User login
Adding melatonin to alprazolam boosts preoperative anxiolysis
SAN FRANCISCO – Adding melatonin to alprazolam significantly decreased preoperative anxiety, compared with either medication alone or with placebo, in a randomized, double-blind trial of 80 patients.
Adult patients undergoing laparoscopic cholecystectomy who reported a preoperative anxiety level of at least 3 cm on a 10-cm Visual Analog Scale (VAS) had average anxiety scores of 5 cm before being randomized to preoperative medication with alprazolam 0.5 mg, melatonin 3 mg, both drugs, or placebo (with 20 patients in each group).
After 1 hour spent in a quiet room following the premedication, VAS scores had fallen by an average of 3 cm in the two-drug group, significantly more than average 2-cm reductions with either drug alone, or a 1-cm decline on placebo, Dr. Krishna Pokharel and her associates reported.
Adding melatonin did not seem to worsen the sedative or amnesiac effects of alprazolam, she reported in a poster presentation at the annual meeting of the American Society of Anesthesiologists.
In the past, some of her patients who had been premedicated with a benzodiazepine before general anesthesia and surgery sometimes became aroused during the procedure, perhaps because benzodiazepines suppress endogenous melatonin levels, Dr. Pokharel said. She hypothesized that adding melatonin might help, and the study results have convinced her institution to routinely add melatonin to alprazolam for surgical premedication in anxious patients, said Dr. Pokharel of B.P. Koirala Institute of Health Sciences, Dharan, Nepal.
Patients were shown different pictures during assessments of anxiety and sedation at various time points before surgery. At 24 hours after surgery, 10 patients on alprazolam plus melatonin could recall the picture they saw 1 hour after taking the presurgical medication, compared with 9 patients on alprazolam alone, 18 patients on melatonin alone, and 16 patients on placebo, the poster reported.
In other results, average scores on a 5-point scale for sedation at 1 hour were 0.5 with melatonin, 1 for each group using alprazolam, and 0 with placebo, among other secondary outcomes. At 24 hours after surgery, five patients in the two-drug group could not remember being transferred to the OR, compared with four patients on alprazolam, one patient on melatonin, and none of the patients on placebo.
All groups scored 2 on a 3-point scale for orientation 1 hour after taking the premedication. The amount of propofol needed to achieve a loss of response to verbal commands at the time of general anesthesia induction averaged 66 mg in the alprazolam plus melatonin group, 59 mg after alprazolam alone, 79 mg after melatonin alone, and 76 mg on placebo.
No patients developed serious adverse events.
Dr. Pokharel reported having no financial disclosures.
On Twitter @sherryboschert
laparoscopic cholecystectomy, Visual Analog Scale, VAS, anxiety, Dr. Krishna Pokharel, the American Society of Anesthesiologists, benzodiazepines,
SAN FRANCISCO – Adding melatonin to alprazolam significantly decreased preoperative anxiety, compared with either medication alone or with placebo, in a randomized, double-blind trial of 80 patients.
Adult patients undergoing laparoscopic cholecystectomy who reported a preoperative anxiety level of at least 3 cm on a 10-cm Visual Analog Scale (VAS) had average anxiety scores of 5 cm before being randomized to preoperative medication with alprazolam 0.5 mg, melatonin 3 mg, both drugs, or placebo (with 20 patients in each group).
After 1 hour spent in a quiet room following the premedication, VAS scores had fallen by an average of 3 cm in the two-drug group, significantly more than average 2-cm reductions with either drug alone, or a 1-cm decline on placebo, Dr. Krishna Pokharel and her associates reported.
Adding melatonin did not seem to worsen the sedative or amnesiac effects of alprazolam, she reported in a poster presentation at the annual meeting of the American Society of Anesthesiologists.
In the past, some of her patients who had been premedicated with a benzodiazepine before general anesthesia and surgery sometimes became aroused during the procedure, perhaps because benzodiazepines suppress endogenous melatonin levels, Dr. Pokharel said. She hypothesized that adding melatonin might help, and the study results have convinced her institution to routinely add melatonin to alprazolam for surgical premedication in anxious patients, said Dr. Pokharel of B.P. Koirala Institute of Health Sciences, Dharan, Nepal.
Patients were shown different pictures during assessments of anxiety and sedation at various time points before surgery. At 24 hours after surgery, 10 patients on alprazolam plus melatonin could recall the picture they saw 1 hour after taking the presurgical medication, compared with 9 patients on alprazolam alone, 18 patients on melatonin alone, and 16 patients on placebo, the poster reported.
In other results, average scores on a 5-point scale for sedation at 1 hour were 0.5 with melatonin, 1 for each group using alprazolam, and 0 with placebo, among other secondary outcomes. At 24 hours after surgery, five patients in the two-drug group could not remember being transferred to the OR, compared with four patients on alprazolam, one patient on melatonin, and none of the patients on placebo.
All groups scored 2 on a 3-point scale for orientation 1 hour after taking the premedication. The amount of propofol needed to achieve a loss of response to verbal commands at the time of general anesthesia induction averaged 66 mg in the alprazolam plus melatonin group, 59 mg after alprazolam alone, 79 mg after melatonin alone, and 76 mg on placebo.
No patients developed serious adverse events.
Dr. Pokharel reported having no financial disclosures.
On Twitter @sherryboschert
SAN FRANCISCO – Adding melatonin to alprazolam significantly decreased preoperative anxiety, compared with either medication alone or with placebo, in a randomized, double-blind trial of 80 patients.
Adult patients undergoing laparoscopic cholecystectomy who reported a preoperative anxiety level of at least 3 cm on a 10-cm Visual Analog Scale (VAS) had average anxiety scores of 5 cm before being randomized to preoperative medication with alprazolam 0.5 mg, melatonin 3 mg, both drugs, or placebo (with 20 patients in each group).
After 1 hour spent in a quiet room following the premedication, VAS scores had fallen by an average of 3 cm in the two-drug group, significantly more than average 2-cm reductions with either drug alone, or a 1-cm decline on placebo, Dr. Krishna Pokharel and her associates reported.
Adding melatonin did not seem to worsen the sedative or amnesiac effects of alprazolam, she reported in a poster presentation at the annual meeting of the American Society of Anesthesiologists.
In the past, some of her patients who had been premedicated with a benzodiazepine before general anesthesia and surgery sometimes became aroused during the procedure, perhaps because benzodiazepines suppress endogenous melatonin levels, Dr. Pokharel said. She hypothesized that adding melatonin might help, and the study results have convinced her institution to routinely add melatonin to alprazolam for surgical premedication in anxious patients, said Dr. Pokharel of B.P. Koirala Institute of Health Sciences, Dharan, Nepal.
Patients were shown different pictures during assessments of anxiety and sedation at various time points before surgery. At 24 hours after surgery, 10 patients on alprazolam plus melatonin could recall the picture they saw 1 hour after taking the presurgical medication, compared with 9 patients on alprazolam alone, 18 patients on melatonin alone, and 16 patients on placebo, the poster reported.
In other results, average scores on a 5-point scale for sedation at 1 hour were 0.5 with melatonin, 1 for each group using alprazolam, and 0 with placebo, among other secondary outcomes. At 24 hours after surgery, five patients in the two-drug group could not remember being transferred to the OR, compared with four patients on alprazolam, one patient on melatonin, and none of the patients on placebo.
All groups scored 2 on a 3-point scale for orientation 1 hour after taking the premedication. The amount of propofol needed to achieve a loss of response to verbal commands at the time of general anesthesia induction averaged 66 mg in the alprazolam plus melatonin group, 59 mg after alprazolam alone, 79 mg after melatonin alone, and 76 mg on placebo.
No patients developed serious adverse events.
Dr. Pokharel reported having no financial disclosures.
On Twitter @sherryboschert
laparoscopic cholecystectomy, Visual Analog Scale, VAS, anxiety, Dr. Krishna Pokharel, the American Society of Anesthesiologists, benzodiazepines,
laparoscopic cholecystectomy, Visual Analog Scale, VAS, anxiety, Dr. Krishna Pokharel, the American Society of Anesthesiologists, benzodiazepines,
AT THE ASA ANNUAL MEETING
Major finding: Anxiety VAS scores at 60 minutes, compared with baseline, fell by 3 cm with melatonin plus alprazolam, 2 cm with either drug alone, or 1 cm with placebo.
Data source: A prospective, randomized, controlled trial of 80 adults undergoing laparoscopic cholecystectomy at one hospital.
Disclosures: Dr. Pokharel reported having no financial disclosures.
Antirheumatic drugs don’t boost surgical infection risk
SAN DIEGO – Rheumatoid arthritis patients undergoing surgery who stayed on their antirheumatic medication perioperatively didn’t have a higher risk of early postoperative infection compared with those who temporarily stopped treatment before surgery, according to findings from a large national Veterans Affairs study.
Rheumatologists are frequently consulted about this issue. Evidence to guide practice has been scarce, however, and until now many rheumatologists and surgeons have taken a conservative approach, reasoning that the immunosuppressive drugs employed in controlling inflammation in rheumatoid arthritis might also increase the risk of surgical wound infection.
A common practice has been to have RA patients stop their medication a month ahead of elective surgery, or at least two drug half-lives beforehand, then start treatment again roughly a month after the operation, or when the wound has healed. The new Veterans Affairs (VA) study findings suggest this practice may be unnecessary, Dr. Zaki Abou Zahr said at the annual meeting of the American College of Rheumatology.
Dr. Bernard Ng, his senior coinvestigator in the study, added that temporarily stopping antirheumatic agents before surgery may actually be harmful in that it increases the risk of a flare of the RA, which in turn would impede postoperative rehabilitation.
But there is a major caveat regarding the VA study: Participation was restricted to RA patients on only a single conventional disease-modifying antirheumatic drug (DMARD) or biologic agent leading up to surgery. This restriction, imposed to make for a more clear-cut analysis, means that the study results can’t be extrapolated to patients on multidrug therapy. And multidrug therapy is quite common. Indeed, slightly more than half of RA patients in the VA health care system are on combination therapy, most often methotrexate plus a biologic agent, noted Dr. Ng, chief of rheumatology at the VA Puget Sound Health Care System, Seattle.
Dr. Abou Zahr presented the retrospective cohort study involving 6,548 RA patients in VA administrative databases, all of whom were on antirheumatic drug monotherapy prior to surgery. The surgery was of all types, including cardiothoracic, gastrointestinal, vascular, and orthopedic, as well as emergent and elective.
The primary endpoints were the rate of wound infections, both superficial and deep, within 30 days post surgery, and the general infection rate – including pneumonia, sepsis, and urinary tract infections – during the same time frame.
Sixty-two percent of the 1,480 RA patients on a single biologic agent did not stop taking it preoperatively. One key study finding was that neither their postoperative wound infection rate nor their general infection rate differed significantly from rates in patients who temporarily halted their biologic agent. The same held true among the 70% of patients on a single conventional DMARD who did not stop taking their medication preoperatively, according to Dr. Abou Zahr of Baylor College of Medicine, Houston.
Dr. Ng said the investigators plan to extend their work to include RA patients on multiple antirheumatic drugs that they do or don’t temporarily stop when undergoing surgery within the VA system. The researchers also plan to take a close look at patients undergoing specific types of surgery to see if the postoperative infection risk in patients who remain on treatment varies according to their operation.
Dr. Fehmida Zahabi, a rheumatologist from Plano, Tex., who chaired a press conference highlighting the VA study findings, said that while she’d like to see a confirmatory study, "I think we’re getting to the point where we’re saying we should cautiously keep these patients on their medications. That’s what the data suggest."
She noted that before the VA study, the very limited evidence available to guide practice in this area centered on a 12-year-old British randomized trial involving RA patients on methotrexate undergoing elective orthopedic surgery. Those assigned to stop the drug from 2 weeks before surgery to 2 weeks post surgery had significantly more infections, surgical complications, and RA flares within 6 weeks after surgery (Ann. Rheum. Dis. 2001;60:214-7).
As for patients on multidrug therapy who are scheduled for surgery, her inclination until evidence becomes available for guidance is to pare down the regimen preoperatively, while keeping the patient on one or two drugs.
The VA study was funded by the Department of Veterans Affairs. Dr. Abou Zahr and Dr. Ng reported having no conflicts of interest.
SAN DIEGO – Rheumatoid arthritis patients undergoing surgery who stayed on their antirheumatic medication perioperatively didn’t have a higher risk of early postoperative infection compared with those who temporarily stopped treatment before surgery, according to findings from a large national Veterans Affairs study.
Rheumatologists are frequently consulted about this issue. Evidence to guide practice has been scarce, however, and until now many rheumatologists and surgeons have taken a conservative approach, reasoning that the immunosuppressive drugs employed in controlling inflammation in rheumatoid arthritis might also increase the risk of surgical wound infection.
A common practice has been to have RA patients stop their medication a month ahead of elective surgery, or at least two drug half-lives beforehand, then start treatment again roughly a month after the operation, or when the wound has healed. The new Veterans Affairs (VA) study findings suggest this practice may be unnecessary, Dr. Zaki Abou Zahr said at the annual meeting of the American College of Rheumatology.
Dr. Bernard Ng, his senior coinvestigator in the study, added that temporarily stopping antirheumatic agents before surgery may actually be harmful in that it increases the risk of a flare of the RA, which in turn would impede postoperative rehabilitation.
But there is a major caveat regarding the VA study: Participation was restricted to RA patients on only a single conventional disease-modifying antirheumatic drug (DMARD) or biologic agent leading up to surgery. This restriction, imposed to make for a more clear-cut analysis, means that the study results can’t be extrapolated to patients on multidrug therapy. And multidrug therapy is quite common. Indeed, slightly more than half of RA patients in the VA health care system are on combination therapy, most often methotrexate plus a biologic agent, noted Dr. Ng, chief of rheumatology at the VA Puget Sound Health Care System, Seattle.
Dr. Abou Zahr presented the retrospective cohort study involving 6,548 RA patients in VA administrative databases, all of whom were on antirheumatic drug monotherapy prior to surgery. The surgery was of all types, including cardiothoracic, gastrointestinal, vascular, and orthopedic, as well as emergent and elective.
The primary endpoints were the rate of wound infections, both superficial and deep, within 30 days post surgery, and the general infection rate – including pneumonia, sepsis, and urinary tract infections – during the same time frame.
Sixty-two percent of the 1,480 RA patients on a single biologic agent did not stop taking it preoperatively. One key study finding was that neither their postoperative wound infection rate nor their general infection rate differed significantly from rates in patients who temporarily halted their biologic agent. The same held true among the 70% of patients on a single conventional DMARD who did not stop taking their medication preoperatively, according to Dr. Abou Zahr of Baylor College of Medicine, Houston.
