User login
Official Newspaper of the American College of Surgeons
New HIPAA requirements
I’m hearing a lot of concern about the impending changes in the Health Insurance Portability and Accountability Act (HIPAA) – which is understandable, since the Department of Health and Human Services has presented them as "the most sweeping ... since [the Act] was first implemented."
But after a careful perusal of the new rules – all 150 three-column pages of them – I can say with a modest degree of confidence that for most physicians, compliance will not be as challenging as some (such as those trying to sell you compliance-related materials) have warned.
However, you can’t simply ignore the new regulations; definitions will be more complex, security breaches more liberally defined, and potential penalties will be stiffer. Herewith the salient points:
• Business associates. The criteria for identifying "business associates" (BAs) remain the same: nonemployees, performing "functions or activities" on behalf of the "covered entity" (your practice), that involve "creating, receiving, maintaining, or transmitting" personal health information (PHI).
Typical BAs include answering and billing services, independent transcriptionists, hardware and software companies, and any other vendors involved in creating or maintaining your medical records. Practice management consultants, attorneys, companies that store or microfilm medical records, and record-shredding services are BAs if they must have direct access to PHI to do their jobs.
Mail carriers, package-delivery people, cleaning services, copier repairmen, bank employees, and the like are not considered BAs, even though they might conceivably come in contact with PHI on occasion. You are required to use "reasonable diligence" in limiting the PHI that these folks may encounter, but you do not need to enter into written BA agreements with them.
Independent contractors who work within your practice – aestheticians and physical therapists, for example – are not considered BAs either, and do not need to sign a BA agreement; just train them, as you do your employees. (I’ll have more on HIPAA and OSHA training in a future column.)
What is new is the additional onus placed on physicians for confidentiality breaches committed by their BAs. It’s not enough to simply have a BA contract. You are expected to use "reasonable diligence" in monitoring the work of your BAs. BAs and their subcontractors are directly responsible for their own actions, but the primary responsibility is ours. Let’s say that a contractor you hire to shred old medical records throws them into a trash bin instead; under the new rules, you must assume the worst-case scenario. Previously, you would only have to notify affected patients (and the government) if there was a "significant risk of financial or reputational harm," but now, any incident involving patient records is assumed to be a breach, and must be reported. Failure to do so could subject your practice, as well as the contractor, to significant fines – as high as $1 million in egregious cases.
• New patient rights. Patients will now be able to restrict the PHI shared with third-party insurers and health plans if they pay for the services themselves. They also have the right to request copies of their electronic health records, and you can bill the actual costs of responding to such a request. If you have EHR, now might be a good time to work out a system for doing this, because the response time has been decreased from 90 to 30 days – even less in some states.
• Marketing limitations. The new rule prohibits third-party-funded marketing to patients for products and services without their prior written authorization. You do not need prior authorization to market your own products and services, even when the communication is funded by a third party, but if there is any such funding, you will need to disclose it.
• Notice of privacy practices (NPP). You will need to revise your NPP to explain your relationships with BAs, and their status under the new rules. You will need to explain the breach notification process, too, as well as the new patient rights mentioned above. You must post your revised NPP in your office, and make copies available there, but you need not mail a copy to every patient.
• Get on it. The rules specify Sept. 23 as the effective date for the new regulations, although you have a year beyond that to revise your existing BA agreements. Extensions are possible, even likely.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J.
I’m hearing a lot of concern about the impending changes in the Health Insurance Portability and Accountability Act (HIPAA) – which is understandable, since the Department of Health and Human Services has presented them as "the most sweeping ... since [the Act] was first implemented."
But after a careful perusal of the new rules – all 150 three-column pages of them – I can say with a modest degree of confidence that for most physicians, compliance will not be as challenging as some (such as those trying to sell you compliance-related materials) have warned.
However, you can’t simply ignore the new regulations; definitions will be more complex, security breaches more liberally defined, and potential penalties will be stiffer. Herewith the salient points:
• Business associates. The criteria for identifying "business associates" (BAs) remain the same: nonemployees, performing "functions or activities" on behalf of the "covered entity" (your practice), that involve "creating, receiving, maintaining, or transmitting" personal health information (PHI).
Typical BAs include answering and billing services, independent transcriptionists, hardware and software companies, and any other vendors involved in creating or maintaining your medical records. Practice management consultants, attorneys, companies that store or microfilm medical records, and record-shredding services are BAs if they must have direct access to PHI to do their jobs.
Mail carriers, package-delivery people, cleaning services, copier repairmen, bank employees, and the like are not considered BAs, even though they might conceivably come in contact with PHI on occasion. You are required to use "reasonable diligence" in limiting the PHI that these folks may encounter, but you do not need to enter into written BA agreements with them.
Independent contractors who work within your practice – aestheticians and physical therapists, for example – are not considered BAs either, and do not need to sign a BA agreement; just train them, as you do your employees. (I’ll have more on HIPAA and OSHA training in a future column.)
What is new is the additional onus placed on physicians for confidentiality breaches committed by their BAs. It’s not enough to simply have a BA contract. You are expected to use "reasonable diligence" in monitoring the work of your BAs. BAs and their subcontractors are directly responsible for their own actions, but the primary responsibility is ours. Let’s say that a contractor you hire to shred old medical records throws them into a trash bin instead; under the new rules, you must assume the worst-case scenario. Previously, you would only have to notify affected patients (and the government) if there was a "significant risk of financial or reputational harm," but now, any incident involving patient records is assumed to be a breach, and must be reported. Failure to do so could subject your practice, as well as the contractor, to significant fines – as high as $1 million in egregious cases.
• New patient rights. Patients will now be able to restrict the PHI shared with third-party insurers and health plans if they pay for the services themselves. They also have the right to request copies of their electronic health records, and you can bill the actual costs of responding to such a request. If you have EHR, now might be a good time to work out a system for doing this, because the response time has been decreased from 90 to 30 days – even less in some states.
• Marketing limitations. The new rule prohibits third-party-funded marketing to patients for products and services without their prior written authorization. You do not need prior authorization to market your own products and services, even when the communication is funded by a third party, but if there is any such funding, you will need to disclose it.
• Notice of privacy practices (NPP). You will need to revise your NPP to explain your relationships with BAs, and their status under the new rules. You will need to explain the breach notification process, too, as well as the new patient rights mentioned above. You must post your revised NPP in your office, and make copies available there, but you need not mail a copy to every patient.
• Get on it. The rules specify Sept. 23 as the effective date for the new regulations, although you have a year beyond that to revise your existing BA agreements. Extensions are possible, even likely.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J.
I’m hearing a lot of concern about the impending changes in the Health Insurance Portability and Accountability Act (HIPAA) – which is understandable, since the Department of Health and Human Services has presented them as "the most sweeping ... since [the Act] was first implemented."
But after a careful perusal of the new rules – all 150 three-column pages of them – I can say with a modest degree of confidence that for most physicians, compliance will not be as challenging as some (such as those trying to sell you compliance-related materials) have warned.
However, you can’t simply ignore the new regulations; definitions will be more complex, security breaches more liberally defined, and potential penalties will be stiffer. Herewith the salient points:
• Business associates. The criteria for identifying "business associates" (BAs) remain the same: nonemployees, performing "functions or activities" on behalf of the "covered entity" (your practice), that involve "creating, receiving, maintaining, or transmitting" personal health information (PHI).
Typical BAs include answering and billing services, independent transcriptionists, hardware and software companies, and any other vendors involved in creating or maintaining your medical records. Practice management consultants, attorneys, companies that store or microfilm medical records, and record-shredding services are BAs if they must have direct access to PHI to do their jobs.
Mail carriers, package-delivery people, cleaning services, copier repairmen, bank employees, and the like are not considered BAs, even though they might conceivably come in contact with PHI on occasion. You are required to use "reasonable diligence" in limiting the PHI that these folks may encounter, but you do not need to enter into written BA agreements with them.
Independent contractors who work within your practice – aestheticians and physical therapists, for example – are not considered BAs either, and do not need to sign a BA agreement; just train them, as you do your employees. (I’ll have more on HIPAA and OSHA training in a future column.)
What is new is the additional onus placed on physicians for confidentiality breaches committed by their BAs. It’s not enough to simply have a BA contract. You are expected to use "reasonable diligence" in monitoring the work of your BAs. BAs and their subcontractors are directly responsible for their own actions, but the primary responsibility is ours. Let’s say that a contractor you hire to shred old medical records throws them into a trash bin instead; under the new rules, you must assume the worst-case scenario. Previously, you would only have to notify affected patients (and the government) if there was a "significant risk of financial or reputational harm," but now, any incident involving patient records is assumed to be a breach, and must be reported. Failure to do so could subject your practice, as well as the contractor, to significant fines – as high as $1 million in egregious cases.
• New patient rights. Patients will now be able to restrict the PHI shared with third-party insurers and health plans if they pay for the services themselves. They also have the right to request copies of their electronic health records, and you can bill the actual costs of responding to such a request. If you have EHR, now might be a good time to work out a system for doing this, because the response time has been decreased from 90 to 30 days – even less in some states.
• Marketing limitations. The new rule prohibits third-party-funded marketing to patients for products and services without their prior written authorization. You do not need prior authorization to market your own products and services, even when the communication is funded by a third party, but if there is any such funding, you will need to disclose it.
• Notice of privacy practices (NPP). You will need to revise your NPP to explain your relationships with BAs, and their status under the new rules. You will need to explain the breach notification process, too, as well as the new patient rights mentioned above. You must post your revised NPP in your office, and make copies available there, but you need not mail a copy to every patient.
• Get on it. The rules specify Sept. 23 as the effective date for the new regulations, although you have a year beyond that to revise your existing BA agreements. Extensions are possible, even likely.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J.
Hypoglycemia linked to increased morbidity risk in pediatric burn patients
LAS VEGAS – Although inpatient glucose levels in critically ill adults are generally kept between 140 and 180 mg/dL, Toronto investigators have found that it might be best to keep pediatric burn patients between 130 and 140 mg/dL.
Morbidity and mortality outcomes were better in that range when 760 children – the majority boys under 10 years old burned over half their bodies, usually by flame – were followed for 2 months after ICU admission.
"We used about 300,000 glucose measurements" during the study "to determine the ideal glucose target. For burn patients, the range of 130-140 mg/dL should be targeted. You avoid hyperglycemia as well as hypoglycemia. [Also,] a major factor to be considered" in burns "is that protein glycosylation starts at around 150 mg/dL; we burn surgeons try to be below that," said lead researcher Dr. Marc Jeschke, director of the burn center at Toronto’s Sunnybrook Health Sciences Centre.
Dr. Jeschke’s study isn’t the first to suggest that range for critically ill children. "There seems to be a signal [across] studies that this is the range we should target in order to see the benefits of glucose control," he said (e.g., J. Pediatr. 2009;155:734-9).
It’s been known that burns cause a hyperglycemic response, especially those in excess of 40% of the body. When not reined in, "you lose more grafts, you have more infections, and you [are more likely to] die," Dr. Jeschke said at the annual meeting of the Surgical Infection Society.
In its investigation, however, his team also found that, as in critically ill adults, hypoglycemia must also be avoided in pediatric burn patients.
Eighty-five patients had one hypoglycemia episode in the study, defined as blood glucose below 60?mg/dL, and 107 had two or more. The remaining 568 children had no episodes.
Twenty-one percent of patients who had hypoglycemic episodes – versus 6.5% of those who did not – developed sepsis; 47.9%, versus 10%, developed multiple organ failure, and a quarter died. Mortality was 3.3% in the nonhypoglycemic group. The differences were statistically significant.
"We [also] found that hypoglycemic patients are more inflammatory and hypermetabolic," Dr. Jeschke said.
Hypoglycemia was associated with larger burns and more inhalation injuries, so the team did a propensity analysis comparing 166 children who had hypoglycemic episodes to 166 with similar injury severities who did not.
Among those matched patients, children were 2.67 more likely to die (95% confidence interval 1.15-6.20) if they had one hypoglycemic episode, 5.58 more likely to die if they had two (95% CI 2.26-13.81), and 9.25 times more likely if they had three (95% CI 4.30-19.88).
Hypoglycemia during sepsis or at time of death was excluded in the analysis. Even so, "we don’t know" if hypoglycemia was the cause of death or a marker for another fatal process, Dr. Jeschke noted.
Whatever the case, the results indicate that just as in sick adults, "glycemic control in [pediatric] burns is an integral part of good clinical outcomes," he said.
Dr. Jeschke said he has no conflicts of interest.
Glycemic control in critically ill patients, both children and adults, has been extensively studied in the past decade. Despite the evidence for harms associated with hyperglycemia such as increased risk of infection, the optimal glucose range for critically ill patients is a moving target. As noted in Dr. Jeschke's study, the risk of mortality in critically ill pediatric burn patients treated with an insulin protocol increased as the number of hypoglycemic episodes (below 60 mg/dL) increased.
Despite the initial rapid adoption of tight glycemic control in critically ill patients, the benefits have not always outweighed the harms. Thus, in implementing glycemic control regimens, attention needs to be focused not only on the treatment of hyperglycemia but also on the avoidance of hypoglycemia in order to ensure good patient outcomes.
Dr. Lillian S. Kao, FACS, is an associate professor of surgery, University of Texas Health Science Center at Houston
Glycemic control in critically ill patients, both children and adults, has been extensively studied in the past decade. Despite the evidence for harms associated with hyperglycemia such as increased risk of infection, the optimal glucose range for critically ill patients is a moving target. As noted in Dr. Jeschke's study, the risk of mortality in critically ill pediatric burn patients treated with an insulin protocol increased as the number of hypoglycemic episodes (below 60 mg/dL) increased.
Despite the initial rapid adoption of tight glycemic control in critically ill patients, the benefits have not always outweighed the harms. Thus, in implementing glycemic control regimens, attention needs to be focused not only on the treatment of hyperglycemia but also on the avoidance of hypoglycemia in order to ensure good patient outcomes.
Dr. Lillian S. Kao, FACS, is an associate professor of surgery, University of Texas Health Science Center at Houston
Glycemic control in critically ill patients, both children and adults, has been extensively studied in the past decade. Despite the evidence for harms associated with hyperglycemia such as increased risk of infection, the optimal glucose range for critically ill patients is a moving target. As noted in Dr. Jeschke's study, the risk of mortality in critically ill pediatric burn patients treated with an insulin protocol increased as the number of hypoglycemic episodes (below 60 mg/dL) increased.
Despite the initial rapid adoption of tight glycemic control in critically ill patients, the benefits have not always outweighed the harms. Thus, in implementing glycemic control regimens, attention needs to be focused not only on the treatment of hyperglycemia but also on the avoidance of hypoglycemia in order to ensure good patient outcomes.
Dr. Lillian S. Kao, FACS, is an associate professor of surgery, University of Texas Health Science Center at Houston
LAS VEGAS – Although inpatient glucose levels in critically ill adults are generally kept between 140 and 180 mg/dL, Toronto investigators have found that it might be best to keep pediatric burn patients between 130 and 140 mg/dL.
Morbidity and mortality outcomes were better in that range when 760 children – the majority boys under 10 years old burned over half their bodies, usually by flame – were followed for 2 months after ICU admission.
"We used about 300,000 glucose measurements" during the study "to determine the ideal glucose target. For burn patients, the range of 130-140 mg/dL should be targeted. You avoid hyperglycemia as well as hypoglycemia. [Also,] a major factor to be considered" in burns "is that protein glycosylation starts at around 150 mg/dL; we burn surgeons try to be below that," said lead researcher Dr. Marc Jeschke, director of the burn center at Toronto’s Sunnybrook Health Sciences Centre.
Dr. Jeschke’s study isn’t the first to suggest that range for critically ill children. "There seems to be a signal [across] studies that this is the range we should target in order to see the benefits of glucose control," he said (e.g., J. Pediatr. 2009;155:734-9).
It’s been known that burns cause a hyperglycemic response, especially those in excess of 40% of the body. When not reined in, "you lose more grafts, you have more infections, and you [are more likely to] die," Dr. Jeschke said at the annual meeting of the Surgical Infection Society.
