the Pediatric Academic Societies annual meeting.
Accelerated Diagnosis
In one study, 80% of the evaluations were conducted within 6 weeks of patient enrollment, according to Corinna Rea, MD, a clinician in the primary care center at Boston Children’s Hospital as well as an assistant professor at Harvard Medical School, Boston, Massachusetts.
This outcome was drawn from a pilot study with 179 children suspected of autism spectrum disorder (ASD) by clinicians in a pediatric clinic. All were under the age of 3 years. In the first step, families completed the Bayley-4 Social-Emotional and Adaptive Behavior Scale.
The next step was a virtual assessment by a trained clinician using the TELE-ADS-PEDs (TAP) tool developed by Vanderbilt University, Nashville, Tennessee. Patients and families participated from their homes. The diagnosis of ASD was made by a psychologist using the patient’s history and data provided by the two assessment tools.
Through this approach, the median time to diagnosis was 30 days, according to Dr. Rea. Relative to a median time of 168 days to diagnosis among patients considered likely to have ASD at Dr. Rea’s center in the year prior to this pilot study, the time was reduced significantly (P < .001).
All patients in the study were subsequently evaluated by traditional methods. One hundred percent of the ASD diagnoses were confirmed with traditional assessment.
On the basis of these data, the accelerated approach “seems efficient and quite accurate,” Dr. Rea reported. When family members were surveyed at the end of the pilot study, 60% were satisfied and 28% were moderately satisfied. Although 59% reported that they would have preferred an in-person assessment, approximately 90% agreed the child’s development was mostly or completely captured in the accelerated assessment.
Dr. Rea pointed out that the psychologists participating in this study offered the opinion that home-based assessments are in their experience better than in-person evaluations due to the more natural behavior of the child in their own environment. However, she said that the diagnostic approach in the pilot study is still being modified, and one of the goals is to make virtual assessment more acceptable to the families.
A Commercialized Diagnostic Approach
A similar approach has been commercialized by a firm called As You Are, according to Steven D. Hicks, MD, PhD, who is an associate professor of pediatrics at Pennsylvania State University College of Medicine, Hershey, Pennsylvania. Dr. Hicks is a principal in the enterprise, which is also assessing ASD virtually.
Trained pediatricians are evaluating patients with multiple tools in addition to TAP, including the Childhood Autism Rating Scale (CARS) and the Diagnostic and Statistical Manual (DSM-V) checklist for ASD. The company, which began offering this diagnostic service in 2022, now employs more than 30 pediatricians who participated in a 1-month training program.
At the 2024 PAS meeting, quality assurance data were presented on 215 (2.2%) of the 9632 children evaluated between February 2023 and March 2024. The diagnostic assessments of these randomly selected children were reviewed by one of three randomly assigned experts (a developmental pediatrician, a child psychologist, or a pediatrician with 7 years’ diagnostic experience) blinded to the initial scoring.
The diagnostic agreement was 94%, according to the data presented, providing a specificity of 90% and a sensitivity of 90% for ASD. The commercialized diagnostic approach is providing a diagnosis in a mean time of 29 days from initial contact, compared with delays that typically exceed 1 year for many children with suspected ASD, according to Dr. Hicks.
Additional Studies Aim at Streamlining Diagnosis
Two additional studies also evaluated strategies to streamline the diagnosis of ASD. Both were positive. In one, the accuracy and time to diagnosis among pediatricians trained in TAP and CARS were compared with those of ASD specialists in a dedicated autism clinic. Both were located at Nemours Children’s Health Center, Wilmington, Delaware.
In this study, presented by Meghan Harrison, DO, an attending pediatrician at Nemours Children’s Health, time to diagnosis among the 39 patients evaluated by pediatricians relative to the 349 patients evaluated at the dedicated ASD center (2.0 vs 5.1 months; P = .001) was significantly shorter. The age at diagnosis in the pediatrician-assessed population (27.5 vs 36.5 months; P < .001) was also significantly younger.
In another study, led by Ashely L. Early, MSW, a clinical social worker at the Medical University of South Carolina, Charleston, South Carolina, switching to a screening tool called the Rapid Interactive Screening Test for Autism in Toddlers (RITA-1) reduced the wait time to evaluation by approximately 5 months relative to previous practice with a more cumbersome screening method.
An ‘Urgent Need’ to Accelerate Diagnosis
In most places in the United States, children suspected of ASD are referred to specialists for confirmation of the diagnosis, which is needed to quality for ASD services, according to Katherine Zuckerman, MD, a professor of pediatrics the Oregon Health and Science University, Portland, Oregon. Dr. Zuckerman, who was moderator of the session in which all four of these abstracts were presented, explained that there is an urgent need to accelerate the time to diagnosis, which involves long delays for many if not most children with ASD. This is important because treatment and supportive services for ASD are almost always dependent on a diagnosis.
“There are tons of data to show that earlier access to ASD services has important patient benefits, including higher IQs,” she said. Other benefits she listed include a better quality of life for the child and the family.
“It can provide a huge reduction in family stress,” she added, suggesting that early interventions favorably modify the trajectory of the disability over time with accruing benefits.
“The lifetime costs of ASD exceed cancer and most other disease, so there are major implications for the cumulative cost of ASD management,” Dr. Zuckerman said. She suggested that the studies presented at the meeting reflect a likely evolution in who evaluates children for ASD and how quickly the evaluation is performed.
Dr. Rea, Dr. Harrison, Dr. Zuckerman, and Ms. Early reported no potential conflicts of interest. In addition to his executive role in As You Are, Dr. Hicks has financial relationships with Quadrant Biosciences and Spectrum Solutions.
TORONTO — , according to a series of studies presented at the Pediatric Academic Societies annual meeting.
Accelerated Diagnosis
In one study, 80% of the evaluations were conducted within 6 weeks of patient enrollment, according to Corinna Rea, MD, a clinician in the primary care center at Boston Children’s Hospital as well as an assistant professor at Harvard Medical School, Boston, Massachusetts.
This outcome was drawn from a pilot study with 179 children suspected of autism spectrum disorder (ASD) by clinicians in a pediatric clinic. All were under the age of 3 years. In the first step, families completed the Bayley-4 Social-Emotional and Adaptive Behavior Scale.
The next step was a virtual assessment by a trained clinician using the TELE-ADS-PEDs (TAP) tool developed by Vanderbilt University, Nashville, Tennessee. Patients and families participated from their homes. The diagnosis of ASD was made by a psychologist using the patient’s history and data provided by the two assessment tools.
Through this approach, the median time to diagnosis was 30 days, according to Dr. Rea. Relative to a median time of 168 days to diagnosis among patients considered likely to have ASD at Dr. Rea’s center in the year prior to this pilot study, the time was reduced significantly (P < .001).
All patients in the study were subsequently evaluated by traditional methods. One hundred percent of the ASD diagnoses were confirmed with traditional assessment.
On the basis of these data, the accelerated approach “seems efficient and quite accurate,” Dr. Rea reported. When family members were surveyed at the end of the pilot study, 60% were satisfied and 28% were moderately satisfied. Although 59% reported that they would have preferred an in-person assessment, approximately 90% agreed the child’s development was mostly or completely captured in the accelerated assessment.
Dr. Rea pointed out that the psychologists participating in this study offered the opinion that home-based assessments are in their experience better than in-person evaluations due to the more natural behavior of the child in their own environment. However, she said that the diagnostic approach in the pilot study is still being modified, and one of the goals is to make virtual assessment more acceptable to the families.
