User login
White AAV patients post highest mortality rates
Age-adjusted mortality from antineutrophil cytoplasmic autoantibody–associated vasculitides (AAV) in the United States declined by nearly 2% each year between 1999 and 2017, based on data from the Centers for Disease Control and Prevention.
Significant morbidity and mortality are associated with untreated AAV, wrote Alexander W. Steinberg, MD, of Saint Joseph Hospital, Denver, Colo., and colleagues.
“Although population data from the United Kingdom have shown decreased AAV-related mortality during the past 20 years, it is unknown whether this pattern has occurred in the United States,” they wrote.
In a study published in Annals of Internal Medicine, the researchers identified 11,316 AAV-related deaths from 1999 to 2017 in the CDC data.
Overall, age-adjusted mortality was 1.86 per 1,000,000 persons, with highest rates among non-Hispanic whites, men, and residents of the Midwest. Mortality from AAV declined by an average of 1.6% in each year of the study period, and changes in subgroups stratified by gender, race, and geographic region were similar.
Mortality increased with age and was highest among individuals aged 75-84 years, but a significant decline in mortality occurred among individuals aged 65-74 years. “The decrease in overall mortality and mortality among persons aged 65 to 74 years may reflect increased longevity due to improved treatment of AAV and common comorbid conditions,” the researchers said.
“Surprisingly, the authors found much lower age-adjusted mortality rates for non-Hispanic black persons (0.77) and moderately lower mortality rates for Hispanic persons (1.57) than for non-Hispanic white persons (2.03),” wrote John R. Stone, MD, PhD, of Creighton University, Omaha, Neb., in an accompanying editorial.
“Suppose the mortality rate differences reported by Steinberg and colleagues are statistically significant, accurately represent death certificate diagnoses, and match people’s racial/ethnic self-identification. The data then show neither that the vasculitides actually have lower mortality rates in blacks or Hispanics compared with whites, nor that the diseases are indeed less frequent in blacks and Hispanics,” he said. “Rather, these differences probably signify how social inequities, social structural violence, and inferior health care access adversely influence diagnosis of rare diseases and promote health inequity,” Dr. Stone added. The findings suggest that clinicians should remain alert to AAV in some ethnic groups to improve diagnostic accuracy, he said.
“Moreover, improved AAV diagnosis in such groups is key to recruiting participants for research investigating whether therapies should differ among populations,” he emphasized.
The study findings were limited by possible under- or overreporting of AAV on death certificates, but they were strengthened by the large sample size, the researchers noted. “We hope that the mortality patterns presented here can be used to direct future research on the driving forces behind these trends,” they said.
Dr. Steinberg had no financial conflicts to disclose. Dr. Stone had no financial conflicts to disclose.
SOURCES: Steinberg AW et al. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-1564; and Stone JR. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-2755.
Age-adjusted mortality from antineutrophil cytoplasmic autoantibody–associated vasculitides (AAV) in the United States declined by nearly 2% each year between 1999 and 2017, based on data from the Centers for Disease Control and Prevention.
Significant morbidity and mortality are associated with untreated AAV, wrote Alexander W. Steinberg, MD, of Saint Joseph Hospital, Denver, Colo., and colleagues.
“Although population data from the United Kingdom have shown decreased AAV-related mortality during the past 20 years, it is unknown whether this pattern has occurred in the United States,” they wrote.
In a study published in Annals of Internal Medicine, the researchers identified 11,316 AAV-related deaths from 1999 to 2017 in the CDC data.
Overall, age-adjusted mortality was 1.86 per 1,000,000 persons, with highest rates among non-Hispanic whites, men, and residents of the Midwest. Mortality from AAV declined by an average of 1.6% in each year of the study period, and changes in subgroups stratified by gender, race, and geographic region were similar.
Mortality increased with age and was highest among individuals aged 75-84 years, but a significant decline in mortality occurred among individuals aged 65-74 years. “The decrease in overall mortality and mortality among persons aged 65 to 74 years may reflect increased longevity due to improved treatment of AAV and common comorbid conditions,” the researchers said.
“Surprisingly, the authors found much lower age-adjusted mortality rates for non-Hispanic black persons (0.77) and moderately lower mortality rates for Hispanic persons (1.57) than for non-Hispanic white persons (2.03),” wrote John R. Stone, MD, PhD, of Creighton University, Omaha, Neb., in an accompanying editorial.
“Suppose the mortality rate differences reported by Steinberg and colleagues are statistically significant, accurately represent death certificate diagnoses, and match people’s racial/ethnic self-identification. The data then show neither that the vasculitides actually have lower mortality rates in blacks or Hispanics compared with whites, nor that the diseases are indeed less frequent in blacks and Hispanics,” he said. “Rather, these differences probably signify how social inequities, social structural violence, and inferior health care access adversely influence diagnosis of rare diseases and promote health inequity,” Dr. Stone added. The findings suggest that clinicians should remain alert to AAV in some ethnic groups to improve diagnostic accuracy, he said.
“Moreover, improved AAV diagnosis in such groups is key to recruiting participants for research investigating whether therapies should differ among populations,” he emphasized.
The study findings were limited by possible under- or overreporting of AAV on death certificates, but they were strengthened by the large sample size, the researchers noted. “We hope that the mortality patterns presented here can be used to direct future research on the driving forces behind these trends,” they said.
Dr. Steinberg had no financial conflicts to disclose. Dr. Stone had no financial conflicts to disclose.
SOURCES: Steinberg AW et al. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-1564; and Stone JR. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-2755.
Age-adjusted mortality from antineutrophil cytoplasmic autoantibody–associated vasculitides (AAV) in the United States declined by nearly 2% each year between 1999 and 2017, based on data from the Centers for Disease Control and Prevention.
Significant morbidity and mortality are associated with untreated AAV, wrote Alexander W. Steinberg, MD, of Saint Joseph Hospital, Denver, Colo., and colleagues.
“Although population data from the United Kingdom have shown decreased AAV-related mortality during the past 20 years, it is unknown whether this pattern has occurred in the United States,” they wrote.
In a study published in Annals of Internal Medicine, the researchers identified 11,316 AAV-related deaths from 1999 to 2017 in the CDC data.
Overall, age-adjusted mortality was 1.86 per 1,000,000 persons, with highest rates among non-Hispanic whites, men, and residents of the Midwest. Mortality from AAV declined by an average of 1.6% in each year of the study period, and changes in subgroups stratified by gender, race, and geographic region were similar.
Mortality increased with age and was highest among individuals aged 75-84 years, but a significant decline in mortality occurred among individuals aged 65-74 years. “The decrease in overall mortality and mortality among persons aged 65 to 74 years may reflect increased longevity due to improved treatment of AAV and common comorbid conditions,” the researchers said.
“Surprisingly, the authors found much lower age-adjusted mortality rates for non-Hispanic black persons (0.77) and moderately lower mortality rates for Hispanic persons (1.57) than for non-Hispanic white persons (2.03),” wrote John R. Stone, MD, PhD, of Creighton University, Omaha, Neb., in an accompanying editorial.
“Suppose the mortality rate differences reported by Steinberg and colleagues are statistically significant, accurately represent death certificate diagnoses, and match people’s racial/ethnic self-identification. The data then show neither that the vasculitides actually have lower mortality rates in blacks or Hispanics compared with whites, nor that the diseases are indeed less frequent in blacks and Hispanics,” he said. “Rather, these differences probably signify how social inequities, social structural violence, and inferior health care access adversely influence diagnosis of rare diseases and promote health inequity,” Dr. Stone added. The findings suggest that clinicians should remain alert to AAV in some ethnic groups to improve diagnostic accuracy, he said.
“Moreover, improved AAV diagnosis in such groups is key to recruiting participants for research investigating whether therapies should differ among populations,” he emphasized.
The study findings were limited by possible under- or overreporting of AAV on death certificates, but they were strengthened by the large sample size, the researchers noted. “We hope that the mortality patterns presented here can be used to direct future research on the driving forces behind these trends,” they said.
Dr. Steinberg had no financial conflicts to disclose. Dr. Stone had no financial conflicts to disclose.
SOURCES: Steinberg AW et al. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-1564; and Stone JR. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-2755.
FROM ANNALS OF INTERNAL MEDICINE
Key clinical point: The mortality rate from antineutrophil cytoplasmic autoantibody–associated vasculitides (AAV) in the United States was 1.86 per 1,000,000 individuals from 1999 to 2017.
Major finding: Age-adjusted mortality from AAV decreased by approximately 2% each year between 1999 and 2017.
Study details: The data come from a review of 11,316 AAV-related deaths.
Disclosures: Dr. Steinberg had no financial conflicts to disclose.
Source: Steinberg AW et al. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-1564.
Clinician burnout can impact quality of care
Burnout among health care professionals has been associated with lower quality of care, but the effect may be smaller than it seems, based on data from a meta-analysis of more than 200,000 clinicians.
Previous studies have reported associations between burnout and lower quality of care, but a standardized approach to analyze bias in the studies is lacking, wrote Daniel S. Tawfik, MD, of Stanford (Calif.) University and colleagues.
In a study published in the Annals of Internal Medicine, the researchers identified 123 publications from 1994 to 2019 with 142 study populations that included 241,553 health care providers.
Emotional exhaustion was the primary predictor for lower quality of care in 75 study populations, and overall burnout and depersonalization were the primary predictors for 56 and 11 study populations, respectively.
In an analysis of 114 unique burnout-quality combinations, 58 showed effects of burnout related to poor-quality care, 6 showed burnout related to high-quality care, and 50 showed no significant effect. Approximately one-third (33%) of the burnout-quality combinations were reported at least three times. In a review of the 46 burnout-quality combinations with primary effect sizes, 24 showed a significant effect of burnout on poor quality of care, 1 showed a significant effect of burnout on high quality of care, and 21 showed no significant effect.
The researchers also tested study bias using the Ioannidis test and found “an excess of observed versus predicted statistically significant studies (73% observed vs. 62%).”
The findings were limited by several factors, including the use of many cross-sectional, observational studies that could not show causality, the researchers noted. However, the results suggest several implications for future research including the need to consider exaggerated effects and reduce bias.
“Although the effect sizes in the published literature are modestly strong, our finding of excess significance implies that the true magnitude may be smaller than reported, and the studies that attempted to lower the risk of bias demonstrate fewer significant associations than the full evidence base,” the researchers noted.
“Whether curtailing burnout improves quality of care, or whether improving quality of care reduces burnout, is not yet known, and adequately powered and designed randomized trials will be indispensable in answering these questions,” they concluded.
The study was supported by the Stanford Maternal and Child Health Research Institute. Dr. Tawfik disclosed grants from Stanford Maternal and Child Health Research Institute during the study period.
SOURCE: Tawfik DS et al. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-1152.
The current meta-analysis is consistent with previous research, but offers nothing new on the relationship between clinician burnout and quality of care, wrote Carolyn S. Dewa, MPH, PhD, Karen Nieuwenhuijsen, PhD, and Jeffrey S. Hoch, PhD, in an accompanying editorial.
Some of the concerns they expressed included variability in the methods used to measure provider burnout, as well as variability in measuring and defining medical error. They suggested that the researchers could have conducted a subgroup analysis based on error definition. “Such analyses might shed light on the types of errors associated with burnout and suggest directions for the design of robust psychometric studies about the error metrics,” they wrote.
The editorialists also expressed concerns about the heterogeneity of the studies included in the review and the potential for confounding. Finally, they noted that the use of observational studies in a meta-analysis can be challenging because “the assessment of observational studies is not straightforward.” They added that knowing the limitations of the studies is important in allowing readers to be confident in the estimates from any meta-analyses.
“Considering the limitations of the available literature, prior reviews, and Tawfik and colleagues’ current meta-analysis, we conclude that higher burnout is associated with lower quality, but we are left without clear answers about the magnitude or clinical significance of the relationship,” they wrote (Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-2760).
Dr. Dewa and Dr. Hoch are affiliated with the University of California, Davis. Dr. Nieuwenhuijsen is affiliated with the University of Amsterdam. The editorialists had no financial conflicts to disclose.
The current meta-analysis is consistent with previous research, but offers nothing new on the relationship between clinician burnout and quality of care, wrote Carolyn S. Dewa, MPH, PhD, Karen Nieuwenhuijsen, PhD, and Jeffrey S. Hoch, PhD, in an accompanying editorial.
Some of the concerns they expressed included variability in the methods used to measure provider burnout, as well as variability in measuring and defining medical error. They suggested that the researchers could have conducted a subgroup analysis based on error definition. “Such analyses might shed light on the types of errors associated with burnout and suggest directions for the design of robust psychometric studies about the error metrics,” they wrote.
