User login
NHLBI expert panel issues guideline on sickle cell disease
The "much anticipated" guideline to help primary care and emergency clinicians improve the management of sickle cell disease includes a consensus treatment protocol for implementing hydroxyurea therapy and more detailed guidance regarding long-term transfusion therapy, according to a summary report published online September 9 in Journal of the American Medical Association.
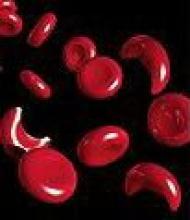
Sickle cell disease (SCD), a life-threatening genetically transmitted disorder affecting 70,000-100,000 Americans, is associated with a wide array of complex acute and chronic complications that require immediate medical attention. But high-quality data on which to base management decisions are sorely lacking, and clinicians get little in the way of guidance from existing recommendations. One result is that "the two most widely available disease-modifying therapies, hydroxyurea and long-term transfusions, are underused, and hematopoietic stem cell transplantation, the only curative approach, has been used in only a small proportion of affected individuals," said Dr. Barbara P. Yawn and her associates on the National Heart, Lung, and Blood Institute expert panel that issued the summary report.
Even this guideline is somewhat rudimentary due to the dearth of good data "in virtually every area related to SCD management," and cannot help but leave "many uncertainties for health professionals caring for individuals with SCD." But it is hoped that this guideline will furnish a critical foundation for future research and will now begin "to facilitate improved and more accessible care for all affected individuals," said Dr. Yawn, director of research at Olmsted Medical Center, Rochester, Minn., and her associates.
The guideline is based on an extensive literature review of more than 13,000 abstracts and articles, which was winnowed to 1,583 original studies regarding SCD. From this, a team of health care professionals in family medicine, internal medicine, pediatric and adult hematology, psychiatry and mental health, transfusion medicine, obstetrics and gynecology, maternal/fetal medicine, and emergency department nursing compiled the guideline as well as the summary, entitled Evidence-Based Management of Sickle Cell Disease: Expert Panel Report 2014 (JAMA 2014 September 9 [doi:10.1001/jama.2014.10517]).
In addition to establishing a protocol for implementing hydroxyurea therapy, the guideline addresses changes in pneumococcal vaccination recommendations for adults and children; annual transcranial Doppler screening coupled with long-term transfusion therapy when necessary to prevent stroke in children aged 2-16 years; rapid initiation of opioids for severe pain during vasoocclusive crises; analgesics and physical therapy for avascular necrosis; ACE inhibitor treatment for adults with microalbuminuria; referral to specialists for screening and treatment of proliferative retinopathy; echocardiography to assess signs of pulmonary hypertension; and monitoring for iron overload in patients receiving transfusion therapy.
Both the summary report and the full guideline are available at http://www.nhlbi.nih.gov/health-pro/guidelines/sickle-cell-disease-guidelines/.
Yawn et al. have made a monumental effort to produce practical, evidence-based guidelines, but they were hampered at every turn by a pervasive lack of good quality evidence on which to base their recommendations. Still missing from this guideline are suggestions for how often and when to screen for kidney disease, how to screen for and treat the common clinical problem of asthma-like symptoms (when standard therapies are contraindicated in SCD), how to advocate for patients with the common sequelae of silent cerebral infarcts, or when to consider hematopoietic stem-cell transplantation.
The expert panel also failed to include representatives from the people most affected by SCD: patients and their families. Failure to listen to the perspective of the families, understand which of these recommendations are important to them, and deal with the obstacles families face in implementing the recommendations is a critically important omission.
Dr. Michael R. DeBaun is in the department of pediatrics at the Vanderbilt-Meharry Center of Excellence in Sickle Cell Disease, Nashville. He made his remarks in an editorial accompanying Dr. Yawn’s report (JAMA 2014:312;1004-5). Dr. DeBaun reported no financial conflicts of interest.
Yawn et al. have made a monumental effort to produce practical, evidence-based guidelines, but they were hampered at every turn by a pervasive lack of good quality evidence on which to base their recommendations. Still missing from this guideline are suggestions for how often and when to screen for kidney disease, how to screen for and treat the common clinical problem of asthma-like symptoms (when standard therapies are contraindicated in SCD), how to advocate for patients with the common sequelae of silent cerebral infarcts, or when to consider hematopoietic stem-cell transplantation.
The expert panel also failed to include representatives from the people most affected by SCD: patients and their families. Failure to listen to the perspective of the families, understand which of these recommendations are important to them, and deal with the obstacles families face in implementing the recommendations is a critically important omission.
Dr. Michael R. DeBaun is in the department of pediatrics at the Vanderbilt-Meharry Center of Excellence in Sickle Cell Disease, Nashville. He made his remarks in an editorial accompanying Dr. Yawn’s report (JAMA 2014:312;1004-5). Dr. DeBaun reported no financial conflicts of interest.
Yawn et al. have made a monumental effort to produce practical, evidence-based guidelines, but they were hampered at every turn by a pervasive lack of good quality evidence on which to base their recommendations. Still missing from this guideline are suggestions for how often and when to screen for kidney disease, how to screen for and treat the common clinical problem of asthma-like symptoms (when standard therapies are contraindicated in SCD), how to advocate for patients with the common sequelae of silent cerebral infarcts, or when to consider hematopoietic stem-cell transplantation.
The expert panel also failed to include representatives from the people most affected by SCD: patients and their families. Failure to listen to the perspective of the families, understand which of these recommendations are important to them, and deal with the obstacles families face in implementing the recommendations is a critically important omission.
Dr. Michael R. DeBaun is in the department of pediatrics at the Vanderbilt-Meharry Center of Excellence in Sickle Cell Disease, Nashville. He made his remarks in an editorial accompanying Dr. Yawn’s report (JAMA 2014:312;1004-5). Dr. DeBaun reported no financial conflicts of interest.
The "much anticipated" guideline to help primary care and emergency clinicians improve the management of sickle cell disease includes a consensus treatment protocol for implementing hydroxyurea therapy and more detailed guidance regarding long-term transfusion therapy, according to a summary report published online September 9 in Journal of the American Medical Association.
Sickle cell disease (SCD), a life-threatening genetically transmitted disorder affecting 70,000-100,000 Americans, is associated with a wide array of complex acute and chronic complications that require immediate medical attention. But high-quality data on which to base management decisions are sorely lacking, and clinicians get little in the way of guidance from existing recommendations. One result is that "the two most widely available disease-modifying therapies, hydroxyurea and long-term transfusions, are underused, and hematopoietic stem cell transplantation, the only curative approach, has been used in only a small proportion of affected individuals," said Dr. Barbara P. Yawn and her associates on the National Heart, Lung, and Blood Institute expert panel that issued the summary report.
Even this guideline is somewhat rudimentary due to the dearth of good data "in virtually every area related to SCD management," and cannot help but leave "many uncertainties for health professionals caring for individuals with SCD." But it is hoped that this guideline will furnish a critical foundation for future research and will now begin "to facilitate improved and more accessible care for all affected individuals," said Dr. Yawn, director of research at Olmsted Medical Center, Rochester, Minn., and her associates.
The guideline is based on an extensive literature review of more than 13,000 abstracts and articles, which was winnowed to 1,583 original studies regarding SCD. From this, a team of health care professionals in family medicine, internal medicine, pediatric and adult hematology, psychiatry and mental health, transfusion medicine, obstetrics and gynecology, maternal/fetal medicine, and emergency department nursing compiled the guideline as well as the summary, entitled Evidence-Based Management of Sickle Cell Disease: Expert Panel Report 2014 (JAMA 2014 September 9 [doi:10.1001/jama.2014.10517]).
In addition to establishing a protocol for implementing hydroxyurea therapy, the guideline addresses changes in pneumococcal vaccination recommendations for adults and children; annual transcranial Doppler screening coupled with long-term transfusion therapy when necessary to prevent stroke in children aged 2-16 years; rapid initiation of opioids for severe pain during vasoocclusive crises; analgesics and physical therapy for avascular necrosis; ACE inhibitor treatment for adults with microalbuminuria; referral to specialists for screening and treatment of proliferative retinopathy; echocardiography to assess signs of pulmonary hypertension; and monitoring for iron overload in patients receiving transfusion therapy.
Both the summary report and the full guideline are available at http://www.nhlbi.nih.gov/health-pro/guidelines/sickle-cell-disease-guidelines/.
The "much anticipated" guideline to help primary care and emergency clinicians improve the management of sickle cell disease includes a consensus treatment protocol for implementing hydroxyurea therapy and more detailed guidance regarding long-term transfusion therapy, according to a summary report published online September 9 in Journal of the American Medical Association.
Sickle cell disease (SCD), a life-threatening genetically transmitted disorder affecting 70,000-100,000 Americans, is associated with a wide array of complex acute and chronic complications that require immediate medical attention. But high-quality data on which to base management decisions are sorely lacking, and clinicians get little in the way of guidance from existing recommendations. One result is that "the two most widely available disease-modifying therapies, hydroxyurea and long-term transfusions, are underused, and hematopoietic stem cell transplantation, the only curative approach, has been used in only a small proportion of affected individuals," said Dr. Barbara P. Yawn and her associates on the National Heart, Lung, and Blood Institute expert panel that issued the summary report.
Even this guideline is somewhat rudimentary due to the dearth of good data "in virtually every area related to SCD management," and cannot help but leave "many uncertainties for health professionals caring for individuals with SCD." But it is hoped that this guideline will furnish a critical foundation for future research and will now begin "to facilitate improved and more accessible care for all affected individuals," said Dr. Yawn, director of research at Olmsted Medical Center, Rochester, Minn., and her associates.
The guideline is based on an extensive literature review of more than 13,000 abstracts and articles, which was winnowed to 1,583 original studies regarding SCD. From this, a team of health care professionals in family medicine, internal medicine, pediatric and adult hematology, psychiatry and mental health, transfusion medicine, obstetrics and gynecology, maternal/fetal medicine, and emergency department nursing compiled the guideline as well as the summary, entitled Evidence-Based Management of Sickle Cell Disease: Expert Panel Report 2014 (JAMA 2014 September 9 [doi:10.1001/jama.2014.10517]).
In addition to establishing a protocol for implementing hydroxyurea therapy, the guideline addresses changes in pneumococcal vaccination recommendations for adults and children; annual transcranial Doppler screening coupled with long-term transfusion therapy when necessary to prevent stroke in children aged 2-16 years; rapid initiation of opioids for severe pain during vasoocclusive crises; analgesics and physical therapy for avascular necrosis; ACE inhibitor treatment for adults with microalbuminuria; referral to specialists for screening and treatment of proliferative retinopathy; echocardiography to assess signs of pulmonary hypertension; and monitoring for iron overload in patients receiving transfusion therapy.
Both the summary report and the full guideline are available at http://www.nhlbi.nih.gov/health-pro/guidelines/sickle-cell-disease-guidelines/.
FROM JAMA
Major finding: The two most widely available disease-modifying therapies for SCD, hydroxyurea and long-term transfusions, are underused, in large part because no evidence-based treatment protocols have been devised until now.
Data source: A review of the literature and compilation of management guidelines "to assist health care professionals in the management of common issues of sickle cell disease."
Disclosures: The National Heart, Lung, and Blood Institute sponsored the development of this guideline. All expert panel members served voluntarily. Many reported numerous ties to industry sources.
USPSTF recommends low-dose aspirin for preeclampsia prevention
The use of low-dose aspirin is advisable after 12 weeks of gestation in asymptomatic pregnant women at high risk for developing preeclampsia, according to a recommendation from the U.S. Preventive Services Task Force.
The recommendation, published online Sept. 8 in the Annals of Internal Medicine, is based on a review of new evidence suggesting that the net benefit of low-dose aspirin for preventing preeclampsia is of substantial magnitude. It updates a 1996 recommendation from the USPSTF, which concluded that there was insufficient evidence at that time to recommend for or against the routine use of aspirin for the prevention of preeclampsia.
The current evidence – including 15 randomized controlled trials used to assess the health benefits of low-dose aspirin, 13 randomized controlled trials used to evaluate preeclampsia incidence, and 19 randomized controlled trials and 2 good-quality observational studies used to evaluate harms associated with low-dose aspirin use – suggests that women at risk may benefit from low-dose aspirin beginning after 12 weeks of gestation.
Preeclampsia complicates 2%-8% of pregnancies worldwide, and accounts for 15% of preterm births and 12% of maternal deaths in the United States, according to the task force.
"The USPSTF found adequate evidence of a reduction in risk for preeclampsia, preterm birth, and IUGR [intrauterine growth restriction] in women at increased risk for preeclampsia who received low-dose aspirin, thus demonstrating substantial benefit. Low-dose aspirin (range, 60-150 mg/day) reduced the risk for preeclampsia by 24% in clinical trials [pooled relative risk, 0.76] and reduced the risk for preterm birth by 14% and IUGR by 20% [pooled relative risk, 0.86 and 0.80, respectively]," the updated recommendation stated (Ann. Intern. Med. 2014 Sept. 8 [doi:10.7326/m14-1884]).
Adequate evidence also indicates that low-dose aspirin is not associated with any increase in the risk of placental abruption, postpartum hemorrhage, fetal intracranial bleeding, or perinatal mortality.
"Evidence on long-term outcomes in offspring exposed in utero to low-dose aspirin is limited, but no developmental harms were identified by age 18 months in the one study reviewed," the task force wrote, concluding – with moderate certainty – that there is a substantial net benefit of daily low-dose aspirin use to reduce the risk for preeclampsia, preterm birth, and IUGR in women at high risk.
The decision to initiate low-dose aspirin therapy in this population is typically based on medical history; there are no validated methods for identifying women at high risk based on biomarkers, clinical diagnostic tests, or medical history. However, as part of the recommendation, the USPSTF provided a pragmatic approach that may help identify those at risk.
"Women with one or more risk factors should receive low-dose aspirin. Women with several moderate risk factors may also benefit from low-dose aspirin," the task force noted, adding that the evidence for the latter approach is less certain, and that clinicians should use clinical judgment and discuss the risks and benefits with patients.
The recommendation applies to asymptomatic women at risk in whom low-dose aspirin is not contraindicated, and defines women at high risk as those with a history of preeclampsia, especially those with an adverse outcome; chronic hypertension, renal disease, type 1 or 2 diabetes, or an autoimmune disease; and those with multifetal gestation, according to the updated recommendation.
Moderate risk factors include nulliparity, obesity, a family history of preeclampsia, age greater than or equal to 35 years, African American race, low socioeconomic status, low birth rate or small for gestational age, greater than 10-year pregnancy interval, or previous adverse pregnancy outcome.
As for appropriate dosing, the most common dosage across studies was 100 mg, but the two largest trials contributing to benefit estimates used 60 mg.
An 81-mg dose was not specifically evaluated, but is commonly available in the United States in tablet form, and is a reasonable dosage for preeclampsia prophylaxis, the task force said.
The updated recommendation is generally in keeping with those of other organizations, including the American College of Obstetricians and Gynecologists, the World Health Organization, the National Institute for Health and Clinical Excellence, the American Heart Association/American Stroke Association, and the American Academy of Family Physicians. For example, ACOG recommends initiating daily low-dose aspirin during the late first trimester in those with a history of early-onset preeclampsia and preterm delivery, or with a history of preeclampsia in more than one prior pregnancy (<cf number="\"2\"">“</cf>American College of Obstetricians and Gynecologists: Hypertension in Pregnancy [Washington, D.C.: American College of Obstetricians and Gynecologists, 2013]), and WHO recommends daily low-dose aspirin as early as 12 weeks for those at high risk ("WHO Recommendations for Prevention and Treatment of Pre-Eclampsia and Eclampsia" [Geneva: World Health Organization, 2011]).
The review by the USPSTF identified several research needs. For example, additional study is needed on the effects of low-dose aspirin on the development of preeclampsia and how patient response is affected by various risk factors. Research is also needed on how to improve clinicians’ ability to identify those at risk, and particularly those who would benefit most from prophylaxis. Study is needed on risk assessment tools, and on populations at particular risk, such as African American and nulliparous women.
Future trials should recruit adequate numbers of women from racial/ethnic populations that are at disproportionate risk.
"Larger studies on aspirin use in the first or early second trimester may improve the evidence base on optimal timing of low-dose aspirin preventive medication. Other areas of research include optimal therapies that individualize the aspirin dosage and timing of administration (e.g., morning vs. bedtime)," they concluded, noting that research is also needed to explore less-well-established risk factors, and to investigate whether preeclampsia prevention with low-dose aspirin affects long-term risk for cardiovascular disease, and whether there is any benefit to continuing low-dose aspirin after delivery in those at high risk.
The use of low-dose aspirin is advisable after 12 weeks of gestation in asymptomatic pregnant women at high risk for developing preeclampsia, according to a recommendation from the U.S. Preventive Services Task Force.
The recommendation, published online Sept. 8 in the Annals of Internal Medicine, is based on a review of new evidence suggesting that the net benefit of low-dose aspirin for preventing preeclampsia is of substantial magnitude. It updates a 1996 recommendation from the USPSTF, which concluded that there was insufficient evidence at that time to recommend for or against the routine use of aspirin for the prevention of preeclampsia.
The current evidence – including 15 randomized controlled trials used to assess the health benefits of low-dose aspirin, 13 randomized controlled trials used to evaluate preeclampsia incidence, and 19 randomized controlled trials and 2 good-quality observational studies used to evaluate harms associated with low-dose aspirin use – suggests that women at risk may benefit from low-dose aspirin beginning after 12 weeks of gestation.
Preeclampsia complicates 2%-8% of pregnancies worldwide, and accounts for 15% of preterm births and 12% of maternal deaths in the United States, according to the task force.
"The USPSTF found adequate evidence of a reduction in risk for preeclampsia, preterm birth, and IUGR [intrauterine growth restriction] in women at increased risk for preeclampsia who received low-dose aspirin, thus demonstrating substantial benefit. Low-dose aspirin (range, 60-150 mg/day) reduced the risk for preeclampsia by 24% in clinical trials [pooled relative risk, 0.76] and reduced the risk for preterm birth by 14% and IUGR by 20% [pooled relative risk, 0.86 and 0.80, respectively]," the updated recommendation stated (Ann. Intern. Med. 2014 Sept. 8 [doi:10.7326/m14-1884]).
Adequate evidence also indicates that low-dose aspirin is not associated with any increase in the risk of placental abruption, postpartum hemorrhage, fetal intracranial bleeding, or perinatal mortality.
"Evidence on long-term outcomes in offspring exposed in utero to low-dose aspirin is limited, but no developmental harms were identified by age 18 months in the one study reviewed," the task force wrote, concluding – with moderate certainty – that there is a substantial net benefit of daily low-dose aspirin use to reduce the risk for preeclampsia, preterm birth, and IUGR in women at high risk.
The decision to initiate low-dose aspirin therapy in this population is typically based on medical history; there are no validated methods for identifying women at high risk based on biomarkers, clinical diagnostic tests, or medical history. However, as part of the recommendation, the USPSTF provided a pragmatic approach that may help identify those at risk.
"Women with one or more risk factors should receive low-dose aspirin. Women with several moderate risk factors may also benefit from low-dose aspirin," the task force noted, adding that the evidence for the latter approach is less certain, and that clinicians should use clinical judgment and discuss the risks and benefits with patients.
The recommendation applies to asymptomatic women at risk in whom low-dose aspirin is not contraindicated, and defines women at high risk as those with a history of preeclampsia, especially those with an adverse outcome; chronic hypertension, renal disease, type 1 or 2 diabetes, or an autoimmune disease; and those with multifetal gestation, according to the updated recommendation.
Moderate risk factors include nulliparity, obesity, a family history of preeclampsia, age greater than or equal to 35 years, African American race, low socioeconomic status, low birth rate or small for gestational age, greater than 10-year pregnancy interval, or previous adverse pregnancy outcome.
As for appropriate dosing, the most common dosage across studies was 100 mg, but the two largest trials contributing to benefit estimates used 60 mg.
An 81-mg dose was not specifically evaluated, but is commonly available in the United States in tablet form, and is a reasonable dosage for preeclampsia prophylaxis, the task force said.
The updated recommendation is generally in keeping with those of other organizations, including the American College of Obstetricians and Gynecologists, the World Health Organization, the National Institute for Health and Clinical Excellence, the American Heart Association/American Stroke Association, and the American Academy of Family Physicians. For example, ACOG recommends initiating daily low-dose aspirin during the late first trimester in those with a history of early-onset preeclampsia and preterm delivery, or with a history of preeclampsia in more than one prior pregnancy (<cf number="\"2\"">“</cf>American College of Obstetricians and Gynecologists: Hypertension in Pregnancy [Washington, D.C.: American College of Obstetricians and Gynecologists, 2013]), and WHO recommends daily low-dose aspirin as early as 12 weeks for those at high risk ("WHO Recommendations for Prevention and Treatment of Pre-Eclampsia and Eclampsia" [Geneva: World Health Organization, 2011]).
The review by the USPSTF identified several research needs. For example, additional study is needed on the effects of low-dose aspirin on the development of preeclampsia and how patient response is affected by various risk factors. Research is also needed on how to improve clinicians’ ability to identify those at risk, and particularly those who would benefit most from prophylaxis. Study is needed on risk assessment tools, and on populations at particular risk, such as African American and nulliparous women.
Future trials should recruit adequate numbers of women from racial/ethnic populations that are at disproportionate risk.
"Larger studies on aspirin use in the first or early second trimester may improve the evidence base on optimal timing of low-dose aspirin preventive medication. Other areas of research include optimal therapies that individualize the aspirin dosage and timing of administration (e.g., morning vs. bedtime)," they concluded, noting that research is also needed to explore less-well-established risk factors, and to investigate whether preeclampsia prevention with low-dose aspirin affects long-term risk for cardiovascular disease, and whether there is any benefit to continuing low-dose aspirin after delivery in those at high risk.
The use of low-dose aspirin is advisable after 12 weeks of gestation in asymptomatic pregnant women at high risk for developing preeclampsia, according to a recommendation from the U.S. Preventive Services Task Force.
The recommendation, published online Sept. 8 in the Annals of Internal Medicine, is based on a review of new evidence suggesting that the net benefit of low-dose aspirin for preventing preeclampsia is of substantial magnitude. It updates a 1996 recommendation from the USPSTF, which concluded that there was insufficient evidence at that time to recommend for or against the routine use of aspirin for the prevention of preeclampsia.
The current evidence – including 15 randomized controlled trials used to assess the health benefits of low-dose aspirin, 13 randomized controlled trials used to evaluate preeclampsia incidence, and 19 randomized controlled trials and 2 good-quality observational studies used to evaluate harms associated with low-dose aspirin use – suggests that women at risk may benefit from low-dose aspirin beginning after 12 weeks of gestation.
