User login
Antibody could treat AML, MM, and NHL
An investigational antibody has demonstrated activity against acute myeloid leukemia (AML), multiple myeloma (MM), and non-Hodgkin lymphoma (NHL), according to researchers.
PF-06747143 is a humanized CXCR4 immunoglobulin G1 (IgG1) antibody that binds to CXCR4 and inhibits both CXCL12-mediated signaling pathways and cell migration.
Whether given alone or in combination with chemotherapy, PF-06747143 demonstrated efficacy in mouse models of NHL, MM, and AML.
Treatment involving PF-06747143—alone or in combination—eradicated more cancer cells than did standard treatment options.
These results were published in Blood Advances. The research was sponsored by Pfizer, Inc., the company developing PF-06747143.
“One of the major limitations we see in treating blood cancers is the failure to clear cancer cells from the bone marrow,” said study author Flavia Pernasetti, PhD, of Pfizer Oncology Research and Development.
“Because the bone marrow allows the cancer cells to flourish, removing these cells is an essential step in treating these malignancies effectively.”
With this goal in mind, Dr Pernasetti and her colleagues looked to the mechanisms that control the movement of cells into the bone marrow (BM) in the first place—the chemokine receptor CXCR4 and its ligand CXCL12.
The researchers created PF-06747143, which attacks and kills cancer cells directly but also removes cancer cells from the BM so they can be killed by other treatments.
Results in NHL
The researchers first tested PF-06747143 in an NHL Ramos xenograft model. Mice received PF-06747143 or a control IgG1 antibody at 10 mg/kg on days 1 and 8.
PF-06747143 significantly inhibited tumor growth compared to the control antibody (P<0.0001). Seventy percent of PF-06747143-treated mice had tumor volumes below their initial size at the end of the study.
PF-06747143 produced a dose-dependent response that was sustained until the end of the study, even after treatment was stopped.
Results in MM
The researchers tested PF-06747143 in a disseminated MM model, in which the OPM2-Luc tumor cells were implanted intravenously and migrated spontaneously to the BM.
Mice received PF-06747143 or IgG1 control at 10 mg/kg weekly for 5 doses. Other mice received melphalan at 1 mg/kg twice a week for a total of 4 cycles.
On day 30, PF-06747143 had significantly inhibited BM tumor growth compared to the control antibody or melphalan (P<0.0001).
PF-06747143-treated mice also had a significant survival benefit. The median survival was 33.5 days for mice that received the control antibody and 36 days for mice treated with melphalan. However, there were no deaths in the PF-06747143-treated mice by day 50, which marked the end of the study (P<0.0001).
The researchers also tested PF-06747143 at a lower dose (1 mg/kg weekly for a total of 7 doses), both alone and in combination with bortezomib (0.5 mg/kg twice a week for a total of 4 cycles).
The median survival was 34 days in the control mice, 44 days in mice that received bortezomib alone, and 47 days in mice that received PF-06747143 alone. However, there were no deaths in the combination arm at day 51, which was the end of the study (P<0.0003).
Results in AML
The researchers tested PF-06747143 in an AML disseminated tumor model using MV4-11 cells.
They compared PF-06747143 (given at 0.1, 1, or 10 mg/kg weekly for 4 doses) to the chemotherapeutic agent daunorubicin (2 mg/kg on days 1, 3, and 5), the FLT3 inhibitor crenolanib (7.5 mg/kg twice a day, on days 11-15 and 25-29), and a control IgG1 antibody (10 mg/kg weekly for 4 doses).
PF-06747143 (at 10 mg/kg), daunorubicin, and crenolanib all significantly reduced the number of tumor cells in the peripheral blood and BM when compared with the control antibody (P<0.05).
PF-06746143 treatment (at 10 mg/kg) reduced the number of AML cells in the BM by 95.9%, while daunorubicin reduced them by 84.5% and crenolanib by 80.5%.
The median survival was 36 days for mice that received PF-06747143 at 0.1 mg/kg, 41 days for mice that received the control antibody, 47 days for mice that received PF-06747143 at 1 mg/kg, and 63 days for mice that received PF-06747143 at 10 mg/kg.
The researchers also found that PF-06747143 had a “strong combinatorial effect” with daunorubicin and cytarabine in a chemotherapy-resistant model of AML. The team noted that only 36% of BM cells are positive for CXCR4 in this model.
Treatment with PF-06747143 alone reduced the percentage of AML cells in the BM to 80%, combination daunorubicin and cytarabine reduced it to 27%, and combination PF-06747143, daunorubicin, and cytarabine reduced the percentage of AML cells in the BM to 0.3%.
“Our preliminary preclinical results are encouraging,” Dr Pernasetti said, “and we are very excited to see how our antibody fares in clinical testing.”
PF-06747143 is currently being evaluated in a phase 1 trial of AML patients. ![]()
An investigational antibody has demonstrated activity against acute myeloid leukemia (AML), multiple myeloma (MM), and non-Hodgkin lymphoma (NHL), according to researchers.
PF-06747143 is a humanized CXCR4 immunoglobulin G1 (IgG1) antibody that binds to CXCR4 and inhibits both CXCL12-mediated signaling pathways and cell migration.
Whether given alone or in combination with chemotherapy, PF-06747143 demonstrated efficacy in mouse models of NHL, MM, and AML.
Treatment involving PF-06747143—alone or in combination—eradicated more cancer cells than did standard treatment options.
These results were published in Blood Advances. The research was sponsored by Pfizer, Inc., the company developing PF-06747143.
“One of the major limitations we see in treating blood cancers is the failure to clear cancer cells from the bone marrow,” said study author Flavia Pernasetti, PhD, of Pfizer Oncology Research and Development.
“Because the bone marrow allows the cancer cells to flourish, removing these cells is an essential step in treating these malignancies effectively.”
With this goal in mind, Dr Pernasetti and her colleagues looked to the mechanisms that control the movement of cells into the bone marrow (BM) in the first place—the chemokine receptor CXCR4 and its ligand CXCL12.
The researchers created PF-06747143, which attacks and kills cancer cells directly but also removes cancer cells from the BM so they can be killed by other treatments.
Results in NHL
The researchers first tested PF-06747143 in an NHL Ramos xenograft model. Mice received PF-06747143 or a control IgG1 antibody at 10 mg/kg on days 1 and 8.
PF-06747143 significantly inhibited tumor growth compared to the control antibody (P<0.0001). Seventy percent of PF-06747143-treated mice had tumor volumes below their initial size at the end of the study.
PF-06747143 produced a dose-dependent response that was sustained until the end of the study, even after treatment was stopped.
Results in MM
The researchers tested PF-06747143 in a disseminated MM model, in which the OPM2-Luc tumor cells were implanted intravenously and migrated spontaneously to the BM.
Mice received PF-06747143 or IgG1 control at 10 mg/kg weekly for 5 doses. Other mice received melphalan at 1 mg/kg twice a week for a total of 4 cycles.
On day 30, PF-06747143 had significantly inhibited BM tumor growth compared to the control antibody or melphalan (P<0.0001).
PF-06747143-treated mice also had a significant survival benefit. The median survival was 33.5 days for mice that received the control antibody and 36 days for mice treated with melphalan. However, there were no deaths in the PF-06747143-treated mice by day 50, which marked the end of the study (P<0.0001).
The researchers also tested PF-06747143 at a lower dose (1 mg/kg weekly for a total of 7 doses), both alone and in combination with bortezomib (0.5 mg/kg twice a week for a total of 4 cycles).
The median survival was 34 days in the control mice, 44 days in mice that received bortezomib alone, and 47 days in mice that received PF-06747143 alone. However, there were no deaths in the combination arm at day 51, which was the end of the study (P<0.0003).
Results in AML
The researchers tested PF-06747143 in an AML disseminated tumor model using MV4-11 cells.
They compared PF-06747143 (given at 0.1, 1, or 10 mg/kg weekly for 4 doses) to the chemotherapeutic agent daunorubicin (2 mg/kg on days 1, 3, and 5), the FLT3 inhibitor crenolanib (7.5 mg/kg twice a day, on days 11-15 and 25-29), and a control IgG1 antibody (10 mg/kg weekly for 4 doses).
PF-06747143 (at 10 mg/kg), daunorubicin, and crenolanib all significantly reduced the number of tumor cells in the peripheral blood and BM when compared with the control antibody (P<0.05).
PF-06746143 treatment (at 10 mg/kg) reduced the number of AML cells in the BM by 95.9%, while daunorubicin reduced them by 84.5% and crenolanib by 80.5%.
The median survival was 36 days for mice that received PF-06747143 at 0.1 mg/kg, 41 days for mice that received the control antibody, 47 days for mice that received PF-06747143 at 1 mg/kg, and 63 days for mice that received PF-06747143 at 10 mg/kg.
The researchers also found that PF-06747143 had a “strong combinatorial effect” with daunorubicin and cytarabine in a chemotherapy-resistant model of AML. The team noted that only 36% of BM cells are positive for CXCR4 in this model.
Treatment with PF-06747143 alone reduced the percentage of AML cells in the BM to 80%, combination daunorubicin and cytarabine reduced it to 27%, and combination PF-06747143, daunorubicin, and cytarabine reduced the percentage of AML cells in the BM to 0.3%.
“Our preliminary preclinical results are encouraging,” Dr Pernasetti said, “and we are very excited to see how our antibody fares in clinical testing.”
PF-06747143 is currently being evaluated in a phase 1 trial of AML patients. ![]()
An investigational antibody has demonstrated activity against acute myeloid leukemia (AML), multiple myeloma (MM), and non-Hodgkin lymphoma (NHL), according to researchers.
PF-06747143 is a humanized CXCR4 immunoglobulin G1 (IgG1) antibody that binds to CXCR4 and inhibits both CXCL12-mediated signaling pathways and cell migration.
Whether given alone or in combination with chemotherapy, PF-06747143 demonstrated efficacy in mouse models of NHL, MM, and AML.
Treatment involving PF-06747143—alone or in combination—eradicated more cancer cells than did standard treatment options.
These results were published in Blood Advances. The research was sponsored by Pfizer, Inc., the company developing PF-06747143.
“One of the major limitations we see in treating blood cancers is the failure to clear cancer cells from the bone marrow,” said study author Flavia Pernasetti, PhD, of Pfizer Oncology Research and Development.
“Because the bone marrow allows the cancer cells to flourish, removing these cells is an essential step in treating these malignancies effectively.”
With this goal in mind, Dr Pernasetti and her colleagues looked to the mechanisms that control the movement of cells into the bone marrow (BM) in the first place—the chemokine receptor CXCR4 and its ligand CXCL12.
The researchers created PF-06747143, which attacks and kills cancer cells directly but also removes cancer cells from the BM so they can be killed by other treatments.
Results in NHL
The researchers first tested PF-06747143 in an NHL Ramos xenograft model. Mice received PF-06747143 or a control IgG1 antibody at 10 mg/kg on days 1 and 8.
PF-06747143 significantly inhibited tumor growth compared to the control antibody (P<0.0001). Seventy percent of PF-06747143-treated mice had tumor volumes below their initial size at the end of the study.
PF-06747143 produced a dose-dependent response that was sustained until the end of the study, even after treatment was stopped.
Results in MM
The researchers tested PF-06747143 in a disseminated MM model, in which the OPM2-Luc tumor cells were implanted intravenously and migrated spontaneously to the BM.
Mice received PF-06747143 or IgG1 control at 10 mg/kg weekly for 5 doses. Other mice received melphalan at 1 mg/kg twice a week for a total of 4 cycles.
On day 30, PF-06747143 had significantly inhibited BM tumor growth compared to the control antibody or melphalan (P<0.0001).
PF-06747143-treated mice also had a significant survival benefit. The median survival was 33.5 days for mice that received the control antibody and 36 days for mice treated with melphalan. However, there were no deaths in the PF-06747143-treated mice by day 50, which marked the end of the study (P<0.0001).
The researchers also tested PF-06747143 at a lower dose (1 mg/kg weekly for a total of 7 doses), both alone and in combination with bortezomib (0.5 mg/kg twice a week for a total of 4 cycles).
The median survival was 34 days in the control mice, 44 days in mice that received bortezomib alone, and 47 days in mice that received PF-06747143 alone. However, there were no deaths in the combination arm at day 51, which was the end of the study (P<0.0003).
Results in AML
The researchers tested PF-06747143 in an AML disseminated tumor model using MV4-11 cells.
They compared PF-06747143 (given at 0.1, 1, or 10 mg/kg weekly for 4 doses) to the chemotherapeutic agent daunorubicin (2 mg/kg on days 1, 3, and 5), the FLT3 inhibitor crenolanib (7.5 mg/kg twice a day, on days 11-15 and 25-29), and a control IgG1 antibody (10 mg/kg weekly for 4 doses).
PF-06747143 (at 10 mg/kg), daunorubicin, and crenolanib all significantly reduced the number of tumor cells in the peripheral blood and BM when compared with the control antibody (P<0.05).
PF-06746143 treatment (at 10 mg/kg) reduced the number of AML cells in the BM by 95.9%, while daunorubicin reduced them by 84.5% and crenolanib by 80.5%.
The median survival was 36 days for mice that received PF-06747143 at 0.1 mg/kg, 41 days for mice that received the control antibody, 47 days for mice that received PF-06747143 at 1 mg/kg, and 63 days for mice that received PF-06747143 at 10 mg/kg.
The researchers also found that PF-06747143 had a “strong combinatorial effect” with daunorubicin and cytarabine in a chemotherapy-resistant model of AML. The team noted that only 36% of BM cells are positive for CXCR4 in this model.
Treatment with PF-06747143 alone reduced the percentage of AML cells in the BM to 80%, combination daunorubicin and cytarabine reduced it to 27%, and combination PF-06747143, daunorubicin, and cytarabine reduced the percentage of AML cells in the BM to 0.3%.
