User login
Kojic Acid
Kojic acid has many uses in dermatologic products, primarily as a skin lightener, but concerns about its irritant properties have limited its role in cosmetics. Research on kojic acid shows both its promise and some evidence to support restrictions on its widespread use.
Kojic acid (5-hydroxy-2[hydroxymethyl]-gamma-pyrone, or C6H6O4), a hydrophilic fungal metabolite derived from various species of Aspergillus, Acetobacter, and Penicillium, is commonly used as a treatment for hyperpigmentation disorders (Biochem. Mol. Biol. Int. 1994;32:731-5; Contact Dermatitis 1998;39:86-7), as a food additive for preventing enzymatic browning, and as an agent to promote the reddening of unripe strawberries (J. Sci. Food. Agr. 1977;28:243). It was discovered as a fungal natural product in 1907 (Nat. Prod. Rep. 2006;23:1046-62). Kojic acid exerts a slow-binding inhibition of tyrosinase activity, mainly by chelating copper (Dermatol. Clin. 2007;25:337-42; J. Pharm. Pharmacol. 1994;46:982-5; Phytother. Res. 2006;20:921-34), and the result is a cutaneous whitening effect.
The efficacy of kojic acid in achieving such an effect is similar to that of hydroquinone, the standard and yet still controversial depigmenting agent (Dermatol. Ther. 2004;17:151-7; Skin Therapy Lett. 2004;9:1-3). Used mainly as a skin-lightening agent, kojic acid also exhibits antibiotic, anti-inflammatory, and anodyne properties (Dermatol. Clin. 2007;25:337-42). In addition, it is used in Asia as a dietary antioxidant (Phytother. Res. 2006;20:921-34; Dermatol. Surg. 1999;25:282-4).
Treatment of Hyperpigmentation
Manufacturers, especially in Japan, have used kojic acid since 1988 in cosmetic agents for its capacity to decrease pigmentation (Semin. Cutan. Med. Surg. 2009;28:77-85; J. Pharm. Pharmacol. 1994;46:982-5). In cosmetic formulations, kojic acid enhances the shelf life of products by dint of its preservative and antibiotic activity (Cent. Eur. J. Public Health. 2004;12 [Suppl]:S16-8). Its stability is one of the advantages of kojic acid over hydroquinone and other skin-lightening ingredients (Regul. Toxicol. Pharmacol. 2001;33:80-101).
In two studies, kojic acid combined with glycolic acid was demonstrated to be more effective than 10% glycolic acid combined with 4% hydroquinone for the treatment of hyperpigmentation (Facial Plast. Surg. 1995;11:15-21; Dermatol. Surg. 1996;22:443-7). In one case, Garcia and Fulton set out to assess and compare the effects on melasma and other pigmentary conditions of a glycolic acid/hydroquinone formulation and a glycolic acid/kojic acid formulation. Wood’s light and UV light photography were used to evaluate the effects of the different compounds, one on each side of the face, in 39 patients. The investigators found no statistically significant differences between the reactions; in all, 28% of the patients experienced marked improvements on the kojic acid side, 21% on the hydroquinone side. The responses to each formulation were equal in 51% of the participants. Although the kojic acid formulation was considered more irritating, the investigators found both formulations effective in treating melasma (Dermatol. Surg. 1996;22:443-7).
Treatment for Melasma
Lim studied the effects on melasma of 2% kojic acid in a gel containing 10% glycolic acid and 2% hydroquinone in 40 Chinese women with epidermal melasma. In this 12-week study, subjects were treated with the test formulation, in randomized fashion, on one side of the face and the same formulation minus kojic acid on the other side. Self-assessment questionnaires every 4 weeks, photographs, and clinical evaluations were used to rate the efficacy of the treatment. Lim found that the addition of kojic acid to the glycolic acid/hydroquinone gel improved melasma. Specifically, more than half of the melasma cleared in 24 of 40 patients who received the kojic acid formulation, compared with 19 of 40 who received the kojic acid–free gel. Two patients experienced complete clearance, in both cases on the side of the face on which the kojic acid gel was used (Dermatol. Surg. 1999;25:282-4). Two years later, Ferioli and colleagues found that combining hydroquinone and kojic acid exerted a synergistic effect, with an equimolecular distribution achieving the optimal result (Int. J. Cosmet. Sci. 2001;23:333-40).
As a lone therapy for the treatment of melasma, however, kojic acid is a member of the arsenal but is one of the last options typically selected (Dermatol. Clin. 2007;25:337-42), because it may be irritating to the skin (Skin Therapy Lett. 2006;11:1-6; Dermatol. Nurs. 2004;16:401-6, 413-6). It can be effective, though, in patients who do not tolerate the first-line products, particularly hydroquinone (Dermatol. Nurs. 2004;16:401-6, 413-6). Furthermore, combining a topical corticosteroid with kojic acid can reduce the irritant qualities of the fungal derivative (Int. J. Dermatol. 1998;37:897-903; Phytother. Res. 2006;20:921-34). In the experimental setting, kojic acid is regularly used as a reference or positive control to test the skin-whitening potential of new agents.
Antiwrinkle Properties
Other applications of kojic acid have also been considered. In 2001, Mitani and colleagues investigated the potential antiwrinkle activity of kojic acid given the iron-chelating properties of the acid and the known association between chronic photodamage and cutaneous iron. Over 20 weeks, the investigators topically applied kojic acid prior to exposing hairless mice to UV radiation. The agent successfully inhibited wrinkle development, epidermal hyperplasia, lower dermis fibrosis, and increases in upper dermis extracellular matrix components (Eur. J. Pharmacol. 2001;411:169-74).
Skin-Lightening Properties
The primary use for kojic acid in dermatology, though, remains skin whitening. Kojic acid is second only to hydroquinone in terms of effectiveness as a skin-lightening agent in topical, over-the-counter products (Dermatol. Ther. 2007;20:308-13), and is the most popular agent for treating melasma in East Asia (Dermatol. Surg. 1999;25:282-4; Dermatol. Ther. 2007;20:308-13).This makes sense, given the increasing regulatory scrutiny of hydroquinone, which has been banned in Europe and is tightly regulated in Asia, while remaining available, however tenuously, in the United States. Kojic acid is also a sensitizer. Mild facial erythema is the primary adverse effect reported in association with the typically well-tolerated fungal metabolite (Dermatol. Clin. 2007;25:353-62), which has been banned and then permitted to return to the market as a skin-lightening agent (Dermatol. Ther. 2007;20:308-13).
Kojic acid products are typically used twice daily for 1 to 2 months or until the patient achieves the desired results. Unfortunately, kojic acid has reportedly provoked contact allergies and is considered to exhibit a high sensitizing potential (Contact Dermatitis 1995;32:9-13). Because preparations containing a 2.5% concentration of kojic acid have been associated with facial dermatitis, a concentration of 1% has become more common. However, there have also been some reports of sensitization linked to 1% creams (Contact Dermatitis 1995;32:9-13). As kojic acid has also been extensively used in foods, there have been many reports on its oral safety. In addition, injecting kojic acid has the potential to induce convulsions (Regul. Toxicol. Pharmacol. 2001;33:80-101).
Possible Link With Tumor Promotion
Despite the success of kojic acid at 1% concentrations, particularly in Japan, some studies have indicated that longer term use of the agent may engender contact dermatitis and erythema (Skin Therapy Lett. 2004;9:1-3; Contact Dermatitis 1998;39:86-7; Contact Dermatitis 1995;32:9-13). In addition, an association between hepatic tumors in heterozygous p53-deficient mice and the topical application of kojic acid has been identified (Toxicol. Sci. 2003;73:287-93; Dermatol. Clin. 2007;25:353-62). In 2003, Japan’s health ministry ordered the removal of kojic acid from the market over fears, based on animal studies, that the fungal metabolite might cause cancer (Nature 2004;432:938).