The editorialists also expressed concerns about the heterogeneity of the studies included in the review and the potential for confounding. Finally, they noted that the use of observational studies in a meta-analysis can be challenging because “the assessment of observational studies is not straightforward.” They added that knowing the limitations of the studies is important in allowing readers to be confident in the estimates from any meta-analyses.
“Considering the limitations of the available literature, prior reviews, and Tawfik and colleagues’ current meta-analysis, we conclude that higher burnout is associated with lower quality, but we are left without clear answers about the magnitude or clinical significance of the relationship,” they wrote (Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-2760).
Dr. Dewa and Dr. Hoch are affiliated with the University of California, Davis. Dr. Nieuwenhuijsen is affiliated with the University of Amsterdam. The editorialists had no financial conflicts to disclose.
The current meta-analysis is consistent with previous research, but offers nothing new on the relationship between clinician burnout and quality of care, wrote Carolyn S. Dewa, MPH, PhD, Karen Nieuwenhuijsen, PhD, and Jeffrey S. Hoch, PhD, in an accompanying editorial.
Some of the concerns they expressed included variability in the methods used to measure provider burnout, as well as variability in measuring and defining medical error. They suggested that the researchers could have conducted a subgroup analysis based on error definition. “Such analyses might shed light on the types of errors associated with burnout and suggest directions for the design of robust psychometric studies about the error metrics,” they wrote.
The editorialists also expressed concerns about the heterogeneity of the studies included in the review and the potential for confounding. Finally, they noted that the use of observational studies in a meta-analysis can be challenging because “the assessment of observational studies is not straightforward.” They added that knowing the limitations of the studies is important in allowing readers to be confident in the estimates from any meta-analyses.
“Considering the limitations of the available literature, prior reviews, and Tawfik and colleagues’ current meta-analysis, we conclude that higher burnout is associated with lower quality, but we are left without clear answers about the magnitude or clinical significance of the relationship,” they wrote (Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-2760).
Dr. Dewa and Dr. Hoch are affiliated with the University of California, Davis. Dr. Nieuwenhuijsen is affiliated with the University of Amsterdam. The editorialists had no financial conflicts to disclose.
Burnout among health care professionals has been associated with lower quality of care, but the effect may be smaller than it seems, based on data from a meta-analysis of more than 200,000 clinicians.
Previous studies have reported associations between burnout and lower quality of care, but a standardized approach to analyze bias in the studies is lacking, wrote Daniel S. Tawfik, MD, of Stanford (Calif.) University and colleagues.
In a study published in the Annals of Internal Medicine, the researchers identified 123 publications from 1994 to 2019 with 142 study populations that included 241,553 health care providers.
Emotional exhaustion was the primary predictor for lower quality of care in 75 study populations, and overall burnout and depersonalization were the primary predictors for 56 and 11 study populations, respectively.
In an analysis of 114 unique burnout-quality combinations, 58 showed effects of burnout related to poor-quality care, 6 showed burnout related to high-quality care, and 50 showed no significant effect. Approximately one-third (33%) of the burnout-quality combinations were reported at least three times. In a review of the 46 burnout-quality combinations with primary effect sizes, 24 showed a significant effect of burnout on poor quality of care, 1 showed a significant effect of burnout on high quality of care, and 21 showed no significant effect.
The researchers also tested study bias using the Ioannidis test and found “an excess of observed versus predicted statistically significant studies (73% observed vs. 62%).”
The findings were limited by several factors, including the use of many cross-sectional, observational studies that could not show causality, the researchers noted. However, the results suggest several implications for future research including the need to consider exaggerated effects and reduce bias.
“Although the effect sizes in the published literature are modestly strong, our finding of excess significance implies that the true magnitude may be smaller than reported, and the studies that attempted to lower the risk of bias demonstrate fewer significant associations than the full evidence base,” the researchers noted.
“Whether curtailing burnout improves quality of care, or whether improving quality of care reduces burnout, is not yet known, and adequately powered and designed randomized trials will be indispensable in answering these questions,” they concluded.
The study was supported by the Stanford Maternal and Child Health Research Institute. Dr. Tawfik disclosed grants from Stanford Maternal and Child Health Research Institute during the study period.
SOURCE: Tawfik DS et al. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-1152.
Burnout among health care professionals has been associated with lower quality of care, but the effect may be smaller than it seems, based on data from a meta-analysis of more than 200,000 clinicians.
Previous studies have reported associations between burnout and lower quality of care, but a standardized approach to analyze bias in the studies is lacking, wrote Daniel S. Tawfik, MD, of Stanford (Calif.) University and colleagues.
In a study published in the Annals of Internal Medicine, the researchers identified 123 publications from 1994 to 2019 with 142 study populations that included 241,553 health care providers.
Emotional exhaustion was the primary predictor for lower quality of care in 75 study populations, and overall burnout and depersonalization were the primary predictors for 56 and 11 study populations, respectively.
In an analysis of 114 unique burnout-quality combinations, 58 showed effects of burnout related to poor-quality care, 6 showed burnout related to high-quality care, and 50 showed no significant effect. Approximately one-third (33%) of the burnout-quality combinations were reported at least three times. In a review of the 46 burnout-quality combinations with primary effect sizes, 24 showed a significant effect of burnout on poor quality of care, 1 showed a significant effect of burnout on high quality of care, and 21 showed no significant effect.
The researchers also tested study bias using the Ioannidis test and found “an excess of observed versus predicted statistically significant studies (73% observed vs. 62%).”
The findings were limited by several factors, including the use of many cross-sectional, observational studies that could not show causality, the researchers noted. However, the results suggest several implications for future research including the need to consider exaggerated effects and reduce bias.
“Although the effect sizes in the published literature are modestly strong, our finding of excess significance implies that the true magnitude may be smaller than reported, and the studies that attempted to lower the risk of bias demonstrate fewer significant associations than the full evidence base,” the researchers noted.
“Whether curtailing burnout improves quality of care, or whether improving quality of care reduces burnout, is not yet known, and adequately powered and designed randomized trials will be indispensable in answering these questions,” they concluded.
The study was supported by the Stanford Maternal and Child Health Research Institute. Dr. Tawfik disclosed grants from Stanford Maternal and Child Health Research Institute during the study period.
SOURCE: Tawfik DS et al. Ann Intern Med. 2019 Oct 8. doi: 10.7326/M19-1152.
FROM THE ANNALS OF INTERNAL MEDICINE
FDA approves trifarotene for treating acne
The Food and Drug Administration has approved trifarotene cream 0.005% for the treatment of acne vulgaris. The product is manufactured by Galderma under the brand name Aklief.
The approval was based on data from a pair of phase 3, randomized trials including 2,420 patients aged 9 years and older. The trials evaluated the effectiveness of the cream in a once-daily topical dose for facial and truncal acne at 12 weeks. Patients showed a significant reduction in the number of inflammatory lesions as early as 2 weeks on the face (including forehead cheeks, nose, and chin) and as early as 4 weeks on the trunk (including back, chest, and shoulders), compared with a control cream. The most common treatment-emergent adverse events were pain, dryness, discoloration, or rash at the site of application. Some patients also reported sunburn.
The complete study findings were published in the June issue of the Journal of the American Academy of Dermatology.
The studies, funded by Galderma, “showed that once-daily trifarotene cream appears effective and safe, with manageable local tolerability, for the treatment for facial and truncal acne,” wrote lead author Jerry Tan, MD, of the University of Western Ontario, London, and colleagues. “The studies provide substantial evidence to support use of this new topical retinoid in facial and truncal acne,” the researchers wrote.
Trifarotene is designed to target the retinoic acid receptor gamma, the most common retinoic acid receptor in the skin, and is the first new retinoid to be approved by the FDA in approximately 2 decades, according to a press release from Galderma.
The product is expected to be available in the United States in November 2019 in a 45-g pump.
The Food and Drug Administration has approved trifarotene cream 0.005% for the treatment of acne vulgaris. The product is manufactured by Galderma under the brand name Aklief.
The approval was based on data from a pair of phase 3, randomized trials including 2,420 patients aged 9 years and older. The trials evaluated the effectiveness of the cream in a once-daily topical dose for facial and truncal acne at 12 weeks. Patients showed a significant reduction in the number of inflammatory lesions as early as 2 weeks on the face (including forehead cheeks, nose, and chin) and as early as 4 weeks on the trunk (including back, chest, and shoulders), compared with a control cream. The most common treatment-emergent adverse events were pain, dryness, discoloration, or rash at the site of application. Some patients also reported sunburn.
The complete study findings were published in the June issue of the Journal of the American Academy of Dermatology.
The studies, funded by Galderma, “showed that once-daily trifarotene cream appears effective and safe, with manageable local tolerability, for the treatment for facial and truncal acne,” wrote lead author Jerry Tan, MD, of the University of Western Ontario, London, and colleagues. “The studies provide substantial evidence to support use of this new topical retinoid in facial and truncal acne,” the researchers wrote.
Trifarotene is designed to target the retinoic acid receptor gamma, the most common retinoic acid receptor in the skin, and is the first new retinoid to be approved by the FDA in approximately 2 decades, according to a press release from Galderma.
The product is expected to be available in the United States in November 2019 in a 45-g pump.
The Food and Drug Administration has approved trifarotene cream 0.005% for the treatment of acne vulgaris. The product is manufactured by Galderma under the brand name Aklief.
The approval was based on data from a pair of phase 3, randomized trials including 2,420 patients aged 9 years and older. The trials evaluated the effectiveness of the cream in a once-daily topical dose for facial and truncal acne at 12 weeks. Patients showed a significant reduction in the number of inflammatory lesions as early as 2 weeks on the face (including forehead cheeks, nose, and chin) and as early as 4 weeks on the trunk (including back, chest, and shoulders), compared with a control cream. The most common treatment-emergent adverse events were pain, dryness, discoloration, or rash at the site of application. Some patients also reported sunburn.
The complete study findings were published in the June issue of the Journal of the American Academy of Dermatology.
The studies, funded by Galderma, “showed that once-daily trifarotene cream appears effective and safe, with manageable local tolerability, for the treatment for facial and truncal acne,” wrote lead author Jerry Tan, MD, of the University of Western Ontario, London, and colleagues. “The studies provide substantial evidence to support use of this new topical retinoid in facial and truncal acne,” the researchers wrote.
Trifarotene is designed to target the retinoic acid receptor gamma, the most common retinoic acid receptor in the skin, and is the first new retinoid to be approved by the FDA in approximately 2 decades, according to a press release from Galderma.
The product is expected to be available in the United States in November 2019 in a 45-g pump.
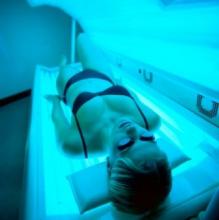
Lifetime indoor tanning raises risk of cutaneous squamous cell carcinoma
Women who accumulated more indoor tanning sessions over time significantly increased their risk for squamous cell cancer over women who never engaged in indoor tanning, based on data from 159,419 women.
Previous research has examined associations between indoor tanning and cutaneous melanoma, but an association between indoor tanning and squamous cell carcinoma (SCC) has not been well studied, wrote Simon Lergenmuller, MSc, of the University of Oslo, and colleagues.
In a prospective cohort study published in JAMA Dermatology, the researchers surveyed 159,419 women from the Norwegian Women and Cancer study. Of these, 95,552 women (69%) reported ever use of indoor tanning. The average age at study inclusion was 50 years. During an average of 17 years’ follow-up, 597 women developed SCC.
Overall, the risk of SCC increased with increasing numbers of indoor tanning sessions. The adjusted hazard ratio for most tanning sessions versus no tanning sessions was 1.83. “The association between cumulative exposure to indoor tanning and SCC risk was the same regardless of duration of use and age at initiation,” the researchers wrote.
The risk of SCC was significantly higher both among women with 10 years or less of tanning bed use and among those with more than 10 years of use, compared with never users (HRs, 1.41 and 1.43, respectively). Similarly, researchers found a significantly higher risk of SCC among women who started indoor tanning at age 30 years or older and those who started younger than 30 years, compared with never users (HRs, 1.36 and HR, 1.51, respectively).
No significant association appeared between age at initiation of indoor tanning and age at the time of SCC diagnosis.
The study findings were limited by several factors including the variation in UV radiation among tanning devices, the lack of data on men, and the retrospective collection of UV exposure data that likely led to some misclassification, the researchers noted.