In its investigation, however, his team also found that, as in critically ill adults, hypoglycemia must also be avoided in pediatric burn patients.
Eighty-five patients had one hypoglycemia episode in the study, defined as blood glucose below 60?mg/dL, and 107 had two or more. The remaining 568 children had no episodes.
Twenty-one percent of patients who had hypoglycemic episodes – versus 6.5% of those who did not – developed sepsis; 47.9%, versus 10%, developed multiple organ failure, and a quarter died. Mortality was 3.3% in the nonhypoglycemic group. The differences were statistically significant.
"We [also] found that hypoglycemic patients are more inflammatory and hypermetabolic," Dr. Jeschke said.
Hypoglycemia was associated with larger burns and more inhalation injuries, so the team did a propensity analysis comparing 166 children who had hypoglycemic episodes to 166 with similar injury severities who did not.
Among those matched patients, children were 2.67 more likely to die (95% confidence interval 1.15-6.20) if they had one hypoglycemic episode, 5.58 more likely to die if they had two (95% CI 2.26-13.81), and 9.25 times more likely if they had three (95% CI 4.30-19.88).
Hypoglycemia during sepsis or at time of death was excluded in the analysis. Even so, "we don’t know" if hypoglycemia was the cause of death or a marker for another fatal process, Dr. Jeschke noted.
Whatever the case, the results indicate that just as in sick adults, "glycemic control in [pediatric] burns is an integral part of good clinical outcomes," he said.
Dr. Jeschke said he has no conflicts of interest.
LAS VEGAS – Although inpatient glucose levels in critically ill adults are generally kept between 140 and 180 mg/dL, Toronto investigators have found that it might be best to keep pediatric burn patients between 130 and 140 mg/dL.
Morbidity and mortality outcomes were better in that range when 760 children – the majority boys under 10 years old burned over half their bodies, usually by flame – were followed for 2 months after ICU admission.
"We used about 300,000 glucose measurements" during the study "to determine the ideal glucose target. For burn patients, the range of 130-140 mg/dL should be targeted. You avoid hyperglycemia as well as hypoglycemia. [Also,] a major factor to be considered" in burns "is that protein glycosylation starts at around 150 mg/dL; we burn surgeons try to be below that," said lead researcher Dr. Marc Jeschke, director of the burn center at Toronto’s Sunnybrook Health Sciences Centre.
Dr. Jeschke’s study isn’t the first to suggest that range for critically ill children. "There seems to be a signal [across] studies that this is the range we should target in order to see the benefits of glucose control," he said (e.g., J. Pediatr. 2009;155:734-9).
It’s been known that burns cause a hyperglycemic response, especially those in excess of 40% of the body. When not reined in, "you lose more grafts, you have more infections, and you [are more likely to] die," Dr. Jeschke said at the annual meeting of the Surgical Infection Society.
In its investigation, however, his team also found that, as in critically ill adults, hypoglycemia must also be avoided in pediatric burn patients.
Eighty-five patients had one hypoglycemia episode in the study, defined as blood glucose below 60?mg/dL, and 107 had two or more. The remaining 568 children had no episodes.
Twenty-one percent of patients who had hypoglycemic episodes – versus 6.5% of those who did not – developed sepsis; 47.9%, versus 10%, developed multiple organ failure, and a quarter died. Mortality was 3.3% in the nonhypoglycemic group. The differences were statistically significant.
"We [also] found that hypoglycemic patients are more inflammatory and hypermetabolic," Dr. Jeschke said.
Hypoglycemia was associated with larger burns and more inhalation injuries, so the team did a propensity analysis comparing 166 children who had hypoglycemic episodes to 166 with similar injury severities who did not.
Among those matched patients, children were 2.67 more likely to die (95% confidence interval 1.15-6.20) if they had one hypoglycemic episode, 5.58 more likely to die if they had two (95% CI 2.26-13.81), and 9.25 times more likely if they had three (95% CI 4.30-19.88).
Hypoglycemia during sepsis or at time of death was excluded in the analysis. Even so, "we don’t know" if hypoglycemia was the cause of death or a marker for another fatal process, Dr. Jeschke noted.
Whatever the case, the results indicate that just as in sick adults, "glycemic control in [pediatric] burns is an integral part of good clinical outcomes," he said.
Dr. Jeschke said he has no conflicts of interest.
AT THE SIS ANNUAL MEETING
Major finding: Severely burned children are almost three times more likely to die if they have even one hypoglycemic episode.
Data Source: Retrospective review of 760 pediatric burn patients.
Disclosures: The lead investigator said he has no disclosures.
Dilation and regurgitation complicate outcomes of ASO for TGA
Neoaortic root dilation and neoaortic valve regurgitation are common complications in infants with transposition of the great arteries who undergo an arterial switch operation for repair, and the risk of developing these changes in the neoaorta increases over time, according to the results of a retrospective database study of patients at Children’s Hospital of Wisconsin.
In addition, when dilation occurs, the dimensions may progressively enlarge over time, making it important to maintain lifelong surveillance of this population, according to a report published the Annals of Thoracic Surgery.
Although perioperative mortality and long-term survival (assessed up to 30 years) has improved in more recent eras for use of an arterial switch operation (ASO) for transposition of the great arteries (TGA), these long-term studies have also shown important late complications that may contribute to late morbidity and the need for reoperation, according to Dr. Jennifer G. Co-Vu and her colleagues at the Medical College of Wisconsin, Milwaukee.
These complications include coronary artery insufficiency, right ventricular outflow tract obstructions, and problems with the native pulmonary root and the pulmonary valve functioning as the neoaortic root and the neoaortic valve, respectively. Dr. Co-Vu and her colleagues performed their study to determine the prevalence of neoaortic root dilation and neoaortic valve regurgitation in patients treated at their institution and to determine risk factors involved in the development of these late complications.
Out of 247 patients with TGA treated with an ASO at the hospital, there were 124 patients who had at least one available postoperative transthoracic echocardiogram at least 1 year after the ASO. Median age of these patients was 0.2 months at the time of their ASO and 7.2 years at their last follow-up; 71% were boys (Ann. Thorac. Surg. 2013;95:1654-9).
Retrospective measurements of the neoaortic annulus and root were performed on all available transthoracic echocardiograms and the severity of neoaortic valve regurgitation was determined by assessing the width of the color Doppler jet of regurgitation measured at the level of the valve in the parasternal long-axis view. A jet width of 1-4 mm was defined as trivial to mild; 4-6 mm was defined as moderate; and greater than 6 mm indicated severe regurgitation, according to the researchers. Significant regurgitation was defined as moderate or severe. Significant neoaortic annulus dilation was defined as a z score of 2.5 or greater.
They evaluated potential risk factors for the development of neoaortic root dilation, annulus dilation, and neoaortic valve regurgitation, including age at ASO, sex, weight, coexisting lesions, prior interventions, and associated operations with the ASO. Coexisting lesions and prior interventions occurred in nearly 60% of the patients. The most common previous intervention was balloon atrial septostomy (54%).
Significant neoaortic root dilation developed in 88 of 124 (66%) of the patients during follow-up, with the probability of being free from a root diameter z score of 2.5 or greater of 84%, 67%, 47% and 32% at 1, 5, 10, and 15 years, respectively. Significant risk factors predicting neoaortic root dilation using multivariate analysis were a history of double outlet right ventricle (DORV), previous pulmonary artery (PA) banding, and length of follow-up. A history of ventricular septal defect (VSD), coarctation, left ventricular outflow tract obstruction, and age at ASO were not significant risk factors.
Significant annulus dilation occurred in 54% of patients, with significant risk factors including a history of VSD, history of DORV, and the presence of a dilated neoaortic root. History of PA banding and length of follow-up were not significant.
Moderate or severe neoaortic valve regurgitation occurred in 17 of 124 (14%) of the patients, with a probability of being free of these levels of regurgitation of 96%, 92%, 89%, and 75% at 1, 5, 10, and 15 years, respectively. The significant risk factors for regurgitation were history of DORV, VSD, left ventricular outflow tract obstruction, and length of follow-up.
No patient in the series reported by the researchers required reintervention on the neoaorta.
Limitations of the study included its retrospective nature; the lack of postoperative echocardiograms on all patients, which raises questions of selection bias; and an inability to account for changes in surgical and postoperative management over time, the authors noted.
"Neoaortic root dilation and neoaortic valve regurgitation are common complications in patients with TGA after repair with ASO. Patients with DORV morphologies or previous PA banding may be at higher risk for these complications," the researchers concluded.
The authors had no relevant disclosures.
Most people living with congenital heart disease are now adults. Unfortunately the majority of these adults, for unclear reasons, are not receiving expert care by congenital heart specialists. Perhaps some of these adults have a misperception that they are cured. Co-Vu and coauthors at the Medical College of Wisconsin confirm that the highly successful arterial switch operation is not a ‘cure.’ Their important, carefully executed echo study demonstrates important progressive increases in measured diameters of the neoaortic annulus and neoaortic root over the first 15 years of life. The authors point out that the dilation has not as yet led to a need for reintervention, and the late prevalence of neoaortic regurgitation is not high, although it too is slowly increasing over time. Their message is a clarion call for lifelong clinical surveillance following an arterial switch operation; a message that should be applied to all patients with congenital heart disease.
Dr. William G. Williams is executive director of the Congenital Heart Surgeons’ Society Data Center, Toronto, and emeritus professor of surgery, University of Toronto, and an associate medical editor for Thoracic Surgery News.
Most people living with congenital heart disease are now adults. Unfortunately the majority of these adults, for unclear reasons, are not receiving expert care by congenital heart specialists. Perhaps some of these adults have a misperception that they are cured. Co-Vu and coauthors at the Medical College of Wisconsin confirm that the highly successful arterial switch operation is not a ‘cure.’ Their important, carefully executed echo study demonstrates important progressive increases in measured diameters of the neoaortic annulus and neoaortic root over the first 15 years of life. The authors point out that the dilation has not as yet led to a need for reintervention, and the late prevalence of neoaortic regurgitation is not high, although it too is slowly increasing over time. Their message is a clarion call for lifelong clinical surveillance following an arterial switch operation; a message that should be applied to all patients with congenital heart disease.
Dr. William G. Williams is executive director of the Congenital Heart Surgeons’ Society Data Center, Toronto, and emeritus professor of surgery, University of Toronto, and an associate medical editor for Thoracic Surgery News.
Most people living with congenital heart disease are now adults. Unfortunately the majority of these adults, for unclear reasons, are not receiving expert care by congenital heart specialists. Perhaps some of these adults have a misperception that they are cured. Co-Vu and coauthors at the Medical College of Wisconsin confirm that the highly successful arterial switch operation is not a ‘cure.’ Their important, carefully executed echo study demonstrates important progressive increases in measured diameters of the neoaortic annulus and neoaortic root over the first 15 years of life. The authors point out that the dilation has not as yet led to a need for reintervention, and the late prevalence of neoaortic regurgitation is not high, although it too is slowly increasing over time. Their message is a clarion call for lifelong clinical surveillance following an arterial switch operation; a message that should be applied to all patients with congenital heart disease.
Dr. William G. Williams is executive director of the Congenital Heart Surgeons’ Society Data Center, Toronto, and emeritus professor of surgery, University of Toronto, and an associate medical editor for Thoracic Surgery News.
Neoaortic root dilation and neoaortic valve regurgitation are common complications in infants with transposition of the great arteries who undergo an arterial switch operation for repair, and the risk of developing these changes in the neoaorta increases over time, according to the results of a retrospective database study of patients at Children’s Hospital of Wisconsin.
In addition, when dilation occurs, the dimensions may progressively enlarge over time, making it important to maintain lifelong surveillance of this population, according to a report published the Annals of Thoracic Surgery.
Although perioperative mortality and long-term survival (assessed up to 30 years) has improved in more recent eras for use of an arterial switch operation (ASO) for transposition of the great arteries (TGA), these long-term studies have also shown important late complications that may contribute to late morbidity and the need for reoperation, according to Dr. Jennifer G. Co-Vu and her colleagues at the Medical College of Wisconsin, Milwaukee.
These complications include coronary artery insufficiency, right ventricular outflow tract obstructions, and problems with the native pulmonary root and the pulmonary valve functioning as the neoaortic root and the neoaortic valve, respectively. Dr. Co-Vu and her colleagues performed their study to determine the prevalence of neoaortic root dilation and neoaortic valve regurgitation in patients treated at their institution and to determine risk factors involved in the development of these late complications.
Out of 247 patients with TGA treated with an ASO at the hospital, there were 124 patients who had at least one available postoperative transthoracic echocardiogram at least 1 year after the ASO. Median age of these patients was 0.2 months at the time of their ASO and 7.2 years at their last follow-up; 71% were boys (Ann. Thorac. Surg. 2013;95:1654-9).
Retrospective measurements of the neoaortic annulus and root were performed on all available transthoracic echocardiograms and the severity of neoaortic valve regurgitation was determined by assessing the width of the color Doppler jet of regurgitation measured at the level of the valve in the parasternal long-axis view. A jet width of 1-4 mm was defined as trivial to mild; 4-6 mm was defined as moderate; and greater than 6 mm indicated severe regurgitation, according to the researchers. Significant regurgitation was defined as moderate or severe. Significant neoaortic annulus dilation was defined as a z score of 2.5 or greater.
They evaluated potential risk factors for the development of neoaortic root dilation, annulus dilation, and neoaortic valve regurgitation, including age at ASO, sex, weight, coexisting lesions, prior interventions, and associated operations with the ASO. Coexisting lesions and prior interventions occurred in nearly 60% of the patients. The most common previous intervention was balloon atrial septostomy (54%).
Significant neoaortic root dilation developed in 88 of 124 (66%) of the patients during follow-up, with the probability of being free from a root diameter z score of 2.5 or greater of 84%, 67%, 47% and 32% at 1, 5, 10, and 15 years, respectively. Significant risk factors predicting neoaortic root dilation using multivariate analysis were a history of double outlet right ventricle (DORV), previous pulmonary artery (PA) banding, and length of follow-up. A history of ventricular septal defect (VSD), coarctation, left ventricular outflow tract obstruction, and age at ASO were not significant risk factors.
Significant annulus dilation occurred in 54% of patients, with significant risk factors including a history of VSD, history of DORV, and the presence of a dilated neoaortic root. History of PA banding and length of follow-up were not significant.
Moderate or severe neoaortic valve regurgitation occurred in 17 of 124 (14%) of the patients, with a probability of being free of these levels of regurgitation of 96%, 92%, 89%, and 75% at 1, 5, 10, and 15 years, respectively. The significant risk factors for regurgitation were history of DORV, VSD, left ventricular outflow tract obstruction, and length of follow-up.
No patient in the series reported by the researchers required reintervention on the neoaorta.
Limitations of the study included its retrospective nature; the lack of postoperative echocardiograms on all patients, which raises questions of selection bias; and an inability to account for changes in surgical and postoperative management over time, the authors noted.
"Neoaortic root dilation and neoaortic valve regurgitation are common complications in patients with TGA after repair with ASO. Patients with DORV morphologies or previous PA banding may be at higher risk for these complications," the researchers concluded.
The authors had no relevant disclosures.
Neoaortic root dilation and neoaortic valve regurgitation are common complications in infants with transposition of the great arteries who undergo an arterial switch operation for repair, and the risk of developing these changes in the neoaorta increases over time, according to the results of a retrospective database study of patients at Children’s Hospital of Wisconsin.
In addition, when dilation occurs, the dimensions may progressively enlarge over time, making it important to maintain lifelong surveillance of this population, according to a report published the Annals of Thoracic Surgery.
Although perioperative mortality and long-term survival (assessed up to 30 years) has improved in more recent eras for use of an arterial switch operation (ASO) for transposition of the great arteries (TGA), these long-term studies have also shown important late complications that may contribute to late morbidity and the need for reoperation, according to Dr. Jennifer G. Co-Vu and her colleagues at the Medical College of Wisconsin, Milwaukee.