In response to such findings and concerns, specifically the link between potential tumor promotion in mouse and rat livers caused by use of kojic acid, Higa and colleagues examined the presence of initiation activity in rat liver and the potential of photogenotoxicity and carcinogenicity in mouse skin in relation to kojic acid. In one of the team’s multiple experiments, a cream containing 1.0% or 3.0% kojic acid was applied twice to the backs of mice in a 24-hour period, and researchers noted that kojic acid failed to induce epidermal cell micronuclei. In addition, a skin carcinogenesis bioassay for initiation-promotion potential revealed the emergence of no skin nodules that were caused by the topical application of 3.0% kojic acid cream to the backs of mice daily for 7 days or five times a week for 19 weeks, administered during either cancer stage. Overall, the investigators concluded that kojic acid posed a minimal risk of photocarcinogenesis in the skin and did not exhibit skin carcinogenesis initiation nor promotion activity. The findings also lent support to the contention that kojic acid is a safe ingredient in cosmeceuticals (J. Toxicol. Sci. 2007;32:143-59). In addition, Lee and colleagues recently reported on derivatives of kojic acid displaying greater efficiency through increased penetration into the skin (Arch. Pharm. (Weinheim) 2006;339:111-4).
Previously, in 2003, Kim and colleagues studied the effects of a stable kojic acid derivative, 5-[(3-aminopropyl)phosphinooxy]-2-(hydroxymethyl)-4H-pyran-4-one (Kojyl-APPA), on tyrosinase activity and melanin production. The investigators found that Kojyl-APPA is not a direct inhibitor of tyrosinase, but is enzymatically converted to kojic acid in cells. However, the derivative was found to suppress tyrosinase activity markedly 24 hours after treatment in normal human melanocytes and demonstrated a 30% inhibition of tyrosinase in situ (although not in vitro). The kojic acid derivative also lowered melanin content to 75% of control in melanoma cells and neomelanin production to 43% of control in normal human melanocytes. Notably, Kojyl-APPA had an eightfold greater capacity to permeate the skin than did kojic acid (Chem. Pharm. Bull. (Tokyo) 2003;51:113-6). A kojic acid derivative found to be eight times more potent than kojic acid as a tyrosinase inhibitor was also synthesized in 2006. The compound produced by Lee and colleagues also displayed strong inhibitory activity toward melanin production (Arch. Pharm. (Weinheim) 2006;33:111-4).
It is worth noting that although kojic acid yields greater stability than does hydroquinone, the fungal derivative does have labile oxidative properties, which are enhanced by light and heat exposure. For that reason, the inclusion of kojic acid in cosmetic formulations has been through its dipalmitic ester (as kojic dipalmitate) (Talanta 2008;75:407-1).
Conclusion
The fungal derivative kojic acid has maintained a significant role in the dermatologic armamentarium for 2 decades as a skin-whitening agent and is best used in combination with other depigmenting ingredients, which enhance the overall effect of the formulation and blunt the irritating effects of kojic acid. Recent evidence has allayed fears regarding long-term carcinogenic effects, but as always, research is ongoing to develop newer, safer derivatives.
Kojic acid has many uses in dermatologic products, primarily as a skin lightener, but concerns about its irritant properties have limited its role in cosmetics. Research on kojic acid shows both its promise and some evidence to support restrictions on its widespread use.
Kojic acid (5-hydroxy-2[hydroxymethyl]-gamma-pyrone, or C6H6O4), a hydrophilic fungal metabolite derived from various species of Aspergillus, Acetobacter, and Penicillium, is commonly used as a treatment for hyperpigmentation disorders (Biochem. Mol. Biol. Int. 1994;32:731-5; Contact Dermatitis 1998;39:86-7), as a food additive for preventing enzymatic browning, and as an agent to promote the reddening of unripe strawberries (J. Sci. Food. Agr. 1977;28:243). It was discovered as a fungal natural product in 1907 (Nat. Prod. Rep. 2006;23:1046-62). Kojic acid exerts a slow-binding inhibition of tyrosinase activity, mainly by chelating copper (Dermatol. Clin. 2007;25:337-42; J. Pharm. Pharmacol. 1994;46:982-5; Phytother. Res. 2006;20:921-34), and the result is a cutaneous whitening effect.
The efficacy of kojic acid in achieving such an effect is similar to that of hydroquinone, the standard and yet still controversial depigmenting agent (Dermatol. Ther. 2004;17:151-7; Skin Therapy Lett. 2004;9:1-3). Used mainly as a skin-lightening agent, kojic acid also exhibits antibiotic, anti-inflammatory, and anodyne properties (Dermatol. Clin. 2007;25:337-42). In addition, it is used in Asia as a dietary antioxidant (Phytother. Res. 2006;20:921-34; Dermatol. Surg. 1999;25:282-4).
Treatment of Hyperpigmentation
Manufacturers, especially in Japan, have used kojic acid since 1988 in cosmetic agents for its capacity to decrease pigmentation (Semin. Cutan. Med. Surg. 2009;28:77-85; J. Pharm. Pharmacol. 1994;46:982-5). In cosmetic formulations, kojic acid enhances the shelf life of products by dint of its preservative and antibiotic activity (Cent. Eur. J. Public Health. 2004;12 [Suppl]:S16-8). Its stability is one of the advantages of kojic acid over hydroquinone and other skin-lightening ingredients (Regul. Toxicol. Pharmacol. 2001;33:80-101).
In two studies, kojic acid combined with glycolic acid was demonstrated to be more effective than 10% glycolic acid combined with 4% hydroquinone for the treatment of hyperpigmentation (Facial Plast. Surg. 1995;11:15-21; Dermatol. Surg. 1996;22:443-7). In one case, Garcia and Fulton set out to assess and compare the effects on melasma and other pigmentary conditions of a glycolic acid/hydroquinone formulation and a glycolic acid/kojic acid formulation. Wood’s light and UV light photography were used to evaluate the effects of the different compounds, one on each side of the face, in 39 patients. The investigators found no statistically significant differences between the reactions; in all, 28% of the patients experienced marked improvements on the kojic acid side, 21% on the hydroquinone side. The responses to each formulation were equal in 51% of the participants. Although the kojic acid formulation was considered more irritating, the investigators found both formulations effective in treating melasma (Dermatol. Surg. 1996;22:443-7).
Treatment for Melasma
Lim studied the effects on melasma of 2% kojic acid in a gel containing 10% glycolic acid and 2% hydroquinone in 40 Chinese women with epidermal melasma. In this 12-week study, subjects were treated with the test formulation, in randomized fashion, on one side of the face and the same formulation minus kojic acid on the other side. Self-assessment questionnaires every 4 weeks, photographs, and clinical evaluations were used to rate the efficacy of the treatment. Lim found that the addition of kojic acid to the glycolic acid/hydroquinone gel improved melasma. Specifically, more than half of the melasma cleared in 24 of 40 patients who received the kojic acid formulation, compared with 19 of 40 who received the kojic acid–free gel. Two patients experienced complete clearance, in both cases on the side of the face on which the kojic acid gel was used (Dermatol. Surg. 1999;25:282-4). Two years later, Ferioli and colleagues found that combining hydroquinone and kojic acid exerted a synergistic effect, with an equimolecular distribution achieving the optimal result (Int. J. Cosmet. Sci. 2001;23:333-40).
As a lone therapy for the treatment of melasma, however, kojic acid is a member of the arsenal but is one of the last options typically selected (Dermatol. Clin. 2007;25:337-42), because it may be irritating to the skin (Skin Therapy Lett. 2006;11:1-6; Dermatol. Nurs. 2004;16:401-6, 413-6). It can be effective, though, in patients who do not tolerate the first-line products, particularly hydroquinone (Dermatol. Nurs. 2004;16:401-6, 413-6). Furthermore, combining a topical corticosteroid with kojic acid can reduce the irritant qualities of the fungal derivative (Int. J. Dermatol. 1998;37:897-903; Phytother. Res. 2006;20:921-34). In the experimental setting, kojic acid is regularly used as a reference or positive control to test the skin-whitening potential of new agents.
Antiwrinkle Properties
Other applications of kojic acid have also been considered. In 2001, Mitani and colleagues investigated the potential antiwrinkle activity of kojic acid given the iron-chelating properties of the acid and the known association between chronic photodamage and cutaneous iron. Over 20 weeks, the investigators topically applied kojic acid prior to exposing hairless mice to UV radiation. The agent successfully inhibited wrinkle development, epidermal hyperplasia, lower dermis fibrosis, and increases in upper dermis extracellular matrix components (Eur. J. Pharmacol. 2001;411:169-74).