Preeclampsia complicates 2%-8% of pregnancies worldwide, and accounts for 15% of preterm births and 12% of maternal deaths in the United States, according to the task force.
"The USPSTF found adequate evidence of a reduction in risk for preeclampsia, preterm birth, and IUGR [intrauterine growth restriction] in women at increased risk for preeclampsia who received low-dose aspirin, thus demonstrating substantial benefit. Low-dose aspirin (range, 60-150 mg/day) reduced the risk for preeclampsia by 24% in clinical trials [pooled relative risk, 0.76] and reduced the risk for preterm birth by 14% and IUGR by 20% [pooled relative risk, 0.86 and 0.80, respectively]," the updated recommendation stated (Ann. Intern. Med. 2014 Sept. 8 [doi:10.7326/m14-1884]).
Adequate evidence also indicates that low-dose aspirin is not associated with any increase in the risk of placental abruption, postpartum hemorrhage, fetal intracranial bleeding, or perinatal mortality.
"Evidence on long-term outcomes in offspring exposed in utero to low-dose aspirin is limited, but no developmental harms were identified by age 18 months in the one study reviewed," the task force wrote, concluding – with moderate certainty – that there is a substantial net benefit of daily low-dose aspirin use to reduce the risk for preeclampsia, preterm birth, and IUGR in women at high risk.
The decision to initiate low-dose aspirin therapy in this population is typically based on medical history; there are no validated methods for identifying women at high risk based on biomarkers, clinical diagnostic tests, or medical history. However, as part of the recommendation, the USPSTF provided a pragmatic approach that may help identify those at risk.
"Women with one or more risk factors should receive low-dose aspirin. Women with several moderate risk factors may also benefit from low-dose aspirin," the task force noted, adding that the evidence for the latter approach is less certain, and that clinicians should use clinical judgment and discuss the risks and benefits with patients.
The recommendation applies to asymptomatic women at risk in whom low-dose aspirin is not contraindicated, and defines women at high risk as those with a history of preeclampsia, especially those with an adverse outcome; chronic hypertension, renal disease, type 1 or 2 diabetes, or an autoimmune disease; and those with multifetal gestation, according to the updated recommendation.
Moderate risk factors include nulliparity, obesity, a family history of preeclampsia, age greater than or equal to 35 years, African American race, low socioeconomic status, low birth rate or small for gestational age, greater than 10-year pregnancy interval, or previous adverse pregnancy outcome.
As for appropriate dosing, the most common dosage across studies was 100 mg, but the two largest trials contributing to benefit estimates used 60 mg.
An 81-mg dose was not specifically evaluated, but is commonly available in the United States in tablet form, and is a reasonable dosage for preeclampsia prophylaxis, the task force said.
The updated recommendation is generally in keeping with those of other organizations, including the American College of Obstetricians and Gynecologists, the World Health Organization, the National Institute for Health and Clinical Excellence, the American Heart Association/American Stroke Association, and the American Academy of Family Physicians. For example, ACOG recommends initiating daily low-dose aspirin during the late first trimester in those with a history of early-onset preeclampsia and preterm delivery, or with a history of preeclampsia in more than one prior pregnancy (<cf number="\"2\"">“</cf>American College of Obstetricians and Gynecologists: Hypertension in Pregnancy [Washington, D.C.: American College of Obstetricians and Gynecologists, 2013]), and WHO recommends daily low-dose aspirin as early as 12 weeks for those at high risk ("WHO Recommendations for Prevention and Treatment of Pre-Eclampsia and Eclampsia" [Geneva: World Health Organization, 2011]).
The review by the USPSTF identified several research needs. For example, additional study is needed on the effects of low-dose aspirin on the development of preeclampsia and how patient response is affected by various risk factors. Research is also needed on how to improve clinicians’ ability to identify those at risk, and particularly those who would benefit most from prophylaxis. Study is needed on risk assessment tools, and on populations at particular risk, such as African American and nulliparous women.
Future trials should recruit adequate numbers of women from racial/ethnic populations that are at disproportionate risk.
"Larger studies on aspirin use in the first or early second trimester may improve the evidence base on optimal timing of low-dose aspirin preventive medication. Other areas of research include optimal therapies that individualize the aspirin dosage and timing of administration (e.g., morning vs. bedtime)," they concluded, noting that research is also needed to explore less-well-established risk factors, and to investigate whether preeclampsia prevention with low-dose aspirin affects long-term risk for cardiovascular disease, and whether there is any benefit to continuing low-dose aspirin after delivery in those at high risk.
FROM ANNALS OF INTERNAL MEDICINE
USPSTF: Offer behavioral counseling to prevent cardiovascular disease
Overweight or obese adults at risk for cardiovascular disease should receive intensive behavioral counseling interventions, according to a recommendation statement by the U. S. Preventive Services Task Force.
After a comprehensive review of the current literature, the USPSTF concluded "with moderate certainty" that interventions promoting a healthful diet and increased physical activity have a moderate net benefit in this patient population, said Dr. Michael L. LeFevre, chair of the task force at the time the recommendation was finalized, and professor of family medicine at the University of Missouri, Columbia.
The recommendation statement issued Aug. 25 is "an update and refinement" of the 2003 USPSTF recommendation on dietary counseling for at-risk adults, this time targeting overweight or obese patients who have additional CVD risk factors such as hypertension, dyslipidemia, impaired fasting glucose, or metabolic syndrome.
The group reviewed 74 trials assessing the effectiveness of behavioral counseling interventions of various intensities. Only 16 reported on direct health outcomes such as CVD events, mortality, or quality of life, the task force noted, so there is inadequate evidence about intensive behavioral counseling’s effect on such outcomes.
A total of 71 trials involving more than 32,000 participants focused on intermediate health outcomes such as lipid levels, blood pressure, glucose levels, weight, and medication use. Overall, intensive counseling interventions made "small but important changes" in these outcomes, with total cholesterol levels decreasing approximately 3-6 mg/dL, LDL cholesterol decreasing by 1.5-5.0 mg/dL, systolic blood pressure decreasing by 1-3 mm Hg, diastolic blood pressure decreasing by 1-2 mm Hg, and fasting glucose levels decreasing by 1-3 mg/dL.
In addition, weight decreased by a mean of approximately 3 kg, and the proportion of patients who participated in moderate-intensity exercise for 150 minutes per week rose from 10% to 25%. However, few of these studies followed patients for more than 1-2 years, so the evidence was inadequate to assess longer-term benefits.
Because very few and mostly minor adverse events were associated with these interventions, they yielded a moderate net benefit.
Most of the intensive behavioral counseling interventions that were assessed averaged 5-16 individual or group sessions during a period of 9-12 months. All included didactic education; in most programs, specially trained professionals (dietitians, nutritionists, physiotherapists, exercise professionals, health educators, and psychologists) provided monitoring and feedback for the participants, devised individualized care plans, and taught problem-solving skills. Many types and combinations of interventions were effective, and almost all were delivered outside the primary care setting.
The recommendation statement is in line with others published by the American Heart Association, the American College of Sports Medicine, and the American Academy of Family Physicians. The AAFP is updating its recommendations regarding behavioral counseling to prevent CVD, Dr. LeFevre and his associates noted.
The USPSTF, funded by but independent of the federal government, makes recommendations about the effectiveness of specific preventive-care services based on evidence of benefits and harms, without considering costs.
Do you refer overweight or obese patients with cardiovascular risk factors for intensive behavioral counseling? Take our Quick Poll on the Family Practice News homepage.
Overweight or obese adults at risk for cardiovascular disease should receive intensive behavioral counseling interventions, according to a recommendation statement by the U. S. Preventive Services Task Force.
After a comprehensive review of the current literature, the USPSTF concluded "with moderate certainty" that interventions promoting a healthful diet and increased physical activity have a moderate net benefit in this patient population, said Dr. Michael L. LeFevre, chair of the task force at the time the recommendation was finalized, and professor of family medicine at the University of Missouri, Columbia.
The recommendation statement issued Aug. 25 is "an update and refinement" of the 2003 USPSTF recommendation on dietary counseling for at-risk adults, this time targeting overweight or obese patients who have additional CVD risk factors such as hypertension, dyslipidemia, impaired fasting glucose, or metabolic syndrome.
The group reviewed 74 trials assessing the effectiveness of behavioral counseling interventions of various intensities. Only 16 reported on direct health outcomes such as CVD events, mortality, or quality of life, the task force noted, so there is inadequate evidence about intensive behavioral counseling’s effect on such outcomes.
A total of 71 trials involving more than 32,000 participants focused on intermediate health outcomes such as lipid levels, blood pressure, glucose levels, weight, and medication use. Overall, intensive counseling interventions made "small but important changes" in these outcomes, with total cholesterol levels decreasing approximately 3-6 mg/dL, LDL cholesterol decreasing by 1.5-5.0 mg/dL, systolic blood pressure decreasing by 1-3 mm Hg, diastolic blood pressure decreasing by 1-2 mm Hg, and fasting glucose levels decreasing by 1-3 mg/dL.
In addition, weight decreased by a mean of approximately 3 kg, and the proportion of patients who participated in moderate-intensity exercise for 150 minutes per week rose from 10% to 25%. However, few of these studies followed patients for more than 1-2 years, so the evidence was inadequate to assess longer-term benefits.
Because very few and mostly minor adverse events were associated with these interventions, they yielded a moderate net benefit.
Most of the intensive behavioral counseling interventions that were assessed averaged 5-16 individual or group sessions during a period of 9-12 months. All included didactic education; in most programs, specially trained professionals (dietitians, nutritionists, physiotherapists, exercise professionals, health educators, and psychologists) provided monitoring and feedback for the participants, devised individualized care plans, and taught problem-solving skills. Many types and combinations of interventions were effective, and almost all were delivered outside the primary care setting.
The recommendation statement is in line with others published by the American Heart Association, the American College of Sports Medicine, and the American Academy of Family Physicians. The AAFP is updating its recommendations regarding behavioral counseling to prevent CVD, Dr. LeFevre and his associates noted.
The USPSTF, funded by but independent of the federal government, makes recommendations about the effectiveness of specific preventive-care services based on evidence of benefits and harms, without considering costs.
Do you refer overweight or obese patients with cardiovascular risk factors for intensive behavioral counseling? Take our Quick Poll on the Family Practice News homepage.
Overweight or obese adults at risk for cardiovascular disease should receive intensive behavioral counseling interventions, according to a recommendation statement by the U. S. Preventive Services Task Force.
After a comprehensive review of the current literature, the USPSTF concluded "with moderate certainty" that interventions promoting a healthful diet and increased physical activity have a moderate net benefit in this patient population, said Dr. Michael L. LeFevre, chair of the task force at the time the recommendation was finalized, and professor of family medicine at the University of Missouri, Columbia.
The recommendation statement issued Aug. 25 is "an update and refinement" of the 2003 USPSTF recommendation on dietary counseling for at-risk adults, this time targeting overweight or obese patients who have additional CVD risk factors such as hypertension, dyslipidemia, impaired fasting glucose, or metabolic syndrome.
The group reviewed 74 trials assessing the effectiveness of behavioral counseling interventions of various intensities. Only 16 reported on direct health outcomes such as CVD events, mortality, or quality of life, the task force noted, so there is inadequate evidence about intensive behavioral counseling’s effect on such outcomes.
A total of 71 trials involving more than 32,000 participants focused on intermediate health outcomes such as lipid levels, blood pressure, glucose levels, weight, and medication use. Overall, intensive counseling interventions made "small but important changes" in these outcomes, with total cholesterol levels decreasing approximately 3-6 mg/dL, LDL cholesterol decreasing by 1.5-5.0 mg/dL, systolic blood pressure decreasing by 1-3 mm Hg, diastolic blood pressure decreasing by 1-2 mm Hg, and fasting glucose levels decreasing by 1-3 mg/dL.
In addition, weight decreased by a mean of approximately 3 kg, and the proportion of patients who participated in moderate-intensity exercise for 150 minutes per week rose from 10% to 25%. However, few of these studies followed patients for more than 1-2 years, so the evidence was inadequate to assess longer-term benefits.
Because very few and mostly minor adverse events were associated with these interventions, they yielded a moderate net benefit.
Most of the intensive behavioral counseling interventions that were assessed averaged 5-16 individual or group sessions during a period of 9-12 months. All included didactic education; in most programs, specially trained professionals (dietitians, nutritionists, physiotherapists, exercise professionals, health educators, and psychologists) provided monitoring and feedback for the participants, devised individualized care plans, and taught problem-solving skills. Many types and combinations of interventions were effective, and almost all were delivered outside the primary care setting.
The recommendation statement is in line with others published by the American Heart Association, the American College of Sports Medicine, and the American Academy of Family Physicians. The AAFP is updating its recommendations regarding behavioral counseling to prevent CVD, Dr. LeFevre and his associates noted.
The USPSTF, funded by but independent of the federal government, makes recommendations about the effectiveness of specific preventive-care services based on evidence of benefits and harms, without considering costs.
Do you refer overweight or obese patients with cardiovascular risk factors for intensive behavioral counseling? Take our Quick Poll on the Family Practice News homepage.
FROM ANNALS OF INTERNAL MEDICINE
Key clinical point: Refer overweight or obese patients at risk of cardiovascular disease for intensive behavioral counseling.
Major Finding: Intensive behavioral counseling interventions made small but important changes in several intermediate health outcomes, with total cholesterol levels decreasing by about 3-6 mg/dL, LDL cholesterol decreasing by 1.5-5.0 mg/dL, systolic blood pressure decreasing by 1-3 mm Hg, diastolic blood pressure decreasing by 1-2 mm Hg, fasting glucose levels decreasing by 1-3 mg/dL, and weight decreasing by a mean of 3 kg.
Data Source: An update and refinement of a 2003 USPSTF recommendation on dietary counseling for overweight/obese adults who have additional risk factors for CVD, based on a comprehensive review of the literature.
Disclosures: The USPSTF, funded by but independent of the federal government, makes recommendations about the effectiveness of specific preventive-care services based on evidence of benefits and harms, without considering costs.
AHA wants e-cigarettes regulated but notes they help some smokers quit
The American Heart Association has released its recommendations regarding the sale and usage of e-cigarettes, cautioning that the devices should be regulated to avoid enticing children to smoke while also saying that e-cigarettes could be used as a way to help some current smokers quit.
The guidelines, published online Aug. 24 in Circulation, state that clinicians "should not discourage" their patients from resorting to e-cigarettes if other approved forms of smoking cessation, such as the nicotine patch, have been exhausted. The AHA warned, however, that further studies are needed to fully understand the effects of e-cigarette usage, stressing that e-cigarettes have not been approved by the Food and Drug Administration as an acceptable smoking cessation device and could contain low amounts of toxic chemicals that would prove more harmful than helpful to patients in the long run.
"E-cigarettes have caused a major shift in the tobacco-control landscape," Aruni Bhatnagar, Ph.D., lead author of the guidelines and chair of cardiovascular medicine at the University of Louisville, Ky., said in a statement. "It’s critical that we rigorously examine the long-term impact of this new technology on public health, cardiovascular disease, and stroke, and pay careful attention to the effect of e-cigarettes on adolescents."
For now, the AHA says that clinicians should tell their patients who use e-cigarettes to set a firm quit date, warning that any device that delivers nicotine into the body is harmful and likely lethal.
"Nicotine is a dangerous and highly addictive chemical no matter what form it takes – conventional cigarettes or some other tobacco product," Dr. Elliott Antman, AHA president, said in the statement. "Every life that has been lost to tobacco addiction" could have been saved, he noted.
To that end, the AHA also called for strong regulations regarding the potential marketability of e-cigarettes to youngsters. The group recommended a federal ban on the sale of e-cigarettes to minors, warning that the devices could become a gateway to actual cigarettes for young people who see e-cigarettes as "high-tech, accessible, and convenient," according to a JAMA Pediatrics study of 40,000 middle and high school students. The AHA also recommended that all existing rules and regulations in place for tobacco-related products should apply to e-cigarettes.
"We must protect future generations from any potential smokescreens in the tobacco product landscape that will cause us to lose precious ground in the fight to make our nation 100% tobacco-free," Dr. Antman said.
According to the AHA, 20 million Americans have lost their lives to tobacco over the last 50 years.
The American Heart Association has released its recommendations regarding the sale and usage of e-cigarettes, cautioning that the devices should be regulated to avoid enticing children to smoke while also saying that e-cigarettes could be used as a way to help some current smokers quit.
The guidelines, published online Aug. 24 in Circulation, state that clinicians "should not discourage" their patients from resorting to e-cigarettes if other approved forms of smoking cessation, such as the nicotine patch, have been exhausted. The AHA warned, however, that further studies are needed to fully understand the effects of e-cigarette usage, stressing that e-cigarettes have not been approved by the Food and Drug Administration as an acceptable smoking cessation device and could contain low amounts of toxic chemicals that would prove more harmful than helpful to patients in the long run.
"E-cigarettes have caused a major shift in the tobacco-control landscape," Aruni Bhatnagar, Ph.D., lead author of the guidelines and chair of cardiovascular medicine at the University of Louisville, Ky., said in a statement. "It’s critical that we rigorously examine the long-term impact of this new technology on public health, cardiovascular disease, and stroke, and pay careful attention to the effect of e-cigarettes on adolescents."
For now, the AHA says that clinicians should tell their patients who use e-cigarettes to set a firm quit date, warning that any device that delivers nicotine into the body is harmful and likely lethal.
"Nicotine is a dangerous and highly addictive chemical no matter what form it takes – conventional cigarettes or some other tobacco product," Dr. Elliott Antman, AHA president, said in the statement. "Every life that has been lost to tobacco addiction" could have been saved, he noted.
To that end, the AHA also called for strong regulations regarding the potential marketability of e-cigarettes to youngsters. The group recommended a federal ban on the sale of e-cigarettes to minors, warning that the devices could become a gateway to actual cigarettes for young people who see e-cigarettes as "high-tech, accessible, and convenient," according to a JAMA Pediatrics study of 40,000 middle and high school students. The AHA also recommended that all existing rules and regulations in place for tobacco-related products should apply to e-cigarettes.
"We must protect future generations from any potential smokescreens in the tobacco product landscape that will cause us to lose precious ground in the fight to make our nation 100% tobacco-free," Dr. Antman said.
According to the AHA, 20 million Americans have lost their lives to tobacco over the last 50 years.
The American Heart Association has released its recommendations regarding the sale and usage of e-cigarettes, cautioning that the devices should be regulated to avoid enticing children to smoke while also saying that e-cigarettes could be used as a way to help some current smokers quit.
The guidelines, published online Aug. 24 in Circulation, state that clinicians "should not discourage" their patients from resorting to e-cigarettes if other approved forms of smoking cessation, such as the nicotine patch, have been exhausted. The AHA warned, however, that further studies are needed to fully understand the effects of e-cigarette usage, stressing that e-cigarettes have not been approved by the Food and Drug Administration as an acceptable smoking cessation device and could contain low amounts of toxic chemicals that would prove more harmful than helpful to patients in the long run.
"E-cigarettes have caused a major shift in the tobacco-control landscape," Aruni Bhatnagar, Ph.D., lead author of the guidelines and chair of cardiovascular medicine at the University of Louisville, Ky., said in a statement. "It’s critical that we rigorously examine the long-term impact of this new technology on public health, cardiovascular disease, and stroke, and pay careful attention to the effect of e-cigarettes on adolescents."
For now, the AHA says that clinicians should tell their patients who use e-cigarettes to set a firm quit date, warning that any device that delivers nicotine into the body is harmful and likely lethal.
"Nicotine is a dangerous and highly addictive chemical no matter what form it takes – conventional cigarettes or some other tobacco product," Dr. Elliott Antman, AHA president, said in the statement. "Every life that has been lost to tobacco addiction" could have been saved, he noted.
To that end, the AHA also called for strong regulations regarding the potential marketability of e-cigarettes to youngsters. The group recommended a federal ban on the sale of e-cigarettes to minors, warning that the devices could become a gateway to actual cigarettes for young people who see e-cigarettes as "high-tech, accessible, and convenient," according to a JAMA Pediatrics study of 40,000 middle and high school students. The AHA also recommended that all existing rules and regulations in place for tobacco-related products should apply to e-cigarettes.
"We must protect future generations from any potential smokescreens in the tobacco product landscape that will cause us to lose precious ground in the fight to make our nation 100% tobacco-free," Dr. Antman said.
According to the AHA, 20 million Americans have lost their lives to tobacco over the last 50 years.
FROM CIRCULATION
Autoantibody profile may affect the number and size of RA bone erosions
Rheumatoid arthritis patients who tested positive for both rheumatoid factor and anticitrullinated protein antibodies showed a greater prevalence and size of bone erosions than did patients who came up negative for both in a prospective cohort study.
High-resolution peripheral quantitative CT revealed a prevalence of around 5.35 bone erosions per patient among 112 who were positive for both rheumatoid factor (RF) and anticitrullinated protein antibodies (ACPAs), compared with 2.49 in 69 who were negative for both of the autoantibodies. Another 29 patients who were ACPA positive and RH negative had 2.41 erosions, while 28 patients who were ACPA negative and RH positive had 2.00 erosions. The size of the bone erosion had a similar pattern, with the greatest volume observed in patients positive for both autoantibodies (7.66 mm3), followed by ACPA-positive patients (6.20 mm3), patients negative for both autoantibodies (3.32 mm3), and RH-positive patients (2.76 mm3).
The size of erosions was also associated with the presence and titer of rheumatoid factor in ACPA-positive but not ACPA-negative patients (Ann. Rheum. Dis. 2014 Aug. 12 [doi:10.1136/annrheumdis-2014-205428]).
"These observations suggest that RF may act as an enhancer of bone loss in patients with RA, and acts as an additive to ACPAs," wrote Dr. Carolin Hecht of the University of Erlangen-Nuremberg (Germany) and colleagues.
The study was supported by the Deutsche Forschungsgemeinschaft, the Bundesministerium fu¨r Bildung und Forschung, the Marie Curie project OSTEOIMMUNE, the TEAM and MASTERSWITCH projects of the European Union, and the IMI-funded project BTCure. There were no other conflicts of interest declared.
Rheumatoid arthritis patients who tested positive for both rheumatoid factor and anticitrullinated protein antibodies showed a greater prevalence and size of bone erosions than did patients who came up negative for both in a prospective cohort study.