Dr. Ng said the investigators plan to extend their work to include RA patients on multiple antirheumatic drugs that they do or don’t temporarily stop when undergoing surgery within the VA system. The researchers also plan to take a close look at patients undergoing specific types of surgery to see if the postoperative infection risk in patients who remain on treatment varies according to their operation.
Dr. Fehmida Zahabi, a rheumatologist from Plano, Tex., who chaired a press conference highlighting the VA study findings, said that while she’d like to see a confirmatory study, "I think we’re getting to the point where we’re saying we should cautiously keep these patients on their medications. That’s what the data suggest."
She noted that before the VA study, the very limited evidence available to guide practice in this area centered on a 12-year-old British randomized trial involving RA patients on methotrexate undergoing elective orthopedic surgery. Those assigned to stop the drug from 2 weeks before surgery to 2 weeks post surgery had significantly more infections, surgical complications, and RA flares within 6 weeks after surgery (Ann. Rheum. Dis. 2001;60:214-7).
As for patients on multidrug therapy who are scheduled for surgery, her inclination until evidence becomes available for guidance is to pare down the regimen preoperatively, while keeping the patient on one or two drugs.
The VA study was funded by the Department of Veterans Affairs. Dr. Abou Zahr and Dr. Ng reported having no conflicts of interest.
SAN DIEGO – Rheumatoid arthritis patients undergoing surgery who stayed on their antirheumatic medication perioperatively didn’t have a higher risk of early postoperative infection compared with those who temporarily stopped treatment before surgery, according to findings from a large national Veterans Affairs study.
Rheumatologists are frequently consulted about this issue. Evidence to guide practice has been scarce, however, and until now many rheumatologists and surgeons have taken a conservative approach, reasoning that the immunosuppressive drugs employed in controlling inflammation in rheumatoid arthritis might also increase the risk of surgical wound infection.
A common practice has been to have RA patients stop their medication a month ahead of elective surgery, or at least two drug half-lives beforehand, then start treatment again roughly a month after the operation, or when the wound has healed. The new Veterans Affairs (VA) study findings suggest this practice may be unnecessary, Dr. Zaki Abou Zahr said at the annual meeting of the American College of Rheumatology.
Dr. Bernard Ng, his senior coinvestigator in the study, added that temporarily stopping antirheumatic agents before surgery may actually be harmful in that it increases the risk of a flare of the RA, which in turn would impede postoperative rehabilitation.
But there is a major caveat regarding the VA study: Participation was restricted to RA patients on only a single conventional disease-modifying antirheumatic drug (DMARD) or biologic agent leading up to surgery. This restriction, imposed to make for a more clear-cut analysis, means that the study results can’t be extrapolated to patients on multidrug therapy. And multidrug therapy is quite common. Indeed, slightly more than half of RA patients in the VA health care system are on combination therapy, most often methotrexate plus a biologic agent, noted Dr. Ng, chief of rheumatology at the VA Puget Sound Health Care System, Seattle.
Dr. Abou Zahr presented the retrospective cohort study involving 6,548 RA patients in VA administrative databases, all of whom were on antirheumatic drug monotherapy prior to surgery. The surgery was of all types, including cardiothoracic, gastrointestinal, vascular, and orthopedic, as well as emergent and elective.
The primary endpoints were the rate of wound infections, both superficial and deep, within 30 days post surgery, and the general infection rate – including pneumonia, sepsis, and urinary tract infections – during the same time frame.
Sixty-two percent of the 1,480 RA patients on a single biologic agent did not stop taking it preoperatively. One key study finding was that neither their postoperative wound infection rate nor their general infection rate differed significantly from rates in patients who temporarily halted their biologic agent. The same held true among the 70% of patients on a single conventional DMARD who did not stop taking their medication preoperatively, according to Dr. Abou Zahr of Baylor College of Medicine, Houston.
Dr. Ng said the investigators plan to extend their work to include RA patients on multiple antirheumatic drugs that they do or don’t temporarily stop when undergoing surgery within the VA system. The researchers also plan to take a close look at patients undergoing specific types of surgery to see if the postoperative infection risk in patients who remain on treatment varies according to their operation.
Dr. Fehmida Zahabi, a rheumatologist from Plano, Tex., who chaired a press conference highlighting the VA study findings, said that while she’d like to see a confirmatory study, "I think we’re getting to the point where we’re saying we should cautiously keep these patients on their medications. That’s what the data suggest."
She noted that before the VA study, the very limited evidence available to guide practice in this area centered on a 12-year-old British randomized trial involving RA patients on methotrexate undergoing elective orthopedic surgery. Those assigned to stop the drug from 2 weeks before surgery to 2 weeks post surgery had significantly more infections, surgical complications, and RA flares within 6 weeks after surgery (Ann. Rheum. Dis. 2001;60:214-7).
As for patients on multidrug therapy who are scheduled for surgery, her inclination until evidence becomes available for guidance is to pare down the regimen preoperatively, while keeping the patient on one or two drugs.
The VA study was funded by the Department of Veterans Affairs. Dr. Abou Zahr and Dr. Ng reported having no conflicts of interest.
AT THE ACR ANNUAL MEETING
Major finding: Rheumatoid arthritis patients who remained on their antirheumatic medication while they underwent various types of surgery did not have a significantly different 30-day wound infection rate than those who stopped treatment temporarily prior to surgery.
Data source: This was a retrospective observational cohort study involving 6,548 rheumatoid arthritis patients undergoing various types of surgery.
Disclosures: The study was funded by the Department of Veterans Affairs. The presenters reported having no financial conflicts.
Laparoscopic gastrostomy associated with better outcomes than open gastrostomy in adults
WASHINGTON – Laparoscopic gastrostomy in adults was associated with fewer complications than open gastrostomy in the same population, according to data presented at the annual clinical congress of the American College of Surgeons.
In a retrospective study of data from 2,883 patients, taken from the 2005-2010 National Surgical Quality Improvement Program (NSQIP) database, Dr. Rachel Van Dusen and her colleagues reviewed a variety of outcomes, including wound, pulmonary, renal, cardiac, and thromboembolic, in patients who underwent either a laparoscopic (n = 382), open (n = 2,112), or percutaneous endoscopic gastrostomy (PEG) (n = 389).
Either laparoscopic or open gastrostomies are performed in patients for whom PEG, the standard of care, is unfeasible. Dr. Van Dusen, of George Washington University, Washington, said that theirs was the first study to measure the association between all three procedures and complications in the adult gastrostomy patient population.
The average age of patients was 58 years in the laparoscopic cohort, 62 years in the open group, and 65 years in the PEG group. The patients were at least 18 years old. The laparoscopic group was 88.8% white and 69.4% female; the open group, 80.7% white and 58.2% female; and the PEG group, 85.2% and 57.6%, respectively.
A stepwise logistic regression analysis of patient characteristics in all three cohorts indicated that at baseline, open gastrostomy patients tended, among other factors, to have serum albumin levels less than 3 g/dL (44%), sepsis (35.7%), diabetes (20.4%), a body mass index of 20 kg/m2 or less (27.8%), and ascites (9.0%); in addition, 27% of patients were undergoing chemotherapy.
In a similar analysis, laparoscopic patients were seen to be less ill at baseline: Only 20.4% had low albumin levels, diabetes and sepsis levels were just under 16%, BMI was between 20 and 40, 2.9% were ascitic, and only 1.3% were receiving chemotherapy.
Complications in each group were reviewed according to either wound or organ system. PEG patients had the fewest overall complications (22.4%), with none that were comparatively significant. However, there were several significant differences in complication rates between the laparoscopic and open gastrostomy cohorts.
Pulmonary complications occurred in 23.2% of the open gastrostomy group, compared with 9.7% of the laparoscopic group (multivariate odds ratio, 1.97). Also in the open gastrostomy group, 2.5% had renal complications, compared with 0.5% of the laparoscopic patients (mOR, 4.48). Sepsis was found in 13.5% of the open group and 5.8% of the laparoscopic group (mOR 1.72).
Open gastrostomy patients, when compared with the PEG group, had twice the odds of experiencing wound events (mOR, 2.10) and a 1.5 times greater chance of having sepsis (mOR, 1.51). No significant differences were found between other complications.
"We surmise that the reason the higher rate of infection was associated with the open gastrostomy [patients] is the increase in fascial violation and the exposure of the soft tissues," said Dr. Van Dusen. "The increase in pulmonary problems may be related to poor pulmonary toilet from more postoperative pain, and more septic issues may be related to more significant fluid shifts during laparotomy."
Dr. Van Dusen concluded that while PEG remains the best method of enteral access, laparoscopic gastrostomy is superior to open gastrostomy.
Dr. Van Dusen did not have any relevant disclosures.
WASHINGTON – Laparoscopic gastrostomy in adults was associated with fewer complications than open gastrostomy in the same population, according to data presented at the annual clinical congress of the American College of Surgeons.
In a retrospective study of data from 2,883 patients, taken from the 2005-2010 National Surgical Quality Improvement Program (NSQIP) database, Dr. Rachel Van Dusen and her colleagues reviewed a variety of outcomes, including wound, pulmonary, renal, cardiac, and thromboembolic, in patients who underwent either a laparoscopic (n = 382), open (n = 2,112), or percutaneous endoscopic gastrostomy (PEG) (n = 389).
Either laparoscopic or open gastrostomies are performed in patients for whom PEG, the standard of care, is unfeasible. Dr. Van Dusen, of George Washington University, Washington, said that theirs was the first study to measure the association between all three procedures and complications in the adult gastrostomy patient population.
The average age of patients was 58 years in the laparoscopic cohort, 62 years in the open group, and 65 years in the PEG group. The patients were at least 18 years old. The laparoscopic group was 88.8% white and 69.4% female; the open group, 80.7% white and 58.2% female; and the PEG group, 85.2% and 57.6%, respectively.
A stepwise logistic regression analysis of patient characteristics in all three cohorts indicated that at baseline, open gastrostomy patients tended, among other factors, to have serum albumin levels less than 3 g/dL (44%), sepsis (35.7%), diabetes (20.4%), a body mass index of 20 kg/m2 or less (27.8%), and ascites (9.0%); in addition, 27% of patients were undergoing chemotherapy.
In a similar analysis, laparoscopic patients were seen to be less ill at baseline: Only 20.4% had low albumin levels, diabetes and sepsis levels were just under 16%, BMI was between 20 and 40, 2.9% were ascitic, and only 1.3% were receiving chemotherapy.
Complications in each group were reviewed according to either wound or organ system. PEG patients had the fewest overall complications (22.4%), with none that were comparatively significant. However, there were several significant differences in complication rates between the laparoscopic and open gastrostomy cohorts.
Pulmonary complications occurred in 23.2% of the open gastrostomy group, compared with 9.7% of the laparoscopic group (multivariate odds ratio, 1.97). Also in the open gastrostomy group, 2.5% had renal complications, compared with 0.5% of the laparoscopic patients (mOR, 4.48). Sepsis was found in 13.5% of the open group and 5.8% of the laparoscopic group (mOR 1.72).
Open gastrostomy patients, when compared with the PEG group, had twice the odds of experiencing wound events (mOR, 2.10) and a 1.5 times greater chance of having sepsis (mOR, 1.51). No significant differences were found between other complications.
"We surmise that the reason the higher rate of infection was associated with the open gastrostomy [patients] is the increase in fascial violation and the exposure of the soft tissues," said Dr. Van Dusen. "The increase in pulmonary problems may be related to poor pulmonary toilet from more postoperative pain, and more septic issues may be related to more significant fluid shifts during laparotomy."
Dr. Van Dusen concluded that while PEG remains the best method of enteral access, laparoscopic gastrostomy is superior to open gastrostomy.
Dr. Van Dusen did not have any relevant disclosures.
WASHINGTON – Laparoscopic gastrostomy in adults was associated with fewer complications than open gastrostomy in the same population, according to data presented at the annual clinical congress of the American College of Surgeons.
In a retrospective study of data from 2,883 patients, taken from the 2005-2010 National Surgical Quality Improvement Program (NSQIP) database, Dr. Rachel Van Dusen and her colleagues reviewed a variety of outcomes, including wound, pulmonary, renal, cardiac, and thromboembolic, in patients who underwent either a laparoscopic (n = 382), open (n = 2,112), or percutaneous endoscopic gastrostomy (PEG) (n = 389).
Either laparoscopic or open gastrostomies are performed in patients for whom PEG, the standard of care, is unfeasible. Dr. Van Dusen, of George Washington University, Washington, said that theirs was the first study to measure the association between all three procedures and complications in the adult gastrostomy patient population.
The average age of patients was 58 years in the laparoscopic cohort, 62 years in the open group, and 65 years in the PEG group. The patients were at least 18 years old. The laparoscopic group was 88.8% white and 69.4% female; the open group, 80.7% white and 58.2% female; and the PEG group, 85.2% and 57.6%, respectively.
A stepwise logistic regression analysis of patient characteristics in all three cohorts indicated that at baseline, open gastrostomy patients tended, among other factors, to have serum albumin levels less than 3 g/dL (44%), sepsis (35.7%), diabetes (20.4%), a body mass index of 20 kg/m2 or less (27.8%), and ascites (9.0%); in addition, 27% of patients were undergoing chemotherapy.
In a similar analysis, laparoscopic patients were seen to be less ill at baseline: Only 20.4% had low albumin levels, diabetes and sepsis levels were just under 16%, BMI was between 20 and 40, 2.9% were ascitic, and only 1.3% were receiving chemotherapy.
Complications in each group were reviewed according to either wound or organ system. PEG patients had the fewest overall complications (22.4%), with none that were comparatively significant. However, there were several significant differences in complication rates between the laparoscopic and open gastrostomy cohorts.
Pulmonary complications occurred in 23.2% of the open gastrostomy group, compared with 9.7% of the laparoscopic group (multivariate odds ratio, 1.97). Also in the open gastrostomy group, 2.5% had renal complications, compared with 0.5% of the laparoscopic patients (mOR, 4.48). Sepsis was found in 13.5% of the open group and 5.8% of the laparoscopic group (mOR 1.72).
Open gastrostomy patients, when compared with the PEG group, had twice the odds of experiencing wound events (mOR, 2.10) and a 1.5 times greater chance of having sepsis (mOR, 1.51). No significant differences were found between other complications.
"We surmise that the reason the higher rate of infection was associated with the open gastrostomy [patients] is the increase in fascial violation and the exposure of the soft tissues," said Dr. Van Dusen. "The increase in pulmonary problems may be related to poor pulmonary toilet from more postoperative pain, and more septic issues may be related to more significant fluid shifts during laparotomy."
Dr. Van Dusen concluded that while PEG remains the best method of enteral access, laparoscopic gastrostomy is superior to open gastrostomy.