Skin-Lightening Properties
The primary use for kojic acid in dermatology, though, remains skin whitening. Kojic acid is second only to hydroquinone in terms of effectiveness as a skin-lightening agent in topical, over-the-counter products (Dermatol. Ther. 2007;20:308-13), and is the most popular agent for treating melasma in East Asia (Dermatol. Surg. 1999;25:282-4; Dermatol. Ther. 2007;20:308-13).This makes sense, given the increasing regulatory scrutiny of hydroquinone, which has been banned in Europe and is tightly regulated in Asia, while remaining available, however tenuously, in the United States. Kojic acid is also a sensitizer. Mild facial erythema is the primary adverse effect reported in association with the typically well-tolerated fungal metabolite (Dermatol. Clin. 2007;25:353-62), which has been banned and then permitted to return to the market as a skin-lightening agent (Dermatol. Ther. 2007;20:308-13).
Kojic acid products are typically used twice daily for 1 to 2 months or until the patient achieves the desired results. Unfortunately, kojic acid has reportedly provoked contact allergies and is considered to exhibit a high sensitizing potential (Contact Dermatitis 1995;32:9-13). Because preparations containing a 2.5% concentration of kojic acid have been associated with facial dermatitis, a concentration of 1% has become more common. However, there have also been some reports of sensitization linked to 1% creams (Contact Dermatitis 1995;32:9-13). As kojic acid has also been extensively used in foods, there have been many reports on its oral safety. In addition, injecting kojic acid has the potential to induce convulsions (Regul. Toxicol. Pharmacol. 2001;33:80-101).
Possible Link With Tumor Promotion
Despite the success of kojic acid at 1% concentrations, particularly in Japan, some studies have indicated that longer term use of the agent may engender contact dermatitis and erythema (Skin Therapy Lett. 2004;9:1-3; Contact Dermatitis 1998;39:86-7; Contact Dermatitis 1995;32:9-13). In addition, an association between hepatic tumors in heterozygous p53-deficient mice and the topical application of kojic acid has been identified (Toxicol. Sci. 2003;73:287-93; Dermatol. Clin. 2007;25:353-62). In 2003, Japan’s health ministry ordered the removal of kojic acid from the market over fears, based on animal studies, that the fungal metabolite might cause cancer (Nature 2004;432:938).
In response to such findings and concerns, specifically the link between potential tumor promotion in mouse and rat livers caused by use of kojic acid, Higa and colleagues examined the presence of initiation activity in rat liver and the potential of photogenotoxicity and carcinogenicity in mouse skin in relation to kojic acid. In one of the team’s multiple experiments, a cream containing 1.0% or 3.0% kojic acid was applied twice to the backs of mice in a 24-hour period, and researchers noted that kojic acid failed to induce epidermal cell micronuclei. In addition, a skin carcinogenesis bioassay for initiation-promotion potential revealed the emergence of no skin nodules that were caused by the topical application of 3.0% kojic acid cream to the backs of mice daily for 7 days or five times a week for 19 weeks, administered during either cancer stage. Overall, the investigators concluded that kojic acid posed a minimal risk of photocarcinogenesis in the skin and did not exhibit skin carcinogenesis initiation nor promotion activity. The findings also lent support to the contention that kojic acid is a safe ingredient in cosmeceuticals (J. Toxicol. Sci. 2007;32:143-59). In addition, Lee and colleagues recently reported on derivatives of kojic acid displaying greater efficiency through increased penetration into the skin (Arch. Pharm. (Weinheim) 2006;339:111-4).
Previously, in 2003, Kim and colleagues studied the effects of a stable kojic acid derivative, 5-[(3-aminopropyl)phosphinooxy]-2-(hydroxymethyl)-4H-pyran-4-one (Kojyl-APPA), on tyrosinase activity and melanin production. The investigators found that Kojyl-APPA is not a direct inhibitor of tyrosinase, but is enzymatically converted to kojic acid in cells. However, the derivative was found to suppress tyrosinase activity markedly 24 hours after treatment in normal human melanocytes and demonstrated a 30% inhibition of tyrosinase in situ (although not in vitro). The kojic acid derivative also lowered melanin content to 75% of control in melanoma cells and neomelanin production to 43% of control in normal human melanocytes. Notably, Kojyl-APPA had an eightfold greater capacity to permeate the skin than did kojic acid (Chem. Pharm. Bull. (Tokyo) 2003;51:113-6). A kojic acid derivative found to be eight times more potent than kojic acid as a tyrosinase inhibitor was also synthesized in 2006. The compound produced by Lee and colleagues also displayed strong inhibitory activity toward melanin production (Arch. Pharm. (Weinheim) 2006;33:111-4).
It is worth noting that although kojic acid yields greater stability than does hydroquinone, the fungal derivative does have labile oxidative properties, which are enhanced by light and heat exposure. For that reason, the inclusion of kojic acid in cosmetic formulations has been through its dipalmitic ester (as kojic dipalmitate) (Talanta 2008;75:407-1).
Conclusion
The fungal derivative kojic acid has maintained a significant role in the dermatologic armamentarium for 2 decades as a skin-whitening agent and is best used in combination with other depigmenting ingredients, which enhance the overall effect of the formulation and blunt the irritating effects of kojic acid. Recent evidence has allayed fears regarding long-term carcinogenic effects, but as always, research is ongoing to develop newer, safer derivatives.
Kojic acid has many uses in dermatologic products, primarily as a skin lightener, but concerns about its irritant properties have limited its role in cosmetics. Research on kojic acid shows both its promise and some evidence to support restrictions on its widespread use.
Kojic acid (5-hydroxy-2[hydroxymethyl]-gamma-pyrone, or C6H6O4), a hydrophilic fungal metabolite derived from various species of Aspergillus, Acetobacter, and Penicillium, is commonly used as a treatment for hyperpigmentation disorders (Biochem. Mol. Biol. Int. 1994;32:731-5; Contact Dermatitis 1998;39:86-7), as a food additive for preventing enzymatic browning, and as an agent to promote the reddening of unripe strawberries (J. Sci. Food. Agr. 1977;28:243). It was discovered as a fungal natural product in 1907 (Nat. Prod. Rep. 2006;23:1046-62). Kojic acid exerts a slow-binding inhibition of tyrosinase activity, mainly by chelating copper (Dermatol. Clin. 2007;25:337-42; J. Pharm. Pharmacol. 1994;46:982-5; Phytother. Res. 2006;20:921-34), and the result is a cutaneous whitening effect.
The efficacy of kojic acid in achieving such an effect is similar to that of hydroquinone, the standard and yet still controversial depigmenting agent (Dermatol. Ther. 2004;17:151-7; Skin Therapy Lett. 2004;9:1-3). Used mainly as a skin-lightening agent, kojic acid also exhibits antibiotic, anti-inflammatory, and anodyne properties (Dermatol. Clin. 2007;25:337-42). In addition, it is used in Asia as a dietary antioxidant (Phytother. Res. 2006;20:921-34; Dermatol. Surg. 1999;25:282-4).
Treatment of Hyperpigmentation
Manufacturers, especially in Japan, have used kojic acid since 1988 in cosmetic agents for its capacity to decrease pigmentation (Semin. Cutan. Med. Surg. 2009;28:77-85; J. Pharm. Pharmacol. 1994;46:982-5). In cosmetic formulations, kojic acid enhances the shelf life of products by dint of its preservative and antibiotic activity (Cent. Eur. J. Public Health. 2004;12 [Suppl]:S16-8). Its stability is one of the advantages of kojic acid over hydroquinone and other skin-lightening ingredients (Regul. Toxicol. Pharmacol. 2001;33:80-101).
In two studies, kojic acid combined with glycolic acid was demonstrated to be more effective than 10% glycolic acid combined with 4% hydroquinone for the treatment of hyperpigmentation (Facial Plast. Surg. 1995;11:15-21; Dermatol. Surg. 1996;22:443-7). In one case, Garcia and Fulton set out to assess and compare the effects on melasma and other pigmentary conditions of a glycolic acid/hydroquinone formulation and a glycolic acid/kojic acid formulation. Wood’s light and UV light photography were used to evaluate the effects of the different compounds, one on each side of the face, in 39 patients. The investigators found no statistically significant differences between the reactions; in all, 28% of the patients experienced marked improvements on the kojic acid side, 21% on the hydroquinone side. The responses to each formulation were equal in 51% of the participants. Although the kojic acid formulation was considered more irritating, the investigators found both formulations effective in treating melasma (Dermatol. Surg. 1996;22:443-7).