However, the results were strengthened by the large sample size and support the association between increased exposure to indoor tanning and increased risk of SCC, they wrote. “Avoidance of indoor tanning may help prevent not only melanoma but also SCC, and our results support the development of policies that regulate indoor tanning.”
The study was supported by the Institute of Basic Medical Sciences, University of Oslo, and the Norwegian Cancer Society. The researchers had no financial conflicts to disclose.
SOURCE: Lergenmuller S et al. JAMA Dermatol. 2019 Oct 2. doi: 10.1001/jamadermatol.2019.2681.
“There is a saying that ‘when prevention works, nothing happens,’ ” wrote Boris D. Lushniak, MD, in an accompanying editorial. Dermatology plays an important role in public health, most notably skin cancer prevention, and the specialty’s efforts to educate the public and raise awareness about skin cancer and its causes are paying off, in combination with government initiatives to reduce exposure to UV radiation. The current study adds to the data on risk factors for skin cancer, and is distinctive in its focus on artificial sources of UV radiation, specifically indoor tanning sources. The relationship between indoor tanning and basal cell carcinoma or squamous cell carcinoma has not been well studied, “so this study fills an important gap,” he noted.
Research on indoor tanning and other skin cancer risk factors can help expand skin cancer prevention efforts and support goals such as the Healthy People 2020 goal of “reducing the proportion of adolescents in grades 9-12 who report using artificial sources of UV light for tanning, and reducing the proportion of adults aged 18 years or older who report using artificial sources of UV light for tanning,” he wrote.
The first-ever Surgeon General’s Call to Action to Prevent Skin Cancer, released in 2014, made skin cancer prevention a priority and offered specific strategies including providing more sun protection in outdoor settings, educating the public about UV exposure, promoting polices to help prevent skin cancer, reducing harm from indoor tanning, and increasing the collection of data related to skin cancer prevention.
The strategies seem to be working, Dr. Lushniak wrote. Based on data from the 2015 Youth Risk Behavior Surveillance System, a significant linear decrease in the use of indoor tanning devices by youth occurred between 2009 and 2015. “Oftentimes we do not appreciate or celebrate the successes of prevention. ... Let’s keep on track on that bold and noble mission of preventing skin cancer,” he added (JAMA Dermatol. 2019 Oct 2. doi: 10.1001/jamadermatol.2019.2680).
Dr. Lushniak is affiliated with the University of Maryland School of Public Health, College Park. He served as acting U.S. Surgeon General from 2013 to 2014, and as U.S. Deputy Surgeon General from 2010 to 2015. He had no financial conflicts to disclose.
“There is a saying that ‘when prevention works, nothing happens,’ ” wrote Boris D. Lushniak, MD, in an accompanying editorial. Dermatology plays an important role in public health, most notably skin cancer prevention, and the specialty’s efforts to educate the public and raise awareness about skin cancer and its causes are paying off, in combination with government initiatives to reduce exposure to UV radiation. The current study adds to the data on risk factors for skin cancer, and is distinctive in its focus on artificial sources of UV radiation, specifically indoor tanning sources. The relationship between indoor tanning and basal cell carcinoma or squamous cell carcinoma has not been well studied, “so this study fills an important gap,” he noted.
Research on indoor tanning and other skin cancer risk factors can help expand skin cancer prevention efforts and support goals such as the Healthy People 2020 goal of “reducing the proportion of adolescents in grades 9-12 who report using artificial sources of UV light for tanning, and reducing the proportion of adults aged 18 years or older who report using artificial sources of UV light for tanning,” he wrote.
The first-ever Surgeon General’s Call to Action to Prevent Skin Cancer, released in 2014, made skin cancer prevention a priority and offered specific strategies including providing more sun protection in outdoor settings, educating the public about UV exposure, promoting polices to help prevent skin cancer, reducing harm from indoor tanning, and increasing the collection of data related to skin cancer prevention.
The strategies seem to be working, Dr. Lushniak wrote. Based on data from the 2015 Youth Risk Behavior Surveillance System, a significant linear decrease in the use of indoor tanning devices by youth occurred between 2009 and 2015. “Oftentimes we do not appreciate or celebrate the successes of prevention. ... Let’s keep on track on that bold and noble mission of preventing skin cancer,” he added (JAMA Dermatol. 2019 Oct 2. doi: 10.1001/jamadermatol.2019.2680).
Dr. Lushniak is affiliated with the University of Maryland School of Public Health, College Park. He served as acting U.S. Surgeon General from 2013 to 2014, and as U.S. Deputy Surgeon General from 2010 to 2015. He had no financial conflicts to disclose.
“There is a saying that ‘when prevention works, nothing happens,’ ” wrote Boris D. Lushniak, MD, in an accompanying editorial. Dermatology plays an important role in public health, most notably skin cancer prevention, and the specialty’s efforts to educate the public and raise awareness about skin cancer and its causes are paying off, in combination with government initiatives to reduce exposure to UV radiation. The current study adds to the data on risk factors for skin cancer, and is distinctive in its focus on artificial sources of UV radiation, specifically indoor tanning sources. The relationship between indoor tanning and basal cell carcinoma or squamous cell carcinoma has not been well studied, “so this study fills an important gap,” he noted.
Research on indoor tanning and other skin cancer risk factors can help expand skin cancer prevention efforts and support goals such as the Healthy People 2020 goal of “reducing the proportion of adolescents in grades 9-12 who report using artificial sources of UV light for tanning, and reducing the proportion of adults aged 18 years or older who report using artificial sources of UV light for tanning,” he wrote.
The first-ever Surgeon General’s Call to Action to Prevent Skin Cancer, released in 2014, made skin cancer prevention a priority and offered specific strategies including providing more sun protection in outdoor settings, educating the public about UV exposure, promoting polices to help prevent skin cancer, reducing harm from indoor tanning, and increasing the collection of data related to skin cancer prevention.
The strategies seem to be working, Dr. Lushniak wrote. Based on data from the 2015 Youth Risk Behavior Surveillance System, a significant linear decrease in the use of indoor tanning devices by youth occurred between 2009 and 2015. “Oftentimes we do not appreciate or celebrate the successes of prevention. ... Let’s keep on track on that bold and noble mission of preventing skin cancer,” he added (JAMA Dermatol. 2019 Oct 2. doi: 10.1001/jamadermatol.2019.2680).
Dr. Lushniak is affiliated with the University of Maryland School of Public Health, College Park. He served as acting U.S. Surgeon General from 2013 to 2014, and as U.S. Deputy Surgeon General from 2010 to 2015. He had no financial conflicts to disclose.
Women who accumulated more indoor tanning sessions over time significantly increased their risk for squamous cell cancer over women who never engaged in indoor tanning, based on data from 159,419 women.
Previous research has examined associations between indoor tanning and cutaneous melanoma, but an association between indoor tanning and squamous cell carcinoma (SCC) has not been well studied, wrote Simon Lergenmuller, MSc, of the University of Oslo, and colleagues.
In a prospective cohort study published in JAMA Dermatology, the researchers surveyed 159,419 women from the Norwegian Women and Cancer study. Of these, 95,552 women (69%) reported ever use of indoor tanning. The average age at study inclusion was 50 years. During an average of 17 years’ follow-up, 597 women developed SCC.
Overall, the risk of SCC increased with increasing numbers of indoor tanning sessions. The adjusted hazard ratio for most tanning sessions versus no tanning sessions was 1.83. “The association between cumulative exposure to indoor tanning and SCC risk was the same regardless of duration of use and age at initiation,” the researchers wrote.
The risk of SCC was significantly higher both among women with 10 years or less of tanning bed use and among those with more than 10 years of use, compared with never users (HRs, 1.41 and 1.43, respectively). Similarly, researchers found a significantly higher risk of SCC among women who started indoor tanning at age 30 years or older and those who started younger than 30 years, compared with never users (HRs, 1.36 and HR, 1.51, respectively).
No significant association appeared between age at initiation of indoor tanning and age at the time of SCC diagnosis.
The study findings were limited by several factors including the variation in UV radiation among tanning devices, the lack of data on men, and the retrospective collection of UV exposure data that likely led to some misclassification, the researchers noted.
However, the results were strengthened by the large sample size and support the association between increased exposure to indoor tanning and increased risk of SCC, they wrote. “Avoidance of indoor tanning may help prevent not only melanoma but also SCC, and our results support the development of policies that regulate indoor tanning.”
The study was supported by the Institute of Basic Medical Sciences, University of Oslo, and the Norwegian Cancer Society. The researchers had no financial conflicts to disclose.
SOURCE: Lergenmuller S et al. JAMA Dermatol. 2019 Oct 2. doi: 10.1001/jamadermatol.2019.2681.
Women who accumulated more indoor tanning sessions over time significantly increased their risk for squamous cell cancer over women who never engaged in indoor tanning, based on data from 159,419 women.
Previous research has examined associations between indoor tanning and cutaneous melanoma, but an association between indoor tanning and squamous cell carcinoma (SCC) has not been well studied, wrote Simon Lergenmuller, MSc, of the University of Oslo, and colleagues.
In a prospective cohort study published in JAMA Dermatology, the researchers surveyed 159,419 women from the Norwegian Women and Cancer study. Of these, 95,552 women (69%) reported ever use of indoor tanning. The average age at study inclusion was 50 years. During an average of 17 years’ follow-up, 597 women developed SCC.
Overall, the risk of SCC increased with increasing numbers of indoor tanning sessions. The adjusted hazard ratio for most tanning sessions versus no tanning sessions was 1.83. “The association between cumulative exposure to indoor tanning and SCC risk was the same regardless of duration of use and age at initiation,” the researchers wrote.
The risk of SCC was significantly higher both among women with 10 years or less of tanning bed use and among those with more than 10 years of use, compared with never users (HRs, 1.41 and 1.43, respectively). Similarly, researchers found a significantly higher risk of SCC among women who started indoor tanning at age 30 years or older and those who started younger than 30 years, compared with never users (HRs, 1.36 and HR, 1.51, respectively).
No significant association appeared between age at initiation of indoor tanning and age at the time of SCC diagnosis.
The study findings were limited by several factors including the variation in UV radiation among tanning devices, the lack of data on men, and the retrospective collection of UV exposure data that likely led to some misclassification, the researchers noted.
However, the results were strengthened by the large sample size and support the association between increased exposure to indoor tanning and increased risk of SCC, they wrote. “Avoidance of indoor tanning may help prevent not only melanoma but also SCC, and our results support the development of policies that regulate indoor tanning.”
The study was supported by the Institute of Basic Medical Sciences, University of Oslo, and the Norwegian Cancer Society. The researchers had no financial conflicts to disclose.
SOURCE: Lergenmuller S et al. JAMA Dermatol. 2019 Oct 2. doi: 10.1001/jamadermatol.2019.2681.
FROM JAMA DERMATOLOGY
Supine sleep in late pregnancy may promote low birth weight
Data from previous studies suggest that impaired uteroplacental flow can affect fetal growth, wrote Ngaire H. Anderson, PhD, of the University of Auckland, N.Z., and colleagues.
“The initial going-to-sleep position is the sleep position that women maintain for the longest duration throughout the night; therefore, going-to-sleep position is likely to have the greatest impact on blood flow to the developing fetus,” they said.
In a study published in JAMA Network Open, the researchers interviewed women with ongoing pregnancies at 28 weeks’ gestation or later to determine their sleeping positions. The mean age of the participants was 30 years. Of the 1,760 women, 3% reported that they usually slept supine during the past 1-4 weeks.
The adjusted mean birth weight was 3,410 g among supine sleepers and 3,554 g among nonsupine sleepers. The primary outcome was an adjusted mean difference in birth weight between infants of supine sleepers and nonsupine sleepers, which was a statistically significant 144 g (P = .009).
The study findings were limited by several factors including the small number of women who were reported supine sleepers, as well as the reliance on self-reports of sleep position, the researchers said.
However, women who had going-to-sleep data for the previous night and the previous month suggest that most women are consistent in their going-to-sleep position, they noted. “It is also biologically plausible that the association of decreased maternal blood flow on birth size with supine maternal position is cumulative over time,” but the researchers were not able to investigate how the duration of supine sleeping might further affect birth weight.
Although it might make additional studies more difficult, a public health campaign to encourage pregnant women to sleep on their side during the third trimester is a safe and easy opportunity to potentially optimize birth weight, they added.
The study was important because of the limited number of high-quality studies on the effects of maternal sleep on perinatal outcomes, Martina Badell, MD of Emory University in Atlanta said in an interview.