Dr. Van Dusen did not have any relevant disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: Open gastrostomy patients were found to have 4.5 times as many renal complications, twice as many wound events, and 50% more pulmonary complications than laparoscopic gastrostomy patients.
Data source: Retrospective study of 2005-2010 NSQIP database of 2,883 patients aged 18 years or older who underwent either open, laparoscopic, or percutaneous endoscopic gastrostomy.
Disclosures: Dr. Van Dusen did not have any relevant disclosures.
Increasing proportion of musculoskeletal infections involve MRSA
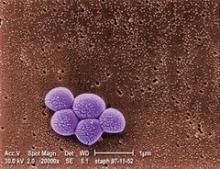
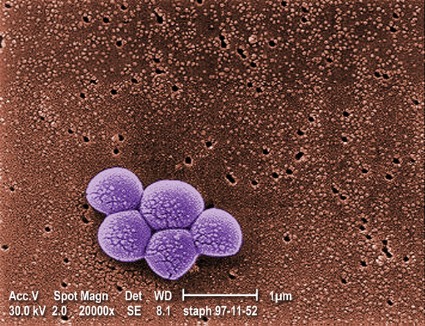
ORLANDO – The proportion of pediatric musculoskeletal infections involving methicillin-resistant Staphylococcus aureus vs. methicillin-sensitive S. aureus has increased dramatically over the past decade, according to a retrospective review of cases.
Between 2001 and 2010, 148 patients at the Children’s Hospital of Philadelphia presented with acute musculoskeletal S. aureus infection, and overall, 37 of those involved methicillin-resistant S. aureus (MRSA), Eric Sarkissian reported at the annual meeting of the American Academy of Pediatrics conference.
The proportion of musculoskeletal cases involving MRSA increased from 12% in 2001-2002 to about 35% in 2010, said Mr. Sarkissian, a 4th-year medical student at Drexel University, Philadelphia.
"Furthermore, we found that MRSA infections were associated with a significantly more complicated hospital stay," Mr. Sarkissian said.
MRSA and methicillin-sensitive S. aureus (MSSA) patients were undergoing magnetic resonance imaging at similar rates, but the average duration of hospitalization was longer for the MRSA patients (13 vs. 8 days), and more MRSA patients required multiple surgical procedures (38% vs. 15%), he said.
In addition, mean presenting C-reactive protein levels were higher in the MRSA vs. MSSA patients (14.7 mg/L vs. 9.8 mg/L), as were infection-related complications, including deep vein thrombosis, septic emboli, septic shock, recurrent infection, and/or avascular necrosis (22% vs. 6%).
MRSA patients also were more often admitted to the ICU for further treatment.
Patients included in this series – the largest known case series of children and adolescents presenting with culture-positive S. aureus osteomyelitis and/or septic arthritis – were consecutive patients with positive cultures of blood, bone, or joint aspirate. Those with postoperative and chronic infections were excluded in an effort to minimize bias caused by nosocomial infections, Mr. Sarkissian noted.
The findings support the ongoing concern that MRSA is evolving and becoming more virulent and invasive over time, compared with MSSA infections. In addition, the findings underscore the need for prompt recognition and aggressive treatment of MRSA musculoskeletal infections, as early recognition is paramount for avoiding sequelae and improving patient outcomes.
"A high index of suspicion is still necessary in the setting of musculoskeletal infections in pediatric patients. Multidisciplinary care provides the most successful opportunity for having improved patient outcomes, and this requires employing broad spectrum antibiotic coverage, using aggressive surgical management, and having an awareness of potential complications," Mr. Sarkissian said.
While clinical prediction models have been developed to help in detecting MRSA infections, outcomes using the models have varied geographically, suggesting that there are unknown regional differences among MRSA cases. It remains to be seen whether available models will be useful for identifying MRSA at presentation, he said.
Mr. Sarkissian reported having no disclosures.
ORLANDO – The proportion of pediatric musculoskeletal infections involving methicillin-resistant Staphylococcus aureus vs. methicillin-sensitive S. aureus has increased dramatically over the past decade, according to a retrospective review of cases.
Between 2001 and 2010, 148 patients at the Children’s Hospital of Philadelphia presented with acute musculoskeletal S. aureus infection, and overall, 37 of those involved methicillin-resistant S. aureus (MRSA), Eric Sarkissian reported at the annual meeting of the American Academy of Pediatrics conference.
The proportion of musculoskeletal cases involving MRSA increased from 12% in 2001-2002 to about 35% in 2010, said Mr. Sarkissian, a 4th-year medical student at Drexel University, Philadelphia.
"Furthermore, we found that MRSA infections were associated with a significantly more complicated hospital stay," Mr. Sarkissian said.
MRSA and methicillin-sensitive S. aureus (MSSA) patients were undergoing magnetic resonance imaging at similar rates, but the average duration of hospitalization was longer for the MRSA patients (13 vs. 8 days), and more MRSA patients required multiple surgical procedures (38% vs. 15%), he said.
In addition, mean presenting C-reactive protein levels were higher in the MRSA vs. MSSA patients (14.7 mg/L vs. 9.8 mg/L), as were infection-related complications, including deep vein thrombosis, septic emboli, septic shock, recurrent infection, and/or avascular necrosis (22% vs. 6%).
MRSA patients also were more often admitted to the ICU for further treatment.
Patients included in this series – the largest known case series of children and adolescents presenting with culture-positive S. aureus osteomyelitis and/or septic arthritis – were consecutive patients with positive cultures of blood, bone, or joint aspirate. Those with postoperative and chronic infections were excluded in an effort to minimize bias caused by nosocomial infections, Mr. Sarkissian noted.
The findings support the ongoing concern that MRSA is evolving and becoming more virulent and invasive over time, compared with MSSA infections. In addition, the findings underscore the need for prompt recognition and aggressive treatment of MRSA musculoskeletal infections, as early recognition is paramount for avoiding sequelae and improving patient outcomes.
"A high index of suspicion is still necessary in the setting of musculoskeletal infections in pediatric patients. Multidisciplinary care provides the most successful opportunity for having improved patient outcomes, and this requires employing broad spectrum antibiotic coverage, using aggressive surgical management, and having an awareness of potential complications," Mr. Sarkissian said.
While clinical prediction models have been developed to help in detecting MRSA infections, outcomes using the models have varied geographically, suggesting that there are unknown regional differences among MRSA cases. It remains to be seen whether available models will be useful for identifying MRSA at presentation, he said.
Mr. Sarkissian reported having no disclosures.
ORLANDO – The proportion of pediatric musculoskeletal infections involving methicillin-resistant Staphylococcus aureus vs. methicillin-sensitive S. aureus has increased dramatically over the past decade, according to a retrospective review of cases.
Between 2001 and 2010, 148 patients at the Children’s Hospital of Philadelphia presented with acute musculoskeletal S. aureus infection, and overall, 37 of those involved methicillin-resistant S. aureus (MRSA), Eric Sarkissian reported at the annual meeting of the American Academy of Pediatrics conference.
The proportion of musculoskeletal cases involving MRSA increased from 12% in 2001-2002 to about 35% in 2010, said Mr. Sarkissian, a 4th-year medical student at Drexel University, Philadelphia.
"Furthermore, we found that MRSA infections were associated with a significantly more complicated hospital stay," Mr. Sarkissian said.
MRSA and methicillin-sensitive S. aureus (MSSA) patients were undergoing magnetic resonance imaging at similar rates, but the average duration of hospitalization was longer for the MRSA patients (13 vs. 8 days), and more MRSA patients required multiple surgical procedures (38% vs. 15%), he said.
In addition, mean presenting C-reactive protein levels were higher in the MRSA vs. MSSA patients (14.7 mg/L vs. 9.8 mg/L), as were infection-related complications, including deep vein thrombosis, septic emboli, septic shock, recurrent infection, and/or avascular necrosis (22% vs. 6%).
MRSA patients also were more often admitted to the ICU for further treatment.
Patients included in this series – the largest known case series of children and adolescents presenting with culture-positive S. aureus osteomyelitis and/or septic arthritis – were consecutive patients with positive cultures of blood, bone, or joint aspirate. Those with postoperative and chronic infections were excluded in an effort to minimize bias caused by nosocomial infections, Mr. Sarkissian noted.
The findings support the ongoing concern that MRSA is evolving and becoming more virulent and invasive over time, compared with MSSA infections. In addition, the findings underscore the need for prompt recognition and aggressive treatment of MRSA musculoskeletal infections, as early recognition is paramount for avoiding sequelae and improving patient outcomes.
"A high index of suspicion is still necessary in the setting of musculoskeletal infections in pediatric patients. Multidisciplinary care provides the most successful opportunity for having improved patient outcomes, and this requires employing broad spectrum antibiotic coverage, using aggressive surgical management, and having an awareness of potential complications," Mr. Sarkissian said.
While clinical prediction models have been developed to help in detecting MRSA infections, outcomes using the models have varied geographically, suggesting that there are unknown regional differences among MRSA cases. It remains to be seen whether available models will be useful for identifying MRSA at presentation, he said.
Mr. Sarkissian reported having no disclosures.
AT THE AAP NATIONAL CONFERENCE
Major finding: The proportion of musculoskeletal infection cases involving MRSA vs. MSSA increased from 12% to 35% between 2001 and 2010.
Data source: A retrospective study of 148 consecutive cases.
Disclosures: Mr. Sarkissian reported having no disclosures.
RYGB showed better nutritional outcomes than duodenal switch
WASHINGTON – Despite better excess weight loss outcomes from the biliopancreatic diversion with duodenal switch, the Roux-en-Y gastric bypass procedure was associated with better nutritional outcomes in the superobese, according to the results of a prospective cohort study presented at this year’s American College of Surgeons Clinical Congress.
Investigators retrospectively analyzed data collected prospectively from 350 consecutive superobese patients, who underwent either biliopancreatic diversion with duodenal switch (BPD/DS; n = 198) or Roux-en-Y gastric bypass surgery (RYGB; n = 152), and compared long-term nutritional outcomes in each cohort. The research was conducted by Dr. Marc Ward and his colleagues at the University of Chicago, who presented the results.
The cohorts were self-selected and equally distributed across the sexes; each group’s mean age was just under 41 years. The mean body mass index (BMI) in the BPD/DS group was 59 kg/m2 and was 56 kg/m2 in RYGB. The preoperative body weight in the BPD/DS group was higher than that in the RYGB group (range, 267 lbs to 597 lbs. vs. 240 lbs to 505 lbs, respectively).
Although the BPD/DS had higher morbidity and mortality rates than did the RYGB, as well as more complications, such as altered bowel habits, the BPD/DS is associated with better comorbidity resolution independent of weight loss, and up to 20% greater excess weight loss in superobese patients. Superobesity is defined as having a BMI of 50 kg/m2 and above.
Because the reduction in intestinal absorptive surface area in BPD/DS is greater than in RYGB, the researchers theorized that the resultant nutritional deficiencies might be clinically significant enough to consider when counseling patients on procedure selection.
At seven postoperative follow-up points between 6 months and 8 years, the investigators obtained a variety of nutritional parameters from each group. Patients were given nutritional supplementation as clinically indicated.
Dr. Ward said that while he and his colleagues expected the BPD/DS group to have lower nutritional values, "We didn’t expect that 75% of our patients would have, at 4 years out, a below-normal level of vitamin A, compared to 23% in the RYGB patients."
There were similar surprises for other nutritional markers: At all time points, the BPD/DS group also had significantly more nutritional deficiencies than did the RYGB group in fat-soluble vitamins D and E, and in minerals selenium and zinc. Between years 1 and 3, iron values were near parity at about 20%, although the BPD/DS group was still more deficient, and at year 8 had more than double the rate of iron deficiency as RYGB patients.
Values for albumin, vitamin B12, ferritin, folate, and parathyroid hormone, however, were not significantly different between the two groups. Dr. Ward said that low nutritional values in patients, "does not necessarily mean they are developing symptoms or can’t be treated with supplementation."
Only one RYGB patient underwent revision because of insufficient weight loss, whereas five BPD/DS patients underwent revision, all for malnutrition.
"It’s absolutely crucial for people who elect to have a duodenal switch operation to have long-term, life-long nutritional follow-up," Dr. Ward told the audience. He also said that clinicians should closely evaluate their patients’ level of commitment to compliance over the long-term when discussing bariatric procedures.
WASHINGTON – Despite better excess weight loss outcomes from the biliopancreatic diversion with duodenal switch, the Roux-en-Y gastric bypass procedure was associated with better nutritional outcomes in the superobese, according to the results of a prospective cohort study presented at this year’s American College of Surgeons Clinical Congress.
Investigators retrospectively analyzed data collected prospectively from 350 consecutive superobese patients, who underwent either biliopancreatic diversion with duodenal switch (BPD/DS; n = 198) or Roux-en-Y gastric bypass surgery (RYGB; n = 152), and compared long-term nutritional outcomes in each cohort. The research was conducted by Dr. Marc Ward and his colleagues at the University of Chicago, who presented the results.
The cohorts were self-selected and equally distributed across the sexes; each group’s mean age was just under 41 years. The mean body mass index (BMI) in the BPD/DS group was 59 kg/m2 and was 56 kg/m2 in RYGB. The preoperative body weight in the BPD/DS group was higher than that in the RYGB group (range, 267 lbs to 597 lbs. vs. 240 lbs to 505 lbs, respectively).
Although the BPD/DS had higher morbidity and mortality rates than did the RYGB, as well as more complications, such as altered bowel habits, the BPD/DS is associated with better comorbidity resolution independent of weight loss, and up to 20% greater excess weight loss in superobese patients. Superobesity is defined as having a BMI of 50 kg/m2 and above.
Because the reduction in intestinal absorptive surface area in BPD/DS is greater than in RYGB, the researchers theorized that the resultant nutritional deficiencies might be clinically significant enough to consider when counseling patients on procedure selection.
At seven postoperative follow-up points between 6 months and 8 years, the investigators obtained a variety of nutritional parameters from each group. Patients were given nutritional supplementation as clinically indicated.
Dr. Ward said that while he and his colleagues expected the BPD/DS group to have lower nutritional values, "We didn’t expect that 75% of our patients would have, at 4 years out, a below-normal level of vitamin A, compared to 23% in the RYGB patients."
There were similar surprises for other nutritional markers: At all time points, the BPD/DS group also had significantly more nutritional deficiencies than did the RYGB group in fat-soluble vitamins D and E, and in minerals selenium and zinc. Between years 1 and 3, iron values were near parity at about 20%, although the BPD/DS group was still more deficient, and at year 8 had more than double the rate of iron deficiency as RYGB patients.
Values for albumin, vitamin B12, ferritin, folate, and parathyroid hormone, however, were not significantly different between the two groups. Dr. Ward said that low nutritional values in patients, "does not necessarily mean they are developing symptoms or can’t be treated with supplementation."
