User login
Emerging treatments for molluscum contagiosum and acne show promise
, but that could soon change, according to Leon H. Kircik, MD.
“The treatment of molluscum is still an unmet need,” Dr. Kircik, clinical professor of dermatology at the Icahn School of Medicine at Mount Sinai, New York, said at the Orlando Dermatology Aesthetic and Clinical Conference. However, a proprietary drug-device combination of cantharidin 0.7% administered through a single-use precision applicator, which has been tested in phase 3 studies, is currently under FDA review. The manufacturer, Verrica Pharmaceuticals resubmitted a new drug application for the product, VP-102, in December 2020.
“VP-102 features a visualization agent so the injector can see which lesions have been treated, as well as a bittering agent to mitigate oral ingestion by children. Complete clearance at 12 weeks ranged from 46% to 54% of patients, while lesion count reduction compared with baseline ranged from 69% to 82%.”
Acne
In August, 2020, clascoterone 1% cream was approved for the treatment of acne in patients 12 years and older, a development that Dr. Kircik said “can be a game changer in acne treatment.” Clascoterone cream 1% exhibits strong, selective anti-androgen activity by targeting androgen receptors in the skin, not systemically. “It limits or blocks transcription of androgen responsive genes, but it also has an anti-inflammatory effect and an anti-sebum effect,” he explained.
According to results from two phase 3 trials of the product, a response of clear or almost clear on the IGA scale at week 12 was achieved in 18.4% of those on treatment vs. 9% of those on vehicle in one study (P less than .001) and 20.3% vs. 6.5%, respectively, in the second study (P less than .001). Clascoterone is also being evaluated for treating androgenetic alopecia.
In Dr. Kircik’s clinical experience, retinoids can be helpful for patients with moderate to severe acne. “We always use them for anticomedogenic effects, but we also know that they have anti-inflammatory effects,” he said. “They actually inhibit toll-like receptor activity. They also inhibit the AP-1 pathway by causing a reduction in inflammatory signaling associated with collagen degradation and scarring.”
The most recent retinoid to be approved for the topical treatment of acne was 0.005% trifarotene cream, in 2019, for patients aged 9 years and older. “But when we got the results, it was not that exciting,” a difference of about 3.6 (mean) inflammatory lesion reduction between the active and the vehicle arm, said Dr. Kircik, medical director of Physicians Skin Care in Louisville, Ky. “According to the package insert, treatment side effects included mild to moderate erythema in 59% of patients, scaling in 65%, dryness in 69%, and stinging/burning in 56%, which makes it difficult to use in our clinical practice.”
The drug was also tested for treating truncal acne. However, one comparative study showed that tazarotene 0.045% lotion spread an average of 36.7 square centimeters farther than the trifarotene cream, which makes the tazarotene lotion easier to use on the chest and back, he said.
Dr. Kircik also discussed 4% minocycline, a hydrophobic, topical foam formulation of minocycline that was approved by the FDA in 2019 for the treatment of moderate to severe acne, for patients aged 9 and older. In a 12-week study that involved 1,488 patients (mean age was about 20 years), investigators observed a 56% reduction in inflammatory lesion count among those treated with minocycline 4%, compared with 43% in the vehicle group.
Dr. Kircik, one of the authors of the study, noted that the hydrophobic composition of minocycline 4% allows for stable and efficient delivery of an inherently unstable active pharmaceutical ingredient such as minocycline. “It’s free of primary irritants such as surfactants and short chain alcohols, which makes it much more tolerable,” he said. “The unique physical foam characteristics facilitate ease of application and absorption at target sites.”
Dr. Kircik reported that he serves as a consultant and/or adviser to numerous pharmaceutical companies, including Galderma, the manufacturer of trifarotene cream.
[email protected]
, but that could soon change, according to Leon H. Kircik, MD.
“The treatment of molluscum is still an unmet need,” Dr. Kircik, clinical professor of dermatology at the Icahn School of Medicine at Mount Sinai, New York, said at the Orlando Dermatology Aesthetic and Clinical Conference. However, a proprietary drug-device combination of cantharidin 0.7% administered through a single-use precision applicator, which has been tested in phase 3 studies, is currently under FDA review. The manufacturer, Verrica Pharmaceuticals resubmitted a new drug application for the product, VP-102, in December 2020.
“VP-102 features a visualization agent so the injector can see which lesions have been treated, as well as a bittering agent to mitigate oral ingestion by children. Complete clearance at 12 weeks ranged from 46% to 54% of patients, while lesion count reduction compared with baseline ranged from 69% to 82%.”
Acne
In August, 2020, clascoterone 1% cream was approved for the treatment of acne in patients 12 years and older, a development that Dr. Kircik said “can be a game changer in acne treatment.” Clascoterone cream 1% exhibits strong, selective anti-androgen activity by targeting androgen receptors in the skin, not systemically. “It limits or blocks transcription of androgen responsive genes, but it also has an anti-inflammatory effect and an anti-sebum effect,” he explained.
According to results from two phase 3 trials of the product, a response of clear or almost clear on the IGA scale at week 12 was achieved in 18.4% of those on treatment vs. 9% of those on vehicle in one study (P less than .001) and 20.3% vs. 6.5%, respectively, in the second study (P less than .001). Clascoterone is also being evaluated for treating androgenetic alopecia.
In Dr. Kircik’s clinical experience, retinoids can be helpful for patients with moderate to severe acne. “We always use them for anticomedogenic effects, but we also know that they have anti-inflammatory effects,” he said. “They actually inhibit toll-like receptor activity. They also inhibit the AP-1 pathway by causing a reduction in inflammatory signaling associated with collagen degradation and scarring.”
The most recent retinoid to be approved for the topical treatment of acne was 0.005% trifarotene cream, in 2019, for patients aged 9 years and older. “But when we got the results, it was not that exciting,” a difference of about 3.6 (mean) inflammatory lesion reduction between the active and the vehicle arm, said Dr. Kircik, medical director of Physicians Skin Care in Louisville, Ky. “According to the package insert, treatment side effects included mild to moderate erythema in 59% of patients, scaling in 65%, dryness in 69%, and stinging/burning in 56%, which makes it difficult to use in our clinical practice.”
The drug was also tested for treating truncal acne. However, one comparative study showed that tazarotene 0.045% lotion spread an average of 36.7 square centimeters farther than the trifarotene cream, which makes the tazarotene lotion easier to use on the chest and back, he said.
Dr. Kircik also discussed 4% minocycline, a hydrophobic, topical foam formulation of minocycline that was approved by the FDA in 2019 for the treatment of moderate to severe acne, for patients aged 9 and older. In a 12-week study that involved 1,488 patients (mean age was about 20 years), investigators observed a 56% reduction in inflammatory lesion count among those treated with minocycline 4%, compared with 43% in the vehicle group.
Dr. Kircik, one of the authors of the study, noted that the hydrophobic composition of minocycline 4% allows for stable and efficient delivery of an inherently unstable active pharmaceutical ingredient such as minocycline. “It’s free of primary irritants such as surfactants and short chain alcohols, which makes it much more tolerable,” he said. “The unique physical foam characteristics facilitate ease of application and absorption at target sites.”
Dr. Kircik reported that he serves as a consultant and/or adviser to numerous pharmaceutical companies, including Galderma, the manufacturer of trifarotene cream.
[email protected]
, but that could soon change, according to Leon H. Kircik, MD.
“The treatment of molluscum is still an unmet need,” Dr. Kircik, clinical professor of dermatology at the Icahn School of Medicine at Mount Sinai, New York, said at the Orlando Dermatology Aesthetic and Clinical Conference. However, a proprietary drug-device combination of cantharidin 0.7% administered through a single-use precision applicator, which has been tested in phase 3 studies, is currently under FDA review. The manufacturer, Verrica Pharmaceuticals resubmitted a new drug application for the product, VP-102, in December 2020.
“VP-102 features a visualization agent so the injector can see which lesions have been treated, as well as a bittering agent to mitigate oral ingestion by children. Complete clearance at 12 weeks ranged from 46% to 54% of patients, while lesion count reduction compared with baseline ranged from 69% to 82%.”
Acne
In August, 2020, clascoterone 1% cream was approved for the treatment of acne in patients 12 years and older, a development that Dr. Kircik said “can be a game changer in acne treatment.” Clascoterone cream 1% exhibits strong, selective anti-androgen activity by targeting androgen receptors in the skin, not systemically. “It limits or blocks transcription of androgen responsive genes, but it also has an anti-inflammatory effect and an anti-sebum effect,” he explained.
According to results from two phase 3 trials of the product, a response of clear or almost clear on the IGA scale at week 12 was achieved in 18.4% of those on treatment vs. 9% of those on vehicle in one study (P less than .001) and 20.3% vs. 6.5%, respectively, in the second study (P less than .001). Clascoterone is also being evaluated for treating androgenetic alopecia.
In Dr. Kircik’s clinical experience, retinoids can be helpful for patients with moderate to severe acne. “We always use them for anticomedogenic effects, but we also know that they have anti-inflammatory effects,” he said. “They actually inhibit toll-like receptor activity. They also inhibit the AP-1 pathway by causing a reduction in inflammatory signaling associated with collagen degradation and scarring.”
The most recent retinoid to be approved for the topical treatment of acne was 0.005% trifarotene cream, in 2019, for patients aged 9 years and older. “But when we got the results, it was not that exciting,” a difference of about 3.6 (mean) inflammatory lesion reduction between the active and the vehicle arm, said Dr. Kircik, medical director of Physicians Skin Care in Louisville, Ky. “According to the package insert, treatment side effects included mild to moderate erythema in 59% of patients, scaling in 65%, dryness in 69%, and stinging/burning in 56%, which makes it difficult to use in our clinical practice.”
The drug was also tested for treating truncal acne. However, one comparative study showed that tazarotene 0.045% lotion spread an average of 36.7 square centimeters farther than the trifarotene cream, which makes the tazarotene lotion easier to use on the chest and back, he said.
Dr. Kircik also discussed 4% minocycline, a hydrophobic, topical foam formulation of minocycline that was approved by the FDA in 2019 for the treatment of moderate to severe acne, for patients aged 9 and older. In a 12-week study that involved 1,488 patients (mean age was about 20 years), investigators observed a 56% reduction in inflammatory lesion count among those treated with minocycline 4%, compared with 43% in the vehicle group.
Dr. Kircik, one of the authors of the study, noted that the hydrophobic composition of minocycline 4% allows for stable and efficient delivery of an inherently unstable active pharmaceutical ingredient such as minocycline. “It’s free of primary irritants such as surfactants and short chain alcohols, which makes it much more tolerable,” he said. “The unique physical foam characteristics facilitate ease of application and absorption at target sites.”
Dr. Kircik reported that he serves as a consultant and/or adviser to numerous pharmaceutical companies, including Galderma, the manufacturer of trifarotene cream.
[email protected]
FROM ODAC 2021
What’s best for filler injection, needle or cannula?
“You may be a needle person or a cannula person, but it doesn’t have to be that way,” he said during the Orlando Dermatology Aesthetic and Clinical Conference. “There are pros and cons of both techniques, but I think there’s a place for both.”
With a sharp needle, placement of the tip is considered precise, especially when delivering a supraperiosteal injection. “From a learning curve, especially for us as dermatologists, it’s easier because we’re used to injecting lidocaine, and we’re using needles on a day-to-day basis for injectables and other applications,” said Dr. Keaney, a dermatologist who is founder and director of SkinDC in Arlington, Va. “However, use of a needle is traumatic; it creates an increased risk of bruising and we’re cutting through tissue. We can potentially puncture a blood vessel and create a vascular event.”
Clinicians may consider filler delivery by sharp needle as being more precise, but in an observational cadaver study of cannula vs. sharp needle for placement of tissue fillers, investigators found an increased risk for spread of filler to more superficial layers along the needle trajectory, as well as a higher risk of intra-arterial injection. “This may explain why, when you’re injecting on a tear trough, you may still get some swelling in the area,” Dr. Keaney said. “You may see some swelling and some product, because it’s tracking along the injection point. One can argue that you can reduce this risk by using a longer needle or cannula.”
With a longer cannula, the blunt tips may act to displace blood vessels rather than to lacerate them. “They allow for greater coverage through fewer injection points and they approach the injection site at a more oblique angle, so it’s harder for the product to track,” he explained. “Cannula patients tend to faint on me a lot more than my needle patients do, so while the cannula may be more comfortable, it can be more nerve-wracking for patients.”
Recent studies have shown that with cannula proficiency, clinicians can achieve results on par with using sharp needles for dermal filler treatments (Dermatol Surg. 2020 Apr;46[4]:465-72; Dermatol Surg. 2012 Feb;38[2]:207-14). A recent head-to-head comparison found no significant differences in the use of needles vs. cannulas for the treatment of the dorsal hand with diluted calcium hydroxylapatite, though patients reported 12% greater satisfaction with the cannula technique (Dermatol Surg. 2020 Oct;46 Suppl 1:S54-61).
“Based on these articles, we can feel comfortable that with proficient use, you can deliver similar results with the cannula as you would with the needle,” said Dr. Keaney, a clinical associate faculty member in the department of dermatology at George Washington University, Washington. “As a result, we are seeing Food and Drug Administration–approved indications for the use of cannulas for dermal fillers: Restylane Silk for lips, Restylane Lyft for cheeks, Juvederm Voluma for cheeks, and Juvederm Voluma for the chin.”
Such emerging data present a conundrum, though. If someone is comfortable injecting dermal filler with needles, why switch to using cannulas? After all, a case study reported arterial penetration with blunt-tipped cannulas using injectables . “Cannulas are not 100% safe,” Dr. Keaney said. “One of my mentors once said, “If a vascular event has not happened to you yet, you have not injected enough. These things can happen even in the most experienced hands, whether you use a needle or a cannula.”
However, safety data from a recently published retrospective study demonstrated that cannulas are less likely to be associated with occlusions compared with needles (a risk of 1 occlusion per 40,882 injections vs. 1 occlusion per 6,410 injections (P less than .001).