“The overall findings suggested a possible small increased risk of small-for-gestational-age babies with supine maternal sleeping, however, the absolute gram difference of 144 grams at term may not be clinically relevant,” she said. In addition, the relatively small number of women who reported supine sleep in late pregnancy suggests that broad public health campaigns or recommendations may not be indicated at this time.
“Also, the percentage of women who are supine sleepers at term is only approximately 3%, and this study didn’t assess reasons for supine sleeping in this small subset of women,” she said. “Further research is needed to assess whether there are specific maternal factors associated with supine sleeping, such as GI symptoms or respiratory difficulties, which could contribute to smaller fetal size rather than the sleep position itself.”
The study was supported by a Trans-Tasman Research Funding Grant by Cure Kids and Red Nose Australia. Six coauthors reported receiving numerous grants from a variety of organizations. Dr. Anderson and the remaining coauthors had no financial conflicts to disclose. Dr. Badell had no relevant financial disclosures.
SOURCE: Anderson NH et al. JAMA Network Open. 2019 Oct 2. doi: 10.1001/jamanetworkopen.2019.12614.
Data from previous studies suggest that impaired uteroplacental flow can affect fetal growth, wrote Ngaire H. Anderson, PhD, of the University of Auckland, N.Z., and colleagues.
“The initial going-to-sleep position is the sleep position that women maintain for the longest duration throughout the night; therefore, going-to-sleep position is likely to have the greatest impact on blood flow to the developing fetus,” they said.
In a study published in JAMA Network Open, the researchers interviewed women with ongoing pregnancies at 28 weeks’ gestation or later to determine their sleeping positions. The mean age of the participants was 30 years. Of the 1,760 women, 3% reported that they usually slept supine during the past 1-4 weeks.
The adjusted mean birth weight was 3,410 g among supine sleepers and 3,554 g among nonsupine sleepers. The primary outcome was an adjusted mean difference in birth weight between infants of supine sleepers and nonsupine sleepers, which was a statistically significant 144 g (P = .009).
The study findings were limited by several factors including the small number of women who were reported supine sleepers, as well as the reliance on self-reports of sleep position, the researchers said.
However, women who had going-to-sleep data for the previous night and the previous month suggest that most women are consistent in their going-to-sleep position, they noted. “It is also biologically plausible that the association of decreased maternal blood flow on birth size with supine maternal position is cumulative over time,” but the researchers were not able to investigate how the duration of supine sleeping might further affect birth weight.
Although it might make additional studies more difficult, a public health campaign to encourage pregnant women to sleep on their side during the third trimester is a safe and easy opportunity to potentially optimize birth weight, they added.
The study was important because of the limited number of high-quality studies on the effects of maternal sleep on perinatal outcomes, Martina Badell, MD of Emory University in Atlanta said in an interview.
“The overall findings suggested a possible small increased risk of small-for-gestational-age babies with supine maternal sleeping, however, the absolute gram difference of 144 grams at term may not be clinically relevant,” she said. In addition, the relatively small number of women who reported supine sleep in late pregnancy suggests that broad public health campaigns or recommendations may not be indicated at this time.
“Also, the percentage of women who are supine sleepers at term is only approximately 3%, and this study didn’t assess reasons for supine sleeping in this small subset of women,” she said. “Further research is needed to assess whether there are specific maternal factors associated with supine sleeping, such as GI symptoms or respiratory difficulties, which could contribute to smaller fetal size rather than the sleep position itself.”
The study was supported by a Trans-Tasman Research Funding Grant by Cure Kids and Red Nose Australia. Six coauthors reported receiving numerous grants from a variety of organizations. Dr. Anderson and the remaining coauthors had no financial conflicts to disclose. Dr. Badell had no relevant financial disclosures.
SOURCE: Anderson NH et al. JAMA Network Open. 2019 Oct 2. doi: 10.1001/jamanetworkopen.2019.12614.
Data from previous studies suggest that impaired uteroplacental flow can affect fetal growth, wrote Ngaire H. Anderson, PhD, of the University of Auckland, N.Z., and colleagues.
“The initial going-to-sleep position is the sleep position that women maintain for the longest duration throughout the night; therefore, going-to-sleep position is likely to have the greatest impact on blood flow to the developing fetus,” they said.
In a study published in JAMA Network Open, the researchers interviewed women with ongoing pregnancies at 28 weeks’ gestation or later to determine their sleeping positions. The mean age of the participants was 30 years. Of the 1,760 women, 3% reported that they usually slept supine during the past 1-4 weeks.
The adjusted mean birth weight was 3,410 g among supine sleepers and 3,554 g among nonsupine sleepers. The primary outcome was an adjusted mean difference in birth weight between infants of supine sleepers and nonsupine sleepers, which was a statistically significant 144 g (P = .009).
The study findings were limited by several factors including the small number of women who were reported supine sleepers, as well as the reliance on self-reports of sleep position, the researchers said.
However, women who had going-to-sleep data for the previous night and the previous month suggest that most women are consistent in their going-to-sleep position, they noted. “It is also biologically plausible that the association of decreased maternal blood flow on birth size with supine maternal position is cumulative over time,” but the researchers were not able to investigate how the duration of supine sleeping might further affect birth weight.
Although it might make additional studies more difficult, a public health campaign to encourage pregnant women to sleep on their side during the third trimester is a safe and easy opportunity to potentially optimize birth weight, they added.
The study was important because of the limited number of high-quality studies on the effects of maternal sleep on perinatal outcomes, Martina Badell, MD of Emory University in Atlanta said in an interview.
“The overall findings suggested a possible small increased risk of small-for-gestational-age babies with supine maternal sleeping, however, the absolute gram difference of 144 grams at term may not be clinically relevant,” she said. In addition, the relatively small number of women who reported supine sleep in late pregnancy suggests that broad public health campaigns or recommendations may not be indicated at this time.
“Also, the percentage of women who are supine sleepers at term is only approximately 3%, and this study didn’t assess reasons for supine sleeping in this small subset of women,” she said. “Further research is needed to assess whether there are specific maternal factors associated with supine sleeping, such as GI symptoms or respiratory difficulties, which could contribute to smaller fetal size rather than the sleep position itself.”
The study was supported by a Trans-Tasman Research Funding Grant by Cure Kids and Red Nose Australia. Six coauthors reported receiving numerous grants from a variety of organizations. Dr. Anderson and the remaining coauthors had no financial conflicts to disclose. Dr. Badell had no relevant financial disclosures.
SOURCE: Anderson NH et al. JAMA Network Open. 2019 Oct 2. doi: 10.1001/jamanetworkopen.2019.12614.
FROM JAMA NETWORK OPEN
Lefamulin found noninferior to moxifloxacin for bacterial pneumonia
Persistent high rates of bacterial resistance to current treatments have created the need for more options, especially for the treatment of community-acquired bacterial pneumonia (CABP), which remains a leading cause of hospitalization and death in the United States, wrote Elizabeth Alexander, MD, of Nabriva Therapeutics in King of Prussia, Penn., and colleagues. Lefamulin, “the first pleuromutilin antibiotic approved for intravenous and oral use in humans,” has demonstrated activity against many CABP-causing pathogens, including some not susceptible to other classes of antimicrobials, they noted.
Findings of Lefamulin Evaluation Against Pneumonia 2 (LEAP2) were published in JAMA. In this study, the researchers randomized 370 patients to 600 mg of oral lefamulin every 12 hours for 5 days and 368 patients to 400 mg of oral moxifloxacin every 24 hours for 7 days.
Early clinical response rates at 96 hours were 90.8% for both medications (difference of 0.1%). In addition, the rates of clinical response success were similar between the groups in both the modified intent-to-treat population (87.5% with lefamulin and 89.1% with moxifloxacin) and the clinically evaluable population (89.7% with lefamulin and 93.6% with moxifloxacin).
Gastrointestinal issues of diarrhea and nausea were the two most frequently reported treatment-emergent adverse events in both groups. Both conditions occurred more often in the lefamulin group, compared with the moxifloxacin group, but the differences were not significant (12.2% vs. 1.1% and 5.2% vs. 1.9%, respectively).
The study findings were limited by several factors including strict exclusion criteria that may limit the generalizability of the results, as well as a lack of testing for viral copathogens, low recovery of resistant pathogens, and possible misclassification of patient ethnicity, the researchers noted.
However, the results were strengthened by the randomized design, inclusion of patients with more severe CABP, and low rate of discontinuation, they said. The data support previous studies of lefamulin. Its lack of cross-resistance to other drug classes, coverage of typical and atypical CABP pathogens, and options for both oral and intravenous use suggest that it “may provide an alternative approach for the treatment of vulnerable patients,” the researchers said.
The study was supported by Nabriva Therapeutics. Dr. Alexander and several coauthors are employees of Nabriva Therapeutics and own stock in the company.
SOURCE: Alexander E et al. JAMA. 2019 Sep 27. doi:10.1001/jama.2019.15468.
“The development and approval of a new antibiotic is a rare occurrence and a reason to celebrate” given the scientific, regulatory, and economic challenges to antibiotic development, wrote Preeti N. Malani, MD, in an accompanying editorial. Lefamulin in both oral and intravenous forms was approved by the Food and Drug Administration in August 2019 for the treatment of community-acquired bacterial pneumonia, Dr. Malani said.
Lefamulin will likely be an expensive option. According to a manufacturer press release, lefamulin may cost $205/day for intravenous treatment and $275/day for oral treatment. “This is severalfold more than moxifloxacin or levofloxacin, which are the most commonly prescribed fluoroquinolones for CABP [community-acquired bacterial pneumonia],” said Dr. Malani. However, the addition of lefamulin to the array of antibiotics is important because of the persistent burden of bacterial pneumonia as an indication for antibiotic use, Dr. Malani emphasized.
Dr. Malani is affiliated with the University of Michigan, Ann Arbor, and serves as an associate editor of JAMA, but had no financial conflicts to disclose. These remarks were taken from an accompanying editorial (JAMA. 2019 Sep 27. doi:10.1001/jama.2019.16215).
“The development and approval of a new antibiotic is a rare occurrence and a reason to celebrate” given the scientific, regulatory, and economic challenges to antibiotic development, wrote Preeti N. Malani, MD, in an accompanying editorial. Lefamulin in both oral and intravenous forms was approved by the Food and Drug Administration in August 2019 for the treatment of community-acquired bacterial pneumonia, Dr. Malani said.
Lefamulin will likely be an expensive option. According to a manufacturer press release, lefamulin may cost $205/day for intravenous treatment and $275/day for oral treatment. “This is severalfold more than moxifloxacin or levofloxacin, which are the most commonly prescribed fluoroquinolones for CABP [community-acquired bacterial pneumonia],” said Dr. Malani. However, the addition of lefamulin to the array of antibiotics is important because of the persistent burden of bacterial pneumonia as an indication for antibiotic use, Dr. Malani emphasized.
Dr. Malani is affiliated with the University of Michigan, Ann Arbor, and serves as an associate editor of JAMA, but had no financial conflicts to disclose. These remarks were taken from an accompanying editorial (JAMA. 2019 Sep 27. doi:10.1001/jama.2019.16215).
“The development and approval of a new antibiotic is a rare occurrence and a reason to celebrate” given the scientific, regulatory, and economic challenges to antibiotic development, wrote Preeti N. Malani, MD, in an accompanying editorial. Lefamulin in both oral and intravenous forms was approved by the Food and Drug Administration in August 2019 for the treatment of community-acquired bacterial pneumonia, Dr. Malani said.
Lefamulin will likely be an expensive option. According to a manufacturer press release, lefamulin may cost $205/day for intravenous treatment and $275/day for oral treatment. “This is severalfold more than moxifloxacin or levofloxacin, which are the most commonly prescribed fluoroquinolones for CABP [community-acquired bacterial pneumonia],” said Dr. Malani. However, the addition of lefamulin to the array of antibiotics is important because of the persistent burden of bacterial pneumonia as an indication for antibiotic use, Dr. Malani emphasized.
Dr. Malani is affiliated with the University of Michigan, Ann Arbor, and serves as an associate editor of JAMA, but had no financial conflicts to disclose. These remarks were taken from an accompanying editorial (JAMA. 2019 Sep 27. doi:10.1001/jama.2019.16215).
Persistent high rates of bacterial resistance to current treatments have created the need for more options, especially for the treatment of community-acquired bacterial pneumonia (CABP), which remains a leading cause of hospitalization and death in the United States, wrote Elizabeth Alexander, MD, of Nabriva Therapeutics in King of Prussia, Penn., and colleagues. Lefamulin, “the first pleuromutilin antibiotic approved for intravenous and oral use in humans,” has demonstrated activity against many CABP-causing pathogens, including some not susceptible to other classes of antimicrobials, they noted.