“Our preliminary preclinical results are encouraging,” Dr Pernasetti said, “and we are very excited to see how our antibody fares in clinical testing.”
PF-06747143 is currently being evaluated in a phase 1 trial of AML patients. ![]()
FDA grants drug orphan designation for AML
The US Food and Drug Administration (FDA) has granted orphan drug designation to SY-1425 for the treatment of acute myeloid leukemia (AML).
SY-1425 is an oral, first-in-class, selective retinoic acid receptor alpha (RARα) agonist. It is currently under investigation in a phase 2 trial of patients with AML and myelodysplastic syndromes (MDS).
“We believe that SY-1425 may provide a meaningful benefit for subsets of AML patients whose disease is driven by abnormally high expression of the RARA or IRF8 genes,” said David A. Roth, MD, chief medical officer at Syros Pharmaceuticals, the company developing SY-1425.
“Receiving orphan drug designation is an important regulatory milestone in the development of SY-1425. We’re pleased with the continued progress of the ongoing phase 2 clinical trial, and we look forward to presenting initial clinical data in the fourth quarter of this year.”
Using its gene control platform, Syros discovered subsets of AML and MDS patients with super-enhancers associated with RARA or IRF8. These super-enhancers are believed to drive overexpression of the RARA or IRF8 genes, locking cells in an immature, undifferentiated, and proliferative state and leading to disease.
In preclinical studies, SY-1425 promoted differentiation of AML cells with high RARA or IRF8 expression and inhibited tumor growth and prolonged survival in patient-derived xenograft models of AML with high RARA expression.
In the ongoing phase 2 trial, researchers are assessing the safety and efficacy of SY-1425 as a single agent in 4 AML and MDS patient populations, as well as SY-1425 in combination with azacitidine in newly diagnosed AML patients who are not suitable candidates for standard chemotherapy.
All patients are prospectively selected using biomarkers for high expression of RARA or IRF8. Additional details about the trial can be found at https://clinicaltrials.gov/ct2/show/NCT02807558.
About orphan designation
The FDA grants orphan designation to products intended to treat, diagnose, or prevent diseases/disorders that affect fewer than 200,000 people in the US.
The designation provides incentives for sponsors to develop products for rare diseases. This may include tax credits toward the cost of clinical trials, prescription drug user fee waivers, and 7 years of market exclusivity if the product is approved. ![]()
The US Food and Drug Administration (FDA) has granted orphan drug designation to SY-1425 for the treatment of acute myeloid leukemia (AML).
SY-1425 is an oral, first-in-class, selective retinoic acid receptor alpha (RARα) agonist. It is currently under investigation in a phase 2 trial of patients with AML and myelodysplastic syndromes (MDS).
“We believe that SY-1425 may provide a meaningful benefit for subsets of AML patients whose disease is driven by abnormally high expression of the RARA or IRF8 genes,” said David A. Roth, MD, chief medical officer at Syros Pharmaceuticals, the company developing SY-1425.
“Receiving orphan drug designation is an important regulatory milestone in the development of SY-1425. We’re pleased with the continued progress of the ongoing phase 2 clinical trial, and we look forward to presenting initial clinical data in the fourth quarter of this year.”
Using its gene control platform, Syros discovered subsets of AML and MDS patients with super-enhancers associated with RARA or IRF8. These super-enhancers are believed to drive overexpression of the RARA or IRF8 genes, locking cells in an immature, undifferentiated, and proliferative state and leading to disease.
In preclinical studies, SY-1425 promoted differentiation of AML cells with high RARA or IRF8 expression and inhibited tumor growth and prolonged survival in patient-derived xenograft models of AML with high RARA expression.
In the ongoing phase 2 trial, researchers are assessing the safety and efficacy of SY-1425 as a single agent in 4 AML and MDS patient populations, as well as SY-1425 in combination with azacitidine in newly diagnosed AML patients who are not suitable candidates for standard chemotherapy.
All patients are prospectively selected using biomarkers for high expression of RARA or IRF8. Additional details about the trial can be found at https://clinicaltrials.gov/ct2/show/NCT02807558.
About orphan designation
The FDA grants orphan designation to products intended to treat, diagnose, or prevent diseases/disorders that affect fewer than 200,000 people in the US.
The designation provides incentives for sponsors to develop products for rare diseases. This may include tax credits toward the cost of clinical trials, prescription drug user fee waivers, and 7 years of market exclusivity if the product is approved. ![]()
The US Food and Drug Administration (FDA) has granted orphan drug designation to SY-1425 for the treatment of acute myeloid leukemia (AML).
SY-1425 is an oral, first-in-class, selective retinoic acid receptor alpha (RARα) agonist. It is currently under investigation in a phase 2 trial of patients with AML and myelodysplastic syndromes (MDS).
“We believe that SY-1425 may provide a meaningful benefit for subsets of AML patients whose disease is driven by abnormally high expression of the RARA or IRF8 genes,” said David A. Roth, MD, chief medical officer at Syros Pharmaceuticals, the company developing SY-1425.
“Receiving orphan drug designation is an important regulatory milestone in the development of SY-1425. We’re pleased with the continued progress of the ongoing phase 2 clinical trial, and we look forward to presenting initial clinical data in the fourth quarter of this year.”
Using its gene control platform, Syros discovered subsets of AML and MDS patients with super-enhancers associated with RARA or IRF8. These super-enhancers are believed to drive overexpression of the RARA or IRF8 genes, locking cells in an immature, undifferentiated, and proliferative state and leading to disease.
In preclinical studies, SY-1425 promoted differentiation of AML cells with high RARA or IRF8 expression and inhibited tumor growth and prolonged survival in patient-derived xenograft models of AML with high RARA expression.
In the ongoing phase 2 trial, researchers are assessing the safety and efficacy of SY-1425 as a single agent in 4 AML and MDS patient populations, as well as SY-1425 in combination with azacitidine in newly diagnosed AML patients who are not suitable candidates for standard chemotherapy.
All patients are prospectively selected using biomarkers for high expression of RARA or IRF8. Additional details about the trial can be found at https://clinicaltrials.gov/ct2/show/NCT02807558.
About orphan designation
The FDA grants orphan designation to products intended to treat, diagnose, or prevent diseases/disorders that affect fewer than 200,000 people in the US.
The designation provides incentives for sponsors to develop products for rare diseases. This may include tax credits toward the cost of clinical trials, prescription drug user fee waivers, and 7 years of market exclusivity if the product is approved. ![]()
BMI z scores fall short for tracking severe obesity
, based on data from nearly 7,000 children in the Bogalusa Heart Study.
The current parameters used in the Centers for Disease Control and Prevention growth charts for children with high body mass index (BMI) “can result in estimates that differ substantially from those that are observed and constrains the maximum BMI z that is attainable at a given sex and age,” wrote David S. Freedman, PhD, of the Centers for Disease Control and Prevention in Atlanta, and Gerald S. Berenson, MD, of Louisiana State University Health Sciences Center, New Orleans, (Pediatrics. 2017;140:e20171072).
The BMI adjusted z score (BMIaz) or the BMI expressed as a percentage of the 95th percentile (%BMIp95) “will provide more accurate information on body size over time among children with very high BMIs,” they said.
In children with severe obesity, BMI z was a weaker measure (r = 0.46) than were measures of %BMIp95 (r = 0.61) or BMIaz scores with no upper boundary (r = 0.65).
BMI z scores were weakest when applied to children younger than 10 years, with correlations of r = 0.36 for BMI z vs. correlations of 0.60 and 0.57 for BMIaz and %BMIp95, respectively.
The results were limited by several factors including the age of the data (40 years ago, when the prevalence of severe obesity was lower, 2% compared with approximately 6% now) and long intervals between exams in some cases (5 years or more), the researchers noted. However, the results suggest that BMI z values “can differ substantially from empirical estimates, have an effective upper limit, and are strongly influenced by sex and age,” they said. As an alternative, the researchers recommended that “very high BMIs should be should expressed as z scores on the basis of linear extrapolations of a fixed SD or as percentage of the CDC 95th percentile,” or using multilevel models that adjust for age and sex.
The researchers had no financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
The use of BMI z scores to assess and track severe obesity in children should be abandoned.
In the study by Freedman et al., BMI z scores, which are extrapolations of BMI measurements, did not correlate well with other measures of adiposity. Their use to assess severe obesity is problematic because large changes in weight and BMI are linked to small changes in BMI z or BMI percentiles.
William H. Dietz, MD, PhD, is at the Sumner M. Redstone Global Center for Prevention and Wellness, Milken Institute School of Public Health at George Washington University in Washington. He had no relevant financial disclosures, but disclosed that he serves on the scientific advisory board for Weight Watchers and is on the board of directors for the Partnership for a Healthier America. He discussed the article by Freedman et al. in an editorial (Pediatrics. 2017;140:e20172148).
The use of BMI z scores to assess and track severe obesity in children should be abandoned.
In the study by Freedman et al., BMI z scores, which are extrapolations of BMI measurements, did not correlate well with other measures of adiposity. Their use to assess severe obesity is problematic because large changes in weight and BMI are linked to small changes in BMI z or BMI percentiles.
William H. Dietz, MD, PhD, is at the Sumner M. Redstone Global Center for Prevention and Wellness, Milken Institute School of Public Health at George Washington University in Washington. He had no relevant financial disclosures, but disclosed that he serves on the scientific advisory board for Weight Watchers and is on the board of directors for the Partnership for a Healthier America. He discussed the article by Freedman et al. in an editorial (Pediatrics. 2017;140:e20172148).
The use of BMI z scores to assess and track severe obesity in children should be abandoned.
In the study by Freedman et al., BMI z scores, which are extrapolations of BMI measurements, did not correlate well with other measures of adiposity. Their use to assess severe obesity is problematic because large changes in weight and BMI are linked to small changes in BMI z or BMI percentiles.
William H. Dietz, MD, PhD, is at the Sumner M. Redstone Global Center for Prevention and Wellness, Milken Institute School of Public Health at George Washington University in Washington. He had no relevant financial disclosures, but disclosed that he serves on the scientific advisory board for Weight Watchers and is on the board of directors for the Partnership for a Healthier America. He discussed the article by Freedman et al. in an editorial (Pediatrics. 2017;140:e20172148).
, based on data from nearly 7,000 children in the Bogalusa Heart Study.
The current parameters used in the Centers for Disease Control and Prevention growth charts for children with high body mass index (BMI) “can result in estimates that differ substantially from those that are observed and constrains the maximum BMI z that is attainable at a given sex and age,” wrote David S. Freedman, PhD, of the Centers for Disease Control and Prevention in Atlanta, and Gerald S. Berenson, MD, of Louisiana State University Health Sciences Center, New Orleans, (Pediatrics. 2017;140:e20171072).
The BMI adjusted z score (BMIaz) or the BMI expressed as a percentage of the 95th percentile (%BMIp95) “will provide more accurate information on body size over time among children with very high BMIs,” they said.
In children with severe obesity, BMI z was a weaker measure (r = 0.46) than were measures of %BMIp95 (r = 0.61) or BMIaz scores with no upper boundary (r = 0.65).
BMI z scores were weakest when applied to children younger than 10 years, with correlations of r = 0.36 for BMI z vs. correlations of 0.60 and 0.57 for BMIaz and %BMIp95, respectively.
The results were limited by several factors including the age of the data (40 years ago, when the prevalence of severe obesity was lower, 2% compared with approximately 6% now) and long intervals between exams in some cases (5 years or more), the researchers noted. However, the results suggest that BMI z values “can differ substantially from empirical estimates, have an effective upper limit, and are strongly influenced by sex and age,” they said. As an alternative, the researchers recommended that “very high BMIs should be should expressed as z scores on the basis of linear extrapolations of a fixed SD or as percentage of the CDC 95th percentile,” or using multilevel models that adjust for age and sex.
The researchers had no financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
, based on data from nearly 7,000 children in the Bogalusa Heart Study.
The current parameters used in the Centers for Disease Control and Prevention growth charts for children with high body mass index (BMI) “can result in estimates that differ substantially from those that are observed and constrains the maximum BMI z that is attainable at a given sex and age,” wrote David S. Freedman, PhD, of the Centers for Disease Control and Prevention in Atlanta, and Gerald S. Berenson, MD, of Louisiana State University Health Sciences Center, New Orleans, (Pediatrics. 2017;140:e20171072).
The BMI adjusted z score (BMIaz) or the BMI expressed as a percentage of the 95th percentile (%BMIp95) “will provide more accurate information on body size over time among children with very high BMIs,” they said.
In children with severe obesity, BMI z was a weaker measure (r = 0.46) than were measures of %BMIp95 (r = 0.61) or BMIaz scores with no upper boundary (r = 0.65).
BMI z scores were weakest when applied to children younger than 10 years, with correlations of r = 0.36 for BMI z vs. correlations of 0.60 and 0.57 for BMIaz and %BMIp95, respectively.
The results were limited by several factors including the age of the data (40 years ago, when the prevalence of severe obesity was lower, 2% compared with approximately 6% now) and long intervals between exams in some cases (5 years or more), the researchers noted. However, the results suggest that BMI z values “can differ substantially from empirical estimates, have an effective upper limit, and are strongly influenced by sex and age,” they said. As an alternative, the researchers recommended that “very high BMIs should be should expressed as z scores on the basis of linear extrapolations of a fixed SD or as percentage of the CDC 95th percentile,” or using multilevel models that adjust for age and sex.
The researchers had no financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
FROM PEDIATRICS
Key clinical point: BMI z scores are weak trackers of severe obesity in children.
Major finding: Correlations were weaker for BMI z scores (r = 0.46) than for metrics of BMI using the 95th percentile or z scores with no upper bound (r = approximately 0.6) over 2.8 years.
Data source: The study is based on longitudinal data from 6,994 children participating in the Bogalusa Heart study, including 247 children with severe obesity.