A Commercialized Diagnostic Approach
A similar approach has been commercialized by a firm called As You Are, according to Steven D. Hicks, MD, PhD, who is an associate professor of pediatrics at Pennsylvania State University College of Medicine, Hershey, Pennsylvania. Dr. Hicks is a principal in the enterprise, which is also assessing ASD virtually.
Trained pediatricians are evaluating patients with multiple tools in addition to TAP, including the Childhood Autism Rating Scale (CARS) and the Diagnostic and Statistical Manual (DSM-V) checklist for ASD. The company, which began offering this diagnostic service in 2022, now employs more than 30 pediatricians who participated in a 1-month training program.
At the 2024 PAS meeting, quality assurance data were presented on 215 (2.2%) of the 9632 children evaluated between February 2023 and March 2024. The diagnostic assessments of these randomly selected children were reviewed by one of three randomly assigned experts (a developmental pediatrician, a child psychologist, or a pediatrician with 7 years’ diagnostic experience) blinded to the initial scoring.
The diagnostic agreement was 94%, according to the data presented, providing a specificity of 90% and a sensitivity of 90% for ASD. The commercialized diagnostic approach is providing a diagnosis in a mean time of 29 days from initial contact, compared with delays that typically exceed 1 year for many children with suspected ASD, according to Dr. Hicks.
Additional Studies Aim at Streamlining Diagnosis
Two additional studies also evaluated strategies to streamline the diagnosis of ASD. Both were positive. In one, the accuracy and time to diagnosis among pediatricians trained in TAP and CARS were compared with those of ASD specialists in a dedicated autism clinic. Both were located at Nemours Children’s Health Center, Wilmington, Delaware.
In this study, presented by Meghan Harrison, DO, an attending pediatrician at Nemours Children’s Health, time to diagnosis among the 39 patients evaluated by pediatricians relative to the 349 patients evaluated at the dedicated ASD center (2.0 vs 5.1 months; P = .001) was significantly shorter. The age at diagnosis in the pediatrician-assessed population (27.5 vs 36.5 months; P < .001) was also significantly younger.
In another study, led by Ashely L. Early, MSW, a clinical social worker at the Medical University of South Carolina, Charleston, South Carolina, switching to a screening tool called the Rapid Interactive Screening Test for Autism in Toddlers (RITA-1) reduced the wait time to evaluation by approximately 5 months relative to previous practice with a more cumbersome screening method.
An ‘Urgent Need’ to Accelerate Diagnosis
In most places in the United States, children suspected of ASD are referred to specialists for confirmation of the diagnosis, which is needed to quality for ASD services, according to Katherine Zuckerman, MD, a professor of pediatrics the Oregon Health and Science University, Portland, Oregon. Dr. Zuckerman, who was moderator of the session in which all four of these abstracts were presented, explained that there is an urgent need to accelerate the time to diagnosis, which involves long delays for many if not most children with ASD. This is important because treatment and supportive services for ASD are almost always dependent on a diagnosis.
“There are tons of data to show that earlier access to ASD services has important patient benefits, including higher IQs,” she said. Other benefits she listed include a better quality of life for the child and the family.
“It can provide a huge reduction in family stress,” she added, suggesting that early interventions favorably modify the trajectory of the disability over time with accruing benefits.
“The lifetime costs of ASD exceed cancer and most other disease, so there are major implications for the cumulative cost of ASD management,” Dr. Zuckerman said. She suggested that the studies presented at the meeting reflect a likely evolution in who evaluates children for ASD and how quickly the evaluation is performed.
Dr. Rea, Dr. Harrison, Dr. Zuckerman, and Ms. Early reported no potential conflicts of interest. In addition to his executive role in As You Are, Dr. Hicks has financial relationships with Quadrant Biosciences and Spectrum Solutions.
FROM PAS 2024
Video Games Marketing Food Impacts Teens’ Eating
, according to research presented on May 12, 2024, at the 31st European Congress on Obesity in Venice, Italy.
The presentation by Rebecca Evans, University of Liverpool, United Kingdom, included findings from three recently published studies and a submitted randomized controlled trial. At the time of the research, the top VGLSPs globally were Twitch (with 77% of the market share by hours watched), YouTube Gaming (15%), and Facebook Gaming Live (7%).
“Endorsement deals for prominent streamers on Twitch can be worth many millions of dollars, and younger people, who are attractive to advertisers, are moving away from television to these more interactive forms of entertainment,” Evans said. “These deals involve collaborating with brands and promoting their products, including foods that are high in fats, salt, and/or sugar.”
To delve more deeply into the extent and consequences of VGLSP advertising for HFSS, the researchers first analyzed 52 hour-long Twitch videos uploaded to gaming platforms by three popular influencers. They found that food cues appeared at an average rate of 2.6 per hour, and the average duration of each cue was 20 minutes.
Most cues (70.7%) were for branded HFSS (80.5%), led by energy drinks (62.4%). Most (97.7%) were not accompanied by an advertising disclosure. Most food cues were either product placement (44.0%) and looping banners (40.6%) or features such as tie-ins, logos, or offers. Notably, these forms of advertising are always visible on the video game screen, so viewers cannot skip over them or close them.
Next, the team did a systematic review and meta-analysis to assess the relationship between exposure to digital game-based or influencer food marketing with food-related outcomes. They found that young people were twice as likely to prefer foods displayed via digital game-based marketing, and that influencer and digital game-based marketing was associated with increased HFSS food consumption of about 37 additional calories in one sitting.
Researchers then surveyed 490 youngsters (mean age, 16.8 years; 70%, female) to explore associations between recall of food marketing of the top VGLSPs and food-related outcomes. Recall was associated with more positive attitudes towards HFSS foods and, in turn, the purchase and consumption of the marketed HFSS foods.
In addition, the researchers conducted a lab-based randomized controlled trial to explore associations between HFSS food marketing via a mock Twitch stream and subsequent snack intake. A total of 91 youngsters (average age, 18 years; 69% women) viewed the mock stream, which contained either an advertisement (an image overlaid on the video featuring a brand logo and product) for an HFSS food, or a non-branded food. They were then offered a snack. Acute exposure to HFSS food marketing was not associated with immediate consumption, but more habitual use of VGLSPs was associated with increased intake of the marketed snack.
The observational studies could not prove cause and effect, and may not be generalizable to all teens, the authors acknowledged. They also noted that some of the findings are based on self-report surveys, which can lead to recall bias and may have affected the results.
Nevertheless, Ms. Evans said, “The high level of exposure to digital marketing of unhealthy food could drive excess calorie consumption and weight gain, particularly in adolescents who are more susceptible to advertising. It is important that digital food marketing restrictions encompass innovative and emerging digital media such as VGLSPs.”
The research formed Ms. Evans’ PhD work, which is funded by the University of Liverpool. Evans and colleagues declared no conflicts of interest.
A version of this article appeared on Medscape.com .
, according to research presented on May 12, 2024, at the 31st European Congress on Obesity in Venice, Italy.
The presentation by Rebecca Evans, University of Liverpool, United Kingdom, included findings from three recently published studies and a submitted randomized controlled trial. At the time of the research, the top VGLSPs globally were Twitch (with 77% of the market share by hours watched), YouTube Gaming (15%), and Facebook Gaming Live (7%).
“Endorsement deals for prominent streamers on Twitch can be worth many millions of dollars, and younger people, who are attractive to advertisers, are moving away from television to these more interactive forms of entertainment,” Evans said. “These deals involve collaborating with brands and promoting their products, including foods that are high in fats, salt, and/or sugar.”
