User login
Doug Brunk is a San Diego-based award-winning reporter who began covering health care in 1991. Before joining the company, he wrote for the health sciences division of Columbia University and was an associate editor at Contemporary Long Term Care magazine when it won a Jesse H. Neal Award. His work has been syndicated by the Los Angeles Times and he is the author of two books related to the University of Kentucky Wildcats men's basketball program. Doug has a master’s degree in magazine journalism from the S.I. Newhouse School of Public Communications at Syracuse University. Follow him on Twitter @dougbrunk.
Psychopathology management skills in childhood epilepsy vary across settings
SAN DIEGO – Behavioral health professionals who work in a school or hospital had better attitudes and felt more comfortable managing psychopathology in children with epilepsy, compared with their counterparts who provided treatment in the community.
However, no statistically significant differences were observed in the attitude, knowledge, or comfort in managing psychopathology among providers in the various disciplines who care for this patient population. The findings come from an online survey of 146 psychologists, clinical counselors, clinical social workers, physicians, and other health care professionals.
"For the past several years there have been many articles coming out regarding the comorbidities in epilepsy, [including] depression, anxiety, cognitive difficulties, issues with memory and learning," Jayne Pacheco-Phillips said during a press briefing at annual meeting of the American Epilepsy Society. "Everyone has started to talk about referring these children early for services. However, no one has looked at what the people who are providing the services know or believe about epilepsy."
Ms. Pacheco-Phillips, a licensed independent social worker in the division of child neurology at Nationwide Children’s Hospital, Columbus, Ohio, and her associates sent a link to an online questionnaire to the clinical directors of nine government-funded agencies that primarily provide services to children and youth in Franklin County, Ohio. Clinical directors then distributed the link to an estimated 500 behavioral health care professionals. The survey included 21 questions based on a Likert scale and was intended to assess the knowledge, attitudes, and the comfort of behavioral health professionals in terms of managing psychopathology in children with epilepsy.
Ms. Pacheco-Phillips reported findings from 146 providers who completed the entire survey, including psychologists, clinical counselors, clinical social workers, physicians, nurses, and those in unlicensed/other roles. Of the 146 respondents, 70 said that they did not know someone with epilepsy while the remaining 76 said they did.
Respondents who provided services in an institution, such as a school or hospital, possessed better attitudes (P = .003) and more comfort in managing psychopathology in children with epilepsy (P = .002), compared with those who provided treatment in the community, such as in families’ homes or in mental health agencies. Respondents who reported having witnessed a seizure had a higher comfort level in managing psychopathology in children (P = .001). Similarly, those who know someone with epilepsy indicated a better attitude (P = .003) and are more comfortable managing psychopathology (P = .007).
"Within the disciplines, we did not find a statistically significant difference in attitudes," Ms. Pacheco-Phillips added. "We were surprised by this. The physicians [surveyed] included psychiatrists and developmental pediatricians. Another interesting point was that 84% of the providers overall indicated that they would be interested in receiving additional education about psychopathology in epilepsy."
One of her coauthors, Dr. Lorie D. Hamiwka, characterized the study findings as important for all epilepsy providers, "because when families come to the clinic, a lot of these comorbidities that we see are more debilitating for children and families than the seizures are themselves," said Dr. Hamiwka, a neurologist at Nationwide Children’s. "They’re often a bigger burden."
Ms. Pacheco-Phillips said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Behavioral health professionals who work in a school or hospital had better attitudes and felt more comfortable managing psychopathology in children with epilepsy, compared with their counterparts who provided treatment in the community.
However, no statistically significant differences were observed in the attitude, knowledge, or comfort in managing psychopathology among providers in the various disciplines who care for this patient population. The findings come from an online survey of 146 psychologists, clinical counselors, clinical social workers, physicians, and other health care professionals.
"For the past several years there have been many articles coming out regarding the comorbidities in epilepsy, [including] depression, anxiety, cognitive difficulties, issues with memory and learning," Jayne Pacheco-Phillips said during a press briefing at annual meeting of the American Epilepsy Society. "Everyone has started to talk about referring these children early for services. However, no one has looked at what the people who are providing the services know or believe about epilepsy."
Ms. Pacheco-Phillips, a licensed independent social worker in the division of child neurology at Nationwide Children’s Hospital, Columbus, Ohio, and her associates sent a link to an online questionnaire to the clinical directors of nine government-funded agencies that primarily provide services to children and youth in Franklin County, Ohio. Clinical directors then distributed the link to an estimated 500 behavioral health care professionals. The survey included 21 questions based on a Likert scale and was intended to assess the knowledge, attitudes, and the comfort of behavioral health professionals in terms of managing psychopathology in children with epilepsy.
Ms. Pacheco-Phillips reported findings from 146 providers who completed the entire survey, including psychologists, clinical counselors, clinical social workers, physicians, nurses, and those in unlicensed/other roles. Of the 146 respondents, 70 said that they did not know someone with epilepsy while the remaining 76 said they did.
Respondents who provided services in an institution, such as a school or hospital, possessed better attitudes (P = .003) and more comfort in managing psychopathology in children with epilepsy (P = .002), compared with those who provided treatment in the community, such as in families’ homes or in mental health agencies. Respondents who reported having witnessed a seizure had a higher comfort level in managing psychopathology in children (P = .001). Similarly, those who know someone with epilepsy indicated a better attitude (P = .003) and are more comfortable managing psychopathology (P = .007).
"Within the disciplines, we did not find a statistically significant difference in attitudes," Ms. Pacheco-Phillips added. "We were surprised by this. The physicians [surveyed] included psychiatrists and developmental pediatricians. Another interesting point was that 84% of the providers overall indicated that they would be interested in receiving additional education about psychopathology in epilepsy."
One of her coauthors, Dr. Lorie D. Hamiwka, characterized the study findings as important for all epilepsy providers, "because when families come to the clinic, a lot of these comorbidities that we see are more debilitating for children and families than the seizures are themselves," said Dr. Hamiwka, a neurologist at Nationwide Children’s. "They’re often a bigger burden."
Ms. Pacheco-Phillips said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Behavioral health professionals who work in a school or hospital had better attitudes and felt more comfortable managing psychopathology in children with epilepsy, compared with their counterparts who provided treatment in the community.
However, no statistically significant differences were observed in the attitude, knowledge, or comfort in managing psychopathology among providers in the various disciplines who care for this patient population. The findings come from an online survey of 146 psychologists, clinical counselors, clinical social workers, physicians, and other health care professionals.
"For the past several years there have been many articles coming out regarding the comorbidities in epilepsy, [including] depression, anxiety, cognitive difficulties, issues with memory and learning," Jayne Pacheco-Phillips said during a press briefing at annual meeting of the American Epilepsy Society. "Everyone has started to talk about referring these children early for services. However, no one has looked at what the people who are providing the services know or believe about epilepsy."
Ms. Pacheco-Phillips, a licensed independent social worker in the division of child neurology at Nationwide Children’s Hospital, Columbus, Ohio, and her associates sent a link to an online questionnaire to the clinical directors of nine government-funded agencies that primarily provide services to children and youth in Franklin County, Ohio. Clinical directors then distributed the link to an estimated 500 behavioral health care professionals. The survey included 21 questions based on a Likert scale and was intended to assess the knowledge, attitudes, and the comfort of behavioral health professionals in terms of managing psychopathology in children with epilepsy.
Ms. Pacheco-Phillips reported findings from 146 providers who completed the entire survey, including psychologists, clinical counselors, clinical social workers, physicians, nurses, and those in unlicensed/other roles. Of the 146 respondents, 70 said that they did not know someone with epilepsy while the remaining 76 said they did.
Respondents who provided services in an institution, such as a school or hospital, possessed better attitudes (P = .003) and more comfort in managing psychopathology in children with epilepsy (P = .002), compared with those who provided treatment in the community, such as in families’ homes or in mental health agencies. Respondents who reported having witnessed a seizure had a higher comfort level in managing psychopathology in children (P = .001). Similarly, those who know someone with epilepsy indicated a better attitude (P = .003) and are more comfortable managing psychopathology (P = .007).
"Within the disciplines, we did not find a statistically significant difference in attitudes," Ms. Pacheco-Phillips added. "We were surprised by this. The physicians [surveyed] included psychiatrists and developmental pediatricians. Another interesting point was that 84% of the providers overall indicated that they would be interested in receiving additional education about psychopathology in epilepsy."
One of her coauthors, Dr. Lorie D. Hamiwka, characterized the study findings as important for all epilepsy providers, "because when families come to the clinic, a lot of these comorbidities that we see are more debilitating for children and families than the seizures are themselves," said Dr. Hamiwka, a neurologist at Nationwide Children’s. "They’re often a bigger burden."
Ms. Pacheco-Phillips said that she had no relevant financial conflicts to disclose.
AT THE ANNUAL MEETING OF THE AMERICAN EPILEPSY SOCIETY
Major Finding: Behavioral health care professionals who provided services in an institution, such as a school or hospital, possessed better attitudes (P = .003) and more comfort in managing psychopathology in children with epilepsy (P = .002), than did those who provided treatment in the community, such as in families’ homes or in mental health agencies.
Data Source: A survey of 146 clinical social workers, physicians, and other behavioral health care providers in the Franklin County, Ohio, region.
Disclosures: Ms. Pacheco-Phillips said that she had no relevant financial conflicts to disclose.
Neurodevelopmental comorbidities common in kids with epilepsy
SAN DIEGO – Nearly one-third of children with epilepsy had neurodevelopmental problems at the onset of unprovoked seizures, results from a large registry study found.
The finding supports the notion that seizures "often appear as part of a broader neurological problem, and that in most cases comorbidities should not be considered consequences of the seizure disorder," researchers led by Dr. Eva Andell wrote in a poster presented at the annual meeting of the American Epilepsy Society.