High-resolution peripheral quantitative CT revealed a prevalence of around 5.35 bone erosions per patient among 112 who were positive for both rheumatoid factor (RF) and anticitrullinated protein antibodies (ACPAs), compared with 2.49 in 69 who were negative for both of the autoantibodies. Another 29 patients who were ACPA positive and RH negative had 2.41 erosions, while 28 patients who were ACPA negative and RH positive had 2.00 erosions. The size of the bone erosion had a similar pattern, with the greatest volume observed in patients positive for both autoantibodies (7.66 mm3), followed by ACPA-positive patients (6.20 mm3), patients negative for both autoantibodies (3.32 mm3), and RH-positive patients (2.76 mm3).
The size of erosions was also associated with the presence and titer of rheumatoid factor in ACPA-positive but not ACPA-negative patients (Ann. Rheum. Dis. 2014 Aug. 12 [doi:10.1136/annrheumdis-2014-205428]).
"These observations suggest that RF may act as an enhancer of bone loss in patients with RA, and acts as an additive to ACPAs," wrote Dr. Carolin Hecht of the University of Erlangen-Nuremberg (Germany) and colleagues.
The study was supported by the Deutsche Forschungsgemeinschaft, the Bundesministerium fu¨r Bildung und Forschung, the Marie Curie project OSTEOIMMUNE, the TEAM and MASTERSWITCH projects of the European Union, and the IMI-funded project BTCure. There were no other conflicts of interest declared.
Rheumatoid arthritis patients who tested positive for both rheumatoid factor and anticitrullinated protein antibodies showed a greater prevalence and size of bone erosions than did patients who came up negative for both in a prospective cohort study.
High-resolution peripheral quantitative CT revealed a prevalence of around 5.35 bone erosions per patient among 112 who were positive for both rheumatoid factor (RF) and anticitrullinated protein antibodies (ACPAs), compared with 2.49 in 69 who were negative for both of the autoantibodies. Another 29 patients who were ACPA positive and RH negative had 2.41 erosions, while 28 patients who were ACPA negative and RH positive had 2.00 erosions. The size of the bone erosion had a similar pattern, with the greatest volume observed in patients positive for both autoantibodies (7.66 mm3), followed by ACPA-positive patients (6.20 mm3), patients negative for both autoantibodies (3.32 mm3), and RH-positive patients (2.76 mm3).
The size of erosions was also associated with the presence and titer of rheumatoid factor in ACPA-positive but not ACPA-negative patients (Ann. Rheum. Dis. 2014 Aug. 12 [doi:10.1136/annrheumdis-2014-205428]).
"These observations suggest that RF may act as an enhancer of bone loss in patients with RA, and acts as an additive to ACPAs," wrote Dr. Carolin Hecht of the University of Erlangen-Nuremberg (Germany) and colleagues.
The study was supported by the Deutsche Forschungsgemeinschaft, the Bundesministerium fu¨r Bildung und Forschung, the Marie Curie project OSTEOIMMUNE, the TEAM and MASTERSWITCH projects of the European Union, and the IMI-funded project BTCure. There were no other conflicts of interest declared.
FROM ANNALS OF THE RHEUMATIC DISEASES
Key clinical point: RF may enhance the loss of bone in patients who are positive for ACPAs.
Major finding: There was a prevalence of around 5.35 bone erosions per patient among 112 who were positive for both rheumatoid factor and anticitrullinated protein antibodies, compared with 2.49 in 69 who were negative for both of the autoantibodies.
Data source: A prospective cohort study in 238 patients with rheumatoid arthritis.
Disclosures: The study was supported by the Deutsche Forschungsgemeinschaft, the Bundesministerium fu¨r Bildung und Forschung, the Marie Curie project OSTEOIMMUNE, the TEAM and MASTERSWITCH projects of the European Union, and the IMI-funded project BTCure.
2012 update of the 2008 American College of Rheumatology recommendations for the use of disease-modifying antirheumatic drugs and biologic agents in the treatment of rheumatoid arthritis
The levels of evidence supporting the recommendations (A-C) are defined at the end of the "Major Recommendations" field.
Recommendations for the Use of Disease-Modifying Antirheumatic Drugs (DMARDs) and Biologic Agents in Patients Who Qualify for Treatment of Rheumatoid Arthritis (RA)
This 2012 American College of Rheumatology (ACR) recommendations update incorporates the evidence from systematic literature review synthesis and recommendations from 2008 and rates updated and new clinical scenarios regarding the use of DMARDs and biologic agents for the treatment of RA. Terms used in the recommendations are defined in Table 2 of the original guideline document. The 2012 recommendations are listed in the 4 sections below and in the following order:
- Indications for and switching DMARDs and biologic agents: early RA (indications, see Figure 1 in the original guideline document) followed by established RA (indications and switching, see Figure 2 in the original guideline document), along with details of the level of evidence supporting these recommendations (see Supplementary Appendix 7, available in the online version at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658
- Use of biologic agents in patients with hepatitis, malignancy, or congestive heart failure (CHF) who qualify for RA management (see Table 4 in the original guideline document)
- Screening for tuberculosis (TB) in patients starting or currently receiving biologic agents as part of their RA therapy (see Figure 3 in the original guideline document)
- Vaccination in patients starting or currently receiving DMARDs or biologic agents as part of their RA therapy (see Table 5 in the original guideline document)
The recommendations in the text below and in Tables 4 and 5 in the original guideline document represent the results of the 2012 update only, whereas Figures 1–3 in the original guideline document also incorporate some of the 2008 ACR RA recommendations that did not change. Areas of uncertainty by the panel (that did not lead to recommendations) are noted in Supplementary Appendix 8 (available in the online version of this article at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658 ![]()
- Indications for Starting, Resuming, Adding, or Switching DMARDs or Biologic Agents
The panel first describes a recommendation targeting remission or low disease activity in RA (section 1A). This is followed by recommendations for DMARD or biologic agent use in early RA (section 1B). Next, the panel provides recommendations for initiating and switching between DMARDs and biologic agents in established RA (section 1C).
1A. Target Low Disease Activity or Remission
The panel recommends targeting either low disease activity (see Table 3 in the original guideline document) or remission (see Table 2 in the original guideline document) in all patients with early RA (see Figure 1 in the original guideline document; level of evidence C) and established RA (see Figure 2 in the original guideline document; level of evidence C) receiving any DMARD or biologic agent.
1B. Early RA (Disease Duration <6 Months)
In patients with early RA, the panel recommends the use of DMARD monotherapy both for low disease activity and for moderate or high disease activity with the absence of poor prognostic features (see Figure 1 in the original guideline document; level of evidence A–C) (details are shown in Supplementary Appendix 7, available in the online version of this article at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658
In patients with early RA, the panel recommends the use of DMARD combination therapy (including double and triple therapy) in patients with moderate or high disease activity plus poor prognostic features (see Figure 1 in the original guideline document; level of evidence A–C).
In patients with early RA, the panel also recommends the use of an anti-tumor necrosis factor (anti-TNF) biologic with or without methotrexate in patients who have high disease activity with poor prognostic features (see Figure 1 in the original guideline document; level of evidence A and B). Infliximab is the only exception and the recommendation is to use it in combination with methotrexate, but not as monotherapy.
1C. Established RA (Disease Duration ≥6 Months or Meeting the 1987 ACR RA Classification Criteria)
The remainder of panel recommendations regarding indications for DMARDs and biologic agents are for patients with established RA. The 3 subsections below define recommendations for initiating and switching therapies in established RA (see Figure 2 in the original guideline document). Where the prognosis is not mentioned, the recommendation to use/switch to a DMARD or a biologic agent applies to all patients, regardless of prognostic features.
Initiating and Switching Among DMARDs
If after 3 months of DMARD monotherapy (in patients without poor prognostic features), a patient deteriorates from low to moderate/high disease activity, then methotrexate, hydroxychloroquine, or leflunomide should be added (see rectangle A of Figure 2 in the original guideline document; level of evidence A and B).
If after 3 months of methotrexate or methotrexate/DMARD combination, a patient still has moderate or high disease activity, then add another non-methotrexate DMARD or switch to a different non-methotrexate DMARD (see rectangle B of Figure 2 in the original guideline document; level of evidence B and C).
Switching from DMARDs to Biologic Agents
If a patient has moderate or high disease activity after 3 months of methotrexate monotherapy or DMARD combination therapy, as an alternative to the DMARD recommendation just noted above, the panel recommends adding or switching to an anti-TNF biologic, abatacept, or rituximab (see rectangles C and D of Figure 2 in the original guideline document; level of evidence A–C).
If after 3 months of intensified DMARD combination therapy or after a second DMARD, a patient still has moderate or high disease activity, add or switch to an anti-TNF biologic (see rectangle C of Figure 2 in the original guideline document; level of evidence C).
Switching Among Biologic Agents Due to Lack of Benefit or Loss of Benefit
If a patient still has moderate or high disease activity after 3 months of anti-TNF biologic therapy and this is due to a lack or loss of benefit, switching to another anti-TNF biologic or a non-TNF biologic is recommended (see rectangles F and G of Figure 2 in the original guideline document; level of evidence B and C).
If a patient still has moderate or high disease activity after 6 months of a non-TNF biologic and the failure is due to a lack or loss of benefit, switch to another non-TNF biologic or an anti-TNF biologic (see rectangles F and G of Figure 2 in the original guideline document; level of evidence B and C). An assessment period of 6 months was chosen rather than 3 months, due to the anticipation that a longer time may be required for efficacy of a non-TNF biologic.
Switching Among Biologic Agents Due to Harms/Adverse Events
If a patient has high disease activity after failing an anti-TNF biologic because of a serious adverse event, switch to a non-TNF biologic (see rectangle E of Figure 2 in the original guideline document; level of evidence C).
If a patient has moderate or high disease activity after failing an anti-TNF biologic because of a nonserious adverse event, switch to another anti-TNF biologic or a non-TNF biologic (see rectangle F of Figure 2 in the original guideline document; level of evidence B and C).
If a patient has moderate or high disease activity after failing a non-TNF biologic because of an adverse event (serious or nonserious), switch to another non-TNF biologic or an anti-TNF biologic (see rectangle F of Figure 2 in the original guideline document; level of evidence C).
- Use of Biologic Agents in RA Patients With Hepatitis, Malignancy, or Chronic Heart Failure (CHF), Qualifying for More Aggressive Treatment (level of evidence C for all recommendations)
Hepatitis B or C
The panel recommends that etanercept could potentially be used in RA patients with hepatitis C requiring RA treatment (see Table 4 in the original guideline document).
The panel also recommends not using biologic agents in RA patients with untreated chronic hepatitis B (disease not treated due to contraindications to treatment or intolerable adverse events) and in RA patients with treated chronic hepatitis B with Child-Pugh class B and higher (see Table 4 in the original guideline document; for details of Child-Pugh classification, see Table 2 in the original guideline document). The panel did not make recommendations regarding the use of any biologic agent for treatment in RA patients with a history of hepatitis B and a positive hepatitis B core antibody.
Malignancies
For patients who have been treated for solid malignancies more than 5 years ago or who have been treated for nonmelanoma skin cancer more than 5 years ago, the panel recommends starting or resuming any biologic agent if those patients would otherwise qualify for this RA management strategy (see Table 4 in the original guideline document).
The panel only recommends starting or resuming rituximab in RA patients with: 1) a previously treated solid malignancy within the last 5 years, 2) a previously treated nonmelanoma skin cancer within the last 5 years, 3) a previously treated melanoma skin cancer, or 4) a previously treated lymphoproliferative malignancy. Little is known about the effects of biologic therapy in patients with a history of a solid cancer within the past 5 years owing to the exclusion of such patients from participation in clinical trials and the lack of studies examining the risk of recurrent cancer in this subgroup of patients.
CHF
The panel recommends not using an anti-TNF biologic in RA patients with CHF that is New York Heart Association (NYHA) class III or IV and who have an ejection fraction of 50% or less (see Table 4 in the original guideline document).
- TB Screening for Biologic Agents (level of evidence C for all recommendations except for initiation of biologic agents in patients being treated for latent TB infection [LTBI], where the level of evidence is B)
The panel recommends screening to identify LTBI in all RA patients being considered for therapy with biologic agents, regardless of the presence of risk factors for LTBI (see diamond A of Figure 3 in the original guideline document). It recommends that clinicians assess the patient's medical history to identify risk factors for TB (specified by the Centers for Disease Control and Prevention [CDC]) (see Table 2 in the original guideline document).
The panel recommends the tuberculin skin test (TST) or interferon-gamma–release assays (IGRAs) as the initial test in all RA patients starting biologic agents, regardless of risk factors for LTBI (see diamond A of Figure 3 in the original guideline document). It recommends the use of the IGRA over the TST in patients who had previously received a bacillus Calmette-Guerin (BCG) vaccination, due to the high false-positive test rates for TST (see Figure 3 in the original guideline document).
The panel recommends that RA patients with a positive initial or repeat TST or IGRA should have a chest radiograph and, if suggestive of active TB, a subsequent sputum examination to check for the presence of active TB (see diamonds B and C of Figure 3 in the original guideline document). RA patients with a negative screening TST or IGRA may not need further evaluation in the absence of risk factors and/or clinical suspicion for TB. Since patients with RA may have false-negative TST or IGRA results due to immunosuppression, a negative TST or IGRA should not be interpreted as excluding the possibility that a patient has LTBI. Accordingly, in immunosuppressed RA patients with risk factors for LTBI and negative initial screening tests, the panel recommends that a repeat TST or IGRA could be considered 1–3 weeks after the initial negative screening (see diamond A of Figure 3 in the original guideline document).
If the RA patient has active or latent TB based on the test results, the panel recommends appropriate antitubercular treatment and consideration of referral to a specialist. Treatment with biologic agents can be initiated or resumed after 1 month of latent TB treatment with antitubercular medications and after completion of the treatment of active TB, as applicable (see Figure 3 in the original guideline document).
The panel recommends annual testing in RA patients who live, travel, or work in situations where TB exposure is likely while they continue treatment with biologic agents (see diamond D of Figure 3 in the original guideline document). Patients who test positive for TST or IGRA at baseline can remain positive for these tests even after successful treatment of TB. These patients need monitoring for clinical signs and symptoms of recurrent TB, since repeating tests will not help in the diagnosis of recurrent TB.
- Vaccination in Patients Starting or Currently Receiving DMARDs or Biologic Agents as Part of Their RA Therapy (level of evidence C for all recommendations)
The panel recommends that all killed (pneumococcal, influenza intramuscular, and hepatitis B), recombinant (human papillomavirus [HPV] vaccine for cervical cancer), and live attenuated (herpes zoster) vaccinations should be undertaken before starting a DMARD or a biologic agent (see Table 5 in the original guideline document).
It also recommends that, if not previously done, vaccination with indicated pneumococcal (killed), influenza intramuscular (killed), hepatitis B (killed), and HPV vaccine (recombinant) should be undertaken in RA patients already taking a DMARD or a biologic agent (see Table 5 in the original guideline document).
The panel recommends vaccination with herpes zoster vaccine in RA patients already taking a DMARD. All vaccines should be given based on age and risk, and physicians should refer to vaccine instructions and CDC recommendations for details about dosing and timing issues related to vaccinations.
Definitions:
Level of Evidence
- Level of Evidence A: Data derived from multiple randomized clinical trials.
- Level of Evidence B: Data derived from a single randomized trial, or nonrandomized studies.
- Level of Evidence C: Only consensus opinion of experts, case studies, or standard-of-care.
Note: Level C evidence often denoted a circumstance where medical literature addressed the general topic under discussion but it did not address the specific clinical situations or scenarios reviewed by the panel.
- 2012 American College of Rheumatology (ACR) recommendations update for the treatment of early rheumatoid arthritis (RA), defined as a disease duration <6 months
- 2012 ACR recommendations update for the treatment of established RA, defined as a disease duration ≥6 months or meeting the 1987 ACR classification criteria
- 2012 ACR recommendations update for tuberculosis (TB) screening with biologic agent use
The levels of evidence supporting the recommendations (A-C) are defined at the end of the "Major Recommendations" field.
Recommendations for the Use of Disease-Modifying Antirheumatic Drugs (DMARDs) and Biologic Agents in Patients Who Qualify for Treatment of Rheumatoid Arthritis (RA)
This 2012 American College of Rheumatology (ACR) recommendations update incorporates the evidence from systematic literature review synthesis and recommendations from 2008 and rates updated and new clinical scenarios regarding the use of DMARDs and biologic agents for the treatment of RA. Terms used in the recommendations are defined in Table 2 of the original guideline document. The 2012 recommendations are listed in the 4 sections below and in the following order:
- Indications for and switching DMARDs and biologic agents: early RA (indications, see Figure 1 in the original guideline document) followed by established RA (indications and switching, see Figure 2 in the original guideline document), along with details of the level of evidence supporting these recommendations (see Supplementary Appendix 7, available in the online version at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658
- Use of biologic agents in patients with hepatitis, malignancy, or congestive heart failure (CHF) who qualify for RA management (see Table 4 in the original guideline document)
- Screening for tuberculosis (TB) in patients starting or currently receiving biologic agents as part of their RA therapy (see Figure 3 in the original guideline document)
- Vaccination in patients starting or currently receiving DMARDs or biologic agents as part of their RA therapy (see Table 5 in the original guideline document)
The recommendations in the text below and in Tables 4 and 5 in the original guideline document represent the results of the 2012 update only, whereas Figures 1–3 in the original guideline document also incorporate some of the 2008 ACR RA recommendations that did not change. Areas of uncertainty by the panel (that did not lead to recommendations) are noted in Supplementary Appendix 8 (available in the online version of this article at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658 ![]()
- Indications for Starting, Resuming, Adding, or Switching DMARDs or Biologic Agents
The panel first describes a recommendation targeting remission or low disease activity in RA (section 1A). This is followed by recommendations for DMARD or biologic agent use in early RA (section 1B). Next, the panel provides recommendations for initiating and switching between DMARDs and biologic agents in established RA (section 1C).
1A. Target Low Disease Activity or Remission
The panel recommends targeting either low disease activity (see Table 3 in the original guideline document) or remission (see Table 2 in the original guideline document) in all patients with early RA (see Figure 1 in the original guideline document; level of evidence C) and established RA (see Figure 2 in the original guideline document; level of evidence C) receiving any DMARD or biologic agent.
1B. Early RA (Disease Duration <6 Months)
In patients with early RA, the panel recommends the use of DMARD monotherapy both for low disease activity and for moderate or high disease activity with the absence of poor prognostic features (see Figure 1 in the original guideline document; level of evidence A–C) (details are shown in Supplementary Appendix 7, available in the online version of this article at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658
In patients with early RA, the panel recommends the use of DMARD combination therapy (including double and triple therapy) in patients with moderate or high disease activity plus poor prognostic features (see Figure 1 in the original guideline document; level of evidence A–C).
In patients with early RA, the panel also recommends the use of an anti-tumor necrosis factor (anti-TNF) biologic with or without methotrexate in patients who have high disease activity with poor prognostic features (see Figure 1 in the original guideline document; level of evidence A and B). Infliximab is the only exception and the recommendation is to use it in combination with methotrexate, but not as monotherapy.
1C. Established RA (Disease Duration ≥6 Months or Meeting the 1987 ACR RA Classification Criteria)
The remainder of panel recommendations regarding indications for DMARDs and biologic agents are for patients with established RA. The 3 subsections below define recommendations for initiating and switching therapies in established RA (see Figure 2 in the original guideline document). Where the prognosis is not mentioned, the recommendation to use/switch to a DMARD or a biologic agent applies to all patients, regardless of prognostic features.
Initiating and Switching Among DMARDs
If after 3 months of DMARD monotherapy (in patients without poor prognostic features), a patient deteriorates from low to moderate/high disease activity, then methotrexate, hydroxychloroquine, or leflunomide should be added (see rectangle A of Figure 2 in the original guideline document; level of evidence A and B).
If after 3 months of methotrexate or methotrexate/DMARD combination, a patient still has moderate or high disease activity, then add another non-methotrexate DMARD or switch to a different non-methotrexate DMARD (see rectangle B of Figure 2 in the original guideline document; level of evidence B and C).
Switching from DMARDs to Biologic Agents
If a patient has moderate or high disease activity after 3 months of methotrexate monotherapy or DMARD combination therapy, as an alternative to the DMARD recommendation just noted above, the panel recommends adding or switching to an anti-TNF biologic, abatacept, or rituximab (see rectangles C and D of Figure 2 in the original guideline document; level of evidence A–C).
If after 3 months of intensified DMARD combination therapy or after a second DMARD, a patient still has moderate or high disease activity, add or switch to an anti-TNF biologic (see rectangle C of Figure 2 in the original guideline document; level of evidence C).
Switching Among Biologic Agents Due to Lack of Benefit or Loss of Benefit
If a patient still has moderate or high disease activity after 3 months of anti-TNF biologic therapy and this is due to a lack or loss of benefit, switching to another anti-TNF biologic or a non-TNF biologic is recommended (see rectangles F and G of Figure 2 in the original guideline document; level of evidence B and C).
If a patient still has moderate or high disease activity after 6 months of a non-TNF biologic and the failure is due to a lack or loss of benefit, switch to another non-TNF biologic or an anti-TNF biologic (see rectangles F and G of Figure 2 in the original guideline document; level of evidence B and C). An assessment period of 6 months was chosen rather than 3 months, due to the anticipation that a longer time may be required for efficacy of a non-TNF biologic.
Switching Among Biologic Agents Due to Harms/Adverse Events
If a patient has high disease activity after failing an anti-TNF biologic because of a serious adverse event, switch to a non-TNF biologic (see rectangle E of Figure 2 in the original guideline document; level of evidence C).
If a patient has moderate or high disease activity after failing an anti-TNF biologic because of a nonserious adverse event, switch to another anti-TNF biologic or a non-TNF biologic (see rectangle F of Figure 2 in the original guideline document; level of evidence B and C).
If a patient has moderate or high disease activity after failing a non-TNF biologic because of an adverse event (serious or nonserious), switch to another non-TNF biologic or an anti-TNF biologic (see rectangle F of Figure 2 in the original guideline document; level of evidence C).
- Use of Biologic Agents in RA Patients With Hepatitis, Malignancy, or Chronic Heart Failure (CHF), Qualifying for More Aggressive Treatment (level of evidence C for all recommendations)
Hepatitis B or C
The panel recommends that etanercept could potentially be used in RA patients with hepatitis C requiring RA treatment (see Table 4 in the original guideline document).
The panel also recommends not using biologic agents in RA patients with untreated chronic hepatitis B (disease not treated due to contraindications to treatment or intolerable adverse events) and in RA patients with treated chronic hepatitis B with Child-Pugh class B and higher (see Table 4 in the original guideline document; for details of Child-Pugh classification, see Table 2 in the original guideline document). The panel did not make recommendations regarding the use of any biologic agent for treatment in RA patients with a history of hepatitis B and a positive hepatitis B core antibody.