Findings of Lefamulin Evaluation Against Pneumonia 2 (LEAP2) were published in JAMA. In this study, the researchers randomized 370 patients to 600 mg of oral lefamulin every 12 hours for 5 days and 368 patients to 400 mg of oral moxifloxacin every 24 hours for 7 days.
Early clinical response rates at 96 hours were 90.8% for both medications (difference of 0.1%). In addition, the rates of clinical response success were similar between the groups in both the modified intent-to-treat population (87.5% with lefamulin and 89.1% with moxifloxacin) and the clinically evaluable population (89.7% with lefamulin and 93.6% with moxifloxacin).
Gastrointestinal issues of diarrhea and nausea were the two most frequently reported treatment-emergent adverse events in both groups. Both conditions occurred more often in the lefamulin group, compared with the moxifloxacin group, but the differences were not significant (12.2% vs. 1.1% and 5.2% vs. 1.9%, respectively).
The study findings were limited by several factors including strict exclusion criteria that may limit the generalizability of the results, as well as a lack of testing for viral copathogens, low recovery of resistant pathogens, and possible misclassification of patient ethnicity, the researchers noted.
However, the results were strengthened by the randomized design, inclusion of patients with more severe CABP, and low rate of discontinuation, they said. The data support previous studies of lefamulin. Its lack of cross-resistance to other drug classes, coverage of typical and atypical CABP pathogens, and options for both oral and intravenous use suggest that it “may provide an alternative approach for the treatment of vulnerable patients,” the researchers said.
The study was supported by Nabriva Therapeutics. Dr. Alexander and several coauthors are employees of Nabriva Therapeutics and own stock in the company.
SOURCE: Alexander E et al. JAMA. 2019 Sep 27. doi:10.1001/jama.2019.15468.
Persistent high rates of bacterial resistance to current treatments have created the need for more options, especially for the treatment of community-acquired bacterial pneumonia (CABP), which remains a leading cause of hospitalization and death in the United States, wrote Elizabeth Alexander, MD, of Nabriva Therapeutics in King of Prussia, Penn., and colleagues. Lefamulin, “the first pleuromutilin antibiotic approved for intravenous and oral use in humans,” has demonstrated activity against many CABP-causing pathogens, including some not susceptible to other classes of antimicrobials, they noted.
Findings of Lefamulin Evaluation Against Pneumonia 2 (LEAP2) were published in JAMA. In this study, the researchers randomized 370 patients to 600 mg of oral lefamulin every 12 hours for 5 days and 368 patients to 400 mg of oral moxifloxacin every 24 hours for 7 days.
Early clinical response rates at 96 hours were 90.8% for both medications (difference of 0.1%). In addition, the rates of clinical response success were similar between the groups in both the modified intent-to-treat population (87.5% with lefamulin and 89.1% with moxifloxacin) and the clinically evaluable population (89.7% with lefamulin and 93.6% with moxifloxacin).
Gastrointestinal issues of diarrhea and nausea were the two most frequently reported treatment-emergent adverse events in both groups. Both conditions occurred more often in the lefamulin group, compared with the moxifloxacin group, but the differences were not significant (12.2% vs. 1.1% and 5.2% vs. 1.9%, respectively).
The study findings were limited by several factors including strict exclusion criteria that may limit the generalizability of the results, as well as a lack of testing for viral copathogens, low recovery of resistant pathogens, and possible misclassification of patient ethnicity, the researchers noted.
However, the results were strengthened by the randomized design, inclusion of patients with more severe CABP, and low rate of discontinuation, they said. The data support previous studies of lefamulin. Its lack of cross-resistance to other drug classes, coverage of typical and atypical CABP pathogens, and options for both oral and intravenous use suggest that it “may provide an alternative approach for the treatment of vulnerable patients,” the researchers said.
The study was supported by Nabriva Therapeutics. Dr. Alexander and several coauthors are employees of Nabriva Therapeutics and own stock in the company.
SOURCE: Alexander E et al. JAMA. 2019 Sep 27. doi:10.1001/jama.2019.15468.
FROM JAMA
IBS complaints differ with diarrhea versus constipation
At least 50% of patients with irritable bowel syndrome (IBS) described their condition as “extremely bothersome” based on survey data from 3,254 individuals. However, differences in the nature of other symptoms among IBS subtypes, namely IBS with diarrhea (IBS-D) and IBS with constipation (IBS-C), have not been well studied, wrote Sarah Ballou, PhD, of Beth Israel Deaconess Medical Center, Boston, and colleagues.
Source: American Gastroenterological Association
In a study published in Clinical Gastroenterology and Hepatology, the researchers reviewed survey results from 1,587 individuals with IBS-D and 1,667 with IBS-C. The average age of the patients was 47 years, 81% were female, and 90% were white.
Approximately 84% of patients with IBS-C and 93% of those with IBS-D reported abdominal pain, the most common symptom in both groups. Overall, 36% of the 1,885 patients employed or in school reported decreased productivity in those settings.
IBS-C patients were significantly more likely to report that their symptoms caused them to avoid sex, feel self-conscious about their bodies, have trouble concentrating, and feel “not like myself,” compared with IBS-D patients (P less than .004 for all).
IBS-D patients were significantly more likely to report that their symptoms caused them to avoid traveling in general, avoid places without bathrooms, avoid leaving the house, and have trouble making plans, compared with IBS-C patients (P less than .004 for all).
The survey also asked respondents what they would give up for 1 month in exchange for 1 month of relief from IBS symptoms. Overall, approximately 60% said they would give up alcohol, 55% said they would give up caffeine, 40% would give up sex, 24.5% would give up their cell phones, and 21.5% would give up the internet, the researchers wrote.
The study findings were limited by several factors, including the absence of survey respondents with mixed-type IBS, the reliance on self-reports, and the potential for recall bias. Also, the study was not designed to assess the impact of other comorbidities and did not include non-IBS controls, the researchers noted.
However, the results suggest that patients with different IBS subtypes struggle differently in areas of daily function, which has implications for treatment, they wrote.
“This study highlights important differences between IBS-C and IBS-D, which could impact the development and refinement of mind-body therapies for IBS, with tailored treatment goals for each IBS subtype. For example, treatment tailored specifically for IBS-D may be more behaviorally focused (e.g., exposure to specific situations outside the home) while treatment for IBS-C may be more cognitively focused (e.g., evaluating self-esteem and beliefs about self and others) in addition to targeting the bowel dysfunction and pain,” they concluded.
The researchers had no financial conflicts to disclose.
SOURCE: Ballou S et al. Clin Gastroenterol Hepatol. 2019 Aug 13. doi: 10.1016/j.cgh.2019.08.016.
Irritable bowel syndrome (IBS) patients experience frequent symptoms of abdominal pain and changes in bowel function, often on a weekly basis.
Both IBS subtypes expressed a willingness to go to considerable lengths in a theoretical “trade-off” to obtain symptom relief. A remarkable percentage of patients were willing to forgo both primitive drives (sex in 40% of respondents) and modern conveniences (cellphones and Internet in more than 20% of respondents) in exchange for IBS relief.
In light of these findings, it is not surprising that previous surveys observed considerable IBS patient acceptance of treatments with higher risks of serious adverse events in return for better symptom control. In recent years, several novel therapies have emerged as effective options for the management of IBS. Of course, these newer IBS medications are more costly, and some have recognized rare, yet potentially serious adverse events. In balance, gastroenterology providers must recall the substantial effect of IBS symptoms on the well-being and daily functioning of the individual and account for this major burden when making IBS treatment recommendations.
Gregory S. Sayuk, MD, MPH, is an associate professor, department of medicine, division of gastroenterology, and department of psychiatry, and associate program director, gastroenterology training, Washington University in St. Louis; and a staff physician, John Cochran VA Medical Center, St. Louis. He has no relevant conflicts.
Irritable bowel syndrome (IBS) patients experience frequent symptoms of abdominal pain and changes in bowel function, often on a weekly basis.
Both IBS subtypes expressed a willingness to go to considerable lengths in a theoretical “trade-off” to obtain symptom relief. A remarkable percentage of patients were willing to forgo both primitive drives (sex in 40% of respondents) and modern conveniences (cellphones and Internet in more than 20% of respondents) in exchange for IBS relief.
In light of these findings, it is not surprising that previous surveys observed considerable IBS patient acceptance of treatments with higher risks of serious adverse events in return for better symptom control. In recent years, several novel therapies have emerged as effective options for the management of IBS. Of course, these newer IBS medications are more costly, and some have recognized rare, yet potentially serious adverse events. In balance, gastroenterology providers must recall the substantial effect of IBS symptoms on the well-being and daily functioning of the individual and account for this major burden when making IBS treatment recommendations.
Gregory S. Sayuk, MD, MPH, is an associate professor, department of medicine, division of gastroenterology, and department of psychiatry, and associate program director, gastroenterology training, Washington University in St. Louis; and a staff physician, John Cochran VA Medical Center, St. Louis. He has no relevant conflicts.
Irritable bowel syndrome (IBS) patients experience frequent symptoms of abdominal pain and changes in bowel function, often on a weekly basis.
Both IBS subtypes expressed a willingness to go to considerable lengths in a theoretical “trade-off” to obtain symptom relief. A remarkable percentage of patients were willing to forgo both primitive drives (sex in 40% of respondents) and modern conveniences (cellphones and Internet in more than 20% of respondents) in exchange for IBS relief.
In light of these findings, it is not surprising that previous surveys observed considerable IBS patient acceptance of treatments with higher risks of serious adverse events in return for better symptom control. In recent years, several novel therapies have emerged as effective options for the management of IBS. Of course, these newer IBS medications are more costly, and some have recognized rare, yet potentially serious adverse events. In balance, gastroenterology providers must recall the substantial effect of IBS symptoms on the well-being and daily functioning of the individual and account for this major burden when making IBS treatment recommendations.
Gregory S. Sayuk, MD, MPH, is an associate professor, department of medicine, division of gastroenterology, and department of psychiatry, and associate program director, gastroenterology training, Washington University in St. Louis; and a staff physician, John Cochran VA Medical Center, St. Louis. He has no relevant conflicts.
At least 50% of patients with irritable bowel syndrome (IBS) described their condition as “extremely bothersome” based on survey data from 3,254 individuals. However, differences in the nature of other symptoms among IBS subtypes, namely IBS with diarrhea (IBS-D) and IBS with constipation (IBS-C), have not been well studied, wrote Sarah Ballou, PhD, of Beth Israel Deaconess Medical Center, Boston, and colleagues.
Source: American Gastroenterological Association
In a study published in Clinical Gastroenterology and Hepatology, the researchers reviewed survey results from 1,587 individuals with IBS-D and 1,667 with IBS-C. The average age of the patients was 47 years, 81% were female, and 90% were white.
Approximately 84% of patients with IBS-C and 93% of those with IBS-D reported abdominal pain, the most common symptom in both groups. Overall, 36% of the 1,885 patients employed or in school reported decreased productivity in those settings.
IBS-C patients were significantly more likely to report that their symptoms caused them to avoid sex, feel self-conscious about their bodies, have trouble concentrating, and feel “not like myself,” compared with IBS-D patients (P less than .004 for all).
IBS-D patients were significantly more likely to report that their symptoms caused them to avoid traveling in general, avoid places without bathrooms, avoid leaving the house, and have trouble making plans, compared with IBS-C patients (P less than .004 for all).
The survey also asked respondents what they would give up for 1 month in exchange for 1 month of relief from IBS symptoms. Overall, approximately 60% said they would give up alcohol, 55% said they would give up caffeine, 40% would give up sex, 24.5% would give up their cell phones, and 21.5% would give up the internet, the researchers wrote.
The study findings were limited by several factors, including the absence of survey respondents with mixed-type IBS, the reliance on self-reports, and the potential for recall bias. Also, the study was not designed to assess the impact of other comorbidities and did not include non-IBS controls, the researchers noted.
However, the results suggest that patients with different IBS subtypes struggle differently in areas of daily function, which has implications for treatment, they wrote.
“This study highlights important differences between IBS-C and IBS-D, which could impact the development and refinement of mind-body therapies for IBS, with tailored treatment goals for each IBS subtype. For example, treatment tailored specifically for IBS-D may be more behaviorally focused (e.g., exposure to specific situations outside the home) while treatment for IBS-C may be more cognitively focused (e.g., evaluating self-esteem and beliefs about self and others) in addition to targeting the bowel dysfunction and pain,” they concluded.
