User login
Exposure to air pollution increases incident breast cancer risk
Key clinical point: Women who were exposed to fine particulate matter, ie, airborne particles with an aerodynamic diameter ≤ 2.5 μm (PM2.5), showed an increased risk of developing breast cancer (BC), particularly estrogen receptor-positive (ER+) BC.
Major finding: As little as a 10 µg/m3 increase in PM2.5 concentration during 1980-1984 increased the incident risk for BC by 8% (hazard ratio [HR] 1.08; 95% CI 1.02-1.13), with the risk being even higher in case of ER+ BC (HR 1.10; 95% CI 1.04-1.17).
Study details: Findings are from an analysis of a prospective, US-based cohort including 196,905 women with no prior history of cancer, of whom 15,870 developed incident BC.
Disclosures: This study was funded by the US National Institutes of Environmental Health Sciences and the US National Cancer Institute Intramural Program. The authors declared no conflicts of interest.
Source: White AJ et al. Ambient fine particulate matter and breast cancer incidence in a large prospective US cohort. J Natl Cancer Inst. 2023 (Sep 11). doi: 10.1093/jnci/djad170
Key clinical point: Women who were exposed to fine particulate matter, ie, airborne particles with an aerodynamic diameter ≤ 2.5 μm (PM2.5), showed an increased risk of developing breast cancer (BC), particularly estrogen receptor-positive (ER+) BC.
Major finding: As little as a 10 µg/m3 increase in PM2.5 concentration during 1980-1984 increased the incident risk for BC by 8% (hazard ratio [HR] 1.08; 95% CI 1.02-1.13), with the risk being even higher in case of ER+ BC (HR 1.10; 95% CI 1.04-1.17).
Study details: Findings are from an analysis of a prospective, US-based cohort including 196,905 women with no prior history of cancer, of whom 15,870 developed incident BC.
Disclosures: This study was funded by the US National Institutes of Environmental Health Sciences and the US National Cancer Institute Intramural Program. The authors declared no conflicts of interest.
Source: White AJ et al. Ambient fine particulate matter and breast cancer incidence in a large prospective US cohort. J Natl Cancer Inst. 2023 (Sep 11). doi: 10.1093/jnci/djad170
Key clinical point: Women who were exposed to fine particulate matter, ie, airborne particles with an aerodynamic diameter ≤ 2.5 μm (PM2.5), showed an increased risk of developing breast cancer (BC), particularly estrogen receptor-positive (ER+) BC.
Major finding: As little as a 10 µg/m3 increase in PM2.5 concentration during 1980-1984 increased the incident risk for BC by 8% (hazard ratio [HR] 1.08; 95% CI 1.02-1.13), with the risk being even higher in case of ER+ BC (HR 1.10; 95% CI 1.04-1.17).
Study details: Findings are from an analysis of a prospective, US-based cohort including 196,905 women with no prior history of cancer, of whom 15,870 developed incident BC.
Disclosures: This study was funded by the US National Institutes of Environmental Health Sciences and the US National Cancer Institute Intramural Program. The authors declared no conflicts of interest.
Source: White AJ et al. Ambient fine particulate matter and breast cancer incidence in a large prospective US cohort. J Natl Cancer Inst. 2023 (Sep 11). doi: 10.1093/jnci/djad170
Doxorubicin chemo increases subsequent BC risk in childhood cancer survivors
Key clinical point: Women who survived cancer during childhood and received ≥ 200 mg/m2 cumulative doxorubicin dose as a part of the treatment may have an increased risk of developing subsequent breast cancer (SBC).
Major finding: A ≥200 mg/m2 cumulative doxorubicin dose vs no doxorubicin treatment led to > 2-fold increase in the risk for SBC (hazard ratio [HR] for 200-299 mg/m2: 2.50, 95% CI 1.85-3.40; HR for 300-399 mg/m2: 2.33, 95% CI 1.68-3.23; and HR for ≥ 400 mg/m2: 2.78, 95% CI 1.99-3.88). Every 100 mg/m2 increase in the cumulative doxorubicin dose increased SBC risk in patients who survived cancer and either received (HR 1.11; 95% CI 1.02-1.21) or did not receive chest radiotherapy (HR 1.26; 95% CI 1.17-1.36).
<Study details: Findings are from an analysis of a pooled cohort including 17,903 females who survived cancer for ≥ 5 years, of whom 782 survivors developed SBC.
Disclosures: This study was supported by the Children Cancer Free Foundation (aka Foundation KiKa, Stichting Kinderen Kankervrij), Amsterdam. The authors declared no conflicts of interest.
Source: Wang Y et al for The International Consortium for Pooled Studies on Subsequent Malignancies after Childhood and Adolescent Cancer. Subsequent female breast cancer risk associated with anthracycline chemotherapy for childhood cancer. Nat Med. 2023;29(9):2268-2277 (Sep 11). doi: 10.1038/s41591-023-02514-1
Key clinical point: Women who survived cancer during childhood and received ≥ 200 mg/m2 cumulative doxorubicin dose as a part of the treatment may have an increased risk of developing subsequent breast cancer (SBC).
Major finding: A ≥200 mg/m2 cumulative doxorubicin dose vs no doxorubicin treatment led to > 2-fold increase in the risk for SBC (hazard ratio [HR] for 200-299 mg/m2: 2.50, 95% CI 1.85-3.40; HR for 300-399 mg/m2: 2.33, 95% CI 1.68-3.23; and HR for ≥ 400 mg/m2: 2.78, 95% CI 1.99-3.88). Every 100 mg/m2 increase in the cumulative doxorubicin dose increased SBC risk in patients who survived cancer and either received (HR 1.11; 95% CI 1.02-1.21) or did not receive chest radiotherapy (HR 1.26; 95% CI 1.17-1.36).
<Study details: Findings are from an analysis of a pooled cohort including 17,903 females who survived cancer for ≥ 5 years, of whom 782 survivors developed SBC.
Disclosures: This study was supported by the Children Cancer Free Foundation (aka Foundation KiKa, Stichting Kinderen Kankervrij), Amsterdam. The authors declared no conflicts of interest.
Source: Wang Y et al for The International Consortium for Pooled Studies on Subsequent Malignancies after Childhood and Adolescent Cancer. Subsequent female breast cancer risk associated with anthracycline chemotherapy for childhood cancer. Nat Med. 2023;29(9):2268-2277 (Sep 11). doi: 10.1038/s41591-023-02514-1
Key clinical point: Women who survived cancer during childhood and received ≥ 200 mg/m2 cumulative doxorubicin dose as a part of the treatment may have an increased risk of developing subsequent breast cancer (SBC).
Major finding: A ≥200 mg/m2 cumulative doxorubicin dose vs no doxorubicin treatment led to > 2-fold increase in the risk for SBC (hazard ratio [HR] for 200-299 mg/m2: 2.50, 95% CI 1.85-3.40; HR for 300-399 mg/m2: 2.33, 95% CI 1.68-3.23; and HR for ≥ 400 mg/m2: 2.78, 95% CI 1.99-3.88). Every 100 mg/m2 increase in the cumulative doxorubicin dose increased SBC risk in patients who survived cancer and either received (HR 1.11; 95% CI 1.02-1.21) or did not receive chest radiotherapy (HR 1.26; 95% CI 1.17-1.36).
<Study details: Findings are from an analysis of a pooled cohort including 17,903 females who survived cancer for ≥ 5 years, of whom 782 survivors developed SBC.
Disclosures: This study was supported by the Children Cancer Free Foundation (aka Foundation KiKa, Stichting Kinderen Kankervrij), Amsterdam. The authors declared no conflicts of interest.
Source: Wang Y et al for The International Consortium for Pooled Studies on Subsequent Malignancies after Childhood and Adolescent Cancer. Subsequent female breast cancer risk associated with anthracycline chemotherapy for childhood cancer. Nat Med. 2023;29(9):2268-2277 (Sep 11). doi: 10.1038/s41591-023-02514-1
Early BC patients with small tumors and negative axillary lymph node ultrasound may skip axillary surgery
Key clinical point: The omission of axillary surgery leads to non-inferior outcomes compared to sentinel lymph node biopsy (SLNB) and may not be necessary in patients with early breast cancer (BC) having a tumor diameter ≤ 2 cm and negative results for preoperative axillary lymph node ultrasonography.
Major finding: The rates of 5-year distant disease-free survival were comparable in patients who underwent SLNB and those who did not undergo axillary surgery (97.7% vs 98.0%; hazard ratio 0.84; noninferiority P = .02).
Study details: Findings are from the phase 3 SOUND trial including 1405 women with BC having a tumor diameter ≤ 2 cm and negative preoperative axillary ultrasonography results who were randomly assigned to undergo either SLNB or no axillary surgery.
Disclosures: This study did not disclose any funding source. Some authors declared receiving personal fees from various sources.
Source: Gentilini OD et al for the SOUND Trial Group. Sentinel lymph node biopsy vs no axillary surgery in patients with small breast cancer and negative results on ultrasonography of axillary lymph nodes: The SOUND randomized clinical trial. JAMA Oncol. 2023 (Sep 21). doi: 10.1001/jamaoncol.2023.3759
Key clinical point: The omission of axillary surgery leads to non-inferior outcomes compared to sentinel lymph node biopsy (SLNB) and may not be necessary in patients with early breast cancer (BC) having a tumor diameter ≤ 2 cm and negative results for preoperative axillary lymph node ultrasonography.
Major finding: The rates of 5-year distant disease-free survival were comparable in patients who underwent SLNB and those who did not undergo axillary surgery (97.7% vs 98.0%; hazard ratio 0.84; noninferiority P = .02).
Study details: Findings are from the phase 3 SOUND trial including 1405 women with BC having a tumor diameter ≤ 2 cm and negative preoperative axillary ultrasonography results who were randomly assigned to undergo either SLNB or no axillary surgery.
Disclosures: This study did not disclose any funding source. Some authors declared receiving personal fees from various sources.
Source: Gentilini OD et al for the SOUND Trial Group. Sentinel lymph node biopsy vs no axillary surgery in patients with small breast cancer and negative results on ultrasonography of axillary lymph nodes: The SOUND randomized clinical trial. JAMA Oncol. 2023 (Sep 21). doi: 10.1001/jamaoncol.2023.3759
Key clinical point: The omission of axillary surgery leads to non-inferior outcomes compared to sentinel lymph node biopsy (SLNB) and may not be necessary in patients with early breast cancer (BC) having a tumor diameter ≤ 2 cm and negative results for preoperative axillary lymph node ultrasonography.
Major finding: The rates of 5-year distant disease-free survival were comparable in patients who underwent SLNB and those who did not undergo axillary surgery (97.7% vs 98.0%; hazard ratio 0.84; noninferiority P = .02).
Study details: Findings are from the phase 3 SOUND trial including 1405 women with BC having a tumor diameter ≤ 2 cm and negative preoperative axillary ultrasonography results who were randomly assigned to undergo either SLNB or no axillary surgery.
Disclosures: This study did not disclose any funding source. Some authors declared receiving personal fees from various sources.
Source: Gentilini OD et al for the SOUND Trial Group. Sentinel lymph node biopsy vs no axillary surgery in patients with small breast cancer and negative results on ultrasonography of axillary lymph nodes: The SOUND randomized clinical trial. JAMA Oncol. 2023 (Sep 21). doi: 10.1001/jamaoncol.2023.3759
Do screening mammograms in women aged 70 and older improve stage at diagnosis or breast cancer–specific mortality?
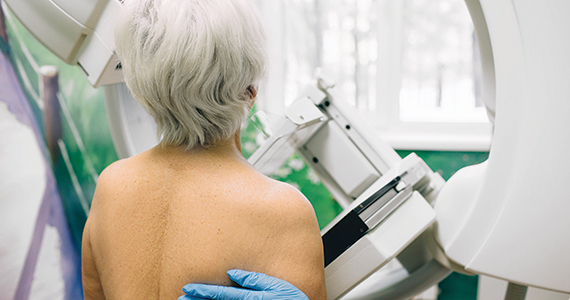
Richman IB, Long JB, Soulos PR, et al. Estimating breast cancer overdiagnosis after screening mammography among older women in the United States. Ann Intern Med. 2023;176:1172-1180. doi:10.7326/M23-0133
EXPERT COMMENTARY
A screening test is performed to detect potential health disorders or diseases in people who do not have any symptoms of disease. The goal of screening is to detect the condition early enough to treat it most effectively, and ultimately to decrease morbidity and mortality related to the disease. Overdiagnosis refers to the finding of a cancer that would not have caused clinical problems during a person’s lifetime.
Current guidelines for the early detection of breast cancer vary considerably, including recommendations for what age to initiate screening, the cadence of screening (annual or biannual), the use of ancillary screening for people with dense breasts, and importantly the upper age limit for which screening is advised. The US Preventive Services Task Force recommends continuing screening to age 74. The American Cancer Society suggests ongoing screening if life expectancy is estimated at more than 10 years, and the American College of Physicians recommends stopping screening at age 75, or younger if life expectancy is less than 10 years. The American College of Obstetricians and Gynecologists states that women at average risk of breast cancer should continue screening mammography until at least age 75.
Overdiagnosis is a difficult concept for clinicians to understand let alone explain to our patients. Recently, Richman and colleagues published the results of their study aimed at estimating overdiagnosis associated with breast cancer screening among older women.1 As Dr. Otis Brawley, former Chief Medical and Scientific Officer of the American Cancer Society and current Distinguished Professor of Oncology and Epidemiology at Johns Hopkins University, states in the editorial that accompanies the study by Richman and colleagues, “Some tumors are not destined to grow, spread, and kill due to their genomics or their microenvironment. A second type of overdiagnosis involves small tumors that do have the potential to grow but will not grow fast enough to bother the patient within their natural lifetime.”2
Although screening mammography in older women results in frequent false positives that require additional imaging as well as biopsies, we have become more aware of the potential of overdiagnosis as an important downside of screening mammography in an elderly population.
Continue to: Details of the study...
Details of the study
Using the SEER registry to identify breast cancers linked to a 5% sample of Medicare beneficiaries, Richman and colleagues (funded by the National Cancer Institute and based at Yale University) conducted a retrospectivecohort study to estimate the likelihood of overdiagnosis associated with screening mammography among older women over 15 years of follow-up. Specifically, they assessed the difference in cumulative incidence of in situ and invasive breast cancer among women aged 70 years and older without a history of breast cancer when screened in 2002. During the subsequent 3 years, participants either continued screening (screened group) or did not (unscreened group). Women were followed through 2017.
Among almost 55,000 women followed, 88% were White, 6% were Black, and 3% were Hispanic. Mean follow-up was 13.7 years among women aged 70 to 74 years at baseline. For those aged 75 to 84 at baseline, mean follow-up was 10 years, and for those aged 85 years and older, mean follow-up was 5.7 years.
Estimated rates of overdiagnosis. Overall, among women aged 70 to 74 at baseline who were eventually diagnosed with breast cancer, the investigators estimated that 31% of these cancers were overdiagnosed. The corresponding percentage of breast cancers estimated to represent overdiagnosis climbed to 47% for those aged 75 to 84 years at baseline and to 54% for those aged 85 years and older at baseline.
The investigators assessed the impact of greater screening among women with a first-degree relative with a diagnosis of breast cancer and determined that this did not explain their results. With respect to cancer stage, the investigators noted that overdiagnosis was more prevalent among in situ and localized invasive cancers compared with those with regional or distant spread. Of note, the incidence of cancer with regional or distant spread was neither higher nor lower among those who were screened. Finally, the investigators did not observe significant differences in breast cancer–specific mortality by screening status.
The proportion of cancers that were overdiagnosed was particularly high among women with in situ as well as those with localized invasive disease. The investigators pointed out that as many as 90% of women aged 80 and older diagnosed with localized cancer undergo surgery, and almost two-thirds of those older than 70 years have radiation therapy for early-stage disease. In addition to the burdens associated with these treatments for overdiagnosed cancers in older women, simply being diagnosed with breast cancer profoundly affects the health and well-being of women, resulting in anxiety and substantial reductions in quality of life.
The authors also noted that some studies suggest that, among breast cancers diagnosed with screening, chemotherapy is less likely to be employed among older women, a screening benefit that must be weighed against the high likelihood of overdiagnosis. However, this benefit is unlikely to be meaningful for the majority of patients in this study who presented with in situ or early invasive lesions since chemotherapy often is not recommended for such women.
Study strengths and limitations
If screening mammography is effective, the incidence of advanced-stage tumors and breast cancer–specific mortality should be reduced in screened populations. Accordingly, in this large, long-term study using reliable sources of data, the findings that the incidence of advanced-stage disease as well as breast cancer–specific mortality were similar in the screened and unscreened cohorts provides powerful evidence that screening mammography is not effective in older women.3
As the authors pointed out, their findings regarding a high prevalence of overdiagnosis associated with screening mammography in older women are consistent with findings of other studies, some of which used different methodology.
The authors acknowledged that some women in their Medicare cohort who initially continued screening likely stopped screening subsequently, while some who initially did not continue screening might have been screened subsequently. They went on to indicate that if patients were completely adherent with subsequent screening (or not getting screened) the likelihood that cancers among screened women were overdiagnosed would be even higher.
Lead-time bias occurs when screening finds a cancer earlier than that cancer would have been diagnosed because of symptoms. This study followed the cohorts over a long timeframe to reduce the possibility that lead time was inappropriately identified as overdiagnosis. They also observed that, among women aged 85 and older, most cohort members had died by the end of study follow-up; accordingly, lead time is not likely to have explained their findings.
Limitations. The authors acknowledged that miscoding the mammogram type (screening vs diagnostic) could result in higher estimates of overdiagnosis. In their most conservative sensitivity analysis, the overdiagnosis rates could be as low as 15% for women aged 70 to 74, 36% for those aged 75 to 84, and 44% for people aged 85 and older.
Because this was an observational cohort study, unmeasured differences in breast cancer risk and underlying health factors may have been confounders. Specifically, people with severe life-threatening conditions that limited their expected life span may have chosen not to undergo regular screening. Although the authors did attempt to adjust for these factors, there may have been unrecognized confounders. This study was designed to estimate overdiagnosis, and therefore the specific benefits and harms of screening could not be addressed based on the data collected. ●
The high prevalence of overdiagnosis and lack of a breast cancer–specific mortality benefit among older women who undergo screening mammography is sobering. Clinician recommendations and shared decision making with our patients regarding screening mammography should take into consideration overdiagnosis and the considerable harms associated with overtreatment. Although we may recognize that overdiagnosed cancers are often indolent tumors with a long presymptomatic phase, in older women, even finding a biologically aggressive cancer may represent overdiagnosis if life expectancy is limited.