Disclosures: The researchers had no relevant financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
PVC phlebitis rates varied widely, depending on assessment tool
Rates of phlebitis associated with peripheral venous catheters (PVC) ranged from less than 1% to 34% depending on which assessment tool researchers used in a large cross-sectional study.
Rates also varied within individual instruments because they included several possible case definitions, Katarina Göransson, PhD, and her associates reported in Lancet Haematology. “We find it concerning that our study shows variation of the proportion of PVCs causing phlebitis both within and across the instruments investigated,” they wrote. “How to best measure phlebitis outcomes is still unclear, since no universally accepted instrument exists that has had rigorous testing. From a work environment and patient safety perspective, clinical staff engaged in PVC management should be aware of the absence of adequately validated instruments for phlebitis assessment.”
There are many tools to measure PVC-related phlebitis, but no consensus on which to use, and past studies have reported rates of anywhere from 2% to 62%. Hypothesizing that instrument variability contributed to this discrepancy, the researchers tested 17 instruments in 1,032 patients who had 1,175 PVCs placed at 12 inpatient units in Sweden. Eight tools used clinical definitions, seven used severity rating systems, and two used scoring systems (Lancet Haematol. 2017 doi: 10.1016/S2352-3026[17]30122-9).
Rates of PVC-induced phlebitis reached 12% (137 cases) when the researchers used case definition tools, up to 31% when they used scoring systems (P less than .0001), and up to 34% when they used severity rating systems (P less than .0001, compared with the 12% rate). “The proportion within instruments ranged from less than 1% to 28%,” they added. “We [also] identified face validity issues, such as use of indistinct or complex measurements and inconsistent measurements or definitions.”
The investigators did not perform a systematic review to identify these instruments, and they did not necessarily use the most recent versions, they noted. Nevertheless, the findings have direct implications for hospital quality control measures, which require using a single validated instrument over time to generate meaningful results, they said. Hence, the investigators recommended developing a joint research program to develop reliable measures of PVC-related adverse events and better support clinicians who are trying to decide whether to remove PVCs.
The investigators reported having no funding sources and no competing interests.
Rates of phlebitis associated with peripheral venous catheters (PVC) ranged from less than 1% to 34% depending on which assessment tool researchers used in a large cross-sectional study.
Rates also varied within individual instruments because they included several possible case definitions, Katarina Göransson, PhD, and her associates reported in Lancet Haematology. “We find it concerning that our study shows variation of the proportion of PVCs causing phlebitis both within and across the instruments investigated,” they wrote. “How to best measure phlebitis outcomes is still unclear, since no universally accepted instrument exists that has had rigorous testing. From a work environment and patient safety perspective, clinical staff engaged in PVC management should be aware of the absence of adequately validated instruments for phlebitis assessment.”
There are many tools to measure PVC-related phlebitis, but no consensus on which to use, and past studies have reported rates of anywhere from 2% to 62%. Hypothesizing that instrument variability contributed to this discrepancy, the researchers tested 17 instruments in 1,032 patients who had 1,175 PVCs placed at 12 inpatient units in Sweden. Eight tools used clinical definitions, seven used severity rating systems, and two used scoring systems (Lancet Haematol. 2017 doi: 10.1016/S2352-3026[17]30122-9).
Rates of PVC-induced phlebitis reached 12% (137 cases) when the researchers used case definition tools, up to 31% when they used scoring systems (P less than .0001), and up to 34% when they used severity rating systems (P less than .0001, compared with the 12% rate). “The proportion within instruments ranged from less than 1% to 28%,” they added. “We [also] identified face validity issues, such as use of indistinct or complex measurements and inconsistent measurements or definitions.”
The investigators did not perform a systematic review to identify these instruments, and they did not necessarily use the most recent versions, they noted. Nevertheless, the findings have direct implications for hospital quality control measures, which require using a single validated instrument over time to generate meaningful results, they said. Hence, the investigators recommended developing a joint research program to develop reliable measures of PVC-related adverse events and better support clinicians who are trying to decide whether to remove PVCs.
The investigators reported having no funding sources and no competing interests.
Rates of phlebitis associated with peripheral venous catheters (PVC) ranged from less than 1% to 34% depending on which assessment tool researchers used in a large cross-sectional study.
Rates also varied within individual instruments because they included several possible case definitions, Katarina Göransson, PhD, and her associates reported in Lancet Haematology. “We find it concerning that our study shows variation of the proportion of PVCs causing phlebitis both within and across the instruments investigated,” they wrote. “How to best measure phlebitis outcomes is still unclear, since no universally accepted instrument exists that has had rigorous testing. From a work environment and patient safety perspective, clinical staff engaged in PVC management should be aware of the absence of adequately validated instruments for phlebitis assessment.”
There are many tools to measure PVC-related phlebitis, but no consensus on which to use, and past studies have reported rates of anywhere from 2% to 62%. Hypothesizing that instrument variability contributed to this discrepancy, the researchers tested 17 instruments in 1,032 patients who had 1,175 PVCs placed at 12 inpatient units in Sweden. Eight tools used clinical definitions, seven used severity rating systems, and two used scoring systems (Lancet Haematol. 2017 doi: 10.1016/S2352-3026[17]30122-9).
Rates of PVC-induced phlebitis reached 12% (137 cases) when the researchers used case definition tools, up to 31% when they used scoring systems (P less than .0001), and up to 34% when they used severity rating systems (P less than .0001, compared with the 12% rate). “The proportion within instruments ranged from less than 1% to 28%,” they added. “We [also] identified face validity issues, such as use of indistinct or complex measurements and inconsistent measurements or definitions.”
The investigators did not perform a systematic review to identify these instruments, and they did not necessarily use the most recent versions, they noted. Nevertheless, the findings have direct implications for hospital quality control measures, which require using a single validated instrument over time to generate meaningful results, they said. Hence, the investigators recommended developing a joint research program to develop reliable measures of PVC-related adverse events and better support clinicians who are trying to decide whether to remove PVCs.
The investigators reported having no funding sources and no competing interests.
FROM LANCET HAEMATOLOGY
Key clinical point: Rates of PVC-induced phlebitis varied widely within and between assessment instruments.
Major finding: Rates were as high as 12% (137 cases) based on the case definition tools, up to 31% based on the scoring systems (P less than .0001), and up to 34% based on the severity rating systems (P less than .0001, compared with the case definition rate).
Data source: A cross-sectional study of 17 instruments used to identify phlebitis associated with peripheral venous catheters.
Disclosures: The investigators reported having no funding sources and no competing interests.
Cognitive decline not seen with lower BP treatment targets
Tighter blood pressure control is not linked to cognitive decline among older adults and may instead be associated with preservation of cognitive function, according to a new analysis.
Further, the cognitive benefits of tighter control are even more pronounced among black patients.
Dr. Hajjar and colleagues report that subjects whose systolic blood pressure (SBP) was maintained at 150 mm Hg or higher during the study period saw significantly greater cognitive decline over 10 years, compared with those treated to levels of 120 mm Hg or lower (JAMA Neurol. 2017 Aug 21; doi: 10.1001/jamaneurol.2017.1863). Furthermore, the investigators noted a differential decrease by blood pressure levels for both cognitive scoring systems, with the greatest decline seen in the group with SBP of 150 mm/Hg or higher and the lowest decrease in the group with 120 mm/Hg or lower (P less than .001 for both).
Black patients saw a greater difference, compared with white patients, between the higher and lower SBP levels in the decrease in cognition. Adjusted differences between the group with 150 mm Hg or higher and those with 120 mm Hg or lower were –0.05 in white patients and –0.08 in black patients for the 3MSE test (P = .03), and –0.07 in white patients and –0.13 in black patients for the DSST (P = .05).
“Almost all guidelines have recommended that target blood pressures be similar for black and white patients,” the investigators wrote in their analysis, adding that “future recommendations for the management of hypertension and cognitive outcomes need to take this racial disparity into consideration.”
The study was funded by the National Institutes on Health and National Institute on Aging. Dr. Hajjar and his colleagues disclosed no conflicts of interest.
Although unanswered questions remain, the data presented by Dr. Hajjar and colleagues add to the existing literature by emphasizing that tight blood pressure control does not appear to lead to poorer cognitive trajectories in older adults and may even be associated with improved cognitive trajectories. An important and unique feature of the data is the diverse population included, with nearly half of the enrollment composed of black individuals. The finding that lower systolic BP was especially protective for black individuals is important, given a noted disparity in rates of dementia among black and white persons. Adding to that the finding that hypertension is more common and more severe in black than in white persons (also supported by the data in this study), and that black persons tend to have more poorly controlled hypertension than do white persons, this outcome points to an important opportunity from a public health standpoint. BP reduction might actually reduce the rates of dementia and reduce the disparities by race with regard to dementia rates; the fact that BP control may require more medications for black than for white patients needs to be considered when monitoring blood pressure levels.
Rebecca F. Gottesman, MD, PhD, of Johns Hopkins University, Baltimore, made these comments in an accompanying editorial (JAMA Neurol. 2017 Aug. 21; doi: 10.1001/jamaneurol.2017.1869). She is an associate editor at JAMA Neurology, and reports no other conflicts of interest.
Although unanswered questions remain, the data presented by Dr. Hajjar and colleagues add to the existing literature by emphasizing that tight blood pressure control does not appear to lead to poorer cognitive trajectories in older adults and may even be associated with improved cognitive trajectories. An important and unique feature of the data is the diverse population included, with nearly half of the enrollment composed of black individuals. The finding that lower systolic BP was especially protective for black individuals is important, given a noted disparity in rates of dementia among black and white persons. Adding to that the finding that hypertension is more common and more severe in black than in white persons (also supported by the data in this study), and that black persons tend to have more poorly controlled hypertension than do white persons, this outcome points to an important opportunity from a public health standpoint. BP reduction might actually reduce the rates of dementia and reduce the disparities by race with regard to dementia rates; the fact that BP control may require more medications for black than for white patients needs to be considered when monitoring blood pressure levels.
Rebecca F. Gottesman, MD, PhD, of Johns Hopkins University, Baltimore, made these comments in an accompanying editorial (JAMA Neurol. 2017 Aug. 21; doi: 10.1001/jamaneurol.2017.1869). She is an associate editor at JAMA Neurology, and reports no other conflicts of interest.
Although unanswered questions remain, the data presented by Dr. Hajjar and colleagues add to the existing literature by emphasizing that tight blood pressure control does not appear to lead to poorer cognitive trajectories in older adults and may even be associated with improved cognitive trajectories. An important and unique feature of the data is the diverse population included, with nearly half of the enrollment composed of black individuals. The finding that lower systolic BP was especially protective for black individuals is important, given a noted disparity in rates of dementia among black and white persons. Adding to that the finding that hypertension is more common and more severe in black than in white persons (also supported by the data in this study), and that black persons tend to have more poorly controlled hypertension than do white persons, this outcome points to an important opportunity from a public health standpoint. BP reduction might actually reduce the rates of dementia and reduce the disparities by race with regard to dementia rates; the fact that BP control may require more medications for black than for white patients needs to be considered when monitoring blood pressure levels.
Rebecca F. Gottesman, MD, PhD, of Johns Hopkins University, Baltimore, made these comments in an accompanying editorial (JAMA Neurol. 2017 Aug. 21; doi: 10.1001/jamaneurol.2017.1869). She is an associate editor at JAMA Neurology, and reports no other conflicts of interest.
Tighter blood pressure control is not linked to cognitive decline among older adults and may instead be associated with preservation of cognitive function, according to a new analysis.
Further, the cognitive benefits of tighter control are even more pronounced among black patients.
Dr. Hajjar and colleagues report that subjects whose systolic blood pressure (SBP) was maintained at 150 mm Hg or higher during the study period saw significantly greater cognitive decline over 10 years, compared with those treated to levels of 120 mm Hg or lower (JAMA Neurol. 2017 Aug 21; doi: 10.1001/jamaneurol.2017.1863). Furthermore, the investigators noted a differential decrease by blood pressure levels for both cognitive scoring systems, with the greatest decline seen in the group with SBP of 150 mm/Hg or higher and the lowest decrease in the group with 120 mm/Hg or lower (P less than .001 for both).
Black patients saw a greater difference, compared with white patients, between the higher and lower SBP levels in the decrease in cognition. Adjusted differences between the group with 150 mm Hg or higher and those with 120 mm Hg or lower were –0.05 in white patients and –0.08 in black patients for the 3MSE test (P = .03), and –0.07 in white patients and –0.13 in black patients for the DSST (P = .05).
“Almost all guidelines have recommended that target blood pressures be similar for black and white patients,” the investigators wrote in their analysis, adding that “future recommendations for the management of hypertension and cognitive outcomes need to take this racial disparity into consideration.”
The study was funded by the National Institutes on Health and National Institute on Aging. Dr. Hajjar and his colleagues disclosed no conflicts of interest.
Tighter blood pressure control is not linked to cognitive decline among older adults and may instead be associated with preservation of cognitive function, according to a new analysis.
Further, the cognitive benefits of tighter control are even more pronounced among black patients.
Dr. Hajjar and colleagues report that subjects whose systolic blood pressure (SBP) was maintained at 150 mm Hg or higher during the study period saw significantly greater cognitive decline over 10 years, compared with those treated to levels of 120 mm Hg or lower (JAMA Neurol. 2017 Aug 21; doi: 10.1001/jamaneurol.2017.1863). Furthermore, the investigators noted a differential decrease by blood pressure levels for both cognitive scoring systems, with the greatest decline seen in the group with SBP of 150 mm/Hg or higher and the lowest decrease in the group with 120 mm/Hg or lower (P less than .001 for both).
Black patients saw a greater difference, compared with white patients, between the higher and lower SBP levels in the decrease in cognition. Adjusted differences between the group with 150 mm Hg or higher and those with 120 mm Hg or lower were –0.05 in white patients and –0.08 in black patients for the 3MSE test (P = .03), and –0.07 in white patients and –0.13 in black patients for the DSST (P = .05).