The researchers had no financial conflicts to disclose.
SOURCE: Ballou S et al. Clin Gastroenterol Hepatol. 2019 Aug 13. doi: 10.1016/j.cgh.2019.08.016.
At least 50% of patients with irritable bowel syndrome (IBS) described their condition as “extremely bothersome” based on survey data from 3,254 individuals. However, differences in the nature of other symptoms among IBS subtypes, namely IBS with diarrhea (IBS-D) and IBS with constipation (IBS-C), have not been well studied, wrote Sarah Ballou, PhD, of Beth Israel Deaconess Medical Center, Boston, and colleagues.
Source: American Gastroenterological Association
In a study published in Clinical Gastroenterology and Hepatology, the researchers reviewed survey results from 1,587 individuals with IBS-D and 1,667 with IBS-C. The average age of the patients was 47 years, 81% were female, and 90% were white.
Approximately 84% of patients with IBS-C and 93% of those with IBS-D reported abdominal pain, the most common symptom in both groups. Overall, 36% of the 1,885 patients employed or in school reported decreased productivity in those settings.
IBS-C patients were significantly more likely to report that their symptoms caused them to avoid sex, feel self-conscious about their bodies, have trouble concentrating, and feel “not like myself,” compared with IBS-D patients (P less than .004 for all).
IBS-D patients were significantly more likely to report that their symptoms caused them to avoid traveling in general, avoid places without bathrooms, avoid leaving the house, and have trouble making plans, compared with IBS-C patients (P less than .004 for all).
The survey also asked respondents what they would give up for 1 month in exchange for 1 month of relief from IBS symptoms. Overall, approximately 60% said they would give up alcohol, 55% said they would give up caffeine, 40% would give up sex, 24.5% would give up their cell phones, and 21.5% would give up the internet, the researchers wrote.
The study findings were limited by several factors, including the absence of survey respondents with mixed-type IBS, the reliance on self-reports, and the potential for recall bias. Also, the study was not designed to assess the impact of other comorbidities and did not include non-IBS controls, the researchers noted.
However, the results suggest that patients with different IBS subtypes struggle differently in areas of daily function, which has implications for treatment, they wrote.
“This study highlights important differences between IBS-C and IBS-D, which could impact the development and refinement of mind-body therapies for IBS, with tailored treatment goals for each IBS subtype. For example, treatment tailored specifically for IBS-D may be more behaviorally focused (e.g., exposure to specific situations outside the home) while treatment for IBS-C may be more cognitively focused (e.g., evaluating self-esteem and beliefs about self and others) in addition to targeting the bowel dysfunction and pain,” they concluded.
The researchers had no financial conflicts to disclose.
SOURCE: Ballou S et al. Clin Gastroenterol Hepatol. 2019 Aug 13. doi: 10.1016/j.cgh.2019.08.016.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Vitamin C infusion falls short for sepsis and ARDS patients
Vitamin C infusion did not improve outcomes related to organ failure, inflammation, or vascular injury for patients with sepsis and acute respiratory distress syndrome, based on data from 167 adults.
“Previous research found that vitamin C attenuates systemic inflammation, corrects sepsis-induced coagulopathy, and attenuates vascular injury,” wrote Alpha A. Fowler III, MD, of Virginia Commonwealth University, Richmond, and colleagues.
To examine the impact of vitamin C infusion on patients with sepsis and acute respiratory distress syndrome (ARDS), the researchers designed the CITRIS-ALI trial, a randomized, double-blind, placebo-controlled study conducted at 7 medical intensive care units in the United States.
In the study, published in JAMA, the researchers randomized 167 adults with sepsis and ARDS to receive high-dose intravenous vitamin C (50 mg/kg in 5% dextrose in water) or placebo (5% dextrose in water only) every 6 hours for 96 hours. The primary outcomes were measures of organ failure based on changes in the modified Sequential Organ Failure Assessment score (mSOFA), inflammation (based on changes in C-reactive protein), and vascular injury based on thrombomodulin.
Overall, no significant differences appeared between the vitamin C and placebo groups, respectively in the three primary outcome measures: change in average SOFA score (3-point change vs. a 3.5-point change) at 96 hours; change in C-reactive protein levels (change of 54.1 mcg/mL vs. 46.1 mcg/mL) at 168 hours; and change in thrombomodulin levels (14.5 ng/mL vs. 13.8 ng/mL) at 168 hours.
The average age of the patients was 55 years, and 54% were men.
The researchers also assessed 46 secondary outcomes. Most of these showed no significant differences between the groups, but 28-day all-cause mortality was significantly lower in the vitamin C group, compared with the placebo group (46.3% vs. 29.8%), the researchers said. Vitamin C also was significantly associated with increased ICU-free days to day 28 and hospital-free days to day 60, compared with placebo.
No significant differences were seen between the groups on 43 other secondary outcomes including ventilator-free days and vasopressor use. However, “these findings were based on analyses that did not account for multiple comparisons and therefore must be considered exploratory,” they said.
“The inability of vitamin C to affect C-reactive protein and thrombomodulin levels in this trial possibly resulted from the advanced stages of sepsis that were present before the development of ARDS,” the researchers noted.
The findings were limited by several factors including the variability in the timing of vitamin C administration and the use of a single high dose of vitamin C, they emphasized. However, the results suggest that further research may be needed to determine the potential of vitamin C for improving outcomes in patients with sepsis and ARDS, they said.
The study was supported by the National Heart, Lung, and Blood Institute, National Center for Advancing Translational Sciences, VCU Wright Center for Translational Science Award, VCU Investigational Drug Services, and McGuff Pharmaceuticals, who supplied the vitamin C free of charge. Dr. Fowler disclosed funding from Virginia Polytechnic Institute and State University, Richmond; the NHLBI; and study materials from McGuff Pharmaceuticals.
SOURCE: Fowler AA et al. JAMA. 2019 Oct 1;322:1261-70. doi:10.1001/jama.2019.11825.
Although none of the primary outcomes was significant, “the difference in mortality is tantalizing and likely to spur much debate,” wrote Emily B. Brant, MD, and Derek C. Angus, MD, in an accompanying editorial.
“However, this outcome was one of many secondary outcomes, and although reported as statistically significant, that finding was without adjustment for multiple comparisons,” they said.
The study was well-designed, and resulted in the collection of considerable patient data, they said. Previous studies have suggested that approximately 40% of sepsis patients are vitamin C deficient, and vitamin C is considered safe and inexpensive, which may be reason to pursue research in this area, they added.
Study design for addition research should keep in mind the timing and dosage that were limitations in the current study; the lack of effect on organ dysfunction may have occurred because vitamin C was given too late, they said.
Researchers planning further evaluation might “reconsider optimal dosing and timing, as well as the likelihood that any potential benefits may only accrue to subsets of patients, given the underlying heterogeneity of sepsis,” they concluded (JAMA. 2019 Oct 1; 322:1257-8).
Dr. Brant and Dr. Angus are affiliated with the department of critical care medicine, University of Pittsburgh. Dr. Angus serves as a associate editor for JAMA and disclosed receiving consulting fees from Ferring, Bristol-Myers Squibb, and Beckman Coulter; holding stock in Alung Technologies; and holding pending patents for selepressin and for proteomic biomarkers of sepsis in elderly patients. Dr. Brant had no financial conflicts to disclose.
Although none of the primary outcomes was significant, “the difference in mortality is tantalizing and likely to spur much debate,” wrote Emily B. Brant, MD, and Derek C. Angus, MD, in an accompanying editorial.
“However, this outcome was one of many secondary outcomes, and although reported as statistically significant, that finding was without adjustment for multiple comparisons,” they said.
The study was well-designed, and resulted in the collection of considerable patient data, they said. Previous studies have suggested that approximately 40% of sepsis patients are vitamin C deficient, and vitamin C is considered safe and inexpensive, which may be reason to pursue research in this area, they added.
Study design for addition research should keep in mind the timing and dosage that were limitations in the current study; the lack of effect on organ dysfunction may have occurred because vitamin C was given too late, they said.
Researchers planning further evaluation might “reconsider optimal dosing and timing, as well as the likelihood that any potential benefits may only accrue to subsets of patients, given the underlying heterogeneity of sepsis,” they concluded (JAMA. 2019 Oct 1; 322:1257-8).
Dr. Brant and Dr. Angus are affiliated with the department of critical care medicine, University of Pittsburgh. Dr. Angus serves as a associate editor for JAMA and disclosed receiving consulting fees from Ferring, Bristol-Myers Squibb, and Beckman Coulter; holding stock in Alung Technologies; and holding pending patents for selepressin and for proteomic biomarkers of sepsis in elderly patients. Dr. Brant had no financial conflicts to disclose.
Although none of the primary outcomes was significant, “the difference in mortality is tantalizing and likely to spur much debate,” wrote Emily B. Brant, MD, and Derek C. Angus, MD, in an accompanying editorial.
“However, this outcome was one of many secondary outcomes, and although reported as statistically significant, that finding was without adjustment for multiple comparisons,” they said.
The study was well-designed, and resulted in the collection of considerable patient data, they said. Previous studies have suggested that approximately 40% of sepsis patients are vitamin C deficient, and vitamin C is considered safe and inexpensive, which may be reason to pursue research in this area, they added.
Study design for addition research should keep in mind the timing and dosage that were limitations in the current study; the lack of effect on organ dysfunction may have occurred because vitamin C was given too late, they said.
Researchers planning further evaluation might “reconsider optimal dosing and timing, as well as the likelihood that any potential benefits may only accrue to subsets of patients, given the underlying heterogeneity of sepsis,” they concluded (JAMA. 2019 Oct 1; 322:1257-8).
Dr. Brant and Dr. Angus are affiliated with the department of critical care medicine, University of Pittsburgh. Dr. Angus serves as a associate editor for JAMA and disclosed receiving consulting fees from Ferring, Bristol-Myers Squibb, and Beckman Coulter; holding stock in Alung Technologies; and holding pending patents for selepressin and for proteomic biomarkers of sepsis in elderly patients. Dr. Brant had no financial conflicts to disclose.
Vitamin C infusion did not improve outcomes related to organ failure, inflammation, or vascular injury for patients with sepsis and acute respiratory distress syndrome, based on data from 167 adults.
“Previous research found that vitamin C attenuates systemic inflammation, corrects sepsis-induced coagulopathy, and attenuates vascular injury,” wrote Alpha A. Fowler III, MD, of Virginia Commonwealth University, Richmond, and colleagues.
To examine the impact of vitamin C infusion on patients with sepsis and acute respiratory distress syndrome (ARDS), the researchers designed the CITRIS-ALI trial, a randomized, double-blind, placebo-controlled study conducted at 7 medical intensive care units in the United States.
In the study, published in JAMA, the researchers randomized 167 adults with sepsis and ARDS to receive high-dose intravenous vitamin C (50 mg/kg in 5% dextrose in water) or placebo (5% dextrose in water only) every 6 hours for 96 hours. The primary outcomes were measures of organ failure based on changes in the modified Sequential Organ Failure Assessment score (mSOFA), inflammation (based on changes in C-reactive protein), and vascular injury based on thrombomodulin.
Overall, no significant differences appeared between the vitamin C and placebo groups, respectively in the three primary outcome measures: change in average SOFA score (3-point change vs. a 3.5-point change) at 96 hours; change in C-reactive protein levels (change of 54.1 mcg/mL vs. 46.1 mcg/mL) at 168 hours; and change in thrombomodulin levels (14.5 ng/mL vs. 13.8 ng/mL) at 168 hours.
The average age of the patients was 55 years, and 54% were men.
The researchers also assessed 46 secondary outcomes. Most of these showed no significant differences between the groups, but 28-day all-cause mortality was significantly lower in the vitamin C group, compared with the placebo group (46.3% vs. 29.8%), the researchers said. Vitamin C also was significantly associated with increased ICU-free days to day 28 and hospital-free days to day 60, compared with placebo.
No significant differences were seen between the groups on 43 other secondary outcomes including ventilator-free days and vasopressor use. However, “these findings were based on analyses that did not account for multiple comparisons and therefore must be considered exploratory,” they said.
“The inability of vitamin C to affect C-reactive protein and thrombomodulin levels in this trial possibly resulted from the advanced stages of sepsis that were present before the development of ARDS,” the researchers noted.