These complications include coronary artery insufficiency, right ventricular outflow tract obstructions, and problems with the native pulmonary root and the pulmonary valve functioning as the neoaortic root and the neoaortic valve, respectively. Dr. Co-Vu and her colleagues performed their study to determine the prevalence of neoaortic root dilation and neoaortic valve regurgitation in patients treated at their institution and to determine risk factors involved in the development of these late complications.
Out of 247 patients with TGA treated with an ASO at the hospital, there were 124 patients who had at least one available postoperative transthoracic echocardiogram at least 1 year after the ASO. Median age of these patients was 0.2 months at the time of their ASO and 7.2 years at their last follow-up; 71% were boys (Ann. Thorac. Surg. 2013;95:1654-9).
Retrospective measurements of the neoaortic annulus and root were performed on all available transthoracic echocardiograms and the severity of neoaortic valve regurgitation was determined by assessing the width of the color Doppler jet of regurgitation measured at the level of the valve in the parasternal long-axis view. A jet width of 1-4 mm was defined as trivial to mild; 4-6 mm was defined as moderate; and greater than 6 mm indicated severe regurgitation, according to the researchers. Significant regurgitation was defined as moderate or severe. Significant neoaortic annulus dilation was defined as a z score of 2.5 or greater.
They evaluated potential risk factors for the development of neoaortic root dilation, annulus dilation, and neoaortic valve regurgitation, including age at ASO, sex, weight, coexisting lesions, prior interventions, and associated operations with the ASO. Coexisting lesions and prior interventions occurred in nearly 60% of the patients. The most common previous intervention was balloon atrial septostomy (54%).
Significant neoaortic root dilation developed in 88 of 124 (66%) of the patients during follow-up, with the probability of being free from a root diameter z score of 2.5 or greater of 84%, 67%, 47% and 32% at 1, 5, 10, and 15 years, respectively. Significant risk factors predicting neoaortic root dilation using multivariate analysis were a history of double outlet right ventricle (DORV), previous pulmonary artery (PA) banding, and length of follow-up. A history of ventricular septal defect (VSD), coarctation, left ventricular outflow tract obstruction, and age at ASO were not significant risk factors.
Significant annulus dilation occurred in 54% of patients, with significant risk factors including a history of VSD, history of DORV, and the presence of a dilated neoaortic root. History of PA banding and length of follow-up were not significant.
Moderate or severe neoaortic valve regurgitation occurred in 17 of 124 (14%) of the patients, with a probability of being free of these levels of regurgitation of 96%, 92%, 89%, and 75% at 1, 5, 10, and 15 years, respectively. The significant risk factors for regurgitation were history of DORV, VSD, left ventricular outflow tract obstruction, and length of follow-up.
No patient in the series reported by the researchers required reintervention on the neoaorta.
Limitations of the study included its retrospective nature; the lack of postoperative echocardiograms on all patients, which raises questions of selection bias; and an inability to account for changes in surgical and postoperative management over time, the authors noted.
"Neoaortic root dilation and neoaortic valve regurgitation are common complications in patients with TGA after repair with ASO. Patients with DORV morphologies or previous PA banding may be at higher risk for these complications," the researchers concluded.
The authors had no relevant disclosures.
FROM ANNALS OF THORACIC SURGERY
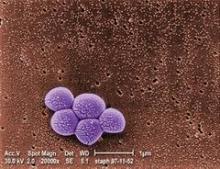
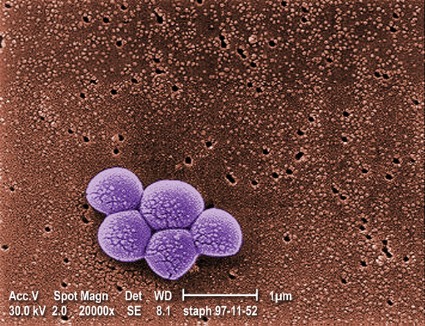
Swab both the nose and throat to catch Staph colonization
LAS VEGAS – It’s a good idea to swab both the throat and nose when looking for Staphylococcus aureus colonization; doing so picks up cases missed by swabbing the nares alone, according to researchers from the Baylor College of Medicine in Houston.
That holds true whether testing is by culture or PCR [polymerase chain reaction], said the lead investigator, Dr. Meredith Knofsky, a surgery resident there.
The team swabbed both areas preoperatively and on the day of surgery in patients undergoing operations involving hardware implants, such as new knees or hips. The 109 samples they obtained were then tested for methicillin-sensitive (MSSA) and methicillin-resistant (MRSA) S. aureus by both MRSA select media culture and the GeneXpert PCR system.
By culture, 7 throat swabs and 18 nares swabs were positive for MRSA; 20 throat and 40 nares swabs were positive for MSSA.
By PCR, 7 throat and 21 nares samples were MRSA positive; 33 throat and 51 nares swabs were positive for MSSA.
The detection rate differences weren’t surprising; PCR is known to be more accurate and the results confirm its greater sensitivity, Dr. Knofsky said at the annual meeting of the Surgical Infection Society.
The bigger finding is that "throat screening identifies additional patients missed by screening the nares alone," she said.
Adding PCR throat testing to PCR nasal screening picked up one additional MRSA and 14 additional MSSA carriers. Similarly, the addition of throat cultures to nares cultures picked up an additional MRSA and eight additional MSSA carriers.
Not infrequently, patients were positive in one location, such as the throat, but not in the other. Although "nasal carrier status of Staphylococcus aureus is an important risk factor for surgical site infections," it’s not known at the moment if that’s also true for carriage limited to the throat, Dr. Knofsky said.
"We have plans to go back and evaluate which of these patients colonized only in the oropharynx actually developed a surgical site infection. It’s important that we invest in evaluating pharyngeal carriage," she said.
In the meantime, session moderator and surgeon Dr. E. Patchen Dellinger of the University of Washington in Seattle, noted that MSSA in the study "was two to three times more common than MRSA; an MSSA infection of implanted hardware is just as devastating to the patient as an MRSA infection. I would like to urge that we not focus on MRSA alone, but consider at least in selected surgical populations seeking and suppressing any Staph that colonizes our surgical patients."
PCR could help with that because it "has the advantage of very rapid answers. The logistics of getting [colonization] information in time to do something [before an operation] is very difficult for us. PCR could make that better, [but it] isn’t standard of care mostly because it costs a lot more" than does culture, he said.
Dr. Knofsky and Dr. Dellinger said they have no relevant disclosures.
LAS VEGAS – It’s a good idea to swab both the throat and nose when looking for Staphylococcus aureus colonization; doing so picks up cases missed by swabbing the nares alone, according to researchers from the Baylor College of Medicine in Houston.
That holds true whether testing is by culture or PCR [polymerase chain reaction], said the lead investigator, Dr. Meredith Knofsky, a surgery resident there.
The team swabbed both areas preoperatively and on the day of surgery in patients undergoing operations involving hardware implants, such as new knees or hips. The 109 samples they obtained were then tested for methicillin-sensitive (MSSA) and methicillin-resistant (MRSA) S. aureus by both MRSA select media culture and the GeneXpert PCR system.
By culture, 7 throat swabs and 18 nares swabs were positive for MRSA; 20 throat and 40 nares swabs were positive for MSSA.
By PCR, 7 throat and 21 nares samples were MRSA positive; 33 throat and 51 nares swabs were positive for MSSA.
The detection rate differences weren’t surprising; PCR is known to be more accurate and the results confirm its greater sensitivity, Dr. Knofsky said at the annual meeting of the Surgical Infection Society.
The bigger finding is that "throat screening identifies additional patients missed by screening the nares alone," she said.
Adding PCR throat testing to PCR nasal screening picked up one additional MRSA and 14 additional MSSA carriers. Similarly, the addition of throat cultures to nares cultures picked up an additional MRSA and eight additional MSSA carriers.
Not infrequently, patients were positive in one location, such as the throat, but not in the other. Although "nasal carrier status of Staphylococcus aureus is an important risk factor for surgical site infections," it’s not known at the moment if that’s also true for carriage limited to the throat, Dr. Knofsky said.
"We have plans to go back and evaluate which of these patients colonized only in the oropharynx actually developed a surgical site infection. It’s important that we invest in evaluating pharyngeal carriage," she said.
In the meantime, session moderator and surgeon Dr. E. Patchen Dellinger of the University of Washington in Seattle, noted that MSSA in the study "was two to three times more common than MRSA; an MSSA infection of implanted hardware is just as devastating to the patient as an MRSA infection. I would like to urge that we not focus on MRSA alone, but consider at least in selected surgical populations seeking and suppressing any Staph that colonizes our surgical patients."
PCR could help with that because it "has the advantage of very rapid answers. The logistics of getting [colonization] information in time to do something [before an operation] is very difficult for us. PCR could make that better, [but it] isn’t standard of care mostly because it costs a lot more" than does culture, he said.
Dr. Knofsky and Dr. Dellinger said they have no relevant disclosures.
LAS VEGAS – It’s a good idea to swab both the throat and nose when looking for Staphylococcus aureus colonization; doing so picks up cases missed by swabbing the nares alone, according to researchers from the Baylor College of Medicine in Houston.
That holds true whether testing is by culture or PCR [polymerase chain reaction], said the lead investigator, Dr. Meredith Knofsky, a surgery resident there.
The team swabbed both areas preoperatively and on the day of surgery in patients undergoing operations involving hardware implants, such as new knees or hips. The 109 samples they obtained were then tested for methicillin-sensitive (MSSA) and methicillin-resistant (MRSA) S. aureus by both MRSA select media culture and the GeneXpert PCR system.
By culture, 7 throat swabs and 18 nares swabs were positive for MRSA; 20 throat and 40 nares swabs were positive for MSSA.
By PCR, 7 throat and 21 nares samples were MRSA positive; 33 throat and 51 nares swabs were positive for MSSA.
The detection rate differences weren’t surprising; PCR is known to be more accurate and the results confirm its greater sensitivity, Dr. Knofsky said at the annual meeting of the Surgical Infection Society.
The bigger finding is that "throat screening identifies additional patients missed by screening the nares alone," she said.
Adding PCR throat testing to PCR nasal screening picked up one additional MRSA and 14 additional MSSA carriers. Similarly, the addition of throat cultures to nares cultures picked up an additional MRSA and eight additional MSSA carriers.
Not infrequently, patients were positive in one location, such as the throat, but not in the other. Although "nasal carrier status of Staphylococcus aureus is an important risk factor for surgical site infections," it’s not known at the moment if that’s also true for carriage limited to the throat, Dr. Knofsky said.
"We have plans to go back and evaluate which of these patients colonized only in the oropharynx actually developed a surgical site infection. It’s important that we invest in evaluating pharyngeal carriage," she said.
In the meantime, session moderator and surgeon Dr. E. Patchen Dellinger of the University of Washington in Seattle, noted that MSSA in the study "was two to three times more common than MRSA; an MSSA infection of implanted hardware is just as devastating to the patient as an MRSA infection. I would like to urge that we not focus on MRSA alone, but consider at least in selected surgical populations seeking and suppressing any Staph that colonizes our surgical patients."
PCR could help with that because it "has the advantage of very rapid answers. The logistics of getting [colonization] information in time to do something [before an operation] is very difficult for us. PCR could make that better, [but it] isn’t standard of care mostly because it costs a lot more" than does culture, he said.
Dr. Knofsky and Dr. Dellinger said they have no relevant disclosures.
AT THE SIS ANNUAL MEETING
Major finding: In an analysis of 109 throat and nares swabs, the addition of PCR throat testing to PCR nasal screening picked up one additional MRSA and 14 additional MSSA carriers. Similarly, the addition of throat cultures to nares cultures picked up an additional MRSA and eight additional MSSA carriers.
Data source: Samples from presurgical patients
Disclosures: The lead investigator said she has no disclosures.
Benefits of laparoscopic over open colectomy decrease with operative time
PHOENIX – The longer a laparoscopic colectomy for cancer takes, the less its advantages over an open colectomy in terms of morbidity and mortality, researchers reported at the annual meeting of the American Society of Colon and Rectal Surgeons.
A team led by Dr. Matthew Bailey, a surgery resident at the University of Kentucky in Lexington, queried the National Surgical Quality Improvement Program (NSQIP) database to identify more than 4,000 patients undergoing right colectomy because of colorectal malignancy.
Results showed that compared with their peers having an open operation lasting 3 hours or less, patients having a laparoscopic operation of this duration were less likely to develop complications and to die. However, when the operations lasted more than 3 hours, there was no longer any significant difference.
Within the laparoscopic group, patients were more likely to have a procedure lasting longer than 3 hours if they had recently received radiation therapy, were morbidly obese, or had peripheral vascular disease.
"We recommend that surgeons consider an open approach if the patient has risk factors for an operative duration greater than 3 hours," Dr. Bailey said. "We also recommend surgeons consider conversion to an open approach when it is anticipated that a laparoscopic right colectomy will exceed 3 hours."
Dr. Walter Peters of Columbia (Mo.) Surgical Associates, who comoderated the session, asked, "Were the laparoscopic procedures lasting more than 3 hours concentrated in a few institutions, or were they spread across the entire NSQIP database?"
The investigators did not assess the institutional distribution, and it may not be possible to tease that information out of NSQIP, Dr. Bailey replied.
Session attendee Dr. Eric Haas, of Colorectal Surgical Associates in Houston asked what percentage of patients had a conversion from laparoscopic to open procedures and whether analyses were conducted according to intention to treat.
"NSQIP unfortunately does not allow you to discern that, there’s no CPT [Current Procedural Terminology] code for conversion," Dr. Bailey said. "We can only assume that cases that were converted laparoscopic to open were most likely ultimately coded as open. So there was no way to perform an intent-to-treat analysis."
Dr. Haas also noted that surgeon experience with laparoscopy may have played a role. "In my own experience, certainly at the beginning of the learning curve phase, I would take 3, maybe 4 hours. And the one risk factor that you can’t put [in analyses] is surgeon," he said. "So were these 3-hour cases because of the learning curve, or were they true 3-hour cases because of the patient factors?"
The NSQIP database captures the surgeon who dictates the operative report and the level of training, the highest-level resident involved, and the specialty of the surgeon (although colorectal surgery is not among the options), according to Dr. Bailey. Still, it is generally not possible to determine who did all or most of the operation.
"We did look at operative time, and it was around 138 minutes, plus-minus, for a laparoscopic right colectomy, with the reported literature being around 187 minutes. So I’m not sure if the reported literature is dated or if, in these over 200 hospitals across the nation, this is realistic of current practice trends," he said.
"The study shows that patients are probably going to have increased complications with longer surgery, whether it’s laparoscopic or open," Dr. Timothy Geiger of Vanderbilt University Medical Center, Nashville, Tenn., the session’s other comoderator, said in an interview. "It was a good study, but it needs a little bit more in-depth look, especially at things like redosing of antibiotics, whether that is done in an appropriate manner. But otherwise, it’s a great kind of intro for us to look at this."
Giving some background to the research, Dr. Bailey noted, "The use of laparoscopy in colon cancer has been shown to be equivalent to open surgery in survival and oncologic outcomes. The question of whether operative time negatively impacts laparoscopic outcomes compared to open surgery outcomes requires further investigation if we are to endorse a laparoscopic approach regardless of procedure length. We postulated that there is an operative duration where the benefits of a laparoscopic approach are negated."
The investigators analyzed data from the NSQIP database for the years 2005 through 2010, identifying patients who had a right colectomy for cancer and excluding those treated on an emergent basis, or having secondary procedures other than enterolysis or mobilization of the splenic flexure.
Analyses were based on 2,141 patients in the laparoscopic group and 2,132 patients in the open group. Procedures lasted longer than 3 hours in 18% of the former and 11% of the latter.
Compared with the open group, the laparoscopic group was younger and had lower American Society of Anesthesiologists scores, higher serum albumin levels, and lower prothrombin time and platelet count.
In unadjusted analysis among patients whose operations lasted 3 hours or less, the laparoscopic group fared better than did the open group in terms of 30-day mortality (1.1% vs 2.6%, P less than .001), cardiopulmonary and cerebrovascular complications (5.4% vs. 8.4%, P less than .001), and infectious complications (9.2% vs. 13.3%, P less than .001).
In contrast, among patients whose operations lasted more than 3 hours, differences in these outcomes were not significant. If anything, there was a trend toward a higher rate of infectious complications with laparoscopy.