Dr. Andell, a pediatrician at Karolinska University, Stockholm, and her associates analyzed data from the Stockholm Incidence Register of Epilepsy, a surveillance system established in 2001 with the intent to identify incident cases of first unprovoked seizures and epilepsy among residents of Northern Stockholm.
The researchers limited their analysis to medical records from the time of first unprovoked seizure and the following 6 months among 766 children aged 0-18 years who were followed through Dec. 31, 2006, and set out to identify potential comorbidities that included developmental delay, language problems, mental retardation, cerebral palsy, autism spectrum disorders, attention-deficit/hyperactivity disorder (ADHD), and psychiatric diagnoses.
"Comorbidities were considered to be present when a relevant defined diagnosis appeared in the medical records or when the records included a clear problem description highly suggestive of a comorbidity," the researchers explained in their abstract.
Of the 766 children, 247 (32%) had one or two of the defined comorbidities at the time of the first recognized seizure or in the following 6 months. Of these, 87 (11%) were diagnosed with, or suspected to have two or more of the following diagnoses: mental retardation, cerebral palsy, autism spectrum disorders, ADHD, and psychiatric diagnoses.
The prevalence of all studied comorbidities was more common in the seizure cohort compared with reported rates in the general pediatric population, especially mental retardation (16% vs. 3%, respectively), cerebral palsy (9% vs. 0.2%), autism spectrum disorders (7% vs. 1%), and ADHD (6% vs. 5%).
In an interview, Dr. Andell advised clinicians to "not to forget to look into whether children with epilepsy have a comorbidity, and to treat the comorbidity as well."
Dr. Andell said she had no relevant financial conflicts to disclose.
SAN DIEGO – Nearly one-third of children with epilepsy had neurodevelopmental problems at the onset of unprovoked seizures, results from a large registry study found.
The finding supports the notion that seizures "often appear as part of a broader neurological problem, and that in most cases comorbidities should not be considered consequences of the seizure disorder," researchers led by Dr. Eva Andell wrote in a poster presented at the annual meeting of the American Epilepsy Society.
Dr. Andell, a pediatrician at Karolinska University, Stockholm, and her associates analyzed data from the Stockholm Incidence Register of Epilepsy, a surveillance system established in 2001 with the intent to identify incident cases of first unprovoked seizures and epilepsy among residents of Northern Stockholm.
The researchers limited their analysis to medical records from the time of first unprovoked seizure and the following 6 months among 766 children aged 0-18 years who were followed through Dec. 31, 2006, and set out to identify potential comorbidities that included developmental delay, language problems, mental retardation, cerebral palsy, autism spectrum disorders, attention-deficit/hyperactivity disorder (ADHD), and psychiatric diagnoses.
"Comorbidities were considered to be present when a relevant defined diagnosis appeared in the medical records or when the records included a clear problem description highly suggestive of a comorbidity," the researchers explained in their abstract.
Of the 766 children, 247 (32%) had one or two of the defined comorbidities at the time of the first recognized seizure or in the following 6 months. Of these, 87 (11%) were diagnosed with, or suspected to have two or more of the following diagnoses: mental retardation, cerebral palsy, autism spectrum disorders, ADHD, and psychiatric diagnoses.
The prevalence of all studied comorbidities was more common in the seizure cohort compared with reported rates in the general pediatric population, especially mental retardation (16% vs. 3%, respectively), cerebral palsy (9% vs. 0.2%), autism spectrum disorders (7% vs. 1%), and ADHD (6% vs. 5%).
In an interview, Dr. Andell advised clinicians to "not to forget to look into whether children with epilepsy have a comorbidity, and to treat the comorbidity as well."
Dr. Andell said she had no relevant financial conflicts to disclose.
SAN DIEGO – Nearly one-third of children with epilepsy had neurodevelopmental problems at the onset of unprovoked seizures, results from a large registry study found.
The finding supports the notion that seizures "often appear as part of a broader neurological problem, and that in most cases comorbidities should not be considered consequences of the seizure disorder," researchers led by Dr. Eva Andell wrote in a poster presented at the annual meeting of the American Epilepsy Society.
Dr. Andell, a pediatrician at Karolinska University, Stockholm, and her associates analyzed data from the Stockholm Incidence Register of Epilepsy, a surveillance system established in 2001 with the intent to identify incident cases of first unprovoked seizures and epilepsy among residents of Northern Stockholm.
The researchers limited their analysis to medical records from the time of first unprovoked seizure and the following 6 months among 766 children aged 0-18 years who were followed through Dec. 31, 2006, and set out to identify potential comorbidities that included developmental delay, language problems, mental retardation, cerebral palsy, autism spectrum disorders, attention-deficit/hyperactivity disorder (ADHD), and psychiatric diagnoses.
"Comorbidities were considered to be present when a relevant defined diagnosis appeared in the medical records or when the records included a clear problem description highly suggestive of a comorbidity," the researchers explained in their abstract.
Of the 766 children, 247 (32%) had one or two of the defined comorbidities at the time of the first recognized seizure or in the following 6 months. Of these, 87 (11%) were diagnosed with, or suspected to have two or more of the following diagnoses: mental retardation, cerebral palsy, autism spectrum disorders, ADHD, and psychiatric diagnoses.
The prevalence of all studied comorbidities was more common in the seizure cohort compared with reported rates in the general pediatric population, especially mental retardation (16% vs. 3%, respectively), cerebral palsy (9% vs. 0.2%), autism spectrum disorders (7% vs. 1%), and ADHD (6% vs. 5%).
In an interview, Dr. Andell advised clinicians to "not to forget to look into whether children with epilepsy have a comorbidity, and to treat the comorbidity as well."
Dr. Andell said she had no relevant financial conflicts to disclose.
AT THE ANNUAL MEETING OF THE AMERICAN EPILEPSY SOCIETY
Major Finding: As early as the time of onset of unprovoked seizures or in the following 6 months, 32% of children had one or more neurodevelopmental comorbidities such as mental retardation and cerebral palsy.
Data Source: A study of 766 children in the Stockholm Incidence Register of Epilepsy who were followed through Dec. 31, 2006.
Disclosures: Dr. Andell said she had no relevant financial conflicts to disclose.
CAT-STARTS mnemonic guides Mohs wound closure
SAN DIEGO – Before he proceeds to close a wound following Mohs surgery, Dr. Howard Steinman employs the mnemonic CAT-STARTS to help him select the repair.
A modification of STARTS, Dr. Steinman uses CAT-STARTS to represent the following factors he considers prior to carrying out the repair: first assess the Cosmetic units, Areas of available skin, and Textures of available skin. Then consider closure options: Second intention and Simple (linear) repairs, Transposition flaps, Advancement flaps, Rotation flaps, Tissue interpolation flaps, and Skin grafts.
"Prior to closing, I draw in the surrounding cosmetic units of the face. Once you’ve done that, you should pay attention to the relaxed skin tension lines," Dr. Steinman said at a meeting sponsored by the American Society for Mohs Surgery.
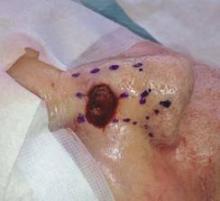
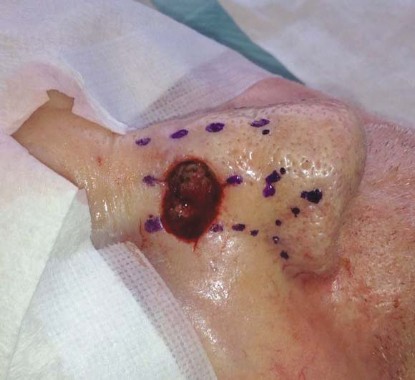
To illustrate, he showed attendees a digital image of a patient’s nasal lesion prior to repair. "I draw in the midline, the side of the nasal dorsum and nasal-jugal lines, and the alar fold," he explained. "Then I look at the skin texture. This case had a mix of sebaceous skin and smooth skin, so I factored that consideration in to my repair."
Candidate wounds for second-intention healing "are small, shallow wounds, usually less than 1 cm in diameter," said Dr. Steinman, who practices dermatology and Mohs surgery in Irving, Tex. "They’re usually less than a half centimeter deep. Second-intention healing is often especially effective for the alar fold and the medial canthus and less effective for the cheeks, chin, and around the lips."
If healing by second intention is not an option, "you want to consider your repair choices, from the simplest to the most complex," he said. Thus, consider simple (linear) repairs. Thereafter, his suggested order of complexity begins with transposition flaps, followed by advancement flaps, rotation flaps, tissue interpolation flaps, and skin grafts.
"The midline of the nose and the midline of the forehead are two of the best places to do linear repairs, as is the cheek and forehead," Dr. Steinman commented. "One thing to remember about straight line repairs is that they cause significant secondary motion perpendicular to the axis of closure. You need to respect that when doing linear repairs near free margins," he added.
If you unable to close a wound in a side-to-side fashion, "a transition flap may be your best option," he continued. "Because rotation flaps require longer, broad incisions, in my view you should often think about an advancement flap as your next choice after transposition flaps in terms of complexity."
Tissue interpolation flaps are reserved "for instances where no local skin flap is a better choice," he said. "The midline forehead flap is excellent for distal nasal defects because you have a broad area of skin and it’s based on a vascular pedicle. Interpolation flaps are two-stage procedures."
He views skin grafts to be a last choice for most wound repairs. "If you do them well and, when needed, laser or abrade them, they often look acceptable, but in my opinion they are the last option for many locations," he said.
Dr. Steinman said that he had no relevant financial conflicts to disclose.
SAN DIEGO – Before he proceeds to close a wound following Mohs surgery, Dr. Howard Steinman employs the mnemonic CAT-STARTS to help him select the repair.
A modification of STARTS, Dr. Steinman uses CAT-STARTS to represent the following factors he considers prior to carrying out the repair: first assess the Cosmetic units, Areas of available skin, and Textures of available skin. Then consider closure options: Second intention and Simple (linear) repairs, Transposition flaps, Advancement flaps, Rotation flaps, Tissue interpolation flaps, and Skin grafts.