The findings were limited by several factors including the variability in the timing of vitamin C administration and the use of a single high dose of vitamin C, they emphasized. However, the results suggest that further research may be needed to determine the potential of vitamin C for improving outcomes in patients with sepsis and ARDS, they said.
The study was supported by the National Heart, Lung, and Blood Institute, National Center for Advancing Translational Sciences, VCU Wright Center for Translational Science Award, VCU Investigational Drug Services, and McGuff Pharmaceuticals, who supplied the vitamin C free of charge. Dr. Fowler disclosed funding from Virginia Polytechnic Institute and State University, Richmond; the NHLBI; and study materials from McGuff Pharmaceuticals.
SOURCE: Fowler AA et al. JAMA. 2019 Oct 1;322:1261-70. doi:10.1001/jama.2019.11825.
Vitamin C infusion did not improve outcomes related to organ failure, inflammation, or vascular injury for patients with sepsis and acute respiratory distress syndrome, based on data from 167 adults.
“Previous research found that vitamin C attenuates systemic inflammation, corrects sepsis-induced coagulopathy, and attenuates vascular injury,” wrote Alpha A. Fowler III, MD, of Virginia Commonwealth University, Richmond, and colleagues.
To examine the impact of vitamin C infusion on patients with sepsis and acute respiratory distress syndrome (ARDS), the researchers designed the CITRIS-ALI trial, a randomized, double-blind, placebo-controlled study conducted at 7 medical intensive care units in the United States.
In the study, published in JAMA, the researchers randomized 167 adults with sepsis and ARDS to receive high-dose intravenous vitamin C (50 mg/kg in 5% dextrose in water) or placebo (5% dextrose in water only) every 6 hours for 96 hours. The primary outcomes were measures of organ failure based on changes in the modified Sequential Organ Failure Assessment score (mSOFA), inflammation (based on changes in C-reactive protein), and vascular injury based on thrombomodulin.
Overall, no significant differences appeared between the vitamin C and placebo groups, respectively in the three primary outcome measures: change in average SOFA score (3-point change vs. a 3.5-point change) at 96 hours; change in C-reactive protein levels (change of 54.1 mcg/mL vs. 46.1 mcg/mL) at 168 hours; and change in thrombomodulin levels (14.5 ng/mL vs. 13.8 ng/mL) at 168 hours.
The average age of the patients was 55 years, and 54% were men.
The researchers also assessed 46 secondary outcomes. Most of these showed no significant differences between the groups, but 28-day all-cause mortality was significantly lower in the vitamin C group, compared with the placebo group (46.3% vs. 29.8%), the researchers said. Vitamin C also was significantly associated with increased ICU-free days to day 28 and hospital-free days to day 60, compared with placebo.
No significant differences were seen between the groups on 43 other secondary outcomes including ventilator-free days and vasopressor use. However, “these findings were based on analyses that did not account for multiple comparisons and therefore must be considered exploratory,” they said.
“The inability of vitamin C to affect C-reactive protein and thrombomodulin levels in this trial possibly resulted from the advanced stages of sepsis that were present before the development of ARDS,” the researchers noted.
The findings were limited by several factors including the variability in the timing of vitamin C administration and the use of a single high dose of vitamin C, they emphasized. However, the results suggest that further research may be needed to determine the potential of vitamin C for improving outcomes in patients with sepsis and ARDS, they said.
The study was supported by the National Heart, Lung, and Blood Institute, National Center for Advancing Translational Sciences, VCU Wright Center for Translational Science Award, VCU Investigational Drug Services, and McGuff Pharmaceuticals, who supplied the vitamin C free of charge. Dr. Fowler disclosed funding from Virginia Polytechnic Institute and State University, Richmond; the NHLBI; and study materials from McGuff Pharmaceuticals.
SOURCE: Fowler AA et al. JAMA. 2019 Oct 1;322:1261-70. doi:10.1001/jama.2019.11825.
FROM JAMA
Key clinical point: Vitamin C infusion failed to improve outcomes for patients with ARDS and sepsis.
Major finding: The average SOFA score to measure organ failure changed by 3 points in the vitamin C group vs. 3.5 points in the placebo group.
Study details: The data come from a randomized trial of 167 adults with ARDS and sepsis.
Disclosures: The study was supported by the National Heart, Lung, and Blood Institute, the National Center for Advancing Translational Sciences, VCU Wright Center for Translational Science Award, VCU Investigational Drug Services, and McGuff Pharmaceuticals, who supplied the vitamin C free of charge. Dr. Fowler disclosed funding from Virginia Tech School of Medicine, the NHLBI, and study materials from McGuff Pharmaceuticals.
Source: Fowler AA et al. JAMA. 2019 Oct 1;322:1261-70. doi: 10.1001/jama.2019.11825.
Fibrosis severity and cirrhosis drive patient-reported outcomes with NASH
Patients with nonalcoholic steatohepatitis (NASH) and advanced fibrosis reported lower quality of life that is worsened in those who develop cirrhosis, based on data from 1,667 individuals.
NASH is becoming an increasingly common cause of liver disease, cirrhosis, and hepatocellular carcinoma and can have a negative effect on patients’ quality of life and other patient-reported outcomes (PROs), but studies of the impact on PROs in these patients are limited, wrote Zobair M. Younossi, MD, of the Inova Health System, Falls Church, Va., and colleagues.
In a study published in Clinical Gastroenterology and Hepatology, the researchers reviewed data from 870 adults with NASH cirrhosis and 797 with NASH and bridging fibrosis. The average age of the patients was 58 years, 73% were white, 40% were male, 52% had cirrhosis, and 74% had diabetes.
The researchers used four tools to assess quality of life: the SF-36 (36-Item Short Form Health Survey), the EQ-5D (Euroqol, a generic health questionnaire), the CLDQ-NASH (Chronic Liver Disease Questionnaire-NASH), and the WPAI:SHP (Work Productivity and Activity Impairment: Specific Health Problem).
The SF-36 score is based on eight domains: physical functioning, role physical, bodily pain, general health, vitality, social functioning, role emotional, and mental health.
Overall, patients with NASH and cirrhosis had significantly lower scores on domains of the SF-36 that related to physical function, compared with bridging fibrosis patients (70.3 vs. 73.6), as well as role physical (71.6 vs. 75.4) and bodily pain (65.0 vs. 68.6). The other areas of significant impairment in NASH patients with cirrhosis, compared with NASH patients with fibrosis, appeared in four domains of the disease-specific CLDQ-NASH: activity, emotional, fatigue, and worry. In addition, the EQ-5D utility score was significantly lower in cirrhosis patients, compared with fibrosis patients.
Older age, male sex, Asian race, and U.S. location of study enrollment were independent predictors of higher PRO scores in a multivariate analysis, while black race, history of smoking, history of diabetes, higher body mass index, cirrhosis, and history of comorbidities that were gastrointestinal, musculoskeletal, psychiatric, or neurologic were independent predictors of lower PRO scores in patients with advanced fibrosis and NASH.
WPAI:SHP scores, which focused on work productivity impairment and absenteeism, were not significantly different between the groups.
The study findings were limited by several factors including the specific nature of the study population and absence of non-NASH controls, the potential of false positives because of the use of self-reports, and the lack of longitudinal data, the researchers said. The results should be verified in a larger, diverse patient population, the researchers noted, but the data highlight the impairment in quality of life and productivity among patients with NASH and “can inform patients, clinicians, payers, and policymakers about the total burden of the disease and also the comprehensive benefit of treatment,” they concluded.
The study was supported by Gilead Sciences. Dr. Younossi disclosed relationships with Gilead Sciences, as well as Intercept, NovoNordisk, BMS, Allergan/Tobira, Terns, Viking, AbbVie, Novartis, and Quest Diagnostics.
SOURCE: Younossi ZM et al. Clin Gastroenterol Hepatol. 2019. doi: 10.1016/j.cgh.2019.02.024.
Patients with nonalcoholic steatohepatitis (NASH) and advanced fibrosis reported lower quality of life that is worsened in those who develop cirrhosis, based on data from 1,667 individuals.
NASH is becoming an increasingly common cause of liver disease, cirrhosis, and hepatocellular carcinoma and can have a negative effect on patients’ quality of life and other patient-reported outcomes (PROs), but studies of the impact on PROs in these patients are limited, wrote Zobair M. Younossi, MD, of the Inova Health System, Falls Church, Va., and colleagues.
In a study published in Clinical Gastroenterology and Hepatology, the researchers reviewed data from 870 adults with NASH cirrhosis and 797 with NASH and bridging fibrosis. The average age of the patients was 58 years, 73% were white, 40% were male, 52% had cirrhosis, and 74% had diabetes.
The researchers used four tools to assess quality of life: the SF-36 (36-Item Short Form Health Survey), the EQ-5D (Euroqol, a generic health questionnaire), the CLDQ-NASH (Chronic Liver Disease Questionnaire-NASH), and the WPAI:SHP (Work Productivity and Activity Impairment: Specific Health Problem).
The SF-36 score is based on eight domains: physical functioning, role physical, bodily pain, general health, vitality, social functioning, role emotional, and mental health.
Overall, patients with NASH and cirrhosis had significantly lower scores on domains of the SF-36 that related to physical function, compared with bridging fibrosis patients (70.3 vs. 73.6), as well as role physical (71.6 vs. 75.4) and bodily pain (65.0 vs. 68.6). The other areas of significant impairment in NASH patients with cirrhosis, compared with NASH patients with fibrosis, appeared in four domains of the disease-specific CLDQ-NASH: activity, emotional, fatigue, and worry. In addition, the EQ-5D utility score was significantly lower in cirrhosis patients, compared with fibrosis patients.
Older age, male sex, Asian race, and U.S. location of study enrollment were independent predictors of higher PRO scores in a multivariate analysis, while black race, history of smoking, history of diabetes, higher body mass index, cirrhosis, and history of comorbidities that were gastrointestinal, musculoskeletal, psychiatric, or neurologic were independent predictors of lower PRO scores in patients with advanced fibrosis and NASH.
WPAI:SHP scores, which focused on work productivity impairment and absenteeism, were not significantly different between the groups.
The study findings were limited by several factors including the specific nature of the study population and absence of non-NASH controls, the potential of false positives because of the use of self-reports, and the lack of longitudinal data, the researchers said. The results should be verified in a larger, diverse patient population, the researchers noted, but the data highlight the impairment in quality of life and productivity among patients with NASH and “can inform patients, clinicians, payers, and policymakers about the total burden of the disease and also the comprehensive benefit of treatment,” they concluded.
The study was supported by Gilead Sciences. Dr. Younossi disclosed relationships with Gilead Sciences, as well as Intercept, NovoNordisk, BMS, Allergan/Tobira, Terns, Viking, AbbVie, Novartis, and Quest Diagnostics.
SOURCE: Younossi ZM et al. Clin Gastroenterol Hepatol. 2019. doi: 10.1016/j.cgh.2019.02.024.
Patients with nonalcoholic steatohepatitis (NASH) and advanced fibrosis reported lower quality of life that is worsened in those who develop cirrhosis, based on data from 1,667 individuals.
NASH is becoming an increasingly common cause of liver disease, cirrhosis, and hepatocellular carcinoma and can have a negative effect on patients’ quality of life and other patient-reported outcomes (PROs), but studies of the impact on PROs in these patients are limited, wrote Zobair M. Younossi, MD, of the Inova Health System, Falls Church, Va., and colleagues.
In a study published in Clinical Gastroenterology and Hepatology, the researchers reviewed data from 870 adults with NASH cirrhosis and 797 with NASH and bridging fibrosis. The average age of the patients was 58 years, 73% were white, 40% were male, 52% had cirrhosis, and 74% had diabetes.
The researchers used four tools to assess quality of life: the SF-36 (36-Item Short Form Health Survey), the EQ-5D (Euroqol, a generic health questionnaire), the CLDQ-NASH (Chronic Liver Disease Questionnaire-NASH), and the WPAI:SHP (Work Productivity and Activity Impairment: Specific Health Problem).
The SF-36 score is based on eight domains: physical functioning, role physical, bodily pain, general health, vitality, social functioning, role emotional, and mental health.
Overall, patients with NASH and cirrhosis had significantly lower scores on domains of the SF-36 that related to physical function, compared with bridging fibrosis patients (70.3 vs. 73.6), as well as role physical (71.6 vs. 75.4) and bodily pain (65.0 vs. 68.6). The other areas of significant impairment in NASH patients with cirrhosis, compared with NASH patients with fibrosis, appeared in four domains of the disease-specific CLDQ-NASH: activity, emotional, fatigue, and worry. In addition, the EQ-5D utility score was significantly lower in cirrhosis patients, compared with fibrosis patients.