Only one RYGB patient underwent revision because of insufficient weight loss, whereas five BPD/DS patients underwent revision, all for malnutrition.
"It’s absolutely crucial for people who elect to have a duodenal switch operation to have long-term, life-long nutritional follow-up," Dr. Ward told the audience. He also said that clinicians should closely evaluate their patients’ level of commitment to compliance over the long-term when discussing bariatric procedures.
WASHINGTON – Despite better excess weight loss outcomes from the biliopancreatic diversion with duodenal switch, the Roux-en-Y gastric bypass procedure was associated with better nutritional outcomes in the superobese, according to the results of a prospective cohort study presented at this year’s American College of Surgeons Clinical Congress.
Investigators retrospectively analyzed data collected prospectively from 350 consecutive superobese patients, who underwent either biliopancreatic diversion with duodenal switch (BPD/DS; n = 198) or Roux-en-Y gastric bypass surgery (RYGB; n = 152), and compared long-term nutritional outcomes in each cohort. The research was conducted by Dr. Marc Ward and his colleagues at the University of Chicago, who presented the results.
The cohorts were self-selected and equally distributed across the sexes; each group’s mean age was just under 41 years. The mean body mass index (BMI) in the BPD/DS group was 59 kg/m2 and was 56 kg/m2 in RYGB. The preoperative body weight in the BPD/DS group was higher than that in the RYGB group (range, 267 lbs to 597 lbs. vs. 240 lbs to 505 lbs, respectively).
Although the BPD/DS had higher morbidity and mortality rates than did the RYGB, as well as more complications, such as altered bowel habits, the BPD/DS is associated with better comorbidity resolution independent of weight loss, and up to 20% greater excess weight loss in superobese patients. Superobesity is defined as having a BMI of 50 kg/m2 and above.
Because the reduction in intestinal absorptive surface area in BPD/DS is greater than in RYGB, the researchers theorized that the resultant nutritional deficiencies might be clinically significant enough to consider when counseling patients on procedure selection.
At seven postoperative follow-up points between 6 months and 8 years, the investigators obtained a variety of nutritional parameters from each group. Patients were given nutritional supplementation as clinically indicated.
Dr. Ward said that while he and his colleagues expected the BPD/DS group to have lower nutritional values, "We didn’t expect that 75% of our patients would have, at 4 years out, a below-normal level of vitamin A, compared to 23% in the RYGB patients."
There were similar surprises for other nutritional markers: At all time points, the BPD/DS group also had significantly more nutritional deficiencies than did the RYGB group in fat-soluble vitamins D and E, and in minerals selenium and zinc. Between years 1 and 3, iron values were near parity at about 20%, although the BPD/DS group was still more deficient, and at year 8 had more than double the rate of iron deficiency as RYGB patients.
Values for albumin, vitamin B12, ferritin, folate, and parathyroid hormone, however, were not significantly different between the two groups. Dr. Ward said that low nutritional values in patients, "does not necessarily mean they are developing symptoms or can’t be treated with supplementation."
Only one RYGB patient underwent revision because of insufficient weight loss, whereas five BPD/DS patients underwent revision, all for malnutrition.
"It’s absolutely crucial for people who elect to have a duodenal switch operation to have long-term, life-long nutritional follow-up," Dr. Ward told the audience. He also said that clinicians should closely evaluate their patients’ level of commitment to compliance over the long-term when discussing bariatric procedures.
AT THE ACS CLINICAL CONGRESS
Major finding: A significantly greater proportion of deficient nutritional values were found in duodenal switch patients at multiple postoperative points than in RYGB patients.
Data source: Retrospective review of prospective database study of 350 consecutive superobese patients tested at clinical follow-up post duodenal switch or RYGB surgery between 2002 and 2005.
Disclosures: Dr. Ward and his colleagues reported no relevant disclosures.
Alvimopan reduces ileus, cuts hospital time in bowel surgery
WASHINGTON – The nonopioid pain reliever alvimopan significantly decreased the incidence of postoperative ileus and shortened hospital stay among bowel surgery patients who took the drug as part of an existing accelerated recovery program.
Compared with patients who took placebo, those who took alvimopan left the hospital about 1 day sooner. In addition to the decrease in ileus, patients experienced a quicker return to normal bowel function, including time to first flatus and first bowel movement, Dr. Robert Moesinger said at the annual clinical congress of the American College of Surgeons.
"Alvimopan augmented the already improved outcomes we had seen with our validated recovery pathway, in both laparoscopic- and open-surgery patients," said Dr. Moesinger of Intermountain Healthcare, Salt Lake City. "Given the very diverse nature of our health care system, with multiple types of hospitals and surgeons, we feel these data are widely applicable and we are very comfortable recommending its routine use for patients having elective bowel surgery."
Dr. Moesinger and his colleagues conducted a randomized, placebo-controlled trial of alvimopan in 248 such patients. Those taking the study drug received 12 mg before surgery; after surgery, they received 12 mg twice a day until discharge.
The primary endpoint was postoperative length of stay. Secondary endpoints included the incidence of postoperative ileus, time to first flatus and first bowel movement, tolerance of solid food, total hospital and pharmacy costs, nasogastric tube reinsertion, 30-day readmission rates, and anastomotic leak.
The patients’ mean age was 61 years. There were no significant differences in any of their baseline demographics or clinical characteristics. Because of a statistical fluke, the placebo group did contain significantly more open-surgery patients than the alvimopan group (34% vs. 20%). The rest of the patients had laparoscopic surgery. Patients had an average of nine doses of the study drug.
The mean length of stay was 4 days in the alvimopan group and 5 in the placebo group – a significant difference.
There was significantly less postoperative ileus in the alvimopan group (2% vs. 10%). Significantly fewer of those taking the study drug needed a nasogastric tube reinserted (2% vs. 9%). The rates of 30-day readmission, reoperation, and anastomotic leak were similar in both groups. The mean time to first bowel movement was about 1 day sooner in the alvimopan group.
The median hospital cost was $10,832 for the alvimopan group and $11,924 for the placebo group – a significant difference. The median total pharmacy cost was $476 vs. $501; this difference was not significant.
Because Cubist Pharmaceuticals, which makes alvimopan, provided the study drug at no cost, the overall cost analysis cannot be considered complete, Dr. Moesinger noted. However, the pharmacy cost for a similar course of the drug would be $84. Figuring that cost into the total saved for each admission ($1,686) still yielded a net financial benefit of $930 per patient, he said.
Dr. Moesinger had no financial disclosures.
Alvimopan (Entereg, Cubist Pharmaceuticals) is an orally administered, peripherally acting mu-opioid receptor antagonist that does not cross the blood-brain barrier. It is designed to reverse opioid-induced changes in the gastrointestinal tract without adversely affecting opioid-induced analgesia.

|
| Dr. Brian E. Lacy |
Alvimopan, the first FDA-approved medication for the treatment of postoperative ileus (POI), was approved in May 2008 with a Risk Evaluation and Mitigation Strategy in place, due to concerns over an increased number of myocardial infarctions in one research study.
Postoperative ileus is the impairment of gastrointestinal motility after abdominal or pelvic surgery, and is an expected complication of major abdominal surgery. It can affect all segments of the gastrointestinal tract and may lead to symptoms of nausea, vomiting, bloating, distention, constipation, and inability to evacuate flatus. Several studies have demonstrated that POI delays hospital discharges, increases the rate of hospital readmission after abdominal surgery, and increases the risk of postoperative complications. As such, POI imposes a significant economic impact on the health care system.
The current study confirms earlier studies involving over 2,000 patients that led to the approval of alvimopan. The current study was a single-center, randomized, double-blind study comparing placebo to alvimopan. Patients randomized to alvimopan (12 mg preoperatively; 12 mg twice daily until discharge) were discharged from the hospital 1 day earlier, were less likely to have a nasogastric tube reinserted, and had a bowel movement 1 day earlier, compared with those patients receiving placebo. The authors reported a significant cost savings per patient.*
These findings are important given the absence of other FDA-approved medications for the treatment of POI and the lack of other effective treatments. Alvimopan is available only to patients who are in hospitals that are registered to use this medication under the EASE (Entereg Access Support and Education) program. This recent study should prompt nonparticipating hospitals to consider routine use of alvimopan in all patients undergoing elective and emergent surgeries at risk for development of POI.
Dr. Brian E. Lacy is a professor of medicine at the Geisel School of Medicine at Dartmouth, Hanover, N.H., and chief of the section of gastroenterology and hepatology at Dartmouth-Hitchcock Medical Center. He has no relevant conflicts of interest.
*CORRECTION 11/21/13: The original version of this story misstated the cost savings per patient.
Alvimopan (Entereg, Cubist Pharmaceuticals) is an orally administered, peripherally acting mu-opioid receptor antagonist that does not cross the blood-brain barrier. It is designed to reverse opioid-induced changes in the gastrointestinal tract without adversely affecting opioid-induced analgesia.

|
| Dr. Brian E. Lacy |
Alvimopan, the first FDA-approved medication for the treatment of postoperative ileus (POI), was approved in May 2008 with a Risk Evaluation and Mitigation Strategy in place, due to concerns over an increased number of myocardial infarctions in one research study.
Postoperative ileus is the impairment of gastrointestinal motility after abdominal or pelvic surgery, and is an expected complication of major abdominal surgery. It can affect all segments of the gastrointestinal tract and may lead to symptoms of nausea, vomiting, bloating, distention, constipation, and inability to evacuate flatus. Several studies have demonstrated that POI delays hospital discharges, increases the rate of hospital readmission after abdominal surgery, and increases the risk of postoperative complications. As such, POI imposes a significant economic impact on the health care system.
The current study confirms earlier studies involving over 2,000 patients that led to the approval of alvimopan. The current study was a single-center, randomized, double-blind study comparing placebo to alvimopan. Patients randomized to alvimopan (12 mg preoperatively; 12 mg twice daily until discharge) were discharged from the hospital 1 day earlier, were less likely to have a nasogastric tube reinserted, and had a bowel movement 1 day earlier, compared with those patients receiving placebo. The authors reported a significant cost savings per patient.*
These findings are important given the absence of other FDA-approved medications for the treatment of POI and the lack of other effective treatments. Alvimopan is available only to patients who are in hospitals that are registered to use this medication under the EASE (Entereg Access Support and Education) program. This recent study should prompt nonparticipating hospitals to consider routine use of alvimopan in all patients undergoing elective and emergent surgeries at risk for development of POI.
Dr. Brian E. Lacy is a professor of medicine at the Geisel School of Medicine at Dartmouth, Hanover, N.H., and chief of the section of gastroenterology and hepatology at Dartmouth-Hitchcock Medical Center. He has no relevant conflicts of interest.
*CORRECTION 11/21/13: The original version of this story misstated the cost savings per patient.
Alvimopan (Entereg, Cubist Pharmaceuticals) is an orally administered, peripherally acting mu-opioid receptor antagonist that does not cross the blood-brain barrier. It is designed to reverse opioid-induced changes in the gastrointestinal tract without adversely affecting opioid-induced analgesia.

|
| Dr. Brian E. Lacy |
Alvimopan, the first FDA-approved medication for the treatment of postoperative ileus (POI), was approved in May 2008 with a Risk Evaluation and Mitigation Strategy in place, due to concerns over an increased number of myocardial infarctions in one research study.
Postoperative ileus is the impairment of gastrointestinal motility after abdominal or pelvic surgery, and is an expected complication of major abdominal surgery. It can affect all segments of the gastrointestinal tract and may lead to symptoms of nausea, vomiting, bloating, distention, constipation, and inability to evacuate flatus. Several studies have demonstrated that POI delays hospital discharges, increases the rate of hospital readmission after abdominal surgery, and increases the risk of postoperative complications. As such, POI imposes a significant economic impact on the health care system.
The current study confirms earlier studies involving over 2,000 patients that led to the approval of alvimopan. The current study was a single-center, randomized, double-blind study comparing placebo to alvimopan. Patients randomized to alvimopan (12 mg preoperatively; 12 mg twice daily until discharge) were discharged from the hospital 1 day earlier, were less likely to have a nasogastric tube reinserted, and had a bowel movement 1 day earlier, compared with those patients receiving placebo. The authors reported a significant cost savings per patient.*
These findings are important given the absence of other FDA-approved medications for the treatment of POI and the lack of other effective treatments. Alvimopan is available only to patients who are in hospitals that are registered to use this medication under the EASE (Entereg Access Support and Education) program. This recent study should prompt nonparticipating hospitals to consider routine use of alvimopan in all patients undergoing elective and emergent surgeries at risk for development of POI.
Dr. Brian E. Lacy is a professor of medicine at the Geisel School of Medicine at Dartmouth, Hanover, N.H., and chief of the section of gastroenterology and hepatology at Dartmouth-Hitchcock Medical Center. He has no relevant conflicts of interest.
*CORRECTION 11/21/13: The original version of this story misstated the cost savings per patient.
WASHINGTON – The nonopioid pain reliever alvimopan significantly decreased the incidence of postoperative ileus and shortened hospital stay among bowel surgery patients who took the drug as part of an existing accelerated recovery program.
Compared with patients who took placebo, those who took alvimopan left the hospital about 1 day sooner. In addition to the decrease in ileus, patients experienced a quicker return to normal bowel function, including time to first flatus and first bowel movement, Dr. Robert Moesinger said at the annual clinical congress of the American College of Surgeons.
"Alvimopan augmented the already improved outcomes we had seen with our validated recovery pathway, in both laparoscopic- and open-surgery patients," said Dr. Moesinger of Intermountain Healthcare, Salt Lake City. "Given the very diverse nature of our health care system, with multiple types of hospitals and surgeons, we feel these data are widely applicable and we are very comfortable recommending its routine use for patients having elective bowel surgery."
Dr. Moesinger and his colleagues conducted a randomized, placebo-controlled trial of alvimopan in 248 such patients. Those taking the study drug received 12 mg before surgery; after surgery, they received 12 mg twice a day until discharge.
The primary endpoint was postoperative length of stay. Secondary endpoints included the incidence of postoperative ileus, time to first flatus and first bowel movement, tolerance of solid food, total hospital and pharmacy costs, nasogastric tube reinsertion, 30-day readmission rates, and anastomotic leak.
The patients’ mean age was 61 years. There were no significant differences in any of their baseline demographics or clinical characteristics. Because of a statistical fluke, the placebo group did contain significantly more open-surgery patients than the alvimopan group (34% vs. 20%). The rest of the patients had laparoscopic surgery. Patients had an average of nine doses of the study drug.
The mean length of stay was 4 days in the alvimopan group and 5 in the placebo group – a significant difference.