BARBARA LEVY, MD, MSCP; ANDREW M. KAUNITZ, MD, MSCP.
- Richman IB, Long JB, Soulos PR, et al. Estimating breast cancer overdiagnosis after screening mammography among older women in the United States. Ann Intern Med. 2023;176:1172-1180. doi:10.7326/M23-0133
- Brawley OW, Ramalingam R. Understanding the varying biological behaviors of breast and other types of cancer to avoid overdiagnosis. Ann Intern Med. 2023;176:1273-1274. doi:10.7326/M23-18953
- Welch HG, Gorski DH, Albertsen PC. Trends in metastatic breast and prostate cancer—lessons in cancer dynamics. N Engl J Med. 2015;373:1685-1687. doi:10.1056/NEJM p1510443

Richman IB, Long JB, Soulos PR, et al. Estimating breast cancer overdiagnosis after screening mammography among older women in the United States. Ann Intern Med. 2023;176:1172-1180. doi:10.7326/M23-0133
EXPERT COMMENTARY
A screening test is performed to detect potential health disorders or diseases in people who do not have any symptoms of disease. The goal of screening is to detect the condition early enough to treat it most effectively, and ultimately to decrease morbidity and mortality related to the disease. Overdiagnosis refers to the finding of a cancer that would not have caused clinical problems during a person’s lifetime.
Current guidelines for the early detection of breast cancer vary considerably, including recommendations for what age to initiate screening, the cadence of screening (annual or biannual), the use of ancillary screening for people with dense breasts, and importantly the upper age limit for which screening is advised. The US Preventive Services Task Force recommends continuing screening to age 74. The American Cancer Society suggests ongoing screening if life expectancy is estimated at more than 10 years, and the American College of Physicians recommends stopping screening at age 75, or younger if life expectancy is less than 10 years. The American College of Obstetricians and Gynecologists states that women at average risk of breast cancer should continue screening mammography until at least age 75.
Overdiagnosis is a difficult concept for clinicians to understand let alone explain to our patients. Recently, Richman and colleagues published the results of their study aimed at estimating overdiagnosis associated with breast cancer screening among older women.1 As Dr. Otis Brawley, former Chief Medical and Scientific Officer of the American Cancer Society and current Distinguished Professor of Oncology and Epidemiology at Johns Hopkins University, states in the editorial that accompanies the study by Richman and colleagues, “Some tumors are not destined to grow, spread, and kill due to their genomics or their microenvironment. A second type of overdiagnosis involves small tumors that do have the potential to grow but will not grow fast enough to bother the patient within their natural lifetime.”2
Although screening mammography in older women results in frequent false positives that require additional imaging as well as biopsies, we have become more aware of the potential of overdiagnosis as an important downside of screening mammography in an elderly population.
Continue to: Details of the study...
Details of the study
Using the SEER registry to identify breast cancers linked to a 5% sample of Medicare beneficiaries, Richman and colleagues (funded by the National Cancer Institute and based at Yale University) conducted a retrospectivecohort study to estimate the likelihood of overdiagnosis associated with screening mammography among older women over 15 years of follow-up. Specifically, they assessed the difference in cumulative incidence of in situ and invasive breast cancer among women aged 70 years and older without a history of breast cancer when screened in 2002. During the subsequent 3 years, participants either continued screening (screened group) or did not (unscreened group). Women were followed through 2017.
Among almost 55,000 women followed, 88% were White, 6% were Black, and 3% were Hispanic. Mean follow-up was 13.7 years among women aged 70 to 74 years at baseline. For those aged 75 to 84 at baseline, mean follow-up was 10 years, and for those aged 85 years and older, mean follow-up was 5.7 years.
Estimated rates of overdiagnosis. Overall, among women aged 70 to 74 at baseline who were eventually diagnosed with breast cancer, the investigators estimated that 31% of these cancers were overdiagnosed. The corresponding percentage of breast cancers estimated to represent overdiagnosis climbed to 47% for those aged 75 to 84 years at baseline and to 54% for those aged 85 years and older at baseline.
The investigators assessed the impact of greater screening among women with a first-degree relative with a diagnosis of breast cancer and determined that this did not explain their results. With respect to cancer stage, the investigators noted that overdiagnosis was more prevalent among in situ and localized invasive cancers compared with those with regional or distant spread. Of note, the incidence of cancer with regional or distant spread was neither higher nor lower among those who were screened. Finally, the investigators did not observe significant differences in breast cancer–specific mortality by screening status.
The proportion of cancers that were overdiagnosed was particularly high among women with in situ as well as those with localized invasive disease. The investigators pointed out that as many as 90% of women aged 80 and older diagnosed with localized cancer undergo surgery, and almost two-thirds of those older than 70 years have radiation therapy for early-stage disease. In addition to the burdens associated with these treatments for overdiagnosed cancers in older women, simply being diagnosed with breast cancer profoundly affects the health and well-being of women, resulting in anxiety and substantial reductions in quality of life.
The authors also noted that some studies suggest that, among breast cancers diagnosed with screening, chemotherapy is less likely to be employed among older women, a screening benefit that must be weighed against the high likelihood of overdiagnosis. However, this benefit is unlikely to be meaningful for the majority of patients in this study who presented with in situ or early invasive lesions since chemotherapy often is not recommended for such women.
Study strengths and limitations
If screening mammography is effective, the incidence of advanced-stage tumors and breast cancer–specific mortality should be reduced in screened populations. Accordingly, in this large, long-term study using reliable sources of data, the findings that the incidence of advanced-stage disease as well as breast cancer–specific mortality were similar in the screened and unscreened cohorts provides powerful evidence that screening mammography is not effective in older women.3
As the authors pointed out, their findings regarding a high prevalence of overdiagnosis associated with screening mammography in older women are consistent with findings of other studies, some of which used different methodology.
The authors acknowledged that some women in their Medicare cohort who initially continued screening likely stopped screening subsequently, while some who initially did not continue screening might have been screened subsequently. They went on to indicate that if patients were completely adherent with subsequent screening (or not getting screened) the likelihood that cancers among screened women were overdiagnosed would be even higher.
Lead-time bias occurs when screening finds a cancer earlier than that cancer would have been diagnosed because of symptoms. This study followed the cohorts over a long timeframe to reduce the possibility that lead time was inappropriately identified as overdiagnosis. They also observed that, among women aged 85 and older, most cohort members had died by the end of study follow-up; accordingly, lead time is not likely to have explained their findings.
Limitations. The authors acknowledged that miscoding the mammogram type (screening vs diagnostic) could result in higher estimates of overdiagnosis. In their most conservative sensitivity analysis, the overdiagnosis rates could be as low as 15% for women aged 70 to 74, 36% for those aged 75 to 84, and 44% for people aged 85 and older.
Because this was an observational cohort study, unmeasured differences in breast cancer risk and underlying health factors may have been confounders. Specifically, people with severe life-threatening conditions that limited their expected life span may have chosen not to undergo regular screening. Although the authors did attempt to adjust for these factors, there may have been unrecognized confounders. This study was designed to estimate overdiagnosis, and therefore the specific benefits and harms of screening could not be addressed based on the data collected. ●
The high prevalence of overdiagnosis and lack of a breast cancer–specific mortality benefit among older women who undergo screening mammography is sobering. Clinician recommendations and shared decision making with our patients regarding screening mammography should take into consideration overdiagnosis and the considerable harms associated with overtreatment. Although we may recognize that overdiagnosed cancers are often indolent tumors with a long presymptomatic phase, in older women, even finding a biologically aggressive cancer may represent overdiagnosis if life expectancy is limited.
BARBARA LEVY, MD, MSCP; ANDREW M. KAUNITZ, MD, MSCP.

Richman IB, Long JB, Soulos PR, et al. Estimating breast cancer overdiagnosis after screening mammography among older women in the United States. Ann Intern Med. 2023;176:1172-1180. doi:10.7326/M23-0133
EXPERT COMMENTARY
A screening test is performed to detect potential health disorders or diseases in people who do not have any symptoms of disease. The goal of screening is to detect the condition early enough to treat it most effectively, and ultimately to decrease morbidity and mortality related to the disease. Overdiagnosis refers to the finding of a cancer that would not have caused clinical problems during a person’s lifetime.
Current guidelines for the early detection of breast cancer vary considerably, including recommendations for what age to initiate screening, the cadence of screening (annual or biannual), the use of ancillary screening for people with dense breasts, and importantly the upper age limit for which screening is advised. The US Preventive Services Task Force recommends continuing screening to age 74. The American Cancer Society suggests ongoing screening if life expectancy is estimated at more than 10 years, and the American College of Physicians recommends stopping screening at age 75, or younger if life expectancy is less than 10 years. The American College of Obstetricians and Gynecologists states that women at average risk of breast cancer should continue screening mammography until at least age 75.
Overdiagnosis is a difficult concept for clinicians to understand let alone explain to our patients. Recently, Richman and colleagues published the results of their study aimed at estimating overdiagnosis associated with breast cancer screening among older women.1 As Dr. Otis Brawley, former Chief Medical and Scientific Officer of the American Cancer Society and current Distinguished Professor of Oncology and Epidemiology at Johns Hopkins University, states in the editorial that accompanies the study by Richman and colleagues, “Some tumors are not destined to grow, spread, and kill due to their genomics or their microenvironment. A second type of overdiagnosis involves small tumors that do have the potential to grow but will not grow fast enough to bother the patient within their natural lifetime.”2
Although screening mammography in older women results in frequent false positives that require additional imaging as well as biopsies, we have become more aware of the potential of overdiagnosis as an important downside of screening mammography in an elderly population.
Continue to: Details of the study...
Details of the study
Using the SEER registry to identify breast cancers linked to a 5% sample of Medicare beneficiaries, Richman and colleagues (funded by the National Cancer Institute and based at Yale University) conducted a retrospectivecohort study to estimate the likelihood of overdiagnosis associated with screening mammography among older women over 15 years of follow-up. Specifically, they assessed the difference in cumulative incidence of in situ and invasive breast cancer among women aged 70 years and older without a history of breast cancer when screened in 2002. During the subsequent 3 years, participants either continued screening (screened group) or did not (unscreened group). Women were followed through 2017.
Among almost 55,000 women followed, 88% were White, 6% were Black, and 3% were Hispanic. Mean follow-up was 13.7 years among women aged 70 to 74 years at baseline. For those aged 75 to 84 at baseline, mean follow-up was 10 years, and for those aged 85 years and older, mean follow-up was 5.7 years.
Estimated rates of overdiagnosis. Overall, among women aged 70 to 74 at baseline who were eventually diagnosed with breast cancer, the investigators estimated that 31% of these cancers were overdiagnosed. The corresponding percentage of breast cancers estimated to represent overdiagnosis climbed to 47% for those aged 75 to 84 years at baseline and to 54% for those aged 85 years and older at baseline.
The investigators assessed the impact of greater screening among women with a first-degree relative with a diagnosis of breast cancer and determined that this did not explain their results. With respect to cancer stage, the investigators noted that overdiagnosis was more prevalent among in situ and localized invasive cancers compared with those with regional or distant spread. Of note, the incidence of cancer with regional or distant spread was neither higher nor lower among those who were screened. Finally, the investigators did not observe significant differences in breast cancer–specific mortality by screening status.
The proportion of cancers that were overdiagnosed was particularly high among women with in situ as well as those with localized invasive disease. The investigators pointed out that as many as 90% of women aged 80 and older diagnosed with localized cancer undergo surgery, and almost two-thirds of those older than 70 years have radiation therapy for early-stage disease. In addition to the burdens associated with these treatments for overdiagnosed cancers in older women, simply being diagnosed with breast cancer profoundly affects the health and well-being of women, resulting in anxiety and substantial reductions in quality of life.
The authors also noted that some studies suggest that, among breast cancers diagnosed with screening, chemotherapy is less likely to be employed among older women, a screening benefit that must be weighed against the high likelihood of overdiagnosis. However, this benefit is unlikely to be meaningful for the majority of patients in this study who presented with in situ or early invasive lesions since chemotherapy often is not recommended for such women.
Study strengths and limitations
If screening mammography is effective, the incidence of advanced-stage tumors and breast cancer–specific mortality should be reduced in screened populations. Accordingly, in this large, long-term study using reliable sources of data, the findings that the incidence of advanced-stage disease as well as breast cancer–specific mortality were similar in the screened and unscreened cohorts provides powerful evidence that screening mammography is not effective in older women.3
As the authors pointed out, their findings regarding a high prevalence of overdiagnosis associated with screening mammography in older women are consistent with findings of other studies, some of which used different methodology.
The authors acknowledged that some women in their Medicare cohort who initially continued screening likely stopped screening subsequently, while some who initially did not continue screening might have been screened subsequently. They went on to indicate that if patients were completely adherent with subsequent screening (or not getting screened) the likelihood that cancers among screened women were overdiagnosed would be even higher.
Lead-time bias occurs when screening finds a cancer earlier than that cancer would have been diagnosed because of symptoms. This study followed the cohorts over a long timeframe to reduce the possibility that lead time was inappropriately identified as overdiagnosis. They also observed that, among women aged 85 and older, most cohort members had died by the end of study follow-up; accordingly, lead time is not likely to have explained their findings.
Limitations. The authors acknowledged that miscoding the mammogram type (screening vs diagnostic) could result in higher estimates of overdiagnosis. In their most conservative sensitivity analysis, the overdiagnosis rates could be as low as 15% for women aged 70 to 74, 36% for those aged 75 to 84, and 44% for people aged 85 and older.
Because this was an observational cohort study, unmeasured differences in breast cancer risk and underlying health factors may have been confounders. Specifically, people with severe life-threatening conditions that limited their expected life span may have chosen not to undergo regular screening. Although the authors did attempt to adjust for these factors, there may have been unrecognized confounders. This study was designed to estimate overdiagnosis, and therefore the specific benefits and harms of screening could not be addressed based on the data collected. ●
The high prevalence of overdiagnosis and lack of a breast cancer–specific mortality benefit among older women who undergo screening mammography is sobering. Clinician recommendations and shared decision making with our patients regarding screening mammography should take into consideration overdiagnosis and the considerable harms associated with overtreatment. Although we may recognize that overdiagnosed cancers are often indolent tumors with a long presymptomatic phase, in older women, even finding a biologically aggressive cancer may represent overdiagnosis if life expectancy is limited.
BARBARA LEVY, MD, MSCP; ANDREW M. KAUNITZ, MD, MSCP.
- Richman IB, Long JB, Soulos PR, et al. Estimating breast cancer overdiagnosis after screening mammography among older women in the United States. Ann Intern Med. 2023;176:1172-1180. doi:10.7326/M23-0133
- Brawley OW, Ramalingam R. Understanding the varying biological behaviors of breast and other types of cancer to avoid overdiagnosis. Ann Intern Med. 2023;176:1273-1274. doi:10.7326/M23-18953
- Welch HG, Gorski DH, Albertsen PC. Trends in metastatic breast and prostate cancer—lessons in cancer dynamics. N Engl J Med. 2015;373:1685-1687. doi:10.1056/NEJM p1510443
- Richman IB, Long JB, Soulos PR, et al. Estimating breast cancer overdiagnosis after screening mammography among older women in the United States. Ann Intern Med. 2023;176:1172-1180. doi:10.7326/M23-0133
- Brawley OW, Ramalingam R. Understanding the varying biological behaviors of breast and other types of cancer to avoid overdiagnosis. Ann Intern Med. 2023;176:1273-1274. doi:10.7326/M23-18953
- Welch HG, Gorski DH, Albertsen PC. Trends in metastatic breast and prostate cancer—lessons in cancer dynamics. N Engl J Med. 2015;373:1685-1687. doi:10.1056/NEJM p1510443
News & Perspectives from Ob.Gyn. News
COMMENTARY
The safety of vaginal estrogen in breast cancer survivors
Currently, more than 3.8 million breast cancer survivors reside in the United States, reflecting high prevalence as well as cure rates for this common malignancy.
When over-the-counter measures including vaginal lubricants and moisturizers are not adequate, vaginal estrogen may be a highly effective treatment for genitourinary syndrome of menopause (GSM), a common condition associated with hypoestrogenism that impairs sexual function and quality of life.
Use of vaginal formulations does not result in systemic levels of estrogen above the normal postmenopausal range. Nonetheless, the U.S. Food and Drug Administration lists a history of breast cancer as a contraindication to the use of all systemic as well as vaginal estrogens.
In premenopausal women, chemotherapy for breast cancer often results in early menopause. Aromatase inhibitors, although effective in preventing recurrent disease in menopausal women, exacerbate GSM. These factors result in a high prevalence of GSM in breast cancer survivors.
Because the safety of vaginal estrogen in the setting of breast cancer is uncertain, investigators at Johns Hopkins conducted a cohort study using claims-based data from more than 200 million U.S. patients that identified women with GSM who had previously been diagnosed with breast cancer. Among some 42,000 women diagnosed with GSM after breast cancer, 5% had three or more prescriptions and were considered vaginal estrogen users.
No significant differences were noted in recurrence-free survival between the vaginal estrogen group and the no estrogen group. At 5 and 10 years of follow-up, use of vaginal estrogen was not associated with higher all-cause mortality. Among women with estrogen receptor–positive tumors, risk for breast cancer recurrence was similar between estrogen users and nonusers.
LATEST NEWS
Older women who get mammograms risk overdiagnosis
TOPLINE:
Women who continue breast cancer screening after age 70 face a considerable risk for overdiagnosis.
METHODOLOGY:
- Overdiagnosis – the risk of detecting and treating cancers that would never have caused issues in a person’s lifetime – is increasingly recognized as a harm of breast cancer screening; however, the scope of the problem among older women remains uncertain.
- To get an idea, investigators linked Medicare claims data with Surveillance, Epidemiology, and End Results (SEER) data for 54,635 women 70 years or older to compare the incidence of breast cancer and breast cancer–specific death among women who continued screening mammography with those who did not.
- The women all had undergone recent screening mammograms and had no history of breast cancer at study entry. Those who had a subsequent mammogram within 3 years were classified as undergoing continued screening while those who did not were classified as not undergoing continued screening.
- Overdiagnosis was defined as the difference in cumulative incidence of breast cancer between screened and unscreened women divided by the cumulative incidence among screened women.
- Results were adjusted for potential confounders, including age, race, and ethnicity.
Continue to: TAKEAWAY...
TAKEAWAY:
- Over 80% of women 70-84 years old and more than 60% of women 85 years or older continued screening.