To delve more deeply into the extent and consequences of VGLSP advertising for HFSS, the researchers first analyzed 52 hour-long Twitch videos uploaded to gaming platforms by three popular influencers. They found that food cues appeared at an average rate of 2.6 per hour, and the average duration of each cue was 20 minutes.
Most cues (70.7%) were for branded HFSS (80.5%), led by energy drinks (62.4%). Most (97.7%) were not accompanied by an advertising disclosure. Most food cues were either product placement (44.0%) and looping banners (40.6%) or features such as tie-ins, logos, or offers. Notably, these forms of advertising are always visible on the video game screen, so viewers cannot skip over them or close them.
Next, the team did a systematic review and meta-analysis to assess the relationship between exposure to digital game-based or influencer food marketing with food-related outcomes. They found that young people were twice as likely to prefer foods displayed via digital game-based marketing, and that influencer and digital game-based marketing was associated with increased HFSS food consumption of about 37 additional calories in one sitting.
Researchers then surveyed 490 youngsters (mean age, 16.8 years; 70%, female) to explore associations between recall of food marketing of the top VGLSPs and food-related outcomes. Recall was associated with more positive attitudes towards HFSS foods and, in turn, the purchase and consumption of the marketed HFSS foods.
In addition, the researchers conducted a lab-based randomized controlled trial to explore associations between HFSS food marketing via a mock Twitch stream and subsequent snack intake. A total of 91 youngsters (average age, 18 years; 69% women) viewed the mock stream, which contained either an advertisement (an image overlaid on the video featuring a brand logo and product) for an HFSS food, or a non-branded food. They were then offered a snack. Acute exposure to HFSS food marketing was not associated with immediate consumption, but more habitual use of VGLSPs was associated with increased intake of the marketed snack.
The observational studies could not prove cause and effect, and may not be generalizable to all teens, the authors acknowledged. They also noted that some of the findings are based on self-report surveys, which can lead to recall bias and may have affected the results.
Nevertheless, Ms. Evans said, “The high level of exposure to digital marketing of unhealthy food could drive excess calorie consumption and weight gain, particularly in adolescents who are more susceptible to advertising. It is important that digital food marketing restrictions encompass innovative and emerging digital media such as VGLSPs.”
The research formed Ms. Evans’ PhD work, which is funded by the University of Liverpool. Evans and colleagues declared no conflicts of interest.
A version of this article appeared on Medscape.com .
, according to research presented on May 12, 2024, at the 31st European Congress on Obesity in Venice, Italy.
The presentation by Rebecca Evans, University of Liverpool, United Kingdom, included findings from three recently published studies and a submitted randomized controlled trial. At the time of the research, the top VGLSPs globally were Twitch (with 77% of the market share by hours watched), YouTube Gaming (15%), and Facebook Gaming Live (7%).
“Endorsement deals for prominent streamers on Twitch can be worth many millions of dollars, and younger people, who are attractive to advertisers, are moving away from television to these more interactive forms of entertainment,” Evans said. “These deals involve collaborating with brands and promoting their products, including foods that are high in fats, salt, and/or sugar.”
To delve more deeply into the extent and consequences of VGLSP advertising for HFSS, the researchers first analyzed 52 hour-long Twitch videos uploaded to gaming platforms by three popular influencers. They found that food cues appeared at an average rate of 2.6 per hour, and the average duration of each cue was 20 minutes.
Most cues (70.7%) were for branded HFSS (80.5%), led by energy drinks (62.4%). Most (97.7%) were not accompanied by an advertising disclosure. Most food cues were either product placement (44.0%) and looping banners (40.6%) or features such as tie-ins, logos, or offers. Notably, these forms of advertising are always visible on the video game screen, so viewers cannot skip over them or close them.
Next, the team did a systematic review and meta-analysis to assess the relationship between exposure to digital game-based or influencer food marketing with food-related outcomes. They found that young people were twice as likely to prefer foods displayed via digital game-based marketing, and that influencer and digital game-based marketing was associated with increased HFSS food consumption of about 37 additional calories in one sitting.
Researchers then surveyed 490 youngsters (mean age, 16.8 years; 70%, female) to explore associations between recall of food marketing of the top VGLSPs and food-related outcomes. Recall was associated with more positive attitudes towards HFSS foods and, in turn, the purchase and consumption of the marketed HFSS foods.
In addition, the researchers conducted a lab-based randomized controlled trial to explore associations between HFSS food marketing via a mock Twitch stream and subsequent snack intake. A total of 91 youngsters (average age, 18 years; 69% women) viewed the mock stream, which contained either an advertisement (an image overlaid on the video featuring a brand logo and product) for an HFSS food, or a non-branded food. They were then offered a snack. Acute exposure to HFSS food marketing was not associated with immediate consumption, but more habitual use of VGLSPs was associated with increased intake of the marketed snack.
The observational studies could not prove cause and effect, and may not be generalizable to all teens, the authors acknowledged. They also noted that some of the findings are based on self-report surveys, which can lead to recall bias and may have affected the results.
Nevertheless, Ms. Evans said, “The high level of exposure to digital marketing of unhealthy food could drive excess calorie consumption and weight gain, particularly in adolescents who are more susceptible to advertising. It is important that digital food marketing restrictions encompass innovative and emerging digital media such as VGLSPs.”
The research formed Ms. Evans’ PhD work, which is funded by the University of Liverpool. Evans and colleagues declared no conflicts of interest.
A version of this article appeared on Medscape.com .
The Inconsistency of Preparticipation Sports Evaluations Raises Issues About Their Utility
TORONTO — There is little consistency in the elements and types of information captured in preparticipation physical evaluations (PPE) for sports among school-aged children, which is complicating efforts to determine if they have value, according to a study presented at the Pediatric Academic Societies annual meeting.
The study concept developed when Tammy Ng, MD, a third-year resident in pediatrics at the University of California, Davis, School of Medicine in Sacramento, was surprised to learn that the American Academy of Pediatrics (AAP) had been issuing a standard-of-care PPE for decades.
Dr. Ng had a long-standing interest in pediatric sports medicine and thought that if she was unfamiliar with this form, which was first developed by the AAP in the 1990s in collaboration with other professional organizations, there must be others who were unaware of this resource.
Assuming that this collaborative effort led by the AAP could serve as a standard of care, Dr. Ng evaluated whether PPEs at her own institution were capturing similar information.
In the most recent (5th) edition of the PPE, which was released in 2019 and is available online, medical history is elicited for numerous organ systems relevant to risk. The questions are not directed to any specific sport; the form does not even provide a question about which sports are being considered.
Little Consistency
In evaluating whether PPEs completed at her institution in the previous year elicited similar information, Dr. Ng sought to match 25 elements of patient history from the AAP form to questions posed in the PPEs completed at her institution, some of which had been supplied by school or sports organizations.
Of the 365 PPE forms completed at Dr. Ng’s institution that met study criteria, only 28.6% addressed all 25 elements in the AAP form (range, 0%-78%). Although more than half asked specifically about a history of respiratory symptoms, fewer than half included inquiries about cardiovascular history. There was also little consistency in the capture of information about other relevant medical history.
According to Dr. Ng, these low percentages were observed even when liberally awarding credit. For one example, she said forms that asked any question about syncope with exercise were credited with seeking information about cardiovascular health even though a yes-or-no response might not be helpful.