There was significantly less postoperative ileus in the alvimopan group (2% vs. 10%). Significantly fewer of those taking the study drug needed a nasogastric tube reinserted (2% vs. 9%). The rates of 30-day readmission, reoperation, and anastomotic leak were similar in both groups. The mean time to first bowel movement was about 1 day sooner in the alvimopan group.
The median hospital cost was $10,832 for the alvimopan group and $11,924 for the placebo group – a significant difference. The median total pharmacy cost was $476 vs. $501; this difference was not significant.
Because Cubist Pharmaceuticals, which makes alvimopan, provided the study drug at no cost, the overall cost analysis cannot be considered complete, Dr. Moesinger noted. However, the pharmacy cost for a similar course of the drug would be $84. Figuring that cost into the total saved for each admission ($1,686) still yielded a net financial benefit of $930 per patient, he said.
Dr. Moesinger had no financial disclosures.
WASHINGTON – The nonopioid pain reliever alvimopan significantly decreased the incidence of postoperative ileus and shortened hospital stay among bowel surgery patients who took the drug as part of an existing accelerated recovery program.
Compared with patients who took placebo, those who took alvimopan left the hospital about 1 day sooner. In addition to the decrease in ileus, patients experienced a quicker return to normal bowel function, including time to first flatus and first bowel movement, Dr. Robert Moesinger said at the annual clinical congress of the American College of Surgeons.
"Alvimopan augmented the already improved outcomes we had seen with our validated recovery pathway, in both laparoscopic- and open-surgery patients," said Dr. Moesinger of Intermountain Healthcare, Salt Lake City. "Given the very diverse nature of our health care system, with multiple types of hospitals and surgeons, we feel these data are widely applicable and we are very comfortable recommending its routine use for patients having elective bowel surgery."
Dr. Moesinger and his colleagues conducted a randomized, placebo-controlled trial of alvimopan in 248 such patients. Those taking the study drug received 12 mg before surgery; after surgery, they received 12 mg twice a day until discharge.
The primary endpoint was postoperative length of stay. Secondary endpoints included the incidence of postoperative ileus, time to first flatus and first bowel movement, tolerance of solid food, total hospital and pharmacy costs, nasogastric tube reinsertion, 30-day readmission rates, and anastomotic leak.
The patients’ mean age was 61 years. There were no significant differences in any of their baseline demographics or clinical characteristics. Because of a statistical fluke, the placebo group did contain significantly more open-surgery patients than the alvimopan group (34% vs. 20%). The rest of the patients had laparoscopic surgery. Patients had an average of nine doses of the study drug.
The mean length of stay was 4 days in the alvimopan group and 5 in the placebo group – a significant difference.
There was significantly less postoperative ileus in the alvimopan group (2% vs. 10%). Significantly fewer of those taking the study drug needed a nasogastric tube reinserted (2% vs. 9%). The rates of 30-day readmission, reoperation, and anastomotic leak were similar in both groups. The mean time to first bowel movement was about 1 day sooner in the alvimopan group.
The median hospital cost was $10,832 for the alvimopan group and $11,924 for the placebo group – a significant difference. The median total pharmacy cost was $476 vs. $501; this difference was not significant.
Because Cubist Pharmaceuticals, which makes alvimopan, provided the study drug at no cost, the overall cost analysis cannot be considered complete, Dr. Moesinger noted. However, the pharmacy cost for a similar course of the drug would be $84. Figuring that cost into the total saved for each admission ($1,686) still yielded a net financial benefit of $930 per patient, he said.
Dr. Moesinger had no financial disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: Compared with placebo, alvimopan given before and after elective bowel surgery reduced the length of stay by 1 day and significantly decreased the incidence of postoperative ileus (2% vs. 10%).
Data source: The randomized placebo-controlled trial comprised 248 patients.
Disclosures: Dr. Moesinger had no financial disclosures.
Long-term data show laparoscopic Roux-en-Y still safer, cheaper than open
WASHINGTON – Fifteen years after having a Roux-en-Y gastric bypass, patients who had laparoscopic surgery were more likely to still be alive, without long-term complications and with a much smaller surgery-related medical bill than those who had open surgery.
Laparoscopic surgery conferred a 44% decrease in the chance of death from any cause, and a 20% decrease in the risk of having a long-term complication related to bariatric surgery, Dr. Anna Weiss reported at the annual clinical congress of the American College of Surgeons.
Her population-based study of 135,000 patients is one of the largest and longest of its kind, allowing it to pick up long-term outcomes trends that have not been detailed before, said Dr. Weiss of the University of California, San Diego.
The study used data from the California Office of Statewide Health Planning and Development. The database assigns every patient a unique identification number and tracks every hospital admission for that patient. Dr. Weiss looked at health outcomes for patients who underwent an open or laparoscopic Roux-en-Y gastric bypass anytime from 1995 to 2009.
The study’s primary outcome was all-cause mortality. Secondary outcomes included the incidence of gallbladder disease, cholecystectomy, marginal ulcer, and reoperation. It also examined the cost of the index surgery and subsequent costs related to the surgery.
She found a significant, time-bound association with the frequency of laparoscopic bypass. In 1995, less than 5% of the procedures were performed laparoscopically. By 2000, that had risen to about 20%. Thereafter, the frequency rose sharply. By 2009, just over 90% of Roux-en-Y procedures were minimally invasive.
About 80% of the patients were women; about 72% were white. They ranged widely in age, with more than 2,000 being 80 years or older at the time of surgery. But, Dr. Weiss said, the majority, about 70%, were aged 30-60 years.
Comorbidities were common and included prior gallbladder disease (20%), hypertension (51%), hyperlipidemia (31%), and diabetes (28%).
Most patients (67%) stayed in the hospital no more than 3 days. However, significantly more patients with laparoscopic surgery had these short stays (90% vs. 44% of the open-surgery group). Significantly more patients in the open-surgery group stayed 4-6 days (33% vs. 8%) and 7 or more days (22% vs. 2%).
Most of the patients had private insurance (80%). Medicare insured 10% and Medi-Cal, 6%. The remainder were self-pay. Significantly more laparoscopic procedures were performed at Centers of Excellence (76% vs. 59% of open procedures).
Overall, the rates of marginal ulcer and reoperations were low (1% each). However, Dr. Weiss noted, other outcomes were much more common, including gallbladder complications (22%) and cholecystectomies (13%). Long-term complications were significantly more common in the open group (10% vs. less than 5%).
By the end of the follow-up period, overall all-cause mortality was 11%. It was significantly less in the laparoscopic group than in the open group (about 5% vs. 20%).
Laparoscopic surgery carried a significantly smaller price tag than open surgery. The mean cost of the index operation was $56,170 for laparoscopic surgery, compared with a mean of $87,026 for open surgery. Over the entire follow-up period, patients who had open surgery racked up about $31,000 more in costs related directly to the procedure. However, Dr. Weiss noted, the standard deviation of lifetime costs ranged from $208,153 for an open procedure vs. $84,299 for a laparoscopic procedure.
Despite these differences, publicly insured patients were much more likely to have had open surgery. Patients with Medicare were significantly more likely to have an open than a laparoscopic procedure (15% vs. 6%), as were patients with Medi-Cal (7% vs. 4%). Patients with private insurance were significantly more likely to have laparoscopic surgery (86% vs. 74%).
In a multivariate analysis, several factors were significantly associated with outcome. Female gender reduced the risk of death by more than 30%. Younger age also portended better outcomes. Compared with patients in their 20s, those in their 50s were three times as likely to have died; those in their 60s, six times as likely, and those in their 70s, almost nine times as likely. The few patients who had surgery in their 80s were 10 times as likely to die as the youngest. However, several commentators pointed out during discussion that age-related all-cause mortality is not a surprising finding in a longitudinal study.
Insurance was also significantly related to outcome. Dr. Weiss used the self-pay group as her reference group. Compared with these patients, Medicare and Medi-Cal patients were twice as likely to have died by the study’s end. "Interestingly, they were no more likely to have long-term complications. However, when they did, these were more serious complications, possibly indicating that overall those with public insurance could have been a sicker group" at baseline.
Longer length of stay was also a significant predictor of mortality, with patients staying a week or longer five times more likely to have died by the end of follow-up than the reference group of those staying 4-6 days. "Interestingly, we also found that patients who stayed 3 days or less were 73% more likely to have died." This probably represented patients who had serious perioperative complications, she suggested.
Having either surgery at a Center of Excellence reduced the risk of mortality by 25%, she added.
Dr. Weiss had no financial disclosures.
WASHINGTON – Fifteen years after having a Roux-en-Y gastric bypass, patients who had laparoscopic surgery were more likely to still be alive, without long-term complications and with a much smaller surgery-related medical bill than those who had open surgery.
Laparoscopic surgery conferred a 44% decrease in the chance of death from any cause, and a 20% decrease in the risk of having a long-term complication related to bariatric surgery, Dr. Anna Weiss reported at the annual clinical congress of the American College of Surgeons.
Her population-based study of 135,000 patients is one of the largest and longest of its kind, allowing it to pick up long-term outcomes trends that have not been detailed before, said Dr. Weiss of the University of California, San Diego.
The study used data from the California Office of Statewide Health Planning and Development. The database assigns every patient a unique identification number and tracks every hospital admission for that patient. Dr. Weiss looked at health outcomes for patients who underwent an open or laparoscopic Roux-en-Y gastric bypass anytime from 1995 to 2009.
The study’s primary outcome was all-cause mortality. Secondary outcomes included the incidence of gallbladder disease, cholecystectomy, marginal ulcer, and reoperation. It also examined the cost of the index surgery and subsequent costs related to the surgery.
She found a significant, time-bound association with the frequency of laparoscopic bypass. In 1995, less than 5% of the procedures were performed laparoscopically. By 2000, that had risen to about 20%. Thereafter, the frequency rose sharply. By 2009, just over 90% of Roux-en-Y procedures were minimally invasive.
About 80% of the patients were women; about 72% were white. They ranged widely in age, with more than 2,000 being 80 years or older at the time of surgery. But, Dr. Weiss said, the majority, about 70%, were aged 30-60 years.
Comorbidities were common and included prior gallbladder disease (20%), hypertension (51%), hyperlipidemia (31%), and diabetes (28%).
Most patients (67%) stayed in the hospital no more than 3 days. However, significantly more patients with laparoscopic surgery had these short stays (90% vs. 44% of the open-surgery group). Significantly more patients in the open-surgery group stayed 4-6 days (33% vs. 8%) and 7 or more days (22% vs. 2%).
Most of the patients had private insurance (80%). Medicare insured 10% and Medi-Cal, 6%. The remainder were self-pay. Significantly more laparoscopic procedures were performed at Centers of Excellence (76% vs. 59% of open procedures).
Overall, the rates of marginal ulcer and reoperations were low (1% each). However, Dr. Weiss noted, other outcomes were much more common, including gallbladder complications (22%) and cholecystectomies (13%). Long-term complications were significantly more common in the open group (10% vs. less than 5%).
By the end of the follow-up period, overall all-cause mortality was 11%. It was significantly less in the laparoscopic group than in the open group (about 5% vs. 20%).
Laparoscopic surgery carried a significantly smaller price tag than open surgery. The mean cost of the index operation was $56,170 for laparoscopic surgery, compared with a mean of $87,026 for open surgery. Over the entire follow-up period, patients who had open surgery racked up about $31,000 more in costs related directly to the procedure. However, Dr. Weiss noted, the standard deviation of lifetime costs ranged from $208,153 for an open procedure vs. $84,299 for a laparoscopic procedure.
Despite these differences, publicly insured patients were much more likely to have had open surgery. Patients with Medicare were significantly more likely to have an open than a laparoscopic procedure (15% vs. 6%), as were patients with Medi-Cal (7% vs. 4%). Patients with private insurance were significantly more likely to have laparoscopic surgery (86% vs. 74%).
In a multivariate analysis, several factors were significantly associated with outcome. Female gender reduced the risk of death by more than 30%. Younger age also portended better outcomes. Compared with patients in their 20s, those in their 50s were three times as likely to have died; those in their 60s, six times as likely, and those in their 70s, almost nine times as likely. The few patients who had surgery in their 80s were 10 times as likely to die as the youngest. However, several commentators pointed out during discussion that age-related all-cause mortality is not a surprising finding in a longitudinal study.
Insurance was also significantly related to outcome. Dr. Weiss used the self-pay group as her reference group. Compared with these patients, Medicare and Medi-Cal patients were twice as likely to have died by the study’s end. "Interestingly, they were no more likely to have long-term complications. However, when they did, these were more serious complications, possibly indicating that overall those with public insurance could have been a sicker group" at baseline.
Longer length of stay was also a significant predictor of mortality, with patients staying a week or longer five times more likely to have died by the end of follow-up than the reference group of those staying 4-6 days. "Interestingly, we also found that patients who stayed 3 days or less were 73% more likely to have died." This probably represented patients who had serious perioperative complications, she suggested.
Having either surgery at a Center of Excellence reduced the risk of mortality by 25%, she added.
Dr. Weiss had no financial disclosures.
WASHINGTON – Fifteen years after having a Roux-en-Y gastric bypass, patients who had laparoscopic surgery were more likely to still be alive, without long-term complications and with a much smaller surgery-related medical bill than those who had open surgery.
Laparoscopic surgery conferred a 44% decrease in the chance of death from any cause, and a 20% decrease in the risk of having a long-term complication related to bariatric surgery, Dr. Anna Weiss reported at the annual clinical congress of the American College of Surgeons.
Her population-based study of 135,000 patients is one of the largest and longest of its kind, allowing it to pick up long-term outcomes trends that have not been detailed before, said Dr. Weiss of the University of California, San Diego.
The study used data from the California Office of Statewide Health Planning and Development. The database assigns every patient a unique identification number and tracks every hospital admission for that patient. Dr. Weiss looked at health outcomes for patients who underwent an open or laparoscopic Roux-en-Y gastric bypass anytime from 1995 to 2009.
The study’s primary outcome was all-cause mortality. Secondary outcomes included the incidence of gallbladder disease, cholecystectomy, marginal ulcer, and reoperation. It also examined the cost of the index surgery and subsequent costs related to the surgery.
She found a significant, time-bound association with the frequency of laparoscopic bypass. In 1995, less than 5% of the procedures were performed laparoscopically. By 2000, that had risen to about 20%. Thereafter, the frequency rose sharply. By 2009, just over 90% of Roux-en-Y procedures were minimally invasive.
About 80% of the patients were women; about 72% were white. They ranged widely in age, with more than 2,000 being 80 years or older at the time of surgery. But, Dr. Weiss said, the majority, about 70%, were aged 30-60 years.
Comorbidities were common and included prior gallbladder disease (20%), hypertension (51%), hyperlipidemia (31%), and diabetes (28%).