- Among women 70-74 years old, the adjusted cumulative incidence of breast cancer was 6.1 cases per 100 screened women vs. 4.2 cases per 100 unscreened women; for women aged 75-84 years old, the cumulative incidence was 4.9 per 100 screened women vs. 2.6 per 100 unscreened women, and for women 85 years and older, the cumulative incidence was 2.8 vs. 1.3 per 100, respectively.
- Estimates of overdiagnosis ranged from 31% of breast cancer cases among screened women in the 70-74 age group to 54% of cases in the 85 and older group.
- The researchers found no statistically significant reduction in breast cancer–specific death associated with screening in any age or life-expectancy group. Overdiagnosis appeared to be driven by in situ and localized invasive breast cancer, not advanced breast cancer.
IN PRACTICE:
The proportion of older women who continue to receive screening mammograms and may experience breast cancer overdiagnosis is “considerable” and “increases with advancing age and with decreasing life expectancy,” the authors conclude. Given potential benefits and harms of screening in this population, “patient preferences, including risk tolerance, comfort with uncertainty, and willingness to undergo treatment, are important for informing screening decisions.”
SOURCE: https://www.acpjournals.org/doi/10.7326/M23-0133
https://www.mdedge.com/obgyn/latest-news
CONFERENCE COVERAGE
Offering HPV vaccine at age 9 linked to greater series completion
BALTIMORE—Receiving the first dose of the human papillomavirus (HPV) vaccine at age 9, rather than bundling it with the Tdap and meningitis vaccines, appears to increase the likelihood that children will complete the HPV vaccine series, according to a retrospective cohort study of commercially insured youth presented at the annual clinical and scientific meeting of the American College of Obstetricians and Gynecologists. The research was published ahead of print in Human Vaccines and Immunotherapeutics.
“These findings are novel because they emphasize starting at age 9, and that is different than prior studies that emphasize bundling of these vaccines,” Kevin Ault, MD, professor and chair of the department of obstetrics and gynecology at Western Michigan University Homer Stryker MD School of Medicine and a former member of the CDC’s Advisory Committee on Immunization Practices, said in an interview.
Dr. Ault was not involved in the study but noted that these findings support the AAP’s recommendation to start the HPV vaccine series at age 9. The Centers for Disease Control and Prevention currently recommends giving the first dose of the HPV vaccine at ages 11-12, at the same time as the Tdap and meningitis vaccines. This recommendation to “bundle” the HPV vaccine with the Tdap and meningitis vaccines aims to facilitate provider-family discussion about the HPV vaccine, ideally reducing parent hesitancy and concerns about the vaccines. Multiple studies have shown improved HPV vaccine uptake when providers offer the HPV vaccine at the same time as the Tdap and meningococcal vaccines.
However, shifts in parents’ attitudes have occurred toward the HPV vaccine since those studies on bundling: Concerns about sexual activity have receded while concerns about safety remain high. The American Academy of Pediatrics and the American Cancer Society both advise starting the HPV vaccine series at age 9, based on evidence showing that more children complete the series when they get the first shot before age 11 compared to getting it at 11 or 12.
COMMENTARY
The safety of vaginal estrogen in breast cancer survivors
Currently, more than 3.8 million breast cancer survivors reside in the United States, reflecting high prevalence as well as cure rates for this common malignancy.
When over-the-counter measures including vaginal lubricants and moisturizers are not adequate, vaginal estrogen may be a highly effective treatment for genitourinary syndrome of menopause (GSM), a common condition associated with hypoestrogenism that impairs sexual function and quality of life.
Use of vaginal formulations does not result in systemic levels of estrogen above the normal postmenopausal range. Nonetheless, the U.S. Food and Drug Administration lists a history of breast cancer as a contraindication to the use of all systemic as well as vaginal estrogens.
In premenopausal women, chemotherapy for breast cancer often results in early menopause. Aromatase inhibitors, although effective in preventing recurrent disease in menopausal women, exacerbate GSM. These factors result in a high prevalence of GSM in breast cancer survivors.
Because the safety of vaginal estrogen in the setting of breast cancer is uncertain, investigators at Johns Hopkins conducted a cohort study using claims-based data from more than 200 million U.S. patients that identified women with GSM who had previously been diagnosed with breast cancer. Among some 42,000 women diagnosed with GSM after breast cancer, 5% had three or more prescriptions and were considered vaginal estrogen users.
No significant differences were noted in recurrence-free survival between the vaginal estrogen group and the no estrogen group. At 5 and 10 years of follow-up, use of vaginal estrogen was not associated with higher all-cause mortality. Among women with estrogen receptor–positive tumors, risk for breast cancer recurrence was similar between estrogen users and nonusers.
LATEST NEWS
Older women who get mammograms risk overdiagnosis
TOPLINE:
Women who continue breast cancer screening after age 70 face a considerable risk for overdiagnosis.
METHODOLOGY:
- Overdiagnosis – the risk of detecting and treating cancers that would never have caused issues in a person’s lifetime – is increasingly recognized as a harm of breast cancer screening; however, the scope of the problem among older women remains uncertain.
- To get an idea, investigators linked Medicare claims data with Surveillance, Epidemiology, and End Results (SEER) data for 54,635 women 70 years or older to compare the incidence of breast cancer and breast cancer–specific death among women who continued screening mammography with those who did not.
- The women all had undergone recent screening mammograms and had no history of breast cancer at study entry. Those who had a subsequent mammogram within 3 years were classified as undergoing continued screening while those who did not were classified as not undergoing continued screening.
- Overdiagnosis was defined as the difference in cumulative incidence of breast cancer between screened and unscreened women divided by the cumulative incidence among screened women.
- Results were adjusted for potential confounders, including age, race, and ethnicity.
Continue to: TAKEAWAY...
TAKEAWAY:
- Over 80% of women 70-84 years old and more than 60% of women 85 years or older continued screening.
- Among women 70-74 years old, the adjusted cumulative incidence of breast cancer was 6.1 cases per 100 screened women vs. 4.2 cases per 100 unscreened women; for women aged 75-84 years old, the cumulative incidence was 4.9 per 100 screened women vs. 2.6 per 100 unscreened women, and for women 85 years and older, the cumulative incidence was 2.8 vs. 1.3 per 100, respectively.
- Estimates of overdiagnosis ranged from 31% of breast cancer cases among screened women in the 70-74 age group to 54% of cases in the 85 and older group.
- The researchers found no statistically significant reduction in breast cancer–specific death associated with screening in any age or life-expectancy group. Overdiagnosis appeared to be driven by in situ and localized invasive breast cancer, not advanced breast cancer.
IN PRACTICE:
The proportion of older women who continue to receive screening mammograms and may experience breast cancer overdiagnosis is “considerable” and “increases with advancing age and with decreasing life expectancy,” the authors conclude. Given potential benefits and harms of screening in this population, “patient preferences, including risk tolerance, comfort with uncertainty, and willingness to undergo treatment, are important for informing screening decisions.”
SOURCE: https://www.acpjournals.org/doi/10.7326/M23-0133
https://www.mdedge.com/obgyn/latest-news
CONFERENCE COVERAGE
Offering HPV vaccine at age 9 linked to greater series completion
BALTIMORE—Receiving the first dose of the human papillomavirus (HPV) vaccine at age 9, rather than bundling it with the Tdap and meningitis vaccines, appears to increase the likelihood that children will complete the HPV vaccine series, according to a retrospective cohort study of commercially insured youth presented at the annual clinical and scientific meeting of the American College of Obstetricians and Gynecologists. The research was published ahead of print in Human Vaccines and Immunotherapeutics.
“These findings are novel because they emphasize starting at age 9, and that is different than prior studies that emphasize bundling of these vaccines,” Kevin Ault, MD, professor and chair of the department of obstetrics and gynecology at Western Michigan University Homer Stryker MD School of Medicine and a former member of the CDC’s Advisory Committee on Immunization Practices, said in an interview.
Dr. Ault was not involved in the study but noted that these findings support the AAP’s recommendation to start the HPV vaccine series at age 9. The Centers for Disease Control and Prevention currently recommends giving the first dose of the HPV vaccine at ages 11-12, at the same time as the Tdap and meningitis vaccines. This recommendation to “bundle” the HPV vaccine with the Tdap and meningitis vaccines aims to facilitate provider-family discussion about the HPV vaccine, ideally reducing parent hesitancy and concerns about the vaccines. Multiple studies have shown improved HPV vaccine uptake when providers offer the HPV vaccine at the same time as the Tdap and meningococcal vaccines.
However, shifts in parents’ attitudes have occurred toward the HPV vaccine since those studies on bundling: Concerns about sexual activity have receded while concerns about safety remain high. The American Academy of Pediatrics and the American Cancer Society both advise starting the HPV vaccine series at age 9, based on evidence showing that more children complete the series when they get the first shot before age 11 compared to getting it at 11 or 12.
COMMENTARY
The safety of vaginal estrogen in breast cancer survivors
Currently, more than 3.8 million breast cancer survivors reside in the United States, reflecting high prevalence as well as cure rates for this common malignancy.
When over-the-counter measures including vaginal lubricants and moisturizers are not adequate, vaginal estrogen may be a highly effective treatment for genitourinary syndrome of menopause (GSM), a common condition associated with hypoestrogenism that impairs sexual function and quality of life.
Use of vaginal formulations does not result in systemic levels of estrogen above the normal postmenopausal range. Nonetheless, the U.S. Food and Drug Administration lists a history of breast cancer as a contraindication to the use of all systemic as well as vaginal estrogens.
In premenopausal women, chemotherapy for breast cancer often results in early menopause. Aromatase inhibitors, although effective in preventing recurrent disease in menopausal women, exacerbate GSM. These factors result in a high prevalence of GSM in breast cancer survivors.
Because the safety of vaginal estrogen in the setting of breast cancer is uncertain, investigators at Johns Hopkins conducted a cohort study using claims-based data from more than 200 million U.S. patients that identified women with GSM who had previously been diagnosed with breast cancer. Among some 42,000 women diagnosed with GSM after breast cancer, 5% had three or more prescriptions and were considered vaginal estrogen users.
No significant differences were noted in recurrence-free survival between the vaginal estrogen group and the no estrogen group. At 5 and 10 years of follow-up, use of vaginal estrogen was not associated with higher all-cause mortality. Among women with estrogen receptor–positive tumors, risk for breast cancer recurrence was similar between estrogen users and nonusers.
LATEST NEWS
Older women who get mammograms risk overdiagnosis
TOPLINE:
Women who continue breast cancer screening after age 70 face a considerable risk for overdiagnosis.
METHODOLOGY:
- Overdiagnosis – the risk of detecting and treating cancers that would never have caused issues in a person’s lifetime – is increasingly recognized as a harm of breast cancer screening; however, the scope of the problem among older women remains uncertain.
- To get an idea, investigators linked Medicare claims data with Surveillance, Epidemiology, and End Results (SEER) data for 54,635 women 70 years or older to compare the incidence of breast cancer and breast cancer–specific death among women who continued screening mammography with those who did not.
- The women all had undergone recent screening mammograms and had no history of breast cancer at study entry. Those who had a subsequent mammogram within 3 years were classified as undergoing continued screening while those who did not were classified as not undergoing continued screening.
- Overdiagnosis was defined as the difference in cumulative incidence of breast cancer between screened and unscreened women divided by the cumulative incidence among screened women.
- Results were adjusted for potential confounders, including age, race, and ethnicity.
Continue to: TAKEAWAY...
TAKEAWAY:
- Over 80% of women 70-84 years old and more than 60% of women 85 years or older continued screening.
- Among women 70-74 years old, the adjusted cumulative incidence of breast cancer was 6.1 cases per 100 screened women vs. 4.2 cases per 100 unscreened women; for women aged 75-84 years old, the cumulative incidence was 4.9 per 100 screened women vs. 2.6 per 100 unscreened women, and for women 85 years and older, the cumulative incidence was 2.8 vs. 1.3 per 100, respectively.
- Estimates of overdiagnosis ranged from 31% of breast cancer cases among screened women in the 70-74 age group to 54% of cases in the 85 and older group.
- The researchers found no statistically significant reduction in breast cancer–specific death associated with screening in any age or life-expectancy group. Overdiagnosis appeared to be driven by in situ and localized invasive breast cancer, not advanced breast cancer.
IN PRACTICE:
The proportion of older women who continue to receive screening mammograms and may experience breast cancer overdiagnosis is “considerable” and “increases with advancing age and with decreasing life expectancy,” the authors conclude. Given potential benefits and harms of screening in this population, “patient preferences, including risk tolerance, comfort with uncertainty, and willingness to undergo treatment, are important for informing screening decisions.”
SOURCE: https://www.acpjournals.org/doi/10.7326/M23-0133
https://www.mdedge.com/obgyn/latest-news
CONFERENCE COVERAGE
Offering HPV vaccine at age 9 linked to greater series completion
BALTIMORE—Receiving the first dose of the human papillomavirus (HPV) vaccine at age 9, rather than bundling it with the Tdap and meningitis vaccines, appears to increase the likelihood that children will complete the HPV vaccine series, according to a retrospective cohort study of commercially insured youth presented at the annual clinical and scientific meeting of the American College of Obstetricians and Gynecologists. The research was published ahead of print in Human Vaccines and Immunotherapeutics.
“These findings are novel because they emphasize starting at age 9, and that is different than prior studies that emphasize bundling of these vaccines,” Kevin Ault, MD, professor and chair of the department of obstetrics and gynecology at Western Michigan University Homer Stryker MD School of Medicine and a former member of the CDC’s Advisory Committee on Immunization Practices, said in an interview.
Dr. Ault was not involved in the study but noted that these findings support the AAP’s recommendation to start the HPV vaccine series at age 9. The Centers for Disease Control and Prevention currently recommends giving the first dose of the HPV vaccine at ages 11-12, at the same time as the Tdap and meningitis vaccines. This recommendation to “bundle” the HPV vaccine with the Tdap and meningitis vaccines aims to facilitate provider-family discussion about the HPV vaccine, ideally reducing parent hesitancy and concerns about the vaccines. Multiple studies have shown improved HPV vaccine uptake when providers offer the HPV vaccine at the same time as the Tdap and meningococcal vaccines.
However, shifts in parents’ attitudes have occurred toward the HPV vaccine since those studies on bundling: Concerns about sexual activity have receded while concerns about safety remain high. The American Academy of Pediatrics and the American Cancer Society both advise starting the HPV vaccine series at age 9, based on evidence showing that more children complete the series when they get the first shot before age 11 compared to getting it at 11 or 12.
Male patients with breast cancer: Special considerations and gender-specific concerns
This transcript has been edited for clarity.
Fatima Cardoso, MD: Today we will be discussing breast cancer in male patients. To join me in this discussion, I have Sharon Giordano and Oliver Bogler. I will ask, to start, that we briefly introduce ourselves.
I’m Fatima Cardoso. I’m a medical oncologist based in Lisbon, Portugal. I have had a special interest in this topic for a couple of years. Sharon?
Sharon H. Giordano, MD, MPH, FASCO: I’m Sharon Giordano. I practice at the University of Texas MD Anderson Cancer Center. I’m also a medical oncologist and treat most of the male breast cancer patients that are seen here.
Oliver Bogler, PhD: I’m Oliver Bogler. I’m a cancer biologist by background and an 11-year survivor of breast cancer. Dr. Giordano was my oncologist during the active phase of my treatment. It’s great to be here with you.
Special considerations surrounding male patients
- Dr. Cardoso: Sharon, when you are treating breast cancer in a male patient, what specific considerations do you have?
- Dr. Giordano: As we all know, breast cancer in men is a rare disease. It makes up about 1 in 1,000 cases of breast cancer.
Often, what we need to do and what we end up doing is extrapolating as much as possible from clinical trials that were conducted in female patients with breast cancer. I think that’s one of the major challenges we face in treating the disease. There have been international efforts to try to put together standardized treatment approaches.
For example, ASCO has created guidelines for the management of male breast cancer. NCCN also has a special page on considerations for treatment of men with breast cancer. I would encourage people to look at those resources if questions do come up on the topic.
Dr. Cardoso: Perhaps we can also mention that the latest clinical trials fortunately have been allowing for male patients to be included, which is very important so that we can start having some data on the new drugs. I think that’s also relevant.
Dr. Giordano: That’s a great point because, historically, most of the trials explicitly excluded men. I don’t know if it was intentional or they just wrote the trials saying “women with breast cancer,” because that’s what most people thought of. I think it’s a great effort by the FDA and by investigators to make sure now that men are included in the trials. That will help build our evidence base.
Dr. Cardoso: Oliver, 11 years ago, you faced the diagnosis and you went through this. Can you speak a little bit about this challenge of going through what is considered a rare disease, but also a disease that is very much associated with the female gender traditionally?
Dr. Bogler: Gladly. For me, it was particularly odd because my wife, at the time that I was diagnosed, was a 5-year survivor of breast cancer. It took me some time to even think that the lump I felt might be the same disease. That seemed very unlikely, statistically, and also odd.
I have to say that I was protected from much of the fish-out-of-water experience that many men have because I both worked and was treated at MD Anderson, where Dr Giordano has a large practice, so my colleagues and my friends were not surprised that a man could get this disease.
Many of the patients I met had that experience, difficulty convincing their primary care physician or even their first-line oncologist that this could be the case. I just want to connect to what you both said, which is that 10 years ago, inclusion of men in clinical trials was not standard. It is a fantastic development to see that because unless we include men, we won’t learn about that type of breast cancer.
Dr. Cardoso: Even if only a few are entering each trial, at least it allows us to see if the drug behaves the same way or if there is any strange behavior of the drug in a male patient. It’s already one step forward. You were going to mention something, Sharon?
Dr. Giordano: I was going to say that, anecdotally, I’ve heard the experience that Oliver referred to, of many men feeling not so much uncomfortable with the diagnosis – although that does happen – but not having an obvious fit within the health care system.
For example, going to get their mammogram as part of their diagnostic workup and whoever might be taking them back saying, “Oh, no, this is Mrs. Jones, not Mr.,” and trying to argue with them that it’s not really meant for them. I had a patient – and this guy had a great sense of humor – who had a biopsy done and the instructions were to place this pink, floral ice pack inside your bra.
Even the materials that we have are gender specific. I think those things all together can certainly contribute to a man feeling like a fish out of water.
Dr. Cardoso: Actually, I fought in my institution because they wanted to call the Breast and Gynecology Unit the Women’s Unit. I said that there is no way you can call it the Women’s Unit because we have male patients. There are small things that we can do in our institutions to try to decrease the stigma and to make it less awkward for a man to be in a waiting room that says Women’s Clinic or something similar to that.
The importance of a support system
Dr. Cardoso: I wanted Oliver, perhaps, to mention experiences that you may have heard from other men. Some men do not feel that comfortable speaking about the disease. Also, some of them do not feel comfortable after treatment to go to the beach, to show the scar, and to show what happens after you have radiation.