Malignancies
For patients who have been treated for solid malignancies more than 5 years ago or who have been treated for nonmelanoma skin cancer more than 5 years ago, the panel recommends starting or resuming any biologic agent if those patients would otherwise qualify for this RA management strategy (see Table 4 in the original guideline document).
The panel only recommends starting or resuming rituximab in RA patients with: 1) a previously treated solid malignancy within the last 5 years, 2) a previously treated nonmelanoma skin cancer within the last 5 years, 3) a previously treated melanoma skin cancer, or 4) a previously treated lymphoproliferative malignancy. Little is known about the effects of biologic therapy in patients with a history of a solid cancer within the past 5 years owing to the exclusion of such patients from participation in clinical trials and the lack of studies examining the risk of recurrent cancer in this subgroup of patients.
CHF
The panel recommends not using an anti-TNF biologic in RA patients with CHF that is New York Heart Association (NYHA) class III or IV and who have an ejection fraction of 50% or less (see Table 4 in the original guideline document).
- TB Screening for Biologic Agents (level of evidence C for all recommendations except for initiation of biologic agents in patients being treated for latent TB infection [LTBI], where the level of evidence is B)
The panel recommends screening to identify LTBI in all RA patients being considered for therapy with biologic agents, regardless of the presence of risk factors for LTBI (see diamond A of Figure 3 in the original guideline document). It recommends that clinicians assess the patient's medical history to identify risk factors for TB (specified by the Centers for Disease Control and Prevention [CDC]) (see Table 2 in the original guideline document).
The panel recommends the tuberculin skin test (TST) or interferon-gamma–release assays (IGRAs) as the initial test in all RA patients starting biologic agents, regardless of risk factors for LTBI (see diamond A of Figure 3 in the original guideline document). It recommends the use of the IGRA over the TST in patients who had previously received a bacillus Calmette-Guerin (BCG) vaccination, due to the high false-positive test rates for TST (see Figure 3 in the original guideline document).
The panel recommends that RA patients with a positive initial or repeat TST or IGRA should have a chest radiograph and, if suggestive of active TB, a subsequent sputum examination to check for the presence of active TB (see diamonds B and C of Figure 3 in the original guideline document). RA patients with a negative screening TST or IGRA may not need further evaluation in the absence of risk factors and/or clinical suspicion for TB. Since patients with RA may have false-negative TST or IGRA results due to immunosuppression, a negative TST or IGRA should not be interpreted as excluding the possibility that a patient has LTBI. Accordingly, in immunosuppressed RA patients with risk factors for LTBI and negative initial screening tests, the panel recommends that a repeat TST or IGRA could be considered 1–3 weeks after the initial negative screening (see diamond A of Figure 3 in the original guideline document).
If the RA patient has active or latent TB based on the test results, the panel recommends appropriate antitubercular treatment and consideration of referral to a specialist. Treatment with biologic agents can be initiated or resumed after 1 month of latent TB treatment with antitubercular medications and after completion of the treatment of active TB, as applicable (see Figure 3 in the original guideline document).
The panel recommends annual testing in RA patients who live, travel, or work in situations where TB exposure is likely while they continue treatment with biologic agents (see diamond D of Figure 3 in the original guideline document). Patients who test positive for TST or IGRA at baseline can remain positive for these tests even after successful treatment of TB. These patients need monitoring for clinical signs and symptoms of recurrent TB, since repeating tests will not help in the diagnosis of recurrent TB.
- Vaccination in Patients Starting or Currently Receiving DMARDs or Biologic Agents as Part of Their RA Therapy (level of evidence C for all recommendations)
The panel recommends that all killed (pneumococcal, influenza intramuscular, and hepatitis B), recombinant (human papillomavirus [HPV] vaccine for cervical cancer), and live attenuated (herpes zoster) vaccinations should be undertaken before starting a DMARD or a biologic agent (see Table 5 in the original guideline document).
It also recommends that, if not previously done, vaccination with indicated pneumococcal (killed), influenza intramuscular (killed), hepatitis B (killed), and HPV vaccine (recombinant) should be undertaken in RA patients already taking a DMARD or a biologic agent (see Table 5 in the original guideline document).
The panel recommends vaccination with herpes zoster vaccine in RA patients already taking a DMARD. All vaccines should be given based on age and risk, and physicians should refer to vaccine instructions and CDC recommendations for details about dosing and timing issues related to vaccinations.
Definitions:
Level of Evidence
- Level of Evidence A: Data derived from multiple randomized clinical trials.
- Level of Evidence B: Data derived from a single randomized trial, or nonrandomized studies.
- Level of Evidence C: Only consensus opinion of experts, case studies, or standard-of-care.
Note: Level C evidence often denoted a circumstance where medical literature addressed the general topic under discussion but it did not address the specific clinical situations or scenarios reviewed by the panel.
- 2012 American College of Rheumatology (ACR) recommendations update for the treatment of early rheumatoid arthritis (RA), defined as a disease duration <6 months
- 2012 ACR recommendations update for the treatment of established RA, defined as a disease duration ≥6 months or meeting the 1987 ACR classification criteria
- 2012 ACR recommendations update for tuberculosis (TB) screening with biologic agent use
The levels of evidence supporting the recommendations (A-C) are defined at the end of the "Major Recommendations" field.
Recommendations for the Use of Disease-Modifying Antirheumatic Drugs (DMARDs) and Biologic Agents in Patients Who Qualify for Treatment of Rheumatoid Arthritis (RA)
This 2012 American College of Rheumatology (ACR) recommendations update incorporates the evidence from systematic literature review synthesis and recommendations from 2008 and rates updated and new clinical scenarios regarding the use of DMARDs and biologic agents for the treatment of RA. Terms used in the recommendations are defined in Table 2 of the original guideline document. The 2012 recommendations are listed in the 4 sections below and in the following order:
- Indications for and switching DMARDs and biologic agents: early RA (indications, see Figure 1 in the original guideline document) followed by established RA (indications and switching, see Figure 2 in the original guideline document), along with details of the level of evidence supporting these recommendations (see Supplementary Appendix 7, available in the online version at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658
- Use of biologic agents in patients with hepatitis, malignancy, or congestive heart failure (CHF) who qualify for RA management (see Table 4 in the original guideline document)
- Screening for tuberculosis (TB) in patients starting or currently receiving biologic agents as part of their RA therapy (see Figure 3 in the original guideline document)
- Vaccination in patients starting or currently receiving DMARDs or biologic agents as part of their RA therapy (see Table 5 in the original guideline document)
The recommendations in the text below and in Tables 4 and 5 in the original guideline document represent the results of the 2012 update only, whereas Figures 1–3 in the original guideline document also incorporate some of the 2008 ACR RA recommendations that did not change. Areas of uncertainty by the panel (that did not lead to recommendations) are noted in Supplementary Appendix 8 (available in the online version of this article at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658 ![]()
- Indications for Starting, Resuming, Adding, or Switching DMARDs or Biologic Agents
The panel first describes a recommendation targeting remission or low disease activity in RA (section 1A). This is followed by recommendations for DMARD or biologic agent use in early RA (section 1B). Next, the panel provides recommendations for initiating and switching between DMARDs and biologic agents in established RA (section 1C).
1A. Target Low Disease Activity or Remission
The panel recommends targeting either low disease activity (see Table 3 in the original guideline document) or remission (see Table 2 in the original guideline document) in all patients with early RA (see Figure 1 in the original guideline document; level of evidence C) and established RA (see Figure 2 in the original guideline document; level of evidence C) receiving any DMARD or biologic agent.
1B. Early RA (Disease Duration <6 Months)
In patients with early RA, the panel recommends the use of DMARD monotherapy both for low disease activity and for moderate or high disease activity with the absence of poor prognostic features (see Figure 1 in the original guideline document; level of evidence A–C) (details are shown in Supplementary Appendix 7, available in the online version of this article at http://onlinelibrary.wiley.com/journal/10.1002/(ISSN)2151-4658
In patients with early RA, the panel recommends the use of DMARD combination therapy (including double and triple therapy) in patients with moderate or high disease activity plus poor prognostic features (see Figure 1 in the original guideline document; level of evidence A–C).
In patients with early RA, the panel also recommends the use of an anti-tumor necrosis factor (anti-TNF) biologic with or without methotrexate in patients who have high disease activity with poor prognostic features (see Figure 1 in the original guideline document; level of evidence A and B). Infliximab is the only exception and the recommendation is to use it in combination with methotrexate, but not as monotherapy.
1C. Established RA (Disease Duration ≥6 Months or Meeting the 1987 ACR RA Classification Criteria)
The remainder of panel recommendations regarding indications for DMARDs and biologic agents are for patients with established RA. The 3 subsections below define recommendations for initiating and switching therapies in established RA (see Figure 2 in the original guideline document). Where the prognosis is not mentioned, the recommendation to use/switch to a DMARD or a biologic agent applies to all patients, regardless of prognostic features.
Initiating and Switching Among DMARDs
If after 3 months of DMARD monotherapy (in patients without poor prognostic features), a patient deteriorates from low to moderate/high disease activity, then methotrexate, hydroxychloroquine, or leflunomide should be added (see rectangle A of Figure 2 in the original guideline document; level of evidence A and B).
If after 3 months of methotrexate or methotrexate/DMARD combination, a patient still has moderate or high disease activity, then add another non-methotrexate DMARD or switch to a different non-methotrexate DMARD (see rectangle B of Figure 2 in the original guideline document; level of evidence B and C).
Switching from DMARDs to Biologic Agents
If a patient has moderate or high disease activity after 3 months of methotrexate monotherapy or DMARD combination therapy, as an alternative to the DMARD recommendation just noted above, the panel recommends adding or switching to an anti-TNF biologic, abatacept, or rituximab (see rectangles C and D of Figure 2 in the original guideline document; level of evidence A–C).
If after 3 months of intensified DMARD combination therapy or after a second DMARD, a patient still has moderate or high disease activity, add or switch to an anti-TNF biologic (see rectangle C of Figure 2 in the original guideline document; level of evidence C).
Switching Among Biologic Agents Due to Lack of Benefit or Loss of Benefit
If a patient still has moderate or high disease activity after 3 months of anti-TNF biologic therapy and this is due to a lack or loss of benefit, switching to another anti-TNF biologic or a non-TNF biologic is recommended (see rectangles F and G of Figure 2 in the original guideline document; level of evidence B and C).
If a patient still has moderate or high disease activity after 6 months of a non-TNF biologic and the failure is due to a lack or loss of benefit, switch to another non-TNF biologic or an anti-TNF biologic (see rectangles F and G of Figure 2 in the original guideline document; level of evidence B and C). An assessment period of 6 months was chosen rather than 3 months, due to the anticipation that a longer time may be required for efficacy of a non-TNF biologic.
Switching Among Biologic Agents Due to Harms/Adverse Events
If a patient has high disease activity after failing an anti-TNF biologic because of a serious adverse event, switch to a non-TNF biologic (see rectangle E of Figure 2 in the original guideline document; level of evidence C).
If a patient has moderate or high disease activity after failing an anti-TNF biologic because of a nonserious adverse event, switch to another anti-TNF biologic or a non-TNF biologic (see rectangle F of Figure 2 in the original guideline document; level of evidence B and C).
If a patient has moderate or high disease activity after failing a non-TNF biologic because of an adverse event (serious or nonserious), switch to another non-TNF biologic or an anti-TNF biologic (see rectangle F of Figure 2 in the original guideline document; level of evidence C).
- Use of Biologic Agents in RA Patients With Hepatitis, Malignancy, or Chronic Heart Failure (CHF), Qualifying for More Aggressive Treatment (level of evidence C for all recommendations)
Hepatitis B or C
The panel recommends that etanercept could potentially be used in RA patients with hepatitis C requiring RA treatment (see Table 4 in the original guideline document).
The panel also recommends not using biologic agents in RA patients with untreated chronic hepatitis B (disease not treated due to contraindications to treatment or intolerable adverse events) and in RA patients with treated chronic hepatitis B with Child-Pugh class B and higher (see Table 4 in the original guideline document; for details of Child-Pugh classification, see Table 2 in the original guideline document). The panel did not make recommendations regarding the use of any biologic agent for treatment in RA patients with a history of hepatitis B and a positive hepatitis B core antibody.
Malignancies
For patients who have been treated for solid malignancies more than 5 years ago or who have been treated for nonmelanoma skin cancer more than 5 years ago, the panel recommends starting or resuming any biologic agent if those patients would otherwise qualify for this RA management strategy (see Table 4 in the original guideline document).
The panel only recommends starting or resuming rituximab in RA patients with: 1) a previously treated solid malignancy within the last 5 years, 2) a previously treated nonmelanoma skin cancer within the last 5 years, 3) a previously treated melanoma skin cancer, or 4) a previously treated lymphoproliferative malignancy. Little is known about the effects of biologic therapy in patients with a history of a solid cancer within the past 5 years owing to the exclusion of such patients from participation in clinical trials and the lack of studies examining the risk of recurrent cancer in this subgroup of patients.
CHF
The panel recommends not using an anti-TNF biologic in RA patients with CHF that is New York Heart Association (NYHA) class III or IV and who have an ejection fraction of 50% or less (see Table 4 in the original guideline document).
- TB Screening for Biologic Agents (level of evidence C for all recommendations except for initiation of biologic agents in patients being treated for latent TB infection [LTBI], where the level of evidence is B)
The panel recommends screening to identify LTBI in all RA patients being considered for therapy with biologic agents, regardless of the presence of risk factors for LTBI (see diamond A of Figure 3 in the original guideline document). It recommends that clinicians assess the patient's medical history to identify risk factors for TB (specified by the Centers for Disease Control and Prevention [CDC]) (see Table 2 in the original guideline document).
The panel recommends the tuberculin skin test (TST) or interferon-gamma–release assays (IGRAs) as the initial test in all RA patients starting biologic agents, regardless of risk factors for LTBI (see diamond A of Figure 3 in the original guideline document). It recommends the use of the IGRA over the TST in patients who had previously received a bacillus Calmette-Guerin (BCG) vaccination, due to the high false-positive test rates for TST (see Figure 3 in the original guideline document).
The panel recommends that RA patients with a positive initial or repeat TST or IGRA should have a chest radiograph and, if suggestive of active TB, a subsequent sputum examination to check for the presence of active TB (see diamonds B and C of Figure 3 in the original guideline document). RA patients with a negative screening TST or IGRA may not need further evaluation in the absence of risk factors and/or clinical suspicion for TB. Since patients with RA may have false-negative TST or IGRA results due to immunosuppression, a negative TST or IGRA should not be interpreted as excluding the possibility that a patient has LTBI. Accordingly, in immunosuppressed RA patients with risk factors for LTBI and negative initial screening tests, the panel recommends that a repeat TST or IGRA could be considered 1–3 weeks after the initial negative screening (see diamond A of Figure 3 in the original guideline document).
If the RA patient has active or latent TB based on the test results, the panel recommends appropriate antitubercular treatment and consideration of referral to a specialist. Treatment with biologic agents can be initiated or resumed after 1 month of latent TB treatment with antitubercular medications and after completion of the treatment of active TB, as applicable (see Figure 3 in the original guideline document).
The panel recommends annual testing in RA patients who live, travel, or work in situations where TB exposure is likely while they continue treatment with biologic agents (see diamond D of Figure 3 in the original guideline document). Patients who test positive for TST or IGRA at baseline can remain positive for these tests even after successful treatment of TB. These patients need monitoring for clinical signs and symptoms of recurrent TB, since repeating tests will not help in the diagnosis of recurrent TB.
- Vaccination in Patients Starting or Currently Receiving DMARDs or Biologic Agents as Part of Their RA Therapy (level of evidence C for all recommendations)
The panel recommends that all killed (pneumococcal, influenza intramuscular, and hepatitis B), recombinant (human papillomavirus [HPV] vaccine for cervical cancer), and live attenuated (herpes zoster) vaccinations should be undertaken before starting a DMARD or a biologic agent (see Table 5 in the original guideline document).
It also recommends that, if not previously done, vaccination with indicated pneumococcal (killed), influenza intramuscular (killed), hepatitis B (killed), and HPV vaccine (recombinant) should be undertaken in RA patients already taking a DMARD or a biologic agent (see Table 5 in the original guideline document).
The panel recommends vaccination with herpes zoster vaccine in RA patients already taking a DMARD. All vaccines should be given based on age and risk, and physicians should refer to vaccine instructions and CDC recommendations for details about dosing and timing issues related to vaccinations.
Definitions:
Level of Evidence
- Level of Evidence A: Data derived from multiple randomized clinical trials.
- Level of Evidence B: Data derived from a single randomized trial, or nonrandomized studies.
- Level of Evidence C: Only consensus opinion of experts, case studies, or standard-of-care.
Note: Level C evidence often denoted a circumstance where medical literature addressed the general topic under discussion but it did not address the specific clinical situations or scenarios reviewed by the panel.
- 2012 American College of Rheumatology (ACR) recommendations update for the treatment of early rheumatoid arthritis (RA), defined as a disease duration <6 months
- 2012 ACR recommendations update for the treatment of established RA, defined as a disease duration ≥6 months or meeting the 1987 ACR classification criteria
- 2012 ACR recommendations update for tuberculosis (TB) screening with biologic agent use
OBJECTIVE:
-To simplify the treatment algorithms for patients with rheumatoid arthritis (RA) and providers
-To provide clinicians with choices for treatments of patients with active RA, both in early and established disease phases
-To provide guidance regarding treatment choices in RA patients with comorbidities such as hepatitis, congestive heart failure (CHF), and malignancy
Guidelines are copyright © 2012 American College of Rheumatology. All rights reserved. The summary is provided by the Agency for Healthcare Research and Quality.
American College of Rheumatology guidelines for screening, treatment, and management of lupus nephritis
Renal Biopsy and Histology
The Task Force Panel recommended that all patients with clinical evidence of active lupus nephritis (LN), previously untreated, undergo renal biopsy (unless strongly contraindicated) so that glomerular disease can be classified by current International Society of Nephrology/Renal Pathology Society (ISN/RPS) classification (level C evidence) (see Table 1 in the original guideline document for ISN/RPS classification of LN). In addition, disease can be evaluated for activity and chronicity and for tubular and vascular changes. Finally, biopsies may identify additional or alternative causes of renal disease, such as tubular necrosis related to medications, hypovolemia, or hypotension. Biopsy is most highly recommended in patients with the characteristics indicated in the following table.
Table. Indications for Renal Biopsy in Patients with Systemic Lupus Erythematosus
| Level of Evidence | |
|---|---|
| Increasing serum creatinine without compelling alternative causes (such as sepsis, hypovolemia, or medication) | C |
| Confirmed proteinuria of ≥1.0 gm per 24 hours (either 24-hour urine specimens or spot protein/creatinine ratios are acceptable) | C |
Combinations of the following, assuming the findings are confirmed in at least two tests done within a short period of time and in the absence of alternative causes:
| C |
RBCs = red blood cells; hpf = high-power field.
The Task Force Panel recommended that treatment be based in large part on the classification of type of LN by these ISN/RPS criteria. As a result, the following recommendations are presented according to the histologic classification of nephritis. The Task Force Panel agreed that class I (minimal mesangial immune deposits on immunofluorescence with normal light microscopy) and class II (mesangial hypercellularity or matrix expansion on light microscopy with immune deposits confined to mesangium on immunofluorescence) generally do not require immunosuppressive treatment (level C evidence). In general, patients with class III (subendothelial immune deposits and proliferative changes in <50% of glomeruli) and class IV (subendothelial deposits and proliferative glomerular changes involving ≥50% of glomeruli) require aggressive therapy with glucocorticoids and immunosuppressive agents. Class V (subepithelial immune deposits and membranous thickening of glomerular capillaries) when combined with class III or IV should be treated in the same manner as class III or IV. Class V alone ("pure membranous LN") may be approached somewhat differently, as indicated below under "Recommendations for Induction of Improvement in Patients with Class V 'Pure Membranous' LN". Histologic class VI (sclerosis of ≥90% of glomeruli) generally requires preparation for renal replacement therapy rather than immunosuppression. The designations "A" and "C" indicate whether active or chronic changes are present; the higher the chronicity the less likely that the nephritis will respond to immunosuppression. However, A or C classifications were not included in the entry criteria for clinical trials in LN published to date, and therefore they are not considered in the recommendations.
Adjunctive Treatments
The Task Force Panel recommended that all systemic lupus erythematosus (SLE) patients with nephritis be treated with a background of hydroxychloroquine (HCQ; level C evidence), unless there is a contraindication.
All LN patients with proteinuria ≥0.5 gm per 24 hours (or equivalent by protein/creatinine ratios on spot urine samples) should have blockade of the renin–angiotensin system, which drives intraglomerular pressure (level A evidence for nondiabetic chronic renal disease). Treatment with either angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs) reduces proteinuria by approximately 30%, and significantly delays doubling of serum creatinine and progression to end-stage renal disease in patients with nondiabetic chronic renal disease. These classes of medications are contraindicated in pregnancy. The use of combination ACE inhibitors/ARB therapies is controversial. ACE inhibitors or ARB treatments are superior to calcium-channel blockers and diuretics alone in preserving renal function in chronic kidney disease.
The Task Force Panel recommended that careful attention be paid to control of hypertension, with a target of ≤130/80 mm Hg (level A evidence for nondiabetic chronic renal disease). The Task Force Panel also recommended that statin therapy be introduced in patients with low-density lipoprotein cholesterol >100 mg/dl (level C evidence). Note that a glomerular filtration rate <60 ml/minute/1.73 m2 (equivalent to a serum creatinine level >1.5 mg/dl or 133 µmoles/liter) is a risk factor for accelerated atherosclerosis. SLE itself is also an independent risk factor for accelerated atherosclerosis.
Finally, the Task Force Panel recommended that women of child-bearing potential with active or prior LN receive counseling regarding pregnancy risks conferred by the disease and its treatments (level C evidence).
Recommendations for Induction of Improvement in Patients with ISN Class III/IV Lupus Glomerulonephritis
The Task Force Panel recommended mycophenolate mofetil (MMF) (2–3 gm total daily orally) or intravenous (IV) cyclophosphamide (CYC) along with glucocorticoids (level A evidence) (see Figure 2 in the original guideline document). MMF and CYC are considered equivalent based on recent high-quality studies, a meta-analysis, and expert opinion. Long-term studies with MMF are not as abundant as those with CYC; data show good results for induction therapy with MMF of 3 gm total dose daily for 6 months, followed by maintenance with lower doses of MMF for 3 years. MMF has been similar in efficacy in all races studied to date (whites, Asians, African Americans, and Latin/Hispanic Americans). The Aspreva Lupus Management Study (ALMS) trial comparing response rates of LN to MMF plus glucocorticoids showed similar improvement in whites, Asians, and other races (primarily African Americans and Hispanics). However, The Task Force Panel voted that Asians compared to non-Asians might require lower doses of MMF for similar efficacy (level C evidence). Therefore, the physician might aim for 3 gm per day total daily highest dose in non-Asians and 2 gm per day in Asians. There is evidence that African Americans and Hispanics with LN respond less well to IV CYC than do patients of white or Asian races. MMF/mycophenolic acid (MPA) may be an initial choice more likely to induce improvement in patients who are African American or Hispanic.