Treatment for Melasma
Lim studied the effects on melasma of 2% kojic acid in a gel containing 10% glycolic acid and 2% hydroquinone in 40 Chinese women with epidermal melasma. In this 12-week study, subjects were treated with the test formulation, in randomized fashion, on one side of the face and the same formulation minus kojic acid on the other side. Self-assessment questionnaires every 4 weeks, photographs, and clinical evaluations were used to rate the efficacy of the treatment. Lim found that the addition of kojic acid to the glycolic acid/hydroquinone gel improved melasma. Specifically, more than half of the melasma cleared in 24 of 40 patients who received the kojic acid formulation, compared with 19 of 40 who received the kojic acid–free gel. Two patients experienced complete clearance, in both cases on the side of the face on which the kojic acid gel was used (Dermatol. Surg. 1999;25:282-4). Two years later, Ferioli and colleagues found that combining hydroquinone and kojic acid exerted a synergistic effect, with an equimolecular distribution achieving the optimal result (Int. J. Cosmet. Sci. 2001;23:333-40).
As a lone therapy for the treatment of melasma, however, kojic acid is a member of the arsenal but is one of the last options typically selected (Dermatol. Clin. 2007;25:337-42), because it may be irritating to the skin (Skin Therapy Lett. 2006;11:1-6; Dermatol. Nurs. 2004;16:401-6, 413-6). It can be effective, though, in patients who do not tolerate the first-line products, particularly hydroquinone (Dermatol. Nurs. 2004;16:401-6, 413-6). Furthermore, combining a topical corticosteroid with kojic acid can reduce the irritant qualities of the fungal derivative (Int. J. Dermatol. 1998;37:897-903; Phytother. Res. 2006;20:921-34). In the experimental setting, kojic acid is regularly used as a reference or positive control to test the skin-whitening potential of new agents.
Antiwrinkle Properties
Other applications of kojic acid have also been considered. In 2001, Mitani and colleagues investigated the potential antiwrinkle activity of kojic acid given the iron-chelating properties of the acid and the known association between chronic photodamage and cutaneous iron. Over 20 weeks, the investigators topically applied kojic acid prior to exposing hairless mice to UV radiation. The agent successfully inhibited wrinkle development, epidermal hyperplasia, lower dermis fibrosis, and increases in upper dermis extracellular matrix components (Eur. J. Pharmacol. 2001;411:169-74).
Skin-Lightening Properties
The primary use for kojic acid in dermatology, though, remains skin whitening. Kojic acid is second only to hydroquinone in terms of effectiveness as a skin-lightening agent in topical, over-the-counter products (Dermatol. Ther. 2007;20:308-13), and is the most popular agent for treating melasma in East Asia (Dermatol. Surg. 1999;25:282-4; Dermatol. Ther. 2007;20:308-13).This makes sense, given the increasing regulatory scrutiny of hydroquinone, which has been banned in Europe and is tightly regulated in Asia, while remaining available, however tenuously, in the United States. Kojic acid is also a sensitizer. Mild facial erythema is the primary adverse effect reported in association with the typically well-tolerated fungal metabolite (Dermatol. Clin. 2007;25:353-62), which has been banned and then permitted to return to the market as a skin-lightening agent (Dermatol. Ther. 2007;20:308-13).
Kojic acid products are typically used twice daily for 1 to 2 months or until the patient achieves the desired results. Unfortunately, kojic acid has reportedly provoked contact allergies and is considered to exhibit a high sensitizing potential (Contact Dermatitis 1995;32:9-13). Because preparations containing a 2.5% concentration of kojic acid have been associated with facial dermatitis, a concentration of 1% has become more common. However, there have also been some reports of sensitization linked to 1% creams (Contact Dermatitis 1995;32:9-13). As kojic acid has also been extensively used in foods, there have been many reports on its oral safety. In addition, injecting kojic acid has the potential to induce convulsions (Regul. Toxicol. Pharmacol. 2001;33:80-101).
Possible Link With Tumor Promotion
Despite the success of kojic acid at 1% concentrations, particularly in Japan, some studies have indicated that longer term use of the agent may engender contact dermatitis and erythema (Skin Therapy Lett. 2004;9:1-3; Contact Dermatitis 1998;39:86-7; Contact Dermatitis 1995;32:9-13). In addition, an association between hepatic tumors in heterozygous p53-deficient mice and the topical application of kojic acid has been identified (Toxicol. Sci. 2003;73:287-93; Dermatol. Clin. 2007;25:353-62). In 2003, Japan’s health ministry ordered the removal of kojic acid from the market over fears, based on animal studies, that the fungal metabolite might cause cancer (Nature 2004;432:938).
In response to such findings and concerns, specifically the link between potential tumor promotion in mouse and rat livers caused by use of kojic acid, Higa and colleagues examined the presence of initiation activity in rat liver and the potential of photogenotoxicity and carcinogenicity in mouse skin in relation to kojic acid. In one of the team’s multiple experiments, a cream containing 1.0% or 3.0% kojic acid was applied twice to the backs of mice in a 24-hour period, and researchers noted that kojic acid failed to induce epidermal cell micronuclei. In addition, a skin carcinogenesis bioassay for initiation-promotion potential revealed the emergence of no skin nodules that were caused by the topical application of 3.0% kojic acid cream to the backs of mice daily for 7 days or five times a week for 19 weeks, administered during either cancer stage. Overall, the investigators concluded that kojic acid posed a minimal risk of photocarcinogenesis in the skin and did not exhibit skin carcinogenesis initiation nor promotion activity. The findings also lent support to the contention that kojic acid is a safe ingredient in cosmeceuticals (J. Toxicol. Sci. 2007;32:143-59). In addition, Lee and colleagues recently reported on derivatives of kojic acid displaying greater efficiency through increased penetration into the skin (Arch. Pharm. (Weinheim) 2006;339:111-4).
Previously, in 2003, Kim and colleagues studied the effects of a stable kojic acid derivative, 5-[(3-aminopropyl)phosphinooxy]-2-(hydroxymethyl)-4H-pyran-4-one (Kojyl-APPA), on tyrosinase activity and melanin production. The investigators found that Kojyl-APPA is not a direct inhibitor of tyrosinase, but is enzymatically converted to kojic acid in cells. However, the derivative was found to suppress tyrosinase activity markedly 24 hours after treatment in normal human melanocytes and demonstrated a 30% inhibition of tyrosinase in situ (although not in vitro). The kojic acid derivative also lowered melanin content to 75% of control in melanoma cells and neomelanin production to 43% of control in normal human melanocytes. Notably, Kojyl-APPA had an eightfold greater capacity to permeate the skin than did kojic acid (Chem. Pharm. Bull. (Tokyo) 2003;51:113-6). A kojic acid derivative found to be eight times more potent than kojic acid as a tyrosinase inhibitor was also synthesized in 2006. The compound produced by Lee and colleagues also displayed strong inhibitory activity toward melanin production (Arch. Pharm. (Weinheim) 2006;33:111-4).
It is worth noting that although kojic acid yields greater stability than does hydroquinone, the fungal derivative does have labile oxidative properties, which are enhanced by light and heat exposure. For that reason, the inclusion of kojic acid in cosmetic formulations has been through its dipalmitic ester (as kojic dipalmitate) (Talanta 2008;75:407-1).
Conclusion
The fungal derivative kojic acid has maintained a significant role in the dermatologic armamentarium for 2 decades as a skin-whitening agent and is best used in combination with other depigmenting ingredients, which enhance the overall effect of the formulation and blunt the irritating effects of kojic acid. Recent evidence has allayed fears regarding long-term carcinogenic effects, but as always, research is ongoing to develop newer, safer derivatives.