“We did not distinguish between syncope before or after exercise and this is relevant,” Dr. Ng said. “Syncope during exercise is more likely to be a predictor of sudden cardiac death, whereas syncope after exercise is more likely to be a vasovagal response to exertion.”
Of the 365 PPEs evaluated, about half were completed by pediatricians and half by family medicine clinicians. The average age of the children was about 14 years. Sixty-three percent were male. Only one third of the forms documented the sport for which a pre-participation screen was being submitted.
While almost all states now require PPEs for children considering participation in sports, few specify what information should be elicited, according to Dr. Ng. She further noted that no major study has shown that PPEs have any role in preventing morbidity or mortality related to sports participation.
Does Heterogeneity Negate Worth?
With such diversity across PPEs, evaluating their role is difficult. For example, with such heterogeneity among forms for the information elicited, there is no reasonable approach for testing their sensitivity in predicting medical complications.
Dr. Ng noted that school-created forms were just as likely as forms from other sources to diverge from the AAP-endorsed PPE and ignore organ systems relevant to risk of medical complications. Yet, if the answer is to use the AAP form, Dr. Ng noted that the first sentence on the form reads, “This form should be placed in the athlete’s medical file and should not be shared with schools or sports organizations.”
Although Dr. Ng acknowledged that providing completed PPEs to third parties raises questions about privacy, she questioned how the information should be used by children, parents, and sports organization administrators for discussing risks if not shared.
This concern was seconded in the discussion following Dr. Ng’s presentation.
“You might be signing off on sports participation, but is this for cheerleading or for football?” asked Daniel C. Worthington, MD, a pediatrician in private practice who has a clinical appointment at Case Western Reserve University School of Medicine, Cleveland. “This makes a huge difference when evaluating if participation is safe.”
He has no issue with completing PPEs for the goal of keeping children safe, but he focused on the inconsistency of how information is collected and distributed.
“The major question is: Does it make any difference?” said Dr. Worthington, referring to the completion of PPEs.
Another participant in the discussion that followed Dr. Ng’s presentation pointed out that the urgent care office in a mall near to his office offers a completed PPE form for a price of $20. In their recommendations, the AAP suggests PPEs be completed by the individual’s primary care physician during a well visit, according to Dr. Ng.
Dr. Ng indicated that PPEs and their purpose deserve a closer look. Based on her data, it is reasonable to assume that the priority for some – whether those requiring or those completing the form — is completing the task rather than meaningful screening of risk.
Dr. Ng and Dr. Worthington report no potential conflicts of interest.
TORONTO — There is little consistency in the elements and types of information captured in preparticipation physical evaluations (PPE) for sports among school-aged children, which is complicating efforts to determine if they have value, according to a study presented at the Pediatric Academic Societies annual meeting.
The study concept developed when Tammy Ng, MD, a third-year resident in pediatrics at the University of California, Davis, School of Medicine in Sacramento, was surprised to learn that the American Academy of Pediatrics (AAP) had been issuing a standard-of-care PPE for decades.
Dr. Ng had a long-standing interest in pediatric sports medicine and thought that if she was unfamiliar with this form, which was first developed by the AAP in the 1990s in collaboration with other professional organizations, there must be others who were unaware of this resource.
Assuming that this collaborative effort led by the AAP could serve as a standard of care, Dr. Ng evaluated whether PPEs at her own institution were capturing similar information.
In the most recent (5th) edition of the PPE, which was released in 2019 and is available online, medical history is elicited for numerous organ systems relevant to risk. The questions are not directed to any specific sport; the form does not even provide a question about which sports are being considered.
Little Consistency
In evaluating whether PPEs completed at her institution in the previous year elicited similar information, Dr. Ng sought to match 25 elements of patient history from the AAP form to questions posed in the PPEs completed at her institution, some of which had been supplied by school or sports organizations.
Of the 365 PPE forms completed at Dr. Ng’s institution that met study criteria, only 28.6% addressed all 25 elements in the AAP form (range, 0%-78%). Although more than half asked specifically about a history of respiratory symptoms, fewer than half included inquiries about cardiovascular history. There was also little consistency in the capture of information about other relevant medical history.
According to Dr. Ng, these low percentages were observed even when liberally awarding credit. For one example, she said forms that asked any question about syncope with exercise were credited with seeking information about cardiovascular health even though a yes-or-no response might not be helpful.
“We did not distinguish between syncope before or after exercise and this is relevant,” Dr. Ng said. “Syncope during exercise is more likely to be a predictor of sudden cardiac death, whereas syncope after exercise is more likely to be a vasovagal response to exertion.”
Of the 365 PPEs evaluated, about half were completed by pediatricians and half by family medicine clinicians. The average age of the children was about 14 years. Sixty-three percent were male. Only one third of the forms documented the sport for which a pre-participation screen was being submitted.
While almost all states now require PPEs for children considering participation in sports, few specify what information should be elicited, according to Dr. Ng. She further noted that no major study has shown that PPEs have any role in preventing morbidity or mortality related to sports participation.
Does Heterogeneity Negate Worth?
With such diversity across PPEs, evaluating their role is difficult. For example, with such heterogeneity among forms for the information elicited, there is no reasonable approach for testing their sensitivity in predicting medical complications.
Dr. Ng noted that school-created forms were just as likely as forms from other sources to diverge from the AAP-endorsed PPE and ignore organ systems relevant to risk of medical complications. Yet, if the answer is to use the AAP form, Dr. Ng noted that the first sentence on the form reads, “This form should be placed in the athlete’s medical file and should not be shared with schools or sports organizations.”
Although Dr. Ng acknowledged that providing completed PPEs to third parties raises questions about privacy, she questioned how the information should be used by children, parents, and sports organization administrators for discussing risks if not shared.
This concern was seconded in the discussion following Dr. Ng’s presentation.
“You might be signing off on sports participation, but is this for cheerleading or for football?” asked Daniel C. Worthington, MD, a pediatrician in private practice who has a clinical appointment at Case Western Reserve University School of Medicine, Cleveland. “This makes a huge difference when evaluating if participation is safe.”
He has no issue with completing PPEs for the goal of keeping children safe, but he focused on the inconsistency of how information is collected and distributed.
“The major question is: Does it make any difference?” said Dr. Worthington, referring to the completion of PPEs.
Another participant in the discussion that followed Dr. Ng’s presentation pointed out that the urgent care office in a mall near to his office offers a completed PPE form for a price of $20. In their recommendations, the AAP suggests PPEs be completed by the individual’s primary care physician during a well visit, according to Dr. Ng.
Dr. Ng indicated that PPEs and their purpose deserve a closer look. Based on her data, it is reasonable to assume that the priority for some – whether those requiring or those completing the form — is completing the task rather than meaningful screening of risk.
Dr. Ng and Dr. Worthington report no potential conflicts of interest.
TORONTO — There is little consistency in the elements and types of information captured in preparticipation physical evaluations (PPE) for sports among school-aged children, which is complicating efforts to determine if they have value, according to a study presented at the Pediatric Academic Societies annual meeting.
The study concept developed when Tammy Ng, MD, a third-year resident in pediatrics at the University of California, Davis, School of Medicine in Sacramento, was surprised to learn that the American Academy of Pediatrics (AAP) had been issuing a standard-of-care PPE for decades.
Dr. Ng had a long-standing interest in pediatric sports medicine and thought that if she was unfamiliar with this form, which was first developed by the AAP in the 1990s in collaboration with other professional organizations, there must be others who were unaware of this resource.