Most patients (67%) stayed in the hospital no more than 3 days. However, significantly more patients with laparoscopic surgery had these short stays (90% vs. 44% of the open-surgery group). Significantly more patients in the open-surgery group stayed 4-6 days (33% vs. 8%) and 7 or more days (22% vs. 2%).
Most of the patients had private insurance (80%). Medicare insured 10% and Medi-Cal, 6%. The remainder were self-pay. Significantly more laparoscopic procedures were performed at Centers of Excellence (76% vs. 59% of open procedures).
Overall, the rates of marginal ulcer and reoperations were low (1% each). However, Dr. Weiss noted, other outcomes were much more common, including gallbladder complications (22%) and cholecystectomies (13%). Long-term complications were significantly more common in the open group (10% vs. less than 5%).
By the end of the follow-up period, overall all-cause mortality was 11%. It was significantly less in the laparoscopic group than in the open group (about 5% vs. 20%).
Laparoscopic surgery carried a significantly smaller price tag than open surgery. The mean cost of the index operation was $56,170 for laparoscopic surgery, compared with a mean of $87,026 for open surgery. Over the entire follow-up period, patients who had open surgery racked up about $31,000 more in costs related directly to the procedure. However, Dr. Weiss noted, the standard deviation of lifetime costs ranged from $208,153 for an open procedure vs. $84,299 for a laparoscopic procedure.
Despite these differences, publicly insured patients were much more likely to have had open surgery. Patients with Medicare were significantly more likely to have an open than a laparoscopic procedure (15% vs. 6%), as were patients with Medi-Cal (7% vs. 4%). Patients with private insurance were significantly more likely to have laparoscopic surgery (86% vs. 74%).
In a multivariate analysis, several factors were significantly associated with outcome. Female gender reduced the risk of death by more than 30%. Younger age also portended better outcomes. Compared with patients in their 20s, those in their 50s were three times as likely to have died; those in their 60s, six times as likely, and those in their 70s, almost nine times as likely. The few patients who had surgery in their 80s were 10 times as likely to die as the youngest. However, several commentators pointed out during discussion that age-related all-cause mortality is not a surprising finding in a longitudinal study.
Insurance was also significantly related to outcome. Dr. Weiss used the self-pay group as her reference group. Compared with these patients, Medicare and Medi-Cal patients were twice as likely to have died by the study’s end. "Interestingly, they were no more likely to have long-term complications. However, when they did, these were more serious complications, possibly indicating that overall those with public insurance could have been a sicker group" at baseline.
Longer length of stay was also a significant predictor of mortality, with patients staying a week or longer five times more likely to have died by the end of follow-up than the reference group of those staying 4-6 days. "Interestingly, we also found that patients who stayed 3 days or less were 73% more likely to have died." This probably represented patients who had serious perioperative complications, she suggested.
Having either surgery at a Center of Excellence reduced the risk of mortality by 25%, she added.
Dr. Weiss had no financial disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: After up to 15 years of follow-up, patients who had laparoscopic gastric bypass were 44% less likely to have died and 20% less likely to have a long-term surgical complication than patients who had an open procedure.
Data source: The longitudinal study comprised data on 135,000 patients treated from 1995 to 2009.
Disclosures: Dr. Weiss had no financial disclosures.
Gastric bypass induces diabetes remission in obese patients
WASHINGTON – Gastric bypass surgery resulted in significantly more weight loss and also improved measures of glycemic control significantly more than did other forms of bariatric surgery, Dr. John Morton reported at the annual clinical congress of the American College of Surgeons.
However, he noted, while remission did correlate with weight loss in patients who had gastric banding or sleeving, it appeared to be independent of weight loss in those who had the bypass surgery. While he didn’t speculate on the reasons for this finding, he did affirm his belief that gastric bypass is the best option for most obese patients with comorbid diabetes.
"I feel very comfortable recommending it" for these patients, said Dr. Morton of the Stanford (Calif.) University. "There are, of course, other clinical conditions to consider when deciding [among] bypass, banding, and sleeve, but if the only consideration is around diabetes, I’m 100% comfortable in recommending it for obese diabetics."
He presented the 1-year follow-up data on 1,792 obese patients who underwent bariatric surgery. Of these, 1,364 had a Roux-en-Y bypass; 264 had a sleeve gastrectomy; and 164 had adjustable gastric banding.
The patients were a mean of about 46 years old. Body mass index was statistically, but not clinically, different between the groups (bypass 47 kg/m2; band 44 kg/m2; sleeve 44 kg/m2). Waist circumference ranged from 51 to 53 inches. About 75% of the group was female and more than half, white.
Overall, about one-third of each group had type 2 diabetes. Most were taking only oral medications. About 5% took only insulin, and about a quarter took both oral agents and insulin. At baseline, the mean HbA1c was more than 7% in each group. The mean fasting insulin was 36 microU/mL in the bypass group, 28 microU/mL in the band group, and 32 microU/mL in the sleeve group.
By 12 months after surgery, patients with diabetes who had bypass had lost the most weight – a mean of 71% of their excess body weight, compared with 38% in the banding group and 50% in the sleeve group.
Those who had the bypass surgery also experienced the biggest change in their HbA1c – dropping almost 16% to a mean of 5.8%. Patients in the other two groups experienced a mean drop of 10%, resulting in HbA1c levels of right around 6%.
Fasting insulin levels also improved significantly more in the bypass group, falling from a baseline mean of 56 microU/mL to 7.8 microU/mL – a decrease of 68%. In the band group, the level fell from 28 microU/mL to 12 microU/mL – a 52% decrease. In the sleeve group, levels fell from 32 microU/mL to 10 microU/mL – a 61% decrease.
"Fasting insulin is also considered an independent marker of cardiac risk," Dr. Morton added, indicating that the risk of cardiovascular problems would fall along with insulin levels.
Blood glucose improved significantly more in the bypass group, falling from a baseline mean of 149 mg/dL to 101 mg/dL – a 22% change. In the band group, the level fell from 140 mg/dL to 125 mg/dL (8%) and in the sleeve group, from 130 mg/dL to 118 mg/dL (5.6%).
A multivariate analysis controlled for surgery type, sex, body mass index, race, age, and insurance status. Of these factors, surgery type was the strongest predictor, with bypass patients three times more likely to achieve that goal than those undergoing banding or sleeve placement.
Dr. Morton did not present his complication data. However, during the discussion period, he said the three procedures were similarly safe. The gastric sleeve group had a higher leak rate than did the other groups, but that remained less than 1%. Readmission rates were comparable, he said, but he did not provide that number.
"Any time you consider this, it has to be a risk/benefit analysis," he said. "It’s our philosophy that for obese patients with severe diabetes, we approach them first with the bypass because it has the most proven track record over time."
Dr. Morton has up to 7 years of data on some of the patients, and said he is now analyzing that. But when questioned about durability, he agreed that diabetes can recur in the rather common scenario of a patient regaining weight. "At the end of the day, though, what’s important is that the obese patient with diabetes gets treatment. All three surgeries demonstrated some improvement, and I believe that any surgery is better than no surgery at all."
Dr. Morton has received research support from Covidien.
WASHINGTON – Gastric bypass surgery resulted in significantly more weight loss and also improved measures of glycemic control significantly more than did other forms of bariatric surgery, Dr. John Morton reported at the annual clinical congress of the American College of Surgeons.
However, he noted, while remission did correlate with weight loss in patients who had gastric banding or sleeving, it appeared to be independent of weight loss in those who had the bypass surgery. While he didn’t speculate on the reasons for this finding, he did affirm his belief that gastric bypass is the best option for most obese patients with comorbid diabetes.
"I feel very comfortable recommending it" for these patients, said Dr. Morton of the Stanford (Calif.) University. "There are, of course, other clinical conditions to consider when deciding [among] bypass, banding, and sleeve, but if the only consideration is around diabetes, I’m 100% comfortable in recommending it for obese diabetics."
He presented the 1-year follow-up data on 1,792 obese patients who underwent bariatric surgery. Of these, 1,364 had a Roux-en-Y bypass; 264 had a sleeve gastrectomy; and 164 had adjustable gastric banding.
The patients were a mean of about 46 years old. Body mass index was statistically, but not clinically, different between the groups (bypass 47 kg/m2; band 44 kg/m2; sleeve 44 kg/m2). Waist circumference ranged from 51 to 53 inches. About 75% of the group was female and more than half, white.
Overall, about one-third of each group had type 2 diabetes. Most were taking only oral medications. About 5% took only insulin, and about a quarter took both oral agents and insulin. At baseline, the mean HbA1c was more than 7% in each group. The mean fasting insulin was 36 microU/mL in the bypass group, 28 microU/mL in the band group, and 32 microU/mL in the sleeve group.
By 12 months after surgery, patients with diabetes who had bypass had lost the most weight – a mean of 71% of their excess body weight, compared with 38% in the banding group and 50% in the sleeve group.
Those who had the bypass surgery also experienced the biggest change in their HbA1c – dropping almost 16% to a mean of 5.8%. Patients in the other two groups experienced a mean drop of 10%, resulting in HbA1c levels of right around 6%.
Fasting insulin levels also improved significantly more in the bypass group, falling from a baseline mean of 56 microU/mL to 7.8 microU/mL – a decrease of 68%. In the band group, the level fell from 28 microU/mL to 12 microU/mL – a 52% decrease. In the sleeve group, levels fell from 32 microU/mL to 10 microU/mL – a 61% decrease.
"Fasting insulin is also considered an independent marker of cardiac risk," Dr. Morton added, indicating that the risk of cardiovascular problems would fall along with insulin levels.
Blood glucose improved significantly more in the bypass group, falling from a baseline mean of 149 mg/dL to 101 mg/dL – a 22% change. In the band group, the level fell from 140 mg/dL to 125 mg/dL (8%) and in the sleeve group, from 130 mg/dL to 118 mg/dL (5.6%).
A multivariate analysis controlled for surgery type, sex, body mass index, race, age, and insurance status. Of these factors, surgery type was the strongest predictor, with bypass patients three times more likely to achieve that goal than those undergoing banding or sleeve placement.
Dr. Morton did not present his complication data. However, during the discussion period, he said the three procedures were similarly safe. The gastric sleeve group had a higher leak rate than did the other groups, but that remained less than 1%. Readmission rates were comparable, he said, but he did not provide that number.
"Any time you consider this, it has to be a risk/benefit analysis," he said. "It’s our philosophy that for obese patients with severe diabetes, we approach them first with the bypass because it has the most proven track record over time."
Dr. Morton has up to 7 years of data on some of the patients, and said he is now analyzing that. But when questioned about durability, he agreed that diabetes can recur in the rather common scenario of a patient regaining weight. "At the end of the day, though, what’s important is that the obese patient with diabetes gets treatment. All three surgeries demonstrated some improvement, and I believe that any surgery is better than no surgery at all."
Dr. Morton has received research support from Covidien.
WASHINGTON – Gastric bypass surgery resulted in significantly more weight loss and also improved measures of glycemic control significantly more than did other forms of bariatric surgery, Dr. John Morton reported at the annual clinical congress of the American College of Surgeons.
However, he noted, while remission did correlate with weight loss in patients who had gastric banding or sleeving, it appeared to be independent of weight loss in those who had the bypass surgery. While he didn’t speculate on the reasons for this finding, he did affirm his belief that gastric bypass is the best option for most obese patients with comorbid diabetes.
"I feel very comfortable recommending it" for these patients, said Dr. Morton of the Stanford (Calif.) University. "There are, of course, other clinical conditions to consider when deciding [among] bypass, banding, and sleeve, but if the only consideration is around diabetes, I’m 100% comfortable in recommending it for obese diabetics."
He presented the 1-year follow-up data on 1,792 obese patients who underwent bariatric surgery. Of these, 1,364 had a Roux-en-Y bypass; 264 had a sleeve gastrectomy; and 164 had adjustable gastric banding.
The patients were a mean of about 46 years old. Body mass index was statistically, but not clinically, different between the groups (bypass 47 kg/m2; band 44 kg/m2; sleeve 44 kg/m2). Waist circumference ranged from 51 to 53 inches. About 75% of the group was female and more than half, white.
Overall, about one-third of each group had type 2 diabetes. Most were taking only oral medications. About 5% took only insulin, and about a quarter took both oral agents and insulin. At baseline, the mean HbA1c was more than 7% in each group. The mean fasting insulin was 36 microU/mL in the bypass group, 28 microU/mL in the band group, and 32 microU/mL in the sleeve group.
By 12 months after surgery, patients with diabetes who had bypass had lost the most weight – a mean of 71% of their excess body weight, compared with 38% in the banding group and 50% in the sleeve group.
Those who had the bypass surgery also experienced the biggest change in their HbA1c – dropping almost 16% to a mean of 5.8%. Patients in the other two groups experienced a mean drop of 10%, resulting in HbA1c levels of right around 6%.
Fasting insulin levels also improved significantly more in the bypass group, falling from a baseline mean of 56 microU/mL to 7.8 microU/mL – a decrease of 68%. In the band group, the level fell from 28 microU/mL to 12 microU/mL – a 52% decrease. In the sleeve group, levels fell from 32 microU/mL to 10 microU/mL – a 61% decrease.
"Fasting insulin is also considered an independent marker of cardiac risk," Dr. Morton added, indicating that the risk of cardiovascular problems would fall along with insulin levels.
Blood glucose improved significantly more in the bypass group, falling from a baseline mean of 149 mg/dL to 101 mg/dL – a 22% change. In the band group, the level fell from 140 mg/dL to 125 mg/dL (8%) and in the sleeve group, from 130 mg/dL to 118 mg/dL (5.6%).
A multivariate analysis controlled for surgery type, sex, body mass index, race, age, and insurance status. Of these factors, surgery type was the strongest predictor, with bypass patients three times more likely to achieve that goal than those undergoing banding or sleeve placement.
Dr. Morton did not present his complication data. However, during the discussion period, he said the three procedures were similarly safe. The gastric sleeve group had a higher leak rate than did the other groups, but that remained less than 1%. Readmission rates were comparable, he said, but he did not provide that number.
"Any time you consider this, it has to be a risk/benefit analysis," he said. "It’s our philosophy that for obese patients with severe diabetes, we approach them first with the bypass because it has the most proven track record over time."
Dr. Morton has up to 7 years of data on some of the patients, and said he is now analyzing that. But when questioned about durability, he agreed that diabetes can recur in the rather common scenario of a patient regaining weight. "At the end of the day, though, what’s important is that the obese patient with diabetes gets treatment. All three surgeries demonstrated some improvement, and I believe that any surgery is better than no surgery at all."
Dr. Morton has received research support from Covidien.
AT THE ACS CLINICAL CONGRESS
Major finding: Obese patients with diabetes lost significantly more weight and had significantly better glycemic control after gastric bypass than after gastric banding or sleeve gastrectomy.