Evaluation of a Kojic Acid, Emblica Extract, and Glycolic Acid Formulation Compared With Hydroquinone 4% for Skin Lightening
Acanthosis Nigricans in a Patient Treated With Palifermin
Acne Scar Patients Give Thumbs Up to CO2 Laser Treatment
Single treatment with a carbon dioxide fractional laser was as effective for acne scars as a nonablative fractional system, according to results of a randomized split-face study.
Fractional lasers are well tolerated and widely used to treat scarring, but patients often need multiple sessions to achieve clinical improvement, reported Dr. S.B. Cho of Yonsei University College of Medicine in Seoul, Korea, and colleagues.
However, previous studies have shown that carbon dioxide fractional laser systems can improve scars in as few as three treatments.
In this study, the researchers directly compared improvements in acne scarring after half of a patient’s face underwent a single treatment with a nonablative 1550-nm erbium-doped fractional photothermolysis system (FPS) and the other half underwent a single treatment with an ablative 10,600-nm carbon dioxide fractional laser system (CO2 FS).
The eight patients in the study were Asian males (Fitzpatrick skin type IV) aged 20 to 23 years with mild to severe atrophic acne scars.
At follow-up 3 months after FPS treatment, six of the eight patients showed clinical improvements of 26%-50% from baseline, one patient showed a clinical improvement of 51%-75%, and one showed no clinical improvement (J. Eur. Acad. Dermatol. Venereol. 2010;24:921-5). As for CO2 FS results at 3 months, five of the eight patients had a 26%-50% clinical improvement from baseline, two patients had a 51%-75% improvement, and one had an improvement of over 76%.
The level of clinical improvement was not affected by the type of acne scar (boxcar, icepick, or rolling).
The average VAS pain score on a scale of 0, no pain, to 10, severe pain, was significantly higher after the CO2 FS treatment, compared with the FPS treatment (7.0 vs. 3.9, respectively). However, patient-reported satisfaction was higher after the CO2 FS treatment. Two patients (25%) were “very satisfied,” four (50%) were “satisfied,” one (12.5%) was “slightly satisfied,” and one (12.5%) was “unsatisfied.” After the FPS treatment, none of the patients were very satisfied, two (25%) were satisfied, five (62.5%) were slightly satisfied, and one (12.5%) was unsatisfied.
Common side effects associated with both treatments included crusting, scaling, and erythema. The average duration of crusting or scaling was significantly longer in the CO2 FS group, compared with the FPS group (7.4 days vs. 2.3 days, respectively). However, the difference in post-therapy erythema was not significantly different between the two groups (11.5 days vs. 7.5 days, respectively).
“We could not completely eliminate the possibility of subject bias as the participants experienced different posttreatment responses with FPS and CO2 FS,” the researchers wrote. But the results suggest that a single treatment with CO2 FS might be more effective than a single treatment with FPS.
Although the findings are not conclusive, given the study’s small size, they could serve as a reference for clinicians choosing among laser options for acne scar treatment, the researchers added.
Dr. Cho and colleagues had no financial conflicts to disclose.
Single treatment with a carbon dioxide fractional laser was as effective for acne scars as a nonablative fractional system, according to results of a randomized split-face study.
Fractional lasers are well tolerated and widely used to treat scarring, but patients often need multiple sessions to achieve clinical improvement, reported Dr. S.B. Cho of Yonsei University College of Medicine in Seoul, Korea, and colleagues.
However, previous studies have shown that carbon dioxide fractional laser systems can improve scars in as few as three treatments.
In this study, the researchers directly compared improvements in acne scarring after half of a patient’s face underwent a single treatment with a nonablative 1550-nm erbium-doped fractional photothermolysis system (FPS) and the other half underwent a single treatment with an ablative 10,600-nm carbon dioxide fractional laser system (CO2 FS).
The eight patients in the study were Asian males (Fitzpatrick skin type IV) aged 20 to 23 years with mild to severe atrophic acne scars.
At follow-up 3 months after FPS treatment, six of the eight patients showed clinical improvements of 26%-50% from baseline, one patient showed a clinical improvement of 51%-75%, and one showed no clinical improvement (J. Eur. Acad. Dermatol. Venereol. 2010;24:921-5). As for CO2 FS results at 3 months, five of the eight patients had a 26%-50% clinical improvement from baseline, two patients had a 51%-75% improvement, and one had an improvement of over 76%.
The level of clinical improvement was not affected by the type of acne scar (boxcar, icepick, or rolling).
The average VAS pain score on a scale of 0, no pain, to 10, severe pain, was significantly higher after the CO2 FS treatment, compared with the FPS treatment (7.0 vs. 3.9, respectively). However, patient-reported satisfaction was higher after the CO2 FS treatment. Two patients (25%) were “very satisfied,” four (50%) were “satisfied,” one (12.5%) was “slightly satisfied,” and one (12.5%) was “unsatisfied.” After the FPS treatment, none of the patients were very satisfied, two (25%) were satisfied, five (62.5%) were slightly satisfied, and one (12.5%) was unsatisfied.
Common side effects associated with both treatments included crusting, scaling, and erythema. The average duration of crusting or scaling was significantly longer in the CO2 FS group, compared with the FPS group (7.4 days vs. 2.3 days, respectively). However, the difference in post-therapy erythema was not significantly different between the two groups (11.5 days vs. 7.5 days, respectively).
“We could not completely eliminate the possibility of subject bias as the participants experienced different posttreatment responses with FPS and CO2 FS,” the researchers wrote. But the results suggest that a single treatment with CO2 FS might be more effective than a single treatment with FPS.
Although the findings are not conclusive, given the study’s small size, they could serve as a reference for clinicians choosing among laser options for acne scar treatment, the researchers added.
Dr. Cho and colleagues had no financial conflicts to disclose.
Single treatment with a carbon dioxide fractional laser was as effective for acne scars as a nonablative fractional system, according to results of a randomized split-face study.
Fractional lasers are well tolerated and widely used to treat scarring, but patients often need multiple sessions to achieve clinical improvement, reported Dr. S.B. Cho of Yonsei University College of Medicine in Seoul, Korea, and colleagues.
However, previous studies have shown that carbon dioxide fractional laser systems can improve scars in as few as three treatments.
In this study, the researchers directly compared improvements in acne scarring after half of a patient’s face underwent a single treatment with a nonablative 1550-nm erbium-doped fractional photothermolysis system (FPS) and the other half underwent a single treatment with an ablative 10,600-nm carbon dioxide fractional laser system (CO2 FS).
The eight patients in the study were Asian males (Fitzpatrick skin type IV) aged 20 to 23 years with mild to severe atrophic acne scars.
At follow-up 3 months after FPS treatment, six of the eight patients showed clinical improvements of 26%-50% from baseline, one patient showed a clinical improvement of 51%-75%, and one showed no clinical improvement (J. Eur. Acad. Dermatol. Venereol. 2010;24:921-5). As for CO2 FS results at 3 months, five of the eight patients had a 26%-50% clinical improvement from baseline, two patients had a 51%-75% improvement, and one had an improvement of over 76%.
The level of clinical improvement was not affected by the type of acne scar (boxcar, icepick, or rolling).
The average VAS pain score on a scale of 0, no pain, to 10, severe pain, was significantly higher after the CO2 FS treatment, compared with the FPS treatment (7.0 vs. 3.9, respectively). However, patient-reported satisfaction was higher after the CO2 FS treatment. Two patients (25%) were “very satisfied,” four (50%) were “satisfied,” one (12.5%) was “slightly satisfied,” and one (12.5%) was “unsatisfied.” After the FPS treatment, none of the patients were very satisfied, two (25%) were satisfied, five (62.5%) were slightly satisfied, and one (12.5%) was unsatisfied.
Common side effects associated with both treatments included crusting, scaling, and erythema. The average duration of crusting or scaling was significantly longer in the CO2 FS group, compared with the FPS group (7.4 days vs. 2.3 days, respectively). However, the difference in post-therapy erythema was not significantly different between the two groups (11.5 days vs. 7.5 days, respectively).
“We could not completely eliminate the possibility of subject bias as the participants experienced different posttreatment responses with FPS and CO2 FS,” the researchers wrote. But the results suggest that a single treatment with CO2 FS might be more effective than a single treatment with FPS.
Although the findings are not conclusive, given the study’s small size, they could serve as a reference for clinicians choosing among laser options for acne scar treatment, the researchers added.