The exact suggested dose of MMF varied based on the clinical scenario: for those with class III/IV without cellular crescents and for those with proteinuria and a stable creatinine for whom a renal biopsy sample cannot be obtained, both 2 gm and 3 gm total daily doses were acceptable to the Task Force Panel, while a dose of 3 gm daily was favored for those with class III/IV and crescents and for those with proteinuria and a recent significant rise in creatinine.
Some evidence suggests that MPA and enteric-coated mycophenolate sodium are less likely than MMF to cause nausea and diarrhea, but this is controversial, and the exact equivalency of the preparations is not firmly established. The Core Expert Panel recommended that MMF and MPA are likely to be equivalent in inducing improvement of LN, with 1,440–2,160 mg total daily dose of MPA roughly equivalent to 2,000–3,000 mg total daily dose of MMF. Some investigators have suggested that serum levels of MPA, the active metabolite of MMF, should be measured at the trough or peak (1 hour after a dose), and treatment of SLE should be guided by these levels. However, there are not enough data at this time to make recommendations for monitoring of drug levels.
There are two regimens of IV CYC recommended by the Task Force Panel: 1) low-dose "Euro-Lupus" CYC (500 mg IV once every 2 weeks for a total of 6 doses), followed by maintenance therapy with daily oral azathioprine (AZA) or daily oral MMF (level B evidence), and 2) high-dose CYC (500–1,000 mg/m2 IV once a month for 6 doses), followed by maintenance treatment with MMF or AZA (level A evidence) (see Figure 2 in the original guideline document). If CYC is being considered for treatment, the Core Expert Panel recommended IV CYC at the low "Euro-Lupus" dose for white patients with Western European or Southern European racial/ethnic backgrounds (level B evidence). In European study patients, the low- and high-dose regimens were equivalent in efficacy, and serious infections were less frequent with the lower doses. The low- and high-dose regimens have not been compared in nonwhite racial groups. Ten years of followup comparing low- and high-dose regimens showed similar rates of LN flares, end-stage renal disease, and doubling of the serum creatinine.
Pulse IV glucocorticoids (500–1,000 mg methylprednisolone daily for 3 doses) in combination with immunosuppressive therapy is recommended by the Task Force Panel, followed by daily oral glucocorticoids (0.5–1 mg/kg/day), followed by a taper to the minimal amount necessary to control disease (level C evidence). There are insufficient data to recommend a specific steroid taper because the nephritis and extrarenal manifestations vary from patient to patient. There was no consensus reached regarding the use of monthly IV methylprednisolone with monthly IV CYC.
Although AZA has been used to treat LN, the Task Force Panel did not recommend it as one of the first choices for induction therapy.
The panel recommends that most patients be followed for 6 months after initiation of induction treatment with either CYC or MMF before making major changes in treatment other than alteration of glucocorticoid doses, unless there is clear evidence of worsening at 3 months (50% or more worsening of proteinuria or serum creatinine; level A evidence).
Fertility issues are often a concern for young SLE patients with nephritis. In a discussion, the Task Force Panel recommended that MMF was preferable to CYC for patients who express a major concern with fertility preservation, since high-dose CYC can cause permanent infertility in both women and men (level A evidence of gonadal toxicity). Six months of high-dose IV CYC was associated with approximately 10% sustained infertility in young women, and higher rates in older women. If 6 months of CYC were followed by quarterly doses, there was a higher rate of infertility. The Task Force Panel did not reach a consensus on the use of leuprolide in patients with SLE receiving CYC as a means to preserve fertility. They also noted that MMF is teratogenic (class D in US Food and Drug Administration [FDA] ranking). Therefore, the physician should be sure that a patient is not pregnant before prescribing MMF or MPA, and the medications should be stopped for at least 6 weeks before pregnancy is attempted.
Recommendations for Induction of Improvement in Patients with Class IV or IV/V Plus Cellular Crescents
The Task Force Panel recommended either CYC or MMF for induction of improvement in this type of LN (level C evidence), along with IV pulses of high-dose glucocorticoid and initiation of oral glucocorticoids at the higher-range dosage, 1 mg/kg/day orally (see Figure 2 in the original guideline document). For the purpose of these recommendations statements, the presence of any crescents on a renal biopsy sample was considered crescentic LN. Until recently, experts have favored high-dose IV CYC for treatment of LN with cellular crescents. In general, the presence of crescents indicates a poorer prognosis, even with appropriate treatment. Further recommendations for a pregnant patient with crescentic glomerulonephritis are provided in the section on "Treatment of LN in Patients Who Are Pregnant," below.
Recommendations for Induction of Improvement in Patients with Class V "Pure Membranous" LN
The Task Force Panel recommends that patients with pure class V LN and with nephrotic range proteinuria be started on prednisone (0.5 mg/kg/day) plus MMF 2–3 gm total daily dose (level A evidence) (see Figure 3 in the original guideline document).
Other therapies for membranous LN have been reported; however, the Task Force Panel did not reach consensus on a recommendation regarding those therapies.
Recommendations for Maintaining Improvement in Patients Who Respond to Induction Therapy
The Task Force Panel recommended that either AZA or MMF be used for maintenance therapy (level A evidence) (see Figure 2 in the original guideline document). The Task Force Panel did not vote on the rate of medication taper during the maintenance phase; to date, there are no adequate data to inform the physician regarding how rapidly AZA or MMF can be tapered or withdrawn.
Recommendations for Changing Therapies in Patients Who Do Not Respond Adequately to Induction Therapy
In patients who fail to respond after 6 months of treatment (based on the treating physician's clinical impression) with glucocorticoids plus MMF or CYC, the Task Force Panel recommends a switch of the immunosuppressive agent from either CYC to MMF, or from MMF to CYC, with these changes accompanied by IV pulses of glucocorticoids for 3 days (level C evidence) (see Figure 2 in the original guideline document). For CYC, either low dose or high dose can be used in white individuals, as discussed above in the section on "Recommendations for Induction of Improvement in Patients with ISN Class III/IV Lupus Glomerulonephritis," above. Evidence to support these opinions is not as strong as evidence for the efficacy of initial induction therapy. The panel also voted that in some cases rituximab can be used in patients whose nephritis fails to improve or worsens after 6 months of one induction therapy, or after the patient has failed both CYC and MMF treatments (level C evidence). The Task Force Panel did not reach consensus regarding the use of calcineurin inhibitors in this setting; however, there is evidence for their efficacy as an induction agent and in refractory disease.
There is evidence in open-label trials that LN may respond to rituximab treatment. Prospective, randomized, placebo-controlled trials did not show a significant difference between rituximab and placebo (on a background of MMF and glucocorticoids) after 1 year of treatment.
Evidence to support the use of cyclosporine or tacrolimus in LN is from open trials and recent prospective clinical trials; additional prospective trials are in progress. In a recent prospective trial, tacrolimus was equivalent to high-dose IV CYC in inducing complete and partial remissions of LN over a 6-month period. In another 4-year–long prospective trial, cyclosporine was similar to AZA in preventing renal flares in patients receiving maintenance therapy.
If nephritis is worsening in patients treated for 3 months with glucocorticoids plus CYC or MMF, the Task Force Panel recommended that the clinician can choose any of the alternative treatments discussed (level C evidence). Although combinations of MMF and calcineurin inhibitors and of rituximab and MMF are being studied and might be considered for those who have failed the recommended induction therapies, data are not robust enough at this time to include them for voting scenarios.
The FDA has approved belimumab for use in seropositive patients with SLE who have active disease in spite of prior therapies.
Identification of Vascular Disease in Patients with SLE and Renal Abnormalities
Several types of vascular involvement can occur in renal tissue of SLE, including vasculitis, fibrinoid necrosis with narrowing of small arteries/arterioles ("bland" vasculopathy), thrombotic microangiopathy, and renal vein thrombosis. In general, vasculitis is treated similarly to the more common forms of LN discussed above. Bland vasculopathy is highly associated with hypertension; it is not clear which comes first, SLE or hypertension. Thrombotic microangiopathy can be associated with a thrombotic thrombocytopenia–like picture. The Task Force Panel recommended that thrombotic microangiopathy be treated primarily with plasma exchange therapy (level C evidence)
Treatment of LN in Patients Who Are Pregnant
The Task Force Panel recommended several approaches for management of LN in women who are pregnant (all level C evidence) (see Figure 4 in the original guideline document). In patients with prior LN but no current evidence of systemic or renal disease activity, no nephritis medications are necessary. Patients with mild systemic activity may be treated with HCQ; this probably reduces activity of SLE during pregnancy. If clinically active nephritis is present, or there is substantial extrarenal disease activity, the clinician may prescribe glucocorticoids at doses necessary to control disease activity, and if necessary AZA can be added. High-dose glucocorticoid therapy in patients with SLE is associated with a high risk of maternal complications such as hypertension and diabetes mellitus. MMF, CYC, and methotrexate should be avoided because they are teratogenic in humans. Although AZA is listed as pregnancy category D in Micromedex, cross-sectional studies have shown that the risk of fetal abnormalities is low. The dose of AZA should not exceed 2 mg/kg in a pregnant woman. For patients with a persistently active nephritis with documented or suspected class III or IV with crescents, consideration of delivery after 28 weeks for a viable fetus is recommended.
Monitoring Activity of LN
Recommendations for monitoring LN are shown in the following table, and result from votes of the Task Force Panel (level C evidence).
Table. Recommended Monitoring of Lupus Nephritis*
| Blood Pressure | Urinalysis | Protein/Creatinine Ratio | Serum Creatinine | C3/C4 Levels | Anti-DNA | |
|---|---|---|---|---|---|---|
| Active nephritis at onset of treatment | 1 | 1 | 1 | 1 | 2† | 3 |
| Previous active nephritis, none currently | 3 | 3 | 3 | 3 | 3 | 6 |
| Pregnant with active GN at onset of treatment | 1 | 1 | 1 | 1 | 1 | 1 |
| Pregnant with previous nephritis, none currently | 1 | 1 | 3 | 3 | 3 | 3 |
| No prior or current nephritis | 3 | 6 | 6 | 6 | 6 | 6 |
*Values are the monthly intervals suggested as the minimum frequency at which the indicated laboratory tests should be measured in the systemic lupus erythematosus scenarios shown in the left-hand column. GN = glomerulonephritis.
†Opinion of authors based on a study published after the Task Force Panel had voted.
Definitions:
Level of Evidence
- Level of Evidence A: Data derived from multiple randomized clinical trials
- Level of Evidence B: Data derived from a single randomized trial, or nonrandomized studies
- Level of Evidence C: Only consensus opinion of experts, case studies, or standard-of-care
- Class III/IV induction therapy for lupus nephritis (LN)
- Treatment of class V LN without proliferative changes and with nephrotic range proteinuria (>3 gm/24 hours)
- Treatment of class III, IV, and V LN in patients who are pregnant
Renal Biopsy and Histology
The Task Force Panel recommended that all patients with clinical evidence of active lupus nephritis (LN), previously untreated, undergo renal biopsy (unless strongly contraindicated) so that glomerular disease can be classified by current International Society of Nephrology/Renal Pathology Society (ISN/RPS) classification (level C evidence) (see Table 1 in the original guideline document for ISN/RPS classification of LN). In addition, disease can be evaluated for activity and chronicity and for tubular and vascular changes. Finally, biopsies may identify additional or alternative causes of renal disease, such as tubular necrosis related to medications, hypovolemia, or hypotension. Biopsy is most highly recommended in patients with the characteristics indicated in the following table.
Table. Indications for Renal Biopsy in Patients with Systemic Lupus Erythematosus
| Level of Evidence | |
|---|---|
| Increasing serum creatinine without compelling alternative causes (such as sepsis, hypovolemia, or medication) | C |
| Confirmed proteinuria of ≥1.0 gm per 24 hours (either 24-hour urine specimens or spot protein/creatinine ratios are acceptable) | C |
Combinations of the following, assuming the findings are confirmed in at least two tests done within a short period of time and in the absence of alternative causes:
| C |
RBCs = red blood cells; hpf = high-power field.
The Task Force Panel recommended that treatment be based in large part on the classification of type of LN by these ISN/RPS criteria. As a result, the following recommendations are presented according to the histologic classification of nephritis. The Task Force Panel agreed that class I (minimal mesangial immune deposits on immunofluorescence with normal light microscopy) and class II (mesangial hypercellularity or matrix expansion on light microscopy with immune deposits confined to mesangium on immunofluorescence) generally do not require immunosuppressive treatment (level C evidence). In general, patients with class III (subendothelial immune deposits and proliferative changes in <50% of glomeruli) and class IV (subendothelial deposits and proliferative glomerular changes involving ≥50% of glomeruli) require aggressive therapy with glucocorticoids and immunosuppressive agents. Class V (subepithelial immune deposits and membranous thickening of glomerular capillaries) when combined with class III or IV should be treated in the same manner as class III or IV. Class V alone ("pure membranous LN") may be approached somewhat differently, as indicated below under "Recommendations for Induction of Improvement in Patients with Class V 'Pure Membranous' LN". Histologic class VI (sclerosis of ≥90% of glomeruli) generally requires preparation for renal replacement therapy rather than immunosuppression. The designations "A" and "C" indicate whether active or chronic changes are present; the higher the chronicity the less likely that the nephritis will respond to immunosuppression. However, A or C classifications were not included in the entry criteria for clinical trials in LN published to date, and therefore they are not considered in the recommendations.
Adjunctive Treatments
The Task Force Panel recommended that all systemic lupus erythematosus (SLE) patients with nephritis be treated with a background of hydroxychloroquine (HCQ; level C evidence), unless there is a contraindication.
All LN patients with proteinuria ≥0.5 gm per 24 hours (or equivalent by protein/creatinine ratios on spot urine samples) should have blockade of the renin–angiotensin system, which drives intraglomerular pressure (level A evidence for nondiabetic chronic renal disease). Treatment with either angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs) reduces proteinuria by approximately 30%, and significantly delays doubling of serum creatinine and progression to end-stage renal disease in patients with nondiabetic chronic renal disease. These classes of medications are contraindicated in pregnancy. The use of combination ACE inhibitors/ARB therapies is controversial. ACE inhibitors or ARB treatments are superior to calcium-channel blockers and diuretics alone in preserving renal function in chronic kidney disease.
The Task Force Panel recommended that careful attention be paid to control of hypertension, with a target of ≤130/80 mm Hg (level A evidence for nondiabetic chronic renal disease). The Task Force Panel also recommended that statin therapy be introduced in patients with low-density lipoprotein cholesterol >100 mg/dl (level C evidence). Note that a glomerular filtration rate <60 ml/minute/1.73 m2 (equivalent to a serum creatinine level >1.5 mg/dl or 133 µmoles/liter) is a risk factor for accelerated atherosclerosis. SLE itself is also an independent risk factor for accelerated atherosclerosis.
Finally, the Task Force Panel recommended that women of child-bearing potential with active or prior LN receive counseling regarding pregnancy risks conferred by the disease and its treatments (level C evidence).
Recommendations for Induction of Improvement in Patients with ISN Class III/IV Lupus Glomerulonephritis
The Task Force Panel recommended mycophenolate mofetil (MMF) (2–3 gm total daily orally) or intravenous (IV) cyclophosphamide (CYC) along with glucocorticoids (level A evidence) (see Figure 2 in the original guideline document). MMF and CYC are considered equivalent based on recent high-quality studies, a meta-analysis, and expert opinion. Long-term studies with MMF are not as abundant as those with CYC; data show good results for induction therapy with MMF of 3 gm total dose daily for 6 months, followed by maintenance with lower doses of MMF for 3 years. MMF has been similar in efficacy in all races studied to date (whites, Asians, African Americans, and Latin/Hispanic Americans). The Aspreva Lupus Management Study (ALMS) trial comparing response rates of LN to MMF plus glucocorticoids showed similar improvement in whites, Asians, and other races (primarily African Americans and Hispanics). However, The Task Force Panel voted that Asians compared to non-Asians might require lower doses of MMF for similar efficacy (level C evidence). Therefore, the physician might aim for 3 gm per day total daily highest dose in non-Asians and 2 gm per day in Asians. There is evidence that African Americans and Hispanics with LN respond less well to IV CYC than do patients of white or Asian races. MMF/mycophenolic acid (MPA) may be an initial choice more likely to induce improvement in patients who are African American or Hispanic.
The exact suggested dose of MMF varied based on the clinical scenario: for those with class III/IV without cellular crescents and for those with proteinuria and a stable creatinine for whom a renal biopsy sample cannot be obtained, both 2 gm and 3 gm total daily doses were acceptable to the Task Force Panel, while a dose of 3 gm daily was favored for those with class III/IV and crescents and for those with proteinuria and a recent significant rise in creatinine.
Some evidence suggests that MPA and enteric-coated mycophenolate sodium are less likely than MMF to cause nausea and diarrhea, but this is controversial, and the exact equivalency of the preparations is not firmly established. The Core Expert Panel recommended that MMF and MPA are likely to be equivalent in inducing improvement of LN, with 1,440–2,160 mg total daily dose of MPA roughly equivalent to 2,000–3,000 mg total daily dose of MMF. Some investigators have suggested that serum levels of MPA, the active metabolite of MMF, should be measured at the trough or peak (1 hour after a dose), and treatment of SLE should be guided by these levels. However, there are not enough data at this time to make recommendations for monitoring of drug levels.
There are two regimens of IV CYC recommended by the Task Force Panel: 1) low-dose "Euro-Lupus" CYC (500 mg IV once every 2 weeks for a total of 6 doses), followed by maintenance therapy with daily oral azathioprine (AZA) or daily oral MMF (level B evidence), and 2) high-dose CYC (500–1,000 mg/m2 IV once a month for 6 doses), followed by maintenance treatment with MMF or AZA (level A evidence) (see Figure 2 in the original guideline document). If CYC is being considered for treatment, the Core Expert Panel recommended IV CYC at the low "Euro-Lupus" dose for white patients with Western European or Southern European racial/ethnic backgrounds (level B evidence). In European study patients, the low- and high-dose regimens were equivalent in efficacy, and serious infections were less frequent with the lower doses. The low- and high-dose regimens have not been compared in nonwhite racial groups. Ten years of followup comparing low- and high-dose regimens showed similar rates of LN flares, end-stage renal disease, and doubling of the serum creatinine.
Pulse IV glucocorticoids (500–1,000 mg methylprednisolone daily for 3 doses) in combination with immunosuppressive therapy is recommended by the Task Force Panel, followed by daily oral glucocorticoids (0.5–1 mg/kg/day), followed by a taper to the minimal amount necessary to control disease (level C evidence). There are insufficient data to recommend a specific steroid taper because the nephritis and extrarenal manifestations vary from patient to patient. There was no consensus reached regarding the use of monthly IV methylprednisolone with monthly IV CYC.
Although AZA has been used to treat LN, the Task Force Panel did not recommend it as one of the first choices for induction therapy.
The panel recommends that most patients be followed for 6 months after initiation of induction treatment with either CYC or MMF before making major changes in treatment other than alteration of glucocorticoid doses, unless there is clear evidence of worsening at 3 months (50% or more worsening of proteinuria or serum creatinine; level A evidence).
Fertility issues are often a concern for young SLE patients with nephritis. In a discussion, the Task Force Panel recommended that MMF was preferable to CYC for patients who express a major concern with fertility preservation, since high-dose CYC can cause permanent infertility in both women and men (level A evidence of gonadal toxicity). Six months of high-dose IV CYC was associated with approximately 10% sustained infertility in young women, and higher rates in older women. If 6 months of CYC were followed by quarterly doses, there was a higher rate of infertility. The Task Force Panel did not reach a consensus on the use of leuprolide in patients with SLE receiving CYC as a means to preserve fertility. They also noted that MMF is teratogenic (class D in US Food and Drug Administration [FDA] ranking). Therefore, the physician should be sure that a patient is not pregnant before prescribing MMF or MPA, and the medications should be stopped for at least 6 weeks before pregnancy is attempted.
Recommendations for Induction of Improvement in Patients with Class IV or IV/V Plus Cellular Crescents
The Task Force Panel recommended either CYC or MMF for induction of improvement in this type of LN (level C evidence), along with IV pulses of high-dose glucocorticoid and initiation of oral glucocorticoids at the higher-range dosage, 1 mg/kg/day orally (see Figure 2 in the original guideline document). For the purpose of these recommendations statements, the presence of any crescents on a renal biopsy sample was considered crescentic LN. Until recently, experts have favored high-dose IV CYC for treatment of LN with cellular crescents. In general, the presence of crescents indicates a poorer prognosis, even with appropriate treatment. Further recommendations for a pregnant patient with crescentic glomerulonephritis are provided in the section on "Treatment of LN in Patients Who Are Pregnant," below.
Recommendations for Induction of Improvement in Patients with Class V "Pure Membranous" LN
The Task Force Panel recommends that patients with pure class V LN and with nephrotic range proteinuria be started on prednisone (0.5 mg/kg/day) plus MMF 2–3 gm total daily dose (level A evidence) (see Figure 3 in the original guideline document).
Other therapies for membranous LN have been reported; however, the Task Force Panel did not reach consensus on a recommendation regarding those therapies.
Recommendations for Maintaining Improvement in Patients Who Respond to Induction Therapy
The Task Force Panel recommended that either AZA or MMF be used for maintenance therapy (level A evidence) (see Figure 2 in the original guideline document). The Task Force Panel did not vote on the rate of medication taper during the maintenance phase; to date, there are no adequate data to inform the physician regarding how rapidly AZA or MMF can be tapered or withdrawn.