Assuming that this collaborative effort led by the AAP could serve as a standard of care, Dr. Ng evaluated whether PPEs at her own institution were capturing similar information.
In the most recent (5th) edition of the PPE, which was released in 2019 and is available online, medical history is elicited for numerous organ systems relevant to risk. The questions are not directed to any specific sport; the form does not even provide a question about which sports are being considered.
Little Consistency
In evaluating whether PPEs completed at her institution in the previous year elicited similar information, Dr. Ng sought to match 25 elements of patient history from the AAP form to questions posed in the PPEs completed at her institution, some of which had been supplied by school or sports organizations.
Of the 365 PPE forms completed at Dr. Ng’s institution that met study criteria, only 28.6% addressed all 25 elements in the AAP form (range, 0%-78%). Although more than half asked specifically about a history of respiratory symptoms, fewer than half included inquiries about cardiovascular history. There was also little consistency in the capture of information about other relevant medical history.
According to Dr. Ng, these low percentages were observed even when liberally awarding credit. For one example, she said forms that asked any question about syncope with exercise were credited with seeking information about cardiovascular health even though a yes-or-no response might not be helpful.
“We did not distinguish between syncope before or after exercise and this is relevant,” Dr. Ng said. “Syncope during exercise is more likely to be a predictor of sudden cardiac death, whereas syncope after exercise is more likely to be a vasovagal response to exertion.”
Of the 365 PPEs evaluated, about half were completed by pediatricians and half by family medicine clinicians. The average age of the children was about 14 years. Sixty-three percent were male. Only one third of the forms documented the sport for which a pre-participation screen was being submitted.
While almost all states now require PPEs for children considering participation in sports, few specify what information should be elicited, according to Dr. Ng. She further noted that no major study has shown that PPEs have any role in preventing morbidity or mortality related to sports participation.
Does Heterogeneity Negate Worth?
With such diversity across PPEs, evaluating their role is difficult. For example, with such heterogeneity among forms for the information elicited, there is no reasonable approach for testing their sensitivity in predicting medical complications.
Dr. Ng noted that school-created forms were just as likely as forms from other sources to diverge from the AAP-endorsed PPE and ignore organ systems relevant to risk of medical complications. Yet, if the answer is to use the AAP form, Dr. Ng noted that the first sentence on the form reads, “This form should be placed in the athlete’s medical file and should not be shared with schools or sports organizations.”
Although Dr. Ng acknowledged that providing completed PPEs to third parties raises questions about privacy, she questioned how the information should be used by children, parents, and sports organization administrators for discussing risks if not shared.
This concern was seconded in the discussion following Dr. Ng’s presentation.
“You might be signing off on sports participation, but is this for cheerleading or for football?” asked Daniel C. Worthington, MD, a pediatrician in private practice who has a clinical appointment at Case Western Reserve University School of Medicine, Cleveland. “This makes a huge difference when evaluating if participation is safe.”
He has no issue with completing PPEs for the goal of keeping children safe, but he focused on the inconsistency of how information is collected and distributed.
“The major question is: Does it make any difference?” said Dr. Worthington, referring to the completion of PPEs.
Another participant in the discussion that followed Dr. Ng’s presentation pointed out that the urgent care office in a mall near to his office offers a completed PPE form for a price of $20. In their recommendations, the AAP suggests PPEs be completed by the individual’s primary care physician during a well visit, according to Dr. Ng.
Dr. Ng indicated that PPEs and their purpose deserve a closer look. Based on her data, it is reasonable to assume that the priority for some – whether those requiring or those completing the form — is completing the task rather than meaningful screening of risk.
Dr. Ng and Dr. Worthington report no potential conflicts of interest.
FROM PAS 2024
Childhood Loneliness Predictive of Subsequent Psychosis?
BUDAPEST, HUNGARY — Self-perceived loneliness during childhood is linked to a more than twofold increased risk for subsequent first-episode psychosis (FEP) — new findings that may point to a novel marker for the disorder.
The association between loneliness and FEP “appears to extend beyond the effects of objective social isolation,” said study presenter Covadonga M. Díaz-Caneja, MD, PhD, Institute of Psychiatry and Mental Health, Hospital General Universitario Gregorio Marañón, Madrid, and “is particularly pronounced in females.”
“These findings suggest the potential of childhood loneliness as an early risk marker for psychosis that could help guide targeted interventions,” she added.
The results were presented at the European Psychiatric Association 2024 Congress.
Isolation a Major Risk Factor
There are two components to isolation, both of which are “major risk factors” for morbidity, mortality, and the onset of mental disorders, said Dr. Díaz-Caneja.
The first is “objective social isolation,” which consists of a demonstrable lack of social connections, including social interactions, contacts, and relationships, while the other is a perceived sense of isolation, or “loneliness,” defined as a “subjective feeling of distress associated with a lack of meaningful relationships,” regardless of the amount of actual social contact an individual experiences.
Childhood loneliness occurs before age 12 and is becoming increasingly prevalent, said Dr. Díaz-Caneja. A recent survey shows that approximately one third of children report they often feel lonely.
Genetic and observational research has shown there is a bidirectional relationship between loneliness and psychosis and that patients with schizophrenia are more likely to report loneliness than is the general population.
Dr. Díaz-Caneja noted that there is no previous research that has assessed the potential association between childhood loneliness and subsequent psychosis.
To investigate, the researchers conducted an observational, case-control study in seven university hospitals in Madrid. It included individuals aged 7-40 years, including FEP patients with a psychosis duration of less than 2 years, and healthy controls from the same geographic areas.
They assessed childhood objective social isolation using the Premorbid Adjustment Scale and examined childhood loneliness with the single item: “Have you ever felt lonely for more than 6 months before the age of 12?”
A range of measures and questionnaires were also administered to assess participants’ symptom scores, alongside the Global Assessment of Functioning (GAF).
Alone vs Lonely
Two hundred eighty-five patients with FEP participated in the study. They had a mean age of 24.5 years, and 32.6% were female. The study also included 261 healthy controls (average age, 25.9 years; 48.7% female).
After the researchers adjusted for age, gender, ethnicity, and socioeconomic status, loneliness during childhood was associated with a significantly increased risk for FEP (odds ratio [OR], 2.17; 95% CI, 1.40-3.51), which increased (OR, 2.70; 95% CI, 1.58-4.62) after further adjustment for objective social isolation.
Further analysis revealed that in those who did not have objective social isolation in childhood, loneliness was associated with a significantly increased risk for FEP (OR, 2.68; 95% CI, 1.56-4.60).
However, the relationship between loneliness and FEP was not significant in participants who were objectively socially isolated during childhood (OR, 0.33; 95% CI, 0.08-1.45).
Compared with males, females reporting loneliness had a markedly increased risk for FEP (OR, 4.74; 95% CI, 2.23-10.05 vs OR, 1.17; 95% CI, 0.63-2.19).
However, females had a reduced risk of receiving a diagnosis of schizophrenia spectrum disorder (OR, 0.155; 95% CI, 0.048-0.506), indicating that loneliness influenced the type of diagnosis, she noted.
There was a significant positive relationship between loneliness in childhood and symptom scores in men, and a negative association with GAF scores in men.
Dr. Díaz-Caneja noted that the study is preliminary and a “work in progress.” The investigators plan to increase the sample size and will conduct more complex analyses, she said.
“We also of course have to bear in mind that it is a cross-sectional study and that there may be some kind of recall biases [because] we are asking patients now about what happened in the past.”