Dr. Cho and colleagues had no financial conflicts to disclose.
Facial Hyperpigmentation Caused by Diltiazem Hydrochloride
A Handheld Broadband UV Phototherapy Module for the Treatment of Patients With Psoriasis and Vitiligo
Cutaneous Manifestations of Diabetes Mellitus: A Case Series
Cultural Competence Key to Treating Skin of Color
NAPLES, Fla. — Vitiligo, keloids, acne keloidalis nuchae, and hair and scalp concerns are among the challenges dermatologists face when treating darker skin, Dr. George Cohen said.
Black skin is prone to adverse pigmentary or hyperproliferative responses to cryotherapy, lasers, and chemical skin treatments. Because of these and other concerns in a growing population of patients with skin types IV through VI, Dr. Cohen suggested dermatologists learn more about recognition and treatment of these important differences.
"We are a more diverse society. Become culturally competent and learn as much as you can," Dr. Cohen said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons. Respect, inquire, and do not make assumptions—those are the three pillars of cultural competence, he said.
Cultural competence is not only good for patients; it can be good for your practice as well. "Access and acceptance are good for us—this creates more demand for services," said Dr. Cohen, of the department of dermatology and cutaneous surgery at the University of South Florida in Tampa.
Vitiligo
Vitiligo is the prototypic pigmentary challenge for patients with skin of color, Dr. Cohen said. Although the etiology is not completely understood, it may be related to the immune system. The challenge for dermatologists is that "some people respond to some things some of the time, so we don't always know who is going to respond," Dr. Cohen said.
The myriad of treatments available for vitiligo include:
- Narrow-band UVB therapy.
- Targeted laser treatment with the XeCL Excimer (308 nm).
- Topical steroids.
- Calcineurin inhibitors.
- Surgery.
- Depigmentation (using medications or 694-nm Q-switched Ruby laser).
- Makeup.
Unfortunately, "none of these work perfectly," he said.
He cited the case of a patient with vitiligo who tried steroids, psoralen and UVA (PUVA), and other treatments to no avail. "He was desperate. He came to me with his family and asked: 'Doctor, can you make me one color?' I told him we can only make him one color—white—that is all we are able to do.
"Sometimes you cannot repigment the patient, and you have to know how to judiciously offer depigmentation. Some might say I robbed him of his culture. I say, no, I didn't, I robbed him of a disfiguring condition," said Dr. Cohen.
More research is clearly warranted to improve treatment options for vitiligo, such as studies to assess the biology of melanocytes, he said.
Keloids
Keloids are another challenge in skin of color patients. The therapeutic approach depends in part on the extent of the patient's condition. For example, a single keloid on the earlobe would be treated differently than more widespread presentation.
Again, more research is warranted on optimal treatments, Dr. Cohen said, because studies in the literature are contradictory and provide no consensus.
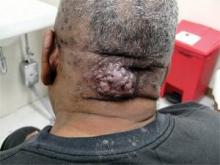
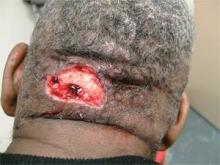
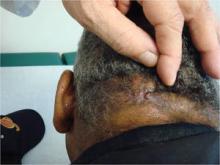
Acne keloidalis nuchae, "the keloids' cousin," most often occur in black men, he said. These nuchae can advance to plaque and form tumors, "and at the very least will need intralesional therapy." One clinical tip is to make an incision only within the keloid, he said.
If a patient presents with an acne keloidalis tumor, simply excise it. Once you get hemostasis, dress the wound with petroleum jelly only, and let it close by the magic of second intention
"I monitor these people. If I see any evidence of regrowth, I treat with triamcinolone early and often," he said.
Hair and Scalp Challenges
Hair and scalp concerns are common in patients with skin of color, Dr. Cohen said. A scalp biopsy is recommended to determine or confirm a diagnosis and to guide the course of clinical treatment.
These presentations can have a great psychosocial impact. "Do not underestimate the effect on patients," he said. Know your limitations and the limitations of therapy, and make sure you communicate those effectively to the patient. Otherwise, both the patient and provider can become frustrated.
Be honest with genetically-susceptible patients who present with scarring on the scalp from physical insult. In this population, scarring results when fibrous tissue replaces hair follicles. "Let them know up front that creams and other nonsense are not going to work," he said.
Contrary to popular belief, Dr. Cohen said, hair transplants are an option in patients with skin of color. "Hair transplants in black patients are not scary— I've been doing them for years and never had keloids," he said.
Black hair is heterogenous, so not everyone has curved follicles. If a skin of color patient has straight follicles, standard hair transplant procedures—for example, with 4-mm donor grafts—would be an option.
Dr. Cohen said that he did not have any relevant financial disclosures.
NAPLES, Fla. — Vitiligo, keloids, acne keloidalis nuchae, and hair and scalp concerns are among the challenges dermatologists face when treating darker skin, Dr. George Cohen said.
Black skin is prone to adverse pigmentary or hyperproliferative responses to cryotherapy, lasers, and chemical skin treatments. Because of these and other concerns in a growing population of patients with skin types IV through VI, Dr. Cohen suggested dermatologists learn more about recognition and treatment of these important differences.
"We are a more diverse society. Become culturally competent and learn as much as you can," Dr. Cohen said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons. Respect, inquire, and do not make assumptions—those are the three pillars of cultural competence, he said.
Cultural competence is not only good for patients; it can be good for your practice as well. "Access and acceptance are good for us—this creates more demand for services," said Dr. Cohen, of the department of dermatology and cutaneous surgery at the University of South Florida in Tampa.
Vitiligo
Vitiligo is the prototypic pigmentary challenge for patients with skin of color, Dr. Cohen said. Although the etiology is not completely understood, it may be related to the immune system. The challenge for dermatologists is that "some people respond to some things some of the time, so we don't always know who is going to respond," Dr. Cohen said.
The myriad of treatments available for vitiligo include:
- Narrow-band UVB therapy.
- Targeted laser treatment with the XeCL Excimer (308 nm).
- Topical steroids.
- Calcineurin inhibitors.
- Surgery.
- Depigmentation (using medications or 694-nm Q-switched Ruby laser).
- Makeup.
Unfortunately, "none of these work perfectly," he said.
He cited the case of a patient with vitiligo who tried steroids, psoralen and UVA (PUVA), and other treatments to no avail. "He was desperate. He came to me with his family and asked: 'Doctor, can you make me one color?' I told him we can only make him one color—white—that is all we are able to do.
"Sometimes you cannot repigment the patient, and you have to know how to judiciously offer depigmentation. Some might say I robbed him of his culture. I say, no, I didn't, I robbed him of a disfiguring condition," said Dr. Cohen.
More research is clearly warranted to improve treatment options for vitiligo, such as studies to assess the biology of melanocytes, he said.
Keloids
Keloids are another challenge in skin of color patients. The therapeutic approach depends in part on the extent of the patient's condition. For example, a single keloid on the earlobe would be treated differently than more widespread presentation.
Again, more research is warranted on optimal treatments, Dr. Cohen said, because studies in the literature are contradictory and provide no consensus.
Acne keloidalis nuchae, "the keloids' cousin," most often occur in black men, he said. These nuchae can advance to plaque and form tumors, "and at the very least will need intralesional therapy." One clinical tip is to make an incision only within the keloid, he said.
If a patient presents with an acne keloidalis tumor, simply excise it. Once you get hemostasis, dress the wound with petroleum jelly only, and let it close by the magic of second intention
"I monitor these people. If I see any evidence of regrowth, I treat with triamcinolone early and often," he said.
Hair and Scalp Challenges
Hair and scalp concerns are common in patients with skin of color, Dr. Cohen said. A scalp biopsy is recommended to determine or confirm a diagnosis and to guide the course of clinical treatment.
These presentations can have a great psychosocial impact. "Do not underestimate the effect on patients," he said. Know your limitations and the limitations of therapy, and make sure you communicate those effectively to the patient. Otherwise, both the patient and provider can become frustrated.
Be honest with genetically-susceptible patients who present with scarring on the scalp from physical insult. In this population, scarring results when fibrous tissue replaces hair follicles. "Let them know up front that creams and other nonsense are not going to work," he said.