"Prior to closing, I draw in the surrounding cosmetic units of the face. Once you’ve done that, you should pay attention to the relaxed skin tension lines," Dr. Steinman said at a meeting sponsored by the American Society for Mohs Surgery.
To illustrate, he showed attendees a digital image of a patient’s nasal lesion prior to repair. "I draw in the midline, the side of the nasal dorsum and nasal-jugal lines, and the alar fold," he explained. "Then I look at the skin texture. This case had a mix of sebaceous skin and smooth skin, so I factored that consideration in to my repair."
Candidate wounds for second-intention healing "are small, shallow wounds, usually less than 1 cm in diameter," said Dr. Steinman, who practices dermatology and Mohs surgery in Irving, Tex. "They’re usually less than a half centimeter deep. Second-intention healing is often especially effective for the alar fold and the medial canthus and less effective for the cheeks, chin, and around the lips."
If healing by second intention is not an option, "you want to consider your repair choices, from the simplest to the most complex," he said. Thus, consider simple (linear) repairs. Thereafter, his suggested order of complexity begins with transposition flaps, followed by advancement flaps, rotation flaps, tissue interpolation flaps, and skin grafts.
"The midline of the nose and the midline of the forehead are two of the best places to do linear repairs, as is the cheek and forehead," Dr. Steinman commented. "One thing to remember about straight line repairs is that they cause significant secondary motion perpendicular to the axis of closure. You need to respect that when doing linear repairs near free margins," he added.
If you unable to close a wound in a side-to-side fashion, "a transition flap may be your best option," he continued. "Because rotation flaps require longer, broad incisions, in my view you should often think about an advancement flap as your next choice after transposition flaps in terms of complexity."
Tissue interpolation flaps are reserved "for instances where no local skin flap is a better choice," he said. "The midline forehead flap is excellent for distal nasal defects because you have a broad area of skin and it’s based on a vascular pedicle. Interpolation flaps are two-stage procedures."
He views skin grafts to be a last choice for most wound repairs. "If you do them well and, when needed, laser or abrade them, they often look acceptable, but in my opinion they are the last option for many locations," he said.
Dr. Steinman said that he had no relevant financial conflicts to disclose.
SAN DIEGO – Before he proceeds to close a wound following Mohs surgery, Dr. Howard Steinman employs the mnemonic CAT-STARTS to help him select the repair.
A modification of STARTS, Dr. Steinman uses CAT-STARTS to represent the following factors he considers prior to carrying out the repair: first assess the Cosmetic units, Areas of available skin, and Textures of available skin. Then consider closure options: Second intention and Simple (linear) repairs, Transposition flaps, Advancement flaps, Rotation flaps, Tissue interpolation flaps, and Skin grafts.
"Prior to closing, I draw in the surrounding cosmetic units of the face. Once you’ve done that, you should pay attention to the relaxed skin tension lines," Dr. Steinman said at a meeting sponsored by the American Society for Mohs Surgery.
To illustrate, he showed attendees a digital image of a patient’s nasal lesion prior to repair. "I draw in the midline, the side of the nasal dorsum and nasal-jugal lines, and the alar fold," he explained. "Then I look at the skin texture. This case had a mix of sebaceous skin and smooth skin, so I factored that consideration in to my repair."
Candidate wounds for second-intention healing "are small, shallow wounds, usually less than 1 cm in diameter," said Dr. Steinman, who practices dermatology and Mohs surgery in Irving, Tex. "They’re usually less than a half centimeter deep. Second-intention healing is often especially effective for the alar fold and the medial canthus and less effective for the cheeks, chin, and around the lips."
If healing by second intention is not an option, "you want to consider your repair choices, from the simplest to the most complex," he said. Thus, consider simple (linear) repairs. Thereafter, his suggested order of complexity begins with transposition flaps, followed by advancement flaps, rotation flaps, tissue interpolation flaps, and skin grafts.
"The midline of the nose and the midline of the forehead are two of the best places to do linear repairs, as is the cheek and forehead," Dr. Steinman commented. "One thing to remember about straight line repairs is that they cause significant secondary motion perpendicular to the axis of closure. You need to respect that when doing linear repairs near free margins," he added.
If you unable to close a wound in a side-to-side fashion, "a transition flap may be your best option," he continued. "Because rotation flaps require longer, broad incisions, in my view you should often think about an advancement flap as your next choice after transposition flaps in terms of complexity."
Tissue interpolation flaps are reserved "for instances where no local skin flap is a better choice," he said. "The midline forehead flap is excellent for distal nasal defects because you have a broad area of skin and it’s based on a vascular pedicle. Interpolation flaps are two-stage procedures."
He views skin grafts to be a last choice for most wound repairs. "If you do them well and, when needed, laser or abrade them, they often look acceptable, but in my opinion they are the last option for many locations," he said.
Dr. Steinman said that he had no relevant financial conflicts to disclose.
EXPERT ANALYSIS FROM A MEETING SPONSORED BY THE AMERICAN SOCIETY FOR MOHS SURGERY
Beta-blockers had no impact on CKD mortality
SAN DIEGO – Beta-blocker use by patients with advanced chronic kidney disease was not associated with a lower risk of all-cause mortality or initiation of chronic dialysis, results from a large study demonstrated.
"The sympathetic nervous system is increased in chronic kidney disease and end-stage renal disease," Dr. Anna Jovanovich said in an interview during a poster session at Kidney Week 2012. "That can be associated with mortality – you can have more arrhythmias when your sympathetic drive is higher. You would think that beta-blockers might help decrease the sympathetic drive and then decrease mortality, but from this observational study we don’t see that association."
Dr. Jovanovich, a second-year renal fellow at the University of Colorado, Denver, and her associates evaluated 1,099 advanced kidney disease patients not yet on dialysis who participated in the Homocysteine in Kidney and End-Stage Renal Disease (HOST) study, conducted between 2001 and 2006.
The mean age of patients was 69 years, 98% were male, 26% were African American, and the mean estimated glomerular filtration rate was 18 mL/min per 1.73 m2. During a mean follow-up of 3 years, 453 patients (41%) died from any cause and 615 (56%) started chronic dialysis.
After adjustment for age, gender, race, smoking status, diabetes, hypertension, cardiovascular disease, body mass index, systolic blood pressure, albumin, and eGFR, baseline beta-blocker use was not associated with lower risk of all-cause mortality (adjusted HR of 1.14; P = .07), nor was it associated with a lower risk of initiation of chronic dialysis (adjusted HR of 0.90).
"This is only an observational study so we can’t draw conclusions, but in a kidney disease patient who has heart failure, I think beta-blockers are an important medication in their armamentarium," she said. "However, in a kidney disease patient without heart failure there may be other blood pressure–lowering medications to try first before you try a beta-blocker."
Dr. Jovanovich said that the findings support those of the Hemodialysis Study (Am. J. Kidney Dis. 2011;58:939-45).
Dr. Jovanovich said that she had no relevant financial conflicts to disclose.
The meeting was sponsored by the American Society of Nephrology.
SAN DIEGO – Beta-blocker use by patients with advanced chronic kidney disease was not associated with a lower risk of all-cause mortality or initiation of chronic dialysis, results from a large study demonstrated.
"The sympathetic nervous system is increased in chronic kidney disease and end-stage renal disease," Dr. Anna Jovanovich said in an interview during a poster session at Kidney Week 2012. "That can be associated with mortality – you can have more arrhythmias when your sympathetic drive is higher. You would think that beta-blockers might help decrease the sympathetic drive and then decrease mortality, but from this observational study we don’t see that association."
Dr. Jovanovich, a second-year renal fellow at the University of Colorado, Denver, and her associates evaluated 1,099 advanced kidney disease patients not yet on dialysis who participated in the Homocysteine in Kidney and End-Stage Renal Disease (HOST) study, conducted between 2001 and 2006.
The mean age of patients was 69 years, 98% were male, 26% were African American, and the mean estimated glomerular filtration rate was 18 mL/min per 1.73 m2. During a mean follow-up of 3 years, 453 patients (41%) died from any cause and 615 (56%) started chronic dialysis.
After adjustment for age, gender, race, smoking status, diabetes, hypertension, cardiovascular disease, body mass index, systolic blood pressure, albumin, and eGFR, baseline beta-blocker use was not associated with lower risk of all-cause mortality (adjusted HR of 1.14; P = .07), nor was it associated with a lower risk of initiation of chronic dialysis (adjusted HR of 0.90).
"This is only an observational study so we can’t draw conclusions, but in a kidney disease patient who has heart failure, I think beta-blockers are an important medication in their armamentarium," she said. "However, in a kidney disease patient without heart failure there may be other blood pressure–lowering medications to try first before you try a beta-blocker."
Dr. Jovanovich said that the findings support those of the Hemodialysis Study (Am. J. Kidney Dis. 2011;58:939-45).
Dr. Jovanovich said that she had no relevant financial conflicts to disclose.
The meeting was sponsored by the American Society of Nephrology.
SAN DIEGO – Beta-blocker use by patients with advanced chronic kidney disease was not associated with a lower risk of all-cause mortality or initiation of chronic dialysis, results from a large study demonstrated.
"The sympathetic nervous system is increased in chronic kidney disease and end-stage renal disease," Dr. Anna Jovanovich said in an interview during a poster session at Kidney Week 2012. "That can be associated with mortality – you can have more arrhythmias when your sympathetic drive is higher. You would think that beta-blockers might help decrease the sympathetic drive and then decrease mortality, but from this observational study we don’t see that association."
Dr. Jovanovich, a second-year renal fellow at the University of Colorado, Denver, and her associates evaluated 1,099 advanced kidney disease patients not yet on dialysis who participated in the Homocysteine in Kidney and End-Stage Renal Disease (HOST) study, conducted between 2001 and 2006.
The mean age of patients was 69 years, 98% were male, 26% were African American, and the mean estimated glomerular filtration rate was 18 mL/min per 1.73 m2. During a mean follow-up of 3 years, 453 patients (41%) died from any cause and 615 (56%) started chronic dialysis.