Older age, male sex, Asian race, and U.S. location of study enrollment were independent predictors of higher PRO scores in a multivariate analysis, while black race, history of smoking, history of diabetes, higher body mass index, cirrhosis, and history of comorbidities that were gastrointestinal, musculoskeletal, psychiatric, or neurologic were independent predictors of lower PRO scores in patients with advanced fibrosis and NASH.
WPAI:SHP scores, which focused on work productivity impairment and absenteeism, were not significantly different between the groups.
The study findings were limited by several factors including the specific nature of the study population and absence of non-NASH controls, the potential of false positives because of the use of self-reports, and the lack of longitudinal data, the researchers said. The results should be verified in a larger, diverse patient population, the researchers noted, but the data highlight the impairment in quality of life and productivity among patients with NASH and “can inform patients, clinicians, payers, and policymakers about the total burden of the disease and also the comprehensive benefit of treatment,” they concluded.
The study was supported by Gilead Sciences. Dr. Younossi disclosed relationships with Gilead Sciences, as well as Intercept, NovoNordisk, BMS, Allergan/Tobira, Terns, Viking, AbbVie, Novartis, and Quest Diagnostics.
SOURCE: Younossi ZM et al. Clin Gastroenterol Hepatol. 2019. doi: 10.1016/j.cgh.2019.02.024.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Clip closure reduced bleeding after large lesion resection
Use of clip closure significantly reduced delayed bleeding in patients who underwent resections for large colorectal lesions, based on data from 235 individuals.
Source: American Gastroenterological Association
“Closure of a mucosal defect with clips after resection has long been considered to reduce the risk of bleeding,” but evidence to support this practice is limited, wrote Eduardo Albéniz, MD, of the Public University of Navarra (Spain), and colleagues.
In a study published in Gastroenterology, the researchers identified 235 consecutive patients who had resections of large nonpedunculated colorectal lesions from May 2016 to June 2018. Patients had an average or high risk of delayed bleeding and were randomized to receive scar closure with either 11-mm through-the-scope clips (119 patients) or no clip (116 patients).
Delayed bleeding occurred in 14 control patients (12.1%), compared with 6 clip patients (5%), for a risk reduction of 7%. The clip group included 68 cases (57%) of complete closure and 33 cases (28%) with partial closure, as well as 18 cases of failure to close (15%); only 1 case of delayed bleeding occurred in the clip group after completion of clip closure. On average, six clips were needed for complete closure.
None of the patients who experienced delayed bleeding required surgical or angiographic intervention, although 15 of the 20 patients with bleeding underwent additional endoscopy. Other adverse events included immediate bleeding in 21 clip patients and 18 controls that was managed with snare soft-tip coagulation. No deaths were reported in connection with the study.
Demographics were similar between the two groups, but the subset of patients with complete closure included more individuals aged 75 years and older and more cases with smaller polyps, compared with other subgroups, the researchers noted.
The study findings were limited by several factors, including the difficulty in predicting delayed bleeding, the potential for selection bias given the timing of patient randomization, the lack of information about polyps that were excluded from treatment, and the difficulty in completely closing the mucosal defects, the researchers noted. However, the results suggest that complete clip closure, despite its challenges, “displays a clear trend to reduce delayed bleeding risk,” and is worth an attempt.
The study was supported by the Spanish Society of Digestive Endoscopy. The researchers had no financial conflicts to disclose. MicroTech (Nanjing, China) contributed the clips used in the study.
SOURCE: Albéniz E et al. Gastroenterology. 2019 Jul 27. doi: 10.1053/j.gastro.2019.07.037.
With the advent of routine submucosal lifting prior to endoscopic mucosal resection, perforation now occurs less commonly; however, delayed bleeding following resection remains problematic given the aging population and increasing use of antithrombotic agents. In this study, clip closure resulted in a decrease in post-polypectomy bleeding in patients deemed to be at high risk (at least 8%) for delayed bleeding.
The protective benefit of clip closure was seen almost exclusively in patients who had complete closure of the defect, which was achieved in only 57% of procedures. Clinical efficacy is largely driven by endoscopist skill level and the ability to achieve complete closure. Notably, defects that were successfully clipped were smaller in size, had better accessibility, and were technically easier. Defining such procedural factors a priori is important and may influence whether one should attempt clip closure if complete clip closure is unlikely. Interestingly, the bleeding rate was higher in the control group in lesions proximal to the transverse colon, where clip closure is likely to be most beneficial and cost effective, based on emerging data. It’s worth noting that the clips used in this study were relatively small (11 mm), and not currently available in the United States, although most endoscopic clips function similarly.
Studies such as this provide evidenced-based medicine to endoscopic practice. Hemostatic clips were introduced nearly 20 years ago without evidence for their effectiveness. Future studies are needed, such as those that compare electrocautery-based resection of high-risk polyps with standard clips to over-the-scope clips, and those that compare electrocautery-based resection to cold snare resection.
Todd H. Baron, MD, is a gastroenterologist based at the University of North Carolina, Chapel Hill. He is a speaker and consultant for Olympus, Boston Scientific, and Cook Endoscopy.
With the advent of routine submucosal lifting prior to endoscopic mucosal resection, perforation now occurs less commonly; however, delayed bleeding following resection remains problematic given the aging population and increasing use of antithrombotic agents. In this study, clip closure resulted in a decrease in post-polypectomy bleeding in patients deemed to be at high risk (at least 8%) for delayed bleeding.
The protective benefit of clip closure was seen almost exclusively in patients who had complete closure of the defect, which was achieved in only 57% of procedures. Clinical efficacy is largely driven by endoscopist skill level and the ability to achieve complete closure. Notably, defects that were successfully clipped were smaller in size, had better accessibility, and were technically easier. Defining such procedural factors a priori is important and may influence whether one should attempt clip closure if complete clip closure is unlikely. Interestingly, the bleeding rate was higher in the control group in lesions proximal to the transverse colon, where clip closure is likely to be most beneficial and cost effective, based on emerging data. It’s worth noting that the clips used in this study were relatively small (11 mm), and not currently available in the United States, although most endoscopic clips function similarly.
Studies such as this provide evidenced-based medicine to endoscopic practice. Hemostatic clips were introduced nearly 20 years ago without evidence for their effectiveness. Future studies are needed, such as those that compare electrocautery-based resection of high-risk polyps with standard clips to over-the-scope clips, and those that compare electrocautery-based resection to cold snare resection.
Todd H. Baron, MD, is a gastroenterologist based at the University of North Carolina, Chapel Hill. He is a speaker and consultant for Olympus, Boston Scientific, and Cook Endoscopy.
With the advent of routine submucosal lifting prior to endoscopic mucosal resection, perforation now occurs less commonly; however, delayed bleeding following resection remains problematic given the aging population and increasing use of antithrombotic agents. In this study, clip closure resulted in a decrease in post-polypectomy bleeding in patients deemed to be at high risk (at least 8%) for delayed bleeding.
The protective benefit of clip closure was seen almost exclusively in patients who had complete closure of the defect, which was achieved in only 57% of procedures. Clinical efficacy is largely driven by endoscopist skill level and the ability to achieve complete closure. Notably, defects that were successfully clipped were smaller in size, had better accessibility, and were technically easier. Defining such procedural factors a priori is important and may influence whether one should attempt clip closure if complete clip closure is unlikely. Interestingly, the bleeding rate was higher in the control group in lesions proximal to the transverse colon, where clip closure is likely to be most beneficial and cost effective, based on emerging data. It’s worth noting that the clips used in this study were relatively small (11 mm), and not currently available in the United States, although most endoscopic clips function similarly.
Studies such as this provide evidenced-based medicine to endoscopic practice. Hemostatic clips were introduced nearly 20 years ago without evidence for their effectiveness. Future studies are needed, such as those that compare electrocautery-based resection of high-risk polyps with standard clips to over-the-scope clips, and those that compare electrocautery-based resection to cold snare resection.
Todd H. Baron, MD, is a gastroenterologist based at the University of North Carolina, Chapel Hill. He is a speaker and consultant for Olympus, Boston Scientific, and Cook Endoscopy.
Use of clip closure significantly reduced delayed bleeding in patients who underwent resections for large colorectal lesions, based on data from 235 individuals.
Source: American Gastroenterological Association
“Closure of a mucosal defect with clips after resection has long been considered to reduce the risk of bleeding,” but evidence to support this practice is limited, wrote Eduardo Albéniz, MD, of the Public University of Navarra (Spain), and colleagues.
In a study published in Gastroenterology, the researchers identified 235 consecutive patients who had resections of large nonpedunculated colorectal lesions from May 2016 to June 2018. Patients had an average or high risk of delayed bleeding and were randomized to receive scar closure with either 11-mm through-the-scope clips (119 patients) or no clip (116 patients).
Delayed bleeding occurred in 14 control patients (12.1%), compared with 6 clip patients (5%), for a risk reduction of 7%. The clip group included 68 cases (57%) of complete closure and 33 cases (28%) with partial closure, as well as 18 cases of failure to close (15%); only 1 case of delayed bleeding occurred in the clip group after completion of clip closure. On average, six clips were needed for complete closure.
None of the patients who experienced delayed bleeding required surgical or angiographic intervention, although 15 of the 20 patients with bleeding underwent additional endoscopy. Other adverse events included immediate bleeding in 21 clip patients and 18 controls that was managed with snare soft-tip coagulation. No deaths were reported in connection with the study.
Demographics were similar between the two groups, but the subset of patients with complete closure included more individuals aged 75 years and older and more cases with smaller polyps, compared with other subgroups, the researchers noted.
The study findings were limited by several factors, including the difficulty in predicting delayed bleeding, the potential for selection bias given the timing of patient randomization, the lack of information about polyps that were excluded from treatment, and the difficulty in completely closing the mucosal defects, the researchers noted. However, the results suggest that complete clip closure, despite its challenges, “displays a clear trend to reduce delayed bleeding risk,” and is worth an attempt.
The study was supported by the Spanish Society of Digestive Endoscopy. The researchers had no financial conflicts to disclose. MicroTech (Nanjing, China) contributed the clips used in the study.
SOURCE: Albéniz E et al. Gastroenterology. 2019 Jul 27. doi: 10.1053/j.gastro.2019.07.037.
Use of clip closure significantly reduced delayed bleeding in patients who underwent resections for large colorectal lesions, based on data from 235 individuals.
Source: American Gastroenterological Association
“Closure of a mucosal defect with clips after resection has long been considered to reduce the risk of bleeding,” but evidence to support this practice is limited, wrote Eduardo Albéniz, MD, of the Public University of Navarra (Spain), and colleagues.
In a study published in Gastroenterology, the researchers identified 235 consecutive patients who had resections of large nonpedunculated colorectal lesions from May 2016 to June 2018. Patients had an average or high risk of delayed bleeding and were randomized to receive scar closure with either 11-mm through-the-scope clips (119 patients) or no clip (116 patients).
Delayed bleeding occurred in 14 control patients (12.1%), compared with 6 clip patients (5%), for a risk reduction of 7%. The clip group included 68 cases (57%) of complete closure and 33 cases (28%) with partial closure, as well as 18 cases of failure to close (15%); only 1 case of delayed bleeding occurred in the clip group after completion of clip closure. On average, six clips were needed for complete closure.
None of the patients who experienced delayed bleeding required surgical or angiographic intervention, although 15 of the 20 patients with bleeding underwent additional endoscopy. Other adverse events included immediate bleeding in 21 clip patients and 18 controls that was managed with snare soft-tip coagulation. No deaths were reported in connection with the study.
Demographics were similar between the two groups, but the subset of patients with complete closure included more individuals aged 75 years and older and more cases with smaller polyps, compared with other subgroups, the researchers noted.
The study findings were limited by several factors, including the difficulty in predicting delayed bleeding, the potential for selection bias given the timing of patient randomization, the lack of information about polyps that were excluded from treatment, and the difficulty in completely closing the mucosal defects, the researchers noted. However, the results suggest that complete clip closure, despite its challenges, “displays a clear trend to reduce delayed bleeding risk,” and is worth an attempt.
The study was supported by the Spanish Society of Digestive Endoscopy. The researchers had no financial conflicts to disclose. MicroTech (Nanjing, China) contributed the clips used in the study.
SOURCE: Albéniz E et al. Gastroenterology. 2019 Jul 27. doi: 10.1053/j.gastro.2019.07.037.
FROM GASTROENTEROLOGY