To assess the role of preoperative risk factors, the investigators looked at NSQIP estimates of morbidity and mortality for all gastrointestinal and abdominal surgery by operative duration and including 37 preoperative risk factors, and found patterns differing from those in the study cohort.
Specifically, these estimates suggested mortality was consistently lower for procedures lasting more then 3 hours, whether laparoscopic or open. And the risk of infectious complications was constant for each type and less for laparoscopy, regardless of the operative duration.
Thus, "there is something other than preoperative risk factors causing an increase in mortality" with longer operative time for laparoscopic procedures in the study cohort, said Dr. Bailey, who disclosed no conflicts of interest related to the research. Also, "the increased infectious complications that we demonstrated are not related to the morbidity risk."
Patients in the laparoscopic group had a significantly higher risk of surgery lasting more than 3 hours if they had recently received radiation therapy (odds ratio, 6.5), were morbidly obese (3.0), or had peripheral vascular disease (2.5).
Hospital length of stay was consistently shorter with the laparoscopic approach, regardless of how long the operation lasted, according to Dr. Bailey.
PHOENIX – The longer a laparoscopic colectomy for cancer takes, the less its advantages over an open colectomy in terms of morbidity and mortality, researchers reported at the annual meeting of the American Society of Colon and Rectal Surgeons.
A team led by Dr. Matthew Bailey, a surgery resident at the University of Kentucky in Lexington, queried the National Surgical Quality Improvement Program (NSQIP) database to identify more than 4,000 patients undergoing right colectomy because of colorectal malignancy.
Results showed that compared with their peers having an open operation lasting 3 hours or less, patients having a laparoscopic operation of this duration were less likely to develop complications and to die. However, when the operations lasted more than 3 hours, there was no longer any significant difference.
Within the laparoscopic group, patients were more likely to have a procedure lasting longer than 3 hours if they had recently received radiation therapy, were morbidly obese, or had peripheral vascular disease.
"We recommend that surgeons consider an open approach if the patient has risk factors for an operative duration greater than 3 hours," Dr. Bailey said. "We also recommend surgeons consider conversion to an open approach when it is anticipated that a laparoscopic right colectomy will exceed 3 hours."
Dr. Walter Peters of Columbia (Mo.) Surgical Associates, who comoderated the session, asked, "Were the laparoscopic procedures lasting more than 3 hours concentrated in a few institutions, or were they spread across the entire NSQIP database?"
The investigators did not assess the institutional distribution, and it may not be possible to tease that information out of NSQIP, Dr. Bailey replied.
Session attendee Dr. Eric Haas, of Colorectal Surgical Associates in Houston asked what percentage of patients had a conversion from laparoscopic to open procedures and whether analyses were conducted according to intention to treat.
"NSQIP unfortunately does not allow you to discern that, there’s no CPT [Current Procedural Terminology] code for conversion," Dr. Bailey said. "We can only assume that cases that were converted laparoscopic to open were most likely ultimately coded as open. So there was no way to perform an intent-to-treat analysis."
Dr. Haas also noted that surgeon experience with laparoscopy may have played a role. "In my own experience, certainly at the beginning of the learning curve phase, I would take 3, maybe 4 hours. And the one risk factor that you can’t put [in analyses] is surgeon," he said. "So were these 3-hour cases because of the learning curve, or were they true 3-hour cases because of the patient factors?"
The NSQIP database captures the surgeon who dictates the operative report and the level of training, the highest-level resident involved, and the specialty of the surgeon (although colorectal surgery is not among the options), according to Dr. Bailey. Still, it is generally not possible to determine who did all or most of the operation.
"We did look at operative time, and it was around 138 minutes, plus-minus, for a laparoscopic right colectomy, with the reported literature being around 187 minutes. So I’m not sure if the reported literature is dated or if, in these over 200 hospitals across the nation, this is realistic of current practice trends," he said.
"The study shows that patients are probably going to have increased complications with longer surgery, whether it’s laparoscopic or open," Dr. Timothy Geiger of Vanderbilt University Medical Center, Nashville, Tenn., the session’s other comoderator, said in an interview. "It was a good study, but it needs a little bit more in-depth look, especially at things like redosing of antibiotics, whether that is done in an appropriate manner. But otherwise, it’s a great kind of intro for us to look at this."
Giving some background to the research, Dr. Bailey noted, "The use of laparoscopy in colon cancer has been shown to be equivalent to open surgery in survival and oncologic outcomes. The question of whether operative time negatively impacts laparoscopic outcomes compared to open surgery outcomes requires further investigation if we are to endorse a laparoscopic approach regardless of procedure length. We postulated that there is an operative duration where the benefits of a laparoscopic approach are negated."
The investigators analyzed data from the NSQIP database for the years 2005 through 2010, identifying patients who had a right colectomy for cancer and excluding those treated on an emergent basis, or having secondary procedures other than enterolysis or mobilization of the splenic flexure.
Analyses were based on 2,141 patients in the laparoscopic group and 2,132 patients in the open group. Procedures lasted longer than 3 hours in 18% of the former and 11% of the latter.
Compared with the open group, the laparoscopic group was younger and had lower American Society of Anesthesiologists scores, higher serum albumin levels, and lower prothrombin time and platelet count.
In unadjusted analysis among patients whose operations lasted 3 hours or less, the laparoscopic group fared better than did the open group in terms of 30-day mortality (1.1% vs 2.6%, P less than .001), cardiopulmonary and cerebrovascular complications (5.4% vs. 8.4%, P less than .001), and infectious complications (9.2% vs. 13.3%, P less than .001).
In contrast, among patients whose operations lasted more than 3 hours, differences in these outcomes were not significant. If anything, there was a trend toward a higher rate of infectious complications with laparoscopy.
To assess the role of preoperative risk factors, the investigators looked at NSQIP estimates of morbidity and mortality for all gastrointestinal and abdominal surgery by operative duration and including 37 preoperative risk factors, and found patterns differing from those in the study cohort.
Specifically, these estimates suggested mortality was consistently lower for procedures lasting more then 3 hours, whether laparoscopic or open. And the risk of infectious complications was constant for each type and less for laparoscopy, regardless of the operative duration.
Thus, "there is something other than preoperative risk factors causing an increase in mortality" with longer operative time for laparoscopic procedures in the study cohort, said Dr. Bailey, who disclosed no conflicts of interest related to the research. Also, "the increased infectious complications that we demonstrated are not related to the morbidity risk."
Patients in the laparoscopic group had a significantly higher risk of surgery lasting more than 3 hours if they had recently received radiation therapy (odds ratio, 6.5), were morbidly obese (3.0), or had peripheral vascular disease (2.5).
Hospital length of stay was consistently shorter with the laparoscopic approach, regardless of how long the operation lasted, according to Dr. Bailey.
PHOENIX – The longer a laparoscopic colectomy for cancer takes, the less its advantages over an open colectomy in terms of morbidity and mortality, researchers reported at the annual meeting of the American Society of Colon and Rectal Surgeons.
A team led by Dr. Matthew Bailey, a surgery resident at the University of Kentucky in Lexington, queried the National Surgical Quality Improvement Program (NSQIP) database to identify more than 4,000 patients undergoing right colectomy because of colorectal malignancy.
Results showed that compared with their peers having an open operation lasting 3 hours or less, patients having a laparoscopic operation of this duration were less likely to develop complications and to die. However, when the operations lasted more than 3 hours, there was no longer any significant difference.
Within the laparoscopic group, patients were more likely to have a procedure lasting longer than 3 hours if they had recently received radiation therapy, were morbidly obese, or had peripheral vascular disease.
"We recommend that surgeons consider an open approach if the patient has risk factors for an operative duration greater than 3 hours," Dr. Bailey said. "We also recommend surgeons consider conversion to an open approach when it is anticipated that a laparoscopic right colectomy will exceed 3 hours."
Dr. Walter Peters of Columbia (Mo.) Surgical Associates, who comoderated the session, asked, "Were the laparoscopic procedures lasting more than 3 hours concentrated in a few institutions, or were they spread across the entire NSQIP database?"
The investigators did not assess the institutional distribution, and it may not be possible to tease that information out of NSQIP, Dr. Bailey replied.
Session attendee Dr. Eric Haas, of Colorectal Surgical Associates in Houston asked what percentage of patients had a conversion from laparoscopic to open procedures and whether analyses were conducted according to intention to treat.
"NSQIP unfortunately does not allow you to discern that, there’s no CPT [Current Procedural Terminology] code for conversion," Dr. Bailey said. "We can only assume that cases that were converted laparoscopic to open were most likely ultimately coded as open. So there was no way to perform an intent-to-treat analysis."
Dr. Haas also noted that surgeon experience with laparoscopy may have played a role. "In my own experience, certainly at the beginning of the learning curve phase, I would take 3, maybe 4 hours. And the one risk factor that you can’t put [in analyses] is surgeon," he said. "So were these 3-hour cases because of the learning curve, or were they true 3-hour cases because of the patient factors?"
The NSQIP database captures the surgeon who dictates the operative report and the level of training, the highest-level resident involved, and the specialty of the surgeon (although colorectal surgery is not among the options), according to Dr. Bailey. Still, it is generally not possible to determine who did all or most of the operation.
"We did look at operative time, and it was around 138 minutes, plus-minus, for a laparoscopic right colectomy, with the reported literature being around 187 minutes. So I’m not sure if the reported literature is dated or if, in these over 200 hospitals across the nation, this is realistic of current practice trends," he said.
"The study shows that patients are probably going to have increased complications with longer surgery, whether it’s laparoscopic or open," Dr. Timothy Geiger of Vanderbilt University Medical Center, Nashville, Tenn., the session’s other comoderator, said in an interview. "It was a good study, but it needs a little bit more in-depth look, especially at things like redosing of antibiotics, whether that is done in an appropriate manner. But otherwise, it’s a great kind of intro for us to look at this."
Giving some background to the research, Dr. Bailey noted, "The use of laparoscopy in colon cancer has been shown to be equivalent to open surgery in survival and oncologic outcomes. The question of whether operative time negatively impacts laparoscopic outcomes compared to open surgery outcomes requires further investigation if we are to endorse a laparoscopic approach regardless of procedure length. We postulated that there is an operative duration where the benefits of a laparoscopic approach are negated."
The investigators analyzed data from the NSQIP database for the years 2005 through 2010, identifying patients who had a right colectomy for cancer and excluding those treated on an emergent basis, or having secondary procedures other than enterolysis or mobilization of the splenic flexure.
Analyses were based on 2,141 patients in the laparoscopic group and 2,132 patients in the open group. Procedures lasted longer than 3 hours in 18% of the former and 11% of the latter.
Compared with the open group, the laparoscopic group was younger and had lower American Society of Anesthesiologists scores, higher serum albumin levels, and lower prothrombin time and platelet count.
In unadjusted analysis among patients whose operations lasted 3 hours or less, the laparoscopic group fared better than did the open group in terms of 30-day mortality (1.1% vs 2.6%, P less than .001), cardiopulmonary and cerebrovascular complications (5.4% vs. 8.4%, P less than .001), and infectious complications (9.2% vs. 13.3%, P less than .001).
In contrast, among patients whose operations lasted more than 3 hours, differences in these outcomes were not significant. If anything, there was a trend toward a higher rate of infectious complications with laparoscopy.
To assess the role of preoperative risk factors, the investigators looked at NSQIP estimates of morbidity and mortality for all gastrointestinal and abdominal surgery by operative duration and including 37 preoperative risk factors, and found patterns differing from those in the study cohort.
Specifically, these estimates suggested mortality was consistently lower for procedures lasting more then 3 hours, whether laparoscopic or open. And the risk of infectious complications was constant for each type and less for laparoscopy, regardless of the operative duration.
Thus, "there is something other than preoperative risk factors causing an increase in mortality" with longer operative time for laparoscopic procedures in the study cohort, said Dr. Bailey, who disclosed no conflicts of interest related to the research. Also, "the increased infectious complications that we demonstrated are not related to the morbidity risk."
Patients in the laparoscopic group had a significantly higher risk of surgery lasting more than 3 hours if they had recently received radiation therapy (odds ratio, 6.5), were morbidly obese (3.0), or had peripheral vascular disease (2.5).
Hospital length of stay was consistently shorter with the laparoscopic approach, regardless of how long the operation lasted, according to Dr. Bailey.
AT THE ASCRS ANNUAL MEETING
Major Finding: The rates of complications and death postoperatively were lower with the laparoscopic approach if the operation lasted 3 hours or less, but not if it lasted longer.
Data Source: A retrospective cohort study of 4,273 cases of laparoscopic or open right colectomy for cancer.
Disclosures: Dr. Bailey disclosed no relevant conflicts of interest.
Bariatric surgery less efficacious in blacks
ORLANDO – Although obesity is more prevalent among blacks, fewer get bariatric surgery, and for those who do, the outcomes are less efficacious than for whites and Hispanics, according to analysis of a national database, examining the influence of ethnicity on bariatric surgery.
"All qualified obese patients, particularly the rapidly growing black population, need improved access to bariatric surgery to reduce mortality," said Dr. Ranjan Sudan, vice chair of education in the department of surgery at Duke University, Durham, N.C. He presented his unpublished abstract at the annual Digestive Disease Week.
Studies have shown that bariatric surgery is an effective treatment for obesity and decreases mortality, but the reason behind the disparity and surgery outcomes is rather nuanced and not so clear (N. Engl. J. Med. 2007;357:753-61).
A 2012 study at the Louisiana State University System, Baton Rouge, found that white females appeared to lose more weight than did black females regardless of the type of bariatric surgery, although both races experienced surgical complications. Also, "black patients may be less likely to undergo bariatric surgery without insurance coverage," the authors wrote (Adv. Ther. 2012;29:970-8).
Meanwhile, a 2012 meta-analysis looking at ethnic differences in weight loss and diabetes remission after bariatric surgery found that for the percentage of excess weight loss, bariatric surgery was more effective in whites than in blacks, regardless of procedure type. "Further studies are needed to investigate the exact mechanisms behind these disparities and to determine whether ethnic differences exist in the remission of comorbidities after bariatric surgery," the authors wrote (Diabetes Care 2012;35:1951-8).
"It could be because of underlying difference in physiology among races," an area that is still poorly-understood, Dr. Vic Velanovich, professor of medicine at the University of South Florida, Tampa, said in an interview. Also, "Is this a problem of geographic variation?" he said, commenting on Dr. Sudan’s findings. "Are blacks getting their health care in such a way that they don’t have access to bariatric surgery? And the third issue is cultural. It could be very well that [the] cultural view of body image is different. So there are a lot of unanswered questions," said Dr. Velanovich, who was not involved in the study.
Dr. Sudan and his colleagues examined the primary Roux-en-Y gastric bypass surgery (RYGB) data from the American Society for Bariatric and Metabolic Surgery database, submitted by more than 1,000 surgeons and 700 hospitals between June 2007 and September 2011.
All patients gave research consent and were eligible for 1-year follow-up.
Of the 135,000 patients, 79% were white, 12% black, and 9% Hispanic. Compared with whites at baseline, black patients were younger (43 years vs. 46 years), heavier (body mass index of 50 kg/m2 vs. 48 kg/m2), and were more often hypertensive (58% vs. 53%).
Among black patients who were undergoing RYGB, 15% were male, compared with 23% white and 22% Hispanic males. More black patients had a history of hypertension (57%), compared with whites (52%) and Hispanics (41%). Hispanic patients had the least comorbid disease burden, said Dr. Sudan.
Meanwhile, more white patients had diabetes (32%), compared with Hispanics (31%) and blacks (30%), at baseline.
Follow up rates were 60% in white patients, 50% in Hispanics, and 49% in blacks.
Overall, the benefits of RYGB were significant in the three groups at 1-year follow-up, but the procedure was less efficient for black patients, according to the analysis.
For instance, although fewer black patients had diabetes at baseline, at 1-year follow-up a higher percentage of them had diabetes with less decline in diabetes rates (from 30% to 13%, decline of 59%), compared with whites (from 32% to 11%; –65%), and Hispanics (from 31% to 12%; –61%.)