Some men actually take it quite heavily, psychologically speaking. Have you encountered some of these men?
Dr. Bogler: Definitely. I think it leads to men not accessing the support opportunities – their family, their friends, or the support groups – and staying away from those because of this feeling of not wanting to share about it. That can be damaging. Cancer treatment is usually a tough road for most people, and the long-term consequences of hormone therapy – most men have hormone-driven disease – can be significant. I agree with you.
I participated in the male breast cancer SCAR Project by David Jay, a famous photographer. One of the high points of my life has been appearing in The New York Times topless, right after my radiation treatment, showing my scar. There are quite a few of us out there who’ve done that.
I’ll just mention in passing the Male Breast Cancer Global Alliance, which is a patient support supergroup, if you will. We’ve got a symposium coming up in November. That’s a great place for men who are early in the stage of their disease, or at any stage, to connect to others who are facing this issue.
Dr. Cardoso: They can also find specific information. This is a really good website where you can find information. One of the most important topics that I’ve heard from my patients is, “I never thought that I could have this disease. I never heard that men could have breast cancer as well.” Information is very crucial.
I believe that if you are well informed, you will also be less scared of the disease. Sources of reliable information are really crucial for patients. Since you mentioned the SCAR Project, we have a similar project here in Portugal that really called attention to the disease. It was very visual and really interesting.
Discussions during and after treatment
Dr. Cardoso: I wanted to say something, and I don’t know if both of you would agree. I think only recently surgeons have started to pay attention to the way they operate on men with breast cancer, and even in considering techniques of breast conservation and oncoplastic surgery. I had the feeling, looking at those photos, that some years ago, it wouldn’t have mattered how they do with the mastectomy scar just because it was a man. This was biased, right?
Just because it was a man, there was no need to pay attention to the aesthetic outcome. That is wrong, in my perspective. I’m very happy to see that now there are surgeons considering other types of breast surgery to conserve as much as possible the aesthetic outcome.
Dr. Bogler: I have to say that I was offered reconstruction at MD Anderson. I declined it. It wasn’t that big a part of my body image. When I raised this issue at home, my kids, who were quite young at the time, just suggested, “Well, Dad, why don’t you just wear a swim shirt?” They came up with a very practical solution for this issue.
I agree with you that it should be an option. I was also offered a nipple tattoo. I have yet to take that up, but maybe one day.
Dr. Cardoso: I’m not sure that we need to go into reconstruction. It also depends on whether a man has gynecomastia, if it’s going to be very asymmetric. There are other techniques to do, and depending on the size of the tumor, we can also do breast conservation, which we have done here in a couple of patients.
It’s quite an interesting approach where, for example, a skin-sparing mastectomy would be less aggressive, let’s say. Sharon?
Dr. Giordano: I completely agree. I’ve noticed increasing attention to the issue over the years that I’ve been in practice. I do think that it’s more front-and-center when the surgeons are having discussions with the patients now.
Also, although it’s still a minority, some do choose to have reconstructive surgery; some have more extensive surgeries, and some maybe have nipple reconstruction or a nipple tattoo. In a few men, like you mentioned, who are somewhat asymmetric, it actually can make a difference even when they’re dressed.
For many men, it’s more that they want to take off their shirt to play basketball or go swimming, and to decrease the feeling of awkwardness or like they have to make an explanation for why they have a nipple missing and a scar across their chest.
Biological aspects of male patients
Dr. Cardoso: Let’s switch gears now to the management, and before that, the biology. Oliver, with your other hat of biology, speak a little bit on what we know so far – whether it is exactly the same disease or there are biological specific characteristics of breast cancer in men.
Dr. Bogler: I should preface this by saying that I spent my career studying brain tumors. That was clearly a mistake.
Dr. Cardoso: It starts with a B. ...
Dr. Bogler: It starts with a B, but it’s the wrong part of the body. The reality is that we don’t really know that much fundamental biology yet, though the picture is changing and it has changed in recent years. Part of the reason is we don’t have many of the tools that we’ve had for the female disease for many years, particularly laboratory models.
On the genetic and transcriptomics front, there has been some really good activity. There was a comprehensive systematic review by Professor Val Speirs from the University of Aberdeen earlier this year that summarized much of the recent data. It showed that there are a handful of molecular hallmarks of the male disease, compared with the female disease, that are worth exploring.
Interestingly enough, one of them is the androgen receptor. It does beg the question of whether hormone-driven disease might not show up quite differently in males and females, where the hormone picture is a little different. I think there’s increasing evidence that there’s information out there to go after.
I will say that I was treated by Dr. Giordano and her colleagues very much like a woman would have been with my disease, and actually, very similarly to my wife. I’ve done well with it, so I would say, in most cases, the current standard of care is very effective but it falls a little short of personalized medicine, particularly when it comes to the hormone component.
Dr. Cardoso: Sharon?
Dr. Giordano: I would add that when I think about it as a clinician, although there’s a large amount of overlap and many similarities, when we’re treating men with breast cancer, almost all of the men have hormone receptor–positive disease, which I think Oliver mentioned earlier. We’re really thinking about endocrine therapy as one of the mainstays of treatment.
Obviously, as he also mentioned, it’s a different biologic background of hormones in a male vs. a female patient. There’s reason to think that some of those treatments could differ. In general, the subtypes are a little bit different. We see very, very few cases of triple-negative breast cancer in men. I think I’ve seen only one or two in my career. The ones I remember were probably radiation induced. They were cancer survivors who’d had chest-wall radiation for previous diseases. Those patients are very uncommon.
We also tend to see that the histology patterns are a little bit different. We tend to see more ductal cancers in men than we do in women as a relative proportion.
One thing that I always try to remember is that the risk for BRCA mutations or underlying germline genetic mutations is higher in men than in women. Just having a diagnosis of male breast cancer is an indication to consider genetic testing or meet with a genetic counselor to look for a BRCA1 or BRCA2 mutation.
Now, most men will not have that. Only roughly 10% of male patients, or maybe a little less, will have a BRCA2 mutation; for BRCA1, it’s more like only 1% or 2%. They’re not that common. Certainly, male breast cancer is recognized as being associated with the BRCA mutations.
Dr. Cardoso: If I have to give a take-home message in terms of biology, it would be that if there is a diagnosis of hormone receptor–negative or HER2-positive disease in a male patient, I would ask for a confirmation of the diagnosis. It’s not that it cannot exist, but it’s so rare that it’s worthwhile to confirm.
You mentioned that triple-negative disease is less than 1%, at about 0.5%, and HER2-positive disease is about 9%-10%. I think it will be very important to keep this in mind and confirm the biology if you have a different diagnosis than ER-positive, HER2-negative. Unfortunately, I received some cases where this was not done, and in fact, it ended up being a technical problem. People can receive the wrong treatment based on that.
Dr. Giordano: I’ve also seen that happen when it’s a metastasis to the breast rather than a primary breast cancer. I completely agree. That’s an excellent point.
Management approaches
Dr. Cardoso: Let’s go now to management and focus on early breast cancer first. Sharon, what are your main take-home messages for a professional who doesn’t see this very often? What does someone need to remember when they manage a male patient who has early breast cancer?
Dr. Giordano: In general, in terms of chemotherapy, we essentially use the same guidelines as we do for women. Most of the male patients will have tumors that are hormone receptor positive. For endocrine therapy, we typically rely on tamoxifen as the standard of care for adjuvant endocrine treatment for breast cancer.
There are some data suggesting that there can be some efficacy of aromatase inhibitors as single agents. In general, and extrapolated from some population-based registry data, the outcomes for men treated with single-agent aromatase inhibitors don’t tend to be as good as for those treated with tamoxifen.
I know that these are not randomized data so there are all the caveats of that, but the best information we have suggests that tamoxifen appears to likely be more effective. Typically, we stay with tamoxifen. If, for some reason, a man cannot tolerate tamoxifen or has a contraindication, then we could use a GnRH agonist along with an aromatase inhibitor.
Dr. Cardoso: I would like to mention that, because it’s ER-positive, HER2-negative disease most of the time, there will be the question as to whether we can use genomic tests. I think it is important that people know that we have much less data regarding the use of Oncotype DX, MammaPrint, or any of the genomic tests in male patients.
We have some data on the distribution of, for example, Oncotype DX or MammaPrint scores. Whether we can use these tests for the decision of chemotherapy, we don’t have much data on that. I’ve seen many people making exactly the same decisions as with female patients, but that’s not really based on very strong evidence.
Dr. Giordano: It’s hard to know what to do with that. There are prognostic data on Oncotype, so the higher-risk tumors do seem to have a worse outcome than the lower-score tumors. You’re right, though; I don’t think we have any predictive information to really show that the Oncotype DX score predicts benefit to chemotherapy.
Having said that, I will sometimes order the test in my practice. If somebody comes back with a score of 5 or a very low-risk score, I will use that in my decision-making.
Dr. Cardoso: There is something we didn’t exactly mention in the diagnosis that may be important. We discussed most men not knowing that they can have breast cancer, and Oliver, you mentioned that sometimes the first-line physicians can think that very often. Usually, we have late diagnosis and that means a higher tumor burden.
Sometimes we have to go to chemotherapy because of locally advanced or very positive axillas and not really because of the biology. That’s one of the reasons to go for chemotherapy in this setting, right?
Dr. Bogler: Yes. I remember that conversation with you, Dr. Giordano. I asked you whether I should do one of these tests. You said, “Don’t worry about it. At stage III, you’re going to have chemo anyway.”
Dr. Cardoso: The problem of these rare diagnoses is the not thinking about it, even from the health professional side, and then having the diagnosis quite late that will demand chemotherapy use.
To clarify to everybody, in terms of distinguishing luminal A–like, luminal B–like, and what that implies in a male patient, we really don’t know if it’s the same as in a female. There have been some very interesting studies from our Nordic country colleagues showing that maybe the subtyping is different. There is likely a male-specific subtype that does not exist in female breast cancer and that probably behaves differently. We still have a large amount of research to do to understand that.
Is there anything else you would like to mention about early breast cancer management?
Dr. Bogler: One of the things that’s probably underexplored is adherence to tamoxifen therapy in men. I do know anecdotally that this is the discussion among men because of the impact on quality of life. I do worry that sometimes men perhaps make the wrong choice, and I think that’s an opportunity for more research. Again, if there were alternative therapies that were perhaps a little less impactful on things like libido, that might be an advance in the field.
Dr. Cardoso: We have been seeing more studies on the issue of quality of life. Noncompliance is also an issue in female patients. We have to acknowledge that. Not everybody is able to keep taking the treatments. Interestingly, when there is a relapse and people had stopped taking the tamoxifen, most of them say, “I stopped because I had not understood exactly how important it is.”
We come back to the importance of explaining that it is the most crucial treatment for this subtype of breast cancer. Again, information is really key.
Sometimes I also use the argument with my patients that the alternative is even worse because if you use an aromatase inhibitor, and you have to use an LHRH agonist, then the implications for your sexual life are even worse. That’s how I try to convince them to stay on tamoxifen.
Let’s finalize with a couple of words on metastatic breast cancer in male patients. Sharon, I’ll start with you again. Is there any difference in the management if you have a patient with metastatic, ER-positive, HER2-negative disease? How do you treat? How do you sequence the available therapies? Is it different from the female patient?
Dr. Giordano: I’d say that, big picture, it’s quite similar. Again, most of the men have hormone receptor–positive disease, so really, the mainstay of treatment and the first treatments are going to be endocrine therapies. We’ll sequence through the endocrine therapies like we do in women. When using aromatase inhibitors, I typically would add a GnRH agonist to that, and I have had that be a very successful therapy, along now with the CDK inhibitors that are also approved.
I don’t think the studies of CDK inhibitors included male patients, but at least palbociclib actually was approved in the United States, based on some real-world evidence of its efficacy. Anecdotally, again, in my clinical practice, that tends to be a really powerful combination of leuprolide, an aromatase inhibitor, and a CDK inhibitor.
I think there’s less information about drugs like fulvestrant, whether that would benefit from combination with a GnRH agonist or whether those should be given as single agents. We just don’t really know. We have a few case series out there.
Similar to the early breast cancer setting, I think it’s really important to remember to check for BRCA1 and BRCA2 mutations. PARP inhibitors could be a part of the treatment plan if those underlying germline mutations are found. Generally, we’re following a similar sequence of endocrine therapies and then, eventually, chemotherapy.
Dr. Cardoso: Maybe, Oliver, you’re also seeing that one consistent finding in the biology study is the importance of the AKT/PI3K/mTOR pathway in male patients with breast cancer, because we now have at least two classes of agents to tackle this pathway. Again, anecdotally – we’re not talking about trials – I’ve been seeing quite interesting responses, for example, to everolimus combined with endocrine therapy.
We have a little less experience with the PI3K inhibitor, but that’s just because of accessibility to the drug. I think this combination is also something to keep in mind that can be quite effective in these patients.
Dr. Bogler: I agree. Those findings are exciting in the context of dealing with something as difficult as metastatic breast cancer. It’s good to know that there’s some information coming and opportunities and options, hopefully, down the road for men facing that problem.
Dr. Cardoso: Sharon, although small numbers, in these cases where there is HER2-positive disease, you would also use the new anti-HER2 agents and more or less the same sequence, right?
Dr. Giordano: Absolutely. It’s not particularly data driven, but yes, I would. If it’s a HER2-positive tumor, I would use the same HER2-targeted therapies that are used for women with breast cancer.
Working toward a balance in patient care
Dr. Cardoso: I would like to add something for all of us to be united in the fight. I don’t know if it happens in the U.S., but in many countries, access to these new agents for male patients is very difficult because of the approval and the labeling. This is why I’m always fighting with those who are proposing that the labeling, again, says “women with breast cancer.”
It is really important that we keep on lobbying and pushing for the labeling to say “patients with breast cancer” so that nobody can withhold access to these new therapies because of gender. In the U.S., maybe you don’t have this problem. There are many European countries where men cannot access, for example, fulvestrant because it has been approved for women with breast cancer.
Dr. Giordano: Thankfully, I have not faced that issue very often. I’ve had occasional issues with getting GnRH agonists approved. Generally, in the U.S., if I provide, for example, the NCCN guideline recommendations, most insurers will cover it. I think it’s often just lack of knowledge.
Dr. Cardoso: It’s something to keep working hard on because for the old drugs that were approved with the wording that still said “women,” we have to keep fighting for accessibility.
I think we had a really nice discussion. I’m going to give you an opportunity for any last words that you want to say on this topic. Perhaps we’ll start with you, Sharon, and we’ll leave the very last word to Oliver.
Dr. Giordano: I would just emphasize the importance of doing research in this area. Hopefully, we will be able to get clinical trials. There are reasons to think that endocrine therapies may behave differently in men and women. We need to continue to work together as a community to collect the data so that we can ultimately improve the outcomes for our patients.
Dr. Bogler: I would echo what you just said, Dr. Giordano. I would like to express my gratitude to both of you. Dr. Giordano, you have a huge practice of men at MD Anderson. You took care of me and many other people I know.
Dr. Cardoso, you are a pioneer of a big registry trial that I am privileged to be working on, trying to gather data on men. You’re both pioneers in this field of working on behalf of people like me. I’m just very grateful for what you do.
Dr. Giordano: Thank you.
Dr. Cardoso: Thank you both for accepting this invitation. We hope that everybody takes more interest in this field. Who knows? Maybe we can find enough funds to run a specific trial for male patients with breast cancer.
Dr. Cardoso is director of the breast unit at Champalimaud Clinical Centre/Champalimaud Foundation, Lisbon. Dr. Giordano is professor of breast medical oncology and chair of health services research at the University of Texas MD Anderson Cancer Center, Houston. Dr. Bogler is a cancer biologist at the Randolph (Vt.) Center. Dr. Cardoso reported conflicts of interest with numerous pharmaceutical companies; Dr. Giordano and Dr. Bogler reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
Fatima Cardoso, MD: Today we will be discussing breast cancer in male patients. To join me in this discussion, I have Sharon Giordano and Oliver Bogler. I will ask, to start, that we briefly introduce ourselves.
I’m Fatima Cardoso. I’m a medical oncologist based in Lisbon, Portugal. I have had a special interest in this topic for a couple of years. Sharon?
Sharon H. Giordano, MD, MPH, FASCO: I’m Sharon Giordano. I practice at the University of Texas MD Anderson Cancer Center. I’m also a medical oncologist and treat most of the male breast cancer patients that are seen here.
Oliver Bogler, PhD: I’m Oliver Bogler. I’m a cancer biologist by background and an 11-year survivor of breast cancer. Dr. Giordano was my oncologist during the active phase of my treatment. It’s great to be here with you.
Special considerations surrounding male patients
- Dr. Cardoso: Sharon, when you are treating breast cancer in a male patient, what specific considerations do you have?
- Dr. Giordano: As we all know, breast cancer in men is a rare disease. It makes up about 1 in 1,000 cases of breast cancer.
Often, what we need to do and what we end up doing is extrapolating as much as possible from clinical trials that were conducted in female patients with breast cancer. I think that’s one of the major challenges we face in treating the disease. There have been international efforts to try to put together standardized treatment approaches.
For example, ASCO has created guidelines for the management of male breast cancer. NCCN also has a special page on considerations for treatment of men with breast cancer. I would encourage people to look at those resources if questions do come up on the topic.
Dr. Cardoso: Perhaps we can also mention that the latest clinical trials fortunately have been allowing for male patients to be included, which is very important so that we can start having some data on the new drugs. I think that’s also relevant.
Dr. Giordano: That’s a great point because, historically, most of the trials explicitly excluded men. I don’t know if it was intentional or they just wrote the trials saying “women with breast cancer,” because that’s what most people thought of. I think it’s a great effort by the FDA and by investigators to make sure now that men are included in the trials. That will help build our evidence base.
Dr. Cardoso: Oliver, 11 years ago, you faced the diagnosis and you went through this. Can you speak a little bit about this challenge of going through what is considered a rare disease, but also a disease that is very much associated with the female gender traditionally?
Dr. Bogler: Gladly. For me, it was particularly odd because my wife, at the time that I was diagnosed, was a 5-year survivor of breast cancer. It took me some time to even think that the lump I felt might be the same disease. That seemed very unlikely, statistically, and also odd.
I have to say that I was protected from much of the fish-out-of-water experience that many men have because I both worked and was treated at MD Anderson, where Dr Giordano has a large practice, so my colleagues and my friends were not surprised that a man could get this disease.