“Almost all guidelines have recommended that target blood pressures be similar for black and white patients,” the investigators wrote in their analysis, adding that “future recommendations for the management of hypertension and cognitive outcomes need to take this racial disparity into consideration.”
The study was funded by the National Institutes on Health and National Institute on Aging. Dr. Hajjar and his colleagues disclosed no conflicts of interest.
FROM JAMA NEUROLOGY
Key clinical point: Treating to more aggressive blood pressure targets does not promote cognitive decline and may help stem it, particularly among black patients.
Major finding: Black patients saw significantly greater decline in cognition over time associated with systolic BP control to 150 mm Hg vs. 120 mm Hg.
Data source: A cohort of 1,700 hypertension-treated patients aged 70-79, about half of them black, drawn from a 10-year observational study of 3,000 patients.
Disclosures: Both the larger cohort and this study were funded by the National Institutes of Health and the National Institute on Aging. None of the investigators declared conflicts of interest.
L-glutamine to prevent sickle cell complications featured in FDA podcast
The recent approval of L-glutamine, marketed as Endari, to reduce the acute complications of sickle cell disease in adult and pediatric patients 5 years of age and older is discussed in the Drug Information Soundcast in Clinical Oncology (DISCO) from a Food and Drug Adminstration podcast series that provides information about new product approvals, emerging safety information for cancer treatments, and other current topics in cancer drug development.
The basis for the approval was discussed in our coverage of the FDA’s Oncologic Drugs Advisory Committee meeting.
This episode of DISCO is hosted by Sanjeeve Bala, MD, and was developed by Abhilasha Nair, MD; Dr. Bala; Kathy M. Robie Suh, MD; Ann T. Farrell, MD; Kirsten B. Goldberg, and Richard Pazdur, MD. All are with the FDA’s Oncology Center of Excellence and the Office of Hematology and Oncology Products. Steven Jackson of the FDA’s Division of Drug Information was the sound producer.
The recent approval of L-glutamine, marketed as Endari, to reduce the acute complications of sickle cell disease in adult and pediatric patients 5 years of age and older is discussed in the Drug Information Soundcast in Clinical Oncology (DISCO) from a Food and Drug Adminstration podcast series that provides information about new product approvals, emerging safety information for cancer treatments, and other current topics in cancer drug development.
The basis for the approval was discussed in our coverage of the FDA’s Oncologic Drugs Advisory Committee meeting.
This episode of DISCO is hosted by Sanjeeve Bala, MD, and was developed by Abhilasha Nair, MD; Dr. Bala; Kathy M. Robie Suh, MD; Ann T. Farrell, MD; Kirsten B. Goldberg, and Richard Pazdur, MD. All are with the FDA’s Oncology Center of Excellence and the Office of Hematology and Oncology Products. Steven Jackson of the FDA’s Division of Drug Information was the sound producer.
The recent approval of L-glutamine, marketed as Endari, to reduce the acute complications of sickle cell disease in adult and pediatric patients 5 years of age and older is discussed in the Drug Information Soundcast in Clinical Oncology (DISCO) from a Food and Drug Adminstration podcast series that provides information about new product approvals, emerging safety information for cancer treatments, and other current topics in cancer drug development.
The basis for the approval was discussed in our coverage of the FDA’s Oncologic Drugs Advisory Committee meeting.
This episode of DISCO is hosted by Sanjeeve Bala, MD, and was developed by Abhilasha Nair, MD; Dr. Bala; Kathy M. Robie Suh, MD; Ann T. Farrell, MD; Kirsten B. Goldberg, and Richard Pazdur, MD. All are with the FDA’s Oncology Center of Excellence and the Office of Hematology and Oncology Products. Steven Jackson of the FDA’s Division of Drug Information was the sound producer.
Acute lobar nephronia often has misleading presentation
MADRID – Acute lobar nephronia needs to be considered in children with high fever, abdominal pain, and markedly elevated acute-phase reactants, even if their urinalysis and ultrasound results are negative, Paula Sanchez-Marcos, MD, reported at the annual meeting of the European Society for Paediatric Infectious Diseases.
She presented a retrospective study of 18 episodes of acute lobar nephronia (ALN) in 16 children seen at the hospital, a tertiary referral center. Six of the children had vesicoureteral reflux or another underlying uropathy. Mean age at diagnosis was 79 months, with a range of 5 to 180 months.
All patients had a fever greater than 38.5° C when they presented with a mean 6-day history of illness. Of the 16 children, 14 had abdominal pain. The mean C-reactive protein level was 197 mg/L, with a WBC count of 21,962 cells/mcL and a neutrophil count of 17,372 cells/mcL.
Urine dipstick was negative in five episodes. However, urine culture was eventually productive in 10 episodes, with Escherichia coli the most commonly isolated microorganism, found in five of these cases.
All patients underwent ultrasound imaging a mean of 1.7 days into their hospital admission, although it established the diagnosis of ALN in only two episodes. Additional imaging with CT had a 91% sensitivity, showing positive results in 10 of 11 cases, while MRI had 100% sensitivity.
Patients received IV antibiotics for a median of 14 days before switching to sequential oral antibiotics for a median of 8.7 days.
Three patients developed renal abscesses, with percutaneous drainage required in two instances. Unilateral renal scarring occurred in 7 of 16 patients.
Dr. Sanchez-Marcos recommended technetium-99m dimercaptosuccinic acid renal scintigraphy as a tool to confirm improvement in response to antimicrobial therapy.
She reported having no financial conflicts regarding her presentation.
MADRID – Acute lobar nephronia needs to be considered in children with high fever, abdominal pain, and markedly elevated acute-phase reactants, even if their urinalysis and ultrasound results are negative, Paula Sanchez-Marcos, MD, reported at the annual meeting of the European Society for Paediatric Infectious Diseases.
She presented a retrospective study of 18 episodes of acute lobar nephronia (ALN) in 16 children seen at the hospital, a tertiary referral center. Six of the children had vesicoureteral reflux or another underlying uropathy. Mean age at diagnosis was 79 months, with a range of 5 to 180 months.
All patients had a fever greater than 38.5° C when they presented with a mean 6-day history of illness. Of the 16 children, 14 had abdominal pain. The mean C-reactive protein level was 197 mg/L, with a WBC count of 21,962 cells/mcL and a neutrophil count of 17,372 cells/mcL.
Urine dipstick was negative in five episodes. However, urine culture was eventually productive in 10 episodes, with Escherichia coli the most commonly isolated microorganism, found in five of these cases.
All patients underwent ultrasound imaging a mean of 1.7 days into their hospital admission, although it established the diagnosis of ALN in only two episodes. Additional imaging with CT had a 91% sensitivity, showing positive results in 10 of 11 cases, while MRI had 100% sensitivity.
Patients received IV antibiotics for a median of 14 days before switching to sequential oral antibiotics for a median of 8.7 days.
Three patients developed renal abscesses, with percutaneous drainage required in two instances. Unilateral renal scarring occurred in 7 of 16 patients.
Dr. Sanchez-Marcos recommended technetium-99m dimercaptosuccinic acid renal scintigraphy as a tool to confirm improvement in response to antimicrobial therapy.
She reported having no financial conflicts regarding her presentation.
MADRID – Acute lobar nephronia needs to be considered in children with high fever, abdominal pain, and markedly elevated acute-phase reactants, even if their urinalysis and ultrasound results are negative, Paula Sanchez-Marcos, MD, reported at the annual meeting of the European Society for Paediatric Infectious Diseases.
She presented a retrospective study of 18 episodes of acute lobar nephronia (ALN) in 16 children seen at the hospital, a tertiary referral center. Six of the children had vesicoureteral reflux or another underlying uropathy. Mean age at diagnosis was 79 months, with a range of 5 to 180 months.
All patients had a fever greater than 38.5° C when they presented with a mean 6-day history of illness. Of the 16 children, 14 had abdominal pain. The mean C-reactive protein level was 197 mg/L, with a WBC count of 21,962 cells/mcL and a neutrophil count of 17,372 cells/mcL.
Urine dipstick was negative in five episodes. However, urine culture was eventually productive in 10 episodes, with Escherichia coli the most commonly isolated microorganism, found in five of these cases.
All patients underwent ultrasound imaging a mean of 1.7 days into their hospital admission, although it established the diagnosis of ALN in only two episodes. Additional imaging with CT had a 91% sensitivity, showing positive results in 10 of 11 cases, while MRI had 100% sensitivity.
Patients received IV antibiotics for a median of 14 days before switching to sequential oral antibiotics for a median of 8.7 days.
Three patients developed renal abscesses, with percutaneous drainage required in two instances. Unilateral renal scarring occurred in 7 of 16 patients.
Dr. Sanchez-Marcos recommended technetium-99m dimercaptosuccinic acid renal scintigraphy as a tool to confirm improvement in response to antimicrobial therapy.
She reported having no financial conflicts regarding her presentation.
AT ESPID 2017
Key clinical point:
Major finding: Urine dipstick results were negative in 5 instances, and ultrasound was negative in 16 cases.
Data source: This was a single-center, retrospective, descriptive study of 18 episodes of acute lobar nephronia in 16 children.
Disclosures: Dr. Sanchez-Marcos reported having no financial conflicts of interest.
Bullous Lesions in a Neonate
The Diagnosis: Incontinentia Pigmenti
The infant's mother was noted to have diffuse hypopigmented patches over the trunk, arms, and legs (present since adolescence) with whorled cicatricial alopecia of the vertex scalp and peg-shaped teeth (Figure). Together, these findings suggested incontinentia pigmenti (IP), which the mother revealed she had been diagnosed with in childhood. The infant's characteristic lesions in the setting of her mother's diagnosed genodermatosis confirmed the diagnosis of IP.
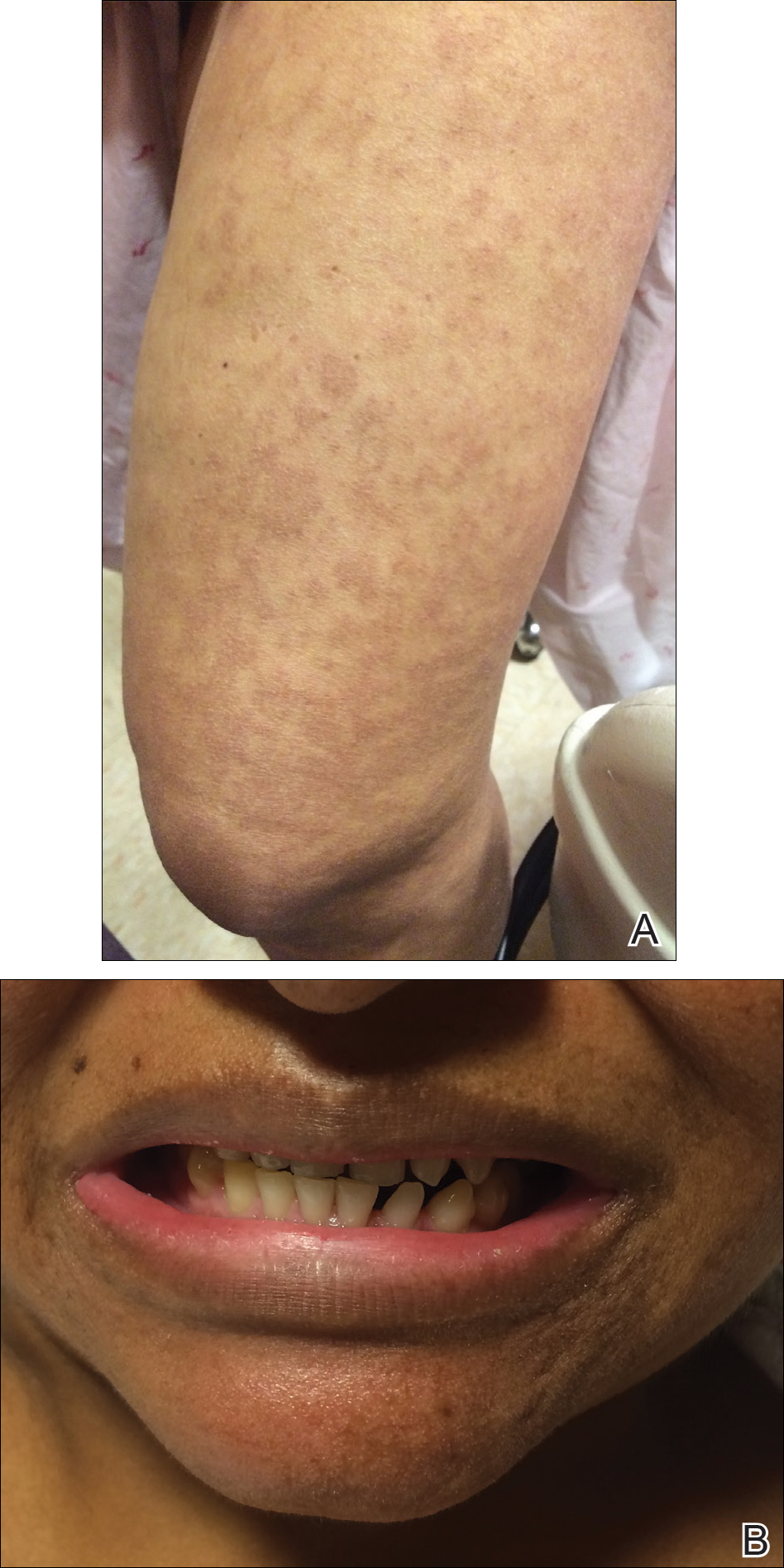
Incontinentia pigmenti is an X-linked dominant disorder that presents with many classic dermatologic, dental, neurologic, and ophthalmologic findings. The causative mutation occurs in IKBKG/NEMO (inhibitor of κ polypeptide gene enhancer in B-cells, kinase γ/nuclear factor-κB essential modulator) gene on Xq28, disabling the resultant protein that normally protects cells from tumor necrosis factor family-induced apoptosis.1 Incontinentia pigmenti usually is lethal in males and causes an unbalanced X-inactivation in surviving female IP patients. Occurring at a rate of 1.2 per 100,000 births,2 IP typically presents in female infants with skin lesions patterned along Blaschko lines that evolve in 4 stages over a lifetime.3 Stage I, presenting in the neonatal period, manifests as vesiculobullous eruptions on the limbs and scalp. Stages II to IV vary in duration from months to years and are comprised of a verrucous stage, a hyperpigmented stage, and a hypopigmented stage, respectively.3 All stages of IP can overlap and coexist.