“Cannulas are generally safer because the blunt tip kind of dissects tissue and pushes vessels away,” he said. “That doesn’t mean it can’t get into a vessel, it just requires greater force to penetrate facial arteries with a cannula. Finer tips may be easier to use.”
Larger cannulas can tear into an arterial wall when the artery wall is relatively fixed, so it cannot slide aside enough to avoid injury, Dr. Keaney continued. “Arterial location perpendicular to cannula trajectory carries the most risk,” he said. Meanwhile, filler-induced blindness, which he characterized as “the worst possible outcome,” is often due to the retrograde embolization of the product. This can occur with injection pressures greater than the sum of the systolic arterial pressure and the frictional forces due to viscous flow.
Dr. Keaney said he uses both needles and cannulas in his clinical practice. “I use a needle to inject on bone if I want to mimic bony projections along the zygomatic arch or jawline or chin,” he said. “I think a needle can get those boluses to develop that projection that you want. If I’m injecting within soft tissue plane, I use a 22 G cannula and keep the cannula moving within the tissue. I inject slowly and less than 0.2 cc per bolus. I compress when injecting on the nose and I’m cautious to inject previous patients who have undergone plastic surgery or in areas of previous scarring.”
Dr. Keaney reported that he is a consultant to and/or an advisory board member for several pharmaceutical companies.
“You may be a needle person or a cannula person, but it doesn’t have to be that way,” he said during the Orlando Dermatology Aesthetic and Clinical Conference. “There are pros and cons of both techniques, but I think there’s a place for both.”
With a sharp needle, placement of the tip is considered precise, especially when delivering a supraperiosteal injection. “From a learning curve, especially for us as dermatologists, it’s easier because we’re used to injecting lidocaine, and we’re using needles on a day-to-day basis for injectables and other applications,” said Dr. Keaney, a dermatologist who is founder and director of SkinDC in Arlington, Va. “However, use of a needle is traumatic; it creates an increased risk of bruising and we’re cutting through tissue. We can potentially puncture a blood vessel and create a vascular event.”
Clinicians may consider filler delivery by sharp needle as being more precise, but in an observational cadaver study of cannula vs. sharp needle for placement of tissue fillers, investigators found an increased risk for spread of filler to more superficial layers along the needle trajectory, as well as a higher risk of intra-arterial injection. “This may explain why, when you’re injecting on a tear trough, you may still get some swelling in the area,” Dr. Keaney said. “You may see some swelling and some product, because it’s tracking along the injection point. One can argue that you can reduce this risk by using a longer needle or cannula.”
With a longer cannula, the blunt tips may act to displace blood vessels rather than to lacerate them. “They allow for greater coverage through fewer injection points and they approach the injection site at a more oblique angle, so it’s harder for the product to track,” he explained. “Cannula patients tend to faint on me a lot more than my needle patients do, so while the cannula may be more comfortable, it can be more nerve-wracking for patients.”
Recent studies have shown that with cannula proficiency, clinicians can achieve results on par with using sharp needles for dermal filler treatments (Dermatol Surg. 2020 Apr;46[4]:465-72; Dermatol Surg. 2012 Feb;38[2]:207-14). A recent head-to-head comparison found no significant differences in the use of needles vs. cannulas for the treatment of the dorsal hand with diluted calcium hydroxylapatite, though patients reported 12% greater satisfaction with the cannula technique (Dermatol Surg. 2020 Oct;46 Suppl 1:S54-61).
“Based on these articles, we can feel comfortable that with proficient use, you can deliver similar results with the cannula as you would with the needle,” said Dr. Keaney, a clinical associate faculty member in the department of dermatology at George Washington University, Washington. “As a result, we are seeing Food and Drug Administration–approved indications for the use of cannulas for dermal fillers: Restylane Silk for lips, Restylane Lyft for cheeks, Juvederm Voluma for cheeks, and Juvederm Voluma for the chin.”
Such emerging data present a conundrum, though. If someone is comfortable injecting dermal filler with needles, why switch to using cannulas? After all, a case study reported arterial penetration with blunt-tipped cannulas using injectables . “Cannulas are not 100% safe,” Dr. Keaney said. “One of my mentors once said, “If a vascular event has not happened to you yet, you have not injected enough. These things can happen even in the most experienced hands, whether you use a needle or a cannula.”
However, safety data from a recently published retrospective study demonstrated that cannulas are less likely to be associated with occlusions compared with needles (a risk of 1 occlusion per 40,882 injections vs. 1 occlusion per 6,410 injections (P less than .001).
“Cannulas are generally safer because the blunt tip kind of dissects tissue and pushes vessels away,” he said. “That doesn’t mean it can’t get into a vessel, it just requires greater force to penetrate facial arteries with a cannula. Finer tips may be easier to use.”
Larger cannulas can tear into an arterial wall when the artery wall is relatively fixed, so it cannot slide aside enough to avoid injury, Dr. Keaney continued. “Arterial location perpendicular to cannula trajectory carries the most risk,” he said. Meanwhile, filler-induced blindness, which he characterized as “the worst possible outcome,” is often due to the retrograde embolization of the product. This can occur with injection pressures greater than the sum of the systolic arterial pressure and the frictional forces due to viscous flow.
Dr. Keaney said he uses both needles and cannulas in his clinical practice. “I use a needle to inject on bone if I want to mimic bony projections along the zygomatic arch or jawline or chin,” he said. “I think a needle can get those boluses to develop that projection that you want. If I’m injecting within soft tissue plane, I use a 22 G cannula and keep the cannula moving within the tissue. I inject slowly and less than 0.2 cc per bolus. I compress when injecting on the nose and I’m cautious to inject previous patients who have undergone plastic surgery or in areas of previous scarring.”
Dr. Keaney reported that he is a consultant to and/or an advisory board member for several pharmaceutical companies.
“You may be a needle person or a cannula person, but it doesn’t have to be that way,” he said during the Orlando Dermatology Aesthetic and Clinical Conference. “There are pros and cons of both techniques, but I think there’s a place for both.”
With a sharp needle, placement of the tip is considered precise, especially when delivering a supraperiosteal injection. “From a learning curve, especially for us as dermatologists, it’s easier because we’re used to injecting lidocaine, and we’re using needles on a day-to-day basis for injectables and other applications,” said Dr. Keaney, a dermatologist who is founder and director of SkinDC in Arlington, Va. “However, use of a needle is traumatic; it creates an increased risk of bruising and we’re cutting through tissue. We can potentially puncture a blood vessel and create a vascular event.”
Clinicians may consider filler delivery by sharp needle as being more precise, but in an observational cadaver study of cannula vs. sharp needle for placement of tissue fillers, investigators found an increased risk for spread of filler to more superficial layers along the needle trajectory, as well as a higher risk of intra-arterial injection. “This may explain why, when you’re injecting on a tear trough, you may still get some swelling in the area,” Dr. Keaney said. “You may see some swelling and some product, because it’s tracking along the injection point. One can argue that you can reduce this risk by using a longer needle or cannula.”
With a longer cannula, the blunt tips may act to displace blood vessels rather than to lacerate them. “They allow for greater coverage through fewer injection points and they approach the injection site at a more oblique angle, so it’s harder for the product to track,” he explained. “Cannula patients tend to faint on me a lot more than my needle patients do, so while the cannula may be more comfortable, it can be more nerve-wracking for patients.”
Recent studies have shown that with cannula proficiency, clinicians can achieve results on par with using sharp needles for dermal filler treatments (Dermatol Surg. 2020 Apr;46[4]:465-72; Dermatol Surg. 2012 Feb;38[2]:207-14). A recent head-to-head comparison found no significant differences in the use of needles vs. cannulas for the treatment of the dorsal hand with diluted calcium hydroxylapatite, though patients reported 12% greater satisfaction with the cannula technique (Dermatol Surg. 2020 Oct;46 Suppl 1:S54-61).
“Based on these articles, we can feel comfortable that with proficient use, you can deliver similar results with the cannula as you would with the needle,” said Dr. Keaney, a clinical associate faculty member in the department of dermatology at George Washington University, Washington. “As a result, we are seeing Food and Drug Administration–approved indications for the use of cannulas for dermal fillers: Restylane Silk for lips, Restylane Lyft for cheeks, Juvederm Voluma for cheeks, and Juvederm Voluma for the chin.”
Such emerging data present a conundrum, though. If someone is comfortable injecting dermal filler with needles, why switch to using cannulas? After all, a case study reported arterial penetration with blunt-tipped cannulas using injectables . “Cannulas are not 100% safe,” Dr. Keaney said. “One of my mentors once said, “If a vascular event has not happened to you yet, you have not injected enough. These things can happen even in the most experienced hands, whether you use a needle or a cannula.”
However, safety data from a recently published retrospective study demonstrated that cannulas are less likely to be associated with occlusions compared with needles (a risk of 1 occlusion per 40,882 injections vs. 1 occlusion per 6,410 injections (P less than .001).
“Cannulas are generally safer because the blunt tip kind of dissects tissue and pushes vessels away,” he said. “That doesn’t mean it can’t get into a vessel, it just requires greater force to penetrate facial arteries with a cannula. Finer tips may be easier to use.”
Larger cannulas can tear into an arterial wall when the artery wall is relatively fixed, so it cannot slide aside enough to avoid injury, Dr. Keaney continued. “Arterial location perpendicular to cannula trajectory carries the most risk,” he said. Meanwhile, filler-induced blindness, which he characterized as “the worst possible outcome,” is often due to the retrograde embolization of the product. This can occur with injection pressures greater than the sum of the systolic arterial pressure and the frictional forces due to viscous flow.
Dr. Keaney said he uses both needles and cannulas in his clinical practice. “I use a needle to inject on bone if I want to mimic bony projections along the zygomatic arch or jawline or chin,” he said. “I think a needle can get those boluses to develop that projection that you want. If I’m injecting within soft tissue plane, I use a 22 G cannula and keep the cannula moving within the tissue. I inject slowly and less than 0.2 cc per bolus. I compress when injecting on the nose and I’m cautious to inject previous patients who have undergone plastic surgery or in areas of previous scarring.”
Dr. Keaney reported that he is a consultant to and/or an advisory board member for several pharmaceutical companies.
FROM ODAC 2021
Expert calls for paradigm shift in lab monitoring of some dermatology drugs
From time to time, Joslyn Kirby, MD, asks other physicians about their experience with certain medications used in dermatology, especially when something new hits the market.
“Sometimes I get an answer like, ‘The last time I used that medicine, my patient needed a liver transplant,’ ” Dr. Kirby, associate professor of dermatology, Penn State University, Hershey, said during the Orlando Dermatology Aesthetic and Clinical Conference. “It’s typically a story of something rare, uncommon, and awful. The challenge with an anecdote is that for all its power, it has a lower level of evidence. But it sticks with us and influences us more than a better level of evidence because it’s a situation and a story that we might relate to.”
Dr. Kirby said that when she thinks about managing side effects from drugs used in dermatology, it usually relates to something common and low-risk such as sore, dry skin with isotretinoin use. In contrast, if there is an uncommon but serious side effect, then mitigation rather than management is key. “I want to mitigate the risk – meaning warn my patient about it or be careful about how I select my patients when it is a serious side effect that happens infrequently,” she said. “The worst combination is a frequent and severe side effect. That is something we should avoid, for sure.”
Isotretinoin
But another aspect of prescribing a new drug for patients can be less clear-cut, Dr. Kirby continued, such as the rationale for routine lab monitoring. She began by discussing one of her male patients with moderate to severe acne. After he failed oral antibiotics and topical retinoids, she recommended isotretinoin, which carries a risk of hypertriglyceridemia-associated pancreatitis. “Early in my career, I was getting a lot of monthly labs in patients on this drug that were totally normal and not influencing my practice,” Dr. Kirby recalled. “We’ve seen studies coming out on isotretinoin lab monitoring, showing us that we can keep our patients safe and that we really don’t need to be checking labs as often, because lab changes are infrequent.”
In one of those studies, researchers evaluated 1,863 patients treated with isotretinoin for acne between Jan. 1, 2008, and June 30, 2017 (J Am Acad Dermatol. 2020 Jan;82[1]:72-9).Over time, fewer than 1% of patients screened developed grade 3 or greater triglyceride testing abnormalities, while fewer than 0.5% developed liver function testing (LFT) abnormalities. Authors of a separate systematic review concluded that for patients on isotretinoin therapy without elevated baseline triglycerides, or risk thereof, monitoring triglycerides is of little value (Br J Dermatol. 2017 Oct;177[4]:960-6). Of the 25 patients in the analysis who developed pancreatitis on isotretinoin, only 3 had elevated triglycerides at baseline.
“I was taught that I need to check triglycerides frequently due to the risk of pancreatitis developing with isotretinoin use,” Dr. Kirby said. “Lipid changes on therapy are expected, but they tend to peak early, meaning the first 3 months of treatment when we’re ramping up from a starting dose to a maintenance dose. It’s rare for somebody to be a late bloomer, meaning that they have totally normal labs in the first 3 months and then suddenly develop an abnormality. People are either going to demonstrate an abnormality early or not have one at all.”
When Dr. Kirby starts patients on isotretinoin, she orders baseline LFTs and a lipid panel and repeats them 60 days later. “If everything is fine or only mildly high, we don’t do more testing, only a review of systems,” she said. “This is valuable to our patients because fear of needles and fainting peak during adolescence.”
Spironolactone
The clinical use of regularly monitoring potassium levels in young women taking spironolactone for acne has also been questioned. The drug has been linked to an increased risk for hyperkalemia, but the prevalence is unclear. “I got a lot of normal potassium levels in these patients [when] I was in training and I really questioned, ‘Why am I doing this? What is the rationale?’ ” Dr. Kirby said.