Many of the patients I met had that experience, difficulty convincing their primary care physician or even their first-line oncologist that this could be the case. I just want to connect to what you both said, which is that 10 years ago, inclusion of men in clinical trials was not standard. It is a fantastic development to see that because unless we include men, we won’t learn about that type of breast cancer.
Dr. Cardoso: Even if only a few are entering each trial, at least it allows us to see if the drug behaves the same way or if there is any strange behavior of the drug in a male patient. It’s already one step forward. You were going to mention something, Sharon?
Dr. Giordano: I was going to say that, anecdotally, I’ve heard the experience that Oliver referred to, of many men feeling not so much uncomfortable with the diagnosis – although that does happen – but not having an obvious fit within the health care system.
For example, going to get their mammogram as part of their diagnostic workup and whoever might be taking them back saying, “Oh, no, this is Mrs. Jones, not Mr.,” and trying to argue with them that it’s not really meant for them. I had a patient – and this guy had a great sense of humor – who had a biopsy done and the instructions were to place this pink, floral ice pack inside your bra.
Even the materials that we have are gender specific. I think those things all together can certainly contribute to a man feeling like a fish out of water.
Dr. Cardoso: Actually, I fought in my institution because they wanted to call the Breast and Gynecology Unit the Women’s Unit. I said that there is no way you can call it the Women’s Unit because we have male patients. There are small things that we can do in our institutions to try to decrease the stigma and to make it less awkward for a man to be in a waiting room that says Women’s Clinic or something similar to that.
The importance of a support system
Dr. Cardoso: I wanted Oliver, perhaps, to mention experiences that you may have heard from other men. Some men do not feel that comfortable speaking about the disease. Also, some of them do not feel comfortable after treatment to go to the beach, to show the scar, and to show what happens after you have radiation.
Some men actually take it quite heavily, psychologically speaking. Have you encountered some of these men?
Dr. Bogler: Definitely. I think it leads to men not accessing the support opportunities – their family, their friends, or the support groups – and staying away from those because of this feeling of not wanting to share about it. That can be damaging. Cancer treatment is usually a tough road for most people, and the long-term consequences of hormone therapy – most men have hormone-driven disease – can be significant. I agree with you.
I participated in the male breast cancer SCAR Project by David Jay, a famous photographer. One of the high points of my life has been appearing in The New York Times topless, right after my radiation treatment, showing my scar. There are quite a few of us out there who’ve done that.
I’ll just mention in passing the Male Breast Cancer Global Alliance, which is a patient support supergroup, if you will. We’ve got a symposium coming up in November. That’s a great place for men who are early in the stage of their disease, or at any stage, to connect to others who are facing this issue.
Dr. Cardoso: They can also find specific information. This is a really good website where you can find information. One of the most important topics that I’ve heard from my patients is, “I never thought that I could have this disease. I never heard that men could have breast cancer as well.” Information is very crucial.
I believe that if you are well informed, you will also be less scared of the disease. Sources of reliable information are really crucial for patients. Since you mentioned the SCAR Project, we have a similar project here in Portugal that really called attention to the disease. It was very visual and really interesting.
Discussions during and after treatment
Dr. Cardoso: I wanted to say something, and I don’t know if both of you would agree. I think only recently surgeons have started to pay attention to the way they operate on men with breast cancer, and even in considering techniques of breast conservation and oncoplastic surgery. I had the feeling, looking at those photos, that some years ago, it wouldn’t have mattered how they do with the mastectomy scar just because it was a man. This was biased, right?
Just because it was a man, there was no need to pay attention to the aesthetic outcome. That is wrong, in my perspective. I’m very happy to see that now there are surgeons considering other types of breast surgery to conserve as much as possible the aesthetic outcome.
Dr. Bogler: I have to say that I was offered reconstruction at MD Anderson. I declined it. It wasn’t that big a part of my body image. When I raised this issue at home, my kids, who were quite young at the time, just suggested, “Well, Dad, why don’t you just wear a swim shirt?” They came up with a very practical solution for this issue.
I agree with you that it should be an option. I was also offered a nipple tattoo. I have yet to take that up, but maybe one day.
Dr. Cardoso: I’m not sure that we need to go into reconstruction. It also depends on whether a man has gynecomastia, if it’s going to be very asymmetric. There are other techniques to do, and depending on the size of the tumor, we can also do breast conservation, which we have done here in a couple of patients.
It’s quite an interesting approach where, for example, a skin-sparing mastectomy would be less aggressive, let’s say. Sharon?
Dr. Giordano: I completely agree. I’ve noticed increasing attention to the issue over the years that I’ve been in practice. I do think that it’s more front-and-center when the surgeons are having discussions with the patients now.
Also, although it’s still a minority, some do choose to have reconstructive surgery; some have more extensive surgeries, and some maybe have nipple reconstruction or a nipple tattoo. In a few men, like you mentioned, who are somewhat asymmetric, it actually can make a difference even when they’re dressed.
For many men, it’s more that they want to take off their shirt to play basketball or go swimming, and to decrease the feeling of awkwardness or like they have to make an explanation for why they have a nipple missing and a scar across their chest.
Biological aspects of male patients
Dr. Cardoso: Let’s switch gears now to the management, and before that, the biology. Oliver, with your other hat of biology, speak a little bit on what we know so far – whether it is exactly the same disease or there are biological specific characteristics of breast cancer in men.
Dr. Bogler: I should preface this by saying that I spent my career studying brain tumors. That was clearly a mistake.
Dr. Cardoso: It starts with a B. ...
Dr. Bogler: It starts with a B, but it’s the wrong part of the body. The reality is that we don’t really know that much fundamental biology yet, though the picture is changing and it has changed in recent years. Part of the reason is we don’t have many of the tools that we’ve had for the female disease for many years, particularly laboratory models.
On the genetic and transcriptomics front, there has been some really good activity. There was a comprehensive systematic review by Professor Val Speirs from the University of Aberdeen earlier this year that summarized much of the recent data. It showed that there are a handful of molecular hallmarks of the male disease, compared with the female disease, that are worth exploring.
Interestingly enough, one of them is the androgen receptor. It does beg the question of whether hormone-driven disease might not show up quite differently in males and females, where the hormone picture is a little different. I think there’s increasing evidence that there’s information out there to go after.
I will say that I was treated by Dr. Giordano and her colleagues very much like a woman would have been with my disease, and actually, very similarly to my wife. I’ve done well with it, so I would say, in most cases, the current standard of care is very effective but it falls a little short of personalized medicine, particularly when it comes to the hormone component.
Dr. Cardoso: Sharon?
Dr. Giordano: I would add that when I think about it as a clinician, although there’s a large amount of overlap and many similarities, when we’re treating men with breast cancer, almost all of the men have hormone receptor–positive disease, which I think Oliver mentioned earlier. We’re really thinking about endocrine therapy as one of the mainstays of treatment.
Obviously, as he also mentioned, it’s a different biologic background of hormones in a male vs. a female patient. There’s reason to think that some of those treatments could differ. In general, the subtypes are a little bit different. We see very, very few cases of triple-negative breast cancer in men. I think I’ve seen only one or two in my career. The ones I remember were probably radiation induced. They were cancer survivors who’d had chest-wall radiation for previous diseases. Those patients are very uncommon.
We also tend to see that the histology patterns are a little bit different. We tend to see more ductal cancers in men than we do in women as a relative proportion.
One thing that I always try to remember is that the risk for BRCA mutations or underlying germline genetic mutations is higher in men than in women. Just having a diagnosis of male breast cancer is an indication to consider genetic testing or meet with a genetic counselor to look for a BRCA1 or BRCA2 mutation.
Now, most men will not have that. Only roughly 10% of male patients, or maybe a little less, will have a BRCA2 mutation; for BRCA1, it’s more like only 1% or 2%. They’re not that common. Certainly, male breast cancer is recognized as being associated with the BRCA mutations.
Dr. Cardoso: If I have to give a take-home message in terms of biology, it would be that if there is a diagnosis of hormone receptor–negative or HER2-positive disease in a male patient, I would ask for a confirmation of the diagnosis. It’s not that it cannot exist, but it’s so rare that it’s worthwhile to confirm.
You mentioned that triple-negative disease is less than 1%, at about 0.5%, and HER2-positive disease is about 9%-10%. I think it will be very important to keep this in mind and confirm the biology if you have a different diagnosis than ER-positive, HER2-negative. Unfortunately, I received some cases where this was not done, and in fact, it ended up being a technical problem. People can receive the wrong treatment based on that.
Dr. Giordano: I’ve also seen that happen when it’s a metastasis to the breast rather than a primary breast cancer. I completely agree. That’s an excellent point.
Management approaches
Dr. Cardoso: Let’s go now to management and focus on early breast cancer first. Sharon, what are your main take-home messages for a professional who doesn’t see this very often? What does someone need to remember when they manage a male patient who has early breast cancer?
Dr. Giordano: In general, in terms of chemotherapy, we essentially use the same guidelines as we do for women. Most of the male patients will have tumors that are hormone receptor positive. For endocrine therapy, we typically rely on tamoxifen as the standard of care for adjuvant endocrine treatment for breast cancer.
There are some data suggesting that there can be some efficacy of aromatase inhibitors as single agents. In general, and extrapolated from some population-based registry data, the outcomes for men treated with single-agent aromatase inhibitors don’t tend to be as good as for those treated with tamoxifen.
I know that these are not randomized data so there are all the caveats of that, but the best information we have suggests that tamoxifen appears to likely be more effective. Typically, we stay with tamoxifen. If, for some reason, a man cannot tolerate tamoxifen or has a contraindication, then we could use a GnRH agonist along with an aromatase inhibitor.
Dr. Cardoso: I would like to mention that, because it’s ER-positive, HER2-negative disease most of the time, there will be the question as to whether we can use genomic tests. I think it is important that people know that we have much less data regarding the use of Oncotype DX, MammaPrint, or any of the genomic tests in male patients.
We have some data on the distribution of, for example, Oncotype DX or MammaPrint scores. Whether we can use these tests for the decision of chemotherapy, we don’t have much data on that. I’ve seen many people making exactly the same decisions as with female patients, but that’s not really based on very strong evidence.
Dr. Giordano: It’s hard to know what to do with that. There are prognostic data on Oncotype, so the higher-risk tumors do seem to have a worse outcome than the lower-score tumors. You’re right, though; I don’t think we have any predictive information to really show that the Oncotype DX score predicts benefit to chemotherapy.
Having said that, I will sometimes order the test in my practice. If somebody comes back with a score of 5 or a very low-risk score, I will use that in my decision-making.
Dr. Cardoso: There is something we didn’t exactly mention in the diagnosis that may be important. We discussed most men not knowing that they can have breast cancer, and Oliver, you mentioned that sometimes the first-line physicians can think that very often. Usually, we have late diagnosis and that means a higher tumor burden.
Sometimes we have to go to chemotherapy because of locally advanced or very positive axillas and not really because of the biology. That’s one of the reasons to go for chemotherapy in this setting, right?
Dr. Bogler: Yes. I remember that conversation with you, Dr. Giordano. I asked you whether I should do one of these tests. You said, “Don’t worry about it. At stage III, you’re going to have chemo anyway.”
Dr. Cardoso: The problem of these rare diagnoses is the not thinking about it, even from the health professional side, and then having the diagnosis quite late that will demand chemotherapy use.
To clarify to everybody, in terms of distinguishing luminal A–like, luminal B–like, and what that implies in a male patient, we really don’t know if it’s the same as in a female. There have been some very interesting studies from our Nordic country colleagues showing that maybe the subtyping is different. There is likely a male-specific subtype that does not exist in female breast cancer and that probably behaves differently. We still have a large amount of research to do to understand that.
Is there anything else you would like to mention about early breast cancer management?
Dr. Bogler: One of the things that’s probably underexplored is adherence to tamoxifen therapy in men. I do know anecdotally that this is the discussion among men because of the impact on quality of life. I do worry that sometimes men perhaps make the wrong choice, and I think that’s an opportunity for more research. Again, if there were alternative therapies that were perhaps a little less impactful on things like libido, that might be an advance in the field.
Dr. Cardoso: We have been seeing more studies on the issue of quality of life. Noncompliance is also an issue in female patients. We have to acknowledge that. Not everybody is able to keep taking the treatments. Interestingly, when there is a relapse and people had stopped taking the tamoxifen, most of them say, “I stopped because I had not understood exactly how important it is.”
We come back to the importance of explaining that it is the most crucial treatment for this subtype of breast cancer. Again, information is really key.
Sometimes I also use the argument with my patients that the alternative is even worse because if you use an aromatase inhibitor, and you have to use an LHRH agonist, then the implications for your sexual life are even worse. That’s how I try to convince them to stay on tamoxifen.
Let’s finalize with a couple of words on metastatic breast cancer in male patients. Sharon, I’ll start with you again. Is there any difference in the management if you have a patient with metastatic, ER-positive, HER2-negative disease? How do you treat? How do you sequence the available therapies? Is it different from the female patient?
Dr. Giordano: I’d say that, big picture, it’s quite similar. Again, most of the men have hormone receptor–positive disease, so really, the mainstay of treatment and the first treatments are going to be endocrine therapies. We’ll sequence through the endocrine therapies like we do in women. When using aromatase inhibitors, I typically would add a GnRH agonist to that, and I have had that be a very successful therapy, along now with the CDK inhibitors that are also approved.
I don’t think the studies of CDK inhibitors included male patients, but at least palbociclib actually was approved in the United States, based on some real-world evidence of its efficacy. Anecdotally, again, in my clinical practice, that tends to be a really powerful combination of leuprolide, an aromatase inhibitor, and a CDK inhibitor.
I think there’s less information about drugs like fulvestrant, whether that would benefit from combination with a GnRH agonist or whether those should be given as single agents. We just don’t really know. We have a few case series out there.
Similar to the early breast cancer setting, I think it’s really important to remember to check for BRCA1 and BRCA2 mutations. PARP inhibitors could be a part of the treatment plan if those underlying germline mutations are found. Generally, we’re following a similar sequence of endocrine therapies and then, eventually, chemotherapy.
Dr. Cardoso: Maybe, Oliver, you’re also seeing that one consistent finding in the biology study is the importance of the AKT/PI3K/mTOR pathway in male patients with breast cancer, because we now have at least two classes of agents to tackle this pathway. Again, anecdotally – we’re not talking about trials – I’ve been seeing quite interesting responses, for example, to everolimus combined with endocrine therapy.
We have a little less experience with the PI3K inhibitor, but that’s just because of accessibility to the drug. I think this combination is also something to keep in mind that can be quite effective in these patients.
Dr. Bogler: I agree. Those findings are exciting in the context of dealing with something as difficult as metastatic breast cancer. It’s good to know that there’s some information coming and opportunities and options, hopefully, down the road for men facing that problem.
Dr. Cardoso: Sharon, although small numbers, in these cases where there is HER2-positive disease, you would also use the new anti-HER2 agents and more or less the same sequence, right?
Dr. Giordano: Absolutely. It’s not particularly data driven, but yes, I would. If it’s a HER2-positive tumor, I would use the same HER2-targeted therapies that are used for women with breast cancer.
Working toward a balance in patient care
Dr. Cardoso: I would like to add something for all of us to be united in the fight. I don’t know if it happens in the U.S., but in many countries, access to these new agents for male patients is very difficult because of the approval and the labeling. This is why I’m always fighting with those who are proposing that the labeling, again, says “women with breast cancer.”
It is really important that we keep on lobbying and pushing for the labeling to say “patients with breast cancer” so that nobody can withhold access to these new therapies because of gender. In the U.S., maybe you don’t have this problem. There are many European countries where men cannot access, for example, fulvestrant because it has been approved for women with breast cancer.
Dr. Giordano: Thankfully, I have not faced that issue very often. I’ve had occasional issues with getting GnRH agonists approved. Generally, in the U.S., if I provide, for example, the NCCN guideline recommendations, most insurers will cover it. I think it’s often just lack of knowledge.
Dr. Cardoso: It’s something to keep working hard on because for the old drugs that were approved with the wording that still said “women,” we have to keep fighting for accessibility.
I think we had a really nice discussion. I’m going to give you an opportunity for any last words that you want to say on this topic. Perhaps we’ll start with you, Sharon, and we’ll leave the very last word to Oliver.
Dr. Giordano: I would just emphasize the importance of doing research in this area. Hopefully, we will be able to get clinical trials. There are reasons to think that endocrine therapies may behave differently in men and women. We need to continue to work together as a community to collect the data so that we can ultimately improve the outcomes for our patients.
Dr. Bogler: I would echo what you just said, Dr. Giordano. I would like to express my gratitude to both of you. Dr. Giordano, you have a huge practice of men at MD Anderson. You took care of me and many other people I know.
Dr. Cardoso, you are a pioneer of a big registry trial that I am privileged to be working on, trying to gather data on men. You’re both pioneers in this field of working on behalf of people like me. I’m just very grateful for what you do.
Dr. Giordano: Thank you.
Dr. Cardoso: Thank you both for accepting this invitation. We hope that everybody takes more interest in this field. Who knows? Maybe we can find enough funds to run a specific trial for male patients with breast cancer.
Dr. Cardoso is director of the breast unit at Champalimaud Clinical Centre/Champalimaud Foundation, Lisbon. Dr. Giordano is professor of breast medical oncology and chair of health services research at the University of Texas MD Anderson Cancer Center, Houston. Dr. Bogler is a cancer biologist at the Randolph (Vt.) Center. Dr. Cardoso reported conflicts of interest with numerous pharmaceutical companies; Dr. Giordano and Dr. Bogler reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
Fatima Cardoso, MD: Today we will be discussing breast cancer in male patients. To join me in this discussion, I have Sharon Giordano and Oliver Bogler. I will ask, to start, that we briefly introduce ourselves.
I’m Fatima Cardoso. I’m a medical oncologist based in Lisbon, Portugal. I have had a special interest in this topic for a couple of years. Sharon?
Sharon H. Giordano, MD, MPH, FASCO: I’m Sharon Giordano. I practice at the University of Texas MD Anderson Cancer Center. I’m also a medical oncologist and treat most of the male breast cancer patients that are seen here.
Oliver Bogler, PhD: I’m Oliver Bogler. I’m a cancer biologist by background and an 11-year survivor of breast cancer. Dr. Giordano was my oncologist during the active phase of my treatment. It’s great to be here with you.
Special considerations surrounding male patients
- Dr. Cardoso: Sharon, when you are treating breast cancer in a male patient, what specific considerations do you have?
- Dr. Giordano: As we all know, breast cancer in men is a rare disease. It makes up about 1 in 1,000 cases of breast cancer.
Often, what we need to do and what we end up doing is extrapolating as much as possible from clinical trials that were conducted in female patients with breast cancer. I think that’s one of the major challenges we face in treating the disease. There have been international efforts to try to put together standardized treatment approaches.