Contrary to popular belief, Dr. Cohen said, hair transplants are an option in patients with skin of color. "Hair transplants in black patients are not scary— I've been doing them for years and never had keloids," he said.
Black hair is heterogenous, so not everyone has curved follicles. If a skin of color patient has straight follicles, standard hair transplant procedures—for example, with 4-mm donor grafts—would be an option.
Dr. Cohen said that he did not have any relevant financial disclosures.
NAPLES, Fla. — Vitiligo, keloids, acne keloidalis nuchae, and hair and scalp concerns are among the challenges dermatologists face when treating darker skin, Dr. George Cohen said.
Black skin is prone to adverse pigmentary or hyperproliferative responses to cryotherapy, lasers, and chemical skin treatments. Because of these and other concerns in a growing population of patients with skin types IV through VI, Dr. Cohen suggested dermatologists learn more about recognition and treatment of these important differences.
"We are a more diverse society. Become culturally competent and learn as much as you can," Dr. Cohen said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons. Respect, inquire, and do not make assumptions—those are the three pillars of cultural competence, he said.
Cultural competence is not only good for patients; it can be good for your practice as well. "Access and acceptance are good for us—this creates more demand for services," said Dr. Cohen, of the department of dermatology and cutaneous surgery at the University of South Florida in Tampa.
Vitiligo
Vitiligo is the prototypic pigmentary challenge for patients with skin of color, Dr. Cohen said. Although the etiology is not completely understood, it may be related to the immune system. The challenge for dermatologists is that "some people respond to some things some of the time, so we don't always know who is going to respond," Dr. Cohen said.
The myriad of treatments available for vitiligo include:
- Narrow-band UVB therapy.
- Targeted laser treatment with the XeCL Excimer (308 nm).
- Topical steroids.
- Calcineurin inhibitors.
- Surgery.
- Depigmentation (using medications or 694-nm Q-switched Ruby laser).
- Makeup.
Unfortunately, "none of these work perfectly," he said.
He cited the case of a patient with vitiligo who tried steroids, psoralen and UVA (PUVA), and other treatments to no avail. "He was desperate. He came to me with his family and asked: 'Doctor, can you make me one color?' I told him we can only make him one color—white—that is all we are able to do.
"Sometimes you cannot repigment the patient, and you have to know how to judiciously offer depigmentation. Some might say I robbed him of his culture. I say, no, I didn't, I robbed him of a disfiguring condition," said Dr. Cohen.
More research is clearly warranted to improve treatment options for vitiligo, such as studies to assess the biology of melanocytes, he said.
Keloids
Keloids are another challenge in skin of color patients. The therapeutic approach depends in part on the extent of the patient's condition. For example, a single keloid on the earlobe would be treated differently than more widespread presentation.
Again, more research is warranted on optimal treatments, Dr. Cohen said, because studies in the literature are contradictory and provide no consensus.
Acne keloidalis nuchae, "the keloids' cousin," most often occur in black men, he said. These nuchae can advance to plaque and form tumors, "and at the very least will need intralesional therapy." One clinical tip is to make an incision only within the keloid, he said.
If a patient presents with an acne keloidalis tumor, simply excise it. Once you get hemostasis, dress the wound with petroleum jelly only, and let it close by the magic of second intention
"I monitor these people. If I see any evidence of regrowth, I treat with triamcinolone early and often," he said.
Hair and Scalp Challenges
Hair and scalp concerns are common in patients with skin of color, Dr. Cohen said. A scalp biopsy is recommended to determine or confirm a diagnosis and to guide the course of clinical treatment.
These presentations can have a great psychosocial impact. "Do not underestimate the effect on patients," he said. Know your limitations and the limitations of therapy, and make sure you communicate those effectively to the patient. Otherwise, both the patient and provider can become frustrated.
Be honest with genetically-susceptible patients who present with scarring on the scalp from physical insult. In this population, scarring results when fibrous tissue replaces hair follicles. "Let them know up front that creams and other nonsense are not going to work," he said.
Contrary to popular belief, Dr. Cohen said, hair transplants are an option in patients with skin of color. "Hair transplants in black patients are not scary— I've been doing them for years and never had keloids," he said.
Black hair is heterogenous, so not everyone has curved follicles. If a skin of color patient has straight follicles, standard hair transplant procedures—for example, with 4-mm donor grafts—would be an option.
Dr. Cohen said that he did not have any relevant financial disclosures.
Tips for Treating Acne Scarring in Darker Skinned Patients
PHOENIX — Educate darker skinned patients who seek treatment for acne scars that there is no remedy to make the scars completely disappear.
"Depending on the patient's skin type, the sensitivity of their skin, and how aggressively you treat them, the risk of hyperpigmentation can be relatively modest, or well over 50%. The expected degree of improvement, on the other hand, even with multiple modalities and multiple treatments, is 40%-50%. I think it's very important to explain that," said Dr. Murad Alam at the annual meeting of the American Society for Laser Medicine and Surgery.
Dr. Alam, chief of cutaneous and aesthetic surgery at Northwestern University, Chicago, said that clinicians face certain challenges in treating acne scars in patients of color, including the risk of exacerbation of active acne, risk of focal or diffuse hyperpigmentation or hypopigmentation, risk of nodularity or surface texture change, and risk of minimal effect.
To mitigate risks, Dr. Alam considers oral antibiotics in patients who have any degree of active acne, "even if they get one or two acne pimples once in a blue moon," he said. "If the acne is more than very mild, you may wish to target that as the primary goal and defer treatment of the acne scarring until the acne is under good control."
If the acne is mild, "you can start oral antibiotics at least 1 month before the acne scarring intervention, so they do have something on board to reduce the risk of an acne flare," he said. "You may also consider pretreatment with bleaching agents. I'm personally not that convinced that pre-treatment is that helpful, but post-treatment with bleaching agents is of definite efficacy in mitigating postinflammatory hyperpigmentation."
As for treatment, nonablative resurfacing with mid-infrared lasers, including 1320-nm, 1450-nm, and 1540-nm devices, has been shown to be effective in patients with lighter skin. "This heating process causes collagen remodeling, and can have a modest effect on so-called rolling scars, which can be quite disfiguring," he said.
Another option is ablative resurfacing with non-CO2 fractional lasers such as the 1550-nm laser. "This is one of the most gentle devices in this category, but even so you have risks of postinflammatory hyperpigmentation," Dr. Alam said. "I like to err on the side of being very modest with regard to fluences. It's much better to do more treatments than to push each individual treatment at the risk of having pigmentary abnormalities."
A more aggressive approach is ablative resurfacing with CO2 fractional lasers, which "should be restricted to patients who are of lighter skin type. If they do choose this [modality], they need to understand the significant risk of postinflammatory hyperpigmentation. I would say that virtually every patient of skin of color who undergoes this treatment will have some degree of postinflammatory hyperpigmentation. In some cases they might consider that worth it if it makes their scarring better and if it can be managed after treatment so it eventually goes away."
Perhaps the most beneficial treatment for acne scars in patients of color, Dr. Alam said, is subdermal manipulation.
In one procedure, known as subcision, clinicians insert a needle with a sphere-like tip, often an 18-guage Nokor needle, underneath the skin. "By debriding the underside of the skin, you can cause some of the acne scars to float upward," he explained. "You want to ensure very good hemostasis before doing this—lidocaine with epinephrine—because you want to avoid bruising during the procedure. If done properly, this can result in modest improvement of rolling scars, and it can be done repeatedly."
Dermal fillers can be used as an adjunct. About a month after subcision procedures Dr. Alam considers collagen for fine defects, hyaluronic acid for medium defects, and calcium hydroxylapatite for deeper defects.
The best way to develop a treatment plan for acne scarring, he said, is to assess the patient's commitment to improvement and their tolerance for adverse events.
"How much annoyance and disfigurement are they willing to tolerate?" Dr. Alam asked. "If both of these are low, you might wish to restrict yourself to subcision with or without fillers, because if done properly, that almost eliminates the risk of adverse events like hyperpigmentation, and it does provide some modest improvement with relatively little cost."
If the patient is highly committed to achieving improvement but is wary of adverse events, "then you might consider subcision and fillers, followed by nonablative laser or repeated low energy non-CO2 fractional laser treatments."