She noted that it’s unclear whether the results can be extrapolated to individuals who are currently experiencing loneliness because “the determinants of loneliness 10 years ago or 15 years ago may be different.”
How, When to Intervene
Session chair Judit Lazáry, MD, PhD, Department of Clinical and Theoretical Mental Health, Kútvölgyi Clinical Center, Semmelweis University, Budapest, Hungary, told this news organization that the association between loneliness and FEP was “not surprising.”
She explained there are a lot of data indicating that premorbid symptoms in childhood are “predictive signs for the later onset of psychosis,” and loneliness may be “a part of that.”
Individuals experiencing loneliness are more anxious and have difficulties in cultivating and maintaining relationships. In addition, they tend to socially isolate, she said.
The key question, said Dr. Lazáry, is: “How can we intervene to prevent the onset of psychosis? What is the point at which we can support the young person?”
This is challenging, she added, because while “you can detect that a kid is always alone, you cannot detect the feeling of loneliness,” and children can’t always easily express themselves.
Another potential confounder is that in adults with current psychosis, the self-perception that they were lonely during childhood may be a consequence of the disorder.
In addition, she said, individuals with psychosis often experience cognitive impairment, which could affect memory reliability.
Nevertheless, said Dr. Lazáry, the study’s findings suggest that a young person reporting loneliness in childhood may be “another symptom that we have to investigate.”
No funding was declared.
Dr. Díaz-Caneja declared a relationship with Angelini, Janssen, and Viatris and grant support from Instituto de Salud Carlos III, the Spanish Ministry of Science and Innovation, and the European Commission.
A version of this article appeared on Medscape.com.
BUDAPEST, HUNGARY — Self-perceived loneliness during childhood is linked to a more than twofold increased risk for subsequent first-episode psychosis (FEP) — new findings that may point to a novel marker for the disorder.
The association between loneliness and FEP “appears to extend beyond the effects of objective social isolation,” said study presenter Covadonga M. Díaz-Caneja, MD, PhD, Institute of Psychiatry and Mental Health, Hospital General Universitario Gregorio Marañón, Madrid, and “is particularly pronounced in females.”
“These findings suggest the potential of childhood loneliness as an early risk marker for psychosis that could help guide targeted interventions,” she added.
The results were presented at the European Psychiatric Association 2024 Congress.
Isolation a Major Risk Factor
There are two components to isolation, both of which are “major risk factors” for morbidity, mortality, and the onset of mental disorders, said Dr. Díaz-Caneja.
The first is “objective social isolation,” which consists of a demonstrable lack of social connections, including social interactions, contacts, and relationships, while the other is a perceived sense of isolation, or “loneliness,” defined as a “subjective feeling of distress associated with a lack of meaningful relationships,” regardless of the amount of actual social contact an individual experiences.
Childhood loneliness occurs before age 12 and is becoming increasingly prevalent, said Dr. Díaz-Caneja. A recent survey shows that approximately one third of children report they often feel lonely.
Genetic and observational research has shown there is a bidirectional relationship between loneliness and psychosis and that patients with schizophrenia are more likely to report loneliness than is the general population.
Dr. Díaz-Caneja noted that there is no previous research that has assessed the potential association between childhood loneliness and subsequent psychosis.
To investigate, the researchers conducted an observational, case-control study in seven university hospitals in Madrid. It included individuals aged 7-40 years, including FEP patients with a psychosis duration of less than 2 years, and healthy controls from the same geographic areas.
They assessed childhood objective social isolation using the Premorbid Adjustment Scale and examined childhood loneliness with the single item: “Have you ever felt lonely for more than 6 months before the age of 12?”
A range of measures and questionnaires were also administered to assess participants’ symptom scores, alongside the Global Assessment of Functioning (GAF).
Alone vs Lonely
Two hundred eighty-five patients with FEP participated in the study. They had a mean age of 24.5 years, and 32.6% were female. The study also included 261 healthy controls (average age, 25.9 years; 48.7% female).
After the researchers adjusted for age, gender, ethnicity, and socioeconomic status, loneliness during childhood was associated with a significantly increased risk for FEP (odds ratio [OR], 2.17; 95% CI, 1.40-3.51), which increased (OR, 2.70; 95% CI, 1.58-4.62) after further adjustment for objective social isolation.
Further analysis revealed that in those who did not have objective social isolation in childhood, loneliness was associated with a significantly increased risk for FEP (OR, 2.68; 95% CI, 1.56-4.60).
However, the relationship between loneliness and FEP was not significant in participants who were objectively socially isolated during childhood (OR, 0.33; 95% CI, 0.08-1.45).
Compared with males, females reporting loneliness had a markedly increased risk for FEP (OR, 4.74; 95% CI, 2.23-10.05 vs OR, 1.17; 95% CI, 0.63-2.19).
However, females had a reduced risk of receiving a diagnosis of schizophrenia spectrum disorder (OR, 0.155; 95% CI, 0.048-0.506), indicating that loneliness influenced the type of diagnosis, she noted.
There was a significant positive relationship between loneliness in childhood and symptom scores in men, and a negative association with GAF scores in men.
Dr. Díaz-Caneja noted that the study is preliminary and a “work in progress.” The investigators plan to increase the sample size and will conduct more complex analyses, she said.
“We also of course have to bear in mind that it is a cross-sectional study and that there may be some kind of recall biases [because] we are asking patients now about what happened in the past.”
She noted that it’s unclear whether the results can be extrapolated to individuals who are currently experiencing loneliness because “the determinants of loneliness 10 years ago or 15 years ago may be different.”
How, When to Intervene
Session chair Judit Lazáry, MD, PhD, Department of Clinical and Theoretical Mental Health, Kútvölgyi Clinical Center, Semmelweis University, Budapest, Hungary, told this news organization that the association between loneliness and FEP was “not surprising.”
She explained there are a lot of data indicating that premorbid symptoms in childhood are “predictive signs for the later onset of psychosis,” and loneliness may be “a part of that.”
Individuals experiencing loneliness are more anxious and have difficulties in cultivating and maintaining relationships. In addition, they tend to socially isolate, she said.
The key question, said Dr. Lazáry, is: “How can we intervene to prevent the onset of psychosis? What is the point at which we can support the young person?”
This is challenging, she added, because while “you can detect that a kid is always alone, you cannot detect the feeling of loneliness,” and children can’t always easily express themselves.
Another potential confounder is that in adults with current psychosis, the self-perception that they were lonely during childhood may be a consequence of the disorder.
In addition, she said, individuals with psychosis often experience cognitive impairment, which could affect memory reliability.
Nevertheless, said Dr. Lazáry, the study’s findings suggest that a young person reporting loneliness in childhood may be “another symptom that we have to investigate.”
No funding was declared.
Dr. Díaz-Caneja declared a relationship with Angelini, Janssen, and Viatris and grant support from Instituto de Salud Carlos III, the Spanish Ministry of Science and Innovation, and the European Commission.
A version of this article appeared on Medscape.com.
BUDAPEST, HUNGARY — Self-perceived loneliness during childhood is linked to a more than twofold increased risk for subsequent first-episode psychosis (FEP) — new findings that may point to a novel marker for the disorder.
The association between loneliness and FEP “appears to extend beyond the effects of objective social isolation,” said study presenter Covadonga M. Díaz-Caneja, MD, PhD, Institute of Psychiatry and Mental Health, Hospital General Universitario Gregorio Marañón, Madrid, and “is particularly pronounced in females.”
“These findings suggest the potential of childhood loneliness as an early risk marker for psychosis that could help guide targeted interventions,” she added.