For example, ASCO has created guidelines for the management of male breast cancer. NCCN also has a special page on considerations for treatment of men with breast cancer. I would encourage people to look at those resources if questions do come up on the topic.
Dr. Cardoso: Perhaps we can also mention that the latest clinical trials fortunately have been allowing for male patients to be included, which is very important so that we can start having some data on the new drugs. I think that’s also relevant.
Dr. Giordano: That’s a great point because, historically, most of the trials explicitly excluded men. I don’t know if it was intentional or they just wrote the trials saying “women with breast cancer,” because that’s what most people thought of. I think it’s a great effort by the FDA and by investigators to make sure now that men are included in the trials. That will help build our evidence base.
Dr. Cardoso: Oliver, 11 years ago, you faced the diagnosis and you went through this. Can you speak a little bit about this challenge of going through what is considered a rare disease, but also a disease that is very much associated with the female gender traditionally?
Dr. Bogler: Gladly. For me, it was particularly odd because my wife, at the time that I was diagnosed, was a 5-year survivor of breast cancer. It took me some time to even think that the lump I felt might be the same disease. That seemed very unlikely, statistically, and also odd.
I have to say that I was protected from much of the fish-out-of-water experience that many men have because I both worked and was treated at MD Anderson, where Dr Giordano has a large practice, so my colleagues and my friends were not surprised that a man could get this disease.
Many of the patients I met had that experience, difficulty convincing their primary care physician or even their first-line oncologist that this could be the case. I just want to connect to what you both said, which is that 10 years ago, inclusion of men in clinical trials was not standard. It is a fantastic development to see that because unless we include men, we won’t learn about that type of breast cancer.
Dr. Cardoso: Even if only a few are entering each trial, at least it allows us to see if the drug behaves the same way or if there is any strange behavior of the drug in a male patient. It’s already one step forward. You were going to mention something, Sharon?
Dr. Giordano: I was going to say that, anecdotally, I’ve heard the experience that Oliver referred to, of many men feeling not so much uncomfortable with the diagnosis – although that does happen – but not having an obvious fit within the health care system.
For example, going to get their mammogram as part of their diagnostic workup and whoever might be taking them back saying, “Oh, no, this is Mrs. Jones, not Mr.,” and trying to argue with them that it’s not really meant for them. I had a patient – and this guy had a great sense of humor – who had a biopsy done and the instructions were to place this pink, floral ice pack inside your bra.
Even the materials that we have are gender specific. I think those things all together can certainly contribute to a man feeling like a fish out of water.
Dr. Cardoso: Actually, I fought in my institution because they wanted to call the Breast and Gynecology Unit the Women’s Unit. I said that there is no way you can call it the Women’s Unit because we have male patients. There are small things that we can do in our institutions to try to decrease the stigma and to make it less awkward for a man to be in a waiting room that says Women’s Clinic or something similar to that.
The importance of a support system
Dr. Cardoso: I wanted Oliver, perhaps, to mention experiences that you may have heard from other men. Some men do not feel that comfortable speaking about the disease. Also, some of them do not feel comfortable after treatment to go to the beach, to show the scar, and to show what happens after you have radiation.
Some men actually take it quite heavily, psychologically speaking. Have you encountered some of these men?
Dr. Bogler: Definitely. I think it leads to men not accessing the support opportunities – their family, their friends, or the support groups – and staying away from those because of this feeling of not wanting to share about it. That can be damaging. Cancer treatment is usually a tough road for most people, and the long-term consequences of hormone therapy – most men have hormone-driven disease – can be significant. I agree with you.
I participated in the male breast cancer SCAR Project by David Jay, a famous photographer. One of the high points of my life has been appearing in The New York Times topless, right after my radiation treatment, showing my scar. There are quite a few of us out there who’ve done that.
I’ll just mention in passing the Male Breast Cancer Global Alliance, which is a patient support supergroup, if you will. We’ve got a symposium coming up in November. That’s a great place for men who are early in the stage of their disease, or at any stage, to connect to others who are facing this issue.
Dr. Cardoso: They can also find specific information. This is a really good website where you can find information. One of the most important topics that I’ve heard from my patients is, “I never thought that I could have this disease. I never heard that men could have breast cancer as well.” Information is very crucial.
I believe that if you are well informed, you will also be less scared of the disease. Sources of reliable information are really crucial for patients. Since you mentioned the SCAR Project, we have a similar project here in Portugal that really called attention to the disease. It was very visual and really interesting.
Discussions during and after treatment
Dr. Cardoso: I wanted to say something, and I don’t know if both of you would agree. I think only recently surgeons have started to pay attention to the way they operate on men with breast cancer, and even in considering techniques of breast conservation and oncoplastic surgery. I had the feeling, looking at those photos, that some years ago, it wouldn’t have mattered how they do with the mastectomy scar just because it was a man. This was biased, right?
Just because it was a man, there was no need to pay attention to the aesthetic outcome. That is wrong, in my perspective. I’m very happy to see that now there are surgeons considering other types of breast surgery to conserve as much as possible the aesthetic outcome.
Dr. Bogler: I have to say that I was offered reconstruction at MD Anderson. I declined it. It wasn’t that big a part of my body image. When I raised this issue at home, my kids, who were quite young at the time, just suggested, “Well, Dad, why don’t you just wear a swim shirt?” They came up with a very practical solution for this issue.
I agree with you that it should be an option. I was also offered a nipple tattoo. I have yet to take that up, but maybe one day.
Dr. Cardoso: I’m not sure that we need to go into reconstruction. It also depends on whether a man has gynecomastia, if it’s going to be very asymmetric. There are other techniques to do, and depending on the size of the tumor, we can also do breast conservation, which we have done here in a couple of patients.
It’s quite an interesting approach where, for example, a skin-sparing mastectomy would be less aggressive, let’s say. Sharon?
Dr. Giordano: I completely agree. I’ve noticed increasing attention to the issue over the years that I’ve been in practice. I do think that it’s more front-and-center when the surgeons are having discussions with the patients now.
Also, although it’s still a minority, some do choose to have reconstructive surgery; some have more extensive surgeries, and some maybe have nipple reconstruction or a nipple tattoo. In a few men, like you mentioned, who are somewhat asymmetric, it actually can make a difference even when they’re dressed.
For many men, it’s more that they want to take off their shirt to play basketball or go swimming, and to decrease the feeling of awkwardness or like they have to make an explanation for why they have a nipple missing and a scar across their chest.
Biological aspects of male patients
Dr. Cardoso: Let’s switch gears now to the management, and before that, the biology. Oliver, with your other hat of biology, speak a little bit on what we know so far – whether it is exactly the same disease or there are biological specific characteristics of breast cancer in men.
Dr. Bogler: I should preface this by saying that I spent my career studying brain tumors. That was clearly a mistake.
Dr. Cardoso: It starts with a B. ...
Dr. Bogler: It starts with a B, but it’s the wrong part of the body. The reality is that we don’t really know that much fundamental biology yet, though the picture is changing and it has changed in recent years. Part of the reason is we don’t have many of the tools that we’ve had for the female disease for many years, particularly laboratory models.
On the genetic and transcriptomics front, there has been some really good activity. There was a comprehensive systematic review by Professor Val Speirs from the University of Aberdeen earlier this year that summarized much of the recent data. It showed that there are a handful of molecular hallmarks of the male disease, compared with the female disease, that are worth exploring.
Interestingly enough, one of them is the androgen receptor. It does beg the question of whether hormone-driven disease might not show up quite differently in males and females, where the hormone picture is a little different. I think there’s increasing evidence that there’s information out there to go after.
I will say that I was treated by Dr. Giordano and her colleagues very much like a woman would have been with my disease, and actually, very similarly to my wife. I’ve done well with it, so I would say, in most cases, the current standard of care is very effective but it falls a little short of personalized medicine, particularly when it comes to the hormone component.
Dr. Cardoso: Sharon?
Dr. Giordano: I would add that when I think about it as a clinician, although there’s a large amount of overlap and many similarities, when we’re treating men with breast cancer, almost all of the men have hormone receptor–positive disease, which I think Oliver mentioned earlier. We’re really thinking about endocrine therapy as one of the mainstays of treatment.
Obviously, as he also mentioned, it’s a different biologic background of hormones in a male vs. a female patient. There’s reason to think that some of those treatments could differ. In general, the subtypes are a little bit different. We see very, very few cases of triple-negative breast cancer in men. I think I’ve seen only one or two in my career. The ones I remember were probably radiation induced. They were cancer survivors who’d had chest-wall radiation for previous diseases. Those patients are very uncommon.
We also tend to see that the histology patterns are a little bit different. We tend to see more ductal cancers in men than we do in women as a relative proportion.
One thing that I always try to remember is that the risk for BRCA mutations or underlying germline genetic mutations is higher in men than in women. Just having a diagnosis of male breast cancer is an indication to consider genetic testing or meet with a genetic counselor to look for a BRCA1 or BRCA2 mutation.
Now, most men will not have that. Only roughly 10% of male patients, or maybe a little less, will have a BRCA2 mutation; for BRCA1, it’s more like only 1% or 2%. They’re not that common. Certainly, male breast cancer is recognized as being associated with the BRCA mutations.
Dr. Cardoso: If I have to give a take-home message in terms of biology, it would be that if there is a diagnosis of hormone receptor–negative or HER2-positive disease in a male patient, I would ask for a confirmation of the diagnosis. It’s not that it cannot exist, but it’s so rare that it’s worthwhile to confirm.
You mentioned that triple-negative disease is less than 1%, at about 0.5%, and HER2-positive disease is about 9%-10%. I think it will be very important to keep this in mind and confirm the biology if you have a different diagnosis than ER-positive, HER2-negative. Unfortunately, I received some cases where this was not done, and in fact, it ended up being a technical problem. People can receive the wrong treatment based on that.
Dr. Giordano: I’ve also seen that happen when it’s a metastasis to the breast rather than a primary breast cancer. I completely agree. That’s an excellent point.
Management approaches
Dr. Cardoso: Let’s go now to management and focus on early breast cancer first. Sharon, what are your main take-home messages for a professional who doesn’t see this very often? What does someone need to remember when they manage a male patient who has early breast cancer?
Dr. Giordano: In general, in terms of chemotherapy, we essentially use the same guidelines as we do for women. Most of the male patients will have tumors that are hormone receptor positive. For endocrine therapy, we typically rely on tamoxifen as the standard of care for adjuvant endocrine treatment for breast cancer.
There are some data suggesting that there can be some efficacy of aromatase inhibitors as single agents. In general, and extrapolated from some population-based registry data, the outcomes for men treated with single-agent aromatase inhibitors don’t tend to be as good as for those treated with tamoxifen.
I know that these are not randomized data so there are all the caveats of that, but the best information we have suggests that tamoxifen appears to likely be more effective. Typically, we stay with tamoxifen. If, for some reason, a man cannot tolerate tamoxifen or has a contraindication, then we could use a GnRH agonist along with an aromatase inhibitor.
Dr. Cardoso: I would like to mention that, because it’s ER-positive, HER2-negative disease most of the time, there will be the question as to whether we can use genomic tests. I think it is important that people know that we have much less data regarding the use of Oncotype DX, MammaPrint, or any of the genomic tests in male patients.
We have some data on the distribution of, for example, Oncotype DX or MammaPrint scores. Whether we can use these tests for the decision of chemotherapy, we don’t have much data on that. I’ve seen many people making exactly the same decisions as with female patients, but that’s not really based on very strong evidence.
Dr. Giordano: It’s hard to know what to do with that. There are prognostic data on Oncotype, so the higher-risk tumors do seem to have a worse outcome than the lower-score tumors. You’re right, though; I don’t think we have any predictive information to really show that the Oncotype DX score predicts benefit to chemotherapy.
Having said that, I will sometimes order the test in my practice. If somebody comes back with a score of 5 or a very low-risk score, I will use that in my decision-making.
Dr. Cardoso: There is something we didn’t exactly mention in the diagnosis that may be important. We discussed most men not knowing that they can have breast cancer, and Oliver, you mentioned that sometimes the first-line physicians can think that very often. Usually, we have late diagnosis and that means a higher tumor burden.
Sometimes we have to go to chemotherapy because of locally advanced or very positive axillas and not really because of the biology. That’s one of the reasons to go for chemotherapy in this setting, right?
Dr. Bogler: Yes. I remember that conversation with you, Dr. Giordano. I asked you whether I should do one of these tests. You said, “Don’t worry about it. At stage III, you’re going to have chemo anyway.”
Dr. Cardoso: The problem of these rare diagnoses is the not thinking about it, even from the health professional side, and then having the diagnosis quite late that will demand chemotherapy use.
To clarify to everybody, in terms of distinguishing luminal A–like, luminal B–like, and what that implies in a male patient, we really don’t know if it’s the same as in a female. There have been some very interesting studies from our Nordic country colleagues showing that maybe the subtyping is different. There is likely a male-specific subtype that does not exist in female breast cancer and that probably behaves differently. We still have a large amount of research to do to understand that.
Is there anything else you would like to mention about early breast cancer management?
Dr. Bogler: One of the things that’s probably underexplored is adherence to tamoxifen therapy in men. I do know anecdotally that this is the discussion among men because of the impact on quality of life. I do worry that sometimes men perhaps make the wrong choice, and I think that’s an opportunity for more research. Again, if there were alternative therapies that were perhaps a little less impactful on things like libido, that might be an advance in the field.
Dr. Cardoso: We have been seeing more studies on the issue of quality of life. Noncompliance is also an issue in female patients. We have to acknowledge that. Not everybody is able to keep taking the treatments. Interestingly, when there is a relapse and people had stopped taking the tamoxifen, most of them say, “I stopped because I had not understood exactly how important it is.”
We come back to the importance of explaining that it is the most crucial treatment for this subtype of breast cancer. Again, information is really key.
Sometimes I also use the argument with my patients that the alternative is even worse because if you use an aromatase inhibitor, and you have to use an LHRH agonist, then the implications for your sexual life are even worse. That’s how I try to convince them to stay on tamoxifen.
Let’s finalize with a couple of words on metastatic breast cancer in male patients. Sharon, I’ll start with you again. Is there any difference in the management if you have a patient with metastatic, ER-positive, HER2-negative disease? How do you treat? How do you sequence the available therapies? Is it different from the female patient?
Dr. Giordano: I’d say that, big picture, it’s quite similar. Again, most of the men have hormone receptor–positive disease, so really, the mainstay of treatment and the first treatments are going to be endocrine therapies. We’ll sequence through the endocrine therapies like we do in women. When using aromatase inhibitors, I typically would add a GnRH agonist to that, and I have had that be a very successful therapy, along now with the CDK inhibitors that are also approved.
I don’t think the studies of CDK inhibitors included male patients, but at least palbociclib actually was approved in the United States, based on some real-world evidence of its efficacy. Anecdotally, again, in my clinical practice, that tends to be a really powerful combination of leuprolide, an aromatase inhibitor, and a CDK inhibitor.
I think there’s less information about drugs like fulvestrant, whether that would benefit from combination with a GnRH agonist or whether those should be given as single agents. We just don’t really know. We have a few case series out there.
Similar to the early breast cancer setting, I think it’s really important to remember to check for BRCA1 and BRCA2 mutations. PARP inhibitors could be a part of the treatment plan if those underlying germline mutations are found. Generally, we’re following a similar sequence of endocrine therapies and then, eventually, chemotherapy.
Dr. Cardoso: Maybe, Oliver, you’re also seeing that one consistent finding in the biology study is the importance of the AKT/PI3K/mTOR pathway in male patients with breast cancer, because we now have at least two classes of agents to tackle this pathway. Again, anecdotally – we’re not talking about trials – I’ve been seeing quite interesting responses, for example, to everolimus combined with endocrine therapy.
We have a little less experience with the PI3K inhibitor, but that’s just because of accessibility to the drug. I think this combination is also something to keep in mind that can be quite effective in these patients.
Dr. Bogler: I agree. Those findings are exciting in the context of dealing with something as difficult as metastatic breast cancer. It’s good to know that there’s some information coming and opportunities and options, hopefully, down the road for men facing that problem.
Dr. Cardoso: Sharon, although small numbers, in these cases where there is HER2-positive disease, you would also use the new anti-HER2 agents and more or less the same sequence, right?
Dr. Giordano: Absolutely. It’s not particularly data driven, but yes, I would. If it’s a HER2-positive tumor, I would use the same HER2-targeted therapies that are used for women with breast cancer.
Working toward a balance in patient care
Dr. Cardoso: I would like to add something for all of us to be united in the fight. I don’t know if it happens in the U.S., but in many countries, access to these new agents for male patients is very difficult because of the approval and the labeling. This is why I’m always fighting with those who are proposing that the labeling, again, says “women with breast cancer.”
It is really important that we keep on lobbying and pushing for the labeling to say “patients with breast cancer” so that nobody can withhold access to these new therapies because of gender. In the U.S., maybe you don’t have this problem. There are many European countries where men cannot access, for example, fulvestrant because it has been approved for women with breast cancer.
Dr. Giordano: Thankfully, I have not faced that issue very often. I’ve had occasional issues with getting GnRH agonists approved. Generally, in the U.S., if I provide, for example, the NCCN guideline recommendations, most insurers will cover it. I think it’s often just lack of knowledge.
Dr. Cardoso: It’s something to keep working hard on because for the old drugs that were approved with the wording that still said “women,” we have to keep fighting for accessibility.
I think we had a really nice discussion. I’m going to give you an opportunity for any last words that you want to say on this topic. Perhaps we’ll start with you, Sharon, and we’ll leave the very last word to Oliver.
Dr. Giordano: I would just emphasize the importance of doing research in this area. Hopefully, we will be able to get clinical trials. There are reasons to think that endocrine therapies may behave differently in men and women. We need to continue to work together as a community to collect the data so that we can ultimately improve the outcomes for our patients.
Dr. Bogler: I would echo what you just said, Dr. Giordano. I would like to express my gratitude to both of you. Dr. Giordano, you have a huge practice of men at MD Anderson. You took care of me and many other people I know.
Dr. Cardoso, you are a pioneer of a big registry trial that I am privileged to be working on, trying to gather data on men. You’re both pioneers in this field of working on behalf of people like me. I’m just very grateful for what you do.
Dr. Giordano: Thank you.
Dr. Cardoso: Thank you both for accepting this invitation. We hope that everybody takes more interest in this field. Who knows? Maybe we can find enough funds to run a specific trial for male patients with breast cancer.