In a study that informed her own practice, researchers reviewed the rate of hyperkalemia in 974 healthy young women taking spironolactone for acne or for an endocrine disorder with associated acne between Dec. 1, 2000, and March 31, 2014 (JAMA Dermatol. 2015 Sep;151[9]:941-4). Of the total of 1,802 serum potassium measurements taken during treatment, 13 (0.72%) were mildly elevated levels and none of the patients had a potassium level above 5.5 mEq/L. Retesting within 1 to 3 weeks in 6 of 13 patients with elevated levels found that potassium levels were normal. “The recommendation for spironolactone in healthy women is not to check the potassium level,” Dr. Kirby said, adding that she does counsel patients about the risk of breast tenderness (which can occur 5% to 40% of the time) and spotting (which can occur in 10% to 20% of patients). Gynecomastia can occur in 10% to 30% of men, which is one of the reasons she does not use spironolactone in male patients.
TB testing and biologics
Whether or not to test for TB in patients with psoriasis taking biologic therapies represents another conundrum, she continued. Patients taking biologics are at risk of reactivation of latent TB infection, but in her experience, package inserts contain language like “perform TB testing at baseline, then periodically,” or “use at baseline, then with active TB symptoms,” and “after treatment is discontinued.”
“What the inserts didn’t recommend was to perform TB testing every year, which is what my routine had been,” Dr. Kirby said. “In the United States, thankfully we don’t have a lot of TB.” In a study that informed her own practice, researchers at a single academic medical center retrospectively reviewed the TB seroconversion rate among 316 patients treated with second-generation biologics (J Am Acad Dermatol. 2020 Oct 1;S0190-9622[20]32676-1. doi: 10.1016/j.jaad.2020.09.075). It found that only six patients (2%) converted and had a positive TB test later during treatment with the biologic. “Of these six people, all had grown up outside the U.S., had traveled outside of the U.S., or were in a group living situation,” said Dr. Kirby, who was not affiliated with the study.
“This informs our rationale for how we can do this testing. If insurance requires it every year, fine. But if they don’t, I ask patients about travel, about their living situation, and how they’re feeling. If everything’s going great, I don’t order TB testing. I do favor the interferon-gamma release assays because they’re a lot more effective than PPDs [purified protein derivative skin tests]. Also, PPDs are difficult for patients who have a low rate of returning to have that test read.”
Terbinafine for onychomycosis
Dr. Kirby also discussed the rationale for ordering regular LFTs in patients taking terbinafine for onychomycosis. “There is a risk of drug-induced liver injury from taking terbinafine, but it’s rare,” she said. “Can we be thoughtful about which patients we expose?”
Evidence suggests that patients with hyperkeratosis greater than 2 mm, with nail matrix involvement, with 50% or more of the nail involved, or having concomitant peripheral vascular disease and diabetes are recalcitrant to treatment with terbinafine
(J Am Acad Dermatol. 2019 Apr;80[4]:853-67). “If we can frame this risk, then we can frame it for our patients,” she said. “We’re more likely to cause liver injury with an antibiotic. When it comes to an oral antifungal, itraconazole is more likely than terbinafine to cause liver injury. The rate of liver injury with terbinafine is only about 2 out of 100,000. It’s five times more likely with itraconazole and 21 times more likely with Augmentin.”
She recommends obtaining a baseline LFT in patients starting terbinafine therapy “to make sure their liver is normal from the start.” In addition, she advised, “let them know that there is a TB seroconversion risk of about 1 in 50,000 people, and that if it happens there would be symptomatic changes. They would maybe notice pruritus and have a darkening in their urine, and they’d have some flu-like symptoms, which would mean stop the drug and get some care.”
Dr. Kirby emphasized that a patient’s propensity for developing drug-induced liver injury from terbinafine use is not predictable from LFT monitoring. “What you’re more likely to find is an asymptomatic LFT rise in about 1% of people,” she said.
She disclosed that she has received honoraria from AbbVie, ChemoCentryx, Incyte, Janssen, Novartis, and UCB Pharma.
From time to time, Joslyn Kirby, MD, asks other physicians about their experience with certain medications used in dermatology, especially when something new hits the market.
“Sometimes I get an answer like, ‘The last time I used that medicine, my patient needed a liver transplant,’ ” Dr. Kirby, associate professor of dermatology, Penn State University, Hershey, said during the Orlando Dermatology Aesthetic and Clinical Conference. “It’s typically a story of something rare, uncommon, and awful. The challenge with an anecdote is that for all its power, it has a lower level of evidence. But it sticks with us and influences us more than a better level of evidence because it’s a situation and a story that we might relate to.”
Dr. Kirby said that when she thinks about managing side effects from drugs used in dermatology, it usually relates to something common and low-risk such as sore, dry skin with isotretinoin use. In contrast, if there is an uncommon but serious side effect, then mitigation rather than management is key. “I want to mitigate the risk – meaning warn my patient about it or be careful about how I select my patients when it is a serious side effect that happens infrequently,” she said. “The worst combination is a frequent and severe side effect. That is something we should avoid, for sure.”
Isotretinoin
But another aspect of prescribing a new drug for patients can be less clear-cut, Dr. Kirby continued, such as the rationale for routine lab monitoring. She began by discussing one of her male patients with moderate to severe acne. After he failed oral antibiotics and topical retinoids, she recommended isotretinoin, which carries a risk of hypertriglyceridemia-associated pancreatitis. “Early in my career, I was getting a lot of monthly labs in patients on this drug that were totally normal and not influencing my practice,” Dr. Kirby recalled. “We’ve seen studies coming out on isotretinoin lab monitoring, showing us that we can keep our patients safe and that we really don’t need to be checking labs as often, because lab changes are infrequent.”
In one of those studies, researchers evaluated 1,863 patients treated with isotretinoin for acne between Jan. 1, 2008, and June 30, 2017 (J Am Acad Dermatol. 2020 Jan;82[1]:72-9).Over time, fewer than 1% of patients screened developed grade 3 or greater triglyceride testing abnormalities, while fewer than 0.5% developed liver function testing (LFT) abnormalities. Authors of a separate systematic review concluded that for patients on isotretinoin therapy without elevated baseline triglycerides, or risk thereof, monitoring triglycerides is of little value (Br J Dermatol. 2017 Oct;177[4]:960-6). Of the 25 patients in the analysis who developed pancreatitis on isotretinoin, only 3 had elevated triglycerides at baseline.
“I was taught that I need to check triglycerides frequently due to the risk of pancreatitis developing with isotretinoin use,” Dr. Kirby said. “Lipid changes on therapy are expected, but they tend to peak early, meaning the first 3 months of treatment when we’re ramping up from a starting dose to a maintenance dose. It’s rare for somebody to be a late bloomer, meaning that they have totally normal labs in the first 3 months and then suddenly develop an abnormality. People are either going to demonstrate an abnormality early or not have one at all.”
When Dr. Kirby starts patients on isotretinoin, she orders baseline LFTs and a lipid panel and repeats them 60 days later. “If everything is fine or only mildly high, we don’t do more testing, only a review of systems,” she said. “This is valuable to our patients because fear of needles and fainting peak during adolescence.”
Spironolactone
The clinical use of regularly monitoring potassium levels in young women taking spironolactone for acne has also been questioned. The drug has been linked to an increased risk for hyperkalemia, but the prevalence is unclear. “I got a lot of normal potassium levels in these patients [when] I was in training and I really questioned, ‘Why am I doing this? What is the rationale?’ ” Dr. Kirby said.
In a study that informed her own practice, researchers reviewed the rate of hyperkalemia in 974 healthy young women taking spironolactone for acne or for an endocrine disorder with associated acne between Dec. 1, 2000, and March 31, 2014 (JAMA Dermatol. 2015 Sep;151[9]:941-4). Of the total of 1,802 serum potassium measurements taken during treatment, 13 (0.72%) were mildly elevated levels and none of the patients had a potassium level above 5.5 mEq/L. Retesting within 1 to 3 weeks in 6 of 13 patients with elevated levels found that potassium levels were normal. “The recommendation for spironolactone in healthy women is not to check the potassium level,” Dr. Kirby said, adding that she does counsel patients about the risk of breast tenderness (which can occur 5% to 40% of the time) and spotting (which can occur in 10% to 20% of patients). Gynecomastia can occur in 10% to 30% of men, which is one of the reasons she does not use spironolactone in male patients.
TB testing and biologics
Whether or not to test for TB in patients with psoriasis taking biologic therapies represents another conundrum, she continued. Patients taking biologics are at risk of reactivation of latent TB infection, but in her experience, package inserts contain language like “perform TB testing at baseline, then periodically,” or “use at baseline, then with active TB symptoms,” and “after treatment is discontinued.”
“What the inserts didn’t recommend was to perform TB testing every year, which is what my routine had been,” Dr. Kirby said. “In the United States, thankfully we don’t have a lot of TB.” In a study that informed her own practice, researchers at a single academic medical center retrospectively reviewed the TB seroconversion rate among 316 patients treated with second-generation biologics (J Am Acad Dermatol. 2020 Oct 1;S0190-9622[20]32676-1. doi: 10.1016/j.jaad.2020.09.075). It found that only six patients (2%) converted and had a positive TB test later during treatment with the biologic. “Of these six people, all had grown up outside the U.S., had traveled outside of the U.S., or were in a group living situation,” said Dr. Kirby, who was not affiliated with the study.
“This informs our rationale for how we can do this testing. If insurance requires it every year, fine. But if they don’t, I ask patients about travel, about their living situation, and how they’re feeling. If everything’s going great, I don’t order TB testing. I do favor the interferon-gamma release assays because they’re a lot more effective than PPDs [purified protein derivative skin tests]. Also, PPDs are difficult for patients who have a low rate of returning to have that test read.”
Terbinafine for onychomycosis
Dr. Kirby also discussed the rationale for ordering regular LFTs in patients taking terbinafine for onychomycosis. “There is a risk of drug-induced liver injury from taking terbinafine, but it’s rare,” she said. “Can we be thoughtful about which patients we expose?”
Evidence suggests that patients with hyperkeratosis greater than 2 mm, with nail matrix involvement, with 50% or more of the nail involved, or having concomitant peripheral vascular disease and diabetes are recalcitrant to treatment with terbinafine
(J Am Acad Dermatol. 2019 Apr;80[4]:853-67). “If we can frame this risk, then we can frame it for our patients,” she said. “We’re more likely to cause liver injury with an antibiotic. When it comes to an oral antifungal, itraconazole is more likely than terbinafine to cause liver injury. The rate of liver injury with terbinafine is only about 2 out of 100,000. It’s five times more likely with itraconazole and 21 times more likely with Augmentin.”
She recommends obtaining a baseline LFT in patients starting terbinafine therapy “to make sure their liver is normal from the start.” In addition, she advised, “let them know that there is a TB seroconversion risk of about 1 in 50,000 people, and that if it happens there would be symptomatic changes. They would maybe notice pruritus and have a darkening in their urine, and they’d have some flu-like symptoms, which would mean stop the drug and get some care.”
Dr. Kirby emphasized that a patient’s propensity for developing drug-induced liver injury from terbinafine use is not predictable from LFT monitoring. “What you’re more likely to find is an asymptomatic LFT rise in about 1% of people,” she said.
She disclosed that she has received honoraria from AbbVie, ChemoCentryx, Incyte, Janssen, Novartis, and UCB Pharma.
From time to time, Joslyn Kirby, MD, asks other physicians about their experience with certain medications used in dermatology, especially when something new hits the market.
“Sometimes I get an answer like, ‘The last time I used that medicine, my patient needed a liver transplant,’ ” Dr. Kirby, associate professor of dermatology, Penn State University, Hershey, said during the Orlando Dermatology Aesthetic and Clinical Conference. “It’s typically a story of something rare, uncommon, and awful. The challenge with an anecdote is that for all its power, it has a lower level of evidence. But it sticks with us and influences us more than a better level of evidence because it’s a situation and a story that we might relate to.”
Dr. Kirby said that when she thinks about managing side effects from drugs used in dermatology, it usually relates to something common and low-risk such as sore, dry skin with isotretinoin use. In contrast, if there is an uncommon but serious side effect, then mitigation rather than management is key. “I want to mitigate the risk – meaning warn my patient about it or be careful about how I select my patients when it is a serious side effect that happens infrequently,” she said. “The worst combination is a frequent and severe side effect. That is something we should avoid, for sure.”
Isotretinoin
But another aspect of prescribing a new drug for patients can be less clear-cut, Dr. Kirby continued, such as the rationale for routine lab monitoring. She began by discussing one of her male patients with moderate to severe acne. After he failed oral antibiotics and topical retinoids, she recommended isotretinoin, which carries a risk of hypertriglyceridemia-associated pancreatitis. “Early in my career, I was getting a lot of monthly labs in patients on this drug that were totally normal and not influencing my practice,” Dr. Kirby recalled. “We’ve seen studies coming out on isotretinoin lab monitoring, showing us that we can keep our patients safe and that we really don’t need to be checking labs as often, because lab changes are infrequent.”
In one of those studies, researchers evaluated 1,863 patients treated with isotretinoin for acne between Jan. 1, 2008, and June 30, 2017 (J Am Acad Dermatol. 2020 Jan;82[1]:72-9).Over time, fewer than 1% of patients screened developed grade 3 or greater triglyceride testing abnormalities, while fewer than 0.5% developed liver function testing (LFT) abnormalities. Authors of a separate systematic review concluded that for patients on isotretinoin therapy without elevated baseline triglycerides, or risk thereof, monitoring triglycerides is of little value (Br J Dermatol. 2017 Oct;177[4]:960-6). Of the 25 patients in the analysis who developed pancreatitis on isotretinoin, only 3 had elevated triglycerides at baseline.
“I was taught that I need to check triglycerides frequently due to the risk of pancreatitis developing with isotretinoin use,” Dr. Kirby said. “Lipid changes on therapy are expected, but they tend to peak early, meaning the first 3 months of treatment when we’re ramping up from a starting dose to a maintenance dose. It’s rare for somebody to be a late bloomer, meaning that they have totally normal labs in the first 3 months and then suddenly develop an abnormality. People are either going to demonstrate an abnormality early or not have one at all.”