Data source: The 1-year follow-up study contained data on 1,792 patients.
Disclosures: Dr. Morton has received research support from Covidien.
Outpatient laparoscopic appendectomy found safe, cost saving
SAN FRANCISCO – Implementing an outpatient laparoscopic appendectomy protocol for uncomplicated appendicitis allowed 88% of 345 cases at one institution to be performed without hospitalizing the patient overnight.
The outpatients went home an average of 171 minutes after completion of the surgery.
Forty patients were admitted (12%) because of pre-existing comorbidities in 15 patients, postoperative morbidity in 6, and a lack of transportation or assistance for 19, Dr. Richard C. Frazee and his associates reported.
Only 4 of the 305 patients who underwent the procedure as outpatients were admitted after going home, for an overall outpatient success rate of 87%, he said at the annual meeting of the American Association for the Surgery of Trauma. Reasons for readmission included fever, nausea and vomiting, partial small bowel obstruction, or deep vein thrombosis.
Morbidity affected 7% of patients in the form of urinary retention, wound infection, operative enterotomy, cecal serosal injury, deep vein thrombosis, or exacerbation of chronic obstructive pulmonary disease. One laparoscopic appendectomy was converted to open surgery; none of the patients died.
This is not the first time Dr. Frazee has presented his institution’s experience with the outpatient laparoscopic appendectomy protocol; he shared similar findings from an earlier series at the same meeting a few years ago. In an interview, he expressed some frustration that more hospitals haven’t adopted similar protocols.
By his rough calculation, 20% of all laparoscopic uncomplicated appendectomies performed in the United States each year cause perforations requiring hospitalization and 80% of the rest are successful outpatient procedures. That means 242,760 patients each year would not be hospitalized overnight for this surgery. Separate data show that the average U.S. length of hospitalization for laparoscopic appendectomy is 2 days, at an average cost of $1,900 per day. Nationwide adoption of an outpatient protocol potentially could avoid over $921 million in annual costs.
"It is time for us to create a change in the standard of care for uncomplicated appendicitis," said Dr. Frazee, chief of acute care surgery at Scott & White Healthcare in Temple, Tex.
His interest in the subject started when his son, an otherwise healthy young adult, complained about having to stay in the hospital after a laparoscopic appendectomy. Dr. Frazee conducted a review of 119 laparoscopic appendectomies at his institution and found that 35% of patients went home the same day, 61% were admitted for a day, and the few others were hospitalized longer. Morbidity was seen in 8%.
He and his colleagues developed an outpatient protocol in July 2010, under which patients undergoing uncomplicated laparoscopic appendectomies would not be admitted unless they were pregnant or younger than 17 years, or if a perforated or gangrenous appendicitis was discovered during the surgery. To qualify for same-day discharge, outpatients had to be able to tolerate intake of liquids, ambulate, urinate, and have adequate respiratory effort. They also had to be hemodynamically stable, have pain controlled with oral analgesics, have nausea and vomiting controlled, show no alteration in mental status from baseline, have the approval of their physician, and have appropriate supervision and assistance at home.
An initial review compared 116 patients treated under the protocol in 2010-2011 with historical controls and found a significant reduction in length of stay without increased morbidity. Under the protocol, 85% of patients were outpatients, compared with 35% in the control group. Postoperative morbidity affected 5% in the protocol group and 8% in the control group, and no patients were readmitted (Am. Surg. 2012;215:101-5).
Since then, the outpatient protocol has been the standard of care at his institution. The current report covers 166 men and 179 women treated under the protocol from July 2010 through December 2012. They had a mean age of 35 years and a mean body mass index of 31 kg/m2. Thirty-two percent had a history of prior abdominal surgery. Comorbidities at baseline included hypertension in 29%, diabetes in 11%, coronary artery disease in 4%, and chronic obstructive pulmonary disease in 1%.
Outpatients were sent home from the day surgery unit or the post–anesthetic care unit. Thirty percent were dismissed between 6 a.m. and noon, 15% went home between noon and 6 p.m., 25% were dismissed between 6 p.m. and midnight, and 30% went home between midnight and 6 a.m.
The investigators now are conducting a follow-up study to assess patient satisfaction with the protocol. "Our impression is that they like going home the same day," but a study will confirm whether this is true or not, he said.
Dr. Frazee reported having no financial disclosures.
This is a well-written paper that continues a series of contributions from the authors addressing management of acute appendicitis. A 1994 paper from the authors prospectively compared laparoscopic with open appendectomy. In 2012, the authors reported and described their protocol for outpatient management of laparoscopic appendectomy, comparing 116 patients with a matched historical cohort group. This paper is an update of the 2012 paper and now includes 345 patients.
They assume that their patients are at home, happy, and doing well after discharge. They may not be. The conclusions would be more valid if patients had completed a questionnaire that stated that they were home and doing well, as other authors have done in studying this disease.
The report provides mean times from the emergency department to the operating room and from completion of surgery to discharge. Median times would be helpful to know.
I congratulate them on a well-presented and well-written paper.
Dr. Andrew Peitzman is professor of surgery and chief of general surgery and of trauma/surgical critical care at the University of Pittsburgh. He gave these comments as the discussant of Dr. Frazee’s study at the meeting.
This is a well-written paper that continues a series of contributions from the authors addressing management of acute appendicitis. A 1994 paper from the authors prospectively compared laparoscopic with open appendectomy. In 2012, the authors reported and described their protocol for outpatient management of laparoscopic appendectomy, comparing 116 patients with a matched historical cohort group. This paper is an update of the 2012 paper and now includes 345 patients.
They assume that their patients are at home, happy, and doing well after discharge. They may not be. The conclusions would be more valid if patients had completed a questionnaire that stated that they were home and doing well, as other authors have done in studying this disease.
The report provides mean times from the emergency department to the operating room and from completion of surgery to discharge. Median times would be helpful to know.
I congratulate them on a well-presented and well-written paper.
Dr. Andrew Peitzman is professor of surgery and chief of general surgery and of trauma/surgical critical care at the University of Pittsburgh. He gave these comments as the discussant of Dr. Frazee’s study at the meeting.
This is a well-written paper that continues a series of contributions from the authors addressing management of acute appendicitis. A 1994 paper from the authors prospectively compared laparoscopic with open appendectomy. In 2012, the authors reported and described their protocol for outpatient management of laparoscopic appendectomy, comparing 116 patients with a matched historical cohort group. This paper is an update of the 2012 paper and now includes 345 patients.
They assume that their patients are at home, happy, and doing well after discharge. They may not be. The conclusions would be more valid if patients had completed a questionnaire that stated that they were home and doing well, as other authors have done in studying this disease.
The report provides mean times from the emergency department to the operating room and from completion of surgery to discharge. Median times would be helpful to know.
I congratulate them on a well-presented and well-written paper.
Dr. Andrew Peitzman is professor of surgery and chief of general surgery and of trauma/surgical critical care at the University of Pittsburgh. He gave these comments as the discussant of Dr. Frazee’s study at the meeting.
SAN FRANCISCO – Implementing an outpatient laparoscopic appendectomy protocol for uncomplicated appendicitis allowed 88% of 345 cases at one institution to be performed without hospitalizing the patient overnight.
The outpatients went home an average of 171 minutes after completion of the surgery.
Forty patients were admitted (12%) because of pre-existing comorbidities in 15 patients, postoperative morbidity in 6, and a lack of transportation or assistance for 19, Dr. Richard C. Frazee and his associates reported.
Only 4 of the 305 patients who underwent the procedure as outpatients were admitted after going home, for an overall outpatient success rate of 87%, he said at the annual meeting of the American Association for the Surgery of Trauma. Reasons for readmission included fever, nausea and vomiting, partial small bowel obstruction, or deep vein thrombosis.
Morbidity affected 7% of patients in the form of urinary retention, wound infection, operative enterotomy, cecal serosal injury, deep vein thrombosis, or exacerbation of chronic obstructive pulmonary disease. One laparoscopic appendectomy was converted to open surgery; none of the patients died.
This is not the first time Dr. Frazee has presented his institution’s experience with the outpatient laparoscopic appendectomy protocol; he shared similar findings from an earlier series at the same meeting a few years ago. In an interview, he expressed some frustration that more hospitals haven’t adopted similar protocols.
By his rough calculation, 20% of all laparoscopic uncomplicated appendectomies performed in the United States each year cause perforations requiring hospitalization and 80% of the rest are successful outpatient procedures. That means 242,760 patients each year would not be hospitalized overnight for this surgery. Separate data show that the average U.S. length of hospitalization for laparoscopic appendectomy is 2 days, at an average cost of $1,900 per day. Nationwide adoption of an outpatient protocol potentially could avoid over $921 million in annual costs.
"It is time for us to create a change in the standard of care for uncomplicated appendicitis," said Dr. Frazee, chief of acute care surgery at Scott & White Healthcare in Temple, Tex.
His interest in the subject started when his son, an otherwise healthy young adult, complained about having to stay in the hospital after a laparoscopic appendectomy. Dr. Frazee conducted a review of 119 laparoscopic appendectomies at his institution and found that 35% of patients went home the same day, 61% were admitted for a day, and the few others were hospitalized longer. Morbidity was seen in 8%.
He and his colleagues developed an outpatient protocol in July 2010, under which patients undergoing uncomplicated laparoscopic appendectomies would not be admitted unless they were pregnant or younger than 17 years, or if a perforated or gangrenous appendicitis was discovered during the surgery. To qualify for same-day discharge, outpatients had to be able to tolerate intake of liquids, ambulate, urinate, and have adequate respiratory effort. They also had to be hemodynamically stable, have pain controlled with oral analgesics, have nausea and vomiting controlled, show no alteration in mental status from baseline, have the approval of their physician, and have appropriate supervision and assistance at home.
An initial review compared 116 patients treated under the protocol in 2010-2011 with historical controls and found a significant reduction in length of stay without increased morbidity. Under the protocol, 85% of patients were outpatients, compared with 35% in the control group. Postoperative morbidity affected 5% in the protocol group and 8% in the control group, and no patients were readmitted (Am. Surg. 2012;215:101-5).
Since then, the outpatient protocol has been the standard of care at his institution. The current report covers 166 men and 179 women treated under the protocol from July 2010 through December 2012. They had a mean age of 35 years and a mean body mass index of 31 kg/m2. Thirty-two percent had a history of prior abdominal surgery. Comorbidities at baseline included hypertension in 29%, diabetes in 11%, coronary artery disease in 4%, and chronic obstructive pulmonary disease in 1%.
Outpatients were sent home from the day surgery unit or the post–anesthetic care unit. Thirty percent were dismissed between 6 a.m. and noon, 15% went home between noon and 6 p.m., 25% were dismissed between 6 p.m. and midnight, and 30% went home between midnight and 6 a.m.
The investigators now are conducting a follow-up study to assess patient satisfaction with the protocol. "Our impression is that they like going home the same day," but a study will confirm whether this is true or not, he said.
Dr. Frazee reported having no financial disclosures.
SAN FRANCISCO – Implementing an outpatient laparoscopic appendectomy protocol for uncomplicated appendicitis allowed 88% of 345 cases at one institution to be performed without hospitalizing the patient overnight.
The outpatients went home an average of 171 minutes after completion of the surgery.
Forty patients were admitted (12%) because of pre-existing comorbidities in 15 patients, postoperative morbidity in 6, and a lack of transportation or assistance for 19, Dr. Richard C. Frazee and his associates reported.
Only 4 of the 305 patients who underwent the procedure as outpatients were admitted after going home, for an overall outpatient success rate of 87%, he said at the annual meeting of the American Association for the Surgery of Trauma. Reasons for readmission included fever, nausea and vomiting, partial small bowel obstruction, or deep vein thrombosis.
Morbidity affected 7% of patients in the form of urinary retention, wound infection, operative enterotomy, cecal serosal injury, deep vein thrombosis, or exacerbation of chronic obstructive pulmonary disease. One laparoscopic appendectomy was converted to open surgery; none of the patients died.
This is not the first time Dr. Frazee has presented his institution’s experience with the outpatient laparoscopic appendectomy protocol; he shared similar findings from an earlier series at the same meeting a few years ago. In an interview, he expressed some frustration that more hospitals haven’t adopted similar protocols.
By his rough calculation, 20% of all laparoscopic uncomplicated appendectomies performed in the United States each year cause perforations requiring hospitalization and 80% of the rest are successful outpatient procedures. That means 242,760 patients each year would not be hospitalized overnight for this surgery. Separate data show that the average U.S. length of hospitalization for laparoscopic appendectomy is 2 days, at an average cost of $1,900 per day. Nationwide adoption of an outpatient protocol potentially could avoid over $921 million in annual costs.
"It is time for us to create a change in the standard of care for uncomplicated appendicitis," said Dr. Frazee, chief of acute care surgery at Scott & White Healthcare in Temple, Tex.
His interest in the subject started when his son, an otherwise healthy young adult, complained about having to stay in the hospital after a laparoscopic appendectomy. Dr. Frazee conducted a review of 119 laparoscopic appendectomies at his institution and found that 35% of patients went home the same day, 61% were admitted for a day, and the few others were hospitalized longer. Morbidity was seen in 8%.
He and his colleagues developed an outpatient protocol in July 2010, under which patients undergoing uncomplicated laparoscopic appendectomies would not be admitted unless they were pregnant or younger than 17 years, or if a perforated or gangrenous appendicitis was discovered during the surgery. To qualify for same-day discharge, outpatients had to be able to tolerate intake of liquids, ambulate, urinate, and have adequate respiratory effort. They also had to be hemodynamically stable, have pain controlled with oral analgesics, have nausea and vomiting controlled, show no alteration in mental status from baseline, have the approval of their physician, and have appropriate supervision and assistance at home.
An initial review compared 116 patients treated under the protocol in 2010-2011 with historical controls and found a significant reduction in length of stay without increased morbidity. Under the protocol, 85% of patients were outpatients, compared with 35% in the control group. Postoperative morbidity affected 5% in the protocol group and 8% in the control group, and no patients were readmitted (Am. Surg. 2012;215:101-5).
Since then, the outpatient protocol has been the standard of care at his institution. The current report covers 166 men and 179 women treated under the protocol from July 2010 through December 2012. They had a mean age of 35 years and a mean body mass index of 31 kg/m2. Thirty-two percent had a history of prior abdominal surgery. Comorbidities at baseline included hypertension in 29%, diabetes in 11%, coronary artery disease in 4%, and chronic obstructive pulmonary disease in 1%.
Outpatients were sent home from the day surgery unit or the post–anesthetic care unit. Thirty percent were dismissed between 6 a.m. and noon, 15% went home between noon and 6 p.m., 25% were dismissed between 6 p.m. and midnight, and 30% went home between midnight and 6 a.m.