The vesiculobullous findings in infants with IP may be mistakenly attributed to other diseases with prominent vesicular or bullous components including herpes simplex virus, epidermolysis bullosa, and infantile acropustulosis. With neonatal herpes simplex virus infection, vesicular skin or mucocutaneous lesions occur 9 to 11 days after birth and can be confirmed by specimen culture or qualitative polymerase chain reaction, while stage I of IP appears within the first 6 to 8 weeks of life and can be present at birth.4 The hallmark of epidermolysis bullosa, caused by mutations in keratins 5 and 14, is blistering erosions of the skin in response to frictional stress,1 thus these lesions do not follow Blaschko lines. Infantile acropustulosis, a nonheritable vesiculopustular eruption of the hands and feet, rarely occurs in the immediate newborn period; it most often appears in the 3- to 6-month age range with recurrent eruptions at 3- to 4-week intervals.5 Focal dermal hypoplasia is another X-linked dominant disorder with blaschkolinear findings at birth that presents with pink or red, angular, atrophic macules, in contrast to the bullous lesions of IP.6
Incontinentia pigmenti may encompass a wide range of systemic symptoms in addition to the classic dermatologic findings. Notably, central nervous system defects are concurrent in up to 40% of IP cases, with seizures, mental retardation, and spastic paresis being the most common sequelae.7 Teeth defects, seen in 35% of patients, include delayed primary dentition and peg-shaped teeth. Many patients will experience ophthalmologic defects including vision problems (16%) and retinopathy (15%).7
The cutaneous eruptions of IP may be treated with topical corticosteroids or topical tacrolimus, and vesicles should be left intact and monitored for signs of infection.8,9 Seizures, if present, should be treated with anticonvulsants, and regular neuropsychiatric monitoring and physical rehabilitation may be warranted. Patients should be regularly monitored for retinopathy beginning at the time of diagnosis. Retinal fibrovascular proliferation is treated with xenon laser photocoagulation to reduce the high risk for retinal detachment in this population.10,11 Older and younger at-risk relatives must be evaluated by genetic testing or thorough physical examination to clarify their disease status and determine the need for additional genetic counseling.
- Bolognia JL, Jorizzo JL, Schaffer JV, eds. Dermatology. 3rd ed. China: Elsevier Saunders; 2012.
- Prevalence and incidence of rare diseases: bibliographic data. Orphanet Report Series, Rare Diseases collection. http://www.orpha.net/orphacom/cahiers/docs/GB/Prevalence_of_rare_diseases_by_alphabetical_list.pdf. Published June 2017. Accessed July 13, 2017.
- Scheuerle AE, Ursini MV. Incontinentia pigmenti. In: Pagon RA, Adam MP, Ardinger HH, et al, eds. GeneReviews. Seattle, WA: University of Washington; 2015. http://www.ncbi.nlm.nih.gov/books/NBK1472/. Accessed July 25, 2017.
- James SH, Kimberlin DW. Neonatal herpes simplex virus infection. Infect Dis Clin North Am. 2015;29:391-400.
- Eichenfield LF, Frieden IJ, Mathes E, et al, eds. Neonatal and Infant Dermatology. Philadelphia, PA: Saunders; 2015.
- Temple IK, MacDowall P, Baraitser M, et al. Focal dermal hypoplasia (Goltz syndrome). J Med Genet. 1990;27:180-187.
- Fusco F, Paciolla M, Conte MI, et al. Incontinentia pigmenti: report on data from 2000 to 2013. Orphanet J Rare Dis. 2014;9:93.
- Jessup CJ, Morgan SC, Cohen LM, et al. Incontinentia pigmenti: treatment of IP with topical tacrolimus. J Drugs Dermatol. 2009;8:944-946.
- Kaya TI, Tursen U, Ikizoglu G. Therapeutic use of topical corticosteroids in the vesiculobullous lesions of incontinentia pigmenti [published online June 1, 2009]. Clin Exp Dermatol. 2009;34:E611-E613.
- Nguyen JK, Brady-Mccreery KM. Laser photocoagulation in preproliferative retinopathy of incontinentia pigmenti. J AAPOS. 2001;5:258-259.
- Chen CJ, Han IC, Tian J, et al. Extended follow-up of treated and untreated retinopathy in incontinentia pigmenti: analysis of peripheral vascular changes and incidence of retinal detachment. JAMA Ophthalmol. 2015;133:542-548.
The Diagnosis: Incontinentia Pigmenti
The infant's mother was noted to have diffuse hypopigmented patches over the trunk, arms, and legs (present since adolescence) with whorled cicatricial alopecia of the vertex scalp and peg-shaped teeth (Figure). Together, these findings suggested incontinentia pigmenti (IP), which the mother revealed she had been diagnosed with in childhood. The infant's characteristic lesions in the setting of her mother's diagnosed genodermatosis confirmed the diagnosis of IP.

Incontinentia pigmenti is an X-linked dominant disorder that presents with many classic dermatologic, dental, neurologic, and ophthalmologic findings. The causative mutation occurs in IKBKG/NEMO (inhibitor of κ polypeptide gene enhancer in B-cells, kinase γ/nuclear factor-κB essential modulator) gene on Xq28, disabling the resultant protein that normally protects cells from tumor necrosis factor family-induced apoptosis.1 Incontinentia pigmenti usually is lethal in males and causes an unbalanced X-inactivation in surviving female IP patients. Occurring at a rate of 1.2 per 100,000 births,2 IP typically presents in female infants with skin lesions patterned along Blaschko lines that evolve in 4 stages over a lifetime.3 Stage I, presenting in the neonatal period, manifests as vesiculobullous eruptions on the limbs and scalp. Stages II to IV vary in duration from months to years and are comprised of a verrucous stage, a hyperpigmented stage, and a hypopigmented stage, respectively.3 All stages of IP can overlap and coexist.
The vesiculobullous findings in infants with IP may be mistakenly attributed to other diseases with prominent vesicular or bullous components including herpes simplex virus, epidermolysis bullosa, and infantile acropustulosis. With neonatal herpes simplex virus infection, vesicular skin or mucocutaneous lesions occur 9 to 11 days after birth and can be confirmed by specimen culture or qualitative polymerase chain reaction, while stage I of IP appears within the first 6 to 8 weeks of life and can be present at birth.4 The hallmark of epidermolysis bullosa, caused by mutations in keratins 5 and 14, is blistering erosions of the skin in response to frictional stress,1 thus these lesions do not follow Blaschko lines. Infantile acropustulosis, a nonheritable vesiculopustular eruption of the hands and feet, rarely occurs in the immediate newborn period; it most often appears in the 3- to 6-month age range with recurrent eruptions at 3- to 4-week intervals.5 Focal dermal hypoplasia is another X-linked dominant disorder with blaschkolinear findings at birth that presents with pink or red, angular, atrophic macules, in contrast to the bullous lesions of IP.6
Incontinentia pigmenti may encompass a wide range of systemic symptoms in addition to the classic dermatologic findings. Notably, central nervous system defects are concurrent in up to 40% of IP cases, with seizures, mental retardation, and spastic paresis being the most common sequelae.7 Teeth defects, seen in 35% of patients, include delayed primary dentition and peg-shaped teeth. Many patients will experience ophthalmologic defects including vision problems (16%) and retinopathy (15%).7
The cutaneous eruptions of IP may be treated with topical corticosteroids or topical tacrolimus, and vesicles should be left intact and monitored for signs of infection.8,9 Seizures, if present, should be treated with anticonvulsants, and regular neuropsychiatric monitoring and physical rehabilitation may be warranted. Patients should be regularly monitored for retinopathy beginning at the time of diagnosis. Retinal fibrovascular proliferation is treated with xenon laser photocoagulation to reduce the high risk for retinal detachment in this population.10,11 Older and younger at-risk relatives must be evaluated by genetic testing or thorough physical examination to clarify their disease status and determine the need for additional genetic counseling.
The Diagnosis: Incontinentia Pigmenti
The infant's mother was noted to have diffuse hypopigmented patches over the trunk, arms, and legs (present since adolescence) with whorled cicatricial alopecia of the vertex scalp and peg-shaped teeth (Figure). Together, these findings suggested incontinentia pigmenti (IP), which the mother revealed she had been diagnosed with in childhood. The infant's characteristic lesions in the setting of her mother's diagnosed genodermatosis confirmed the diagnosis of IP.

Incontinentia pigmenti is an X-linked dominant disorder that presents with many classic dermatologic, dental, neurologic, and ophthalmologic findings. The causative mutation occurs in IKBKG/NEMO (inhibitor of κ polypeptide gene enhancer in B-cells, kinase γ/nuclear factor-κB essential modulator) gene on Xq28, disabling the resultant protein that normally protects cells from tumor necrosis factor family-induced apoptosis.1 Incontinentia pigmenti usually is lethal in males and causes an unbalanced X-inactivation in surviving female IP patients. Occurring at a rate of 1.2 per 100,000 births,2 IP typically presents in female infants with skin lesions patterned along Blaschko lines that evolve in 4 stages over a lifetime.3 Stage I, presenting in the neonatal period, manifests as vesiculobullous eruptions on the limbs and scalp. Stages II to IV vary in duration from months to years and are comprised of a verrucous stage, a hyperpigmented stage, and a hypopigmented stage, respectively.3 All stages of IP can overlap and coexist.
The vesiculobullous findings in infants with IP may be mistakenly attributed to other diseases with prominent vesicular or bullous components including herpes simplex virus, epidermolysis bullosa, and infantile acropustulosis. With neonatal herpes simplex virus infection, vesicular skin or mucocutaneous lesions occur 9 to 11 days after birth and can be confirmed by specimen culture or qualitative polymerase chain reaction, while stage I of IP appears within the first 6 to 8 weeks of life and can be present at birth.4 The hallmark of epidermolysis bullosa, caused by mutations in keratins 5 and 14, is blistering erosions of the skin in response to frictional stress,1 thus these lesions do not follow Blaschko lines. Infantile acropustulosis, a nonheritable vesiculopustular eruption of the hands and feet, rarely occurs in the immediate newborn period; it most often appears in the 3- to 6-month age range with recurrent eruptions at 3- to 4-week intervals.5 Focal dermal hypoplasia is another X-linked dominant disorder with blaschkolinear findings at birth that presents with pink or red, angular, atrophic macules, in contrast to the bullous lesions of IP.6
Incontinentia pigmenti may encompass a wide range of systemic symptoms in addition to the classic dermatologic findings. Notably, central nervous system defects are concurrent in up to 40% of IP cases, with seizures, mental retardation, and spastic paresis being the most common sequelae.7 Teeth defects, seen in 35% of patients, include delayed primary dentition and peg-shaped teeth. Many patients will experience ophthalmologic defects including vision problems (16%) and retinopathy (15%).7
The cutaneous eruptions of IP may be treated with topical corticosteroids or topical tacrolimus, and vesicles should be left intact and monitored for signs of infection.8,9 Seizures, if present, should be treated with anticonvulsants, and regular neuropsychiatric monitoring and physical rehabilitation may be warranted. Patients should be regularly monitored for retinopathy beginning at the time of diagnosis. Retinal fibrovascular proliferation is treated with xenon laser photocoagulation to reduce the high risk for retinal detachment in this population.10,11 Older and younger at-risk relatives must be evaluated by genetic testing or thorough physical examination to clarify their disease status and determine the need for additional genetic counseling.
- Bolognia JL, Jorizzo JL, Schaffer JV, eds. Dermatology. 3rd ed. China: Elsevier Saunders; 2012.
- Prevalence and incidence of rare diseases: bibliographic data. Orphanet Report Series, Rare Diseases collection. http://www.orpha.net/orphacom/cahiers/docs/GB/Prevalence_of_rare_diseases_by_alphabetical_list.pdf. Published June 2017. Accessed July 13, 2017.
- Scheuerle AE, Ursini MV. Incontinentia pigmenti. In: Pagon RA, Adam MP, Ardinger HH, et al, eds. GeneReviews. Seattle, WA: University of Washington; 2015. http://www.ncbi.nlm.nih.gov/books/NBK1472/. Accessed July 25, 2017.
- James SH, Kimberlin DW. Neonatal herpes simplex virus infection. Infect Dis Clin North Am. 2015;29:391-400.
- Eichenfield LF, Frieden IJ, Mathes E, et al, eds. Neonatal and Infant Dermatology. Philadelphia, PA: Saunders; 2015.
- Temple IK, MacDowall P, Baraitser M, et al. Focal dermal hypoplasia (Goltz syndrome). J Med Genet. 1990;27:180-187.
- Fusco F, Paciolla M, Conte MI, et al. Incontinentia pigmenti: report on data from 2000 to 2013. Orphanet J Rare Dis. 2014;9:93.
- Jessup CJ, Morgan SC, Cohen LM, et al. Incontinentia pigmenti: treatment of IP with topical tacrolimus. J Drugs Dermatol. 2009;8:944-946.
- Kaya TI, Tursen U, Ikizoglu G. Therapeutic use of topical corticosteroids in the vesiculobullous lesions of incontinentia pigmenti [published online June 1, 2009]. Clin Exp Dermatol. 2009;34:E611-E613.
- Nguyen JK, Brady-Mccreery KM. Laser photocoagulation in preproliferative retinopathy of incontinentia pigmenti. J AAPOS. 2001;5:258-259.