When Dr. Kirby starts patients on isotretinoin, she orders baseline LFTs and a lipid panel and repeats them 60 days later. “If everything is fine or only mildly high, we don’t do more testing, only a review of systems,” she said. “This is valuable to our patients because fear of needles and fainting peak during adolescence.”
Spironolactone
The clinical use of regularly monitoring potassium levels in young women taking spironolactone for acne has also been questioned. The drug has been linked to an increased risk for hyperkalemia, but the prevalence is unclear. “I got a lot of normal potassium levels in these patients [when] I was in training and I really questioned, ‘Why am I doing this? What is the rationale?’ ” Dr. Kirby said.
In a study that informed her own practice, researchers reviewed the rate of hyperkalemia in 974 healthy young women taking spironolactone for acne or for an endocrine disorder with associated acne between Dec. 1, 2000, and March 31, 2014 (JAMA Dermatol. 2015 Sep;151[9]:941-4). Of the total of 1,802 serum potassium measurements taken during treatment, 13 (0.72%) were mildly elevated levels and none of the patients had a potassium level above 5.5 mEq/L. Retesting within 1 to 3 weeks in 6 of 13 patients with elevated levels found that potassium levels were normal. “The recommendation for spironolactone in healthy women is not to check the potassium level,” Dr. Kirby said, adding that she does counsel patients about the risk of breast tenderness (which can occur 5% to 40% of the time) and spotting (which can occur in 10% to 20% of patients). Gynecomastia can occur in 10% to 30% of men, which is one of the reasons she does not use spironolactone in male patients.
TB testing and biologics
Whether or not to test for TB in patients with psoriasis taking biologic therapies represents another conundrum, she continued. Patients taking biologics are at risk of reactivation of latent TB infection, but in her experience, package inserts contain language like “perform TB testing at baseline, then periodically,” or “use at baseline, then with active TB symptoms,” and “after treatment is discontinued.”
“What the inserts didn’t recommend was to perform TB testing every year, which is what my routine had been,” Dr. Kirby said. “In the United States, thankfully we don’t have a lot of TB.” In a study that informed her own practice, researchers at a single academic medical center retrospectively reviewed the TB seroconversion rate among 316 patients treated with second-generation biologics (J Am Acad Dermatol. 2020 Oct 1;S0190-9622[20]32676-1. doi: 10.1016/j.jaad.2020.09.075). It found that only six patients (2%) converted and had a positive TB test later during treatment with the biologic. “Of these six people, all had grown up outside the U.S., had traveled outside of the U.S., or were in a group living situation,” said Dr. Kirby, who was not affiliated with the study.
“This informs our rationale for how we can do this testing. If insurance requires it every year, fine. But if they don’t, I ask patients about travel, about their living situation, and how they’re feeling. If everything’s going great, I don’t order TB testing. I do favor the interferon-gamma release assays because they’re a lot more effective than PPDs [purified protein derivative skin tests]. Also, PPDs are difficult for patients who have a low rate of returning to have that test read.”
Terbinafine for onychomycosis
Dr. Kirby also discussed the rationale for ordering regular LFTs in patients taking terbinafine for onychomycosis. “There is a risk of drug-induced liver injury from taking terbinafine, but it’s rare,” she said. “Can we be thoughtful about which patients we expose?”
Evidence suggests that patients with hyperkeratosis greater than 2 mm, with nail matrix involvement, with 50% or more of the nail involved, or having concomitant peripheral vascular disease and diabetes are recalcitrant to treatment with terbinafine
(J Am Acad Dermatol. 2019 Apr;80[4]:853-67). “If we can frame this risk, then we can frame it for our patients,” she said. “We’re more likely to cause liver injury with an antibiotic. When it comes to an oral antifungal, itraconazole is more likely than terbinafine to cause liver injury. The rate of liver injury with terbinafine is only about 2 out of 100,000. It’s five times more likely with itraconazole and 21 times more likely with Augmentin.”
She recommends obtaining a baseline LFT in patients starting terbinafine therapy “to make sure their liver is normal from the start.” In addition, she advised, “let them know that there is a TB seroconversion risk of about 1 in 50,000 people, and that if it happens there would be symptomatic changes. They would maybe notice pruritus and have a darkening in their urine, and they’d have some flu-like symptoms, which would mean stop the drug and get some care.”
Dr. Kirby emphasized that a patient’s propensity for developing drug-induced liver injury from terbinafine use is not predictable from LFT monitoring. “What you’re more likely to find is an asymptomatic LFT rise in about 1% of people,” she said.
She disclosed that she has received honoraria from AbbVie, ChemoCentryx, Incyte, Janssen, Novartis, and UCB Pharma.
FROM ODAC 2021
Expert shares hyperhidrosis treatment pearls
Even though over-the-counter topical antiperspirants are a common go-to treatment for primary axillary hyperhidrosis, a large survey commissioned by the International Hyperhidrosis Society showed that, while OTC aluminum products are the most recommended, they offer the least satisfaction to patients.
Of the 1,985 survey respondents who self-identified as having excessive sweating, those who received treatment were most satisfied with injections and least satisfied with prescription and OTC antiperspirants and liposuction. “It’s important to recognize that, while these are not invasive, they’re simple, you need to keep up with it, and they’re really not that effective for primary hyperhidrosis,” Adam Friedman, MD, said during the virtual Orlando Dermatology Aesthetic and Clinical Conference.
A major development came in 2018, when the Food and Drug Administration approved topical glycopyrronium tosylate for the treatment of primary axillary hyperhidrosis in adults and in children as young as age 9. It marked the first topical anticholinergic approved for the condition. Results from the pivotal phase 2 ATMOS-1 and ATMOS-2 randomized, controlled trials found that, after 4 weeks of daily use, 53%-66% of patients reported a 4-point improvement or greater on the ASDD item 2, which is defined as the worst sweating they experienced in a 24-hour period on an 11-point scale.
“Patients want to know: How quickly am I going to see improvement? The answer to this can be central to treatment compliance,” said Dr. Friedman, professor and interim chair of dermatology at the George Washington University, Washington. “We have data showing that 23%-29% of patients using glycopyrronium tosylate met that primary outcome within 1 week of use. So, you can tell patients: ‘Help is on the way. You may see a response relatively soon.’ ”
The most common adverse events in the two trials were dry mouth, which affected 24% of patients, followed by mydriasis (7%), and oropharyngeal pain (6%). He advises patients to apply it once at night. “I tell my patients make this the last thing you do during your nighttime routine,” said Dr. Friedman, who coauthored a case-based clinical algorithm for approaching primary hyperhidrosis patients.
“Open it up, one swipe to the right [underarm], flip it over, one wipe of the left [underarm], toss the towelette, and wash your hands thoroughly. You don’t need to remove axillary hair or occlude the area. I tell them they may find some improvement within one week of daily use, but I give realistic expectations, usually 2-3 weeks. Tell them about the potential for side effects, which certainly can happen,” he said.
Investigators are evaluating how this product could be delivered to other body sites. Dr. Friedman said that he uses glycopyrronium tosylate off label for palmar and plantar hyperhidrosis. He advises patients to rub their hands or feet the cloth until it dries, toss the towelette, apply an occlusive agent like Aquaphor followed by gloves/socks for at least an hour, and then wash their hands or feet. “If they can keep the gloves or socks on overnight, that’s fine, but that’s very rare,” Dr. Friedman added.
“Typically, an hour or 2 of occlusive covering will get the product in where it needs to be. The upside of this product is that it’s noninvasive, there’s minimal irritation, it’s effective, and FDA approved. On the downside, it’s a long-term therapy. This is forever, so cost can be an issue, and you have to think about the anticholinergic effects as well.”
Iontophoresis is a first-line treatment for moderate to severe palmar and plantar hyperhidrosis. It’s also effective for mild hyperhidrosis with limited side effects, but it’s cumbersome, he said, requiring thrice-weekly treatment of each palm or sole for approximately 30 minutes to a controlled electric current at 15-20 mA with tap water.
There are no systemic agents approved for hyperhidrosis, only case reports or small case series. For now, the two commonly used anticholinergics are glycopyrrolate and oxybutynin. Glycopyrrolate comes in 1- and 2-mg capsules. “You can break the tablets easily and it’s pretty cheap, with an estimated cost of 2 mg/day at $756 per year,” Dr. Friedman said. “I typically start patients on 1 mg twice per day for a week, then ask how they’re doing. If they notice improvement, have minimal side effects but think they can do better, then I increase it by 1 mg and reassess. I give them autonomy, and at most, want them to max out at 6 mg per day. There is an oral solution for kids, which can make this a little more accessible.”
He prescribes oxybutynin infrequently but considers it effective. “Most patients respond to 5- to 10-mg/day dosing, but doses up to 15 or 20 mg daily may be required,” he noted.
For persistent flushing with hyperhidrosis, Dr. Friedman typically recommends treatment with clonidine. “I start patients pretty low, sometimes 0.05 mg twice per day.”
For patients who sweat because of social phobias and performance anxiety, he typically recommends treatment with a beta-adrenergic blocker. “These are highly lipophilic, so I advise patients not to take them with food,” he said. “The peak concentration is 1-1.5 hours. Usually, I start at 10 mg and I have people do a test run at home. I also take a baseline blood pressure in the office to make sure they’re not hypotensive.” The use of beta-adrenergic blockers is contraindicated in patients with bradycardia, atrioventricular block, and asthma. They can also exacerbate psoriasis.
On Sept. 20, 2020, Brickell Biotech announced the approval of sofpironium bromide gel, 5%, in Japan for the treatment of primary axillary hyperhidrosis. Sofpironium bromide is an analog of glycopyrrolate “that gets metabolized very quickly in order to limit systemic absorption of the active agent and therefore mitigate side effects,” Dr. Friedman said.
A recently published Japanese study found that 54% of patients with primary axillary hyperhidrosis who received sofpironium bromide experienced a 1- or 2-point improvement on the Hyperhidrosis Disease Severity Scale and a 50% or greater reduction in gravimetric sweat production from baseline to week 6 of treatment, compared with 36% of patients in the control group (P = .003). According to Dr. Friedman, a 15% formulation of this product is being studied in the United States, “but the experience in Japan with the 5% formulation should give us some real-world information about this product,” he said. “Out of the gate, we’re going to know something about how it’s being used.”
Dr. Friedman reported that he serves as a consultant and/or advisor to numerous pharmaceutical companies, including some that produce cannabinoids. He is also a speaker for Regeneron, Abbvie, Novartis, LRP, Dermira, and Brickel Biotech, and has received grants from Pfizer, the Dermatology Foundation, Almirall, and Janssen.
Even though over-the-counter topical antiperspirants are a common go-to treatment for primary axillary hyperhidrosis, a large survey commissioned by the International Hyperhidrosis Society showed that, while OTC aluminum products are the most recommended, they offer the least satisfaction to patients.
Of the 1,985 survey respondents who self-identified as having excessive sweating, those who received treatment were most satisfied with injections and least satisfied with prescription and OTC antiperspirants and liposuction. “It’s important to recognize that, while these are not invasive, they’re simple, you need to keep up with it, and they’re really not that effective for primary hyperhidrosis,” Adam Friedman, MD, said during the virtual Orlando Dermatology Aesthetic and Clinical Conference.
A major development came in 2018, when the Food and Drug Administration approved topical glycopyrronium tosylate for the treatment of primary axillary hyperhidrosis in adults and in children as young as age 9. It marked the first topical anticholinergic approved for the condition. Results from the pivotal phase 2 ATMOS-1 and ATMOS-2 randomized, controlled trials found that, after 4 weeks of daily use, 53%-66% of patients reported a 4-point improvement or greater on the ASDD item 2, which is defined as the worst sweating they experienced in a 24-hour period on an 11-point scale.
“Patients want to know: How quickly am I going to see improvement? The answer to this can be central to treatment compliance,” said Dr. Friedman, professor and interim chair of dermatology at the George Washington University, Washington. “We have data showing that 23%-29% of patients using glycopyrronium tosylate met that primary outcome within 1 week of use. So, you can tell patients: ‘Help is on the way. You may see a response relatively soon.’ ”
The most common adverse events in the two trials were dry mouth, which affected 24% of patients, followed by mydriasis (7%), and oropharyngeal pain (6%). He advises patients to apply it once at night. “I tell my patients make this the last thing you do during your nighttime routine,” said Dr. Friedman, who coauthored a case-based clinical algorithm for approaching primary hyperhidrosis patients.
“Open it up, one swipe to the right [underarm], flip it over, one wipe of the left [underarm], toss the towelette, and wash your hands thoroughly. You don’t need to remove axillary hair or occlude the area. I tell them they may find some improvement within one week of daily use, but I give realistic expectations, usually 2-3 weeks. Tell them about the potential for side effects, which certainly can happen,” he said.
Investigators are evaluating how this product could be delivered to other body sites. Dr. Friedman said that he uses glycopyrronium tosylate off label for palmar and plantar hyperhidrosis. He advises patients to rub their hands or feet the cloth until it dries, toss the towelette, apply an occlusive agent like Aquaphor followed by gloves/socks for at least an hour, and then wash their hands or feet. “If they can keep the gloves or socks on overnight, that’s fine, but that’s very rare,” Dr. Friedman added.
“Typically, an hour or 2 of occlusive covering will get the product in where it needs to be. The upside of this product is that it’s noninvasive, there’s minimal irritation, it’s effective, and FDA approved. On the downside, it’s a long-term therapy. This is forever, so cost can be an issue, and you have to think about the anticholinergic effects as well.”
Iontophoresis is a first-line treatment for moderate to severe palmar and plantar hyperhidrosis. It’s also effective for mild hyperhidrosis with limited side effects, but it’s cumbersome, he said, requiring thrice-weekly treatment of each palm or sole for approximately 30 minutes to a controlled electric current at 15-20 mA with tap water.