The investigators now are conducting a follow-up study to assess patient satisfaction with the protocol. "Our impression is that they like going home the same day," but a study will confirm whether this is true or not, he said.
Dr. Frazee reported having no financial disclosures.
AT THE AAST ANNUAL MEETING
Major finding: Outpatient laparoscopic uncomplicated appendectomies increased from 35% to 88% of the procedures under the outpatient protocol.
Data source: Review of 345 outpatient procedures at one institution from July 2010 through December 2012, compared with historical controls.
Disclosures: Dr. Frazee reported having no financial disclosures.
VTE rate does not accurately measure quality of care
Postoperative venous thromboembolism rates may not be an effective way of measuring hospital quality, according to Dr. Karl Y. Bilimoria and his colleagues.
The investigators calculated patient-level rates of venous thromboembolism as well as rates of imaging for VTE using data from the American Hospital Association and Medicare Compare from 2009-2010 from nearly 1 million patients discharged from 2,786 hospitals after a major surgery.
They sought to determine the association between hospital adherence to VTE reduction protocols (Surgical Care Improvement Project for VTE or SCIP-VTE-2) and risk-adjusted rates of VTE as measured by Patient Safety Indicator 12 (PSI-12) from the Agency for Healthcare Research and Quality. They also looked at how overall hospital quality scores correlated with VTE prophylaxis and risk-adjusted VTE scores.
Their findings were presented at the annual clinical congress of the American College of Surgeons and simultaneously published Oct. 7 in JAMA (2013 Oct. 7 [doi:10.1001/jama.2013.280048]).
Hospitals that adhered consistently to VTE reduction protocols paradoxically had higher PSI-12 scores, although not significantly so (P = .03). Hospitals with higher overall quality scores also adhered to VTE reduction protocols at a higher rate (93.3% in the lowest quartile vs. 95.5% in the highest) and had significantly higher risk-adjusted VTE event scores (P less than .001).
"Most important, hospital VTE rates were associated with the intensity of detecting VTE with imaging studies," the investigators said. Mean VTE diagnostic imaging rates ranged from 32/1,000 in the lowest quartile to 167/1,000 in the highest.
Hospitals with the lowest imaging rates diagnosed 5.0 VTEs per 1,000 discharges, compared with hospitals with the highest imaging rates diagnosing 13.5 VTEs per 1,000 discharges.
In effect, PSI-12 scores the use of VTE imaging by hospitals instead of the quality of care provided, the investigators said. Further, surveillance bias impedes quality performance improvements; thus, decision making becomes more difficult for "patients seeking to identify a high-quality hospital."
In an accompanying editorial, Dr. Edwin H. Livingston, deputy editor of JAMA, noted that hypervigilance of VTEs might further worsen care in that "the very high compliance rate with VTE prophylaxis might result from many patients receiving treatments from which they are not likely to benefit. This is because current process measures were based on older guidelines that overestimated the benefits of VTE prophylaxis" (JAMA 2013 Oct. 7 [doi:10.1001/jama.2013.280049]).
For that reason, Dr. Livingston recommended that public reporting of VTEs be "reconsidered or curtailed because few hospitals have sufficient numbers of patients to show statistically significant effects of prophylactic measures on VTE rates."
The study was funded by the AHRQ and Northwestern University. Dr. Bilimoria has received honoraria from hospitals, professional societies, and continuing medical education companies for presentation on quality improvement.
Measuring outcomes in general and safety events in particular is a complex proposition. This is particularly true when using patient safety indicators (PSIs) and hospital-acquired conditions (HACs) as outcome metrics to compare performance across organizations.

|
| Dr. Robert Pendleton |
In addition to the usual challenging nuances such as severity of illness adjustment, these indicators rely on accurate documentation and coding and as the Agency for Healthcare Research and Quality states: PSIs identify "potential in-hospital complications and adverse events following surgeries, procedures, and childbirth."
This is well meaning when an analytic team uses these metrics as part of a comprehensive quality and patient safety program to identify potential internal improvement opportunities. However, there are real limitations when using these metrics as outcomes that are tied to public reporting initiatives, payment incentives, and rankings.
The study in this weeks JAMA by Bilimoria and colleagues highlights another limitation of some of these metrics- that of surveillance bias. Using PSI-12 (postoperative venous thromboembolism) risk-adjusted VTE rates were shown to correlate positively with intensity of imaging use (surveillance) and inversely with other measures of quality such as structure or process.
Thus, those with the highest VTE rates did everything right, but also looked for events more often.
This finding complicates the use of PSI-12 as an indicator to compare outcomes across healthcare systems. However, when used as an internal driver in the context of other local metrics of quality and safety, the original intent of PSI-12 as an indicator of potential hospital complications does not change.
This highlights the importance of health care systems in
understanding the strengths and limitations of quality and safety metrics and
in developing the analytic capabilities to turn data points into real
opportunities to deliver better care, rather than going down the proverbial
rabbit hole.
Yet, regulatory agencies should also recognize that using imperfect metrics as a part of payment-reform initiatives needs to be done with extreme caution or there will be unintended consequences that do not lead to our collective goal of exceptional value in healthcare for our patients.
Dr. Robert Pendleton is chief medical quality officer for University of Utah Health Care, Salt Lake City.
Measuring outcomes in general and safety events in particular is a complex proposition. This is particularly true when using patient safety indicators (PSIs) and hospital-acquired conditions (HACs) as outcome metrics to compare performance across organizations.

|
| Dr. Robert Pendleton |
In addition to the usual challenging nuances such as severity of illness adjustment, these indicators rely on accurate documentation and coding and as the Agency for Healthcare Research and Quality states: PSIs identify "potential in-hospital complications and adverse events following surgeries, procedures, and childbirth."
This is well meaning when an analytic team uses these metrics as part of a comprehensive quality and patient safety program to identify potential internal improvement opportunities. However, there are real limitations when using these metrics as outcomes that are tied to public reporting initiatives, payment incentives, and rankings.
The study in this weeks JAMA by Bilimoria and colleagues highlights another limitation of some of these metrics- that of surveillance bias. Using PSI-12 (postoperative venous thromboembolism) risk-adjusted VTE rates were shown to correlate positively with intensity of imaging use (surveillance) and inversely with other measures of quality such as structure or process.
Thus, those with the highest VTE rates did everything right, but also looked for events more often.
This finding complicates the use of PSI-12 as an indicator to compare outcomes across healthcare systems. However, when used as an internal driver in the context of other local metrics of quality and safety, the original intent of PSI-12 as an indicator of potential hospital complications does not change.
This highlights the importance of health care systems in
understanding the strengths and limitations of quality and safety metrics and
in developing the analytic capabilities to turn data points into real
opportunities to deliver better care, rather than going down the proverbial
rabbit hole.
Yet, regulatory agencies should also recognize that using imperfect metrics as a part of payment-reform initiatives needs to be done with extreme caution or there will be unintended consequences that do not lead to our collective goal of exceptional value in healthcare for our patients.
Dr. Robert Pendleton is chief medical quality officer for University of Utah Health Care, Salt Lake City.
Measuring outcomes in general and safety events in particular is a complex proposition. This is particularly true when using patient safety indicators (PSIs) and hospital-acquired conditions (HACs) as outcome metrics to compare performance across organizations.

|
| Dr. Robert Pendleton |
In addition to the usual challenging nuances such as severity of illness adjustment, these indicators rely on accurate documentation and coding and as the Agency for Healthcare Research and Quality states: PSIs identify "potential in-hospital complications and adverse events following surgeries, procedures, and childbirth."
This is well meaning when an analytic team uses these metrics as part of a comprehensive quality and patient safety program to identify potential internal improvement opportunities. However, there are real limitations when using these metrics as outcomes that are tied to public reporting initiatives, payment incentives, and rankings.
The study in this weeks JAMA by Bilimoria and colleagues highlights another limitation of some of these metrics- that of surveillance bias. Using PSI-12 (postoperative venous thromboembolism) risk-adjusted VTE rates were shown to correlate positively with intensity of imaging use (surveillance) and inversely with other measures of quality such as structure or process.
Thus, those with the highest VTE rates did everything right, but also looked for events more often.
This finding complicates the use of PSI-12 as an indicator to compare outcomes across healthcare systems. However, when used as an internal driver in the context of other local metrics of quality and safety, the original intent of PSI-12 as an indicator of potential hospital complications does not change.
This highlights the importance of health care systems in
understanding the strengths and limitations of quality and safety metrics and
in developing the analytic capabilities to turn data points into real
opportunities to deliver better care, rather than going down the proverbial
rabbit hole.
Yet, regulatory agencies should also recognize that using imperfect metrics as a part of payment-reform initiatives needs to be done with extreme caution or there will be unintended consequences that do not lead to our collective goal of exceptional value in healthcare for our patients.
Dr. Robert Pendleton is chief medical quality officer for University of Utah Health Care, Salt Lake City.
Postoperative venous thromboembolism rates may not be an effective way of measuring hospital quality, according to Dr. Karl Y. Bilimoria and his colleagues.
The investigators calculated patient-level rates of venous thromboembolism as well as rates of imaging for VTE using data from the American Hospital Association and Medicare Compare from 2009-2010 from nearly 1 million patients discharged from 2,786 hospitals after a major surgery.
They sought to determine the association between hospital adherence to VTE reduction protocols (Surgical Care Improvement Project for VTE or SCIP-VTE-2) and risk-adjusted rates of VTE as measured by Patient Safety Indicator 12 (PSI-12) from the Agency for Healthcare Research and Quality. They also looked at how overall hospital quality scores correlated with VTE prophylaxis and risk-adjusted VTE scores.
Their findings were presented at the annual clinical congress of the American College of Surgeons and simultaneously published Oct. 7 in JAMA (2013 Oct. 7 [doi:10.1001/jama.2013.280048]).
Hospitals that adhered consistently to VTE reduction protocols paradoxically had higher PSI-12 scores, although not significantly so (P = .03). Hospitals with higher overall quality scores also adhered to VTE reduction protocols at a higher rate (93.3% in the lowest quartile vs. 95.5% in the highest) and had significantly higher risk-adjusted VTE event scores (P less than .001).
"Most important, hospital VTE rates were associated with the intensity of detecting VTE with imaging studies," the investigators said. Mean VTE diagnostic imaging rates ranged from 32/1,000 in the lowest quartile to 167/1,000 in the highest.
Hospitals with the lowest imaging rates diagnosed 5.0 VTEs per 1,000 discharges, compared with hospitals with the highest imaging rates diagnosing 13.5 VTEs per 1,000 discharges.
In effect, PSI-12 scores the use of VTE imaging by hospitals instead of the quality of care provided, the investigators said. Further, surveillance bias impedes quality performance improvements; thus, decision making becomes more difficult for "patients seeking to identify a high-quality hospital."
In an accompanying editorial, Dr. Edwin H. Livingston, deputy editor of JAMA, noted that hypervigilance of VTEs might further worsen care in that "the very high compliance rate with VTE prophylaxis might result from many patients receiving treatments from which they are not likely to benefit. This is because current process measures were based on older guidelines that overestimated the benefits of VTE prophylaxis" (JAMA 2013 Oct. 7 [doi:10.1001/jama.2013.280049]).
For that reason, Dr. Livingston recommended that public reporting of VTEs be "reconsidered or curtailed because few hospitals have sufficient numbers of patients to show statistically significant effects of prophylactic measures on VTE rates."
The study was funded by the AHRQ and Northwestern University. Dr. Bilimoria has received honoraria from hospitals, professional societies, and continuing medical education companies for presentation on quality improvement.
Postoperative venous thromboembolism rates may not be an effective way of measuring hospital quality, according to Dr. Karl Y. Bilimoria and his colleagues.
The investigators calculated patient-level rates of venous thromboembolism as well as rates of imaging for VTE using data from the American Hospital Association and Medicare Compare from 2009-2010 from nearly 1 million patients discharged from 2,786 hospitals after a major surgery.
They sought to determine the association between hospital adherence to VTE reduction protocols (Surgical Care Improvement Project for VTE or SCIP-VTE-2) and risk-adjusted rates of VTE as measured by Patient Safety Indicator 12 (PSI-12) from the Agency for Healthcare Research and Quality. They also looked at how overall hospital quality scores correlated with VTE prophylaxis and risk-adjusted VTE scores.
Their findings were presented at the annual clinical congress of the American College of Surgeons and simultaneously published Oct. 7 in JAMA (2013 Oct. 7 [doi:10.1001/jama.2013.280048]).
Hospitals that adhered consistently to VTE reduction protocols paradoxically had higher PSI-12 scores, although not significantly so (P = .03). Hospitals with higher overall quality scores also adhered to VTE reduction protocols at a higher rate (93.3% in the lowest quartile vs. 95.5% in the highest) and had significantly higher risk-adjusted VTE event scores (P less than .001).
"Most important, hospital VTE rates were associated with the intensity of detecting VTE with imaging studies," the investigators said. Mean VTE diagnostic imaging rates ranged from 32/1,000 in the lowest quartile to 167/1,000 in the highest.
Hospitals with the lowest imaging rates diagnosed 5.0 VTEs per 1,000 discharges, compared with hospitals with the highest imaging rates diagnosing 13.5 VTEs per 1,000 discharges.
In effect, PSI-12 scores the use of VTE imaging by hospitals instead of the quality of care provided, the investigators said. Further, surveillance bias impedes quality performance improvements; thus, decision making becomes more difficult for "patients seeking to identify a high-quality hospital."
In an accompanying editorial, Dr. Edwin H. Livingston, deputy editor of JAMA, noted that hypervigilance of VTEs might further worsen care in that "the very high compliance rate with VTE prophylaxis might result from many patients receiving treatments from which they are not likely to benefit. This is because current process measures were based on older guidelines that overestimated the benefits of VTE prophylaxis" (JAMA 2013 Oct. 7 [doi:10.1001/jama.2013.280049]).
For that reason, Dr. Livingston recommended that public reporting of VTEs be "reconsidered or curtailed because few hospitals have sufficient numbers of patients to show statistically significant effects of prophylactic measures on VTE rates."
The study was funded by the AHRQ and Northwestern University. Dr. Bilimoria has received honoraria from hospitals, professional societies, and continuing medical education companies for presentation on quality improvement.
FROM THE ACS CLINICAL CONGRESS
Major finding: Hospitals that adhered consistently to VTE reduction protocols had higher rates of VTE, although not significantly so (P = .03).
Data source: Study of hospital risk-adjusted VTE prophylaxis adherence rates to postoperative VTE event rates in 2,786 hospitals.
Disclosures: The study was funded by the AHRQ and Northwestern University. Dr. Bilimoria has received honoraria from hospitals, professional societies, and continuing medical education companies for presentation on quality improvement.