- Chen CJ, Han IC, Tian J, et al. Extended follow-up of treated and untreated retinopathy in incontinentia pigmenti: analysis of peripheral vascular changes and incidence of retinal detachment. JAMA Ophthalmol. 2015;133:542-548.
- Bolognia JL, Jorizzo JL, Schaffer JV, eds. Dermatology. 3rd ed. China: Elsevier Saunders; 2012.
- Prevalence and incidence of rare diseases: bibliographic data. Orphanet Report Series, Rare Diseases collection. http://www.orpha.net/orphacom/cahiers/docs/GB/Prevalence_of_rare_diseases_by_alphabetical_list.pdf. Published June 2017. Accessed July 13, 2017.
- Scheuerle AE, Ursini MV. Incontinentia pigmenti. In: Pagon RA, Adam MP, Ardinger HH, et al, eds. GeneReviews. Seattle, WA: University of Washington; 2015. http://www.ncbi.nlm.nih.gov/books/NBK1472/. Accessed July 25, 2017.
- James SH, Kimberlin DW. Neonatal herpes simplex virus infection. Infect Dis Clin North Am. 2015;29:391-400.
- Eichenfield LF, Frieden IJ, Mathes E, et al, eds. Neonatal and Infant Dermatology. Philadelphia, PA: Saunders; 2015.
- Temple IK, MacDowall P, Baraitser M, et al. Focal dermal hypoplasia (Goltz syndrome). J Med Genet. 1990;27:180-187.
- Fusco F, Paciolla M, Conte MI, et al. Incontinentia pigmenti: report on data from 2000 to 2013. Orphanet J Rare Dis. 2014;9:93.
- Jessup CJ, Morgan SC, Cohen LM, et al. Incontinentia pigmenti: treatment of IP with topical tacrolimus. J Drugs Dermatol. 2009;8:944-946.
- Kaya TI, Tursen U, Ikizoglu G. Therapeutic use of topical corticosteroids in the vesiculobullous lesions of incontinentia pigmenti [published online June 1, 2009]. Clin Exp Dermatol. 2009;34:E611-E613.
- Nguyen JK, Brady-Mccreery KM. Laser photocoagulation in preproliferative retinopathy of incontinentia pigmenti. J AAPOS. 2001;5:258-259.
- Chen CJ, Han IC, Tian J, et al. Extended follow-up of treated and untreated retinopathy in incontinentia pigmenti: analysis of peripheral vascular changes and incidence of retinal detachment. JAMA Ophthalmol. 2015;133:542-548.
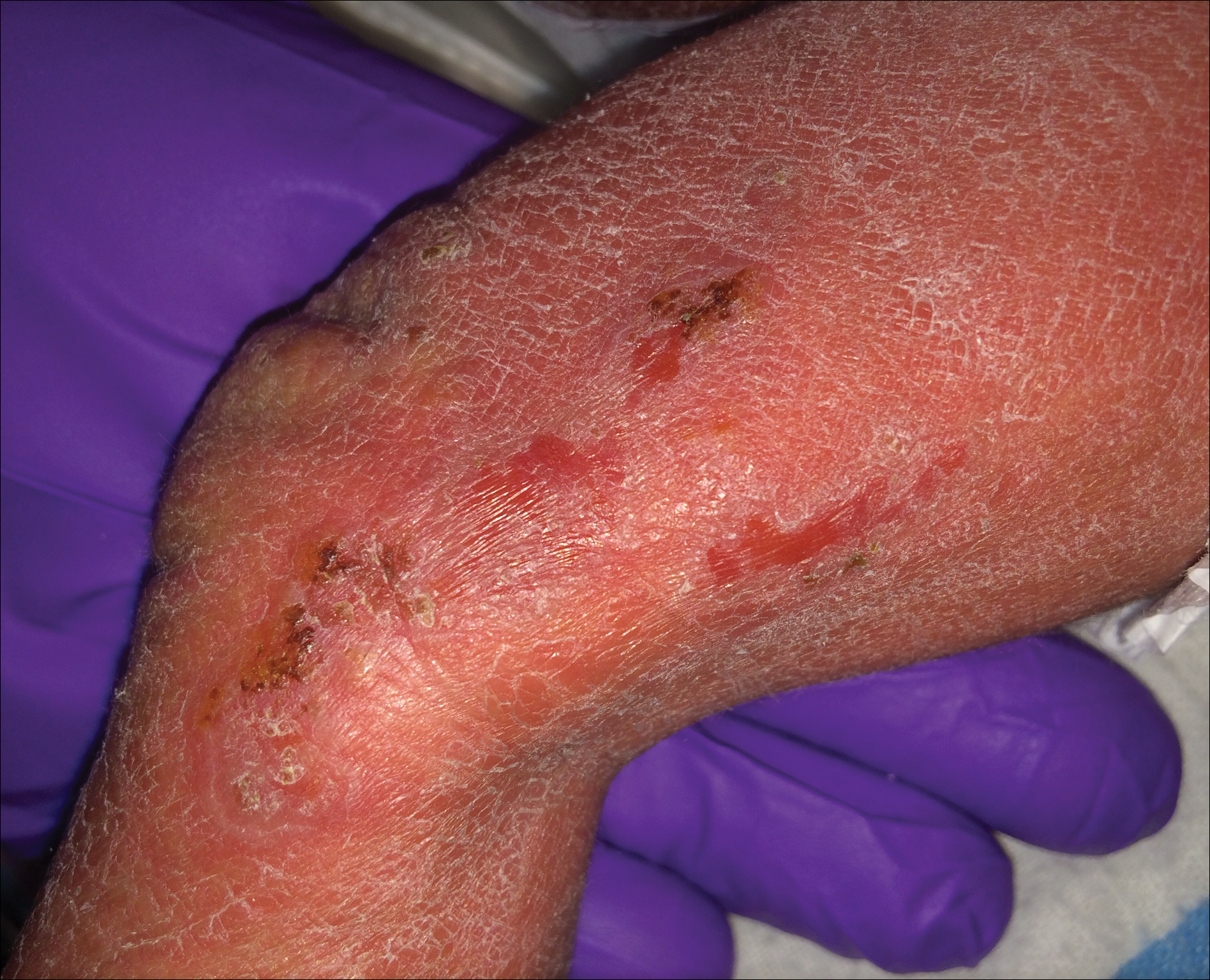
A 1-day-old Hispanic female infant was born via uncomplicated vaginal delivery at 41 weeks' gestation after a normal pregnancy. Linear plaques containing multiple ruptured vesicles and bullae following Blaschko lines were noted on the right medial thigh and anterior arm. The infant was afebrile and generally well-appearing.
Pediatric Pearls From the AAD Annual Meeting
This article exhibits key pediatric dermatology pearls garnered at the 2017 Annual Meeting of the American Academy of Dermatology (AAD) in Orlando, Florida (March 3–7, 2017). Highlights from both the Society for Pediatric Dermatology pre-AAD meeting (March 2, 2017) and the AAD general meeting sessions are included. This discussion is intended to help maximize care of our pediatric patients in dermatology and present high-yield take-home points from the AAD that can be readily transferred to our patient care.
“New Tools for Your Therapeutic Toolbox” by Erin Mathes, MD (University of California, San Francisco)
During this lecture at the Society for Pediatric Dermatology meeting, Dr. Mathes discussed a randomized controlled trial that took place in 2014 in both the United States and the United Kingdom to assess skin barrier enhancement to reduce the incidence of atopic dermatitis (AD) in 124 high-risk infants.1 The high-risk infants had either a parent or sibling with physician-diagnosed AD, asthma, or rhinitis, or a first-degree relative with an aforementioned condition. Full-body emollient therapy was applied at least once daily within 3 weeks of birth for 6 months, while the control arm did not use emollient. Parents were allowed to choose from the following emollients: sunflower seed oil, moisturizing cream, or ointment. The primary outcome was the incidence of AD at 6 months. The authors found a 43% incidence of AD in the control group compared to 22% in the emollient group, amounting to a relative risk reduction of approximately 50%.1
Emollients in AD are hypothesized to help through the enhanced barrier function and decreased penetration of irritant substances and allergens. This study is vital given the ease of use of emollients and the foreseeable substantial impact on reduced health care costs associated with the decreased incidence of AD.
Take-Home Point
Full-body emollient therapy within 3 weeks of birth may reduce the incidence of AD in high-risk infants.
Dr. Mathes also discussed the novel topical phosphodiesterase 4 inhibitor crisaborole and its emerging role in AD. She reviewed the results of a large phase 3 trial of crisaborole therapy for patients aged 2 years or older with mild to moderate AD.2 Crisaborole ointment was applied twice daily for 28 days. The primary outcome measured was an investigator static global assessment score of clear or almost clear, which is a score for AD based on the degree of erythema, presence of oozing and crusting, and presence of induration or papulation. Overall, 32.8% of patients treated with crisaborole achieved success compared to 25.4% of vehicle-treated patients. The control patients were still given a vehicle to apply, which can function as therapy to help repair the barrier of AD and thus theoretically reduced the percentage gap between patients who met success with and without crisaborole therapy. Furthermore, only 4% of patients reported adverse effects such as burning and stinging with application of crisaborole in contrast to topical calcineurin inhibitors, which can elicit symptoms up to 50% of the time.2 In summary, this lecture reviewed the first new topical treatment for AD in 15 years.
Take-Home Point
Crisaborole ointment is a novel topical phosphodiesterase 4 inhibitor approved for mild to moderate AD in patients 2 years of age and older.
“The Truth About Pediatric Contact Dermatitis” by Sharon Jacob, MD (Loma Linda University, California)
In this session, Dr. Jacob discussed how she approaches pediatric patients with suspected contact dermatitis and elaborated on the common allergens unique to this patient population. Furthermore, she explained the substantial role of nickel in pediatric contact dermatitis, citing a study performed in Denmark and the United States, which tested 212 toys for nickel using the dimethylglyoxime test and found that 34.4% of toys did in fact release nickel.3 Additional studies have shown that nickel released from children’s toys is deposited on the skin, even with short contact times such as 30 minutes on one or more occasions within 2 weeks.3,4 She is currently evaluating the presence of nickel in locales frequented by children such as schools, libraries, and supermarkets. Interestingly, she anecdotally found that a pediatric eczematous eruption in a spiralized distribution of the legs can be attributed to the presence of nickel in school chairs, and the morphology is secondary to children wrapping their legs around the chairs. In conclusion, she reiterated that nickel continues to be the top allergen among pediatric patients, and states that additional allergens for patch testing in this population are unique to their adult counterparts.
Take-Home Point
Nickel is an ubiquitous allergen for pediatric contact dermatitis; additionally, the list of allergens for patch testing should be tailored to this patient population.
“When to Image, When to Sedate” by Annette Wagner, MD (Northwestern Medicine, Chicago, Illinois)
This lecture was a 3-part discussion on the safety of general anesthesia in children, when to image children, and when sedation may be worth the risk. Dr. Wagner shared her pearls for when children younger than 3 years may benefit from dermatologic procedures that involve general anesthesia. Large congenital lesions of the scalp or face that require tissue expansion or multiple stages may be best performed at a younger age due to the flexibility of the infant scalp, providing the best outcome. Additional considerations include a questionable malignant diagnosis in which a punch biopsy is not enough, rapidly growing facial lesions, Spitz nevi of the face, congenital lesions with no available therapy, and nonhealing refractory lesions causing severe pain. The general rule proposed was intervention for single procedures lasting less than 1 hour that otherwise would result in a worse outcome if postponed. Finally, she concluded to always advocate for your patient, to wait if the outcome will be the same regardless of timing, and to be frank about not knowing the risks of general anesthesia in this population. The resource, SmartTots (http://smarttots.org) provides current consensus statements and ongoing research on the use and safety of general anesthesia in children.
Take-Home Point
General sedation may be considered for short pediatric procedures that will result in a worse outcome if postponed.
“Highlights From the Pediatric Literature” by Katherine Marks, DO (Geisinger, Danville and Wilkes-Barre, Pennsylvania)
Dr. Marks discussed numerous emerging pediatric dermatology articles. One article looked at 40 infants with proliferating infantile hemangiomas (IHs) who had timolol gel 0.5% applied twice daily.5 The primary outcomes were the urinary excretion and serum levels of timolol as well as the clinical response to therapy measured by a visual analog scale at monthly visits. A urinalysis collected 3 to 4 hours after timolol application was found to be positive in 83% (20/24) of the tested patients; the first 3 positive infants were then sent to have their serum timolol levels drawn and also were found to be positive, though substantially small levels (median, 0.16 ng/mL). The 3 patients tested had small IHs on the face with no ulceration. None of these patients experienced adverse effects and all of the IHs significantly (P<.001) improved with therapy. The authors stated that even though the absorption was minimal, it is wise to be cognizant about the use of timolol in certain patient demographics such as preterm or young infants with large ulcerating IHs.5
Take-Home Point
Systemic absorption with topical timolol occurs, albeit substantially small; be judicious about giving this medication in select patient populations with ulcerated hemangiomas.
Acknowledgment
The author thanks the presenters for their review and contributions to this article.
- Simpson EL, Chalmers JR, Hanifin JM, et al. Emollient enhancement of the skin barrier from birth offers effective atopic dermatitis prevention. J Allergy Clin Immunol. 2014;134:818-823.
- Paller AS, Tom WL, Lebwohl MG, et al. Efficacy and safety of crisaborole ointment, a novel phosphodiesterase 4 inhibitor for the topical treatment of AD in children and adults [published online July 11, 2016]. J Am Acad Dermatol. 2016;75:494-503.
- Jensen P, Hamann D, Hamann CR, et al. Nickel and cobalt release from children’s toys purchased in Denmark and the United States. Dermatitis. 2014;25:356-365.