There are no systemic agents approved for hyperhidrosis, only case reports or small case series. For now, the two commonly used anticholinergics are glycopyrrolate and oxybutynin. Glycopyrrolate comes in 1- and 2-mg capsules. “You can break the tablets easily and it’s pretty cheap, with an estimated cost of 2 mg/day at $756 per year,” Dr. Friedman said. “I typically start patients on 1 mg twice per day for a week, then ask how they’re doing. If they notice improvement, have minimal side effects but think they can do better, then I increase it by 1 mg and reassess. I give them autonomy, and at most, want them to max out at 6 mg per day. There is an oral solution for kids, which can make this a little more accessible.”
He prescribes oxybutynin infrequently but considers it effective. “Most patients respond to 5- to 10-mg/day dosing, but doses up to 15 or 20 mg daily may be required,” he noted.
For persistent flushing with hyperhidrosis, Dr. Friedman typically recommends treatment with clonidine. “I start patients pretty low, sometimes 0.05 mg twice per day.”
For patients who sweat because of social phobias and performance anxiety, he typically recommends treatment with a beta-adrenergic blocker. “These are highly lipophilic, so I advise patients not to take them with food,” he said. “The peak concentration is 1-1.5 hours. Usually, I start at 10 mg and I have people do a test run at home. I also take a baseline blood pressure in the office to make sure they’re not hypotensive.” The use of beta-adrenergic blockers is contraindicated in patients with bradycardia, atrioventricular block, and asthma. They can also exacerbate psoriasis.
On Sept. 20, 2020, Brickell Biotech announced the approval of sofpironium bromide gel, 5%, in Japan for the treatment of primary axillary hyperhidrosis. Sofpironium bromide is an analog of glycopyrrolate “that gets metabolized very quickly in order to limit systemic absorption of the active agent and therefore mitigate side effects,” Dr. Friedman said.
A recently published Japanese study found that 54% of patients with primary axillary hyperhidrosis who received sofpironium bromide experienced a 1- or 2-point improvement on the Hyperhidrosis Disease Severity Scale and a 50% or greater reduction in gravimetric sweat production from baseline to week 6 of treatment, compared with 36% of patients in the control group (P = .003). According to Dr. Friedman, a 15% formulation of this product is being studied in the United States, “but the experience in Japan with the 5% formulation should give us some real-world information about this product,” he said. “Out of the gate, we’re going to know something about how it’s being used.”
Dr. Friedman reported that he serves as a consultant and/or advisor to numerous pharmaceutical companies, including some that produce cannabinoids. He is also a speaker for Regeneron, Abbvie, Novartis, LRP, Dermira, and Brickel Biotech, and has received grants from Pfizer, the Dermatology Foundation, Almirall, and Janssen.
Even though over-the-counter topical antiperspirants are a common go-to treatment for primary axillary hyperhidrosis, a large survey commissioned by the International Hyperhidrosis Society showed that, while OTC aluminum products are the most recommended, they offer the least satisfaction to patients.
Of the 1,985 survey respondents who self-identified as having excessive sweating, those who received treatment were most satisfied with injections and least satisfied with prescription and OTC antiperspirants and liposuction. “It’s important to recognize that, while these are not invasive, they’re simple, you need to keep up with it, and they’re really not that effective for primary hyperhidrosis,” Adam Friedman, MD, said during the virtual Orlando Dermatology Aesthetic and Clinical Conference.
A major development came in 2018, when the Food and Drug Administration approved topical glycopyrronium tosylate for the treatment of primary axillary hyperhidrosis in adults and in children as young as age 9. It marked the first topical anticholinergic approved for the condition. Results from the pivotal phase 2 ATMOS-1 and ATMOS-2 randomized, controlled trials found that, after 4 weeks of daily use, 53%-66% of patients reported a 4-point improvement or greater on the ASDD item 2, which is defined as the worst sweating they experienced in a 24-hour period on an 11-point scale.
“Patients want to know: How quickly am I going to see improvement? The answer to this can be central to treatment compliance,” said Dr. Friedman, professor and interim chair of dermatology at the George Washington University, Washington. “We have data showing that 23%-29% of patients using glycopyrronium tosylate met that primary outcome within 1 week of use. So, you can tell patients: ‘Help is on the way. You may see a response relatively soon.’ ”
The most common adverse events in the two trials were dry mouth, which affected 24% of patients, followed by mydriasis (7%), and oropharyngeal pain (6%). He advises patients to apply it once at night. “I tell my patients make this the last thing you do during your nighttime routine,” said Dr. Friedman, who coauthored a case-based clinical algorithm for approaching primary hyperhidrosis patients.
“Open it up, one swipe to the right [underarm], flip it over, one wipe of the left [underarm], toss the towelette, and wash your hands thoroughly. You don’t need to remove axillary hair or occlude the area. I tell them they may find some improvement within one week of daily use, but I give realistic expectations, usually 2-3 weeks. Tell them about the potential for side effects, which certainly can happen,” he said.
Investigators are evaluating how this product could be delivered to other body sites. Dr. Friedman said that he uses glycopyrronium tosylate off label for palmar and plantar hyperhidrosis. He advises patients to rub their hands or feet the cloth until it dries, toss the towelette, apply an occlusive agent like Aquaphor followed by gloves/socks for at least an hour, and then wash their hands or feet. “If they can keep the gloves or socks on overnight, that’s fine, but that’s very rare,” Dr. Friedman added.
“Typically, an hour or 2 of occlusive covering will get the product in where it needs to be. The upside of this product is that it’s noninvasive, there’s minimal irritation, it’s effective, and FDA approved. On the downside, it’s a long-term therapy. This is forever, so cost can be an issue, and you have to think about the anticholinergic effects as well.”
Iontophoresis is a first-line treatment for moderate to severe palmar and plantar hyperhidrosis. It’s also effective for mild hyperhidrosis with limited side effects, but it’s cumbersome, he said, requiring thrice-weekly treatment of each palm or sole for approximately 30 minutes to a controlled electric current at 15-20 mA with tap water.
There are no systemic agents approved for hyperhidrosis, only case reports or small case series. For now, the two commonly used anticholinergics are glycopyrrolate and oxybutynin. Glycopyrrolate comes in 1- and 2-mg capsules. “You can break the tablets easily and it’s pretty cheap, with an estimated cost of 2 mg/day at $756 per year,” Dr. Friedman said. “I typically start patients on 1 mg twice per day for a week, then ask how they’re doing. If they notice improvement, have minimal side effects but think they can do better, then I increase it by 1 mg and reassess. I give them autonomy, and at most, want them to max out at 6 mg per day. There is an oral solution for kids, which can make this a little more accessible.”
He prescribes oxybutynin infrequently but considers it effective. “Most patients respond to 5- to 10-mg/day dosing, but doses up to 15 or 20 mg daily may be required,” he noted.
For persistent flushing with hyperhidrosis, Dr. Friedman typically recommends treatment with clonidine. “I start patients pretty low, sometimes 0.05 mg twice per day.”
For patients who sweat because of social phobias and performance anxiety, he typically recommends treatment with a beta-adrenergic blocker. “These are highly lipophilic, so I advise patients not to take them with food,” he said. “The peak concentration is 1-1.5 hours. Usually, I start at 10 mg and I have people do a test run at home. I also take a baseline blood pressure in the office to make sure they’re not hypotensive.” The use of beta-adrenergic blockers is contraindicated in patients with bradycardia, atrioventricular block, and asthma. They can also exacerbate psoriasis.
On Sept. 20, 2020, Brickell Biotech announced the approval of sofpironium bromide gel, 5%, in Japan for the treatment of primary axillary hyperhidrosis. Sofpironium bromide is an analog of glycopyrrolate “that gets metabolized very quickly in order to limit systemic absorption of the active agent and therefore mitigate side effects,” Dr. Friedman said.
A recently published Japanese study found that 54% of patients with primary axillary hyperhidrosis who received sofpironium bromide experienced a 1- or 2-point improvement on the Hyperhidrosis Disease Severity Scale and a 50% or greater reduction in gravimetric sweat production from baseline to week 6 of treatment, compared with 36% of patients in the control group (P = .003). According to Dr. Friedman, a 15% formulation of this product is being studied in the United States, “but the experience in Japan with the 5% formulation should give us some real-world information about this product,” he said. “Out of the gate, we’re going to know something about how it’s being used.”
Dr. Friedman reported that he serves as a consultant and/or advisor to numerous pharmaceutical companies, including some that produce cannabinoids. He is also a speaker for Regeneron, Abbvie, Novartis, LRP, Dermira, and Brickel Biotech, and has received grants from Pfizer, the Dermatology Foundation, Almirall, and Janssen.
FROM ODAC 2021
How to choose the best aesthetic devices when launching your career
When a new body contouring device hit the market a few years ago, Nazanin Saedi, MD, had an opportunity to become the first Philadelphia area dermatologist to add the technology to her practice.
“I thought about it, but it didn’t make sense because it wasn’t something important to my patient population,” Dr. Saedi, who directs the Jefferson Laser Surgery and Cosmetic Dermatology Center in Philadelphia, said during the Orlando Dermatology Aesthetic and Clinical Conference. “If I’m not going to have the patient demand and make money from it, then it just doesn’t make sense.”
That experience illustrates one of many pearls of advice that Dr. Saedi shared during . “Include additional questions in new patient intake forms or online forms to get a sense of what your patient population is interested in,” she advised. “It’s important to understand that before you start to offer new services. Don’t just depend on social media to inform you of the latest trends and what people are doing across the country, because if you purchase something that is very popular on social media for people in New York or L.A., that might not be the best for your practice.”
According to market trends from the American Society for Dermatologic Surgery, 3.5 million laser-, light-, and energy-based procedures were performed in 2018. The top five were for wrinkles (809,166), sun damage (786,856), facial redness (612,367), excess hair (385,466), and melasma (226,007). “Considering this data, when you start a practice, do you buy something for wrinkles or for sun damage right away?” Dr. Saedi asked. “Maybe, but you really need to gauge the market that you practice in. You also want to consider your own skill set and what other dermatologists in your area are offering. If you don’t want to do aggressive procedures, then purchasing a fractional CO2 laser might not be the best device to start off with. If you are not comfortable dealing with those patients, and potential infections and scarring, then that’s not the right treatment for you. You have to reflect on and identify what you’re comfortable learning and doing and managing.”
Taking time to investigate the services offered by dermatologists and med spas within a few miles of your practice can help you avoid redundancy. “Learn the techniques and the small nuances that will give you a little bit of finesse and make you an expert, to set you apart from other practices,” said Dr. Saedi, who coauthored a chapter in the book, “The Business of Dermatology” (New York: Thieme Medical Publishers, 2020). “I always recommend treating your staff and members of your family, to understand how you can tweak treatments to get the most out of them. Once you treat your staff, they are walking advertisements for what you do. They can also counsel patients, walking them through the healing process after a procedure, so they can know what to expect.”
Appropriate planning and preparation can help avoid acquiring the wrong device, she continued. This includes patient demand, scheduling availability, office space, overhead costs, and the level of staff training. She recommends buying one device at a time and clearing profitability from that device before purchasing another, “because it can be a burden on your practice to have multiple devices all at once,” she said. “You also have to think about the hidden costs – the maintenance and the service contracts. That can exceed $10,000 per year, so consider that when you’re looking to purchase a new device.”
Most people buy laser-, light-, and energy-based devices, but renting for a stretch can help you test the waters without a significant long-term investment. “It might not be the newest laser, but it can help you gauge how much of demand you have for that service to see if you have the patient base to make that larger step of purchasing the device,” she said. “If you buy a new device, make sure that it’s not a counterfeit and that you still have a company service contract. There are many third-party companies selling pre-owned laser aesthetics. Make sure you’re getting the authentic device and that there is some kind of a service contract with the actual manufacturer so they can help fix it when things break down.”
When Dr. Saedi counsels residents about purchasing devices, she typically recommends these five categories in order of preference: vascular, pigment, hair, resurfacing, and body contouring/skin tightening. “If you can cover vascular, pigment, and some kind of textural improvement, you can treat about 90% of aesthetic patients who come through your door,” she said. “Sure, there are some who may want skin tightening that you may not be able to offer with laser resurfacing, but you’re going to be able capture a high patient population by offering these services,” she added. That is why a lot of people end up getting a platform with attachable handpieces, “where you can have one system that is able to offer many different services right off the bat.”
She advised factoring in the amount of time it takes for a procedure and how much time it will take up in a certain room. “That will affect your revenue as well. Are you going to delegate this, or is this something you will do on your own? Take that into account.”
Above all, don’t rush your device purchase. “Some laser company sales representatives may pressure you at the end of a quarter by saying, ‘This is the best deal I’m going to offer you. You’re never going to get a deal like this ever again,’ ” she said. “I advise people to do multiple demos so you’re not just doing a demo for a day and seeing one or two patients. Treat the same patients again a month later. Do multiple demos so that you can feel comfortable. Talk to dermatologists who have the device, who have real experience with it, so you can have the most amount of information moving forward.”
Dr. Saedi reported that she has received equipment from Alma, Aerolase, Cartessa, and Cynosure. She is a consultant to and/or an advisory board member for those companies, as well as for Alastin.
When a new body contouring device hit the market a few years ago, Nazanin Saedi, MD, had an opportunity to become the first Philadelphia area dermatologist to add the technology to her practice.
“I thought about it, but it didn’t make sense because it wasn’t something important to my patient population,” Dr. Saedi, who directs the Jefferson Laser Surgery and Cosmetic Dermatology Center in Philadelphia, said during the Orlando Dermatology Aesthetic and Clinical Conference. “If I’m not going to have the patient demand and make money from it, then it just doesn’t make sense.”
That experience illustrates one of many pearls of advice that Dr. Saedi shared during . “Include additional questions in new patient intake forms or online forms to get a sense of what your patient population is interested in,” she advised. “It’s important to understand that before you start to offer new services. Don’t just depend on social media to inform you of the latest trends and what people are doing across the country, because if you purchase something that is very popular on social media for people in New York or L.A., that might not be the best for your practice.”