After adjustment for age, gender, race, smoking status, diabetes, hypertension, cardiovascular disease, body mass index, systolic blood pressure, albumin, and eGFR, baseline beta-blocker use was not associated with lower risk of all-cause mortality (adjusted HR of 1.14; P = .07), nor was it associated with a lower risk of initiation of chronic dialysis (adjusted HR of 0.90).
"This is only an observational study so we can’t draw conclusions, but in a kidney disease patient who has heart failure, I think beta-blockers are an important medication in their armamentarium," she said. "However, in a kidney disease patient without heart failure there may be other blood pressure–lowering medications to try first before you try a beta-blocker."
Dr. Jovanovich said that the findings support those of the Hemodialysis Study (Am. J. Kidney Dis. 2011;58:939-45).
Dr. Jovanovich said that she had no relevant financial conflicts to disclose.
The meeting was sponsored by the American Society of Nephrology.
AT KIDNEY WEEK 2012
Major Finding: Beta-blocker use was not associated with a lower risk of all-cause mortality (adjusted HR of 1.14; P = .07) in patients with advanced kidney disease.
Data Source: A study of 1,099 patients not yet on dialysis who participated in the Homocysteine in Kidney and End-Stage Renal Disease (HOST) study.
Disclosures: Dr. Jovanovich said that she had no relevant financial conflicts to disclose.
Follow AIDET to guide patient expectations
SAN DIEGO – When performing dermatologic surgery, "fulfilling the expectations of patients and their families is the key to satisfaction," Dr. Howard K. Steinman said at a meeting sponsored by the American Society for Mohs Surgery.
"The yin and the yang of keeping patients satisfied involves fulfilling their expectations and satisfying their unmet expectations," Dr. Steinman said. "You have to do both. The trouble is, patient expectations are often unknown, vague, or inaccurate, or they’re irrational and unachievable. These types of expectations are dangerous and often the result of significant dissatisfaction, and unfortunately, litigation and complaints to medical boards."
Examples of nonspecific expectations include remarks such as "I want to look 10 years younger," "I hate my face," "I want to look like this picture," "what do you think I need, doctor?" and "my spouse wants me to have this fixed."
In these instances, expectations need to be modified before treatment, Dr. Steinman emphasized. This is all part of the consultation.
Dr. Steinman, who practices dermatology in Irving, Tex., shared techniques that help him to stay effective, centered, and calm while satisfying patient expectations.
To track these techniques, he advised using the mnemonic AIDET, which he learned during his post as director of dermatologic and skin surgery at Scott & White Clinic in Temple, Tex. AIDET stands for acknowledge, introduce, duration, explanation, and thank you.
The "acknowledge" component of AIDET involves a visible, audible, or tactile sign acknowledging the patient’s presence and an introduction. "Every person entering the exam room or operating room should introduce themselves to the patient," Dr. Steinman said. If loved ones accompany the patient, "I’ll introduce myself to them also, and ask how they’re related. I then go on to explain my role, my background and experience, and my intention to provide excellent service."
Next, provide an estimated time frame for how long the procedure will take. For example, during Mohs surgery cases, "I’ll take the specimen out, but before I leave the room I’ll say, ‘please have a seat in the waiting room. It’s going to be about 45 minutes until your slides are ready’ – even though this usually only takes 20-25 minutes. Overestimate the time so patients don’t become disappointed."
The "explanation" component of the mnemonic is crucial, Dr. Steinman said. He makes it a point to explain what he’s going to do during the procedure and asks the patient if he or she has any questions before he starts. "If the procedure is going to hurt, let the patient know," he said. "Offer to narrate what you’re doing if the patient finds that helpful. Keep the patient informed. Explain all tasks, sounds, smells, processes, and procedures, and have your staff do the same." For example, if the procedure involves cauterizing tissue, Dr. Steinman will tell the patient, "I’m going to start cauterizing. There is going to be a bad smell. You may want to breathe through your mouth."
Finally, thank patients "for the opportunity to care for them, for their time, their patience (if they had to wait), and for choosing you," he said.
Dr. Steinman said that he had no relevant financial conflicts to disclose.
SAN DIEGO – When performing dermatologic surgery, "fulfilling the expectations of patients and their families is the key to satisfaction," Dr. Howard K. Steinman said at a meeting sponsored by the American Society for Mohs Surgery.
"The yin and the yang of keeping patients satisfied involves fulfilling their expectations and satisfying their unmet expectations," Dr. Steinman said. "You have to do both. The trouble is, patient expectations are often unknown, vague, or inaccurate, or they’re irrational and unachievable. These types of expectations are dangerous and often the result of significant dissatisfaction, and unfortunately, litigation and complaints to medical boards."
Examples of nonspecific expectations include remarks such as "I want to look 10 years younger," "I hate my face," "I want to look like this picture," "what do you think I need, doctor?" and "my spouse wants me to have this fixed."
In these instances, expectations need to be modified before treatment, Dr. Steinman emphasized. This is all part of the consultation.
Dr. Steinman, who practices dermatology in Irving, Tex., shared techniques that help him to stay effective, centered, and calm while satisfying patient expectations.
To track these techniques, he advised using the mnemonic AIDET, which he learned during his post as director of dermatologic and skin surgery at Scott & White Clinic in Temple, Tex. AIDET stands for acknowledge, introduce, duration, explanation, and thank you.
The "acknowledge" component of AIDET involves a visible, audible, or tactile sign acknowledging the patient’s presence and an introduction. "Every person entering the exam room or operating room should introduce themselves to the patient," Dr. Steinman said. If loved ones accompany the patient, "I’ll introduce myself to them also, and ask how they’re related. I then go on to explain my role, my background and experience, and my intention to provide excellent service."
Next, provide an estimated time frame for how long the procedure will take. For example, during Mohs surgery cases, "I’ll take the specimen out, but before I leave the room I’ll say, ‘please have a seat in the waiting room. It’s going to be about 45 minutes until your slides are ready’ – even though this usually only takes 20-25 minutes. Overestimate the time so patients don’t become disappointed."
The "explanation" component of the mnemonic is crucial, Dr. Steinman said. He makes it a point to explain what he’s going to do during the procedure and asks the patient if he or she has any questions before he starts. "If the procedure is going to hurt, let the patient know," he said. "Offer to narrate what you’re doing if the patient finds that helpful. Keep the patient informed. Explain all tasks, sounds, smells, processes, and procedures, and have your staff do the same." For example, if the procedure involves cauterizing tissue, Dr. Steinman will tell the patient, "I’m going to start cauterizing. There is going to be a bad smell. You may want to breathe through your mouth."
Finally, thank patients "for the opportunity to care for them, for their time, their patience (if they had to wait), and for choosing you," he said.
Dr. Steinman said that he had no relevant financial conflicts to disclose.
SAN DIEGO – When performing dermatologic surgery, "fulfilling the expectations of patients and their families is the key to satisfaction," Dr. Howard K. Steinman said at a meeting sponsored by the American Society for Mohs Surgery.
"The yin and the yang of keeping patients satisfied involves fulfilling their expectations and satisfying their unmet expectations," Dr. Steinman said. "You have to do both. The trouble is, patient expectations are often unknown, vague, or inaccurate, or they’re irrational and unachievable. These types of expectations are dangerous and often the result of significant dissatisfaction, and unfortunately, litigation and complaints to medical boards."
Examples of nonspecific expectations include remarks such as "I want to look 10 years younger," "I hate my face," "I want to look like this picture," "what do you think I need, doctor?" and "my spouse wants me to have this fixed."
In these instances, expectations need to be modified before treatment, Dr. Steinman emphasized. This is all part of the consultation.
Dr. Steinman, who practices dermatology in Irving, Tex., shared techniques that help him to stay effective, centered, and calm while satisfying patient expectations.
To track these techniques, he advised using the mnemonic AIDET, which he learned during his post as director of dermatologic and skin surgery at Scott & White Clinic in Temple, Tex. AIDET stands for acknowledge, introduce, duration, explanation, and thank you.
The "acknowledge" component of AIDET involves a visible, audible, or tactile sign acknowledging the patient’s presence and an introduction. "Every person entering the exam room or operating room should introduce themselves to the patient," Dr. Steinman said. If loved ones accompany the patient, "I’ll introduce myself to them also, and ask how they’re related. I then go on to explain my role, my background and experience, and my intention to provide excellent service."
Next, provide an estimated time frame for how long the procedure will take. For example, during Mohs surgery cases, "I’ll take the specimen out, but before I leave the room I’ll say, ‘please have a seat in the waiting room. It’s going to be about 45 minutes until your slides are ready’ – even though this usually only takes 20-25 minutes. Overestimate the time so patients don’t become disappointed."
The "explanation" component of the mnemonic is crucial, Dr. Steinman said. He makes it a point to explain what he’s going to do during the procedure and asks the patient if he or she has any questions before he starts. "If the procedure is going to hurt, let the patient know," he said. "Offer to narrate what you’re doing if the patient finds that helpful. Keep the patient informed. Explain all tasks, sounds, smells, processes, and procedures, and have your staff do the same." For example, if the procedure involves cauterizing tissue, Dr. Steinman will tell the patient, "I’m going to start cauterizing. There is going to be a bad smell. You may want to breathe through your mouth."
Finally, thank patients "for the opportunity to care for them, for their time, their patience (if they had to wait), and for choosing you," he said.
Dr. Steinman said that he had no relevant financial conflicts to disclose.
EXPERT ANALYSIS FROM A MEETING SPONSORED BY THE AMERICAN SOCIETY FOR MOHS SURGERY
Exercise intervention boosted walking in CKD patients
SAN DIEGO – A 12-week exercise program improved the physical capacity of patients with stage 3 and 4 chronic kidney disease, results from a single-center demonstrated.