Black patients also had less decline in the mean body mass index (–30%), compared with whites (–34%), and Hispanics (–32%). Their hypertension also declined less (–35%) than in whites (–49%), and Hispanics (–50%).
The mortality rates within 30 days were similar for all three group (0.23%-0.26%), but black patients had a higher rate of total adverse events (22%), compared with whites and Hispanics (17% each).
The study has some limitations, said Dr. Sudan. Some of the data is self-reported, and researchers did not stratify disease severity by ethnicity.
Recent studies shows that grade 2 or higher obesity (BMI of 35 or more) is most prevalent among blacks (26%), compared with whites (15%) and Hispanics (15%). The overall rate for all ethnicities is 15.5%. (JAMA 2012;307:491-7). Black women also have the highest rate of grade 2 or higher obesity (31%), followed by black men (21%), Hispanic women (18%), white women (17%), white men (12%), and Hispanic men (11.4%).
Dr. Sudan also pointed out that the black population has higher rates of hypertension and diabetes, compared with Hispanics and whites, while more white patients (56%) control their hypertension, compared with blacks (48%) and Hispanics (41%) (NCHS Data Brief 2012;107:1-8).
"Hypertension control is very important because hypertension is a risk factor for cardiovascular mortality," said Dr. Sudan. "If the medical control is not good, then we certainly want to consider bariatric surgery."
Dr. Sudan said the he’s planning on examining the database for geographic distribution and socioeconomic factors.
Dr. Sudan and Dr. Velanovich said they had no disclosures.
On Twitter @NaseemSMiller
This review of over 135,000 patients provided insight into the demographics of bariatric surgery patients. From a disparity perspective it was not surprising that fewer black patients received bariatric surgery and even fewer black patients paid cash for their surgery. It is well known that obesity and its associated comorbidities are more prevalent among minorities, lower socioeconomic classes, and less educated groups. It is also well known that black patients are under-represented as weight loss surgery patients.
A very important outcome not discussed in detail was the overall success of weight loss surgery in blacks and whites. Did the 4% difference in weight loss result in more failures in the black group? How was success after weight loss surgery defined? On multivariate analysis, was being black, or being in a lower socioeconomic class or in a less educated group, regardless of race, independent risk factors for weight loss surgery failure at 1 year? Or was weight loss surgery successful regardless of these variables?
A large database review may not provide information regarding the success of preoperative and postoperative behavioral modification programs. Were blacks less likely to complete a program because of costs? If so, this may represent a difference in socioeconomic status and not physiology. It is well known that compliance with nutrition and exercise has a short- and long-term effect on weight loss before and after surgery. Nutritional supplements and exercise programs are rarely covered by insurance and thus represent another cost that may result in a disparity in access not related to physiology, culture, or geography.
Finally, can the differences in this study be directly attributed to a demographic as diverse as the black race? For this conclusion, it would be necessary to differentiate and determine the value of the various ethnic origins (West Indies vs. West Africa) and geographic cultures (New York vs. Mississippi) that exist in the study population.
Terrence M. Fullum, M.D., professor of surgery, Howard University College of Medicine; chief, Division of General, Minimally Invasive, and Bariatric Surgery; and Director, Howard University Center for Wellness and Weight Loss Surgery, Howard University Hospital, Washington. He has no disclosures.
This review of over 135,000 patients provided insight into the demographics of bariatric surgery patients. From a disparity perspective it was not surprising that fewer black patients received bariatric surgery and even fewer black patients paid cash for their surgery. It is well known that obesity and its associated comorbidities are more prevalent among minorities, lower socioeconomic classes, and less educated groups. It is also well known that black patients are under-represented as weight loss surgery patients.
A very important outcome not discussed in detail was the overall success of weight loss surgery in blacks and whites. Did the 4% difference in weight loss result in more failures in the black group? How was success after weight loss surgery defined? On multivariate analysis, was being black, or being in a lower socioeconomic class or in a less educated group, regardless of race, independent risk factors for weight loss surgery failure at 1 year? Or was weight loss surgery successful regardless of these variables?
A large database review may not provide information regarding the success of preoperative and postoperative behavioral modification programs. Were blacks less likely to complete a program because of costs? If so, this may represent a difference in socioeconomic status and not physiology. It is well known that compliance with nutrition and exercise has a short- and long-term effect on weight loss before and after surgery. Nutritional supplements and exercise programs are rarely covered by insurance and thus represent another cost that may result in a disparity in access not related to physiology, culture, or geography.
Finally, can the differences in this study be directly attributed to a demographic as diverse as the black race? For this conclusion, it would be necessary to differentiate and determine the value of the various ethnic origins (West Indies vs. West Africa) and geographic cultures (New York vs. Mississippi) that exist in the study population.
Terrence M. Fullum, M.D., professor of surgery, Howard University College of Medicine; chief, Division of General, Minimally Invasive, and Bariatric Surgery; and Director, Howard University Center for Wellness and Weight Loss Surgery, Howard University Hospital, Washington. He has no disclosures.
This review of over 135,000 patients provided insight into the demographics of bariatric surgery patients. From a disparity perspective it was not surprising that fewer black patients received bariatric surgery and even fewer black patients paid cash for their surgery. It is well known that obesity and its associated comorbidities are more prevalent among minorities, lower socioeconomic classes, and less educated groups. It is also well known that black patients are under-represented as weight loss surgery patients.
A very important outcome not discussed in detail was the overall success of weight loss surgery in blacks and whites. Did the 4% difference in weight loss result in more failures in the black group? How was success after weight loss surgery defined? On multivariate analysis, was being black, or being in a lower socioeconomic class or in a less educated group, regardless of race, independent risk factors for weight loss surgery failure at 1 year? Or was weight loss surgery successful regardless of these variables?
A large database review may not provide information regarding the success of preoperative and postoperative behavioral modification programs. Were blacks less likely to complete a program because of costs? If so, this may represent a difference in socioeconomic status and not physiology. It is well known that compliance with nutrition and exercise has a short- and long-term effect on weight loss before and after surgery. Nutritional supplements and exercise programs are rarely covered by insurance and thus represent another cost that may result in a disparity in access not related to physiology, culture, or geography.
Finally, can the differences in this study be directly attributed to a demographic as diverse as the black race? For this conclusion, it would be necessary to differentiate and determine the value of the various ethnic origins (West Indies vs. West Africa) and geographic cultures (New York vs. Mississippi) that exist in the study population.
Terrence M. Fullum, M.D., professor of surgery, Howard University College of Medicine; chief, Division of General, Minimally Invasive, and Bariatric Surgery; and Director, Howard University Center for Wellness and Weight Loss Surgery, Howard University Hospital, Washington. He has no disclosures.
ORLANDO – Although obesity is more prevalent among blacks, fewer get bariatric surgery, and for those who do, the outcomes are less efficacious than for whites and Hispanics, according to analysis of a national database, examining the influence of ethnicity on bariatric surgery.
"All qualified obese patients, particularly the rapidly growing black population, need improved access to bariatric surgery to reduce mortality," said Dr. Ranjan Sudan, vice chair of education in the department of surgery at Duke University, Durham, N.C. He presented his unpublished abstract at the annual Digestive Disease Week.
Studies have shown that bariatric surgery is an effective treatment for obesity and decreases mortality, but the reason behind the disparity and surgery outcomes is rather nuanced and not so clear (N. Engl. J. Med. 2007;357:753-61).
A 2012 study at the Louisiana State University System, Baton Rouge, found that white females appeared to lose more weight than did black females regardless of the type of bariatric surgery, although both races experienced surgical complications. Also, "black patients may be less likely to undergo bariatric surgery without insurance coverage," the authors wrote (Adv. Ther. 2012;29:970-8).
Meanwhile, a 2012 meta-analysis looking at ethnic differences in weight loss and diabetes remission after bariatric surgery found that for the percentage of excess weight loss, bariatric surgery was more effective in whites than in blacks, regardless of procedure type. "Further studies are needed to investigate the exact mechanisms behind these disparities and to determine whether ethnic differences exist in the remission of comorbidities after bariatric surgery," the authors wrote (Diabetes Care 2012;35:1951-8).
"It could be because of underlying difference in physiology among races," an area that is still poorly-understood, Dr. Vic Velanovich, professor of medicine at the University of South Florida, Tampa, said in an interview. Also, "Is this a problem of geographic variation?" he said, commenting on Dr. Sudan’s findings. "Are blacks getting their health care in such a way that they don’t have access to bariatric surgery? And the third issue is cultural. It could be very well that [the] cultural view of body image is different. So there are a lot of unanswered questions," said Dr. Velanovich, who was not involved in the study.
Dr. Sudan and his colleagues examined the primary Roux-en-Y gastric bypass surgery (RYGB) data from the American Society for Bariatric and Metabolic Surgery database, submitted by more than 1,000 surgeons and 700 hospitals between June 2007 and September 2011.
All patients gave research consent and were eligible for 1-year follow-up.
Of the 135,000 patients, 79% were white, 12% black, and 9% Hispanic. Compared with whites at baseline, black patients were younger (43 years vs. 46 years), heavier (body mass index of 50 kg/m2 vs. 48 kg/m2), and were more often hypertensive (58% vs. 53%).
Among black patients who were undergoing RYGB, 15% were male, compared with 23% white and 22% Hispanic males. More black patients had a history of hypertension (57%), compared with whites (52%) and Hispanics (41%). Hispanic patients had the least comorbid disease burden, said Dr. Sudan.
Meanwhile, more white patients had diabetes (32%), compared with Hispanics (31%) and blacks (30%), at baseline.
Follow up rates were 60% in white patients, 50% in Hispanics, and 49% in blacks.
Overall, the benefits of RYGB were significant in the three groups at 1-year follow-up, but the procedure was less efficient for black patients, according to the analysis.
For instance, although fewer black patients had diabetes at baseline, at 1-year follow-up a higher percentage of them had diabetes with less decline in diabetes rates (from 30% to 13%, decline of 59%), compared with whites (from 32% to 11%; –65%), and Hispanics (from 31% to 12%; –61%.)
Black patients also had less decline in the mean body mass index (–30%), compared with whites (–34%), and Hispanics (–32%). Their hypertension also declined less (–35%) than in whites (–49%), and Hispanics (–50%).
The mortality rates within 30 days were similar for all three group (0.23%-0.26%), but black patients had a higher rate of total adverse events (22%), compared with whites and Hispanics (17% each).
The study has some limitations, said Dr. Sudan. Some of the data is self-reported, and researchers did not stratify disease severity by ethnicity.
Recent studies shows that grade 2 or higher obesity (BMI of 35 or more) is most prevalent among blacks (26%), compared with whites (15%) and Hispanics (15%). The overall rate for all ethnicities is 15.5%. (JAMA 2012;307:491-7). Black women also have the highest rate of grade 2 or higher obesity (31%), followed by black men (21%), Hispanic women (18%), white women (17%), white men (12%), and Hispanic men (11.4%).
Dr. Sudan also pointed out that the black population has higher rates of hypertension and diabetes, compared with Hispanics and whites, while more white patients (56%) control their hypertension, compared with blacks (48%) and Hispanics (41%) (NCHS Data Brief 2012;107:1-8).
"Hypertension control is very important because hypertension is a risk factor for cardiovascular mortality," said Dr. Sudan. "If the medical control is not good, then we certainly want to consider bariatric surgery."
Dr. Sudan said the he’s planning on examining the database for geographic distribution and socioeconomic factors.
Dr. Sudan and Dr. Velanovich said they had no disclosures.
On Twitter @NaseemSMiller
ORLANDO – Although obesity is more prevalent among blacks, fewer get bariatric surgery, and for those who do, the outcomes are less efficacious than for whites and Hispanics, according to analysis of a national database, examining the influence of ethnicity on bariatric surgery.
"All qualified obese patients, particularly the rapidly growing black population, need improved access to bariatric surgery to reduce mortality," said Dr. Ranjan Sudan, vice chair of education in the department of surgery at Duke University, Durham, N.C. He presented his unpublished abstract at the annual Digestive Disease Week.
Studies have shown that bariatric surgery is an effective treatment for obesity and decreases mortality, but the reason behind the disparity and surgery outcomes is rather nuanced and not so clear (N. Engl. J. Med. 2007;357:753-61).
A 2012 study at the Louisiana State University System, Baton Rouge, found that white females appeared to lose more weight than did black females regardless of the type of bariatric surgery, although both races experienced surgical complications. Also, "black patients may be less likely to undergo bariatric surgery without insurance coverage," the authors wrote (Adv. Ther. 2012;29:970-8).
Meanwhile, a 2012 meta-analysis looking at ethnic differences in weight loss and diabetes remission after bariatric surgery found that for the percentage of excess weight loss, bariatric surgery was more effective in whites than in blacks, regardless of procedure type. "Further studies are needed to investigate the exact mechanisms behind these disparities and to determine whether ethnic differences exist in the remission of comorbidities after bariatric surgery," the authors wrote (Diabetes Care 2012;35:1951-8).
"It could be because of underlying difference in physiology among races," an area that is still poorly-understood, Dr. Vic Velanovich, professor of medicine at the University of South Florida, Tampa, said in an interview. Also, "Is this a problem of geographic variation?" he said, commenting on Dr. Sudan’s findings. "Are blacks getting their health care in such a way that they don’t have access to bariatric surgery? And the third issue is cultural. It could be very well that [the] cultural view of body image is different. So there are a lot of unanswered questions," said Dr. Velanovich, who was not involved in the study.
Dr. Sudan and his colleagues examined the primary Roux-en-Y gastric bypass surgery (RYGB) data from the American Society for Bariatric and Metabolic Surgery database, submitted by more than 1,000 surgeons and 700 hospitals between June 2007 and September 2011.
All patients gave research consent and were eligible for 1-year follow-up.
Of the 135,000 patients, 79% were white, 12% black, and 9% Hispanic. Compared with whites at baseline, black patients were younger (43 years vs. 46 years), heavier (body mass index of 50 kg/m2 vs. 48 kg/m2), and were more often hypertensive (58% vs. 53%).
Among black patients who were undergoing RYGB, 15% were male, compared with 23% white and 22% Hispanic males. More black patients had a history of hypertension (57%), compared with whites (52%) and Hispanics (41%). Hispanic patients had the least comorbid disease burden, said Dr. Sudan.
Meanwhile, more white patients had diabetes (32%), compared with Hispanics (31%) and blacks (30%), at baseline.
Follow up rates were 60% in white patients, 50% in Hispanics, and 49% in blacks.
Overall, the benefits of RYGB were significant in the three groups at 1-year follow-up, but the procedure was less efficient for black patients, according to the analysis.
For instance, although fewer black patients had diabetes at baseline, at 1-year follow-up a higher percentage of them had diabetes with less decline in diabetes rates (from 30% to 13%, decline of 59%), compared with whites (from 32% to 11%; –65%), and Hispanics (from 31% to 12%; –61%.)
Black patients also had less decline in the mean body mass index (–30%), compared with whites (–34%), and Hispanics (–32%). Their hypertension also declined less (–35%) than in whites (–49%), and Hispanics (–50%).
The mortality rates within 30 days were similar for all three group (0.23%-0.26%), but black patients had a higher rate of total adverse events (22%), compared with whites and Hispanics (17% each).
The study has some limitations, said Dr. Sudan. Some of the data is self-reported, and researchers did not stratify disease severity by ethnicity.
Recent studies shows that grade 2 or higher obesity (BMI of 35 or more) is most prevalent among blacks (26%), compared with whites (15%) and Hispanics (15%). The overall rate for all ethnicities is 15.5%. (JAMA 2012;307:491-7). Black women also have the highest rate of grade 2 or higher obesity (31%), followed by black men (21%), Hispanic women (18%), white women (17%), white men (12%), and Hispanic men (11.4%).
Dr. Sudan also pointed out that the black population has higher rates of hypertension and diabetes, compared with Hispanics and whites, while more white patients (56%) control their hypertension, compared with blacks (48%) and Hispanics (41%) (NCHS Data Brief 2012;107:1-8).