According to market trends from the American Society for Dermatologic Surgery, 3.5 million laser-, light-, and energy-based procedures were performed in 2018. The top five were for wrinkles (809,166), sun damage (786,856), facial redness (612,367), excess hair (385,466), and melasma (226,007). “Considering this data, when you start a practice, do you buy something for wrinkles or for sun damage right away?” Dr. Saedi asked. “Maybe, but you really need to gauge the market that you practice in. You also want to consider your own skill set and what other dermatologists in your area are offering. If you don’t want to do aggressive procedures, then purchasing a fractional CO2 laser might not be the best device to start off with. If you are not comfortable dealing with those patients, and potential infections and scarring, then that’s not the right treatment for you. You have to reflect on and identify what you’re comfortable learning and doing and managing.”
Taking time to investigate the services offered by dermatologists and med spas within a few miles of your practice can help you avoid redundancy. “Learn the techniques and the small nuances that will give you a little bit of finesse and make you an expert, to set you apart from other practices,” said Dr. Saedi, who coauthored a chapter in the book, “The Business of Dermatology” (New York: Thieme Medical Publishers, 2020). “I always recommend treating your staff and members of your family, to understand how you can tweak treatments to get the most out of them. Once you treat your staff, they are walking advertisements for what you do. They can also counsel patients, walking them through the healing process after a procedure, so they can know what to expect.”
Appropriate planning and preparation can help avoid acquiring the wrong device, she continued. This includes patient demand, scheduling availability, office space, overhead costs, and the level of staff training. She recommends buying one device at a time and clearing profitability from that device before purchasing another, “because it can be a burden on your practice to have multiple devices all at once,” she said. “You also have to think about the hidden costs – the maintenance and the service contracts. That can exceed $10,000 per year, so consider that when you’re looking to purchase a new device.”
Most people buy laser-, light-, and energy-based devices, but renting for a stretch can help you test the waters without a significant long-term investment. “It might not be the newest laser, but it can help you gauge how much of demand you have for that service to see if you have the patient base to make that larger step of purchasing the device,” she said. “If you buy a new device, make sure that it’s not a counterfeit and that you still have a company service contract. There are many third-party companies selling pre-owned laser aesthetics. Make sure you’re getting the authentic device and that there is some kind of a service contract with the actual manufacturer so they can help fix it when things break down.”
When Dr. Saedi counsels residents about purchasing devices, she typically recommends these five categories in order of preference: vascular, pigment, hair, resurfacing, and body contouring/skin tightening. “If you can cover vascular, pigment, and some kind of textural improvement, you can treat about 90% of aesthetic patients who come through your door,” she said. “Sure, there are some who may want skin tightening that you may not be able to offer with laser resurfacing, but you’re going to be able capture a high patient population by offering these services,” she added. That is why a lot of people end up getting a platform with attachable handpieces, “where you can have one system that is able to offer many different services right off the bat.”
She advised factoring in the amount of time it takes for a procedure and how much time it will take up in a certain room. “That will affect your revenue as well. Are you going to delegate this, or is this something you will do on your own? Take that into account.”
Above all, don’t rush your device purchase. “Some laser company sales representatives may pressure you at the end of a quarter by saying, ‘This is the best deal I’m going to offer you. You’re never going to get a deal like this ever again,’ ” she said. “I advise people to do multiple demos so you’re not just doing a demo for a day and seeing one or two patients. Treat the same patients again a month later. Do multiple demos so that you can feel comfortable. Talk to dermatologists who have the device, who have real experience with it, so you can have the most amount of information moving forward.”
Dr. Saedi reported that she has received equipment from Alma, Aerolase, Cartessa, and Cynosure. She is a consultant to and/or an advisory board member for those companies, as well as for Alastin.
When a new body contouring device hit the market a few years ago, Nazanin Saedi, MD, had an opportunity to become the first Philadelphia area dermatologist to add the technology to her practice.
“I thought about it, but it didn’t make sense because it wasn’t something important to my patient population,” Dr. Saedi, who directs the Jefferson Laser Surgery and Cosmetic Dermatology Center in Philadelphia, said during the Orlando Dermatology Aesthetic and Clinical Conference. “If I’m not going to have the patient demand and make money from it, then it just doesn’t make sense.”
That experience illustrates one of many pearls of advice that Dr. Saedi shared during . “Include additional questions in new patient intake forms or online forms to get a sense of what your patient population is interested in,” she advised. “It’s important to understand that before you start to offer new services. Don’t just depend on social media to inform you of the latest trends and what people are doing across the country, because if you purchase something that is very popular on social media for people in New York or L.A., that might not be the best for your practice.”
According to market trends from the American Society for Dermatologic Surgery, 3.5 million laser-, light-, and energy-based procedures were performed in 2018. The top five were for wrinkles (809,166), sun damage (786,856), facial redness (612,367), excess hair (385,466), and melasma (226,007). “Considering this data, when you start a practice, do you buy something for wrinkles or for sun damage right away?” Dr. Saedi asked. “Maybe, but you really need to gauge the market that you practice in. You also want to consider your own skill set and what other dermatologists in your area are offering. If you don’t want to do aggressive procedures, then purchasing a fractional CO2 laser might not be the best device to start off with. If you are not comfortable dealing with those patients, and potential infections and scarring, then that’s not the right treatment for you. You have to reflect on and identify what you’re comfortable learning and doing and managing.”
Taking time to investigate the services offered by dermatologists and med spas within a few miles of your practice can help you avoid redundancy. “Learn the techniques and the small nuances that will give you a little bit of finesse and make you an expert, to set you apart from other practices,” said Dr. Saedi, who coauthored a chapter in the book, “The Business of Dermatology” (New York: Thieme Medical Publishers, 2020). “I always recommend treating your staff and members of your family, to understand how you can tweak treatments to get the most out of them. Once you treat your staff, they are walking advertisements for what you do. They can also counsel patients, walking them through the healing process after a procedure, so they can know what to expect.”
Appropriate planning and preparation can help avoid acquiring the wrong device, she continued. This includes patient demand, scheduling availability, office space, overhead costs, and the level of staff training. She recommends buying one device at a time and clearing profitability from that device before purchasing another, “because it can be a burden on your practice to have multiple devices all at once,” she said. “You also have to think about the hidden costs – the maintenance and the service contracts. That can exceed $10,000 per year, so consider that when you’re looking to purchase a new device.”
Most people buy laser-, light-, and energy-based devices, but renting for a stretch can help you test the waters without a significant long-term investment. “It might not be the newest laser, but it can help you gauge how much of demand you have for that service to see if you have the patient base to make that larger step of purchasing the device,” she said. “If you buy a new device, make sure that it’s not a counterfeit and that you still have a company service contract. There are many third-party companies selling pre-owned laser aesthetics. Make sure you’re getting the authentic device and that there is some kind of a service contract with the actual manufacturer so they can help fix it when things break down.”
When Dr. Saedi counsels residents about purchasing devices, she typically recommends these five categories in order of preference: vascular, pigment, hair, resurfacing, and body contouring/skin tightening. “If you can cover vascular, pigment, and some kind of textural improvement, you can treat about 90% of aesthetic patients who come through your door,” she said. “Sure, there are some who may want skin tightening that you may not be able to offer with laser resurfacing, but you’re going to be able capture a high patient population by offering these services,” she added. That is why a lot of people end up getting a platform with attachable handpieces, “where you can have one system that is able to offer many different services right off the bat.”
She advised factoring in the amount of time it takes for a procedure and how much time it will take up in a certain room. “That will affect your revenue as well. Are you going to delegate this, or is this something you will do on your own? Take that into account.”
Above all, don’t rush your device purchase. “Some laser company sales representatives may pressure you at the end of a quarter by saying, ‘This is the best deal I’m going to offer you. You’re never going to get a deal like this ever again,’ ” she said. “I advise people to do multiple demos so you’re not just doing a demo for a day and seeing one or two patients. Treat the same patients again a month later. Do multiple demos so that you can feel comfortable. Talk to dermatologists who have the device, who have real experience with it, so you can have the most amount of information moving forward.”
Dr. Saedi reported that she has received equipment from Alma, Aerolase, Cartessa, and Cynosure. She is a consultant to and/or an advisory board member for those companies, as well as for Alastin.
FROM ODAC 2021
Diagnosing, treating delayed nodules an imperfect science, expert says
When a is no easy task.
“It’s sometime very difficult to distinguish between the two,” Terrence Keaney, MD, said during the Orlando Dermatology Aesthetic and Clinical Conference. “Classically, an early-onset infection presents as a suppurative mass that’s fluctuant and tender. The challenge with delayed-onset infection is that it often does not tend to be fluctuant. It doesn’t resemble the classic infection you see in regular dermatology practice.”
Dr. Keaney, a dermatologist who is founder and director of SkinDC in Arlington, Va., said that the source of delayed infection could stem from inoculation at the time of injection – primarily via the skin microflora. “There are also rare case reports of mycobacterial infections from watered gauze,” which he said is why he does not use watered gauze in his practice. “This risk reinforces the importance of filler hygiene when you’re using dermal fillers. Isopropyl alcohol is often not enough. A lot of practices use chlorhexidine, avoiding its use around the eyes, to reduce the skin flora. Hypochlorous acid is another safe antiseptic for the face. You also want to be very careful with the needle or cannula tip not to touch your glove and to minimize going in and out of the skin so you’re not seeding the filler with bacteria.”
Other potential sources of a delayed infection described in the literature include a dental abscess, pimple popping, and subsequent injections from acupuncture or hyaluronidase.
When patients present with a nonfluctuant delayed nodule that shows no obvious signs of infection, however, the root cause can stump clinicians. “Is this infectious or not?” asked Dr. Keaney, who is also clinical associate faculty in the department of dermatology at George Washington University, Washington. “Is this a focus on chronic inflammation in response to the product, or is this a collection of chronic bacteria, a biofilm too large to be engulfed by a single cell?” A review of the topic found that three risk factors for the development of biofilms include the surface area of product (large boluses of filler), longevity of the product, and inadequate sterilization technique.
Dr. Keaney said that biofilms create an impaired immune system penetration, which boosts their resistance to antibiotics by 1,000-fold. “These bacteria also have a reduced growth rate, an altered microenvironment, and altered gene expression, so it makes it difficult to clear these biofilms.”
To determine if a delayed nodule is infectious or not, performing a biopsy with polymerase chain reaction (PCR) analysis of tissue samples is ideal. “This would amplify the DNA by electrophoresis,” Dr. Keaney continued. “The problem is, it is often difficult to find labs to perform PCR. Also, you’re likely going to have to biopsy someone’s face. The patient is likely already upset that they have a delayed nodule. Ideally, you would want to avoid having to do a punch biopsy of a patient’s lip, tear trough, temple, or chin. The flip side of the coin is, how do you accurately determine if this is a noninfectious delayed nodule? If it is noninfectious, what is the mechanism of action?”
According to Dr. Keaney, short hyaluronic acid (HA) fragments can act as substrates for cell trafficking and can activate macrophages, dendritic cells, and T cells. In an analysis of immune cell response that used in vitro cell-based assays and was presented during a poster session at the 2018 Anti-Aging Medicine World Congress, researchers found no evidence of inflammatory or immune response to HA used for dermal fillers, regardless of size or formulation. However, physiologic degradation of HA to intermediate/small fragments tends to occur 4-5 months after injection.
“The hypothesis is that proinflammatory HA fragments may prime the immune system for an inflammatory response in the setting of a triggering event,” Dr. Keaney said. “The presence of an inflammatory reaction triggers an immune response to the HA fragments. Possible triggers include infections, dental procedures, and immunizations.”
The American Society for Dermatologic Surgery (ASDS) recently published a guidance regarding SARS-CoV-2 mRNA vaccine side effects in dermal filler patients after three patients developed a reaction to the Moderna vaccine, in clinical trials. “One patient, a 29-year-old, had previous angioedema from a flu vaccine, so the question is: Is it truly a delayed nodule or an immunologic reaction to the ingredients in the vaccine?” Dr. Keaney said. Two other patients, a 51-year-old female and a 46-year-old female, developed facial swelling that were believed to be related to a previous filler injection. Both cases resolved.
“Is the COVID vaccine more of an immunologic trigger than other vaccines?” Dr. Keaney asked. “Are we going to see this more frequently? We may. We just don’t know the denominator. We do not know how many patients in the Moderna or Pfizer vaccine studies had been previously treated with dermal fillers. In patients who have had previous filler treatments, I’m still advising them to get the COVID vaccine if they can.”
Dr. Keaney’s algorithm for treating a delayed nodule that is fluctuant starts with culturing any exudate and beginning a course of empiric antibiotic therapy. “If it’s a nonfluctuant delayed nodule where you’re not sure if it’s related to a biofilm or to an immunologic reaction, there are multiple global consensus papers about this challenging condition in the medical literature,” he said. “Among the papers, there is no consensus treatment, even among consensus panels. They often recommend multiple antibiotic regimens when biofilm is the suspected culprit. For a noninfectious delayed nodule, they recommend prednisone or anti-inflammatory medications. If the nodule is recalcitrant to anti-inflammatory treatments, consider adding empiric antibiotic therapy or dissolve the product.”
In other specialties, the No. 1 priority of a biofilm infection is to get rid of the implant. In orthopedics, for example, the surgeon may remove the artificial joint, Dr. Keaney said. “If that delayed nodule is not responding to comprehensive antibiotic therapy or prednisone anti-inflammatories, you may consider dissolving the filler. The challenge is, there is wide variation in the ability of different hyaluronidase [products] and fillers to dissolve. Another concern is that you may make smaller, more immunogenic HA fragments by dissolving the filler.”