Dr. Cardoso is director of the breast unit at Champalimaud Clinical Centre/Champalimaud Foundation, Lisbon. Dr. Giordano is professor of breast medical oncology and chair of health services research at the University of Texas MD Anderson Cancer Center, Houston. Dr. Bogler is a cancer biologist at the Randolph (Vt.) Center. Dr. Cardoso reported conflicts of interest with numerous pharmaceutical companies; Dr. Giordano and Dr. Bogler reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
What the first authorized DNA cancer risk test can and can’t tell you
A novel DNA test system that assesses a person’s genetic predisposition for certain cancers – the first of its kind granted marketing authorization by the Food and Drug Administration – may become a valuable new public health tool.
The Common Hereditary Cancers Panel (Invitae) was approved late September following FDA review under the De Novo process, a regulatory pathway for new types of low- to moderate-risk devices.
Validation of the prescription-only in vitro test was based on assessments of more than 9,000 clinical samples, which demonstrated accuracy of at least 99% for all tested variants in 47 genes known to be associated with an increased risk of developing certain cancers, including breast, ovarian, uterine, prostate, colorectal, gastric, pancreatic as well as melanoma.
How the test system works
Next-generation sequencing assesses germline human genomic DNA extracted from a single blood sample collected at the point of care, such as a doctor’s office, and is sent to a laboratory for analysis.
Specifically, the system aims to detect substitutions, small insertion and deletion alterations, and copy number variants in the panel of 47 targeted genes.
Jeff Shuren, MD, JD, director of the FDA’s Center for Devices and Radiological health, explained in an FDA press release announcing the marketing authorization.
Clinical interpretation is based on evidence from the published literature, prediction programs, public databases, and Invitae’s own variants database, the FDA statement explained.
What the test can do
Not only can the Common Hereditary Cancer Panel identify genetic variants that increase an individual’s risk of certain cancers, the panel can also help identify potential cancer-related hereditary variants in patients already diagnosed with cancer.
The most clinically significant genes the test system can detect include BRCA1 and BRCA2, which have known associations with hereditary breast and ovarian cancer syndrome; Lynch syndrome–associated genes including MLH1, MSH2, MSH6, PMS2, and EPCAM; CDH1, which is largely associated with hereditary diffuse gastric cancer and lobular breast cancer; and STK11, which is associated with Peutz-Jeghers syndrome.
“Patients should speak with a health care professional, such as a genetic counselor, to discuss any personal/family history of cancer, as such information can be helpful in interpreting test results,” the FDA advised.
What the test can’t do
The test is not intended to identify or evaluate all known genes tied to a person’s potential predisposition for cancer. The test is also not intended for cancer screening or prenatal testing.
For these reasons, and because genetics are not the only factor associated with developing cancer, negative test results could lead to misunderstanding among some patients about their cancer risk.
“Results are intended to be interpreted within the context of additional laboratory results, family history, and clinical findings,” the company wrote in a statement.
Test safety
Risks associated with the test include the possibility of false positive and false negative results and the potential for people to misunderstand what the results mean about their risk for cancer.
A false sense of assurance after a false negative result might, for instance, lead patients to forgo recommended surveillance or clinical management, whereas false positive test results could lead to inappropriate decision-making and undesirable consequences.
“These risks are mitigated by the analytical performance validation, clinical validation, and appropriate labeling of this test,” the agency explained.
Along with the De Novo authorization, the FDA is establishing special controls to define requirements for these tests. For instance, accuracy must be 99% or higher for positive agreement and at least 99.9% for negative agreement with a validated, independent method.
Public health implications
The information gleaned from this tool can “help guide physicians to provide appropriate monitoring and potential therapy, based on discovered variants,” Dr. Shuren said.
The marketing authorization of Invitae’s test established a new regulatory category, which “means that subsequent devices of the same type with the same intended use may go through FDA’s 510(k) premarket process,” the FDA explained.
A version of this article first appeared on Medscape.com.
A novel DNA test system that assesses a person’s genetic predisposition for certain cancers – the first of its kind granted marketing authorization by the Food and Drug Administration – may become a valuable new public health tool.
The Common Hereditary Cancers Panel (Invitae) was approved late September following FDA review under the De Novo process, a regulatory pathway for new types of low- to moderate-risk devices.
Validation of the prescription-only in vitro test was based on assessments of more than 9,000 clinical samples, which demonstrated accuracy of at least 99% for all tested variants in 47 genes known to be associated with an increased risk of developing certain cancers, including breast, ovarian, uterine, prostate, colorectal, gastric, pancreatic as well as melanoma.
How the test system works
Next-generation sequencing assesses germline human genomic DNA extracted from a single blood sample collected at the point of care, such as a doctor’s office, and is sent to a laboratory for analysis.
Specifically, the system aims to detect substitutions, small insertion and deletion alterations, and copy number variants in the panel of 47 targeted genes.
Jeff Shuren, MD, JD, director of the FDA’s Center for Devices and Radiological health, explained in an FDA press release announcing the marketing authorization.
Clinical interpretation is based on evidence from the published literature, prediction programs, public databases, and Invitae’s own variants database, the FDA statement explained.
What the test can do
Not only can the Common Hereditary Cancer Panel identify genetic variants that increase an individual’s risk of certain cancers, the panel can also help identify potential cancer-related hereditary variants in patients already diagnosed with cancer.
The most clinically significant genes the test system can detect include BRCA1 and BRCA2, which have known associations with hereditary breast and ovarian cancer syndrome; Lynch syndrome–associated genes including MLH1, MSH2, MSH6, PMS2, and EPCAM; CDH1, which is largely associated with hereditary diffuse gastric cancer and lobular breast cancer; and STK11, which is associated with Peutz-Jeghers syndrome.
“Patients should speak with a health care professional, such as a genetic counselor, to discuss any personal/family history of cancer, as such information can be helpful in interpreting test results,” the FDA advised.
What the test can’t do
The test is not intended to identify or evaluate all known genes tied to a person’s potential predisposition for cancer. The test is also not intended for cancer screening or prenatal testing.
For these reasons, and because genetics are not the only factor associated with developing cancer, negative test results could lead to misunderstanding among some patients about their cancer risk.
“Results are intended to be interpreted within the context of additional laboratory results, family history, and clinical findings,” the company wrote in a statement.
Test safety
Risks associated with the test include the possibility of false positive and false negative results and the potential for people to misunderstand what the results mean about their risk for cancer.
A false sense of assurance after a false negative result might, for instance, lead patients to forgo recommended surveillance or clinical management, whereas false positive test results could lead to inappropriate decision-making and undesirable consequences.
“These risks are mitigated by the analytical performance validation, clinical validation, and appropriate labeling of this test,” the agency explained.
Along with the De Novo authorization, the FDA is establishing special controls to define requirements for these tests. For instance, accuracy must be 99% or higher for positive agreement and at least 99.9% for negative agreement with a validated, independent method.
Public health implications
The information gleaned from this tool can “help guide physicians to provide appropriate monitoring and potential therapy, based on discovered variants,” Dr. Shuren said.
The marketing authorization of Invitae’s test established a new regulatory category, which “means that subsequent devices of the same type with the same intended use may go through FDA’s 510(k) premarket process,” the FDA explained.
A version of this article first appeared on Medscape.com.
A novel DNA test system that assesses a person’s genetic predisposition for certain cancers – the first of its kind granted marketing authorization by the Food and Drug Administration – may become a valuable new public health tool.
The Common Hereditary Cancers Panel (Invitae) was approved late September following FDA review under the De Novo process, a regulatory pathway for new types of low- to moderate-risk devices.
Validation of the prescription-only in vitro test was based on assessments of more than 9,000 clinical samples, which demonstrated accuracy of at least 99% for all tested variants in 47 genes known to be associated with an increased risk of developing certain cancers, including breast, ovarian, uterine, prostate, colorectal, gastric, pancreatic as well as melanoma.
How the test system works
Next-generation sequencing assesses germline human genomic DNA extracted from a single blood sample collected at the point of care, such as a doctor’s office, and is sent to a laboratory for analysis.
Specifically, the system aims to detect substitutions, small insertion and deletion alterations, and copy number variants in the panel of 47 targeted genes.
Jeff Shuren, MD, JD, director of the FDA’s Center for Devices and Radiological health, explained in an FDA press release announcing the marketing authorization.
Clinical interpretation is based on evidence from the published literature, prediction programs, public databases, and Invitae’s own variants database, the FDA statement explained.
What the test can do
Not only can the Common Hereditary Cancer Panel identify genetic variants that increase an individual’s risk of certain cancers, the panel can also help identify potential cancer-related hereditary variants in patients already diagnosed with cancer.
The most clinically significant genes the test system can detect include BRCA1 and BRCA2, which have known associations with hereditary breast and ovarian cancer syndrome; Lynch syndrome–associated genes including MLH1, MSH2, MSH6, PMS2, and EPCAM; CDH1, which is largely associated with hereditary diffuse gastric cancer and lobular breast cancer; and STK11, which is associated with Peutz-Jeghers syndrome.
“Patients should speak with a health care professional, such as a genetic counselor, to discuss any personal/family history of cancer, as such information can be helpful in interpreting test results,” the FDA advised.
What the test can’t do
The test is not intended to identify or evaluate all known genes tied to a person’s potential predisposition for cancer. The test is also not intended for cancer screening or prenatal testing.
For these reasons, and because genetics are not the only factor associated with developing cancer, negative test results could lead to misunderstanding among some patients about their cancer risk.
“Results are intended to be interpreted within the context of additional laboratory results, family history, and clinical findings,” the company wrote in a statement.
Test safety
Risks associated with the test include the possibility of false positive and false negative results and the potential for people to misunderstand what the results mean about their risk for cancer.
A false sense of assurance after a false negative result might, for instance, lead patients to forgo recommended surveillance or clinical management, whereas false positive test results could lead to inappropriate decision-making and undesirable consequences.
“These risks are mitigated by the analytical performance validation, clinical validation, and appropriate labeling of this test,” the agency explained.
Along with the De Novo authorization, the FDA is establishing special controls to define requirements for these tests. For instance, accuracy must be 99% or higher for positive agreement and at least 99.9% for negative agreement with a validated, independent method.
Public health implications
The information gleaned from this tool can “help guide physicians to provide appropriate monitoring and potential therapy, based on discovered variants,” Dr. Shuren said.
The marketing authorization of Invitae’s test established a new regulatory category, which “means that subsequent devices of the same type with the same intended use may go through FDA’s 510(k) premarket process,” the FDA explained.
A version of this article first appeared on Medscape.com.
Breast reconstruction post mastectomy: What matters most to women?
TOPLINE:
, a new survey suggests.
METHODOLOGY:
- As many as 40% of women feel dissatisfied after breast reconstruction because of unexpected outcomes that are poorly aligned with their personal preferences. Identifying what women value when considering breast reconstruction surgery could improve shared decision-making.
- Researchers used an adaptive choice-based conjoint analysis, a survey-based method used in marketing research, to identify attributes of breast reconstruction that are most important to women considering it.
- A total of 406 women completed the survey, which assessed the relative importance of breast appearance (flap or implant), abdominal morbidity, recovery time, additional operations, and complications of breast reconstruction.
- The survey included 105 women from Duke University, Durham, N.C., who had a new diagnosis of, or genetic predisposition to, breast cancer and were considering mastectomy with reconstruction. The survey also included another 301 women, identified through the Love Research Army registry, who had a history of breast cancer or a genetic predisposition.
TAKEAWAY:
- Overall, the risk for abdominal morbidity was most important to patients (mean relative importance, 28%); women also rated the chance for major complications (RI, 25%), the number of additional surgeries (RI, 23%), breast appearance (RI, 13%), and recovery time (RI, 11%) as important factors.
- Most women preferred implant-based reconstruction (85%), and these women cared most about abdominal morbidity (RI, 30%), risk for complications (RI, 26%), and added operations (RI, 21%).
- Women who preferred flap reconstruction cared most about additional operations (RI, 31%), followed by breast appearance (RI, 27%) and risk of complications (RI, 18%), which suggests that the appearance of the reconstruction procedure was particularly important, the authors noted.
- Participants who preferred the flap appearance were willing to accept an increased risk for abdominal morbidity and a slightly higher risk for complications; among the participants who preferred the implant option, one-third actually preferred the flap appearance.
IN PRACTICE:
“This study provides information on how women value different aspects of their care when making decisions for breast reconstruction,” the authors conclude, adding that “developing decision aids that elicit individual-level preferences and align patient values with treatment may provide an avenue to improve patient-centered care.”
SOURCE:
The study, led by first author Ronnie Shammas, MD, of Duke University, Durham, N.C., was published online in JAMA Surgery.
LIMITATIONS:
The attributes included in the survey may not represent all factors that women consider during the decision-making process. The cohort was composed of predominately upper-middle class and White women, which may reflect an increased preference toward implant, compared with flap reconstruction, as suggested in previous studies.
DISCLOSURES:
Funding for the research was provided by a grant from the National Endowment for Plastic Surgery awarded by the Plastic Surgery Foundation. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
TOPLINE:
, a new survey suggests.
METHODOLOGY:
- As many as 40% of women feel dissatisfied after breast reconstruction because of unexpected outcomes that are poorly aligned with their personal preferences. Identifying what women value when considering breast reconstruction surgery could improve shared decision-making.
- Researchers used an adaptive choice-based conjoint analysis, a survey-based method used in marketing research, to identify attributes of breast reconstruction that are most important to women considering it.
- A total of 406 women completed the survey, which assessed the relative importance of breast appearance (flap or implant), abdominal morbidity, recovery time, additional operations, and complications of breast reconstruction.
- The survey included 105 women from Duke University, Durham, N.C., who had a new diagnosis of, or genetic predisposition to, breast cancer and were considering mastectomy with reconstruction. The survey also included another 301 women, identified through the Love Research Army registry, who had a history of breast cancer or a genetic predisposition.
TAKEAWAY:
- Overall, the risk for abdominal morbidity was most important to patients (mean relative importance, 28%); women also rated the chance for major complications (RI, 25%), the number of additional surgeries (RI, 23%), breast appearance (RI, 13%), and recovery time (RI, 11%) as important factors.
- Most women preferred implant-based reconstruction (85%), and these women cared most about abdominal morbidity (RI, 30%), risk for complications (RI, 26%), and added operations (RI, 21%).
- Women who preferred flap reconstruction cared most about additional operations (RI, 31%), followed by breast appearance (RI, 27%) and risk of complications (RI, 18%), which suggests that the appearance of the reconstruction procedure was particularly important, the authors noted.
- Participants who preferred the flap appearance were willing to accept an increased risk for abdominal morbidity and a slightly higher risk for complications; among the participants who preferred the implant option, one-third actually preferred the flap appearance.
IN PRACTICE:
“This study provides information on how women value different aspects of their care when making decisions for breast reconstruction,” the authors conclude, adding that “developing decision aids that elicit individual-level preferences and align patient values with treatment may provide an avenue to improve patient-centered care.”
SOURCE:
The study, led by first author Ronnie Shammas, MD, of Duke University, Durham, N.C., was published online in JAMA Surgery.
LIMITATIONS:
The attributes included in the survey may not represent all factors that women consider during the decision-making process. The cohort was composed of predominately upper-middle class and White women, which may reflect an increased preference toward implant, compared with flap reconstruction, as suggested in previous studies.
DISCLOSURES:
Funding for the research was provided by a grant from the National Endowment for Plastic Surgery awarded by the Plastic Surgery Foundation. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
TOPLINE:
, a new survey suggests.
METHODOLOGY:
- As many as 40% of women feel dissatisfied after breast reconstruction because of unexpected outcomes that are poorly aligned with their personal preferences. Identifying what women value when considering breast reconstruction surgery could improve shared decision-making.
- Researchers used an adaptive choice-based conjoint analysis, a survey-based method used in marketing research, to identify attributes of breast reconstruction that are most important to women considering it.
- A total of 406 women completed the survey, which assessed the relative importance of breast appearance (flap or implant), abdominal morbidity, recovery time, additional operations, and complications of breast reconstruction.
- The survey included 105 women from Duke University, Durham, N.C., who had a new diagnosis of, or genetic predisposition to, breast cancer and were considering mastectomy with reconstruction. The survey also included another 301 women, identified through the Love Research Army registry, who had a history of breast cancer or a genetic predisposition.
TAKEAWAY:
- Overall, the risk for abdominal morbidity was most important to patients (mean relative importance, 28%); women also rated the chance for major complications (RI, 25%), the number of additional surgeries (RI, 23%), breast appearance (RI, 13%), and recovery time (RI, 11%) as important factors.
- Most women preferred implant-based reconstruction (85%), and these women cared most about abdominal morbidity (RI, 30%), risk for complications (RI, 26%), and added operations (RI, 21%).
- Women who preferred flap reconstruction cared most about additional operations (RI, 31%), followed by breast appearance (RI, 27%) and risk of complications (RI, 18%), which suggests that the appearance of the reconstruction procedure was particularly important, the authors noted.
- Participants who preferred the flap appearance were willing to accept an increased risk for abdominal morbidity and a slightly higher risk for complications; among the participants who preferred the implant option, one-third actually preferred the flap appearance.
IN PRACTICE:
“This study provides information on how women value different aspects of their care when making decisions for breast reconstruction,” the authors conclude, adding that “developing decision aids that elicit individual-level preferences and align patient values with treatment may provide an avenue to improve patient-centered care.”
SOURCE:
The study, led by first author Ronnie Shammas, MD, of Duke University, Durham, N.C., was published online in JAMA Surgery.
LIMITATIONS:
The attributes included in the survey may not represent all factors that women consider during the decision-making process. The cohort was composed of predominately upper-middle class and White women, which may reflect an increased preference toward implant, compared with flap reconstruction, as suggested in previous studies.
DISCLOSURES:
Funding for the research was provided by a grant from the National Endowment for Plastic Surgery awarded by the Plastic Surgery Foundation. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
This is how you get patients back for follow-up cancer testing
according to authors of a new study published in the Journal of the American Medical Association.
Results from the clustered, randomized clinical trial indicate that systems-based interventions, such as automating reminders in electronic health records (EHRs), outreach in the form of phone calls or letters, and assistance with barriers to health care, such as housing insecurity, can increase the number of patients who complete appropriate diagnostic follow-up after an abnormal result.
Patients who received an EHR reminder, outreach call or letter, and additional calls to screen for and assist with nine barriers to health care – housing insecurity, food insecurity, paying for basic utilities, family caregiving, legal issues, transportation, financial compensation for treatment, education, and employment – completed follow-up within 120 days of study enrollment at a rate of 31.4%. The follow-up rate was 31% for those who received only an EHR reminder and outreach, 22.7% for those who received only an EHR reminder, and 22.9% for those who received usual care.