"Hypertension control is very important because hypertension is a risk factor for cardiovascular mortality," said Dr. Sudan. "If the medical control is not good, then we certainly want to consider bariatric surgery."
Dr. Sudan said the he’s planning on examining the database for geographic distribution and socioeconomic factors.
Dr. Sudan and Dr. Velanovich said they had no disclosures.
On Twitter @NaseemSMiller
AT THE ANNUAL DDW
Major finding: Black patients had a smaller decline in the mean body mass index (–30%), compared with whites (–34%), and Hispanics (–32%). Their hypertension also decreased less (–35%) than in whites (49%), and Hispanics (–50%).
Data source: The primary RYGB surgery data from the American Society for Bariatric and Metabolic Surgery database, including 135,000 patients, submitted by more than 1,000 surgeons and 700 hospitals between June 2007 and September 2011.
Disclosures: Dr. Sudan and Dr. Velanovich said they had no disclosures.
HHS fundraising probe expands: The Policy & Practice Podcast
If the recent scandals related to the Internal Revenue Service, the Benghazi attack aftermath, and the search for government leakers isn’t enough for you, there’s a nice juicy health care scandal in the mix, too.
A handful of congressional committees are investigating telephone calls made by Health and Human Services Secretary Kathleen Sebelius to help bolster the work of the nonprofit group Enroll America. At a congressional hearing held June 4, Ms. Sebelius got specific about what she did and did not do and why she thinks it’s not only legal, but also ethical.
Ms. Sebelius made five phone calls as part of ongoing effort to engage private partners in fostering enrollment in the health insurance exchanges coming online later this year. Ms. Sebelius said that three of the calls were to organizations regulated by HHS: Ascension Health, Kaiser Permanente, and Johnson & Johnson. She did not ask any of these organizations to give money but did discuss with them the virtues of Enroll America, she told lawmakers. However, she testified that she did ask officials at the Robert Wood Johnson Foundation and H&R Block, organizations not regulated by HHS, to contribute to Enroll America, although she didn’t suggest a particular dollar figure.
Ms. Sebelius said she was within her legal rights under the Public Health Service Act to solicit funds for the effort from any organization, even those regulated by her agency. However, she said she drew her own line where she felt it to be proper.
While the Secretary’s testimony provided some clarity on the situation, Republicans in Congress are far from satisfied with her explanation. They are expanding their investigations into who else made calls on behalf of Enroll America and if anyone in the White House was involved in the decision to steer money that way.
Grilling Ms. Sebelius isn’t the only item on the congressional agenda. Lawmakers are also moving forward with plans to permanently replace Medicare’s Sustainable Growth Rate formula. The House GOP is pushing draft legislation that would put a greater emphasis on quality of care. But some detractors say it relies too much on the existing fee-for-service system. Either way, lawmakers say they will have a bipartisan bill on the president’s desk in just a few months.
Check out this week’s Policy & Practice podcast for all this and more on the adoption of electronic health records.
On Twitter @MaryEllenNY
If the recent scandals related to the Internal Revenue Service, the Benghazi attack aftermath, and the search for government leakers isn’t enough for you, there’s a nice juicy health care scandal in the mix, too.
A handful of congressional committees are investigating telephone calls made by Health and Human Services Secretary Kathleen Sebelius to help bolster the work of the nonprofit group Enroll America. At a congressional hearing held June 4, Ms. Sebelius got specific about what she did and did not do and why she thinks it’s not only legal, but also ethical.
Ms. Sebelius made five phone calls as part of ongoing effort to engage private partners in fostering enrollment in the health insurance exchanges coming online later this year. Ms. Sebelius said that three of the calls were to organizations regulated by HHS: Ascension Health, Kaiser Permanente, and Johnson & Johnson. She did not ask any of these organizations to give money but did discuss with them the virtues of Enroll America, she told lawmakers. However, she testified that she did ask officials at the Robert Wood Johnson Foundation and H&R Block, organizations not regulated by HHS, to contribute to Enroll America, although she didn’t suggest a particular dollar figure.
Ms. Sebelius said she was within her legal rights under the Public Health Service Act to solicit funds for the effort from any organization, even those regulated by her agency. However, she said she drew her own line where she felt it to be proper.
While the Secretary’s testimony provided some clarity on the situation, Republicans in Congress are far from satisfied with her explanation. They are expanding their investigations into who else made calls on behalf of Enroll America and if anyone in the White House was involved in the decision to steer money that way.
Grilling Ms. Sebelius isn’t the only item on the congressional agenda. Lawmakers are also moving forward with plans to permanently replace Medicare’s Sustainable Growth Rate formula. The House GOP is pushing draft legislation that would put a greater emphasis on quality of care. But some detractors say it relies too much on the existing fee-for-service system. Either way, lawmakers say they will have a bipartisan bill on the president’s desk in just a few months.
Check out this week’s Policy & Practice podcast for all this and more on the adoption of electronic health records.
On Twitter @MaryEllenNY
If the recent scandals related to the Internal Revenue Service, the Benghazi attack aftermath, and the search for government leakers isn’t enough for you, there’s a nice juicy health care scandal in the mix, too.
A handful of congressional committees are investigating telephone calls made by Health and Human Services Secretary Kathleen Sebelius to help bolster the work of the nonprofit group Enroll America. At a congressional hearing held June 4, Ms. Sebelius got specific about what she did and did not do and why she thinks it’s not only legal, but also ethical.
Ms. Sebelius made five phone calls as part of ongoing effort to engage private partners in fostering enrollment in the health insurance exchanges coming online later this year. Ms. Sebelius said that three of the calls were to organizations regulated by HHS: Ascension Health, Kaiser Permanente, and Johnson & Johnson. She did not ask any of these organizations to give money but did discuss with them the virtues of Enroll America, she told lawmakers. However, she testified that she did ask officials at the Robert Wood Johnson Foundation and H&R Block, organizations not regulated by HHS, to contribute to Enroll America, although she didn’t suggest a particular dollar figure.
Ms. Sebelius said she was within her legal rights under the Public Health Service Act to solicit funds for the effort from any organization, even those regulated by her agency. However, she said she drew her own line where she felt it to be proper.
While the Secretary’s testimony provided some clarity on the situation, Republicans in Congress are far from satisfied with her explanation. They are expanding their investigations into who else made calls on behalf of Enroll America and if anyone in the White House was involved in the decision to steer money that way.
Grilling Ms. Sebelius isn’t the only item on the congressional agenda. Lawmakers are also moving forward with plans to permanently replace Medicare’s Sustainable Growth Rate formula. The House GOP is pushing draft legislation that would put a greater emphasis on quality of care. But some detractors say it relies too much on the existing fee-for-service system. Either way, lawmakers say they will have a bipartisan bill on the president’s desk in just a few months.
Check out this week’s Policy & Practice podcast for all this and more on the adoption of electronic health records.
On Twitter @MaryEllenNY
Antibacterial envelope may limit cardiac device infections
DENVER – Encasing implantable cardioverter-defibrillators and cardiac resynchronization therapy devices in a proprietary antibiotic-impregnated envelope during implantation was associated with a low 90-day major infection rate in an interim analysis of a large prospective multicenter study.
The CITADEL/CENTURION study involves 1,000 patients who underwent ICD or CRT device replacement using the antibacterial envelope at 55 U.S. centers. A major device infection – defined as an infection involving the device pocket, deep tissue, or endocarditis – occurred in one patient through 3 months of prospective follow-up, for an infection incidence of 0.1%, Dr. Charles Henrikson reported at the annual meeting of the Heart Rhythm Society.
CITADEL/CENTURION is not a randomized trial. Instead, the control group consists of 533 Canadian patients in a published study, all of whom underwent ICD or CRT replacement because of device advisories or recalls. The major device infection rate in this retrospective study (JAMA 2006;295:1907-11) during a mean 2.7 months following device replacement was 1.9%, or roughly 19-fold greater than in CITADEL/CENTURION, noted Dr. Henrikson of Oregon Health and Science University, Portland.
Device replacement is a known risk factor for major device infections, which carry a substantial toll in terms of morbidity, mortality, and expense.
The antibacterial envelope, known as AIGISRx, has received Food and Drug Administration approval and is commercially available. The antibacterial envelope is designed to prevent device migration as well as infections. "It changes the device from something that’s slick and slides right in into something with an incredibly high coefficient of friction, so you need to make a larger pocket to put it in. That’s why we’re paying a lot of attention to the hematoma rate," according to Dr. Henrikson.
The device consists of a nonresorbable polypropylene mesh coated with a resorbable polymer layer, which releases rifampin and minocycline for 7-10 days. These two antibiotics are active against the pathogens that cause most device infections, including both methicillin-sensitive and -resistant Staphylococcus aureus as well as S. epidermis.
The indication for device replacement in CITADEL/CENTURION was end of battery life in about three-quarters of patients, with device upgrades and lead revisions accounting for nearly all of the rest. Explantation because of device infection was a contraindication to study participation. All subjects were on perioperative prophylactic antibiotics, as were the historical controls.
The chief device-related complication recorded during the study was major pocket hematoma requiring a change in patient management, typically open drainage or transfusion. The complication occurred in 1.5% of patients, as compared to 2.25% of the historical controls.
Two of the 1,000 patients developed generalized rashes thought by independent reviewers to be possibly related to AIGISRx.
The plan is to monitor CITADEL/CENTURION participants for device infections and mechanical complications through 12 months, Dr. Henrikson explained. Only the 3-month data were available for presentation at a late-breaking clinical trials session during Heart Rhythm 2013.
CITADEL/CENTURION is sponsored by TYRX, which markets AIGISRx. Dr. Henrikson reported having received research support from the company.
DENVER – Encasing implantable cardioverter-defibrillators and cardiac resynchronization therapy devices in a proprietary antibiotic-impregnated envelope during implantation was associated with a low 90-day major infection rate in an interim analysis of a large prospective multicenter study.
The CITADEL/CENTURION study involves 1,000 patients who underwent ICD or CRT device replacement using the antibacterial envelope at 55 U.S. centers. A major device infection – defined as an infection involving the device pocket, deep tissue, or endocarditis – occurred in one patient through 3 months of prospective follow-up, for an infection incidence of 0.1%, Dr. Charles Henrikson reported at the annual meeting of the Heart Rhythm Society.
CITADEL/CENTURION is not a randomized trial. Instead, the control group consists of 533 Canadian patients in a published study, all of whom underwent ICD or CRT replacement because of device advisories or recalls. The major device infection rate in this retrospective study (JAMA 2006;295:1907-11) during a mean 2.7 months following device replacement was 1.9%, or roughly 19-fold greater than in CITADEL/CENTURION, noted Dr. Henrikson of Oregon Health and Science University, Portland.
Device replacement is a known risk factor for major device infections, which carry a substantial toll in terms of morbidity, mortality, and expense.
The antibacterial envelope, known as AIGISRx, has received Food and Drug Administration approval and is commercially available. The antibacterial envelope is designed to prevent device migration as well as infections. "It changes the device from something that’s slick and slides right in into something with an incredibly high coefficient of friction, so you need to make a larger pocket to put it in. That’s why we’re paying a lot of attention to the hematoma rate," according to Dr. Henrikson.
The device consists of a nonresorbable polypropylene mesh coated with a resorbable polymer layer, which releases rifampin and minocycline for 7-10 days. These two antibiotics are active against the pathogens that cause most device infections, including both methicillin-sensitive and -resistant Staphylococcus aureus as well as S. epidermis.
The indication for device replacement in CITADEL/CENTURION was end of battery life in about three-quarters of patients, with device upgrades and lead revisions accounting for nearly all of the rest. Explantation because of device infection was a contraindication to study participation. All subjects were on perioperative prophylactic antibiotics, as were the historical controls.
The chief device-related complication recorded during the study was major pocket hematoma requiring a change in patient management, typically open drainage or transfusion. The complication occurred in 1.5% of patients, as compared to 2.25% of the historical controls.
Two of the 1,000 patients developed generalized rashes thought by independent reviewers to be possibly related to AIGISRx.
The plan is to monitor CITADEL/CENTURION participants for device infections and mechanical complications through 12 months, Dr. Henrikson explained. Only the 3-month data were available for presentation at a late-breaking clinical trials session during Heart Rhythm 2013.
CITADEL/CENTURION is sponsored by TYRX, which markets AIGISRx. Dr. Henrikson reported having received research support from the company.
DENVER – Encasing implantable cardioverter-defibrillators and cardiac resynchronization therapy devices in a proprietary antibiotic-impregnated envelope during implantation was associated with a low 90-day major infection rate in an interim analysis of a large prospective multicenter study.
The CITADEL/CENTURION study involves 1,000 patients who underwent ICD or CRT device replacement using the antibacterial envelope at 55 U.S. centers. A major device infection – defined as an infection involving the device pocket, deep tissue, or endocarditis – occurred in one patient through 3 months of prospective follow-up, for an infection incidence of 0.1%, Dr. Charles Henrikson reported at the annual meeting of the Heart Rhythm Society.
CITADEL/CENTURION is not a randomized trial. Instead, the control group consists of 533 Canadian patients in a published study, all of whom underwent ICD or CRT replacement because of device advisories or recalls. The major device infection rate in this retrospective study (JAMA 2006;295:1907-11) during a mean 2.7 months following device replacement was 1.9%, or roughly 19-fold greater than in CITADEL/CENTURION, noted Dr. Henrikson of Oregon Health and Science University, Portland.
Device replacement is a known risk factor for major device infections, which carry a substantial toll in terms of morbidity, mortality, and expense.
The antibacterial envelope, known as AIGISRx, has received Food and Drug Administration approval and is commercially available. The antibacterial envelope is designed to prevent device migration as well as infections. "It changes the device from something that’s slick and slides right in into something with an incredibly high coefficient of friction, so you need to make a larger pocket to put it in. That’s why we’re paying a lot of attention to the hematoma rate," according to Dr. Henrikson.
The device consists of a nonresorbable polypropylene mesh coated with a resorbable polymer layer, which releases rifampin and minocycline for 7-10 days. These two antibiotics are active against the pathogens that cause most device infections, including both methicillin-sensitive and -resistant Staphylococcus aureus as well as S. epidermis.
The indication for device replacement in CITADEL/CENTURION was end of battery life in about three-quarters of patients, with device upgrades and lead revisions accounting for nearly all of the rest. Explantation because of device infection was a contraindication to study participation. All subjects were on perioperative prophylactic antibiotics, as were the historical controls.
The chief device-related complication recorded during the study was major pocket hematoma requiring a change in patient management, typically open drainage or transfusion. The complication occurred in 1.5% of patients, as compared to 2.25% of the historical controls.
Two of the 1,000 patients developed generalized rashes thought by independent reviewers to be possibly related to AIGISRx.
The plan is to monitor CITADEL/CENTURION participants for device infections and mechanical complications through 12 months, Dr. Henrikson explained. Only the 3-month data were available for presentation at a late-breaking clinical trials session during Heart Rhythm 2013.
CITADEL/CENTURION is sponsored by TYRX, which markets AIGISRx. Dr. Henrikson reported having received research support from the company.
AT HEART RHYTHM 2013
Major finding: A major device infection – defined as an infection involving the device pocket, deep tissue, or endocarditis – occurred in one patient, for an infection incidence of 0.1%.
Data source: Three months of data from 1,000 patients in CITADEL/CENTURION study, an ongoing multicenter, prospective study.
Disclosures: The study is sponsored by TYRX, which markets the AIGISRx antibacterial envelope. The presenter reported receiving research support from the company.
Postop care program cuts pneumonia, unplanned intubation
A multidisciplinary postoperative care program of patient and staff education, early patient mobilization, and pulmonary interventions has begun to reduce the excessive rate of postsurgical pulmonary complications at a large urban safety-net hospital, according to a report published online June 5 in JAMA Surgery (formerly Archives of Surgery).
"We are eager to monitor our outcomes over a longer period, and we are stimulated by the possibility that postoperative complications may be diminished by adherence to simple, inexpensive, easily performed patient care strategies," said Dr. Michael R. Cassidy of the department of surgery, Boston University Medical Center, and his associates.