- Overgaard LE, Engebretsen KA, Jensen P, et al. Nickel released from children’s toys is deposited on the skin. Contact Dermatitis. 2016;74:380-381.
- Weibel L, Barysch MJ, Scheer HS, et al. Topical timolol for infantile hemangiomas: evidence for efficacy and degree of systemic absorption [published online February 3, 2016]. Pediatr Dermatol. 2016;33:184-190.
This article exhibits key pediatric dermatology pearls garnered at the 2017 Annual Meeting of the American Academy of Dermatology (AAD) in Orlando, Florida (March 3–7, 2017). Highlights from both the Society for Pediatric Dermatology pre-AAD meeting (March 2, 2017) and the AAD general meeting sessions are included. This discussion is intended to help maximize care of our pediatric patients in dermatology and present high-yield take-home points from the AAD that can be readily transferred to our patient care.
“New Tools for Your Therapeutic Toolbox” by Erin Mathes, MD (University of California, San Francisco)
During this lecture at the Society for Pediatric Dermatology meeting, Dr. Mathes discussed a randomized controlled trial that took place in 2014 in both the United States and the United Kingdom to assess skin barrier enhancement to reduce the incidence of atopic dermatitis (AD) in 124 high-risk infants.1 The high-risk infants had either a parent or sibling with physician-diagnosed AD, asthma, or rhinitis, or a first-degree relative with an aforementioned condition. Full-body emollient therapy was applied at least once daily within 3 weeks of birth for 6 months, while the control arm did not use emollient. Parents were allowed to choose from the following emollients: sunflower seed oil, moisturizing cream, or ointment. The primary outcome was the incidence of AD at 6 months. The authors found a 43% incidence of AD in the control group compared to 22% in the emollient group, amounting to a relative risk reduction of approximately 50%.1
Emollients in AD are hypothesized to help through the enhanced barrier function and decreased penetration of irritant substances and allergens. This study is vital given the ease of use of emollients and the foreseeable substantial impact on reduced health care costs associated with the decreased incidence of AD.
Take-Home Point
Full-body emollient therapy within 3 weeks of birth may reduce the incidence of AD in high-risk infants.
Dr. Mathes also discussed the novel topical phosphodiesterase 4 inhibitor crisaborole and its emerging role in AD. She reviewed the results of a large phase 3 trial of crisaborole therapy for patients aged 2 years or older with mild to moderate AD.2 Crisaborole ointment was applied twice daily for 28 days. The primary outcome measured was an investigator static global assessment score of clear or almost clear, which is a score for AD based on the degree of erythema, presence of oozing and crusting, and presence of induration or papulation. Overall, 32.8% of patients treated with crisaborole achieved success compared to 25.4% of vehicle-treated patients. The control patients were still given a vehicle to apply, which can function as therapy to help repair the barrier of AD and thus theoretically reduced the percentage gap between patients who met success with and without crisaborole therapy. Furthermore, only 4% of patients reported adverse effects such as burning and stinging with application of crisaborole in contrast to topical calcineurin inhibitors, which can elicit symptoms up to 50% of the time.2 In summary, this lecture reviewed the first new topical treatment for AD in 15 years.
Take-Home Point
Crisaborole ointment is a novel topical phosphodiesterase 4 inhibitor approved for mild to moderate AD in patients 2 years of age and older.
“The Truth About Pediatric Contact Dermatitis” by Sharon Jacob, MD (Loma Linda University, California)
In this session, Dr. Jacob discussed how she approaches pediatric patients with suspected contact dermatitis and elaborated on the common allergens unique to this patient population. Furthermore, she explained the substantial role of nickel in pediatric contact dermatitis, citing a study performed in Denmark and the United States, which tested 212 toys for nickel using the dimethylglyoxime test and found that 34.4% of toys did in fact release nickel.3 Additional studies have shown that nickel released from children’s toys is deposited on the skin, even with short contact times such as 30 minutes on one or more occasions within 2 weeks.3,4 She is currently evaluating the presence of nickel in locales frequented by children such as schools, libraries, and supermarkets. Interestingly, she anecdotally found that a pediatric eczematous eruption in a spiralized distribution of the legs can be attributed to the presence of nickel in school chairs, and the morphology is secondary to children wrapping their legs around the chairs. In conclusion, she reiterated that nickel continues to be the top allergen among pediatric patients, and states that additional allergens for patch testing in this population are unique to their adult counterparts.
Take-Home Point
Nickel is an ubiquitous allergen for pediatric contact dermatitis; additionally, the list of allergens for patch testing should be tailored to this patient population.
“When to Image, When to Sedate” by Annette Wagner, MD (Northwestern Medicine, Chicago, Illinois)
This lecture was a 3-part discussion on the safety of general anesthesia in children, when to image children, and when sedation may be worth the risk. Dr. Wagner shared her pearls for when children younger than 3 years may benefit from dermatologic procedures that involve general anesthesia. Large congenital lesions of the scalp or face that require tissue expansion or multiple stages may be best performed at a younger age due to the flexibility of the infant scalp, providing the best outcome. Additional considerations include a questionable malignant diagnosis in which a punch biopsy is not enough, rapidly growing facial lesions, Spitz nevi of the face, congenital lesions with no available therapy, and nonhealing refractory lesions causing severe pain. The general rule proposed was intervention for single procedures lasting less than 1 hour that otherwise would result in a worse outcome if postponed. Finally, she concluded to always advocate for your patient, to wait if the outcome will be the same regardless of timing, and to be frank about not knowing the risks of general anesthesia in this population. The resource, SmartTots (http://smarttots.org) provides current consensus statements and ongoing research on the use and safety of general anesthesia in children.
Take-Home Point
General sedation may be considered for short pediatric procedures that will result in a worse outcome if postponed.
“Highlights From the Pediatric Literature” by Katherine Marks, DO (Geisinger, Danville and Wilkes-Barre, Pennsylvania)
Dr. Marks discussed numerous emerging pediatric dermatology articles. One article looked at 40 infants with proliferating infantile hemangiomas (IHs) who had timolol gel 0.5% applied twice daily.5 The primary outcomes were the urinary excretion and serum levels of timolol as well as the clinical response to therapy measured by a visual analog scale at monthly visits. A urinalysis collected 3 to 4 hours after timolol application was found to be positive in 83% (20/24) of the tested patients; the first 3 positive infants were then sent to have their serum timolol levels drawn and also were found to be positive, though substantially small levels (median, 0.16 ng/mL). The 3 patients tested had small IHs on the face with no ulceration. None of these patients experienced adverse effects and all of the IHs significantly (P<.001) improved with therapy. The authors stated that even though the absorption was minimal, it is wise to be cognizant about the use of timolol in certain patient demographics such as preterm or young infants with large ulcerating IHs.5
Take-Home Point
Systemic absorption with topical timolol occurs, albeit substantially small; be judicious about giving this medication in select patient populations with ulcerated hemangiomas.
Acknowledgment
The author thanks the presenters for their review and contributions to this article.
This article exhibits key pediatric dermatology pearls garnered at the 2017 Annual Meeting of the American Academy of Dermatology (AAD) in Orlando, Florida (March 3–7, 2017). Highlights from both the Society for Pediatric Dermatology pre-AAD meeting (March 2, 2017) and the AAD general meeting sessions are included. This discussion is intended to help maximize care of our pediatric patients in dermatology and present high-yield take-home points from the AAD that can be readily transferred to our patient care.
“New Tools for Your Therapeutic Toolbox” by Erin Mathes, MD (University of California, San Francisco)
During this lecture at the Society for Pediatric Dermatology meeting, Dr. Mathes discussed a randomized controlled trial that took place in 2014 in both the United States and the United Kingdom to assess skin barrier enhancement to reduce the incidence of atopic dermatitis (AD) in 124 high-risk infants.1 The high-risk infants had either a parent or sibling with physician-diagnosed AD, asthma, or rhinitis, or a first-degree relative with an aforementioned condition. Full-body emollient therapy was applied at least once daily within 3 weeks of birth for 6 months, while the control arm did not use emollient. Parents were allowed to choose from the following emollients: sunflower seed oil, moisturizing cream, or ointment. The primary outcome was the incidence of AD at 6 months. The authors found a 43% incidence of AD in the control group compared to 22% in the emollient group, amounting to a relative risk reduction of approximately 50%.1
Emollients in AD are hypothesized to help through the enhanced barrier function and decreased penetration of irritant substances and allergens. This study is vital given the ease of use of emollients and the foreseeable substantial impact on reduced health care costs associated with the decreased incidence of AD.
Take-Home Point
Full-body emollient therapy within 3 weeks of birth may reduce the incidence of AD in high-risk infants.
Dr. Mathes also discussed the novel topical phosphodiesterase 4 inhibitor crisaborole and its emerging role in AD. She reviewed the results of a large phase 3 trial of crisaborole therapy for patients aged 2 years or older with mild to moderate AD.2 Crisaborole ointment was applied twice daily for 28 days. The primary outcome measured was an investigator static global assessment score of clear or almost clear, which is a score for AD based on the degree of erythema, presence of oozing and crusting, and presence of induration or papulation. Overall, 32.8% of patients treated with crisaborole achieved success compared to 25.4% of vehicle-treated patients. The control patients were still given a vehicle to apply, which can function as therapy to help repair the barrier of AD and thus theoretically reduced the percentage gap between patients who met success with and without crisaborole therapy. Furthermore, only 4% of patients reported adverse effects such as burning and stinging with application of crisaborole in contrast to topical calcineurin inhibitors, which can elicit symptoms up to 50% of the time.2 In summary, this lecture reviewed the first new topical treatment for AD in 15 years.
Take-Home Point
Crisaborole ointment is a novel topical phosphodiesterase 4 inhibitor approved for mild to moderate AD in patients 2 years of age and older.
“The Truth About Pediatric Contact Dermatitis” by Sharon Jacob, MD (Loma Linda University, California)
In this session, Dr. Jacob discussed how she approaches pediatric patients with suspected contact dermatitis and elaborated on the common allergens unique to this patient population. Furthermore, she explained the substantial role of nickel in pediatric contact dermatitis, citing a study performed in Denmark and the United States, which tested 212 toys for nickel using the dimethylglyoxime test and found that 34.4% of toys did in fact release nickel.3 Additional studies have shown that nickel released from children’s toys is deposited on the skin, even with short contact times such as 30 minutes on one or more occasions within 2 weeks.3,4 She is currently evaluating the presence of nickel in locales frequented by children such as schools, libraries, and supermarkets. Interestingly, she anecdotally found that a pediatric eczematous eruption in a spiralized distribution of the legs can be attributed to the presence of nickel in school chairs, and the morphology is secondary to children wrapping their legs around the chairs. In conclusion, she reiterated that nickel continues to be the top allergen among pediatric patients, and states that additional allergens for patch testing in this population are unique to their adult counterparts.
Take-Home Point
Nickel is an ubiquitous allergen for pediatric contact dermatitis; additionally, the list of allergens for patch testing should be tailored to this patient population.
“When to Image, When to Sedate” by Annette Wagner, MD (Northwestern Medicine, Chicago, Illinois)
This lecture was a 3-part discussion on the safety of general anesthesia in children, when to image children, and when sedation may be worth the risk. Dr. Wagner shared her pearls for when children younger than 3 years may benefit from dermatologic procedures that involve general anesthesia. Large congenital lesions of the scalp or face that require tissue expansion or multiple stages may be best performed at a younger age due to the flexibility of the infant scalp, providing the best outcome. Additional considerations include a questionable malignant diagnosis in which a punch biopsy is not enough, rapidly growing facial lesions, Spitz nevi of the face, congenital lesions with no available therapy, and nonhealing refractory lesions causing severe pain. The general rule proposed was intervention for single procedures lasting less than 1 hour that otherwise would result in a worse outcome if postponed. Finally, she concluded to always advocate for your patient, to wait if the outcome will be the same regardless of timing, and to be frank about not knowing the risks of general anesthesia in this population. The resource, SmartTots (http://smarttots.org) provides current consensus statements and ongoing research on the use and safety of general anesthesia in children.
Take-Home Point
General sedation may be considered for short pediatric procedures that will result in a worse outcome if postponed.
“Highlights From the Pediatric Literature” by Katherine Marks, DO (Geisinger, Danville and Wilkes-Barre, Pennsylvania)
Dr. Marks discussed numerous emerging pediatric dermatology articles. One article looked at 40 infants with proliferating infantile hemangiomas (IHs) who had timolol gel 0.5% applied twice daily.5 The primary outcomes were the urinary excretion and serum levels of timolol as well as the clinical response to therapy measured by a visual analog scale at monthly visits. A urinalysis collected 3 to 4 hours after timolol application was found to be positive in 83% (20/24) of the tested patients; the first 3 positive infants were then sent to have their serum timolol levels drawn and also were found to be positive, though substantially small levels (median, 0.16 ng/mL). The 3 patients tested had small IHs on the face with no ulceration. None of these patients experienced adverse effects and all of the IHs significantly (P<.001) improved with therapy. The authors stated that even though the absorption was minimal, it is wise to be cognizant about the use of timolol in certain patient demographics such as preterm or young infants with large ulcerating IHs.5
Take-Home Point
Systemic absorption with topical timolol occurs, albeit substantially small; be judicious about giving this medication in select patient populations with ulcerated hemangiomas.
Acknowledgment
The author thanks the presenters for their review and contributions to this article.
- Simpson EL, Chalmers JR, Hanifin JM, et al. Emollient enhancement of the skin barrier from birth offers effective atopic dermatitis prevention. J Allergy Clin Immunol. 2014;134:818-823.
- Paller AS, Tom WL, Lebwohl MG, et al. Efficacy and safety of crisaborole ointment, a novel phosphodiesterase 4 inhibitor for the topical treatment of AD in children and adults [published online July 11, 2016]. J Am Acad Dermatol. 2016;75:494-503.