One approach for vascular occlusions introduced by Claudio DeLorenzi, MD, a plastic surgeon in private practice in Kitchener, Ontario, is to dissolve dermal fillers with high-dose pulsed hyaluronidase using up to 1,500 IU every hour. “In the U.S., hyaluronidase comes in 150-200-unit sizes,” Dr. Keaney said. “In my practice, it’s not enough to have one bottle of hyaluronidase. You need around 15-20 bottles to be able to treat for a vascular incident, but if you have a delayed nodule you may also have to use high doses of hyaluronidase.”
Dr. Keaney reported that he is a consultant to and/or an advisory board member for several pharmaceutical companies.
When a is no easy task.
“It’s sometime very difficult to distinguish between the two,” Terrence Keaney, MD, said during the Orlando Dermatology Aesthetic and Clinical Conference. “Classically, an early-onset infection presents as a suppurative mass that’s fluctuant and tender. The challenge with delayed-onset infection is that it often does not tend to be fluctuant. It doesn’t resemble the classic infection you see in regular dermatology practice.”
Dr. Keaney, a dermatologist who is founder and director of SkinDC in Arlington, Va., said that the source of delayed infection could stem from inoculation at the time of injection – primarily via the skin microflora. “There are also rare case reports of mycobacterial infections from watered gauze,” which he said is why he does not use watered gauze in his practice. “This risk reinforces the importance of filler hygiene when you’re using dermal fillers. Isopropyl alcohol is often not enough. A lot of practices use chlorhexidine, avoiding its use around the eyes, to reduce the skin flora. Hypochlorous acid is another safe antiseptic for the face. You also want to be very careful with the needle or cannula tip not to touch your glove and to minimize going in and out of the skin so you’re not seeding the filler with bacteria.”
Other potential sources of a delayed infection described in the literature include a dental abscess, pimple popping, and subsequent injections from acupuncture or hyaluronidase.
When patients present with a nonfluctuant delayed nodule that shows no obvious signs of infection, however, the root cause can stump clinicians. “Is this infectious or not?” asked Dr. Keaney, who is also clinical associate faculty in the department of dermatology at George Washington University, Washington. “Is this a focus on chronic inflammation in response to the product, or is this a collection of chronic bacteria, a biofilm too large to be engulfed by a single cell?” A review of the topic found that three risk factors for the development of biofilms include the surface area of product (large boluses of filler), longevity of the product, and inadequate sterilization technique.
Dr. Keaney said that biofilms create an impaired immune system penetration, which boosts their resistance to antibiotics by 1,000-fold. “These bacteria also have a reduced growth rate, an altered microenvironment, and altered gene expression, so it makes it difficult to clear these biofilms.”
To determine if a delayed nodule is infectious or not, performing a biopsy with polymerase chain reaction (PCR) analysis of tissue samples is ideal. “This would amplify the DNA by electrophoresis,” Dr. Keaney continued. “The problem is, it is often difficult to find labs to perform PCR. Also, you’re likely going to have to biopsy someone’s face. The patient is likely already upset that they have a delayed nodule. Ideally, you would want to avoid having to do a punch biopsy of a patient’s lip, tear trough, temple, or chin. The flip side of the coin is, how do you accurately determine if this is a noninfectious delayed nodule? If it is noninfectious, what is the mechanism of action?”
According to Dr. Keaney, short hyaluronic acid (HA) fragments can act as substrates for cell trafficking and can activate macrophages, dendritic cells, and T cells. In an analysis of immune cell response that used in vitro cell-based assays and was presented during a poster session at the 2018 Anti-Aging Medicine World Congress, researchers found no evidence of inflammatory or immune response to HA used for dermal fillers, regardless of size or formulation. However, physiologic degradation of HA to intermediate/small fragments tends to occur 4-5 months after injection.
“The hypothesis is that proinflammatory HA fragments may prime the immune system for an inflammatory response in the setting of a triggering event,” Dr. Keaney said. “The presence of an inflammatory reaction triggers an immune response to the HA fragments. Possible triggers include infections, dental procedures, and immunizations.”
The American Society for Dermatologic Surgery (ASDS) recently published a guidance regarding SARS-CoV-2 mRNA vaccine side effects in dermal filler patients after three patients developed a reaction to the Moderna vaccine, in clinical trials. “One patient, a 29-year-old, had previous angioedema from a flu vaccine, so the question is: Is it truly a delayed nodule or an immunologic reaction to the ingredients in the vaccine?” Dr. Keaney said. Two other patients, a 51-year-old female and a 46-year-old female, developed facial swelling that were believed to be related to a previous filler injection. Both cases resolved.
“Is the COVID vaccine more of an immunologic trigger than other vaccines?” Dr. Keaney asked. “Are we going to see this more frequently? We may. We just don’t know the denominator. We do not know how many patients in the Moderna or Pfizer vaccine studies had been previously treated with dermal fillers. In patients who have had previous filler treatments, I’m still advising them to get the COVID vaccine if they can.”
Dr. Keaney’s algorithm for treating a delayed nodule that is fluctuant starts with culturing any exudate and beginning a course of empiric antibiotic therapy. “If it’s a nonfluctuant delayed nodule where you’re not sure if it’s related to a biofilm or to an immunologic reaction, there are multiple global consensus papers about this challenging condition in the medical literature,” he said. “Among the papers, there is no consensus treatment, even among consensus panels. They often recommend multiple antibiotic regimens when biofilm is the suspected culprit. For a noninfectious delayed nodule, they recommend prednisone or anti-inflammatory medications. If the nodule is recalcitrant to anti-inflammatory treatments, consider adding empiric antibiotic therapy or dissolve the product.”
In other specialties, the No. 1 priority of a biofilm infection is to get rid of the implant. In orthopedics, for example, the surgeon may remove the artificial joint, Dr. Keaney said. “If that delayed nodule is not responding to comprehensive antibiotic therapy or prednisone anti-inflammatories, you may consider dissolving the filler. The challenge is, there is wide variation in the ability of different hyaluronidase [products] and fillers to dissolve. Another concern is that you may make smaller, more immunogenic HA fragments by dissolving the filler.”
One approach for vascular occlusions introduced by Claudio DeLorenzi, MD, a plastic surgeon in private practice in Kitchener, Ontario, is to dissolve dermal fillers with high-dose pulsed hyaluronidase using up to 1,500 IU every hour. “In the U.S., hyaluronidase comes in 150-200-unit sizes,” Dr. Keaney said. “In my practice, it’s not enough to have one bottle of hyaluronidase. You need around 15-20 bottles to be able to treat for a vascular incident, but if you have a delayed nodule you may also have to use high doses of hyaluronidase.”
Dr. Keaney reported that he is a consultant to and/or an advisory board member for several pharmaceutical companies.
When a is no easy task.
“It’s sometime very difficult to distinguish between the two,” Terrence Keaney, MD, said during the Orlando Dermatology Aesthetic and Clinical Conference. “Classically, an early-onset infection presents as a suppurative mass that’s fluctuant and tender. The challenge with delayed-onset infection is that it often does not tend to be fluctuant. It doesn’t resemble the classic infection you see in regular dermatology practice.”
Dr. Keaney, a dermatologist who is founder and director of SkinDC in Arlington, Va., said that the source of delayed infection could stem from inoculation at the time of injection – primarily via the skin microflora. “There are also rare case reports of mycobacterial infections from watered gauze,” which he said is why he does not use watered gauze in his practice. “This risk reinforces the importance of filler hygiene when you’re using dermal fillers. Isopropyl alcohol is often not enough. A lot of practices use chlorhexidine, avoiding its use around the eyes, to reduce the skin flora. Hypochlorous acid is another safe antiseptic for the face. You also want to be very careful with the needle or cannula tip not to touch your glove and to minimize going in and out of the skin so you’re not seeding the filler with bacteria.”
Other potential sources of a delayed infection described in the literature include a dental abscess, pimple popping, and subsequent injections from acupuncture or hyaluronidase.
When patients present with a nonfluctuant delayed nodule that shows no obvious signs of infection, however, the root cause can stump clinicians. “Is this infectious or not?” asked Dr. Keaney, who is also clinical associate faculty in the department of dermatology at George Washington University, Washington. “Is this a focus on chronic inflammation in response to the product, or is this a collection of chronic bacteria, a biofilm too large to be engulfed by a single cell?” A review of the topic found that three risk factors for the development of biofilms include the surface area of product (large boluses of filler), longevity of the product, and inadequate sterilization technique.
Dr. Keaney said that biofilms create an impaired immune system penetration, which boosts their resistance to antibiotics by 1,000-fold. “These bacteria also have a reduced growth rate, an altered microenvironment, and altered gene expression, so it makes it difficult to clear these biofilms.”
To determine if a delayed nodule is infectious or not, performing a biopsy with polymerase chain reaction (PCR) analysis of tissue samples is ideal. “This would amplify the DNA by electrophoresis,” Dr. Keaney continued. “The problem is, it is often difficult to find labs to perform PCR. Also, you’re likely going to have to biopsy someone’s face. The patient is likely already upset that they have a delayed nodule. Ideally, you would want to avoid having to do a punch biopsy of a patient’s lip, tear trough, temple, or chin. The flip side of the coin is, how do you accurately determine if this is a noninfectious delayed nodule? If it is noninfectious, what is the mechanism of action?”
According to Dr. Keaney, short hyaluronic acid (HA) fragments can act as substrates for cell trafficking and can activate macrophages, dendritic cells, and T cells. In an analysis of immune cell response that used in vitro cell-based assays and was presented during a poster session at the 2018 Anti-Aging Medicine World Congress, researchers found no evidence of inflammatory or immune response to HA used for dermal fillers, regardless of size or formulation. However, physiologic degradation of HA to intermediate/small fragments tends to occur 4-5 months after injection.
“The hypothesis is that proinflammatory HA fragments may prime the immune system for an inflammatory response in the setting of a triggering event,” Dr. Keaney said. “The presence of an inflammatory reaction triggers an immune response to the HA fragments. Possible triggers include infections, dental procedures, and immunizations.”
The American Society for Dermatologic Surgery (ASDS) recently published a guidance regarding SARS-CoV-2 mRNA vaccine side effects in dermal filler patients after three patients developed a reaction to the Moderna vaccine, in clinical trials. “One patient, a 29-year-old, had previous angioedema from a flu vaccine, so the question is: Is it truly a delayed nodule or an immunologic reaction to the ingredients in the vaccine?” Dr. Keaney said. Two other patients, a 51-year-old female and a 46-year-old female, developed facial swelling that were believed to be related to a previous filler injection. Both cases resolved.
“Is the COVID vaccine more of an immunologic trigger than other vaccines?” Dr. Keaney asked. “Are we going to see this more frequently? We may. We just don’t know the denominator. We do not know how many patients in the Moderna or Pfizer vaccine studies had been previously treated with dermal fillers. In patients who have had previous filler treatments, I’m still advising them to get the COVID vaccine if they can.”
Dr. Keaney’s algorithm for treating a delayed nodule that is fluctuant starts with culturing any exudate and beginning a course of empiric antibiotic therapy. “If it’s a nonfluctuant delayed nodule where you’re not sure if it’s related to a biofilm or to an immunologic reaction, there are multiple global consensus papers about this challenging condition in the medical literature,” he said. “Among the papers, there is no consensus treatment, even among consensus panels. They often recommend multiple antibiotic regimens when biofilm is the suspected culprit. For a noninfectious delayed nodule, they recommend prednisone or anti-inflammatory medications. If the nodule is recalcitrant to anti-inflammatory treatments, consider adding empiric antibiotic therapy or dissolve the product.”
In other specialties, the No. 1 priority of a biofilm infection is to get rid of the implant. In orthopedics, for example, the surgeon may remove the artificial joint, Dr. Keaney said. “If that delayed nodule is not responding to comprehensive antibiotic therapy or prednisone anti-inflammatories, you may consider dissolving the filler. The challenge is, there is wide variation in the ability of different hyaluronidase [products] and fillers to dissolve. Another concern is that you may make smaller, more immunogenic HA fragments by dissolving the filler.”
One approach for vascular occlusions introduced by Claudio DeLorenzi, MD, a plastic surgeon in private practice in Kitchener, Ontario, is to dissolve dermal fillers with high-dose pulsed hyaluronidase using up to 1,500 IU every hour. “In the U.S., hyaluronidase comes in 150-200-unit sizes,” Dr. Keaney said. “In my practice, it’s not enough to have one bottle of hyaluronidase. You need around 15-20 bottles to be able to treat for a vascular incident, but if you have a delayed nodule you may also have to use high doses of hyaluronidase.”
Dr. Keaney reported that he is a consultant to and/or an advisory board member for several pharmaceutical companies.
FROM ODAC 2021
Expert offers tips for sorting out pink lesions on dermoscopy
Even in the most experienced hands, .