Recommendations for Changing Therapies in Patients Who Do Not Respond Adequately to Induction Therapy
In patients who fail to respond after 6 months of treatment (based on the treating physician's clinical impression) with glucocorticoids plus MMF or CYC, the Task Force Panel recommends a switch of the immunosuppressive agent from either CYC to MMF, or from MMF to CYC, with these changes accompanied by IV pulses of glucocorticoids for 3 days (level C evidence) (see Figure 2 in the original guideline document). For CYC, either low dose or high dose can be used in white individuals, as discussed above in the section on "Recommendations for Induction of Improvement in Patients with ISN Class III/IV Lupus Glomerulonephritis," above. Evidence to support these opinions is not as strong as evidence for the efficacy of initial induction therapy. The panel also voted that in some cases rituximab can be used in patients whose nephritis fails to improve or worsens after 6 months of one induction therapy, or after the patient has failed both CYC and MMF treatments (level C evidence). The Task Force Panel did not reach consensus regarding the use of calcineurin inhibitors in this setting; however, there is evidence for their efficacy as an induction agent and in refractory disease.
There is evidence in open-label trials that LN may respond to rituximab treatment. Prospective, randomized, placebo-controlled trials did not show a significant difference between rituximab and placebo (on a background of MMF and glucocorticoids) after 1 year of treatment.
Evidence to support the use of cyclosporine or tacrolimus in LN is from open trials and recent prospective clinical trials; additional prospective trials are in progress. In a recent prospective trial, tacrolimus was equivalent to high-dose IV CYC in inducing complete and partial remissions of LN over a 6-month period. In another 4-year–long prospective trial, cyclosporine was similar to AZA in preventing renal flares in patients receiving maintenance therapy.
If nephritis is worsening in patients treated for 3 months with glucocorticoids plus CYC or MMF, the Task Force Panel recommended that the clinician can choose any of the alternative treatments discussed (level C evidence). Although combinations of MMF and calcineurin inhibitors and of rituximab and MMF are being studied and might be considered for those who have failed the recommended induction therapies, data are not robust enough at this time to include them for voting scenarios.
The FDA has approved belimumab for use in seropositive patients with SLE who have active disease in spite of prior therapies.
Identification of Vascular Disease in Patients with SLE and Renal Abnormalities
Several types of vascular involvement can occur in renal tissue of SLE, including vasculitis, fibrinoid necrosis with narrowing of small arteries/arterioles ("bland" vasculopathy), thrombotic microangiopathy, and renal vein thrombosis. In general, vasculitis is treated similarly to the more common forms of LN discussed above. Bland vasculopathy is highly associated with hypertension; it is not clear which comes first, SLE or hypertension. Thrombotic microangiopathy can be associated with a thrombotic thrombocytopenia–like picture. The Task Force Panel recommended that thrombotic microangiopathy be treated primarily with plasma exchange therapy (level C evidence)
Treatment of LN in Patients Who Are Pregnant
The Task Force Panel recommended several approaches for management of LN in women who are pregnant (all level C evidence) (see Figure 4 in the original guideline document). In patients with prior LN but no current evidence of systemic or renal disease activity, no nephritis medications are necessary. Patients with mild systemic activity may be treated with HCQ; this probably reduces activity of SLE during pregnancy. If clinically active nephritis is present, or there is substantial extrarenal disease activity, the clinician may prescribe glucocorticoids at doses necessary to control disease activity, and if necessary AZA can be added. High-dose glucocorticoid therapy in patients with SLE is associated with a high risk of maternal complications such as hypertension and diabetes mellitus. MMF, CYC, and methotrexate should be avoided because they are teratogenic in humans. Although AZA is listed as pregnancy category D in Micromedex, cross-sectional studies have shown that the risk of fetal abnormalities is low. The dose of AZA should not exceed 2 mg/kg in a pregnant woman. For patients with a persistently active nephritis with documented or suspected class III or IV with crescents, consideration of delivery after 28 weeks for a viable fetus is recommended.
Monitoring Activity of LN
Recommendations for monitoring LN are shown in the following table, and result from votes of the Task Force Panel (level C evidence).
Table. Recommended Monitoring of Lupus Nephritis*
| Blood Pressure | Urinalysis | Protein/Creatinine Ratio | Serum Creatinine | C3/C4 Levels | Anti-DNA | |
|---|---|---|---|---|---|---|
| Active nephritis at onset of treatment | 1 | 1 | 1 | 1 | 2† | 3 |
| Previous active nephritis, none currently | 3 | 3 | 3 | 3 | 3 | 6 |
| Pregnant with active GN at onset of treatment | 1 | 1 | 1 | 1 | 1 | 1 |
| Pregnant with previous nephritis, none currently | 1 | 1 | 3 | 3 | 3 | 3 |
| No prior or current nephritis | 3 | 6 | 6 | 6 | 6 | 6 |
*Values are the monthly intervals suggested as the minimum frequency at which the indicated laboratory tests should be measured in the systemic lupus erythematosus scenarios shown in the left-hand column. GN = glomerulonephritis.
†Opinion of authors based on a study published after the Task Force Panel had voted.
Definitions:
Level of Evidence
- Level of Evidence A: Data derived from multiple randomized clinical trials
- Level of Evidence B: Data derived from a single randomized trial, or nonrandomized studies
- Level of Evidence C: Only consensus opinion of experts, case studies, or standard-of-care
- Class III/IV induction therapy for lupus nephritis (LN)
- Treatment of class V LN without proliferative changes and with nephrotic range proteinuria (>3 gm/24 hours)
- Treatment of class III, IV, and V LN in patients who are pregnant
Renal Biopsy and Histology
The Task Force Panel recommended that all patients with clinical evidence of active lupus nephritis (LN), previously untreated, undergo renal biopsy (unless strongly contraindicated) so that glomerular disease can be classified by current International Society of Nephrology/Renal Pathology Society (ISN/RPS) classification (level C evidence) (see Table 1 in the original guideline document for ISN/RPS classification of LN). In addition, disease can be evaluated for activity and chronicity and for tubular and vascular changes. Finally, biopsies may identify additional or alternative causes of renal disease, such as tubular necrosis related to medications, hypovolemia, or hypotension. Biopsy is most highly recommended in patients with the characteristics indicated in the following table.
Table. Indications for Renal Biopsy in Patients with Systemic Lupus Erythematosus
| Level of Evidence | |
|---|---|
| Increasing serum creatinine without compelling alternative causes (such as sepsis, hypovolemia, or medication) | C |
| Confirmed proteinuria of ≥1.0 gm per 24 hours (either 24-hour urine specimens or spot protein/creatinine ratios are acceptable) | C |
Combinations of the following, assuming the findings are confirmed in at least two tests done within a short period of time and in the absence of alternative causes:
| C |
RBCs = red blood cells; hpf = high-power field.
The Task Force Panel recommended that treatment be based in large part on the classification of type of LN by these ISN/RPS criteria. As a result, the following recommendations are presented according to the histologic classification of nephritis. The Task Force Panel agreed that class I (minimal mesangial immune deposits on immunofluorescence with normal light microscopy) and class II (mesangial hypercellularity or matrix expansion on light microscopy with immune deposits confined to mesangium on immunofluorescence) generally do not require immunosuppressive treatment (level C evidence). In general, patients with class III (subendothelial immune deposits and proliferative changes in <50% of glomeruli) and class IV (subendothelial deposits and proliferative glomerular changes involving ≥50% of glomeruli) require aggressive therapy with glucocorticoids and immunosuppressive agents. Class V (subepithelial immune deposits and membranous thickening of glomerular capillaries) when combined with class III or IV should be treated in the same manner as class III or IV. Class V alone ("pure membranous LN") may be approached somewhat differently, as indicated below under "Recommendations for Induction of Improvement in Patients with Class V 'Pure Membranous' LN". Histologic class VI (sclerosis of ≥90% of glomeruli) generally requires preparation for renal replacement therapy rather than immunosuppression. The designations "A" and "C" indicate whether active or chronic changes are present; the higher the chronicity the less likely that the nephritis will respond to immunosuppression. However, A or C classifications were not included in the entry criteria for clinical trials in LN published to date, and therefore they are not considered in the recommendations.
Adjunctive Treatments
The Task Force Panel recommended that all systemic lupus erythematosus (SLE) patients with nephritis be treated with a background of hydroxychloroquine (HCQ; level C evidence), unless there is a contraindication.
All LN patients with proteinuria ≥0.5 gm per 24 hours (or equivalent by protein/creatinine ratios on spot urine samples) should have blockade of the renin–angiotensin system, which drives intraglomerular pressure (level A evidence for nondiabetic chronic renal disease). Treatment with either angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs) reduces proteinuria by approximately 30%, and significantly delays doubling of serum creatinine and progression to end-stage renal disease in patients with nondiabetic chronic renal disease. These classes of medications are contraindicated in pregnancy. The use of combination ACE inhibitors/ARB therapies is controversial. ACE inhibitors or ARB treatments are superior to calcium-channel blockers and diuretics alone in preserving renal function in chronic kidney disease.
The Task Force Panel recommended that careful attention be paid to control of hypertension, with a target of ≤130/80 mm Hg (level A evidence for nondiabetic chronic renal disease). The Task Force Panel also recommended that statin therapy be introduced in patients with low-density lipoprotein cholesterol >100 mg/dl (level C evidence). Note that a glomerular filtration rate <60 ml/minute/1.73 m2 (equivalent to a serum creatinine level >1.5 mg/dl or 133 µmoles/liter) is a risk factor for accelerated atherosclerosis. SLE itself is also an independent risk factor for accelerated atherosclerosis.
Finally, the Task Force Panel recommended that women of child-bearing potential with active or prior LN receive counseling regarding pregnancy risks conferred by the disease and its treatments (level C evidence).
Recommendations for Induction of Improvement in Patients with ISN Class III/IV Lupus Glomerulonephritis
The Task Force Panel recommended mycophenolate mofetil (MMF) (2–3 gm total daily orally) or intravenous (IV) cyclophosphamide (CYC) along with glucocorticoids (level A evidence) (see Figure 2 in the original guideline document). MMF and CYC are considered equivalent based on recent high-quality studies, a meta-analysis, and expert opinion. Long-term studies with MMF are not as abundant as those with CYC; data show good results for induction therapy with MMF of 3 gm total dose daily for 6 months, followed by maintenance with lower doses of MMF for 3 years. MMF has been similar in efficacy in all races studied to date (whites, Asians, African Americans, and Latin/Hispanic Americans). The Aspreva Lupus Management Study (ALMS) trial comparing response rates of LN to MMF plus glucocorticoids showed similar improvement in whites, Asians, and other races (primarily African Americans and Hispanics). However, The Task Force Panel voted that Asians compared to non-Asians might require lower doses of MMF for similar efficacy (level C evidence). Therefore, the physician might aim for 3 gm per day total daily highest dose in non-Asians and 2 gm per day in Asians. There is evidence that African Americans and Hispanics with LN respond less well to IV CYC than do patients of white or Asian races. MMF/mycophenolic acid (MPA) may be an initial choice more likely to induce improvement in patients who are African American or Hispanic.
The exact suggested dose of MMF varied based on the clinical scenario: for those with class III/IV without cellular crescents and for those with proteinuria and a stable creatinine for whom a renal biopsy sample cannot be obtained, both 2 gm and 3 gm total daily doses were acceptable to the Task Force Panel, while a dose of 3 gm daily was favored for those with class III/IV and crescents and for those with proteinuria and a recent significant rise in creatinine.
Some evidence suggests that MPA and enteric-coated mycophenolate sodium are less likely than MMF to cause nausea and diarrhea, but this is controversial, and the exact equivalency of the preparations is not firmly established. The Core Expert Panel recommended that MMF and MPA are likely to be equivalent in inducing improvement of LN, with 1,440–2,160 mg total daily dose of MPA roughly equivalent to 2,000–3,000 mg total daily dose of MMF. Some investigators have suggested that serum levels of MPA, the active metabolite of MMF, should be measured at the trough or peak (1 hour after a dose), and treatment of SLE should be guided by these levels. However, there are not enough data at this time to make recommendations for monitoring of drug levels.
There are two regimens of IV CYC recommended by the Task Force Panel: 1) low-dose "Euro-Lupus" CYC (500 mg IV once every 2 weeks for a total of 6 doses), followed by maintenance therapy with daily oral azathioprine (AZA) or daily oral MMF (level B evidence), and 2) high-dose CYC (500–1,000 mg/m2 IV once a month for 6 doses), followed by maintenance treatment with MMF or AZA (level A evidence) (see Figure 2 in the original guideline document). If CYC is being considered for treatment, the Core Expert Panel recommended IV CYC at the low "Euro-Lupus" dose for white patients with Western European or Southern European racial/ethnic backgrounds (level B evidence). In European study patients, the low- and high-dose regimens were equivalent in efficacy, and serious infections were less frequent with the lower doses. The low- and high-dose regimens have not been compared in nonwhite racial groups. Ten years of followup comparing low- and high-dose regimens showed similar rates of LN flares, end-stage renal disease, and doubling of the serum creatinine.
Pulse IV glucocorticoids (500–1,000 mg methylprednisolone daily for 3 doses) in combination with immunosuppressive therapy is recommended by the Task Force Panel, followed by daily oral glucocorticoids (0.5–1 mg/kg/day), followed by a taper to the minimal amount necessary to control disease (level C evidence). There are insufficient data to recommend a specific steroid taper because the nephritis and extrarenal manifestations vary from patient to patient. There was no consensus reached regarding the use of monthly IV methylprednisolone with monthly IV CYC.
Although AZA has been used to treat LN, the Task Force Panel did not recommend it as one of the first choices for induction therapy.
The panel recommends that most patients be followed for 6 months after initiation of induction treatment with either CYC or MMF before making major changes in treatment other than alteration of glucocorticoid doses, unless there is clear evidence of worsening at 3 months (50% or more worsening of proteinuria or serum creatinine; level A evidence).
Fertility issues are often a concern for young SLE patients with nephritis. In a discussion, the Task Force Panel recommended that MMF was preferable to CYC for patients who express a major concern with fertility preservation, since high-dose CYC can cause permanent infertility in both women and men (level A evidence of gonadal toxicity). Six months of high-dose IV CYC was associated with approximately 10% sustained infertility in young women, and higher rates in older women. If 6 months of CYC were followed by quarterly doses, there was a higher rate of infertility. The Task Force Panel did not reach a consensus on the use of leuprolide in patients with SLE receiving CYC as a means to preserve fertility. They also noted that MMF is teratogenic (class D in US Food and Drug Administration [FDA] ranking). Therefore, the physician should be sure that a patient is not pregnant before prescribing MMF or MPA, and the medications should be stopped for at least 6 weeks before pregnancy is attempted.
Recommendations for Induction of Improvement in Patients with Class IV or IV/V Plus Cellular Crescents
The Task Force Panel recommended either CYC or MMF for induction of improvement in this type of LN (level C evidence), along with IV pulses of high-dose glucocorticoid and initiation of oral glucocorticoids at the higher-range dosage, 1 mg/kg/day orally (see Figure 2 in the original guideline document). For the purpose of these recommendations statements, the presence of any crescents on a renal biopsy sample was considered crescentic LN. Until recently, experts have favored high-dose IV CYC for treatment of LN with cellular crescents. In general, the presence of crescents indicates a poorer prognosis, even with appropriate treatment. Further recommendations for a pregnant patient with crescentic glomerulonephritis are provided in the section on "Treatment of LN in Patients Who Are Pregnant," below.
Recommendations for Induction of Improvement in Patients with Class V "Pure Membranous" LN
The Task Force Panel recommends that patients with pure class V LN and with nephrotic range proteinuria be started on prednisone (0.5 mg/kg/day) plus MMF 2–3 gm total daily dose (level A evidence) (see Figure 3 in the original guideline document).
Other therapies for membranous LN have been reported; however, the Task Force Panel did not reach consensus on a recommendation regarding those therapies.
Recommendations for Maintaining Improvement in Patients Who Respond to Induction Therapy
The Task Force Panel recommended that either AZA or MMF be used for maintenance therapy (level A evidence) (see Figure 2 in the original guideline document). The Task Force Panel did not vote on the rate of medication taper during the maintenance phase; to date, there are no adequate data to inform the physician regarding how rapidly AZA or MMF can be tapered or withdrawn.
Recommendations for Changing Therapies in Patients Who Do Not Respond Adequately to Induction Therapy
In patients who fail to respond after 6 months of treatment (based on the treating physician's clinical impression) with glucocorticoids plus MMF or CYC, the Task Force Panel recommends a switch of the immunosuppressive agent from either CYC to MMF, or from MMF to CYC, with these changes accompanied by IV pulses of glucocorticoids for 3 days (level C evidence) (see Figure 2 in the original guideline document). For CYC, either low dose or high dose can be used in white individuals, as discussed above in the section on "Recommendations for Induction of Improvement in Patients with ISN Class III/IV Lupus Glomerulonephritis," above. Evidence to support these opinions is not as strong as evidence for the efficacy of initial induction therapy. The panel also voted that in some cases rituximab can be used in patients whose nephritis fails to improve or worsens after 6 months of one induction therapy, or after the patient has failed both CYC and MMF treatments (level C evidence). The Task Force Panel did not reach consensus regarding the use of calcineurin inhibitors in this setting; however, there is evidence for their efficacy as an induction agent and in refractory disease.
There is evidence in open-label trials that LN may respond to rituximab treatment. Prospective, randomized, placebo-controlled trials did not show a significant difference between rituximab and placebo (on a background of MMF and glucocorticoids) after 1 year of treatment.
Evidence to support the use of cyclosporine or tacrolimus in LN is from open trials and recent prospective clinical trials; additional prospective trials are in progress. In a recent prospective trial, tacrolimus was equivalent to high-dose IV CYC in inducing complete and partial remissions of LN over a 6-month period. In another 4-year–long prospective trial, cyclosporine was similar to AZA in preventing renal flares in patients receiving maintenance therapy.
If nephritis is worsening in patients treated for 3 months with glucocorticoids plus CYC or MMF, the Task Force Panel recommended that the clinician can choose any of the alternative treatments discussed (level C evidence). Although combinations of MMF and calcineurin inhibitors and of rituximab and MMF are being studied and might be considered for those who have failed the recommended induction therapies, data are not robust enough at this time to include them for voting scenarios.
The FDA has approved belimumab for use in seropositive patients with SLE who have active disease in spite of prior therapies.
Identification of Vascular Disease in Patients with SLE and Renal Abnormalities
Several types of vascular involvement can occur in renal tissue of SLE, including vasculitis, fibrinoid necrosis with narrowing of small arteries/arterioles ("bland" vasculopathy), thrombotic microangiopathy, and renal vein thrombosis. In general, vasculitis is treated similarly to the more common forms of LN discussed above. Bland vasculopathy is highly associated with hypertension; it is not clear which comes first, SLE or hypertension. Thrombotic microangiopathy can be associated with a thrombotic thrombocytopenia–like picture. The Task Force Panel recommended that thrombotic microangiopathy be treated primarily with plasma exchange therapy (level C evidence)
Treatment of LN in Patients Who Are Pregnant
The Task Force Panel recommended several approaches for management of LN in women who are pregnant (all level C evidence) (see Figure 4 in the original guideline document). In patients with prior LN but no current evidence of systemic or renal disease activity, no nephritis medications are necessary. Patients with mild systemic activity may be treated with HCQ; this probably reduces activity of SLE during pregnancy. If clinically active nephritis is present, or there is substantial extrarenal disease activity, the clinician may prescribe glucocorticoids at doses necessary to control disease activity, and if necessary AZA can be added. High-dose glucocorticoid therapy in patients with SLE is associated with a high risk of maternal complications such as hypertension and diabetes mellitus. MMF, CYC, and methotrexate should be avoided because they are teratogenic in humans. Although AZA is listed as pregnancy category D in Micromedex, cross-sectional studies have shown that the risk of fetal abnormalities is low. The dose of AZA should not exceed 2 mg/kg in a pregnant woman. For patients with a persistently active nephritis with documented or suspected class III or IV with crescents, consideration of delivery after 28 weeks for a viable fetus is recommended.
Monitoring Activity of LN
Recommendations for monitoring LN are shown in the following table, and result from votes of the Task Force Panel (level C evidence).
Table. Recommended Monitoring of Lupus Nephritis*
| Blood Pressure | Urinalysis | Protein/Creatinine Ratio | Serum Creatinine | C3/C4 Levels | Anti-DNA | |
|---|---|---|---|---|---|---|
| Active nephritis at onset of treatment | 1 | 1 | 1 | 1 | 2† | 3 |
| Previous active nephritis, none currently | 3 | 3 | 3 | 3 | 3 | 6 |
| Pregnant with active GN at onset of treatment | 1 | 1 | 1 | 1 | 1 | 1 |
| Pregnant with previous nephritis, none currently | 1 | 1 | 3 | 3 | 3 | 3 |
| No prior or current nephritis | 3 | 6 | 6 | 6 | 6 | 6 |
*Values are the monthly intervals suggested as the minimum frequency at which the indicated laboratory tests should be measured in the systemic lupus erythematosus scenarios shown in the left-hand column. GN = glomerulonephritis.
†Opinion of authors based on a study published after the Task Force Panel had voted.
Definitions:
Level of Evidence
- Level of Evidence A: Data derived from multiple randomized clinical trials
- Level of Evidence B: Data derived from a single randomized trial, or nonrandomized studies
- Level of Evidence C: Only consensus opinion of experts, case studies, or standard-of-care
- Class III/IV induction therapy for lupus nephritis (LN)
- Treatment of class V LN without proliferative changes and with nephrotic range proteinuria (>3 gm/24 hours)
- Treatment of class III, IV, and V LN in patients who are pregnant
OBJECTIVE: To provide a new set of management recommendations for lupus nephritis (LN) for adults with lupus nephritis (LN), particularly to those receiving care in the United States.
Guidelines are copyright © 2012 American College of Rheumatology. All rights reserved. The summary is provided by the Agency for Healthcare Research and Quality.
More patients with multidrug-resistant TB respond quickly to bedaquiline
Adding bedaquiline to a five-drug background regimen for multidrug-resistant pulmonary tuberculosis significantly accelerated the time at which sputum cultures showed clearance of Mycobacterium tuberculosis in a phase IIb clinical trial, which was published online Aug. 21 in the New England Journal of Medicine.
The addition of 6 months of oral bedaquiline – a diarylquinoline that inhibits mycobacterial ATP synthase and depletes cellular energy stores – also significantly increased the number of patients who achieved such culture conversion (a surrogate for clinical cure), compared with adding placebo, in this industry-sponsored study. Bedaquiline "is the first antituberculosis drug with a new mechanism of action to be approved for use in multidrug-resistant TB in 40 years," said Dr. Andreas H. Diacon of the National Research Foundation Centre of Excellence for Biomedical Tuberculosis Research at Stellenbosch University in Cape Town, South Africa, and his associates.
Bedaquiline was approved in 2012 under the Food and Drug Administration’s accelerated-approval regulations for drugs that provide meaningful therapeutic benefit over existing therapies for serious or life-threatening conditions. The drug is approved only for patients for whom an effective treatment regimen cannot be constructed without it, a population in whom the benefits outweigh the risks.