The intervention also improved patient perceptions of general health, vitality, and physical functioning. "We believe that renal rehabilitation exercise programs can be integrated into standard chronic kidney disease treatment," Dr. Ana Paula Rossi, a nephrology fellow at Maine Medical Center, Portland, said at Kidney Week 2012.
"We need longer follow-up and larger studies to determine if this will translate into decreased mortality rates and slow the progression of CKD," she said.
In a 12-week study conducted in 2011, Dr. Rossi and her associates randomized 48 patients with stage 3 and 4 CKD to usual care and 59 patients to an exercise intervention, which consisted of guided exercise at a cardiac rehabilitation facility two times per week for 3 months. Patients were encouraged to exercise an additional day per week on their own.
Exercise consisted of treadmill walking and/or stationary cycling. The duration was increased by 2-3 minutes per session, with the ultimate goal of 60 minutes of continuous exercise. Patients also did weight training with upper and lower extremity extensions and flexions with free weights. They started with one set of 10 repetitions per exercise, which was increased to a goal of three sets of 15 repetitions before the weight was increased. They also did stretching exercises.
Outcomes included the results of the 6-minute walk test (the number of feet walked per 6 minutes), the sit-to-stand test in which the patient is asked to sit and stand up 10 times (time reported is the percentage of age-predicted time), and the gait-speed test, a measurement of centimeters per second walked over a distance of 20 feet. To assess quality of life, the researchers administered the RAND 36-item Short Form Health Survey.
Patients with ongoing angina or transient ischemic attacks were excluded from the study, as were those with chronic lung disease resulting in significant shortness of breath or oxygen desaturation at rest, and those with lower-extremity amputation with no prosthesis or with an orthopedic disorder severely exacerbated by activity.
Patients in both groups were around 69 years old and had similar baseline reported levels of activity.
After the 12-week study period, the usual care group had no significant improvements in the three main outcomes. Patients in the exercise intervention group had significant improvements in the 6-minute walk test (19%, from 1,117 to 1,327 feet per 6 minutes; P = less than .0001) and in the sit-to-stand test (29%, from 68% to 97% of age predicted; P = .0004), but not in the gait-speed test (183 vs. 171 cm; P = .06).
Compared with their counterparts in the usual care group, patients in the intervention group reported significant improvements in energy (P = .01), physical functioning (P less than .01), and in general health (P = .03). Neither group experienced significant improvements in pain, emotional well-being, or in social functioning.
The study was funded by the Maine Medical Center Research Institute. Dr. Rossi said that she had no relevant financial conflicts to disclose.
The meeting was sponsored by the American Society of Nephrology.
SAN DIEGO – A 12-week exercise program improved the physical capacity of patients with stage 3 and 4 chronic kidney disease, results from a single-center demonstrated.
The intervention also improved patient perceptions of general health, vitality, and physical functioning. "We believe that renal rehabilitation exercise programs can be integrated into standard chronic kidney disease treatment," Dr. Ana Paula Rossi, a nephrology fellow at Maine Medical Center, Portland, said at Kidney Week 2012.
"We need longer follow-up and larger studies to determine if this will translate into decreased mortality rates and slow the progression of CKD," she said.
In a 12-week study conducted in 2011, Dr. Rossi and her associates randomized 48 patients with stage 3 and 4 CKD to usual care and 59 patients to an exercise intervention, which consisted of guided exercise at a cardiac rehabilitation facility two times per week for 3 months. Patients were encouraged to exercise an additional day per week on their own.
Exercise consisted of treadmill walking and/or stationary cycling. The duration was increased by 2-3 minutes per session, with the ultimate goal of 60 minutes of continuous exercise. Patients also did weight training with upper and lower extremity extensions and flexions with free weights. They started with one set of 10 repetitions per exercise, which was increased to a goal of three sets of 15 repetitions before the weight was increased. They also did stretching exercises.
Outcomes included the results of the 6-minute walk test (the number of feet walked per 6 minutes), the sit-to-stand test in which the patient is asked to sit and stand up 10 times (time reported is the percentage of age-predicted time), and the gait-speed test, a measurement of centimeters per second walked over a distance of 20 feet. To assess quality of life, the researchers administered the RAND 36-item Short Form Health Survey.
Patients with ongoing angina or transient ischemic attacks were excluded from the study, as were those with chronic lung disease resulting in significant shortness of breath or oxygen desaturation at rest, and those with lower-extremity amputation with no prosthesis or with an orthopedic disorder severely exacerbated by activity.
Patients in both groups were around 69 years old and had similar baseline reported levels of activity.
After the 12-week study period, the usual care group had no significant improvements in the three main outcomes. Patients in the exercise intervention group had significant improvements in the 6-minute walk test (19%, from 1,117 to 1,327 feet per 6 minutes; P = less than .0001) and in the sit-to-stand test (29%, from 68% to 97% of age predicted; P = .0004), but not in the gait-speed test (183 vs. 171 cm; P = .06).
Compared with their counterparts in the usual care group, patients in the intervention group reported significant improvements in energy (P = .01), physical functioning (P less than .01), and in general health (P = .03). Neither group experienced significant improvements in pain, emotional well-being, or in social functioning.
The study was funded by the Maine Medical Center Research Institute. Dr. Rossi said that she had no relevant financial conflicts to disclose.
The meeting was sponsored by the American Society of Nephrology.
SAN DIEGO – A 12-week exercise program improved the physical capacity of patients with stage 3 and 4 chronic kidney disease, results from a single-center demonstrated.
The intervention also improved patient perceptions of general health, vitality, and physical functioning. "We believe that renal rehabilitation exercise programs can be integrated into standard chronic kidney disease treatment," Dr. Ana Paula Rossi, a nephrology fellow at Maine Medical Center, Portland, said at Kidney Week 2012.
"We need longer follow-up and larger studies to determine if this will translate into decreased mortality rates and slow the progression of CKD," she said.
In a 12-week study conducted in 2011, Dr. Rossi and her associates randomized 48 patients with stage 3 and 4 CKD to usual care and 59 patients to an exercise intervention, which consisted of guided exercise at a cardiac rehabilitation facility two times per week for 3 months. Patients were encouraged to exercise an additional day per week on their own.
Exercise consisted of treadmill walking and/or stationary cycling. The duration was increased by 2-3 minutes per session, with the ultimate goal of 60 minutes of continuous exercise. Patients also did weight training with upper and lower extremity extensions and flexions with free weights. They started with one set of 10 repetitions per exercise, which was increased to a goal of three sets of 15 repetitions before the weight was increased. They also did stretching exercises.
Outcomes included the results of the 6-minute walk test (the number of feet walked per 6 minutes), the sit-to-stand test in which the patient is asked to sit and stand up 10 times (time reported is the percentage of age-predicted time), and the gait-speed test, a measurement of centimeters per second walked over a distance of 20 feet. To assess quality of life, the researchers administered the RAND 36-item Short Form Health Survey.
Patients with ongoing angina or transient ischemic attacks were excluded from the study, as were those with chronic lung disease resulting in significant shortness of breath or oxygen desaturation at rest, and those with lower-extremity amputation with no prosthesis or with an orthopedic disorder severely exacerbated by activity.
Patients in both groups were around 69 years old and had similar baseline reported levels of activity.
After the 12-week study period, the usual care group had no significant improvements in the three main outcomes. Patients in the exercise intervention group had significant improvements in the 6-minute walk test (19%, from 1,117 to 1,327 feet per 6 minutes; P = less than .0001) and in the sit-to-stand test (29%, from 68% to 97% of age predicted; P = .0004), but not in the gait-speed test (183 vs. 171 cm; P = .06).
Compared with their counterparts in the usual care group, patients in the intervention group reported significant improvements in energy (P = .01), physical functioning (P less than .01), and in general health (P = .03). Neither group experienced significant improvements in pain, emotional well-being, or in social functioning.
The study was funded by the Maine Medical Center Research Institute. Dr. Rossi said that she had no relevant financial conflicts to disclose.
The meeting was sponsored by the American Society of Nephrology.
AT KIDNEY WEEK 2012
Major Finding: After 12 weeks, patients in the exercise intervention group had a 19% improvement in the 6-minute walk test and a 29% improvement in the sit-to-stand test.
Data Source: A single center study of 107 stage 3 and 4 chronic kidney disease patients randomized to usual care or an exercise intervention.
Disclosures: The study was funded by the Maine Medical Center Research Institute. Dr. Rossi said that she had no relevant financial conflicts to disclose.
Certain Factors Predict Dialysis Patients' Return to Work
SAN DIEGO – Being catheter free and having a serum albumin level of at least 4 g/dL were among the quality indicators associated with the ability of dialysis patients to return to work, judging from the results of a large study.
"There has been limited attention to employment issues in this patient population," Nancy G. Kutner, Ph.D., said in an interview during a poster session at Kidney Week 2012. "There has been a general impression that most people aren’t going to even try to resume employment – even those who were employed immediately before starting dialysis."
Dr. Kutner, professor of rehabilitation medicine at Emory University, Atlanta, and her associates enrolled 509 patients who were on hemodialysis treatment for 3 months or longer during 2009-2011 for a U.S. Renal Data System study conducted in seven outpatient clinics in San Francisco and seven in Atlanta. The patients were between the ages of 18 and 64 years, and they responded to the question: "Are you now able to work for pay (full-time or part-time)?"
Using a logistic regression model adjusted for age, gender, race, educational level, diabetes, congestive heart failure, presence of symptoms of depression, length of time on dialysis, and facility clustering, the researchers investigated whether incremental achievement of certain hemodialysis quality indicator (HD QI) goals were correlated with patient-reported ability to work. The HD QI goals were standardized Kt/V of 1.2 or greater; being catheter free; and having a hemoglobin level of 10-12 g/dL, a serum albumin level of 4 g/dL or greater, and a serum phosphorus level of 3.5 mg/dL to 5.5 mg/dL.