- Jensen P, Hamann D, Hamann CR, et al. Nickel and cobalt release from children’s toys purchased in Denmark and the United States. Dermatitis. 2014;25:356-365.
- Overgaard LE, Engebretsen KA, Jensen P, et al. Nickel released from children’s toys is deposited on the skin. Contact Dermatitis. 2016;74:380-381.
- Weibel L, Barysch MJ, Scheer HS, et al. Topical timolol for infantile hemangiomas: evidence for efficacy and degree of systemic absorption [published online February 3, 2016]. Pediatr Dermatol. 2016;33:184-190.
- Simpson EL, Chalmers JR, Hanifin JM, et al. Emollient enhancement of the skin barrier from birth offers effective atopic dermatitis prevention. J Allergy Clin Immunol. 2014;134:818-823.
- Paller AS, Tom WL, Lebwohl MG, et al. Efficacy and safety of crisaborole ointment, a novel phosphodiesterase 4 inhibitor for the topical treatment of AD in children and adults [published online July 11, 2016]. J Am Acad Dermatol. 2016;75:494-503.
- Jensen P, Hamann D, Hamann CR, et al. Nickel and cobalt release from children’s toys purchased in Denmark and the United States. Dermatitis. 2014;25:356-365.
- Overgaard LE, Engebretsen KA, Jensen P, et al. Nickel released from children’s toys is deposited on the skin. Contact Dermatitis. 2016;74:380-381.
- Weibel L, Barysch MJ, Scheer HS, et al. Topical timolol for infantile hemangiomas: evidence for efficacy and degree of systemic absorption [published online February 3, 2016]. Pediatr Dermatol. 2016;33:184-190.
Inotuzumab ozogamicin tied to sinusoidal obstruction syndrome in ALL
Inotuzumab ozogamicin therapy significantly increased the risk of sinusoidal obstruction syndrome (veno-occlusive disease) among adults with relapsed or refractory B-cell precursor acute lymphoblastic leukemia (ALL), especially when they also received follow-up hematopoietic stem cell transplantation, according to a safety analysis from the INO-VATE trial.
After a median of 9 weeks of treatment, 13% of 164 patients who received inotuzumab ozogamicin (Besponsa, Wyeth/Pfizer) developed sinusoidal obstruction syndrome, compared with less than 1% of 143 patients who received standard care, reported Hagop M. Kantarjian, MD, of the University of Texas MD Anderson Cancer Center in Houston, and his associates (Lancet Haematol. 2017 Jul 4. doi: 10.1016/ S2352-3026[17]30103-5).
Follow-up treatment with HSCT increased the risk of sinusoidal obstruction syndrome in both the intervention (22%) and standard-care (3%) groups. Among patients who did not undergo HSCT, rates of this adverse event were 3% and 0%, respectively. Five patients died from sinusoidal obstruction syndrome, all of whom received both inotuzumab ozogamicin and HSCT. The findings earned the newly approved regimen a boxed warning for severe hepatotoxicity.
The open-label, phase 3, multicenter INO-VATE study included 326 adults with CD22-positive, Philadelphia chromosome–negative or Philadelphia chromosome–positive relapsed or refractory B-cell precursor ALL. The safety analysis included 305 patients. Rates of treatment-emergent hepatotoxicities, of all grades, were 51% with inotuzumab ozogamicin and 34% with standard care. Most adverse hepatic events were grade 1-2 liver-related laboratory abnormalities, but 8% of inotuzumab ozogamicin recipients developed grade 3 or higher sinusoidal obstruction syndrome, versus less than 1% of the control group.
“After follow-up HSCT, the frequency of sinusoidal obstruction syndrome was 50% or higher in the following subgroups: patients aged 65 years or older, patients with last available pre-HSCT serum bilirubin concentration more than or equal to the upper limit of normal, and patients who received conditioning regimens with two alkylating agents,” Dr. Kantarjian and his fellow investigators wrote. Conditioning regimens that included thiotepa markedly increased the risk of sinusoidal obstruction syndrome. Additional risk factors included HSCT before study enrollment, history of liver disease, and a final pre-HSCT platelet count of less than 100 × 109 platelets per L.
Rates of sinusoidal obstruction syndrome were 42% with four to six cycles of inotuzumab ozogamicin, 23% with three cycles, 19% with two cycles, and 8% with one cycle, said the investigators. In multivariate analysis, conditioning with two alkylating agents (P = .02 compared with one alkylating agent) and pre-HSCT bilirubin of at least the upper limit of normal (P = .01) significantly increased the risk of sinusoidal obstruction syndrome during or after treatment with inotuzumab ozogamicin.
Notably, inotuzumab ozogamicin did not significantly increase the chances of survival compared with standard care among patients who also received follow-up HSCT (hazard ratio, 1.3; 97.5% confidence interval, 0.66 to 2.3; P = 0.77). Among HSCT recipients, the chances of surviving to 24 months were 39% (95% CI, 28%-50%) with inotuzumab ozogamicin and 29% (11%-49%) with standard care. Nonetheless, HSCT “offers possibility of cure in the relapsed or recurrent [ALL] setting,” the researchers wrote. Clinicians should be especially wary of sinusoidal obstruction syndrome if patients are 65 years or older, received HSCT before inotuzumab ozogamicin treatment, or have a baseline history of liver disease, they said. Strategies to minimize risk include shortening the duration of inotuzumab ozogamicin treatment and avoiding conditioning regimens that contain two alkylating agents.
Pfizer funded and collaborated in the trial. Dr. Kantarjian disclosed ties to Pfizer and numerous other pharmaceutical companies.
Inotuzumab ozogamicin therapy significantly increased the risk of sinusoidal obstruction syndrome (veno-occlusive disease) among adults with relapsed or refractory B-cell precursor acute lymphoblastic leukemia (ALL), especially when they also received follow-up hematopoietic stem cell transplantation, according to a safety analysis from the INO-VATE trial.
After a median of 9 weeks of treatment, 13% of 164 patients who received inotuzumab ozogamicin (Besponsa, Wyeth/Pfizer) developed sinusoidal obstruction syndrome, compared with less than 1% of 143 patients who received standard care, reported Hagop M. Kantarjian, MD, of the University of Texas MD Anderson Cancer Center in Houston, and his associates (Lancet Haematol. 2017 Jul 4. doi: 10.1016/ S2352-3026[17]30103-5).
Follow-up treatment with HSCT increased the risk of sinusoidal obstruction syndrome in both the intervention (22%) and standard-care (3%) groups. Among patients who did not undergo HSCT, rates of this adverse event were 3% and 0%, respectively. Five patients died from sinusoidal obstruction syndrome, all of whom received both inotuzumab ozogamicin and HSCT. The findings earned the newly approved regimen a boxed warning for severe hepatotoxicity.
The open-label, phase 3, multicenter INO-VATE study included 326 adults with CD22-positive, Philadelphia chromosome–negative or Philadelphia chromosome–positive relapsed or refractory B-cell precursor ALL. The safety analysis included 305 patients. Rates of treatment-emergent hepatotoxicities, of all grades, were 51% with inotuzumab ozogamicin and 34% with standard care. Most adverse hepatic events were grade 1-2 liver-related laboratory abnormalities, but 8% of inotuzumab ozogamicin recipients developed grade 3 or higher sinusoidal obstruction syndrome, versus less than 1% of the control group.
“After follow-up HSCT, the frequency of sinusoidal obstruction syndrome was 50% or higher in the following subgroups: patients aged 65 years or older, patients with last available pre-HSCT serum bilirubin concentration more than or equal to the upper limit of normal, and patients who received conditioning regimens with two alkylating agents,” Dr. Kantarjian and his fellow investigators wrote. Conditioning regimens that included thiotepa markedly increased the risk of sinusoidal obstruction syndrome. Additional risk factors included HSCT before study enrollment, history of liver disease, and a final pre-HSCT platelet count of less than 100 × 109 platelets per L.
Rates of sinusoidal obstruction syndrome were 42% with four to six cycles of inotuzumab ozogamicin, 23% with three cycles, 19% with two cycles, and 8% with one cycle, said the investigators. In multivariate analysis, conditioning with two alkylating agents (P = .02 compared with one alkylating agent) and pre-HSCT bilirubin of at least the upper limit of normal (P = .01) significantly increased the risk of sinusoidal obstruction syndrome during or after treatment with inotuzumab ozogamicin.
Notably, inotuzumab ozogamicin did not significantly increase the chances of survival compared with standard care among patients who also received follow-up HSCT (hazard ratio, 1.3; 97.5% confidence interval, 0.66 to 2.3; P = 0.77). Among HSCT recipients, the chances of surviving to 24 months were 39% (95% CI, 28%-50%) with inotuzumab ozogamicin and 29% (11%-49%) with standard care. Nonetheless, HSCT “offers possibility of cure in the relapsed or recurrent [ALL] setting,” the researchers wrote. Clinicians should be especially wary of sinusoidal obstruction syndrome if patients are 65 years or older, received HSCT before inotuzumab ozogamicin treatment, or have a baseline history of liver disease, they said. Strategies to minimize risk include shortening the duration of inotuzumab ozogamicin treatment and avoiding conditioning regimens that contain two alkylating agents.
Pfizer funded and collaborated in the trial. Dr. Kantarjian disclosed ties to Pfizer and numerous other pharmaceutical companies.
Inotuzumab ozogamicin therapy significantly increased the risk of sinusoidal obstruction syndrome (veno-occlusive disease) among adults with relapsed or refractory B-cell precursor acute lymphoblastic leukemia (ALL), especially when they also received follow-up hematopoietic stem cell transplantation, according to a safety analysis from the INO-VATE trial.
After a median of 9 weeks of treatment, 13% of 164 patients who received inotuzumab ozogamicin (Besponsa, Wyeth/Pfizer) developed sinusoidal obstruction syndrome, compared with less than 1% of 143 patients who received standard care, reported Hagop M. Kantarjian, MD, of the University of Texas MD Anderson Cancer Center in Houston, and his associates (Lancet Haematol. 2017 Jul 4. doi: 10.1016/ S2352-3026[17]30103-5).
Follow-up treatment with HSCT increased the risk of sinusoidal obstruction syndrome in both the intervention (22%) and standard-care (3%) groups. Among patients who did not undergo HSCT, rates of this adverse event were 3% and 0%, respectively. Five patients died from sinusoidal obstruction syndrome, all of whom received both inotuzumab ozogamicin and HSCT. The findings earned the newly approved regimen a boxed warning for severe hepatotoxicity.
The open-label, phase 3, multicenter INO-VATE study included 326 adults with CD22-positive, Philadelphia chromosome–negative or Philadelphia chromosome–positive relapsed or refractory B-cell precursor ALL. The safety analysis included 305 patients. Rates of treatment-emergent hepatotoxicities, of all grades, were 51% with inotuzumab ozogamicin and 34% with standard care. Most adverse hepatic events were grade 1-2 liver-related laboratory abnormalities, but 8% of inotuzumab ozogamicin recipients developed grade 3 or higher sinusoidal obstruction syndrome, versus less than 1% of the control group.
“After follow-up HSCT, the frequency of sinusoidal obstruction syndrome was 50% or higher in the following subgroups: patients aged 65 years or older, patients with last available pre-HSCT serum bilirubin concentration more than or equal to the upper limit of normal, and patients who received conditioning regimens with two alkylating agents,” Dr. Kantarjian and his fellow investigators wrote. Conditioning regimens that included thiotepa markedly increased the risk of sinusoidal obstruction syndrome. Additional risk factors included HSCT before study enrollment, history of liver disease, and a final pre-HSCT platelet count of less than 100 × 109 platelets per L.
Rates of sinusoidal obstruction syndrome were 42% with four to six cycles of inotuzumab ozogamicin, 23% with three cycles, 19% with two cycles, and 8% with one cycle, said the investigators. In multivariate analysis, conditioning with two alkylating agents (P = .02 compared with one alkylating agent) and pre-HSCT bilirubin of at least the upper limit of normal (P = .01) significantly increased the risk of sinusoidal obstruction syndrome during or after treatment with inotuzumab ozogamicin.
Notably, inotuzumab ozogamicin did not significantly increase the chances of survival compared with standard care among patients who also received follow-up HSCT (hazard ratio, 1.3; 97.5% confidence interval, 0.66 to 2.3; P = 0.77). Among HSCT recipients, the chances of surviving to 24 months were 39% (95% CI, 28%-50%) with inotuzumab ozogamicin and 29% (11%-49%) with standard care. Nonetheless, HSCT “offers possibility of cure in the relapsed or recurrent [ALL] setting,” the researchers wrote. Clinicians should be especially wary of sinusoidal obstruction syndrome if patients are 65 years or older, received HSCT before inotuzumab ozogamicin treatment, or have a baseline history of liver disease, they said. Strategies to minimize risk include shortening the duration of inotuzumab ozogamicin treatment and avoiding conditioning regimens that contain two alkylating agents.
Pfizer funded and collaborated in the trial. Dr. Kantarjian disclosed ties to Pfizer and numerous other pharmaceutical companies.
FROM LANCET HAEMATOLOGY
Key clinical point: Treatment with inotuzumab ozogamicin (Besponsa, Wyeth/Pfizer) led to sinusoidal obstructive syndrome (veno-occlusive disease), especially after follow-up hematopoietic stem cell transplantation, compared with standard care for relapsed or refractory acute lymphoblastic leukemia.
Major finding: After a median of 9 weeks of treatment, rates of sinusoidal obstructive syndrome were 13% among inotuzumab ozogamicin recipients overall, 22% among those who also received HSCT, and less than 1% in the standard-care group.
Data source: A prespecified safety analysis of INO-VATE, an open-label, phase 3, multicenter trial of 326 adults with Philadelphia chromosome–negative or Philadelphia chromosome–positive relapsed or refractory B-cell precursor ALL.
Disclosures: Pfizer funded and collaborated in the trial. Dr. Kantarjian disclosed ties to Pfizer and numerous other pharmaceutical companies.