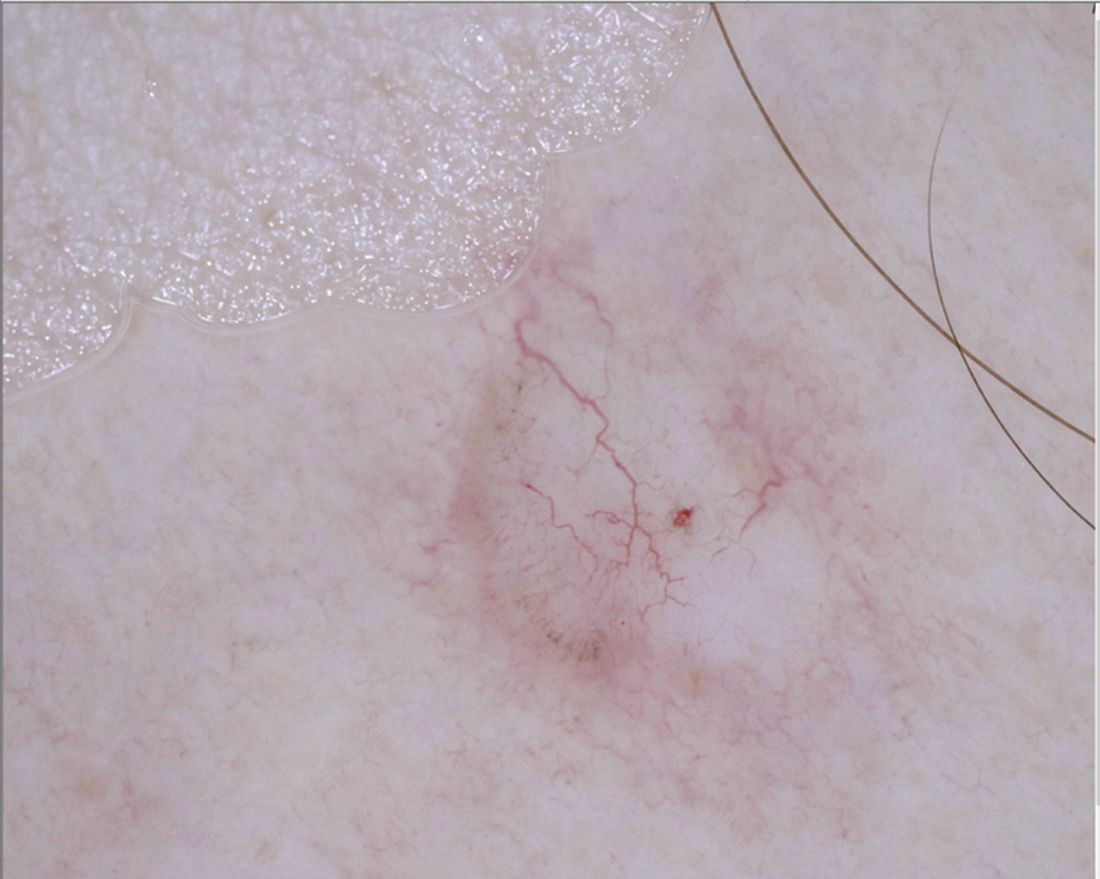
“For me, pink lesions are challenging,” Jennifer A. Stein, MD, PhD, said during the virtual Orlando Dermatology Aesthetic and Clinical Conference. “How can dermoscopy help us distinguish between Spitz nevus, melanoma, clear cell acanthoma, psoriasis, basal cell carcinoma, and squamous cell carcinoma?”
Dr. Stein, professor of dermatology at New York University, offered four tips. First, look for the shiny white perpendicular lines, otherwise known as the chrysalis or crystalline pattern. “You can only see this feature when you’re looking with polarized light,” she said. “This is why you want a dermatoscope that has polarized light, and better yet, one that you’re able to turn on and off, the hybrid kind, because then you can convince yourself that you’re looking at this feature, because it blinks on and off.”
The differential diagnosis for white shiny perpendicular lines includes dermatofibroma/scars (which is most common), Spitz and atypical genital nevi, BCC, and melanoma. “Dermatofibromas sometimes have white circles or rings in the center,” Dr. Stein said. “In BCC, the lines aren’t always perpendicular. Sometimes it’s more of a blotch or strands.”
A second tip for managing a pink lesion on dermoscopy is to look for any brown color. “When you see that combo together you have to worry,” she said. “When you see pigment network on dermoscopy, you have to put melanoma in your differential. If you see shiny white lines in something that is melanocytic, there’s a 98% specificity for melanoma.”
A third tip she offered for managing pink lesions is to check the blood vessels for clues. “For years, I was just naming the vessels based on making the diagnosis and then deciding, ‘that’s a basal cell carcinoma; those must be branching vessels,’ ” said Dr. Stein, who manages NYU’s medical dermatology faculty group practice.
However, blood vessel patterns differ. For example, branching or arborizing vessels are suggestive of BCC. “These vessels are very crisp-looking on dermoscopy,” she said. “They’re all in the same plane of focus and they look like they were drawn in with a fine point marker. That’s different from other blood vessel patterns.” She also pointed out that superficial basal cells have short, fine telangiectasias. “When you put on the polarized light, the clue is the white, shiny structures,” she said.
Dotted vessels, meanwhile, appear on dermoscopy as small red dots aligned perpendicular to the skin surface. The differential includes inflammatory lesions like psoriasis, stasis, and trauma; clear cell acanthoma (characterized by a “string of pearls” arrangement), nevi, and melanoma. “I find dermoscopy most useful in diagnosing SCC – especially squamous cell in situ,” she said. “Important clinical clues suggestive of SCC or melanoma include a solitary lesion, it’s new, it’s growing, and it’s not going away with a topical steroid.”
An additional pattern to be aware of are hairpin vessels, which are looped and feature a sharp bend at one end. These are often seen in seborrheic keratoses. “You can’t count on the hairpin vessels alone, because you can see this in anything keratotic, such as in keratoacanthoma (at the periphery with a yellow keratotic center), warts, SCC, BCC, as well as in dermal nevi and Spitz nevi,” said Dr. Stein, who recommended dermoscopedia.org as resource.
Comma vessels, meanwhile, appear in dermal or compound nevi. She described these as “slightly curved vessels that are much less in focus than branched vessels, because they come in and out of the plane of focus,” she said. “If you put your dermatoscope on top of the nevus and wobble it around you can appreciate the curve. If you look at it from the side, it looks like a curve. If you look at it straight on it will look more like a line. If you look at from the end it will look like a dot.”
Another vessel type she discussed are linear irregular and polymorphous vessels, which she described as “any combination of different types of vessels. We get most worried when we see dotted and linear irregular vessels together. In that case, you worry about melanoma. These can also be seen in nevi and other tumors, such as BCC.”
Dr. Stein’s fourth tip of the presentation was a reminder to consider dermoscopy as one piece of the clinical exam. “Always think about the lesion in context of the rest of the clinical picture and history,” she said. “Don’t get discouraged if it’s hard; just keep practicing. Look for any brown and use your clinical clues to put together to make the right decision.”
She disclosed that NYU receives compensation from MoleSafe for her telemedicine dermoscopic diagnoses.
Even in the most experienced hands, .

“For me, pink lesions are challenging,” Jennifer A. Stein, MD, PhD, said during the virtual Orlando Dermatology Aesthetic and Clinical Conference. “How can dermoscopy help us distinguish between Spitz nevus, melanoma, clear cell acanthoma, psoriasis, basal cell carcinoma, and squamous cell carcinoma?”
Dr. Stein, professor of dermatology at New York University, offered four tips. First, look for the shiny white perpendicular lines, otherwise known as the chrysalis or crystalline pattern. “You can only see this feature when you’re looking with polarized light,” she said. “This is why you want a dermatoscope that has polarized light, and better yet, one that you’re able to turn on and off, the hybrid kind, because then you can convince yourself that you’re looking at this feature, because it blinks on and off.”
The differential diagnosis for white shiny perpendicular lines includes dermatofibroma/scars (which is most common), Spitz and atypical genital nevi, BCC, and melanoma. “Dermatofibromas sometimes have white circles or rings in the center,” Dr. Stein said. “In BCC, the lines aren’t always perpendicular. Sometimes it’s more of a blotch or strands.”
A second tip for managing a pink lesion on dermoscopy is to look for any brown color. “When you see that combo together you have to worry,” she said. “When you see pigment network on dermoscopy, you have to put melanoma in your differential. If you see shiny white lines in something that is melanocytic, there’s a 98% specificity for melanoma.”
A third tip she offered for managing pink lesions is to check the blood vessels for clues. “For years, I was just naming the vessels based on making the diagnosis and then deciding, ‘that’s a basal cell carcinoma; those must be branching vessels,’ ” said Dr. Stein, who manages NYU’s medical dermatology faculty group practice.
However, blood vessel patterns differ. For example, branching or arborizing vessels are suggestive of BCC. “These vessels are very crisp-looking on dermoscopy,” she said. “They’re all in the same plane of focus and they look like they were drawn in with a fine point marker. That’s different from other blood vessel patterns.” She also pointed out that superficial basal cells have short, fine telangiectasias. “When you put on the polarized light, the clue is the white, shiny structures,” she said.
Dotted vessels, meanwhile, appear on dermoscopy as small red dots aligned perpendicular to the skin surface. The differential includes inflammatory lesions like psoriasis, stasis, and trauma; clear cell acanthoma (characterized by a “string of pearls” arrangement), nevi, and melanoma. “I find dermoscopy most useful in diagnosing SCC – especially squamous cell in situ,” she said. “Important clinical clues suggestive of SCC or melanoma include a solitary lesion, it’s new, it’s growing, and it’s not going away with a topical steroid.”
An additional pattern to be aware of are hairpin vessels, which are looped and feature a sharp bend at one end. These are often seen in seborrheic keratoses. “You can’t count on the hairpin vessels alone, because you can see this in anything keratotic, such as in keratoacanthoma (at the periphery with a yellow keratotic center), warts, SCC, BCC, as well as in dermal nevi and Spitz nevi,” said Dr. Stein, who recommended dermoscopedia.org as resource.
Comma vessels, meanwhile, appear in dermal or compound nevi. She described these as “slightly curved vessels that are much less in focus than branched vessels, because they come in and out of the plane of focus,” she said. “If you put your dermatoscope on top of the nevus and wobble it around you can appreciate the curve. If you look at it from the side, it looks like a curve. If you look at it straight on it will look more like a line. If you look at from the end it will look like a dot.”
Another vessel type she discussed are linear irregular and polymorphous vessels, which she described as “any combination of different types of vessels. We get most worried when we see dotted and linear irregular vessels together. In that case, you worry about melanoma. These can also be seen in nevi and other tumors, such as BCC.”
Dr. Stein’s fourth tip of the presentation was a reminder to consider dermoscopy as one piece of the clinical exam. “Always think about the lesion in context of the rest of the clinical picture and history,” she said. “Don’t get discouraged if it’s hard; just keep practicing. Look for any brown and use your clinical clues to put together to make the right decision.”
She disclosed that NYU receives compensation from MoleSafe for her telemedicine dermoscopic diagnoses.
Even in the most experienced hands, .

“For me, pink lesions are challenging,” Jennifer A. Stein, MD, PhD, said during the virtual Orlando Dermatology Aesthetic and Clinical Conference. “How can dermoscopy help us distinguish between Spitz nevus, melanoma, clear cell acanthoma, psoriasis, basal cell carcinoma, and squamous cell carcinoma?”
Dr. Stein, professor of dermatology at New York University, offered four tips. First, look for the shiny white perpendicular lines, otherwise known as the chrysalis or crystalline pattern. “You can only see this feature when you’re looking with polarized light,” she said. “This is why you want a dermatoscope that has polarized light, and better yet, one that you’re able to turn on and off, the hybrid kind, because then you can convince yourself that you’re looking at this feature, because it blinks on and off.”
The differential diagnosis for white shiny perpendicular lines includes dermatofibroma/scars (which is most common), Spitz and atypical genital nevi, BCC, and melanoma. “Dermatofibromas sometimes have white circles or rings in the center,” Dr. Stein said. “In BCC, the lines aren’t always perpendicular. Sometimes it’s more of a blotch or strands.”
A second tip for managing a pink lesion on dermoscopy is to look for any brown color. “When you see that combo together you have to worry,” she said. “When you see pigment network on dermoscopy, you have to put melanoma in your differential. If you see shiny white lines in something that is melanocytic, there’s a 98% specificity for melanoma.”
A third tip she offered for managing pink lesions is to check the blood vessels for clues. “For years, I was just naming the vessels based on making the diagnosis and then deciding, ‘that’s a basal cell carcinoma; those must be branching vessels,’ ” said Dr. Stein, who manages NYU’s medical dermatology faculty group practice.
However, blood vessel patterns differ. For example, branching or arborizing vessels are suggestive of BCC. “These vessels are very crisp-looking on dermoscopy,” she said. “They’re all in the same plane of focus and they look like they were drawn in with a fine point marker. That’s different from other blood vessel patterns.” She also pointed out that superficial basal cells have short, fine telangiectasias. “When you put on the polarized light, the clue is the white, shiny structures,” she said.
Dotted vessels, meanwhile, appear on dermoscopy as small red dots aligned perpendicular to the skin surface. The differential includes inflammatory lesions like psoriasis, stasis, and trauma; clear cell acanthoma (characterized by a “string of pearls” arrangement), nevi, and melanoma. “I find dermoscopy most useful in diagnosing SCC – especially squamous cell in situ,” she said. “Important clinical clues suggestive of SCC or melanoma include a solitary lesion, it’s new, it’s growing, and it’s not going away with a topical steroid.”
An additional pattern to be aware of are hairpin vessels, which are looped and feature a sharp bend at one end. These are often seen in seborrheic keratoses. “You can’t count on the hairpin vessels alone, because you can see this in anything keratotic, such as in keratoacanthoma (at the periphery with a yellow keratotic center), warts, SCC, BCC, as well as in dermal nevi and Spitz nevi,” said Dr. Stein, who recommended dermoscopedia.org as resource.
Comma vessels, meanwhile, appear in dermal or compound nevi. She described these as “slightly curved vessels that are much less in focus than branched vessels, because they come in and out of the plane of focus,” she said. “If you put your dermatoscope on top of the nevus and wobble it around you can appreciate the curve. If you look at it from the side, it looks like a curve. If you look at it straight on it will look more like a line. If you look at from the end it will look like a dot.”
Another vessel type she discussed are linear irregular and polymorphous vessels, which she described as “any combination of different types of vessels. We get most worried when we see dotted and linear irregular vessels together. In that case, you worry about melanoma. These can also be seen in nevi and other tumors, such as BCC.”
Dr. Stein’s fourth tip of the presentation was a reminder to consider dermoscopy as one piece of the clinical exam. “Always think about the lesion in context of the rest of the clinical picture and history,” she said. “Don’t get discouraged if it’s hard; just keep practicing. Look for any brown and use your clinical clues to put together to make the right decision.”
She disclosed that NYU receives compensation from MoleSafe for her telemedicine dermoscopic diagnoses.
FROM ODAC 2021