The results were presented at the European Psychiatric Association 2024 Congress.
Isolation a Major Risk Factor
There are two components to isolation, both of which are “major risk factors” for morbidity, mortality, and the onset of mental disorders, said Dr. Díaz-Caneja.
The first is “objective social isolation,” which consists of a demonstrable lack of social connections, including social interactions, contacts, and relationships, while the other is a perceived sense of isolation, or “loneliness,” defined as a “subjective feeling of distress associated with a lack of meaningful relationships,” regardless of the amount of actual social contact an individual experiences.
Childhood loneliness occurs before age 12 and is becoming increasingly prevalent, said Dr. Díaz-Caneja. A recent survey shows that approximately one third of children report they often feel lonely.
Genetic and observational research has shown there is a bidirectional relationship between loneliness and psychosis and that patients with schizophrenia are more likely to report loneliness than is the general population.
Dr. Díaz-Caneja noted that there is no previous research that has assessed the potential association between childhood loneliness and subsequent psychosis.
To investigate, the researchers conducted an observational, case-control study in seven university hospitals in Madrid. It included individuals aged 7-40 years, including FEP patients with a psychosis duration of less than 2 years, and healthy controls from the same geographic areas.
They assessed childhood objective social isolation using the Premorbid Adjustment Scale and examined childhood loneliness with the single item: “Have you ever felt lonely for more than 6 months before the age of 12?”
A range of measures and questionnaires were also administered to assess participants’ symptom scores, alongside the Global Assessment of Functioning (GAF).
Alone vs Lonely
Two hundred eighty-five patients with FEP participated in the study. They had a mean age of 24.5 years, and 32.6% were female. The study also included 261 healthy controls (average age, 25.9 years; 48.7% female).
After the researchers adjusted for age, gender, ethnicity, and socioeconomic status, loneliness during childhood was associated with a significantly increased risk for FEP (odds ratio [OR], 2.17; 95% CI, 1.40-3.51), which increased (OR, 2.70; 95% CI, 1.58-4.62) after further adjustment for objective social isolation.
Further analysis revealed that in those who did not have objective social isolation in childhood, loneliness was associated with a significantly increased risk for FEP (OR, 2.68; 95% CI, 1.56-4.60).
However, the relationship between loneliness and FEP was not significant in participants who were objectively socially isolated during childhood (OR, 0.33; 95% CI, 0.08-1.45).
Compared with males, females reporting loneliness had a markedly increased risk for FEP (OR, 4.74; 95% CI, 2.23-10.05 vs OR, 1.17; 95% CI, 0.63-2.19).
However, females had a reduced risk of receiving a diagnosis of schizophrenia spectrum disorder (OR, 0.155; 95% CI, 0.048-0.506), indicating that loneliness influenced the type of diagnosis, she noted.
There was a significant positive relationship between loneliness in childhood and symptom scores in men, and a negative association with GAF scores in men.
Dr. Díaz-Caneja noted that the study is preliminary and a “work in progress.” The investigators plan to increase the sample size and will conduct more complex analyses, she said.
“We also of course have to bear in mind that it is a cross-sectional study and that there may be some kind of recall biases [because] we are asking patients now about what happened in the past.”
She noted that it’s unclear whether the results can be extrapolated to individuals who are currently experiencing loneliness because “the determinants of loneliness 10 years ago or 15 years ago may be different.”
How, When to Intervene
Session chair Judit Lazáry, MD, PhD, Department of Clinical and Theoretical Mental Health, Kútvölgyi Clinical Center, Semmelweis University, Budapest, Hungary, told this news organization that the association between loneliness and FEP was “not surprising.”
She explained there are a lot of data indicating that premorbid symptoms in childhood are “predictive signs for the later onset of psychosis,” and loneliness may be “a part of that.”
Individuals experiencing loneliness are more anxious and have difficulties in cultivating and maintaining relationships. In addition, they tend to socially isolate, she said.
The key question, said Dr. Lazáry, is: “How can we intervene to prevent the onset of psychosis? What is the point at which we can support the young person?”
This is challenging, she added, because while “you can detect that a kid is always alone, you cannot detect the feeling of loneliness,” and children can’t always easily express themselves.
Another potential confounder is that in adults with current psychosis, the self-perception that they were lonely during childhood may be a consequence of the disorder.
In addition, she said, individuals with psychosis often experience cognitive impairment, which could affect memory reliability.
Nevertheless, said Dr. Lazáry, the study’s findings suggest that a young person reporting loneliness in childhood may be “another symptom that we have to investigate.”
No funding was declared.
Dr. Díaz-Caneja declared a relationship with Angelini, Janssen, and Viatris and grant support from Instituto de Salud Carlos III, the Spanish Ministry of Science and Innovation, and the European Commission.
A version of this article appeared on Medscape.com.
First Consensus Statement on Improving Healthcare for Children with Neurodevelopmental Disabilities
The statement was published in Pediatrics.
The disparities in healthcare culture, mindset, and practice often start in childhood for young people with conditions including autism spectrum disorder (ASD), intellectual disability, and attention-deficit/hyperactivity disorder (ADHD), wrote co–first authors Carol Weitzman, MD, co-director of the Autism Spectrum Center at Boston Children’s Hospital, Boston, Massachusetts, and Cy Nadler, PhD, section chief of Autism Psychology at Children’s Mercy in Kansas City, Missouri, and colleagues.
Without better access to safe and appropriate care, people with NDDs experience more seclusion, accidents, restraints, and injury in healthcare encounters, the researchers wrote.
‘Accessible, Humane, Effective Care’
“At the heart of this consensus statement is an affirmation that all people are entitled to healthcare that is accessible, humane, and effective,” they wrote.
The consensus statement was developed as part of the Supporting Access for Everyone (SAFE) Initiative, launched by the Developmental Behavioral Pediatric Research Network and the Association of University Centers on Disability. The consensus panel comprised professionals, caregivers, and adults with NDDs. After a 2-day public forum, the consensus panel held a conference and developed a statement on SAFE care, an NDD Health Care Bill of Rights and Transition Considerations. They developed 10 statements across five domains: training; communication; access and planning; diversity, equity, inclusion, belonging, and anti-ableism; and policy and structural change.
Asking the Patient ‘What do You Need?’
One theme in the statement that may have the most impact is “the importance of asking the person in front of you what they need,” and building a care plan around that, said senior author Marilyn Augustyn, MD, Director of the Division of Developmental and Behavioral Pediatrics at Boston University Chobanian & Avedisian School of Medicine, Boston, Massachusetts. “The medical community hasn’t done that very well for individuals with neurodevelopmental disabilities.”
Dr. Weitzman added: “Traditionally in healthcare settings, we’ve asked people to check their disabilities at the door.” Many people with neurodevelopmental disabilities often have “invisible disabilities,” she said, explaining that patients may have accommodation needs that aren’t immediately obvious, but could improve their access to care, so asking them what they need is critical.
Examples of ‘Ableism’
The consensus statement also calls attention to structural “ableism” or policies or practices that favor able-bodied people over those with disabilities and details the need for more training and changed policies.
The paper gives some examples of ableism, such as inappropriately excluding people with NDDs from research; staff assuming nonspeaking patients have no capacity for communication; or lack of awareness of sensory needs before using cold stethoscopes or flashing direct light into eyes.
Dr. Weitzman says this work is just the beginning of a complex process. It is intended to be the driver for developing curriculum to train all clinicians and others working with patients about neurodevelopmental disabilities. The hope is it will lead to more research to formalize best practices and make policies mandatory rather than optional.