The mean age of the patients was 50 years, and 61% were male. Of the 509 patients, 36% said that they were able to work and 13% were actually employed. The mean number of HD QI goals met was 3.31, and the patients’ likelihood of reporting being able to work increased with an increasing number of QI goals met (odds ratio 1.28; P = .02). "Achieving a quality indicator goal is likely a joint process between the provider and the patient," said Dr. Kutner, who directs the USRDS Rehabilitation/QoL Special Studies Center at Emory.
"The end result seems to be that as more of these goals are met, it furthers the potential for work and rehabilitation. This is very encouraging," she said at the meeting, which was sponsored by the American Society of Nephrology.
Compared with their counterparts who reported being unable to work, a higher proportion of those who reported being able to work met the QI goals of Kt/V of 1.2 or greater (92% vs. 90%, respectively), being catheter free (84% vs. 74%), having a hemoglobin level of 10-12 g/dL (62% vs. 60%), and having a serum albumin of 4.0 g/dL or greater (59% vs. 49%). The proportion of those reporting a serum phosphorus level of 3.5-5.5 mg/dL was similar between the two groups (48% vs. 50%).
Dr. Kutner said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Being catheter free and having a serum albumin level of at least 4 g/dL were among the quality indicators associated with the ability of dialysis patients to return to work, judging from the results of a large study.
"There has been limited attention to employment issues in this patient population," Nancy G. Kutner, Ph.D., said in an interview during a poster session at Kidney Week 2012. "There has been a general impression that most people aren’t going to even try to resume employment – even those who were employed immediately before starting dialysis."
Dr. Kutner, professor of rehabilitation medicine at Emory University, Atlanta, and her associates enrolled 509 patients who were on hemodialysis treatment for 3 months or longer during 2009-2011 for a U.S. Renal Data System study conducted in seven outpatient clinics in San Francisco and seven in Atlanta. The patients were between the ages of 18 and 64 years, and they responded to the question: "Are you now able to work for pay (full-time or part-time)?"
Using a logistic regression model adjusted for age, gender, race, educational level, diabetes, congestive heart failure, presence of symptoms of depression, length of time on dialysis, and facility clustering, the researchers investigated whether incremental achievement of certain hemodialysis quality indicator (HD QI) goals were correlated with patient-reported ability to work. The HD QI goals were standardized Kt/V of 1.2 or greater; being catheter free; and having a hemoglobin level of 10-12 g/dL, a serum albumin level of 4 g/dL or greater, and a serum phosphorus level of 3.5 mg/dL to 5.5 mg/dL.
The mean age of the patients was 50 years, and 61% were male. Of the 509 patients, 36% said that they were able to work and 13% were actually employed. The mean number of HD QI goals met was 3.31, and the patients’ likelihood of reporting being able to work increased with an increasing number of QI goals met (odds ratio 1.28; P = .02). "Achieving a quality indicator goal is likely a joint process between the provider and the patient," said Dr. Kutner, who directs the USRDS Rehabilitation/QoL Special Studies Center at Emory.
"The end result seems to be that as more of these goals are met, it furthers the potential for work and rehabilitation. This is very encouraging," she said at the meeting, which was sponsored by the American Society of Nephrology.
Compared with their counterparts who reported being unable to work, a higher proportion of those who reported being able to work met the QI goals of Kt/V of 1.2 or greater (92% vs. 90%, respectively), being catheter free (84% vs. 74%), having a hemoglobin level of 10-12 g/dL (62% vs. 60%), and having a serum albumin of 4.0 g/dL or greater (59% vs. 49%). The proportion of those reporting a serum phosphorus level of 3.5-5.5 mg/dL was similar between the two groups (48% vs. 50%).
Dr. Kutner said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Being catheter free and having a serum albumin level of at least 4 g/dL were among the quality indicators associated with the ability of dialysis patients to return to work, judging from the results of a large study.
"There has been limited attention to employment issues in this patient population," Nancy G. Kutner, Ph.D., said in an interview during a poster session at Kidney Week 2012. "There has been a general impression that most people aren’t going to even try to resume employment – even those who were employed immediately before starting dialysis."
Dr. Kutner, professor of rehabilitation medicine at Emory University, Atlanta, and her associates enrolled 509 patients who were on hemodialysis treatment for 3 months or longer during 2009-2011 for a U.S. Renal Data System study conducted in seven outpatient clinics in San Francisco and seven in Atlanta. The patients were between the ages of 18 and 64 years, and they responded to the question: "Are you now able to work for pay (full-time or part-time)?"
Using a logistic regression model adjusted for age, gender, race, educational level, diabetes, congestive heart failure, presence of symptoms of depression, length of time on dialysis, and facility clustering, the researchers investigated whether incremental achievement of certain hemodialysis quality indicator (HD QI) goals were correlated with patient-reported ability to work. The HD QI goals were standardized Kt/V of 1.2 or greater; being catheter free; and having a hemoglobin level of 10-12 g/dL, a serum albumin level of 4 g/dL or greater, and a serum phosphorus level of 3.5 mg/dL to 5.5 mg/dL.
The mean age of the patients was 50 years, and 61% were male. Of the 509 patients, 36% said that they were able to work and 13% were actually employed. The mean number of HD QI goals met was 3.31, and the patients’ likelihood of reporting being able to work increased with an increasing number of QI goals met (odds ratio 1.28; P = .02). "Achieving a quality indicator goal is likely a joint process between the provider and the patient," said Dr. Kutner, who directs the USRDS Rehabilitation/QoL Special Studies Center at Emory.
"The end result seems to be that as more of these goals are met, it furthers the potential for work and rehabilitation. This is very encouraging," she said at the meeting, which was sponsored by the American Society of Nephrology.
Compared with their counterparts who reported being unable to work, a higher proportion of those who reported being able to work met the QI goals of Kt/V of 1.2 or greater (92% vs. 90%, respectively), being catheter free (84% vs. 74%), having a hemoglobin level of 10-12 g/dL (62% vs. 60%), and having a serum albumin of 4.0 g/dL or greater (59% vs. 49%). The proportion of those reporting a serum phosphorus level of 3.5-5.5 mg/dL was similar between the two groups (48% vs. 50%).
Dr. Kutner said that she had no relevant financial conflicts to disclose.
AT KIDNEY WEEK 2012
Major Finding: Compared with dialysis patients who reported being unable to work, a higher proportion of those who were able to work met the hemodialysis quality indicator goals of Kt/V of 1.2 or greater (92% vs. 90%, respectively), being catheter free (84% vs. 74%), having a hemoglobin level of 10-12 g/dL (62% vs. 60%), and having a serum albumin of 4.0 g/dL or greater (59% vs. 49%).
Data Source: The analysis involved 509 patients who were on hemodialysis treatment for 3 months or longer during 2009-2011 for a U.S. Renal Data System study conducted in seven outpatient clinics in San Francisco and seven in Atlanta.
Disclosures: Dr. Kutner said that she had no relevant financial conflicts.
Metabolic bone disease markers poor in CKD patients with HF
SAN DIEGO – Levels of calcium, phosphorus, and parathyroid hormone are poorer in patients with heart failure at each stage of chronic kidney disease, results from a large study showed.
The finding "raises more questions than it answers," Dr. Claudine T. Jurkovitz said in an interview during a poster session at Kidney Week 2012. "The question is, are these patients less well managed for their metabolic bone disease than the patients without HF? If so, why? Is it because their HF is so severe, or is it because the nephrologists count on cardiologists or primary care physicians to treat the patients’ metabolic bone disease also? And do cardiologists identify metabolic bone disease in patients with HF?"
Dr. Jurkovitz, a physician scientist with Christiana Care Health System in Newark, Del., and her associates compared the management of CKD-associated metabolic bone disease between patients with and without HF who were treated at a local nephrology practice between 2000 and 2010. They evaluated the medical records of 11,883 patients with CKD stage 3 and above, and excluded dialysis and transplant patients. The researchers calculated average calcium, phosphorus, and intact parathyroid hormone (iPTH) by radioimmunoassay for each patient, and used multilinear regressions to determine the effects of CKD and HF on calcium, phosphorus, and iPTH after controlling for age, race, and gender.
The mean follow-up of the 11,883 patients was 4 years. Of these, nearly one-quarter (24%) had HF at baseline, while 76% had stage 3 CKD, 22% had stage 4 CKD, and 2% had stage 5 CKD. Patients with HF were slightly older, with a mean of 69 years, than were their counterparts without HF, who had a mean 66 years.
Dr. Jurkovitz and her associates found that the adjusted mean for calcium was significantly lower in patients with HF at each CKD stage. The interaction between CKD and HF was statistically significant. The adjusted means for phosphorus and iPTH were significantly higher in patients with HF at each CKD stage, while the interactions between CKD and HF were not significant.
"Physicians need to be concerned about the management of chronic kidney disease in their patients with HF, and the management of metabolic bone disease addressed on a case by case basis in a dialogue between the cardiologists, nephrologists, and primary care physicians," she concluded.
The meeting was sponsored by the American Society of Nephrology. Dr. Jurkovitz said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Levels of calcium, phosphorus, and parathyroid hormone are poorer in patients with heart failure at each stage of chronic kidney disease, results from a large study showed.
The finding "raises more questions than it answers," Dr. Claudine T. Jurkovitz said in an interview during a poster session at Kidney Week 2012. "The question is, are these patients less well managed for their metabolic bone disease than the patients without HF? If so, why? Is it because their HF is so severe, or is it because the nephrologists count on cardiologists or primary care physicians to treat the patients’ metabolic bone disease also? And do cardiologists identify metabolic bone disease in patients with HF?"
Dr. Jurkovitz, a physician scientist with Christiana Care Health System in Newark, Del., and her associates compared the management of CKD-associated metabolic bone disease between patients with and without HF who were treated at a local nephrology practice between 2000 and 2010. They evaluated the medical records of 11,883 patients with CKD stage 3 and above, and excluded dialysis and transplant patients. The researchers calculated average calcium, phosphorus, and intact parathyroid hormone (iPTH) by radioimmunoassay for each patient, and used multilinear regressions to determine the effects of CKD and HF on calcium, phosphorus, and iPTH after controlling for age, race, and gender.