In the trial, 160 adults with multidrug-resistant pulmonary TB were randomly assigned to receive either oral bedaquiline (79 patients) or matching placebo tablets (81 patients) for 24 weeks at medical centers in Brazil, India, Latvia, Peru, the Philippines, Russia, South Africa, and Thailand, in addition to the five-drug background regimen of antituberculosis drugs preferred at each location. They continued the background therapy for a further 96 weeks and had a final follow-up exam at the conclusion of that treatment. Sixty participants (38%) left the study prematurely, usually because of withdrawal of consent, adverse effects, nonadherence, loss to follow-up, and pregnancy. The number of and reasons for these discontinuations were similar between the two study groups.
The primary endpoint of the study was the median time to sputum conversion. This was significantly faster in the intervention group (83 days) than in the control group (125 days) in both the modified intention-to-treat analysis and the full intention-to-treat analysis. Moreover, more patients in the intervention group (79%) than in the placebo group (58%) showed culture conversion at 24 weeks, as well as at 120 weeks (62% vs 44%). And according to the World Health Organization definition of "cure," nearly twice as many patients in the bedaquiline group (58%) were cured as in the placebo group (32%) at 120 weeks, Dr. Diacon and his associates said (N. Engl. J. Med. 2014;371:723-32 [doi:10.1056/NEJMoa1313865]).
Fewer patients taking bedaquiline (2) than taking placebo (16) developed new resistance to at least one antituberculosis agent during the study. Rates, types, and severity of adverse events were comparable between the two study groups. However, mortality was significantly higher with bedaquiline (10 patients, 13% mortality) than with placebo (2 patients, 2% mortality), for reasons that are not yet understood but do not appear to be related to the study drug.
"A planned phase III study will enroll a larger number of patients, including HIV-positive patients receiving antiretroviral therapy," the investigators noted.
This study was funded by Janssen Pharmaceuticals. Dr. Diacon reported no financial conflicts of interest. His associates reported ties to Janssen; to its parent company, Johnson & Johnson; and to Quintiles.
The Food and Drug Administration approved the limited use of bedaquiline despite the unexpected finding of significantly increased mortality in the intervention group (13%) than in the control group (2%), because the length of time between the last receipt of bedaquiline and death – 329 days – makes it difficult to discern a mechanism by which the drug could be directly related to the deaths, even if bedaquiline’s long half-life is taken into consideration.
This imbalance in mortality is an important concern. However, 1 of the 10 deaths that occurred in patients who received bedaquiline was because of a motor vehicle accident, 5 were from disease progression (as were both deaths in the placebo group), and the remaining 4 had no apparent commonality. A confirmatory trial, a condition of the accelerated approval of the drug, should shed more light on this discrepancy in mortality.
Dr. Edward Cox and Dr. Katherine Laessig are in the Office of Antimicrobial Products and the Office of New Drugs, the Center for Drug Evaluation and Research, at the FDA. They made their remarks in a perspective piece accompanying Dr. Diacon’s report (N. Engl. J. Med. 2014;371:689-91 [doi:10.1056/NEJMp1314385]). They reported no financial conflicts of interest.
The Food and Drug Administration approved the limited use of bedaquiline despite the unexpected finding of significantly increased mortality in the intervention group (13%) than in the control group (2%), because the length of time between the last receipt of bedaquiline and death – 329 days – makes it difficult to discern a mechanism by which the drug could be directly related to the deaths, even if bedaquiline’s long half-life is taken into consideration.
This imbalance in mortality is an important concern. However, 1 of the 10 deaths that occurred in patients who received bedaquiline was because of a motor vehicle accident, 5 were from disease progression (as were both deaths in the placebo group), and the remaining 4 had no apparent commonality. A confirmatory trial, a condition of the accelerated approval of the drug, should shed more light on this discrepancy in mortality.
Dr. Edward Cox and Dr. Katherine Laessig are in the Office of Antimicrobial Products and the Office of New Drugs, the Center for Drug Evaluation and Research, at the FDA. They made their remarks in a perspective piece accompanying Dr. Diacon’s report (N. Engl. J. Med. 2014;371:689-91 [doi:10.1056/NEJMp1314385]). They reported no financial conflicts of interest.
The Food and Drug Administration approved the limited use of bedaquiline despite the unexpected finding of significantly increased mortality in the intervention group (13%) than in the control group (2%), because the length of time between the last receipt of bedaquiline and death – 329 days – makes it difficult to discern a mechanism by which the drug could be directly related to the deaths, even if bedaquiline’s long half-life is taken into consideration.
This imbalance in mortality is an important concern. However, 1 of the 10 deaths that occurred in patients who received bedaquiline was because of a motor vehicle accident, 5 were from disease progression (as were both deaths in the placebo group), and the remaining 4 had no apparent commonality. A confirmatory trial, a condition of the accelerated approval of the drug, should shed more light on this discrepancy in mortality.
Dr. Edward Cox and Dr. Katherine Laessig are in the Office of Antimicrobial Products and the Office of New Drugs, the Center for Drug Evaluation and Research, at the FDA. They made their remarks in a perspective piece accompanying Dr. Diacon’s report (N. Engl. J. Med. 2014;371:689-91 [doi:10.1056/NEJMp1314385]). They reported no financial conflicts of interest.
Adding bedaquiline to a five-drug background regimen for multidrug-resistant pulmonary tuberculosis significantly accelerated the time at which sputum cultures showed clearance of Mycobacterium tuberculosis in a phase IIb clinical trial, which was published online Aug. 21 in the New England Journal of Medicine.
The addition of 6 months of oral bedaquiline – a diarylquinoline that inhibits mycobacterial ATP synthase and depletes cellular energy stores – also significantly increased the number of patients who achieved such culture conversion (a surrogate for clinical cure), compared with adding placebo, in this industry-sponsored study. Bedaquiline "is the first antituberculosis drug with a new mechanism of action to be approved for use in multidrug-resistant TB in 40 years," said Dr. Andreas H. Diacon of the National Research Foundation Centre of Excellence for Biomedical Tuberculosis Research at Stellenbosch University in Cape Town, South Africa, and his associates.
Bedaquiline was approved in 2012 under the Food and Drug Administration’s accelerated-approval regulations for drugs that provide meaningful therapeutic benefit over existing therapies for serious or life-threatening conditions. The drug is approved only for patients for whom an effective treatment regimen cannot be constructed without it, a population in whom the benefits outweigh the risks.
In the trial, 160 adults with multidrug-resistant pulmonary TB were randomly assigned to receive either oral bedaquiline (79 patients) or matching placebo tablets (81 patients) for 24 weeks at medical centers in Brazil, India, Latvia, Peru, the Philippines, Russia, South Africa, and Thailand, in addition to the five-drug background regimen of antituberculosis drugs preferred at each location. They continued the background therapy for a further 96 weeks and had a final follow-up exam at the conclusion of that treatment. Sixty participants (38%) left the study prematurely, usually because of withdrawal of consent, adverse effects, nonadherence, loss to follow-up, and pregnancy. The number of and reasons for these discontinuations were similar between the two study groups.
The primary endpoint of the study was the median time to sputum conversion. This was significantly faster in the intervention group (83 days) than in the control group (125 days) in both the modified intention-to-treat analysis and the full intention-to-treat analysis. Moreover, more patients in the intervention group (79%) than in the placebo group (58%) showed culture conversion at 24 weeks, as well as at 120 weeks (62% vs 44%). And according to the World Health Organization definition of "cure," nearly twice as many patients in the bedaquiline group (58%) were cured as in the placebo group (32%) at 120 weeks, Dr. Diacon and his associates said (N. Engl. J. Med. 2014;371:723-32 [doi:10.1056/NEJMoa1313865]).
Fewer patients taking bedaquiline (2) than taking placebo (16) developed new resistance to at least one antituberculosis agent during the study. Rates, types, and severity of adverse events were comparable between the two study groups. However, mortality was significantly higher with bedaquiline (10 patients, 13% mortality) than with placebo (2 patients, 2% mortality), for reasons that are not yet understood but do not appear to be related to the study drug.
"A planned phase III study will enroll a larger number of patients, including HIV-positive patients receiving antiretroviral therapy," the investigators noted.
This study was funded by Janssen Pharmaceuticals. Dr. Diacon reported no financial conflicts of interest. His associates reported ties to Janssen; to its parent company, Johnson & Johnson; and to Quintiles.
Adding bedaquiline to a five-drug background regimen for multidrug-resistant pulmonary tuberculosis significantly accelerated the time at which sputum cultures showed clearance of Mycobacterium tuberculosis in a phase IIb clinical trial, which was published online Aug. 21 in the New England Journal of Medicine.
The addition of 6 months of oral bedaquiline – a diarylquinoline that inhibits mycobacterial ATP synthase and depletes cellular energy stores – also significantly increased the number of patients who achieved such culture conversion (a surrogate for clinical cure), compared with adding placebo, in this industry-sponsored study. Bedaquiline "is the first antituberculosis drug with a new mechanism of action to be approved for use in multidrug-resistant TB in 40 years," said Dr. Andreas H. Diacon of the National Research Foundation Centre of Excellence for Biomedical Tuberculosis Research at Stellenbosch University in Cape Town, South Africa, and his associates.
Bedaquiline was approved in 2012 under the Food and Drug Administration’s accelerated-approval regulations for drugs that provide meaningful therapeutic benefit over existing therapies for serious or life-threatening conditions. The drug is approved only for patients for whom an effective treatment regimen cannot be constructed without it, a population in whom the benefits outweigh the risks.
In the trial, 160 adults with multidrug-resistant pulmonary TB were randomly assigned to receive either oral bedaquiline (79 patients) or matching placebo tablets (81 patients) for 24 weeks at medical centers in Brazil, India, Latvia, Peru, the Philippines, Russia, South Africa, and Thailand, in addition to the five-drug background regimen of antituberculosis drugs preferred at each location. They continued the background therapy for a further 96 weeks and had a final follow-up exam at the conclusion of that treatment. Sixty participants (38%) left the study prematurely, usually because of withdrawal of consent, adverse effects, nonadherence, loss to follow-up, and pregnancy. The number of and reasons for these discontinuations were similar between the two study groups.
The primary endpoint of the study was the median time to sputum conversion. This was significantly faster in the intervention group (83 days) than in the control group (125 days) in both the modified intention-to-treat analysis and the full intention-to-treat analysis. Moreover, more patients in the intervention group (79%) than in the placebo group (58%) showed culture conversion at 24 weeks, as well as at 120 weeks (62% vs 44%). And according to the World Health Organization definition of "cure," nearly twice as many patients in the bedaquiline group (58%) were cured as in the placebo group (32%) at 120 weeks, Dr. Diacon and his associates said (N. Engl. J. Med. 2014;371:723-32 [doi:10.1056/NEJMoa1313865]).
Fewer patients taking bedaquiline (2) than taking placebo (16) developed new resistance to at least one antituberculosis agent during the study. Rates, types, and severity of adverse events were comparable between the two study groups. However, mortality was significantly higher with bedaquiline (10 patients, 13% mortality) than with placebo (2 patients, 2% mortality), for reasons that are not yet understood but do not appear to be related to the study drug.
"A planned phase III study will enroll a larger number of patients, including HIV-positive patients receiving antiretroviral therapy," the investigators noted.
This study was funded by Janssen Pharmaceuticals. Dr. Diacon reported no financial conflicts of interest. His associates reported ties to Janssen; to its parent company, Johnson & Johnson; and to Quintiles.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Bedaquiline may offer an alternative treatment for multidrug-resistant TB.
Major finding: The primary endpoint of the study – the median time to sputum conversion – was significantly faster in the intervention group (83 days) than in the control group (125 days), and more patients in the intervention group (79%) than in the placebo group (58%) showed culture conversion at 24 weeks, as well as at 120 weeks (62% vs 44%).
Data source: A randomized, double-blind, placebo-controlled, phase IIb clinical trial involving 160 adults with multidrug-resistant pulmonary TB treated for 24 weeks in eight countries.
Disclosures: This study was funded by Janssen Pharmaceuticals. Dr. Diacon reported no financial conflicts of interest. His associates reported ties to Janssen; to its parent company, Johnson & Johnson; and to Quintiles.
Evidence-based guideline update: vagus nerve stimulation for the treatment of epilepsy: Report of the Guideline Development Subcommittee of the American Academy of Neurology
In Children with Epilepsy, Is Using Adjunctive Vagus Nerve Stimulation (VNS) Therapy for Seizure Frequency Reduction Better Than Not Using Adjunctive VNS therapy for Seizure Frequency Reduction?
Conclusion
Based on data from 14 Class III studies, VNS is possibly effective in achieving >50% seizure frequency reduction (responder rate). In the pooled analysis of 481 children, the responder rate was 55% (95% confidence interval [CI] 51%–59%), but there was significant heterogeneity in the data. Two of the 16 studies were not included in the analysis because either they did not provide information about responder rate or they included a significant number (>20%) of adults in their population. The pooled seizure freedom rate was 7% (95% CI 5%–10%).
Recommendation
VNS may be considered as adjunctive treatment for children with partial or generalized epilepsy (Level C).
Clinical Context
VNS may be considered a possibly effective option after a child with medication-resistant epilepsy has been declared a poor surgical candidate or has had unsuccessful surgery.
In Patients with Lennox-Gastaut Syndrome (LGS), Is Using Adjunctive VNS Therapy for Seizure Frequency Reduction Better Than Not Using Adjunctive VNS Therapy for Seizure Frequency Reduction?
Conclusion
Based on data from 4 Class III studies, VNS is possibly effective in achieving >50% seizure frequency reduction in patients with LGS. The pooled analysis of 113 patients with LGS (including data from articles with multiple seizure types where LGS data were parsed out) yielded a 55% (95% CI 46%–64%) responder rate.
Recommendation
VNS may be considered in patients with LGS (Level C).
Clinical Context
The responder rate for patients with LGS does not appear to differ from that of the general population of patients with medication-resistant epilepsy.
In Patients with Epilepsy, Is Using VNS Associated with Mood Improvement?
Conclusion
Based on data from 2 Class III studies, VNS is possibly effective for mood improvement in adults with epilepsy.
Recommendation
In adult patients receiving VNS for epilepsy, improvement in mood may be an additional benefit (Level C).
Clinical Context
Depression is a common comorbidity for people with epilepsy. VNS may provide an additional benefit by improving mood in some patients; however, the potential for mood improvement should be considered a secondary rather than a primary reason for VNS implantation. The evidence does not clearly support an independent effect on mood in this complex population.
In Patients with Epilepsy, Is VNS Use Associated with Reduced Seizure Frequency Over Time?
Conclusion
Based on data from 2 Class III studies, VNS is possibly associated with an increase in ≥50% seizure frequency reduction rates of 7% from 1 to 5 years postimplantation.
Recommendation
VNS may be considered progressively effective in patients over multiple years of exposure (Level C).
Clinical Context
The loss of medication efficacy over time is a challenging aspect of epilepsy management. The evidence of maintained efficacy in the long term and the trend toward improvement over time make VNS an option.
In Patients Undergoing VNS Therapy, Does Rapid Stimulation (Usual VNS Settings Are 7 Seconds "On" and 30 Seconds "Off") Improve Seizure Frequency More Often Than Standard Stimulation Settings (30 Seconds "On" and 300 Seconds "Off")?
Conclusion
These 3 Class III studies were underpowered to detect a difference in efficacy between rapid stimulation (7 seconds "on," 30 seconds "off") used either after standard stimulation (30 seconds "on," 300 seconds "off") was unsuccessful or as an initial treatment setting.
Recommendation
Optimal VNS settings are still unknown, and the evidence is insufficient to support a recommendation for the use of standard stimulation vs. rapid stimulation to reduce seizure occurrence (Level U).
Clinical Context
Rapid cycling increases the duty cycle and hastens the need for battery replacement; therefore, when used, the efficacy of rapid cycling should be carefully assessed.
In Patients Undergoing VNS Therapy, Does Using Additional Magnet-Activated Stimulation Trains for Auras or at Seizure Onset Interrupt Seizures Relative to Not Using Additional Magnet-Induced Stimulation Trains for Auras or at Seizure Onset?
Conclusion
Based on data from 2 Class III studies, seizure abortion with magnet-activated stimulation is possibly associated with overall response to VNS therapy. Based on 3 Class III studies, magnet-activated stimulation may be expected to abort seizures one-fourth to two-thirds of the time when used during seizure auras (one Class III study omitted because it was not generalizable).
Recommendation
Patients may be counseled that VNS magnet activation may be associated with seizure abortion when used at the time of seizure auras (Level C) and that seizure abortion with magnet use may be associated with overall response to VNS treatment (Level C).
In Patients Undergoing VNS Therapy, Have New Safety Concerns Emerged Since the Last Assessment?
Clinical Context
Current physician attention to intraoperative rhythm disturbances from VNS use need not be changed. The paroxysmal nature of epilepsy poses a challenge for identifying a cardiac rhythm disturbance as device-related rather than as an additional seizure manifestation. Video electroencephalogram (EEG) and electrocardiogram (ECG) monitoring of new-onset events that might be cardiac-related would be warranted to exclude this possibility in what is likely to be a small number of patients. Reduced sudden unexpected death in epilepsy (SUDEP) rates over time is an important finding associated with VNS therapy; in a cohort of 1,819 individuals followed 3,176.3 person-years from VNS implantation, the SUDEP rate was 5.5 per 1,000 over the first 2 years but only 1.7 per 1,000 thereafter. The clinical importance of the effect of VNS on sleep apnea and treatment is unclear, but caution regarding VNS use in this setting is suggested.
In Children Undergoing VNS Therapy, Do Adverse Events (AEs) Differ from Those in Adults?
Clinical Context
Children may have greater risk for wound infection than adults due to behaviors more common in children. Extra vigilance in monitoring for occurrence of site infection in children should be undertaken.
Definitions:
Classification of Evidence for Therapeutic Intervention
Class I: A randomized, controlled clinical trial of the intervention of interest with masked or objective outcome assessment, in a representative population. Relevant baseline characteristics are presented and substantially equivalent among treatment groups or there is appropriate statistical adjustment for differences.
The following are also required:
- Concealed allocation
- Primary outcome(s) clearly defined
- Exclusion/inclusion criteria clearly defined
- Adequate accounting for dropouts (with at least 80% of enrolled subjects completing the study) and crossovers with numbers sufficiently low to have minimal potential for bias.
- For noninferiority or equivalence trials claiming to prove efficacy for one or both drugs, the following are also required*
- The authors explicitly state the clinically meaningful difference to be excluded by defining the threshold for equivalence or noninferiority.
- The standard treatment used in the study is substantially similar to that used in previous studies establishing efficacy of the standard treatment (e.g., for a drug, the mode of administration, dose and dosage adjustments are similar to those previously shown to be effective).
- The inclusion and exclusion criteria for patient selection and the outcomes of patients on the standard treatment are comparable to those of previous studies establishing efficacy of the standard treatment.
- The interpretation of the results of the study is based upon a per protocol analysis that takes into account dropouts or crossovers.
Class II: A randomized controlled clinical trial of the intervention of interest in a representative population with masked or objective outcome assessment that lacks one criteria a–e above or a prospective matched cohort study with masked or objective outcome assessment in a representative population that meets b–e above. Relevant baseline characteristics are presented and substantially equivalent among treatment groups or there is appropriate statistical adjustment for differences.
Class III: All other controlled trials (including well-defined natural history controls or patients serving as own controls) in a representative population, where outcome is independently assessed, or independently derived by objective outcome measurement.**
Class IV: Studies not meeting Class I, II, or III criteria including consensus or expert opinion.
*Note that numbers 1-3 in Class Ie are required for Class II in equivalence trials. If any one of the three is missing, the class is automatically downgraded to Class III.
**Objective outcome measurement: an outcome measure that is unlikely to be affected by an observer's (patient, treating physician, investigator) expectation or bias (e.g., blood tests, administrative outcome data).
Classification of Recommendations
Level A = Established as effective, ineffective or harmful (or established as useful/predictive or not useful/predictive) for the given condition in the specified population. (Level A rating requires at least two consistent Class I studies.*)
Level B = Probably effective, ineffective or harmful (or probably useful/predictive or not useful/predictive) for the given condition in the specified population. (Level B rating requires at least one Class I study or two consistent Class II studies.)
Level C = Possibly effective, ineffective or harmful (or possibly useful/predictive or not useful/predictive) for the given condition in the specified population. (Level C rating requires at least one Class II study or two consistent Class III studies.)
Level U = Data inadequate or conflicting; given current knowledge, treatment (test, predictor) is unproven.
*In exceptional cases, one convincing Class I study may suffice for an "A" recommendation if 1) all criteria are met, 2) the magnitude of effect is large (relative rate improved outcome >5 and the lower limit of the confidence interval is >2).
In Children with Epilepsy, Is Using Adjunctive Vagus Nerve Stimulation (VNS) Therapy for Seizure Frequency Reduction Better Than Not Using Adjunctive VNS therapy for Seizure Frequency Reduction?
Conclusion
Based on data from 14 Class III studies, VNS is possibly effective in achieving >50% seizure frequency reduction (responder rate). In the pooled analysis of 481 children, the responder rate was 55% (95% confidence interval [CI] 51%–59%), but there was significant heterogeneity in the data. Two of the 16 studies were not included in the analysis because either they did not provide information about responder rate or they included a significant number (>20%) of adults in their population. The pooled seizure freedom rate was 7% (95% CI 5%–10%).
Recommendation
VNS may be considered as adjunctive treatment for children with partial or generalized epilepsy (Level C).
Clinical Context
VNS may be considered a possibly effective option after a child with medication-resistant epilepsy has been declared a poor surgical candidate or has had unsuccessful surgery.
In Patients with Lennox-Gastaut Syndrome (LGS), Is Using Adjunctive VNS Therapy for Seizure Frequency Reduction Better Than Not Using Adjunctive VNS Therapy for Seizure Frequency Reduction?
Conclusion
Based on data from 4 Class III studies, VNS is possibly effective in achieving >50% seizure frequency reduction in patients with LGS. The pooled analysis of 113 patients with LGS (including data from articles with multiple seizure types where LGS data were parsed out) yielded a 55% (95% CI 46%–64%) responder rate.
Recommendation
VNS may be considered in patients with LGS (Level C).
Clinical Context
The responder rate for patients with LGS does not appear to differ from that of the general population of patients with medication-resistant epilepsy.
In Patients with Epilepsy, Is Using VNS Associated with Mood Improvement?
Conclusion
Based on data from 2 Class III studies, VNS is possibly effective for mood improvement in adults with epilepsy.