When data collected in the National Surgical Quality Improvement Program (NSQIP) revealed that their center "was a high outlier for all measured postoperative pulmonary complications," the investigators formed a multidisciplinary group to address the problem.
BUMC is the largest safety-net facility in New England. The annual income of more than half of its patients is below $20,420, approximately 25% of its patients do not speak English, and 70% belong to racial or ethnic minorities, the investigators noted.
The committee included representatives from the hospital’s departments of surgery, nursing, and quality improvement, as well as from the units on respiratory therapy, preoperative assessment, infection control, and physical therapy. To devise a program to reduce the incidence of adverse pulmonary complications, these members reviewed the sparse literature regarding prevention of postoperative pneumonia and audited postsurgical pulmonary practices at their medical center.
The audit found that patients received no formal preoperative education about the importance of lung expansion, mobility, and other strategies to prevent pulmonary complications, and that families usually weren’t included in whatever minimal education did take place. In addition, physicians’ orders for nurses regarding postoperative pulmonary care "were irregular or absent."
The program that was then developed was given the acronym "I COUGH" to help physicians, nurses, patients, and families remember its key principles: Incentive spirometry, Coughing and deep breathing, Oral care, Understanding, Getting out of bed frequently, and Head-of-the-bed elevation. It was intended for all patients on the general surgery and vascular surgery services.
I COUGH included brochures, a video, and posters to educate patients, families, nurses, and physicians about the importance of pulmonary care. Proper use of incentive spirometry was demonstrated, the use of mouthwash and toothbrushing was recommended at least twice a day, and elevation of the head of the bed to at least 30 degrees was advocated. All this information was reinforced at preoperative clinic visits and in the preoperative holding area just before surgery. Nursing staff also reiterated the information after the procedures, as did surgeons, attending physicians, and house staff during rounds.
The effort also included standardized electronic physician order sets with "specific and detailed orders for all elements of the I COUGH program." These included instructions for patients to perform deep breathing and coughing every 2 hours; for patients to perform incentive spirometry 10 times every hour while awake; for nurses to document incentive spirometry volume every 4 hours and to ensure that the head of the patient’s bed was elevated to at least 30 degrees; for patients to walk at least once on the day of operation unless contraindicated; and for patients to get out of bed and sit in a chair for a while at least 3 times per day.
Dr. Cassidy and his associates then compared data collected during the year before I COUGH was implemented to that collected during the year afterward.
Before I COUGH, 80% of 250 patients were in bed at the time of the audit, with only 19.6% seated in a chair or walking. After I COUGH, 69.1% of 250 patients were out of bed. Before I COUGH, only 52.8% of patients had an incentive spirometer within reach and an unknown number were using it appropriately, whereas afterward 77.2% of patients had the device within reach and were using it appropriately. Both findings were statistically significant.
The incidence of postoperative pneumonia was 2.6% before I COUGH, which dropped to 1.6% in the year afterward (P = .09). Similarly, the incidence of unplanned intubations was 2.0% before I COUGH, which decreased to 1.2% afterward, the authors reported (JAMA Surg. 2013 June 5 [doi: 10.1001/jamasurg.2013.358]).
These successes are due in part to the involvement of the multidisciplinary team at all stages of development of the I COUGH program, the investigators said.
"We have not imposed a standard of care by mandate, but instead have involved nursing leadership and practicing ward and ICU nurses in the process of redefining the culture.
"We found that involvement of representatives of each discipline significantly increased acceptance of the I COUGH program, and instilled a sense of commitment and pride that could not have been achieved by simply instituting and enforcing a policy without input from all parties involved," Dr. Cassidy and his colleagues added.
While the study had several limitations, including variations in data-gathering techniques and NSQIP reporting protocols, the investigators pointed to "substantial differences in nursing practice documented between the audits before and after I COUGH implementation."
"We believe that a favorable change in practice occurred as a result of our program," they wrote.
The investigators reported having no financial conflicts of interest.
Bruce J. Leavitt, M.D., commented: The reductions in postoperative pneumonia and unplanned intubations fell short of statistical significance in this study, but the investigators still demonstrated many positive outcomes, said Dr. Bruce J. Leavitt.
"Cassidy and his colleagues have shown that creating a multidisciplinary team that implements simple measures involving the pulmonary care of the surgical patient can improve outcomes and lower medical costs," he noted.
Bruce J. Leavitt, M.D., is in the department of surgery at Fletcher Allen Health Care, Burlington, Vt. He reported having no financial conflicts of interest. These remarks were taken from his invited critique accompanying Dr. Cassidy’s report (JAMA Surg. 2013 June 5 [doi: 10.1001/jamasurg.2013.375]).
Bruce J. Leavitt, M.D., commented: The reductions in postoperative pneumonia and unplanned intubations fell short of statistical significance in this study, but the investigators still demonstrated many positive outcomes, said Dr. Bruce J. Leavitt.
"Cassidy and his colleagues have shown that creating a multidisciplinary team that implements simple measures involving the pulmonary care of the surgical patient can improve outcomes and lower medical costs," he noted.
Bruce J. Leavitt, M.D., is in the department of surgery at Fletcher Allen Health Care, Burlington, Vt. He reported having no financial conflicts of interest. These remarks were taken from his invited critique accompanying Dr. Cassidy’s report (JAMA Surg. 2013 June 5 [doi: 10.1001/jamasurg.2013.375]).
Bruce J. Leavitt, M.D., commented: The reductions in postoperative pneumonia and unplanned intubations fell short of statistical significance in this study, but the investigators still demonstrated many positive outcomes, said Dr. Bruce J. Leavitt.
"Cassidy and his colleagues have shown that creating a multidisciplinary team that implements simple measures involving the pulmonary care of the surgical patient can improve outcomes and lower medical costs," he noted.
Bruce J. Leavitt, M.D., is in the department of surgery at Fletcher Allen Health Care, Burlington, Vt. He reported having no financial conflicts of interest. These remarks were taken from his invited critique accompanying Dr. Cassidy’s report (JAMA Surg. 2013 June 5 [doi: 10.1001/jamasurg.2013.375]).
A multidisciplinary postoperative care program of patient and staff education, early patient mobilization, and pulmonary interventions has begun to reduce the excessive rate of postsurgical pulmonary complications at a large urban safety-net hospital, according to a report published online June 5 in JAMA Surgery (formerly Archives of Surgery).
"We are eager to monitor our outcomes over a longer period, and we are stimulated by the possibility that postoperative complications may be diminished by adherence to simple, inexpensive, easily performed patient care strategies," said Dr. Michael R. Cassidy of the department of surgery, Boston University Medical Center, and his associates.
When data collected in the National Surgical Quality Improvement Program (NSQIP) revealed that their center "was a high outlier for all measured postoperative pulmonary complications," the investigators formed a multidisciplinary group to address the problem.
BUMC is the largest safety-net facility in New England. The annual income of more than half of its patients is below $20,420, approximately 25% of its patients do not speak English, and 70% belong to racial or ethnic minorities, the investigators noted.
The committee included representatives from the hospital’s departments of surgery, nursing, and quality improvement, as well as from the units on respiratory therapy, preoperative assessment, infection control, and physical therapy. To devise a program to reduce the incidence of adverse pulmonary complications, these members reviewed the sparse literature regarding prevention of postoperative pneumonia and audited postsurgical pulmonary practices at their medical center.
The audit found that patients received no formal preoperative education about the importance of lung expansion, mobility, and other strategies to prevent pulmonary complications, and that families usually weren’t included in whatever minimal education did take place. In addition, physicians’ orders for nurses regarding postoperative pulmonary care "were irregular or absent."
The program that was then developed was given the acronym "I COUGH" to help physicians, nurses, patients, and families remember its key principles: Incentive spirometry, Coughing and deep breathing, Oral care, Understanding, Getting out of bed frequently, and Head-of-the-bed elevation. It was intended for all patients on the general surgery and vascular surgery services.
I COUGH included brochures, a video, and posters to educate patients, families, nurses, and physicians about the importance of pulmonary care. Proper use of incentive spirometry was demonstrated, the use of mouthwash and toothbrushing was recommended at least twice a day, and elevation of the head of the bed to at least 30 degrees was advocated. All this information was reinforced at preoperative clinic visits and in the preoperative holding area just before surgery. Nursing staff also reiterated the information after the procedures, as did surgeons, attending physicians, and house staff during rounds.
The effort also included standardized electronic physician order sets with "specific and detailed orders for all elements of the I COUGH program." These included instructions for patients to perform deep breathing and coughing every 2 hours; for patients to perform incentive spirometry 10 times every hour while awake; for nurses to document incentive spirometry volume every 4 hours and to ensure that the head of the patient’s bed was elevated to at least 30 degrees; for patients to walk at least once on the day of operation unless contraindicated; and for patients to get out of bed and sit in a chair for a while at least 3 times per day.
Dr. Cassidy and his associates then compared data collected during the year before I COUGH was implemented to that collected during the year afterward.
Before I COUGH, 80% of 250 patients were in bed at the time of the audit, with only 19.6% seated in a chair or walking. After I COUGH, 69.1% of 250 patients were out of bed. Before I COUGH, only 52.8% of patients had an incentive spirometer within reach and an unknown number were using it appropriately, whereas afterward 77.2% of patients had the device within reach and were using it appropriately. Both findings were statistically significant.
The incidence of postoperative pneumonia was 2.6% before I COUGH, which dropped to 1.6% in the year afterward (P = .09). Similarly, the incidence of unplanned intubations was 2.0% before I COUGH, which decreased to 1.2% afterward, the authors reported (JAMA Surg. 2013 June 5 [doi: 10.1001/jamasurg.2013.358]).
These successes are due in part to the involvement of the multidisciplinary team at all stages of development of the I COUGH program, the investigators said.
"We have not imposed a standard of care by mandate, but instead have involved nursing leadership and practicing ward and ICU nurses in the process of redefining the culture.
"We found that involvement of representatives of each discipline significantly increased acceptance of the I COUGH program, and instilled a sense of commitment and pride that could not have been achieved by simply instituting and enforcing a policy without input from all parties involved," Dr. Cassidy and his colleagues added.
While the study had several limitations, including variations in data-gathering techniques and NSQIP reporting protocols, the investigators pointed to "substantial differences in nursing practice documented between the audits before and after I COUGH implementation."
"We believe that a favorable change in practice occurred as a result of our program," they wrote.
The investigators reported having no financial conflicts of interest.
A multidisciplinary postoperative care program of patient and staff education, early patient mobilization, and pulmonary interventions has begun to reduce the excessive rate of postsurgical pulmonary complications at a large urban safety-net hospital, according to a report published online June 5 in JAMA Surgery (formerly Archives of Surgery).
"We are eager to monitor our outcomes over a longer period, and we are stimulated by the possibility that postoperative complications may be diminished by adherence to simple, inexpensive, easily performed patient care strategies," said Dr. Michael R. Cassidy of the department of surgery, Boston University Medical Center, and his associates.
When data collected in the National Surgical Quality Improvement Program (NSQIP) revealed that their center "was a high outlier for all measured postoperative pulmonary complications," the investigators formed a multidisciplinary group to address the problem.
BUMC is the largest safety-net facility in New England. The annual income of more than half of its patients is below $20,420, approximately 25% of its patients do not speak English, and 70% belong to racial or ethnic minorities, the investigators noted.
The committee included representatives from the hospital’s departments of surgery, nursing, and quality improvement, as well as from the units on respiratory therapy, preoperative assessment, infection control, and physical therapy. To devise a program to reduce the incidence of adverse pulmonary complications, these members reviewed the sparse literature regarding prevention of postoperative pneumonia and audited postsurgical pulmonary practices at their medical center.
The audit found that patients received no formal preoperative education about the importance of lung expansion, mobility, and other strategies to prevent pulmonary complications, and that families usually weren’t included in whatever minimal education did take place. In addition, physicians’ orders for nurses regarding postoperative pulmonary care "were irregular or absent."
The program that was then developed was given the acronym "I COUGH" to help physicians, nurses, patients, and families remember its key principles: Incentive spirometry, Coughing and deep breathing, Oral care, Understanding, Getting out of bed frequently, and Head-of-the-bed elevation. It was intended for all patients on the general surgery and vascular surgery services.
I COUGH included brochures, a video, and posters to educate patients, families, nurses, and physicians about the importance of pulmonary care. Proper use of incentive spirometry was demonstrated, the use of mouthwash and toothbrushing was recommended at least twice a day, and elevation of the head of the bed to at least 30 degrees was advocated. All this information was reinforced at preoperative clinic visits and in the preoperative holding area just before surgery. Nursing staff also reiterated the information after the procedures, as did surgeons, attending physicians, and house staff during rounds.
The effort also included standardized electronic physician order sets with "specific and detailed orders for all elements of the I COUGH program." These included instructions for patients to perform deep breathing and coughing every 2 hours; for patients to perform incentive spirometry 10 times every hour while awake; for nurses to document incentive spirometry volume every 4 hours and to ensure that the head of the patient’s bed was elevated to at least 30 degrees; for patients to walk at least once on the day of operation unless contraindicated; and for patients to get out of bed and sit in a chair for a while at least 3 times per day.
Dr. Cassidy and his associates then compared data collected during the year before I COUGH was implemented to that collected during the year afterward.
Before I COUGH, 80% of 250 patients were in bed at the time of the audit, with only 19.6% seated in a chair or walking. After I COUGH, 69.1% of 250 patients were out of bed. Before I COUGH, only 52.8% of patients had an incentive spirometer within reach and an unknown number were using it appropriately, whereas afterward 77.2% of patients had the device within reach and were using it appropriately. Both findings were statistically significant.
The incidence of postoperative pneumonia was 2.6% before I COUGH, which dropped to 1.6% in the year afterward (P = .09). Similarly, the incidence of unplanned intubations was 2.0% before I COUGH, which decreased to 1.2% afterward, the authors reported (JAMA Surg. 2013 June 5 [doi: 10.1001/jamasurg.2013.358]).
These successes are due in part to the involvement of the multidisciplinary team at all stages of development of the I COUGH program, the investigators said.
"We have not imposed a standard of care by mandate, but instead have involved nursing leadership and practicing ward and ICU nurses in the process of redefining the culture.
"We found that involvement of representatives of each discipline significantly increased acceptance of the I COUGH program, and instilled a sense of commitment and pride that could not have been achieved by simply instituting and enforcing a policy without input from all parties involved," Dr. Cassidy and his colleagues added.
While the study had several limitations, including variations in data-gathering techniques and NSQIP reporting protocols, the investigators pointed to "substantial differences in nursing practice documented between the audits before and after I COUGH implementation."
"We believe that a favorable change in practice occurred as a result of our program," they wrote.
The investigators reported having no financial conflicts of interest.
FROM JAMA SURGERY
Major finding: Before I COUGH, 52.8% of patients had an incentive spirometer within reach; an unknown number were using it appropriately. Afterward, 77.2% had the device within reach and were using it appropriately.
Data source: A comparison of postoperative complications between 250 patients hospitalized before I COUGH was implemented and 250 hospitalized afterward.
Disclosures: The investigators reported having no financial conflicts of interest.
Rates of adjuvant therapy for pancreatic cancer still low
ORLANDO – The rates of adjuvant therapy and the use of surgery for resectable stage I and II pancreatic cancer have remained lower than expected, while nonsurgical therapy for the stage II disease has significantly increased, according to an analysis of a national cancer database.
The analysis showed that more patients with stage I and II resectable disease are receiving chemotherapy in addition to surgery, and fewer are undergoing chemoradiation.
But, "despite all the evidence in favor of adjuvant therapy, its use remains unacceptably low," said Siavash Raigani, a second-year medical student at Case Western Reserve University, Cleveland, who presented the abstract at the annual Digestive Disease Week.
Depending on hospital setting and stage, somewhere between one-third and two-thirds of the patients did not receive adjuvant therapy, Mr. Raigani reported.
The analysis also showed that nonsurgical therapy for the disease continues to be used at a high rate, with 43% of stage I and 60% of stage II pancreatic cancer patients undergoing surgery, "which is lower than expected," said Mr. Raigani.
The analysis reflects what previous studies have shown.