The mean follow-up of the 11,883 patients was 4 years. Of these, nearly one-quarter (24%) had HF at baseline, while 76% had stage 3 CKD, 22% had stage 4 CKD, and 2% had stage 5 CKD. Patients with HF were slightly older, with a mean of 69 years, than were their counterparts without HF, who had a mean 66 years.
Dr. Jurkovitz and her associates found that the adjusted mean for calcium was significantly lower in patients with HF at each CKD stage. The interaction between CKD and HF was statistically significant. The adjusted means for phosphorus and iPTH were significantly higher in patients with HF at each CKD stage, while the interactions between CKD and HF were not significant.
"Physicians need to be concerned about the management of chronic kidney disease in their patients with HF, and the management of metabolic bone disease addressed on a case by case basis in a dialogue between the cardiologists, nephrologists, and primary care physicians," she concluded.
The meeting was sponsored by the American Society of Nephrology. Dr. Jurkovitz said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Levels of calcium, phosphorus, and parathyroid hormone are poorer in patients with heart failure at each stage of chronic kidney disease, results from a large study showed.
The finding "raises more questions than it answers," Dr. Claudine T. Jurkovitz said in an interview during a poster session at Kidney Week 2012. "The question is, are these patients less well managed for their metabolic bone disease than the patients without HF? If so, why? Is it because their HF is so severe, or is it because the nephrologists count on cardiologists or primary care physicians to treat the patients’ metabolic bone disease also? And do cardiologists identify metabolic bone disease in patients with HF?"
Dr. Jurkovitz, a physician scientist with Christiana Care Health System in Newark, Del., and her associates compared the management of CKD-associated metabolic bone disease between patients with and without HF who were treated at a local nephrology practice between 2000 and 2010. They evaluated the medical records of 11,883 patients with CKD stage 3 and above, and excluded dialysis and transplant patients. The researchers calculated average calcium, phosphorus, and intact parathyroid hormone (iPTH) by radioimmunoassay for each patient, and used multilinear regressions to determine the effects of CKD and HF on calcium, phosphorus, and iPTH after controlling for age, race, and gender.
The mean follow-up of the 11,883 patients was 4 years. Of these, nearly one-quarter (24%) had HF at baseline, while 76% had stage 3 CKD, 22% had stage 4 CKD, and 2% had stage 5 CKD. Patients with HF were slightly older, with a mean of 69 years, than were their counterparts without HF, who had a mean 66 years.
Dr. Jurkovitz and her associates found that the adjusted mean for calcium was significantly lower in patients with HF at each CKD stage. The interaction between CKD and HF was statistically significant. The adjusted means for phosphorus and iPTH were significantly higher in patients with HF at each CKD stage, while the interactions between CKD and HF were not significant.
"Physicians need to be concerned about the management of chronic kidney disease in their patients with HF, and the management of metabolic bone disease addressed on a case by case basis in a dialogue between the cardiologists, nephrologists, and primary care physicians," she concluded.
The meeting was sponsored by the American Society of Nephrology. Dr. Jurkovitz said that she had no relevant financial conflicts to disclose.
AT KIDNEY WEEK 2012
Major Finding: The adjusted mean for serum calcium was significantly lower in patients with heart failure at each CKD stage, while the adjusted means for serum phosphorus and parathyroid hormone by immunoassay were significantly higher in patients with HF at each CKD stage.
Data Source: This was a study of 11,883 patients with CKD stage 3 and above who were treated at a single nephrology practice during 2000-2010.
Disclosures: The meeting was sponsored by the American Society of Nephrology. Dr. Jurkovitz said that she had no relevant financial conflicts to disclose.
Antibiotic Stewardship Crucial in Special Pediatric Populations
SAN DIEGO – Antibiotic stewardship is important for every patient population, but it’s especially crucial in the care of infants hospitalized in the neonatal intensive care unit and in infants and children with cystic fibrosis, Dr. Lisa Saiman said at IDWeek 2012.
The use of antibiotics in these two pediatric populations "is clearly different," said Dr. Saiman, professor of clinical pediatrics at Columbia University Medical Center, N.Y. "In the NICU, approximately 80% of preterm babies will get IV antibiotics for early-onset sepsis and 20%-30% for late-onset sepsis. In the CF population, everybody gets antibiotics throughout their entire lives. In the NICU, we use relatively few agents because of concerns about toxicity and dosing, while in the CF population the number of agents used is enormous."
Both of these patient populations "have existing networks consisting of care centers of excellence and very motivated providers," noted Dr. Saiman, who is also the hospital epidemiologist for Morgan Stanley Children’s Hospital of New York-Presbyterian. "In the United States, it’s estimated that about 500,000 infants are hospitalized in the neonatal ICU each year, and there are about 30,000 people with CF, making this a rare disease."
In a published study of 323 courses of antibiotics administered in the NICU, Dr. Saiman and her associates found that 35% of infants received at least 1 day of inappropriate antibiotics (Pediatr. Infect. Dis. J. 2009;28:1047-51). The consequences of inappropriate antibiotic use in these two patient populations are potentially dire. In NICU patients, Dr. Saiman said, this practice could result in necrotizing endocarditis, candidemia, nephrotoxicity, ototoxicity, and drug-drug interactions. In CF patients, inappropriate antibiotic use could lead to the emergence of multidrug-resistant strains of Pseudomonas aeruginosa and of other organisms, life-threatening allergies, nephrotoxicity, ototoxicity, hepatotoxicity, phototoxicity, Clostridium difficile infection, and drug-drug interactions.
To optimize antibiotic prescribing practices in these two patient populations, Dr. Saiman advised obtaining "buy-in from key stakeholders from the beginning. Review and implement evidence-based practices to develop local guidelines. Obtain local data and provide feedback to your care teams."
Dr. Saiman disclosed that she served on the advisory boards of Novartis, Vertex, and Insmed. She has also received funding from the CF Foundation.
IDWeek is the combined annual meetings of the Infectious Diseases Society of America, the Society for Healthcare Epidemiology of America, the HIV Medicine Association, and the Pediatric Infectious Diseases Society.
SAN DIEGO – Antibiotic stewardship is important for every patient population, but it’s especially crucial in the care of infants hospitalized in the neonatal intensive care unit and in infants and children with cystic fibrosis, Dr. Lisa Saiman said at IDWeek 2012.
The use of antibiotics in these two pediatric populations "is clearly different," said Dr. Saiman, professor of clinical pediatrics at Columbia University Medical Center, N.Y. "In the NICU, approximately 80% of preterm babies will get IV antibiotics for early-onset sepsis and 20%-30% for late-onset sepsis. In the CF population, everybody gets antibiotics throughout their entire lives. In the NICU, we use relatively few agents because of concerns about toxicity and dosing, while in the CF population the number of agents used is enormous."
Both of these patient populations "have existing networks consisting of care centers of excellence and very motivated providers," noted Dr. Saiman, who is also the hospital epidemiologist for Morgan Stanley Children’s Hospital of New York-Presbyterian. "In the United States, it’s estimated that about 500,000 infants are hospitalized in the neonatal ICU each year, and there are about 30,000 people with CF, making this a rare disease."
In a published study of 323 courses of antibiotics administered in the NICU, Dr. Saiman and her associates found that 35% of infants received at least 1 day of inappropriate antibiotics (Pediatr. Infect. Dis. J. 2009;28:1047-51). The consequences of inappropriate antibiotic use in these two patient populations are potentially dire. In NICU patients, Dr. Saiman said, this practice could result in necrotizing endocarditis, candidemia, nephrotoxicity, ototoxicity, and drug-drug interactions. In CF patients, inappropriate antibiotic use could lead to the emergence of multidrug-resistant strains of Pseudomonas aeruginosa and of other organisms, life-threatening allergies, nephrotoxicity, ototoxicity, hepatotoxicity, phototoxicity, Clostridium difficile infection, and drug-drug interactions.
To optimize antibiotic prescribing practices in these two patient populations, Dr. Saiman advised obtaining "buy-in from key stakeholders from the beginning. Review and implement evidence-based practices to develop local guidelines. Obtain local data and provide feedback to your care teams."
Dr. Saiman disclosed that she served on the advisory boards of Novartis, Vertex, and Insmed. She has also received funding from the CF Foundation.
IDWeek is the combined annual meetings of the Infectious Diseases Society of America, the Society for Healthcare Epidemiology of America, the HIV Medicine Association, and the Pediatric Infectious Diseases Society.
SAN DIEGO – Antibiotic stewardship is important for every patient population, but it’s especially crucial in the care of infants hospitalized in the neonatal intensive care unit and in infants and children with cystic fibrosis, Dr. Lisa Saiman said at IDWeek 2012.
The use of antibiotics in these two pediatric populations "is clearly different," said Dr. Saiman, professor of clinical pediatrics at Columbia University Medical Center, N.Y. "In the NICU, approximately 80% of preterm babies will get IV antibiotics for early-onset sepsis and 20%-30% for late-onset sepsis. In the CF population, everybody gets antibiotics throughout their entire lives. In the NICU, we use relatively few agents because of concerns about toxicity and dosing, while in the CF population the number of agents used is enormous."
Both of these patient populations "have existing networks consisting of care centers of excellence and very motivated providers," noted Dr. Saiman, who is also the hospital epidemiologist for Morgan Stanley Children’s Hospital of New York-Presbyterian. "In the United States, it’s estimated that about 500,000 infants are hospitalized in the neonatal ICU each year, and there are about 30,000 people with CF, making this a rare disease."