Recommendation
In adult patients receiving VNS for epilepsy, improvement in mood may be an additional benefit (Level C).
Clinical Context
Depression is a common comorbidity for people with epilepsy. VNS may provide an additional benefit by improving mood in some patients; however, the potential for mood improvement should be considered a secondary rather than a primary reason for VNS implantation. The evidence does not clearly support an independent effect on mood in this complex population.
In Patients with Epilepsy, Is VNS Use Associated with Reduced Seizure Frequency Over Time?
Conclusion
Based on data from 2 Class III studies, VNS is possibly associated with an increase in ≥50% seizure frequency reduction rates of 7% from 1 to 5 years postimplantation.
Recommendation
VNS may be considered progressively effective in patients over multiple years of exposure (Level C).
Clinical Context
The loss of medication efficacy over time is a challenging aspect of epilepsy management. The evidence of maintained efficacy in the long term and the trend toward improvement over time make VNS an option.
In Patients Undergoing VNS Therapy, Does Rapid Stimulation (Usual VNS Settings Are 7 Seconds "On" and 30 Seconds "Off") Improve Seizure Frequency More Often Than Standard Stimulation Settings (30 Seconds "On" and 300 Seconds "Off")?
Conclusion
These 3 Class III studies were underpowered to detect a difference in efficacy between rapid stimulation (7 seconds "on," 30 seconds "off") used either after standard stimulation (30 seconds "on," 300 seconds "off") was unsuccessful or as an initial treatment setting.
Recommendation
Optimal VNS settings are still unknown, and the evidence is insufficient to support a recommendation for the use of standard stimulation vs. rapid stimulation to reduce seizure occurrence (Level U).
Clinical Context
Rapid cycling increases the duty cycle and hastens the need for battery replacement; therefore, when used, the efficacy of rapid cycling should be carefully assessed.
In Patients Undergoing VNS Therapy, Does Using Additional Magnet-Activated Stimulation Trains for Auras or at Seizure Onset Interrupt Seizures Relative to Not Using Additional Magnet-Induced Stimulation Trains for Auras or at Seizure Onset?
Conclusion
Based on data from 2 Class III studies, seizure abortion with magnet-activated stimulation is possibly associated with overall response to VNS therapy. Based on 3 Class III studies, magnet-activated stimulation may be expected to abort seizures one-fourth to two-thirds of the time when used during seizure auras (one Class III study omitted because it was not generalizable).
Recommendation
Patients may be counseled that VNS magnet activation may be associated with seizure abortion when used at the time of seizure auras (Level C) and that seizure abortion with magnet use may be associated with overall response to VNS treatment (Level C).
In Patients Undergoing VNS Therapy, Have New Safety Concerns Emerged Since the Last Assessment?
Clinical Context
Current physician attention to intraoperative rhythm disturbances from VNS use need not be changed. The paroxysmal nature of epilepsy poses a challenge for identifying a cardiac rhythm disturbance as device-related rather than as an additional seizure manifestation. Video electroencephalogram (EEG) and electrocardiogram (ECG) monitoring of new-onset events that might be cardiac-related would be warranted to exclude this possibility in what is likely to be a small number of patients. Reduced sudden unexpected death in epilepsy (SUDEP) rates over time is an important finding associated with VNS therapy; in a cohort of 1,819 individuals followed 3,176.3 person-years from VNS implantation, the SUDEP rate was 5.5 per 1,000 over the first 2 years but only 1.7 per 1,000 thereafter. The clinical importance of the effect of VNS on sleep apnea and treatment is unclear, but caution regarding VNS use in this setting is suggested.
In Children Undergoing VNS Therapy, Do Adverse Events (AEs) Differ from Those in Adults?
Clinical Context
Children may have greater risk for wound infection than adults due to behaviors more common in children. Extra vigilance in monitoring for occurrence of site infection in children should be undertaken.
Definitions:
Classification of Evidence for Therapeutic Intervention
Class I: A randomized, controlled clinical trial of the intervention of interest with masked or objective outcome assessment, in a representative population. Relevant baseline characteristics are presented and substantially equivalent among treatment groups or there is appropriate statistical adjustment for differences.
The following are also required:
- Concealed allocation
- Primary outcome(s) clearly defined
- Exclusion/inclusion criteria clearly defined
- Adequate accounting for dropouts (with at least 80% of enrolled subjects completing the study) and crossovers with numbers sufficiently low to have minimal potential for bias.
- For noninferiority or equivalence trials claiming to prove efficacy for one or both drugs, the following are also required*
- The authors explicitly state the clinically meaningful difference to be excluded by defining the threshold for equivalence or noninferiority.
- The standard treatment used in the study is substantially similar to that used in previous studies establishing efficacy of the standard treatment (e.g., for a drug, the mode of administration, dose and dosage adjustments are similar to those previously shown to be effective).
- The inclusion and exclusion criteria for patient selection and the outcomes of patients on the standard treatment are comparable to those of previous studies establishing efficacy of the standard treatment.
- The interpretation of the results of the study is based upon a per protocol analysis that takes into account dropouts or crossovers.
Class II: A randomized controlled clinical trial of the intervention of interest in a representative population with masked or objective outcome assessment that lacks one criteria a–e above or a prospective matched cohort study with masked or objective outcome assessment in a representative population that meets b–e above. Relevant baseline characteristics are presented and substantially equivalent among treatment groups or there is appropriate statistical adjustment for differences.
Class III: All other controlled trials (including well-defined natural history controls or patients serving as own controls) in a representative population, where outcome is independently assessed, or independently derived by objective outcome measurement.**
Class IV: Studies not meeting Class I, II, or III criteria including consensus or expert opinion.
*Note that numbers 1-3 in Class Ie are required for Class II in equivalence trials. If any one of the three is missing, the class is automatically downgraded to Class III.
**Objective outcome measurement: an outcome measure that is unlikely to be affected by an observer's (patient, treating physician, investigator) expectation or bias (e.g., blood tests, administrative outcome data).
Classification of Recommendations
Level A = Established as effective, ineffective or harmful (or established as useful/predictive or not useful/predictive) for the given condition in the specified population. (Level A rating requires at least two consistent Class I studies.*)
Level B = Probably effective, ineffective or harmful (or probably useful/predictive or not useful/predictive) for the given condition in the specified population. (Level B rating requires at least one Class I study or two consistent Class II studies.)
Level C = Possibly effective, ineffective or harmful (or possibly useful/predictive or not useful/predictive) for the given condition in the specified population. (Level C rating requires at least one Class II study or two consistent Class III studies.)
Level U = Data inadequate or conflicting; given current knowledge, treatment (test, predictor) is unproven.
*In exceptional cases, one convincing Class I study may suffice for an "A" recommendation if 1) all criteria are met, 2) the magnitude of effect is large (relative rate improved outcome >5 and the lower limit of the confidence interval is >2).
In Children with Epilepsy, Is Using Adjunctive Vagus Nerve Stimulation (VNS) Therapy for Seizure Frequency Reduction Better Than Not Using Adjunctive VNS therapy for Seizure Frequency Reduction?
Conclusion
Based on data from 14 Class III studies, VNS is possibly effective in achieving >50% seizure frequency reduction (responder rate). In the pooled analysis of 481 children, the responder rate was 55% (95% confidence interval [CI] 51%–59%), but there was significant heterogeneity in the data. Two of the 16 studies were not included in the analysis because either they did not provide information about responder rate or they included a significant number (>20%) of adults in their population. The pooled seizure freedom rate was 7% (95% CI 5%–10%).
Recommendation
VNS may be considered as adjunctive treatment for children with partial or generalized epilepsy (Level C).
Clinical Context
VNS may be considered a possibly effective option after a child with medication-resistant epilepsy has been declared a poor surgical candidate or has had unsuccessful surgery.
In Patients with Lennox-Gastaut Syndrome (LGS), Is Using Adjunctive VNS Therapy for Seizure Frequency Reduction Better Than Not Using Adjunctive VNS Therapy for Seizure Frequency Reduction?
Conclusion
Based on data from 4 Class III studies, VNS is possibly effective in achieving >50% seizure frequency reduction in patients with LGS. The pooled analysis of 113 patients with LGS (including data from articles with multiple seizure types where LGS data were parsed out) yielded a 55% (95% CI 46%–64%) responder rate.
Recommendation
VNS may be considered in patients with LGS (Level C).
Clinical Context
The responder rate for patients with LGS does not appear to differ from that of the general population of patients with medication-resistant epilepsy.
In Patients with Epilepsy, Is Using VNS Associated with Mood Improvement?
Conclusion
Based on data from 2 Class III studies, VNS is possibly effective for mood improvement in adults with epilepsy.
Recommendation
In adult patients receiving VNS for epilepsy, improvement in mood may be an additional benefit (Level C).
Clinical Context
Depression is a common comorbidity for people with epilepsy. VNS may provide an additional benefit by improving mood in some patients; however, the potential for mood improvement should be considered a secondary rather than a primary reason for VNS implantation. The evidence does not clearly support an independent effect on mood in this complex population.
In Patients with Epilepsy, Is VNS Use Associated with Reduced Seizure Frequency Over Time?
Conclusion
Based on data from 2 Class III studies, VNS is possibly associated with an increase in ≥50% seizure frequency reduction rates of 7% from 1 to 5 years postimplantation.
Recommendation
VNS may be considered progressively effective in patients over multiple years of exposure (Level C).
Clinical Context
The loss of medication efficacy over time is a challenging aspect of epilepsy management. The evidence of maintained efficacy in the long term and the trend toward improvement over time make VNS an option.
In Patients Undergoing VNS Therapy, Does Rapid Stimulation (Usual VNS Settings Are 7 Seconds "On" and 30 Seconds "Off") Improve Seizure Frequency More Often Than Standard Stimulation Settings (30 Seconds "On" and 300 Seconds "Off")?
Conclusion
These 3 Class III studies were underpowered to detect a difference in efficacy between rapid stimulation (7 seconds "on," 30 seconds "off") used either after standard stimulation (30 seconds "on," 300 seconds "off") was unsuccessful or as an initial treatment setting.
Recommendation
Optimal VNS settings are still unknown, and the evidence is insufficient to support a recommendation for the use of standard stimulation vs. rapid stimulation to reduce seizure occurrence (Level U).
Clinical Context
Rapid cycling increases the duty cycle and hastens the need for battery replacement; therefore, when used, the efficacy of rapid cycling should be carefully assessed.
In Patients Undergoing VNS Therapy, Does Using Additional Magnet-Activated Stimulation Trains for Auras or at Seizure Onset Interrupt Seizures Relative to Not Using Additional Magnet-Induced Stimulation Trains for Auras or at Seizure Onset?
Conclusion
Based on data from 2 Class III studies, seizure abortion with magnet-activated stimulation is possibly associated with overall response to VNS therapy. Based on 3 Class III studies, magnet-activated stimulation may be expected to abort seizures one-fourth to two-thirds of the time when used during seizure auras (one Class III study omitted because it was not generalizable).
Recommendation
Patients may be counseled that VNS magnet activation may be associated with seizure abortion when used at the time of seizure auras (Level C) and that seizure abortion with magnet use may be associated with overall response to VNS treatment (Level C).
In Patients Undergoing VNS Therapy, Have New Safety Concerns Emerged Since the Last Assessment?
Clinical Context
Current physician attention to intraoperative rhythm disturbances from VNS use need not be changed. The paroxysmal nature of epilepsy poses a challenge for identifying a cardiac rhythm disturbance as device-related rather than as an additional seizure manifestation. Video electroencephalogram (EEG) and electrocardiogram (ECG) monitoring of new-onset events that might be cardiac-related would be warranted to exclude this possibility in what is likely to be a small number of patients. Reduced sudden unexpected death in epilepsy (SUDEP) rates over time is an important finding associated with VNS therapy; in a cohort of 1,819 individuals followed 3,176.3 person-years from VNS implantation, the SUDEP rate was 5.5 per 1,000 over the first 2 years but only 1.7 per 1,000 thereafter. The clinical importance of the effect of VNS on sleep apnea and treatment is unclear, but caution regarding VNS use in this setting is suggested.
In Children Undergoing VNS Therapy, Do Adverse Events (AEs) Differ from Those in Adults?
Clinical Context
Children may have greater risk for wound infection than adults due to behaviors more common in children. Extra vigilance in monitoring for occurrence of site infection in children should be undertaken.
Definitions:
Classification of Evidence for Therapeutic Intervention
Class I: A randomized, controlled clinical trial of the intervention of interest with masked or objective outcome assessment, in a representative population. Relevant baseline characteristics are presented and substantially equivalent among treatment groups or there is appropriate statistical adjustment for differences.
The following are also required:
- Concealed allocation
- Primary outcome(s) clearly defined
- Exclusion/inclusion criteria clearly defined
- Adequate accounting for dropouts (with at least 80% of enrolled subjects completing the study) and crossovers with numbers sufficiently low to have minimal potential for bias.
- For noninferiority or equivalence trials claiming to prove efficacy for one or both drugs, the following are also required*
- The authors explicitly state the clinically meaningful difference to be excluded by defining the threshold for equivalence or noninferiority.
- The standard treatment used in the study is substantially similar to that used in previous studies establishing efficacy of the standard treatment (e.g., for a drug, the mode of administration, dose and dosage adjustments are similar to those previously shown to be effective).
- The inclusion and exclusion criteria for patient selection and the outcomes of patients on the standard treatment are comparable to those of previous studies establishing efficacy of the standard treatment.
- The interpretation of the results of the study is based upon a per protocol analysis that takes into account dropouts or crossovers.
Class II: A randomized controlled clinical trial of the intervention of interest in a representative population with masked or objective outcome assessment that lacks one criteria a–e above or a prospective matched cohort study with masked or objective outcome assessment in a representative population that meets b–e above. Relevant baseline characteristics are presented and substantially equivalent among treatment groups or there is appropriate statistical adjustment for differences.
Class III: All other controlled trials (including well-defined natural history controls or patients serving as own controls) in a representative population, where outcome is independently assessed, or independently derived by objective outcome measurement.**
Class IV: Studies not meeting Class I, II, or III criteria including consensus or expert opinion.
*Note that numbers 1-3 in Class Ie are required for Class II in equivalence trials. If any one of the three is missing, the class is automatically downgraded to Class III.
**Objective outcome measurement: an outcome measure that is unlikely to be affected by an observer's (patient, treating physician, investigator) expectation or bias (e.g., blood tests, administrative outcome data).
Classification of Recommendations
Level A = Established as effective, ineffective or harmful (or established as useful/predictive or not useful/predictive) for the given condition in the specified population. (Level A rating requires at least two consistent Class I studies.*)
Level B = Probably effective, ineffective or harmful (or probably useful/predictive or not useful/predictive) for the given condition in the specified population. (Level B rating requires at least one Class I study or two consistent Class II studies.)
Level C = Possibly effective, ineffective or harmful (or possibly useful/predictive or not useful/predictive) for the given condition in the specified population. (Level C rating requires at least one Class II study or two consistent Class III studies.)
Level U = Data inadequate or conflicting; given current knowledge, treatment (test, predictor) is unproven.
*In exceptional cases, one convincing Class I study may suffice for an "A" recommendation if 1) all criteria are met, 2) the magnitude of effect is large (relative rate improved outcome >5 and the lower limit of the confidence interval is >2).
OBJECTIVE: To evaluate the evidence since the 1999 assessment regarding efficacy and safety of vagus nerve stimulation (VNS) for epilepsy, currently approved as adjunctive therapy for partial-onset seizures in patients >12 years.
METHODS: We reviewed the literature and identified relevant published studies. We classified these studies according to the American Academy of Neurology evidence-based methodology.
Guidelines are copyright © 2014 American Academy of Neurology. All rights reserved. The summary is provided by the Agency for Healthcare Research and Quality.
Management of acute atrial fibrillation and atrial flutter in non-pregnant hospitalized adults.
Major Recommendations Note from the University of Michigan Health System (UMHS) and the National Guideline Clearinghouse (NGC): The following guidance was current as of May 2014. Because UMHS occasionally releases minor revisions to its guidance based on new information, users may wish to consult the original guideline document Note from NGC: The following key points summarize the content of the guideline. Refer to the full text of the original guideline document for detailed information on each of the screening procedures. The strength of recommendation (I-III) and levels of evidence (A-D) are defined at the end of the "Major Recommendations" field. Key Points Clinical Presentation Patients presenting with palpitations, irregular pulse, chest pain, dyspnea, fatigue, lightheadedness, syncope, cardio-embolic disease and new or recurrent heart failure should be evaluated for atrial fibrillation/atrial flutter (AF/AFL). While AF may be asymptomatic and found incidentally, AFL is usually highly symptomatic. Diagnosis Electrocardiogram (ECG) is essential in the diagnosis of AF/AFL. The initial evaluation is summarized in Table 1 in the original guideline document and should include:
Treatment Initial treatment of AF/AFL depends on hemodynamic stability. Unstable AF/AFL (refer to Figure 1 in the original guideline document):
Stable AF/AFL (refer to Figure 2 in the original guideline document):
Definitions: Levels of Evidence
Strength of Recommendation
Clinical Algorithm(s) The following algorithms are provided in the original guideline document:
An algorithm titled "Management of acute atrial fibrillation/flutter after thoracic surgery" is also provided in Appendix C in the original guideline document. |
Evidence Supporting the Recommendations Type of Evidence Supporting the Recommendations The type of supporting evidence is identified and graded for selected recommendations (see the "Major Recommendations" field). Conclusions were based on prospective randomized clinical trials (RCTs) if available, to the exclusion of other data; if RCTs were not available, observational studies were admitted to consideration. If no such data were available for a given link in the problem formulation, expert opinion was used to estimate effect size. |
Benefits/Harms of Implementing the Guideline Recommendations Potential Benefits It is hoped that standardization of care will result in improved patient outcomes, shorter length of hospital stay, lower readmission rates, and overall cost savings for the system. Potential Harms
Refer to Table 4 and Appendices A and B in the original guideline document for more information on specific drugs. |
Major Recommendations Note from the University of Michigan Health System (UMHS) and the National Guideline Clearinghouse (NGC): The following guidance was current as of May 2014. Because UMHS occasionally releases minor revisions to its guidance based on new information, users may wish to consult the original guideline document Note from NGC: The following key points summarize the content of the guideline. Refer to the full text of the original guideline document for detailed information on each of the screening procedures. The strength of recommendation (I-III) and levels of evidence (A-D) are defined at the end of the "Major Recommendations" field. Key Points Clinical Presentation Patients presenting with palpitations, irregular pulse, chest pain, dyspnea, fatigue, lightheadedness, syncope, cardio-embolic disease and new or recurrent heart failure should be evaluated for atrial fibrillation/atrial flutter (AF/AFL). While AF may be asymptomatic and found incidentally, AFL is usually highly symptomatic. Diagnosis Electrocardiogram (ECG) is essential in the diagnosis of AF/AFL. The initial evaluation is summarized in Table 1 in the original guideline document and should include:
Treatment Initial treatment of AF/AFL depends on hemodynamic stability. Unstable AF/AFL (refer to Figure 1 in the original guideline document):
Stable AF/AFL (refer to Figure 2 in the original guideline document):
Definitions: Levels of Evidence
Strength of Recommendation
Clinical Algorithm(s) The following algorithms are provided in the original guideline document:
An algorithm titled "Management of acute atrial fibrillation/flutter after thoracic surgery" is also provided in Appendix C in the original guideline document. |
Evidence Supporting the Recommendations Type of Evidence Supporting the Recommendations The type of supporting evidence is identified and graded for selected recommendations (see the "Major Recommendations" field). Conclusions were based on prospective randomized clinical trials (RCTs) if available, to the exclusion of other data; if RCTs were not available, observational studies were admitted to consideration. If no such data were available for a given link in the problem formulation, expert opinion was used to estimate effect size. |
Benefits/Harms of Implementing the Guideline Recommendations Potential Benefits It is hoped that standardization of care will result in improved patient outcomes, shorter length of hospital stay, lower readmission rates, and overall cost savings for the system. Potential Harms
Refer to Table 4 and Appendices A and B in the original guideline document for more information on specific drugs. |
Major Recommendations Note from the University of Michigan Health System (UMHS) and the National Guideline Clearinghouse (NGC): The following guidance was current as of May 2014. Because UMHS occasionally releases minor revisions to its guidance based on new information, users may wish to consult the original guideline document Note from NGC: The following key points summarize the content of the guideline. Refer to the full text of the original guideline document for detailed information on each of the screening procedures. The strength of recommendation (I-III) and levels of evidence (A-D) are defined at the end of the "Major Recommendations" field. Key Points Clinical Presentation Patients presenting with palpitations, irregular pulse, chest pain, dyspnea, fatigue, lightheadedness, syncope, cardio-embolic disease and new or recurrent heart failure should be evaluated for atrial fibrillation/atrial flutter (AF/AFL). While AF may be asymptomatic and found incidentally, AFL is usually highly symptomatic. Diagnosis Electrocardiogram (ECG) is essential in the diagnosis of AF/AFL. The initial evaluation is summarized in Table 1 in the original guideline document and should include:
Treatment Initial treatment of AF/AFL depends on hemodynamic stability. Unstable AF/AFL (refer to Figure 1 in the original guideline document):
Stable AF/AFL (refer to Figure 2 in the original guideline document):
Definitions: Levels of Evidence
Strength of Recommendation
Clinical Algorithm(s) The following algorithms are provided in the original guideline document:
An algorithm titled "Management of acute atrial fibrillation/flutter after thoracic surgery" is also provided in Appendix C in the original guideline document. |
Evidence Supporting the Recommendations Type of Evidence Supporting the Recommendations The type of supporting evidence is identified and graded for selected recommendations (see the "Major Recommendations" field). Conclusions were based on prospective randomized clinical trials (RCTs) if available, to the exclusion of other data; if RCTs were not available, observational studies were admitted to consideration. If no such data were available for a given link in the problem formulation, expert opinion was used to estimate effect size. |
Benefits/Harms of Implementing the Guideline Recommendations Potential Benefits It is hoped that standardization of care will result in improved patient outcomes, shorter length of hospital stay, lower readmission rates, and overall cost savings for the system. Potential Harms
Refer to Table 4 and Appendices A and B in the original guideline document for more information on specific drugs. |
OBJECTIVE: To provide an evidence-based blue print for the acute care of patients with atrial fibrillation (AF) and atrial flutter (AFL) at the University of Michigan Health System and to assure consistent care delivery for patients with AF across the inpatient services.
Guidelines are copyright © 2014 University of Michigan Health System. All rights reserved. The summary is provided by the Agency for Healthcare Research and Quality.