The urgency in highlighting these issues is partly related to the prevalence of children and adolescents with neurodevelopmental disabilities, which the paper states is approximately 1 in 6.
But there are personal reasons as well for the team who developed the statement.
“We just believe that it is just a human right,” Dr. Weitzman said. “Having a neurodevelopmental disability does not make you any less entitled to good care. “
Dr. Augustyn added, “The children I’ve had the honor of caring for for the last 30 years deserve all this care and more. I think it’s time.”
This work was supported by the Developmental Behavioral Pediatric Research Network and the Association of University Centers on Disability. Dr. Weitzman is a past consultant for Helios/Meliora. The other authors report no relevant financial relationships.
The statement was published in Pediatrics.
The disparities in healthcare culture, mindset, and practice often start in childhood for young people with conditions including autism spectrum disorder (ASD), intellectual disability, and attention-deficit/hyperactivity disorder (ADHD), wrote co–first authors Carol Weitzman, MD, co-director of the Autism Spectrum Center at Boston Children’s Hospital, Boston, Massachusetts, and Cy Nadler, PhD, section chief of Autism Psychology at Children’s Mercy in Kansas City, Missouri, and colleagues.
Without better access to safe and appropriate care, people with NDDs experience more seclusion, accidents, restraints, and injury in healthcare encounters, the researchers wrote.
‘Accessible, Humane, Effective Care’
“At the heart of this consensus statement is an affirmation that all people are entitled to healthcare that is accessible, humane, and effective,” they wrote.
The consensus statement was developed as part of the Supporting Access for Everyone (SAFE) Initiative, launched by the Developmental Behavioral Pediatric Research Network and the Association of University Centers on Disability. The consensus panel comprised professionals, caregivers, and adults with NDDs. After a 2-day public forum, the consensus panel held a conference and developed a statement on SAFE care, an NDD Health Care Bill of Rights and Transition Considerations. They developed 10 statements across five domains: training; communication; access and planning; diversity, equity, inclusion, belonging, and anti-ableism; and policy and structural change.
Asking the Patient ‘What do You Need?’
One theme in the statement that may have the most impact is “the importance of asking the person in front of you what they need,” and building a care plan around that, said senior author Marilyn Augustyn, MD, Director of the Division of Developmental and Behavioral Pediatrics at Boston University Chobanian & Avedisian School of Medicine, Boston, Massachusetts. “The medical community hasn’t done that very well for individuals with neurodevelopmental disabilities.”
Dr. Weitzman added: “Traditionally in healthcare settings, we’ve asked people to check their disabilities at the door.” Many people with neurodevelopmental disabilities often have “invisible disabilities,” she said, explaining that patients may have accommodation needs that aren’t immediately obvious, but could improve their access to care, so asking them what they need is critical.
Examples of ‘Ableism’
The consensus statement also calls attention to structural “ableism” or policies or practices that favor able-bodied people over those with disabilities and details the need for more training and changed policies.
The paper gives some examples of ableism, such as inappropriately excluding people with NDDs from research; staff assuming nonspeaking patients have no capacity for communication; or lack of awareness of sensory needs before using cold stethoscopes or flashing direct light into eyes.
Dr. Weitzman says this work is just the beginning of a complex process. It is intended to be the driver for developing curriculum to train all clinicians and others working with patients about neurodevelopmental disabilities. The hope is it will lead to more research to formalize best practices and make policies mandatory rather than optional.
The urgency in highlighting these issues is partly related to the prevalence of children and adolescents with neurodevelopmental disabilities, which the paper states is approximately 1 in 6.
But there are personal reasons as well for the team who developed the statement.
“We just believe that it is just a human right,” Dr. Weitzman said. “Having a neurodevelopmental disability does not make you any less entitled to good care. “
Dr. Augustyn added, “The children I’ve had the honor of caring for for the last 30 years deserve all this care and more. I think it’s time.”
This work was supported by the Developmental Behavioral Pediatric Research Network and the Association of University Centers on Disability. Dr. Weitzman is a past consultant for Helios/Meliora. The other authors report no relevant financial relationships.
The statement was published in Pediatrics.
The disparities in healthcare culture, mindset, and practice often start in childhood for young people with conditions including autism spectrum disorder (ASD), intellectual disability, and attention-deficit/hyperactivity disorder (ADHD), wrote co–first authors Carol Weitzman, MD, co-director of the Autism Spectrum Center at Boston Children’s Hospital, Boston, Massachusetts, and Cy Nadler, PhD, section chief of Autism Psychology at Children’s Mercy in Kansas City, Missouri, and colleagues.
Without better access to safe and appropriate care, people with NDDs experience more seclusion, accidents, restraints, and injury in healthcare encounters, the researchers wrote.
‘Accessible, Humane, Effective Care’
“At the heart of this consensus statement is an affirmation that all people are entitled to healthcare that is accessible, humane, and effective,” they wrote.
The consensus statement was developed as part of the Supporting Access for Everyone (SAFE) Initiative, launched by the Developmental Behavioral Pediatric Research Network and the Association of University Centers on Disability. The consensus panel comprised professionals, caregivers, and adults with NDDs. After a 2-day public forum, the consensus panel held a conference and developed a statement on SAFE care, an NDD Health Care Bill of Rights and Transition Considerations. They developed 10 statements across five domains: training; communication; access and planning; diversity, equity, inclusion, belonging, and anti-ableism; and policy and structural change.
Asking the Patient ‘What do You Need?’
One theme in the statement that may have the most impact is “the importance of asking the person in front of you what they need,” and building a care plan around that, said senior author Marilyn Augustyn, MD, Director of the Division of Developmental and Behavioral Pediatrics at Boston University Chobanian & Avedisian School of Medicine, Boston, Massachusetts. “The medical community hasn’t done that very well for individuals with neurodevelopmental disabilities.”
Dr. Weitzman added: “Traditionally in healthcare settings, we’ve asked people to check their disabilities at the door.” Many people with neurodevelopmental disabilities often have “invisible disabilities,” she said, explaining that patients may have accommodation needs that aren’t immediately obvious, but could improve their access to care, so asking them what they need is critical.
Examples of ‘Ableism’
The consensus statement also calls attention to structural “ableism” or policies or practices that favor able-bodied people over those with disabilities and details the need for more training and changed policies.
The paper gives some examples of ableism, such as inappropriately excluding people with NDDs from research; staff assuming nonspeaking patients have no capacity for communication; or lack of awareness of sensory needs before using cold stethoscopes or flashing direct light into eyes.
Dr. Weitzman says this work is just the beginning of a complex process. It is intended to be the driver for developing curriculum to train all clinicians and others working with patients about neurodevelopmental disabilities. The hope is it will lead to more research to formalize best practices and make policies mandatory rather than optional.
The urgency in highlighting these issues is partly related to the prevalence of children and adolescents with neurodevelopmental disabilities, which the paper states is approximately 1 in 6.
But there are personal reasons as well for the team who developed the statement.
“We just believe that it is just a human right,” Dr. Weitzman said. “Having a neurodevelopmental disability does not make you any less entitled to good care. “
Dr. Augustyn added, “The children I’ve had the honor of caring for for the last 30 years deserve all this care and more. I think it’s time.”
This work was supported by the Developmental Behavioral Pediatric Research Network and the Association of University Centers on Disability. Dr. Weitzman is a past consultant for Helios/Meliora. The other authors report no relevant financial relationships.