In those rare patients with a high tolerance for adverse events, he said, consider CO2 fractional laser treatments "at very modest settings."
Dr. Alam said that he had no relevant financial conflicts.
PHOENIX — Educate darker skinned patients who seek treatment for acne scars that there is no remedy to make the scars completely disappear.
"Depending on the patient's skin type, the sensitivity of their skin, and how aggressively you treat them, the risk of hyperpigmentation can be relatively modest, or well over 50%. The expected degree of improvement, on the other hand, even with multiple modalities and multiple treatments, is 40%-50%. I think it's very important to explain that," said Dr. Murad Alam at the annual meeting of the American Society for Laser Medicine and Surgery.
Dr. Alam, chief of cutaneous and aesthetic surgery at Northwestern University, Chicago, said that clinicians face certain challenges in treating acne scars in patients of color, including the risk of exacerbation of active acne, risk of focal or diffuse hyperpigmentation or hypopigmentation, risk of nodularity or surface texture change, and risk of minimal effect.
To mitigate risks, Dr. Alam considers oral antibiotics in patients who have any degree of active acne, "even if they get one or two acne pimples once in a blue moon," he said. "If the acne is more than very mild, you may wish to target that as the primary goal and defer treatment of the acne scarring until the acne is under good control."
If the acne is mild, "you can start oral antibiotics at least 1 month before the acne scarring intervention, so they do have something on board to reduce the risk of an acne flare," he said. "You may also consider pretreatment with bleaching agents. I'm personally not that convinced that pre-treatment is that helpful, but post-treatment with bleaching agents is of definite efficacy in mitigating postinflammatory hyperpigmentation."
As for treatment, nonablative resurfacing with mid-infrared lasers, including 1320-nm, 1450-nm, and 1540-nm devices, has been shown to be effective in patients with lighter skin. "This heating process causes collagen remodeling, and can have a modest effect on so-called rolling scars, which can be quite disfiguring," he said.
Another option is ablative resurfacing with non-CO2 fractional lasers such as the 1550-nm laser. "This is one of the most gentle devices in this category, but even so you have risks of postinflammatory hyperpigmentation," Dr. Alam said. "I like to err on the side of being very modest with regard to fluences. It's much better to do more treatments than to push each individual treatment at the risk of having pigmentary abnormalities."
A more aggressive approach is ablative resurfacing with CO2 fractional lasers, which "should be restricted to patients who are of lighter skin type. If they do choose this [modality], they need to understand the significant risk of postinflammatory hyperpigmentation. I would say that virtually every patient of skin of color who undergoes this treatment will have some degree of postinflammatory hyperpigmentation. In some cases they might consider that worth it if it makes their scarring better and if it can be managed after treatment so it eventually goes away."
Perhaps the most beneficial treatment for acne scars in patients of color, Dr. Alam said, is subdermal manipulation.
In one procedure, known as subcision, clinicians insert a needle with a sphere-like tip, often an 18-guage Nokor needle, underneath the skin. "By debriding the underside of the skin, you can cause some of the acne scars to float upward," he explained. "You want to ensure very good hemostasis before doing this—lidocaine with epinephrine—because you want to avoid bruising during the procedure. If done properly, this can result in modest improvement of rolling scars, and it can be done repeatedly."
Dermal fillers can be used as an adjunct. About a month after subcision procedures Dr. Alam considers collagen for fine defects, hyaluronic acid for medium defects, and calcium hydroxylapatite for deeper defects.
The best way to develop a treatment plan for acne scarring, he said, is to assess the patient's commitment to improvement and their tolerance for adverse events.
"How much annoyance and disfigurement are they willing to tolerate?" Dr. Alam asked. "If both of these are low, you might wish to restrict yourself to subcision with or without fillers, because if done properly, that almost eliminates the risk of adverse events like hyperpigmentation, and it does provide some modest improvement with relatively little cost."
If the patient is highly committed to achieving improvement but is wary of adverse events, "then you might consider subcision and fillers, followed by nonablative laser or repeated low energy non-CO2 fractional laser treatments."
In those rare patients with a high tolerance for adverse events, he said, consider CO2 fractional laser treatments "at very modest settings."
Dr. Alam said that he had no relevant financial conflicts.
PHOENIX — Educate darker skinned patients who seek treatment for acne scars that there is no remedy to make the scars completely disappear.
"Depending on the patient's skin type, the sensitivity of their skin, and how aggressively you treat them, the risk of hyperpigmentation can be relatively modest, or well over 50%. The expected degree of improvement, on the other hand, even with multiple modalities and multiple treatments, is 40%-50%. I think it's very important to explain that," said Dr. Murad Alam at the annual meeting of the American Society for Laser Medicine and Surgery.
Dr. Alam, chief of cutaneous and aesthetic surgery at Northwestern University, Chicago, said that clinicians face certain challenges in treating acne scars in patients of color, including the risk of exacerbation of active acne, risk of focal or diffuse hyperpigmentation or hypopigmentation, risk of nodularity or surface texture change, and risk of minimal effect.
To mitigate risks, Dr. Alam considers oral antibiotics in patients who have any degree of active acne, "even if they get one or two acne pimples once in a blue moon," he said. "If the acne is more than very mild, you may wish to target that as the primary goal and defer treatment of the acne scarring until the acne is under good control."
If the acne is mild, "you can start oral antibiotics at least 1 month before the acne scarring intervention, so they do have something on board to reduce the risk of an acne flare," he said. "You may also consider pretreatment with bleaching agents. I'm personally not that convinced that pre-treatment is that helpful, but post-treatment with bleaching agents is of definite efficacy in mitigating postinflammatory hyperpigmentation."
As for treatment, nonablative resurfacing with mid-infrared lasers, including 1320-nm, 1450-nm, and 1540-nm devices, has been shown to be effective in patients with lighter skin. "This heating process causes collagen remodeling, and can have a modest effect on so-called rolling scars, which can be quite disfiguring," he said.
Another option is ablative resurfacing with non-CO2 fractional lasers such as the 1550-nm laser. "This is one of the most gentle devices in this category, but even so you have risks of postinflammatory hyperpigmentation," Dr. Alam said. "I like to err on the side of being very modest with regard to fluences. It's much better to do more treatments than to push each individual treatment at the risk of having pigmentary abnormalities."
A more aggressive approach is ablative resurfacing with CO2 fractional lasers, which "should be restricted to patients who are of lighter skin type. If they do choose this [modality], they need to understand the significant risk of postinflammatory hyperpigmentation. I would say that virtually every patient of skin of color who undergoes this treatment will have some degree of postinflammatory hyperpigmentation. In some cases they might consider that worth it if it makes their scarring better and if it can be managed after treatment so it eventually goes away."
Perhaps the most beneficial treatment for acne scars in patients of color, Dr. Alam said, is subdermal manipulation.
In one procedure, known as subcision, clinicians insert a needle with a sphere-like tip, often an 18-guage Nokor needle, underneath the skin. "By debriding the underside of the skin, you can cause some of the acne scars to float upward," he explained. "You want to ensure very good hemostasis before doing this—lidocaine with epinephrine—because you want to avoid bruising during the procedure. If done properly, this can result in modest improvement of rolling scars, and it can be done repeatedly."
Dermal fillers can be used as an adjunct. About a month after subcision procedures Dr. Alam considers collagen for fine defects, hyaluronic acid for medium defects, and calcium hydroxylapatite for deeper defects.
The best way to develop a treatment plan for acne scarring, he said, is to assess the patient's commitment to improvement and their tolerance for adverse events.
"How much annoyance and disfigurement are they willing to tolerate?" Dr. Alam asked. "If both of these are low, you might wish to restrict yourself to subcision with or without fillers, because if done properly, that almost eliminates the risk of adverse events like hyperpigmentation, and it does provide some modest improvement with relatively little cost."
If the patient is highly committed to achieving improvement but is wary of adverse events, "then you might consider subcision and fillers, followed by nonablative laser or repeated low energy non-CO2 fractional laser treatments."
In those rare patients with a high tolerance for adverse events, he said, consider CO2 fractional laser treatments "at very modest settings."
Dr. Alam said that he had no relevant financial conflicts.