“The benefits of cancer screening won’t be fully realized without systems to ensure timely follow-up of abnormal results,” said Anna Tosteson, ScD, director of the Dartmouth Institute for Health Policy and Clinical Practice in Lebanon, N.H., a coauthor of the study.
Current payment incentives and quality-of-care indicators focus on getting people in for screening but should also address completion of screening – meaning timely and appropriate follow-up of results that could be indicative of cancer, Dr. Tosteson said.
“There’s a disconnect if you have screening rates that are high but once people have an abnormal result, which is potentially one step closer to a cancer diagnosis, there are no systems in place to help clinicians track them,” said study coauthor Jennifer Haas, MD, director of the Center for Primary Care Research at Massachusetts General Hospital in Boston.
In a 2016 study, researchers found that follow-up rates after abnormal cancer screenings varied widely. While 95.6% of patients with abnormal breast cancer screenings underwent timely follow-up testing, only 68.1% of patients with colorectal abnormalities and 44.8% of patients with cervical abnormalities did so.
Researchers for the new study used guideline recommendations and specialist input to create automated EHR algorithms that determined a follow-up period and diagnostic test.
They put the algorithm into practice with 11,980 patients who were part of 44 primary care practices within three health networks between August 2020 and December 2021. All patients had received abnormal test results for colorectal, breast, cervical, or lung cancer in varying risk categories.
All patients received usual care from their providers, which consisted of a “hodgepodge of whatever their clinic usually does,” Dr. Haas said. Without standards and systems in place for follow-up, the burden of testing and tracking patients with abnormal results typically falls on the primary care provider.
The researchers intervened only when patients were overdue for completion of follow-up. They then staggered the interventions sequentially.
All study participants received an automated, algorithm-triggered EHR reminder for follow-up in their patient portal along with routine health maintenance reminders. To view the reminder, patients had to log into their portal. Participants in the outreach and outreach and navigation groups also received a phone call, an EHR message, or a physical letter 2 weeks after receiving an EHR notification if they hadn’t completed follow-up. Research assistants performed the outreach after having been prompted by the algorithm.
After another 4 weeks, those in the EHR, outreach, and navigation group received a call from a patient navigator who helped them address nine barriers to health care, chiefly by providing them with referrals to free resources.
Among patients who received navigation, outcomes were not significantly better than among those who received EHR and outreach, indicating social determinants of health did not significantly affect the population studied or that the modest approach to navigation and the resources provided were insufficient, Dr. Haas said.
The complexity of an automated platform that encompasses many types of cancers, test results, and other data elements could prove difficult to apply in settings with less infrastructure, said Steven Atlas, MD, MPH, director of the Practice-Based Research and Quality Improvement Network in the division of general internal medicine at Mass General.
“I think there’s a role for the federal government to take on these initiatives,” Dr. Atlas said. Government intervention could help create “national IT systems to create standards for creating code for what an abnormal result is and how it should be followed,” he said.
While interventions improved patient follow-up, the overall rates were still low.
“What concerns me is that despite the various interventions implemented to encourage and support patients to return for follow-up testing, over 60% of patients still did not return for the recommended testing,” said Joann G. Elmore, MD, MPH, professor of medicine at the University of California, Los Angeles. Dr. Elmore was not involved with the study.
The research took place during the COVID-19 pandemic, which may have reduced follow-up, the study authors wrote. Still, given that previous research has shown that follow-up tends to be low, the rates highlight “the need to understand factors associated with not completing follow-up that go beyond reminder effort,” they wrote. These include a need for patient education about the meaning of test results and what follow-up procedures involve.
The study was supported by the National Cancer Institute and the American Cancer Society. The authors have disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
according to authors of a new study published in the Journal of the American Medical Association.
Results from the clustered, randomized clinical trial indicate that systems-based interventions, such as automating reminders in electronic health records (EHRs), outreach in the form of phone calls or letters, and assistance with barriers to health care, such as housing insecurity, can increase the number of patients who complete appropriate diagnostic follow-up after an abnormal result.
Patients who received an EHR reminder, outreach call or letter, and additional calls to screen for and assist with nine barriers to health care – housing insecurity, food insecurity, paying for basic utilities, family caregiving, legal issues, transportation, financial compensation for treatment, education, and employment – completed follow-up within 120 days of study enrollment at a rate of 31.4%. The follow-up rate was 31% for those who received only an EHR reminder and outreach, 22.7% for those who received only an EHR reminder, and 22.9% for those who received usual care.
“The benefits of cancer screening won’t be fully realized without systems to ensure timely follow-up of abnormal results,” said Anna Tosteson, ScD, director of the Dartmouth Institute for Health Policy and Clinical Practice in Lebanon, N.H., a coauthor of the study.
Current payment incentives and quality-of-care indicators focus on getting people in for screening but should also address completion of screening – meaning timely and appropriate follow-up of results that could be indicative of cancer, Dr. Tosteson said.
“There’s a disconnect if you have screening rates that are high but once people have an abnormal result, which is potentially one step closer to a cancer diagnosis, there are no systems in place to help clinicians track them,” said study coauthor Jennifer Haas, MD, director of the Center for Primary Care Research at Massachusetts General Hospital in Boston.
In a 2016 study, researchers found that follow-up rates after abnormal cancer screenings varied widely. While 95.6% of patients with abnormal breast cancer screenings underwent timely follow-up testing, only 68.1% of patients with colorectal abnormalities and 44.8% of patients with cervical abnormalities did so.
Researchers for the new study used guideline recommendations and specialist input to create automated EHR algorithms that determined a follow-up period and diagnostic test.
They put the algorithm into practice with 11,980 patients who were part of 44 primary care practices within three health networks between August 2020 and December 2021. All patients had received abnormal test results for colorectal, breast, cervical, or lung cancer in varying risk categories.
All patients received usual care from their providers, which consisted of a “hodgepodge of whatever their clinic usually does,” Dr. Haas said. Without standards and systems in place for follow-up, the burden of testing and tracking patients with abnormal results typically falls on the primary care provider.
The researchers intervened only when patients were overdue for completion of follow-up. They then staggered the interventions sequentially.
All study participants received an automated, algorithm-triggered EHR reminder for follow-up in their patient portal along with routine health maintenance reminders. To view the reminder, patients had to log into their portal. Participants in the outreach and outreach and navigation groups also received a phone call, an EHR message, or a physical letter 2 weeks after receiving an EHR notification if they hadn’t completed follow-up. Research assistants performed the outreach after having been prompted by the algorithm.
After another 4 weeks, those in the EHR, outreach, and navigation group received a call from a patient navigator who helped them address nine barriers to health care, chiefly by providing them with referrals to free resources.
Among patients who received navigation, outcomes were not significantly better than among those who received EHR and outreach, indicating social determinants of health did not significantly affect the population studied or that the modest approach to navigation and the resources provided were insufficient, Dr. Haas said.
The complexity of an automated platform that encompasses many types of cancers, test results, and other data elements could prove difficult to apply in settings with less infrastructure, said Steven Atlas, MD, MPH, director of the Practice-Based Research and Quality Improvement Network in the division of general internal medicine at Mass General.
“I think there’s a role for the federal government to take on these initiatives,” Dr. Atlas said. Government intervention could help create “national IT systems to create standards for creating code for what an abnormal result is and how it should be followed,” he said.
While interventions improved patient follow-up, the overall rates were still low.
“What concerns me is that despite the various interventions implemented to encourage and support patients to return for follow-up testing, over 60% of patients still did not return for the recommended testing,” said Joann G. Elmore, MD, MPH, professor of medicine at the University of California, Los Angeles. Dr. Elmore was not involved with the study.
The research took place during the COVID-19 pandemic, which may have reduced follow-up, the study authors wrote. Still, given that previous research has shown that follow-up tends to be low, the rates highlight “the need to understand factors associated with not completing follow-up that go beyond reminder effort,” they wrote. These include a need for patient education about the meaning of test results and what follow-up procedures involve.
The study was supported by the National Cancer Institute and the American Cancer Society. The authors have disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
according to authors of a new study published in the Journal of the American Medical Association.
Results from the clustered, randomized clinical trial indicate that systems-based interventions, such as automating reminders in electronic health records (EHRs), outreach in the form of phone calls or letters, and assistance with barriers to health care, such as housing insecurity, can increase the number of patients who complete appropriate diagnostic follow-up after an abnormal result.
Patients who received an EHR reminder, outreach call or letter, and additional calls to screen for and assist with nine barriers to health care – housing insecurity, food insecurity, paying for basic utilities, family caregiving, legal issues, transportation, financial compensation for treatment, education, and employment – completed follow-up within 120 days of study enrollment at a rate of 31.4%. The follow-up rate was 31% for those who received only an EHR reminder and outreach, 22.7% for those who received only an EHR reminder, and 22.9% for those who received usual care.
“The benefits of cancer screening won’t be fully realized without systems to ensure timely follow-up of abnormal results,” said Anna Tosteson, ScD, director of the Dartmouth Institute for Health Policy and Clinical Practice in Lebanon, N.H., a coauthor of the study.
Current payment incentives and quality-of-care indicators focus on getting people in for screening but should also address completion of screening – meaning timely and appropriate follow-up of results that could be indicative of cancer, Dr. Tosteson said.
“There’s a disconnect if you have screening rates that are high but once people have an abnormal result, which is potentially one step closer to a cancer diagnosis, there are no systems in place to help clinicians track them,” said study coauthor Jennifer Haas, MD, director of the Center for Primary Care Research at Massachusetts General Hospital in Boston.
In a 2016 study, researchers found that follow-up rates after abnormal cancer screenings varied widely. While 95.6% of patients with abnormal breast cancer screenings underwent timely follow-up testing, only 68.1% of patients with colorectal abnormalities and 44.8% of patients with cervical abnormalities did so.
Researchers for the new study used guideline recommendations and specialist input to create automated EHR algorithms that determined a follow-up period and diagnostic test.
They put the algorithm into practice with 11,980 patients who were part of 44 primary care practices within three health networks between August 2020 and December 2021. All patients had received abnormal test results for colorectal, breast, cervical, or lung cancer in varying risk categories.
All patients received usual care from their providers, which consisted of a “hodgepodge of whatever their clinic usually does,” Dr. Haas said. Without standards and systems in place for follow-up, the burden of testing and tracking patients with abnormal results typically falls on the primary care provider.
The researchers intervened only when patients were overdue for completion of follow-up. They then staggered the interventions sequentially.
All study participants received an automated, algorithm-triggered EHR reminder for follow-up in their patient portal along with routine health maintenance reminders. To view the reminder, patients had to log into their portal. Participants in the outreach and outreach and navigation groups also received a phone call, an EHR message, or a physical letter 2 weeks after receiving an EHR notification if they hadn’t completed follow-up. Research assistants performed the outreach after having been prompted by the algorithm.
After another 4 weeks, those in the EHR, outreach, and navigation group received a call from a patient navigator who helped them address nine barriers to health care, chiefly by providing them with referrals to free resources.
Among patients who received navigation, outcomes were not significantly better than among those who received EHR and outreach, indicating social determinants of health did not significantly affect the population studied or that the modest approach to navigation and the resources provided were insufficient, Dr. Haas said.
The complexity of an automated platform that encompasses many types of cancers, test results, and other data elements could prove difficult to apply in settings with less infrastructure, said Steven Atlas, MD, MPH, director of the Practice-Based Research and Quality Improvement Network in the division of general internal medicine at Mass General.
“I think there’s a role for the federal government to take on these initiatives,” Dr. Atlas said. Government intervention could help create “national IT systems to create standards for creating code for what an abnormal result is and how it should be followed,” he said.
While interventions improved patient follow-up, the overall rates were still low.
“What concerns me is that despite the various interventions implemented to encourage and support patients to return for follow-up testing, over 60% of patients still did not return for the recommended testing,” said Joann G. Elmore, MD, MPH, professor of medicine at the University of California, Los Angeles. Dr. Elmore was not involved with the study.
The research took place during the COVID-19 pandemic, which may have reduced follow-up, the study authors wrote. Still, given that previous research has shown that follow-up tends to be low, the rates highlight “the need to understand factors associated with not completing follow-up that go beyond reminder effort,” they wrote. These include a need for patient education about the meaning of test results and what follow-up procedures involve.
The study was supported by the National Cancer Institute and the American Cancer Society. The authors have disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
FROM JAMA
Does surgery improve survival in metastatic breast cancer?
TOPLINE:
METHODOLOGY:
- Given conflicting results from prospective trials and improved outcomes reported in retrospective studies, removing the primary tumor in patients with metastatic breast cancer remains common practice but also “controversial,” the authors explained.
- To clarify whether to remove the primary tumor in metastatic breast cancer, investigators performed a meta-analysis of the five randomized clinical trials evaluating the issue.
- The five trials, published from 2015 to 2023, included 1,381 women with de novo metastatic breast cancer; half had their primary tumor removed, half did not.
TAKEAWAY:
- The analysis revealed no overall survival benefit for patients who underwent surgical excision of their primary breast tumor (hazard ratio [HR], 0.93; 95% confidence interval [CI], 0.76-1.14).
- Surgery was not associated with an overall survival benefit in subgroup analyses by receptor status, pattern of metastasis (bone vs. viscera or oligometastatic vs nonoligometastatic disease), number of metastatic sites, or location of metastatic lesions.
- The one possible exception: Surgery did appear to improve overall survival in younger, premenopausal women (HR, 0.74; 95% CI 0.58-0.94), but “the lack of uniform definitions and inconsistent trial results suggest that this subgroup analysis should be viewed as exploratory and requiring further validation,” the authors said.
- Breast surgery was associated with improved local progression-free survival (HR, 0.37) but not distant progression-free survival or patient-reported quality of life.
IN PRACTICE:
“We conclude that surgical excision of the primary tumor in case of de novo metastatic breast cancer is not associated with improved patient survival,” with a “potential exception” among younger patients, the authors said. “As such, besides the need to palliate local symptoms, surgery should not be routinely offered to patients with metastatic disease.”
SOURCE:
The work, led by Guillermo Villacampa of the SOLTI Breast Cancer Research Group in Barcelona, was published Sept. 12 in The Oncologist.
LIMITATIONS:
The five trials had various weaknesses, including imbalances in patient characteristics, protocol violations regarding planned and administered treatment, and missing information on associations between surgical margins and outcomes.
DISCLOSURES:
There was no funding for the work. Investigators reported speaker fees, consultant fees, and/or research funding from various companies, including Merck, AstraZeneca, Pfizer, and Novartis.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Given conflicting results from prospective trials and improved outcomes reported in retrospective studies, removing the primary tumor in patients with metastatic breast cancer remains common practice but also “controversial,” the authors explained.
- To clarify whether to remove the primary tumor in metastatic breast cancer, investigators performed a meta-analysis of the five randomized clinical trials evaluating the issue.
- The five trials, published from 2015 to 2023, included 1,381 women with de novo metastatic breast cancer; half had their primary tumor removed, half did not.
TAKEAWAY:
- The analysis revealed no overall survival benefit for patients who underwent surgical excision of their primary breast tumor (hazard ratio [HR], 0.93; 95% confidence interval [CI], 0.76-1.14).
- Surgery was not associated with an overall survival benefit in subgroup analyses by receptor status, pattern of metastasis (bone vs. viscera or oligometastatic vs nonoligometastatic disease), number of metastatic sites, or location of metastatic lesions.
- The one possible exception: Surgery did appear to improve overall survival in younger, premenopausal women (HR, 0.74; 95% CI 0.58-0.94), but “the lack of uniform definitions and inconsistent trial results suggest that this subgroup analysis should be viewed as exploratory and requiring further validation,” the authors said.
- Breast surgery was associated with improved local progression-free survival (HR, 0.37) but not distant progression-free survival or patient-reported quality of life.
IN PRACTICE:
“We conclude that surgical excision of the primary tumor in case of de novo metastatic breast cancer is not associated with improved patient survival,” with a “potential exception” among younger patients, the authors said. “As such, besides the need to palliate local symptoms, surgery should not be routinely offered to patients with metastatic disease.”
SOURCE:
The work, led by Guillermo Villacampa of the SOLTI Breast Cancer Research Group in Barcelona, was published Sept. 12 in The Oncologist.
LIMITATIONS:
The five trials had various weaknesses, including imbalances in patient characteristics, protocol violations regarding planned and administered treatment, and missing information on associations between surgical margins and outcomes.
DISCLOSURES:
There was no funding for the work. Investigators reported speaker fees, consultant fees, and/or research funding from various companies, including Merck, AstraZeneca, Pfizer, and Novartis.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Given conflicting results from prospective trials and improved outcomes reported in retrospective studies, removing the primary tumor in patients with metastatic breast cancer remains common practice but also “controversial,” the authors explained.
- To clarify whether to remove the primary tumor in metastatic breast cancer, investigators performed a meta-analysis of the five randomized clinical trials evaluating the issue.
- The five trials, published from 2015 to 2023, included 1,381 women with de novo metastatic breast cancer; half had their primary tumor removed, half did not.
TAKEAWAY:
- The analysis revealed no overall survival benefit for patients who underwent surgical excision of their primary breast tumor (hazard ratio [HR], 0.93; 95% confidence interval [CI], 0.76-1.14).
- Surgery was not associated with an overall survival benefit in subgroup analyses by receptor status, pattern of metastasis (bone vs. viscera or oligometastatic vs nonoligometastatic disease), number of metastatic sites, or location of metastatic lesions.
- The one possible exception: Surgery did appear to improve overall survival in younger, premenopausal women (HR, 0.74; 95% CI 0.58-0.94), but “the lack of uniform definitions and inconsistent trial results suggest that this subgroup analysis should be viewed as exploratory and requiring further validation,” the authors said.
- Breast surgery was associated with improved local progression-free survival (HR, 0.37) but not distant progression-free survival or patient-reported quality of life.
IN PRACTICE:
“We conclude that surgical excision of the primary tumor in case of de novo metastatic breast cancer is not associated with improved patient survival,” with a “potential exception” among younger patients, the authors said. “As such, besides the need to palliate local symptoms, surgery should not be routinely offered to patients with metastatic disease.”
SOURCE:
The work, led by Guillermo Villacampa of the SOLTI Breast Cancer Research Group in Barcelona, was published Sept. 12 in The Oncologist.
LIMITATIONS:
The five trials had various weaknesses, including imbalances in patient characteristics, protocol violations regarding planned and administered treatment, and missing information on associations between surgical margins and outcomes.
DISCLOSURES:
There was no funding for the work. Investigators reported speaker fees, consultant fees, and/or research funding from various companies, including Merck, AstraZeneca, Pfizer, and Novartis.
A version of this article first appeared on Medscape.com.