In 2007, Dr. Karl Y. Bilimoria and his colleagues analyzed the National Cancer Data Base (NCDB) for the years between 1995 and 2004 and found "the striking underuse of pancreatectomy in the United States. Of early stage pancreatic cancer patients without any identifiable contraindications, 38.2% failed to undergo surgery." (Ann. Surg. 2007;246:173-80).
"What’s more startling is that there has been no improvement in the years since Dr. Bilimoria brought this to our attention several years ago and the authors should be commended for not letting this issue rest," said Dr. John D. Allendorf of Columbia University Medical Center, New York, who called Mr. Raigani’s analysis "impressive."
Mr. Raigani and his colleagues analyzed the NCDB, selecting 47,000 patients diagnosed with stage I and II pancreatic cancer between 2003 and 2010. They analyzed the database on initial treatment – surgery alone, surgery plus chemotherapy, or surgery plus chemoradiation – and collected data on the hospital setting, community hospital or teaching-research hospital.
Results showed that there was no significant change in surgical resection rates for stage I pancreatic cancer during the study period, but there was a significant different between the two hospital settings, with 53% of patients receiving surgery in teaching hospitals, compared with 32% in community hospitals in 2010.
Similarly, the use of surgery for treatment of stage II disease didn’t change significantly over time, but a significant difference remained between teaching hospitals (60%) and community hospitals (52%) in 2010.
One issue in pancreatic cancer keeps coming up over and over again, said Dr. Vic Velanovich, professor of medicine at the University of South Florida, Tampa. "We know who is a resectable candidate based on pathologic criteria, but what we don’t know is should they be getting an operation based on associated comorbidities," he said.
The other issue has to do with where patients are getting these operations done. "The teaching hospitals or high-volume hospitals are all going to have lower mortalities. But the opposite side of that coin is if you’re at a smaller hospital, where your predicted mortality is higher, perhaps by not operating on those patient, you’re actually saving lives, because you’re not subjecting them to postoperative mortality just because of that operation," said Dr. Velanovich, who moderated the abstract session.
Meanwhile, the use of chemotherapy plus surgery for treatment of stage I and II disease increased more than twofold at both types of hospital (P less than .0001). In contrast, use of chemoradiation plus surgery decreased by roughly 30% in both types of hospitals (P less than .05), the authors reported.
The analysis showed that in community hospitals, the rate of chemotherapy for patients with stage I disease receiving surgery increased from 5% to 14%, while the chemoradiation rates decreased from 34% to 19% during the study period. For stage II patients, the rate of chemotherapy increased from 9% to 27%, and chemoradiation rates decreased from 53% to 39% (P less than .0001 for all).
In teaching hospitals, the rate of chemotherapy for stage I patients increased from 6% to 16%, while the chemoradiation rate decreased from 30% to 19% between 2003 and 2010. For stage II patients, the rate of chemotherapy increased from 9% to 32%, while chemoradiation rates decreased from 42% to 30% (P less than .0001 for all).
Mr. Raigani said the increase in the use of chemotherapy concurrent with the decrease in the use of chemoradiation in addition to surgery correlates temporally with the publication of more trials examining chemotherapy only. However, the use of adjuvant chemoradiation was still more common in the United States as of 2010. Among stage I patients, 44% received chemotherapy, compared with 56% receiving chemoradiation. In stage II patients, those rates were 47% and 53%, respectively.
Meanwhile, the use of surgery alone as first-course treatment for stage II pancreatic cancer decreased by nearly 25% at both hospital settings (P less than .0001 for both). There was no significant change in rates of surgery alone in stage I disease.
Nonsurgical treatment of stage II disease was "surprisingly high," the authors reported. It increased from 31% to 36% at teaching-research hospitals and from 41% to 43% at community hospitals (P less than .0001). There was no significant change in the use of nonsurgical therapy for stage I cancer at either hospital setting during the analysis period, although the difference based on hospital setting remained significant (44% in teaching hospitals vs. 63% in community hospitals, P less than .0001).
Mr. Raigani said some of the possible factors leading to nonsurgical therapy – in addition to age, race, and insurance type – are lack of referral because of the pessimistic view on pancreatic cancer survival and an evaluation by a surgeon inexperienced in pancreas surgery.
The analysis had several limitations, according to the authors. The NCDB provides data in aggregate form and not at an individual level, which limits the predictive factor analysis. Also, NDCB does not distinguish between adjuvant and neoadjuvant therapy.
Mr. Raigani and Dr. Velanovich had no disclosures. Dr. Allendorf is a consultant for Covidien.
On Twitter @NaseemSMiller
Dr. Karl Y. Bilimoria, National Cancer Data Base, pancreatectomy, Dr. John D. Allendorf,
ORLANDO – The rates of adjuvant therapy and the use of surgery for resectable stage I and II pancreatic cancer have remained lower than expected, while nonsurgical therapy for the stage II disease has significantly increased, according to an analysis of a national cancer database.
The analysis showed that more patients with stage I and II resectable disease are receiving chemotherapy in addition to surgery, and fewer are undergoing chemoradiation.
But, "despite all the evidence in favor of adjuvant therapy, its use remains unacceptably low," said Siavash Raigani, a second-year medical student at Case Western Reserve University, Cleveland, who presented the abstract at the annual Digestive Disease Week.
Depending on hospital setting and stage, somewhere between one-third and two-thirds of the patients did not receive adjuvant therapy, Mr. Raigani reported.
The analysis also showed that nonsurgical therapy for the disease continues to be used at a high rate, with 43% of stage I and 60% of stage II pancreatic cancer patients undergoing surgery, "which is lower than expected," said Mr. Raigani.
The analysis reflects what previous studies have shown.
In 2007, Dr. Karl Y. Bilimoria and his colleagues analyzed the National Cancer Data Base (NCDB) for the years between 1995 and 2004 and found "the striking underuse of pancreatectomy in the United States. Of early stage pancreatic cancer patients without any identifiable contraindications, 38.2% failed to undergo surgery." (Ann. Surg. 2007;246:173-80).
"What’s more startling is that there has been no improvement in the years since Dr. Bilimoria brought this to our attention several years ago and the authors should be commended for not letting this issue rest," said Dr. John D. Allendorf of Columbia University Medical Center, New York, who called Mr. Raigani’s analysis "impressive."
Mr. Raigani and his colleagues analyzed the NCDB, selecting 47,000 patients diagnosed with stage I and II pancreatic cancer between 2003 and 2010. They analyzed the database on initial treatment – surgery alone, surgery plus chemotherapy, or surgery plus chemoradiation – and collected data on the hospital setting, community hospital or teaching-research hospital.
Results showed that there was no significant change in surgical resection rates for stage I pancreatic cancer during the study period, but there was a significant different between the two hospital settings, with 53% of patients receiving surgery in teaching hospitals, compared with 32% in community hospitals in 2010.
Similarly, the use of surgery for treatment of stage II disease didn’t change significantly over time, but a significant difference remained between teaching hospitals (60%) and community hospitals (52%) in 2010.
One issue in pancreatic cancer keeps coming up over and over again, said Dr. Vic Velanovich, professor of medicine at the University of South Florida, Tampa. "We know who is a resectable candidate based on pathologic criteria, but what we don’t know is should they be getting an operation based on associated comorbidities," he said.
The other issue has to do with where patients are getting these operations done. "The teaching hospitals or high-volume hospitals are all going to have lower mortalities. But the opposite side of that coin is if you’re at a smaller hospital, where your predicted mortality is higher, perhaps by not operating on those patient, you’re actually saving lives, because you’re not subjecting them to postoperative mortality just because of that operation," said Dr. Velanovich, who moderated the abstract session.
Meanwhile, the use of chemotherapy plus surgery for treatment of stage I and II disease increased more than twofold at both types of hospital (P less than .0001). In contrast, use of chemoradiation plus surgery decreased by roughly 30% in both types of hospitals (P less than .05), the authors reported.
The analysis showed that in community hospitals, the rate of chemotherapy for patients with stage I disease receiving surgery increased from 5% to 14%, while the chemoradiation rates decreased from 34% to 19% during the study period. For stage II patients, the rate of chemotherapy increased from 9% to 27%, and chemoradiation rates decreased from 53% to 39% (P less than .0001 for all).
In teaching hospitals, the rate of chemotherapy for stage I patients increased from 6% to 16%, while the chemoradiation rate decreased from 30% to 19% between 2003 and 2010. For stage II patients, the rate of chemotherapy increased from 9% to 32%, while chemoradiation rates decreased from 42% to 30% (P less than .0001 for all).
Mr. Raigani said the increase in the use of chemotherapy concurrent with the decrease in the use of chemoradiation in addition to surgery correlates temporally with the publication of more trials examining chemotherapy only. However, the use of adjuvant chemoradiation was still more common in the United States as of 2010. Among stage I patients, 44% received chemotherapy, compared with 56% receiving chemoradiation. In stage II patients, those rates were 47% and 53%, respectively.
Meanwhile, the use of surgery alone as first-course treatment for stage II pancreatic cancer decreased by nearly 25% at both hospital settings (P less than .0001 for both). There was no significant change in rates of surgery alone in stage I disease.
Nonsurgical treatment of stage II disease was "surprisingly high," the authors reported. It increased from 31% to 36% at teaching-research hospitals and from 41% to 43% at community hospitals (P less than .0001). There was no significant change in the use of nonsurgical therapy for stage I cancer at either hospital setting during the analysis period, although the difference based on hospital setting remained significant (44% in teaching hospitals vs. 63% in community hospitals, P less than .0001).
Mr. Raigani said some of the possible factors leading to nonsurgical therapy – in addition to age, race, and insurance type – are lack of referral because of the pessimistic view on pancreatic cancer survival and an evaluation by a surgeon inexperienced in pancreas surgery.
The analysis had several limitations, according to the authors. The NCDB provides data in aggregate form and not at an individual level, which limits the predictive factor analysis. Also, NDCB does not distinguish between adjuvant and neoadjuvant therapy.
Mr. Raigani and Dr. Velanovich had no disclosures. Dr. Allendorf is a consultant for Covidien.
On Twitter @NaseemSMiller
ORLANDO – The rates of adjuvant therapy and the use of surgery for resectable stage I and II pancreatic cancer have remained lower than expected, while nonsurgical therapy for the stage II disease has significantly increased, according to an analysis of a national cancer database.
The analysis showed that more patients with stage I and II resectable disease are receiving chemotherapy in addition to surgery, and fewer are undergoing chemoradiation.
But, "despite all the evidence in favor of adjuvant therapy, its use remains unacceptably low," said Siavash Raigani, a second-year medical student at Case Western Reserve University, Cleveland, who presented the abstract at the annual Digestive Disease Week.
Depending on hospital setting and stage, somewhere between one-third and two-thirds of the patients did not receive adjuvant therapy, Mr. Raigani reported.
The analysis also showed that nonsurgical therapy for the disease continues to be used at a high rate, with 43% of stage I and 60% of stage II pancreatic cancer patients undergoing surgery, "which is lower than expected," said Mr. Raigani.
The analysis reflects what previous studies have shown.
In 2007, Dr. Karl Y. Bilimoria and his colleagues analyzed the National Cancer Data Base (NCDB) for the years between 1995 and 2004 and found "the striking underuse of pancreatectomy in the United States. Of early stage pancreatic cancer patients without any identifiable contraindications, 38.2% failed to undergo surgery." (Ann. Surg. 2007;246:173-80).
"What’s more startling is that there has been no improvement in the years since Dr. Bilimoria brought this to our attention several years ago and the authors should be commended for not letting this issue rest," said Dr. John D. Allendorf of Columbia University Medical Center, New York, who called Mr. Raigani’s analysis "impressive."
Mr. Raigani and his colleagues analyzed the NCDB, selecting 47,000 patients diagnosed with stage I and II pancreatic cancer between 2003 and 2010. They analyzed the database on initial treatment – surgery alone, surgery plus chemotherapy, or surgery plus chemoradiation – and collected data on the hospital setting, community hospital or teaching-research hospital.
Results showed that there was no significant change in surgical resection rates for stage I pancreatic cancer during the study period, but there was a significant different between the two hospital settings, with 53% of patients receiving surgery in teaching hospitals, compared with 32% in community hospitals in 2010.
Similarly, the use of surgery for treatment of stage II disease didn’t change significantly over time, but a significant difference remained between teaching hospitals (60%) and community hospitals (52%) in 2010.
One issue in pancreatic cancer keeps coming up over and over again, said Dr. Vic Velanovich, professor of medicine at the University of South Florida, Tampa. "We know who is a resectable candidate based on pathologic criteria, but what we don’t know is should they be getting an operation based on associated comorbidities," he said.
The other issue has to do with where patients are getting these operations done. "The teaching hospitals or high-volume hospitals are all going to have lower mortalities. But the opposite side of that coin is if you’re at a smaller hospital, where your predicted mortality is higher, perhaps by not operating on those patient, you’re actually saving lives, because you’re not subjecting them to postoperative mortality just because of that operation," said Dr. Velanovich, who moderated the abstract session.
Meanwhile, the use of chemotherapy plus surgery for treatment of stage I and II disease increased more than twofold at both types of hospital (P less than .0001). In contrast, use of chemoradiation plus surgery decreased by roughly 30% in both types of hospitals (P less than .05), the authors reported.
The analysis showed that in community hospitals, the rate of chemotherapy for patients with stage I disease receiving surgery increased from 5% to 14%, while the chemoradiation rates decreased from 34% to 19% during the study period. For stage II patients, the rate of chemotherapy increased from 9% to 27%, and chemoradiation rates decreased from 53% to 39% (P less than .0001 for all).
In teaching hospitals, the rate of chemotherapy for stage I patients increased from 6% to 16%, while the chemoradiation rate decreased from 30% to 19% between 2003 and 2010. For stage II patients, the rate of chemotherapy increased from 9% to 32%, while chemoradiation rates decreased from 42% to 30% (P less than .0001 for all).
Mr. Raigani said the increase in the use of chemotherapy concurrent with the decrease in the use of chemoradiation in addition to surgery correlates temporally with the publication of more trials examining chemotherapy only. However, the use of adjuvant chemoradiation was still more common in the United States as of 2010. Among stage I patients, 44% received chemotherapy, compared with 56% receiving chemoradiation. In stage II patients, those rates were 47% and 53%, respectively.
Meanwhile, the use of surgery alone as first-course treatment for stage II pancreatic cancer decreased by nearly 25% at both hospital settings (P less than .0001 for both). There was no significant change in rates of surgery alone in stage I disease.
Nonsurgical treatment of stage II disease was "surprisingly high," the authors reported. It increased from 31% to 36% at teaching-research hospitals and from 41% to 43% at community hospitals (P less than .0001). There was no significant change in the use of nonsurgical therapy for stage I cancer at either hospital setting during the analysis period, although the difference based on hospital setting remained significant (44% in teaching hospitals vs. 63% in community hospitals, P less than .0001).
Mr. Raigani said some of the possible factors leading to nonsurgical therapy – in addition to age, race, and insurance type – are lack of referral because of the pessimistic view on pancreatic cancer survival and an evaluation by a surgeon inexperienced in pancreas surgery.
The analysis had several limitations, according to the authors. The NCDB provides data in aggregate form and not at an individual level, which limits the predictive factor analysis. Also, NDCB does not distinguish between adjuvant and neoadjuvant therapy.
Mr. Raigani and Dr. Velanovich had no disclosures. Dr. Allendorf is a consultant for Covidien.
On Twitter @NaseemSMiller
Dr. Karl Y. Bilimoria, National Cancer Data Base, pancreatectomy, Dr. John D. Allendorf,
Dr. Karl Y. Bilimoria, National Cancer Data Base, pancreatectomy, Dr. John D. Allendorf,
AT DDW 2013
Major finding: The use of surgery alone as first course treatment for stage II pancreatic cancer decreased by nearly 25% at teaching and community hospitals (P less than .0001 for both).
Data source: Analysis of the National Cancer Data Base, selecting 47,000 patients diagnosed with stage I and II pancreatic cancer between 2003 and 2010.
Disclosures: Mr. Raigani and Dr. Velanovich had no disclosures. Dr. Allendorf is a consultant for Covidien.