In a published study of 323 courses of antibiotics administered in the NICU, Dr. Saiman and her associates found that 35% of infants received at least 1 day of inappropriate antibiotics (Pediatr. Infect. Dis. J. 2009;28:1047-51). The consequences of inappropriate antibiotic use in these two patient populations are potentially dire. In NICU patients, Dr. Saiman said, this practice could result in necrotizing endocarditis, candidemia, nephrotoxicity, ototoxicity, and drug-drug interactions. In CF patients, inappropriate antibiotic use could lead to the emergence of multidrug-resistant strains of Pseudomonas aeruginosa and of other organisms, life-threatening allergies, nephrotoxicity, ototoxicity, hepatotoxicity, phototoxicity, Clostridium difficile infection, and drug-drug interactions.
To optimize antibiotic prescribing practices in these two patient populations, Dr. Saiman advised obtaining "buy-in from key stakeholders from the beginning. Review and implement evidence-based practices to develop local guidelines. Obtain local data and provide feedback to your care teams."
Dr. Saiman disclosed that she served on the advisory boards of Novartis, Vertex, and Insmed. She has also received funding from the CF Foundation.
IDWeek is the combined annual meetings of the Infectious Diseases Society of America, the Society for Healthcare Epidemiology of America, the HIV Medicine Association, and the Pediatric Infectious Diseases Society.
EXPERT ANALYSIS FROM IDWEEK 2012
Study Finds Long-Term Benefits of DBS in Refractory Epilepsy
SAN DIEGO – Bilateral stimulation of the anterior nuclei of the thalamus led to a median reduction in partial-onset seizure frequency of 69% after a follow-up period of 5 years in the ongoing multicenter, double-blind, randomized SANTE trial.
"We were surprised that these patients still showed improvement, despite the fact that they had failed so many other treatments, including surgery," Dr. Vicenta Salanova said during a press briefing at the annual meeting of the American Epilepsy Society. "We were happy to see that."
Based on SANTE (Stimulation of the Anterior Nucleus of Thalamus for Epilepsy) trial results to date, deep brain stimulation (DBS) therapy for medically refractory partial and secondarily generalized seizures has been approved in Europe and in Canada, but it remains investigational in the United States. In 2010, the SANTE trial’s sponsor, Medtronic, submitted a premarket approval application for DBS therapy in epilepsy with the Food and Drug Administration, but both parties "are still in discussions," said Dr. Salanova, professor of neurology and director of the Indiana University School of Medicine Comprehensive Epilepsy Program in Indianapolis. "We hope that, based on the results we have shown, this will eventually be approved in the United States."
The researchers reported on 110 participants aged 18-65 years with at least six partial or secondarily generalized seizures per month who had failed treatment with at least three antiepileptic drugs. Patients with an IQ of less than 70 and those who were unable to complete neuropsychological testing or had progressive neurologic lesions were excluded from the analysis. After a baseline period of 3 months, the researchers used a stereotactic technique to implant DBS electrodes in the anterior nuclei of the thalamus bilaterally. One month after implantation, study participants were randomized to stimulation at 5 V or to no stimulation. After 3 months of blinded treatment, all patients received stimulation. Long-term follow-up began at 13 months with stimulation parameters adjusted at the investigators’ discretion. Primary analysis was performed on patients with at least 70 days of seizure diary data.
Dr. Salanova reported that by the end of the blinded treatment phase, the median seizure frequency reduction was 40% in patients who underwent DBS, compared with 14.5% in controls. Over time, patients in the DBS group demonstrated stepwise improvements in the median percent reduction of seizures from baseline, to 41% at 1 year, 56% at 2 years, and 69% at 5 years. Responder rates, defined as a 50% or greater reduction in seizure frequency, also progressively improved over time to 43% at 1 year, 54% at 2 years, and 69% at 5 years.
The researchers also found that over the entire study period 16% of patients were seizure-free for at least 6 months. They observed no unanticipated adverse device effects or symptomatic intracranial hemorrhages. Both the Liverpool Seizure Severity Scale and Quality of Life in Epilepsy-31 inventory also showed statistically significant improvement over baseline by 1 year, which continued to be significant at 5 years (P less than .001).
Medtronic sponsored the study. Dr. Salanova said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Bilateral stimulation of the anterior nuclei of the thalamus led to a median reduction in partial-onset seizure frequency of 69% after a follow-up period of 5 years in the ongoing multicenter, double-blind, randomized SANTE trial.
"We were surprised that these patients still showed improvement, despite the fact that they had failed so many other treatments, including surgery," Dr. Vicenta Salanova said during a press briefing at the annual meeting of the American Epilepsy Society. "We were happy to see that."
Based on SANTE (Stimulation of the Anterior Nucleus of Thalamus for Epilepsy) trial results to date, deep brain stimulation (DBS) therapy for medically refractory partial and secondarily generalized seizures has been approved in Europe and in Canada, but it remains investigational in the United States. In 2010, the SANTE trial’s sponsor, Medtronic, submitted a premarket approval application for DBS therapy in epilepsy with the Food and Drug Administration, but both parties "are still in discussions," said Dr. Salanova, professor of neurology and director of the Indiana University School of Medicine Comprehensive Epilepsy Program in Indianapolis. "We hope that, based on the results we have shown, this will eventually be approved in the United States."
The researchers reported on 110 participants aged 18-65 years with at least six partial or secondarily generalized seizures per month who had failed treatment with at least three antiepileptic drugs. Patients with an IQ of less than 70 and those who were unable to complete neuropsychological testing or had progressive neurologic lesions were excluded from the analysis. After a baseline period of 3 months, the researchers used a stereotactic technique to implant DBS electrodes in the anterior nuclei of the thalamus bilaterally. One month after implantation, study participants were randomized to stimulation at 5 V or to no stimulation. After 3 months of blinded treatment, all patients received stimulation. Long-term follow-up began at 13 months with stimulation parameters adjusted at the investigators’ discretion. Primary analysis was performed on patients with at least 70 days of seizure diary data.
Dr. Salanova reported that by the end of the blinded treatment phase, the median seizure frequency reduction was 40% in patients who underwent DBS, compared with 14.5% in controls. Over time, patients in the DBS group demonstrated stepwise improvements in the median percent reduction of seizures from baseline, to 41% at 1 year, 56% at 2 years, and 69% at 5 years. Responder rates, defined as a 50% or greater reduction in seizure frequency, also progressively improved over time to 43% at 1 year, 54% at 2 years, and 69% at 5 years.
The researchers also found that over the entire study period 16% of patients were seizure-free for at least 6 months. They observed no unanticipated adverse device effects or symptomatic intracranial hemorrhages. Both the Liverpool Seizure Severity Scale and Quality of Life in Epilepsy-31 inventory also showed statistically significant improvement over baseline by 1 year, which continued to be significant at 5 years (P less than .001).
Medtronic sponsored the study. Dr. Salanova said that she had no relevant financial conflicts to disclose.
SAN DIEGO – Bilateral stimulation of the anterior nuclei of the thalamus led to a median reduction in partial-onset seizure frequency of 69% after a follow-up period of 5 years in the ongoing multicenter, double-blind, randomized SANTE trial.
"We were surprised that these patients still showed improvement, despite the fact that they had failed so many other treatments, including surgery," Dr. Vicenta Salanova said during a press briefing at the annual meeting of the American Epilepsy Society. "We were happy to see that."
Based on SANTE (Stimulation of the Anterior Nucleus of Thalamus for Epilepsy) trial results to date, deep brain stimulation (DBS) therapy for medically refractory partial and secondarily generalized seizures has been approved in Europe and in Canada, but it remains investigational in the United States. In 2010, the SANTE trial’s sponsor, Medtronic, submitted a premarket approval application for DBS therapy in epilepsy with the Food and Drug Administration, but both parties "are still in discussions," said Dr. Salanova, professor of neurology and director of the Indiana University School of Medicine Comprehensive Epilepsy Program in Indianapolis. "We hope that, based on the results we have shown, this will eventually be approved in the United States."
The researchers reported on 110 participants aged 18-65 years with at least six partial or secondarily generalized seizures per month who had failed treatment with at least three antiepileptic drugs. Patients with an IQ of less than 70 and those who were unable to complete neuropsychological testing or had progressive neurologic lesions were excluded from the analysis. After a baseline period of 3 months, the researchers used a stereotactic technique to implant DBS electrodes in the anterior nuclei of the thalamus bilaterally. One month after implantation, study participants were randomized to stimulation at 5 V or to no stimulation. After 3 months of blinded treatment, all patients received stimulation. Long-term follow-up began at 13 months with stimulation parameters adjusted at the investigators’ discretion. Primary analysis was performed on patients with at least 70 days of seizure diary data.
Dr. Salanova reported that by the end of the blinded treatment phase, the median seizure frequency reduction was 40% in patients who underwent DBS, compared with 14.5% in controls. Over time, patients in the DBS group demonstrated stepwise improvements in the median percent reduction of seizures from baseline, to 41% at 1 year, 56% at 2 years, and 69% at 5 years. Responder rates, defined as a 50% or greater reduction in seizure frequency, also progressively improved over time to 43% at 1 year, 54% at 2 years, and 69% at 5 years.
The researchers also found that over the entire study period 16% of patients were seizure-free for at least 6 months. They observed no unanticipated adverse device effects or symptomatic intracranial hemorrhages. Both the Liverpool Seizure Severity Scale and Quality of Life in Epilepsy-31 inventory also showed statistically significant improvement over baseline by 1 year, which continued to be significant at 5 years (P less than .001).
Medtronic sponsored the study. Dr. Salanova said that she had no relevant financial conflicts to disclose.
AT THE ANNUAL MEETING OF THE AMERICAN EPILEPSY SOCIETY
Major Finding: Bilateral deep brain stimulation of the anterior nucleus of the thalamus demonstrated stepwise improvements in the median percent reduction of partial-onset seizures from baseline to 41% at 1 year, 56% at 2 years, and 69% at 5 years.
Data Source: This was a 5-year follow-up analysis of 110 patients enrolled in the Stimulation of the Anterior Nucleus of Thalamus for Epilepsy (SANTE) trial, an ongoing multicenter, double-blind, randomized study.
Disclosures: Medtronic sponsored the study. Dr. Salanova said that she had no relevant financial conflicts to disclose.